User login
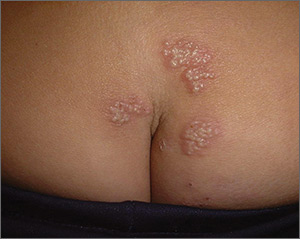
Based on the appearance and location of the lesions, a diagnosis of recurrent herpes simplex virus-2 (HSV-2) was made. HSV-2 is generally a genital eruption but can also occur on the buttocks, especially in women. (Our patient was not aware that she’d had a genital primary HSV-2 infection.) HSV-2 infects an estimated 5% to 25% of adults in western nations. In 2012, approximately 417 million people ages 15 to 49 were living with HSV-2 worldwide, including 19 million who were newly infected.
Following a genital primary infection, HSV-2 lies dormant in the sacral nerve root ganglia, which innervate both the genitals and sacrum. Reactivation can thus result in recurrences anywhere over the sacral dermatome. The sacral area is the most common nongenital site for recurrent HSV-2. Reactivation of HSV-2 is more common and more severe in patients with human immunodeficiency virus infection.
The mainstay of treatment for HSV is antiviral therapy with acyclovir. Famciclovir and valacyclovir can be used, as well. These antivirals inhibit viral DNA replication, shorten duration of symptoms, increase lesion healing, and decrease viral shedding time. They are generally safe; the main adverse effects of oral therapy are nausea, vomiting, and diarrhea.
In general, nongenital recurrences of HSV are treated the same as genital recurrences. Dosing during prodromal symptoms or at the first sign of a recurrence is recommended for maximum efficacy. Suppressive therapy can be effective in patients who experience frequent recurrences and is generally recommended for 6 months to a year (or longer). Patients should also be warned that because of increased genital viral shedding during sacral recurrences, they should avoid sexual contact during outbreaks.
After a discussion about the benefits and risks of antiviral suppression, the patient decided she was ready to proceed with treatment. The physician prescribed oral valacyclovir 1 g daily for treatment and suppression. She had no recurrences over the next year.
Adapted from: Flowers H, Brodell RT. Recurrent vesicular rash over the sacrum. J Fam Pract. 2015;64:577-579.

Based on the appearance and location of the lesions, a diagnosis of recurrent herpes simplex virus-2 (HSV-2) was made. HSV-2 is generally a genital eruption but can also occur on the buttocks, especially in women. (Our patient was not aware that she’d had a genital primary HSV-2 infection.) HSV-2 infects an estimated 5% to 25% of adults in western nations. In 2012, approximately 417 million people ages 15 to 49 were living with HSV-2 worldwide, including 19 million who were newly infected.
Following a genital primary infection, HSV-2 lies dormant in the sacral nerve root ganglia, which innervate both the genitals and sacrum. Reactivation can thus result in recurrences anywhere over the sacral dermatome. The sacral area is the most common nongenital site for recurrent HSV-2. Reactivation of HSV-2 is more common and more severe in patients with human immunodeficiency virus infection.
The mainstay of treatment for HSV is antiviral therapy with acyclovir. Famciclovir and valacyclovir can be used, as well. These antivirals inhibit viral DNA replication, shorten duration of symptoms, increase lesion healing, and decrease viral shedding time. They are generally safe; the main adverse effects of oral therapy are nausea, vomiting, and diarrhea.
In general, nongenital recurrences of HSV are treated the same as genital recurrences. Dosing during prodromal symptoms or at the first sign of a recurrence is recommended for maximum efficacy. Suppressive therapy can be effective in patients who experience frequent recurrences and is generally recommended for 6 months to a year (or longer). Patients should also be warned that because of increased genital viral shedding during sacral recurrences, they should avoid sexual contact during outbreaks.
After a discussion about the benefits and risks of antiviral suppression, the patient decided she was ready to proceed with treatment. The physician prescribed oral valacyclovir 1 g daily for treatment and suppression. She had no recurrences over the next year.
Adapted from: Flowers H, Brodell RT. Recurrent vesicular rash over the sacrum. J Fam Pract. 2015;64:577-579.

Based on the appearance and location of the lesions, a diagnosis of recurrent herpes simplex virus-2 (HSV-2) was made. HSV-2 is generally a genital eruption but can also occur on the buttocks, especially in women. (Our patient was not aware that she’d had a genital primary HSV-2 infection.) HSV-2 infects an estimated 5% to 25% of adults in western nations. In 2012, approximately 417 million people ages 15 to 49 were living with HSV-2 worldwide, including 19 million who were newly infected.
Following a genital primary infection, HSV-2 lies dormant in the sacral nerve root ganglia, which innervate both the genitals and sacrum. Reactivation can thus result in recurrences anywhere over the sacral dermatome. The sacral area is the most common nongenital site for recurrent HSV-2. Reactivation of HSV-2 is more common and more severe in patients with human immunodeficiency virus infection.
The mainstay of treatment for HSV is antiviral therapy with acyclovir. Famciclovir and valacyclovir can be used, as well. These antivirals inhibit viral DNA replication, shorten duration of symptoms, increase lesion healing, and decrease viral shedding time. They are generally safe; the main adverse effects of oral therapy are nausea, vomiting, and diarrhea.
In general, nongenital recurrences of HSV are treated the same as genital recurrences. Dosing during prodromal symptoms or at the first sign of a recurrence is recommended for maximum efficacy. Suppressive therapy can be effective in patients who experience frequent recurrences and is generally recommended for 6 months to a year (or longer). Patients should also be warned that because of increased genital viral shedding during sacral recurrences, they should avoid sexual contact during outbreaks.
After a discussion about the benefits and risks of antiviral suppression, the patient decided she was ready to proceed with treatment. The physician prescribed oral valacyclovir 1 g daily for treatment and suppression. She had no recurrences over the next year.
Adapted from: Flowers H, Brodell RT. Recurrent vesicular rash over the sacrum. J Fam Pract. 2015;64:577-579.