User login
ANSWER
The correct answer is tuberous sclerosis (choice “d”), a genetic disorder affecting cellular differentiation and proliferation. As a result, hamartomas commonly form in organs such as the brain.
Von Recklinghausen disease (choice “a”; also known as neurofibromatosis type 1) presents with hyperpigmented macules and patches called café au lait macules. These and other findings differentiate it considerably from tuberous sclerosis.
“No unifying explanation” (choice “b”) is incorrect, because, as stated above, there is a unifying explanation for these findings!
Vitiligo (choice “c”) involves hypopigmented macules and patches. However, it does not present with some of the other findings seen in this case.
DISCUSSION
Tuberous sclerosis was first described in 1862 by von Recklinghausen, who noted the collection of findings we now term tuberous sclerosis complex (TSC) due to the wide variation in presentation.
In the United States, TSC occurs in an estimated one in 6,000 to one in 30,000 newborns. Usually, it manifests when the child is between ages 2 and 6, but genetic penetrance is highly variable—a major reason for the shift to the use of the term complex with this condition. (This case, with its late presentation, illustrates this variability.)
In about 60% of cases, TSC is transmitted in autosomal dominant mode, although at least 20% of cases may be due to spontaneous mutations. It has not shown any racial or gender predilections. Up to 90% of TSC patients will present with seizures, and 60% to 70% of those affected will demonstrate some developmental disability.
Skin is affected in at least 70% of TSC cases. This patient typifies the common dermatologic findings: dart-shaped hypopigmented macules (known as mountain ash leaf spots) and fleshy facial papules in the nasolabial region (originally called adenoma sebaceum and now called angiofibromas). Periungal fibromas are also common. Other major diagnostic criteria for TSC include cortical tubers seen on imaging and retinal hamartomas. Minor diagnostic criteria include pits in dental enamel and gingival fibromas.
Definitive diagnosis depends on identification of either two major manifestations or one major and two minor findings. There are no blood tests to confirm the diagnosis. In terms of treatment, the various elements that comprise TSC can be dealt with (eg, control of seizures and destruction or modification of skin lesions).
This patient received a diagnosis of TSC. She was returned to her primary care provider, who referred her for additional imaging of her lungs and heart and for ophthalmologic evaluation of her retinas. Genetic counseling was also arranged. With her seizures under control, she was able to continue matriculation through high school.
ANSWER
The correct answer is tuberous sclerosis (choice “d”), a genetic disorder affecting cellular differentiation and proliferation. As a result, hamartomas commonly form in organs such as the brain.
Von Recklinghausen disease (choice “a”; also known as neurofibromatosis type 1) presents with hyperpigmented macules and patches called café au lait macules. These and other findings differentiate it considerably from tuberous sclerosis.
“No unifying explanation” (choice “b”) is incorrect, because, as stated above, there is a unifying explanation for these findings!
Vitiligo (choice “c”) involves hypopigmented macules and patches. However, it does not present with some of the other findings seen in this case.
DISCUSSION
Tuberous sclerosis was first described in 1862 by von Recklinghausen, who noted the collection of findings we now term tuberous sclerosis complex (TSC) due to the wide variation in presentation.
In the United States, TSC occurs in an estimated one in 6,000 to one in 30,000 newborns. Usually, it manifests when the child is between ages 2 and 6, but genetic penetrance is highly variable—a major reason for the shift to the use of the term complex with this condition. (This case, with its late presentation, illustrates this variability.)
In about 60% of cases, TSC is transmitted in autosomal dominant mode, although at least 20% of cases may be due to spontaneous mutations. It has not shown any racial or gender predilections. Up to 90% of TSC patients will present with seizures, and 60% to 70% of those affected will demonstrate some developmental disability.
Skin is affected in at least 70% of TSC cases. This patient typifies the common dermatologic findings: dart-shaped hypopigmented macules (known as mountain ash leaf spots) and fleshy facial papules in the nasolabial region (originally called adenoma sebaceum and now called angiofibromas). Periungal fibromas are also common. Other major diagnostic criteria for TSC include cortical tubers seen on imaging and retinal hamartomas. Minor diagnostic criteria include pits in dental enamel and gingival fibromas.
Definitive diagnosis depends on identification of either two major manifestations or one major and two minor findings. There are no blood tests to confirm the diagnosis. In terms of treatment, the various elements that comprise TSC can be dealt with (eg, control of seizures and destruction or modification of skin lesions).
This patient received a diagnosis of TSC. She was returned to her primary care provider, who referred her for additional imaging of her lungs and heart and for ophthalmologic evaluation of her retinas. Genetic counseling was also arranged. With her seizures under control, she was able to continue matriculation through high school.
ANSWER
The correct answer is tuberous sclerosis (choice “d”), a genetic disorder affecting cellular differentiation and proliferation. As a result, hamartomas commonly form in organs such as the brain.
Von Recklinghausen disease (choice “a”; also known as neurofibromatosis type 1) presents with hyperpigmented macules and patches called café au lait macules. These and other findings differentiate it considerably from tuberous sclerosis.
“No unifying explanation” (choice “b”) is incorrect, because, as stated above, there is a unifying explanation for these findings!
Vitiligo (choice “c”) involves hypopigmented macules and patches. However, it does not present with some of the other findings seen in this case.
DISCUSSION
Tuberous sclerosis was first described in 1862 by von Recklinghausen, who noted the collection of findings we now term tuberous sclerosis complex (TSC) due to the wide variation in presentation.
In the United States, TSC occurs in an estimated one in 6,000 to one in 30,000 newborns. Usually, it manifests when the child is between ages 2 and 6, but genetic penetrance is highly variable—a major reason for the shift to the use of the term complex with this condition. (This case, with its late presentation, illustrates this variability.)
In about 60% of cases, TSC is transmitted in autosomal dominant mode, although at least 20% of cases may be due to spontaneous mutations. It has not shown any racial or gender predilections. Up to 90% of TSC patients will present with seizures, and 60% to 70% of those affected will demonstrate some developmental disability.
Skin is affected in at least 70% of TSC cases. This patient typifies the common dermatologic findings: dart-shaped hypopigmented macules (known as mountain ash leaf spots) and fleshy facial papules in the nasolabial region (originally called adenoma sebaceum and now called angiofibromas). Periungal fibromas are also common. Other major diagnostic criteria for TSC include cortical tubers seen on imaging and retinal hamartomas. Minor diagnostic criteria include pits in dental enamel and gingival fibromas.
Definitive diagnosis depends on identification of either two major manifestations or one major and two minor findings. There are no blood tests to confirm the diagnosis. In terms of treatment, the various elements that comprise TSC can be dealt with (eg, control of seizures and destruction or modification of skin lesions).
This patient received a diagnosis of TSC. She was returned to her primary care provider, who referred her for additional imaging of her lungs and heart and for ophthalmologic evaluation of her retinas. Genetic counseling was also arranged. With her seizures under control, she was able to continue matriculation through high school.
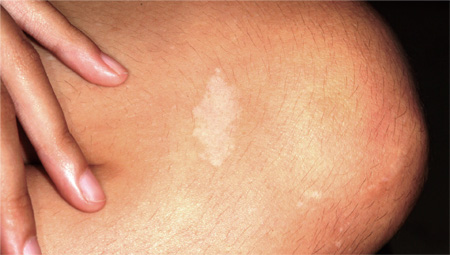
The parents of this 16-year-old girl first noticed the “spots” on their daughter’s thigh when she was 2. At that time, they expressed mild concern to the child’s pediatrician, who advised them to watch the lesions for change. In the absence of any, the spots were essentially ignored. But recently—and alarmingly—the patient experienced two grand mal seizures. Three months ago, she was hospitalized and underwent a thorough examination and workup, including imaging studies of the brain. These revealed presumed neural tumors, which are being followed with serial imaging. In the meantime, her primary care provider recommends a visit to dermatology for evaluation of the child’s skin—including the aforementioned spots on her thigh. Her parents deny any family history of similar problems with skin or seizures. The spots are located on the patient’s right lateral thigh. The largest is a dart-shaped 4 x 2.5–cm hypopigmented patch. It is surrounded by much smaller (< 1 cm in diameter) but similarly hypopigmented macules. The large lesion is symmetrical but has slightly serrated borders. Examination elsewhere reveals periungual fibromas on two of 10 fingers. Odd fleshy papules are noted in the bilateral nasolabial areas.
