User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
Powered by CHEST Physician, Clinician Reviews, MDedge Family Medicine, Internal Medicine News, and The Journal of Clinical Outcomes Management.
Breaking the glass ceiling: Women in pulmonary medicine face both barriers and opportunities
SAN ANTONIO – Women in medicine have made great strides in cracking the glass ceiling, but it’s not shattered yet, said Stephanie M. Levine, MD, FCCP, the incoming president of CHEST.
At a session on women in medicine at the annual meeting of the American College of Chest Physicians, Dr. Levine discussed the challenges of breaking through the metaphorical invisible barrier. The “glass ceiling” refers to multiple ways in which women lack equality with men in medicine: leadership roles, positions and titles, progress in academic medicine, gaps in salaries and compensation, and overall gender parity in specialties.
For example, according to data from the American Association of Medical Colleges for 2017-2018, women comprise 50% of medical school graduates but only 34% of the physician workforce and 22% of leadership roles. Women are 13% less likely to be promoted to professor. They receive salaries an average 21% lower than those of their male peers, said Dr. Levine, professor of medicine and director of the pulmonary/critical care fellowship program at the University of Texas, San Antonio.
Disparities exist particularly within specialties and subspecialties, she said. Women make 85% of what men earn in primary care but, in the specialties, only 75% of what men earn. Among active fellow trainees in the areas of medicine most represented by CHEST, one-third (32%) of critical care physicians and less than a third (29%) of pulmonary physicians are female.
Why the lag in specialty parity?
The reasons for these disparities are complex, Dr. Levine argued, but the problem is not insurmountable. They begin, in a sense, with the problem itself: When there are fewer mentors, role models, sponsors, and leaders, and less overall representation of women in the first place, it is harder for women to advance.
One male audience member, for example, asked how his department could recruit more women, because most turned down interviews despite the fact that more women than men were being invited. “How many women are in your leadership?” Dr. Levine asked. He acknowledged that there were none – and therein lies the likely problem. Applicants are looking for female representation in leadership.
Gender bias and discrimination certainly play a role among peers, leadership, and even patients. Patients referring to female physicians by their first names and asking questions such as “Are you my nurse?” are subtle but cutting examples of the ways in which they reveal implicit bias and reinforce gender stereotypes, Dr. Levine said to weary nods of agreement among the attendees.
Implicit, unconscious bias is also built into the culture of a place and the way things have always been done. Lack of equity in salary, space to work, support, and promotion all compound one another. Work-life integration challenges often do not favor women. Studies have shown that in the hiring process, CVs with female names do not receive as much attention as do CVs with male names, Dr. Levine noted.
Some of the challenges lie with the way women themselves do or do not advocate for themselves. Research has long shown that women do not negotiate as well – or at all – compared with men. Women tend to be less aggressive in seeking higher compensation and leadership roles, possibly because of existing implicit bias against female assertiveness in general.
The catch-22 is that being more assertive or direct can lead others to interpret a woman as being rude or brusk, as one audience member noted when she described how colleagues perceive her simple, direct tone as seeming “upset.”
Conscious bias remains alive and well: The stereotypes that women are caretakers and men are take-charge dominators persist and can reinforce gender disparities in leadership roles.
Women also must make calculations and trade-offs between their academic promotion clocks and their biologic clocks, Dr. Levine explained.
“The 30s are great for both academic and biologic productivity,” she told attendees. The typical age for a person’s first National Institutes of Health Research Project grant (R01) is in the early 40s.
How to improve gender equality
Women bring diverse skills and perspectives to the table, Dr. Levine explained. Women tend to have stronger collaborative skills and greater compassion and empathy, for example. They tend to be less hierarchal and better at mentoring and empowerment, she said.
There are many ways to poke more cracks in the ceiling, starting with diversity and inclusion officers who make it a priority to focus on parity. Formal programs can educate staff and colleagues about implicit bias so that they might more easily recognize it when it kicks in, and training for gatekeepers can lead to more proportional hiring of women at every level.
Institutions should review their policies – salary inequities, diversity in promotion, processes for selecting leaders – and set formal interventional goals that are then evaluated in honest, documented annual reviews.
Some of these policies should address work-life balance as well: Offering part-time and flexible work options during early child-rearing years helps not only mothers, but also fathers who are now taking a more active role in parenting. Slowing or prorating the promotion clock can help those building families, and shifting meetings away from times such as 7:00 a.m. and 6:00 p.m. allow mothers and fathers alike to get their kids to and from school and attend children’s events.
Sponsorship of women is an important strategy in breaking the glass ceiling, Dr. Levine said. Sponsors can support women with untapped leadership potential and do the necessary networking and introductions that help make that advance happen. And it must be done by sponsors with power and influence, including men, Dr. Levine said.
Men can play important roles in promoting gender parity by suggesting women for key roles, leadership positions, and committees and also notifying women of upcoming opportunities, such as editorial board spots and other hot jobs. For women who aspire to be leaders, men can seek to convey leadership skills that may be needed to chair committees and other groups. Search committees need to expand beyond looking for “token women,” she said.
Dr. Levine illustrated her address with her own story. She described how many of these strategies had helped her career and how many male supervisors, mentors, and colleagues helped her, including introducing her to other male leaders who then offered her opportunities to contribute to the American College of Chest Physicians. She ran for CHEST president twice before being elected on her third run in September. She is the fifth woman to lead CHEST.
“Don’t give up,” she encouraged women in the audience, telling them to advocate for themselves and to encourage, mentor, and sponsor their female fellows and junior faculty.
“This will result in closing the gaps and will help women achieve leadership roles and competitive salaries as well as work-life integration,” Dr. Levine said.
SAN ANTONIO – Women in medicine have made great strides in cracking the glass ceiling, but it’s not shattered yet, said Stephanie M. Levine, MD, FCCP, the incoming president of CHEST.
At a session on women in medicine at the annual meeting of the American College of Chest Physicians, Dr. Levine discussed the challenges of breaking through the metaphorical invisible barrier. The “glass ceiling” refers to multiple ways in which women lack equality with men in medicine: leadership roles, positions and titles, progress in academic medicine, gaps in salaries and compensation, and overall gender parity in specialties.
For example, according to data from the American Association of Medical Colleges for 2017-2018, women comprise 50% of medical school graduates but only 34% of the physician workforce and 22% of leadership roles. Women are 13% less likely to be promoted to professor. They receive salaries an average 21% lower than those of their male peers, said Dr. Levine, professor of medicine and director of the pulmonary/critical care fellowship program at the University of Texas, San Antonio.
Disparities exist particularly within specialties and subspecialties, she said. Women make 85% of what men earn in primary care but, in the specialties, only 75% of what men earn. Among active fellow trainees in the areas of medicine most represented by CHEST, one-third (32%) of critical care physicians and less than a third (29%) of pulmonary physicians are female.
Why the lag in specialty parity?
The reasons for these disparities are complex, Dr. Levine argued, but the problem is not insurmountable. They begin, in a sense, with the problem itself: When there are fewer mentors, role models, sponsors, and leaders, and less overall representation of women in the first place, it is harder for women to advance.
One male audience member, for example, asked how his department could recruit more women, because most turned down interviews despite the fact that more women than men were being invited. “How many women are in your leadership?” Dr. Levine asked. He acknowledged that there were none – and therein lies the likely problem. Applicants are looking for female representation in leadership.
Gender bias and discrimination certainly play a role among peers, leadership, and even patients. Patients referring to female physicians by their first names and asking questions such as “Are you my nurse?” are subtle but cutting examples of the ways in which they reveal implicit bias and reinforce gender stereotypes, Dr. Levine said to weary nods of agreement among the attendees.
Implicit, unconscious bias is also built into the culture of a place and the way things have always been done. Lack of equity in salary, space to work, support, and promotion all compound one another. Work-life integration challenges often do not favor women. Studies have shown that in the hiring process, CVs with female names do not receive as much attention as do CVs with male names, Dr. Levine noted.
Some of the challenges lie with the way women themselves do or do not advocate for themselves. Research has long shown that women do not negotiate as well – or at all – compared with men. Women tend to be less aggressive in seeking higher compensation and leadership roles, possibly because of existing implicit bias against female assertiveness in general.
The catch-22 is that being more assertive or direct can lead others to interpret a woman as being rude or brusk, as one audience member noted when she described how colleagues perceive her simple, direct tone as seeming “upset.”
Conscious bias remains alive and well: The stereotypes that women are caretakers and men are take-charge dominators persist and can reinforce gender disparities in leadership roles.
Women also must make calculations and trade-offs between their academic promotion clocks and their biologic clocks, Dr. Levine explained.
“The 30s are great for both academic and biologic productivity,” she told attendees. The typical age for a person’s first National Institutes of Health Research Project grant (R01) is in the early 40s.
How to improve gender equality
Women bring diverse skills and perspectives to the table, Dr. Levine explained. Women tend to have stronger collaborative skills and greater compassion and empathy, for example. They tend to be less hierarchal and better at mentoring and empowerment, she said.
There are many ways to poke more cracks in the ceiling, starting with diversity and inclusion officers who make it a priority to focus on parity. Formal programs can educate staff and colleagues about implicit bias so that they might more easily recognize it when it kicks in, and training for gatekeepers can lead to more proportional hiring of women at every level.
Institutions should review their policies – salary inequities, diversity in promotion, processes for selecting leaders – and set formal interventional goals that are then evaluated in honest, documented annual reviews.
Some of these policies should address work-life balance as well: Offering part-time and flexible work options during early child-rearing years helps not only mothers, but also fathers who are now taking a more active role in parenting. Slowing or prorating the promotion clock can help those building families, and shifting meetings away from times such as 7:00 a.m. and 6:00 p.m. allow mothers and fathers alike to get their kids to and from school and attend children’s events.
Sponsorship of women is an important strategy in breaking the glass ceiling, Dr. Levine said. Sponsors can support women with untapped leadership potential and do the necessary networking and introductions that help make that advance happen. And it must be done by sponsors with power and influence, including men, Dr. Levine said.
Men can play important roles in promoting gender parity by suggesting women for key roles, leadership positions, and committees and also notifying women of upcoming opportunities, such as editorial board spots and other hot jobs. For women who aspire to be leaders, men can seek to convey leadership skills that may be needed to chair committees and other groups. Search committees need to expand beyond looking for “token women,” she said.
Dr. Levine illustrated her address with her own story. She described how many of these strategies had helped her career and how many male supervisors, mentors, and colleagues helped her, including introducing her to other male leaders who then offered her opportunities to contribute to the American College of Chest Physicians. She ran for CHEST president twice before being elected on her third run in September. She is the fifth woman to lead CHEST.
“Don’t give up,” she encouraged women in the audience, telling them to advocate for themselves and to encourage, mentor, and sponsor their female fellows and junior faculty.
“This will result in closing the gaps and will help women achieve leadership roles and competitive salaries as well as work-life integration,” Dr. Levine said.
SAN ANTONIO – Women in medicine have made great strides in cracking the glass ceiling, but it’s not shattered yet, said Stephanie M. Levine, MD, FCCP, the incoming president of CHEST.
At a session on women in medicine at the annual meeting of the American College of Chest Physicians, Dr. Levine discussed the challenges of breaking through the metaphorical invisible barrier. The “glass ceiling” refers to multiple ways in which women lack equality with men in medicine: leadership roles, positions and titles, progress in academic medicine, gaps in salaries and compensation, and overall gender parity in specialties.
For example, according to data from the American Association of Medical Colleges for 2017-2018, women comprise 50% of medical school graduates but only 34% of the physician workforce and 22% of leadership roles. Women are 13% less likely to be promoted to professor. They receive salaries an average 21% lower than those of their male peers, said Dr. Levine, professor of medicine and director of the pulmonary/critical care fellowship program at the University of Texas, San Antonio.
Disparities exist particularly within specialties and subspecialties, she said. Women make 85% of what men earn in primary care but, in the specialties, only 75% of what men earn. Among active fellow trainees in the areas of medicine most represented by CHEST, one-third (32%) of critical care physicians and less than a third (29%) of pulmonary physicians are female.
Why the lag in specialty parity?
The reasons for these disparities are complex, Dr. Levine argued, but the problem is not insurmountable. They begin, in a sense, with the problem itself: When there are fewer mentors, role models, sponsors, and leaders, and less overall representation of women in the first place, it is harder for women to advance.
One male audience member, for example, asked how his department could recruit more women, because most turned down interviews despite the fact that more women than men were being invited. “How many women are in your leadership?” Dr. Levine asked. He acknowledged that there were none – and therein lies the likely problem. Applicants are looking for female representation in leadership.
Gender bias and discrimination certainly play a role among peers, leadership, and even patients. Patients referring to female physicians by their first names and asking questions such as “Are you my nurse?” are subtle but cutting examples of the ways in which they reveal implicit bias and reinforce gender stereotypes, Dr. Levine said to weary nods of agreement among the attendees.
Implicit, unconscious bias is also built into the culture of a place and the way things have always been done. Lack of equity in salary, space to work, support, and promotion all compound one another. Work-life integration challenges often do not favor women. Studies have shown that in the hiring process, CVs with female names do not receive as much attention as do CVs with male names, Dr. Levine noted.
Some of the challenges lie with the way women themselves do or do not advocate for themselves. Research has long shown that women do not negotiate as well – or at all – compared with men. Women tend to be less aggressive in seeking higher compensation and leadership roles, possibly because of existing implicit bias against female assertiveness in general.
The catch-22 is that being more assertive or direct can lead others to interpret a woman as being rude or brusk, as one audience member noted when she described how colleagues perceive her simple, direct tone as seeming “upset.”
Conscious bias remains alive and well: The stereotypes that women are caretakers and men are take-charge dominators persist and can reinforce gender disparities in leadership roles.
Women also must make calculations and trade-offs between their academic promotion clocks and their biologic clocks, Dr. Levine explained.
“The 30s are great for both academic and biologic productivity,” she told attendees. The typical age for a person’s first National Institutes of Health Research Project grant (R01) is in the early 40s.
How to improve gender equality
Women bring diverse skills and perspectives to the table, Dr. Levine explained. Women tend to have stronger collaborative skills and greater compassion and empathy, for example. They tend to be less hierarchal and better at mentoring and empowerment, she said.
There are many ways to poke more cracks in the ceiling, starting with diversity and inclusion officers who make it a priority to focus on parity. Formal programs can educate staff and colleagues about implicit bias so that they might more easily recognize it when it kicks in, and training for gatekeepers can lead to more proportional hiring of women at every level.
Institutions should review their policies – salary inequities, diversity in promotion, processes for selecting leaders – and set formal interventional goals that are then evaluated in honest, documented annual reviews.
Some of these policies should address work-life balance as well: Offering part-time and flexible work options during early child-rearing years helps not only mothers, but also fathers who are now taking a more active role in parenting. Slowing or prorating the promotion clock can help those building families, and shifting meetings away from times such as 7:00 a.m. and 6:00 p.m. allow mothers and fathers alike to get their kids to and from school and attend children’s events.
Sponsorship of women is an important strategy in breaking the glass ceiling, Dr. Levine said. Sponsors can support women with untapped leadership potential and do the necessary networking and introductions that help make that advance happen. And it must be done by sponsors with power and influence, including men, Dr. Levine said.
Men can play important roles in promoting gender parity by suggesting women for key roles, leadership positions, and committees and also notifying women of upcoming opportunities, such as editorial board spots and other hot jobs. For women who aspire to be leaders, men can seek to convey leadership skills that may be needed to chair committees and other groups. Search committees need to expand beyond looking for “token women,” she said.
Dr. Levine illustrated her address with her own story. She described how many of these strategies had helped her career and how many male supervisors, mentors, and colleagues helped her, including introducing her to other male leaders who then offered her opportunities to contribute to the American College of Chest Physicians. She ran for CHEST president twice before being elected on her third run in September. She is the fifth woman to lead CHEST.
“Don’t give up,” she encouraged women in the audience, telling them to advocate for themselves and to encourage, mentor, and sponsor their female fellows and junior faculty.
“This will result in closing the gaps and will help women achieve leadership roles and competitive salaries as well as work-life integration,” Dr. Levine said.
REPORTING FROM CHEST 2018
Genetic risk factor found for RA-associated interstitial lung disease
CHICAGO – Rheumatoid arthritis–associated interstitial lung disease and idiopathic pulmonary fibrosis without RA share a common genetic underpinning whose hallmark is a gain-of-function MUC5B gene promoter variant that cranks up mucin production in the lungs, Pierre-Antoine Juge, MD, reported at the annual meeting of the American College of Rheumatology.
He presented a seven-country genetic case-control study of 620 patients with RA-associated interstitial lung disease (RA-ILD), 614 with RA but no ILD, and 5,448 unaffected controls. The key finding was that the MUC5B promoter variant rs35705950, already known to be the strongest genetic risk factor for idiopathic pulmonary fibrosis (IPF), also contributes substantially to the risk of RA-ILD.
Indeed, the presence of the MUC5B promoter variant in patients with RA proved to be associated with substantially higher risk of RA-ILD than the previously recognized risk factors for RA-ILD, including cigarette smoking and the human leukocyte antigen locus for RA, according to Dr. Juge, a rheumatologist at Bichat Hospital–Claude Bernard and Paris Diderot University.
MUC5B encodes for mucin production in the lungs. The increased risk of RA-ILD conferred by the presence of the MUC5B promoter variant was confined to the 41% of RA-ILD patients with a pattern of usual interstitial pneumonia (UIP) or possible UIP on high-resolution CT. The presence of the MUC5B promoter variant in RA patients was independently associated with an adjusted 6.1-fold increased risk of ILD with a UIP pattern on imaging – marked by honeycombing, reticular abnormalities, and subpleural involvement – compared with RA patients who didn’t possess the gain-of-function MUC5B variant. The risk of other types of RA-ILD wasn’t affected by the presence or absence of the MUC5B variant.
The MUC5B promoter variant was not a risk factor for development of RA.
These findings have potentially important implications for clinical practice, given that clinically significant ILD is present in about 10% of all RA patients and occult ILD is detectable using high-resolution CT in up to half of individuals with RA, Dr. Juge observed. Detection of the MUC5B promoter variant could be used to screen patients with RA for preclinical ILD. Also, there is now a sound rationale to study drugs known to be effective for IPF as potential treatments for RA-ILD, he said.
Dr. Juge reported having no financial conflicts regarding the study, which was sponsored by the National Institutes of Health, the U.S. Department of Defense, the French Rheumatology Society, the Japanese Society for the Promotion of Science, Fondation Arthritis, and the Nina Ireland Program for Lung Health.
In conjunction with his presentation in Chicago, the study was published online in the New England Journal of Medicine (doi: 10.1056/NEJMoa1801562).
SOURCE: Juge P-A et al. Arthritis Rheumatol. 2018;70(Suppl 10): Abstract 1819.
CHICAGO – Rheumatoid arthritis–associated interstitial lung disease and idiopathic pulmonary fibrosis without RA share a common genetic underpinning whose hallmark is a gain-of-function MUC5B gene promoter variant that cranks up mucin production in the lungs, Pierre-Antoine Juge, MD, reported at the annual meeting of the American College of Rheumatology.
He presented a seven-country genetic case-control study of 620 patients with RA-associated interstitial lung disease (RA-ILD), 614 with RA but no ILD, and 5,448 unaffected controls. The key finding was that the MUC5B promoter variant rs35705950, already known to be the strongest genetic risk factor for idiopathic pulmonary fibrosis (IPF), also contributes substantially to the risk of RA-ILD.
Indeed, the presence of the MUC5B promoter variant in patients with RA proved to be associated with substantially higher risk of RA-ILD than the previously recognized risk factors for RA-ILD, including cigarette smoking and the human leukocyte antigen locus for RA, according to Dr. Juge, a rheumatologist at Bichat Hospital–Claude Bernard and Paris Diderot University.
MUC5B encodes for mucin production in the lungs. The increased risk of RA-ILD conferred by the presence of the MUC5B promoter variant was confined to the 41% of RA-ILD patients with a pattern of usual interstitial pneumonia (UIP) or possible UIP on high-resolution CT. The presence of the MUC5B promoter variant in RA patients was independently associated with an adjusted 6.1-fold increased risk of ILD with a UIP pattern on imaging – marked by honeycombing, reticular abnormalities, and subpleural involvement – compared with RA patients who didn’t possess the gain-of-function MUC5B variant. The risk of other types of RA-ILD wasn’t affected by the presence or absence of the MUC5B variant.
The MUC5B promoter variant was not a risk factor for development of RA.
These findings have potentially important implications for clinical practice, given that clinically significant ILD is present in about 10% of all RA patients and occult ILD is detectable using high-resolution CT in up to half of individuals with RA, Dr. Juge observed. Detection of the MUC5B promoter variant could be used to screen patients with RA for preclinical ILD. Also, there is now a sound rationale to study drugs known to be effective for IPF as potential treatments for RA-ILD, he said.
Dr. Juge reported having no financial conflicts regarding the study, which was sponsored by the National Institutes of Health, the U.S. Department of Defense, the French Rheumatology Society, the Japanese Society for the Promotion of Science, Fondation Arthritis, and the Nina Ireland Program for Lung Health.
In conjunction with his presentation in Chicago, the study was published online in the New England Journal of Medicine (doi: 10.1056/NEJMoa1801562).
SOURCE: Juge P-A et al. Arthritis Rheumatol. 2018;70(Suppl 10): Abstract 1819.
CHICAGO – Rheumatoid arthritis–associated interstitial lung disease and idiopathic pulmonary fibrosis without RA share a common genetic underpinning whose hallmark is a gain-of-function MUC5B gene promoter variant that cranks up mucin production in the lungs, Pierre-Antoine Juge, MD, reported at the annual meeting of the American College of Rheumatology.
He presented a seven-country genetic case-control study of 620 patients with RA-associated interstitial lung disease (RA-ILD), 614 with RA but no ILD, and 5,448 unaffected controls. The key finding was that the MUC5B promoter variant rs35705950, already known to be the strongest genetic risk factor for idiopathic pulmonary fibrosis (IPF), also contributes substantially to the risk of RA-ILD.
Indeed, the presence of the MUC5B promoter variant in patients with RA proved to be associated with substantially higher risk of RA-ILD than the previously recognized risk factors for RA-ILD, including cigarette smoking and the human leukocyte antigen locus for RA, according to Dr. Juge, a rheumatologist at Bichat Hospital–Claude Bernard and Paris Diderot University.
MUC5B encodes for mucin production in the lungs. The increased risk of RA-ILD conferred by the presence of the MUC5B promoter variant was confined to the 41% of RA-ILD patients with a pattern of usual interstitial pneumonia (UIP) or possible UIP on high-resolution CT. The presence of the MUC5B promoter variant in RA patients was independently associated with an adjusted 6.1-fold increased risk of ILD with a UIP pattern on imaging – marked by honeycombing, reticular abnormalities, and subpleural involvement – compared with RA patients who didn’t possess the gain-of-function MUC5B variant. The risk of other types of RA-ILD wasn’t affected by the presence or absence of the MUC5B variant.
The MUC5B promoter variant was not a risk factor for development of RA.
These findings have potentially important implications for clinical practice, given that clinically significant ILD is present in about 10% of all RA patients and occult ILD is detectable using high-resolution CT in up to half of individuals with RA, Dr. Juge observed. Detection of the MUC5B promoter variant could be used to screen patients with RA for preclinical ILD. Also, there is now a sound rationale to study drugs known to be effective for IPF as potential treatments for RA-ILD, he said.
Dr. Juge reported having no financial conflicts regarding the study, which was sponsored by the National Institutes of Health, the U.S. Department of Defense, the French Rheumatology Society, the Japanese Society for the Promotion of Science, Fondation Arthritis, and the Nina Ireland Program for Lung Health.
In conjunction with his presentation in Chicago, the study was published online in the New England Journal of Medicine (doi: 10.1056/NEJMoa1801562).
SOURCE: Juge P-A et al. Arthritis Rheumatol. 2018;70(Suppl 10): Abstract 1819.
REPORTING FROM THE ACR ANNUAL MEETING
Mepolizumab shows efficacy in bronchiectasis with eosinophilia
PARIS – according to a small case series of patients presented as a late-breaking study at the annual congress of the European Respiratory Society.
“The message is that it is important to think of all of the etiologies and treatable traits in patients with bronchiectasis, and do not forget eosinophilia, because this can be treated,” reported Jessica Rademacher, MD, of the Clinic for Pulmonology at Hannover (Germany) Medical School.
Mepolizumab is a monoclonal antibody that targets interleukin-5, an important signaling protein for eosinophil recruitment, and is approved for use in asthma with eosinophilia. Larger, controlled trials are needed to confirm its efficacy in bronchiectasis, but the clinical improvements after 6 months of treatment in a series of 12 patients at Dr. Rademacher’s center were impressive.
Bronchiectasis patients were selected for treatment with mepolizumab if they had been poorly controlled on conventional therapies and they had an eosinophil count of greater than 300 cells/mm3. Of 328 patients with bronchiectasis that are being followed at Dr. Rademacher’s center, 7% met these criteria. Dr. Rademacher presented data on 12 who had been followed for at least 6 months.
In these patients, the median eosinophil count fell from a median baseline of 1,000 cells/mm3 to 100 cells/mm3 at 6 months (P = .0012). The median annualized rate of exacerbations fell from three per year to one per year, and the median Modified Medical Research Council Dyspnea Scale score fell from 2 to 0 (P = .004).
“There was a steroid-sparing effect in all seven patients who were taking oral corticosteroids at baseline. Five stopped oral steroids completely,” Dr. Rademacher reported.
A visual analog scale ranging from 1 to 10 with higher scores representing improvement showed patient-rated quality of life improved from 4 to 6.5 (P = .01). Dr. Rademacher emphasized this outcome because “improved quality of life is really what we are trying to achieve.”
Mepolizumab was well tolerated. In one patient who developed pneumonia, mepolizumab was discontinued, but it was restarted when the infection resolved, because the pneumonia was not considered mepolizumab related.
Although Dr. Rademacher acknowledged the possibility that at least some of the patients in this case series had overlapping asthma, she emphasized that they were selected from a referral population that had a comprehensive workup and that this overlap has been rarely reported.
There is evidence that anti–interleukin-5 therapies such as mepolizumab are effective in respiratory diseases when eosinophilia is present, according to Dr. Rademacher. For example, she cited reports of clinical improvement in chronic obstructive pulmonary disease and granulomatosis with polyangiitis patients with high eosinophil counts. In bronchiectasis, which has many causes, it may be particularly important to select relevant targets.
“There is an important variability in the presentation of bronchiectasis. Not all these patients have reduced lung function,” she said. Rather, the most significant symptoms for a patient may be sputum or cough. She suggested that the goals are to identify underlying causes of symptoms and which may be treatable.
According to these data, eosinophilia may be one of the treatable causes in a small but significant proportion of patients with bronchiectasis. A trial of mepolizumab may be reasonable in patients inadequately controlled on inhaled anti-inflammatory drugs. “If they do not profit from this therapy, then stop,” she added.
Dr. Rademacher acknowledged that data from this small case series are “not enough to say that [mepolizumab] is an option for these patients,” but she believes the consistency of benefit in this small series will encourage the trials needed to confirm that this approach is safe and effective.
Dr. Rademacher reported no disclosures relevant to the report.
PARIS – according to a small case series of patients presented as a late-breaking study at the annual congress of the European Respiratory Society.
“The message is that it is important to think of all of the etiologies and treatable traits in patients with bronchiectasis, and do not forget eosinophilia, because this can be treated,” reported Jessica Rademacher, MD, of the Clinic for Pulmonology at Hannover (Germany) Medical School.
Mepolizumab is a monoclonal antibody that targets interleukin-5, an important signaling protein for eosinophil recruitment, and is approved for use in asthma with eosinophilia. Larger, controlled trials are needed to confirm its efficacy in bronchiectasis, but the clinical improvements after 6 months of treatment in a series of 12 patients at Dr. Rademacher’s center were impressive.
Bronchiectasis patients were selected for treatment with mepolizumab if they had been poorly controlled on conventional therapies and they had an eosinophil count of greater than 300 cells/mm3. Of 328 patients with bronchiectasis that are being followed at Dr. Rademacher’s center, 7% met these criteria. Dr. Rademacher presented data on 12 who had been followed for at least 6 months.
In these patients, the median eosinophil count fell from a median baseline of 1,000 cells/mm3 to 100 cells/mm3 at 6 months (P = .0012). The median annualized rate of exacerbations fell from three per year to one per year, and the median Modified Medical Research Council Dyspnea Scale score fell from 2 to 0 (P = .004).
“There was a steroid-sparing effect in all seven patients who were taking oral corticosteroids at baseline. Five stopped oral steroids completely,” Dr. Rademacher reported.
A visual analog scale ranging from 1 to 10 with higher scores representing improvement showed patient-rated quality of life improved from 4 to 6.5 (P = .01). Dr. Rademacher emphasized this outcome because “improved quality of life is really what we are trying to achieve.”
Mepolizumab was well tolerated. In one patient who developed pneumonia, mepolizumab was discontinued, but it was restarted when the infection resolved, because the pneumonia was not considered mepolizumab related.
Although Dr. Rademacher acknowledged the possibility that at least some of the patients in this case series had overlapping asthma, she emphasized that they were selected from a referral population that had a comprehensive workup and that this overlap has been rarely reported.
There is evidence that anti–interleukin-5 therapies such as mepolizumab are effective in respiratory diseases when eosinophilia is present, according to Dr. Rademacher. For example, she cited reports of clinical improvement in chronic obstructive pulmonary disease and granulomatosis with polyangiitis patients with high eosinophil counts. In bronchiectasis, which has many causes, it may be particularly important to select relevant targets.
“There is an important variability in the presentation of bronchiectasis. Not all these patients have reduced lung function,” she said. Rather, the most significant symptoms for a patient may be sputum or cough. She suggested that the goals are to identify underlying causes of symptoms and which may be treatable.
According to these data, eosinophilia may be one of the treatable causes in a small but significant proportion of patients with bronchiectasis. A trial of mepolizumab may be reasonable in patients inadequately controlled on inhaled anti-inflammatory drugs. “If they do not profit from this therapy, then stop,” she added.
Dr. Rademacher acknowledged that data from this small case series are “not enough to say that [mepolizumab] is an option for these patients,” but she believes the consistency of benefit in this small series will encourage the trials needed to confirm that this approach is safe and effective.
Dr. Rademacher reported no disclosures relevant to the report.
PARIS – according to a small case series of patients presented as a late-breaking study at the annual congress of the European Respiratory Society.
“The message is that it is important to think of all of the etiologies and treatable traits in patients with bronchiectasis, and do not forget eosinophilia, because this can be treated,” reported Jessica Rademacher, MD, of the Clinic for Pulmonology at Hannover (Germany) Medical School.
Mepolizumab is a monoclonal antibody that targets interleukin-5, an important signaling protein for eosinophil recruitment, and is approved for use in asthma with eosinophilia. Larger, controlled trials are needed to confirm its efficacy in bronchiectasis, but the clinical improvements after 6 months of treatment in a series of 12 patients at Dr. Rademacher’s center were impressive.
Bronchiectasis patients were selected for treatment with mepolizumab if they had been poorly controlled on conventional therapies and they had an eosinophil count of greater than 300 cells/mm3. Of 328 patients with bronchiectasis that are being followed at Dr. Rademacher’s center, 7% met these criteria. Dr. Rademacher presented data on 12 who had been followed for at least 6 months.
In these patients, the median eosinophil count fell from a median baseline of 1,000 cells/mm3 to 100 cells/mm3 at 6 months (P = .0012). The median annualized rate of exacerbations fell from three per year to one per year, and the median Modified Medical Research Council Dyspnea Scale score fell from 2 to 0 (P = .004).
“There was a steroid-sparing effect in all seven patients who were taking oral corticosteroids at baseline. Five stopped oral steroids completely,” Dr. Rademacher reported.
A visual analog scale ranging from 1 to 10 with higher scores representing improvement showed patient-rated quality of life improved from 4 to 6.5 (P = .01). Dr. Rademacher emphasized this outcome because “improved quality of life is really what we are trying to achieve.”
Mepolizumab was well tolerated. In one patient who developed pneumonia, mepolizumab was discontinued, but it was restarted when the infection resolved, because the pneumonia was not considered mepolizumab related.
Although Dr. Rademacher acknowledged the possibility that at least some of the patients in this case series had overlapping asthma, she emphasized that they were selected from a referral population that had a comprehensive workup and that this overlap has been rarely reported.
There is evidence that anti–interleukin-5 therapies such as mepolizumab are effective in respiratory diseases when eosinophilia is present, according to Dr. Rademacher. For example, she cited reports of clinical improvement in chronic obstructive pulmonary disease and granulomatosis with polyangiitis patients with high eosinophil counts. In bronchiectasis, which has many causes, it may be particularly important to select relevant targets.
“There is an important variability in the presentation of bronchiectasis. Not all these patients have reduced lung function,” she said. Rather, the most significant symptoms for a patient may be sputum or cough. She suggested that the goals are to identify underlying causes of symptoms and which may be treatable.
According to these data, eosinophilia may be one of the treatable causes in a small but significant proportion of patients with bronchiectasis. A trial of mepolizumab may be reasonable in patients inadequately controlled on inhaled anti-inflammatory drugs. “If they do not profit from this therapy, then stop,” she added.
Dr. Rademacher acknowledged that data from this small case series are “not enough to say that [mepolizumab] is an option for these patients,” but she believes the consistency of benefit in this small series will encourage the trials needed to confirm that this approach is safe and effective.
Dr. Rademacher reported no disclosures relevant to the report.
REPORTING FROM THE Ers congress 2018
Key clinical point: Although tested in a small case series, mepolizumab was highly effective for bronchiectasis presenting with eosinophilia.
Major finding: At 6 months, the median Modified Medical Research Council Dyspnea Scale score decreased from 2 at baseline to 0 (P = .004).
Study details: A case series of 12 patients from a single center.
Disclosures: Dr. Rademacher reported no financial relationships relevant to this report.
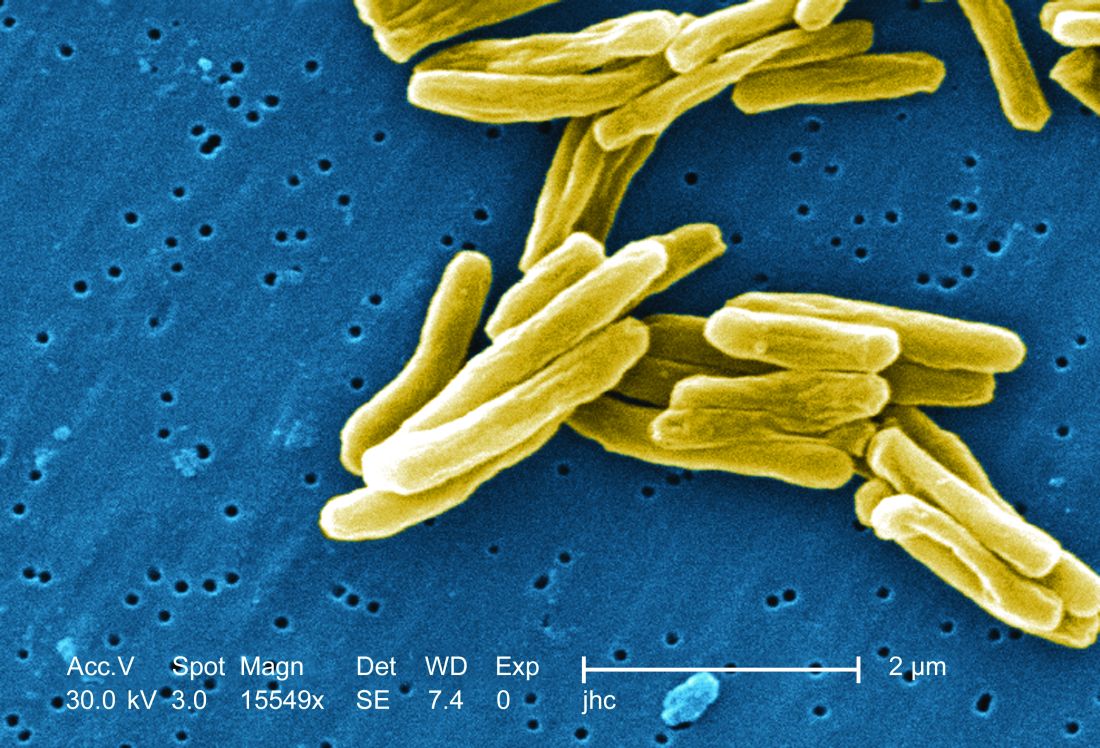
TB vaccine shows promise in previously infected
san francisco – A new The vaccine showed efficacy in young adults – an important finding because models suggest that inducing immunity in adolescents and young adults would be the fastest and most cost-effective approach to dealing with the global TB epidemic.
The study recruited adults who had previously been exposed to Mycobacterium tuberculosis, a population that receives no benefit from the long-standing bacillus Calmette-Guérin (BCG) vaccine. The overall efficacy of protection was 54%. “There isn’t any vaccine that’s been demonstrated to work in people who are already infected. It’s also the first vaccine to show this level of statistically significant protection in adults, and it’s adults who are the major transmitters of tuberculosis. The modeling has shown that even a vaccine that could protect infected adults at 20% vaccine efficacy would have a substantial impact on the epidemic and be cost effective,” said Ann Ginsberg, MD, PhD, chief medical officer at Aeras, which developed the vaccine and is now testing it in partnership with GlaxoSmithKline.
The results of the study were presented at ID Week 2018 and published in the New England Journal of Medicine (2018 Sep 25. doi: 10.1056/NEJMoa1803484).
The results address a major weakness of the BCG vaccine, which is that some studies have shown it offers little benefit to subjects who are already infected with the disease, which is the case for about a quarter of the world’s population, according to Dr. Ginsberg. The probable explanation is that previous infection with M. tuberculosis or a related bacteria is common in some populations and that this exposure grants some protection against progression to active disease.
The researchers tested the M72/AS01E vaccine, which includes two M. tuberculosis antigens that were identified from patients who had controlled their infection and also the AS01 adjuvant, which contains two immunostimulating agents and is a component of a developmental malaria vaccine and the recombinant zoster vaccine Shingrix.
In Kenya, South Africa, and Zambia, the researchers randomized 3,330 participants (mean age, 28.9 years; 43% female) to receive two doses 1 month apart of either vaccine or placebo. After a mean follow-up of 2.3 years, the protocol efficacy analysis showed that the vaccine had an efficacy rate of 54.0% (P = .04) for pulmonary tuberculosis.
The vaccine had greater efficacy in men (75.2%; P = .03) than it did in women (27.4%; P = .52) and among individuals aged 25 years or younger (84.4%; P = .01) than it did among older subjects (10.2%, P = .82).
The frequency of serious adverse events was similar between the vaccine (1.6%) and the placebo group (1.8%). Unsolicited reports of adverse events were more common in the vaccine group than the placebo group (67.4% vs. 45.4%, respectively), driven largely by more reports of injection site reactions and flu-like symptoms. Solicited reports of adverse events were highlighted by a greater frequency of injection site pain in the vaccine group (81.8% vs. 34.4%). A total of 24.3% of the vaccine recipients reported grade 3 pain, compared with 3.3% in the placebo arm. Rates of fatigue, headache, malaise, or myalgia were also higher in the vaccine group, as was fever.
All of the subjects in the vaccine group had seroconversion at month 2, and 99% remained seroconverted at 12 months.
Next, the researchers plan to conduct studies in HIV-infected individuals and to proceed with phase III trials.
The trial was funded by GlaxoSmithKline Biologicals and Aeras. Dr. Ginsberg is an employee of Aeras.
SOURCE: Ginsberg A et al. IDWeek 2018, Abstract 120
san francisco – A new The vaccine showed efficacy in young adults – an important finding because models suggest that inducing immunity in adolescents and young adults would be the fastest and most cost-effective approach to dealing with the global TB epidemic.
The study recruited adults who had previously been exposed to Mycobacterium tuberculosis, a population that receives no benefit from the long-standing bacillus Calmette-Guérin (BCG) vaccine. The overall efficacy of protection was 54%. “There isn’t any vaccine that’s been demonstrated to work in people who are already infected. It’s also the first vaccine to show this level of statistically significant protection in adults, and it’s adults who are the major transmitters of tuberculosis. The modeling has shown that even a vaccine that could protect infected adults at 20% vaccine efficacy would have a substantial impact on the epidemic and be cost effective,” said Ann Ginsberg, MD, PhD, chief medical officer at Aeras, which developed the vaccine and is now testing it in partnership with GlaxoSmithKline.
The results of the study were presented at ID Week 2018 and published in the New England Journal of Medicine (2018 Sep 25. doi: 10.1056/NEJMoa1803484).
The results address a major weakness of the BCG vaccine, which is that some studies have shown it offers little benefit to subjects who are already infected with the disease, which is the case for about a quarter of the world’s population, according to Dr. Ginsberg. The probable explanation is that previous infection with M. tuberculosis or a related bacteria is common in some populations and that this exposure grants some protection against progression to active disease.
The researchers tested the M72/AS01E vaccine, which includes two M. tuberculosis antigens that were identified from patients who had controlled their infection and also the AS01 adjuvant, which contains two immunostimulating agents and is a component of a developmental malaria vaccine and the recombinant zoster vaccine Shingrix.
In Kenya, South Africa, and Zambia, the researchers randomized 3,330 participants (mean age, 28.9 years; 43% female) to receive two doses 1 month apart of either vaccine or placebo. After a mean follow-up of 2.3 years, the protocol efficacy analysis showed that the vaccine had an efficacy rate of 54.0% (P = .04) for pulmonary tuberculosis.
The vaccine had greater efficacy in men (75.2%; P = .03) than it did in women (27.4%; P = .52) and among individuals aged 25 years or younger (84.4%; P = .01) than it did among older subjects (10.2%, P = .82).
The frequency of serious adverse events was similar between the vaccine (1.6%) and the placebo group (1.8%). Unsolicited reports of adverse events were more common in the vaccine group than the placebo group (67.4% vs. 45.4%, respectively), driven largely by more reports of injection site reactions and flu-like symptoms. Solicited reports of adverse events were highlighted by a greater frequency of injection site pain in the vaccine group (81.8% vs. 34.4%). A total of 24.3% of the vaccine recipients reported grade 3 pain, compared with 3.3% in the placebo arm. Rates of fatigue, headache, malaise, or myalgia were also higher in the vaccine group, as was fever.
All of the subjects in the vaccine group had seroconversion at month 2, and 99% remained seroconverted at 12 months.
Next, the researchers plan to conduct studies in HIV-infected individuals and to proceed with phase III trials.
The trial was funded by GlaxoSmithKline Biologicals and Aeras. Dr. Ginsberg is an employee of Aeras.
SOURCE: Ginsberg A et al. IDWeek 2018, Abstract 120
san francisco – A new The vaccine showed efficacy in young adults – an important finding because models suggest that inducing immunity in adolescents and young adults would be the fastest and most cost-effective approach to dealing with the global TB epidemic.
The study recruited adults who had previously been exposed to Mycobacterium tuberculosis, a population that receives no benefit from the long-standing bacillus Calmette-Guérin (BCG) vaccine. The overall efficacy of protection was 54%. “There isn’t any vaccine that’s been demonstrated to work in people who are already infected. It’s also the first vaccine to show this level of statistically significant protection in adults, and it’s adults who are the major transmitters of tuberculosis. The modeling has shown that even a vaccine that could protect infected adults at 20% vaccine efficacy would have a substantial impact on the epidemic and be cost effective,” said Ann Ginsberg, MD, PhD, chief medical officer at Aeras, which developed the vaccine and is now testing it in partnership with GlaxoSmithKline.
The results of the study were presented at ID Week 2018 and published in the New England Journal of Medicine (2018 Sep 25. doi: 10.1056/NEJMoa1803484).
The results address a major weakness of the BCG vaccine, which is that some studies have shown it offers little benefit to subjects who are already infected with the disease, which is the case for about a quarter of the world’s population, according to Dr. Ginsberg. The probable explanation is that previous infection with M. tuberculosis or a related bacteria is common in some populations and that this exposure grants some protection against progression to active disease.
The researchers tested the M72/AS01E vaccine, which includes two M. tuberculosis antigens that were identified from patients who had controlled their infection and also the AS01 adjuvant, which contains two immunostimulating agents and is a component of a developmental malaria vaccine and the recombinant zoster vaccine Shingrix.
In Kenya, South Africa, and Zambia, the researchers randomized 3,330 participants (mean age, 28.9 years; 43% female) to receive two doses 1 month apart of either vaccine or placebo. After a mean follow-up of 2.3 years, the protocol efficacy analysis showed that the vaccine had an efficacy rate of 54.0% (P = .04) for pulmonary tuberculosis.
The vaccine had greater efficacy in men (75.2%; P = .03) than it did in women (27.4%; P = .52) and among individuals aged 25 years or younger (84.4%; P = .01) than it did among older subjects (10.2%, P = .82).
The frequency of serious adverse events was similar between the vaccine (1.6%) and the placebo group (1.8%). Unsolicited reports of adverse events were more common in the vaccine group than the placebo group (67.4% vs. 45.4%, respectively), driven largely by more reports of injection site reactions and flu-like symptoms. Solicited reports of adverse events were highlighted by a greater frequency of injection site pain in the vaccine group (81.8% vs. 34.4%). A total of 24.3% of the vaccine recipients reported grade 3 pain, compared with 3.3% in the placebo arm. Rates of fatigue, headache, malaise, or myalgia were also higher in the vaccine group, as was fever.
All of the subjects in the vaccine group had seroconversion at month 2, and 99% remained seroconverted at 12 months.
Next, the researchers plan to conduct studies in HIV-infected individuals and to proceed with phase III trials.
The trial was funded by GlaxoSmithKline Biologicals and Aeras. Dr. Ginsberg is an employee of Aeras.
SOURCE: Ginsberg A et al. IDWeek 2018, Abstract 120
REPORTING FROM IDWEEK 2018
Key clinical point: The vaccine is the first to show efficacy in patients previously exposed to the TB bacterium.
Major finding: The vaccine had a protective efficacy of 54%.
Study details: Randomized, controlled trial with 3,330 participants.
Disclosures: The trial was funded by GlaxoSmithKline Biologicals and Aeras. Dr. Ginsberg is an employee of Aeras.
Source: Ginsberg A et al. IDWeek 2018, Abstract 120.
Next-gen triple correctors look safe and effective for cystic fibrosis
Adding a next-generation corrector to dual corrector-potentiator therapy is safe and effective in cystic fibrosis patients with one or two Phe508del alleles, results of two randomized phase 2, proof-of-concept clinical trials suggest.
The were reported in the New England Journal of Medicine.
Both triple combinations improved lung function for patients heterozygous for the Phe508del cystic fibrosis transmembrane conductance regulator (CFTR) mutation and a minimal function mutation (Phe508del-MF) who had not previously received CFTR modulators, according to the investigators, who reported results simultaneously at the North American Cystic Fibrosis Conference in Denver.
These therapies also were effective in patients homozygous for Phe508del CFTR mutation (Phe508del-Phe508del) who had previously been treated with tezacaftor-ivacaftor, the results show.
No dose-limiting side effects or toxic effects were observed in the phase 2 studies, which included 4-week treatment periods.
“These trials provide proof of the concept that targeting the Phe508del CFTR protein with a triple-combination corrector–potentiator regimen can restore CFTR function and has the potential to represent a clinical advance for patients with cystic fibrosis who harbor either one or two Phe508del alleles, approximately 9 of every 10 patients with the disease,” Steven M. Rowe, MD, of the University of Alabama at Birmingham and his coauthors said in the report on VX-659 phase 2 study.
In that report, 63 patients with the Phe508del-MF genotype were randomized to one of three VX-659 doses in combination with tezacaftor and ivacaftor versus triple placebo for 4 weeks, while 29 Phe508del-Phe508del patients underwent a 4-week tezacaftor-ivacaftor run-in phase before starting 4 weeks of the triple combination.
The primary efficacy endpoint of the study was the absolute increase in percentage of predicted forced expiratory volume in 1 second (FEV1).
In the Phe508del-MF patients, adding VX-659 improved that endpoint by up to 13.3 points versus baseline (P less than .001), whereas the absolute change was just 0.4 in the placebo group, the report shows. In the Phe508del-phe508del group, there was a 9.7-point increase over baseline.
Similarly, the companion study on VX-445, reported by Jennifer L. Taylor‑Cousar, MD, of National Jewish Health, Denver, and her colleagues, showed an increase in percentage of predicted FEV1 of up to 13.8 points for Phe508del-MF patients (P less than .001), and an increase of 11.0 points in the Phe508del-Phe508del group (P less than .001).
Those results suggest that targeting the Phe508del CFTR mutation with a combination of two correctors and a potentiator can produce effective CFTR function in patients who have these forms of cystic fibrosis, according to Dr. Taylor-Cousar and her colleagues.
“Lung function was improved by a magnitude similar to that achieved with the CFTR modulator ivacaftor in patients with gating mutations, in whom treatment has been disease modifying,” the researchers wrote in their report.
Sweat chloride concentrations were reduced and respiratory domain scores were improved in patients receiving triple therapy, investigators reported.
Triple therapy improved Phe508del CFTR protein processing and trafficking, and chloride transport more so than any two agents in combination, according in vitro results, also described in the studies.
Phase 3 trials of these compounds are now underway, they said.
Both studies were supported by Vertex Pharmaceuticals, which received funding from the Cystic Fibrosis Foundation for the development of both VX-445 and VX-659. Dr. Rowe and Dr. Taylor-Cousar reported grants, personal fees, and nonfinancial support from Vertex while conducting the study. Study authors also reported disclosures related to AstraZeneca, Novartis, Bayer, Proteostasis, Gilead, Galapagos/AbbVie, and Celtaxsys, among other entities. Full disclosures for all authors were provided in the journal.
SOURCES: Keating D et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807120; Davies JC et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807119.
These recent investigations show that triple combination therapy improves lung function more than double combination therapy in patients with cystic fibrosis and Phe508del mutations, according to Fernando Holguin, MD, of the division of pulmonary sciences and critical care at the University of Colorado, Aurora.
“These reports represent a major breakthrough in cystic fibrosis therapeutics, with the potential for improving health and possibly survival in all patients who carry the most common cystic fibrosis transmembrane conductance regulator [CFTR] mutation,” Dr. Holguin said in an editorial.
Neither study reported dose-limiting side effects or toxicity, and only three patients in the VX-445 study stopped treatment due to adverse events, he remarked in his editorial.
However, it remains to be seen whether the lung function improvements will be maintained for longer treatment periods, he said. Patients in the phase 2 studies received a total of 4 weeks of the trial regimen, according to the reports. Also unknown is whether the new therapies will reduce exacerbation rates, or impact outcomes such as weight gain.
“These questions should soon be answered in the ongoing phase 3 trials of these regimens,” he added.
These comments are excerpted from an editorial by Dr. Holguin that accompanied the study (N Eng J Med. Oct 18; doi: 10.1056/NEJMe1811996). Dr. Holguin reported that he had no disclosures related to his editorial.
These recent investigations show that triple combination therapy improves lung function more than double combination therapy in patients with cystic fibrosis and Phe508del mutations, according to Fernando Holguin, MD, of the division of pulmonary sciences and critical care at the University of Colorado, Aurora.
“These reports represent a major breakthrough in cystic fibrosis therapeutics, with the potential for improving health and possibly survival in all patients who carry the most common cystic fibrosis transmembrane conductance regulator [CFTR] mutation,” Dr. Holguin said in an editorial.
Neither study reported dose-limiting side effects or toxicity, and only three patients in the VX-445 study stopped treatment due to adverse events, he remarked in his editorial.
However, it remains to be seen whether the lung function improvements will be maintained for longer treatment periods, he said. Patients in the phase 2 studies received a total of 4 weeks of the trial regimen, according to the reports. Also unknown is whether the new therapies will reduce exacerbation rates, or impact outcomes such as weight gain.
“These questions should soon be answered in the ongoing phase 3 trials of these regimens,” he added.
These comments are excerpted from an editorial by Dr. Holguin that accompanied the study (N Eng J Med. Oct 18; doi: 10.1056/NEJMe1811996). Dr. Holguin reported that he had no disclosures related to his editorial.
These recent investigations show that triple combination therapy improves lung function more than double combination therapy in patients with cystic fibrosis and Phe508del mutations, according to Fernando Holguin, MD, of the division of pulmonary sciences and critical care at the University of Colorado, Aurora.
“These reports represent a major breakthrough in cystic fibrosis therapeutics, with the potential for improving health and possibly survival in all patients who carry the most common cystic fibrosis transmembrane conductance regulator [CFTR] mutation,” Dr. Holguin said in an editorial.
Neither study reported dose-limiting side effects or toxicity, and only three patients in the VX-445 study stopped treatment due to adverse events, he remarked in his editorial.
However, it remains to be seen whether the lung function improvements will be maintained for longer treatment periods, he said. Patients in the phase 2 studies received a total of 4 weeks of the trial regimen, according to the reports. Also unknown is whether the new therapies will reduce exacerbation rates, or impact outcomes such as weight gain.
“These questions should soon be answered in the ongoing phase 3 trials of these regimens,” he added.
These comments are excerpted from an editorial by Dr. Holguin that accompanied the study (N Eng J Med. Oct 18; doi: 10.1056/NEJMe1811996). Dr. Holguin reported that he had no disclosures related to his editorial.
Adding a next-generation corrector to dual corrector-potentiator therapy is safe and effective in cystic fibrosis patients with one or two Phe508del alleles, results of two randomized phase 2, proof-of-concept clinical trials suggest.
The were reported in the New England Journal of Medicine.
Both triple combinations improved lung function for patients heterozygous for the Phe508del cystic fibrosis transmembrane conductance regulator (CFTR) mutation and a minimal function mutation (Phe508del-MF) who had not previously received CFTR modulators, according to the investigators, who reported results simultaneously at the North American Cystic Fibrosis Conference in Denver.
These therapies also were effective in patients homozygous for Phe508del CFTR mutation (Phe508del-Phe508del) who had previously been treated with tezacaftor-ivacaftor, the results show.
No dose-limiting side effects or toxic effects were observed in the phase 2 studies, which included 4-week treatment periods.
“These trials provide proof of the concept that targeting the Phe508del CFTR protein with a triple-combination corrector–potentiator regimen can restore CFTR function and has the potential to represent a clinical advance for patients with cystic fibrosis who harbor either one or two Phe508del alleles, approximately 9 of every 10 patients with the disease,” Steven M. Rowe, MD, of the University of Alabama at Birmingham and his coauthors said in the report on VX-659 phase 2 study.
In that report, 63 patients with the Phe508del-MF genotype were randomized to one of three VX-659 doses in combination with tezacaftor and ivacaftor versus triple placebo for 4 weeks, while 29 Phe508del-Phe508del patients underwent a 4-week tezacaftor-ivacaftor run-in phase before starting 4 weeks of the triple combination.
The primary efficacy endpoint of the study was the absolute increase in percentage of predicted forced expiratory volume in 1 second (FEV1).
In the Phe508del-MF patients, adding VX-659 improved that endpoint by up to 13.3 points versus baseline (P less than .001), whereas the absolute change was just 0.4 in the placebo group, the report shows. In the Phe508del-phe508del group, there was a 9.7-point increase over baseline.
Similarly, the companion study on VX-445, reported by Jennifer L. Taylor‑Cousar, MD, of National Jewish Health, Denver, and her colleagues, showed an increase in percentage of predicted FEV1 of up to 13.8 points for Phe508del-MF patients (P less than .001), and an increase of 11.0 points in the Phe508del-Phe508del group (P less than .001).
Those results suggest that targeting the Phe508del CFTR mutation with a combination of two correctors and a potentiator can produce effective CFTR function in patients who have these forms of cystic fibrosis, according to Dr. Taylor-Cousar and her colleagues.
“Lung function was improved by a magnitude similar to that achieved with the CFTR modulator ivacaftor in patients with gating mutations, in whom treatment has been disease modifying,” the researchers wrote in their report.
Sweat chloride concentrations were reduced and respiratory domain scores were improved in patients receiving triple therapy, investigators reported.
Triple therapy improved Phe508del CFTR protein processing and trafficking, and chloride transport more so than any two agents in combination, according in vitro results, also described in the studies.
Phase 3 trials of these compounds are now underway, they said.
Both studies were supported by Vertex Pharmaceuticals, which received funding from the Cystic Fibrosis Foundation for the development of both VX-445 and VX-659. Dr. Rowe and Dr. Taylor-Cousar reported grants, personal fees, and nonfinancial support from Vertex while conducting the study. Study authors also reported disclosures related to AstraZeneca, Novartis, Bayer, Proteostasis, Gilead, Galapagos/AbbVie, and Celtaxsys, among other entities. Full disclosures for all authors were provided in the journal.
SOURCES: Keating D et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807120; Davies JC et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807119.
Adding a next-generation corrector to dual corrector-potentiator therapy is safe and effective in cystic fibrosis patients with one or two Phe508del alleles, results of two randomized phase 2, proof-of-concept clinical trials suggest.
The were reported in the New England Journal of Medicine.
Both triple combinations improved lung function for patients heterozygous for the Phe508del cystic fibrosis transmembrane conductance regulator (CFTR) mutation and a minimal function mutation (Phe508del-MF) who had not previously received CFTR modulators, according to the investigators, who reported results simultaneously at the North American Cystic Fibrosis Conference in Denver.
These therapies also were effective in patients homozygous for Phe508del CFTR mutation (Phe508del-Phe508del) who had previously been treated with tezacaftor-ivacaftor, the results show.
No dose-limiting side effects or toxic effects were observed in the phase 2 studies, which included 4-week treatment periods.
“These trials provide proof of the concept that targeting the Phe508del CFTR protein with a triple-combination corrector–potentiator regimen can restore CFTR function and has the potential to represent a clinical advance for patients with cystic fibrosis who harbor either one or two Phe508del alleles, approximately 9 of every 10 patients with the disease,” Steven M. Rowe, MD, of the University of Alabama at Birmingham and his coauthors said in the report on VX-659 phase 2 study.
In that report, 63 patients with the Phe508del-MF genotype were randomized to one of three VX-659 doses in combination with tezacaftor and ivacaftor versus triple placebo for 4 weeks, while 29 Phe508del-Phe508del patients underwent a 4-week tezacaftor-ivacaftor run-in phase before starting 4 weeks of the triple combination.
The primary efficacy endpoint of the study was the absolute increase in percentage of predicted forced expiratory volume in 1 second (FEV1).
In the Phe508del-MF patients, adding VX-659 improved that endpoint by up to 13.3 points versus baseline (P less than .001), whereas the absolute change was just 0.4 in the placebo group, the report shows. In the Phe508del-phe508del group, there was a 9.7-point increase over baseline.
Similarly, the companion study on VX-445, reported by Jennifer L. Taylor‑Cousar, MD, of National Jewish Health, Denver, and her colleagues, showed an increase in percentage of predicted FEV1 of up to 13.8 points for Phe508del-MF patients (P less than .001), and an increase of 11.0 points in the Phe508del-Phe508del group (P less than .001).
Those results suggest that targeting the Phe508del CFTR mutation with a combination of two correctors and a potentiator can produce effective CFTR function in patients who have these forms of cystic fibrosis, according to Dr. Taylor-Cousar and her colleagues.
“Lung function was improved by a magnitude similar to that achieved with the CFTR modulator ivacaftor in patients with gating mutations, in whom treatment has been disease modifying,” the researchers wrote in their report.
Sweat chloride concentrations were reduced and respiratory domain scores were improved in patients receiving triple therapy, investigators reported.
Triple therapy improved Phe508del CFTR protein processing and trafficking, and chloride transport more so than any two agents in combination, according in vitro results, also described in the studies.
Phase 3 trials of these compounds are now underway, they said.
Both studies were supported by Vertex Pharmaceuticals, which received funding from the Cystic Fibrosis Foundation for the development of both VX-445 and VX-659. Dr. Rowe and Dr. Taylor-Cousar reported grants, personal fees, and nonfinancial support from Vertex while conducting the study. Study authors also reported disclosures related to AstraZeneca, Novartis, Bayer, Proteostasis, Gilead, Galapagos/AbbVie, and Celtaxsys, among other entities. Full disclosures for all authors were provided in the journal.
SOURCES: Keating D et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807120; Davies JC et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807119.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Adding the next-generation correctors VX-445 or VX-659 to tezacaftor-ivacaftor was safe and improved lung function in patients with one or two Phe508del alleles.
Major finding: Improvements of up to 13.8 points over baseline were noted in absolute increase in percentage of predicted FEV1, the primary efficacy endpoint of the investigations.
Study details: Companion phase 2, randomized proof-of-concept studies included a total of 117 and 123 patients with cystic fibrosis.
Disclosures: Both studies were supported by Vertex Pharmaceuticals. Lead investigators reported grants, personal fees, and nonfinancial support from Vertex during the study. Other disclosures reported were related to AstraZeneca, Novartis, Bayer, Gilead, and Galapagos/AbbVie, among others.
Sources: Keating D et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807120; Davies JC et al. N Engl J Med. 2018 Oct 18. doi: 10.1056/NEJMoa1807119.
Macitentan brought down arterial pressure in PoPH trial
PARIS – In a multicenter, placebo-controlled including the primary endpoint of pulmonary vascular resistance, according to a late-breaking presentation at the annual congress of the European Respiratory Society.
“This is the first randomized, controlled trial that enrolled only patients with PoPH, and it demonstrates that a therapy used in pulmonary arterial hypertension improves hemodynamics in PoPH,” reported Olivier Sitbon, MD, of the Centre des Maladies Vasculaires Pulmonaires, Université de Paris–Sud, Clamart, France.
PoPH, defined by accompanying portal hypertension, is a variant on pulmonary arterial hypertension (PAH). Liver dysfunction is common but not required for a diagnosis. Although patients often receive therapies known to be effective in PAH, such as drugs in the endothelin receptor antagonist class, prostanoids, or phosphodiesterase-5 inhibitors, there “are very limited data” demonstrating efficacy of any drug specifically for patients with PoPH, according to Dr. Sitbon. One reason is that PoPH has been an exclusion criterion in large PAH treatment trials.
In PORTICO, a double-blind trial presented by Dr. Sitbon, 85 PoPH patients were randomized to 10 mg macitentan or placebo. Essentially, all were in World Health Organization functional class II or III with a median 6-minute walk distance (6MWD) of about 385 meters. During the trial, patients were permitted to remain on baseline therapies, including prostanoids and phosphodiesterase-5 inhibitors when doses had been stable for at least 3 months prior to randomization.
The primary endpoint was change in pulmonary vascular resistance (PVR) at 12 weeks. Other hemodynamic changes, such as change in cardiac index and total pulmonary resistance, were included in secondary endpoints along with change in WHO class and change in 6MWD.
When compared at 12 weeks with a model-adjusted ratio of geometric means, the ratio of PVR for the treatment to experimental arms was 0.65, which was a 35% relative improvement (P less than .0001) with macitentan.
The relative reduction from baseline in total arterial pressure was also highly significant favoring macitentan (–199.8 vs. –18.3 dyne/sec per cm–5; P less than .0001). Mean pulmonary pressure was slightly increased at the end of 12 weeks relative to baseline in the placebo group (+0.4 mm Hg) but fell 6.4 mm Hg in the treatment group (P less than .0001). In addition, cardiac index improved substantially on macitentan but not on placebo (0.6 vs. 0.1 L/min per m2; P = .0009).
However, there were no significant differences at the end of 12 weeks between groups for change from baseline in WHO functional class or 6MWD. Change in hepatic venous pressure gradient was evaluated in patients with liver disease, but macitentan was not associated with any effect on this parameter.
Macitentan was well tolerated overall. Although one patient experienced a equal to or greater than three times the upper limit of normal elevation of liver enzymes, Dr. Sitbon reported that there were no other hepatic safety concerns. Overall, he characterized the safety of macitentan in PoPH as “consistent with that previously observed in PAH.”
Larger and longer-term trials are needed to evaluate the impact of treatment on clinical events, but Dr. Sitbon indicated that these results demonstrate acceptable safety and tolerability and a favorable effect on hemodynamics. He further suggested that this randomized study provides a first step toward establishing an evidence-based treatment in this disease.
Dr. Sitbon reported financial relationships with Bayer, GlaxoSmithKline, and Actelion, the sponsor of this trial.
PARIS – In a multicenter, placebo-controlled including the primary endpoint of pulmonary vascular resistance, according to a late-breaking presentation at the annual congress of the European Respiratory Society.
“This is the first randomized, controlled trial that enrolled only patients with PoPH, and it demonstrates that a therapy used in pulmonary arterial hypertension improves hemodynamics in PoPH,” reported Olivier Sitbon, MD, of the Centre des Maladies Vasculaires Pulmonaires, Université de Paris–Sud, Clamart, France.
PoPH, defined by accompanying portal hypertension, is a variant on pulmonary arterial hypertension (PAH). Liver dysfunction is common but not required for a diagnosis. Although patients often receive therapies known to be effective in PAH, such as drugs in the endothelin receptor antagonist class, prostanoids, or phosphodiesterase-5 inhibitors, there “are very limited data” demonstrating efficacy of any drug specifically for patients with PoPH, according to Dr. Sitbon. One reason is that PoPH has been an exclusion criterion in large PAH treatment trials.
In PORTICO, a double-blind trial presented by Dr. Sitbon, 85 PoPH patients were randomized to 10 mg macitentan or placebo. Essentially, all were in World Health Organization functional class II or III with a median 6-minute walk distance (6MWD) of about 385 meters. During the trial, patients were permitted to remain on baseline therapies, including prostanoids and phosphodiesterase-5 inhibitors when doses had been stable for at least 3 months prior to randomization.
The primary endpoint was change in pulmonary vascular resistance (PVR) at 12 weeks. Other hemodynamic changes, such as change in cardiac index and total pulmonary resistance, were included in secondary endpoints along with change in WHO class and change in 6MWD.
When compared at 12 weeks with a model-adjusted ratio of geometric means, the ratio of PVR for the treatment to experimental arms was 0.65, which was a 35% relative improvement (P less than .0001) with macitentan.
The relative reduction from baseline in total arterial pressure was also highly significant favoring macitentan (–199.8 vs. –18.3 dyne/sec per cm–5; P less than .0001). Mean pulmonary pressure was slightly increased at the end of 12 weeks relative to baseline in the placebo group (+0.4 mm Hg) but fell 6.4 mm Hg in the treatment group (P less than .0001). In addition, cardiac index improved substantially on macitentan but not on placebo (0.6 vs. 0.1 L/min per m2; P = .0009).
However, there were no significant differences at the end of 12 weeks between groups for change from baseline in WHO functional class or 6MWD. Change in hepatic venous pressure gradient was evaluated in patients with liver disease, but macitentan was not associated with any effect on this parameter.
Macitentan was well tolerated overall. Although one patient experienced a equal to or greater than three times the upper limit of normal elevation of liver enzymes, Dr. Sitbon reported that there were no other hepatic safety concerns. Overall, he characterized the safety of macitentan in PoPH as “consistent with that previously observed in PAH.”
Larger and longer-term trials are needed to evaluate the impact of treatment on clinical events, but Dr. Sitbon indicated that these results demonstrate acceptable safety and tolerability and a favorable effect on hemodynamics. He further suggested that this randomized study provides a first step toward establishing an evidence-based treatment in this disease.
Dr. Sitbon reported financial relationships with Bayer, GlaxoSmithKline, and Actelion, the sponsor of this trial.
PARIS – In a multicenter, placebo-controlled including the primary endpoint of pulmonary vascular resistance, according to a late-breaking presentation at the annual congress of the European Respiratory Society.
“This is the first randomized, controlled trial that enrolled only patients with PoPH, and it demonstrates that a therapy used in pulmonary arterial hypertension improves hemodynamics in PoPH,” reported Olivier Sitbon, MD, of the Centre des Maladies Vasculaires Pulmonaires, Université de Paris–Sud, Clamart, France.
PoPH, defined by accompanying portal hypertension, is a variant on pulmonary arterial hypertension (PAH). Liver dysfunction is common but not required for a diagnosis. Although patients often receive therapies known to be effective in PAH, such as drugs in the endothelin receptor antagonist class, prostanoids, or phosphodiesterase-5 inhibitors, there “are very limited data” demonstrating efficacy of any drug specifically for patients with PoPH, according to Dr. Sitbon. One reason is that PoPH has been an exclusion criterion in large PAH treatment trials.
In PORTICO, a double-blind trial presented by Dr. Sitbon, 85 PoPH patients were randomized to 10 mg macitentan or placebo. Essentially, all were in World Health Organization functional class II or III with a median 6-minute walk distance (6MWD) of about 385 meters. During the trial, patients were permitted to remain on baseline therapies, including prostanoids and phosphodiesterase-5 inhibitors when doses had been stable for at least 3 months prior to randomization.
The primary endpoint was change in pulmonary vascular resistance (PVR) at 12 weeks. Other hemodynamic changes, such as change in cardiac index and total pulmonary resistance, were included in secondary endpoints along with change in WHO class and change in 6MWD.
When compared at 12 weeks with a model-adjusted ratio of geometric means, the ratio of PVR for the treatment to experimental arms was 0.65, which was a 35% relative improvement (P less than .0001) with macitentan.
The relative reduction from baseline in total arterial pressure was also highly significant favoring macitentan (–199.8 vs. –18.3 dyne/sec per cm–5; P less than .0001). Mean pulmonary pressure was slightly increased at the end of 12 weeks relative to baseline in the placebo group (+0.4 mm Hg) but fell 6.4 mm Hg in the treatment group (P less than .0001). In addition, cardiac index improved substantially on macitentan but not on placebo (0.6 vs. 0.1 L/min per m2; P = .0009).
However, there were no significant differences at the end of 12 weeks between groups for change from baseline in WHO functional class or 6MWD. Change in hepatic venous pressure gradient was evaluated in patients with liver disease, but macitentan was not associated with any effect on this parameter.
Macitentan was well tolerated overall. Although one patient experienced a equal to or greater than three times the upper limit of normal elevation of liver enzymes, Dr. Sitbon reported that there were no other hepatic safety concerns. Overall, he characterized the safety of macitentan in PoPH as “consistent with that previously observed in PAH.”
Larger and longer-term trials are needed to evaluate the impact of treatment on clinical events, but Dr. Sitbon indicated that these results demonstrate acceptable safety and tolerability and a favorable effect on hemodynamics. He further suggested that this randomized study provides a first step toward establishing an evidence-based treatment in this disease.
Dr. Sitbon reported financial relationships with Bayer, GlaxoSmithKline, and Actelion, the sponsor of this trial.
Key clinical point: Compared with placebo, macitentan improves hemodynamic parameters in patients with portopulmonary hypertension.
Major finding: In a 12-week trial, macitentan reduced pulmonary vascular resistance by 35% (P less than 0.0001).
Study details: A double-blind, multicenter, placebo-controlled trial.
Disclosures: Dr. Sitbon reported financial relationships with Bayer, GlaxoSmithKline, and Actelion, the sponsor of this trial.
Two-thirds of COPD patients not using inhalers correctly
SAN ANTONIO – Two-thirds of U.S. adults with (MDIs), according to new research. About half of patients failed to inhale slowly and deeply to ensure they received the appropriate dose, and about 40% of patients failed to hold their breath for 5-10 seconds afterward so that the medication made its way to their lungs, the findings show.
“There’s a need to educate patients on proper inhalation technique to optimize the appropriate delivery of medication,” Maryam Navaie, DrPH, of Advance Health Solutions in New York told attendees at the annual meeting of the American College of Chest Physicians. She also urged practitioners to think more carefully about what devices to prescribe to patients based on their own personal attributes.
“Nebulizer devices may be a better consideration for patients who have difficulty performing the necessary steps required by handheld inhalers,” Dr. Navaie said.
She and fellow researchers conducted a systematic review to gain more insights into the errors and difficulties experienced by U.S. adults using MDIs for COPD or asthma. They combed through PubMed, EMBASE, PsycINFO, Cochrane, and Google Scholar databases for English language studies about MDI-related errors in U.S. adult COPD or asthma patients published between January 2003 and February 2017.
The researchers included only randomized controlled trials and cross-sectional and observational studies, and they excluded studies with combined error rates across multiple devices so they could better parse out the data. They also used baseline rates only in studies that involved an intervention to reduce errors.
The researchers defined the proportion of overall MDI errors as “the percentage of patients who made errors in equal to or greater than 20% of inhalation steps.” They computed pooled estimates and created forest plots for both overall errors and for errors according to each step in using an MDI.
The eight studies they identified involved 1,221 patients, with ages ranging from a mean 48 to 82 years, 53% of whom were female. Nearly two-thirds of the patients had COPD (63.6%) while 36.4% had asthma. Most of the devices studied were MDIs alone (68.8%), while 31.2% included a spacer.
The pooled weighted average revealed a 66.5% error rate, that is, two-thirds of all the patients were making at least two errors during the 10 steps involved in using their device. The researchers then used individual error rates data in five studies to calculate the overall error rate for each step in using MDIs. The most common error, made by 73.8% of people in those five studies, was failing to attach the inhaler to the spacer. In addition, 68.7% of patients were failing to exhale fully and away from the inhaler before inhaling, and 47.8% were inhaling too fast instead of inhaling deeply.
“So these [findings] actually give you [some specific] ideas of how we could help improve patients’ ability to use the device properly,” Dr. Navaie told attendees, adding that these data can inform patient education needs and interventions.
Based on the data from those five studies, the error rates for all 10 steps to using an MDI were as follows:
- Failed to shake inhaler before use (37.9%).
- Failed to attach inhaler to spacer (73.8%).
- Failed to exhale fully and away from inhaler before inhalation (68.7%).
- Failed to place mouthpiece between teeth and sealed lips (7.4%).
- Failed to actuate once during inhalation (24.4%).
- Inhalation too fast, not deep (47.8%).
- Failed to hold breath for 5-10 seconds (40.1%).
- Failed to remove the inhaler/spacer from mouth (11.3%).
- Failed to exhale after inhalation (33.2%).
- Failed to repeat steps for second puff (36.7%).
Dr. Navaie also noted the investigators were surprised to learn that physicians themselves sometimes make several of these errors in explaining to patients how to use their devices.
“I think for the reps and other people who go out and visit doctors, it’s important to think about making sure the clinicians are using the devices properly,” Dr. Navaie said. She pointed out the potential for patients to forget steps between visits.
“One of the things a lot of our clinicians and key opinion leaders told us during the course of this study is that you shouldn’t just educate the patient at the time you are scripting the device but repeatedly because patients forget,” she said. She recommended having patients demonstrate their use of the device at each visit. If patients continue to struggle, it may be worth considering other therapies, such as a nebulizer, for patients unable to regularly use their devices correctly.
The meta-analysis was limited by the sparse research available in general on MDI errors in the U.S. adult population, so the data on error rates for each individual step may not be broadly generalizable. The studies also did not distinguish between rates among users with asthma vs. users with COPD. Further, too few data exist on associations between MDI errors and health outcomes to have a clear picture of the clinical implications of regularly making multiple errors in MDI use.
Dr. Navaie is employed by Advance Health Solutions, which received Sunovion Pharmaceuticals funding for the study.
SOURCE: Navaie M et al. CHEST 2018. doi: 10.1016/j.chest.2018.08.705.
SAN ANTONIO – Two-thirds of U.S. adults with (MDIs), according to new research. About half of patients failed to inhale slowly and deeply to ensure they received the appropriate dose, and about 40% of patients failed to hold their breath for 5-10 seconds afterward so that the medication made its way to their lungs, the findings show.
“There’s a need to educate patients on proper inhalation technique to optimize the appropriate delivery of medication,” Maryam Navaie, DrPH, of Advance Health Solutions in New York told attendees at the annual meeting of the American College of Chest Physicians. She also urged practitioners to think more carefully about what devices to prescribe to patients based on their own personal attributes.
“Nebulizer devices may be a better consideration for patients who have difficulty performing the necessary steps required by handheld inhalers,” Dr. Navaie said.
She and fellow researchers conducted a systematic review to gain more insights into the errors and difficulties experienced by U.S. adults using MDIs for COPD or asthma. They combed through PubMed, EMBASE, PsycINFO, Cochrane, and Google Scholar databases for English language studies about MDI-related errors in U.S. adult COPD or asthma patients published between January 2003 and February 2017.
The researchers included only randomized controlled trials and cross-sectional and observational studies, and they excluded studies with combined error rates across multiple devices so they could better parse out the data. They also used baseline rates only in studies that involved an intervention to reduce errors.
The researchers defined the proportion of overall MDI errors as “the percentage of patients who made errors in equal to or greater than 20% of inhalation steps.” They computed pooled estimates and created forest plots for both overall errors and for errors according to each step in using an MDI.
The eight studies they identified involved 1,221 patients, with ages ranging from a mean 48 to 82 years, 53% of whom were female. Nearly two-thirds of the patients had COPD (63.6%) while 36.4% had asthma. Most of the devices studied were MDIs alone (68.8%), while 31.2% included a spacer.
The pooled weighted average revealed a 66.5% error rate, that is, two-thirds of all the patients were making at least two errors during the 10 steps involved in using their device. The researchers then used individual error rates data in five studies to calculate the overall error rate for each step in using MDIs. The most common error, made by 73.8% of people in those five studies, was failing to attach the inhaler to the spacer. In addition, 68.7% of patients were failing to exhale fully and away from the inhaler before inhaling, and 47.8% were inhaling too fast instead of inhaling deeply.
“So these [findings] actually give you [some specific] ideas of how we could help improve patients’ ability to use the device properly,” Dr. Navaie told attendees, adding that these data can inform patient education needs and interventions.
Based on the data from those five studies, the error rates for all 10 steps to using an MDI were as follows:
- Failed to shake inhaler before use (37.9%).
- Failed to attach inhaler to spacer (73.8%).
- Failed to exhale fully and away from inhaler before inhalation (68.7%).
- Failed to place mouthpiece between teeth and sealed lips (7.4%).
- Failed to actuate once during inhalation (24.4%).
- Inhalation too fast, not deep (47.8%).
- Failed to hold breath for 5-10 seconds (40.1%).
- Failed to remove the inhaler/spacer from mouth (11.3%).
- Failed to exhale after inhalation (33.2%).
- Failed to repeat steps for second puff (36.7%).
Dr. Navaie also noted the investigators were surprised to learn that physicians themselves sometimes make several of these errors in explaining to patients how to use their devices.
“I think for the reps and other people who go out and visit doctors, it’s important to think about making sure the clinicians are using the devices properly,” Dr. Navaie said. She pointed out the potential for patients to forget steps between visits.
“One of the things a lot of our clinicians and key opinion leaders told us during the course of this study is that you shouldn’t just educate the patient at the time you are scripting the device but repeatedly because patients forget,” she said. She recommended having patients demonstrate their use of the device at each visit. If patients continue to struggle, it may be worth considering other therapies, such as a nebulizer, for patients unable to regularly use their devices correctly.
The meta-analysis was limited by the sparse research available in general on MDI errors in the U.S. adult population, so the data on error rates for each individual step may not be broadly generalizable. The studies also did not distinguish between rates among users with asthma vs. users with COPD. Further, too few data exist on associations between MDI errors and health outcomes to have a clear picture of the clinical implications of regularly making multiple errors in MDI use.
Dr. Navaie is employed by Advance Health Solutions, which received Sunovion Pharmaceuticals funding for the study.
SOURCE: Navaie M et al. CHEST 2018. doi: 10.1016/j.chest.2018.08.705.
SAN ANTONIO – Two-thirds of U.S. adults with (MDIs), according to new research. About half of patients failed to inhale slowly and deeply to ensure they received the appropriate dose, and about 40% of patients failed to hold their breath for 5-10 seconds afterward so that the medication made its way to their lungs, the findings show.
“There’s a need to educate patients on proper inhalation technique to optimize the appropriate delivery of medication,” Maryam Navaie, DrPH, of Advance Health Solutions in New York told attendees at the annual meeting of the American College of Chest Physicians. She also urged practitioners to think more carefully about what devices to prescribe to patients based on their own personal attributes.
“Nebulizer devices may be a better consideration for patients who have difficulty performing the necessary steps required by handheld inhalers,” Dr. Navaie said.
She and fellow researchers conducted a systematic review to gain more insights into the errors and difficulties experienced by U.S. adults using MDIs for COPD or asthma. They combed through PubMed, EMBASE, PsycINFO, Cochrane, and Google Scholar databases for English language studies about MDI-related errors in U.S. adult COPD or asthma patients published between January 2003 and February 2017.
The researchers included only randomized controlled trials and cross-sectional and observational studies, and they excluded studies with combined error rates across multiple devices so they could better parse out the data. They also used baseline rates only in studies that involved an intervention to reduce errors.
The researchers defined the proportion of overall MDI errors as “the percentage of patients who made errors in equal to or greater than 20% of inhalation steps.” They computed pooled estimates and created forest plots for both overall errors and for errors according to each step in using an MDI.
The eight studies they identified involved 1,221 patients, with ages ranging from a mean 48 to 82 years, 53% of whom were female. Nearly two-thirds of the patients had COPD (63.6%) while 36.4% had asthma. Most of the devices studied were MDIs alone (68.8%), while 31.2% included a spacer.
The pooled weighted average revealed a 66.5% error rate, that is, two-thirds of all the patients were making at least two errors during the 10 steps involved in using their device. The researchers then used individual error rates data in five studies to calculate the overall error rate for each step in using MDIs. The most common error, made by 73.8% of people in those five studies, was failing to attach the inhaler to the spacer. In addition, 68.7% of patients were failing to exhale fully and away from the inhaler before inhaling, and 47.8% were inhaling too fast instead of inhaling deeply.
“So these [findings] actually give you [some specific] ideas of how we could help improve patients’ ability to use the device properly,” Dr. Navaie told attendees, adding that these data can inform patient education needs and interventions.
Based on the data from those five studies, the error rates for all 10 steps to using an MDI were as follows:
- Failed to shake inhaler before use (37.9%).
- Failed to attach inhaler to spacer (73.8%).
- Failed to exhale fully and away from inhaler before inhalation (68.7%).
- Failed to place mouthpiece between teeth and sealed lips (7.4%).
- Failed to actuate once during inhalation (24.4%).
- Inhalation too fast, not deep (47.8%).
- Failed to hold breath for 5-10 seconds (40.1%).
- Failed to remove the inhaler/spacer from mouth (11.3%).
- Failed to exhale after inhalation (33.2%).
- Failed to repeat steps for second puff (36.7%).
Dr. Navaie also noted the investigators were surprised to learn that physicians themselves sometimes make several of these errors in explaining to patients how to use their devices.
“I think for the reps and other people who go out and visit doctors, it’s important to think about making sure the clinicians are using the devices properly,” Dr. Navaie said. She pointed out the potential for patients to forget steps between visits.
“One of the things a lot of our clinicians and key opinion leaders told us during the course of this study is that you shouldn’t just educate the patient at the time you are scripting the device but repeatedly because patients forget,” she said. She recommended having patients demonstrate their use of the device at each visit. If patients continue to struggle, it may be worth considering other therapies, such as a nebulizer, for patients unable to regularly use their devices correctly.
The meta-analysis was limited by the sparse research available in general on MDI errors in the U.S. adult population, so the data on error rates for each individual step may not be broadly generalizable. The studies also did not distinguish between rates among users with asthma vs. users with COPD. Further, too few data exist on associations between MDI errors and health outcomes to have a clear picture of the clinical implications of regularly making multiple errors in MDI use.
Dr. Navaie is employed by Advance Health Solutions, which received Sunovion Pharmaceuticals funding for the study.
SOURCE: Navaie M et al. CHEST 2018. doi: 10.1016/j.chest.2018.08.705.
REPORTING FROM CHEST 2018
Key clinical point: 67% of US adult patients with COPD or asthma report making errors in using metered-dose inhalers.
Major finding: 69% of patients do not exhale fully and away from the inhaler before inhalation; 50% do not inhale slowly and deeply.
Study details: Meta-analysis of eight studies involving 1,221 U.S. adult patients with COPD or asthma who use metered-dose inhalers.
Disclosures: Dr. Navaie is employed by Advance Health Solutions, which received Sunovion Pharmaceuticals funding for the study.
Source: Navaie M et al. CHEST 2018. doi: 10.1016/j.chest.2018.08.705.
Nasal cannula device may be an option for severe COPD
PARIS – As an alternative to noninvasive ventilator devices (NIV), a battery-powered high-flow nasal cannula delivering heated air improves exercise tolerance as measured with the 6-minute walking distance (6MWD), according to a crossover trial presented at the annual congress of the European Respiratory Society.
Not least important, these preliminary results show treatment with the device to be well tolerated, a potential advantage over NIV, according to Ms. Rossi, who cited published studies suggesting up to 35% of patients are intolerant to ambulatory NIV therapy.
In the study, 12 clinically stable COPD patients with a 6MWD of less than 300 m and dyspnea at a low level of exertion were enrolled. In random order on 2 consecutive days, patients were evaluated with the 6MWD test while fitted with the high-flow nasal cannula (HFNC) or while breathing room air.
The HFNC device delivers heated and humidified oxygen, which has been previously shown by the same group to improve oxygen saturation (Respir Med. 2016;118:128-32). In this study, the oxygen fraction (FiO2) of the air delivered by the proprietary HFNC device, marketed under the name AIRVO2 (Fisher & Paykel), was the same as the room air during the control exam.
In both tests, the patients performed the 6MWD while pushing a cart holding the device and the battery power source.
The mean 6MWD was 306 m using HFNC versus 267 m during the control test (P less than .05), even though the mean and nadir blood oxygenation (SpO2) levels were the same. However, the postexertion respiratory rate was significantly lower (P less than .05) when HFNC was used, Ms. Rossi reported. The inspiratory capacity was unchanged.
The improved levels of oxygen saturation (SaO2) demonstrated previously with high flows of humidified oxygen provided the basis for this preliminary crossover study, but a larger multicenter randomized trial was initiated last year. In that study with a planned enrollment of 160 COPD patients, the comparison will be between HFNC and usual oxygen delivered by a venturi mask. The primary outcome of the study, which will be completed early in 2019, is endurance improvement.
“COPD patients with severe dyspnea are frequently unable to achieve a workload that leads to improved exercise tolerance, with a result of reduced daily physical activities,” Ms. Rossi explained. She indicated that the HFNC, which is now being evaluated at several institutions, might be an important alternative to NIV in permitting patients to achieve adequate mobility.
The device is likely to be improved with technological advances, according to Ms. Rossi. She acknowledged that the current battery is heavy and the duration of the charge is relatively short, but she characterized this device as “good fit” for patients with very severe COPD. Only 8% of patients failed to complete this study.
Dr. Rossi reports no financial relationships relevant to this study.
PARIS – As an alternative to noninvasive ventilator devices (NIV), a battery-powered high-flow nasal cannula delivering heated air improves exercise tolerance as measured with the 6-minute walking distance (6MWD), according to a crossover trial presented at the annual congress of the European Respiratory Society.
Not least important, these preliminary results show treatment with the device to be well tolerated, a potential advantage over NIV, according to Ms. Rossi, who cited published studies suggesting up to 35% of patients are intolerant to ambulatory NIV therapy.
In the study, 12 clinically stable COPD patients with a 6MWD of less than 300 m and dyspnea at a low level of exertion were enrolled. In random order on 2 consecutive days, patients were evaluated with the 6MWD test while fitted with the high-flow nasal cannula (HFNC) or while breathing room air.
The HFNC device delivers heated and humidified oxygen, which has been previously shown by the same group to improve oxygen saturation (Respir Med. 2016;118:128-32). In this study, the oxygen fraction (FiO2) of the air delivered by the proprietary HFNC device, marketed under the name AIRVO2 (Fisher & Paykel), was the same as the room air during the control exam.
In both tests, the patients performed the 6MWD while pushing a cart holding the device and the battery power source.
The mean 6MWD was 306 m using HFNC versus 267 m during the control test (P less than .05), even though the mean and nadir blood oxygenation (SpO2) levels were the same. However, the postexertion respiratory rate was significantly lower (P less than .05) when HFNC was used, Ms. Rossi reported. The inspiratory capacity was unchanged.
The improved levels of oxygen saturation (SaO2) demonstrated previously with high flows of humidified oxygen provided the basis for this preliminary crossover study, but a larger multicenter randomized trial was initiated last year. In that study with a planned enrollment of 160 COPD patients, the comparison will be between HFNC and usual oxygen delivered by a venturi mask. The primary outcome of the study, which will be completed early in 2019, is endurance improvement.
“COPD patients with severe dyspnea are frequently unable to achieve a workload that leads to improved exercise tolerance, with a result of reduced daily physical activities,” Ms. Rossi explained. She indicated that the HFNC, which is now being evaluated at several institutions, might be an important alternative to NIV in permitting patients to achieve adequate mobility.
The device is likely to be improved with technological advances, according to Ms. Rossi. She acknowledged that the current battery is heavy and the duration of the charge is relatively short, but she characterized this device as “good fit” for patients with very severe COPD. Only 8% of patients failed to complete this study.
Dr. Rossi reports no financial relationships relevant to this study.
PARIS – As an alternative to noninvasive ventilator devices (NIV), a battery-powered high-flow nasal cannula delivering heated air improves exercise tolerance as measured with the 6-minute walking distance (6MWD), according to a crossover trial presented at the annual congress of the European Respiratory Society.
Not least important, these preliminary results show treatment with the device to be well tolerated, a potential advantage over NIV, according to Ms. Rossi, who cited published studies suggesting up to 35% of patients are intolerant to ambulatory NIV therapy.
In the study, 12 clinically stable COPD patients with a 6MWD of less than 300 m and dyspnea at a low level of exertion were enrolled. In random order on 2 consecutive days, patients were evaluated with the 6MWD test while fitted with the high-flow nasal cannula (HFNC) or while breathing room air.
The HFNC device delivers heated and humidified oxygen, which has been previously shown by the same group to improve oxygen saturation (Respir Med. 2016;118:128-32). In this study, the oxygen fraction (FiO2) of the air delivered by the proprietary HFNC device, marketed under the name AIRVO2 (Fisher & Paykel), was the same as the room air during the control exam.
In both tests, the patients performed the 6MWD while pushing a cart holding the device and the battery power source.
The mean 6MWD was 306 m using HFNC versus 267 m during the control test (P less than .05), even though the mean and nadir blood oxygenation (SpO2) levels were the same. However, the postexertion respiratory rate was significantly lower (P less than .05) when HFNC was used, Ms. Rossi reported. The inspiratory capacity was unchanged.
The improved levels of oxygen saturation (SaO2) demonstrated previously with high flows of humidified oxygen provided the basis for this preliminary crossover study, but a larger multicenter randomized trial was initiated last year. In that study with a planned enrollment of 160 COPD patients, the comparison will be between HFNC and usual oxygen delivered by a venturi mask. The primary outcome of the study, which will be completed early in 2019, is endurance improvement.
“COPD patients with severe dyspnea are frequently unable to achieve a workload that leads to improved exercise tolerance, with a result of reduced daily physical activities,” Ms. Rossi explained. She indicated that the HFNC, which is now being evaluated at several institutions, might be an important alternative to NIV in permitting patients to achieve adequate mobility.
The device is likely to be improved with technological advances, according to Ms. Rossi. She acknowledged that the current battery is heavy and the duration of the charge is relatively short, but she characterized this device as “good fit” for patients with very severe COPD. Only 8% of patients failed to complete this study.
Dr. Rossi reports no financial relationships relevant to this study.
REPORTNG FROM THE ERS CONGRESS 2018
Key clinical point: A battery-powered high-flow nasal cannula device improved the exercise capacity of patients with severe COPD.
Major finding: In a crossover study, the high-flow nasal cannula relative to no device increased mean 6-minute walking distance 39 m (15%).
Study details: Prospective crossover study.
Disclosures: Dr. Rossi reports no financial relationships relevant to this study.
Suicide risk doubled in COPD patients taking benzodiazepines
Patients with chronic obstructive pulmonary disease (COPD) who are taking benzodiazepines have a more than doubled risk of suicide, compared with similar patients not taking the medications.
The risk of all-cause mortality in , according to the results of research published in the Annals of the American Thoracic Society.
Benzodiazepines were often prescribed for people with COPD to manage chronic symptoms of anxiety, dyspnea, and insomnia that affect quality of life, Lucas M. Donovan, MD, of the division of pulmonary, critical care, and sleep medicine at the University of Washington, Seattle, and his colleagues noted.
However, there were documented concerns that the class of medications could lead to respiratory depression and increase the risk of exacerbations. According to the authors, one particular area of controversy was the long-term use of benzodiazepines, with up to 40% of COPD patients using them on a long-term basis against the advice of clinical guidelines.
They noted that benzodiazepines were also often used to treat dyspnea, a fact which had the potential to introduce confounding into research as the symptom was linked to increased mortality, nonfatal respiratory events, and suicidal ideation.
“One strategy to reduce confounding is to examine risks of benzodiazepines in a sample of patients who are likely to be prescribed benzodiazepines to manage nonrespiratory symptoms, and patients with comorbid posttraumatic stress disorder (PTSD) provide one such opportunity,” they wrote.
In the current study, the research team therefore used data from a nationwide cohort of patients with comorbid COPD and PTSD identified from the Veteran’s Health Administration administrative data between 2010 and 2012. The primary outcome was all-cause mortality in the 2 years following index among propensity-matched veterans with long-term benzodiazepine use, compared with nonusers.
Of 44,555 patients with COPD and PTSD included in the analysis, 29,237 had no benzodiazepine use, 4,782 patients had short-term use (less than 90 days’ supply), and 10,536 patients had long-term use (equal to or more than 90 days).
With a matched sample of 19,552 patients who did not receive benzodiazepines, the risk of all-cause mortality was not significantly different among those with long-term benzodiazepine use relative to those without use (hazard ratio, 1.06; 95% confidence interval, 0.95-1.18).
Furthermore, the specific relative risks of death related to obstructive lung disease and accidental overdose did not differ between the two groups.
Among matched and unmatched patients, short-term benzodiazepine use (HR, 1.16; 95% CI, 1.05-1.28), but not long-term use (HR, 1.03; 95% CI, 0.94-1.13) was associated with increased mortality. However, the authors said it was “worth noting that the associations with short-term use were found in analyses with unmatched patients and may be confounded by the specific episodic reasons for short-term benzodiazepine use such as acute illnesses not captured in our data.”
According to the research team, the most “consistent” and “striking” finding in their analysis was the link between benzodiazepine use and suicide.
They saw a substantially greater risk for death by suicide among those with long-term benzodiazepine use (HR, 2.33; 95% CI, 1.14-4.79). After adjusting all analyses by propensity score for any benzodiazepine exposure, individuals with both short-term and long-term use of benzodiazepines were at a greater risk of suicide (short-term: HR, 2.46; 95% CI, 1.16-5.26; long-term: HR, 2.35; 95% CI, 1.33-4.16).
“Similar to other estimates of the suicide rate within the veteran population (0.3 per 1,000 person-years), the rate of suicide among those without benzodiazepine use (0.4-0.5 per 1,000 person-years) in our sample was greater than the rate in the civilian population (0.1 per 1,000 person-years). However the risk of suicide was substantially greater among those with short- and long-term benzodiazepine use (1.1 per 1,000 person-years),” they wrote.
The use of long-acting benzodiazepines, such as diazepam, chlordiazepoxide, and flurazepam, was also positively associated with suicide (HR for every 10 days of exposure, 1.07; 95% CI, 1.01-1.13), and higher prescribed doses were associated with an increased risk of accidental overdose (HR for every 10 mg of diazepam equivalents, 1.19; 95% CI, 1.07-1.31).
The findings suggested that long-acting agents could pose a particular suicide risk but also “may relate to the sustained half-life of medication or the more severe and sustained mental health symptoms that prompt the use of long-acting agents,” the investigators wrote.
Concomitant opioid use was associated with increased risk of overall mortality (HR for every 10 days of exposure, 1.02; 95% CI, 1.01-1.02) and accidental overdose (HR, 1.11; 95% CI, 1.04-1.18). Individuals with long-term benzodiazepine use also had a higher rate of psychiatric admissions (incidence rate ratio, 1.37; 95% CI, 1.14-1.65).
The researchers concluded that, overall, their results did not suggest that discontinuation of long-term benzodiazepines would reduce overall mortality or death related to obstructive lung disease or overdose.
However, they advised that providers consider discontinuing benzodiazepines in patients already at high suicide risk as well as avoiding the concomitant use of opioids.
“Furthermore, providers should be aware of the risks that new benzodiazepine prescriptions may present to patients with COPD and PTSD without prior exposure to these medications,” they added.
The study was funded by several National Institutes of Heath grants, the ASPIRE (Academic Sleep Pulmonary Integrated Research/Clinical) Fellowship, and a VA grant.
SOURCE: Donovan LM et al. Ann Am Thorac Soc. 2018 Oct 12. doi: 10.1513/AnnalsATS.201802-145OC. Epub ahead of print.
Patients with chronic obstructive pulmonary disease (COPD) who are taking benzodiazepines have a more than doubled risk of suicide, compared with similar patients not taking the medications.
The risk of all-cause mortality in , according to the results of research published in the Annals of the American Thoracic Society.
Benzodiazepines were often prescribed for people with COPD to manage chronic symptoms of anxiety, dyspnea, and insomnia that affect quality of life, Lucas M. Donovan, MD, of the division of pulmonary, critical care, and sleep medicine at the University of Washington, Seattle, and his colleagues noted.
However, there were documented concerns that the class of medications could lead to respiratory depression and increase the risk of exacerbations. According to the authors, one particular area of controversy was the long-term use of benzodiazepines, with up to 40% of COPD patients using them on a long-term basis against the advice of clinical guidelines.
They noted that benzodiazepines were also often used to treat dyspnea, a fact which had the potential to introduce confounding into research as the symptom was linked to increased mortality, nonfatal respiratory events, and suicidal ideation.
“One strategy to reduce confounding is to examine risks of benzodiazepines in a sample of patients who are likely to be prescribed benzodiazepines to manage nonrespiratory symptoms, and patients with comorbid posttraumatic stress disorder (PTSD) provide one such opportunity,” they wrote.
In the current study, the research team therefore used data from a nationwide cohort of patients with comorbid COPD and PTSD identified from the Veteran’s Health Administration administrative data between 2010 and 2012. The primary outcome was all-cause mortality in the 2 years following index among propensity-matched veterans with long-term benzodiazepine use, compared with nonusers.
Of 44,555 patients with COPD and PTSD included in the analysis, 29,237 had no benzodiazepine use, 4,782 patients had short-term use (less than 90 days’ supply), and 10,536 patients had long-term use (equal to or more than 90 days).
With a matched sample of 19,552 patients who did not receive benzodiazepines, the risk of all-cause mortality was not significantly different among those with long-term benzodiazepine use relative to those without use (hazard ratio, 1.06; 95% confidence interval, 0.95-1.18).
Furthermore, the specific relative risks of death related to obstructive lung disease and accidental overdose did not differ between the two groups.
Among matched and unmatched patients, short-term benzodiazepine use (HR, 1.16; 95% CI, 1.05-1.28), but not long-term use (HR, 1.03; 95% CI, 0.94-1.13) was associated with increased mortality. However, the authors said it was “worth noting that the associations with short-term use were found in analyses with unmatched patients and may be confounded by the specific episodic reasons for short-term benzodiazepine use such as acute illnesses not captured in our data.”
According to the research team, the most “consistent” and “striking” finding in their analysis was the link between benzodiazepine use and suicide.
They saw a substantially greater risk for death by suicide among those with long-term benzodiazepine use (HR, 2.33; 95% CI, 1.14-4.79). After adjusting all analyses by propensity score for any benzodiazepine exposure, individuals with both short-term and long-term use of benzodiazepines were at a greater risk of suicide (short-term: HR, 2.46; 95% CI, 1.16-5.26; long-term: HR, 2.35; 95% CI, 1.33-4.16).
“Similar to other estimates of the suicide rate within the veteran population (0.3 per 1,000 person-years), the rate of suicide among those without benzodiazepine use (0.4-0.5 per 1,000 person-years) in our sample was greater than the rate in the civilian population (0.1 per 1,000 person-years). However the risk of suicide was substantially greater among those with short- and long-term benzodiazepine use (1.1 per 1,000 person-years),” they wrote.
The use of long-acting benzodiazepines, such as diazepam, chlordiazepoxide, and flurazepam, was also positively associated with suicide (HR for every 10 days of exposure, 1.07; 95% CI, 1.01-1.13), and higher prescribed doses were associated with an increased risk of accidental overdose (HR for every 10 mg of diazepam equivalents, 1.19; 95% CI, 1.07-1.31).
The findings suggested that long-acting agents could pose a particular suicide risk but also “may relate to the sustained half-life of medication or the more severe and sustained mental health symptoms that prompt the use of long-acting agents,” the investigators wrote.
Concomitant opioid use was associated with increased risk of overall mortality (HR for every 10 days of exposure, 1.02; 95% CI, 1.01-1.02) and accidental overdose (HR, 1.11; 95% CI, 1.04-1.18). Individuals with long-term benzodiazepine use also had a higher rate of psychiatric admissions (incidence rate ratio, 1.37; 95% CI, 1.14-1.65).
The researchers concluded that, overall, their results did not suggest that discontinuation of long-term benzodiazepines would reduce overall mortality or death related to obstructive lung disease or overdose.
However, they advised that providers consider discontinuing benzodiazepines in patients already at high suicide risk as well as avoiding the concomitant use of opioids.
“Furthermore, providers should be aware of the risks that new benzodiazepine prescriptions may present to patients with COPD and PTSD without prior exposure to these medications,” they added.
The study was funded by several National Institutes of Heath grants, the ASPIRE (Academic Sleep Pulmonary Integrated Research/Clinical) Fellowship, and a VA grant.
SOURCE: Donovan LM et al. Ann Am Thorac Soc. 2018 Oct 12. doi: 10.1513/AnnalsATS.201802-145OC. Epub ahead of print.
Patients with chronic obstructive pulmonary disease (COPD) who are taking benzodiazepines have a more than doubled risk of suicide, compared with similar patients not taking the medications.
The risk of all-cause mortality in , according to the results of research published in the Annals of the American Thoracic Society.
Benzodiazepines were often prescribed for people with COPD to manage chronic symptoms of anxiety, dyspnea, and insomnia that affect quality of life, Lucas M. Donovan, MD, of the division of pulmonary, critical care, and sleep medicine at the University of Washington, Seattle, and his colleagues noted.
However, there were documented concerns that the class of medications could lead to respiratory depression and increase the risk of exacerbations. According to the authors, one particular area of controversy was the long-term use of benzodiazepines, with up to 40% of COPD patients using them on a long-term basis against the advice of clinical guidelines.
They noted that benzodiazepines were also often used to treat dyspnea, a fact which had the potential to introduce confounding into research as the symptom was linked to increased mortality, nonfatal respiratory events, and suicidal ideation.
“One strategy to reduce confounding is to examine risks of benzodiazepines in a sample of patients who are likely to be prescribed benzodiazepines to manage nonrespiratory symptoms, and patients with comorbid posttraumatic stress disorder (PTSD) provide one such opportunity,” they wrote.
In the current study, the research team therefore used data from a nationwide cohort of patients with comorbid COPD and PTSD identified from the Veteran’s Health Administration administrative data between 2010 and 2012. The primary outcome was all-cause mortality in the 2 years following index among propensity-matched veterans with long-term benzodiazepine use, compared with nonusers.
Of 44,555 patients with COPD and PTSD included in the analysis, 29,237 had no benzodiazepine use, 4,782 patients had short-term use (less than 90 days’ supply), and 10,536 patients had long-term use (equal to or more than 90 days).
With a matched sample of 19,552 patients who did not receive benzodiazepines, the risk of all-cause mortality was not significantly different among those with long-term benzodiazepine use relative to those without use (hazard ratio, 1.06; 95% confidence interval, 0.95-1.18).
Furthermore, the specific relative risks of death related to obstructive lung disease and accidental overdose did not differ between the two groups.
Among matched and unmatched patients, short-term benzodiazepine use (HR, 1.16; 95% CI, 1.05-1.28), but not long-term use (HR, 1.03; 95% CI, 0.94-1.13) was associated with increased mortality. However, the authors said it was “worth noting that the associations with short-term use were found in analyses with unmatched patients and may be confounded by the specific episodic reasons for short-term benzodiazepine use such as acute illnesses not captured in our data.”
According to the research team, the most “consistent” and “striking” finding in their analysis was the link between benzodiazepine use and suicide.
They saw a substantially greater risk for death by suicide among those with long-term benzodiazepine use (HR, 2.33; 95% CI, 1.14-4.79). After adjusting all analyses by propensity score for any benzodiazepine exposure, individuals with both short-term and long-term use of benzodiazepines were at a greater risk of suicide (short-term: HR, 2.46; 95% CI, 1.16-5.26; long-term: HR, 2.35; 95% CI, 1.33-4.16).
“Similar to other estimates of the suicide rate within the veteran population (0.3 per 1,000 person-years), the rate of suicide among those without benzodiazepine use (0.4-0.5 per 1,000 person-years) in our sample was greater than the rate in the civilian population (0.1 per 1,000 person-years). However the risk of suicide was substantially greater among those with short- and long-term benzodiazepine use (1.1 per 1,000 person-years),” they wrote.
The use of long-acting benzodiazepines, such as diazepam, chlordiazepoxide, and flurazepam, was also positively associated with suicide (HR for every 10 days of exposure, 1.07; 95% CI, 1.01-1.13), and higher prescribed doses were associated with an increased risk of accidental overdose (HR for every 10 mg of diazepam equivalents, 1.19; 95% CI, 1.07-1.31).
The findings suggested that long-acting agents could pose a particular suicide risk but also “may relate to the sustained half-life of medication or the more severe and sustained mental health symptoms that prompt the use of long-acting agents,” the investigators wrote.
Concomitant opioid use was associated with increased risk of overall mortality (HR for every 10 days of exposure, 1.02; 95% CI, 1.01-1.02) and accidental overdose (HR, 1.11; 95% CI, 1.04-1.18). Individuals with long-term benzodiazepine use also had a higher rate of psychiatric admissions (incidence rate ratio, 1.37; 95% CI, 1.14-1.65).
The researchers concluded that, overall, their results did not suggest that discontinuation of long-term benzodiazepines would reduce overall mortality or death related to obstructive lung disease or overdose.
However, they advised that providers consider discontinuing benzodiazepines in patients already at high suicide risk as well as avoiding the concomitant use of opioids.
“Furthermore, providers should be aware of the risks that new benzodiazepine prescriptions may present to patients with COPD and PTSD without prior exposure to these medications,” they added.
The study was funded by several National Institutes of Heath grants, the ASPIRE (Academic Sleep Pulmonary Integrated Research/Clinical) Fellowship, and a VA grant.
SOURCE: Donovan LM et al. Ann Am Thorac Soc. 2018 Oct 12. doi: 10.1513/AnnalsATS.201802-145OC. Epub ahead of print.
FROM ANNALS OF THE AMERICAN THORACIC SOCIETY
Key clinical point: Health care providers should consider discontinuing benzodiazepines among COPD patients already at high suicide risk and should avoid concomitant opioid use.
Major finding: A strong risk of suicide was associated with benzodiazepine use among patients with COPD (HR, 2.33; 95% CI, 1.14-4.79).
Study details: A nationwide cohort of patients with comorbid COPD and PTSD identified from Veteran’s Health Administration administrative data between 2010 and 2012.
Disclosures: The study was funded by several National Institutes of Health grants, the ASPIRE (Academic Sleep Pulmonary Integrated Research/Clinical) Fellowship, and a VA grant.
Source: Donovan LM et al. Ann Am Thorac Soc. 2018 Oct 12. doi: 10.1513/AnnalsATS.201802-145OC. Epub ahead of print.
Dupilumab offers extra benefits to asthmatic teens
SAN ANTONIO – For adolescents with asthma, treatment with the biologic agent dupilumab provided benefits that were at least comparable with what was seen in adults, results from a retrospective analysis of a randomized, phase 3 study suggest.
Adolescents had reduced asthma exacerbations in line with what was seen in adults and had improvements in lung function that were at a greater magnitude than adults, according to study coauthor Neil M.H. Graham, MD, of Regeneron Pharmaceuticals, Tarrytown, N.Y.
“We think, overall, it’s a very good treatment response from this drug in this high-risk population, and it is generally well tolerated, as we’ve seen in other studies,” Dr. Graham said in a podium presentation at the annual meeting of the American College of Chest Physicians.
Dr. Graham presented results of an analysis of the 1,902-patient, phase 3 Liberty Asthma QUEST trial, published in May 2018 in the New England Journal of Medicine.
Top-line results of QUEST showed that treatment with dupilumab, a fully human anti–IL-4Ra monoclonal antibody, resulted in significantly lower rates of severe asthma exacerbation, along with improved lung function, in patients aged 12 years and older with moderate to severe asthma.
Now, this retrospective analysis shows that, in adolescents, improvements from baseline to week 12 in forced expiratory volume in 1 second (FEV1) were significant and at a greater magnitude than in adults, according to Dr. Graham and his coinvestigators.
The improvement over 12 weeks in FEV1 for adolescents was 0.36 L and 0.27 L, respectively, for the 200- and 300-mg doses of dupilumab (P less than .05 vs. placebo for both), Dr. Graham and his coinvestigators reported. In adults, the improvement was 0.12 L.
The annualized exacerbation rate dropped by 46.4% for those adolescents who received 200 mg dupilumab, though there was no treatment effect versus placebo for dupilumab 300 mg; the investigators said the lack of effect in this retrospective analysis could have been caused by imbalances in prior event rates or the small sample size.
A total of 107 out of 1,902 patients in QUEST were adolescents, and of those, 68 were randomly assigned to dupilumab, according to the report. Injection site reaction was the most common adverse event in adolescents in both dosing groups.
Dr. Graham reported disclosures related to his employment with Regeneron. Study coauthors reported disclosures related to Regeneron, AstraZeneca, Sanofi, Teva Pharmaceutical, GlaxoSmithKline, Boehringer Ingelheim, Merck, Genentech, and others.
SOURCE: Graham NMH et al. CHEST. 2018 Oct. doi: 10.1016/j.chest.2018.08.022.
SAN ANTONIO – For adolescents with asthma, treatment with the biologic agent dupilumab provided benefits that were at least comparable with what was seen in adults, results from a retrospective analysis of a randomized, phase 3 study suggest.
Adolescents had reduced asthma exacerbations in line with what was seen in adults and had improvements in lung function that were at a greater magnitude than adults, according to study coauthor Neil M.H. Graham, MD, of Regeneron Pharmaceuticals, Tarrytown, N.Y.
“We think, overall, it’s a very good treatment response from this drug in this high-risk population, and it is generally well tolerated, as we’ve seen in other studies,” Dr. Graham said in a podium presentation at the annual meeting of the American College of Chest Physicians.
Dr. Graham presented results of an analysis of the 1,902-patient, phase 3 Liberty Asthma QUEST trial, published in May 2018 in the New England Journal of Medicine.
Top-line results of QUEST showed that treatment with dupilumab, a fully human anti–IL-4Ra monoclonal antibody, resulted in significantly lower rates of severe asthma exacerbation, along with improved lung function, in patients aged 12 years and older with moderate to severe asthma.
Now, this retrospective analysis shows that, in adolescents, improvements from baseline to week 12 in forced expiratory volume in 1 second (FEV1) were significant and at a greater magnitude than in adults, according to Dr. Graham and his coinvestigators.
The improvement over 12 weeks in FEV1 for adolescents was 0.36 L and 0.27 L, respectively, for the 200- and 300-mg doses of dupilumab (P less than .05 vs. placebo for both), Dr. Graham and his coinvestigators reported. In adults, the improvement was 0.12 L.
The annualized exacerbation rate dropped by 46.4% for those adolescents who received 200 mg dupilumab, though there was no treatment effect versus placebo for dupilumab 300 mg; the investigators said the lack of effect in this retrospective analysis could have been caused by imbalances in prior event rates or the small sample size.
A total of 107 out of 1,902 patients in QUEST were adolescents, and of those, 68 were randomly assigned to dupilumab, according to the report. Injection site reaction was the most common adverse event in adolescents in both dosing groups.
Dr. Graham reported disclosures related to his employment with Regeneron. Study coauthors reported disclosures related to Regeneron, AstraZeneca, Sanofi, Teva Pharmaceutical, GlaxoSmithKline, Boehringer Ingelheim, Merck, Genentech, and others.
SOURCE: Graham NMH et al. CHEST. 2018 Oct. doi: 10.1016/j.chest.2018.08.022.
SAN ANTONIO – For adolescents with asthma, treatment with the biologic agent dupilumab provided benefits that were at least comparable with what was seen in adults, results from a retrospective analysis of a randomized, phase 3 study suggest.
Adolescents had reduced asthma exacerbations in line with what was seen in adults and had improvements in lung function that were at a greater magnitude than adults, according to study coauthor Neil M.H. Graham, MD, of Regeneron Pharmaceuticals, Tarrytown, N.Y.
“We think, overall, it’s a very good treatment response from this drug in this high-risk population, and it is generally well tolerated, as we’ve seen in other studies,” Dr. Graham said in a podium presentation at the annual meeting of the American College of Chest Physicians.
Dr. Graham presented results of an analysis of the 1,902-patient, phase 3 Liberty Asthma QUEST trial, published in May 2018 in the New England Journal of Medicine.
Top-line results of QUEST showed that treatment with dupilumab, a fully human anti–IL-4Ra monoclonal antibody, resulted in significantly lower rates of severe asthma exacerbation, along with improved lung function, in patients aged 12 years and older with moderate to severe asthma.
Now, this retrospective analysis shows that, in adolescents, improvements from baseline to week 12 in forced expiratory volume in 1 second (FEV1) were significant and at a greater magnitude than in adults, according to Dr. Graham and his coinvestigators.
The improvement over 12 weeks in FEV1 for adolescents was 0.36 L and 0.27 L, respectively, for the 200- and 300-mg doses of dupilumab (P less than .05 vs. placebo for both), Dr. Graham and his coinvestigators reported. In adults, the improvement was 0.12 L.
The annualized exacerbation rate dropped by 46.4% for those adolescents who received 200 mg dupilumab, though there was no treatment effect versus placebo for dupilumab 300 mg; the investigators said the lack of effect in this retrospective analysis could have been caused by imbalances in prior event rates or the small sample size.
A total of 107 out of 1,902 patients in QUEST were adolescents, and of those, 68 were randomly assigned to dupilumab, according to the report. Injection site reaction was the most common adverse event in adolescents in both dosing groups.
Dr. Graham reported disclosures related to his employment with Regeneron. Study coauthors reported disclosures related to Regeneron, AstraZeneca, Sanofi, Teva Pharmaceutical, GlaxoSmithKline, Boehringer Ingelheim, Merck, Genentech, and others.
SOURCE: Graham NMH et al. CHEST. 2018 Oct. doi: 10.1016/j.chest.2018.08.022.
REPORTING FROM CHEST 2018
Key clinical point: Dupilumab’s benefits in adolescents with moderate to severe asthma are at least comparable with what has been reported in adults.
Major finding: The improvement over 12 weeks in forced expiratory volume in 1 second for adolescents was 0.36 L and 0.27 L, respectively, for the 200- and 300-mg doses of dupilumab versus 0.12 L for adults.
Study details: A retrospective analysis of 1,902 patients (including 107 adolescents) in Liberty Asthma QUEST, a recently reported randomized, phase 3 trial.
Disclosures: Several study coauthors reported employment with Regeneron. Dr. Graham reported disclosures related to his employment with Regeneron. Other reported disclosures were related to AstraZeneca, Sanofi, Teva Pharmaceutical, GlaxoSmithKline, Boehringer Ingelheim, Merck, and Genentech, among other entities.
Source: Graham NMH et al. CHEST. 2018 Oct. doi: 10.1016/j/chest.2018.08.002.