User login
Method enables complex, large-scale genetic analysis

Image by Spencer Phillips
A new algorithm makes it possible to perform genetic analyses on as many as 500,000 individuals—and many traits—at the same time, according to an article in Nature Methods.
The authors noted that determining how genetic variations affect health and disease involves analyzing associations between many different variants and multiple traits and making the best use of data from large cohorts that include hundreds of thousands of individuals.
“It is very challenging to identify genetic variants that underlie phenotypes, or traits, and, usually, we do this by analyzing each phenotype and each variant one by one,” explained Oliver Stegle, PhD, of the European Molecular Biology Laboratory-European Bioinformatics Institute in Cambridge, UK.
“But the simple models we use to do this are too simplistic to uncover the complex dependencies between sets of genetic variants and disease phenotypes.”
On the other hand, complex models that reveal the combined action of many different variants have involved so much computation that it would take a year to run a single complex query. But Dr Stegle and his colleagues said their algorithm can change that.
“The breakthrough here is that we’ve made it possible to perform an integrative analysis involving many variants and phenotypes at the same speed as current approaches,” Dr Stegle said.
He and his colleagues tested their new method, called mtSet, on data from 2 studies and compared the results with existing tools used for genetic analysis. The researchers found that mtSet was substantially faster than existing methods and could explain a larger proportion of traits in terms of the genetics that drive them.
The team said mtSet will allow researchers to explore several variants of a gene at once, while comparing them with several related phenotypes. This makes it easier to pinpoint which genes—or locations on genes—are involved in a particular function.
“What’s important about this work is that it improves statistical power and provides the tools people need to analyze multiple traits in very large cohorts,” Dr Stegle said. “Our algorithm can be used to study up to half a million individuals. That hasn’t been possible until now.” ![]()

Image by Spencer Phillips
A new algorithm makes it possible to perform genetic analyses on as many as 500,000 individuals—and many traits—at the same time, according to an article in Nature Methods.
The authors noted that determining how genetic variations affect health and disease involves analyzing associations between many different variants and multiple traits and making the best use of data from large cohorts that include hundreds of thousands of individuals.
“It is very challenging to identify genetic variants that underlie phenotypes, or traits, and, usually, we do this by analyzing each phenotype and each variant one by one,” explained Oliver Stegle, PhD, of the European Molecular Biology Laboratory-European Bioinformatics Institute in Cambridge, UK.
“But the simple models we use to do this are too simplistic to uncover the complex dependencies between sets of genetic variants and disease phenotypes.”
On the other hand, complex models that reveal the combined action of many different variants have involved so much computation that it would take a year to run a single complex query. But Dr Stegle and his colleagues said their algorithm can change that.
“The breakthrough here is that we’ve made it possible to perform an integrative analysis involving many variants and phenotypes at the same speed as current approaches,” Dr Stegle said.
He and his colleagues tested their new method, called mtSet, on data from 2 studies and compared the results with existing tools used for genetic analysis. The researchers found that mtSet was substantially faster than existing methods and could explain a larger proportion of traits in terms of the genetics that drive them.
The team said mtSet will allow researchers to explore several variants of a gene at once, while comparing them with several related phenotypes. This makes it easier to pinpoint which genes—or locations on genes—are involved in a particular function.
“What’s important about this work is that it improves statistical power and provides the tools people need to analyze multiple traits in very large cohorts,” Dr Stegle said. “Our algorithm can be used to study up to half a million individuals. That hasn’t been possible until now.” ![]()

Image by Spencer Phillips
A new algorithm makes it possible to perform genetic analyses on as many as 500,000 individuals—and many traits—at the same time, according to an article in Nature Methods.
The authors noted that determining how genetic variations affect health and disease involves analyzing associations between many different variants and multiple traits and making the best use of data from large cohorts that include hundreds of thousands of individuals.
“It is very challenging to identify genetic variants that underlie phenotypes, or traits, and, usually, we do this by analyzing each phenotype and each variant one by one,” explained Oliver Stegle, PhD, of the European Molecular Biology Laboratory-European Bioinformatics Institute in Cambridge, UK.
“But the simple models we use to do this are too simplistic to uncover the complex dependencies between sets of genetic variants and disease phenotypes.”
On the other hand, complex models that reveal the combined action of many different variants have involved so much computation that it would take a year to run a single complex query. But Dr Stegle and his colleagues said their algorithm can change that.
“The breakthrough here is that we’ve made it possible to perform an integrative analysis involving many variants and phenotypes at the same speed as current approaches,” Dr Stegle said.
He and his colleagues tested their new method, called mtSet, on data from 2 studies and compared the results with existing tools used for genetic analysis. The researchers found that mtSet was substantially faster than existing methods and could explain a larger proportion of traits in terms of the genetics that drive them.
The team said mtSet will allow researchers to explore several variants of a gene at once, while comparing them with several related phenotypes. This makes it easier to pinpoint which genes—or locations on genes—are involved in a particular function.
“What’s important about this work is that it improves statistical power and provides the tools people need to analyze multiple traits in very large cohorts,” Dr Stegle said. “Our algorithm can be used to study up to half a million individuals. That hasn’t been possible until now.” ![]()
Targeting IL-1β could limit damage after joint bleed

Photo by Rhoda Baer
ROME, ITALY—Interleukin-1β (IL-1β) is a crucial factor in the development of blood-induced cartilage damage, according to research presented at the European League Against Rheumatism Annual Congress (EULAR 2015).
This discovery suggests that therapeutically targeting IL-1β could provide a new way to protect cartilage after a joint bleed, which can occur after joint trauma, major joint surgery, or due to hemophilia.
Whatever the cause, joint bleeds are expected to lead to an inflammatory response in the joint and to significant destruction of joint cartilage. So a treatment that could limit the damage from a joint bleed could potentially minimize future disability.
“As therapeutic agents opposing the activity of IL-1β are readily available, further research is now warranted to investigate whether an IL-1β antagonist would be effective in preventing and treating joint damage as a result of bleeding into the joint,” said study investigator Simon Mastbergen, PhD, of the University Medical Centre Utrecht in the Netherlands.
“Findings also suggest that the quicker treatment is initiated, the less damage to the joint may be sustained.”
Dr Mastbergen and his colleagues presented these findings at EULAR 2015 as abstract OP0262.
The researchers had cultured healthy human cartilage samples for 4 days in the presence or absence of 50% whole blood. They then added an IL-1β monoclonal antibody (mAb), an IL-1 receptor antagonist (IL-1RA), or a TNF-α mAb during blood exposure and assessed subsequent cartilage damage.
The IL-1β mAb and IL-1RA protected cartilage from blood-induced damage in a dose- and time-dependent manner. Early administration after blood exposure was the most beneficial. And, when the treatments were given at higher concentrations, there was near-complete normalization of cartilage.
The researchers said these effects were accompanied by a reduction in IL-1β and IL-6 production. The level of IL-1β was 74 pg/mL in whole-blood culture, but levels were undetectable after the IL-1RA was added (P=0.028). The level of IL-6 was 21,347 pg/mL in whole-blood culture, 27 pg/mL after the IL-1RA was added, and 289 pg/mL after the IL-1β mAb was added (P=0.028 for both).
However, TNF-α levels were unaffected by the IL-1RA or IL-1β mAb. TNF-α levels wer 35 pg/mL in whole-blood culture and 37 pg/mL after the addition of the IL-1RA or IL-1β mAb (P=0.753 for both).
Of course, the TNF-α mAb inhibited the effects of TNF-α on cartilage, but the mAb had no significant effect on blood-induced cartilage damage.
“This would appear to rule out TNF-α inhibitors, a class of drug currently used to treat various forms of arthritis, for this new indication,” Dr Mastbergen said. ![]()

Photo by Rhoda Baer
ROME, ITALY—Interleukin-1β (IL-1β) is a crucial factor in the development of blood-induced cartilage damage, according to research presented at the European League Against Rheumatism Annual Congress (EULAR 2015).
This discovery suggests that therapeutically targeting IL-1β could provide a new way to protect cartilage after a joint bleed, which can occur after joint trauma, major joint surgery, or due to hemophilia.
Whatever the cause, joint bleeds are expected to lead to an inflammatory response in the joint and to significant destruction of joint cartilage. So a treatment that could limit the damage from a joint bleed could potentially minimize future disability.
“As therapeutic agents opposing the activity of IL-1β are readily available, further research is now warranted to investigate whether an IL-1β antagonist would be effective in preventing and treating joint damage as a result of bleeding into the joint,” said study investigator Simon Mastbergen, PhD, of the University Medical Centre Utrecht in the Netherlands.
“Findings also suggest that the quicker treatment is initiated, the less damage to the joint may be sustained.”
Dr Mastbergen and his colleagues presented these findings at EULAR 2015 as abstract OP0262.
The researchers had cultured healthy human cartilage samples for 4 days in the presence or absence of 50% whole blood. They then added an IL-1β monoclonal antibody (mAb), an IL-1 receptor antagonist (IL-1RA), or a TNF-α mAb during blood exposure and assessed subsequent cartilage damage.
The IL-1β mAb and IL-1RA protected cartilage from blood-induced damage in a dose- and time-dependent manner. Early administration after blood exposure was the most beneficial. And, when the treatments were given at higher concentrations, there was near-complete normalization of cartilage.
The researchers said these effects were accompanied by a reduction in IL-1β and IL-6 production. The level of IL-1β was 74 pg/mL in whole-blood culture, but levels were undetectable after the IL-1RA was added (P=0.028). The level of IL-6 was 21,347 pg/mL in whole-blood culture, 27 pg/mL after the IL-1RA was added, and 289 pg/mL after the IL-1β mAb was added (P=0.028 for both).
However, TNF-α levels were unaffected by the IL-1RA or IL-1β mAb. TNF-α levels wer 35 pg/mL in whole-blood culture and 37 pg/mL after the addition of the IL-1RA or IL-1β mAb (P=0.753 for both).
Of course, the TNF-α mAb inhibited the effects of TNF-α on cartilage, but the mAb had no significant effect on blood-induced cartilage damage.
“This would appear to rule out TNF-α inhibitors, a class of drug currently used to treat various forms of arthritis, for this new indication,” Dr Mastbergen said. ![]()

Photo by Rhoda Baer
ROME, ITALY—Interleukin-1β (IL-1β) is a crucial factor in the development of blood-induced cartilage damage, according to research presented at the European League Against Rheumatism Annual Congress (EULAR 2015).
This discovery suggests that therapeutically targeting IL-1β could provide a new way to protect cartilage after a joint bleed, which can occur after joint trauma, major joint surgery, or due to hemophilia.
Whatever the cause, joint bleeds are expected to lead to an inflammatory response in the joint and to significant destruction of joint cartilage. So a treatment that could limit the damage from a joint bleed could potentially minimize future disability.
“As therapeutic agents opposing the activity of IL-1β are readily available, further research is now warranted to investigate whether an IL-1β antagonist would be effective in preventing and treating joint damage as a result of bleeding into the joint,” said study investigator Simon Mastbergen, PhD, of the University Medical Centre Utrecht in the Netherlands.
“Findings also suggest that the quicker treatment is initiated, the less damage to the joint may be sustained.”
Dr Mastbergen and his colleagues presented these findings at EULAR 2015 as abstract OP0262.
The researchers had cultured healthy human cartilage samples for 4 days in the presence or absence of 50% whole blood. They then added an IL-1β monoclonal antibody (mAb), an IL-1 receptor antagonist (IL-1RA), or a TNF-α mAb during blood exposure and assessed subsequent cartilage damage.
The IL-1β mAb and IL-1RA protected cartilage from blood-induced damage in a dose- and time-dependent manner. Early administration after blood exposure was the most beneficial. And, when the treatments were given at higher concentrations, there was near-complete normalization of cartilage.
The researchers said these effects were accompanied by a reduction in IL-1β and IL-6 production. The level of IL-1β was 74 pg/mL in whole-blood culture, but levels were undetectable after the IL-1RA was added (P=0.028). The level of IL-6 was 21,347 pg/mL in whole-blood culture, 27 pg/mL after the IL-1RA was added, and 289 pg/mL after the IL-1β mAb was added (P=0.028 for both).
However, TNF-α levels were unaffected by the IL-1RA or IL-1β mAb. TNF-α levels wer 35 pg/mL in whole-blood culture and 37 pg/mL after the addition of the IL-1RA or IL-1β mAb (P=0.753 for both).
Of course, the TNF-α mAb inhibited the effects of TNF-α on cartilage, but the mAb had no significant effect on blood-induced cartilage damage.
“This would appear to rule out TNF-α inhibitors, a class of drug currently used to treat various forms of arthritis, for this new indication,” Dr Mastbergen said. ![]()
Team identifies new target for malaria vaccine

Photo courtesy of the CDC
Researchers say they have located a new, more precise target for a mosquito-based vaccine to block the transmission of malaria.
The team created a 3-D crystal structure of AnAPN1, a protein found in the gut of the Anopheles mosquito that is considered essential to malaria transmission.
In studying the entire protein, the researchers found that previous incarnations of a proposed vaccine included irrelevant regions of AnAPN1.
Rhoel R. Dinglasan, PhD, of the Johns Hopkins Bloomberg School of Public Health in Baltimore, Maryland, and his colleagues described this work in Nature Structural & Molecular Biology.
AnAPN1 is found on the apical surface of the Anopheles gambiae midgut and is potentially a receptor for the Plasmodium parasite. As a vaccine antigen, AnAPN1 prompts antibody production, but only some of these antibodies block parasite transmission.
“This dilution of the overall antibody response to AnAPN1 is problematic,” Dr Dinglasan said. “To further improve vaccine immunogenicity at the preclinical stage, we need to immuno-focus the antibody response to only the critical, transmission-blocking regions of the protein.”
Using the Australian Synchrotron, the researchers were able to visualize the crystal structure of AnAPN1 for the first time. This allowed the team to pinpoint the binding site of AnAPN1 antibodies that can and cannot block parasite development.
“We now know much more about which parts of the AnAPN1 protein are involved in generating transmission-blocking antibodies and have a new hypothesis as to how they might work,” said Natalie Borg, PhD, of Monash University in Clayton, Victoria, Australia.
The researchers identified a particularly potent antibody, 4H5B7, and tested it in blood samples from children carrying the Plasmodium falciparum parasite. 4H5B7 exhibited “complete transmission-blocking activity” against these naturally circulating strains of P falciparum.
The team said their data indicate the mechanism underlying this activity is the recognition of a conformation-dependent epitope that is predominantly found on peptide 4, which is part of peptide 7 on domain 1 of AnAPN1.
These findings suggest that, previously, researchers were asking the immune system to target too many regions on AnAPN1, which diluted the response to the relevant regions of the protein. ![]()

Photo courtesy of the CDC
Researchers say they have located a new, more precise target for a mosquito-based vaccine to block the transmission of malaria.
The team created a 3-D crystal structure of AnAPN1, a protein found in the gut of the Anopheles mosquito that is considered essential to malaria transmission.
In studying the entire protein, the researchers found that previous incarnations of a proposed vaccine included irrelevant regions of AnAPN1.
Rhoel R. Dinglasan, PhD, of the Johns Hopkins Bloomberg School of Public Health in Baltimore, Maryland, and his colleagues described this work in Nature Structural & Molecular Biology.
AnAPN1 is found on the apical surface of the Anopheles gambiae midgut and is potentially a receptor for the Plasmodium parasite. As a vaccine antigen, AnAPN1 prompts antibody production, but only some of these antibodies block parasite transmission.
“This dilution of the overall antibody response to AnAPN1 is problematic,” Dr Dinglasan said. “To further improve vaccine immunogenicity at the preclinical stage, we need to immuno-focus the antibody response to only the critical, transmission-blocking regions of the protein.”
Using the Australian Synchrotron, the researchers were able to visualize the crystal structure of AnAPN1 for the first time. This allowed the team to pinpoint the binding site of AnAPN1 antibodies that can and cannot block parasite development.
“We now know much more about which parts of the AnAPN1 protein are involved in generating transmission-blocking antibodies and have a new hypothesis as to how they might work,” said Natalie Borg, PhD, of Monash University in Clayton, Victoria, Australia.
The researchers identified a particularly potent antibody, 4H5B7, and tested it in blood samples from children carrying the Plasmodium falciparum parasite. 4H5B7 exhibited “complete transmission-blocking activity” against these naturally circulating strains of P falciparum.
The team said their data indicate the mechanism underlying this activity is the recognition of a conformation-dependent epitope that is predominantly found on peptide 4, which is part of peptide 7 on domain 1 of AnAPN1.
These findings suggest that, previously, researchers were asking the immune system to target too many regions on AnAPN1, which diluted the response to the relevant regions of the protein. ![]()

Photo courtesy of the CDC
Researchers say they have located a new, more precise target for a mosquito-based vaccine to block the transmission of malaria.
The team created a 3-D crystal structure of AnAPN1, a protein found in the gut of the Anopheles mosquito that is considered essential to malaria transmission.
In studying the entire protein, the researchers found that previous incarnations of a proposed vaccine included irrelevant regions of AnAPN1.
Rhoel R. Dinglasan, PhD, of the Johns Hopkins Bloomberg School of Public Health in Baltimore, Maryland, and his colleagues described this work in Nature Structural & Molecular Biology.
AnAPN1 is found on the apical surface of the Anopheles gambiae midgut and is potentially a receptor for the Plasmodium parasite. As a vaccine antigen, AnAPN1 prompts antibody production, but only some of these antibodies block parasite transmission.
“This dilution of the overall antibody response to AnAPN1 is problematic,” Dr Dinglasan said. “To further improve vaccine immunogenicity at the preclinical stage, we need to immuno-focus the antibody response to only the critical, transmission-blocking regions of the protein.”
Using the Australian Synchrotron, the researchers were able to visualize the crystal structure of AnAPN1 for the first time. This allowed the team to pinpoint the binding site of AnAPN1 antibodies that can and cannot block parasite development.
“We now know much more about which parts of the AnAPN1 protein are involved in generating transmission-blocking antibodies and have a new hypothesis as to how they might work,” said Natalie Borg, PhD, of Monash University in Clayton, Victoria, Australia.
The researchers identified a particularly potent antibody, 4H5B7, and tested it in blood samples from children carrying the Plasmodium falciparum parasite. 4H5B7 exhibited “complete transmission-blocking activity” against these naturally circulating strains of P falciparum.
The team said their data indicate the mechanism underlying this activity is the recognition of a conformation-dependent epitope that is predominantly found on peptide 4, which is part of peptide 7 on domain 1 of AnAPN1.
These findings suggest that, previously, researchers were asking the immune system to target too many regions on AnAPN1, which diluted the response to the relevant regions of the protein. ![]()
VTE may cause mental health problems

Photo by Jiri Hodan
DUBROVNIK, CROATIA—Results of a large study suggest patients who develop a venous thromboembolism (VTE) may have more mental health problems than their healthy peers.
One in 5 patients in the study purchased psychotropic drugs within 5 years of developing a VTE, a rate that was more than double that of age- and sex-matched control subjects.
Anette Arbjerg Højen, of Aalborg University Hospital in Denmark, presented these findings at EuroHeartCare 2015 (abstract 22).
“We know that other chronic medical illnesses in youth can lead to emotional and behavioral problems,” Arbjerg Højen said. “However, until now, VTE has been considered an acute condition that occurs in older people. There is no follow-up of [young VTE] patients regarding their mental health, and no studies have been done on this issue.”
So she and her colleagues investigated the mental health prognosis of young VTE patients using data from 4 nationwide registries: the Danish Civil Registration System, the Danish National Patient Register, the Danish National Prescription Registry, and the Danish Medical Birth Registry.
The investigators identified 4132 patients, ages 13 to 33, who had a first VTE between 1997 and 2010. The team then matched these patients by sex and birth year to a control group of 19,292 people without VTE.
All study participants were followed for their first purchase of psychotropic drugs, including antidepressants, anti-anxiety medications, sedatives, and antipsychotics.
The researchers used the purchase of psychotropic drugs as a proxy measure for mental health status and compared the measure between the two groups. The team used regression analysis to exclude non-VTE-related causes of psychotropic drug purchase, such as postpartum depression.
Results showed the VTE patients were much more likely to purchase psychotropic drugs than control subjects. Among VTE patients, the risk of purchasing psychotropic drugs following their diagnosis was 7.1% after 1 year and 22.1% after 5 years.
The excess risk for VTE patients relative to the controls was 4.7% after 1 year and 10.8% after 5 years. When the investigators adjusted for the effect of recent pregnancy or recent provocations, the risk differences became 4.1% after 1 year and 9.6% after 5 years.
“Most of the drugs prescribed were antidepressants,” Arbjerg Højen said. “These young patients struggle a lot with the fear of VTE recurrence. They are scared that, if it strikes again, it could become a pulmonary embolism and they might die.”
“Our study only included patients who received a prescription for psychotropic drugs. There will be others who were not prescribed medication because of their young age, so the group with mental health problems could be much larger than what we found.”
“Our study looked at mental health up to 5 years and not just in the immediate period after the VTE event, suggesting that it is not just a short-term panic. We don’t know how long mental health problems in VTE patients last, but we do know that these patients will always be at high risk of recurrent VTE, so there is a possibility that their depression or anxiety could be life-long if untreated.”
“Most young VTE patients are monitored by their general practitioner for 3 to 6 months because they are on oral anticoagulant treatment, but, after that, there is generally no long-term follow up. Our study points to the need for treating VTE as a chronic condition with serious mental health consequences requiring specialist care.” ![]()

Photo by Jiri Hodan
DUBROVNIK, CROATIA—Results of a large study suggest patients who develop a venous thromboembolism (VTE) may have more mental health problems than their healthy peers.
One in 5 patients in the study purchased psychotropic drugs within 5 years of developing a VTE, a rate that was more than double that of age- and sex-matched control subjects.
Anette Arbjerg Højen, of Aalborg University Hospital in Denmark, presented these findings at EuroHeartCare 2015 (abstract 22).
“We know that other chronic medical illnesses in youth can lead to emotional and behavioral problems,” Arbjerg Højen said. “However, until now, VTE has been considered an acute condition that occurs in older people. There is no follow-up of [young VTE] patients regarding their mental health, and no studies have been done on this issue.”
So she and her colleagues investigated the mental health prognosis of young VTE patients using data from 4 nationwide registries: the Danish Civil Registration System, the Danish National Patient Register, the Danish National Prescription Registry, and the Danish Medical Birth Registry.
The investigators identified 4132 patients, ages 13 to 33, who had a first VTE between 1997 and 2010. The team then matched these patients by sex and birth year to a control group of 19,292 people without VTE.
All study participants were followed for their first purchase of psychotropic drugs, including antidepressants, anti-anxiety medications, sedatives, and antipsychotics.
The researchers used the purchase of psychotropic drugs as a proxy measure for mental health status and compared the measure between the two groups. The team used regression analysis to exclude non-VTE-related causes of psychotropic drug purchase, such as postpartum depression.
Results showed the VTE patients were much more likely to purchase psychotropic drugs than control subjects. Among VTE patients, the risk of purchasing psychotropic drugs following their diagnosis was 7.1% after 1 year and 22.1% after 5 years.
The excess risk for VTE patients relative to the controls was 4.7% after 1 year and 10.8% after 5 years. When the investigators adjusted for the effect of recent pregnancy or recent provocations, the risk differences became 4.1% after 1 year and 9.6% after 5 years.
“Most of the drugs prescribed were antidepressants,” Arbjerg Højen said. “These young patients struggle a lot with the fear of VTE recurrence. They are scared that, if it strikes again, it could become a pulmonary embolism and they might die.”
“Our study only included patients who received a prescription for psychotropic drugs. There will be others who were not prescribed medication because of their young age, so the group with mental health problems could be much larger than what we found.”
“Our study looked at mental health up to 5 years and not just in the immediate period after the VTE event, suggesting that it is not just a short-term panic. We don’t know how long mental health problems in VTE patients last, but we do know that these patients will always be at high risk of recurrent VTE, so there is a possibility that their depression or anxiety could be life-long if untreated.”
“Most young VTE patients are monitored by their general practitioner for 3 to 6 months because they are on oral anticoagulant treatment, but, after that, there is generally no long-term follow up. Our study points to the need for treating VTE as a chronic condition with serious mental health consequences requiring specialist care.” ![]()

Photo by Jiri Hodan
DUBROVNIK, CROATIA—Results of a large study suggest patients who develop a venous thromboembolism (VTE) may have more mental health problems than their healthy peers.
One in 5 patients in the study purchased psychotropic drugs within 5 years of developing a VTE, a rate that was more than double that of age- and sex-matched control subjects.
Anette Arbjerg Højen, of Aalborg University Hospital in Denmark, presented these findings at EuroHeartCare 2015 (abstract 22).
“We know that other chronic medical illnesses in youth can lead to emotional and behavioral problems,” Arbjerg Højen said. “However, until now, VTE has been considered an acute condition that occurs in older people. There is no follow-up of [young VTE] patients regarding their mental health, and no studies have been done on this issue.”
So she and her colleagues investigated the mental health prognosis of young VTE patients using data from 4 nationwide registries: the Danish Civil Registration System, the Danish National Patient Register, the Danish National Prescription Registry, and the Danish Medical Birth Registry.
The investigators identified 4132 patients, ages 13 to 33, who had a first VTE between 1997 and 2010. The team then matched these patients by sex and birth year to a control group of 19,292 people without VTE.
All study participants were followed for their first purchase of psychotropic drugs, including antidepressants, anti-anxiety medications, sedatives, and antipsychotics.
The researchers used the purchase of psychotropic drugs as a proxy measure for mental health status and compared the measure between the two groups. The team used regression analysis to exclude non-VTE-related causes of psychotropic drug purchase, such as postpartum depression.
Results showed the VTE patients were much more likely to purchase psychotropic drugs than control subjects. Among VTE patients, the risk of purchasing psychotropic drugs following their diagnosis was 7.1% after 1 year and 22.1% after 5 years.
The excess risk for VTE patients relative to the controls was 4.7% after 1 year and 10.8% after 5 years. When the investigators adjusted for the effect of recent pregnancy or recent provocations, the risk differences became 4.1% after 1 year and 9.6% after 5 years.
“Most of the drugs prescribed were antidepressants,” Arbjerg Højen said. “These young patients struggle a lot with the fear of VTE recurrence. They are scared that, if it strikes again, it could become a pulmonary embolism and they might die.”
“Our study only included patients who received a prescription for psychotropic drugs. There will be others who were not prescribed medication because of their young age, so the group with mental health problems could be much larger than what we found.”
“Our study looked at mental health up to 5 years and not just in the immediate period after the VTE event, suggesting that it is not just a short-term panic. We don’t know how long mental health problems in VTE patients last, but we do know that these patients will always be at high risk of recurrent VTE, so there is a possibility that their depression or anxiety could be life-long if untreated.”
“Most young VTE patients are monitored by their general practitioner for 3 to 6 months because they are on oral anticoagulant treatment, but, after that, there is generally no long-term follow up. Our study points to the need for treating VTE as a chronic condition with serious mental health consequences requiring specialist care.” ![]()
Assay could guide therapy for MM, other cancers

showing multiple myeloma
Researchers say they have created a microenvironment in a dish that can be used to anticipate a multiple myeloma (MM) patient’s response to treatment.
The team developed an assay that involves co-culturing MM cells with their surrounding nontumor cells, all from the same patient, in a microscale petri dish.
The researchers then treated the tumor cells with bortezomib, and, after 3 days, they could determine whether the drug was effective or not.
The team described this research in Integrative Biology.
They compared the results of their ex vivo tests with the success or failure rates of actual MM patients who received bortezomib, and 100% of the ex vivo test results matched the patients’ results.
The researchers therefore believe this assay could save many MM patients the psychological stress of having to try multiple drugs until they find the most effective one. The assay could reduce clinicians’ need for this trial-and-error approach while lowering the cost of treatment, the team said.
Study author Chorom Pak, PhD, of the University of Toronto in Ontario, Canada, has founded a service-based company called Lynx Biosciences based on these findings. Now, she and her colleagues are planning to conduct a prospective trial in which they will use the ex vivo tests to identify responsive and nonresponsive patients.
The researchers believe this work could have wide-ranging implications for the treatment of MM and other malignancies, but their work is far from over.
“This is only one type of cancer, one particular drug, and we’re a long way from implementing this and helping patients in a widespread way,” said study author David Beebe, PhD, of the University of Wisconsin Carbone Cancer Center in Madison.
“But it’s happening. This is an exciting time in this area, and we’re definitely going to see more of this.” ![]()

showing multiple myeloma
Researchers say they have created a microenvironment in a dish that can be used to anticipate a multiple myeloma (MM) patient’s response to treatment.
The team developed an assay that involves co-culturing MM cells with their surrounding nontumor cells, all from the same patient, in a microscale petri dish.
The researchers then treated the tumor cells with bortezomib, and, after 3 days, they could determine whether the drug was effective or not.
The team described this research in Integrative Biology.
They compared the results of their ex vivo tests with the success or failure rates of actual MM patients who received bortezomib, and 100% of the ex vivo test results matched the patients’ results.
The researchers therefore believe this assay could save many MM patients the psychological stress of having to try multiple drugs until they find the most effective one. The assay could reduce clinicians’ need for this trial-and-error approach while lowering the cost of treatment, the team said.
Study author Chorom Pak, PhD, of the University of Toronto in Ontario, Canada, has founded a service-based company called Lynx Biosciences based on these findings. Now, she and her colleagues are planning to conduct a prospective trial in which they will use the ex vivo tests to identify responsive and nonresponsive patients.
The researchers believe this work could have wide-ranging implications for the treatment of MM and other malignancies, but their work is far from over.
“This is only one type of cancer, one particular drug, and we’re a long way from implementing this and helping patients in a widespread way,” said study author David Beebe, PhD, of the University of Wisconsin Carbone Cancer Center in Madison.
“But it’s happening. This is an exciting time in this area, and we’re definitely going to see more of this.” ![]()

showing multiple myeloma
Researchers say they have created a microenvironment in a dish that can be used to anticipate a multiple myeloma (MM) patient’s response to treatment.
The team developed an assay that involves co-culturing MM cells with their surrounding nontumor cells, all from the same patient, in a microscale petri dish.
The researchers then treated the tumor cells with bortezomib, and, after 3 days, they could determine whether the drug was effective or not.
The team described this research in Integrative Biology.
They compared the results of their ex vivo tests with the success or failure rates of actual MM patients who received bortezomib, and 100% of the ex vivo test results matched the patients’ results.
The researchers therefore believe this assay could save many MM patients the psychological stress of having to try multiple drugs until they find the most effective one. The assay could reduce clinicians’ need for this trial-and-error approach while lowering the cost of treatment, the team said.
Study author Chorom Pak, PhD, of the University of Toronto in Ontario, Canada, has founded a service-based company called Lynx Biosciences based on these findings. Now, she and her colleagues are planning to conduct a prospective trial in which they will use the ex vivo tests to identify responsive and nonresponsive patients.
The researchers believe this work could have wide-ranging implications for the treatment of MM and other malignancies, but their work is far from over.
“This is only one type of cancer, one particular drug, and we’re a long way from implementing this and helping patients in a widespread way,” said study author David Beebe, PhD, of the University of Wisconsin Carbone Cancer Center in Madison.
“But it’s happening. This is an exciting time in this area, and we’re definitely going to see more of this.” ![]()
New trial design accounts for patient behavior

Photo by Esther Dyson
New research suggests patient behavior can have a serious impact on the effectiveness of a treatment, and procedures used in double-blind randomized controlled trials (DBRCTs) may not allow researchers to assess the effects of behavior on treatment.
To solve this problem, a group of investigators has proposed a new trial design, called a two-by-two trial, that can account for behavior-treatment interactions.
They described this design in PLOS ONE.
Study rationale
The study authors pointed out that patient behaviors can directly relate to a trial. For example, a patient who believes in the drug might religiously stick to his or her treatment regimen, while someone more skeptical might skip a few doses.
Alternatively, patient behaviors may relate to how the person acts in general, such as preferences in diet, exercise, and social engagement. And in the design of today’s standard trials, these behaviors are not accounted for, said author Erik Snowberg, PhD, of the California Institute of Technology in Pasadena.
He noted that DBRCTs typically assign patients to an experimental group that receives the new treatment and a control group that does not. As the trial is double-blinded, neither the subjects nor their doctors know who falls into which group.
However, patients do know their probability of getting the treatment, and that 50% likelihood of getting the new treatment might not be enough to encourage a patient to change behaviors that could influence the efficacy of the drug, Dr Snowberg said.
For example, if a subject wants to lose weight and knows he has a high probability—a 70% chance—of being in the experimental group for a new weight loss drug, he may be more likely to take the drug as directed and to make other healthy lifestyle choices that can contribute to weight loss. As a result, he might lose more weight, boosting the apparent effectiveness of the drug.
However, if the subject knows he only has a 30% chance of being in the experimental group, he might be less motivated to both take the drug as directed and to make those other changes. As a result, he might lose less weight—even if he is in the treatment group—and the same drug would seem less effective.
“Most medical research just wants to know if a drug will work or not,” Dr Snowberg said. “We wanted to go a step further, designing new trials that would take into account the way people behave. As social scientists, we naturally turned to the mathematical tools of formal social science to do this.”
New trial design
Dr Snowberg and his colleagues found that, with the two-by-two trial, they can tease out the effects of behavior and the interaction of behavior and treatment, as well as the effects of treatment alone. The new trial design, which still randomizes treatment, also randomizes the probability of treatment, which can change a patient’s behavior.
In a two-by-two trial, instead of patients first being assigned to either the experimental or control groups, they are randomly assigned to either a “high probability of treatment” group or a “low probability of treatment” group.
The patients in the high probability group are then randomized to either the treatment or the control group, giving them a 70% chance of receiving the treatment. Patients in the low probability group are also randomized to treatment or control, and their likelihood of receiving the treatment is 30%. The patients are then informed of their probability of treatment.
By randomizing both the treatment and the probability of treatment, researchers can quantify the effects of treatment, the effects of behavior, and the effects of the interaction between treatment and behavior, Dr Snowberg said. And determining each is essential for understanding the overall efficacy of treatment.
“It’s a very small change to the design of the trial, but it’s important,” he said. “The effect of a treatment has these two constituent parts: pure treatment effect and the treatment-behavior interaction. Standard blind trials just randomize the likelihood of treatment, so you can’t see this interaction. Although you can’t just tell someone to randomize their behavior, we found a way that you can randomize the probability that a patient will get something that will change their behavior.”
Testing the design
Because it is difficult to implement new trial design changes in active trials, Dr Snowberg and his colleagues wanted to first test their idea with a meta-analysis of data from previous clinical trials. They devised a new mathematical formula that can be used to analyze DBRCT data.
The formula teases out the health outcomes resulting from treatment alone as well as outcomes resulting from an interaction between treatment and behavior.
The investigators used the formula to analyze 6 DBRCTs evaluating the antidepressants imipramine (a tricyclic antidepressant also known as Tofranil) and paroxetine (a selective serotonin reuptake inhibitor sold as Paxil).
First, the researchers wanted to see if there was evidence that patients behave differently when they have a high probability of treatment and when they have a low probability of treatment.
The trials recorded how many patients dropped out of the study, so this was the behavior Dr Snowberg and his colleagues analyzed. They found that, in trials where patients happened to have a relatively high probability of treatment—near 70%—the dropout rate was significantly lower than in trials where patients had a lower probability of treatment—around 50%.
Although the team did not have any specific behaviors to analyze, other than dropping out of the study, they also wanted to determine if behavior in general could have added to the effect of the treatments.
Using their statistical techniques, the investigators found that imipramine seemed to have a pure treatment effect but no effect from the interaction between treatment and behavior. That is, the drug seemed to work fine, regardless of any behavioral differences that may have been present.
The researchers also found that paroxetine seemed to have no effect from the treatment alone or behavior alone. However, an interaction between the treatment and behavior did effectively decrease depression.
Because this study was conducted in the past, the investigators could not determine which specific behavior was responsible for the interaction, but with the mathematical formula, they were able to tell that this behavior was necessary for the drug to be effective.
In their paper, Dr Snowberg and his colleagues speculate how a situation like this might come about.
“Maybe there is a drug, for instance, that makes people feel better in social situations, and if you’re in the high probability group, then maybe you’d be more willing to go out to parties to see if the drug helps you talk to people,” Dr Snowberg explained.
“Your behavior drives you to go to the party, and once you’re at the party, the drug helps you feel comfortable talking to people. That would be an example of an interaction effect. You couldn’t get that if people just took this drug alone at home.”
Although this specific example is just speculation, Dr Snowberg said the researchers’ actual results reveal that some behavior or set of behaviors interact with paroxetine to effectively treat depression. And, without this behavior, the drug appears to be ineffective.
“Normally, what you get when you run a standard blind trial is some sort of mishmash of the treatment effect and the treatment-behavior interaction effect,” Dr Snowberg said. “But knowing the full interaction effect is important.”
“Our work indicates that clinical trials underestimate the efficacy of a drug where behavior matters. It may be the case that 50% probability isn’t high enough for people to change any of their behaviors, especially if it’s a really uncertain new treatment. Then, it’s just going to look like the drug doesn’t work, and that isn’t the case.”
Because the meta-analysis supported the team’s hypothesis—that the interaction between treatment and behavior can have an effect on health outcomes—the next step is incorporating these new ideas into an active clinical trial.
Dr Snowberg said the best fit would be a drug trial for a condition, such as a mental health disorder or an addiction, that is known to be associated with behavior. At the very least, he hopes these results will lead the medical research community to a conversation about ways to improve the DBRCT. ![]()

Photo by Esther Dyson
New research suggests patient behavior can have a serious impact on the effectiveness of a treatment, and procedures used in double-blind randomized controlled trials (DBRCTs) may not allow researchers to assess the effects of behavior on treatment.
To solve this problem, a group of investigators has proposed a new trial design, called a two-by-two trial, that can account for behavior-treatment interactions.
They described this design in PLOS ONE.
Study rationale
The study authors pointed out that patient behaviors can directly relate to a trial. For example, a patient who believes in the drug might religiously stick to his or her treatment regimen, while someone more skeptical might skip a few doses.
Alternatively, patient behaviors may relate to how the person acts in general, such as preferences in diet, exercise, and social engagement. And in the design of today’s standard trials, these behaviors are not accounted for, said author Erik Snowberg, PhD, of the California Institute of Technology in Pasadena.
He noted that DBRCTs typically assign patients to an experimental group that receives the new treatment and a control group that does not. As the trial is double-blinded, neither the subjects nor their doctors know who falls into which group.
However, patients do know their probability of getting the treatment, and that 50% likelihood of getting the new treatment might not be enough to encourage a patient to change behaviors that could influence the efficacy of the drug, Dr Snowberg said.
For example, if a subject wants to lose weight and knows he has a high probability—a 70% chance—of being in the experimental group for a new weight loss drug, he may be more likely to take the drug as directed and to make other healthy lifestyle choices that can contribute to weight loss. As a result, he might lose more weight, boosting the apparent effectiveness of the drug.
However, if the subject knows he only has a 30% chance of being in the experimental group, he might be less motivated to both take the drug as directed and to make those other changes. As a result, he might lose less weight—even if he is in the treatment group—and the same drug would seem less effective.
“Most medical research just wants to know if a drug will work or not,” Dr Snowberg said. “We wanted to go a step further, designing new trials that would take into account the way people behave. As social scientists, we naturally turned to the mathematical tools of formal social science to do this.”
New trial design
Dr Snowberg and his colleagues found that, with the two-by-two trial, they can tease out the effects of behavior and the interaction of behavior and treatment, as well as the effects of treatment alone. The new trial design, which still randomizes treatment, also randomizes the probability of treatment, which can change a patient’s behavior.
In a two-by-two trial, instead of patients first being assigned to either the experimental or control groups, they are randomly assigned to either a “high probability of treatment” group or a “low probability of treatment” group.
The patients in the high probability group are then randomized to either the treatment or the control group, giving them a 70% chance of receiving the treatment. Patients in the low probability group are also randomized to treatment or control, and their likelihood of receiving the treatment is 30%. The patients are then informed of their probability of treatment.
By randomizing both the treatment and the probability of treatment, researchers can quantify the effects of treatment, the effects of behavior, and the effects of the interaction between treatment and behavior, Dr Snowberg said. And determining each is essential for understanding the overall efficacy of treatment.
“It’s a very small change to the design of the trial, but it’s important,” he said. “The effect of a treatment has these two constituent parts: pure treatment effect and the treatment-behavior interaction. Standard blind trials just randomize the likelihood of treatment, so you can’t see this interaction. Although you can’t just tell someone to randomize their behavior, we found a way that you can randomize the probability that a patient will get something that will change their behavior.”
Testing the design
Because it is difficult to implement new trial design changes in active trials, Dr Snowberg and his colleagues wanted to first test their idea with a meta-analysis of data from previous clinical trials. They devised a new mathematical formula that can be used to analyze DBRCT data.
The formula teases out the health outcomes resulting from treatment alone as well as outcomes resulting from an interaction between treatment and behavior.
The investigators used the formula to analyze 6 DBRCTs evaluating the antidepressants imipramine (a tricyclic antidepressant also known as Tofranil) and paroxetine (a selective serotonin reuptake inhibitor sold as Paxil).
First, the researchers wanted to see if there was evidence that patients behave differently when they have a high probability of treatment and when they have a low probability of treatment.
The trials recorded how many patients dropped out of the study, so this was the behavior Dr Snowberg and his colleagues analyzed. They found that, in trials where patients happened to have a relatively high probability of treatment—near 70%—the dropout rate was significantly lower than in trials where patients had a lower probability of treatment—around 50%.
Although the team did not have any specific behaviors to analyze, other than dropping out of the study, they also wanted to determine if behavior in general could have added to the effect of the treatments.
Using their statistical techniques, the investigators found that imipramine seemed to have a pure treatment effect but no effect from the interaction between treatment and behavior. That is, the drug seemed to work fine, regardless of any behavioral differences that may have been present.
The researchers also found that paroxetine seemed to have no effect from the treatment alone or behavior alone. However, an interaction between the treatment and behavior did effectively decrease depression.
Because this study was conducted in the past, the investigators could not determine which specific behavior was responsible for the interaction, but with the mathematical formula, they were able to tell that this behavior was necessary for the drug to be effective.
In their paper, Dr Snowberg and his colleagues speculate how a situation like this might come about.
“Maybe there is a drug, for instance, that makes people feel better in social situations, and if you’re in the high probability group, then maybe you’d be more willing to go out to parties to see if the drug helps you talk to people,” Dr Snowberg explained.
“Your behavior drives you to go to the party, and once you’re at the party, the drug helps you feel comfortable talking to people. That would be an example of an interaction effect. You couldn’t get that if people just took this drug alone at home.”
Although this specific example is just speculation, Dr Snowberg said the researchers’ actual results reveal that some behavior or set of behaviors interact with paroxetine to effectively treat depression. And, without this behavior, the drug appears to be ineffective.
“Normally, what you get when you run a standard blind trial is some sort of mishmash of the treatment effect and the treatment-behavior interaction effect,” Dr Snowberg said. “But knowing the full interaction effect is important.”
“Our work indicates that clinical trials underestimate the efficacy of a drug where behavior matters. It may be the case that 50% probability isn’t high enough for people to change any of their behaviors, especially if it’s a really uncertain new treatment. Then, it’s just going to look like the drug doesn’t work, and that isn’t the case.”
Because the meta-analysis supported the team’s hypothesis—that the interaction between treatment and behavior can have an effect on health outcomes—the next step is incorporating these new ideas into an active clinical trial.
Dr Snowberg said the best fit would be a drug trial for a condition, such as a mental health disorder or an addiction, that is known to be associated with behavior. At the very least, he hopes these results will lead the medical research community to a conversation about ways to improve the DBRCT. ![]()

Photo by Esther Dyson
New research suggests patient behavior can have a serious impact on the effectiveness of a treatment, and procedures used in double-blind randomized controlled trials (DBRCTs) may not allow researchers to assess the effects of behavior on treatment.
To solve this problem, a group of investigators has proposed a new trial design, called a two-by-two trial, that can account for behavior-treatment interactions.
They described this design in PLOS ONE.
Study rationale
The study authors pointed out that patient behaviors can directly relate to a trial. For example, a patient who believes in the drug might religiously stick to his or her treatment regimen, while someone more skeptical might skip a few doses.
Alternatively, patient behaviors may relate to how the person acts in general, such as preferences in diet, exercise, and social engagement. And in the design of today’s standard trials, these behaviors are not accounted for, said author Erik Snowberg, PhD, of the California Institute of Technology in Pasadena.
He noted that DBRCTs typically assign patients to an experimental group that receives the new treatment and a control group that does not. As the trial is double-blinded, neither the subjects nor their doctors know who falls into which group.
However, patients do know their probability of getting the treatment, and that 50% likelihood of getting the new treatment might not be enough to encourage a patient to change behaviors that could influence the efficacy of the drug, Dr Snowberg said.
For example, if a subject wants to lose weight and knows he has a high probability—a 70% chance—of being in the experimental group for a new weight loss drug, he may be more likely to take the drug as directed and to make other healthy lifestyle choices that can contribute to weight loss. As a result, he might lose more weight, boosting the apparent effectiveness of the drug.
However, if the subject knows he only has a 30% chance of being in the experimental group, he might be less motivated to both take the drug as directed and to make those other changes. As a result, he might lose less weight—even if he is in the treatment group—and the same drug would seem less effective.
“Most medical research just wants to know if a drug will work or not,” Dr Snowberg said. “We wanted to go a step further, designing new trials that would take into account the way people behave. As social scientists, we naturally turned to the mathematical tools of formal social science to do this.”
New trial design
Dr Snowberg and his colleagues found that, with the two-by-two trial, they can tease out the effects of behavior and the interaction of behavior and treatment, as well as the effects of treatment alone. The new trial design, which still randomizes treatment, also randomizes the probability of treatment, which can change a patient’s behavior.
In a two-by-two trial, instead of patients first being assigned to either the experimental or control groups, they are randomly assigned to either a “high probability of treatment” group or a “low probability of treatment” group.
The patients in the high probability group are then randomized to either the treatment or the control group, giving them a 70% chance of receiving the treatment. Patients in the low probability group are also randomized to treatment or control, and their likelihood of receiving the treatment is 30%. The patients are then informed of their probability of treatment.
By randomizing both the treatment and the probability of treatment, researchers can quantify the effects of treatment, the effects of behavior, and the effects of the interaction between treatment and behavior, Dr Snowberg said. And determining each is essential for understanding the overall efficacy of treatment.
“It’s a very small change to the design of the trial, but it’s important,” he said. “The effect of a treatment has these two constituent parts: pure treatment effect and the treatment-behavior interaction. Standard blind trials just randomize the likelihood of treatment, so you can’t see this interaction. Although you can’t just tell someone to randomize their behavior, we found a way that you can randomize the probability that a patient will get something that will change their behavior.”
Testing the design
Because it is difficult to implement new trial design changes in active trials, Dr Snowberg and his colleagues wanted to first test their idea with a meta-analysis of data from previous clinical trials. They devised a new mathematical formula that can be used to analyze DBRCT data.
The formula teases out the health outcomes resulting from treatment alone as well as outcomes resulting from an interaction between treatment and behavior.
The investigators used the formula to analyze 6 DBRCTs evaluating the antidepressants imipramine (a tricyclic antidepressant also known as Tofranil) and paroxetine (a selective serotonin reuptake inhibitor sold as Paxil).
First, the researchers wanted to see if there was evidence that patients behave differently when they have a high probability of treatment and when they have a low probability of treatment.
The trials recorded how many patients dropped out of the study, so this was the behavior Dr Snowberg and his colleagues analyzed. They found that, in trials where patients happened to have a relatively high probability of treatment—near 70%—the dropout rate was significantly lower than in trials where patients had a lower probability of treatment—around 50%.
Although the team did not have any specific behaviors to analyze, other than dropping out of the study, they also wanted to determine if behavior in general could have added to the effect of the treatments.
Using their statistical techniques, the investigators found that imipramine seemed to have a pure treatment effect but no effect from the interaction between treatment and behavior. That is, the drug seemed to work fine, regardless of any behavioral differences that may have been present.
The researchers also found that paroxetine seemed to have no effect from the treatment alone or behavior alone. However, an interaction between the treatment and behavior did effectively decrease depression.
Because this study was conducted in the past, the investigators could not determine which specific behavior was responsible for the interaction, but with the mathematical formula, they were able to tell that this behavior was necessary for the drug to be effective.
In their paper, Dr Snowberg and his colleagues speculate how a situation like this might come about.
“Maybe there is a drug, for instance, that makes people feel better in social situations, and if you’re in the high probability group, then maybe you’d be more willing to go out to parties to see if the drug helps you talk to people,” Dr Snowberg explained.
“Your behavior drives you to go to the party, and once you’re at the party, the drug helps you feel comfortable talking to people. That would be an example of an interaction effect. You couldn’t get that if people just took this drug alone at home.”
Although this specific example is just speculation, Dr Snowberg said the researchers’ actual results reveal that some behavior or set of behaviors interact with paroxetine to effectively treat depression. And, without this behavior, the drug appears to be ineffective.
“Normally, what you get when you run a standard blind trial is some sort of mishmash of the treatment effect and the treatment-behavior interaction effect,” Dr Snowberg said. “But knowing the full interaction effect is important.”
“Our work indicates that clinical trials underestimate the efficacy of a drug where behavior matters. It may be the case that 50% probability isn’t high enough for people to change any of their behaviors, especially if it’s a really uncertain new treatment. Then, it’s just going to look like the drug doesn’t work, and that isn’t the case.”
Because the meta-analysis supported the team’s hypothesis—that the interaction between treatment and behavior can have an effect on health outcomes—the next step is incorporating these new ideas into an active clinical trial.
Dr Snowberg said the best fit would be a drug trial for a condition, such as a mental health disorder or an addiction, that is known to be associated with behavior. At the very least, he hopes these results will lead the medical research community to a conversation about ways to improve the DBRCT. ![]()
Program helped reduce VTE in trauma patients

Photo by Piotr Bodzek
Data from a statewide quality collaborative helped the University of Michigan Trauma Service reduce its annual rate of venous thromboembolism (VTE), according to an article published in the Journal of the American College of Surgeons.
The data suggested that changing first-line VTE prophylaxis from unfractionated heparin to enoxaparin would decrease the incidence of VTE, and it did. The annual VTE incidence fell from about 36 cases to about 14.
Researchers said this study should not be interpreted as a head-to-head comparison of unfractionated heparin and enoxaparin as VTE prophylaxis in trauma patients. Instead, it should be seen as a model of how hospitals and physicians can use quality improvement data in a real-world setting.
Existing medical evidence has shown that both heparin and enoxaparin can be effective in preventing VTE, depending on factors such as how the agents are dosed and administered.
“Based on our data, the enoxaparin regimen was more effective than heparin,” said study author David A. Machado-Aranda, MD, of the University of Michigan in Ann Arbor.
“Now, this result could be different in another institution, another collaborative, another geographical area, or another patient population based on the circumstances encountered.”
Dr Machado-Aranda and his colleagues participate in the Michigan Trauma Quality Improvement Program (MTQIP), a statewide program of 27 ACS Level 1 and 2 trauma centers.
The program showed the researchers that the rate of VTE was higher for the University of Michigan Trauma Service than the collaborative average.
A closer look at the data revealed that VTE rates among trauma patients who received unfractionated heparin were twice as high as rates for patients who received enoxaparin.
After the University of Michigan Trauma Service switched from using unfractionated heparin to enoxaparin as first-line VTE prophylaxis, the rate of VTE dropped from 6.2% to 2.6%.
“What we’ve done is to use the collaborative as our ‘mission control’ to see where we’re heading and what our trajectory is,” Dr Machado-Aranda said. “Once we saw ourselves deviating from a favorable trajectory, we used the data derived from the collaborative to investigate our problem.”
“We also accessed many different resources to review best practices, receive suggestions from other collaborative participants, and perform root-cause analysis. An action plan was formulated, approved, and implemented to get our trauma service off of an unfavorable trajectory for VTE complications.”
Dr Machado-Aranda noted that the trauma team encountered some challenges in changing the protocol for VTE prophylaxis. Hospital administration and other departments were concerned about the higher cost of enoxaparin.
In the end, “the increased costs of using enoxaparin were more than offset by savings generated by reducing the rate of venous thromboembolism complications,” he said.
The trauma surgeons also found they had to review the data with the neurosurgeons and orthopedic surgeons on staff to understand and alleviate their concerns about enoxaparin and potential higher rates of bleeding complications.
The neurosurgical group had previously published a study that showed higher rates of intracranial bleeding in patients undergoing brain tumor surgery who received enoxaparin rather than sequential compression devices alone.
“These results became extrapolated into the trauma setting, and it took us some time convincing our neurosurgeons to consider changing their practice for trauma patients,” Dr Machado-Aranda said. ![]()

Photo by Piotr Bodzek
Data from a statewide quality collaborative helped the University of Michigan Trauma Service reduce its annual rate of venous thromboembolism (VTE), according to an article published in the Journal of the American College of Surgeons.
The data suggested that changing first-line VTE prophylaxis from unfractionated heparin to enoxaparin would decrease the incidence of VTE, and it did. The annual VTE incidence fell from about 36 cases to about 14.
Researchers said this study should not be interpreted as a head-to-head comparison of unfractionated heparin and enoxaparin as VTE prophylaxis in trauma patients. Instead, it should be seen as a model of how hospitals and physicians can use quality improvement data in a real-world setting.
Existing medical evidence has shown that both heparin and enoxaparin can be effective in preventing VTE, depending on factors such as how the agents are dosed and administered.
“Based on our data, the enoxaparin regimen was more effective than heparin,” said study author David A. Machado-Aranda, MD, of the University of Michigan in Ann Arbor.
“Now, this result could be different in another institution, another collaborative, another geographical area, or another patient population based on the circumstances encountered.”
Dr Machado-Aranda and his colleagues participate in the Michigan Trauma Quality Improvement Program (MTQIP), a statewide program of 27 ACS Level 1 and 2 trauma centers.
The program showed the researchers that the rate of VTE was higher for the University of Michigan Trauma Service than the collaborative average.
A closer look at the data revealed that VTE rates among trauma patients who received unfractionated heparin were twice as high as rates for patients who received enoxaparin.
After the University of Michigan Trauma Service switched from using unfractionated heparin to enoxaparin as first-line VTE prophylaxis, the rate of VTE dropped from 6.2% to 2.6%.
“What we’ve done is to use the collaborative as our ‘mission control’ to see where we’re heading and what our trajectory is,” Dr Machado-Aranda said. “Once we saw ourselves deviating from a favorable trajectory, we used the data derived from the collaborative to investigate our problem.”
“We also accessed many different resources to review best practices, receive suggestions from other collaborative participants, and perform root-cause analysis. An action plan was formulated, approved, and implemented to get our trauma service off of an unfavorable trajectory for VTE complications.”
Dr Machado-Aranda noted that the trauma team encountered some challenges in changing the protocol for VTE prophylaxis. Hospital administration and other departments were concerned about the higher cost of enoxaparin.
In the end, “the increased costs of using enoxaparin were more than offset by savings generated by reducing the rate of venous thromboembolism complications,” he said.
The trauma surgeons also found they had to review the data with the neurosurgeons and orthopedic surgeons on staff to understand and alleviate their concerns about enoxaparin and potential higher rates of bleeding complications.
The neurosurgical group had previously published a study that showed higher rates of intracranial bleeding in patients undergoing brain tumor surgery who received enoxaparin rather than sequential compression devices alone.
“These results became extrapolated into the trauma setting, and it took us some time convincing our neurosurgeons to consider changing their practice for trauma patients,” Dr Machado-Aranda said. ![]()

Photo by Piotr Bodzek
Data from a statewide quality collaborative helped the University of Michigan Trauma Service reduce its annual rate of venous thromboembolism (VTE), according to an article published in the Journal of the American College of Surgeons.
The data suggested that changing first-line VTE prophylaxis from unfractionated heparin to enoxaparin would decrease the incidence of VTE, and it did. The annual VTE incidence fell from about 36 cases to about 14.
Researchers said this study should not be interpreted as a head-to-head comparison of unfractionated heparin and enoxaparin as VTE prophylaxis in trauma patients. Instead, it should be seen as a model of how hospitals and physicians can use quality improvement data in a real-world setting.
Existing medical evidence has shown that both heparin and enoxaparin can be effective in preventing VTE, depending on factors such as how the agents are dosed and administered.
“Based on our data, the enoxaparin regimen was more effective than heparin,” said study author David A. Machado-Aranda, MD, of the University of Michigan in Ann Arbor.
“Now, this result could be different in another institution, another collaborative, another geographical area, or another patient population based on the circumstances encountered.”
Dr Machado-Aranda and his colleagues participate in the Michigan Trauma Quality Improvement Program (MTQIP), a statewide program of 27 ACS Level 1 and 2 trauma centers.
The program showed the researchers that the rate of VTE was higher for the University of Michigan Trauma Service than the collaborative average.
A closer look at the data revealed that VTE rates among trauma patients who received unfractionated heparin were twice as high as rates for patients who received enoxaparin.
After the University of Michigan Trauma Service switched from using unfractionated heparin to enoxaparin as first-line VTE prophylaxis, the rate of VTE dropped from 6.2% to 2.6%.
“What we’ve done is to use the collaborative as our ‘mission control’ to see where we’re heading and what our trajectory is,” Dr Machado-Aranda said. “Once we saw ourselves deviating from a favorable trajectory, we used the data derived from the collaborative to investigate our problem.”
“We also accessed many different resources to review best practices, receive suggestions from other collaborative participants, and perform root-cause analysis. An action plan was formulated, approved, and implemented to get our trauma service off of an unfavorable trajectory for VTE complications.”
Dr Machado-Aranda noted that the trauma team encountered some challenges in changing the protocol for VTE prophylaxis. Hospital administration and other departments were concerned about the higher cost of enoxaparin.
In the end, “the increased costs of using enoxaparin were more than offset by savings generated by reducing the rate of venous thromboembolism complications,” he said.
The trauma surgeons also found they had to review the data with the neurosurgeons and orthopedic surgeons on staff to understand and alleviate their concerns about enoxaparin and potential higher rates of bleeding complications.
The neurosurgical group had previously published a study that showed higher rates of intracranial bleeding in patients undergoing brain tumor surgery who received enoxaparin rather than sequential compression devices alone.
“These results became extrapolated into the trauma setting, and it took us some time convincing our neurosurgeons to consider changing their practice for trauma patients,” Dr Machado-Aranda said.
Molecule accelerates recovery after BMT

Photo by Chad McNeeley
A small molecule may be able to accelerate cell recovery in bone marrow transplant (BMT) recipients and patients with liver or colon disease, researchers believe.
The molecule, SW033291, inhibits 15-PGDH, a prostaglandin-degrading enzyme that regulates tissue regeneration in multiple organs.
SW033291 accelerated hematopoietic recovery in mice that received BMTs and promoted tissue regeneration in mice with liver or colon injuries.
“We propose that SW033291 will be useful in accelerating recovery of bone marrow cells following a bone marrow transplant and may also be a treatment for colitis,” said James Willson, MD, of the University of Texas Southwestern Medical Center in Dallas.
He and his colleagues described their work with SW033291 in Science.
To examine the effects of inhibiting 15-PGDH on the bone marrow, the researchers conducted experiments with 15-PGDH-knockout mice and SW033291-treated mice, comparing them to control mice.
The team saw a 43% increase in neutrophil counts and a 39% increase in bone marrow Sca-1+ C-kit+ Lin– (SKL) cells in 15-PGDH knockout compared to wild-type mice. There were no significant differences in counts of other peripheral blood cells, bone marrow cellularity, or counts of bone marrow Sca-1+ C-kit+ Lin– CD48– CD150+ (SLAM) cells.
SW033291-treated mice had double the peripheral neutrophil counts of controls, a 65% increase in marrow SKL cells, and a 71% increase in marrow SLAM cells.
Results of additional experiments indicated that SW033291 works by increasing PGE2 levels in the bone marrow, and PGE2 functions through the EP2 and EP4 receptors to induce expression of CXCL12 and SCF.
The researchers also tested whether SW033291 could increase the bone marrow’s ability to attract and support new hematopoietic stem cells after BMT in mice. They found that BMT recipients treated with SW033291 had a 2- to 3-fold increase in the number of donor cells that homed to their bone marrow, compared to vehicle-treated BMT recipients.
The researchers said this SW033291-induced homing of transplanted bone marrow cells was driven, at least in part, by the induction of CXCL12 expression in CD45– nonmyeloid cells that were already resident in the bone marrow of recipient mice.
These results suggest 15-PGDH inhibition causes an increase in bone marrow PGE2, which induces the expression of bone marrow CXCL12 and SCF, and these cytokines alter the bone marrow microenvironment to better support the homing of transplanted cells.
The researchers also evaluated whether 15-PGDH inhibition promotes hematopoietic recovery after BMT. They studied lethally irradiated mice that received 200,000 strain-matched donor bone marrow cells, which were insufficient to reconstitute hematopoiesis in the mice.
When the mice were treated with SW033291, they survived for more than 30 days. All control mice, on the other hand, died between days 6 and 14.
For the last of their BMT experiments, the researchers examined the effect of SW033291 on mice transplanted with 500,000 bone marrow cells.
All SW033291-treated mice and 63% of control mice survived for 30 days, which allowed the team to compare hematopoietic recovery between the two groups. They found that SW033291 significantly accelerated the recovery of neutrophils, platelets, and red blood cells.
Experiments in mice with liver or colon injuries suggested that SW033291 can aid recovery in these models as well.

Photo by Chad McNeeley
A small molecule may be able to accelerate cell recovery in bone marrow transplant (BMT) recipients and patients with liver or colon disease, researchers believe.
The molecule, SW033291, inhibits 15-PGDH, a prostaglandin-degrading enzyme that regulates tissue regeneration in multiple organs.
SW033291 accelerated hematopoietic recovery in mice that received BMTs and promoted tissue regeneration in mice with liver or colon injuries.
“We propose that SW033291 will be useful in accelerating recovery of bone marrow cells following a bone marrow transplant and may also be a treatment for colitis,” said James Willson, MD, of the University of Texas Southwestern Medical Center in Dallas.
He and his colleagues described their work with SW033291 in Science.
To examine the effects of inhibiting 15-PGDH on the bone marrow, the researchers conducted experiments with 15-PGDH-knockout mice and SW033291-treated mice, comparing them to control mice.
The team saw a 43% increase in neutrophil counts and a 39% increase in bone marrow Sca-1+ C-kit+ Lin– (SKL) cells in 15-PGDH knockout compared to wild-type mice. There were no significant differences in counts of other peripheral blood cells, bone marrow cellularity, or counts of bone marrow Sca-1+ C-kit+ Lin– CD48– CD150+ (SLAM) cells.
SW033291-treated mice had double the peripheral neutrophil counts of controls, a 65% increase in marrow SKL cells, and a 71% increase in marrow SLAM cells.
Results of additional experiments indicated that SW033291 works by increasing PGE2 levels in the bone marrow, and PGE2 functions through the EP2 and EP4 receptors to induce expression of CXCL12 and SCF.
The researchers also tested whether SW033291 could increase the bone marrow’s ability to attract and support new hematopoietic stem cells after BMT in mice. They found that BMT recipients treated with SW033291 had a 2- to 3-fold increase in the number of donor cells that homed to their bone marrow, compared to vehicle-treated BMT recipients.
The researchers said this SW033291-induced homing of transplanted bone marrow cells was driven, at least in part, by the induction of CXCL12 expression in CD45– nonmyeloid cells that were already resident in the bone marrow of recipient mice.
These results suggest 15-PGDH inhibition causes an increase in bone marrow PGE2, which induces the expression of bone marrow CXCL12 and SCF, and these cytokines alter the bone marrow microenvironment to better support the homing of transplanted cells.
The researchers also evaluated whether 15-PGDH inhibition promotes hematopoietic recovery after BMT. They studied lethally irradiated mice that received 200,000 strain-matched donor bone marrow cells, which were insufficient to reconstitute hematopoiesis in the mice.
When the mice were treated with SW033291, they survived for more than 30 days. All control mice, on the other hand, died between days 6 and 14.
For the last of their BMT experiments, the researchers examined the effect of SW033291 on mice transplanted with 500,000 bone marrow cells.
All SW033291-treated mice and 63% of control mice survived for 30 days, which allowed the team to compare hematopoietic recovery between the two groups. They found that SW033291 significantly accelerated the recovery of neutrophils, platelets, and red blood cells.
Experiments in mice with liver or colon injuries suggested that SW033291 can aid recovery in these models as well.

Photo by Chad McNeeley
A small molecule may be able to accelerate cell recovery in bone marrow transplant (BMT) recipients and patients with liver or colon disease, researchers believe.
The molecule, SW033291, inhibits 15-PGDH, a prostaglandin-degrading enzyme that regulates tissue regeneration in multiple organs.
SW033291 accelerated hematopoietic recovery in mice that received BMTs and promoted tissue regeneration in mice with liver or colon injuries.
“We propose that SW033291 will be useful in accelerating recovery of bone marrow cells following a bone marrow transplant and may also be a treatment for colitis,” said James Willson, MD, of the University of Texas Southwestern Medical Center in Dallas.
He and his colleagues described their work with SW033291 in Science.
To examine the effects of inhibiting 15-PGDH on the bone marrow, the researchers conducted experiments with 15-PGDH-knockout mice and SW033291-treated mice, comparing them to control mice.
The team saw a 43% increase in neutrophil counts and a 39% increase in bone marrow Sca-1+ C-kit+ Lin– (SKL) cells in 15-PGDH knockout compared to wild-type mice. There were no significant differences in counts of other peripheral blood cells, bone marrow cellularity, or counts of bone marrow Sca-1+ C-kit+ Lin– CD48– CD150+ (SLAM) cells.
SW033291-treated mice had double the peripheral neutrophil counts of controls, a 65% increase in marrow SKL cells, and a 71% increase in marrow SLAM cells.
Results of additional experiments indicated that SW033291 works by increasing PGE2 levels in the bone marrow, and PGE2 functions through the EP2 and EP4 receptors to induce expression of CXCL12 and SCF.
The researchers also tested whether SW033291 could increase the bone marrow’s ability to attract and support new hematopoietic stem cells after BMT in mice. They found that BMT recipients treated with SW033291 had a 2- to 3-fold increase in the number of donor cells that homed to their bone marrow, compared to vehicle-treated BMT recipients.
The researchers said this SW033291-induced homing of transplanted bone marrow cells was driven, at least in part, by the induction of CXCL12 expression in CD45– nonmyeloid cells that were already resident in the bone marrow of recipient mice.
These results suggest 15-PGDH inhibition causes an increase in bone marrow PGE2, which induces the expression of bone marrow CXCL12 and SCF, and these cytokines alter the bone marrow microenvironment to better support the homing of transplanted cells.
The researchers also evaluated whether 15-PGDH inhibition promotes hematopoietic recovery after BMT. They studied lethally irradiated mice that received 200,000 strain-matched donor bone marrow cells, which were insufficient to reconstitute hematopoiesis in the mice.
When the mice were treated with SW033291, they survived for more than 30 days. All control mice, on the other hand, died between days 6 and 14.
For the last of their BMT experiments, the researchers examined the effect of SW033291 on mice transplanted with 500,000 bone marrow cells.
All SW033291-treated mice and 63% of control mice survived for 30 days, which allowed the team to compare hematopoietic recovery between the two groups. They found that SW033291 significantly accelerated the recovery of neutrophils, platelets, and red blood cells.
Experiments in mice with liver or colon injuries suggested that SW033291 can aid recovery in these models as well.
Modern housing may reduce malaria risk

Photo by James Gathany
Living in a “modern” house may reduce a person’s risk of contracting malaria, according to research published in Malaria Journal.
As insecticide and drug resistance are on the rise, researchers wanted to determine how making changes to housing might aid the fight against malaria.
So they reviewed 90 studies conducted in Africa, Asia, and South America, comparing the incidence of malaria among people who live in “traditional” and “modern” houses.
The traditional houses consisted of mud, stone, bamboo, or wood walls; thatched, mud, or wood roofs; and earth or wood floors. The modern houses had closed eaves, ceilings, screened doors, and windows.
The researchers found that residents of modern homes were 47% less likely to be infected with malaria than those living in traditional houses. And residents of modern homes were 45% to 65% less likely to have clinical malaria (fever with infection).
“Housing improvements were traditionally an important pillar of public health, but they remain underexploited in malaria control,” said study author Lucy Tusting, of the London School of Hygiene & Tropical Medicine in the UK.
“Good housing can block mosquitoes from entering homes and prevent them from transmitting malaria to the people who live there. Our study suggests housing could be an important tool in tackling malaria. This is a welcome finding at a time when we are facing increasing resistance to our most effective insecticides and drugs.”
“We now need to pinpoint which housing features can reduce mosquito entry in different settings, to incorporate these into local housing designs, and to assess the impact on malaria in large-scale field trials.”
The researchers noted that the effectiveness of improving housing will vary depending on the location. While many mosquitoes enter homes to bite humans at night, outdoor malaria transmission is more common in some places. So interventions centered on the home will have less of an impact in these areas.
The researchers also conceded that the studies eligible for inclusion in this review were of low quality. However, they said the consistency of the findings indicate that housing is an important risk factor for malaria.

Photo by James Gathany
Living in a “modern” house may reduce a person’s risk of contracting malaria, according to research published in Malaria Journal.
As insecticide and drug resistance are on the rise, researchers wanted to determine how making changes to housing might aid the fight against malaria.
So they reviewed 90 studies conducted in Africa, Asia, and South America, comparing the incidence of malaria among people who live in “traditional” and “modern” houses.
The traditional houses consisted of mud, stone, bamboo, or wood walls; thatched, mud, or wood roofs; and earth or wood floors. The modern houses had closed eaves, ceilings, screened doors, and windows.
The researchers found that residents of modern homes were 47% less likely to be infected with malaria than those living in traditional houses. And residents of modern homes were 45% to 65% less likely to have clinical malaria (fever with infection).
“Housing improvements were traditionally an important pillar of public health, but they remain underexploited in malaria control,” said study author Lucy Tusting, of the London School of Hygiene & Tropical Medicine in the UK.
“Good housing can block mosquitoes from entering homes and prevent them from transmitting malaria to the people who live there. Our study suggests housing could be an important tool in tackling malaria. This is a welcome finding at a time when we are facing increasing resistance to our most effective insecticides and drugs.”
“We now need to pinpoint which housing features can reduce mosquito entry in different settings, to incorporate these into local housing designs, and to assess the impact on malaria in large-scale field trials.”
The researchers noted that the effectiveness of improving housing will vary depending on the location. While many mosquitoes enter homes to bite humans at night, outdoor malaria transmission is more common in some places. So interventions centered on the home will have less of an impact in these areas.
The researchers also conceded that the studies eligible for inclusion in this review were of low quality. However, they said the consistency of the findings indicate that housing is an important risk factor for malaria.

Photo by James Gathany
Living in a “modern” house may reduce a person’s risk of contracting malaria, according to research published in Malaria Journal.
As insecticide and drug resistance are on the rise, researchers wanted to determine how making changes to housing might aid the fight against malaria.
So they reviewed 90 studies conducted in Africa, Asia, and South America, comparing the incidence of malaria among people who live in “traditional” and “modern” houses.
The traditional houses consisted of mud, stone, bamboo, or wood walls; thatched, mud, or wood roofs; and earth or wood floors. The modern houses had closed eaves, ceilings, screened doors, and windows.
The researchers found that residents of modern homes were 47% less likely to be infected with malaria than those living in traditional houses. And residents of modern homes were 45% to 65% less likely to have clinical malaria (fever with infection).
“Housing improvements were traditionally an important pillar of public health, but they remain underexploited in malaria control,” said study author Lucy Tusting, of the London School of Hygiene & Tropical Medicine in the UK.
“Good housing can block mosquitoes from entering homes and prevent them from transmitting malaria to the people who live there. Our study suggests housing could be an important tool in tackling malaria. This is a welcome finding at a time when we are facing increasing resistance to our most effective insecticides and drugs.”
“We now need to pinpoint which housing features can reduce mosquito entry in different settings, to incorporate these into local housing designs, and to assess the impact on malaria in large-scale field trials.”
The researchers noted that the effectiveness of improving housing will vary depending on the location. While many mosquitoes enter homes to bite humans at night, outdoor malaria transmission is more common in some places. So interventions centered on the home will have less of an impact in these areas.
The researchers also conceded that the studies eligible for inclusion in this review were of low quality. However, they said the consistency of the findings indicate that housing is an important risk factor for malaria.
Viral protein protects EBV-infected B cells
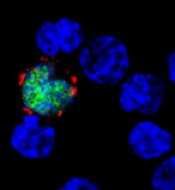
expresses the ligand (red)
that activates NKG2D, while
uninfected cells (blue) do not
Benjamin Chaigne-Delalande
A study published in PLOS Pathogens sheds new light on why the immune system cannot eliminate Epstein-Barr virus (EBV) or the risk of cancer associated with the virus.
Researchers investigated the immune system’s response against EBV, focusing on the role of LMP2A.
This viral protein is present in latently infected B cells and in many EBV-associated cancers, which have somehow escaped detection and elimination by the immune system.
Andreas Moosmann, PhD, of the Helmholtz-Zentrum in Munich, Germany, and his colleagues studied an engineered EBV virus that cannot make LMP2A and compared this mutant virus with the normal one.
The researchers infected human B cells with normal and LMP2A-deficient EBV. Because EBV transforms these cells, the team was able to examine lymphoblastic cell lines that contained either virus.
They found that LMP2A counteracts the recognition of EBV-infected B cells by EBV-specific, CD8+ killer T cells. In contrast, EBV-transformed cells without LMP2A are more efficiently identified, and the T cells’ ability to recognize and kill the EBV-infected B cells is enhanced.
The researchers examined the mechanism underlying the LMP2A-mediated evasion and found several ways in which it interferes with the recognition of EBV-infected cells.
First, LMP2A reduced the levels of several EBV proteins whose fragments are recognized by CD8+ T cells on the surface of the cell targeted for killing.
Second, LMP2A disturbs the expression of cellular molecules on infected B cells that interact with NKG2D, a host molecule on the surface of CD8+ T cells that aids their activation, thereby weakening the immune response against EBV-infected cells.
The researchers said these results suggest a functional immunomodulatory effect for the EBV protein LMP2A and show that LMP2A mediates the partial escape of infected B cells from recognition by CD8+ T cells.
The team also said similar immune evasion mechanisms may operate in different types of LMP2A-expressing cancers caused by EBV.

expresses the ligand (red)
that activates NKG2D, while
uninfected cells (blue) do not
Benjamin Chaigne-Delalande
A study published in PLOS Pathogens sheds new light on why the immune system cannot eliminate Epstein-Barr virus (EBV) or the risk of cancer associated with the virus.
Researchers investigated the immune system’s response against EBV, focusing on the role of LMP2A.
This viral protein is present in latently infected B cells and in many EBV-associated cancers, which have somehow escaped detection and elimination by the immune system.
Andreas Moosmann, PhD, of the Helmholtz-Zentrum in Munich, Germany, and his colleagues studied an engineered EBV virus that cannot make LMP2A and compared this mutant virus with the normal one.
The researchers infected human B cells with normal and LMP2A-deficient EBV. Because EBV transforms these cells, the team was able to examine lymphoblastic cell lines that contained either virus.
They found that LMP2A counteracts the recognition of EBV-infected B cells by EBV-specific, CD8+ killer T cells. In contrast, EBV-transformed cells without LMP2A are more efficiently identified, and the T cells’ ability to recognize and kill the EBV-infected B cells is enhanced.
The researchers examined the mechanism underlying the LMP2A-mediated evasion and found several ways in which it interferes with the recognition of EBV-infected cells.
First, LMP2A reduced the levels of several EBV proteins whose fragments are recognized by CD8+ T cells on the surface of the cell targeted for killing.
Second, LMP2A disturbs the expression of cellular molecules on infected B cells that interact with NKG2D, a host molecule on the surface of CD8+ T cells that aids their activation, thereby weakening the immune response against EBV-infected cells.
The researchers said these results suggest a functional immunomodulatory effect for the EBV protein LMP2A and show that LMP2A mediates the partial escape of infected B cells from recognition by CD8+ T cells.
The team also said similar immune evasion mechanisms may operate in different types of LMP2A-expressing cancers caused by EBV.

expresses the ligand (red)
that activates NKG2D, while
uninfected cells (blue) do not
Benjamin Chaigne-Delalande
A study published in PLOS Pathogens sheds new light on why the immune system cannot eliminate Epstein-Barr virus (EBV) or the risk of cancer associated with the virus.
Researchers investigated the immune system’s response against EBV, focusing on the role of LMP2A.
This viral protein is present in latently infected B cells and in many EBV-associated cancers, which have somehow escaped detection and elimination by the immune system.
Andreas Moosmann, PhD, of the Helmholtz-Zentrum in Munich, Germany, and his colleagues studied an engineered EBV virus that cannot make LMP2A and compared this mutant virus with the normal one.
The researchers infected human B cells with normal and LMP2A-deficient EBV. Because EBV transforms these cells, the team was able to examine lymphoblastic cell lines that contained either virus.
They found that LMP2A counteracts the recognition of EBV-infected B cells by EBV-specific, CD8+ killer T cells. In contrast, EBV-transformed cells without LMP2A are more efficiently identified, and the T cells’ ability to recognize and kill the EBV-infected B cells is enhanced.
The researchers examined the mechanism underlying the LMP2A-mediated evasion and found several ways in which it interferes with the recognition of EBV-infected cells.
First, LMP2A reduced the levels of several EBV proteins whose fragments are recognized by CD8+ T cells on the surface of the cell targeted for killing.
Second, LMP2A disturbs the expression of cellular molecules on infected B cells that interact with NKG2D, a host molecule on the surface of CD8+ T cells that aids their activation, thereby weakening the immune response against EBV-infected cells.
The researchers said these results suggest a functional immunomodulatory effect for the EBV protein LMP2A and show that LMP2A mediates the partial escape of infected B cells from recognition by CD8+ T cells.
The team also said similar immune evasion mechanisms may operate in different types of LMP2A-expressing cancers caused by EBV.