User login
ANSWER
The correct answer is acrodermatitis of Hallopeau (choice “c”).
DISCUSSION
Acrodermatitis of Hallopeau (ADH), a rare form of pustular psoriasis, affects the distal digits with changes typified by this patient’s case. It is notoriously difficult to treat, although the advent of the “biologic age” appears to offer a quantum leap in terms of effective treatment alternatives.
Prompt referral to dermatology is needed for ADH to be readily diagnosed and treated. Because ADH is both rare and obscure, it’s not surprising that so many patients suffer for years due to an incorrect diagnosis. And even when correctly diagnosed, treatment is far from satisfactory. For example, methotrexate is commonly used for psoriasis vulgaris but rarely improves ADH—nor do topical steroids or vitamin D–derived topicals.
The 3 other items in the differential would not explain the patient’s condition: (1) Except in cases of immunosuppression, we would not expect Candida (choice “a”) or any other yeast infection to manifest in this manner. (2) Atypical mycobacteria (choice “b”)—such as Mycobacterium marinum—can cause skin infections, but not in a chronically relapsing manner. Moreover, this patient was given minocycline, which would have quickly cleared or at least improved his condition. (3) Pityriasis rubra pilaris (choice “d”) is an unusual papulosquamous disease that can affect nails, but its manifestation would not be as limited as this patient’s was.
TREATMENT
Because the patient’s symptoms are sometimes severe enough to interfere with almost all daily activities, he is clearly in need of prompt treatment. In more severe cases, a short course of cyclosporine followed by a biologic can be an option. For this patient, adalimumab was used. Although it is too early to tell, we expect him to be much improved within a few months.
ANSWER
The correct answer is acrodermatitis of Hallopeau (choice “c”).
DISCUSSION
Acrodermatitis of Hallopeau (ADH), a rare form of pustular psoriasis, affects the distal digits with changes typified by this patient’s case. It is notoriously difficult to treat, although the advent of the “biologic age” appears to offer a quantum leap in terms of effective treatment alternatives.
Prompt referral to dermatology is needed for ADH to be readily diagnosed and treated. Because ADH is both rare and obscure, it’s not surprising that so many patients suffer for years due to an incorrect diagnosis. And even when correctly diagnosed, treatment is far from satisfactory. For example, methotrexate is commonly used for psoriasis vulgaris but rarely improves ADH—nor do topical steroids or vitamin D–derived topicals.
The 3 other items in the differential would not explain the patient’s condition: (1) Except in cases of immunosuppression, we would not expect Candida (choice “a”) or any other yeast infection to manifest in this manner. (2) Atypical mycobacteria (choice “b”)—such as Mycobacterium marinum—can cause skin infections, but not in a chronically relapsing manner. Moreover, this patient was given minocycline, which would have quickly cleared or at least improved his condition. (3) Pityriasis rubra pilaris (choice “d”) is an unusual papulosquamous disease that can affect nails, but its manifestation would not be as limited as this patient’s was.
TREATMENT
Because the patient’s symptoms are sometimes severe enough to interfere with almost all daily activities, he is clearly in need of prompt treatment. In more severe cases, a short course of cyclosporine followed by a biologic can be an option. For this patient, adalimumab was used. Although it is too early to tell, we expect him to be much improved within a few months.
ANSWER
The correct answer is acrodermatitis of Hallopeau (choice “c”).
DISCUSSION
Acrodermatitis of Hallopeau (ADH), a rare form of pustular psoriasis, affects the distal digits with changes typified by this patient’s case. It is notoriously difficult to treat, although the advent of the “biologic age” appears to offer a quantum leap in terms of effective treatment alternatives.
Prompt referral to dermatology is needed for ADH to be readily diagnosed and treated. Because ADH is both rare and obscure, it’s not surprising that so many patients suffer for years due to an incorrect diagnosis. And even when correctly diagnosed, treatment is far from satisfactory. For example, methotrexate is commonly used for psoriasis vulgaris but rarely improves ADH—nor do topical steroids or vitamin D–derived topicals.
The 3 other items in the differential would not explain the patient’s condition: (1) Except in cases of immunosuppression, we would not expect Candida (choice “a”) or any other yeast infection to manifest in this manner. (2) Atypical mycobacteria (choice “b”)—such as Mycobacterium marinum—can cause skin infections, but not in a chronically relapsing manner. Moreover, this patient was given minocycline, which would have quickly cleared or at least improved his condition. (3) Pityriasis rubra pilaris (choice “d”) is an unusual papulosquamous disease that can affect nails, but its manifestation would not be as limited as this patient’s was.
TREATMENT
Because the patient’s symptoms are sometimes severe enough to interfere with almost all daily activities, he is clearly in need of prompt treatment. In more severe cases, a short course of cyclosporine followed by a biologic can be an option. For this patient, adalimumab was used. Although it is too early to tell, we expect him to be much improved within a few months.

For years, a 29-year-old man has been troubled by persistent painful outbreaks on his right thumb and forefinger and left great toe. The condition sometimes prevents him from engaging in daily activities. Several health care providers—none a dermatology specialist—attempted to treat him with topical and oral antifungals (clotrimazole and terbinafine), topical steroids (triamcinolone and clobetasol), and oral antibiotics (including minocycline)—none of which had an impact.
His latest provider, a podiatrist, was sure the problem was fungal in origin and prescribed another course of antifungal treatment. When this failed to produce a benefit, the podiatrist conceded that he was at a loss and referred the patient to dermatology.
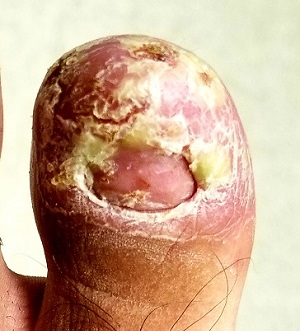
On physical exam, the 3 affected digits show similar characteristics: the skin is covered by dense, tenacious scaling on a dark red base. Small pustules are noted on these areas in addition to marked dystrophy of the adjacent nails. Bacterial and fungal cultures of the pustular fluid show no growth.
The rest of the patient’s skin—elbows, oral mucosa, knees, and scalp—show no noteworthy changes. He has no other skin problems. There is no family history of psoriasis or other skin conditions.