User login
Natalizumab mobilizes latent JC virus in mononuclear cells in MS
Researchers have detected John Cunningham virus DNA in the mononuclear cells of patients with multiple sclerosis who have been treated with natalizumab, suggesting a possible mechanism to explain the association of natalizumab with the development of progressive multifocal leukoencephalopathy.
The results from the study, published online March 24 in JAMA Neurology, also suggest that some patients who test seronegative for antibodies against John Cunningham virus (JCV) and undergo treatment with natalizumab have cell-associated viremia that goes undetected by current assays.
More than 440 cases of progressive multifocal leukoencephalopathy (PML) have been reported since the monoclonal antibody natalizumab was reintroduced in 2006 for the treatment of relapsing-remitting forms of multiple sclerosis (MS), and approximately 11 new cases are reported each month.
"Natalizumab is known to promote mobilization of hematopoietic stem cells from the bone marrow, a putative site for JCV latency, into the peripheral circulation, resulting in higher-than-normal physiological levels of CD34-positive cells for months to years after treatment," wrote Dr. Elliot M. Frohman from the University of Texas Southwestern Medical Center, Dallas, and his colleagues.
"The observation of JCV latency within these characterized mononuclear cells makes a direct mechanistic link between natalizumab and the occurrence of PML."
Researchers collected peripheral blood samples from 26 MS patients at baseline before initiation of natalizumab, and at approximately 3-month intervals over the next 10 monthly infusions. They also collected blood samples at a single time point from 23 MS patients who had received 24 or more natalizumab infusions and 19 healthy age- and sex-matched controls (JAMA Neurol. 2014 March 24 [doi: 10.1001/jamaneurol.2014.63]).
They found JCV DNA in half of the 26 MS patients with baseline and follow-up blood samples at one or more points, and significantly more MS patients had detectable JCV DNA in either the CD19-positive or CD34-positive cell compartments, compared with the healthy volunteers.
However, the investigators observed a low viral copy number, as compared with what would usually be seen in virus excreted in urine, regardless of which cell compartment the viral DNA was detected in. The viral copy numbers were generally higher in patients treated for longer periods.
"The low viral copy number in our study is consistent with a latent or a persistent infection," the investigators wrote. "In previous work, a cell culture model had shown that even a low level of persistence of JCV has significance because JCV can be transferred to other cells."
Of 23 MS patients overall who had cell-associated viremia, 14 were seronegative for antibodies against JC virus. One healthy control patient who had cell-associated viremia also tested seronegative. The investigators cautioned that serology alone may not be enough to identify all patients with prior exposure to JCV.
"Other measures of JCV infection may be of equal importance and should be considered, including T-cell responses, a rise in antibody titer indicating active infection, and the presence of JCV DNA variants in peripheral circulation, particularly in cell compartments."
The study was supported by intramural research funds within the National Institute of Neurological Disorders and Stroke and the National Institute of Allergy and Infectious Disease and a grant from the National Multiple Sclerosis Society. Four researchers declared that they received speaking and consultancy fees, honoraria, and grant support from a range of pharmaceutical companies that market drugs for MS, including Biogen Idec, manufacturer of natalizumab.
Researchers have detected John Cunningham virus DNA in the mononuclear cells of patients with multiple sclerosis who have been treated with natalizumab, suggesting a possible mechanism to explain the association of natalizumab with the development of progressive multifocal leukoencephalopathy.
The results from the study, published online March 24 in JAMA Neurology, also suggest that some patients who test seronegative for antibodies against John Cunningham virus (JCV) and undergo treatment with natalizumab have cell-associated viremia that goes undetected by current assays.
More than 440 cases of progressive multifocal leukoencephalopathy (PML) have been reported since the monoclonal antibody natalizumab was reintroduced in 2006 for the treatment of relapsing-remitting forms of multiple sclerosis (MS), and approximately 11 new cases are reported each month.
"Natalizumab is known to promote mobilization of hematopoietic stem cells from the bone marrow, a putative site for JCV latency, into the peripheral circulation, resulting in higher-than-normal physiological levels of CD34-positive cells for months to years after treatment," wrote Dr. Elliot M. Frohman from the University of Texas Southwestern Medical Center, Dallas, and his colleagues.
"The observation of JCV latency within these characterized mononuclear cells makes a direct mechanistic link between natalizumab and the occurrence of PML."
Researchers collected peripheral blood samples from 26 MS patients at baseline before initiation of natalizumab, and at approximately 3-month intervals over the next 10 monthly infusions. They also collected blood samples at a single time point from 23 MS patients who had received 24 or more natalizumab infusions and 19 healthy age- and sex-matched controls (JAMA Neurol. 2014 March 24 [doi: 10.1001/jamaneurol.2014.63]).
They found JCV DNA in half of the 26 MS patients with baseline and follow-up blood samples at one or more points, and significantly more MS patients had detectable JCV DNA in either the CD19-positive or CD34-positive cell compartments, compared with the healthy volunteers.
However, the investigators observed a low viral copy number, as compared with what would usually be seen in virus excreted in urine, regardless of which cell compartment the viral DNA was detected in. The viral copy numbers were generally higher in patients treated for longer periods.
"The low viral copy number in our study is consistent with a latent or a persistent infection," the investigators wrote. "In previous work, a cell culture model had shown that even a low level of persistence of JCV has significance because JCV can be transferred to other cells."
Of 23 MS patients overall who had cell-associated viremia, 14 were seronegative for antibodies against JC virus. One healthy control patient who had cell-associated viremia also tested seronegative. The investigators cautioned that serology alone may not be enough to identify all patients with prior exposure to JCV.
"Other measures of JCV infection may be of equal importance and should be considered, including T-cell responses, a rise in antibody titer indicating active infection, and the presence of JCV DNA variants in peripheral circulation, particularly in cell compartments."
The study was supported by intramural research funds within the National Institute of Neurological Disorders and Stroke and the National Institute of Allergy and Infectious Disease and a grant from the National Multiple Sclerosis Society. Four researchers declared that they received speaking and consultancy fees, honoraria, and grant support from a range of pharmaceutical companies that market drugs for MS, including Biogen Idec, manufacturer of natalizumab.
Researchers have detected John Cunningham virus DNA in the mononuclear cells of patients with multiple sclerosis who have been treated with natalizumab, suggesting a possible mechanism to explain the association of natalizumab with the development of progressive multifocal leukoencephalopathy.
The results from the study, published online March 24 in JAMA Neurology, also suggest that some patients who test seronegative for antibodies against John Cunningham virus (JCV) and undergo treatment with natalizumab have cell-associated viremia that goes undetected by current assays.
More than 440 cases of progressive multifocal leukoencephalopathy (PML) have been reported since the monoclonal antibody natalizumab was reintroduced in 2006 for the treatment of relapsing-remitting forms of multiple sclerosis (MS), and approximately 11 new cases are reported each month.
"Natalizumab is known to promote mobilization of hematopoietic stem cells from the bone marrow, a putative site for JCV latency, into the peripheral circulation, resulting in higher-than-normal physiological levels of CD34-positive cells for months to years after treatment," wrote Dr. Elliot M. Frohman from the University of Texas Southwestern Medical Center, Dallas, and his colleagues.
"The observation of JCV latency within these characterized mononuclear cells makes a direct mechanistic link between natalizumab and the occurrence of PML."
Researchers collected peripheral blood samples from 26 MS patients at baseline before initiation of natalizumab, and at approximately 3-month intervals over the next 10 monthly infusions. They also collected blood samples at a single time point from 23 MS patients who had received 24 or more natalizumab infusions and 19 healthy age- and sex-matched controls (JAMA Neurol. 2014 March 24 [doi: 10.1001/jamaneurol.2014.63]).
They found JCV DNA in half of the 26 MS patients with baseline and follow-up blood samples at one or more points, and significantly more MS patients had detectable JCV DNA in either the CD19-positive or CD34-positive cell compartments, compared with the healthy volunteers.
However, the investigators observed a low viral copy number, as compared with what would usually be seen in virus excreted in urine, regardless of which cell compartment the viral DNA was detected in. The viral copy numbers were generally higher in patients treated for longer periods.
"The low viral copy number in our study is consistent with a latent or a persistent infection," the investigators wrote. "In previous work, a cell culture model had shown that even a low level of persistence of JCV has significance because JCV can be transferred to other cells."
Of 23 MS patients overall who had cell-associated viremia, 14 were seronegative for antibodies against JC virus. One healthy control patient who had cell-associated viremia also tested seronegative. The investigators cautioned that serology alone may not be enough to identify all patients with prior exposure to JCV.
"Other measures of JCV infection may be of equal importance and should be considered, including T-cell responses, a rise in antibody titer indicating active infection, and the presence of JCV DNA variants in peripheral circulation, particularly in cell compartments."
The study was supported by intramural research funds within the National Institute of Neurological Disorders and Stroke and the National Institute of Allergy and Infectious Disease and a grant from the National Multiple Sclerosis Society. Four researchers declared that they received speaking and consultancy fees, honoraria, and grant support from a range of pharmaceutical companies that market drugs for MS, including Biogen Idec, manufacturer of natalizumab.
FROM JAMA NEUROLOGY
Major finding: Of 23 MS patients with cell-associated JC virus viremia, 14 tested seronegative for antibodies against the virus.
Data source: A prospective observational study in 49 multiple sclerosis patients treated with natalizumab and 19 healthy controls.
Disclosures: The study was supported by intramural research funds within the National Institute of Neurological Disorders and Stroke and the National Institute of Allergy and Infectious Disease and a grant from the National Multiple Sclerosis Society. Four researchers declared that they received speaking and consultancy fees, honoraria, and grant support from a range of pharmaceutical companies that market drugs for MS, including Biogen Idec, manufacturer of natalizumab.
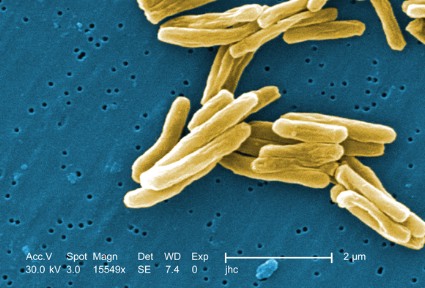
First estimates of multidrug-resistant tuberculosis in children made
The risk of multidrug-resistant tuberculosis appears similar in children and treatment-naive adults, according to a study published online ahead of World Tuberculosis Day, which is March 24.
This study provides the first global and regional estimates of the incidence of drug-resistant disease in children.
Researchers led by Helen E. Jenkins, Ph.D., of Brigham and Women’s Hospital, Boston, calculated the incidence of tuberculosis in children and conducted a systematic review to estimate the risk of multidrug-resistant disease. They concluded that nearly 1 million children developed tuberculosis in 2010 – a figure substantially higher than the 2011 World Health Organization estimates. Of those, nearly 32,000 had multidrug-resistant disease.
The highest concentrations of pediatric tuberculosis and drug-resistant disease were in Southeast Asia, according to Dr. Jenkins and her associates (Lancet 2014 March 24 [doi: 10.1016/S0140-6736(14)60195-1]).
In an accompanying editorial, Dr. Ben J. Marais of the Marie Bashir Institute for Infectious Diseases and Biosecurity, University of Sydney, Australia, called the study the "most rigorous effort to date to provide contextualized estimates of both tuberculosis and multidrug-resistant tuberculosis incidence in children," and said it was likely to provide a benchmark for future studies in the area.
"Given that treatment outcomes for children with multidrug-resistant tuberculosis are excellent (clinical cure rates in excess of 80%), every effort should be made to reduce the massive case-detection gap and address the vast unmet need for diagnosis and treatment," he said (Lancet 2014 March 24 [doi: 10.1016/S0140-6736(14)60489-X]).
The authors and Dr. Marais declared that they had no competing interests. Funding for the study was provided by awards from the U.S. National Institute of General Medical Sciences and the National Institute of Allergy and Infectious Diseases, as well as various fellowships.
The risk of multidrug-resistant tuberculosis appears similar in children and treatment-naive adults, according to a study published online ahead of World Tuberculosis Day, which is March 24.
This study provides the first global and regional estimates of the incidence of drug-resistant disease in children.
Researchers led by Helen E. Jenkins, Ph.D., of Brigham and Women’s Hospital, Boston, calculated the incidence of tuberculosis in children and conducted a systematic review to estimate the risk of multidrug-resistant disease. They concluded that nearly 1 million children developed tuberculosis in 2010 – a figure substantially higher than the 2011 World Health Organization estimates. Of those, nearly 32,000 had multidrug-resistant disease.
The highest concentrations of pediatric tuberculosis and drug-resistant disease were in Southeast Asia, according to Dr. Jenkins and her associates (Lancet 2014 March 24 [doi: 10.1016/S0140-6736(14)60195-1]).
In an accompanying editorial, Dr. Ben J. Marais of the Marie Bashir Institute for Infectious Diseases and Biosecurity, University of Sydney, Australia, called the study the "most rigorous effort to date to provide contextualized estimates of both tuberculosis and multidrug-resistant tuberculosis incidence in children," and said it was likely to provide a benchmark for future studies in the area.
"Given that treatment outcomes for children with multidrug-resistant tuberculosis are excellent (clinical cure rates in excess of 80%), every effort should be made to reduce the massive case-detection gap and address the vast unmet need for diagnosis and treatment," he said (Lancet 2014 March 24 [doi: 10.1016/S0140-6736(14)60489-X]).
The authors and Dr. Marais declared that they had no competing interests. Funding for the study was provided by awards from the U.S. National Institute of General Medical Sciences and the National Institute of Allergy and Infectious Diseases, as well as various fellowships.
The risk of multidrug-resistant tuberculosis appears similar in children and treatment-naive adults, according to a study published online ahead of World Tuberculosis Day, which is March 24.
This study provides the first global and regional estimates of the incidence of drug-resistant disease in children.
Researchers led by Helen E. Jenkins, Ph.D., of Brigham and Women’s Hospital, Boston, calculated the incidence of tuberculosis in children and conducted a systematic review to estimate the risk of multidrug-resistant disease. They concluded that nearly 1 million children developed tuberculosis in 2010 – a figure substantially higher than the 2011 World Health Organization estimates. Of those, nearly 32,000 had multidrug-resistant disease.
The highest concentrations of pediatric tuberculosis and drug-resistant disease were in Southeast Asia, according to Dr. Jenkins and her associates (Lancet 2014 March 24 [doi: 10.1016/S0140-6736(14)60195-1]).
In an accompanying editorial, Dr. Ben J. Marais of the Marie Bashir Institute for Infectious Diseases and Biosecurity, University of Sydney, Australia, called the study the "most rigorous effort to date to provide contextualized estimates of both tuberculosis and multidrug-resistant tuberculosis incidence in children," and said it was likely to provide a benchmark for future studies in the area.
"Given that treatment outcomes for children with multidrug-resistant tuberculosis are excellent (clinical cure rates in excess of 80%), every effort should be made to reduce the massive case-detection gap and address the vast unmet need for diagnosis and treatment," he said (Lancet 2014 March 24 [doi: 10.1016/S0140-6736(14)60489-X]).
The authors and Dr. Marais declared that they had no competing interests. Funding for the study was provided by awards from the U.S. National Institute of General Medical Sciences and the National Institute of Allergy and Infectious Diseases, as well as various fellowships.
FROM THE LANCET
Major finding: A study has estimated nearly 32,000 children developed multidrug-resistant tuberculosis in 2010, finding the risk of multidrug-resistance is similar in children and in treatment-naive adults.
Data source: Systematic review and modeling using age-specific regional notification data.
Disclosures: The authors and Dr. Marais declared that they had no competing interests. Funding for the study was provided by awards from the National Institute of General Medical Sciences and the National Institute of Allergy and Infectious Diseases, as well as various fellowships.
Glycerol phenylbutyrate reduces hepatic encephalopathy events in cirrhosis
Glycerol phenylbutyrate significantly reduced the number of cirrhosis patients experiencing hepatic encephalopathy and the time to first event, a phase II trial has shown.
The randomized, double-blind placebo-controlled trial in 178 patients with cirrhosis found that only 21% of patients treated with glycerol phenylbutyrate (GPB) had a hepatic encephalopathy (HE) event compared with 36% of the placebo group (P =.02).
Treatment with 6 mL of oral GPB twice daily also significantly reduced the time to a first HE event (HR 0.56, 95% CI 0.32-0.99, P less than .05), in particular, more severe West Haven grade 2 events, according to a study published in the March issue of Hepatology.
The HE group also had significantly fewer total events (35 vs. 57, P less than .05), and treatment was associated with a nonsignificant reduction in HE hospitalizations (13 vs. 25; P = .06)
The treatment effect was more pronounced in the 119 patients not taking the antibiotic rifaximin at entry; among patients taking rifaximin there were no differences between the treatment arms in the number of patients experiencing an HE event, time to event, or total number of events (Hepatology 2014;59:1073-83).
Glycerol phenylbutyrate is currently approved for the treatment of urea cycle disorders and other inherited disorders characterized by an excess of ammonia in the blood.
This study followed a previous 4-week, open-label study that suggested this dose of GPB was well tolerated and lowered ammonia levels in patients with cirrhosis and HE.
"Though elevated blood ammonia has long been suspected as important, the evidence is largely correlative, other factors have been postulated, and evidence against ammonia has been reported," wrote Dr. Don C. Rockey of the Medical University of South Carolina, Charleston, and his colleagues.
In the current study, "GPB significantly lowered plasma ammonia and correlated strongly with HE events when assessed either at baseline or during the study."
Baseline ammonia levels were also higher among patients who subsequently experienced an HE event compared with those who did not, prompting the authors to suggest that elevated blood ammonia level does in fact play an important role in the pathogenesis of recurrent, overt HE.
Researchers reported similar types of adverse events in the two treatment arms and a similar frequency of these events, although serious adverse events and study drug discontinuations associated with adverse events occurred slightly more often in the GPB group.
"There were no treatment-related effects on liver biochemical tests, including alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), bilirubin, international normalized ratio (INR), or MELD [score]," the investigators wrote.
They concluced that "that GPB reduced the likelihood of HE events in patients with preexisting HE, and ... that it deserves further study as a potential therapeutic for these patients."
The study was funded by Hyperion Therapeutics. There were no other conflicts of interest declared.
The publication by Dr. Rockey and his colleagues describes the findings of a randomized, double-blind controlled trial using glycerol phenylbutyrate to treat hepatic encephalopathy. The study design essentially enrolled patients who had at least two "bouts of HE in the previous 6 months." This drug is given orally and promotes excretion of waste nitrogen through the kidneys in the form of urinary phenylacetylglutamine. It has been approved and used for the treatment of hyperammonemia in patients with urea cycle defects.

|
| Dr. Kevin D. Mullen |
In light of all the issues involved, the authors appear to have conducted the study in a satisfactory fashion. The 50% of enrollees coming from Russia and the Ukraine reflects the difficulty in enrolling patients in the United States. This must have posed some difficulties in running the study such as standardization of the ammonia assays. Nonetheless, this is an important study demonstrating that this agent has a measurable degree of efficacy in the control of HE. Further studies are needed to verify the findings with more and larger randomized controlled trials.
Dr. Kevin D. Mullen, professor of medicine, Case Western Reserve University, Metrohealth Medical Center, Cleveland. He has consulted for Salix and Abbott.
The publication by Dr. Rockey and his colleagues describes the findings of a randomized, double-blind controlled trial using glycerol phenylbutyrate to treat hepatic encephalopathy. The study design essentially enrolled patients who had at least two "bouts of HE in the previous 6 months." This drug is given orally and promotes excretion of waste nitrogen through the kidneys in the form of urinary phenylacetylglutamine. It has been approved and used for the treatment of hyperammonemia in patients with urea cycle defects.

|
| Dr. Kevin D. Mullen |
In light of all the issues involved, the authors appear to have conducted the study in a satisfactory fashion. The 50% of enrollees coming from Russia and the Ukraine reflects the difficulty in enrolling patients in the United States. This must have posed some difficulties in running the study such as standardization of the ammonia assays. Nonetheless, this is an important study demonstrating that this agent has a measurable degree of efficacy in the control of HE. Further studies are needed to verify the findings with more and larger randomized controlled trials.
Dr. Kevin D. Mullen, professor of medicine, Case Western Reserve University, Metrohealth Medical Center, Cleveland. He has consulted for Salix and Abbott.
The publication by Dr. Rockey and his colleagues describes the findings of a randomized, double-blind controlled trial using glycerol phenylbutyrate to treat hepatic encephalopathy. The study design essentially enrolled patients who had at least two "bouts of HE in the previous 6 months." This drug is given orally and promotes excretion of waste nitrogen through the kidneys in the form of urinary phenylacetylglutamine. It has been approved and used for the treatment of hyperammonemia in patients with urea cycle defects.

|
| Dr. Kevin D. Mullen |
In light of all the issues involved, the authors appear to have conducted the study in a satisfactory fashion. The 50% of enrollees coming from Russia and the Ukraine reflects the difficulty in enrolling patients in the United States. This must have posed some difficulties in running the study such as standardization of the ammonia assays. Nonetheless, this is an important study demonstrating that this agent has a measurable degree of efficacy in the control of HE. Further studies are needed to verify the findings with more and larger randomized controlled trials.
Dr. Kevin D. Mullen, professor of medicine, Case Western Reserve University, Metrohealth Medical Center, Cleveland. He has consulted for Salix and Abbott.
Glycerol phenylbutyrate significantly reduced the number of cirrhosis patients experiencing hepatic encephalopathy and the time to first event, a phase II trial has shown.
The randomized, double-blind placebo-controlled trial in 178 patients with cirrhosis found that only 21% of patients treated with glycerol phenylbutyrate (GPB) had a hepatic encephalopathy (HE) event compared with 36% of the placebo group (P =.02).
Treatment with 6 mL of oral GPB twice daily also significantly reduced the time to a first HE event (HR 0.56, 95% CI 0.32-0.99, P less than .05), in particular, more severe West Haven grade 2 events, according to a study published in the March issue of Hepatology.
The HE group also had significantly fewer total events (35 vs. 57, P less than .05), and treatment was associated with a nonsignificant reduction in HE hospitalizations (13 vs. 25; P = .06)
The treatment effect was more pronounced in the 119 patients not taking the antibiotic rifaximin at entry; among patients taking rifaximin there were no differences between the treatment arms in the number of patients experiencing an HE event, time to event, or total number of events (Hepatology 2014;59:1073-83).
Glycerol phenylbutyrate is currently approved for the treatment of urea cycle disorders and other inherited disorders characterized by an excess of ammonia in the blood.
This study followed a previous 4-week, open-label study that suggested this dose of GPB was well tolerated and lowered ammonia levels in patients with cirrhosis and HE.
"Though elevated blood ammonia has long been suspected as important, the evidence is largely correlative, other factors have been postulated, and evidence against ammonia has been reported," wrote Dr. Don C. Rockey of the Medical University of South Carolina, Charleston, and his colleagues.
In the current study, "GPB significantly lowered plasma ammonia and correlated strongly with HE events when assessed either at baseline or during the study."
Baseline ammonia levels were also higher among patients who subsequently experienced an HE event compared with those who did not, prompting the authors to suggest that elevated blood ammonia level does in fact play an important role in the pathogenesis of recurrent, overt HE.
Researchers reported similar types of adverse events in the two treatment arms and a similar frequency of these events, although serious adverse events and study drug discontinuations associated with adverse events occurred slightly more often in the GPB group.
"There were no treatment-related effects on liver biochemical tests, including alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), bilirubin, international normalized ratio (INR), or MELD [score]," the investigators wrote.
They concluced that "that GPB reduced the likelihood of HE events in patients with preexisting HE, and ... that it deserves further study as a potential therapeutic for these patients."
The study was funded by Hyperion Therapeutics. There were no other conflicts of interest declared.
Glycerol phenylbutyrate significantly reduced the number of cirrhosis patients experiencing hepatic encephalopathy and the time to first event, a phase II trial has shown.
The randomized, double-blind placebo-controlled trial in 178 patients with cirrhosis found that only 21% of patients treated with glycerol phenylbutyrate (GPB) had a hepatic encephalopathy (HE) event compared with 36% of the placebo group (P =.02).
Treatment with 6 mL of oral GPB twice daily also significantly reduced the time to a first HE event (HR 0.56, 95% CI 0.32-0.99, P less than .05), in particular, more severe West Haven grade 2 events, according to a study published in the March issue of Hepatology.
The HE group also had significantly fewer total events (35 vs. 57, P less than .05), and treatment was associated with a nonsignificant reduction in HE hospitalizations (13 vs. 25; P = .06)
The treatment effect was more pronounced in the 119 patients not taking the antibiotic rifaximin at entry; among patients taking rifaximin there were no differences between the treatment arms in the number of patients experiencing an HE event, time to event, or total number of events (Hepatology 2014;59:1073-83).
Glycerol phenylbutyrate is currently approved for the treatment of urea cycle disorders and other inherited disorders characterized by an excess of ammonia in the blood.
This study followed a previous 4-week, open-label study that suggested this dose of GPB was well tolerated and lowered ammonia levels in patients with cirrhosis and HE.
"Though elevated blood ammonia has long been suspected as important, the evidence is largely correlative, other factors have been postulated, and evidence against ammonia has been reported," wrote Dr. Don C. Rockey of the Medical University of South Carolina, Charleston, and his colleagues.
In the current study, "GPB significantly lowered plasma ammonia and correlated strongly with HE events when assessed either at baseline or during the study."
Baseline ammonia levels were also higher among patients who subsequently experienced an HE event compared with those who did not, prompting the authors to suggest that elevated blood ammonia level does in fact play an important role in the pathogenesis of recurrent, overt HE.
Researchers reported similar types of adverse events in the two treatment arms and a similar frequency of these events, although serious adverse events and study drug discontinuations associated with adverse events occurred slightly more often in the GPB group.
"There were no treatment-related effects on liver biochemical tests, including alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), bilirubin, international normalized ratio (INR), or MELD [score]," the investigators wrote.
They concluced that "that GPB reduced the likelihood of HE events in patients with preexisting HE, and ... that it deserves further study as a potential therapeutic for these patients."
The study was funded by Hyperion Therapeutics. There were no other conflicts of interest declared.
Major finding: Glycerol phenylbutyrate significantly reduces the number of cirrhosis patients experiencing hepatic encephalopathy and the time to first event, particularly among patients not taking rifaximin.
Data source: A randomized, placebo-controlled, double-blind phase II trial in 178 patients with cirrhosis.
Disclosures: The study was funded by Hyperion Therapeutics.
Plasma biomarker panel predicts amnestic MCI or Alzheimer’s
Researchers have identified a panel of 10 lipid metabolites that can predict the development of either amnestic mild cognitive impairment or Alzheimer’s disease within 2-3 years with 90% sensitivity and 90% specificity.
"The defined ten-metabolite profile features PCs [phosphatidylcholines] and ACs [acylcarnitines], phospholipids that have essential structural and functional roles in the integrity and functionality of cell membranes," Dr. Mark Mapstone of the University of Rochester (N.Y.) and his colleagues wrote in Nature Medicine.
Of the 525 healthy, community-dwelling individuals aged 70 years and older enrolled in the observational study, 74 met the criteria for amnestic mild cognitive impairment (aMCI) or mild Alzheimer’s disease during the 5-year follow-up period – 46 who were incidental at entry to the study and 28 who converted over a mean time of 2.1 years (Nat. Med. 2014 March 9 [doi:10.1038/nm.3466]).
In the third year of the study, the investigators conducted untargeted metabolomic and lipidomic analysis on blood samples from 53 participants with either aMCI or Alzheimer’s disease, including 18 converters and 53 cognitively normal controls. Blood samples from the converters were taken before and after conversion.
Analysis revealed a number of amino acids and phospholipids that were significantly different between the two groups, and a further targeted analysis showed that the converter group had significantly lower plasma levels of serotonin, phenylalanine, proline, lysine, phosphatidylcholine, taurine, and acylcarnitine.
In particular, Dr. Mapstone and his associates identified a set of 10 metabolites that comprised phosphatidylcholines, lysophosphatidylcholine, and acylcarnitines, which were each found at much lower levels in the plasma of the converter group before conversion than in the plasma of the cognitively normal group. Apolipoprotein E epsilon-4 allele status did not have a significant effect on the classification of converters to aMCI or AD or the normal controls.
"These metabolites remained depleted after phenoconversion to aMCI/AD ... and were similar to the levels in the aMCI/AD group," the researchers reported.
"We posit that this ten–phospholipid biomarker panel, consisting of PC and AC species, reveals the breakdown of neural cell membranes in those individuals destined to phenoconvert from cognitive intactness to aMCI or AD and may mark the transition between preclinical states where synaptic dysfunction and early neurodegeneration give rise to subtle cognitive changes," Dr. Mapstone and his coworkers wrote.
Commenting on the study, Dr. Richard J. Caselli, professor of neurology at the Mayo Clinic in Scottsdale, Ariz., and clinical core director of the Arizona Alzheimer’s Disease Center, said that lipidomic studies represent a different approach from the usual proteomic and genomic approaches, although it was not possible to say whether any one approach would be more valid than another.
Dr. Caselli, however, said that a test using blood samples would have its advantages.
"Blood tests are always easier and often cheaper than spinal taps or PET scans (or any other brain imaging procedure) [and] they can also be repeated more easily to track disease progression," Dr. Caselli said.
"For patients with overt symptoms, even at the MCI stage, PET scans are quite sensitive. The problem is they are expensive and not always covered by insurance, so a less expensive and equally reliable blood test would certainly be welcome," he added.
The investigators and Dr. Caselli had no conflicts of interest to declare.
Researchers have identified a panel of 10 lipid metabolites that can predict the development of either amnestic mild cognitive impairment or Alzheimer’s disease within 2-3 years with 90% sensitivity and 90% specificity.
"The defined ten-metabolite profile features PCs [phosphatidylcholines] and ACs [acylcarnitines], phospholipids that have essential structural and functional roles in the integrity and functionality of cell membranes," Dr. Mark Mapstone of the University of Rochester (N.Y.) and his colleagues wrote in Nature Medicine.
Of the 525 healthy, community-dwelling individuals aged 70 years and older enrolled in the observational study, 74 met the criteria for amnestic mild cognitive impairment (aMCI) or mild Alzheimer’s disease during the 5-year follow-up period – 46 who were incidental at entry to the study and 28 who converted over a mean time of 2.1 years (Nat. Med. 2014 March 9 [doi:10.1038/nm.3466]).
In the third year of the study, the investigators conducted untargeted metabolomic and lipidomic analysis on blood samples from 53 participants with either aMCI or Alzheimer’s disease, including 18 converters and 53 cognitively normal controls. Blood samples from the converters were taken before and after conversion.
Analysis revealed a number of amino acids and phospholipids that were significantly different between the two groups, and a further targeted analysis showed that the converter group had significantly lower plasma levels of serotonin, phenylalanine, proline, lysine, phosphatidylcholine, taurine, and acylcarnitine.
In particular, Dr. Mapstone and his associates identified a set of 10 metabolites that comprised phosphatidylcholines, lysophosphatidylcholine, and acylcarnitines, which were each found at much lower levels in the plasma of the converter group before conversion than in the plasma of the cognitively normal group. Apolipoprotein E epsilon-4 allele status did not have a significant effect on the classification of converters to aMCI or AD or the normal controls.
"These metabolites remained depleted after phenoconversion to aMCI/AD ... and were similar to the levels in the aMCI/AD group," the researchers reported.
"We posit that this ten–phospholipid biomarker panel, consisting of PC and AC species, reveals the breakdown of neural cell membranes in those individuals destined to phenoconvert from cognitive intactness to aMCI or AD and may mark the transition between preclinical states where synaptic dysfunction and early neurodegeneration give rise to subtle cognitive changes," Dr. Mapstone and his coworkers wrote.
Commenting on the study, Dr. Richard J. Caselli, professor of neurology at the Mayo Clinic in Scottsdale, Ariz., and clinical core director of the Arizona Alzheimer’s Disease Center, said that lipidomic studies represent a different approach from the usual proteomic and genomic approaches, although it was not possible to say whether any one approach would be more valid than another.
Dr. Caselli, however, said that a test using blood samples would have its advantages.
"Blood tests are always easier and often cheaper than spinal taps or PET scans (or any other brain imaging procedure) [and] they can also be repeated more easily to track disease progression," Dr. Caselli said.
"For patients with overt symptoms, even at the MCI stage, PET scans are quite sensitive. The problem is they are expensive and not always covered by insurance, so a less expensive and equally reliable blood test would certainly be welcome," he added.
The investigators and Dr. Caselli had no conflicts of interest to declare.
Researchers have identified a panel of 10 lipid metabolites that can predict the development of either amnestic mild cognitive impairment or Alzheimer’s disease within 2-3 years with 90% sensitivity and 90% specificity.
"The defined ten-metabolite profile features PCs [phosphatidylcholines] and ACs [acylcarnitines], phospholipids that have essential structural and functional roles in the integrity and functionality of cell membranes," Dr. Mark Mapstone of the University of Rochester (N.Y.) and his colleagues wrote in Nature Medicine.
Of the 525 healthy, community-dwelling individuals aged 70 years and older enrolled in the observational study, 74 met the criteria for amnestic mild cognitive impairment (aMCI) or mild Alzheimer’s disease during the 5-year follow-up period – 46 who were incidental at entry to the study and 28 who converted over a mean time of 2.1 years (Nat. Med. 2014 March 9 [doi:10.1038/nm.3466]).
In the third year of the study, the investigators conducted untargeted metabolomic and lipidomic analysis on blood samples from 53 participants with either aMCI or Alzheimer’s disease, including 18 converters and 53 cognitively normal controls. Blood samples from the converters were taken before and after conversion.
Analysis revealed a number of amino acids and phospholipids that were significantly different between the two groups, and a further targeted analysis showed that the converter group had significantly lower plasma levels of serotonin, phenylalanine, proline, lysine, phosphatidylcholine, taurine, and acylcarnitine.
In particular, Dr. Mapstone and his associates identified a set of 10 metabolites that comprised phosphatidylcholines, lysophosphatidylcholine, and acylcarnitines, which were each found at much lower levels in the plasma of the converter group before conversion than in the plasma of the cognitively normal group. Apolipoprotein E epsilon-4 allele status did not have a significant effect on the classification of converters to aMCI or AD or the normal controls.
"These metabolites remained depleted after phenoconversion to aMCI/AD ... and were similar to the levels in the aMCI/AD group," the researchers reported.
"We posit that this ten–phospholipid biomarker panel, consisting of PC and AC species, reveals the breakdown of neural cell membranes in those individuals destined to phenoconvert from cognitive intactness to aMCI or AD and may mark the transition between preclinical states where synaptic dysfunction and early neurodegeneration give rise to subtle cognitive changes," Dr. Mapstone and his coworkers wrote.
Commenting on the study, Dr. Richard J. Caselli, professor of neurology at the Mayo Clinic in Scottsdale, Ariz., and clinical core director of the Arizona Alzheimer’s Disease Center, said that lipidomic studies represent a different approach from the usual proteomic and genomic approaches, although it was not possible to say whether any one approach would be more valid than another.
Dr. Caselli, however, said that a test using blood samples would have its advantages.
"Blood tests are always easier and often cheaper than spinal taps or PET scans (or any other brain imaging procedure) [and] they can also be repeated more easily to track disease progression," Dr. Caselli said.
"For patients with overt symptoms, even at the MCI stage, PET scans are quite sensitive. The problem is they are expensive and not always covered by insurance, so a less expensive and equally reliable blood test would certainly be welcome," he added.
The investigators and Dr. Caselli had no conflicts of interest to declare.
FROM NATURE MEDICINE
Major finding: A panel of 10 plasma lipid biomarkers can predict the development of either amnestic mild cognitive impairment or Alzheimer’s disease within 2-3 years in healthy adults with 90% sensitivity and 90% specificity.
Data source: A 5-year, prospective, observational study of 525 healthy older adults, including 74 who developed mild cognitive impairment or Alzheimer’s disease during follow-up.
Disclosures: No conflicts of interest were declared.
Stem cell transplantation effective in aggressive relapsing-remitting MS
Autologous hematopoietic stem cell transplantation was an effective treatment option for aggressive multiple sclerosis, particularly in patients with inflammatory activity at baseline, in a study of the Swedish experience with the procedure since it was first performed there in 2004.
A prospective, observational study of 41 patients with MS treated with autologous hematopoietic stem cell transplantation (HCST) showed a 5-year, relapse-free survival rate of 87% and disease-free survival of 68%. The data also showed a magnetic resonance imaging (MRI) event-free survival rate of 85% and expanded disability status scale (EDSS) score progression-free survival of 77%.
"We know that HSCT causes a profound renewal of the immune system and not just long-lasting immune suppression," wrote first author Dr. Joachim Burman from Uppsala (Sweden) University Hospital and his colleagues. "At least part of the effect is likely related to removal of autoreactive cells, but some of these cells probably escape the treatment and remain after HSCT."
Autologous HSCT has been used to treat MS for nearly two decades and was initially used to treat progressive forms of MS, but when the procedure did not stop deterioration in patients with progressive disease, researchers found that it could be effective in treating highly aggressive relapsing-remitting MS. However, no randomized controlled trial has been performed, few case series have been published, and systematic safety and efficacy follow-up data for relapsing-remitting MS are scarce, the authors noted.
In the study, patients with ongoing inflammatory activity at baseline showed the most significant treatment response, and 79% of these patients had no new MRI lesions, relapses, or EDSS score progression following treatment.
The EDSS score improved in relapsing-remitting patients from a median of 5.5 at the time of HSCT to 3.25 at 1 year and 3 at 2 years, and in those with progressive forms of MS the median score stayed at 6.5 at those three time points.
Of the 41 patients, 34 had relapsing-remitting MS and 7 had other progressive forms of MS. All of the patients had at least 1 year of follow-up, and the mean duration was 47.4 months (J. Neurol. Neurosurg. Psychiatr. 2014 Feb. 19 [doi: 10.1136/jnnp-2013-307207]).
Researchers noted that new disease activity, when it did occur, was predominantly seen during the first 2 years after treatment, and no patient who remained disease-free during the first 3 years – meaning no relapses, no new MRI lesions, and no EDSS progression – went on to have a clinical relapse or develop new MRI lesions.
No deaths were associated with the treatment, although almost all patients experienced acute toxicity during hospitalization. The most common long-term side effects were herpes zoster reactivation (15%) and thyroid disease (8.4%).
The research was supported by the Swedish Association of Persons with Neurological Disabilities, the MÅH Ländell Foundation, and Uppsala University Hospital. The authors declared individual funding, support, and grants from a range of pharmaceutical companies.
Autologous hematopoietic stem cell transplantation was an effective treatment option for aggressive multiple sclerosis, particularly in patients with inflammatory activity at baseline, in a study of the Swedish experience with the procedure since it was first performed there in 2004.
A prospective, observational study of 41 patients with MS treated with autologous hematopoietic stem cell transplantation (HCST) showed a 5-year, relapse-free survival rate of 87% and disease-free survival of 68%. The data also showed a magnetic resonance imaging (MRI) event-free survival rate of 85% and expanded disability status scale (EDSS) score progression-free survival of 77%.
"We know that HSCT causes a profound renewal of the immune system and not just long-lasting immune suppression," wrote first author Dr. Joachim Burman from Uppsala (Sweden) University Hospital and his colleagues. "At least part of the effect is likely related to removal of autoreactive cells, but some of these cells probably escape the treatment and remain after HSCT."
Autologous HSCT has been used to treat MS for nearly two decades and was initially used to treat progressive forms of MS, but when the procedure did not stop deterioration in patients with progressive disease, researchers found that it could be effective in treating highly aggressive relapsing-remitting MS. However, no randomized controlled trial has been performed, few case series have been published, and systematic safety and efficacy follow-up data for relapsing-remitting MS are scarce, the authors noted.
In the study, patients with ongoing inflammatory activity at baseline showed the most significant treatment response, and 79% of these patients had no new MRI lesions, relapses, or EDSS score progression following treatment.
The EDSS score improved in relapsing-remitting patients from a median of 5.5 at the time of HSCT to 3.25 at 1 year and 3 at 2 years, and in those with progressive forms of MS the median score stayed at 6.5 at those three time points.
Of the 41 patients, 34 had relapsing-remitting MS and 7 had other progressive forms of MS. All of the patients had at least 1 year of follow-up, and the mean duration was 47.4 months (J. Neurol. Neurosurg. Psychiatr. 2014 Feb. 19 [doi: 10.1136/jnnp-2013-307207]).
Researchers noted that new disease activity, when it did occur, was predominantly seen during the first 2 years after treatment, and no patient who remained disease-free during the first 3 years – meaning no relapses, no new MRI lesions, and no EDSS progression – went on to have a clinical relapse or develop new MRI lesions.
No deaths were associated with the treatment, although almost all patients experienced acute toxicity during hospitalization. The most common long-term side effects were herpes zoster reactivation (15%) and thyroid disease (8.4%).
The research was supported by the Swedish Association of Persons with Neurological Disabilities, the MÅH Ländell Foundation, and Uppsala University Hospital. The authors declared individual funding, support, and grants from a range of pharmaceutical companies.
Autologous hematopoietic stem cell transplantation was an effective treatment option for aggressive multiple sclerosis, particularly in patients with inflammatory activity at baseline, in a study of the Swedish experience with the procedure since it was first performed there in 2004.
A prospective, observational study of 41 patients with MS treated with autologous hematopoietic stem cell transplantation (HCST) showed a 5-year, relapse-free survival rate of 87% and disease-free survival of 68%. The data also showed a magnetic resonance imaging (MRI) event-free survival rate of 85% and expanded disability status scale (EDSS) score progression-free survival of 77%.
"We know that HSCT causes a profound renewal of the immune system and not just long-lasting immune suppression," wrote first author Dr. Joachim Burman from Uppsala (Sweden) University Hospital and his colleagues. "At least part of the effect is likely related to removal of autoreactive cells, but some of these cells probably escape the treatment and remain after HSCT."
Autologous HSCT has been used to treat MS for nearly two decades and was initially used to treat progressive forms of MS, but when the procedure did not stop deterioration in patients with progressive disease, researchers found that it could be effective in treating highly aggressive relapsing-remitting MS. However, no randomized controlled trial has been performed, few case series have been published, and systematic safety and efficacy follow-up data for relapsing-remitting MS are scarce, the authors noted.
In the study, patients with ongoing inflammatory activity at baseline showed the most significant treatment response, and 79% of these patients had no new MRI lesions, relapses, or EDSS score progression following treatment.
The EDSS score improved in relapsing-remitting patients from a median of 5.5 at the time of HSCT to 3.25 at 1 year and 3 at 2 years, and in those with progressive forms of MS the median score stayed at 6.5 at those three time points.
Of the 41 patients, 34 had relapsing-remitting MS and 7 had other progressive forms of MS. All of the patients had at least 1 year of follow-up, and the mean duration was 47.4 months (J. Neurol. Neurosurg. Psychiatr. 2014 Feb. 19 [doi: 10.1136/jnnp-2013-307207]).
Researchers noted that new disease activity, when it did occur, was predominantly seen during the first 2 years after treatment, and no patient who remained disease-free during the first 3 years – meaning no relapses, no new MRI lesions, and no EDSS progression – went on to have a clinical relapse or develop new MRI lesions.
No deaths were associated with the treatment, although almost all patients experienced acute toxicity during hospitalization. The most common long-term side effects were herpes zoster reactivation (15%) and thyroid disease (8.4%).
The research was supported by the Swedish Association of Persons with Neurological Disabilities, the MÅH Ländell Foundation, and Uppsala University Hospital. The authors declared individual funding, support, and grants from a range of pharmaceutical companies.
FROM THE JOURNAL OF NEUROLOGY, NEUROSURGERY AND PSYCHIATRY
Major finding: Autologous hematopoietic stem cell transplantation in multiple sclerosis showed a 5-year, relapse-free survival rate of 87% and disease-free survival of 68%.
Data source: A prospective, observational study in 41 patients with aggressive MS.
Disclosures: The research was supported by the Swedish Association of Persons with Neurological Disabilities, the MÅH Ländell Foundation, and Uppsala University Hospital. The authors declared individual funding, support, and grants from a range of pharmaceutical companies.
TNF inhibitors reduce coronary artery disease risk in rheumatoid arthritis
Use of tumor necrosis factor–alpha inhibitors was associated with a significant reduction in the risk of coronary artery disease in patients with rheumatoid arthritis, particularly with longer term use of the drugs, in a retrospective cohort study.
The study of 2,101 patients with incident RA diagnosed during 2001-2011 showed that those treated with a tumor necrosis factor–alpha (TNF-alpha) inhibitor alone or with methotrexate had 55% lower relative risk (95% CI, 0.21-0.96) of coronary artery disease than did a reference group treated with non-methotrexate, nonbiologic, disease-modifying antirheumatic drugs (DMARDs).
Patients treated with methotrexate alone or in combination with other nonbiologic DMARDs showed a nonsignificant 46% reduction (95% CI, 0.27-1.09) in the incidence of coronary artery disease, compared with the reference group (Arthritis Care Res. 2014;66:355-63).
There were similar trends in reduction of the risk of cardiovascular disease (CVD, defined as a composite of coronary artery disease, stroke, transient ischemic attack, abdominal aortic aneurysm, peripheral arterial disease, or arterial revascularization procedure), but these did not reach statistical significance. However, the authors suggested this and the methotrexate result may have been from inadequate power.
"These findings indicate that the benefits of TNF inhibitors may extend beyond their effects on joint disease and are associated with reduction in the leading comorbidity in RA, namely CVD," wrote Dr. Androniki Bili from Geisinger Medical Center, Danville, Pa., and her colleagues.
"These benefits should be considered when weighing the risks and benefits of using these costly medications in the treatment of RA," they wrote
Patients enrolled in the study had no history of CVD prior to treatment, and the model was adjusted for a range of confounders, including age, sex, race, smoking, blood pressure, diabetes, and other cardiovascular risk factors. Median follow-up was 3.4 years.
Patients taking TNF-alpha inhibitors for 16.1 months or more had a relative risk of 0.18 for coronary artery disease (95% CI, 0.06-0.50) and 0.31 for CVD (95% CI, 0.15-0.65). There was a similar but not statistically significant trend for use of methotrexate at 23.4 months.
Subgroup analysis showed that the incidence of coronary artery disease was even lower among patients without diabetes mellitus (hazard ratio, 0.39; 95% CI, 0.15-0.98) and among rheumatoid factor–positive patients (HR, 0.38; 95% CI, 0.15-0.95), compared with the reference group.
Rheumatoid arthritis is associated with increased cardiovascular morbidity, independent of traditional cardiovascular risk factors, that is thought to be partly mediated by chronic, systemic inflammation, the researchers said.
This has led to considerable interest in the potential of medication such as TNF-alpha inhibitors in reducing this risk, particularly in light of several observational studies suggesting a reduced risk of CVD among patients treated with methotrexate.
One author was coinvestigator on two AstraZeneca clinical trials in rheumatoid arthritis, but there were no other conflicts of interest declared.
Use of tumor necrosis factor–alpha inhibitors was associated with a significant reduction in the risk of coronary artery disease in patients with rheumatoid arthritis, particularly with longer term use of the drugs, in a retrospective cohort study.
The study of 2,101 patients with incident RA diagnosed during 2001-2011 showed that those treated with a tumor necrosis factor–alpha (TNF-alpha) inhibitor alone or with methotrexate had 55% lower relative risk (95% CI, 0.21-0.96) of coronary artery disease than did a reference group treated with non-methotrexate, nonbiologic, disease-modifying antirheumatic drugs (DMARDs).
Patients treated with methotrexate alone or in combination with other nonbiologic DMARDs showed a nonsignificant 46% reduction (95% CI, 0.27-1.09) in the incidence of coronary artery disease, compared with the reference group (Arthritis Care Res. 2014;66:355-63).
There were similar trends in reduction of the risk of cardiovascular disease (CVD, defined as a composite of coronary artery disease, stroke, transient ischemic attack, abdominal aortic aneurysm, peripheral arterial disease, or arterial revascularization procedure), but these did not reach statistical significance. However, the authors suggested this and the methotrexate result may have been from inadequate power.
"These findings indicate that the benefits of TNF inhibitors may extend beyond their effects on joint disease and are associated with reduction in the leading comorbidity in RA, namely CVD," wrote Dr. Androniki Bili from Geisinger Medical Center, Danville, Pa., and her colleagues.
"These benefits should be considered when weighing the risks and benefits of using these costly medications in the treatment of RA," they wrote
Patients enrolled in the study had no history of CVD prior to treatment, and the model was adjusted for a range of confounders, including age, sex, race, smoking, blood pressure, diabetes, and other cardiovascular risk factors. Median follow-up was 3.4 years.
Patients taking TNF-alpha inhibitors for 16.1 months or more had a relative risk of 0.18 for coronary artery disease (95% CI, 0.06-0.50) and 0.31 for CVD (95% CI, 0.15-0.65). There was a similar but not statistically significant trend for use of methotrexate at 23.4 months.
Subgroup analysis showed that the incidence of coronary artery disease was even lower among patients without diabetes mellitus (hazard ratio, 0.39; 95% CI, 0.15-0.98) and among rheumatoid factor–positive patients (HR, 0.38; 95% CI, 0.15-0.95), compared with the reference group.
Rheumatoid arthritis is associated with increased cardiovascular morbidity, independent of traditional cardiovascular risk factors, that is thought to be partly mediated by chronic, systemic inflammation, the researchers said.
This has led to considerable interest in the potential of medication such as TNF-alpha inhibitors in reducing this risk, particularly in light of several observational studies suggesting a reduced risk of CVD among patients treated with methotrexate.
One author was coinvestigator on two AstraZeneca clinical trials in rheumatoid arthritis, but there were no other conflicts of interest declared.
Use of tumor necrosis factor–alpha inhibitors was associated with a significant reduction in the risk of coronary artery disease in patients with rheumatoid arthritis, particularly with longer term use of the drugs, in a retrospective cohort study.
The study of 2,101 patients with incident RA diagnosed during 2001-2011 showed that those treated with a tumor necrosis factor–alpha (TNF-alpha) inhibitor alone or with methotrexate had 55% lower relative risk (95% CI, 0.21-0.96) of coronary artery disease than did a reference group treated with non-methotrexate, nonbiologic, disease-modifying antirheumatic drugs (DMARDs).
Patients treated with methotrexate alone or in combination with other nonbiologic DMARDs showed a nonsignificant 46% reduction (95% CI, 0.27-1.09) in the incidence of coronary artery disease, compared with the reference group (Arthritis Care Res. 2014;66:355-63).
There were similar trends in reduction of the risk of cardiovascular disease (CVD, defined as a composite of coronary artery disease, stroke, transient ischemic attack, abdominal aortic aneurysm, peripheral arterial disease, or arterial revascularization procedure), but these did not reach statistical significance. However, the authors suggested this and the methotrexate result may have been from inadequate power.
"These findings indicate that the benefits of TNF inhibitors may extend beyond their effects on joint disease and are associated with reduction in the leading comorbidity in RA, namely CVD," wrote Dr. Androniki Bili from Geisinger Medical Center, Danville, Pa., and her colleagues.
"These benefits should be considered when weighing the risks and benefits of using these costly medications in the treatment of RA," they wrote
Patients enrolled in the study had no history of CVD prior to treatment, and the model was adjusted for a range of confounders, including age, sex, race, smoking, blood pressure, diabetes, and other cardiovascular risk factors. Median follow-up was 3.4 years.
Patients taking TNF-alpha inhibitors for 16.1 months or more had a relative risk of 0.18 for coronary artery disease (95% CI, 0.06-0.50) and 0.31 for CVD (95% CI, 0.15-0.65). There was a similar but not statistically significant trend for use of methotrexate at 23.4 months.
Subgroup analysis showed that the incidence of coronary artery disease was even lower among patients without diabetes mellitus (hazard ratio, 0.39; 95% CI, 0.15-0.98) and among rheumatoid factor–positive patients (HR, 0.38; 95% CI, 0.15-0.95), compared with the reference group.
Rheumatoid arthritis is associated with increased cardiovascular morbidity, independent of traditional cardiovascular risk factors, that is thought to be partly mediated by chronic, systemic inflammation, the researchers said.
This has led to considerable interest in the potential of medication such as TNF-alpha inhibitors in reducing this risk, particularly in light of several observational studies suggesting a reduced risk of CVD among patients treated with methotrexate.
One author was coinvestigator on two AstraZeneca clinical trials in rheumatoid arthritis, but there were no other conflicts of interest declared.
FROM ARTHRITIS CARE AND RESEARCH
Major finding: Treatment with TNF-alpha inhibitors more than halves the risk of coronary artery disease in patients with rheumatoid arthritis, in particular among RF-positive patients and those without diabetes mellitus.
Data source: A retrospective cohort study of 2,101 patients with rheumatoid arthritis.
Disclosures: One author was coinvestigator on two AstraZeneca clinical trials in rheumatoid arthritis but there were no other conflicts of interest declared.
Aggressive secondary squamous carcinoma appeared during BRAF inhibitor targeted therapy
A woman undergoing BRAF inhibitor targeted therapy for advanced melanoma has presented with invasive spindle cell squamous carcinoma masquerading as a secondary cutaneous squamous cell carcinoma, highlighting the importance of histologic evaluation of these lesions.
"Secondary cutaneous squamous cell carcinomas (cSCCs) are adverse effects of BRAF inhibitor targeted therapy for advanced melanoma," wrote Dr. Daniel N. Cohen and his associates online Feb. 26 in JAMA Dermatology.
The most commonly seen histologic type of secondary cutaneous squamous cell carcinomas is keratoacanthoma-like cSCC (cSCC-KA), which is thought to have a low risk of metastasis or recurrence, said lead author Dr. Cohen of the Vanderbilt University Medical Center, Nashville, Tenn.
In this case report, however, a woman in her 50s with BRAF-mutant metastatic melanoma developed more than 100 new cutaneous squamous proliferations across her face, trunk, and extremities within 4 weeks of starting treatment with the BRAF inhibitor dabrafenib as part of a clinical trial, with some lesions appearing to be a more aggressive type upon analysis.
The lesions began as acrochordons on her face and extremities, as well as new nevi on her torso and axilla. She also developed fever, chills, and fatigue and had enlarging, tender, and bleeding lesions on her trunk and extremities.
Seven large, tender, and indurated lesions were removed using a deep scoop shave biopsy, revealing a biphasic malignant growth pattern (JAMA Dermatology 2014 Feb 26 [doi:10.1001/jamadermatol.2013.7784]).
"The superficial portion demonstrated conventional cSCC-KA features of hyperkeratosis, epidermal acanthosis, and central core of glassy eosinophilic keratin with pseudopapillomatosis and a base with focal invasive lobules of cytologically atypical keratinocytes, consistent with previously reported cSCC-KA" the study authors reported.
However, they added, "in stark contrast to prior reports, the deep aspects of 6 of 7 lesions showed invasive spindled and epithelioid cells with monomorphic elongated nuclei with condensed chromatin and mitoses consistent with spindle cell squamous carcinoma, an aggressive subtype of squamous cell carcinoma."
The cells were strongly immunoreactive for cytokeratin CK5/6 and CK903, and both the squamous and spindle components were vimentin reactive and showed increased proliferation index. In contrast to the usual pattern of a spindle cell melanoma, the spindle tumor cells were also MART-1 and S100 negative.
The authors said this was the first known report of invasive spindle cell squamous carcinoma that mimicked keratoacanthoma-like secondary SCC appearing during BRAF inhibitor therapy and suggested that the discovery has implications for management of secondary squamous cell carcinoma.
"Because the clinical appearance of cSCC-KA and the spindle cell squamous carcinomas in our patient are indistinguishable, histologic evaluation of the entire lesion (via saucerization biopsy or incisional biopsy) is vital to prevent inadequate treatment of a deeply invasive process with a probable higher malignant potential," Dr. Cohen and his associates wrote.
The patient stopped BRAF inhibitor therapy and had no recurrence or new development of cutaneous secondary SCCs. A single later recurrence of melanoma was resected but she remains disease free.
One author declared a consultancy with Bristol-Myers Squibb and Genentech, as well as grant support from Genentech. There were no other financial disclosures reported.
A woman undergoing BRAF inhibitor targeted therapy for advanced melanoma has presented with invasive spindle cell squamous carcinoma masquerading as a secondary cutaneous squamous cell carcinoma, highlighting the importance of histologic evaluation of these lesions.
"Secondary cutaneous squamous cell carcinomas (cSCCs) are adverse effects of BRAF inhibitor targeted therapy for advanced melanoma," wrote Dr. Daniel N. Cohen and his associates online Feb. 26 in JAMA Dermatology.
The most commonly seen histologic type of secondary cutaneous squamous cell carcinomas is keratoacanthoma-like cSCC (cSCC-KA), which is thought to have a low risk of metastasis or recurrence, said lead author Dr. Cohen of the Vanderbilt University Medical Center, Nashville, Tenn.
In this case report, however, a woman in her 50s with BRAF-mutant metastatic melanoma developed more than 100 new cutaneous squamous proliferations across her face, trunk, and extremities within 4 weeks of starting treatment with the BRAF inhibitor dabrafenib as part of a clinical trial, with some lesions appearing to be a more aggressive type upon analysis.
The lesions began as acrochordons on her face and extremities, as well as new nevi on her torso and axilla. She also developed fever, chills, and fatigue and had enlarging, tender, and bleeding lesions on her trunk and extremities.
Seven large, tender, and indurated lesions were removed using a deep scoop shave biopsy, revealing a biphasic malignant growth pattern (JAMA Dermatology 2014 Feb 26 [doi:10.1001/jamadermatol.2013.7784]).
"The superficial portion demonstrated conventional cSCC-KA features of hyperkeratosis, epidermal acanthosis, and central core of glassy eosinophilic keratin with pseudopapillomatosis and a base with focal invasive lobules of cytologically atypical keratinocytes, consistent with previously reported cSCC-KA" the study authors reported.
However, they added, "in stark contrast to prior reports, the deep aspects of 6 of 7 lesions showed invasive spindled and epithelioid cells with monomorphic elongated nuclei with condensed chromatin and mitoses consistent with spindle cell squamous carcinoma, an aggressive subtype of squamous cell carcinoma."
The cells were strongly immunoreactive for cytokeratin CK5/6 and CK903, and both the squamous and spindle components were vimentin reactive and showed increased proliferation index. In contrast to the usual pattern of a spindle cell melanoma, the spindle tumor cells were also MART-1 and S100 negative.
The authors said this was the first known report of invasive spindle cell squamous carcinoma that mimicked keratoacanthoma-like secondary SCC appearing during BRAF inhibitor therapy and suggested that the discovery has implications for management of secondary squamous cell carcinoma.
"Because the clinical appearance of cSCC-KA and the spindle cell squamous carcinomas in our patient are indistinguishable, histologic evaluation of the entire lesion (via saucerization biopsy or incisional biopsy) is vital to prevent inadequate treatment of a deeply invasive process with a probable higher malignant potential," Dr. Cohen and his associates wrote.
The patient stopped BRAF inhibitor therapy and had no recurrence or new development of cutaneous secondary SCCs. A single later recurrence of melanoma was resected but she remains disease free.
One author declared a consultancy with Bristol-Myers Squibb and Genentech, as well as grant support from Genentech. There were no other financial disclosures reported.
A woman undergoing BRAF inhibitor targeted therapy for advanced melanoma has presented with invasive spindle cell squamous carcinoma masquerading as a secondary cutaneous squamous cell carcinoma, highlighting the importance of histologic evaluation of these lesions.
"Secondary cutaneous squamous cell carcinomas (cSCCs) are adverse effects of BRAF inhibitor targeted therapy for advanced melanoma," wrote Dr. Daniel N. Cohen and his associates online Feb. 26 in JAMA Dermatology.
The most commonly seen histologic type of secondary cutaneous squamous cell carcinomas is keratoacanthoma-like cSCC (cSCC-KA), which is thought to have a low risk of metastasis or recurrence, said lead author Dr. Cohen of the Vanderbilt University Medical Center, Nashville, Tenn.
In this case report, however, a woman in her 50s with BRAF-mutant metastatic melanoma developed more than 100 new cutaneous squamous proliferations across her face, trunk, and extremities within 4 weeks of starting treatment with the BRAF inhibitor dabrafenib as part of a clinical trial, with some lesions appearing to be a more aggressive type upon analysis.
The lesions began as acrochordons on her face and extremities, as well as new nevi on her torso and axilla. She also developed fever, chills, and fatigue and had enlarging, tender, and bleeding lesions on her trunk and extremities.
Seven large, tender, and indurated lesions were removed using a deep scoop shave biopsy, revealing a biphasic malignant growth pattern (JAMA Dermatology 2014 Feb 26 [doi:10.1001/jamadermatol.2013.7784]).
"The superficial portion demonstrated conventional cSCC-KA features of hyperkeratosis, epidermal acanthosis, and central core of glassy eosinophilic keratin with pseudopapillomatosis and a base with focal invasive lobules of cytologically atypical keratinocytes, consistent with previously reported cSCC-KA" the study authors reported.
However, they added, "in stark contrast to prior reports, the deep aspects of 6 of 7 lesions showed invasive spindled and epithelioid cells with monomorphic elongated nuclei with condensed chromatin and mitoses consistent with spindle cell squamous carcinoma, an aggressive subtype of squamous cell carcinoma."
The cells were strongly immunoreactive for cytokeratin CK5/6 and CK903, and both the squamous and spindle components were vimentin reactive and showed increased proliferation index. In contrast to the usual pattern of a spindle cell melanoma, the spindle tumor cells were also MART-1 and S100 negative.
The authors said this was the first known report of invasive spindle cell squamous carcinoma that mimicked keratoacanthoma-like secondary SCC appearing during BRAF inhibitor therapy and suggested that the discovery has implications for management of secondary squamous cell carcinoma.
"Because the clinical appearance of cSCC-KA and the spindle cell squamous carcinomas in our patient are indistinguishable, histologic evaluation of the entire lesion (via saucerization biopsy or incisional biopsy) is vital to prevent inadequate treatment of a deeply invasive process with a probable higher malignant potential," Dr. Cohen and his associates wrote.
The patient stopped BRAF inhibitor therapy and had no recurrence or new development of cutaneous secondary SCCs. A single later recurrence of melanoma was resected but she remains disease free.
One author declared a consultancy with Bristol-Myers Squibb and Genentech, as well as grant support from Genentech. There were no other financial disclosures reported.
FROM JAMA DERMATOLOGY
Major finding: A woman undergoing BRAF inhibitor targeted therapy for advanced melanoma has presented with invasive spindle cell squamous carcinoma masquerading as a secondary cutaneous squamous cell carcinoma.
Data source: Case report.
Disclosures: One author declared a consultancy with Bristol-Myers Squibb and Genentech, as well as grant support from Genentech. There were no other financial disclosures reported.
Postsurgical withdrawal of antiepileptic drugs raises only short-term seizure risk
Withdrawing antiepileptic medication after temporal lobe epilepsy surgery may increase the risk of breakthrough seizures in the short term but does not alter long-term remission rates, a retrospective, observational cohort study found.
Two years after surgery, 69% of patients whose medication was discontinued at 1 year were completely seizure free, compared with 72% of those whose medication was reduced at 1 year and 79% of those whose medication was unchanged, Dr. Ruta Yardi of the Cleveland Clinic and her colleagues reported in Annals of Clinical and Translational Neurology (Ann. Clin. Transl. Neurol. 2014;1:115-23 [doi:10.1002/acn3.35]).
The authors said that there is long-standing debate on how to manage antiepilepsy medication after surgery, with concerns about breakthrough seizures being countered by patient desire to cease medication, concerns about polytherapy toxicity, and the rising cost of medication. There is little, however, by way of guidance on postoperative antiepileptic medication management.
"Our findings suggest though that postoperative AED [antiepileptic drug] management in this [temporal lobe epilepsy] cohort may reflect a compromise between needing to relieve patients from significant medication-related side effects and confidence about surgical success," Dr. Yardi and her associates wrote.
The researchers reviewed 609 patients (86% adults) who underwent temporal lobe epilepsy surgery during 1995-2011 and who had previously failed at least two antiepileptic drugs. Data on the exact dates of medication regimen change were available for 311 patients, including 253 who reduced their medication and 127 who stopped it entirely.
The study showed that long-term remission rates were similar in both the discontinuation groups (82% remission when medications were withdrawn after 1 year and 90% for medications withdrawn after 2 years) and the "unchanged" groups.
Patients who experienced seizures while their antiepileptic medication was being reduced, however, were less likely to achieve remission (50% remission rate) than were those who experienced breakthrough seizures after complete discontinuation of their medication (70%; P = .0001). Of the patients who experienced breakthrough seizures while their antiepileptic medications were being reduced, only 65% achieved 2-year remission.
"Patients with brain tumors (and thus an easily ascertainable complete removal of the epileptic focus) were at least twice as likely as those with any other epilepsy pathology to have their AEDs completely discontinued after surgery, while those with spikes on postoperative EEG (and thus an easily ascertainable presence of an epileptic focus) were almost twice as likely to continue their AEDs unchanged," the investigators wrote.
Among the 311 patients for whom data on medication change were available, the mean interval from surgery to starting withdrawal of medication was 1.34 years. This interval was longer in patients who had more than 20 preoperative seizures per month but tended to be shorter in children.
The mean interval from surgery to the latest change in medication was 1.64 years, and again, this interval was shorter in children (0.95 years vs. 1.76 years in adults, P = .002).
The authors declared having no conflicts of interest.
Withdrawing antiepileptic medication after temporal lobe epilepsy surgery may increase the risk of breakthrough seizures in the short term but does not alter long-term remission rates, a retrospective, observational cohort study found.
Two years after surgery, 69% of patients whose medication was discontinued at 1 year were completely seizure free, compared with 72% of those whose medication was reduced at 1 year and 79% of those whose medication was unchanged, Dr. Ruta Yardi of the Cleveland Clinic and her colleagues reported in Annals of Clinical and Translational Neurology (Ann. Clin. Transl. Neurol. 2014;1:115-23 [doi:10.1002/acn3.35]).
The authors said that there is long-standing debate on how to manage antiepilepsy medication after surgery, with concerns about breakthrough seizures being countered by patient desire to cease medication, concerns about polytherapy toxicity, and the rising cost of medication. There is little, however, by way of guidance on postoperative antiepileptic medication management.
"Our findings suggest though that postoperative AED [antiepileptic drug] management in this [temporal lobe epilepsy] cohort may reflect a compromise between needing to relieve patients from significant medication-related side effects and confidence about surgical success," Dr. Yardi and her associates wrote.
The researchers reviewed 609 patients (86% adults) who underwent temporal lobe epilepsy surgery during 1995-2011 and who had previously failed at least two antiepileptic drugs. Data on the exact dates of medication regimen change were available for 311 patients, including 253 who reduced their medication and 127 who stopped it entirely.
The study showed that long-term remission rates were similar in both the discontinuation groups (82% remission when medications were withdrawn after 1 year and 90% for medications withdrawn after 2 years) and the "unchanged" groups.
Patients who experienced seizures while their antiepileptic medication was being reduced, however, were less likely to achieve remission (50% remission rate) than were those who experienced breakthrough seizures after complete discontinuation of their medication (70%; P = .0001). Of the patients who experienced breakthrough seizures while their antiepileptic medications were being reduced, only 65% achieved 2-year remission.
"Patients with brain tumors (and thus an easily ascertainable complete removal of the epileptic focus) were at least twice as likely as those with any other epilepsy pathology to have their AEDs completely discontinued after surgery, while those with spikes on postoperative EEG (and thus an easily ascertainable presence of an epileptic focus) were almost twice as likely to continue their AEDs unchanged," the investigators wrote.
Among the 311 patients for whom data on medication change were available, the mean interval from surgery to starting withdrawal of medication was 1.34 years. This interval was longer in patients who had more than 20 preoperative seizures per month but tended to be shorter in children.
The mean interval from surgery to the latest change in medication was 1.64 years, and again, this interval was shorter in children (0.95 years vs. 1.76 years in adults, P = .002).
The authors declared having no conflicts of interest.
Withdrawing antiepileptic medication after temporal lobe epilepsy surgery may increase the risk of breakthrough seizures in the short term but does not alter long-term remission rates, a retrospective, observational cohort study found.
Two years after surgery, 69% of patients whose medication was discontinued at 1 year were completely seizure free, compared with 72% of those whose medication was reduced at 1 year and 79% of those whose medication was unchanged, Dr. Ruta Yardi of the Cleveland Clinic and her colleagues reported in Annals of Clinical and Translational Neurology (Ann. Clin. Transl. Neurol. 2014;1:115-23 [doi:10.1002/acn3.35]).
The authors said that there is long-standing debate on how to manage antiepilepsy medication after surgery, with concerns about breakthrough seizures being countered by patient desire to cease medication, concerns about polytherapy toxicity, and the rising cost of medication. There is little, however, by way of guidance on postoperative antiepileptic medication management.
"Our findings suggest though that postoperative AED [antiepileptic drug] management in this [temporal lobe epilepsy] cohort may reflect a compromise between needing to relieve patients from significant medication-related side effects and confidence about surgical success," Dr. Yardi and her associates wrote.
The researchers reviewed 609 patients (86% adults) who underwent temporal lobe epilepsy surgery during 1995-2011 and who had previously failed at least two antiepileptic drugs. Data on the exact dates of medication regimen change were available for 311 patients, including 253 who reduced their medication and 127 who stopped it entirely.
The study showed that long-term remission rates were similar in both the discontinuation groups (82% remission when medications were withdrawn after 1 year and 90% for medications withdrawn after 2 years) and the "unchanged" groups.
Patients who experienced seizures while their antiepileptic medication was being reduced, however, were less likely to achieve remission (50% remission rate) than were those who experienced breakthrough seizures after complete discontinuation of their medication (70%; P = .0001). Of the patients who experienced breakthrough seizures while their antiepileptic medications were being reduced, only 65% achieved 2-year remission.
"Patients with brain tumors (and thus an easily ascertainable complete removal of the epileptic focus) were at least twice as likely as those with any other epilepsy pathology to have their AEDs completely discontinued after surgery, while those with spikes on postoperative EEG (and thus an easily ascertainable presence of an epileptic focus) were almost twice as likely to continue their AEDs unchanged," the investigators wrote.
Among the 311 patients for whom data on medication change were available, the mean interval from surgery to starting withdrawal of medication was 1.34 years. This interval was longer in patients who had more than 20 preoperative seizures per month but tended to be shorter in children.
The mean interval from surgery to the latest change in medication was 1.64 years, and again, this interval was shorter in children (0.95 years vs. 1.76 years in adults, P = .002).
The authors declared having no conflicts of interest.
FROM ANNALS OF CLINICAL AND TRANSLATIONAL NEUROLOGY
Major finding: Two years after surgery, 69% of patients whose medication was discontinued at 1 year were completely seizure free, compared with 72% of those whose medication was reduced at 1 year and 79% of those whose medication was unchanged.
Data source: A retrospective, observational cohort study of 609 patients who underwent temporal lobe epilepsy surgery.
Disclosures: The authors declared having no conflicts of interest.
Increased mortality persists in drug-resistant epilepsy
Drug-resistant epilepsy is associated with a significant increase in mortality that persists for decades after diagnosis, particularly among individuals with a known etiology, according to data from a retrospective, multicenter cohort study.
Dr. Brian Callaghan of the University of Michigan, Ann Arbor, and his colleagues identified 433 patients with drug-resistant epilepsy, which was defined as one or more seizures per month for 3 months prior to inclusion and failure on at least two antiepileptic drugs prior to the index date.
The authors said that a consensus exists, based on previous studies, that patients with epilepsy have increased mortality, compared with the general population. However, these studies also suggest that this mortality decreases over time.
"Ours is a prevalent cohort of drug-resistant epilepsy, and mortality was evaluated after the period of increased mortality risk in an incident cohort with epilepsy (i.e., the first 5 years after diagnosis)," the investigators wrote in their report.
"In our study, we also demonstrate increased mortality. Thus, in this group with a median duration of epilepsy at entry of 25 years, elevated mortality persists."
Over the 6-year follow-up period, there were 33 deaths (7.6%). However, in patients with a known etiology, the case fatality rate was 10.1%, compared with 5.1% among patients with unknown etiology, the researchers reported (J. Neurol. Neurosurg. Psychiatry 2014 Feb. 19 [doi:10.1136/jnnp-2013-307074]).
Among those whose epilepsy had a known etiology, the case fatality rate was 45.5% for progressive etiologies and 8.2% for remote etiologies (P less than .001).
The standardized mortality ratio for the entire cohort was 2.4 (95% confidence interval, 1.7-3.3), while for those with a remote or progressive etiology, the ratio was 3.1 (95% CI, 2.0-4.6), and 1.7 (95% CI, 0.8-2.8) for those with an unknown etiology.
The majority of patients had focal epilepsy (82.5%), 10.6% had symptomatic generalized epilepsy, 5.8% had genetic generalized epilepsy, and 1.2% had another epilepsy syndrome.
Ten of the 33 deaths were definitely or potentially epilepsy related, including 5 cases of sudden unexplained death in epilepsy (3 with unknown and 2 with known etiology), 3 cases of status epilepticus, 1 accident, and 1 suicide.
Ten patients who died had known active cancer at the index date, two other patients had known neurodegenerative conditions, and seven deaths were linked to the underlying cause of the epilepsy such as brain tumors and strokes.
The remaining 16 deaths were unrelated to epilepsy or the underlying etiology.
"The two clinical factors associated with an increased risk of death were older age at study entry and ‘symptomatic generalized epilepsy syndrome’ (in pre-2010 terminology)," the researchers wrote.
"Gender, age of epilepsy onset, and number of [antiepileptic drugs] failed were not associated with mortality, providing further evidence that epilepsy syndrome and etiology are the most important risk factors for death."
The authors also noted that in 11 of the 33 deaths, the epileptologist did not know that the patient had died, and 12% of patients recorded on their medical charts as lost to follow-up were in fact dead.
Some authors reported grant funding and support from a range of pharmaceutical companies, including Lundbeck, Vertex Pharmaceuticals, SK Life Science, Pfizer, Medtronic, GlaxoSmithKline, Eisai, Cyberonics, Neuropace, and Upsher-Smith.
Drug-resistant epilepsy is associated with a significant increase in mortality that persists for decades after diagnosis, particularly among individuals with a known etiology, according to data from a retrospective, multicenter cohort study.
Dr. Brian Callaghan of the University of Michigan, Ann Arbor, and his colleagues identified 433 patients with drug-resistant epilepsy, which was defined as one or more seizures per month for 3 months prior to inclusion and failure on at least two antiepileptic drugs prior to the index date.
The authors said that a consensus exists, based on previous studies, that patients with epilepsy have increased mortality, compared with the general population. However, these studies also suggest that this mortality decreases over time.
"Ours is a prevalent cohort of drug-resistant epilepsy, and mortality was evaluated after the period of increased mortality risk in an incident cohort with epilepsy (i.e., the first 5 years after diagnosis)," the investigators wrote in their report.
"In our study, we also demonstrate increased mortality. Thus, in this group with a median duration of epilepsy at entry of 25 years, elevated mortality persists."
Over the 6-year follow-up period, there were 33 deaths (7.6%). However, in patients with a known etiology, the case fatality rate was 10.1%, compared with 5.1% among patients with unknown etiology, the researchers reported (J. Neurol. Neurosurg. Psychiatry 2014 Feb. 19 [doi:10.1136/jnnp-2013-307074]).
Among those whose epilepsy had a known etiology, the case fatality rate was 45.5% for progressive etiologies and 8.2% for remote etiologies (P less than .001).
The standardized mortality ratio for the entire cohort was 2.4 (95% confidence interval, 1.7-3.3), while for those with a remote or progressive etiology, the ratio was 3.1 (95% CI, 2.0-4.6), and 1.7 (95% CI, 0.8-2.8) for those with an unknown etiology.
The majority of patients had focal epilepsy (82.5%), 10.6% had symptomatic generalized epilepsy, 5.8% had genetic generalized epilepsy, and 1.2% had another epilepsy syndrome.
Ten of the 33 deaths were definitely or potentially epilepsy related, including 5 cases of sudden unexplained death in epilepsy (3 with unknown and 2 with known etiology), 3 cases of status epilepticus, 1 accident, and 1 suicide.
Ten patients who died had known active cancer at the index date, two other patients had known neurodegenerative conditions, and seven deaths were linked to the underlying cause of the epilepsy such as brain tumors and strokes.
The remaining 16 deaths were unrelated to epilepsy or the underlying etiology.
"The two clinical factors associated with an increased risk of death were older age at study entry and ‘symptomatic generalized epilepsy syndrome’ (in pre-2010 terminology)," the researchers wrote.
"Gender, age of epilepsy onset, and number of [antiepileptic drugs] failed were not associated with mortality, providing further evidence that epilepsy syndrome and etiology are the most important risk factors for death."
The authors also noted that in 11 of the 33 deaths, the epileptologist did not know that the patient had died, and 12% of patients recorded on their medical charts as lost to follow-up were in fact dead.
Some authors reported grant funding and support from a range of pharmaceutical companies, including Lundbeck, Vertex Pharmaceuticals, SK Life Science, Pfizer, Medtronic, GlaxoSmithKline, Eisai, Cyberonics, Neuropace, and Upsher-Smith.
Drug-resistant epilepsy is associated with a significant increase in mortality that persists for decades after diagnosis, particularly among individuals with a known etiology, according to data from a retrospective, multicenter cohort study.
Dr. Brian Callaghan of the University of Michigan, Ann Arbor, and his colleagues identified 433 patients with drug-resistant epilepsy, which was defined as one or more seizures per month for 3 months prior to inclusion and failure on at least two antiepileptic drugs prior to the index date.
The authors said that a consensus exists, based on previous studies, that patients with epilepsy have increased mortality, compared with the general population. However, these studies also suggest that this mortality decreases over time.
"Ours is a prevalent cohort of drug-resistant epilepsy, and mortality was evaluated after the period of increased mortality risk in an incident cohort with epilepsy (i.e., the first 5 years after diagnosis)," the investigators wrote in their report.
"In our study, we also demonstrate increased mortality. Thus, in this group with a median duration of epilepsy at entry of 25 years, elevated mortality persists."
Over the 6-year follow-up period, there were 33 deaths (7.6%). However, in patients with a known etiology, the case fatality rate was 10.1%, compared with 5.1% among patients with unknown etiology, the researchers reported (J. Neurol. Neurosurg. Psychiatry 2014 Feb. 19 [doi:10.1136/jnnp-2013-307074]).
Among those whose epilepsy had a known etiology, the case fatality rate was 45.5% for progressive etiologies and 8.2% for remote etiologies (P less than .001).
The standardized mortality ratio for the entire cohort was 2.4 (95% confidence interval, 1.7-3.3), while for those with a remote or progressive etiology, the ratio was 3.1 (95% CI, 2.0-4.6), and 1.7 (95% CI, 0.8-2.8) for those with an unknown etiology.
The majority of patients had focal epilepsy (82.5%), 10.6% had symptomatic generalized epilepsy, 5.8% had genetic generalized epilepsy, and 1.2% had another epilepsy syndrome.
Ten of the 33 deaths were definitely or potentially epilepsy related, including 5 cases of sudden unexplained death in epilepsy (3 with unknown and 2 with known etiology), 3 cases of status epilepticus, 1 accident, and 1 suicide.
Ten patients who died had known active cancer at the index date, two other patients had known neurodegenerative conditions, and seven deaths were linked to the underlying cause of the epilepsy such as brain tumors and strokes.
The remaining 16 deaths were unrelated to epilepsy or the underlying etiology.
"The two clinical factors associated with an increased risk of death were older age at study entry and ‘symptomatic generalized epilepsy syndrome’ (in pre-2010 terminology)," the researchers wrote.
"Gender, age of epilepsy onset, and number of [antiepileptic drugs] failed were not associated with mortality, providing further evidence that epilepsy syndrome and etiology are the most important risk factors for death."
The authors also noted that in 11 of the 33 deaths, the epileptologist did not know that the patient had died, and 12% of patients recorded on their medical charts as lost to follow-up were in fact dead.
Some authors reported grant funding and support from a range of pharmaceutical companies, including Lundbeck, Vertex Pharmaceuticals, SK Life Science, Pfizer, Medtronic, GlaxoSmithKline, Eisai, Cyberonics, Neuropace, and Upsher-Smith.
FROM JOURNAL OF NEUROLOGY, NEUROSURGERY & PSYCHIATRY
Major finding: Drug-resistant epilepsy is associated with an increase in mortality (standardized mortality ratio, 2.4), especially among individuals with a known etiology (SMR, 3.1), which persists long after diagnosis.
Data source: A retrospective cohort study of 433 patients with drug-resistant epilepsy.
Disclosures: Some authors reported grant funding and support from a range of pharmaceutical companies, including Lundbeck, Vertex Pharmaceuticals, SK Life Science, Pfizer, Medtronic, GlaxoSmithKline, Eisai, Cyberonics, Neuropace, and Upsher-Smith.
Microvascular complications increase with diabetes duration but not age
MELBOURNE – A diagnosis of type 2 diabetes before age 50 was associated with an increased risk of microvascular complications, based on a secondary analysis of data from the international ADVANCE trial.
In ADVANCE, the risk of microvascular complications, such as eye and kidney disease, increased with disease duration but not with patient age. The risk of macrovascular complications, such as myocardial infarction, stroke, and cardiovascular events, as well as all-cause mortality, increased with both patient age and disease duration, Dr. John Chalmers, principal investigator for ADVANCE, said at the World Diabetes Congress.
"The findings tell you that if you get [type 2 diabetes] early, you’re in for a rougher time. If you’re younger at the time of diagnosis, then you may have a slightly more progressive, aggressive, resistant-to-treatment form of type 2 diabetes. It’s important to be aware of that, to control the glucose and to keep looking at the kidneys and eyes," said Dr. Chalmers, senior director of the George Institute, Sydney, and emeritus professor of medicine at the University of Sydney.
ADVANCE is a randomized trial across 20 countries of blood pressure lowering and intensive versus standard glucose control in 11,140 adults with type 2 diabetes who were followed up for 5 years. Mean age at study entry was 66 years, and average diabetes duration was 7.9 years. However when patients were stratified in 5-year increments of disease duration, researchers observed that the average age for each increment was roughly the same, around 66 years.
"You might guess a priori that people with the longest duration might be the oldest, but they’re not necessarily," Dr. Chalmers said in an interview.
In ADVANCE, 7.5% of patients with disease duration of less than 5 years had a history of major microvascular disease, as did 18.6% of those with disease duration of more than 15 years. The patients with the longest duration of disease – more than 15 years – started at a mean age of 47, and those with less than 5 years’ disease duration started at a mean age of 63.
The study also noted that those with the longest duration of disease had the highest mean hemoglobin A1c at baseline, 7.9%, compared with 7.2% in patients with less than 5 years’ disease duration.
"Major macrovascular events rise steeply as patients get older and as the duration of diabetes increases; they both have independent effects," he said. "The microvascular complications are more influenced by the glycemic burden, whereas the macrovascular events are probably more affected by the traditional risk factors of blood pressure, cholesterol, and smoking."
The ADVANCE study was partly funded by Servier, the maker of Preterax (perindopril arginine plus indapamide). Dr. Chalmers declared that he received research grants and honoraria from Servier as the principal investigator for the study.
MELBOURNE – A diagnosis of type 2 diabetes before age 50 was associated with an increased risk of microvascular complications, based on a secondary analysis of data from the international ADVANCE trial.
In ADVANCE, the risk of microvascular complications, such as eye and kidney disease, increased with disease duration but not with patient age. The risk of macrovascular complications, such as myocardial infarction, stroke, and cardiovascular events, as well as all-cause mortality, increased with both patient age and disease duration, Dr. John Chalmers, principal investigator for ADVANCE, said at the World Diabetes Congress.
"The findings tell you that if you get [type 2 diabetes] early, you’re in for a rougher time. If you’re younger at the time of diagnosis, then you may have a slightly more progressive, aggressive, resistant-to-treatment form of type 2 diabetes. It’s important to be aware of that, to control the glucose and to keep looking at the kidneys and eyes," said Dr. Chalmers, senior director of the George Institute, Sydney, and emeritus professor of medicine at the University of Sydney.
ADVANCE is a randomized trial across 20 countries of blood pressure lowering and intensive versus standard glucose control in 11,140 adults with type 2 diabetes who were followed up for 5 years. Mean age at study entry was 66 years, and average diabetes duration was 7.9 years. However when patients were stratified in 5-year increments of disease duration, researchers observed that the average age for each increment was roughly the same, around 66 years.
"You might guess a priori that people with the longest duration might be the oldest, but they’re not necessarily," Dr. Chalmers said in an interview.
In ADVANCE, 7.5% of patients with disease duration of less than 5 years had a history of major microvascular disease, as did 18.6% of those with disease duration of more than 15 years. The patients with the longest duration of disease – more than 15 years – started at a mean age of 47, and those with less than 5 years’ disease duration started at a mean age of 63.
The study also noted that those with the longest duration of disease had the highest mean hemoglobin A1c at baseline, 7.9%, compared with 7.2% in patients with less than 5 years’ disease duration.
"Major macrovascular events rise steeply as patients get older and as the duration of diabetes increases; they both have independent effects," he said. "The microvascular complications are more influenced by the glycemic burden, whereas the macrovascular events are probably more affected by the traditional risk factors of blood pressure, cholesterol, and smoking."
The ADVANCE study was partly funded by Servier, the maker of Preterax (perindopril arginine plus indapamide). Dr. Chalmers declared that he received research grants and honoraria from Servier as the principal investigator for the study.
MELBOURNE – A diagnosis of type 2 diabetes before age 50 was associated with an increased risk of microvascular complications, based on a secondary analysis of data from the international ADVANCE trial.
In ADVANCE, the risk of microvascular complications, such as eye and kidney disease, increased with disease duration but not with patient age. The risk of macrovascular complications, such as myocardial infarction, stroke, and cardiovascular events, as well as all-cause mortality, increased with both patient age and disease duration, Dr. John Chalmers, principal investigator for ADVANCE, said at the World Diabetes Congress.
"The findings tell you that if you get [type 2 diabetes] early, you’re in for a rougher time. If you’re younger at the time of diagnosis, then you may have a slightly more progressive, aggressive, resistant-to-treatment form of type 2 diabetes. It’s important to be aware of that, to control the glucose and to keep looking at the kidneys and eyes," said Dr. Chalmers, senior director of the George Institute, Sydney, and emeritus professor of medicine at the University of Sydney.
ADVANCE is a randomized trial across 20 countries of blood pressure lowering and intensive versus standard glucose control in 11,140 adults with type 2 diabetes who were followed up for 5 years. Mean age at study entry was 66 years, and average diabetes duration was 7.9 years. However when patients were stratified in 5-year increments of disease duration, researchers observed that the average age for each increment was roughly the same, around 66 years.
"You might guess a priori that people with the longest duration might be the oldest, but they’re not necessarily," Dr. Chalmers said in an interview.
In ADVANCE, 7.5% of patients with disease duration of less than 5 years had a history of major microvascular disease, as did 18.6% of those with disease duration of more than 15 years. The patients with the longest duration of disease – more than 15 years – started at a mean age of 47, and those with less than 5 years’ disease duration started at a mean age of 63.
The study also noted that those with the longest duration of disease had the highest mean hemoglobin A1c at baseline, 7.9%, compared with 7.2% in patients with less than 5 years’ disease duration.
"Major macrovascular events rise steeply as patients get older and as the duration of diabetes increases; they both have independent effects," he said. "The microvascular complications are more influenced by the glycemic burden, whereas the macrovascular events are probably more affected by the traditional risk factors of blood pressure, cholesterol, and smoking."
The ADVANCE study was partly funded by Servier, the maker of Preterax (perindopril arginine plus indapamide). Dr. Chalmers declared that he received research grants and honoraria from Servier as the principal investigator for the study.
AT THE WORLD DIABETES CONGRESS
Major finding: In ADVANCE, 7.5% of patients with disease duration of less than 5 years had a history of major microvascular disease, as did 18.6% of those with disease duration of more than 15 years.
Data source: Secondary analysis of data from 11,140 adults with type 2 diabetes who were followed up for 5 years in the ADVANCE trial.
Disclosures: The ADVANCE study was partly funded by Servier, the maker of Preterax (perindopril arginine plus indapamide). Dr. Chalmers declared that he received research grants and honoraria from Servier as the principal investigator for the study.