User login
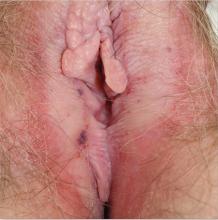
1. A 62-year-old woman reports anogenital itching with pain on scratching and has developed introital dyspareunia. Physical exam reveals a well-demarcated white plaque of thickened, crinkled skin. A wet mount shows parabasal cells and no lactobacilli.
Diagnosis: Lichen sclerosus is a skin disease found most often on the vulva of postmenopausal women, although it also can affect prepubertal children and reproductive-age women. Lichen sclerosus is multifactorial in pathogenesis, including prominent autoimmune factors, local environmental factors, and genetic predisposition.1
Although there is no cure for lichen sclerosus, the symptoms and clinical abnormalities usually can be well managed with ultra-potent topical corticosteroids. However, scarring and architectural changes are not reversible. Moreover, poorly controlled lichen sclerosus exhibits malignant transformation on anogenital skin in about 3% of affected patients.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
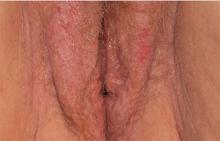
2. A 34-year-old patient reports excruciating itching, with disruption of daily activities and sleep. She has been treated for candidiasis on multiple occasions, but her wet mount and confirmatory culture are negative. Physical exam reveals a pink, lichenified plaque with excoriation.
Diagnosis: Lichen simplex chronicus (formerly called squamous hyperplasia or hyperplastic dystrophy, and also known as eczema, neurodermatitis, or localized atopic dermatitis) occurs when irritation from any cause produces itching in a predisposed person. The subsequent scratching and rubbing both produce the rash and exacerbate the irritation that drives the itching, even after the original cause is gone. The rubbing and scratching perpetuate the irritation and itching, producing the “itch-scratch” cycle.
The appearance of lichen simplex chronicus is produced by rubbing (where the skin thickens and lichenifies) or scratching (where the skin becomes red with linear erosions, called excoriations, caused by fingernails).
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
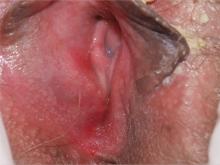
3. A 36-year-old has a history of chronic yeast infection with introital burning, discharge, and dyspareunia. She is otherwise healthy, except for irritable bowel syndrome and fibromyalgia. A mild patchy redness appears on the vestibule and surrounding modified mucous membranes. Gentle probing triggers exquisite pain in the vestibule, with slight extension to the labia minora. Lactobacilli are abundant.
Diagnosis: Vulvodynia is a genital pain syndrome defined as sensations of chronic burning, irritation, rawness, and soreness in the absence of objective disease and infection that could explain the discomfort. Vulvodynia occurs in approximately 7% to 8% of women.
Vulvodynia generally is believed to be a multifactorial symptom, occurring as a result of pelvic floor dysfunction and neuropathic pain, with anxiety/depression issues exacerbating symptoms. Some recent studies have shown the presence of biochemical mediators of inflammation in the absence of clinical and histologic inflammation. Discomfort often is worsened by infections or the application of common irritants (creams, panty liners, soaps, some topical anesthetics). Estrogen deficiency is another common exacerbating factor.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
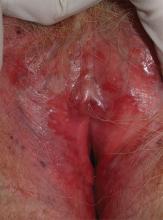
4. A 73-year-old patient has longstanding introital itching and rawness, with dyspareunia. Topical estradiol cream intravaginally three times weekly with weekly fluconazole has not helped. The physical reveals deep red patches and erosions of the vestibule and anterior mucosal membranes, with loss of the labia minora. An oral exam shows deep redness of the gingivae and erosions of the buccal mucosae, with surrounding white, lacy papules.
Diagnosis: After correlating the vulvar and oral findings, you make a diagnosis of lichen planus. Erosive multimucosal lichen planus is a disease of cell-mediated immunity that overwhelmingly affects menopausal women. The most common surfaces involved are the mouth, vagina, rectal mucosa, and vulva; usually, at least two surfaces are affected. The esophagus, extra-auditory canals, nasal mucosa, and eyes also can be involved. Dry, extragenital skin usually is not affected in the setting of erosive vulvovaginal lichen planus.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
1. A 62-year-old woman reports anogenital itching with pain on scratching and has developed introital dyspareunia. Physical exam reveals a well-demarcated white plaque of thickened, crinkled skin. A wet mount shows parabasal cells and no lactobacilli.
Diagnosis: Lichen sclerosus is a skin disease found most often on the vulva of postmenopausal women, although it also can affect prepubertal children and reproductive-age women. Lichen sclerosus is multifactorial in pathogenesis, including prominent autoimmune factors, local environmental factors, and genetic predisposition.1
Although there is no cure for lichen sclerosus, the symptoms and clinical abnormalities usually can be well managed with ultra-potent topical corticosteroids. However, scarring and architectural changes are not reversible. Moreover, poorly controlled lichen sclerosus exhibits malignant transformation on anogenital skin in about 3% of affected patients.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
2. A 34-year-old patient reports excruciating itching, with disruption of daily activities and sleep. She has been treated for candidiasis on multiple occasions, but her wet mount and confirmatory culture are negative. Physical exam reveals a pink, lichenified plaque with excoriation.
Diagnosis: Lichen simplex chronicus (formerly called squamous hyperplasia or hyperplastic dystrophy, and also known as eczema, neurodermatitis, or localized atopic dermatitis) occurs when irritation from any cause produces itching in a predisposed person. The subsequent scratching and rubbing both produce the rash and exacerbate the irritation that drives the itching, even after the original cause is gone. The rubbing and scratching perpetuate the irritation and itching, producing the “itch-scratch” cycle.
The appearance of lichen simplex chronicus is produced by rubbing (where the skin thickens and lichenifies) or scratching (where the skin becomes red with linear erosions, called excoriations, caused by fingernails).
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
3. A 36-year-old has a history of chronic yeast infection with introital burning, discharge, and dyspareunia. She is otherwise healthy, except for irritable bowel syndrome and fibromyalgia. A mild patchy redness appears on the vestibule and surrounding modified mucous membranes. Gentle probing triggers exquisite pain in the vestibule, with slight extension to the labia minora. Lactobacilli are abundant.
Diagnosis: Vulvodynia is a genital pain syndrome defined as sensations of chronic burning, irritation, rawness, and soreness in the absence of objective disease and infection that could explain the discomfort. Vulvodynia occurs in approximately 7% to 8% of women.
Vulvodynia generally is believed to be a multifactorial symptom, occurring as a result of pelvic floor dysfunction and neuropathic pain, with anxiety/depression issues exacerbating symptoms. Some recent studies have shown the presence of biochemical mediators of inflammation in the absence of clinical and histologic inflammation. Discomfort often is worsened by infections or the application of common irritants (creams, panty liners, soaps, some topical anesthetics). Estrogen deficiency is another common exacerbating factor.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
4. A 73-year-old patient has longstanding introital itching and rawness, with dyspareunia. Topical estradiol cream intravaginally three times weekly with weekly fluconazole has not helped. The physical reveals deep red patches and erosions of the vestibule and anterior mucosal membranes, with loss of the labia minora. An oral exam shows deep redness of the gingivae and erosions of the buccal mucosae, with surrounding white, lacy papules.
Diagnosis: After correlating the vulvar and oral findings, you make a diagnosis of lichen planus. Erosive multimucosal lichen planus is a disease of cell-mediated immunity that overwhelmingly affects menopausal women. The most common surfaces involved are the mouth, vagina, rectal mucosa, and vulva; usually, at least two surfaces are affected. The esophagus, extra-auditory canals, nasal mucosa, and eyes also can be involved. Dry, extragenital skin usually is not affected in the setting of erosive vulvovaginal lichen planus.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
1. A 62-year-old woman reports anogenital itching with pain on scratching and has developed introital dyspareunia. Physical exam reveals a well-demarcated white plaque of thickened, crinkled skin. A wet mount shows parabasal cells and no lactobacilli.
Diagnosis: Lichen sclerosus is a skin disease found most often on the vulva of postmenopausal women, although it also can affect prepubertal children and reproductive-age women. Lichen sclerosus is multifactorial in pathogenesis, including prominent autoimmune factors, local environmental factors, and genetic predisposition.1
Although there is no cure for lichen sclerosus, the symptoms and clinical abnormalities usually can be well managed with ultra-potent topical corticosteroids. However, scarring and architectural changes are not reversible. Moreover, poorly controlled lichen sclerosus exhibits malignant transformation on anogenital skin in about 3% of affected patients.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
2. A 34-year-old patient reports excruciating itching, with disruption of daily activities and sleep. She has been treated for candidiasis on multiple occasions, but her wet mount and confirmatory culture are negative. Physical exam reveals a pink, lichenified plaque with excoriation.
Diagnosis: Lichen simplex chronicus (formerly called squamous hyperplasia or hyperplastic dystrophy, and also known as eczema, neurodermatitis, or localized atopic dermatitis) occurs when irritation from any cause produces itching in a predisposed person. The subsequent scratching and rubbing both produce the rash and exacerbate the irritation that drives the itching, even after the original cause is gone. The rubbing and scratching perpetuate the irritation and itching, producing the “itch-scratch” cycle.
The appearance of lichen simplex chronicus is produced by rubbing (where the skin thickens and lichenifies) or scratching (where the skin becomes red with linear erosions, called excoriations, caused by fingernails).
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
3. A 36-year-old has a history of chronic yeast infection with introital burning, discharge, and dyspareunia. She is otherwise healthy, except for irritable bowel syndrome and fibromyalgia. A mild patchy redness appears on the vestibule and surrounding modified mucous membranes. Gentle probing triggers exquisite pain in the vestibule, with slight extension to the labia minora. Lactobacilli are abundant.
Diagnosis: Vulvodynia is a genital pain syndrome defined as sensations of chronic burning, irritation, rawness, and soreness in the absence of objective disease and infection that could explain the discomfort. Vulvodynia occurs in approximately 7% to 8% of women.
Vulvodynia generally is believed to be a multifactorial symptom, occurring as a result of pelvic floor dysfunction and neuropathic pain, with anxiety/depression issues exacerbating symptoms. Some recent studies have shown the presence of biochemical mediators of inflammation in the absence of clinical and histologic inflammation. Discomfort often is worsened by infections or the application of common irritants (creams, panty liners, soaps, some topical anesthetics). Estrogen deficiency is another common exacerbating factor.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.
For the next photograph, proceed to the next page >>
4. A 73-year-old patient has longstanding introital itching and rawness, with dyspareunia. Topical estradiol cream intravaginally three times weekly with weekly fluconazole has not helped. The physical reveals deep red patches and erosions of the vestibule and anterior mucosal membranes, with loss of the labia minora. An oral exam shows deep redness of the gingivae and erosions of the buccal mucosae, with surrounding white, lacy papules.
Diagnosis: After correlating the vulvar and oral findings, you make a diagnosis of lichen planus. Erosive multimucosal lichen planus is a disease of cell-mediated immunity that overwhelmingly affects menopausal women. The most common surfaces involved are the mouth, vagina, rectal mucosa, and vulva; usually, at least two surfaces are affected. The esophagus, extra-auditory canals, nasal mucosa, and eyes also can be involved. Dry, extragenital skin usually is not affected in the setting of erosive vulvovaginal lichen planus.
For more information on this case, see “Chronic vulvar symptoms and dermatologic disruptions: How to make the correct diagnosis.” OBG Manag. 2014;26(5):30-49.