User login
By Catalina Matiz, M.D., and David Ginsberg
Nummular eczema
Nummular eczema is not an uncommon dermatosis that presents in pediatric and adult patients; its name, which derives from the Latin word nummulus (coin-like), refers to the coined-shape plaques that characterize this condition. It also has been referred to as discoid eczema and nummular dermatitis.1
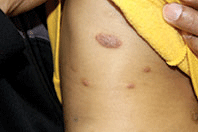
The lesions begin as erythematous papules and vesicles that extend into larger oval or circular plaques that often become crusted, and can later progress to dry and scaly plaques.1,2 Patients often complain of intense pruritus.1 The lesions can be single or multiple, and more commonly occur on the extensor extremities as well as the trunk, and rarely affect the neck and the head.1-3 The pathophysiology of nummular eczema is not fully understood. It can occur in patients that exhibit atopic manifestations such as atopic dermatitis and other allergies, but there has been no clear link found between nummular eczema and atopy.3,4
Many theories exist implicating causative factors including Staphylococcus aureus colonization and xerosis.1 Similarly, some physicians believe that patch testing can be useful in these patients because of the potential for exacerbation caused by environmental allergens, but there is still no agreement on the ultimate cause.5 There is a higher incidence in males than females, and in the pediatric population, it is more common among “school aged” children between the ages of 2-12.6 Overall, nummular eczema is more commonly seen in adults, but it can occur at any age.2,3,6
Differential diagnosis
Nummular eczema is commonly mistaken as tinea corporis.1 The coined shape lesions, from which nummular eczema gets its name, can resemble the characteristic annular shape plaques of “ring worm,” but a potassium hydroxide (KOH) test or a fungal culture are simple ways to differentiate between the two conditions.
Nummular eczema occasionally can be confused for psoriasis as both entities can present with oval plaques. Psoriasis lesions tend to be pinker and less erythematous than nummular eczema lesions and most psoriasis plaques present with a characteristic silver scale.7 Clinically, nummular eczema is frequently associated with extreme pruritus, while in psoriasis the pruritus is less prominent.7
A biopsy would yield a more definitive diagnosis in difficult cases. Histologically, nummular eczema resembles other forms of spongiotic dermatitis, while psoriasis has very distinct histological features.7 Differentiating between contact dermatitis and nummular eczema relies on a thorough history of known allergies and potential exposure to environmental allergens. If history alone does not yield a definitive diagnosis and a suspicion for contact allergy is high, patch testing could help support one diagnosis over the other.5
Treatment
The generally accepted first line therapy includes mid to high potency topical corticosteroids in an ointment preparation or else under occlusion.1,4 Other topical agents used include tar preparations and calcineurin inhibitors.4 Intralesional corticosteroid injection can be used to treat isolated lesions that fail to respond to topical treatments.4
As with almost all manifestations of dermatitis, general gentle skin care measures and daily moisturizing are recommended.1 For more severe cases in older children, narrow-band UVB light therapy can be helpful.1 Due to their efficacy in treatment of other forms of refractory dermatitis, systemic therapy with cyclosporine, azathioprine, mycophenolate mofetil, and methotrexate can be used in cases in which phototherapy fails or is not accessible.4
In cases recalcitrant to topical therapies, secondary staphylococcal infection always should be ruled out and treated with systemic antimicrobials such as first generation cephalosporins.1
References
- Eczematous eruptions in childhood in “Hurwitz Clinical Pediatric Dermatology,” 4th ed. (New York, N.Y.: Elsevier, pp. 59-60
- Acta Derm Venereol. 1961;41:453-60.
- Acta Derm Venereol. 1969;49(2):189-96.
- Australas J Dermatol. 2010 May;51(2):128-30.
- Contact Dermatitis. 1997 May;36(5):261-4.
- Ped Dermatol. 2012 Oct;29(5):580-3.
- Dermatol Ther. 2006 Mar-Apr;19(2):73-82.
Dr. Matiz is assistant professor of dermatology at Rady Children’s Hospital San Diego–University of California, San Diego and Mr. Ginsberg is a research associate at the hospital. Dr. Matiz and Mr. Ginsberg said they have no relevant financial disclosures.
By Catalina Matiz, M.D., and David Ginsberg
Nummular eczema
Nummular eczema is not an uncommon dermatosis that presents in pediatric and adult patients; its name, which derives from the Latin word nummulus (coin-like), refers to the coined-shape plaques that characterize this condition. It also has been referred to as discoid eczema and nummular dermatitis.1
The lesions begin as erythematous papules and vesicles that extend into larger oval or circular plaques that often become crusted, and can later progress to dry and scaly plaques.1,2 Patients often complain of intense pruritus.1 The lesions can be single or multiple, and more commonly occur on the extensor extremities as well as the trunk, and rarely affect the neck and the head.1-3 The pathophysiology of nummular eczema is not fully understood. It can occur in patients that exhibit atopic manifestations such as atopic dermatitis and other allergies, but there has been no clear link found between nummular eczema and atopy.3,4
Many theories exist implicating causative factors including Staphylococcus aureus colonization and xerosis.1 Similarly, some physicians believe that patch testing can be useful in these patients because of the potential for exacerbation caused by environmental allergens, but there is still no agreement on the ultimate cause.5 There is a higher incidence in males than females, and in the pediatric population, it is more common among “school aged” children between the ages of 2-12.6 Overall, nummular eczema is more commonly seen in adults, but it can occur at any age.2,3,6
Differential diagnosis
Nummular eczema is commonly mistaken as tinea corporis.1 The coined shape lesions, from which nummular eczema gets its name, can resemble the characteristic annular shape plaques of “ring worm,” but a potassium hydroxide (KOH) test or a fungal culture are simple ways to differentiate between the two conditions.
Nummular eczema occasionally can be confused for psoriasis as both entities can present with oval plaques. Psoriasis lesions tend to be pinker and less erythematous than nummular eczema lesions and most psoriasis plaques present with a characteristic silver scale.7 Clinically, nummular eczema is frequently associated with extreme pruritus, while in psoriasis the pruritus is less prominent.7
A biopsy would yield a more definitive diagnosis in difficult cases. Histologically, nummular eczema resembles other forms of spongiotic dermatitis, while psoriasis has very distinct histological features.7 Differentiating between contact dermatitis and nummular eczema relies on a thorough history of known allergies and potential exposure to environmental allergens. If history alone does not yield a definitive diagnosis and a suspicion for contact allergy is high, patch testing could help support one diagnosis over the other.5
Treatment
The generally accepted first line therapy includes mid to high potency topical corticosteroids in an ointment preparation or else under occlusion.1,4 Other topical agents used include tar preparations and calcineurin inhibitors.4 Intralesional corticosteroid injection can be used to treat isolated lesions that fail to respond to topical treatments.4
As with almost all manifestations of dermatitis, general gentle skin care measures and daily moisturizing are recommended.1 For more severe cases in older children, narrow-band UVB light therapy can be helpful.1 Due to their efficacy in treatment of other forms of refractory dermatitis, systemic therapy with cyclosporine, azathioprine, mycophenolate mofetil, and methotrexate can be used in cases in which phototherapy fails or is not accessible.4
In cases recalcitrant to topical therapies, secondary staphylococcal infection always should be ruled out and treated with systemic antimicrobials such as first generation cephalosporins.1
References
- Eczematous eruptions in childhood in “Hurwitz Clinical Pediatric Dermatology,” 4th ed. (New York, N.Y.: Elsevier, pp. 59-60
- Acta Derm Venereol. 1961;41:453-60.
- Acta Derm Venereol. 1969;49(2):189-96.
- Australas J Dermatol. 2010 May;51(2):128-30.
- Contact Dermatitis. 1997 May;36(5):261-4.
- Ped Dermatol. 2012 Oct;29(5):580-3.
- Dermatol Ther. 2006 Mar-Apr;19(2):73-82.
Dr. Matiz is assistant professor of dermatology at Rady Children’s Hospital San Diego–University of California, San Diego and Mr. Ginsberg is a research associate at the hospital. Dr. Matiz and Mr. Ginsberg said they have no relevant financial disclosures.
By Catalina Matiz, M.D., and David Ginsberg
Nummular eczema
Nummular eczema is not an uncommon dermatosis that presents in pediatric and adult patients; its name, which derives from the Latin word nummulus (coin-like), refers to the coined-shape plaques that characterize this condition. It also has been referred to as discoid eczema and nummular dermatitis.1
The lesions begin as erythematous papules and vesicles that extend into larger oval or circular plaques that often become crusted, and can later progress to dry and scaly plaques.1,2 Patients often complain of intense pruritus.1 The lesions can be single or multiple, and more commonly occur on the extensor extremities as well as the trunk, and rarely affect the neck and the head.1-3 The pathophysiology of nummular eczema is not fully understood. It can occur in patients that exhibit atopic manifestations such as atopic dermatitis and other allergies, but there has been no clear link found between nummular eczema and atopy.3,4
Many theories exist implicating causative factors including Staphylococcus aureus colonization and xerosis.1 Similarly, some physicians believe that patch testing can be useful in these patients because of the potential for exacerbation caused by environmental allergens, but there is still no agreement on the ultimate cause.5 There is a higher incidence in males than females, and in the pediatric population, it is more common among “school aged” children between the ages of 2-12.6 Overall, nummular eczema is more commonly seen in adults, but it can occur at any age.2,3,6
Differential diagnosis
Nummular eczema is commonly mistaken as tinea corporis.1 The coined shape lesions, from which nummular eczema gets its name, can resemble the characteristic annular shape plaques of “ring worm,” but a potassium hydroxide (KOH) test or a fungal culture are simple ways to differentiate between the two conditions.
Nummular eczema occasionally can be confused for psoriasis as both entities can present with oval plaques. Psoriasis lesions tend to be pinker and less erythematous than nummular eczema lesions and most psoriasis plaques present with a characteristic silver scale.7 Clinically, nummular eczema is frequently associated with extreme pruritus, while in psoriasis the pruritus is less prominent.7
A biopsy would yield a more definitive diagnosis in difficult cases. Histologically, nummular eczema resembles other forms of spongiotic dermatitis, while psoriasis has very distinct histological features.7 Differentiating between contact dermatitis and nummular eczema relies on a thorough history of known allergies and potential exposure to environmental allergens. If history alone does not yield a definitive diagnosis and a suspicion for contact allergy is high, patch testing could help support one diagnosis over the other.5
Treatment
The generally accepted first line therapy includes mid to high potency topical corticosteroids in an ointment preparation or else under occlusion.1,4 Other topical agents used include tar preparations and calcineurin inhibitors.4 Intralesional corticosteroid injection can be used to treat isolated lesions that fail to respond to topical treatments.4
As with almost all manifestations of dermatitis, general gentle skin care measures and daily moisturizing are recommended.1 For more severe cases in older children, narrow-band UVB light therapy can be helpful.1 Due to their efficacy in treatment of other forms of refractory dermatitis, systemic therapy with cyclosporine, azathioprine, mycophenolate mofetil, and methotrexate can be used in cases in which phototherapy fails or is not accessible.4
In cases recalcitrant to topical therapies, secondary staphylococcal infection always should be ruled out and treated with systemic antimicrobials such as first generation cephalosporins.1
References
- Eczematous eruptions in childhood in “Hurwitz Clinical Pediatric Dermatology,” 4th ed. (New York, N.Y.: Elsevier, pp. 59-60
- Acta Derm Venereol. 1961;41:453-60.
- Acta Derm Venereol. 1969;49(2):189-96.
- Australas J Dermatol. 2010 May;51(2):128-30.
- Contact Dermatitis. 1997 May;36(5):261-4.
- Ped Dermatol. 2012 Oct;29(5):580-3.
- Dermatol Ther. 2006 Mar-Apr;19(2):73-82.
Dr. Matiz is assistant professor of dermatology at Rady Children’s Hospital San Diego–University of California, San Diego and Mr. Ginsberg is a research associate at the hospital. Dr. Matiz and Mr. Ginsberg said they have no relevant financial disclosures.
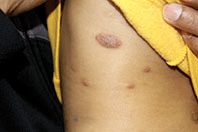
A 9-month-old male with no significant previous medical history presents with a very itchy rash that has been present for 6 weeks. His mother reports that the lesions began as small red bumps on the extremities and his torso, that developed over the course of a few weeks into large round, red, very pruritic plaques. He has been treated with an antifungal cream for several weeks without resolution, and most recently his mother has been applying hydrocortisone 2.5% cream with no improvement either. On exam, the patient is a well appearing infant, who is visibly irritated due to the pruritus accompanying his rash. There are several 1-cm to 4-cm round and oval dry, scaly, erythematous plaques on the trunk (see photo) and a few on the extremities. There is no generalized xerosis.