User login
Doug Brunk is a San Diego-based award-winning reporter who began covering health care in 1991. Before joining the company, he wrote for the health sciences division of Columbia University and was an associate editor at Contemporary Long Term Care magazine when it won a Jesse H. Neal Award. His work has been syndicated by the Los Angeles Times and he is the author of two books related to the University of Kentucky Wildcats men's basketball program. Doug has a master’s degree in magazine journalism from the S.I. Newhouse School of Public Communications at Syracuse University. Follow him on Twitter @dougbrunk.
Study Find Advantages With Meso-Rex Bypass
PALM DESERT, CALIF. – Compared with portosystemic shunting in the management of extrahepatic portal vein obstruction, mesenterico-left portal vein bypass restores portal circulation and achieves superior relief of thrombocytopenia and certain metabolic symptoms, results from a single-center study showed.
"For surgeons who still perform portosystemic shunts as a first-line operation for extrahepatic portal vein obstruction, we hope that this evidence provides further proof of the advantages of doing the mesenterico-left portal vein bypass," Dr. Timothy B. Lautz said at the annual meeting of the American Pediatric Surgical Association.
Modern surgical options for extrahepatic portal vein obstruction include the distal splenorenal shunt and the mesenterico-left portal vein bypass (meso-Rex). "The distal splenorenal shunt preserves the spleen but diverts the splenic portion of portal flow into the systemic circulation," said Dr. Lautz of the department of surgery at Children’s Memorial Hospital, the primary pediatric teaching hospital of Northwestern University, Chicago.
"The meso-Rex bypass, on the other hand, is a totally restorative procedure that diverts all portal flow around the area of obstruction and into the intrahepatic left portal vein," he said.
In an effort to compare the two procedures, Dr. Lautz and senior author Dr. Riccardo A. Superina evaluated 91 consecutive patients who underwent an operation for extrahepatic portal vein obstruction at the hospital between 1998 and 2009. Their mean age was 7 years, and 58% were male. Meso-Rex bypass was the treatment of choice in all cases, but portosytemic shunts were reserved for those with anatomic or technical constraints that prevented meso-Rex. Analysis was limited to patients with at least 1 year of postoperative follow-up.
Dr. Lautz reported that 72 patients underwent the meso-Rex procedure (group 1) and 19 underwent portosystemic shunts (group 2). Prior to surgery, patients in both groups experienced growth retardation, thrombocytopenia, hyperammonemia, and impaired synthetic function.
Following surgery, variceal bleeding resolved in 59 of the group-1 patients and in 13 group-2 patients who manifested this symptom preoperatively. In addition, group-1 patients had significantly better improvements compared with group-2 patients in weight for age z-score (+0.76 vs. +0.13, respectively; P = .048), platelet count (+77,700 vs. +29,000 per mL; P = 0.006), international normalized ratio (-0.23 vs. +0.22; P = .002), and serum ammonia (-25.5 vs. +18 micromol/L; P = .002).
"The meso-Rex bypass and portosystemic shunts are both effective at relieving portal hypertensive bleeding," Dr. Lautz concluded. "By restoring normal physiologic portal venous circulation, the meso-Rex bypass better relieves hypersplenism, liver dysfunction, and growth impairment."
Dr. Lautz said he had no relevant financial disclosures to make.
The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Compared with portosystemic shunting in the management of extrahepatic portal vein obstruction, mesenterico-left portal vein bypass restores portal circulation and achieves superior relief of thrombocytopenia and certain metabolic symptoms, results from a single-center study showed.
"For surgeons who still perform portosystemic shunts as a first-line operation for extrahepatic portal vein obstruction, we hope that this evidence provides further proof of the advantages of doing the mesenterico-left portal vein bypass," Dr. Timothy B. Lautz said at the annual meeting of the American Pediatric Surgical Association.
Modern surgical options for extrahepatic portal vein obstruction include the distal splenorenal shunt and the mesenterico-left portal vein bypass (meso-Rex). "The distal splenorenal shunt preserves the spleen but diverts the splenic portion of portal flow into the systemic circulation," said Dr. Lautz of the department of surgery at Children’s Memorial Hospital, the primary pediatric teaching hospital of Northwestern University, Chicago.
"The meso-Rex bypass, on the other hand, is a totally restorative procedure that diverts all portal flow around the area of obstruction and into the intrahepatic left portal vein," he said.
In an effort to compare the two procedures, Dr. Lautz and senior author Dr. Riccardo A. Superina evaluated 91 consecutive patients who underwent an operation for extrahepatic portal vein obstruction at the hospital between 1998 and 2009. Their mean age was 7 years, and 58% were male. Meso-Rex bypass was the treatment of choice in all cases, but portosytemic shunts were reserved for those with anatomic or technical constraints that prevented meso-Rex. Analysis was limited to patients with at least 1 year of postoperative follow-up.
Dr. Lautz reported that 72 patients underwent the meso-Rex procedure (group 1) and 19 underwent portosystemic shunts (group 2). Prior to surgery, patients in both groups experienced growth retardation, thrombocytopenia, hyperammonemia, and impaired synthetic function.
Following surgery, variceal bleeding resolved in 59 of the group-1 patients and in 13 group-2 patients who manifested this symptom preoperatively. In addition, group-1 patients had significantly better improvements compared with group-2 patients in weight for age z-score (+0.76 vs. +0.13, respectively; P = .048), platelet count (+77,700 vs. +29,000 per mL; P = 0.006), international normalized ratio (-0.23 vs. +0.22; P = .002), and serum ammonia (-25.5 vs. +18 micromol/L; P = .002).
"The meso-Rex bypass and portosystemic shunts are both effective at relieving portal hypertensive bleeding," Dr. Lautz concluded. "By restoring normal physiologic portal venous circulation, the meso-Rex bypass better relieves hypersplenism, liver dysfunction, and growth impairment."
Dr. Lautz said he had no relevant financial disclosures to make.
The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Compared with portosystemic shunting in the management of extrahepatic portal vein obstruction, mesenterico-left portal vein bypass restores portal circulation and achieves superior relief of thrombocytopenia and certain metabolic symptoms, results from a single-center study showed.
"For surgeons who still perform portosystemic shunts as a first-line operation for extrahepatic portal vein obstruction, we hope that this evidence provides further proof of the advantages of doing the mesenterico-left portal vein bypass," Dr. Timothy B. Lautz said at the annual meeting of the American Pediatric Surgical Association.
Modern surgical options for extrahepatic portal vein obstruction include the distal splenorenal shunt and the mesenterico-left portal vein bypass (meso-Rex). "The distal splenorenal shunt preserves the spleen but diverts the splenic portion of portal flow into the systemic circulation," said Dr. Lautz of the department of surgery at Children’s Memorial Hospital, the primary pediatric teaching hospital of Northwestern University, Chicago.
"The meso-Rex bypass, on the other hand, is a totally restorative procedure that diverts all portal flow around the area of obstruction and into the intrahepatic left portal vein," he said.
In an effort to compare the two procedures, Dr. Lautz and senior author Dr. Riccardo A. Superina evaluated 91 consecutive patients who underwent an operation for extrahepatic portal vein obstruction at the hospital between 1998 and 2009. Their mean age was 7 years, and 58% were male. Meso-Rex bypass was the treatment of choice in all cases, but portosytemic shunts were reserved for those with anatomic or technical constraints that prevented meso-Rex. Analysis was limited to patients with at least 1 year of postoperative follow-up.
Dr. Lautz reported that 72 patients underwent the meso-Rex procedure (group 1) and 19 underwent portosystemic shunts (group 2). Prior to surgery, patients in both groups experienced growth retardation, thrombocytopenia, hyperammonemia, and impaired synthetic function.
Following surgery, variceal bleeding resolved in 59 of the group-1 patients and in 13 group-2 patients who manifested this symptom preoperatively. In addition, group-1 patients had significantly better improvements compared with group-2 patients in weight for age z-score (+0.76 vs. +0.13, respectively; P = .048), platelet count (+77,700 vs. +29,000 per mL; P = 0.006), international normalized ratio (-0.23 vs. +0.22; P = .002), and serum ammonia (-25.5 vs. +18 micromol/L; P = .002).
"The meso-Rex bypass and portosystemic shunts are both effective at relieving portal hypertensive bleeding," Dr. Lautz concluded. "By restoring normal physiologic portal venous circulation, the meso-Rex bypass better relieves hypersplenism, liver dysfunction, and growth impairment."
Dr. Lautz said he had no relevant financial disclosures to make.
The meeting was supported by a grant from Elsevier, which owns this news organization.
FROM THE ANNUAL MEETING OF THE AMERICAN PEDIATRIC SURGICAL ASSOCIATION
SDEF: When to Discard and Replace Lasers, Factors Considered
DANA POINT, CALIF. - Between 1985 and 2011, Dr. Gordon Sasaki retired or discarded an estimated 15 devices used for aesthetic plastic surgery, including two erbium lasers, three CO2 lasers, and an external radiofrequency system for tissue lifting.
Factors that played into the dismissal of these devices included obsolescence of technology, the rise of improved, similar technologies, and competing devices in the office.
At the Summit in Aesthetic Medicine sponsored by Skin Disease Education Foundation (SDEF), Dr. Sasaki, clinical professor of plastic surgery at Loma Linda (Calif.) University Medical Center, shared why he chose to retire or let go of certain devices and embrace others.
Sometimes he stopped working with a device after comparing the cost of buying or leasing it with its positive return on investment, he said. Other factors he considered included the cost of disposable equipment, warranty renewals, and unanticipated costs for reparative procedures when a patient had unsatisfactory results or complications.
One device Dr. Sasaki retired was a high frequency eradicator, which is a low-powered, nongrounded electrosurgical device used for desiccation of subdermal lesions and fulguration of superficial lesions. His rationale included its cost to purchase ($1,000-$1,500), cost of the disposable tip ($1.50 each), and nontransportability from room to room.
He replaced it with the Medi-Pak handheld battery-powered cautery device, which achieves acceptable results yet costs only $9.95 per device, has no disposable components, and can be used multiple times until loss of battery power. After battery power loss, a new device is purchased.
Dr. Sasaki, who has a private aesthetic plastic surgery practice in Pasadena, Calif., also retired a nonablative monopolar radiofrequency device he used for tissue lifting and volumetric heating of dermis, septae, and fat. The initial cost of the second-generation device was $65,000, with a warranty that ranged from $2,800 to $3,300 per year. The annual cost of disposable tips added another $450-$949 per year. "Although the device produced satisfactory results in some patients, it also had unpredictable responses, as well as patient and operator fatigue, especially for body contouring procedures," he said. "There was low patient request for this device, and new, improved technology became available."
He put aside the nonablative radiofrequency device in favor of a multilevel focused and imaged ultrasonic tissue lifting device that provides an imaging level of treatment, precise thermal coagulation points, and more predictable patient responses. In his experience, 80%-90% of his patients showed clinical improvement by 3 months, and results tend to last 1-1.5 years. "There is minimal to moderate pain during treatment, and there is a high patient request for this procedure," Dr. Sasaki said.
Costs of the unit, including a 3-year warranty, were $87,500, he said. Additional warranties cost $10,000 per year, and the cost of a disposable transducer amounts to $2,100, which can last for at least four patient treatments, depending on the area of treatment.
Dr. Sasaki said that he currently shares a fractional CO2 resurfacing laser, in part because of its high purchase cost ($152,000, plus $240 for a box of 30 disposable tips), but also because of patient and operator fatigue, complex patient recovery, unpredictable and unsatisfactory patient responses, and low patient requests for the technology.
As a substitute for selected patients, Dr. Sasaki uses croton oil peels for patients who request facial resurfacing. Concentrations ranging from 0.0125% to 0.4% can be prepared, he said, and the procedure does not require application of a topical or local anesthesia. Costs are reasonable. In his practice a 1-ounce container of phenol costs $23.75 and a 1-ounce container of croton oil costs $106. "The preferred treatments are in patients with Fitzpatrick I-IV skin types," he said. "There are predictable and satisfactory patient responses."
Dr. Sasaki disclosed that he has been a paid consultant for many laser and device companies.
SDEF and this news organization are owned by Elsevier.
DANA POINT, CALIF. - Between 1985 and 2011, Dr. Gordon Sasaki retired or discarded an estimated 15 devices used for aesthetic plastic surgery, including two erbium lasers, three CO2 lasers, and an external radiofrequency system for tissue lifting.
Factors that played into the dismissal of these devices included obsolescence of technology, the rise of improved, similar technologies, and competing devices in the office.
At the Summit in Aesthetic Medicine sponsored by Skin Disease Education Foundation (SDEF), Dr. Sasaki, clinical professor of plastic surgery at Loma Linda (Calif.) University Medical Center, shared why he chose to retire or let go of certain devices and embrace others.
Sometimes he stopped working with a device after comparing the cost of buying or leasing it with its positive return on investment, he said. Other factors he considered included the cost of disposable equipment, warranty renewals, and unanticipated costs for reparative procedures when a patient had unsatisfactory results or complications.
One device Dr. Sasaki retired was a high frequency eradicator, which is a low-powered, nongrounded electrosurgical device used for desiccation of subdermal lesions and fulguration of superficial lesions. His rationale included its cost to purchase ($1,000-$1,500), cost of the disposable tip ($1.50 each), and nontransportability from room to room.
He replaced it with the Medi-Pak handheld battery-powered cautery device, which achieves acceptable results yet costs only $9.95 per device, has no disposable components, and can be used multiple times until loss of battery power. After battery power loss, a new device is purchased.
Dr. Sasaki, who has a private aesthetic plastic surgery practice in Pasadena, Calif., also retired a nonablative monopolar radiofrequency device he used for tissue lifting and volumetric heating of dermis, septae, and fat. The initial cost of the second-generation device was $65,000, with a warranty that ranged from $2,800 to $3,300 per year. The annual cost of disposable tips added another $450-$949 per year. "Although the device produced satisfactory results in some patients, it also had unpredictable responses, as well as patient and operator fatigue, especially for body contouring procedures," he said. "There was low patient request for this device, and new, improved technology became available."
He put aside the nonablative radiofrequency device in favor of a multilevel focused and imaged ultrasonic tissue lifting device that provides an imaging level of treatment, precise thermal coagulation points, and more predictable patient responses. In his experience, 80%-90% of his patients showed clinical improvement by 3 months, and results tend to last 1-1.5 years. "There is minimal to moderate pain during treatment, and there is a high patient request for this procedure," Dr. Sasaki said.
Costs of the unit, including a 3-year warranty, were $87,500, he said. Additional warranties cost $10,000 per year, and the cost of a disposable transducer amounts to $2,100, which can last for at least four patient treatments, depending on the area of treatment.
Dr. Sasaki said that he currently shares a fractional CO2 resurfacing laser, in part because of its high purchase cost ($152,000, plus $240 for a box of 30 disposable tips), but also because of patient and operator fatigue, complex patient recovery, unpredictable and unsatisfactory patient responses, and low patient requests for the technology.
As a substitute for selected patients, Dr. Sasaki uses croton oil peels for patients who request facial resurfacing. Concentrations ranging from 0.0125% to 0.4% can be prepared, he said, and the procedure does not require application of a topical or local anesthesia. Costs are reasonable. In his practice a 1-ounce container of phenol costs $23.75 and a 1-ounce container of croton oil costs $106. "The preferred treatments are in patients with Fitzpatrick I-IV skin types," he said. "There are predictable and satisfactory patient responses."
Dr. Sasaki disclosed that he has been a paid consultant for many laser and device companies.
SDEF and this news organization are owned by Elsevier.
DANA POINT, CALIF. - Between 1985 and 2011, Dr. Gordon Sasaki retired or discarded an estimated 15 devices used for aesthetic plastic surgery, including two erbium lasers, three CO2 lasers, and an external radiofrequency system for tissue lifting.
Factors that played into the dismissal of these devices included obsolescence of technology, the rise of improved, similar technologies, and competing devices in the office.
At the Summit in Aesthetic Medicine sponsored by Skin Disease Education Foundation (SDEF), Dr. Sasaki, clinical professor of plastic surgery at Loma Linda (Calif.) University Medical Center, shared why he chose to retire or let go of certain devices and embrace others.
Sometimes he stopped working with a device after comparing the cost of buying or leasing it with its positive return on investment, he said. Other factors he considered included the cost of disposable equipment, warranty renewals, and unanticipated costs for reparative procedures when a patient had unsatisfactory results or complications.
One device Dr. Sasaki retired was a high frequency eradicator, which is a low-powered, nongrounded electrosurgical device used for desiccation of subdermal lesions and fulguration of superficial lesions. His rationale included its cost to purchase ($1,000-$1,500), cost of the disposable tip ($1.50 each), and nontransportability from room to room.
He replaced it with the Medi-Pak handheld battery-powered cautery device, which achieves acceptable results yet costs only $9.95 per device, has no disposable components, and can be used multiple times until loss of battery power. After battery power loss, a new device is purchased.
Dr. Sasaki, who has a private aesthetic plastic surgery practice in Pasadena, Calif., also retired a nonablative monopolar radiofrequency device he used for tissue lifting and volumetric heating of dermis, septae, and fat. The initial cost of the second-generation device was $65,000, with a warranty that ranged from $2,800 to $3,300 per year. The annual cost of disposable tips added another $450-$949 per year. "Although the device produced satisfactory results in some patients, it also had unpredictable responses, as well as patient and operator fatigue, especially for body contouring procedures," he said. "There was low patient request for this device, and new, improved technology became available."
He put aside the nonablative radiofrequency device in favor of a multilevel focused and imaged ultrasonic tissue lifting device that provides an imaging level of treatment, precise thermal coagulation points, and more predictable patient responses. In his experience, 80%-90% of his patients showed clinical improvement by 3 months, and results tend to last 1-1.5 years. "There is minimal to moderate pain during treatment, and there is a high patient request for this procedure," Dr. Sasaki said.
Costs of the unit, including a 3-year warranty, were $87,500, he said. Additional warranties cost $10,000 per year, and the cost of a disposable transducer amounts to $2,100, which can last for at least four patient treatments, depending on the area of treatment.
Dr. Sasaki said that he currently shares a fractional CO2 resurfacing laser, in part because of its high purchase cost ($152,000, plus $240 for a box of 30 disposable tips), but also because of patient and operator fatigue, complex patient recovery, unpredictable and unsatisfactory patient responses, and low patient requests for the technology.
As a substitute for selected patients, Dr. Sasaki uses croton oil peels for patients who request facial resurfacing. Concentrations ranging from 0.0125% to 0.4% can be prepared, he said, and the procedure does not require application of a topical or local anesthesia. Costs are reasonable. In his practice a 1-ounce container of phenol costs $23.75 and a 1-ounce container of croton oil costs $106. "The preferred treatments are in patients with Fitzpatrick I-IV skin types," he said. "There are predictable and satisfactory patient responses."
Dr. Sasaki disclosed that he has been a paid consultant for many laser and device companies.
SDEF and this news organization are owned by Elsevier.
EXPERT ANALYSIS FROM THE SDEF SUMMIT IN AESTHETIC MEDICINE
SDEF: Fractionated Radiofrequency Smoothes Wrinkles, New Findings Show
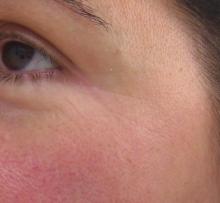
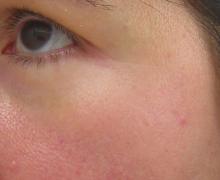
DANA POINT, CALIF. – In the clinical experience of Dr. George J. Hruza, bipolar fractionated radiofrequency provides good wrinkle effacement, especially in the periorbital area.
"The benefits of bipolar fractionated radiofrequency include a limited downtime, no adverse events are seen, and any skin type can be treated," Dr. Hruza said at the Summit in Aesthetic Medicine sponsored by Skin Disease Education Foundation (SDEF).
Dr. Hruza, clinical professor of dermatology at St. Louis University, presented findings from a study of 22 adults with Fitzpatrick skin types I-IV who were treated with bipolar fractionated radiofrequency for visible wrinkles and/or elastosis. He and his associates used the Food and Drug Administration–cleared eMatrix radiofrequency device (Syneron) to treat two of the following facial regions per patient: the periorbital region, the perioral region, the cheeks, and the forehead.
Both 64 and 144 pin tips were used; energy was delivered at a range of 2-14 joules per pulse, or 20 J/double pulse, for a maximum duration of 50 milliseconds per pulse. Each patient underwent three treatments at 3 weeks apart. Topical anesthesia was used, and the patients were followed up a month after the last treatment.
Photographic analysis at the 1-month follow-up revealed that fine lines, smoothness, tightness, and brightness improved in about half of the patients by at least 40%. Periorbital photographic results demonstrated a mean improvement in fine lines of at least 30%, with almost all patients showing clinically significant improvement. A 6-month follow-up study of the patients showed persistence of the improvement.
Dr. Hruza noted that patients may experience micro peeling for 2-4 days after undergoing bipolar fractionated radiofrequency.
An emerging technology for deeper skin lesions is dermal bipolar fractionated radiofrequency, which delivers radiofrequency energy within the dermis via micro-needle electrode pairs. "Ninety-six percent of energy is absorbed in the dermis, and the thermal profile is confined along and between the needles," Dr. Hruza said. "This creates a controlled lesion and a fractionated zone of thermal injury."
Tumescent anesthesia is recommended for bipolar dermal fractionated radiofrequency, he said, because it protects deeper skin structures and reduces bleeding. The procedure typically requires 100-300 insertions in the lower face and upper neck. The needle entry points typically close in 2 hours.
Dr. Hruza said that he had no relevant disclosures.
SDEF and this news organization are owned by Elsevier.
DANA POINT, CALIF. – In the clinical experience of Dr. George J. Hruza, bipolar fractionated radiofrequency provides good wrinkle effacement, especially in the periorbital area.
"The benefits of bipolar fractionated radiofrequency include a limited downtime, no adverse events are seen, and any skin type can be treated," Dr. Hruza said at the Summit in Aesthetic Medicine sponsored by Skin Disease Education Foundation (SDEF).
Dr. Hruza, clinical professor of dermatology at St. Louis University, presented findings from a study of 22 adults with Fitzpatrick skin types I-IV who were treated with bipolar fractionated radiofrequency for visible wrinkles and/or elastosis. He and his associates used the Food and Drug Administration–cleared eMatrix radiofrequency device (Syneron) to treat two of the following facial regions per patient: the periorbital region, the perioral region, the cheeks, and the forehead.
Both 64 and 144 pin tips were used; energy was delivered at a range of 2-14 joules per pulse, or 20 J/double pulse, for a maximum duration of 50 milliseconds per pulse. Each patient underwent three treatments at 3 weeks apart. Topical anesthesia was used, and the patients were followed up a month after the last treatment.
Photographic analysis at the 1-month follow-up revealed that fine lines, smoothness, tightness, and brightness improved in about half of the patients by at least 40%. Periorbital photographic results demonstrated a mean improvement in fine lines of at least 30%, with almost all patients showing clinically significant improvement. A 6-month follow-up study of the patients showed persistence of the improvement.
Dr. Hruza noted that patients may experience micro peeling for 2-4 days after undergoing bipolar fractionated radiofrequency.
An emerging technology for deeper skin lesions is dermal bipolar fractionated radiofrequency, which delivers radiofrequency energy within the dermis via micro-needle electrode pairs. "Ninety-six percent of energy is absorbed in the dermis, and the thermal profile is confined along and between the needles," Dr. Hruza said. "This creates a controlled lesion and a fractionated zone of thermal injury."
Tumescent anesthesia is recommended for bipolar dermal fractionated radiofrequency, he said, because it protects deeper skin structures and reduces bleeding. The procedure typically requires 100-300 insertions in the lower face and upper neck. The needle entry points typically close in 2 hours.
Dr. Hruza said that he had no relevant disclosures.
SDEF and this news organization are owned by Elsevier.
DANA POINT, CALIF. – In the clinical experience of Dr. George J. Hruza, bipolar fractionated radiofrequency provides good wrinkle effacement, especially in the periorbital area.
"The benefits of bipolar fractionated radiofrequency include a limited downtime, no adverse events are seen, and any skin type can be treated," Dr. Hruza said at the Summit in Aesthetic Medicine sponsored by Skin Disease Education Foundation (SDEF).
Dr. Hruza, clinical professor of dermatology at St. Louis University, presented findings from a study of 22 adults with Fitzpatrick skin types I-IV who were treated with bipolar fractionated radiofrequency for visible wrinkles and/or elastosis. He and his associates used the Food and Drug Administration–cleared eMatrix radiofrequency device (Syneron) to treat two of the following facial regions per patient: the periorbital region, the perioral region, the cheeks, and the forehead.
Both 64 and 144 pin tips were used; energy was delivered at a range of 2-14 joules per pulse, or 20 J/double pulse, for a maximum duration of 50 milliseconds per pulse. Each patient underwent three treatments at 3 weeks apart. Topical anesthesia was used, and the patients were followed up a month after the last treatment.
Photographic analysis at the 1-month follow-up revealed that fine lines, smoothness, tightness, and brightness improved in about half of the patients by at least 40%. Periorbital photographic results demonstrated a mean improvement in fine lines of at least 30%, with almost all patients showing clinically significant improvement. A 6-month follow-up study of the patients showed persistence of the improvement.
Dr. Hruza noted that patients may experience micro peeling for 2-4 days after undergoing bipolar fractionated radiofrequency.
An emerging technology for deeper skin lesions is dermal bipolar fractionated radiofrequency, which delivers radiofrequency energy within the dermis via micro-needle electrode pairs. "Ninety-six percent of energy is absorbed in the dermis, and the thermal profile is confined along and between the needles," Dr. Hruza said. "This creates a controlled lesion and a fractionated zone of thermal injury."
Tumescent anesthesia is recommended for bipolar dermal fractionated radiofrequency, he said, because it protects deeper skin structures and reduces bleeding. The procedure typically requires 100-300 insertions in the lower face and upper neck. The needle entry points typically close in 2 hours.
Dr. Hruza said that he had no relevant disclosures.
SDEF and this news organization are owned by Elsevier.
FROM THE SDEF SUMMIT IN AESTHETIC MEDICINE
Major Finding: Photographic analysis at 1 month follow-up revealed that fine lines, smoothness, tightness, and brightness improved in about half of patients by at least 40%.
Data Source: A study of 22 adults with Fitzpatrick skin types I-IV who were treated with bipolar fractionated radiofrequency for visible wrinkles and/or elastosis.
Disclosures: Dr. Hruza said that he had no relevant disclosures. SDEF and this news organization are owned by Elsevier.
SDEF: Remain Skeptical Over Efficacy of Noninvasive Fat Removal Devices
DANA POINT, CALIF. – Practice skepticism when it comes to the efficacy of noninvasive fat removal devices, advised Dr. Matthew A. Avram.
"Fat removal has a long history of 'snake oil' salesmanship," Dr. Avram said at the Summit in Aesthetic Medicine, which was sponsored by Skin Disease Education Foundation (SDEF). "You can count on this to continue, because many of these devices do little, if anything. It is important to critically assess these technologies in this emerging field."
Focused Ultrasound
Dr. Avram, faculty director for procedural dermatology training at Harvard Medical School and director of the dermatology laser and cosmetic center at Massachusetts General Hospital, both in Boston, discussed the evidence surrounding devices for noninvasive fat reduction.
One non–Food and Drug Administration–cleared modality being studied is focused ultrasound, which delivers mechanical, nonthermal energy to the thigh, abdomen, and flanks. A study of 30 patients who were treated once a month for 3 months demonstrated a circumference reduction of 2-4 cm in the treated sites (Lasers Surg. Med. 2007;39:315-23). Liver function tests, a lipid panel, and liver ultrasound showed no adverse systemic effects from the procedure.
However, Dr. Avram noted that the study is limited because there was no untreated control group and that circumference "is an inherently imprecise measure of improvement that can be manipulated." MRI would prove objective improvement, he said, but it was not performed in this trial.
In a subsequent study from Hong Kong, 53 patients underwent treatment once a month for 3 months for body contouring (Lasers Surg. Med. 2009; 41:751-9). No significant changes were observed in circumference and caliper measurements, and patients rated their satisfaction as poor.
High-Intensity Focused Ultrasound
High-intensity focused ultrasound, which is also not FDA cleared, involves the rapid heating of adipocytes that are purported to produce coagulative necrosis and cell death in adipose tissue. A retrospective chart review of the modality that was used in 85 patients who underwent one treatment session showed a mean 4.6 cm decrease in waist circumference after 3 months (Aesth. Plast. Surg. 2010;34:577-82). Adverse events that lasted 4-12 weeks occurred in 12% of subjects and included prolonged tenderness, ecchymosis, nodules, and edema, as well as procedural pain in one patient, which required discontinuation of the procedure.
Dr. Avram called high-intensity focused ultrasound a promising technology, "but it's difficult to assess its efficacy. Further study of this technology is needed."
Monopolar Radiofrequency
Monopolar radiofrequency, conventionally used for tissue tightening of the face, has produced lipoatrophy with aggressive settings as a complication. "Perhaps this can be harnessed to effectively treat fat," he said, noting that clinical studies are currently underway.
Low-Level Light Therapy
Low-level light therapy, an FDA-cleared modality for fat removal, uses a multiple head, low-level diode laser at an energy level of 635 nm, which is "roughly equivalent to a laser pointer," Dr. Avram said. In one randomized trial, 59 patients received three treatments of the technology or sham treatment per week for 2 weeks (Lasers Surg. Med. 2009;41:799-809). At 2 weeks, mean circumference reductions in the treatment group were 0.98 inches at the waist, 1.05 inches at the hip, and 0.85 inches at the right thigh and 0.65 inches at the left thigh. Circumference increased in the 2 weeks following treatment.
Dr. Avram said the study was poorly designed because there was no untreated control group, the duration of treatment was only 2 weeks, and there was no ultrasound or other noninvasive evidence of decreased fat layer. "Treat with extreme skepticism," he advised.
Cryolipolysis
Perhaps the most promising technology is cryolipolysis, he said, which is FDA cleared for noninvasive fat removal. Cryolipolysis involves the noninvasive cooling of fat to selectively cause cell death without damage to surrounding tissue.
The mechanism of action of cryolipolysis is believed to involve selective crystallization of lipids in fat cells at temperatures near freezing. "Apoptotic fat cell death is followed by slow dissolution of the fat cell and a gradual release of lipids," Dr. Avram explained. "The inflammatory process results in fat layer reduction over 2-4 months."
When human studies of the technology were first conducted in 2008, enrollment was restricted to 32 patients whose "love handles" were treated at a cooling intensity factor (CIF) of 33 for 60 minutes, and progressed to higher rates of energy extractions for 45 minutes per application site. One side was treated; the untreated contralateral side served as the control.
Efficacy was evaluated at 4 months post treatment via visual assessment as a primary end point, as well as ultrasound and histology. The ultrasound results demonstrated an average 23% decrease in fat layer thickness.
"In this initial group of 32 love handle patients treated once, discernible changes were seen on the treated side vs. baseline of the treated side, and compared to the untreated contralateral control," Dr. Avram said of the findings presented during a poster session at the 2008 annual meeting of the American Society for Dermatologic Surgery. "This unique study design [using each patient as his or her own control], provided very powerful evidence that this was a true treatment effect rather than a change in the patient's diet or exercise pattern during the 4 months after this single procedure exposure."
Common effects after cryolipolysis include redness, which lasts minutes to a few hours; bruising, which may last for a few weeks; and temporary dulling of sensation in the treated area, which typically resolves in 1-8 weeks. No postprocedural changes in pigmentation or laboratory abnormalities have been observed, he said.
About 1 in 2,000 patients experiences severe pain beginning 3-7 days post treatment, which translates into 26 reported cases out of 60,000 treatments. "We are not sure why these occur, but these cases completely resolve with no sequelae," Dr. Avram said.
He emphasized that cryolipolysis is not a replacement for liposuction. "It is not a weight-loss device," he said. "It's best suited for local fat removal resistant to exercise in relatively fit patients."
Dr. Avram disclosed holding stock options in Zeltiq Aesthetics, which manufactures cryolipolysis equipment. SDEF and this news organization are owned by Elsevier.
DANA POINT, CALIF. – Practice skepticism when it comes to the efficacy of noninvasive fat removal devices, advised Dr. Matthew A. Avram.
"Fat removal has a long history of 'snake oil' salesmanship," Dr. Avram said at the Summit in Aesthetic Medicine, which was sponsored by Skin Disease Education Foundation (SDEF). "You can count on this to continue, because many of these devices do little, if anything. It is important to critically assess these technologies in this emerging field."
Focused Ultrasound
Dr. Avram, faculty director for procedural dermatology training at Harvard Medical School and director of the dermatology laser and cosmetic center at Massachusetts General Hospital, both in Boston, discussed the evidence surrounding devices for noninvasive fat reduction.
One non–Food and Drug Administration–cleared modality being studied is focused ultrasound, which delivers mechanical, nonthermal energy to the thigh, abdomen, and flanks. A study of 30 patients who were treated once a month for 3 months demonstrated a circumference reduction of 2-4 cm in the treated sites (Lasers Surg. Med. 2007;39:315-23). Liver function tests, a lipid panel, and liver ultrasound showed no adverse systemic effects from the procedure.
However, Dr. Avram noted that the study is limited because there was no untreated control group and that circumference "is an inherently imprecise measure of improvement that can be manipulated." MRI would prove objective improvement, he said, but it was not performed in this trial.
In a subsequent study from Hong Kong, 53 patients underwent treatment once a month for 3 months for body contouring (Lasers Surg. Med. 2009; 41:751-9). No significant changes were observed in circumference and caliper measurements, and patients rated their satisfaction as poor.
High-Intensity Focused Ultrasound
High-intensity focused ultrasound, which is also not FDA cleared, involves the rapid heating of adipocytes that are purported to produce coagulative necrosis and cell death in adipose tissue. A retrospective chart review of the modality that was used in 85 patients who underwent one treatment session showed a mean 4.6 cm decrease in waist circumference after 3 months (Aesth. Plast. Surg. 2010;34:577-82). Adverse events that lasted 4-12 weeks occurred in 12% of subjects and included prolonged tenderness, ecchymosis, nodules, and edema, as well as procedural pain in one patient, which required discontinuation of the procedure.
Dr. Avram called high-intensity focused ultrasound a promising technology, "but it's difficult to assess its efficacy. Further study of this technology is needed."
Monopolar Radiofrequency
Monopolar radiofrequency, conventionally used for tissue tightening of the face, has produced lipoatrophy with aggressive settings as a complication. "Perhaps this can be harnessed to effectively treat fat," he said, noting that clinical studies are currently underway.
Low-Level Light Therapy
Low-level light therapy, an FDA-cleared modality for fat removal, uses a multiple head, low-level diode laser at an energy level of 635 nm, which is "roughly equivalent to a laser pointer," Dr. Avram said. In one randomized trial, 59 patients received three treatments of the technology or sham treatment per week for 2 weeks (Lasers Surg. Med. 2009;41:799-809). At 2 weeks, mean circumference reductions in the treatment group were 0.98 inches at the waist, 1.05 inches at the hip, and 0.85 inches at the right thigh and 0.65 inches at the left thigh. Circumference increased in the 2 weeks following treatment.
Dr. Avram said the study was poorly designed because there was no untreated control group, the duration of treatment was only 2 weeks, and there was no ultrasound or other noninvasive evidence of decreased fat layer. "Treat with extreme skepticism," he advised.
Cryolipolysis
Perhaps the most promising technology is cryolipolysis, he said, which is FDA cleared for noninvasive fat removal. Cryolipolysis involves the noninvasive cooling of fat to selectively cause cell death without damage to surrounding tissue.
The mechanism of action of cryolipolysis is believed to involve selective crystallization of lipids in fat cells at temperatures near freezing. "Apoptotic fat cell death is followed by slow dissolution of the fat cell and a gradual release of lipids," Dr. Avram explained. "The inflammatory process results in fat layer reduction over 2-4 months."
When human studies of the technology were first conducted in 2008, enrollment was restricted to 32 patients whose "love handles" were treated at a cooling intensity factor (CIF) of 33 for 60 minutes, and progressed to higher rates of energy extractions for 45 minutes per application site. One side was treated; the untreated contralateral side served as the control.
Efficacy was evaluated at 4 months post treatment via visual assessment as a primary end point, as well as ultrasound and histology. The ultrasound results demonstrated an average 23% decrease in fat layer thickness.
"In this initial group of 32 love handle patients treated once, discernible changes were seen on the treated side vs. baseline of the treated side, and compared to the untreated contralateral control," Dr. Avram said of the findings presented during a poster session at the 2008 annual meeting of the American Society for Dermatologic Surgery. "This unique study design [using each patient as his or her own control], provided very powerful evidence that this was a true treatment effect rather than a change in the patient's diet or exercise pattern during the 4 months after this single procedure exposure."
Common effects after cryolipolysis include redness, which lasts minutes to a few hours; bruising, which may last for a few weeks; and temporary dulling of sensation in the treated area, which typically resolves in 1-8 weeks. No postprocedural changes in pigmentation or laboratory abnormalities have been observed, he said.
About 1 in 2,000 patients experiences severe pain beginning 3-7 days post treatment, which translates into 26 reported cases out of 60,000 treatments. "We are not sure why these occur, but these cases completely resolve with no sequelae," Dr. Avram said.
He emphasized that cryolipolysis is not a replacement for liposuction. "It is not a weight-loss device," he said. "It's best suited for local fat removal resistant to exercise in relatively fit patients."
Dr. Avram disclosed holding stock options in Zeltiq Aesthetics, which manufactures cryolipolysis equipment. SDEF and this news organization are owned by Elsevier.
DANA POINT, CALIF. – Practice skepticism when it comes to the efficacy of noninvasive fat removal devices, advised Dr. Matthew A. Avram.
"Fat removal has a long history of 'snake oil' salesmanship," Dr. Avram said at the Summit in Aesthetic Medicine, which was sponsored by Skin Disease Education Foundation (SDEF). "You can count on this to continue, because many of these devices do little, if anything. It is important to critically assess these technologies in this emerging field."
Focused Ultrasound
Dr. Avram, faculty director for procedural dermatology training at Harvard Medical School and director of the dermatology laser and cosmetic center at Massachusetts General Hospital, both in Boston, discussed the evidence surrounding devices for noninvasive fat reduction.
One non–Food and Drug Administration–cleared modality being studied is focused ultrasound, which delivers mechanical, nonthermal energy to the thigh, abdomen, and flanks. A study of 30 patients who were treated once a month for 3 months demonstrated a circumference reduction of 2-4 cm in the treated sites (Lasers Surg. Med. 2007;39:315-23). Liver function tests, a lipid panel, and liver ultrasound showed no adverse systemic effects from the procedure.
However, Dr. Avram noted that the study is limited because there was no untreated control group and that circumference "is an inherently imprecise measure of improvement that can be manipulated." MRI would prove objective improvement, he said, but it was not performed in this trial.
In a subsequent study from Hong Kong, 53 patients underwent treatment once a month for 3 months for body contouring (Lasers Surg. Med. 2009; 41:751-9). No significant changes were observed in circumference and caliper measurements, and patients rated their satisfaction as poor.
High-Intensity Focused Ultrasound
High-intensity focused ultrasound, which is also not FDA cleared, involves the rapid heating of adipocytes that are purported to produce coagulative necrosis and cell death in adipose tissue. A retrospective chart review of the modality that was used in 85 patients who underwent one treatment session showed a mean 4.6 cm decrease in waist circumference after 3 months (Aesth. Plast. Surg. 2010;34:577-82). Adverse events that lasted 4-12 weeks occurred in 12% of subjects and included prolonged tenderness, ecchymosis, nodules, and edema, as well as procedural pain in one patient, which required discontinuation of the procedure.
Dr. Avram called high-intensity focused ultrasound a promising technology, "but it's difficult to assess its efficacy. Further study of this technology is needed."
Monopolar Radiofrequency
Monopolar radiofrequency, conventionally used for tissue tightening of the face, has produced lipoatrophy with aggressive settings as a complication. "Perhaps this can be harnessed to effectively treat fat," he said, noting that clinical studies are currently underway.
Low-Level Light Therapy
Low-level light therapy, an FDA-cleared modality for fat removal, uses a multiple head, low-level diode laser at an energy level of 635 nm, which is "roughly equivalent to a laser pointer," Dr. Avram said. In one randomized trial, 59 patients received three treatments of the technology or sham treatment per week for 2 weeks (Lasers Surg. Med. 2009;41:799-809). At 2 weeks, mean circumference reductions in the treatment group were 0.98 inches at the waist, 1.05 inches at the hip, and 0.85 inches at the right thigh and 0.65 inches at the left thigh. Circumference increased in the 2 weeks following treatment.
Dr. Avram said the study was poorly designed because there was no untreated control group, the duration of treatment was only 2 weeks, and there was no ultrasound or other noninvasive evidence of decreased fat layer. "Treat with extreme skepticism," he advised.
Cryolipolysis
Perhaps the most promising technology is cryolipolysis, he said, which is FDA cleared for noninvasive fat removal. Cryolipolysis involves the noninvasive cooling of fat to selectively cause cell death without damage to surrounding tissue.
The mechanism of action of cryolipolysis is believed to involve selective crystallization of lipids in fat cells at temperatures near freezing. "Apoptotic fat cell death is followed by slow dissolution of the fat cell and a gradual release of lipids," Dr. Avram explained. "The inflammatory process results in fat layer reduction over 2-4 months."
When human studies of the technology were first conducted in 2008, enrollment was restricted to 32 patients whose "love handles" were treated at a cooling intensity factor (CIF) of 33 for 60 minutes, and progressed to higher rates of energy extractions for 45 minutes per application site. One side was treated; the untreated contralateral side served as the control.
Efficacy was evaluated at 4 months post treatment via visual assessment as a primary end point, as well as ultrasound and histology. The ultrasound results demonstrated an average 23% decrease in fat layer thickness.
"In this initial group of 32 love handle patients treated once, discernible changes were seen on the treated side vs. baseline of the treated side, and compared to the untreated contralateral control," Dr. Avram said of the findings presented during a poster session at the 2008 annual meeting of the American Society for Dermatologic Surgery. "This unique study design [using each patient as his or her own control], provided very powerful evidence that this was a true treatment effect rather than a change in the patient's diet or exercise pattern during the 4 months after this single procedure exposure."
Common effects after cryolipolysis include redness, which lasts minutes to a few hours; bruising, which may last for a few weeks; and temporary dulling of sensation in the treated area, which typically resolves in 1-8 weeks. No postprocedural changes in pigmentation or laboratory abnormalities have been observed, he said.
About 1 in 2,000 patients experiences severe pain beginning 3-7 days post treatment, which translates into 26 reported cases out of 60,000 treatments. "We are not sure why these occur, but these cases completely resolve with no sequelae," Dr. Avram said.
He emphasized that cryolipolysis is not a replacement for liposuction. "It is not a weight-loss device," he said. "It's best suited for local fat removal resistant to exercise in relatively fit patients."
Dr. Avram disclosed holding stock options in Zeltiq Aesthetics, which manufactures cryolipolysis equipment. SDEF and this news organization are owned by Elsevier.
EXPERT ANALYISIS FROM THE SDEF SUMMIT IN AESTHETIC MEDICINE
Infliximab Increases Post-IPAA Complications in Children
PALM DESERT, CALIF. – Children treated with infliximab prior to ileal pouch anal anastomosis for chronic ulcerative colitis experienced nearly twice as many postoperative complications, compared with controls, but the long-term outcomes were similar between the two groups, results from a single-center study showed.
Infliximab, an anti–tumor necrosis factor–alpha antibody, has become increasingly popular for the treatment of ulcerative colitis and was approved by the Food and Drug Administration for use in moderate and severe disease in 2005. "Since that time, there have been a multitude of conflicting reports regarding infliximab’s potential to cause postoperative infections," Dr. Raelene Kennedy said at the annual meeting of the American Pediatric Surgical Association. "However, there has been a lack of data specific to the pediatric population."
Dr. Kennedy of the Mayo Clinic, Rochester, Minn., and her pediatric surgery associates retrospectively studied 38 patients aged 18 years and younger who underwent ileal pouch anal anastomosis (IPAA) for chronic ulcerative colitis at the Mayo Clinic in 2003-2008. Of these, 11 patients received infliximab within 8 weeks prior to surgery. The control group included 27 patients who were well matched in terms of age and sex. "However, preoperative albumin levels were slightly lower in the infliximab group (3.4 vs. 4 g/dL)," she said. "This may suggest that our infliximab group had more severe disease."
Use of other medications was similar between the two groups, except that a significantly greater proportion of patients in the infliximab group vs. the control group used thiopurines (91% vs. 41%, respectively).
Operative technique for the groups varied. Overall, most patients underwent a two-stage procedure, but 33% of control group patients underwent three-stage procedures, whereas none in the infliximab group did. Additionally, a laparoscopic approach was used for all patients in the infliximab group, compared with 63% of the control group.
Overall complications following IPAA were more frequent in the infliximab group than in the control group (55% vs. 26%, respectively), but this did not reach statistical significance. Small-bowel obstruction was significantly higher in the infliximab group, compared with the control group (55% vs. 7%), as was the rate of wound infections (18% vs. 7%). The rate of postoperative leaks between the two groups was similar (9% vs. 7%, respectively).
Compared with controls, a greater proportion of patients in the infliximab group had leak/abscess, small-bowel obstruction, wound infection, or pouchitis 30 days after ileostomy closure (36% vs. 19%), but there were no differences in the rates of complications between the two groups at postoperative year 1 (64% in the infliximab group vs. 62% in the control group). Pouchitis accounted for nearly all of the late complications in both groups.
"From this, we can conclude that children treated with infliximab prior to surgery are at increased risk for postoperative complications following their pouch procedures," Dr. Kennedy said. "Specifically, these children are at increased risk for small-bowel obstruction and wound infection. However, long-term outcomes remain similar to [those of] children who were not treated with infliximab."
She acknowledged certain limitations of the study, including its small sample size. "Larger pediatric studies are required to further evaluate these findings," she said.
Currently, Dr. Kennedy and her associates recommend discontinuing infliximab at least 8 weeks prior to IPAA when possible. "For patients who are currently being treated with infliximab, we recommend total abdominal colectomy with temporary end ileostomy followed by IPAA at a later date," she said.
Dr. Kennedy said that she had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Children treated with infliximab prior to ileal pouch anal anastomosis for chronic ulcerative colitis experienced nearly twice as many postoperative complications, compared with controls, but the long-term outcomes were similar between the two groups, results from a single-center study showed.
Infliximab, an anti–tumor necrosis factor–alpha antibody, has become increasingly popular for the treatment of ulcerative colitis and was approved by the Food and Drug Administration for use in moderate and severe disease in 2005. "Since that time, there have been a multitude of conflicting reports regarding infliximab’s potential to cause postoperative infections," Dr. Raelene Kennedy said at the annual meeting of the American Pediatric Surgical Association. "However, there has been a lack of data specific to the pediatric population."
Dr. Kennedy of the Mayo Clinic, Rochester, Minn., and her pediatric surgery associates retrospectively studied 38 patients aged 18 years and younger who underwent ileal pouch anal anastomosis (IPAA) for chronic ulcerative colitis at the Mayo Clinic in 2003-2008. Of these, 11 patients received infliximab within 8 weeks prior to surgery. The control group included 27 patients who were well matched in terms of age and sex. "However, preoperative albumin levels were slightly lower in the infliximab group (3.4 vs. 4 g/dL)," she said. "This may suggest that our infliximab group had more severe disease."
Use of other medications was similar between the two groups, except that a significantly greater proportion of patients in the infliximab group vs. the control group used thiopurines (91% vs. 41%, respectively).
Operative technique for the groups varied. Overall, most patients underwent a two-stage procedure, but 33% of control group patients underwent three-stage procedures, whereas none in the infliximab group did. Additionally, a laparoscopic approach was used for all patients in the infliximab group, compared with 63% of the control group.
Overall complications following IPAA were more frequent in the infliximab group than in the control group (55% vs. 26%, respectively), but this did not reach statistical significance. Small-bowel obstruction was significantly higher in the infliximab group, compared with the control group (55% vs. 7%), as was the rate of wound infections (18% vs. 7%). The rate of postoperative leaks between the two groups was similar (9% vs. 7%, respectively).
Compared with controls, a greater proportion of patients in the infliximab group had leak/abscess, small-bowel obstruction, wound infection, or pouchitis 30 days after ileostomy closure (36% vs. 19%), but there were no differences in the rates of complications between the two groups at postoperative year 1 (64% in the infliximab group vs. 62% in the control group). Pouchitis accounted for nearly all of the late complications in both groups.
"From this, we can conclude that children treated with infliximab prior to surgery are at increased risk for postoperative complications following their pouch procedures," Dr. Kennedy said. "Specifically, these children are at increased risk for small-bowel obstruction and wound infection. However, long-term outcomes remain similar to [those of] children who were not treated with infliximab."
She acknowledged certain limitations of the study, including its small sample size. "Larger pediatric studies are required to further evaluate these findings," she said.
Currently, Dr. Kennedy and her associates recommend discontinuing infliximab at least 8 weeks prior to IPAA when possible. "For patients who are currently being treated with infliximab, we recommend total abdominal colectomy with temporary end ileostomy followed by IPAA at a later date," she said.
Dr. Kennedy said that she had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Children treated with infliximab prior to ileal pouch anal anastomosis for chronic ulcerative colitis experienced nearly twice as many postoperative complications, compared with controls, but the long-term outcomes were similar between the two groups, results from a single-center study showed.
Infliximab, an anti–tumor necrosis factor–alpha antibody, has become increasingly popular for the treatment of ulcerative colitis and was approved by the Food and Drug Administration for use in moderate and severe disease in 2005. "Since that time, there have been a multitude of conflicting reports regarding infliximab’s potential to cause postoperative infections," Dr. Raelene Kennedy said at the annual meeting of the American Pediatric Surgical Association. "However, there has been a lack of data specific to the pediatric population."
Dr. Kennedy of the Mayo Clinic, Rochester, Minn., and her pediatric surgery associates retrospectively studied 38 patients aged 18 years and younger who underwent ileal pouch anal anastomosis (IPAA) for chronic ulcerative colitis at the Mayo Clinic in 2003-2008. Of these, 11 patients received infliximab within 8 weeks prior to surgery. The control group included 27 patients who were well matched in terms of age and sex. "However, preoperative albumin levels were slightly lower in the infliximab group (3.4 vs. 4 g/dL)," she said. "This may suggest that our infliximab group had more severe disease."
Use of other medications was similar between the two groups, except that a significantly greater proportion of patients in the infliximab group vs. the control group used thiopurines (91% vs. 41%, respectively).
Operative technique for the groups varied. Overall, most patients underwent a two-stage procedure, but 33% of control group patients underwent three-stage procedures, whereas none in the infliximab group did. Additionally, a laparoscopic approach was used for all patients in the infliximab group, compared with 63% of the control group.
Overall complications following IPAA were more frequent in the infliximab group than in the control group (55% vs. 26%, respectively), but this did not reach statistical significance. Small-bowel obstruction was significantly higher in the infliximab group, compared with the control group (55% vs. 7%), as was the rate of wound infections (18% vs. 7%). The rate of postoperative leaks between the two groups was similar (9% vs. 7%, respectively).
Compared with controls, a greater proportion of patients in the infliximab group had leak/abscess, small-bowel obstruction, wound infection, or pouchitis 30 days after ileostomy closure (36% vs. 19%), but there were no differences in the rates of complications between the two groups at postoperative year 1 (64% in the infliximab group vs. 62% in the control group). Pouchitis accounted for nearly all of the late complications in both groups.
"From this, we can conclude that children treated with infliximab prior to surgery are at increased risk for postoperative complications following their pouch procedures," Dr. Kennedy said. "Specifically, these children are at increased risk for small-bowel obstruction and wound infection. However, long-term outcomes remain similar to [those of] children who were not treated with infliximab."
She acknowledged certain limitations of the study, including its small sample size. "Larger pediatric studies are required to further evaluate these findings," she said.
Currently, Dr. Kennedy and her associates recommend discontinuing infliximab at least 8 weeks prior to IPAA when possible. "For patients who are currently being treated with infliximab, we recommend total abdominal colectomy with temporary end ileostomy followed by IPAA at a later date," she said.
Dr. Kennedy said that she had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
FROM THE ANNUAL MEETING OF THE AMERICAN PEDIATRIC SURGICAL ASSOCIATION
Infliximab Increases Post-IPAA Complications in Children
PALM DESERT, CALIF. – Children treated with infliximab prior to ileal pouch anal anastomosis for chronic ulcerative colitis experienced nearly twice as many postoperative complications, compared with controls, but the long-term outcomes were similar between the two groups, results from a single-center study showed.
Infliximab, an anti–tumor necrosis factor–alpha antibody, has become increasingly popular for the treatment of ulcerative colitis and was approved by the Food and Drug Administration for use in moderate and severe disease in 2005. "Since that time, there have been a multitude of conflicting reports regarding infliximab’s potential to cause postoperative infections," Dr. Raelene Kennedy said at the annual meeting of the American Pediatric Surgical Association. "However, there has been a lack of data specific to the pediatric population."
Dr. Kennedy of the Mayo Clinic, Rochester, Minn., and her pediatric surgery associates retrospectively studied 38 patients aged 18 years and younger who underwent ileal pouch anal anastomosis (IPAA) for chronic ulcerative colitis at the Mayo Clinic in 2003-2008. Of these, 11 patients received infliximab within 8 weeks prior to surgery. The control group included 27 patients who were well matched in terms of age and sex. "However, preoperative albumin levels were slightly lower in the infliximab group (3.4 vs. 4 g/dL)," she said. "This may suggest that our infliximab group had more severe disease."
Use of other medications was similar between the two groups, except that a significantly greater proportion of patients in the infliximab group vs. the control group used thiopurines (91% vs. 41%, respectively).
Operative technique for the groups varied. Overall, most patients underwent a two-stage procedure, but 33% of control group patients underwent three-stage procedures, whereas none in the infliximab group did. Additionally, a laparoscopic approach was used for all patients in the infliximab group, compared with 63% of the control group.
Overall complications following IPAA were more frequent in the infliximab group than in the control group (55% vs. 26%, respectively), but this did not reach statistical significance. Small-bowel obstruction was significantly higher in the infliximab group, compared with the control group (55% vs. 7%), as was the rate of wound infections (18% vs. 7%). The rate of postoperative leaks between the two groups was similar (9% vs. 7%, respectively).
Compared with controls, a greater proportion of patients in the infliximab group had leak/abscess, small-bowel obstruction, wound infection, or pouchitis 30 days after ileostomy closure (36% vs. 19%), but there were no differences in the rates of complications between the two groups at postoperative year 1 (64% in the infliximab group vs. 62% in the control group). Pouchitis accounted for nearly all of the late complications in both groups.
"From this, we can conclude that children treated with infliximab prior to surgery are at increased risk for postoperative complications following their pouch procedures," Dr. Kennedy said. "Specifically, these children are at increased risk for small-bowel obstruction and wound infection. However, long-term outcomes remain similar to [those of] children who were not treated with infliximab."
She acknowledged certain limitations of the study, including its small sample size. "Larger pediatric studies are required to further evaluate these findings," she said.
Currently, Dr. Kennedy and her associates recommend discontinuing infliximab at least 8 weeks prior to IPAA when possible. "For patients who are currently being treated with infliximab, we recommend total abdominal colectomy with temporary end ileostomy followed by IPAA at a later date," she said.
Dr. Kennedy said that she had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Children treated with infliximab prior to ileal pouch anal anastomosis for chronic ulcerative colitis experienced nearly twice as many postoperative complications, compared with controls, but the long-term outcomes were similar between the two groups, results from a single-center study showed.
Infliximab, an anti–tumor necrosis factor–alpha antibody, has become increasingly popular for the treatment of ulcerative colitis and was approved by the Food and Drug Administration for use in moderate and severe disease in 2005. "Since that time, there have been a multitude of conflicting reports regarding infliximab’s potential to cause postoperative infections," Dr. Raelene Kennedy said at the annual meeting of the American Pediatric Surgical Association. "However, there has been a lack of data specific to the pediatric population."
Dr. Kennedy of the Mayo Clinic, Rochester, Minn., and her pediatric surgery associates retrospectively studied 38 patients aged 18 years and younger who underwent ileal pouch anal anastomosis (IPAA) for chronic ulcerative colitis at the Mayo Clinic in 2003-2008. Of these, 11 patients received infliximab within 8 weeks prior to surgery. The control group included 27 patients who were well matched in terms of age and sex. "However, preoperative albumin levels were slightly lower in the infliximab group (3.4 vs. 4 g/dL)," she said. "This may suggest that our infliximab group had more severe disease."
Use of other medications was similar between the two groups, except that a significantly greater proportion of patients in the infliximab group vs. the control group used thiopurines (91% vs. 41%, respectively).
Operative technique for the groups varied. Overall, most patients underwent a two-stage procedure, but 33% of control group patients underwent three-stage procedures, whereas none in the infliximab group did. Additionally, a laparoscopic approach was used for all patients in the infliximab group, compared with 63% of the control group.
Overall complications following IPAA were more frequent in the infliximab group than in the control group (55% vs. 26%, respectively), but this did not reach statistical significance. Small-bowel obstruction was significantly higher in the infliximab group, compared with the control group (55% vs. 7%), as was the rate of wound infections (18% vs. 7%). The rate of postoperative leaks between the two groups was similar (9% vs. 7%, respectively).
Compared with controls, a greater proportion of patients in the infliximab group had leak/abscess, small-bowel obstruction, wound infection, or pouchitis 30 days after ileostomy closure (36% vs. 19%), but there were no differences in the rates of complications between the two groups at postoperative year 1 (64% in the infliximab group vs. 62% in the control group). Pouchitis accounted for nearly all of the late complications in both groups.
"From this, we can conclude that children treated with infliximab prior to surgery are at increased risk for postoperative complications following their pouch procedures," Dr. Kennedy said. "Specifically, these children are at increased risk for small-bowel obstruction and wound infection. However, long-term outcomes remain similar to [those of] children who were not treated with infliximab."
She acknowledged certain limitations of the study, including its small sample size. "Larger pediatric studies are required to further evaluate these findings," she said.
Currently, Dr. Kennedy and her associates recommend discontinuing infliximab at least 8 weeks prior to IPAA when possible. "For patients who are currently being treated with infliximab, we recommend total abdominal colectomy with temporary end ileostomy followed by IPAA at a later date," she said.
Dr. Kennedy said that she had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Children treated with infliximab prior to ileal pouch anal anastomosis for chronic ulcerative colitis experienced nearly twice as many postoperative complications, compared with controls, but the long-term outcomes were similar between the two groups, results from a single-center study showed.
Infliximab, an anti–tumor necrosis factor–alpha antibody, has become increasingly popular for the treatment of ulcerative colitis and was approved by the Food and Drug Administration for use in moderate and severe disease in 2005. "Since that time, there have been a multitude of conflicting reports regarding infliximab’s potential to cause postoperative infections," Dr. Raelene Kennedy said at the annual meeting of the American Pediatric Surgical Association. "However, there has been a lack of data specific to the pediatric population."
Dr. Kennedy of the Mayo Clinic, Rochester, Minn., and her pediatric surgery associates retrospectively studied 38 patients aged 18 years and younger who underwent ileal pouch anal anastomosis (IPAA) for chronic ulcerative colitis at the Mayo Clinic in 2003-2008. Of these, 11 patients received infliximab within 8 weeks prior to surgery. The control group included 27 patients who were well matched in terms of age and sex. "However, preoperative albumin levels were slightly lower in the infliximab group (3.4 vs. 4 g/dL)," she said. "This may suggest that our infliximab group had more severe disease."
Use of other medications was similar between the two groups, except that a significantly greater proportion of patients in the infliximab group vs. the control group used thiopurines (91% vs. 41%, respectively).
Operative technique for the groups varied. Overall, most patients underwent a two-stage procedure, but 33% of control group patients underwent three-stage procedures, whereas none in the infliximab group did. Additionally, a laparoscopic approach was used for all patients in the infliximab group, compared with 63% of the control group.
Overall complications following IPAA were more frequent in the infliximab group than in the control group (55% vs. 26%, respectively), but this did not reach statistical significance. Small-bowel obstruction was significantly higher in the infliximab group, compared with the control group (55% vs. 7%), as was the rate of wound infections (18% vs. 7%). The rate of postoperative leaks between the two groups was similar (9% vs. 7%, respectively).
Compared with controls, a greater proportion of patients in the infliximab group had leak/abscess, small-bowel obstruction, wound infection, or pouchitis 30 days after ileostomy closure (36% vs. 19%), but there were no differences in the rates of complications between the two groups at postoperative year 1 (64% in the infliximab group vs. 62% in the control group). Pouchitis accounted for nearly all of the late complications in both groups.
"From this, we can conclude that children treated with infliximab prior to surgery are at increased risk for postoperative complications following their pouch procedures," Dr. Kennedy said. "Specifically, these children are at increased risk for small-bowel obstruction and wound infection. However, long-term outcomes remain similar to [those of] children who were not treated with infliximab."
She acknowledged certain limitations of the study, including its small sample size. "Larger pediatric studies are required to further evaluate these findings," she said.
Currently, Dr. Kennedy and her associates recommend discontinuing infliximab at least 8 weeks prior to IPAA when possible. "For patients who are currently being treated with infliximab, we recommend total abdominal colectomy with temporary end ileostomy followed by IPAA at a later date," she said.
Dr. Kennedy said that she had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
FROM THE ANNUAL MEETING OF THE AMERICAN PEDIATRIC SURGICAL ASSOCIATION
Major Finding: Overall complications following IPAA for chronic ulcerative colitis were more frequent in children who were treated preoperatively with infliximab, compared with controls (55% vs. 26%, respectively), but this did not reach statistical significance.
Data Source: A review of 38 patients aged 18 years and younger who underwent IPAA for chronic ulcerative colitis at the Mayo Clinic in 2003-2008.
Disclosures: Dr. Kennedy said that she had no relevant financial conflicts to disclose.
Survey Tackles Competence of Interpreting Medical Findings in Child Sexual Abuse
DENVER – When it comes to accurately interpreting medical findings in suspected cases of child sexual abuse, experience isn’t the only factor.
Physicians who have completed a fellowship in child abuse pediatrics appear to fare best, as do clinicians who have an expert review their cases at least quarterly, and those who read the Quarterly Update, a newsletter with reviews of published medical journal articles in the field of child abuse.
These findings come from a Web-based survey administered between July and December of 2007, Dr. Joyce A. Adams reported at the annual meeting of the Pediatric Academic Societies. The purpose of the survey was to assess clinicians’ ability to recognize and interpret children’s normal and abnormal anogenital findings from magnified photographs, and to determine which factors in education, clinical experience, and oversight correlate with correct responses to the survey questions.
Study participants were sent an invitation via Listservs of the American Academy of Pediatrics section on child abuse and neglect, the Ray Helfer Society, the American Pediatric Association child abuse special interest group, and forensic nurses who examine children, said Dr. Adams of the University of California, San Diego.
The 45-question survey covered 20 cases and included questions on the identification and interpretation of findings in photos, clinical management of cases, and knowledge of medical literature. It also asked participants about their profession, specialty, experience, practice variables, frequency of expert review of cases, memberships in organizations, and related continuing medical education activities.
Dr. Adams reported on findings from 197 completed surveys. More than half (60%) were from physicians, followed by registered nurses (22%) and advanced practice nurses (17%). The remaining 1% of respondents consisted of one physician assistant and one researcher. In all, 51 of the respondents (26%) indicated that they had completed an earlier version of the survey that had been presented at previous child abuse medical conferences.
Correct answers to the survey were agreed upon by an independent panel of Helfer Society members in 2010. The expert panel could not agree on the answers to four of the survey questions, leaving a total of 41 questions to be included in the study. Each question was worth 1 point, with a perfect score being 41.
The mean total score for first-time survey takers was 32, compared with 35 for those who had completed an earlier version of the survey. Dr. Adams and her associates limited all further analyses to the 146 first-time survey takers. They conducted analysis of means, bivariate analysis, and multivariate analysis to identify variables significantly associated with higher survey scores.
Total number of examinations performed and number of examinations performed monthly were significantly associated with a higher total score on the survey. Other factors – such as having completed a fellowship in child abuse pediatrics, being a member of the Ray Helfer Society, attending workshops on sexual abuse evaluation, being a member of the American Professional Society on the Abuse of Children, and reading the Quarterly Update – contributed positively to total score. Using multivariate analysis, researchers found that the three significant contributors to higher total score were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Dr. Adams also reported that non–child abuse physicians, sexual assault nurse examiners, and advanced practice nurses who examined fewer than five children monthly for sexual abuse correctly answered fewer than 70% of the questions.
Dr. Adams acknowledged certain limitations of the study, including the fact that it was a convenience sample and that competence in performing child sexual abuse medical evaluations "involves much more than being able to identify a finding and interpret it, although in my view, that is an important part," she said. "It’s clear that we need additional studies to determine the appropriate content and the frequency of educational programs for people who do this work, and the best methods to ensure that individuals have their cases reviewed by an expert."
Dr. Adams said that she had no relevant financial disclosures.
DENVER – When it comes to accurately interpreting medical findings in suspected cases of child sexual abuse, experience isn’t the only factor.
Physicians who have completed a fellowship in child abuse pediatrics appear to fare best, as do clinicians who have an expert review their cases at least quarterly, and those who read the Quarterly Update, a newsletter with reviews of published medical journal articles in the field of child abuse.
These findings come from a Web-based survey administered between July and December of 2007, Dr. Joyce A. Adams reported at the annual meeting of the Pediatric Academic Societies. The purpose of the survey was to assess clinicians’ ability to recognize and interpret children’s normal and abnormal anogenital findings from magnified photographs, and to determine which factors in education, clinical experience, and oversight correlate with correct responses to the survey questions.
Study participants were sent an invitation via Listservs of the American Academy of Pediatrics section on child abuse and neglect, the Ray Helfer Society, the American Pediatric Association child abuse special interest group, and forensic nurses who examine children, said Dr. Adams of the University of California, San Diego.
The 45-question survey covered 20 cases and included questions on the identification and interpretation of findings in photos, clinical management of cases, and knowledge of medical literature. It also asked participants about their profession, specialty, experience, practice variables, frequency of expert review of cases, memberships in organizations, and related continuing medical education activities.
Dr. Adams reported on findings from 197 completed surveys. More than half (60%) were from physicians, followed by registered nurses (22%) and advanced practice nurses (17%). The remaining 1% of respondents consisted of one physician assistant and one researcher. In all, 51 of the respondents (26%) indicated that they had completed an earlier version of the survey that had been presented at previous child abuse medical conferences.
Correct answers to the survey were agreed upon by an independent panel of Helfer Society members in 2010. The expert panel could not agree on the answers to four of the survey questions, leaving a total of 41 questions to be included in the study. Each question was worth 1 point, with a perfect score being 41.
The mean total score for first-time survey takers was 32, compared with 35 for those who had completed an earlier version of the survey. Dr. Adams and her associates limited all further analyses to the 146 first-time survey takers. They conducted analysis of means, bivariate analysis, and multivariate analysis to identify variables significantly associated with higher survey scores.
Total number of examinations performed and number of examinations performed monthly were significantly associated with a higher total score on the survey. Other factors – such as having completed a fellowship in child abuse pediatrics, being a member of the Ray Helfer Society, attending workshops on sexual abuse evaluation, being a member of the American Professional Society on the Abuse of Children, and reading the Quarterly Update – contributed positively to total score. Using multivariate analysis, researchers found that the three significant contributors to higher total score were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Dr. Adams also reported that non–child abuse physicians, sexual assault nurse examiners, and advanced practice nurses who examined fewer than five children monthly for sexual abuse correctly answered fewer than 70% of the questions.
Dr. Adams acknowledged certain limitations of the study, including the fact that it was a convenience sample and that competence in performing child sexual abuse medical evaluations "involves much more than being able to identify a finding and interpret it, although in my view, that is an important part," she said. "It’s clear that we need additional studies to determine the appropriate content and the frequency of educational programs for people who do this work, and the best methods to ensure that individuals have their cases reviewed by an expert."
Dr. Adams said that she had no relevant financial disclosures.
DENVER – When it comes to accurately interpreting medical findings in suspected cases of child sexual abuse, experience isn’t the only factor.
Physicians who have completed a fellowship in child abuse pediatrics appear to fare best, as do clinicians who have an expert review their cases at least quarterly, and those who read the Quarterly Update, a newsletter with reviews of published medical journal articles in the field of child abuse.
These findings come from a Web-based survey administered between July and December of 2007, Dr. Joyce A. Adams reported at the annual meeting of the Pediatric Academic Societies. The purpose of the survey was to assess clinicians’ ability to recognize and interpret children’s normal and abnormal anogenital findings from magnified photographs, and to determine which factors in education, clinical experience, and oversight correlate with correct responses to the survey questions.
Study participants were sent an invitation via Listservs of the American Academy of Pediatrics section on child abuse and neglect, the Ray Helfer Society, the American Pediatric Association child abuse special interest group, and forensic nurses who examine children, said Dr. Adams of the University of California, San Diego.
The 45-question survey covered 20 cases and included questions on the identification and interpretation of findings in photos, clinical management of cases, and knowledge of medical literature. It also asked participants about their profession, specialty, experience, practice variables, frequency of expert review of cases, memberships in organizations, and related continuing medical education activities.
Dr. Adams reported on findings from 197 completed surveys. More than half (60%) were from physicians, followed by registered nurses (22%) and advanced practice nurses (17%). The remaining 1% of respondents consisted of one physician assistant and one researcher. In all, 51 of the respondents (26%) indicated that they had completed an earlier version of the survey that had been presented at previous child abuse medical conferences.
Correct answers to the survey were agreed upon by an independent panel of Helfer Society members in 2010. The expert panel could not agree on the answers to four of the survey questions, leaving a total of 41 questions to be included in the study. Each question was worth 1 point, with a perfect score being 41.
The mean total score for first-time survey takers was 32, compared with 35 for those who had completed an earlier version of the survey. Dr. Adams and her associates limited all further analyses to the 146 first-time survey takers. They conducted analysis of means, bivariate analysis, and multivariate analysis to identify variables significantly associated with higher survey scores.
Total number of examinations performed and number of examinations performed monthly were significantly associated with a higher total score on the survey. Other factors – such as having completed a fellowship in child abuse pediatrics, being a member of the Ray Helfer Society, attending workshops on sexual abuse evaluation, being a member of the American Professional Society on the Abuse of Children, and reading the Quarterly Update – contributed positively to total score. Using multivariate analysis, researchers found that the three significant contributors to higher total score were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Dr. Adams also reported that non–child abuse physicians, sexual assault nurse examiners, and advanced practice nurses who examined fewer than five children monthly for sexual abuse correctly answered fewer than 70% of the questions.
Dr. Adams acknowledged certain limitations of the study, including the fact that it was a convenience sample and that competence in performing child sexual abuse medical evaluations "involves much more than being able to identify a finding and interpret it, although in my view, that is an important part," she said. "It’s clear that we need additional studies to determine the appropriate content and the frequency of educational programs for people who do this work, and the best methods to ensure that individuals have their cases reviewed by an expert."
Dr. Adams said that she had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE PEDIATRIC ACADEMIC SOCIETIES
Major Finding: On multivariate analysis, the three significant contributors to a higher total score on a survey of interpreting medical findings on child sexual abuse cases were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Data Source: Responses of 197 clinicians to a 45-question survey that included questions on the identification and interpretation of child sexual abuse findings in photos, the clinical management of cases, and knowledge of medical literature.
Disclosures: Dr. Adams said that she had no relevant financial disclosures.
Survey Tackles Competence of Interpreting Medical Findings in Child Sexual Abuse
DENVER – When it comes to accurately interpreting medical findings in suspected cases of child sexual abuse, experience isn’t the only factor.
Physicians who have completed a fellowship in child abuse pediatrics appear to fare best, as do clinicians who have an expert review their cases at least quarterly, and those who read the Quarterly Update, a newsletter with reviews of published medical journal articles in the field of child abuse.
These findings come from a Web-based survey administered between July and December of 2007, Dr. Joyce A. Adams reported at the annual meeting of the Pediatric Academic Societies. The purpose of the survey was to assess clinicians’ ability to recognize and interpret children’s normal and abnormal anogenital findings from magnified photographs, and to determine which factors in education, clinical experience, and oversight correlate with correct responses to the survey questions.
Study participants were sent an invitation via Listservs of the American Academy of Pediatrics section on child abuse and neglect, the Ray Helfer Society, the American Pediatric Association child abuse special interest group, and forensic nurses who examine children, said Dr. Adams of the University of California, San Diego.
The 45-question survey covered 20 cases and included questions on the identification and interpretation of findings in photos, clinical management of cases, and knowledge of medical literature. It also asked participants about their profession, specialty, experience, practice variables, frequency of expert review of cases, memberships in organizations, and related continuing medical education activities.
Dr. Adams reported on findings from 197 completed surveys. More than half (60%) were from physicians, followed by registered nurses (22%) and advanced practice nurses (17%). The remaining 1% of respondents consisted of one physician assistant and one researcher. In all, 51 of the respondents (26%) indicated that they had completed an earlier version of the survey that had been presented at previous child abuse medical conferences.
Correct answers to the survey were agreed upon by an independent panel of Helfer Society members in 2010. The expert panel could not agree on the answers to four of the survey questions, leaving a total of 41 questions to be included in the study. Each question was worth 1 point, with a perfect score being 41.
The mean total score for first-time survey takers was 32, compared with 35 for those who had completed an earlier version of the survey. Dr. Adams and her associates limited all further analyses to the 146 first-time survey takers. They conducted analysis of means, bivariate analysis, and multivariate analysis to identify variables significantly associated with higher survey scores.
Total number of examinations performed and number of examinations performed monthly were significantly associated with a higher total score on the survey. Other factors – such as having completed a fellowship in child abuse pediatrics, being a member of the Ray Helfer Society, attending workshops on sexual abuse evaluation, being a member of the American Professional Society on the Abuse of Children, and reading the Quarterly Update – contributed positively to total score. Using multivariate analysis, researchers found that the three significant contributors to higher total score were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Dr. Adams also reported that non–child abuse physicians, sexual assault nurse examiners, and advanced practice nurses who examined fewer than five children monthly for sexual abuse correctly answered fewer than 70% of the questions.
Dr. Adams acknowledged certain limitations of the study, including the fact that it was a convenience sample and that competence in performing child sexual abuse medical evaluations "involves much more than being able to identify a finding and interpret it, although in my view, that is an important part," she said. "It’s clear that we need additional studies to determine the appropriate content and the frequency of educational programs for people who do this work, and the best methods to ensure that individuals have their cases reviewed by an expert."
Dr. Adams said that she had no relevant financial disclosures.
DENVER – When it comes to accurately interpreting medical findings in suspected cases of child sexual abuse, experience isn’t the only factor.
Physicians who have completed a fellowship in child abuse pediatrics appear to fare best, as do clinicians who have an expert review their cases at least quarterly, and those who read the Quarterly Update, a newsletter with reviews of published medical journal articles in the field of child abuse.
These findings come from a Web-based survey administered between July and December of 2007, Dr. Joyce A. Adams reported at the annual meeting of the Pediatric Academic Societies. The purpose of the survey was to assess clinicians’ ability to recognize and interpret children’s normal and abnormal anogenital findings from magnified photographs, and to determine which factors in education, clinical experience, and oversight correlate with correct responses to the survey questions.
Study participants were sent an invitation via Listservs of the American Academy of Pediatrics section on child abuse and neglect, the Ray Helfer Society, the American Pediatric Association child abuse special interest group, and forensic nurses who examine children, said Dr. Adams of the University of California, San Diego.
The 45-question survey covered 20 cases and included questions on the identification and interpretation of findings in photos, clinical management of cases, and knowledge of medical literature. It also asked participants about their profession, specialty, experience, practice variables, frequency of expert review of cases, memberships in organizations, and related continuing medical education activities.
Dr. Adams reported on findings from 197 completed surveys. More than half (60%) were from physicians, followed by registered nurses (22%) and advanced practice nurses (17%). The remaining 1% of respondents consisted of one physician assistant and one researcher. In all, 51 of the respondents (26%) indicated that they had completed an earlier version of the survey that had been presented at previous child abuse medical conferences.
Correct answers to the survey were agreed upon by an independent panel of Helfer Society members in 2010. The expert panel could not agree on the answers to four of the survey questions, leaving a total of 41 questions to be included in the study. Each question was worth 1 point, with a perfect score being 41.
The mean total score for first-time survey takers was 32, compared with 35 for those who had completed an earlier version of the survey. Dr. Adams and her associates limited all further analyses to the 146 first-time survey takers. They conducted analysis of means, bivariate analysis, and multivariate analysis to identify variables significantly associated with higher survey scores.
Total number of examinations performed and number of examinations performed monthly were significantly associated with a higher total score on the survey. Other factors – such as having completed a fellowship in child abuse pediatrics, being a member of the Ray Helfer Society, attending workshops on sexual abuse evaluation, being a member of the American Professional Society on the Abuse of Children, and reading the Quarterly Update – contributed positively to total score. Using multivariate analysis, researchers found that the three significant contributors to higher total score were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Dr. Adams also reported that non–child abuse physicians, sexual assault nurse examiners, and advanced practice nurses who examined fewer than five children monthly for sexual abuse correctly answered fewer than 70% of the questions.
Dr. Adams acknowledged certain limitations of the study, including the fact that it was a convenience sample and that competence in performing child sexual abuse medical evaluations "involves much more than being able to identify a finding and interpret it, although in my view, that is an important part," she said. "It’s clear that we need additional studies to determine the appropriate content and the frequency of educational programs for people who do this work, and the best methods to ensure that individuals have their cases reviewed by an expert."
Dr. Adams said that she had no relevant financial disclosures.
DENVER – When it comes to accurately interpreting medical findings in suspected cases of child sexual abuse, experience isn’t the only factor.
Physicians who have completed a fellowship in child abuse pediatrics appear to fare best, as do clinicians who have an expert review their cases at least quarterly, and those who read the Quarterly Update, a newsletter with reviews of published medical journal articles in the field of child abuse.
These findings come from a Web-based survey administered between July and December of 2007, Dr. Joyce A. Adams reported at the annual meeting of the Pediatric Academic Societies. The purpose of the survey was to assess clinicians’ ability to recognize and interpret children’s normal and abnormal anogenital findings from magnified photographs, and to determine which factors in education, clinical experience, and oversight correlate with correct responses to the survey questions.
Study participants were sent an invitation via Listservs of the American Academy of Pediatrics section on child abuse and neglect, the Ray Helfer Society, the American Pediatric Association child abuse special interest group, and forensic nurses who examine children, said Dr. Adams of the University of California, San Diego.
The 45-question survey covered 20 cases and included questions on the identification and interpretation of findings in photos, clinical management of cases, and knowledge of medical literature. It also asked participants about their profession, specialty, experience, practice variables, frequency of expert review of cases, memberships in organizations, and related continuing medical education activities.
Dr. Adams reported on findings from 197 completed surveys. More than half (60%) were from physicians, followed by registered nurses (22%) and advanced practice nurses (17%). The remaining 1% of respondents consisted of one physician assistant and one researcher. In all, 51 of the respondents (26%) indicated that they had completed an earlier version of the survey that had been presented at previous child abuse medical conferences.
Correct answers to the survey were agreed upon by an independent panel of Helfer Society members in 2010. The expert panel could not agree on the answers to four of the survey questions, leaving a total of 41 questions to be included in the study. Each question was worth 1 point, with a perfect score being 41.
The mean total score for first-time survey takers was 32, compared with 35 for those who had completed an earlier version of the survey. Dr. Adams and her associates limited all further analyses to the 146 first-time survey takers. They conducted analysis of means, bivariate analysis, and multivariate analysis to identify variables significantly associated with higher survey scores.
Total number of examinations performed and number of examinations performed monthly were significantly associated with a higher total score on the survey. Other factors – such as having completed a fellowship in child abuse pediatrics, being a member of the Ray Helfer Society, attending workshops on sexual abuse evaluation, being a member of the American Professional Society on the Abuse of Children, and reading the Quarterly Update – contributed positively to total score. Using multivariate analysis, researchers found that the three significant contributors to higher total score were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Dr. Adams also reported that non–child abuse physicians, sexual assault nurse examiners, and advanced practice nurses who examined fewer than five children monthly for sexual abuse correctly answered fewer than 70% of the questions.
Dr. Adams acknowledged certain limitations of the study, including the fact that it was a convenience sample and that competence in performing child sexual abuse medical evaluations "involves much more than being able to identify a finding and interpret it, although in my view, that is an important part," she said. "It’s clear that we need additional studies to determine the appropriate content and the frequency of educational programs for people who do this work, and the best methods to ensure that individuals have their cases reviewed by an expert."
Dr. Adams said that she had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE PEDIATRIC ACADEMIC SOCIETIES
Major Finding: On multivariate analysis, the three significant contributors to a higher total score on a survey of interpreting medical findings on child sexual abuse cases were being a child abuse pediatrician, having cases reviewed by an expert at least quarterly, and reading the Quarterly Update.
Data Source: Responses of 197 clinicians to a 45-question survey that included questions on the identification and interpretation of child sexual abuse findings in photos, the clinical management of cases, and knowledge of medical literature.
Disclosures: Dr. Adams said that she had no relevant financial disclosures.
Venovenous ECMO Improves Survival for Select Pediatric Patients
PALM DESERT, CALIF. – Venoarterial extracorporeal circulation membrane oxygenation appears to be the primary mode of treatment for septic patients, but new research suggests that venovenous ECMO confers a significant survival benefit in select noncardiac pediatric patients with sepsis.
"ECMO is used as a last resort in sepsis, but to date there is really no consensus on the best mode of ECMO to be used" in these patients," Dr. Sean C. Skinner said at the annual meeting of the American Pediatric Surgical Association.
To compare venoarterial (VA) with venovenous (VV) ECMO in septic pediatric patients, Dr. Skinner and his associates analyzed Extracorporeal Life Support Organization (ELSO) registry data from 1990 to 2008 in patients younger than age 18 years with a primary, secondary, or discharge diagnosis of sepsis. Patients with congenital heart diagnoses were excluded. The primary outcome was survival.
Patients were grouped by modality (VA vs. VV ECMO) and by three age categories: neonates to 1 month of age, children aged 1 month to 12 years of age, and adolescents older than age 12 years. To assess the patients’ severity of illness, the investigators examined pre-ECMO vasoactive medication and any advanced respiratory support that was provided. Univariate and multivariate analyses were performed.
Of the 4,332 ECMO runs that were analyzed during the study period, 3,256 (75%) were VA and 1,076 (25%) were VV, said Dr. Skinner, a pediatric surgeon at the University of Kentucky, Lexington. Overall survival was 68% and was significantly higher in the VV group, compared with the VA group (79% vs. 64%, respectively). Survival also decreased significantly with age, from 75% of neonates to 40% of children aged 1 month–12 years and 31% of adolescents.
Dr. Skinner reported that there was survival benefit favoring VV in all three age groups. The rate of survival was 83% in neonates who underwent VV vs. 70% in neonates who underwent VA. Survival rates were 64% vs. 37%, respectively, in children 1 month–12 years of age, and were 43% vs. 29%, respectively, in adolescents.
After adjusting for age group, vasoactive medication use, and any advanced respiratory support provided, the investigators found a significant survival benefit to VV ECMO, with an odds ratio for mortality of 2.06 in VA ECMO patients. Advanced age and use of vasoactive medications remain independent mortality risk factors after adjustment (OR, 4.07 for children vs. neonates; OR, 5.84 for adolescents vs. neonates; and OR, 1.28 for those on vasoactive medications vs. those who were not).
Dr. Skinner acknowledged certain limitations of the study: The ELSO registry consists of retrospective data, it was not possible to control for selection bias, and there was limited adjustment for severity of illness.
"We believe that there is a survival benefit in VV vs. VA ECMO in select septic pediatric patients who do not have any underlying congenital heart disease," he concluded. "Patients who have severe cardiac depression may benefit from VA ECMO, but when possible, septic patients can be tried on VV ECMO as a primary modality in a safe manner."
Dr. Skinner said that he had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Venoarterial extracorporeal circulation membrane oxygenation appears to be the primary mode of treatment for septic patients, but new research suggests that venovenous ECMO confers a significant survival benefit in select noncardiac pediatric patients with sepsis.
"ECMO is used as a last resort in sepsis, but to date there is really no consensus on the best mode of ECMO to be used" in these patients," Dr. Sean C. Skinner said at the annual meeting of the American Pediatric Surgical Association.
To compare venoarterial (VA) with venovenous (VV) ECMO in septic pediatric patients, Dr. Skinner and his associates analyzed Extracorporeal Life Support Organization (ELSO) registry data from 1990 to 2008 in patients younger than age 18 years with a primary, secondary, or discharge diagnosis of sepsis. Patients with congenital heart diagnoses were excluded. The primary outcome was survival.
Patients were grouped by modality (VA vs. VV ECMO) and by three age categories: neonates to 1 month of age, children aged 1 month to 12 years of age, and adolescents older than age 12 years. To assess the patients’ severity of illness, the investigators examined pre-ECMO vasoactive medication and any advanced respiratory support that was provided. Univariate and multivariate analyses were performed.
Of the 4,332 ECMO runs that were analyzed during the study period, 3,256 (75%) were VA and 1,076 (25%) were VV, said Dr. Skinner, a pediatric surgeon at the University of Kentucky, Lexington. Overall survival was 68% and was significantly higher in the VV group, compared with the VA group (79% vs. 64%, respectively). Survival also decreased significantly with age, from 75% of neonates to 40% of children aged 1 month–12 years and 31% of adolescents.
Dr. Skinner reported that there was survival benefit favoring VV in all three age groups. The rate of survival was 83% in neonates who underwent VV vs. 70% in neonates who underwent VA. Survival rates were 64% vs. 37%, respectively, in children 1 month–12 years of age, and were 43% vs. 29%, respectively, in adolescents.
After adjusting for age group, vasoactive medication use, and any advanced respiratory support provided, the investigators found a significant survival benefit to VV ECMO, with an odds ratio for mortality of 2.06 in VA ECMO patients. Advanced age and use of vasoactive medications remain independent mortality risk factors after adjustment (OR, 4.07 for children vs. neonates; OR, 5.84 for adolescents vs. neonates; and OR, 1.28 for those on vasoactive medications vs. those who were not).
Dr. Skinner acknowledged certain limitations of the study: The ELSO registry consists of retrospective data, it was not possible to control for selection bias, and there was limited adjustment for severity of illness.
"We believe that there is a survival benefit in VV vs. VA ECMO in select septic pediatric patients who do not have any underlying congenital heart disease," he concluded. "Patients who have severe cardiac depression may benefit from VA ECMO, but when possible, septic patients can be tried on VV ECMO as a primary modality in a safe manner."
Dr. Skinner said that he had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Venoarterial extracorporeal circulation membrane oxygenation appears to be the primary mode of treatment for septic patients, but new research suggests that venovenous ECMO confers a significant survival benefit in select noncardiac pediatric patients with sepsis.
"ECMO is used as a last resort in sepsis, but to date there is really no consensus on the best mode of ECMO to be used" in these patients," Dr. Sean C. Skinner said at the annual meeting of the American Pediatric Surgical Association.
To compare venoarterial (VA) with venovenous (VV) ECMO in septic pediatric patients, Dr. Skinner and his associates analyzed Extracorporeal Life Support Organization (ELSO) registry data from 1990 to 2008 in patients younger than age 18 years with a primary, secondary, or discharge diagnosis of sepsis. Patients with congenital heart diagnoses were excluded. The primary outcome was survival.
Patients were grouped by modality (VA vs. VV ECMO) and by three age categories: neonates to 1 month of age, children aged 1 month to 12 years of age, and adolescents older than age 12 years. To assess the patients’ severity of illness, the investigators examined pre-ECMO vasoactive medication and any advanced respiratory support that was provided. Univariate and multivariate analyses were performed.
Of the 4,332 ECMO runs that were analyzed during the study period, 3,256 (75%) were VA and 1,076 (25%) were VV, said Dr. Skinner, a pediatric surgeon at the University of Kentucky, Lexington. Overall survival was 68% and was significantly higher in the VV group, compared with the VA group (79% vs. 64%, respectively). Survival also decreased significantly with age, from 75% of neonates to 40% of children aged 1 month–12 years and 31% of adolescents.
Dr. Skinner reported that there was survival benefit favoring VV in all three age groups. The rate of survival was 83% in neonates who underwent VV vs. 70% in neonates who underwent VA. Survival rates were 64% vs. 37%, respectively, in children 1 month–12 years of age, and were 43% vs. 29%, respectively, in adolescents.
After adjusting for age group, vasoactive medication use, and any advanced respiratory support provided, the investigators found a significant survival benefit to VV ECMO, with an odds ratio for mortality of 2.06 in VA ECMO patients. Advanced age and use of vasoactive medications remain independent mortality risk factors after adjustment (OR, 4.07 for children vs. neonates; OR, 5.84 for adolescents vs. neonates; and OR, 1.28 for those on vasoactive medications vs. those who were not).
Dr. Skinner acknowledged certain limitations of the study: The ELSO registry consists of retrospective data, it was not possible to control for selection bias, and there was limited adjustment for severity of illness.
"We believe that there is a survival benefit in VV vs. VA ECMO in select septic pediatric patients who do not have any underlying congenital heart disease," he concluded. "Patients who have severe cardiac depression may benefit from VA ECMO, but when possible, septic patients can be tried on VV ECMO as a primary modality in a safe manner."
Dr. Skinner said that he had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
FROM THE ANNUAL MEETING OF THE AMERICAN PEDIATRIC SURGICAL ASSOCIATION
Venovenous ECMO Improves Survival for Select Pediatric Patients
PALM DESERT, CALIF. – Venoarterial extracorporeal circulation membrane oxygenation appears to be the primary mode of treatment for septic patients, but new research suggests that venovenous ECMO confers a significant survival benefit in select noncardiac pediatric patients with sepsis.
"ECMO is used as a last resort in sepsis, but to date there is really no consensus on the best mode of ECMO to be used" in these patients," Dr. Sean C. Skinner said at the annual meeting of the American Pediatric Surgical Association.
To compare venoarterial (VA) with venovenous (VV) ECMO in septic pediatric patients, Dr. Skinner and his associates analyzed Extracorporeal Life Support Organization (ELSO) registry data from 1990 to 2008 in patients younger than age 18 years with a primary, secondary, or discharge diagnosis of sepsis. Patients with congenital heart diagnoses were excluded. The primary outcome was survival.
Patients were grouped by modality (VA vs. VV ECMO) and by three age categories: neonates to 1 month of age, children aged 1 month to 12 years of age, and adolescents older than age 12 years. To assess the patients’ severity of illness, the investigators examined pre-ECMO vasoactive medication and any advanced respiratory support that was provided. Univariate and multivariate analyses were performed.
Of the 4,332 ECMO runs that were analyzed during the study period, 3,256 (75%) were VA and 1,076 (25%) were VV, said Dr. Skinner, a pediatric surgeon at the University of Kentucky, Lexington. Overall survival was 68% and was significantly higher in the VV group, compared with the VA group (79% vs. 64%, respectively). Survival also decreased significantly with age, from 75% of neonates to 40% of children aged 1 month–12 years and 31% of adolescents.
Dr. Skinner reported that there was survival benefit favoring VV in all three age groups. The rate of survival was 83% in neonates who underwent VV vs. 70% in neonates who underwent VA. Survival rates were 64% vs. 37%, respectively, in children 1 month–12 years of age, and were 43% vs. 29%, respectively, in adolescents.
After adjusting for age group, vasoactive medication use, and any advanced respiratory support provided, the investigators found a significant survival benefit to VV ECMO, with an odds ratio for mortality of 2.06 in VA ECMO patients. Advanced age and use of vasoactive medications remain independent mortality risk factors after adjustment (OR, 4.07 for children vs. neonates; OR, 5.84 for adolescents vs. neonates; and OR, 1.28 for those on vasoactive medications vs. those who were not).
Dr. Skinner acknowledged certain limitations of the study: The ELSO registry consists of retrospective data, it was not possible to control for selection bias, and there was limited adjustment for severity of illness.
"We believe that there is a survival benefit in VV vs. VA ECMO in select septic pediatric patients who do not have any underlying congenital heart disease," he concluded. "Patients who have severe cardiac depression may benefit from VA ECMO, but when possible, septic patients can be tried on VV ECMO as a primary modality in a safe manner."
Dr. Skinner said that he had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Venoarterial extracorporeal circulation membrane oxygenation appears to be the primary mode of treatment for septic patients, but new research suggests that venovenous ECMO confers a significant survival benefit in select noncardiac pediatric patients with sepsis.
"ECMO is used as a last resort in sepsis, but to date there is really no consensus on the best mode of ECMO to be used" in these patients," Dr. Sean C. Skinner said at the annual meeting of the American Pediatric Surgical Association.
To compare venoarterial (VA) with venovenous (VV) ECMO in septic pediatric patients, Dr. Skinner and his associates analyzed Extracorporeal Life Support Organization (ELSO) registry data from 1990 to 2008 in patients younger than age 18 years with a primary, secondary, or discharge diagnosis of sepsis. Patients with congenital heart diagnoses were excluded. The primary outcome was survival.
Patients were grouped by modality (VA vs. VV ECMO) and by three age categories: neonates to 1 month of age, children aged 1 month to 12 years of age, and adolescents older than age 12 years. To assess the patients’ severity of illness, the investigators examined pre-ECMO vasoactive medication and any advanced respiratory support that was provided. Univariate and multivariate analyses were performed.
Of the 4,332 ECMO runs that were analyzed during the study period, 3,256 (75%) were VA and 1,076 (25%) were VV, said Dr. Skinner, a pediatric surgeon at the University of Kentucky, Lexington. Overall survival was 68% and was significantly higher in the VV group, compared with the VA group (79% vs. 64%, respectively). Survival also decreased significantly with age, from 75% of neonates to 40% of children aged 1 month–12 years and 31% of adolescents.
Dr. Skinner reported that there was survival benefit favoring VV in all three age groups. The rate of survival was 83% in neonates who underwent VV vs. 70% in neonates who underwent VA. Survival rates were 64% vs. 37%, respectively, in children 1 month–12 years of age, and were 43% vs. 29%, respectively, in adolescents.
After adjusting for age group, vasoactive medication use, and any advanced respiratory support provided, the investigators found a significant survival benefit to VV ECMO, with an odds ratio for mortality of 2.06 in VA ECMO patients. Advanced age and use of vasoactive medications remain independent mortality risk factors after adjustment (OR, 4.07 for children vs. neonates; OR, 5.84 for adolescents vs. neonates; and OR, 1.28 for those on vasoactive medications vs. those who were not).
Dr. Skinner acknowledged certain limitations of the study: The ELSO registry consists of retrospective data, it was not possible to control for selection bias, and there was limited adjustment for severity of illness.
"We believe that there is a survival benefit in VV vs. VA ECMO in select septic pediatric patients who do not have any underlying congenital heart disease," he concluded. "Patients who have severe cardiac depression may benefit from VA ECMO, but when possible, septic patients can be tried on VV ECMO as a primary modality in a safe manner."
Dr. Skinner said that he had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
PALM DESERT, CALIF. – Venoarterial extracorporeal circulation membrane oxygenation appears to be the primary mode of treatment for septic patients, but new research suggests that venovenous ECMO confers a significant survival benefit in select noncardiac pediatric patients with sepsis.
"ECMO is used as a last resort in sepsis, but to date there is really no consensus on the best mode of ECMO to be used" in these patients," Dr. Sean C. Skinner said at the annual meeting of the American Pediatric Surgical Association.
To compare venoarterial (VA) with venovenous (VV) ECMO in septic pediatric patients, Dr. Skinner and his associates analyzed Extracorporeal Life Support Organization (ELSO) registry data from 1990 to 2008 in patients younger than age 18 years with a primary, secondary, or discharge diagnosis of sepsis. Patients with congenital heart diagnoses were excluded. The primary outcome was survival.
Patients were grouped by modality (VA vs. VV ECMO) and by three age categories: neonates to 1 month of age, children aged 1 month to 12 years of age, and adolescents older than age 12 years. To assess the patients’ severity of illness, the investigators examined pre-ECMO vasoactive medication and any advanced respiratory support that was provided. Univariate and multivariate analyses were performed.
Of the 4,332 ECMO runs that were analyzed during the study period, 3,256 (75%) were VA and 1,076 (25%) were VV, said Dr. Skinner, a pediatric surgeon at the University of Kentucky, Lexington. Overall survival was 68% and was significantly higher in the VV group, compared with the VA group (79% vs. 64%, respectively). Survival also decreased significantly with age, from 75% of neonates to 40% of children aged 1 month–12 years and 31% of adolescents.
Dr. Skinner reported that there was survival benefit favoring VV in all three age groups. The rate of survival was 83% in neonates who underwent VV vs. 70% in neonates who underwent VA. Survival rates were 64% vs. 37%, respectively, in children 1 month–12 years of age, and were 43% vs. 29%, respectively, in adolescents.
After adjusting for age group, vasoactive medication use, and any advanced respiratory support provided, the investigators found a significant survival benefit to VV ECMO, with an odds ratio for mortality of 2.06 in VA ECMO patients. Advanced age and use of vasoactive medications remain independent mortality risk factors after adjustment (OR, 4.07 for children vs. neonates; OR, 5.84 for adolescents vs. neonates; and OR, 1.28 for those on vasoactive medications vs. those who were not).
Dr. Skinner acknowledged certain limitations of the study: The ELSO registry consists of retrospective data, it was not possible to control for selection bias, and there was limited adjustment for severity of illness.
"We believe that there is a survival benefit in VV vs. VA ECMO in select septic pediatric patients who do not have any underlying congenital heart disease," he concluded. "Patients who have severe cardiac depression may benefit from VA ECMO, but when possible, septic patients can be tried on VV ECMO as a primary modality in a safe manner."
Dr. Skinner said that he had no relevant financial conflicts to disclose. The meeting was supported by a grant from Elsevier, which owns this news organization.
FROM THE ANNUAL MEETING OF THE AMERICAN PEDIATRIC SURGICAL ASSOCIATION
Major Finding: There was a significant survival benefit to the venovenous (VV) mode of ECMO in noncardiac pediatric patients with sepsis, with an odds ratio for mortality of 2.06 in the venoarterial (VA) mode of ECMO.
Data Source: A study of 4,332 ECMO runs that compared VA with VV ECMO in septic pediatric patients.
Disclosures: Dr. Skinner said that he had no relevant financial disclosures to make. The meeting was supported by a grant from Elsevier, which owns this news organization.