User login
ANSWER
The one incorrect answer is yeast infection (choice “c”). All the others should be included in the list of possible explanations. Given the inherent dryness and relatively low temperature of the affected area, as well as the nonresponse to imidazole cream, candida is quite unlikely.
DISCUSSION
The only way this patient could acquire a yeast infection in this area is if she were immunosuppressed. Eyelid dermatitis is seen daily in derm practices; patients are often referred by frustrated primary care providers who are unable to help.
This problem is almost never seen in male patients, which suggests the involvement of makeup, eye shadow, or skin care products, especially cleansers. But even when these are changed or eliminated, the problem often continues.
Here’s why: Women—especially those with sensitive skin in general—will often manifest that sensitivity in areas where skin is the thinnest and most accessible, and therefore the most easily damaged. Once the problem starts, it is difficult for these women to leave it alone. They scratch it, rub it, and often apply multiple products to it, all of which only serves to worsen it.
In contrast, most men use no products at all on their faces, let alone “eye creams” or special cleansers. The male version of this problem is the equally ubiquitous chronic anterior scrotal rash—which develops for many of the same reasons.
Many of these women also happen to have a history of atopic dermatitis, which not only means extraordinarily sensitive skin all over the body but also tends to involve unusually dry skin (xerosis). These women have multiple allergies to contactants, such as nickel and nail polish.
TREATMENT
As the cycle of applying different (unhelpful) products to the problem area continues, women are increasingly likely to use products with irritating ingredients. If they are to get any relief, this cycle must be broken.
I usually prescribe hydrocortisone 2.5% ointment (not the cream, which has a drying effect) or tacrolimus 0.1% ointment (either treatment to be used twice a day), plus once-a-day application of the greasiest moisturizer they can stand (eg, petroleum jelly) over the affected area.
They can use this same approach with future episodes, although there must be strict limits on the duration (two weeks) and frequency of the application. Overuse of the steroid can lead to glaucoma and permanent thinning of already thin skin.
Obviously, it would be of great utility if the patient were in fact found to be allergic to nail polish, but in my experience, most women have eliminated that as a potential cause before they get to a dermatology provider. The same goes for makeup.
The eyelid dermatitis patient certainly could be suffering from seborrhea or psoriasis; however, in such cases, the same itch-scratch-itch cycle often results, and the treatment would be identical.
ANSWER
The one incorrect answer is yeast infection (choice “c”). All the others should be included in the list of possible explanations. Given the inherent dryness and relatively low temperature of the affected area, as well as the nonresponse to imidazole cream, candida is quite unlikely.
DISCUSSION
The only way this patient could acquire a yeast infection in this area is if she were immunosuppressed. Eyelid dermatitis is seen daily in derm practices; patients are often referred by frustrated primary care providers who are unable to help.
This problem is almost never seen in male patients, which suggests the involvement of makeup, eye shadow, or skin care products, especially cleansers. But even when these are changed or eliminated, the problem often continues.
Here’s why: Women—especially those with sensitive skin in general—will often manifest that sensitivity in areas where skin is the thinnest and most accessible, and therefore the most easily damaged. Once the problem starts, it is difficult for these women to leave it alone. They scratch it, rub it, and often apply multiple products to it, all of which only serves to worsen it.
In contrast, most men use no products at all on their faces, let alone “eye creams” or special cleansers. The male version of this problem is the equally ubiquitous chronic anterior scrotal rash—which develops for many of the same reasons.
Many of these women also happen to have a history of atopic dermatitis, which not only means extraordinarily sensitive skin all over the body but also tends to involve unusually dry skin (xerosis). These women have multiple allergies to contactants, such as nickel and nail polish.
TREATMENT
As the cycle of applying different (unhelpful) products to the problem area continues, women are increasingly likely to use products with irritating ingredients. If they are to get any relief, this cycle must be broken.
I usually prescribe hydrocortisone 2.5% ointment (not the cream, which has a drying effect) or tacrolimus 0.1% ointment (either treatment to be used twice a day), plus once-a-day application of the greasiest moisturizer they can stand (eg, petroleum jelly) over the affected area.
They can use this same approach with future episodes, although there must be strict limits on the duration (two weeks) and frequency of the application. Overuse of the steroid can lead to glaucoma and permanent thinning of already thin skin.
Obviously, it would be of great utility if the patient were in fact found to be allergic to nail polish, but in my experience, most women have eliminated that as a potential cause before they get to a dermatology provider. The same goes for makeup.
The eyelid dermatitis patient certainly could be suffering from seborrhea or psoriasis; however, in such cases, the same itch-scratch-itch cycle often results, and the treatment would be identical.
ANSWER
The one incorrect answer is yeast infection (choice “c”). All the others should be included in the list of possible explanations. Given the inherent dryness and relatively low temperature of the affected area, as well as the nonresponse to imidazole cream, candida is quite unlikely.
DISCUSSION
The only way this patient could acquire a yeast infection in this area is if she were immunosuppressed. Eyelid dermatitis is seen daily in derm practices; patients are often referred by frustrated primary care providers who are unable to help.
This problem is almost never seen in male patients, which suggests the involvement of makeup, eye shadow, or skin care products, especially cleansers. But even when these are changed or eliminated, the problem often continues.
Here’s why: Women—especially those with sensitive skin in general—will often manifest that sensitivity in areas where skin is the thinnest and most accessible, and therefore the most easily damaged. Once the problem starts, it is difficult for these women to leave it alone. They scratch it, rub it, and often apply multiple products to it, all of which only serves to worsen it.
In contrast, most men use no products at all on their faces, let alone “eye creams” or special cleansers. The male version of this problem is the equally ubiquitous chronic anterior scrotal rash—which develops for many of the same reasons.
Many of these women also happen to have a history of atopic dermatitis, which not only means extraordinarily sensitive skin all over the body but also tends to involve unusually dry skin (xerosis). These women have multiple allergies to contactants, such as nickel and nail polish.
TREATMENT
As the cycle of applying different (unhelpful) products to the problem area continues, women are increasingly likely to use products with irritating ingredients. If they are to get any relief, this cycle must be broken.
I usually prescribe hydrocortisone 2.5% ointment (not the cream, which has a drying effect) or tacrolimus 0.1% ointment (either treatment to be used twice a day), plus once-a-day application of the greasiest moisturizer they can stand (eg, petroleum jelly) over the affected area.
They can use this same approach with future episodes, although there must be strict limits on the duration (two weeks) and frequency of the application. Overuse of the steroid can lead to glaucoma and permanent thinning of already thin skin.
Obviously, it would be of great utility if the patient were in fact found to be allergic to nail polish, but in my experience, most women have eliminated that as a potential cause before they get to a dermatology provider. The same goes for makeup.
The eyelid dermatitis patient certainly could be suffering from seborrhea or psoriasis; however, in such cases, the same itch-scratch-itch cycle often results, and the treatment would be identical.
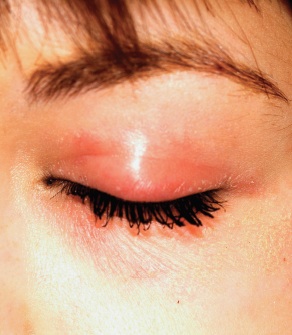
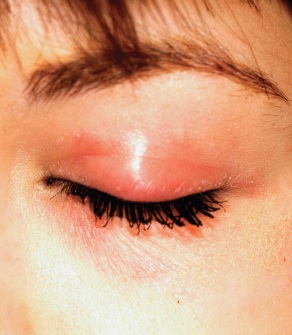
A 22-year-old woman is evaluated for a recurring itchy rash on both the upper and lower bilateral eyelids, which has been present for months. Her eyes themselves are unaffected, but the skin around them is highly irritated. The patient has already seen a number of providers who prescribed or recommended several remedies, including hydrocortisone creams, imidazole creams, and OTC moisturizers. Since none of these has proved helpful, she presents to the dermatology clinic. Her medical history includes seasonal allergies and “sensitive skin”; by the latter, she means frequent rashes or irritation brought on by various products, such as shampoos and conditioners. During this occurrence, as in several previous episodes, she has changed eye shadow and other makeup, to no avail. The patient denies any history of psoriasis, seborrhea, or other skin disease. On examination, a brisk red, dry, wrinkly rash covering the above-mentioned areas is noted. No rash is seen elsewhere, and there are no signs of psoriasis or seborrhea in any of the locations where they typically appear.