User login
ANSWER
All of the above choices are correct and, in fact, were seen on this patient. These findings served to confirm the diagnosis of tuberous sclerosis.
DISCUSSION
Also called Bourneville’s disease or epiloia (an acronym for epilepsy, low intelligence, and adenoma sebaceum—all major findings in this disease), tuberous sclerosis (TS) occurs in one of 10,000 births and affects both genders equally. It is considered a genodermatosis, with 75% of cases related to spontaneous mutations and 25% to autosomal dominant transmission. Two separate genes have been identified.
The earliest skin finding in these patients is that of hypopigmented macules, especially the so-called mountain ash leaf spots typically seen on the trunk and extremities—better observed sometimes with the aid of a Wood’s lamp.
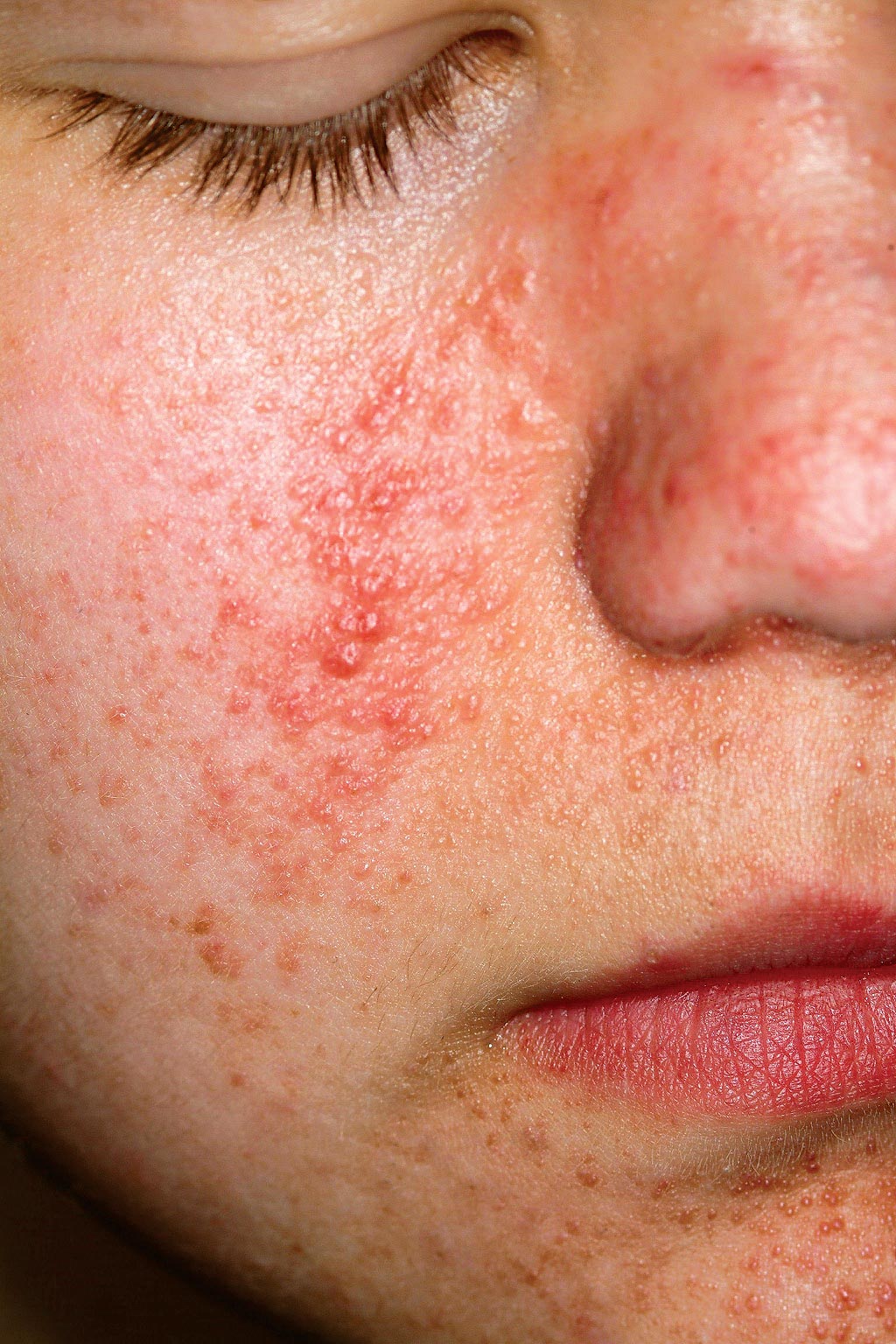
Another common early finding is that of seizures, occurring in 75% of TS patients with central nervous system lesions. Facial angiofibromas, called adenoma sebaceum, also appear in early childhood, increase during adolescence, and are permanent. About 80% of affected patients will eventually develop the connective tissue nevus called shagreen patch, which usually occurs on the low back.
Conical smooth papular projections originating from the nail folds of fingers and toes appear at puberty in a high percentage of TS patients and are permanent. Redundant and sometimes papular lesions are seen in the gingival mucosa. Numerous other signs of the disease—in lungs, heart, and bony tissue—have been described.
The acronym mentioned above, epiloia, has been largely abandoned, in part because it suggests that low intelligence with TS patients is inevitable. The truth is, many patients, such as this one, function quite normally, typifying the variable penetrance of the genetic changes so common to TS.
TREATMENT
The main focus for this patient is to get his seizures under control and arrange for proper follow-up, as well as genetic counseling. Unfortunately, there is no effective treatment for the facial lesions.
ANSWER
All of the above choices are correct and, in fact, were seen on this patient. These findings served to confirm the diagnosis of tuberous sclerosis.
DISCUSSION
Also called Bourneville’s disease or epiloia (an acronym for epilepsy, low intelligence, and adenoma sebaceum—all major findings in this disease), tuberous sclerosis (TS) occurs in one of 10,000 births and affects both genders equally. It is considered a genodermatosis, with 75% of cases related to spontaneous mutations and 25% to autosomal dominant transmission. Two separate genes have been identified.
The earliest skin finding in these patients is that of hypopigmented macules, especially the so-called mountain ash leaf spots typically seen on the trunk and extremities—better observed sometimes with the aid of a Wood’s lamp.
Another common early finding is that of seizures, occurring in 75% of TS patients with central nervous system lesions. Facial angiofibromas, called adenoma sebaceum, also appear in early childhood, increase during adolescence, and are permanent. About 80% of affected patients will eventually develop the connective tissue nevus called shagreen patch, which usually occurs on the low back.
Conical smooth papular projections originating from the nail folds of fingers and toes appear at puberty in a high percentage of TS patients and are permanent. Redundant and sometimes papular lesions are seen in the gingival mucosa. Numerous other signs of the disease—in lungs, heart, and bony tissue—have been described.
The acronym mentioned above, epiloia, has been largely abandoned, in part because it suggests that low intelligence with TS patients is inevitable. The truth is, many patients, such as this one, function quite normally, typifying the variable penetrance of the genetic changes so common to TS.
TREATMENT
The main focus for this patient is to get his seizures under control and arrange for proper follow-up, as well as genetic counseling. Unfortunately, there is no effective treatment for the facial lesions.
ANSWER
All of the above choices are correct and, in fact, were seen on this patient. These findings served to confirm the diagnosis of tuberous sclerosis.
DISCUSSION
Also called Bourneville’s disease or epiloia (an acronym for epilepsy, low intelligence, and adenoma sebaceum—all major findings in this disease), tuberous sclerosis (TS) occurs in one of 10,000 births and affects both genders equally. It is considered a genodermatosis, with 75% of cases related to spontaneous mutations and 25% to autosomal dominant transmission. Two separate genes have been identified.
The earliest skin finding in these patients is that of hypopigmented macules, especially the so-called mountain ash leaf spots typically seen on the trunk and extremities—better observed sometimes with the aid of a Wood’s lamp.
Another common early finding is that of seizures, occurring in 75% of TS patients with central nervous system lesions. Facial angiofibromas, called adenoma sebaceum, also appear in early childhood, increase during adolescence, and are permanent. About 80% of affected patients will eventually develop the connective tissue nevus called shagreen patch, which usually occurs on the low back.
Conical smooth papular projections originating from the nail folds of fingers and toes appear at puberty in a high percentage of TS patients and are permanent. Redundant and sometimes papular lesions are seen in the gingival mucosa. Numerous other signs of the disease—in lungs, heart, and bony tissue—have been described.
The acronym mentioned above, epiloia, has been largely abandoned, in part because it suggests that low intelligence with TS patients is inevitable. The truth is, many patients, such as this one, function quite normally, typifying the variable penetrance of the genetic changes so common to TS.
TREATMENT
The main focus for this patient is to get his seizures under control and arrange for proper follow-up, as well as genetic counseling. Unfortunately, there is no effective treatment for the facial lesions.
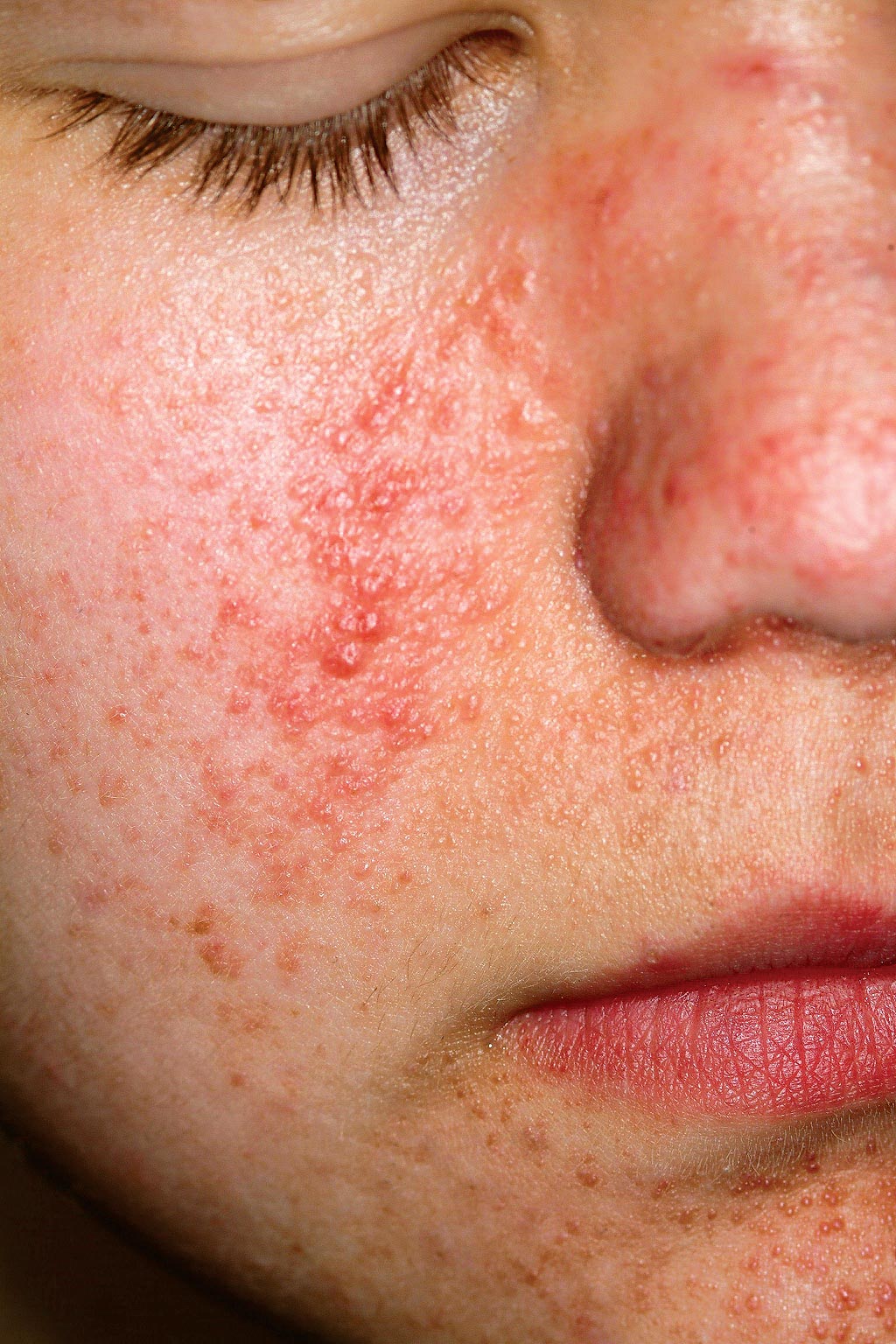
A 14-year-old boy is seen for “acne” that has been unresponsive to oral and topical antibiotics. There is no family history of acne, but the boy has a history of unexplained grand mal seizures. The dermatologic condition, which has been present since an early age, has been variously diagnosed as warts and molluscum contagiosum, as well as acne. However, since none of the treatments offered has been successful, the patient is referred to dermatology. On examination, you note a dense collection of fleshy papules in bilateral nasolabial areas, thinning out around the mouth.