User login
Larry Beresford is an Oakland, Calif.-based freelance medical journalist with a breadth of experience writing about the policy, financial, clinical, management and human aspects of hospice, palliative care, end-of-life care, death, and dying. He is a longtime contributor to The Hospitalist, for which he covers re-admissions, pain management, palliative care, physician stress and burnout, quality improvement, waste prevention, practice management, innovation, and technology. He also contributes to Medscape. Learn more about his work at www.larryberesford.com; follow him on Twitter @larryberesford.
Proof of Concept
Published research on hospitalist quality, cost-effectiveness, and other outcomes, such as a recent study in Archives of Internal Medicine (2009;169(15):1389-1394) that shows hospitalists achieve higher scores on three quality-of-care measures, can provide ammunition for HM leaders trying to justify their programs’ worth to hospital administrators, says one HM group leader.
In the study, Lenny Lopez, MD, MPH, and colleagues at Massachusetts General Hospital examined Hospital Quality Alliance data from 3,619 hospitals, 40% of which had hospitalists. They compared composite measures of quality of care for acute myocardial infarction, congestive heart failure, and pneumonia, and found that scores were higher for the hospitals with hospitalist programs.
Such studies help shed light on the central questions of hospitalists’ value, says Julia Wright, MD, FHM, head of the hospital medicine section at the University of Wisconsin in Madison. Initially, the question was whether the hospitalist model was even viable, which Dr. Wright believes has been laid to rest. The next questions involved efficiency and bottom-line issues—such as length of stay—and a strong case has been made overall for HM’s cost-effectiveness, she says. Quality of care has been harder to demonstrate, but newer quality measures make it easier to report, Dr. Wright adds.
Dr. Wright says the Lopez study, which highlights hospitalists’ ability to conform to guidelines, will be valuable to hospitalist groups. “We do talk with our administration about these questions, although we focus more on alignment of goals and mission, occasionally citing articles like this,” she says. “More important is to be aware of the core quality issues and have metrics of our own.”
Then again, programs just starting out might find the research essential, she says.
“Hospitalists participate in any number of quality initiatives,” Dr. Wright adds. “A lot of their data could be published and added to the small library of research on hospital medicine’s contributions to quality.”
Published research on hospitalist quality, cost-effectiveness, and other outcomes, such as a recent study in Archives of Internal Medicine (2009;169(15):1389-1394) that shows hospitalists achieve higher scores on three quality-of-care measures, can provide ammunition for HM leaders trying to justify their programs’ worth to hospital administrators, says one HM group leader.
In the study, Lenny Lopez, MD, MPH, and colleagues at Massachusetts General Hospital examined Hospital Quality Alliance data from 3,619 hospitals, 40% of which had hospitalists. They compared composite measures of quality of care for acute myocardial infarction, congestive heart failure, and pneumonia, and found that scores were higher for the hospitals with hospitalist programs.
Such studies help shed light on the central questions of hospitalists’ value, says Julia Wright, MD, FHM, head of the hospital medicine section at the University of Wisconsin in Madison. Initially, the question was whether the hospitalist model was even viable, which Dr. Wright believes has been laid to rest. The next questions involved efficiency and bottom-line issues—such as length of stay—and a strong case has been made overall for HM’s cost-effectiveness, she says. Quality of care has been harder to demonstrate, but newer quality measures make it easier to report, Dr. Wright adds.
Dr. Wright says the Lopez study, which highlights hospitalists’ ability to conform to guidelines, will be valuable to hospitalist groups. “We do talk with our administration about these questions, although we focus more on alignment of goals and mission, occasionally citing articles like this,” she says. “More important is to be aware of the core quality issues and have metrics of our own.”
Then again, programs just starting out might find the research essential, she says.
“Hospitalists participate in any number of quality initiatives,” Dr. Wright adds. “A lot of their data could be published and added to the small library of research on hospital medicine’s contributions to quality.”
Published research on hospitalist quality, cost-effectiveness, and other outcomes, such as a recent study in Archives of Internal Medicine (2009;169(15):1389-1394) that shows hospitalists achieve higher scores on three quality-of-care measures, can provide ammunition for HM leaders trying to justify their programs’ worth to hospital administrators, says one HM group leader.
In the study, Lenny Lopez, MD, MPH, and colleagues at Massachusetts General Hospital examined Hospital Quality Alliance data from 3,619 hospitals, 40% of which had hospitalists. They compared composite measures of quality of care for acute myocardial infarction, congestive heart failure, and pneumonia, and found that scores were higher for the hospitals with hospitalist programs.
Such studies help shed light on the central questions of hospitalists’ value, says Julia Wright, MD, FHM, head of the hospital medicine section at the University of Wisconsin in Madison. Initially, the question was whether the hospitalist model was even viable, which Dr. Wright believes has been laid to rest. The next questions involved efficiency and bottom-line issues—such as length of stay—and a strong case has been made overall for HM’s cost-effectiveness, she says. Quality of care has been harder to demonstrate, but newer quality measures make it easier to report, Dr. Wright adds.
Dr. Wright says the Lopez study, which highlights hospitalists’ ability to conform to guidelines, will be valuable to hospitalist groups. “We do talk with our administration about these questions, although we focus more on alignment of goals and mission, occasionally citing articles like this,” she says. “More important is to be aware of the core quality issues and have metrics of our own.”
Then again, programs just starting out might find the research essential, she says.
“Hospitalists participate in any number of quality initiatives,” Dr. Wright adds. “A lot of their data could be published and added to the small library of research on hospital medicine’s contributions to quality.”
Back to Basics
Most primary care physicians will tell you it’s getting harder to maintain a traditional medical practice with a foot in both the outpatient and inpatient realms. Caseload demands, inadequate reimbursement, and other professional and medical pressures are forcing primary care physicians to choose one setting or the other.
For those interested in exploring the field of hospital medicine, a unique, three-day, hands-on training course at the University of California-San Francisco (UCSF) Medical Center offered an opportunity to address some of the gaps in their inpatient clinical knowledge and skills, which either were not sufficiently covered in residency training or have atrophied from lack of practice.
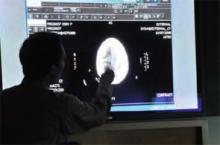
The hospitalist “mini-college” allowed working hospitalists and prospective hospitalists to practice short neurological exams on real patients, use ultrasound to guide needle placements, interpret radiologic evidence, engage in diagnostic reasoning exercises, and even conduct online medical information searches, all under the watchful eyes of UCSF faculty. The course was limited to 27 participants to maximize small group interactions. It emphasized clinical practice needs identified in surveys of hospitalists and assessments by the faculty, led by Robert M. Wachter, MD, professor and chief of the division of hospital medicine at UCSF, a former SHM president, and author of the blog “Wachter’s World” (www.wachtersworld.com).
Participants in this intensive course were a mix of working hospitalists in stable positions seeking to enhance their clinical practice, and physicians in various stages of transition—in or out of hospitalist positions. More than half of the participants are in their first hospitalist job and have worked in the field for less than two years, according to attendee surveys. Two-thirds say they are pretty satisfied and 24% say they are very satisfied with their work, according to the survey. Most say they love the clinical aspects best, but others express frustrations with caseload pressures and ownership changes at their practices.
“For me, being a doctor always meant being a primary care doctor, and I find great joy working in both the inpatient and outpatient settings. But primary care is becoming a losing proposition,” says Ronald Distajo, MD, who has maintained a primary clinic practice for Cambridge Health Alliance in Cambridge, Mass., for the past three years—all the while moonlighting as a hospitalist for the health system.
With student loans, long hours, and relatively low pay in the outpatient setting, Dr. Distajo plans to find full-time work as a hospitalist. At the mini-college, he received a phone call informing him the outpatient clinic he practices in will close by the end of the year. The UCSF course seemed like a timely opportunity to bolster his inpatient management skills in areas he believes he could benefit from a refresher. “They’ve done a good job of picking all of them,” Dr. Distajo says.
Another mini-college participant in transition, Madeleine Martindale, MD, was looking to hear what “hospitalists in other places are doing, to confirm and validate my own experience.” Dr. Martindale recently left a hospitalist position in Anchorage, Alaska, in part because of high caseloads. “A lot of the topics presented here will help me. I also wanted to learn more about the range of responsibilities expected in hospital medicine.”
With few work settings for hospitalists in Alaska, Dr. Martindale is planning to become a traveling hospitalist in the lower 48 states next year. She is hoping to devote part of the year to practicing medicine in a high-altitude clinic, as she prepares to staff a clinic in Nepal operated by the Himalayan Rescue Association. She also plans to serve as the support physician—stationed mainly at base camp—for a two-month Mount Everest climb. “There are a lot of hospitalist services and places to practice, if I’m willing to leave Alaska,” she says. “I feel inspired to hear hospitalists who love their jobs and are interested in quality of care and safety.”
Student and Staff Member
Mini-college participants were issued temporary visitor privileges at UCSF, name badges and lab coats. “So much of our planning for this experience was about getting [participants] into the hospital, and to offer [them] a set of knowledge and skills that may be new or taught in a new way, which [they] can apply in [their own] hospitals,” says Arpana R. Vidyarthi, MD, a hospitalist at UCSF and mini-college co-chair.
The first session, hosted by Gurpreet Dhaliwal, MD, assistant professor of medicine, nocturnist, and recipient of a distinguished teaching award at UCSF, led participants through an exercise in clinical reasoning, using a challenging case to exercise diagnostic skills. “When you leave medical training, the assumption is that you’re done, and you will get better and better on the job somehow through experience,” Dr. Dhaliwal explained. However, there is little in the literature addressing how doctors actually get better and what separates those who continue to improve from those who plateau in their careers. “What are the things doctors do to put themselves in the upper 10% of diagnosticians? We know from other fields that innate smartness rarely counts the most, and that expertise is not something that necessarily comes with experience.”
Dr. Dhaliwal recommends a program of “progressive reinvestment” in diagnostics—a deliberate practice of challenging mental processes and learning something new from every case. He also suggests regularly seeking feedback from peers, tracking down what happened to patients treated and whether the discharge diagnosis matched the hospitalist’s initial assessment, and even practicing diagnostic skills with sample cases like the New England Journal of Medicine’s “Case Records of the Massachusetts General Hospital.”
Participants broke into small groups to visit hospital wards with UCSF neurologists and intensivists, discuss actual cases and practice their examination skills at the bedside. H. Quinny Cheng, MD, a hospitalist and director of the UCSF’s medical consultation and neurosurgery co-management services, walked them through current research and controversies in the pre-operative evaluation and management of surgical patients, including recent data on the use of anti-coagulants, beta blockers, deep vein thrombosis prophylaxis, and drug-eluting coronary artery stents. UCSF respiratory therapist Brian Daniel, RRT, reviewed recent advances in ventilator equipment, including the high-flow nasal cannula.
S. Andrew Josephson, MD, a neurologist and director of the neuro-hospitalist program at UCSF, says hospitalists generally do not have time for full neurological workups on their patients. He suggests high-yield results can be derived from quick assessments of patients’ language, gait, and visual fields.
“I thought the neurology session was fantastic,” says participant Marcus Zachary, MD, group leader for Cogent Healthcare of California at St. Francis Memorial Hospital in San Francisco. “I know across the country hospitalists are being asked to bear a heavy load in this area, and we’re not really prepared. Neurologists don’t want to come into the hospital, and hospitalists increasingly are plugging the gap.”
Dr. Wachter convened a Department of Hospital Medicine case conference discussion of a real patient. He also led a simulated root cause analysis discussion of an actual medical error, which occurred at UCSF when the wrong patient was given an unnecessary cardiovascular physiology procedure scheduled for a different patient with a similar sounding name. Organized discussion of medical errors, led by UCSF hospitalists, take place weekly at the medical center.
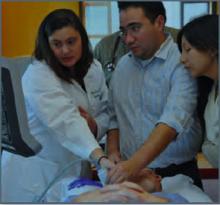
In a hands-on procedure workshop in the library, Diane Sliwka, MD, who developed the hospitalist procedure service at UCSF, introduced the clinical benefits of using ultrasound diagnostic imaging to guide routine central line placements, paracentesis, and thoracentesis in hospitalized patients. She reviewed the basics of frequency, contrast, and sterile technique with ultrasound, and the visual and spatial orientation necessary to interpret the image on the screen. Participants used the equipment to locate pockets of ascites in the abdomen of a UCSF patient and frequent training volunteer known to have pleural effusions. Participants also practiced needle insertion technique with actual hospital equipment on prepared chicken carcasses.
“Ultrasound does enhance the safety of bedside procedures. Ultrasound basics are learnable with practice and give a new dimension of ‘sight’ to common bedside procedures,” Dr. Sliwka explained to the participants, 70% of whom had not used ultrasound for bedside procedures. “Where it’s available, you can learn to do it with a bit of practice.”
Attendee Moira Ogden, MD, hospitalist at Terrebonne General Medical Center in Houma, La., is interested in bringing ultrasound-guided procedures into her practice, although she fears access to the equipment may not be easy to obtain. “I want to start using them; I just need to know the cost,” she says.
Mini-college Motives
“We’ve been at it for a year with our new hospitalist program,” Dr. Ogden said. “There’s such a difference between academic medicine and practice in the community. In my hospital, it’s very busy, although we’ve really just scratched the surface. It’s hard to keep up with the literature, and when I saw the flyer for this course, it looked so in-depth—almost like a re-introduction to hospital medicine.”
“Part of it was just plain curiosity—what is this going to be about? What do they see as blind spots for hospitalists in their day-to-day jobs?” asks Dr. Zachary, a six-year hospitalist, discussing his interest in attending the UCSF mini-college. “For the most part, my sense of the gaps has been dead-on.”
Kevin Leary, MD, internal medicine faculty at Walter Reed Army Medical Center in Washington, D.C., is not a hospitalist, although his position with the teaching service is similar in many ways. “My goal in coming here is to learn more about the field of hospital medicine and to meet physicians who are hospitalists,” Dr. Leary explains. “When I leave my role in the military service, I would get a lot of job satisfaction out of becoming a hospitalist.”
Charles Oppong, MD, a native of Ghana who now lives in Los Angeles with his wife and infant daughter, is waiting for his application for a California medical license to be processed and currently works part-time as a hospitalist in Circleville, Ohio, and in LaCrosse, Wis. “Personally, I enjoy caring for patients in the inpatient setting. I like the challenges of keeping my medical skills current,” he says. “I heard about UCSF and its famous hospitalist program, and when they sent me a flyer, I saw all of these topics to improve my inpatient management skills.”
Organizers of the mini-college are attempting to give participants an opportunity to re-experience “what it was like in residency to participate in rounds with a truly spectacular teacher. With the teaching resources we have here at UCSF, we have the capacity to offer that kind of experience,” Dr. Wachter says.
“Those of us who stay in academic settings are constantly jazzed by our interactions with young people, who tend to ask a lot of questions,” he adds. “For many other hospitalists, they don’t have much opportunity to step back and recapture what brought them to the field in the first place. That’s what I hoped to capture with the mini-college. If we can do that, then we’ve succeeded.” TH
Larry Beresford is a medical writer based in Oakland, Calif.
Most primary care physicians will tell you it’s getting harder to maintain a traditional medical practice with a foot in both the outpatient and inpatient realms. Caseload demands, inadequate reimbursement, and other professional and medical pressures are forcing primary care physicians to choose one setting or the other.
For those interested in exploring the field of hospital medicine, a unique, three-day, hands-on training course at the University of California-San Francisco (UCSF) Medical Center offered an opportunity to address some of the gaps in their inpatient clinical knowledge and skills, which either were not sufficiently covered in residency training or have atrophied from lack of practice.
The hospitalist “mini-college” allowed working hospitalists and prospective hospitalists to practice short neurological exams on real patients, use ultrasound to guide needle placements, interpret radiologic evidence, engage in diagnostic reasoning exercises, and even conduct online medical information searches, all under the watchful eyes of UCSF faculty. The course was limited to 27 participants to maximize small group interactions. It emphasized clinical practice needs identified in surveys of hospitalists and assessments by the faculty, led by Robert M. Wachter, MD, professor and chief of the division of hospital medicine at UCSF, a former SHM president, and author of the blog “Wachter’s World” (www.wachtersworld.com).
Participants in this intensive course were a mix of working hospitalists in stable positions seeking to enhance their clinical practice, and physicians in various stages of transition—in or out of hospitalist positions. More than half of the participants are in their first hospitalist job and have worked in the field for less than two years, according to attendee surveys. Two-thirds say they are pretty satisfied and 24% say they are very satisfied with their work, according to the survey. Most say they love the clinical aspects best, but others express frustrations with caseload pressures and ownership changes at their practices.
“For me, being a doctor always meant being a primary care doctor, and I find great joy working in both the inpatient and outpatient settings. But primary care is becoming a losing proposition,” says Ronald Distajo, MD, who has maintained a primary clinic practice for Cambridge Health Alliance in Cambridge, Mass., for the past three years—all the while moonlighting as a hospitalist for the health system.
With student loans, long hours, and relatively low pay in the outpatient setting, Dr. Distajo plans to find full-time work as a hospitalist. At the mini-college, he received a phone call informing him the outpatient clinic he practices in will close by the end of the year. The UCSF course seemed like a timely opportunity to bolster his inpatient management skills in areas he believes he could benefit from a refresher. “They’ve done a good job of picking all of them,” Dr. Distajo says.
Another mini-college participant in transition, Madeleine Martindale, MD, was looking to hear what “hospitalists in other places are doing, to confirm and validate my own experience.” Dr. Martindale recently left a hospitalist position in Anchorage, Alaska, in part because of high caseloads. “A lot of the topics presented here will help me. I also wanted to learn more about the range of responsibilities expected in hospital medicine.”
With few work settings for hospitalists in Alaska, Dr. Martindale is planning to become a traveling hospitalist in the lower 48 states next year. She is hoping to devote part of the year to practicing medicine in a high-altitude clinic, as she prepares to staff a clinic in Nepal operated by the Himalayan Rescue Association. She also plans to serve as the support physician—stationed mainly at base camp—for a two-month Mount Everest climb. “There are a lot of hospitalist services and places to practice, if I’m willing to leave Alaska,” she says. “I feel inspired to hear hospitalists who love their jobs and are interested in quality of care and safety.”
Student and Staff Member
Mini-college participants were issued temporary visitor privileges at UCSF, name badges and lab coats. “So much of our planning for this experience was about getting [participants] into the hospital, and to offer [them] a set of knowledge and skills that may be new or taught in a new way, which [they] can apply in [their own] hospitals,” says Arpana R. Vidyarthi, MD, a hospitalist at UCSF and mini-college co-chair.
The first session, hosted by Gurpreet Dhaliwal, MD, assistant professor of medicine, nocturnist, and recipient of a distinguished teaching award at UCSF, led participants through an exercise in clinical reasoning, using a challenging case to exercise diagnostic skills. “When you leave medical training, the assumption is that you’re done, and you will get better and better on the job somehow through experience,” Dr. Dhaliwal explained. However, there is little in the literature addressing how doctors actually get better and what separates those who continue to improve from those who plateau in their careers. “What are the things doctors do to put themselves in the upper 10% of diagnosticians? We know from other fields that innate smartness rarely counts the most, and that expertise is not something that necessarily comes with experience.”
Dr. Dhaliwal recommends a program of “progressive reinvestment” in diagnostics—a deliberate practice of challenging mental processes and learning something new from every case. He also suggests regularly seeking feedback from peers, tracking down what happened to patients treated and whether the discharge diagnosis matched the hospitalist’s initial assessment, and even practicing diagnostic skills with sample cases like the New England Journal of Medicine’s “Case Records of the Massachusetts General Hospital.”
Participants broke into small groups to visit hospital wards with UCSF neurologists and intensivists, discuss actual cases and practice their examination skills at the bedside. H. Quinny Cheng, MD, a hospitalist and director of the UCSF’s medical consultation and neurosurgery co-management services, walked them through current research and controversies in the pre-operative evaluation and management of surgical patients, including recent data on the use of anti-coagulants, beta blockers, deep vein thrombosis prophylaxis, and drug-eluting coronary artery stents. UCSF respiratory therapist Brian Daniel, RRT, reviewed recent advances in ventilator equipment, including the high-flow nasal cannula.
S. Andrew Josephson, MD, a neurologist and director of the neuro-hospitalist program at UCSF, says hospitalists generally do not have time for full neurological workups on their patients. He suggests high-yield results can be derived from quick assessments of patients’ language, gait, and visual fields.
“I thought the neurology session was fantastic,” says participant Marcus Zachary, MD, group leader for Cogent Healthcare of California at St. Francis Memorial Hospital in San Francisco. “I know across the country hospitalists are being asked to bear a heavy load in this area, and we’re not really prepared. Neurologists don’t want to come into the hospital, and hospitalists increasingly are plugging the gap.”
Dr. Wachter convened a Department of Hospital Medicine case conference discussion of a real patient. He also led a simulated root cause analysis discussion of an actual medical error, which occurred at UCSF when the wrong patient was given an unnecessary cardiovascular physiology procedure scheduled for a different patient with a similar sounding name. Organized discussion of medical errors, led by UCSF hospitalists, take place weekly at the medical center.
In a hands-on procedure workshop in the library, Diane Sliwka, MD, who developed the hospitalist procedure service at UCSF, introduced the clinical benefits of using ultrasound diagnostic imaging to guide routine central line placements, paracentesis, and thoracentesis in hospitalized patients. She reviewed the basics of frequency, contrast, and sterile technique with ultrasound, and the visual and spatial orientation necessary to interpret the image on the screen. Participants used the equipment to locate pockets of ascites in the abdomen of a UCSF patient and frequent training volunteer known to have pleural effusions. Participants also practiced needle insertion technique with actual hospital equipment on prepared chicken carcasses.
“Ultrasound does enhance the safety of bedside procedures. Ultrasound basics are learnable with practice and give a new dimension of ‘sight’ to common bedside procedures,” Dr. Sliwka explained to the participants, 70% of whom had not used ultrasound for bedside procedures. “Where it’s available, you can learn to do it with a bit of practice.”
Attendee Moira Ogden, MD, hospitalist at Terrebonne General Medical Center in Houma, La., is interested in bringing ultrasound-guided procedures into her practice, although she fears access to the equipment may not be easy to obtain. “I want to start using them; I just need to know the cost,” she says.
Mini-college Motives
“We’ve been at it for a year with our new hospitalist program,” Dr. Ogden said. “There’s such a difference between academic medicine and practice in the community. In my hospital, it’s very busy, although we’ve really just scratched the surface. It’s hard to keep up with the literature, and when I saw the flyer for this course, it looked so in-depth—almost like a re-introduction to hospital medicine.”
“Part of it was just plain curiosity—what is this going to be about? What do they see as blind spots for hospitalists in their day-to-day jobs?” asks Dr. Zachary, a six-year hospitalist, discussing his interest in attending the UCSF mini-college. “For the most part, my sense of the gaps has been dead-on.”
Kevin Leary, MD, internal medicine faculty at Walter Reed Army Medical Center in Washington, D.C., is not a hospitalist, although his position with the teaching service is similar in many ways. “My goal in coming here is to learn more about the field of hospital medicine and to meet physicians who are hospitalists,” Dr. Leary explains. “When I leave my role in the military service, I would get a lot of job satisfaction out of becoming a hospitalist.”
Charles Oppong, MD, a native of Ghana who now lives in Los Angeles with his wife and infant daughter, is waiting for his application for a California medical license to be processed and currently works part-time as a hospitalist in Circleville, Ohio, and in LaCrosse, Wis. “Personally, I enjoy caring for patients in the inpatient setting. I like the challenges of keeping my medical skills current,” he says. “I heard about UCSF and its famous hospitalist program, and when they sent me a flyer, I saw all of these topics to improve my inpatient management skills.”
Organizers of the mini-college are attempting to give participants an opportunity to re-experience “what it was like in residency to participate in rounds with a truly spectacular teacher. With the teaching resources we have here at UCSF, we have the capacity to offer that kind of experience,” Dr. Wachter says.
“Those of us who stay in academic settings are constantly jazzed by our interactions with young people, who tend to ask a lot of questions,” he adds. “For many other hospitalists, they don’t have much opportunity to step back and recapture what brought them to the field in the first place. That’s what I hoped to capture with the mini-college. If we can do that, then we’ve succeeded.” TH
Larry Beresford is a medical writer based in Oakland, Calif.
Most primary care physicians will tell you it’s getting harder to maintain a traditional medical practice with a foot in both the outpatient and inpatient realms. Caseload demands, inadequate reimbursement, and other professional and medical pressures are forcing primary care physicians to choose one setting or the other.
For those interested in exploring the field of hospital medicine, a unique, three-day, hands-on training course at the University of California-San Francisco (UCSF) Medical Center offered an opportunity to address some of the gaps in their inpatient clinical knowledge and skills, which either were not sufficiently covered in residency training or have atrophied from lack of practice.
The hospitalist “mini-college” allowed working hospitalists and prospective hospitalists to practice short neurological exams on real patients, use ultrasound to guide needle placements, interpret radiologic evidence, engage in diagnostic reasoning exercises, and even conduct online medical information searches, all under the watchful eyes of UCSF faculty. The course was limited to 27 participants to maximize small group interactions. It emphasized clinical practice needs identified in surveys of hospitalists and assessments by the faculty, led by Robert M. Wachter, MD, professor and chief of the division of hospital medicine at UCSF, a former SHM president, and author of the blog “Wachter’s World” (www.wachtersworld.com).
Participants in this intensive course were a mix of working hospitalists in stable positions seeking to enhance their clinical practice, and physicians in various stages of transition—in or out of hospitalist positions. More than half of the participants are in their first hospitalist job and have worked in the field for less than two years, according to attendee surveys. Two-thirds say they are pretty satisfied and 24% say they are very satisfied with their work, according to the survey. Most say they love the clinical aspects best, but others express frustrations with caseload pressures and ownership changes at their practices.
“For me, being a doctor always meant being a primary care doctor, and I find great joy working in both the inpatient and outpatient settings. But primary care is becoming a losing proposition,” says Ronald Distajo, MD, who has maintained a primary clinic practice for Cambridge Health Alliance in Cambridge, Mass., for the past three years—all the while moonlighting as a hospitalist for the health system.
With student loans, long hours, and relatively low pay in the outpatient setting, Dr. Distajo plans to find full-time work as a hospitalist. At the mini-college, he received a phone call informing him the outpatient clinic he practices in will close by the end of the year. The UCSF course seemed like a timely opportunity to bolster his inpatient management skills in areas he believes he could benefit from a refresher. “They’ve done a good job of picking all of them,” Dr. Distajo says.
Another mini-college participant in transition, Madeleine Martindale, MD, was looking to hear what “hospitalists in other places are doing, to confirm and validate my own experience.” Dr. Martindale recently left a hospitalist position in Anchorage, Alaska, in part because of high caseloads. “A lot of the topics presented here will help me. I also wanted to learn more about the range of responsibilities expected in hospital medicine.”
With few work settings for hospitalists in Alaska, Dr. Martindale is planning to become a traveling hospitalist in the lower 48 states next year. She is hoping to devote part of the year to practicing medicine in a high-altitude clinic, as she prepares to staff a clinic in Nepal operated by the Himalayan Rescue Association. She also plans to serve as the support physician—stationed mainly at base camp—for a two-month Mount Everest climb. “There are a lot of hospitalist services and places to practice, if I’m willing to leave Alaska,” she says. “I feel inspired to hear hospitalists who love their jobs and are interested in quality of care and safety.”
Student and Staff Member
Mini-college participants were issued temporary visitor privileges at UCSF, name badges and lab coats. “So much of our planning for this experience was about getting [participants] into the hospital, and to offer [them] a set of knowledge and skills that may be new or taught in a new way, which [they] can apply in [their own] hospitals,” says Arpana R. Vidyarthi, MD, a hospitalist at UCSF and mini-college co-chair.
The first session, hosted by Gurpreet Dhaliwal, MD, assistant professor of medicine, nocturnist, and recipient of a distinguished teaching award at UCSF, led participants through an exercise in clinical reasoning, using a challenging case to exercise diagnostic skills. “When you leave medical training, the assumption is that you’re done, and you will get better and better on the job somehow through experience,” Dr. Dhaliwal explained. However, there is little in the literature addressing how doctors actually get better and what separates those who continue to improve from those who plateau in their careers. “What are the things doctors do to put themselves in the upper 10% of diagnosticians? We know from other fields that innate smartness rarely counts the most, and that expertise is not something that necessarily comes with experience.”
Dr. Dhaliwal recommends a program of “progressive reinvestment” in diagnostics—a deliberate practice of challenging mental processes and learning something new from every case. He also suggests regularly seeking feedback from peers, tracking down what happened to patients treated and whether the discharge diagnosis matched the hospitalist’s initial assessment, and even practicing diagnostic skills with sample cases like the New England Journal of Medicine’s “Case Records of the Massachusetts General Hospital.”
Participants broke into small groups to visit hospital wards with UCSF neurologists and intensivists, discuss actual cases and practice their examination skills at the bedside. H. Quinny Cheng, MD, a hospitalist and director of the UCSF’s medical consultation and neurosurgery co-management services, walked them through current research and controversies in the pre-operative evaluation and management of surgical patients, including recent data on the use of anti-coagulants, beta blockers, deep vein thrombosis prophylaxis, and drug-eluting coronary artery stents. UCSF respiratory therapist Brian Daniel, RRT, reviewed recent advances in ventilator equipment, including the high-flow nasal cannula.
S. Andrew Josephson, MD, a neurologist and director of the neuro-hospitalist program at UCSF, says hospitalists generally do not have time for full neurological workups on their patients. He suggests high-yield results can be derived from quick assessments of patients’ language, gait, and visual fields.
“I thought the neurology session was fantastic,” says participant Marcus Zachary, MD, group leader for Cogent Healthcare of California at St. Francis Memorial Hospital in San Francisco. “I know across the country hospitalists are being asked to bear a heavy load in this area, and we’re not really prepared. Neurologists don’t want to come into the hospital, and hospitalists increasingly are plugging the gap.”
Dr. Wachter convened a Department of Hospital Medicine case conference discussion of a real patient. He also led a simulated root cause analysis discussion of an actual medical error, which occurred at UCSF when the wrong patient was given an unnecessary cardiovascular physiology procedure scheduled for a different patient with a similar sounding name. Organized discussion of medical errors, led by UCSF hospitalists, take place weekly at the medical center.
In a hands-on procedure workshop in the library, Diane Sliwka, MD, who developed the hospitalist procedure service at UCSF, introduced the clinical benefits of using ultrasound diagnostic imaging to guide routine central line placements, paracentesis, and thoracentesis in hospitalized patients. She reviewed the basics of frequency, contrast, and sterile technique with ultrasound, and the visual and spatial orientation necessary to interpret the image on the screen. Participants used the equipment to locate pockets of ascites in the abdomen of a UCSF patient and frequent training volunteer known to have pleural effusions. Participants also practiced needle insertion technique with actual hospital equipment on prepared chicken carcasses.
“Ultrasound does enhance the safety of bedside procedures. Ultrasound basics are learnable with practice and give a new dimension of ‘sight’ to common bedside procedures,” Dr. Sliwka explained to the participants, 70% of whom had not used ultrasound for bedside procedures. “Where it’s available, you can learn to do it with a bit of practice.”
Attendee Moira Ogden, MD, hospitalist at Terrebonne General Medical Center in Houma, La., is interested in bringing ultrasound-guided procedures into her practice, although she fears access to the equipment may not be easy to obtain. “I want to start using them; I just need to know the cost,” she says.
Mini-college Motives
“We’ve been at it for a year with our new hospitalist program,” Dr. Ogden said. “There’s such a difference between academic medicine and practice in the community. In my hospital, it’s very busy, although we’ve really just scratched the surface. It’s hard to keep up with the literature, and when I saw the flyer for this course, it looked so in-depth—almost like a re-introduction to hospital medicine.”
“Part of it was just plain curiosity—what is this going to be about? What do they see as blind spots for hospitalists in their day-to-day jobs?” asks Dr. Zachary, a six-year hospitalist, discussing his interest in attending the UCSF mini-college. “For the most part, my sense of the gaps has been dead-on.”
Kevin Leary, MD, internal medicine faculty at Walter Reed Army Medical Center in Washington, D.C., is not a hospitalist, although his position with the teaching service is similar in many ways. “My goal in coming here is to learn more about the field of hospital medicine and to meet physicians who are hospitalists,” Dr. Leary explains. “When I leave my role in the military service, I would get a lot of job satisfaction out of becoming a hospitalist.”
Charles Oppong, MD, a native of Ghana who now lives in Los Angeles with his wife and infant daughter, is waiting for his application for a California medical license to be processed and currently works part-time as a hospitalist in Circleville, Ohio, and in LaCrosse, Wis. “Personally, I enjoy caring for patients in the inpatient setting. I like the challenges of keeping my medical skills current,” he says. “I heard about UCSF and its famous hospitalist program, and when they sent me a flyer, I saw all of these topics to improve my inpatient management skills.”
Organizers of the mini-college are attempting to give participants an opportunity to re-experience “what it was like in residency to participate in rounds with a truly spectacular teacher. With the teaching resources we have here at UCSF, we have the capacity to offer that kind of experience,” Dr. Wachter says.
“Those of us who stay in academic settings are constantly jazzed by our interactions with young people, who tend to ask a lot of questions,” he adds. “For many other hospitalists, they don’t have much opportunity to step back and recapture what brought them to the field in the first place. That’s what I hoped to capture with the mini-college. If we can do that, then we’ve succeeded.” TH
Larry Beresford is a medical writer based in Oakland, Calif.
Coat Tales
Russ Cucina, MD, MS, a hospitalist at the University of California San Francisco (UCSF) Medical Center, and a colleague once spent a week wearing pedometers on the job to study how much ground they covered in the course of managing their patient caseloads in a huge hospital like UCSF. The result: an average of four miles walked per day.
“The usual productivity infrastructure for physicians in their offices is simply not as available to hospitalists, or isn’t under our control,” Dr. Cucina says. There may be networked computer terminals throughout the hospital, but how many there are, how accessible they are, and how much competition there is for them varies. Hospitalists may have their own offices, desks or shared office space, depending on institutional commitments, but these may be a trek from patient care areas.
As a result, they must bring essential tools of their trade on their persons. Some carry a briefcase or wear a fanny pack, but more often these essential tools are stuffed into every available pocket of their medical lab coats.
Dr. Cucina’s short list of essentials is typical of working hospitalists. It includes his “smart phone,” combining a personal digital assistant (PDA) and cell phone, pens, a reflex hammer, a tuning fork for testing neurologic sensitivities, a stethoscope, swabs for sterilizing the stethoscope, a stash of large hospital gloves (which can be a hard size to find), and a bulky and awkward—but secure—prescription pad in a cardstock wrapper.
He also totes a stack of 3-by-5-inch index cards held together with a steel ring—one card for each active patient, updated daily by hand with medication changes, lab results and other information provided by the residents. “I have tried higher-tech approaches,” he explains. “I am the hospital’s associate medical director for information technology, and I need to keep up to date and try new things, including the various applications for keeping patient lists on line. But nothing has yet beaten out hand-written index cards for efficiency and ease of use. The time it takes to input this information electronically just isn’t worth it.”
Hospitalists say additional medical tools, such as an otoscope or ophthalmoscope, could be helpful but may pile on too much bulk and weight. “I’m often challenged to find one on the floor when I really need it,” Dr. Cucina says. Portable scopes are also quite valuable and at some risk for disappearing from an unattended lab coat in the highly trafficked hospital setting.
PDA Is No Panacea
For many hospitalists, one key to efficient mobility on the job is the PDA or laptop computer, with basic references such as UpToDate, Epocrates, Tarascon Pocket Pharmacopoeia, or the Washington Manual of Medical Therapeutics, either loaded or accessed via the Internet. PDAs involve serious compromises balancing size and weight with ease of keyboard use, ease of reading the screen, and memory or processing speed. (See “Tackle Technology,” November 2007, p. 22 for a discussion of how hospitalists use portable computing devices on the job.)
“We’ve come a long way from tongue depressors and otoscopes,” says William Ford, MD, program medical director for Cogent Healthcare’s large and expanding hospitalist group based at Temple University, Collegeville, Pa. “Some of us at Temple, depending on the service, carry one or more cell phones and between one and three pagers, in a pocket or attached to a belt.” The doctors may have their own PDAs, but Cogent no longer supplies them, having converted to a Web-based tool that offers a variety of practice management resources accessed by laptop computers via the Internet.
Dr. Cucina believes the technology is evolving toward a tablet device that will integrate more of the resource databases hospitalists need in their daily practice with other essential functions, such as lab results, billing, and communications with primary physicians—all in a user-friendly scale and format. In the meantime, there’s still a lot that has to be stuffed into pockets.
Some hospitalists also prefer to hold favorite reference resources, such as the pocket-sized Sanford Guide to Antimicrobial Therapy in their hands. That also involves tradeoffs, notes Michelle Pezzani, MD, hospitalist at El Camino Hospital in Mountain View, Calif.
“I tried carrying a book bag over my shoulder, but I felt like a school kid,” Dr. Pezzani relates. “I also noticed that the more reference books I had stuffed into my pockets, the less confidence other people seemed to have in me as a physician.” Not to mention that her pockets ripped open from the weight. She even developed a sore neck from her ergonomically unbalanced, overstuffed lab coat.
“Although I love being a hospitalist, it’s getting to the point where I feel disorganized because I have no real home base,” Dr. Pezzani laments. She finds her hospitalist group’s shared office—a converted labor-and-delivery room with no windows and three desktop computers for nine doctors—less than ideal. She spends as little time as possible there.
“My life would be easier if I didn’t have to carry my office in my pockets—my ink-stained pockets,” she says. “I can’t carry my laptop around with me because of the neck pain, so I asked the hospital to give me a locker closer to the middle of the building. It has also become a kind of science for me to transfer a few personal essentials into a little satchel with a string that I wear around my neck,” since a purse is not feasible.
Love/Hate Situation
Dr. Cucina uses an online custom supplier of medical lab coats with extra, zippered pockets on the inside and outside. He’s careful not to let the lab coat of out his sight when he takes it off.
Randy Ferrance, MD, a hospitalist in internal medicine and pediatrics at Riverside Tappahannock Hospital in Tappahannock, Va., acknowledges his own love-hate relationship with the lab coat. In his pockets, he carries a stack of 3-by-5-inch index cards, an 8.5-by-11-inch hospital census sheet, folded over, a prescription pad, a highlighter pen and spare pens, the ubiquitous stethoscope, an EKG caliper, a reflex hammer with microfilament test for diabetes, and a pocket Sanford Guide.
“I’d love to ditch the lab coat,” Dr. Ferrance says. “I often take it off when I sit down and sometimes end up leaving it behind, such as in the medical dictation area. I never want to wear one when I’m talking to a child. But for a lot of families of patients who are critically ill, it is a symbol, almost like the armor of the knighthood of medicine. You have to read each family, but for some, you lose credibility when you take it off. They’re looking for everything that medicine can offer, and the lab coat gives them more confidence in you.”
Dr. Ferrance appreciates the smaller size of his 47-bed hospital, where he is never a long walk from anyplace. He frequently returns during the day to his office, which he doesn’t have to share with other doctors. He uses it for family conferences and to store larger manuals, his laptop, and diagnostic kits.
He also values his Treo Smart phone, which incorporates a variety of programs, including a drug reference, billing program, lab reports on active patients, pediatric growth chart program, pneumonia severity index calculator, a medical calculator, Geriatrics At Your Fingertips, the Harriet Lane Handbook: A Manual for Pediatric House Officers, the American Association of Pediatrics’ Redbook comprehensive online infectious disease resource, hospice eligibility criteria, a camera—“to take pictures of odd lesions”—and access to e-mail and sports scores.
Although a briefcase is one more thing to lug around and risk losing, Julia Wright, MD, director of hospital medicine at the University of Wisconsin Hospital in Madison, says she carries a bag that is a woman’s version of a briefcase, with her laptop and active administrative files required for her growing administrative duties as director of an academic hospitalist group.
“There are advantages to being mobile, but disadvantages as well,” Dr. Wright says. “You just can’t get everything done. I get between 50 and 60 phone pages a day, and a lot of curbside consults, as well.” The medical center is restructuring teaching services so a hospitalist’s assigned patients would be more often concentrated in one area, with less running from floor to floor, as well as exploring new office facilities for the hospitalist group.
Currently, 11 University of Wisconsin hospitalists share a room with five cubicles. “I’ve put my pictures up on the wall anyway, and I keep my files, stapler, and office supplies there. A couple of my partners keep their reference books there. What I like about sharing space like this is it can help with communication and collegiality within the group. We do a lot of patient hand-offs there. But as we grow and it becomes more crowded, we’re going to need some more dedicated space.” TH
Larry Beresford is a medical writer based in California.
Russ Cucina, MD, MS, a hospitalist at the University of California San Francisco (UCSF) Medical Center, and a colleague once spent a week wearing pedometers on the job to study how much ground they covered in the course of managing their patient caseloads in a huge hospital like UCSF. The result: an average of four miles walked per day.
“The usual productivity infrastructure for physicians in their offices is simply not as available to hospitalists, or isn’t under our control,” Dr. Cucina says. There may be networked computer terminals throughout the hospital, but how many there are, how accessible they are, and how much competition there is for them varies. Hospitalists may have their own offices, desks or shared office space, depending on institutional commitments, but these may be a trek from patient care areas.
As a result, they must bring essential tools of their trade on their persons. Some carry a briefcase or wear a fanny pack, but more often these essential tools are stuffed into every available pocket of their medical lab coats.
Dr. Cucina’s short list of essentials is typical of working hospitalists. It includes his “smart phone,” combining a personal digital assistant (PDA) and cell phone, pens, a reflex hammer, a tuning fork for testing neurologic sensitivities, a stethoscope, swabs for sterilizing the stethoscope, a stash of large hospital gloves (which can be a hard size to find), and a bulky and awkward—but secure—prescription pad in a cardstock wrapper.
He also totes a stack of 3-by-5-inch index cards held together with a steel ring—one card for each active patient, updated daily by hand with medication changes, lab results and other information provided by the residents. “I have tried higher-tech approaches,” he explains. “I am the hospital’s associate medical director for information technology, and I need to keep up to date and try new things, including the various applications for keeping patient lists on line. But nothing has yet beaten out hand-written index cards for efficiency and ease of use. The time it takes to input this information electronically just isn’t worth it.”
Hospitalists say additional medical tools, such as an otoscope or ophthalmoscope, could be helpful but may pile on too much bulk and weight. “I’m often challenged to find one on the floor when I really need it,” Dr. Cucina says. Portable scopes are also quite valuable and at some risk for disappearing from an unattended lab coat in the highly trafficked hospital setting.
PDA Is No Panacea
For many hospitalists, one key to efficient mobility on the job is the PDA or laptop computer, with basic references such as UpToDate, Epocrates, Tarascon Pocket Pharmacopoeia, or the Washington Manual of Medical Therapeutics, either loaded or accessed via the Internet. PDAs involve serious compromises balancing size and weight with ease of keyboard use, ease of reading the screen, and memory or processing speed. (See “Tackle Technology,” November 2007, p. 22 for a discussion of how hospitalists use portable computing devices on the job.)
“We’ve come a long way from tongue depressors and otoscopes,” says William Ford, MD, program medical director for Cogent Healthcare’s large and expanding hospitalist group based at Temple University, Collegeville, Pa. “Some of us at Temple, depending on the service, carry one or more cell phones and between one and three pagers, in a pocket or attached to a belt.” The doctors may have their own PDAs, but Cogent no longer supplies them, having converted to a Web-based tool that offers a variety of practice management resources accessed by laptop computers via the Internet.
Dr. Cucina believes the technology is evolving toward a tablet device that will integrate more of the resource databases hospitalists need in their daily practice with other essential functions, such as lab results, billing, and communications with primary physicians—all in a user-friendly scale and format. In the meantime, there’s still a lot that has to be stuffed into pockets.
Some hospitalists also prefer to hold favorite reference resources, such as the pocket-sized Sanford Guide to Antimicrobial Therapy in their hands. That also involves tradeoffs, notes Michelle Pezzani, MD, hospitalist at El Camino Hospital in Mountain View, Calif.
“I tried carrying a book bag over my shoulder, but I felt like a school kid,” Dr. Pezzani relates. “I also noticed that the more reference books I had stuffed into my pockets, the less confidence other people seemed to have in me as a physician.” Not to mention that her pockets ripped open from the weight. She even developed a sore neck from her ergonomically unbalanced, overstuffed lab coat.
“Although I love being a hospitalist, it’s getting to the point where I feel disorganized because I have no real home base,” Dr. Pezzani laments. She finds her hospitalist group’s shared office—a converted labor-and-delivery room with no windows and three desktop computers for nine doctors—less than ideal. She spends as little time as possible there.
“My life would be easier if I didn’t have to carry my office in my pockets—my ink-stained pockets,” she says. “I can’t carry my laptop around with me because of the neck pain, so I asked the hospital to give me a locker closer to the middle of the building. It has also become a kind of science for me to transfer a few personal essentials into a little satchel with a string that I wear around my neck,” since a purse is not feasible.
Love/Hate Situation
Dr. Cucina uses an online custom supplier of medical lab coats with extra, zippered pockets on the inside and outside. He’s careful not to let the lab coat of out his sight when he takes it off.
Randy Ferrance, MD, a hospitalist in internal medicine and pediatrics at Riverside Tappahannock Hospital in Tappahannock, Va., acknowledges his own love-hate relationship with the lab coat. In his pockets, he carries a stack of 3-by-5-inch index cards, an 8.5-by-11-inch hospital census sheet, folded over, a prescription pad, a highlighter pen and spare pens, the ubiquitous stethoscope, an EKG caliper, a reflex hammer with microfilament test for diabetes, and a pocket Sanford Guide.
“I’d love to ditch the lab coat,” Dr. Ferrance says. “I often take it off when I sit down and sometimes end up leaving it behind, such as in the medical dictation area. I never want to wear one when I’m talking to a child. But for a lot of families of patients who are critically ill, it is a symbol, almost like the armor of the knighthood of medicine. You have to read each family, but for some, you lose credibility when you take it off. They’re looking for everything that medicine can offer, and the lab coat gives them more confidence in you.”
Dr. Ferrance appreciates the smaller size of his 47-bed hospital, where he is never a long walk from anyplace. He frequently returns during the day to his office, which he doesn’t have to share with other doctors. He uses it for family conferences and to store larger manuals, his laptop, and diagnostic kits.
He also values his Treo Smart phone, which incorporates a variety of programs, including a drug reference, billing program, lab reports on active patients, pediatric growth chart program, pneumonia severity index calculator, a medical calculator, Geriatrics At Your Fingertips, the Harriet Lane Handbook: A Manual for Pediatric House Officers, the American Association of Pediatrics’ Redbook comprehensive online infectious disease resource, hospice eligibility criteria, a camera—“to take pictures of odd lesions”—and access to e-mail and sports scores.
Although a briefcase is one more thing to lug around and risk losing, Julia Wright, MD, director of hospital medicine at the University of Wisconsin Hospital in Madison, says she carries a bag that is a woman’s version of a briefcase, with her laptop and active administrative files required for her growing administrative duties as director of an academic hospitalist group.
“There are advantages to being mobile, but disadvantages as well,” Dr. Wright says. “You just can’t get everything done. I get between 50 and 60 phone pages a day, and a lot of curbside consults, as well.” The medical center is restructuring teaching services so a hospitalist’s assigned patients would be more often concentrated in one area, with less running from floor to floor, as well as exploring new office facilities for the hospitalist group.
Currently, 11 University of Wisconsin hospitalists share a room with five cubicles. “I’ve put my pictures up on the wall anyway, and I keep my files, stapler, and office supplies there. A couple of my partners keep their reference books there. What I like about sharing space like this is it can help with communication and collegiality within the group. We do a lot of patient hand-offs there. But as we grow and it becomes more crowded, we’re going to need some more dedicated space.” TH
Larry Beresford is a medical writer based in California.
Russ Cucina, MD, MS, a hospitalist at the University of California San Francisco (UCSF) Medical Center, and a colleague once spent a week wearing pedometers on the job to study how much ground they covered in the course of managing their patient caseloads in a huge hospital like UCSF. The result: an average of four miles walked per day.
“The usual productivity infrastructure for physicians in their offices is simply not as available to hospitalists, or isn’t under our control,” Dr. Cucina says. There may be networked computer terminals throughout the hospital, but how many there are, how accessible they are, and how much competition there is for them varies. Hospitalists may have their own offices, desks or shared office space, depending on institutional commitments, but these may be a trek from patient care areas.
As a result, they must bring essential tools of their trade on their persons. Some carry a briefcase or wear a fanny pack, but more often these essential tools are stuffed into every available pocket of their medical lab coats.
Dr. Cucina’s short list of essentials is typical of working hospitalists. It includes his “smart phone,” combining a personal digital assistant (PDA) and cell phone, pens, a reflex hammer, a tuning fork for testing neurologic sensitivities, a stethoscope, swabs for sterilizing the stethoscope, a stash of large hospital gloves (which can be a hard size to find), and a bulky and awkward—but secure—prescription pad in a cardstock wrapper.
He also totes a stack of 3-by-5-inch index cards held together with a steel ring—one card for each active patient, updated daily by hand with medication changes, lab results and other information provided by the residents. “I have tried higher-tech approaches,” he explains. “I am the hospital’s associate medical director for information technology, and I need to keep up to date and try new things, including the various applications for keeping patient lists on line. But nothing has yet beaten out hand-written index cards for efficiency and ease of use. The time it takes to input this information electronically just isn’t worth it.”
Hospitalists say additional medical tools, such as an otoscope or ophthalmoscope, could be helpful but may pile on too much bulk and weight. “I’m often challenged to find one on the floor when I really need it,” Dr. Cucina says. Portable scopes are also quite valuable and at some risk for disappearing from an unattended lab coat in the highly trafficked hospital setting.
PDA Is No Panacea
For many hospitalists, one key to efficient mobility on the job is the PDA or laptop computer, with basic references such as UpToDate, Epocrates, Tarascon Pocket Pharmacopoeia, or the Washington Manual of Medical Therapeutics, either loaded or accessed via the Internet. PDAs involve serious compromises balancing size and weight with ease of keyboard use, ease of reading the screen, and memory or processing speed. (See “Tackle Technology,” November 2007, p. 22 for a discussion of how hospitalists use portable computing devices on the job.)
“We’ve come a long way from tongue depressors and otoscopes,” says William Ford, MD, program medical director for Cogent Healthcare’s large and expanding hospitalist group based at Temple University, Collegeville, Pa. “Some of us at Temple, depending on the service, carry one or more cell phones and between one and three pagers, in a pocket or attached to a belt.” The doctors may have their own PDAs, but Cogent no longer supplies them, having converted to a Web-based tool that offers a variety of practice management resources accessed by laptop computers via the Internet.
Dr. Cucina believes the technology is evolving toward a tablet device that will integrate more of the resource databases hospitalists need in their daily practice with other essential functions, such as lab results, billing, and communications with primary physicians—all in a user-friendly scale and format. In the meantime, there’s still a lot that has to be stuffed into pockets.
Some hospitalists also prefer to hold favorite reference resources, such as the pocket-sized Sanford Guide to Antimicrobial Therapy in their hands. That also involves tradeoffs, notes Michelle Pezzani, MD, hospitalist at El Camino Hospital in Mountain View, Calif.
“I tried carrying a book bag over my shoulder, but I felt like a school kid,” Dr. Pezzani relates. “I also noticed that the more reference books I had stuffed into my pockets, the less confidence other people seemed to have in me as a physician.” Not to mention that her pockets ripped open from the weight. She even developed a sore neck from her ergonomically unbalanced, overstuffed lab coat.
“Although I love being a hospitalist, it’s getting to the point where I feel disorganized because I have no real home base,” Dr. Pezzani laments. She finds her hospitalist group’s shared office—a converted labor-and-delivery room with no windows and three desktop computers for nine doctors—less than ideal. She spends as little time as possible there.
“My life would be easier if I didn’t have to carry my office in my pockets—my ink-stained pockets,” she says. “I can’t carry my laptop around with me because of the neck pain, so I asked the hospital to give me a locker closer to the middle of the building. It has also become a kind of science for me to transfer a few personal essentials into a little satchel with a string that I wear around my neck,” since a purse is not feasible.
Love/Hate Situation
Dr. Cucina uses an online custom supplier of medical lab coats with extra, zippered pockets on the inside and outside. He’s careful not to let the lab coat of out his sight when he takes it off.
Randy Ferrance, MD, a hospitalist in internal medicine and pediatrics at Riverside Tappahannock Hospital in Tappahannock, Va., acknowledges his own love-hate relationship with the lab coat. In his pockets, he carries a stack of 3-by-5-inch index cards, an 8.5-by-11-inch hospital census sheet, folded over, a prescription pad, a highlighter pen and spare pens, the ubiquitous stethoscope, an EKG caliper, a reflex hammer with microfilament test for diabetes, and a pocket Sanford Guide.
“I’d love to ditch the lab coat,” Dr. Ferrance says. “I often take it off when I sit down and sometimes end up leaving it behind, such as in the medical dictation area. I never want to wear one when I’m talking to a child. But for a lot of families of patients who are critically ill, it is a symbol, almost like the armor of the knighthood of medicine. You have to read each family, but for some, you lose credibility when you take it off. They’re looking for everything that medicine can offer, and the lab coat gives them more confidence in you.”
Dr. Ferrance appreciates the smaller size of his 47-bed hospital, where he is never a long walk from anyplace. He frequently returns during the day to his office, which he doesn’t have to share with other doctors. He uses it for family conferences and to store larger manuals, his laptop, and diagnostic kits.
He also values his Treo Smart phone, which incorporates a variety of programs, including a drug reference, billing program, lab reports on active patients, pediatric growth chart program, pneumonia severity index calculator, a medical calculator, Geriatrics At Your Fingertips, the Harriet Lane Handbook: A Manual for Pediatric House Officers, the American Association of Pediatrics’ Redbook comprehensive online infectious disease resource, hospice eligibility criteria, a camera—“to take pictures of odd lesions”—and access to e-mail and sports scores.
Although a briefcase is one more thing to lug around and risk losing, Julia Wright, MD, director of hospital medicine at the University of Wisconsin Hospital in Madison, says she carries a bag that is a woman’s version of a briefcase, with her laptop and active administrative files required for her growing administrative duties as director of an academic hospitalist group.
“There are advantages to being mobile, but disadvantages as well,” Dr. Wright says. “You just can’t get everything done. I get between 50 and 60 phone pages a day, and a lot of curbside consults, as well.” The medical center is restructuring teaching services so a hospitalist’s assigned patients would be more often concentrated in one area, with less running from floor to floor, as well as exploring new office facilities for the hospitalist group.
Currently, 11 University of Wisconsin hospitalists share a room with five cubicles. “I’ve put my pictures up on the wall anyway, and I keep my files, stapler, and office supplies there. A couple of my partners keep their reference books there. What I like about sharing space like this is it can help with communication and collegiality within the group. We do a lot of patient hand-offs there. But as we grow and it becomes more crowded, we’re going to need some more dedicated space.” TH
Larry Beresford is a medical writer based in California.
Weekend Effect Persists
Recent research published in the Journal of the American Medical Association (JAMA) highlights a continued hospital care issue identified in previous studies: worse patient outcomes from in-hospital cardiac arrests occur at night or on the weekend.1
An analysis of 86,748 adult cardiac events between January 2000 and February 2007 in 507 hospitals participating in the National Registry of Cardiopulmonary Resuscitation (NRCPR) compared outcomes at night (from 11 p.m. to 6:59 a.m.) and weekends (from 11 p.m. Friday to 6:59 a.m. Monday) with day/evening shifts. The primary measure of survival to discharge and secondary outcomes from in-hospital cardiac arrests were significantly worse during nights and weekends. In essence, heart attack patients were 41% more likely to survive if treated during daytime weekday hours.
“This was the first comprehensive, large-scale study in a cross section of hospitals across the country of heart attack survival differences between shifts,” says lead author Mary Ann Peberdy, MD, of Virginia Commonwealth University in Richmond. “We adjusted for a variety of potentially confounding factors and patient characteristics, none of which explained the worse outcomes nights and weekends.”
The national database was not designed to provide an explanation for its findings, which may be due to multiple patient, event or hospital factors. “We can’t exclude physiological factors of patients or of staff working on the night shift,” Dr. Peberdy explains. “But I think we need to focus on process issues. We know that hospitals simply do not run the same way at night. Things are different—more errors, more accidents, more needle sticks, less people around. Those who work the night shift may also be less experienced,” and early identification of heart attacks is critical to positive outcome.
The JAMA results confirm previous research documenting worse outcomes on nights and weekends. Single-site studies and a smaller study of heart attack survival in New Jersey hospitals for weekend versus weekday admissions found similar trends.2
Stroke patients who enter the hospital at night or over the weekend are more likely to die in the hospital than those admitted during daytime hours (7 a.m. to 6 p.m.) on weekdays, according to two studies presented at the American Heart Association’s International Stroke Conference in New Orleans in February 2008.3 Those differences were particularly striking for hemorrhagic strokes. Similar outcomes also have been reported for pulmonary embolisms.
Shift Differences
Different studies have approached this issue in different ways, comparing business hours (e.g., 7 a.m. to 6 p.m.) with evenings, nights, and weekends, or days and evenings up to 11 p.m. with nights. Weekends are compared to weekdays but also to weekend nights.
The size of the hospital did not explain the shift differences found in Dr. Peberdy’s study. For hospitalists trying to address the underlying problems of after-hours quality, the size of the hospital is relevant. Only larger hospitals can afford hospitalist groups large enough to cover night and weekend shifts. For those that can, are all members of the group taking their turns at night, does this duty fall to the junior members, or is the group lucky enough to employ nocturnists who want to work at night? (See The Hospitalist, May 2006, p. 27, for an article on nocturnists in hospital medicine.) Whether the hospital has an academic emphasis also can influence who responds to crises after hours—attendings or house staff (in other words, sleep-deprived residents).
If hospitalists work nights, they are more likely to notice what isn’t available or what doesn’t work as well as what contributes to nocturnal quality problems and what might help to compensate for these differences. Even if hospitalists are not present in the facility at night, technology can help guide appropriate response to cardiac crises, suggests David Grace, MD, area medical officer for the Schumacher Group’s Hospital Medicine Division and a hospitalist at Southwest Medical Center in Lafayette, La.
“Several weeks ago a patient in the hospital was having chest pains,” he recalls. “A nurse called me at home and I ordered an electrocardiogram.” The electrocardiogram’s (EKG) computer program indicated “nonspecific changes” in the patient’s cardiac function, but Dr. Grace asked the nurse to scan the printout and send it to his Web-based fax number.
“I looked at the EKG on my PDA,” he continues. “It was subtle, but it seemed to me that this patient was having a myocardial infarction[MI]. I told the nurse to do the blood work for a suspected MI, give the patient an aspirin and take another EKG, which more clearly showed the MI. If I had not had the ability to look at the printout, I would have had to trust the nurse’s observation or the EKG computer program. As it was, we caught it early and the patient did well.”
Cooperation and Staffing
“I have lived it. I certainly understand the research showing different outcomes from MIs at night,” Dr. Grace observes. “At night, patients are usually asleep, so processes that begin with early warning signals, such as chest pains, may go further down the path before they are identified, especially if the patient has taken a sleeping pill. Often, nurse-to-patient staffing ratios are dramatically different at night—and somewhat reduced on weekends. I’ve also worked in hospitals where on weekends, unless it was a true life-threatening emergency, you could not get an MRI. So if you ordered one on a Saturday, it wouldn’t happen until Monday. There are things you pick up on the MRI that you miss on the CT scan; for example, bleeding, which can affect your management of the patient.”
“I would not be surprised to hear of worse survival for any of these acute decompensations—it goes for acute GI bleeds, stroke, and hemorrhage, as well as MIs,” adds Steven Liu, MD, of Emory University Eastside Medical Center in Atlanta. “We dealt with the problem in this hospital five years ago and addressed a lot of these quality issues by partnering with hospital administration and specialists.”
On weekends, many services may be less available or not available at all in the hospital, from interventional radiology to physical therapy. If patients have fewer contacts with different hospital personnel, it is more likely that subtle early signs of acute problems will go unnoticed until later.
“At my hospital, the interventional radiology [IR] department is not open 24 hours,” says Erica Grabscheid, MD, associate director of the hospitalist program at Beth Israel Hospital in New York City. If a peripherally inserted central catheter needs to be placed on the weekend but IR is not available, the patient may have to wait until Monday morning. Alternatives for the hospitalist, Dr. Grabscheid says, are to become skilled at line placement or to collect data for the hospital’s administrators on the costs of not having 24-hour IR.
Jeffrey Robinson, MD, hospitalist group leader for Intermountain Medical Center in Salt Lake City, Utah, believes staffing is an essential part of the equation. He says Intermountain Health has made a commitment to do what’s necessary for quality patient care—including adequate staffing. “Every time we feel we’re stretched, we add more hospitalist shifts, including weekends and holidays. I feel we give good patient care from the physician side. Obstacles have more to do with ancillaries, but we’ve made great progress in addressing these, as well.”
At one time, interventional radiology only was available in the hospital five days a week, Dr. Robinson notes. “You couldn’t get feeding tubes placed or certain other interventional procedures. But with the commitment of radiology and the hiring power of Intermountain Health, we now have 24-hour availability. MRIs have been harder to cover after hours, but there is now an on-call team for MRIs.”
In each case, hospitalists were important advocates for expanding the hours of availability, Dr. Robinson says: “We needed to gather data and look at results for patients staying over the weekend. We also got expanded case management, so that nursing home placements could happen on Saturdays and Sundays.” TH
Larry Beresford is a medical writer based in California.
References
- Peberdy MA, Ornato JP, Larkin GL, et al. Survival from in-hospital cardiac arrest during nights and weekends. JAMA. 2008; 99(7):785-792.
- Kostis WS, Demissie K, Marcella SW, Shao YH, Wilson AC, Moreyra AE. Weekend versus weekday admission and mortality from myocardial infarction. N Engl J Med. 2007; 356(11):1099-1109.
- American Heart Association. Deaths higher in stroke patients who enter hospital at night, weekends. Available at www.sciencedaily.com/releases/2008/02/080220161720/htm. Accessed March 13, 2008.
Recent research published in the Journal of the American Medical Association (JAMA) highlights a continued hospital care issue identified in previous studies: worse patient outcomes from in-hospital cardiac arrests occur at night or on the weekend.1
An analysis of 86,748 adult cardiac events between January 2000 and February 2007 in 507 hospitals participating in the National Registry of Cardiopulmonary Resuscitation (NRCPR) compared outcomes at night (from 11 p.m. to 6:59 a.m.) and weekends (from 11 p.m. Friday to 6:59 a.m. Monday) with day/evening shifts. The primary measure of survival to discharge and secondary outcomes from in-hospital cardiac arrests were significantly worse during nights and weekends. In essence, heart attack patients were 41% more likely to survive if treated during daytime weekday hours.
“This was the first comprehensive, large-scale study in a cross section of hospitals across the country of heart attack survival differences between shifts,” says lead author Mary Ann Peberdy, MD, of Virginia Commonwealth University in Richmond. “We adjusted for a variety of potentially confounding factors and patient characteristics, none of which explained the worse outcomes nights and weekends.”
The national database was not designed to provide an explanation for its findings, which may be due to multiple patient, event or hospital factors. “We can’t exclude physiological factors of patients or of staff working on the night shift,” Dr. Peberdy explains. “But I think we need to focus on process issues. We know that hospitals simply do not run the same way at night. Things are different—more errors, more accidents, more needle sticks, less people around. Those who work the night shift may also be less experienced,” and early identification of heart attacks is critical to positive outcome.
The JAMA results confirm previous research documenting worse outcomes on nights and weekends. Single-site studies and a smaller study of heart attack survival in New Jersey hospitals for weekend versus weekday admissions found similar trends.2
Stroke patients who enter the hospital at night or over the weekend are more likely to die in the hospital than those admitted during daytime hours (7 a.m. to 6 p.m.) on weekdays, according to two studies presented at the American Heart Association’s International Stroke Conference in New Orleans in February 2008.3 Those differences were particularly striking for hemorrhagic strokes. Similar outcomes also have been reported for pulmonary embolisms.
Shift Differences
Different studies have approached this issue in different ways, comparing business hours (e.g., 7 a.m. to 6 p.m.) with evenings, nights, and weekends, or days and evenings up to 11 p.m. with nights. Weekends are compared to weekdays but also to weekend nights.
The size of the hospital did not explain the shift differences found in Dr. Peberdy’s study. For hospitalists trying to address the underlying problems of after-hours quality, the size of the hospital is relevant. Only larger hospitals can afford hospitalist groups large enough to cover night and weekend shifts. For those that can, are all members of the group taking their turns at night, does this duty fall to the junior members, or is the group lucky enough to employ nocturnists who want to work at night? (See The Hospitalist, May 2006, p. 27, for an article on nocturnists in hospital medicine.) Whether the hospital has an academic emphasis also can influence who responds to crises after hours—attendings or house staff (in other words, sleep-deprived residents).
If hospitalists work nights, they are more likely to notice what isn’t available or what doesn’t work as well as what contributes to nocturnal quality problems and what might help to compensate for these differences. Even if hospitalists are not present in the facility at night, technology can help guide appropriate response to cardiac crises, suggests David Grace, MD, area medical officer for the Schumacher Group’s Hospital Medicine Division and a hospitalist at Southwest Medical Center in Lafayette, La.
“Several weeks ago a patient in the hospital was having chest pains,” he recalls. “A nurse called me at home and I ordered an electrocardiogram.” The electrocardiogram’s (EKG) computer program indicated “nonspecific changes” in the patient’s cardiac function, but Dr. Grace asked the nurse to scan the printout and send it to his Web-based fax number.
“I looked at the EKG on my PDA,” he continues. “It was subtle, but it seemed to me that this patient was having a myocardial infarction[MI]. I told the nurse to do the blood work for a suspected MI, give the patient an aspirin and take another EKG, which more clearly showed the MI. If I had not had the ability to look at the printout, I would have had to trust the nurse’s observation or the EKG computer program. As it was, we caught it early and the patient did well.”
Cooperation and Staffing
“I have lived it. I certainly understand the research showing different outcomes from MIs at night,” Dr. Grace observes. “At night, patients are usually asleep, so processes that begin with early warning signals, such as chest pains, may go further down the path before they are identified, especially if the patient has taken a sleeping pill. Often, nurse-to-patient staffing ratios are dramatically different at night—and somewhat reduced on weekends. I’ve also worked in hospitals where on weekends, unless it was a true life-threatening emergency, you could not get an MRI. So if you ordered one on a Saturday, it wouldn’t happen until Monday. There are things you pick up on the MRI that you miss on the CT scan; for example, bleeding, which can affect your management of the patient.”
“I would not be surprised to hear of worse survival for any of these acute decompensations—it goes for acute GI bleeds, stroke, and hemorrhage, as well as MIs,” adds Steven Liu, MD, of Emory University Eastside Medical Center in Atlanta. “We dealt with the problem in this hospital five years ago and addressed a lot of these quality issues by partnering with hospital administration and specialists.”
On weekends, many services may be less available or not available at all in the hospital, from interventional radiology to physical therapy. If patients have fewer contacts with different hospital personnel, it is more likely that subtle early signs of acute problems will go unnoticed until later.
“At my hospital, the interventional radiology [IR] department is not open 24 hours,” says Erica Grabscheid, MD, associate director of the hospitalist program at Beth Israel Hospital in New York City. If a peripherally inserted central catheter needs to be placed on the weekend but IR is not available, the patient may have to wait until Monday morning. Alternatives for the hospitalist, Dr. Grabscheid says, are to become skilled at line placement or to collect data for the hospital’s administrators on the costs of not having 24-hour IR.
Jeffrey Robinson, MD, hospitalist group leader for Intermountain Medical Center in Salt Lake City, Utah, believes staffing is an essential part of the equation. He says Intermountain Health has made a commitment to do what’s necessary for quality patient care—including adequate staffing. “Every time we feel we’re stretched, we add more hospitalist shifts, including weekends and holidays. I feel we give good patient care from the physician side. Obstacles have more to do with ancillaries, but we’ve made great progress in addressing these, as well.”
At one time, interventional radiology only was available in the hospital five days a week, Dr. Robinson notes. “You couldn’t get feeding tubes placed or certain other interventional procedures. But with the commitment of radiology and the hiring power of Intermountain Health, we now have 24-hour availability. MRIs have been harder to cover after hours, but there is now an on-call team for MRIs.”
In each case, hospitalists were important advocates for expanding the hours of availability, Dr. Robinson says: “We needed to gather data and look at results for patients staying over the weekend. We also got expanded case management, so that nursing home placements could happen on Saturdays and Sundays.” TH
Larry Beresford is a medical writer based in California.
References
- Peberdy MA, Ornato JP, Larkin GL, et al. Survival from in-hospital cardiac arrest during nights and weekends. JAMA. 2008; 99(7):785-792.
- Kostis WS, Demissie K, Marcella SW, Shao YH, Wilson AC, Moreyra AE. Weekend versus weekday admission and mortality from myocardial infarction. N Engl J Med. 2007; 356(11):1099-1109.
- American Heart Association. Deaths higher in stroke patients who enter hospital at night, weekends. Available at www.sciencedaily.com/releases/2008/02/080220161720/htm. Accessed March 13, 2008.
Recent research published in the Journal of the American Medical Association (JAMA) highlights a continued hospital care issue identified in previous studies: worse patient outcomes from in-hospital cardiac arrests occur at night or on the weekend.1
An analysis of 86,748 adult cardiac events between January 2000 and February 2007 in 507 hospitals participating in the National Registry of Cardiopulmonary Resuscitation (NRCPR) compared outcomes at night (from 11 p.m. to 6:59 a.m.) and weekends (from 11 p.m. Friday to 6:59 a.m. Monday) with day/evening shifts. The primary measure of survival to discharge and secondary outcomes from in-hospital cardiac arrests were significantly worse during nights and weekends. In essence, heart attack patients were 41% more likely to survive if treated during daytime weekday hours.
“This was the first comprehensive, large-scale study in a cross section of hospitals across the country of heart attack survival differences between shifts,” says lead author Mary Ann Peberdy, MD, of Virginia Commonwealth University in Richmond. “We adjusted for a variety of potentially confounding factors and patient characteristics, none of which explained the worse outcomes nights and weekends.”
The national database was not designed to provide an explanation for its findings, which may be due to multiple patient, event or hospital factors. “We can’t exclude physiological factors of patients or of staff working on the night shift,” Dr. Peberdy explains. “But I think we need to focus on process issues. We know that hospitals simply do not run the same way at night. Things are different—more errors, more accidents, more needle sticks, less people around. Those who work the night shift may also be less experienced,” and early identification of heart attacks is critical to positive outcome.
The JAMA results confirm previous research documenting worse outcomes on nights and weekends. Single-site studies and a smaller study of heart attack survival in New Jersey hospitals for weekend versus weekday admissions found similar trends.2
Stroke patients who enter the hospital at night or over the weekend are more likely to die in the hospital than those admitted during daytime hours (7 a.m. to 6 p.m.) on weekdays, according to two studies presented at the American Heart Association’s International Stroke Conference in New Orleans in February 2008.3 Those differences were particularly striking for hemorrhagic strokes. Similar outcomes also have been reported for pulmonary embolisms.
Shift Differences
Different studies have approached this issue in different ways, comparing business hours (e.g., 7 a.m. to 6 p.m.) with evenings, nights, and weekends, or days and evenings up to 11 p.m. with nights. Weekends are compared to weekdays but also to weekend nights.
The size of the hospital did not explain the shift differences found in Dr. Peberdy’s study. For hospitalists trying to address the underlying problems of after-hours quality, the size of the hospital is relevant. Only larger hospitals can afford hospitalist groups large enough to cover night and weekend shifts. For those that can, are all members of the group taking their turns at night, does this duty fall to the junior members, or is the group lucky enough to employ nocturnists who want to work at night? (See The Hospitalist, May 2006, p. 27, for an article on nocturnists in hospital medicine.) Whether the hospital has an academic emphasis also can influence who responds to crises after hours—attendings or house staff (in other words, sleep-deprived residents).
If hospitalists work nights, they are more likely to notice what isn’t available or what doesn’t work as well as what contributes to nocturnal quality problems and what might help to compensate for these differences. Even if hospitalists are not present in the facility at night, technology can help guide appropriate response to cardiac crises, suggests David Grace, MD, area medical officer for the Schumacher Group’s Hospital Medicine Division and a hospitalist at Southwest Medical Center in Lafayette, La.
“Several weeks ago a patient in the hospital was having chest pains,” he recalls. “A nurse called me at home and I ordered an electrocardiogram.” The electrocardiogram’s (EKG) computer program indicated “nonspecific changes” in the patient’s cardiac function, but Dr. Grace asked the nurse to scan the printout and send it to his Web-based fax number.
“I looked at the EKG on my PDA,” he continues. “It was subtle, but it seemed to me that this patient was having a myocardial infarction[MI]. I told the nurse to do the blood work for a suspected MI, give the patient an aspirin and take another EKG, which more clearly showed the MI. If I had not had the ability to look at the printout, I would have had to trust the nurse’s observation or the EKG computer program. As it was, we caught it early and the patient did well.”
Cooperation and Staffing
“I have lived it. I certainly understand the research showing different outcomes from MIs at night,” Dr. Grace observes. “At night, patients are usually asleep, so processes that begin with early warning signals, such as chest pains, may go further down the path before they are identified, especially if the patient has taken a sleeping pill. Often, nurse-to-patient staffing ratios are dramatically different at night—and somewhat reduced on weekends. I’ve also worked in hospitals where on weekends, unless it was a true life-threatening emergency, you could not get an MRI. So if you ordered one on a Saturday, it wouldn’t happen until Monday. There are things you pick up on the MRI that you miss on the CT scan; for example, bleeding, which can affect your management of the patient.”
“I would not be surprised to hear of worse survival for any of these acute decompensations—it goes for acute GI bleeds, stroke, and hemorrhage, as well as MIs,” adds Steven Liu, MD, of Emory University Eastside Medical Center in Atlanta. “We dealt with the problem in this hospital five years ago and addressed a lot of these quality issues by partnering with hospital administration and specialists.”
On weekends, many services may be less available or not available at all in the hospital, from interventional radiology to physical therapy. If patients have fewer contacts with different hospital personnel, it is more likely that subtle early signs of acute problems will go unnoticed until later.
“At my hospital, the interventional radiology [IR] department is not open 24 hours,” says Erica Grabscheid, MD, associate director of the hospitalist program at Beth Israel Hospital in New York City. If a peripherally inserted central catheter needs to be placed on the weekend but IR is not available, the patient may have to wait until Monday morning. Alternatives for the hospitalist, Dr. Grabscheid says, are to become skilled at line placement or to collect data for the hospital’s administrators on the costs of not having 24-hour IR.
Jeffrey Robinson, MD, hospitalist group leader for Intermountain Medical Center in Salt Lake City, Utah, believes staffing is an essential part of the equation. He says Intermountain Health has made a commitment to do what’s necessary for quality patient care—including adequate staffing. “Every time we feel we’re stretched, we add more hospitalist shifts, including weekends and holidays. I feel we give good patient care from the physician side. Obstacles have more to do with ancillaries, but we’ve made great progress in addressing these, as well.”
At one time, interventional radiology only was available in the hospital five days a week, Dr. Robinson notes. “You couldn’t get feeding tubes placed or certain other interventional procedures. But with the commitment of radiology and the hiring power of Intermountain Health, we now have 24-hour availability. MRIs have been harder to cover after hours, but there is now an on-call team for MRIs.”
In each case, hospitalists were important advocates for expanding the hours of availability, Dr. Robinson says: “We needed to gather data and look at results for patients staying over the weekend. We also got expanded case management, so that nursing home placements could happen on Saturdays and Sundays.” TH
Larry Beresford is a medical writer based in California.
References
- Peberdy MA, Ornato JP, Larkin GL, et al. Survival from in-hospital cardiac arrest during nights and weekends. JAMA. 2008; 99(7):785-792.
- Kostis WS, Demissie K, Marcella SW, Shao YH, Wilson AC, Moreyra AE. Weekend versus weekday admission and mortality from myocardial infarction. N Engl J Med. 2007; 356(11):1099-1109.
- American Heart Association. Deaths higher in stroke patients who enter hospital at night, weekends. Available at www.sciencedaily.com/releases/2008/02/080220161720/htm. Accessed March 13, 2008.
High-Tech Nightmare
Joseph Heaton, MD, a hospitalist with Kaiser Permanente practicing at Exempla Good Samaritan Medical Center in Lafayette, Colo., has spent the past three years helping develop an electronic medical record for the hospital.
The project includes computerized physician order entry (CPOE), which was rolled out Oct. 2. He estimates he has dedicated anywhere from 20% to 50% of his time to technology implementation.
“I’ve been the physician champion for the project, working alongside the IT (information technology) development team,” Dr. Heaton explains. “I was chosen not for any particular computer expertise but because of other leadership roles I have played as a hospitalist and my involvement in quality projects. I see CPOE and electronic medical records as obvious extensions of the other quality projects hospitalists participate in.”
Dr. Heaton’s experience in implementing a CPOE system highlights the barriers faced by those charged with advancing technology critical to hospital medicine.
He says he has learned a lot about computers along the way, but the technology is a snap compared with the challenges of managing change and making sure physicians are in tune with the new system.
“Not only was I representing other hospitalists, but also a broader group of physicians with privileges at the hospital, as well as other employees, including nurses and pharmacists,” he says. “Much of what I did was to translate language about workflow from the clinicians to IT, and then report back to the clinicians.”
But it wasn’t as easy at it sounds.
“Unfortunately, in this institution there is no single, agreed-upon communications venue for reaching all of the physicians who practice at the hospital,” says Dr. Heaton. “So we’ve had to use e-mail, voice mail, noon bag-lunch demos, mailings, departmental meetings and classes—multiple opportunities to make sure that physicians feel informed. That way, when they show up for their actual training in how to use the system, they’re not still asking questions like, ‘Why are we doing this?’ ”
Blessing or Curse?
CPOE, of course, refers to the process by which physicians and other clinicians directly enter medical orders into a computer application. CPOE can be independent of other computer applications or part of an electronic medical record or other computer system.
Standardized order sets, decision support tools, and other customized methods can make hospitalists’ jobs easier—if the system is well-designed. It’s not uncommon for CPOE to add time-consuming new tasks and functions. For example, hospitalists may be asked to enter information they’ve not previously been asked to supply. But CPOE is also touted as a way to reduce medical errors and improve quality.
“It’s a good thing to do,” Dr. Heaton concludes. “Six weeks into the implementation of CPOE here, medication delivery is much faster. There are efficiencies to be had. For the most part, the high-volume users, including hospitalists, are fine with it, even if they’re not taking full advantage of the system’s capabilities.”
But Campbell, et al., describe a number of unintended adverse consequences that have followed CPOE implementation.1 These downsides include unfavorable workflow issues, continuous demands for system change, untoward changes in communications patterns and practices, generation of new kinds of medical errors, and negative emotional responses to the system by clinicians. Physician resistance can derail costly, complex CPOE projects.
A widely cited example of such barriers comes from Cedars-Sinai Medical Center in Los Angeles. An institution known for its pioneering medical techniques and technologies, Cedars-Sinai was forced in 2003 to shut down implementation of CPOE after three months because of a full-blown staff rebellion, according to an article in The Washington Post.2 Various explanations have been offered for this failure, including inadequate training for users, intrusive decision support queries, and other provider frustrations with the system. The hospital’s public relations department declined a request to comment for this article or provide an update on the current status of CPOE at Cedars-Sinai.
Doing the Best We Can
The importance of CPOE to hospitalists is illustrated by Duane Spaulding, MD, FACP, president and executive contracting officer for Advantage Inpatient Medical Specialists, practicing at Penrose-St. Francis Hospital in Colorado Springs, Colo. Half of his 11-member hospitalist group could be considered “power users” of the hospital’s current, DOS-based CPOE system—but Dr. Spaulding is No. 1. “I enter more CPOE orders than any of the other 600-plus physicians on staff here,” he says.
For some hospitalists, computers are a passion. For others, “they are just a tool for getting from Point A to Point B,” he says. “I have probably spent 1,500 hours over the past decade on committee after committee, putting together computerized order sets and screens and the like.”
Dr. Spaulding says the hospital’s current, antiquated system can be laborious to work with: “I can only do 50% of my orders on the system.” At the end of last year, Centura—the hospital’s parent health system—was preparing to implement a regional electronic medical record integrating CPOE and other applications.
“It is a gargantuan change,” he says. With rollout planned in phases, hospitalists at Penrose-St. Francis will lose access to CPOE for an estimated six to nine months, although the new CPOE system eventually will be accessed on a tablet PC.
Amid this stressful transition to new technology, the hospitalists have been trying to do the best they can with available resources, Dr. Spaulding notes. “We have come up with a paper-based Plan B for entering all of our orders until we get access to the new CPOE system,” he says. “We have been reminding everyone in the group how important it is to take care of each other, such as by putting in a PRN order set for every new patient, because we know we all will be taking our turn on-call.”
Arieh Rosenbaum, MD, hospitalist at California Pacific Medical Center (CPMC) in San Francisco, has for years been involved in technology issues at his hospital, which is developing a new electronic medical record with CPOE. It will replace a 15-year-old, DOS-based CPOE system he describes as “powerful but clunky.” However, CPMC’s parent, Sutter Health, is rolling out the new computer system gradually across its 40 Northern California facilities. It won’t reach CPMC until 2011.
“It’s an incredibly complex project,” Dr. Rosenbaum says. “To Sutter’s credit, they’re trying very hard to get physicians’ input, establishing structures for gathering feedback at the corporate and local levels. I am one of the physicians who will be involved at the local level, both building the clinical content and interface as well as gaining physicians’ acceptance and participation.”
Success depends on how the new system relates to physicians’ workflow. “Everybody knows the benefits of CPOE, but there are mitigating factors, such as what to do when the system crashes,” he says. “Hospitalists are the people who will be interacting with the new system the most. It’s our job to be leaders and to be aware that this is in our future.”
Head-On Approach
Timothy Hartzog, MD, a pediatric hospitalist and medical director of information technology/CPOE at Medical College of South Carolina (MUSC), Charleston, urges hospitalists to take CPOE seriously and view it as an opportunity.
“Implementation of CPOE, or electronic medical records, can be one of the most fundamental changes a hospital makes—affecting the workflow of everybody who works there,” he says. “As physicians, we each work a little differently. With the standardization imposed by CPOE, it’s going to make some physicians a little crazy, no matter how well it’s implemented.”
Dr. Hartzog encourages hospitalists to set aside any doubts they may have and get involved in creating workable CPOE solutions.
“Hospitalists don’t have to be experts in technology,” he stresses. “If you learned medicine, you can learn the technology—if you’re willing to put in some time, read a couple of books, take some training, and work with your IT people. Tackle CPOE head on—make sure your voice is heard. Be part of the build. But you need to have time dedicated for the IT project, and you need to do the work. If you are not present and if other people on the development group don’t know you and hear you speak, decisions will be made when you’re not in the room.”
For some physicians, Dr. Hartzog says, it could even be fun. “Especially if we can actually make the system work for us. We can actually create something that makes life better for our group.” TH
Larry Beresford is a regular contributor to The Hospitalist.
References
- Campbell EM, Sittig, DF, Ash JS, et al. Types of unintended consequences related to computerized provider order entry. J Am Med Inform Assoc. 2006 Sept-Oct;13(5):547-556.
- Connolly C. Cedars-Sinai doctors cling to pen and paper. The Washington Post, March 21, 2005:A1.
Joseph Heaton, MD, a hospitalist with Kaiser Permanente practicing at Exempla Good Samaritan Medical Center in Lafayette, Colo., has spent the past three years helping develop an electronic medical record for the hospital.
The project includes computerized physician order entry (CPOE), which was rolled out Oct. 2. He estimates he has dedicated anywhere from 20% to 50% of his time to technology implementation.
“I’ve been the physician champion for the project, working alongside the IT (information technology) development team,” Dr. Heaton explains. “I was chosen not for any particular computer expertise but because of other leadership roles I have played as a hospitalist and my involvement in quality projects. I see CPOE and electronic medical records as obvious extensions of the other quality projects hospitalists participate in.”
Dr. Heaton’s experience in implementing a CPOE system highlights the barriers faced by those charged with advancing technology critical to hospital medicine.
He says he has learned a lot about computers along the way, but the technology is a snap compared with the challenges of managing change and making sure physicians are in tune with the new system.
“Not only was I representing other hospitalists, but also a broader group of physicians with privileges at the hospital, as well as other employees, including nurses and pharmacists,” he says. “Much of what I did was to translate language about workflow from the clinicians to IT, and then report back to the clinicians.”
But it wasn’t as easy at it sounds.
“Unfortunately, in this institution there is no single, agreed-upon communications venue for reaching all of the physicians who practice at the hospital,” says Dr. Heaton. “So we’ve had to use e-mail, voice mail, noon bag-lunch demos, mailings, departmental meetings and classes—multiple opportunities to make sure that physicians feel informed. That way, when they show up for their actual training in how to use the system, they’re not still asking questions like, ‘Why are we doing this?’ ”
Blessing or Curse?
CPOE, of course, refers to the process by which physicians and other clinicians directly enter medical orders into a computer application. CPOE can be independent of other computer applications or part of an electronic medical record or other computer system.
Standardized order sets, decision support tools, and other customized methods can make hospitalists’ jobs easier—if the system is well-designed. It’s not uncommon for CPOE to add time-consuming new tasks and functions. For example, hospitalists may be asked to enter information they’ve not previously been asked to supply. But CPOE is also touted as a way to reduce medical errors and improve quality.
“It’s a good thing to do,” Dr. Heaton concludes. “Six weeks into the implementation of CPOE here, medication delivery is much faster. There are efficiencies to be had. For the most part, the high-volume users, including hospitalists, are fine with it, even if they’re not taking full advantage of the system’s capabilities.”
But Campbell, et al., describe a number of unintended adverse consequences that have followed CPOE implementation.1 These downsides include unfavorable workflow issues, continuous demands for system change, untoward changes in communications patterns and practices, generation of new kinds of medical errors, and negative emotional responses to the system by clinicians. Physician resistance can derail costly, complex CPOE projects.
A widely cited example of such barriers comes from Cedars-Sinai Medical Center in Los Angeles. An institution known for its pioneering medical techniques and technologies, Cedars-Sinai was forced in 2003 to shut down implementation of CPOE after three months because of a full-blown staff rebellion, according to an article in The Washington Post.2 Various explanations have been offered for this failure, including inadequate training for users, intrusive decision support queries, and other provider frustrations with the system. The hospital’s public relations department declined a request to comment for this article or provide an update on the current status of CPOE at Cedars-Sinai.
Doing the Best We Can
The importance of CPOE to hospitalists is illustrated by Duane Spaulding, MD, FACP, president and executive contracting officer for Advantage Inpatient Medical Specialists, practicing at Penrose-St. Francis Hospital in Colorado Springs, Colo. Half of his 11-member hospitalist group could be considered “power users” of the hospital’s current, DOS-based CPOE system—but Dr. Spaulding is No. 1. “I enter more CPOE orders than any of the other 600-plus physicians on staff here,” he says.
For some hospitalists, computers are a passion. For others, “they are just a tool for getting from Point A to Point B,” he says. “I have probably spent 1,500 hours over the past decade on committee after committee, putting together computerized order sets and screens and the like.”
Dr. Spaulding says the hospital’s current, antiquated system can be laborious to work with: “I can only do 50% of my orders on the system.” At the end of last year, Centura—the hospital’s parent health system—was preparing to implement a regional electronic medical record integrating CPOE and other applications.
“It is a gargantuan change,” he says. With rollout planned in phases, hospitalists at Penrose-St. Francis will lose access to CPOE for an estimated six to nine months, although the new CPOE system eventually will be accessed on a tablet PC.
Amid this stressful transition to new technology, the hospitalists have been trying to do the best they can with available resources, Dr. Spaulding notes. “We have come up with a paper-based Plan B for entering all of our orders until we get access to the new CPOE system,” he says. “We have been reminding everyone in the group how important it is to take care of each other, such as by putting in a PRN order set for every new patient, because we know we all will be taking our turn on-call.”
Arieh Rosenbaum, MD, hospitalist at California Pacific Medical Center (CPMC) in San Francisco, has for years been involved in technology issues at his hospital, which is developing a new electronic medical record with CPOE. It will replace a 15-year-old, DOS-based CPOE system he describes as “powerful but clunky.” However, CPMC’s parent, Sutter Health, is rolling out the new computer system gradually across its 40 Northern California facilities. It won’t reach CPMC until 2011.
“It’s an incredibly complex project,” Dr. Rosenbaum says. “To Sutter’s credit, they’re trying very hard to get physicians’ input, establishing structures for gathering feedback at the corporate and local levels. I am one of the physicians who will be involved at the local level, both building the clinical content and interface as well as gaining physicians’ acceptance and participation.”
Success depends on how the new system relates to physicians’ workflow. “Everybody knows the benefits of CPOE, but there are mitigating factors, such as what to do when the system crashes,” he says. “Hospitalists are the people who will be interacting with the new system the most. It’s our job to be leaders and to be aware that this is in our future.”
Head-On Approach
Timothy Hartzog, MD, a pediatric hospitalist and medical director of information technology/CPOE at Medical College of South Carolina (MUSC), Charleston, urges hospitalists to take CPOE seriously and view it as an opportunity.
“Implementation of CPOE, or electronic medical records, can be one of the most fundamental changes a hospital makes—affecting the workflow of everybody who works there,” he says. “As physicians, we each work a little differently. With the standardization imposed by CPOE, it’s going to make some physicians a little crazy, no matter how well it’s implemented.”
Dr. Hartzog encourages hospitalists to set aside any doubts they may have and get involved in creating workable CPOE solutions.
“Hospitalists don’t have to be experts in technology,” he stresses. “If you learned medicine, you can learn the technology—if you’re willing to put in some time, read a couple of books, take some training, and work with your IT people. Tackle CPOE head on—make sure your voice is heard. Be part of the build. But you need to have time dedicated for the IT project, and you need to do the work. If you are not present and if other people on the development group don’t know you and hear you speak, decisions will be made when you’re not in the room.”
For some physicians, Dr. Hartzog says, it could even be fun. “Especially if we can actually make the system work for us. We can actually create something that makes life better for our group.” TH
Larry Beresford is a regular contributor to The Hospitalist.
References
- Campbell EM, Sittig, DF, Ash JS, et al. Types of unintended consequences related to computerized provider order entry. J Am Med Inform Assoc. 2006 Sept-Oct;13(5):547-556.
- Connolly C. Cedars-Sinai doctors cling to pen and paper. The Washington Post, March 21, 2005:A1.
Joseph Heaton, MD, a hospitalist with Kaiser Permanente practicing at Exempla Good Samaritan Medical Center in Lafayette, Colo., has spent the past three years helping develop an electronic medical record for the hospital.
The project includes computerized physician order entry (CPOE), which was rolled out Oct. 2. He estimates he has dedicated anywhere from 20% to 50% of his time to technology implementation.
“I’ve been the physician champion for the project, working alongside the IT (information technology) development team,” Dr. Heaton explains. “I was chosen not for any particular computer expertise but because of other leadership roles I have played as a hospitalist and my involvement in quality projects. I see CPOE and electronic medical records as obvious extensions of the other quality projects hospitalists participate in.”
Dr. Heaton’s experience in implementing a CPOE system highlights the barriers faced by those charged with advancing technology critical to hospital medicine.
He says he has learned a lot about computers along the way, but the technology is a snap compared with the challenges of managing change and making sure physicians are in tune with the new system.
“Not only was I representing other hospitalists, but also a broader group of physicians with privileges at the hospital, as well as other employees, including nurses and pharmacists,” he says. “Much of what I did was to translate language about workflow from the clinicians to IT, and then report back to the clinicians.”
But it wasn’t as easy at it sounds.
“Unfortunately, in this institution there is no single, agreed-upon communications venue for reaching all of the physicians who practice at the hospital,” says Dr. Heaton. “So we’ve had to use e-mail, voice mail, noon bag-lunch demos, mailings, departmental meetings and classes—multiple opportunities to make sure that physicians feel informed. That way, when they show up for their actual training in how to use the system, they’re not still asking questions like, ‘Why are we doing this?’ ”
Blessing or Curse?
CPOE, of course, refers to the process by which physicians and other clinicians directly enter medical orders into a computer application. CPOE can be independent of other computer applications or part of an electronic medical record or other computer system.
Standardized order sets, decision support tools, and other customized methods can make hospitalists’ jobs easier—if the system is well-designed. It’s not uncommon for CPOE to add time-consuming new tasks and functions. For example, hospitalists may be asked to enter information they’ve not previously been asked to supply. But CPOE is also touted as a way to reduce medical errors and improve quality.
“It’s a good thing to do,” Dr. Heaton concludes. “Six weeks into the implementation of CPOE here, medication delivery is much faster. There are efficiencies to be had. For the most part, the high-volume users, including hospitalists, are fine with it, even if they’re not taking full advantage of the system’s capabilities.”
But Campbell, et al., describe a number of unintended adverse consequences that have followed CPOE implementation.1 These downsides include unfavorable workflow issues, continuous demands for system change, untoward changes in communications patterns and practices, generation of new kinds of medical errors, and negative emotional responses to the system by clinicians. Physician resistance can derail costly, complex CPOE projects.
A widely cited example of such barriers comes from Cedars-Sinai Medical Center in Los Angeles. An institution known for its pioneering medical techniques and technologies, Cedars-Sinai was forced in 2003 to shut down implementation of CPOE after three months because of a full-blown staff rebellion, according to an article in The Washington Post.2 Various explanations have been offered for this failure, including inadequate training for users, intrusive decision support queries, and other provider frustrations with the system. The hospital’s public relations department declined a request to comment for this article or provide an update on the current status of CPOE at Cedars-Sinai.
Doing the Best We Can
The importance of CPOE to hospitalists is illustrated by Duane Spaulding, MD, FACP, president and executive contracting officer for Advantage Inpatient Medical Specialists, practicing at Penrose-St. Francis Hospital in Colorado Springs, Colo. Half of his 11-member hospitalist group could be considered “power users” of the hospital’s current, DOS-based CPOE system—but Dr. Spaulding is No. 1. “I enter more CPOE orders than any of the other 600-plus physicians on staff here,” he says.
For some hospitalists, computers are a passion. For others, “they are just a tool for getting from Point A to Point B,” he says. “I have probably spent 1,500 hours over the past decade on committee after committee, putting together computerized order sets and screens and the like.”
Dr. Spaulding says the hospital’s current, antiquated system can be laborious to work with: “I can only do 50% of my orders on the system.” At the end of last year, Centura—the hospital’s parent health system—was preparing to implement a regional electronic medical record integrating CPOE and other applications.
“It is a gargantuan change,” he says. With rollout planned in phases, hospitalists at Penrose-St. Francis will lose access to CPOE for an estimated six to nine months, although the new CPOE system eventually will be accessed on a tablet PC.
Amid this stressful transition to new technology, the hospitalists have been trying to do the best they can with available resources, Dr. Spaulding notes. “We have come up with a paper-based Plan B for entering all of our orders until we get access to the new CPOE system,” he says. “We have been reminding everyone in the group how important it is to take care of each other, such as by putting in a PRN order set for every new patient, because we know we all will be taking our turn on-call.”
Arieh Rosenbaum, MD, hospitalist at California Pacific Medical Center (CPMC) in San Francisco, has for years been involved in technology issues at his hospital, which is developing a new electronic medical record with CPOE. It will replace a 15-year-old, DOS-based CPOE system he describes as “powerful but clunky.” However, CPMC’s parent, Sutter Health, is rolling out the new computer system gradually across its 40 Northern California facilities. It won’t reach CPMC until 2011.
“It’s an incredibly complex project,” Dr. Rosenbaum says. “To Sutter’s credit, they’re trying very hard to get physicians’ input, establishing structures for gathering feedback at the corporate and local levels. I am one of the physicians who will be involved at the local level, both building the clinical content and interface as well as gaining physicians’ acceptance and participation.”
Success depends on how the new system relates to physicians’ workflow. “Everybody knows the benefits of CPOE, but there are mitigating factors, such as what to do when the system crashes,” he says. “Hospitalists are the people who will be interacting with the new system the most. It’s our job to be leaders and to be aware that this is in our future.”
Head-On Approach
Timothy Hartzog, MD, a pediatric hospitalist and medical director of information technology/CPOE at Medical College of South Carolina (MUSC), Charleston, urges hospitalists to take CPOE seriously and view it as an opportunity.
“Implementation of CPOE, or electronic medical records, can be one of the most fundamental changes a hospital makes—affecting the workflow of everybody who works there,” he says. “As physicians, we each work a little differently. With the standardization imposed by CPOE, it’s going to make some physicians a little crazy, no matter how well it’s implemented.”
Dr. Hartzog encourages hospitalists to set aside any doubts they may have and get involved in creating workable CPOE solutions.
“Hospitalists don’t have to be experts in technology,” he stresses. “If you learned medicine, you can learn the technology—if you’re willing to put in some time, read a couple of books, take some training, and work with your IT people. Tackle CPOE head on—make sure your voice is heard. Be part of the build. But you need to have time dedicated for the IT project, and you need to do the work. If you are not present and if other people on the development group don’t know you and hear you speak, decisions will be made when you’re not in the room.”
For some physicians, Dr. Hartzog says, it could even be fun. “Especially if we can actually make the system work for us. We can actually create something that makes life better for our group.” TH
Larry Beresford is a regular contributor to The Hospitalist.
References
- Campbell EM, Sittig, DF, Ash JS, et al. Types of unintended consequences related to computerized provider order entry. J Am Med Inform Assoc. 2006 Sept-Oct;13(5):547-556.
- Connolly C. Cedars-Sinai doctors cling to pen and paper. The Washington Post, March 21, 2005:A1.
Know Your Neurology
Although hospitalists may work alongside neurological specialists, they are increasingly on their own when responding to neurological emergencies, such as strokes, in hospitalized patients.
There are times the neurologist may be in the clinic, out of the hospital after hours, or otherwise unavailable, so responsibility for managing neurological conditions falls back on the hospitalist. But he or she may not have received sufficient exposure to neurology during medical training.
S. Andrew Josephson, MD, of the neurovascular division, director of the neurohospitalist program and assistant professor of neurology at the University of California-San Francisco (UCSF), regularly speaks on neurological issues to hospitalist audiences.
“I ask how many hospitalists in the room are primary caregivers for stroke in their hospital, and a surprising proportion raise their hands,” he says. “We do a good job of teaching neurology residents and fellows how to treat strokes. But it is important that we train internal medicine doctors as well, as they are seeing the majority of these patients nationwide.”
Depending on the setting, there may be wide variation in the hospitalist’s responsibility for neurological cases. “Here at UCSF, hospitalists almost never see stroke patients because we have a dedicated stroke service staffed by neurology attendings and residents,” Dr. Josephson says. “But at many community hospitals, they [care for neurological patients] all the time.”
David Likosky, MD, director of the stroke program at Evergreen Hospital Medical Center in Kirkland, Wash., concurs. “Neurology training in internal medicine residencies can be fairly limited,” he says. “After entering practice, these doctors are on the front lines in the hospital managing patients, many times without readily available neurologist backup.”
Dr. Likosky’s colleague at Evergreen, hospitalist Tony Yen, MD, says there are several neurological issues hospitalists are likely to encounter on a regular basis.
“Often the first responder to a stroke is the emergency department [ED] doctor or the hospitalist,” notes Dr. Yen. “Strokes are a time-critical, high-volume condition for our community hospitalist practice.”
Another important diagnosis is uncontrolled seizure (status epilepticus) that is unremitting for 10 minutes or more. Prompt response is critical.
Dr. Yen recalls the case of a young woman who collapsed while playing soccer. She was brought to the hospital and found to have suffered a brain-stem stroke. Physicians had three hours from the onset of symptoms to decide whether the patient was a candidate for tissue plasminogen activator (t-PA), a thrombolytic clot buster.
“I worked alongside the interventional radiologist and neurologist,” Dr. Yen recalls. “We were able to quickly establish a definitive diagnosis and then treat with intra-arterial t-PA.” The patient had a prolonged stay in intensive care and was on a ventilator for a couple of weeks but eventually recovered and walked out of the hospital.
Common Conditions
Stroke: The most common neurological emergency hospitalists are likely to see, whether on the floor or through the ED, is acute stroke, Dr. Josephson notes. “The evaluation of stroke requires a non-contrast computed tomography (CT) scan of the head to exclude intracerebral hemorrhage,” he says. “You can’t tell by looking at the patient whether it’s an ischemic stroke, the more common variety, or hemorrhagic stroke. But the difference is crucial because drugs to treat ischemic stroke can make hemorrhage worse. We view stroke as such a time-sensitive emergency that it always gets priority in the radiology department.”
It is also important to ascertain, as much as possible, when symptoms first began or when the patient was last observed to be normal. The treatment of choice in the first three hours following an ischemic stroke is intravenous t-PA. From hours three through six or eight, endovascular therapies (intra-arterial thrombolysis or mechanical clot retrieval) are an option. Signs suggesting a possible stroke include a new unilateral weakness, one-sided numbness, vertigo or imbalance, visual changes, inability to talk, and new headaches—although indications of a stroke can be subtle. The National Institutes of Health has issued a stroke scale, with training modules, accessible at www.strokecenter.org/trials/scales/nihss.html.
Seizures: Prolonged seizures that don’t resolve on their own within a reasonable amount of time require attention because the longer they last, the more likely they are to cause brain damage, Dr. Josephson says. Medications to treat the seizure work more effectively the earlier they are administered. He recommends a protocol for treating status epilepticus that starts with lorazepam (Ativan), proceeds to fosphenytoin (Cerebyx), and is followed by a general anesthetic such as midazolam (Versed) or propofol (Diprivan).
Intracranial pressure (ICP): This could be the result of a stroke or hemorrhage, brain tumor, or trauma. Fast action to control ICP is important because permanent brain injury can result. “I emphasize to hospitalists who are used to targeting ICP that it is better to look at cerebral perfusion pressure (CPP),” Dr. Josephson says, offering the following equation: CPP equals mean arterial pressure minus ICP. He also emphasizes raising the head of the patient’s bed, hyperventilation in early stages of treatment, and using osmotic agents such as mannitol to remove water from the brain.
Neuro-muscular emergencies: Acute disorders of the peripheral nerves, including Guillain-Barre Syndrome (an autoimmune neuropathy often triggered by infection), present a subacute onset of weakness and numbness. “We have good treatments for Guillain-Barre, such as plasmapheresis and administration of intravenous immunoglobulin,” Dr. Josephson says. “But recognition is important because the breathing may be affected. If the disorder reaches the diaphragm, it could kill the patient.” Disorders such as Guillain-Barre commonly present with ascending weakness, from the toes up.
A lumbar puncture (demonstrating few if any cells with an elevated protein) or an electromyogram (EMG) may be required for diagnosis. Hospitalists also are urged to watch for impending respiratory weakness, which can be measured by forced vital capacity or mean inspiratory flow. “Consider this diagnosis for anyone presenting with general weakness,” he says.
Exams on the Run
There is a standard technique for assessing and diagnosing neurological conditions, called the neurological examination. Unfortunately, a full, detailed neurological exam can be time-consuming and unrealistic, given caseload demands and field judgments required from the working hospitalist.
“As a hospitalist, you don’t have to perform an hourlong neurological examination,” Dr. Josephson says. “But for patients presenting neurological symptoms, you need to do a screening examination tied to their specific complaint. Your hypothesis-driven exam can be done in a few minutes if you know which elements are high-yield screening tests.”
These brief screening tests can be part of a routine assessment of the patient, Dr. Likosky adds.
Hospitalists can learn a lot just by walking into the patient’s room. “The bulk of such a neurological exam can be performed while talking to the patient, if you pay attention,” he notes. “There may be subtle signs of weakness. For example, when the patient is lying in bed, the feet should point straight up.” Note if one foot points to the side, or if the patient uses both sides of the face equally when talking.
“You can do sensory exams and test reflexes very briefly, as well,” Dr. Likosky says. “If those issues are on your radar screen, you can do much of the screening work in a stepwise fashion. The rest depends on clinical observation.”
There is not a huge spectrum of neurological disorders likely to confront the hospitalist, but it is important to know about the most common conditions and remember that time is of the essence, Dr. Likosky says. “Most neurological conditions are garden variety, but keep in mind the differential diagnoses, for example, for weakness and headache—common conditions that may rarely have an uncommon cause.”
Beef Up Training
Heather A. Harris, MD, a hospitalist at UCSF, illustrates the divide between academic medical centers and community hospitals when it comes to management of neurological diseases. She did her internal medicine training at UCSF and in 2003 went to a community hospital, Eden Medical Center in suburban Castro Valley, Calif., to help establish a hospitalist group. Suddenly, she was seeing lots of neurological cases.
“I’ll be frank: My internal medicine training at a wonderful medical institution had not prepared me for the reality that many new hospitalists face regarding neurological disorders,” says Dr. Harris. “You may see strokes as a resident, but it’s very different when you are the physician primarily managing strokes as they roll in. Yes, you may have a neurologist back-up, but they can’t always come in right away. The first time you see a patient with a stroke, it can be quite intimidating. You’re really learning on the fly. Plus, stroke management has advanced substantially in the last few years and there may be controversy, for example, over the use of t-PA in a community hospital setting.”
Feeling that her exposure to neurology was insufficient, Dr. Harris sought additional training at SHM meetings and talked to hospitalist colleagues in other community settings. “Hospitalists like me were trying to beef up our neurological knowledge and skill set.”
Dr. Harris developed a keen personal interest in neurology. In 2007, she returned to UCSF, where many of the hospitalists rarely see neurological patients. But she joined a new co-management service where hospitalists work alongside neuro-surgeons, helping manage the inevitable medical issues that arise in these patients.
Based on her first-hand appreciation for what hospitalists in community settings need to learn, Dr. Harris is also part of a team developing a new, hands-on training curriculum at UCSF for working hospitalists from community settings. That team is making sure neurology is adequately covered in UCSF’s curriculum.
“My overall experience is that if you’re going to be a hospitalist in a community setting, you’ll have to face a wide range of neurological emergencies,” Dr. Harris concludes. “It behooves us as hospitalists to learn the skill sets to manage these issues. There are also medical-legal issues that may put hospitalists out on a limb for doing too much too far outside of their knowledge and training. These are issues for SHM and our specialty to address.” TH
Larry Beresford is a regular contributor to The Hospitalist.
Although hospitalists may work alongside neurological specialists, they are increasingly on their own when responding to neurological emergencies, such as strokes, in hospitalized patients.
There are times the neurologist may be in the clinic, out of the hospital after hours, or otherwise unavailable, so responsibility for managing neurological conditions falls back on the hospitalist. But he or she may not have received sufficient exposure to neurology during medical training.
S. Andrew Josephson, MD, of the neurovascular division, director of the neurohospitalist program and assistant professor of neurology at the University of California-San Francisco (UCSF), regularly speaks on neurological issues to hospitalist audiences.
“I ask how many hospitalists in the room are primary caregivers for stroke in their hospital, and a surprising proportion raise their hands,” he says. “We do a good job of teaching neurology residents and fellows how to treat strokes. But it is important that we train internal medicine doctors as well, as they are seeing the majority of these patients nationwide.”
Depending on the setting, there may be wide variation in the hospitalist’s responsibility for neurological cases. “Here at UCSF, hospitalists almost never see stroke patients because we have a dedicated stroke service staffed by neurology attendings and residents,” Dr. Josephson says. “But at many community hospitals, they [care for neurological patients] all the time.”
David Likosky, MD, director of the stroke program at Evergreen Hospital Medical Center in Kirkland, Wash., concurs. “Neurology training in internal medicine residencies can be fairly limited,” he says. “After entering practice, these doctors are on the front lines in the hospital managing patients, many times without readily available neurologist backup.”
Dr. Likosky’s colleague at Evergreen, hospitalist Tony Yen, MD, says there are several neurological issues hospitalists are likely to encounter on a regular basis.
“Often the first responder to a stroke is the emergency department [ED] doctor or the hospitalist,” notes Dr. Yen. “Strokes are a time-critical, high-volume condition for our community hospitalist practice.”
Another important diagnosis is uncontrolled seizure (status epilepticus) that is unremitting for 10 minutes or more. Prompt response is critical.
Dr. Yen recalls the case of a young woman who collapsed while playing soccer. She was brought to the hospital and found to have suffered a brain-stem stroke. Physicians had three hours from the onset of symptoms to decide whether the patient was a candidate for tissue plasminogen activator (t-PA), a thrombolytic clot buster.
“I worked alongside the interventional radiologist and neurologist,” Dr. Yen recalls. “We were able to quickly establish a definitive diagnosis and then treat with intra-arterial t-PA.” The patient had a prolonged stay in intensive care and was on a ventilator for a couple of weeks but eventually recovered and walked out of the hospital.
Common Conditions
Stroke: The most common neurological emergency hospitalists are likely to see, whether on the floor or through the ED, is acute stroke, Dr. Josephson notes. “The evaluation of stroke requires a non-contrast computed tomography (CT) scan of the head to exclude intracerebral hemorrhage,” he says. “You can’t tell by looking at the patient whether it’s an ischemic stroke, the more common variety, or hemorrhagic stroke. But the difference is crucial because drugs to treat ischemic stroke can make hemorrhage worse. We view stroke as such a time-sensitive emergency that it always gets priority in the radiology department.”
It is also important to ascertain, as much as possible, when symptoms first began or when the patient was last observed to be normal. The treatment of choice in the first three hours following an ischemic stroke is intravenous t-PA. From hours three through six or eight, endovascular therapies (intra-arterial thrombolysis or mechanical clot retrieval) are an option. Signs suggesting a possible stroke include a new unilateral weakness, one-sided numbness, vertigo or imbalance, visual changes, inability to talk, and new headaches—although indications of a stroke can be subtle. The National Institutes of Health has issued a stroke scale, with training modules, accessible at www.strokecenter.org/trials/scales/nihss.html.
Seizures: Prolonged seizures that don’t resolve on their own within a reasonable amount of time require attention because the longer they last, the more likely they are to cause brain damage, Dr. Josephson says. Medications to treat the seizure work more effectively the earlier they are administered. He recommends a protocol for treating status epilepticus that starts with lorazepam (Ativan), proceeds to fosphenytoin (Cerebyx), and is followed by a general anesthetic such as midazolam (Versed) or propofol (Diprivan).
Intracranial pressure (ICP): This could be the result of a stroke or hemorrhage, brain tumor, or trauma. Fast action to control ICP is important because permanent brain injury can result. “I emphasize to hospitalists who are used to targeting ICP that it is better to look at cerebral perfusion pressure (CPP),” Dr. Josephson says, offering the following equation: CPP equals mean arterial pressure minus ICP. He also emphasizes raising the head of the patient’s bed, hyperventilation in early stages of treatment, and using osmotic agents such as mannitol to remove water from the brain.
Neuro-muscular emergencies: Acute disorders of the peripheral nerves, including Guillain-Barre Syndrome (an autoimmune neuropathy often triggered by infection), present a subacute onset of weakness and numbness. “We have good treatments for Guillain-Barre, such as plasmapheresis and administration of intravenous immunoglobulin,” Dr. Josephson says. “But recognition is important because the breathing may be affected. If the disorder reaches the diaphragm, it could kill the patient.” Disorders such as Guillain-Barre commonly present with ascending weakness, from the toes up.
A lumbar puncture (demonstrating few if any cells with an elevated protein) or an electromyogram (EMG) may be required for diagnosis. Hospitalists also are urged to watch for impending respiratory weakness, which can be measured by forced vital capacity or mean inspiratory flow. “Consider this diagnosis for anyone presenting with general weakness,” he says.
Exams on the Run
There is a standard technique for assessing and diagnosing neurological conditions, called the neurological examination. Unfortunately, a full, detailed neurological exam can be time-consuming and unrealistic, given caseload demands and field judgments required from the working hospitalist.
“As a hospitalist, you don’t have to perform an hourlong neurological examination,” Dr. Josephson says. “But for patients presenting neurological symptoms, you need to do a screening examination tied to their specific complaint. Your hypothesis-driven exam can be done in a few minutes if you know which elements are high-yield screening tests.”
These brief screening tests can be part of a routine assessment of the patient, Dr. Likosky adds.
Hospitalists can learn a lot just by walking into the patient’s room. “The bulk of such a neurological exam can be performed while talking to the patient, if you pay attention,” he notes. “There may be subtle signs of weakness. For example, when the patient is lying in bed, the feet should point straight up.” Note if one foot points to the side, or if the patient uses both sides of the face equally when talking.
“You can do sensory exams and test reflexes very briefly, as well,” Dr. Likosky says. “If those issues are on your radar screen, you can do much of the screening work in a stepwise fashion. The rest depends on clinical observation.”
There is not a huge spectrum of neurological disorders likely to confront the hospitalist, but it is important to know about the most common conditions and remember that time is of the essence, Dr. Likosky says. “Most neurological conditions are garden variety, but keep in mind the differential diagnoses, for example, for weakness and headache—common conditions that may rarely have an uncommon cause.”
Beef Up Training
Heather A. Harris, MD, a hospitalist at UCSF, illustrates the divide between academic medical centers and community hospitals when it comes to management of neurological diseases. She did her internal medicine training at UCSF and in 2003 went to a community hospital, Eden Medical Center in suburban Castro Valley, Calif., to help establish a hospitalist group. Suddenly, she was seeing lots of neurological cases.
“I’ll be frank: My internal medicine training at a wonderful medical institution had not prepared me for the reality that many new hospitalists face regarding neurological disorders,” says Dr. Harris. “You may see strokes as a resident, but it’s very different when you are the physician primarily managing strokes as they roll in. Yes, you may have a neurologist back-up, but they can’t always come in right away. The first time you see a patient with a stroke, it can be quite intimidating. You’re really learning on the fly. Plus, stroke management has advanced substantially in the last few years and there may be controversy, for example, over the use of t-PA in a community hospital setting.”
Feeling that her exposure to neurology was insufficient, Dr. Harris sought additional training at SHM meetings and talked to hospitalist colleagues in other community settings. “Hospitalists like me were trying to beef up our neurological knowledge and skill set.”
Dr. Harris developed a keen personal interest in neurology. In 2007, she returned to UCSF, where many of the hospitalists rarely see neurological patients. But she joined a new co-management service where hospitalists work alongside neuro-surgeons, helping manage the inevitable medical issues that arise in these patients.
Based on her first-hand appreciation for what hospitalists in community settings need to learn, Dr. Harris is also part of a team developing a new, hands-on training curriculum at UCSF for working hospitalists from community settings. That team is making sure neurology is adequately covered in UCSF’s curriculum.
“My overall experience is that if you’re going to be a hospitalist in a community setting, you’ll have to face a wide range of neurological emergencies,” Dr. Harris concludes. “It behooves us as hospitalists to learn the skill sets to manage these issues. There are also medical-legal issues that may put hospitalists out on a limb for doing too much too far outside of their knowledge and training. These are issues for SHM and our specialty to address.” TH
Larry Beresford is a regular contributor to The Hospitalist.
Although hospitalists may work alongside neurological specialists, they are increasingly on their own when responding to neurological emergencies, such as strokes, in hospitalized patients.
There are times the neurologist may be in the clinic, out of the hospital after hours, or otherwise unavailable, so responsibility for managing neurological conditions falls back on the hospitalist. But he or she may not have received sufficient exposure to neurology during medical training.
S. Andrew Josephson, MD, of the neurovascular division, director of the neurohospitalist program and assistant professor of neurology at the University of California-San Francisco (UCSF), regularly speaks on neurological issues to hospitalist audiences.
“I ask how many hospitalists in the room are primary caregivers for stroke in their hospital, and a surprising proportion raise their hands,” he says. “We do a good job of teaching neurology residents and fellows how to treat strokes. But it is important that we train internal medicine doctors as well, as they are seeing the majority of these patients nationwide.”
Depending on the setting, there may be wide variation in the hospitalist’s responsibility for neurological cases. “Here at UCSF, hospitalists almost never see stroke patients because we have a dedicated stroke service staffed by neurology attendings and residents,” Dr. Josephson says. “But at many community hospitals, they [care for neurological patients] all the time.”
David Likosky, MD, director of the stroke program at Evergreen Hospital Medical Center in Kirkland, Wash., concurs. “Neurology training in internal medicine residencies can be fairly limited,” he says. “After entering practice, these doctors are on the front lines in the hospital managing patients, many times without readily available neurologist backup.”
Dr. Likosky’s colleague at Evergreen, hospitalist Tony Yen, MD, says there are several neurological issues hospitalists are likely to encounter on a regular basis.
“Often the first responder to a stroke is the emergency department [ED] doctor or the hospitalist,” notes Dr. Yen. “Strokes are a time-critical, high-volume condition for our community hospitalist practice.”
Another important diagnosis is uncontrolled seizure (status epilepticus) that is unremitting for 10 minutes or more. Prompt response is critical.
Dr. Yen recalls the case of a young woman who collapsed while playing soccer. She was brought to the hospital and found to have suffered a brain-stem stroke. Physicians had three hours from the onset of symptoms to decide whether the patient was a candidate for tissue plasminogen activator (t-PA), a thrombolytic clot buster.
“I worked alongside the interventional radiologist and neurologist,” Dr. Yen recalls. “We were able to quickly establish a definitive diagnosis and then treat with intra-arterial t-PA.” The patient had a prolonged stay in intensive care and was on a ventilator for a couple of weeks but eventually recovered and walked out of the hospital.
Common Conditions
Stroke: The most common neurological emergency hospitalists are likely to see, whether on the floor or through the ED, is acute stroke, Dr. Josephson notes. “The evaluation of stroke requires a non-contrast computed tomography (CT) scan of the head to exclude intracerebral hemorrhage,” he says. “You can’t tell by looking at the patient whether it’s an ischemic stroke, the more common variety, or hemorrhagic stroke. But the difference is crucial because drugs to treat ischemic stroke can make hemorrhage worse. We view stroke as such a time-sensitive emergency that it always gets priority in the radiology department.”
It is also important to ascertain, as much as possible, when symptoms first began or when the patient was last observed to be normal. The treatment of choice in the first three hours following an ischemic stroke is intravenous t-PA. From hours three through six or eight, endovascular therapies (intra-arterial thrombolysis or mechanical clot retrieval) are an option. Signs suggesting a possible stroke include a new unilateral weakness, one-sided numbness, vertigo or imbalance, visual changes, inability to talk, and new headaches—although indications of a stroke can be subtle. The National Institutes of Health has issued a stroke scale, with training modules, accessible at www.strokecenter.org/trials/scales/nihss.html.
Seizures: Prolonged seizures that don’t resolve on their own within a reasonable amount of time require attention because the longer they last, the more likely they are to cause brain damage, Dr. Josephson says. Medications to treat the seizure work more effectively the earlier they are administered. He recommends a protocol for treating status epilepticus that starts with lorazepam (Ativan), proceeds to fosphenytoin (Cerebyx), and is followed by a general anesthetic such as midazolam (Versed) or propofol (Diprivan).
Intracranial pressure (ICP): This could be the result of a stroke or hemorrhage, brain tumor, or trauma. Fast action to control ICP is important because permanent brain injury can result. “I emphasize to hospitalists who are used to targeting ICP that it is better to look at cerebral perfusion pressure (CPP),” Dr. Josephson says, offering the following equation: CPP equals mean arterial pressure minus ICP. He also emphasizes raising the head of the patient’s bed, hyperventilation in early stages of treatment, and using osmotic agents such as mannitol to remove water from the brain.
Neuro-muscular emergencies: Acute disorders of the peripheral nerves, including Guillain-Barre Syndrome (an autoimmune neuropathy often triggered by infection), present a subacute onset of weakness and numbness. “We have good treatments for Guillain-Barre, such as plasmapheresis and administration of intravenous immunoglobulin,” Dr. Josephson says. “But recognition is important because the breathing may be affected. If the disorder reaches the diaphragm, it could kill the patient.” Disorders such as Guillain-Barre commonly present with ascending weakness, from the toes up.
A lumbar puncture (demonstrating few if any cells with an elevated protein) or an electromyogram (EMG) may be required for diagnosis. Hospitalists also are urged to watch for impending respiratory weakness, which can be measured by forced vital capacity or mean inspiratory flow. “Consider this diagnosis for anyone presenting with general weakness,” he says.
Exams on the Run
There is a standard technique for assessing and diagnosing neurological conditions, called the neurological examination. Unfortunately, a full, detailed neurological exam can be time-consuming and unrealistic, given caseload demands and field judgments required from the working hospitalist.
“As a hospitalist, you don’t have to perform an hourlong neurological examination,” Dr. Josephson says. “But for patients presenting neurological symptoms, you need to do a screening examination tied to their specific complaint. Your hypothesis-driven exam can be done in a few minutes if you know which elements are high-yield screening tests.”
These brief screening tests can be part of a routine assessment of the patient, Dr. Likosky adds.
Hospitalists can learn a lot just by walking into the patient’s room. “The bulk of such a neurological exam can be performed while talking to the patient, if you pay attention,” he notes. “There may be subtle signs of weakness. For example, when the patient is lying in bed, the feet should point straight up.” Note if one foot points to the side, or if the patient uses both sides of the face equally when talking.
“You can do sensory exams and test reflexes very briefly, as well,” Dr. Likosky says. “If those issues are on your radar screen, you can do much of the screening work in a stepwise fashion. The rest depends on clinical observation.”
There is not a huge spectrum of neurological disorders likely to confront the hospitalist, but it is important to know about the most common conditions and remember that time is of the essence, Dr. Likosky says. “Most neurological conditions are garden variety, but keep in mind the differential diagnoses, for example, for weakness and headache—common conditions that may rarely have an uncommon cause.”
Beef Up Training
Heather A. Harris, MD, a hospitalist at UCSF, illustrates the divide between academic medical centers and community hospitals when it comes to management of neurological diseases. She did her internal medicine training at UCSF and in 2003 went to a community hospital, Eden Medical Center in suburban Castro Valley, Calif., to help establish a hospitalist group. Suddenly, she was seeing lots of neurological cases.
“I’ll be frank: My internal medicine training at a wonderful medical institution had not prepared me for the reality that many new hospitalists face regarding neurological disorders,” says Dr. Harris. “You may see strokes as a resident, but it’s very different when you are the physician primarily managing strokes as they roll in. Yes, you may have a neurologist back-up, but they can’t always come in right away. The first time you see a patient with a stroke, it can be quite intimidating. You’re really learning on the fly. Plus, stroke management has advanced substantially in the last few years and there may be controversy, for example, over the use of t-PA in a community hospital setting.”
Feeling that her exposure to neurology was insufficient, Dr. Harris sought additional training at SHM meetings and talked to hospitalist colleagues in other community settings. “Hospitalists like me were trying to beef up our neurological knowledge and skill set.”
Dr. Harris developed a keen personal interest in neurology. In 2007, she returned to UCSF, where many of the hospitalists rarely see neurological patients. But she joined a new co-management service where hospitalists work alongside neuro-surgeons, helping manage the inevitable medical issues that arise in these patients.
Based on her first-hand appreciation for what hospitalists in community settings need to learn, Dr. Harris is also part of a team developing a new, hands-on training curriculum at UCSF for working hospitalists from community settings. That team is making sure neurology is adequately covered in UCSF’s curriculum.
“My overall experience is that if you’re going to be a hospitalist in a community setting, you’ll have to face a wide range of neurological emergencies,” Dr. Harris concludes. “It behooves us as hospitalists to learn the skill sets to manage these issues. There are also medical-legal issues that may put hospitalists out on a limb for doing too much too far outside of their knowledge and training. These are issues for SHM and our specialty to address.” TH
Larry Beresford is a regular contributor to The Hospitalist.
Tackle Technology
Dennis Deruelle, MD, a hospitalist at University Community Hospital in Tampa, Fla., once needed reliable medical information in a hurry while treating a young woman admitted to the hospital with cellulitis.
The woman was later diagnosed with methicillin-resistant staphylococcus aureus (MRSA). After Dr. Deruelle administered prochlorperazine (Compazine), she had a severe dystonic reaction.
“She was going rigid right before my eyes,” Dr. Deruelle says. There was no instantly accessible hospital clearinghouse of medical information, although he had called the pharmacy department and was waiting for a call back. So he opened his laptop and turned to an aid available to anyone with a computer and Internet access: Google. “I immediately looked up information on reactions to Compazine and the correct dose for counteracting it. I administered the dose, and within minutes [the patient] was getting better.”
Dr. Deruelle is not alone among physicians in answering medical questions with Google. (See The Hospitalist, July 2007, p. 33.)
He has been interested in medical applications of computer technology for years and serves on SHM’s advisory committee on technology. He receives tech support from his employer, IPC-The Hospitalist Company, based in North Hollywood, Calif. IPC offers its physicians a Web-accessible network called IPC Link—a “virtual office” to help with billing, medical decision support, reference software, continuing medical education, and even blogs written by company CEO Adam Singer, MD.
But Dr. Deruelle has also developed his own applications, including an off-the-shelf voice recognition software loaded onto his company-supplied, 2.5-lb. Tablet PC. He uses it to dictate brief notes to give attending physicians a heads-up about patients being discharged. These notes are uploaded to the company’s network, which automatically generates a fax to the attending within minutes.
The formal discharge summary, produced by the hospital’s medical transcription department, may take 48 hours to arrive.
Dr. Deruelle has wireless Internet access at four of the five hospitals he visits as a hospitalist practice leader.
“As soon as I walk in the door I’m ‘hot,’ ” he says. At the fifth hospital, he uses workstation computers to connect with IPC Link.
Array of Options
A dizzying range of communications technology is available to working hospitalists, typically accessed through personal digital assistants (PDAs), smartphones, computer tablets, pocket PCs, and laptops.
The Palm Pilot, introduced in 1996, is a well-known example of this technology, as are the Palm Treo and BlackBerry. PDAs combine the functions of cell phones, video phones, cameras, video recorders, media players, Web browsers, reference tools, bar code scanners, and global positioning system (GPS) devices—all in a palm-size package.
Hardware and supporting software vary in terms of ease of use, in particular, the ability to interface with the Web or the hospital, practice, or employer network the physician needs to connect with.
The technology is evolving rapidly. But anomalies abound, such as dependence on the fax machine as a staple of communication with attending physicians. Through all of these changes, hospitalists are responsible for learning what works and how best to take advantage of the technology to make their jobs easier.
Hospitalists also vary tremendously in terms of their comfort levels and openness to new technology.
“There is a considerable gap between those of us who ‘Palm’ and those who don’t,” says Timothy Hartzog, MD, pediatric hospitalist at Medical University of South Carolina (MUSC) in Charleston and a medical technology consultant. “Physicians want their patient data in different ways. Some want it printed out or in a paper chart.”
—Steven Liu, MD, of Emory University Medical Center in Atlanta
But implementation of technology, such as hospital electronic health records or computerized physician order entry, inevitably changes their relationships with information technology and patient information.
Some hospitalists, like Dr. Deruelle, are interested in what communication technology can bring their work and how to adapt it to their needs. Others, like Dr. Hartzog, medical director of Information Technology at MUSC, have taken added responsibilities for technology within their institutions.
And a few, such as Steven Liu, MD, of Emory University Medical Center in Atlanta, have taken their interest in computer technology a step further. In 1999, Dr. Liu founded Ingenious Med, an Atlanta software company that offers a suite of inpatient practice management applications to working hospitalists.
“Often the hospitalist is already on the forefront of technology,” Dr. Liu says. “The demographic is typically younger and techno-savvy. They may get tapped by their hospitals to help customize the electronic health record to make sure it satisfies the needs of clinicians. Conversely, if an electronic project does not involve strong physician feedback and collaboration, physicians can be the Achilles’ heel impeding successful implementation. Even though they are the ones who stand to gain most from the potential efficiency, physicians will not adopt technology that does not fit their workflow.”
State of the Art?
Russell Cucina, MD, MS, a hospitalist at the University of California-San Francisco Medical Center, San Francisco, is also the associate medical director for information technology at UCSF.
Dr. Cucina quips that a good example of a state-of-the-art, stand-alone patient data management system offering rapid data entry, long battery life, and high mobility is the paper index card, the longtime standard for making rounding notes.
“Plenty of doctors, including me, use it every day,” he says. But growing numbers of hospitalists also use PDAs, smartphones, and laptops to access information and support applications. Among the plethora of reference applications readily available to physicians by PDA or laptop are UpToDate, Epocrates, the Pocket Sanford Guide to Anti-Microbial Therapy, and Merck Medicus.
“I use many different resources as a hospitalist,” Dr. Cucina says. “I Google all the time.” Hospitalists still have opportunities to innovate, although increasingly their “home-grown” solutions will compete with multinational technology conglomerates entering the medical market.
The use of technology and equipment also varies depending on whether the hospitalist is employed by the hospital or part of an independent medical group.
Another factor is whether that hospital is academic, community-based, or part of a system like the Veterans Affairs or a staff-model HMO such as Kaiser Permanente. But all hospitalists are used to working on the run, Dr. Cucina says. And in their daily jobs, workflow is everything.
Tech in Use
“I use medical technology on the job to a moderate degree,” reports Latha Sivaprasad, MD, a hospitalist at Beth Israel Medical Center in New York City. “This is my sixth year working as a hospitalist, and for the first five years I didn’t use a specific device. Now I have a Palm-based program with MD Everywhere, Epocrates, UpToDate, and the ability to do billing. The hospital’s tech support staff trained us on the new system and how to use the PDA for tasks like developing rounding lists, accessing our colleagues’ lists and creating system-based memos.”
Dr. Sivaprasad also has GPS in her car, a cell phone, and a laptop at home. “We probably aren’t using medical technology as much as we could,” she says. “Many physicians still write prescriptions by hand. I’ve never used voice-recognition software. In a previous hospital, we used the hospital’s transcription service for dictated notes.”
Karim Godamunne, MD, MBA, a hospitalist with Eagle Hospital Physicians and a practice medical director at South Fulton Medical Center in Atlanta, uses a PDA at work for billing.
“I don’t use the PDA intensively,’’ he says. “I’d like to see our hospital create a wireless network like the one I have at home. Our sister hospital has wireless.” He notes, however, that there are computer workstations for him to use at his hospital.
Dr. Godamunne’s group has a practice coordinator who faxes discharge summaries to attending physicians.
“Fax is kind of what they expect these days,” he says. “I’m not sure e-mail would be as reliable for the community we serve. I’d be concerned that the attendings wouldn’t read their e-mails.” He says he sometimes gives written notes to patients at discharge with instructions to hand the note to their physician on their next office visit.
Michelle Pezzani, MD, is part of a 10-member hospital medicine group that practices at El Camino Hospital in Mountain View, Calif., in the heart of Silicon Valley. The hospital tries to stay on the cutting edge with technology, and its hospitalists were given Microsoft XP Tablet laptops a few years ago. “I access the Web two to four times a day at work,” Dr. Pezzani says. “It helps keep us current. The great thing about the laptop is I also take it home with me, and I can use it to check or reorder labs from home. We’re all connected to the hospital’s Intranet from home.”
“One of the issues we’re struggling with is how to achieve the best sign-out possible,” with up to four hospitalists on the day shift checking out and handing over patient responsibilities to the night shift, Dr. Pezzani says. For her, the ideal sign-out is face to face because it permits asking questions and reading nonverbal cues about how sick the patients really are. However, the logistics of multiple physicians and patients makes this ideal difficult to achieve.
Second best (if all group members used a Palm Pilot), would be to send sign-outs via text messaging—although that would also present logistical challenges. “Texting is easier,” she says. “You know who is sending the message. We could beam the written sign-out to each other in a matter of seconds, making it quick and easy. Furthermore, any day-to-day changes on a specific patient would be easy to amend and easy to send. It’s also a quick way to let a colleague know, ‘I need you right now!’ ”
The hospitalists at El Camino use voicemail to record sign-outs. But these messages can take a long time to record and play back, multiplied by the four physicians signing out. “Ideally, there would be a different voice mail for every patient, so I wouldn’t have to listen to patients A, B, C, D, and E to get to the pertinent information about patient F, who is crashing upstairs,” she says. Dr. Pezzani’s group is still exploring how to balance these considerations.
She says her hospitalist group is tight-knit and collaborative. “We leave our cell phones on all the time and answer each other’s calls after hours,” she says. “For example, I’m now on vacation with my family in San Diego and I have gotten at least two calls a day from my partners, either business related, or something like: ‘Do you remember that patient you admitted? Can you give me some information on them?’”
The Wired Hospital
Dr. Cucina is excited about the extra large, easy-to-grip handle on the 3-lb. Motion Computing C5 portable PC that UCSF hospitalists are field-testing. He’s also intrigued by the ever-expanding opportunities for interfacing with the hospital’s technology.
In August he gave a tour of Unit 13L at UCSF’s Moffitt/Long Hospital, a new ward that opened in June and is being used as a technology demonstration site.
The 32-bed unit has a narrow corridor lined with 10 computer workstations for the nurses. All 10 are in use. In an adjacent cubicle, several physicians are typing on their laptops.
On the unit, portable vital signs monitors are attached to rolling stands that also have docking ports for the laptops, offering real-time point-of-care acquisition of vital-signs data directly into the hospital’s medical record.
A nurse or physician can grab the big-handled Tablet PC and run to another room while remaining connected to the patient’s vital signs. The docking ports in patients’ rooms are also linked to a 37-inch, high-definition television. “A clinician can show the patient radiographic studies here or bring up interactive patient education programs,” he explains.
One of the most exciting potentials for this emerging technology is to find ways for embedding medical decision support in physicians’ workflow. “We know that the barriers to physicians routinely consulting decision support applications are high,” Dr. Cucina says.
For Dr. Deruelle, who had to look outside of hospital channels to answer his question about a dystonic patient, medicine has a serious information gap. “I believe we will move to where the technology will put that information at my fingertips,” he says. “Why aren’t we there yet? Not enough people are using the technology, and we don’t agree on what information should be included. But I think we can start with basic things and work up from there. What excites me is that we’re closing the information gap—although medicine is still in the Stone Age compared with other professions.” TH
Larry Beresford is a frequent contributor to The Hospitalist.
Dennis Deruelle, MD, a hospitalist at University Community Hospital in Tampa, Fla., once needed reliable medical information in a hurry while treating a young woman admitted to the hospital with cellulitis.
The woman was later diagnosed with methicillin-resistant staphylococcus aureus (MRSA). After Dr. Deruelle administered prochlorperazine (Compazine), she had a severe dystonic reaction.
“She was going rigid right before my eyes,” Dr. Deruelle says. There was no instantly accessible hospital clearinghouse of medical information, although he had called the pharmacy department and was waiting for a call back. So he opened his laptop and turned to an aid available to anyone with a computer and Internet access: Google. “I immediately looked up information on reactions to Compazine and the correct dose for counteracting it. I administered the dose, and within minutes [the patient] was getting better.”
Dr. Deruelle is not alone among physicians in answering medical questions with Google. (See The Hospitalist, July 2007, p. 33.)
He has been interested in medical applications of computer technology for years and serves on SHM’s advisory committee on technology. He receives tech support from his employer, IPC-The Hospitalist Company, based in North Hollywood, Calif. IPC offers its physicians a Web-accessible network called IPC Link—a “virtual office” to help with billing, medical decision support, reference software, continuing medical education, and even blogs written by company CEO Adam Singer, MD.
But Dr. Deruelle has also developed his own applications, including an off-the-shelf voice recognition software loaded onto his company-supplied, 2.5-lb. Tablet PC. He uses it to dictate brief notes to give attending physicians a heads-up about patients being discharged. These notes are uploaded to the company’s network, which automatically generates a fax to the attending within minutes.
The formal discharge summary, produced by the hospital’s medical transcription department, may take 48 hours to arrive.
Dr. Deruelle has wireless Internet access at four of the five hospitals he visits as a hospitalist practice leader.
“As soon as I walk in the door I’m ‘hot,’ ” he says. At the fifth hospital, he uses workstation computers to connect with IPC Link.
Array of Options
A dizzying range of communications technology is available to working hospitalists, typically accessed through personal digital assistants (PDAs), smartphones, computer tablets, pocket PCs, and laptops.
The Palm Pilot, introduced in 1996, is a well-known example of this technology, as are the Palm Treo and BlackBerry. PDAs combine the functions of cell phones, video phones, cameras, video recorders, media players, Web browsers, reference tools, bar code scanners, and global positioning system (GPS) devices—all in a palm-size package.
Hardware and supporting software vary in terms of ease of use, in particular, the ability to interface with the Web or the hospital, practice, or employer network the physician needs to connect with.
The technology is evolving rapidly. But anomalies abound, such as dependence on the fax machine as a staple of communication with attending physicians. Through all of these changes, hospitalists are responsible for learning what works and how best to take advantage of the technology to make their jobs easier.
Hospitalists also vary tremendously in terms of their comfort levels and openness to new technology.
“There is a considerable gap between those of us who ‘Palm’ and those who don’t,” says Timothy Hartzog, MD, pediatric hospitalist at Medical University of South Carolina (MUSC) in Charleston and a medical technology consultant. “Physicians want their patient data in different ways. Some want it printed out or in a paper chart.”
—Steven Liu, MD, of Emory University Medical Center in Atlanta
But implementation of technology, such as hospital electronic health records or computerized physician order entry, inevitably changes their relationships with information technology and patient information.
Some hospitalists, like Dr. Deruelle, are interested in what communication technology can bring their work and how to adapt it to their needs. Others, like Dr. Hartzog, medical director of Information Technology at MUSC, have taken added responsibilities for technology within their institutions.
And a few, such as Steven Liu, MD, of Emory University Medical Center in Atlanta, have taken their interest in computer technology a step further. In 1999, Dr. Liu founded Ingenious Med, an Atlanta software company that offers a suite of inpatient practice management applications to working hospitalists.
“Often the hospitalist is already on the forefront of technology,” Dr. Liu says. “The demographic is typically younger and techno-savvy. They may get tapped by their hospitals to help customize the electronic health record to make sure it satisfies the needs of clinicians. Conversely, if an electronic project does not involve strong physician feedback and collaboration, physicians can be the Achilles’ heel impeding successful implementation. Even though they are the ones who stand to gain most from the potential efficiency, physicians will not adopt technology that does not fit their workflow.”
State of the Art?
Russell Cucina, MD, MS, a hospitalist at the University of California-San Francisco Medical Center, San Francisco, is also the associate medical director for information technology at UCSF.
Dr. Cucina quips that a good example of a state-of-the-art, stand-alone patient data management system offering rapid data entry, long battery life, and high mobility is the paper index card, the longtime standard for making rounding notes.
“Plenty of doctors, including me, use it every day,” he says. But growing numbers of hospitalists also use PDAs, smartphones, and laptops to access information and support applications. Among the plethora of reference applications readily available to physicians by PDA or laptop are UpToDate, Epocrates, the Pocket Sanford Guide to Anti-Microbial Therapy, and Merck Medicus.
“I use many different resources as a hospitalist,” Dr. Cucina says. “I Google all the time.” Hospitalists still have opportunities to innovate, although increasingly their “home-grown” solutions will compete with multinational technology conglomerates entering the medical market.
The use of technology and equipment also varies depending on whether the hospitalist is employed by the hospital or part of an independent medical group.
Another factor is whether that hospital is academic, community-based, or part of a system like the Veterans Affairs or a staff-model HMO such as Kaiser Permanente. But all hospitalists are used to working on the run, Dr. Cucina says. And in their daily jobs, workflow is everything.
Tech in Use
“I use medical technology on the job to a moderate degree,” reports Latha Sivaprasad, MD, a hospitalist at Beth Israel Medical Center in New York City. “This is my sixth year working as a hospitalist, and for the first five years I didn’t use a specific device. Now I have a Palm-based program with MD Everywhere, Epocrates, UpToDate, and the ability to do billing. The hospital’s tech support staff trained us on the new system and how to use the PDA for tasks like developing rounding lists, accessing our colleagues’ lists and creating system-based memos.”
Dr. Sivaprasad also has GPS in her car, a cell phone, and a laptop at home. “We probably aren’t using medical technology as much as we could,” she says. “Many physicians still write prescriptions by hand. I’ve never used voice-recognition software. In a previous hospital, we used the hospital’s transcription service for dictated notes.”
Karim Godamunne, MD, MBA, a hospitalist with Eagle Hospital Physicians and a practice medical director at South Fulton Medical Center in Atlanta, uses a PDA at work for billing.
“I don’t use the PDA intensively,’’ he says. “I’d like to see our hospital create a wireless network like the one I have at home. Our sister hospital has wireless.” He notes, however, that there are computer workstations for him to use at his hospital.
Dr. Godamunne’s group has a practice coordinator who faxes discharge summaries to attending physicians.
“Fax is kind of what they expect these days,” he says. “I’m not sure e-mail would be as reliable for the community we serve. I’d be concerned that the attendings wouldn’t read their e-mails.” He says he sometimes gives written notes to patients at discharge with instructions to hand the note to their physician on their next office visit.
Michelle Pezzani, MD, is part of a 10-member hospital medicine group that practices at El Camino Hospital in Mountain View, Calif., in the heart of Silicon Valley. The hospital tries to stay on the cutting edge with technology, and its hospitalists were given Microsoft XP Tablet laptops a few years ago. “I access the Web two to four times a day at work,” Dr. Pezzani says. “It helps keep us current. The great thing about the laptop is I also take it home with me, and I can use it to check or reorder labs from home. We’re all connected to the hospital’s Intranet from home.”
“One of the issues we’re struggling with is how to achieve the best sign-out possible,” with up to four hospitalists on the day shift checking out and handing over patient responsibilities to the night shift, Dr. Pezzani says. For her, the ideal sign-out is face to face because it permits asking questions and reading nonverbal cues about how sick the patients really are. However, the logistics of multiple physicians and patients makes this ideal difficult to achieve.
Second best (if all group members used a Palm Pilot), would be to send sign-outs via text messaging—although that would also present logistical challenges. “Texting is easier,” she says. “You know who is sending the message. We could beam the written sign-out to each other in a matter of seconds, making it quick and easy. Furthermore, any day-to-day changes on a specific patient would be easy to amend and easy to send. It’s also a quick way to let a colleague know, ‘I need you right now!’ ”
The hospitalists at El Camino use voicemail to record sign-outs. But these messages can take a long time to record and play back, multiplied by the four physicians signing out. “Ideally, there would be a different voice mail for every patient, so I wouldn’t have to listen to patients A, B, C, D, and E to get to the pertinent information about patient F, who is crashing upstairs,” she says. Dr. Pezzani’s group is still exploring how to balance these considerations.
She says her hospitalist group is tight-knit and collaborative. “We leave our cell phones on all the time and answer each other’s calls after hours,” she says. “For example, I’m now on vacation with my family in San Diego and I have gotten at least two calls a day from my partners, either business related, or something like: ‘Do you remember that patient you admitted? Can you give me some information on them?’”
The Wired Hospital
Dr. Cucina is excited about the extra large, easy-to-grip handle on the 3-lb. Motion Computing C5 portable PC that UCSF hospitalists are field-testing. He’s also intrigued by the ever-expanding opportunities for interfacing with the hospital’s technology.
In August he gave a tour of Unit 13L at UCSF’s Moffitt/Long Hospital, a new ward that opened in June and is being used as a technology demonstration site.
The 32-bed unit has a narrow corridor lined with 10 computer workstations for the nurses. All 10 are in use. In an adjacent cubicle, several physicians are typing on their laptops.
On the unit, portable vital signs monitors are attached to rolling stands that also have docking ports for the laptops, offering real-time point-of-care acquisition of vital-signs data directly into the hospital’s medical record.
A nurse or physician can grab the big-handled Tablet PC and run to another room while remaining connected to the patient’s vital signs. The docking ports in patients’ rooms are also linked to a 37-inch, high-definition television. “A clinician can show the patient radiographic studies here or bring up interactive patient education programs,” he explains.
One of the most exciting potentials for this emerging technology is to find ways for embedding medical decision support in physicians’ workflow. “We know that the barriers to physicians routinely consulting decision support applications are high,” Dr. Cucina says.
For Dr. Deruelle, who had to look outside of hospital channels to answer his question about a dystonic patient, medicine has a serious information gap. “I believe we will move to where the technology will put that information at my fingertips,” he says. “Why aren’t we there yet? Not enough people are using the technology, and we don’t agree on what information should be included. But I think we can start with basic things and work up from there. What excites me is that we’re closing the information gap—although medicine is still in the Stone Age compared with other professions.” TH
Larry Beresford is a frequent contributor to The Hospitalist.
Dennis Deruelle, MD, a hospitalist at University Community Hospital in Tampa, Fla., once needed reliable medical information in a hurry while treating a young woman admitted to the hospital with cellulitis.
The woman was later diagnosed with methicillin-resistant staphylococcus aureus (MRSA). After Dr. Deruelle administered prochlorperazine (Compazine), she had a severe dystonic reaction.
“She was going rigid right before my eyes,” Dr. Deruelle says. There was no instantly accessible hospital clearinghouse of medical information, although he had called the pharmacy department and was waiting for a call back. So he opened his laptop and turned to an aid available to anyone with a computer and Internet access: Google. “I immediately looked up information on reactions to Compazine and the correct dose for counteracting it. I administered the dose, and within minutes [the patient] was getting better.”
Dr. Deruelle is not alone among physicians in answering medical questions with Google. (See The Hospitalist, July 2007, p. 33.)
He has been interested in medical applications of computer technology for years and serves on SHM’s advisory committee on technology. He receives tech support from his employer, IPC-The Hospitalist Company, based in North Hollywood, Calif. IPC offers its physicians a Web-accessible network called IPC Link—a “virtual office” to help with billing, medical decision support, reference software, continuing medical education, and even blogs written by company CEO Adam Singer, MD.
But Dr. Deruelle has also developed his own applications, including an off-the-shelf voice recognition software loaded onto his company-supplied, 2.5-lb. Tablet PC. He uses it to dictate brief notes to give attending physicians a heads-up about patients being discharged. These notes are uploaded to the company’s network, which automatically generates a fax to the attending within minutes.
The formal discharge summary, produced by the hospital’s medical transcription department, may take 48 hours to arrive.
Dr. Deruelle has wireless Internet access at four of the five hospitals he visits as a hospitalist practice leader.
“As soon as I walk in the door I’m ‘hot,’ ” he says. At the fifth hospital, he uses workstation computers to connect with IPC Link.
Array of Options
A dizzying range of communications technology is available to working hospitalists, typically accessed through personal digital assistants (PDAs), smartphones, computer tablets, pocket PCs, and laptops.
The Palm Pilot, introduced in 1996, is a well-known example of this technology, as are the Palm Treo and BlackBerry. PDAs combine the functions of cell phones, video phones, cameras, video recorders, media players, Web browsers, reference tools, bar code scanners, and global positioning system (GPS) devices—all in a palm-size package.
Hardware and supporting software vary in terms of ease of use, in particular, the ability to interface with the Web or the hospital, practice, or employer network the physician needs to connect with.
The technology is evolving rapidly. But anomalies abound, such as dependence on the fax machine as a staple of communication with attending physicians. Through all of these changes, hospitalists are responsible for learning what works and how best to take advantage of the technology to make their jobs easier.
Hospitalists also vary tremendously in terms of their comfort levels and openness to new technology.
“There is a considerable gap between those of us who ‘Palm’ and those who don’t,” says Timothy Hartzog, MD, pediatric hospitalist at Medical University of South Carolina (MUSC) in Charleston and a medical technology consultant. “Physicians want their patient data in different ways. Some want it printed out or in a paper chart.”
—Steven Liu, MD, of Emory University Medical Center in Atlanta
But implementation of technology, such as hospital electronic health records or computerized physician order entry, inevitably changes their relationships with information technology and patient information.
Some hospitalists, like Dr. Deruelle, are interested in what communication technology can bring their work and how to adapt it to their needs. Others, like Dr. Hartzog, medical director of Information Technology at MUSC, have taken added responsibilities for technology within their institutions.
And a few, such as Steven Liu, MD, of Emory University Medical Center in Atlanta, have taken their interest in computer technology a step further. In 1999, Dr. Liu founded Ingenious Med, an Atlanta software company that offers a suite of inpatient practice management applications to working hospitalists.
“Often the hospitalist is already on the forefront of technology,” Dr. Liu says. “The demographic is typically younger and techno-savvy. They may get tapped by their hospitals to help customize the electronic health record to make sure it satisfies the needs of clinicians. Conversely, if an electronic project does not involve strong physician feedback and collaboration, physicians can be the Achilles’ heel impeding successful implementation. Even though they are the ones who stand to gain most from the potential efficiency, physicians will not adopt technology that does not fit their workflow.”
State of the Art?
Russell Cucina, MD, MS, a hospitalist at the University of California-San Francisco Medical Center, San Francisco, is also the associate medical director for information technology at UCSF.
Dr. Cucina quips that a good example of a state-of-the-art, stand-alone patient data management system offering rapid data entry, long battery life, and high mobility is the paper index card, the longtime standard for making rounding notes.
“Plenty of doctors, including me, use it every day,” he says. But growing numbers of hospitalists also use PDAs, smartphones, and laptops to access information and support applications. Among the plethora of reference applications readily available to physicians by PDA or laptop are UpToDate, Epocrates, the Pocket Sanford Guide to Anti-Microbial Therapy, and Merck Medicus.
“I use many different resources as a hospitalist,” Dr. Cucina says. “I Google all the time.” Hospitalists still have opportunities to innovate, although increasingly their “home-grown” solutions will compete with multinational technology conglomerates entering the medical market.
The use of technology and equipment also varies depending on whether the hospitalist is employed by the hospital or part of an independent medical group.
Another factor is whether that hospital is academic, community-based, or part of a system like the Veterans Affairs or a staff-model HMO such as Kaiser Permanente. But all hospitalists are used to working on the run, Dr. Cucina says. And in their daily jobs, workflow is everything.
Tech in Use
“I use medical technology on the job to a moderate degree,” reports Latha Sivaprasad, MD, a hospitalist at Beth Israel Medical Center in New York City. “This is my sixth year working as a hospitalist, and for the first five years I didn’t use a specific device. Now I have a Palm-based program with MD Everywhere, Epocrates, UpToDate, and the ability to do billing. The hospital’s tech support staff trained us on the new system and how to use the PDA for tasks like developing rounding lists, accessing our colleagues’ lists and creating system-based memos.”
Dr. Sivaprasad also has GPS in her car, a cell phone, and a laptop at home. “We probably aren’t using medical technology as much as we could,” she says. “Many physicians still write prescriptions by hand. I’ve never used voice-recognition software. In a previous hospital, we used the hospital’s transcription service for dictated notes.”
Karim Godamunne, MD, MBA, a hospitalist with Eagle Hospital Physicians and a practice medical director at South Fulton Medical Center in Atlanta, uses a PDA at work for billing.
“I don’t use the PDA intensively,’’ he says. “I’d like to see our hospital create a wireless network like the one I have at home. Our sister hospital has wireless.” He notes, however, that there are computer workstations for him to use at his hospital.
Dr. Godamunne’s group has a practice coordinator who faxes discharge summaries to attending physicians.
“Fax is kind of what they expect these days,” he says. “I’m not sure e-mail would be as reliable for the community we serve. I’d be concerned that the attendings wouldn’t read their e-mails.” He says he sometimes gives written notes to patients at discharge with instructions to hand the note to their physician on their next office visit.
Michelle Pezzani, MD, is part of a 10-member hospital medicine group that practices at El Camino Hospital in Mountain View, Calif., in the heart of Silicon Valley. The hospital tries to stay on the cutting edge with technology, and its hospitalists were given Microsoft XP Tablet laptops a few years ago. “I access the Web two to four times a day at work,” Dr. Pezzani says. “It helps keep us current. The great thing about the laptop is I also take it home with me, and I can use it to check or reorder labs from home. We’re all connected to the hospital’s Intranet from home.”
“One of the issues we’re struggling with is how to achieve the best sign-out possible,” with up to four hospitalists on the day shift checking out and handing over patient responsibilities to the night shift, Dr. Pezzani says. For her, the ideal sign-out is face to face because it permits asking questions and reading nonverbal cues about how sick the patients really are. However, the logistics of multiple physicians and patients makes this ideal difficult to achieve.
Second best (if all group members used a Palm Pilot), would be to send sign-outs via text messaging—although that would also present logistical challenges. “Texting is easier,” she says. “You know who is sending the message. We could beam the written sign-out to each other in a matter of seconds, making it quick and easy. Furthermore, any day-to-day changes on a specific patient would be easy to amend and easy to send. It’s also a quick way to let a colleague know, ‘I need you right now!’ ”
The hospitalists at El Camino use voicemail to record sign-outs. But these messages can take a long time to record and play back, multiplied by the four physicians signing out. “Ideally, there would be a different voice mail for every patient, so I wouldn’t have to listen to patients A, B, C, D, and E to get to the pertinent information about patient F, who is crashing upstairs,” she says. Dr. Pezzani’s group is still exploring how to balance these considerations.
She says her hospitalist group is tight-knit and collaborative. “We leave our cell phones on all the time and answer each other’s calls after hours,” she says. “For example, I’m now on vacation with my family in San Diego and I have gotten at least two calls a day from my partners, either business related, or something like: ‘Do you remember that patient you admitted? Can you give me some information on them?’”
The Wired Hospital
Dr. Cucina is excited about the extra large, easy-to-grip handle on the 3-lb. Motion Computing C5 portable PC that UCSF hospitalists are field-testing. He’s also intrigued by the ever-expanding opportunities for interfacing with the hospital’s technology.
In August he gave a tour of Unit 13L at UCSF’s Moffitt/Long Hospital, a new ward that opened in June and is being used as a technology demonstration site.
The 32-bed unit has a narrow corridor lined with 10 computer workstations for the nurses. All 10 are in use. In an adjacent cubicle, several physicians are typing on their laptops.
On the unit, portable vital signs monitors are attached to rolling stands that also have docking ports for the laptops, offering real-time point-of-care acquisition of vital-signs data directly into the hospital’s medical record.
A nurse or physician can grab the big-handled Tablet PC and run to another room while remaining connected to the patient’s vital signs. The docking ports in patients’ rooms are also linked to a 37-inch, high-definition television. “A clinician can show the patient radiographic studies here or bring up interactive patient education programs,” he explains.
One of the most exciting potentials for this emerging technology is to find ways for embedding medical decision support in physicians’ workflow. “We know that the barriers to physicians routinely consulting decision support applications are high,” Dr. Cucina says.
For Dr. Deruelle, who had to look outside of hospital channels to answer his question about a dystonic patient, medicine has a serious information gap. “I believe we will move to where the technology will put that information at my fingertips,” he says. “Why aren’t we there yet? Not enough people are using the technology, and we don’t agree on what information should be included. But I think we can start with basic things and work up from there. What excites me is that we’re closing the information gap—although medicine is still in the Stone Age compared with other professions.” TH
Larry Beresford is a frequent contributor to The Hospitalist.
Methadone: Handle with Care
Few topics in hospital-based pain management generate such diverse viewpoints as the use of methadone as an analgesic. Increasingly ordered by hospice physicians and some hospitalists as a tool for managing difficult pain cases, it is also coming under scrutiny for risks related to cardiac complications, respiratory depression, and the challenges of determining appropriate doses.
For some, the risks are grave enough to contraindicate methadone prescription for use in routine hospital practice, unless the hospitalist is well-versed in its use and has access to a pharmacist or other pain expert to review medication orders. Hospitalists should also be aware of the Food and Drug Administration’s strongly worded November 2006 Public Health Advisory, “Methadone Use for Pain Control May Result in Death and Life-Threatening Changes in Breathing and Heart Beat.”1
The FDA stopped short of recommending against the use of methadone as an analgesic, but it admonished physicians to use caution when prescribing it for patients unused to the drug—particularly during drug initiation, conversion from another opioid, or titration upward. Patients should be cautioned to take the drug exactly as prescribed. The advisory also recommended a new maximum initial dose of 30 mg per day (typically prescribed 10 mg tid), when initiating methadone for pain management.
Jean Youngwerth, MD, associate program director of the University of Colorado at Denver and Health Sciences Center, is well aware of the benefits and risks of prescribing methadone in her dual roles as hospitalist and palliative care consultant. “It is a great analgesic, becoming a lot more popular in recent years,” Dr. Youngwerth says. “It’s also ridiculously cheap [often under a dollar a day], which is an important consideration for some of our patients returning home with chronic pain. For other patients, it’s an extra analgesic tool, giving good pain relief, especially for refractory somatic or neuropathic pain.”
But methadone also has downsides. “Its pharmaco-kinetics are so complex and poorly understood that people unfamiliar with prescribing it can get in trouble in a hurry,” Dr. Youngwerth says. “You can kill people with oversedation. I do not prescribe it in my hospitalist practice and I discourage other hospitalists from prescribing it for their patients without consulting a pain or palliative care specialist. You don’t see its maximal effects until at least three to four days out, and that’s usually too long for the hospitalist. When I start palliative care patients on methadone, I normally keep them in the hospital for three or four days so that I can monitor the effects.”
Dr. Youngwerth believes her experience in pain management justifies prescribing methadone for palliative care patients. Even so, she always calls one of the local physician pain experts she works with or a hospital pharmacist to make sure she is ordering it safely and correctly. “I don’t think doctors should be scared off by all the bad publicity about methadone, but they need to realize these are valid concerns,” she says. “People run into problems when they assume that it is just another opioid.”
Hospitalists must recognize the stark realities of using the drug.
“Methadone is the easiest opioid to kill someone with,” says Gail Gazelle, MD, palliative care physician with MD Can Help and Harvard Medical School in Boston. “At the same time, its unique properties can give analgesic effects you can get from no other drug.”
For hospitalists, these issues are complicated by their short involvement with hospitalized patients, who are quickly prepped for discharge back to various community settings and living situations.
Dr. Gazelle wonders, “Is a short hospital stay the right place to initiate methadone treatment, given all of the complications?” If the answer is yes, communicating with the attending and agreeing on a plan for its continued use after discharge from the hospital are essential.
Although narcotic abuse is notoriously difficult to manage, with high relapse rates in every setting, methadone maintenance therapy (MMT) has been shown to reduce overall rates of abuse of other drugs, overdose and death, criminal activity, needle sharing, and commercial sex work. Methadone maintenance is a long-term strategy. The drug is provided as a substitute, not a cure, for narcotic abuse. Patients may continue to receive their daily maintenance dose for years. One-year retention rates in several large studies of MMT have ranged from 25% to 60%, while rates of relapse after leaving MMT are high. Stopping methadone use poses the same challenges as quitting any narcotic and should only be done under a doctor’s care.
Methadone is also used to treat heroin withdrawal, an issue for some hospitalized patients. Prescribing methadone for maintenance therapy is limited to federally licensed methadone treatment programs.
Complications
There are several critical facets of this drug hospitalists must be aware of:
Unpredictable half-life: Methadone, relative to other opioids, has high lipid solubility, slow metabolism, and a typical half-life ranging from 15 to 60 hours—although it can be longer. Methadone’s analgesic effect is shorter-lived, so analgesic doses should be given two, three, or four times daily. But the longer half-life means it can take three days or more after the initial dose before the drug’s full effect—on respiration for example—is known. That is why therapeutic doses can build to toxic levels. There is also wide variation in its effects among patients. Guidelines suggest titrating methadone upward for increased analgesic effect should not be attempted until at least three days after the first dose.
Respiratory depression: This is an issue when the drug is initiated in an opioid-naïve patient or is too rapidly titrated. Deaths from methadone have been seen at doses once considered safe. Physicians are cautioned to start patients on low doses while using other, short-acting opioids for breakthrough pain and frequently assessing for signs of overdose or respiratory depression, such as difficulty in breathing, shallow breathing, extreme sleepiness, or inability to think, talk, or walk normally.
Effect on heart arrhythmias: Methadone can prolong the QTc interval in heart function, leading to a potentially serious cardiac abnormality known as torsade de pointes. The potential for cardiac deaths is another complicating factor that may contraindicate methadone for patients at risk for developing a prolonged QTc interval, including patients with cardiac hypertrophy, hypokalemia, or hypomagnesemia, or a history of cardiac conduction abnormalities or taking medications affecting cardiac conduction. A current EKG may be an appropriate precaution when initiating methadone in elderly patients who have a cardiac history or are receiving methadone in high doses or by intravenous administration.
Drug interactions: The list of drugs that interact with methadone is long, with potential for unwanted side effects and increased or decreased potency. This list includes most anti-retroviral treatments for HIV; sedatives, tranquilizers, barbiturates, seizure medications, muscle relaxants, or any central nervous system depressants; certain steroids and anti-fungals; even over-the-counter cough and cold medications. Also watch for medications that treat irregular heartbeat or prolong the QTc interval. Pharmaceutical company labels for methadone, as well as the FDA advisory, contain a more complete list of drugs that interact with methadone. Always review with patients the other medications they take, including over-the-counter medications and alternative treatments.
Other complications: Methadone should not be prescribed when opioids in general are contraindicated. It can be a management challenge to convert patients from methadone back to other opioids. Another complication of prescribing methadone is the negative publicity it has received in recent years, combined with the stigma of its associations with drug treatment. Some patients, families, or attending physicians may be leery of using it as a pain reliever. It may not be worth titrating methadone to the correct dose in the hospital if it is going to be discontinued post-discharge.
A series of articles in The Charleston (W.Va.) Gazette starting in June 2006 alerted many to the fact methadone is listed by medical examiners nationwide as a cause of death more often than any other prescription pain reliever.10 Methadone was implicated in nearly 4,000 deaths in 2006, four times as many as in 1999. Most of the deaths were considered accidental, and many involved combinations with other drugs—although some were in patients taking methadone as prescribed.
Hospitalists can expect that the diverse caseloads they see likely will include some patients taking methadone. Some may be getting it as an analgesic prescribed by a community physician, pain clinic, or hospice. Others in MMT and receiving a daily dose to manage their addiction disorder may present at the hospital with a different medical problem and perhaps new pain issues.
The hospitalist should not take it for granted that patients on MMT are not also intoxicated or abusing methadone or other drugs, says Michael Weaver, MD, pain and addiction specialist at Virginia Commonwealth University Medical Center in Richmond. Nor should they assume MMT doses are providing adequate analgesia.
“The bottom line in all of these situations is communication,” Dr. Weaver says. Talk to the medical director of the methadone clinic or the community physician who prescribed methadone as an analgesic. Verify the patient’s status, confirm dosage, and discuss the pain issues that need to be addressed—while recognizing pain relief is an appropriate expectation of any hospitalized patient, regardless of drug history or treatment.
Generally, Dr. Weaver says, the maintenance dose of methadone would continue during the hospital stay, and a different analgesic would be ordered for the pain—although the clinic physician may have other ideas. Changing methadone dose or schedule—or attempting to wean a patient off methadone—is not a decision a hospitalist should make unilaterally.11
Methadone’s Merits
Why would a hospitalist want to prescribe a drug that comes with so many caveats?
Carol Jessop, MD, a hospitalist and palliative care consultant at Alta Bates Summit Medical Center in Berkeley, Calif., uses methadone—often in combination with the anti-depressant desipramine or the anticonvulsant gabapentin—to treat complex regional pain syndromes and neuropathic pain.
Dr. Jessop carefully assesses patients for neuropathic pain, listening for descriptors such as burning, stinging, or numbing. These are the patients for whom she most often receives palliative care consultations, often following years of out-of-control pain or lack of response to high doses of other opioids. “My job is much easier now that I understand the difference between nocioceptive and neuropathic pain,” she notes.
“I think methadone is magic, perhaps due to its effect on the NMDA (n-methyl, d-asparte) receptors,” Dr. Jessop says. “I’m also convinced from my clinical experience that there can be nerve healing going on when these pain syndromes are effectively treated. I had a patient with horrible phantom pain following multiple hip surgeries and amputation of his leg. He was referred by a family practitioner, who said, ‘I cannot get this man’s pain under control.’ ” The patient’s pain is now controlled with methadone, 30 mg three times a day. He rarely needs to take his hydromorphone (Dilaudid) for breakthrough pain, and he is able to use his prosthetic leg—which would have been unthinkable before.
Dr. Jessop believes low doses of methadone—even lower than the conversion charts recommend—can have a big effect. “I don’t have problems with methadone because I’m so careful in prescribing it,” she says. “I also work closely with the attending physician and give patients my cell phone number when they return home. It is important to get the family involved and to be clear about the risks and benefits.”
Brad Stuart, MD, senior medical director of Sutter VNA and Hospice in Northern California, also believes methadone can be a wonderful pain management tool. “There is no substitute, in my estimation, to adding a little methadone to the opioid regimen—even just 5 mg of liquid three times a day—for difficult neuropathic pain cases,” Dr. Stuart says. “It’s true that you don’t want to raise the dose too quickly. But I find that it’s unusual not to see benefit in these kinds of patients. I disagree with those who would advise hospitalists to stay away from methadone for treating refractory neuropathic pain. If you start slow and go slow, the risks are small relative to the gain.”
Eduardo Bruera, MD, a palliative care physician at M.D. Anderson Cancer Center in Houston, is another believer in methadone for difficult pain cases, although he emphasizes that his experience is limited to the pain associated with cancer. Dr. Bruera does not use methadone as a first-line analgesic, but he finds it effective when other opioids have not been. “Patients who continue to have a lot of pain after multiple escalating opioid doses or signs of opioid toxicity may be signaling that the opioid you’re using is not working,” he says. “If we make three or four dose changes without response, it’s time to change the opioid.”
Dr. Bruera acknowledges that persuasive research studies to establish methadone’s purported efficacy in treating neuropathic pain have not been conducted. “Unfortunately, methadone is an orphan drug, so we don’t know who would pay for those studies. Should we consider it as a first-line opioid for cancer pain? Again, that is an unanswered question.”
Dr. Bruera has been involved in a number of the few published studies and reviews of methadone’s analgesic efficacy, and he is engaged in ongoing orphan drug status research.12, 13
Methadone as Analgesic
Stephen Bekanich, MD, hospitalist and palliative care consultant at the University of Utah Medical Center in Salt Lake City, falls in the middle range of opinions on methadone.
“From the hospitalist’s standpoint, there are downsides,” Dr. Bekanich says. “People who don’t understand how to titrate it may change doses on a daily basis or more often, which is dangerous. They may not understand the dosing equivalents or pay enough attention to drug interactions.
“Of all the opioids, careful assessment and follow-up may be the most important with methadone. Always make sure you have concrete post-discharge plans. If I didn’t have a pharmacist to collaborate with, as a hospitalist I’d probably stay away from it. But it’s different when I put on my palliative care hat.”
Rachelle Bernacki, MD, a hospitalist, palliative care physician and geriatrician at the University of California-San Francisco Medical Center, agrees methadone can be a useful analgesic—particularly when other opioids have failed to relieve the pain. “But I don’t start with it; I may add a small dose of methadone to the existing regimen for complex pain,” she says.
“I caution my residents not to try methadone without consulting with someone familiar with the drug,” explains Dr. Bernacki, who adds that she is fortunate to work with a pharmacist at UCSF who is an expert in pain management and palliative medicine. “Having taught residents, I can confirm that there is a lot of confusion about its use. But I have also used methadone in my outpatient geriatric practice—with fantastic results.”
Paresh Patel, MD, a hospitalist at VCU Medical Center, says he and his colleagues use methadone as a second-line analgesic when pain is not well managed with morphine. He always keeps an eye out for the risks, including potential interactions with psychiatric medications and the need to look at EKGs.
Dr. Patel says conversion from other opioids is one of the biggest challenges in using methadone. He is not satisfied with the various published opioid conversion charts and relies on experience and trial and error. “I always wait 48 hours before titrating up,” he says.
More research is needed in this area, Dr. Patel says, and he is thinking of getting involved in a methadone research project. TH
Larry Beresford is a frequent contributor to The Hospitalist.
References
- Food and Drug Administration. FDA Public Health Advisory: Methadone use for pain control may result in death and life-threatening changes in breathing and heart beat. Available at: www.fda.gov/cder/drug/advisory/methadone.htm. Last accessed June 4, 2007.
- Moulin DE, Palma D, Watling C, et al. Methadone in the management of intractable neuropathic noncancer pain. Can J Neurol Sci. 2005 Aug: 32(3); 340-343.
- Altier N, Dion D, Boulanger A, et al. Management of chronic neuropathic pain with methadone: A review of 13 cases. Clin J Pain. 2005 Jul-Aug;21(4):364-369.
- Morley JS, Bridson J, Nash TP, et al. Low-dose methadone has an analgesic effect in neuropathic pain: A double-blind randomized controlled crossover trial. Palliat Med. 2003 Oct;17(7):576-587.
- Lawlor PG, Turner KS, Hanson J, et al. Dose ratio between morphine and methadone in patients with cancer pain: A retrospective study. Cancer. 1998 Mar;82(6):1167-1173.
- Ripamonti C, De Conno F, Groff L, et al. Equianal-gesic dose/ratio between methadone and other opioid agonists in cancer pain: Comparison of two clinical experiences. Ann Oncol. 1998 Jan;9(1):79-83.
- Gazelle G, Fine PG. Fast Fact and Concept #75: Methadone for the treatment of pain. End-of-Life/Palliative Education Resource Center, Medical College of Wisconsin, Milwaukee, www.eperc.mcw.edu/ff_index.htm; and Roxane Laboratories, Inc., label for dolophine hydrochloride CH (methadone hydrochloride tablets).
- American Methadone Treatment Association. 1998 Methadone Maintenance Program and Patient Census in the U.S., New York, NY, April 1999.
- Office of National Drug Control Policy. Fact sheet. Available at: www.whitehousedrugpolicy.gov. Last accessed June 4, 2007.
- Finn S, Tuckwiller T. The Killer Cure. The Charlotte (W. Va.) Gazette. Available at: www.wvgazette.com. Last accessed June 29, 2007.
- Weaver MF, Schnoll SH. Opioid treatment of chronic pain in patients with addiction. J Pain Palliat Care Pharmacother. 2002:16(3);5-26.
- Bruera E, Sweeney C. Methadone use in cancer patients with pain: A review. J Palliat Med. 2002 Feb;5(1):127-137.
- Bruera E, Palmer JL, Bosnjak S, et al. Methadone versus morphine as a first-line strong opioid for cancer pain: A randomized, double-blind study. J Clin Oncol. 2004 Jan 1;22(1):185-192.
Few topics in hospital-based pain management generate such diverse viewpoints as the use of methadone as an analgesic. Increasingly ordered by hospice physicians and some hospitalists as a tool for managing difficult pain cases, it is also coming under scrutiny for risks related to cardiac complications, respiratory depression, and the challenges of determining appropriate doses.
For some, the risks are grave enough to contraindicate methadone prescription for use in routine hospital practice, unless the hospitalist is well-versed in its use and has access to a pharmacist or other pain expert to review medication orders. Hospitalists should also be aware of the Food and Drug Administration’s strongly worded November 2006 Public Health Advisory, “Methadone Use for Pain Control May Result in Death and Life-Threatening Changes in Breathing and Heart Beat.”1
The FDA stopped short of recommending against the use of methadone as an analgesic, but it admonished physicians to use caution when prescribing it for patients unused to the drug—particularly during drug initiation, conversion from another opioid, or titration upward. Patients should be cautioned to take the drug exactly as prescribed. The advisory also recommended a new maximum initial dose of 30 mg per day (typically prescribed 10 mg tid), when initiating methadone for pain management.
Jean Youngwerth, MD, associate program director of the University of Colorado at Denver and Health Sciences Center, is well aware of the benefits and risks of prescribing methadone in her dual roles as hospitalist and palliative care consultant. “It is a great analgesic, becoming a lot more popular in recent years,” Dr. Youngwerth says. “It’s also ridiculously cheap [often under a dollar a day], which is an important consideration for some of our patients returning home with chronic pain. For other patients, it’s an extra analgesic tool, giving good pain relief, especially for refractory somatic or neuropathic pain.”
But methadone also has downsides. “Its pharmaco-kinetics are so complex and poorly understood that people unfamiliar with prescribing it can get in trouble in a hurry,” Dr. Youngwerth says. “You can kill people with oversedation. I do not prescribe it in my hospitalist practice and I discourage other hospitalists from prescribing it for their patients without consulting a pain or palliative care specialist. You don’t see its maximal effects until at least three to four days out, and that’s usually too long for the hospitalist. When I start palliative care patients on methadone, I normally keep them in the hospital for three or four days so that I can monitor the effects.”
Dr. Youngwerth believes her experience in pain management justifies prescribing methadone for palliative care patients. Even so, she always calls one of the local physician pain experts she works with or a hospital pharmacist to make sure she is ordering it safely and correctly. “I don’t think doctors should be scared off by all the bad publicity about methadone, but they need to realize these are valid concerns,” she says. “People run into problems when they assume that it is just another opioid.”
Hospitalists must recognize the stark realities of using the drug.
“Methadone is the easiest opioid to kill someone with,” says Gail Gazelle, MD, palliative care physician with MD Can Help and Harvard Medical School in Boston. “At the same time, its unique properties can give analgesic effects you can get from no other drug.”
For hospitalists, these issues are complicated by their short involvement with hospitalized patients, who are quickly prepped for discharge back to various community settings and living situations.
Dr. Gazelle wonders, “Is a short hospital stay the right place to initiate methadone treatment, given all of the complications?” If the answer is yes, communicating with the attending and agreeing on a plan for its continued use after discharge from the hospital are essential.
Although narcotic abuse is notoriously difficult to manage, with high relapse rates in every setting, methadone maintenance therapy (MMT) has been shown to reduce overall rates of abuse of other drugs, overdose and death, criminal activity, needle sharing, and commercial sex work. Methadone maintenance is a long-term strategy. The drug is provided as a substitute, not a cure, for narcotic abuse. Patients may continue to receive their daily maintenance dose for years. One-year retention rates in several large studies of MMT have ranged from 25% to 60%, while rates of relapse after leaving MMT are high. Stopping methadone use poses the same challenges as quitting any narcotic and should only be done under a doctor’s care.
Methadone is also used to treat heroin withdrawal, an issue for some hospitalized patients. Prescribing methadone for maintenance therapy is limited to federally licensed methadone treatment programs.
Complications
There are several critical facets of this drug hospitalists must be aware of:
Unpredictable half-life: Methadone, relative to other opioids, has high lipid solubility, slow metabolism, and a typical half-life ranging from 15 to 60 hours—although it can be longer. Methadone’s analgesic effect is shorter-lived, so analgesic doses should be given two, three, or four times daily. But the longer half-life means it can take three days or more after the initial dose before the drug’s full effect—on respiration for example—is known. That is why therapeutic doses can build to toxic levels. There is also wide variation in its effects among patients. Guidelines suggest titrating methadone upward for increased analgesic effect should not be attempted until at least three days after the first dose.
Respiratory depression: This is an issue when the drug is initiated in an opioid-naïve patient or is too rapidly titrated. Deaths from methadone have been seen at doses once considered safe. Physicians are cautioned to start patients on low doses while using other, short-acting opioids for breakthrough pain and frequently assessing for signs of overdose or respiratory depression, such as difficulty in breathing, shallow breathing, extreme sleepiness, or inability to think, talk, or walk normally.
Effect on heart arrhythmias: Methadone can prolong the QTc interval in heart function, leading to a potentially serious cardiac abnormality known as torsade de pointes. The potential for cardiac deaths is another complicating factor that may contraindicate methadone for patients at risk for developing a prolonged QTc interval, including patients with cardiac hypertrophy, hypokalemia, or hypomagnesemia, or a history of cardiac conduction abnormalities or taking medications affecting cardiac conduction. A current EKG may be an appropriate precaution when initiating methadone in elderly patients who have a cardiac history or are receiving methadone in high doses or by intravenous administration.
Drug interactions: The list of drugs that interact with methadone is long, with potential for unwanted side effects and increased or decreased potency. This list includes most anti-retroviral treatments for HIV; sedatives, tranquilizers, barbiturates, seizure medications, muscle relaxants, or any central nervous system depressants; certain steroids and anti-fungals; even over-the-counter cough and cold medications. Also watch for medications that treat irregular heartbeat or prolong the QTc interval. Pharmaceutical company labels for methadone, as well as the FDA advisory, contain a more complete list of drugs that interact with methadone. Always review with patients the other medications they take, including over-the-counter medications and alternative treatments.
Other complications: Methadone should not be prescribed when opioids in general are contraindicated. It can be a management challenge to convert patients from methadone back to other opioids. Another complication of prescribing methadone is the negative publicity it has received in recent years, combined with the stigma of its associations with drug treatment. Some patients, families, or attending physicians may be leery of using it as a pain reliever. It may not be worth titrating methadone to the correct dose in the hospital if it is going to be discontinued post-discharge.
A series of articles in The Charleston (W.Va.) Gazette starting in June 2006 alerted many to the fact methadone is listed by medical examiners nationwide as a cause of death more often than any other prescription pain reliever.10 Methadone was implicated in nearly 4,000 deaths in 2006, four times as many as in 1999. Most of the deaths were considered accidental, and many involved combinations with other drugs—although some were in patients taking methadone as prescribed.
Hospitalists can expect that the diverse caseloads they see likely will include some patients taking methadone. Some may be getting it as an analgesic prescribed by a community physician, pain clinic, or hospice. Others in MMT and receiving a daily dose to manage their addiction disorder may present at the hospital with a different medical problem and perhaps new pain issues.
The hospitalist should not take it for granted that patients on MMT are not also intoxicated or abusing methadone or other drugs, says Michael Weaver, MD, pain and addiction specialist at Virginia Commonwealth University Medical Center in Richmond. Nor should they assume MMT doses are providing adequate analgesia.
“The bottom line in all of these situations is communication,” Dr. Weaver says. Talk to the medical director of the methadone clinic or the community physician who prescribed methadone as an analgesic. Verify the patient’s status, confirm dosage, and discuss the pain issues that need to be addressed—while recognizing pain relief is an appropriate expectation of any hospitalized patient, regardless of drug history or treatment.
Generally, Dr. Weaver says, the maintenance dose of methadone would continue during the hospital stay, and a different analgesic would be ordered for the pain—although the clinic physician may have other ideas. Changing methadone dose or schedule—or attempting to wean a patient off methadone—is not a decision a hospitalist should make unilaterally.11
Methadone’s Merits
Why would a hospitalist want to prescribe a drug that comes with so many caveats?
Carol Jessop, MD, a hospitalist and palliative care consultant at Alta Bates Summit Medical Center in Berkeley, Calif., uses methadone—often in combination with the anti-depressant desipramine or the anticonvulsant gabapentin—to treat complex regional pain syndromes and neuropathic pain.
Dr. Jessop carefully assesses patients for neuropathic pain, listening for descriptors such as burning, stinging, or numbing. These are the patients for whom she most often receives palliative care consultations, often following years of out-of-control pain or lack of response to high doses of other opioids. “My job is much easier now that I understand the difference between nocioceptive and neuropathic pain,” she notes.
“I think methadone is magic, perhaps due to its effect on the NMDA (n-methyl, d-asparte) receptors,” Dr. Jessop says. “I’m also convinced from my clinical experience that there can be nerve healing going on when these pain syndromes are effectively treated. I had a patient with horrible phantom pain following multiple hip surgeries and amputation of his leg. He was referred by a family practitioner, who said, ‘I cannot get this man’s pain under control.’ ” The patient’s pain is now controlled with methadone, 30 mg three times a day. He rarely needs to take his hydromorphone (Dilaudid) for breakthrough pain, and he is able to use his prosthetic leg—which would have been unthinkable before.
Dr. Jessop believes low doses of methadone—even lower than the conversion charts recommend—can have a big effect. “I don’t have problems with methadone because I’m so careful in prescribing it,” she says. “I also work closely with the attending physician and give patients my cell phone number when they return home. It is important to get the family involved and to be clear about the risks and benefits.”
Brad Stuart, MD, senior medical director of Sutter VNA and Hospice in Northern California, also believes methadone can be a wonderful pain management tool. “There is no substitute, in my estimation, to adding a little methadone to the opioid regimen—even just 5 mg of liquid three times a day—for difficult neuropathic pain cases,” Dr. Stuart says. “It’s true that you don’t want to raise the dose too quickly. But I find that it’s unusual not to see benefit in these kinds of patients. I disagree with those who would advise hospitalists to stay away from methadone for treating refractory neuropathic pain. If you start slow and go slow, the risks are small relative to the gain.”
Eduardo Bruera, MD, a palliative care physician at M.D. Anderson Cancer Center in Houston, is another believer in methadone for difficult pain cases, although he emphasizes that his experience is limited to the pain associated with cancer. Dr. Bruera does not use methadone as a first-line analgesic, but he finds it effective when other opioids have not been. “Patients who continue to have a lot of pain after multiple escalating opioid doses or signs of opioid toxicity may be signaling that the opioid you’re using is not working,” he says. “If we make three or four dose changes without response, it’s time to change the opioid.”
Dr. Bruera acknowledges that persuasive research studies to establish methadone’s purported efficacy in treating neuropathic pain have not been conducted. “Unfortunately, methadone is an orphan drug, so we don’t know who would pay for those studies. Should we consider it as a first-line opioid for cancer pain? Again, that is an unanswered question.”
Dr. Bruera has been involved in a number of the few published studies and reviews of methadone’s analgesic efficacy, and he is engaged in ongoing orphan drug status research.12, 13
Methadone as Analgesic
Stephen Bekanich, MD, hospitalist and palliative care consultant at the University of Utah Medical Center in Salt Lake City, falls in the middle range of opinions on methadone.
“From the hospitalist’s standpoint, there are downsides,” Dr. Bekanich says. “People who don’t understand how to titrate it may change doses on a daily basis or more often, which is dangerous. They may not understand the dosing equivalents or pay enough attention to drug interactions.
“Of all the opioids, careful assessment and follow-up may be the most important with methadone. Always make sure you have concrete post-discharge plans. If I didn’t have a pharmacist to collaborate with, as a hospitalist I’d probably stay away from it. But it’s different when I put on my palliative care hat.”
Rachelle Bernacki, MD, a hospitalist, palliative care physician and geriatrician at the University of California-San Francisco Medical Center, agrees methadone can be a useful analgesic—particularly when other opioids have failed to relieve the pain. “But I don’t start with it; I may add a small dose of methadone to the existing regimen for complex pain,” she says.
“I caution my residents not to try methadone without consulting with someone familiar with the drug,” explains Dr. Bernacki, who adds that she is fortunate to work with a pharmacist at UCSF who is an expert in pain management and palliative medicine. “Having taught residents, I can confirm that there is a lot of confusion about its use. But I have also used methadone in my outpatient geriatric practice—with fantastic results.”
Paresh Patel, MD, a hospitalist at VCU Medical Center, says he and his colleagues use methadone as a second-line analgesic when pain is not well managed with morphine. He always keeps an eye out for the risks, including potential interactions with psychiatric medications and the need to look at EKGs.
Dr. Patel says conversion from other opioids is one of the biggest challenges in using methadone. He is not satisfied with the various published opioid conversion charts and relies on experience and trial and error. “I always wait 48 hours before titrating up,” he says.
More research is needed in this area, Dr. Patel says, and he is thinking of getting involved in a methadone research project. TH
Larry Beresford is a frequent contributor to The Hospitalist.
References
- Food and Drug Administration. FDA Public Health Advisory: Methadone use for pain control may result in death and life-threatening changes in breathing and heart beat. Available at: www.fda.gov/cder/drug/advisory/methadone.htm. Last accessed June 4, 2007.
- Moulin DE, Palma D, Watling C, et al. Methadone in the management of intractable neuropathic noncancer pain. Can J Neurol Sci. 2005 Aug: 32(3); 340-343.
- Altier N, Dion D, Boulanger A, et al. Management of chronic neuropathic pain with methadone: A review of 13 cases. Clin J Pain. 2005 Jul-Aug;21(4):364-369.
- Morley JS, Bridson J, Nash TP, et al. Low-dose methadone has an analgesic effect in neuropathic pain: A double-blind randomized controlled crossover trial. Palliat Med. 2003 Oct;17(7):576-587.
- Lawlor PG, Turner KS, Hanson J, et al. Dose ratio between morphine and methadone in patients with cancer pain: A retrospective study. Cancer. 1998 Mar;82(6):1167-1173.
- Ripamonti C, De Conno F, Groff L, et al. Equianal-gesic dose/ratio between methadone and other opioid agonists in cancer pain: Comparison of two clinical experiences. Ann Oncol. 1998 Jan;9(1):79-83.
- Gazelle G, Fine PG. Fast Fact and Concept #75: Methadone for the treatment of pain. End-of-Life/Palliative Education Resource Center, Medical College of Wisconsin, Milwaukee, www.eperc.mcw.edu/ff_index.htm; and Roxane Laboratories, Inc., label for dolophine hydrochloride CH (methadone hydrochloride tablets).
- American Methadone Treatment Association. 1998 Methadone Maintenance Program and Patient Census in the U.S., New York, NY, April 1999.
- Office of National Drug Control Policy. Fact sheet. Available at: www.whitehousedrugpolicy.gov. Last accessed June 4, 2007.
- Finn S, Tuckwiller T. The Killer Cure. The Charlotte (W. Va.) Gazette. Available at: www.wvgazette.com. Last accessed June 29, 2007.
- Weaver MF, Schnoll SH. Opioid treatment of chronic pain in patients with addiction. J Pain Palliat Care Pharmacother. 2002:16(3);5-26.
- Bruera E, Sweeney C. Methadone use in cancer patients with pain: A review. J Palliat Med. 2002 Feb;5(1):127-137.
- Bruera E, Palmer JL, Bosnjak S, et al. Methadone versus morphine as a first-line strong opioid for cancer pain: A randomized, double-blind study. J Clin Oncol. 2004 Jan 1;22(1):185-192.
Few topics in hospital-based pain management generate such diverse viewpoints as the use of methadone as an analgesic. Increasingly ordered by hospice physicians and some hospitalists as a tool for managing difficult pain cases, it is also coming under scrutiny for risks related to cardiac complications, respiratory depression, and the challenges of determining appropriate doses.
For some, the risks are grave enough to contraindicate methadone prescription for use in routine hospital practice, unless the hospitalist is well-versed in its use and has access to a pharmacist or other pain expert to review medication orders. Hospitalists should also be aware of the Food and Drug Administration’s strongly worded November 2006 Public Health Advisory, “Methadone Use for Pain Control May Result in Death and Life-Threatening Changes in Breathing and Heart Beat.”1
The FDA stopped short of recommending against the use of methadone as an analgesic, but it admonished physicians to use caution when prescribing it for patients unused to the drug—particularly during drug initiation, conversion from another opioid, or titration upward. Patients should be cautioned to take the drug exactly as prescribed. The advisory also recommended a new maximum initial dose of 30 mg per day (typically prescribed 10 mg tid), when initiating methadone for pain management.
Jean Youngwerth, MD, associate program director of the University of Colorado at Denver and Health Sciences Center, is well aware of the benefits and risks of prescribing methadone in her dual roles as hospitalist and palliative care consultant. “It is a great analgesic, becoming a lot more popular in recent years,” Dr. Youngwerth says. “It’s also ridiculously cheap [often under a dollar a day], which is an important consideration for some of our patients returning home with chronic pain. For other patients, it’s an extra analgesic tool, giving good pain relief, especially for refractory somatic or neuropathic pain.”
But methadone also has downsides. “Its pharmaco-kinetics are so complex and poorly understood that people unfamiliar with prescribing it can get in trouble in a hurry,” Dr. Youngwerth says. “You can kill people with oversedation. I do not prescribe it in my hospitalist practice and I discourage other hospitalists from prescribing it for their patients without consulting a pain or palliative care specialist. You don’t see its maximal effects until at least three to four days out, and that’s usually too long for the hospitalist. When I start palliative care patients on methadone, I normally keep them in the hospital for three or four days so that I can monitor the effects.”
Dr. Youngwerth believes her experience in pain management justifies prescribing methadone for palliative care patients. Even so, she always calls one of the local physician pain experts she works with or a hospital pharmacist to make sure she is ordering it safely and correctly. “I don’t think doctors should be scared off by all the bad publicity about methadone, but they need to realize these are valid concerns,” she says. “People run into problems when they assume that it is just another opioid.”
Hospitalists must recognize the stark realities of using the drug.
“Methadone is the easiest opioid to kill someone with,” says Gail Gazelle, MD, palliative care physician with MD Can Help and Harvard Medical School in Boston. “At the same time, its unique properties can give analgesic effects you can get from no other drug.”
For hospitalists, these issues are complicated by their short involvement with hospitalized patients, who are quickly prepped for discharge back to various community settings and living situations.
Dr. Gazelle wonders, “Is a short hospital stay the right place to initiate methadone treatment, given all of the complications?” If the answer is yes, communicating with the attending and agreeing on a plan for its continued use after discharge from the hospital are essential.
Although narcotic abuse is notoriously difficult to manage, with high relapse rates in every setting, methadone maintenance therapy (MMT) has been shown to reduce overall rates of abuse of other drugs, overdose and death, criminal activity, needle sharing, and commercial sex work. Methadone maintenance is a long-term strategy. The drug is provided as a substitute, not a cure, for narcotic abuse. Patients may continue to receive their daily maintenance dose for years. One-year retention rates in several large studies of MMT have ranged from 25% to 60%, while rates of relapse after leaving MMT are high. Stopping methadone use poses the same challenges as quitting any narcotic and should only be done under a doctor’s care.
Methadone is also used to treat heroin withdrawal, an issue for some hospitalized patients. Prescribing methadone for maintenance therapy is limited to federally licensed methadone treatment programs.
Complications
There are several critical facets of this drug hospitalists must be aware of:
Unpredictable half-life: Methadone, relative to other opioids, has high lipid solubility, slow metabolism, and a typical half-life ranging from 15 to 60 hours—although it can be longer. Methadone’s analgesic effect is shorter-lived, so analgesic doses should be given two, three, or four times daily. But the longer half-life means it can take three days or more after the initial dose before the drug’s full effect—on respiration for example—is known. That is why therapeutic doses can build to toxic levels. There is also wide variation in its effects among patients. Guidelines suggest titrating methadone upward for increased analgesic effect should not be attempted until at least three days after the first dose.
Respiratory depression: This is an issue when the drug is initiated in an opioid-naïve patient or is too rapidly titrated. Deaths from methadone have been seen at doses once considered safe. Physicians are cautioned to start patients on low doses while using other, short-acting opioids for breakthrough pain and frequently assessing for signs of overdose or respiratory depression, such as difficulty in breathing, shallow breathing, extreme sleepiness, or inability to think, talk, or walk normally.
Effect on heart arrhythmias: Methadone can prolong the QTc interval in heart function, leading to a potentially serious cardiac abnormality known as torsade de pointes. The potential for cardiac deaths is another complicating factor that may contraindicate methadone for patients at risk for developing a prolonged QTc interval, including patients with cardiac hypertrophy, hypokalemia, or hypomagnesemia, or a history of cardiac conduction abnormalities or taking medications affecting cardiac conduction. A current EKG may be an appropriate precaution when initiating methadone in elderly patients who have a cardiac history or are receiving methadone in high doses or by intravenous administration.
Drug interactions: The list of drugs that interact with methadone is long, with potential for unwanted side effects and increased or decreased potency. This list includes most anti-retroviral treatments for HIV; sedatives, tranquilizers, barbiturates, seizure medications, muscle relaxants, or any central nervous system depressants; certain steroids and anti-fungals; even over-the-counter cough and cold medications. Also watch for medications that treat irregular heartbeat or prolong the QTc interval. Pharmaceutical company labels for methadone, as well as the FDA advisory, contain a more complete list of drugs that interact with methadone. Always review with patients the other medications they take, including over-the-counter medications and alternative treatments.
Other complications: Methadone should not be prescribed when opioids in general are contraindicated. It can be a management challenge to convert patients from methadone back to other opioids. Another complication of prescribing methadone is the negative publicity it has received in recent years, combined with the stigma of its associations with drug treatment. Some patients, families, or attending physicians may be leery of using it as a pain reliever. It may not be worth titrating methadone to the correct dose in the hospital if it is going to be discontinued post-discharge.
A series of articles in The Charleston (W.Va.) Gazette starting in June 2006 alerted many to the fact methadone is listed by medical examiners nationwide as a cause of death more often than any other prescription pain reliever.10 Methadone was implicated in nearly 4,000 deaths in 2006, four times as many as in 1999. Most of the deaths were considered accidental, and many involved combinations with other drugs—although some were in patients taking methadone as prescribed.
Hospitalists can expect that the diverse caseloads they see likely will include some patients taking methadone. Some may be getting it as an analgesic prescribed by a community physician, pain clinic, or hospice. Others in MMT and receiving a daily dose to manage their addiction disorder may present at the hospital with a different medical problem and perhaps new pain issues.
The hospitalist should not take it for granted that patients on MMT are not also intoxicated or abusing methadone or other drugs, says Michael Weaver, MD, pain and addiction specialist at Virginia Commonwealth University Medical Center in Richmond. Nor should they assume MMT doses are providing adequate analgesia.
“The bottom line in all of these situations is communication,” Dr. Weaver says. Talk to the medical director of the methadone clinic or the community physician who prescribed methadone as an analgesic. Verify the patient’s status, confirm dosage, and discuss the pain issues that need to be addressed—while recognizing pain relief is an appropriate expectation of any hospitalized patient, regardless of drug history or treatment.
Generally, Dr. Weaver says, the maintenance dose of methadone would continue during the hospital stay, and a different analgesic would be ordered for the pain—although the clinic physician may have other ideas. Changing methadone dose or schedule—or attempting to wean a patient off methadone—is not a decision a hospitalist should make unilaterally.11
Methadone’s Merits
Why would a hospitalist want to prescribe a drug that comes with so many caveats?
Carol Jessop, MD, a hospitalist and palliative care consultant at Alta Bates Summit Medical Center in Berkeley, Calif., uses methadone—often in combination with the anti-depressant desipramine or the anticonvulsant gabapentin—to treat complex regional pain syndromes and neuropathic pain.
Dr. Jessop carefully assesses patients for neuropathic pain, listening for descriptors such as burning, stinging, or numbing. These are the patients for whom she most often receives palliative care consultations, often following years of out-of-control pain or lack of response to high doses of other opioids. “My job is much easier now that I understand the difference between nocioceptive and neuropathic pain,” she notes.
“I think methadone is magic, perhaps due to its effect on the NMDA (n-methyl, d-asparte) receptors,” Dr. Jessop says. “I’m also convinced from my clinical experience that there can be nerve healing going on when these pain syndromes are effectively treated. I had a patient with horrible phantom pain following multiple hip surgeries and amputation of his leg. He was referred by a family practitioner, who said, ‘I cannot get this man’s pain under control.’ ” The patient’s pain is now controlled with methadone, 30 mg three times a day. He rarely needs to take his hydromorphone (Dilaudid) for breakthrough pain, and he is able to use his prosthetic leg—which would have been unthinkable before.
Dr. Jessop believes low doses of methadone—even lower than the conversion charts recommend—can have a big effect. “I don’t have problems with methadone because I’m so careful in prescribing it,” she says. “I also work closely with the attending physician and give patients my cell phone number when they return home. It is important to get the family involved and to be clear about the risks and benefits.”
Brad Stuart, MD, senior medical director of Sutter VNA and Hospice in Northern California, also believes methadone can be a wonderful pain management tool. “There is no substitute, in my estimation, to adding a little methadone to the opioid regimen—even just 5 mg of liquid three times a day—for difficult neuropathic pain cases,” Dr. Stuart says. “It’s true that you don’t want to raise the dose too quickly. But I find that it’s unusual not to see benefit in these kinds of patients. I disagree with those who would advise hospitalists to stay away from methadone for treating refractory neuropathic pain. If you start slow and go slow, the risks are small relative to the gain.”
Eduardo Bruera, MD, a palliative care physician at M.D. Anderson Cancer Center in Houston, is another believer in methadone for difficult pain cases, although he emphasizes that his experience is limited to the pain associated with cancer. Dr. Bruera does not use methadone as a first-line analgesic, but he finds it effective when other opioids have not been. “Patients who continue to have a lot of pain after multiple escalating opioid doses or signs of opioid toxicity may be signaling that the opioid you’re using is not working,” he says. “If we make three or four dose changes without response, it’s time to change the opioid.”
Dr. Bruera acknowledges that persuasive research studies to establish methadone’s purported efficacy in treating neuropathic pain have not been conducted. “Unfortunately, methadone is an orphan drug, so we don’t know who would pay for those studies. Should we consider it as a first-line opioid for cancer pain? Again, that is an unanswered question.”
Dr. Bruera has been involved in a number of the few published studies and reviews of methadone’s analgesic efficacy, and he is engaged in ongoing orphan drug status research.12, 13
Methadone as Analgesic
Stephen Bekanich, MD, hospitalist and palliative care consultant at the University of Utah Medical Center in Salt Lake City, falls in the middle range of opinions on methadone.
“From the hospitalist’s standpoint, there are downsides,” Dr. Bekanich says. “People who don’t understand how to titrate it may change doses on a daily basis or more often, which is dangerous. They may not understand the dosing equivalents or pay enough attention to drug interactions.
“Of all the opioids, careful assessment and follow-up may be the most important with methadone. Always make sure you have concrete post-discharge plans. If I didn’t have a pharmacist to collaborate with, as a hospitalist I’d probably stay away from it. But it’s different when I put on my palliative care hat.”
Rachelle Bernacki, MD, a hospitalist, palliative care physician and geriatrician at the University of California-San Francisco Medical Center, agrees methadone can be a useful analgesic—particularly when other opioids have failed to relieve the pain. “But I don’t start with it; I may add a small dose of methadone to the existing regimen for complex pain,” she says.
“I caution my residents not to try methadone without consulting with someone familiar with the drug,” explains Dr. Bernacki, who adds that she is fortunate to work with a pharmacist at UCSF who is an expert in pain management and palliative medicine. “Having taught residents, I can confirm that there is a lot of confusion about its use. But I have also used methadone in my outpatient geriatric practice—with fantastic results.”
Paresh Patel, MD, a hospitalist at VCU Medical Center, says he and his colleagues use methadone as a second-line analgesic when pain is not well managed with morphine. He always keeps an eye out for the risks, including potential interactions with psychiatric medications and the need to look at EKGs.
Dr. Patel says conversion from other opioids is one of the biggest challenges in using methadone. He is not satisfied with the various published opioid conversion charts and relies on experience and trial and error. “I always wait 48 hours before titrating up,” he says.
More research is needed in this area, Dr. Patel says, and he is thinking of getting involved in a methadone research project. TH
Larry Beresford is a frequent contributor to The Hospitalist.
References
- Food and Drug Administration. FDA Public Health Advisory: Methadone use for pain control may result in death and life-threatening changes in breathing and heart beat. Available at: www.fda.gov/cder/drug/advisory/methadone.htm. Last accessed June 4, 2007.
- Moulin DE, Palma D, Watling C, et al. Methadone in the management of intractable neuropathic noncancer pain. Can J Neurol Sci. 2005 Aug: 32(3); 340-343.
- Altier N, Dion D, Boulanger A, et al. Management of chronic neuropathic pain with methadone: A review of 13 cases. Clin J Pain. 2005 Jul-Aug;21(4):364-369.
- Morley JS, Bridson J, Nash TP, et al. Low-dose methadone has an analgesic effect in neuropathic pain: A double-blind randomized controlled crossover trial. Palliat Med. 2003 Oct;17(7):576-587.
- Lawlor PG, Turner KS, Hanson J, et al. Dose ratio between morphine and methadone in patients with cancer pain: A retrospective study. Cancer. 1998 Mar;82(6):1167-1173.
- Ripamonti C, De Conno F, Groff L, et al. Equianal-gesic dose/ratio between methadone and other opioid agonists in cancer pain: Comparison of two clinical experiences. Ann Oncol. 1998 Jan;9(1):79-83.
- Gazelle G, Fine PG. Fast Fact and Concept #75: Methadone for the treatment of pain. End-of-Life/Palliative Education Resource Center, Medical College of Wisconsin, Milwaukee, www.eperc.mcw.edu/ff_index.htm; and Roxane Laboratories, Inc., label for dolophine hydrochloride CH (methadone hydrochloride tablets).
- American Methadone Treatment Association. 1998 Methadone Maintenance Program and Patient Census in the U.S., New York, NY, April 1999.
- Office of National Drug Control Policy. Fact sheet. Available at: www.whitehousedrugpolicy.gov. Last accessed June 4, 2007.
- Finn S, Tuckwiller T. The Killer Cure. The Charlotte (W. Va.) Gazette. Available at: www.wvgazette.com. Last accessed June 29, 2007.
- Weaver MF, Schnoll SH. Opioid treatment of chronic pain in patients with addiction. J Pain Palliat Care Pharmacother. 2002:16(3);5-26.
- Bruera E, Sweeney C. Methadone use in cancer patients with pain: A review. J Palliat Med. 2002 Feb;5(1):127-137.
- Bruera E, Palmer JL, Bosnjak S, et al. Methadone versus morphine as a first-line strong opioid for cancer pain: A randomized, double-blind study. J Clin Oncol. 2004 Jan 1;22(1):185-192.
Pain at the Pump
Patient-controlled analgesia (PCA), well accepted and widely used to quickly ease post-operative and acute pain, is safe and effective—in skilled hands. But there are complications, caveats, and safety concerns hospitalists should consider to incorporate this tool into their pain management routines and hospital protocols.
Studies show patients prefer the PCA compared with other analgesic routes.1-2 Less clear is whether it is more effective or leads to lower opioid use.
Some hospitalists use the PCA for their patients with pain—others defer to anesthesiologists, pain services, or palliative care consultants to manage the PCA and its multifaceted dosing requirements.
“There are a lot of misconceptions about the PCA,” says Deb Gordon, RN, MS, FAAN, senior clinical nurse specialist and pain consultant at the University of Wisconsin (UW) Medical Center in Madison. “There is a misunderstanding that the PCA is a magic black box for pain relief,” which can lead to its overuse. As a general rule of pain management, patients prefer the oral route of analgesic administration, Gordon says, unless that is a problem or rapid titration is needed.
“I don’t think [the PCA is] rocket science—it’s just a tool to deliver analgesics conveniently,” Gordon says. “I think every hospitalist should learn how to use the PCA, but there are always nuances of how to titrate opioids by any route.” UW has implemented PCA protocols, which staff can use for ballpark dosing recommendations.
How Hospitalists Use the PCA
The PCA delivers pain medication intravenously via a computerized pump with a button the patient can press when needed—without waiting for busy nurses to answer a call button and then confirm, prepare, and administer an analgesic treatment.
Hospitalists at UW, including Rob Hoffman, MD, often order the PCA. “It’s very well-liked by patients, who are not dependent on a busy nurse to get their analgesics administered,” Dr. Hoffman says. “The biggest concern, involving overdosing patients who are opioid-naïve, may be somewhat overblown. I haven’t experienced problems with my patients being over narcotized, but I start with a low dose and monitor them frequently.”
PCA technology can tabulate how much analgesic the patient has received during the previous 24 hours, Dr. Hoffman notes. “You know that’s a safe dose for the patient, and you can use it to make the transition to oral medications,” he says.
“Most of the patients I have on PCAs are palliative care patients,” says Rachelle Bernacki, MD, MS, a hospitalist, palliative care physician, and geriatrician at the University of California-San Francisco Medical Center. “I use it somewhat differently for the patients in my hospitalist practice—for example, for those who are experiencing intermittent, unpredictable episodes of abdominal pain. It’s also useful for patients with a need to feel in control of their situation. For constant, predictable pain, it’s better to use an around-the-clock schedule. I also send certain patients home on PCAs, especially if they are going to hospice care.”
Dr. Bernacki notes that some of her patients kiss the PCA button as if it were a long-lost friend, including one she recalls who had a bowel obstruction and had not found relief prior to starting on the PCA. But she also recalls a patient for whom the PCA was not a solution. “He was Cantonese-speaking,” she says. “Despite the presence of an interpreter and several attempts at education, he was never able to understand the connection between the PCA button and relief for his pain. We just couldn’t cross the cultural and language barriers.”
Hospitalists probably underuse the PCA, says Mahmood Shahlapour, MD, hospitalist and palliative care consultant at Chandler Regional Hospital in Chandler, Ariz. “Some hospitalists may feel uncomfortable with it,” he says. “I think it’s important for hospitalists to try to get more experience and comfort to be able to use it for the right patient and the right setting.”
What Is the PCA?
PCA technology as we know it today was pioneered in the early 1970s. Now it’s routine for post-surgical pain management. It is used for patients who have trouble taking oral medications or who need rapid response to acute pain crises. Increasingly, it is also used for patients with moderate to severe chronic pain related to cancer or who are being followed by hospice or palliative care services.
PCA refers both to the process of patient self-administration of parenteral analgesics and to the computerized infusion pump that makes this control possible. Recent advances in pain management also include patient-controlled epidural and transdermal analgesia systems—and other new pain modalities continue to be developed.3 Patients unable to operate the equipment themselves—for example, neonates or infants—may receive nurse-controlled analgesia, but experts say this should only be done within carefully defined parameters.
With the more typical intravenous PCA, the computerized pump allows for a number of variables, including:
- An initial bolus or loading dose to bring the pain under immediate control—an important but sometimes overlooked consideration in the successful use of PCAs;
- The patient-initiated or demand dose, available to the patient at the press of a button;
- The delay interval or lockout, typically between six and 15 minutes, allowing the analgesic to achieve its peak effect before another dose can be administered. The number of unsuccessful demands by patients during lockout periods is important for the physician to know;
- A continuous infusion or basal rate to provide continuous pain relief, although this may be contraindicated for opioid-naïve patients starting on PCAs.4 For those receiving opioids for chronic pain, the basal rate could be their current analgesic dose converted to the intravenous equivalent. Alternatively, the patient could receive this dose in a long-acting oral analgesic, with the PCA used for incidental or breakthrough pain. A basal rate also helps patients sleep, their pain controlled without having to wake up to press for a dose;
- A maximum volume of drug to be administered within a defined period of one, four, eight, or 24 hours, calculated to prevent an opioid overdose—regardless of how many times the PCA button gets pushed; and
- Monitoring devices such as pulse oximeter or end-tidal carbon dioxide monitor may be part of the PCA system to help warn of emerging respiratory depression.
The fundamental challenge for physicians lies in balancing the loading, basal, and patient-initiated doses with an appropriate maximum to make sure the patient gets adequate pain relief but doesn’t overdose. This is a more complex, multifaceted mathematical formula than ordering opioids to be administered two, three, or four times a day.
A basic safeguard of the PCA for preventing overdose is that when the opioid analgesic starts to make the patient drowsy, he or she is likely to stop pressing the button for another dose. However, for this to work, the PCA must be patient-controlled. If a nurse or family member pushes the button on the patient’s behalf out of a well-meaning desire to keep pain in check, this raises the risk of overdose.
In the past few years, several national quality and safety organizations have issued alerts about the danger of such patient-controlled analgesia by proxy. The Institute for Safe Medication Practices (ISMP) in Huntington Valley, Pa., issued two safety alerts in July 2003 discussing how potentially life-threatening errors can occur with PCAs and offering ways to prevent such errors.
U.S. Pharmacopeia’s summer 2004 USP Quality Review also offered safety recommendations based on analysis of medical errors directly resulting from PCA by proxy. The Joint Commission issued a Sentinel Alert on Dec. 20, 2004, noting that “serious adverse effects can occur when family members, caregivers or clinicians who are not authorized become involved in administering the analgesic for the patient by proxy.”5 Earlier this year the American Society for Pain Management Nursing issued clinical practice recommendations for how nurses can deal with the problem of PCA by proxy.6
Well-designed hospital PCA protocols will address this problem by including clear instructions to family members not to push the button for the patient, with an explanation of why this can be dangerous. Printed brochures and signs in the patient’s room are also helpful.
The Need for Training
“Physicians, as a rule, don’t receive adequate training in the PCA,” says Jean Youngwerth, MD, hospitalist, palliative care consultant and fellowship associate director at the University of Colorado Health Sciences Center in Denver. “Then you’re expected to know how to use it. There clearly is a need for this kind of training in the basics of the PCA, but a brief in-service should be sufficient.”
Dan Johnson, MD, regional department chief for palliative care for Kaiser-Permanente in Colorado, says the level of experience with the PCA is highly variable among physicians he works with. “Some know how to use the PCA and actually do it quite well. Many others are not adequately trained,” he says. “When I test residents with a few questions, they customarily do very poorly. Some of the answers I see make me nervous.”
Dr. Johnson offers a refresher on the PCA for hospitalists in the Denver area who attend an annual palliative care retreat. Those who come regularly seem to retain the information he offers. “If I were in a hospital that had not rolled out PCA standing orders, I’d make sure that there were educational units provided for hospitalists,” he says. “I’d also investigate how to develop standing orders for the hospital.” TH
Larry Beresford is a frequent contributor to The Hospitalist.
References
- Hudcova J, McNicol E, Quah C, et al. Patient controlled opioid analgesia versus conventional opioid analgesia for postoperative pain. Cochrane Database Syst Rev. 2006;4.
- Ballantyne JC, Carr DB, Chalmers TC. Postoperative patient-controlled analgesia: Meta-analyses of initial randomized controlled trials. J Clin Anesth. 1993 May/June;5(3):182-193.
- D’Arcy Y. New pain management options: Delivery systems and techniques. Nursing. 2007 February; 37(2):26-27.
- Pasero C, McCaffery M. Safe use of a continuous infusion with IV PCA. J PeriAnesthesia Nursing. 2004 Feb;19(1):42-45.
- Joint Commission. Patient-controlled analgesia by proxy. Available at www.jointcommission.org/SentinelEvents/SentinelEventAlert/sea_33.htm. Last accessed July 12, 2007.
- Wuhrman E, Cooney MF, Dunwoody CJ, et al. Authorized and unauthorized (“PCA by Proxy”) dosing of analgesic infusion pumps: Position statement with clinical practice recommendations. Pain Manag Nurs. 2007 Mar;8(1):4-11.
- Prommer E. Fast Fact and Concept #92, Patient controlled analgesia in palliative care. End-of-Life/ Palliative Education Resource Center, Medical College of Wisconsin, Milwaukee:www.eperc.mcw.edu/ff_index.htm.
- Owen H, Plummer JL, Armstrong I, et al. Variables of patient-controlled analgesia. 1. Bolus size. Anaesthesia.1989 Jan.;44(1):7-10.
- Vicente KJ, Kada-Bekhaled K, Hillel G, et al. Programming errors contribute to death from patient-controlled analgesia. Can J Anesth. 2003;50:328-332.
Patient-controlled analgesia (PCA), well accepted and widely used to quickly ease post-operative and acute pain, is safe and effective—in skilled hands. But there are complications, caveats, and safety concerns hospitalists should consider to incorporate this tool into their pain management routines and hospital protocols.
Studies show patients prefer the PCA compared with other analgesic routes.1-2 Less clear is whether it is more effective or leads to lower opioid use.
Some hospitalists use the PCA for their patients with pain—others defer to anesthesiologists, pain services, or palliative care consultants to manage the PCA and its multifaceted dosing requirements.
“There are a lot of misconceptions about the PCA,” says Deb Gordon, RN, MS, FAAN, senior clinical nurse specialist and pain consultant at the University of Wisconsin (UW) Medical Center in Madison. “There is a misunderstanding that the PCA is a magic black box for pain relief,” which can lead to its overuse. As a general rule of pain management, patients prefer the oral route of analgesic administration, Gordon says, unless that is a problem or rapid titration is needed.
“I don’t think [the PCA is] rocket science—it’s just a tool to deliver analgesics conveniently,” Gordon says. “I think every hospitalist should learn how to use the PCA, but there are always nuances of how to titrate opioids by any route.” UW has implemented PCA protocols, which staff can use for ballpark dosing recommendations.
How Hospitalists Use the PCA
The PCA delivers pain medication intravenously via a computerized pump with a button the patient can press when needed—without waiting for busy nurses to answer a call button and then confirm, prepare, and administer an analgesic treatment.
Hospitalists at UW, including Rob Hoffman, MD, often order the PCA. “It’s very well-liked by patients, who are not dependent on a busy nurse to get their analgesics administered,” Dr. Hoffman says. “The biggest concern, involving overdosing patients who are opioid-naïve, may be somewhat overblown. I haven’t experienced problems with my patients being over narcotized, but I start with a low dose and monitor them frequently.”
PCA technology can tabulate how much analgesic the patient has received during the previous 24 hours, Dr. Hoffman notes. “You know that’s a safe dose for the patient, and you can use it to make the transition to oral medications,” he says.
“Most of the patients I have on PCAs are palliative care patients,” says Rachelle Bernacki, MD, MS, a hospitalist, palliative care physician, and geriatrician at the University of California-San Francisco Medical Center. “I use it somewhat differently for the patients in my hospitalist practice—for example, for those who are experiencing intermittent, unpredictable episodes of abdominal pain. It’s also useful for patients with a need to feel in control of their situation. For constant, predictable pain, it’s better to use an around-the-clock schedule. I also send certain patients home on PCAs, especially if they are going to hospice care.”
Dr. Bernacki notes that some of her patients kiss the PCA button as if it were a long-lost friend, including one she recalls who had a bowel obstruction and had not found relief prior to starting on the PCA. But she also recalls a patient for whom the PCA was not a solution. “He was Cantonese-speaking,” she says. “Despite the presence of an interpreter and several attempts at education, he was never able to understand the connection between the PCA button and relief for his pain. We just couldn’t cross the cultural and language barriers.”
Hospitalists probably underuse the PCA, says Mahmood Shahlapour, MD, hospitalist and palliative care consultant at Chandler Regional Hospital in Chandler, Ariz. “Some hospitalists may feel uncomfortable with it,” he says. “I think it’s important for hospitalists to try to get more experience and comfort to be able to use it for the right patient and the right setting.”
What Is the PCA?
PCA technology as we know it today was pioneered in the early 1970s. Now it’s routine for post-surgical pain management. It is used for patients who have trouble taking oral medications or who need rapid response to acute pain crises. Increasingly, it is also used for patients with moderate to severe chronic pain related to cancer or who are being followed by hospice or palliative care services.
PCA refers both to the process of patient self-administration of parenteral analgesics and to the computerized infusion pump that makes this control possible. Recent advances in pain management also include patient-controlled epidural and transdermal analgesia systems—and other new pain modalities continue to be developed.3 Patients unable to operate the equipment themselves—for example, neonates or infants—may receive nurse-controlled analgesia, but experts say this should only be done within carefully defined parameters.
With the more typical intravenous PCA, the computerized pump allows for a number of variables, including:
- An initial bolus or loading dose to bring the pain under immediate control—an important but sometimes overlooked consideration in the successful use of PCAs;
- The patient-initiated or demand dose, available to the patient at the press of a button;
- The delay interval or lockout, typically between six and 15 minutes, allowing the analgesic to achieve its peak effect before another dose can be administered. The number of unsuccessful demands by patients during lockout periods is important for the physician to know;
- A continuous infusion or basal rate to provide continuous pain relief, although this may be contraindicated for opioid-naïve patients starting on PCAs.4 For those receiving opioids for chronic pain, the basal rate could be their current analgesic dose converted to the intravenous equivalent. Alternatively, the patient could receive this dose in a long-acting oral analgesic, with the PCA used for incidental or breakthrough pain. A basal rate also helps patients sleep, their pain controlled without having to wake up to press for a dose;
- A maximum volume of drug to be administered within a defined period of one, four, eight, or 24 hours, calculated to prevent an opioid overdose—regardless of how many times the PCA button gets pushed; and
- Monitoring devices such as pulse oximeter or end-tidal carbon dioxide monitor may be part of the PCA system to help warn of emerging respiratory depression.
The fundamental challenge for physicians lies in balancing the loading, basal, and patient-initiated doses with an appropriate maximum to make sure the patient gets adequate pain relief but doesn’t overdose. This is a more complex, multifaceted mathematical formula than ordering opioids to be administered two, three, or four times a day.
A basic safeguard of the PCA for preventing overdose is that when the opioid analgesic starts to make the patient drowsy, he or she is likely to stop pressing the button for another dose. However, for this to work, the PCA must be patient-controlled. If a nurse or family member pushes the button on the patient’s behalf out of a well-meaning desire to keep pain in check, this raises the risk of overdose.
In the past few years, several national quality and safety organizations have issued alerts about the danger of such patient-controlled analgesia by proxy. The Institute for Safe Medication Practices (ISMP) in Huntington Valley, Pa., issued two safety alerts in July 2003 discussing how potentially life-threatening errors can occur with PCAs and offering ways to prevent such errors.
U.S. Pharmacopeia’s summer 2004 USP Quality Review also offered safety recommendations based on analysis of medical errors directly resulting from PCA by proxy. The Joint Commission issued a Sentinel Alert on Dec. 20, 2004, noting that “serious adverse effects can occur when family members, caregivers or clinicians who are not authorized become involved in administering the analgesic for the patient by proxy.”5 Earlier this year the American Society for Pain Management Nursing issued clinical practice recommendations for how nurses can deal with the problem of PCA by proxy.6
Well-designed hospital PCA protocols will address this problem by including clear instructions to family members not to push the button for the patient, with an explanation of why this can be dangerous. Printed brochures and signs in the patient’s room are also helpful.
The Need for Training
“Physicians, as a rule, don’t receive adequate training in the PCA,” says Jean Youngwerth, MD, hospitalist, palliative care consultant and fellowship associate director at the University of Colorado Health Sciences Center in Denver. “Then you’re expected to know how to use it. There clearly is a need for this kind of training in the basics of the PCA, but a brief in-service should be sufficient.”
Dan Johnson, MD, regional department chief for palliative care for Kaiser-Permanente in Colorado, says the level of experience with the PCA is highly variable among physicians he works with. “Some know how to use the PCA and actually do it quite well. Many others are not adequately trained,” he says. “When I test residents with a few questions, they customarily do very poorly. Some of the answers I see make me nervous.”
Dr. Johnson offers a refresher on the PCA for hospitalists in the Denver area who attend an annual palliative care retreat. Those who come regularly seem to retain the information he offers. “If I were in a hospital that had not rolled out PCA standing orders, I’d make sure that there were educational units provided for hospitalists,” he says. “I’d also investigate how to develop standing orders for the hospital.” TH
Larry Beresford is a frequent contributor to The Hospitalist.
References
- Hudcova J, McNicol E, Quah C, et al. Patient controlled opioid analgesia versus conventional opioid analgesia for postoperative pain. Cochrane Database Syst Rev. 2006;4.
- Ballantyne JC, Carr DB, Chalmers TC. Postoperative patient-controlled analgesia: Meta-analyses of initial randomized controlled trials. J Clin Anesth. 1993 May/June;5(3):182-193.
- D’Arcy Y. New pain management options: Delivery systems and techniques. Nursing. 2007 February; 37(2):26-27.
- Pasero C, McCaffery M. Safe use of a continuous infusion with IV PCA. J PeriAnesthesia Nursing. 2004 Feb;19(1):42-45.
- Joint Commission. Patient-controlled analgesia by proxy. Available at www.jointcommission.org/SentinelEvents/SentinelEventAlert/sea_33.htm. Last accessed July 12, 2007.
- Wuhrman E, Cooney MF, Dunwoody CJ, et al. Authorized and unauthorized (“PCA by Proxy”) dosing of analgesic infusion pumps: Position statement with clinical practice recommendations. Pain Manag Nurs. 2007 Mar;8(1):4-11.
- Prommer E. Fast Fact and Concept #92, Patient controlled analgesia in palliative care. End-of-Life/ Palliative Education Resource Center, Medical College of Wisconsin, Milwaukee:www.eperc.mcw.edu/ff_index.htm.
- Owen H, Plummer JL, Armstrong I, et al. Variables of patient-controlled analgesia. 1. Bolus size. Anaesthesia.1989 Jan.;44(1):7-10.
- Vicente KJ, Kada-Bekhaled K, Hillel G, et al. Programming errors contribute to death from patient-controlled analgesia. Can J Anesth. 2003;50:328-332.
Patient-controlled analgesia (PCA), well accepted and widely used to quickly ease post-operative and acute pain, is safe and effective—in skilled hands. But there are complications, caveats, and safety concerns hospitalists should consider to incorporate this tool into their pain management routines and hospital protocols.
Studies show patients prefer the PCA compared with other analgesic routes.1-2 Less clear is whether it is more effective or leads to lower opioid use.
Some hospitalists use the PCA for their patients with pain—others defer to anesthesiologists, pain services, or palliative care consultants to manage the PCA and its multifaceted dosing requirements.
“There are a lot of misconceptions about the PCA,” says Deb Gordon, RN, MS, FAAN, senior clinical nurse specialist and pain consultant at the University of Wisconsin (UW) Medical Center in Madison. “There is a misunderstanding that the PCA is a magic black box for pain relief,” which can lead to its overuse. As a general rule of pain management, patients prefer the oral route of analgesic administration, Gordon says, unless that is a problem or rapid titration is needed.
“I don’t think [the PCA is] rocket science—it’s just a tool to deliver analgesics conveniently,” Gordon says. “I think every hospitalist should learn how to use the PCA, but there are always nuances of how to titrate opioids by any route.” UW has implemented PCA protocols, which staff can use for ballpark dosing recommendations.
How Hospitalists Use the PCA
The PCA delivers pain medication intravenously via a computerized pump with a button the patient can press when needed—without waiting for busy nurses to answer a call button and then confirm, prepare, and administer an analgesic treatment.
Hospitalists at UW, including Rob Hoffman, MD, often order the PCA. “It’s very well-liked by patients, who are not dependent on a busy nurse to get their analgesics administered,” Dr. Hoffman says. “The biggest concern, involving overdosing patients who are opioid-naïve, may be somewhat overblown. I haven’t experienced problems with my patients being over narcotized, but I start with a low dose and monitor them frequently.”
PCA technology can tabulate how much analgesic the patient has received during the previous 24 hours, Dr. Hoffman notes. “You know that’s a safe dose for the patient, and you can use it to make the transition to oral medications,” he says.
“Most of the patients I have on PCAs are palliative care patients,” says Rachelle Bernacki, MD, MS, a hospitalist, palliative care physician, and geriatrician at the University of California-San Francisco Medical Center. “I use it somewhat differently for the patients in my hospitalist practice—for example, for those who are experiencing intermittent, unpredictable episodes of abdominal pain. It’s also useful for patients with a need to feel in control of their situation. For constant, predictable pain, it’s better to use an around-the-clock schedule. I also send certain patients home on PCAs, especially if they are going to hospice care.”
Dr. Bernacki notes that some of her patients kiss the PCA button as if it were a long-lost friend, including one she recalls who had a bowel obstruction and had not found relief prior to starting on the PCA. But she also recalls a patient for whom the PCA was not a solution. “He was Cantonese-speaking,” she says. “Despite the presence of an interpreter and several attempts at education, he was never able to understand the connection between the PCA button and relief for his pain. We just couldn’t cross the cultural and language barriers.”
Hospitalists probably underuse the PCA, says Mahmood Shahlapour, MD, hospitalist and palliative care consultant at Chandler Regional Hospital in Chandler, Ariz. “Some hospitalists may feel uncomfortable with it,” he says. “I think it’s important for hospitalists to try to get more experience and comfort to be able to use it for the right patient and the right setting.”
What Is the PCA?
PCA technology as we know it today was pioneered in the early 1970s. Now it’s routine for post-surgical pain management. It is used for patients who have trouble taking oral medications or who need rapid response to acute pain crises. Increasingly, it is also used for patients with moderate to severe chronic pain related to cancer or who are being followed by hospice or palliative care services.
PCA refers both to the process of patient self-administration of parenteral analgesics and to the computerized infusion pump that makes this control possible. Recent advances in pain management also include patient-controlled epidural and transdermal analgesia systems—and other new pain modalities continue to be developed.3 Patients unable to operate the equipment themselves—for example, neonates or infants—may receive nurse-controlled analgesia, but experts say this should only be done within carefully defined parameters.
With the more typical intravenous PCA, the computerized pump allows for a number of variables, including:
- An initial bolus or loading dose to bring the pain under immediate control—an important but sometimes overlooked consideration in the successful use of PCAs;
- The patient-initiated or demand dose, available to the patient at the press of a button;
- The delay interval or lockout, typically between six and 15 minutes, allowing the analgesic to achieve its peak effect before another dose can be administered. The number of unsuccessful demands by patients during lockout periods is important for the physician to know;
- A continuous infusion or basal rate to provide continuous pain relief, although this may be contraindicated for opioid-naïve patients starting on PCAs.4 For those receiving opioids for chronic pain, the basal rate could be their current analgesic dose converted to the intravenous equivalent. Alternatively, the patient could receive this dose in a long-acting oral analgesic, with the PCA used for incidental or breakthrough pain. A basal rate also helps patients sleep, their pain controlled without having to wake up to press for a dose;
- A maximum volume of drug to be administered within a defined period of one, four, eight, or 24 hours, calculated to prevent an opioid overdose—regardless of how many times the PCA button gets pushed; and
- Monitoring devices such as pulse oximeter or end-tidal carbon dioxide monitor may be part of the PCA system to help warn of emerging respiratory depression.
The fundamental challenge for physicians lies in balancing the loading, basal, and patient-initiated doses with an appropriate maximum to make sure the patient gets adequate pain relief but doesn’t overdose. This is a more complex, multifaceted mathematical formula than ordering opioids to be administered two, three, or four times a day.
A basic safeguard of the PCA for preventing overdose is that when the opioid analgesic starts to make the patient drowsy, he or she is likely to stop pressing the button for another dose. However, for this to work, the PCA must be patient-controlled. If a nurse or family member pushes the button on the patient’s behalf out of a well-meaning desire to keep pain in check, this raises the risk of overdose.
In the past few years, several national quality and safety organizations have issued alerts about the danger of such patient-controlled analgesia by proxy. The Institute for Safe Medication Practices (ISMP) in Huntington Valley, Pa., issued two safety alerts in July 2003 discussing how potentially life-threatening errors can occur with PCAs and offering ways to prevent such errors.
U.S. Pharmacopeia’s summer 2004 USP Quality Review also offered safety recommendations based on analysis of medical errors directly resulting from PCA by proxy. The Joint Commission issued a Sentinel Alert on Dec. 20, 2004, noting that “serious adverse effects can occur when family members, caregivers or clinicians who are not authorized become involved in administering the analgesic for the patient by proxy.”5 Earlier this year the American Society for Pain Management Nursing issued clinical practice recommendations for how nurses can deal with the problem of PCA by proxy.6
Well-designed hospital PCA protocols will address this problem by including clear instructions to family members not to push the button for the patient, with an explanation of why this can be dangerous. Printed brochures and signs in the patient’s room are also helpful.
The Need for Training
“Physicians, as a rule, don’t receive adequate training in the PCA,” says Jean Youngwerth, MD, hospitalist, palliative care consultant and fellowship associate director at the University of Colorado Health Sciences Center in Denver. “Then you’re expected to know how to use it. There clearly is a need for this kind of training in the basics of the PCA, but a brief in-service should be sufficient.”
Dan Johnson, MD, regional department chief for palliative care for Kaiser-Permanente in Colorado, says the level of experience with the PCA is highly variable among physicians he works with. “Some know how to use the PCA and actually do it quite well. Many others are not adequately trained,” he says. “When I test residents with a few questions, they customarily do very poorly. Some of the answers I see make me nervous.”
Dr. Johnson offers a refresher on the PCA for hospitalists in the Denver area who attend an annual palliative care retreat. Those who come regularly seem to retain the information he offers. “If I were in a hospital that had not rolled out PCA standing orders, I’d make sure that there were educational units provided for hospitalists,” he says. “I’d also investigate how to develop standing orders for the hospital.” TH
Larry Beresford is a frequent contributor to The Hospitalist.
References
- Hudcova J, McNicol E, Quah C, et al. Patient controlled opioid analgesia versus conventional opioid analgesia for postoperative pain. Cochrane Database Syst Rev. 2006;4.
- Ballantyne JC, Carr DB, Chalmers TC. Postoperative patient-controlled analgesia: Meta-analyses of initial randomized controlled trials. J Clin Anesth. 1993 May/June;5(3):182-193.
- D’Arcy Y. New pain management options: Delivery systems and techniques. Nursing. 2007 February; 37(2):26-27.
- Pasero C, McCaffery M. Safe use of a continuous infusion with IV PCA. J PeriAnesthesia Nursing. 2004 Feb;19(1):42-45.
- Joint Commission. Patient-controlled analgesia by proxy. Available at www.jointcommission.org/SentinelEvents/SentinelEventAlert/sea_33.htm. Last accessed July 12, 2007.
- Wuhrman E, Cooney MF, Dunwoody CJ, et al. Authorized and unauthorized (“PCA by Proxy”) dosing of analgesic infusion pumps: Position statement with clinical practice recommendations. Pain Manag Nurs. 2007 Mar;8(1):4-11.
- Prommer E. Fast Fact and Concept #92, Patient controlled analgesia in palliative care. End-of-Life/ Palliative Education Resource Center, Medical College of Wisconsin, Milwaukee:www.eperc.mcw.edu/ff_index.htm.
- Owen H, Plummer JL, Armstrong I, et al. Variables of patient-controlled analgesia. 1. Bolus size. Anaesthesia.1989 Jan.;44(1):7-10.
- Vicente KJ, Kada-Bekhaled K, Hillel G, et al. Programming errors contribute to death from patient-controlled analgesia. Can J Anesth. 2003;50:328-332.
Heal the Whole Hurt
Note: This is Part 3 of The Hospitalist’s series on pain and hospital medicine. Part 1 appeared on p. 45 of the April issue, and Part 2 appeared on p. 33 of the June issue.
Hospitalists face demands for pain care every day. Usually, the general pain principles described in the first two articles in this series and the use of a few opioid analgesics with which the hospitalist has become familiar can supply relief.
But what about the more difficult cases in which psychosocial influences or a history of substance abuse complicates the patient’s pain? Perhaps it is a chronic pain case that has never been adequately addressed, or the patient keeps turning up in the emergency department (ED) complaining of out-of-control pain. Other examples of difficult-to-manage pain include complex regional pain syndrome, post-herpetic neuralgia, other neuropathic pains, sickle cell anemia, and patients at high risk of opioid toxicity.
These cases are like a leaky bucket for the hospital—costly, frustrating, unsatisfying to the patient, and prone to bad outcomes, says Jerry Wesch, PhD, director of the pain service for the Alexian Brothers Health System in greater Chicago. “These are the patients who tend to bedevil everybody in the hospital,” he says.
Dealing with such patients is a demanding task.
“You don’t have chronic pain without a psycho-social-spiritual overlay,” adds Scott Fishman, MD, chief of the Division of Pain Medicine at University of California-Davis in Sacramento. “Their emotional lives are deteriorating. They can’t sleep, they’re depressed, and their physical functioning is also deteriorating. There are all kinds of situations that demand use of a full spectrum of bio-psycho-social interventions in addition to opioid analgesics.”
These complex, unresolved cases are likely to have emotional, social, or spiritual manifestations. But what does that mean to a busy hospitalist with a short window of opportunity to address patients’ pain before pointing them toward discharge? A psychologist, social worker, or chaplain may have something to contribute to pain management. Meanwhile, the rest of the caseload is clamoring for the hospitalist’s attention.
Make Pain Management Multidisciplinary
A dizzying array of pain modalities can be brought to bear on complex pain cases. These range from opioid analgesics to a variety of adjuvant non-opioid medications to interventional techniques involving surgery, spinal injections, nerve blocks, nerve stimulation, and nerve destruction techniques.
There are also complementary methodologies (e.g., acupuncture) that have been shown to reduce the volume of narcotics needed for pain control, even though how they work is not well understood.
But how many hospitalists call on acupuncturists, hypnotists, or teachers of guided-imagery meditation for their patients? Many of these techniques are more appropriately initiated in the outpatient setting, but the hospitalist still has a responsibility to make sure “frequent fliers” with complex pain complaints get connected post-discharge to a pain service that can offer long-term relief. The challenge is applying the acute treatment models of the hospital to chronic pain syndromes that are not optimally addressed in crisis mode.
Jonathan Weston, MD, a hospitalist at Penrose Hospital in Colorado Springs, Colo., says these difficult, chronic pain cases are the bane of the hospitalist’s working life. These patients show up at night in the ED saying, “ ‘I’m in so much pain, please don’t send me home,’ ” he says. “The emergency physician puts them on an IV drip and their pain is relieved for the moment, but only one facet of that pain has been addressed.”
The emergency physician—also under caseload pressure— decides the easiest disposition is to admit the patient and dump the problem on the hospitalist. “They’re out of their pain medications at home, and when you call the attending you are told that they are drug seekers,” Dr. Weston relates. “These patients take a lot of energy. They can be manipulative. We can’t do right for them. It’s not satisfying. We don’t want to round on them. The way we hospitalists manage these patients sometimes reflects not only the patient’s personality, but our personality as well.”
Hospitalists don’t just treat these patients’ pain, they also address their suffering, he says.
High-quality pain management is multidisciplinary, Dr. Weston notes, because pain is multifactorial. The hospitalist occupies an important coordinating position and is charged with responsibility for the whole person during that patient’s brief hospital stay. But there are limits to what the hospitalist can accomplish. A palliative care team or an acute pain service can make important contributions to hospitalized patients’ pain. So can social workers, psychologists, pharmacists, and chaplains. But it is the hospitalist’s responsibility to coordinate these pieces of the pain puzzle for patients on service.
In many hospitals, the palliative care service has been set up to consult on pain, suffering, and clarification of treatment goals for patients nearing the end of life. These services vary from institution to institution in terms of whether they prefer to focus on end-of-life issues or are comfortable fielding other kinds of chronic pain questions. Acute pain services equally vary in terms of whether their focus is primarily on surgical pain “interventions” or on a multidisciplinary approach to pain management.
Ideally, Dr. Weston says, a major hospital would have both services available as resources to the hospitalist. Or, if there is only one of them, it should have a broad approach to pain management. Otherwise, it is up to the hospitalist to pull together a virtual pain team to provide a multidisciplinary response to complex pain.
“I am also board certified in hospice and palliative medicine,” Dr. Weston says. “I can use my medical knowledge to try to get the patient comfortable on oral meds so that they can go home. And I can personally make an appointment for them within 48 hours of discharge with their attending physician or a pain specialist. But for too many patients, this connection never happens.”
“Pain management in general is a hard thing to deal with,” adds Lauren Fraser, MD, regional chief of the department of hospital medicine for Kaiser Permanente Colorado in Denver. “It’s frustrating because you want to do the right thing,” she says. “We need first of all to rule out anything we can fix that might be causing the pain. Then we’re dealing with the patient’s quality of life and the disabling effects of pain. Each patient and family has a different need, and when you meet with them one-on-one you’re dealing with all of it.”
Dr. Fraser doesn’t have access to an acute pain service in her current setting, “although we have interventional folks to put in the PCAs and epidurals. We generally are able to get the services we need, although there would be an advantage to having an identified multidisciplinary pain service to provide the coordination.”
A “Pain Hospitalist”
Jerry Wesch, director of the pain program at Alexian Brothers Hospital Network in Arlington Heights, Ill., recently posted a job listing on the Internet seeking a pain management physician. He is looking for a doctor with an interest in comprehensive, interdisciplinary team management of chronic pain who is “able to function as a pain hospitalist.”
Although the details of this new position are still being finalized and a pain hospitalist would function with a different focus than a generalist hospitalist, Wesch suggests the role has important analogies with what hospitalists like Dr. Weston face in coordinating a virtual team of multidisciplinary pain resources.
Wesch is building an inpatient pain service comprising the pain physician, two nurse practitioners, and a part-time psychologist with full-time presence in two Alexian Brothers acute hospitals. This team would work closely with hospitalists, the palliative care service, and ancillary services such as physical therapy and chaplains.
“This should make us ideal collaborators with the hospitalists, who can just walk down the hall and initiate a pain consult,” he explains. “We’re all working toward the same goal, which is to improve efficiency, medical management, quality of care, and patient satisfaction. A good hospitalist is also my best ally in building a multidisciplinary pain service.”
In other settings, however, it will be the hospitalist’s responsibility to build the relationships that bring these pain resources together.
Deb Gordon, RN, MS, FAAN, senior clinical nurse specialist at the University of Wisconsin Medical Center in Madison, also sees herself functioning like a hospitalist in addressing pain issues. “I manage a clinical pain consultation service. I see patients every day,” she says. “I’m also in staff development, helping professionals in the hospital learn to manage pain better, and using quality improvement techniques to take what we know about pain management to support people like hospitalists at the bedside.”
Since 1990, an interdisciplinary quality improvement pain management group has been meeting at the UW medical center to improve the institution’s response to pain patients. Gordon believes pain is a natural target for hospital quality-improvement activities because it touches on the domains of quality identified by groups such as the Institute of Medicine in Washington, D.C., and the Institute for Healthcare Improvement in Cambridge, Mass.
Limits in the Hospital Setting
Even with a vast array of pain modalities, hospitalists face inherent limitations in addressing pain challenges within the hospital, starting with caseload pressures and short lengths of stay. Many of the approaches that might offer long-term solutions to the patient’s chronic pain syndrome belong in the outpatient setting, adds John Massey, MD, president and medical director of Nebraska Pain Consultants in Lincoln.
Dr. Massey sees chronic pain cases that have been refractory to treatment, both at his clinic and as a consultant in the hospital. Inevitably there is a psychological overlay to these cases, he says. That doesn’t mean the patient’s pain isn’t real, but if high doses of analgesics have failed to bring the pain under control, then a different approach is needed—one that includes behavioral techniques and involves the patient not as a passive recipient of treatment, but an active participant in his or her own pain management and coping strategies.
“There are ways to treat, for example, back pain that require finding a specific nerve in the spine responsible for the pain,” says Dr. Massey. “If I can locate that nerve, there are things that I can do, like radio frequency neuro-ablation. But this requires three separate visits to the pain clinic to make an accurate diagnosis. I’m often consulted by hospitalists and there are things I can do to put a finger in the dike. But I try to add another perspective to my discussion with the hospitalist, pointing out that many of the best pain management modalities are done on an outpatient basis.”
What can be achieved in the hospital often is more of a Band-Aid, sometimes even a step backward in terms of the lifestyle changes necessary to get patients out of their passive response to their chronic pain, Dr. Massey says.
The hospitalist’s job is to see what can be done to make patients more comfortable and then send them home with a referral to the pain service, if that is indicated. “I’m happy to help with an intervention in the hospital but, ultimately, we’d like the patient to be less dependent on opioids to treat their pain,” says Dr. Massey. “I know that nothing I can do will really change the situation until I get them out of the hospital and can initiate physical therapy and behavioral interventions.”
There are no shortcuts to permanent pain relief, which can be long, slow, hard work using evidence-based medicine, Dr. Massey says. But it also involves a frank discussion with the patient, which may be hard in the hospital.
“One of the questions we ask patients is: How many times have you visited the emergency room for pain?” says Dr. Massey. “If the answer is more than four in a year, there are likely to be psychological co-morbidities. The challenge for the hospitalist is, ‘How can I arrest this acute pain episode, and then what can I contribute to helping the patient find the help he or she needs to prevent the next episode?’ That means trying to establish rapport and pointing the person to appropriate follow-up pain resources. If you go too hard too fast, the patient may reject what you’re offering. But if you do nothing, you’re facilitating a continued passive approach that doesn’t lead to meaningful solutions.”
Dr. Massey recently saw a woman who had been in the ED 48 times in the previous year for pain that had a major behavioral component. The hospital hired him after the 48th visit to find a different approach to controlling the patient’s pain.
Make Pain a Priority
“My hospitalist group meets regularly to discuss difficult topics, and pain often comes up,” says Stephen Bekanich, MD, hospitalist and palliative care physician at the University of Utah Medical Center in Salt Lake City. “The more you can focus on pain, the more time you spend making it a priority, you are sending a message: This is important to me. You communicate to nurses and other staff that you take pain seriously.”
Dr. Fishman concurs. “Ultimately, it is an issue of priorities and how to prioritize what gets done in the hospital,” he says. “Why would a health professional ever categorize pain relief as a lower priority? We have wandered far from our compassionate mission as doctors when that happens.
“In the real world, when there is no one else to do it, and no pain clinics available, the responsibility for pain management falls on the provider at the front lines, often the emergency physician and the hospitalist. Hospitalists are becoming de facto pain specialists for patients with chronic and terminal conditions. These patients are looking for support, comfort, and redirection. This can also be one of the most rewarding aspects of hospital practice. It really brings you back to the roots of medicine.” TH
Larry Beresford is a regular contributor to The Hospitalist.
Note: This is Part 3 of The Hospitalist’s series on pain and hospital medicine. Part 1 appeared on p. 45 of the April issue, and Part 2 appeared on p. 33 of the June issue.
Hospitalists face demands for pain care every day. Usually, the general pain principles described in the first two articles in this series and the use of a few opioid analgesics with which the hospitalist has become familiar can supply relief.
But what about the more difficult cases in which psychosocial influences or a history of substance abuse complicates the patient’s pain? Perhaps it is a chronic pain case that has never been adequately addressed, or the patient keeps turning up in the emergency department (ED) complaining of out-of-control pain. Other examples of difficult-to-manage pain include complex regional pain syndrome, post-herpetic neuralgia, other neuropathic pains, sickle cell anemia, and patients at high risk of opioid toxicity.
These cases are like a leaky bucket for the hospital—costly, frustrating, unsatisfying to the patient, and prone to bad outcomes, says Jerry Wesch, PhD, director of the pain service for the Alexian Brothers Health System in greater Chicago. “These are the patients who tend to bedevil everybody in the hospital,” he says.
Dealing with such patients is a demanding task.
“You don’t have chronic pain without a psycho-social-spiritual overlay,” adds Scott Fishman, MD, chief of the Division of Pain Medicine at University of California-Davis in Sacramento. “Their emotional lives are deteriorating. They can’t sleep, they’re depressed, and their physical functioning is also deteriorating. There are all kinds of situations that demand use of a full spectrum of bio-psycho-social interventions in addition to opioid analgesics.”
These complex, unresolved cases are likely to have emotional, social, or spiritual manifestations. But what does that mean to a busy hospitalist with a short window of opportunity to address patients’ pain before pointing them toward discharge? A psychologist, social worker, or chaplain may have something to contribute to pain management. Meanwhile, the rest of the caseload is clamoring for the hospitalist’s attention.
Make Pain Management Multidisciplinary
A dizzying array of pain modalities can be brought to bear on complex pain cases. These range from opioid analgesics to a variety of adjuvant non-opioid medications to interventional techniques involving surgery, spinal injections, nerve blocks, nerve stimulation, and nerve destruction techniques.
There are also complementary methodologies (e.g., acupuncture) that have been shown to reduce the volume of narcotics needed for pain control, even though how they work is not well understood.
But how many hospitalists call on acupuncturists, hypnotists, or teachers of guided-imagery meditation for their patients? Many of these techniques are more appropriately initiated in the outpatient setting, but the hospitalist still has a responsibility to make sure “frequent fliers” with complex pain complaints get connected post-discharge to a pain service that can offer long-term relief. The challenge is applying the acute treatment models of the hospital to chronic pain syndromes that are not optimally addressed in crisis mode.
Jonathan Weston, MD, a hospitalist at Penrose Hospital in Colorado Springs, Colo., says these difficult, chronic pain cases are the bane of the hospitalist’s working life. These patients show up at night in the ED saying, “ ‘I’m in so much pain, please don’t send me home,’ ” he says. “The emergency physician puts them on an IV drip and their pain is relieved for the moment, but only one facet of that pain has been addressed.”
The emergency physician—also under caseload pressure— decides the easiest disposition is to admit the patient and dump the problem on the hospitalist. “They’re out of their pain medications at home, and when you call the attending you are told that they are drug seekers,” Dr. Weston relates. “These patients take a lot of energy. They can be manipulative. We can’t do right for them. It’s not satisfying. We don’t want to round on them. The way we hospitalists manage these patients sometimes reflects not only the patient’s personality, but our personality as well.”
Hospitalists don’t just treat these patients’ pain, they also address their suffering, he says.
High-quality pain management is multidisciplinary, Dr. Weston notes, because pain is multifactorial. The hospitalist occupies an important coordinating position and is charged with responsibility for the whole person during that patient’s brief hospital stay. But there are limits to what the hospitalist can accomplish. A palliative care team or an acute pain service can make important contributions to hospitalized patients’ pain. So can social workers, psychologists, pharmacists, and chaplains. But it is the hospitalist’s responsibility to coordinate these pieces of the pain puzzle for patients on service.
In many hospitals, the palliative care service has been set up to consult on pain, suffering, and clarification of treatment goals for patients nearing the end of life. These services vary from institution to institution in terms of whether they prefer to focus on end-of-life issues or are comfortable fielding other kinds of chronic pain questions. Acute pain services equally vary in terms of whether their focus is primarily on surgical pain “interventions” or on a multidisciplinary approach to pain management.
Ideally, Dr. Weston says, a major hospital would have both services available as resources to the hospitalist. Or, if there is only one of them, it should have a broad approach to pain management. Otherwise, it is up to the hospitalist to pull together a virtual pain team to provide a multidisciplinary response to complex pain.
“I am also board certified in hospice and palliative medicine,” Dr. Weston says. “I can use my medical knowledge to try to get the patient comfortable on oral meds so that they can go home. And I can personally make an appointment for them within 48 hours of discharge with their attending physician or a pain specialist. But for too many patients, this connection never happens.”
“Pain management in general is a hard thing to deal with,” adds Lauren Fraser, MD, regional chief of the department of hospital medicine for Kaiser Permanente Colorado in Denver. “It’s frustrating because you want to do the right thing,” she says. “We need first of all to rule out anything we can fix that might be causing the pain. Then we’re dealing with the patient’s quality of life and the disabling effects of pain. Each patient and family has a different need, and when you meet with them one-on-one you’re dealing with all of it.”
Dr. Fraser doesn’t have access to an acute pain service in her current setting, “although we have interventional folks to put in the PCAs and epidurals. We generally are able to get the services we need, although there would be an advantage to having an identified multidisciplinary pain service to provide the coordination.”
A “Pain Hospitalist”
Jerry Wesch, director of the pain program at Alexian Brothers Hospital Network in Arlington Heights, Ill., recently posted a job listing on the Internet seeking a pain management physician. He is looking for a doctor with an interest in comprehensive, interdisciplinary team management of chronic pain who is “able to function as a pain hospitalist.”
Although the details of this new position are still being finalized and a pain hospitalist would function with a different focus than a generalist hospitalist, Wesch suggests the role has important analogies with what hospitalists like Dr. Weston face in coordinating a virtual team of multidisciplinary pain resources.
Wesch is building an inpatient pain service comprising the pain physician, two nurse practitioners, and a part-time psychologist with full-time presence in two Alexian Brothers acute hospitals. This team would work closely with hospitalists, the palliative care service, and ancillary services such as physical therapy and chaplains.
“This should make us ideal collaborators with the hospitalists, who can just walk down the hall and initiate a pain consult,” he explains. “We’re all working toward the same goal, which is to improve efficiency, medical management, quality of care, and patient satisfaction. A good hospitalist is also my best ally in building a multidisciplinary pain service.”
In other settings, however, it will be the hospitalist’s responsibility to build the relationships that bring these pain resources together.
Deb Gordon, RN, MS, FAAN, senior clinical nurse specialist at the University of Wisconsin Medical Center in Madison, also sees herself functioning like a hospitalist in addressing pain issues. “I manage a clinical pain consultation service. I see patients every day,” she says. “I’m also in staff development, helping professionals in the hospital learn to manage pain better, and using quality improvement techniques to take what we know about pain management to support people like hospitalists at the bedside.”
Since 1990, an interdisciplinary quality improvement pain management group has been meeting at the UW medical center to improve the institution’s response to pain patients. Gordon believes pain is a natural target for hospital quality-improvement activities because it touches on the domains of quality identified by groups such as the Institute of Medicine in Washington, D.C., and the Institute for Healthcare Improvement in Cambridge, Mass.
Limits in the Hospital Setting
Even with a vast array of pain modalities, hospitalists face inherent limitations in addressing pain challenges within the hospital, starting with caseload pressures and short lengths of stay. Many of the approaches that might offer long-term solutions to the patient’s chronic pain syndrome belong in the outpatient setting, adds John Massey, MD, president and medical director of Nebraska Pain Consultants in Lincoln.
Dr. Massey sees chronic pain cases that have been refractory to treatment, both at his clinic and as a consultant in the hospital. Inevitably there is a psychological overlay to these cases, he says. That doesn’t mean the patient’s pain isn’t real, but if high doses of analgesics have failed to bring the pain under control, then a different approach is needed—one that includes behavioral techniques and involves the patient not as a passive recipient of treatment, but an active participant in his or her own pain management and coping strategies.
“There are ways to treat, for example, back pain that require finding a specific nerve in the spine responsible for the pain,” says Dr. Massey. “If I can locate that nerve, there are things that I can do, like radio frequency neuro-ablation. But this requires three separate visits to the pain clinic to make an accurate diagnosis. I’m often consulted by hospitalists and there are things I can do to put a finger in the dike. But I try to add another perspective to my discussion with the hospitalist, pointing out that many of the best pain management modalities are done on an outpatient basis.”
What can be achieved in the hospital often is more of a Band-Aid, sometimes even a step backward in terms of the lifestyle changes necessary to get patients out of their passive response to their chronic pain, Dr. Massey says.
The hospitalist’s job is to see what can be done to make patients more comfortable and then send them home with a referral to the pain service, if that is indicated. “I’m happy to help with an intervention in the hospital but, ultimately, we’d like the patient to be less dependent on opioids to treat their pain,” says Dr. Massey. “I know that nothing I can do will really change the situation until I get them out of the hospital and can initiate physical therapy and behavioral interventions.”
There are no shortcuts to permanent pain relief, which can be long, slow, hard work using evidence-based medicine, Dr. Massey says. But it also involves a frank discussion with the patient, which may be hard in the hospital.
“One of the questions we ask patients is: How many times have you visited the emergency room for pain?” says Dr. Massey. “If the answer is more than four in a year, there are likely to be psychological co-morbidities. The challenge for the hospitalist is, ‘How can I arrest this acute pain episode, and then what can I contribute to helping the patient find the help he or she needs to prevent the next episode?’ That means trying to establish rapport and pointing the person to appropriate follow-up pain resources. If you go too hard too fast, the patient may reject what you’re offering. But if you do nothing, you’re facilitating a continued passive approach that doesn’t lead to meaningful solutions.”
Dr. Massey recently saw a woman who had been in the ED 48 times in the previous year for pain that had a major behavioral component. The hospital hired him after the 48th visit to find a different approach to controlling the patient’s pain.
Make Pain a Priority
“My hospitalist group meets regularly to discuss difficult topics, and pain often comes up,” says Stephen Bekanich, MD, hospitalist and palliative care physician at the University of Utah Medical Center in Salt Lake City. “The more you can focus on pain, the more time you spend making it a priority, you are sending a message: This is important to me. You communicate to nurses and other staff that you take pain seriously.”
Dr. Fishman concurs. “Ultimately, it is an issue of priorities and how to prioritize what gets done in the hospital,” he says. “Why would a health professional ever categorize pain relief as a lower priority? We have wandered far from our compassionate mission as doctors when that happens.
“In the real world, when there is no one else to do it, and no pain clinics available, the responsibility for pain management falls on the provider at the front lines, often the emergency physician and the hospitalist. Hospitalists are becoming de facto pain specialists for patients with chronic and terminal conditions. These patients are looking for support, comfort, and redirection. This can also be one of the most rewarding aspects of hospital practice. It really brings you back to the roots of medicine.” TH
Larry Beresford is a regular contributor to The Hospitalist.
Note: This is Part 3 of The Hospitalist’s series on pain and hospital medicine. Part 1 appeared on p. 45 of the April issue, and Part 2 appeared on p. 33 of the June issue.
Hospitalists face demands for pain care every day. Usually, the general pain principles described in the first two articles in this series and the use of a few opioid analgesics with which the hospitalist has become familiar can supply relief.
But what about the more difficult cases in which psychosocial influences or a history of substance abuse complicates the patient’s pain? Perhaps it is a chronic pain case that has never been adequately addressed, or the patient keeps turning up in the emergency department (ED) complaining of out-of-control pain. Other examples of difficult-to-manage pain include complex regional pain syndrome, post-herpetic neuralgia, other neuropathic pains, sickle cell anemia, and patients at high risk of opioid toxicity.
These cases are like a leaky bucket for the hospital—costly, frustrating, unsatisfying to the patient, and prone to bad outcomes, says Jerry Wesch, PhD, director of the pain service for the Alexian Brothers Health System in greater Chicago. “These are the patients who tend to bedevil everybody in the hospital,” he says.
Dealing with such patients is a demanding task.
“You don’t have chronic pain without a psycho-social-spiritual overlay,” adds Scott Fishman, MD, chief of the Division of Pain Medicine at University of California-Davis in Sacramento. “Their emotional lives are deteriorating. They can’t sleep, they’re depressed, and their physical functioning is also deteriorating. There are all kinds of situations that demand use of a full spectrum of bio-psycho-social interventions in addition to opioid analgesics.”
These complex, unresolved cases are likely to have emotional, social, or spiritual manifestations. But what does that mean to a busy hospitalist with a short window of opportunity to address patients’ pain before pointing them toward discharge? A psychologist, social worker, or chaplain may have something to contribute to pain management. Meanwhile, the rest of the caseload is clamoring for the hospitalist’s attention.
Make Pain Management Multidisciplinary
A dizzying array of pain modalities can be brought to bear on complex pain cases. These range from opioid analgesics to a variety of adjuvant non-opioid medications to interventional techniques involving surgery, spinal injections, nerve blocks, nerve stimulation, and nerve destruction techniques.
There are also complementary methodologies (e.g., acupuncture) that have been shown to reduce the volume of narcotics needed for pain control, even though how they work is not well understood.
But how many hospitalists call on acupuncturists, hypnotists, or teachers of guided-imagery meditation for their patients? Many of these techniques are more appropriately initiated in the outpatient setting, but the hospitalist still has a responsibility to make sure “frequent fliers” with complex pain complaints get connected post-discharge to a pain service that can offer long-term relief. The challenge is applying the acute treatment models of the hospital to chronic pain syndromes that are not optimally addressed in crisis mode.
Jonathan Weston, MD, a hospitalist at Penrose Hospital in Colorado Springs, Colo., says these difficult, chronic pain cases are the bane of the hospitalist’s working life. These patients show up at night in the ED saying, “ ‘I’m in so much pain, please don’t send me home,’ ” he says. “The emergency physician puts them on an IV drip and their pain is relieved for the moment, but only one facet of that pain has been addressed.”
The emergency physician—also under caseload pressure— decides the easiest disposition is to admit the patient and dump the problem on the hospitalist. “They’re out of their pain medications at home, and when you call the attending you are told that they are drug seekers,” Dr. Weston relates. “These patients take a lot of energy. They can be manipulative. We can’t do right for them. It’s not satisfying. We don’t want to round on them. The way we hospitalists manage these patients sometimes reflects not only the patient’s personality, but our personality as well.”
Hospitalists don’t just treat these patients’ pain, they also address their suffering, he says.
High-quality pain management is multidisciplinary, Dr. Weston notes, because pain is multifactorial. The hospitalist occupies an important coordinating position and is charged with responsibility for the whole person during that patient’s brief hospital stay. But there are limits to what the hospitalist can accomplish. A palliative care team or an acute pain service can make important contributions to hospitalized patients’ pain. So can social workers, psychologists, pharmacists, and chaplains. But it is the hospitalist’s responsibility to coordinate these pieces of the pain puzzle for patients on service.
In many hospitals, the palliative care service has been set up to consult on pain, suffering, and clarification of treatment goals for patients nearing the end of life. These services vary from institution to institution in terms of whether they prefer to focus on end-of-life issues or are comfortable fielding other kinds of chronic pain questions. Acute pain services equally vary in terms of whether their focus is primarily on surgical pain “interventions” or on a multidisciplinary approach to pain management.
Ideally, Dr. Weston says, a major hospital would have both services available as resources to the hospitalist. Or, if there is only one of them, it should have a broad approach to pain management. Otherwise, it is up to the hospitalist to pull together a virtual pain team to provide a multidisciplinary response to complex pain.
“I am also board certified in hospice and palliative medicine,” Dr. Weston says. “I can use my medical knowledge to try to get the patient comfortable on oral meds so that they can go home. And I can personally make an appointment for them within 48 hours of discharge with their attending physician or a pain specialist. But for too many patients, this connection never happens.”
“Pain management in general is a hard thing to deal with,” adds Lauren Fraser, MD, regional chief of the department of hospital medicine for Kaiser Permanente Colorado in Denver. “It’s frustrating because you want to do the right thing,” she says. “We need first of all to rule out anything we can fix that might be causing the pain. Then we’re dealing with the patient’s quality of life and the disabling effects of pain. Each patient and family has a different need, and when you meet with them one-on-one you’re dealing with all of it.”
Dr. Fraser doesn’t have access to an acute pain service in her current setting, “although we have interventional folks to put in the PCAs and epidurals. We generally are able to get the services we need, although there would be an advantage to having an identified multidisciplinary pain service to provide the coordination.”
A “Pain Hospitalist”
Jerry Wesch, director of the pain program at Alexian Brothers Hospital Network in Arlington Heights, Ill., recently posted a job listing on the Internet seeking a pain management physician. He is looking for a doctor with an interest in comprehensive, interdisciplinary team management of chronic pain who is “able to function as a pain hospitalist.”
Although the details of this new position are still being finalized and a pain hospitalist would function with a different focus than a generalist hospitalist, Wesch suggests the role has important analogies with what hospitalists like Dr. Weston face in coordinating a virtual team of multidisciplinary pain resources.
Wesch is building an inpatient pain service comprising the pain physician, two nurse practitioners, and a part-time psychologist with full-time presence in two Alexian Brothers acute hospitals. This team would work closely with hospitalists, the palliative care service, and ancillary services such as physical therapy and chaplains.
“This should make us ideal collaborators with the hospitalists, who can just walk down the hall and initiate a pain consult,” he explains. “We’re all working toward the same goal, which is to improve efficiency, medical management, quality of care, and patient satisfaction. A good hospitalist is also my best ally in building a multidisciplinary pain service.”
In other settings, however, it will be the hospitalist’s responsibility to build the relationships that bring these pain resources together.
Deb Gordon, RN, MS, FAAN, senior clinical nurse specialist at the University of Wisconsin Medical Center in Madison, also sees herself functioning like a hospitalist in addressing pain issues. “I manage a clinical pain consultation service. I see patients every day,” she says. “I’m also in staff development, helping professionals in the hospital learn to manage pain better, and using quality improvement techniques to take what we know about pain management to support people like hospitalists at the bedside.”
Since 1990, an interdisciplinary quality improvement pain management group has been meeting at the UW medical center to improve the institution’s response to pain patients. Gordon believes pain is a natural target for hospital quality-improvement activities because it touches on the domains of quality identified by groups such as the Institute of Medicine in Washington, D.C., and the Institute for Healthcare Improvement in Cambridge, Mass.
Limits in the Hospital Setting
Even with a vast array of pain modalities, hospitalists face inherent limitations in addressing pain challenges within the hospital, starting with caseload pressures and short lengths of stay. Many of the approaches that might offer long-term solutions to the patient’s chronic pain syndrome belong in the outpatient setting, adds John Massey, MD, president and medical director of Nebraska Pain Consultants in Lincoln.
Dr. Massey sees chronic pain cases that have been refractory to treatment, both at his clinic and as a consultant in the hospital. Inevitably there is a psychological overlay to these cases, he says. That doesn’t mean the patient’s pain isn’t real, but if high doses of analgesics have failed to bring the pain under control, then a different approach is needed—one that includes behavioral techniques and involves the patient not as a passive recipient of treatment, but an active participant in his or her own pain management and coping strategies.
“There are ways to treat, for example, back pain that require finding a specific nerve in the spine responsible for the pain,” says Dr. Massey. “If I can locate that nerve, there are things that I can do, like radio frequency neuro-ablation. But this requires three separate visits to the pain clinic to make an accurate diagnosis. I’m often consulted by hospitalists and there are things I can do to put a finger in the dike. But I try to add another perspective to my discussion with the hospitalist, pointing out that many of the best pain management modalities are done on an outpatient basis.”
What can be achieved in the hospital often is more of a Band-Aid, sometimes even a step backward in terms of the lifestyle changes necessary to get patients out of their passive response to their chronic pain, Dr. Massey says.
The hospitalist’s job is to see what can be done to make patients more comfortable and then send them home with a referral to the pain service, if that is indicated. “I’m happy to help with an intervention in the hospital but, ultimately, we’d like the patient to be less dependent on opioids to treat their pain,” says Dr. Massey. “I know that nothing I can do will really change the situation until I get them out of the hospital and can initiate physical therapy and behavioral interventions.”
There are no shortcuts to permanent pain relief, which can be long, slow, hard work using evidence-based medicine, Dr. Massey says. But it also involves a frank discussion with the patient, which may be hard in the hospital.
“One of the questions we ask patients is: How many times have you visited the emergency room for pain?” says Dr. Massey. “If the answer is more than four in a year, there are likely to be psychological co-morbidities. The challenge for the hospitalist is, ‘How can I arrest this acute pain episode, and then what can I contribute to helping the patient find the help he or she needs to prevent the next episode?’ That means trying to establish rapport and pointing the person to appropriate follow-up pain resources. If you go too hard too fast, the patient may reject what you’re offering. But if you do nothing, you’re facilitating a continued passive approach that doesn’t lead to meaningful solutions.”
Dr. Massey recently saw a woman who had been in the ED 48 times in the previous year for pain that had a major behavioral component. The hospital hired him after the 48th visit to find a different approach to controlling the patient’s pain.
Make Pain a Priority
“My hospitalist group meets regularly to discuss difficult topics, and pain often comes up,” says Stephen Bekanich, MD, hospitalist and palliative care physician at the University of Utah Medical Center in Salt Lake City. “The more you can focus on pain, the more time you spend making it a priority, you are sending a message: This is important to me. You communicate to nurses and other staff that you take pain seriously.”
Dr. Fishman concurs. “Ultimately, it is an issue of priorities and how to prioritize what gets done in the hospital,” he says. “Why would a health professional ever categorize pain relief as a lower priority? We have wandered far from our compassionate mission as doctors when that happens.
“In the real world, when there is no one else to do it, and no pain clinics available, the responsibility for pain management falls on the provider at the front lines, often the emergency physician and the hospitalist. Hospitalists are becoming de facto pain specialists for patients with chronic and terminal conditions. These patients are looking for support, comfort, and redirection. This can also be one of the most rewarding aspects of hospital practice. It really brings you back to the roots of medicine.” TH
Larry Beresford is a regular contributor to The Hospitalist.