User login
Dr. Catalina Matiz and David Ginsberg discuss the diagnosis and treatment of phytophotodermatitis.
Phytophotodermatitis
The term phytophotodermatitis was first used in 1942 by Robert Klaber, but knowledge of this condition dates back as far as 1500 BC.1,2 It is a nonimmune reaction caused by exposure to chemicals called furocoumarins and psoralens, found in a variety of plants and fruits such as lemons, limes, celery, parsnips, figs, carrots, dill, mustard, and rindweed.1,2
When these chemicals get in contact with the skin and are then exposed to UV light from the sun, a phototoxic reaction occurs. This reaction leads to cell membrane damage and cell death, which after the acute insult has resolved results in postinflammatory hyperpigmentation that may last months and is not responsive to bleaching skin treatments.1,2
Studies have shown that long-wave length UV radiation is the best trigger to induce this irritating reaction.2 There have been rare reports of photosensitivity reactions due to ingestion of large quantities of plants containing furocoumarins and psoralens.3 Plants known to cause phytophotodermatitis are found in almost every country across the globe, and exposure does not have to just be to the fruit, but contact with the leaves or sap also can induce the reaction.2-4 Typically after contact with the plant, followed by sun exposure, erythema will begin within 1 to 2 days, followed by bullae and vesicles, which tend to coalesce and burst over the following days. The patient is left with hyperpigmentation.2-4
Differential diagnosis
This condition can be difficult to diagnose and is often confused with type IV hypersensitivity reaction, eczema, herpes simplex virus (HSV), and burns, potentially leading to suspicion of child abuse.4,5 A thorough and detailed history is essential to correctly making the diagnosis and ruling out other potential causes.
Because the cause in children is often due to exposure to certain plants, unsupervised time outdoors leading to a rash may lead parents to think of poison ivy or poison oak, which are type IV hypersensitivity reactions.4,5 Although the rash may appear in a similar time course, the evolution to hyperpigmented patches is a distinguishing feature that helps to make the diagnosis of phytophotodermatitis.4 The postinflammatory hyperpigmentation, along with the clinical course, also can help differentiate it from burns and HSV infections, which it sometimes is mistaken for due to the bullous and vesicular lesions.4,5
Treatment
Counseling for avoidance of the exposure in the future is the most important aspect of treatment in order to prevent recurrences. Depending on the extent of the inflammatory reaction prior to the hyperpigmentation, no treatment may be needed for mild cases, but for more extreme bullous reactions, systemic steroids may be used.4
Topical corticosteroids and sun avoidance are the mainstays for treating mild to moderate cases. UV avoidance can be difficult because the long wave-length UV radiation that causes this reaction is not blocked by windows, and therefore it is important to keep affected areas covered even while indoors during daylight hours.4
There is no effective treatment for the hyperpigmented lesions. Patients need to be informed that this may resolve in months.
References
- Br J Dermatol. 1942;54(7):193-211.
- Clin Dermatol. 1986 Apr-Jun;4(2):102-21.
- Arch Dermatol. 1990 Oct;126(10):1334-6.
- J Am Acad Dermatol. 2007 Nov;57(5 Suppl):S88-91.
- Arch Fam Med. 2000 Jan;9(1):88.
Dr. Matiz is assistant professor of dermatology at Rady Children’s Hospital San Diego–University of California, San Diego, and Mr. Ginsberg is a research associate at the hospital. Dr. Matiz and Mr. Ginsberg said they have no relevant financial disclosures.
Dr. Catalina Matiz and David Ginsberg discuss the diagnosis and treatment of phytophotodermatitis.
Phytophotodermatitis
The term phytophotodermatitis was first used in 1942 by Robert Klaber, but knowledge of this condition dates back as far as 1500 BC.1,2 It is a nonimmune reaction caused by exposure to chemicals called furocoumarins and psoralens, found in a variety of plants and fruits such as lemons, limes, celery, parsnips, figs, carrots, dill, mustard, and rindweed.1,2
When these chemicals get in contact with the skin and are then exposed to UV light from the sun, a phototoxic reaction occurs. This reaction leads to cell membrane damage and cell death, which after the acute insult has resolved results in postinflammatory hyperpigmentation that may last months and is not responsive to bleaching skin treatments.1,2
Studies have shown that long-wave length UV radiation is the best trigger to induce this irritating reaction.2 There have been rare reports of photosensitivity reactions due to ingestion of large quantities of plants containing furocoumarins and psoralens.3 Plants known to cause phytophotodermatitis are found in almost every country across the globe, and exposure does not have to just be to the fruit, but contact with the leaves or sap also can induce the reaction.2-4 Typically after contact with the plant, followed by sun exposure, erythema will begin within 1 to 2 days, followed by bullae and vesicles, which tend to coalesce and burst over the following days. The patient is left with hyperpigmentation.2-4
Differential diagnosis
This condition can be difficult to diagnose and is often confused with type IV hypersensitivity reaction, eczema, herpes simplex virus (HSV), and burns, potentially leading to suspicion of child abuse.4,5 A thorough and detailed history is essential to correctly making the diagnosis and ruling out other potential causes.
Because the cause in children is often due to exposure to certain plants, unsupervised time outdoors leading to a rash may lead parents to think of poison ivy or poison oak, which are type IV hypersensitivity reactions.4,5 Although the rash may appear in a similar time course, the evolution to hyperpigmented patches is a distinguishing feature that helps to make the diagnosis of phytophotodermatitis.4 The postinflammatory hyperpigmentation, along with the clinical course, also can help differentiate it from burns and HSV infections, which it sometimes is mistaken for due to the bullous and vesicular lesions.4,5
Treatment
Counseling for avoidance of the exposure in the future is the most important aspect of treatment in order to prevent recurrences. Depending on the extent of the inflammatory reaction prior to the hyperpigmentation, no treatment may be needed for mild cases, but for more extreme bullous reactions, systemic steroids may be used.4
Topical corticosteroids and sun avoidance are the mainstays for treating mild to moderate cases. UV avoidance can be difficult because the long wave-length UV radiation that causes this reaction is not blocked by windows, and therefore it is important to keep affected areas covered even while indoors during daylight hours.4
There is no effective treatment for the hyperpigmented lesions. Patients need to be informed that this may resolve in months.
References
- Br J Dermatol. 1942;54(7):193-211.
- Clin Dermatol. 1986 Apr-Jun;4(2):102-21.
- Arch Dermatol. 1990 Oct;126(10):1334-6.
- J Am Acad Dermatol. 2007 Nov;57(5 Suppl):S88-91.
- Arch Fam Med. 2000 Jan;9(1):88.
Dr. Matiz is assistant professor of dermatology at Rady Children’s Hospital San Diego–University of California, San Diego, and Mr. Ginsberg is a research associate at the hospital. Dr. Matiz and Mr. Ginsberg said they have no relevant financial disclosures.
Dr. Catalina Matiz and David Ginsberg discuss the diagnosis and treatment of phytophotodermatitis.
Phytophotodermatitis
The term phytophotodermatitis was first used in 1942 by Robert Klaber, but knowledge of this condition dates back as far as 1500 BC.1,2 It is a nonimmune reaction caused by exposure to chemicals called furocoumarins and psoralens, found in a variety of plants and fruits such as lemons, limes, celery, parsnips, figs, carrots, dill, mustard, and rindweed.1,2
When these chemicals get in contact with the skin and are then exposed to UV light from the sun, a phototoxic reaction occurs. This reaction leads to cell membrane damage and cell death, which after the acute insult has resolved results in postinflammatory hyperpigmentation that may last months and is not responsive to bleaching skin treatments.1,2
Studies have shown that long-wave length UV radiation is the best trigger to induce this irritating reaction.2 There have been rare reports of photosensitivity reactions due to ingestion of large quantities of plants containing furocoumarins and psoralens.3 Plants known to cause phytophotodermatitis are found in almost every country across the globe, and exposure does not have to just be to the fruit, but contact with the leaves or sap also can induce the reaction.2-4 Typically after contact with the plant, followed by sun exposure, erythema will begin within 1 to 2 days, followed by bullae and vesicles, which tend to coalesce and burst over the following days. The patient is left with hyperpigmentation.2-4
Differential diagnosis
This condition can be difficult to diagnose and is often confused with type IV hypersensitivity reaction, eczema, herpes simplex virus (HSV), and burns, potentially leading to suspicion of child abuse.4,5 A thorough and detailed history is essential to correctly making the diagnosis and ruling out other potential causes.
Because the cause in children is often due to exposure to certain plants, unsupervised time outdoors leading to a rash may lead parents to think of poison ivy or poison oak, which are type IV hypersensitivity reactions.4,5 Although the rash may appear in a similar time course, the evolution to hyperpigmented patches is a distinguishing feature that helps to make the diagnosis of phytophotodermatitis.4 The postinflammatory hyperpigmentation, along with the clinical course, also can help differentiate it from burns and HSV infections, which it sometimes is mistaken for due to the bullous and vesicular lesions.4,5
Treatment
Counseling for avoidance of the exposure in the future is the most important aspect of treatment in order to prevent recurrences. Depending on the extent of the inflammatory reaction prior to the hyperpigmentation, no treatment may be needed for mild cases, but for more extreme bullous reactions, systemic steroids may be used.4
Topical corticosteroids and sun avoidance are the mainstays for treating mild to moderate cases. UV avoidance can be difficult because the long wave-length UV radiation that causes this reaction is not blocked by windows, and therefore it is important to keep affected areas covered even while indoors during daylight hours.4
There is no effective treatment for the hyperpigmented lesions. Patients need to be informed that this may resolve in months.
References
- Br J Dermatol. 1942;54(7):193-211.
- Clin Dermatol. 1986 Apr-Jun;4(2):102-21.
- Arch Dermatol. 1990 Oct;126(10):1334-6.
- J Am Acad Dermatol. 2007 Nov;57(5 Suppl):S88-91.
- Arch Fam Med. 2000 Jan;9(1):88.
Dr. Matiz is assistant professor of dermatology at Rady Children’s Hospital San Diego–University of California, San Diego, and Mr. Ginsberg is a research associate at the hospital. Dr. Matiz and Mr. Ginsberg said they have no relevant financial disclosures.
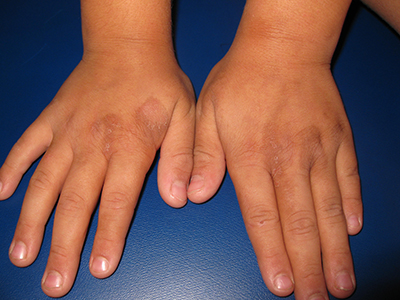
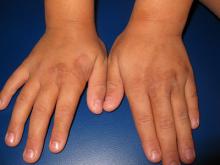
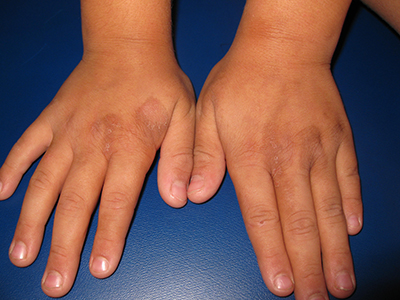
An 8-year-old healthy female presents with a 7-day history of a rash on the dorsum of her hands bilaterally. Her mother reports that it began as redness and swelling followed by blisters. She also reports that after the blisters popped and the redness went away, she noticed some darkened areas around where the blisters had been. The patient reports that there was some slight stinging and burning when the rash first appeared, which has been improving with time. She has had no fevers and has not been ill. The family has a dog, the patient has one older sibling who has atopic dermatitis, and the mother has asthma. The mother reports they live on a farm, and they have a vegetable and flower garden where the daughter plays every afternoon. She has no known allergies. The mother denies any recent travels or family history of bullous disease. Physical exam The patient is a well-appearing child who is attentive and in no apparent distress. On exam, there are several non-tender hyperpigmented patches between 1 cm and 3 cm on the dorsum of the hands, and intertriginous areas with overlying erosions. There are no other lesions on the skin. She is afebrile.