User login
A 72-year-old man self-refers to dermatology at the insistence of his wife, who wants confirmation of her assertion that he needs to use a moisturizer on his arms. “They’re just so dry!” she says. “They’d look so much better if he’d use moisturizer every day, like I do.”
Her husband says he tried it and it didn’t help, so he stopped. “Besides, I can’t stand the greasy feeling it leaves behind!”
The patient claims to be in decent health aside from mild arthritis. He is retired from his job with the local power company, which kept him outdoors for many years. His employer required workers to wear long-sleeved khaki shirts, but, like all his fellow employees, the patient rolled up the sleeves in hot weather, exposing his forearms.
EXAMINATION
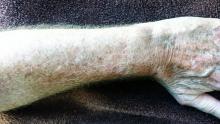
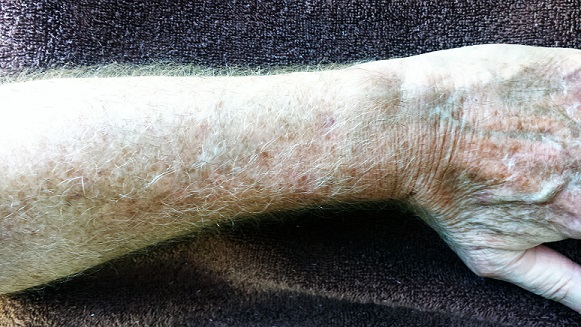
The patient has type II skin, blue eyes, and light brown hair. The skin on the dorsa of both arms is flecked with innumerable tan to orange macules from the mid forearms to (and including) the hands. Many old scars are seen in these same areas.
Closer examination reveals that the skin in these areas is quite thin and dry. Fine telangiectasias and focal scaling are also noted. The effect is much less pronounced from about the elbow up and is totally absent on both volar forearms.
What is the diagnosis?
DISCUSSION
The patient’s admittedly dry skin is not his primary problem, and all the moisturizers in the world will not make much difference. The term we use for his problem is dermatoheliosis , literally “sun condition,” which includes predictable indicators of past overexposure to UV sources. Specific lesions include solar lentigines, the tan to orange freckles that are commonly called “age spots” or “liver spots.” (Given enough sun exposure, a 25-year-old can develop solar lentigines, so age is not the cause. Likewise, the liver is not involved at all.)
Chronic overexposure to the sun thins the skin (solar atrophy), making it more susceptible to minor trauma and resultant scarring and also making the tortuous red blood vessels (telangiectasias) visible. Other indications of sun damage include actinic keratoses (flaky white papules), solar elastosis (creamy yellow to white “chicken skin”), and solar purpura. The combination of these superimposed colors (white, red, tan, orange, pink) in the context of dermatoheliosis is sometimes termed poikilodermatous change.
Although dermatoheliosis is a problem in terms of the potential for skin cancer and for cosmetic reasons, it will not be helped much by moisturizers. Sunscreen, too, will have minimal impact so long after the damage has been done. Laser resurfacing could erase most of these skin changes, but it would also knock out all the normal skin pigment, making the area contrast sharply with the rest of the patient’s skin.
A combination of fade cream (4% hydroquinone, applied bid) and sunscreen could reduce the brown discoloration to a degree. Twice-daily application of 5-fluorouracil cream for two weeks would erase much of the redness, but only for a few months. Various other methods have been tried with modest success.
The main outcome of this patient’s visit was to establish the need for periodic examination. His wife’s opinion notwithstanding, the utility of moisturizers is dubious.
TAKE-HOME LEARNING POINTS
• Dermatoheliosis is the collective term for skin changes associated with chronic overexposure to the sun.
• The white, red, pink, and yellow discoloration seen on this kind of sun-damaged skin is known as poikilodermatous change.
• In addition to poikiloderma, patients with advanced dermatoheliosis also have solar atrophy, multiple scars, telangiectasias, actinic keratoses, dry skin, and often solar purpura.
• Moisturizers play a minimal role in treating dermatoheliosis (providing skin-smoothing effects, if anything).
• Such patients need to be examined periodically for skin cancer.
• Younger patients with dermatoheliosis are well advised to use better sun protection.
A 72-year-old man self-refers to dermatology at the insistence of his wife, who wants confirmation of her assertion that he needs to use a moisturizer on his arms. “They’re just so dry!” she says. “They’d look so much better if he’d use moisturizer every day, like I do.”
Her husband says he tried it and it didn’t help, so he stopped. “Besides, I can’t stand the greasy feeling it leaves behind!”
The patient claims to be in decent health aside from mild arthritis. He is retired from his job with the local power company, which kept him outdoors for many years. His employer required workers to wear long-sleeved khaki shirts, but, like all his fellow employees, the patient rolled up the sleeves in hot weather, exposing his forearms.
EXAMINATION
The patient has type II skin, blue eyes, and light brown hair. The skin on the dorsa of both arms is flecked with innumerable tan to orange macules from the mid forearms to (and including) the hands. Many old scars are seen in these same areas.
Closer examination reveals that the skin in these areas is quite thin and dry. Fine telangiectasias and focal scaling are also noted. The effect is much less pronounced from about the elbow up and is totally absent on both volar forearms.
What is the diagnosis?
DISCUSSION
The patient’s admittedly dry skin is not his primary problem, and all the moisturizers in the world will not make much difference. The term we use for his problem is dermatoheliosis , literally “sun condition,” which includes predictable indicators of past overexposure to UV sources. Specific lesions include solar lentigines, the tan to orange freckles that are commonly called “age spots” or “liver spots.” (Given enough sun exposure, a 25-year-old can develop solar lentigines, so age is not the cause. Likewise, the liver is not involved at all.)
Chronic overexposure to the sun thins the skin (solar atrophy), making it more susceptible to minor trauma and resultant scarring and also making the tortuous red blood vessels (telangiectasias) visible. Other indications of sun damage include actinic keratoses (flaky white papules), solar elastosis (creamy yellow to white “chicken skin”), and solar purpura. The combination of these superimposed colors (white, red, tan, orange, pink) in the context of dermatoheliosis is sometimes termed poikilodermatous change.
Although dermatoheliosis is a problem in terms of the potential for skin cancer and for cosmetic reasons, it will not be helped much by moisturizers. Sunscreen, too, will have minimal impact so long after the damage has been done. Laser resurfacing could erase most of these skin changes, but it would also knock out all the normal skin pigment, making the area contrast sharply with the rest of the patient’s skin.
A combination of fade cream (4% hydroquinone, applied bid) and sunscreen could reduce the brown discoloration to a degree. Twice-daily application of 5-fluorouracil cream for two weeks would erase much of the redness, but only for a few months. Various other methods have been tried with modest success.
The main outcome of this patient’s visit was to establish the need for periodic examination. His wife’s opinion notwithstanding, the utility of moisturizers is dubious.
TAKE-HOME LEARNING POINTS
• Dermatoheliosis is the collective term for skin changes associated with chronic overexposure to the sun.
• The white, red, pink, and yellow discoloration seen on this kind of sun-damaged skin is known as poikilodermatous change.
• In addition to poikiloderma, patients with advanced dermatoheliosis also have solar atrophy, multiple scars, telangiectasias, actinic keratoses, dry skin, and often solar purpura.
• Moisturizers play a minimal role in treating dermatoheliosis (providing skin-smoothing effects, if anything).
• Such patients need to be examined periodically for skin cancer.
• Younger patients with dermatoheliosis are well advised to use better sun protection.
A 72-year-old man self-refers to dermatology at the insistence of his wife, who wants confirmation of her assertion that he needs to use a moisturizer on his arms. “They’re just so dry!” she says. “They’d look so much better if he’d use moisturizer every day, like I do.”
Her husband says he tried it and it didn’t help, so he stopped. “Besides, I can’t stand the greasy feeling it leaves behind!”
The patient claims to be in decent health aside from mild arthritis. He is retired from his job with the local power company, which kept him outdoors for many years. His employer required workers to wear long-sleeved khaki shirts, but, like all his fellow employees, the patient rolled up the sleeves in hot weather, exposing his forearms.
EXAMINATION
The patient has type II skin, blue eyes, and light brown hair. The skin on the dorsa of both arms is flecked with innumerable tan to orange macules from the mid forearms to (and including) the hands. Many old scars are seen in these same areas.
Closer examination reveals that the skin in these areas is quite thin and dry. Fine telangiectasias and focal scaling are also noted. The effect is much less pronounced from about the elbow up and is totally absent on both volar forearms.
What is the diagnosis?
DISCUSSION
The patient’s admittedly dry skin is not his primary problem, and all the moisturizers in the world will not make much difference. The term we use for his problem is dermatoheliosis , literally “sun condition,” which includes predictable indicators of past overexposure to UV sources. Specific lesions include solar lentigines, the tan to orange freckles that are commonly called “age spots” or “liver spots.” (Given enough sun exposure, a 25-year-old can develop solar lentigines, so age is not the cause. Likewise, the liver is not involved at all.)
Chronic overexposure to the sun thins the skin (solar atrophy), making it more susceptible to minor trauma and resultant scarring and also making the tortuous red blood vessels (telangiectasias) visible. Other indications of sun damage include actinic keratoses (flaky white papules), solar elastosis (creamy yellow to white “chicken skin”), and solar purpura. The combination of these superimposed colors (white, red, tan, orange, pink) in the context of dermatoheliosis is sometimes termed poikilodermatous change.
Although dermatoheliosis is a problem in terms of the potential for skin cancer and for cosmetic reasons, it will not be helped much by moisturizers. Sunscreen, too, will have minimal impact so long after the damage has been done. Laser resurfacing could erase most of these skin changes, but it would also knock out all the normal skin pigment, making the area contrast sharply with the rest of the patient’s skin.
A combination of fade cream (4% hydroquinone, applied bid) and sunscreen could reduce the brown discoloration to a degree. Twice-daily application of 5-fluorouracil cream for two weeks would erase much of the redness, but only for a few months. Various other methods have been tried with modest success.
The main outcome of this patient’s visit was to establish the need for periodic examination. His wife’s opinion notwithstanding, the utility of moisturizers is dubious.
TAKE-HOME LEARNING POINTS
• Dermatoheliosis is the collective term for skin changes associated with chronic overexposure to the sun.
• The white, red, pink, and yellow discoloration seen on this kind of sun-damaged skin is known as poikilodermatous change.
• In addition to poikiloderma, patients with advanced dermatoheliosis also have solar atrophy, multiple scars, telangiectasias, actinic keratoses, dry skin, and often solar purpura.
• Moisturizers play a minimal role in treating dermatoheliosis (providing skin-smoothing effects, if anything).
• Such patients need to be examined periodically for skin cancer.
• Younger patients with dermatoheliosis are well advised to use better sun protection.