User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Hepatitis C Infection Rates Rising in Women, Young Children
Rates of hepatitis C virus detection increased in U.S. women aged 15-44 years and in children less than 2 years old from 2011 to 2014, according to investigators from the Centers for Disease Control and Prevention.
A report published July 21 in Morbidity and Mortality Weekly Report revealed hepatitis C virus (HCV) detection rates (detection via antibody or RNA positivity) that were determined using data collected from Quest Diagnostics for Kentucky and for the United States. In Kentucky, the rate of HCV detection in women aged 15-44 increased 213% over the study period, from 275 to 862 cases per 100,000 people, and for the entire U.S., the rate of detection increased by 22% from 139 to 169 cases per 100,000 people (65[28]:705-10).
The rate of HCV testing for children under 2 years old in Kentucky increased 151% over the study period, rising from 403 to 1,011 per 100,000 people, and the rate of children born to HCV-positive mothers increased from 0.71% to 1.59%. Nationwide, the HCV testing rate for children under 2 years old increased 14% from 310 to 353 per 100,000, and the rate of children born to HCV-positive mothers increased from 0.19% to 0.32%.
“These findings underscore the importance of providing primary prevention services and following current recommendations to identify persons at risk for HCV infection and test accordingly; doing so among pregnant women would improve early identification of HCV-infected infants and linkage of the mother and infant to care and treatment,” the CDC investigators said.
Rates of hepatitis C virus detection increased in U.S. women aged 15-44 years and in children less than 2 years old from 2011 to 2014, according to investigators from the Centers for Disease Control and Prevention.
A report published July 21 in Morbidity and Mortality Weekly Report revealed hepatitis C virus (HCV) detection rates (detection via antibody or RNA positivity) that were determined using data collected from Quest Diagnostics for Kentucky and for the United States. In Kentucky, the rate of HCV detection in women aged 15-44 increased 213% over the study period, from 275 to 862 cases per 100,000 people, and for the entire U.S., the rate of detection increased by 22% from 139 to 169 cases per 100,000 people (65[28]:705-10).
The rate of HCV testing for children under 2 years old in Kentucky increased 151% over the study period, rising from 403 to 1,011 per 100,000 people, and the rate of children born to HCV-positive mothers increased from 0.71% to 1.59%. Nationwide, the HCV testing rate for children under 2 years old increased 14% from 310 to 353 per 100,000, and the rate of children born to HCV-positive mothers increased from 0.19% to 0.32%.
“These findings underscore the importance of providing primary prevention services and following current recommendations to identify persons at risk for HCV infection and test accordingly; doing so among pregnant women would improve early identification of HCV-infected infants and linkage of the mother and infant to care and treatment,” the CDC investigators said.
Rates of hepatitis C virus detection increased in U.S. women aged 15-44 years and in children less than 2 years old from 2011 to 2014, according to investigators from the Centers for Disease Control and Prevention.
A report published July 21 in Morbidity and Mortality Weekly Report revealed hepatitis C virus (HCV) detection rates (detection via antibody or RNA positivity) that were determined using data collected from Quest Diagnostics for Kentucky and for the United States. In Kentucky, the rate of HCV detection in women aged 15-44 increased 213% over the study period, from 275 to 862 cases per 100,000 people, and for the entire U.S., the rate of detection increased by 22% from 139 to 169 cases per 100,000 people (65[28]:705-10).
The rate of HCV testing for children under 2 years old in Kentucky increased 151% over the study period, rising from 403 to 1,011 per 100,000 people, and the rate of children born to HCV-positive mothers increased from 0.71% to 1.59%. Nationwide, the HCV testing rate for children under 2 years old increased 14% from 310 to 353 per 100,000, and the rate of children born to HCV-positive mothers increased from 0.19% to 0.32%.
“These findings underscore the importance of providing primary prevention services and following current recommendations to identify persons at risk for HCV infection and test accordingly; doing so among pregnant women would improve early identification of HCV-infected infants and linkage of the mother and infant to care and treatment,” the CDC investigators said.
FROM MMWR
Hepatitis C infection rates rising in women, young children
Rates of hepatitis C virus detection increased in U.S. women aged 15-44 years and in children less than 2 years old from 2011 to 2014, according to investigators from the Centers for Disease Control and Prevention.
A report published July 21 in Morbidity and Mortality Weekly Report revealed hepatitis C virus (HCV) detection rates (detection via antibody or RNA positivity) that were determined using data collected from Quest Diagnostics for Kentucky and for the United States. In Kentucky, the rate of HCV detection in women aged 15-44 increased 213% over the study period, from 275 to 862 cases per 100,000 people, and for the entire U.S., the rate of detection increased by 22% from 139 to 169 cases per 100,000 people (65[28]:705-10).
The rate of HCV testing for children under 2 years old in Kentucky increased 151% over the study period, rising from 403 to 1,011 per 100,000 people, and the rate of children born to HCV-positive mothers increased from 0.71% to 1.59%. Nationwide, the HCV testing rate for children under 2 years old increased 14% from 310 to 353 per 100,000, and the rate of children born to HCV-positive mothers increased from 0.19% to 0.32%.
“These findings underscore the importance of providing primary prevention services and following current recommendations to identify persons at risk for HCV infection and test accordingly; doing so among pregnant women would improve early identification of HCV-infected infants and linkage of the mother and infant to care and treatment,” the CDC investigators said.
Rates of hepatitis C virus detection increased in U.S. women aged 15-44 years and in children less than 2 years old from 2011 to 2014, according to investigators from the Centers for Disease Control and Prevention.
A report published July 21 in Morbidity and Mortality Weekly Report revealed hepatitis C virus (HCV) detection rates (detection via antibody or RNA positivity) that were determined using data collected from Quest Diagnostics for Kentucky and for the United States. In Kentucky, the rate of HCV detection in women aged 15-44 increased 213% over the study period, from 275 to 862 cases per 100,000 people, and for the entire U.S., the rate of detection increased by 22% from 139 to 169 cases per 100,000 people (65[28]:705-10).
The rate of HCV testing for children under 2 years old in Kentucky increased 151% over the study period, rising from 403 to 1,011 per 100,000 people, and the rate of children born to HCV-positive mothers increased from 0.71% to 1.59%. Nationwide, the HCV testing rate for children under 2 years old increased 14% from 310 to 353 per 100,000, and the rate of children born to HCV-positive mothers increased from 0.19% to 0.32%.
“These findings underscore the importance of providing primary prevention services and following current recommendations to identify persons at risk for HCV infection and test accordingly; doing so among pregnant women would improve early identification of HCV-infected infants and linkage of the mother and infant to care and treatment,” the CDC investigators said.
Rates of hepatitis C virus detection increased in U.S. women aged 15-44 years and in children less than 2 years old from 2011 to 2014, according to investigators from the Centers for Disease Control and Prevention.
A report published July 21 in Morbidity and Mortality Weekly Report revealed hepatitis C virus (HCV) detection rates (detection via antibody or RNA positivity) that were determined using data collected from Quest Diagnostics for Kentucky and for the United States. In Kentucky, the rate of HCV detection in women aged 15-44 increased 213% over the study period, from 275 to 862 cases per 100,000 people, and for the entire U.S., the rate of detection increased by 22% from 139 to 169 cases per 100,000 people (65[28]:705-10).
The rate of HCV testing for children under 2 years old in Kentucky increased 151% over the study period, rising from 403 to 1,011 per 100,000 people, and the rate of children born to HCV-positive mothers increased from 0.71% to 1.59%. Nationwide, the HCV testing rate for children under 2 years old increased 14% from 310 to 353 per 100,000, and the rate of children born to HCV-positive mothers increased from 0.19% to 0.32%.
“These findings underscore the importance of providing primary prevention services and following current recommendations to identify persons at risk for HCV infection and test accordingly; doing so among pregnant women would improve early identification of HCV-infected infants and linkage of the mother and infant to care and treatment,” the CDC investigators said.
FROM MMWR
HPV vaccination rates not improved by increased awareness
Increased awareness did not increase adolescent HPV vaccination rates in a high-risk population, according to Jessica Fishman, PhD, of the University of Pennsylvania, Philadelphia, and her associates.
The study sample included 211 low-income adolescents, aged 13-18 years, and 149 parents of different adolescents, aged 9-18 years, who had not been vaccinated for HPV. In the adolescent group, 3% received an HPV vaccination after 3 months, 9% received a vaccination after 6 months, and 15% received a vaccination after 1 year. In the parent group, 5% had their daughters vaccinated after 3 months, 10% had their daughters vaccinated after 6 months, and 13% had their daughters vaccinated after 1 year.
Awareness was measured using a questionnaire asking about individual awareness of HPV, cervical cancer, HPV vaccination, and news or advertising about HPV vaccination. Both adolescents and parents were most aware of cervical cancer (73% and 94%, respectively) and least aware of news about HPV advertising (51% and 66%, respectively). A total of 14% of adolescents and 4% of parents had no awareness of any questionnaire item, while 32% of adolescents and 57% of parents had awareness of all items.
Probability of vaccination was less than 0.5 for all levels of awareness, and accuracy of HPV vaccination prediction models was poor, Dr. Fishman and her associates noted.
“For this high-risk population where vaccination is rare, evidence-based behavioral interventions are urgently needed. Ideally, interventions will target variables associated with vaccination. Interventions that do not target actual determinants can have no effect or even a ‘boomerang’ effect that increases unhealthy behavior,” the investigators concluded.
Find the full study in Pediatrics (doi: 10.1542/peds.2015-2048).
Increased awareness did not increase adolescent HPV vaccination rates in a high-risk population, according to Jessica Fishman, PhD, of the University of Pennsylvania, Philadelphia, and her associates.
The study sample included 211 low-income adolescents, aged 13-18 years, and 149 parents of different adolescents, aged 9-18 years, who had not been vaccinated for HPV. In the adolescent group, 3% received an HPV vaccination after 3 months, 9% received a vaccination after 6 months, and 15% received a vaccination after 1 year. In the parent group, 5% had their daughters vaccinated after 3 months, 10% had their daughters vaccinated after 6 months, and 13% had their daughters vaccinated after 1 year.
Awareness was measured using a questionnaire asking about individual awareness of HPV, cervical cancer, HPV vaccination, and news or advertising about HPV vaccination. Both adolescents and parents were most aware of cervical cancer (73% and 94%, respectively) and least aware of news about HPV advertising (51% and 66%, respectively). A total of 14% of adolescents and 4% of parents had no awareness of any questionnaire item, while 32% of adolescents and 57% of parents had awareness of all items.
Probability of vaccination was less than 0.5 for all levels of awareness, and accuracy of HPV vaccination prediction models was poor, Dr. Fishman and her associates noted.
“For this high-risk population where vaccination is rare, evidence-based behavioral interventions are urgently needed. Ideally, interventions will target variables associated with vaccination. Interventions that do not target actual determinants can have no effect or even a ‘boomerang’ effect that increases unhealthy behavior,” the investigators concluded.
Find the full study in Pediatrics (doi: 10.1542/peds.2015-2048).
Increased awareness did not increase adolescent HPV vaccination rates in a high-risk population, according to Jessica Fishman, PhD, of the University of Pennsylvania, Philadelphia, and her associates.
The study sample included 211 low-income adolescents, aged 13-18 years, and 149 parents of different adolescents, aged 9-18 years, who had not been vaccinated for HPV. In the adolescent group, 3% received an HPV vaccination after 3 months, 9% received a vaccination after 6 months, and 15% received a vaccination after 1 year. In the parent group, 5% had their daughters vaccinated after 3 months, 10% had their daughters vaccinated after 6 months, and 13% had their daughters vaccinated after 1 year.
Awareness was measured using a questionnaire asking about individual awareness of HPV, cervical cancer, HPV vaccination, and news or advertising about HPV vaccination. Both adolescents and parents were most aware of cervical cancer (73% and 94%, respectively) and least aware of news about HPV advertising (51% and 66%, respectively). A total of 14% of adolescents and 4% of parents had no awareness of any questionnaire item, while 32% of adolescents and 57% of parents had awareness of all items.
Probability of vaccination was less than 0.5 for all levels of awareness, and accuracy of HPV vaccination prediction models was poor, Dr. Fishman and her associates noted.
“For this high-risk population where vaccination is rare, evidence-based behavioral interventions are urgently needed. Ideally, interventions will target variables associated with vaccination. Interventions that do not target actual determinants can have no effect or even a ‘boomerang’ effect that increases unhealthy behavior,” the investigators concluded.
Find the full study in Pediatrics (doi: 10.1542/peds.2015-2048).
FROM PEDIATRICS
PCR better at diagnosing fungal chronic rhinosinusitis than cultures
ITS1/ITS2 polymerase chain reaction sequencing was significantly better at identifying fungal chronic rhinosinusitis (CRS) than were cultures, according to Dr. Pauline Comacle and her associates.
A total of 70 samples from 61 patients with CRS were tested via the use of polymerase chain reaction (PCR) testing and cultures. Fungal CRS was identified in 42 patients, of whom 37 had a fungus ball, 3 had allergic fungal CRS, and 2 had unspecified fungal CRS. ITS1/ITS2 PCR sequencing successfully identified fungal CRS in all patients, while cultures were positive for fungal CRS in 20 of the 42 patients.
Aspergillus fumigatus was the most common fungus in the study, occurring in 69% of patients. Cladosporium cladosporoides occurred in 9.5% of patients, and A. nidulans, A. flavus, and Scedosporium species each occurred in 7% of patients.
“This study nicely shows that molecular methods are powerful tools for the diagnosis of chronic rhinosinusitis and help in characterizing the accurate epidemiology of fungal CRS,” the investigators concluded.
Find the full study in Medical Mycology (doi: 10.1093/mmy/myw041).
ITS1/ITS2 polymerase chain reaction sequencing was significantly better at identifying fungal chronic rhinosinusitis (CRS) than were cultures, according to Dr. Pauline Comacle and her associates.
A total of 70 samples from 61 patients with CRS were tested via the use of polymerase chain reaction (PCR) testing and cultures. Fungal CRS was identified in 42 patients, of whom 37 had a fungus ball, 3 had allergic fungal CRS, and 2 had unspecified fungal CRS. ITS1/ITS2 PCR sequencing successfully identified fungal CRS in all patients, while cultures were positive for fungal CRS in 20 of the 42 patients.
Aspergillus fumigatus was the most common fungus in the study, occurring in 69% of patients. Cladosporium cladosporoides occurred in 9.5% of patients, and A. nidulans, A. flavus, and Scedosporium species each occurred in 7% of patients.
“This study nicely shows that molecular methods are powerful tools for the diagnosis of chronic rhinosinusitis and help in characterizing the accurate epidemiology of fungal CRS,” the investigators concluded.
Find the full study in Medical Mycology (doi: 10.1093/mmy/myw041).
ITS1/ITS2 polymerase chain reaction sequencing was significantly better at identifying fungal chronic rhinosinusitis (CRS) than were cultures, according to Dr. Pauline Comacle and her associates.
A total of 70 samples from 61 patients with CRS were tested via the use of polymerase chain reaction (PCR) testing and cultures. Fungal CRS was identified in 42 patients, of whom 37 had a fungus ball, 3 had allergic fungal CRS, and 2 had unspecified fungal CRS. ITS1/ITS2 PCR sequencing successfully identified fungal CRS in all patients, while cultures were positive for fungal CRS in 20 of the 42 patients.
Aspergillus fumigatus was the most common fungus in the study, occurring in 69% of patients. Cladosporium cladosporoides occurred in 9.5% of patients, and A. nidulans, A. flavus, and Scedosporium species each occurred in 7% of patients.
“This study nicely shows that molecular methods are powerful tools for the diagnosis of chronic rhinosinusitis and help in characterizing the accurate epidemiology of fungal CRS,” the investigators concluded.
Find the full study in Medical Mycology (doi: 10.1093/mmy/myw041).
FROM MEDICAL MYCOLOGY
Dexlansoprazole Approved to Treat Heartburn in Younger Patients
The Food and Drug Administration has approved dexlansoprazole (Dexilant) for gastroesophageal reflux disease patients aged 12-17 years, according to a press release from Takeda Pharmaceuticals.
FDA approval of dexlansoprazole for this age group is based on adequate and well controlled studies proving its efficacy in adults, as well data on safety, pharmacokinetics, and efficacy in children 12-17 years. Dexlansoprazole is approved for younger patients to maintain healing of erosive esophagus and heartburn relief for 16 weeks, healing all grades of EE for 8 weeks, and treating heartburn associated with GERD for 4 weeks.
Ddexlansoprazole is a proton pump inhibitor, prescribed to relieve heartburn associated with GERD and maintain healed erosive esophagus. The most common side effects seen in individuals aged 12-17 were headache, abdominal pain, diarrhea, nasopharyngitis, and oropharyngeal pain.
“Takeda is pleased with the FDA’s approval to expand the access of Dexilant to younger patients with GERD. This new approval provides an alternative treatment option for appropriate patients with this condition. With our more than 20 years of experience in gastroenterology, we remain dedicated to all patients living with these conditions,” noted Thomas Gibbs, senior vice president of general medicine at Takeda.
Find the full press release on the Takeda Pharmaceuticals website.
The Food and Drug Administration has approved dexlansoprazole (Dexilant) for gastroesophageal reflux disease patients aged 12-17 years, according to a press release from Takeda Pharmaceuticals.
FDA approval of dexlansoprazole for this age group is based on adequate and well controlled studies proving its efficacy in adults, as well data on safety, pharmacokinetics, and efficacy in children 12-17 years. Dexlansoprazole is approved for younger patients to maintain healing of erosive esophagus and heartburn relief for 16 weeks, healing all grades of EE for 8 weeks, and treating heartburn associated with GERD for 4 weeks.
Ddexlansoprazole is a proton pump inhibitor, prescribed to relieve heartburn associated with GERD and maintain healed erosive esophagus. The most common side effects seen in individuals aged 12-17 were headache, abdominal pain, diarrhea, nasopharyngitis, and oropharyngeal pain.
“Takeda is pleased with the FDA’s approval to expand the access of Dexilant to younger patients with GERD. This new approval provides an alternative treatment option for appropriate patients with this condition. With our more than 20 years of experience in gastroenterology, we remain dedicated to all patients living with these conditions,” noted Thomas Gibbs, senior vice president of general medicine at Takeda.
Find the full press release on the Takeda Pharmaceuticals website.
The Food and Drug Administration has approved dexlansoprazole (Dexilant) for gastroesophageal reflux disease patients aged 12-17 years, according to a press release from Takeda Pharmaceuticals.
FDA approval of dexlansoprazole for this age group is based on adequate and well controlled studies proving its efficacy in adults, as well data on safety, pharmacokinetics, and efficacy in children 12-17 years. Dexlansoprazole is approved for younger patients to maintain healing of erosive esophagus and heartburn relief for 16 weeks, healing all grades of EE for 8 weeks, and treating heartburn associated with GERD for 4 weeks.
Ddexlansoprazole is a proton pump inhibitor, prescribed to relieve heartburn associated with GERD and maintain healed erosive esophagus. The most common side effects seen in individuals aged 12-17 were headache, abdominal pain, diarrhea, nasopharyngitis, and oropharyngeal pain.
“Takeda is pleased with the FDA’s approval to expand the access of Dexilant to younger patients with GERD. This new approval provides an alternative treatment option for appropriate patients with this condition. With our more than 20 years of experience in gastroenterology, we remain dedicated to all patients living with these conditions,” noted Thomas Gibbs, senior vice president of general medicine at Takeda.
Find the full press release on the Takeda Pharmaceuticals website.
Dexlansoprazole approved to treat heartburn in younger patients
The Food and Drug Administration has approved dexlansoprazole (Dexilant) for gastroesophageal reflux disease patients aged 12-17 years, according to a press release from Takeda Pharmaceuticals.
FDA approval of dexlansoprazole for this age group is based on adequate and well controlled studies proving its efficacy in adults, as well data on safety, pharmacokinetics, and efficacy in children 12-17 years. Dexlansoprazole is approved for younger patients to maintain healing of erosive esophagus and heartburn relief for 16 weeks, healing all grades of EE for 8 weeks, and treating heartburn associated with GERD for 4 weeks.
Ddexlansoprazole is a proton pump inhibitor, prescribed to relieve heartburn associated with GERD and maintain healed erosive esophagus. The most common side effects seen in individuals aged 12-17 were headache, abdominal pain, diarrhea, nasopharyngitis, and oropharyngeal pain.
“Takeda is pleased with the FDA’s approval to expand the access of Dexilant to younger patients with GERD. This new approval provides an alternative treatment option for appropriate patients with this condition. With our more than 20 years of experience in gastroenterology, we remain dedicated to all patients living with these conditions,” noted Thomas Gibbs, senior vice president of general medicine at Takeda.
Find the full press release on the Takeda Pharmaceuticals website.
The Food and Drug Administration has approved dexlansoprazole (Dexilant) for gastroesophageal reflux disease patients aged 12-17 years, according to a press release from Takeda Pharmaceuticals.
FDA approval of dexlansoprazole for this age group is based on adequate and well controlled studies proving its efficacy in adults, as well data on safety, pharmacokinetics, and efficacy in children 12-17 years. Dexlansoprazole is approved for younger patients to maintain healing of erosive esophagus and heartburn relief for 16 weeks, healing all grades of EE for 8 weeks, and treating heartburn associated with GERD for 4 weeks.
Ddexlansoprazole is a proton pump inhibitor, prescribed to relieve heartburn associated with GERD and maintain healed erosive esophagus. The most common side effects seen in individuals aged 12-17 were headache, abdominal pain, diarrhea, nasopharyngitis, and oropharyngeal pain.
“Takeda is pleased with the FDA’s approval to expand the access of Dexilant to younger patients with GERD. This new approval provides an alternative treatment option for appropriate patients with this condition. With our more than 20 years of experience in gastroenterology, we remain dedicated to all patients living with these conditions,” noted Thomas Gibbs, senior vice president of general medicine at Takeda.
Find the full press release on the Takeda Pharmaceuticals website.
The Food and Drug Administration has approved dexlansoprazole (Dexilant) for gastroesophageal reflux disease patients aged 12-17 years, according to a press release from Takeda Pharmaceuticals.
FDA approval of dexlansoprazole for this age group is based on adequate and well controlled studies proving its efficacy in adults, as well data on safety, pharmacokinetics, and efficacy in children 12-17 years. Dexlansoprazole is approved for younger patients to maintain healing of erosive esophagus and heartburn relief for 16 weeks, healing all grades of EE for 8 weeks, and treating heartburn associated with GERD for 4 weeks.
Ddexlansoprazole is a proton pump inhibitor, prescribed to relieve heartburn associated with GERD and maintain healed erosive esophagus. The most common side effects seen in individuals aged 12-17 were headache, abdominal pain, diarrhea, nasopharyngitis, and oropharyngeal pain.
“Takeda is pleased with the FDA’s approval to expand the access of Dexilant to younger patients with GERD. This new approval provides an alternative treatment option for appropriate patients with this condition. With our more than 20 years of experience in gastroenterology, we remain dedicated to all patients living with these conditions,” noted Thomas Gibbs, senior vice president of general medicine at Takeda.
Find the full press release on the Takeda Pharmaceuticals website.
Radiographic vertebral fractures common in ankylosing spondylitis patients
Radiographic vertebral fractures occur frequently in patients with ankylosing spondylitis, according to Dr. Fiona Maas and her associates.
At baseline, 59 (20%) of the 292 patients included in a prospective cohort study had radiographic vertebral fractures. During a 2-year follow-up period, 15 patients developed new fractures and 7 patients experienced an increase in severity of current fractures. A significant majority of fractures were defined as mild, and most were located in the mid-thoracic and thoracolumbar regions of the spine.
Fractures were more likely in patients who were older, had a higher body mass index, had smoked for long durations, had larger occiput-to-wall distances, had more spinal radiographic damage, and had lower hip bone mineral density (BMD). Patients who developed new fractures during the study period were older and had lower hip BMD. Incidence and prevalence of fractures was reduced in patients who were receiving nonsteroidal anti-inflammatory drugs (NSAIDs) at baseline.
“The influence of anti-inflammatory drugs (e.g. NSAIDs, TNF-alpha inhibitors), anti-osteoporotic treatment (e.g. calcium/vitamin D supplements, bisphosphonates), and lifestyle changes (e.g. smoking cessation, body weight control, physical exercise) on the development of vertebral fractures in AS should be further investigated in a large study population with long-term follow-up,” the investigators concluded.
Find the full study in Arthritis Care & Research (doi: 10.1002/acr.22980).
Radiographic vertebral fractures occur frequently in patients with ankylosing spondylitis, according to Dr. Fiona Maas and her associates.
At baseline, 59 (20%) of the 292 patients included in a prospective cohort study had radiographic vertebral fractures. During a 2-year follow-up period, 15 patients developed new fractures and 7 patients experienced an increase in severity of current fractures. A significant majority of fractures were defined as mild, and most were located in the mid-thoracic and thoracolumbar regions of the spine.
Fractures were more likely in patients who were older, had a higher body mass index, had smoked for long durations, had larger occiput-to-wall distances, had more spinal radiographic damage, and had lower hip bone mineral density (BMD). Patients who developed new fractures during the study period were older and had lower hip BMD. Incidence and prevalence of fractures was reduced in patients who were receiving nonsteroidal anti-inflammatory drugs (NSAIDs) at baseline.
“The influence of anti-inflammatory drugs (e.g. NSAIDs, TNF-alpha inhibitors), anti-osteoporotic treatment (e.g. calcium/vitamin D supplements, bisphosphonates), and lifestyle changes (e.g. smoking cessation, body weight control, physical exercise) on the development of vertebral fractures in AS should be further investigated in a large study population with long-term follow-up,” the investigators concluded.
Find the full study in Arthritis Care & Research (doi: 10.1002/acr.22980).
Radiographic vertebral fractures occur frequently in patients with ankylosing spondylitis, according to Dr. Fiona Maas and her associates.
At baseline, 59 (20%) of the 292 patients included in a prospective cohort study had radiographic vertebral fractures. During a 2-year follow-up period, 15 patients developed new fractures and 7 patients experienced an increase in severity of current fractures. A significant majority of fractures were defined as mild, and most were located in the mid-thoracic and thoracolumbar regions of the spine.
Fractures were more likely in patients who were older, had a higher body mass index, had smoked for long durations, had larger occiput-to-wall distances, had more spinal radiographic damage, and had lower hip bone mineral density (BMD). Patients who developed new fractures during the study period were older and had lower hip BMD. Incidence and prevalence of fractures was reduced in patients who were receiving nonsteroidal anti-inflammatory drugs (NSAIDs) at baseline.
“The influence of anti-inflammatory drugs (e.g. NSAIDs, TNF-alpha inhibitors), anti-osteoporotic treatment (e.g. calcium/vitamin D supplements, bisphosphonates), and lifestyle changes (e.g. smoking cessation, body weight control, physical exercise) on the development of vertebral fractures in AS should be further investigated in a large study population with long-term follow-up,” the investigators concluded.
Find the full study in Arthritis Care & Research (doi: 10.1002/acr.22980).
FROM ARTHRITIS CARE & RESEARCH
Telephone triage system can help predict dengue outbreaks
Data collected by a telephone-based hotline system can be used to effectively predict outbreaks of dengue in developing countries weeks ahead of time, according to researchers in Pakistan.
After an outbreak of dengue in Lahore, Pakistan, in 2011, a phone-based helpline system was set up by the province of Punjab to combat the epidemic and to improve surveillance and rapid response capabilities. The system received more than 300,000 calls from September 2011 through the end of 2013, and during the three peaks of dengue cases during that time, calls to the help center strongly correlated to an increase in suspected dengue cases.
While calls correlated to outbreaks, the call system alone left some gaps. During the first peak in 2013, when campaign awareness activity was low, comparatively fewer calls were received. The model used in Punjab also factored in weather, and successfully predicted increases in dengue cases at a subcity level 2-3 weeks in advance. As a result, total case incidence in Punjab decreased from 21,000 in 2011 to 257 in 2012 and to 1,600 in 2013.
“Our system has helped public health officials to take early actions to contain the spread of the disease and provide hospitals an early warning of dengue cases in their vicinity. We believe that this system can also be used for a broad array of diseases beyond dengue and can easily be replicated in other developing countries at low costs,” the investigators concluded.
Read the full study in Science Advances (doi: 10.1126/sciadv.1501215).
Data collected by a telephone-based hotline system can be used to effectively predict outbreaks of dengue in developing countries weeks ahead of time, according to researchers in Pakistan.
After an outbreak of dengue in Lahore, Pakistan, in 2011, a phone-based helpline system was set up by the province of Punjab to combat the epidemic and to improve surveillance and rapid response capabilities. The system received more than 300,000 calls from September 2011 through the end of 2013, and during the three peaks of dengue cases during that time, calls to the help center strongly correlated to an increase in suspected dengue cases.
While calls correlated to outbreaks, the call system alone left some gaps. During the first peak in 2013, when campaign awareness activity was low, comparatively fewer calls were received. The model used in Punjab also factored in weather, and successfully predicted increases in dengue cases at a subcity level 2-3 weeks in advance. As a result, total case incidence in Punjab decreased from 21,000 in 2011 to 257 in 2012 and to 1,600 in 2013.
“Our system has helped public health officials to take early actions to contain the spread of the disease and provide hospitals an early warning of dengue cases in their vicinity. We believe that this system can also be used for a broad array of diseases beyond dengue and can easily be replicated in other developing countries at low costs,” the investigators concluded.
Read the full study in Science Advances (doi: 10.1126/sciadv.1501215).
Data collected by a telephone-based hotline system can be used to effectively predict outbreaks of dengue in developing countries weeks ahead of time, according to researchers in Pakistan.
After an outbreak of dengue in Lahore, Pakistan, in 2011, a phone-based helpline system was set up by the province of Punjab to combat the epidemic and to improve surveillance and rapid response capabilities. The system received more than 300,000 calls from September 2011 through the end of 2013, and during the three peaks of dengue cases during that time, calls to the help center strongly correlated to an increase in suspected dengue cases.
While calls correlated to outbreaks, the call system alone left some gaps. During the first peak in 2013, when campaign awareness activity was low, comparatively fewer calls were received. The model used in Punjab also factored in weather, and successfully predicted increases in dengue cases at a subcity level 2-3 weeks in advance. As a result, total case incidence in Punjab decreased from 21,000 in 2011 to 257 in 2012 and to 1,600 in 2013.
“Our system has helped public health officials to take early actions to contain the spread of the disease and provide hospitals an early warning of dengue cases in their vicinity. We believe that this system can also be used for a broad array of diseases beyond dengue and can easily be replicated in other developing countries at low costs,” the investigators concluded.
Read the full study in Science Advances (doi: 10.1126/sciadv.1501215).
FROM SCIENCE ADVANCES
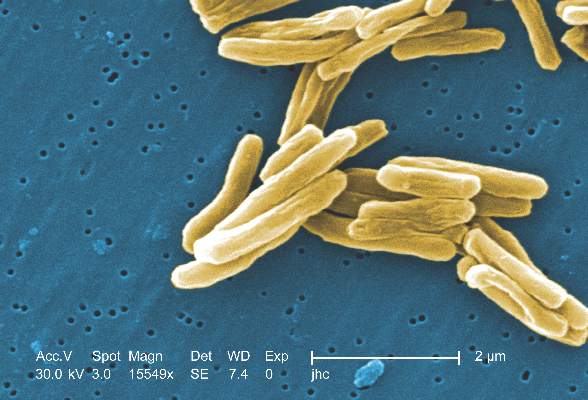
MPT64 rapid test may miss TB caused by M. africanum strain
Tuberculosis caused by Mycobacterium africanum West Africa 2 is significantly less likely to be detected by a MPT64 rapid antigen test than is M. tuberculosis, according to a research team based in the Gambia.
A total of 173 MGIT culture-positive sputum samples were included in the study, and the initial MPT64 test was negative in 23 samples. Just over 90% of M. tuberculosis (MTB) samples converted to positive on day 0, while only 78.4% of M. africanum West Africa 2 (MAF2) samples converted. After 10 days, 97.5% of MTB samples were positive, while conversion of MAF2 samples remained low at 84.3%.
In a comparison of the mRNA transcript from samples of six MTB and five MAF2 patients who had not been treated for TB, the MTP64 gene was about 2.5 times more abundant in the MTB samples than the MAF2 samples. No association was found between conversion to positivity and sex, age, therapy, or mycobacterial growth units.
“Given the relatively low cost, limited technical expertise, and shorter turnaround time associated with using rapid speciation tests, compared to alternative speciation methods, MPT64 rapid tests will likely remain one of the preferred options for timely diagnosis of suspected TB despite the possibility of false negative results. Therefore, a negative MPT64 result would require confirmation by an alternative method, such as molecular tests or culture on p-nitrobenzoic acid, depending on laboratory infrastructure and resources,” the investigators noted.
Read the full study in PLoS Neglected Tropical Diseases (doi:10.1371/journal.pntd.0004801).
Tuberculosis caused by Mycobacterium africanum West Africa 2 is significantly less likely to be detected by a MPT64 rapid antigen test than is M. tuberculosis, according to a research team based in the Gambia.
A total of 173 MGIT culture-positive sputum samples were included in the study, and the initial MPT64 test was negative in 23 samples. Just over 90% of M. tuberculosis (MTB) samples converted to positive on day 0, while only 78.4% of M. africanum West Africa 2 (MAF2) samples converted. After 10 days, 97.5% of MTB samples were positive, while conversion of MAF2 samples remained low at 84.3%.
In a comparison of the mRNA transcript from samples of six MTB and five MAF2 patients who had not been treated for TB, the MTP64 gene was about 2.5 times more abundant in the MTB samples than the MAF2 samples. No association was found between conversion to positivity and sex, age, therapy, or mycobacterial growth units.
“Given the relatively low cost, limited technical expertise, and shorter turnaround time associated with using rapid speciation tests, compared to alternative speciation methods, MPT64 rapid tests will likely remain one of the preferred options for timely diagnosis of suspected TB despite the possibility of false negative results. Therefore, a negative MPT64 result would require confirmation by an alternative method, such as molecular tests or culture on p-nitrobenzoic acid, depending on laboratory infrastructure and resources,” the investigators noted.
Read the full study in PLoS Neglected Tropical Diseases (doi:10.1371/journal.pntd.0004801).
Tuberculosis caused by Mycobacterium africanum West Africa 2 is significantly less likely to be detected by a MPT64 rapid antigen test than is M. tuberculosis, according to a research team based in the Gambia.
A total of 173 MGIT culture-positive sputum samples were included in the study, and the initial MPT64 test was negative in 23 samples. Just over 90% of M. tuberculosis (MTB) samples converted to positive on day 0, while only 78.4% of M. africanum West Africa 2 (MAF2) samples converted. After 10 days, 97.5% of MTB samples were positive, while conversion of MAF2 samples remained low at 84.3%.
In a comparison of the mRNA transcript from samples of six MTB and five MAF2 patients who had not been treated for TB, the MTP64 gene was about 2.5 times more abundant in the MTB samples than the MAF2 samples. No association was found between conversion to positivity and sex, age, therapy, or mycobacterial growth units.
“Given the relatively low cost, limited technical expertise, and shorter turnaround time associated with using rapid speciation tests, compared to alternative speciation methods, MPT64 rapid tests will likely remain one of the preferred options for timely diagnosis of suspected TB despite the possibility of false negative results. Therefore, a negative MPT64 result would require confirmation by an alternative method, such as molecular tests or culture on p-nitrobenzoic acid, depending on laboratory infrastructure and resources,” the investigators noted.
Read the full study in PLoS Neglected Tropical Diseases (doi:10.1371/journal.pntd.0004801).
FROM PLOS NEGLECTED TROPICAL DISEASES
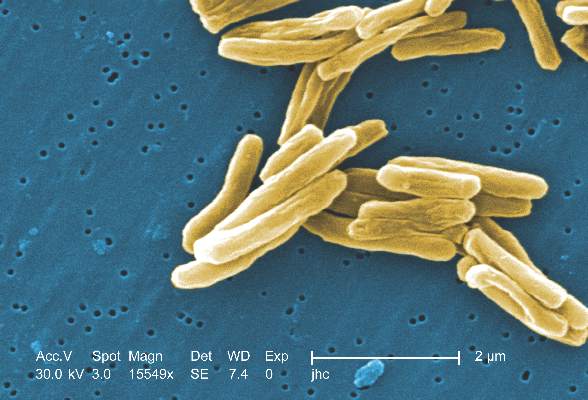
MPT64 rapid test may miss TB caused by M. africanum strain
Tuberculosis caused by Mycobacterium africanum West Africa 2 is significantly less likely to be detected by a MPT64 rapid antigen test than is M. tuberculosis, according to a research team based in the Gambia.
A total of 173 MGIT culture-positive sputum samples were included in the study, and the initial MPT64 test was negative in 23 samples. Just over 90% of M. tuberculosis (MTB) samples converted to positive on day 0, while only 78.4% of M. africanum West Africa 2 (MAF2) samples converted. After 10 days, 97.5% of MTB samples were positive, while conversion of MAF2 samples remained low at 84.3%.
In a comparison of the mRNA transcript from samples of six MTB and five MAF2 patients who had not been treated for TB, the MTP64 gene was about 2.5 times more abundant in the MTB samples than the MAF2 samples. No association was found between conversion to positivity and sex, age, therapy, or mycobacterial growth units.
“Given the relatively low cost, limited technical expertise, and shorter turnaround time associated with using rapid speciation tests, compared to alternative speciation methods, MPT64 rapid tests will likely remain one of the preferred options for timely diagnosis of suspected TB despite the possibility of false negative results. Therefore, a negative MPT64 result would require confirmation by an alternative method, such as molecular tests or culture on p-nitrobenzoic acid, depending on laboratory infrastructure and resources,” the investigators noted.
Read the full study in PLoS Neglected Tropical Diseases (doi:10.1371/journal.pntd.0004801).
Tuberculosis caused by Mycobacterium africanum West Africa 2 is significantly less likely to be detected by a MPT64 rapid antigen test than is M. tuberculosis, according to a research team based in the Gambia.
A total of 173 MGIT culture-positive sputum samples were included in the study, and the initial MPT64 test was negative in 23 samples. Just over 90% of M. tuberculosis (MTB) samples converted to positive on day 0, while only 78.4% of M. africanum West Africa 2 (MAF2) samples converted. After 10 days, 97.5% of MTB samples were positive, while conversion of MAF2 samples remained low at 84.3%.
In a comparison of the mRNA transcript from samples of six MTB and five MAF2 patients who had not been treated for TB, the MTP64 gene was about 2.5 times more abundant in the MTB samples than the MAF2 samples. No association was found between conversion to positivity and sex, age, therapy, or mycobacterial growth units.
“Given the relatively low cost, limited technical expertise, and shorter turnaround time associated with using rapid speciation tests, compared to alternative speciation methods, MPT64 rapid tests will likely remain one of the preferred options for timely diagnosis of suspected TB despite the possibility of false negative results. Therefore, a negative MPT64 result would require confirmation by an alternative method, such as molecular tests or culture on p-nitrobenzoic acid, depending on laboratory infrastructure and resources,” the investigators noted.
Read the full study in PLoS Neglected Tropical Diseases (doi:10.1371/journal.pntd.0004801).
Tuberculosis caused by Mycobacterium africanum West Africa 2 is significantly less likely to be detected by a MPT64 rapid antigen test than is M. tuberculosis, according to a research team based in the Gambia.
A total of 173 MGIT culture-positive sputum samples were included in the study, and the initial MPT64 test was negative in 23 samples. Just over 90% of M. tuberculosis (MTB) samples converted to positive on day 0, while only 78.4% of M. africanum West Africa 2 (MAF2) samples converted. After 10 days, 97.5% of MTB samples were positive, while conversion of MAF2 samples remained low at 84.3%.
In a comparison of the mRNA transcript from samples of six MTB and five MAF2 patients who had not been treated for TB, the MTP64 gene was about 2.5 times more abundant in the MTB samples than the MAF2 samples. No association was found between conversion to positivity and sex, age, therapy, or mycobacterial growth units.
“Given the relatively low cost, limited technical expertise, and shorter turnaround time associated with using rapid speciation tests, compared to alternative speciation methods, MPT64 rapid tests will likely remain one of the preferred options for timely diagnosis of suspected TB despite the possibility of false negative results. Therefore, a negative MPT64 result would require confirmation by an alternative method, such as molecular tests or culture on p-nitrobenzoic acid, depending on laboratory infrastructure and resources,” the investigators noted.
Read the full study in PLoS Neglected Tropical Diseases (doi:10.1371/journal.pntd.0004801).
FROM PLOS NEGLECTED TROPICAL DISEASES