User login
A 43-year-old Hispanic man has a very itchy rash on his left leg. It manifested within a few weeks of the patient starting a new job, one that involved working more hours than he had previously and on rotating shifts, which interfered with his sleep schedule.
For several years, he tried using different products—mostly OTC creams—on it, with no success. Increasingly annoyed by the rash, he finally consulted his family physician, who prescribed a combination clotrimazole/betamethasone cream. This helped a bit, but over time, the rash steadily worsened, and his primary care provider referred him to dermatology.
The patient claims to be otherwise healthy, with no history of atopy. He takes no prescription medications. He admits finding it difficult to refrain from scratching his legs.
EXAMINATION
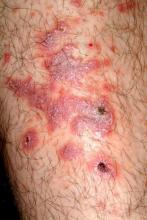
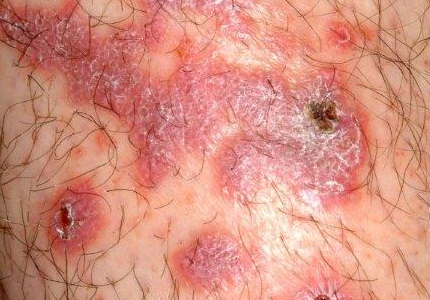
There are large, slightly purplish, hypertrophic papulosquamous plaques of up to 8 cm on both anterior tibial areas. His arms, trunk, and wrists are rash-free, and his oral mucosal surfaces show no obvious signs of disease.
Punch biopsy shows a hypertrophic epidermis. There is marked obliteration of the dermoepidermal junction by a dense bandlike layer of lymphocytic infiltrate, associated with vacuolar change and necrotic keratinocytes in the basal layer of the epidermis.
DISCUSSION
This is a classic clinical and histologic picture of a dermatosis commonly seen in dermatology offices: lichen planus (LP). As is often the case, by the time the patient gets to dermatology, the clinical picture can be confused and atypical. But there is much to learn from such a case.
LP is the prototypical interface lichenoid dermatitis, which can be depended on to present in certain identifiable ways. In this case, what suggested this diagnosis was the word “puzzling.” It’s the perfect example of the intuitive, somewhat subjective side of dermatologic diagnosis: When I see a condition that baffles me momentarily, my puzzled reaction becomes meaningful because the word puzzling starts with a “p.” Lichen planus has long been associated with an extremely useful mnemonic device known as “The Ps.” Besides puzzling, it can stand for purple, plaquish, polygonal (ie, not round), prurtitic, papular, penile (LP has a predilection for this area), and planar (ie, flat-topped).
But it’s the “puzzling” aspect that unlocks the entrance to “The Ps,” and that in turn leads to consideration of this diagnosis. In this case, LP was not totally obvious, but a biopsy confirmed my clinical suspicions by demonstrating the classic findings associated with it.
An LP-like eruption can be provoked by drugs, such as the antimalarials, gold compounds, and penicillamine. It has also been associated with hepatitis C. But in my experience, the most common trigger appears to be stress, since it’s a rare case that doesn’t involve some. (I’ll happily concede that this is my opinion and not established fact.)
This patient’s LP demonstrated two common variants: For one, the darker the patient’s skin, the deeper the purple color of the LP—sometimes to the point of obscuring the diagnosis.
As if that were not enough to confuse the examiner, there was an element of lichen simplex chronicus (LSC; also known as neurodermatitis), which instigates the “itch-scratch-itch” cycle. By its nature, LSC tends to hyperpigmentation (brown). By definition, it involves hypertrophy of the epidermis secondary to scratching. But there is always a primary cause; sometimes mere dry skin will trigger it, or insect bites, eczema, or even psoriasis. This confuses the issue, but the biopsy will establish the true basis for the patient’s condition.
The more common presentation of LP is that of a collection of flat-topped (“planar”), pruritic, purplish papules on the volar wrist, ankles, and sacral area. The surfaces of these lesions often demonstrate a faintly white, shiny surface. LP can also appear on oral mucosal surfaces, where it has a totally different, lacy-white look. In these areas, it tends to burn and not itch. LP appears to have a predilection for the penile glans, where it presents as an annular purplish plaque that sits astride the proximal glans, spilling over onto the coronal area.
LP can present as a widespread generalized eruption mimicking granuloma annulare and secondary syphilis. The differential for simple, classic LP includes psoriasis, granuloma annulare and pityriasis rosea.
Treatment of LP is with topical steroid creams or ointments, tailored in terms of strength to the area of involvement. For example, a class II or III corticosteroid would be used on areas with thicker skin and a class IV or V on thinner skin. Stubborn, solitary plaques can be treated with intralesional steroid injection (2.5 to 10 mg/cc triamcinolone solution).
TAKE-HOME LEARNING POINTS
• Lichen planus (LP) is common and typically presents on the volar wrists, dorsal ankles, and sacrum.
• In a minority of cases, LP can present on the legs as a hypertrophic, plaquish condition with secondary features of lichen simplex chronicus.
• A mnemonic device (“The Ps”) describes LP: papular, pruritic, purple, planar, polygonal, plaquish, and (perhaps most importantly) “puzzling.”
• LP can present as an annular plaque on the penile glans.
• LP has a pathognomic histologic picture on biopsy.
A 43-year-old Hispanic man has a very itchy rash on his left leg. It manifested within a few weeks of the patient starting a new job, one that involved working more hours than he had previously and on rotating shifts, which interfered with his sleep schedule.
For several years, he tried using different products—mostly OTC creams—on it, with no success. Increasingly annoyed by the rash, he finally consulted his family physician, who prescribed a combination clotrimazole/betamethasone cream. This helped a bit, but over time, the rash steadily worsened, and his primary care provider referred him to dermatology.
The patient claims to be otherwise healthy, with no history of atopy. He takes no prescription medications. He admits finding it difficult to refrain from scratching his legs.
EXAMINATION
There are large, slightly purplish, hypertrophic papulosquamous plaques of up to 8 cm on both anterior tibial areas. His arms, trunk, and wrists are rash-free, and his oral mucosal surfaces show no obvious signs of disease.
Punch biopsy shows a hypertrophic epidermis. There is marked obliteration of the dermoepidermal junction by a dense bandlike layer of lymphocytic infiltrate, associated with vacuolar change and necrotic keratinocytes in the basal layer of the epidermis.
DISCUSSION
This is a classic clinical and histologic picture of a dermatosis commonly seen in dermatology offices: lichen planus (LP). As is often the case, by the time the patient gets to dermatology, the clinical picture can be confused and atypical. But there is much to learn from such a case.
LP is the prototypical interface lichenoid dermatitis, which can be depended on to present in certain identifiable ways. In this case, what suggested this diagnosis was the word “puzzling.” It’s the perfect example of the intuitive, somewhat subjective side of dermatologic diagnosis: When I see a condition that baffles me momentarily, my puzzled reaction becomes meaningful because the word puzzling starts with a “p.” Lichen planus has long been associated with an extremely useful mnemonic device known as “The Ps.” Besides puzzling, it can stand for purple, plaquish, polygonal (ie, not round), prurtitic, papular, penile (LP has a predilection for this area), and planar (ie, flat-topped).
But it’s the “puzzling” aspect that unlocks the entrance to “The Ps,” and that in turn leads to consideration of this diagnosis. In this case, LP was not totally obvious, but a biopsy confirmed my clinical suspicions by demonstrating the classic findings associated with it.
An LP-like eruption can be provoked by drugs, such as the antimalarials, gold compounds, and penicillamine. It has also been associated with hepatitis C. But in my experience, the most common trigger appears to be stress, since it’s a rare case that doesn’t involve some. (I’ll happily concede that this is my opinion and not established fact.)
This patient’s LP demonstrated two common variants: For one, the darker the patient’s skin, the deeper the purple color of the LP—sometimes to the point of obscuring the diagnosis.
As if that were not enough to confuse the examiner, there was an element of lichen simplex chronicus (LSC; also known as neurodermatitis), which instigates the “itch-scratch-itch” cycle. By its nature, LSC tends to hyperpigmentation (brown). By definition, it involves hypertrophy of the epidermis secondary to scratching. But there is always a primary cause; sometimes mere dry skin will trigger it, or insect bites, eczema, or even psoriasis. This confuses the issue, but the biopsy will establish the true basis for the patient’s condition.
The more common presentation of LP is that of a collection of flat-topped (“planar”), pruritic, purplish papules on the volar wrist, ankles, and sacral area. The surfaces of these lesions often demonstrate a faintly white, shiny surface. LP can also appear on oral mucosal surfaces, where it has a totally different, lacy-white look. In these areas, it tends to burn and not itch. LP appears to have a predilection for the penile glans, where it presents as an annular purplish plaque that sits astride the proximal glans, spilling over onto the coronal area.
LP can present as a widespread generalized eruption mimicking granuloma annulare and secondary syphilis. The differential for simple, classic LP includes psoriasis, granuloma annulare and pityriasis rosea.
Treatment of LP is with topical steroid creams or ointments, tailored in terms of strength to the area of involvement. For example, a class II or III corticosteroid would be used on areas with thicker skin and a class IV or V on thinner skin. Stubborn, solitary plaques can be treated with intralesional steroid injection (2.5 to 10 mg/cc triamcinolone solution).
TAKE-HOME LEARNING POINTS
• Lichen planus (LP) is common and typically presents on the volar wrists, dorsal ankles, and sacrum.
• In a minority of cases, LP can present on the legs as a hypertrophic, plaquish condition with secondary features of lichen simplex chronicus.
• A mnemonic device (“The Ps”) describes LP: papular, pruritic, purple, planar, polygonal, plaquish, and (perhaps most importantly) “puzzling.”
• LP can present as an annular plaque on the penile glans.
• LP has a pathognomic histologic picture on biopsy.
A 43-year-old Hispanic man has a very itchy rash on his left leg. It manifested within a few weeks of the patient starting a new job, one that involved working more hours than he had previously and on rotating shifts, which interfered with his sleep schedule.
For several years, he tried using different products—mostly OTC creams—on it, with no success. Increasingly annoyed by the rash, he finally consulted his family physician, who prescribed a combination clotrimazole/betamethasone cream. This helped a bit, but over time, the rash steadily worsened, and his primary care provider referred him to dermatology.
The patient claims to be otherwise healthy, with no history of atopy. He takes no prescription medications. He admits finding it difficult to refrain from scratching his legs.
EXAMINATION
There are large, slightly purplish, hypertrophic papulosquamous plaques of up to 8 cm on both anterior tibial areas. His arms, trunk, and wrists are rash-free, and his oral mucosal surfaces show no obvious signs of disease.
Punch biopsy shows a hypertrophic epidermis. There is marked obliteration of the dermoepidermal junction by a dense bandlike layer of lymphocytic infiltrate, associated with vacuolar change and necrotic keratinocytes in the basal layer of the epidermis.
DISCUSSION
This is a classic clinical and histologic picture of a dermatosis commonly seen in dermatology offices: lichen planus (LP). As is often the case, by the time the patient gets to dermatology, the clinical picture can be confused and atypical. But there is much to learn from such a case.
LP is the prototypical interface lichenoid dermatitis, which can be depended on to present in certain identifiable ways. In this case, what suggested this diagnosis was the word “puzzling.” It’s the perfect example of the intuitive, somewhat subjective side of dermatologic diagnosis: When I see a condition that baffles me momentarily, my puzzled reaction becomes meaningful because the word puzzling starts with a “p.” Lichen planus has long been associated with an extremely useful mnemonic device known as “The Ps.” Besides puzzling, it can stand for purple, plaquish, polygonal (ie, not round), prurtitic, papular, penile (LP has a predilection for this area), and planar (ie, flat-topped).
But it’s the “puzzling” aspect that unlocks the entrance to “The Ps,” and that in turn leads to consideration of this diagnosis. In this case, LP was not totally obvious, but a biopsy confirmed my clinical suspicions by demonstrating the classic findings associated with it.
An LP-like eruption can be provoked by drugs, such as the antimalarials, gold compounds, and penicillamine. It has also been associated with hepatitis C. But in my experience, the most common trigger appears to be stress, since it’s a rare case that doesn’t involve some. (I’ll happily concede that this is my opinion and not established fact.)
This patient’s LP demonstrated two common variants: For one, the darker the patient’s skin, the deeper the purple color of the LP—sometimes to the point of obscuring the diagnosis.
As if that were not enough to confuse the examiner, there was an element of lichen simplex chronicus (LSC; also known as neurodermatitis), which instigates the “itch-scratch-itch” cycle. By its nature, LSC tends to hyperpigmentation (brown). By definition, it involves hypertrophy of the epidermis secondary to scratching. But there is always a primary cause; sometimes mere dry skin will trigger it, or insect bites, eczema, or even psoriasis. This confuses the issue, but the biopsy will establish the true basis for the patient’s condition.
The more common presentation of LP is that of a collection of flat-topped (“planar”), pruritic, purplish papules on the volar wrist, ankles, and sacral area. The surfaces of these lesions often demonstrate a faintly white, shiny surface. LP can also appear on oral mucosal surfaces, where it has a totally different, lacy-white look. In these areas, it tends to burn and not itch. LP appears to have a predilection for the penile glans, where it presents as an annular purplish plaque that sits astride the proximal glans, spilling over onto the coronal area.
LP can present as a widespread generalized eruption mimicking granuloma annulare and secondary syphilis. The differential for simple, classic LP includes psoriasis, granuloma annulare and pityriasis rosea.
Treatment of LP is with topical steroid creams or ointments, tailored in terms of strength to the area of involvement. For example, a class II or III corticosteroid would be used on areas with thicker skin and a class IV or V on thinner skin. Stubborn, solitary plaques can be treated with intralesional steroid injection (2.5 to 10 mg/cc triamcinolone solution).
TAKE-HOME LEARNING POINTS
• Lichen planus (LP) is common and typically presents on the volar wrists, dorsal ankles, and sacrum.
• In a minority of cases, LP can present on the legs as a hypertrophic, plaquish condition with secondary features of lichen simplex chronicus.
• A mnemonic device (“The Ps”) describes LP: papular, pruritic, purple, planar, polygonal, plaquish, and (perhaps most importantly) “puzzling.”
• LP can present as an annular plaque on the penile glans.
• LP has a pathognomic histologic picture on biopsy.