User login
By Ellen S. Haddock and Lawrence F. Eichenfield, MD
Terra firma-forme dermatosis
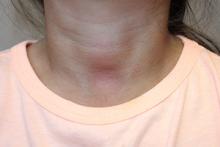
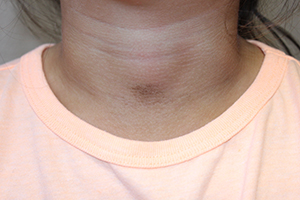
The easy removal of this patient’s persistent skin discoloration with an alcohol wipe confirms the diagnosis of terra firma-forme dermatosis. Terra firma-forme dermatosis is a benign skin condition in which dirt-like plaques develop on the skin despite normal hygiene. They cannot be removed with soap and water, but are removed easily with alcohol.
Terra firma means “solid earth” in Latin and refers to the dirt-like appearance of the lesion.1,2 The condition typically presents with brown or black hyperkeratotic plaques or papules. The hyperpigmented lesions may be papillomatous, verrucous (warty), or have a reticulated (net-like) distribution.3 The condition is usually asymptomatic but occasionally itchy.1 In the largest published series of 31 patients by Berk et al., the neck, ankles, and face were most commonly affected, but the condition can occur anywhere on the body.4 Lesions may be single or multiple and tend to be symmetrically distributed.4 The condition seems to be most common in young adults and adolescents, but can occur at any age and affects both genders equally.2,5
It seems to occur more commonly in darker skin, heavier patients, and concave body areas.3,6 The condition can last for months (median duration of 4 months in Berk et al.’s series), and by the time patients present to a physician they usually have tried aggressive scrubbing with multiple different soaps.4 As in this case, it is not uncommon for patients to receive an unnecessary work-up for diabetes due to concern for acanthosis nigricans.4 This work-up can be avoided if practitioners attempt removal with 70% isopropyl alcohol before ordering the diabetic work-up.
Biopsies are not typically performed (and should be abandoned if the lesion disappears when the site is cleansed with alcohol in preparation for biopsy), but hematoxylin and eosin staining shows lamellar hyperkeratosis, orthokeratotic whorls, and increased melanin in the basal layer and hyperkeratotic areas. Keratin globules are seen throughout the stratum corneum.7
Electron microscopy shows that the keratin lamellae is immature in some places, with incomplete keratinization and retention of desmosomal attachments.7 Overall, the histology is nonspecific and may be indistinguishable from other benign papillomatous conditions including confluent and reticulated papillomatosis (CARP), acanthosis nigricans, and epidermal nevi.6
Differential diagnosis
Clinically, the lesion may appear very similar to the brown velvety plaques of acanthosis nigricans, but the latter can be quickly ruled out if the lesion disappears when cleansed with alcohol. The differential diagnosis also includes dermatosis neglecta, CARP, hyperpigmented tinea versicolor, and dirty neck syndrome of atopic dermatitis.4,7
Dermatosis neglecta is caused by poor hygiene with insufficient skin cleaning. In contrast with terra firma-forme dermatitis, it can be removed with soap and water. Patients with dermatosis neglecta lack a history of aggressive attempts at removal by scrubbing. Dermatosis neglecta looks similar to terra firma-forme dermatosis, but may have a waxy “cornflake-like” scale.2 It is most common in the elderly, but also can be seen in children, especially if they have had a cast or brace that prevented washing an area.8
CARP may present as brown hyperkeratotic or verrucous papules, but typically occurs on the trunk and has a reticulated pattern, which is less common in terra firma-forme dermatosis. Typically, it cannot be removed completely with alcohol10-12 and tends to respond best to treatment with minocycline.11
Hyperpigmented tinea versicolor lesions are usually more discrete and have fine scale, which becomes more prominent when the lesions are scraped. When analyzed with KOH under a microscope, hyphae and spores looking like spaghetti and meatballs can be seen.
Dirty neck syndrome is acquired hyperpigmentation that may develop on the neck of patients with atopic dermatitis. It cannot be removed with alcohol.4 It may result from frictional melanosis with melanin incontinence and post-inflammatory hyperpigmentation.12 The hyperpigmentation is patchy or rippled,12 whereas terra firma-forme dermatosis more often presents as plaques.
Etiology
The cause of terra firma-forme dermatosis is uncertain. It is thought to be a disorder of keratinocyte retention, in which delayed keratinocyte maturation causes prolonged cell-to-cell adhesion that impairs shedding.7,8 Discoloration may be due to retained melanin as well as sebum and dirt that build up along with excess keratinocytes.7-9 Alcohol is a better solvent for this retained material than soap and water. Patients using heavy emollients or oily soaps for conditions like atopic dermatitis may be relatively predisposed to the condition if emollients or oily soaps are not removed completely by bathing; the combination of underlying scale and retained skin care products may make skin more adhesive, disrupting normal keratinocyte shedding and allowing dirt and sebum to accumulate.1 Atopic dermatitis was the most common comorbid condition for terra firma-forme dermatosis in Berk et al.’s series (12 of 31 patients).4
Treatment
Wiping with 70% isopropyl alcohol is both diagnostic and therapeutic, removing the lesion completely. Recurrence is uncommon but possible.3 In rare instances of regularly recurrent lesions, the area can be wiped prophylactically with alcohol weekly.1
References
- Indian J Dermatol Venereol Leprol. 2012 May-Jun;78(3):358-60.
- Pediatr Dermatol. 2011 Jan-Feb;28(1):79-81.
- Dermatol Pract Concept. 2015 Jul; 5(3): 29-33.
- Pediatr Dermatol. 2012 May-Jun;29(3):297-300.
- Eur J Intern Med. 2016 Feb. doi: 10.1016/j.ejim.2016.02.009.
- J Cutan Pathol. 2012 Feb;39(2):300-1.
- Arch Dermatol. 1987;123(5):567-9.
- Pediatr Dermatol. 2015;32(2):e50-3.
- Arch Dermatol. 2010;146(6):679-80.
- Arch Dermatol. 2011 Feb;147(2):247-8.
- Am J Clin Dermatol. 2006;7(5):305-313.
- Dermatology. 2014;229:174-182.
Ms. Haddock is a medical student at the University of California, San Diego, and a research associate at Rady Children’s Hospital–San Diego. Dr. Eichenfield is chief of pediatric and adolescent dermatology at Rady Children’s Hospital–San Diego and professor of dermatology and pediatrics at the University of California, San Diego. Dr. Eichenfield and Ms. Haddock state they have no relevant financial disclosures. Email them at [email protected].
By Ellen S. Haddock and Lawrence F. Eichenfield, MD
Terra firma-forme dermatosis
The easy removal of this patient’s persistent skin discoloration with an alcohol wipe confirms the diagnosis of terra firma-forme dermatosis. Terra firma-forme dermatosis is a benign skin condition in which dirt-like plaques develop on the skin despite normal hygiene. They cannot be removed with soap and water, but are removed easily with alcohol.
Terra firma means “solid earth” in Latin and refers to the dirt-like appearance of the lesion.1,2 The condition typically presents with brown or black hyperkeratotic plaques or papules. The hyperpigmented lesions may be papillomatous, verrucous (warty), or have a reticulated (net-like) distribution.3 The condition is usually asymptomatic but occasionally itchy.1 In the largest published series of 31 patients by Berk et al., the neck, ankles, and face were most commonly affected, but the condition can occur anywhere on the body.4 Lesions may be single or multiple and tend to be symmetrically distributed.4 The condition seems to be most common in young adults and adolescents, but can occur at any age and affects both genders equally.2,5
It seems to occur more commonly in darker skin, heavier patients, and concave body areas.3,6 The condition can last for months (median duration of 4 months in Berk et al.’s series), and by the time patients present to a physician they usually have tried aggressive scrubbing with multiple different soaps.4 As in this case, it is not uncommon for patients to receive an unnecessary work-up for diabetes due to concern for acanthosis nigricans.4 This work-up can be avoided if practitioners attempt removal with 70% isopropyl alcohol before ordering the diabetic work-up.
Biopsies are not typically performed (and should be abandoned if the lesion disappears when the site is cleansed with alcohol in preparation for biopsy), but hematoxylin and eosin staining shows lamellar hyperkeratosis, orthokeratotic whorls, and increased melanin in the basal layer and hyperkeratotic areas. Keratin globules are seen throughout the stratum corneum.7
Electron microscopy shows that the keratin lamellae is immature in some places, with incomplete keratinization and retention of desmosomal attachments.7 Overall, the histology is nonspecific and may be indistinguishable from other benign papillomatous conditions including confluent and reticulated papillomatosis (CARP), acanthosis nigricans, and epidermal nevi.6
Differential diagnosis
Clinically, the lesion may appear very similar to the brown velvety plaques of acanthosis nigricans, but the latter can be quickly ruled out if the lesion disappears when cleansed with alcohol. The differential diagnosis also includes dermatosis neglecta, CARP, hyperpigmented tinea versicolor, and dirty neck syndrome of atopic dermatitis.4,7
Dermatosis neglecta is caused by poor hygiene with insufficient skin cleaning. In contrast with terra firma-forme dermatitis, it can be removed with soap and water. Patients with dermatosis neglecta lack a history of aggressive attempts at removal by scrubbing. Dermatosis neglecta looks similar to terra firma-forme dermatosis, but may have a waxy “cornflake-like” scale.2 It is most common in the elderly, but also can be seen in children, especially if they have had a cast or brace that prevented washing an area.8
CARP may present as brown hyperkeratotic or verrucous papules, but typically occurs on the trunk and has a reticulated pattern, which is less common in terra firma-forme dermatosis. Typically, it cannot be removed completely with alcohol10-12 and tends to respond best to treatment with minocycline.11
Hyperpigmented tinea versicolor lesions are usually more discrete and have fine scale, which becomes more prominent when the lesions are scraped. When analyzed with KOH under a microscope, hyphae and spores looking like spaghetti and meatballs can be seen.
Dirty neck syndrome is acquired hyperpigmentation that may develop on the neck of patients with atopic dermatitis. It cannot be removed with alcohol.4 It may result from frictional melanosis with melanin incontinence and post-inflammatory hyperpigmentation.12 The hyperpigmentation is patchy or rippled,12 whereas terra firma-forme dermatosis more often presents as plaques.
Etiology
The cause of terra firma-forme dermatosis is uncertain. It is thought to be a disorder of keratinocyte retention, in which delayed keratinocyte maturation causes prolonged cell-to-cell adhesion that impairs shedding.7,8 Discoloration may be due to retained melanin as well as sebum and dirt that build up along with excess keratinocytes.7-9 Alcohol is a better solvent for this retained material than soap and water. Patients using heavy emollients or oily soaps for conditions like atopic dermatitis may be relatively predisposed to the condition if emollients or oily soaps are not removed completely by bathing; the combination of underlying scale and retained skin care products may make skin more adhesive, disrupting normal keratinocyte shedding and allowing dirt and sebum to accumulate.1 Atopic dermatitis was the most common comorbid condition for terra firma-forme dermatosis in Berk et al.’s series (12 of 31 patients).4
Treatment
Wiping with 70% isopropyl alcohol is both diagnostic and therapeutic, removing the lesion completely. Recurrence is uncommon but possible.3 In rare instances of regularly recurrent lesions, the area can be wiped prophylactically with alcohol weekly.1
References
- Indian J Dermatol Venereol Leprol. 2012 May-Jun;78(3):358-60.
- Pediatr Dermatol. 2011 Jan-Feb;28(1):79-81.
- Dermatol Pract Concept. 2015 Jul; 5(3): 29-33.
- Pediatr Dermatol. 2012 May-Jun;29(3):297-300.
- Eur J Intern Med. 2016 Feb. doi: 10.1016/j.ejim.2016.02.009.
- J Cutan Pathol. 2012 Feb;39(2):300-1.
- Arch Dermatol. 1987;123(5):567-9.
- Pediatr Dermatol. 2015;32(2):e50-3.
- Arch Dermatol. 2010;146(6):679-80.
- Arch Dermatol. 2011 Feb;147(2):247-8.
- Am J Clin Dermatol. 2006;7(5):305-313.
- Dermatology. 2014;229:174-182.
Ms. Haddock is a medical student at the University of California, San Diego, and a research associate at Rady Children’s Hospital–San Diego. Dr. Eichenfield is chief of pediatric and adolescent dermatology at Rady Children’s Hospital–San Diego and professor of dermatology and pediatrics at the University of California, San Diego. Dr. Eichenfield and Ms. Haddock state they have no relevant financial disclosures. Email them at [email protected].
By Ellen S. Haddock and Lawrence F. Eichenfield, MD
Terra firma-forme dermatosis
The easy removal of this patient’s persistent skin discoloration with an alcohol wipe confirms the diagnosis of terra firma-forme dermatosis. Terra firma-forme dermatosis is a benign skin condition in which dirt-like plaques develop on the skin despite normal hygiene. They cannot be removed with soap and water, but are removed easily with alcohol.
Terra firma means “solid earth” in Latin and refers to the dirt-like appearance of the lesion.1,2 The condition typically presents with brown or black hyperkeratotic plaques or papules. The hyperpigmented lesions may be papillomatous, verrucous (warty), or have a reticulated (net-like) distribution.3 The condition is usually asymptomatic but occasionally itchy.1 In the largest published series of 31 patients by Berk et al., the neck, ankles, and face were most commonly affected, but the condition can occur anywhere on the body.4 Lesions may be single or multiple and tend to be symmetrically distributed.4 The condition seems to be most common in young adults and adolescents, but can occur at any age and affects both genders equally.2,5
It seems to occur more commonly in darker skin, heavier patients, and concave body areas.3,6 The condition can last for months (median duration of 4 months in Berk et al.’s series), and by the time patients present to a physician they usually have tried aggressive scrubbing with multiple different soaps.4 As in this case, it is not uncommon for patients to receive an unnecessary work-up for diabetes due to concern for acanthosis nigricans.4 This work-up can be avoided if practitioners attempt removal with 70% isopropyl alcohol before ordering the diabetic work-up.
Biopsies are not typically performed (and should be abandoned if the lesion disappears when the site is cleansed with alcohol in preparation for biopsy), but hematoxylin and eosin staining shows lamellar hyperkeratosis, orthokeratotic whorls, and increased melanin in the basal layer and hyperkeratotic areas. Keratin globules are seen throughout the stratum corneum.7
Electron microscopy shows that the keratin lamellae is immature in some places, with incomplete keratinization and retention of desmosomal attachments.7 Overall, the histology is nonspecific and may be indistinguishable from other benign papillomatous conditions including confluent and reticulated papillomatosis (CARP), acanthosis nigricans, and epidermal nevi.6
Differential diagnosis
Clinically, the lesion may appear very similar to the brown velvety plaques of acanthosis nigricans, but the latter can be quickly ruled out if the lesion disappears when cleansed with alcohol. The differential diagnosis also includes dermatosis neglecta, CARP, hyperpigmented tinea versicolor, and dirty neck syndrome of atopic dermatitis.4,7
Dermatosis neglecta is caused by poor hygiene with insufficient skin cleaning. In contrast with terra firma-forme dermatitis, it can be removed with soap and water. Patients with dermatosis neglecta lack a history of aggressive attempts at removal by scrubbing. Dermatosis neglecta looks similar to terra firma-forme dermatosis, but may have a waxy “cornflake-like” scale.2 It is most common in the elderly, but also can be seen in children, especially if they have had a cast or brace that prevented washing an area.8
CARP may present as brown hyperkeratotic or verrucous papules, but typically occurs on the trunk and has a reticulated pattern, which is less common in terra firma-forme dermatosis. Typically, it cannot be removed completely with alcohol10-12 and tends to respond best to treatment with minocycline.11
Hyperpigmented tinea versicolor lesions are usually more discrete and have fine scale, which becomes more prominent when the lesions are scraped. When analyzed with KOH under a microscope, hyphae and spores looking like spaghetti and meatballs can be seen.
Dirty neck syndrome is acquired hyperpigmentation that may develop on the neck of patients with atopic dermatitis. It cannot be removed with alcohol.4 It may result from frictional melanosis with melanin incontinence and post-inflammatory hyperpigmentation.12 The hyperpigmentation is patchy or rippled,12 whereas terra firma-forme dermatosis more often presents as plaques.
Etiology
The cause of terra firma-forme dermatosis is uncertain. It is thought to be a disorder of keratinocyte retention, in which delayed keratinocyte maturation causes prolonged cell-to-cell adhesion that impairs shedding.7,8 Discoloration may be due to retained melanin as well as sebum and dirt that build up along with excess keratinocytes.7-9 Alcohol is a better solvent for this retained material than soap and water. Patients using heavy emollients or oily soaps for conditions like atopic dermatitis may be relatively predisposed to the condition if emollients or oily soaps are not removed completely by bathing; the combination of underlying scale and retained skin care products may make skin more adhesive, disrupting normal keratinocyte shedding and allowing dirt and sebum to accumulate.1 Atopic dermatitis was the most common comorbid condition for terra firma-forme dermatosis in Berk et al.’s series (12 of 31 patients).4
Treatment
Wiping with 70% isopropyl alcohol is both diagnostic and therapeutic, removing the lesion completely. Recurrence is uncommon but possible.3 In rare instances of regularly recurrent lesions, the area can be wiped prophylactically with alcohol weekly.1
References
- Indian J Dermatol Venereol Leprol. 2012 May-Jun;78(3):358-60.
- Pediatr Dermatol. 2011 Jan-Feb;28(1):79-81.
- Dermatol Pract Concept. 2015 Jul; 5(3): 29-33.
- Pediatr Dermatol. 2012 May-Jun;29(3):297-300.
- Eur J Intern Med. 2016 Feb. doi: 10.1016/j.ejim.2016.02.009.
- J Cutan Pathol. 2012 Feb;39(2):300-1.
- Arch Dermatol. 1987;123(5):567-9.
- Pediatr Dermatol. 2015;32(2):e50-3.
- Arch Dermatol. 2010;146(6):679-80.
- Arch Dermatol. 2011 Feb;147(2):247-8.
- Am J Clin Dermatol. 2006;7(5):305-313.
- Dermatology. 2014;229:174-182.
Ms. Haddock is a medical student at the University of California, San Diego, and a research associate at Rady Children’s Hospital–San Diego. Dr. Eichenfield is chief of pediatric and adolescent dermatology at Rady Children’s Hospital–San Diego and professor of dermatology and pediatrics at the University of California, San Diego. Dr. Eichenfield and Ms. Haddock state they have no relevant financial disclosures. Email them at [email protected].
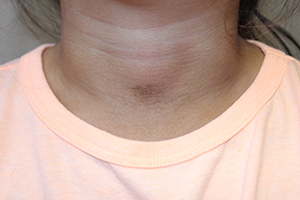
A 4-year-old girl presented for evaluation of a localized hyperpigmented rash of 4 months duration. The family noticed a localized, brown discoloration on her anterior neck. It was asymptomatic. Her mother tried scrubbing the area with several different soaps and baby wipes, but noted no change. Her medical history is notable for atopic dermatitis, well controlled with intermittent topical corticosteroids, and reactive airway disease. There is a family history of atopic dermatitis and type 2 diabetes. On physical exam, the patient is a non-obese (BMI 16 kg/m2) female with a 4 x 3–cm hyperpigmented, rough, slightly elevated plaque on her anterior neck. (See Before photo.) On close inspection, the plaque appears to be composed of hyperpigmented rugations. Viewed through a dermatoscope, the lesion’s polygonal brownish pigmentation looks like cobblestones (Can Med Assoc J. 2016;188[4]:285).The patient had no discoloration on the posterior neck, axillae, groin, or other locations. Blood work, ordered by a practitioner concerned about possible acanthosis nigricans, revealed: • CBC: within normal limits • Glucose: 82 mg/dL (normal 60-110) • Insulin: 3 mU/mL (normal less than 17) • Cholesterol: 136 mg/dL (normal less than 200) • Triglycerides: 79 mg/dL (normal 32-116) • Thyroid-stimulating hormone: 1.72 uIU/mL (normal 0.35-5) Rubbing the hyperpigmented area with a 70% isopropyl alcohol swab in clinic removed it completely.