User login
The stubborn focal eruption on this 6-year-old boy’s left fourth finger remains unaffected after a one-week course of oral cephalexin, so his pediatrician refers him to dermatology. The problem initially manifested as a cluster of tiny blisters, which tingled a bit but didn’t hurt. When redness developed around it, the patient’s mother brought him for evaluation.
The boy experienced the same problem in the same location almost exactly a year ago. It was treated the same way and within a week or two had resolved.
The child is otherwise reasonably healthy, despite being allergy-prone. He has a history of seasonal allergies and is susceptible to skin infections, such as staph.
EXAMINATION
On the dorsal aspect of his finger are grouped vesicles on an erythematous base, measuring about 1 cm altogether. Several of these demonstrate central umbilication, and several are filled with pus. The erythema is minimal, and there is no tenderness on palpation. Palpation of the epitrochlear area reveals a tiny, nontender node.
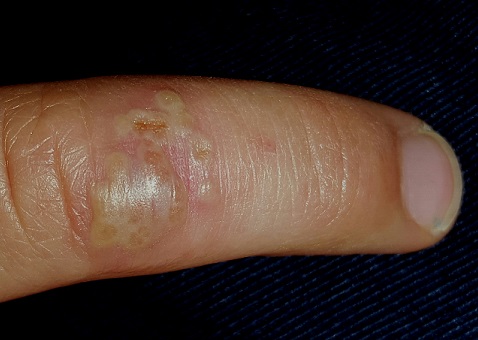
What is the diagnosis?
DISCUSSION
Herpetic whitlow (HW), while uncommon, is far from rare. Essentially a cold sore occurring away from the usual labial/facial location, HW presents with premonitory symptoms of itch, tingle, and slight pain, followed by the appearance of grouped vesicles on an erythematous base. The vesicles are often umbillicated, as with most herpetic conditions. And, like most herpes simplex–related outbreaks, HW tends to recur in the same location—an extremely useful piece of information.
Its appearance on unusual areas can cause confusion, but herpes simplex can manifest almost anywhere: toes, legs, nipples, the tips of ears, and even the eye. On the thicker skin of fingers, these vesicles may be a bit harder to recognize than they would be on a penis or lip.
Because it is often assumed that pus designates a bacterial infection, its presence in this situation can be puzzling. But pus is really just a collection of dead white cells, often seen in conditions unrelated to bacteria (eg, psoriasis).
One additional factor played a role in the diagnosis of this condition. Atopic children (with seasonal allergies, asthma, eczema, and other related phenomena) are exceptionally susceptible to skin infections of all kinds, including bacterial, viral, and fungal. Further evaluation revealed that this child had a history of molluscum contagiosum and impetigo.
If the nature of this outbreak had been unclear, it could have been cultured (though it could take a week or two to get results) or even biopsied. The latter option would have shown the cytopathic effects of the virus.
No treatment was possible, nor was it necessary. HW has to be treated within the first day or two of the outbreak to be effective. Since this patient’s outbreaks only occur once a year, he does not need prophylactic treatment. Over time, as he and his immune system mature, he can be expected to have fewer attacks.
In terms of contagion, he represents no more threat to others than a child with a cold sore or a wart.
TAKE-HOME LEARNING POINTS
• Herpetic whitlow (HW), although commonly found on fingers, can occur almost anywhere.
• The causative organism is herpes simplex; each episode begins with premonitory symptoms, followed within a few days by the appearance of grouped vesicles on an erythematous base. After a week or two, the episode resolves.
• Herpes infections of all kinds in immunocompetent patients tend to recur in the same places repeatedly.
• Atopy predisposes to skin infections of all kinds.
• Pus is not necessarily an indication of bacterial infection; it is often seen in viral infections.
The stubborn focal eruption on this 6-year-old boy’s left fourth finger remains unaffected after a one-week course of oral cephalexin, so his pediatrician refers him to dermatology. The problem initially manifested as a cluster of tiny blisters, which tingled a bit but didn’t hurt. When redness developed around it, the patient’s mother brought him for evaluation.
The boy experienced the same problem in the same location almost exactly a year ago. It was treated the same way and within a week or two had resolved.
The child is otherwise reasonably healthy, despite being allergy-prone. He has a history of seasonal allergies and is susceptible to skin infections, such as staph.
EXAMINATION
On the dorsal aspect of his finger are grouped vesicles on an erythematous base, measuring about 1 cm altogether. Several of these demonstrate central umbilication, and several are filled with pus. The erythema is minimal, and there is no tenderness on palpation. Palpation of the epitrochlear area reveals a tiny, nontender node.

What is the diagnosis?
DISCUSSION
Herpetic whitlow (HW), while uncommon, is far from rare. Essentially a cold sore occurring away from the usual labial/facial location, HW presents with premonitory symptoms of itch, tingle, and slight pain, followed by the appearance of grouped vesicles on an erythematous base. The vesicles are often umbillicated, as with most herpetic conditions. And, like most herpes simplex–related outbreaks, HW tends to recur in the same location—an extremely useful piece of information.
Its appearance on unusual areas can cause confusion, but herpes simplex can manifest almost anywhere: toes, legs, nipples, the tips of ears, and even the eye. On the thicker skin of fingers, these vesicles may be a bit harder to recognize than they would be on a penis or lip.
Because it is often assumed that pus designates a bacterial infection, its presence in this situation can be puzzling. But pus is really just a collection of dead white cells, often seen in conditions unrelated to bacteria (eg, psoriasis).
One additional factor played a role in the diagnosis of this condition. Atopic children (with seasonal allergies, asthma, eczema, and other related phenomena) are exceptionally susceptible to skin infections of all kinds, including bacterial, viral, and fungal. Further evaluation revealed that this child had a history of molluscum contagiosum and impetigo.
If the nature of this outbreak had been unclear, it could have been cultured (though it could take a week or two to get results) or even biopsied. The latter option would have shown the cytopathic effects of the virus.
No treatment was possible, nor was it necessary. HW has to be treated within the first day or two of the outbreak to be effective. Since this patient’s outbreaks only occur once a year, he does not need prophylactic treatment. Over time, as he and his immune system mature, he can be expected to have fewer attacks.
In terms of contagion, he represents no more threat to others than a child with a cold sore or a wart.
TAKE-HOME LEARNING POINTS
• Herpetic whitlow (HW), although commonly found on fingers, can occur almost anywhere.
• The causative organism is herpes simplex; each episode begins with premonitory symptoms, followed within a few days by the appearance of grouped vesicles on an erythematous base. After a week or two, the episode resolves.
• Herpes infections of all kinds in immunocompetent patients tend to recur in the same places repeatedly.
• Atopy predisposes to skin infections of all kinds.
• Pus is not necessarily an indication of bacterial infection; it is often seen in viral infections.
The stubborn focal eruption on this 6-year-old boy’s left fourth finger remains unaffected after a one-week course of oral cephalexin, so his pediatrician refers him to dermatology. The problem initially manifested as a cluster of tiny blisters, which tingled a bit but didn’t hurt. When redness developed around it, the patient’s mother brought him for evaluation.
The boy experienced the same problem in the same location almost exactly a year ago. It was treated the same way and within a week or two had resolved.
The child is otherwise reasonably healthy, despite being allergy-prone. He has a history of seasonal allergies and is susceptible to skin infections, such as staph.
EXAMINATION
On the dorsal aspect of his finger are grouped vesicles on an erythematous base, measuring about 1 cm altogether. Several of these demonstrate central umbilication, and several are filled with pus. The erythema is minimal, and there is no tenderness on palpation. Palpation of the epitrochlear area reveals a tiny, nontender node.

What is the diagnosis?
DISCUSSION
Herpetic whitlow (HW), while uncommon, is far from rare. Essentially a cold sore occurring away from the usual labial/facial location, HW presents with premonitory symptoms of itch, tingle, and slight pain, followed by the appearance of grouped vesicles on an erythematous base. The vesicles are often umbillicated, as with most herpetic conditions. And, like most herpes simplex–related outbreaks, HW tends to recur in the same location—an extremely useful piece of information.
Its appearance on unusual areas can cause confusion, but herpes simplex can manifest almost anywhere: toes, legs, nipples, the tips of ears, and even the eye. On the thicker skin of fingers, these vesicles may be a bit harder to recognize than they would be on a penis or lip.
Because it is often assumed that pus designates a bacterial infection, its presence in this situation can be puzzling. But pus is really just a collection of dead white cells, often seen in conditions unrelated to bacteria (eg, psoriasis).
One additional factor played a role in the diagnosis of this condition. Atopic children (with seasonal allergies, asthma, eczema, and other related phenomena) are exceptionally susceptible to skin infections of all kinds, including bacterial, viral, and fungal. Further evaluation revealed that this child had a history of molluscum contagiosum and impetigo.
If the nature of this outbreak had been unclear, it could have been cultured (though it could take a week or two to get results) or even biopsied. The latter option would have shown the cytopathic effects of the virus.
No treatment was possible, nor was it necessary. HW has to be treated within the first day or two of the outbreak to be effective. Since this patient’s outbreaks only occur once a year, he does not need prophylactic treatment. Over time, as he and his immune system mature, he can be expected to have fewer attacks.
In terms of contagion, he represents no more threat to others than a child with a cold sore or a wart.
TAKE-HOME LEARNING POINTS
• Herpetic whitlow (HW), although commonly found on fingers, can occur almost anywhere.
• The causative organism is herpes simplex; each episode begins with premonitory symptoms, followed within a few days by the appearance of grouped vesicles on an erythematous base. After a week or two, the episode resolves.
• Herpes infections of all kinds in immunocompetent patients tend to recur in the same places repeatedly.
• Atopy predisposes to skin infections of all kinds.
• Pus is not necessarily an indication of bacterial infection; it is often seen in viral infections.