User login
DLBCL tied to metabolic disruption

Researchers say they have found evidence linking disrupted metabolism and diffuse large B-cell lymphoma (DLBCL).
“The link between metabolism and cancer has been proposed or inferred to exist for a long time, but what is more scarce is evidence for a direct connection—genetic mutations in metabolic enzymes,” said Ricardo C.T. Aguiar, MD, PhD, of the University of Texas Health Science Center at San Antonio.
“We have discovered a metabolic imbalance that is oncogenic or pro-cancer.”
Dr Aguiar and his colleagues described this discovery in Nature Communications.
The team found that the gene encoding the enzyme D2-hydroxyglutarate dehydrogenase (D2HGDH) is mutated in DLBCL.
The mutated lymphoma cell displays a deficiency of a metabolite called alpha-ketoglutarate (α-KG), which is needed in steady levels for cells to be healthy.
“When the levels of α-KG are abnormally low, another class of enzymes called dioxygenases don‘t function properly, resulting in a host of additional disturbances,” Dr Aguiar said.
He added that α-KG has been identified as a critical regulator of aging and stem cell maintenance. So the implications of his group’s findings are not limited to cancer biology. ![]()

Researchers say they have found evidence linking disrupted metabolism and diffuse large B-cell lymphoma (DLBCL).
“The link between metabolism and cancer has been proposed or inferred to exist for a long time, but what is more scarce is evidence for a direct connection—genetic mutations in metabolic enzymes,” said Ricardo C.T. Aguiar, MD, PhD, of the University of Texas Health Science Center at San Antonio.
“We have discovered a metabolic imbalance that is oncogenic or pro-cancer.”
Dr Aguiar and his colleagues described this discovery in Nature Communications.
The team found that the gene encoding the enzyme D2-hydroxyglutarate dehydrogenase (D2HGDH) is mutated in DLBCL.
The mutated lymphoma cell displays a deficiency of a metabolite called alpha-ketoglutarate (α-KG), which is needed in steady levels for cells to be healthy.
“When the levels of α-KG are abnormally low, another class of enzymes called dioxygenases don‘t function properly, resulting in a host of additional disturbances,” Dr Aguiar said.
He added that α-KG has been identified as a critical regulator of aging and stem cell maintenance. So the implications of his group’s findings are not limited to cancer biology. ![]()

Researchers say they have found evidence linking disrupted metabolism and diffuse large B-cell lymphoma (DLBCL).
“The link between metabolism and cancer has been proposed or inferred to exist for a long time, but what is more scarce is evidence for a direct connection—genetic mutations in metabolic enzymes,” said Ricardo C.T. Aguiar, MD, PhD, of the University of Texas Health Science Center at San Antonio.
“We have discovered a metabolic imbalance that is oncogenic or pro-cancer.”
Dr Aguiar and his colleagues described this discovery in Nature Communications.
The team found that the gene encoding the enzyme D2-hydroxyglutarate dehydrogenase (D2HGDH) is mutated in DLBCL.
The mutated lymphoma cell displays a deficiency of a metabolite called alpha-ketoglutarate (α-KG), which is needed in steady levels for cells to be healthy.
“When the levels of α-KG are abnormally low, another class of enzymes called dioxygenases don‘t function properly, resulting in a host of additional disturbances,” Dr Aguiar said.
He added that α-KG has been identified as a critical regulator of aging and stem cell maintenance. So the implications of his group’s findings are not limited to cancer biology. ![]()
Modified T cells may improve auto-SCT outcomes in MM

Photo from Penn Medicine
Infusions of modified autologous T cells may improve responses in multiple myeloma (MM) patients undergoing autologous stem cell transplant (auto-SCT), according to research published in Nature Medicine.
Researchers said patients who received the T cells—which were engineered to express an affinity-enhanced T-cell receptor (TCR)—after auto-SCT had a better response rate than is expected for MM patients undergoing auto-SCT. At day 100, the overall response rate was 90%.
The researchers also said the T cells were safe. There were no treatment-related deaths, and all 7 serious adverse events were resolved.
“This study shows us that these TCR-specific T cells are safe and feasible . . . , but it also revealed encouraging antitumor activity and showed impressive, durable T-cell persistence,” said study author Carl June, MD, of the Perelman School of Medicine at the University of Pennsylvania in Philadelphia.
The research was a collaboration between the University of Maryland School of Medicine, the Perelman School of Medicine, and Adaptimmune, a clinical stage biopharmaceutical company that owns the core TCR technology and funded the study.
The study included 20 evaluable patients with advanced MM. They received an average of 2.4 billion autologous T cells 2 days after undergoing auto-SCT.
The T cells were engineered to express an affinity-enhanced TCR recognizing a naturally processed peptide shared by the cancer-testis antigens NY-ESO-1 and LAGE-1. Up to 60% of advanced myelomas have been reported to express NY-ESO-1 and/or LAGE-1, which is correlated with tumor proliferation and poorer outcomes.
Response and survival
“The majority of patients who participated in this trial had a meaningful degree of clinical benefit,” said study author Aaron P. Rapoport, MD, of the University of Maryland School of Medicine in Baltimore.
“Even patients who later relapsed after achieving a complete response to treatment or didn’t have a complete response had periods of disease control that I believe they would not have otherwise experienced. Some patients are still in remission after nearly 3 years.”
Treatment responses were as follows:
| Outcome | Prior
to infusion |
Day
42 |
Day
100 |
Day
180 |
|---|---|---|---|---|
| Complete
response (CR) |
1 | 2 | ||
| Stringent
CR |
1 | 2 | 2 | |
| Near
CR |
1 | 6 | 11 | 8 |
| Very
good partial response |
2 | 7 | 2 | 2 |
| Partial
response |
6 | 4 | 2 | 1 |
| Stable
disease |
6 | 2 | 1 | 1 |
| Progressive
disease |
5 | 1 | 3 |
A subset of patients received lenalidomide maintenance after day 100, and 1 patient had died by the 180-day mark, as a result of disease progression.
The researchers noted that relapse was associated with a loss of the engineered T cells, which suggests methods for sustaining long-term persistence of the cells could improve outcomes.
At a median follow up of 21.1 months, 75% of patients were still alive, 50% were progression-free, and 25% had died after disease progression.
At a median follow up of 30.1 months, the median progression-free survival was 19.1 months, and the median overall survival was 32.1 months.
Adverse events
There were no treatment-related deaths, and all 7 serious adverse events were resolved. The serious events included grade 3 gastrointestinal graft-vs-host disease (GVHD), grade 3 hypoxia, grade 3 dehydration, grade 4 neutropenia, grade 4 hyponatremia, grade 4 hypotension, and grade 4 pancytopenia.
There were 17 adverse events that were considered probably related to treatment. These were gastrointestinal GVHD (3 grade 3), skin GVHD (2 grade 2), fatigue (1 grade 1), fever (2 grade 1-2), rash (3 grade 1-3), diarrhea (2 grade 1-2), sinus tachycardia (1 grade 1), injection site reaction/extravasation changes (1 grade 1), weakness (1 grade 1), and hypotension (1 grade 3).
“This study suggests that treatment with engineered T cells is not only safe but of potential clinical benefit to patients with certain types of aggressive multiple myeloma,” Dr Rapoport said. “Our findings provide a strong foundation for further research in the field of cellular immunotherapy for myeloma to help achieve even better results for our patients.” ![]()

Photo from Penn Medicine
Infusions of modified autologous T cells may improve responses in multiple myeloma (MM) patients undergoing autologous stem cell transplant (auto-SCT), according to research published in Nature Medicine.
Researchers said patients who received the T cells—which were engineered to express an affinity-enhanced T-cell receptor (TCR)—after auto-SCT had a better response rate than is expected for MM patients undergoing auto-SCT. At day 100, the overall response rate was 90%.
The researchers also said the T cells were safe. There were no treatment-related deaths, and all 7 serious adverse events were resolved.
“This study shows us that these TCR-specific T cells are safe and feasible . . . , but it also revealed encouraging antitumor activity and showed impressive, durable T-cell persistence,” said study author Carl June, MD, of the Perelman School of Medicine at the University of Pennsylvania in Philadelphia.
The research was a collaboration between the University of Maryland School of Medicine, the Perelman School of Medicine, and Adaptimmune, a clinical stage biopharmaceutical company that owns the core TCR technology and funded the study.
The study included 20 evaluable patients with advanced MM. They received an average of 2.4 billion autologous T cells 2 days after undergoing auto-SCT.
The T cells were engineered to express an affinity-enhanced TCR recognizing a naturally processed peptide shared by the cancer-testis antigens NY-ESO-1 and LAGE-1. Up to 60% of advanced myelomas have been reported to express NY-ESO-1 and/or LAGE-1, which is correlated with tumor proliferation and poorer outcomes.
Response and survival
“The majority of patients who participated in this trial had a meaningful degree of clinical benefit,” said study author Aaron P. Rapoport, MD, of the University of Maryland School of Medicine in Baltimore.
“Even patients who later relapsed after achieving a complete response to treatment or didn’t have a complete response had periods of disease control that I believe they would not have otherwise experienced. Some patients are still in remission after nearly 3 years.”
Treatment responses were as follows:
| Outcome | Prior
to infusion |
Day
42 |
Day
100 |
Day
180 |
|---|---|---|---|---|
| Complete
response (CR) |
1 | 2 | ||
| Stringent
CR |
1 | 2 | 2 | |
| Near
CR |
1 | 6 | 11 | 8 |
| Very
good partial response |
2 | 7 | 2 | 2 |
| Partial
response |
6 | 4 | 2 | 1 |
| Stable
disease |
6 | 2 | 1 | 1 |
| Progressive
disease |
5 | 1 | 3 |
A subset of patients received lenalidomide maintenance after day 100, and 1 patient had died by the 180-day mark, as a result of disease progression.
The researchers noted that relapse was associated with a loss of the engineered T cells, which suggests methods for sustaining long-term persistence of the cells could improve outcomes.
At a median follow up of 21.1 months, 75% of patients were still alive, 50% were progression-free, and 25% had died after disease progression.
At a median follow up of 30.1 months, the median progression-free survival was 19.1 months, and the median overall survival was 32.1 months.
Adverse events
There were no treatment-related deaths, and all 7 serious adverse events were resolved. The serious events included grade 3 gastrointestinal graft-vs-host disease (GVHD), grade 3 hypoxia, grade 3 dehydration, grade 4 neutropenia, grade 4 hyponatremia, grade 4 hypotension, and grade 4 pancytopenia.
There were 17 adverse events that were considered probably related to treatment. These were gastrointestinal GVHD (3 grade 3), skin GVHD (2 grade 2), fatigue (1 grade 1), fever (2 grade 1-2), rash (3 grade 1-3), diarrhea (2 grade 1-2), sinus tachycardia (1 grade 1), injection site reaction/extravasation changes (1 grade 1), weakness (1 grade 1), and hypotension (1 grade 3).
“This study suggests that treatment with engineered T cells is not only safe but of potential clinical benefit to patients with certain types of aggressive multiple myeloma,” Dr Rapoport said. “Our findings provide a strong foundation for further research in the field of cellular immunotherapy for myeloma to help achieve even better results for our patients.” ![]()

Photo from Penn Medicine
Infusions of modified autologous T cells may improve responses in multiple myeloma (MM) patients undergoing autologous stem cell transplant (auto-SCT), according to research published in Nature Medicine.
Researchers said patients who received the T cells—which were engineered to express an affinity-enhanced T-cell receptor (TCR)—after auto-SCT had a better response rate than is expected for MM patients undergoing auto-SCT. At day 100, the overall response rate was 90%.
The researchers also said the T cells were safe. There were no treatment-related deaths, and all 7 serious adverse events were resolved.
“This study shows us that these TCR-specific T cells are safe and feasible . . . , but it also revealed encouraging antitumor activity and showed impressive, durable T-cell persistence,” said study author Carl June, MD, of the Perelman School of Medicine at the University of Pennsylvania in Philadelphia.
The research was a collaboration between the University of Maryland School of Medicine, the Perelman School of Medicine, and Adaptimmune, a clinical stage biopharmaceutical company that owns the core TCR technology and funded the study.
The study included 20 evaluable patients with advanced MM. They received an average of 2.4 billion autologous T cells 2 days after undergoing auto-SCT.
The T cells were engineered to express an affinity-enhanced TCR recognizing a naturally processed peptide shared by the cancer-testis antigens NY-ESO-1 and LAGE-1. Up to 60% of advanced myelomas have been reported to express NY-ESO-1 and/or LAGE-1, which is correlated with tumor proliferation and poorer outcomes.
Response and survival
“The majority of patients who participated in this trial had a meaningful degree of clinical benefit,” said study author Aaron P. Rapoport, MD, of the University of Maryland School of Medicine in Baltimore.
“Even patients who later relapsed after achieving a complete response to treatment or didn’t have a complete response had periods of disease control that I believe they would not have otherwise experienced. Some patients are still in remission after nearly 3 years.”
Treatment responses were as follows:
| Outcome | Prior
to infusion |
Day
42 |
Day
100 |
Day
180 |
|---|---|---|---|---|
| Complete
response (CR) |
1 | 2 | ||
| Stringent
CR |
1 | 2 | 2 | |
| Near
CR |
1 | 6 | 11 | 8 |
| Very
good partial response |
2 | 7 | 2 | 2 |
| Partial
response |
6 | 4 | 2 | 1 |
| Stable
disease |
6 | 2 | 1 | 1 |
| Progressive
disease |
5 | 1 | 3 |
A subset of patients received lenalidomide maintenance after day 100, and 1 patient had died by the 180-day mark, as a result of disease progression.
The researchers noted that relapse was associated with a loss of the engineered T cells, which suggests methods for sustaining long-term persistence of the cells could improve outcomes.
At a median follow up of 21.1 months, 75% of patients were still alive, 50% were progression-free, and 25% had died after disease progression.
At a median follow up of 30.1 months, the median progression-free survival was 19.1 months, and the median overall survival was 32.1 months.
Adverse events
There were no treatment-related deaths, and all 7 serious adverse events were resolved. The serious events included grade 3 gastrointestinal graft-vs-host disease (GVHD), grade 3 hypoxia, grade 3 dehydration, grade 4 neutropenia, grade 4 hyponatremia, grade 4 hypotension, and grade 4 pancytopenia.
There were 17 adverse events that were considered probably related to treatment. These were gastrointestinal GVHD (3 grade 3), skin GVHD (2 grade 2), fatigue (1 grade 1), fever (2 grade 1-2), rash (3 grade 1-3), diarrhea (2 grade 1-2), sinus tachycardia (1 grade 1), injection site reaction/extravasation changes (1 grade 1), weakness (1 grade 1), and hypotension (1 grade 3).
“This study suggests that treatment with engineered T cells is not only safe but of potential clinical benefit to patients with certain types of aggressive multiple myeloma,” Dr Rapoport said. “Our findings provide a strong foundation for further research in the field of cellular immunotherapy for myeloma to help achieve even better results for our patients.” ![]()
Response to ibrutinib varies by DLBCL subtype

Photo by Larry Young
Responses to the BTK inhibitor ibrutinib differ according to a patient’s subtype of diffuse large B-cell lymphoma (DLBCL), results of a phase 1/2 trial suggest.
The study showed that patients with activated B-cell-like (ABC) DLBCL were more likely to respond to ibrutinib than patients with germinal center B-cell-like (GCB) DLBCL.
“This is the first clinical study to demonstrate the importance of precision medicine in lymphomas,” said Wyndham Wilson, MD, PhD, of the National Cancer Institute in Bethesda, Maryland.
Dr Wilson and his colleagues described the trial in Nature Medicine. The research, which was sponsored by Pharmacyclics, Inc. (the company developing ibrutinib), was previously presented at EHA 2013.
The trial enrolled 80 patients with relapsed or refractory DLBCL. All patients received ibrutinib. Tumor responses occurred in 25% of patients. There were 8 complete responses and 12 partial responses.
After a median follow-up of 11.5 months, the median progression-free survival was 1.6 months, and the median overall survival was 6.4 months.
An analysis of outcomes by disease subtype showed that ibrutinib produced complete or partial responses in 37% (14/38) of patients with ABC DLBCL but only 5% (1/20) of patients with GCB DLBCL.
The researchers speculated that ABC tumors may produce abnormal B-cell receptor signals that promote the survival of cancer cells by activating BTK, which would account for the sensitivity of ABC tumors to ibrutinib.
Based on this study’s results, researchers are conducting an international phase 3 trial of standard chemotherapy with or without ibrutinib in patients with DLBCL, excluding the GCB subtype (NCT01855750).
This is the first time a phase 3 trial has been designed to selectively enroll patients with a particular molecular subtype of DLBCL. The study’s objective is to determine if the addition of ibrutinib to standard chemotherapy can increase the cure rate of patients with ABC DLBCL. ![]()

Photo by Larry Young
Responses to the BTK inhibitor ibrutinib differ according to a patient’s subtype of diffuse large B-cell lymphoma (DLBCL), results of a phase 1/2 trial suggest.
The study showed that patients with activated B-cell-like (ABC) DLBCL were more likely to respond to ibrutinib than patients with germinal center B-cell-like (GCB) DLBCL.
“This is the first clinical study to demonstrate the importance of precision medicine in lymphomas,” said Wyndham Wilson, MD, PhD, of the National Cancer Institute in Bethesda, Maryland.
Dr Wilson and his colleagues described the trial in Nature Medicine. The research, which was sponsored by Pharmacyclics, Inc. (the company developing ibrutinib), was previously presented at EHA 2013.
The trial enrolled 80 patients with relapsed or refractory DLBCL. All patients received ibrutinib. Tumor responses occurred in 25% of patients. There were 8 complete responses and 12 partial responses.
After a median follow-up of 11.5 months, the median progression-free survival was 1.6 months, and the median overall survival was 6.4 months.
An analysis of outcomes by disease subtype showed that ibrutinib produced complete or partial responses in 37% (14/38) of patients with ABC DLBCL but only 5% (1/20) of patients with GCB DLBCL.
The researchers speculated that ABC tumors may produce abnormal B-cell receptor signals that promote the survival of cancer cells by activating BTK, which would account for the sensitivity of ABC tumors to ibrutinib.
Based on this study’s results, researchers are conducting an international phase 3 trial of standard chemotherapy with or without ibrutinib in patients with DLBCL, excluding the GCB subtype (NCT01855750).
This is the first time a phase 3 trial has been designed to selectively enroll patients with a particular molecular subtype of DLBCL. The study’s objective is to determine if the addition of ibrutinib to standard chemotherapy can increase the cure rate of patients with ABC DLBCL. ![]()

Photo by Larry Young
Responses to the BTK inhibitor ibrutinib differ according to a patient’s subtype of diffuse large B-cell lymphoma (DLBCL), results of a phase 1/2 trial suggest.
The study showed that patients with activated B-cell-like (ABC) DLBCL were more likely to respond to ibrutinib than patients with germinal center B-cell-like (GCB) DLBCL.
“This is the first clinical study to demonstrate the importance of precision medicine in lymphomas,” said Wyndham Wilson, MD, PhD, of the National Cancer Institute in Bethesda, Maryland.
Dr Wilson and his colleagues described the trial in Nature Medicine. The research, which was sponsored by Pharmacyclics, Inc. (the company developing ibrutinib), was previously presented at EHA 2013.
The trial enrolled 80 patients with relapsed or refractory DLBCL. All patients received ibrutinib. Tumor responses occurred in 25% of patients. There were 8 complete responses and 12 partial responses.
After a median follow-up of 11.5 months, the median progression-free survival was 1.6 months, and the median overall survival was 6.4 months.
An analysis of outcomes by disease subtype showed that ibrutinib produced complete or partial responses in 37% (14/38) of patients with ABC DLBCL but only 5% (1/20) of patients with GCB DLBCL.
The researchers speculated that ABC tumors may produce abnormal B-cell receptor signals that promote the survival of cancer cells by activating BTK, which would account for the sensitivity of ABC tumors to ibrutinib.
Based on this study’s results, researchers are conducting an international phase 3 trial of standard chemotherapy with or without ibrutinib in patients with DLBCL, excluding the GCB subtype (NCT01855750).
This is the first time a phase 3 trial has been designed to selectively enroll patients with a particular molecular subtype of DLBCL. The study’s objective is to determine if the addition of ibrutinib to standard chemotherapy can increase the cure rate of patients with ABC DLBCL. ![]()
Testosterone therapy doesn’t increase VTE risk
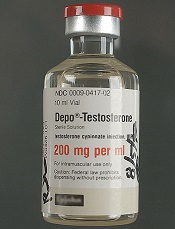
for intramuscular injection
Contrary to previous findings, a new study suggests there is no link between testosterone therapy and venous thromboembolism (VTE).
Investigators analyzed more than 30,000 commercially insured men who were age 40 and older, comparing men with VTE to those without the
condition.
Results indicated that exposure to testosterone therapy did not confer an increased risk of VTE.
The investigators reported these results in Mayo Clinic Proceedings.
“In 2014, the [US Food and Drug Administration] required manufacturers to add a warning about potential risks of VTE to the label of all approved testosterone products,” said Jacques Baillargeon, PhD, of the University of Texas Medical Branch at Galveston.
“The warning, however, is based primarily on post-marketing drug surveillance and case reports. To date, there have been no published, comparative, large-scale studies examining the association of testosterone therapy and the risk of VTE.”
With that in mind, Dr Baillargeon and his colleagues conducted a case-control study of 30,572 men age 40 and older. The men were enrolled in one of the nation’s largest commercial insurance programs between January 1, 2007 and December 31, 2012.
Cases were defined as men who had a primary diagnosis of VTE and received an anticoagulant or an intravascular vena cava filter in the 60 days following their diagnoses.
Each case was matched with 3 control subjects by age, geographic region, diagnosis of low testosterone, and diagnosis of any underlying coagulopathy.
The investigators found that being exposed to testosterone therapy in the previous 15 days was not associated with an increased risk of VTE. The adjusted odds ratio was 0.90 for 15 days, and findings were similar for exposure within 30 days and 60 days.
Dr Baillargeon and his colleagues also looked at specific routes of administration for testosterone therapy—topical creams, transdermal patches, and intramuscular injections.
The team found no increased risk of VTE with any of these methods. The adjusted odds ratios were 0.80 for topical, 0.91 for transdermal, and 1.15 for intramuscular administration.
“It is important to acknowledge, for a man who has medically diagnosed low testosterone, that there are clear risks to not receiving testosterone therapy, including osteoporosis, sexual dysfunction, increased amounts of fat tissue, decreased lean muscle mass, possible metabolic syndrome, and cardiovascular disease,” Dr Baillargeon said.
“It’s also important to note that further research needs to be conducted to rigorously assess the long-term risks of testosterone therapy. These findings may help to inform the benefit-risk assessment for men with testosterone deficiency considering treatment.” ![]()

for intramuscular injection
Contrary to previous findings, a new study suggests there is no link between testosterone therapy and venous thromboembolism (VTE).
Investigators analyzed more than 30,000 commercially insured men who were age 40 and older, comparing men with VTE to those without the
condition.
Results indicated that exposure to testosterone therapy did not confer an increased risk of VTE.
The investigators reported these results in Mayo Clinic Proceedings.
“In 2014, the [US Food and Drug Administration] required manufacturers to add a warning about potential risks of VTE to the label of all approved testosterone products,” said Jacques Baillargeon, PhD, of the University of Texas Medical Branch at Galveston.
“The warning, however, is based primarily on post-marketing drug surveillance and case reports. To date, there have been no published, comparative, large-scale studies examining the association of testosterone therapy and the risk of VTE.”
With that in mind, Dr Baillargeon and his colleagues conducted a case-control study of 30,572 men age 40 and older. The men were enrolled in one of the nation’s largest commercial insurance programs between January 1, 2007 and December 31, 2012.
Cases were defined as men who had a primary diagnosis of VTE and received an anticoagulant or an intravascular vena cava filter in the 60 days following their diagnoses.
Each case was matched with 3 control subjects by age, geographic region, diagnosis of low testosterone, and diagnosis of any underlying coagulopathy.
The investigators found that being exposed to testosterone therapy in the previous 15 days was not associated with an increased risk of VTE. The adjusted odds ratio was 0.90 for 15 days, and findings were similar for exposure within 30 days and 60 days.
Dr Baillargeon and his colleagues also looked at specific routes of administration for testosterone therapy—topical creams, transdermal patches, and intramuscular injections.
The team found no increased risk of VTE with any of these methods. The adjusted odds ratios were 0.80 for topical, 0.91 for transdermal, and 1.15 for intramuscular administration.
“It is important to acknowledge, for a man who has medically diagnosed low testosterone, that there are clear risks to not receiving testosterone therapy, including osteoporosis, sexual dysfunction, increased amounts of fat tissue, decreased lean muscle mass, possible metabolic syndrome, and cardiovascular disease,” Dr Baillargeon said.
“It’s also important to note that further research needs to be conducted to rigorously assess the long-term risks of testosterone therapy. These findings may help to inform the benefit-risk assessment for men with testosterone deficiency considering treatment.” ![]()

for intramuscular injection
Contrary to previous findings, a new study suggests there is no link between testosterone therapy and venous thromboembolism (VTE).
Investigators analyzed more than 30,000 commercially insured men who were age 40 and older, comparing men with VTE to those without the
condition.
Results indicated that exposure to testosterone therapy did not confer an increased risk of VTE.
The investigators reported these results in Mayo Clinic Proceedings.
“In 2014, the [US Food and Drug Administration] required manufacturers to add a warning about potential risks of VTE to the label of all approved testosterone products,” said Jacques Baillargeon, PhD, of the University of Texas Medical Branch at Galveston.
“The warning, however, is based primarily on post-marketing drug surveillance and case reports. To date, there have been no published, comparative, large-scale studies examining the association of testosterone therapy and the risk of VTE.”
With that in mind, Dr Baillargeon and his colleagues conducted a case-control study of 30,572 men age 40 and older. The men were enrolled in one of the nation’s largest commercial insurance programs between January 1, 2007 and December 31, 2012.
Cases were defined as men who had a primary diagnosis of VTE and received an anticoagulant or an intravascular vena cava filter in the 60 days following their diagnoses.
Each case was matched with 3 control subjects by age, geographic region, diagnosis of low testosterone, and diagnosis of any underlying coagulopathy.
The investigators found that being exposed to testosterone therapy in the previous 15 days was not associated with an increased risk of VTE. The adjusted odds ratio was 0.90 for 15 days, and findings were similar for exposure within 30 days and 60 days.
Dr Baillargeon and his colleagues also looked at specific routes of administration for testosterone therapy—topical creams, transdermal patches, and intramuscular injections.
The team found no increased risk of VTE with any of these methods. The adjusted odds ratios were 0.80 for topical, 0.91 for transdermal, and 1.15 for intramuscular administration.
“It is important to acknowledge, for a man who has medically diagnosed low testosterone, that there are clear risks to not receiving testosterone therapy, including osteoporosis, sexual dysfunction, increased amounts of fat tissue, decreased lean muscle mass, possible metabolic syndrome, and cardiovascular disease,” Dr Baillargeon said.
“It’s also important to note that further research needs to be conducted to rigorously assess the long-term risks of testosterone therapy. These findings may help to inform the benefit-risk assessment for men with testosterone deficiency considering treatment.” ![]()
A new way to treat ITP?

Photo courtesy of
St. Michael’s Hospital
New research appears to explain why symptoms and treatment responses vary in patients with immune thrombocytopenia (ITP). The work has also revealed a new potential treatment option.
Researchers previously thought that all ITP antibodies lead platelets to the spleen for destruction.
But the new study, published in Nature Communications, has shown that some ITP antibodies destroy platelets in the liver.
“Every existing treatment for ITP has been dedicated to stopping antibodies from destroying platelets in the spleen, but we’ve discovered that some antibodies actually destroy platelets in the liver,” said study author Heyu Ni, MD, of St. Michael’s Hospital in Toronto, Ontario, Canada.
The discovery was made by analyzing mice treated with two monoclonal antibodies, each targeting a different protein on the surface of platelets—GPIb or GPIIbIIIa.
The researchers found that antibodies targeting GPIb lead to platelet destruction in the liver, and those targeting GPIIbIIIa cause platelet destruction in the spleen.
“By detecting the specific antibodies present in someone with ITP, we may be able to detect where and how the immune system will attack,” Dr Ni said. “And because we now know the liver’s immune response destroys platelets covered with GPIb, we may be able to design new therapies to stop this type of platelet destruction.”
Dr Ni noted that sialidase inhibitors such as oseltamivir phosphate (Tamiflu) may be able to inhibit the liver’s immune response to the platelets. In fact, he and his colleagues used human blood samples to test whether Tamiflu might inhibit antibodies targeting GPIb.
“Using healthy blood samples and ITP antibodies in a test tube, we showed that Tamiflu may impede platelet destruction for those with antibodies that target GPIb,” Dr Ni said.
Based on an early abstract of this research, some ITP patients around the world have been treated with oseltamivir phosphate. These patients were extremely resistant to existing treatments targeting the spleen, and their ITP was considered life-threatening.
Although these instances of experimental treatment have been successful, Dr Ni said more research is needed to verify the safety and efficacy of this approach. ![]()

Photo courtesy of
St. Michael’s Hospital
New research appears to explain why symptoms and treatment responses vary in patients with immune thrombocytopenia (ITP). The work has also revealed a new potential treatment option.
Researchers previously thought that all ITP antibodies lead platelets to the spleen for destruction.
But the new study, published in Nature Communications, has shown that some ITP antibodies destroy platelets in the liver.
“Every existing treatment for ITP has been dedicated to stopping antibodies from destroying platelets in the spleen, but we’ve discovered that some antibodies actually destroy platelets in the liver,” said study author Heyu Ni, MD, of St. Michael’s Hospital in Toronto, Ontario, Canada.
The discovery was made by analyzing mice treated with two monoclonal antibodies, each targeting a different protein on the surface of platelets—GPIb or GPIIbIIIa.
The researchers found that antibodies targeting GPIb lead to platelet destruction in the liver, and those targeting GPIIbIIIa cause platelet destruction in the spleen.
“By detecting the specific antibodies present in someone with ITP, we may be able to detect where and how the immune system will attack,” Dr Ni said. “And because we now know the liver’s immune response destroys platelets covered with GPIb, we may be able to design new therapies to stop this type of platelet destruction.”
Dr Ni noted that sialidase inhibitors such as oseltamivir phosphate (Tamiflu) may be able to inhibit the liver’s immune response to the platelets. In fact, he and his colleagues used human blood samples to test whether Tamiflu might inhibit antibodies targeting GPIb.
“Using healthy blood samples and ITP antibodies in a test tube, we showed that Tamiflu may impede platelet destruction for those with antibodies that target GPIb,” Dr Ni said.
Based on an early abstract of this research, some ITP patients around the world have been treated with oseltamivir phosphate. These patients were extremely resistant to existing treatments targeting the spleen, and their ITP was considered life-threatening.
Although these instances of experimental treatment have been successful, Dr Ni said more research is needed to verify the safety and efficacy of this approach. ![]()

Photo courtesy of
St. Michael’s Hospital
New research appears to explain why symptoms and treatment responses vary in patients with immune thrombocytopenia (ITP). The work has also revealed a new potential treatment option.
Researchers previously thought that all ITP antibodies lead platelets to the spleen for destruction.
But the new study, published in Nature Communications, has shown that some ITP antibodies destroy platelets in the liver.
“Every existing treatment for ITP has been dedicated to stopping antibodies from destroying platelets in the spleen, but we’ve discovered that some antibodies actually destroy platelets in the liver,” said study author Heyu Ni, MD, of St. Michael’s Hospital in Toronto, Ontario, Canada.
The discovery was made by analyzing mice treated with two monoclonal antibodies, each targeting a different protein on the surface of platelets—GPIb or GPIIbIIIa.
The researchers found that antibodies targeting GPIb lead to platelet destruction in the liver, and those targeting GPIIbIIIa cause platelet destruction in the spleen.
“By detecting the specific antibodies present in someone with ITP, we may be able to detect where and how the immune system will attack,” Dr Ni said. “And because we now know the liver’s immune response destroys platelets covered with GPIb, we may be able to design new therapies to stop this type of platelet destruction.”
Dr Ni noted that sialidase inhibitors such as oseltamivir phosphate (Tamiflu) may be able to inhibit the liver’s immune response to the platelets. In fact, he and his colleagues used human blood samples to test whether Tamiflu might inhibit antibodies targeting GPIb.
“Using healthy blood samples and ITP antibodies in a test tube, we showed that Tamiflu may impede platelet destruction for those with antibodies that target GPIb,” Dr Ni said.
Based on an early abstract of this research, some ITP patients around the world have been treated with oseltamivir phosphate. These patients were extremely resistant to existing treatments targeting the spleen, and their ITP was considered life-threatening.
Although these instances of experimental treatment have been successful, Dr Ni said more research is needed to verify the safety and efficacy of this approach. ![]()
Group creates mouse model of RUNX1-mutated AML

Researchers have developed a mouse model to help them understand why patients with RUNX1-mutated acute myeloid leukemia (AML) respond poorly to chemotherapy.
Approximately 15% of AML patients harbor a mutation in the RUNX1 gene.
In these patients, anthracycline/cytarabine-based chemotherapy does not eradicate AML cells from the bone marrow.
But scientists don’t fully understand the underlying mechanisms protecting these residual cells.
Jason H. Mendler, MD, PhD, of the University of Rochester Medical Center in Rochester, New York, and his colleagues have suggested that a genetically defined mouse model of RUNX1-mutated AML is the ideal platform to investigate the cellular mechanisms protecting residual AML cells in this disease subtype.
“Like all cancers, leukemia is not a one-size-fits-all, and, therefore, it’s important to find better ways to study high-risk subtypes of the disease,” Dr Mendler said. “We believe our mouse model will allow us to quickly define new ways to target this challenging disease.”
Dr Mendler and his colleagues described their model in PLOS ONE.
The researchers began with a patient-derived cell line of RUNX1-mutated, cytogenetically normal AML. They injected these cells into NOD-SCID-γ mice and observed leukemic engraftment in the bone marrow, spleen, and peripheral blood within 6 weeks.
When the researchers treated the mice with anthracycline/cytarabine-based chemotherapy, they saw AML clearance in the spleen and peripheral blood. But leukemic cells remained in the bone marrow.
Dr Mendler and his colleagues also found their mouse model contained mutations in 5 genes aside from RUNX1—ASXL1, CEBPA, GATA2, NRAS, and SETBP1.
The team said further investigation will be focused on identifying the interplay of genes and pathways that are critical to mediating chemotherapy resistance in this model. ![]()

Researchers have developed a mouse model to help them understand why patients with RUNX1-mutated acute myeloid leukemia (AML) respond poorly to chemotherapy.
Approximately 15% of AML patients harbor a mutation in the RUNX1 gene.
In these patients, anthracycline/cytarabine-based chemotherapy does not eradicate AML cells from the bone marrow.
But scientists don’t fully understand the underlying mechanisms protecting these residual cells.
Jason H. Mendler, MD, PhD, of the University of Rochester Medical Center in Rochester, New York, and his colleagues have suggested that a genetically defined mouse model of RUNX1-mutated AML is the ideal platform to investigate the cellular mechanisms protecting residual AML cells in this disease subtype.
“Like all cancers, leukemia is not a one-size-fits-all, and, therefore, it’s important to find better ways to study high-risk subtypes of the disease,” Dr Mendler said. “We believe our mouse model will allow us to quickly define new ways to target this challenging disease.”
Dr Mendler and his colleagues described their model in PLOS ONE.
The researchers began with a patient-derived cell line of RUNX1-mutated, cytogenetically normal AML. They injected these cells into NOD-SCID-γ mice and observed leukemic engraftment in the bone marrow, spleen, and peripheral blood within 6 weeks.
When the researchers treated the mice with anthracycline/cytarabine-based chemotherapy, they saw AML clearance in the spleen and peripheral blood. But leukemic cells remained in the bone marrow.
Dr Mendler and his colleagues also found their mouse model contained mutations in 5 genes aside from RUNX1—ASXL1, CEBPA, GATA2, NRAS, and SETBP1.
The team said further investigation will be focused on identifying the interplay of genes and pathways that are critical to mediating chemotherapy resistance in this model. ![]()

Researchers have developed a mouse model to help them understand why patients with RUNX1-mutated acute myeloid leukemia (AML) respond poorly to chemotherapy.
Approximately 15% of AML patients harbor a mutation in the RUNX1 gene.
In these patients, anthracycline/cytarabine-based chemotherapy does not eradicate AML cells from the bone marrow.
But scientists don’t fully understand the underlying mechanisms protecting these residual cells.
Jason H. Mendler, MD, PhD, of the University of Rochester Medical Center in Rochester, New York, and his colleagues have suggested that a genetically defined mouse model of RUNX1-mutated AML is the ideal platform to investigate the cellular mechanisms protecting residual AML cells in this disease subtype.
“Like all cancers, leukemia is not a one-size-fits-all, and, therefore, it’s important to find better ways to study high-risk subtypes of the disease,” Dr Mendler said. “We believe our mouse model will allow us to quickly define new ways to target this challenging disease.”
Dr Mendler and his colleagues described their model in PLOS ONE.
The researchers began with a patient-derived cell line of RUNX1-mutated, cytogenetically normal AML. They injected these cells into NOD-SCID-γ mice and observed leukemic engraftment in the bone marrow, spleen, and peripheral blood within 6 weeks.
When the researchers treated the mice with anthracycline/cytarabine-based chemotherapy, they saw AML clearance in the spleen and peripheral blood. But leukemic cells remained in the bone marrow.
Dr Mendler and his colleagues also found their mouse model contained mutations in 5 genes aside from RUNX1—ASXL1, CEBPA, GATA2, NRAS, and SETBP1.
The team said further investigation will be focused on identifying the interplay of genes and pathways that are critical to mediating chemotherapy resistance in this model. ![]()
FDA approves patch for treating hemorrhage
Image by James Weaver
The US Food and Drug Administration (FDA) has granted 501(k) clearance for the Hemogrip Patch, a product used to treat uncontrolled hemorrhage.
The patch is designed to control bleeding that occurs when accessing veins or arteries for various medical treatments and applications.
The Hemogrip platform technology is based on chitosan, a natural biopolymer found in the exoskeleton of crustaceans.
Chitosan is biocompatible, anti-microbial, and durable under a range of environmental conditions.
When applied to wounds, Hemogrip creates a nano-scale, 3-dimensional mesh, rapidly coagulating blood and stopping blood loss.
Hemogrip technology has proven effective in a study of swine, halting uncontrolled hemorrhage in a model of lethal arterial injury. Other in vivo research showed that Hemogrip’s hemostatic effects are reversible.
The Hemogrip Patch is under development by the medical device company Remedium Technologies, a spin-out of the University of Maryland. ![]()

Image by James Weaver
The US Food and Drug Administration (FDA) has granted 501(k) clearance for the Hemogrip Patch, a product used to treat uncontrolled hemorrhage.
The patch is designed to control bleeding that occurs when accessing veins or arteries for various medical treatments and applications.
The Hemogrip platform technology is based on chitosan, a natural biopolymer found in the exoskeleton of crustaceans.
Chitosan is biocompatible, anti-microbial, and durable under a range of environmental conditions.
When applied to wounds, Hemogrip creates a nano-scale, 3-dimensional mesh, rapidly coagulating blood and stopping blood loss.
Hemogrip technology has proven effective in a study of swine, halting uncontrolled hemorrhage in a model of lethal arterial injury. Other in vivo research showed that Hemogrip’s hemostatic effects are reversible.
The Hemogrip Patch is under development by the medical device company Remedium Technologies, a spin-out of the University of Maryland. ![]()

Image by James Weaver
The US Food and Drug Administration (FDA) has granted 501(k) clearance for the Hemogrip Patch, a product used to treat uncontrolled hemorrhage.
The patch is designed to control bleeding that occurs when accessing veins or arteries for various medical treatments and applications.
The Hemogrip platform technology is based on chitosan, a natural biopolymer found in the exoskeleton of crustaceans.
Chitosan is biocompatible, anti-microbial, and durable under a range of environmental conditions.
When applied to wounds, Hemogrip creates a nano-scale, 3-dimensional mesh, rapidly coagulating blood and stopping blood loss.
Hemogrip technology has proven effective in a study of swine, halting uncontrolled hemorrhage in a model of lethal arterial injury. Other in vivo research showed that Hemogrip’s hemostatic effects are reversible.
The Hemogrip Patch is under development by the medical device company Remedium Technologies, a spin-out of the University of Maryland.
Pegylated rFVIII product produces favorable results in hemophilia A

An investigational recombinant factor VIII (rFVIII) product can safely treat and prevent bleeding in previously treated patients with hemophilia A, according to researchers.
The product, BAX 855, is a pegylated version of ADVATE, a full-length rFVIII product already approved to treat hemophilia A.
BAX 855 was designed to have a longer half-life than ADVATE, thereby allowing for fewer prophylactic infusions without affecting hemostatic efficacy.
Results of a phase 1 study showed that BAX 855 had a longer half-life and mean residence time than ADVATE. And results of a phase 2/3 study showed that twice-weekly prophylactic treatment with BAX 855 lowered the median annualized bleed rate (ABR) when compared to on-demand treatment with BAX 855.
None of the patients who received BAX 855 in either study developed inhibitors, and there were no serious adverse events (AEs) that were considered treatment-related.
Results from both trials were published in Blood. The research was funded by Baxalta, a spin-off of Baxter Healthcare Corporation.
Study characteristics
The phase 1 study included 19 previously treated patients with severe hemophilia A and a median age of 29 (range, 18-60). The patients received single infusions of ADVATE followed by BAX 855 (after a wash-out period) at 30 IU/kg or 60 IU/kg.
In the phase 2/3 trial, researchers evaluated BAX 855 in 137 previously treated patients with hemophilia A. These patients also had a median age of 29 (range, 12-58).
They were assigned to either twice-weekly prophylaxis (40-50 IU/kg, n=120) or on-demand treatment (10-60 IU/kg, n=17) with BAX 855. One hundred and twenty-six patients completed the study.
Pharmacokinetics and safety
In the phase 1 study, the mean residence time was higher with BAX 855 than with ADVATE—1.4-fold higher in the 30 IU/kg arm and 1.5-fold higher in the 60 IU/kg arm. The mean half-life was higher with BAX 855 as well—1.4-fold higher in the 30 IU/kg arm and 1.5-fold in the 60 IU/kg arm.
Results were similar in the phase 2/3 trial.
None of the subjects in the phase 1 study experienced a serious AE after their single infusion of BAX 855. Eight patients experienced a total of 11 non-serious AEs, none of which were considered related to BAX 855.
In the phase 2/3 study, there were 171 AEs in 73 patients who received BAX 855 for about 6 months. There were 7 AEs (occurring in 6 patients) that were considered possibly related to BAX 855. These included diarrhea, nausea, headache, and flushing.
There were 5 serious AEs (occurring in 5 patients) that were not considered treatment-related. These included osteoarthritis, herpes zoster infection, humerus fracture, neuroendocrine carcinoma, and muscle hemorrhage.
Efficacy: Prophylaxis and on-demand
The researchers only assessed the efficacy of BAX 855 prophylaxis and on-demand treatment in the phase 2/3 study.
Patients received a median dose of 44.6 IU/kg per prophylactic infusion. The mean reduction in dosing frequency from pre-study prophylaxis was 26.7%, and 70.4% of patients were able to reduce the frequency of dosing by 30% or more. This is roughly equivalent to at least 1 less prophylactic infusion per week.
Patients who received prophylaxis had a 90% reduction in ABR compared to those who received on-demand treatment. The median ABR was 1.9 in the prophylactic arm and 41.5 in the on-demand arm.
The ABRs for joint bleeds or spontaneous/unknown bleeds were both 0 in the prophylactic arm, compared to 38.1 and 21.6, respectively, in the on-demand treatment arm.
Patients who received on-demand treatment were given a median dose of 30.87 IU/kg per episode and 29.19 IU/kg for the maintenance of hemostasis.
Of the 518 bleeding episodes reported during the study, 95.9% were treated with 1 or 2 infusions of BAX 855. The mean number of infusions required to treat a bleeding episode was 1.2.

An investigational recombinant factor VIII (rFVIII) product can safely treat and prevent bleeding in previously treated patients with hemophilia A, according to researchers.
The product, BAX 855, is a pegylated version of ADVATE, a full-length rFVIII product already approved to treat hemophilia A.
BAX 855 was designed to have a longer half-life than ADVATE, thereby allowing for fewer prophylactic infusions without affecting hemostatic efficacy.
Results of a phase 1 study showed that BAX 855 had a longer half-life and mean residence time than ADVATE. And results of a phase 2/3 study showed that twice-weekly prophylactic treatment with BAX 855 lowered the median annualized bleed rate (ABR) when compared to on-demand treatment with BAX 855.
None of the patients who received BAX 855 in either study developed inhibitors, and there were no serious adverse events (AEs) that were considered treatment-related.
Results from both trials were published in Blood. The research was funded by Baxalta, a spin-off of Baxter Healthcare Corporation.
Study characteristics
The phase 1 study included 19 previously treated patients with severe hemophilia A and a median age of 29 (range, 18-60). The patients received single infusions of ADVATE followed by BAX 855 (after a wash-out period) at 30 IU/kg or 60 IU/kg.
In the phase 2/3 trial, researchers evaluated BAX 855 in 137 previously treated patients with hemophilia A. These patients also had a median age of 29 (range, 12-58).
They were assigned to either twice-weekly prophylaxis (40-50 IU/kg, n=120) or on-demand treatment (10-60 IU/kg, n=17) with BAX 855. One hundred and twenty-six patients completed the study.
Pharmacokinetics and safety
In the phase 1 study, the mean residence time was higher with BAX 855 than with ADVATE—1.4-fold higher in the 30 IU/kg arm and 1.5-fold higher in the 60 IU/kg arm. The mean half-life was higher with BAX 855 as well—1.4-fold higher in the 30 IU/kg arm and 1.5-fold in the 60 IU/kg arm.
Results were similar in the phase 2/3 trial.
None of the subjects in the phase 1 study experienced a serious AE after their single infusion of BAX 855. Eight patients experienced a total of 11 non-serious AEs, none of which were considered related to BAX 855.
In the phase 2/3 study, there were 171 AEs in 73 patients who received BAX 855 for about 6 months. There were 7 AEs (occurring in 6 patients) that were considered possibly related to BAX 855. These included diarrhea, nausea, headache, and flushing.
There were 5 serious AEs (occurring in 5 patients) that were not considered treatment-related. These included osteoarthritis, herpes zoster infection, humerus fracture, neuroendocrine carcinoma, and muscle hemorrhage.
Efficacy: Prophylaxis and on-demand
The researchers only assessed the efficacy of BAX 855 prophylaxis and on-demand treatment in the phase 2/3 study.
Patients received a median dose of 44.6 IU/kg per prophylactic infusion. The mean reduction in dosing frequency from pre-study prophylaxis was 26.7%, and 70.4% of patients were able to reduce the frequency of dosing by 30% or more. This is roughly equivalent to at least 1 less prophylactic infusion per week.
Patients who received prophylaxis had a 90% reduction in ABR compared to those who received on-demand treatment. The median ABR was 1.9 in the prophylactic arm and 41.5 in the on-demand arm.
The ABRs for joint bleeds or spontaneous/unknown bleeds were both 0 in the prophylactic arm, compared to 38.1 and 21.6, respectively, in the on-demand treatment arm.
Patients who received on-demand treatment were given a median dose of 30.87 IU/kg per episode and 29.19 IU/kg for the maintenance of hemostasis.
Of the 518 bleeding episodes reported during the study, 95.9% were treated with 1 or 2 infusions of BAX 855. The mean number of infusions required to treat a bleeding episode was 1.2.

An investigational recombinant factor VIII (rFVIII) product can safely treat and prevent bleeding in previously treated patients with hemophilia A, according to researchers.
The product, BAX 855, is a pegylated version of ADVATE, a full-length rFVIII product already approved to treat hemophilia A.
BAX 855 was designed to have a longer half-life than ADVATE, thereby allowing for fewer prophylactic infusions without affecting hemostatic efficacy.
Results of a phase 1 study showed that BAX 855 had a longer half-life and mean residence time than ADVATE. And results of a phase 2/3 study showed that twice-weekly prophylactic treatment with BAX 855 lowered the median annualized bleed rate (ABR) when compared to on-demand treatment with BAX 855.
None of the patients who received BAX 855 in either study developed inhibitors, and there were no serious adverse events (AEs) that were considered treatment-related.
Results from both trials were published in Blood. The research was funded by Baxalta, a spin-off of Baxter Healthcare Corporation.
Study characteristics
The phase 1 study included 19 previously treated patients with severe hemophilia A and a median age of 29 (range, 18-60). The patients received single infusions of ADVATE followed by BAX 855 (after a wash-out period) at 30 IU/kg or 60 IU/kg.
In the phase 2/3 trial, researchers evaluated BAX 855 in 137 previously treated patients with hemophilia A. These patients also had a median age of 29 (range, 12-58).
They were assigned to either twice-weekly prophylaxis (40-50 IU/kg, n=120) or on-demand treatment (10-60 IU/kg, n=17) with BAX 855. One hundred and twenty-six patients completed the study.
Pharmacokinetics and safety
In the phase 1 study, the mean residence time was higher with BAX 855 than with ADVATE—1.4-fold higher in the 30 IU/kg arm and 1.5-fold higher in the 60 IU/kg arm. The mean half-life was higher with BAX 855 as well—1.4-fold higher in the 30 IU/kg arm and 1.5-fold in the 60 IU/kg arm.
Results were similar in the phase 2/3 trial.
None of the subjects in the phase 1 study experienced a serious AE after their single infusion of BAX 855. Eight patients experienced a total of 11 non-serious AEs, none of which were considered related to BAX 855.
In the phase 2/3 study, there were 171 AEs in 73 patients who received BAX 855 for about 6 months. There were 7 AEs (occurring in 6 patients) that were considered possibly related to BAX 855. These included diarrhea, nausea, headache, and flushing.
There were 5 serious AEs (occurring in 5 patients) that were not considered treatment-related. These included osteoarthritis, herpes zoster infection, humerus fracture, neuroendocrine carcinoma, and muscle hemorrhage.
Efficacy: Prophylaxis and on-demand
The researchers only assessed the efficacy of BAX 855 prophylaxis and on-demand treatment in the phase 2/3 study.
Patients received a median dose of 44.6 IU/kg per prophylactic infusion. The mean reduction in dosing frequency from pre-study prophylaxis was 26.7%, and 70.4% of patients were able to reduce the frequency of dosing by 30% or more. This is roughly equivalent to at least 1 less prophylactic infusion per week.
Patients who received prophylaxis had a 90% reduction in ABR compared to those who received on-demand treatment. The median ABR was 1.9 in the prophylactic arm and 41.5 in the on-demand arm.
The ABRs for joint bleeds or spontaneous/unknown bleeds were both 0 in the prophylactic arm, compared to 38.1 and 21.6, respectively, in the on-demand treatment arm.
Patients who received on-demand treatment were given a median dose of 30.87 IU/kg per episode and 29.19 IU/kg for the maintenance of hemostasis.
Of the 518 bleeding episodes reported during the study, 95.9% were treated with 1 or 2 infusions of BAX 855. The mean number of infusions required to treat a bleeding episode was 1.2.
Rivaroxaban safe, effective after ED admission

Photo courtesy of the CDC
Patients admitted to the emergency department (ED) for venous thromboembolism (VTE) can be placed on oral anticoagulation and discharged immediately, according to research published in Academic Emergency Medicine.
The study showed that patients who received anticoagulation with rivaroxaban, were discharged from the ED right away, and did not undergo weekly monitoring had a low rate of VTE recurrence and major or clinically relevant bleeding.
A related study suggested this approach was less costly than standard treatment with heparin and warfarin.
The prospect of being able to send patients home from the ED on the day of admission is a quality of life issue, according to Jeffrey A. Kline, MD, a professor at the Indiana University School of Medicine in Indianapolis and an author of both studies.
“We really do empower the patient more with [rivaroxaban],” he said. “Patients say treatment with no injections is a much better option. [Rivaroxaban] takes a condition that is life-threatening and makes it something the patient can control.”
Safety and efficacy
For the first study, Dr Kline and his colleagues evaluated 106 low-risk patients who were diagnosed with deep vein thrombosis (DVT) or pulmonary embolism (PE) at 2 metropolitan EDs.
The patients were admitted between March 2013 and April 2014. Seventy-one patients had DVT, 30 had PE, and 5 had both.
The standard of care for these patients is heparin injections, followed by oral warfarin and close monitoring to ensure safe dosage levels.
But patients in this study received rivaroxaban, which does not require blood monitoring, and were released from the hospital on the day of admission. The patients did undergo follow up-monitoring at 2 weeks, 5 weeks, 3 months, and 6 months.
The researchers followed patients for a mean of 389 days (range, 213 to 594 days). None of the patients had a VTE recurrence, major bleeding, or clinically relevant bleeding while on therapy.
However, 3 patients (2.8%) experienced DVT recurrence within a year of stopping treatment. All 3 had completed their prescribed treatment.
“This study is about giving patients a new option,” Dr Kline said. “Treating patients at home for blood clots was found to have fewer errors than the standard of care and better outcomes. Patients [receiving standard therapy] have to be taught to give themselves injections, and it scares them to death. Almost everyone has taken a pill, so there is no learning curve for patients [with rivaroxaban].”
Treatment costs
In the second study, Dr Kline and his colleagues compared costs associated with standard treatment and rivaroxaban. Total hospital charges with the rivaroxaban protocol were about half the cost of charges for standard therapy.
The researchers evaluated 97 patients, matching them for age, sex, and the severity of their illness. At 6 months after ED admission, the median cost was $4787 (interquartile range=$3042 to $7596) for the rivaroxaban group and $11,128 (interquartile range=$8110 to $23,390) for the group treated with standard care (P<0.001).
Among patients with PE, costs were 57% lower in the rivaroxaban group than the standard therapy group (P<0.001). For patients with DVT, costs were 56% lower in the rivaroxaban group (P=0.003).

Photo courtesy of the CDC
Patients admitted to the emergency department (ED) for venous thromboembolism (VTE) can be placed on oral anticoagulation and discharged immediately, according to research published in Academic Emergency Medicine.
The study showed that patients who received anticoagulation with rivaroxaban, were discharged from the ED right away, and did not undergo weekly monitoring had a low rate of VTE recurrence and major or clinically relevant bleeding.
A related study suggested this approach was less costly than standard treatment with heparin and warfarin.
The prospect of being able to send patients home from the ED on the day of admission is a quality of life issue, according to Jeffrey A. Kline, MD, a professor at the Indiana University School of Medicine in Indianapolis and an author of both studies.
“We really do empower the patient more with [rivaroxaban],” he said. “Patients say treatment with no injections is a much better option. [Rivaroxaban] takes a condition that is life-threatening and makes it something the patient can control.”
Safety and efficacy
For the first study, Dr Kline and his colleagues evaluated 106 low-risk patients who were diagnosed with deep vein thrombosis (DVT) or pulmonary embolism (PE) at 2 metropolitan EDs.
The patients were admitted between March 2013 and April 2014. Seventy-one patients had DVT, 30 had PE, and 5 had both.
The standard of care for these patients is heparin injections, followed by oral warfarin and close monitoring to ensure safe dosage levels.
But patients in this study received rivaroxaban, which does not require blood monitoring, and were released from the hospital on the day of admission. The patients did undergo follow up-monitoring at 2 weeks, 5 weeks, 3 months, and 6 months.
The researchers followed patients for a mean of 389 days (range, 213 to 594 days). None of the patients had a VTE recurrence, major bleeding, or clinically relevant bleeding while on therapy.
However, 3 patients (2.8%) experienced DVT recurrence within a year of stopping treatment. All 3 had completed their prescribed treatment.
“This study is about giving patients a new option,” Dr Kline said. “Treating patients at home for blood clots was found to have fewer errors than the standard of care and better outcomes. Patients [receiving standard therapy] have to be taught to give themselves injections, and it scares them to death. Almost everyone has taken a pill, so there is no learning curve for patients [with rivaroxaban].”
Treatment costs
In the second study, Dr Kline and his colleagues compared costs associated with standard treatment and rivaroxaban. Total hospital charges with the rivaroxaban protocol were about half the cost of charges for standard therapy.
The researchers evaluated 97 patients, matching them for age, sex, and the severity of their illness. At 6 months after ED admission, the median cost was $4787 (interquartile range=$3042 to $7596) for the rivaroxaban group and $11,128 (interquartile range=$8110 to $23,390) for the group treated with standard care (P<0.001).
Among patients with PE, costs were 57% lower in the rivaroxaban group than the standard therapy group (P<0.001). For patients with DVT, costs were 56% lower in the rivaroxaban group (P=0.003).

Photo courtesy of the CDC
Patients admitted to the emergency department (ED) for venous thromboembolism (VTE) can be placed on oral anticoagulation and discharged immediately, according to research published in Academic Emergency Medicine.
The study showed that patients who received anticoagulation with rivaroxaban, were discharged from the ED right away, and did not undergo weekly monitoring had a low rate of VTE recurrence and major or clinically relevant bleeding.
A related study suggested this approach was less costly than standard treatment with heparin and warfarin.
The prospect of being able to send patients home from the ED on the day of admission is a quality of life issue, according to Jeffrey A. Kline, MD, a professor at the Indiana University School of Medicine in Indianapolis and an author of both studies.
“We really do empower the patient more with [rivaroxaban],” he said. “Patients say treatment with no injections is a much better option. [Rivaroxaban] takes a condition that is life-threatening and makes it something the patient can control.”
Safety and efficacy
For the first study, Dr Kline and his colleagues evaluated 106 low-risk patients who were diagnosed with deep vein thrombosis (DVT) or pulmonary embolism (PE) at 2 metropolitan EDs.
The patients were admitted between March 2013 and April 2014. Seventy-one patients had DVT, 30 had PE, and 5 had both.
The standard of care for these patients is heparin injections, followed by oral warfarin and close monitoring to ensure safe dosage levels.
But patients in this study received rivaroxaban, which does not require blood monitoring, and were released from the hospital on the day of admission. The patients did undergo follow up-monitoring at 2 weeks, 5 weeks, 3 months, and 6 months.
The researchers followed patients for a mean of 389 days (range, 213 to 594 days). None of the patients had a VTE recurrence, major bleeding, or clinically relevant bleeding while on therapy.
However, 3 patients (2.8%) experienced DVT recurrence within a year of stopping treatment. All 3 had completed their prescribed treatment.
“This study is about giving patients a new option,” Dr Kline said. “Treating patients at home for blood clots was found to have fewer errors than the standard of care and better outcomes. Patients [receiving standard therapy] have to be taught to give themselves injections, and it scares them to death. Almost everyone has taken a pill, so there is no learning curve for patients [with rivaroxaban].”
Treatment costs
In the second study, Dr Kline and his colleagues compared costs associated with standard treatment and rivaroxaban. Total hospital charges with the rivaroxaban protocol were about half the cost of charges for standard therapy.
The researchers evaluated 97 patients, matching them for age, sex, and the severity of their illness. At 6 months after ED admission, the median cost was $4787 (interquartile range=$3042 to $7596) for the rivaroxaban group and $11,128 (interquartile range=$8110 to $23,390) for the group treated with standard care (P<0.001).
Among patients with PE, costs were 57% lower in the rivaroxaban group than the standard therapy group (P<0.001). For patients with DVT, costs were 56% lower in the rivaroxaban group (P=0.003).
Polyphenols may enhance doxorubicin treatment

Photo by Rhoda Baer
New research suggests the polyphenols resveratrol and quercetin could be used to augment treatment with the anthracycline doxorubicin.
Investigators found they could increase the bioavailability of resveratrol and quercetin using copolymers that make the compounds water soluble and allow for their injection into the blood stream.
The team then showed the compounds synergize with doxorubicin while also reducing cardiac toxicity.
Although doxorubicin has proven effective against lymphomas, leukemias, and other cancers, the drug can only be used for a limited time because it confers cardiotoxicity.
The co-administration of resveratrol and quercetin might allow for much more extensive use of doxorubicin, while at the same time improving its efficacy and demonstrating the polyphenols’ own anticancer properties, investigators said.
They described research supporting this idea in the Journal of Controlled Release.
“This has great potential to improve chemotherapeutic cancer treatment,” said Adam Alani, PhD, of Oregon State University in Portland.
“The co-administration of high levels of resveratrol and quercetin, in both in vitro and in vivo studies, shows that it significantly reduces the cardiac toxicity of [doxorubicin]. And these compounds have a synergistic effect that enhances the efficacy of the cancer drug, by sensitizing the cancer cells to the effects of the drug.”
Dr Alani said further research may demonstrate that these compounds can completely eliminate the cardiotoxicity of doxorubicin, as they scavenge the toxic free radicals produced by this drug.
It’s also possible, he said, that administration of these natural polyphenols could have value in cancer therapy by themselves or in combination with a wider range of other chemotherapeutic drugs.
Increasing bioavailability
Resveratrol is a natural compound found in foods such as grapes, red wine, green tea, berries, and dark chocolate. Quercetin reaches some of its highest natural levels in capers, some berries, and leafy greens.
When consumed via food or taken as supplements, these polyphenol compounds reach only a tiny fraction of the level that’s possible with direct injection. Such injection was not possible until Dr Alani and his colleagues adapted the use of polymeric micelles.
Specifically, the investigators combined resveratrol and quercetin in Pluronic F127 micelles (mRQ). Pluronics are triblock copolymers consisting of a polypropylene oxide chain flanked with 2 polyethylene oxide chains that can self-assemble into polymeric micelles. The micelles have hydrophobic cores that help solubilize compounds with poor aqueous solubility.
“There are several advantages with this system,” Dr Alani said. “We can finally reach clinical levels of these polyphenols in the body. We can load both the compounds at one time to help control the cardiotoxicity of the cancer drug, and we can help the polyphenols accumulate in cancer cells where they have their own anticancer properties.”
In combination with doxorubicin
The investigators prepared mRQ micelles that were capable of retaining 1.1 mg/mL of resveratrol and 1.42 mg/mL of quercetin. They then tested mRQ in combination with doxorubicin in human ovarian cancer cells (SKOV-3) and rat cardiomyocytes (H9C2).
The team found that a resveratrol-quercetin-doxorubicin ratio of 10:10:1 was synergistic in SKOV-3 cells and antagonistic in H9C2 cells.
mRQ did not interfere with doxorubicin’s caspase activity in SKOV-3 cells but significantly decreased the activity in H9C2 cells. Likewise, there were no changes in the generation of reactive oxygen species in SKOV-3 cells, but there was significant scavenging in H9C2 cells.
The investigators also administered doxorubicin, with or without mRQ, to healthy mice and found that mRQ “conferred full cardioprotection.”
Dr Alani noted that previous research suggested resveratrol and quercetin are safe when given at high concentrations, but additional research is needed.

Photo by Rhoda Baer
New research suggests the polyphenols resveratrol and quercetin could be used to augment treatment with the anthracycline doxorubicin.
Investigators found they could increase the bioavailability of resveratrol and quercetin using copolymers that make the compounds water soluble and allow for their injection into the blood stream.
The team then showed the compounds synergize with doxorubicin while also reducing cardiac toxicity.
Although doxorubicin has proven effective against lymphomas, leukemias, and other cancers, the drug can only be used for a limited time because it confers cardiotoxicity.
The co-administration of resveratrol and quercetin might allow for much more extensive use of doxorubicin, while at the same time improving its efficacy and demonstrating the polyphenols’ own anticancer properties, investigators said.
They described research supporting this idea in the Journal of Controlled Release.
“This has great potential to improve chemotherapeutic cancer treatment,” said Adam Alani, PhD, of Oregon State University in Portland.
“The co-administration of high levels of resveratrol and quercetin, in both in vitro and in vivo studies, shows that it significantly reduces the cardiac toxicity of [doxorubicin]. And these compounds have a synergistic effect that enhances the efficacy of the cancer drug, by sensitizing the cancer cells to the effects of the drug.”
Dr Alani said further research may demonstrate that these compounds can completely eliminate the cardiotoxicity of doxorubicin, as they scavenge the toxic free radicals produced by this drug.
It’s also possible, he said, that administration of these natural polyphenols could have value in cancer therapy by themselves or in combination with a wider range of other chemotherapeutic drugs.
Increasing bioavailability
Resveratrol is a natural compound found in foods such as grapes, red wine, green tea, berries, and dark chocolate. Quercetin reaches some of its highest natural levels in capers, some berries, and leafy greens.
When consumed via food or taken as supplements, these polyphenol compounds reach only a tiny fraction of the level that’s possible with direct injection. Such injection was not possible until Dr Alani and his colleagues adapted the use of polymeric micelles.
Specifically, the investigators combined resveratrol and quercetin in Pluronic F127 micelles (mRQ). Pluronics are triblock copolymers consisting of a polypropylene oxide chain flanked with 2 polyethylene oxide chains that can self-assemble into polymeric micelles. The micelles have hydrophobic cores that help solubilize compounds with poor aqueous solubility.
“There are several advantages with this system,” Dr Alani said. “We can finally reach clinical levels of these polyphenols in the body. We can load both the compounds at one time to help control the cardiotoxicity of the cancer drug, and we can help the polyphenols accumulate in cancer cells where they have their own anticancer properties.”
In combination with doxorubicin
The investigators prepared mRQ micelles that were capable of retaining 1.1 mg/mL of resveratrol and 1.42 mg/mL of quercetin. They then tested mRQ in combination with doxorubicin in human ovarian cancer cells (SKOV-3) and rat cardiomyocytes (H9C2).
The team found that a resveratrol-quercetin-doxorubicin ratio of 10:10:1 was synergistic in SKOV-3 cells and antagonistic in H9C2 cells.
mRQ did not interfere with doxorubicin’s caspase activity in SKOV-3 cells but significantly decreased the activity in H9C2 cells. Likewise, there were no changes in the generation of reactive oxygen species in SKOV-3 cells, but there was significant scavenging in H9C2 cells.
The investigators also administered doxorubicin, with or without mRQ, to healthy mice and found that mRQ “conferred full cardioprotection.”
Dr Alani noted that previous research suggested resveratrol and quercetin are safe when given at high concentrations, but additional research is needed.

Photo by Rhoda Baer
New research suggests the polyphenols resveratrol and quercetin could be used to augment treatment with the anthracycline doxorubicin.
Investigators found they could increase the bioavailability of resveratrol and quercetin using copolymers that make the compounds water soluble and allow for their injection into the blood stream.
The team then showed the compounds synergize with doxorubicin while also reducing cardiac toxicity.
Although doxorubicin has proven effective against lymphomas, leukemias, and other cancers, the drug can only be used for a limited time because it confers cardiotoxicity.
The co-administration of resveratrol and quercetin might allow for much more extensive use of doxorubicin, while at the same time improving its efficacy and demonstrating the polyphenols’ own anticancer properties, investigators said.
They described research supporting this idea in the Journal of Controlled Release.
“This has great potential to improve chemotherapeutic cancer treatment,” said Adam Alani, PhD, of Oregon State University in Portland.
“The co-administration of high levels of resveratrol and quercetin, in both in vitro and in vivo studies, shows that it significantly reduces the cardiac toxicity of [doxorubicin]. And these compounds have a synergistic effect that enhances the efficacy of the cancer drug, by sensitizing the cancer cells to the effects of the drug.”
Dr Alani said further research may demonstrate that these compounds can completely eliminate the cardiotoxicity of doxorubicin, as they scavenge the toxic free radicals produced by this drug.
It’s also possible, he said, that administration of these natural polyphenols could have value in cancer therapy by themselves or in combination with a wider range of other chemotherapeutic drugs.
Increasing bioavailability
Resveratrol is a natural compound found in foods such as grapes, red wine, green tea, berries, and dark chocolate. Quercetin reaches some of its highest natural levels in capers, some berries, and leafy greens.
When consumed via food or taken as supplements, these polyphenol compounds reach only a tiny fraction of the level that’s possible with direct injection. Such injection was not possible until Dr Alani and his colleagues adapted the use of polymeric micelles.
Specifically, the investigators combined resveratrol and quercetin in Pluronic F127 micelles (mRQ). Pluronics are triblock copolymers consisting of a polypropylene oxide chain flanked with 2 polyethylene oxide chains that can self-assemble into polymeric micelles. The micelles have hydrophobic cores that help solubilize compounds with poor aqueous solubility.
“There are several advantages with this system,” Dr Alani said. “We can finally reach clinical levels of these polyphenols in the body. We can load both the compounds at one time to help control the cardiotoxicity of the cancer drug, and we can help the polyphenols accumulate in cancer cells where they have their own anticancer properties.”
In combination with doxorubicin
The investigators prepared mRQ micelles that were capable of retaining 1.1 mg/mL of resveratrol and 1.42 mg/mL of quercetin. They then tested mRQ in combination with doxorubicin in human ovarian cancer cells (SKOV-3) and rat cardiomyocytes (H9C2).
The team found that a resveratrol-quercetin-doxorubicin ratio of 10:10:1 was synergistic in SKOV-3 cells and antagonistic in H9C2 cells.
mRQ did not interfere with doxorubicin’s caspase activity in SKOV-3 cells but significantly decreased the activity in H9C2 cells. Likewise, there were no changes in the generation of reactive oxygen species in SKOV-3 cells, but there was significant scavenging in H9C2 cells.
The investigators also administered doxorubicin, with or without mRQ, to healthy mice and found that mRQ “conferred full cardioprotection.”
Dr Alani noted that previous research suggested resveratrol and quercetin are safe when given at high concentrations, but additional research is needed.