User login
ANSWER
The correct answer is to perform a punch biopsy (choice “b”). This will help establish the exact nature of the problem, which will dictate rational treatment.
The patient doesn’t have acne, so the suggested treatment options (choices “a,” “c,” and “d”) would be of no use. With cryotherapy, furthermore, there is a risk of leaving a permanent blemish on her skin.
DISCUSSION
A sample of one lesion was obtained via 3-mm punch biopsy and the resulting defect closed with a single suture. Pathologic examination showed the specimen to be a vellus hair cyst (VHC). In this case, it was one of many, making the diagnosis eruptive vellus hair cysts.
VHC, which can be acquired or inherited, typically manifests in the first two decades of life. In this developmental abnormality, a gradual disruption occurs between the proximal and distal portions of the vellus hair follicle, usually at the level of the infundibulum. As a result, the characteristic papule (which holds the retained hair) forms and the hair bulb atrophies.
The lesions may be solitary or appear in clusters on the body; they are easily mistaken for acne, milia, or even molluscum. As this case demonstrates, biopsy is often necessary to establish the correct diagnosis.
One final note about biopsy: It is best to incise each lesion with an 18-gauge needle tip or #11 blade and express the contents. This tedious process causes some discomfort for the patient, but it is quite effective and, if done correctly, should not leave a permanent mark on the skin.
ANSWER
The correct answer is to perform a punch biopsy (choice “b”). This will help establish the exact nature of the problem, which will dictate rational treatment.
The patient doesn’t have acne, so the suggested treatment options (choices “a,” “c,” and “d”) would be of no use. With cryotherapy, furthermore, there is a risk of leaving a permanent blemish on her skin.
DISCUSSION
A sample of one lesion was obtained via 3-mm punch biopsy and the resulting defect closed with a single suture. Pathologic examination showed the specimen to be a vellus hair cyst (VHC). In this case, it was one of many, making the diagnosis eruptive vellus hair cysts.
VHC, which can be acquired or inherited, typically manifests in the first two decades of life. In this developmental abnormality, a gradual disruption occurs between the proximal and distal portions of the vellus hair follicle, usually at the level of the infundibulum. As a result, the characteristic papule (which holds the retained hair) forms and the hair bulb atrophies.
The lesions may be solitary or appear in clusters on the body; they are easily mistaken for acne, milia, or even molluscum. As this case demonstrates, biopsy is often necessary to establish the correct diagnosis.
One final note about biopsy: It is best to incise each lesion with an 18-gauge needle tip or #11 blade and express the contents. This tedious process causes some discomfort for the patient, but it is quite effective and, if done correctly, should not leave a permanent mark on the skin.
ANSWER
The correct answer is to perform a punch biopsy (choice “b”). This will help establish the exact nature of the problem, which will dictate rational treatment.
The patient doesn’t have acne, so the suggested treatment options (choices “a,” “c,” and “d”) would be of no use. With cryotherapy, furthermore, there is a risk of leaving a permanent blemish on her skin.
DISCUSSION
A sample of one lesion was obtained via 3-mm punch biopsy and the resulting defect closed with a single suture. Pathologic examination showed the specimen to be a vellus hair cyst (VHC). In this case, it was one of many, making the diagnosis eruptive vellus hair cysts.
VHC, which can be acquired or inherited, typically manifests in the first two decades of life. In this developmental abnormality, a gradual disruption occurs between the proximal and distal portions of the vellus hair follicle, usually at the level of the infundibulum. As a result, the characteristic papule (which holds the retained hair) forms and the hair bulb atrophies.
The lesions may be solitary or appear in clusters on the body; they are easily mistaken for acne, milia, or even molluscum. As this case demonstrates, biopsy is often necessary to establish the correct diagnosis.
One final note about biopsy: It is best to incise each lesion with an 18-gauge needle tip or #11 blade and express the contents. This tedious process causes some discomfort for the patient, but it is quite effective and, if done correctly, should not leave a permanent mark on the skin.
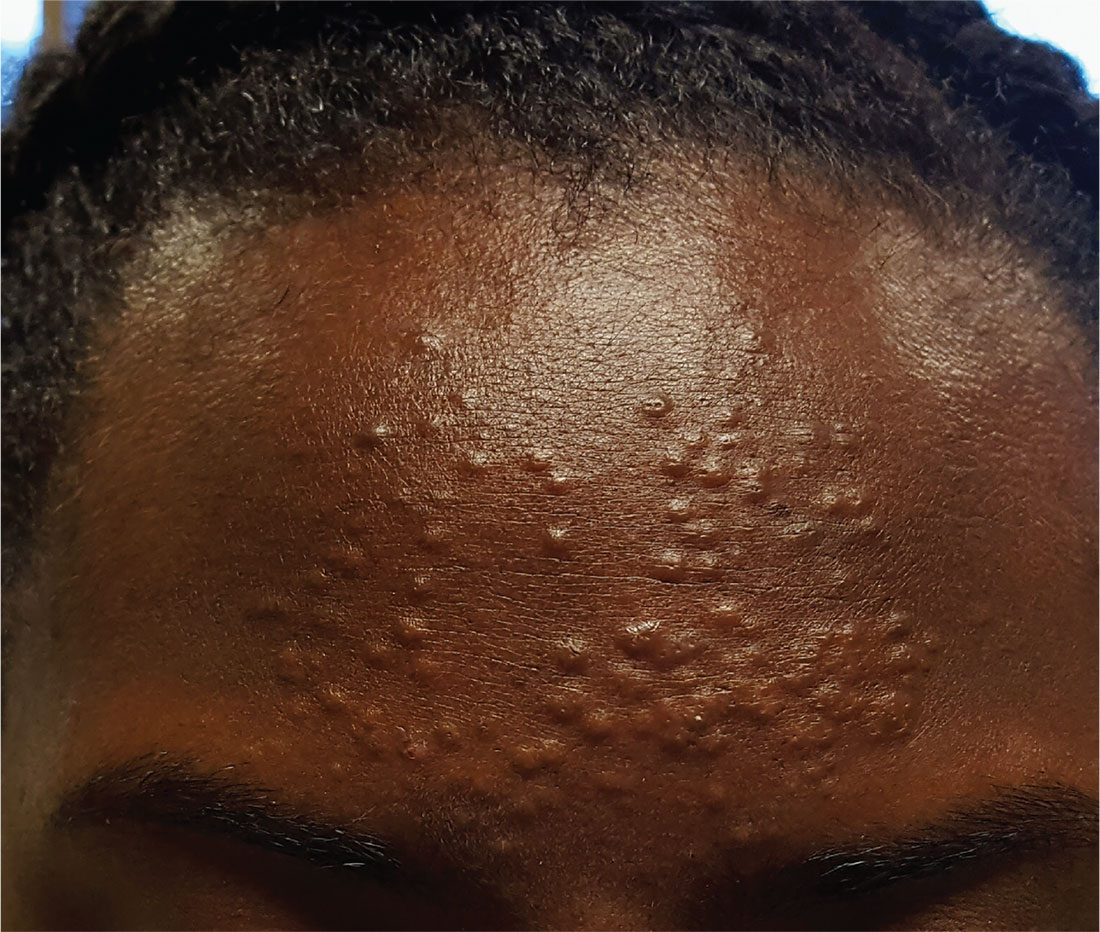
A 13-year-old African-American girl is brought in by her mother for evaluation of lesions that manifested on her forehead several years ago. Over time, the lesions have multiplied from just a few papules to a current total of about 30. Attempted treatment with topical benzoyl peroxide and two retinoids (tazarotene and adapalene)—for a presumptive diagnosis of acne—has yielded no improvement.
The lesions are quite obvious but asymptomatic; they are not tender, inflamed, or pustulant. The soft, 2- to 3-mm intradermal papules are grouped in a fairly round 7-cm area of the patient’s forehead. No punctum is seen with any of the lesions.
The child’s type V skin is otherwise clear, with no sign of acne. Her hair, teeth, and nails appear normal. According to her mother, the patient is healthy apart from this eruption.
