User login
Bivalirudin provides no net benefit in PCI, doc says

Photo by Frank C. Muller
Results of a large meta-analysis indicate that bivalirudin may not be appropriate thromboprophylaxis for patients undergoing percutaneous coronary intervention (PCI).
Investigators found that bivalirudin was associated with an increased risk of stent thrombosis, when compared to an active control group.
Bivalirudin did confer a lower risk of major bleeding and cardiac death than the other anticoagulants studied.
But the drug had “no discernible impact” on all-cause mortality, according to the investigators.
“The take-home message is that, essentially, we didn’t find a net benefit with bivalirudin,” said Behnood Bikdeli, MD, of Yale-New Haven Hospital in Connecticut.
He and his colleagues detailed this discovery in Thrombosis Research.
The team analyzed data from 25 trials involving 41,243 PCI patients. The trials compared bivalirudin to other anticoagulants—largely unfractionated heparin, with or without other agents.
Compared with the active control group, bivalirudin use was associated with a significantly increased risk of definite stent thrombosis (risk ratio[RR]=1.73, P<0.001) and a significantly decreased risk of major bleeding (RR=0.59, P<0.001) and cardiac death (RR=0.72, P=0.05).
The risk of acute myocardial infarction was similar between the 2 groups (RR=1.00, P=0.96), as was the risk of all-cause mortality (RR=0.96, P=0.69).
The investigators said these results were consistent across a wide set of subgroup and sensitivity analyses.
“In our extensive analyses, we could not identify any patient subgroups that had less bleeding but no increase in the risk of clots, or stent thrombosis [with bivalirudin],” Dr Bikdeli said.
“This expensive medication, which is being used in a widespread manner, is not doing a slam-dunk better job. We might need more studies to see if a select minority of patients could potentially fare better with it.” ![]()

Photo by Frank C. Muller
Results of a large meta-analysis indicate that bivalirudin may not be appropriate thromboprophylaxis for patients undergoing percutaneous coronary intervention (PCI).
Investigators found that bivalirudin was associated with an increased risk of stent thrombosis, when compared to an active control group.
Bivalirudin did confer a lower risk of major bleeding and cardiac death than the other anticoagulants studied.
But the drug had “no discernible impact” on all-cause mortality, according to the investigators.
“The take-home message is that, essentially, we didn’t find a net benefit with bivalirudin,” said Behnood Bikdeli, MD, of Yale-New Haven Hospital in Connecticut.
He and his colleagues detailed this discovery in Thrombosis Research.
The team analyzed data from 25 trials involving 41,243 PCI patients. The trials compared bivalirudin to other anticoagulants—largely unfractionated heparin, with or without other agents.
Compared with the active control group, bivalirudin use was associated with a significantly increased risk of definite stent thrombosis (risk ratio[RR]=1.73, P<0.001) and a significantly decreased risk of major bleeding (RR=0.59, P<0.001) and cardiac death (RR=0.72, P=0.05).
The risk of acute myocardial infarction was similar between the 2 groups (RR=1.00, P=0.96), as was the risk of all-cause mortality (RR=0.96, P=0.69).
The investigators said these results were consistent across a wide set of subgroup and sensitivity analyses.
“In our extensive analyses, we could not identify any patient subgroups that had less bleeding but no increase in the risk of clots, or stent thrombosis [with bivalirudin],” Dr Bikdeli said.
“This expensive medication, which is being used in a widespread manner, is not doing a slam-dunk better job. We might need more studies to see if a select minority of patients could potentially fare better with it.” ![]()

Photo by Frank C. Muller
Results of a large meta-analysis indicate that bivalirudin may not be appropriate thromboprophylaxis for patients undergoing percutaneous coronary intervention (PCI).
Investigators found that bivalirudin was associated with an increased risk of stent thrombosis, when compared to an active control group.
Bivalirudin did confer a lower risk of major bleeding and cardiac death than the other anticoagulants studied.
But the drug had “no discernible impact” on all-cause mortality, according to the investigators.
“The take-home message is that, essentially, we didn’t find a net benefit with bivalirudin,” said Behnood Bikdeli, MD, of Yale-New Haven Hospital in Connecticut.
He and his colleagues detailed this discovery in Thrombosis Research.
The team analyzed data from 25 trials involving 41,243 PCI patients. The trials compared bivalirudin to other anticoagulants—largely unfractionated heparin, with or without other agents.
Compared with the active control group, bivalirudin use was associated with a significantly increased risk of definite stent thrombosis (risk ratio[RR]=1.73, P<0.001) and a significantly decreased risk of major bleeding (RR=0.59, P<0.001) and cardiac death (RR=0.72, P=0.05).
The risk of acute myocardial infarction was similar between the 2 groups (RR=1.00, P=0.96), as was the risk of all-cause mortality (RR=0.96, P=0.69).
The investigators said these results were consistent across a wide set of subgroup and sensitivity analyses.
“In our extensive analyses, we could not identify any patient subgroups that had less bleeding but no increase in the risk of clots, or stent thrombosis [with bivalirudin],” Dr Bikdeli said.
“This expensive medication, which is being used in a widespread manner, is not doing a slam-dunk better job. We might need more studies to see if a select minority of patients could potentially fare better with it.” ![]()
CT after unexplained VTE unnecessary, study suggests
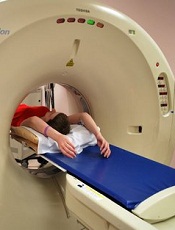
Photo by Angela Mary Butler
TORONTO—A CT scan of the abdomen and pelvis does not improve cancer detection in people with unexplained venous thromboembolism (VTE), results of the SOME trial suggest.
“Unexplained blood clots have long been thought of as a possible early warning sign of cancer, with previous studies suggesting that up to 10% of patients with unexplained clots will be diagnosed with cancer within the year,” said Marc Carrier, MD, of Ottawa Hospital Research Institute in Ontario, Canada.
“Some clinical guidelines recommend a CT scan of the abdomen and pelvis in these patients, in addition to other cancer screening, but there has been very little evidence to know if the added CT scan is helpful. We did this study to find out.”
Dr Carrier and his colleagues described this research in an article published in NEJM and in a presentation given at the 2015 ISTH Congress (abstract LB001*).
The trial involved 854 patients treated at 9 Canadian centers who had an unexplained VTE—deep vein thrombosis, pulmonary embolism, or both.
The patients were randomized to receive basic cancer screening or basic cancer screening plus a CT scan of the abdomen and pelvis. Basic cancer screening included blood work and a chest X-ray, in addition to gender-specific screening (such as a breast exam, Pap smear, and prostate exam) if it had not been conducted in the last year.
Overall, 33 patients (3.9%) had a new diagnosis of occult cancer during the 1-year follow-up period.
There was no significant difference in the rate of diagnosis between the patients who received only basic screening and the patients who underwent CT as well—3.2% (14/431) and 4.5% (19/423), respectively (P=0.28).
Likewise, there was no significant difference in the number of cancers that were not diagnosed by the screening strategies. Basic screening failed to uncover 4 cancers (29%), and basic screening plus CT failed to reveal 5 cancers (26%, P=1.0).
In addition, there was no significant difference between the screening strategies in the time to cancer diagnosis or cancer-related mortality. The mean time to cancer diagnosis was 4.2 months in the basic screening group and 4.0 months in the CT group (P=0.88). And the rate of cancer-related mortality was 1.4% and 0.9%, respectively (P=0.75).
“Although it is tempting to believe that more cancer screening is always better, our study shows that this is not necessarily the case,” Dr Carrier said. “And in fact, unnecessary CT scanning has real risks. It can cause stress and anxiety in patients, as well as radiation exposure, and it can lead to over-investigation of false-positive findings. Our study means many patients will now be able to avoid this.”
That could lead to significant savings for the healthcare system, according to the researchers. For example, approximately 30,000 Canadians suffer from an unexplained VTE every year, and a CT scan costs approximately $300. So avoiding unnecessary CT scans could result in a potential saving of $9 million per year in Canada alone. ![]()
*Information in the abstract differs from that presented at the meeting.

Photo by Angela Mary Butler
TORONTO—A CT scan of the abdomen and pelvis does not improve cancer detection in people with unexplained venous thromboembolism (VTE), results of the SOME trial suggest.
“Unexplained blood clots have long been thought of as a possible early warning sign of cancer, with previous studies suggesting that up to 10% of patients with unexplained clots will be diagnosed with cancer within the year,” said Marc Carrier, MD, of Ottawa Hospital Research Institute in Ontario, Canada.
“Some clinical guidelines recommend a CT scan of the abdomen and pelvis in these patients, in addition to other cancer screening, but there has been very little evidence to know if the added CT scan is helpful. We did this study to find out.”
Dr Carrier and his colleagues described this research in an article published in NEJM and in a presentation given at the 2015 ISTH Congress (abstract LB001*).
The trial involved 854 patients treated at 9 Canadian centers who had an unexplained VTE—deep vein thrombosis, pulmonary embolism, or both.
The patients were randomized to receive basic cancer screening or basic cancer screening plus a CT scan of the abdomen and pelvis. Basic cancer screening included blood work and a chest X-ray, in addition to gender-specific screening (such as a breast exam, Pap smear, and prostate exam) if it had not been conducted in the last year.
Overall, 33 patients (3.9%) had a new diagnosis of occult cancer during the 1-year follow-up period.
There was no significant difference in the rate of diagnosis between the patients who received only basic screening and the patients who underwent CT as well—3.2% (14/431) and 4.5% (19/423), respectively (P=0.28).
Likewise, there was no significant difference in the number of cancers that were not diagnosed by the screening strategies. Basic screening failed to uncover 4 cancers (29%), and basic screening plus CT failed to reveal 5 cancers (26%, P=1.0).
In addition, there was no significant difference between the screening strategies in the time to cancer diagnosis or cancer-related mortality. The mean time to cancer diagnosis was 4.2 months in the basic screening group and 4.0 months in the CT group (P=0.88). And the rate of cancer-related mortality was 1.4% and 0.9%, respectively (P=0.75).
“Although it is tempting to believe that more cancer screening is always better, our study shows that this is not necessarily the case,” Dr Carrier said. “And in fact, unnecessary CT scanning has real risks. It can cause stress and anxiety in patients, as well as radiation exposure, and it can lead to over-investigation of false-positive findings. Our study means many patients will now be able to avoid this.”
That could lead to significant savings for the healthcare system, according to the researchers. For example, approximately 30,000 Canadians suffer from an unexplained VTE every year, and a CT scan costs approximately $300. So avoiding unnecessary CT scans could result in a potential saving of $9 million per year in Canada alone. ![]()
*Information in the abstract differs from that presented at the meeting.

Photo by Angela Mary Butler
TORONTO—A CT scan of the abdomen and pelvis does not improve cancer detection in people with unexplained venous thromboembolism (VTE), results of the SOME trial suggest.
“Unexplained blood clots have long been thought of as a possible early warning sign of cancer, with previous studies suggesting that up to 10% of patients with unexplained clots will be diagnosed with cancer within the year,” said Marc Carrier, MD, of Ottawa Hospital Research Institute in Ontario, Canada.
“Some clinical guidelines recommend a CT scan of the abdomen and pelvis in these patients, in addition to other cancer screening, but there has been very little evidence to know if the added CT scan is helpful. We did this study to find out.”
Dr Carrier and his colleagues described this research in an article published in NEJM and in a presentation given at the 2015 ISTH Congress (abstract LB001*).
The trial involved 854 patients treated at 9 Canadian centers who had an unexplained VTE—deep vein thrombosis, pulmonary embolism, or both.
The patients were randomized to receive basic cancer screening or basic cancer screening plus a CT scan of the abdomen and pelvis. Basic cancer screening included blood work and a chest X-ray, in addition to gender-specific screening (such as a breast exam, Pap smear, and prostate exam) if it had not been conducted in the last year.
Overall, 33 patients (3.9%) had a new diagnosis of occult cancer during the 1-year follow-up period.
There was no significant difference in the rate of diagnosis between the patients who received only basic screening and the patients who underwent CT as well—3.2% (14/431) and 4.5% (19/423), respectively (P=0.28).
Likewise, there was no significant difference in the number of cancers that were not diagnosed by the screening strategies. Basic screening failed to uncover 4 cancers (29%), and basic screening plus CT failed to reveal 5 cancers (26%, P=1.0).
In addition, there was no significant difference between the screening strategies in the time to cancer diagnosis or cancer-related mortality. The mean time to cancer diagnosis was 4.2 months in the basic screening group and 4.0 months in the CT group (P=0.88). And the rate of cancer-related mortality was 1.4% and 0.9%, respectively (P=0.75).
“Although it is tempting to believe that more cancer screening is always better, our study shows that this is not necessarily the case,” Dr Carrier said. “And in fact, unnecessary CT scanning has real risks. It can cause stress and anxiety in patients, as well as radiation exposure, and it can lead to over-investigation of false-positive findings. Our study means many patients will now be able to avoid this.”
That could lead to significant savings for the healthcare system, according to the researchers. For example, approximately 30,000 Canadians suffer from an unexplained VTE every year, and a CT scan costs approximately $300. So avoiding unnecessary CT scans could result in a potential saving of $9 million per year in Canada alone. ![]()
*Information in the abstract differs from that presented at the meeting.
Targeted agent shows early promise for NHL

follicular lymphoma
LUGANO—An anti-CD37 antibody-radionuclide conjugate provides sustained efficacy and a manageable safety profile in patients with relapsed, CD37+ non-Hodgkin lymphoma (NHL), according to researchers.
The drug, 177Lu-DOTA-HH1 (Betalutin), consists of the tumor-specific antibody HH1, which targets the CD37 antigen on the surface of NHL cells, conjugated to the β-emitting isotope lutetium-177 (Lu-177) via the chemical linker DOTA.
In an ongoing, phase 1/2 trial, Betalutin has produced responses in 7 of 12 evaluable patients with relapsed NHL, and 5 of those responses are ongoing.
Grade 3/4 adverse events (AEs) were largely hematologic in nature, and many were transient and reversible. However, grade 3/4 AEs occurred at all 3 dose levels investigated in this study, as did serious AEs.
Arne Kolstad, MD, PhD, of Oslo University Hospital in Norway, and his colleagues reported these results at the 13th International Conference on Malignant Lymphoma (abstract 287*). The study was sponsored by Nordic Nanovector, the company developing Betalutin.
Thus far, the researchers have evaluated 13 patients with relapsed, CD37+ NHL. Twelve patients had a primary diagnosis of follicular lymphoma, and 1 had mantle cell lymphoma (MCL). The patients’ median age was 68 (range, 41-78), and they had received 1 to 8 prior treatments.
In this dose-finding study, the researchers investigated 3 dose levels of Betalutin. Four patients received Betalutin at 10 MBq/kg biweekly, 6 received 15 MBq/kg biweekly, and 3 (including the MCL patient) received 20 MBq/kg biweekly.
All patients received 50 mg of HH1 prior to Betalutin. Patients also received rituximab at 375 mg/m2 on days -28 and -21 (prior to Betalutin on day 0).
Safety and dosing
Dose-limiting toxicities occurred at the 20 MBq/kg biweekly dose, so researchers said 15 MBq/kg biweekly, with HH1 pre-dosing, is the current recommended dose of Betalutin.
Treatment-emergent grade 3 AEs in the 10 MBq/kg group included thrombocytopenia (n=1), neutropenia (n=2), pneumonia (n=1), and pulmonary embolism (n=1). There were no grade 4 AEs in this group.
In the 15 MBq/kg group, 2 patients had grade 3 thrombocytopenia, and 1 had grade 4. One patient each had grade 3 and 4 neutropenia.
Grade 3/4 AEs in the 20 MBq/kg group included grade 4 thrombocytopenia (n=3), grade 3 (n=1) and grade 4 (n=2) neutropenia, and grade 3 epistaxis (n=1).
Serious AEs included pulmonary embolism (1 in the 10 MBq/kg group), pneumonia (1 in the 10 MBq/kg group), atrial fibrillation (2 in the 15 MBq/kg group), thrombocytopenia (1 in the 20 MBq/kg group), and epistaxis (1 in the 20 MBq/kg group).
The researchers said all hematologic AEs were transient and reversible. They also pointed out that 6 patients in this trial have been followed for a year or more, and there have been no secondary malignancies or other events that would suggest long-term toxicity.
Efficacy and next steps
Twelve patients were evaluable for efficacy. Seven patients responded to treatment, including 4 complete responses (CRs) and 3 partial responses. Two patients had stable disease, and 3 progressed. Eight patients had a 50% or greater reduction in tumor volume.
The median response duration has not been reached, and 5 patients’ responses are ongoing. The duration of response in these patients ranges from 6 months to more than 21 months. All 4 patients who achieved a CR (including the MCL patient) are still in CR.
The researchers concluded that Betalutin delivers a highly favorable response rate, with durable clinical responses, and the drug has a predictable and manageable safety profile.
They have opened a new arm of this study to evaluate the safety and efficacy of Betalutin at 15 MBq/kg biweekly and 17.5 MBq/kg biweekly without HH1 pre-dosing. ![]()
*Information in the abstract differs from that presented at the meeting.

follicular lymphoma
LUGANO—An anti-CD37 antibody-radionuclide conjugate provides sustained efficacy and a manageable safety profile in patients with relapsed, CD37+ non-Hodgkin lymphoma (NHL), according to researchers.
The drug, 177Lu-DOTA-HH1 (Betalutin), consists of the tumor-specific antibody HH1, which targets the CD37 antigen on the surface of NHL cells, conjugated to the β-emitting isotope lutetium-177 (Lu-177) via the chemical linker DOTA.
In an ongoing, phase 1/2 trial, Betalutin has produced responses in 7 of 12 evaluable patients with relapsed NHL, and 5 of those responses are ongoing.
Grade 3/4 adverse events (AEs) were largely hematologic in nature, and many were transient and reversible. However, grade 3/4 AEs occurred at all 3 dose levels investigated in this study, as did serious AEs.
Arne Kolstad, MD, PhD, of Oslo University Hospital in Norway, and his colleagues reported these results at the 13th International Conference on Malignant Lymphoma (abstract 287*). The study was sponsored by Nordic Nanovector, the company developing Betalutin.
Thus far, the researchers have evaluated 13 patients with relapsed, CD37+ NHL. Twelve patients had a primary diagnosis of follicular lymphoma, and 1 had mantle cell lymphoma (MCL). The patients’ median age was 68 (range, 41-78), and they had received 1 to 8 prior treatments.
In this dose-finding study, the researchers investigated 3 dose levels of Betalutin. Four patients received Betalutin at 10 MBq/kg biweekly, 6 received 15 MBq/kg biweekly, and 3 (including the MCL patient) received 20 MBq/kg biweekly.
All patients received 50 mg of HH1 prior to Betalutin. Patients also received rituximab at 375 mg/m2 on days -28 and -21 (prior to Betalutin on day 0).
Safety and dosing
Dose-limiting toxicities occurred at the 20 MBq/kg biweekly dose, so researchers said 15 MBq/kg biweekly, with HH1 pre-dosing, is the current recommended dose of Betalutin.
Treatment-emergent grade 3 AEs in the 10 MBq/kg group included thrombocytopenia (n=1), neutropenia (n=2), pneumonia (n=1), and pulmonary embolism (n=1). There were no grade 4 AEs in this group.
In the 15 MBq/kg group, 2 patients had grade 3 thrombocytopenia, and 1 had grade 4. One patient each had grade 3 and 4 neutropenia.
Grade 3/4 AEs in the 20 MBq/kg group included grade 4 thrombocytopenia (n=3), grade 3 (n=1) and grade 4 (n=2) neutropenia, and grade 3 epistaxis (n=1).
Serious AEs included pulmonary embolism (1 in the 10 MBq/kg group), pneumonia (1 in the 10 MBq/kg group), atrial fibrillation (2 in the 15 MBq/kg group), thrombocytopenia (1 in the 20 MBq/kg group), and epistaxis (1 in the 20 MBq/kg group).
The researchers said all hematologic AEs were transient and reversible. They also pointed out that 6 patients in this trial have been followed for a year or more, and there have been no secondary malignancies or other events that would suggest long-term toxicity.
Efficacy and next steps
Twelve patients were evaluable for efficacy. Seven patients responded to treatment, including 4 complete responses (CRs) and 3 partial responses. Two patients had stable disease, and 3 progressed. Eight patients had a 50% or greater reduction in tumor volume.
The median response duration has not been reached, and 5 patients’ responses are ongoing. The duration of response in these patients ranges from 6 months to more than 21 months. All 4 patients who achieved a CR (including the MCL patient) are still in CR.
The researchers concluded that Betalutin delivers a highly favorable response rate, with durable clinical responses, and the drug has a predictable and manageable safety profile.
They have opened a new arm of this study to evaluate the safety and efficacy of Betalutin at 15 MBq/kg biweekly and 17.5 MBq/kg biweekly without HH1 pre-dosing. ![]()
*Information in the abstract differs from that presented at the meeting.

follicular lymphoma
LUGANO—An anti-CD37 antibody-radionuclide conjugate provides sustained efficacy and a manageable safety profile in patients with relapsed, CD37+ non-Hodgkin lymphoma (NHL), according to researchers.
The drug, 177Lu-DOTA-HH1 (Betalutin), consists of the tumor-specific antibody HH1, which targets the CD37 antigen on the surface of NHL cells, conjugated to the β-emitting isotope lutetium-177 (Lu-177) via the chemical linker DOTA.
In an ongoing, phase 1/2 trial, Betalutin has produced responses in 7 of 12 evaluable patients with relapsed NHL, and 5 of those responses are ongoing.
Grade 3/4 adverse events (AEs) were largely hematologic in nature, and many were transient and reversible. However, grade 3/4 AEs occurred at all 3 dose levels investigated in this study, as did serious AEs.
Arne Kolstad, MD, PhD, of Oslo University Hospital in Norway, and his colleagues reported these results at the 13th International Conference on Malignant Lymphoma (abstract 287*). The study was sponsored by Nordic Nanovector, the company developing Betalutin.
Thus far, the researchers have evaluated 13 patients with relapsed, CD37+ NHL. Twelve patients had a primary diagnosis of follicular lymphoma, and 1 had mantle cell lymphoma (MCL). The patients’ median age was 68 (range, 41-78), and they had received 1 to 8 prior treatments.
In this dose-finding study, the researchers investigated 3 dose levels of Betalutin. Four patients received Betalutin at 10 MBq/kg biweekly, 6 received 15 MBq/kg biweekly, and 3 (including the MCL patient) received 20 MBq/kg biweekly.
All patients received 50 mg of HH1 prior to Betalutin. Patients also received rituximab at 375 mg/m2 on days -28 and -21 (prior to Betalutin on day 0).
Safety and dosing
Dose-limiting toxicities occurred at the 20 MBq/kg biweekly dose, so researchers said 15 MBq/kg biweekly, with HH1 pre-dosing, is the current recommended dose of Betalutin.
Treatment-emergent grade 3 AEs in the 10 MBq/kg group included thrombocytopenia (n=1), neutropenia (n=2), pneumonia (n=1), and pulmonary embolism (n=1). There were no grade 4 AEs in this group.
In the 15 MBq/kg group, 2 patients had grade 3 thrombocytopenia, and 1 had grade 4. One patient each had grade 3 and 4 neutropenia.
Grade 3/4 AEs in the 20 MBq/kg group included grade 4 thrombocytopenia (n=3), grade 3 (n=1) and grade 4 (n=2) neutropenia, and grade 3 epistaxis (n=1).
Serious AEs included pulmonary embolism (1 in the 10 MBq/kg group), pneumonia (1 in the 10 MBq/kg group), atrial fibrillation (2 in the 15 MBq/kg group), thrombocytopenia (1 in the 20 MBq/kg group), and epistaxis (1 in the 20 MBq/kg group).
The researchers said all hematologic AEs were transient and reversible. They also pointed out that 6 patients in this trial have been followed for a year or more, and there have been no secondary malignancies or other events that would suggest long-term toxicity.
Efficacy and next steps
Twelve patients were evaluable for efficacy. Seven patients responded to treatment, including 4 complete responses (CRs) and 3 partial responses. Two patients had stable disease, and 3 progressed. Eight patients had a 50% or greater reduction in tumor volume.
The median response duration has not been reached, and 5 patients’ responses are ongoing. The duration of response in these patients ranges from 6 months to more than 21 months. All 4 patients who achieved a CR (including the MCL patient) are still in CR.
The researchers concluded that Betalutin delivers a highly favorable response rate, with durable clinical responses, and the drug has a predictable and manageable safety profile.
They have opened a new arm of this study to evaluate the safety and efficacy of Betalutin at 15 MBq/kg biweekly and 17.5 MBq/kg biweekly without HH1 pre-dosing. ![]()
*Information in the abstract differs from that presented at the meeting.
Inactivating an enzyme can eradicate T-ALL

Preclinical research suggests that inactivating a single enzyme could eradicate or prevent T-cell acute lymphoblastic leukemia (T-ALL).
The researchers knew that T-ALL onset is linked to microRNAs, and most are generated with the help of the enzyme Dicer1.
Now, the team has found evidence to suggest that Dicer1 is crucial for the development of T-ALL, and inhibiting Dicer1 can actually prevent the disease altogether.
They reported these findings in Blood.
The researchers used mice that were genetically modified to develop T-ALL and in which Dicer1 could be abrogated. The team “switched off” Dicer1 in the mice at different stages of T-ALL development to see what role the enzyme plays in disease evolution.
Switching Dicer1 off at an early stage completely prevented T-ALL. In mice where Dicer1 was completely abrogated, T-ALL cells were entirely eliminated, allowing all the mice to survive.
The researchers were able to confirm this effect by monitoring the few residual leukemic cells taken from these animals.
“You can actually see the cancer cells dying off after Dicer1 has been abrogated,” said study author Freddy Radtke, PhD, of Ecole Polytechnique Fédérale de Lausanne in Lausanne, Switzerland.
He and his colleagues found that the key to this cell death is Dicer1’s role in producing microRNAs. The team discovered that a previously unrecognized microRNA, miR-21, was deregulated in both mouse and human T-ALL.
In the context of T-ALL, miR-21 inhibits the tumor suppressor gene Pdcd4. Without Dicer1, there is no miR-21 to do this, which allows Pdcd4 to fight the disease.
This study is the first to conclusively demonstrate that Dicer1 plays a role in T-ALL, the researchers said. The work paves the way for a new set of treatment for this malignancy and possibly others.
However, the team also noted that it can be challenging to target cells of interest when dealing with molecules that are so fundamental to the cell’s life.
“We can’t just go shutting down Dicer1 across the board,” Dr Radtke explained. “Otherwise, we’ll end up killing healthy cells as well.”
His lab is now focused on tackling this obstacle. ![]()

Preclinical research suggests that inactivating a single enzyme could eradicate or prevent T-cell acute lymphoblastic leukemia (T-ALL).
The researchers knew that T-ALL onset is linked to microRNAs, and most are generated with the help of the enzyme Dicer1.
Now, the team has found evidence to suggest that Dicer1 is crucial for the development of T-ALL, and inhibiting Dicer1 can actually prevent the disease altogether.
They reported these findings in Blood.
The researchers used mice that were genetically modified to develop T-ALL and in which Dicer1 could be abrogated. The team “switched off” Dicer1 in the mice at different stages of T-ALL development to see what role the enzyme plays in disease evolution.
Switching Dicer1 off at an early stage completely prevented T-ALL. In mice where Dicer1 was completely abrogated, T-ALL cells were entirely eliminated, allowing all the mice to survive.
The researchers were able to confirm this effect by monitoring the few residual leukemic cells taken from these animals.
“You can actually see the cancer cells dying off after Dicer1 has been abrogated,” said study author Freddy Radtke, PhD, of Ecole Polytechnique Fédérale de Lausanne in Lausanne, Switzerland.
He and his colleagues found that the key to this cell death is Dicer1’s role in producing microRNAs. The team discovered that a previously unrecognized microRNA, miR-21, was deregulated in both mouse and human T-ALL.
In the context of T-ALL, miR-21 inhibits the tumor suppressor gene Pdcd4. Without Dicer1, there is no miR-21 to do this, which allows Pdcd4 to fight the disease.
This study is the first to conclusively demonstrate that Dicer1 plays a role in T-ALL, the researchers said. The work paves the way for a new set of treatment for this malignancy and possibly others.
However, the team also noted that it can be challenging to target cells of interest when dealing with molecules that are so fundamental to the cell’s life.
“We can’t just go shutting down Dicer1 across the board,” Dr Radtke explained. “Otherwise, we’ll end up killing healthy cells as well.”
His lab is now focused on tackling this obstacle. ![]()

Preclinical research suggests that inactivating a single enzyme could eradicate or prevent T-cell acute lymphoblastic leukemia (T-ALL).
The researchers knew that T-ALL onset is linked to microRNAs, and most are generated with the help of the enzyme Dicer1.
Now, the team has found evidence to suggest that Dicer1 is crucial for the development of T-ALL, and inhibiting Dicer1 can actually prevent the disease altogether.
They reported these findings in Blood.
The researchers used mice that were genetically modified to develop T-ALL and in which Dicer1 could be abrogated. The team “switched off” Dicer1 in the mice at different stages of T-ALL development to see what role the enzyme plays in disease evolution.
Switching Dicer1 off at an early stage completely prevented T-ALL. In mice where Dicer1 was completely abrogated, T-ALL cells were entirely eliminated, allowing all the mice to survive.
The researchers were able to confirm this effect by monitoring the few residual leukemic cells taken from these animals.
“You can actually see the cancer cells dying off after Dicer1 has been abrogated,” said study author Freddy Radtke, PhD, of Ecole Polytechnique Fédérale de Lausanne in Lausanne, Switzerland.
He and his colleagues found that the key to this cell death is Dicer1’s role in producing microRNAs. The team discovered that a previously unrecognized microRNA, miR-21, was deregulated in both mouse and human T-ALL.
In the context of T-ALL, miR-21 inhibits the tumor suppressor gene Pdcd4. Without Dicer1, there is no miR-21 to do this, which allows Pdcd4 to fight the disease.
This study is the first to conclusively demonstrate that Dicer1 plays a role in T-ALL, the researchers said. The work paves the way for a new set of treatment for this malignancy and possibly others.
However, the team also noted that it can be challenging to target cells of interest when dealing with molecules that are so fundamental to the cell’s life.
“We can’t just go shutting down Dicer1 across the board,” Dr Radtke explained. “Otherwise, we’ll end up killing healthy cells as well.”
His lab is now focused on tackling this obstacle. ![]()
Drug reverses anticoagulant effect of dabigatran
TORONTO—Interim results of a phase 3 study suggest idarucizumab, a humanized antibody fragment, can reverse the anticoagulant effect of
dabigatran in real-world situations.
In the RE-VERSE AD trial, idarucizumab normalized diluted thrombin time (dTT) and ecarin clotting time (ECT) in a majority of patients with uncontrolled or life-threatening bleeding complications and most patients who required emergency surgery or an invasive procedure.
In addition, researchers said there were no safety concerns related to idarucizumab. However, 23% of patients in this trial experienced serious adverse events, 20% of patients died, and several patients had thrombotic or bleeding events.
These results have been published in NEJM and presented at the 2015 ISTH Congress (abstract LB005). The study was sponsored by Boehringer Ingelheim, the company developing idarucizumab and dabigatran.
“The interim analysis from RE-VERSE AD is important for healthcare professionals as it provides the first insights into the effect of a specific reversal agent to a non-vitamin K antagonist oral anticoagulant during real-world emergency situations,” said study investigator Charles Pollack, MD, of the University of Pennsylvania in Philadelphia.
Because RE-VERSE AD was designed to evaluate how idarucizumab would perform in real-world situations, severely ill or injured patients were eligible for enrollment. The interim analysis included data from 90 patients in emergency settings who were taking dabigatran and required reversal.
The patients were divided into 2 groups: those with uncontrolled or life-threatening bleeding complications, such as intracranial hemorrhage or severe trauma (group A, n=51), and patients requiring emergency surgery or an invasive procedure (group B, n=39).
The primary endpoint of the study is the degree to which 5 g of idarucizumab reversed the anticoagulant effect of dabigatran within 4 hours, measured by dTT and ECT.
The researchers were able to evaluate the percentage of reversal by dTT in 68 patients (40 in group A and 28 in group B) and the percentage of reversal by ECT in 81 patients (47 in group A and 34 in group B).
The dTT was normalized in 98% of evaluable patients in group A and 93% in group B. The ECT was normalized in 89% of evaluable patients in group A and 88% in group B.
At 12 hours and 24 hours, the dTT was below the upper limit of the normal range in 90% of evaluable patients in group A and 81% in group B. The ECT was below the upper limit of the normal range in 72% of evaluable group A patients and 54% of evaluable group B patients.
Among the 35 evaluable patients in group A, hemostasis was restored at a median of 11.4 hours. Among the 36 patients in group B who underwent a procedure, 33 had normal intraoperative hemostasis. Two patients had mildly abnormal hemostasis, and 1 patient had moderately abnormal hemostasis.
“As observed in earlier research in volunteers, idarucizumab reversed the anticoagulant effect of dabigatran in patients completely within minutes, even in those rare critical care situations studied in RE-VERSE AD,” Dr Pollack said.
“These data demonstrate that use of idarucizumab can help physicians focus on other vital aspects of emergency management beyond anticoagulant reversal in dabigatran-treated patients.”
Twenty-one patients (13 in group A and 8 in group B) experienced serious adverse events during the study.
This included 18 events that led to death, 5 thrombotic events, 2 cases of gastrointestinal hemorrhage, a postoperative wound infection, a case of delirium, a case of right ventricular failure, and a case of pulmonary edema. (Some patients had more than one serious adverse event.) ![]()
TORONTO—Interim results of a phase 3 study suggest idarucizumab, a humanized antibody fragment, can reverse the anticoagulant effect of
dabigatran in real-world situations.
In the RE-VERSE AD trial, idarucizumab normalized diluted thrombin time (dTT) and ecarin clotting time (ECT) in a majority of patients with uncontrolled or life-threatening bleeding complications and most patients who required emergency surgery or an invasive procedure.
In addition, researchers said there were no safety concerns related to idarucizumab. However, 23% of patients in this trial experienced serious adverse events, 20% of patients died, and several patients had thrombotic or bleeding events.
These results have been published in NEJM and presented at the 2015 ISTH Congress (abstract LB005). The study was sponsored by Boehringer Ingelheim, the company developing idarucizumab and dabigatran.
“The interim analysis from RE-VERSE AD is important for healthcare professionals as it provides the first insights into the effect of a specific reversal agent to a non-vitamin K antagonist oral anticoagulant during real-world emergency situations,” said study investigator Charles Pollack, MD, of the University of Pennsylvania in Philadelphia.
Because RE-VERSE AD was designed to evaluate how idarucizumab would perform in real-world situations, severely ill or injured patients were eligible for enrollment. The interim analysis included data from 90 patients in emergency settings who were taking dabigatran and required reversal.
The patients were divided into 2 groups: those with uncontrolled or life-threatening bleeding complications, such as intracranial hemorrhage or severe trauma (group A, n=51), and patients requiring emergency surgery or an invasive procedure (group B, n=39).
The primary endpoint of the study is the degree to which 5 g of idarucizumab reversed the anticoagulant effect of dabigatran within 4 hours, measured by dTT and ECT.
The researchers were able to evaluate the percentage of reversal by dTT in 68 patients (40 in group A and 28 in group B) and the percentage of reversal by ECT in 81 patients (47 in group A and 34 in group B).
The dTT was normalized in 98% of evaluable patients in group A and 93% in group B. The ECT was normalized in 89% of evaluable patients in group A and 88% in group B.
At 12 hours and 24 hours, the dTT was below the upper limit of the normal range in 90% of evaluable patients in group A and 81% in group B. The ECT was below the upper limit of the normal range in 72% of evaluable group A patients and 54% of evaluable group B patients.
Among the 35 evaluable patients in group A, hemostasis was restored at a median of 11.4 hours. Among the 36 patients in group B who underwent a procedure, 33 had normal intraoperative hemostasis. Two patients had mildly abnormal hemostasis, and 1 patient had moderately abnormal hemostasis.
“As observed in earlier research in volunteers, idarucizumab reversed the anticoagulant effect of dabigatran in patients completely within minutes, even in those rare critical care situations studied in RE-VERSE AD,” Dr Pollack said.
“These data demonstrate that use of idarucizumab can help physicians focus on other vital aspects of emergency management beyond anticoagulant reversal in dabigatran-treated patients.”
Twenty-one patients (13 in group A and 8 in group B) experienced serious adverse events during the study.
This included 18 events that led to death, 5 thrombotic events, 2 cases of gastrointestinal hemorrhage, a postoperative wound infection, a case of delirium, a case of right ventricular failure, and a case of pulmonary edema. (Some patients had more than one serious adverse event.) ![]()
TORONTO—Interim results of a phase 3 study suggest idarucizumab, a humanized antibody fragment, can reverse the anticoagulant effect of
dabigatran in real-world situations.
In the RE-VERSE AD trial, idarucizumab normalized diluted thrombin time (dTT) and ecarin clotting time (ECT) in a majority of patients with uncontrolled or life-threatening bleeding complications and most patients who required emergency surgery or an invasive procedure.
In addition, researchers said there were no safety concerns related to idarucizumab. However, 23% of patients in this trial experienced serious adverse events, 20% of patients died, and several patients had thrombotic or bleeding events.
These results have been published in NEJM and presented at the 2015 ISTH Congress (abstract LB005). The study was sponsored by Boehringer Ingelheim, the company developing idarucizumab and dabigatran.
“The interim analysis from RE-VERSE AD is important for healthcare professionals as it provides the first insights into the effect of a specific reversal agent to a non-vitamin K antagonist oral anticoagulant during real-world emergency situations,” said study investigator Charles Pollack, MD, of the University of Pennsylvania in Philadelphia.
Because RE-VERSE AD was designed to evaluate how idarucizumab would perform in real-world situations, severely ill or injured patients were eligible for enrollment. The interim analysis included data from 90 patients in emergency settings who were taking dabigatran and required reversal.
The patients were divided into 2 groups: those with uncontrolled or life-threatening bleeding complications, such as intracranial hemorrhage or severe trauma (group A, n=51), and patients requiring emergency surgery or an invasive procedure (group B, n=39).
The primary endpoint of the study is the degree to which 5 g of idarucizumab reversed the anticoagulant effect of dabigatran within 4 hours, measured by dTT and ECT.
The researchers were able to evaluate the percentage of reversal by dTT in 68 patients (40 in group A and 28 in group B) and the percentage of reversal by ECT in 81 patients (47 in group A and 34 in group B).
The dTT was normalized in 98% of evaluable patients in group A and 93% in group B. The ECT was normalized in 89% of evaluable patients in group A and 88% in group B.
At 12 hours and 24 hours, the dTT was below the upper limit of the normal range in 90% of evaluable patients in group A and 81% in group B. The ECT was below the upper limit of the normal range in 72% of evaluable group A patients and 54% of evaluable group B patients.
Among the 35 evaluable patients in group A, hemostasis was restored at a median of 11.4 hours. Among the 36 patients in group B who underwent a procedure, 33 had normal intraoperative hemostasis. Two patients had mildly abnormal hemostasis, and 1 patient had moderately abnormal hemostasis.
“As observed in earlier research in volunteers, idarucizumab reversed the anticoagulant effect of dabigatran in patients completely within minutes, even in those rare critical care situations studied in RE-VERSE AD,” Dr Pollack said.
“These data demonstrate that use of idarucizumab can help physicians focus on other vital aspects of emergency management beyond anticoagulant reversal in dabigatran-treated patients.”
Twenty-one patients (13 in group A and 8 in group B) experienced serious adverse events during the study.
This included 18 events that led to death, 5 thrombotic events, 2 cases of gastrointestinal hemorrhage, a postoperative wound infection, a case of delirium, a case of right ventricular failure, and a case of pulmonary edema. (Some patients had more than one serious adverse event.) ![]()
Bridge therapy not necessary in AFib, team says

TORONTO—Bridge anticoagulant therapy appears to be unnecessary in patients with atrial fibrillation (AFib) undergoing elective surgery, according to researchers.
In the BRIDGE study, AFib patients who stopped all anticoagulant therapy before elective surgery had no higher risk of thrombosis and a lower risk of major bleeding than patients who were given bridge therapy with low-molecular weight heparin after stopping warfarin.
This research was presented at the 2015 ISTH Congress (abstract LB002) and published in NEJM.
“Bridging has been controversial because there has been a lack of data demonstrating that it’s necessary, so people don’t know what to do,” said study author Thomas L. Ortel, MD, PhD, of Duke University Medical Center in Durham, North Carolina.
“You can go to 5 different doctors, and some will bridge, and others won’t. It just depends on what they feel they can safely do. This trial gives a firm answer to that question.”
The trial enrolled 1884 patients with AFib and atrial flutter. Roughly half received bridge therapy with dalteparin, and the other half received a placebo while halting their warfarin for up to 13 days around their elective surgeries. Patients were followed for up to 37 days after their procedures.
Among patients who stopped all anticoagulant therapy, the incidence of arterial thrombosis was 0.4%, compared to 0.3% for patients who received bridge therapy (P=0.01 for noninferiority).
Major bleeding events were significantly less common among the non-bridging group. They occurred in 1.3% of patients who were not on anticoagulant therapy and 3.2% of patients who received bridge therapy (P=0.005 for superiority).
“Bridging does not improve the outcome for stroke prevention but increases the risk of major bleeding complications,” Dr Ortel said. “That’s the counter balance. We’re not doing patients any good, and we are potentially hurting them.”
Dr Ortel noted that these findings are specific to AFib patients who take warfarin and should not be generalized to other types of patients or other anticoagulants. But the results will be taken into consideration by organizations that develop guidelines.
“This is the first study to provide high-quality clinical trial data demonstrating that, for patients with atrial fibrillation who need a procedure and who need to come off warfarin, they can simply stop and restart,” Dr Ortel said. “They do not need to be bridged.” ![]()

TORONTO—Bridge anticoagulant therapy appears to be unnecessary in patients with atrial fibrillation (AFib) undergoing elective surgery, according to researchers.
In the BRIDGE study, AFib patients who stopped all anticoagulant therapy before elective surgery had no higher risk of thrombosis and a lower risk of major bleeding than patients who were given bridge therapy with low-molecular weight heparin after stopping warfarin.
This research was presented at the 2015 ISTH Congress (abstract LB002) and published in NEJM.
“Bridging has been controversial because there has been a lack of data demonstrating that it’s necessary, so people don’t know what to do,” said study author Thomas L. Ortel, MD, PhD, of Duke University Medical Center in Durham, North Carolina.
“You can go to 5 different doctors, and some will bridge, and others won’t. It just depends on what they feel they can safely do. This trial gives a firm answer to that question.”
The trial enrolled 1884 patients with AFib and atrial flutter. Roughly half received bridge therapy with dalteparin, and the other half received a placebo while halting their warfarin for up to 13 days around their elective surgeries. Patients were followed for up to 37 days after their procedures.
Among patients who stopped all anticoagulant therapy, the incidence of arterial thrombosis was 0.4%, compared to 0.3% for patients who received bridge therapy (P=0.01 for noninferiority).
Major bleeding events were significantly less common among the non-bridging group. They occurred in 1.3% of patients who were not on anticoagulant therapy and 3.2% of patients who received bridge therapy (P=0.005 for superiority).
“Bridging does not improve the outcome for stroke prevention but increases the risk of major bleeding complications,” Dr Ortel said. “That’s the counter balance. We’re not doing patients any good, and we are potentially hurting them.”
Dr Ortel noted that these findings are specific to AFib patients who take warfarin and should not be generalized to other types of patients or other anticoagulants. But the results will be taken into consideration by organizations that develop guidelines.
“This is the first study to provide high-quality clinical trial data demonstrating that, for patients with atrial fibrillation who need a procedure and who need to come off warfarin, they can simply stop and restart,” Dr Ortel said. “They do not need to be bridged.” ![]()

TORONTO—Bridge anticoagulant therapy appears to be unnecessary in patients with atrial fibrillation (AFib) undergoing elective surgery, according to researchers.
In the BRIDGE study, AFib patients who stopped all anticoagulant therapy before elective surgery had no higher risk of thrombosis and a lower risk of major bleeding than patients who were given bridge therapy with low-molecular weight heparin after stopping warfarin.
This research was presented at the 2015 ISTH Congress (abstract LB002) and published in NEJM.
“Bridging has been controversial because there has been a lack of data demonstrating that it’s necessary, so people don’t know what to do,” said study author Thomas L. Ortel, MD, PhD, of Duke University Medical Center in Durham, North Carolina.
“You can go to 5 different doctors, and some will bridge, and others won’t. It just depends on what they feel they can safely do. This trial gives a firm answer to that question.”
The trial enrolled 1884 patients with AFib and atrial flutter. Roughly half received bridge therapy with dalteparin, and the other half received a placebo while halting their warfarin for up to 13 days around their elective surgeries. Patients were followed for up to 37 days after their procedures.
Among patients who stopped all anticoagulant therapy, the incidence of arterial thrombosis was 0.4%, compared to 0.3% for patients who received bridge therapy (P=0.01 for noninferiority).
Major bleeding events were significantly less common among the non-bridging group. They occurred in 1.3% of patients who were not on anticoagulant therapy and 3.2% of patients who received bridge therapy (P=0.005 for superiority).
“Bridging does not improve the outcome for stroke prevention but increases the risk of major bleeding complications,” Dr Ortel said. “That’s the counter balance. We’re not doing patients any good, and we are potentially hurting them.”
Dr Ortel noted that these findings are specific to AFib patients who take warfarin and should not be generalized to other types of patients or other anticoagulants. But the results will be taken into consideration by organizations that develop guidelines.
“This is the first study to provide high-quality clinical trial data demonstrating that, for patients with atrial fibrillation who need a procedure and who need to come off warfarin, they can simply stop and restart,” Dr Ortel said. “They do not need to be bridged.” ![]()
FDA grants vaccine orphan designation for MM

The US Food and Drug Administration (FDA) has granted a novel vaccine orphan designation as a treatment for multiple myeloma (MM).
The vaccine, known as ImMucin, targets the signal peptide domain of the MUC1 tumor antigen.
ImMucin works by “teaching” the immune system to identify and destroy cells that display a short, specific, 21-mer portion from MUC1, which appears on 90% of all cancer cells but not in patients’ blood.
Results of a phase 1/2 trial suggested that ImMucin was safe and active in MM patients. The trial included 15 MUC1-positive patients who had residual or biochemically progressive disease after autologous stem cell transplant.
The patients received 6 or 12 bi-weekly intradermal doses of ImMucin co-administered with human granulocyte-macrophage colony-stimulating factor.
The researchers said the vaccine was well-tolerated, as all adverse events were temporary, grade 1-2 in nature, and resolved spontaneously.
There was a significant decrease in soluble MUC1 levels in 9 patients, and 11 patients had stable disease or clinical improvement that persisted for 17.5 months to more than 41.3 months.
A follow-on study (which is ongoing) in patients who responded to ImMucin has shown that some patients can go more than 4 years without requiring any further treatment for their disease.
ImMucin is under development by Vaxil Biotherapeutics Ltd. The vaccine also has orphan designation as a treatment for MM in the European Union.
About orphan designation
The FDA grants orphan designation to encourage companies to develop therapies for diseases that affect fewer than 200,000 individuals in the US.
Orphan designation provides a company with research and development tax credits, an opportunity to obtain grant funding, exemption from FDA application fees, and other benefits.
If the FDA approves ImMucin to treat patients with MM, orphan designation will provide Vaxil Biotherapeutics with 7 years of marketing exclusivity in the US. ![]()

The US Food and Drug Administration (FDA) has granted a novel vaccine orphan designation as a treatment for multiple myeloma (MM).
The vaccine, known as ImMucin, targets the signal peptide domain of the MUC1 tumor antigen.
ImMucin works by “teaching” the immune system to identify and destroy cells that display a short, specific, 21-mer portion from MUC1, which appears on 90% of all cancer cells but not in patients’ blood.
Results of a phase 1/2 trial suggested that ImMucin was safe and active in MM patients. The trial included 15 MUC1-positive patients who had residual or biochemically progressive disease after autologous stem cell transplant.
The patients received 6 or 12 bi-weekly intradermal doses of ImMucin co-administered with human granulocyte-macrophage colony-stimulating factor.
The researchers said the vaccine was well-tolerated, as all adverse events were temporary, grade 1-2 in nature, and resolved spontaneously.
There was a significant decrease in soluble MUC1 levels in 9 patients, and 11 patients had stable disease or clinical improvement that persisted for 17.5 months to more than 41.3 months.
A follow-on study (which is ongoing) in patients who responded to ImMucin has shown that some patients can go more than 4 years without requiring any further treatment for their disease.
ImMucin is under development by Vaxil Biotherapeutics Ltd. The vaccine also has orphan designation as a treatment for MM in the European Union.
About orphan designation
The FDA grants orphan designation to encourage companies to develop therapies for diseases that affect fewer than 200,000 individuals in the US.
Orphan designation provides a company with research and development tax credits, an opportunity to obtain grant funding, exemption from FDA application fees, and other benefits.
If the FDA approves ImMucin to treat patients with MM, orphan designation will provide Vaxil Biotherapeutics with 7 years of marketing exclusivity in the US. ![]()

The US Food and Drug Administration (FDA) has granted a novel vaccine orphan designation as a treatment for multiple myeloma (MM).
The vaccine, known as ImMucin, targets the signal peptide domain of the MUC1 tumor antigen.
ImMucin works by “teaching” the immune system to identify and destroy cells that display a short, specific, 21-mer portion from MUC1, which appears on 90% of all cancer cells but not in patients’ blood.
Results of a phase 1/2 trial suggested that ImMucin was safe and active in MM patients. The trial included 15 MUC1-positive patients who had residual or biochemically progressive disease after autologous stem cell transplant.
The patients received 6 or 12 bi-weekly intradermal doses of ImMucin co-administered with human granulocyte-macrophage colony-stimulating factor.
The researchers said the vaccine was well-tolerated, as all adverse events were temporary, grade 1-2 in nature, and resolved spontaneously.
There was a significant decrease in soluble MUC1 levels in 9 patients, and 11 patients had stable disease or clinical improvement that persisted for 17.5 months to more than 41.3 months.
A follow-on study (which is ongoing) in patients who responded to ImMucin has shown that some patients can go more than 4 years without requiring any further treatment for their disease.
ImMucin is under development by Vaxil Biotherapeutics Ltd. The vaccine also has orphan designation as a treatment for MM in the European Union.
About orphan designation
The FDA grants orphan designation to encourage companies to develop therapies for diseases that affect fewer than 200,000 individuals in the US.
Orphan designation provides a company with research and development tax credits, an opportunity to obtain grant funding, exemption from FDA application fees, and other benefits.
If the FDA approves ImMucin to treat patients with MM, orphan designation will provide Vaxil Biotherapeutics with 7 years of marketing exclusivity in the US.
EZH2 inhibitor proves active in rel/ref NHL

LUGANO—The EZH2 inhibitor tazemetostat (EPZ-6438) has shown “meaningful clinical activity” as monotherapy in patients with advanced non-Hodgkin lymphoma (NHL), according to researchers.
In a phase 1 trial, 9 of the 15 evaluable NHL patients achieved an objective response to tazemetostat.
This included 2 ongoing complete responses (CRs), 1 in a patient with diffuse large B-cell lymphoma (DLBCL) and 1 in a patient with follicular lymphoma (FL).
It also included a partial response (PR) in the first treated patient with an EZH2 mutation.
And researchers said the drug was largely well-tolerated, as most adverse events were grade 1 or 2.
“The breadth, depth, and durability of responses seen in NHL patients among multiple histologies continue to impress, as does the safety and tolerability of tazemetostat in this phase 1 study,” said Vincent Ribrag, MD, of Institut Gustave Roussy in Villejuif, France.
“Among the patients in the dose-escalation cohorts, we have seen a noteworthy deepening of responses over time, and, in the first treated patient with an EZH2 tumor mutation, we have seen a partial response, which is very encouraging.”
Dr Ribrag presented these results at the 13th International Conference on Malignant Lymphoma (abstract 145*). The study, which was previously presented at the 26th EORTC-NCI-AACR Symposium on Molecular Targets and Cancer Therapeutics, was sponsored by Epizyme, Inc., the company developing tazemetostat.
The phase 1 trial has enrolled 19 patients with relapsed or refractory B-cell NHL and 26 patients with advanced solid tumors.
Researchers have evaluated 5 cohorts of patients in the dose-escalation portion of the study—100 mg, 200 mg, 400 mg, 800 mg, and 1600 mg—and 2 cohorts—800 mg and 1600 mg—in the dose-expansion phase. All doses of tazemetostat were given twice daily.
The 19 NHL patients had a median age of 61 (range, 24-84) and were heavily pretreated. Eighty-five percent had received 3 or more prior therapies, and 37% had received 5 or more prior therapies.
Thirty-seven percent of patients were refractory to their last prior regimen, and 26% had received a prior autologous hematopoietic stem cell transplant.
Dosing and efficacy
As of June 8, 2015, 15 NHL patients were evaluable for efficacy. Nine had achieved an objective response, including 2 patients with an ongoing CR. All responses were observed between 2 and 10 months on therapy.
Five of the 9 evaluable patients with DLBCL achieved an objective response. One DLBCL patient with a CR remains on study at 18 months of treatment.
Three of 5 evaluable patients with follicular lymphoma (FL) achieved an objective response. One FL patient with a CR remains on study at 13 months, and 1 FL patient with a PR remains on study at 13 months.
The only patient with marginal zone lymphoma achieved a PR and continues on study at 11 months.
One of the 14 patients evaluated for EZH2 status has a specific EZH2 tumor mutation (Y646H). This patient, who had DLBCL that relapsed or was refractory to 6 previous treatment regimens, achieved a PR after 16 weeks of therapy and remains on study.
The recommended phase 2 dose of tazemetostat is 800 mg twice daily.
Adverse events and next steps
All of the 45 enrolled patients were evaluable for safety. Treatment-related adverse events included asthenia (n=10), nausea (n=6), dyspepsia (n=5), thrombocytopenia (n=4), anorexia (n=4), anemia (n=4), vomiting (n=3), constipation (n=2), muscle spasm (n=2), hypertension (n=2), neutropenia (n=2), and elevated transaminase (n=1).
There were 5 grade 3 or higher adverse events related to treatment, including grade 3 anorexia, grade 3 hypertension, grade 3 transaminase elevation, grade 4 thrombocytopenia, and grade 4 neutropenia.
Epizyme plans to report a further update from this trial by the end of this year. The company is now enrolling patients in a phase 2 study of tazemetostat monotherapy in patients with relapsed or refractory NHL, stratified by cell of origin and EZH2 mutation status.
Epizyme is also planning a phase 2 trial of tazemetostat in adults with INI1-deficient solid tumors, a phase 1 study of pediatric patients with INI1-deficient solid tumors, a combination study of tazemetostat with R-CHOP in patients with DLBCL, and a combination study of tazemetostat with a B-cell signaling agent or other emerging targeted therapies for B-cell lymphomas.
*Information in the abstract differs from that presented at the meeting.

LUGANO—The EZH2 inhibitor tazemetostat (EPZ-6438) has shown “meaningful clinical activity” as monotherapy in patients with advanced non-Hodgkin lymphoma (NHL), according to researchers.
In a phase 1 trial, 9 of the 15 evaluable NHL patients achieved an objective response to tazemetostat.
This included 2 ongoing complete responses (CRs), 1 in a patient with diffuse large B-cell lymphoma (DLBCL) and 1 in a patient with follicular lymphoma (FL).
It also included a partial response (PR) in the first treated patient with an EZH2 mutation.
And researchers said the drug was largely well-tolerated, as most adverse events were grade 1 or 2.
“The breadth, depth, and durability of responses seen in NHL patients among multiple histologies continue to impress, as does the safety and tolerability of tazemetostat in this phase 1 study,” said Vincent Ribrag, MD, of Institut Gustave Roussy in Villejuif, France.
“Among the patients in the dose-escalation cohorts, we have seen a noteworthy deepening of responses over time, and, in the first treated patient with an EZH2 tumor mutation, we have seen a partial response, which is very encouraging.”
Dr Ribrag presented these results at the 13th International Conference on Malignant Lymphoma (abstract 145*). The study, which was previously presented at the 26th EORTC-NCI-AACR Symposium on Molecular Targets and Cancer Therapeutics, was sponsored by Epizyme, Inc., the company developing tazemetostat.
The phase 1 trial has enrolled 19 patients with relapsed or refractory B-cell NHL and 26 patients with advanced solid tumors.
Researchers have evaluated 5 cohorts of patients in the dose-escalation portion of the study—100 mg, 200 mg, 400 mg, 800 mg, and 1600 mg—and 2 cohorts—800 mg and 1600 mg—in the dose-expansion phase. All doses of tazemetostat were given twice daily.
The 19 NHL patients had a median age of 61 (range, 24-84) and were heavily pretreated. Eighty-five percent had received 3 or more prior therapies, and 37% had received 5 or more prior therapies.
Thirty-seven percent of patients were refractory to their last prior regimen, and 26% had received a prior autologous hematopoietic stem cell transplant.
Dosing and efficacy
As of June 8, 2015, 15 NHL patients were evaluable for efficacy. Nine had achieved an objective response, including 2 patients with an ongoing CR. All responses were observed between 2 and 10 months on therapy.
Five of the 9 evaluable patients with DLBCL achieved an objective response. One DLBCL patient with a CR remains on study at 18 months of treatment.
Three of 5 evaluable patients with follicular lymphoma (FL) achieved an objective response. One FL patient with a CR remains on study at 13 months, and 1 FL patient with a PR remains on study at 13 months.
The only patient with marginal zone lymphoma achieved a PR and continues on study at 11 months.
One of the 14 patients evaluated for EZH2 status has a specific EZH2 tumor mutation (Y646H). This patient, who had DLBCL that relapsed or was refractory to 6 previous treatment regimens, achieved a PR after 16 weeks of therapy and remains on study.
The recommended phase 2 dose of tazemetostat is 800 mg twice daily.
Adverse events and next steps
All of the 45 enrolled patients were evaluable for safety. Treatment-related adverse events included asthenia (n=10), nausea (n=6), dyspepsia (n=5), thrombocytopenia (n=4), anorexia (n=4), anemia (n=4), vomiting (n=3), constipation (n=2), muscle spasm (n=2), hypertension (n=2), neutropenia (n=2), and elevated transaminase (n=1).
There were 5 grade 3 or higher adverse events related to treatment, including grade 3 anorexia, grade 3 hypertension, grade 3 transaminase elevation, grade 4 thrombocytopenia, and grade 4 neutropenia.
Epizyme plans to report a further update from this trial by the end of this year. The company is now enrolling patients in a phase 2 study of tazemetostat monotherapy in patients with relapsed or refractory NHL, stratified by cell of origin and EZH2 mutation status.
Epizyme is also planning a phase 2 trial of tazemetostat in adults with INI1-deficient solid tumors, a phase 1 study of pediatric patients with INI1-deficient solid tumors, a combination study of tazemetostat with R-CHOP in patients with DLBCL, and a combination study of tazemetostat with a B-cell signaling agent or other emerging targeted therapies for B-cell lymphomas.
*Information in the abstract differs from that presented at the meeting.

LUGANO—The EZH2 inhibitor tazemetostat (EPZ-6438) has shown “meaningful clinical activity” as monotherapy in patients with advanced non-Hodgkin lymphoma (NHL), according to researchers.
In a phase 1 trial, 9 of the 15 evaluable NHL patients achieved an objective response to tazemetostat.
This included 2 ongoing complete responses (CRs), 1 in a patient with diffuse large B-cell lymphoma (DLBCL) and 1 in a patient with follicular lymphoma (FL).
It also included a partial response (PR) in the first treated patient with an EZH2 mutation.
And researchers said the drug was largely well-tolerated, as most adverse events were grade 1 or 2.
“The breadth, depth, and durability of responses seen in NHL patients among multiple histologies continue to impress, as does the safety and tolerability of tazemetostat in this phase 1 study,” said Vincent Ribrag, MD, of Institut Gustave Roussy in Villejuif, France.
“Among the patients in the dose-escalation cohorts, we have seen a noteworthy deepening of responses over time, and, in the first treated patient with an EZH2 tumor mutation, we have seen a partial response, which is very encouraging.”
Dr Ribrag presented these results at the 13th International Conference on Malignant Lymphoma (abstract 145*). The study, which was previously presented at the 26th EORTC-NCI-AACR Symposium on Molecular Targets and Cancer Therapeutics, was sponsored by Epizyme, Inc., the company developing tazemetostat.
The phase 1 trial has enrolled 19 patients with relapsed or refractory B-cell NHL and 26 patients with advanced solid tumors.
Researchers have evaluated 5 cohorts of patients in the dose-escalation portion of the study—100 mg, 200 mg, 400 mg, 800 mg, and 1600 mg—and 2 cohorts—800 mg and 1600 mg—in the dose-expansion phase. All doses of tazemetostat were given twice daily.
The 19 NHL patients had a median age of 61 (range, 24-84) and were heavily pretreated. Eighty-five percent had received 3 or more prior therapies, and 37% had received 5 or more prior therapies.
Thirty-seven percent of patients were refractory to their last prior regimen, and 26% had received a prior autologous hematopoietic stem cell transplant.
Dosing and efficacy
As of June 8, 2015, 15 NHL patients were evaluable for efficacy. Nine had achieved an objective response, including 2 patients with an ongoing CR. All responses were observed between 2 and 10 months on therapy.
Five of the 9 evaluable patients with DLBCL achieved an objective response. One DLBCL patient with a CR remains on study at 18 months of treatment.
Three of 5 evaluable patients with follicular lymphoma (FL) achieved an objective response. One FL patient with a CR remains on study at 13 months, and 1 FL patient with a PR remains on study at 13 months.
The only patient with marginal zone lymphoma achieved a PR and continues on study at 11 months.
One of the 14 patients evaluated for EZH2 status has a specific EZH2 tumor mutation (Y646H). This patient, who had DLBCL that relapsed or was refractory to 6 previous treatment regimens, achieved a PR after 16 weeks of therapy and remains on study.
The recommended phase 2 dose of tazemetostat is 800 mg twice daily.
Adverse events and next steps
All of the 45 enrolled patients were evaluable for safety. Treatment-related adverse events included asthenia (n=10), nausea (n=6), dyspepsia (n=5), thrombocytopenia (n=4), anorexia (n=4), anemia (n=4), vomiting (n=3), constipation (n=2), muscle spasm (n=2), hypertension (n=2), neutropenia (n=2), and elevated transaminase (n=1).
There were 5 grade 3 or higher adverse events related to treatment, including grade 3 anorexia, grade 3 hypertension, grade 3 transaminase elevation, grade 4 thrombocytopenia, and grade 4 neutropenia.
Epizyme plans to report a further update from this trial by the end of this year. The company is now enrolling patients in a phase 2 study of tazemetostat monotherapy in patients with relapsed or refractory NHL, stratified by cell of origin and EZH2 mutation status.
Epizyme is also planning a phase 2 trial of tazemetostat in adults with INI1-deficient solid tumors, a phase 1 study of pediatric patients with INI1-deficient solid tumors, a combination study of tazemetostat with R-CHOP in patients with DLBCL, and a combination study of tazemetostat with a B-cell signaling agent or other emerging targeted therapies for B-cell lymphomas.
*Information in the abstract differs from that presented at the meeting.
Combo shows promise for heavily pretreated MM
Image by Louis Heiser
and Robert Ackland
VIENNA—Combining a novel agent with dexamethasone can produce successful results where other treatments have failed, according to a presentation at the 20th Congress of the European Hematology Association.
Researchers tested low-dose dexamethasone in combination with melflufen, a peptidase-targeted therapy and antiangiogenic compound, in a phase 1/2 study of patients with relapsed or relapsed-refractory multiple myeloma (MM).
The treatment produced an overall response rate of 52%, and, although grade 3/4 hematologic adverse events were common, there were few serious adverse events related to melflufen.
These results were presented at the meeting as abstract P285.* The research was sponsored by Oncopeptides AB, the company developing melflufen.
Drug dosing and patient characteristics
In the phase 1 portion of this study, researchers evaluated 4 dose levels of melflufen—15 mg, 25 mg, 40 mg, and 55 mg—on day 1 with 40 mg of dexamethasone on days 1, 8, and 15 of 21-day cycles in a standard 3+3 design. Eight cycles of therapy were planned, but patients could continue on treatment if they experienced a clinical benefit.
There were no-dose limiting toxicities (DLTs) when melflufen was given at the 3 lower doses. However, 4 of the 6 patients who received the 55 mg dose experienced DLTs of prolonged and severe neutropenia and thrombocytopenia.
So the researchers said the MTD of melflufen, when combined with 40 mg of weekly dexamethasone, was 40 mg every 21 days.
In the ongoing phase 2 portion of the study, 29 patients have received melflufen at the MTD. The median time from the patients’ MM diagnosis to the first dose of melflufen was 5.5 years (range, 1-15), and their median number of prior therapies was 4 (range, 2-11).
Nineteen of the patients were refractory to an immunomodulatory drug (IMiD) or a proteasome inhibitor (PI); 11 were refractory to an alkylator; 10 were refractory to both an IMiD and a PI; and 5 were refractory to an IMiD, a PI, and an alkylator.
Safety data
Among the 29 patients in the phase 2 portion of the study, 22 had treatment-related grade 3-4 adverse events. These included thrombocytopenia (59%), neutropenia (48%), anemia (31%), leukopenia (21%), asthenia (7%), fatigue (7%), hyperglycemia (7%), and pyrexia/fever (7%).
To date, 12 serious adverse events have been reported in 8 of the phase 2 patients. Three events in 3 patients were considered related to melflufen—2 cases of febrile neutropenia and 1 case of pyrexia.
Fifteen patients discontinued therapy, 8 due to adverse events, 6 due to disease progression, and 1 after completing all planned cycles of treatment.
Efficacy data
Twenty-one patients were evaluable for efficacy according to the protocol, meaning they had received 2 or more cycles of therapy and completed response assessments after cycle 2.
Four patients withdrew from treatment after 1 cycle due to rapid disease progression and were included in a second response assessment (n=25). It was too early to evaluate the remaining 4 patients.
Among the 21 protocol-evaluable patients, the overall response rate was 52%, and the clinical benefit rate was 67%. Eleven patients achieved a partial response, 3 had a minimal response, 6 had stable disease, and 1 had progressive disease.
Among all 25 evaluable patients, the overall response rate was 44%, and the clinical benefit rate was 56%.
The median progression-free survival for these patients was 7.6 months (range, 3.4 months to not reached).
The researchers said enrollment in this trial is ongoing, with the goal of reaching 55 patients to further characterize the safety and efficacy of melflufen in heavily pretreated MM patients.
*Information in the abstract differs from that presented at the meeting.

Image by Louis Heiser
and Robert Ackland
VIENNA—Combining a novel agent with dexamethasone can produce successful results where other treatments have failed, according to a presentation at the 20th Congress of the European Hematology Association.
Researchers tested low-dose dexamethasone in combination with melflufen, a peptidase-targeted therapy and antiangiogenic compound, in a phase 1/2 study of patients with relapsed or relapsed-refractory multiple myeloma (MM).
The treatment produced an overall response rate of 52%, and, although grade 3/4 hematologic adverse events were common, there were few serious adverse events related to melflufen.
These results were presented at the meeting as abstract P285.* The research was sponsored by Oncopeptides AB, the company developing melflufen.
Drug dosing and patient characteristics
In the phase 1 portion of this study, researchers evaluated 4 dose levels of melflufen—15 mg, 25 mg, 40 mg, and 55 mg—on day 1 with 40 mg of dexamethasone on days 1, 8, and 15 of 21-day cycles in a standard 3+3 design. Eight cycles of therapy were planned, but patients could continue on treatment if they experienced a clinical benefit.
There were no-dose limiting toxicities (DLTs) when melflufen was given at the 3 lower doses. However, 4 of the 6 patients who received the 55 mg dose experienced DLTs of prolonged and severe neutropenia and thrombocytopenia.
So the researchers said the MTD of melflufen, when combined with 40 mg of weekly dexamethasone, was 40 mg every 21 days.
In the ongoing phase 2 portion of the study, 29 patients have received melflufen at the MTD. The median time from the patients’ MM diagnosis to the first dose of melflufen was 5.5 years (range, 1-15), and their median number of prior therapies was 4 (range, 2-11).
Nineteen of the patients were refractory to an immunomodulatory drug (IMiD) or a proteasome inhibitor (PI); 11 were refractory to an alkylator; 10 were refractory to both an IMiD and a PI; and 5 were refractory to an IMiD, a PI, and an alkylator.
Safety data
Among the 29 patients in the phase 2 portion of the study, 22 had treatment-related grade 3-4 adverse events. These included thrombocytopenia (59%), neutropenia (48%), anemia (31%), leukopenia (21%), asthenia (7%), fatigue (7%), hyperglycemia (7%), and pyrexia/fever (7%).
To date, 12 serious adverse events have been reported in 8 of the phase 2 patients. Three events in 3 patients were considered related to melflufen—2 cases of febrile neutropenia and 1 case of pyrexia.
Fifteen patients discontinued therapy, 8 due to adverse events, 6 due to disease progression, and 1 after completing all planned cycles of treatment.
Efficacy data
Twenty-one patients were evaluable for efficacy according to the protocol, meaning they had received 2 or more cycles of therapy and completed response assessments after cycle 2.
Four patients withdrew from treatment after 1 cycle due to rapid disease progression and were included in a second response assessment (n=25). It was too early to evaluate the remaining 4 patients.
Among the 21 protocol-evaluable patients, the overall response rate was 52%, and the clinical benefit rate was 67%. Eleven patients achieved a partial response, 3 had a minimal response, 6 had stable disease, and 1 had progressive disease.
Among all 25 evaluable patients, the overall response rate was 44%, and the clinical benefit rate was 56%.
The median progression-free survival for these patients was 7.6 months (range, 3.4 months to not reached).
The researchers said enrollment in this trial is ongoing, with the goal of reaching 55 patients to further characterize the safety and efficacy of melflufen in heavily pretreated MM patients.
*Information in the abstract differs from that presented at the meeting.

Image by Louis Heiser
and Robert Ackland
VIENNA—Combining a novel agent with dexamethasone can produce successful results where other treatments have failed, according to a presentation at the 20th Congress of the European Hematology Association.
Researchers tested low-dose dexamethasone in combination with melflufen, a peptidase-targeted therapy and antiangiogenic compound, in a phase 1/2 study of patients with relapsed or relapsed-refractory multiple myeloma (MM).
The treatment produced an overall response rate of 52%, and, although grade 3/4 hematologic adverse events were common, there were few serious adverse events related to melflufen.
These results were presented at the meeting as abstract P285.* The research was sponsored by Oncopeptides AB, the company developing melflufen.
Drug dosing and patient characteristics
In the phase 1 portion of this study, researchers evaluated 4 dose levels of melflufen—15 mg, 25 mg, 40 mg, and 55 mg—on day 1 with 40 mg of dexamethasone on days 1, 8, and 15 of 21-day cycles in a standard 3+3 design. Eight cycles of therapy were planned, but patients could continue on treatment if they experienced a clinical benefit.
There were no-dose limiting toxicities (DLTs) when melflufen was given at the 3 lower doses. However, 4 of the 6 patients who received the 55 mg dose experienced DLTs of prolonged and severe neutropenia and thrombocytopenia.
So the researchers said the MTD of melflufen, when combined with 40 mg of weekly dexamethasone, was 40 mg every 21 days.
In the ongoing phase 2 portion of the study, 29 patients have received melflufen at the MTD. The median time from the patients’ MM diagnosis to the first dose of melflufen was 5.5 years (range, 1-15), and their median number of prior therapies was 4 (range, 2-11).
Nineteen of the patients were refractory to an immunomodulatory drug (IMiD) or a proteasome inhibitor (PI); 11 were refractory to an alkylator; 10 were refractory to both an IMiD and a PI; and 5 were refractory to an IMiD, a PI, and an alkylator.
Safety data
Among the 29 patients in the phase 2 portion of the study, 22 had treatment-related grade 3-4 adverse events. These included thrombocytopenia (59%), neutropenia (48%), anemia (31%), leukopenia (21%), asthenia (7%), fatigue (7%), hyperglycemia (7%), and pyrexia/fever (7%).
To date, 12 serious adverse events have been reported in 8 of the phase 2 patients. Three events in 3 patients were considered related to melflufen—2 cases of febrile neutropenia and 1 case of pyrexia.
Fifteen patients discontinued therapy, 8 due to adverse events, 6 due to disease progression, and 1 after completing all planned cycles of treatment.
Efficacy data
Twenty-one patients were evaluable for efficacy according to the protocol, meaning they had received 2 or more cycles of therapy and completed response assessments after cycle 2.
Four patients withdrew from treatment after 1 cycle due to rapid disease progression and were included in a second response assessment (n=25). It was too early to evaluate the remaining 4 patients.
Among the 21 protocol-evaluable patients, the overall response rate was 52%, and the clinical benefit rate was 67%. Eleven patients achieved a partial response, 3 had a minimal response, 6 had stable disease, and 1 had progressive disease.
Among all 25 evaluable patients, the overall response rate was 44%, and the clinical benefit rate was 56%.
The median progression-free survival for these patients was 7.6 months (range, 3.4 months to not reached).
The researchers said enrollment in this trial is ongoing, with the goal of reaching 55 patients to further characterize the safety and efficacy of melflufen in heavily pretreated MM patients.
*Information in the abstract differs from that presented at the meeting.
FDA approves antiplatelet drug for PCI patients
Photo courtesy of
The Medicines Company
The US Food and Drug Administration (FDA) has approved the intravenous antiplatelet agent cangrelor (Kengreal) for use in adults undergoing percutaneous coronary intervention (PCI).
The drug can now be used to reduce periprocedural thrombotic events in patients who have not been treated with a P2Y12 inhibitor and are not receiving a glycoprotein IIb/IIIa inhibitor.
The FDA’s approval of cangrelor was based on results of the CHAMPION PHOENIX trial.
In this phase 3 trial, researchers compared cangrelor to clopidogrel in 11,145 patients undergoing PCI.
The study’s primary efficacy endpoint was the incidence of death, myocardial infarction, ischemia-driven revascularization, or stent thrombosis.
At 48 hours, 4.7% of patients in the cangrelor arm had met this endpoint, compared to 5.9% of patients in the clopidogrel arm (P=0.005). At 30 days, the incidence was 6.0% in the cangrelor arm and 7.0% in the clopidogrel arm (P=0.03).
The study’s primary safety endpoint was severe bleeding according to GUSTO criteria. At 48 hours, major bleeding had occurred in 0.16% of patients in the cangrelor arm and 0.11% of patients in the clopidogrel arm (P=0.44).
Major bleeding occurred in 4.3% of patients on cangrelor and 2.5% of patients on clopidogrel (P<0.001). And minor bleeding occurred in 11.8% of patients on cangrelor and 8.6% of patients on clopidogrel (P<0.001).
Cangrelor is manufactured by The Medicines Company, which is based in Parsippany, New Jersey.

Photo courtesy of
The Medicines Company
The US Food and Drug Administration (FDA) has approved the intravenous antiplatelet agent cangrelor (Kengreal) for use in adults undergoing percutaneous coronary intervention (PCI).
The drug can now be used to reduce periprocedural thrombotic events in patients who have not been treated with a P2Y12 inhibitor and are not receiving a glycoprotein IIb/IIIa inhibitor.
The FDA’s approval of cangrelor was based on results of the CHAMPION PHOENIX trial.
In this phase 3 trial, researchers compared cangrelor to clopidogrel in 11,145 patients undergoing PCI.
The study’s primary efficacy endpoint was the incidence of death, myocardial infarction, ischemia-driven revascularization, or stent thrombosis.
At 48 hours, 4.7% of patients in the cangrelor arm had met this endpoint, compared to 5.9% of patients in the clopidogrel arm (P=0.005). At 30 days, the incidence was 6.0% in the cangrelor arm and 7.0% in the clopidogrel arm (P=0.03).
The study’s primary safety endpoint was severe bleeding according to GUSTO criteria. At 48 hours, major bleeding had occurred in 0.16% of patients in the cangrelor arm and 0.11% of patients in the clopidogrel arm (P=0.44).
Major bleeding occurred in 4.3% of patients on cangrelor and 2.5% of patients on clopidogrel (P<0.001). And minor bleeding occurred in 11.8% of patients on cangrelor and 8.6% of patients on clopidogrel (P<0.001).
Cangrelor is manufactured by The Medicines Company, which is based in Parsippany, New Jersey.

Photo courtesy of
The Medicines Company
The US Food and Drug Administration (FDA) has approved the intravenous antiplatelet agent cangrelor (Kengreal) for use in adults undergoing percutaneous coronary intervention (PCI).
The drug can now be used to reduce periprocedural thrombotic events in patients who have not been treated with a P2Y12 inhibitor and are not receiving a glycoprotein IIb/IIIa inhibitor.
The FDA’s approval of cangrelor was based on results of the CHAMPION PHOENIX trial.
In this phase 3 trial, researchers compared cangrelor to clopidogrel in 11,145 patients undergoing PCI.
The study’s primary efficacy endpoint was the incidence of death, myocardial infarction, ischemia-driven revascularization, or stent thrombosis.
At 48 hours, 4.7% of patients in the cangrelor arm had met this endpoint, compared to 5.9% of patients in the clopidogrel arm (P=0.005). At 30 days, the incidence was 6.0% in the cangrelor arm and 7.0% in the clopidogrel arm (P=0.03).
The study’s primary safety endpoint was severe bleeding according to GUSTO criteria. At 48 hours, major bleeding had occurred in 0.16% of patients in the cangrelor arm and 0.11% of patients in the clopidogrel arm (P=0.44).
Major bleeding occurred in 4.3% of patients on cangrelor and 2.5% of patients on clopidogrel (P<0.001). And minor bleeding occurred in 11.8% of patients on cangrelor and 8.6% of patients on clopidogrel (P<0.001).
Cangrelor is manufactured by The Medicines Company, which is based in Parsippany, New Jersey.