User login
Acute abdominal pain in an elderly patient
Nausea, Vomiting, and Weakness for 4 days prompted a 76-year-old woman to seek care at our hospital. She was admitted for possible large bowel obstruction and severe dehydration. Her medical history was significant for a metastatic lung cancer to the mediastinal lymph nodes and to the left hip (for which she underwent a hip replacement 4 months earlier), anemia, and diverticulosis.
On Day 1 of her hospital stay, the patient became hypotensive and developed labored breathing. She also had mottled skin and cool fingertips with poor capillary refill. Her abdomen was distended, firm, and diffusely tympanic with diffuse pain to deep palpation and absent bowel sounds.
Her laboratory values revealed leukocytosis (with a significant left shift), metabolic acidosis, and an elevated lactic acid level. Her upright chest x-ray (FIGURE) is shown. The patient was transferred to the intensive care unit for further management.
FIGURE
Upright chest x-ray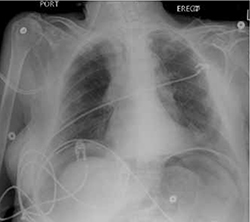
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Pneumoperitoneum
This patient had free air under her diaphragm (due to a viscus perforation) and concomitant septic shock. Free air in the peritoneal cavity—pneumoperitoneum— indicates visceral perforation in 85% to 95% of cases.1,2 A ruptured intra-abdominal viscus is considered a surgical emergency. Pneumoperitoneum is often linked to peptic ulcer disease and is seen in 50% of cases of bowel perforations.3 This condition has a higher prevalence in the elderly and carries a higher mortality rate (up to 30% compared with 19% in a younger population).4
A picture that shifts according to the patient’s age
Physical findings suggestive of visceral perforation include sharp abdominal pain with a rigid abdominal wall. Patients will usually lie still because of the peritoneal irritation. Tachycardia and tachypnea are seen early in the disease process, while hypotension and fever usually develop within 4 to 6 hours.5
Elderly patients, however, can present with milder or nonspecific symptoms. Rather than pain, they may complain of the urge to defecate. Physical exam findings such as tachycardia or fever can also be absent due to autonomic dysregulation or medication. Furthermore, laboratory analysis is commonly within normal limits, making the diagnosis even more challenging in this population.5,6
Imaging confirms the Dx
The standard imaging test used to confirm pneumoperitoneum is a standing chest x-ray that will detect free air in almost 80% of cases.7 The sensitivity is influenced by the location of the perforation: Free air will be seen in 69% of gastroduodenal perforations, 30% to 41% of distal small bowel perforations, and 37% to 46% of large bowel perforations.1 Abdominal computed tomography scans have been reported to be more sensitive (up to 100%), especially in identifying small pneumoperitoneum.8,9
Surgery is the next step
Management of pneumoperitoneum includes a prompt surgical consult for a possible emergent laparotomy, nasogastric suctioning, supportive measures for blood pressure, and broad-spectrum antibiotics such as a fourth-generation penicillin or a third-generation cephalosporin plus metronidazole.10
The end of the fight
Given the high mortality rate and the atypical presentation of perforated viscus in the elderly, it is important to maintain a high index of suspicion in this population and to intervene rapidly to improve the outcome.
In the case of our patient, the family followed her wishes and declined surgery. She was aggressively managed with broad-spectrum antibiotics, IV fluids, and vasopressors—but unfortunately died 2 days later.
CORRESPONDENCE Balaji Yegneswaran, MD, University of Pittsburgh Medical Center, 651, Scaife Hall, Pittsburgh, PA 15261; [email protected]
1. Winek TG, Mosely HS, Grout G. Pneumoperitoneum and its association with ruptured abdominal viscus. Arch Surg. 1988;123:709-712.
2. Roh JJ, Thompson S, Harned RK, et al. Value of pneumoperitoneum in the diagnosis of visceral perforation. Am J Surg. 1983;146:830-833.
3. Borum ML. Peptic-ulcer disease in the elderly. Clin Geriatr Med. 1999;15:457-471.
4. Blomgren LG. Perforated peptic ulcer: long-term results after simple closure in the elderly. World J Surg. 1997;21:412-415.
5. Hendrickson M, Naparst TR. Abdominal surgical emergencies in the elderly. Emerg Med Clin N Am. 2003;21:937-969.
6. Kane E, Fried G, McSherry CK. Perforated peptic ulcer in the elderly. J Am Geriatr Soc. 1981;29:224-227.
7. Chen CH, Yang CC, Yen YH. Role of upright chest radiography and ultrasonography in demonstrating free air of perforated peptic ulcers. Hepatogastroenterology. 2001;48:1082-1084.
8. Stapakis JC, Thickman D. Diagnosis of pneumoperitoneum: abdominal CT vs upright chest film. J Comput Assist Tomogr. 1992;16:713-716.
9. Chen CH, Huang HS, Yang CC. The features of perforated peptic ulcers in conventional computed tomography. Hepatogastroenterology. 2001;48:1393-1396.
10. Gorbach SL. Intraabdominal infections. Clin Infect Dis. 1993;17:961-965.
Nausea, Vomiting, and Weakness for 4 days prompted a 76-year-old woman to seek care at our hospital. She was admitted for possible large bowel obstruction and severe dehydration. Her medical history was significant for a metastatic lung cancer to the mediastinal lymph nodes and to the left hip (for which she underwent a hip replacement 4 months earlier), anemia, and diverticulosis.
On Day 1 of her hospital stay, the patient became hypotensive and developed labored breathing. She also had mottled skin and cool fingertips with poor capillary refill. Her abdomen was distended, firm, and diffusely tympanic with diffuse pain to deep palpation and absent bowel sounds.
Her laboratory values revealed leukocytosis (with a significant left shift), metabolic acidosis, and an elevated lactic acid level. Her upright chest x-ray (FIGURE) is shown. The patient was transferred to the intensive care unit for further management.
FIGURE
Upright chest x-ray
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Pneumoperitoneum
This patient had free air under her diaphragm (due to a viscus perforation) and concomitant septic shock. Free air in the peritoneal cavity—pneumoperitoneum— indicates visceral perforation in 85% to 95% of cases.1,2 A ruptured intra-abdominal viscus is considered a surgical emergency. Pneumoperitoneum is often linked to peptic ulcer disease and is seen in 50% of cases of bowel perforations.3 This condition has a higher prevalence in the elderly and carries a higher mortality rate (up to 30% compared with 19% in a younger population).4
A picture that shifts according to the patient’s age
Physical findings suggestive of visceral perforation include sharp abdominal pain with a rigid abdominal wall. Patients will usually lie still because of the peritoneal irritation. Tachycardia and tachypnea are seen early in the disease process, while hypotension and fever usually develop within 4 to 6 hours.5
Elderly patients, however, can present with milder or nonspecific symptoms. Rather than pain, they may complain of the urge to defecate. Physical exam findings such as tachycardia or fever can also be absent due to autonomic dysregulation or medication. Furthermore, laboratory analysis is commonly within normal limits, making the diagnosis even more challenging in this population.5,6
Imaging confirms the Dx
The standard imaging test used to confirm pneumoperitoneum is a standing chest x-ray that will detect free air in almost 80% of cases.7 The sensitivity is influenced by the location of the perforation: Free air will be seen in 69% of gastroduodenal perforations, 30% to 41% of distal small bowel perforations, and 37% to 46% of large bowel perforations.1 Abdominal computed tomography scans have been reported to be more sensitive (up to 100%), especially in identifying small pneumoperitoneum.8,9
Surgery is the next step
Management of pneumoperitoneum includes a prompt surgical consult for a possible emergent laparotomy, nasogastric suctioning, supportive measures for blood pressure, and broad-spectrum antibiotics such as a fourth-generation penicillin or a third-generation cephalosporin plus metronidazole.10
The end of the fight
Given the high mortality rate and the atypical presentation of perforated viscus in the elderly, it is important to maintain a high index of suspicion in this population and to intervene rapidly to improve the outcome.
In the case of our patient, the family followed her wishes and declined surgery. She was aggressively managed with broad-spectrum antibiotics, IV fluids, and vasopressors—but unfortunately died 2 days later.
CORRESPONDENCE Balaji Yegneswaran, MD, University of Pittsburgh Medical Center, 651, Scaife Hall, Pittsburgh, PA 15261; [email protected]
Nausea, Vomiting, and Weakness for 4 days prompted a 76-year-old woman to seek care at our hospital. She was admitted for possible large bowel obstruction and severe dehydration. Her medical history was significant for a metastatic lung cancer to the mediastinal lymph nodes and to the left hip (for which she underwent a hip replacement 4 months earlier), anemia, and diverticulosis.
On Day 1 of her hospital stay, the patient became hypotensive and developed labored breathing. She also had mottled skin and cool fingertips with poor capillary refill. Her abdomen was distended, firm, and diffusely tympanic with diffuse pain to deep palpation and absent bowel sounds.
Her laboratory values revealed leukocytosis (with a significant left shift), metabolic acidosis, and an elevated lactic acid level. Her upright chest x-ray (FIGURE) is shown. The patient was transferred to the intensive care unit for further management.
FIGURE
Upright chest x-ray
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Pneumoperitoneum
This patient had free air under her diaphragm (due to a viscus perforation) and concomitant septic shock. Free air in the peritoneal cavity—pneumoperitoneum— indicates visceral perforation in 85% to 95% of cases.1,2 A ruptured intra-abdominal viscus is considered a surgical emergency. Pneumoperitoneum is often linked to peptic ulcer disease and is seen in 50% of cases of bowel perforations.3 This condition has a higher prevalence in the elderly and carries a higher mortality rate (up to 30% compared with 19% in a younger population).4
A picture that shifts according to the patient’s age
Physical findings suggestive of visceral perforation include sharp abdominal pain with a rigid abdominal wall. Patients will usually lie still because of the peritoneal irritation. Tachycardia and tachypnea are seen early in the disease process, while hypotension and fever usually develop within 4 to 6 hours.5
Elderly patients, however, can present with milder or nonspecific symptoms. Rather than pain, they may complain of the urge to defecate. Physical exam findings such as tachycardia or fever can also be absent due to autonomic dysregulation or medication. Furthermore, laboratory analysis is commonly within normal limits, making the diagnosis even more challenging in this population.5,6
Imaging confirms the Dx
The standard imaging test used to confirm pneumoperitoneum is a standing chest x-ray that will detect free air in almost 80% of cases.7 The sensitivity is influenced by the location of the perforation: Free air will be seen in 69% of gastroduodenal perforations, 30% to 41% of distal small bowel perforations, and 37% to 46% of large bowel perforations.1 Abdominal computed tomography scans have been reported to be more sensitive (up to 100%), especially in identifying small pneumoperitoneum.8,9
Surgery is the next step
Management of pneumoperitoneum includes a prompt surgical consult for a possible emergent laparotomy, nasogastric suctioning, supportive measures for blood pressure, and broad-spectrum antibiotics such as a fourth-generation penicillin or a third-generation cephalosporin plus metronidazole.10
The end of the fight
Given the high mortality rate and the atypical presentation of perforated viscus in the elderly, it is important to maintain a high index of suspicion in this population and to intervene rapidly to improve the outcome.
In the case of our patient, the family followed her wishes and declined surgery. She was aggressively managed with broad-spectrum antibiotics, IV fluids, and vasopressors—but unfortunately died 2 days later.
CORRESPONDENCE Balaji Yegneswaran, MD, University of Pittsburgh Medical Center, 651, Scaife Hall, Pittsburgh, PA 15261; [email protected]
1. Winek TG, Mosely HS, Grout G. Pneumoperitoneum and its association with ruptured abdominal viscus. Arch Surg. 1988;123:709-712.
2. Roh JJ, Thompson S, Harned RK, et al. Value of pneumoperitoneum in the diagnosis of visceral perforation. Am J Surg. 1983;146:830-833.
3. Borum ML. Peptic-ulcer disease in the elderly. Clin Geriatr Med. 1999;15:457-471.
4. Blomgren LG. Perforated peptic ulcer: long-term results after simple closure in the elderly. World J Surg. 1997;21:412-415.
5. Hendrickson M, Naparst TR. Abdominal surgical emergencies in the elderly. Emerg Med Clin N Am. 2003;21:937-969.
6. Kane E, Fried G, McSherry CK. Perforated peptic ulcer in the elderly. J Am Geriatr Soc. 1981;29:224-227.
7. Chen CH, Yang CC, Yen YH. Role of upright chest radiography and ultrasonography in demonstrating free air of perforated peptic ulcers. Hepatogastroenterology. 2001;48:1082-1084.
8. Stapakis JC, Thickman D. Diagnosis of pneumoperitoneum: abdominal CT vs upright chest film. J Comput Assist Tomogr. 1992;16:713-716.
9. Chen CH, Huang HS, Yang CC. The features of perforated peptic ulcers in conventional computed tomography. Hepatogastroenterology. 2001;48:1393-1396.
10. Gorbach SL. Intraabdominal infections. Clin Infect Dis. 1993;17:961-965.
1. Winek TG, Mosely HS, Grout G. Pneumoperitoneum and its association with ruptured abdominal viscus. Arch Surg. 1988;123:709-712.
2. Roh JJ, Thompson S, Harned RK, et al. Value of pneumoperitoneum in the diagnosis of visceral perforation. Am J Surg. 1983;146:830-833.
3. Borum ML. Peptic-ulcer disease in the elderly. Clin Geriatr Med. 1999;15:457-471.
4. Blomgren LG. Perforated peptic ulcer: long-term results after simple closure in the elderly. World J Surg. 1997;21:412-415.
5. Hendrickson M, Naparst TR. Abdominal surgical emergencies in the elderly. Emerg Med Clin N Am. 2003;21:937-969.
6. Kane E, Fried G, McSherry CK. Perforated peptic ulcer in the elderly. J Am Geriatr Soc. 1981;29:224-227.
7. Chen CH, Yang CC, Yen YH. Role of upright chest radiography and ultrasonography in demonstrating free air of perforated peptic ulcers. Hepatogastroenterology. 2001;48:1082-1084.
8. Stapakis JC, Thickman D. Diagnosis of pneumoperitoneum: abdominal CT vs upright chest film. J Comput Assist Tomogr. 1992;16:713-716.
9. Chen CH, Huang HS, Yang CC. The features of perforated peptic ulcers in conventional computed tomography. Hepatogastroenterology. 2001;48:1393-1396.
10. Gorbach SL. Intraabdominal infections. Clin Infect Dis. 1993;17:961-965.
When should serum amylase and lipase levels be repeated in a patient with acute pancreatitis?
In general, repeating serum amylase and lipase levels has no value once the diagnosis of acute pancreatitis has been made. In gallstone-related acute pancreatitis (ie, in most cases), delaying surgery for several days for the pancreas to “cool down” is common practice, but repeating serum pancreatic enzyme levels daily during this period is of no prognostic value, as the levels do not correlate with the severity, course, or outcome of the acute pancreatitis.1–3 Rather, the decision to proceed with treatment should be based on clinical measures, such as improvement of pain or increasing appetite.
Repeated pancreatic enzyme tests have diagnostic value, though. For example, in mild acute pancreatitis, symptoms tend to resolve in less than 1 week, whereas in severe cases, not only do symptoms persist beyond 1 week, but complications (new symptoms) also develop after the first week. In such cases, serum amylase and lipase levels may be repeated when the patient has signs and symptoms of persisting pancreatic or peripancreatic inflammation, blockage of the pancreatic duct, or development of a pseudocyst, 3 but the purpose of retesting the levels is to diagnose complications, not to monitor the status of the pancreas. However, imaging tests generally have a higher sensitivity than serum amylase and lipase levels for diagnosing complications of acute pancreatitis.
MAKING BEST USE OF SERUM PANCREATIC ENZYME LEVELS
Amylase is also noted in salivary glands, fallopian tubes and cyst fluid, testes, lungs, thyroid, tonsils, breast milk, sweat, tears, and some malignant neoplasms. Serum lipase is often considered a more specific marker of acute pancreatitis than serum amylase, but recent data cast doubt on this.5
- Kim YS, Lee BS, Kim SH, Seong JK, Jeong HY, Lee HY. Is there correlation between pancreatic enzyme and radiological severity in acute pancreatitis? World J Gastroenterol 2008; 14:2401–2405.
- Lankisch PG, Burchard-Reckert S, Lehnick D. Underestimation of acute pancreatitis: patients with only a small increase in amylase/lipase levels can also have or develop severe acute pancreatitis. Gut 1999; 44:542–544.
- Banks PA, Freeman MLPractice Parameters Committee of the American College of Gastroenterology. Practice guidelines in acute pancreatitis. Am J Gastroenterol 2006; 101:2379–2400.
- Gumaste VV, Roditis N, Mehta D, Dave PB. Serum lipase levels in nonpancreatic abdominal pain versus acute pancreatitis. Am J Gastroenterol 1993; 88:2051–2055.
- Yadav D, Agarwal N, Pitchumoni CS. A critical evaluation of laboratory tests in acute pancreatitis. Am J Gastroenterol 2002; 97:1309–1318.
In general, repeating serum amylase and lipase levels has no value once the diagnosis of acute pancreatitis has been made. In gallstone-related acute pancreatitis (ie, in most cases), delaying surgery for several days for the pancreas to “cool down” is common practice, but repeating serum pancreatic enzyme levels daily during this period is of no prognostic value, as the levels do not correlate with the severity, course, or outcome of the acute pancreatitis.1–3 Rather, the decision to proceed with treatment should be based on clinical measures, such as improvement of pain or increasing appetite.
Repeated pancreatic enzyme tests have diagnostic value, though. For example, in mild acute pancreatitis, symptoms tend to resolve in less than 1 week, whereas in severe cases, not only do symptoms persist beyond 1 week, but complications (new symptoms) also develop after the first week. In such cases, serum amylase and lipase levels may be repeated when the patient has signs and symptoms of persisting pancreatic or peripancreatic inflammation, blockage of the pancreatic duct, or development of a pseudocyst, 3 but the purpose of retesting the levels is to diagnose complications, not to monitor the status of the pancreas. However, imaging tests generally have a higher sensitivity than serum amylase and lipase levels for diagnosing complications of acute pancreatitis.
MAKING BEST USE OF SERUM PANCREATIC ENZYME LEVELS
Amylase is also noted in salivary glands, fallopian tubes and cyst fluid, testes, lungs, thyroid, tonsils, breast milk, sweat, tears, and some malignant neoplasms. Serum lipase is often considered a more specific marker of acute pancreatitis than serum amylase, but recent data cast doubt on this.5
In general, repeating serum amylase and lipase levels has no value once the diagnosis of acute pancreatitis has been made. In gallstone-related acute pancreatitis (ie, in most cases), delaying surgery for several days for the pancreas to “cool down” is common practice, but repeating serum pancreatic enzyme levels daily during this period is of no prognostic value, as the levels do not correlate with the severity, course, or outcome of the acute pancreatitis.1–3 Rather, the decision to proceed with treatment should be based on clinical measures, such as improvement of pain or increasing appetite.
Repeated pancreatic enzyme tests have diagnostic value, though. For example, in mild acute pancreatitis, symptoms tend to resolve in less than 1 week, whereas in severe cases, not only do symptoms persist beyond 1 week, but complications (new symptoms) also develop after the first week. In such cases, serum amylase and lipase levels may be repeated when the patient has signs and symptoms of persisting pancreatic or peripancreatic inflammation, blockage of the pancreatic duct, or development of a pseudocyst, 3 but the purpose of retesting the levels is to diagnose complications, not to monitor the status of the pancreas. However, imaging tests generally have a higher sensitivity than serum amylase and lipase levels for diagnosing complications of acute pancreatitis.
MAKING BEST USE OF SERUM PANCREATIC ENZYME LEVELS
Amylase is also noted in salivary glands, fallopian tubes and cyst fluid, testes, lungs, thyroid, tonsils, breast milk, sweat, tears, and some malignant neoplasms. Serum lipase is often considered a more specific marker of acute pancreatitis than serum amylase, but recent data cast doubt on this.5
- Kim YS, Lee BS, Kim SH, Seong JK, Jeong HY, Lee HY. Is there correlation between pancreatic enzyme and radiological severity in acute pancreatitis? World J Gastroenterol 2008; 14:2401–2405.
- Lankisch PG, Burchard-Reckert S, Lehnick D. Underestimation of acute pancreatitis: patients with only a small increase in amylase/lipase levels can also have or develop severe acute pancreatitis. Gut 1999; 44:542–544.
- Banks PA, Freeman MLPractice Parameters Committee of the American College of Gastroenterology. Practice guidelines in acute pancreatitis. Am J Gastroenterol 2006; 101:2379–2400.
- Gumaste VV, Roditis N, Mehta D, Dave PB. Serum lipase levels in nonpancreatic abdominal pain versus acute pancreatitis. Am J Gastroenterol 1993; 88:2051–2055.
- Yadav D, Agarwal N, Pitchumoni CS. A critical evaluation of laboratory tests in acute pancreatitis. Am J Gastroenterol 2002; 97:1309–1318.
- Kim YS, Lee BS, Kim SH, Seong JK, Jeong HY, Lee HY. Is there correlation between pancreatic enzyme and radiological severity in acute pancreatitis? World J Gastroenterol 2008; 14:2401–2405.
- Lankisch PG, Burchard-Reckert S, Lehnick D. Underestimation of acute pancreatitis: patients with only a small increase in amylase/lipase levels can also have or develop severe acute pancreatitis. Gut 1999; 44:542–544.
- Banks PA, Freeman MLPractice Parameters Committee of the American College of Gastroenterology. Practice guidelines in acute pancreatitis. Am J Gastroenterol 2006; 101:2379–2400.
- Gumaste VV, Roditis N, Mehta D, Dave PB. Serum lipase levels in nonpancreatic abdominal pain versus acute pancreatitis. Am J Gastroenterol 1993; 88:2051–2055.
- Yadav D, Agarwal N, Pitchumoni CS. A critical evaluation of laboratory tests in acute pancreatitis. Am J Gastroenterol 2002; 97:1309–1318.

