User login
New Rules for Value-Based Purchasing, Readmission Penalties, Admissions
October is the beginning of a new year—in this case, fiscal-year 2014 for the Centers for Medicare & Medicaid Services (CMS). It’s a time when the new rules kick in. This month, we’ll look at some highlights, focusing on the new developments affecting your practice. Because you are held accountable for hospital-side performance on programs such as hospital value-based purchasing (HVBP) and the Readmissions Reduction Program, a working knowledge of the 2014 edition of the programs is crucial.
Close the Loop on HVBP
How will your hospital get paid under the 2014 version of HVBP? This past July, your hospital received a report outlining how its Medicare payments will be affected based on your hospital’s performance on process of care (heart failure, pneumonia, myocardial infarction, and surgery), patient experience (HCAHPS), and outcomes (30-day mortality for heart failure, pneumonia, and myocardial infarction).
Here are two hypothetical hospitals and how their performance in the program affects their 2014 payment. As background, in 2014, all hospitals have their base diagnosis related group (DRG) payments reduced by 1.25% for HVBP. They can earn back some, all, or an amount in excess of the 1.25% based on their performance. Payment is based on performance during the April 1 to Dec. 31, 2012, period. Under HVBP, CMS incentive payments occur at the level of individual patients, each of which is assigned a DRG.
Let’s look at two examples:
Hospital 1
- Base DRG payment reduction: 1.25% (all hospitals).
- Portion of base DRG earned back based on performance (process/patient experience/outcome metrics): 1.48%.
- Net change in base DRG payment: +0.23%.
Hospital 2
- Base DRG payment reduction: 1.25% (all hospitals).
- Portion of base DRG earned back based on performance (process/patient experience/outcome metrics): 1.08%.
- Net change in base DRG payment: -0.17%.
Hospital 1 performed relatively well, getting a bump of 0.23% in its base DRG rate. Hospital 2 did not perform so well, so it took a 0.17% hit on its base DRG rate.
In order to determine total dollars made or lost for your hospital, one multiplies the total number of eligible Medicare inpatients for 2014 times the base DRG payment times the percent change in base DRG payment. If Hospital 1 has 10,000 eligible patients in 2014 and a base DRG payment of $5,000, the value is 10,000 x $5,000 x 0.0023 (0.23%) = $115,000 gained. Hospital 2, with the same number of patients and base DRG payment, loses (10,000 x $5,000 x 0.0017 = $85,000).
Readmissions and Penalties
For 2014, CMS is adding 30-day readmissions for COPD to readmissions for heart failure, pneumonia, and myocardial infarction for its penalty program. CMS added COPD because it is the fourth-leading cause of readmissions, according to a recent Medicare Payment Advisory Commission report, and because there is wide variation in the rates (from 18% to 25%) of COPD hospital readmissions.
For 2014, CMS raises the ceiling on readmission penalties to a maximum of 2% of reimbursement for all of a hospital’s Medicare inpatients. (The maximum hit during the first round of readmission penalties, which began in October 2012, was 1%.) More than 2,200 U.S. hospitals will face some financial penalty for excess 30-day readmissions.
Disappointingly, CMS did not add a risk adjustment for socioeconomic status despite being under pressure to do so. There is growing evidence that these factors have a major impact on readmission rates.1,2
New Definition of an Admission
Amidst confusion from many and major blowback from beneficiaries saddled with large out-of-pocket expenses for observation stays and subsequent skilled-nursing-facility stays, CMS is clarifying the definition of an inpatient admission. The agency will define an admission as a hospital stay that spans at least two midnights. If a patient is in the hospital for a shorter period of time, CMS will deem the patient to be on observation status, unless medical record documentation supports a physician’s expectation “that the beneficiary would need care spanning at least two midnights” but unanticipated events led to a shorter stay.
Plan of Attack
For HVBP, make contact with your director of quality to understand your hospital’s performance and payment for 2014. If you have incentive compensation riding on HVBP, make sure you understand how your employer or contracted hospital is calculating the payout (because, for example, the performance period was in 2012!) and that your hospitalist group understands the payout calculation.
For COPD readmissions prevention, ensure patients have a home management plan; appropriate specialist follow-up and that they understand medication use, including inhalers and supplemental oxygen; and that you consider early referral for pulmonary rehabilitation for eligible patients.
For the new definition of inpatient admission, work with your hospital’s physician advisor and case management to ensure your group is getting appropriate guidance on documentation requirements. You are probably being held accountable for your hospital’s total number of observation hours, so remember to track these metrics following implementation of the new rule, as they (hopefully) should decrease. If they do, take some of the credit!
References
- Joynt KE, Orav EJ, Jha AK. Thirty-day readmission rates for Medicare beneficiaries by race and site of care. JAMA. 2011;305(7):675-681.
- Lindenauer PK, Lagu T, Rothberg MB, et al. Income inequality and 30 day outcomes after acute myocardial infarction, heart failure, and pneumonia: retrospective cohort study. BMJ. 2013;346:f521.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is co-founder and past president of SHM. Email him at [email protected].
October is the beginning of a new year—in this case, fiscal-year 2014 for the Centers for Medicare & Medicaid Services (CMS). It’s a time when the new rules kick in. This month, we’ll look at some highlights, focusing on the new developments affecting your practice. Because you are held accountable for hospital-side performance on programs such as hospital value-based purchasing (HVBP) and the Readmissions Reduction Program, a working knowledge of the 2014 edition of the programs is crucial.
Close the Loop on HVBP
How will your hospital get paid under the 2014 version of HVBP? This past July, your hospital received a report outlining how its Medicare payments will be affected based on your hospital’s performance on process of care (heart failure, pneumonia, myocardial infarction, and surgery), patient experience (HCAHPS), and outcomes (30-day mortality for heart failure, pneumonia, and myocardial infarction).
Here are two hypothetical hospitals and how their performance in the program affects their 2014 payment. As background, in 2014, all hospitals have their base diagnosis related group (DRG) payments reduced by 1.25% for HVBP. They can earn back some, all, or an amount in excess of the 1.25% based on their performance. Payment is based on performance during the April 1 to Dec. 31, 2012, period. Under HVBP, CMS incentive payments occur at the level of individual patients, each of which is assigned a DRG.
Let’s look at two examples:
Hospital 1
- Base DRG payment reduction: 1.25% (all hospitals).
- Portion of base DRG earned back based on performance (process/patient experience/outcome metrics): 1.48%.
- Net change in base DRG payment: +0.23%.
Hospital 2
- Base DRG payment reduction: 1.25% (all hospitals).
- Portion of base DRG earned back based on performance (process/patient experience/outcome metrics): 1.08%.
- Net change in base DRG payment: -0.17%.
Hospital 1 performed relatively well, getting a bump of 0.23% in its base DRG rate. Hospital 2 did not perform so well, so it took a 0.17% hit on its base DRG rate.
In order to determine total dollars made or lost for your hospital, one multiplies the total number of eligible Medicare inpatients for 2014 times the base DRG payment times the percent change in base DRG payment. If Hospital 1 has 10,000 eligible patients in 2014 and a base DRG payment of $5,000, the value is 10,000 x $5,000 x 0.0023 (0.23%) = $115,000 gained. Hospital 2, with the same number of patients and base DRG payment, loses (10,000 x $5,000 x 0.0017 = $85,000).
Readmissions and Penalties
For 2014, CMS is adding 30-day readmissions for COPD to readmissions for heart failure, pneumonia, and myocardial infarction for its penalty program. CMS added COPD because it is the fourth-leading cause of readmissions, according to a recent Medicare Payment Advisory Commission report, and because there is wide variation in the rates (from 18% to 25%) of COPD hospital readmissions.
For 2014, CMS raises the ceiling on readmission penalties to a maximum of 2% of reimbursement for all of a hospital’s Medicare inpatients. (The maximum hit during the first round of readmission penalties, which began in October 2012, was 1%.) More than 2,200 U.S. hospitals will face some financial penalty for excess 30-day readmissions.
Disappointingly, CMS did not add a risk adjustment for socioeconomic status despite being under pressure to do so. There is growing evidence that these factors have a major impact on readmission rates.1,2
New Definition of an Admission
Amidst confusion from many and major blowback from beneficiaries saddled with large out-of-pocket expenses for observation stays and subsequent skilled-nursing-facility stays, CMS is clarifying the definition of an inpatient admission. The agency will define an admission as a hospital stay that spans at least two midnights. If a patient is in the hospital for a shorter period of time, CMS will deem the patient to be on observation status, unless medical record documentation supports a physician’s expectation “that the beneficiary would need care spanning at least two midnights” but unanticipated events led to a shorter stay.
Plan of Attack
For HVBP, make contact with your director of quality to understand your hospital’s performance and payment for 2014. If you have incentive compensation riding on HVBP, make sure you understand how your employer or contracted hospital is calculating the payout (because, for example, the performance period was in 2012!) and that your hospitalist group understands the payout calculation.
For COPD readmissions prevention, ensure patients have a home management plan; appropriate specialist follow-up and that they understand medication use, including inhalers and supplemental oxygen; and that you consider early referral for pulmonary rehabilitation for eligible patients.
For the new definition of inpatient admission, work with your hospital’s physician advisor and case management to ensure your group is getting appropriate guidance on documentation requirements. You are probably being held accountable for your hospital’s total number of observation hours, so remember to track these metrics following implementation of the new rule, as they (hopefully) should decrease. If they do, take some of the credit!
References
- Joynt KE, Orav EJ, Jha AK. Thirty-day readmission rates for Medicare beneficiaries by race and site of care. JAMA. 2011;305(7):675-681.
- Lindenauer PK, Lagu T, Rothberg MB, et al. Income inequality and 30 day outcomes after acute myocardial infarction, heart failure, and pneumonia: retrospective cohort study. BMJ. 2013;346:f521.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is co-founder and past president of SHM. Email him at [email protected].
October is the beginning of a new year—in this case, fiscal-year 2014 for the Centers for Medicare & Medicaid Services (CMS). It’s a time when the new rules kick in. This month, we’ll look at some highlights, focusing on the new developments affecting your practice. Because you are held accountable for hospital-side performance on programs such as hospital value-based purchasing (HVBP) and the Readmissions Reduction Program, a working knowledge of the 2014 edition of the programs is crucial.
Close the Loop on HVBP
How will your hospital get paid under the 2014 version of HVBP? This past July, your hospital received a report outlining how its Medicare payments will be affected based on your hospital’s performance on process of care (heart failure, pneumonia, myocardial infarction, and surgery), patient experience (HCAHPS), and outcomes (30-day mortality for heart failure, pneumonia, and myocardial infarction).
Here are two hypothetical hospitals and how their performance in the program affects their 2014 payment. As background, in 2014, all hospitals have their base diagnosis related group (DRG) payments reduced by 1.25% for HVBP. They can earn back some, all, or an amount in excess of the 1.25% based on their performance. Payment is based on performance during the April 1 to Dec. 31, 2012, period. Under HVBP, CMS incentive payments occur at the level of individual patients, each of which is assigned a DRG.
Let’s look at two examples:
Hospital 1
- Base DRG payment reduction: 1.25% (all hospitals).
- Portion of base DRG earned back based on performance (process/patient experience/outcome metrics): 1.48%.
- Net change in base DRG payment: +0.23%.
Hospital 2
- Base DRG payment reduction: 1.25% (all hospitals).
- Portion of base DRG earned back based on performance (process/patient experience/outcome metrics): 1.08%.
- Net change in base DRG payment: -0.17%.
Hospital 1 performed relatively well, getting a bump of 0.23% in its base DRG rate. Hospital 2 did not perform so well, so it took a 0.17% hit on its base DRG rate.
In order to determine total dollars made or lost for your hospital, one multiplies the total number of eligible Medicare inpatients for 2014 times the base DRG payment times the percent change in base DRG payment. If Hospital 1 has 10,000 eligible patients in 2014 and a base DRG payment of $5,000, the value is 10,000 x $5,000 x 0.0023 (0.23%) = $115,000 gained. Hospital 2, with the same number of patients and base DRG payment, loses (10,000 x $5,000 x 0.0017 = $85,000).
Readmissions and Penalties
For 2014, CMS is adding 30-day readmissions for COPD to readmissions for heart failure, pneumonia, and myocardial infarction for its penalty program. CMS added COPD because it is the fourth-leading cause of readmissions, according to a recent Medicare Payment Advisory Commission report, and because there is wide variation in the rates (from 18% to 25%) of COPD hospital readmissions.
For 2014, CMS raises the ceiling on readmission penalties to a maximum of 2% of reimbursement for all of a hospital’s Medicare inpatients. (The maximum hit during the first round of readmission penalties, which began in October 2012, was 1%.) More than 2,200 U.S. hospitals will face some financial penalty for excess 30-day readmissions.
Disappointingly, CMS did not add a risk adjustment for socioeconomic status despite being under pressure to do so. There is growing evidence that these factors have a major impact on readmission rates.1,2
New Definition of an Admission
Amidst confusion from many and major blowback from beneficiaries saddled with large out-of-pocket expenses for observation stays and subsequent skilled-nursing-facility stays, CMS is clarifying the definition of an inpatient admission. The agency will define an admission as a hospital stay that spans at least two midnights. If a patient is in the hospital for a shorter period of time, CMS will deem the patient to be on observation status, unless medical record documentation supports a physician’s expectation “that the beneficiary would need care spanning at least two midnights” but unanticipated events led to a shorter stay.
Plan of Attack
For HVBP, make contact with your director of quality to understand your hospital’s performance and payment for 2014. If you have incentive compensation riding on HVBP, make sure you understand how your employer or contracted hospital is calculating the payout (because, for example, the performance period was in 2012!) and that your hospitalist group understands the payout calculation.
For COPD readmissions prevention, ensure patients have a home management plan; appropriate specialist follow-up and that they understand medication use, including inhalers and supplemental oxygen; and that you consider early referral for pulmonary rehabilitation for eligible patients.
For the new definition of inpatient admission, work with your hospital’s physician advisor and case management to ensure your group is getting appropriate guidance on documentation requirements. You are probably being held accountable for your hospital’s total number of observation hours, so remember to track these metrics following implementation of the new rule, as they (hopefully) should decrease. If they do, take some of the credit!
References
- Joynt KE, Orav EJ, Jha AK. Thirty-day readmission rates for Medicare beneficiaries by race and site of care. JAMA. 2011;305(7):675-681.
- Lindenauer PK, Lagu T, Rothberg MB, et al. Income inequality and 30 day outcomes after acute myocardial infarction, heart failure, and pneumonia: retrospective cohort study. BMJ. 2013;346:f521.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is co-founder and past president of SHM. Email him at [email protected].
Society of Hospital Medicine’s MARQUIS Initiative Highlights Need For Improved Medication Reconciliation

–Jeffrey Schnipper, MD, MPH, FHM
What is the best possible medication history? How is it done? Who should do it? When should it be done during a patient’s journey in and out of the hospital? What medication discrepancies—and potential adverse drug events—are most likely?
Those are questions veteran hospitalist Jason Stein, MD, tried to answer during an HM13 breakout session on medication reconciliation at the Gaylord National Resort and Conference Center in National Harbor, Md.
“How do you know as the discharging provider if the medication list you’re looking at is gold or garbage?” said Dr. Stein, associate director for quality improvement (QI) at Emory University in Atlanta and a mentor for SHM’s Multi-Center Medication Reconciliation Quality Improvement Study (MARQUIS) quality-research initiative.
The concept of the “best possible medication history” (BPMH) originated with patient-safety expert Edward Etchells, MD, MSc, at Sunnybrook Health Sciences Centre in Toronto. The concept is outlined on a pocket reminder card for MARQUIS participants, explained co-presenter and principal investigator Jeffrey Schnipper MD, MPH, FHM, a hospitalist at Brigham & Women’s Hospital in Boston.
“Sometimes it’s impossible to know what the patient was or wasn’t taking, but it doesn’t mean you don’t do your best,” he said, adding that hospitalists should attempt to get at least one reliable, corroborating source of information for a patient’s medical history.
Sometimes it is necessary to speak to family members or the community pharmacy, Dr. Schnipper said, because many patients can’t remember all of the drugs they are taking. Trying to do medication reconciliation at the time of discharge when BPMH has not been done can lead to more work for the provider, medication errors, or rehospitalizations. Ideally, knowledge of what the patient was taking before admission, as well as the patient’s health literacy and adherence history, should be gathered and documented once, early, and well during the hospitalization by a trained provider, according to Dr. Schnipper.
An SHM survey, however, showed 50% to 70% percent of front-line providers have never received BPMH training, and 60% say they are not given the time.
“Not knowing means a diligent provider would need to take a BPMH at discharge, which is a waste,” Dr. Stein said. It would be nice to tell from the electronic health record whether a true BPMH had been taken for every hospitalized patient—or at least every high-risk patient—but this goal is not well-supported by current information technology, MARQUIS investigators said they have learned.
The MARQUIS program was launched in 2011 with a grant from the federal Agency for Healthcare Research and Quality. It began with a thorough review of the literature on medication reconciliation and the development of a toolkit of best practices. In 2012, six pilot sites were offered a menu of 11 MARQUIS medication-reconciliation interventions to choose from and help in implementing them from an SHM mentor, with expertise in both QI and medication safety.
Participating sites have mobilized high-level hospital leadership and utilize a local champion, usually a hospitalist, tools for assessing high-risk patients, medication-reconciliation assistants or counselors, and pharmacist involvement. Different sites have employed different professional staff to take medication histories.
Dr. Schnipper said he expects another round of MARQUIS-mentored implementation, probably in 2014, after data from the first round have been analyzed. The program is tracking such outcomes as the number of potentially harmful, unintentional medication discrepancies per patient at participating sites.
The MARQUIS toolkit is available on the SHM website at www.hospitalmedicine.org/marquis.
Larry Beresford is a freelance writer in San Francisco.

–Jeffrey Schnipper, MD, MPH, FHM
What is the best possible medication history? How is it done? Who should do it? When should it be done during a patient’s journey in and out of the hospital? What medication discrepancies—and potential adverse drug events—are most likely?
Those are questions veteran hospitalist Jason Stein, MD, tried to answer during an HM13 breakout session on medication reconciliation at the Gaylord National Resort and Conference Center in National Harbor, Md.
“How do you know as the discharging provider if the medication list you’re looking at is gold or garbage?” said Dr. Stein, associate director for quality improvement (QI) at Emory University in Atlanta and a mentor for SHM’s Multi-Center Medication Reconciliation Quality Improvement Study (MARQUIS) quality-research initiative.
The concept of the “best possible medication history” (BPMH) originated with patient-safety expert Edward Etchells, MD, MSc, at Sunnybrook Health Sciences Centre in Toronto. The concept is outlined on a pocket reminder card for MARQUIS participants, explained co-presenter and principal investigator Jeffrey Schnipper MD, MPH, FHM, a hospitalist at Brigham & Women’s Hospital in Boston.
“Sometimes it’s impossible to know what the patient was or wasn’t taking, but it doesn’t mean you don’t do your best,” he said, adding that hospitalists should attempt to get at least one reliable, corroborating source of information for a patient’s medical history.
Sometimes it is necessary to speak to family members or the community pharmacy, Dr. Schnipper said, because many patients can’t remember all of the drugs they are taking. Trying to do medication reconciliation at the time of discharge when BPMH has not been done can lead to more work for the provider, medication errors, or rehospitalizations. Ideally, knowledge of what the patient was taking before admission, as well as the patient’s health literacy and adherence history, should be gathered and documented once, early, and well during the hospitalization by a trained provider, according to Dr. Schnipper.
An SHM survey, however, showed 50% to 70% percent of front-line providers have never received BPMH training, and 60% say they are not given the time.
“Not knowing means a diligent provider would need to take a BPMH at discharge, which is a waste,” Dr. Stein said. It would be nice to tell from the electronic health record whether a true BPMH had been taken for every hospitalized patient—or at least every high-risk patient—but this goal is not well-supported by current information technology, MARQUIS investigators said they have learned.
The MARQUIS program was launched in 2011 with a grant from the federal Agency for Healthcare Research and Quality. It began with a thorough review of the literature on medication reconciliation and the development of a toolkit of best practices. In 2012, six pilot sites were offered a menu of 11 MARQUIS medication-reconciliation interventions to choose from and help in implementing them from an SHM mentor, with expertise in both QI and medication safety.
Participating sites have mobilized high-level hospital leadership and utilize a local champion, usually a hospitalist, tools for assessing high-risk patients, medication-reconciliation assistants or counselors, and pharmacist involvement. Different sites have employed different professional staff to take medication histories.
Dr. Schnipper said he expects another round of MARQUIS-mentored implementation, probably in 2014, after data from the first round have been analyzed. The program is tracking such outcomes as the number of potentially harmful, unintentional medication discrepancies per patient at participating sites.
The MARQUIS toolkit is available on the SHM website at www.hospitalmedicine.org/marquis.
Larry Beresford is a freelance writer in San Francisco.

–Jeffrey Schnipper, MD, MPH, FHM
What is the best possible medication history? How is it done? Who should do it? When should it be done during a patient’s journey in and out of the hospital? What medication discrepancies—and potential adverse drug events—are most likely?
Those are questions veteran hospitalist Jason Stein, MD, tried to answer during an HM13 breakout session on medication reconciliation at the Gaylord National Resort and Conference Center in National Harbor, Md.
“How do you know as the discharging provider if the medication list you’re looking at is gold or garbage?” said Dr. Stein, associate director for quality improvement (QI) at Emory University in Atlanta and a mentor for SHM’s Multi-Center Medication Reconciliation Quality Improvement Study (MARQUIS) quality-research initiative.
The concept of the “best possible medication history” (BPMH) originated with patient-safety expert Edward Etchells, MD, MSc, at Sunnybrook Health Sciences Centre in Toronto. The concept is outlined on a pocket reminder card for MARQUIS participants, explained co-presenter and principal investigator Jeffrey Schnipper MD, MPH, FHM, a hospitalist at Brigham & Women’s Hospital in Boston.
“Sometimes it’s impossible to know what the patient was or wasn’t taking, but it doesn’t mean you don’t do your best,” he said, adding that hospitalists should attempt to get at least one reliable, corroborating source of information for a patient’s medical history.
Sometimes it is necessary to speak to family members or the community pharmacy, Dr. Schnipper said, because many patients can’t remember all of the drugs they are taking. Trying to do medication reconciliation at the time of discharge when BPMH has not been done can lead to more work for the provider, medication errors, or rehospitalizations. Ideally, knowledge of what the patient was taking before admission, as well as the patient’s health literacy and adherence history, should be gathered and documented once, early, and well during the hospitalization by a trained provider, according to Dr. Schnipper.
An SHM survey, however, showed 50% to 70% percent of front-line providers have never received BPMH training, and 60% say they are not given the time.
“Not knowing means a diligent provider would need to take a BPMH at discharge, which is a waste,” Dr. Stein said. It would be nice to tell from the electronic health record whether a true BPMH had been taken for every hospitalized patient—or at least every high-risk patient—but this goal is not well-supported by current information technology, MARQUIS investigators said they have learned.
The MARQUIS program was launched in 2011 with a grant from the federal Agency for Healthcare Research and Quality. It began with a thorough review of the literature on medication reconciliation and the development of a toolkit of best practices. In 2012, six pilot sites were offered a menu of 11 MARQUIS medication-reconciliation interventions to choose from and help in implementing them from an SHM mentor, with expertise in both QI and medication safety.
Participating sites have mobilized high-level hospital leadership and utilize a local champion, usually a hospitalist, tools for assessing high-risk patients, medication-reconciliation assistants or counselors, and pharmacist involvement. Different sites have employed different professional staff to take medication histories.
Dr. Schnipper said he expects another round of MARQUIS-mentored implementation, probably in 2014, after data from the first round have been analyzed. The program is tracking such outcomes as the number of potentially harmful, unintentional medication discrepancies per patient at participating sites.
The MARQUIS toolkit is available on the SHM website at www.hospitalmedicine.org/marquis.
Larry Beresford is a freelance writer in San Francisco.
Little Resistance to Rising Hospital-Acquired Infections
Antibiotic resistance to hospital-acquired infections (HAIs) is rising at faster rates than predicted in 2008 by the Centers for Disease Control and Prevention (CDC), according to an analysis of privately gathered data reported in a recent commentary in Antimicrobial Agents and Chemotherapy, concluding that resistance is “at crisis levels.”3
Antibiotic-resistant microbes infect more than 2 million Americans each year and kill more than 100,000.
“We must act to find new weapons in the global battle against deadly superbugs,” particularly three common HAIs: acinetobacter, E. coli, and klebsiella, said co-author Brad Spellberg, MD, infectious-disease specialist at Harbor-UCLA Medical Center in Los Angeles.
A recent fact sheet from the Alliance for Aging Research notes that older patients, who represent 45% of HAIs annually, carry a higher burden of illness and less favorable outcomes than younger patients.4
Meanwhile, a study of the ICUs at 43 Hospital Corporation of America hospitals, published in the New England Journal of Medicine, provides support for treating all ICU patients with universal precautions for methicillin-resistant Staphylococcus aureus (MRSA).5 Washing all ICU patients with antibiotic soap and administering nasal antibiotics reduced all types of bloodstream infections by 44% and proved more effective than the common practice of screening patients for MRSA first, then treating those testing positive.
Another recent resource for HAIs is the “Eliminating Catheter-Associated Urinary Tract Infections” guide from the American Hospital Association’s Hospitals in Pursuit of Excellence unit.6 The booklet recommends an evidence-based, three-step action plan derived from AHA’s On the CUSP: Stop CAUTI project, and is available free on the AHA website. It has an accompanying webinar, which outlines the business case for eliminating catheter-associated urinary tract infections (CAUTIs) and the importance of hospital culture in achieving sustainability.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
Antibiotic resistance to hospital-acquired infections (HAIs) is rising at faster rates than predicted in 2008 by the Centers for Disease Control and Prevention (CDC), according to an analysis of privately gathered data reported in a recent commentary in Antimicrobial Agents and Chemotherapy, concluding that resistance is “at crisis levels.”3
Antibiotic-resistant microbes infect more than 2 million Americans each year and kill more than 100,000.
“We must act to find new weapons in the global battle against deadly superbugs,” particularly three common HAIs: acinetobacter, E. coli, and klebsiella, said co-author Brad Spellberg, MD, infectious-disease specialist at Harbor-UCLA Medical Center in Los Angeles.
A recent fact sheet from the Alliance for Aging Research notes that older patients, who represent 45% of HAIs annually, carry a higher burden of illness and less favorable outcomes than younger patients.4
Meanwhile, a study of the ICUs at 43 Hospital Corporation of America hospitals, published in the New England Journal of Medicine, provides support for treating all ICU patients with universal precautions for methicillin-resistant Staphylococcus aureus (MRSA).5 Washing all ICU patients with antibiotic soap and administering nasal antibiotics reduced all types of bloodstream infections by 44% and proved more effective than the common practice of screening patients for MRSA first, then treating those testing positive.
Another recent resource for HAIs is the “Eliminating Catheter-Associated Urinary Tract Infections” guide from the American Hospital Association’s Hospitals in Pursuit of Excellence unit.6 The booklet recommends an evidence-based, three-step action plan derived from AHA’s On the CUSP: Stop CAUTI project, and is available free on the AHA website. It has an accompanying webinar, which outlines the business case for eliminating catheter-associated urinary tract infections (CAUTIs) and the importance of hospital culture in achieving sustainability.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
Antibiotic resistance to hospital-acquired infections (HAIs) is rising at faster rates than predicted in 2008 by the Centers for Disease Control and Prevention (CDC), according to an analysis of privately gathered data reported in a recent commentary in Antimicrobial Agents and Chemotherapy, concluding that resistance is “at crisis levels.”3
Antibiotic-resistant microbes infect more than 2 million Americans each year and kill more than 100,000.
“We must act to find new weapons in the global battle against deadly superbugs,” particularly three common HAIs: acinetobacter, E. coli, and klebsiella, said co-author Brad Spellberg, MD, infectious-disease specialist at Harbor-UCLA Medical Center in Los Angeles.
A recent fact sheet from the Alliance for Aging Research notes that older patients, who represent 45% of HAIs annually, carry a higher burden of illness and less favorable outcomes than younger patients.4
Meanwhile, a study of the ICUs at 43 Hospital Corporation of America hospitals, published in the New England Journal of Medicine, provides support for treating all ICU patients with universal precautions for methicillin-resistant Staphylococcus aureus (MRSA).5 Washing all ICU patients with antibiotic soap and administering nasal antibiotics reduced all types of bloodstream infections by 44% and proved more effective than the common practice of screening patients for MRSA first, then treating those testing positive.
Another recent resource for HAIs is the “Eliminating Catheter-Associated Urinary Tract Infections” guide from the American Hospital Association’s Hospitals in Pursuit of Excellence unit.6 The booklet recommends an evidence-based, three-step action plan derived from AHA’s On the CUSP: Stop CAUTI project, and is available free on the AHA website. It has an accompanying webinar, which outlines the business case for eliminating catheter-associated urinary tract infections (CAUTIs) and the importance of hospital culture in achieving sustainability.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
Boston Hospital Earns Quality Award
In July, four U.S. hospitals were recognized for their leadership and innovation in quality improvement (QI) and safety—as defined by the Institute of Medicine (IOM)—through the American Hospital Association’s McKesson Quest for Quality Prize.2 Beth Israel Deaconess Medical Center (BIDMC) in Boston was awarded the overall prize for its sustainable approach and hospitalwide commitment to pursuing IOM’s quality aims for safe, effective, efficient, timely, patient-centered, and equitable health care.
The award, presented since 2002, is supported by healthcare-services company McKesson Corp., based in San Francisco.
Key to BIDMC’s success is the clear message of its top leadership’s commitment to quality and a strong partnership with the medical community, says Kenneth Sands, MD, MPH, BIDMC’s senior vice president for healthcare quality. “That includes an official vote by the hospital’s board to adopt IOM’s definition of quality. And everyone here participates in the quality process,” he says.
Each year, the hospital holds a quality symposium featuring QI projects solicited from across the organization. This year’s poster contest recognized three winners, one from the finance department, one from an ICU, and a third from the hospital cafeteria (it tracked the percentage of days that fresh fish is offered as a healthy menu choice).
“To see these three winners standing together on the podium sends a powerful message,” Dr. Sands says. “These are not quality-improvement experts, but front-line staff.”
Another quality initiative involves a hospitalist leader trying to promote “conversation readiness” for a hospital staff’s ability to respond to patients’ expressed desires to complete advance directives, then make sure these documents get captured in the medical record.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
In July, four U.S. hospitals were recognized for their leadership and innovation in quality improvement (QI) and safety—as defined by the Institute of Medicine (IOM)—through the American Hospital Association’s McKesson Quest for Quality Prize.2 Beth Israel Deaconess Medical Center (BIDMC) in Boston was awarded the overall prize for its sustainable approach and hospitalwide commitment to pursuing IOM’s quality aims for safe, effective, efficient, timely, patient-centered, and equitable health care.
The award, presented since 2002, is supported by healthcare-services company McKesson Corp., based in San Francisco.
Key to BIDMC’s success is the clear message of its top leadership’s commitment to quality and a strong partnership with the medical community, says Kenneth Sands, MD, MPH, BIDMC’s senior vice president for healthcare quality. “That includes an official vote by the hospital’s board to adopt IOM’s definition of quality. And everyone here participates in the quality process,” he says.
Each year, the hospital holds a quality symposium featuring QI projects solicited from across the organization. This year’s poster contest recognized three winners, one from the finance department, one from an ICU, and a third from the hospital cafeteria (it tracked the percentage of days that fresh fish is offered as a healthy menu choice).
“To see these three winners standing together on the podium sends a powerful message,” Dr. Sands says. “These are not quality-improvement experts, but front-line staff.”
Another quality initiative involves a hospitalist leader trying to promote “conversation readiness” for a hospital staff’s ability to respond to patients’ expressed desires to complete advance directives, then make sure these documents get captured in the medical record.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
In July, four U.S. hospitals were recognized for their leadership and innovation in quality improvement (QI) and safety—as defined by the Institute of Medicine (IOM)—through the American Hospital Association’s McKesson Quest for Quality Prize.2 Beth Israel Deaconess Medical Center (BIDMC) in Boston was awarded the overall prize for its sustainable approach and hospitalwide commitment to pursuing IOM’s quality aims for safe, effective, efficient, timely, patient-centered, and equitable health care.
The award, presented since 2002, is supported by healthcare-services company McKesson Corp., based in San Francisco.
Key to BIDMC’s success is the clear message of its top leadership’s commitment to quality and a strong partnership with the medical community, says Kenneth Sands, MD, MPH, BIDMC’s senior vice president for healthcare quality. “That includes an official vote by the hospital’s board to adopt IOM’s definition of quality. And everyone here participates in the quality process,” he says.
Each year, the hospital holds a quality symposium featuring QI projects solicited from across the organization. This year’s poster contest recognized three winners, one from the finance department, one from an ICU, and a third from the hospital cafeteria (it tracked the percentage of days that fresh fish is offered as a healthy menu choice).
“To see these three winners standing together on the podium sends a powerful message,” Dr. Sands says. “These are not quality-improvement experts, but front-line staff.”
Another quality initiative involves a hospitalist leader trying to promote “conversation readiness” for a hospital staff’s ability to respond to patients’ expressed desires to complete advance directives, then make sure these documents get captured in the medical record.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
Post-Discharge Phone Calls Prevent Hospital Readmissions
Two RIV posters presented at HM13 from University of California at San Francisco (UCSF) hospitalists analyzed outcomes from post-discharge phone calls to patients and found that those who were reached and interviewed by a call nurse had a 33% lower all-cause readmission rate.
UCSF joined SHM’s Project BOOST quality initiative in 2009 and adopted its recommendation to call patients within 72 hours of their hospital discharge, according to co-author Michelle Mourad, MD, assistant professor of clinical medicine and a UCSF hospitalist. “We reached out to about 60% to 70% of our patients with a standard script to address issues associated with readmissions,” Dr. Mourad explains. “We were also lucky enough to build a computer program with quantifiable outcomes in the database.”1
Researchers broke the data down into three categories: those called and interviewed by the nurse; those called who didn’t answer the phone or had a wrong number; and those who were never called due to errors in the administrative list of discharged patients. Interpreting the results is complicated, Dr. Mourad says, because of the challenges of separating factors leading to patients answering the survey from those that affect their readmission risk.
“These phone calls weren’t done in isolation and were part of our overall bridging interventions for patients going home from the hospital,” she says. “We designed the intervention to help people, and we found that 43% of those reached had at least one issue identified in the call for which the nurse tried to help.”
However, whether patients reported post-discharge issues and their responses to specific questions within the interview were not associated with readmission rates. “Does that mean the nurses’ calls are not helping? It either means the nurses are effectively managing these issues to prevent readmissions or that the factors affecting readmissions are more complicated than we currently understand,” Dr. Mourad says.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
Two RIV posters presented at HM13 from University of California at San Francisco (UCSF) hospitalists analyzed outcomes from post-discharge phone calls to patients and found that those who were reached and interviewed by a call nurse had a 33% lower all-cause readmission rate.
UCSF joined SHM’s Project BOOST quality initiative in 2009 and adopted its recommendation to call patients within 72 hours of their hospital discharge, according to co-author Michelle Mourad, MD, assistant professor of clinical medicine and a UCSF hospitalist. “We reached out to about 60% to 70% of our patients with a standard script to address issues associated with readmissions,” Dr. Mourad explains. “We were also lucky enough to build a computer program with quantifiable outcomes in the database.”1
Researchers broke the data down into three categories: those called and interviewed by the nurse; those called who didn’t answer the phone or had a wrong number; and those who were never called due to errors in the administrative list of discharged patients. Interpreting the results is complicated, Dr. Mourad says, because of the challenges of separating factors leading to patients answering the survey from those that affect their readmission risk.
“These phone calls weren’t done in isolation and were part of our overall bridging interventions for patients going home from the hospital,” she says. “We designed the intervention to help people, and we found that 43% of those reached had at least one issue identified in the call for which the nurse tried to help.”
However, whether patients reported post-discharge issues and their responses to specific questions within the interview were not associated with readmission rates. “Does that mean the nurses’ calls are not helping? It either means the nurses are effectively managing these issues to prevent readmissions or that the factors affecting readmissions are more complicated than we currently understand,” Dr. Mourad says.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
Two RIV posters presented at HM13 from University of California at San Francisco (UCSF) hospitalists analyzed outcomes from post-discharge phone calls to patients and found that those who were reached and interviewed by a call nurse had a 33% lower all-cause readmission rate.
UCSF joined SHM’s Project BOOST quality initiative in 2009 and adopted its recommendation to call patients within 72 hours of their hospital discharge, according to co-author Michelle Mourad, MD, assistant professor of clinical medicine and a UCSF hospitalist. “We reached out to about 60% to 70% of our patients with a standard script to address issues associated with readmissions,” Dr. Mourad explains. “We were also lucky enough to build a computer program with quantifiable outcomes in the database.”1
Researchers broke the data down into three categories: those called and interviewed by the nurse; those called who didn’t answer the phone or had a wrong number; and those who were never called due to errors in the administrative list of discharged patients. Interpreting the results is complicated, Dr. Mourad says, because of the challenges of separating factors leading to patients answering the survey from those that affect their readmission risk.
“These phone calls weren’t done in isolation and were part of our overall bridging interventions for patients going home from the hospital,” she says. “We designed the intervention to help people, and we found that 43% of those reached had at least one issue identified in the call for which the nurse tried to help.”
However, whether patients reported post-discharge issues and their responses to specific questions within the interview were not associated with readmission rates. “Does that mean the nurses’ calls are not helping? It either means the nurses are effectively managing these issues to prevent readmissions or that the factors affecting readmissions are more complicated than we currently understand,” Dr. Mourad says.
Larry Beresford is a freelance writer in San Francisco.
References
- Harrison J, Quinn K, Mourad M. Is anyone home? The association between being reached for a post-discharge telephone call and 30-day hospital readmission. Harrison J, Quinn K, Mourad M. Any questions? The relationship between responses to post-discharge call questions and 30-day hospital readmissions [abstracts]. Journal of Hospital Medicine, 2013, 8 Suppl 1.
- Institute of Medicine. Crossing the quality chasm: a new health system for the 21st century. Institute of Medicine website. Available at: http://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf. Accessed Sept. 9, 2013.
- Shlaes DM, Sahm D, Opiela C, Spellberg B. Commentary: the FDA reboot of antibiotic development. Antimicrob Agents Chemother. 29 Jul 2013 [Epub ahead of print].
- Alliance for Aging Research. HAIs growing problem, group says. Alliance for Aging Research website. Available at: http://www.agingresearch.org/content/article/detail/33504. Accessed Sept. 9, 2013.
- Huang SS, Septimus E, Kleinman K, et al. Targeted versus universal decolonization to prevent ICU infection. N Engl J Med. 2013;368:2255-2265.
- Hospitals in Pursuit of Excellence. Eliminating catheter-associated urinary tract infections. Hospitals in Pursuit of Excellence website. Available at: http://www.hpoe.org/Reports-HPOE/eliminating_catheter_associated_urinary_tract_infection.pdf. Accessed Sept. 9, 2013.
- Center to Advance Palliative Care. Growth of palliative care in U.S. hospitals 2013 snapshot. Center to Advance Palliative Care website. Available at: http://www.capc.org/capc-growth-analysis-snapshot-2013.pdf. Accessed Sept. 9, 2013.
What Is the Best Empiric Therapy for Community-Acquired Cellulitis?
Editor’s note: This month’s KCQ first appeared in July 2009, and since that time it has been one of our website’s most-read articles, generating 23,000-plus pageviews.
Case
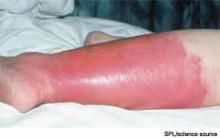
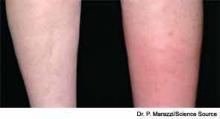
A previously healthy 55-year-old white female presents to the ED with a three-day history of pain and erythema in her right hand. Examination reveals fluctuance as well. She is diagnosed with an abscess with surrounding cellulitis. The abscess is incised, drained, and cultured, and she is sent home on oral trimethoprim/sulfamethoxazole. The following day, her cellulitis has worsened. She is hospitalized and commenced on intravenous vancomycin. What is the best empiric therapy for community-acquired cellulitis?
Background
Cellulitis is defined as a skin and soft-tissue infection (SSTI), which develops as a result of bacterial entry via breaches in the skin barrier. Typically, it involves the dermis and subcutaneous tissue and is associated with local tenderness, erythema, swelling and fever. Cellulitis usually affects the lower extremities, but it can affect other locations, resulting in diagnoses such as periorbital, abdominal wall, buccal, and perianal cellulitis.1,2
Gram-positive organisms, especially Staphylococcus aureus and beta hemolytic streptococci, are the most common causes of cellulitis. Although it is less common, cellulitis can be caused by gram-negative organisms. The recent significant increase in the prevalence of SSTIs due to community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) has led to changes in the selection of antibiotics that were most commonly utilized to empirically treat cellulitis.
The diagnosis of cellulitis is based primarily on clinical manifestations. Due to low diagnostic yields, blood cultures, needle aspiration, or punch biopsy specimens usually are not helpful in the setting of simple cellulitis.3 Therefore, antibiotic therapy is almost universally started empirically. Starting appropriate initial antibiotic therapy improves patient outcomes by reducing mortality rates, length of stay, and inpatient costs.4
Cellulitis incidence is about two cases per 1,000 patient-years.5 This rather high incidence, coupled with escalating rates of SSTIs due to CA-MRSA, demands reliable and cost-effective treatment strategies for the management of community-acquired cellulitis.
Review of the Data
The treatment of community-acquired cellulitis was straightforward until the past decade, as physicians saw a significant increase in CA-MRSA incidence.6 MRSA was reported initially in 1961, only two years after methicillin was introduced into clinical practice.7,8 Subsequently, MRSA prevalence increased dramatically, and by the beginning of this decade, more than 50% of the Staphylococcus aureus hospital strains were resistant to methicillin.8 Furthermore, 60% to 80% of community-acquired Staphylococcus aureus strains in the U.S. are methicillin-resistant.8
The two major types of MRSA infections are healthcare-acquired (HA-MRSA) and community-acquired (CA-MRSA). The HA-MRSA infection group is further subdivided into those strains that develop during a period of hospitalization and those that develop following contact with healthcare facilities (e.g. hospitalization or surgery within the previous year). This subgroup includes HA-MRSA infections in hemodialysis patients, residents of long-term-care facilities, and individuals who have a vascular catheter or other indwelling device.9,10
CA-MRSA infections, on the other hand, occur in individuals who have not had any contact with healthcare facilities. Higher rates of CA-MRSA infection are observed in settings where individuals have close contact with each other, including military trainees, athletes involved in contact sports, patients age 65 and older, men who have sex with other men, and parenteral substance abusers.8,11-13 However, in view of the high prevalence of CA-MRSA in the U.S., most patients, including those without any apparent risk factors, are at risk.8
HA-MRSA has the ability to survive on inanimate objects for extended time periods, increasing the likelihood of transmission to persons who come into contact with those objects. Although evidence has not confirmed that CA-MRSA has a similar capacity, it seems plausible that such spread does contribute to the propagation of CA-MRSA.12
The increasing importance of CA-MRSA also is evident in hospital settings, where it is replacing HA-MRSA as the most common type of Staphylococcus aureus. Because CA-MRSA tends to be susceptible to a larger number of antibiotics than HA-MRSA is, this has led to a reduced incidence of multidrug resistance. Fortunately, unlike HA-MRSA, CA-MRSA is susceptible to non-beta-lactam antibiotics, including tetracyclines, sulfonamides, and clindamycin.9
CA-MRSA most often causes SSTIs, and a tender abscess is a typical presentation.8 Patients commonly misinterpret early skin lesions as an insect or spider bite.12,14 When cutaneous CA-MRSA presents as an abscess, an incision and drainage procedure is essential for adequate treatment of the infection. For some CA-MRSA infections, particularly those characterized by the presence of a relatively small abscess, it might be adequate to do only an incision and drainage procedure, and not administer antibiotics.8,15 However, in most instances, especially when there is an area of cellulitis around the abscess, the initiation of antibiotic therapy improves patients’ clinical outcomes.9,16
When there is no apparent drainable purulent fluid collection, which often occurs with cellulitis, antibiotics should be the mainstay of therapy. The decision about which antibiotic to start can present some challenges, because the organism causing the cellulitis usually is not identified. This is because blood cultures are positive in less than 5% of cases. Also, positive culture results from needle aspiration are only helpful 5% to 40% of the time. Meanwhile, culture of punch biopsy specimens yields a pathogen in only 20% to 30% of cases.3,17-19
Due to increased CA-MRSA incidence, cephalexin should not be prescribed to treat cellulitis in the outpatient setting because it does not provide coverage for the pathogen.13 Instead, oral antibiotics (e.g. clindamycin or trimethoprim/sulfamethoxazole) should be prescribed. Doxycycline, minocycline, rifampin (usually prescribed in combination with fusidic acid to prevent resistance development), and linezolid are additional therapeutic options.
Trimethoprim/sulfamethoxazole and clindamycin have several advantages: good oral bioavailability, familiarity to physicians, and general affordability. A disadvantage to using both trimethoprim/sulfamethoxazole and doxycycline is that they provide inadequate coverage for group A streptococci, which are a common cause of cellulitis. Therefore, the simultaneous use of a beta-lactam antibiotic with either of these medications may improve outcomes for “nonpurulent” cellulitis.13,15 Linezolid has proven effective for SSTIs caused by MRSA, even though it is not bactericidal.
Excellent oral bioavailability of this drug is an attractive characteristic, as it facilitates the transition from the use of intravenous to oral antibiotic therapy later in a patient’s hospital course. Although oral linezolid has been studied in clinical trials and provides good coverage for MRSA, its use in the outpatient setting is relatively limited, largely due to its significant cost.20 In 2008, the cost of 10 days of treatment with oral linezolid was $1,286.80. In comparison, the generic trimethoprim/sulfamethoxazole cost $9.40, and generic clindamycin cost $95.10.8 The lack of routine availability in many outpatient pharmacies also hinders the widespread use of linezolid.13
To date, with the exception of linezolid, no randomized prospective clinical trials clearly demonstrate the efficacy of the oral agents that are commonly used for the outpatient treatment of cellulitis.20
When patients require hospitalization for the optimal treatment of cellulitis, it is important to select a parenteral antibiotic that provides coverage for MRSA.8 Vancomycin, daptomycin, linezolid, and tigecycline are the most commonly used agents.6
In the inpatient setting, failure to initiate appropriate medical therapy can result in longer hospital admissions, which significantly increase inpatient costs. Inadequate antibiotic therapy creates a significant financial burden and has been associated with increased mortality.4 Historically, vancomycin is used whenever a MRSA infection is suspected. However, there is concern about the declining efficacy of vancomycin related to a gradual increase in the rate of relative resistance—a minimal inhibitory concentration (MIC) increase—in MRSA strains. This MIC creep is noted in some medical centers and can lead to a failure to respond to vancomycin.13,20
Daptomycin is rapidly bactericidal against MRSA; in some institutions, its use may be preferred over vancomycin because the former antibiotic is associated with a significantly more rapid clinical response, which may shorten the required length of hospitalization.21 The once-daily dosing requirement for daptomycin allows for ease of use in both hospital and outpatient settings, and therefore may facilitate early hospital discharge or prevent the need for hospitalization altogether. Clinical experience also suggests potential economic advantages with the use of daptomycin.22
Tigecycline is a bacteriostatic antibiotic that achieves low serum concentrations. However, it penetrates the skin well and has a similar effectiveness to combination therapy with vancomycin and aztreonam. Thus far, tigecycline is not widely used for the treatment of MRSA infections, and it has been suggested that it may be preferred for polymicrobial infections or for patients who exhibit allergies to more commonly used agents.8
When selecting an antibiotic therapy, cost considerations play an important role in the decision-making process. For intravenous agents commonly used to treat CA-MRSA infections, the 2008 cost for 10 days of treatment with generic vancomycin was $182.80; daptomycin cost $1,660.80. For tigecycline and linezolid, the same duration of treatment cost $1,362 and $1,560, respectively.8
Back to the Case
Our patient, an otherwise healthy female, presented with no apparent risk factors for developing a CA-MRSA SSTI. However, more detailed history revealed that she regularly used sports equipment at her local fitness center. Based on her clinical presentation and concerns about the high local prevalence of CA-MRSA, an incision and drainage procedure was performed, and she was started empirically on IV vancomycin. She had a positive clinical response to this treatment.
Wound culture results confirmed CA-MRSA abscess and cellulitis, susceptible to trimethoprim/sulfamethoxazole. She was discharged on the oral formulation of this antibiotic to complete a 10-day course of treatment, including the days she received intravenous antibiotics.
Few well-designed trials have compared different lengths of cellulitis therapy. Most authorities recommend five to 10 days of treatment; however, longer courses might be required for more severe or complicated diseases.
Bottom line
Because of the high prevalence of CA-MRSA, initial antibiotic therapy for the treatment of community-acquired cellulitis must provide coverage for this organism.
Dr. Clarke is a hospitalist and assistant professor of medicine at Emory University School of Medicine, Atlanta. Dr. Dressler is a professor of medicine, hospital medicine associate division director for education, and associate program director for the J. Willis Hurst Internal Medicine Residency Program. Dr. Purohit, formerly an instructor in clinical medicine at Emory, is a hospitalist at WakeMed Health and Hospitals in Raleigh, N.C.
References
- Barzilai A, Choen HA. Isolation of group A streptococci from children with perianal cellulitis and from their siblings. Pediatr Infect Dis J. 1998;17(4):358-360.
- Thorsteinsdottir B, Tleyjeh IM, Baddour LM. Abdominal wall cellulitis in the morbidly obese. Scand J Infect Dis. 2005;37(8):605-608.
- Swartz MN. Clinical practice. Cellulitis. N Engl J Med. 2004;350(9):904-912.
- Edelsberg J, Berger A, Weber DJ, et al. Clinical and economic consequences of failure of initial antibiotic therapy for hospitalized patients with complicated skin and skin-structure infections. Infect Control Hosp Epidemiol. 2008;29(2):160-169.
- McNamara DR, Tleyjeh IM, Berbari EF, et al. Incidence of lower extremity cellulitis: a population-based study in Olmsted County, Minnesota. Mayo Clin Proc. 2007;82(7):817-821.
- Moellering RC. Current treatment options for community-acquired methicillin-resistant Staphylococcus aureus infection. Clin Infect Dis. 2008;46(7):1032-1037.
- Chambers HF. The changing epidemiology of Staphylococcus aureus. Emerg Infect Dis. 2001;7(2):178-182.
- Moellering RC. A 39-year-old man with a skin infection. JAMA. 2008;299(1):79-87.
- Ruhe J, Smith N, Bradsher RW, Menon A. Community-onset methicillin-resistant Staphylococcus aureus skin and soft tissue infections: impact of antimicrobial therapy on outcome. Clin Infect Dis. 2007;44(6):777-784.
- David MZ, Glikman D, Crawford SE, et al. What is community-associated methicillin-resistant Staphylococcus aureus? J Infect Dis. 2008;197(9):1235-1243.
- Iyer S, Jones DH. Community-acquired methicillin-resistant Staphylococcus aureus skin infection: a retrospective analysis of clinical presentation and treatment of a local outbreak. J Am Acad Dermatol. 2004;50(6):854-858.
- Centers for Disease Control and Prevention. Methicillin-resistant Staphylococcus aureus skin or soft tissue infections in a state prison—Mississippi, 2000. MMWR Morb Mortal Wkly Rep. 2001;50(42):919-922.
- Daum RS. Clinical practice. Skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. N Engl J Med. 2007;357(4):380-390.
- Dominguez TJ. It’s not a spider bite, it’s community-acquired methicillin-resistant Staphylococcus aureus. J Am Board Fam Pract. 2004;17(3):220-226.
- Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med. 2006;355(7):666-674.
- Jetton L. Therapy for methicillin-resistant Staphylococcus aureus. N Engl J Med. 2006;355(20):2153-2155.
- Hook EW, Hooton TM, Horton CA, et al. Microbiologic evaluation of cutaneous cellulitis in adults. Arch Intern Med. 1986;146(2):295-297. Duvanel T, Auckenthaler R, Rohner P, Harms M,
- Saurat JH. Quantitative cultures of biopsy specimens from cutaneous cellulitis. Arch Intern Med. 1989;149(2):293-296.
- Newell PM, Norden CW. Value of needle aspiration in bacteriologic diagnosis of cellulitis in adults. J Clin Microbiol. 1988; 26(3):401-404.
- Loffler CA, Macdougall C. Update on prevalence and treatment of methicillin-resistant Staphylococcus aureus infections. Expert Rev Anti Infect Ther. 2007;5(6):961-981.
- Davis SL, McKinnon PS, Hall LM, et al. Daptomycin versus vancomycin for complicated skin and skin structure infections: clinical and economic outcomes. Pharmacotherapy. 2007;27(12):1611-1618.
- Seaton RA. Daptomycin: rationale and role in the management of skin and soft tissue infections. J Antimicrob Chemother. 2008;62(Suppl 3):iii15-23.
Editor’s note: This month’s KCQ first appeared in July 2009, and since that time it has been one of our website’s most-read articles, generating 23,000-plus pageviews.
Case
A previously healthy 55-year-old white female presents to the ED with a three-day history of pain and erythema in her right hand. Examination reveals fluctuance as well. She is diagnosed with an abscess with surrounding cellulitis. The abscess is incised, drained, and cultured, and she is sent home on oral trimethoprim/sulfamethoxazole. The following day, her cellulitis has worsened. She is hospitalized and commenced on intravenous vancomycin. What is the best empiric therapy for community-acquired cellulitis?
Background
Cellulitis is defined as a skin and soft-tissue infection (SSTI), which develops as a result of bacterial entry via breaches in the skin barrier. Typically, it involves the dermis and subcutaneous tissue and is associated with local tenderness, erythema, swelling and fever. Cellulitis usually affects the lower extremities, but it can affect other locations, resulting in diagnoses such as periorbital, abdominal wall, buccal, and perianal cellulitis.1,2
Gram-positive organisms, especially Staphylococcus aureus and beta hemolytic streptococci, are the most common causes of cellulitis. Although it is less common, cellulitis can be caused by gram-negative organisms. The recent significant increase in the prevalence of SSTIs due to community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) has led to changes in the selection of antibiotics that were most commonly utilized to empirically treat cellulitis.
The diagnosis of cellulitis is based primarily on clinical manifestations. Due to low diagnostic yields, blood cultures, needle aspiration, or punch biopsy specimens usually are not helpful in the setting of simple cellulitis.3 Therefore, antibiotic therapy is almost universally started empirically. Starting appropriate initial antibiotic therapy improves patient outcomes by reducing mortality rates, length of stay, and inpatient costs.4
Cellulitis incidence is about two cases per 1,000 patient-years.5 This rather high incidence, coupled with escalating rates of SSTIs due to CA-MRSA, demands reliable and cost-effective treatment strategies for the management of community-acquired cellulitis.
Review of the Data
The treatment of community-acquired cellulitis was straightforward until the past decade, as physicians saw a significant increase in CA-MRSA incidence.6 MRSA was reported initially in 1961, only two years after methicillin was introduced into clinical practice.7,8 Subsequently, MRSA prevalence increased dramatically, and by the beginning of this decade, more than 50% of the Staphylococcus aureus hospital strains were resistant to methicillin.8 Furthermore, 60% to 80% of community-acquired Staphylococcus aureus strains in the U.S. are methicillin-resistant.8
The two major types of MRSA infections are healthcare-acquired (HA-MRSA) and community-acquired (CA-MRSA). The HA-MRSA infection group is further subdivided into those strains that develop during a period of hospitalization and those that develop following contact with healthcare facilities (e.g. hospitalization or surgery within the previous year). This subgroup includes HA-MRSA infections in hemodialysis patients, residents of long-term-care facilities, and individuals who have a vascular catheter or other indwelling device.9,10
CA-MRSA infections, on the other hand, occur in individuals who have not had any contact with healthcare facilities. Higher rates of CA-MRSA infection are observed in settings where individuals have close contact with each other, including military trainees, athletes involved in contact sports, patients age 65 and older, men who have sex with other men, and parenteral substance abusers.8,11-13 However, in view of the high prevalence of CA-MRSA in the U.S., most patients, including those without any apparent risk factors, are at risk.8
HA-MRSA has the ability to survive on inanimate objects for extended time periods, increasing the likelihood of transmission to persons who come into contact with those objects. Although evidence has not confirmed that CA-MRSA has a similar capacity, it seems plausible that such spread does contribute to the propagation of CA-MRSA.12
The increasing importance of CA-MRSA also is evident in hospital settings, where it is replacing HA-MRSA as the most common type of Staphylococcus aureus. Because CA-MRSA tends to be susceptible to a larger number of antibiotics than HA-MRSA is, this has led to a reduced incidence of multidrug resistance. Fortunately, unlike HA-MRSA, CA-MRSA is susceptible to non-beta-lactam antibiotics, including tetracyclines, sulfonamides, and clindamycin.9
CA-MRSA most often causes SSTIs, and a tender abscess is a typical presentation.8 Patients commonly misinterpret early skin lesions as an insect or spider bite.12,14 When cutaneous CA-MRSA presents as an abscess, an incision and drainage procedure is essential for adequate treatment of the infection. For some CA-MRSA infections, particularly those characterized by the presence of a relatively small abscess, it might be adequate to do only an incision and drainage procedure, and not administer antibiotics.8,15 However, in most instances, especially when there is an area of cellulitis around the abscess, the initiation of antibiotic therapy improves patients’ clinical outcomes.9,16
When there is no apparent drainable purulent fluid collection, which often occurs with cellulitis, antibiotics should be the mainstay of therapy. The decision about which antibiotic to start can present some challenges, because the organism causing the cellulitis usually is not identified. This is because blood cultures are positive in less than 5% of cases. Also, positive culture results from needle aspiration are only helpful 5% to 40% of the time. Meanwhile, culture of punch biopsy specimens yields a pathogen in only 20% to 30% of cases.3,17-19
Due to increased CA-MRSA incidence, cephalexin should not be prescribed to treat cellulitis in the outpatient setting because it does not provide coverage for the pathogen.13 Instead, oral antibiotics (e.g. clindamycin or trimethoprim/sulfamethoxazole) should be prescribed. Doxycycline, minocycline, rifampin (usually prescribed in combination with fusidic acid to prevent resistance development), and linezolid are additional therapeutic options.
Trimethoprim/sulfamethoxazole and clindamycin have several advantages: good oral bioavailability, familiarity to physicians, and general affordability. A disadvantage to using both trimethoprim/sulfamethoxazole and doxycycline is that they provide inadequate coverage for group A streptococci, which are a common cause of cellulitis. Therefore, the simultaneous use of a beta-lactam antibiotic with either of these medications may improve outcomes for “nonpurulent” cellulitis.13,15 Linezolid has proven effective for SSTIs caused by MRSA, even though it is not bactericidal.
Excellent oral bioavailability of this drug is an attractive characteristic, as it facilitates the transition from the use of intravenous to oral antibiotic therapy later in a patient’s hospital course. Although oral linezolid has been studied in clinical trials and provides good coverage for MRSA, its use in the outpatient setting is relatively limited, largely due to its significant cost.20 In 2008, the cost of 10 days of treatment with oral linezolid was $1,286.80. In comparison, the generic trimethoprim/sulfamethoxazole cost $9.40, and generic clindamycin cost $95.10.8 The lack of routine availability in many outpatient pharmacies also hinders the widespread use of linezolid.13
To date, with the exception of linezolid, no randomized prospective clinical trials clearly demonstrate the efficacy of the oral agents that are commonly used for the outpatient treatment of cellulitis.20
When patients require hospitalization for the optimal treatment of cellulitis, it is important to select a parenteral antibiotic that provides coverage for MRSA.8 Vancomycin, daptomycin, linezolid, and tigecycline are the most commonly used agents.6
In the inpatient setting, failure to initiate appropriate medical therapy can result in longer hospital admissions, which significantly increase inpatient costs. Inadequate antibiotic therapy creates a significant financial burden and has been associated with increased mortality.4 Historically, vancomycin is used whenever a MRSA infection is suspected. However, there is concern about the declining efficacy of vancomycin related to a gradual increase in the rate of relative resistance—a minimal inhibitory concentration (MIC) increase—in MRSA strains. This MIC creep is noted in some medical centers and can lead to a failure to respond to vancomycin.13,20
Daptomycin is rapidly bactericidal against MRSA; in some institutions, its use may be preferred over vancomycin because the former antibiotic is associated with a significantly more rapid clinical response, which may shorten the required length of hospitalization.21 The once-daily dosing requirement for daptomycin allows for ease of use in both hospital and outpatient settings, and therefore may facilitate early hospital discharge or prevent the need for hospitalization altogether. Clinical experience also suggests potential economic advantages with the use of daptomycin.22
Tigecycline is a bacteriostatic antibiotic that achieves low serum concentrations. However, it penetrates the skin well and has a similar effectiveness to combination therapy with vancomycin and aztreonam. Thus far, tigecycline is not widely used for the treatment of MRSA infections, and it has been suggested that it may be preferred for polymicrobial infections or for patients who exhibit allergies to more commonly used agents.8
When selecting an antibiotic therapy, cost considerations play an important role in the decision-making process. For intravenous agents commonly used to treat CA-MRSA infections, the 2008 cost for 10 days of treatment with generic vancomycin was $182.80; daptomycin cost $1,660.80. For tigecycline and linezolid, the same duration of treatment cost $1,362 and $1,560, respectively.8
Back to the Case
Our patient, an otherwise healthy female, presented with no apparent risk factors for developing a CA-MRSA SSTI. However, more detailed history revealed that she regularly used sports equipment at her local fitness center. Based on her clinical presentation and concerns about the high local prevalence of CA-MRSA, an incision and drainage procedure was performed, and she was started empirically on IV vancomycin. She had a positive clinical response to this treatment.
Wound culture results confirmed CA-MRSA abscess and cellulitis, susceptible to trimethoprim/sulfamethoxazole. She was discharged on the oral formulation of this antibiotic to complete a 10-day course of treatment, including the days she received intravenous antibiotics.
Few well-designed trials have compared different lengths of cellulitis therapy. Most authorities recommend five to 10 days of treatment; however, longer courses might be required for more severe or complicated diseases.
Bottom line
Because of the high prevalence of CA-MRSA, initial antibiotic therapy for the treatment of community-acquired cellulitis must provide coverage for this organism.
Dr. Clarke is a hospitalist and assistant professor of medicine at Emory University School of Medicine, Atlanta. Dr. Dressler is a professor of medicine, hospital medicine associate division director for education, and associate program director for the J. Willis Hurst Internal Medicine Residency Program. Dr. Purohit, formerly an instructor in clinical medicine at Emory, is a hospitalist at WakeMed Health and Hospitals in Raleigh, N.C.
References
- Barzilai A, Choen HA. Isolation of group A streptococci from children with perianal cellulitis and from their siblings. Pediatr Infect Dis J. 1998;17(4):358-360.
- Thorsteinsdottir B, Tleyjeh IM, Baddour LM. Abdominal wall cellulitis in the morbidly obese. Scand J Infect Dis. 2005;37(8):605-608.
- Swartz MN. Clinical practice. Cellulitis. N Engl J Med. 2004;350(9):904-912.
- Edelsberg J, Berger A, Weber DJ, et al. Clinical and economic consequences of failure of initial antibiotic therapy for hospitalized patients with complicated skin and skin-structure infections. Infect Control Hosp Epidemiol. 2008;29(2):160-169.
- McNamara DR, Tleyjeh IM, Berbari EF, et al. Incidence of lower extremity cellulitis: a population-based study in Olmsted County, Minnesota. Mayo Clin Proc. 2007;82(7):817-821.
- Moellering RC. Current treatment options for community-acquired methicillin-resistant Staphylococcus aureus infection. Clin Infect Dis. 2008;46(7):1032-1037.
- Chambers HF. The changing epidemiology of Staphylococcus aureus. Emerg Infect Dis. 2001;7(2):178-182.
- Moellering RC. A 39-year-old man with a skin infection. JAMA. 2008;299(1):79-87.
- Ruhe J, Smith N, Bradsher RW, Menon A. Community-onset methicillin-resistant Staphylococcus aureus skin and soft tissue infections: impact of antimicrobial therapy on outcome. Clin Infect Dis. 2007;44(6):777-784.
- David MZ, Glikman D, Crawford SE, et al. What is community-associated methicillin-resistant Staphylococcus aureus? J Infect Dis. 2008;197(9):1235-1243.
- Iyer S, Jones DH. Community-acquired methicillin-resistant Staphylococcus aureus skin infection: a retrospective analysis of clinical presentation and treatment of a local outbreak. J Am Acad Dermatol. 2004;50(6):854-858.
- Centers for Disease Control and Prevention. Methicillin-resistant Staphylococcus aureus skin or soft tissue infections in a state prison—Mississippi, 2000. MMWR Morb Mortal Wkly Rep. 2001;50(42):919-922.
- Daum RS. Clinical practice. Skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. N Engl J Med. 2007;357(4):380-390.
- Dominguez TJ. It’s not a spider bite, it’s community-acquired methicillin-resistant Staphylococcus aureus. J Am Board Fam Pract. 2004;17(3):220-226.
- Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med. 2006;355(7):666-674.
- Jetton L. Therapy for methicillin-resistant Staphylococcus aureus. N Engl J Med. 2006;355(20):2153-2155.
- Hook EW, Hooton TM, Horton CA, et al. Microbiologic evaluation of cutaneous cellulitis in adults. Arch Intern Med. 1986;146(2):295-297. Duvanel T, Auckenthaler R, Rohner P, Harms M,
- Saurat JH. Quantitative cultures of biopsy specimens from cutaneous cellulitis. Arch Intern Med. 1989;149(2):293-296.
- Newell PM, Norden CW. Value of needle aspiration in bacteriologic diagnosis of cellulitis in adults. J Clin Microbiol. 1988; 26(3):401-404.
- Loffler CA, Macdougall C. Update on prevalence and treatment of methicillin-resistant Staphylococcus aureus infections. Expert Rev Anti Infect Ther. 2007;5(6):961-981.
- Davis SL, McKinnon PS, Hall LM, et al. Daptomycin versus vancomycin for complicated skin and skin structure infections: clinical and economic outcomes. Pharmacotherapy. 2007;27(12):1611-1618.
- Seaton RA. Daptomycin: rationale and role in the management of skin and soft tissue infections. J Antimicrob Chemother. 2008;62(Suppl 3):iii15-23.
Editor’s note: This month’s KCQ first appeared in July 2009, and since that time it has been one of our website’s most-read articles, generating 23,000-plus pageviews.
Case
A previously healthy 55-year-old white female presents to the ED with a three-day history of pain and erythema in her right hand. Examination reveals fluctuance as well. She is diagnosed with an abscess with surrounding cellulitis. The abscess is incised, drained, and cultured, and she is sent home on oral trimethoprim/sulfamethoxazole. The following day, her cellulitis has worsened. She is hospitalized and commenced on intravenous vancomycin. What is the best empiric therapy for community-acquired cellulitis?
Background
Cellulitis is defined as a skin and soft-tissue infection (SSTI), which develops as a result of bacterial entry via breaches in the skin barrier. Typically, it involves the dermis and subcutaneous tissue and is associated with local tenderness, erythema, swelling and fever. Cellulitis usually affects the lower extremities, but it can affect other locations, resulting in diagnoses such as periorbital, abdominal wall, buccal, and perianal cellulitis.1,2
Gram-positive organisms, especially Staphylococcus aureus and beta hemolytic streptococci, are the most common causes of cellulitis. Although it is less common, cellulitis can be caused by gram-negative organisms. The recent significant increase in the prevalence of SSTIs due to community-acquired methicillin-resistant Staphylococcus aureus (CA-MRSA) has led to changes in the selection of antibiotics that were most commonly utilized to empirically treat cellulitis.
The diagnosis of cellulitis is based primarily on clinical manifestations. Due to low diagnostic yields, blood cultures, needle aspiration, or punch biopsy specimens usually are not helpful in the setting of simple cellulitis.3 Therefore, antibiotic therapy is almost universally started empirically. Starting appropriate initial antibiotic therapy improves patient outcomes by reducing mortality rates, length of stay, and inpatient costs.4
Cellulitis incidence is about two cases per 1,000 patient-years.5 This rather high incidence, coupled with escalating rates of SSTIs due to CA-MRSA, demands reliable and cost-effective treatment strategies for the management of community-acquired cellulitis.
Review of the Data
The treatment of community-acquired cellulitis was straightforward until the past decade, as physicians saw a significant increase in CA-MRSA incidence.6 MRSA was reported initially in 1961, only two years after methicillin was introduced into clinical practice.7,8 Subsequently, MRSA prevalence increased dramatically, and by the beginning of this decade, more than 50% of the Staphylococcus aureus hospital strains were resistant to methicillin.8 Furthermore, 60% to 80% of community-acquired Staphylococcus aureus strains in the U.S. are methicillin-resistant.8
The two major types of MRSA infections are healthcare-acquired (HA-MRSA) and community-acquired (CA-MRSA). The HA-MRSA infection group is further subdivided into those strains that develop during a period of hospitalization and those that develop following contact with healthcare facilities (e.g. hospitalization or surgery within the previous year). This subgroup includes HA-MRSA infections in hemodialysis patients, residents of long-term-care facilities, and individuals who have a vascular catheter or other indwelling device.9,10
CA-MRSA infections, on the other hand, occur in individuals who have not had any contact with healthcare facilities. Higher rates of CA-MRSA infection are observed in settings where individuals have close contact with each other, including military trainees, athletes involved in contact sports, patients age 65 and older, men who have sex with other men, and parenteral substance abusers.8,11-13 However, in view of the high prevalence of CA-MRSA in the U.S., most patients, including those without any apparent risk factors, are at risk.8
HA-MRSA has the ability to survive on inanimate objects for extended time periods, increasing the likelihood of transmission to persons who come into contact with those objects. Although evidence has not confirmed that CA-MRSA has a similar capacity, it seems plausible that such spread does contribute to the propagation of CA-MRSA.12
The increasing importance of CA-MRSA also is evident in hospital settings, where it is replacing HA-MRSA as the most common type of Staphylococcus aureus. Because CA-MRSA tends to be susceptible to a larger number of antibiotics than HA-MRSA is, this has led to a reduced incidence of multidrug resistance. Fortunately, unlike HA-MRSA, CA-MRSA is susceptible to non-beta-lactam antibiotics, including tetracyclines, sulfonamides, and clindamycin.9
CA-MRSA most often causes SSTIs, and a tender abscess is a typical presentation.8 Patients commonly misinterpret early skin lesions as an insect or spider bite.12,14 When cutaneous CA-MRSA presents as an abscess, an incision and drainage procedure is essential for adequate treatment of the infection. For some CA-MRSA infections, particularly those characterized by the presence of a relatively small abscess, it might be adequate to do only an incision and drainage procedure, and not administer antibiotics.8,15 However, in most instances, especially when there is an area of cellulitis around the abscess, the initiation of antibiotic therapy improves patients’ clinical outcomes.9,16
When there is no apparent drainable purulent fluid collection, which often occurs with cellulitis, antibiotics should be the mainstay of therapy. The decision about which antibiotic to start can present some challenges, because the organism causing the cellulitis usually is not identified. This is because blood cultures are positive in less than 5% of cases. Also, positive culture results from needle aspiration are only helpful 5% to 40% of the time. Meanwhile, culture of punch biopsy specimens yields a pathogen in only 20% to 30% of cases.3,17-19
Due to increased CA-MRSA incidence, cephalexin should not be prescribed to treat cellulitis in the outpatient setting because it does not provide coverage for the pathogen.13 Instead, oral antibiotics (e.g. clindamycin or trimethoprim/sulfamethoxazole) should be prescribed. Doxycycline, minocycline, rifampin (usually prescribed in combination with fusidic acid to prevent resistance development), and linezolid are additional therapeutic options.
Trimethoprim/sulfamethoxazole and clindamycin have several advantages: good oral bioavailability, familiarity to physicians, and general affordability. A disadvantage to using both trimethoprim/sulfamethoxazole and doxycycline is that they provide inadequate coverage for group A streptococci, which are a common cause of cellulitis. Therefore, the simultaneous use of a beta-lactam antibiotic with either of these medications may improve outcomes for “nonpurulent” cellulitis.13,15 Linezolid has proven effective for SSTIs caused by MRSA, even though it is not bactericidal.
Excellent oral bioavailability of this drug is an attractive characteristic, as it facilitates the transition from the use of intravenous to oral antibiotic therapy later in a patient’s hospital course. Although oral linezolid has been studied in clinical trials and provides good coverage for MRSA, its use in the outpatient setting is relatively limited, largely due to its significant cost.20 In 2008, the cost of 10 days of treatment with oral linezolid was $1,286.80. In comparison, the generic trimethoprim/sulfamethoxazole cost $9.40, and generic clindamycin cost $95.10.8 The lack of routine availability in many outpatient pharmacies also hinders the widespread use of linezolid.13
To date, with the exception of linezolid, no randomized prospective clinical trials clearly demonstrate the efficacy of the oral agents that are commonly used for the outpatient treatment of cellulitis.20
When patients require hospitalization for the optimal treatment of cellulitis, it is important to select a parenteral antibiotic that provides coverage for MRSA.8 Vancomycin, daptomycin, linezolid, and tigecycline are the most commonly used agents.6
In the inpatient setting, failure to initiate appropriate medical therapy can result in longer hospital admissions, which significantly increase inpatient costs. Inadequate antibiotic therapy creates a significant financial burden and has been associated with increased mortality.4 Historically, vancomycin is used whenever a MRSA infection is suspected. However, there is concern about the declining efficacy of vancomycin related to a gradual increase in the rate of relative resistance—a minimal inhibitory concentration (MIC) increase—in MRSA strains. This MIC creep is noted in some medical centers and can lead to a failure to respond to vancomycin.13,20
Daptomycin is rapidly bactericidal against MRSA; in some institutions, its use may be preferred over vancomycin because the former antibiotic is associated with a significantly more rapid clinical response, which may shorten the required length of hospitalization.21 The once-daily dosing requirement for daptomycin allows for ease of use in both hospital and outpatient settings, and therefore may facilitate early hospital discharge or prevent the need for hospitalization altogether. Clinical experience also suggests potential economic advantages with the use of daptomycin.22
Tigecycline is a bacteriostatic antibiotic that achieves low serum concentrations. However, it penetrates the skin well and has a similar effectiveness to combination therapy with vancomycin and aztreonam. Thus far, tigecycline is not widely used for the treatment of MRSA infections, and it has been suggested that it may be preferred for polymicrobial infections or for patients who exhibit allergies to more commonly used agents.8
When selecting an antibiotic therapy, cost considerations play an important role in the decision-making process. For intravenous agents commonly used to treat CA-MRSA infections, the 2008 cost for 10 days of treatment with generic vancomycin was $182.80; daptomycin cost $1,660.80. For tigecycline and linezolid, the same duration of treatment cost $1,362 and $1,560, respectively.8
Back to the Case
Our patient, an otherwise healthy female, presented with no apparent risk factors for developing a CA-MRSA SSTI. However, more detailed history revealed that she regularly used sports equipment at her local fitness center. Based on her clinical presentation and concerns about the high local prevalence of CA-MRSA, an incision and drainage procedure was performed, and she was started empirically on IV vancomycin. She had a positive clinical response to this treatment.
Wound culture results confirmed CA-MRSA abscess and cellulitis, susceptible to trimethoprim/sulfamethoxazole. She was discharged on the oral formulation of this antibiotic to complete a 10-day course of treatment, including the days she received intravenous antibiotics.
Few well-designed trials have compared different lengths of cellulitis therapy. Most authorities recommend five to 10 days of treatment; however, longer courses might be required for more severe or complicated diseases.
Bottom line
Because of the high prevalence of CA-MRSA, initial antibiotic therapy for the treatment of community-acquired cellulitis must provide coverage for this organism.
Dr. Clarke is a hospitalist and assistant professor of medicine at Emory University School of Medicine, Atlanta. Dr. Dressler is a professor of medicine, hospital medicine associate division director for education, and associate program director for the J. Willis Hurst Internal Medicine Residency Program. Dr. Purohit, formerly an instructor in clinical medicine at Emory, is a hospitalist at WakeMed Health and Hospitals in Raleigh, N.C.
References
- Barzilai A, Choen HA. Isolation of group A streptococci from children with perianal cellulitis and from their siblings. Pediatr Infect Dis J. 1998;17(4):358-360.
- Thorsteinsdottir B, Tleyjeh IM, Baddour LM. Abdominal wall cellulitis in the morbidly obese. Scand J Infect Dis. 2005;37(8):605-608.
- Swartz MN. Clinical practice. Cellulitis. N Engl J Med. 2004;350(9):904-912.
- Edelsberg J, Berger A, Weber DJ, et al. Clinical and economic consequences of failure of initial antibiotic therapy for hospitalized patients with complicated skin and skin-structure infections. Infect Control Hosp Epidemiol. 2008;29(2):160-169.
- McNamara DR, Tleyjeh IM, Berbari EF, et al. Incidence of lower extremity cellulitis: a population-based study in Olmsted County, Minnesota. Mayo Clin Proc. 2007;82(7):817-821.
- Moellering RC. Current treatment options for community-acquired methicillin-resistant Staphylococcus aureus infection. Clin Infect Dis. 2008;46(7):1032-1037.
- Chambers HF. The changing epidemiology of Staphylococcus aureus. Emerg Infect Dis. 2001;7(2):178-182.
- Moellering RC. A 39-year-old man with a skin infection. JAMA. 2008;299(1):79-87.
- Ruhe J, Smith N, Bradsher RW, Menon A. Community-onset methicillin-resistant Staphylococcus aureus skin and soft tissue infections: impact of antimicrobial therapy on outcome. Clin Infect Dis. 2007;44(6):777-784.
- David MZ, Glikman D, Crawford SE, et al. What is community-associated methicillin-resistant Staphylococcus aureus? J Infect Dis. 2008;197(9):1235-1243.
- Iyer S, Jones DH. Community-acquired methicillin-resistant Staphylococcus aureus skin infection: a retrospective analysis of clinical presentation and treatment of a local outbreak. J Am Acad Dermatol. 2004;50(6):854-858.
- Centers for Disease Control and Prevention. Methicillin-resistant Staphylococcus aureus skin or soft tissue infections in a state prison—Mississippi, 2000. MMWR Morb Mortal Wkly Rep. 2001;50(42):919-922.
- Daum RS. Clinical practice. Skin and soft-tissue infections caused by methicillin-resistant Staphylococcus aureus. N Engl J Med. 2007;357(4):380-390.
- Dominguez TJ. It’s not a spider bite, it’s community-acquired methicillin-resistant Staphylococcus aureus. J Am Board Fam Pract. 2004;17(3):220-226.
- Moran GJ, Krishnadasan A, Gorwitz RJ, et al. Methicillin-resistant S. aureus infections among patients in the emergency department. N Engl J Med. 2006;355(7):666-674.
- Jetton L. Therapy for methicillin-resistant Staphylococcus aureus. N Engl J Med. 2006;355(20):2153-2155.
- Hook EW, Hooton TM, Horton CA, et al. Microbiologic evaluation of cutaneous cellulitis in adults. Arch Intern Med. 1986;146(2):295-297. Duvanel T, Auckenthaler R, Rohner P, Harms M,
- Saurat JH. Quantitative cultures of biopsy specimens from cutaneous cellulitis. Arch Intern Med. 1989;149(2):293-296.
- Newell PM, Norden CW. Value of needle aspiration in bacteriologic diagnosis of cellulitis in adults. J Clin Microbiol. 1988; 26(3):401-404.
- Loffler CA, Macdougall C. Update on prevalence and treatment of methicillin-resistant Staphylococcus aureus infections. Expert Rev Anti Infect Ther. 2007;5(6):961-981.
- Davis SL, McKinnon PS, Hall LM, et al. Daptomycin versus vancomycin for complicated skin and skin structure infections: clinical and economic outcomes. Pharmacotherapy. 2007;27(12):1611-1618.
- Seaton RA. Daptomycin: rationale and role in the management of skin and soft tissue infections. J Antimicrob Chemother. 2008;62(Suppl 3):iii15-23.
ACCF/AHA 2013 Guidelines for Managing Heart Failure
Background
Heart failure (HF) is the No. 1 cause of both hospitalization and readmission among Americans 65 years and older.1 Hospitalizations in the HF population are associated with poor patient outcomes (30% mortality in the following year) and high costs, accounting for approximately 70% of the $32 billion spent on HF care annually in the United States.1 In 2009, the Centers for Medicare & Medicaid Services (CMS) introduced the 30-day, risk-standardized, all-cause readmission for HF as an indicator of quality and efficiency of care, which has since been incorporated into Medicare’s value-based purchasing program.2
HF is a complex syndrome that is associated with multiple comorbidities. Appropriate to these issues, management is multifaceted and involves care across the spectrum of disease:
- Diagnosing and treating underlying causes;
- Minimizing exacerbants;
- Optimizing management of comorbidities;
- Addressing psychosocial and environmental issues beyond the hospital; and
- Confronting end-of-life care.
In order to address this continuum of disease management, the American College of Cardiology Foundation (ACCF) and the American Heart Association (AHA) simultaneously released a new Guideline for the Management of HF in June in the Journal of the American College of Cardiology and Circulation.3,4 This update was developed in collaboration with the American Academy of Family Physicians, American College of Chest Physicians, Heart Rhythm Society, and the International Society for Heart and Lung Transplantation. The goals of the document are to improve quality of care, optimize patient outcomes, and advance the efficient use of healthcare resources. The guideline includes important recommendations for overall care, but particularly for hospital-based care and transitions of care that are largely the purview of hospitalists.
Guideline Update
The 2013 guideline is the third revision of the original guideline that was released in 2000. Despite being a complete rewrite of the 2009 HF guideline, the updated document contains relatively few changes to the recommendations that are Class I (should be performed) and III (no benefit or harm). The most significant randomized controlled trials in HF patients that have been published since the 2009 guideline include EMPHASIS-HF5 and MADIT-CRT/RAFT, which expand indications for aldosterone antagonists (AA) and cardiac resyncronization therapy (CRT), respectively, to patients with mild symptoms.5,6,7 Additionally, the WARCEF trial was published, which failed to demonstrate a significant difference in death, ischemic stroke, or intracerebral hemorrhage between treatment with warfarin or aspirin in patients with HF and reduced left ventricular ejection fraction (LVEF) in sinus rhythm.8
The most notable updates from the 2009 guideline include (* = Class I and III indications):
- The definition of HF has been revised to include: 1) HF with reduced ejection fraction (HFrEF; LVEF ≤40%), 2) HF failure with preserved ejection fraction (HFpEF; LVEF ≥50%), 3) HFpEF, borderline (LVEF 41-49%), and 4) HFpEF, improved (LVEF >40%).
- In the hospitalized patient, measurement of brain natriuretic peptide (BNP) or NT-proBNP is useful to support clinical judgment for the diagnosis of acutely decompensated HF, especially in the setting of uncertainty for the diagnosis.*
- AA should be used in patients with New York Heart Association (NYHA) functional Class II-IV and LVEF ≤35% unless contraindicated (creatinine ≤2.5 mg/dL in men, ≤2.0 mg/dL in women, and potassium <5.0 mEq/L).*
- CRT is indicated for patients who have LVEF of 35% or less, sinus rhythm, left bundle-branch block with a QRS duration of ³150 ms, and NYHA functional Class II-IV on guideline-directed medical therapy (GDMT).*
- Anticoagulation should not be used in patients with chronic HFrEF without atrial fibrillation, prior thromboembolic event, or cardioembolic source.*
- Transitions of care and GDMT can be improved by employing the following: 1) use of performance-improvement systems to identify HF patients, 2) development of multidisciplinary HF disease-management programs for patients at high risk of readmission, and 3) placing phone calls to the patient within three days of discharge and scheduling a follow-up visit within seven to 14 days.
Analysis
Overall, the new guideline provides a thorough reassessment and expert analysis on the diagnosis and management of HF for both inpatient and outpatient care. The authors introduce the phrase “guideline-directed medical therapy” (GDMT) to emphasize the smaller set of recommendations that constitute optimal medical therapy for HF patients. This designation, encompassing primarily Class I recommendations, helps providers rapidly determine the optimal treatment course for an individual patient. The mainstay of GDMT in HFrEF patients remains angiotensin-converting enzyme inhibitors (ACE-I), angiotensin receptor blockers (ARB) when ACE-I-intolerant, beta-blockers, and, in select patients, AA, hydralazine-nitrates, and diuretics.
A major shift in focus is seen in the new guideline with a greater emphasis on improved patient-centered outcomes across the spectrum of the disease. HF requires a continuum of care, from screening and genetic testing of family members of patients with idiopathic cardiomyopathy to conversations about palliative care and hospice. To this end, the authors highlight quality of life, shared decision-making, care coordination, transitions of care, and appropriateness of palliative care in a chronic disease state.
Further, the guideline expands upon previous recommendations for compliance with performance and quality metrics. Quality of care and adherence to performance measures of HF patients are becoming increasingly recognized, particularly in the hospital setting. The guideline offers recommendations for transitions of care in the hospitalized patient, which utilize systems of care coordination to ensure an evidence-based plan of care that includes the achievement of GDMT goals, effective management of comorbid conditions, timely follow-up, and appropriate dietary and physical activities.
HM Takeaways
HF is one of the most common, most challenging diseases managed by hospitalists. The 2013 ACCF/AHA Guideline for the Management of HF, while providing a comprehensive summary of evidence with recommendations for the totality of care for these patients throughout the course of the disease, places heavy emphasis on management during hospitalization and transitions. This includes repositioning of performance measures involving GDMT to better ensure optimal use of proven therapies in HFrEF, evidence-based steps to reduce readmissions, and greater recognition of the role of palliative care for patients with advanced disease.
Drs. McIlvennan and Allen are cardiologists in the Department of Medicine at the University of Colorado School of Medicine in Denver. Dr. Allen also works in the Colorado Health Outcomes Program.
References available at the-hospitalist.org.
Background
Heart failure (HF) is the No. 1 cause of both hospitalization and readmission among Americans 65 years and older.1 Hospitalizations in the HF population are associated with poor patient outcomes (30% mortality in the following year) and high costs, accounting for approximately 70% of the $32 billion spent on HF care annually in the United States.1 In 2009, the Centers for Medicare & Medicaid Services (CMS) introduced the 30-day, risk-standardized, all-cause readmission for HF as an indicator of quality and efficiency of care, which has since been incorporated into Medicare’s value-based purchasing program.2
HF is a complex syndrome that is associated with multiple comorbidities. Appropriate to these issues, management is multifaceted and involves care across the spectrum of disease:
- Diagnosing and treating underlying causes;
- Minimizing exacerbants;
- Optimizing management of comorbidities;
- Addressing psychosocial and environmental issues beyond the hospital; and
- Confronting end-of-life care.
In order to address this continuum of disease management, the American College of Cardiology Foundation (ACCF) and the American Heart Association (AHA) simultaneously released a new Guideline for the Management of HF in June in the Journal of the American College of Cardiology and Circulation.3,4 This update was developed in collaboration with the American Academy of Family Physicians, American College of Chest Physicians, Heart Rhythm Society, and the International Society for Heart and Lung Transplantation. The goals of the document are to improve quality of care, optimize patient outcomes, and advance the efficient use of healthcare resources. The guideline includes important recommendations for overall care, but particularly for hospital-based care and transitions of care that are largely the purview of hospitalists.
Guideline Update
The 2013 guideline is the third revision of the original guideline that was released in 2000. Despite being a complete rewrite of the 2009 HF guideline, the updated document contains relatively few changes to the recommendations that are Class I (should be performed) and III (no benefit or harm). The most significant randomized controlled trials in HF patients that have been published since the 2009 guideline include EMPHASIS-HF5 and MADIT-CRT/RAFT, which expand indications for aldosterone antagonists (AA) and cardiac resyncronization therapy (CRT), respectively, to patients with mild symptoms.5,6,7 Additionally, the WARCEF trial was published, which failed to demonstrate a significant difference in death, ischemic stroke, or intracerebral hemorrhage between treatment with warfarin or aspirin in patients with HF and reduced left ventricular ejection fraction (LVEF) in sinus rhythm.8
The most notable updates from the 2009 guideline include (* = Class I and III indications):
- The definition of HF has been revised to include: 1) HF with reduced ejection fraction (HFrEF; LVEF ≤40%), 2) HF failure with preserved ejection fraction (HFpEF; LVEF ≥50%), 3) HFpEF, borderline (LVEF 41-49%), and 4) HFpEF, improved (LVEF >40%).
- In the hospitalized patient, measurement of brain natriuretic peptide (BNP) or NT-proBNP is useful to support clinical judgment for the diagnosis of acutely decompensated HF, especially in the setting of uncertainty for the diagnosis.*
- AA should be used in patients with New York Heart Association (NYHA) functional Class II-IV and LVEF ≤35% unless contraindicated (creatinine ≤2.5 mg/dL in men, ≤2.0 mg/dL in women, and potassium <5.0 mEq/L).*
- CRT is indicated for patients who have LVEF of 35% or less, sinus rhythm, left bundle-branch block with a QRS duration of ³150 ms, and NYHA functional Class II-IV on guideline-directed medical therapy (GDMT).*
- Anticoagulation should not be used in patients with chronic HFrEF without atrial fibrillation, prior thromboembolic event, or cardioembolic source.*
- Transitions of care and GDMT can be improved by employing the following: 1) use of performance-improvement systems to identify HF patients, 2) development of multidisciplinary HF disease-management programs for patients at high risk of readmission, and 3) placing phone calls to the patient within three days of discharge and scheduling a follow-up visit within seven to 14 days.
Analysis
Overall, the new guideline provides a thorough reassessment and expert analysis on the diagnosis and management of HF for both inpatient and outpatient care. The authors introduce the phrase “guideline-directed medical therapy” (GDMT) to emphasize the smaller set of recommendations that constitute optimal medical therapy for HF patients. This designation, encompassing primarily Class I recommendations, helps providers rapidly determine the optimal treatment course for an individual patient. The mainstay of GDMT in HFrEF patients remains angiotensin-converting enzyme inhibitors (ACE-I), angiotensin receptor blockers (ARB) when ACE-I-intolerant, beta-blockers, and, in select patients, AA, hydralazine-nitrates, and diuretics.
A major shift in focus is seen in the new guideline with a greater emphasis on improved patient-centered outcomes across the spectrum of the disease. HF requires a continuum of care, from screening and genetic testing of family members of patients with idiopathic cardiomyopathy to conversations about palliative care and hospice. To this end, the authors highlight quality of life, shared decision-making, care coordination, transitions of care, and appropriateness of palliative care in a chronic disease state.
Further, the guideline expands upon previous recommendations for compliance with performance and quality metrics. Quality of care and adherence to performance measures of HF patients are becoming increasingly recognized, particularly in the hospital setting. The guideline offers recommendations for transitions of care in the hospitalized patient, which utilize systems of care coordination to ensure an evidence-based plan of care that includes the achievement of GDMT goals, effective management of comorbid conditions, timely follow-up, and appropriate dietary and physical activities.
HM Takeaways
HF is one of the most common, most challenging diseases managed by hospitalists. The 2013 ACCF/AHA Guideline for the Management of HF, while providing a comprehensive summary of evidence with recommendations for the totality of care for these patients throughout the course of the disease, places heavy emphasis on management during hospitalization and transitions. This includes repositioning of performance measures involving GDMT to better ensure optimal use of proven therapies in HFrEF, evidence-based steps to reduce readmissions, and greater recognition of the role of palliative care for patients with advanced disease.
Drs. McIlvennan and Allen are cardiologists in the Department of Medicine at the University of Colorado School of Medicine in Denver. Dr. Allen also works in the Colorado Health Outcomes Program.
References available at the-hospitalist.org.
Background
Heart failure (HF) is the No. 1 cause of both hospitalization and readmission among Americans 65 years and older.1 Hospitalizations in the HF population are associated with poor patient outcomes (30% mortality in the following year) and high costs, accounting for approximately 70% of the $32 billion spent on HF care annually in the United States.1 In 2009, the Centers for Medicare & Medicaid Services (CMS) introduced the 30-day, risk-standardized, all-cause readmission for HF as an indicator of quality and efficiency of care, which has since been incorporated into Medicare’s value-based purchasing program.2
HF is a complex syndrome that is associated with multiple comorbidities. Appropriate to these issues, management is multifaceted and involves care across the spectrum of disease:
- Diagnosing and treating underlying causes;
- Minimizing exacerbants;
- Optimizing management of comorbidities;
- Addressing psychosocial and environmental issues beyond the hospital; and
- Confronting end-of-life care.
In order to address this continuum of disease management, the American College of Cardiology Foundation (ACCF) and the American Heart Association (AHA) simultaneously released a new Guideline for the Management of HF in June in the Journal of the American College of Cardiology and Circulation.3,4 This update was developed in collaboration with the American Academy of Family Physicians, American College of Chest Physicians, Heart Rhythm Society, and the International Society for Heart and Lung Transplantation. The goals of the document are to improve quality of care, optimize patient outcomes, and advance the efficient use of healthcare resources. The guideline includes important recommendations for overall care, but particularly for hospital-based care and transitions of care that are largely the purview of hospitalists.
Guideline Update
The 2013 guideline is the third revision of the original guideline that was released in 2000. Despite being a complete rewrite of the 2009 HF guideline, the updated document contains relatively few changes to the recommendations that are Class I (should be performed) and III (no benefit or harm). The most significant randomized controlled trials in HF patients that have been published since the 2009 guideline include EMPHASIS-HF5 and MADIT-CRT/RAFT, which expand indications for aldosterone antagonists (AA) and cardiac resyncronization therapy (CRT), respectively, to patients with mild symptoms.5,6,7 Additionally, the WARCEF trial was published, which failed to demonstrate a significant difference in death, ischemic stroke, or intracerebral hemorrhage between treatment with warfarin or aspirin in patients with HF and reduced left ventricular ejection fraction (LVEF) in sinus rhythm.8
The most notable updates from the 2009 guideline include (* = Class I and III indications):
- The definition of HF has been revised to include: 1) HF with reduced ejection fraction (HFrEF; LVEF ≤40%), 2) HF failure with preserved ejection fraction (HFpEF; LVEF ≥50%), 3) HFpEF, borderline (LVEF 41-49%), and 4) HFpEF, improved (LVEF >40%).
- In the hospitalized patient, measurement of brain natriuretic peptide (BNP) or NT-proBNP is useful to support clinical judgment for the diagnosis of acutely decompensated HF, especially in the setting of uncertainty for the diagnosis.*
- AA should be used in patients with New York Heart Association (NYHA) functional Class II-IV and LVEF ≤35% unless contraindicated (creatinine ≤2.5 mg/dL in men, ≤2.0 mg/dL in women, and potassium <5.0 mEq/L).*
- CRT is indicated for patients who have LVEF of 35% or less, sinus rhythm, left bundle-branch block with a QRS duration of ³150 ms, and NYHA functional Class II-IV on guideline-directed medical therapy (GDMT).*
- Anticoagulation should not be used in patients with chronic HFrEF without atrial fibrillation, prior thromboembolic event, or cardioembolic source.*
- Transitions of care and GDMT can be improved by employing the following: 1) use of performance-improvement systems to identify HF patients, 2) development of multidisciplinary HF disease-management programs for patients at high risk of readmission, and 3) placing phone calls to the patient within three days of discharge and scheduling a follow-up visit within seven to 14 days.
Analysis
Overall, the new guideline provides a thorough reassessment and expert analysis on the diagnosis and management of HF for both inpatient and outpatient care. The authors introduce the phrase “guideline-directed medical therapy” (GDMT) to emphasize the smaller set of recommendations that constitute optimal medical therapy for HF patients. This designation, encompassing primarily Class I recommendations, helps providers rapidly determine the optimal treatment course for an individual patient. The mainstay of GDMT in HFrEF patients remains angiotensin-converting enzyme inhibitors (ACE-I), angiotensin receptor blockers (ARB) when ACE-I-intolerant, beta-blockers, and, in select patients, AA, hydralazine-nitrates, and diuretics.
A major shift in focus is seen in the new guideline with a greater emphasis on improved patient-centered outcomes across the spectrum of the disease. HF requires a continuum of care, from screening and genetic testing of family members of patients with idiopathic cardiomyopathy to conversations about palliative care and hospice. To this end, the authors highlight quality of life, shared decision-making, care coordination, transitions of care, and appropriateness of palliative care in a chronic disease state.
Further, the guideline expands upon previous recommendations for compliance with performance and quality metrics. Quality of care and adherence to performance measures of HF patients are becoming increasingly recognized, particularly in the hospital setting. The guideline offers recommendations for transitions of care in the hospitalized patient, which utilize systems of care coordination to ensure an evidence-based plan of care that includes the achievement of GDMT goals, effective management of comorbid conditions, timely follow-up, and appropriate dietary and physical activities.
HM Takeaways
HF is one of the most common, most challenging diseases managed by hospitalists. The 2013 ACCF/AHA Guideline for the Management of HF, while providing a comprehensive summary of evidence with recommendations for the totality of care for these patients throughout the course of the disease, places heavy emphasis on management during hospitalization and transitions. This includes repositioning of performance measures involving GDMT to better ensure optimal use of proven therapies in HFrEF, evidence-based steps to reduce readmissions, and greater recognition of the role of palliative care for patients with advanced disease.
Drs. McIlvennan and Allen are cardiologists in the Department of Medicine at the University of Colorado School of Medicine in Denver. Dr. Allen also works in the Colorado Health Outcomes Program.
References available at the-hospitalist.org.
SHM Introduces Discounted PQRS Through New Learning Portal
First, SHM’s new Learning Portal was the one-stop shop for free and discounted continuing medical education (CME) credits online. Now, the Learning Portal can help hospitalists report into the physician quality reporting system (PQRS) at a discounted individual rate.
And the time to start reporting measures in PQRS is now.
The PQRS was developed by the Centers for Medicare & Medicaid Services (CMS) in 2007 as a voluntary reporting program that provides a financial incentive to physicians and other eligible professionals who report data on quality measures for covered services furnished to Medicare beneficiaries. Starting in 2013, reporting in PQRS becomes mandatory for all eligible professionals.
SHM has encouraged its members to participate in the PQRS since the system’s inception in 2007. With the exciting launch of the SHM Learning Portal, it is easier than ever to get started. If you or your group are not currently reporting, there are still incentive payments available in 2013 and 2014. Beginning in 2015, there will be a penalty for not reporting quality measures based on 2013 performance.
Access the PQRIwizard through the SHM Learning Portal
SHM has secured a significant discount for members to report PQRS through the PQRIwizard. Located within the SHM Learning Portal, this online tool is a fast, convenient, and cost-effective solution to help collect and report quality measures data for the PQRS program. Similar to online tax-preparation software, the PQRIwizard guides you through a few easy steps to help rapidly collect, validate, report, and submit your results to CMS. The tool is powered by the CECity Registry, a CMS-qualified registry for PQRS reporting.
What Measures Are Available?
The SHM PQRIwizard features six individual quality measures in the areas of stroke and stroke rehabilitation, including measures on screening for dysphagia and thrombolytic therapy. To report on any of these measures, simply select three measures and report on 80 percent of your Medicare Part B fee-for-services patients who apply to the measures you selected.
PQRIwizard has a built-in progress monitor that validates your report by checking for missing data. The monitor also tracks your data to provide you with continuous feedback regarding valid patients. The system even calculates your measures and provides a printable report of your measure results in real time.
First, SHM’s new Learning Portal was the one-stop shop for free and discounted continuing medical education (CME) credits online. Now, the Learning Portal can help hospitalists report into the physician quality reporting system (PQRS) at a discounted individual rate.
And the time to start reporting measures in PQRS is now.
The PQRS was developed by the Centers for Medicare & Medicaid Services (CMS) in 2007 as a voluntary reporting program that provides a financial incentive to physicians and other eligible professionals who report data on quality measures for covered services furnished to Medicare beneficiaries. Starting in 2013, reporting in PQRS becomes mandatory for all eligible professionals.
SHM has encouraged its members to participate in the PQRS since the system’s inception in 2007. With the exciting launch of the SHM Learning Portal, it is easier than ever to get started. If you or your group are not currently reporting, there are still incentive payments available in 2013 and 2014. Beginning in 2015, there will be a penalty for not reporting quality measures based on 2013 performance.
Access the PQRIwizard through the SHM Learning Portal
SHM has secured a significant discount for members to report PQRS through the PQRIwizard. Located within the SHM Learning Portal, this online tool is a fast, convenient, and cost-effective solution to help collect and report quality measures data for the PQRS program. Similar to online tax-preparation software, the PQRIwizard guides you through a few easy steps to help rapidly collect, validate, report, and submit your results to CMS. The tool is powered by the CECity Registry, a CMS-qualified registry for PQRS reporting.
What Measures Are Available?
The SHM PQRIwizard features six individual quality measures in the areas of stroke and stroke rehabilitation, including measures on screening for dysphagia and thrombolytic therapy. To report on any of these measures, simply select three measures and report on 80 percent of your Medicare Part B fee-for-services patients who apply to the measures you selected.
PQRIwizard has a built-in progress monitor that validates your report by checking for missing data. The monitor also tracks your data to provide you with continuous feedback regarding valid patients. The system even calculates your measures and provides a printable report of your measure results in real time.
First, SHM’s new Learning Portal was the one-stop shop for free and discounted continuing medical education (CME) credits online. Now, the Learning Portal can help hospitalists report into the physician quality reporting system (PQRS) at a discounted individual rate.
And the time to start reporting measures in PQRS is now.
The PQRS was developed by the Centers for Medicare & Medicaid Services (CMS) in 2007 as a voluntary reporting program that provides a financial incentive to physicians and other eligible professionals who report data on quality measures for covered services furnished to Medicare beneficiaries. Starting in 2013, reporting in PQRS becomes mandatory for all eligible professionals.
SHM has encouraged its members to participate in the PQRS since the system’s inception in 2007. With the exciting launch of the SHM Learning Portal, it is easier than ever to get started. If you or your group are not currently reporting, there are still incentive payments available in 2013 and 2014. Beginning in 2015, there will be a penalty for not reporting quality measures based on 2013 performance.
Access the PQRIwizard through the SHM Learning Portal
SHM has secured a significant discount for members to report PQRS through the PQRIwizard. Located within the SHM Learning Portal, this online tool is a fast, convenient, and cost-effective solution to help collect and report quality measures data for the PQRS program. Similar to online tax-preparation software, the PQRIwizard guides you through a few easy steps to help rapidly collect, validate, report, and submit your results to CMS. The tool is powered by the CECity Registry, a CMS-qualified registry for PQRS reporting.
What Measures Are Available?
The SHM PQRIwizard features six individual quality measures in the areas of stroke and stroke rehabilitation, including measures on screening for dysphagia and thrombolytic therapy. To report on any of these measures, simply select three measures and report on 80 percent of your Medicare Part B fee-for-services patients who apply to the measures you selected.
PQRIwizard has a built-in progress monitor that validates your report by checking for missing data. The monitor also tracks your data to provide you with continuous feedback regarding valid patients. The system even calculates your measures and provides a printable report of your measure results in real time.
Hospitalist Groups Extract New Solutions Via Data Mining
One hospital wanted to reduce readmissions among patients with congestive heart failure. Another hoped to improve upon its sepsis mortality rates. A third sought to determine whether its doctors were providing cost-effective care for pneumonia patients. All of them adopted the same type of technology to help identify a solution.
As the healthcare industry tilts toward accountable care, pay for performance and an increasingly
cost-conscious mindset, hospitalists and other providers are tapping into a fast-growing analytical tool collectively known as data mining to help make sense of the growing mounds of information. Although no single technology can be considered a cure-all, HM leaders are so optimistic about data mining’s potential to address cost, outcome, and performance issues that some have labeled it a “game changer” for hospitalists.
Karim Godamunne, MD, MBA, SFHM, chief medical officer at North Fulton Hospital in Roswell, Ga., and a member of SHM’s Practice Management Committee, says he can’t overstate the importance of hospitalists’ involvement in physician data mining. “From my perspective, we’re looking to hospitalists to help drive this quality-utilization bandwagon, to be the real leaders in it,” he says. With the tremendous value that can be generated through understanding and using the information, “it’s good for your group and can be good to your hospital as a whole.”
So what is data mining? The technology fully emerged in the mid-1990s as a way to help scientists analyze large and often disparate bodies of data, present relevant information in new ways, and illuminate previously unknown relationships.1 In the healthcare industry, early adopters realized that the insights gleaned from data mining could help inform their clinical decision-making; organizations used the new tools to help predict health insurance fraud and identify at-risk patients, for example.
Cynthia Burghard, research director of Accountable Care IT Strategies at IDC Health Insights in Framingham, Mass., says researchers in academic medical centers initially conducted most of the clinical analytical work. Within the past few years, however, the increasing availability of data has allowed more hospitals to begin analyzing chronic disease, readmissions, and other areas of concern. In addition, Burghard says, new tools based on natural language processing are giving hospitals better access to unstructured clinical data, such as notes written by doctors and nurses.
“What I’m seeing both in my surveys as well as in conversations with hospitals is that analytics is the top of the investment priority for both hospitals and health plans,” Burghard says. According to IDC estimates, total spending for clinical analytics in the U.S. reached $3.7 billion in 2012 and is expected to grow to $5.14 billion by 2016. Much of the growth, she notes, is being driven by healthcare reform. “If your mandate is to manage populations of patients, it behooves you to know who those patients are and what their illnesses are, and to monitor what you’re doing for them,” she says.
Practice Improvement
Accordingly, a major goal of all this data-mining technology is to change practice behavior in a way that achieves the triple aim of improving quality of care, controlling costs, and bettering patient outcomes.
A growing number of companies are releasing tools that can compile and analyze the separate bits of information captured from claims and billing systems, Medicare reporting requirements, internal benchmarks, and other sources. Unlike passive data sources, such as Medicare’s Hospital Compare website, more active analytics can help their users zoom down to the level of an individual doctor or patient, pan out to the level of a hospitalist group, or expand out even more for a broader comparison among peer institutions.
Some newer data-mining tools with names like CRIMSON, Truven, Iodine, and Imagine are billing themselves as hospitalist-friendly performance-improvement aids and giving individual providers the ability to access and analyze the data themselves. A few of these applications can even provide real-time data via mobile devices (see “Physician Performance Aids,”).
Thomas Frederickson, MD, MBA, SFHM, medical director of the HM service at Alegent Creighton Health in Omaha, Neb., and a member of SHM’s Practice Management Committee, sees the biggest potential of this data-mining technology in its ability to help drive practice consistency. “You can use the database to analyze practice patterns of large groups, or even individuals, and see where variability exists,” he says. “And then, based on that, you can analyze why the variability exists and begin to address whether it’s variability that’s clinically indicated or not.”
When Alegent Creighton Health was scrutinizing the care of its pneumonia patients, for example, officials could compare the number of chest X-rays per pneumonia patient by hospital or across the entire CRIMSON database. At a deeper level, the officials could see how often individual providers ordered the tests compared to their peers. For outliers, they could follow up to determine whether the variability was warranted.
As champions of process improvement, Dr. Frederickson says, hospitalists can make particularly good use of database analytics. “It’s part of the process of making hospitalists invaluable to their hospitals and their systems,” he says. “Part of that is building up expertise on process improvement and safety, and familiarity with these kinds of tools is one thing that will help us do that.”
North Fulton Hospital used CRIMSON to analyze how its doctors care for patients with sepsis and to establish new benchmarks. Dr. Godamunne says the tools allowed the hospital to track its doctors’ progress over time and identify potential problems. “If a patient with sepsis is staying too long, you can see who admitted the patient and see if, a few months ago, the same physician was having similar problems,” he says. Similarly, the hospital was able to track the top DRGs resulting in excess length of stay among patients, to identify potential bottlenecks in the care and discharge processes.
Some tools require only two-day training sessions for basic proficiency, though more advanced manipulations often require a bigger commitment, like the 12-week training session that Dr. Godamunne completed. That training included one hour of online learning and one hour of homework every week, and most of the cases highlighted during his coursework, he says, focused on hospitalists—another sign of the major role he believes HM will play in harnessing data to improve performance quality.

—Thomas Frederickson, MD, MBA, SFHM, medical director, hospital medicine service, Alegent Creighton Health, Omaha, Neb., SHM Practice Management Committee member
Slow—Construction Ahead
The best information is meaningful, individualized, and timely, says Steven Deitelzweig, MD, SFHM, system chairman for hospital medicine and medical director of regional business development at Ochsner Health System in New Orleans. “If you get something back six months after you’ve delivered the care, you’ll have a limited opportunity to improve, versus if you get it back in a week or two, or ideally, in real time,” says Dr. Deitelzweig, chair of SHM’s Practice Management Committee.
In examining length of stay, Dr. Deitelzweig says doctors could use data mining to look at time-stamped elements of patient flow and the timeliness of provider response: how patients go through the ED, and when they receive written orders or lab results. “It could be really powerful, and right now it’s a little bit of a black hole,” he says.
Based on her conversations with hospital executives and leaders, however, Burghard cautions that some real-time mobile applications, although technologically impressive, may be less useful or necessary in practice. “If it’s performance measurement, why do you need that in real time? It’s not going to change your behavior in the moment,” she says. “What you may want to get is an alert that your patient, who is in the hospital, has had some sort of negative event.”
Data mining has other potential limitations. “There’s always going to be questions of attribution, and you need to have clinical knowledge of your location,” Dr. Godamunne says. And data mining is only as good as the data that have been documented, underscoring the importance of securing provider cooperation.
Dr. Frederickson says physician acceptance, in fact, might be one of the biggest obstacles—a major reason why he recommends introducing the technology slowly and explaining why and how it will be used. If introduced too quickly and without adequate explanation about what a hospital or health system hopes to accomplish, he says, “there certainly is the potential for suspicion.” The key, he says, is to emphasize that the tools provide a valuable mechanism for gleaning new insights into doctors’ practice patterns, “not something that’s going to be used against them.”
Paul Roscoe, CEO of the Washington, D.C.-based Advisory Board Company's Crimson division, agrees that personally engaging physicians is essential for a good return on investment in analytical tools like his company’s suite of CRIMSON products. “If you can’t work with the physicians to get them to understand the data and actively use the data in their practice patterns, it becomes a bit meaningless,” he says.

—Karim Godamunne, MD, MBA, SFHM, chief medical officer, North Fulton Hospital, Roswell, Ga., SHM Practice Management Committee member
Roscoe sees big opportunities in prospectively examining information while a patient is still in the hospital and when a change of course by providers could avert a bad outcome. “Suggesting a set of interventions that they could do differently is really the value-add,” he says. But he cautions that those suggestions must be worded carefully to avoid alienating physicians.
“If doctors don’t feel like they’re being judged, they’ll engage with you,” Roscoe says.
Similar nuances can affect how users perceive the tools themselves. After hearing feedback from members that the words “data mining” didn’t conjure trust and confidence, the Advisory Board Company dropped the phrase altogether in favor of “data analytics,” “physician engagement,” and similar descriptors. “It’s simple things like that that can very quickly either turn a physician on or off,” Roscoe says.
Once users take the time to understand data-mining tools and how they can be properly harnessed, advocates say, the technology can lead to a host of unanticipated benefits. When a hospital bills the federal government for a Medicare patient, for example, it must submit an HCC code that describes the patient’s condition. By doing a better job of mining the data, Burghard says, a hospital can more accurately reflect that patient’s contdition. For example, if a hospital is treating a diabetic who comes in with a broken leg, the hospital could receive a lower payment rate if it does not properly identify and record both conditions.
And by using the tools prospectively, Burghard says, “I think there’s the opportunity to make a quantum leap from what we’re doing today. We usually just report on facts, and usually retrospectively. With some of the new technology that’s available, the healthcare industry can begin to do discovery analytics—you’re identifying insights, patterns, and relationships.”
Better integration of computerized physician order entry with data-mining ports, Dr. Godamunne predicts, will allow for much better attribution and finer parsing of the data. As the transparency increases, though, hospitalists will have to adapt to a new reality in which stronger analytical tools may point out individual outliers. And that level of detail, in turn, will require some hospitalists to justify why they’re different than their peers.
Even so, Roscoe says, he’s found that hospitalists are very open to using data to improve performance and that they make up a high percentage of CRIMSON users. “There isn’t a physician group that is in a better position to help drive this quality- and data-driven culture,” he says.
Bryn Nelson is a freelance medical writer in Seattle.
Reference
One hospital wanted to reduce readmissions among patients with congestive heart failure. Another hoped to improve upon its sepsis mortality rates. A third sought to determine whether its doctors were providing cost-effective care for pneumonia patients. All of them adopted the same type of technology to help identify a solution.
As the healthcare industry tilts toward accountable care, pay for performance and an increasingly
cost-conscious mindset, hospitalists and other providers are tapping into a fast-growing analytical tool collectively known as data mining to help make sense of the growing mounds of information. Although no single technology can be considered a cure-all, HM leaders are so optimistic about data mining’s potential to address cost, outcome, and performance issues that some have labeled it a “game changer” for hospitalists.
Karim Godamunne, MD, MBA, SFHM, chief medical officer at North Fulton Hospital in Roswell, Ga., and a member of SHM’s Practice Management Committee, says he can’t overstate the importance of hospitalists’ involvement in physician data mining. “From my perspective, we’re looking to hospitalists to help drive this quality-utilization bandwagon, to be the real leaders in it,” he says. With the tremendous value that can be generated through understanding and using the information, “it’s good for your group and can be good to your hospital as a whole.”
So what is data mining? The technology fully emerged in the mid-1990s as a way to help scientists analyze large and often disparate bodies of data, present relevant information in new ways, and illuminate previously unknown relationships.1 In the healthcare industry, early adopters realized that the insights gleaned from data mining could help inform their clinical decision-making; organizations used the new tools to help predict health insurance fraud and identify at-risk patients, for example.
Cynthia Burghard, research director of Accountable Care IT Strategies at IDC Health Insights in Framingham, Mass., says researchers in academic medical centers initially conducted most of the clinical analytical work. Within the past few years, however, the increasing availability of data has allowed more hospitals to begin analyzing chronic disease, readmissions, and other areas of concern. In addition, Burghard says, new tools based on natural language processing are giving hospitals better access to unstructured clinical data, such as notes written by doctors and nurses.
“What I’m seeing both in my surveys as well as in conversations with hospitals is that analytics is the top of the investment priority for both hospitals and health plans,” Burghard says. According to IDC estimates, total spending for clinical analytics in the U.S. reached $3.7 billion in 2012 and is expected to grow to $5.14 billion by 2016. Much of the growth, she notes, is being driven by healthcare reform. “If your mandate is to manage populations of patients, it behooves you to know who those patients are and what their illnesses are, and to monitor what you’re doing for them,” she says.
Practice Improvement
Accordingly, a major goal of all this data-mining technology is to change practice behavior in a way that achieves the triple aim of improving quality of care, controlling costs, and bettering patient outcomes.
A growing number of companies are releasing tools that can compile and analyze the separate bits of information captured from claims and billing systems, Medicare reporting requirements, internal benchmarks, and other sources. Unlike passive data sources, such as Medicare’s Hospital Compare website, more active analytics can help their users zoom down to the level of an individual doctor or patient, pan out to the level of a hospitalist group, or expand out even more for a broader comparison among peer institutions.
Some newer data-mining tools with names like CRIMSON, Truven, Iodine, and Imagine are billing themselves as hospitalist-friendly performance-improvement aids and giving individual providers the ability to access and analyze the data themselves. A few of these applications can even provide real-time data via mobile devices (see “Physician Performance Aids,”).
Thomas Frederickson, MD, MBA, SFHM, medical director of the HM service at Alegent Creighton Health in Omaha, Neb., and a member of SHM’s Practice Management Committee, sees the biggest potential of this data-mining technology in its ability to help drive practice consistency. “You can use the database to analyze practice patterns of large groups, or even individuals, and see where variability exists,” he says. “And then, based on that, you can analyze why the variability exists and begin to address whether it’s variability that’s clinically indicated or not.”
When Alegent Creighton Health was scrutinizing the care of its pneumonia patients, for example, officials could compare the number of chest X-rays per pneumonia patient by hospital or across the entire CRIMSON database. At a deeper level, the officials could see how often individual providers ordered the tests compared to their peers. For outliers, they could follow up to determine whether the variability was warranted.
As champions of process improvement, Dr. Frederickson says, hospitalists can make particularly good use of database analytics. “It’s part of the process of making hospitalists invaluable to their hospitals and their systems,” he says. “Part of that is building up expertise on process improvement and safety, and familiarity with these kinds of tools is one thing that will help us do that.”
North Fulton Hospital used CRIMSON to analyze how its doctors care for patients with sepsis and to establish new benchmarks. Dr. Godamunne says the tools allowed the hospital to track its doctors’ progress over time and identify potential problems. “If a patient with sepsis is staying too long, you can see who admitted the patient and see if, a few months ago, the same physician was having similar problems,” he says. Similarly, the hospital was able to track the top DRGs resulting in excess length of stay among patients, to identify potential bottlenecks in the care and discharge processes.
Some tools require only two-day training sessions for basic proficiency, though more advanced manipulations often require a bigger commitment, like the 12-week training session that Dr. Godamunne completed. That training included one hour of online learning and one hour of homework every week, and most of the cases highlighted during his coursework, he says, focused on hospitalists—another sign of the major role he believes HM will play in harnessing data to improve performance quality.

—Thomas Frederickson, MD, MBA, SFHM, medical director, hospital medicine service, Alegent Creighton Health, Omaha, Neb., SHM Practice Management Committee member
Slow—Construction Ahead
The best information is meaningful, individualized, and timely, says Steven Deitelzweig, MD, SFHM, system chairman for hospital medicine and medical director of regional business development at Ochsner Health System in New Orleans. “If you get something back six months after you’ve delivered the care, you’ll have a limited opportunity to improve, versus if you get it back in a week or two, or ideally, in real time,” says Dr. Deitelzweig, chair of SHM’s Practice Management Committee.
In examining length of stay, Dr. Deitelzweig says doctors could use data mining to look at time-stamped elements of patient flow and the timeliness of provider response: how patients go through the ED, and when they receive written orders or lab results. “It could be really powerful, and right now it’s a little bit of a black hole,” he says.
Based on her conversations with hospital executives and leaders, however, Burghard cautions that some real-time mobile applications, although technologically impressive, may be less useful or necessary in practice. “If it’s performance measurement, why do you need that in real time? It’s not going to change your behavior in the moment,” she says. “What you may want to get is an alert that your patient, who is in the hospital, has had some sort of negative event.”
Data mining has other potential limitations. “There’s always going to be questions of attribution, and you need to have clinical knowledge of your location,” Dr. Godamunne says. And data mining is only as good as the data that have been documented, underscoring the importance of securing provider cooperation.
Dr. Frederickson says physician acceptance, in fact, might be one of the biggest obstacles—a major reason why he recommends introducing the technology slowly and explaining why and how it will be used. If introduced too quickly and without adequate explanation about what a hospital or health system hopes to accomplish, he says, “there certainly is the potential for suspicion.” The key, he says, is to emphasize that the tools provide a valuable mechanism for gleaning new insights into doctors’ practice patterns, “not something that’s going to be used against them.”
Paul Roscoe, CEO of the Washington, D.C.-based Advisory Board Company's Crimson division, agrees that personally engaging physicians is essential for a good return on investment in analytical tools like his company’s suite of CRIMSON products. “If you can’t work with the physicians to get them to understand the data and actively use the data in their practice patterns, it becomes a bit meaningless,” he says.

—Karim Godamunne, MD, MBA, SFHM, chief medical officer, North Fulton Hospital, Roswell, Ga., SHM Practice Management Committee member
Roscoe sees big opportunities in prospectively examining information while a patient is still in the hospital and when a change of course by providers could avert a bad outcome. “Suggesting a set of interventions that they could do differently is really the value-add,” he says. But he cautions that those suggestions must be worded carefully to avoid alienating physicians.
“If doctors don’t feel like they’re being judged, they’ll engage with you,” Roscoe says.
Similar nuances can affect how users perceive the tools themselves. After hearing feedback from members that the words “data mining” didn’t conjure trust and confidence, the Advisory Board Company dropped the phrase altogether in favor of “data analytics,” “physician engagement,” and similar descriptors. “It’s simple things like that that can very quickly either turn a physician on or off,” Roscoe says.
Once users take the time to understand data-mining tools and how they can be properly harnessed, advocates say, the technology can lead to a host of unanticipated benefits. When a hospital bills the federal government for a Medicare patient, for example, it must submit an HCC code that describes the patient’s condition. By doing a better job of mining the data, Burghard says, a hospital can more accurately reflect that patient’s contdition. For example, if a hospital is treating a diabetic who comes in with a broken leg, the hospital could receive a lower payment rate if it does not properly identify and record both conditions.
And by using the tools prospectively, Burghard says, “I think there’s the opportunity to make a quantum leap from what we’re doing today. We usually just report on facts, and usually retrospectively. With some of the new technology that’s available, the healthcare industry can begin to do discovery analytics—you’re identifying insights, patterns, and relationships.”
Better integration of computerized physician order entry with data-mining ports, Dr. Godamunne predicts, will allow for much better attribution and finer parsing of the data. As the transparency increases, though, hospitalists will have to adapt to a new reality in which stronger analytical tools may point out individual outliers. And that level of detail, in turn, will require some hospitalists to justify why they’re different than their peers.
Even so, Roscoe says, he’s found that hospitalists are very open to using data to improve performance and that they make up a high percentage of CRIMSON users. “There isn’t a physician group that is in a better position to help drive this quality- and data-driven culture,” he says.
Bryn Nelson is a freelance medical writer in Seattle.
Reference
One hospital wanted to reduce readmissions among patients with congestive heart failure. Another hoped to improve upon its sepsis mortality rates. A third sought to determine whether its doctors were providing cost-effective care for pneumonia patients. All of them adopted the same type of technology to help identify a solution.
As the healthcare industry tilts toward accountable care, pay for performance and an increasingly
cost-conscious mindset, hospitalists and other providers are tapping into a fast-growing analytical tool collectively known as data mining to help make sense of the growing mounds of information. Although no single technology can be considered a cure-all, HM leaders are so optimistic about data mining’s potential to address cost, outcome, and performance issues that some have labeled it a “game changer” for hospitalists.
Karim Godamunne, MD, MBA, SFHM, chief medical officer at North Fulton Hospital in Roswell, Ga., and a member of SHM’s Practice Management Committee, says he can’t overstate the importance of hospitalists’ involvement in physician data mining. “From my perspective, we’re looking to hospitalists to help drive this quality-utilization bandwagon, to be the real leaders in it,” he says. With the tremendous value that can be generated through understanding and using the information, “it’s good for your group and can be good to your hospital as a whole.”
So what is data mining? The technology fully emerged in the mid-1990s as a way to help scientists analyze large and often disparate bodies of data, present relevant information in new ways, and illuminate previously unknown relationships.1 In the healthcare industry, early adopters realized that the insights gleaned from data mining could help inform their clinical decision-making; organizations used the new tools to help predict health insurance fraud and identify at-risk patients, for example.
Cynthia Burghard, research director of Accountable Care IT Strategies at IDC Health Insights in Framingham, Mass., says researchers in academic medical centers initially conducted most of the clinical analytical work. Within the past few years, however, the increasing availability of data has allowed more hospitals to begin analyzing chronic disease, readmissions, and other areas of concern. In addition, Burghard says, new tools based on natural language processing are giving hospitals better access to unstructured clinical data, such as notes written by doctors and nurses.
“What I’m seeing both in my surveys as well as in conversations with hospitals is that analytics is the top of the investment priority for both hospitals and health plans,” Burghard says. According to IDC estimates, total spending for clinical analytics in the U.S. reached $3.7 billion in 2012 and is expected to grow to $5.14 billion by 2016. Much of the growth, she notes, is being driven by healthcare reform. “If your mandate is to manage populations of patients, it behooves you to know who those patients are and what their illnesses are, and to monitor what you’re doing for them,” she says.
Practice Improvement
Accordingly, a major goal of all this data-mining technology is to change practice behavior in a way that achieves the triple aim of improving quality of care, controlling costs, and bettering patient outcomes.
A growing number of companies are releasing tools that can compile and analyze the separate bits of information captured from claims and billing systems, Medicare reporting requirements, internal benchmarks, and other sources. Unlike passive data sources, such as Medicare’s Hospital Compare website, more active analytics can help their users zoom down to the level of an individual doctor or patient, pan out to the level of a hospitalist group, or expand out even more for a broader comparison among peer institutions.
Some newer data-mining tools with names like CRIMSON, Truven, Iodine, and Imagine are billing themselves as hospitalist-friendly performance-improvement aids and giving individual providers the ability to access and analyze the data themselves. A few of these applications can even provide real-time data via mobile devices (see “Physician Performance Aids,”).
Thomas Frederickson, MD, MBA, SFHM, medical director of the HM service at Alegent Creighton Health in Omaha, Neb., and a member of SHM’s Practice Management Committee, sees the biggest potential of this data-mining technology in its ability to help drive practice consistency. “You can use the database to analyze practice patterns of large groups, or even individuals, and see where variability exists,” he says. “And then, based on that, you can analyze why the variability exists and begin to address whether it’s variability that’s clinically indicated or not.”
When Alegent Creighton Health was scrutinizing the care of its pneumonia patients, for example, officials could compare the number of chest X-rays per pneumonia patient by hospital or across the entire CRIMSON database. At a deeper level, the officials could see how often individual providers ordered the tests compared to their peers. For outliers, they could follow up to determine whether the variability was warranted.
As champions of process improvement, Dr. Frederickson says, hospitalists can make particularly good use of database analytics. “It’s part of the process of making hospitalists invaluable to their hospitals and their systems,” he says. “Part of that is building up expertise on process improvement and safety, and familiarity with these kinds of tools is one thing that will help us do that.”
North Fulton Hospital used CRIMSON to analyze how its doctors care for patients with sepsis and to establish new benchmarks. Dr. Godamunne says the tools allowed the hospital to track its doctors’ progress over time and identify potential problems. “If a patient with sepsis is staying too long, you can see who admitted the patient and see if, a few months ago, the same physician was having similar problems,” he says. Similarly, the hospital was able to track the top DRGs resulting in excess length of stay among patients, to identify potential bottlenecks in the care and discharge processes.
Some tools require only two-day training sessions for basic proficiency, though more advanced manipulations often require a bigger commitment, like the 12-week training session that Dr. Godamunne completed. That training included one hour of online learning and one hour of homework every week, and most of the cases highlighted during his coursework, he says, focused on hospitalists—another sign of the major role he believes HM will play in harnessing data to improve performance quality.

—Thomas Frederickson, MD, MBA, SFHM, medical director, hospital medicine service, Alegent Creighton Health, Omaha, Neb., SHM Practice Management Committee member
Slow—Construction Ahead
The best information is meaningful, individualized, and timely, says Steven Deitelzweig, MD, SFHM, system chairman for hospital medicine and medical director of regional business development at Ochsner Health System in New Orleans. “If you get something back six months after you’ve delivered the care, you’ll have a limited opportunity to improve, versus if you get it back in a week or two, or ideally, in real time,” says Dr. Deitelzweig, chair of SHM’s Practice Management Committee.
In examining length of stay, Dr. Deitelzweig says doctors could use data mining to look at time-stamped elements of patient flow and the timeliness of provider response: how patients go through the ED, and when they receive written orders or lab results. “It could be really powerful, and right now it’s a little bit of a black hole,” he says.
Based on her conversations with hospital executives and leaders, however, Burghard cautions that some real-time mobile applications, although technologically impressive, may be less useful or necessary in practice. “If it’s performance measurement, why do you need that in real time? It’s not going to change your behavior in the moment,” she says. “What you may want to get is an alert that your patient, who is in the hospital, has had some sort of negative event.”
Data mining has other potential limitations. “There’s always going to be questions of attribution, and you need to have clinical knowledge of your location,” Dr. Godamunne says. And data mining is only as good as the data that have been documented, underscoring the importance of securing provider cooperation.
Dr. Frederickson says physician acceptance, in fact, might be one of the biggest obstacles—a major reason why he recommends introducing the technology slowly and explaining why and how it will be used. If introduced too quickly and without adequate explanation about what a hospital or health system hopes to accomplish, he says, “there certainly is the potential for suspicion.” The key, he says, is to emphasize that the tools provide a valuable mechanism for gleaning new insights into doctors’ practice patterns, “not something that’s going to be used against them.”
Paul Roscoe, CEO of the Washington, D.C.-based Advisory Board Company's Crimson division, agrees that personally engaging physicians is essential for a good return on investment in analytical tools like his company’s suite of CRIMSON products. “If you can’t work with the physicians to get them to understand the data and actively use the data in their practice patterns, it becomes a bit meaningless,” he says.

—Karim Godamunne, MD, MBA, SFHM, chief medical officer, North Fulton Hospital, Roswell, Ga., SHM Practice Management Committee member
Roscoe sees big opportunities in prospectively examining information while a patient is still in the hospital and when a change of course by providers could avert a bad outcome. “Suggesting a set of interventions that they could do differently is really the value-add,” he says. But he cautions that those suggestions must be worded carefully to avoid alienating physicians.
“If doctors don’t feel like they’re being judged, they’ll engage with you,” Roscoe says.
Similar nuances can affect how users perceive the tools themselves. After hearing feedback from members that the words “data mining” didn’t conjure trust and confidence, the Advisory Board Company dropped the phrase altogether in favor of “data analytics,” “physician engagement,” and similar descriptors. “It’s simple things like that that can very quickly either turn a physician on or off,” Roscoe says.
Once users take the time to understand data-mining tools and how they can be properly harnessed, advocates say, the technology can lead to a host of unanticipated benefits. When a hospital bills the federal government for a Medicare patient, for example, it must submit an HCC code that describes the patient’s condition. By doing a better job of mining the data, Burghard says, a hospital can more accurately reflect that patient’s contdition. For example, if a hospital is treating a diabetic who comes in with a broken leg, the hospital could receive a lower payment rate if it does not properly identify and record both conditions.
And by using the tools prospectively, Burghard says, “I think there’s the opportunity to make a quantum leap from what we’re doing today. We usually just report on facts, and usually retrospectively. With some of the new technology that’s available, the healthcare industry can begin to do discovery analytics—you’re identifying insights, patterns, and relationships.”
Better integration of computerized physician order entry with data-mining ports, Dr. Godamunne predicts, will allow for much better attribution and finer parsing of the data. As the transparency increases, though, hospitalists will have to adapt to a new reality in which stronger analytical tools may point out individual outliers. And that level of detail, in turn, will require some hospitalists to justify why they’re different than their peers.
Even so, Roscoe says, he’s found that hospitalists are very open to using data to improve performance and that they make up a high percentage of CRIMSON users. “There isn’t a physician group that is in a better position to help drive this quality- and data-driven culture,” he says.
Bryn Nelson is a freelance medical writer in Seattle.
Reference
Study Investigator Explains Why Copper Surfaces Can Help Prevent Infections
Click here to listen to more of our interview with Dr. Schmidt
Click here to listen to more of our interview with Dr. Schmidt
Click here to listen to more of our interview with Dr. Schmidt