User login
CDC Released Voluntary Guidelines to Help Lower Opioid and Abuse of Painkillers
(Reuters) - Addressing a growing "epidemic" of opioid overdoses and abuse of the prescribed painkillers in the United States, the Centers for Disease Control and Prevention on Tuesday released voluntary guidelines that instruct primary care doctors to sharply deter use of the medicines for chronic pain.
"Overprescribing opioids, largely for chronic pain, is a key driver of America's drug-overdose epidemic," said CDC Director Tom Frieden. Sales of the prescription therapies have quadrupled since 1999, causing 165,000 fatal overdoses over the same period and now growing at more than 40 per day, according to the agency.
Primary care doctors who treat adults for chronic pain in outpatient settings account for nearly half of all opioid prescriptions, the CDC said. It defined chronic pain as lasting longer than three months, or past the typical time it takes for normal tissue healing.
The new guidelines recommend non-opioids, including acetaminophen and ibuprofen, as preferred therapy for chronic pain unless patients have active cancer or are receiving palliative or end-of-life care.
When opioids are used, the lowest possible dose should be prescribed to reduce risks of opioid abuse and overdose and patients should then be closely monitored, according to the CDC guidelines. The drugs should also be combined with non-drug approaches to controlling pain, like physical therapy and exercise, the agency said.
Moreover, when starting opioid therapy for chronic pain, doctors should prescribe immediate-release formulations instead of long-acting versions, the guidelines say. They recommend doctors avoid prescribing opioids with sedatives called benzodiazepines.
When prescribed for acute, or short-term pain, doctors should prescribe the lowest effective dose of immediate release opioids.
"Three days or less will often be sufficient; more than seven days will rarely be needed," the guidelines say.
Some studies suggest only 5 percent of patients prescribed opioids receive them for chronic pain, but they account for 70 percent of overall opioid prescriptions and the majority of overdoses.
For the vast majority of patients taking opioids for chronic pain, risks from the drugs will outweigh benefits, Frieden said. "The prescription overdose epidemic is doctor-driven," Frieden said, adding it can be reversed if doctors rein in their prescriptions of the painkillers.
The American College of Physicians on Tuesday said the new guidelines provide important guidance "at a time when many communities are being devastated by the adverse impact of opioid misuse."
The most widely used opioids include hydrocodone, which is the main active ingredient of Vicodin, and oxycodone, an active ingredient of OxyContin and Percocet. They are synthetic narcotics which work by binding to opioid receptors in the brain and are mostly available in pill form.
Nearly two million Americans aged 12 or older either abused or were dependent on prescription opioids in 2014, the CDC said.
Opioids also include heroin, an illegal injectable drug which has become a far cheaper alternative to oral opioids on the streets of many U.S. communities, causing many overdoses.
Other U.S. health officials on Tuesday said first responders should have wider access to naloxone, a drug that can reverse opioid overdoses.
SHM offers a safe opioid prescribing implementation guideline. The Implementation Toolkit, Reducing Adverse Drug Events related to Opioids, or RADEO, provides step-by step instructions for hospitals to implement a successful QI program to make opioid prescribing safer, with fewer adverse events, and much less likely to result in dangerous sedation, respiratory depression and death. Its scope is for hospitalized patients.
(Reuters) - Addressing a growing "epidemic" of opioid overdoses and abuse of the prescribed painkillers in the United States, the Centers for Disease Control and Prevention on Tuesday released voluntary guidelines that instruct primary care doctors to sharply deter use of the medicines for chronic pain.
"Overprescribing opioids, largely for chronic pain, is a key driver of America's drug-overdose epidemic," said CDC Director Tom Frieden. Sales of the prescription therapies have quadrupled since 1999, causing 165,000 fatal overdoses over the same period and now growing at more than 40 per day, according to the agency.
Primary care doctors who treat adults for chronic pain in outpatient settings account for nearly half of all opioid prescriptions, the CDC said. It defined chronic pain as lasting longer than three months, or past the typical time it takes for normal tissue healing.
The new guidelines recommend non-opioids, including acetaminophen and ibuprofen, as preferred therapy for chronic pain unless patients have active cancer or are receiving palliative or end-of-life care.
When opioids are used, the lowest possible dose should be prescribed to reduce risks of opioid abuse and overdose and patients should then be closely monitored, according to the CDC guidelines. The drugs should also be combined with non-drug approaches to controlling pain, like physical therapy and exercise, the agency said.
Moreover, when starting opioid therapy for chronic pain, doctors should prescribe immediate-release formulations instead of long-acting versions, the guidelines say. They recommend doctors avoid prescribing opioids with sedatives called benzodiazepines.
When prescribed for acute, or short-term pain, doctors should prescribe the lowest effective dose of immediate release opioids.
"Three days or less will often be sufficient; more than seven days will rarely be needed," the guidelines say.
Some studies suggest only 5 percent of patients prescribed opioids receive them for chronic pain, but they account for 70 percent of overall opioid prescriptions and the majority of overdoses.
For the vast majority of patients taking opioids for chronic pain, risks from the drugs will outweigh benefits, Frieden said. "The prescription overdose epidemic is doctor-driven," Frieden said, adding it can be reversed if doctors rein in their prescriptions of the painkillers.
The American College of Physicians on Tuesday said the new guidelines provide important guidance "at a time when many communities are being devastated by the adverse impact of opioid misuse."
The most widely used opioids include hydrocodone, which is the main active ingredient of Vicodin, and oxycodone, an active ingredient of OxyContin and Percocet. They are synthetic narcotics which work by binding to opioid receptors in the brain and are mostly available in pill form.
Nearly two million Americans aged 12 or older either abused or were dependent on prescription opioids in 2014, the CDC said.
Opioids also include heroin, an illegal injectable drug which has become a far cheaper alternative to oral opioids on the streets of many U.S. communities, causing many overdoses.
Other U.S. health officials on Tuesday said first responders should have wider access to naloxone, a drug that can reverse opioid overdoses.
SHM offers a safe opioid prescribing implementation guideline. The Implementation Toolkit, Reducing Adverse Drug Events related to Opioids, or RADEO, provides step-by step instructions for hospitals to implement a successful QI program to make opioid prescribing safer, with fewer adverse events, and much less likely to result in dangerous sedation, respiratory depression and death. Its scope is for hospitalized patients.
(Reuters) - Addressing a growing "epidemic" of opioid overdoses and abuse of the prescribed painkillers in the United States, the Centers for Disease Control and Prevention on Tuesday released voluntary guidelines that instruct primary care doctors to sharply deter use of the medicines for chronic pain.
"Overprescribing opioids, largely for chronic pain, is a key driver of America's drug-overdose epidemic," said CDC Director Tom Frieden. Sales of the prescription therapies have quadrupled since 1999, causing 165,000 fatal overdoses over the same period and now growing at more than 40 per day, according to the agency.
Primary care doctors who treat adults for chronic pain in outpatient settings account for nearly half of all opioid prescriptions, the CDC said. It defined chronic pain as lasting longer than three months, or past the typical time it takes for normal tissue healing.
The new guidelines recommend non-opioids, including acetaminophen and ibuprofen, as preferred therapy for chronic pain unless patients have active cancer or are receiving palliative or end-of-life care.
When opioids are used, the lowest possible dose should be prescribed to reduce risks of opioid abuse and overdose and patients should then be closely monitored, according to the CDC guidelines. The drugs should also be combined with non-drug approaches to controlling pain, like physical therapy and exercise, the agency said.
Moreover, when starting opioid therapy for chronic pain, doctors should prescribe immediate-release formulations instead of long-acting versions, the guidelines say. They recommend doctors avoid prescribing opioids with sedatives called benzodiazepines.
When prescribed for acute, or short-term pain, doctors should prescribe the lowest effective dose of immediate release opioids.
"Three days or less will often be sufficient; more than seven days will rarely be needed," the guidelines say.
Some studies suggest only 5 percent of patients prescribed opioids receive them for chronic pain, but they account for 70 percent of overall opioid prescriptions and the majority of overdoses.
For the vast majority of patients taking opioids for chronic pain, risks from the drugs will outweigh benefits, Frieden said. "The prescription overdose epidemic is doctor-driven," Frieden said, adding it can be reversed if doctors rein in their prescriptions of the painkillers.
The American College of Physicians on Tuesday said the new guidelines provide important guidance "at a time when many communities are being devastated by the adverse impact of opioid misuse."
The most widely used opioids include hydrocodone, which is the main active ingredient of Vicodin, and oxycodone, an active ingredient of OxyContin and Percocet. They are synthetic narcotics which work by binding to opioid receptors in the brain and are mostly available in pill form.
Nearly two million Americans aged 12 or older either abused or were dependent on prescription opioids in 2014, the CDC said.
Opioids also include heroin, an illegal injectable drug which has become a far cheaper alternative to oral opioids on the streets of many U.S. communities, causing many overdoses.
Other U.S. health officials on Tuesday said first responders should have wider access to naloxone, a drug that can reverse opioid overdoses.
SHM offers a safe opioid prescribing implementation guideline. The Implementation Toolkit, Reducing Adverse Drug Events related to Opioids, or RADEO, provides step-by step instructions for hospitals to implement a successful QI program to make opioid prescribing safer, with fewer adverse events, and much less likely to result in dangerous sedation, respiratory depression and death. Its scope is for hospitalized patients.
Hospital Medicine 2016 Brims with Lively Talks, Record Crowds in San Diego
Yes, it rained some in dry San Diego—for the first time in a month, according to locals. But that was the extent of the disappointment at HM16—SHM’s annual meeting highlighted by inspiring words from the U.S. surgeon general, a fellow hospitalist.
Read more about the speakers at HM16.
HM16 featured fascinating perspectives from giants in the field, vigorous panel discussions, lively workshops, streamlined how-to’s, encouraging work-life talks, and practical presentations on management.
And a record-breaking crowd continued the field’s trajectory of expansion.
“You were 4,000 strong this year,” said assistant course director Leonard Feldman, MD, SFHM. “Next year, let’s try for five.”
Yes, it rained some in dry San Diego—for the first time in a month, according to locals. But that was the extent of the disappointment at HM16—SHM’s annual meeting highlighted by inspiring words from the U.S. surgeon general, a fellow hospitalist.
Read more about the speakers at HM16.
HM16 featured fascinating perspectives from giants in the field, vigorous panel discussions, lively workshops, streamlined how-to’s, encouraging work-life talks, and practical presentations on management.
And a record-breaking crowd continued the field’s trajectory of expansion.
“You were 4,000 strong this year,” said assistant course director Leonard Feldman, MD, SFHM. “Next year, let’s try for five.”
Yes, it rained some in dry San Diego—for the first time in a month, according to locals. But that was the extent of the disappointment at HM16—SHM’s annual meeting highlighted by inspiring words from the U.S. surgeon general, a fellow hospitalist.
Read more about the speakers at HM16.
HM16 featured fascinating perspectives from giants in the field, vigorous panel discussions, lively workshops, streamlined how-to’s, encouraging work-life talks, and practical presentations on management.
And a record-breaking crowd continued the field’s trajectory of expansion.
“You were 4,000 strong this year,” said assistant course director Leonard Feldman, MD, SFHM. “Next year, let’s try for five.”
Community Partnerships, Data Key to Readmission Reduction in Diverse Populations
“We found it wasn’t on a bus route,” says Janice Finder, RN, MSN, director of the hospital’s Transitions in Care program and a part of SHM’s Project BOOST, which focuses on successful discharge outcomes. So in collaboration with the Texas Department of Aging and Disability Services, the hospital provided cab vouchers for these patients to travel to and from appointments.
The hospital also realized that to improve the chances its large Hispanic diabetic population remained healthy, it would need to tailor its disease management efforts to their culture, particularly when it came to diet.
“Their eating habits are very different, and we want to ensure they have meals based on what they actually eat,” Finder says.
These are exactly the kinds of approaches a new guide developed for the Centers for Medicare & Medicaid Services (CMS) by the Disparities Solutions Center (DSC), based at Massachusetts General Hospital (MGH) in Boston, is looking to promote in an effort to reduce unnecessary hospital readmissions.1 CMS recently made the Guide to Preventing Readmissions among Racially and Ethnically Diverse Medicare Beneficiaries available on its website.
“We know readmissions is an issue for diverse populations, that they are more likely than their white counterparts to be admitted within 30 days of discharge,” says Aswita Tan-McGrory, MBA, MSPH, deputy director of DSC within the Mongan Institute for Health Policy at MGH. “So there was a good business case for creating this guide.”
Keys to Success
Within the guide is a collection of evidence-based information, case studies, and seven recommendations the DSC team assembled to assist hospital leaders looking to reduce readmissions among some of the nation’s highest-risk populations.
While Tan-McGrory acknowledges it may be impractical for hospitals to adopt each recommendation, she says they can pick and choose which they can most effectively adopt.
“We put together these seven steps and looked for who does this really well, and the honest truth is not very many are,” she says. “It’s a complicated process, but it’s some guidance because there really wasn’t anything out there.”
Included in the recommendations: Create a “strong radar” (engage in robust data collection), identify root causes, begin to think about discharge at admission, deploy a team, consider systems and social determinants, focus on culturally competent communication, and foster community partnerships.
“It’s not just medication reconciliation or discharge instructions in a different language,” Tan-McGrory says. “What happens when a patient gets home?”
These types of questions are important because CMS now penalizes hospitals for what it deems excessive avoidable readmissions within 30 days of discharge. In 2016, hospitals can lose up to 3% of their Medicare payments under the Hospital Readmissions Reduction Program.
In 2014, nearly 18% of Medicare patients were admitted within a month of discharge at a cost of $26 billion.2 According to the new guide, Agency for Healthcare Research and Quality data indicate African-American and Hispanic patients make up a higher share of these readmissions, in part because they are disproportionately affected by chronic high-readmission-risk diseases like congestive heart failure.
Social Determinants
Though it’s challenging for healthcare providers, one way to reduce readmissions is to address the social determinants of health, Tan-McGrory says.
“Hospitals have felt in the past that it’s not their domain, but their patients are coming back,” she says. “How do you address people’s isolation at home? How can you send them from the hospital when no one is there to follow up or take care of them?”
The answers may lie in part on building community partnerships, something in which Finder’s hospital has successfully engaged. For example, the hospital has teamed with its local United Way to work with Asian patients on issues related to pain management and palliative care.
At Berkshire Medical Center, a 300-bed community teaching hospital in western Massachusetts, electronic health software helps staff flag patients at admission for potential readmission risks. Looking briefly at the new guide, William DeMarco, DO, SFHM, chief of hospital medicine (and also part of Project BOOST), noticed several new areas they may be able to incorporate into the system.
But adequate data collection and interpretation to help understand these disparities is not always possible, particularly for readmissions, Dr. DeMarco says.
However, as in one of the case studies examined in the DCS guide, Berkshire recently began to identify its high utilizers, pairing multidisciplinary teams with individual primary care providers in order to help meet these patients’ needs.
“It can take several hours for one patient, coordinating and getting a lot of people together,” Dr. DeMarco says. “It’s the only way to accomplish that goal, but it’s very resource intensive.”
Although hospitals traditionally focus on what they can do within their four walls, providers are becoming increasingly aware that the social determinants of health—like transportation, dietary choices, and language barriers—deeply impact some racial and ethnically diverse populations. Now, CMS thinks it’s worth paying closer attention. TH
Kelly April Tyrrell is a freelance writer in Madison, Wis.
References
- Betancourt JR, Tan-McGrory A, Kenst KS. Guide to preventing readmissions among racially and ethnically diverse medicare beneficiaries. Prepared by the Disparities Solutions Center, Mongan Institute for Health Policy at Massachusetts General Hospital. Baltimore, MD: Centers for Medicare & Medicaid Services Office of Minority Health; September 2015.
- Rau J. Medicare fines 2,610 hospitals in third round of readmission penalties. Kaiser Health News. Available at: http://kaiserhealthnews.org/news/medicare-readmissions-penalties-2015/. Accessed February 15, 2016.
“We found it wasn’t on a bus route,” says Janice Finder, RN, MSN, director of the hospital’s Transitions in Care program and a part of SHM’s Project BOOST, which focuses on successful discharge outcomes. So in collaboration with the Texas Department of Aging and Disability Services, the hospital provided cab vouchers for these patients to travel to and from appointments.
The hospital also realized that to improve the chances its large Hispanic diabetic population remained healthy, it would need to tailor its disease management efforts to their culture, particularly when it came to diet.
“Their eating habits are very different, and we want to ensure they have meals based on what they actually eat,” Finder says.
These are exactly the kinds of approaches a new guide developed for the Centers for Medicare & Medicaid Services (CMS) by the Disparities Solutions Center (DSC), based at Massachusetts General Hospital (MGH) in Boston, is looking to promote in an effort to reduce unnecessary hospital readmissions.1 CMS recently made the Guide to Preventing Readmissions among Racially and Ethnically Diverse Medicare Beneficiaries available on its website.
“We know readmissions is an issue for diverse populations, that they are more likely than their white counterparts to be admitted within 30 days of discharge,” says Aswita Tan-McGrory, MBA, MSPH, deputy director of DSC within the Mongan Institute for Health Policy at MGH. “So there was a good business case for creating this guide.”
Keys to Success
Within the guide is a collection of evidence-based information, case studies, and seven recommendations the DSC team assembled to assist hospital leaders looking to reduce readmissions among some of the nation’s highest-risk populations.
While Tan-McGrory acknowledges it may be impractical for hospitals to adopt each recommendation, she says they can pick and choose which they can most effectively adopt.
“We put together these seven steps and looked for who does this really well, and the honest truth is not very many are,” she says. “It’s a complicated process, but it’s some guidance because there really wasn’t anything out there.”
Included in the recommendations: Create a “strong radar” (engage in robust data collection), identify root causes, begin to think about discharge at admission, deploy a team, consider systems and social determinants, focus on culturally competent communication, and foster community partnerships.
“It’s not just medication reconciliation or discharge instructions in a different language,” Tan-McGrory says. “What happens when a patient gets home?”
These types of questions are important because CMS now penalizes hospitals for what it deems excessive avoidable readmissions within 30 days of discharge. In 2016, hospitals can lose up to 3% of their Medicare payments under the Hospital Readmissions Reduction Program.
In 2014, nearly 18% of Medicare patients were admitted within a month of discharge at a cost of $26 billion.2 According to the new guide, Agency for Healthcare Research and Quality data indicate African-American and Hispanic patients make up a higher share of these readmissions, in part because they are disproportionately affected by chronic high-readmission-risk diseases like congestive heart failure.
Social Determinants
Though it’s challenging for healthcare providers, one way to reduce readmissions is to address the social determinants of health, Tan-McGrory says.
“Hospitals have felt in the past that it’s not their domain, but their patients are coming back,” she says. “How do you address people’s isolation at home? How can you send them from the hospital when no one is there to follow up or take care of them?”
The answers may lie in part on building community partnerships, something in which Finder’s hospital has successfully engaged. For example, the hospital has teamed with its local United Way to work with Asian patients on issues related to pain management and palliative care.
At Berkshire Medical Center, a 300-bed community teaching hospital in western Massachusetts, electronic health software helps staff flag patients at admission for potential readmission risks. Looking briefly at the new guide, William DeMarco, DO, SFHM, chief of hospital medicine (and also part of Project BOOST), noticed several new areas they may be able to incorporate into the system.
But adequate data collection and interpretation to help understand these disparities is not always possible, particularly for readmissions, Dr. DeMarco says.
However, as in one of the case studies examined in the DCS guide, Berkshire recently began to identify its high utilizers, pairing multidisciplinary teams with individual primary care providers in order to help meet these patients’ needs.
“It can take several hours for one patient, coordinating and getting a lot of people together,” Dr. DeMarco says. “It’s the only way to accomplish that goal, but it’s very resource intensive.”
Although hospitals traditionally focus on what they can do within their four walls, providers are becoming increasingly aware that the social determinants of health—like transportation, dietary choices, and language barriers—deeply impact some racial and ethnically diverse populations. Now, CMS thinks it’s worth paying closer attention. TH
Kelly April Tyrrell is a freelance writer in Madison, Wis.
References
- Betancourt JR, Tan-McGrory A, Kenst KS. Guide to preventing readmissions among racially and ethnically diverse medicare beneficiaries. Prepared by the Disparities Solutions Center, Mongan Institute for Health Policy at Massachusetts General Hospital. Baltimore, MD: Centers for Medicare & Medicaid Services Office of Minority Health; September 2015.
- Rau J. Medicare fines 2,610 hospitals in third round of readmission penalties. Kaiser Health News. Available at: http://kaiserhealthnews.org/news/medicare-readmissions-penalties-2015/. Accessed February 15, 2016.
“We found it wasn’t on a bus route,” says Janice Finder, RN, MSN, director of the hospital’s Transitions in Care program and a part of SHM’s Project BOOST, which focuses on successful discharge outcomes. So in collaboration with the Texas Department of Aging and Disability Services, the hospital provided cab vouchers for these patients to travel to and from appointments.
The hospital also realized that to improve the chances its large Hispanic diabetic population remained healthy, it would need to tailor its disease management efforts to their culture, particularly when it came to diet.
“Their eating habits are very different, and we want to ensure they have meals based on what they actually eat,” Finder says.
These are exactly the kinds of approaches a new guide developed for the Centers for Medicare & Medicaid Services (CMS) by the Disparities Solutions Center (DSC), based at Massachusetts General Hospital (MGH) in Boston, is looking to promote in an effort to reduce unnecessary hospital readmissions.1 CMS recently made the Guide to Preventing Readmissions among Racially and Ethnically Diverse Medicare Beneficiaries available on its website.
“We know readmissions is an issue for diverse populations, that they are more likely than their white counterparts to be admitted within 30 days of discharge,” says Aswita Tan-McGrory, MBA, MSPH, deputy director of DSC within the Mongan Institute for Health Policy at MGH. “So there was a good business case for creating this guide.”
Keys to Success
Within the guide is a collection of evidence-based information, case studies, and seven recommendations the DSC team assembled to assist hospital leaders looking to reduce readmissions among some of the nation’s highest-risk populations.
While Tan-McGrory acknowledges it may be impractical for hospitals to adopt each recommendation, she says they can pick and choose which they can most effectively adopt.
“We put together these seven steps and looked for who does this really well, and the honest truth is not very many are,” she says. “It’s a complicated process, but it’s some guidance because there really wasn’t anything out there.”
Included in the recommendations: Create a “strong radar” (engage in robust data collection), identify root causes, begin to think about discharge at admission, deploy a team, consider systems and social determinants, focus on culturally competent communication, and foster community partnerships.
“It’s not just medication reconciliation or discharge instructions in a different language,” Tan-McGrory says. “What happens when a patient gets home?”
These types of questions are important because CMS now penalizes hospitals for what it deems excessive avoidable readmissions within 30 days of discharge. In 2016, hospitals can lose up to 3% of their Medicare payments under the Hospital Readmissions Reduction Program.
In 2014, nearly 18% of Medicare patients were admitted within a month of discharge at a cost of $26 billion.2 According to the new guide, Agency for Healthcare Research and Quality data indicate African-American and Hispanic patients make up a higher share of these readmissions, in part because they are disproportionately affected by chronic high-readmission-risk diseases like congestive heart failure.
Social Determinants
Though it’s challenging for healthcare providers, one way to reduce readmissions is to address the social determinants of health, Tan-McGrory says.
“Hospitals have felt in the past that it’s not their domain, but their patients are coming back,” she says. “How do you address people’s isolation at home? How can you send them from the hospital when no one is there to follow up or take care of them?”
The answers may lie in part on building community partnerships, something in which Finder’s hospital has successfully engaged. For example, the hospital has teamed with its local United Way to work with Asian patients on issues related to pain management and palliative care.
At Berkshire Medical Center, a 300-bed community teaching hospital in western Massachusetts, electronic health software helps staff flag patients at admission for potential readmission risks. Looking briefly at the new guide, William DeMarco, DO, SFHM, chief of hospital medicine (and also part of Project BOOST), noticed several new areas they may be able to incorporate into the system.
But adequate data collection and interpretation to help understand these disparities is not always possible, particularly for readmissions, Dr. DeMarco says.
However, as in one of the case studies examined in the DCS guide, Berkshire recently began to identify its high utilizers, pairing multidisciplinary teams with individual primary care providers in order to help meet these patients’ needs.
“It can take several hours for one patient, coordinating and getting a lot of people together,” Dr. DeMarco says. “It’s the only way to accomplish that goal, but it’s very resource intensive.”
Although hospitals traditionally focus on what they can do within their four walls, providers are becoming increasingly aware that the social determinants of health—like transportation, dietary choices, and language barriers—deeply impact some racial and ethnically diverse populations. Now, CMS thinks it’s worth paying closer attention. TH
Kelly April Tyrrell is a freelance writer in Madison, Wis.
References
- Betancourt JR, Tan-McGrory A, Kenst KS. Guide to preventing readmissions among racially and ethnically diverse medicare beneficiaries. Prepared by the Disparities Solutions Center, Mongan Institute for Health Policy at Massachusetts General Hospital. Baltimore, MD: Centers for Medicare & Medicaid Services Office of Minority Health; September 2015.
- Rau J. Medicare fines 2,610 hospitals in third round of readmission penalties. Kaiser Health News. Available at: http://kaiserhealthnews.org/news/medicare-readmissions-penalties-2015/. Accessed February 15, 2016.
'Everything We Say and Do': Soliciting Goals from Our Patients and Their Families
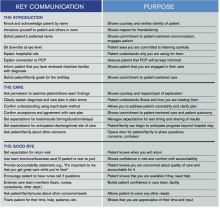
Editor’s note: “Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Each article will focus on how the contributor applies one ormore of the “key communication” tactics in practice to maintain provider accountability for “Everything we say and do that affects our patients’ thoughts, feelings and well-being.”
Read more from the “Everything We Say and Do” series.
What I Say and Do
Why I Do It
The literature shows that, in most cases, doctors interrupt within 18 to 23 seconds and that when we interrupt, patients often never get back to what they were saying, the course of their story changes, and our diagnostic accuracy decreases. I also do it because I learn things that I wouldn’t otherwise know, and my patients feel heard and treated with respect. Listening has a healing effect, and in medicine, it can be equally if not more therapeutic than the medicines and clinical care we provide. I find that it helps me to be a more effective doctor, one who is helping my patient in the way that is most meaningful and helpful to them. It is very easy to navigate an encounter from the physician point of view and to make assumptions about what people want and need from me, but in reality, what is most important to me is not always what is most important to them.
Allowing patients to tell me what is important shows them respect and also sets me up for success as I am more likely to know and meet their needs. Doing this up front saves time by preventing the “doorknob” questions on the way out. The human connection that follows keeps me connected to my purpose as a doctor. People often worry that listening will take too much time, but we know from the literature that most patients will talk for no more than 90 seconds. It’s really a very short amount of time for a gold mine of information.
How I Do It
Before I jump into my agenda, I make sure to know what is on the patient’s and family’s mind. What is most important to them to address? Once we have agreed on what we will be discussing or doing with our time in a way that includes both what I and the patient/family find important, I start by asking the patient to tell me everything about the first item at hand. I do not interrupt by asking questions, making comments, or “fixing.” I approach them with authentic curiosity, encouraging more without directing what they say.
I start with, “I’m here to talk to you about _____, but first, can you tell me what you’d like to make sure we talk about today?” Or, “Tell me a list of things that you’d like to make sure we talk about today.”
I follow that with, “What else?” until there is nothing else. Once we have negotiated what we will discuss, I say, “Tell me all about _______.” I do not interrupt or think about my response while I am listening. My only response is to use nonverbal continuers (“Uh huh,” “mmmm”), reflections (“That sounds really hard”), verbal continuers (“Tell me more”), empathic statements (“I can see why you would feel that way”), and body language that shows I am with them (sitting at eye level, facing them, looking at them rather than at my phone, pager or a computer screen.)
All of this happens before I jump into any of my own focused or clarifying questions.
Dr. Sliwka is medical director of patient and provider experience, medical director of the Goldman Medical Service, and associate clinical professor of medicine in the Division of Hospital Medicine at the UCSF Medical Center in San Francisco.
Table 1.
Editor’s note: “Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Each article will focus on how the contributor applies one ormore of the “key communication” tactics in practice to maintain provider accountability for “Everything we say and do that affects our patients’ thoughts, feelings and well-being.”
Read more from the “Everything We Say and Do” series.
What I Say and Do
Why I Do It
The literature shows that, in most cases, doctors interrupt within 18 to 23 seconds and that when we interrupt, patients often never get back to what they were saying, the course of their story changes, and our diagnostic accuracy decreases. I also do it because I learn things that I wouldn’t otherwise know, and my patients feel heard and treated with respect. Listening has a healing effect, and in medicine, it can be equally if not more therapeutic than the medicines and clinical care we provide. I find that it helps me to be a more effective doctor, one who is helping my patient in the way that is most meaningful and helpful to them. It is very easy to navigate an encounter from the physician point of view and to make assumptions about what people want and need from me, but in reality, what is most important to me is not always what is most important to them.
Allowing patients to tell me what is important shows them respect and also sets me up for success as I am more likely to know and meet their needs. Doing this up front saves time by preventing the “doorknob” questions on the way out. The human connection that follows keeps me connected to my purpose as a doctor. People often worry that listening will take too much time, but we know from the literature that most patients will talk for no more than 90 seconds. It’s really a very short amount of time for a gold mine of information.
How I Do It
Before I jump into my agenda, I make sure to know what is on the patient’s and family’s mind. What is most important to them to address? Once we have agreed on what we will be discussing or doing with our time in a way that includes both what I and the patient/family find important, I start by asking the patient to tell me everything about the first item at hand. I do not interrupt by asking questions, making comments, or “fixing.” I approach them with authentic curiosity, encouraging more without directing what they say.
I start with, “I’m here to talk to you about _____, but first, can you tell me what you’d like to make sure we talk about today?” Or, “Tell me a list of things that you’d like to make sure we talk about today.”
I follow that with, “What else?” until there is nothing else. Once we have negotiated what we will discuss, I say, “Tell me all about _______.” I do not interrupt or think about my response while I am listening. My only response is to use nonverbal continuers (“Uh huh,” “mmmm”), reflections (“That sounds really hard”), verbal continuers (“Tell me more”), empathic statements (“I can see why you would feel that way”), and body language that shows I am with them (sitting at eye level, facing them, looking at them rather than at my phone, pager or a computer screen.)
All of this happens before I jump into any of my own focused or clarifying questions.
Dr. Sliwka is medical director of patient and provider experience, medical director of the Goldman Medical Service, and associate clinical professor of medicine in the Division of Hospital Medicine at the UCSF Medical Center in San Francisco.
Table 1.
Editor’s note: “Everything We Say and Do” is an informational series developed by SHM’s Patient Experience Committee to provide readers with thoughtful and actionable communication tactics that have great potential to positively impact patients’ experience of care. Each article will focus on how the contributor applies one ormore of the “key communication” tactics in practice to maintain provider accountability for “Everything we say and do that affects our patients’ thoughts, feelings and well-being.”
Read more from the “Everything We Say and Do” series.
What I Say and Do
Why I Do It
The literature shows that, in most cases, doctors interrupt within 18 to 23 seconds and that when we interrupt, patients often never get back to what they were saying, the course of their story changes, and our diagnostic accuracy decreases. I also do it because I learn things that I wouldn’t otherwise know, and my patients feel heard and treated with respect. Listening has a healing effect, and in medicine, it can be equally if not more therapeutic than the medicines and clinical care we provide. I find that it helps me to be a more effective doctor, one who is helping my patient in the way that is most meaningful and helpful to them. It is very easy to navigate an encounter from the physician point of view and to make assumptions about what people want and need from me, but in reality, what is most important to me is not always what is most important to them.
Allowing patients to tell me what is important shows them respect and also sets me up for success as I am more likely to know and meet their needs. Doing this up front saves time by preventing the “doorknob” questions on the way out. The human connection that follows keeps me connected to my purpose as a doctor. People often worry that listening will take too much time, but we know from the literature that most patients will talk for no more than 90 seconds. It’s really a very short amount of time for a gold mine of information.
How I Do It
Before I jump into my agenda, I make sure to know what is on the patient’s and family’s mind. What is most important to them to address? Once we have agreed on what we will be discussing or doing with our time in a way that includes both what I and the patient/family find important, I start by asking the patient to tell me everything about the first item at hand. I do not interrupt by asking questions, making comments, or “fixing.” I approach them with authentic curiosity, encouraging more without directing what they say.
I start with, “I’m here to talk to you about _____, but first, can you tell me what you’d like to make sure we talk about today?” Or, “Tell me a list of things that you’d like to make sure we talk about today.”
I follow that with, “What else?” until there is nothing else. Once we have negotiated what we will discuss, I say, “Tell me all about _______.” I do not interrupt or think about my response while I am listening. My only response is to use nonverbal continuers (“Uh huh,” “mmmm”), reflections (“That sounds really hard”), verbal continuers (“Tell me more”), empathic statements (“I can see why you would feel that way”), and body language that shows I am with them (sitting at eye level, facing them, looking at them rather than at my phone, pager or a computer screen.)
All of this happens before I jump into any of my own focused or clarifying questions.
Dr. Sliwka is medical director of patient and provider experience, medical director of the Goldman Medical Service, and associate clinical professor of medicine in the Division of Hospital Medicine at the UCSF Medical Center in San Francisco.
Table 1.
Study Suggests Growing Up in a Stress-Free Environment Lowers your Risk of Heart Attacks
(Reuters Health) - Kids who live in a stress-free environment may grow up to be adults with a lower risk of heart attacks than their peers who experience social, emotional or financial difficulties during childhood, a Finnish study suggests.
Researchers assessed psychosocial factors in 311 kids at age 12 and 18. Then, at age 28, they looked for coronary artery calcification.
The adults who had high psychosocial wellbeing as kids were 15% less likely to have calcium deposits clogging their arteries as adults, the study found.
"This study suggests that childhood psychosocial factors may have long-term consequences on cardiovascular health," lead study author Dr. Markus Juonala of the University of Turku in Finland said by email.
To understand the connection between how kids feel growing up and how their arteries look decades later, Juonala and colleagues analyzed data gathered from 1980 to 2008 as part of the Cardiovascular Risk in Young Finns Study.
Among other things, this study measured psychosocial wellbeing by looking at family income and education levels, parents' job status, parents' mental health and history of smoking or substance abuse, parents' weight and exercise habits, stressful events such as divorce, death or moves, as well as the child's level of aggressive or anti-social behaviors and ability to interact with other people.
In addition, researchers analyzed results from computed tomography (CT) scans assessing coronary artery calcification. Overall, 55 participants, or about 18%, had at least some calcification in their arteries, researchers report in JAMA Pediatrics, March 14.
Among this group with calcification, 28 participants had low levels of buildup, 20 had moderate amounts of calcium and 7 had substantial deposits, the study found.
Even after accounting for adult circumstances like psychosocial factors and risk factors for heart disease like obesity, smoking, hypertension and elevated cholesterol, the research team still found well-being during childhood was associated with reduced coronary artery calcification in adulthood.
The study is observational and doesn't prove childhood stress causes clogged arteries or heart attacks, only that the two things are related, the authors note.
It's possible, however, that stress during childhood might trigger changes in metabolic functioning and inflammation that later contribute to calcium deposits in the arteries, the researchers point out.
It's also possible that happier kids may develop healthier habits like better diets and more rigorous exercise routines that help keep arteries unclogged and lower their risk of heart disease later in life.
"The take-home message for parents is to understand that stress in childhood may have many adverse effects and that they should help their children avoid stress," said Dr. Stephen Daniels, a researcher at the University of Colorado School of Medicine and pediatrician-in-chief at Children's Hospital Colorado.
Parents may not always be able to eliminate stress, however, particularly the stress that can come from environmental factors like lower socioeconomic status, Daniels, who wasn't involved in the study, added by email.
When children grow up with stress, they can still take charge of their health as adults to lower their risk of heart disease, Daniels noted.
"For an adult who had a stressful childhood, the best approach is to be aware of their cardiovascular risk status and to reduce their risk by improving diet and physical activity and avoiding cigarette smoking," Daniels added. "Where risk factors exist, such as high blood pressure, they should be appropriately treated."
(Reuters Health) - Kids who live in a stress-free environment may grow up to be adults with a lower risk of heart attacks than their peers who experience social, emotional or financial difficulties during childhood, a Finnish study suggests.
Researchers assessed psychosocial factors in 311 kids at age 12 and 18. Then, at age 28, they looked for coronary artery calcification.
The adults who had high psychosocial wellbeing as kids were 15% less likely to have calcium deposits clogging their arteries as adults, the study found.
"This study suggests that childhood psychosocial factors may have long-term consequences on cardiovascular health," lead study author Dr. Markus Juonala of the University of Turku in Finland said by email.
To understand the connection between how kids feel growing up and how their arteries look decades later, Juonala and colleagues analyzed data gathered from 1980 to 2008 as part of the Cardiovascular Risk in Young Finns Study.
Among other things, this study measured psychosocial wellbeing by looking at family income and education levels, parents' job status, parents' mental health and history of smoking or substance abuse, parents' weight and exercise habits, stressful events such as divorce, death or moves, as well as the child's level of aggressive or anti-social behaviors and ability to interact with other people.
In addition, researchers analyzed results from computed tomography (CT) scans assessing coronary artery calcification. Overall, 55 participants, or about 18%, had at least some calcification in their arteries, researchers report in JAMA Pediatrics, March 14.
Among this group with calcification, 28 participants had low levels of buildup, 20 had moderate amounts of calcium and 7 had substantial deposits, the study found.
Even after accounting for adult circumstances like psychosocial factors and risk factors for heart disease like obesity, smoking, hypertension and elevated cholesterol, the research team still found well-being during childhood was associated with reduced coronary artery calcification in adulthood.
The study is observational and doesn't prove childhood stress causes clogged arteries or heart attacks, only that the two things are related, the authors note.
It's possible, however, that stress during childhood might trigger changes in metabolic functioning and inflammation that later contribute to calcium deposits in the arteries, the researchers point out.
It's also possible that happier kids may develop healthier habits like better diets and more rigorous exercise routines that help keep arteries unclogged and lower their risk of heart disease later in life.
"The take-home message for parents is to understand that stress in childhood may have many adverse effects and that they should help their children avoid stress," said Dr. Stephen Daniels, a researcher at the University of Colorado School of Medicine and pediatrician-in-chief at Children's Hospital Colorado.
Parents may not always be able to eliminate stress, however, particularly the stress that can come from environmental factors like lower socioeconomic status, Daniels, who wasn't involved in the study, added by email.
When children grow up with stress, they can still take charge of their health as adults to lower their risk of heart disease, Daniels noted.
"For an adult who had a stressful childhood, the best approach is to be aware of their cardiovascular risk status and to reduce their risk by improving diet and physical activity and avoiding cigarette smoking," Daniels added. "Where risk factors exist, such as high blood pressure, they should be appropriately treated."
(Reuters Health) - Kids who live in a stress-free environment may grow up to be adults with a lower risk of heart attacks than their peers who experience social, emotional or financial difficulties during childhood, a Finnish study suggests.
Researchers assessed psychosocial factors in 311 kids at age 12 and 18. Then, at age 28, they looked for coronary artery calcification.
The adults who had high psychosocial wellbeing as kids were 15% less likely to have calcium deposits clogging their arteries as adults, the study found.
"This study suggests that childhood psychosocial factors may have long-term consequences on cardiovascular health," lead study author Dr. Markus Juonala of the University of Turku in Finland said by email.
To understand the connection between how kids feel growing up and how their arteries look decades later, Juonala and colleagues analyzed data gathered from 1980 to 2008 as part of the Cardiovascular Risk in Young Finns Study.
Among other things, this study measured psychosocial wellbeing by looking at family income and education levels, parents' job status, parents' mental health and history of smoking or substance abuse, parents' weight and exercise habits, stressful events such as divorce, death or moves, as well as the child's level of aggressive or anti-social behaviors and ability to interact with other people.
In addition, researchers analyzed results from computed tomography (CT) scans assessing coronary artery calcification. Overall, 55 participants, or about 18%, had at least some calcification in their arteries, researchers report in JAMA Pediatrics, March 14.
Among this group with calcification, 28 participants had low levels of buildup, 20 had moderate amounts of calcium and 7 had substantial deposits, the study found.
Even after accounting for adult circumstances like psychosocial factors and risk factors for heart disease like obesity, smoking, hypertension and elevated cholesterol, the research team still found well-being during childhood was associated with reduced coronary artery calcification in adulthood.
The study is observational and doesn't prove childhood stress causes clogged arteries or heart attacks, only that the two things are related, the authors note.
It's possible, however, that stress during childhood might trigger changes in metabolic functioning and inflammation that later contribute to calcium deposits in the arteries, the researchers point out.
It's also possible that happier kids may develop healthier habits like better diets and more rigorous exercise routines that help keep arteries unclogged and lower their risk of heart disease later in life.
"The take-home message for parents is to understand that stress in childhood may have many adverse effects and that they should help their children avoid stress," said Dr. Stephen Daniels, a researcher at the University of Colorado School of Medicine and pediatrician-in-chief at Children's Hospital Colorado.
Parents may not always be able to eliminate stress, however, particularly the stress that can come from environmental factors like lower socioeconomic status, Daniels, who wasn't involved in the study, added by email.
When children grow up with stress, they can still take charge of their health as adults to lower their risk of heart disease, Daniels noted.
"For an adult who had a stressful childhood, the best approach is to be aware of their cardiovascular risk status and to reduce their risk by improving diet and physical activity and avoiding cigarette smoking," Daniels added. "Where risk factors exist, such as high blood pressure, they should be appropriately treated."
Hospitalist Engagement Benchmarking Service Returns for 2016
Engaged hospitalists drive quality care, and SHM has the tools to help you assess the level of engagement of hospitalists in your hospital medicine group. SHM offered a Hospitalist Engagement Benchmarking Service in 2015 and analyzed engagement of approximately 1,500 hospitalists. Organizational climate, care quality, autonomy, effective motivation, and burnout risk are just a few of the domains that were benchmarked.
“The engagement survey opened conversations about everything from how we relate to the C-suite to what we can do to sustain teamwork,” says Erin Stucky Fisher, MD, MHM, pediatric hospitalist at Rady Children’s Hospital-San Diego. “[It] highlighted what was working well and identified what needs work.”
More than 80% of respondents indicated that they will utilize the service again and plan to recommend it to a colleague. Help ensure hospitalists are engaged in your hospital medicine group by registering now for the next cohort at www.hospitalmedicine.org/engage. TH
Brett Radler is SHM’s communications coordinator.
Engaged hospitalists drive quality care, and SHM has the tools to help you assess the level of engagement of hospitalists in your hospital medicine group. SHM offered a Hospitalist Engagement Benchmarking Service in 2015 and analyzed engagement of approximately 1,500 hospitalists. Organizational climate, care quality, autonomy, effective motivation, and burnout risk are just a few of the domains that were benchmarked.
“The engagement survey opened conversations about everything from how we relate to the C-suite to what we can do to sustain teamwork,” says Erin Stucky Fisher, MD, MHM, pediatric hospitalist at Rady Children’s Hospital-San Diego. “[It] highlighted what was working well and identified what needs work.”
More than 80% of respondents indicated that they will utilize the service again and plan to recommend it to a colleague. Help ensure hospitalists are engaged in your hospital medicine group by registering now for the next cohort at www.hospitalmedicine.org/engage. TH
Brett Radler is SHM’s communications coordinator.
Engaged hospitalists drive quality care, and SHM has the tools to help you assess the level of engagement of hospitalists in your hospital medicine group. SHM offered a Hospitalist Engagement Benchmarking Service in 2015 and analyzed engagement of approximately 1,500 hospitalists. Organizational climate, care quality, autonomy, effective motivation, and burnout risk are just a few of the domains that were benchmarked.
“The engagement survey opened conversations about everything from how we relate to the C-suite to what we can do to sustain teamwork,” says Erin Stucky Fisher, MD, MHM, pediatric hospitalist at Rady Children’s Hospital-San Diego. “[It] highlighted what was working well and identified what needs work.”
More than 80% of respondents indicated that they will utilize the service again and plan to recommend it to a colleague. Help ensure hospitalists are engaged in your hospital medicine group by registering now for the next cohort at www.hospitalmedicine.org/engage. TH
Brett Radler is SHM’s communications coordinator.
Leadership Academy 2016 heads to Florida in October
Ever wish you had more leadership training in medical school or your residency programs? Feel a bit overwhelmed when developing operational plans for your hospital or negotiating important contracts? Join SHM in sunny Lake Buena Vista, Fla., October 24–27, for its esteemed Leadership Academy (www.shmleadershipacademy.org). SHM Leadership Academy prepares clinicians, academicians, and administrators with vital leadership skills traditionally not taught throughout the course of medical training, tailored specifically to hospital medicine.
“SHM’s Leadership Academy teaches leadership skills for individuals all across the spectrum of the hospital team. My experience helped me to raise the bar not only to benefit myself but also my institution and especially my patients,” says Ron Greeno, MD, MHM. “I highly recommend this experience to any hospital medicine professionals who aspire to take their leadership skills to the next level.”
All three courses run concurrently over the span of the four days and are led by world-renowned faculty. This expanded meeting will provide attendees with unprecedented networking opportunities with hundreds of colleagues and enhanced career development.
Available Leadership Academy courses include:
- Leadership Foundations, a four-day course that serves as the first step in your leadership journey. Attendees learn how to evaluate personal leadership strengths and weaknesses, create and execute a communication strategy for key team members, understand key hospital drivers, examine how hospital metrics are derived, and much more. Attendees are divided into smaller moderated groups to ensure meaningful, relevant application of concepts to hands-on activities.
- Advanced Leadership: Influential Management, a course that builds skills around driving culture change through specific leadership behaviors and actions, financial storytelling, engaging in effective professional negotiation activities with proven techniques, and more through world-renowned faculty and applied exercises.
(Prerequisite: Leadership Foundations or an advanced management degree upon course director approval)
- Advanced Leadership: Mastering Teamwork, a course developed in response to high demand from previous Leadership Academy attendees. Participants learn how to critically assess program growth opportunities and develop operational plans; utilize the principles of SWARM intelligence; lead, manage, and motivate teams in complex hospital environments; and develop effective communication strategies.
(Prerequisite: Leadership Foundations or an advanced management degree upon course director approval.)
SHM members receive reduced rates for course tuition. For more information on how to register, visit www.SHMLeadershipAcademy.org.
Ever wish you had more leadership training in medical school or your residency programs? Feel a bit overwhelmed when developing operational plans for your hospital or negotiating important contracts? Join SHM in sunny Lake Buena Vista, Fla., October 24–27, for its esteemed Leadership Academy (www.shmleadershipacademy.org). SHM Leadership Academy prepares clinicians, academicians, and administrators with vital leadership skills traditionally not taught throughout the course of medical training, tailored specifically to hospital medicine.
“SHM’s Leadership Academy teaches leadership skills for individuals all across the spectrum of the hospital team. My experience helped me to raise the bar not only to benefit myself but also my institution and especially my patients,” says Ron Greeno, MD, MHM. “I highly recommend this experience to any hospital medicine professionals who aspire to take their leadership skills to the next level.”
All three courses run concurrently over the span of the four days and are led by world-renowned faculty. This expanded meeting will provide attendees with unprecedented networking opportunities with hundreds of colleagues and enhanced career development.
Available Leadership Academy courses include:
- Leadership Foundations, a four-day course that serves as the first step in your leadership journey. Attendees learn how to evaluate personal leadership strengths and weaknesses, create and execute a communication strategy for key team members, understand key hospital drivers, examine how hospital metrics are derived, and much more. Attendees are divided into smaller moderated groups to ensure meaningful, relevant application of concepts to hands-on activities.
- Advanced Leadership: Influential Management, a course that builds skills around driving culture change through specific leadership behaviors and actions, financial storytelling, engaging in effective professional negotiation activities with proven techniques, and more through world-renowned faculty and applied exercises.
(Prerequisite: Leadership Foundations or an advanced management degree upon course director approval)
- Advanced Leadership: Mastering Teamwork, a course developed in response to high demand from previous Leadership Academy attendees. Participants learn how to critically assess program growth opportunities and develop operational plans; utilize the principles of SWARM intelligence; lead, manage, and motivate teams in complex hospital environments; and develop effective communication strategies.
(Prerequisite: Leadership Foundations or an advanced management degree upon course director approval.)
SHM members receive reduced rates for course tuition. For more information on how to register, visit www.SHMLeadershipAcademy.org.
Ever wish you had more leadership training in medical school or your residency programs? Feel a bit overwhelmed when developing operational plans for your hospital or negotiating important contracts? Join SHM in sunny Lake Buena Vista, Fla., October 24–27, for its esteemed Leadership Academy (www.shmleadershipacademy.org). SHM Leadership Academy prepares clinicians, academicians, and administrators with vital leadership skills traditionally not taught throughout the course of medical training, tailored specifically to hospital medicine.
“SHM’s Leadership Academy teaches leadership skills for individuals all across the spectrum of the hospital team. My experience helped me to raise the bar not only to benefit myself but also my institution and especially my patients,” says Ron Greeno, MD, MHM. “I highly recommend this experience to any hospital medicine professionals who aspire to take their leadership skills to the next level.”
All three courses run concurrently over the span of the four days and are led by world-renowned faculty. This expanded meeting will provide attendees with unprecedented networking opportunities with hundreds of colleagues and enhanced career development.
Available Leadership Academy courses include:
- Leadership Foundations, a four-day course that serves as the first step in your leadership journey. Attendees learn how to evaluate personal leadership strengths and weaknesses, create and execute a communication strategy for key team members, understand key hospital drivers, examine how hospital metrics are derived, and much more. Attendees are divided into smaller moderated groups to ensure meaningful, relevant application of concepts to hands-on activities.
- Advanced Leadership: Influential Management, a course that builds skills around driving culture change through specific leadership behaviors and actions, financial storytelling, engaging in effective professional negotiation activities with proven techniques, and more through world-renowned faculty and applied exercises.
(Prerequisite: Leadership Foundations or an advanced management degree upon course director approval)
- Advanced Leadership: Mastering Teamwork, a course developed in response to high demand from previous Leadership Academy attendees. Participants learn how to critically assess program growth opportunities and develop operational plans; utilize the principles of SWARM intelligence; lead, manage, and motivate teams in complex hospital environments; and develop effective communication strategies.
(Prerequisite: Leadership Foundations or an advanced management degree upon course director approval.)
SHM members receive reduced rates for course tuition. For more information on how to register, visit www.SHMLeadershipAcademy.org.
Researchers Say Procalcitonin is Linked to Shorter Treatment and Reduced Mortality in Critically Ill
NEW YORK (Reuters Health) - Use of the marker procalcitonin to guide antibacterial therapy in the critically ill is associated with shorter treatment and reduced mortality, according to Dutch researchers.
As Dr. Evelien de Jong told Reuters Health by email, "Antibiotic overconsumption is one of the largest threats to medicine in the near future. Our study is the largest randomized controlled trial of antibiotic reduction in intensive care units (ICUs) and will, hopefully, contribute to a more individualized antibiotic duration per patient and an overall reduction of antibiotic use."
In a February 29 online paper in the Lancet Infectious Diseases, Dr. de Jong, of VU University Medical Center, Amsterdam, and colleagues noted that a "drop in procalcitonin concentration might help (clinicians) to discontinue antibiotic use in a more timely fashion" than reliance on biomarkers such as C-reactive protein.
To investigate, the researchers studied 1,575 ICU patients who received antibiotics and were randomized to procalcitonin-guided antibiotic discontinuation or standard of care. Fifteen were excluded from the procalcitonin group and 14 were excluded from the standard care group.
"In the procalcitonin-guided group, a non-binding advice to discontinue antibiotics was provided if procalcitonin concentration had decreased by 80% or more of its peak value or to 0.5 ug/L or lower," the authors reported.
In all, 538 (71%) of 761 patients in the procalcitonin-guided group and 457 (58%) of 785 patients in the standard-of-care group completed their antibiotic treatment in the ICU.
Median consumption of antibiotics was 7.5 daily defined doses in the procalcitonin group, significantly less than the 9.3 daily defined doses in the standard-of-care group, for a mean group absolute difference of 2.69 (p<0.0001).
Median duration of treatment was also significantly shorter in the procalcitonin-guided group (five versus seven days), for a mean group absolute difference of 1.22 (p<0.0001).
Mortality at 28 days was also significantly less than in the standard-of-care group. This was 20% versus 27% in intention-to-treat analysis. At one year, corresponding per protocol proportions were 36% and 43%.
Overall, the researchers concluded, "Procalcitonin concentrations might help physicians in deciding whether or not the presumed infection is truly bacterial, leading to more adequate diagnosis and treatment, the cornerstones of antibiotic stewardship."
Commenting by email, Dr. Philipp Schuetz, coauthor of an accompanying editorial, told Reuters Health, "This well-done and large landmark trial proves that procalcitonin-guided care reduces unnecessary antibiotic courses in critical care patients with assumed or proven infection and thereby improves patient outcomes, namely overall survival."
Dr. Schuetz, of the University of Basel, Switzerland, concluded, "We should now adapt our guidelines and start to (adopt) more widespread use of procalcitonin protocols in clinical practice to slow emergence of bacterial resistance and improve sepsis care."
NEW YORK (Reuters Health) - Use of the marker procalcitonin to guide antibacterial therapy in the critically ill is associated with shorter treatment and reduced mortality, according to Dutch researchers.
As Dr. Evelien de Jong told Reuters Health by email, "Antibiotic overconsumption is one of the largest threats to medicine in the near future. Our study is the largest randomized controlled trial of antibiotic reduction in intensive care units (ICUs) and will, hopefully, contribute to a more individualized antibiotic duration per patient and an overall reduction of antibiotic use."
In a February 29 online paper in the Lancet Infectious Diseases, Dr. de Jong, of VU University Medical Center, Amsterdam, and colleagues noted that a "drop in procalcitonin concentration might help (clinicians) to discontinue antibiotic use in a more timely fashion" than reliance on biomarkers such as C-reactive protein.
To investigate, the researchers studied 1,575 ICU patients who received antibiotics and were randomized to procalcitonin-guided antibiotic discontinuation or standard of care. Fifteen were excluded from the procalcitonin group and 14 were excluded from the standard care group.
"In the procalcitonin-guided group, a non-binding advice to discontinue antibiotics was provided if procalcitonin concentration had decreased by 80% or more of its peak value or to 0.5 ug/L or lower," the authors reported.
In all, 538 (71%) of 761 patients in the procalcitonin-guided group and 457 (58%) of 785 patients in the standard-of-care group completed their antibiotic treatment in the ICU.
Median consumption of antibiotics was 7.5 daily defined doses in the procalcitonin group, significantly less than the 9.3 daily defined doses in the standard-of-care group, for a mean group absolute difference of 2.69 (p<0.0001).
Median duration of treatment was also significantly shorter in the procalcitonin-guided group (five versus seven days), for a mean group absolute difference of 1.22 (p<0.0001).
Mortality at 28 days was also significantly less than in the standard-of-care group. This was 20% versus 27% in intention-to-treat analysis. At one year, corresponding per protocol proportions were 36% and 43%.
Overall, the researchers concluded, "Procalcitonin concentrations might help physicians in deciding whether or not the presumed infection is truly bacterial, leading to more adequate diagnosis and treatment, the cornerstones of antibiotic stewardship."
Commenting by email, Dr. Philipp Schuetz, coauthor of an accompanying editorial, told Reuters Health, "This well-done and large landmark trial proves that procalcitonin-guided care reduces unnecessary antibiotic courses in critical care patients with assumed or proven infection and thereby improves patient outcomes, namely overall survival."
Dr. Schuetz, of the University of Basel, Switzerland, concluded, "We should now adapt our guidelines and start to (adopt) more widespread use of procalcitonin protocols in clinical practice to slow emergence of bacterial resistance and improve sepsis care."
NEW YORK (Reuters Health) - Use of the marker procalcitonin to guide antibacterial therapy in the critically ill is associated with shorter treatment and reduced mortality, according to Dutch researchers.
As Dr. Evelien de Jong told Reuters Health by email, "Antibiotic overconsumption is one of the largest threats to medicine in the near future. Our study is the largest randomized controlled trial of antibiotic reduction in intensive care units (ICUs) and will, hopefully, contribute to a more individualized antibiotic duration per patient and an overall reduction of antibiotic use."
In a February 29 online paper in the Lancet Infectious Diseases, Dr. de Jong, of VU University Medical Center, Amsterdam, and colleagues noted that a "drop in procalcitonin concentration might help (clinicians) to discontinue antibiotic use in a more timely fashion" than reliance on biomarkers such as C-reactive protein.
To investigate, the researchers studied 1,575 ICU patients who received antibiotics and were randomized to procalcitonin-guided antibiotic discontinuation or standard of care. Fifteen were excluded from the procalcitonin group and 14 were excluded from the standard care group.
"In the procalcitonin-guided group, a non-binding advice to discontinue antibiotics was provided if procalcitonin concentration had decreased by 80% or more of its peak value or to 0.5 ug/L or lower," the authors reported.
In all, 538 (71%) of 761 patients in the procalcitonin-guided group and 457 (58%) of 785 patients in the standard-of-care group completed their antibiotic treatment in the ICU.
Median consumption of antibiotics was 7.5 daily defined doses in the procalcitonin group, significantly less than the 9.3 daily defined doses in the standard-of-care group, for a mean group absolute difference of 2.69 (p<0.0001).
Median duration of treatment was also significantly shorter in the procalcitonin-guided group (five versus seven days), for a mean group absolute difference of 1.22 (p<0.0001).
Mortality at 28 days was also significantly less than in the standard-of-care group. This was 20% versus 27% in intention-to-treat analysis. At one year, corresponding per protocol proportions were 36% and 43%.
Overall, the researchers concluded, "Procalcitonin concentrations might help physicians in deciding whether or not the presumed infection is truly bacterial, leading to more adequate diagnosis and treatment, the cornerstones of antibiotic stewardship."
Commenting by email, Dr. Philipp Schuetz, coauthor of an accompanying editorial, told Reuters Health, "This well-done and large landmark trial proves that procalcitonin-guided care reduces unnecessary antibiotic courses in critical care patients with assumed or proven infection and thereby improves patient outcomes, namely overall survival."
Dr. Schuetz, of the University of Basel, Switzerland, concluded, "We should now adapt our guidelines and start to (adopt) more widespread use of procalcitonin protocols in clinical practice to slow emergence of bacterial resistance and improve sepsis care."
VTEP Guidelines Can Be Systematically Implemented in Pediatric Inpatients
Clinical question: Can venous thromboembolism prophylaxis (VTEP) guidelines be systematically implemented in a pediatric inpatient population?
Background: VTEP for hospitalized adult medical patients has been characterized in the literature as being safe and efficacious, although mortality benefits are unclear.1 Systematic risk stratification based on electronic medical records (EMRs) with resultant implementation of pharmacologic and mechanical thromboprophylaxis has been shown to improve appropriate VTEP ordering in the adult inpatient population.2
Although the incidence of VTE is known to be increasing in the pediatric population, systematic VTEP implementation in hospitalized children is not well-described. Prior studies have shown the safety of systematic VTEP implementation through a protocol identifying high-risk pediatric inpatients with resultant initiation of appropriate VTEP. 3,4
Risk stratification in prior studies has taken into consideration risk factors such as altered mobility, presence of a central venous catheter (CVC), spinal cord injury (SCI), major lower-extremity orthopedic surgery, major trauma, active malignancy, acute infection, obesity, estrogen use, inflammatory bowel disease (IBD), prior VTE, and family history of VTE.4
Study design: Prospective cohort study using QI methodology.
Setting: A 455-bed, tertiary, freestanding children’s hospital.
Synopsis: After reviewing current literature for VTEP in adults and children and existing institutional pathways for VTEP in adults, traumatic brain injury, and SCI, a multidisciplinary committee formulated VTEP guidelines for 12- to 17-year-old patients. Pharmacologic prophylaxis was considered appropriate in the absence of contraindications and only if CVC and altered mobility were present as risk factors. Using a previously published logistic regression model evaluating VTE risk factors, patients were further categorized as high, moderate, or low risk.
Initial risk-factor categorization was via EMR-based order set, where risk factors were displayed, but subsequently was performed by an integrated tool based on an initial screening form completed by providers upon admission. Logic rules applied by the EMR led to specific VTEP recommendations, which were then selectable by the provider.
Over the first 17 months of EMR tool use, 148 patients on average were admitted each month. VTEP screening rates via the EMR tool increased from 48% in the first month to 81% in the final month. Despite EMR tool usage, VTEP orders did not always correlate with recommendations. Although not a stated objective of the study, none of the screened patients developed a VTE (compared to three cases of VTE in patients between 12 and 17 years of age the year prior).
Bottom line: VTEP guidelines can be systematically implemented via an EMR-based tool in a pediatric inpatient population.
Citation: Mahajerin A, Webber E, Morris J, Taylor K, Saysana M. Development and implementation results of a venous thromboembolism prophylaxis guideline in a tertiary care pediatric hospital. Hosp Pediatr. 2015;5(12):630-636.
References
- Spyropoulos AC, Mahan C. Venous thromboembolism prophylaxis in the medical patient: controversies and perspectives. Am J Med. 2009;122(12):1077-1084.
- Kahn SR, Morrison DR, Cohen JM, et al. Interventions for implementation of thromboprophylaxis in hospitalized medical and surgical patients at risk for venous thromboembolism. Cochrane Database Syst Rev. 2013;7:CD008201.
- Takemoto CM, Sohi S, Desai K, et al. Hospital-associated venous thromboembolism in children: incidence and clinical characteristics. J Pediatr. 2014;164(2):332-338.
- Raffini L, Trimarchi T, Beliveau J, Davis D. Thromboprophylaxis in a pediatric hospital: a patient-safety and quality-improvement initiative. Pediatrics. 2011;127(5):e1326-1332.

Clinical question: Can venous thromboembolism prophylaxis (VTEP) guidelines be systematically implemented in a pediatric inpatient population?
Background: VTEP for hospitalized adult medical patients has been characterized in the literature as being safe and efficacious, although mortality benefits are unclear.1 Systematic risk stratification based on electronic medical records (EMRs) with resultant implementation of pharmacologic and mechanical thromboprophylaxis has been shown to improve appropriate VTEP ordering in the adult inpatient population.2
Although the incidence of VTE is known to be increasing in the pediatric population, systematic VTEP implementation in hospitalized children is not well-described. Prior studies have shown the safety of systematic VTEP implementation through a protocol identifying high-risk pediatric inpatients with resultant initiation of appropriate VTEP. 3,4
Risk stratification in prior studies has taken into consideration risk factors such as altered mobility, presence of a central venous catheter (CVC), spinal cord injury (SCI), major lower-extremity orthopedic surgery, major trauma, active malignancy, acute infection, obesity, estrogen use, inflammatory bowel disease (IBD), prior VTE, and family history of VTE.4
Study design: Prospective cohort study using QI methodology.
Setting: A 455-bed, tertiary, freestanding children’s hospital.
Synopsis: After reviewing current literature for VTEP in adults and children and existing institutional pathways for VTEP in adults, traumatic brain injury, and SCI, a multidisciplinary committee formulated VTEP guidelines for 12- to 17-year-old patients. Pharmacologic prophylaxis was considered appropriate in the absence of contraindications and only if CVC and altered mobility were present as risk factors. Using a previously published logistic regression model evaluating VTE risk factors, patients were further categorized as high, moderate, or low risk.
Initial risk-factor categorization was via EMR-based order set, where risk factors were displayed, but subsequently was performed by an integrated tool based on an initial screening form completed by providers upon admission. Logic rules applied by the EMR led to specific VTEP recommendations, which were then selectable by the provider.
Over the first 17 months of EMR tool use, 148 patients on average were admitted each month. VTEP screening rates via the EMR tool increased from 48% in the first month to 81% in the final month. Despite EMR tool usage, VTEP orders did not always correlate with recommendations. Although not a stated objective of the study, none of the screened patients developed a VTE (compared to three cases of VTE in patients between 12 and 17 years of age the year prior).
Bottom line: VTEP guidelines can be systematically implemented via an EMR-based tool in a pediatric inpatient population.
Citation: Mahajerin A, Webber E, Morris J, Taylor K, Saysana M. Development and implementation results of a venous thromboembolism prophylaxis guideline in a tertiary care pediatric hospital. Hosp Pediatr. 2015;5(12):630-636.
References
- Spyropoulos AC, Mahan C. Venous thromboembolism prophylaxis in the medical patient: controversies and perspectives. Am J Med. 2009;122(12):1077-1084.
- Kahn SR, Morrison DR, Cohen JM, et al. Interventions for implementation of thromboprophylaxis in hospitalized medical and surgical patients at risk for venous thromboembolism. Cochrane Database Syst Rev. 2013;7:CD008201.
- Takemoto CM, Sohi S, Desai K, et al. Hospital-associated venous thromboembolism in children: incidence and clinical characteristics. J Pediatr. 2014;164(2):332-338.
- Raffini L, Trimarchi T, Beliveau J, Davis D. Thromboprophylaxis in a pediatric hospital: a patient-safety and quality-improvement initiative. Pediatrics. 2011;127(5):e1326-1332.

Clinical question: Can venous thromboembolism prophylaxis (VTEP) guidelines be systematically implemented in a pediatric inpatient population?
Background: VTEP for hospitalized adult medical patients has been characterized in the literature as being safe and efficacious, although mortality benefits are unclear.1 Systematic risk stratification based on electronic medical records (EMRs) with resultant implementation of pharmacologic and mechanical thromboprophylaxis has been shown to improve appropriate VTEP ordering in the adult inpatient population.2
Although the incidence of VTE is known to be increasing in the pediatric population, systematic VTEP implementation in hospitalized children is not well-described. Prior studies have shown the safety of systematic VTEP implementation through a protocol identifying high-risk pediatric inpatients with resultant initiation of appropriate VTEP. 3,4
Risk stratification in prior studies has taken into consideration risk factors such as altered mobility, presence of a central venous catheter (CVC), spinal cord injury (SCI), major lower-extremity orthopedic surgery, major trauma, active malignancy, acute infection, obesity, estrogen use, inflammatory bowel disease (IBD), prior VTE, and family history of VTE.4
Study design: Prospective cohort study using QI methodology.
Setting: A 455-bed, tertiary, freestanding children’s hospital.
Synopsis: After reviewing current literature for VTEP in adults and children and existing institutional pathways for VTEP in adults, traumatic brain injury, and SCI, a multidisciplinary committee formulated VTEP guidelines for 12- to 17-year-old patients. Pharmacologic prophylaxis was considered appropriate in the absence of contraindications and only if CVC and altered mobility were present as risk factors. Using a previously published logistic regression model evaluating VTE risk factors, patients were further categorized as high, moderate, or low risk.
Initial risk-factor categorization was via EMR-based order set, where risk factors were displayed, but subsequently was performed by an integrated tool based on an initial screening form completed by providers upon admission. Logic rules applied by the EMR led to specific VTEP recommendations, which were then selectable by the provider.
Over the first 17 months of EMR tool use, 148 patients on average were admitted each month. VTEP screening rates via the EMR tool increased from 48% in the first month to 81% in the final month. Despite EMR tool usage, VTEP orders did not always correlate with recommendations. Although not a stated objective of the study, none of the screened patients developed a VTE (compared to three cases of VTE in patients between 12 and 17 years of age the year prior).
Bottom line: VTEP guidelines can be systematically implemented via an EMR-based tool in a pediatric inpatient population.
Citation: Mahajerin A, Webber E, Morris J, Taylor K, Saysana M. Development and implementation results of a venous thromboembolism prophylaxis guideline in a tertiary care pediatric hospital. Hosp Pediatr. 2015;5(12):630-636.
References
- Spyropoulos AC, Mahan C. Venous thromboembolism prophylaxis in the medical patient: controversies and perspectives. Am J Med. 2009;122(12):1077-1084.
- Kahn SR, Morrison DR, Cohen JM, et al. Interventions for implementation of thromboprophylaxis in hospitalized medical and surgical patients at risk for venous thromboembolism. Cochrane Database Syst Rev. 2013;7:CD008201.
- Takemoto CM, Sohi S, Desai K, et al. Hospital-associated venous thromboembolism in children: incidence and clinical characteristics. J Pediatr. 2014;164(2):332-338.
- Raffini L, Trimarchi T, Beliveau J, Davis D. Thromboprophylaxis in a pediatric hospital: a patient-safety and quality-improvement initiative. Pediatrics. 2011;127(5):e1326-1332.

Questions Have Been Raised about Potential Risks from Using Abbott Laboratories' Novel Coronary Stent
(Reuters) - U.S. government scientists have raised questions about the potential risks to patients of heart attacks and blood clots from Abbott Laboratories' novel coronary stent that dissolves after it is implanted.
Abbott is seeking U.S. approval to sell the stent, called Absorb, as an alternative to metal stents currently used in percutaneous coronary intervention. Unlike traditional stents that remain in place after implantation, Absorb is designed to disappear within three years of the procedure.
U.S. Food and Drug Administration staff, in documents released before an advisory panel meets on Tuesday to consider whether to recommend approval of the device, said they would ask the outside experts about data showing more heart attack and stent-related blood clots compared with Abbott's drug-coated metal Xience stent.
FDA said it also will ask the panel to address risks associated with the device when used in smaller arteries.
A large clinical trial released in October concluded that the Absorb stent, which is made of a plastic similar to dissolving sutures, was comparable to Xience in overall safety and effectiveness. Although Xience appeared to be numerically better than Absorb at one year on a variety of secondary measures, the differences were not considered statistically significant.
"These results are from physicians using a new therapy for the first time. Consequently, we expect them to improve with time and experience," said Abbott spokesman Jonathon Hamilton.
In the Absorb III clinical study, patients with small vessels comprised less than 20 percent of the total and experienced relatively low rates of adverse events even though many had known risk factors, including diabetes, Hamilton said.
More than 125,000 patients already have been treated with Absorb in more than 100 countries where it is commercially available.
If approved in the United States, Absorb would compete with Xience, the market-leading stent, and with Medtronic Plc's Resolute stent and Boston Scientific's Synergy and Promus stents. Synergy's polymer coating used to deliver a drug disappears over time, leaving a bare metal stent in place.
Wells Fargo analyst Larry Biegelsen said he expects Absorb to get a positive recommendation from the advisory panel, followed by FDA approval later this year.
"In the U.S., we estimate Absorb will capture about 5 percent of the total drug-eluting stent market, although our estimate may prove conservative if the post-approval data and experience with Absorb improves," Biegelsen wrote in a note to clients.
(Reuters) - U.S. government scientists have raised questions about the potential risks to patients of heart attacks and blood clots from Abbott Laboratories' novel coronary stent that dissolves after it is implanted.
Abbott is seeking U.S. approval to sell the stent, called Absorb, as an alternative to metal stents currently used in percutaneous coronary intervention. Unlike traditional stents that remain in place after implantation, Absorb is designed to disappear within three years of the procedure.
U.S. Food and Drug Administration staff, in documents released before an advisory panel meets on Tuesday to consider whether to recommend approval of the device, said they would ask the outside experts about data showing more heart attack and stent-related blood clots compared with Abbott's drug-coated metal Xience stent.
FDA said it also will ask the panel to address risks associated with the device when used in smaller arteries.
A large clinical trial released in October concluded that the Absorb stent, which is made of a plastic similar to dissolving sutures, was comparable to Xience in overall safety and effectiveness. Although Xience appeared to be numerically better than Absorb at one year on a variety of secondary measures, the differences were not considered statistically significant.
"These results are from physicians using a new therapy for the first time. Consequently, we expect them to improve with time and experience," said Abbott spokesman Jonathon Hamilton.
In the Absorb III clinical study, patients with small vessels comprised less than 20 percent of the total and experienced relatively low rates of adverse events even though many had known risk factors, including diabetes, Hamilton said.
More than 125,000 patients already have been treated with Absorb in more than 100 countries where it is commercially available.
If approved in the United States, Absorb would compete with Xience, the market-leading stent, and with Medtronic Plc's Resolute stent and Boston Scientific's Synergy and Promus stents. Synergy's polymer coating used to deliver a drug disappears over time, leaving a bare metal stent in place.
Wells Fargo analyst Larry Biegelsen said he expects Absorb to get a positive recommendation from the advisory panel, followed by FDA approval later this year.
"In the U.S., we estimate Absorb will capture about 5 percent of the total drug-eluting stent market, although our estimate may prove conservative if the post-approval data and experience with Absorb improves," Biegelsen wrote in a note to clients.
(Reuters) - U.S. government scientists have raised questions about the potential risks to patients of heart attacks and blood clots from Abbott Laboratories' novel coronary stent that dissolves after it is implanted.
Abbott is seeking U.S. approval to sell the stent, called Absorb, as an alternative to metal stents currently used in percutaneous coronary intervention. Unlike traditional stents that remain in place after implantation, Absorb is designed to disappear within three years of the procedure.
U.S. Food and Drug Administration staff, in documents released before an advisory panel meets on Tuesday to consider whether to recommend approval of the device, said they would ask the outside experts about data showing more heart attack and stent-related blood clots compared with Abbott's drug-coated metal Xience stent.
FDA said it also will ask the panel to address risks associated with the device when used in smaller arteries.
A large clinical trial released in October concluded that the Absorb stent, which is made of a plastic similar to dissolving sutures, was comparable to Xience in overall safety and effectiveness. Although Xience appeared to be numerically better than Absorb at one year on a variety of secondary measures, the differences were not considered statistically significant.
"These results are from physicians using a new therapy for the first time. Consequently, we expect them to improve with time and experience," said Abbott spokesman Jonathon Hamilton.
In the Absorb III clinical study, patients with small vessels comprised less than 20 percent of the total and experienced relatively low rates of adverse events even though many had known risk factors, including diabetes, Hamilton said.
More than 125,000 patients already have been treated with Absorb in more than 100 countries where it is commercially available.
If approved in the United States, Absorb would compete with Xience, the market-leading stent, and with Medtronic Plc's Resolute stent and Boston Scientific's Synergy and Promus stents. Synergy's polymer coating used to deliver a drug disappears over time, leaving a bare metal stent in place.
Wells Fargo analyst Larry Biegelsen said he expects Absorb to get a positive recommendation from the advisory panel, followed by FDA approval later this year.
"In the U.S., we estimate Absorb will capture about 5 percent of the total drug-eluting stent market, although our estimate may prove conservative if the post-approval data and experience with Absorb improves," Biegelsen wrote in a note to clients.