User login
NICE releases guideline on sepsis

Photo courtesy of the CDC
The National Institute for Health and Care Excellence (NICE) has published a new draft guideline to help healthcare professionals recognize sepsis and provide early treatment.
Although treatable in many cases, sepsis can be difficult to recognize and diagnose.
A recent study* of more than 3000 patients treated at UK hospitals revealed delays in identifying sepsis in more than a third of cases.
“There are around 123,000 cases of sepsis in England every year, and, unfortunately, thousands of people die after developing the condition,” said Mark Baker, director of the centre for clinical practice at NICE.
“Many of these deaths might be prevented if sepsis was recognized quickly and treatment started early. We know that when hospitals are well-prepared, clinicians do better at responding to patients with sepsis. However, recent reports have revealed that a third of hospitals have no formal protocols for recognizing and responding to sepsis.”
NICE created its draft guidance with that in mind. The guidance provides recommendations to aid in the recognition, diagnosis, and early management of sepsis, including:
- What signs and symptoms to look out for
- How to identify patients at high risk of developing sepsis
- Which tests to use to diagnose and monitor patients
- How to care for people with suspected sepsis outside of the hospital
- When patients should be referred for emergency care
- Appropriate use of antibiotics and other supportive treatments, such as fluids and oxygen
- The type of information that should be given to patients, families, and caregivers.
“We want all healthcare professionals to see sepsis as an immediate, life-threatening condition and make sure there are systems in place across the NHS for it to be recognized and treated as an emergency,” Baker said.
“This new guideline will be the first to provide evidence-based best practice advice on how to quickly identify and treat people with sepsis. We now urge all healthcare professionals and organizations with an interest in this area to comment on the proposed recommendations.”
The draft version of this guideline has been published for consultation. Organizations can register as a stakeholder on the NICE website and have until February 22, 2016, to submit their comments. Individuals are advised to pass comments through a registered stakeholder organization that most closely represents them. ![]()
*Published in “Just Say Sepsis!”—a report by the National Confidential Enquiry into Patient Outcome and Death.

Photo courtesy of the CDC
The National Institute for Health and Care Excellence (NICE) has published a new draft guideline to help healthcare professionals recognize sepsis and provide early treatment.
Although treatable in many cases, sepsis can be difficult to recognize and diagnose.
A recent study* of more than 3000 patients treated at UK hospitals revealed delays in identifying sepsis in more than a third of cases.
“There are around 123,000 cases of sepsis in England every year, and, unfortunately, thousands of people die after developing the condition,” said Mark Baker, director of the centre for clinical practice at NICE.
“Many of these deaths might be prevented if sepsis was recognized quickly and treatment started early. We know that when hospitals are well-prepared, clinicians do better at responding to patients with sepsis. However, recent reports have revealed that a third of hospitals have no formal protocols for recognizing and responding to sepsis.”
NICE created its draft guidance with that in mind. The guidance provides recommendations to aid in the recognition, diagnosis, and early management of sepsis, including:
- What signs and symptoms to look out for
- How to identify patients at high risk of developing sepsis
- Which tests to use to diagnose and monitor patients
- How to care for people with suspected sepsis outside of the hospital
- When patients should be referred for emergency care
- Appropriate use of antibiotics and other supportive treatments, such as fluids and oxygen
- The type of information that should be given to patients, families, and caregivers.
“We want all healthcare professionals to see sepsis as an immediate, life-threatening condition and make sure there are systems in place across the NHS for it to be recognized and treated as an emergency,” Baker said.
“This new guideline will be the first to provide evidence-based best practice advice on how to quickly identify and treat people with sepsis. We now urge all healthcare professionals and organizations with an interest in this area to comment on the proposed recommendations.”
The draft version of this guideline has been published for consultation. Organizations can register as a stakeholder on the NICE website and have until February 22, 2016, to submit their comments. Individuals are advised to pass comments through a registered stakeholder organization that most closely represents them. ![]()
*Published in “Just Say Sepsis!”—a report by the National Confidential Enquiry into Patient Outcome and Death.

Photo courtesy of the CDC
The National Institute for Health and Care Excellence (NICE) has published a new draft guideline to help healthcare professionals recognize sepsis and provide early treatment.
Although treatable in many cases, sepsis can be difficult to recognize and diagnose.
A recent study* of more than 3000 patients treated at UK hospitals revealed delays in identifying sepsis in more than a third of cases.
“There are around 123,000 cases of sepsis in England every year, and, unfortunately, thousands of people die after developing the condition,” said Mark Baker, director of the centre for clinical practice at NICE.
“Many of these deaths might be prevented if sepsis was recognized quickly and treatment started early. We know that when hospitals are well-prepared, clinicians do better at responding to patients with sepsis. However, recent reports have revealed that a third of hospitals have no formal protocols for recognizing and responding to sepsis.”
NICE created its draft guidance with that in mind. The guidance provides recommendations to aid in the recognition, diagnosis, and early management of sepsis, including:
- What signs and symptoms to look out for
- How to identify patients at high risk of developing sepsis
- Which tests to use to diagnose and monitor patients
- How to care for people with suspected sepsis outside of the hospital
- When patients should be referred for emergency care
- Appropriate use of antibiotics and other supportive treatments, such as fluids and oxygen
- The type of information that should be given to patients, families, and caregivers.
“We want all healthcare professionals to see sepsis as an immediate, life-threatening condition and make sure there are systems in place across the NHS for it to be recognized and treated as an emergency,” Baker said.
“This new guideline will be the first to provide evidence-based best practice advice on how to quickly identify and treat people with sepsis. We now urge all healthcare professionals and organizations with an interest in this area to comment on the proposed recommendations.”
The draft version of this guideline has been published for consultation. Organizations can register as a stakeholder on the NICE website and have until February 22, 2016, to submit their comments. Individuals are advised to pass comments through a registered stakeholder organization that most closely represents them. ![]()
*Published in “Just Say Sepsis!”—a report by the National Confidential Enquiry into Patient Outcome and Death.
Cancer survival tied to reduction in treatment

Photo by Bill Branson
Results of a large study suggest that long-term survivors of childhood cancer are living longer, partly due to a reduction in the use of certain treatments.
The 15-year death rate among the more than 34,000 childhood cancer survivors studied decreased steadily from 1970 onward.
And this decline coincided with changes in pediatric cancer therapy, including reductions in the use and dose of radiation therapy and anthracyclines.
These therapies are known to put cancer survivors at increased risk for developing second malignancies, heart failure, and other serious health problems.
“This study is the first to show that younger survivors from more recent treatment eras are less likely to die from the late effects of cancer treatment and more likely to enjoy longer lives,” said study author Greg Armstrong, MD, of St. Jude Children's Research Hospital in Memphis, Tennessee.
He and his colleagues reported these results in NEJM.
The study included 34,033 subjects who had been diagnosed with cancer and received treatment between 1970 and 1999 when they were age 20 or younger. All patients lived at least 5 years after their cancers were discovered and were considered long-term survivors.
Changes in mortality
At a median follow-up of 21 years (range, 5 to 38), there were 3958 deaths. Forty-one percent of deaths (n=1618) were considered health-related. This included 746 deaths from subsequent neoplasms, 241 from cardiac causes, 137 from pulmonary causes, and 494 from other causes.
The 15-year death rate (death from any cause) fell from 12.4% in the early 1970s to 6% in the 1990s (P<0.001). During the same period, the rate of death from health-related causes fell from 3.5% to 2.1% (P<0.001).
The researchers said there were significant reductions across treatment eras in the rates of death from any health-related cause among patients with acute lymphoblastic leukemia (ALL), Hodgkin lymphoma (HL), Wilms’ tumor, and astrocytoma, but not among patients with other cancers.
The rate of health-related death among ALL patients fell from 3.2% in the early 1970s to 2.1% in the 1990s (P<0.001). The rate fell from 5.3% to 2.6% (P=0.006) for HL patients, from 2.6% to 0.4% (P=0.005) for Wilms’ tumor patients, and from 4.7% to 1.8% (P=0.02) for astrocytoma patients.
The researchers said these reductions in mortality were attributable to decreases in the rates of death from subsequent neoplasm (P<0.001), cardiac causes (P<0.001), and pulmonary causes (P=0.04).
Treatment changes
The overall use of anthracyclines fell from 73% in the 1970s to 42% in the 1990s. And the use of any radiation decreased from 77% to 41%.
The use of cranial radiotherapy for ALL fell from 85% to 19%. The use of abdominal radiotherapy for Wilms’ tumor decreased from 78% to 43%. And the use of chest radiotherapy for HL fell from 87% to 61%.
The researchers noted that temporal reductions in 15-year rates of death from health-related causes followed temporal reductions in therapeutic exposure for patients with ALL, HL, Wilms’ tumor, and astrocytoma.
However, when the team adjusted their analysis for therapy (eg, anthracycline dose), the effect of the treatment era on the relative rate of death from health-related causes was attenuated in ALL (unadjusted relative rate=0.88, adjusted relative rate=1.02) and Wilms’ tumor (0.68 and 0.80, respectively) but not in HL (0.79 in both models) and astrocytoma (0.81 and 0.82, respectively).
Still, the researchers said the results of this study suggest the strategy of lowering therapeutic exposure has contributed to the decline in late mortality among 5-year survivors of childhood cancer. ![]()

Photo by Bill Branson
Results of a large study suggest that long-term survivors of childhood cancer are living longer, partly due to a reduction in the use of certain treatments.
The 15-year death rate among the more than 34,000 childhood cancer survivors studied decreased steadily from 1970 onward.
And this decline coincided with changes in pediatric cancer therapy, including reductions in the use and dose of radiation therapy and anthracyclines.
These therapies are known to put cancer survivors at increased risk for developing second malignancies, heart failure, and other serious health problems.
“This study is the first to show that younger survivors from more recent treatment eras are less likely to die from the late effects of cancer treatment and more likely to enjoy longer lives,” said study author Greg Armstrong, MD, of St. Jude Children's Research Hospital in Memphis, Tennessee.
He and his colleagues reported these results in NEJM.
The study included 34,033 subjects who had been diagnosed with cancer and received treatment between 1970 and 1999 when they were age 20 or younger. All patients lived at least 5 years after their cancers were discovered and were considered long-term survivors.
Changes in mortality
At a median follow-up of 21 years (range, 5 to 38), there were 3958 deaths. Forty-one percent of deaths (n=1618) were considered health-related. This included 746 deaths from subsequent neoplasms, 241 from cardiac causes, 137 from pulmonary causes, and 494 from other causes.
The 15-year death rate (death from any cause) fell from 12.4% in the early 1970s to 6% in the 1990s (P<0.001). During the same period, the rate of death from health-related causes fell from 3.5% to 2.1% (P<0.001).
The researchers said there were significant reductions across treatment eras in the rates of death from any health-related cause among patients with acute lymphoblastic leukemia (ALL), Hodgkin lymphoma (HL), Wilms’ tumor, and astrocytoma, but not among patients with other cancers.
The rate of health-related death among ALL patients fell from 3.2% in the early 1970s to 2.1% in the 1990s (P<0.001). The rate fell from 5.3% to 2.6% (P=0.006) for HL patients, from 2.6% to 0.4% (P=0.005) for Wilms’ tumor patients, and from 4.7% to 1.8% (P=0.02) for astrocytoma patients.
The researchers said these reductions in mortality were attributable to decreases in the rates of death from subsequent neoplasm (P<0.001), cardiac causes (P<0.001), and pulmonary causes (P=0.04).
Treatment changes
The overall use of anthracyclines fell from 73% in the 1970s to 42% in the 1990s. And the use of any radiation decreased from 77% to 41%.
The use of cranial radiotherapy for ALL fell from 85% to 19%. The use of abdominal radiotherapy for Wilms’ tumor decreased from 78% to 43%. And the use of chest radiotherapy for HL fell from 87% to 61%.
The researchers noted that temporal reductions in 15-year rates of death from health-related causes followed temporal reductions in therapeutic exposure for patients with ALL, HL, Wilms’ tumor, and astrocytoma.
However, when the team adjusted their analysis for therapy (eg, anthracycline dose), the effect of the treatment era on the relative rate of death from health-related causes was attenuated in ALL (unadjusted relative rate=0.88, adjusted relative rate=1.02) and Wilms’ tumor (0.68 and 0.80, respectively) but not in HL (0.79 in both models) and astrocytoma (0.81 and 0.82, respectively).
Still, the researchers said the results of this study suggest the strategy of lowering therapeutic exposure has contributed to the decline in late mortality among 5-year survivors of childhood cancer. ![]()

Photo by Bill Branson
Results of a large study suggest that long-term survivors of childhood cancer are living longer, partly due to a reduction in the use of certain treatments.
The 15-year death rate among the more than 34,000 childhood cancer survivors studied decreased steadily from 1970 onward.
And this decline coincided with changes in pediatric cancer therapy, including reductions in the use and dose of radiation therapy and anthracyclines.
These therapies are known to put cancer survivors at increased risk for developing second malignancies, heart failure, and other serious health problems.
“This study is the first to show that younger survivors from more recent treatment eras are less likely to die from the late effects of cancer treatment and more likely to enjoy longer lives,” said study author Greg Armstrong, MD, of St. Jude Children's Research Hospital in Memphis, Tennessee.
He and his colleagues reported these results in NEJM.
The study included 34,033 subjects who had been diagnosed with cancer and received treatment between 1970 and 1999 when they were age 20 or younger. All patients lived at least 5 years after their cancers were discovered and were considered long-term survivors.
Changes in mortality
At a median follow-up of 21 years (range, 5 to 38), there were 3958 deaths. Forty-one percent of deaths (n=1618) were considered health-related. This included 746 deaths from subsequent neoplasms, 241 from cardiac causes, 137 from pulmonary causes, and 494 from other causes.
The 15-year death rate (death from any cause) fell from 12.4% in the early 1970s to 6% in the 1990s (P<0.001). During the same period, the rate of death from health-related causes fell from 3.5% to 2.1% (P<0.001).
The researchers said there were significant reductions across treatment eras in the rates of death from any health-related cause among patients with acute lymphoblastic leukemia (ALL), Hodgkin lymphoma (HL), Wilms’ tumor, and astrocytoma, but not among patients with other cancers.
The rate of health-related death among ALL patients fell from 3.2% in the early 1970s to 2.1% in the 1990s (P<0.001). The rate fell from 5.3% to 2.6% (P=0.006) for HL patients, from 2.6% to 0.4% (P=0.005) for Wilms’ tumor patients, and from 4.7% to 1.8% (P=0.02) for astrocytoma patients.
The researchers said these reductions in mortality were attributable to decreases in the rates of death from subsequent neoplasm (P<0.001), cardiac causes (P<0.001), and pulmonary causes (P=0.04).
Treatment changes
The overall use of anthracyclines fell from 73% in the 1970s to 42% in the 1990s. And the use of any radiation decreased from 77% to 41%.
The use of cranial radiotherapy for ALL fell from 85% to 19%. The use of abdominal radiotherapy for Wilms’ tumor decreased from 78% to 43%. And the use of chest radiotherapy for HL fell from 87% to 61%.
The researchers noted that temporal reductions in 15-year rates of death from health-related causes followed temporal reductions in therapeutic exposure for patients with ALL, HL, Wilms’ tumor, and astrocytoma.
However, when the team adjusted their analysis for therapy (eg, anthracycline dose), the effect of the treatment era on the relative rate of death from health-related causes was attenuated in ALL (unadjusted relative rate=0.88, adjusted relative rate=1.02) and Wilms’ tumor (0.68 and 0.80, respectively) but not in HL (0.79 in both models) and astrocytoma (0.81 and 0.82, respectively).
Still, the researchers said the results of this study suggest the strategy of lowering therapeutic exposure has contributed to the decline in late mortality among 5-year survivors of childhood cancer. ![]()
Kinase could be therapeutic target for Fanconi anemia

The protein kinase CHK1 may be a therapeutic target for Fanconi anemia (FA), according to researchers.
They studied induced pluripotent stem cells (iPSCs) derived from FA patients and found the FA DNA repair pathway was essential for the cells’ proliferation and survival.
The team also discovered that CHK1 played a “crucial” role in iPSCs’ sensitivity to accrued DNA damage, and inhibiting CHK1 allowed FA-deficient iPSCs to grow
normally.
The team relayed these findings in Stem Cell Reports.
“This study provides an experimental platform to test new therapies that could prevent pre- and post-natal Fanconi anemia conditions, which have no cure and limited treatment options,” said study author Susanne Wells, PhD, of the Cincinnati Children’s Hospital Medical Center in Ohio.
“Our findings also raise a number of important questions, so there is a lot more to be done.”
For this study, Dr Wells and her colleagues used iPSCs reprogrammed from mature skin and connective tissue cells donated by FA patients. The cells had a defective FA DNA repair pathway.
The researchers studied the iPSCs in culture and injected them into humanized mouse models, monitoring their genetic, molecular, and developmental progression.
Even with defective FA DNA repair, the iPSCs retained their ability to transform into different tissues, and humanized mice injected with the defective cells started to form teratomas.
However, the DNA repair defect started to kill off the iPSCs by blocking cell division and causing apoptosis.
The researchers noticed that CHK1, which serves as a DNA regulatory checkpoint during cell division, was hyperactive in the iPSCs, which hastened their death.
So the team used pharmacologic inhibitors of CHK1 to block the hyperactive enzyme at a critical stage of the stem cell cycle. This allowed them to override what are usually unfixable errors in the FA repair pathway.
After targeted treatment, FA-pathway-deficient iPSCs resumed dividing and expanding normally.
The researchers said that, to their surprise, the resumption of cell growth occurred without what they had expected to be massive chromosome abnormalities. Because of this, they speculate that a compensating DNA repair process is engaged in the reinvigorated cells.
Because this unidentified repair process may also rescue the DNA repair defect in the different tissue types affected by FA, Dr Wells and her colleagues believe their study may point to an approach that treats all clinical manifestations of the disease, including anemia and cancer.
“A key question for us is, ‘What type of DNA repair kicks in under these conditions, and is it error-free or error-prone?’” Dr Wells explained. “A novel mode of emergency DNA repair might indeed be discovered in the [iPSCs]. We believe some type of compensatory DNA repair must be driven by CHK1 inhibition when cells have FA pathway loss. Otherwise, the cells would have died off very quickly.”
The researchers plan to follow up this study with additional testing in humanized and genetic mouse models. They said they will attempt to improve embryonic development and post-birth fitness in FA-pathway-deficient mice with timed application of a CHK1 inhibitor.
The team will monitor the mice as they age and use genetic sequencing to screen for disease-causing mutations. And they will look for evidence of a DNA repair process (either novel or existing) in the FA-deficient mice. ![]()

The protein kinase CHK1 may be a therapeutic target for Fanconi anemia (FA), according to researchers.
They studied induced pluripotent stem cells (iPSCs) derived from FA patients and found the FA DNA repair pathway was essential for the cells’ proliferation and survival.
The team also discovered that CHK1 played a “crucial” role in iPSCs’ sensitivity to accrued DNA damage, and inhibiting CHK1 allowed FA-deficient iPSCs to grow
normally.
The team relayed these findings in Stem Cell Reports.
“This study provides an experimental platform to test new therapies that could prevent pre- and post-natal Fanconi anemia conditions, which have no cure and limited treatment options,” said study author Susanne Wells, PhD, of the Cincinnati Children’s Hospital Medical Center in Ohio.
“Our findings also raise a number of important questions, so there is a lot more to be done.”
For this study, Dr Wells and her colleagues used iPSCs reprogrammed from mature skin and connective tissue cells donated by FA patients. The cells had a defective FA DNA repair pathway.
The researchers studied the iPSCs in culture and injected them into humanized mouse models, monitoring their genetic, molecular, and developmental progression.
Even with defective FA DNA repair, the iPSCs retained their ability to transform into different tissues, and humanized mice injected with the defective cells started to form teratomas.
However, the DNA repair defect started to kill off the iPSCs by blocking cell division and causing apoptosis.
The researchers noticed that CHK1, which serves as a DNA regulatory checkpoint during cell division, was hyperactive in the iPSCs, which hastened their death.
So the team used pharmacologic inhibitors of CHK1 to block the hyperactive enzyme at a critical stage of the stem cell cycle. This allowed them to override what are usually unfixable errors in the FA repair pathway.
After targeted treatment, FA-pathway-deficient iPSCs resumed dividing and expanding normally.
The researchers said that, to their surprise, the resumption of cell growth occurred without what they had expected to be massive chromosome abnormalities. Because of this, they speculate that a compensating DNA repair process is engaged in the reinvigorated cells.
Because this unidentified repair process may also rescue the DNA repair defect in the different tissue types affected by FA, Dr Wells and her colleagues believe their study may point to an approach that treats all clinical manifestations of the disease, including anemia and cancer.
“A key question for us is, ‘What type of DNA repair kicks in under these conditions, and is it error-free or error-prone?’” Dr Wells explained. “A novel mode of emergency DNA repair might indeed be discovered in the [iPSCs]. We believe some type of compensatory DNA repair must be driven by CHK1 inhibition when cells have FA pathway loss. Otherwise, the cells would have died off very quickly.”
The researchers plan to follow up this study with additional testing in humanized and genetic mouse models. They said they will attempt to improve embryonic development and post-birth fitness in FA-pathway-deficient mice with timed application of a CHK1 inhibitor.
The team will monitor the mice as they age and use genetic sequencing to screen for disease-causing mutations. And they will look for evidence of a DNA repair process (either novel or existing) in the FA-deficient mice. ![]()

The protein kinase CHK1 may be a therapeutic target for Fanconi anemia (FA), according to researchers.
They studied induced pluripotent stem cells (iPSCs) derived from FA patients and found the FA DNA repair pathway was essential for the cells’ proliferation and survival.
The team also discovered that CHK1 played a “crucial” role in iPSCs’ sensitivity to accrued DNA damage, and inhibiting CHK1 allowed FA-deficient iPSCs to grow
normally.
The team relayed these findings in Stem Cell Reports.
“This study provides an experimental platform to test new therapies that could prevent pre- and post-natal Fanconi anemia conditions, which have no cure and limited treatment options,” said study author Susanne Wells, PhD, of the Cincinnati Children’s Hospital Medical Center in Ohio.
“Our findings also raise a number of important questions, so there is a lot more to be done.”
For this study, Dr Wells and her colleagues used iPSCs reprogrammed from mature skin and connective tissue cells donated by FA patients. The cells had a defective FA DNA repair pathway.
The researchers studied the iPSCs in culture and injected them into humanized mouse models, monitoring their genetic, molecular, and developmental progression.
Even with defective FA DNA repair, the iPSCs retained their ability to transform into different tissues, and humanized mice injected with the defective cells started to form teratomas.
However, the DNA repair defect started to kill off the iPSCs by blocking cell division and causing apoptosis.
The researchers noticed that CHK1, which serves as a DNA regulatory checkpoint during cell division, was hyperactive in the iPSCs, which hastened their death.
So the team used pharmacologic inhibitors of CHK1 to block the hyperactive enzyme at a critical stage of the stem cell cycle. This allowed them to override what are usually unfixable errors in the FA repair pathway.
After targeted treatment, FA-pathway-deficient iPSCs resumed dividing and expanding normally.
The researchers said that, to their surprise, the resumption of cell growth occurred without what they had expected to be massive chromosome abnormalities. Because of this, they speculate that a compensating DNA repair process is engaged in the reinvigorated cells.
Because this unidentified repair process may also rescue the DNA repair defect in the different tissue types affected by FA, Dr Wells and her colleagues believe their study may point to an approach that treats all clinical manifestations of the disease, including anemia and cancer.
“A key question for us is, ‘What type of DNA repair kicks in under these conditions, and is it error-free or error-prone?’” Dr Wells explained. “A novel mode of emergency DNA repair might indeed be discovered in the [iPSCs]. We believe some type of compensatory DNA repair must be driven by CHK1 inhibition when cells have FA pathway loss. Otherwise, the cells would have died off very quickly.”
The researchers plan to follow up this study with additional testing in humanized and genetic mouse models. They said they will attempt to improve embryonic development and post-birth fitness in FA-pathway-deficient mice with timed application of a CHK1 inhibitor.
The team will monitor the mice as they age and use genetic sequencing to screen for disease-causing mutations. And they will look for evidence of a DNA repair process (either novel or existing) in the FA-deficient mice. ![]()
Team identifies potential target for XLP-1

Image courtesy of NIAID
A protein called diacylglycerol kinase alpha (DGKα) could be a therapeutic target for X-linked lymphoproliferative disease (XLP-1), according to research published in Science Translational Medicine.
Researchers have known for some time that XLP-1 is a heritable disorder caused by germline mutations in SH2D1A.
When this gene is affected, it leads to defects in an adaptor molecule known as SAP (signaling lymphocytic activation molecule-associated protein), which regulates T-cell receptor signaling and triggers cytotoxic T cells to self-destruct when they are no longer needed.
Without an effective SAP adaptor molecule, apoptosis is impaired, and DGKα is activated.
With the current study, researchers wanted to determine whether the over-activation of DGKα might contribute to the reduced apoptosis observed in T cells in patients with XLP-1 and the accumulation of T cells that occurs following infection with Epstein-Barr virus.
“Patients with X-linked lymphoproliferative disease are prone to severe Epstein-Barr virus infection due to a weakened immune system,” explained study author Kim Nichols, MD, of St. Jude Children’s Research Hospital in Memphis, Tennessee.
“Infection with Epstein-Barr virus can have potentially fatal consequences for these patients. This severe disease is a double-edged sword. On the one hand, the immune system is significantly weakened. However, detrimental side effects occur due to the expansion and hyper-activation of T cells.”
“[W]e wanted to establish the biochemical mechanism underlying these changes so that we could develop better treatments for X-linked lymphoproliferative disease patients experiencing hyper-inflammation.”
Studying T cells from XLP-1 patients, the researchers found that SAP and DGKα are both crucial for the regulation of T-cell death. Loss of SAP, which normally inhibits DGKα, led to unrestrained DGKα activity, resulting in impaired T-cell receptor signaling and resistance to apoptosis.
Pharmacologic inhibition of DGKα restored the sensitivity of XLP-1 T cells to cell death. Using small interfering RNA to knockout DGKα in cultured XLP-1 T cells had the same results.
And pharmacologic inhibition of DGKα curtailed the expansion of T cells in virus-infected mice that served as a model organism to study XLP-1.
Treating the mice with a DGKα inhibitor restored T cells’ sensitivity to cell death by boosting the expression of pro-apoptotic proteins, which prevented excessive T-cell buildup and reduced the severity of the disease.
“Our findings suggest that inhibition of DGKα could reverse some of the life-threatening effects linked to Epstein-Barr virus infection of patients with X-linked lymphoproliferative disease,” Dr Nichols concluded. ![]()

Image courtesy of NIAID
A protein called diacylglycerol kinase alpha (DGKα) could be a therapeutic target for X-linked lymphoproliferative disease (XLP-1), according to research published in Science Translational Medicine.
Researchers have known for some time that XLP-1 is a heritable disorder caused by germline mutations in SH2D1A.
When this gene is affected, it leads to defects in an adaptor molecule known as SAP (signaling lymphocytic activation molecule-associated protein), which regulates T-cell receptor signaling and triggers cytotoxic T cells to self-destruct when they are no longer needed.
Without an effective SAP adaptor molecule, apoptosis is impaired, and DGKα is activated.
With the current study, researchers wanted to determine whether the over-activation of DGKα might contribute to the reduced apoptosis observed in T cells in patients with XLP-1 and the accumulation of T cells that occurs following infection with Epstein-Barr virus.
“Patients with X-linked lymphoproliferative disease are prone to severe Epstein-Barr virus infection due to a weakened immune system,” explained study author Kim Nichols, MD, of St. Jude Children’s Research Hospital in Memphis, Tennessee.
“Infection with Epstein-Barr virus can have potentially fatal consequences for these patients. This severe disease is a double-edged sword. On the one hand, the immune system is significantly weakened. However, detrimental side effects occur due to the expansion and hyper-activation of T cells.”
“[W]e wanted to establish the biochemical mechanism underlying these changes so that we could develop better treatments for X-linked lymphoproliferative disease patients experiencing hyper-inflammation.”
Studying T cells from XLP-1 patients, the researchers found that SAP and DGKα are both crucial for the regulation of T-cell death. Loss of SAP, which normally inhibits DGKα, led to unrestrained DGKα activity, resulting in impaired T-cell receptor signaling and resistance to apoptosis.
Pharmacologic inhibition of DGKα restored the sensitivity of XLP-1 T cells to cell death. Using small interfering RNA to knockout DGKα in cultured XLP-1 T cells had the same results.
And pharmacologic inhibition of DGKα curtailed the expansion of T cells in virus-infected mice that served as a model organism to study XLP-1.
Treating the mice with a DGKα inhibitor restored T cells’ sensitivity to cell death by boosting the expression of pro-apoptotic proteins, which prevented excessive T-cell buildup and reduced the severity of the disease.
“Our findings suggest that inhibition of DGKα could reverse some of the life-threatening effects linked to Epstein-Barr virus infection of patients with X-linked lymphoproliferative disease,” Dr Nichols concluded. ![]()

Image courtesy of NIAID
A protein called diacylglycerol kinase alpha (DGKα) could be a therapeutic target for X-linked lymphoproliferative disease (XLP-1), according to research published in Science Translational Medicine.
Researchers have known for some time that XLP-1 is a heritable disorder caused by germline mutations in SH2D1A.
When this gene is affected, it leads to defects in an adaptor molecule known as SAP (signaling lymphocytic activation molecule-associated protein), which regulates T-cell receptor signaling and triggers cytotoxic T cells to self-destruct when they are no longer needed.
Without an effective SAP adaptor molecule, apoptosis is impaired, and DGKα is activated.
With the current study, researchers wanted to determine whether the over-activation of DGKα might contribute to the reduced apoptosis observed in T cells in patients with XLP-1 and the accumulation of T cells that occurs following infection with Epstein-Barr virus.
“Patients with X-linked lymphoproliferative disease are prone to severe Epstein-Barr virus infection due to a weakened immune system,” explained study author Kim Nichols, MD, of St. Jude Children’s Research Hospital in Memphis, Tennessee.
“Infection with Epstein-Barr virus can have potentially fatal consequences for these patients. This severe disease is a double-edged sword. On the one hand, the immune system is significantly weakened. However, detrimental side effects occur due to the expansion and hyper-activation of T cells.”
“[W]e wanted to establish the biochemical mechanism underlying these changes so that we could develop better treatments for X-linked lymphoproliferative disease patients experiencing hyper-inflammation.”
Studying T cells from XLP-1 patients, the researchers found that SAP and DGKα are both crucial for the regulation of T-cell death. Loss of SAP, which normally inhibits DGKα, led to unrestrained DGKα activity, resulting in impaired T-cell receptor signaling and resistance to apoptosis.
Pharmacologic inhibition of DGKα restored the sensitivity of XLP-1 T cells to cell death. Using small interfering RNA to knockout DGKα in cultured XLP-1 T cells had the same results.
And pharmacologic inhibition of DGKα curtailed the expansion of T cells in virus-infected mice that served as a model organism to study XLP-1.
Treating the mice with a DGKα inhibitor restored T cells’ sensitivity to cell death by boosting the expression of pro-apoptotic proteins, which prevented excessive T-cell buildup and reduced the severity of the disease.
“Our findings suggest that inhibition of DGKα could reverse some of the life-threatening effects linked to Epstein-Barr virus infection of patients with X-linked lymphoproliferative disease,” Dr Nichols concluded. ![]()
A new tool for studying sepsis

Photo by Ingela Björck
Researchers have reported using mass spectrometry to measure hundreds of proteins in a single blood sample.
And they used the resulting protein patterns to determine the severity of sepsis in animal models. They were also able to determine which organs had been damaged in these mice.
The researchers said they’ve been able to map the majority of proteins found in vital organs and list which proteins are specific to each organ.
“If you see in a blood sample that the amount of proteins from a specific organ increases, it indicates damage to this organ,” explained study author Erik Malmström, of Lund University in Sweden.
“The method provides an understanding of the molecular events that take place during the course of a disease and the possibility, using the same analysis, to study how different organs are affected.”
The researchers described this work in Nature Communications.
The group believes their study of hundreds of different proteins could eventually be used to select other important proteins that can serve as biomarkers for different aspects of sepsis.
First and foremost, however, they think their method will be an important research tool.
“There is so much we don’t know about sepsis,” Malmström said. “Why do not all patients react the same way? Why do some organs suffer the most damage in some patients and not in others? Do different bacteria cause the disease to progress? Can you divide patients into different subgroups, or bacteria, or does each new combination of patients and bacteria lead to a specific form of sepsis?”
The current study was conducted in animals, but the researchers are now moving on to human tissue. They have obtained samples of healthy tissue from various organs and are comparing protein patterns of these samples with patterns in corresponding tissues from sepsis patients. ![]()

Photo by Ingela Björck
Researchers have reported using mass spectrometry to measure hundreds of proteins in a single blood sample.
And they used the resulting protein patterns to determine the severity of sepsis in animal models. They were also able to determine which organs had been damaged in these mice.
The researchers said they’ve been able to map the majority of proteins found in vital organs and list which proteins are specific to each organ.
“If you see in a blood sample that the amount of proteins from a specific organ increases, it indicates damage to this organ,” explained study author Erik Malmström, of Lund University in Sweden.
“The method provides an understanding of the molecular events that take place during the course of a disease and the possibility, using the same analysis, to study how different organs are affected.”
The researchers described this work in Nature Communications.
The group believes their study of hundreds of different proteins could eventually be used to select other important proteins that can serve as biomarkers for different aspects of sepsis.
First and foremost, however, they think their method will be an important research tool.
“There is so much we don’t know about sepsis,” Malmström said. “Why do not all patients react the same way? Why do some organs suffer the most damage in some patients and not in others? Do different bacteria cause the disease to progress? Can you divide patients into different subgroups, or bacteria, or does each new combination of patients and bacteria lead to a specific form of sepsis?”
The current study was conducted in animals, but the researchers are now moving on to human tissue. They have obtained samples of healthy tissue from various organs and are comparing protein patterns of these samples with patterns in corresponding tissues from sepsis patients. ![]()

Photo by Ingela Björck
Researchers have reported using mass spectrometry to measure hundreds of proteins in a single blood sample.
And they used the resulting protein patterns to determine the severity of sepsis in animal models. They were also able to determine which organs had been damaged in these mice.
The researchers said they’ve been able to map the majority of proteins found in vital organs and list which proteins are specific to each organ.
“If you see in a blood sample that the amount of proteins from a specific organ increases, it indicates damage to this organ,” explained study author Erik Malmström, of Lund University in Sweden.
“The method provides an understanding of the molecular events that take place during the course of a disease and the possibility, using the same analysis, to study how different organs are affected.”
The researchers described this work in Nature Communications.
The group believes their study of hundreds of different proteins could eventually be used to select other important proteins that can serve as biomarkers for different aspects of sepsis.
First and foremost, however, they think their method will be an important research tool.
“There is so much we don’t know about sepsis,” Malmström said. “Why do not all patients react the same way? Why do some organs suffer the most damage in some patients and not in others? Do different bacteria cause the disease to progress? Can you divide patients into different subgroups, or bacteria, or does each new combination of patients and bacteria lead to a specific form of sepsis?”
The current study was conducted in animals, but the researchers are now moving on to human tissue. They have obtained samples of healthy tissue from various organs and are comparing protein patterns of these samples with patterns in corresponding tissues from sepsis patients. ![]()
Predicting transformation from MDS to AML

Photo courtesy of
McMaster University
Research published in Cancer Cell suggests a molecular signature can be used to predict which patients with myelodysplastic syndromes (MDS) will develop acute myeloid leukemia (AML).
Investigators found that progressive removal of glycogen synthase kinase-3 (GSK-3) signaling via GSK-3β deletion in hematopoietic stem cells (HSCs) results in an MDS-like state.
And when both GSK-3β and GSK-3α are deleted, AML develops.
“We’ve found that the transition from healthy to cancerous blood stem cells happens in clear, compartmentalized steps,” said study author Mick Bhatia, PhD, of McMaster University in Hamilton, Ontario, Canada. “We’ve identified 2 steps in that staircase.”
Specifically, the investigators found that deleting GSK-3β in HSCs led to the generation of self-renewing cells dubbed MDS-initiating cells. These cells proved capable of sustaining MDS in vivo.
Next, the team found that GSK-3β deletion drives Wnt/Akt/mTOR signaling and can induce AML in the absence of GSK-3α.
They noted that GSK-3α has no biological impact on hematopoiesis, but GSK-3α deletion is necessary for the evolution of MDS to AML that occurs in the absence of GSK-3β.
The investigators then defined a molecular signature of GSK-3β-deficient HSCs that could predict transformation to AML in patients with MDS.
The team tested the utility of this 63-gene signature using blood samples that were previously collected from patients with MDS, some of whom ultimately developed AML. The results showed the signature could accurately predict which patients would develop AML and which would not.
“[O]ur next step is to go beyond better predictive measures for the development of a blood cancer and use this predictive gene expression as a target for drugs to prevent AML from developing altogether,” Dr Bhatia said. “This will be part of a new era of genetic-based drug discovery.” ![]()

Photo courtesy of
McMaster University
Research published in Cancer Cell suggests a molecular signature can be used to predict which patients with myelodysplastic syndromes (MDS) will develop acute myeloid leukemia (AML).
Investigators found that progressive removal of glycogen synthase kinase-3 (GSK-3) signaling via GSK-3β deletion in hematopoietic stem cells (HSCs) results in an MDS-like state.
And when both GSK-3β and GSK-3α are deleted, AML develops.
“We’ve found that the transition from healthy to cancerous blood stem cells happens in clear, compartmentalized steps,” said study author Mick Bhatia, PhD, of McMaster University in Hamilton, Ontario, Canada. “We’ve identified 2 steps in that staircase.”
Specifically, the investigators found that deleting GSK-3β in HSCs led to the generation of self-renewing cells dubbed MDS-initiating cells. These cells proved capable of sustaining MDS in vivo.
Next, the team found that GSK-3β deletion drives Wnt/Akt/mTOR signaling and can induce AML in the absence of GSK-3α.
They noted that GSK-3α has no biological impact on hematopoiesis, but GSK-3α deletion is necessary for the evolution of MDS to AML that occurs in the absence of GSK-3β.
The investigators then defined a molecular signature of GSK-3β-deficient HSCs that could predict transformation to AML in patients with MDS.
The team tested the utility of this 63-gene signature using blood samples that were previously collected from patients with MDS, some of whom ultimately developed AML. The results showed the signature could accurately predict which patients would develop AML and which would not.
“[O]ur next step is to go beyond better predictive measures for the development of a blood cancer and use this predictive gene expression as a target for drugs to prevent AML from developing altogether,” Dr Bhatia said. “This will be part of a new era of genetic-based drug discovery.” ![]()

Photo courtesy of
McMaster University
Research published in Cancer Cell suggests a molecular signature can be used to predict which patients with myelodysplastic syndromes (MDS) will develop acute myeloid leukemia (AML).
Investigators found that progressive removal of glycogen synthase kinase-3 (GSK-3) signaling via GSK-3β deletion in hematopoietic stem cells (HSCs) results in an MDS-like state.
And when both GSK-3β and GSK-3α are deleted, AML develops.
“We’ve found that the transition from healthy to cancerous blood stem cells happens in clear, compartmentalized steps,” said study author Mick Bhatia, PhD, of McMaster University in Hamilton, Ontario, Canada. “We’ve identified 2 steps in that staircase.”
Specifically, the investigators found that deleting GSK-3β in HSCs led to the generation of self-renewing cells dubbed MDS-initiating cells. These cells proved capable of sustaining MDS in vivo.
Next, the team found that GSK-3β deletion drives Wnt/Akt/mTOR signaling and can induce AML in the absence of GSK-3α.
They noted that GSK-3α has no biological impact on hematopoiesis, but GSK-3α deletion is necessary for the evolution of MDS to AML that occurs in the absence of GSK-3β.
The investigators then defined a molecular signature of GSK-3β-deficient HSCs that could predict transformation to AML in patients with MDS.
The team tested the utility of this 63-gene signature using blood samples that were previously collected from patients with MDS, some of whom ultimately developed AML. The results showed the signature could accurately predict which patients would develop AML and which would not.
“[O]ur next step is to go beyond better predictive measures for the development of a blood cancer and use this predictive gene expression as a target for drugs to prevent AML from developing altogether,” Dr Bhatia said. “This will be part of a new era of genetic-based drug discovery.” ![]()
Fewer doses of malaria drug just as effective

Photo by Sarah Mattison
A trial of African children suggests that 3 doses of artesunate can be just as effective as 5 doses for treating severe malaria.
A 3-dose intramuscular (IM) artesunate regimen proved noninferior to 5 doses of IM artesunate.
However, a 3-dose intravenous (IV) artesunate regimen was not as effective.
Peter Kremsner, MD, of Eberhard Karls Universität Tübingen in Germany, and his colleagues reported these results in PLOS Medicine.
The World Health Organization recommends that patients with severe malaria be given a 5-dose regimen of IV or IM artesunate at the time of admission (0 hours) and at 12, 24, 48, and 72 hours. However, in resource-limited settings, administering 5 doses on schedule can be challenging.
So Dr Kremsner and his colleagues wanted to determine if 3 doses of artesunate would be just as effective. They conducted an open-label, randomized, controlled trial investigating the efficacy of 3-dose IV or IM artesunate at 0, 24, and 48 hours.
The researchers enrolled 1047 children (0.5 to 10 years of age) who had severe malaria and were treated at 7 different sites in 5 African countries. The children were randomized to receive a total artesunate dose of 12 mg/kg as a control regimen of 5 IM injections (n=348) or 3 injections of 4 mg/kg either IM (n=348) or IV (n=351).
Of these children, 1002 received treatment per-protocol—331 in the 5-dose group, 338 in the 3-dose IM group, and 333 in the 3-dose IV group.
Seventy-eight percent of patients in the 3-dose IM group had about 99% parasite clearance at 24 hours, as did 79% of patients in the 5-dose IM group, a result that met a preset criterion for noninferiority (P=0.02).
However, the 3-dose IV regimen did not meet the noninferiority criterion. Seventy-four percent of these children had about 99% parasite clearance at 24 hours (P=0.24).
Twenty-two percent of the entire study population developed delayed anemia, but there was no difference in the incidence of this adverse event between the treatment arms.
The researchers said further studies are needed to clarify whether treatment with artesunate or the malaria infection itself was responsible for the delayed anemia. And patients receiving the drug should be monitored for this complication.
The team also said their findings suggest a 3-dose IM artesunate regimen can be effective against severe malaria in children, but this study did have limitations. For instance, due to practical constraints, the primary endpoint was parasite clearance at 24 hours rather than survival. ![]()

Photo by Sarah Mattison
A trial of African children suggests that 3 doses of artesunate can be just as effective as 5 doses for treating severe malaria.
A 3-dose intramuscular (IM) artesunate regimen proved noninferior to 5 doses of IM artesunate.
However, a 3-dose intravenous (IV) artesunate regimen was not as effective.
Peter Kremsner, MD, of Eberhard Karls Universität Tübingen in Germany, and his colleagues reported these results in PLOS Medicine.
The World Health Organization recommends that patients with severe malaria be given a 5-dose regimen of IV or IM artesunate at the time of admission (0 hours) and at 12, 24, 48, and 72 hours. However, in resource-limited settings, administering 5 doses on schedule can be challenging.
So Dr Kremsner and his colleagues wanted to determine if 3 doses of artesunate would be just as effective. They conducted an open-label, randomized, controlled trial investigating the efficacy of 3-dose IV or IM artesunate at 0, 24, and 48 hours.
The researchers enrolled 1047 children (0.5 to 10 years of age) who had severe malaria and were treated at 7 different sites in 5 African countries. The children were randomized to receive a total artesunate dose of 12 mg/kg as a control regimen of 5 IM injections (n=348) or 3 injections of 4 mg/kg either IM (n=348) or IV (n=351).
Of these children, 1002 received treatment per-protocol—331 in the 5-dose group, 338 in the 3-dose IM group, and 333 in the 3-dose IV group.
Seventy-eight percent of patients in the 3-dose IM group had about 99% parasite clearance at 24 hours, as did 79% of patients in the 5-dose IM group, a result that met a preset criterion for noninferiority (P=0.02).
However, the 3-dose IV regimen did not meet the noninferiority criterion. Seventy-four percent of these children had about 99% parasite clearance at 24 hours (P=0.24).
Twenty-two percent of the entire study population developed delayed anemia, but there was no difference in the incidence of this adverse event between the treatment arms.
The researchers said further studies are needed to clarify whether treatment with artesunate or the malaria infection itself was responsible for the delayed anemia. And patients receiving the drug should be monitored for this complication.
The team also said their findings suggest a 3-dose IM artesunate regimen can be effective against severe malaria in children, but this study did have limitations. For instance, due to practical constraints, the primary endpoint was parasite clearance at 24 hours rather than survival. ![]()

Photo by Sarah Mattison
A trial of African children suggests that 3 doses of artesunate can be just as effective as 5 doses for treating severe malaria.
A 3-dose intramuscular (IM) artesunate regimen proved noninferior to 5 doses of IM artesunate.
However, a 3-dose intravenous (IV) artesunate regimen was not as effective.
Peter Kremsner, MD, of Eberhard Karls Universität Tübingen in Germany, and his colleagues reported these results in PLOS Medicine.
The World Health Organization recommends that patients with severe malaria be given a 5-dose regimen of IV or IM artesunate at the time of admission (0 hours) and at 12, 24, 48, and 72 hours. However, in resource-limited settings, administering 5 doses on schedule can be challenging.
So Dr Kremsner and his colleagues wanted to determine if 3 doses of artesunate would be just as effective. They conducted an open-label, randomized, controlled trial investigating the efficacy of 3-dose IV or IM artesunate at 0, 24, and 48 hours.
The researchers enrolled 1047 children (0.5 to 10 years of age) who had severe malaria and were treated at 7 different sites in 5 African countries. The children were randomized to receive a total artesunate dose of 12 mg/kg as a control regimen of 5 IM injections (n=348) or 3 injections of 4 mg/kg either IM (n=348) or IV (n=351).
Of these children, 1002 received treatment per-protocol—331 in the 5-dose group, 338 in the 3-dose IM group, and 333 in the 3-dose IV group.
Seventy-eight percent of patients in the 3-dose IM group had about 99% parasite clearance at 24 hours, as did 79% of patients in the 5-dose IM group, a result that met a preset criterion for noninferiority (P=0.02).
However, the 3-dose IV regimen did not meet the noninferiority criterion. Seventy-four percent of these children had about 99% parasite clearance at 24 hours (P=0.24).
Twenty-two percent of the entire study population developed delayed anemia, but there was no difference in the incidence of this adverse event between the treatment arms.
The researchers said further studies are needed to clarify whether treatment with artesunate or the malaria infection itself was responsible for the delayed anemia. And patients receiving the drug should be monitored for this complication.
The team also said their findings suggest a 3-dose IM artesunate regimen can be effective against severe malaria in children, but this study did have limitations. For instance, due to practical constraints, the primary endpoint was parasite clearance at 24 hours rather than survival.
Drug gets priority review as CLL treatment

Image by Mary Ann Thompson
Despite previous safety concerns, the US Food and Drug Administration (FDA) has granted priority review for the BCL-2 inhibitor venetoclax.
The FDA is reviewing the drug as a potential treatment for patients with chronic lymphocytic leukemia (CLL), including those with 17p deletion, who have received at least 1 prior therapy.
A priority review designation is granted to drugs thought to have the potential to provide significant improvements in the treatment, prevention, or diagnosis of a disease.
The designation means the FDA’s goal is to take action on a drug application within 6 months, compared to 10 months under standard review.
Venetoclax has proven active against CLL and other hematologic malignancies, but it is known to induce tumor lysis syndrome (TLS). In fact, TLS-related deaths temporarily halted enrollment in trials of venetoclax. But researchers discovered ways to reduce the risk of TLS, and the trials continued.
Venetoclax received breakthrough therapy designation from the FDA last year for the treatment of patients with relapsed or refractory CLL and 17p deletion. This designation is designed to expedite the development and review of medicines intended to treat serious or life-threatening diseases.
The new drug application for venetoclax is based, in part, on data from the phase 2 M13-982 study, which were just presented at the 2015 ASH Annual Meeting.
Phase 2 trial
M13-982 is an open-label, single-arm, multicenter study in which researchers are evaluating the efficacy and safety of venetoclax in patients with relapsed, refractory, or previously untreated CLL with 17p deletion.
The study included 107 patients with relapsed or refractory disease, and all but 1 had 17p deletion. An additional 50 patients with relapsed, refractory, or previously untreated disease have been enrolled in the safety expansion cohort.
The primary endpoint of the study is overall response rate as determined by an independent review committee, and secondary endpoints include complete response, partial response, duration of response, progression-free survival, and overall survival. The level of minimal residual disease (MRD) in peripheral blood and/or bone marrow was assessed in a subset of patients.
The study met its primary endpoint, with an overall response rate of 79.4% among the 107 patients with relapsed or refractory disease. In addition, 7.5% of patients achieved a complete response, with or without complete recovery of blood counts in the bone marrow.
Forty-five patients had an assessment for MRD in the blood. Of these, 18 patients achieved MRD-negativity. Ten of these 18 patients also had bone marrow assessments, and 6 were MRD-negative.
At 1 year, 84.7% of all responses and 94.4% of MRD-negative responses were maintained. The 1-year progression-free survival and overall survival rates were 72% and 86.7%, respectively.
The most common serious adverse events were pyrexia (7%), autoimmune hemolytic anemia (7%), pneumonia (6%), and febrile neutropenia (5%). The most common grade 3-4 adverse events were neutropenia (40%), infection (20%), anemia (18%), and thrombocytopenia (15%).
Laboratory TLS was reported in 5 patients. None had clinical consequences.
Venetoclax is under development by AbbVie and Genentech/Roche.

Image by Mary Ann Thompson
Despite previous safety concerns, the US Food and Drug Administration (FDA) has granted priority review for the BCL-2 inhibitor venetoclax.
The FDA is reviewing the drug as a potential treatment for patients with chronic lymphocytic leukemia (CLL), including those with 17p deletion, who have received at least 1 prior therapy.
A priority review designation is granted to drugs thought to have the potential to provide significant improvements in the treatment, prevention, or diagnosis of a disease.
The designation means the FDA’s goal is to take action on a drug application within 6 months, compared to 10 months under standard review.
Venetoclax has proven active against CLL and other hematologic malignancies, but it is known to induce tumor lysis syndrome (TLS). In fact, TLS-related deaths temporarily halted enrollment in trials of venetoclax. But researchers discovered ways to reduce the risk of TLS, and the trials continued.
Venetoclax received breakthrough therapy designation from the FDA last year for the treatment of patients with relapsed or refractory CLL and 17p deletion. This designation is designed to expedite the development and review of medicines intended to treat serious or life-threatening diseases.
The new drug application for venetoclax is based, in part, on data from the phase 2 M13-982 study, which were just presented at the 2015 ASH Annual Meeting.
Phase 2 trial
M13-982 is an open-label, single-arm, multicenter study in which researchers are evaluating the efficacy and safety of venetoclax in patients with relapsed, refractory, or previously untreated CLL with 17p deletion.
The study included 107 patients with relapsed or refractory disease, and all but 1 had 17p deletion. An additional 50 patients with relapsed, refractory, or previously untreated disease have been enrolled in the safety expansion cohort.
The primary endpoint of the study is overall response rate as determined by an independent review committee, and secondary endpoints include complete response, partial response, duration of response, progression-free survival, and overall survival. The level of minimal residual disease (MRD) in peripheral blood and/or bone marrow was assessed in a subset of patients.
The study met its primary endpoint, with an overall response rate of 79.4% among the 107 patients with relapsed or refractory disease. In addition, 7.5% of patients achieved a complete response, with or without complete recovery of blood counts in the bone marrow.
Forty-five patients had an assessment for MRD in the blood. Of these, 18 patients achieved MRD-negativity. Ten of these 18 patients also had bone marrow assessments, and 6 were MRD-negative.
At 1 year, 84.7% of all responses and 94.4% of MRD-negative responses were maintained. The 1-year progression-free survival and overall survival rates were 72% and 86.7%, respectively.
The most common serious adverse events were pyrexia (7%), autoimmune hemolytic anemia (7%), pneumonia (6%), and febrile neutropenia (5%). The most common grade 3-4 adverse events were neutropenia (40%), infection (20%), anemia (18%), and thrombocytopenia (15%).
Laboratory TLS was reported in 5 patients. None had clinical consequences.
Venetoclax is under development by AbbVie and Genentech/Roche.

Image by Mary Ann Thompson
Despite previous safety concerns, the US Food and Drug Administration (FDA) has granted priority review for the BCL-2 inhibitor venetoclax.
The FDA is reviewing the drug as a potential treatment for patients with chronic lymphocytic leukemia (CLL), including those with 17p deletion, who have received at least 1 prior therapy.
A priority review designation is granted to drugs thought to have the potential to provide significant improvements in the treatment, prevention, or diagnosis of a disease.
The designation means the FDA’s goal is to take action on a drug application within 6 months, compared to 10 months under standard review.
Venetoclax has proven active against CLL and other hematologic malignancies, but it is known to induce tumor lysis syndrome (TLS). In fact, TLS-related deaths temporarily halted enrollment in trials of venetoclax. But researchers discovered ways to reduce the risk of TLS, and the trials continued.
Venetoclax received breakthrough therapy designation from the FDA last year for the treatment of patients with relapsed or refractory CLL and 17p deletion. This designation is designed to expedite the development and review of medicines intended to treat serious or life-threatening diseases.
The new drug application for venetoclax is based, in part, on data from the phase 2 M13-982 study, which were just presented at the 2015 ASH Annual Meeting.
Phase 2 trial
M13-982 is an open-label, single-arm, multicenter study in which researchers are evaluating the efficacy and safety of venetoclax in patients with relapsed, refractory, or previously untreated CLL with 17p deletion.
The study included 107 patients with relapsed or refractory disease, and all but 1 had 17p deletion. An additional 50 patients with relapsed, refractory, or previously untreated disease have been enrolled in the safety expansion cohort.
The primary endpoint of the study is overall response rate as determined by an independent review committee, and secondary endpoints include complete response, partial response, duration of response, progression-free survival, and overall survival. The level of minimal residual disease (MRD) in peripheral blood and/or bone marrow was assessed in a subset of patients.
The study met its primary endpoint, with an overall response rate of 79.4% among the 107 patients with relapsed or refractory disease. In addition, 7.5% of patients achieved a complete response, with or without complete recovery of blood counts in the bone marrow.
Forty-five patients had an assessment for MRD in the blood. Of these, 18 patients achieved MRD-negativity. Ten of these 18 patients also had bone marrow assessments, and 6 were MRD-negative.
At 1 year, 84.7% of all responses and 94.4% of MRD-negative responses were maintained. The 1-year progression-free survival and overall survival rates were 72% and 86.7%, respectively.
The most common serious adverse events were pyrexia (7%), autoimmune hemolytic anemia (7%), pneumonia (6%), and febrile neutropenia (5%). The most common grade 3-4 adverse events were neutropenia (40%), infection (20%), anemia (18%), and thrombocytopenia (15%).
Laboratory TLS was reported in 5 patients. None had clinical consequences.
Venetoclax is under development by AbbVie and Genentech/Roche.
PBSCs used to treat BMF despite drawbacks
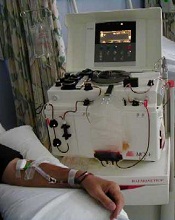
Photo from the Canterbury
District Health Board
Although studies have suggested that peripheral blood stem cells (PBSCs) are not the ideal graft source for patients with bone marrow failure (BMF), new research suggests transplant centers worldwide are still using PBSCs in these patients.
The study included data on more than 3000 hematopoietic stem cell transplants (HSCTs) performed in patients with BMF.
The numbers revealed that PBSCs were most-used in the Asia-Pacific region, Africa, and the Eastern Mediterranean region. But they were also used in Europe and the Americas.
Ayami Yoshimi, MD, PhD, of the University of Freiburg, Germany, and colleagues disclosed these findings in a letter to JAMA.
The researchers noted that bone marrow is the recommended graft source for HSCT in patients with BMF, as studies have shown that PBSCs are associated with higher rates of graft-vs-host disease and lower rates of survival.
With this in mind, the team examined the graft sources used in patients with BMF who underwent HSCTs from 2009 through 2010. The researchers looked at 194 World Health Organization member states and found that 74 had reported at least 1 HSCT during that time period.
Of the 114,217 transplants performed, there were 3282 allogeneic HSCTs in patients with BMF. Overall, the most-used graft source was bone marrow (54%), followed by PBSCs (41%), and then cord blood (5%).
Bone marrow was used most commonly in the Americas (75%) and in Europe (60%) but not in the Eastern Mediterranean region and Africa (46%) or in the Asia-Pacific region (41%; excluding Japan, 19%).
The researchers also looked at graft source according to donor type, both overall and by region, but they excluded the 180 cord blood transplants from this analysis.
The team found that, among patients who had a related donor, 57% received bone marrow and 43% received PBSCs.
For related HSCTs in the Americas, 75% of patients received bone marrow and 25% received PBSCs. In Europe, 63% received bone marrow and 37% received PBSCs. In the Eastern Mediterranean and Africa, 47% received bone marrow and 53% received PBSCs. And in the Asia-Pacific region, 37% received bone marrow and 63% received PBSCs.
Among patients who had unrelated donors, 57% received bone marrow and 43% received PBSCs.
For unrelated HSCTs in the Americas, 74% of patients received bone marrow and 26% received PBSCs. In Europe, 56% received bone marrow and 44% received PBSCs. In the Asia-Pacific region, 47% received bone marrow and 53% received PBSCs. And in the Eastern Mediterranean and Africa, 100% received PBSCs.
The use of bone marrow increased from 20% in countries with low and low-middle incomes to 50% in countries with high-middle incomes and 64% in countries with high incomes (P<0.001). There was a significant association between gross national income per capita and stem cell source (P=0.002).
The researchers speculated that PBSCs are still used in BMF patients, despite the disadvantages, because transplant centers routinely obtain PBSCs for other indications, cell separators are available at any transplant center, and PBSC transplants can be performed at a lower cost than bone marrow transplants.
The team said the association between graft source and income supports the idea that short-term financial considerations are important.
So transplant organizations and authorities should help foster regional-accredited bone marrow harvest centers for patients with nonmalignant disorders. And unrelated donor registries should provide information on the necessity of bone marrow donation for patients with BMF.

Photo from the Canterbury
District Health Board
Although studies have suggested that peripheral blood stem cells (PBSCs) are not the ideal graft source for patients with bone marrow failure (BMF), new research suggests transplant centers worldwide are still using PBSCs in these patients.
The study included data on more than 3000 hematopoietic stem cell transplants (HSCTs) performed in patients with BMF.
The numbers revealed that PBSCs were most-used in the Asia-Pacific region, Africa, and the Eastern Mediterranean region. But they were also used in Europe and the Americas.
Ayami Yoshimi, MD, PhD, of the University of Freiburg, Germany, and colleagues disclosed these findings in a letter to JAMA.
The researchers noted that bone marrow is the recommended graft source for HSCT in patients with BMF, as studies have shown that PBSCs are associated with higher rates of graft-vs-host disease and lower rates of survival.
With this in mind, the team examined the graft sources used in patients with BMF who underwent HSCTs from 2009 through 2010. The researchers looked at 194 World Health Organization member states and found that 74 had reported at least 1 HSCT during that time period.
Of the 114,217 transplants performed, there were 3282 allogeneic HSCTs in patients with BMF. Overall, the most-used graft source was bone marrow (54%), followed by PBSCs (41%), and then cord blood (5%).
Bone marrow was used most commonly in the Americas (75%) and in Europe (60%) but not in the Eastern Mediterranean region and Africa (46%) or in the Asia-Pacific region (41%; excluding Japan, 19%).
The researchers also looked at graft source according to donor type, both overall and by region, but they excluded the 180 cord blood transplants from this analysis.
The team found that, among patients who had a related donor, 57% received bone marrow and 43% received PBSCs.
For related HSCTs in the Americas, 75% of patients received bone marrow and 25% received PBSCs. In Europe, 63% received bone marrow and 37% received PBSCs. In the Eastern Mediterranean and Africa, 47% received bone marrow and 53% received PBSCs. And in the Asia-Pacific region, 37% received bone marrow and 63% received PBSCs.
Among patients who had unrelated donors, 57% received bone marrow and 43% received PBSCs.
For unrelated HSCTs in the Americas, 74% of patients received bone marrow and 26% received PBSCs. In Europe, 56% received bone marrow and 44% received PBSCs. In the Asia-Pacific region, 47% received bone marrow and 53% received PBSCs. And in the Eastern Mediterranean and Africa, 100% received PBSCs.
The use of bone marrow increased from 20% in countries with low and low-middle incomes to 50% in countries with high-middle incomes and 64% in countries with high incomes (P<0.001). There was a significant association between gross national income per capita and stem cell source (P=0.002).
The researchers speculated that PBSCs are still used in BMF patients, despite the disadvantages, because transplant centers routinely obtain PBSCs for other indications, cell separators are available at any transplant center, and PBSC transplants can be performed at a lower cost than bone marrow transplants.
The team said the association between graft source and income supports the idea that short-term financial considerations are important.
So transplant organizations and authorities should help foster regional-accredited bone marrow harvest centers for patients with nonmalignant disorders. And unrelated donor registries should provide information on the necessity of bone marrow donation for patients with BMF.

Photo from the Canterbury
District Health Board
Although studies have suggested that peripheral blood stem cells (PBSCs) are not the ideal graft source for patients with bone marrow failure (BMF), new research suggests transplant centers worldwide are still using PBSCs in these patients.
The study included data on more than 3000 hematopoietic stem cell transplants (HSCTs) performed in patients with BMF.
The numbers revealed that PBSCs were most-used in the Asia-Pacific region, Africa, and the Eastern Mediterranean region. But they were also used in Europe and the Americas.
Ayami Yoshimi, MD, PhD, of the University of Freiburg, Germany, and colleagues disclosed these findings in a letter to JAMA.
The researchers noted that bone marrow is the recommended graft source for HSCT in patients with BMF, as studies have shown that PBSCs are associated with higher rates of graft-vs-host disease and lower rates of survival.
With this in mind, the team examined the graft sources used in patients with BMF who underwent HSCTs from 2009 through 2010. The researchers looked at 194 World Health Organization member states and found that 74 had reported at least 1 HSCT during that time period.
Of the 114,217 transplants performed, there were 3282 allogeneic HSCTs in patients with BMF. Overall, the most-used graft source was bone marrow (54%), followed by PBSCs (41%), and then cord blood (5%).
Bone marrow was used most commonly in the Americas (75%) and in Europe (60%) but not in the Eastern Mediterranean region and Africa (46%) or in the Asia-Pacific region (41%; excluding Japan, 19%).
The researchers also looked at graft source according to donor type, both overall and by region, but they excluded the 180 cord blood transplants from this analysis.
The team found that, among patients who had a related donor, 57% received bone marrow and 43% received PBSCs.
For related HSCTs in the Americas, 75% of patients received bone marrow and 25% received PBSCs. In Europe, 63% received bone marrow and 37% received PBSCs. In the Eastern Mediterranean and Africa, 47% received bone marrow and 53% received PBSCs. And in the Asia-Pacific region, 37% received bone marrow and 63% received PBSCs.
Among patients who had unrelated donors, 57% received bone marrow and 43% received PBSCs.
For unrelated HSCTs in the Americas, 74% of patients received bone marrow and 26% received PBSCs. In Europe, 56% received bone marrow and 44% received PBSCs. In the Asia-Pacific region, 47% received bone marrow and 53% received PBSCs. And in the Eastern Mediterranean and Africa, 100% received PBSCs.
The use of bone marrow increased from 20% in countries with low and low-middle incomes to 50% in countries with high-middle incomes and 64% in countries with high incomes (P<0.001). There was a significant association between gross national income per capita and stem cell source (P=0.002).
The researchers speculated that PBSCs are still used in BMF patients, despite the disadvantages, because transplant centers routinely obtain PBSCs for other indications, cell separators are available at any transplant center, and PBSC transplants can be performed at a lower cost than bone marrow transplants.
The team said the association between graft source and income supports the idea that short-term financial considerations are important.
So transplant organizations and authorities should help foster regional-accredited bone marrow harvest centers for patients with nonmalignant disorders. And unrelated donor registries should provide information on the necessity of bone marrow donation for patients with BMF.
Team identifies new mechanism of megakaryocyte differentiation
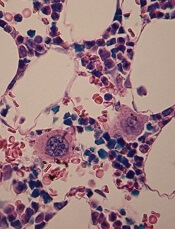
in the bone marrow
Investigators have discovered a new mechanism of megakaryocyte differentiation, according to a paper published in eLife.
They found that overexpression of the methyltransferase enzyme PRMT1 in acute megakaryocytic leukemia blocks megakaryocyte differentiation by downregulating levels of the RNA-binding protein RBM15.
The team therefore believes that targeting PRMT1 could restore megakaryocyte differentiation in this malignancy.
They also think their findings could lead to new approaches for researching and treating other hematologic malignancies and solid tumors.
Xinyang Zhao, PhD, of the University of Alabama at Birmingham, and his colleagues began this study looking at PRMT1, which attaches a methyl group onto specific arginine amino acid residues of target proteins.
The investigators screened for proteins that were tagged with methyl groups by PRMT1 and selected one of them—RBM15—for further study. RBM15 was of interest because a mutant fusion of RBM15 and MKL1 proteins is associated with acute megakaryoblastic leukemia.
The team discovered that when a cell’s PRMT1 levels are high, a greater proportion of RBM15 is tagged with methyl groups on certain arginine residues. This tagging causes a ligase called CNOT4 to mark RBM15 with another tag, ubiquitin, which marks the protein for transport to the cell’s garbage removal machinery.
The methyl-tagged RBM15 proteins rapidly disappear, even though the amount of RBM15 messenger RNA does not change. Thus, the expression levels of PRMT1 inversely affect the amount of RBM15.
When the concentration of RBM15 is low, megakaryocytic progenitor cells cannot move forward to differentiation. But when the concentration of RBM15 is high enough, the progenitor cells differentiate into mature megakaryocytes.
The investigators also found that RBM15 binds to intron regions of the pre-messenger RNA for genes known to be important in megakaryocyte differentiation, including 3 transcription factors—RUNX1, GATA1, and TAL1—that are important for normal and abnormal hematopoiesis.
And RBM15 appears to recruit the splicing factor SF3B1 to correctly splice exons. When RBM15 is low, one or more exons are not correctly spliced.
The team said this is a new mechanism for cell differentiation, initiated by methylation of RNA-binding proteins.
“The regulation of alternative splicing by RBM15 through SF3B1 is an exciting and novel pathway that clearly participates in the decision of a megakaryocyte to grow or differentiate,” said John Crispino, PhD, of the Northwestern University Feinberg School of Medicine in Chicago, Illinois, who was not involved in this study.
“These findings suggest that modulation of RBM15 activity by suppressing PRMT1 activity may change the splicing pattern of megakaryocytic tumor cells and facilitate their differentiation.”
The investigators also believe RBM15 may have broader functions in cells. They found that RBM15 binds directly to the pre-messenger RNA of 1257 genes. Among them are genes involved in metabolic regulation.
In agreement with this finding, the team discovered that overexpression of PRMT1 or reduced expression of RBM15 enhances the creation of more mitochondria.
The investigators have further identified metabolic pathways regulated by PRMT1 in leukemia cells. They said these data, in a manuscript under preparation, will further link tumorigenesis to metabolic pathways.
The team also noted that SF3B1 contains mutations in more than 70% of myelodysplastic syndrome patients and 20% of chronic lymphocytic leukemia patients, and mutated SF3B1 appears in other hematologic malignancies as well.
So the investigators believe that understanding the PRMT1-RBM15 axis can shed new light on SF3B1-mutated hematologic malignancies and may lead to targeting PRMT1 as a novel therapy for myelodysplastic syndromes. The team is already testing PRMT1 inhibitors.

in the bone marrow
Investigators have discovered a new mechanism of megakaryocyte differentiation, according to a paper published in eLife.
They found that overexpression of the methyltransferase enzyme PRMT1 in acute megakaryocytic leukemia blocks megakaryocyte differentiation by downregulating levels of the RNA-binding protein RBM15.
The team therefore believes that targeting PRMT1 could restore megakaryocyte differentiation in this malignancy.
They also think their findings could lead to new approaches for researching and treating other hematologic malignancies and solid tumors.
Xinyang Zhao, PhD, of the University of Alabama at Birmingham, and his colleagues began this study looking at PRMT1, which attaches a methyl group onto specific arginine amino acid residues of target proteins.
The investigators screened for proteins that were tagged with methyl groups by PRMT1 and selected one of them—RBM15—for further study. RBM15 was of interest because a mutant fusion of RBM15 and MKL1 proteins is associated with acute megakaryoblastic leukemia.
The team discovered that when a cell’s PRMT1 levels are high, a greater proportion of RBM15 is tagged with methyl groups on certain arginine residues. This tagging causes a ligase called CNOT4 to mark RBM15 with another tag, ubiquitin, which marks the protein for transport to the cell’s garbage removal machinery.
The methyl-tagged RBM15 proteins rapidly disappear, even though the amount of RBM15 messenger RNA does not change. Thus, the expression levels of PRMT1 inversely affect the amount of RBM15.
When the concentration of RBM15 is low, megakaryocytic progenitor cells cannot move forward to differentiation. But when the concentration of RBM15 is high enough, the progenitor cells differentiate into mature megakaryocytes.
The investigators also found that RBM15 binds to intron regions of the pre-messenger RNA for genes known to be important in megakaryocyte differentiation, including 3 transcription factors—RUNX1, GATA1, and TAL1—that are important for normal and abnormal hematopoiesis.
And RBM15 appears to recruit the splicing factor SF3B1 to correctly splice exons. When RBM15 is low, one or more exons are not correctly spliced.
The team said this is a new mechanism for cell differentiation, initiated by methylation of RNA-binding proteins.
“The regulation of alternative splicing by RBM15 through SF3B1 is an exciting and novel pathway that clearly participates in the decision of a megakaryocyte to grow or differentiate,” said John Crispino, PhD, of the Northwestern University Feinberg School of Medicine in Chicago, Illinois, who was not involved in this study.
“These findings suggest that modulation of RBM15 activity by suppressing PRMT1 activity may change the splicing pattern of megakaryocytic tumor cells and facilitate their differentiation.”
The investigators also believe RBM15 may have broader functions in cells. They found that RBM15 binds directly to the pre-messenger RNA of 1257 genes. Among them are genes involved in metabolic regulation.
In agreement with this finding, the team discovered that overexpression of PRMT1 or reduced expression of RBM15 enhances the creation of more mitochondria.
The investigators have further identified metabolic pathways regulated by PRMT1 in leukemia cells. They said these data, in a manuscript under preparation, will further link tumorigenesis to metabolic pathways.
The team also noted that SF3B1 contains mutations in more than 70% of myelodysplastic syndrome patients and 20% of chronic lymphocytic leukemia patients, and mutated SF3B1 appears in other hematologic malignancies as well.
So the investigators believe that understanding the PRMT1-RBM15 axis can shed new light on SF3B1-mutated hematologic malignancies and may lead to targeting PRMT1 as a novel therapy for myelodysplastic syndromes. The team is already testing PRMT1 inhibitors.

in the bone marrow
Investigators have discovered a new mechanism of megakaryocyte differentiation, according to a paper published in eLife.
They found that overexpression of the methyltransferase enzyme PRMT1 in acute megakaryocytic leukemia blocks megakaryocyte differentiation by downregulating levels of the RNA-binding protein RBM15.
The team therefore believes that targeting PRMT1 could restore megakaryocyte differentiation in this malignancy.
They also think their findings could lead to new approaches for researching and treating other hematologic malignancies and solid tumors.
Xinyang Zhao, PhD, of the University of Alabama at Birmingham, and his colleagues began this study looking at PRMT1, which attaches a methyl group onto specific arginine amino acid residues of target proteins.
The investigators screened for proteins that were tagged with methyl groups by PRMT1 and selected one of them—RBM15—for further study. RBM15 was of interest because a mutant fusion of RBM15 and MKL1 proteins is associated with acute megakaryoblastic leukemia.
The team discovered that when a cell’s PRMT1 levels are high, a greater proportion of RBM15 is tagged with methyl groups on certain arginine residues. This tagging causes a ligase called CNOT4 to mark RBM15 with another tag, ubiquitin, which marks the protein for transport to the cell’s garbage removal machinery.
The methyl-tagged RBM15 proteins rapidly disappear, even though the amount of RBM15 messenger RNA does not change. Thus, the expression levels of PRMT1 inversely affect the amount of RBM15.
When the concentration of RBM15 is low, megakaryocytic progenitor cells cannot move forward to differentiation. But when the concentration of RBM15 is high enough, the progenitor cells differentiate into mature megakaryocytes.
The investigators also found that RBM15 binds to intron regions of the pre-messenger RNA for genes known to be important in megakaryocyte differentiation, including 3 transcription factors—RUNX1, GATA1, and TAL1—that are important for normal and abnormal hematopoiesis.
And RBM15 appears to recruit the splicing factor SF3B1 to correctly splice exons. When RBM15 is low, one or more exons are not correctly spliced.
The team said this is a new mechanism for cell differentiation, initiated by methylation of RNA-binding proteins.
“The regulation of alternative splicing by RBM15 through SF3B1 is an exciting and novel pathway that clearly participates in the decision of a megakaryocyte to grow or differentiate,” said John Crispino, PhD, of the Northwestern University Feinberg School of Medicine in Chicago, Illinois, who was not involved in this study.
“These findings suggest that modulation of RBM15 activity by suppressing PRMT1 activity may change the splicing pattern of megakaryocytic tumor cells and facilitate their differentiation.”
The investigators also believe RBM15 may have broader functions in cells. They found that RBM15 binds directly to the pre-messenger RNA of 1257 genes. Among them are genes involved in metabolic regulation.
In agreement with this finding, the team discovered that overexpression of PRMT1 or reduced expression of RBM15 enhances the creation of more mitochondria.
The investigators have further identified metabolic pathways regulated by PRMT1 in leukemia cells. They said these data, in a manuscript under preparation, will further link tumorigenesis to metabolic pathways.
The team also noted that SF3B1 contains mutations in more than 70% of myelodysplastic syndrome patients and 20% of chronic lymphocytic leukemia patients, and mutated SF3B1 appears in other hematologic malignancies as well.
So the investigators believe that understanding the PRMT1-RBM15 axis can shed new light on SF3B1-mutated hematologic malignancies and may lead to targeting PRMT1 as a novel therapy for myelodysplastic syndromes. The team is already testing PRMT1 inhibitors.