User login
Home pesticide exposure linked to childhood cancers

in his garden
Researchers have linked residential pesticide exposure to childhood cancers, but the estimated risks vary according to the cancer type, the type of pesticide, and where it is applied.
The investigators conducted a meta-analysis of published studies and found that childhood exposure to indoor pesticides was associated with a
significantly increased risk of all the cancers analyzed, as well as leukemia and lymphoma individually.
Overall, exposure to outdoor pesticides was not associated with an increased risk of childhood cancers. However, herbicide exposure was linked to an increased risk of leukemia and all cancers combined.
Mei Chen, PhD, of the Harvard T.H. Chan School of Public Health in Boston, Massachusetts, and colleagues conducted this meta-analysis and reported the results in Pediatrics.
The team searched for observational studies published in PubMed before February 2014 and ultimately included 16 studies in their analysis.
They assessed exposure to indoor pesticides and indoor insecticides (a subgroup of indoor pesticides), as well as exposure to outdoor pesticides, which included outdoor insecticides, herbicides, and fungicides.
The cancer types analyzed were leukemia, lymphoma, brain tumors, neuroblastoma, Wilms tumor, and soft tissue sarcoma.
Indoor pesticides
When the investigators analyzed all cancer types together, they found a significantly increased risk of childhood cancers associated with exposure to indoor pesticides (odds ratio [OR]=1.40).
Likewise, there was a significantly increased risk for leukemia (OR=1.48), acute leukemia (OR=1.59), lymphoma (OR=1.43), and all hematopoietic malignancies (leukemias and lymphomas, OR=1.47).
But the increased risk of childhood brain tumors was not statistically significant, and the other cancers were not analyzed separately.
Exposure to indoor insecticides was associated with a significant increase in the risk of leukemia (OR=1.47), acute leukemia (OR=1.59), lymphoma (OR=1.43), and all hematopoietic malignancies (OR=1.46).
Outdoor pesticides
There was no significant association between exposure to outdoor pesticides or outdoor insecticides and any of the cancer types. And there were not enough studies on fungicides to assess the risk of cancers associated with their use.
However, there was a significant association between exposure to herbicide and all childhood cancers (OR=1.35) as well as leukemia (OR=1.26).
The investigators said these results suggest cancer risks are related to the type of pesticides used and where they are applied.
And although additional research is needed to confirm the association between pesticide exposure and childhood cancers, steps should be taken to limit exposure to pesticides during childhood. ![]()

in his garden
Researchers have linked residential pesticide exposure to childhood cancers, but the estimated risks vary according to the cancer type, the type of pesticide, and where it is applied.
The investigators conducted a meta-analysis of published studies and found that childhood exposure to indoor pesticides was associated with a
significantly increased risk of all the cancers analyzed, as well as leukemia and lymphoma individually.
Overall, exposure to outdoor pesticides was not associated with an increased risk of childhood cancers. However, herbicide exposure was linked to an increased risk of leukemia and all cancers combined.
Mei Chen, PhD, of the Harvard T.H. Chan School of Public Health in Boston, Massachusetts, and colleagues conducted this meta-analysis and reported the results in Pediatrics.
The team searched for observational studies published in PubMed before February 2014 and ultimately included 16 studies in their analysis.
They assessed exposure to indoor pesticides and indoor insecticides (a subgroup of indoor pesticides), as well as exposure to outdoor pesticides, which included outdoor insecticides, herbicides, and fungicides.
The cancer types analyzed were leukemia, lymphoma, brain tumors, neuroblastoma, Wilms tumor, and soft tissue sarcoma.
Indoor pesticides
When the investigators analyzed all cancer types together, they found a significantly increased risk of childhood cancers associated with exposure to indoor pesticides (odds ratio [OR]=1.40).
Likewise, there was a significantly increased risk for leukemia (OR=1.48), acute leukemia (OR=1.59), lymphoma (OR=1.43), and all hematopoietic malignancies (leukemias and lymphomas, OR=1.47).
But the increased risk of childhood brain tumors was not statistically significant, and the other cancers were not analyzed separately.
Exposure to indoor insecticides was associated with a significant increase in the risk of leukemia (OR=1.47), acute leukemia (OR=1.59), lymphoma (OR=1.43), and all hematopoietic malignancies (OR=1.46).
Outdoor pesticides
There was no significant association between exposure to outdoor pesticides or outdoor insecticides and any of the cancer types. And there were not enough studies on fungicides to assess the risk of cancers associated with their use.
However, there was a significant association between exposure to herbicide and all childhood cancers (OR=1.35) as well as leukemia (OR=1.26).
The investigators said these results suggest cancer risks are related to the type of pesticides used and where they are applied.
And although additional research is needed to confirm the association between pesticide exposure and childhood cancers, steps should be taken to limit exposure to pesticides during childhood. ![]()

in his garden
Researchers have linked residential pesticide exposure to childhood cancers, but the estimated risks vary according to the cancer type, the type of pesticide, and where it is applied.
The investigators conducted a meta-analysis of published studies and found that childhood exposure to indoor pesticides was associated with a
significantly increased risk of all the cancers analyzed, as well as leukemia and lymphoma individually.
Overall, exposure to outdoor pesticides was not associated with an increased risk of childhood cancers. However, herbicide exposure was linked to an increased risk of leukemia and all cancers combined.
Mei Chen, PhD, of the Harvard T.H. Chan School of Public Health in Boston, Massachusetts, and colleagues conducted this meta-analysis and reported the results in Pediatrics.
The team searched for observational studies published in PubMed before February 2014 and ultimately included 16 studies in their analysis.
They assessed exposure to indoor pesticides and indoor insecticides (a subgroup of indoor pesticides), as well as exposure to outdoor pesticides, which included outdoor insecticides, herbicides, and fungicides.
The cancer types analyzed were leukemia, lymphoma, brain tumors, neuroblastoma, Wilms tumor, and soft tissue sarcoma.
Indoor pesticides
When the investigators analyzed all cancer types together, they found a significantly increased risk of childhood cancers associated with exposure to indoor pesticides (odds ratio [OR]=1.40).
Likewise, there was a significantly increased risk for leukemia (OR=1.48), acute leukemia (OR=1.59), lymphoma (OR=1.43), and all hematopoietic malignancies (leukemias and lymphomas, OR=1.47).
But the increased risk of childhood brain tumors was not statistically significant, and the other cancers were not analyzed separately.
Exposure to indoor insecticides was associated with a significant increase in the risk of leukemia (OR=1.47), acute leukemia (OR=1.59), lymphoma (OR=1.43), and all hematopoietic malignancies (OR=1.46).
Outdoor pesticides
There was no significant association between exposure to outdoor pesticides or outdoor insecticides and any of the cancer types. And there were not enough studies on fungicides to assess the risk of cancers associated with their use.
However, there was a significant association between exposure to herbicide and all childhood cancers (OR=1.35) as well as leukemia (OR=1.26).
The investigators said these results suggest cancer risks are related to the type of pesticides used and where they are applied.
And although additional research is needed to confirm the association between pesticide exposure and childhood cancers, steps should be taken to limit exposure to pesticides during childhood. ![]()
Platelet mimics provide targeted drug delivery
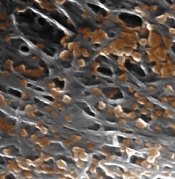
nanoparticles binding to the
lining of a damaged artery
Image courtesy of the
Zhang Research Group
Nanoparticles disguised as human platelets can provide targeted drug delivery, according to research published in Nature.
The nanoparticles are made of a biodegradable polymer coated with human platelet membranes.
This coating allows the nanoparticles to circulate in the bloodstream without being attacked by the immune system and to preferentially bind to damaged blood vessels and certain pathogens.
Murine experiments showed that these platelet-mimicking nanoparticles can deliver drugs to targeted sites, thereby increasing the therapeutic effect.
“Because of their targeting ability, platelet-mimicking nanoparticles can directly provide a much higher dose of medication specifically to diseased areas without saturating the entire body with drugs,” said study author Liangfang Zhang, PhD, of the University of California San Diego.
Creating the platelet mimics
To make the nanoparticles, Dr Zhang and his colleagues first separated platelets from whole blood samples using a centrifuge. The platelets were then processed to isolate the membranes from the platelets.
Next, the platelet membranes were broken up into much smaller pieces and fused to the surface of the nanoparticle cores. The resulting platelet-membrane-coated nanoparticles were approximately 100 nanometers in diameter.
This cloaking technology is based on a strategy Dr Zhang’s group had developed to cloak nanoparticles in red blood cell membranes. The researchers previously demonstrated that nanoparticles disguised as red blood cells are capable of removing toxins from the bloodstream.
With the current work, the researchers were able to produce platelet mimics that contain the complete set of surface receptors, antigens, and proteins naturally present on platelet membranes.
“Our technique takes advantage of the unique natural properties of human platelet membranes, which have a natural preference to bind to certain tissues and organisms in the body,” Dr Zhang said.
This targeting ability, which red blood cell membranes do not have, makes platelet membranes extremely useful for targeted drug delivery, according to the researchers.
Platelet mimics at work
The researchers packed the platelet-mimicking nanoparticles with docetaxel, a drug used to prevent scar tissue formation in the lining of damaged blood vessels, and administered them to rats afflicted with injured arteries.
The docetaxel-containing nanoparticles collected at the damaged sites of arteries and healed them.
The researchers then injected nanoparticles containing one-sixth the clinical dose of the antibiotic vancomycin into a group of mice systemically infected with methicillin-resistant Staphylococcus aureus bacteria.
Bacterial counts in the organs of these mice were up to 1000 times lower than in mice treated with the clinical dose of vancomycin alone.
“Our platelet-mimicking nanoparticles can increase the therapeutic efficacy of antibiotics because they can focus treatment on the bacteria locally without spreading drugs to healthy tissues and organs throughout the rest of the body,” Dr Zhang said. “We hope to develop platelet-mimicking nanoparticles into new treatments for systemic bacterial infections and cardiovascular disease.”
Dr Zhang noted that this drug delivery technique could potentially be used in other diseases as well, including cancers. ![]()

nanoparticles binding to the
lining of a damaged artery
Image courtesy of the
Zhang Research Group
Nanoparticles disguised as human platelets can provide targeted drug delivery, according to research published in Nature.
The nanoparticles are made of a biodegradable polymer coated with human platelet membranes.
This coating allows the nanoparticles to circulate in the bloodstream without being attacked by the immune system and to preferentially bind to damaged blood vessels and certain pathogens.
Murine experiments showed that these platelet-mimicking nanoparticles can deliver drugs to targeted sites, thereby increasing the therapeutic effect.
“Because of their targeting ability, platelet-mimicking nanoparticles can directly provide a much higher dose of medication specifically to diseased areas without saturating the entire body with drugs,” said study author Liangfang Zhang, PhD, of the University of California San Diego.
Creating the platelet mimics
To make the nanoparticles, Dr Zhang and his colleagues first separated platelets from whole blood samples using a centrifuge. The platelets were then processed to isolate the membranes from the platelets.
Next, the platelet membranes were broken up into much smaller pieces and fused to the surface of the nanoparticle cores. The resulting platelet-membrane-coated nanoparticles were approximately 100 nanometers in diameter.
This cloaking technology is based on a strategy Dr Zhang’s group had developed to cloak nanoparticles in red blood cell membranes. The researchers previously demonstrated that nanoparticles disguised as red blood cells are capable of removing toxins from the bloodstream.
With the current work, the researchers were able to produce platelet mimics that contain the complete set of surface receptors, antigens, and proteins naturally present on platelet membranes.
“Our technique takes advantage of the unique natural properties of human platelet membranes, which have a natural preference to bind to certain tissues and organisms in the body,” Dr Zhang said.
This targeting ability, which red blood cell membranes do not have, makes platelet membranes extremely useful for targeted drug delivery, according to the researchers.
Platelet mimics at work
The researchers packed the platelet-mimicking nanoparticles with docetaxel, a drug used to prevent scar tissue formation in the lining of damaged blood vessels, and administered them to rats afflicted with injured arteries.
The docetaxel-containing nanoparticles collected at the damaged sites of arteries and healed them.
The researchers then injected nanoparticles containing one-sixth the clinical dose of the antibiotic vancomycin into a group of mice systemically infected with methicillin-resistant Staphylococcus aureus bacteria.
Bacterial counts in the organs of these mice were up to 1000 times lower than in mice treated with the clinical dose of vancomycin alone.
“Our platelet-mimicking nanoparticles can increase the therapeutic efficacy of antibiotics because they can focus treatment on the bacteria locally without spreading drugs to healthy tissues and organs throughout the rest of the body,” Dr Zhang said. “We hope to develop platelet-mimicking nanoparticles into new treatments for systemic bacterial infections and cardiovascular disease.”
Dr Zhang noted that this drug delivery technique could potentially be used in other diseases as well, including cancers. ![]()

nanoparticles binding to the
lining of a damaged artery
Image courtesy of the
Zhang Research Group
Nanoparticles disguised as human platelets can provide targeted drug delivery, according to research published in Nature.
The nanoparticles are made of a biodegradable polymer coated with human platelet membranes.
This coating allows the nanoparticles to circulate in the bloodstream without being attacked by the immune system and to preferentially bind to damaged blood vessels and certain pathogens.
Murine experiments showed that these platelet-mimicking nanoparticles can deliver drugs to targeted sites, thereby increasing the therapeutic effect.
“Because of their targeting ability, platelet-mimicking nanoparticles can directly provide a much higher dose of medication specifically to diseased areas without saturating the entire body with drugs,” said study author Liangfang Zhang, PhD, of the University of California San Diego.
Creating the platelet mimics
To make the nanoparticles, Dr Zhang and his colleagues first separated platelets from whole blood samples using a centrifuge. The platelets were then processed to isolate the membranes from the platelets.
Next, the platelet membranes were broken up into much smaller pieces and fused to the surface of the nanoparticle cores. The resulting platelet-membrane-coated nanoparticles were approximately 100 nanometers in diameter.
This cloaking technology is based on a strategy Dr Zhang’s group had developed to cloak nanoparticles in red blood cell membranes. The researchers previously demonstrated that nanoparticles disguised as red blood cells are capable of removing toxins from the bloodstream.
With the current work, the researchers were able to produce platelet mimics that contain the complete set of surface receptors, antigens, and proteins naturally present on platelet membranes.
“Our technique takes advantage of the unique natural properties of human platelet membranes, which have a natural preference to bind to certain tissues and organisms in the body,” Dr Zhang said.
This targeting ability, which red blood cell membranes do not have, makes platelet membranes extremely useful for targeted drug delivery, according to the researchers.
Platelet mimics at work
The researchers packed the platelet-mimicking nanoparticles with docetaxel, a drug used to prevent scar tissue formation in the lining of damaged blood vessels, and administered them to rats afflicted with injured arteries.
The docetaxel-containing nanoparticles collected at the damaged sites of arteries and healed them.
The researchers then injected nanoparticles containing one-sixth the clinical dose of the antibiotic vancomycin into a group of mice systemically infected with methicillin-resistant Staphylococcus aureus bacteria.
Bacterial counts in the organs of these mice were up to 1000 times lower than in mice treated with the clinical dose of vancomycin alone.
“Our platelet-mimicking nanoparticles can increase the therapeutic efficacy of antibiotics because they can focus treatment on the bacteria locally without spreading drugs to healthy tissues and organs throughout the rest of the body,” Dr Zhang said. “We hope to develop platelet-mimicking nanoparticles into new treatments for systemic bacterial infections and cardiovascular disease.”
Dr Zhang noted that this drug delivery technique could potentially be used in other diseases as well, including cancers. ![]()
FDA approves product for hemophilia A
The US Food and Drug Administration (FDA) has approved the recombinant factor VIII product simoctocog alfa (Nuwiq) for adults and children with hemophilia A.
The approval includes on-demand treatment and control of bleeding episodes, routine prophylaxis to reduce the frequency of bleeding episodes, and perioperative management of bleeding.
Simoctocog alfa is the first B-domain-deleted recombinant factor VIII product derived from a human cell line—not chemically modified or fused with another protein—designed to treat hemophilia A.
Simoctocog alfa is already approved for use in the European Union, Argentina, Australia, and Canada.
In the US, simoctocog alfa is being developed by Octapharma USA, a subsidiary of Octapharma AG.
According to Octapharma USA, simoctocog alfa should be available in the US by early 2016. The company plans to offer hemophilia A patients educational and support services in connection with the product.
Trials of simoctocog alfa
Simoctocog alfa has been evaluated for safety in 5 prospective trials and for efficacy in 3 prospective studies.
A total of 135 previously treated patients with severe hemophilia A have received simoctocog alfa across all the studies. This includes 74 adults, 3 adolescents between ages 12 and 17, and 58 pediatric patients between ages 2 and 11.
The patients were treated with a total of 16,134 infusions over 15,950 exposure days.
In a study of adults, the overall prophylactic efficacy of simoctocog alfa for spontaneous bleeds was rated “excellent” or “good” in 92% of patients. In a study of children, prophylactic efficacy for spontaneous bleeds was rated “excellent” or “good” in 97% of patients.
The mean annualized bleeding rates for spontaneous bleeds during prophylaxis were approximately 1.5 in children and 1.2 in adults.
For hemophilia A patients receiving simoctocog alfa prophylaxis compared to on-demand treatment, the annualized bleeding rates were reduced 96% for adults and 93% for children.
Treatment of breakthrough bleeds during simoctocog alfa prophylaxis was rated as “excellent” or “good” in 100% of bleeds (30/30) in adults and 82% of bleeds (89/108) in children.
For on-demand treatment with simoctocog alfa in 20 adults and 2 adolescents, efficacy for the treatment of bleeds was considered “excellent” or “good” in 94% of bleeds (931/986).
The overall efficacy in surgical prophylaxis was rated “excellent” or “good” in 97% of procedures using simoctocog alfa (32/33).
For all the trials of simoctocog alfa, there were 7 adverse events reported. Each of these events occurred once, with a rate of 0.7% across all 135 patients. The events were paresthesia, headache, injection site inflammation, injection site pain, back pain, vertigo, and dry mouth.
Non-neutralizing anti-factor VIII antibodies (without inhibitory activity as measured by the modified Bethesda assay) were reported in 4 patients (3%). Three of the 4 patients had pre-existing non-neutralizing antibodies prior to simoctocog alfa exposure.
For more details on simoctocog alfa, see the full prescribing information, available at www.octapharmausa.com. ![]()
The US Food and Drug Administration (FDA) has approved the recombinant factor VIII product simoctocog alfa (Nuwiq) for adults and children with hemophilia A.
The approval includes on-demand treatment and control of bleeding episodes, routine prophylaxis to reduce the frequency of bleeding episodes, and perioperative management of bleeding.
Simoctocog alfa is the first B-domain-deleted recombinant factor VIII product derived from a human cell line—not chemically modified or fused with another protein—designed to treat hemophilia A.
Simoctocog alfa is already approved for use in the European Union, Argentina, Australia, and Canada.
In the US, simoctocog alfa is being developed by Octapharma USA, a subsidiary of Octapharma AG.
According to Octapharma USA, simoctocog alfa should be available in the US by early 2016. The company plans to offer hemophilia A patients educational and support services in connection with the product.
Trials of simoctocog alfa
Simoctocog alfa has been evaluated for safety in 5 prospective trials and for efficacy in 3 prospective studies.
A total of 135 previously treated patients with severe hemophilia A have received simoctocog alfa across all the studies. This includes 74 adults, 3 adolescents between ages 12 and 17, and 58 pediatric patients between ages 2 and 11.
The patients were treated with a total of 16,134 infusions over 15,950 exposure days.
In a study of adults, the overall prophylactic efficacy of simoctocog alfa for spontaneous bleeds was rated “excellent” or “good” in 92% of patients. In a study of children, prophylactic efficacy for spontaneous bleeds was rated “excellent” or “good” in 97% of patients.
The mean annualized bleeding rates for spontaneous bleeds during prophylaxis were approximately 1.5 in children and 1.2 in adults.
For hemophilia A patients receiving simoctocog alfa prophylaxis compared to on-demand treatment, the annualized bleeding rates were reduced 96% for adults and 93% for children.
Treatment of breakthrough bleeds during simoctocog alfa prophylaxis was rated as “excellent” or “good” in 100% of bleeds (30/30) in adults and 82% of bleeds (89/108) in children.
For on-demand treatment with simoctocog alfa in 20 adults and 2 adolescents, efficacy for the treatment of bleeds was considered “excellent” or “good” in 94% of bleeds (931/986).
The overall efficacy in surgical prophylaxis was rated “excellent” or “good” in 97% of procedures using simoctocog alfa (32/33).
For all the trials of simoctocog alfa, there were 7 adverse events reported. Each of these events occurred once, with a rate of 0.7% across all 135 patients. The events were paresthesia, headache, injection site inflammation, injection site pain, back pain, vertigo, and dry mouth.
Non-neutralizing anti-factor VIII antibodies (without inhibitory activity as measured by the modified Bethesda assay) were reported in 4 patients (3%). Three of the 4 patients had pre-existing non-neutralizing antibodies prior to simoctocog alfa exposure.
For more details on simoctocog alfa, see the full prescribing information, available at www.octapharmausa.com. ![]()
The US Food and Drug Administration (FDA) has approved the recombinant factor VIII product simoctocog alfa (Nuwiq) for adults and children with hemophilia A.
The approval includes on-demand treatment and control of bleeding episodes, routine prophylaxis to reduce the frequency of bleeding episodes, and perioperative management of bleeding.
Simoctocog alfa is the first B-domain-deleted recombinant factor VIII product derived from a human cell line—not chemically modified or fused with another protein—designed to treat hemophilia A.
Simoctocog alfa is already approved for use in the European Union, Argentina, Australia, and Canada.
In the US, simoctocog alfa is being developed by Octapharma USA, a subsidiary of Octapharma AG.
According to Octapharma USA, simoctocog alfa should be available in the US by early 2016. The company plans to offer hemophilia A patients educational and support services in connection with the product.
Trials of simoctocog alfa
Simoctocog alfa has been evaluated for safety in 5 prospective trials and for efficacy in 3 prospective studies.
A total of 135 previously treated patients with severe hemophilia A have received simoctocog alfa across all the studies. This includes 74 adults, 3 adolescents between ages 12 and 17, and 58 pediatric patients between ages 2 and 11.
The patients were treated with a total of 16,134 infusions over 15,950 exposure days.
In a study of adults, the overall prophylactic efficacy of simoctocog alfa for spontaneous bleeds was rated “excellent” or “good” in 92% of patients. In a study of children, prophylactic efficacy for spontaneous bleeds was rated “excellent” or “good” in 97% of patients.
The mean annualized bleeding rates for spontaneous bleeds during prophylaxis were approximately 1.5 in children and 1.2 in adults.
For hemophilia A patients receiving simoctocog alfa prophylaxis compared to on-demand treatment, the annualized bleeding rates were reduced 96% for adults and 93% for children.
Treatment of breakthrough bleeds during simoctocog alfa prophylaxis was rated as “excellent” or “good” in 100% of bleeds (30/30) in adults and 82% of bleeds (89/108) in children.
For on-demand treatment with simoctocog alfa in 20 adults and 2 adolescents, efficacy for the treatment of bleeds was considered “excellent” or “good” in 94% of bleeds (931/986).
The overall efficacy in surgical prophylaxis was rated “excellent” or “good” in 97% of procedures using simoctocog alfa (32/33).
For all the trials of simoctocog alfa, there were 7 adverse events reported. Each of these events occurred once, with a rate of 0.7% across all 135 patients. The events were paresthesia, headache, injection site inflammation, injection site pain, back pain, vertigo, and dry mouth.
Non-neutralizing anti-factor VIII antibodies (without inhibitory activity as measured by the modified Bethesda assay) were reported in 4 patients (3%). Three of the 4 patients had pre-existing non-neutralizing antibodies prior to simoctocog alfa exposure.
For more details on simoctocog alfa, see the full prescribing information, available at www.octapharmausa.com. ![]()
Studies help explain resistance to BET inhibitors
Image by Robert Paulson
Two groups of researchers have reported results that help explain how leukemia resists treatment with BET inhibitors.
One group was able to grow and maintain leukemia stem cells (LSCs) in vitro, and their subsequent experiments showed how LSCs react to BET inhibition.
The other group found evidence to suggest that by measuring Wnt signaling markers, we might be able to predict which patients will respond to BET inhibition.
Both groups described their research in letters to Nature.
“[T]he risk of resistance developing is common in any cancer treatment,” said Mark Dawson, PhD, a researcher at Peter MacCallum Cancer Centre in East Melbourne, Victoria, Australia and an author of the LSC study.
“Knowing precisely how that happens in advance puts us one step ahead in outmaneuvering the disease. Being able to grow and maintain leukemia
stem cells in vitro also gives us unprecedented access and insight into how they work so we can find new and better ways to target and destroy them.”
In their study, Dr Dawson and his colleagues assessed BET inhibitor resistance in a model of acute myeloid leukemia.
The team transduced murine hematopoietic stem and progenitor cells with MLL–AF9 and treated the cells with the BET inhibitor I-BET or dimethylsulfoxide (vehicle). They then isolated individual blast colonies to generate 4 vehicle-treated and 5 I-BET-resistant cell lines.
The researchers found that resistance to I-BET also conferred resistance to the chemically distinct BET inhibitor JQ1 and to genetic knockdown of BET proteins.
Further investigation revealed that resistance to BET inhibitors emerges from LSCs, both ex vivo and in vivo. And that resistance is, in part, a result of increased Wnt/β-catenin signaling.
The researchers noted that not all LSCs are intrinsically resistant to BET inhibition, but a small proportion of them are either transcriptionally primed or display rapid transcriptional plasticity to survive the initial BET inhibitor challenge. The team said these cells then thrive and become the dominant population.
These findings are consistent with results of the other study, conducted by Johannes Zuber, MD, of the Research Institute of Molecular Pathology in Vienna, Austria, and his colleagues.
With this study, the researchers set out to determine why only certain leukemia subtypes are sensitive to BET inhibitors. Their experiments revealed that loss of the PRC2 complex, which is known to inactivate genes during normal development, can render leukemia cells resistant to BET inhibitors.
By further characterizing these resistant cells, the team found that MYC and other BRD4-regulated genes (which are turned off by BET inhibitors) were back on again. So the leukemia cells had found a way to activate these genes in the absence of BRD4.
The researchers then compared leukemia cells that had acquired resistance during BET inhibitor treatment to leukemia cells that were resistant in the first place.
In both cases, the cells used similar pathways to turn critical genes such as MYC back on and thereby escape the effects of BET inhibition. A pathway that proved particularly important was the Wnt signaling pathway, which is known to activate MYC in cancers.
To determine whether this knowledge could be used to predict which patients will respond to BET inhibitors, the researchers measured Wnt signaling markers in samples from leukemia patients.
The team found that cells with low Wnt activity were sensitive to BET inhibitors, while high Wnt activity was associated with resistance.
Specifically, the researchers quantified 9 Wnt-associated transcripts in sensitive and resistant samples. Three of these transcripts—TCF4, CCND2, and HOXB4—were significantly overexpressed in resistant samples.
So the team used these 3 transcripts to establish a “resistance index” that, they believe, may provide a first step toward developing a predictive biomarker.
The researchers said, collectively, their study reveals that leukemia cells can become resistant to BET inhibitors by rewiring the regulation of critical BRD4 target genes. This transcriptional plasticity highlights an emerging mode of drug resistance that is distinct from established resistance mechanisms such as mutations in binding pockets or drug elimination through efflux pumps.
Dr Zuber and his colleagues believe that a better understanding of these adaptation mechanisms will lead to combination therapies that will ultimately “outsmart” cancer cells.
“We now have learned that cancer cells can adapt to targeted therapies, but their repertoire of escape routes is quite limited,” Dr Zuber said. “A better understanding of the common escape routes will allow us to predict the next effective targeted therapy so that we are always one step ahead of the cancer cell.” ![]()

Image by Robert Paulson
Two groups of researchers have reported results that help explain how leukemia resists treatment with BET inhibitors.
One group was able to grow and maintain leukemia stem cells (LSCs) in vitro, and their subsequent experiments showed how LSCs react to BET inhibition.
The other group found evidence to suggest that by measuring Wnt signaling markers, we might be able to predict which patients will respond to BET inhibition.
Both groups described their research in letters to Nature.
“[T]he risk of resistance developing is common in any cancer treatment,” said Mark Dawson, PhD, a researcher at Peter MacCallum Cancer Centre in East Melbourne, Victoria, Australia and an author of the LSC study.
“Knowing precisely how that happens in advance puts us one step ahead in outmaneuvering the disease. Being able to grow and maintain leukemia
stem cells in vitro also gives us unprecedented access and insight into how they work so we can find new and better ways to target and destroy them.”
In their study, Dr Dawson and his colleagues assessed BET inhibitor resistance in a model of acute myeloid leukemia.
The team transduced murine hematopoietic stem and progenitor cells with MLL–AF9 and treated the cells with the BET inhibitor I-BET or dimethylsulfoxide (vehicle). They then isolated individual blast colonies to generate 4 vehicle-treated and 5 I-BET-resistant cell lines.
The researchers found that resistance to I-BET also conferred resistance to the chemically distinct BET inhibitor JQ1 and to genetic knockdown of BET proteins.
Further investigation revealed that resistance to BET inhibitors emerges from LSCs, both ex vivo and in vivo. And that resistance is, in part, a result of increased Wnt/β-catenin signaling.
The researchers noted that not all LSCs are intrinsically resistant to BET inhibition, but a small proportion of them are either transcriptionally primed or display rapid transcriptional plasticity to survive the initial BET inhibitor challenge. The team said these cells then thrive and become the dominant population.
These findings are consistent with results of the other study, conducted by Johannes Zuber, MD, of the Research Institute of Molecular Pathology in Vienna, Austria, and his colleagues.
With this study, the researchers set out to determine why only certain leukemia subtypes are sensitive to BET inhibitors. Their experiments revealed that loss of the PRC2 complex, which is known to inactivate genes during normal development, can render leukemia cells resistant to BET inhibitors.
By further characterizing these resistant cells, the team found that MYC and other BRD4-regulated genes (which are turned off by BET inhibitors) were back on again. So the leukemia cells had found a way to activate these genes in the absence of BRD4.
The researchers then compared leukemia cells that had acquired resistance during BET inhibitor treatment to leukemia cells that were resistant in the first place.
In both cases, the cells used similar pathways to turn critical genes such as MYC back on and thereby escape the effects of BET inhibition. A pathway that proved particularly important was the Wnt signaling pathway, which is known to activate MYC in cancers.
To determine whether this knowledge could be used to predict which patients will respond to BET inhibitors, the researchers measured Wnt signaling markers in samples from leukemia patients.
The team found that cells with low Wnt activity were sensitive to BET inhibitors, while high Wnt activity was associated with resistance.
Specifically, the researchers quantified 9 Wnt-associated transcripts in sensitive and resistant samples. Three of these transcripts—TCF4, CCND2, and HOXB4—were significantly overexpressed in resistant samples.
So the team used these 3 transcripts to establish a “resistance index” that, they believe, may provide a first step toward developing a predictive biomarker.
The researchers said, collectively, their study reveals that leukemia cells can become resistant to BET inhibitors by rewiring the regulation of critical BRD4 target genes. This transcriptional plasticity highlights an emerging mode of drug resistance that is distinct from established resistance mechanisms such as mutations in binding pockets or drug elimination through efflux pumps.
Dr Zuber and his colleagues believe that a better understanding of these adaptation mechanisms will lead to combination therapies that will ultimately “outsmart” cancer cells.
“We now have learned that cancer cells can adapt to targeted therapies, but their repertoire of escape routes is quite limited,” Dr Zuber said. “A better understanding of the common escape routes will allow us to predict the next effective targeted therapy so that we are always one step ahead of the cancer cell.” ![]()

Image by Robert Paulson
Two groups of researchers have reported results that help explain how leukemia resists treatment with BET inhibitors.
One group was able to grow and maintain leukemia stem cells (LSCs) in vitro, and their subsequent experiments showed how LSCs react to BET inhibition.
The other group found evidence to suggest that by measuring Wnt signaling markers, we might be able to predict which patients will respond to BET inhibition.
Both groups described their research in letters to Nature.
“[T]he risk of resistance developing is common in any cancer treatment,” said Mark Dawson, PhD, a researcher at Peter MacCallum Cancer Centre in East Melbourne, Victoria, Australia and an author of the LSC study.
“Knowing precisely how that happens in advance puts us one step ahead in outmaneuvering the disease. Being able to grow and maintain leukemia
stem cells in vitro also gives us unprecedented access and insight into how they work so we can find new and better ways to target and destroy them.”
In their study, Dr Dawson and his colleagues assessed BET inhibitor resistance in a model of acute myeloid leukemia.
The team transduced murine hematopoietic stem and progenitor cells with MLL–AF9 and treated the cells with the BET inhibitor I-BET or dimethylsulfoxide (vehicle). They then isolated individual blast colonies to generate 4 vehicle-treated and 5 I-BET-resistant cell lines.
The researchers found that resistance to I-BET also conferred resistance to the chemically distinct BET inhibitor JQ1 and to genetic knockdown of BET proteins.
Further investigation revealed that resistance to BET inhibitors emerges from LSCs, both ex vivo and in vivo. And that resistance is, in part, a result of increased Wnt/β-catenin signaling.
The researchers noted that not all LSCs are intrinsically resistant to BET inhibition, but a small proportion of them are either transcriptionally primed or display rapid transcriptional plasticity to survive the initial BET inhibitor challenge. The team said these cells then thrive and become the dominant population.
These findings are consistent with results of the other study, conducted by Johannes Zuber, MD, of the Research Institute of Molecular Pathology in Vienna, Austria, and his colleagues.
With this study, the researchers set out to determine why only certain leukemia subtypes are sensitive to BET inhibitors. Their experiments revealed that loss of the PRC2 complex, which is known to inactivate genes during normal development, can render leukemia cells resistant to BET inhibitors.
By further characterizing these resistant cells, the team found that MYC and other BRD4-regulated genes (which are turned off by BET inhibitors) were back on again. So the leukemia cells had found a way to activate these genes in the absence of BRD4.
The researchers then compared leukemia cells that had acquired resistance during BET inhibitor treatment to leukemia cells that were resistant in the first place.
In both cases, the cells used similar pathways to turn critical genes such as MYC back on and thereby escape the effects of BET inhibition. A pathway that proved particularly important was the Wnt signaling pathway, which is known to activate MYC in cancers.
To determine whether this knowledge could be used to predict which patients will respond to BET inhibitors, the researchers measured Wnt signaling markers in samples from leukemia patients.
The team found that cells with low Wnt activity were sensitive to BET inhibitors, while high Wnt activity was associated with resistance.
Specifically, the researchers quantified 9 Wnt-associated transcripts in sensitive and resistant samples. Three of these transcripts—TCF4, CCND2, and HOXB4—were significantly overexpressed in resistant samples.
So the team used these 3 transcripts to establish a “resistance index” that, they believe, may provide a first step toward developing a predictive biomarker.
The researchers said, collectively, their study reveals that leukemia cells can become resistant to BET inhibitors by rewiring the regulation of critical BRD4 target genes. This transcriptional plasticity highlights an emerging mode of drug resistance that is distinct from established resistance mechanisms such as mutations in binding pockets or drug elimination through efflux pumps.
Dr Zuber and his colleagues believe that a better understanding of these adaptation mechanisms will lead to combination therapies that will ultimately “outsmart” cancer cells.
“We now have learned that cancer cells can adapt to targeted therapies, but their repertoire of escape routes is quite limited,” Dr Zuber said. “A better understanding of the common escape routes will allow us to predict the next effective targeted therapy so that we are always one step ahead of the cancer cell.” ![]()
Plant-derived compound shows activity against NHL

The active compound in a plant extract has shown promise for treating non-Hodgkin lymphomas (NHLs), according to researchers.
The compound, withaferin A, is a steroidal lactone isolated from the Ayruvedic medicinal plant Ashwagandha (Withania somnifera).
Withaferin A has previously exhibited activity against a range of solid tumor malignancies, but its effects in NHLs and other hematologic malignancies have not been well-studied.
So Subbarao Bondada, PhD, of the University of Kentucky in Lexington, and his colleagues tested withaferin A in NHLs and reported their results in Cancer Biology and Therapy.
Withaferin A exhibited activity in several human B-cell lymphoma cell lines—the diffuse large B-cell lymphoma (DLBCL) cell lines LY-3, LY-10, and SudHL-6; the Burkitt lymphoma cell lines Raji and Ramos; and the mantle cell lymphoma cell line MINO.
Ramos was the most sensitive to withaferin A, and the mantle cell lymphoma cell line JEKO was the most resistant. The researchers said they are still investigating this resistance.
Withaferin A also inhibited the growth of the murine immature B-cell lymphoma cell line BKS-2 and the germinal center lymphoma cell line A20-Luc/YFP.
Further investigation revealed that withaferin A induces cell-cycle arrest, prompts apoptosis, inhibits NF-kB nuclear translocation, and reduces the expression of pro-survival signals in B-cell lymphomas.
The researchers also found evidence to suggest that withaferin A inhibits the activity of Hsp90. Although Hsp90 levels were unaltered in withaferin-A-treated lymphoma cells, the team observed a “robust” increase in Hsp70 expression levels (which suggests a decrease in Hsp90 function).
Finally, the researchers tested withaferin A in mice injected with the murine DLBCL line A20-Luc. The treatment proved active against A20-Luc cells but did not affect other proliferating cells.
Mice treated with withaferin A had a significant reduction in tumor size, compared to placebo-treated mice, on days 10 and 13 (P<0.05).
Based on these results, the researchers concluded that withaferin A may hold promise for treating NHL, particularly DLBCL.
“It may be possible to develop orally administered versions of withaferin A that could be used in lymphoma patients with fewer side effects than current chemotherapy regimens,” Dr Bondada said.
He and his colleagues are now testing withaferin A in chronic lymphocytic leukemia. ![]()

The active compound in a plant extract has shown promise for treating non-Hodgkin lymphomas (NHLs), according to researchers.
The compound, withaferin A, is a steroidal lactone isolated from the Ayruvedic medicinal plant Ashwagandha (Withania somnifera).
Withaferin A has previously exhibited activity against a range of solid tumor malignancies, but its effects in NHLs and other hematologic malignancies have not been well-studied.
So Subbarao Bondada, PhD, of the University of Kentucky in Lexington, and his colleagues tested withaferin A in NHLs and reported their results in Cancer Biology and Therapy.
Withaferin A exhibited activity in several human B-cell lymphoma cell lines—the diffuse large B-cell lymphoma (DLBCL) cell lines LY-3, LY-10, and SudHL-6; the Burkitt lymphoma cell lines Raji and Ramos; and the mantle cell lymphoma cell line MINO.
Ramos was the most sensitive to withaferin A, and the mantle cell lymphoma cell line JEKO was the most resistant. The researchers said they are still investigating this resistance.
Withaferin A also inhibited the growth of the murine immature B-cell lymphoma cell line BKS-2 and the germinal center lymphoma cell line A20-Luc/YFP.
Further investigation revealed that withaferin A induces cell-cycle arrest, prompts apoptosis, inhibits NF-kB nuclear translocation, and reduces the expression of pro-survival signals in B-cell lymphomas.
The researchers also found evidence to suggest that withaferin A inhibits the activity of Hsp90. Although Hsp90 levels were unaltered in withaferin-A-treated lymphoma cells, the team observed a “robust” increase in Hsp70 expression levels (which suggests a decrease in Hsp90 function).
Finally, the researchers tested withaferin A in mice injected with the murine DLBCL line A20-Luc. The treatment proved active against A20-Luc cells but did not affect other proliferating cells.
Mice treated with withaferin A had a significant reduction in tumor size, compared to placebo-treated mice, on days 10 and 13 (P<0.05).
Based on these results, the researchers concluded that withaferin A may hold promise for treating NHL, particularly DLBCL.
“It may be possible to develop orally administered versions of withaferin A that could be used in lymphoma patients with fewer side effects than current chemotherapy regimens,” Dr Bondada said.
He and his colleagues are now testing withaferin A in chronic lymphocytic leukemia. ![]()

The active compound in a plant extract has shown promise for treating non-Hodgkin lymphomas (NHLs), according to researchers.
The compound, withaferin A, is a steroidal lactone isolated from the Ayruvedic medicinal plant Ashwagandha (Withania somnifera).
Withaferin A has previously exhibited activity against a range of solid tumor malignancies, but its effects in NHLs and other hematologic malignancies have not been well-studied.
So Subbarao Bondada, PhD, of the University of Kentucky in Lexington, and his colleagues tested withaferin A in NHLs and reported their results in Cancer Biology and Therapy.
Withaferin A exhibited activity in several human B-cell lymphoma cell lines—the diffuse large B-cell lymphoma (DLBCL) cell lines LY-3, LY-10, and SudHL-6; the Burkitt lymphoma cell lines Raji and Ramos; and the mantle cell lymphoma cell line MINO.
Ramos was the most sensitive to withaferin A, and the mantle cell lymphoma cell line JEKO was the most resistant. The researchers said they are still investigating this resistance.
Withaferin A also inhibited the growth of the murine immature B-cell lymphoma cell line BKS-2 and the germinal center lymphoma cell line A20-Luc/YFP.
Further investigation revealed that withaferin A induces cell-cycle arrest, prompts apoptosis, inhibits NF-kB nuclear translocation, and reduces the expression of pro-survival signals in B-cell lymphomas.
The researchers also found evidence to suggest that withaferin A inhibits the activity of Hsp90. Although Hsp90 levels were unaltered in withaferin-A-treated lymphoma cells, the team observed a “robust” increase in Hsp70 expression levels (which suggests a decrease in Hsp90 function).
Finally, the researchers tested withaferin A in mice injected with the murine DLBCL line A20-Luc. The treatment proved active against A20-Luc cells but did not affect other proliferating cells.
Mice treated with withaferin A had a significant reduction in tumor size, compared to placebo-treated mice, on days 10 and 13 (P<0.05).
Based on these results, the researchers concluded that withaferin A may hold promise for treating NHL, particularly DLBCL.
“It may be possible to develop orally administered versions of withaferin A that could be used in lymphoma patients with fewer side effects than current chemotherapy regimens,” Dr Bondada said.
He and his colleagues are now testing withaferin A in chronic lymphocytic leukemia. ![]()
Tool can guide allocation of research resources

Photo by Bill Branson
Scientists say they have developed a tool that can guide the allocation of resources for biomedical research in an unbiased way.
The tool, called the Research Opportunity Index (ROI), measures disparities between resources dedicated to a disease and its relative burden on society.
This reveals diseases that receive a disproportionate share of resources and opportunities for high-impact investment or the realignment of existing resources.
The ROI was designed to provide an unbiased, data-driven framework to help scientific and political communities assess resource investment and identify unmet medical needs.
The tool is described in a letter to Nature Biotechnology.
“The misalignment of resources in biomedical research could be likened to poor budgeting of household finances,” said Andrey Rzhetsky, PhD, of the University of Chicago in Illinois.
“It would be bad to spend all your money on food, for example, and have nothing for rent. Resources are finite, and attention to each problem, ideally, should be proportional to the need.”
With this in mind, Dr Rzhetsky and his colleagues created the ROI. They used it to estimate the societal burden of 1400 medical conditions in the US over a 12-year timespan, based on frequency of diagnosis and healthcare insurance costs, as well as research publications, awarded grants, and clinical trials for each condition.
The tool revealed misalignments, which allowed the scientists to create an “investment portfolio” of the resources dedicated to each disease, relative to its burden on the US healthcare system.
The team found that breast cancer, for example, stands out as a disease with higher dedicated resources than its relative societal burden. On the opposite end of the spectrum, Hashimoto’s thyroiditis is among the conditions with the most investment potential.
While Hashimoto’s disease has nearly the same incidence among women as breast cancer, there were only 16 open clinical trials for Hashimoto’s disease as of August 2015, according to a list on clinicaltrials.gov. Breast cancer had 2205 open trials.
Dr Rzhetsky and his colleagues acknowledge that the question of what makes a condition more deserving of funding than any other ailment is complex and multifaceted. But the team hopes this new tool can aid decisions on how best to allocate funds and other resources.
By providing a framework based on unbiased quantitative analytics and big data, they hope to identify diseases that are high-impact and rewarding targets for additional investment.
“Some diseases stick in the public’s attention,” Dr Rzhetsky said. “We have a distorted map of the frequency and importance of events from media and articles, and, without special efforts to reconcile the reality, we are inherently biased.”
The team is now working to incorporate other models of funding distribution into their tool to account for additional variables.
For example, the “trendy model,” which supports investment for diseases with large emotional impact, suggests that even though this reduces funding for other diseases, there may still be benefits as basic science discoveries are added to the scientific and medical community. ![]()

Photo by Bill Branson
Scientists say they have developed a tool that can guide the allocation of resources for biomedical research in an unbiased way.
The tool, called the Research Opportunity Index (ROI), measures disparities between resources dedicated to a disease and its relative burden on society.
This reveals diseases that receive a disproportionate share of resources and opportunities for high-impact investment or the realignment of existing resources.
The ROI was designed to provide an unbiased, data-driven framework to help scientific and political communities assess resource investment and identify unmet medical needs.
The tool is described in a letter to Nature Biotechnology.
“The misalignment of resources in biomedical research could be likened to poor budgeting of household finances,” said Andrey Rzhetsky, PhD, of the University of Chicago in Illinois.
“It would be bad to spend all your money on food, for example, and have nothing for rent. Resources are finite, and attention to each problem, ideally, should be proportional to the need.”
With this in mind, Dr Rzhetsky and his colleagues created the ROI. They used it to estimate the societal burden of 1400 medical conditions in the US over a 12-year timespan, based on frequency of diagnosis and healthcare insurance costs, as well as research publications, awarded grants, and clinical trials for each condition.
The tool revealed misalignments, which allowed the scientists to create an “investment portfolio” of the resources dedicated to each disease, relative to its burden on the US healthcare system.
The team found that breast cancer, for example, stands out as a disease with higher dedicated resources than its relative societal burden. On the opposite end of the spectrum, Hashimoto’s thyroiditis is among the conditions with the most investment potential.
While Hashimoto’s disease has nearly the same incidence among women as breast cancer, there were only 16 open clinical trials for Hashimoto’s disease as of August 2015, according to a list on clinicaltrials.gov. Breast cancer had 2205 open trials.
Dr Rzhetsky and his colleagues acknowledge that the question of what makes a condition more deserving of funding than any other ailment is complex and multifaceted. But the team hopes this new tool can aid decisions on how best to allocate funds and other resources.
By providing a framework based on unbiased quantitative analytics and big data, they hope to identify diseases that are high-impact and rewarding targets for additional investment.
“Some diseases stick in the public’s attention,” Dr Rzhetsky said. “We have a distorted map of the frequency and importance of events from media and articles, and, without special efforts to reconcile the reality, we are inherently biased.”
The team is now working to incorporate other models of funding distribution into their tool to account for additional variables.
For example, the “trendy model,” which supports investment for diseases with large emotional impact, suggests that even though this reduces funding for other diseases, there may still be benefits as basic science discoveries are added to the scientific and medical community. ![]()

Photo by Bill Branson
Scientists say they have developed a tool that can guide the allocation of resources for biomedical research in an unbiased way.
The tool, called the Research Opportunity Index (ROI), measures disparities between resources dedicated to a disease and its relative burden on society.
This reveals diseases that receive a disproportionate share of resources and opportunities for high-impact investment or the realignment of existing resources.
The ROI was designed to provide an unbiased, data-driven framework to help scientific and political communities assess resource investment and identify unmet medical needs.
The tool is described in a letter to Nature Biotechnology.
“The misalignment of resources in biomedical research could be likened to poor budgeting of household finances,” said Andrey Rzhetsky, PhD, of the University of Chicago in Illinois.
“It would be bad to spend all your money on food, for example, and have nothing for rent. Resources are finite, and attention to each problem, ideally, should be proportional to the need.”
With this in mind, Dr Rzhetsky and his colleagues created the ROI. They used it to estimate the societal burden of 1400 medical conditions in the US over a 12-year timespan, based on frequency of diagnosis and healthcare insurance costs, as well as research publications, awarded grants, and clinical trials for each condition.
The tool revealed misalignments, which allowed the scientists to create an “investment portfolio” of the resources dedicated to each disease, relative to its burden on the US healthcare system.
The team found that breast cancer, for example, stands out as a disease with higher dedicated resources than its relative societal burden. On the opposite end of the spectrum, Hashimoto’s thyroiditis is among the conditions with the most investment potential.
While Hashimoto’s disease has nearly the same incidence among women as breast cancer, there were only 16 open clinical trials for Hashimoto’s disease as of August 2015, according to a list on clinicaltrials.gov. Breast cancer had 2205 open trials.
Dr Rzhetsky and his colleagues acknowledge that the question of what makes a condition more deserving of funding than any other ailment is complex and multifaceted. But the team hopes this new tool can aid decisions on how best to allocate funds and other resources.
By providing a framework based on unbiased quantitative analytics and big data, they hope to identify diseases that are high-impact and rewarding targets for additional investment.
“Some diseases stick in the public’s attention,” Dr Rzhetsky said. “We have a distorted map of the frequency and importance of events from media and articles, and, without special efforts to reconcile the reality, we are inherently biased.”
The team is now working to incorporate other models of funding distribution into their tool to account for additional variables.
For example, the “trendy model,” which supports investment for diseases with large emotional impact, suggests that even though this reduces funding for other diseases, there may still be benefits as basic science discoveries are added to the scientific and medical community. ![]()
Gene linked to aggressive AML

Photo courtesy of NIH
The gene FOXC1 is associated with aggressive acute myeloid leukemia (AML), according to research published in Cancer Cell.
Researchers said tissue-inappropriate derepression of FOXC1 has functional consequences and prognostic significance in AML.
They found evidence suggesting that FOXC1 enhances clonogenic potential, helps block monocyte/macrophage differentiation, accelerates leukemia onset in mice, and leads to inferior survival in AML patients.
“This is an important finding which helps us understand how acute myeloid leukemia develops and why some cases of AML are more aggressive than others,” said study author Tim Somervaille, MBBS, PhD, of The University of Manchester in the UK.
“Here, instead of being faulty or mutated, this normal gene is turned on in the wrong place at the wrong time, which makes the cancer grow more rapidly. There are certain situations where this gene is necessary, as in the development of the eye and skeleton before birth, but when it’s switched on in the wrong tissue, it causes more aggressive forms of leukemia.”
Dr Somervaille and his colleagues said FOXC1 is expressed in at least 20% of human AML cases but not in normal hematopoietic populations.
The researchers analyzed levels of transcription factor genes in data from published studies to identify transcription regulators expressed in human AML hematopoietic stem and progenitor cells (HSPCs) but not normal HSPCs. In these studies, FOXC1 was among the genes that were most highly upregulated in AML HSPCs.
Further investigation revealed that FOXC1 expression is associated with mutations in NPM1 and t(6;9) but no other recurring mutations in AML.
When Dr Somervaille and his colleagues conducted experiments with human AML cells, they found that FOXC1 “contributes to oncogenic potential by maintaining differentiation block and clonogenic activity.”
In vitro experiments with normal HSPCs showed that FOXC1 expression temporarily impairs myeloid differentiation. In mice, expression of FOXC1 in normal HSPCs reduced donor:recipient chimerism in the blood and skewed differentiation toward the myeloid lineage and away from the B-cell lineage.
By comparing samples from AML patients, the researchers found that FOXC1 expression is associated with high HOX gene expression.
Subsequent experiments showed that FOXC1 collaborates with HOXA9 to enhance clonogenic potential and cell-cycle progression, help block monocyte/macrophage and B-lineage differentiation, and accelerate the onset of symptomatic leukemia in mice.
To determine if the same effects occur in humans, the researchers again analyzed data from AML patients. The results indicated that FOXC1 expression helps block monocyte/macrophage differentiation and leads to inferior survival.
Dr Somervaille and his colleagues said these findings may have therapeutic implications, as previous research has shown that, in basal-like breast cancer, high FOXC1 expression renders cells more susceptible to pharmacological inhibition of NF-kB. But additional research is needed to investigate therapeutic implications for AML. ![]()

Photo courtesy of NIH
The gene FOXC1 is associated with aggressive acute myeloid leukemia (AML), according to research published in Cancer Cell.
Researchers said tissue-inappropriate derepression of FOXC1 has functional consequences and prognostic significance in AML.
They found evidence suggesting that FOXC1 enhances clonogenic potential, helps block monocyte/macrophage differentiation, accelerates leukemia onset in mice, and leads to inferior survival in AML patients.
“This is an important finding which helps us understand how acute myeloid leukemia develops and why some cases of AML are more aggressive than others,” said study author Tim Somervaille, MBBS, PhD, of The University of Manchester in the UK.
“Here, instead of being faulty or mutated, this normal gene is turned on in the wrong place at the wrong time, which makes the cancer grow more rapidly. There are certain situations where this gene is necessary, as in the development of the eye and skeleton before birth, but when it’s switched on in the wrong tissue, it causes more aggressive forms of leukemia.”
Dr Somervaille and his colleagues said FOXC1 is expressed in at least 20% of human AML cases but not in normal hematopoietic populations.
The researchers analyzed levels of transcription factor genes in data from published studies to identify transcription regulators expressed in human AML hematopoietic stem and progenitor cells (HSPCs) but not normal HSPCs. In these studies, FOXC1 was among the genes that were most highly upregulated in AML HSPCs.
Further investigation revealed that FOXC1 expression is associated with mutations in NPM1 and t(6;9) but no other recurring mutations in AML.
When Dr Somervaille and his colleagues conducted experiments with human AML cells, they found that FOXC1 “contributes to oncogenic potential by maintaining differentiation block and clonogenic activity.”
In vitro experiments with normal HSPCs showed that FOXC1 expression temporarily impairs myeloid differentiation. In mice, expression of FOXC1 in normal HSPCs reduced donor:recipient chimerism in the blood and skewed differentiation toward the myeloid lineage and away from the B-cell lineage.
By comparing samples from AML patients, the researchers found that FOXC1 expression is associated with high HOX gene expression.
Subsequent experiments showed that FOXC1 collaborates with HOXA9 to enhance clonogenic potential and cell-cycle progression, help block monocyte/macrophage and B-lineage differentiation, and accelerate the onset of symptomatic leukemia in mice.
To determine if the same effects occur in humans, the researchers again analyzed data from AML patients. The results indicated that FOXC1 expression helps block monocyte/macrophage differentiation and leads to inferior survival.
Dr Somervaille and his colleagues said these findings may have therapeutic implications, as previous research has shown that, in basal-like breast cancer, high FOXC1 expression renders cells more susceptible to pharmacological inhibition of NF-kB. But additional research is needed to investigate therapeutic implications for AML. ![]()

Photo courtesy of NIH
The gene FOXC1 is associated with aggressive acute myeloid leukemia (AML), according to research published in Cancer Cell.
Researchers said tissue-inappropriate derepression of FOXC1 has functional consequences and prognostic significance in AML.
They found evidence suggesting that FOXC1 enhances clonogenic potential, helps block monocyte/macrophage differentiation, accelerates leukemia onset in mice, and leads to inferior survival in AML patients.
“This is an important finding which helps us understand how acute myeloid leukemia develops and why some cases of AML are more aggressive than others,” said study author Tim Somervaille, MBBS, PhD, of The University of Manchester in the UK.
“Here, instead of being faulty or mutated, this normal gene is turned on in the wrong place at the wrong time, which makes the cancer grow more rapidly. There are certain situations where this gene is necessary, as in the development of the eye and skeleton before birth, but when it’s switched on in the wrong tissue, it causes more aggressive forms of leukemia.”
Dr Somervaille and his colleagues said FOXC1 is expressed in at least 20% of human AML cases but not in normal hematopoietic populations.
The researchers analyzed levels of transcription factor genes in data from published studies to identify transcription regulators expressed in human AML hematopoietic stem and progenitor cells (HSPCs) but not normal HSPCs. In these studies, FOXC1 was among the genes that were most highly upregulated in AML HSPCs.
Further investigation revealed that FOXC1 expression is associated with mutations in NPM1 and t(6;9) but no other recurring mutations in AML.
When Dr Somervaille and his colleagues conducted experiments with human AML cells, they found that FOXC1 “contributes to oncogenic potential by maintaining differentiation block and clonogenic activity.”
In vitro experiments with normal HSPCs showed that FOXC1 expression temporarily impairs myeloid differentiation. In mice, expression of FOXC1 in normal HSPCs reduced donor:recipient chimerism in the blood and skewed differentiation toward the myeloid lineage and away from the B-cell lineage.
By comparing samples from AML patients, the researchers found that FOXC1 expression is associated with high HOX gene expression.
Subsequent experiments showed that FOXC1 collaborates with HOXA9 to enhance clonogenic potential and cell-cycle progression, help block monocyte/macrophage and B-lineage differentiation, and accelerate the onset of symptomatic leukemia in mice.
To determine if the same effects occur in humans, the researchers again analyzed data from AML patients. The results indicated that FOXC1 expression helps block monocyte/macrophage differentiation and leads to inferior survival.
Dr Somervaille and his colleagues said these findings may have therapeutic implications, as previous research has shown that, in basal-like breast cancer, high FOXC1 expression renders cells more susceptible to pharmacological inhibition of NF-kB. But additional research is needed to investigate therapeutic implications for AML. ![]()
Living near dams increases malaria risk, study shows

Photo courtesy of the
International Water
Management Institute
More than 1 million people in sub-Saharan Africa will contract malaria this year because they live near a large dam, according to a study published in Malaria Journal.
For the first time, researchers correlated the location of large dams in sub-Saharan Africa with the incidence of malaria.
And they found evidence to suggest that construction of an expected 78 major new dams over the next few years will lead to an additional 56,000 malaria cases annually.
The researchers said these findings have major implications for new dam projects and how health impacts should be assessed prior to construction.
“Dams are at the center of much development planning in Africa,” said study author Solomon Kibret, a graduate student at the University of New England in Armidale, New South Wales, Australia.
“While dams clearly bring many benefits—contributing to economic growth, poverty alleviation, and food security—adverse malaria impacts need to be addressed or they will undermine the sustainability of Africa’s drive for development.”
As part of the CGIAR Research Program on Water, Land, and Ecosystems, Kibret and colleagues looked at 1268 dams in sub-Saharan Africa. Of these, just under two-thirds (n=723) are in malarious areas.
The researchers compared detailed maps of malaria incidence with the dam sites. The number of annual malaria cases associated with the dams was estimated by comparing the number of cases for communities less than 5 kilometers from the dam reservoir with the number of cases for communities further away.
The team found that 15 million people live within 5 kilometers of dam reservoirs and are therefore at risk of contracting malaria. And at least 1.1 million malaria cases annually are linked to the presence of the dams.
“Our study showed that the population at risk of malaria around dams is at least 4 times greater than previously estimated,” Kibret said, noting that the authors were conservative in all their analyses.
The risk is particularly high in areas of sub-Saharan Africa with “unstable” malaria transmission, where malaria is seasonal. The study indicated that the impact of dams on malaria in unstable areas could either lead to intensified malaria transmission or change the nature of transmission from seasonal to perennial.
Explaining the risk
Previous research revealed increases in malaria incidence near major sub-Saharan dams such as the Akosombo Dam in Ghana, the Koka Dam in Ethiopia, and the Kamburu Dam in Kenya. But until now, no attempt has been made to assess the cumulative effect of large dam-building on malaria.
Malaria is transmitted by the Anopheles mosquito, which needs slow-moving or stagnant water in which to breed. Dam reservoirs, particularly shallow puddles that often form along shorelines, provide a perfect environment for the insects to multiply. Thus, dam construction can intensify transmission and shift patterns of malaria infection.
Many African countries are planning new dams to help drive economic growth and increase water security. Improved water storage for growing populations, irrigation, and hydropower generation are needed for a fast-developing continent, but the researchers warn that building new dams has potential costs as well as benefits.
“Dams are an important option for governments anxious to develop,” said study author Matthew McCartney, PhD, of the International Water Management Institute in Vientiane, Laos.
“But it is unethical that people living close to them pay the price of that development through increased suffering and, possibly in extreme cases, loss of life due to disease.”
Lowering the risk
The researchers noted that, despite growing evidence of the impact of dams on malaria, there is scant evidence of their negative impacts being fully offset.
The team therefore made recommendations for managing the increased malaria risk. They said dam reservoirs could be more effectively designed and managed to reduce mosquito breeding. For instance, one option is to adopt operating schedules that, at critical times, dry out shoreline areas where mosquitoes tend to breed.
The researchers said dam developers should also consider increasing investment in integrated malaria intervention programs that include measures such as bed net distribution. Other environmental controls, such as introducing fish that eat mosquito larva in dam reservoirs, could also help reduce malaria cases in some instances.
“The bottom line is that adverse malaria impacts of dams routinely receive recognition in Environmental Impact Assessments, and areas around dams are frequently earmarked for intensive control efforts,” said study author Jonathan Lautze, PhD, of the International Water Management Institute in Pretoria, South Africa.
“The findings of our work hammer home the reality that this recognition and effort—well-intentioned though it may be—is simply not sufficient. Given the need for water resources development in Africa, malaria control around dams requires interdisciplinary cooperation, particularly between water and health communities. Malaria must be addressed while planning, designing, and operating African dams.” ![]()

Photo courtesy of the
International Water
Management Institute
More than 1 million people in sub-Saharan Africa will contract malaria this year because they live near a large dam, according to a study published in Malaria Journal.
For the first time, researchers correlated the location of large dams in sub-Saharan Africa with the incidence of malaria.
And they found evidence to suggest that construction of an expected 78 major new dams over the next few years will lead to an additional 56,000 malaria cases annually.
The researchers said these findings have major implications for new dam projects and how health impacts should be assessed prior to construction.
“Dams are at the center of much development planning in Africa,” said study author Solomon Kibret, a graduate student at the University of New England in Armidale, New South Wales, Australia.
“While dams clearly bring many benefits—contributing to economic growth, poverty alleviation, and food security—adverse malaria impacts need to be addressed or they will undermine the sustainability of Africa’s drive for development.”
As part of the CGIAR Research Program on Water, Land, and Ecosystems, Kibret and colleagues looked at 1268 dams in sub-Saharan Africa. Of these, just under two-thirds (n=723) are in malarious areas.
The researchers compared detailed maps of malaria incidence with the dam sites. The number of annual malaria cases associated with the dams was estimated by comparing the number of cases for communities less than 5 kilometers from the dam reservoir with the number of cases for communities further away.
The team found that 15 million people live within 5 kilometers of dam reservoirs and are therefore at risk of contracting malaria. And at least 1.1 million malaria cases annually are linked to the presence of the dams.
“Our study showed that the population at risk of malaria around dams is at least 4 times greater than previously estimated,” Kibret said, noting that the authors were conservative in all their analyses.
The risk is particularly high in areas of sub-Saharan Africa with “unstable” malaria transmission, where malaria is seasonal. The study indicated that the impact of dams on malaria in unstable areas could either lead to intensified malaria transmission or change the nature of transmission from seasonal to perennial.
Explaining the risk
Previous research revealed increases in malaria incidence near major sub-Saharan dams such as the Akosombo Dam in Ghana, the Koka Dam in Ethiopia, and the Kamburu Dam in Kenya. But until now, no attempt has been made to assess the cumulative effect of large dam-building on malaria.
Malaria is transmitted by the Anopheles mosquito, which needs slow-moving or stagnant water in which to breed. Dam reservoirs, particularly shallow puddles that often form along shorelines, provide a perfect environment for the insects to multiply. Thus, dam construction can intensify transmission and shift patterns of malaria infection.
Many African countries are planning new dams to help drive economic growth and increase water security. Improved water storage for growing populations, irrigation, and hydropower generation are needed for a fast-developing continent, but the researchers warn that building new dams has potential costs as well as benefits.
“Dams are an important option for governments anxious to develop,” said study author Matthew McCartney, PhD, of the International Water Management Institute in Vientiane, Laos.
“But it is unethical that people living close to them pay the price of that development through increased suffering and, possibly in extreme cases, loss of life due to disease.”
Lowering the risk
The researchers noted that, despite growing evidence of the impact of dams on malaria, there is scant evidence of their negative impacts being fully offset.
The team therefore made recommendations for managing the increased malaria risk. They said dam reservoirs could be more effectively designed and managed to reduce mosquito breeding. For instance, one option is to adopt operating schedules that, at critical times, dry out shoreline areas where mosquitoes tend to breed.
The researchers said dam developers should also consider increasing investment in integrated malaria intervention programs that include measures such as bed net distribution. Other environmental controls, such as introducing fish that eat mosquito larva in dam reservoirs, could also help reduce malaria cases in some instances.
“The bottom line is that adverse malaria impacts of dams routinely receive recognition in Environmental Impact Assessments, and areas around dams are frequently earmarked for intensive control efforts,” said study author Jonathan Lautze, PhD, of the International Water Management Institute in Pretoria, South Africa.
“The findings of our work hammer home the reality that this recognition and effort—well-intentioned though it may be—is simply not sufficient. Given the need for water resources development in Africa, malaria control around dams requires interdisciplinary cooperation, particularly between water and health communities. Malaria must be addressed while planning, designing, and operating African dams.” ![]()

Photo courtesy of the
International Water
Management Institute
More than 1 million people in sub-Saharan Africa will contract malaria this year because they live near a large dam, according to a study published in Malaria Journal.
For the first time, researchers correlated the location of large dams in sub-Saharan Africa with the incidence of malaria.
And they found evidence to suggest that construction of an expected 78 major new dams over the next few years will lead to an additional 56,000 malaria cases annually.
The researchers said these findings have major implications for new dam projects and how health impacts should be assessed prior to construction.
“Dams are at the center of much development planning in Africa,” said study author Solomon Kibret, a graduate student at the University of New England in Armidale, New South Wales, Australia.
“While dams clearly bring many benefits—contributing to economic growth, poverty alleviation, and food security—adverse malaria impacts need to be addressed or they will undermine the sustainability of Africa’s drive for development.”
As part of the CGIAR Research Program on Water, Land, and Ecosystems, Kibret and colleagues looked at 1268 dams in sub-Saharan Africa. Of these, just under two-thirds (n=723) are in malarious areas.
The researchers compared detailed maps of malaria incidence with the dam sites. The number of annual malaria cases associated with the dams was estimated by comparing the number of cases for communities less than 5 kilometers from the dam reservoir with the number of cases for communities further away.
The team found that 15 million people live within 5 kilometers of dam reservoirs and are therefore at risk of contracting malaria. And at least 1.1 million malaria cases annually are linked to the presence of the dams.
“Our study showed that the population at risk of malaria around dams is at least 4 times greater than previously estimated,” Kibret said, noting that the authors were conservative in all their analyses.
The risk is particularly high in areas of sub-Saharan Africa with “unstable” malaria transmission, where malaria is seasonal. The study indicated that the impact of dams on malaria in unstable areas could either lead to intensified malaria transmission or change the nature of transmission from seasonal to perennial.
Explaining the risk
Previous research revealed increases in malaria incidence near major sub-Saharan dams such as the Akosombo Dam in Ghana, the Koka Dam in Ethiopia, and the Kamburu Dam in Kenya. But until now, no attempt has been made to assess the cumulative effect of large dam-building on malaria.
Malaria is transmitted by the Anopheles mosquito, which needs slow-moving or stagnant water in which to breed. Dam reservoirs, particularly shallow puddles that often form along shorelines, provide a perfect environment for the insects to multiply. Thus, dam construction can intensify transmission and shift patterns of malaria infection.
Many African countries are planning new dams to help drive economic growth and increase water security. Improved water storage for growing populations, irrigation, and hydropower generation are needed for a fast-developing continent, but the researchers warn that building new dams has potential costs as well as benefits.
“Dams are an important option for governments anxious to develop,” said study author Matthew McCartney, PhD, of the International Water Management Institute in Vientiane, Laos.
“But it is unethical that people living close to them pay the price of that development through increased suffering and, possibly in extreme cases, loss of life due to disease.”
Lowering the risk
The researchers noted that, despite growing evidence of the impact of dams on malaria, there is scant evidence of their negative impacts being fully offset.
The team therefore made recommendations for managing the increased malaria risk. They said dam reservoirs could be more effectively designed and managed to reduce mosquito breeding. For instance, one option is to adopt operating schedules that, at critical times, dry out shoreline areas where mosquitoes tend to breed.
The researchers said dam developers should also consider increasing investment in integrated malaria intervention programs that include measures such as bed net distribution. Other environmental controls, such as introducing fish that eat mosquito larva in dam reservoirs, could also help reduce malaria cases in some instances.
“The bottom line is that adverse malaria impacts of dams routinely receive recognition in Environmental Impact Assessments, and areas around dams are frequently earmarked for intensive control efforts,” said study author Jonathan Lautze, PhD, of the International Water Management Institute in Pretoria, South Africa.
“The findings of our work hammer home the reality that this recognition and effort—well-intentioned though it may be—is simply not sufficient. Given the need for water resources development in Africa, malaria control around dams requires interdisciplinary cooperation, particularly between water and health communities. Malaria must be addressed while planning, designing, and operating African dams.”
Doc stresses importance of vitamin K shots

Photo by Vera Kratochvil
Cases of vitamin K-deficiency bleeding (VKDB) reported in infants have healthcare professionals concerned about parents refusing vitamin K shots for their newborns.
Some parents have been declining the shots in what is believed to be an extension of the anti-vaccination movement.
But avoiding vitamin K shots can result in dire consequences for newborns, said DeeAnne Jackson, MD, of the University of Alabama at Birmingham.
“Newborns have been receiving vitamin K booster injections since 1961 to prevent internal bleeding,” Dr Jackson noted. “These injections are necessary because babies have very low levels of vitamin K at birth, which can lead to serious bleeding problems if not supplemented. It is an essential nutrient babies need to assist the body in blood clot formation.”
In a recent issue of the Journal of Emergency Medicine, doctors in Ohio documented a case where a 10-week-old child had profound anemia and intracranial bleeding after the child’s parents refused both the vitamin K shot and the hepatitis B vaccine.
The parents brought the child to the emergency room when the mother noticed flecks of blood in the baby’s stool. Emergency physicians were able to stop the intracranial bleeding before it became severe with an infusion of vitamin K.
A previous report published in 2013 revealed 4 cases of VKDB at a hospital in Nashville, Tennessee. These incidents were directly related to newborns not receiving their vitamin K shot.
When the US Centers for Disease Control and Prevention investigated this issue, the agency found that 28% of parents with babies born at private birthing centers in Nashville had refused the shot.
An update published in 2014 detailed 5 cases of late VKDB treated at the aforementioned hospital between February and September 2013 and 2 additional infants who had severe vitamin K deficiency but no bleeding.
Dr Jackson believes incidents like these might be avoided by better communication between parents and healthcare professionals.
“I would encourage parents who may be nervous about vitamin K shots or vaccines to start these conversations prior to their baby’s delivery so they can learn more about why these treatments are recommended ahead of time,” she said.
“You really shouldn’t wait to see if your baby needs a vitamin K shot after birth, because delaying medical care can lead to serious and life-threatening consequences.”

Photo by Vera Kratochvil
Cases of vitamin K-deficiency bleeding (VKDB) reported in infants have healthcare professionals concerned about parents refusing vitamin K shots for their newborns.
Some parents have been declining the shots in what is believed to be an extension of the anti-vaccination movement.
But avoiding vitamin K shots can result in dire consequences for newborns, said DeeAnne Jackson, MD, of the University of Alabama at Birmingham.
“Newborns have been receiving vitamin K booster injections since 1961 to prevent internal bleeding,” Dr Jackson noted. “These injections are necessary because babies have very low levels of vitamin K at birth, which can lead to serious bleeding problems if not supplemented. It is an essential nutrient babies need to assist the body in blood clot formation.”
In a recent issue of the Journal of Emergency Medicine, doctors in Ohio documented a case where a 10-week-old child had profound anemia and intracranial bleeding after the child’s parents refused both the vitamin K shot and the hepatitis B vaccine.
The parents brought the child to the emergency room when the mother noticed flecks of blood in the baby’s stool. Emergency physicians were able to stop the intracranial bleeding before it became severe with an infusion of vitamin K.
A previous report published in 2013 revealed 4 cases of VKDB at a hospital in Nashville, Tennessee. These incidents were directly related to newborns not receiving their vitamin K shot.
When the US Centers for Disease Control and Prevention investigated this issue, the agency found that 28% of parents with babies born at private birthing centers in Nashville had refused the shot.
An update published in 2014 detailed 5 cases of late VKDB treated at the aforementioned hospital between February and September 2013 and 2 additional infants who had severe vitamin K deficiency but no bleeding.
Dr Jackson believes incidents like these might be avoided by better communication between parents and healthcare professionals.
“I would encourage parents who may be nervous about vitamin K shots or vaccines to start these conversations prior to their baby’s delivery so they can learn more about why these treatments are recommended ahead of time,” she said.
“You really shouldn’t wait to see if your baby needs a vitamin K shot after birth, because delaying medical care can lead to serious and life-threatening consequences.”

Photo by Vera Kratochvil
Cases of vitamin K-deficiency bleeding (VKDB) reported in infants have healthcare professionals concerned about parents refusing vitamin K shots for their newborns.
Some parents have been declining the shots in what is believed to be an extension of the anti-vaccination movement.
But avoiding vitamin K shots can result in dire consequences for newborns, said DeeAnne Jackson, MD, of the University of Alabama at Birmingham.
“Newborns have been receiving vitamin K booster injections since 1961 to prevent internal bleeding,” Dr Jackson noted. “These injections are necessary because babies have very low levels of vitamin K at birth, which can lead to serious bleeding problems if not supplemented. It is an essential nutrient babies need to assist the body in blood clot formation.”
In a recent issue of the Journal of Emergency Medicine, doctors in Ohio documented a case where a 10-week-old child had profound anemia and intracranial bleeding after the child’s parents refused both the vitamin K shot and the hepatitis B vaccine.
The parents brought the child to the emergency room when the mother noticed flecks of blood in the baby’s stool. Emergency physicians were able to stop the intracranial bleeding before it became severe with an infusion of vitamin K.
A previous report published in 2013 revealed 4 cases of VKDB at a hospital in Nashville, Tennessee. These incidents were directly related to newborns not receiving their vitamin K shot.
When the US Centers for Disease Control and Prevention investigated this issue, the agency found that 28% of parents with babies born at private birthing centers in Nashville had refused the shot.
An update published in 2014 detailed 5 cases of late VKDB treated at the aforementioned hospital between February and September 2013 and 2 additional infants who had severe vitamin K deficiency but no bleeding.
Dr Jackson believes incidents like these might be avoided by better communication between parents and healthcare professionals.
“I would encourage parents who may be nervous about vitamin K shots or vaccines to start these conversations prior to their baby’s delivery so they can learn more about why these treatments are recommended ahead of time,” she said.
“You really shouldn’t wait to see if your baby needs a vitamin K shot after birth, because delaying medical care can lead to serious and life-threatening consequences.”
Group creates guide for PICC use

A group of international experts has created a guide to promote the appropriate use of peripherally inserted central catheters (PICCs) in adults.
The guide, called Michigan Appropriateness Guide for Intravenous Catheters (MAGIC), was published in Annals of Internal Medicine.
MAGIC is based on a review of evidence and was designed to give clinicians an easy-to-use framework to pick the right venous access device for each patient.
“PICCs, or peripherally inserted central catheters, have become especially convenient to place, and their use has gone up dramatically, as have the complications from them,” said guideline author Vineet Chopra, MD, of the University of Michigan in Ann Arbor.
“The easiest way to prevent these complications is not to place a PICC in the first place. So we set out to determine when the use of a PICC is appropriate and when other choices are the best.”
The experts reviewed 665 scenarios in which PICCs were used. Their use was deemed appropriate in 38% (n=253) of cases and inappropriate in 43% (n=288). In 19% (n=124) of cases, the experts could not agree or were unsure about whether PICC use was appropriate.
The experts said that, in patients with cancer, PICCs are appropriate for irritant or vesicant infusion, regardless of the duration of use.
On the other hand, they said PICC use is inappropriate for peripherally compatible infusions when the proposed duration of use is 5 days or fewer. And when the duration is between 6 days and 14 days, midline and ultrasonography-guided peripheral intravenous catheters should be used over PICCs.
The experts also said that nontunneled central venous catheters should be used over PICCs in critically ill patients when the duration of use is likely to be 14 days or fewer.
How MAGIC happened
The panel of 15 experts included doctors and nurses from a range of fields where PICCs and other such devices are commonly used, such as vascular nursing, critical care, infectious disease, and oncology. Also participating was a patient who had suffered complications from various intravenous devices and still lives with the consequences.
The panel evaluated the scenarios and supporting medical literature, and made its recommendations, using the RAND/UCLA Appropriateness Method.
The panel did not consider pediatric use of PICCs and other vascular access devices, but they hope their work could provide a framework for a similar effort in pediatrics.
Putting MAGIC to the test
MAGIC is getting its first test in 47 Michigan hospitals taking part in a patient safety project known as the Michigan Hospital Medicine Safety Consortium.
Researchers also plan to test ways to deploy MAGIC across the Veterans Affairs health system, working with the VA National Center for Patient Safety and the No Preventable Harms Campaign.
Even as they evaluate MAGIC’s ability to improve appropriate use of different devices and reduce complications, the team behind the new guide hopes other clinicians will begin using it.
“IV devices of all kinds are being put into patients without much thought about risks, benefits, or alternatives,” Dr Chopra said. “At the end of the day, we hope MAGIC will give providers the information they need to make a good decision for their patient, one that will render these devices appropriate and safe.”
Dr Chopra and his colleagues have also launched a website, improvepicc.com, that provides links to research on PICCs and other resources for clinicians.

A group of international experts has created a guide to promote the appropriate use of peripherally inserted central catheters (PICCs) in adults.
The guide, called Michigan Appropriateness Guide for Intravenous Catheters (MAGIC), was published in Annals of Internal Medicine.
MAGIC is based on a review of evidence and was designed to give clinicians an easy-to-use framework to pick the right venous access device for each patient.
“PICCs, or peripherally inserted central catheters, have become especially convenient to place, and their use has gone up dramatically, as have the complications from them,” said guideline author Vineet Chopra, MD, of the University of Michigan in Ann Arbor.
“The easiest way to prevent these complications is not to place a PICC in the first place. So we set out to determine when the use of a PICC is appropriate and when other choices are the best.”
The experts reviewed 665 scenarios in which PICCs were used. Their use was deemed appropriate in 38% (n=253) of cases and inappropriate in 43% (n=288). In 19% (n=124) of cases, the experts could not agree or were unsure about whether PICC use was appropriate.
The experts said that, in patients with cancer, PICCs are appropriate for irritant or vesicant infusion, regardless of the duration of use.
On the other hand, they said PICC use is inappropriate for peripherally compatible infusions when the proposed duration of use is 5 days or fewer. And when the duration is between 6 days and 14 days, midline and ultrasonography-guided peripheral intravenous catheters should be used over PICCs.
The experts also said that nontunneled central venous catheters should be used over PICCs in critically ill patients when the duration of use is likely to be 14 days or fewer.
How MAGIC happened
The panel of 15 experts included doctors and nurses from a range of fields where PICCs and other such devices are commonly used, such as vascular nursing, critical care, infectious disease, and oncology. Also participating was a patient who had suffered complications from various intravenous devices and still lives with the consequences.
The panel evaluated the scenarios and supporting medical literature, and made its recommendations, using the RAND/UCLA Appropriateness Method.
The panel did not consider pediatric use of PICCs and other vascular access devices, but they hope their work could provide a framework for a similar effort in pediatrics.
Putting MAGIC to the test
MAGIC is getting its first test in 47 Michigan hospitals taking part in a patient safety project known as the Michigan Hospital Medicine Safety Consortium.
Researchers also plan to test ways to deploy MAGIC across the Veterans Affairs health system, working with the VA National Center for Patient Safety and the No Preventable Harms Campaign.
Even as they evaluate MAGIC’s ability to improve appropriate use of different devices and reduce complications, the team behind the new guide hopes other clinicians will begin using it.
“IV devices of all kinds are being put into patients without much thought about risks, benefits, or alternatives,” Dr Chopra said. “At the end of the day, we hope MAGIC will give providers the information they need to make a good decision for their patient, one that will render these devices appropriate and safe.”
Dr Chopra and his colleagues have also launched a website, improvepicc.com, that provides links to research on PICCs and other resources for clinicians.

A group of international experts has created a guide to promote the appropriate use of peripherally inserted central catheters (PICCs) in adults.
The guide, called Michigan Appropriateness Guide for Intravenous Catheters (MAGIC), was published in Annals of Internal Medicine.
MAGIC is based on a review of evidence and was designed to give clinicians an easy-to-use framework to pick the right venous access device for each patient.
“PICCs, or peripherally inserted central catheters, have become especially convenient to place, and their use has gone up dramatically, as have the complications from them,” said guideline author Vineet Chopra, MD, of the University of Michigan in Ann Arbor.
“The easiest way to prevent these complications is not to place a PICC in the first place. So we set out to determine when the use of a PICC is appropriate and when other choices are the best.”
The experts reviewed 665 scenarios in which PICCs were used. Their use was deemed appropriate in 38% (n=253) of cases and inappropriate in 43% (n=288). In 19% (n=124) of cases, the experts could not agree or were unsure about whether PICC use was appropriate.
The experts said that, in patients with cancer, PICCs are appropriate for irritant or vesicant infusion, regardless of the duration of use.
On the other hand, they said PICC use is inappropriate for peripherally compatible infusions when the proposed duration of use is 5 days or fewer. And when the duration is between 6 days and 14 days, midline and ultrasonography-guided peripheral intravenous catheters should be used over PICCs.
The experts also said that nontunneled central venous catheters should be used over PICCs in critically ill patients when the duration of use is likely to be 14 days or fewer.
How MAGIC happened
The panel of 15 experts included doctors and nurses from a range of fields where PICCs and other such devices are commonly used, such as vascular nursing, critical care, infectious disease, and oncology. Also participating was a patient who had suffered complications from various intravenous devices and still lives with the consequences.
The panel evaluated the scenarios and supporting medical literature, and made its recommendations, using the RAND/UCLA Appropriateness Method.
The panel did not consider pediatric use of PICCs and other vascular access devices, but they hope their work could provide a framework for a similar effort in pediatrics.
Putting MAGIC to the test
MAGIC is getting its first test in 47 Michigan hospitals taking part in a patient safety project known as the Michigan Hospital Medicine Safety Consortium.
Researchers also plan to test ways to deploy MAGIC across the Veterans Affairs health system, working with the VA National Center for Patient Safety and the No Preventable Harms Campaign.
Even as they evaluate MAGIC’s ability to improve appropriate use of different devices and reduce complications, the team behind the new guide hopes other clinicians will begin using it.
“IV devices of all kinds are being put into patients without much thought about risks, benefits, or alternatives,” Dr Chopra said. “At the end of the day, we hope MAGIC will give providers the information they need to make a good decision for their patient, one that will render these devices appropriate and safe.”
Dr Chopra and his colleagues have also launched a website, improvepicc.com, that provides links to research on PICCs and other resources for clinicians.