User login
HSC self-renewal depends on surroundings

in the bone marrow
Scientists say that, using a model of the hematopoietic system, they have determined which signaling pathways play an essential role in the self-renewal of hematopoietic stem cells (HSCs).
They found that a particularly important role in this process is the interactive communication with surrounding tissue cells in the bone marrow.
Robert Oostendorp, PhD, of Klinikum Rechts der Isar der Technischen Universität München in Munich, Germany, and his colleagues described these findings in Stem Cell Reports.
The team noted that, in steady-state conditions, HSCs are maintained as slow-dividing clones of quiescent cells. However, when stress occurs, such as an accident that leads to substantial blood loss or the defense against a pathogen requires more blood cells in the course of an infection, HSCs are activated.
In response, the entire hematopoietic system switches from “standby” mode into a state of alert. The activated HSCs generate new blood cells to counteract the blood loss or combat the pathogen. At the same time, self-renewal keeps the stem cell pool replenished.
This switch is accompanied by a complex communication process between the HSCs and tissue cells—an area that had not previously been examined in depth.
“In our study, we set out to establish which tissue signals are important to stem cell maintenance and functionality, and which HSC signals influence the microenvironment,” Dr Oostendorp said.
He and his colleagues used mixed cultures of tissue cells and HSCs to investigate how these cell types interact.
The scientists analyzed factors that are upregulated or downregulated in the interplay between tissue cells and HSCs. And they linked these findings with the signaling pathways described in existing literature.
The team then consolidated this information in a bioinformatics computer model. And they conducted extensive cell experiments to confirm the computer-generated signaling pathway model.
“The outcome was very interesting indeed,” Dr Oostendorp said. “The entire system operates in a feedback loop. In ‘alert’ mode, the stem cells first influence the behavior of the tissue cells, which, in turn, impact on the stem cells, triggering the self-renewal step.”
In alert mode, HSCs emit signaling substances, which induce tissue cells to release the connective tissue growth factor (CTGF) messenger. This is essential to maintain the HSCs through self-renewal. In the absence of CTGF, HSCs age and cannot replenish the stem cell pool.
“Our findings could prove significant in treating leukemia,” Dr Oostendorp noted. “In this condition, the stem cells are hyperactive, and their division is unchecked. Leukemic blood cells are in a constant state of alert, so we would expect a similar interplay with the tissue cells.”
To date, however, the focus here has been limited to stem cells as the actual source of the defect.
“Given what we know now about feedback loops, it would be important to integrate the surrounding cells in therapeutic approaches too, since they exert a strong influence on stem cell division,” Dr Oostendorp concluded. ![]()

in the bone marrow
Scientists say that, using a model of the hematopoietic system, they have determined which signaling pathways play an essential role in the self-renewal of hematopoietic stem cells (HSCs).
They found that a particularly important role in this process is the interactive communication with surrounding tissue cells in the bone marrow.
Robert Oostendorp, PhD, of Klinikum Rechts der Isar der Technischen Universität München in Munich, Germany, and his colleagues described these findings in Stem Cell Reports.
The team noted that, in steady-state conditions, HSCs are maintained as slow-dividing clones of quiescent cells. However, when stress occurs, such as an accident that leads to substantial blood loss or the defense against a pathogen requires more blood cells in the course of an infection, HSCs are activated.
In response, the entire hematopoietic system switches from “standby” mode into a state of alert. The activated HSCs generate new blood cells to counteract the blood loss or combat the pathogen. At the same time, self-renewal keeps the stem cell pool replenished.
This switch is accompanied by a complex communication process between the HSCs and tissue cells—an area that had not previously been examined in depth.
“In our study, we set out to establish which tissue signals are important to stem cell maintenance and functionality, and which HSC signals influence the microenvironment,” Dr Oostendorp said.
He and his colleagues used mixed cultures of tissue cells and HSCs to investigate how these cell types interact.
The scientists analyzed factors that are upregulated or downregulated in the interplay between tissue cells and HSCs. And they linked these findings with the signaling pathways described in existing literature.
The team then consolidated this information in a bioinformatics computer model. And they conducted extensive cell experiments to confirm the computer-generated signaling pathway model.
“The outcome was very interesting indeed,” Dr Oostendorp said. “The entire system operates in a feedback loop. In ‘alert’ mode, the stem cells first influence the behavior of the tissue cells, which, in turn, impact on the stem cells, triggering the self-renewal step.”
In alert mode, HSCs emit signaling substances, which induce tissue cells to release the connective tissue growth factor (CTGF) messenger. This is essential to maintain the HSCs through self-renewal. In the absence of CTGF, HSCs age and cannot replenish the stem cell pool.
“Our findings could prove significant in treating leukemia,” Dr Oostendorp noted. “In this condition, the stem cells are hyperactive, and their division is unchecked. Leukemic blood cells are in a constant state of alert, so we would expect a similar interplay with the tissue cells.”
To date, however, the focus here has been limited to stem cells as the actual source of the defect.
“Given what we know now about feedback loops, it would be important to integrate the surrounding cells in therapeutic approaches too, since they exert a strong influence on stem cell division,” Dr Oostendorp concluded. ![]()

in the bone marrow
Scientists say that, using a model of the hematopoietic system, they have determined which signaling pathways play an essential role in the self-renewal of hematopoietic stem cells (HSCs).
They found that a particularly important role in this process is the interactive communication with surrounding tissue cells in the bone marrow.
Robert Oostendorp, PhD, of Klinikum Rechts der Isar der Technischen Universität München in Munich, Germany, and his colleagues described these findings in Stem Cell Reports.
The team noted that, in steady-state conditions, HSCs are maintained as slow-dividing clones of quiescent cells. However, when stress occurs, such as an accident that leads to substantial blood loss or the defense against a pathogen requires more blood cells in the course of an infection, HSCs are activated.
In response, the entire hematopoietic system switches from “standby” mode into a state of alert. The activated HSCs generate new blood cells to counteract the blood loss or combat the pathogen. At the same time, self-renewal keeps the stem cell pool replenished.
This switch is accompanied by a complex communication process between the HSCs and tissue cells—an area that had not previously been examined in depth.
“In our study, we set out to establish which tissue signals are important to stem cell maintenance and functionality, and which HSC signals influence the microenvironment,” Dr Oostendorp said.
He and his colleagues used mixed cultures of tissue cells and HSCs to investigate how these cell types interact.
The scientists analyzed factors that are upregulated or downregulated in the interplay between tissue cells and HSCs. And they linked these findings with the signaling pathways described in existing literature.
The team then consolidated this information in a bioinformatics computer model. And they conducted extensive cell experiments to confirm the computer-generated signaling pathway model.
“The outcome was very interesting indeed,” Dr Oostendorp said. “The entire system operates in a feedback loop. In ‘alert’ mode, the stem cells first influence the behavior of the tissue cells, which, in turn, impact on the stem cells, triggering the self-renewal step.”
In alert mode, HSCs emit signaling substances, which induce tissue cells to release the connective tissue growth factor (CTGF) messenger. This is essential to maintain the HSCs through self-renewal. In the absence of CTGF, HSCs age and cannot replenish the stem cell pool.
“Our findings could prove significant in treating leukemia,” Dr Oostendorp noted. “In this condition, the stem cells are hyperactive, and their division is unchecked. Leukemic blood cells are in a constant state of alert, so we would expect a similar interplay with the tissue cells.”
To date, however, the focus here has been limited to stem cells as the actual source of the defect.
“Given what we know now about feedback loops, it would be important to integrate the surrounding cells in therapeutic approaches too, since they exert a strong influence on stem cell division,” Dr Oostendorp concluded. ![]()
Experiment reveals new method of RBC production

Photo courtesy of
Josh Barney/University of
Virginia Health System
An unexpected result of a lab experiment has led researchers to a new way to trigger red blood cell (RBC) production.
They found that engaging a stress receptor on type 1 conventional dendritic cells can induce stress erythropoiesis in mice.
The team believes that, eventually, this method could be used to turn on RBC production in humans when necessary, perhaps to replace a blood transfusion or as a stop-gap measure when a transfusion is delayed.
Thomas J. Braciale, MD, PhD, of the University of Virginia in Charlottesville, and his colleagues conducted this research and reported the results in The Journal of Clinical Investigation.
The team was not investigating RBC production when they made their discovery. They were looking into the role of dendritic cells in the lungs.
Dendritic cells have traditionally been thought to be sensors of infection and inflammation, but a lab test involving the flu virus produced an unexpected effect in mice that ultimately revealed a new aspect to the cells’ function.
The researchers injected mice with the flu virus and an αCD24 monoclonal antibody, which resulted in splenomegaly. The team was baffled at this outcome, so they repeated the experiment, only to get the same results.
“We did it again, and I didn’t believe it, and we did it again, and I didn’t believe it,” Dr Braciale recalled. “I asked whether you needed flu to infect the mice when you injected this antibody. So the postdoc did the experiment, and he just injected the antibody without flu-injecting the mice—giant spleens. After much consultation, after talking with my colleagues in pathology, we decided we were inducing stress erythropoiesis.”
Specifically, the researchers found that engaging CD24 on type 1 conventional dendritic cells upregulates expression of the Kit ligand stem cell factor, which results in Kit-mediated proliferative expansion of early erythroid progenitors and transient reticulocytosis.
“In a very basic way, what we’ve discovered is that the process of regulating stress in the body is mediated—certainly in part, at least—by these dendritic cells,” Dr Braciale explained. “And stress can be a variety of different stresses.”
“It doesn’t have to be infection. It doesn’t have to be inflammation. It can be anemia. It can be hemorrhage. And these cells act to initiate this response that, until this report, there’s been really no evidence that [dendritic] cells ever participate in making red blood cells.”
More work is needed before this approach to RBC production can be tested in humans. However, Dr Braciale is optimistic, based on the findings so far.
“We’re very excited to see where this goes,” he said. “We know that the same things can be done in humans in the following sense. There are mice called humanized mice. These are mice that are engineered so they have a human blood system. And if you inject these mice with this antibody, they’ll make red blood cells.” ![]()

Photo courtesy of
Josh Barney/University of
Virginia Health System
An unexpected result of a lab experiment has led researchers to a new way to trigger red blood cell (RBC) production.
They found that engaging a stress receptor on type 1 conventional dendritic cells can induce stress erythropoiesis in mice.
The team believes that, eventually, this method could be used to turn on RBC production in humans when necessary, perhaps to replace a blood transfusion or as a stop-gap measure when a transfusion is delayed.
Thomas J. Braciale, MD, PhD, of the University of Virginia in Charlottesville, and his colleagues conducted this research and reported the results in The Journal of Clinical Investigation.
The team was not investigating RBC production when they made their discovery. They were looking into the role of dendritic cells in the lungs.
Dendritic cells have traditionally been thought to be sensors of infection and inflammation, but a lab test involving the flu virus produced an unexpected effect in mice that ultimately revealed a new aspect to the cells’ function.
The researchers injected mice with the flu virus and an αCD24 monoclonal antibody, which resulted in splenomegaly. The team was baffled at this outcome, so they repeated the experiment, only to get the same results.
“We did it again, and I didn’t believe it, and we did it again, and I didn’t believe it,” Dr Braciale recalled. “I asked whether you needed flu to infect the mice when you injected this antibody. So the postdoc did the experiment, and he just injected the antibody without flu-injecting the mice—giant spleens. After much consultation, after talking with my colleagues in pathology, we decided we were inducing stress erythropoiesis.”
Specifically, the researchers found that engaging CD24 on type 1 conventional dendritic cells upregulates expression of the Kit ligand stem cell factor, which results in Kit-mediated proliferative expansion of early erythroid progenitors and transient reticulocytosis.
“In a very basic way, what we’ve discovered is that the process of regulating stress in the body is mediated—certainly in part, at least—by these dendritic cells,” Dr Braciale explained. “And stress can be a variety of different stresses.”
“It doesn’t have to be infection. It doesn’t have to be inflammation. It can be anemia. It can be hemorrhage. And these cells act to initiate this response that, until this report, there’s been really no evidence that [dendritic] cells ever participate in making red blood cells.”
More work is needed before this approach to RBC production can be tested in humans. However, Dr Braciale is optimistic, based on the findings so far.
“We’re very excited to see where this goes,” he said. “We know that the same things can be done in humans in the following sense. There are mice called humanized mice. These are mice that are engineered so they have a human blood system. And if you inject these mice with this antibody, they’ll make red blood cells.” ![]()

Photo courtesy of
Josh Barney/University of
Virginia Health System
An unexpected result of a lab experiment has led researchers to a new way to trigger red blood cell (RBC) production.
They found that engaging a stress receptor on type 1 conventional dendritic cells can induce stress erythropoiesis in mice.
The team believes that, eventually, this method could be used to turn on RBC production in humans when necessary, perhaps to replace a blood transfusion or as a stop-gap measure when a transfusion is delayed.
Thomas J. Braciale, MD, PhD, of the University of Virginia in Charlottesville, and his colleagues conducted this research and reported the results in The Journal of Clinical Investigation.
The team was not investigating RBC production when they made their discovery. They were looking into the role of dendritic cells in the lungs.
Dendritic cells have traditionally been thought to be sensors of infection and inflammation, but a lab test involving the flu virus produced an unexpected effect in mice that ultimately revealed a new aspect to the cells’ function.
The researchers injected mice with the flu virus and an αCD24 monoclonal antibody, which resulted in splenomegaly. The team was baffled at this outcome, so they repeated the experiment, only to get the same results.
“We did it again, and I didn’t believe it, and we did it again, and I didn’t believe it,” Dr Braciale recalled. “I asked whether you needed flu to infect the mice when you injected this antibody. So the postdoc did the experiment, and he just injected the antibody without flu-injecting the mice—giant spleens. After much consultation, after talking with my colleagues in pathology, we decided we were inducing stress erythropoiesis.”
Specifically, the researchers found that engaging CD24 on type 1 conventional dendritic cells upregulates expression of the Kit ligand stem cell factor, which results in Kit-mediated proliferative expansion of early erythroid progenitors and transient reticulocytosis.
“In a very basic way, what we’ve discovered is that the process of regulating stress in the body is mediated—certainly in part, at least—by these dendritic cells,” Dr Braciale explained. “And stress can be a variety of different stresses.”
“It doesn’t have to be infection. It doesn’t have to be inflammation. It can be anemia. It can be hemorrhage. And these cells act to initiate this response that, until this report, there’s been really no evidence that [dendritic] cells ever participate in making red blood cells.”
More work is needed before this approach to RBC production can be tested in humans. However, Dr Braciale is optimistic, based on the findings so far.
“We’re very excited to see where this goes,” he said. “We know that the same things can be done in humans in the following sense. There are mice called humanized mice. These are mice that are engineered so they have a human blood system. And if you inject these mice with this antibody, they’ll make red blood cells.” ![]()
EC expands indication for azacitidine in AML

The European Commission (EC) has expanded the approved indication for azacitidine for injection (Vidaza) in acute myeloid leukemia (AML).
Now, the drug is approved to treat AML patients age 65 and older who are ineligible for hematopoietic stem cell transplant (HSCT) and have more than 30% myeloblasts according to the WHO classification.
Previously, HSCT-ineligible elderly AML patients could only receive azacitidine if they had less than 30% blasts.
Because this new indication for azacitidine is thought to bring significant clinical benefit in comparison with existing therapies, the drug will receive extended market protection in all its indications for an additional year throughout the European Economic Area.
In addition to the aforementioned AML indications, azacitidine is approved in the European Economic Area to treat HSCT-ineligible adults with intermediate-2- and high-risk myelodysplastic syndromes and HSCT-ineligible adults who have chronic myelomonocytic leukemia and 10%-29% marrow blasts without myeloproliferative disorder.
Azacitidine is marketed as Vidaza by Celgene.
AML-001 trial
The EC’s recommendation to expand the indication of azacitidine in AML was based on data from the AML-001 trial. This randomized study included patients age 65 and older with newly diagnosed or secondary AML with greater than 30% blasts.
Patients were pre-selected to receive 1 of 3 regimens per investigator’s choice. This included intensive chemotherapy (standard 7+3 regimen), low-dose cytarabine (20 mg subcutaneously twice a day for 10 days of each 28-day cycle), or best supportive care only.
Patients were then randomized to receive either azacitidine (75 mg/m2/day subcutaneously for 7 days of each 28-day cycle, n=241) or their predetermined conventional care regimen (CCR, n=247).
Median overall survival, the study’s primary endpoint, was 10.4 months for patients receiving azacitidine and 6.5 months for patients receiving CCR (hazard ratio=0.85, P=0.1009).
One-year survival rates with azacitidine and CCR were 46.5% and 34.2%, respectively.
Grade 3/4 anemia occurred in 16% of patients who received azacitidine, 5% who received best supportive care, 23% who received low-dose cytarabine, and 14% who received intensive chemotherapy.
Grade 3/4 neutropenia occurred in 26%, 5%, 25%, and 33% of patients, respectively. Grade 3/4 febrile neutropenia occurred in 28%, 28%, 30%, and 31%, respectively. And grade 3/4 thrombocytopenia occurred in 24%, 5%, 28%, and 21%, respectively. ![]()

The European Commission (EC) has expanded the approved indication for azacitidine for injection (Vidaza) in acute myeloid leukemia (AML).
Now, the drug is approved to treat AML patients age 65 and older who are ineligible for hematopoietic stem cell transplant (HSCT) and have more than 30% myeloblasts according to the WHO classification.
Previously, HSCT-ineligible elderly AML patients could only receive azacitidine if they had less than 30% blasts.
Because this new indication for azacitidine is thought to bring significant clinical benefit in comparison with existing therapies, the drug will receive extended market protection in all its indications for an additional year throughout the European Economic Area.
In addition to the aforementioned AML indications, azacitidine is approved in the European Economic Area to treat HSCT-ineligible adults with intermediate-2- and high-risk myelodysplastic syndromes and HSCT-ineligible adults who have chronic myelomonocytic leukemia and 10%-29% marrow blasts without myeloproliferative disorder.
Azacitidine is marketed as Vidaza by Celgene.
AML-001 trial
The EC’s recommendation to expand the indication of azacitidine in AML was based on data from the AML-001 trial. This randomized study included patients age 65 and older with newly diagnosed or secondary AML with greater than 30% blasts.
Patients were pre-selected to receive 1 of 3 regimens per investigator’s choice. This included intensive chemotherapy (standard 7+3 regimen), low-dose cytarabine (20 mg subcutaneously twice a day for 10 days of each 28-day cycle), or best supportive care only.
Patients were then randomized to receive either azacitidine (75 mg/m2/day subcutaneously for 7 days of each 28-day cycle, n=241) or their predetermined conventional care regimen (CCR, n=247).
Median overall survival, the study’s primary endpoint, was 10.4 months for patients receiving azacitidine and 6.5 months for patients receiving CCR (hazard ratio=0.85, P=0.1009).
One-year survival rates with azacitidine and CCR were 46.5% and 34.2%, respectively.
Grade 3/4 anemia occurred in 16% of patients who received azacitidine, 5% who received best supportive care, 23% who received low-dose cytarabine, and 14% who received intensive chemotherapy.
Grade 3/4 neutropenia occurred in 26%, 5%, 25%, and 33% of patients, respectively. Grade 3/4 febrile neutropenia occurred in 28%, 28%, 30%, and 31%, respectively. And grade 3/4 thrombocytopenia occurred in 24%, 5%, 28%, and 21%, respectively. ![]()

The European Commission (EC) has expanded the approved indication for azacitidine for injection (Vidaza) in acute myeloid leukemia (AML).
Now, the drug is approved to treat AML patients age 65 and older who are ineligible for hematopoietic stem cell transplant (HSCT) and have more than 30% myeloblasts according to the WHO classification.
Previously, HSCT-ineligible elderly AML patients could only receive azacitidine if they had less than 30% blasts.
Because this new indication for azacitidine is thought to bring significant clinical benefit in comparison with existing therapies, the drug will receive extended market protection in all its indications for an additional year throughout the European Economic Area.
In addition to the aforementioned AML indications, azacitidine is approved in the European Economic Area to treat HSCT-ineligible adults with intermediate-2- and high-risk myelodysplastic syndromes and HSCT-ineligible adults who have chronic myelomonocytic leukemia and 10%-29% marrow blasts without myeloproliferative disorder.
Azacitidine is marketed as Vidaza by Celgene.
AML-001 trial
The EC’s recommendation to expand the indication of azacitidine in AML was based on data from the AML-001 trial. This randomized study included patients age 65 and older with newly diagnosed or secondary AML with greater than 30% blasts.
Patients were pre-selected to receive 1 of 3 regimens per investigator’s choice. This included intensive chemotherapy (standard 7+3 regimen), low-dose cytarabine (20 mg subcutaneously twice a day for 10 days of each 28-day cycle), or best supportive care only.
Patients were then randomized to receive either azacitidine (75 mg/m2/day subcutaneously for 7 days of each 28-day cycle, n=241) or their predetermined conventional care regimen (CCR, n=247).
Median overall survival, the study’s primary endpoint, was 10.4 months for patients receiving azacitidine and 6.5 months for patients receiving CCR (hazard ratio=0.85, P=0.1009).
One-year survival rates with azacitidine and CCR were 46.5% and 34.2%, respectively.
Grade 3/4 anemia occurred in 16% of patients who received azacitidine, 5% who received best supportive care, 23% who received low-dose cytarabine, and 14% who received intensive chemotherapy.
Grade 3/4 neutropenia occurred in 26%, 5%, 25%, and 33% of patients, respectively. Grade 3/4 febrile neutropenia occurred in 28%, 28%, 30%, and 31%, respectively. And grade 3/4 thrombocytopenia occurred in 24%, 5%, 28%, and 21%, respectively. ![]()
France to lift lifetime ban on MSM blood donors
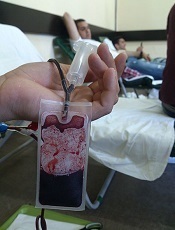
Photo by Михаило Јовановић
France is planning to lift its lifetime ban on blood donations from men who have sex with men (MSM), and the change is set to take effect next year.
French officials say that, beginning in Spring 2016, an MSM will be able to donate whole blood in France if he has not had sex with another man in the last 12
months.
An MSM will be allowed to donate plasma if he has been abstinent or had only 1 sexual partner in the last 4 months.
Experts will analyze the impact of this policy change for about a year. If there has been no increase in health risks, the policy may be relaxed further, and MSM donors may be treated the same as non-MSM donors.
Non-MSM individuals in France are deferred from donating blood if they have had more than 1 sexual partner in the last 4 months.
Studies recently conducted in Canada and the UK have suggested that lifting restrictions on MSM blood donors does not
increase the risk of sexually transmitted infections affecting the blood
supply.
France’s lifetime ban on MSM blood donation was enacted in 1983 in an attempt to counter the spread of HIV/AIDS.
Hundreds of people died in France in the 1980s after HIV-tainted blood was distributed by the French National Blood Transfusion Center. HIV-positive blood donations were exported as well, which led to hundreds of additional deaths in other countries.
Bans lifting worldwide
In lifting its lifetime ban on MSM blood donors, France is following the lead of other countries within and outside of Europe.
England, Scotland, Wales, Sweden, and the Netherlands have all lifted their bans on MSM blood donors and changed to a 12-month deferral period. Australia, Japan, and New Zealand also have 12-month deferral periods for MSM blood donors.
South Africa has a 6-month deferral period for MSMs, while Italy and Spain have no policy specific to MSM blood donors. All donors are screened for high-risk sexual practices, and deferrals are made accordingly.
The US and Canada are currently considering adopting a 12-month deferral policy for MSM blood donors. The lifetime ban is still in place in the US, but Canada has a 5-year deferral period for MSMs. ![]()

Photo by Михаило Јовановић
France is planning to lift its lifetime ban on blood donations from men who have sex with men (MSM), and the change is set to take effect next year.
French officials say that, beginning in Spring 2016, an MSM will be able to donate whole blood in France if he has not had sex with another man in the last 12
months.
An MSM will be allowed to donate plasma if he has been abstinent or had only 1 sexual partner in the last 4 months.
Experts will analyze the impact of this policy change for about a year. If there has been no increase in health risks, the policy may be relaxed further, and MSM donors may be treated the same as non-MSM donors.
Non-MSM individuals in France are deferred from donating blood if they have had more than 1 sexual partner in the last 4 months.
Studies recently conducted in Canada and the UK have suggested that lifting restrictions on MSM blood donors does not
increase the risk of sexually transmitted infections affecting the blood
supply.
France’s lifetime ban on MSM blood donation was enacted in 1983 in an attempt to counter the spread of HIV/AIDS.
Hundreds of people died in France in the 1980s after HIV-tainted blood was distributed by the French National Blood Transfusion Center. HIV-positive blood donations were exported as well, which led to hundreds of additional deaths in other countries.
Bans lifting worldwide
In lifting its lifetime ban on MSM blood donors, France is following the lead of other countries within and outside of Europe.
England, Scotland, Wales, Sweden, and the Netherlands have all lifted their bans on MSM blood donors and changed to a 12-month deferral period. Australia, Japan, and New Zealand also have 12-month deferral periods for MSM blood donors.
South Africa has a 6-month deferral period for MSMs, while Italy and Spain have no policy specific to MSM blood donors. All donors are screened for high-risk sexual practices, and deferrals are made accordingly.
The US and Canada are currently considering adopting a 12-month deferral policy for MSM blood donors. The lifetime ban is still in place in the US, but Canada has a 5-year deferral period for MSMs. ![]()

Photo by Михаило Јовановић
France is planning to lift its lifetime ban on blood donations from men who have sex with men (MSM), and the change is set to take effect next year.
French officials say that, beginning in Spring 2016, an MSM will be able to donate whole blood in France if he has not had sex with another man in the last 12
months.
An MSM will be allowed to donate plasma if he has been abstinent or had only 1 sexual partner in the last 4 months.
Experts will analyze the impact of this policy change for about a year. If there has been no increase in health risks, the policy may be relaxed further, and MSM donors may be treated the same as non-MSM donors.
Non-MSM individuals in France are deferred from donating blood if they have had more than 1 sexual partner in the last 4 months.
Studies recently conducted in Canada and the UK have suggested that lifting restrictions on MSM blood donors does not
increase the risk of sexually transmitted infections affecting the blood
supply.
France’s lifetime ban on MSM blood donation was enacted in 1983 in an attempt to counter the spread of HIV/AIDS.
Hundreds of people died in France in the 1980s after HIV-tainted blood was distributed by the French National Blood Transfusion Center. HIV-positive blood donations were exported as well, which led to hundreds of additional deaths in other countries.
Bans lifting worldwide
In lifting its lifetime ban on MSM blood donors, France is following the lead of other countries within and outside of Europe.
England, Scotland, Wales, Sweden, and the Netherlands have all lifted their bans on MSM blood donors and changed to a 12-month deferral period. Australia, Japan, and New Zealand also have 12-month deferral periods for MSM blood donors.
South Africa has a 6-month deferral period for MSMs, while Italy and Spain have no policy specific to MSM blood donors. All donors are screened for high-risk sexual practices, and deferrals are made accordingly.
The US and Canada are currently considering adopting a 12-month deferral policy for MSM blood donors. The lifetime ban is still in place in the US, but Canada has a 5-year deferral period for MSMs. ![]()
Duo solves mystery regarding FVIII

Turner and Joel Moake
Photo from Rice University
A pair of researchers solved a long-standing mystery about where factor VIII (FVIII) is made, stored, and deployed in the body, according to an article published in PLOS ONE.
The duo found that FVIII is synthesized in glomerular microvascular endothelial cells (GMVECs) and human umbilical vein endothelial cells (HUVECs).
FVIII and von Willebrand factor (VWF) are stored in Weibel-Palade bodies (WPBs) in both of these cell types. And stimulated GMVECs and HUVECs secrete cell-anchored, ultra-large VWF strings with FVIII bound to them.
The researchers said these findings may lead to improved therapy for hemophilia A.
“Great clinical advances have been made over the past 50 years, in spite of our lack of understanding of where FVIII was made and stored,” said study author Joel Moake, MD, of Rice University in Houston, Texas.
“Understanding how the body makes, stores, and deploys the protein will be increasingly important in the future as physicians look to develop gene therapies that could free patients from a reliance on regular injections of FVIII.”
The FVIII research in Dr Moake’s lab began in early 2014 and was based on a hunch by lead author Nancy Turner, who specializes in the study of endothelial cells.
“Endothelial cells are the gate-controllers for the blood system, and, to me, they make all the exciting proteins,” she said. “They’re right on the surface next to the blood, and they constantly interact with the plasma. Similar to circulating cells, they produce their own defensive proteins to fight infections.”
Though Turner had not previously studied FVIII, she had done extensive experiments on VWF, which is made in endothelial cells and stored in WPBs. And VWF and FVIII are often bound together.
Based on her prior work, Turner was intrigued by a pair of 2014 studies that examined FVIII in mouse endothelial cells and showed that FVIII was produced in the endothelial cells within the liver, and not in the liver cells.
“They stopped short of saying that FVIII was stored in endothelial cells, but they suggested the possibility,” she said. “One of the papers was very elegant, and I liked it a lot, but it made a statement that really bothered me.”
The paper explained that FVIII had been found in a half-dozen types of endothelial cell types, but never HUVECs, the type of endothelial cell found in large veins.
“HUVECs are the generic human endothelial cells that [researchers] use the first time they do anything,” Turner said. “They’re cheap. They’re easy to work with, and they’ve been the model for endothelial cells for, I don’t know, at least 50 years.”
“So far, everything I’ve ever looked at in endothelial cells has been consistent. The different types might have different amounts of something, but they’re very similar. There hasn’t been anything that was wholly different from one type to another. Not yet. So I thought, ‘OK, fine. I’m already doing gene-expression experiments. I might as well just throw FVIII in there and see.”
The experiments she was conducting involved both HUVECs and GMVECs, which are found in the smallest capillaries of the kidney. Turner was conducting an extensive analysis to see how protein production differed in the 2 varieties.
She examined the cells for FVIII messenger RNA and found that it was present, which meant it was possible the cells were making the protein. She then ordered a fluorescent antibody designed to detect FVIII.
“I did the experiment and looked, and not only was it there, but it was bright, easy to see, and it worked perfectly the first time,” Turner said. “I thought, ‘What have people been doing for 20 or 30 years? Why couldn’t they see this?’ And then I thought, ‘This was too easy. No one is going to believe me.’”
So Turner set about running controls to rule out mistakes. Were the antibodies interfering with one another? Was there any contamination? Was the microscope working correctly? Could the reading be a false-positive, an inadvertent result of another reaction she hadn’t expected?
“No. 1, I had to convince myself,” she said. “I am always skeptical if something is too easy. I have reviewed many, many papers, and I can always find what people do wrong.”
Once she had convinced herself, she and Dr Moake had to convince the paper’s referees. As she’d expected, they were skeptical. She said the bulk of the work over the past year involved doing a number of controls to remove any doubts about the findings.
In the end, the research confirmed that FVIII was made in both HUVECs and GMVECs. Moreover, Turner found that FVIII, like VWF, is both stored and secreted from WPBs.
Dr Moake said the discovery has clear implications for any future treatments that aim to repair genetic defects in patients with hemophilia A.
“Now that we recognize that FVIII is normally synthesized in endothelial cells and stored in Weibel-Palade bodies,” Dr Moake said, “those become the precise, most effective physiological targets for gene delivery.” ![]()

Turner and Joel Moake
Photo from Rice University
A pair of researchers solved a long-standing mystery about where factor VIII (FVIII) is made, stored, and deployed in the body, according to an article published in PLOS ONE.
The duo found that FVIII is synthesized in glomerular microvascular endothelial cells (GMVECs) and human umbilical vein endothelial cells (HUVECs).
FVIII and von Willebrand factor (VWF) are stored in Weibel-Palade bodies (WPBs) in both of these cell types. And stimulated GMVECs and HUVECs secrete cell-anchored, ultra-large VWF strings with FVIII bound to them.
The researchers said these findings may lead to improved therapy for hemophilia A.
“Great clinical advances have been made over the past 50 years, in spite of our lack of understanding of where FVIII was made and stored,” said study author Joel Moake, MD, of Rice University in Houston, Texas.
“Understanding how the body makes, stores, and deploys the protein will be increasingly important in the future as physicians look to develop gene therapies that could free patients from a reliance on regular injections of FVIII.”
The FVIII research in Dr Moake’s lab began in early 2014 and was based on a hunch by lead author Nancy Turner, who specializes in the study of endothelial cells.
“Endothelial cells are the gate-controllers for the blood system, and, to me, they make all the exciting proteins,” she said. “They’re right on the surface next to the blood, and they constantly interact with the plasma. Similar to circulating cells, they produce their own defensive proteins to fight infections.”
Though Turner had not previously studied FVIII, she had done extensive experiments on VWF, which is made in endothelial cells and stored in WPBs. And VWF and FVIII are often bound together.
Based on her prior work, Turner was intrigued by a pair of 2014 studies that examined FVIII in mouse endothelial cells and showed that FVIII was produced in the endothelial cells within the liver, and not in the liver cells.
“They stopped short of saying that FVIII was stored in endothelial cells, but they suggested the possibility,” she said. “One of the papers was very elegant, and I liked it a lot, but it made a statement that really bothered me.”
The paper explained that FVIII had been found in a half-dozen types of endothelial cell types, but never HUVECs, the type of endothelial cell found in large veins.
“HUVECs are the generic human endothelial cells that [researchers] use the first time they do anything,” Turner said. “They’re cheap. They’re easy to work with, and they’ve been the model for endothelial cells for, I don’t know, at least 50 years.”
“So far, everything I’ve ever looked at in endothelial cells has been consistent. The different types might have different amounts of something, but they’re very similar. There hasn’t been anything that was wholly different from one type to another. Not yet. So I thought, ‘OK, fine. I’m already doing gene-expression experiments. I might as well just throw FVIII in there and see.”
The experiments she was conducting involved both HUVECs and GMVECs, which are found in the smallest capillaries of the kidney. Turner was conducting an extensive analysis to see how protein production differed in the 2 varieties.
She examined the cells for FVIII messenger RNA and found that it was present, which meant it was possible the cells were making the protein. She then ordered a fluorescent antibody designed to detect FVIII.
“I did the experiment and looked, and not only was it there, but it was bright, easy to see, and it worked perfectly the first time,” Turner said. “I thought, ‘What have people been doing for 20 or 30 years? Why couldn’t they see this?’ And then I thought, ‘This was too easy. No one is going to believe me.’”
So Turner set about running controls to rule out mistakes. Were the antibodies interfering with one another? Was there any contamination? Was the microscope working correctly? Could the reading be a false-positive, an inadvertent result of another reaction she hadn’t expected?
“No. 1, I had to convince myself,” she said. “I am always skeptical if something is too easy. I have reviewed many, many papers, and I can always find what people do wrong.”
Once she had convinced herself, she and Dr Moake had to convince the paper’s referees. As she’d expected, they were skeptical. She said the bulk of the work over the past year involved doing a number of controls to remove any doubts about the findings.
In the end, the research confirmed that FVIII was made in both HUVECs and GMVECs. Moreover, Turner found that FVIII, like VWF, is both stored and secreted from WPBs.
Dr Moake said the discovery has clear implications for any future treatments that aim to repair genetic defects in patients with hemophilia A.
“Now that we recognize that FVIII is normally synthesized in endothelial cells and stored in Weibel-Palade bodies,” Dr Moake said, “those become the precise, most effective physiological targets for gene delivery.” ![]()

Turner and Joel Moake
Photo from Rice University
A pair of researchers solved a long-standing mystery about where factor VIII (FVIII) is made, stored, and deployed in the body, according to an article published in PLOS ONE.
The duo found that FVIII is synthesized in glomerular microvascular endothelial cells (GMVECs) and human umbilical vein endothelial cells (HUVECs).
FVIII and von Willebrand factor (VWF) are stored in Weibel-Palade bodies (WPBs) in both of these cell types. And stimulated GMVECs and HUVECs secrete cell-anchored, ultra-large VWF strings with FVIII bound to them.
The researchers said these findings may lead to improved therapy for hemophilia A.
“Great clinical advances have been made over the past 50 years, in spite of our lack of understanding of where FVIII was made and stored,” said study author Joel Moake, MD, of Rice University in Houston, Texas.
“Understanding how the body makes, stores, and deploys the protein will be increasingly important in the future as physicians look to develop gene therapies that could free patients from a reliance on regular injections of FVIII.”
The FVIII research in Dr Moake’s lab began in early 2014 and was based on a hunch by lead author Nancy Turner, who specializes in the study of endothelial cells.
“Endothelial cells are the gate-controllers for the blood system, and, to me, they make all the exciting proteins,” she said. “They’re right on the surface next to the blood, and they constantly interact with the plasma. Similar to circulating cells, they produce their own defensive proteins to fight infections.”
Though Turner had not previously studied FVIII, she had done extensive experiments on VWF, which is made in endothelial cells and stored in WPBs. And VWF and FVIII are often bound together.
Based on her prior work, Turner was intrigued by a pair of 2014 studies that examined FVIII in mouse endothelial cells and showed that FVIII was produced in the endothelial cells within the liver, and not in the liver cells.
“They stopped short of saying that FVIII was stored in endothelial cells, but they suggested the possibility,” she said. “One of the papers was very elegant, and I liked it a lot, but it made a statement that really bothered me.”
The paper explained that FVIII had been found in a half-dozen types of endothelial cell types, but never HUVECs, the type of endothelial cell found in large veins.
“HUVECs are the generic human endothelial cells that [researchers] use the first time they do anything,” Turner said. “They’re cheap. They’re easy to work with, and they’ve been the model for endothelial cells for, I don’t know, at least 50 years.”
“So far, everything I’ve ever looked at in endothelial cells has been consistent. The different types might have different amounts of something, but they’re very similar. There hasn’t been anything that was wholly different from one type to another. Not yet. So I thought, ‘OK, fine. I’m already doing gene-expression experiments. I might as well just throw FVIII in there and see.”
The experiments she was conducting involved both HUVECs and GMVECs, which are found in the smallest capillaries of the kidney. Turner was conducting an extensive analysis to see how protein production differed in the 2 varieties.
She examined the cells for FVIII messenger RNA and found that it was present, which meant it was possible the cells were making the protein. She then ordered a fluorescent antibody designed to detect FVIII.
“I did the experiment and looked, and not only was it there, but it was bright, easy to see, and it worked perfectly the first time,” Turner said. “I thought, ‘What have people been doing for 20 or 30 years? Why couldn’t they see this?’ And then I thought, ‘This was too easy. No one is going to believe me.’”
So Turner set about running controls to rule out mistakes. Were the antibodies interfering with one another? Was there any contamination? Was the microscope working correctly? Could the reading be a false-positive, an inadvertent result of another reaction she hadn’t expected?
“No. 1, I had to convince myself,” she said. “I am always skeptical if something is too easy. I have reviewed many, many papers, and I can always find what people do wrong.”
Once she had convinced herself, she and Dr Moake had to convince the paper’s referees. As she’d expected, they were skeptical. She said the bulk of the work over the past year involved doing a number of controls to remove any doubts about the findings.
In the end, the research confirmed that FVIII was made in both HUVECs and GMVECs. Moreover, Turner found that FVIII, like VWF, is both stored and secreted from WPBs.
Dr Moake said the discovery has clear implications for any future treatments that aim to repair genetic defects in patients with hemophilia A.
“Now that we recognize that FVIII is normally synthesized in endothelial cells and stored in Weibel-Palade bodies,” Dr Moake said, “those become the precise, most effective physiological targets for gene delivery.” ![]()
A new category of cytopenias

New research suggests that clonality may underlie the cytopenias observed in patients with idiopathic cytopenias of undetermined significance (ICUS).
So researchers say these patients should be classified as having clonal cytopenias of undetermined significance (CCUS).
The team believes that recognition of CCUS as a clinical entity would help identify it as a formally defined diagnostic group and could aid future studies.
“We don’t know to what extent patients who have low blood counts and mutations are at increased risk of developing an overt malignancy,” said Rafael Bejar, MD, PhD, of the UCSD Moores Cancer Center in La Jolla, California.
“We hope that by defining CCUS, future studies will follow these patients to learn what these mutations mean for their future, as their genetically abnormal cells may represent early stages of subsequent blood cancers.”
Dr Bejar and his colleagues defined CCUS in Blood. Their research was funded, in part, by Genoptix Medical Laboratory, and several study authors are employees of Genoptix.
The researchers prospectively examined bone marrow samples from 144 patients with unexplained cytopenias. Seventeen percent of these patients were diagnosed with myelodysplastic syndromes (MDS), 15% with ICUS and some evidence of dysplasia, and 69% with ICUS and no dysplasia.
The team then sequenced patient samples looking for mutations in 22 frequently mutated myeloid malignancy genes. They identified somatic mutations in 71% of MDS patients, 62% of patients with ICUS and some dysplasia, and 20% of ICUS patients with no dysplasia.
Overall, 35% of ICUS patients carried a somatic mutation or chromosomal abnormality indicative of clonal hematopoiesis.
To build upon these findings, the researchers performed a retrospective analysis of data from 91 patients with lower-risk MDS and 249 patients with ICUS.
The team identified mutations in 79% of patients with MDS, 45% of patients with ICUS and dysplasia, and 17% of patients with ICUS and no dysplasia.
The researchers said the spectrum of mutated genes was similar among the 3 groups. The exception was SF3B1, which was rarely mutated in patients without dysplasia.
The team added that variant allele fractions were comparable between clonal ICUS (CCUS) and MDS, and the same was true for the patients’ mean age and blood counts. But CCUS was a more frequent diagnosis than MDS.
Dr Bejar and his colleagues said larger, carefully controlled studies will be needed to confirm the findings of this research. ![]()

New research suggests that clonality may underlie the cytopenias observed in patients with idiopathic cytopenias of undetermined significance (ICUS).
So researchers say these patients should be classified as having clonal cytopenias of undetermined significance (CCUS).
The team believes that recognition of CCUS as a clinical entity would help identify it as a formally defined diagnostic group and could aid future studies.
“We don’t know to what extent patients who have low blood counts and mutations are at increased risk of developing an overt malignancy,” said Rafael Bejar, MD, PhD, of the UCSD Moores Cancer Center in La Jolla, California.
“We hope that by defining CCUS, future studies will follow these patients to learn what these mutations mean for their future, as their genetically abnormal cells may represent early stages of subsequent blood cancers.”
Dr Bejar and his colleagues defined CCUS in Blood. Their research was funded, in part, by Genoptix Medical Laboratory, and several study authors are employees of Genoptix.
The researchers prospectively examined bone marrow samples from 144 patients with unexplained cytopenias. Seventeen percent of these patients were diagnosed with myelodysplastic syndromes (MDS), 15% with ICUS and some evidence of dysplasia, and 69% with ICUS and no dysplasia.
The team then sequenced patient samples looking for mutations in 22 frequently mutated myeloid malignancy genes. They identified somatic mutations in 71% of MDS patients, 62% of patients with ICUS and some dysplasia, and 20% of ICUS patients with no dysplasia.
Overall, 35% of ICUS patients carried a somatic mutation or chromosomal abnormality indicative of clonal hematopoiesis.
To build upon these findings, the researchers performed a retrospective analysis of data from 91 patients with lower-risk MDS and 249 patients with ICUS.
The team identified mutations in 79% of patients with MDS, 45% of patients with ICUS and dysplasia, and 17% of patients with ICUS and no dysplasia.
The researchers said the spectrum of mutated genes was similar among the 3 groups. The exception was SF3B1, which was rarely mutated in patients without dysplasia.
The team added that variant allele fractions were comparable between clonal ICUS (CCUS) and MDS, and the same was true for the patients’ mean age and blood counts. But CCUS was a more frequent diagnosis than MDS.
Dr Bejar and his colleagues said larger, carefully controlled studies will be needed to confirm the findings of this research. ![]()

New research suggests that clonality may underlie the cytopenias observed in patients with idiopathic cytopenias of undetermined significance (ICUS).
So researchers say these patients should be classified as having clonal cytopenias of undetermined significance (CCUS).
The team believes that recognition of CCUS as a clinical entity would help identify it as a formally defined diagnostic group and could aid future studies.
“We don’t know to what extent patients who have low blood counts and mutations are at increased risk of developing an overt malignancy,” said Rafael Bejar, MD, PhD, of the UCSD Moores Cancer Center in La Jolla, California.
“We hope that by defining CCUS, future studies will follow these patients to learn what these mutations mean for their future, as their genetically abnormal cells may represent early stages of subsequent blood cancers.”
Dr Bejar and his colleagues defined CCUS in Blood. Their research was funded, in part, by Genoptix Medical Laboratory, and several study authors are employees of Genoptix.
The researchers prospectively examined bone marrow samples from 144 patients with unexplained cytopenias. Seventeen percent of these patients were diagnosed with myelodysplastic syndromes (MDS), 15% with ICUS and some evidence of dysplasia, and 69% with ICUS and no dysplasia.
The team then sequenced patient samples looking for mutations in 22 frequently mutated myeloid malignancy genes. They identified somatic mutations in 71% of MDS patients, 62% of patients with ICUS and some dysplasia, and 20% of ICUS patients with no dysplasia.
Overall, 35% of ICUS patients carried a somatic mutation or chromosomal abnormality indicative of clonal hematopoiesis.
To build upon these findings, the researchers performed a retrospective analysis of data from 91 patients with lower-risk MDS and 249 patients with ICUS.
The team identified mutations in 79% of patients with MDS, 45% of patients with ICUS and dysplasia, and 17% of patients with ICUS and no dysplasia.
The researchers said the spectrum of mutated genes was similar among the 3 groups. The exception was SF3B1, which was rarely mutated in patients without dysplasia.
The team added that variant allele fractions were comparable between clonal ICUS (CCUS) and MDS, and the same was true for the patients’ mean age and blood counts. But CCUS was a more frequent diagnosis than MDS.
Dr Bejar and his colleagues said larger, carefully controlled studies will be needed to confirm the findings of this research. ![]()
Autophagy works in nucleus to ward off cancer

Image by Sarah Pfau
Autophagy works in the cell nucleus to guard against the start of cancer, according to research published in Nature.
The study showed, for the first time, that autophagy is used to digest nuclear material in mammalian cells.
“We found that the molecular machinery of autophagy guides the degradation of components of the nuclear lamina in mammals,” said study author Shelley Berger, PhD, of the University of Pennsylvania in Philadelphia.
The nuclear lamina is a network of protein filaments lining the inside of the membrane of the nucleus. It provides mechanical support to the nucleus and regulates gene expression by making some areas of the genome less or more available to be transcribed into messenger RNA.
Previous studies showed that the autophagy protein LC3 can be found in the nucleus, but it was not clear why, as the protein was thought to be functional in the cytoplasm. Study author Zhixun Dou, PhD, came to the Berger lab with this in mind.
At the same time, Peter Adams, PhD, from the University of Glasgow in Scotland, published a study on the breakdown of the nuclear lamina in which he observed a peculiar protrusion, or blebbing, of the nuclear envelope into the cytoplasm. These blebs contained DNA, nuclear lamina proteins, and chromatin.
This evidence led the Berger and Adams labs to work together to find out what was going on.
Using biochemical and sequencing methods, Dr Dou found that laminB1, a key component of the nuclear lamina, and LC3 were contacting each other in the same places on chromatin.
In fact, LC3 and laminB1 are physically bound to each other. LC3 directly interacts with lamin B1 and binds to lamin-associated domains on chromatin.
Autophagy in cancer and aging
The investigators found that, in response to cellular stress that can cause cancer, LC3, chromatin, and laminB1 migrate from the nucleus—via the nuclear blebs—into the cytoplasm and are eventually targeted for disposal.
This breakdown of laminB1 and other nuclear material leads to senescence. The Berger and Adams labs have been studying senescence in conjunction with cancer for quite some time. One way human cells protect themselves from becoming cancerous is to accelerate aging via senescence so the cells can no longer replicate.
The team showed that when a cell’s DNA is damaged or an oncogene is activated (both of which can cause cancer), a normal cell triggers the digestion of nuclear lamina by autophagy, which promotes senescence. Inhibiting this digestion of nuclear material weakens the senescence program and leads to cancerous growth of cells.
“The nucleus is the headquarters of a cell,” Dr Dou said. “When a cell receives a danger alarm, amazingly, it deliberately messes up its headquarters, with the consequence that many functions are completely stopped for the cell. Our study suggests this new function of autophagy is a guarding mechanism that protects cells from becoming cancerous.”
The investigators noted that senescence is associated with normal aging, and senescent cells accumulate in aged tissues, which impair the normal functions of the tissue and contribute to age-related diseases. While autophagy in the nucleus is able to restrain cancer, this machinery is improperly turned on during normal aging.
“There is a short-term ‘tactical’ advantage, but a long-term ‘strategic’ defeat,” Dr Berger explained. “This mechanism makes a normal cell, even without cancer stress, get old much faster, and in a detrimental way.”
In support of this notion, the investigators found that, in late-middle-aged normal cells, blocking the autophagy-driven breakdown of the nuclear lamina can make cells live 60% longer. In fact, the team said the age extension is equivalent to a 70-year-old person living to over 110 years old.
Looking toward the future, the investigators reason that specific manipulation of the nuclear digestion by autophagy holds promise to intervene in age-related diseases.
The team showed that blocking a peptide, which inhibits LC3-laminB1 interaction, is able to slow cell aging. The implications are that a small molecule could be made to stop the long-term “strategic defeat” of the senescence pathway, and to treat age-related diseases, especially those related to chronic inflammation.
Such a molecule might also be able to ameliorate the side effects of chemotherapy or radiation therapy in cancer patients. Drs Dou and Berger are actively investigating this possibility. ![]()

Image by Sarah Pfau
Autophagy works in the cell nucleus to guard against the start of cancer, according to research published in Nature.
The study showed, for the first time, that autophagy is used to digest nuclear material in mammalian cells.
“We found that the molecular machinery of autophagy guides the degradation of components of the nuclear lamina in mammals,” said study author Shelley Berger, PhD, of the University of Pennsylvania in Philadelphia.
The nuclear lamina is a network of protein filaments lining the inside of the membrane of the nucleus. It provides mechanical support to the nucleus and regulates gene expression by making some areas of the genome less or more available to be transcribed into messenger RNA.
Previous studies showed that the autophagy protein LC3 can be found in the nucleus, but it was not clear why, as the protein was thought to be functional in the cytoplasm. Study author Zhixun Dou, PhD, came to the Berger lab with this in mind.
At the same time, Peter Adams, PhD, from the University of Glasgow in Scotland, published a study on the breakdown of the nuclear lamina in which he observed a peculiar protrusion, or blebbing, of the nuclear envelope into the cytoplasm. These blebs contained DNA, nuclear lamina proteins, and chromatin.
This evidence led the Berger and Adams labs to work together to find out what was going on.
Using biochemical and sequencing methods, Dr Dou found that laminB1, a key component of the nuclear lamina, and LC3 were contacting each other in the same places on chromatin.
In fact, LC3 and laminB1 are physically bound to each other. LC3 directly interacts with lamin B1 and binds to lamin-associated domains on chromatin.
Autophagy in cancer and aging
The investigators found that, in response to cellular stress that can cause cancer, LC3, chromatin, and laminB1 migrate from the nucleus—via the nuclear blebs—into the cytoplasm and are eventually targeted for disposal.
This breakdown of laminB1 and other nuclear material leads to senescence. The Berger and Adams labs have been studying senescence in conjunction with cancer for quite some time. One way human cells protect themselves from becoming cancerous is to accelerate aging via senescence so the cells can no longer replicate.
The team showed that when a cell’s DNA is damaged or an oncogene is activated (both of which can cause cancer), a normal cell triggers the digestion of nuclear lamina by autophagy, which promotes senescence. Inhibiting this digestion of nuclear material weakens the senescence program and leads to cancerous growth of cells.
“The nucleus is the headquarters of a cell,” Dr Dou said. “When a cell receives a danger alarm, amazingly, it deliberately messes up its headquarters, with the consequence that many functions are completely stopped for the cell. Our study suggests this new function of autophagy is a guarding mechanism that protects cells from becoming cancerous.”
The investigators noted that senescence is associated with normal aging, and senescent cells accumulate in aged tissues, which impair the normal functions of the tissue and contribute to age-related diseases. While autophagy in the nucleus is able to restrain cancer, this machinery is improperly turned on during normal aging.
“There is a short-term ‘tactical’ advantage, but a long-term ‘strategic’ defeat,” Dr Berger explained. “This mechanism makes a normal cell, even without cancer stress, get old much faster, and in a detrimental way.”
In support of this notion, the investigators found that, in late-middle-aged normal cells, blocking the autophagy-driven breakdown of the nuclear lamina can make cells live 60% longer. In fact, the team said the age extension is equivalent to a 70-year-old person living to over 110 years old.
Looking toward the future, the investigators reason that specific manipulation of the nuclear digestion by autophagy holds promise to intervene in age-related diseases.
The team showed that blocking a peptide, which inhibits LC3-laminB1 interaction, is able to slow cell aging. The implications are that a small molecule could be made to stop the long-term “strategic defeat” of the senescence pathway, and to treat age-related diseases, especially those related to chronic inflammation.
Such a molecule might also be able to ameliorate the side effects of chemotherapy or radiation therapy in cancer patients. Drs Dou and Berger are actively investigating this possibility. ![]()

Image by Sarah Pfau
Autophagy works in the cell nucleus to guard against the start of cancer, according to research published in Nature.
The study showed, for the first time, that autophagy is used to digest nuclear material in mammalian cells.
“We found that the molecular machinery of autophagy guides the degradation of components of the nuclear lamina in mammals,” said study author Shelley Berger, PhD, of the University of Pennsylvania in Philadelphia.
The nuclear lamina is a network of protein filaments lining the inside of the membrane of the nucleus. It provides mechanical support to the nucleus and regulates gene expression by making some areas of the genome less or more available to be transcribed into messenger RNA.
Previous studies showed that the autophagy protein LC3 can be found in the nucleus, but it was not clear why, as the protein was thought to be functional in the cytoplasm. Study author Zhixun Dou, PhD, came to the Berger lab with this in mind.
At the same time, Peter Adams, PhD, from the University of Glasgow in Scotland, published a study on the breakdown of the nuclear lamina in which he observed a peculiar protrusion, or blebbing, of the nuclear envelope into the cytoplasm. These blebs contained DNA, nuclear lamina proteins, and chromatin.
This evidence led the Berger and Adams labs to work together to find out what was going on.
Using biochemical and sequencing methods, Dr Dou found that laminB1, a key component of the nuclear lamina, and LC3 were contacting each other in the same places on chromatin.
In fact, LC3 and laminB1 are physically bound to each other. LC3 directly interacts with lamin B1 and binds to lamin-associated domains on chromatin.
Autophagy in cancer and aging
The investigators found that, in response to cellular stress that can cause cancer, LC3, chromatin, and laminB1 migrate from the nucleus—via the nuclear blebs—into the cytoplasm and are eventually targeted for disposal.
This breakdown of laminB1 and other nuclear material leads to senescence. The Berger and Adams labs have been studying senescence in conjunction with cancer for quite some time. One way human cells protect themselves from becoming cancerous is to accelerate aging via senescence so the cells can no longer replicate.
The team showed that when a cell’s DNA is damaged or an oncogene is activated (both of which can cause cancer), a normal cell triggers the digestion of nuclear lamina by autophagy, which promotes senescence. Inhibiting this digestion of nuclear material weakens the senescence program and leads to cancerous growth of cells.
“The nucleus is the headquarters of a cell,” Dr Dou said. “When a cell receives a danger alarm, amazingly, it deliberately messes up its headquarters, with the consequence that many functions are completely stopped for the cell. Our study suggests this new function of autophagy is a guarding mechanism that protects cells from becoming cancerous.”
The investigators noted that senescence is associated with normal aging, and senescent cells accumulate in aged tissues, which impair the normal functions of the tissue and contribute to age-related diseases. While autophagy in the nucleus is able to restrain cancer, this machinery is improperly turned on during normal aging.
“There is a short-term ‘tactical’ advantage, but a long-term ‘strategic’ defeat,” Dr Berger explained. “This mechanism makes a normal cell, even without cancer stress, get old much faster, and in a detrimental way.”
In support of this notion, the investigators found that, in late-middle-aged normal cells, blocking the autophagy-driven breakdown of the nuclear lamina can make cells live 60% longer. In fact, the team said the age extension is equivalent to a 70-year-old person living to over 110 years old.
Looking toward the future, the investigators reason that specific manipulation of the nuclear digestion by autophagy holds promise to intervene in age-related diseases.
The team showed that blocking a peptide, which inhibits LC3-laminB1 interaction, is able to slow cell aging. The implications are that a small molecule could be made to stop the long-term “strategic defeat” of the senescence pathway, and to treat age-related diseases, especially those related to chronic inflammation.
Such a molecule might also be able to ameliorate the side effects of chemotherapy or radiation therapy in cancer patients. Drs Dou and Berger are actively investigating this possibility.
Protocol could improve massive blood transfusion
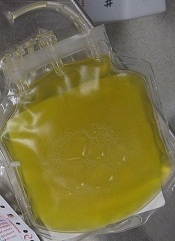
An “early and aggressive” approach to massive blood transfusion can save lives in military combat zones and may provide the same benefit in civilian trauma care as well, according to an article published in the AANA Journal.
The article describes 2 patients who required massive transfusions due to multiple gunshot wounds sustained while in combat zones.
One patient received an inadequate amount of blood products and ultimately died.
But the other patient benefitted from a protocol change to ensure an adequate amount of blood products was delivered quickly.
David Gaskin, CRNA, of Huntsville Memorial Hospital in Texas, and his colleagues described these cases in the journal.
The authors noted that, while providing care in a combat zone, the transfusion of packed red blood cells (PRBC) and fresh frozen plasma (FFP) is performed in a 1:1 ratio. However, the packaging and thawing techniques of the plasma can delay the delivery of blood products and prevent a patient from receiving enough blood.
Another issue in a military environment is the challenge of effectively communicating with live donors on site, which can cause delays in obtaining fresh blood supplies. Both of these issues can have life-threatening consequences for patients.
This is what happened with the first patient described in the article. The 38-year-old man sustained multiple gunshot wounds to the left side of the chest, left side of the back, and flank.
The surgical team was unable to maintain a high ratio of PRBCs to plasma and to infuse an adequate quantity of fresh whole blood (FWB) into this patient. He received 26 units of PRBCs, 5 units of FFP, 3 units of FWB, and 1 unit of cryoprecipitate.
The patient experienced trauma-induced coagulopathy, acidosis, and hypothermia. He died within 2 hours of presentation.
Because of this death, the team identified and implemented a protocol to keep 4 FFP units thawed and ready for immediate use at all times. They also identified and prescreened additional blood donors and implemented a phone roster and base-wide overhead system to enable rapid notification of these donors.
The second patient described in the article benefitted from these changes. This 23-year-old male sustained a gunshot wound to the left lower aspect of the abdomen and multiple gunshot wounds to bilateral lower extremities.
The “early and aggressive” use of FWB and plasma provided the necessary endogenous clotting factors and platelets to promote hemostasis in this patient. He received 18 units of PRBCs, 18 units of FFP, 2 units of cryoprecipitate, and 24 units of FWB.
Gaskin and his colleagues said these results suggest that efforts to incorporate a similar resuscitation strategy into civilian practice may improve outcomes, but it warrants continued study.

An “early and aggressive” approach to massive blood transfusion can save lives in military combat zones and may provide the same benefit in civilian trauma care as well, according to an article published in the AANA Journal.
The article describes 2 patients who required massive transfusions due to multiple gunshot wounds sustained while in combat zones.
One patient received an inadequate amount of blood products and ultimately died.
But the other patient benefitted from a protocol change to ensure an adequate amount of blood products was delivered quickly.
David Gaskin, CRNA, of Huntsville Memorial Hospital in Texas, and his colleagues described these cases in the journal.
The authors noted that, while providing care in a combat zone, the transfusion of packed red blood cells (PRBC) and fresh frozen plasma (FFP) is performed in a 1:1 ratio. However, the packaging and thawing techniques of the plasma can delay the delivery of blood products and prevent a patient from receiving enough blood.
Another issue in a military environment is the challenge of effectively communicating with live donors on site, which can cause delays in obtaining fresh blood supplies. Both of these issues can have life-threatening consequences for patients.
This is what happened with the first patient described in the article. The 38-year-old man sustained multiple gunshot wounds to the left side of the chest, left side of the back, and flank.
The surgical team was unable to maintain a high ratio of PRBCs to plasma and to infuse an adequate quantity of fresh whole blood (FWB) into this patient. He received 26 units of PRBCs, 5 units of FFP, 3 units of FWB, and 1 unit of cryoprecipitate.
The patient experienced trauma-induced coagulopathy, acidosis, and hypothermia. He died within 2 hours of presentation.
Because of this death, the team identified and implemented a protocol to keep 4 FFP units thawed and ready for immediate use at all times. They also identified and prescreened additional blood donors and implemented a phone roster and base-wide overhead system to enable rapid notification of these donors.
The second patient described in the article benefitted from these changes. This 23-year-old male sustained a gunshot wound to the left lower aspect of the abdomen and multiple gunshot wounds to bilateral lower extremities.
The “early and aggressive” use of FWB and plasma provided the necessary endogenous clotting factors and platelets to promote hemostasis in this patient. He received 18 units of PRBCs, 18 units of FFP, 2 units of cryoprecipitate, and 24 units of FWB.
Gaskin and his colleagues said these results suggest that efforts to incorporate a similar resuscitation strategy into civilian practice may improve outcomes, but it warrants continued study.

An “early and aggressive” approach to massive blood transfusion can save lives in military combat zones and may provide the same benefit in civilian trauma care as well, according to an article published in the AANA Journal.
The article describes 2 patients who required massive transfusions due to multiple gunshot wounds sustained while in combat zones.
One patient received an inadequate amount of blood products and ultimately died.
But the other patient benefitted from a protocol change to ensure an adequate amount of blood products was delivered quickly.
David Gaskin, CRNA, of Huntsville Memorial Hospital in Texas, and his colleagues described these cases in the journal.
The authors noted that, while providing care in a combat zone, the transfusion of packed red blood cells (PRBC) and fresh frozen plasma (FFP) is performed in a 1:1 ratio. However, the packaging and thawing techniques of the plasma can delay the delivery of blood products and prevent a patient from receiving enough blood.
Another issue in a military environment is the challenge of effectively communicating with live donors on site, which can cause delays in obtaining fresh blood supplies. Both of these issues can have life-threatening consequences for patients.
This is what happened with the first patient described in the article. The 38-year-old man sustained multiple gunshot wounds to the left side of the chest, left side of the back, and flank.
The surgical team was unable to maintain a high ratio of PRBCs to plasma and to infuse an adequate quantity of fresh whole blood (FWB) into this patient. He received 26 units of PRBCs, 5 units of FFP, 3 units of FWB, and 1 unit of cryoprecipitate.
The patient experienced trauma-induced coagulopathy, acidosis, and hypothermia. He died within 2 hours of presentation.
Because of this death, the team identified and implemented a protocol to keep 4 FFP units thawed and ready for immediate use at all times. They also identified and prescreened additional blood donors and implemented a phone roster and base-wide overhead system to enable rapid notification of these donors.
The second patient described in the article benefitted from these changes. This 23-year-old male sustained a gunshot wound to the left lower aspect of the abdomen and multiple gunshot wounds to bilateral lower extremities.
The “early and aggressive” use of FWB and plasma provided the necessary endogenous clotting factors and platelets to promote hemostasis in this patient. He received 18 units of PRBCs, 18 units of FFP, 2 units of cryoprecipitate, and 24 units of FWB.
Gaskin and his colleagues said these results suggest that efforts to incorporate a similar resuscitation strategy into civilian practice may improve outcomes, but it warrants continued study.
Drug gets orphan designation for BPDCN

The European Medicines Agency (EMA) has granted orphan drug designation to SL-401 for the treatment of blastic plasmacytoid dendritic cell neoplasm (BPDCN).
SL-401 is a targeted therapy directed to the interleukin-3 receptor (IL-3R), which is present on cancer stem cells and tumor bulk in a range of hematologic malignancies.
The drug is composed of human IL-3 coupled to a truncated diphtheria toxin payload that inhibits protein synthesis.
SL-401 already has orphan designation from the EMA to treat acute myeloid leukemia (AML) and from the US Food and Drug Administration (FDA) for the treatment of AML and BPDCN. The drug is under development by Stemline Therapeutics, Inc.
SL-401 research
At ASH 2012 (abstract 3625), researchers reported results with SL-401 in a study of patients with AML, BPDCN, and myelodysplastic syndromes (MDS).
At that time, the study had enrolled 80 patients, including 59 with relapsed or refractory AML, 11 with de novo AML unfit for chemotherapy, 7 with high-risk MDS, and 3 with relapsed/refractory BPDCN.
Patients received a single cycle of SL-401 as a 15-minute intravenous infusion in 1 of 2 dosing regimens to determine the maximum tolerated dose (MTD) and assess antitumor activity.
With regimen A, 45 patients received doses ranging from 4 μg/kg to 12.5 μg/kg every other day for up to 6 doses. With regimen B, 35 patients received doses ranging from 7.1 μg/kg to 22.1 μg/kg daily for up to 5 doses.
Of the 59 patients with relapsed/refractory AML, 2 achieved complete responses (CRs), 5 had partial responses (PRs), and 8 had minor responses (MRs). One CR lasted more than 8 months, and the other lasted more than 25 months.
Of the 11 patients with AML who were not candidates for chemotherapy, 2 had PRs and 1 had an MR. Among the 7 patients with high-risk MDS, there was 1 PR and 1 MR.
And among the 3 patients with BPDCN, there were 2 CRs. One CR lasted more than 2 months, and the other lasted more than 4 months.
The MTD was not achieved with regimen A, but the MTD for regimen B was 16.6 μg/kg/day. The dose-limiting toxicities were a gastrointestinal bleed (n=1), transaminase and creatinine kinase elevations (n=1), and capillary leak syndrome (n=3). There was no evidence of treatment-related bone marrow suppression.
Last year, researchers reported additional results in BPDCN patients (Frankel et al, Blood 2014).
Eleven BPDCN patients received a single course of SL-401 (at 12.5 μg/kg intravenously over 15 minutes) daily for up to 5 doses. Three patients who had initial responses to SL-401 received a second course while in relapse.
Seven of 9 evaluable (78%) patients responded to a single course of SL-401. There were 5 CRs and 2 PRs. The median duration of responses was 5 months (range, 1-20+ months).
The most common adverse events were transient and included fever, chills, hypotension, edema, hypoalbuminemia, thrombocytopenia, and transaminasemia.
Three multicenter clinical trials of SL-401 are currently open in the following indications:
- BPDCN and relapsed/refractory AML
- AML patients in first complete remission with minimal residual disease
- Four types of advanced, high-risk myeloproliferative neoplasms, including systemic mastocytosis, advanced symptomatic hypereosinophilic disorder, myelofibrosis, and chronic myelomonocytic leukemia.
Additional SL-401 studies are planned for patients with myeloma, lymphomas, and other leukemias.
About orphan designation
In the European Union, orphan designation is granted to therapies intended to treat a life-threatening or chronically debilitating condition that affects no more than 5 in 10,000 persons and where no satisfactory treatment is available.
Companies that obtain orphan designation for a drug in the European Union benefit from a number of incentives, including protocol assistance, a type of scientific advice specific for designated orphan medicines, and 10 years of market exclusivity once the medicine is on the market. Fee reductions are also available, depending on the status of the sponsor and the type of service required.
The FDA grants orphan designation to drugs that are intended to treat diseases or conditions affecting fewer than 200,000 patients in the US.
In the US, orphan designation provides the sponsor of a drug with various development incentives, including opportunities to apply for research-related tax credits and grant funding, assistance in designing clinical trials, and 7 years of US market exclusivity if the drug is approved.

The European Medicines Agency (EMA) has granted orphan drug designation to SL-401 for the treatment of blastic plasmacytoid dendritic cell neoplasm (BPDCN).
SL-401 is a targeted therapy directed to the interleukin-3 receptor (IL-3R), which is present on cancer stem cells and tumor bulk in a range of hematologic malignancies.
The drug is composed of human IL-3 coupled to a truncated diphtheria toxin payload that inhibits protein synthesis.
SL-401 already has orphan designation from the EMA to treat acute myeloid leukemia (AML) and from the US Food and Drug Administration (FDA) for the treatment of AML and BPDCN. The drug is under development by Stemline Therapeutics, Inc.
SL-401 research
At ASH 2012 (abstract 3625), researchers reported results with SL-401 in a study of patients with AML, BPDCN, and myelodysplastic syndromes (MDS).
At that time, the study had enrolled 80 patients, including 59 with relapsed or refractory AML, 11 with de novo AML unfit for chemotherapy, 7 with high-risk MDS, and 3 with relapsed/refractory BPDCN.
Patients received a single cycle of SL-401 as a 15-minute intravenous infusion in 1 of 2 dosing regimens to determine the maximum tolerated dose (MTD) and assess antitumor activity.
With regimen A, 45 patients received doses ranging from 4 μg/kg to 12.5 μg/kg every other day for up to 6 doses. With regimen B, 35 patients received doses ranging from 7.1 μg/kg to 22.1 μg/kg daily for up to 5 doses.
Of the 59 patients with relapsed/refractory AML, 2 achieved complete responses (CRs), 5 had partial responses (PRs), and 8 had minor responses (MRs). One CR lasted more than 8 months, and the other lasted more than 25 months.
Of the 11 patients with AML who were not candidates for chemotherapy, 2 had PRs and 1 had an MR. Among the 7 patients with high-risk MDS, there was 1 PR and 1 MR.
And among the 3 patients with BPDCN, there were 2 CRs. One CR lasted more than 2 months, and the other lasted more than 4 months.
The MTD was not achieved with regimen A, but the MTD for regimen B was 16.6 μg/kg/day. The dose-limiting toxicities were a gastrointestinal bleed (n=1), transaminase and creatinine kinase elevations (n=1), and capillary leak syndrome (n=3). There was no evidence of treatment-related bone marrow suppression.
Last year, researchers reported additional results in BPDCN patients (Frankel et al, Blood 2014).
Eleven BPDCN patients received a single course of SL-401 (at 12.5 μg/kg intravenously over 15 minutes) daily for up to 5 doses. Three patients who had initial responses to SL-401 received a second course while in relapse.
Seven of 9 evaluable (78%) patients responded to a single course of SL-401. There were 5 CRs and 2 PRs. The median duration of responses was 5 months (range, 1-20+ months).
The most common adverse events were transient and included fever, chills, hypotension, edema, hypoalbuminemia, thrombocytopenia, and transaminasemia.
Three multicenter clinical trials of SL-401 are currently open in the following indications:
- BPDCN and relapsed/refractory AML
- AML patients in first complete remission with minimal residual disease
- Four types of advanced, high-risk myeloproliferative neoplasms, including systemic mastocytosis, advanced symptomatic hypereosinophilic disorder, myelofibrosis, and chronic myelomonocytic leukemia.
Additional SL-401 studies are planned for patients with myeloma, lymphomas, and other leukemias.
About orphan designation
In the European Union, orphan designation is granted to therapies intended to treat a life-threatening or chronically debilitating condition that affects no more than 5 in 10,000 persons and where no satisfactory treatment is available.
Companies that obtain orphan designation for a drug in the European Union benefit from a number of incentives, including protocol assistance, a type of scientific advice specific for designated orphan medicines, and 10 years of market exclusivity once the medicine is on the market. Fee reductions are also available, depending on the status of the sponsor and the type of service required.
The FDA grants orphan designation to drugs that are intended to treat diseases or conditions affecting fewer than 200,000 patients in the US.
In the US, orphan designation provides the sponsor of a drug with various development incentives, including opportunities to apply for research-related tax credits and grant funding, assistance in designing clinical trials, and 7 years of US market exclusivity if the drug is approved.

The European Medicines Agency (EMA) has granted orphan drug designation to SL-401 for the treatment of blastic plasmacytoid dendritic cell neoplasm (BPDCN).
SL-401 is a targeted therapy directed to the interleukin-3 receptor (IL-3R), which is present on cancer stem cells and tumor bulk in a range of hematologic malignancies.
The drug is composed of human IL-3 coupled to a truncated diphtheria toxin payload that inhibits protein synthesis.
SL-401 already has orphan designation from the EMA to treat acute myeloid leukemia (AML) and from the US Food and Drug Administration (FDA) for the treatment of AML and BPDCN. The drug is under development by Stemline Therapeutics, Inc.
SL-401 research
At ASH 2012 (abstract 3625), researchers reported results with SL-401 in a study of patients with AML, BPDCN, and myelodysplastic syndromes (MDS).
At that time, the study had enrolled 80 patients, including 59 with relapsed or refractory AML, 11 with de novo AML unfit for chemotherapy, 7 with high-risk MDS, and 3 with relapsed/refractory BPDCN.
Patients received a single cycle of SL-401 as a 15-minute intravenous infusion in 1 of 2 dosing regimens to determine the maximum tolerated dose (MTD) and assess antitumor activity.
With regimen A, 45 patients received doses ranging from 4 μg/kg to 12.5 μg/kg every other day for up to 6 doses. With regimen B, 35 patients received doses ranging from 7.1 μg/kg to 22.1 μg/kg daily for up to 5 doses.
Of the 59 patients with relapsed/refractory AML, 2 achieved complete responses (CRs), 5 had partial responses (PRs), and 8 had minor responses (MRs). One CR lasted more than 8 months, and the other lasted more than 25 months.
Of the 11 patients with AML who were not candidates for chemotherapy, 2 had PRs and 1 had an MR. Among the 7 patients with high-risk MDS, there was 1 PR and 1 MR.
And among the 3 patients with BPDCN, there were 2 CRs. One CR lasted more than 2 months, and the other lasted more than 4 months.
The MTD was not achieved with regimen A, but the MTD for regimen B was 16.6 μg/kg/day. The dose-limiting toxicities were a gastrointestinal bleed (n=1), transaminase and creatinine kinase elevations (n=1), and capillary leak syndrome (n=3). There was no evidence of treatment-related bone marrow suppression.
Last year, researchers reported additional results in BPDCN patients (Frankel et al, Blood 2014).
Eleven BPDCN patients received a single course of SL-401 (at 12.5 μg/kg intravenously over 15 minutes) daily for up to 5 doses. Three patients who had initial responses to SL-401 received a second course while in relapse.
Seven of 9 evaluable (78%) patients responded to a single course of SL-401. There were 5 CRs and 2 PRs. The median duration of responses was 5 months (range, 1-20+ months).
The most common adverse events were transient and included fever, chills, hypotension, edema, hypoalbuminemia, thrombocytopenia, and transaminasemia.
Three multicenter clinical trials of SL-401 are currently open in the following indications:
- BPDCN and relapsed/refractory AML
- AML patients in first complete remission with minimal residual disease
- Four types of advanced, high-risk myeloproliferative neoplasms, including systemic mastocytosis, advanced symptomatic hypereosinophilic disorder, myelofibrosis, and chronic myelomonocytic leukemia.
Additional SL-401 studies are planned for patients with myeloma, lymphomas, and other leukemias.
About orphan designation
In the European Union, orphan designation is granted to therapies intended to treat a life-threatening or chronically debilitating condition that affects no more than 5 in 10,000 persons and where no satisfactory treatment is available.
Companies that obtain orphan designation for a drug in the European Union benefit from a number of incentives, including protocol assistance, a type of scientific advice specific for designated orphan medicines, and 10 years of market exclusivity once the medicine is on the market. Fee reductions are also available, depending on the status of the sponsor and the type of service required.
The FDA grants orphan designation to drugs that are intended to treat diseases or conditions affecting fewer than 200,000 patients in the US.
In the US, orphan designation provides the sponsor of a drug with various development incentives, including opportunities to apply for research-related tax credits and grant funding, assistance in designing clinical trials, and 7 years of US market exclusivity if the drug is approved.
MM-related ESRD on the decline
Photo by Anna Frodesiak
New research suggests the risk of end-stage renal disease (ESRD) caused by multiple myeloma (MM) is declining, and survival is lengthening for patients who do develop ESRD due to MM.
Researchers said these findings are encouraging, but efforts are still needed to develop effective MM treatments with fewer side effects.
They noted that MM treatment has changed substantially in the last decade.
But it hasn’t been clear whether the burden of ESRD due to MM has changed or whether survival has improved for patients with ESRD due to MM.
To gain some insight, Robert Foley, MD, of the University of Minnesota in Minneapolis, and his colleagues examined data from the US Renal Data System database spanning the period from 2001 to 2010.
They reported their findings in the Journal of the American Society of Nephrology.
The team found that, of the 1,069,343 patients with ESRD who were on renal replacement therapy (RRT), 12,703 had developed ESRD due to MM.
However, the incidence of ESRD from MM decreased from 2001 to 2010. Compared to 2001-2002 (1.00), the standardized incidence ratios of ESRD due to MM were 0.96 for 2003-2004 (P<0.05), 0.99 for 2005-2006 (P>0.05), 0.89 for 2007-2008 (P<0.001), and 0.82 for 2009-2010 (P<0.001).
The demography-adjusted incidence ratio for ESRD due to MM decreased (P<0.05) between 2001-2002 and 2009-2010 in the overall population and in most of the subgroups examined.
The exceptions were patients younger than 40, Hispanic patients, and those belonging to the “other” race category. (The race categories were “white,” “black,” and “other,” while the ethnicity categories were “Hispanic” and “non-Hispanic.”)
The data also showed improvements in survival over time among patients with ESRD due to MM.
Compared to 2001-2002, the adjusted hazard ratios (AHRs) for death were 1.02 for 2003-2004 (P=0.5), 0.93 for 2005-2006 (P=0.02), 0.86 for 2007-2008 (P<0.001), and 0.74 for 2009-2010 (P<0.001). (This analysis was adjusted for age, sex, race, ethnicity, ischemic heart disease, diabetes, mode of RRT, estimated glomerular filtration rate, body mass index, serum albumin, and hemoglobin.)
AHRs for death were highest in the first year after RRT initiation (AHR=2.6; P<0.001) and decreased in year 3 (AHR=1.59; P<0.001).
The AHR for death in patients with ESRD due to MM compared to those with ESRD due to all other causes was 2.05 (P<0.001).
“Myeloma is the commonest malignancy leading to kidney failure,” Dr Foley said. “It’s encouraging that we found that kidney failure due to multiple myeloma declined considerably over the last decade.”

Photo by Anna Frodesiak
New research suggests the risk of end-stage renal disease (ESRD) caused by multiple myeloma (MM) is declining, and survival is lengthening for patients who do develop ESRD due to MM.
Researchers said these findings are encouraging, but efforts are still needed to develop effective MM treatments with fewer side effects.
They noted that MM treatment has changed substantially in the last decade.
But it hasn’t been clear whether the burden of ESRD due to MM has changed or whether survival has improved for patients with ESRD due to MM.
To gain some insight, Robert Foley, MD, of the University of Minnesota in Minneapolis, and his colleagues examined data from the US Renal Data System database spanning the period from 2001 to 2010.
They reported their findings in the Journal of the American Society of Nephrology.
The team found that, of the 1,069,343 patients with ESRD who were on renal replacement therapy (RRT), 12,703 had developed ESRD due to MM.
However, the incidence of ESRD from MM decreased from 2001 to 2010. Compared to 2001-2002 (1.00), the standardized incidence ratios of ESRD due to MM were 0.96 for 2003-2004 (P<0.05), 0.99 for 2005-2006 (P>0.05), 0.89 for 2007-2008 (P<0.001), and 0.82 for 2009-2010 (P<0.001).
The demography-adjusted incidence ratio for ESRD due to MM decreased (P<0.05) between 2001-2002 and 2009-2010 in the overall population and in most of the subgroups examined.
The exceptions were patients younger than 40, Hispanic patients, and those belonging to the “other” race category. (The race categories were “white,” “black,” and “other,” while the ethnicity categories were “Hispanic” and “non-Hispanic.”)
The data also showed improvements in survival over time among patients with ESRD due to MM.
Compared to 2001-2002, the adjusted hazard ratios (AHRs) for death were 1.02 for 2003-2004 (P=0.5), 0.93 for 2005-2006 (P=0.02), 0.86 for 2007-2008 (P<0.001), and 0.74 for 2009-2010 (P<0.001). (This analysis was adjusted for age, sex, race, ethnicity, ischemic heart disease, diabetes, mode of RRT, estimated glomerular filtration rate, body mass index, serum albumin, and hemoglobin.)
AHRs for death were highest in the first year after RRT initiation (AHR=2.6; P<0.001) and decreased in year 3 (AHR=1.59; P<0.001).
The AHR for death in patients with ESRD due to MM compared to those with ESRD due to all other causes was 2.05 (P<0.001).
“Myeloma is the commonest malignancy leading to kidney failure,” Dr Foley said. “It’s encouraging that we found that kidney failure due to multiple myeloma declined considerably over the last decade.”

Photo by Anna Frodesiak
New research suggests the risk of end-stage renal disease (ESRD) caused by multiple myeloma (MM) is declining, and survival is lengthening for patients who do develop ESRD due to MM.
Researchers said these findings are encouraging, but efforts are still needed to develop effective MM treatments with fewer side effects.
They noted that MM treatment has changed substantially in the last decade.
But it hasn’t been clear whether the burden of ESRD due to MM has changed or whether survival has improved for patients with ESRD due to MM.
To gain some insight, Robert Foley, MD, of the University of Minnesota in Minneapolis, and his colleagues examined data from the US Renal Data System database spanning the period from 2001 to 2010.
They reported their findings in the Journal of the American Society of Nephrology.
The team found that, of the 1,069,343 patients with ESRD who were on renal replacement therapy (RRT), 12,703 had developed ESRD due to MM.
However, the incidence of ESRD from MM decreased from 2001 to 2010. Compared to 2001-2002 (1.00), the standardized incidence ratios of ESRD due to MM were 0.96 for 2003-2004 (P<0.05), 0.99 for 2005-2006 (P>0.05), 0.89 for 2007-2008 (P<0.001), and 0.82 for 2009-2010 (P<0.001).
The demography-adjusted incidence ratio for ESRD due to MM decreased (P<0.05) between 2001-2002 and 2009-2010 in the overall population and in most of the subgroups examined.
The exceptions were patients younger than 40, Hispanic patients, and those belonging to the “other” race category. (The race categories were “white,” “black,” and “other,” while the ethnicity categories were “Hispanic” and “non-Hispanic.”)
The data also showed improvements in survival over time among patients with ESRD due to MM.
Compared to 2001-2002, the adjusted hazard ratios (AHRs) for death were 1.02 for 2003-2004 (P=0.5), 0.93 for 2005-2006 (P=0.02), 0.86 for 2007-2008 (P<0.001), and 0.74 for 2009-2010 (P<0.001). (This analysis was adjusted for age, sex, race, ethnicity, ischemic heart disease, diabetes, mode of RRT, estimated glomerular filtration rate, body mass index, serum albumin, and hemoglobin.)
AHRs for death were highest in the first year after RRT initiation (AHR=2.6; P<0.001) and decreased in year 3 (AHR=1.59; P<0.001).
The AHR for death in patients with ESRD due to MM compared to those with ESRD due to all other causes was 2.05 (P<0.001).
“Myeloma is the commonest malignancy leading to kidney failure,” Dr Foley said. “It’s encouraging that we found that kidney failure due to multiple myeloma declined considerably over the last decade.”