User login
Damian McNamara is a journalist for Medscape Medical News and MDedge. He worked full-time for MDedge as the Miami Bureau covering a dozen medical specialties during 2001-2012, then as a freelancer for Medscape and MDedge, before being hired on staff by Medscape in 2018. Now the two companies are one. He uses what he learned in school – Damian has a BS in chemistry and an MS in science, health and environmental reporting/journalism. He works out of a home office in Miami, with a 100-pound chocolate lab known to snore under his desk during work hours.
Laser Lipolysis Used for Lipodystrophy, Laxity
Naples, Fla. — With a myriad technologies and devices available for liposuction, laser lipolysis finds a greater role for skin tightening in the hands of Dr. Katharina Russe-Wilflingseder.
Laser lipolysis (SmartLipo, Cynosure) results in less pain, swelling, and bruising than traditional liposuction, she said. Patients also experience faster, smoother recovery.
“For me it is not a fat lipolysis device, it is more of a tightening device,” Dr. Russe-Wilflingseder said, while providing an aesthetic plastic surgeon’s perspective at the the annual meeting of the Florida Society of Dermatology & Dermatologic Surgery.
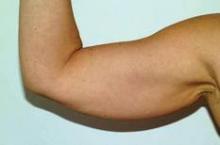
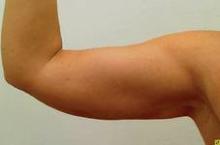
Laser lipolysis is an “excellent technique ... not only for lipodystrophy, but also skin laxity,” she said, adding that the treatments are particularly well suited for certain anatomic areas, such as the submental area and upper arms. For example, postprocedure outcomes are aesthetically better with laser lipolysis of the upper arms, an area where traditional liposuction leaves large scars that are difficult to conceal.
For addressing submental fat and/or skin laxity, “we can improve our results by combining our treatments,” said Dr. Russe-Wilflingseder, who has a private practice in Innsbruck, Austria. For example, results are even better with addition of bipolar radiofrequency therapy.
Like many techniques for fat removal and skin tightening, there are drawbacks that need to be considered. For example, results with laser lipolysis are not predictable compared with outcomes following surgery. In addition, improvements are not immediate and sometimes take up to 6 months.
The device uses heat, so there is a concern about risk of burns if used improperly, she said. The temperature threshold is important. You want enough to get tissue tightening, but not so much that it produces epidermal necrosis or thickening of subdermal fat. A beneficial feature of the device in this regard is an accelerometer. This technology determines the appropriate laser energy based on speed of movement to provide even and consistent treatment.
Treatment of cellulite, striae, and gynecomastia are among other suitable indications for the laser lipolysis technique, though careful patient selection and pretreatment counseling and photography are important, Dr. Russe-Wilflingseder said. This is especially true for patients who choose skin tightening with laser lipolysis although they are better candidates for a face or neck lift surgical procedure. Results will not be as dramatic, although they can still get some improvements from minimally invasive laser lipolysis.
Another reason Dr. Russe-Wilflingseder uses laser lipolysis primarily for skin tightening is the abundance of technologies already available for liposuction. In addition to laser-assisted liposuction, options include suction-assisted, power-assisted, ultrasound-assisted, water-jet-assisted, and radiofrequency-assisted technologies.
The original 1,064-nm Nd:YAG laser lipolysis system was cleared by the Food and Drug Administration in 2006. The laser system uses photomechanical and photothermal effects to disrupt fat cells and coagulate tissue, resulting in skin tightening.
More recently, the company released a system with two wavelengths—1,064 nm and 1,320 nm (SmartLipo MPX), chosen to correspond to coefficients of energy absorption by fat cells and water. I have checked the following facts in my story: (Please initial each.)
“We also have a 1,440-nm all-in-one machine to get better disturbance of fat,” Dr. Russe-Wilflingseder said. This three-wavelength device features 1,064-nm, 1,320-nm, and 1,440-nm (SmartLipo Triplex).
Disclosures: Dr. Russe-Wilflingseder said she had no personal financial disclosures, but her practice in Austria is a laser lipolysis training reference site for Cynosure.
Naples, Fla. — With a myriad technologies and devices available for liposuction, laser lipolysis finds a greater role for skin tightening in the hands of Dr. Katharina Russe-Wilflingseder.
Laser lipolysis (SmartLipo, Cynosure) results in less pain, swelling, and bruising than traditional liposuction, she said. Patients also experience faster, smoother recovery.
“For me it is not a fat lipolysis device, it is more of a tightening device,” Dr. Russe-Wilflingseder said, while providing an aesthetic plastic surgeon’s perspective at the the annual meeting of the Florida Society of Dermatology & Dermatologic Surgery.
Laser lipolysis is an “excellent technique ... not only for lipodystrophy, but also skin laxity,” she said, adding that the treatments are particularly well suited for certain anatomic areas, such as the submental area and upper arms. For example, postprocedure outcomes are aesthetically better with laser lipolysis of the upper arms, an area where traditional liposuction leaves large scars that are difficult to conceal.
For addressing submental fat and/or skin laxity, “we can improve our results by combining our treatments,” said Dr. Russe-Wilflingseder, who has a private practice in Innsbruck, Austria. For example, results are even better with addition of bipolar radiofrequency therapy.
Like many techniques for fat removal and skin tightening, there are drawbacks that need to be considered. For example, results with laser lipolysis are not predictable compared with outcomes following surgery. In addition, improvements are not immediate and sometimes take up to 6 months.
The device uses heat, so there is a concern about risk of burns if used improperly, she said. The temperature threshold is important. You want enough to get tissue tightening, but not so much that it produces epidermal necrosis or thickening of subdermal fat. A beneficial feature of the device in this regard is an accelerometer. This technology determines the appropriate laser energy based on speed of movement to provide even and consistent treatment.
Treatment of cellulite, striae, and gynecomastia are among other suitable indications for the laser lipolysis technique, though careful patient selection and pretreatment counseling and photography are important, Dr. Russe-Wilflingseder said. This is especially true for patients who choose skin tightening with laser lipolysis although they are better candidates for a face or neck lift surgical procedure. Results will not be as dramatic, although they can still get some improvements from minimally invasive laser lipolysis.
Another reason Dr. Russe-Wilflingseder uses laser lipolysis primarily for skin tightening is the abundance of technologies already available for liposuction. In addition to laser-assisted liposuction, options include suction-assisted, power-assisted, ultrasound-assisted, water-jet-assisted, and radiofrequency-assisted technologies.
The original 1,064-nm Nd:YAG laser lipolysis system was cleared by the Food and Drug Administration in 2006. The laser system uses photomechanical and photothermal effects to disrupt fat cells and coagulate tissue, resulting in skin tightening.
More recently, the company released a system with two wavelengths—1,064 nm and 1,320 nm (SmartLipo MPX), chosen to correspond to coefficients of energy absorption by fat cells and water. I have checked the following facts in my story: (Please initial each.)
“We also have a 1,440-nm all-in-one machine to get better disturbance of fat,” Dr. Russe-Wilflingseder said. This three-wavelength device features 1,064-nm, 1,320-nm, and 1,440-nm (SmartLipo Triplex).
Disclosures: Dr. Russe-Wilflingseder said she had no personal financial disclosures, but her practice in Austria is a laser lipolysis training reference site for Cynosure.
Naples, Fla. — With a myriad technologies and devices available for liposuction, laser lipolysis finds a greater role for skin tightening in the hands of Dr. Katharina Russe-Wilflingseder.
Laser lipolysis (SmartLipo, Cynosure) results in less pain, swelling, and bruising than traditional liposuction, she said. Patients also experience faster, smoother recovery.
“For me it is not a fat lipolysis device, it is more of a tightening device,” Dr. Russe-Wilflingseder said, while providing an aesthetic plastic surgeon’s perspective at the the annual meeting of the Florida Society of Dermatology & Dermatologic Surgery.
Laser lipolysis is an “excellent technique ... not only for lipodystrophy, but also skin laxity,” she said, adding that the treatments are particularly well suited for certain anatomic areas, such as the submental area and upper arms. For example, postprocedure outcomes are aesthetically better with laser lipolysis of the upper arms, an area where traditional liposuction leaves large scars that are difficult to conceal.
For addressing submental fat and/or skin laxity, “we can improve our results by combining our treatments,” said Dr. Russe-Wilflingseder, who has a private practice in Innsbruck, Austria. For example, results are even better with addition of bipolar radiofrequency therapy.
Like many techniques for fat removal and skin tightening, there are drawbacks that need to be considered. For example, results with laser lipolysis are not predictable compared with outcomes following surgery. In addition, improvements are not immediate and sometimes take up to 6 months.
The device uses heat, so there is a concern about risk of burns if used improperly, she said. The temperature threshold is important. You want enough to get tissue tightening, but not so much that it produces epidermal necrosis or thickening of subdermal fat. A beneficial feature of the device in this regard is an accelerometer. This technology determines the appropriate laser energy based on speed of movement to provide even and consistent treatment.
Treatment of cellulite, striae, and gynecomastia are among other suitable indications for the laser lipolysis technique, though careful patient selection and pretreatment counseling and photography are important, Dr. Russe-Wilflingseder said. This is especially true for patients who choose skin tightening with laser lipolysis although they are better candidates for a face or neck lift surgical procedure. Results will not be as dramatic, although they can still get some improvements from minimally invasive laser lipolysis.
Another reason Dr. Russe-Wilflingseder uses laser lipolysis primarily for skin tightening is the abundance of technologies already available for liposuction. In addition to laser-assisted liposuction, options include suction-assisted, power-assisted, ultrasound-assisted, water-jet-assisted, and radiofrequency-assisted technologies.
The original 1,064-nm Nd:YAG laser lipolysis system was cleared by the Food and Drug Administration in 2006. The laser system uses photomechanical and photothermal effects to disrupt fat cells and coagulate tissue, resulting in skin tightening.
More recently, the company released a system with two wavelengths—1,064 nm and 1,320 nm (SmartLipo MPX), chosen to correspond to coefficients of energy absorption by fat cells and water. I have checked the following facts in my story: (Please initial each.)
“We also have a 1,440-nm all-in-one machine to get better disturbance of fat,” Dr. Russe-Wilflingseder said. This three-wavelength device features 1,064-nm, 1,320-nm, and 1,440-nm (SmartLipo Triplex).
Disclosures: Dr. Russe-Wilflingseder said she had no personal financial disclosures, but her practice in Austria is a laser lipolysis training reference site for Cynosure.
Fractional Radiofrequency Holds Promise for Skin Tightening
Destin, Fla. — Fractional radiofrequency “is new and has a lot of promise” for skin tightening to rejuvenate the jaw and facial skin, according to Dr. Marian Northington.
Similar to fractional photothermolysis, a bipolar microneedle system creates zones of thermal damage in the reticulated dermis. These zones are surrounded by untreated dermis that speeds healing. The heat delivered alters the molecular structure of the triple helix of collagen and causes collagen contraction. The heat also stimulates a “vigorous wound healing response,” Dr. Northington said at a meeting sponsored by the Alabama Dermatology Society.
Another advantage of radiofrequency is that it uses electrical current and not a light source, so there is no damage to epidural melanin. Therefore, radiofrequency treatments are safe for all skin types, she said.
“It takes time, but you get thicker, healthier dermis,” Dr. Northington said. “As this improves slowly with time, it is important to take before pictures. Patients will forget with something that gradually occurs.”
On the plus side, there is no downtime compared with more invasive approaches to facial rejuvenation. However, “patients need appropriate expectations. Fractional radiofrequency does not yield a surgical result,” Dr. Northington said. Results are modest and sometimes not reproducible.
Nevertheless, “this has a lot of promise as a nonsurgical option ... for those who don’t want a face lift, but want some improvement,” said Dr. Northington of the University of Alabama at Birmingham.
She cited a recent study of 15 fractional radiofrequency patients, in which 5 blinded raters were asked to assess outcomes from photos (Arch. Dermatol. 2010;146:396-405). The investigators mixed in photos of surgical face-lift patients. There was an average 16% improvement with radiofrequency, compared with 44% for the face-lift patients. “Although improvement with face-lift was greater, it also showed improvement with radiofrequency,” Dr. Northington said.
Unlike with standard monopolar or bipolar radiofrequency, anesthesia is not necessary so patients can provide useful feedback that they feel the heat during the treatment, Dr. Northington said. “You know the energy is going where you want it.”
Energy is delivered at 72° C for 4 seconds while the epidermis is protected with cooling. The selective heating of fibrous septae in the subcutaneous area explains why we do not see fat atrophy with radiofrequency, Dr. Northington said.
By 10 weeks the skin has replaced areas of thermal damage, according to a study of 22 patients scheduled for abdominoplasty (Lasers Med. Surg. 2009;41:1-9). “This gives us insight into what happens to the tissue. Look how much thicker all this interstitial collagen is ... with no evidence of fat necrosis or fat atrophy,” she said.
In addition, the study investigators found a significant increase in elastin in 10 weeks. “This is the first study to show this can happen in human skin. This is very exciting. It really demonstrates what this radiofrequency can do and where it’s going in the future,” Dr. Northington said.
Regarding all the advances in radiofrequency technology, Dr. Northington said, “If results are more consistent, [fractional radiofrequency] will be a real player in future for nonsurgical rejuvenation.”
Disclosures: Dr. Northington said she had no relevant disclosures.
Destin, Fla. — Fractional radiofrequency “is new and has a lot of promise” for skin tightening to rejuvenate the jaw and facial skin, according to Dr. Marian Northington.
Similar to fractional photothermolysis, a bipolar microneedle system creates zones of thermal damage in the reticulated dermis. These zones are surrounded by untreated dermis that speeds healing. The heat delivered alters the molecular structure of the triple helix of collagen and causes collagen contraction. The heat also stimulates a “vigorous wound healing response,” Dr. Northington said at a meeting sponsored by the Alabama Dermatology Society.
Another advantage of radiofrequency is that it uses electrical current and not a light source, so there is no damage to epidural melanin. Therefore, radiofrequency treatments are safe for all skin types, she said.
“It takes time, but you get thicker, healthier dermis,” Dr. Northington said. “As this improves slowly with time, it is important to take before pictures. Patients will forget with something that gradually occurs.”
On the plus side, there is no downtime compared with more invasive approaches to facial rejuvenation. However, “patients need appropriate expectations. Fractional radiofrequency does not yield a surgical result,” Dr. Northington said. Results are modest and sometimes not reproducible.
Nevertheless, “this has a lot of promise as a nonsurgical option ... for those who don’t want a face lift, but want some improvement,” said Dr. Northington of the University of Alabama at Birmingham.
She cited a recent study of 15 fractional radiofrequency patients, in which 5 blinded raters were asked to assess outcomes from photos (Arch. Dermatol. 2010;146:396-405). The investigators mixed in photos of surgical face-lift patients. There was an average 16% improvement with radiofrequency, compared with 44% for the face-lift patients. “Although improvement with face-lift was greater, it also showed improvement with radiofrequency,” Dr. Northington said.
Unlike with standard monopolar or bipolar radiofrequency, anesthesia is not necessary so patients can provide useful feedback that they feel the heat during the treatment, Dr. Northington said. “You know the energy is going where you want it.”
Energy is delivered at 72° C for 4 seconds while the epidermis is protected with cooling. The selective heating of fibrous septae in the subcutaneous area explains why we do not see fat atrophy with radiofrequency, Dr. Northington said.
By 10 weeks the skin has replaced areas of thermal damage, according to a study of 22 patients scheduled for abdominoplasty (Lasers Med. Surg. 2009;41:1-9). “This gives us insight into what happens to the tissue. Look how much thicker all this interstitial collagen is ... with no evidence of fat necrosis or fat atrophy,” she said.
In addition, the study investigators found a significant increase in elastin in 10 weeks. “This is the first study to show this can happen in human skin. This is very exciting. It really demonstrates what this radiofrequency can do and where it’s going in the future,” Dr. Northington said.
Regarding all the advances in radiofrequency technology, Dr. Northington said, “If results are more consistent, [fractional radiofrequency] will be a real player in future for nonsurgical rejuvenation.”
Disclosures: Dr. Northington said she had no relevant disclosures.
Destin, Fla. — Fractional radiofrequency “is new and has a lot of promise” for skin tightening to rejuvenate the jaw and facial skin, according to Dr. Marian Northington.
Similar to fractional photothermolysis, a bipolar microneedle system creates zones of thermal damage in the reticulated dermis. These zones are surrounded by untreated dermis that speeds healing. The heat delivered alters the molecular structure of the triple helix of collagen and causes collagen contraction. The heat also stimulates a “vigorous wound healing response,” Dr. Northington said at a meeting sponsored by the Alabama Dermatology Society.
Another advantage of radiofrequency is that it uses electrical current and not a light source, so there is no damage to epidural melanin. Therefore, radiofrequency treatments are safe for all skin types, she said.
“It takes time, but you get thicker, healthier dermis,” Dr. Northington said. “As this improves slowly with time, it is important to take before pictures. Patients will forget with something that gradually occurs.”
On the plus side, there is no downtime compared with more invasive approaches to facial rejuvenation. However, “patients need appropriate expectations. Fractional radiofrequency does not yield a surgical result,” Dr. Northington said. Results are modest and sometimes not reproducible.
Nevertheless, “this has a lot of promise as a nonsurgical option ... for those who don’t want a face lift, but want some improvement,” said Dr. Northington of the University of Alabama at Birmingham.
She cited a recent study of 15 fractional radiofrequency patients, in which 5 blinded raters were asked to assess outcomes from photos (Arch. Dermatol. 2010;146:396-405). The investigators mixed in photos of surgical face-lift patients. There was an average 16% improvement with radiofrequency, compared with 44% for the face-lift patients. “Although improvement with face-lift was greater, it also showed improvement with radiofrequency,” Dr. Northington said.
Unlike with standard monopolar or bipolar radiofrequency, anesthesia is not necessary so patients can provide useful feedback that they feel the heat during the treatment, Dr. Northington said. “You know the energy is going where you want it.”
Energy is delivered at 72° C for 4 seconds while the epidermis is protected with cooling. The selective heating of fibrous septae in the subcutaneous area explains why we do not see fat atrophy with radiofrequency, Dr. Northington said.
By 10 weeks the skin has replaced areas of thermal damage, according to a study of 22 patients scheduled for abdominoplasty (Lasers Med. Surg. 2009;41:1-9). “This gives us insight into what happens to the tissue. Look how much thicker all this interstitial collagen is ... with no evidence of fat necrosis or fat atrophy,” she said.
In addition, the study investigators found a significant increase in elastin in 10 weeks. “This is the first study to show this can happen in human skin. This is very exciting. It really demonstrates what this radiofrequency can do and where it’s going in the future,” Dr. Northington said.
Regarding all the advances in radiofrequency technology, Dr. Northington said, “If results are more consistent, [fractional radiofrequency] will be a real player in future for nonsurgical rejuvenation.”
Disclosures: Dr. Northington said she had no relevant disclosures.
Autologous Fat Injections Advised for Lipofilling
Naples, Fla. — Dermatologists can treat a range of anatomic areas with autologous fat injections—both to address aesthetic concerns and to optimize outcomes after reconstructive plastic surgery, Dr. Katharina Russe-Wilflingseder said.
Lipofilling is an appropriate technique to augment nasolabial folds, cheeks, and hands, as well as for aesthetic improvement after reconstruction breast surgery, for example. The advantages to this approach outweigh the drawbacks, although both should be considered, she said at the Annual Meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Dr. Russe-Wilflingseder recommended standard wet suction aspiration of a patient’s fat with a 2.5-mm to 3-mm cannula. She also is an advocate of minimal processing, or immediate reinjection of unwashed fat, using a 1.4-mm cannula.
“It is an excellent technique—I rarely use any fillers any more,” said Dr. Russe-Wilflingseder, an aesthetic plastic surgeon in private practice in Innsbruck, Austria.
She turned to the literature to answer some basic questions about autologous fat transplantation technique. For example, the “donor site does not seem to be important for cell survival,” she said. “It should be based on your own decision, the adiposity of donor site, and on the patient’s nomination.”
Some physicians ask whether liposuction or excision is best for fat harvesting. “If we look at the literature, this does not make a difference,” she commented. Excision or gentle aspiration is the generally recommended harvesting technique.
Most reports suggest a short and gentle centrifuge is the optimal processing technique. However, Dr. Russe-Wilflingseder keeps it even simpler. She uses a 10-cc filter syringe to immediately re-inject unwashed fat. “We believe it is very important to leave everything inside.”
Her strategy is to re-inject tiny amounts, using multiple passes and applying the autologous fat to different layers using a fine cannula.
In addition, more fat is preferred to less, she said. “We believe it is better to overcorrect than to undercorrect” in part because a sufficient amount of fat is necessary for revascularization, which takes up to 7-21 days.
Redness of the skin the day after the operation is a common adverse event, Dr. Russe-Wilflingseder said. As with any invasive procedure, there is a risk of infection as well. Otherwise, “there are nearly no side effects.”
An inability to predict the stability and longevity of the fat grafts is another potential drawback to autologous lipofilling, she said. “Our experience is that about 50% [of injected fat] stays alive” in the long term. Another concern is the availability of donor site adiposity. For example, more fat is required to correct after reconstructive breast surgery. One patient, for example, required two treatments with a total 100 cc of fat.
On the plus side, fat injections can improve not only volume but the appearance of scarring after breast tumor resection. Other advantages relate to the “ideal properties” of autologous fat: It is easily available, adaptable, and takes little time to harvest and re-inject, Dr. Russe-Wilflingseder said.
She reported success with many different applications to fill soft tissue and contour defects, some done in combination with submental tissue tightening or carbon dioxide laser resurfacing. For example, 10 to 20 cc of autologous fat injected in the upper nasolabial folds yields great long-term results, she said. For another patient, 10 cc of fat rejuvenated the appearance of their hands. “The quality of the skin improves a lot after the lipofilling.”
Disclosures: Dr. Russe-Wilflingseder said she had no relevant financial disclosures.
Naples, Fla. — Dermatologists can treat a range of anatomic areas with autologous fat injections—both to address aesthetic concerns and to optimize outcomes after reconstructive plastic surgery, Dr. Katharina Russe-Wilflingseder said.
Lipofilling is an appropriate technique to augment nasolabial folds, cheeks, and hands, as well as for aesthetic improvement after reconstruction breast surgery, for example. The advantages to this approach outweigh the drawbacks, although both should be considered, she said at the Annual Meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Dr. Russe-Wilflingseder recommended standard wet suction aspiration of a patient’s fat with a 2.5-mm to 3-mm cannula. She also is an advocate of minimal processing, or immediate reinjection of unwashed fat, using a 1.4-mm cannula.
“It is an excellent technique—I rarely use any fillers any more,” said Dr. Russe-Wilflingseder, an aesthetic plastic surgeon in private practice in Innsbruck, Austria.
She turned to the literature to answer some basic questions about autologous fat transplantation technique. For example, the “donor site does not seem to be important for cell survival,” she said. “It should be based on your own decision, the adiposity of donor site, and on the patient’s nomination.”
Some physicians ask whether liposuction or excision is best for fat harvesting. “If we look at the literature, this does not make a difference,” she commented. Excision or gentle aspiration is the generally recommended harvesting technique.
Most reports suggest a short and gentle centrifuge is the optimal processing technique. However, Dr. Russe-Wilflingseder keeps it even simpler. She uses a 10-cc filter syringe to immediately re-inject unwashed fat. “We believe it is very important to leave everything inside.”
Her strategy is to re-inject tiny amounts, using multiple passes and applying the autologous fat to different layers using a fine cannula.
In addition, more fat is preferred to less, she said. “We believe it is better to overcorrect than to undercorrect” in part because a sufficient amount of fat is necessary for revascularization, which takes up to 7-21 days.
Redness of the skin the day after the operation is a common adverse event, Dr. Russe-Wilflingseder said. As with any invasive procedure, there is a risk of infection as well. Otherwise, “there are nearly no side effects.”
An inability to predict the stability and longevity of the fat grafts is another potential drawback to autologous lipofilling, she said. “Our experience is that about 50% [of injected fat] stays alive” in the long term. Another concern is the availability of donor site adiposity. For example, more fat is required to correct after reconstructive breast surgery. One patient, for example, required two treatments with a total 100 cc of fat.
On the plus side, fat injections can improve not only volume but the appearance of scarring after breast tumor resection. Other advantages relate to the “ideal properties” of autologous fat: It is easily available, adaptable, and takes little time to harvest and re-inject, Dr. Russe-Wilflingseder said.
She reported success with many different applications to fill soft tissue and contour defects, some done in combination with submental tissue tightening or carbon dioxide laser resurfacing. For example, 10 to 20 cc of autologous fat injected in the upper nasolabial folds yields great long-term results, she said. For another patient, 10 cc of fat rejuvenated the appearance of their hands. “The quality of the skin improves a lot after the lipofilling.”
Disclosures: Dr. Russe-Wilflingseder said she had no relevant financial disclosures.
Naples, Fla. — Dermatologists can treat a range of anatomic areas with autologous fat injections—both to address aesthetic concerns and to optimize outcomes after reconstructive plastic surgery, Dr. Katharina Russe-Wilflingseder said.
Lipofilling is an appropriate technique to augment nasolabial folds, cheeks, and hands, as well as for aesthetic improvement after reconstruction breast surgery, for example. The advantages to this approach outweigh the drawbacks, although both should be considered, she said at the Annual Meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Dr. Russe-Wilflingseder recommended standard wet suction aspiration of a patient’s fat with a 2.5-mm to 3-mm cannula. She also is an advocate of minimal processing, or immediate reinjection of unwashed fat, using a 1.4-mm cannula.
“It is an excellent technique—I rarely use any fillers any more,” said Dr. Russe-Wilflingseder, an aesthetic plastic surgeon in private practice in Innsbruck, Austria.
She turned to the literature to answer some basic questions about autologous fat transplantation technique. For example, the “donor site does not seem to be important for cell survival,” she said. “It should be based on your own decision, the adiposity of donor site, and on the patient’s nomination.”
Some physicians ask whether liposuction or excision is best for fat harvesting. “If we look at the literature, this does not make a difference,” she commented. Excision or gentle aspiration is the generally recommended harvesting technique.
Most reports suggest a short and gentle centrifuge is the optimal processing technique. However, Dr. Russe-Wilflingseder keeps it even simpler. She uses a 10-cc filter syringe to immediately re-inject unwashed fat. “We believe it is very important to leave everything inside.”
Her strategy is to re-inject tiny amounts, using multiple passes and applying the autologous fat to different layers using a fine cannula.
In addition, more fat is preferred to less, she said. “We believe it is better to overcorrect than to undercorrect” in part because a sufficient amount of fat is necessary for revascularization, which takes up to 7-21 days.
Redness of the skin the day after the operation is a common adverse event, Dr. Russe-Wilflingseder said. As with any invasive procedure, there is a risk of infection as well. Otherwise, “there are nearly no side effects.”
An inability to predict the stability and longevity of the fat grafts is another potential drawback to autologous lipofilling, she said. “Our experience is that about 50% [of injected fat] stays alive” in the long term. Another concern is the availability of donor site adiposity. For example, more fat is required to correct after reconstructive breast surgery. One patient, for example, required two treatments with a total 100 cc of fat.
On the plus side, fat injections can improve not only volume but the appearance of scarring after breast tumor resection. Other advantages relate to the “ideal properties” of autologous fat: It is easily available, adaptable, and takes little time to harvest and re-inject, Dr. Russe-Wilflingseder said.
She reported success with many different applications to fill soft tissue and contour defects, some done in combination with submental tissue tightening or carbon dioxide laser resurfacing. For example, 10 to 20 cc of autologous fat injected in the upper nasolabial folds yields great long-term results, she said. For another patient, 10 cc of fat rejuvenated the appearance of their hands. “The quality of the skin improves a lot after the lipofilling.”
Disclosures: Dr. Russe-Wilflingseder said she had no relevant financial disclosures.
Survey of Primary Care Docs Suggests Greater Need for Bipolar Disorder Education
BOCA RATON, Fla. – Many family physicians do not feel adequately prepared to diagnose and treat bipolar disorder, based on a survey of 77 family physicians.
“When these mentally ill patients ... present in a primary care setting, it is a critical opportunity to intervene,” according to Purvi Kobawala Smith.
Diagnosis and management of bipolar disorder can be complex, given that patients can present with severe depression, severe mania, mixed mood states, rapid cycling, and/or comorbidities. This might explain in part the results of previous studies suggesting that bipolar disorder often can be misunderstood or misdiagnosed in primary care settings (JAMA 2005; 293;956-63; J. Clin. Psychiatry 2003;64:53-9).
“Many [patients] get misdiagnosed with depression and get sent down an entirely wrong treatment path,” Ms. Smith said in an interview at her poster during the New Clinical Drug Evaluation Unit meeting sponsored by the National Institute of Mental Health.
To evaluate family physicians’ educational needs regarding this disorder, Ms. Smith and her colleagues mailed surveys to 900 family physicians in January 2009. The 77 respondents (a 9% response rate) rated their own preparedness regarding screening for bipolar disorder, discussion of comorbidities, evaluation of the phase of bipolar disorder based on symptoms, discussion of psychotherapy and pharmacologic options, and development of a treatment plan.
“By and large, the majority rated themselves as ‘not very prepared’ or ‘somewhat prepared,’” said Ms. Smith, scientific director for a medical education company in Ramsey, N.J.
More than half felt this way, for example, when asked about their ability to assess for bipolar disorder using a screening tool or interviewing techniques (36 of 69 respondents, or 52%). Another 36% felt prepared and 12%, very prepared.
Regarding discussion of comorbidities, 53% of 68 felt they were not very prepared or were only somewhat prepared, 41% were prepared, and 6% were very prepared.
Regarding diagnosis of the phase of the disorder based on symptoms, 51% of 69 physicians felt not very or somewhat prepared, 39% felt prepared, and 10% felt very prepared.
Respondents rated themselves as less prepared to discuss psychotherapy options. For example, 64% of 67 physicians said they were not very prepared or were only somewhat prepared. Another 30% said they were prepared and only 6% were very prepared.
More family physicians said they were prepared or very prepared to discuss pharmacologic treatments: In all, 58% were not very prepared or only somewhat prepared, 33% were prepared, and 9% were very prepared.
Mood symptoms are common in primary care practices, Ms. Smith said. About 23% of their patients regularly complain of mood symptoms, according to 59 family physicians who answered this question.
Primary care physicians play an integral role in the initiation of treatment, especially when there are no psychiatrists in the local community for referral, Ms. Smith said. But she acknowledged that learning more about bipolar disorder may not be easy: “This is a challenge for primary care physicians, given their [time] constraints.”
Along with Dr. Jennifer Payne of the department of psychiatry and behavioral sciences at Johns Hopkins University in Baltimore, who was the lead investigator of the study, Ms. Smith and others developed a free online course. Dr. Payne is the course director.
The survey and online course are supported by a grant from Eli Lilly and Co. Ms. Smith said she had no relevant disclosures. Dr. Payne is a consultant for AstraZeneca and Wyeth and receives honoraria from Wyeth.
BOCA RATON, Fla. – Many family physicians do not feel adequately prepared to diagnose and treat bipolar disorder, based on a survey of 77 family physicians.
“When these mentally ill patients ... present in a primary care setting, it is a critical opportunity to intervene,” according to Purvi Kobawala Smith.
Diagnosis and management of bipolar disorder can be complex, given that patients can present with severe depression, severe mania, mixed mood states, rapid cycling, and/or comorbidities. This might explain in part the results of previous studies suggesting that bipolar disorder often can be misunderstood or misdiagnosed in primary care settings (JAMA 2005; 293;956-63; J. Clin. Psychiatry 2003;64:53-9).
“Many [patients] get misdiagnosed with depression and get sent down an entirely wrong treatment path,” Ms. Smith said in an interview at her poster during the New Clinical Drug Evaluation Unit meeting sponsored by the National Institute of Mental Health.
To evaluate family physicians’ educational needs regarding this disorder, Ms. Smith and her colleagues mailed surveys to 900 family physicians in January 2009. The 77 respondents (a 9% response rate) rated their own preparedness regarding screening for bipolar disorder, discussion of comorbidities, evaluation of the phase of bipolar disorder based on symptoms, discussion of psychotherapy and pharmacologic options, and development of a treatment plan.
“By and large, the majority rated themselves as ‘not very prepared’ or ‘somewhat prepared,’” said Ms. Smith, scientific director for a medical education company in Ramsey, N.J.
More than half felt this way, for example, when asked about their ability to assess for bipolar disorder using a screening tool or interviewing techniques (36 of 69 respondents, or 52%). Another 36% felt prepared and 12%, very prepared.
Regarding discussion of comorbidities, 53% of 68 felt they were not very prepared or were only somewhat prepared, 41% were prepared, and 6% were very prepared.
Regarding diagnosis of the phase of the disorder based on symptoms, 51% of 69 physicians felt not very or somewhat prepared, 39% felt prepared, and 10% felt very prepared.
Respondents rated themselves as less prepared to discuss psychotherapy options. For example, 64% of 67 physicians said they were not very prepared or were only somewhat prepared. Another 30% said they were prepared and only 6% were very prepared.
More family physicians said they were prepared or very prepared to discuss pharmacologic treatments: In all, 58% were not very prepared or only somewhat prepared, 33% were prepared, and 9% were very prepared.
Mood symptoms are common in primary care practices, Ms. Smith said. About 23% of their patients regularly complain of mood symptoms, according to 59 family physicians who answered this question.
Primary care physicians play an integral role in the initiation of treatment, especially when there are no psychiatrists in the local community for referral, Ms. Smith said. But she acknowledged that learning more about bipolar disorder may not be easy: “This is a challenge for primary care physicians, given their [time] constraints.”
Along with Dr. Jennifer Payne of the department of psychiatry and behavioral sciences at Johns Hopkins University in Baltimore, who was the lead investigator of the study, Ms. Smith and others developed a free online course. Dr. Payne is the course director.
The survey and online course are supported by a grant from Eli Lilly and Co. Ms. Smith said she had no relevant disclosures. Dr. Payne is a consultant for AstraZeneca and Wyeth and receives honoraria from Wyeth.
BOCA RATON, Fla. – Many family physicians do not feel adequately prepared to diagnose and treat bipolar disorder, based on a survey of 77 family physicians.
“When these mentally ill patients ... present in a primary care setting, it is a critical opportunity to intervene,” according to Purvi Kobawala Smith.
Diagnosis and management of bipolar disorder can be complex, given that patients can present with severe depression, severe mania, mixed mood states, rapid cycling, and/or comorbidities. This might explain in part the results of previous studies suggesting that bipolar disorder often can be misunderstood or misdiagnosed in primary care settings (JAMA 2005; 293;956-63; J. Clin. Psychiatry 2003;64:53-9).
“Many [patients] get misdiagnosed with depression and get sent down an entirely wrong treatment path,” Ms. Smith said in an interview at her poster during the New Clinical Drug Evaluation Unit meeting sponsored by the National Institute of Mental Health.
To evaluate family physicians’ educational needs regarding this disorder, Ms. Smith and her colleagues mailed surveys to 900 family physicians in January 2009. The 77 respondents (a 9% response rate) rated their own preparedness regarding screening for bipolar disorder, discussion of comorbidities, evaluation of the phase of bipolar disorder based on symptoms, discussion of psychotherapy and pharmacologic options, and development of a treatment plan.
“By and large, the majority rated themselves as ‘not very prepared’ or ‘somewhat prepared,’” said Ms. Smith, scientific director for a medical education company in Ramsey, N.J.
More than half felt this way, for example, when asked about their ability to assess for bipolar disorder using a screening tool or interviewing techniques (36 of 69 respondents, or 52%). Another 36% felt prepared and 12%, very prepared.
Regarding discussion of comorbidities, 53% of 68 felt they were not very prepared or were only somewhat prepared, 41% were prepared, and 6% were very prepared.
Regarding diagnosis of the phase of the disorder based on symptoms, 51% of 69 physicians felt not very or somewhat prepared, 39% felt prepared, and 10% felt very prepared.
Respondents rated themselves as less prepared to discuss psychotherapy options. For example, 64% of 67 physicians said they were not very prepared or were only somewhat prepared. Another 30% said they were prepared and only 6% were very prepared.
More family physicians said they were prepared or very prepared to discuss pharmacologic treatments: In all, 58% were not very prepared or only somewhat prepared, 33% were prepared, and 9% were very prepared.
Mood symptoms are common in primary care practices, Ms. Smith said. About 23% of their patients regularly complain of mood symptoms, according to 59 family physicians who answered this question.
Primary care physicians play an integral role in the initiation of treatment, especially when there are no psychiatrists in the local community for referral, Ms. Smith said. But she acknowledged that learning more about bipolar disorder may not be easy: “This is a challenge for primary care physicians, given their [time] constraints.”
Along with Dr. Jennifer Payne of the department of psychiatry and behavioral sciences at Johns Hopkins University in Baltimore, who was the lead investigator of the study, Ms. Smith and others developed a free online course. Dr. Payne is the course director.
The survey and online course are supported by a grant from Eli Lilly and Co. Ms. Smith said she had no relevant disclosures. Dr. Payne is a consultant for AstraZeneca and Wyeth and receives honoraria from Wyeth.
Major Finding: Survey finds 52% of 69 family physicians feel “not very prepared” or “somewhat prepared” to screen for bipolar disorder, 36% feel “prepared,” and 12% feel “very prepared.”
Data Source: Survey mailed to family physicians nationwide in January 2009.
Disclosures: The survey and online course are supported by a grant from Eli Lilly. Ms. Smith said she had no relevant disclosures. Dr. Payne is a consultant for AstraZeneca and Wyeth and receives honoraria from Wyeth.
Avoiding Pitfalls, Complications in Reconstructive Surgery
Naples, Fla. - Before you start dermatologic reconstructive surgery, know the potential adverse events well, Dr. Keyvan Nouri said.
“It is important to be aware of complications, how to prevent them, and if they do occur, how to manage them,” he said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Bleeding, hematoma, nerve damage, infection, and contact dermatitis are among the adverse sequelae possible after surgery, Dr. Nouri said.
Acute bleeding is one of the most common complications in the immediate postoperative period, for example. Patients taking medications that alter hemostasis -- including aspirin, heparin, or warfarin -- are at higher risk, as are people with hypertension. “We don’t normally check blood pressure ... but [this] may be something you want to consider before surgery,” said Dr. Nouri, director of Mohs, Dermatologic and Laser Surgery at the University of Miami Leonard M. Miller School of Medicine.
To prevent medication-related bleeding, consult the prescribing physician to suggest discontinuation of the agent(s) prior to surgery, Dr. Nouri said. “We as dermatologists really have no role for stopping aspirin, Plavix, etc., beforehand.”
Strategies dermatologic surgeons can employ to minimize bleeding include use of sutures to ligate vessels, use of meticulous hemostasis during a procedure, and use of absorbable gel sponges to collect oozing from muscle and fascia, Dr. Nouri said. Also, observe areas at risk for bleeding for 10-15 minutes prior to closure if using uninterrupted sutures.
Pressure dressings help postoperatively. “Instruct patients to keep them on at least 48 hours,” he said.
A hematoma is another possible surgical complication. This “should be managed by urgently removing sutures and draining the hematoma,” Dr. Nouri said. If the bleeding does not stop, reopen the wound until you achieve hemostasis. If you place a drain to facilitate drainage, remember to remove it within 48 hours to avoid a heightened risk of infection.
Ecchymoses, another surgical complication, can be common, Dr. Nouri said, particularly when operating around the eyes or forehead. It results from blood passing through soft tissue planes. Instruct patients to apply ice on a regular basis postoperatively to minimize this effect.
Knowing your anatomy is essential to avoid damage to nerves or vital organs during surgery, Dr. Nouri said. “Know the facial danger zones.” The temporal area and angle of the jaw are examples. If the temporal nerve is damaged, the patient might be unable to lift their eyebrow after surgery. Also, an asymmetrical smile can result from damage to the submandibular branch at the angle of the jaw, he said.
Tendons also can be cut during surgery. Keep in mind that tendons become more superficial as you go more distally on the hands or lower extremities. “If a tendon is cut, we cannot repair it,” Dr. Nouri said. “The patient needs to be referred.”
The good news regarding contact dermatitis is it “used to happen a lot more in derm surgery,” Dr. Nouri said. Topical antibiotics, tapes and wound dressings, and nickel-plated surgical instruments can cause contact allergies. Watch for red, pruritic, or occasionally, vesiculated and crusted plaques. One tip is that pruritus is common with contact dermatitis, versus tenderness associated with infection.
Acute infections are rare in most dermatologic surgery patients, although immunosuppressed patients or those with uncontrolled diabetes are at higher risk, Dr. Nouri said. Malnutrition, obesity, smoking, and chronic use of steroids are other risk factors.
Also, remember to instruct patients not to shave prior to surgery. “Shaving less than 24 hours prior to surgery increases the risk of infection many times,” he noted.
Dermatologic surgery on a lower extremity carries a higher risk for infection, Dr. Nouri said. “Whenever I operate on someone’s legs, I use prophylactic antibiotics.”
Know that these and other adverse outcomes from surgery can occur, Dr. Nouri said. “Following the principles of tissue closure and antiseptic techniques will minimize these complications.”
Disclosures: Dr. Nouri said he had no relevant financial disclosures.
Naples, Fla. - Before you start dermatologic reconstructive surgery, know the potential adverse events well, Dr. Keyvan Nouri said.
“It is important to be aware of complications, how to prevent them, and if they do occur, how to manage them,” he said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Bleeding, hematoma, nerve damage, infection, and contact dermatitis are among the adverse sequelae possible after surgery, Dr. Nouri said.
Acute bleeding is one of the most common complications in the immediate postoperative period, for example. Patients taking medications that alter hemostasis -- including aspirin, heparin, or warfarin -- are at higher risk, as are people with hypertension. “We don’t normally check blood pressure ... but [this] may be something you want to consider before surgery,” said Dr. Nouri, director of Mohs, Dermatologic and Laser Surgery at the University of Miami Leonard M. Miller School of Medicine.
To prevent medication-related bleeding, consult the prescribing physician to suggest discontinuation of the agent(s) prior to surgery, Dr. Nouri said. “We as dermatologists really have no role for stopping aspirin, Plavix, etc., beforehand.”
Strategies dermatologic surgeons can employ to minimize bleeding include use of sutures to ligate vessels, use of meticulous hemostasis during a procedure, and use of absorbable gel sponges to collect oozing from muscle and fascia, Dr. Nouri said. Also, observe areas at risk for bleeding for 10-15 minutes prior to closure if using uninterrupted sutures.
Pressure dressings help postoperatively. “Instruct patients to keep them on at least 48 hours,” he said.
A hematoma is another possible surgical complication. This “should be managed by urgently removing sutures and draining the hematoma,” Dr. Nouri said. If the bleeding does not stop, reopen the wound until you achieve hemostasis. If you place a drain to facilitate drainage, remember to remove it within 48 hours to avoid a heightened risk of infection.
Ecchymoses, another surgical complication, can be common, Dr. Nouri said, particularly when operating around the eyes or forehead. It results from blood passing through soft tissue planes. Instruct patients to apply ice on a regular basis postoperatively to minimize this effect.
Knowing your anatomy is essential to avoid damage to nerves or vital organs during surgery, Dr. Nouri said. “Know the facial danger zones.” The temporal area and angle of the jaw are examples. If the temporal nerve is damaged, the patient might be unable to lift their eyebrow after surgery. Also, an asymmetrical smile can result from damage to the submandibular branch at the angle of the jaw, he said.
Tendons also can be cut during surgery. Keep in mind that tendons become more superficial as you go more distally on the hands or lower extremities. “If a tendon is cut, we cannot repair it,” Dr. Nouri said. “The patient needs to be referred.”
The good news regarding contact dermatitis is it “used to happen a lot more in derm surgery,” Dr. Nouri said. Topical antibiotics, tapes and wound dressings, and nickel-plated surgical instruments can cause contact allergies. Watch for red, pruritic, or occasionally, vesiculated and crusted plaques. One tip is that pruritus is common with contact dermatitis, versus tenderness associated with infection.
Acute infections are rare in most dermatologic surgery patients, although immunosuppressed patients or those with uncontrolled diabetes are at higher risk, Dr. Nouri said. Malnutrition, obesity, smoking, and chronic use of steroids are other risk factors.
Also, remember to instruct patients not to shave prior to surgery. “Shaving less than 24 hours prior to surgery increases the risk of infection many times,” he noted.
Dermatologic surgery on a lower extremity carries a higher risk for infection, Dr. Nouri said. “Whenever I operate on someone’s legs, I use prophylactic antibiotics.”
Know that these and other adverse outcomes from surgery can occur, Dr. Nouri said. “Following the principles of tissue closure and antiseptic techniques will minimize these complications.”
Disclosures: Dr. Nouri said he had no relevant financial disclosures.
Naples, Fla. - Before you start dermatologic reconstructive surgery, know the potential adverse events well, Dr. Keyvan Nouri said.
“It is important to be aware of complications, how to prevent them, and if they do occur, how to manage them,” he said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons
Bleeding, hematoma, nerve damage, infection, and contact dermatitis are among the adverse sequelae possible after surgery, Dr. Nouri said.
Acute bleeding is one of the most common complications in the immediate postoperative period, for example. Patients taking medications that alter hemostasis -- including aspirin, heparin, or warfarin -- are at higher risk, as are people with hypertension. “We don’t normally check blood pressure ... but [this] may be something you want to consider before surgery,” said Dr. Nouri, director of Mohs, Dermatologic and Laser Surgery at the University of Miami Leonard M. Miller School of Medicine.
To prevent medication-related bleeding, consult the prescribing physician to suggest discontinuation of the agent(s) prior to surgery, Dr. Nouri said. “We as dermatologists really have no role for stopping aspirin, Plavix, etc., beforehand.”
Strategies dermatologic surgeons can employ to minimize bleeding include use of sutures to ligate vessels, use of meticulous hemostasis during a procedure, and use of absorbable gel sponges to collect oozing from muscle and fascia, Dr. Nouri said. Also, observe areas at risk for bleeding for 10-15 minutes prior to closure if using uninterrupted sutures.
Pressure dressings help postoperatively. “Instruct patients to keep them on at least 48 hours,” he said.
A hematoma is another possible surgical complication. This “should be managed by urgently removing sutures and draining the hematoma,” Dr. Nouri said. If the bleeding does not stop, reopen the wound until you achieve hemostasis. If you place a drain to facilitate drainage, remember to remove it within 48 hours to avoid a heightened risk of infection.
Ecchymoses, another surgical complication, can be common, Dr. Nouri said, particularly when operating around the eyes or forehead. It results from blood passing through soft tissue planes. Instruct patients to apply ice on a regular basis postoperatively to minimize this effect.
Knowing your anatomy is essential to avoid damage to nerves or vital organs during surgery, Dr. Nouri said. “Know the facial danger zones.” The temporal area and angle of the jaw are examples. If the temporal nerve is damaged, the patient might be unable to lift their eyebrow after surgery. Also, an asymmetrical smile can result from damage to the submandibular branch at the angle of the jaw, he said.
Tendons also can be cut during surgery. Keep in mind that tendons become more superficial as you go more distally on the hands or lower extremities. “If a tendon is cut, we cannot repair it,” Dr. Nouri said. “The patient needs to be referred.”
The good news regarding contact dermatitis is it “used to happen a lot more in derm surgery,” Dr. Nouri said. Topical antibiotics, tapes and wound dressings, and nickel-plated surgical instruments can cause contact allergies. Watch for red, pruritic, or occasionally, vesiculated and crusted plaques. One tip is that pruritus is common with contact dermatitis, versus tenderness associated with infection.
Acute infections are rare in most dermatologic surgery patients, although immunosuppressed patients or those with uncontrolled diabetes are at higher risk, Dr. Nouri said. Malnutrition, obesity, smoking, and chronic use of steroids are other risk factors.
Also, remember to instruct patients not to shave prior to surgery. “Shaving less than 24 hours prior to surgery increases the risk of infection many times,” he noted.
Dermatologic surgery on a lower extremity carries a higher risk for infection, Dr. Nouri said. “Whenever I operate on someone’s legs, I use prophylactic antibiotics.”
Know that these and other adverse outcomes from surgery can occur, Dr. Nouri said. “Following the principles of tissue closure and antiseptic techniques will minimize these complications.”
Disclosures: Dr. Nouri said he had no relevant financial disclosures.
Cryolipolysis Offers Results for Fat Removal
Naples, Fla. - Effective, noninvasive fat removal is here, according to Dr. Mathew Avram.
"Efficacy is limited but it is real," he said regarding cryolipolysis, a noninvasive cooling and removal of subcutaneous fat.
It is important for dermatologists to assess all emerging noninvasive fat-reduction technologies critically.
"Patients will ask you about this," Dr. Avram said. "There is a lot of snake-oil salesmanship in this field."
Cryolipolysis (CoolSculpting, Zeltiq Aesthetics) selectively kills fat cells at temperatures above freezing without affecting surrounding tissues. This selective crystallization of fat cells leads to apoptotic death and, ultimately, gradual dissolution of fat over 2-4 months, Dr. Avram said.
In 2009, researchers reported a 22% reduction in "love handles" on the side treated with cryolipolysis, compared with the side with no treatment at 4 months in an unpublished study with 32 participants.
"Whether or not that is clinically relevant is up to you to decide," Dr. Avram said at the meeting.
Results of animal studies are more robust. For example, one study conducted by researchers at the Wellman Center for Photomedicine in Boston demonstrated a 40% decrease in fat layer of pigs over 90 days on ultrasound and gross pathology (Laser Surg. Med. 2008;40:595-604).
Cryolipolysis has been approved by the Food and Drug Administration for various skin cooling applications during dermatology procedures, but the CoolSculpting device is not FDA cleared for marketing as a fat removal device, Dr. Avram said, although regulatory approval for noninvasive fat reduction is pending.
Cryolipolysis is not a weight loss device, nor is it intended as a replacement for liposuction, said Dr. Avram, director of the Massachusetts General Hospital Dermatology Laser and Cosmetic Center.
Cryolipolysis is best suited for local fat removal in areas resistant to exercise, such as love handles or the lower abdomen, Dr. Avram said, and "patient selection is crucial." Relatively thin, weight-stable people who have localized fat areas and realistic expectations are appropriate candidates. "Otherwise, patients will be disappointed. We avoid that with very careful patient selection," he said.
"We got this device at Mass General a few months ago," said Dr. Avram, who tried it himself.
Dr. R. Rox Anderson applied the gel sheet "over my love handle area [and] left it on for an hour," he said, noting that it got a little cold and the area became anesthetized after 7-8 minutes.
He reported a minor urticarial plaque on the area immediately after treatment. Redness for a few minutes to a few hours is a common postprocedure effect, as is bruising for up to a few weeks, although "not all will get it," Dr. Avram said.
A temporary dulling of sensation in the treated area that typically resolves in 1-8 weeks can also occur. No changes in pigmentation have been reported.
Dermatologists are the perfect physicians to perform cryolipolysis, Dr. Avram said. "Subcutaneous fat is a fundamental part of dermatology, and the fact that it has not been claimed by any specialty makes it ours."
Disclosures: Dr. Avram said he owns stock options and is a consultant for Zeltiq Aesthetics, Inc.
Naples, Fla. - Effective, noninvasive fat removal is here, according to Dr. Mathew Avram.
"Efficacy is limited but it is real," he said regarding cryolipolysis, a noninvasive cooling and removal of subcutaneous fat.
It is important for dermatologists to assess all emerging noninvasive fat-reduction technologies critically.
"Patients will ask you about this," Dr. Avram said. "There is a lot of snake-oil salesmanship in this field."
Cryolipolysis (CoolSculpting, Zeltiq Aesthetics) selectively kills fat cells at temperatures above freezing without affecting surrounding tissues. This selective crystallization of fat cells leads to apoptotic death and, ultimately, gradual dissolution of fat over 2-4 months, Dr. Avram said.
In 2009, researchers reported a 22% reduction in "love handles" on the side treated with cryolipolysis, compared with the side with no treatment at 4 months in an unpublished study with 32 participants.
"Whether or not that is clinically relevant is up to you to decide," Dr. Avram said at the meeting.
Results of animal studies are more robust. For example, one study conducted by researchers at the Wellman Center for Photomedicine in Boston demonstrated a 40% decrease in fat layer of pigs over 90 days on ultrasound and gross pathology (Laser Surg. Med. 2008;40:595-604).
Cryolipolysis has been approved by the Food and Drug Administration for various skin cooling applications during dermatology procedures, but the CoolSculpting device is not FDA cleared for marketing as a fat removal device, Dr. Avram said, although regulatory approval for noninvasive fat reduction is pending.
Cryolipolysis is not a weight loss device, nor is it intended as a replacement for liposuction, said Dr. Avram, director of the Massachusetts General Hospital Dermatology Laser and Cosmetic Center.
Cryolipolysis is best suited for local fat removal in areas resistant to exercise, such as love handles or the lower abdomen, Dr. Avram said, and "patient selection is crucial." Relatively thin, weight-stable people who have localized fat areas and realistic expectations are appropriate candidates. "Otherwise, patients will be disappointed. We avoid that with very careful patient selection," he said.
"We got this device at Mass General a few months ago," said Dr. Avram, who tried it himself.
Dr. R. Rox Anderson applied the gel sheet "over my love handle area [and] left it on for an hour," he said, noting that it got a little cold and the area became anesthetized after 7-8 minutes.
He reported a minor urticarial plaque on the area immediately after treatment. Redness for a few minutes to a few hours is a common postprocedure effect, as is bruising for up to a few weeks, although "not all will get it," Dr. Avram said.
A temporary dulling of sensation in the treated area that typically resolves in 1-8 weeks can also occur. No changes in pigmentation have been reported.
Dermatologists are the perfect physicians to perform cryolipolysis, Dr. Avram said. "Subcutaneous fat is a fundamental part of dermatology, and the fact that it has not been claimed by any specialty makes it ours."
Disclosures: Dr. Avram said he owns stock options and is a consultant for Zeltiq Aesthetics, Inc.
Naples, Fla. - Effective, noninvasive fat removal is here, according to Dr. Mathew Avram.
"Efficacy is limited but it is real," he said regarding cryolipolysis, a noninvasive cooling and removal of subcutaneous fat.
It is important for dermatologists to assess all emerging noninvasive fat-reduction technologies critically.
"Patients will ask you about this," Dr. Avram said. "There is a lot of snake-oil salesmanship in this field."
Cryolipolysis (CoolSculpting, Zeltiq Aesthetics) selectively kills fat cells at temperatures above freezing without affecting surrounding tissues. This selective crystallization of fat cells leads to apoptotic death and, ultimately, gradual dissolution of fat over 2-4 months, Dr. Avram said.
In 2009, researchers reported a 22% reduction in "love handles" on the side treated with cryolipolysis, compared with the side with no treatment at 4 months in an unpublished study with 32 participants.
"Whether or not that is clinically relevant is up to you to decide," Dr. Avram said at the meeting.
Results of animal studies are more robust. For example, one study conducted by researchers at the Wellman Center for Photomedicine in Boston demonstrated a 40% decrease in fat layer of pigs over 90 days on ultrasound and gross pathology (Laser Surg. Med. 2008;40:595-604).
Cryolipolysis has been approved by the Food and Drug Administration for various skin cooling applications during dermatology procedures, but the CoolSculpting device is not FDA cleared for marketing as a fat removal device, Dr. Avram said, although regulatory approval for noninvasive fat reduction is pending.
Cryolipolysis is not a weight loss device, nor is it intended as a replacement for liposuction, said Dr. Avram, director of the Massachusetts General Hospital Dermatology Laser and Cosmetic Center.
Cryolipolysis is best suited for local fat removal in areas resistant to exercise, such as love handles or the lower abdomen, Dr. Avram said, and "patient selection is crucial." Relatively thin, weight-stable people who have localized fat areas and realistic expectations are appropriate candidates. "Otherwise, patients will be disappointed. We avoid that with very careful patient selection," he said.
"We got this device at Mass General a few months ago," said Dr. Avram, who tried it himself.
Dr. R. Rox Anderson applied the gel sheet "over my love handle area [and] left it on for an hour," he said, noting that it got a little cold and the area became anesthetized after 7-8 minutes.
He reported a minor urticarial plaque on the area immediately after treatment. Redness for a few minutes to a few hours is a common postprocedure effect, as is bruising for up to a few weeks, although "not all will get it," Dr. Avram said.
A temporary dulling of sensation in the treated area that typically resolves in 1-8 weeks can also occur. No changes in pigmentation have been reported.
Dermatologists are the perfect physicians to perform cryolipolysis, Dr. Avram said. "Subcutaneous fat is a fundamental part of dermatology, and the fact that it has not been claimed by any specialty makes it ours."
Disclosures: Dr. Avram said he owns stock options and is a consultant for Zeltiq Aesthetics, Inc.
Expert analysis from the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery
Tips to Improve Derm Surgery Cutting and Suturing
DESTIN, Fla. — It might look easy, but getting a perfect result after dermatologic surgery takes skill and experience, Dr. Christopher J. Miller said.
For dermatologists who are relatively new to incision, excision, and undermining, there are multiple opportunities to assess your expertise during and after surgery. These “quality control checkpoints” include the assessment of incision depth and uniformity of the cut, as well as using your fingers to check for any gaps in your suture line, Dr. Miller said.
Results 1 week after surgery, in particular, provide important feedback on your surgical technique, he said. The goal at 1-week suture removal is wound edges that are sealed and blended together well with minimal inflammation.
“It takes a lot of work to figure out how to do that,” he said.
Recognize that technical errors in the early stages of excision affect subsequent results, said Dr. Miller, director of dermatologic surgery at the University of Pennsylvania, Philadelphia.
-- Incision. Avoid the tendency to bevel edges during incision, because this prevents proper apposition. The goal is for a vertical wound with no internal bevel, so ensure that your scalpel remains perpendicular to the skin.
“If those wound edges cannot come together … you will be forced to have tension on the wound,” which almost guarantees that track marks will develop along the wound, Dr. Miller said.
And make sure you incise all the way through the dermis when you make your ellipse. “This is really your quality control checkpoint.” Applying pressure toward the outward edge of the ellipse is a way to minimize the formation of a bevel, he added.
“No matter what you do, the dermis and epidermis will retract more than the fat. There will always be a little bit of fat popping into the wound,” Dr. Miller said. Take the extra step and remove any excess fat after you undermine; otherwise it will impede your wound edges.
-- Excision. When it is time for excision, remove your ellipse in a uniform plane, Dr. Miller said. The tendency with a scalpel is to go deeper. “What I like to use, which is more reproducible, is scissors at a 45° angle to make a sharp cut. You’ll get a release. Then go across like a plane on a landing strip and you will get a uniform depth of excision.”
Dr. Miller said he generally targets the plane between the upper layer of more organized fat lobules and the less organized lower layer above the fascia. “You are not going to go to the fascia all the time. You might choose to stay just under the dermis—it depends on the size of your incision,” he said. Check for uniform thickness once you excise—this is another quality control checkpoint.
-- Undermining. Which instrument you use to perform your retraction is important for undermining. Forceps, for example, can cause tissue trauma. “I prefer blunt-tip scissors and skin hooks,” Dr. Miller said. Be careful not to place the hooks too superficially or too close to the edge of the wound, he said. Instead, place the hook deeper and apply counterpressure with your finger.
“Understanding the anatomy is really going to drive where you choose to undermine,” Dr. Miller said. For example, remember that the superficial musculoaponeurotic system (SMAS) envelopes the muscles of facial expression. “Your motor nerves are always protected by this SMAS. You cannot cut the motor nerves if you remain above the SMAS. There will still be sensory nerves going to the skin.”
“If you are tentative, stay up higher in the fat on the lateral sides of the face,” Dr. Miller said.
Again, remove any extraneous fat that pops in under the wound edges after you undermine, Dr. Miller suggested. The questions to ask at this point are: Is the dermis clearly visible? Are the wound edges clean and vertical?
When it comes to suturing, Dr. Miller recommended the buried vertical mattress suture. It is a heart-shaped loop, similar to the superficial mattress suture. “The suture ideally is biting your reticular dermis, as far away as possible from the wound edge. This will give you wiggle room,” Dr. Miller said. “If it is too high, up near the epidermal edge, it is harder to adjust.”
Another quality control checkpoint comes after you finish throwing the needle toward the center of wound. Let go of your retracting instrument. “If it snaps back toward your needle, you are at the right depth,” Dr. Miller said.
Finally, “precise, deep sutures are key to the ideal scar,” Dr. Miller said. To confirm the adequacy of your sutures, perform the pull test. “Place your fingers on either side, and if you get a gap [the two wound edges come apart], then you need another deep suture.”
Dr. Miller had no relevant financial disclosures.
DESTIN, Fla. — It might look easy, but getting a perfect result after dermatologic surgery takes skill and experience, Dr. Christopher J. Miller said.
For dermatologists who are relatively new to incision, excision, and undermining, there are multiple opportunities to assess your expertise during and after surgery. These “quality control checkpoints” include the assessment of incision depth and uniformity of the cut, as well as using your fingers to check for any gaps in your suture line, Dr. Miller said.
Results 1 week after surgery, in particular, provide important feedback on your surgical technique, he said. The goal at 1-week suture removal is wound edges that are sealed and blended together well with minimal inflammation.
“It takes a lot of work to figure out how to do that,” he said.
Recognize that technical errors in the early stages of excision affect subsequent results, said Dr. Miller, director of dermatologic surgery at the University of Pennsylvania, Philadelphia.
-- Incision. Avoid the tendency to bevel edges during incision, because this prevents proper apposition. The goal is for a vertical wound with no internal bevel, so ensure that your scalpel remains perpendicular to the skin.
“If those wound edges cannot come together … you will be forced to have tension on the wound,” which almost guarantees that track marks will develop along the wound, Dr. Miller said.
And make sure you incise all the way through the dermis when you make your ellipse. “This is really your quality control checkpoint.” Applying pressure toward the outward edge of the ellipse is a way to minimize the formation of a bevel, he added.
“No matter what you do, the dermis and epidermis will retract more than the fat. There will always be a little bit of fat popping into the wound,” Dr. Miller said. Take the extra step and remove any excess fat after you undermine; otherwise it will impede your wound edges.
-- Excision. When it is time for excision, remove your ellipse in a uniform plane, Dr. Miller said. The tendency with a scalpel is to go deeper. “What I like to use, which is more reproducible, is scissors at a 45° angle to make a sharp cut. You’ll get a release. Then go across like a plane on a landing strip and you will get a uniform depth of excision.”
Dr. Miller said he generally targets the plane between the upper layer of more organized fat lobules and the less organized lower layer above the fascia. “You are not going to go to the fascia all the time. You might choose to stay just under the dermis—it depends on the size of your incision,” he said. Check for uniform thickness once you excise—this is another quality control checkpoint.
-- Undermining. Which instrument you use to perform your retraction is important for undermining. Forceps, for example, can cause tissue trauma. “I prefer blunt-tip scissors and skin hooks,” Dr. Miller said. Be careful not to place the hooks too superficially or too close to the edge of the wound, he said. Instead, place the hook deeper and apply counterpressure with your finger.
“Understanding the anatomy is really going to drive where you choose to undermine,” Dr. Miller said. For example, remember that the superficial musculoaponeurotic system (SMAS) envelopes the muscles of facial expression. “Your motor nerves are always protected by this SMAS. You cannot cut the motor nerves if you remain above the SMAS. There will still be sensory nerves going to the skin.”
“If you are tentative, stay up higher in the fat on the lateral sides of the face,” Dr. Miller said.
Again, remove any extraneous fat that pops in under the wound edges after you undermine, Dr. Miller suggested. The questions to ask at this point are: Is the dermis clearly visible? Are the wound edges clean and vertical?
When it comes to suturing, Dr. Miller recommended the buried vertical mattress suture. It is a heart-shaped loop, similar to the superficial mattress suture. “The suture ideally is biting your reticular dermis, as far away as possible from the wound edge. This will give you wiggle room,” Dr. Miller said. “If it is too high, up near the epidermal edge, it is harder to adjust.”
Another quality control checkpoint comes after you finish throwing the needle toward the center of wound. Let go of your retracting instrument. “If it snaps back toward your needle, you are at the right depth,” Dr. Miller said.
Finally, “precise, deep sutures are key to the ideal scar,” Dr. Miller said. To confirm the adequacy of your sutures, perform the pull test. “Place your fingers on either side, and if you get a gap [the two wound edges come apart], then you need another deep suture.”
Dr. Miller had no relevant financial disclosures.
DESTIN, Fla. — It might look easy, but getting a perfect result after dermatologic surgery takes skill and experience, Dr. Christopher J. Miller said.
For dermatologists who are relatively new to incision, excision, and undermining, there are multiple opportunities to assess your expertise during and after surgery. These “quality control checkpoints” include the assessment of incision depth and uniformity of the cut, as well as using your fingers to check for any gaps in your suture line, Dr. Miller said.
Results 1 week after surgery, in particular, provide important feedback on your surgical technique, he said. The goal at 1-week suture removal is wound edges that are sealed and blended together well with minimal inflammation.
“It takes a lot of work to figure out how to do that,” he said.
Recognize that technical errors in the early stages of excision affect subsequent results, said Dr. Miller, director of dermatologic surgery at the University of Pennsylvania, Philadelphia.
-- Incision. Avoid the tendency to bevel edges during incision, because this prevents proper apposition. The goal is for a vertical wound with no internal bevel, so ensure that your scalpel remains perpendicular to the skin.
“If those wound edges cannot come together … you will be forced to have tension on the wound,” which almost guarantees that track marks will develop along the wound, Dr. Miller said.
And make sure you incise all the way through the dermis when you make your ellipse. “This is really your quality control checkpoint.” Applying pressure toward the outward edge of the ellipse is a way to minimize the formation of a bevel, he added.
“No matter what you do, the dermis and epidermis will retract more than the fat. There will always be a little bit of fat popping into the wound,” Dr. Miller said. Take the extra step and remove any excess fat after you undermine; otherwise it will impede your wound edges.
-- Excision. When it is time for excision, remove your ellipse in a uniform plane, Dr. Miller said. The tendency with a scalpel is to go deeper. “What I like to use, which is more reproducible, is scissors at a 45° angle to make a sharp cut. You’ll get a release. Then go across like a plane on a landing strip and you will get a uniform depth of excision.”
Dr. Miller said he generally targets the plane between the upper layer of more organized fat lobules and the less organized lower layer above the fascia. “You are not going to go to the fascia all the time. You might choose to stay just under the dermis—it depends on the size of your incision,” he said. Check for uniform thickness once you excise—this is another quality control checkpoint.
-- Undermining. Which instrument you use to perform your retraction is important for undermining. Forceps, for example, can cause tissue trauma. “I prefer blunt-tip scissors and skin hooks,” Dr. Miller said. Be careful not to place the hooks too superficially or too close to the edge of the wound, he said. Instead, place the hook deeper and apply counterpressure with your finger.
“Understanding the anatomy is really going to drive where you choose to undermine,” Dr. Miller said. For example, remember that the superficial musculoaponeurotic system (SMAS) envelopes the muscles of facial expression. “Your motor nerves are always protected by this SMAS. You cannot cut the motor nerves if you remain above the SMAS. There will still be sensory nerves going to the skin.”
“If you are tentative, stay up higher in the fat on the lateral sides of the face,” Dr. Miller said.
Again, remove any extraneous fat that pops in under the wound edges after you undermine, Dr. Miller suggested. The questions to ask at this point are: Is the dermis clearly visible? Are the wound edges clean and vertical?
When it comes to suturing, Dr. Miller recommended the buried vertical mattress suture. It is a heart-shaped loop, similar to the superficial mattress suture. “The suture ideally is biting your reticular dermis, as far away as possible from the wound edge. This will give you wiggle room,” Dr. Miller said. “If it is too high, up near the epidermal edge, it is harder to adjust.”
Another quality control checkpoint comes after you finish throwing the needle toward the center of wound. Let go of your retracting instrument. “If it snaps back toward your needle, you are at the right depth,” Dr. Miller said.
Finally, “precise, deep sutures are key to the ideal scar,” Dr. Miller said. To confirm the adequacy of your sutures, perform the pull test. “Place your fingers on either side, and if you get a gap [the two wound edges come apart], then you need another deep suture.”
Dr. Miller had no relevant financial disclosures.
From a Meeting Sponsored by the Alabama Dermatology Society
Anatomical Tips Optimize Volume Replacement
Frozen Sections for Mohs Surgery Can be Used to Treat Melanoma
DESTIN, Fla. - When it comes to melanoma treatment, one of the most effective strategies - excision - is what dermatologists do best, Dr. Christopher J. Miller said.
"Getting the tumor out is the one thing we are good at [with melanoma]. And we have tools to be better at it," he emphasized.
Histostains, including melanoma antigen recognized by T cells 1 (MART-1), are one such tool. "These stains have revolutionized our ability to treat melanoma using frozen sections," said Dr. Miller, director of dermatologic surgery at the University of Pennsylvania in Philadelphia.
Dr. Miller said he hopes MART-1 staining will change a belief in dermatology that detection of residual disease is less accurate with use of frozen sections after Mohs surgery, compared with use of permanent sections after staged excision, also known as "slow Mohs."
"That is a dogma that is holding back the transition to using frozen sections," Dr. Miller noted at the annual meeting of the Alabama Dermatology Society.
There are data to indicate this is a safe practice, Dr. Miller said, including a large study of 625 patients with melanoma in the head and neck area, "an anatomic location with historically high recurrence and metastasis rates and poor survival rates." Mohs surgery using frozen sections resulted in complete melanoma removal in 97%, with 5-year local recurrence and metastasis rates, and disease-specific survival rates comparable to or better than those for historical controls (J. Am. Acad. Dermatol. 2005;52:92-100).
"And the proof is in the high cure rates all of us are getting with Mohs surgery using frozen sections and immunostains," he said.
"If you compare the frozen sections with MART-1 to the permanent sections with MART-1, we’re making the same calls," emphasized Dr. Miller.
Several studies support a finding that MART-1 imparts equivalence in terms of residual disease detection between frozen sections and permanent sections (Dermatol. Surg. 2009;35:207-13; J. Am. Acad. Dermatol. 2002;46:78-84).
With frozen sections, the Mohs surgeon (not a pathologist) checks for evidence of residual disease, results are immediate, and multiple stages of surgery can be performed on the same day. In contrast, slow Mohs requires that permanent sections processed in formalin be sent to a pathologist for evaluation. "And you have to coordinate a lot of logistics because you have to make sure the pathologist is ready to read these slides when they are available, and the patient is ready to come back right when you know your answer," Dr. Miller said. Typical turnaround time for pathology results is 24-48 hours.
Both Mohs with frozen sections and slow Mohs with permanent sections demonstrate excellent cure rates in studies, Dr. Miller said. Recurrences were in the range of 0%-2.6% in a review study (Cancer Control 2008;15:216-24).
"So they are both reliable methods in experienced hands," he noted. Importantly, both Mohs techniques permit examination of 100% of the excised margin for residual disease, Dr. Miller said. "That is what determines how certain you will be that the cancer is removed."
There are dermatologists who remain unconvinced about the benefits of frozen sections, Dr. Miller said. "I’d invite anybody to spend time with me treating these melanomas in my clinic. I’m sure I can convince them that with high-quality sections and attentive [histotechnicians] who are true experts in these stains, we can have stains that are of excellent quality that can give our patients the highest cure rates," he said in a follow-up interview.
Recognition that melanoma is a microscopic disease is important, Dr. Miller noted. "Let's accept we cannot see subclinical spread in every case. Twenty percent of the time we don’t get it all with what we think is an appropriate margin. Surgeons are having to go back for a second stage to remove tumor that wasn’t visible to them."
Dr. Miller's surgical approach to melanoma is Mohs with frozen sections. He supplements a standard hematoxylin and eosin (H&E) stain with a MART-1 immunostain for each patient. This strategy "has allowed me in multiple cases to detect melanocytes I probably would have missed had I used hematoxylin and eosin alone."
Dr. Miller also recommended an online tool that calculates the likelihood for survival from localized melanoma or regional metastatic disease based on clinical and patient characteristics. A blog posting on this easy-to-use tool is available.
For advice from Dr. Miller on the management of patients with thin melanomas, including why sentinel lymph node biopsies remain controversial in this population, watch a video interview.
Dr. Miller said he had no relevant financial disclosures.
DESTIN, Fla. - When it comes to melanoma treatment, one of the most effective strategies - excision - is what dermatologists do best, Dr. Christopher J. Miller said.
"Getting the tumor out is the one thing we are good at [with melanoma]. And we have tools to be better at it," he emphasized.
Histostains, including melanoma antigen recognized by T cells 1 (MART-1), are one such tool. "These stains have revolutionized our ability to treat melanoma using frozen sections," said Dr. Miller, director of dermatologic surgery at the University of Pennsylvania in Philadelphia.
Dr. Miller said he hopes MART-1 staining will change a belief in dermatology that detection of residual disease is less accurate with use of frozen sections after Mohs surgery, compared with use of permanent sections after staged excision, also known as "slow Mohs."
"That is a dogma that is holding back the transition to using frozen sections," Dr. Miller noted at the annual meeting of the Alabama Dermatology Society.
There are data to indicate this is a safe practice, Dr. Miller said, including a large study of 625 patients with melanoma in the head and neck area, "an anatomic location with historically high recurrence and metastasis rates and poor survival rates." Mohs surgery using frozen sections resulted in complete melanoma removal in 97%, with 5-year local recurrence and metastasis rates, and disease-specific survival rates comparable to or better than those for historical controls (J. Am. Acad. Dermatol. 2005;52:92-100).
"And the proof is in the high cure rates all of us are getting with Mohs surgery using frozen sections and immunostains," he said.
"If you compare the frozen sections with MART-1 to the permanent sections with MART-1, we’re making the same calls," emphasized Dr. Miller.
Several studies support a finding that MART-1 imparts equivalence in terms of residual disease detection between frozen sections and permanent sections (Dermatol. Surg. 2009;35:207-13; J. Am. Acad. Dermatol. 2002;46:78-84).
With frozen sections, the Mohs surgeon (not a pathologist) checks for evidence of residual disease, results are immediate, and multiple stages of surgery can be performed on the same day. In contrast, slow Mohs requires that permanent sections processed in formalin be sent to a pathologist for evaluation. "And you have to coordinate a lot of logistics because you have to make sure the pathologist is ready to read these slides when they are available, and the patient is ready to come back right when you know your answer," Dr. Miller said. Typical turnaround time for pathology results is 24-48 hours.
Both Mohs with frozen sections and slow Mohs with permanent sections demonstrate excellent cure rates in studies, Dr. Miller said. Recurrences were in the range of 0%-2.6% in a review study (Cancer Control 2008;15:216-24).
"So they are both reliable methods in experienced hands," he noted. Importantly, both Mohs techniques permit examination of 100% of the excised margin for residual disease, Dr. Miller said. "That is what determines how certain you will be that the cancer is removed."
There are dermatologists who remain unconvinced about the benefits of frozen sections, Dr. Miller said. "I’d invite anybody to spend time with me treating these melanomas in my clinic. I’m sure I can convince them that with high-quality sections and attentive [histotechnicians] who are true experts in these stains, we can have stains that are of excellent quality that can give our patients the highest cure rates," he said in a follow-up interview.
Recognition that melanoma is a microscopic disease is important, Dr. Miller noted. "Let's accept we cannot see subclinical spread in every case. Twenty percent of the time we don’t get it all with what we think is an appropriate margin. Surgeons are having to go back for a second stage to remove tumor that wasn’t visible to them."
Dr. Miller's surgical approach to melanoma is Mohs with frozen sections. He supplements a standard hematoxylin and eosin (H&E) stain with a MART-1 immunostain for each patient. This strategy "has allowed me in multiple cases to detect melanocytes I probably would have missed had I used hematoxylin and eosin alone."
Dr. Miller also recommended an online tool that calculates the likelihood for survival from localized melanoma or regional metastatic disease based on clinical and patient characteristics. A blog posting on this easy-to-use tool is available.
For advice from Dr. Miller on the management of patients with thin melanomas, including why sentinel lymph node biopsies remain controversial in this population, watch a video interview.
Dr. Miller said he had no relevant financial disclosures.
DESTIN, Fla. - When it comes to melanoma treatment, one of the most effective strategies - excision - is what dermatologists do best, Dr. Christopher J. Miller said.
"Getting the tumor out is the one thing we are good at [with melanoma]. And we have tools to be better at it," he emphasized.
Histostains, including melanoma antigen recognized by T cells 1 (MART-1), are one such tool. "These stains have revolutionized our ability to treat melanoma using frozen sections," said Dr. Miller, director of dermatologic surgery at the University of Pennsylvania in Philadelphia.
Dr. Miller said he hopes MART-1 staining will change a belief in dermatology that detection of residual disease is less accurate with use of frozen sections after Mohs surgery, compared with use of permanent sections after staged excision, also known as "slow Mohs."
"That is a dogma that is holding back the transition to using frozen sections," Dr. Miller noted at the annual meeting of the Alabama Dermatology Society.
There are data to indicate this is a safe practice, Dr. Miller said, including a large study of 625 patients with melanoma in the head and neck area, "an anatomic location with historically high recurrence and metastasis rates and poor survival rates." Mohs surgery using frozen sections resulted in complete melanoma removal in 97%, with 5-year local recurrence and metastasis rates, and disease-specific survival rates comparable to or better than those for historical controls (J. Am. Acad. Dermatol. 2005;52:92-100).
"And the proof is in the high cure rates all of us are getting with Mohs surgery using frozen sections and immunostains," he said.
"If you compare the frozen sections with MART-1 to the permanent sections with MART-1, we’re making the same calls," emphasized Dr. Miller.
Several studies support a finding that MART-1 imparts equivalence in terms of residual disease detection between frozen sections and permanent sections (Dermatol. Surg. 2009;35:207-13; J. Am. Acad. Dermatol. 2002;46:78-84).
With frozen sections, the Mohs surgeon (not a pathologist) checks for evidence of residual disease, results are immediate, and multiple stages of surgery can be performed on the same day. In contrast, slow Mohs requires that permanent sections processed in formalin be sent to a pathologist for evaluation. "And you have to coordinate a lot of logistics because you have to make sure the pathologist is ready to read these slides when they are available, and the patient is ready to come back right when you know your answer," Dr. Miller said. Typical turnaround time for pathology results is 24-48 hours.
Both Mohs with frozen sections and slow Mohs with permanent sections demonstrate excellent cure rates in studies, Dr. Miller said. Recurrences were in the range of 0%-2.6% in a review study (Cancer Control 2008;15:216-24).
"So they are both reliable methods in experienced hands," he noted. Importantly, both Mohs techniques permit examination of 100% of the excised margin for residual disease, Dr. Miller said. "That is what determines how certain you will be that the cancer is removed."
There are dermatologists who remain unconvinced about the benefits of frozen sections, Dr. Miller said. "I’d invite anybody to spend time with me treating these melanomas in my clinic. I’m sure I can convince them that with high-quality sections and attentive [histotechnicians] who are true experts in these stains, we can have stains that are of excellent quality that can give our patients the highest cure rates," he said in a follow-up interview.
Recognition that melanoma is a microscopic disease is important, Dr. Miller noted. "Let's accept we cannot see subclinical spread in every case. Twenty percent of the time we don’t get it all with what we think is an appropriate margin. Surgeons are having to go back for a second stage to remove tumor that wasn’t visible to them."
Dr. Miller's surgical approach to melanoma is Mohs with frozen sections. He supplements a standard hematoxylin and eosin (H&E) stain with a MART-1 immunostain for each patient. This strategy "has allowed me in multiple cases to detect melanocytes I probably would have missed had I used hematoxylin and eosin alone."
Dr. Miller also recommended an online tool that calculates the likelihood for survival from localized melanoma or regional metastatic disease based on clinical and patient characteristics. A blog posting on this easy-to-use tool is available.
For advice from Dr. Miller on the management of patients with thin melanomas, including why sentinel lymph node biopsies remain controversial in this population, watch a video interview.
Dr. Miller said he had no relevant financial disclosures.
Functional Abdominal Pain in Children: What to Watch for
MIAMI — Outcomes are optimized when a biopsychosocial approach is used to manage children with functional abdominal pain, according to Dr. Basil J. Zitelli.
Acknowledge the patient's perceptions of their own well-being and that the “pain is real,” he said. Also recognize that negative clinical tests do not invalidate a child's perception of the illness.
Try to identify the location and cause of the pain, rule out other possible causes, and counsel the patient and family throughout the disease process, said Dr. Zitelli, chief of the Paul C. Gaffney Diagnostic Referral Service at the Children's Hospital of Pittsburgh and professor of pediatrics at the University of Pittsburgh.
In addition, educate parents that their own anxiety can worsen a functional gastrointestinal disorder (FGID) in their child.
The following clinical red flags, diagnostic criteria, and conditions that indicate when referral to a specialist may be warranted were among the tips Dr. Zitelli offered attendees at the pediatric update:
▸ Red flags or FGID alarm symptoms include multiple organ involvement, gastrointestinal bleeding, weight loss, mouth ulcers, and liver disease.
▸ The location of pain can be another red flag. In general, pain that is periumbicular in children younger than 8 years suggests FGID. The farther away from the umbilicus, the greater the chance of underlying disease, Dr. Zitelli noted.
▸ If the pain is epigastric, the stomach, esophagus, duodenum, or pancreas may be involved; there may also be dyspepsia and/or Helicobacter pylori involvement.
▸ Right upper quadrant pain suggests hepatobiliary disease or involvement of the pancreas head.
▸ Right lower quadrant pain suggests the appendix, cecum, ovary, and/or rectosigmoid may be involved. Such pain also points to irritable bowel syndrome (IBS).
▸ Left lower quadrant pain also suggests rectosigmoid involvement and IBS, as well as pain caused by ulcerative colitis.
“I also do a rectal examination looking for fissures, tags, or other abnormalities,” Dr. Zitelli said.
Take a detailed family history specific to GI disorders, he advised. Also ask about any initiating events or exacerbating factors for the patient. For example, is the pain associated with eating or defecation? Has there been difficulty in the home—a loss of a family member or marital discord? Has there been any abuse or violence inflicted upon or directly observed by the child?
Before the release of Rome III criteria in 2006, the bias used to be that FGID was “not real,” was “in your head,” or was “nonorganic,” said Dr. Zitelli.
The Rome III criteria allow for more specific diagnoses. The criteria classify pediatric FGID into functional abdominal pain, functional dyspepsia, IBS, and abdominal migraine. Pain has to occur at least once a week for 2 months or more to meet the criteria. The exception is abdominal migraine, where more than two episodes in 12 months are required.
“Abdominal migraine is different, paroxysmal, acute, severe, noncolicky, and periumbicular pain lasting several hours,” Dr. Zitelli said. A patient can have anorexia, nausea/vomiting, and pallor and be healthy between episodes. “This is important,” he noted.
Helpful tests include a complete blood count, erythrocyte sedimentation rate, and C-reactive protein (CRP) assay. However, Dr. Zitelli said, “CRP may not be elevated in patients with ulcerative colitis or a large percentage of children with Crohn's disease.” If specifically indicated, additional tests for transaminases, lipase, celiac studies, and urinalysis may be useful.
However, it is important to avoid overtesting, Dr. Zitelli said. “There is a temptation to do test after test after test. We must be careful as physicians not to become part of the pathologic process by endless testing.” He added that “if FGID [diagnosis] can be made using Rome III criteria, no extensive labs are needed.”
A trial of empiric therapy can be initiated, Dr. Zitelli said. For example, a 2-week trial of a proton pump inhibitor or H2 blocker for a child with upper abdominal pain or polyethylene glycol 3350 for the child with lower abdominal pain may be indicated.
A low-lactose diet, low-fructose diet, and addition of dietary fiber are other possible interventions. Also consider use of complementary or alternative medicines, but “make sure they are safe and only adjunctive therapies,” he said.
Antidepressants may be of some value. For example, tricyclic antidepressants can modulate pain, can alter mood, and may enhance gastrointestinal motility. So they could be helpful for those with constipation.
“If there is no improvement, referral to a pediatric specialist may be warranted,” Dr. Zitelli said.
Many of the recommendations Dr. Zitelli provided are summarized in reports in the May 2009 Pediatric Annals (for example, 38:241-2, 253-8, 279-82). He recommended that pediatricians review this issue for additional information and guidance on FGID.
Disclosures: Dr. Zitelli disclosed that he receives royalties from Elsevier for book publishing.
For more information on the pediatric Rome III Criteria, visit www.romecriteria.org
MIAMI — Outcomes are optimized when a biopsychosocial approach is used to manage children with functional abdominal pain, according to Dr. Basil J. Zitelli.
Acknowledge the patient's perceptions of their own well-being and that the “pain is real,” he said. Also recognize that negative clinical tests do not invalidate a child's perception of the illness.
Try to identify the location and cause of the pain, rule out other possible causes, and counsel the patient and family throughout the disease process, said Dr. Zitelli, chief of the Paul C. Gaffney Diagnostic Referral Service at the Children's Hospital of Pittsburgh and professor of pediatrics at the University of Pittsburgh.
In addition, educate parents that their own anxiety can worsen a functional gastrointestinal disorder (FGID) in their child.
The following clinical red flags, diagnostic criteria, and conditions that indicate when referral to a specialist may be warranted were among the tips Dr. Zitelli offered attendees at the pediatric update:
▸ Red flags or FGID alarm symptoms include multiple organ involvement, gastrointestinal bleeding, weight loss, mouth ulcers, and liver disease.
▸ The location of pain can be another red flag. In general, pain that is periumbicular in children younger than 8 years suggests FGID. The farther away from the umbilicus, the greater the chance of underlying disease, Dr. Zitelli noted.
▸ If the pain is epigastric, the stomach, esophagus, duodenum, or pancreas may be involved; there may also be dyspepsia and/or Helicobacter pylori involvement.
▸ Right upper quadrant pain suggests hepatobiliary disease or involvement of the pancreas head.
▸ Right lower quadrant pain suggests the appendix, cecum, ovary, and/or rectosigmoid may be involved. Such pain also points to irritable bowel syndrome (IBS).
▸ Left lower quadrant pain also suggests rectosigmoid involvement and IBS, as well as pain caused by ulcerative colitis.
“I also do a rectal examination looking for fissures, tags, or other abnormalities,” Dr. Zitelli said.
Take a detailed family history specific to GI disorders, he advised. Also ask about any initiating events or exacerbating factors for the patient. For example, is the pain associated with eating or defecation? Has there been difficulty in the home—a loss of a family member or marital discord? Has there been any abuse or violence inflicted upon or directly observed by the child?
Before the release of Rome III criteria in 2006, the bias used to be that FGID was “not real,” was “in your head,” or was “nonorganic,” said Dr. Zitelli.
The Rome III criteria allow for more specific diagnoses. The criteria classify pediatric FGID into functional abdominal pain, functional dyspepsia, IBS, and abdominal migraine. Pain has to occur at least once a week for 2 months or more to meet the criteria. The exception is abdominal migraine, where more than two episodes in 12 months are required.
“Abdominal migraine is different, paroxysmal, acute, severe, noncolicky, and periumbicular pain lasting several hours,” Dr. Zitelli said. A patient can have anorexia, nausea/vomiting, and pallor and be healthy between episodes. “This is important,” he noted.
Helpful tests include a complete blood count, erythrocyte sedimentation rate, and C-reactive protein (CRP) assay. However, Dr. Zitelli said, “CRP may not be elevated in patients with ulcerative colitis or a large percentage of children with Crohn's disease.” If specifically indicated, additional tests for transaminases, lipase, celiac studies, and urinalysis may be useful.
However, it is important to avoid overtesting, Dr. Zitelli said. “There is a temptation to do test after test after test. We must be careful as physicians not to become part of the pathologic process by endless testing.” He added that “if FGID [diagnosis] can be made using Rome III criteria, no extensive labs are needed.”
A trial of empiric therapy can be initiated, Dr. Zitelli said. For example, a 2-week trial of a proton pump inhibitor or H2 blocker for a child with upper abdominal pain or polyethylene glycol 3350 for the child with lower abdominal pain may be indicated.
A low-lactose diet, low-fructose diet, and addition of dietary fiber are other possible interventions. Also consider use of complementary or alternative medicines, but “make sure they are safe and only adjunctive therapies,” he said.
Antidepressants may be of some value. For example, tricyclic antidepressants can modulate pain, can alter mood, and may enhance gastrointestinal motility. So they could be helpful for those with constipation.
“If there is no improvement, referral to a pediatric specialist may be warranted,” Dr. Zitelli said.
Many of the recommendations Dr. Zitelli provided are summarized in reports in the May 2009 Pediatric Annals (for example, 38:241-2, 253-8, 279-82). He recommended that pediatricians review this issue for additional information and guidance on FGID.
Disclosures: Dr. Zitelli disclosed that he receives royalties from Elsevier for book publishing.
For more information on the pediatric Rome III Criteria, visit www.romecriteria.org
MIAMI — Outcomes are optimized when a biopsychosocial approach is used to manage children with functional abdominal pain, according to Dr. Basil J. Zitelli.
Acknowledge the patient's perceptions of their own well-being and that the “pain is real,” he said. Also recognize that negative clinical tests do not invalidate a child's perception of the illness.
Try to identify the location and cause of the pain, rule out other possible causes, and counsel the patient and family throughout the disease process, said Dr. Zitelli, chief of the Paul C. Gaffney Diagnostic Referral Service at the Children's Hospital of Pittsburgh and professor of pediatrics at the University of Pittsburgh.
In addition, educate parents that their own anxiety can worsen a functional gastrointestinal disorder (FGID) in their child.
The following clinical red flags, diagnostic criteria, and conditions that indicate when referral to a specialist may be warranted were among the tips Dr. Zitelli offered attendees at the pediatric update:
▸ Red flags or FGID alarm symptoms include multiple organ involvement, gastrointestinal bleeding, weight loss, mouth ulcers, and liver disease.
▸ The location of pain can be another red flag. In general, pain that is periumbicular in children younger than 8 years suggests FGID. The farther away from the umbilicus, the greater the chance of underlying disease, Dr. Zitelli noted.
▸ If the pain is epigastric, the stomach, esophagus, duodenum, or pancreas may be involved; there may also be dyspepsia and/or Helicobacter pylori involvement.
▸ Right upper quadrant pain suggests hepatobiliary disease or involvement of the pancreas head.
▸ Right lower quadrant pain suggests the appendix, cecum, ovary, and/or rectosigmoid may be involved. Such pain also points to irritable bowel syndrome (IBS).
▸ Left lower quadrant pain also suggests rectosigmoid involvement and IBS, as well as pain caused by ulcerative colitis.
“I also do a rectal examination looking for fissures, tags, or other abnormalities,” Dr. Zitelli said.
Take a detailed family history specific to GI disorders, he advised. Also ask about any initiating events or exacerbating factors for the patient. For example, is the pain associated with eating or defecation? Has there been difficulty in the home—a loss of a family member or marital discord? Has there been any abuse or violence inflicted upon or directly observed by the child?
Before the release of Rome III criteria in 2006, the bias used to be that FGID was “not real,” was “in your head,” or was “nonorganic,” said Dr. Zitelli.
The Rome III criteria allow for more specific diagnoses. The criteria classify pediatric FGID into functional abdominal pain, functional dyspepsia, IBS, and abdominal migraine. Pain has to occur at least once a week for 2 months or more to meet the criteria. The exception is abdominal migraine, where more than two episodes in 12 months are required.
“Abdominal migraine is different, paroxysmal, acute, severe, noncolicky, and periumbicular pain lasting several hours,” Dr. Zitelli said. A patient can have anorexia, nausea/vomiting, and pallor and be healthy between episodes. “This is important,” he noted.
Helpful tests include a complete blood count, erythrocyte sedimentation rate, and C-reactive protein (CRP) assay. However, Dr. Zitelli said, “CRP may not be elevated in patients with ulcerative colitis or a large percentage of children with Crohn's disease.” If specifically indicated, additional tests for transaminases, lipase, celiac studies, and urinalysis may be useful.
However, it is important to avoid overtesting, Dr. Zitelli said. “There is a temptation to do test after test after test. We must be careful as physicians not to become part of the pathologic process by endless testing.” He added that “if FGID [diagnosis] can be made using Rome III criteria, no extensive labs are needed.”
A trial of empiric therapy can be initiated, Dr. Zitelli said. For example, a 2-week trial of a proton pump inhibitor or H2 blocker for a child with upper abdominal pain or polyethylene glycol 3350 for the child with lower abdominal pain may be indicated.
A low-lactose diet, low-fructose diet, and addition of dietary fiber are other possible interventions. Also consider use of complementary or alternative medicines, but “make sure they are safe and only adjunctive therapies,” he said.
Antidepressants may be of some value. For example, tricyclic antidepressants can modulate pain, can alter mood, and may enhance gastrointestinal motility. So they could be helpful for those with constipation.
“If there is no improvement, referral to a pediatric specialist may be warranted,” Dr. Zitelli said.
Many of the recommendations Dr. Zitelli provided are summarized in reports in the May 2009 Pediatric Annals (for example, 38:241-2, 253-8, 279-82). He recommended that pediatricians review this issue for additional information and guidance on FGID.
Disclosures: Dr. Zitelli disclosed that he receives royalties from Elsevier for book publishing.
For more information on the pediatric Rome III Criteria, visit www.romecriteria.org