User login
The Hospitalist only
Tips for Hospitalists on Spending More of Their Time at the Top of Their License
Hospitalists spend too little time working at the top of their license. Put differently, I think a hospitalist often spends only about 1.5 to two hours in a 10- or 12-hour workday making use of the knowledge base and skills developed in training. (I wrote about this and referenced some hospitalist time-motion studies in my December 2010 column.)
The remaining hours are typically spent in activities such as figuring out which surgeon is on call and tracking her down, managing patient lists, filling out paper or electronic forms, explaining observation status to patients, and so on.
When I first became a hospitalist in the 1980s, there was already a lot of talk about the paperwork burden faced by doctors across all specialties. I recall the gnashing of teeth that ensued—lots of articles and seminars, and it seems to me even a few legislative proposals, focused on the topic. It appears that nearly every recruitment ad at the time mentioned something like “Let us take care of running the business, so you can focus solely on patient care.” Clearly, doctors were seeking relief from the burden of nonclinical work even back then.
I can’t recall reading or hearing anyone talk about the “paperwork” burden of physician practice in the past few years. This isn’t because things have gotten better; in fact, I think the burden of “non-doctoring activities” has steadily increased. We hear less about the problem of excessive paperwork simply because, more recently, it has been framed differently—it is now typically referred to as the problem of too little time spent practicing at the top of license.
Search the Internet for “top of license” and a number of interesting things turn up. Most are healthcare related—maybe other professions don’t use the term—and there are just as many links referring to nurses as physicians. Much is written about the need for primary care physicians to spend more time working at the top of their license, but I couldn’t find anything addressing this issue specifically for hospitalists.
What Can Be Done?
Moving your work as a hospitalist more to the top of your license isn’t a simple thing, and our whole field will need to work on this over time. The most effective interventions will vary some from place to place, but here are some ideas that may be relevant for many hospitalist groups.
Medication reconciliation. I fully support the idea of careful medication reconciliation, but, given that such a large portion of hospitalist patients are on so many medications, this is a time-consuming task. And, in many or most hospitals, the task suffers from diffusion of responsibility; for example, the ED nurse makes only a half-hearted attempt to get an accurate list, and the hospitalist believes that whatever the ED nurse entered into the record regarding patient medications is probably the best obtainable list.
A pharmacy technician stationed in the ED and charged with recording the best obtainable list of medicines on patient arrival can address both of these problems (for more information, the American Society of Health-System Pharmacists offers webinars and other resources on this topic). This would include calling family members, pharmacies, and physician offices for clarification in some cases. Hospitalists working in such an environment nearly always say it is extremely valuable in reducing inaccuracies in the pre-hospital medication list, as well as saving hospitalists time when they are admitting patients.
Unfortunately, hospitals may resist adding pharmacy technicians because of the expense or, in some cases, because of concerns that such work may exceed the legal scope of work for technicians.
Post-hospital appointments. I think arranging post-hospital appointments should be no more difficult for the hospitalist than ordering a complete blood count (CBC). It shouldn’t matter whether I want the patient to follow up with the PCP he has been seeing for years, or see a neurologist or diabetes educator as a new patient consult. Any treating doctor in the hospital should be able to arrange such post-hospital visits with just a click or two in the EHR, or a stroke of the pen. And the patient should leave the hospital with a written date and time of the appointment that has been made for them.
Few hospitals can reliably provide this, however, so, all too often, hospitalists spend their time calling clerical staff at outpatient clinics to arrange appointments, writing them down, and delivering them to patients. This is far from what anyone would consider top of license work. (I wrote a little more about this in last month’s column.)
Medicare benefits specialist. Many hospitalists end up spending significant time explaining to patients and families the reason a patient is on observation status and trying to defuse the resulting frustration and anger. As I stated in my November 2014 column, I think observation status is so frustrating to patients that it is often the root cause of complaints about care and, potentially, the source of malpractice suits.
Physicians have an unavoidable role in determining observation versus inpatient status, but I think hospitals should work hard to ensure that someone other than the doctor is available to explain to patients and families the reason for observation status, along with its implications, and to provide sympathy for their frustrations. This allows the doctor to stay focused on clinical care.
Limit reliance on a “triage hospitalist.” Hospitalist groups larger than about 20 providers often have one provider devoted through much of a daytime shift to triaging and assigning new referrals across all providers working that day. For larger practices, this triage work may consume all of the provider’s shift, so that person has no time left for clinical care. It is hard for me to see this as top of license work that only a physician or advanced practice clinician can do. In my December 2010 column, I provided some potential alternatives to dedicating a physician or other provider to a triage role.
Your list of important changes that are needed to move hospitalists toward more time spent working at the top of their license will likely differ a lot from the issues above. But every group could benefit from deliberately thinking about what would be most valuable for them and trying to make that a reality.

Hospitalists spend too little time working at the top of their license. Put differently, I think a hospitalist often spends only about 1.5 to two hours in a 10- or 12-hour workday making use of the knowledge base and skills developed in training. (I wrote about this and referenced some hospitalist time-motion studies in my December 2010 column.)
The remaining hours are typically spent in activities such as figuring out which surgeon is on call and tracking her down, managing patient lists, filling out paper or electronic forms, explaining observation status to patients, and so on.
When I first became a hospitalist in the 1980s, there was already a lot of talk about the paperwork burden faced by doctors across all specialties. I recall the gnashing of teeth that ensued—lots of articles and seminars, and it seems to me even a few legislative proposals, focused on the topic. It appears that nearly every recruitment ad at the time mentioned something like “Let us take care of running the business, so you can focus solely on patient care.” Clearly, doctors were seeking relief from the burden of nonclinical work even back then.
I can’t recall reading or hearing anyone talk about the “paperwork” burden of physician practice in the past few years. This isn’t because things have gotten better; in fact, I think the burden of “non-doctoring activities” has steadily increased. We hear less about the problem of excessive paperwork simply because, more recently, it has been framed differently—it is now typically referred to as the problem of too little time spent practicing at the top of license.
Search the Internet for “top of license” and a number of interesting things turn up. Most are healthcare related—maybe other professions don’t use the term—and there are just as many links referring to nurses as physicians. Much is written about the need for primary care physicians to spend more time working at the top of their license, but I couldn’t find anything addressing this issue specifically for hospitalists.
What Can Be Done?
Moving your work as a hospitalist more to the top of your license isn’t a simple thing, and our whole field will need to work on this over time. The most effective interventions will vary some from place to place, but here are some ideas that may be relevant for many hospitalist groups.
Medication reconciliation. I fully support the idea of careful medication reconciliation, but, given that such a large portion of hospitalist patients are on so many medications, this is a time-consuming task. And, in many or most hospitals, the task suffers from diffusion of responsibility; for example, the ED nurse makes only a half-hearted attempt to get an accurate list, and the hospitalist believes that whatever the ED nurse entered into the record regarding patient medications is probably the best obtainable list.
A pharmacy technician stationed in the ED and charged with recording the best obtainable list of medicines on patient arrival can address both of these problems (for more information, the American Society of Health-System Pharmacists offers webinars and other resources on this topic). This would include calling family members, pharmacies, and physician offices for clarification in some cases. Hospitalists working in such an environment nearly always say it is extremely valuable in reducing inaccuracies in the pre-hospital medication list, as well as saving hospitalists time when they are admitting patients.
Unfortunately, hospitals may resist adding pharmacy technicians because of the expense or, in some cases, because of concerns that such work may exceed the legal scope of work for technicians.
Post-hospital appointments. I think arranging post-hospital appointments should be no more difficult for the hospitalist than ordering a complete blood count (CBC). It shouldn’t matter whether I want the patient to follow up with the PCP he has been seeing for years, or see a neurologist or diabetes educator as a new patient consult. Any treating doctor in the hospital should be able to arrange such post-hospital visits with just a click or two in the EHR, or a stroke of the pen. And the patient should leave the hospital with a written date and time of the appointment that has been made for them.
Few hospitals can reliably provide this, however, so, all too often, hospitalists spend their time calling clerical staff at outpatient clinics to arrange appointments, writing them down, and delivering them to patients. This is far from what anyone would consider top of license work. (I wrote a little more about this in last month’s column.)
Medicare benefits specialist. Many hospitalists end up spending significant time explaining to patients and families the reason a patient is on observation status and trying to defuse the resulting frustration and anger. As I stated in my November 2014 column, I think observation status is so frustrating to patients that it is often the root cause of complaints about care and, potentially, the source of malpractice suits.
Physicians have an unavoidable role in determining observation versus inpatient status, but I think hospitals should work hard to ensure that someone other than the doctor is available to explain to patients and families the reason for observation status, along with its implications, and to provide sympathy for their frustrations. This allows the doctor to stay focused on clinical care.
Limit reliance on a “triage hospitalist.” Hospitalist groups larger than about 20 providers often have one provider devoted through much of a daytime shift to triaging and assigning new referrals across all providers working that day. For larger practices, this triage work may consume all of the provider’s shift, so that person has no time left for clinical care. It is hard for me to see this as top of license work that only a physician or advanced practice clinician can do. In my December 2010 column, I provided some potential alternatives to dedicating a physician or other provider to a triage role.
Your list of important changes that are needed to move hospitalists toward more time spent working at the top of their license will likely differ a lot from the issues above. But every group could benefit from deliberately thinking about what would be most valuable for them and trying to make that a reality.

Hospitalists spend too little time working at the top of their license. Put differently, I think a hospitalist often spends only about 1.5 to two hours in a 10- or 12-hour workday making use of the knowledge base and skills developed in training. (I wrote about this and referenced some hospitalist time-motion studies in my December 2010 column.)
The remaining hours are typically spent in activities such as figuring out which surgeon is on call and tracking her down, managing patient lists, filling out paper or electronic forms, explaining observation status to patients, and so on.
When I first became a hospitalist in the 1980s, there was already a lot of talk about the paperwork burden faced by doctors across all specialties. I recall the gnashing of teeth that ensued—lots of articles and seminars, and it seems to me even a few legislative proposals, focused on the topic. It appears that nearly every recruitment ad at the time mentioned something like “Let us take care of running the business, so you can focus solely on patient care.” Clearly, doctors were seeking relief from the burden of nonclinical work even back then.
I can’t recall reading or hearing anyone talk about the “paperwork” burden of physician practice in the past few years. This isn’t because things have gotten better; in fact, I think the burden of “non-doctoring activities” has steadily increased. We hear less about the problem of excessive paperwork simply because, more recently, it has been framed differently—it is now typically referred to as the problem of too little time spent practicing at the top of license.
Search the Internet for “top of license” and a number of interesting things turn up. Most are healthcare related—maybe other professions don’t use the term—and there are just as many links referring to nurses as physicians. Much is written about the need for primary care physicians to spend more time working at the top of their license, but I couldn’t find anything addressing this issue specifically for hospitalists.
What Can Be Done?
Moving your work as a hospitalist more to the top of your license isn’t a simple thing, and our whole field will need to work on this over time. The most effective interventions will vary some from place to place, but here are some ideas that may be relevant for many hospitalist groups.
Medication reconciliation. I fully support the idea of careful medication reconciliation, but, given that such a large portion of hospitalist patients are on so many medications, this is a time-consuming task. And, in many or most hospitals, the task suffers from diffusion of responsibility; for example, the ED nurse makes only a half-hearted attempt to get an accurate list, and the hospitalist believes that whatever the ED nurse entered into the record regarding patient medications is probably the best obtainable list.
A pharmacy technician stationed in the ED and charged with recording the best obtainable list of medicines on patient arrival can address both of these problems (for more information, the American Society of Health-System Pharmacists offers webinars and other resources on this topic). This would include calling family members, pharmacies, and physician offices for clarification in some cases. Hospitalists working in such an environment nearly always say it is extremely valuable in reducing inaccuracies in the pre-hospital medication list, as well as saving hospitalists time when they are admitting patients.
Unfortunately, hospitals may resist adding pharmacy technicians because of the expense or, in some cases, because of concerns that such work may exceed the legal scope of work for technicians.
Post-hospital appointments. I think arranging post-hospital appointments should be no more difficult for the hospitalist than ordering a complete blood count (CBC). It shouldn’t matter whether I want the patient to follow up with the PCP he has been seeing for years, or see a neurologist or diabetes educator as a new patient consult. Any treating doctor in the hospital should be able to arrange such post-hospital visits with just a click or two in the EHR, or a stroke of the pen. And the patient should leave the hospital with a written date and time of the appointment that has been made for them.
Few hospitals can reliably provide this, however, so, all too often, hospitalists spend their time calling clerical staff at outpatient clinics to arrange appointments, writing them down, and delivering them to patients. This is far from what anyone would consider top of license work. (I wrote a little more about this in last month’s column.)
Medicare benefits specialist. Many hospitalists end up spending significant time explaining to patients and families the reason a patient is on observation status and trying to defuse the resulting frustration and anger. As I stated in my November 2014 column, I think observation status is so frustrating to patients that it is often the root cause of complaints about care and, potentially, the source of malpractice suits.
Physicians have an unavoidable role in determining observation versus inpatient status, but I think hospitals should work hard to ensure that someone other than the doctor is available to explain to patients and families the reason for observation status, along with its implications, and to provide sympathy for their frustrations. This allows the doctor to stay focused on clinical care.
Limit reliance on a “triage hospitalist.” Hospitalist groups larger than about 20 providers often have one provider devoted through much of a daytime shift to triaging and assigning new referrals across all providers working that day. For larger practices, this triage work may consume all of the provider’s shift, so that person has no time left for clinical care. It is hard for me to see this as top of license work that only a physician or advanced practice clinician can do. In my December 2010 column, I provided some potential alternatives to dedicating a physician or other provider to a triage role.
Your list of important changes that are needed to move hospitalists toward more time spent working at the top of their license will likely differ a lot from the issues above. But every group could benefit from deliberately thinking about what would be most valuable for them and trying to make that a reality.

Specialty Hospitalists May Be Coming to Your Hospital Soon
Nearly 20 years ago, Bob Wachter, MD, coined the term “hospitalist,” defining a new specialty caring for the hospitalized medical patient. Since that time, we’ve seen rapid growth in the numbers of physicians who identify themselves as hospitalists, dominated by training in internal medicine and, to a lesser extent, family practice and pediatrics.
But, what about other specialty hospitalists, trained in the medicine or surgical specialties? How much of a presence do they have in our institutions today and in which specialties? To help us better understand this, a new question in 2014 State of Hospital Medicine survey asked whether specialty hospitalists practice in your hospital or health system.

—Carolyn Sites, DO, FHM
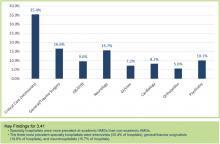
Results show the top three specialty hospitalists to be critical care, at (35.4%), followed by general surgery/trauma (16.6%) and neurology (15.7%), based on the responses of survey participants representing hospital medicine groups (HMGs) that care for adults only. Other specialties included obstetrics (OB), psychiatry, GI, cardiology, and orthopedics (see Figure 1).
Perhaps not too surprising, the greatest number of specialty hospitalists are found in university and academic settings. These are our primary training centers, offering fellowship programs and further subspecialization programs. Much like in our own field of hospital medicine, some academic centers have created one-year fellowships for those interested in specific hospital specialty fields, such as OB hospitalist.
For reasons that are less clear, the survey also shows percentages are highest in the western U.S. and lowest in the East.
Critical care hospitalists, also known as intensivists, dominate the spectrum, being present in academic and nonacademic centers, regardless of the employment model of the medical hospitalists at those facilities. This is not unexpected, given the Leapfrog Group’s endorsement of ICU physician staffing with intensivists.
What’s driving the other specialty hospitalist fields? I suspect the reasons are similar to those of our own specialty. OB and neuro hospitalists at my health system cite the challenges of managing outpatient and inpatient practices, the higher inpatient acuity and focused skill set that are required, immediate availability demands, and work-life balance as key factors. Further drivers include external quality/safety governing agencies or groups, such as the Leapfrog example above, or The Joint Commission’s requirements for certification as a Comprehensive Stroke Center with neurointensive care units.
Much like our own field’s exponential growth, we are likely to see further expansion of specialty hospitalists over the next several years. It will be interesting to watch how much and how fast this occurs, and what impact and influence these groups will bring to the care of the hospitalized patient. I’m already looking forward to next year’s SOHM report to see those results.
Dr. Sites is regional medical director of hospital medicine at Providence Health Systems in Oregon and a member of the SHM Practice Analysis Committee.
Nearly 20 years ago, Bob Wachter, MD, coined the term “hospitalist,” defining a new specialty caring for the hospitalized medical patient. Since that time, we’ve seen rapid growth in the numbers of physicians who identify themselves as hospitalists, dominated by training in internal medicine and, to a lesser extent, family practice and pediatrics.
But, what about other specialty hospitalists, trained in the medicine or surgical specialties? How much of a presence do they have in our institutions today and in which specialties? To help us better understand this, a new question in 2014 State of Hospital Medicine survey asked whether specialty hospitalists practice in your hospital or health system.

—Carolyn Sites, DO, FHM
Results show the top three specialty hospitalists to be critical care, at (35.4%), followed by general surgery/trauma (16.6%) and neurology (15.7%), based on the responses of survey participants representing hospital medicine groups (HMGs) that care for adults only. Other specialties included obstetrics (OB), psychiatry, GI, cardiology, and orthopedics (see Figure 1).
Perhaps not too surprising, the greatest number of specialty hospitalists are found in university and academic settings. These are our primary training centers, offering fellowship programs and further subspecialization programs. Much like in our own field of hospital medicine, some academic centers have created one-year fellowships for those interested in specific hospital specialty fields, such as OB hospitalist.
For reasons that are less clear, the survey also shows percentages are highest in the western U.S. and lowest in the East.
Critical care hospitalists, also known as intensivists, dominate the spectrum, being present in academic and nonacademic centers, regardless of the employment model of the medical hospitalists at those facilities. This is not unexpected, given the Leapfrog Group’s endorsement of ICU physician staffing with intensivists.
What’s driving the other specialty hospitalist fields? I suspect the reasons are similar to those of our own specialty. OB and neuro hospitalists at my health system cite the challenges of managing outpatient and inpatient practices, the higher inpatient acuity and focused skill set that are required, immediate availability demands, and work-life balance as key factors. Further drivers include external quality/safety governing agencies or groups, such as the Leapfrog example above, or The Joint Commission’s requirements for certification as a Comprehensive Stroke Center with neurointensive care units.
Much like our own field’s exponential growth, we are likely to see further expansion of specialty hospitalists over the next several years. It will be interesting to watch how much and how fast this occurs, and what impact and influence these groups will bring to the care of the hospitalized patient. I’m already looking forward to next year’s SOHM report to see those results.
Dr. Sites is regional medical director of hospital medicine at Providence Health Systems in Oregon and a member of the SHM Practice Analysis Committee.
Nearly 20 years ago, Bob Wachter, MD, coined the term “hospitalist,” defining a new specialty caring for the hospitalized medical patient. Since that time, we’ve seen rapid growth in the numbers of physicians who identify themselves as hospitalists, dominated by training in internal medicine and, to a lesser extent, family practice and pediatrics.
But, what about other specialty hospitalists, trained in the medicine or surgical specialties? How much of a presence do they have in our institutions today and in which specialties? To help us better understand this, a new question in 2014 State of Hospital Medicine survey asked whether specialty hospitalists practice in your hospital or health system.

—Carolyn Sites, DO, FHM
Results show the top three specialty hospitalists to be critical care, at (35.4%), followed by general surgery/trauma (16.6%) and neurology (15.7%), based on the responses of survey participants representing hospital medicine groups (HMGs) that care for adults only. Other specialties included obstetrics (OB), psychiatry, GI, cardiology, and orthopedics (see Figure 1).
Perhaps not too surprising, the greatest number of specialty hospitalists are found in university and academic settings. These are our primary training centers, offering fellowship programs and further subspecialization programs. Much like in our own field of hospital medicine, some academic centers have created one-year fellowships for those interested in specific hospital specialty fields, such as OB hospitalist.
For reasons that are less clear, the survey also shows percentages are highest in the western U.S. and lowest in the East.
Critical care hospitalists, also known as intensivists, dominate the spectrum, being present in academic and nonacademic centers, regardless of the employment model of the medical hospitalists at those facilities. This is not unexpected, given the Leapfrog Group’s endorsement of ICU physician staffing with intensivists.
What’s driving the other specialty hospitalist fields? I suspect the reasons are similar to those of our own specialty. OB and neuro hospitalists at my health system cite the challenges of managing outpatient and inpatient practices, the higher inpatient acuity and focused skill set that are required, immediate availability demands, and work-life balance as key factors. Further drivers include external quality/safety governing agencies or groups, such as the Leapfrog example above, or The Joint Commission’s requirements for certification as a Comprehensive Stroke Center with neurointensive care units.
Much like our own field’s exponential growth, we are likely to see further expansion of specialty hospitalists over the next several years. It will be interesting to watch how much and how fast this occurs, and what impact and influence these groups will bring to the care of the hospitalized patient. I’m already looking forward to next year’s SOHM report to see those results.
Dr. Sites is regional medical director of hospital medicine at Providence Health Systems in Oregon and a member of the SHM Practice Analysis Committee.
Hospitalists Choose Quality Metrics Most Important to Them
Fantasy sports, hospital medicine, and quality metrics. Those were the unique elements of an RIV poster presented by Noppon Setji, MD, medical director of the Duke University Medical Center’s hospital medicine program in Durham, N.C., at HM15.
Dr. Setji, who participates in a fantasy football league for physicians, says he aimed to apply the approaches of fantasy sports leagues to hospitalist quality metrics.1 Dr. Setji wanted to find a way to recognize high-performing hospitalists in his group on a regular basis, beyond the group metrics that had been reported to faculty members—and to create greater accountability and evaluate physicians’ performance over time.
A team developed a survey instrument compiling common clinical process and outcome measures for hospitalists, and faculty members were asked to rate how important the various metrics were to them individually as indicators of physician performance. Their responses were combined into a weighted, composite hospital medicine provider performance score, which reflects the relative value practicing hospitalists assign to available performance measures. Results are easily tabulated on an Excel spreadsheet, Dr. Setji says.
Every three months—or football quarter—the top overall performer is awarded two bottles of wine and possession of the traveling trophy.
“We’re always looking for ways to measure our performance,” Dr. Setji says, “and we all want to know how we’re doing relative to our peers.”
Reference
- Setji NP, Bae JG, Griffith BC, Daley C. Fantasy physician leagues? Introducing the physician equivalent of the Qbr (Quarterly Metric-Based Rating) [abstract]. J Hosp Med. 2015;10(suppl 2).
Fantasy sports, hospital medicine, and quality metrics. Those were the unique elements of an RIV poster presented by Noppon Setji, MD, medical director of the Duke University Medical Center’s hospital medicine program in Durham, N.C., at HM15.
Dr. Setji, who participates in a fantasy football league for physicians, says he aimed to apply the approaches of fantasy sports leagues to hospitalist quality metrics.1 Dr. Setji wanted to find a way to recognize high-performing hospitalists in his group on a regular basis, beyond the group metrics that had been reported to faculty members—and to create greater accountability and evaluate physicians’ performance over time.
A team developed a survey instrument compiling common clinical process and outcome measures for hospitalists, and faculty members were asked to rate how important the various metrics were to them individually as indicators of physician performance. Their responses were combined into a weighted, composite hospital medicine provider performance score, which reflects the relative value practicing hospitalists assign to available performance measures. Results are easily tabulated on an Excel spreadsheet, Dr. Setji says.
Every three months—or football quarter—the top overall performer is awarded two bottles of wine and possession of the traveling trophy.
“We’re always looking for ways to measure our performance,” Dr. Setji says, “and we all want to know how we’re doing relative to our peers.”
Reference
- Setji NP, Bae JG, Griffith BC, Daley C. Fantasy physician leagues? Introducing the physician equivalent of the Qbr (Quarterly Metric-Based Rating) [abstract]. J Hosp Med. 2015;10(suppl 2).
Fantasy sports, hospital medicine, and quality metrics. Those were the unique elements of an RIV poster presented by Noppon Setji, MD, medical director of the Duke University Medical Center’s hospital medicine program in Durham, N.C., at HM15.
Dr. Setji, who participates in a fantasy football league for physicians, says he aimed to apply the approaches of fantasy sports leagues to hospitalist quality metrics.1 Dr. Setji wanted to find a way to recognize high-performing hospitalists in his group on a regular basis, beyond the group metrics that had been reported to faculty members—and to create greater accountability and evaluate physicians’ performance over time.
A team developed a survey instrument compiling common clinical process and outcome measures for hospitalists, and faculty members were asked to rate how important the various metrics were to them individually as indicators of physician performance. Their responses were combined into a weighted, composite hospital medicine provider performance score, which reflects the relative value practicing hospitalists assign to available performance measures. Results are easily tabulated on an Excel spreadsheet, Dr. Setji says.
Every three months—or football quarter—the top overall performer is awarded two bottles of wine and possession of the traveling trophy.
“We’re always looking for ways to measure our performance,” Dr. Setji says, “and we all want to know how we’re doing relative to our peers.”
Reference
- Setji NP, Bae JG, Griffith BC, Daley C. Fantasy physician leagues? Introducing the physician equivalent of the Qbr (Quarterly Metric-Based Rating) [abstract]. J Hosp Med. 2015;10(suppl 2).
Small Bowel Block in Elderly Merits Full Hospitalization
NEW YORK (Reuters Health) - The "vast majority" of elderly patients admitted with small bowel obstruction (SBO) are hospitalized for more than two days, and the diagnosis alone should allow appropriate Medicare coverage, according to a new study.
In a paper online July 1 in Annals of Surgery, Dr. Zara Cooper, of Brigham and Women's Hospital, Boston, and colleagues noted that their study was prompted by the Two-Midnight Rule established by the Centers for Medicare & Medicaid Services (CMS) in 2013.
The authors explained that if a physician expects a patient to need a hospital stay that crosses two midnights and thus admits the patient, related costs may be covered. However, shorter stays are deemed as observational and can raise the possibility of non-reimbursement for hospitals.
For example, if someone is admitted as an inpatient, but discharged in less than two days, payment will be made only if it can be documented that a longer stay was reasonably expected and unforeseen circumstances led to the shorter stay. Hospital stays that are incorrectly classified or have improperly documented changes in admission status will not be paid.
However, Dr. Cooper told Reuters Health by email, "Older patients with SBO, a very common diagnosis, should be presumed to be admitted for more than two midnights and hospitals should not get penalized."
She and her colleagues pointed out that SBO accounts for about 15% of surgical admissions to U.S. hospitals and more than $1 billion in annual hospital charges. However, diagnosis requires surgeons to observe patients to determine if surgery is warranted.
Thus, the authors wrote, "It is critically important for surgeons to correctly assign admission status for patients with SBO to ensure that hospitals are reimbursed appropriately, and patients are not unduly burdened."
The investigators examined data on 855 older patients admitted with SBO from 2006 and 2013. Of these, 816 (95%) stayed for two midnights or longer. This was true of all patients aged 85 years or older (n=108, approximately 13%).
The only significant difference in clinical characteristics was the presence of inflammatory bowel disease. Of five such patients, only one stayed for less than two midnights.
"Based on our study and others," the investigators wrote, "we propose that hospital admission for SBO in elderly patients is sufficient justification for the reasonable expectation" of the required length of stay for reimbursement.
This also may be true of other conditions. Dr. Cooper concluded, "More studies like this are needed in surgical patients to better understand the impact of CMS admission guidelines. The rule may not make sense in certain populations, leading to heavy and unfair penalties for hospitals."
The authors reported no disclosures.
NEW YORK (Reuters Health) - The "vast majority" of elderly patients admitted with small bowel obstruction (SBO) are hospitalized for more than two days, and the diagnosis alone should allow appropriate Medicare coverage, according to a new study.
In a paper online July 1 in Annals of Surgery, Dr. Zara Cooper, of Brigham and Women's Hospital, Boston, and colleagues noted that their study was prompted by the Two-Midnight Rule established by the Centers for Medicare & Medicaid Services (CMS) in 2013.
The authors explained that if a physician expects a patient to need a hospital stay that crosses two midnights and thus admits the patient, related costs may be covered. However, shorter stays are deemed as observational and can raise the possibility of non-reimbursement for hospitals.
For example, if someone is admitted as an inpatient, but discharged in less than two days, payment will be made only if it can be documented that a longer stay was reasonably expected and unforeseen circumstances led to the shorter stay. Hospital stays that are incorrectly classified or have improperly documented changes in admission status will not be paid.
However, Dr. Cooper told Reuters Health by email, "Older patients with SBO, a very common diagnosis, should be presumed to be admitted for more than two midnights and hospitals should not get penalized."
She and her colleagues pointed out that SBO accounts for about 15% of surgical admissions to U.S. hospitals and more than $1 billion in annual hospital charges. However, diagnosis requires surgeons to observe patients to determine if surgery is warranted.
Thus, the authors wrote, "It is critically important for surgeons to correctly assign admission status for patients with SBO to ensure that hospitals are reimbursed appropriately, and patients are not unduly burdened."
The investigators examined data on 855 older patients admitted with SBO from 2006 and 2013. Of these, 816 (95%) stayed for two midnights or longer. This was true of all patients aged 85 years or older (n=108, approximately 13%).
The only significant difference in clinical characteristics was the presence of inflammatory bowel disease. Of five such patients, only one stayed for less than two midnights.
"Based on our study and others," the investigators wrote, "we propose that hospital admission for SBO in elderly patients is sufficient justification for the reasonable expectation" of the required length of stay for reimbursement.
This also may be true of other conditions. Dr. Cooper concluded, "More studies like this are needed in surgical patients to better understand the impact of CMS admission guidelines. The rule may not make sense in certain populations, leading to heavy and unfair penalties for hospitals."
The authors reported no disclosures.
NEW YORK (Reuters Health) - The "vast majority" of elderly patients admitted with small bowel obstruction (SBO) are hospitalized for more than two days, and the diagnosis alone should allow appropriate Medicare coverage, according to a new study.
In a paper online July 1 in Annals of Surgery, Dr. Zara Cooper, of Brigham and Women's Hospital, Boston, and colleagues noted that their study was prompted by the Two-Midnight Rule established by the Centers for Medicare & Medicaid Services (CMS) in 2013.
The authors explained that if a physician expects a patient to need a hospital stay that crosses two midnights and thus admits the patient, related costs may be covered. However, shorter stays are deemed as observational and can raise the possibility of non-reimbursement for hospitals.
For example, if someone is admitted as an inpatient, but discharged in less than two days, payment will be made only if it can be documented that a longer stay was reasonably expected and unforeseen circumstances led to the shorter stay. Hospital stays that are incorrectly classified or have improperly documented changes in admission status will not be paid.
However, Dr. Cooper told Reuters Health by email, "Older patients with SBO, a very common diagnosis, should be presumed to be admitted for more than two midnights and hospitals should not get penalized."
She and her colleagues pointed out that SBO accounts for about 15% of surgical admissions to U.S. hospitals and more than $1 billion in annual hospital charges. However, diagnosis requires surgeons to observe patients to determine if surgery is warranted.
Thus, the authors wrote, "It is critically important for surgeons to correctly assign admission status for patients with SBO to ensure that hospitals are reimbursed appropriately, and patients are not unduly burdened."
The investigators examined data on 855 older patients admitted with SBO from 2006 and 2013. Of these, 816 (95%) stayed for two midnights or longer. This was true of all patients aged 85 years or older (n=108, approximately 13%).
The only significant difference in clinical characteristics was the presence of inflammatory bowel disease. Of five such patients, only one stayed for less than two midnights.
"Based on our study and others," the investigators wrote, "we propose that hospital admission for SBO in elderly patients is sufficient justification for the reasonable expectation" of the required length of stay for reimbursement.
This also may be true of other conditions. Dr. Cooper concluded, "More studies like this are needed in surgical patients to better understand the impact of CMS admission guidelines. The rule may not make sense in certain populations, leading to heavy and unfair penalties for hospitals."
The authors reported no disclosures.
LISTEN NOW: Hospitalist, Edwin Lopez, PA-C, on Post-Acute Care in the U.S. Health System
Edwin Lopez, PA-C, of St. Elizabeth Hospital in Enumclaw, Wash., offers his views on post-acute care in the U.S. health system, and how his work as a hospitalist has expanded to the nursing home across the street.
Edwin Lopez, PA-C, of St. Elizabeth Hospital in Enumclaw, Wash., offers his views on post-acute care in the U.S. health system, and how his work as a hospitalist has expanded to the nursing home across the street.
Edwin Lopez, PA-C, of St. Elizabeth Hospital in Enumclaw, Wash., offers his views on post-acute care in the U.S. health system, and how his work as a hospitalist has expanded to the nursing home across the street.
Hospital Medicine's Old Practices Become New Again
The musty collections of National Geographic magazines once found in so many basements are largely gone. Replacing them are dusty sets of the Advisory Board binders and booklets found in hospital administration offices around the country. I think the same principle drives the impulse to collect both publications—the idea that they contain worthwhile information that one day will be reviewed. But I think it’s more likely they will be ignored until it is time to move and someone has to decide what to do with the painfully heavy pile of paper.
Lots of old and largely forgotten things are making a comeback in healthcare. I suppose this is always happening, but I sense we’re now experiencing more of this than usual. It’s a renaissance of sorts.
I first heard about fecal transplant for Clostridium difficile infection (instilling a “better” microbiome in the hope of realizing many benefits) about six or eight years ago. Although I was sure this was a new idea, my retired internist father told me this had been around when he was in training. Wikipedia says that four Colorado surgeons published a paper about it in 1958 and that the Chinese were doing this 1,600 years ago.
PCPs Visit Hospitalized Patients
Writing in the NEJM earlier this year, Goroll and Hunt proposed that primary care physicians visit their hospitalized patients in the role of consultant while the hospitalist remains attending. As they note, this idea surfaced as soon as the hospitalist model began taking hold. Back then, we usually referred to it as a “social visit” by the PCP. Anecdotal experience from my work with hundreds of hospitalist groups tells me that such visits have all but disappeared. But nearly every such PCP visit on a patient I’ve cared for has seemed worthwhile; in many cases, these hospital calls simply reassure a nervous patient or family member, and occasionally they ensure that the PCP and I arrive at a more effective plan of care than we might otherwise.
Perhaps new forms of healthcare reimbursement, accountable care, and population health may make “continuity visits” economically viable for PCPs. Wouldn’t it be interesting if PCP visits to hospitalized patients and hospitalist visits to outpatients, such as those occurring in a pre-op clinic or a skilled nursing facility, become commonplace? The trick in all of this will be to ensure the right amount of overlap, or shared visits, between PCP and hospitalist without expensive duplication of effort or errors stemming from too many cooks in the kitchen.
Post-Hospital Follow-Up Schedules
When I began practicing as a hospitalist in the 1980s, doctors routinely wrote orders similar to this one: “Have patient follow up with Dr. Smith (PCP or specialist) in 1-2 weeks.” The unit secretary or other hospital clerical staff would contact the physician’s office to schedule the appointment, and the patient would leave the hospital with a written reminder in hand. My sense is that nearly all hospitals had been doing this for decades; somehow this practice has nearly disappeared over the last 10-20 years, however, and I sometimes hear this old practice discussed as a new idea.
I think making sure the patient has a follow-up appointment in hand when leaving the hospital is likely good for clinical outcomes, readmissions, and patient satisfaction. In my view, it is hardly worth lots of research to prove the benefit of what should be a relatively low-cost intervention. Why not just have providers write orders detailing follow-up with a specific doctor or clinic and a timeframe, and have unit secretaries communicate with outpatient clinics to schedule the appointments and ensure that the details are provided to the patient, maybe via an EHR-generated after visit summary? Seems pretty easy, right?
Turns out it isn’t easy at all for most hospitals. Lots of energetic hospitalists have taken on a project like this, only to run into so many brick walls. One hospitalist told me recently that the unit secretary’s labor union at her hospital refused to allow it. So some hospitals have turned to a single person, or a small group of people, who make appointments for all hospital patients. Some hospitalist groups have one of their own staff make appointments for hospitalist patients. This relieves the unit secretaries of the task but requires additional funding for the salaries of these people.
Maybe, at some time not so far off, EHRs will be so user-friendly and patients/families so accustomed to using them that it will be common for patients/families to arrange the appointments on their own. It could even be a required step—a hard stop—in the discharge process.
Whatever emerges as the most common method of making these appointments, I think it is safe to say this old practice will become “new” and common within the next few years.
Multidisciplinary Rounds
While working as an orderly in the 1970s, I would often visit with the nurses in their break room. When a doctor arrived to make rounds on the floor, the RN would jump up, stub out her cigarette, and round with the doctor. I sometimes tagged along as an observer. The nurse let the doctor know just how the patient had been doing and provided test results and any other relevant information the doctor might need. The doctor would provide orders, and sometimes the nurse wrote them into the chart (think of today’s medical scribes). Although their interaction was much less collaborative than is typical today, they did ask lots of questions of one another to clarify ambiguities.
I think these 1970s caregivers were doing effective multidisciplinary rounds. But by the late 1980s or so, as both doctor and nurse became busier, they stopped rounding together.
I smile when I hear descriptions of this “new” idea of doctor and nurse (and often other caregivers) rounding together. Today’s hospital culture is less hierarchical than the 1970s, though some would say it still has a ways to go, so teamwork and multidisciplinary rounds may yield more benefit than decades ago. But the idea of rounding together certainly isn’t new.
As we try to figure out the best way to thrive in a rapidly changing healthcare environment, we may find value in returning to the old ways of doing some things.

The musty collections of National Geographic magazines once found in so many basements are largely gone. Replacing them are dusty sets of the Advisory Board binders and booklets found in hospital administration offices around the country. I think the same principle drives the impulse to collect both publications—the idea that they contain worthwhile information that one day will be reviewed. But I think it’s more likely they will be ignored until it is time to move and someone has to decide what to do with the painfully heavy pile of paper.
Lots of old and largely forgotten things are making a comeback in healthcare. I suppose this is always happening, but I sense we’re now experiencing more of this than usual. It’s a renaissance of sorts.
I first heard about fecal transplant for Clostridium difficile infection (instilling a “better” microbiome in the hope of realizing many benefits) about six or eight years ago. Although I was sure this was a new idea, my retired internist father told me this had been around when he was in training. Wikipedia says that four Colorado surgeons published a paper about it in 1958 and that the Chinese were doing this 1,600 years ago.
PCPs Visit Hospitalized Patients
Writing in the NEJM earlier this year, Goroll and Hunt proposed that primary care physicians visit their hospitalized patients in the role of consultant while the hospitalist remains attending. As they note, this idea surfaced as soon as the hospitalist model began taking hold. Back then, we usually referred to it as a “social visit” by the PCP. Anecdotal experience from my work with hundreds of hospitalist groups tells me that such visits have all but disappeared. But nearly every such PCP visit on a patient I’ve cared for has seemed worthwhile; in many cases, these hospital calls simply reassure a nervous patient or family member, and occasionally they ensure that the PCP and I arrive at a more effective plan of care than we might otherwise.
Perhaps new forms of healthcare reimbursement, accountable care, and population health may make “continuity visits” economically viable for PCPs. Wouldn’t it be interesting if PCP visits to hospitalized patients and hospitalist visits to outpatients, such as those occurring in a pre-op clinic or a skilled nursing facility, become commonplace? The trick in all of this will be to ensure the right amount of overlap, or shared visits, between PCP and hospitalist without expensive duplication of effort or errors stemming from too many cooks in the kitchen.
Post-Hospital Follow-Up Schedules
When I began practicing as a hospitalist in the 1980s, doctors routinely wrote orders similar to this one: “Have patient follow up with Dr. Smith (PCP or specialist) in 1-2 weeks.” The unit secretary or other hospital clerical staff would contact the physician’s office to schedule the appointment, and the patient would leave the hospital with a written reminder in hand. My sense is that nearly all hospitals had been doing this for decades; somehow this practice has nearly disappeared over the last 10-20 years, however, and I sometimes hear this old practice discussed as a new idea.
I think making sure the patient has a follow-up appointment in hand when leaving the hospital is likely good for clinical outcomes, readmissions, and patient satisfaction. In my view, it is hardly worth lots of research to prove the benefit of what should be a relatively low-cost intervention. Why not just have providers write orders detailing follow-up with a specific doctor or clinic and a timeframe, and have unit secretaries communicate with outpatient clinics to schedule the appointments and ensure that the details are provided to the patient, maybe via an EHR-generated after visit summary? Seems pretty easy, right?
Turns out it isn’t easy at all for most hospitals. Lots of energetic hospitalists have taken on a project like this, only to run into so many brick walls. One hospitalist told me recently that the unit secretary’s labor union at her hospital refused to allow it. So some hospitals have turned to a single person, or a small group of people, who make appointments for all hospital patients. Some hospitalist groups have one of their own staff make appointments for hospitalist patients. This relieves the unit secretaries of the task but requires additional funding for the salaries of these people.
Maybe, at some time not so far off, EHRs will be so user-friendly and patients/families so accustomed to using them that it will be common for patients/families to arrange the appointments on their own. It could even be a required step—a hard stop—in the discharge process.
Whatever emerges as the most common method of making these appointments, I think it is safe to say this old practice will become “new” and common within the next few years.
Multidisciplinary Rounds
While working as an orderly in the 1970s, I would often visit with the nurses in their break room. When a doctor arrived to make rounds on the floor, the RN would jump up, stub out her cigarette, and round with the doctor. I sometimes tagged along as an observer. The nurse let the doctor know just how the patient had been doing and provided test results and any other relevant information the doctor might need. The doctor would provide orders, and sometimes the nurse wrote them into the chart (think of today’s medical scribes). Although their interaction was much less collaborative than is typical today, they did ask lots of questions of one another to clarify ambiguities.
I think these 1970s caregivers were doing effective multidisciplinary rounds. But by the late 1980s or so, as both doctor and nurse became busier, they stopped rounding together.
I smile when I hear descriptions of this “new” idea of doctor and nurse (and often other caregivers) rounding together. Today’s hospital culture is less hierarchical than the 1970s, though some would say it still has a ways to go, so teamwork and multidisciplinary rounds may yield more benefit than decades ago. But the idea of rounding together certainly isn’t new.
As we try to figure out the best way to thrive in a rapidly changing healthcare environment, we may find value in returning to the old ways of doing some things.

The musty collections of National Geographic magazines once found in so many basements are largely gone. Replacing them are dusty sets of the Advisory Board binders and booklets found in hospital administration offices around the country. I think the same principle drives the impulse to collect both publications—the idea that they contain worthwhile information that one day will be reviewed. But I think it’s more likely they will be ignored until it is time to move and someone has to decide what to do with the painfully heavy pile of paper.
Lots of old and largely forgotten things are making a comeback in healthcare. I suppose this is always happening, but I sense we’re now experiencing more of this than usual. It’s a renaissance of sorts.
I first heard about fecal transplant for Clostridium difficile infection (instilling a “better” microbiome in the hope of realizing many benefits) about six or eight years ago. Although I was sure this was a new idea, my retired internist father told me this had been around when he was in training. Wikipedia says that four Colorado surgeons published a paper about it in 1958 and that the Chinese were doing this 1,600 years ago.
PCPs Visit Hospitalized Patients
Writing in the NEJM earlier this year, Goroll and Hunt proposed that primary care physicians visit their hospitalized patients in the role of consultant while the hospitalist remains attending. As they note, this idea surfaced as soon as the hospitalist model began taking hold. Back then, we usually referred to it as a “social visit” by the PCP. Anecdotal experience from my work with hundreds of hospitalist groups tells me that such visits have all but disappeared. But nearly every such PCP visit on a patient I’ve cared for has seemed worthwhile; in many cases, these hospital calls simply reassure a nervous patient or family member, and occasionally they ensure that the PCP and I arrive at a more effective plan of care than we might otherwise.
Perhaps new forms of healthcare reimbursement, accountable care, and population health may make “continuity visits” economically viable for PCPs. Wouldn’t it be interesting if PCP visits to hospitalized patients and hospitalist visits to outpatients, such as those occurring in a pre-op clinic or a skilled nursing facility, become commonplace? The trick in all of this will be to ensure the right amount of overlap, or shared visits, between PCP and hospitalist without expensive duplication of effort or errors stemming from too many cooks in the kitchen.
Post-Hospital Follow-Up Schedules
When I began practicing as a hospitalist in the 1980s, doctors routinely wrote orders similar to this one: “Have patient follow up with Dr. Smith (PCP or specialist) in 1-2 weeks.” The unit secretary or other hospital clerical staff would contact the physician’s office to schedule the appointment, and the patient would leave the hospital with a written reminder in hand. My sense is that nearly all hospitals had been doing this for decades; somehow this practice has nearly disappeared over the last 10-20 years, however, and I sometimes hear this old practice discussed as a new idea.
I think making sure the patient has a follow-up appointment in hand when leaving the hospital is likely good for clinical outcomes, readmissions, and patient satisfaction. In my view, it is hardly worth lots of research to prove the benefit of what should be a relatively low-cost intervention. Why not just have providers write orders detailing follow-up with a specific doctor or clinic and a timeframe, and have unit secretaries communicate with outpatient clinics to schedule the appointments and ensure that the details are provided to the patient, maybe via an EHR-generated after visit summary? Seems pretty easy, right?
Turns out it isn’t easy at all for most hospitals. Lots of energetic hospitalists have taken on a project like this, only to run into so many brick walls. One hospitalist told me recently that the unit secretary’s labor union at her hospital refused to allow it. So some hospitals have turned to a single person, or a small group of people, who make appointments for all hospital patients. Some hospitalist groups have one of their own staff make appointments for hospitalist patients. This relieves the unit secretaries of the task but requires additional funding for the salaries of these people.
Maybe, at some time not so far off, EHRs will be so user-friendly and patients/families so accustomed to using them that it will be common for patients/families to arrange the appointments on their own. It could even be a required step—a hard stop—in the discharge process.
Whatever emerges as the most common method of making these appointments, I think it is safe to say this old practice will become “new” and common within the next few years.
Multidisciplinary Rounds
While working as an orderly in the 1970s, I would often visit with the nurses in their break room. When a doctor arrived to make rounds on the floor, the RN would jump up, stub out her cigarette, and round with the doctor. I sometimes tagged along as an observer. The nurse let the doctor know just how the patient had been doing and provided test results and any other relevant information the doctor might need. The doctor would provide orders, and sometimes the nurse wrote them into the chart (think of today’s medical scribes). Although their interaction was much less collaborative than is typical today, they did ask lots of questions of one another to clarify ambiguities.
I think these 1970s caregivers were doing effective multidisciplinary rounds. But by the late 1980s or so, as both doctor and nurse became busier, they stopped rounding together.
I smile when I hear descriptions of this “new” idea of doctor and nurse (and often other caregivers) rounding together. Today’s hospital culture is less hierarchical than the 1970s, though some would say it still has a ways to go, so teamwork and multidisciplinary rounds may yield more benefit than decades ago. But the idea of rounding together certainly isn’t new.
As we try to figure out the best way to thrive in a rapidly changing healthcare environment, we may find value in returning to the old ways of doing some things.

ICD-10 Medical Coding System Likely to Improve Documentation, Reimbursement
ICD-10 is the system that will replace ICD-9 for all parties covered by the Health Insurance Portability and Accountability Act (HIPAA). ICD-10 contains a code set used for inpatient procedural reporting and a code set used for diagnosis reporting. Physicians billing for professional services will only be affected when reporting diagnoses codes on their claims, but both physician and hospital selection of ICD-10 codes relies heavily on physician documentation. Therefore, documentation must be scrutinized. The most widely noted impact ICD-10 will have on documentation is increased specificity, with enhanced reporting of the patient’s presenting problem(s). Expanding from a pool of 14,000 3/5-digit codes to 69,000 7-digit codes, and accommodating this change, are daunting tasks. These anticipated burdens make it hard for physicians to recognize the positive effects ICD-10 may create, such as:1
- Better clinical decisions as better data is documented, collected, and evaluated;
- Improved protocol and clinical pathway design for various health conditions;
- Improved public health reporting and tracking of illnesses and severity over time;
- Better definition of patient conditions, providing improved matching of professional resources and care teams and increasing communications between providers;
- Support in practice transition to risk-sharing models with more precise data for patients and populations;
- Provision of clear objective data for credentialing and privileges, and support for professional Maintenance of Certification reporting across specialties;
- Better documentation of patient complexity and level of care, supporting reimbursement and measures for quality and efficiency reporting; and
- Reduction in audit risk exposure by encouraging the use of diagnosis codes with a greater degree of specificity as supported by the clinical documentation.
With the Oct. 1 implementation date rapidly approaching, physicians need to ask themselves, “Am I prepared?”
Getting Started
Everyone has a role and responsibility in transitioning to ICD-10. Active participation by all involved parties guarantees a more successful outcome. Practice administration must ensure that each aspect of implementation is reviewed and appropriately addressed. If not already done, immediate steps should be taken to verify the products and services that affect implementation. These include:
- Payer mix and related contracts: Entities not covered by HIPAA (e.g. workers’ compensation and auto insurance companies) may choose not to implement ICD-10. Since ICD-9 will no longer be maintained post-ICD-10 implementation, it is in the best interest of non-covered entities to use the new coding system.2 For payers who are required to transition to ICD-10, it is important to identify whether patient eligibility, claim processing, and/or payment timelines will be affected, as well as fee schedules or capitated rates.
- Vendor readiness: Physician groups may use a variety of vendors to assist with different aspects of the revenue cycle, including an electronic health record (e.g. documenting services and transmitting physician orders/prescriptions); a practice management system (e.g. scheduling and registering patients); a billing service (e.g. processing patient claims and payments); and a clearinghouse (e.g. verifying patient eligibility and obtaining authorizations). Know when software and/or hardware upgrades are available and if there are additional upgrade fees. Identify vendors that provide support services, training, and tools or templates to ease the transition. Most importantly, inquire about a testing period for products and applications to ensure functionality and adequate feedback on use of the system(s).
- Internal coding and billing resources. Identify physicians and staff who use ICD-9 codes and need to know ICD-10 codes in order to fulfill their responsibilities. Both physicians and staff can assist in identifying common clinical scenarios and the most frequently used ICD-9 codes, in order to develop a list of common ICD-10 specialty codes. Payer coverage policies currently include ICD-10 codes for provider review and comparison. Revise current forms/templates that include diagnosis codes to reflect this updated information. Schedule ICD-10 training for clinicians, office managers, billers, coders, and other key staff. Coding professionals recommend that training take place approximately six months prior to the ICD-10 compliance deadline.3 Training sessions are available from consultants, professional societies, payers, and other entities. Cost varies depending upon the type and length of training. CMS provides some free services, but in-depth training or certification for at least one practice member should be considered.
Once training is completed, dual coding is an option. Dual coding is the process by which both ICD-9 codes and ICD-10 codes are selected during the coding process. Some practices rely on independent selection of each code, while others rely on the General Equivalence Mappings (GEMs). GEMs were developed to assist industry migration to ICD-10. They are intended to be used primarily for translations of code lists or code tables used by an application or other coded data when codes in one code set are the only source of information; they are not intended as a substitution for direct use of ICD-9-CM and ICD-10-CM/PCS.4 Manual coding enhances coding efficiency and also identifies physician documentation deficiencies. Dual coding should begin as soon as possible, prior to October 1.
End-to-end testing is an opportunity to submit test claims to CMS with ICD-10 codes; providers will receive a remittance advice that explains the adjudication of the claims.5 This testing is limited to a small group of providers who were required to register in April, and its final week is July 20-24.
Provide Feedback
The importance of feedback is often understated. Many physician practices do not have the time to plan ahead and, as a result, find themselves in a reactive rather than proactive role. Over the next couple of months, find the time and resources to audit physician documentation based on ICD-10 criteria. Ask yourself whether or not the information contains enough specificity to select the best possible code, or does code selection default to an “unspecified” code?
Avoid “unspecified” codes when possible in preparation for payer policy revisions that are aimed at reducing or eliminating these types of codes. If the documentation lacks detail, educate physicians on the missing elements.
Review ICD-10 code sets with physicians to improve their understanding of the new system. For example, diabetes mellitus is identified in ICD-9 as one category (250.xx), with digits to specify Type I or Type II, controlled vs. uncontrolled, with or without complications. ICD-10 separates diabetes into categories of Type I (E10) or Type II (E11), with subcategories to identify complications and affected body systems, thereby expanding the volume of codes and corresponding documentation criteria.6
Post-implementation feedback will become even more important. Monitor claim denials for invalid codes and medical necessity issues (i.e., valid codes not included for coverage). If the medical necessity denials are a result of inaccurate code selection related to insufficient documentation details, provider education will be crucial in resolving these errors. Continuing education to strengthen and update staff skills is imperative.
CMS has developed many tools and resources to promote a successful transition and assess your ICD-10 preparedness. Physician practices can develop an “action plan,” learn basic ICD-10 concepts, and much more.
Carol Pohlig is a billing and coding expert with the University of Pennsylvania Medical Center, Philadelphia. She is also on the faculty of SHM’s inpatient coding course.
References
- Centers for Medicare and Medicaid Services. Road to 10: the small physician practice’s route to ICD-10? Accessed June 6, 2015.
- Department of Health and Human Services. Centers for Medicare and Medicaid Services. Medicare Learning Network: ICD-10-CM/PCS Myths and Facts. Accessed June 6, 2015.
- Centers for Medicare and Medicaid Services. ICD-10: ICD-10 Basics for Medical Practices. Accessed June 6, 2015.
- American Health Information Management Association (AHIMA). Putting the ICD-10-CM/PCS GEMs into practice. Accessed June 6, 2015.
- Novitas Solutions. Medicare JL, Part B. ICD-10 Implementation. Accessed June 6, 2015.
- Centers for Medicare and Medicaid Services. ICD-10 Coding and Diabetes. Accessed June 6, 2015.
ICD-10 is the system that will replace ICD-9 for all parties covered by the Health Insurance Portability and Accountability Act (HIPAA). ICD-10 contains a code set used for inpatient procedural reporting and a code set used for diagnosis reporting. Physicians billing for professional services will only be affected when reporting diagnoses codes on their claims, but both physician and hospital selection of ICD-10 codes relies heavily on physician documentation. Therefore, documentation must be scrutinized. The most widely noted impact ICD-10 will have on documentation is increased specificity, with enhanced reporting of the patient’s presenting problem(s). Expanding from a pool of 14,000 3/5-digit codes to 69,000 7-digit codes, and accommodating this change, are daunting tasks. These anticipated burdens make it hard for physicians to recognize the positive effects ICD-10 may create, such as:1
- Better clinical decisions as better data is documented, collected, and evaluated;
- Improved protocol and clinical pathway design for various health conditions;
- Improved public health reporting and tracking of illnesses and severity over time;
- Better definition of patient conditions, providing improved matching of professional resources and care teams and increasing communications between providers;
- Support in practice transition to risk-sharing models with more precise data for patients and populations;
- Provision of clear objective data for credentialing and privileges, and support for professional Maintenance of Certification reporting across specialties;
- Better documentation of patient complexity and level of care, supporting reimbursement and measures for quality and efficiency reporting; and
- Reduction in audit risk exposure by encouraging the use of diagnosis codes with a greater degree of specificity as supported by the clinical documentation.
With the Oct. 1 implementation date rapidly approaching, physicians need to ask themselves, “Am I prepared?”
Getting Started
Everyone has a role and responsibility in transitioning to ICD-10. Active participation by all involved parties guarantees a more successful outcome. Practice administration must ensure that each aspect of implementation is reviewed and appropriately addressed. If not already done, immediate steps should be taken to verify the products and services that affect implementation. These include:
- Payer mix and related contracts: Entities not covered by HIPAA (e.g. workers’ compensation and auto insurance companies) may choose not to implement ICD-10. Since ICD-9 will no longer be maintained post-ICD-10 implementation, it is in the best interest of non-covered entities to use the new coding system.2 For payers who are required to transition to ICD-10, it is important to identify whether patient eligibility, claim processing, and/or payment timelines will be affected, as well as fee schedules or capitated rates.
- Vendor readiness: Physician groups may use a variety of vendors to assist with different aspects of the revenue cycle, including an electronic health record (e.g. documenting services and transmitting physician orders/prescriptions); a practice management system (e.g. scheduling and registering patients); a billing service (e.g. processing patient claims and payments); and a clearinghouse (e.g. verifying patient eligibility and obtaining authorizations). Know when software and/or hardware upgrades are available and if there are additional upgrade fees. Identify vendors that provide support services, training, and tools or templates to ease the transition. Most importantly, inquire about a testing period for products and applications to ensure functionality and adequate feedback on use of the system(s).
- Internal coding and billing resources. Identify physicians and staff who use ICD-9 codes and need to know ICD-10 codes in order to fulfill their responsibilities. Both physicians and staff can assist in identifying common clinical scenarios and the most frequently used ICD-9 codes, in order to develop a list of common ICD-10 specialty codes. Payer coverage policies currently include ICD-10 codes for provider review and comparison. Revise current forms/templates that include diagnosis codes to reflect this updated information. Schedule ICD-10 training for clinicians, office managers, billers, coders, and other key staff. Coding professionals recommend that training take place approximately six months prior to the ICD-10 compliance deadline.3 Training sessions are available from consultants, professional societies, payers, and other entities. Cost varies depending upon the type and length of training. CMS provides some free services, but in-depth training or certification for at least one practice member should be considered.
Once training is completed, dual coding is an option. Dual coding is the process by which both ICD-9 codes and ICD-10 codes are selected during the coding process. Some practices rely on independent selection of each code, while others rely on the General Equivalence Mappings (GEMs). GEMs were developed to assist industry migration to ICD-10. They are intended to be used primarily for translations of code lists or code tables used by an application or other coded data when codes in one code set are the only source of information; they are not intended as a substitution for direct use of ICD-9-CM and ICD-10-CM/PCS.4 Manual coding enhances coding efficiency and also identifies physician documentation deficiencies. Dual coding should begin as soon as possible, prior to October 1.
End-to-end testing is an opportunity to submit test claims to CMS with ICD-10 codes; providers will receive a remittance advice that explains the adjudication of the claims.5 This testing is limited to a small group of providers who were required to register in April, and its final week is July 20-24.
Provide Feedback
The importance of feedback is often understated. Many physician practices do not have the time to plan ahead and, as a result, find themselves in a reactive rather than proactive role. Over the next couple of months, find the time and resources to audit physician documentation based on ICD-10 criteria. Ask yourself whether or not the information contains enough specificity to select the best possible code, or does code selection default to an “unspecified” code?
Avoid “unspecified” codes when possible in preparation for payer policy revisions that are aimed at reducing or eliminating these types of codes. If the documentation lacks detail, educate physicians on the missing elements.
Review ICD-10 code sets with physicians to improve their understanding of the new system. For example, diabetes mellitus is identified in ICD-9 as one category (250.xx), with digits to specify Type I or Type II, controlled vs. uncontrolled, with or without complications. ICD-10 separates diabetes into categories of Type I (E10) or Type II (E11), with subcategories to identify complications and affected body systems, thereby expanding the volume of codes and corresponding documentation criteria.6
Post-implementation feedback will become even more important. Monitor claim denials for invalid codes and medical necessity issues (i.e., valid codes not included for coverage). If the medical necessity denials are a result of inaccurate code selection related to insufficient documentation details, provider education will be crucial in resolving these errors. Continuing education to strengthen and update staff skills is imperative.
CMS has developed many tools and resources to promote a successful transition and assess your ICD-10 preparedness. Physician practices can develop an “action plan,” learn basic ICD-10 concepts, and much more.
Carol Pohlig is a billing and coding expert with the University of Pennsylvania Medical Center, Philadelphia. She is also on the faculty of SHM’s inpatient coding course.
References
- Centers for Medicare and Medicaid Services. Road to 10: the small physician practice’s route to ICD-10? Accessed June 6, 2015.
- Department of Health and Human Services. Centers for Medicare and Medicaid Services. Medicare Learning Network: ICD-10-CM/PCS Myths and Facts. Accessed June 6, 2015.
- Centers for Medicare and Medicaid Services. ICD-10: ICD-10 Basics for Medical Practices. Accessed June 6, 2015.
- American Health Information Management Association (AHIMA). Putting the ICD-10-CM/PCS GEMs into practice. Accessed June 6, 2015.
- Novitas Solutions. Medicare JL, Part B. ICD-10 Implementation. Accessed June 6, 2015.
- Centers for Medicare and Medicaid Services. ICD-10 Coding and Diabetes. Accessed June 6, 2015.
ICD-10 is the system that will replace ICD-9 for all parties covered by the Health Insurance Portability and Accountability Act (HIPAA). ICD-10 contains a code set used for inpatient procedural reporting and a code set used for diagnosis reporting. Physicians billing for professional services will only be affected when reporting diagnoses codes on their claims, but both physician and hospital selection of ICD-10 codes relies heavily on physician documentation. Therefore, documentation must be scrutinized. The most widely noted impact ICD-10 will have on documentation is increased specificity, with enhanced reporting of the patient’s presenting problem(s). Expanding from a pool of 14,000 3/5-digit codes to 69,000 7-digit codes, and accommodating this change, are daunting tasks. These anticipated burdens make it hard for physicians to recognize the positive effects ICD-10 may create, such as:1
- Better clinical decisions as better data is documented, collected, and evaluated;
- Improved protocol and clinical pathway design for various health conditions;
- Improved public health reporting and tracking of illnesses and severity over time;
- Better definition of patient conditions, providing improved matching of professional resources and care teams and increasing communications between providers;
- Support in practice transition to risk-sharing models with more precise data for patients and populations;
- Provision of clear objective data for credentialing and privileges, and support for professional Maintenance of Certification reporting across specialties;
- Better documentation of patient complexity and level of care, supporting reimbursement and measures for quality and efficiency reporting; and
- Reduction in audit risk exposure by encouraging the use of diagnosis codes with a greater degree of specificity as supported by the clinical documentation.
With the Oct. 1 implementation date rapidly approaching, physicians need to ask themselves, “Am I prepared?”
Getting Started
Everyone has a role and responsibility in transitioning to ICD-10. Active participation by all involved parties guarantees a more successful outcome. Practice administration must ensure that each aspect of implementation is reviewed and appropriately addressed. If not already done, immediate steps should be taken to verify the products and services that affect implementation. These include:
- Payer mix and related contracts: Entities not covered by HIPAA (e.g. workers’ compensation and auto insurance companies) may choose not to implement ICD-10. Since ICD-9 will no longer be maintained post-ICD-10 implementation, it is in the best interest of non-covered entities to use the new coding system.2 For payers who are required to transition to ICD-10, it is important to identify whether patient eligibility, claim processing, and/or payment timelines will be affected, as well as fee schedules or capitated rates.
- Vendor readiness: Physician groups may use a variety of vendors to assist with different aspects of the revenue cycle, including an electronic health record (e.g. documenting services and transmitting physician orders/prescriptions); a practice management system (e.g. scheduling and registering patients); a billing service (e.g. processing patient claims and payments); and a clearinghouse (e.g. verifying patient eligibility and obtaining authorizations). Know when software and/or hardware upgrades are available and if there are additional upgrade fees. Identify vendors that provide support services, training, and tools or templates to ease the transition. Most importantly, inquire about a testing period for products and applications to ensure functionality and adequate feedback on use of the system(s).
- Internal coding and billing resources. Identify physicians and staff who use ICD-9 codes and need to know ICD-10 codes in order to fulfill their responsibilities. Both physicians and staff can assist in identifying common clinical scenarios and the most frequently used ICD-9 codes, in order to develop a list of common ICD-10 specialty codes. Payer coverage policies currently include ICD-10 codes for provider review and comparison. Revise current forms/templates that include diagnosis codes to reflect this updated information. Schedule ICD-10 training for clinicians, office managers, billers, coders, and other key staff. Coding professionals recommend that training take place approximately six months prior to the ICD-10 compliance deadline.3 Training sessions are available from consultants, professional societies, payers, and other entities. Cost varies depending upon the type and length of training. CMS provides some free services, but in-depth training or certification for at least one practice member should be considered.
Once training is completed, dual coding is an option. Dual coding is the process by which both ICD-9 codes and ICD-10 codes are selected during the coding process. Some practices rely on independent selection of each code, while others rely on the General Equivalence Mappings (GEMs). GEMs were developed to assist industry migration to ICD-10. They are intended to be used primarily for translations of code lists or code tables used by an application or other coded data when codes in one code set are the only source of information; they are not intended as a substitution for direct use of ICD-9-CM and ICD-10-CM/PCS.4 Manual coding enhances coding efficiency and also identifies physician documentation deficiencies. Dual coding should begin as soon as possible, prior to October 1.
End-to-end testing is an opportunity to submit test claims to CMS with ICD-10 codes; providers will receive a remittance advice that explains the adjudication of the claims.5 This testing is limited to a small group of providers who were required to register in April, and its final week is July 20-24.
Provide Feedback
The importance of feedback is often understated. Many physician practices do not have the time to plan ahead and, as a result, find themselves in a reactive rather than proactive role. Over the next couple of months, find the time and resources to audit physician documentation based on ICD-10 criteria. Ask yourself whether or not the information contains enough specificity to select the best possible code, or does code selection default to an “unspecified” code?
Avoid “unspecified” codes when possible in preparation for payer policy revisions that are aimed at reducing or eliminating these types of codes. If the documentation lacks detail, educate physicians on the missing elements.
Review ICD-10 code sets with physicians to improve their understanding of the new system. For example, diabetes mellitus is identified in ICD-9 as one category (250.xx), with digits to specify Type I or Type II, controlled vs. uncontrolled, with or without complications. ICD-10 separates diabetes into categories of Type I (E10) or Type II (E11), with subcategories to identify complications and affected body systems, thereby expanding the volume of codes and corresponding documentation criteria.6
Post-implementation feedback will become even more important. Monitor claim denials for invalid codes and medical necessity issues (i.e., valid codes not included for coverage). If the medical necessity denials are a result of inaccurate code selection related to insufficient documentation details, provider education will be crucial in resolving these errors. Continuing education to strengthen and update staff skills is imperative.
CMS has developed many tools and resources to promote a successful transition and assess your ICD-10 preparedness. Physician practices can develop an “action plan,” learn basic ICD-10 concepts, and much more.
Carol Pohlig is a billing and coding expert with the University of Pennsylvania Medical Center, Philadelphia. She is also on the faculty of SHM’s inpatient coding course.
References
- Centers for Medicare and Medicaid Services. Road to 10: the small physician practice’s route to ICD-10? Accessed June 6, 2015.
- Department of Health and Human Services. Centers for Medicare and Medicaid Services. Medicare Learning Network: ICD-10-CM/PCS Myths and Facts. Accessed June 6, 2015.
- Centers for Medicare and Medicaid Services. ICD-10: ICD-10 Basics for Medical Practices. Accessed June 6, 2015.
- American Health Information Management Association (AHIMA). Putting the ICD-10-CM/PCS GEMs into practice. Accessed June 6, 2015.
- Novitas Solutions. Medicare JL, Part B. ICD-10 Implementation. Accessed June 6, 2015.
- Centers for Medicare and Medicaid Services. ICD-10 Coding and Diabetes. Accessed June 6, 2015.
Post-Acute Patient Care Offers Opportunities for Non-Physicians
More than in the inpatient setting, post-acute care offers opportunities for nurse practitioners and physician assistants to play important clinical and administrative roles. Physician assistant (PA) Edwin Lopez, PA-C, is chief of an eight-member HM group—four doctors, four PAs—that provides coverage at St. Elizabeth, a rural critical access hospital in Enumclaw, Wash., population 10,669, and in the 80-bed SNF located across the street. Lopez was recruited to establish the HM group “in the shadow of Mt. Rainier” about eight years ago, at a time when the hospital’s parent, CHI Franciscan Health System, was trying to rebuild its quality and reputation while planning a new building.
He succeeded, dramatically improving its performance on HCAHPS surveys and other metrics; however, hospital readmissions then emerged as an issue.
“I began to realize, with our little facility’s large population of elderly patients with multiple chronic problems—typically the highest cohort for readmissions—all the gains we had made could be lost if we didn’t do something about this problem,” Lopez says. “I ran the numbers and found that the nursing home across the street readmitted 35% of patients discharged from our hospital.”
It took a year to get the larger system’s approval, but Lopez’s hospitalist group manages all the patients transferred to the nearby nursing home, with daily visits by the doctor and/or PA on duty.
“We started the program in January 2014, and, in one year, readmissions went from 35% down to 7%,” he says. “We developed culturally from the very beginning as a PA/MD collaborative model. The doctor doesn’t need to see the more routine patients with more common conditions but instead is freed up to focus on higher-acuity, more complex patients.”
In Dr. Tollman’s opinion, physician extenders “own” the post-acute realm, because of the demand for their care.
“There just aren’t going to be enough doctors for all of the patients who need to be seen,” he says, “and the amount of money for this care isn’t enough for these facilities to employ groups of doctors.”
Emily Rosenbaum, PA-C, works for Northwest Community Healthcare in Arlington Heights, Ill. She is the lone PA working with eight physician hospitalists. Much of her work is in a rehabilitation facility across the street from Northwest Community Hospital.
“I see all of the new admissions, although under my scope of practice I can’t bill for the initial visit. But I do the follow-ups, see patients that have been in rehab for 30 days or less, and put out [clinical] fires in the facility,” she says.
Rosenbaum works at the hospital part of her day taking care of acute patients, then works with the hospitalist assigned to the rehabilitation facility.
“It’s easier for me to go back and forth and keep my finger on the patients’ pulse,” she says. “As there are more demands on doctors on the acute side, it’s natural for the NP and PA to step up and take a larger role on the post-acute side.”
More than in the inpatient setting, post-acute care offers opportunities for nurse practitioners and physician assistants to play important clinical and administrative roles. Physician assistant (PA) Edwin Lopez, PA-C, is chief of an eight-member HM group—four doctors, four PAs—that provides coverage at St. Elizabeth, a rural critical access hospital in Enumclaw, Wash., population 10,669, and in the 80-bed SNF located across the street. Lopez was recruited to establish the HM group “in the shadow of Mt. Rainier” about eight years ago, at a time when the hospital’s parent, CHI Franciscan Health System, was trying to rebuild its quality and reputation while planning a new building.
He succeeded, dramatically improving its performance on HCAHPS surveys and other metrics; however, hospital readmissions then emerged as an issue.
“I began to realize, with our little facility’s large population of elderly patients with multiple chronic problems—typically the highest cohort for readmissions—all the gains we had made could be lost if we didn’t do something about this problem,” Lopez says. “I ran the numbers and found that the nursing home across the street readmitted 35% of patients discharged from our hospital.”
It took a year to get the larger system’s approval, but Lopez’s hospitalist group manages all the patients transferred to the nearby nursing home, with daily visits by the doctor and/or PA on duty.
“We started the program in January 2014, and, in one year, readmissions went from 35% down to 7%,” he says. “We developed culturally from the very beginning as a PA/MD collaborative model. The doctor doesn’t need to see the more routine patients with more common conditions but instead is freed up to focus on higher-acuity, more complex patients.”
In Dr. Tollman’s opinion, physician extenders “own” the post-acute realm, because of the demand for their care.
“There just aren’t going to be enough doctors for all of the patients who need to be seen,” he says, “and the amount of money for this care isn’t enough for these facilities to employ groups of doctors.”
Emily Rosenbaum, PA-C, works for Northwest Community Healthcare in Arlington Heights, Ill. She is the lone PA working with eight physician hospitalists. Much of her work is in a rehabilitation facility across the street from Northwest Community Hospital.
“I see all of the new admissions, although under my scope of practice I can’t bill for the initial visit. But I do the follow-ups, see patients that have been in rehab for 30 days or less, and put out [clinical] fires in the facility,” she says.
Rosenbaum works at the hospital part of her day taking care of acute patients, then works with the hospitalist assigned to the rehabilitation facility.
“It’s easier for me to go back and forth and keep my finger on the patients’ pulse,” she says. “As there are more demands on doctors on the acute side, it’s natural for the NP and PA to step up and take a larger role on the post-acute side.”
More than in the inpatient setting, post-acute care offers opportunities for nurse practitioners and physician assistants to play important clinical and administrative roles. Physician assistant (PA) Edwin Lopez, PA-C, is chief of an eight-member HM group—four doctors, four PAs—that provides coverage at St. Elizabeth, a rural critical access hospital in Enumclaw, Wash., population 10,669, and in the 80-bed SNF located across the street. Lopez was recruited to establish the HM group “in the shadow of Mt. Rainier” about eight years ago, at a time when the hospital’s parent, CHI Franciscan Health System, was trying to rebuild its quality and reputation while planning a new building.
He succeeded, dramatically improving its performance on HCAHPS surveys and other metrics; however, hospital readmissions then emerged as an issue.
“I began to realize, with our little facility’s large population of elderly patients with multiple chronic problems—typically the highest cohort for readmissions—all the gains we had made could be lost if we didn’t do something about this problem,” Lopez says. “I ran the numbers and found that the nursing home across the street readmitted 35% of patients discharged from our hospital.”
It took a year to get the larger system’s approval, but Lopez’s hospitalist group manages all the patients transferred to the nearby nursing home, with daily visits by the doctor and/or PA on duty.
“We started the program in January 2014, and, in one year, readmissions went from 35% down to 7%,” he says. “We developed culturally from the very beginning as a PA/MD collaborative model. The doctor doesn’t need to see the more routine patients with more common conditions but instead is freed up to focus on higher-acuity, more complex patients.”
In Dr. Tollman’s opinion, physician extenders “own” the post-acute realm, because of the demand for their care.
“There just aren’t going to be enough doctors for all of the patients who need to be seen,” he says, “and the amount of money for this care isn’t enough for these facilities to employ groups of doctors.”
Emily Rosenbaum, PA-C, works for Northwest Community Healthcare in Arlington Heights, Ill. She is the lone PA working with eight physician hospitalists. Much of her work is in a rehabilitation facility across the street from Northwest Community Hospital.
“I see all of the new admissions, although under my scope of practice I can’t bill for the initial visit. But I do the follow-ups, see patients that have been in rehab for 30 days or less, and put out [clinical] fires in the facility,” she says.
Rosenbaum works at the hospital part of her day taking care of acute patients, then works with the hospitalist assigned to the rehabilitation facility.
“It’s easier for me to go back and forth and keep my finger on the patients’ pulse,” she says. “As there are more demands on doctors on the acute side, it’s natural for the NP and PA to step up and take a larger role on the post-acute side.”
11 Things Gastroenterologists Think Hospitalists Need to Know
So many symptoms that are staples of gastroenterology—chest pain, nausea, diarrhea—are mainstay causes for hospitalization that it might be worth fine-tuning how well you handle patients with gastroenterology disorders.
The Hospitalist asked several gastroenterologists for their guidance on better care and their suggestions for correcting some common mistakes that they encounter. Here are their tips:
1 Fluid resuscitation is crucial for pancreatitis patients.
It’s very important to rehydrate these patients within the first 24 hours, because those who remain underhydrated can have a worse prognosis, says Robert Coben, MD, academic coordinator for the Gastroentestinal Fellowship Program at Thomas Jefferson University Hospital in Philadelphia. On occasion, physicians are reluctant to give extra fluids to these patients, he says, particularly if they have heart failure or suffer kidney problems. A 70-kg patient should be receiving about 200 cc per hour, he notes.
“Sometimes we’ll walk in the room and they’re getting 80 cc an hour,” Dr. Coben says.
“These patients…need to be flooded with fluids,” says Rajeev Jain, MD, chief of gastroenterology at Presbyterian Hospital of Dallas, partner at Texas Digestive Disease Consultants, and chair of the Practice Management and Economics Committee of the American Gastroenterological Association. “We’re talking sometimes liters and liters of IV normal saline or lactated Ringer’s (solution) in a 24-hour period.”1
Marcelo Vela, MD, a gastroenterologist and hepatologist at the Mayo Clinic in Scottsdale, Ariz., and an associate editor with Clinical Gastroenterology and Hepatology, says Ringer’s solution is a better choice than normal saline.2
“If you’re going to start IV fluids on somebody who’s coming in with acute pancreatitis, Ringer’s solution has been shown to be superior to saline in randomized controlled trials,” Dr. Vela says. “It reduces systemic inflammation.”
2 Gastrointestinal bleeding decisions
When inpatients have gastrointestinal bleeding, the hospitalist often has to assess its severity and make the call on whether a patient needs the ICU.
“The most important thing for that is obviously the vital signs,” says John Pandolfino, MD, chief of the division of medicine–gastroenterology and hepatology at Northwestern University Feinberg School of Medicine in Chicago. “If people are tachycardic and they’re not responding to hydration and blood transfusion, that usually means it’s a pretty active bleed and they need to go to the intensive care unit. If you have somebody who’s GI bleeding and they’re coagulopathic (i.e., they’re on anti-coagulation because they have a valve and they need anti-coagulation or they have cancer or bad cardiovascular disease), those are the people that you should have a low threshold for sending to the intensive care unit with a GI bleed; those are the people who are at a very high mortality [risk].”
He added that those with an ulcer, with a visible vessel, are at a high-risk of a rebleed and should spend some time in the ICU.
“Those people should be evaluated in the intensive care unit for at least 24 hours, maybe even 72 hours,” Dr. Pandolfino says, “and they should have IV PPI [proton pump inhibitor] therapy.”
3 Endoscopy has very low yield for diagnosis of reflux.
“Endoscopy has good yield for mucosa abnormalities on inspection of the esophageal mucosa, but it does not give you a diagnosis of reflux, especially on patients who have already been treated with a PPI,” says Prakash Gyawali, MD, MRCP, professor of gastroenterology at Washington University in St. Louis, Mo. “So, usually, in those settings, obtaining a consult or trying to decide exactly what you’re looking for to explain the symptoms has better yield than an endoscopy.”
Sometimes a pH study is needed, but that has to be planned, because patients may have to be taken off of a PPI in advance. That means those studies are not easy to set up in the hospital and might best be arranged by the gastroenterologist, Dr. Gyawali says.
4 In cases of acute diarrhea, order a stool sample right away.
That will help guide care from the gastroenterologist, if and when the gastroenterologist is called in, Dr. Pandolfino says.
“One of the things that is frustrating for the gastroenterologist is that we get called initially, but really the hospitalist should be getting stool studies, and they should have at least a very good idea of what they need from us,” he says. “Because, really, endoscopy is not usually needed very often in diagnosis of acute diarrhea.”
Broad-range stool studies, a good history and physical, and examining labs for a possible chronic inflammatory process or anemia are good ways to begin to assess patients with diarrhea, he says. Clostridium difficile colitis has to be considered as well, Dr. Pandolfino says.
Endoscopy is more helpful in evaluating acute diarrhea in those with bloody diarrhea suspected of having inflammatory bowel disease or an infectious diarrhea but on whom cultures have come back negative. For those with compromised immune systems, endoscopy could be done earlier, as well.
“So for us, I think we really need to get into the picture a little bit after the patient has been brought into the hospital and the stool study is negative, unless they’re an immune-compromised patient,” Dr. Pandolfino says.
5 When—and how—to test the stool.
If a patient develops diarrhea while already in the hospital, the only stool test needed is C. diff.
“They shouldn’t be developing a viral diarrhea, they shouldn’t be developing an infectious diarrhea—let’s say, from E. coli or Salmonella—unless they literally developed it a couple hours after getting in,” Dr. Jain says. “It should either be C. diff or a side effect of some medication. … We don’t need to spend the extra money, which is of low-value care to send for OVA and parasites, or bacterial pathogens and so forth.”
Dr. Jain says he thinks such testing is being done more appropriately of late.
“But I still will see multiple stool tests sent on somebody who’s been in the hospital for a week and then develops diarrhea,” he explains.
6 Gastroenterologists do not need to be consulted for every C. diff infection.
“I think that we really should get involved when patients are either not responding or when they’re very ill,” Dr. Pandolfino says.
Hospitalists should consider whether patients are on antibiotics or a PPI and whether or not they need to stay on those medications. Also, medications that slow motility (i.e., loperamide) should be avoided, if possible.
“We don’t want it to linger,” Dr. Pandolfino says. “One of the basic mechanisms of how we get rid of pathogens is to expel them with diarrhea.
“But you certainly don’t want the patient to be uncomfortable to the point where they’re having 20 to 30 bowel movements a day.”
In non-severe patients who have some diarrhea, abdominal pain, nausea, and vomiting—but are able to keep food down—the specialists might not have to be called in, and patients can just be treated with oral metronidazole or oral vancomycin fairly simply, he says.
For those who seem severely ill with a dilating colon, are in nearly a septic state, and have very severe diarrhea, the gastroenterologist should probably be called in, he says.

7 For patients with a possible GI bleed and black stools, do an exam before calling in the gastroenterologist.
The exam should determine what the stool color is and whether it is heme-positive, and the patient’s blood count should be evaluated, Dr. Coben says.
Frequently, “the consultant’s the one who ends up doing the rectal exam and checking that,” he says. “Sometimes we find that [the patient is] really not bleeding,” and it was just a case of a hospitalist taking the patient’s word that they were bleeding.
Being on iron therapy or taking Pepto-Bismol can turn the stool black, and the stool might not really be black; colors can sometimes be open to interpretation.
But he cautions that colon cancer could be the cause for a GI bleed.
“We’ve had it happen a few times where this occurred,” he says. “The patient was discharged, and they really didn’t get proper follow-up, and it ended up that they had a colon cancer. It kind of delayed that diagnosis. So I think you have to be aware of [the fact that], especially in somebody over the age of 40 or 50, if they have an iron-deficiency, anemia, or heme-positive stool, the first thing you really need to exclude is a colon cancer.”
8 Minimize CT scans in early evaluation and management of acute pancreatitis patients.
“The reason for that is they tend to be intravascularly volume-depleted,” Dr. Jain says. “So [with] the IV contrast, there’s an increased risk of developing kidney failure. It’s also been associated with increased risk of necrotizing pancreatitis.”
Dr. Jain notes that when he is consulted on this kind of patient, he will order a sonogram. If it doesn’t show gallstones, and there’s no clear reason for the pancreatitis, he will want a CT scan, but he will wait a few days until the patient is fluid-resuscitated.
Dr. Jain says that this is a problem more often seen in the ED—where 90% of patients with acute pancreatitis have already gotten the CT scan—and less so among hospitalists, but it’s still worth the reminder.
A CT scan right away is justified to rule out something such as a perforation, but not in the case of classic symptoms of acute pancreatitis, he adds.
9 Actively bleeding patients?
It’s smart to give patients a unit of packed red blood cells more quickly if they’re actively bleeding. Even over just one hour is OK, Dr. Jain says.
“Even if they have underlying heart failure, if they’re volume-depleted, they need that volume,” Dr. Jain explains. “Sometimes you’ll see that it takes eight hours to get two units of blood in. That’s inadequate.”
Another point worth a reminder, he says: Two large-bore peripheral IV’s are “much, much better” than a central or PICC line to deliver IV fluid resuscitation.
“Sometimes hospitalists order barium studies because these can be done the same day, whereas with endoscopy, patients need to be put on a schedule and have to be NPO [nothing by mouth] overnight.” —Prakash Gyawali, MD, MRCP
10 Don’t be too quick to order barium studies, especially in patients with dysphagia.
“The problem with that is it takes much longer to do an endoscopy if barium is put in the esophagus, because we usually wait until the barium clears,” Dr. Gyawali says. “And inpatient evaluation of new-onset dysphagia should be endoscopy first, and not barium, because biopsies need to be taken to rule out eosinophilic esophagitis.
“Sometimes hospitalists order barium studies because these can be done the same day, whereas with endoscopy, patients need to be put on a schedule and have to be NPO [nothing by mouth] overnight.”
11 Gastric-emptying studies should be outpatient.
Gastric-emptying studies are often better done when patients are not in a hospital, experts say, because they might be on medications that would interfere with the study.
“A common issue, not just among hospitalists but also gastroenterologists, is that patients may be on a bunch of medicines that would affect stomach-emptying while they are in-house for some other problem,” Dr. Gyawali says. “A lot of times, these patients with pain may get narcotics. They may be on medicines to prevent them from throwing up. … And all of these will slow down gastric emptying.”
With an abnormal test result, “you are left to decide whether that is a real abnormality or whether the medicines the patients were on impacted the abnormality.”
If emptying was significantly prolonged, the test may have some value, “but then it probably will need to be corroborated with symptoms and with endoscopic findings.”
Thomas Collins is a freelance writer in South Florida.
References
- Warndorf MG, Kurtzman JT, Bartel MJ, et al. Early fluid resuscitation reduces morbidity among patients with acute pancreatitis. Clin Gastroenterol Hepatol. 2011;9(8):705-709.
- Wu BU, Hwang JQ, Gardner TH, et al. Lactated Ringer’s solution reduces systemic inflammation compared with saline in patients with acute pancreatitis. Clin Gastroenterol Hepatol. 2011;9(8):710-717.
So many symptoms that are staples of gastroenterology—chest pain, nausea, diarrhea—are mainstay causes for hospitalization that it might be worth fine-tuning how well you handle patients with gastroenterology disorders.
The Hospitalist asked several gastroenterologists for their guidance on better care and their suggestions for correcting some common mistakes that they encounter. Here are their tips:
1 Fluid resuscitation is crucial for pancreatitis patients.
It’s very important to rehydrate these patients within the first 24 hours, because those who remain underhydrated can have a worse prognosis, says Robert Coben, MD, academic coordinator for the Gastroentestinal Fellowship Program at Thomas Jefferson University Hospital in Philadelphia. On occasion, physicians are reluctant to give extra fluids to these patients, he says, particularly if they have heart failure or suffer kidney problems. A 70-kg patient should be receiving about 200 cc per hour, he notes.
“Sometimes we’ll walk in the room and they’re getting 80 cc an hour,” Dr. Coben says.
“These patients…need to be flooded with fluids,” says Rajeev Jain, MD, chief of gastroenterology at Presbyterian Hospital of Dallas, partner at Texas Digestive Disease Consultants, and chair of the Practice Management and Economics Committee of the American Gastroenterological Association. “We’re talking sometimes liters and liters of IV normal saline or lactated Ringer’s (solution) in a 24-hour period.”1
Marcelo Vela, MD, a gastroenterologist and hepatologist at the Mayo Clinic in Scottsdale, Ariz., and an associate editor with Clinical Gastroenterology and Hepatology, says Ringer’s solution is a better choice than normal saline.2
“If you’re going to start IV fluids on somebody who’s coming in with acute pancreatitis, Ringer’s solution has been shown to be superior to saline in randomized controlled trials,” Dr. Vela says. “It reduces systemic inflammation.”
2 Gastrointestinal bleeding decisions
When inpatients have gastrointestinal bleeding, the hospitalist often has to assess its severity and make the call on whether a patient needs the ICU.
“The most important thing for that is obviously the vital signs,” says John Pandolfino, MD, chief of the division of medicine–gastroenterology and hepatology at Northwestern University Feinberg School of Medicine in Chicago. “If people are tachycardic and they’re not responding to hydration and blood transfusion, that usually means it’s a pretty active bleed and they need to go to the intensive care unit. If you have somebody who’s GI bleeding and they’re coagulopathic (i.e., they’re on anti-coagulation because they have a valve and they need anti-coagulation or they have cancer or bad cardiovascular disease), those are the people that you should have a low threshold for sending to the intensive care unit with a GI bleed; those are the people who are at a very high mortality [risk].”
He added that those with an ulcer, with a visible vessel, are at a high-risk of a rebleed and should spend some time in the ICU.
“Those people should be evaluated in the intensive care unit for at least 24 hours, maybe even 72 hours,” Dr. Pandolfino says, “and they should have IV PPI [proton pump inhibitor] therapy.”
3 Endoscopy has very low yield for diagnosis of reflux.
“Endoscopy has good yield for mucosa abnormalities on inspection of the esophageal mucosa, but it does not give you a diagnosis of reflux, especially on patients who have already been treated with a PPI,” says Prakash Gyawali, MD, MRCP, professor of gastroenterology at Washington University in St. Louis, Mo. “So, usually, in those settings, obtaining a consult or trying to decide exactly what you’re looking for to explain the symptoms has better yield than an endoscopy.”
Sometimes a pH study is needed, but that has to be planned, because patients may have to be taken off of a PPI in advance. That means those studies are not easy to set up in the hospital and might best be arranged by the gastroenterologist, Dr. Gyawali says.
4 In cases of acute diarrhea, order a stool sample right away.
That will help guide care from the gastroenterologist, if and when the gastroenterologist is called in, Dr. Pandolfino says.
“One of the things that is frustrating for the gastroenterologist is that we get called initially, but really the hospitalist should be getting stool studies, and they should have at least a very good idea of what they need from us,” he says. “Because, really, endoscopy is not usually needed very often in diagnosis of acute diarrhea.”
Broad-range stool studies, a good history and physical, and examining labs for a possible chronic inflammatory process or anemia are good ways to begin to assess patients with diarrhea, he says. Clostridium difficile colitis has to be considered as well, Dr. Pandolfino says.
Endoscopy is more helpful in evaluating acute diarrhea in those with bloody diarrhea suspected of having inflammatory bowel disease or an infectious diarrhea but on whom cultures have come back negative. For those with compromised immune systems, endoscopy could be done earlier, as well.
“So for us, I think we really need to get into the picture a little bit after the patient has been brought into the hospital and the stool study is negative, unless they’re an immune-compromised patient,” Dr. Pandolfino says.
5 When—and how—to test the stool.
If a patient develops diarrhea while already in the hospital, the only stool test needed is C. diff.
“They shouldn’t be developing a viral diarrhea, they shouldn’t be developing an infectious diarrhea—let’s say, from E. coli or Salmonella—unless they literally developed it a couple hours after getting in,” Dr. Jain says. “It should either be C. diff or a side effect of some medication. … We don’t need to spend the extra money, which is of low-value care to send for OVA and parasites, or bacterial pathogens and so forth.”
Dr. Jain says he thinks such testing is being done more appropriately of late.
“But I still will see multiple stool tests sent on somebody who’s been in the hospital for a week and then develops diarrhea,” he explains.
6 Gastroenterologists do not need to be consulted for every C. diff infection.
“I think that we really should get involved when patients are either not responding or when they’re very ill,” Dr. Pandolfino says.
Hospitalists should consider whether patients are on antibiotics or a PPI and whether or not they need to stay on those medications. Also, medications that slow motility (i.e., loperamide) should be avoided, if possible.
“We don’t want it to linger,” Dr. Pandolfino says. “One of the basic mechanisms of how we get rid of pathogens is to expel them with diarrhea.
“But you certainly don’t want the patient to be uncomfortable to the point where they’re having 20 to 30 bowel movements a day.”
In non-severe patients who have some diarrhea, abdominal pain, nausea, and vomiting—but are able to keep food down—the specialists might not have to be called in, and patients can just be treated with oral metronidazole or oral vancomycin fairly simply, he says.
For those who seem severely ill with a dilating colon, are in nearly a septic state, and have very severe diarrhea, the gastroenterologist should probably be called in, he says.

7 For patients with a possible GI bleed and black stools, do an exam before calling in the gastroenterologist.
The exam should determine what the stool color is and whether it is heme-positive, and the patient’s blood count should be evaluated, Dr. Coben says.
Frequently, “the consultant’s the one who ends up doing the rectal exam and checking that,” he says. “Sometimes we find that [the patient is] really not bleeding,” and it was just a case of a hospitalist taking the patient’s word that they were bleeding.
Being on iron therapy or taking Pepto-Bismol can turn the stool black, and the stool might not really be black; colors can sometimes be open to interpretation.
But he cautions that colon cancer could be the cause for a GI bleed.
“We’ve had it happen a few times where this occurred,” he says. “The patient was discharged, and they really didn’t get proper follow-up, and it ended up that they had a colon cancer. It kind of delayed that diagnosis. So I think you have to be aware of [the fact that], especially in somebody over the age of 40 or 50, if they have an iron-deficiency, anemia, or heme-positive stool, the first thing you really need to exclude is a colon cancer.”
8 Minimize CT scans in early evaluation and management of acute pancreatitis patients.
“The reason for that is they tend to be intravascularly volume-depleted,” Dr. Jain says. “So [with] the IV contrast, there’s an increased risk of developing kidney failure. It’s also been associated with increased risk of necrotizing pancreatitis.”
Dr. Jain notes that when he is consulted on this kind of patient, he will order a sonogram. If it doesn’t show gallstones, and there’s no clear reason for the pancreatitis, he will want a CT scan, but he will wait a few days until the patient is fluid-resuscitated.
Dr. Jain says that this is a problem more often seen in the ED—where 90% of patients with acute pancreatitis have already gotten the CT scan—and less so among hospitalists, but it’s still worth the reminder.
A CT scan right away is justified to rule out something such as a perforation, but not in the case of classic symptoms of acute pancreatitis, he adds.
9 Actively bleeding patients?
It’s smart to give patients a unit of packed red blood cells more quickly if they’re actively bleeding. Even over just one hour is OK, Dr. Jain says.
“Even if they have underlying heart failure, if they’re volume-depleted, they need that volume,” Dr. Jain explains. “Sometimes you’ll see that it takes eight hours to get two units of blood in. That’s inadequate.”
Another point worth a reminder, he says: Two large-bore peripheral IV’s are “much, much better” than a central or PICC line to deliver IV fluid resuscitation.
“Sometimes hospitalists order barium studies because these can be done the same day, whereas with endoscopy, patients need to be put on a schedule and have to be NPO [nothing by mouth] overnight.” —Prakash Gyawali, MD, MRCP
10 Don’t be too quick to order barium studies, especially in patients with dysphagia.
“The problem with that is it takes much longer to do an endoscopy if barium is put in the esophagus, because we usually wait until the barium clears,” Dr. Gyawali says. “And inpatient evaluation of new-onset dysphagia should be endoscopy first, and not barium, because biopsies need to be taken to rule out eosinophilic esophagitis.
“Sometimes hospitalists order barium studies because these can be done the same day, whereas with endoscopy, patients need to be put on a schedule and have to be NPO [nothing by mouth] overnight.”
11 Gastric-emptying studies should be outpatient.
Gastric-emptying studies are often better done when patients are not in a hospital, experts say, because they might be on medications that would interfere with the study.
“A common issue, not just among hospitalists but also gastroenterologists, is that patients may be on a bunch of medicines that would affect stomach-emptying while they are in-house for some other problem,” Dr. Gyawali says. “A lot of times, these patients with pain may get narcotics. They may be on medicines to prevent them from throwing up. … And all of these will slow down gastric emptying.”
With an abnormal test result, “you are left to decide whether that is a real abnormality or whether the medicines the patients were on impacted the abnormality.”
If emptying was significantly prolonged, the test may have some value, “but then it probably will need to be corroborated with symptoms and with endoscopic findings.”
Thomas Collins is a freelance writer in South Florida.
References
- Warndorf MG, Kurtzman JT, Bartel MJ, et al. Early fluid resuscitation reduces morbidity among patients with acute pancreatitis. Clin Gastroenterol Hepatol. 2011;9(8):705-709.
- Wu BU, Hwang JQ, Gardner TH, et al. Lactated Ringer’s solution reduces systemic inflammation compared with saline in patients with acute pancreatitis. Clin Gastroenterol Hepatol. 2011;9(8):710-717.
So many symptoms that are staples of gastroenterology—chest pain, nausea, diarrhea—are mainstay causes for hospitalization that it might be worth fine-tuning how well you handle patients with gastroenterology disorders.
The Hospitalist asked several gastroenterologists for their guidance on better care and their suggestions for correcting some common mistakes that they encounter. Here are their tips:
1 Fluid resuscitation is crucial for pancreatitis patients.
It’s very important to rehydrate these patients within the first 24 hours, because those who remain underhydrated can have a worse prognosis, says Robert Coben, MD, academic coordinator for the Gastroentestinal Fellowship Program at Thomas Jefferson University Hospital in Philadelphia. On occasion, physicians are reluctant to give extra fluids to these patients, he says, particularly if they have heart failure or suffer kidney problems. A 70-kg patient should be receiving about 200 cc per hour, he notes.
“Sometimes we’ll walk in the room and they’re getting 80 cc an hour,” Dr. Coben says.
“These patients…need to be flooded with fluids,” says Rajeev Jain, MD, chief of gastroenterology at Presbyterian Hospital of Dallas, partner at Texas Digestive Disease Consultants, and chair of the Practice Management and Economics Committee of the American Gastroenterological Association. “We’re talking sometimes liters and liters of IV normal saline or lactated Ringer’s (solution) in a 24-hour period.”1
Marcelo Vela, MD, a gastroenterologist and hepatologist at the Mayo Clinic in Scottsdale, Ariz., and an associate editor with Clinical Gastroenterology and Hepatology, says Ringer’s solution is a better choice than normal saline.2
“If you’re going to start IV fluids on somebody who’s coming in with acute pancreatitis, Ringer’s solution has been shown to be superior to saline in randomized controlled trials,” Dr. Vela says. “It reduces systemic inflammation.”
2 Gastrointestinal bleeding decisions
When inpatients have gastrointestinal bleeding, the hospitalist often has to assess its severity and make the call on whether a patient needs the ICU.
“The most important thing for that is obviously the vital signs,” says John Pandolfino, MD, chief of the division of medicine–gastroenterology and hepatology at Northwestern University Feinberg School of Medicine in Chicago. “If people are tachycardic and they’re not responding to hydration and blood transfusion, that usually means it’s a pretty active bleed and they need to go to the intensive care unit. If you have somebody who’s GI bleeding and they’re coagulopathic (i.e., they’re on anti-coagulation because they have a valve and they need anti-coagulation or they have cancer or bad cardiovascular disease), those are the people that you should have a low threshold for sending to the intensive care unit with a GI bleed; those are the people who are at a very high mortality [risk].”
He added that those with an ulcer, with a visible vessel, are at a high-risk of a rebleed and should spend some time in the ICU.
“Those people should be evaluated in the intensive care unit for at least 24 hours, maybe even 72 hours,” Dr. Pandolfino says, “and they should have IV PPI [proton pump inhibitor] therapy.”
3 Endoscopy has very low yield for diagnosis of reflux.
“Endoscopy has good yield for mucosa abnormalities on inspection of the esophageal mucosa, but it does not give you a diagnosis of reflux, especially on patients who have already been treated with a PPI,” says Prakash Gyawali, MD, MRCP, professor of gastroenterology at Washington University in St. Louis, Mo. “So, usually, in those settings, obtaining a consult or trying to decide exactly what you’re looking for to explain the symptoms has better yield than an endoscopy.”
Sometimes a pH study is needed, but that has to be planned, because patients may have to be taken off of a PPI in advance. That means those studies are not easy to set up in the hospital and might best be arranged by the gastroenterologist, Dr. Gyawali says.
4 In cases of acute diarrhea, order a stool sample right away.
That will help guide care from the gastroenterologist, if and when the gastroenterologist is called in, Dr. Pandolfino says.
“One of the things that is frustrating for the gastroenterologist is that we get called initially, but really the hospitalist should be getting stool studies, and they should have at least a very good idea of what they need from us,” he says. “Because, really, endoscopy is not usually needed very often in diagnosis of acute diarrhea.”
Broad-range stool studies, a good history and physical, and examining labs for a possible chronic inflammatory process or anemia are good ways to begin to assess patients with diarrhea, he says. Clostridium difficile colitis has to be considered as well, Dr. Pandolfino says.
Endoscopy is more helpful in evaluating acute diarrhea in those with bloody diarrhea suspected of having inflammatory bowel disease or an infectious diarrhea but on whom cultures have come back negative. For those with compromised immune systems, endoscopy could be done earlier, as well.
“So for us, I think we really need to get into the picture a little bit after the patient has been brought into the hospital and the stool study is negative, unless they’re an immune-compromised patient,” Dr. Pandolfino says.
5 When—and how—to test the stool.
If a patient develops diarrhea while already in the hospital, the only stool test needed is C. diff.
“They shouldn’t be developing a viral diarrhea, they shouldn’t be developing an infectious diarrhea—let’s say, from E. coli or Salmonella—unless they literally developed it a couple hours after getting in,” Dr. Jain says. “It should either be C. diff or a side effect of some medication. … We don’t need to spend the extra money, which is of low-value care to send for OVA and parasites, or bacterial pathogens and so forth.”
Dr. Jain says he thinks such testing is being done more appropriately of late.
“But I still will see multiple stool tests sent on somebody who’s been in the hospital for a week and then develops diarrhea,” he explains.
6 Gastroenterologists do not need to be consulted for every C. diff infection.
“I think that we really should get involved when patients are either not responding or when they’re very ill,” Dr. Pandolfino says.
Hospitalists should consider whether patients are on antibiotics or a PPI and whether or not they need to stay on those medications. Also, medications that slow motility (i.e., loperamide) should be avoided, if possible.
“We don’t want it to linger,” Dr. Pandolfino says. “One of the basic mechanisms of how we get rid of pathogens is to expel them with diarrhea.
“But you certainly don’t want the patient to be uncomfortable to the point where they’re having 20 to 30 bowel movements a day.”
In non-severe patients who have some diarrhea, abdominal pain, nausea, and vomiting—but are able to keep food down—the specialists might not have to be called in, and patients can just be treated with oral metronidazole or oral vancomycin fairly simply, he says.
For those who seem severely ill with a dilating colon, are in nearly a septic state, and have very severe diarrhea, the gastroenterologist should probably be called in, he says.

7 For patients with a possible GI bleed and black stools, do an exam before calling in the gastroenterologist.
The exam should determine what the stool color is and whether it is heme-positive, and the patient’s blood count should be evaluated, Dr. Coben says.
Frequently, “the consultant’s the one who ends up doing the rectal exam and checking that,” he says. “Sometimes we find that [the patient is] really not bleeding,” and it was just a case of a hospitalist taking the patient’s word that they were bleeding.
Being on iron therapy or taking Pepto-Bismol can turn the stool black, and the stool might not really be black; colors can sometimes be open to interpretation.
But he cautions that colon cancer could be the cause for a GI bleed.
“We’ve had it happen a few times where this occurred,” he says. “The patient was discharged, and they really didn’t get proper follow-up, and it ended up that they had a colon cancer. It kind of delayed that diagnosis. So I think you have to be aware of [the fact that], especially in somebody over the age of 40 or 50, if they have an iron-deficiency, anemia, or heme-positive stool, the first thing you really need to exclude is a colon cancer.”
8 Minimize CT scans in early evaluation and management of acute pancreatitis patients.
“The reason for that is they tend to be intravascularly volume-depleted,” Dr. Jain says. “So [with] the IV contrast, there’s an increased risk of developing kidney failure. It’s also been associated with increased risk of necrotizing pancreatitis.”
Dr. Jain notes that when he is consulted on this kind of patient, he will order a sonogram. If it doesn’t show gallstones, and there’s no clear reason for the pancreatitis, he will want a CT scan, but he will wait a few days until the patient is fluid-resuscitated.
Dr. Jain says that this is a problem more often seen in the ED—where 90% of patients with acute pancreatitis have already gotten the CT scan—and less so among hospitalists, but it’s still worth the reminder.
A CT scan right away is justified to rule out something such as a perforation, but not in the case of classic symptoms of acute pancreatitis, he adds.
9 Actively bleeding patients?
It’s smart to give patients a unit of packed red blood cells more quickly if they’re actively bleeding. Even over just one hour is OK, Dr. Jain says.
“Even if they have underlying heart failure, if they’re volume-depleted, they need that volume,” Dr. Jain explains. “Sometimes you’ll see that it takes eight hours to get two units of blood in. That’s inadequate.”
Another point worth a reminder, he says: Two large-bore peripheral IV’s are “much, much better” than a central or PICC line to deliver IV fluid resuscitation.
“Sometimes hospitalists order barium studies because these can be done the same day, whereas with endoscopy, patients need to be put on a schedule and have to be NPO [nothing by mouth] overnight.” —Prakash Gyawali, MD, MRCP
10 Don’t be too quick to order barium studies, especially in patients with dysphagia.
“The problem with that is it takes much longer to do an endoscopy if barium is put in the esophagus, because we usually wait until the barium clears,” Dr. Gyawali says. “And inpatient evaluation of new-onset dysphagia should be endoscopy first, and not barium, because biopsies need to be taken to rule out eosinophilic esophagitis.
“Sometimes hospitalists order barium studies because these can be done the same day, whereas with endoscopy, patients need to be put on a schedule and have to be NPO [nothing by mouth] overnight.”
11 Gastric-emptying studies should be outpatient.
Gastric-emptying studies are often better done when patients are not in a hospital, experts say, because they might be on medications that would interfere with the study.
“A common issue, not just among hospitalists but also gastroenterologists, is that patients may be on a bunch of medicines that would affect stomach-emptying while they are in-house for some other problem,” Dr. Gyawali says. “A lot of times, these patients with pain may get narcotics. They may be on medicines to prevent them from throwing up. … And all of these will slow down gastric emptying.”
With an abnormal test result, “you are left to decide whether that is a real abnormality or whether the medicines the patients were on impacted the abnormality.”
If emptying was significantly prolonged, the test may have some value, “but then it probably will need to be corroborated with symptoms and with endoscopic findings.”
Thomas Collins is a freelance writer in South Florida.
References
- Warndorf MG, Kurtzman JT, Bartel MJ, et al. Early fluid resuscitation reduces morbidity among patients with acute pancreatitis. Clin Gastroenterol Hepatol. 2011;9(8):705-709.
- Wu BU, Hwang JQ, Gardner TH, et al. Lactated Ringer’s solution reduces systemic inflammation compared with saline in patients with acute pancreatitis. Clin Gastroenterol Hepatol. 2011;9(8):710-717.
LISTEN NOW: Hospitalist Manya Gupta on Choosing Wisely
Excerpt of our interviews with Choosing Wisely, hospitalist Manya Gupta, MD, an assistant professor in the department of internal medicine of Rush University Medical Center in Chicago, discusses an example of a Choosing Wisely program.
Excerpt of our interviews with Choosing Wisely, hospitalist Manya Gupta, MD, an assistant professor in the department of internal medicine of Rush University Medical Center in Chicago, discusses an example of a Choosing Wisely program.
Excerpt of our interviews with Choosing Wisely, hospitalist Manya Gupta, MD, an assistant professor in the department of internal medicine of Rush University Medical Center in Chicago, discusses an example of a Choosing Wisely program.