User login
Official news magazine of the Society of Hospital Medicine
Copyright by Society of Hospital Medicine or related companies. All rights reserved. ISSN 1553-085X
nav[contains(@class, 'nav-ce-stack nav-ce-stack__large-screen')]
header[@id='header']
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'main-prefix')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
div[contains(@class, 'view-medstat-quiz-listing-panes')]
div[contains(@class, 'pane-article-sidebar-latest-news')]
div[contains(@class, 'pane-pub-article-hospitalist')]


More U.S. Babies Born Addicted to Opiates
(Reuters Health) - The proportion of U.S. babies born suffering from withdrawal syndrome after exposure to heroin or prescription opiates in utero has more than doubled in less than a decade, a study suggests.
Nationally, the rate of neonatal abstinence syndrome involving mothers' use of opiates - which includes heroin as well as prescription narcotics like codeine and Vicodin - surged from 2.8 cases for every 1,000 births in 2009 to 7.3 cases for every 1,000 births in 2013, the study found.
At least some of this surge in the case count is due to drug policies designed to crack down on prescription drug abuse and combat the methamphetamine epidemic, said lead study author Dr. Joshua Brown, a pharmacy researcher at the University of Kentucky in Lexington.
"The drug policies of the early 2000s were effective in reducing supply - we have seen a decrease in methamphetamine abuse and there have been reductions in some aspects of prescription drug abuse," Brown said by email. "However, the indirect results, mainly the increase in heroin abuse, were likely not anticipated and we are just starting to see these."
The findings of the current study add to a growing body of evidence pointing to a surge in births of babies suffering from opiate withdrawal. One report last month from the U.S. Centers for Disease Control and Prevention found an even bigger spike over a longer period, from 1.5 cases for every 1,000 births in 1999 to 6 cases per 1,000 in 2013.
CDC researchers also found wide variation in neonatal abstinence syndrome by state, ranging in 2013 from 0.7 cases for every 1,000 births in Hawaii to 33.4 cases per 1,000 in West Virginia.
"We know that certain states are harder hit by the opioid/heroin abuse epidemic, with about 10 states contributing half of all neonatal abstinence syndrome cases," Brown said. "These states are often more rural and impoverished areas of the U.S. such as Mississippi, Alabama, and West Virginia."
Brown and colleagues looked at Kentucky in particular. Here, the rate of neonatal abstinence syndrome climbed from 5 cases for every 1,000 births in 2008 to 21.2 cases per 1,000 births in 2014, researchers report in JAMA Pediatrics, online September 26.
While the study didn't look at health outcomes for babies born suffering from drug withdrawal, these infants often require intensive medical care. (See Reuters' 2015 special report "Helpless and Hooked" here.)
These babies may have central nervous system issues like seizures and tremors, gastrointestinal problems and feeding difficulties, breathing challenges, as well as unstable body temperatures.
Typically, they remain in the hospital for several weeks after birth and receive low doses of methadone, Brown said.
Treatment can ease withdrawal symptoms in newborns, but can't necessarily address developmental problems these infants may have later on, said Dr. William Carey, a pediatrics researcher at pediatrics at Mayo Clinic Children's Center in Rochester, Minnesota.
"While abuse of prescription opiates has declined, the use of illicit opiates has increased such that there may be a zero-sum game at best," Carey, who wasn't involved in the study, said by email. "Since maternal use of either prescription opiates or illicit opiates is associated with withdrawal in newborns, it is reasonable to think that any increase in the overall use of opiates would be linked to an increase in the rate of neonatal abstinence syndrome."
(Reuters Health) - The proportion of U.S. babies born suffering from withdrawal syndrome after exposure to heroin or prescription opiates in utero has more than doubled in less than a decade, a study suggests.
Nationally, the rate of neonatal abstinence syndrome involving mothers' use of opiates - which includes heroin as well as prescription narcotics like codeine and Vicodin - surged from 2.8 cases for every 1,000 births in 2009 to 7.3 cases for every 1,000 births in 2013, the study found.
At least some of this surge in the case count is due to drug policies designed to crack down on prescription drug abuse and combat the methamphetamine epidemic, said lead study author Dr. Joshua Brown, a pharmacy researcher at the University of Kentucky in Lexington.
"The drug policies of the early 2000s were effective in reducing supply - we have seen a decrease in methamphetamine abuse and there have been reductions in some aspects of prescription drug abuse," Brown said by email. "However, the indirect results, mainly the increase in heroin abuse, were likely not anticipated and we are just starting to see these."
The findings of the current study add to a growing body of evidence pointing to a surge in births of babies suffering from opiate withdrawal. One report last month from the U.S. Centers for Disease Control and Prevention found an even bigger spike over a longer period, from 1.5 cases for every 1,000 births in 1999 to 6 cases per 1,000 in 2013.
CDC researchers also found wide variation in neonatal abstinence syndrome by state, ranging in 2013 from 0.7 cases for every 1,000 births in Hawaii to 33.4 cases per 1,000 in West Virginia.
"We know that certain states are harder hit by the opioid/heroin abuse epidemic, with about 10 states contributing half of all neonatal abstinence syndrome cases," Brown said. "These states are often more rural and impoverished areas of the U.S. such as Mississippi, Alabama, and West Virginia."
Brown and colleagues looked at Kentucky in particular. Here, the rate of neonatal abstinence syndrome climbed from 5 cases for every 1,000 births in 2008 to 21.2 cases per 1,000 births in 2014, researchers report in JAMA Pediatrics, online September 26.
While the study didn't look at health outcomes for babies born suffering from drug withdrawal, these infants often require intensive medical care. (See Reuters' 2015 special report "Helpless and Hooked" here.)
These babies may have central nervous system issues like seizures and tremors, gastrointestinal problems and feeding difficulties, breathing challenges, as well as unstable body temperatures.
Typically, they remain in the hospital for several weeks after birth and receive low doses of methadone, Brown said.
Treatment can ease withdrawal symptoms in newborns, but can't necessarily address developmental problems these infants may have later on, said Dr. William Carey, a pediatrics researcher at pediatrics at Mayo Clinic Children's Center in Rochester, Minnesota.
"While abuse of prescription opiates has declined, the use of illicit opiates has increased such that there may be a zero-sum game at best," Carey, who wasn't involved in the study, said by email. "Since maternal use of either prescription opiates or illicit opiates is associated with withdrawal in newborns, it is reasonable to think that any increase in the overall use of opiates would be linked to an increase in the rate of neonatal abstinence syndrome."
(Reuters Health) - The proportion of U.S. babies born suffering from withdrawal syndrome after exposure to heroin or prescription opiates in utero has more than doubled in less than a decade, a study suggests.
Nationally, the rate of neonatal abstinence syndrome involving mothers' use of opiates - which includes heroin as well as prescription narcotics like codeine and Vicodin - surged from 2.8 cases for every 1,000 births in 2009 to 7.3 cases for every 1,000 births in 2013, the study found.
At least some of this surge in the case count is due to drug policies designed to crack down on prescription drug abuse and combat the methamphetamine epidemic, said lead study author Dr. Joshua Brown, a pharmacy researcher at the University of Kentucky in Lexington.
"The drug policies of the early 2000s were effective in reducing supply - we have seen a decrease in methamphetamine abuse and there have been reductions in some aspects of prescription drug abuse," Brown said by email. "However, the indirect results, mainly the increase in heroin abuse, were likely not anticipated and we are just starting to see these."
The findings of the current study add to a growing body of evidence pointing to a surge in births of babies suffering from opiate withdrawal. One report last month from the U.S. Centers for Disease Control and Prevention found an even bigger spike over a longer period, from 1.5 cases for every 1,000 births in 1999 to 6 cases per 1,000 in 2013.
CDC researchers also found wide variation in neonatal abstinence syndrome by state, ranging in 2013 from 0.7 cases for every 1,000 births in Hawaii to 33.4 cases per 1,000 in West Virginia.
"We know that certain states are harder hit by the opioid/heroin abuse epidemic, with about 10 states contributing half of all neonatal abstinence syndrome cases," Brown said. "These states are often more rural and impoverished areas of the U.S. such as Mississippi, Alabama, and West Virginia."
Brown and colleagues looked at Kentucky in particular. Here, the rate of neonatal abstinence syndrome climbed from 5 cases for every 1,000 births in 2008 to 21.2 cases per 1,000 births in 2014, researchers report in JAMA Pediatrics, online September 26.
While the study didn't look at health outcomes for babies born suffering from drug withdrawal, these infants often require intensive medical care. (See Reuters' 2015 special report "Helpless and Hooked" here.)
These babies may have central nervous system issues like seizures and tremors, gastrointestinal problems and feeding difficulties, breathing challenges, as well as unstable body temperatures.
Typically, they remain in the hospital for several weeks after birth and receive low doses of methadone, Brown said.
Treatment can ease withdrawal symptoms in newborns, but can't necessarily address developmental problems these infants may have later on, said Dr. William Carey, a pediatrics researcher at pediatrics at Mayo Clinic Children's Center in Rochester, Minnesota.
"While abuse of prescription opiates has declined, the use of illicit opiates has increased such that there may be a zero-sum game at best," Carey, who wasn't involved in the study, said by email. "Since maternal use of either prescription opiates or illicit opiates is associated with withdrawal in newborns, it is reasonable to think that any increase in the overall use of opiates would be linked to an increase in the rate of neonatal abstinence syndrome."
VIDEO: MOC + Me: Maintenance of Certification in Hospital Medicine
Dr. Marianne Green and Dr. Jeffrey Wiese, two members of the ABIM Council, talk about ABIM's Maintenance of Certification process, and the importance of professional assessment. Dr. Green works on Internal Medicine MOC, Dr. Wiese was part of the team that developed the Focused Practice in Hospital Medicine MOC.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Dr. Marianne Green and Dr. Jeffrey Wiese, two members of the ABIM Council, talk about ABIM's Maintenance of Certification process, and the importance of professional assessment. Dr. Green works on Internal Medicine MOC, Dr. Wiese was part of the team that developed the Focused Practice in Hospital Medicine MOC.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Dr. Marianne Green and Dr. Jeffrey Wiese, two members of the ABIM Council, talk about ABIM's Maintenance of Certification process, and the importance of professional assessment. Dr. Green works on Internal Medicine MOC, Dr. Wiese was part of the team that developed the Focused Practice in Hospital Medicine MOC.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
The State of Hospital Medicine Is Strong
Editor's Note: Listen to Dr. Smith share more of his views on the State of Hospital Medicine report.
2016 is the “Year of the Hospitalist,” a sobriquet meant as a proud nod to the specialty’s maturation as a fixture in hospitals across the country. Hospital medicine is no longer the new kid on the block as it has assumed care for the vast majority of hospitalized patients nationwide.
One could understand then if the ever-rising salaries hospitalists have commanded for 20 years might have finally plateaued, particularly as tightening budgets have C-suite administrators looking to trim costs.
Think again.
“Growth suggests that there is still a huge demand,” says Leslie Flores, MHA, a partner in Nelson Flores Hospital Medicine Consultants and a member of SHM’s Practice Analysis Committee. “The demand for hospitalists still exceeds the supply, and so recruiting hospitalists, particularly to nonurban areas, is really challenging and is requiring more money.”
The SoHM is a biennial partnership between SHM and MGMA that provides HM group leaders and rank-and-file hospitalists a litany of benchmarks for salaries, workloads, and everything that informs those two topics. Call it the specialty’s empirical roadmap.
“Often, compensation information relative to staffing information is proprietary, so hospitalists are in a position where they are dependent upon their hospital stakeholders to have access to this information, but they are also the same stakeholders with whom they negotiate their contracts,” says G. Randy Smith, MD, MS, FRCP(Edin), SFHM, an assistant professor in the Division of Hospital Medicine at Northwestern University Feinberg School of Medicine in Chicago and a member of SHM’s Practice Analysis Committee. “The State of Hospital Medicine report by SHM provides an opportunity for hospitalists to have an independent view of the compensation and workforce distribution factors that can impact negotiations with their hospital stakeholders. It’s a very powerful tool.”
Compensation Data
Rachel Lovins, MD, SFHM, CPE, voraciously reads every SoHM report because she uses its keynote compensation data to benchmark what she should pay her staff.
“I make a promise to my group,” says Dr. Lovins, chief of hospital medicine and vice chair of the Department of Medicine at Middlesex Hospital in Middletown, Conn. “I promise them that we will always be at or above what is standard for our areas. So for me, I have to look every time.”
Promises like that are getting more expensive to keep.
Hospitalists in the East region earn a median compensation of $245,977, up 3.1% from the $238,676 figure reported in 2014. But the East, where the bulk of the country’s population lives and where competition for hospitalists is typically lessened, is by far the lowest-paid region.
Hospitalists in the South continue to earn the most, with a median compensation of $301,833, up a whopping 16.9% from $258,020 from 2013. Hospitalists in the West earned a median of $275,658 (up 10.3% from $249,894), while Midwestern hospitalists saw a median compensation of $285,213 (up 8.9% from $261,868).
In addition to year-over-year growth, HM is also seeing outsized growth as compared with family medicine physicians, according to MGMA data. From 2011 to 2015, family medicine hospitalists saw an average compensation increase of 4.7%, bringing the average salary to $285,213. During the same period, family medicine physicians who are not hospitalists and don’t practice obstetrics saw an average annual compensation increase of only 3%, bringing the average salary to $230,456.
“The hospitalist can save the hospital considerable amounts of money because of their ability to better manage the patient and improve the quality of care at the same time,” says David Gans, MSHA, FACMPE, MGMA’s senior fellow of industry affairs. “Hospitals, they have recognized that, and therefore, there is considerable competition for recruiting and retaining hospitalists.”
To that end, 96.3% of HM groups (HMGs) received financial support in addition to their professional fee revenue. That’s up from 89% of HMGs that relied last year on their host hospitals. The median support is $157,535 per full-time employee (FTE), up just 1%. Correspondingly, SoHM reported 8.5% of HMGs received enough income from professional fee revenue to cover expenses, up from 6% two years ago.
Industry watchers predicted that, in two years, fee revenue would have to rise to offset hospitals’ inability to pay. The early returns seem to show that bearing out.
“We’re pretty close to that breaking point,” Flores says. “When we go around the country and do consulting work, we are hearing many more hospital leaders telling us, ‘We’re concerned about how much money this program is costing us, and we are getting to the point where we can’t afford it.’”
Productivity Stalls
While compensation continues to climb, productivity flattened out in this year’s report.
Median relative value units (RVUs) dipped slightly from the figure reported in 2014, to 4,252 from 4,297. But the tally is still ahead of 2012’s total of 4,159. Median collection-to-work RVUs also ticked down from 2014’s tally, to $50.29 from $51.50 in 2013.
Flores largely attributes the falling metrics of productivity to the evolution of HMGs that have standardized their scheduling to the point that most HMGs now offer vacation time.
“So the number of groups that are working 182 days is fewer, and we see a lot more groups that are working something like 168 days or 172 days,” she says. “And if a hospitalist works fewer shifts, even if they see the same number of patients per shift, they’re going to generate less productivity over the course of the year, so that’s part of it.”
Andrew White, MD, SFHM, director of the HM service at the University of Washington Medical Center in Seattle, says the report’s value is in avoiding a myopic approach to how HMGs operate. For example, RVUs are an important metric of productivity, but not all shifts should be expected to produce the same.
For example, it’d be valuable to use the report to see how hard your nocturnists are working compared with other sites, says Dr. White, also a member of the Practice Analysis Committee.
“The fundamental issue with working at night is that not everybody wants to do it, and so you have to recognize that it’s a pain to do and you have to either pay those people more, have them work less, or acknowledge that they’re going to be less productive,” he says. “We use the survey to assess all three of those things and then can work with our nocturnists to reach an agreement about a fair approach to their job structure that’s actually informed by national benchmarks. That process has helped us to pick, for example, how many nights per year they should work or what their salaries should look like compared to the day hospitalists.”
Dr. White says that because the report is comprehensive and includes broad participation, he’s able to use it as a benchmark to make hiring and service structure decisions.
“It also helps me to keep abreast of some trends that may be occurring in the broader workplace that we aren’t participating in but maybe should be or should be thinking about,” he says.
The report’s subsections are also critical for comparing one HMG to others, Dr. White says.
“Obviously, there is the aggregate data there to look at the average program,” he says. “But really as a hospitalist group leader, you want to know what are other programs like mine doing, and it allows you to drill down into that data.”
Survey Limitations
Any hospitalist worth their weight in scrubs knows that any medical study is only as good as its limitations. And while SoHM is a trove of valuable data information, Flores always cautions against taking data points as gospel.
“People should understand what the numbers are telling us, what goes into those numbers, and take them not with a grain of salt but take them for what they are,” she says.
For example, Flores says, look at productivity metrics per shift. Day shifts have traditionally driven that figure, and those shifts are typically busy. But night shifts have fewer patients and less productivity.
“So as more and more hospitals get 24-hour in-house coverage and have doctors working low-productivity night shifts, that [productivity] number might fall,” she says.
That sort of nuanced analysis of productivity can’t be found anywhere else, says Dr. Lovins.
These are “data that we don’t normally get from our administration,” she says, “information on things like staffing and patient loads, and how much more the director makes than the people that work for the director, and how much more nighttime people make than daytime people make. There is no other way for me to get that information, and it’s very important to make sure that our program is fair.”
Aside from fair, the data points are essential talking points as HMGs negotiate contracts and other arrangements with their administrators.
“It’s a reference point so that everybody feels like we’re using data from a national source that everyone can agree upon as fair,” says Dr. White.
In Dr. White’s case, he doesn’t have many local academic programs to benchmark against. And comparing to private, for-profit hospitals isn’t the proverbial apples-to-apples comparison. Having vetted regional and national figures for comparison is incredibly valuable, particularly since he doesn’t have to compile the data.
“If I had to go call all those group leaders and figure out what they were doing, it would be pretty exhausting,” he says.
Alternative Payment Models
Dr. Smith says that one area where the report will become even more valuable over the next few years is addressing alternative payment models (APMs). In particular, HM leaders say they’re excited about being drivers in one of the largest APMs: the Bundled Payments for Care Improvement (BCPI) initiative. In short, the program covers 48 defined episodes of care, including medical and surgical, that could begin three days prior to admission and stretch 30, 60, or 90 days post-discharge.
Dr. Smith thinks it’s still a bit too early to see from the report how APMs have affected compensation.
“We’re still relatively in the early days of bundled-payment models, so in that regard, the State of Hospital Medicine Report still represents very much a starting point with regard to where hospital medicine groups will find themselves as they start to encounter challenges,” he says.
Perhaps more important, Gans doesn’t expect that the maturation of APMs will result in decreased compensation for hospitalists.
“In a hospital environment where the hospital is being reimbursed a set amount for a complete hospital admission and follow-up care and potential readmissions, that is an episodic payment already,” he says. “Consequently, the incentive is there today to better manage the patient and to attain the care coordination and care management necessary for that patient to be discharged and not readmitted.”
In fact, the SHM/MGMA data tell him that the basic economic theory of supply and demand continues to drive hospitalist compensation even 20 years after the field was given its name. He says rising compensation, even as more practices look to hire nurse practitioners or physician assistants as less expensive alternatives, shows no sign of letting up.
“I think demand will continue to be there,” Gans adds. “There may be in the long run some lessening of demand for hospitalists, but I don’t see that for years.”
Richard Quinn is a freelance writer in New Jersey.
Editor's Note: Listen to Dr. Smith share more of his views on the State of Hospital Medicine report.
2016 is the “Year of the Hospitalist,” a sobriquet meant as a proud nod to the specialty’s maturation as a fixture in hospitals across the country. Hospital medicine is no longer the new kid on the block as it has assumed care for the vast majority of hospitalized patients nationwide.
One could understand then if the ever-rising salaries hospitalists have commanded for 20 years might have finally plateaued, particularly as tightening budgets have C-suite administrators looking to trim costs.
Think again.
“Growth suggests that there is still a huge demand,” says Leslie Flores, MHA, a partner in Nelson Flores Hospital Medicine Consultants and a member of SHM’s Practice Analysis Committee. “The demand for hospitalists still exceeds the supply, and so recruiting hospitalists, particularly to nonurban areas, is really challenging and is requiring more money.”
The SoHM is a biennial partnership between SHM and MGMA that provides HM group leaders and rank-and-file hospitalists a litany of benchmarks for salaries, workloads, and everything that informs those two topics. Call it the specialty’s empirical roadmap.
“Often, compensation information relative to staffing information is proprietary, so hospitalists are in a position where they are dependent upon their hospital stakeholders to have access to this information, but they are also the same stakeholders with whom they negotiate their contracts,” says G. Randy Smith, MD, MS, FRCP(Edin), SFHM, an assistant professor in the Division of Hospital Medicine at Northwestern University Feinberg School of Medicine in Chicago and a member of SHM’s Practice Analysis Committee. “The State of Hospital Medicine report by SHM provides an opportunity for hospitalists to have an independent view of the compensation and workforce distribution factors that can impact negotiations with their hospital stakeholders. It’s a very powerful tool.”
Compensation Data
Rachel Lovins, MD, SFHM, CPE, voraciously reads every SoHM report because she uses its keynote compensation data to benchmark what she should pay her staff.
“I make a promise to my group,” says Dr. Lovins, chief of hospital medicine and vice chair of the Department of Medicine at Middlesex Hospital in Middletown, Conn. “I promise them that we will always be at or above what is standard for our areas. So for me, I have to look every time.”
Promises like that are getting more expensive to keep.
Hospitalists in the East region earn a median compensation of $245,977, up 3.1% from the $238,676 figure reported in 2014. But the East, where the bulk of the country’s population lives and where competition for hospitalists is typically lessened, is by far the lowest-paid region.
Hospitalists in the South continue to earn the most, with a median compensation of $301,833, up a whopping 16.9% from $258,020 from 2013. Hospitalists in the West earned a median of $275,658 (up 10.3% from $249,894), while Midwestern hospitalists saw a median compensation of $285,213 (up 8.9% from $261,868).
In addition to year-over-year growth, HM is also seeing outsized growth as compared with family medicine physicians, according to MGMA data. From 2011 to 2015, family medicine hospitalists saw an average compensation increase of 4.7%, bringing the average salary to $285,213. During the same period, family medicine physicians who are not hospitalists and don’t practice obstetrics saw an average annual compensation increase of only 3%, bringing the average salary to $230,456.
“The hospitalist can save the hospital considerable amounts of money because of their ability to better manage the patient and improve the quality of care at the same time,” says David Gans, MSHA, FACMPE, MGMA’s senior fellow of industry affairs. “Hospitals, they have recognized that, and therefore, there is considerable competition for recruiting and retaining hospitalists.”
To that end, 96.3% of HM groups (HMGs) received financial support in addition to their professional fee revenue. That’s up from 89% of HMGs that relied last year on their host hospitals. The median support is $157,535 per full-time employee (FTE), up just 1%. Correspondingly, SoHM reported 8.5% of HMGs received enough income from professional fee revenue to cover expenses, up from 6% two years ago.
Industry watchers predicted that, in two years, fee revenue would have to rise to offset hospitals’ inability to pay. The early returns seem to show that bearing out.
“We’re pretty close to that breaking point,” Flores says. “When we go around the country and do consulting work, we are hearing many more hospital leaders telling us, ‘We’re concerned about how much money this program is costing us, and we are getting to the point where we can’t afford it.’”
Productivity Stalls
While compensation continues to climb, productivity flattened out in this year’s report.
Median relative value units (RVUs) dipped slightly from the figure reported in 2014, to 4,252 from 4,297. But the tally is still ahead of 2012’s total of 4,159. Median collection-to-work RVUs also ticked down from 2014’s tally, to $50.29 from $51.50 in 2013.
Flores largely attributes the falling metrics of productivity to the evolution of HMGs that have standardized their scheduling to the point that most HMGs now offer vacation time.
“So the number of groups that are working 182 days is fewer, and we see a lot more groups that are working something like 168 days or 172 days,” she says. “And if a hospitalist works fewer shifts, even if they see the same number of patients per shift, they’re going to generate less productivity over the course of the year, so that’s part of it.”
Andrew White, MD, SFHM, director of the HM service at the University of Washington Medical Center in Seattle, says the report’s value is in avoiding a myopic approach to how HMGs operate. For example, RVUs are an important metric of productivity, but not all shifts should be expected to produce the same.
For example, it’d be valuable to use the report to see how hard your nocturnists are working compared with other sites, says Dr. White, also a member of the Practice Analysis Committee.
“The fundamental issue with working at night is that not everybody wants to do it, and so you have to recognize that it’s a pain to do and you have to either pay those people more, have them work less, or acknowledge that they’re going to be less productive,” he says. “We use the survey to assess all three of those things and then can work with our nocturnists to reach an agreement about a fair approach to their job structure that’s actually informed by national benchmarks. That process has helped us to pick, for example, how many nights per year they should work or what their salaries should look like compared to the day hospitalists.”
Dr. White says that because the report is comprehensive and includes broad participation, he’s able to use it as a benchmark to make hiring and service structure decisions.
“It also helps me to keep abreast of some trends that may be occurring in the broader workplace that we aren’t participating in but maybe should be or should be thinking about,” he says.
The report’s subsections are also critical for comparing one HMG to others, Dr. White says.
“Obviously, there is the aggregate data there to look at the average program,” he says. “But really as a hospitalist group leader, you want to know what are other programs like mine doing, and it allows you to drill down into that data.”
Survey Limitations
Any hospitalist worth their weight in scrubs knows that any medical study is only as good as its limitations. And while SoHM is a trove of valuable data information, Flores always cautions against taking data points as gospel.
“People should understand what the numbers are telling us, what goes into those numbers, and take them not with a grain of salt but take them for what they are,” she says.
For example, Flores says, look at productivity metrics per shift. Day shifts have traditionally driven that figure, and those shifts are typically busy. But night shifts have fewer patients and less productivity.
“So as more and more hospitals get 24-hour in-house coverage and have doctors working low-productivity night shifts, that [productivity] number might fall,” she says.
That sort of nuanced analysis of productivity can’t be found anywhere else, says Dr. Lovins.
These are “data that we don’t normally get from our administration,” she says, “information on things like staffing and patient loads, and how much more the director makes than the people that work for the director, and how much more nighttime people make than daytime people make. There is no other way for me to get that information, and it’s very important to make sure that our program is fair.”
Aside from fair, the data points are essential talking points as HMGs negotiate contracts and other arrangements with their administrators.
“It’s a reference point so that everybody feels like we’re using data from a national source that everyone can agree upon as fair,” says Dr. White.
In Dr. White’s case, he doesn’t have many local academic programs to benchmark against. And comparing to private, for-profit hospitals isn’t the proverbial apples-to-apples comparison. Having vetted regional and national figures for comparison is incredibly valuable, particularly since he doesn’t have to compile the data.
“If I had to go call all those group leaders and figure out what they were doing, it would be pretty exhausting,” he says.
Alternative Payment Models
Dr. Smith says that one area where the report will become even more valuable over the next few years is addressing alternative payment models (APMs). In particular, HM leaders say they’re excited about being drivers in one of the largest APMs: the Bundled Payments for Care Improvement (BCPI) initiative. In short, the program covers 48 defined episodes of care, including medical and surgical, that could begin three days prior to admission and stretch 30, 60, or 90 days post-discharge.
Dr. Smith thinks it’s still a bit too early to see from the report how APMs have affected compensation.
“We’re still relatively in the early days of bundled-payment models, so in that regard, the State of Hospital Medicine Report still represents very much a starting point with regard to where hospital medicine groups will find themselves as they start to encounter challenges,” he says.
Perhaps more important, Gans doesn’t expect that the maturation of APMs will result in decreased compensation for hospitalists.
“In a hospital environment where the hospital is being reimbursed a set amount for a complete hospital admission and follow-up care and potential readmissions, that is an episodic payment already,” he says. “Consequently, the incentive is there today to better manage the patient and to attain the care coordination and care management necessary for that patient to be discharged and not readmitted.”
In fact, the SHM/MGMA data tell him that the basic economic theory of supply and demand continues to drive hospitalist compensation even 20 years after the field was given its name. He says rising compensation, even as more practices look to hire nurse practitioners or physician assistants as less expensive alternatives, shows no sign of letting up.
“I think demand will continue to be there,” Gans adds. “There may be in the long run some lessening of demand for hospitalists, but I don’t see that for years.”
Richard Quinn is a freelance writer in New Jersey.
Editor's Note: Listen to Dr. Smith share more of his views on the State of Hospital Medicine report.
2016 is the “Year of the Hospitalist,” a sobriquet meant as a proud nod to the specialty’s maturation as a fixture in hospitals across the country. Hospital medicine is no longer the new kid on the block as it has assumed care for the vast majority of hospitalized patients nationwide.
One could understand then if the ever-rising salaries hospitalists have commanded for 20 years might have finally plateaued, particularly as tightening budgets have C-suite administrators looking to trim costs.
Think again.
“Growth suggests that there is still a huge demand,” says Leslie Flores, MHA, a partner in Nelson Flores Hospital Medicine Consultants and a member of SHM’s Practice Analysis Committee. “The demand for hospitalists still exceeds the supply, and so recruiting hospitalists, particularly to nonurban areas, is really challenging and is requiring more money.”
The SoHM is a biennial partnership between SHM and MGMA that provides HM group leaders and rank-and-file hospitalists a litany of benchmarks for salaries, workloads, and everything that informs those two topics. Call it the specialty’s empirical roadmap.
“Often, compensation information relative to staffing information is proprietary, so hospitalists are in a position where they are dependent upon their hospital stakeholders to have access to this information, but they are also the same stakeholders with whom they negotiate their contracts,” says G. Randy Smith, MD, MS, FRCP(Edin), SFHM, an assistant professor in the Division of Hospital Medicine at Northwestern University Feinberg School of Medicine in Chicago and a member of SHM’s Practice Analysis Committee. “The State of Hospital Medicine report by SHM provides an opportunity for hospitalists to have an independent view of the compensation and workforce distribution factors that can impact negotiations with their hospital stakeholders. It’s a very powerful tool.”
Compensation Data
Rachel Lovins, MD, SFHM, CPE, voraciously reads every SoHM report because she uses its keynote compensation data to benchmark what she should pay her staff.
“I make a promise to my group,” says Dr. Lovins, chief of hospital medicine and vice chair of the Department of Medicine at Middlesex Hospital in Middletown, Conn. “I promise them that we will always be at or above what is standard for our areas. So for me, I have to look every time.”
Promises like that are getting more expensive to keep.
Hospitalists in the East region earn a median compensation of $245,977, up 3.1% from the $238,676 figure reported in 2014. But the East, where the bulk of the country’s population lives and where competition for hospitalists is typically lessened, is by far the lowest-paid region.
Hospitalists in the South continue to earn the most, with a median compensation of $301,833, up a whopping 16.9% from $258,020 from 2013. Hospitalists in the West earned a median of $275,658 (up 10.3% from $249,894), while Midwestern hospitalists saw a median compensation of $285,213 (up 8.9% from $261,868).
In addition to year-over-year growth, HM is also seeing outsized growth as compared with family medicine physicians, according to MGMA data. From 2011 to 2015, family medicine hospitalists saw an average compensation increase of 4.7%, bringing the average salary to $285,213. During the same period, family medicine physicians who are not hospitalists and don’t practice obstetrics saw an average annual compensation increase of only 3%, bringing the average salary to $230,456.
“The hospitalist can save the hospital considerable amounts of money because of their ability to better manage the patient and improve the quality of care at the same time,” says David Gans, MSHA, FACMPE, MGMA’s senior fellow of industry affairs. “Hospitals, they have recognized that, and therefore, there is considerable competition for recruiting and retaining hospitalists.”
To that end, 96.3% of HM groups (HMGs) received financial support in addition to their professional fee revenue. That’s up from 89% of HMGs that relied last year on their host hospitals. The median support is $157,535 per full-time employee (FTE), up just 1%. Correspondingly, SoHM reported 8.5% of HMGs received enough income from professional fee revenue to cover expenses, up from 6% two years ago.
Industry watchers predicted that, in two years, fee revenue would have to rise to offset hospitals’ inability to pay. The early returns seem to show that bearing out.
“We’re pretty close to that breaking point,” Flores says. “When we go around the country and do consulting work, we are hearing many more hospital leaders telling us, ‘We’re concerned about how much money this program is costing us, and we are getting to the point where we can’t afford it.’”
Productivity Stalls
While compensation continues to climb, productivity flattened out in this year’s report.
Median relative value units (RVUs) dipped slightly from the figure reported in 2014, to 4,252 from 4,297. But the tally is still ahead of 2012’s total of 4,159. Median collection-to-work RVUs also ticked down from 2014’s tally, to $50.29 from $51.50 in 2013.
Flores largely attributes the falling metrics of productivity to the evolution of HMGs that have standardized their scheduling to the point that most HMGs now offer vacation time.
“So the number of groups that are working 182 days is fewer, and we see a lot more groups that are working something like 168 days or 172 days,” she says. “And if a hospitalist works fewer shifts, even if they see the same number of patients per shift, they’re going to generate less productivity over the course of the year, so that’s part of it.”
Andrew White, MD, SFHM, director of the HM service at the University of Washington Medical Center in Seattle, says the report’s value is in avoiding a myopic approach to how HMGs operate. For example, RVUs are an important metric of productivity, but not all shifts should be expected to produce the same.
For example, it’d be valuable to use the report to see how hard your nocturnists are working compared with other sites, says Dr. White, also a member of the Practice Analysis Committee.
“The fundamental issue with working at night is that not everybody wants to do it, and so you have to recognize that it’s a pain to do and you have to either pay those people more, have them work less, or acknowledge that they’re going to be less productive,” he says. “We use the survey to assess all three of those things and then can work with our nocturnists to reach an agreement about a fair approach to their job structure that’s actually informed by national benchmarks. That process has helped us to pick, for example, how many nights per year they should work or what their salaries should look like compared to the day hospitalists.”
Dr. White says that because the report is comprehensive and includes broad participation, he’s able to use it as a benchmark to make hiring and service structure decisions.
“It also helps me to keep abreast of some trends that may be occurring in the broader workplace that we aren’t participating in but maybe should be or should be thinking about,” he says.
The report’s subsections are also critical for comparing one HMG to others, Dr. White says.
“Obviously, there is the aggregate data there to look at the average program,” he says. “But really as a hospitalist group leader, you want to know what are other programs like mine doing, and it allows you to drill down into that data.”
Survey Limitations
Any hospitalist worth their weight in scrubs knows that any medical study is only as good as its limitations. And while SoHM is a trove of valuable data information, Flores always cautions against taking data points as gospel.
“People should understand what the numbers are telling us, what goes into those numbers, and take them not with a grain of salt but take them for what they are,” she says.
For example, Flores says, look at productivity metrics per shift. Day shifts have traditionally driven that figure, and those shifts are typically busy. But night shifts have fewer patients and less productivity.
“So as more and more hospitals get 24-hour in-house coverage and have doctors working low-productivity night shifts, that [productivity] number might fall,” she says.
That sort of nuanced analysis of productivity can’t be found anywhere else, says Dr. Lovins.
These are “data that we don’t normally get from our administration,” she says, “information on things like staffing and patient loads, and how much more the director makes than the people that work for the director, and how much more nighttime people make than daytime people make. There is no other way for me to get that information, and it’s very important to make sure that our program is fair.”
Aside from fair, the data points are essential talking points as HMGs negotiate contracts and other arrangements with their administrators.
“It’s a reference point so that everybody feels like we’re using data from a national source that everyone can agree upon as fair,” says Dr. White.
In Dr. White’s case, he doesn’t have many local academic programs to benchmark against. And comparing to private, for-profit hospitals isn’t the proverbial apples-to-apples comparison. Having vetted regional and national figures for comparison is incredibly valuable, particularly since he doesn’t have to compile the data.
“If I had to go call all those group leaders and figure out what they were doing, it would be pretty exhausting,” he says.
Alternative Payment Models
Dr. Smith says that one area where the report will become even more valuable over the next few years is addressing alternative payment models (APMs). In particular, HM leaders say they’re excited about being drivers in one of the largest APMs: the Bundled Payments for Care Improvement (BCPI) initiative. In short, the program covers 48 defined episodes of care, including medical and surgical, that could begin three days prior to admission and stretch 30, 60, or 90 days post-discharge.
Dr. Smith thinks it’s still a bit too early to see from the report how APMs have affected compensation.
“We’re still relatively in the early days of bundled-payment models, so in that regard, the State of Hospital Medicine Report still represents very much a starting point with regard to where hospital medicine groups will find themselves as they start to encounter challenges,” he says.
Perhaps more important, Gans doesn’t expect that the maturation of APMs will result in decreased compensation for hospitalists.
“In a hospital environment where the hospital is being reimbursed a set amount for a complete hospital admission and follow-up care and potential readmissions, that is an episodic payment already,” he says. “Consequently, the incentive is there today to better manage the patient and to attain the care coordination and care management necessary for that patient to be discharged and not readmitted.”
In fact, the SHM/MGMA data tell him that the basic economic theory of supply and demand continues to drive hospitalist compensation even 20 years after the field was given its name. He says rising compensation, even as more practices look to hire nurse practitioners or physician assistants as less expensive alternatives, shows no sign of letting up.
“I think demand will continue to be there,” Gans adds. “There may be in the long run some lessening of demand for hospitalists, but I don’t see that for years.”
Richard Quinn is a freelance writer in New Jersey.
LETTER: The Value of a Structured On-Boarding Peer Mentorship Program
To demonstrate the impact of a structured peer mentorship program in a large size service-oriented hospitalist group with 71 full-time hospitalist and 21 full-time APPs serving a daily census of 400 patients, we piloted a structured peer mentorship project from June 2015 until December 2015 with 10 new hospitalist hires. Each new hire was paired with a senior hospitalist colleague for a total of four weeks over a period of two months and the outcomes were measured through a 10-question anonymous survey at the end of 90 days. The survey response rate was 80%. The questions pertained to the effectiveness of mentorship program, practice group culture orientation, adherence to high-yield patient satisfaction behaviors related to Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey, work efficiency, job satisfaction, navigating through various hospital floors, efficient clinical staff communication, hand of care sign-out process, understanding of various hospitalist shifts and open-ended feedback.
Our results revealed that 100% of the new hires recommended to continue the on-boarding mentorship program on a permanent basis and 95% of the responses on the Likert scale were either very positive or positive. The total cost of the mentorship program was estimated to be 2-3 moon-lighting shifts ($2400-$3600) for the group. This cost was mainly associated with extra staffing needed during the first half of the shadowing week since the mentor was carrying half of the daily census. The marginal benefits of the program were far more and long lasting than the short-term cost. The program assisted in early acclimatization to the practice group culture, provider engagement and satisfaction and early productivity. It also has the potential to increase retention in a high-turnover hospitalist work field. We conclude that effective peer mentorship can play an important role in the organizational success of a large hospitalist program. Successful mentoring programs require proper understanding, planning, resource allocation, implementation and evaluation. From increased morale to increased productivity, the benefits are numerous. Mentoring is a tangible way to show employees that they are valued and that the organization’s future includes them.
— Muhammad Nabeel, MD, FACP, Clinical Assistant Professor, College of Human Medicine, Michigan State University, GRMEP; Hospitalist, Spectrum Health Medical Group, Grand Rapids, MI
— Rashelle Ludolph, MHA, MBA (Second Author), Director Operations, Acute Care Medicine, Spectrum Health Medical Group, Grand Rapids, MI
To demonstrate the impact of a structured peer mentorship program in a large size service-oriented hospitalist group with 71 full-time hospitalist and 21 full-time APPs serving a daily census of 400 patients, we piloted a structured peer mentorship project from June 2015 until December 2015 with 10 new hospitalist hires. Each new hire was paired with a senior hospitalist colleague for a total of four weeks over a period of two months and the outcomes were measured through a 10-question anonymous survey at the end of 90 days. The survey response rate was 80%. The questions pertained to the effectiveness of mentorship program, practice group culture orientation, adherence to high-yield patient satisfaction behaviors related to Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey, work efficiency, job satisfaction, navigating through various hospital floors, efficient clinical staff communication, hand of care sign-out process, understanding of various hospitalist shifts and open-ended feedback.
Our results revealed that 100% of the new hires recommended to continue the on-boarding mentorship program on a permanent basis and 95% of the responses on the Likert scale were either very positive or positive. The total cost of the mentorship program was estimated to be 2-3 moon-lighting shifts ($2400-$3600) for the group. This cost was mainly associated with extra staffing needed during the first half of the shadowing week since the mentor was carrying half of the daily census. The marginal benefits of the program were far more and long lasting than the short-term cost. The program assisted in early acclimatization to the practice group culture, provider engagement and satisfaction and early productivity. It also has the potential to increase retention in a high-turnover hospitalist work field. We conclude that effective peer mentorship can play an important role in the organizational success of a large hospitalist program. Successful mentoring programs require proper understanding, planning, resource allocation, implementation and evaluation. From increased morale to increased productivity, the benefits are numerous. Mentoring is a tangible way to show employees that they are valued and that the organization’s future includes them.
— Muhammad Nabeel, MD, FACP, Clinical Assistant Professor, College of Human Medicine, Michigan State University, GRMEP; Hospitalist, Spectrum Health Medical Group, Grand Rapids, MI
— Rashelle Ludolph, MHA, MBA (Second Author), Director Operations, Acute Care Medicine, Spectrum Health Medical Group, Grand Rapids, MI
To demonstrate the impact of a structured peer mentorship program in a large size service-oriented hospitalist group with 71 full-time hospitalist and 21 full-time APPs serving a daily census of 400 patients, we piloted a structured peer mentorship project from June 2015 until December 2015 with 10 new hospitalist hires. Each new hire was paired with a senior hospitalist colleague for a total of four weeks over a period of two months and the outcomes were measured through a 10-question anonymous survey at the end of 90 days. The survey response rate was 80%. The questions pertained to the effectiveness of mentorship program, practice group culture orientation, adherence to high-yield patient satisfaction behaviors related to Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey, work efficiency, job satisfaction, navigating through various hospital floors, efficient clinical staff communication, hand of care sign-out process, understanding of various hospitalist shifts and open-ended feedback.
Our results revealed that 100% of the new hires recommended to continue the on-boarding mentorship program on a permanent basis and 95% of the responses on the Likert scale were either very positive or positive. The total cost of the mentorship program was estimated to be 2-3 moon-lighting shifts ($2400-$3600) for the group. This cost was mainly associated with extra staffing needed during the first half of the shadowing week since the mentor was carrying half of the daily census. The marginal benefits of the program were far more and long lasting than the short-term cost. The program assisted in early acclimatization to the practice group culture, provider engagement and satisfaction and early productivity. It also has the potential to increase retention in a high-turnover hospitalist work field. We conclude that effective peer mentorship can play an important role in the organizational success of a large hospitalist program. Successful mentoring programs require proper understanding, planning, resource allocation, implementation and evaluation. From increased morale to increased productivity, the benefits are numerous. Mentoring is a tangible way to show employees that they are valued and that the organization’s future includes them.
— Muhammad Nabeel, MD, FACP, Clinical Assistant Professor, College of Human Medicine, Michigan State University, GRMEP; Hospitalist, Spectrum Health Medical Group, Grand Rapids, MI
— Rashelle Ludolph, MHA, MBA (Second Author), Director Operations, Acute Care Medicine, Spectrum Health Medical Group, Grand Rapids, MI
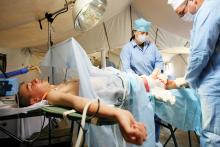
Wartime Lessons Inform Civilian Medicine
Recent wars have led to innovations in military trauma care that can be applied to civilians, say the authors of a JAMA Viewpoint published in June.1
During the Afghanistan and Iraq wars, the percentage of wounded soldiers who died as a result of their injuries reached its lowest point in recorded history, writes lead author Donald M. Berwick, MD, MPP, of the Institute for Healthcare Improvement in Cambridge, Mass., along with colleagues from the National Academies of Sciences, Engineering, and Medicine in Washington, D.C.
“Effective bleeding-control measures, improved resuscitation techniques, and aggressive neurocritical care interventions are among many advances that saved lives on the battlefield that otherwise would have been lost,” they write.
The reduction in injury-related deaths is in part due to the Military Health System and its Joint Trauma System embracing a culture of continuous performance improvement and an agile approach, a model called “focused empiricism,” the authors say. A new report from the National Academies of Sciences, Engineering, and Medicine clarifies the components of such a learning health system, which can also be applied to civilian care:
- Leadership and a culture of learning: “A learning health system must be stewarded by leadership committed to nurturing a culture of continuous learning and improvement. ... Such a system should unite military and civilian trauma care leaders around a common, core aim established at the highest level in the nation; namely, to achieve zero preventable deaths after injury and minimize trauma-related disability.”
- Transparency and incentives for quality trauma care: “Trauma care practitioners at all levels, including trauma surgeons and other physicians, nurses, technicians, and prehospital care personnel, should have access to data on their performance relative to that of their peers.”
- Systems for ensuring an expert trauma care workforce: “A joint, integrated network of military and civilian trauma centers should be created as a training platform to prepare and sustain an expert workforce and to promote the translation of best practices between sectors.”
The progress made by the military’s trauma system could be lost, the writers conclude, without concerted efforts to disseminate and maintain the advances. The authors note that in the United States, there are nearly 150,000 deaths from trauma each year, and injury is the third-leading cause of death.
The “hundreds of thousands of civilians who have sustained trauma deserve the benefits of care improvements achieved in military medicine,” they conclude.
Reference
- Berwick DM, Downey AS, Cornett EA. A national trauma care system to achieve zero preventable deaths after injury: recommendations from a National Academies of Sciences, Engineering, and Medicine report [published online ahead of print June 17, 2006]. JAMA. doi:10.1001/jama.2016.8524.
Quick Byte
Rating RTLS Options
The healthcare industry typically uses real-time location systems (RTLS) to help improve care quality, workflow efficiency, and bottom lines, according to a recent article in HealthcareITNews. The research firm KLAS rated 11 RTLS vendors and gave Centrak the highest overall performance score, beating competitors including AwarePoint, Cerner, GE Healthcare, and Intelligent Insights.
Reference
- Siwicki B. KLAS ranks real-time location systems from AwarePoint, Cerner, CenTrak, Versus and others. HealthcareITNews website. Accessed July 13, 2016.
Recent wars have led to innovations in military trauma care that can be applied to civilians, say the authors of a JAMA Viewpoint published in June.1
During the Afghanistan and Iraq wars, the percentage of wounded soldiers who died as a result of their injuries reached its lowest point in recorded history, writes lead author Donald M. Berwick, MD, MPP, of the Institute for Healthcare Improvement in Cambridge, Mass., along with colleagues from the National Academies of Sciences, Engineering, and Medicine in Washington, D.C.
“Effective bleeding-control measures, improved resuscitation techniques, and aggressive neurocritical care interventions are among many advances that saved lives on the battlefield that otherwise would have been lost,” they write.
The reduction in injury-related deaths is in part due to the Military Health System and its Joint Trauma System embracing a culture of continuous performance improvement and an agile approach, a model called “focused empiricism,” the authors say. A new report from the National Academies of Sciences, Engineering, and Medicine clarifies the components of such a learning health system, which can also be applied to civilian care:
- Leadership and a culture of learning: “A learning health system must be stewarded by leadership committed to nurturing a culture of continuous learning and improvement. ... Such a system should unite military and civilian trauma care leaders around a common, core aim established at the highest level in the nation; namely, to achieve zero preventable deaths after injury and minimize trauma-related disability.”
- Transparency and incentives for quality trauma care: “Trauma care practitioners at all levels, including trauma surgeons and other physicians, nurses, technicians, and prehospital care personnel, should have access to data on their performance relative to that of their peers.”
- Systems for ensuring an expert trauma care workforce: “A joint, integrated network of military and civilian trauma centers should be created as a training platform to prepare and sustain an expert workforce and to promote the translation of best practices between sectors.”
The progress made by the military’s trauma system could be lost, the writers conclude, without concerted efforts to disseminate and maintain the advances. The authors note that in the United States, there are nearly 150,000 deaths from trauma each year, and injury is the third-leading cause of death.
The “hundreds of thousands of civilians who have sustained trauma deserve the benefits of care improvements achieved in military medicine,” they conclude.
Reference
- Berwick DM, Downey AS, Cornett EA. A national trauma care system to achieve zero preventable deaths after injury: recommendations from a National Academies of Sciences, Engineering, and Medicine report [published online ahead of print June 17, 2006]. JAMA. doi:10.1001/jama.2016.8524.
Quick Byte
Rating RTLS Options
The healthcare industry typically uses real-time location systems (RTLS) to help improve care quality, workflow efficiency, and bottom lines, according to a recent article in HealthcareITNews. The research firm KLAS rated 11 RTLS vendors and gave Centrak the highest overall performance score, beating competitors including AwarePoint, Cerner, GE Healthcare, and Intelligent Insights.
Reference
- Siwicki B. KLAS ranks real-time location systems from AwarePoint, Cerner, CenTrak, Versus and others. HealthcareITNews website. Accessed July 13, 2016.
Recent wars have led to innovations in military trauma care that can be applied to civilians, say the authors of a JAMA Viewpoint published in June.1
During the Afghanistan and Iraq wars, the percentage of wounded soldiers who died as a result of their injuries reached its lowest point in recorded history, writes lead author Donald M. Berwick, MD, MPP, of the Institute for Healthcare Improvement in Cambridge, Mass., along with colleagues from the National Academies of Sciences, Engineering, and Medicine in Washington, D.C.
“Effective bleeding-control measures, improved resuscitation techniques, and aggressive neurocritical care interventions are among many advances that saved lives on the battlefield that otherwise would have been lost,” they write.
The reduction in injury-related deaths is in part due to the Military Health System and its Joint Trauma System embracing a culture of continuous performance improvement and an agile approach, a model called “focused empiricism,” the authors say. A new report from the National Academies of Sciences, Engineering, and Medicine clarifies the components of such a learning health system, which can also be applied to civilian care:
- Leadership and a culture of learning: “A learning health system must be stewarded by leadership committed to nurturing a culture of continuous learning and improvement. ... Such a system should unite military and civilian trauma care leaders around a common, core aim established at the highest level in the nation; namely, to achieve zero preventable deaths after injury and minimize trauma-related disability.”
- Transparency and incentives for quality trauma care: “Trauma care practitioners at all levels, including trauma surgeons and other physicians, nurses, technicians, and prehospital care personnel, should have access to data on their performance relative to that of their peers.”
- Systems for ensuring an expert trauma care workforce: “A joint, integrated network of military and civilian trauma centers should be created as a training platform to prepare and sustain an expert workforce and to promote the translation of best practices between sectors.”
The progress made by the military’s trauma system could be lost, the writers conclude, without concerted efforts to disseminate and maintain the advances. The authors note that in the United States, there are nearly 150,000 deaths from trauma each year, and injury is the third-leading cause of death.
The “hundreds of thousands of civilians who have sustained trauma deserve the benefits of care improvements achieved in military medicine,” they conclude.
Reference
- Berwick DM, Downey AS, Cornett EA. A national trauma care system to achieve zero preventable deaths after injury: recommendations from a National Academies of Sciences, Engineering, and Medicine report [published online ahead of print June 17, 2006]. JAMA. doi:10.1001/jama.2016.8524.
Quick Byte
Rating RTLS Options
The healthcare industry typically uses real-time location systems (RTLS) to help improve care quality, workflow efficiency, and bottom lines, according to a recent article in HealthcareITNews. The research firm KLAS rated 11 RTLS vendors and gave Centrak the highest overall performance score, beating competitors including AwarePoint, Cerner, GE Healthcare, and Intelligent Insights.
Reference
- Siwicki B. KLAS ranks real-time location systems from AwarePoint, Cerner, CenTrak, Versus and others. HealthcareITNews website. Accessed July 13, 2016.
Delirium ABCDEF Bundle Program Implementation Toolkit Now Available
The Baylor Research Institute and SHM joined forces to provide a new resource to help accelerate adoption of a specific set of patient safety practices (collectively termed the ABCDEF bundle) to mitigate delirium in the ICU. This guide will allow you to impact care at both the individual patient and the institutional levels. It is intended for the broad, multidisciplinary spectrum of personnel involved in hospital-based quality improvement and patient safety efforts, ranging from frontline care providers to executive leaders. View the toolkit and download the guide at www.hospitalmedicine.org/delirium.
The Baylor Research Institute and SHM joined forces to provide a new resource to help accelerate adoption of a specific set of patient safety practices (collectively termed the ABCDEF bundle) to mitigate delirium in the ICU. This guide will allow you to impact care at both the individual patient and the institutional levels. It is intended for the broad, multidisciplinary spectrum of personnel involved in hospital-based quality improvement and patient safety efforts, ranging from frontline care providers to executive leaders. View the toolkit and download the guide at www.hospitalmedicine.org/delirium.
The Baylor Research Institute and SHM joined forces to provide a new resource to help accelerate adoption of a specific set of patient safety practices (collectively termed the ABCDEF bundle) to mitigate delirium in the ICU. This guide will allow you to impact care at both the individual patient and the institutional levels. It is intended for the broad, multidisciplinary spectrum of personnel involved in hospital-based quality improvement and patient safety efforts, ranging from frontline care providers to executive leaders. View the toolkit and download the guide at www.hospitalmedicine.org/delirium.
Become an SHM Ambassador for a Chance at Free Registration to HM17
- A $35 credit toward 2017–2018 dues when recruiting 1 new member.
- A $50 credit toward 2017–2018 dues when recruiting 2–4 new members.
- A $75 credit toward 2017–2018 dues when recruiting 5–9 new members.
- A $125 credit toward 2017–2018 dues when recruiting 10+ new members.
For each member recruited, referrers will receive one entry into a grand-prize drawing to receive complimentary registration to Hospital Medicine 2017 in Las Vegas.
- A $35 credit toward 2017–2018 dues when recruiting 1 new member.
- A $50 credit toward 2017–2018 dues when recruiting 2–4 new members.
- A $75 credit toward 2017–2018 dues when recruiting 5–9 new members.
- A $125 credit toward 2017–2018 dues when recruiting 10+ new members.
For each member recruited, referrers will receive one entry into a grand-prize drawing to receive complimentary registration to Hospital Medicine 2017 in Las Vegas.
- A $35 credit toward 2017–2018 dues when recruiting 1 new member.
- A $50 credit toward 2017–2018 dues when recruiting 2–4 new members.
- A $75 credit toward 2017–2018 dues when recruiting 5–9 new members.
- A $125 credit toward 2017–2018 dues when recruiting 10+ new members.
For each member recruited, referrers will receive one entry into a grand-prize drawing to receive complimentary registration to Hospital Medicine 2017 in Las Vegas.
6 Tips for Community Hospitalists Initiating QI Projects
The Society of Hospital Medicine asserts that one of the key principles of an effective hospital medicine group is demonstrating a commitment to continuous quality improvement (QI) and actively participating in initiatives directed at quality and patient safety.1 Large hospitalist groups expect their physicians to contribute to the QI initiatives of the hospitals they staff. But as any hospitalist practicing in a community setting can tell you, QI is much easier said than done.
Acknowledge, Overcome the Obstacles
One of the first hurdles hospitalists must overcome when initiating a QI program is finding the time in their schedule as well as obtaining the time commitment from group leadership and fellow clinicians.
“If a hospitalist has no dedicated time and is working clinically, it is difficult to find time to organize a study,” says Kenneth Epstein, MD, chief medical officer of Hospitalist Consultants, the hospitalist management division of ECI Healthcare Partners, in Traverse City, Mich.
However, many national hospitalist management groups, including ECI and IPC Healthcare of North Hollywood, Calif., expect their clinicians to be continuously engaged in QI projects relative to their facility.
Beyond time, an even tougher obstacle to surmount is a lack of training, according to Kerry Weiner, MD, IPC chief medical officer. He says that each of IPC’s clinical practice leaders must participate in a one-year training program that includes a QI project conducted within their facility and mentored by University of California, San Francisco faculty.
David Nash, MD, founding dean of Jefferson College of Population Health in Philadelphia, says The Joint Commission, as part of its accreditation process, requires hospitals to robustly review errors and “have a performance improvement system in place.” He believes the only way community hospitals can successfully undertake this effort is to make sure hospitalists have adequate training in quality and safety.
Training is available from SHM via its Quality and Safety Educators Academy as well as the American Association for Physician Leadership and the Institute for Healthcare Improvement. However, Dr. Nash recommends graduate-level programs in quality and safety available at several schools including Jefferson, Northwestern University in Chicago, and George Washington University in Washington, D.C.
Yet another hurdle is access to data. Many community hospitals have limited financial and human resources to collect accurate data to use for choosing an area to focus on and measuring improvement.
“Despite all the money invested in electronic medical records, finding timely and accurate data is still challenging,” says Jasen Gundersen, MD, president of Knoxville, Tenn.–based TeamHealth Acute Care Services. “The data may exist, but a community hospital may be limited when it comes to finding people to mine, configure, and analyze the data. Community hospitals tend to be focused on publically reported, whole-hospital data.
“If your project is not related to these metrics, you may have trouble getting quality department support.”
Dr. Weiner echoes that sentiment, noting most community hospitals “react to bad metrics, such as low HCAHPS scores. To get the most support possible,” he says, “design a QI program that people see as a genuine problem that needs to be fixed using their resources.”
Get Involved
Experience is another barrier to community-based QI projects. Dr. Gundersen believes that hospitalists who want to get involved in quality should first join a QI committee.
“One of the best ways to effect change in a hospital is to get to know the players—who’s who, who does what, and who is willing to help,” he says.
Arnu Mohan, MD, chief medical officer of hospital medicine at ApolloMD in Atlanta, agrees with gaining experience before setting out on your own.
“Joining a QI committee is almost never a bad idea,” Dr. Mohan says. “You’ll meet people who can support your work, get insight into the needs of the institution, be exposed to other work being done, and better understand the resources available.”
Choose Your Project Carefully
Dr. Gundersen recommends that before settling on a QI project, hospitalists should first consider what their career goals are.
“Ask yourself why you want to do it,” he says. “Do you have the ambition to become a medical director or chief quality officer? In that case, you need a few QI projects under your belt, and you want to choose a system-wide project. Or is there just something in your everyday life that frustrates you so much you must fix it?”
If the project that compels the clinician is not aligned with the needs of the hospital, “it is worthy of a discussion to make sure you are working on the right project,” he adds. “Is the hospitalist off base, or does the administration need to pay more attention to what is happening on the floor?”
Obtain Buy-in
A QI project has a greater chance at being successful if the participants have a high level of interest in the initiative and there is visible support from the administration: high-level people making public statements, making appearances at QI team meetings, and diverting resources such as information technology and process mapping support to sustain the project. This will only happen if community-based hospitalists are successful at selling their project to the C-suite.
“When you approach senior management, you have only 15 minutes to get their attention about your project,” Dr. Weiner says. “You need to show them that you are bringing part of the solution and your idea will affect their bottom line.”
Jeff Brady, MD, director of the Center for Quality Improvement and Patient Safety, says organization commitment is key to any patient safety initiative.
“In addition to the active engagement of leaders who focus on safety and quality, an organization’s culture is another factor that can either enable or thwart progress toward improving the care they deliver,” he says. “AHRQ [the Agency for Healthcare Research and Quality] developed a collection of instruments—AHRQ Surveys on Patient Safety Culture—to help organizations assess and better understand facilitators and barriers their organizations may encounter as they work to improve safety and quality.”2
Politics also can be a factor. Dr. Gundersen points out that smaller hospitals typically are used to “doing things one way.”
“They may not be receptive to changes a QI program would initiate,” he says. “You have to figure out a way to enlist people to move the project forward. Your ability to drive and influence change may be your most important quality as a physician leader.”
Dr. Mohan believes that the best approach is to find a mentor who has worked on QI initiatives before and can champion your efforts.
“You will need the support of the hospital to access required data, change processes, and implement new tools,” he says. “Many hospitals will have a chief medical officer, chief quality officer, or director of QI who can serve as an important ally to mobilize resources on your behalf.”
Go Beyond Hospital Medicine
Even with administrative support, it is better to assemble a team than attempt to go it alone. Successful QI projects, Dr. Mohan says, tend to be team efforts.
“Finding a community of people who will support your work is critical,” he adds. “A multidisciplinary team, including areas such as nursing, therapy, and administration, that engages people who will complement one another increases the likelihood of success.
“That said, multidisciplinary teams have their challenges. They can be unwieldy to lead and without clear roles and responsibilities. I would recommend a group of two to five people who are passionate about the issue you are trying to solve. And be clear from the beginning what each person’s role is within the group.”
Support can also be found in areas outside of the medical staff.
“Key people in other hospital departments can assist with supplying data, financial solutions, and institutional support,” Dr. Mohan says. “These people may be in various departments, such as quality improvement and case management.
“In the current era of value-based purchasing, where Medicare reimbursement is tied to quality metrics, it’s advantageous to show potential financial impact of the QI initiative on hospital revenue, so assistance by the CFO or others in finance may be helpful.”
Dr. Gundersen suggests hospitalists seek out a “lateral mentor,” someone in a department outside the medical staff who is looking for change and can offer resources.
“For example, physicians are looking for quality improvement, and those in the finance department are looking for good economic return. Physicians can explain medical reasons things need to be done, and the finance people can explain the impact of these choices,” he says. “Working together, they can improve both quality and the bottom line.”
Lateral mentoring also is an effective way to meet the challenge of obtaining accurate data, as it opens up the potential to mine data from various departments.
“At different institutions, data may reside in different departments,” Dr. Epstein says. “For example, patient satisfaction may reside with the CMO, core measures or readmissions may reside with the quality management department, and length of stay may be the purview of the finance department.”
Connections in other departments could be the source of your best data, according to Dr. Epstein.
Consider Incentives, Penalties
In addition to buy-in from administration and professionals in other departments, hospitalists also need the commitment of fellow clinicians. Dr. Weiner believes the only way to do this is through financial incentives.
“In a community setting, start with a meaningful reward for improvement. It must be enough that the hospitalist makes the QI project a priority,” he says.
Dr. Weiner also recommends a small penalty for non-participation.
“Most providers realize QI is just good practice, but for some individuals, you need a consequence. It must be part of the system so it isn’t personal,” Dr. Weiner says. “One way is to mandate that if you do not participate, not only do you not get any of the incentive pay, you might lose some of a productivity bonus. You need to be creative when thinking about how to promote QI.”
In the community hospital setting, Dr. Weiner says, practicality ultimately rules.
“The community hospital has real problems to deal with, so don’t make your project pie-in-the-sky,” he says. “Tie it to the bottom line of the hospital if you can. That’s where you start.” TH
Maybelle Cowan-Lincoln is a freelance writer in New Jersey.
References
- Cawley P, Deitelzweig S, Flores L. The key principles and characteristics of an effective hospital medicine group: as assessment guide for hospitals and hospitalists. J Hosp Med. 2014;9:123-128.
- Surveys on patient safety culture. AHRQ website. Accessed October 12, 2015.
- AHRQ Quality Indicators Toolkit for Hospitals: fact sheet. AHRQ website. Accessed October 10, 2015.
- Practice facilitation handbook. AHRQ website. Accessed on September 25, 2015.
- 5. SHM signature programs. SHM website. Accessed October 10, 2015.
The Society of Hospital Medicine asserts that one of the key principles of an effective hospital medicine group is demonstrating a commitment to continuous quality improvement (QI) and actively participating in initiatives directed at quality and patient safety.1 Large hospitalist groups expect their physicians to contribute to the QI initiatives of the hospitals they staff. But as any hospitalist practicing in a community setting can tell you, QI is much easier said than done.
Acknowledge, Overcome the Obstacles
One of the first hurdles hospitalists must overcome when initiating a QI program is finding the time in their schedule as well as obtaining the time commitment from group leadership and fellow clinicians.
“If a hospitalist has no dedicated time and is working clinically, it is difficult to find time to organize a study,” says Kenneth Epstein, MD, chief medical officer of Hospitalist Consultants, the hospitalist management division of ECI Healthcare Partners, in Traverse City, Mich.
However, many national hospitalist management groups, including ECI and IPC Healthcare of North Hollywood, Calif., expect their clinicians to be continuously engaged in QI projects relative to their facility.
Beyond time, an even tougher obstacle to surmount is a lack of training, according to Kerry Weiner, MD, IPC chief medical officer. He says that each of IPC’s clinical practice leaders must participate in a one-year training program that includes a QI project conducted within their facility and mentored by University of California, San Francisco faculty.
David Nash, MD, founding dean of Jefferson College of Population Health in Philadelphia, says The Joint Commission, as part of its accreditation process, requires hospitals to robustly review errors and “have a performance improvement system in place.” He believes the only way community hospitals can successfully undertake this effort is to make sure hospitalists have adequate training in quality and safety.
Training is available from SHM via its Quality and Safety Educators Academy as well as the American Association for Physician Leadership and the Institute for Healthcare Improvement. However, Dr. Nash recommends graduate-level programs in quality and safety available at several schools including Jefferson, Northwestern University in Chicago, and George Washington University in Washington, D.C.
Yet another hurdle is access to data. Many community hospitals have limited financial and human resources to collect accurate data to use for choosing an area to focus on and measuring improvement.
“Despite all the money invested in electronic medical records, finding timely and accurate data is still challenging,” says Jasen Gundersen, MD, president of Knoxville, Tenn.–based TeamHealth Acute Care Services. “The data may exist, but a community hospital may be limited when it comes to finding people to mine, configure, and analyze the data. Community hospitals tend to be focused on publically reported, whole-hospital data.
“If your project is not related to these metrics, you may have trouble getting quality department support.”
Dr. Weiner echoes that sentiment, noting most community hospitals “react to bad metrics, such as low HCAHPS scores. To get the most support possible,” he says, “design a QI program that people see as a genuine problem that needs to be fixed using their resources.”
Get Involved
Experience is another barrier to community-based QI projects. Dr. Gundersen believes that hospitalists who want to get involved in quality should first join a QI committee.
“One of the best ways to effect change in a hospital is to get to know the players—who’s who, who does what, and who is willing to help,” he says.
Arnu Mohan, MD, chief medical officer of hospital medicine at ApolloMD in Atlanta, agrees with gaining experience before setting out on your own.
“Joining a QI committee is almost never a bad idea,” Dr. Mohan says. “You’ll meet people who can support your work, get insight into the needs of the institution, be exposed to other work being done, and better understand the resources available.”
Choose Your Project Carefully
Dr. Gundersen recommends that before settling on a QI project, hospitalists should first consider what their career goals are.
“Ask yourself why you want to do it,” he says. “Do you have the ambition to become a medical director or chief quality officer? In that case, you need a few QI projects under your belt, and you want to choose a system-wide project. Or is there just something in your everyday life that frustrates you so much you must fix it?”
If the project that compels the clinician is not aligned with the needs of the hospital, “it is worthy of a discussion to make sure you are working on the right project,” he adds. “Is the hospitalist off base, or does the administration need to pay more attention to what is happening on the floor?”
Obtain Buy-in
A QI project has a greater chance at being successful if the participants have a high level of interest in the initiative and there is visible support from the administration: high-level people making public statements, making appearances at QI team meetings, and diverting resources such as information technology and process mapping support to sustain the project. This will only happen if community-based hospitalists are successful at selling their project to the C-suite.
“When you approach senior management, you have only 15 minutes to get their attention about your project,” Dr. Weiner says. “You need to show them that you are bringing part of the solution and your idea will affect their bottom line.”
Jeff Brady, MD, director of the Center for Quality Improvement and Patient Safety, says organization commitment is key to any patient safety initiative.
“In addition to the active engagement of leaders who focus on safety and quality, an organization’s culture is another factor that can either enable or thwart progress toward improving the care they deliver,” he says. “AHRQ [the Agency for Healthcare Research and Quality] developed a collection of instruments—AHRQ Surveys on Patient Safety Culture—to help organizations assess and better understand facilitators and barriers their organizations may encounter as they work to improve safety and quality.”2
Politics also can be a factor. Dr. Gundersen points out that smaller hospitals typically are used to “doing things one way.”
“They may not be receptive to changes a QI program would initiate,” he says. “You have to figure out a way to enlist people to move the project forward. Your ability to drive and influence change may be your most important quality as a physician leader.”
Dr. Mohan believes that the best approach is to find a mentor who has worked on QI initiatives before and can champion your efforts.
“You will need the support of the hospital to access required data, change processes, and implement new tools,” he says. “Many hospitals will have a chief medical officer, chief quality officer, or director of QI who can serve as an important ally to mobilize resources on your behalf.”
Go Beyond Hospital Medicine
Even with administrative support, it is better to assemble a team than attempt to go it alone. Successful QI projects, Dr. Mohan says, tend to be team efforts.
“Finding a community of people who will support your work is critical,” he adds. “A multidisciplinary team, including areas such as nursing, therapy, and administration, that engages people who will complement one another increases the likelihood of success.
“That said, multidisciplinary teams have their challenges. They can be unwieldy to lead and without clear roles and responsibilities. I would recommend a group of two to five people who are passionate about the issue you are trying to solve. And be clear from the beginning what each person’s role is within the group.”
Support can also be found in areas outside of the medical staff.
“Key people in other hospital departments can assist with supplying data, financial solutions, and institutional support,” Dr. Mohan says. “These people may be in various departments, such as quality improvement and case management.
“In the current era of value-based purchasing, where Medicare reimbursement is tied to quality metrics, it’s advantageous to show potential financial impact of the QI initiative on hospital revenue, so assistance by the CFO or others in finance may be helpful.”
Dr. Gundersen suggests hospitalists seek out a “lateral mentor,” someone in a department outside the medical staff who is looking for change and can offer resources.
“For example, physicians are looking for quality improvement, and those in the finance department are looking for good economic return. Physicians can explain medical reasons things need to be done, and the finance people can explain the impact of these choices,” he says. “Working together, they can improve both quality and the bottom line.”
Lateral mentoring also is an effective way to meet the challenge of obtaining accurate data, as it opens up the potential to mine data from various departments.
“At different institutions, data may reside in different departments,” Dr. Epstein says. “For example, patient satisfaction may reside with the CMO, core measures or readmissions may reside with the quality management department, and length of stay may be the purview of the finance department.”
Connections in other departments could be the source of your best data, according to Dr. Epstein.
Consider Incentives, Penalties
In addition to buy-in from administration and professionals in other departments, hospitalists also need the commitment of fellow clinicians. Dr. Weiner believes the only way to do this is through financial incentives.
“In a community setting, start with a meaningful reward for improvement. It must be enough that the hospitalist makes the QI project a priority,” he says.
Dr. Weiner also recommends a small penalty for non-participation.
“Most providers realize QI is just good practice, but for some individuals, you need a consequence. It must be part of the system so it isn’t personal,” Dr. Weiner says. “One way is to mandate that if you do not participate, not only do you not get any of the incentive pay, you might lose some of a productivity bonus. You need to be creative when thinking about how to promote QI.”
In the community hospital setting, Dr. Weiner says, practicality ultimately rules.
“The community hospital has real problems to deal with, so don’t make your project pie-in-the-sky,” he says. “Tie it to the bottom line of the hospital if you can. That’s where you start.” TH
Maybelle Cowan-Lincoln is a freelance writer in New Jersey.
References
- Cawley P, Deitelzweig S, Flores L. The key principles and characteristics of an effective hospital medicine group: as assessment guide for hospitals and hospitalists. J Hosp Med. 2014;9:123-128.
- Surveys on patient safety culture. AHRQ website. Accessed October 12, 2015.
- AHRQ Quality Indicators Toolkit for Hospitals: fact sheet. AHRQ website. Accessed October 10, 2015.
- Practice facilitation handbook. AHRQ website. Accessed on September 25, 2015.
- 5. SHM signature programs. SHM website. Accessed October 10, 2015.
The Society of Hospital Medicine asserts that one of the key principles of an effective hospital medicine group is demonstrating a commitment to continuous quality improvement (QI) and actively participating in initiatives directed at quality and patient safety.1 Large hospitalist groups expect their physicians to contribute to the QI initiatives of the hospitals they staff. But as any hospitalist practicing in a community setting can tell you, QI is much easier said than done.
Acknowledge, Overcome the Obstacles
One of the first hurdles hospitalists must overcome when initiating a QI program is finding the time in their schedule as well as obtaining the time commitment from group leadership and fellow clinicians.
“If a hospitalist has no dedicated time and is working clinically, it is difficult to find time to organize a study,” says Kenneth Epstein, MD, chief medical officer of Hospitalist Consultants, the hospitalist management division of ECI Healthcare Partners, in Traverse City, Mich.
However, many national hospitalist management groups, including ECI and IPC Healthcare of North Hollywood, Calif., expect their clinicians to be continuously engaged in QI projects relative to their facility.
Beyond time, an even tougher obstacle to surmount is a lack of training, according to Kerry Weiner, MD, IPC chief medical officer. He says that each of IPC’s clinical practice leaders must participate in a one-year training program that includes a QI project conducted within their facility and mentored by University of California, San Francisco faculty.
David Nash, MD, founding dean of Jefferson College of Population Health in Philadelphia, says The Joint Commission, as part of its accreditation process, requires hospitals to robustly review errors and “have a performance improvement system in place.” He believes the only way community hospitals can successfully undertake this effort is to make sure hospitalists have adequate training in quality and safety.
Training is available from SHM via its Quality and Safety Educators Academy as well as the American Association for Physician Leadership and the Institute for Healthcare Improvement. However, Dr. Nash recommends graduate-level programs in quality and safety available at several schools including Jefferson, Northwestern University in Chicago, and George Washington University in Washington, D.C.
Yet another hurdle is access to data. Many community hospitals have limited financial and human resources to collect accurate data to use for choosing an area to focus on and measuring improvement.
“Despite all the money invested in electronic medical records, finding timely and accurate data is still challenging,” says Jasen Gundersen, MD, president of Knoxville, Tenn.–based TeamHealth Acute Care Services. “The data may exist, but a community hospital may be limited when it comes to finding people to mine, configure, and analyze the data. Community hospitals tend to be focused on publically reported, whole-hospital data.
“If your project is not related to these metrics, you may have trouble getting quality department support.”
Dr. Weiner echoes that sentiment, noting most community hospitals “react to bad metrics, such as low HCAHPS scores. To get the most support possible,” he says, “design a QI program that people see as a genuine problem that needs to be fixed using their resources.”
Get Involved
Experience is another barrier to community-based QI projects. Dr. Gundersen believes that hospitalists who want to get involved in quality should first join a QI committee.
“One of the best ways to effect change in a hospital is to get to know the players—who’s who, who does what, and who is willing to help,” he says.
Arnu Mohan, MD, chief medical officer of hospital medicine at ApolloMD in Atlanta, agrees with gaining experience before setting out on your own.
“Joining a QI committee is almost never a bad idea,” Dr. Mohan says. “You’ll meet people who can support your work, get insight into the needs of the institution, be exposed to other work being done, and better understand the resources available.”
Choose Your Project Carefully
Dr. Gundersen recommends that before settling on a QI project, hospitalists should first consider what their career goals are.
“Ask yourself why you want to do it,” he says. “Do you have the ambition to become a medical director or chief quality officer? In that case, you need a few QI projects under your belt, and you want to choose a system-wide project. Or is there just something in your everyday life that frustrates you so much you must fix it?”
If the project that compels the clinician is not aligned with the needs of the hospital, “it is worthy of a discussion to make sure you are working on the right project,” he adds. “Is the hospitalist off base, or does the administration need to pay more attention to what is happening on the floor?”
Obtain Buy-in
A QI project has a greater chance at being successful if the participants have a high level of interest in the initiative and there is visible support from the administration: high-level people making public statements, making appearances at QI team meetings, and diverting resources such as information technology and process mapping support to sustain the project. This will only happen if community-based hospitalists are successful at selling their project to the C-suite.
“When you approach senior management, you have only 15 minutes to get their attention about your project,” Dr. Weiner says. “You need to show them that you are bringing part of the solution and your idea will affect their bottom line.”
Jeff Brady, MD, director of the Center for Quality Improvement and Patient Safety, says organization commitment is key to any patient safety initiative.
“In addition to the active engagement of leaders who focus on safety and quality, an organization’s culture is another factor that can either enable or thwart progress toward improving the care they deliver,” he says. “AHRQ [the Agency for Healthcare Research and Quality] developed a collection of instruments—AHRQ Surveys on Patient Safety Culture—to help organizations assess and better understand facilitators and barriers their organizations may encounter as they work to improve safety and quality.”2
Politics also can be a factor. Dr. Gundersen points out that smaller hospitals typically are used to “doing things one way.”
“They may not be receptive to changes a QI program would initiate,” he says. “You have to figure out a way to enlist people to move the project forward. Your ability to drive and influence change may be your most important quality as a physician leader.”
Dr. Mohan believes that the best approach is to find a mentor who has worked on QI initiatives before and can champion your efforts.
“You will need the support of the hospital to access required data, change processes, and implement new tools,” he says. “Many hospitals will have a chief medical officer, chief quality officer, or director of QI who can serve as an important ally to mobilize resources on your behalf.”
Go Beyond Hospital Medicine
Even with administrative support, it is better to assemble a team than attempt to go it alone. Successful QI projects, Dr. Mohan says, tend to be team efforts.
“Finding a community of people who will support your work is critical,” he adds. “A multidisciplinary team, including areas such as nursing, therapy, and administration, that engages people who will complement one another increases the likelihood of success.
“That said, multidisciplinary teams have their challenges. They can be unwieldy to lead and without clear roles and responsibilities. I would recommend a group of two to five people who are passionate about the issue you are trying to solve. And be clear from the beginning what each person’s role is within the group.”
Support can also be found in areas outside of the medical staff.
“Key people in other hospital departments can assist with supplying data, financial solutions, and institutional support,” Dr. Mohan says. “These people may be in various departments, such as quality improvement and case management.
“In the current era of value-based purchasing, where Medicare reimbursement is tied to quality metrics, it’s advantageous to show potential financial impact of the QI initiative on hospital revenue, so assistance by the CFO or others in finance may be helpful.”
Dr. Gundersen suggests hospitalists seek out a “lateral mentor,” someone in a department outside the medical staff who is looking for change and can offer resources.
“For example, physicians are looking for quality improvement, and those in the finance department are looking for good economic return. Physicians can explain medical reasons things need to be done, and the finance people can explain the impact of these choices,” he says. “Working together, they can improve both quality and the bottom line.”
Lateral mentoring also is an effective way to meet the challenge of obtaining accurate data, as it opens up the potential to mine data from various departments.
“At different institutions, data may reside in different departments,” Dr. Epstein says. “For example, patient satisfaction may reside with the CMO, core measures or readmissions may reside with the quality management department, and length of stay may be the purview of the finance department.”
Connections in other departments could be the source of your best data, according to Dr. Epstein.
Consider Incentives, Penalties
In addition to buy-in from administration and professionals in other departments, hospitalists also need the commitment of fellow clinicians. Dr. Weiner believes the only way to do this is through financial incentives.
“In a community setting, start with a meaningful reward for improvement. It must be enough that the hospitalist makes the QI project a priority,” he says.
Dr. Weiner also recommends a small penalty for non-participation.
“Most providers realize QI is just good practice, but for some individuals, you need a consequence. It must be part of the system so it isn’t personal,” Dr. Weiner says. “One way is to mandate that if you do not participate, not only do you not get any of the incentive pay, you might lose some of a productivity bonus. You need to be creative when thinking about how to promote QI.”
In the community hospital setting, Dr. Weiner says, practicality ultimately rules.
“The community hospital has real problems to deal with, so don’t make your project pie-in-the-sky,” he says. “Tie it to the bottom line of the hospital if you can. That’s where you start.” TH
Maybelle Cowan-Lincoln is a freelance writer in New Jersey.
References
- Cawley P, Deitelzweig S, Flores L. The key principles and characteristics of an effective hospital medicine group: as assessment guide for hospitals and hospitalists. J Hosp Med. 2014;9:123-128.
- Surveys on patient safety culture. AHRQ website. Accessed October 12, 2015.
- AHRQ Quality Indicators Toolkit for Hospitals: fact sheet. AHRQ website. Accessed October 10, 2015.
- Practice facilitation handbook. AHRQ website. Accessed on September 25, 2015.
- 5. SHM signature programs. SHM website. Accessed October 10, 2015.
Health Official Warns Zika Could Spread across U.S. Gulf
(Reuters) - One of the top U.S. public health officials on Sunday warned that the mosquito-borne Zika virus could extend its reach across the U.S. Gulf Coast after officials last week confirmed it as active in the popular tourist destination of Miami Beach.
The possibility of transmission in Gulf States such as Louisiana and Texas will likely fuel concerns that the virus, which has been shown to cause microcephaly, could spread across the continental United States, even though officials have played down such an outcome.
Concern has mounted since confirmation that Zika has expanded into a second region of the tourist hub of Miami-Dade County in Florida. Miami's Wynwood arts neighborhood last month became the site of the first locally transmitted cases of Zika in the continental United States.
"It would not be surprising we would see additional cases perhaps in other Gulf Coast states," Dr. Anthony Fauci, director of the allergy and infectious diseases unit of the National Institutes of Health (NIH), said in an interview on Sunday morning with ABC News.
Fauci noted that record flooding this month in Louisiana - which has killed at least 13 people and damaged some 60,000 homes damaged - has boosted the likelihood Zika will spread into that state.
"There's going to be a lot of problems getting rid of standing water" that could stymie the mosquito control efforts that are the best way to control Zika's spread, he said.
The connection between Zika and microcephaly first came to light last fall in Brazil, which has now confirmed 1,835 cases of microcephaly that it considers to be related to Zika infections in the mothers.
On Friday, Florida Governor Rick Scott confirmed that state health officials had identified five cases of Zika believed to be contracted in Miami Beach.
The U.S. Centers for Disease Control and Prevention told pregnant women they should avoid the trendy area and suggested those especially worried about exposure might consider avoiding all of Miami-Dade County.
NIH's Fauci on Sunday said the conditions of most of the country make it unlikely there would be a "diffuse, broad outbreak," even though officials need to prepare for that possibility.
He compared it with diseases such as dengue, which is endemic in certain tropical and subtropical regions of the world but rarely occurs in the continental United States. In Miami's Wynwood area, experts have seen "substantial" knockdowns of mosquito populations.
Still, its containment is more complicated because Zika can be sexually transmitted, Fauci said.
"This is something that could hang around for a year or two," he said.
The World Health Organization has said there is strong scientific consensus that Zika can also cause Guillain-Barre syndrome.
(c) Copyright Thomson Reuters 2016.
(Reuters) - One of the top U.S. public health officials on Sunday warned that the mosquito-borne Zika virus could extend its reach across the U.S. Gulf Coast after officials last week confirmed it as active in the popular tourist destination of Miami Beach.
The possibility of transmission in Gulf States such as Louisiana and Texas will likely fuel concerns that the virus, which has been shown to cause microcephaly, could spread across the continental United States, even though officials have played down such an outcome.
Concern has mounted since confirmation that Zika has expanded into a second region of the tourist hub of Miami-Dade County in Florida. Miami's Wynwood arts neighborhood last month became the site of the first locally transmitted cases of Zika in the continental United States.
"It would not be surprising we would see additional cases perhaps in other Gulf Coast states," Dr. Anthony Fauci, director of the allergy and infectious diseases unit of the National Institutes of Health (NIH), said in an interview on Sunday morning with ABC News.
Fauci noted that record flooding this month in Louisiana - which has killed at least 13 people and damaged some 60,000 homes damaged - has boosted the likelihood Zika will spread into that state.
"There's going to be a lot of problems getting rid of standing water" that could stymie the mosquito control efforts that are the best way to control Zika's spread, he said.
The connection between Zika and microcephaly first came to light last fall in Brazil, which has now confirmed 1,835 cases of microcephaly that it considers to be related to Zika infections in the mothers.
On Friday, Florida Governor Rick Scott confirmed that state health officials had identified five cases of Zika believed to be contracted in Miami Beach.
The U.S. Centers for Disease Control and Prevention told pregnant women they should avoid the trendy area and suggested those especially worried about exposure might consider avoiding all of Miami-Dade County.
NIH's Fauci on Sunday said the conditions of most of the country make it unlikely there would be a "diffuse, broad outbreak," even though officials need to prepare for that possibility.
He compared it with diseases such as dengue, which is endemic in certain tropical and subtropical regions of the world but rarely occurs in the continental United States. In Miami's Wynwood area, experts have seen "substantial" knockdowns of mosquito populations.
Still, its containment is more complicated because Zika can be sexually transmitted, Fauci said.
"This is something that could hang around for a year or two," he said.
The World Health Organization has said there is strong scientific consensus that Zika can also cause Guillain-Barre syndrome.
(c) Copyright Thomson Reuters 2016.
(Reuters) - One of the top U.S. public health officials on Sunday warned that the mosquito-borne Zika virus could extend its reach across the U.S. Gulf Coast after officials last week confirmed it as active in the popular tourist destination of Miami Beach.
The possibility of transmission in Gulf States such as Louisiana and Texas will likely fuel concerns that the virus, which has been shown to cause microcephaly, could spread across the continental United States, even though officials have played down such an outcome.
Concern has mounted since confirmation that Zika has expanded into a second region of the tourist hub of Miami-Dade County in Florida. Miami's Wynwood arts neighborhood last month became the site of the first locally transmitted cases of Zika in the continental United States.
"It would not be surprising we would see additional cases perhaps in other Gulf Coast states," Dr. Anthony Fauci, director of the allergy and infectious diseases unit of the National Institutes of Health (NIH), said in an interview on Sunday morning with ABC News.
Fauci noted that record flooding this month in Louisiana - which has killed at least 13 people and damaged some 60,000 homes damaged - has boosted the likelihood Zika will spread into that state.
"There's going to be a lot of problems getting rid of standing water" that could stymie the mosquito control efforts that are the best way to control Zika's spread, he said.
The connection between Zika and microcephaly first came to light last fall in Brazil, which has now confirmed 1,835 cases of microcephaly that it considers to be related to Zika infections in the mothers.
On Friday, Florida Governor Rick Scott confirmed that state health officials had identified five cases of Zika believed to be contracted in Miami Beach.
The U.S. Centers for Disease Control and Prevention told pregnant women they should avoid the trendy area and suggested those especially worried about exposure might consider avoiding all of Miami-Dade County.
NIH's Fauci on Sunday said the conditions of most of the country make it unlikely there would be a "diffuse, broad outbreak," even though officials need to prepare for that possibility.
He compared it with diseases such as dengue, which is endemic in certain tropical and subtropical regions of the world but rarely occurs in the continental United States. In Miami's Wynwood area, experts have seen "substantial" knockdowns of mosquito populations.
Still, its containment is more complicated because Zika can be sexually transmitted, Fauci said.
"This is something that could hang around for a year or two," he said.
The World Health Organization has said there is strong scientific consensus that Zika can also cause Guillain-Barre syndrome.
(c) Copyright Thomson Reuters 2016.
LETTER: Engaging the Next Generation: Hospital Medicine Student Interest Groups
Since the inception of hospital medicine, we are seeing unprecedented levels of reliance on hospitalists for educating and leading the next generation of physicians toward better care. A 2008 survey of internal medicine programs reported that learners gave hospitalists higher scores in the areas of attending rounds quality and the teaching of cost-effective care, in addition to providing an overall better learning experience as compared with non-hospitalist attendings.1
As successful educators, the development of mentorship programs has been shown to improve professional satisfaction and academic productivity in hospitalist communities.2, 3 Unfortunately, most of these programs failed to consider medical schools as valuable targets for outreach, education and support. By limiting vertical integration of training and mentorship, the hospitalist community is keeping itself from realizing its potential in building a pipeline for shaping the leaders of tomorrow’s healthcare sector.
A Hospital Medicine Student Interest Group (HM-SIG) is an organization composed of medical, nurse practitioner or physician assistant students interested in exploring future careers in hospital medicine. The goals of an HM-SIG are multidimensional: (1) introduce students to, or cultivate prior interest in, a career in hospital medicine, (2) provide opportunities for mentorship with faculty, (3) develop a community of future hospitalists, and (4) facilitate student involvement in institutional, local, regional and national hospital medicine projects on patient safety, high-value care and quality improvement.
Since starting the first medical school HM-SIG chapter in 2015, our efforts have led to significant changes in the way students are exposed not only to hospital medicine as a career, but to the tools and the mindset of hospitalists for improving care as well. In the fall of 2015, after brief discussions on the merits of and opportunities in hospital medicine, we selected a dedicated group of individuals and built our executive board. We collectively defined our goals and designed an 18-month plan to create student-led programming, coordinate mentorship opportunities with faculty and build a research pipeline for future medical students to have easier access to quality improvement work within the Loyola University Stritch School of Medicine. Within the first 6 months, we hosted a panel discussion with our hospitalist faculty, facilitated a quality improvement workshop to teach the lean methodology and rolled out a shadowing program that has given students deeper insight into the day in the life of a hospitalist. We’ve also developed a lecture series that has guided curriculum changes in quality improvement, and organized a student-led regional hospital medicine conference for nurse practitioners, physician assistants, medical students and internal medicine residents.
Without any representation from within the medical student community, student exposure to the hospitalist career is entirely dependent on the resources and availability of the affiliate hospital’s department of hospital medicine. With an investment in hospital medicine student interest groups at medical schools, SHM will equip students to become articulate advocates for the profession and SHM as a community.
References
- Goldenberg J, Glasheen JJ. Hospitalist educators: future of inpatient internal medicine training. Mt Sinai J Med 2008;75:430-5.
2. Pane LA, Davis AB, Ottolini MC. Career satisfaction and the role of mentorship: a survey of pediatric hospitalists. Hosp Pediatr. 2012;2(3):141-8.
3. Leary JC, Schainker EG, Leyenaar JK. The unwritten rules of mentorship: Facilitators of and barriers to effective mentorship in pediatric hospital medicine. Hospital Pediatrics. 2016;6(4):219-225; DOI: 10.1542/hpeds.2015-0108
Since the inception of hospital medicine, we are seeing unprecedented levels of reliance on hospitalists for educating and leading the next generation of physicians toward better care. A 2008 survey of internal medicine programs reported that learners gave hospitalists higher scores in the areas of attending rounds quality and the teaching of cost-effective care, in addition to providing an overall better learning experience as compared with non-hospitalist attendings.1
As successful educators, the development of mentorship programs has been shown to improve professional satisfaction and academic productivity in hospitalist communities.2, 3 Unfortunately, most of these programs failed to consider medical schools as valuable targets for outreach, education and support. By limiting vertical integration of training and mentorship, the hospitalist community is keeping itself from realizing its potential in building a pipeline for shaping the leaders of tomorrow’s healthcare sector.
A Hospital Medicine Student Interest Group (HM-SIG) is an organization composed of medical, nurse practitioner or physician assistant students interested in exploring future careers in hospital medicine. The goals of an HM-SIG are multidimensional: (1) introduce students to, or cultivate prior interest in, a career in hospital medicine, (2) provide opportunities for mentorship with faculty, (3) develop a community of future hospitalists, and (4) facilitate student involvement in institutional, local, regional and national hospital medicine projects on patient safety, high-value care and quality improvement.
Since starting the first medical school HM-SIG chapter in 2015, our efforts have led to significant changes in the way students are exposed not only to hospital medicine as a career, but to the tools and the mindset of hospitalists for improving care as well. In the fall of 2015, after brief discussions on the merits of and opportunities in hospital medicine, we selected a dedicated group of individuals and built our executive board. We collectively defined our goals and designed an 18-month plan to create student-led programming, coordinate mentorship opportunities with faculty and build a research pipeline for future medical students to have easier access to quality improvement work within the Loyola University Stritch School of Medicine. Within the first 6 months, we hosted a panel discussion with our hospitalist faculty, facilitated a quality improvement workshop to teach the lean methodology and rolled out a shadowing program that has given students deeper insight into the day in the life of a hospitalist. We’ve also developed a lecture series that has guided curriculum changes in quality improvement, and organized a student-led regional hospital medicine conference for nurse practitioners, physician assistants, medical students and internal medicine residents.
Without any representation from within the medical student community, student exposure to the hospitalist career is entirely dependent on the resources and availability of the affiliate hospital’s department of hospital medicine. With an investment in hospital medicine student interest groups at medical schools, SHM will equip students to become articulate advocates for the profession and SHM as a community.
References
- Goldenberg J, Glasheen JJ. Hospitalist educators: future of inpatient internal medicine training. Mt Sinai J Med 2008;75:430-5.
2. Pane LA, Davis AB, Ottolini MC. Career satisfaction and the role of mentorship: a survey of pediatric hospitalists. Hosp Pediatr. 2012;2(3):141-8.
3. Leary JC, Schainker EG, Leyenaar JK. The unwritten rules of mentorship: Facilitators of and barriers to effective mentorship in pediatric hospital medicine. Hospital Pediatrics. 2016;6(4):219-225; DOI: 10.1542/hpeds.2015-0108
Since the inception of hospital medicine, we are seeing unprecedented levels of reliance on hospitalists for educating and leading the next generation of physicians toward better care. A 2008 survey of internal medicine programs reported that learners gave hospitalists higher scores in the areas of attending rounds quality and the teaching of cost-effective care, in addition to providing an overall better learning experience as compared with non-hospitalist attendings.1
As successful educators, the development of mentorship programs has been shown to improve professional satisfaction and academic productivity in hospitalist communities.2, 3 Unfortunately, most of these programs failed to consider medical schools as valuable targets for outreach, education and support. By limiting vertical integration of training and mentorship, the hospitalist community is keeping itself from realizing its potential in building a pipeline for shaping the leaders of tomorrow’s healthcare sector.
A Hospital Medicine Student Interest Group (HM-SIG) is an organization composed of medical, nurse practitioner or physician assistant students interested in exploring future careers in hospital medicine. The goals of an HM-SIG are multidimensional: (1) introduce students to, or cultivate prior interest in, a career in hospital medicine, (2) provide opportunities for mentorship with faculty, (3) develop a community of future hospitalists, and (4) facilitate student involvement in institutional, local, regional and national hospital medicine projects on patient safety, high-value care and quality improvement.
Since starting the first medical school HM-SIG chapter in 2015, our efforts have led to significant changes in the way students are exposed not only to hospital medicine as a career, but to the tools and the mindset of hospitalists for improving care as well. In the fall of 2015, after brief discussions on the merits of and opportunities in hospital medicine, we selected a dedicated group of individuals and built our executive board. We collectively defined our goals and designed an 18-month plan to create student-led programming, coordinate mentorship opportunities with faculty and build a research pipeline for future medical students to have easier access to quality improvement work within the Loyola University Stritch School of Medicine. Within the first 6 months, we hosted a panel discussion with our hospitalist faculty, facilitated a quality improvement workshop to teach the lean methodology and rolled out a shadowing program that has given students deeper insight into the day in the life of a hospitalist. We’ve also developed a lecture series that has guided curriculum changes in quality improvement, and organized a student-led regional hospital medicine conference for nurse practitioners, physician assistants, medical students and internal medicine residents.
Without any representation from within the medical student community, student exposure to the hospitalist career is entirely dependent on the resources and availability of the affiliate hospital’s department of hospital medicine. With an investment in hospital medicine student interest groups at medical schools, SHM will equip students to become articulate advocates for the profession and SHM as a community.
References
- Goldenberg J, Glasheen JJ. Hospitalist educators: future of inpatient internal medicine training. Mt Sinai J Med 2008;75:430-5.
2. Pane LA, Davis AB, Ottolini MC. Career satisfaction and the role of mentorship: a survey of pediatric hospitalists. Hosp Pediatr. 2012;2(3):141-8.
3. Leary JC, Schainker EG, Leyenaar JK. The unwritten rules of mentorship: Facilitators of and barriers to effective mentorship in pediatric hospital medicine. Hospital Pediatrics. 2016;6(4):219-225; DOI: 10.1542/hpeds.2015-0108