User login
Trends in value-based care favor hospitalists, expert says
Value-based care’s ascendancy equals increased opportunities for hospitalists who know how to wield informatics, speak the language of systems improvement, and have an ability to function as a commodity within a health system, according to the dean of hospital medicine.
“If I were a betting man, I’d say there is no way value-based care can happen without hospitalists,” Robert Wachter, MD, MHM, said during a leadership summit at this year’s annual meeting of the Society of Hospital Medicine. Dr. Wachter is the New York Times bestselling author of “The Digital Doctor: Hope, Hype, and Harm at the Dawn of Medicine’s Computer Age.” He also is a professor and chair of the department of medicine at the University of California, San Francisco.
“There will be talk about closing hospitals and building competencies in ambulatory care. That’s the first 5 minutes, but then there is the realization people are still going to get sick, representing a massive amount of cost, and as far as I can tell, there is no alternative to having hospitals for this,” Dr. Wachter said. “Hospitalists will come out just fine.”
This will be true particularly for hospitalists who understand that electronic health records companies have helped health systems collect massive amounts of data but do not offer help for how those data can be applied to drive better outcomes and improve performance ratings, according to Dr. Wachter.
“These companies have no competencies in data analytics or data visualization,” Dr. Wachter said. “I am hopeful because Silicon Valley has woken up to the possibilities of this and are looking for ways to partner with health care. … The world of improving value, safety, and patient experience is going to be a world enabled by thoughtful use of informatics. So, if you don’t have those competencies, I think it’s important to grow them over time.”
Speaking the language of “lean” or that of other systematic strategies for improvement will also increase the value a hospitalist can bring to an organization, according to Dr. Wachter, who said that as hospital senior leadership and frontline personnel work together to implement system improvement, new leadership roles for hospitalists, ranging from chief patient experience officer to chief quality officers, and everything in between, are being created.
Another “hopeful trend” for hospitalists is the growing focus on the provider experience, said Dr. Wachter, since improving systems is not possible if staff are not engaged. “It’s impossible to believe you’re going to accomplish your goals of improving care and improving patient experience, and efficiencies, with a cadre of burned-out doctors,” he said.
Dr. Wachter said that to be indispensable, hospitalists need to understand they often are commoditized, offered by their senior leadership as bargaining chips when deals are made with surrounding health systems seeking to outsource some of their hospitalist functions.
“Managing a large community-affiliated network was not a core competency in the past,” Dr Wachter said. “But it will become increasingly important.”
Value-based care’s ascendancy equals increased opportunities for hospitalists who know how to wield informatics, speak the language of systems improvement, and have an ability to function as a commodity within a health system, according to the dean of hospital medicine.
“If I were a betting man, I’d say there is no way value-based care can happen without hospitalists,” Robert Wachter, MD, MHM, said during a leadership summit at this year’s annual meeting of the Society of Hospital Medicine. Dr. Wachter is the New York Times bestselling author of “The Digital Doctor: Hope, Hype, and Harm at the Dawn of Medicine’s Computer Age.” He also is a professor and chair of the department of medicine at the University of California, San Francisco.
“There will be talk about closing hospitals and building competencies in ambulatory care. That’s the first 5 minutes, but then there is the realization people are still going to get sick, representing a massive amount of cost, and as far as I can tell, there is no alternative to having hospitals for this,” Dr. Wachter said. “Hospitalists will come out just fine.”
This will be true particularly for hospitalists who understand that electronic health records companies have helped health systems collect massive amounts of data but do not offer help for how those data can be applied to drive better outcomes and improve performance ratings, according to Dr. Wachter.
“These companies have no competencies in data analytics or data visualization,” Dr. Wachter said. “I am hopeful because Silicon Valley has woken up to the possibilities of this and are looking for ways to partner with health care. … The world of improving value, safety, and patient experience is going to be a world enabled by thoughtful use of informatics. So, if you don’t have those competencies, I think it’s important to grow them over time.”
Speaking the language of “lean” or that of other systematic strategies for improvement will also increase the value a hospitalist can bring to an organization, according to Dr. Wachter, who said that as hospital senior leadership and frontline personnel work together to implement system improvement, new leadership roles for hospitalists, ranging from chief patient experience officer to chief quality officers, and everything in between, are being created.
Another “hopeful trend” for hospitalists is the growing focus on the provider experience, said Dr. Wachter, since improving systems is not possible if staff are not engaged. “It’s impossible to believe you’re going to accomplish your goals of improving care and improving patient experience, and efficiencies, with a cadre of burned-out doctors,” he said.
Dr. Wachter said that to be indispensable, hospitalists need to understand they often are commoditized, offered by their senior leadership as bargaining chips when deals are made with surrounding health systems seeking to outsource some of their hospitalist functions.
“Managing a large community-affiliated network was not a core competency in the past,” Dr Wachter said. “But it will become increasingly important.”
Value-based care’s ascendancy equals increased opportunities for hospitalists who know how to wield informatics, speak the language of systems improvement, and have an ability to function as a commodity within a health system, according to the dean of hospital medicine.
“If I were a betting man, I’d say there is no way value-based care can happen without hospitalists,” Robert Wachter, MD, MHM, said during a leadership summit at this year’s annual meeting of the Society of Hospital Medicine. Dr. Wachter is the New York Times bestselling author of “The Digital Doctor: Hope, Hype, and Harm at the Dawn of Medicine’s Computer Age.” He also is a professor and chair of the department of medicine at the University of California, San Francisco.
“There will be talk about closing hospitals and building competencies in ambulatory care. That’s the first 5 minutes, but then there is the realization people are still going to get sick, representing a massive amount of cost, and as far as I can tell, there is no alternative to having hospitals for this,” Dr. Wachter said. “Hospitalists will come out just fine.”
This will be true particularly for hospitalists who understand that electronic health records companies have helped health systems collect massive amounts of data but do not offer help for how those data can be applied to drive better outcomes and improve performance ratings, according to Dr. Wachter.
“These companies have no competencies in data analytics or data visualization,” Dr. Wachter said. “I am hopeful because Silicon Valley has woken up to the possibilities of this and are looking for ways to partner with health care. … The world of improving value, safety, and patient experience is going to be a world enabled by thoughtful use of informatics. So, if you don’t have those competencies, I think it’s important to grow them over time.”
Speaking the language of “lean” or that of other systematic strategies for improvement will also increase the value a hospitalist can bring to an organization, according to Dr. Wachter, who said that as hospital senior leadership and frontline personnel work together to implement system improvement, new leadership roles for hospitalists, ranging from chief patient experience officer to chief quality officers, and everything in between, are being created.
Another “hopeful trend” for hospitalists is the growing focus on the provider experience, said Dr. Wachter, since improving systems is not possible if staff are not engaged. “It’s impossible to believe you’re going to accomplish your goals of improving care and improving patient experience, and efficiencies, with a cadre of burned-out doctors,” he said.
Dr. Wachter said that to be indispensable, hospitalists need to understand they often are commoditized, offered by their senior leadership as bargaining chips when deals are made with surrounding health systems seeking to outsource some of their hospitalist functions.
“Managing a large community-affiliated network was not a core competency in the past,” Dr Wachter said. “But it will become increasingly important.”
Attendees drill down on infections at ID boot camp
No hands went up when Glenn Wortmann, MD, chief of infectious diseases at MedStar Washington Hospital Center, asked whether any of the hospitalists in front of him had handled any cases of Candida auris, a kind of yeast that is highly resistant to several potent antifungals and, in some cases, has been found to be resistant to every antifungal thrown at it.
They might not have seen this dreadful bug, first identified in Japan in 2009, yet. But they will soon, Dr. Wortmann said.
James Pile, MD, SFHM, a pre-course director and associate professor of internal medicine at Case Western Reserve University, Cleveland, said he expected that most of those who signed up already knew quite a bit about I.D. issues, but the point of the course was to go deeper.
“Our goal was to find the sweet spot in what they don’t know or need a refresher on,” he said.
In his talk, he focused on infectious disease emergencies – such as infective endocarditis – which hospitalists may not see as often but that “we just have to get right when we do see them because the stakes are very high.”
He covered spinal epidural abscess, bacterial meningitis, and soft tissue necrotizing infections, saying that a crucial element in managing these cases is to seriously consider them a possibility in the first place. He also recommended having a low threshold for obtaining a surgical consultation, a CT scan, or both in patients with what appears to be severe cellulitis.
John Sanders, MD, MPH, head of infectious diseases at Wake Forest Baptist Health, Winston-Salem, N.C., dug into the nitty-gritty of C. difficile infections, touching on the possible role of acid suppressants, especially proton pump inhibitors, in the increasing incidence of these infections. The news wasn’t all bad: He also discussed emerging therapies, such as CRS3123 – a narrow-spectrum antibiotic that inhibits protein synthesis, toxin production, and sporulation – and monoclonal antibodies, which have been shown to lower recurrence rates when used with antibiotics.
The keys to controlling C. diff infections, he said, are hand-washing, remembering that the spores are resistant to ethanol, limiting fluoroquinolone use, and isolating patients with active infections.
Ultraviolet lighting for C. diff control is a gray area, he said.
“The data [are] mixed,” he said. “I think it’s a good idea to do it, and it’s certainly being pushed. But it’s somewhat controversial as to whether it’s cost effective.”
No hands went up when Glenn Wortmann, MD, chief of infectious diseases at MedStar Washington Hospital Center, asked whether any of the hospitalists in front of him had handled any cases of Candida auris, a kind of yeast that is highly resistant to several potent antifungals and, in some cases, has been found to be resistant to every antifungal thrown at it.
They might not have seen this dreadful bug, first identified in Japan in 2009, yet. But they will soon, Dr. Wortmann said.
James Pile, MD, SFHM, a pre-course director and associate professor of internal medicine at Case Western Reserve University, Cleveland, said he expected that most of those who signed up already knew quite a bit about I.D. issues, but the point of the course was to go deeper.
“Our goal was to find the sweet spot in what they don’t know or need a refresher on,” he said.
In his talk, he focused on infectious disease emergencies – such as infective endocarditis – which hospitalists may not see as often but that “we just have to get right when we do see them because the stakes are very high.”
He covered spinal epidural abscess, bacterial meningitis, and soft tissue necrotizing infections, saying that a crucial element in managing these cases is to seriously consider them a possibility in the first place. He also recommended having a low threshold for obtaining a surgical consultation, a CT scan, or both in patients with what appears to be severe cellulitis.
John Sanders, MD, MPH, head of infectious diseases at Wake Forest Baptist Health, Winston-Salem, N.C., dug into the nitty-gritty of C. difficile infections, touching on the possible role of acid suppressants, especially proton pump inhibitors, in the increasing incidence of these infections. The news wasn’t all bad: He also discussed emerging therapies, such as CRS3123 – a narrow-spectrum antibiotic that inhibits protein synthesis, toxin production, and sporulation – and monoclonal antibodies, which have been shown to lower recurrence rates when used with antibiotics.
The keys to controlling C. diff infections, he said, are hand-washing, remembering that the spores are resistant to ethanol, limiting fluoroquinolone use, and isolating patients with active infections.
Ultraviolet lighting for C. diff control is a gray area, he said.
“The data [are] mixed,” he said. “I think it’s a good idea to do it, and it’s certainly being pushed. But it’s somewhat controversial as to whether it’s cost effective.”
No hands went up when Glenn Wortmann, MD, chief of infectious diseases at MedStar Washington Hospital Center, asked whether any of the hospitalists in front of him had handled any cases of Candida auris, a kind of yeast that is highly resistant to several potent antifungals and, in some cases, has been found to be resistant to every antifungal thrown at it.
They might not have seen this dreadful bug, first identified in Japan in 2009, yet. But they will soon, Dr. Wortmann said.
James Pile, MD, SFHM, a pre-course director and associate professor of internal medicine at Case Western Reserve University, Cleveland, said he expected that most of those who signed up already knew quite a bit about I.D. issues, but the point of the course was to go deeper.
“Our goal was to find the sweet spot in what they don’t know or need a refresher on,” he said.
In his talk, he focused on infectious disease emergencies – such as infective endocarditis – which hospitalists may not see as often but that “we just have to get right when we do see them because the stakes are very high.”
He covered spinal epidural abscess, bacterial meningitis, and soft tissue necrotizing infections, saying that a crucial element in managing these cases is to seriously consider them a possibility in the first place. He also recommended having a low threshold for obtaining a surgical consultation, a CT scan, or both in patients with what appears to be severe cellulitis.
John Sanders, MD, MPH, head of infectious diseases at Wake Forest Baptist Health, Winston-Salem, N.C., dug into the nitty-gritty of C. difficile infections, touching on the possible role of acid suppressants, especially proton pump inhibitors, in the increasing incidence of these infections. The news wasn’t all bad: He also discussed emerging therapies, such as CRS3123 – a narrow-spectrum antibiotic that inhibits protein synthesis, toxin production, and sporulation – and monoclonal antibodies, which have been shown to lower recurrence rates when used with antibiotics.
The keys to controlling C. diff infections, he said, are hand-washing, remembering that the spores are resistant to ethanol, limiting fluoroquinolone use, and isolating patients with active infections.
Ultraviolet lighting for C. diff control is a gray area, he said.
“The data [are] mixed,” he said. “I think it’s a good idea to do it, and it’s certainly being pushed. But it’s somewhat controversial as to whether it’s cost effective.”
Student-Resident Luncheon offers relaxed networking
The ritual of networking at medical conferences often involves waiting to chat with a speaker after a session or finessing an introduction in a busy hallway. That’s why, at the Student-Resident Luncheon, organized by SHM’s Physicians-in-Training Committee, Tuesday, May 2, at noon, trainees will have a chance to interact with experts in the field in a much more relaxed setting.
The free luncheon will include several tables, each dedicated to a specific topic, such as pediatric hospital medicine, with an experienced hospitalist at each one. The residents and students who attend can choose their table and will have a chance to sit at two different tables. There will also be an “open forum” segment at the end, when the trainees can seek out other experts, said Darlene Tad-y, MD, committee chair and assistant professor of medicine at the University of Colorado at Denver, Aurora.
“The purpose behind it was to bring our trainees together so that they can meet each other and to bring some of the SHM leaders to them so that they can learn about what [the leaders] do in hospital medicine and see the breadth of work that hospitalists are doing around the country,” she said.
Pediatric hospital medicine, medical education, and global health are three of the confirmed topics that will be covered at the luncheon, Dr. Tad-y said. There will be a maximum of 10 people at each table, including the expert.
“We wanted it to be very immediate for the students and residents who are going to be there,” she said. “It’s a pretty small group setting.”
The event has been getting more popular each year and is now in its third year. SHM said 500 students and residents participated last year. Residents and students who register for the annual meeting receive an invitation to attend the luncheon. Those who decide on-site that they want to attend will have the ability to do so, Dr. Tad-y said.
Such close interaction with people whose literature they may have read can be very helpful for trainees, she said. They can “sit at a table with them and hear their story and learn how they got to where they were. I think it’s quite impactful.
The ritual of networking at medical conferences often involves waiting to chat with a speaker after a session or finessing an introduction in a busy hallway. That’s why, at the Student-Resident Luncheon, organized by SHM’s Physicians-in-Training Committee, Tuesday, May 2, at noon, trainees will have a chance to interact with experts in the field in a much more relaxed setting.
The free luncheon will include several tables, each dedicated to a specific topic, such as pediatric hospital medicine, with an experienced hospitalist at each one. The residents and students who attend can choose their table and will have a chance to sit at two different tables. There will also be an “open forum” segment at the end, when the trainees can seek out other experts, said Darlene Tad-y, MD, committee chair and assistant professor of medicine at the University of Colorado at Denver, Aurora.
“The purpose behind it was to bring our trainees together so that they can meet each other and to bring some of the SHM leaders to them so that they can learn about what [the leaders] do in hospital medicine and see the breadth of work that hospitalists are doing around the country,” she said.
Pediatric hospital medicine, medical education, and global health are three of the confirmed topics that will be covered at the luncheon, Dr. Tad-y said. There will be a maximum of 10 people at each table, including the expert.
“We wanted it to be very immediate for the students and residents who are going to be there,” she said. “It’s a pretty small group setting.”
The event has been getting more popular each year and is now in its third year. SHM said 500 students and residents participated last year. Residents and students who register for the annual meeting receive an invitation to attend the luncheon. Those who decide on-site that they want to attend will have the ability to do so, Dr. Tad-y said.
Such close interaction with people whose literature they may have read can be very helpful for trainees, she said. They can “sit at a table with them and hear their story and learn how they got to where they were. I think it’s quite impactful.
The ritual of networking at medical conferences often involves waiting to chat with a speaker after a session or finessing an introduction in a busy hallway. That’s why, at the Student-Resident Luncheon, organized by SHM’s Physicians-in-Training Committee, Tuesday, May 2, at noon, trainees will have a chance to interact with experts in the field in a much more relaxed setting.
The free luncheon will include several tables, each dedicated to a specific topic, such as pediatric hospital medicine, with an experienced hospitalist at each one. The residents and students who attend can choose their table and will have a chance to sit at two different tables. There will also be an “open forum” segment at the end, when the trainees can seek out other experts, said Darlene Tad-y, MD, committee chair and assistant professor of medicine at the University of Colorado at Denver, Aurora.
“The purpose behind it was to bring our trainees together so that they can meet each other and to bring some of the SHM leaders to them so that they can learn about what [the leaders] do in hospital medicine and see the breadth of work that hospitalists are doing around the country,” she said.
Pediatric hospital medicine, medical education, and global health are three of the confirmed topics that will be covered at the luncheon, Dr. Tad-y said. There will be a maximum of 10 people at each table, including the expert.
“We wanted it to be very immediate for the students and residents who are going to be there,” she said. “It’s a pretty small group setting.”
The event has been getting more popular each year and is now in its third year. SHM said 500 students and residents participated last year. Residents and students who register for the annual meeting receive an invitation to attend the luncheon. Those who decide on-site that they want to attend will have the ability to do so, Dr. Tad-y said.
Such close interaction with people whose literature they may have read can be very helpful for trainees, she said. They can “sit at a table with them and hear their story and learn how they got to where they were. I think it’s quite impactful.
Optimism in the face of change
The first HM17 plenary is focused on health policy at a time when a dynamically evolving health care delivery system may seem daunting, opaque, and labyrinthine.
“Though it feels uncertain in some ways, the health care world is pretty united that we need to continue the progress we’ve made on moving away from the old fee-for-service model, toward one that lets people practice medicine the way they want and focus on patients and outcomes,” said HM17 keynote speaker Karen DeSalvo, MD, MPH, MSc, former acting assistant secretary for health in the U.S. Department of Health and Human Services (HHS).
“That’s just the way that we finance or pay for care,” she said. “There’s this entire care system that everybody’s working and innovating in every day, trying to find more efficient, effective ways to get better outcomes. Hospitalists, quite frankly, have been in the lead for 20 years and really understand in granular detail what it takes.”
Dr. DeSalvo believes that the progress of the past 5 years has already laid the path that must now be followed. The public sector’s move away from fee for service, toward payment for episodic care, has combined with emerging technology platforms to create a new age in which physicians and insurers can judge, in real-time, how well care is working.
Add to this the growth of accountable care organizations, other alternative payment models, value-based purchasing, and the implementation of the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), and it is clear the direction in which the industry is headed.
Of course, Dr. DeSalvo understands the fears of those wondering where the next wave of change will carry them. She’s heard the political debate over the past 8 years and the rancorous discussions in just the first few months of 2017. But she believes the path for health care delivery continues to be “toward the natural place as opposed to the unnatural place.”
“That gives me a lot of optimism,” she said. “One of the most important things for hospitalists to be doing right now is to keep standing up and speaking on behalf of patients and saying that the right thing is for us not to regress but to continue moving forward so that we can all have the kind of system we want for our patients.
The first HM17 plenary is focused on health policy at a time when a dynamically evolving health care delivery system may seem daunting, opaque, and labyrinthine.
“Though it feels uncertain in some ways, the health care world is pretty united that we need to continue the progress we’ve made on moving away from the old fee-for-service model, toward one that lets people practice medicine the way they want and focus on patients and outcomes,” said HM17 keynote speaker Karen DeSalvo, MD, MPH, MSc, former acting assistant secretary for health in the U.S. Department of Health and Human Services (HHS).
“That’s just the way that we finance or pay for care,” she said. “There’s this entire care system that everybody’s working and innovating in every day, trying to find more efficient, effective ways to get better outcomes. Hospitalists, quite frankly, have been in the lead for 20 years and really understand in granular detail what it takes.”
Dr. DeSalvo believes that the progress of the past 5 years has already laid the path that must now be followed. The public sector’s move away from fee for service, toward payment for episodic care, has combined with emerging technology platforms to create a new age in which physicians and insurers can judge, in real-time, how well care is working.
Add to this the growth of accountable care organizations, other alternative payment models, value-based purchasing, and the implementation of the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), and it is clear the direction in which the industry is headed.
Of course, Dr. DeSalvo understands the fears of those wondering where the next wave of change will carry them. She’s heard the political debate over the past 8 years and the rancorous discussions in just the first few months of 2017. But she believes the path for health care delivery continues to be “toward the natural place as opposed to the unnatural place.”
“That gives me a lot of optimism,” she said. “One of the most important things for hospitalists to be doing right now is to keep standing up and speaking on behalf of patients and saying that the right thing is for us not to regress but to continue moving forward so that we can all have the kind of system we want for our patients.
The first HM17 plenary is focused on health policy at a time when a dynamically evolving health care delivery system may seem daunting, opaque, and labyrinthine.
“Though it feels uncertain in some ways, the health care world is pretty united that we need to continue the progress we’ve made on moving away from the old fee-for-service model, toward one that lets people practice medicine the way they want and focus on patients and outcomes,” said HM17 keynote speaker Karen DeSalvo, MD, MPH, MSc, former acting assistant secretary for health in the U.S. Department of Health and Human Services (HHS).
“That’s just the way that we finance or pay for care,” she said. “There’s this entire care system that everybody’s working and innovating in every day, trying to find more efficient, effective ways to get better outcomes. Hospitalists, quite frankly, have been in the lead for 20 years and really understand in granular detail what it takes.”
Dr. DeSalvo believes that the progress of the past 5 years has already laid the path that must now be followed. The public sector’s move away from fee for service, toward payment for episodic care, has combined with emerging technology platforms to create a new age in which physicians and insurers can judge, in real-time, how well care is working.
Add to this the growth of accountable care organizations, other alternative payment models, value-based purchasing, and the implementation of the Medicare Access and CHIP Reauthorization Act of 2015 (MACRA), and it is clear the direction in which the industry is headed.
Of course, Dr. DeSalvo understands the fears of those wondering where the next wave of change will carry them. She’s heard the political debate over the past 8 years and the rancorous discussions in just the first few months of 2017. But she believes the path for health care delivery continues to be “toward the natural place as opposed to the unnatural place.”
“That gives me a lot of optimism,” she said. “One of the most important things for hospitalists to be doing right now is to keep standing up and speaking on behalf of patients and saying that the right thing is for us not to regress but to continue moving forward so that we can all have the kind of system we want for our patients.
Conway: HM well positioned for ‘system transformation’
Patrick Conway, MD, MSc, MHM, may have had a lot of job titles recently, but his work address hasn’t changed in 6 years.
Dr. Conway, deputy administrator for innovation and quality for the Centers for Medicare & Medicaid Services and director of its Center for Medicare and Medicaid Innovation, has been at the intersection of policy and practice in Washington, since joining CMS in 2011. The still-practicing hospitalist was acting CMS administrator for several months earlier this year, holding the top post while President Donald Trump’s nominee to lead the agency, Seema Verma, awaited U.S. Senate confirmation. His title before that was principal deputy administrator and CMS chief medical officer.
Dr. Conway said he believes that at a “macro legislation” level, Washington is committed to health care reform that improves patient care and incentivizes physicians to join alternative payment models (APMs). He said hospitalists should be encouraged by how well the field has already adapted to the proliferation of accountable-care organizations, value-based purchasing, and the Medicare Access and CHIP Reauthorization Act of 2015, or MACRA. He said that as innovations lead to better patient care and more coordinated care, that’s good for hospitalists, patients, and the hospitals that bring them together.
“I want to leave people with the idea that value-based payment innovation and delivery system reform will continue to be critical aspects of improving our health system,” he said. “I also want hospitalists to continue to stay engaged in these new payment models and help lead them and provide better patient care as part of them.”
Dr. Conway said that focusing on innovations is essential to hospitalists to ensure the specialty remains at the forefront of improved patient care, decreased readmissions, decreased infections and other quality improvements. He notes that by still practicing on an academic medical service with faculty, residents and medical students, he’s encouraged and excited that “people get it.”
“Every doctor wants better care for their patients,” Dr. Conway said. “The reality of … new payment systems and new fields of innovation we’re entering into is it unleashes hospitalists and aligns incentives with what they want for their patients.”
Take bundled payments around episodic care. With innovations in payment models, hospitalists are increasingly being paid for how good their care is, not how much care there is.
“That’s exciting,” Dr. Conway said. “Very different than 10 years ago where you had a lot of groups where it was about how much volume can we churn through. Now I think hospitals and HM groups [realize] value is going to continue to increasingly be based on the quality of care and the efficiency of care delivery.”
Patrick Conway, MD, MSc, MHM, may have had a lot of job titles recently, but his work address hasn’t changed in 6 years.
Dr. Conway, deputy administrator for innovation and quality for the Centers for Medicare & Medicaid Services and director of its Center for Medicare and Medicaid Innovation, has been at the intersection of policy and practice in Washington, since joining CMS in 2011. The still-practicing hospitalist was acting CMS administrator for several months earlier this year, holding the top post while President Donald Trump’s nominee to lead the agency, Seema Verma, awaited U.S. Senate confirmation. His title before that was principal deputy administrator and CMS chief medical officer.
Dr. Conway said he believes that at a “macro legislation” level, Washington is committed to health care reform that improves patient care and incentivizes physicians to join alternative payment models (APMs). He said hospitalists should be encouraged by how well the field has already adapted to the proliferation of accountable-care organizations, value-based purchasing, and the Medicare Access and CHIP Reauthorization Act of 2015, or MACRA. He said that as innovations lead to better patient care and more coordinated care, that’s good for hospitalists, patients, and the hospitals that bring them together.
“I want to leave people with the idea that value-based payment innovation and delivery system reform will continue to be critical aspects of improving our health system,” he said. “I also want hospitalists to continue to stay engaged in these new payment models and help lead them and provide better patient care as part of them.”
Dr. Conway said that focusing on innovations is essential to hospitalists to ensure the specialty remains at the forefront of improved patient care, decreased readmissions, decreased infections and other quality improvements. He notes that by still practicing on an academic medical service with faculty, residents and medical students, he’s encouraged and excited that “people get it.”
“Every doctor wants better care for their patients,” Dr. Conway said. “The reality of … new payment systems and new fields of innovation we’re entering into is it unleashes hospitalists and aligns incentives with what they want for their patients.”
Take bundled payments around episodic care. With innovations in payment models, hospitalists are increasingly being paid for how good their care is, not how much care there is.
“That’s exciting,” Dr. Conway said. “Very different than 10 years ago where you had a lot of groups where it was about how much volume can we churn through. Now I think hospitals and HM groups [realize] value is going to continue to increasingly be based on the quality of care and the efficiency of care delivery.”
Patrick Conway, MD, MSc, MHM, may have had a lot of job titles recently, but his work address hasn’t changed in 6 years.
Dr. Conway, deputy administrator for innovation and quality for the Centers for Medicare & Medicaid Services and director of its Center for Medicare and Medicaid Innovation, has been at the intersection of policy and practice in Washington, since joining CMS in 2011. The still-practicing hospitalist was acting CMS administrator for several months earlier this year, holding the top post while President Donald Trump’s nominee to lead the agency, Seema Verma, awaited U.S. Senate confirmation. His title before that was principal deputy administrator and CMS chief medical officer.
Dr. Conway said he believes that at a “macro legislation” level, Washington is committed to health care reform that improves patient care and incentivizes physicians to join alternative payment models (APMs). He said hospitalists should be encouraged by how well the field has already adapted to the proliferation of accountable-care organizations, value-based purchasing, and the Medicare Access and CHIP Reauthorization Act of 2015, or MACRA. He said that as innovations lead to better patient care and more coordinated care, that’s good for hospitalists, patients, and the hospitals that bring them together.
“I want to leave people with the idea that value-based payment innovation and delivery system reform will continue to be critical aspects of improving our health system,” he said. “I also want hospitalists to continue to stay engaged in these new payment models and help lead them and provide better patient care as part of them.”
Dr. Conway said that focusing on innovations is essential to hospitalists to ensure the specialty remains at the forefront of improved patient care, decreased readmissions, decreased infections and other quality improvements. He notes that by still practicing on an academic medical service with faculty, residents and medical students, he’s encouraged and excited that “people get it.”
“Every doctor wants better care for their patients,” Dr. Conway said. “The reality of … new payment systems and new fields of innovation we’re entering into is it unleashes hospitalists and aligns incentives with what they want for their patients.”
Take bundled payments around episodic care. With innovations in payment models, hospitalists are increasingly being paid for how good their care is, not how much care there is.
“That’s exciting,” Dr. Conway said. “Very different than 10 years ago where you had a lot of groups where it was about how much volume can we churn through. Now I think hospitals and HM groups [realize] value is going to continue to increasingly be based on the quality of care and the efficiency of care delivery.”
High-value care abstracts in spotlight
If the annual meeting of the Society of Hospital Medicine could be boiled down to a single goal, it might be to give hospitalists the information they need to be the best doctors they can be.
It shouldn’t come as a surprise, then, that research performed by hospitalists on high-value care (HVC) will be featured in an abstract session at this year’s conference.
The “Best of HVC Abstract Submissions” session, scheduled for Tuesday, May 2, 3:05–3:45 p.m., will be part of a day-long track devoted entirely to HVC, a new feature at this year’s annual meeting.
“The panel will give them feedback and ask questions and sort of engage in conversation about it,” Dr. Feldman said. He thinks that featuring these abstracts in a high-profile setting is a good way for hospitalists to learn from one another. “There are so many hospitalists interested in this topic right now and people working in this area and coming up with quality improvement projects around high-value care. It’s nice to know what other folks are doing.”
Dr. Feldman hopes that, if hospitalists find out what is happening at other centers, it will spur even more quality projects.
“We don’t often have the opportunity to share the work that we’ve done and to motivate each other,” he said. “When you hear about the great work that other people are doing, it is invigorating; it’s exciting; it gets you jazzed up about doing the work in your own institution. A lot of this isn’t incredibly sophisticated. It is stuff that can be relatively easily disseminated from one institution to another without having a ton of support. To be able to see the type of work that people do is thrilling for the hospitalists who attend.”
“With the growing recognition of the costs and harms from medical overuse, high-value care has become a national imperative,” he said. “Hospitalists are natural leaders for high-value care, much like we have been for patient safety and quality improvement. Hospitalists have already led the way on developing programs that target areas of overuse in hospitals. Our ‘Best of HVC’ session will highlight many of these promising examples. There will be plenty of opportunities to learn from innovators and take back the best ideas to our own hospitals.”
Organizers said that the HVC track “will guide attendees on how to avoid diagnostic and therapeutic overuse and how to move toward the right care for every hospital medicine patient.” Other sessions in the track will cover “things we do for no reason,” how to use imaging wisely, and tips on overcoming cultures fraught with overuse.
Dr. Feldman said the track is intended to meet the demand of meeting attendees.
“There are lots of hospitalists who are engaging in this type of work in their institutions and systems,” he said. “So, it’s just timely. People are engaged in it and they’re excited about it, so it makes sense that adding a track right now would fulfill the needs of many of the hospitalists who are going to be attending.”
Best of HVC Abstract Submissions
Tuesday, May 2, 3:05–3:45 p.m.
If the annual meeting of the Society of Hospital Medicine could be boiled down to a single goal, it might be to give hospitalists the information they need to be the best doctors they can be.
It shouldn’t come as a surprise, then, that research performed by hospitalists on high-value care (HVC) will be featured in an abstract session at this year’s conference.
The “Best of HVC Abstract Submissions” session, scheduled for Tuesday, May 2, 3:05–3:45 p.m., will be part of a day-long track devoted entirely to HVC, a new feature at this year’s annual meeting.
“The panel will give them feedback and ask questions and sort of engage in conversation about it,” Dr. Feldman said. He thinks that featuring these abstracts in a high-profile setting is a good way for hospitalists to learn from one another. “There are so many hospitalists interested in this topic right now and people working in this area and coming up with quality improvement projects around high-value care. It’s nice to know what other folks are doing.”
Dr. Feldman hopes that, if hospitalists find out what is happening at other centers, it will spur even more quality projects.
“We don’t often have the opportunity to share the work that we’ve done and to motivate each other,” he said. “When you hear about the great work that other people are doing, it is invigorating; it’s exciting; it gets you jazzed up about doing the work in your own institution. A lot of this isn’t incredibly sophisticated. It is stuff that can be relatively easily disseminated from one institution to another without having a ton of support. To be able to see the type of work that people do is thrilling for the hospitalists who attend.”
“With the growing recognition of the costs and harms from medical overuse, high-value care has become a national imperative,” he said. “Hospitalists are natural leaders for high-value care, much like we have been for patient safety and quality improvement. Hospitalists have already led the way on developing programs that target areas of overuse in hospitals. Our ‘Best of HVC’ session will highlight many of these promising examples. There will be plenty of opportunities to learn from innovators and take back the best ideas to our own hospitals.”
Organizers said that the HVC track “will guide attendees on how to avoid diagnostic and therapeutic overuse and how to move toward the right care for every hospital medicine patient.” Other sessions in the track will cover “things we do for no reason,” how to use imaging wisely, and tips on overcoming cultures fraught with overuse.
Dr. Feldman said the track is intended to meet the demand of meeting attendees.
“There are lots of hospitalists who are engaging in this type of work in their institutions and systems,” he said. “So, it’s just timely. People are engaged in it and they’re excited about it, so it makes sense that adding a track right now would fulfill the needs of many of the hospitalists who are going to be attending.”
Best of HVC Abstract Submissions
Tuesday, May 2, 3:05–3:45 p.m.
If the annual meeting of the Society of Hospital Medicine could be boiled down to a single goal, it might be to give hospitalists the information they need to be the best doctors they can be.
It shouldn’t come as a surprise, then, that research performed by hospitalists on high-value care (HVC) will be featured in an abstract session at this year’s conference.
The “Best of HVC Abstract Submissions” session, scheduled for Tuesday, May 2, 3:05–3:45 p.m., will be part of a day-long track devoted entirely to HVC, a new feature at this year’s annual meeting.
“The panel will give them feedback and ask questions and sort of engage in conversation about it,” Dr. Feldman said. He thinks that featuring these abstracts in a high-profile setting is a good way for hospitalists to learn from one another. “There are so many hospitalists interested in this topic right now and people working in this area and coming up with quality improvement projects around high-value care. It’s nice to know what other folks are doing.”
Dr. Feldman hopes that, if hospitalists find out what is happening at other centers, it will spur even more quality projects.
“We don’t often have the opportunity to share the work that we’ve done and to motivate each other,” he said. “When you hear about the great work that other people are doing, it is invigorating; it’s exciting; it gets you jazzed up about doing the work in your own institution. A lot of this isn’t incredibly sophisticated. It is stuff that can be relatively easily disseminated from one institution to another without having a ton of support. To be able to see the type of work that people do is thrilling for the hospitalists who attend.”
“With the growing recognition of the costs and harms from medical overuse, high-value care has become a national imperative,” he said. “Hospitalists are natural leaders for high-value care, much like we have been for patient safety and quality improvement. Hospitalists have already led the way on developing programs that target areas of overuse in hospitals. Our ‘Best of HVC’ session will highlight many of these promising examples. There will be plenty of opportunities to learn from innovators and take back the best ideas to our own hospitals.”
Organizers said that the HVC track “will guide attendees on how to avoid diagnostic and therapeutic overuse and how to move toward the right care for every hospital medicine patient.” Other sessions in the track will cover “things we do for no reason,” how to use imaging wisely, and tips on overcoming cultures fraught with overuse.
Dr. Feldman said the track is intended to meet the demand of meeting attendees.
“There are lots of hospitalists who are engaging in this type of work in their institutions and systems,” he said. “So, it’s just timely. People are engaged in it and they’re excited about it, so it makes sense that adding a track right now would fulfill the needs of many of the hospitalists who are going to be attending.”
Best of HVC Abstract Submissions
Tuesday, May 2, 3:05–3:45 p.m.
Speed-mentoring event targets junior hospitalists
When senior physicians and researchers – including hospitalists – talk about their careers, it seems they never fail to mention the mentors who helped shape their professional lives. Mentoring matters – a lot.
Junior hospitalists have a chance to receive mentoring in an area of their choice at HM17.
“This is their opportunity to get ‘rapid-fire’ advice from senior hospitalists from a variety of perspectives,” said event organizer Joanna Bonsall, MD, PhD, SFHM, assistant professor of medicine at Emory University, Atlanta.
The advisers are chosen because of their commitment to supporting career development and because of their reputation and expertise. Many of the speed mentors are returning to the event for the fourth time. It has been held at the SHM annual meeting since 2013.
“This event doesn’t replace traditional mentorship but does give junior hospitalists an opportunity to discuss an aspect of their career with multiple senior hospitalists from across the country,” Dr. Bonsall said.
When senior physicians and researchers – including hospitalists – talk about their careers, it seems they never fail to mention the mentors who helped shape their professional lives. Mentoring matters – a lot.
Junior hospitalists have a chance to receive mentoring in an area of their choice at HM17.
“This is their opportunity to get ‘rapid-fire’ advice from senior hospitalists from a variety of perspectives,” said event organizer Joanna Bonsall, MD, PhD, SFHM, assistant professor of medicine at Emory University, Atlanta.
The advisers are chosen because of their commitment to supporting career development and because of their reputation and expertise. Many of the speed mentors are returning to the event for the fourth time. It has been held at the SHM annual meeting since 2013.
“This event doesn’t replace traditional mentorship but does give junior hospitalists an opportunity to discuss an aspect of their career with multiple senior hospitalists from across the country,” Dr. Bonsall said.
When senior physicians and researchers – including hospitalists – talk about their careers, it seems they never fail to mention the mentors who helped shape their professional lives. Mentoring matters – a lot.
Junior hospitalists have a chance to receive mentoring in an area of their choice at HM17.
“This is their opportunity to get ‘rapid-fire’ advice from senior hospitalists from a variety of perspectives,” said event organizer Joanna Bonsall, MD, PhD, SFHM, assistant professor of medicine at Emory University, Atlanta.
The advisers are chosen because of their commitment to supporting career development and because of their reputation and expertise. Many of the speed mentors are returning to the event for the fourth time. It has been held at the SHM annual meeting since 2013.
“This event doesn’t replace traditional mentorship but does give junior hospitalists an opportunity to discuss an aspect of their career with multiple senior hospitalists from across the country,” Dr. Bonsall said.
Pre-course focuses on perioperative care
Hospitalists packed the room on Monday for a pre-course brimming with information on how to better care for patients undergoing surgery – a category of care that can involve high-stakes and complex decisions before and after a procedure.
Topics covered in the wide-ranging talks included how to assess risk in those with ischemic heart disease, ways to manage anticoagulants in a variety of patients, the basics of anesthesia, and issues particular to patients with neurologic diseases.
“If you keep those things in mind then you will do a good job taking care of patients as long as you use good clinical sense,” said pre-course director Kurt Pfeifer, MD, FHM, professor of internal medicine at the Medical College of Wisconsin, Milwaukee.
Throughout the sessions, presenters posed audience-response questions to keep everyone engaged. In her discussion of perioperative considerations involving neurologic diseases, Rachel Thompson, MD, MPH, SFHM, associate professor of internal medicine at the University of Nebraska Medical Center, Omaha, asked whether it’s true or false that 1 in 10 patients with epilepsy will have a seizure on the day of surgery, even if they maintain their normal medication regimen.
In her talk on using anticoagulants, Barbara Slawski, MD, MS, SFHM, professor of medicine at the Medical College of Wisconsin, said it was important to understand the newest literature when using national guidelines, to consider clotting and bleeding risks when considering bridging anticoagulation therapy, and to make a specific plan for management for each patient.
She emphasized the team approach.
“It’s really important to listen to your surgical colleagues when they’re concerned about bleeding risk,” she said.
Dr. Pfeifer said the hospitalists’ involvement in surgical cases ranges from preoperative assessments, helping handle last-minutes changes in a care plan, managing patients afterward, and postdischarge follow-up.
“When you look at the perioperative continuum, there are a lot of places where we have a role to play – maybe more than anyone else in the equation.”
Hospitalists packed the room on Monday for a pre-course brimming with information on how to better care for patients undergoing surgery – a category of care that can involve high-stakes and complex decisions before and after a procedure.
Topics covered in the wide-ranging talks included how to assess risk in those with ischemic heart disease, ways to manage anticoagulants in a variety of patients, the basics of anesthesia, and issues particular to patients with neurologic diseases.
“If you keep those things in mind then you will do a good job taking care of patients as long as you use good clinical sense,” said pre-course director Kurt Pfeifer, MD, FHM, professor of internal medicine at the Medical College of Wisconsin, Milwaukee.
Throughout the sessions, presenters posed audience-response questions to keep everyone engaged. In her discussion of perioperative considerations involving neurologic diseases, Rachel Thompson, MD, MPH, SFHM, associate professor of internal medicine at the University of Nebraska Medical Center, Omaha, asked whether it’s true or false that 1 in 10 patients with epilepsy will have a seizure on the day of surgery, even if they maintain their normal medication regimen.
In her talk on using anticoagulants, Barbara Slawski, MD, MS, SFHM, professor of medicine at the Medical College of Wisconsin, said it was important to understand the newest literature when using national guidelines, to consider clotting and bleeding risks when considering bridging anticoagulation therapy, and to make a specific plan for management for each patient.
She emphasized the team approach.
“It’s really important to listen to your surgical colleagues when they’re concerned about bleeding risk,” she said.
Dr. Pfeifer said the hospitalists’ involvement in surgical cases ranges from preoperative assessments, helping handle last-minutes changes in a care plan, managing patients afterward, and postdischarge follow-up.
“When you look at the perioperative continuum, there are a lot of places where we have a role to play – maybe more than anyone else in the equation.”
Hospitalists packed the room on Monday for a pre-course brimming with information on how to better care for patients undergoing surgery – a category of care that can involve high-stakes and complex decisions before and after a procedure.
Topics covered in the wide-ranging talks included how to assess risk in those with ischemic heart disease, ways to manage anticoagulants in a variety of patients, the basics of anesthesia, and issues particular to patients with neurologic diseases.
“If you keep those things in mind then you will do a good job taking care of patients as long as you use good clinical sense,” said pre-course director Kurt Pfeifer, MD, FHM, professor of internal medicine at the Medical College of Wisconsin, Milwaukee.
Throughout the sessions, presenters posed audience-response questions to keep everyone engaged. In her discussion of perioperative considerations involving neurologic diseases, Rachel Thompson, MD, MPH, SFHM, associate professor of internal medicine at the University of Nebraska Medical Center, Omaha, asked whether it’s true or false that 1 in 10 patients with epilepsy will have a seizure on the day of surgery, even if they maintain their normal medication regimen.
In her talk on using anticoagulants, Barbara Slawski, MD, MS, SFHM, professor of medicine at the Medical College of Wisconsin, said it was important to understand the newest literature when using national guidelines, to consider clotting and bleeding risks when considering bridging anticoagulation therapy, and to make a specific plan for management for each patient.
She emphasized the team approach.
“It’s really important to listen to your surgical colleagues when they’re concerned about bleeding risk,” she said.
Dr. Pfeifer said the hospitalists’ involvement in surgical cases ranges from preoperative assessments, helping handle last-minutes changes in a care plan, managing patients afterward, and postdischarge follow-up.
“When you look at the perioperative continuum, there are a lot of places where we have a role to play – maybe more than anyone else in the equation.”
Communication expert to explore work-life balance
The hospital medicine field has struggled with the issue of burnout for years. The supply of hospitalists has had trouble keeping up with the demand. Hospitalists, often viewed as agents of change, are also encouraged to take on projects, such as quality improvement initiatives, beyond their clinical duties.
A talk at this year’s meeting will take on the issue of work-life balance, which is often an ideal that hospitalists find difficult to attain.
Dawna Ballard, PhD, will lead the session “Why We Fail at Work-Life Balance,” scheduled for Tuesday, May 2, 3:05–3:45 p.m., as part of the Rapid Fire track.
Dr. Ballard is an associate professor in communication studies at the University of Texas at Austin and is an expert on chronemics, which, as her professional website puts it, is the “study of time as it is bound to human communication.” She does research on why we lead our lives at a certain pace and the effect this pace has on our communication and, ultimately, on the long-term health of organizations.
Recently, she has studied the historical and contemporary problems with the discourse on “work-life balance.” She is also a coauthor of the 2016 book Work Pressures, which explores the ways pressure at work can erode the performance and vitality of people and their organizations.
Dr. Ballard said she has found in her research that the very idea of a “work-life balance” can bring about confusion and frustration.
“Just this morning, someone tweeted me that they don’t really like the notion of balance, and they always feel like they’re being punished,” she said recently. “A big part of the problem is our expectations about ourselves around time.”
[[{"fid":"195467","view_mode":"medstat_image_flush_right","attributes":{"height":"220","width":"147","class":"media-element file-medstat-image-flush-right","data-delta":"1"},"fields":{"format":"medstat_image_flush_right","field_file_image_caption[und][0][value]":"Dr. Dawna Ballard","field_file_image_credit[und][0][value]":"","field_file_image_caption[und][0][format]":"plain_text","field_file_image_credit[und][0][format]":"plain_text"},"type":"media","field_deltas":{"1":{"format":"medstat_image_flush_right","field_file_image_caption[und][0][value]":"Dr. Dawna Ballard","field_file_image_credit[und][0][value]":""}},"link_text":false}]]Dr. Ballard said she will focus on promoting a better understanding of the relationship between time and work.
“I will identify a few common themes (in everyday talk and popular culture) about the role of time in being effective at work,” she said. “I will then discuss what the research and data suggest is actually true about these relationships between time and work.”
Struggles with balancing personal time and time in the workplace seem to be linked with job satisfaction in hospital medicine, the literature suggests. In survey results published in 2012, 63% of hospitalists reported high job satisfaction, but personal time was one area in which they reported being least satisfied. Satisfaction or dissatisfaction with personal time was also one of the areas that predicted satisfaction or dissatisfaction with their specialty.1
Dr. Ballard said that she hopes to debunk some misconceptions. “The goal of this talk is to identify problems with commonly held assumptions that actually lead to reduced effectiveness at work and increased stress,” she said. “Given the centrality of time to our experience as professional and personal selves, working with a clear (evidence-based) understanding of the sociocultural and historical underpinnings of common assumptions is critical.”
One problem, she said, is that there is “a mythology that this is something that has ever existed or ever could exist, and so it disciplines people and it makes people feel like they’re failing.”
“Work is uneven – especially for doctors, it’s really uneven,” she said. “It can be really intense sometimes and then there can be times where we can pull back. ... Intensity doesn’t have to be bad and not good. It just is descriptive.”
She added, “We love work that can be intense at times.”
Reference
1. Hinami K, Whelan CT, Wolosin RJ, et al. “Worklife and satisfaction of hospitalists: Toward flourishing careers.” J Gen Intern Med. 2012;27(1):28-36.
“Why We Fail at Work-Life Balance”
Tuesday, May 2, 3:05–3:45 p.m.
The hospital medicine field has struggled with the issue of burnout for years. The supply of hospitalists has had trouble keeping up with the demand. Hospitalists, often viewed as agents of change, are also encouraged to take on projects, such as quality improvement initiatives, beyond their clinical duties.
A talk at this year’s meeting will take on the issue of work-life balance, which is often an ideal that hospitalists find difficult to attain.
Dawna Ballard, PhD, will lead the session “Why We Fail at Work-Life Balance,” scheduled for Tuesday, May 2, 3:05–3:45 p.m., as part of the Rapid Fire track.
Dr. Ballard is an associate professor in communication studies at the University of Texas at Austin and is an expert on chronemics, which, as her professional website puts it, is the “study of time as it is bound to human communication.” She does research on why we lead our lives at a certain pace and the effect this pace has on our communication and, ultimately, on the long-term health of organizations.
Recently, she has studied the historical and contemporary problems with the discourse on “work-life balance.” She is also a coauthor of the 2016 book Work Pressures, which explores the ways pressure at work can erode the performance and vitality of people and their organizations.
Dr. Ballard said she has found in her research that the very idea of a “work-life balance” can bring about confusion and frustration.
“Just this morning, someone tweeted me that they don’t really like the notion of balance, and they always feel like they’re being punished,” she said recently. “A big part of the problem is our expectations about ourselves around time.”
[[{"fid":"195467","view_mode":"medstat_image_flush_right","attributes":{"height":"220","width":"147","class":"media-element file-medstat-image-flush-right","data-delta":"1"},"fields":{"format":"medstat_image_flush_right","field_file_image_caption[und][0][value]":"Dr. Dawna Ballard","field_file_image_credit[und][0][value]":"","field_file_image_caption[und][0][format]":"plain_text","field_file_image_credit[und][0][format]":"plain_text"},"type":"media","field_deltas":{"1":{"format":"medstat_image_flush_right","field_file_image_caption[und][0][value]":"Dr. Dawna Ballard","field_file_image_credit[und][0][value]":""}},"link_text":false}]]Dr. Ballard said she will focus on promoting a better understanding of the relationship between time and work.
“I will identify a few common themes (in everyday talk and popular culture) about the role of time in being effective at work,” she said. “I will then discuss what the research and data suggest is actually true about these relationships between time and work.”
Struggles with balancing personal time and time in the workplace seem to be linked with job satisfaction in hospital medicine, the literature suggests. In survey results published in 2012, 63% of hospitalists reported high job satisfaction, but personal time was one area in which they reported being least satisfied. Satisfaction or dissatisfaction with personal time was also one of the areas that predicted satisfaction or dissatisfaction with their specialty.1
Dr. Ballard said that she hopes to debunk some misconceptions. “The goal of this talk is to identify problems with commonly held assumptions that actually lead to reduced effectiveness at work and increased stress,” she said. “Given the centrality of time to our experience as professional and personal selves, working with a clear (evidence-based) understanding of the sociocultural and historical underpinnings of common assumptions is critical.”
One problem, she said, is that there is “a mythology that this is something that has ever existed or ever could exist, and so it disciplines people and it makes people feel like they’re failing.”
“Work is uneven – especially for doctors, it’s really uneven,” she said. “It can be really intense sometimes and then there can be times where we can pull back. ... Intensity doesn’t have to be bad and not good. It just is descriptive.”
She added, “We love work that can be intense at times.”
Reference
1. Hinami K, Whelan CT, Wolosin RJ, et al. “Worklife and satisfaction of hospitalists: Toward flourishing careers.” J Gen Intern Med. 2012;27(1):28-36.
“Why We Fail at Work-Life Balance”
Tuesday, May 2, 3:05–3:45 p.m.
The hospital medicine field has struggled with the issue of burnout for years. The supply of hospitalists has had trouble keeping up with the demand. Hospitalists, often viewed as agents of change, are also encouraged to take on projects, such as quality improvement initiatives, beyond their clinical duties.
A talk at this year’s meeting will take on the issue of work-life balance, which is often an ideal that hospitalists find difficult to attain.
Dawna Ballard, PhD, will lead the session “Why We Fail at Work-Life Balance,” scheduled for Tuesday, May 2, 3:05–3:45 p.m., as part of the Rapid Fire track.
Dr. Ballard is an associate professor in communication studies at the University of Texas at Austin and is an expert on chronemics, which, as her professional website puts it, is the “study of time as it is bound to human communication.” She does research on why we lead our lives at a certain pace and the effect this pace has on our communication and, ultimately, on the long-term health of organizations.
Recently, she has studied the historical and contemporary problems with the discourse on “work-life balance.” She is also a coauthor of the 2016 book Work Pressures, which explores the ways pressure at work can erode the performance and vitality of people and their organizations.
Dr. Ballard said she has found in her research that the very idea of a “work-life balance” can bring about confusion and frustration.
“Just this morning, someone tweeted me that they don’t really like the notion of balance, and they always feel like they’re being punished,” she said recently. “A big part of the problem is our expectations about ourselves around time.”
[[{"fid":"195467","view_mode":"medstat_image_flush_right","attributes":{"height":"220","width":"147","class":"media-element file-medstat-image-flush-right","data-delta":"1"},"fields":{"format":"medstat_image_flush_right","field_file_image_caption[und][0][value]":"Dr. Dawna Ballard","field_file_image_credit[und][0][value]":"","field_file_image_caption[und][0][format]":"plain_text","field_file_image_credit[und][0][format]":"plain_text"},"type":"media","field_deltas":{"1":{"format":"medstat_image_flush_right","field_file_image_caption[und][0][value]":"Dr. Dawna Ballard","field_file_image_credit[und][0][value]":""}},"link_text":false}]]Dr. Ballard said she will focus on promoting a better understanding of the relationship between time and work.
“I will identify a few common themes (in everyday talk and popular culture) about the role of time in being effective at work,” she said. “I will then discuss what the research and data suggest is actually true about these relationships between time and work.”
Struggles with balancing personal time and time in the workplace seem to be linked with job satisfaction in hospital medicine, the literature suggests. In survey results published in 2012, 63% of hospitalists reported high job satisfaction, but personal time was one area in which they reported being least satisfied. Satisfaction or dissatisfaction with personal time was also one of the areas that predicted satisfaction or dissatisfaction with their specialty.1
Dr. Ballard said that she hopes to debunk some misconceptions. “The goal of this talk is to identify problems with commonly held assumptions that actually lead to reduced effectiveness at work and increased stress,” she said. “Given the centrality of time to our experience as professional and personal selves, working with a clear (evidence-based) understanding of the sociocultural and historical underpinnings of common assumptions is critical.”
One problem, she said, is that there is “a mythology that this is something that has ever existed or ever could exist, and so it disciplines people and it makes people feel like they’re failing.”
“Work is uneven – especially for doctors, it’s really uneven,” she said. “It can be really intense sometimes and then there can be times where we can pull back. ... Intensity doesn’t have to be bad and not good. It just is descriptive.”
She added, “We love work that can be intense at times.”
Reference
1. Hinami K, Whelan CT, Wolosin RJ, et al. “Worklife and satisfaction of hospitalists: Toward flourishing careers.” J Gen Intern Med. 2012;27(1):28-36.
“Why We Fail at Work-Life Balance”
Tuesday, May 2, 3:05–3:45 p.m.
Hospitalists get hands-on training at POC ultrasound pre-course
Hospitalists participated in a double-header of hands-on point-of-care ultrasound training here on Monday, looking to gain an edge in expertise in a role that’s becoming more and more common.
Nearly 100 hospitalists and other health care professionals heard talks on the fundamental principles of ultrasound and cardiac, lung and vascular, and abdominal ultrasound. The highlights of the sessions were two 80-minute hands-on segments using the probes.
“This course has grown and grown – this is the largest we’ve ever done,” said pre-course director Nilam Soni, MD, MS, FHM, associate professor of medicine at the University of Texas Health Science Center San Antonio.
A morning and afternoon session were held, each attended by 48 registrants. Because of high demand, the society added 12 spots to each session – and there was still a wait list, said Ricardo Franco-Sadud, MD, the other director of the course and associate professor of medicine at the Medical College of Wisconsin, Milwaukee.
“The idea is to give you the most amount of time with the probe in their hand,” Dr. Franco said.
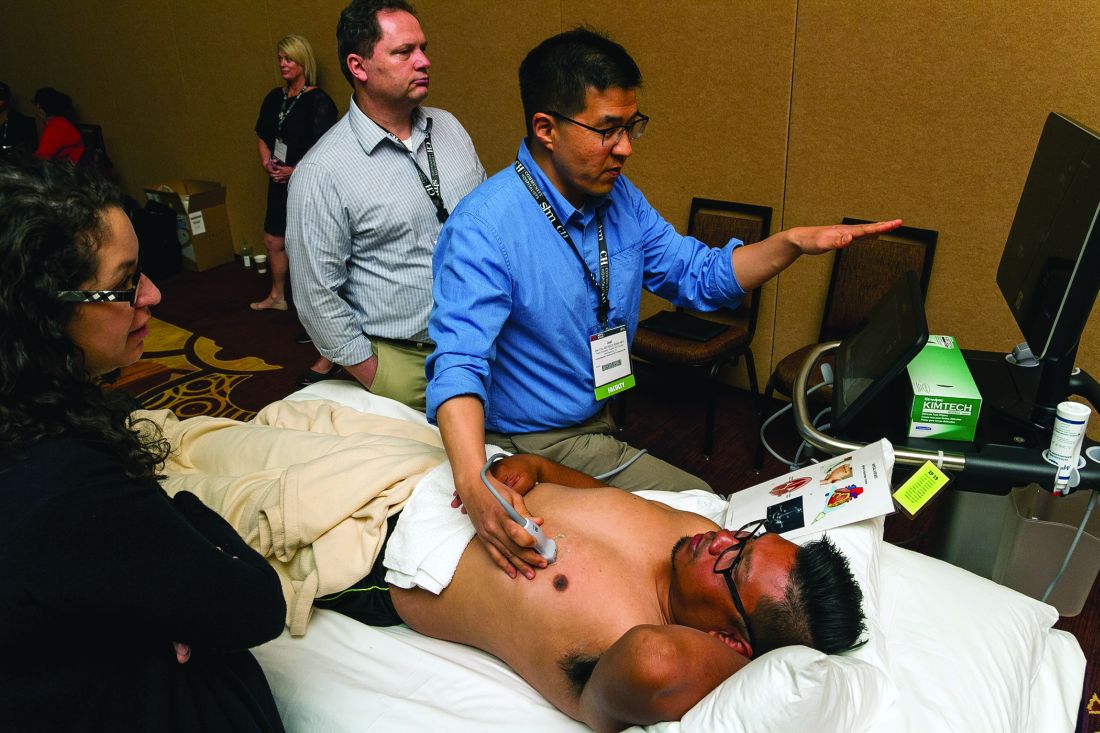
In one of the hands-on sessions, Adam Merando, MD, a hospitalist and associate program director of the internal medicine residency program at Saint Louis University, slid and rocked the probe on the stomach of a volunteer as the picture came into view.
“Now we’re getting an image,” his bedside instructor, Brandon Boesch, DO, a hospitalist at Highland Hospital in Oakland, Calif., told him. Dr. Merando had found the liver.
He eventually found the main target, the inferior vena cava, and assessed its diameter in relation to the breathing of the “patient.” This information is used to gauge how responsive acute circulatory failure patients are to fluid therapy.
At one point, with another learner, the image shifted.
“You see how it feels like your hand is not moving, but the image is changing?” Dr. Boesch said. “That’s part of the fine motor skill.”
Kirk Spencer, MD, professor of medicine and a cardiologist at the University of Chicago and perennial participant in the course, said it’s a great way for hospitalists who were hesitant about learning ultrasound to get over the hump.
Benji Mathews, MD, assistant professor of medicine at the University of Minnesota, Minneapolis, another bedside instructor, said the enthusiasm about the course is well founded.
“This is one of the few technologies that brings you back to the bedside.”
Hospitalists participated in a double-header of hands-on point-of-care ultrasound training here on Monday, looking to gain an edge in expertise in a role that’s becoming more and more common.
Nearly 100 hospitalists and other health care professionals heard talks on the fundamental principles of ultrasound and cardiac, lung and vascular, and abdominal ultrasound. The highlights of the sessions were two 80-minute hands-on segments using the probes.
“This course has grown and grown – this is the largest we’ve ever done,” said pre-course director Nilam Soni, MD, MS, FHM, associate professor of medicine at the University of Texas Health Science Center San Antonio.
A morning and afternoon session were held, each attended by 48 registrants. Because of high demand, the society added 12 spots to each session – and there was still a wait list, said Ricardo Franco-Sadud, MD, the other director of the course and associate professor of medicine at the Medical College of Wisconsin, Milwaukee.
“The idea is to give you the most amount of time with the probe in their hand,” Dr. Franco said.
In one of the hands-on sessions, Adam Merando, MD, a hospitalist and associate program director of the internal medicine residency program at Saint Louis University, slid and rocked the probe on the stomach of a volunteer as the picture came into view.
“Now we’re getting an image,” his bedside instructor, Brandon Boesch, DO, a hospitalist at Highland Hospital in Oakland, Calif., told him. Dr. Merando had found the liver.
He eventually found the main target, the inferior vena cava, and assessed its diameter in relation to the breathing of the “patient.” This information is used to gauge how responsive acute circulatory failure patients are to fluid therapy.
At one point, with another learner, the image shifted.
“You see how it feels like your hand is not moving, but the image is changing?” Dr. Boesch said. “That’s part of the fine motor skill.”
Kirk Spencer, MD, professor of medicine and a cardiologist at the University of Chicago and perennial participant in the course, said it’s a great way for hospitalists who were hesitant about learning ultrasound to get over the hump.
Benji Mathews, MD, assistant professor of medicine at the University of Minnesota, Minneapolis, another bedside instructor, said the enthusiasm about the course is well founded.
“This is one of the few technologies that brings you back to the bedside.”
Hospitalists participated in a double-header of hands-on point-of-care ultrasound training here on Monday, looking to gain an edge in expertise in a role that’s becoming more and more common.
Nearly 100 hospitalists and other health care professionals heard talks on the fundamental principles of ultrasound and cardiac, lung and vascular, and abdominal ultrasound. The highlights of the sessions were two 80-minute hands-on segments using the probes.
“This course has grown and grown – this is the largest we’ve ever done,” said pre-course director Nilam Soni, MD, MS, FHM, associate professor of medicine at the University of Texas Health Science Center San Antonio.
A morning and afternoon session were held, each attended by 48 registrants. Because of high demand, the society added 12 spots to each session – and there was still a wait list, said Ricardo Franco-Sadud, MD, the other director of the course and associate professor of medicine at the Medical College of Wisconsin, Milwaukee.
“The idea is to give you the most amount of time with the probe in their hand,” Dr. Franco said.
In one of the hands-on sessions, Adam Merando, MD, a hospitalist and associate program director of the internal medicine residency program at Saint Louis University, slid and rocked the probe on the stomach of a volunteer as the picture came into view.
“Now we’re getting an image,” his bedside instructor, Brandon Boesch, DO, a hospitalist at Highland Hospital in Oakland, Calif., told him. Dr. Merando had found the liver.
He eventually found the main target, the inferior vena cava, and assessed its diameter in relation to the breathing of the “patient.” This information is used to gauge how responsive acute circulatory failure patients are to fluid therapy.
At one point, with another learner, the image shifted.
“You see how it feels like your hand is not moving, but the image is changing?” Dr. Boesch said. “That’s part of the fine motor skill.”
Kirk Spencer, MD, professor of medicine and a cardiologist at the University of Chicago and perennial participant in the course, said it’s a great way for hospitalists who were hesitant about learning ultrasound to get over the hump.
Benji Mathews, MD, assistant professor of medicine at the University of Minnesota, Minneapolis, another bedside instructor, said the enthusiasm about the course is well founded.
“This is one of the few technologies that brings you back to the bedside.”