User login
VTE guidelines recommend NOACs over VKA therapy

Photo courtesy of NIGMS
The American College of Chest Physicians has released a new edition of guidelines for the treatment of patients with venous thromboembolism (VTE).
This 10th edition of the guidelines, published in CHEST, includes 54 recommendations. However, only 20 of these recommendations were deemed “strong,” and none were based on high-quality evidence.
“The guideline presents stronger recommendations and weaker suggestions for treatment based on the best available evidence and identifies gaps in our knowledge and areas for future research,” said lead author Clive Kearon, MD, PhD, of McMaster University in Hamilton, Ontario, Canada.
One of the key recommendations in the guidelines is a preference for novel oral anticoagulants (NOACs) over vitamin K antagonist (VKA) therapy for initial and long-term treatment of VTE in patients without cancer.
The guideline authors say that, since the publication of the 9th edition, studies have shown that NOACs are as effective as VKA therapy, and NOACs confer a reduced risk of bleeding and increased convenience for patients and healthcare providers.
As long-term anticoagulant therapy for patients without cancer, the guideline authors suggest dabigatran, rivaroxaban, apixaban, or edoxaban over VKA therapy. But they suggest VKA therapy over low-molecular-weight heparin.
For patients with VTE and cancer, the guideline authors suggest low-molecular-weight heparin over VKA, dabigatran, rivaroxaban, apixaban, or edoxaban.
The guidelines advise against an inferior vena cava filter for patients with VTE who are receiving anticoagulant treatment.
Another change to guideline recommendations from the 9th edition to the 10th edition concerns the routine use of compression stockings. Based on recent evidence, the 10th edition advises against routinely using compression stockings to prevent post-thrombotic syndrome in patients with acute deep vein thrombosis (DVT).
The 10th edition also suggests which patients diagnosed with isolated subsegmental pulmonary embolism (PE) should, and should not, receive anticoagulant therapy.
For subsegmental PE and no proximal DVT, the guidelines suggest clinical surveillance over anticoagulation if patients have a low risk of recurrent VTE and anticoagulation over clinical surveillance if patients have a high risk of recurrence.
The guidelines suggest thrombolytic therapy for patients with PE and hypotension and systemic therapy over catheter-directed thrombolysis.
To date, the updated guidelines have been endorsed by the American Association for Clinical Chemistry, American College of Clinical Pharmacy, International Society for Thrombosis and Haemostasis, and American Society of Health-System Pharmacists. ![]()

Photo courtesy of NIGMS
The American College of Chest Physicians has released a new edition of guidelines for the treatment of patients with venous thromboembolism (VTE).
This 10th edition of the guidelines, published in CHEST, includes 54 recommendations. However, only 20 of these recommendations were deemed “strong,” and none were based on high-quality evidence.
“The guideline presents stronger recommendations and weaker suggestions for treatment based on the best available evidence and identifies gaps in our knowledge and areas for future research,” said lead author Clive Kearon, MD, PhD, of McMaster University in Hamilton, Ontario, Canada.
One of the key recommendations in the guidelines is a preference for novel oral anticoagulants (NOACs) over vitamin K antagonist (VKA) therapy for initial and long-term treatment of VTE in patients without cancer.
The guideline authors say that, since the publication of the 9th edition, studies have shown that NOACs are as effective as VKA therapy, and NOACs confer a reduced risk of bleeding and increased convenience for patients and healthcare providers.
As long-term anticoagulant therapy for patients without cancer, the guideline authors suggest dabigatran, rivaroxaban, apixaban, or edoxaban over VKA therapy. But they suggest VKA therapy over low-molecular-weight heparin.
For patients with VTE and cancer, the guideline authors suggest low-molecular-weight heparin over VKA, dabigatran, rivaroxaban, apixaban, or edoxaban.
The guidelines advise against an inferior vena cava filter for patients with VTE who are receiving anticoagulant treatment.
Another change to guideline recommendations from the 9th edition to the 10th edition concerns the routine use of compression stockings. Based on recent evidence, the 10th edition advises against routinely using compression stockings to prevent post-thrombotic syndrome in patients with acute deep vein thrombosis (DVT).
The 10th edition also suggests which patients diagnosed with isolated subsegmental pulmonary embolism (PE) should, and should not, receive anticoagulant therapy.
For subsegmental PE and no proximal DVT, the guidelines suggest clinical surveillance over anticoagulation if patients have a low risk of recurrent VTE and anticoagulation over clinical surveillance if patients have a high risk of recurrence.
The guidelines suggest thrombolytic therapy for patients with PE and hypotension and systemic therapy over catheter-directed thrombolysis.
To date, the updated guidelines have been endorsed by the American Association for Clinical Chemistry, American College of Clinical Pharmacy, International Society for Thrombosis and Haemostasis, and American Society of Health-System Pharmacists. ![]()

Photo courtesy of NIGMS
The American College of Chest Physicians has released a new edition of guidelines for the treatment of patients with venous thromboembolism (VTE).
This 10th edition of the guidelines, published in CHEST, includes 54 recommendations. However, only 20 of these recommendations were deemed “strong,” and none were based on high-quality evidence.
“The guideline presents stronger recommendations and weaker suggestions for treatment based on the best available evidence and identifies gaps in our knowledge and areas for future research,” said lead author Clive Kearon, MD, PhD, of McMaster University in Hamilton, Ontario, Canada.
One of the key recommendations in the guidelines is a preference for novel oral anticoagulants (NOACs) over vitamin K antagonist (VKA) therapy for initial and long-term treatment of VTE in patients without cancer.
The guideline authors say that, since the publication of the 9th edition, studies have shown that NOACs are as effective as VKA therapy, and NOACs confer a reduced risk of bleeding and increased convenience for patients and healthcare providers.
As long-term anticoagulant therapy for patients without cancer, the guideline authors suggest dabigatran, rivaroxaban, apixaban, or edoxaban over VKA therapy. But they suggest VKA therapy over low-molecular-weight heparin.
For patients with VTE and cancer, the guideline authors suggest low-molecular-weight heparin over VKA, dabigatran, rivaroxaban, apixaban, or edoxaban.
The guidelines advise against an inferior vena cava filter for patients with VTE who are receiving anticoagulant treatment.
Another change to guideline recommendations from the 9th edition to the 10th edition concerns the routine use of compression stockings. Based on recent evidence, the 10th edition advises against routinely using compression stockings to prevent post-thrombotic syndrome in patients with acute deep vein thrombosis (DVT).
The 10th edition also suggests which patients diagnosed with isolated subsegmental pulmonary embolism (PE) should, and should not, receive anticoagulant therapy.
For subsegmental PE and no proximal DVT, the guidelines suggest clinical surveillance over anticoagulation if patients have a low risk of recurrent VTE and anticoagulation over clinical surveillance if patients have a high risk of recurrence.
The guidelines suggest thrombolytic therapy for patients with PE and hypotension and systemic therapy over catheter-directed thrombolysis.
To date, the updated guidelines have been endorsed by the American Association for Clinical Chemistry, American College of Clinical Pharmacy, International Society for Thrombosis and Haemostasis, and American Society of Health-System Pharmacists. ![]()
US cancer stats: The good and the bad

patient and her father
Photo by Rhoda Baer
The American Cancer Society’s 2016 report on cancer in the US suggests that, in recent years, overall trends in cancer incidence have remained stable for women and declined for men.
However, the rates of certain malignancies are on the rise. This includes some leukemia subtypes for men and women, as well as myeloma for men.
Leukemia is the leading cause of cancer death for men ages 20 to 39, but leukemia is no longer the leading cause of cancer death among children and adolescents (of both genders).
These and other data are included in the report, which is published in CA: A Cancer Journal for Clinicians.
The report estimates there will be 1,685,210 new cancer cases and 595,690 cancer deaths in the US in 2016. This includes 81,080 new lymphoma cases and 21,270 lymphoma deaths, 60,140 new leukemia cases and 24,400 leukemia deaths, and 30,330 new myeloma cases and 12,650 myeloma deaths.
Cancer incidence over time
The report suggests the overall cancer incidence for women has been stable from 1998 to 2012. But the incidence for men has declined by 3.1% per year from 2009 to 2012, with one-half of the drop in men due to recent rapid declines in prostate cancer diagnoses as prostate-specific antigen testing decreases.
Incidence rates increased from 2003 to 2012 among both men and women for some leukemia subtypes and for cancers of the tongue, tonsil, small intestine, liver, pancreas, kidney, renal pelvis, and thyroid.
Incidence rates increased in men for melanoma, myeloma, and cancers of the breast, testis, and oropharynx. Among women, incidence rates increased for cancers of the anus, vulva, and uterine corpus.
Cancer deaths
The rate of cancer deaths in the US has dropped 23% from its peak in 1991 to 2012. The incidence of cancer death was 215.1 per 100,000 in 1991 and 166.4 per 100,000 in 2012.
The decline is larger in men (28% since 1990) than in women (19% since 1991). Over the past decade of data, the rate dropped by 1.8% per year in men and 1.4% per year in women.
The decline in cancer death rates over the past 2 decades is driven by continued decreases in death rates for the 4 major cancer sites: lung, breast, prostate, and colon/rectum.
Breast cancer is the leading cause of cancer death in women ages 20 to 59, while lung cancer is the leading cause of cancer death in women 60 and older.
Among men, leukemia is the leading cause of cancer death for those ages 20 to 39, whereas lung cancer ranks first among men 40 and older.
Among children and adolescents (0-19), brain cancer has surpassed leukemia as the leading cause of cancer death, a result of more rapid therapeutic advances against leukemia.
The report also features an analysis of leading causes of death by state. It shows that, even as cancer remains the second leading cause of death nationwide, steep drops in deaths from heart disease have made cancer the leading cause of death in 21 states: Alaska, Arizona, Colorado, Delaware, Florida, Georgia, Idaho, Kansas, Maine, Massachusetts, Minnesota, Montana, Nebraska, New Hampshire, New Mexico, North Carolina, Oregon, South Carolina, Vermont, Virginia, and Washington.
In addition, cancer is the leading cause of death among adults ages 40 to 79 and among both Hispanics and Asian/Pacific Islanders, who together make up one-quarter of the US population.
Heart disease remains the top cause of death overall in the US. In 2012, there were 599,711 (24%) deaths from heart disease, compared to 582,623 (23%) deaths from cancer.
“We’re gratified to see cancer death rates continuing to drop,” said Otis W. Brawley, MD, chief medical officer of the American Cancer Society.
“But the fact that cancer is nonetheless becoming the top cause of death in many populations is a strong reminder that the fight is not over.” ![]()

patient and her father
Photo by Rhoda Baer
The American Cancer Society’s 2016 report on cancer in the US suggests that, in recent years, overall trends in cancer incidence have remained stable for women and declined for men.
However, the rates of certain malignancies are on the rise. This includes some leukemia subtypes for men and women, as well as myeloma for men.
Leukemia is the leading cause of cancer death for men ages 20 to 39, but leukemia is no longer the leading cause of cancer death among children and adolescents (of both genders).
These and other data are included in the report, which is published in CA: A Cancer Journal for Clinicians.
The report estimates there will be 1,685,210 new cancer cases and 595,690 cancer deaths in the US in 2016. This includes 81,080 new lymphoma cases and 21,270 lymphoma deaths, 60,140 new leukemia cases and 24,400 leukemia deaths, and 30,330 new myeloma cases and 12,650 myeloma deaths.
Cancer incidence over time
The report suggests the overall cancer incidence for women has been stable from 1998 to 2012. But the incidence for men has declined by 3.1% per year from 2009 to 2012, with one-half of the drop in men due to recent rapid declines in prostate cancer diagnoses as prostate-specific antigen testing decreases.
Incidence rates increased from 2003 to 2012 among both men and women for some leukemia subtypes and for cancers of the tongue, tonsil, small intestine, liver, pancreas, kidney, renal pelvis, and thyroid.
Incidence rates increased in men for melanoma, myeloma, and cancers of the breast, testis, and oropharynx. Among women, incidence rates increased for cancers of the anus, vulva, and uterine corpus.
Cancer deaths
The rate of cancer deaths in the US has dropped 23% from its peak in 1991 to 2012. The incidence of cancer death was 215.1 per 100,000 in 1991 and 166.4 per 100,000 in 2012.
The decline is larger in men (28% since 1990) than in women (19% since 1991). Over the past decade of data, the rate dropped by 1.8% per year in men and 1.4% per year in women.
The decline in cancer death rates over the past 2 decades is driven by continued decreases in death rates for the 4 major cancer sites: lung, breast, prostate, and colon/rectum.
Breast cancer is the leading cause of cancer death in women ages 20 to 59, while lung cancer is the leading cause of cancer death in women 60 and older.
Among men, leukemia is the leading cause of cancer death for those ages 20 to 39, whereas lung cancer ranks first among men 40 and older.
Among children and adolescents (0-19), brain cancer has surpassed leukemia as the leading cause of cancer death, a result of more rapid therapeutic advances against leukemia.
The report also features an analysis of leading causes of death by state. It shows that, even as cancer remains the second leading cause of death nationwide, steep drops in deaths from heart disease have made cancer the leading cause of death in 21 states: Alaska, Arizona, Colorado, Delaware, Florida, Georgia, Idaho, Kansas, Maine, Massachusetts, Minnesota, Montana, Nebraska, New Hampshire, New Mexico, North Carolina, Oregon, South Carolina, Vermont, Virginia, and Washington.
In addition, cancer is the leading cause of death among adults ages 40 to 79 and among both Hispanics and Asian/Pacific Islanders, who together make up one-quarter of the US population.
Heart disease remains the top cause of death overall in the US. In 2012, there were 599,711 (24%) deaths from heart disease, compared to 582,623 (23%) deaths from cancer.
“We’re gratified to see cancer death rates continuing to drop,” said Otis W. Brawley, MD, chief medical officer of the American Cancer Society.
“But the fact that cancer is nonetheless becoming the top cause of death in many populations is a strong reminder that the fight is not over.” ![]()

patient and her father
Photo by Rhoda Baer
The American Cancer Society’s 2016 report on cancer in the US suggests that, in recent years, overall trends in cancer incidence have remained stable for women and declined for men.
However, the rates of certain malignancies are on the rise. This includes some leukemia subtypes for men and women, as well as myeloma for men.
Leukemia is the leading cause of cancer death for men ages 20 to 39, but leukemia is no longer the leading cause of cancer death among children and adolescents (of both genders).
These and other data are included in the report, which is published in CA: A Cancer Journal for Clinicians.
The report estimates there will be 1,685,210 new cancer cases and 595,690 cancer deaths in the US in 2016. This includes 81,080 new lymphoma cases and 21,270 lymphoma deaths, 60,140 new leukemia cases and 24,400 leukemia deaths, and 30,330 new myeloma cases and 12,650 myeloma deaths.
Cancer incidence over time
The report suggests the overall cancer incidence for women has been stable from 1998 to 2012. But the incidence for men has declined by 3.1% per year from 2009 to 2012, with one-half of the drop in men due to recent rapid declines in prostate cancer diagnoses as prostate-specific antigen testing decreases.
Incidence rates increased from 2003 to 2012 among both men and women for some leukemia subtypes and for cancers of the tongue, tonsil, small intestine, liver, pancreas, kidney, renal pelvis, and thyroid.
Incidence rates increased in men for melanoma, myeloma, and cancers of the breast, testis, and oropharynx. Among women, incidence rates increased for cancers of the anus, vulva, and uterine corpus.
Cancer deaths
The rate of cancer deaths in the US has dropped 23% from its peak in 1991 to 2012. The incidence of cancer death was 215.1 per 100,000 in 1991 and 166.4 per 100,000 in 2012.
The decline is larger in men (28% since 1990) than in women (19% since 1991). Over the past decade of data, the rate dropped by 1.8% per year in men and 1.4% per year in women.
The decline in cancer death rates over the past 2 decades is driven by continued decreases in death rates for the 4 major cancer sites: lung, breast, prostate, and colon/rectum.
Breast cancer is the leading cause of cancer death in women ages 20 to 59, while lung cancer is the leading cause of cancer death in women 60 and older.
Among men, leukemia is the leading cause of cancer death for those ages 20 to 39, whereas lung cancer ranks first among men 40 and older.
Among children and adolescents (0-19), brain cancer has surpassed leukemia as the leading cause of cancer death, a result of more rapid therapeutic advances against leukemia.
The report also features an analysis of leading causes of death by state. It shows that, even as cancer remains the second leading cause of death nationwide, steep drops in deaths from heart disease have made cancer the leading cause of death in 21 states: Alaska, Arizona, Colorado, Delaware, Florida, Georgia, Idaho, Kansas, Maine, Massachusetts, Minnesota, Montana, Nebraska, New Hampshire, New Mexico, North Carolina, Oregon, South Carolina, Vermont, Virginia, and Washington.
In addition, cancer is the leading cause of death among adults ages 40 to 79 and among both Hispanics and Asian/Pacific Islanders, who together make up one-quarter of the US population.
Heart disease remains the top cause of death overall in the US. In 2012, there were 599,711 (24%) deaths from heart disease, compared to 582,623 (23%) deaths from cancer.
“We’re gratified to see cancer death rates continuing to drop,” said Otis W. Brawley, MD, chief medical officer of the American Cancer Society.
“But the fact that cancer is nonetheless becoming the top cause of death in many populations is a strong reminder that the fight is not over.” ![]()
Drug produces ‘encouraging efficacy’ in MM

© ASCO/Todd Buchanan
Single-agent daratumumab has exhibited “encouraging efficacy” and a “favorable safety profile” in patients with heavily pretreated and refractory multiple myeloma (MM), according to investigators from the phase 2 SIRIUS trial.
The drug produced an overall response rate of 30% in MM patients who had received 3 or more prior lines of therapy. The median progression-free survival was close to 4 months, and the median overall survival was nearly 18 months.
Thirty percent of patients had treatment-emergent serious adverse events (AEs), and 23% had grade 3 or 4 treatment-emergent serious AEs.
“This represents the first single-agent activity we have for a monoclonal antibody in treating multiple myeloma,” said study author Sagar Lonial, MD, of Emory University School of Medicine in Atlanta, Georgia.
“The future hope for daratumumab is in our ability to bring this active agent to earlier lines of therapy and combine it with drugs where you may get synergy.”
Dr Lonial and his colleagues reported results from the ongoing SIRIUS trial in The Lancet. Results from the trial were previously presented at the 2015 ASCO Annual Meeting. The research was funded by Janssen Research & Development, the company developing daratumumab.
In part 1 of the trial, 34 MM patients were randomized to receive either 8 mg/kg of daratumumab once every 4 weeks or 16 mg/kg once a week for 8 weeks, then once every 2 weeks for 16 weeks and once every 4 weeks after that, until disease progression or unacceptable toxicity.
In part 2, an additional 90 MM patients were enrolled and received 16 mg/kg of daratumumab on the same dosing schedule as in part 1.
Dr Lonial and his colleagues reported results for all patients who received 16 mg/kg of daratumumab. At the first interim analysis, the 8 mg/kg arm did not meet the criteria for expansion because the overall response rate was 11.1%.
The 106 patients who received the 16 mg/kg dose of daratumumab had received a median of 5 prior lines of therapy, including a proteasome inhibitor and an immunomodulatory drug. Ninety-seven percent of these patients were refractory to their last line of therapy, and 95% were refractory to both a proteasome inhibitor and an immunomodulatory drug.
Response and survival
According to an independent review committee, 29.2% of patients responded to daratumumab. Eighteen patients had a partial response, 10 had a very good partial response, and 3 had a stringent complete response.
The median duration of response was 7.4 months, and the median time to first response was 1 month.
The median overall survival was 17.5 months, and the 12-month overall survival was 64.8%. The median progression-free survival was 3.7 months.
Safety
The most common AEs were fatigue (40%), anemia (33%), nausea (29%), thrombocytopenia (25%), neutropenia (23%), back pain (22%), and cough (21%). Thirty percent of patients experienced serious AEs, and 23% had serious grade 3/4 AEs.
Infusion-related reactions were reported in 42% of patients and were predominantly grade 1 or 2 (5% grade 3; no grade 4). The most common infusion-related reactions were nasal congestion (12%), throat irritation (7%), cough (6%), dyspnea (6%), chills (6%), and vomiting (6%)—all of which were treated with standard of care and slower infusion rates.
None of the patients discontinued daratumumab because of drug-related treatment-emergent AEs, infusion-related reactions, or death. However, 5% of patients discontinued treatment because of treatment-emergent AEs—2 cases of progressive disease and 1 case each of H1N1 influenza, hypercalcemia, and spinal cord compression.
Twenty-nine percent of patients died after treatment—27% due to progressive disease and 2% due to AEs. The 2 AEs were cardiorespiratory failure secondary to H1N1 influenza complications and general health deterioration secondary to complications of aspiration pneumonia. ![]()

© ASCO/Todd Buchanan
Single-agent daratumumab has exhibited “encouraging efficacy” and a “favorable safety profile” in patients with heavily pretreated and refractory multiple myeloma (MM), according to investigators from the phase 2 SIRIUS trial.
The drug produced an overall response rate of 30% in MM patients who had received 3 or more prior lines of therapy. The median progression-free survival was close to 4 months, and the median overall survival was nearly 18 months.
Thirty percent of patients had treatment-emergent serious adverse events (AEs), and 23% had grade 3 or 4 treatment-emergent serious AEs.
“This represents the first single-agent activity we have for a monoclonal antibody in treating multiple myeloma,” said study author Sagar Lonial, MD, of Emory University School of Medicine in Atlanta, Georgia.
“The future hope for daratumumab is in our ability to bring this active agent to earlier lines of therapy and combine it with drugs where you may get synergy.”
Dr Lonial and his colleagues reported results from the ongoing SIRIUS trial in The Lancet. Results from the trial were previously presented at the 2015 ASCO Annual Meeting. The research was funded by Janssen Research & Development, the company developing daratumumab.
In part 1 of the trial, 34 MM patients were randomized to receive either 8 mg/kg of daratumumab once every 4 weeks or 16 mg/kg once a week for 8 weeks, then once every 2 weeks for 16 weeks and once every 4 weeks after that, until disease progression or unacceptable toxicity.
In part 2, an additional 90 MM patients were enrolled and received 16 mg/kg of daratumumab on the same dosing schedule as in part 1.
Dr Lonial and his colleagues reported results for all patients who received 16 mg/kg of daratumumab. At the first interim analysis, the 8 mg/kg arm did not meet the criteria for expansion because the overall response rate was 11.1%.
The 106 patients who received the 16 mg/kg dose of daratumumab had received a median of 5 prior lines of therapy, including a proteasome inhibitor and an immunomodulatory drug. Ninety-seven percent of these patients were refractory to their last line of therapy, and 95% were refractory to both a proteasome inhibitor and an immunomodulatory drug.
Response and survival
According to an independent review committee, 29.2% of patients responded to daratumumab. Eighteen patients had a partial response, 10 had a very good partial response, and 3 had a stringent complete response.
The median duration of response was 7.4 months, and the median time to first response was 1 month.
The median overall survival was 17.5 months, and the 12-month overall survival was 64.8%. The median progression-free survival was 3.7 months.
Safety
The most common AEs were fatigue (40%), anemia (33%), nausea (29%), thrombocytopenia (25%), neutropenia (23%), back pain (22%), and cough (21%). Thirty percent of patients experienced serious AEs, and 23% had serious grade 3/4 AEs.
Infusion-related reactions were reported in 42% of patients and were predominantly grade 1 or 2 (5% grade 3; no grade 4). The most common infusion-related reactions were nasal congestion (12%), throat irritation (7%), cough (6%), dyspnea (6%), chills (6%), and vomiting (6%)—all of which were treated with standard of care and slower infusion rates.
None of the patients discontinued daratumumab because of drug-related treatment-emergent AEs, infusion-related reactions, or death. However, 5% of patients discontinued treatment because of treatment-emergent AEs—2 cases of progressive disease and 1 case each of H1N1 influenza, hypercalcemia, and spinal cord compression.
Twenty-nine percent of patients died after treatment—27% due to progressive disease and 2% due to AEs. The 2 AEs were cardiorespiratory failure secondary to H1N1 influenza complications and general health deterioration secondary to complications of aspiration pneumonia. ![]()

© ASCO/Todd Buchanan
Single-agent daratumumab has exhibited “encouraging efficacy” and a “favorable safety profile” in patients with heavily pretreated and refractory multiple myeloma (MM), according to investigators from the phase 2 SIRIUS trial.
The drug produced an overall response rate of 30% in MM patients who had received 3 or more prior lines of therapy. The median progression-free survival was close to 4 months, and the median overall survival was nearly 18 months.
Thirty percent of patients had treatment-emergent serious adverse events (AEs), and 23% had grade 3 or 4 treatment-emergent serious AEs.
“This represents the first single-agent activity we have for a monoclonal antibody in treating multiple myeloma,” said study author Sagar Lonial, MD, of Emory University School of Medicine in Atlanta, Georgia.
“The future hope for daratumumab is in our ability to bring this active agent to earlier lines of therapy and combine it with drugs where you may get synergy.”
Dr Lonial and his colleagues reported results from the ongoing SIRIUS trial in The Lancet. Results from the trial were previously presented at the 2015 ASCO Annual Meeting. The research was funded by Janssen Research & Development, the company developing daratumumab.
In part 1 of the trial, 34 MM patients were randomized to receive either 8 mg/kg of daratumumab once every 4 weeks or 16 mg/kg once a week for 8 weeks, then once every 2 weeks for 16 weeks and once every 4 weeks after that, until disease progression or unacceptable toxicity.
In part 2, an additional 90 MM patients were enrolled and received 16 mg/kg of daratumumab on the same dosing schedule as in part 1.
Dr Lonial and his colleagues reported results for all patients who received 16 mg/kg of daratumumab. At the first interim analysis, the 8 mg/kg arm did not meet the criteria for expansion because the overall response rate was 11.1%.
The 106 patients who received the 16 mg/kg dose of daratumumab had received a median of 5 prior lines of therapy, including a proteasome inhibitor and an immunomodulatory drug. Ninety-seven percent of these patients were refractory to their last line of therapy, and 95% were refractory to both a proteasome inhibitor and an immunomodulatory drug.
Response and survival
According to an independent review committee, 29.2% of patients responded to daratumumab. Eighteen patients had a partial response, 10 had a very good partial response, and 3 had a stringent complete response.
The median duration of response was 7.4 months, and the median time to first response was 1 month.
The median overall survival was 17.5 months, and the 12-month overall survival was 64.8%. The median progression-free survival was 3.7 months.
Safety
The most common AEs were fatigue (40%), anemia (33%), nausea (29%), thrombocytopenia (25%), neutropenia (23%), back pain (22%), and cough (21%). Thirty percent of patients experienced serious AEs, and 23% had serious grade 3/4 AEs.
Infusion-related reactions were reported in 42% of patients and were predominantly grade 1 or 2 (5% grade 3; no grade 4). The most common infusion-related reactions were nasal congestion (12%), throat irritation (7%), cough (6%), dyspnea (6%), chills (6%), and vomiting (6%)—all of which were treated with standard of care and slower infusion rates.
None of the patients discontinued daratumumab because of drug-related treatment-emergent AEs, infusion-related reactions, or death. However, 5% of patients discontinued treatment because of treatment-emergent AEs—2 cases of progressive disease and 1 case each of H1N1 influenza, hypercalcemia, and spinal cord compression.
Twenty-nine percent of patients died after treatment—27% due to progressive disease and 2% due to AEs. The 2 AEs were cardiorespiratory failure secondary to H1N1 influenza complications and general health deterioration secondary to complications of aspiration pneumonia. ![]()
Study links leukemia to low UVB exposure

People residing at higher latitudes, with lower exposure to sunlight/ultraviolet B (UVB) rays, have at least a 2-fold greater risk of developing leukemia than equatorial populations, according to research published in PLOS ONE.
“These results suggest that much of the burden of leukemia worldwide is due to the epidemic of vitamin D deficiency we are experiencing in winter in populations distant from the equator,” said Cedric Garland, DrPH, of the University of California San Diego in La Jolla, California.
“People who live in areas with low solar ultraviolet B exposure tend to have low levels of vitamin D metabolites in their blood. These low levels place them at high risk of certain cancers, including leukemia.”
Dr Garland and his colleagues analyzed age-adjusted incidence rates of leukemia in 172 countries and compared that information with cloud cover data from the International Satellite Cloud Climatology Project.
The team found that leukemia rates were highest in countries relatively closer to the poles, such as Australia, New Zealand, Chile, Ireland, Canada, and the United States.
And leukemia rates were lowest in countries closer to the equator, such as Bolivia, Samoa, Madagascar, and Nigeria.
The researchers also discovered that leukemia incidence was inversely associated with cloud-adjusted UVB irradiance in males (P≤0.01) and females (P≤0.01) in both hemispheres.
The association persisted in males (P≤0.05) and females (P≤0.01) after the team controlled for elevation and life expectancy.
The researchers said it’s plausible that the association is due to vitamin D deficiency.
This study follows similar investigations by Dr Garland and his colleagues in which they looked at other cancers, including breast, colon, pancreas, bladder, and multiple myeloma. In each study, the team found that reduced UVB radiation exposure and lower vitamin D levels were associated with higher risks of cancer.
“These studies do not necessarily provide final evidence,” Dr Garland said, “but they have been helpful in the past in identifying associations that have helped minimize cancer risk.” ![]()

People residing at higher latitudes, with lower exposure to sunlight/ultraviolet B (UVB) rays, have at least a 2-fold greater risk of developing leukemia than equatorial populations, according to research published in PLOS ONE.
“These results suggest that much of the burden of leukemia worldwide is due to the epidemic of vitamin D deficiency we are experiencing in winter in populations distant from the equator,” said Cedric Garland, DrPH, of the University of California San Diego in La Jolla, California.
“People who live in areas with low solar ultraviolet B exposure tend to have low levels of vitamin D metabolites in their blood. These low levels place them at high risk of certain cancers, including leukemia.”
Dr Garland and his colleagues analyzed age-adjusted incidence rates of leukemia in 172 countries and compared that information with cloud cover data from the International Satellite Cloud Climatology Project.
The team found that leukemia rates were highest in countries relatively closer to the poles, such as Australia, New Zealand, Chile, Ireland, Canada, and the United States.
And leukemia rates were lowest in countries closer to the equator, such as Bolivia, Samoa, Madagascar, and Nigeria.
The researchers also discovered that leukemia incidence was inversely associated with cloud-adjusted UVB irradiance in males (P≤0.01) and females (P≤0.01) in both hemispheres.
The association persisted in males (P≤0.05) and females (P≤0.01) after the team controlled for elevation and life expectancy.
The researchers said it’s plausible that the association is due to vitamin D deficiency.
This study follows similar investigations by Dr Garland and his colleagues in which they looked at other cancers, including breast, colon, pancreas, bladder, and multiple myeloma. In each study, the team found that reduced UVB radiation exposure and lower vitamin D levels were associated with higher risks of cancer.
“These studies do not necessarily provide final evidence,” Dr Garland said, “but they have been helpful in the past in identifying associations that have helped minimize cancer risk.” ![]()

People residing at higher latitudes, with lower exposure to sunlight/ultraviolet B (UVB) rays, have at least a 2-fold greater risk of developing leukemia than equatorial populations, according to research published in PLOS ONE.
“These results suggest that much of the burden of leukemia worldwide is due to the epidemic of vitamin D deficiency we are experiencing in winter in populations distant from the equator,” said Cedric Garland, DrPH, of the University of California San Diego in La Jolla, California.
“People who live in areas with low solar ultraviolet B exposure tend to have low levels of vitamin D metabolites in their blood. These low levels place them at high risk of certain cancers, including leukemia.”
Dr Garland and his colleagues analyzed age-adjusted incidence rates of leukemia in 172 countries and compared that information with cloud cover data from the International Satellite Cloud Climatology Project.
The team found that leukemia rates were highest in countries relatively closer to the poles, such as Australia, New Zealand, Chile, Ireland, Canada, and the United States.
And leukemia rates were lowest in countries closer to the equator, such as Bolivia, Samoa, Madagascar, and Nigeria.
The researchers also discovered that leukemia incidence was inversely associated with cloud-adjusted UVB irradiance in males (P≤0.01) and females (P≤0.01) in both hemispheres.
The association persisted in males (P≤0.05) and females (P≤0.01) after the team controlled for elevation and life expectancy.
The researchers said it’s plausible that the association is due to vitamin D deficiency.
This study follows similar investigations by Dr Garland and his colleagues in which they looked at other cancers, including breast, colon, pancreas, bladder, and multiple myeloma. In each study, the team found that reduced UVB radiation exposure and lower vitamin D levels were associated with higher risks of cancer.
“These studies do not necessarily provide final evidence,” Dr Garland said, “but they have been helpful in the past in identifying associations that have helped minimize cancer risk.” ![]()
How microbes drive progression of CTCL

New research indicates that toxins in Staphylococcus bacteria help malignant cells gain control over healthy cells in patients with cutaneous T-cell lymphoma (CTCL).
Investigators found that staphylococcal enterotoxin-A (SEA) induces STAT3 activation and IL-17 expression in malignant T cells via engagement of non-malignant CD4 T cells.
As STAT3 activation has been implicated in CTCL pathogenesis, the discovery suggests bacterial toxins play a key role in activating an oncogenic pathway in CTCL.
“We have gained important insight into the processes that activate cancer cells and make them grow,” said Niels Oedum, MD, of the University of Copenhagen in Denmark.
“[CTCL] patients’ frequent bacterial infections might not be a mere side effect of the disease. On the contrary, toxins in the bacteria actually ‘benefit’ cancer cells. Our next step is examining whether combatting infections can slow down the growth of cancer cells and thus stop the disease.”
Dr Oedum and his colleagues described their research in Blood.
The investigators knew that, in CTCL, CD4 T cells become malignant and turn parasitic on the rest of the immune system. In addition to using healthy cells to do their work for them, the malignant cells slowly destroy the skin’s immune defense mechanism.
The team’s new discoveries indicate that bacterial toxins in some patients enable malignant cells to send off signals that obstruct and change the immune defense mechanism, which would otherwise fight the malignant cells. What was believed to be an overly active immune defense mechanism could, in other words, turn out to be a malignant infection brought on by bacteria, which only worsens the disease.
Dr Oedum and his colleagues found that SEA-positive bacteria isolatated from the skin of CTCL patients stimulated activation of STAT3 and upregulation of IL-17 in malignant and non-malignant T cells.
Malignant T cells expressing an SEA non-responsive T-cell receptor V beta chain did not respond to SEA when cultured alone but exhibited STAT3 activation and IL-17 expression in co-cultures with SEA-responsive, non-malignant T cells.
The investigators found evidence to suggest the response is induced via IL-2Rg cytokines and a JAK3-dependent pathway in malignant T cells. The JAK3 inhibitor tofacitinib inhibited SEA-induced IL-17 production in co-cultures of malignant and non-malignant T cells.
Dr Oedum and his colleagues plan to continue their work investigating how bacteria might affect the balance between the immune defense mechanism and the disease in patients with CTCL.
In the long-term, the investigators’ aim is to understand how bacteria and their toxins can worsen CTCL, knowledge that may be used to develop new targeted treatments.
As only some of the bacteria produce toxins, the team said it will also be important to develop methods to determine which patients may benefit from treatment with antibiotics. ![]()

New research indicates that toxins in Staphylococcus bacteria help malignant cells gain control over healthy cells in patients with cutaneous T-cell lymphoma (CTCL).
Investigators found that staphylococcal enterotoxin-A (SEA) induces STAT3 activation and IL-17 expression in malignant T cells via engagement of non-malignant CD4 T cells.
As STAT3 activation has been implicated in CTCL pathogenesis, the discovery suggests bacterial toxins play a key role in activating an oncogenic pathway in CTCL.
“We have gained important insight into the processes that activate cancer cells and make them grow,” said Niels Oedum, MD, of the University of Copenhagen in Denmark.
“[CTCL] patients’ frequent bacterial infections might not be a mere side effect of the disease. On the contrary, toxins in the bacteria actually ‘benefit’ cancer cells. Our next step is examining whether combatting infections can slow down the growth of cancer cells and thus stop the disease.”
Dr Oedum and his colleagues described their research in Blood.
The investigators knew that, in CTCL, CD4 T cells become malignant and turn parasitic on the rest of the immune system. In addition to using healthy cells to do their work for them, the malignant cells slowly destroy the skin’s immune defense mechanism.
The team’s new discoveries indicate that bacterial toxins in some patients enable malignant cells to send off signals that obstruct and change the immune defense mechanism, which would otherwise fight the malignant cells. What was believed to be an overly active immune defense mechanism could, in other words, turn out to be a malignant infection brought on by bacteria, which only worsens the disease.
Dr Oedum and his colleagues found that SEA-positive bacteria isolatated from the skin of CTCL patients stimulated activation of STAT3 and upregulation of IL-17 in malignant and non-malignant T cells.
Malignant T cells expressing an SEA non-responsive T-cell receptor V beta chain did not respond to SEA when cultured alone but exhibited STAT3 activation and IL-17 expression in co-cultures with SEA-responsive, non-malignant T cells.
The investigators found evidence to suggest the response is induced via IL-2Rg cytokines and a JAK3-dependent pathway in malignant T cells. The JAK3 inhibitor tofacitinib inhibited SEA-induced IL-17 production in co-cultures of malignant and non-malignant T cells.
Dr Oedum and his colleagues plan to continue their work investigating how bacteria might affect the balance between the immune defense mechanism and the disease in patients with CTCL.
In the long-term, the investigators’ aim is to understand how bacteria and their toxins can worsen CTCL, knowledge that may be used to develop new targeted treatments.
As only some of the bacteria produce toxins, the team said it will also be important to develop methods to determine which patients may benefit from treatment with antibiotics. ![]()

New research indicates that toxins in Staphylococcus bacteria help malignant cells gain control over healthy cells in patients with cutaneous T-cell lymphoma (CTCL).
Investigators found that staphylococcal enterotoxin-A (SEA) induces STAT3 activation and IL-17 expression in malignant T cells via engagement of non-malignant CD4 T cells.
As STAT3 activation has been implicated in CTCL pathogenesis, the discovery suggests bacterial toxins play a key role in activating an oncogenic pathway in CTCL.
“We have gained important insight into the processes that activate cancer cells and make them grow,” said Niels Oedum, MD, of the University of Copenhagen in Denmark.
“[CTCL] patients’ frequent bacterial infections might not be a mere side effect of the disease. On the contrary, toxins in the bacteria actually ‘benefit’ cancer cells. Our next step is examining whether combatting infections can slow down the growth of cancer cells and thus stop the disease.”
Dr Oedum and his colleagues described their research in Blood.
The investigators knew that, in CTCL, CD4 T cells become malignant and turn parasitic on the rest of the immune system. In addition to using healthy cells to do their work for them, the malignant cells slowly destroy the skin’s immune defense mechanism.
The team’s new discoveries indicate that bacterial toxins in some patients enable malignant cells to send off signals that obstruct and change the immune defense mechanism, which would otherwise fight the malignant cells. What was believed to be an overly active immune defense mechanism could, in other words, turn out to be a malignant infection brought on by bacteria, which only worsens the disease.
Dr Oedum and his colleagues found that SEA-positive bacteria isolatated from the skin of CTCL patients stimulated activation of STAT3 and upregulation of IL-17 in malignant and non-malignant T cells.
Malignant T cells expressing an SEA non-responsive T-cell receptor V beta chain did not respond to SEA when cultured alone but exhibited STAT3 activation and IL-17 expression in co-cultures with SEA-responsive, non-malignant T cells.
The investigators found evidence to suggest the response is induced via IL-2Rg cytokines and a JAK3-dependent pathway in malignant T cells. The JAK3 inhibitor tofacitinib inhibited SEA-induced IL-17 production in co-cultures of malignant and non-malignant T cells.
Dr Oedum and his colleagues plan to continue their work investigating how bacteria might affect the balance between the immune defense mechanism and the disease in patients with CTCL.
In the long-term, the investigators’ aim is to understand how bacteria and their toxins can worsen CTCL, knowledge that may be used to develop new targeted treatments.
As only some of the bacteria produce toxins, the team said it will also be important to develop methods to determine which patients may benefit from treatment with antibiotics. ![]()
Cutting costs for cancer pts with comorbidities

Photo courtesy of the CDC
Patients with incurable cancer and multiple comorbidities who consulted with a palliative care team within 2 days of hospitalization had significant savings in hospital costs, according to a new study.
The study also showed that the higher number of comorbidities a patient had, the greater the reduction in direct hospital costs with early palliative care as opposed to standard care.
Previous studies have shown a link between palliative care and lower costs, but this is the first to examine whether the effect of palliative care consultation varies by the number of co-existing chronic conditions.
“We already know that coordinated, patient-centered palliative care improves care quality, enhances survival, and reduces costs for persons with cancer,” said R. Sean Morrison, MD, of the Icahn School of Medicine at Mount Sinai in New York, New York.
“Our latest research now shows the strong association between cost and the number of co-occurring conditions. Among patients with advanced cancer and other serious illnesses, aggressive treatments are often inconsistent with patients’ wishes and are associated with worse quality of life compared to other treatments. It is imperative that policymakers act to expand access to palliative care.”
Dr Morrison and his colleagues described their research in Health Affairs.
The study included 906 patients with advanced cancer and multiple comorbidities who were treated at 6 hospitals. One hundred and ninety-three patients were seen by a palliative care team within 2 days of hospitalization, while the remaining 713 patients received usual care.
Patients from the palliative care group had significantly lower total direct hospital costs if they had multimorbidity. For patients with a comorbidity score of 0–1, the estimated mean treatment effect was not significant.
However, patients with a comorbidity score of 2–3 had a 22% reduction in costs, or a reduction of $2321. Patients with a score of 4 or higher had a cost reduction of 32%, or $3515.
“The fact that we found greater cost savings for cancer patients with more comorbidities than for those with fewer comorbidities raises the question of whether similar results would be observed in patients with other serious illnesses and multimorbidity,” said Peter May, of Trinity College Dublin in Ireland.
“Future research is also needed to determine when in the course of illness palliative care is most cost-effective.” ![]()

Photo courtesy of the CDC
Patients with incurable cancer and multiple comorbidities who consulted with a palliative care team within 2 days of hospitalization had significant savings in hospital costs, according to a new study.
The study also showed that the higher number of comorbidities a patient had, the greater the reduction in direct hospital costs with early palliative care as opposed to standard care.
Previous studies have shown a link between palliative care and lower costs, but this is the first to examine whether the effect of palliative care consultation varies by the number of co-existing chronic conditions.
“We already know that coordinated, patient-centered palliative care improves care quality, enhances survival, and reduces costs for persons with cancer,” said R. Sean Morrison, MD, of the Icahn School of Medicine at Mount Sinai in New York, New York.
“Our latest research now shows the strong association between cost and the number of co-occurring conditions. Among patients with advanced cancer and other serious illnesses, aggressive treatments are often inconsistent with patients’ wishes and are associated with worse quality of life compared to other treatments. It is imperative that policymakers act to expand access to palliative care.”
Dr Morrison and his colleagues described their research in Health Affairs.
The study included 906 patients with advanced cancer and multiple comorbidities who were treated at 6 hospitals. One hundred and ninety-three patients were seen by a palliative care team within 2 days of hospitalization, while the remaining 713 patients received usual care.
Patients from the palliative care group had significantly lower total direct hospital costs if they had multimorbidity. For patients with a comorbidity score of 0–1, the estimated mean treatment effect was not significant.
However, patients with a comorbidity score of 2–3 had a 22% reduction in costs, or a reduction of $2321. Patients with a score of 4 or higher had a cost reduction of 32%, or $3515.
“The fact that we found greater cost savings for cancer patients with more comorbidities than for those with fewer comorbidities raises the question of whether similar results would be observed in patients with other serious illnesses and multimorbidity,” said Peter May, of Trinity College Dublin in Ireland.
“Future research is also needed to determine when in the course of illness palliative care is most cost-effective.” ![]()

Photo courtesy of the CDC
Patients with incurable cancer and multiple comorbidities who consulted with a palliative care team within 2 days of hospitalization had significant savings in hospital costs, according to a new study.
The study also showed that the higher number of comorbidities a patient had, the greater the reduction in direct hospital costs with early palliative care as opposed to standard care.
Previous studies have shown a link between palliative care and lower costs, but this is the first to examine whether the effect of palliative care consultation varies by the number of co-existing chronic conditions.
“We already know that coordinated, patient-centered palliative care improves care quality, enhances survival, and reduces costs for persons with cancer,” said R. Sean Morrison, MD, of the Icahn School of Medicine at Mount Sinai in New York, New York.
“Our latest research now shows the strong association between cost and the number of co-occurring conditions. Among patients with advanced cancer and other serious illnesses, aggressive treatments are often inconsistent with patients’ wishes and are associated with worse quality of life compared to other treatments. It is imperative that policymakers act to expand access to palliative care.”
Dr Morrison and his colleagues described their research in Health Affairs.
The study included 906 patients with advanced cancer and multiple comorbidities who were treated at 6 hospitals. One hundred and ninety-three patients were seen by a palliative care team within 2 days of hospitalization, while the remaining 713 patients received usual care.
Patients from the palliative care group had significantly lower total direct hospital costs if they had multimorbidity. For patients with a comorbidity score of 0–1, the estimated mean treatment effect was not significant.
However, patients with a comorbidity score of 2–3 had a 22% reduction in costs, or a reduction of $2321. Patients with a score of 4 or higher had a cost reduction of 32%, or $3515.
“The fact that we found greater cost savings for cancer patients with more comorbidities than for those with fewer comorbidities raises the question of whether similar results would be observed in patients with other serious illnesses and multimorbidity,” said Peter May, of Trinity College Dublin in Ireland.
“Future research is also needed to determine when in the course of illness palliative care is most cost-effective.” ![]()
Cardiac abnormalities among childhood cancer survivors

Photo by Bill Branson
A new study has provided additional insight into the development of cardiac abnormalities in adult survivors of childhood cancer.
Researchers analyzed more than 1800 cancer survivors who were exposed to cardiotoxic therapies as children.
The team said they found evidence of cardiac abnormalities in a substantial number of these subjects, many of whom were younger and did not exhibit symptoms of abnormalities.
Daniel A. Mulrooney, MD, of St. Jude Children’s Research Hospital in Memphis, Tennessee, and his colleagues reported these findings in Annals of Internal Medicine.
The team assessed cardiac outcomes among 1853 subjects who were 18 and older and had received cancer-related cardiotoxic therapy at least 10 years earlier.
The subjects were pretty evenly split along gender lines (52.3% male), their median age at cancer diagnosis was 8 (range, 0 to 24), and their median age at evaluation was 31 (range, 18 to 60).
At evaluation, 7.4% of subjects had cardiomyopathy (newly identified in 4.7%), 3.8% had coronary artery disease (newly identified in 2.2%), 28% had valvular regurgitation or stenosis (newly identified in 24.8%), and 4.4% had conduction or rhythm abnormalities (newly identified in 1.4%). All but 5 subjects were asymptomatic.
Multivariable analysis suggested the odds of developing cardiomyopathy were significantly associated with being male (odds ratio [OR]=1.9), receiving anthracycline doses of 250 mg/m2 or greater (OR=2.7), having cardiac radiation exposure greater than 1500 cGy (OR=1.9), and having hypertension (OR=3.0).
Being younger at diagnosis was associated with higher odds of valvular disease. The ORs were 1.5 for patients who were 0 to 4 years of age at diagnosis and 1.3 for patients who were 5 to 9 at diagnosis.
Receiving higher radiation doses was associated with higher odds of valvular disease as well. But associations between radiation and valvular disease varied according to a patient’s anthracycline exposure (interaction P<0.001). The highest odds were among survivors with the highest doses of radiation exposure and any anthracycline exposure (OR=4.5).
The researchers also noted a reduction in the OR for valvular disease among obese patients (OR=0.4) and those with dyslipidemia (OR=0.7).
The team said there were not enough cases of coronary artery disease and conduction or rhythm abnormalities to support a fully adjusted multivariable model. However, it seemed these outcomes were more common with older age (≥40 years) and among patients with cardiac radiation doses of 1500 cGy or greater.
The researchers said this study revealed “considerable cardiovascular disease” in a large cohort of adult survivors of childhood cancer, which suggests a substantial future healthcare burden.
The team believes their findings could guide stratification of risk factors, screening practices, health counseling, and potential therapeutic measures aimed at changing the disease trajectory in this young adult population. ![]()

Photo by Bill Branson
A new study has provided additional insight into the development of cardiac abnormalities in adult survivors of childhood cancer.
Researchers analyzed more than 1800 cancer survivors who were exposed to cardiotoxic therapies as children.
The team said they found evidence of cardiac abnormalities in a substantial number of these subjects, many of whom were younger and did not exhibit symptoms of abnormalities.
Daniel A. Mulrooney, MD, of St. Jude Children’s Research Hospital in Memphis, Tennessee, and his colleagues reported these findings in Annals of Internal Medicine.
The team assessed cardiac outcomes among 1853 subjects who were 18 and older and had received cancer-related cardiotoxic therapy at least 10 years earlier.
The subjects were pretty evenly split along gender lines (52.3% male), their median age at cancer diagnosis was 8 (range, 0 to 24), and their median age at evaluation was 31 (range, 18 to 60).
At evaluation, 7.4% of subjects had cardiomyopathy (newly identified in 4.7%), 3.8% had coronary artery disease (newly identified in 2.2%), 28% had valvular regurgitation or stenosis (newly identified in 24.8%), and 4.4% had conduction or rhythm abnormalities (newly identified in 1.4%). All but 5 subjects were asymptomatic.
Multivariable analysis suggested the odds of developing cardiomyopathy were significantly associated with being male (odds ratio [OR]=1.9), receiving anthracycline doses of 250 mg/m2 or greater (OR=2.7), having cardiac radiation exposure greater than 1500 cGy (OR=1.9), and having hypertension (OR=3.0).
Being younger at diagnosis was associated with higher odds of valvular disease. The ORs were 1.5 for patients who were 0 to 4 years of age at diagnosis and 1.3 for patients who were 5 to 9 at diagnosis.
Receiving higher radiation doses was associated with higher odds of valvular disease as well. But associations between radiation and valvular disease varied according to a patient’s anthracycline exposure (interaction P<0.001). The highest odds were among survivors with the highest doses of radiation exposure and any anthracycline exposure (OR=4.5).
The researchers also noted a reduction in the OR for valvular disease among obese patients (OR=0.4) and those with dyslipidemia (OR=0.7).
The team said there were not enough cases of coronary artery disease and conduction or rhythm abnormalities to support a fully adjusted multivariable model. However, it seemed these outcomes were more common with older age (≥40 years) and among patients with cardiac radiation doses of 1500 cGy or greater.
The researchers said this study revealed “considerable cardiovascular disease” in a large cohort of adult survivors of childhood cancer, which suggests a substantial future healthcare burden.
The team believes their findings could guide stratification of risk factors, screening practices, health counseling, and potential therapeutic measures aimed at changing the disease trajectory in this young adult population. ![]()

Photo by Bill Branson
A new study has provided additional insight into the development of cardiac abnormalities in adult survivors of childhood cancer.
Researchers analyzed more than 1800 cancer survivors who were exposed to cardiotoxic therapies as children.
The team said they found evidence of cardiac abnormalities in a substantial number of these subjects, many of whom were younger and did not exhibit symptoms of abnormalities.
Daniel A. Mulrooney, MD, of St. Jude Children’s Research Hospital in Memphis, Tennessee, and his colleagues reported these findings in Annals of Internal Medicine.
The team assessed cardiac outcomes among 1853 subjects who were 18 and older and had received cancer-related cardiotoxic therapy at least 10 years earlier.
The subjects were pretty evenly split along gender lines (52.3% male), their median age at cancer diagnosis was 8 (range, 0 to 24), and their median age at evaluation was 31 (range, 18 to 60).
At evaluation, 7.4% of subjects had cardiomyopathy (newly identified in 4.7%), 3.8% had coronary artery disease (newly identified in 2.2%), 28% had valvular regurgitation or stenosis (newly identified in 24.8%), and 4.4% had conduction or rhythm abnormalities (newly identified in 1.4%). All but 5 subjects were asymptomatic.
Multivariable analysis suggested the odds of developing cardiomyopathy were significantly associated with being male (odds ratio [OR]=1.9), receiving anthracycline doses of 250 mg/m2 or greater (OR=2.7), having cardiac radiation exposure greater than 1500 cGy (OR=1.9), and having hypertension (OR=3.0).
Being younger at diagnosis was associated with higher odds of valvular disease. The ORs were 1.5 for patients who were 0 to 4 years of age at diagnosis and 1.3 for patients who were 5 to 9 at diagnosis.
Receiving higher radiation doses was associated with higher odds of valvular disease as well. But associations between radiation and valvular disease varied according to a patient’s anthracycline exposure (interaction P<0.001). The highest odds were among survivors with the highest doses of radiation exposure and any anthracycline exposure (OR=4.5).
The researchers also noted a reduction in the OR for valvular disease among obese patients (OR=0.4) and those with dyslipidemia (OR=0.7).
The team said there were not enough cases of coronary artery disease and conduction or rhythm abnormalities to support a fully adjusted multivariable model. However, it seemed these outcomes were more common with older age (≥40 years) and among patients with cardiac radiation doses of 1500 cGy or greater.
The researchers said this study revealed “considerable cardiovascular disease” in a large cohort of adult survivors of childhood cancer, which suggests a substantial future healthcare burden.
The team believes their findings could guide stratification of risk factors, screening practices, health counseling, and potential therapeutic measures aimed at changing the disease trajectory in this young adult population.
Novel delivery system could treat MCL
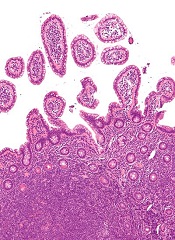
Researchers say they have developed a system for delivering therapy at the site of mantle cell lymphoma (MCL).
The system harnesses nanoparticles coated with “GPS” antibodies that navigate toward cancerous cells, where they offload cyclin D1-blockers in the form of small interfering RNAs (siRNAs).
Experiments showed the system can halt the proliferation of cyclin D1 in both animal models and samples from MCL patients.
Dan Peer, PhD, of Tel Aviv University in Israel, and his colleagues reported these results in PNAS.
“MCL has a genetic hallmark,” Dr Peer noted. “In 85% of cases, the characteristic that defines this aggressive and prototypic B-cell lymphoma is the heightened activity of the gene CCND1, which leads to the extreme overexpression—a 3000- to 15,000-fold increase—of cyclin D1, a protein that controls the proliferation of cells. Downregulation of cyclin D1 using siRNAs is a potential therapeutic approach to this malignancy.”
For this research, Dr Peer and his colleagues designed lipid-based nanoparticles (LNPs) coated with anti-CD38 monoclonal antibodies that were taken up by human MCL cells in the bone marrow of affected mice.
When loaded with siRNAs against cyclin D1, the targeting LNPs induced gene silencing in MCL cells and prolonged the survival of tumor-bearing mice, with no observed adverse effects.
“In MCL, cyclin D1 is the exclusive cause of the overproduction of B lymphocytes, the cells responsible for generating antibodies,” Dr Peer said. “This makes the protein a perfect target for RNA therapy by siRNAs.”
“Normal, healthy cells don’t express the gene, so therapies that destroy the gene will only attack cancer cells. The RNA interference we have developed targets the faulty cyclin D1 within the cancerous cells. And when the cells are inhibited from proliferating, they sense they are being targeted and begin to die off.”
Dr Peer and his colleagues believe this work presents new opportunities for treating MCL and other similar B-cell malignancies.
“This research makes a definite contribution to the revolution of personalized medicine, whereby you tailor the drug based on the genetic profile of patient,” Dr Peer said. “In this case, MCL is a disease with a specific genetic hallmark, so you can sequence the patient to identify the mutation(s) and design RNA blockers to be placed inside a nanovehicle.”
“While the targeting antibodies—the ‘GPS’—can be used to target many different B-cell malignancies, the drug itself is designed to silence this specific disease. However, the delivery system can be used to accommodate any disease with a genetic profile. This could be the future. We are seeing it happen before our very eyes.”

Researchers say they have developed a system for delivering therapy at the site of mantle cell lymphoma (MCL).
The system harnesses nanoparticles coated with “GPS” antibodies that navigate toward cancerous cells, where they offload cyclin D1-blockers in the form of small interfering RNAs (siRNAs).
Experiments showed the system can halt the proliferation of cyclin D1 in both animal models and samples from MCL patients.
Dan Peer, PhD, of Tel Aviv University in Israel, and his colleagues reported these results in PNAS.
“MCL has a genetic hallmark,” Dr Peer noted. “In 85% of cases, the characteristic that defines this aggressive and prototypic B-cell lymphoma is the heightened activity of the gene CCND1, which leads to the extreme overexpression—a 3000- to 15,000-fold increase—of cyclin D1, a protein that controls the proliferation of cells. Downregulation of cyclin D1 using siRNAs is a potential therapeutic approach to this malignancy.”
For this research, Dr Peer and his colleagues designed lipid-based nanoparticles (LNPs) coated with anti-CD38 monoclonal antibodies that were taken up by human MCL cells in the bone marrow of affected mice.
When loaded with siRNAs against cyclin D1, the targeting LNPs induced gene silencing in MCL cells and prolonged the survival of tumor-bearing mice, with no observed adverse effects.
“In MCL, cyclin D1 is the exclusive cause of the overproduction of B lymphocytes, the cells responsible for generating antibodies,” Dr Peer said. “This makes the protein a perfect target for RNA therapy by siRNAs.”
“Normal, healthy cells don’t express the gene, so therapies that destroy the gene will only attack cancer cells. The RNA interference we have developed targets the faulty cyclin D1 within the cancerous cells. And when the cells are inhibited from proliferating, they sense they are being targeted and begin to die off.”
Dr Peer and his colleagues believe this work presents new opportunities for treating MCL and other similar B-cell malignancies.
“This research makes a definite contribution to the revolution of personalized medicine, whereby you tailor the drug based on the genetic profile of patient,” Dr Peer said. “In this case, MCL is a disease with a specific genetic hallmark, so you can sequence the patient to identify the mutation(s) and design RNA blockers to be placed inside a nanovehicle.”
“While the targeting antibodies—the ‘GPS’—can be used to target many different B-cell malignancies, the drug itself is designed to silence this specific disease. However, the delivery system can be used to accommodate any disease with a genetic profile. This could be the future. We are seeing it happen before our very eyes.”

Researchers say they have developed a system for delivering therapy at the site of mantle cell lymphoma (MCL).
The system harnesses nanoparticles coated with “GPS” antibodies that navigate toward cancerous cells, where they offload cyclin D1-blockers in the form of small interfering RNAs (siRNAs).
Experiments showed the system can halt the proliferation of cyclin D1 in both animal models and samples from MCL patients.
Dan Peer, PhD, of Tel Aviv University in Israel, and his colleagues reported these results in PNAS.
“MCL has a genetic hallmark,” Dr Peer noted. “In 85% of cases, the characteristic that defines this aggressive and prototypic B-cell lymphoma is the heightened activity of the gene CCND1, which leads to the extreme overexpression—a 3000- to 15,000-fold increase—of cyclin D1, a protein that controls the proliferation of cells. Downregulation of cyclin D1 using siRNAs is a potential therapeutic approach to this malignancy.”
For this research, Dr Peer and his colleagues designed lipid-based nanoparticles (LNPs) coated with anti-CD38 monoclonal antibodies that were taken up by human MCL cells in the bone marrow of affected mice.
When loaded with siRNAs against cyclin D1, the targeting LNPs induced gene silencing in MCL cells and prolonged the survival of tumor-bearing mice, with no observed adverse effects.
“In MCL, cyclin D1 is the exclusive cause of the overproduction of B lymphocytes, the cells responsible for generating antibodies,” Dr Peer said. “This makes the protein a perfect target for RNA therapy by siRNAs.”
“Normal, healthy cells don’t express the gene, so therapies that destroy the gene will only attack cancer cells. The RNA interference we have developed targets the faulty cyclin D1 within the cancerous cells. And when the cells are inhibited from proliferating, they sense they are being targeted and begin to die off.”
Dr Peer and his colleagues believe this work presents new opportunities for treating MCL and other similar B-cell malignancies.
“This research makes a definite contribution to the revolution of personalized medicine, whereby you tailor the drug based on the genetic profile of patient,” Dr Peer said. “In this case, MCL is a disease with a specific genetic hallmark, so you can sequence the patient to identify the mutation(s) and design RNA blockers to be placed inside a nanovehicle.”
“While the targeting antibodies—the ‘GPS’—can be used to target many different B-cell malignancies, the drug itself is designed to silence this specific disease. However, the delivery system can be used to accommodate any disease with a genetic profile. This could be the future. We are seeing it happen before our very eyes.”
Paste may reduce radiation-induced fibrosis

woman for radiation
Photo by Rhoda Baer
A topical paste can reduce fibrosis caused by radiation therapy, according to preclinical research published in The FASEB Journal.
The study addressed a type of fibrosis called radiation dermatitis, in which radiation applied to the skin causes the buildup of fibrotic tissue and skin thickening.
To test their topical paste, researchers mimicked the development of radiation dermatitis in mice.
They exposed the mice’s skin to a single dose of 40 Gy, an amount of radiation similar to what patients undergoing anticancer radiation typically receive over 5 weeks.
Some of the irradiated animals were wild-type mice, while others were genetically engineered to lack the A2A receptor (A2AR). The researchers had previously shown that occupancy of A2AR induces collagen production.
The wild-type mice went on to receive placebo or daily treatment with ZM241385, a paste made with the research team’s patented A2AR blocker. The paste contains 2.5 milligrams of active ingredient per milliliter of 3% carboxymethyl cellulose, a gum “binder.”
A month after exposure, wild-type mice that received placebo had a nearly 2-fold increase in the amount of collagen and skin thickness. These mice also experienced epithelial hyperplasia.
On the other hand, mice treated with ZM241385 accumulated only 10% more skin-thickening collagen. ZM241385 treatment reduced the number of myofibroblasts, collagen fibrils, proliferating keratinocytes, and angiogenesis when compared to placebo. And the paste prevented epithelial hyperplasia.
Like ZM241385-treated mice, A2AR knockout mice did not have the excessive collagen production and skin thickening observed in placebo-treated wild-type mice. The knockout mice also exhibited reductions in myofibroblast content, angiogenesis, and epithelial hyperplasia.
The researchers noted that radiation-induced changes in the dermis and epidermis were accompanied by an infiltrate of T cells, which was prevented in both ZM241385-treated and A2AR knockout mice.
“Our latest study is the first to demonstrate that blocking or deleting the A2A receptor can be useful in reducing radiation-induced scarring in skin,” said study author Bruce Cronstein, MD, of New York University School of Medicine in New York, New York.
“The study also suggests that adenosine A2A receptor antagonists may have broad applications as drug therapies for preventing fibrosis and scarring, not just in the liver but also in the skin.”
If further experiments prove successful, Dr Cronstein said, clinicians treating early stage cancers with radiation could eventually prescribe an A2AR inhibitor paste to prevent fibrosis. He said his team next plans to study the mechanism underlying A2AR’s role in fibrosis.

woman for radiation
Photo by Rhoda Baer
A topical paste can reduce fibrosis caused by radiation therapy, according to preclinical research published in The FASEB Journal.
The study addressed a type of fibrosis called radiation dermatitis, in which radiation applied to the skin causes the buildup of fibrotic tissue and skin thickening.
To test their topical paste, researchers mimicked the development of radiation dermatitis in mice.
They exposed the mice’s skin to a single dose of 40 Gy, an amount of radiation similar to what patients undergoing anticancer radiation typically receive over 5 weeks.
Some of the irradiated animals were wild-type mice, while others were genetically engineered to lack the A2A receptor (A2AR). The researchers had previously shown that occupancy of A2AR induces collagen production.
The wild-type mice went on to receive placebo or daily treatment with ZM241385, a paste made with the research team’s patented A2AR blocker. The paste contains 2.5 milligrams of active ingredient per milliliter of 3% carboxymethyl cellulose, a gum “binder.”
A month after exposure, wild-type mice that received placebo had a nearly 2-fold increase in the amount of collagen and skin thickness. These mice also experienced epithelial hyperplasia.
On the other hand, mice treated with ZM241385 accumulated only 10% more skin-thickening collagen. ZM241385 treatment reduced the number of myofibroblasts, collagen fibrils, proliferating keratinocytes, and angiogenesis when compared to placebo. And the paste prevented epithelial hyperplasia.
Like ZM241385-treated mice, A2AR knockout mice did not have the excessive collagen production and skin thickening observed in placebo-treated wild-type mice. The knockout mice also exhibited reductions in myofibroblast content, angiogenesis, and epithelial hyperplasia.
The researchers noted that radiation-induced changes in the dermis and epidermis were accompanied by an infiltrate of T cells, which was prevented in both ZM241385-treated and A2AR knockout mice.
“Our latest study is the first to demonstrate that blocking or deleting the A2A receptor can be useful in reducing radiation-induced scarring in skin,” said study author Bruce Cronstein, MD, of New York University School of Medicine in New York, New York.
“The study also suggests that adenosine A2A receptor antagonists may have broad applications as drug therapies for preventing fibrosis and scarring, not just in the liver but also in the skin.”
If further experiments prove successful, Dr Cronstein said, clinicians treating early stage cancers with radiation could eventually prescribe an A2AR inhibitor paste to prevent fibrosis. He said his team next plans to study the mechanism underlying A2AR’s role in fibrosis.

woman for radiation
Photo by Rhoda Baer
A topical paste can reduce fibrosis caused by radiation therapy, according to preclinical research published in The FASEB Journal.
The study addressed a type of fibrosis called radiation dermatitis, in which radiation applied to the skin causes the buildup of fibrotic tissue and skin thickening.
To test their topical paste, researchers mimicked the development of radiation dermatitis in mice.
They exposed the mice’s skin to a single dose of 40 Gy, an amount of radiation similar to what patients undergoing anticancer radiation typically receive over 5 weeks.
Some of the irradiated animals were wild-type mice, while others were genetically engineered to lack the A2A receptor (A2AR). The researchers had previously shown that occupancy of A2AR induces collagen production.
The wild-type mice went on to receive placebo or daily treatment with ZM241385, a paste made with the research team’s patented A2AR blocker. The paste contains 2.5 milligrams of active ingredient per milliliter of 3% carboxymethyl cellulose, a gum “binder.”
A month after exposure, wild-type mice that received placebo had a nearly 2-fold increase in the amount of collagen and skin thickness. These mice also experienced epithelial hyperplasia.
On the other hand, mice treated with ZM241385 accumulated only 10% more skin-thickening collagen. ZM241385 treatment reduced the number of myofibroblasts, collagen fibrils, proliferating keratinocytes, and angiogenesis when compared to placebo. And the paste prevented epithelial hyperplasia.
Like ZM241385-treated mice, A2AR knockout mice did not have the excessive collagen production and skin thickening observed in placebo-treated wild-type mice. The knockout mice also exhibited reductions in myofibroblast content, angiogenesis, and epithelial hyperplasia.
The researchers noted that radiation-induced changes in the dermis and epidermis were accompanied by an infiltrate of T cells, which was prevented in both ZM241385-treated and A2AR knockout mice.
“Our latest study is the first to demonstrate that blocking or deleting the A2A receptor can be useful in reducing radiation-induced scarring in skin,” said study author Bruce Cronstein, MD, of New York University School of Medicine in New York, New York.
“The study also suggests that adenosine A2A receptor antagonists may have broad applications as drug therapies for preventing fibrosis and scarring, not just in the liver but also in the skin.”
If further experiments prove successful, Dr Cronstein said, clinicians treating early stage cancers with radiation could eventually prescribe an A2AR inhibitor paste to prevent fibrosis. He said his team next plans to study the mechanism underlying A2AR’s role in fibrosis.
Why cancer cells thrive when blood sugar is high

Photo by Andre Karwath
New research has revealed a mechanism that allows cancer cells to respond and grow rapidly when blood sugar levels rise.
This may help to explain why people who develop conditions in which they have chronically high blood sugar levels, such as obesity, also have an increased risk of developing certain cancers.
Susumu Hirabayashi, PhD, of Imperial College London in the UK, and Ross Cagan, PhD, of Mount Sinai Hospital in New York, New York, described the mechanism in eLife.
In a study published 2 years ago, the pair engineered fruit flies (Drosophila melanogaster) to activate the genes Ras and Src, which are activated in a range of malignancies.
The researchers activated Ras and Src in the flies’ developing eye tissue. Flies that were fed a normal diet grew small, benign tumors. But when flies were fed a high-sugar diet, they developed large, malignant tumors.
In flies fed a high-sugar diet, the normal cells became insulin-resistant, but the tumor cells didn’t. The tumor cells actually became more sensitive to insulin because they turned on a metabolic switch that triggered them to produce extra receptors for insulin. But this study did not explain how the tumor cells turned on this metabolic switch.
Now, after studying the same flies in more detail, Drs Hirabayashi and Cagan have found the tumor cells detect glucose availability indirectly, through a protein called salt-inducible kinase (SIK). When glucose levels are high, SIK sends a signal along the Hippo signaling pathway.
The Hippo signaling pathway is known to play a role in controlling cell growth. When it’s turned on, it keeps cell growth under control, but if it’s turned off, the cell can continue growing and may ultimately develop into a tumor.
Drs Hirabayashi and Cagan found that SIK acts like a sugar sensor, turning the Hippo signaling pathway off in response to raised glucose levels. This allows the tumor cells to continue to grow.
“Ras and Src co-activated tumors use SIK to sense that there’s lots of glucose available outside of their cells and to tell the cells to take advantage of that,” Dr Hirabayashi said. “Together, Ras and Src co-activated tumors use SIK to efficiently respond to glucose availability and ensure the tumors grow in nutrient-rich conditions such as obesity. We still don’t know if tumors caused by other genes respond to sugar in the same way.”
“Our results suggest that if we can develop drugs to target SIK, and stop it from alerting cancer cells in this way, then we may be able to stop cancer cells from thriving in an insulin-resistant environment and break the connection between obesity and cancer.”

Photo by Andre Karwath
New research has revealed a mechanism that allows cancer cells to respond and grow rapidly when blood sugar levels rise.
This may help to explain why people who develop conditions in which they have chronically high blood sugar levels, such as obesity, also have an increased risk of developing certain cancers.
Susumu Hirabayashi, PhD, of Imperial College London in the UK, and Ross Cagan, PhD, of Mount Sinai Hospital in New York, New York, described the mechanism in eLife.
In a study published 2 years ago, the pair engineered fruit flies (Drosophila melanogaster) to activate the genes Ras and Src, which are activated in a range of malignancies.
The researchers activated Ras and Src in the flies’ developing eye tissue. Flies that were fed a normal diet grew small, benign tumors. But when flies were fed a high-sugar diet, they developed large, malignant tumors.
In flies fed a high-sugar diet, the normal cells became insulin-resistant, but the tumor cells didn’t. The tumor cells actually became more sensitive to insulin because they turned on a metabolic switch that triggered them to produce extra receptors for insulin. But this study did not explain how the tumor cells turned on this metabolic switch.
Now, after studying the same flies in more detail, Drs Hirabayashi and Cagan have found the tumor cells detect glucose availability indirectly, through a protein called salt-inducible kinase (SIK). When glucose levels are high, SIK sends a signal along the Hippo signaling pathway.
The Hippo signaling pathway is known to play a role in controlling cell growth. When it’s turned on, it keeps cell growth under control, but if it’s turned off, the cell can continue growing and may ultimately develop into a tumor.
Drs Hirabayashi and Cagan found that SIK acts like a sugar sensor, turning the Hippo signaling pathway off in response to raised glucose levels. This allows the tumor cells to continue to grow.
“Ras and Src co-activated tumors use SIK to sense that there’s lots of glucose available outside of their cells and to tell the cells to take advantage of that,” Dr Hirabayashi said. “Together, Ras and Src co-activated tumors use SIK to efficiently respond to glucose availability and ensure the tumors grow in nutrient-rich conditions such as obesity. We still don’t know if tumors caused by other genes respond to sugar in the same way.”
“Our results suggest that if we can develop drugs to target SIK, and stop it from alerting cancer cells in this way, then we may be able to stop cancer cells from thriving in an insulin-resistant environment and break the connection between obesity and cancer.”

Photo by Andre Karwath
New research has revealed a mechanism that allows cancer cells to respond and grow rapidly when blood sugar levels rise.
This may help to explain why people who develop conditions in which they have chronically high blood sugar levels, such as obesity, also have an increased risk of developing certain cancers.
Susumu Hirabayashi, PhD, of Imperial College London in the UK, and Ross Cagan, PhD, of Mount Sinai Hospital in New York, New York, described the mechanism in eLife.
In a study published 2 years ago, the pair engineered fruit flies (Drosophila melanogaster) to activate the genes Ras and Src, which are activated in a range of malignancies.
The researchers activated Ras and Src in the flies’ developing eye tissue. Flies that were fed a normal diet grew small, benign tumors. But when flies were fed a high-sugar diet, they developed large, malignant tumors.
In flies fed a high-sugar diet, the normal cells became insulin-resistant, but the tumor cells didn’t. The tumor cells actually became more sensitive to insulin because they turned on a metabolic switch that triggered them to produce extra receptors for insulin. But this study did not explain how the tumor cells turned on this metabolic switch.
Now, after studying the same flies in more detail, Drs Hirabayashi and Cagan have found the tumor cells detect glucose availability indirectly, through a protein called salt-inducible kinase (SIK). When glucose levels are high, SIK sends a signal along the Hippo signaling pathway.
The Hippo signaling pathway is known to play a role in controlling cell growth. When it’s turned on, it keeps cell growth under control, but if it’s turned off, the cell can continue growing and may ultimately develop into a tumor.
Drs Hirabayashi and Cagan found that SIK acts like a sugar sensor, turning the Hippo signaling pathway off in response to raised glucose levels. This allows the tumor cells to continue to grow.
“Ras and Src co-activated tumors use SIK to sense that there’s lots of glucose available outside of their cells and to tell the cells to take advantage of that,” Dr Hirabayashi said. “Together, Ras and Src co-activated tumors use SIK to efficiently respond to glucose availability and ensure the tumors grow in nutrient-rich conditions such as obesity. We still don’t know if tumors caused by other genes respond to sugar in the same way.”
“Our results suggest that if we can develop drugs to target SIK, and stop it from alerting cancer cells in this way, then we may be able to stop cancer cells from thriving in an insulin-resistant environment and break the connection between obesity and cancer.”