User login
Consider C. difficile early in children with cancer with GI symptoms
Children with cancer are at increased risk of potentially life-threatening Clostridioides difficile infections (CDI), and Brianna Murphy, DO, reported at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
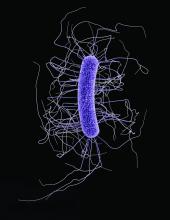
CDI are characterized by diarrhea, fever, and loss of appetite. The clinical features are caused by the release of toxins A and B by this gram-positive bacterium. In pediatric groups, CDI are a leading cause of antibiotic-associated gastric illness. This in turn can lead to a protracted stay in hospital and increases risk of mortality. The rising incidence in the United States over the last 2 decades prompted Dr. Murphy, a pediatric hematology oncology fellow working at the department of pediatric research at the University of Texas MD Anderson Cancer Center, Houston, to investigate further. A search of the literature found limited information regarding CDI and pediatric oncology patients.
Recognized factors for contracting CDI include the presence of other illnesses, a weakened immune system because of drugs or disease, enteral nutrition, usage of medicines such as proton pump inhibitors which decrease gastric acid production, and classically, treatment with broad spectrum antibiotics.
Dr. Murphy’s study included patients aged 1-18 years, all of whom had a cancer diagnosis and a positive stool culture for C. difficile. Presenting symptoms were three or more loose stools per day or acute onset ileus. The study evaluated data for the years 2000-2017 and included 11,366 children; 207 CDI (0.98%) cases were identified among pediatric oncology patients during the study period. This compares with historical data showing an incidence of 0.14% among hospitalized children in general.
Malignancy data were then subdivided into three groups: hematologic, nonneural solid tumors (NNST), and neural tumors. Hematologic malignancies had a CDI prevalence higher than the average for oncologic patients at 5.4%. Inside this group those suffering with acute myeloid leukemia had a rate of 10.5%. In the NNST and neural tumor groups, CDI rates were lower and closer to the overall average.
Dr. Murphy then looked at her patient population in more detail. Poor clinical outcomes (PCOs) were defined as severe, refractory, recurrent, or multiple infections. Severe CDI included features such as toxic megacolon, gastrointestinal perforation, or need for surgical intervention. Refractory CDI were defined as continuation of symptoms beyond 7 days of appropriate therapy, and recurrent CDI were classed as reinfection within 8 weeks of a previous CDI. Ultimately, 51% of patients in this study died. Patients with severe CDI experienced increased mortality (P = .02). There was no difference shown when looking at the type of cancer, age, gender, or patient ethnicity.
Next, Dr. Murphy looked for associations. Hematologic and biochemical testing identified that elevated creatinine was statistically associated with the likelihood of PCOs, compared with leukocytosis and neutropenia, particularly in the NNST group. Treatment modality also was studied. Here radiation therapy was the only treatment shown to increase PCOs in patients with CDI. One-fifth (22%) of radiation therapy recipients experienced multiple CDI, compared with 12% of the total population.
In commenting on her paper, Louis Bent, MD, from the Netherlands raised the issue of deaths in septic patients. What was the origin of the responsible organism, for example from the GI tract or from central lines, and were patients receiving appropriate antibiotic treatment?
Dr. Kelly responded that sepsis was generally believed to occur as a result of infection with mixed bacterial translocation through the bowel wall, notably Escherichia coli. Patients were usually on a cocktail of antibiotics targeting CDI, but also other infections illustrating the serious nature of the situation.
Dr. Murphy had no financial conflicts of interest to declare.
Children with cancer are at increased risk of potentially life-threatening Clostridioides difficile infections (CDI), and Brianna Murphy, DO, reported at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
CDI are characterized by diarrhea, fever, and loss of appetite. The clinical features are caused by the release of toxins A and B by this gram-positive bacterium. In pediatric groups, CDI are a leading cause of antibiotic-associated gastric illness. This in turn can lead to a protracted stay in hospital and increases risk of mortality. The rising incidence in the United States over the last 2 decades prompted Dr. Murphy, a pediatric hematology oncology fellow working at the department of pediatric research at the University of Texas MD Anderson Cancer Center, Houston, to investigate further. A search of the literature found limited information regarding CDI and pediatric oncology patients.
Recognized factors for contracting CDI include the presence of other illnesses, a weakened immune system because of drugs or disease, enteral nutrition, usage of medicines such as proton pump inhibitors which decrease gastric acid production, and classically, treatment with broad spectrum antibiotics.
Dr. Murphy’s study included patients aged 1-18 years, all of whom had a cancer diagnosis and a positive stool culture for C. difficile. Presenting symptoms were three or more loose stools per day or acute onset ileus. The study evaluated data for the years 2000-2017 and included 11,366 children; 207 CDI (0.98%) cases were identified among pediatric oncology patients during the study period. This compares with historical data showing an incidence of 0.14% among hospitalized children in general.
Malignancy data were then subdivided into three groups: hematologic, nonneural solid tumors (NNST), and neural tumors. Hematologic malignancies had a CDI prevalence higher than the average for oncologic patients at 5.4%. Inside this group those suffering with acute myeloid leukemia had a rate of 10.5%. In the NNST and neural tumor groups, CDI rates were lower and closer to the overall average.
Dr. Murphy then looked at her patient population in more detail. Poor clinical outcomes (PCOs) were defined as severe, refractory, recurrent, or multiple infections. Severe CDI included features such as toxic megacolon, gastrointestinal perforation, or need for surgical intervention. Refractory CDI were defined as continuation of symptoms beyond 7 days of appropriate therapy, and recurrent CDI were classed as reinfection within 8 weeks of a previous CDI. Ultimately, 51% of patients in this study died. Patients with severe CDI experienced increased mortality (P = .02). There was no difference shown when looking at the type of cancer, age, gender, or patient ethnicity.
Next, Dr. Murphy looked for associations. Hematologic and biochemical testing identified that elevated creatinine was statistically associated with the likelihood of PCOs, compared with leukocytosis and neutropenia, particularly in the NNST group. Treatment modality also was studied. Here radiation therapy was the only treatment shown to increase PCOs in patients with CDI. One-fifth (22%) of radiation therapy recipients experienced multiple CDI, compared with 12% of the total population.
In commenting on her paper, Louis Bent, MD, from the Netherlands raised the issue of deaths in septic patients. What was the origin of the responsible organism, for example from the GI tract or from central lines, and were patients receiving appropriate antibiotic treatment?
Dr. Kelly responded that sepsis was generally believed to occur as a result of infection with mixed bacterial translocation through the bowel wall, notably Escherichia coli. Patients were usually on a cocktail of antibiotics targeting CDI, but also other infections illustrating the serious nature of the situation.
Dr. Murphy had no financial conflicts of interest to declare.
Children with cancer are at increased risk of potentially life-threatening Clostridioides difficile infections (CDI), and Brianna Murphy, DO, reported at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
CDI are characterized by diarrhea, fever, and loss of appetite. The clinical features are caused by the release of toxins A and B by this gram-positive bacterium. In pediatric groups, CDI are a leading cause of antibiotic-associated gastric illness. This in turn can lead to a protracted stay in hospital and increases risk of mortality. The rising incidence in the United States over the last 2 decades prompted Dr. Murphy, a pediatric hematology oncology fellow working at the department of pediatric research at the University of Texas MD Anderson Cancer Center, Houston, to investigate further. A search of the literature found limited information regarding CDI and pediatric oncology patients.
Recognized factors for contracting CDI include the presence of other illnesses, a weakened immune system because of drugs or disease, enteral nutrition, usage of medicines such as proton pump inhibitors which decrease gastric acid production, and classically, treatment with broad spectrum antibiotics.
Dr. Murphy’s study included patients aged 1-18 years, all of whom had a cancer diagnosis and a positive stool culture for C. difficile. Presenting symptoms were three or more loose stools per day or acute onset ileus. The study evaluated data for the years 2000-2017 and included 11,366 children; 207 CDI (0.98%) cases were identified among pediatric oncology patients during the study period. This compares with historical data showing an incidence of 0.14% among hospitalized children in general.
Malignancy data were then subdivided into three groups: hematologic, nonneural solid tumors (NNST), and neural tumors. Hematologic malignancies had a CDI prevalence higher than the average for oncologic patients at 5.4%. Inside this group those suffering with acute myeloid leukemia had a rate of 10.5%. In the NNST and neural tumor groups, CDI rates were lower and closer to the overall average.
Dr. Murphy then looked at her patient population in more detail. Poor clinical outcomes (PCOs) were defined as severe, refractory, recurrent, or multiple infections. Severe CDI included features such as toxic megacolon, gastrointestinal perforation, or need for surgical intervention. Refractory CDI were defined as continuation of symptoms beyond 7 days of appropriate therapy, and recurrent CDI were classed as reinfection within 8 weeks of a previous CDI. Ultimately, 51% of patients in this study died. Patients with severe CDI experienced increased mortality (P = .02). There was no difference shown when looking at the type of cancer, age, gender, or patient ethnicity.
Next, Dr. Murphy looked for associations. Hematologic and biochemical testing identified that elevated creatinine was statistically associated with the likelihood of PCOs, compared with leukocytosis and neutropenia, particularly in the NNST group. Treatment modality also was studied. Here radiation therapy was the only treatment shown to increase PCOs in patients with CDI. One-fifth (22%) of radiation therapy recipients experienced multiple CDI, compared with 12% of the total population.
In commenting on her paper, Louis Bent, MD, from the Netherlands raised the issue of deaths in septic patients. What was the origin of the responsible organism, for example from the GI tract or from central lines, and were patients receiving appropriate antibiotic treatment?
Dr. Kelly responded that sepsis was generally believed to occur as a result of infection with mixed bacterial translocation through the bowel wall, notably Escherichia coli. Patients were usually on a cocktail of antibiotics targeting CDI, but also other infections illustrating the serious nature of the situation.
Dr. Murphy had no financial conflicts of interest to declare.
FROM ESPID 2020
Should we use antibiotics to treat sore throats?
The use of antibiotics to treat a sore throat remains contentious, with guidelines from around the world providing contradictory advice. This topic generated a lively debate at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
Lauri Ivaska, MD, of the department of pediatrics and adolescent medicine at Turku (Finland) University Hospital, argued for the use of antibiotics, while Borbála Zsigmond, MD, of Heim Pál Children’s Hospital in Budapest, made the case against their use. Interestingly, this debate occurred against the background of a poll conducted before the debate, which found that only 11% of the audience voted in favor of using antibiotics to treat sore throats.
Both speakers began by exploring their approach to the treatment of a recent clinical case involving a 4-year-old girl presenting with sore throat. Dr. Ivaska stressed the difference between a sore throat, pharyngitis, and tonsillitis: the latter two refer to a physical finding, while the former is a subjective symptom.
International guidelines differ on the subject
The debate moved to discussing the international guidelines for treating pharyngitis and tonsillitis. Dr. Zsigmond believes that these are flawed and unhelpful, arguing that they differ depending on what part of the world a physician is practicing in. For example, the 2012 Infectious Diseases Society of America guidelines recommend using best clinical judgment and then backing this up by testing. If testing proves positive for group A Streptococcus pyogenes (GAS), the physician should universally treat. By comparison, the European Society of Clinical Microbiology and Infectious Diseases Sore Throat Guideline Group focuses on severity rather than the cause of the infection. If the case is deemed to be serious, antibiotics can be prescribed without a positive test.
Sore throat is frequently associated with a common cold. In a recent study, more that 80% of students with an acute viral respiratory tract infection had soreness at the beginning of their illness.
Reporting from his own research, Dr. Ivaska argued that viruses can be detected in almost two-thirds of children with pharyngitis using polymerase chain reaction analysis. He thinks antibiotics should be reserved for those 30%-40% of patients with a confirmed GAS infection. The potential role of Fusobacterium necrophorum was raised, but there is no evidence of the benefits of antibiotic treatment in such cases.
There are diagnostic aids for GAS infection
It was suggested that, instead of concentrating on sore throat, the debate should be about whether to use antibiotics to treat GAS infection. But how can the diagnosis be confirmed simply in a clinical setting? Dr. Ivaska recommended adopting diagnostic aids such as Centor, McIsaac, and FeverPAIN, which award scores for several common disease features – the higher the score, the more likely a patient is to be suffering from a GAS infection.
Dr. Zsigmond also likes scoring symptoms but believes they are often inaccurate, especially in young children. She pointed to a report that examined the use of the Centor tool among 441 children attending a pediatric ED. The authors concluded that the Centor criteria were ineffective in predicting a positive GAS culture in throat swabs taken from symptomatic patients.
When are antibiotics warranted?
It is widely accepted that antibiotics should be avoided for viral infections. Returning to the case described at the start of this debate, Dr. Zsigmond calculated that her patient with a 2-day history of sore throat, elevated temperature, pussy tonsils, and enlarged cervical lymph glands but no cough or rhinitis had a FeverPAIN score of 4-5 and a Centor score of 4, meaning that, according to the European guidelines, she should receive antibiotic treatment. However, viral swabs proved positive for adenovirus.
Dr. Ivaska responded with his recent experiences of a similar case, where a 5-year-old boy had a FeverPAIN score of 4-5 and Centor score of 3. Cultures from his throat were GAS positive, illustrating the problem of differentiating between bacterial and viral infections.
But does a GAS-positive pharyngeal culture necessarily mean that antibiotic treatment is indicated? Dr. Ivaska believes it does, citing the importance of preventing serious complications such as rheumatic fever. Dr. Zsigmind countered by pointing out the low levels of acute rheumatic fever in developed nations. In her own country, Hungary, there has not been a case in the last 30 years. Giving antibiotics for historical reasons cannot, in her view, be justified.
Dr. Ivaska responded that perhaps this is because of early treatment in children with sore throats.
Another complication of tonsillitis is quinsy. Dr. Zsigmond cited a study showing that there is no statistically significant evidence demonstrating that antibiotics prevent quinsy. She attributed this to quinsy appearing quickly, typically within 2 days. Delay in seeking help means that the window to treat is often missed. However, should symptoms present early, there is no statistical evidence that prior antibiotic use can prevent quinsy. Also, given the rarity of this condition, prevention would mean excessive use of antibiotics.
Are there other possible benefits of antibiotic treatment in patients with a sore throat? Dr. Ivaska referred to a Cochrane review that found a shortening in duration of throat soreness and fever. Furthermore, compared with placebo, antibiotics reduced the incidence of suppurative complications such as acute otitis media and sinusitis following a sore throat. Other studies have also pointed to the potential benefits of reduced transmission in families where one member with pharyngitis was GAS positive.
As the debate ended, Dr. Zsigmond reported evidence of global antibiotic overprescribing for sore throat ranging from 53% in Europe to 94% in Australia. She also highlighted risks such as altered gut flora, drug resistance, and rashes.
Robin Marlow from the University of Bristol (England), PhD, MBBS, commented that “one of the most enjoyable parts of the ESPID meeting is hearing different viewpoints rationally explained from across the world. As [antibiotic prescription for a sore throat is] a clinical conundrum that faces pediatricians every day, I thought this debate was a really great example of how, despite our different health care systems and ways of working, we are all striving together to improve children’s health using the best evidence available.”
The presenters had no financial conflicts of interest to declare.
The use of antibiotics to treat a sore throat remains contentious, with guidelines from around the world providing contradictory advice. This topic generated a lively debate at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
Lauri Ivaska, MD, of the department of pediatrics and adolescent medicine at Turku (Finland) University Hospital, argued for the use of antibiotics, while Borbála Zsigmond, MD, of Heim Pál Children’s Hospital in Budapest, made the case against their use. Interestingly, this debate occurred against the background of a poll conducted before the debate, which found that only 11% of the audience voted in favor of using antibiotics to treat sore throats.
Both speakers began by exploring their approach to the treatment of a recent clinical case involving a 4-year-old girl presenting with sore throat. Dr. Ivaska stressed the difference between a sore throat, pharyngitis, and tonsillitis: the latter two refer to a physical finding, while the former is a subjective symptom.
International guidelines differ on the subject
The debate moved to discussing the international guidelines for treating pharyngitis and tonsillitis. Dr. Zsigmond believes that these are flawed and unhelpful, arguing that they differ depending on what part of the world a physician is practicing in. For example, the 2012 Infectious Diseases Society of America guidelines recommend using best clinical judgment and then backing this up by testing. If testing proves positive for group A Streptococcus pyogenes (GAS), the physician should universally treat. By comparison, the European Society of Clinical Microbiology and Infectious Diseases Sore Throat Guideline Group focuses on severity rather than the cause of the infection. If the case is deemed to be serious, antibiotics can be prescribed without a positive test.
Sore throat is frequently associated with a common cold. In a recent study, more that 80% of students with an acute viral respiratory tract infection had soreness at the beginning of their illness.
Reporting from his own research, Dr. Ivaska argued that viruses can be detected in almost two-thirds of children with pharyngitis using polymerase chain reaction analysis. He thinks antibiotics should be reserved for those 30%-40% of patients with a confirmed GAS infection. The potential role of Fusobacterium necrophorum was raised, but there is no evidence of the benefits of antibiotic treatment in such cases.
There are diagnostic aids for GAS infection
It was suggested that, instead of concentrating on sore throat, the debate should be about whether to use antibiotics to treat GAS infection. But how can the diagnosis be confirmed simply in a clinical setting? Dr. Ivaska recommended adopting diagnostic aids such as Centor, McIsaac, and FeverPAIN, which award scores for several common disease features – the higher the score, the more likely a patient is to be suffering from a GAS infection.
Dr. Zsigmond also likes scoring symptoms but believes they are often inaccurate, especially in young children. She pointed to a report that examined the use of the Centor tool among 441 children attending a pediatric ED. The authors concluded that the Centor criteria were ineffective in predicting a positive GAS culture in throat swabs taken from symptomatic patients.
When are antibiotics warranted?
It is widely accepted that antibiotics should be avoided for viral infections. Returning to the case described at the start of this debate, Dr. Zsigmond calculated that her patient with a 2-day history of sore throat, elevated temperature, pussy tonsils, and enlarged cervical lymph glands but no cough or rhinitis had a FeverPAIN score of 4-5 and a Centor score of 4, meaning that, according to the European guidelines, she should receive antibiotic treatment. However, viral swabs proved positive for adenovirus.
Dr. Ivaska responded with his recent experiences of a similar case, where a 5-year-old boy had a FeverPAIN score of 4-5 and Centor score of 3. Cultures from his throat were GAS positive, illustrating the problem of differentiating between bacterial and viral infections.
But does a GAS-positive pharyngeal culture necessarily mean that antibiotic treatment is indicated? Dr. Ivaska believes it does, citing the importance of preventing serious complications such as rheumatic fever. Dr. Zsigmind countered by pointing out the low levels of acute rheumatic fever in developed nations. In her own country, Hungary, there has not been a case in the last 30 years. Giving antibiotics for historical reasons cannot, in her view, be justified.
Dr. Ivaska responded that perhaps this is because of early treatment in children with sore throats.
Another complication of tonsillitis is quinsy. Dr. Zsigmond cited a study showing that there is no statistically significant evidence demonstrating that antibiotics prevent quinsy. She attributed this to quinsy appearing quickly, typically within 2 days. Delay in seeking help means that the window to treat is often missed. However, should symptoms present early, there is no statistical evidence that prior antibiotic use can prevent quinsy. Also, given the rarity of this condition, prevention would mean excessive use of antibiotics.
Are there other possible benefits of antibiotic treatment in patients with a sore throat? Dr. Ivaska referred to a Cochrane review that found a shortening in duration of throat soreness and fever. Furthermore, compared with placebo, antibiotics reduced the incidence of suppurative complications such as acute otitis media and sinusitis following a sore throat. Other studies have also pointed to the potential benefits of reduced transmission in families where one member with pharyngitis was GAS positive.
As the debate ended, Dr. Zsigmond reported evidence of global antibiotic overprescribing for sore throat ranging from 53% in Europe to 94% in Australia. She also highlighted risks such as altered gut flora, drug resistance, and rashes.
Robin Marlow from the University of Bristol (England), PhD, MBBS, commented that “one of the most enjoyable parts of the ESPID meeting is hearing different viewpoints rationally explained from across the world. As [antibiotic prescription for a sore throat is] a clinical conundrum that faces pediatricians every day, I thought this debate was a really great example of how, despite our different health care systems and ways of working, we are all striving together to improve children’s health using the best evidence available.”
The presenters had no financial conflicts of interest to declare.
The use of antibiotics to treat a sore throat remains contentious, with guidelines from around the world providing contradictory advice. This topic generated a lively debate at the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year.
Lauri Ivaska, MD, of the department of pediatrics and adolescent medicine at Turku (Finland) University Hospital, argued for the use of antibiotics, while Borbála Zsigmond, MD, of Heim Pál Children’s Hospital in Budapest, made the case against their use. Interestingly, this debate occurred against the background of a poll conducted before the debate, which found that only 11% of the audience voted in favor of using antibiotics to treat sore throats.
Both speakers began by exploring their approach to the treatment of a recent clinical case involving a 4-year-old girl presenting with sore throat. Dr. Ivaska stressed the difference between a sore throat, pharyngitis, and tonsillitis: the latter two refer to a physical finding, while the former is a subjective symptom.
International guidelines differ on the subject
The debate moved to discussing the international guidelines for treating pharyngitis and tonsillitis. Dr. Zsigmond believes that these are flawed and unhelpful, arguing that they differ depending on what part of the world a physician is practicing in. For example, the 2012 Infectious Diseases Society of America guidelines recommend using best clinical judgment and then backing this up by testing. If testing proves positive for group A Streptococcus pyogenes (GAS), the physician should universally treat. By comparison, the European Society of Clinical Microbiology and Infectious Diseases Sore Throat Guideline Group focuses on severity rather than the cause of the infection. If the case is deemed to be serious, antibiotics can be prescribed without a positive test.
Sore throat is frequently associated with a common cold. In a recent study, more that 80% of students with an acute viral respiratory tract infection had soreness at the beginning of their illness.
Reporting from his own research, Dr. Ivaska argued that viruses can be detected in almost two-thirds of children with pharyngitis using polymerase chain reaction analysis. He thinks antibiotics should be reserved for those 30%-40% of patients with a confirmed GAS infection. The potential role of Fusobacterium necrophorum was raised, but there is no evidence of the benefits of antibiotic treatment in such cases.
There are diagnostic aids for GAS infection
It was suggested that, instead of concentrating on sore throat, the debate should be about whether to use antibiotics to treat GAS infection. But how can the diagnosis be confirmed simply in a clinical setting? Dr. Ivaska recommended adopting diagnostic aids such as Centor, McIsaac, and FeverPAIN, which award scores for several common disease features – the higher the score, the more likely a patient is to be suffering from a GAS infection.
Dr. Zsigmond also likes scoring symptoms but believes they are often inaccurate, especially in young children. She pointed to a report that examined the use of the Centor tool among 441 children attending a pediatric ED. The authors concluded that the Centor criteria were ineffective in predicting a positive GAS culture in throat swabs taken from symptomatic patients.
When are antibiotics warranted?
It is widely accepted that antibiotics should be avoided for viral infections. Returning to the case described at the start of this debate, Dr. Zsigmond calculated that her patient with a 2-day history of sore throat, elevated temperature, pussy tonsils, and enlarged cervical lymph glands but no cough or rhinitis had a FeverPAIN score of 4-5 and a Centor score of 4, meaning that, according to the European guidelines, she should receive antibiotic treatment. However, viral swabs proved positive for adenovirus.
Dr. Ivaska responded with his recent experiences of a similar case, where a 5-year-old boy had a FeverPAIN score of 4-5 and Centor score of 3. Cultures from his throat were GAS positive, illustrating the problem of differentiating between bacterial and viral infections.
But does a GAS-positive pharyngeal culture necessarily mean that antibiotic treatment is indicated? Dr. Ivaska believes it does, citing the importance of preventing serious complications such as rheumatic fever. Dr. Zsigmind countered by pointing out the low levels of acute rheumatic fever in developed nations. In her own country, Hungary, there has not been a case in the last 30 years. Giving antibiotics for historical reasons cannot, in her view, be justified.
Dr. Ivaska responded that perhaps this is because of early treatment in children with sore throats.
Another complication of tonsillitis is quinsy. Dr. Zsigmond cited a study showing that there is no statistically significant evidence demonstrating that antibiotics prevent quinsy. She attributed this to quinsy appearing quickly, typically within 2 days. Delay in seeking help means that the window to treat is often missed. However, should symptoms present early, there is no statistical evidence that prior antibiotic use can prevent quinsy. Also, given the rarity of this condition, prevention would mean excessive use of antibiotics.
Are there other possible benefits of antibiotic treatment in patients with a sore throat? Dr. Ivaska referred to a Cochrane review that found a shortening in duration of throat soreness and fever. Furthermore, compared with placebo, antibiotics reduced the incidence of suppurative complications such as acute otitis media and sinusitis following a sore throat. Other studies have also pointed to the potential benefits of reduced transmission in families where one member with pharyngitis was GAS positive.
As the debate ended, Dr. Zsigmond reported evidence of global antibiotic overprescribing for sore throat ranging from 53% in Europe to 94% in Australia. She also highlighted risks such as altered gut flora, drug resistance, and rashes.
Robin Marlow from the University of Bristol (England), PhD, MBBS, commented that “one of the most enjoyable parts of the ESPID meeting is hearing different viewpoints rationally explained from across the world. As [antibiotic prescription for a sore throat is] a clinical conundrum that faces pediatricians every day, I thought this debate was a really great example of how, despite our different health care systems and ways of working, we are all striving together to improve children’s health using the best evidence available.”
The presenters had no financial conflicts of interest to declare.
FROM ESPID 2020