User login
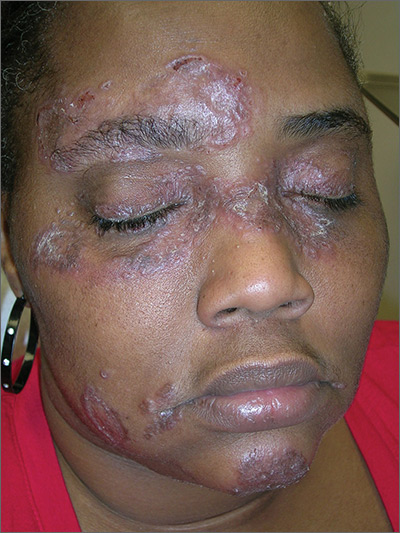
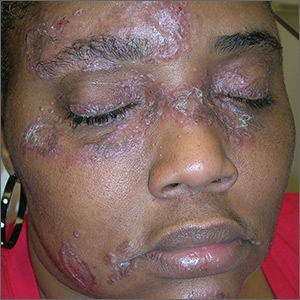
The FP suspected that the patient had sarcoidosis, based on the infiltrated plaques and their distribution on her face. The appearance of the lesions was similar to images he’d seen online of lupus pernio, a pathognomonic finding of sarcoidosis. The FP recommended a punch biopsy of one of the lesions, and the patient consented.
(See the Watch & Learn video on “Punch biopsy.”)
The FP also sent the patient for a chest x-ray, which showed bilateral hilar adenopathy consistent with sarcoidosis. Histopathology of the biopsy also showed sarcoidosis. Chest radiographic involvement is seen in almost 90% of patients with sarcoidosis and is used in staging the disease. Stage I disease shows bilateral hilar lymphadenopathy (BHL). Stage II disease shows BHL plus pulmonary infiltrates. Stage III disease shows pulmonary infiltrates without BHL. Stage IV disease shows pulmonary fibrosis. In this case, the patient had stage I disease.
The FP prescribed topical 0.1% triamcinolone ointment in an 80 g tube and instructed the patient to apply it to all of the areas involved. Although this medication typically comes in a 15 g or 30 g tube, the FP knew that these quantities would be insufficient. He had also read that a mid-potency steroid would be permissible on the face for this diagnosis. Not having any experience with sarcoidosis, the FP referred the patient to Dermatology and Pulmonology.
The dermatologist started the patient on oral prednisone 40 mg/d and awaited the completion of the patient’s baseline labs before beginning a steroid sparing agent such as methotrexate. Treatments for sarcoidosis include topical steroids, systemic steroids, methotrexate, azathioprine, and biologics (with adalimumab and infliximab having the greatest evidence for effectiveness).
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Bae E, Bae Y, Sarabi K, et al. Sarcoidosis. In: Usatine R, Smith M, Mayeaux EJ, et al. Color Atlas and Synopsis of Family Medicine. 3rd ed. New York, NY: McGraw-Hill; 2019:1153-1160.
To learn more about the newest 3rd edition of the Color Atlas and Synopsis of Family Medicine, see: https://www.amazon.com/Color-Atlas-Synopsis-Family-Medicine/dp/1259862046/
You can get the Color Atlas of Family Medicine app by clicking on this link: usatinemedia.com

The FP suspected that the patient had sarcoidosis, based on the infiltrated plaques and their distribution on her face. The appearance of the lesions was similar to images he’d seen online of lupus pernio, a pathognomonic finding of sarcoidosis. The FP recommended a punch biopsy of one of the lesions, and the patient consented.
(See the Watch & Learn video on “Punch biopsy.”)
The FP also sent the patient for a chest x-ray, which showed bilateral hilar adenopathy consistent with sarcoidosis. Histopathology of the biopsy also showed sarcoidosis. Chest radiographic involvement is seen in almost 90% of patients with sarcoidosis and is used in staging the disease. Stage I disease shows bilateral hilar lymphadenopathy (BHL). Stage II disease shows BHL plus pulmonary infiltrates. Stage III disease shows pulmonary infiltrates without BHL. Stage IV disease shows pulmonary fibrosis. In this case, the patient had stage I disease.
The FP prescribed topical 0.1% triamcinolone ointment in an 80 g tube and instructed the patient to apply it to all of the areas involved. Although this medication typically comes in a 15 g or 30 g tube, the FP knew that these quantities would be insufficient. He had also read that a mid-potency steroid would be permissible on the face for this diagnosis. Not having any experience with sarcoidosis, the FP referred the patient to Dermatology and Pulmonology.
The dermatologist started the patient on oral prednisone 40 mg/d and awaited the completion of the patient’s baseline labs before beginning a steroid sparing agent such as methotrexate. Treatments for sarcoidosis include topical steroids, systemic steroids, methotrexate, azathioprine, and biologics (with adalimumab and infliximab having the greatest evidence for effectiveness).
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Bae E, Bae Y, Sarabi K, et al. Sarcoidosis. In: Usatine R, Smith M, Mayeaux EJ, et al. Color Atlas and Synopsis of Family Medicine. 3rd ed. New York, NY: McGraw-Hill; 2019:1153-1160.
To learn more about the newest 3rd edition of the Color Atlas and Synopsis of Family Medicine, see: https://www.amazon.com/Color-Atlas-Synopsis-Family-Medicine/dp/1259862046/
You can get the Color Atlas of Family Medicine app by clicking on this link: usatinemedia.com

The FP suspected that the patient had sarcoidosis, based on the infiltrated plaques and their distribution on her face. The appearance of the lesions was similar to images he’d seen online of lupus pernio, a pathognomonic finding of sarcoidosis. The FP recommended a punch biopsy of one of the lesions, and the patient consented.
(See the Watch & Learn video on “Punch biopsy.”)
The FP also sent the patient for a chest x-ray, which showed bilateral hilar adenopathy consistent with sarcoidosis. Histopathology of the biopsy also showed sarcoidosis. Chest radiographic involvement is seen in almost 90% of patients with sarcoidosis and is used in staging the disease. Stage I disease shows bilateral hilar lymphadenopathy (BHL). Stage II disease shows BHL plus pulmonary infiltrates. Stage III disease shows pulmonary infiltrates without BHL. Stage IV disease shows pulmonary fibrosis. In this case, the patient had stage I disease.
The FP prescribed topical 0.1% triamcinolone ointment in an 80 g tube and instructed the patient to apply it to all of the areas involved. Although this medication typically comes in a 15 g or 30 g tube, the FP knew that these quantities would be insufficient. He had also read that a mid-potency steroid would be permissible on the face for this diagnosis. Not having any experience with sarcoidosis, the FP referred the patient to Dermatology and Pulmonology.
The dermatologist started the patient on oral prednisone 40 mg/d and awaited the completion of the patient’s baseline labs before beginning a steroid sparing agent such as methotrexate. Treatments for sarcoidosis include topical steroids, systemic steroids, methotrexate, azathioprine, and biologics (with adalimumab and infliximab having the greatest evidence for effectiveness).
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Bae E, Bae Y, Sarabi K, et al. Sarcoidosis. In: Usatine R, Smith M, Mayeaux EJ, et al. Color Atlas and Synopsis of Family Medicine. 3rd ed. New York, NY: McGraw-Hill; 2019:1153-1160.
To learn more about the newest 3rd edition of the Color Atlas and Synopsis of Family Medicine, see: https://www.amazon.com/Color-Atlas-Synopsis-Family-Medicine/dp/1259862046/
You can get the Color Atlas of Family Medicine app by clicking on this link: usatinemedia.com