User login
A nonhealing oral ulcer in a man with HIV
A 44-year-old man presented with a 3-week history of a painless, nonhealing ulcer affecting the mucosa in the right angle of the mouth. He reported no fever, weight loss, or systemic symptoms of chronic disease. His medical history included chronic hepatitis C infection and human immunodeficiency virus (HIV) infection; his antiretroviral regimen for HIV was abacavir, lamivudine, and darunavir. His CD4+ T-cell count was 153 cells/mm3, and his viral load was 154.88 copies/mL. He formerly used injected drugs, and he currently smoked 20 cigarettes a day. He had no history of periodontal disease.
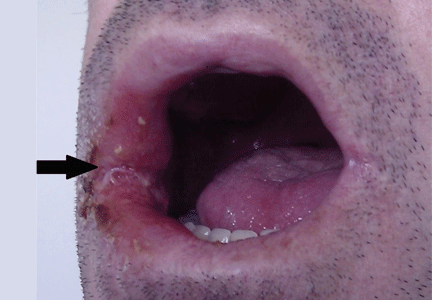
Oral examination showed poor oral hygiene and a solitary ulcerated lesion with an infiltrated base and indurated borders in the right oral commissure (Figure 1). There was also soft-tissue induration in the ipsilateral cheek. He had no other oral lesions or signs of neck lymphadenopathy.
Based on the clinical examination, a provisional diagnosis of malignancy was suspected, and an incisional biopsy of the ulcer was done. The findings on histopathologic study of the biopsy specimen (below; Figure 2) led to additional evaluation with chest radiography and thoracic computed tomography (Figure 3).
FURTHER WORKUP
Histologic study of the biopsy specimen showed ulcerated mucosa with extensive granulomatous inflammation and with caseation necrosis. Ziehl-Neelsen staining demonstrated a few acid-fast bacilli. The patient was then evaluated for pulmonary tuberculosis.
Chest radiography showed pulmonary infiltrates in both bases and the upper right lobe and cavitation in the upper left lobe. Thoracic computed tomography confirmed the presence of multiple cavitated lesions in both left and right lung fields. Sputum cultures were positive for Mycobacterium tuberculosis, an organism sensitive to several agents. Laboratory investigations that included blood cell counts, biochemical tests, and liver and kidney function tests were normal, with the exception of a low lymphocyte count.
ORAL TUBERCULOSIS SECONDARY TO ACTIVE PULMONARY TUBERCULOSIS
Even though the incidence of extrapulmonary tuberculosis has been increasing worldwide in recent years, cutaneous manifestations are uncommon (2% to 10%) and are seen mainly in immunosuppressed patients with coexisting tuberculosis infection of internal organs.1 Oral manifestations of tuberculosis are extremely rare, accounting for 2% of cases of cutaneous manifestations.1,2 For this reason and because of its clinical heterogeneity, oral tuberculosis is often not considered in the differential diagnosis of oral lesions.
The differential diagnosis of oral ulcers in patients with HIV includes adverse drug reactions (eg, nevirapine-induced Stevens-Johnson syndrome); oral ulcers and necrotizing gingivitis related to HIV-associated neutropenia; aphthous ulcers; oral ulcers in reactive arthritis; malignancies such as lymphoma, Kaposi sarcoma, and squamous cell carcinoma; and infections such as candidiasis, herpes simplex virus, cytomegalovirus, primary syphilis, mucosal leishmaniasis, histoplasmosis, and periorificial tuberculosis. Periorificial tuberculosis is more commonly seen in HIV patients, in whom extrapulmonary forms of tuberculosis are frequent.3
Oral tuberculosis is often mistaken for a malignancy such as squamous cell carcinoma; in fact, carcinoma coexists with tubercular ulcer in up to 3% of patients.2 The typical clinical presentation of oral tuberculosis is one or more painful or painless ulcers with irregular borders, usually localized on the tongue (nearly half of cases4), and less frequently affecting the lip, buccal mucosa, gingiva, soft palate, and extraction sockets. It can also present as a nodule, fissure, vesicle, tuberculoma, tubercular papilloma, or periapical granuloma.2,5
Oral tuberculosis may be primary but is more commonly secondary to internal-organ tuberculosis. Secondary disease is seen in patients with pulmonary forms (affecting 0.05% to 1.5% of patients with pulmonary tuberculosis1,2) because of autoinoculation by infected sputum or hematogenous spread.1,4,5
Clinicians should consider oral tuberculosis in the differential diagnosis of a nonhealing ulcer of the mouth, particularly in an immunosuppressed patient such as ours. It is also important to highlight the necessity of searching for a primary site of infection, more frequently in the lungs.
- Kiliç A, Gül U, Gönül M, Soylu S, Cakmak SK, Demiriz M. Orificial tuberculosis of the lip: a case report and review of the literature. Int J Dermatol 2009; 48:178–180.
- Ram H, Kumar S, Mehrotra S, Mohommad S. Tubercular ulcer: mimicking squamous cell carcinoma of buccal mucosa. J Maxillofac Oral Surg 2012; 11:105–108.
- Frezzini C, Leao JC, Porter S. Current trends of HIV disease of the mouth. J Oral Pathol Med 2005; 34:513–531.
- Chauhan V, Mahesh DM, Panda P, Mahajan S, Thakur S. Tuberculosis cutis orificialis (TBCO): a rare manifestation of tuberculosis. J Assoc Physicians India 2012; 60:126–127.
- Kannan S, Thakkar P, Dcruz AK. Tuberculosis masquerading as oral malignancy. Indian J Med Paediatr Oncol 2011; 32:180–182.
A 44-year-old man presented with a 3-week history of a painless, nonhealing ulcer affecting the mucosa in the right angle of the mouth. He reported no fever, weight loss, or systemic symptoms of chronic disease. His medical history included chronic hepatitis C infection and human immunodeficiency virus (HIV) infection; his antiretroviral regimen for HIV was abacavir, lamivudine, and darunavir. His CD4+ T-cell count was 153 cells/mm3, and his viral load was 154.88 copies/mL. He formerly used injected drugs, and he currently smoked 20 cigarettes a day. He had no history of periodontal disease.
Oral examination showed poor oral hygiene and a solitary ulcerated lesion with an infiltrated base and indurated borders in the right oral commissure (Figure 1). There was also soft-tissue induration in the ipsilateral cheek. He had no other oral lesions or signs of neck lymphadenopathy.
Based on the clinical examination, a provisional diagnosis of malignancy was suspected, and an incisional biopsy of the ulcer was done. The findings on histopathologic study of the biopsy specimen (below; Figure 2) led to additional evaluation with chest radiography and thoracic computed tomography (Figure 3).
FURTHER WORKUP
Histologic study of the biopsy specimen showed ulcerated mucosa with extensive granulomatous inflammation and with caseation necrosis. Ziehl-Neelsen staining demonstrated a few acid-fast bacilli. The patient was then evaluated for pulmonary tuberculosis.
Chest radiography showed pulmonary infiltrates in both bases and the upper right lobe and cavitation in the upper left lobe. Thoracic computed tomography confirmed the presence of multiple cavitated lesions in both left and right lung fields. Sputum cultures were positive for Mycobacterium tuberculosis, an organism sensitive to several agents. Laboratory investigations that included blood cell counts, biochemical tests, and liver and kidney function tests were normal, with the exception of a low lymphocyte count.
ORAL TUBERCULOSIS SECONDARY TO ACTIVE PULMONARY TUBERCULOSIS
Even though the incidence of extrapulmonary tuberculosis has been increasing worldwide in recent years, cutaneous manifestations are uncommon (2% to 10%) and are seen mainly in immunosuppressed patients with coexisting tuberculosis infection of internal organs.1 Oral manifestations of tuberculosis are extremely rare, accounting for 2% of cases of cutaneous manifestations.1,2 For this reason and because of its clinical heterogeneity, oral tuberculosis is often not considered in the differential diagnosis of oral lesions.
The differential diagnosis of oral ulcers in patients with HIV includes adverse drug reactions (eg, nevirapine-induced Stevens-Johnson syndrome); oral ulcers and necrotizing gingivitis related to HIV-associated neutropenia; aphthous ulcers; oral ulcers in reactive arthritis; malignancies such as lymphoma, Kaposi sarcoma, and squamous cell carcinoma; and infections such as candidiasis, herpes simplex virus, cytomegalovirus, primary syphilis, mucosal leishmaniasis, histoplasmosis, and periorificial tuberculosis. Periorificial tuberculosis is more commonly seen in HIV patients, in whom extrapulmonary forms of tuberculosis are frequent.3
Oral tuberculosis is often mistaken for a malignancy such as squamous cell carcinoma; in fact, carcinoma coexists with tubercular ulcer in up to 3% of patients.2 The typical clinical presentation of oral tuberculosis is one or more painful or painless ulcers with irregular borders, usually localized on the tongue (nearly half of cases4), and less frequently affecting the lip, buccal mucosa, gingiva, soft palate, and extraction sockets. It can also present as a nodule, fissure, vesicle, tuberculoma, tubercular papilloma, or periapical granuloma.2,5
Oral tuberculosis may be primary but is more commonly secondary to internal-organ tuberculosis. Secondary disease is seen in patients with pulmonary forms (affecting 0.05% to 1.5% of patients with pulmonary tuberculosis1,2) because of autoinoculation by infected sputum or hematogenous spread.1,4,5
Clinicians should consider oral tuberculosis in the differential diagnosis of a nonhealing ulcer of the mouth, particularly in an immunosuppressed patient such as ours. It is also important to highlight the necessity of searching for a primary site of infection, more frequently in the lungs.
A 44-year-old man presented with a 3-week history of a painless, nonhealing ulcer affecting the mucosa in the right angle of the mouth. He reported no fever, weight loss, or systemic symptoms of chronic disease. His medical history included chronic hepatitis C infection and human immunodeficiency virus (HIV) infection; his antiretroviral regimen for HIV was abacavir, lamivudine, and darunavir. His CD4+ T-cell count was 153 cells/mm3, and his viral load was 154.88 copies/mL. He formerly used injected drugs, and he currently smoked 20 cigarettes a day. He had no history of periodontal disease.
Oral examination showed poor oral hygiene and a solitary ulcerated lesion with an infiltrated base and indurated borders in the right oral commissure (Figure 1). There was also soft-tissue induration in the ipsilateral cheek. He had no other oral lesions or signs of neck lymphadenopathy.
Based on the clinical examination, a provisional diagnosis of malignancy was suspected, and an incisional biopsy of the ulcer was done. The findings on histopathologic study of the biopsy specimen (below; Figure 2) led to additional evaluation with chest radiography and thoracic computed tomography (Figure 3).
FURTHER WORKUP
Histologic study of the biopsy specimen showed ulcerated mucosa with extensive granulomatous inflammation and with caseation necrosis. Ziehl-Neelsen staining demonstrated a few acid-fast bacilli. The patient was then evaluated for pulmonary tuberculosis.
Chest radiography showed pulmonary infiltrates in both bases and the upper right lobe and cavitation in the upper left lobe. Thoracic computed tomography confirmed the presence of multiple cavitated lesions in both left and right lung fields. Sputum cultures were positive for Mycobacterium tuberculosis, an organism sensitive to several agents. Laboratory investigations that included blood cell counts, biochemical tests, and liver and kidney function tests were normal, with the exception of a low lymphocyte count.
ORAL TUBERCULOSIS SECONDARY TO ACTIVE PULMONARY TUBERCULOSIS
Even though the incidence of extrapulmonary tuberculosis has been increasing worldwide in recent years, cutaneous manifestations are uncommon (2% to 10%) and are seen mainly in immunosuppressed patients with coexisting tuberculosis infection of internal organs.1 Oral manifestations of tuberculosis are extremely rare, accounting for 2% of cases of cutaneous manifestations.1,2 For this reason and because of its clinical heterogeneity, oral tuberculosis is often not considered in the differential diagnosis of oral lesions.
The differential diagnosis of oral ulcers in patients with HIV includes adverse drug reactions (eg, nevirapine-induced Stevens-Johnson syndrome); oral ulcers and necrotizing gingivitis related to HIV-associated neutropenia; aphthous ulcers; oral ulcers in reactive arthritis; malignancies such as lymphoma, Kaposi sarcoma, and squamous cell carcinoma; and infections such as candidiasis, herpes simplex virus, cytomegalovirus, primary syphilis, mucosal leishmaniasis, histoplasmosis, and periorificial tuberculosis. Periorificial tuberculosis is more commonly seen in HIV patients, in whom extrapulmonary forms of tuberculosis are frequent.3
Oral tuberculosis is often mistaken for a malignancy such as squamous cell carcinoma; in fact, carcinoma coexists with tubercular ulcer in up to 3% of patients.2 The typical clinical presentation of oral tuberculosis is one or more painful or painless ulcers with irregular borders, usually localized on the tongue (nearly half of cases4), and less frequently affecting the lip, buccal mucosa, gingiva, soft palate, and extraction sockets. It can also present as a nodule, fissure, vesicle, tuberculoma, tubercular papilloma, or periapical granuloma.2,5
Oral tuberculosis may be primary but is more commonly secondary to internal-organ tuberculosis. Secondary disease is seen in patients with pulmonary forms (affecting 0.05% to 1.5% of patients with pulmonary tuberculosis1,2) because of autoinoculation by infected sputum or hematogenous spread.1,4,5
Clinicians should consider oral tuberculosis in the differential diagnosis of a nonhealing ulcer of the mouth, particularly in an immunosuppressed patient such as ours. It is also important to highlight the necessity of searching for a primary site of infection, more frequently in the lungs.
- Kiliç A, Gül U, Gönül M, Soylu S, Cakmak SK, Demiriz M. Orificial tuberculosis of the lip: a case report and review of the literature. Int J Dermatol 2009; 48:178–180.
- Ram H, Kumar S, Mehrotra S, Mohommad S. Tubercular ulcer: mimicking squamous cell carcinoma of buccal mucosa. J Maxillofac Oral Surg 2012; 11:105–108.
- Frezzini C, Leao JC, Porter S. Current trends of HIV disease of the mouth. J Oral Pathol Med 2005; 34:513–531.
- Chauhan V, Mahesh DM, Panda P, Mahajan S, Thakur S. Tuberculosis cutis orificialis (TBCO): a rare manifestation of tuberculosis. J Assoc Physicians India 2012; 60:126–127.
- Kannan S, Thakkar P, Dcruz AK. Tuberculosis masquerading as oral malignancy. Indian J Med Paediatr Oncol 2011; 32:180–182.
- Kiliç A, Gül U, Gönül M, Soylu S, Cakmak SK, Demiriz M. Orificial tuberculosis of the lip: a case report and review of the literature. Int J Dermatol 2009; 48:178–180.
- Ram H, Kumar S, Mehrotra S, Mohommad S. Tubercular ulcer: mimicking squamous cell carcinoma of buccal mucosa. J Maxillofac Oral Surg 2012; 11:105–108.
- Frezzini C, Leao JC, Porter S. Current trends of HIV disease of the mouth. J Oral Pathol Med 2005; 34:513–531.
- Chauhan V, Mahesh DM, Panda P, Mahajan S, Thakur S. Tuberculosis cutis orificialis (TBCO): a rare manifestation of tuberculosis. J Assoc Physicians India 2012; 60:126–127.
- Kannan S, Thakkar P, Dcruz AK. Tuberculosis masquerading as oral malignancy. Indian J Med Paediatr Oncol 2011; 32:180–182.