User login
Intervention reduces CLABSIs in pediatric patients

Staphylococcus infection
Photo by Bill Branson
NASHVILLE—A single-center study has shown that incorporating antimicrobial cloths into an infection-prevention protocol can reduce the incidence of central line-associated bloodstream infections (CLABSIs) in pediatric patients.
After the hospital implemented daily “baths” with disposable cloths containing 2% chlorhexidine gluconate (CHG), its CLABSI incidence fell 59% over a 6-month period.
The details of this experience were presented at the APIC 2015 Annual Conference (abstract 013).
The study was conducted at Riley Hospital for Children at Indiana University Health in Indianapolis. The hospital previously used CHG for daily bathing in the hematology/oncology unit and found it successfully reduced CLABSIs there.
This prompted infection preventionists to consider implementing the practice hospital-wide, regardless of whether patients had central-line catheters.
The infection-prevention team worked with nursing staff, parents, and hospital leadership to adopt daily CHG bathing for all patients and to strengthen adherence to a bundle of prevention practices already in place for patients with central lines.
In addition to daily bathing with CHG-impregnated wipes, the strategies included daily linen changes, assessment of central-line dressings, ensuring use of the appropriate technique for giving medications, and regular tubing and cap changes on the lines.
“We took great care to ensure successful implementation of the new bathing regimen,” said Adam N. Karcz, an infection preventionist at the hospital.
“By educating everyone on the care team, including parents, and standardizing bathing procedures, we were able to dramatically reduce infections and save healthcare dollars in just 6 months.”
Bathing compliance increased from 45% to 81% during the 6-month study period. During the control period—6 months prior to implementation—the 269-bed hospital had 22 CLABSIs. During the implementation period, there were 9 CLABSIs.
The hospital also experienced a 56% drop in the number of methicillin-resistant Staphylococcus aureus (MRSA) infections during this time period.
The reduction in healthcare-associated infections during the implementation period represents a potential cost savings of $297,999. ![]()

Staphylococcus infection
Photo by Bill Branson
NASHVILLE—A single-center study has shown that incorporating antimicrobial cloths into an infection-prevention protocol can reduce the incidence of central line-associated bloodstream infections (CLABSIs) in pediatric patients.
After the hospital implemented daily “baths” with disposable cloths containing 2% chlorhexidine gluconate (CHG), its CLABSI incidence fell 59% over a 6-month period.
The details of this experience were presented at the APIC 2015 Annual Conference (abstract 013).
The study was conducted at Riley Hospital for Children at Indiana University Health in Indianapolis. The hospital previously used CHG for daily bathing in the hematology/oncology unit and found it successfully reduced CLABSIs there.
This prompted infection preventionists to consider implementing the practice hospital-wide, regardless of whether patients had central-line catheters.
The infection-prevention team worked with nursing staff, parents, and hospital leadership to adopt daily CHG bathing for all patients and to strengthen adherence to a bundle of prevention practices already in place for patients with central lines.
In addition to daily bathing with CHG-impregnated wipes, the strategies included daily linen changes, assessment of central-line dressings, ensuring use of the appropriate technique for giving medications, and regular tubing and cap changes on the lines.
“We took great care to ensure successful implementation of the new bathing regimen,” said Adam N. Karcz, an infection preventionist at the hospital.
“By educating everyone on the care team, including parents, and standardizing bathing procedures, we were able to dramatically reduce infections and save healthcare dollars in just 6 months.”
Bathing compliance increased from 45% to 81% during the 6-month study period. During the control period—6 months prior to implementation—the 269-bed hospital had 22 CLABSIs. During the implementation period, there were 9 CLABSIs.
The hospital also experienced a 56% drop in the number of methicillin-resistant Staphylococcus aureus (MRSA) infections during this time period.
The reduction in healthcare-associated infections during the implementation period represents a potential cost savings of $297,999. ![]()

Staphylococcus infection
Photo by Bill Branson
NASHVILLE—A single-center study has shown that incorporating antimicrobial cloths into an infection-prevention protocol can reduce the incidence of central line-associated bloodstream infections (CLABSIs) in pediatric patients.
After the hospital implemented daily “baths” with disposable cloths containing 2% chlorhexidine gluconate (CHG), its CLABSI incidence fell 59% over a 6-month period.
The details of this experience were presented at the APIC 2015 Annual Conference (abstract 013).
The study was conducted at Riley Hospital for Children at Indiana University Health in Indianapolis. The hospital previously used CHG for daily bathing in the hematology/oncology unit and found it successfully reduced CLABSIs there.
This prompted infection preventionists to consider implementing the practice hospital-wide, regardless of whether patients had central-line catheters.
The infection-prevention team worked with nursing staff, parents, and hospital leadership to adopt daily CHG bathing for all patients and to strengthen adherence to a bundle of prevention practices already in place for patients with central lines.
In addition to daily bathing with CHG-impregnated wipes, the strategies included daily linen changes, assessment of central-line dressings, ensuring use of the appropriate technique for giving medications, and regular tubing and cap changes on the lines.
“We took great care to ensure successful implementation of the new bathing regimen,” said Adam N. Karcz, an infection preventionist at the hospital.
“By educating everyone on the care team, including parents, and standardizing bathing procedures, we were able to dramatically reduce infections and save healthcare dollars in just 6 months.”
Bathing compliance increased from 45% to 81% during the 6-month study period. During the control period—6 months prior to implementation—the 269-bed hospital had 22 CLABSIs. During the implementation period, there were 9 CLABSIs.
The hospital also experienced a 56% drop in the number of methicillin-resistant Staphylococcus aureus (MRSA) infections during this time period.
The reduction in healthcare-associated infections during the implementation period represents a potential cost savings of $297,999. ![]()
Anticoagulant antidote effective in healthy volunteers
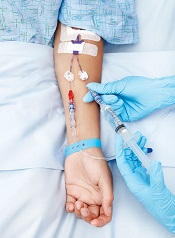
TORONTO—An antidote to factor Xa inhibitors can safely reverse the anticoagulant effect of apixaban in healthy volunteers, results of the ANNEXA-A study suggest.
The first part of this study showed that a bolus of the antidote, andexanet alfa, was effective. And none of the volunteers had serious adverse events, thrombotic events, or antibodies to factor X or Xa.
In the second part of the study, researchers tested a bolus and a 2-hour infusion of andexanet alfa.
The drug normalized coagulation parameters immediately post-bolus, and this effect was sustained during the infusion. The reversal of anti-factor Xa activity lasted 1 to 2 hours post-infusion.
As in part 1, there were no serious adverse events or thrombotic events, and none of the subjects developed antibodies to factor X or Xa.
Mark Crowther, MD, of McMaster University in Hamilton, Ontario, Canada, presented details on part 2 of ANNEXA-A at the ISTH 2015 Congress (abstract LB004). The trial was sponsored by Portola Pharmaceuticals, Inc., the company developing andexanet alfa.
The goal of the randomized, double-blind ANNEXA-A study was to evaluate the safety and efficacy of andexanet alfa in reversing apixaban-induced anticoagulation in healthy volunteers ages 50 to 75.
In part 1, 33 healthy volunteers received apixaban at 5 mg twice daily for 4 days and were then randomized in a 3:1 ratio to andexanet alfa administered as a 400 mg intravenous bolus (n=24) or to placebo (n=9). Results from this part of the study were presented at the American Heart Association 2014 Scientific Sessions.
In the second part of the study, 32 healthy volunteers received apixaban at 5 mg twice daily for 4 days and were then randomized in a 3:1 ratio to andexanet alfa administered as a 400 mg intravenous bolus followed by a continuous infusion of 4 mg/min for 120 minutes (n=24) or to placebo (n=8).
Safety
One subject in the andexanet alfa arm discontinued treatment during the infusion due to mild hives. The subject did not have any other allergic
manifestations or cardiorespiratory effects.
Six subjects had mild infusion-related reactions, 4 (16.7%) in the andexanet alfa arm and 2 (25%) in the placebo arm.
None of the subjects had an increase in D-dimer (more than 2 times the upper limit of normal) on more than 1 day.
The majority of andexanet-alfa-treated subjects had transient elevation of F1 and F2, but, in all cases, levels returned to less than or equal to 2 times the upper limit of normal by the fourth day.
Efficacy
Twenty-three subjects in the andexanet alfa arm and all 8 subjects in the placebo arm were evaluable for efficacy.
All evaluable subjects in the andexanet alfa arm had an 80% or greater reduction in anti-factor Xa activity post-infusion nadir, compared to none of the subjects on placebo (P<0.0001).
The mean percent change in anti-factor Xa activity from baseline to post-infusion nadir was 92% in the andexanet alfa arm (P<0.0001 vs placebo). And the mean percent change from baseline to post-bolus nadir was 93% (P<0.0001 vs placebo).
The mean change in free apixaban concentration from baseline to post-infusion nadir was 1.39 ng/mL in the andexanet alfa arm (P=0.0002 vs placebo).
Thrombin generation was restored to the day 1, pre-apixaban baseline range in all 23 subjects on andexanet alfa (P<0.0001). And there was no long-term effect on thrombin generation.
The researchers said andexanet alfa demonstrated rapid onset and offset of action. Furthermore, it seems that either a bolus dose alone or a bolus plus infusion can reverse apixaban’s anticoagulant activity, which could provide flexibility for bleeding patients.
Andexanet alfa is also under investigation as an antidote to rivaroxaban, edoxaban, enoxaparin, and betrixaban. ![]()

TORONTO—An antidote to factor Xa inhibitors can safely reverse the anticoagulant effect of apixaban in healthy volunteers, results of the ANNEXA-A study suggest.
The first part of this study showed that a bolus of the antidote, andexanet alfa, was effective. And none of the volunteers had serious adverse events, thrombotic events, or antibodies to factor X or Xa.
In the second part of the study, researchers tested a bolus and a 2-hour infusion of andexanet alfa.
The drug normalized coagulation parameters immediately post-bolus, and this effect was sustained during the infusion. The reversal of anti-factor Xa activity lasted 1 to 2 hours post-infusion.
As in part 1, there were no serious adverse events or thrombotic events, and none of the subjects developed antibodies to factor X or Xa.
Mark Crowther, MD, of McMaster University in Hamilton, Ontario, Canada, presented details on part 2 of ANNEXA-A at the ISTH 2015 Congress (abstract LB004). The trial was sponsored by Portola Pharmaceuticals, Inc., the company developing andexanet alfa.
The goal of the randomized, double-blind ANNEXA-A study was to evaluate the safety and efficacy of andexanet alfa in reversing apixaban-induced anticoagulation in healthy volunteers ages 50 to 75.
In part 1, 33 healthy volunteers received apixaban at 5 mg twice daily for 4 days and were then randomized in a 3:1 ratio to andexanet alfa administered as a 400 mg intravenous bolus (n=24) or to placebo (n=9). Results from this part of the study were presented at the American Heart Association 2014 Scientific Sessions.
In the second part of the study, 32 healthy volunteers received apixaban at 5 mg twice daily for 4 days and were then randomized in a 3:1 ratio to andexanet alfa administered as a 400 mg intravenous bolus followed by a continuous infusion of 4 mg/min for 120 minutes (n=24) or to placebo (n=8).
Safety
One subject in the andexanet alfa arm discontinued treatment during the infusion due to mild hives. The subject did not have any other allergic
manifestations or cardiorespiratory effects.
Six subjects had mild infusion-related reactions, 4 (16.7%) in the andexanet alfa arm and 2 (25%) in the placebo arm.
None of the subjects had an increase in D-dimer (more than 2 times the upper limit of normal) on more than 1 day.
The majority of andexanet-alfa-treated subjects had transient elevation of F1 and F2, but, in all cases, levels returned to less than or equal to 2 times the upper limit of normal by the fourth day.
Efficacy
Twenty-three subjects in the andexanet alfa arm and all 8 subjects in the placebo arm were evaluable for efficacy.
All evaluable subjects in the andexanet alfa arm had an 80% or greater reduction in anti-factor Xa activity post-infusion nadir, compared to none of the subjects on placebo (P<0.0001).
The mean percent change in anti-factor Xa activity from baseline to post-infusion nadir was 92% in the andexanet alfa arm (P<0.0001 vs placebo). And the mean percent change from baseline to post-bolus nadir was 93% (P<0.0001 vs placebo).
The mean change in free apixaban concentration from baseline to post-infusion nadir was 1.39 ng/mL in the andexanet alfa arm (P=0.0002 vs placebo).
Thrombin generation was restored to the day 1, pre-apixaban baseline range in all 23 subjects on andexanet alfa (P<0.0001). And there was no long-term effect on thrombin generation.
The researchers said andexanet alfa demonstrated rapid onset and offset of action. Furthermore, it seems that either a bolus dose alone or a bolus plus infusion can reverse apixaban’s anticoagulant activity, which could provide flexibility for bleeding patients.
Andexanet alfa is also under investigation as an antidote to rivaroxaban, edoxaban, enoxaparin, and betrixaban. ![]()

TORONTO—An antidote to factor Xa inhibitors can safely reverse the anticoagulant effect of apixaban in healthy volunteers, results of the ANNEXA-A study suggest.
The first part of this study showed that a bolus of the antidote, andexanet alfa, was effective. And none of the volunteers had serious adverse events, thrombotic events, or antibodies to factor X or Xa.
In the second part of the study, researchers tested a bolus and a 2-hour infusion of andexanet alfa.
The drug normalized coagulation parameters immediately post-bolus, and this effect was sustained during the infusion. The reversal of anti-factor Xa activity lasted 1 to 2 hours post-infusion.
As in part 1, there were no serious adverse events or thrombotic events, and none of the subjects developed antibodies to factor X or Xa.
Mark Crowther, MD, of McMaster University in Hamilton, Ontario, Canada, presented details on part 2 of ANNEXA-A at the ISTH 2015 Congress (abstract LB004). The trial was sponsored by Portola Pharmaceuticals, Inc., the company developing andexanet alfa.
The goal of the randomized, double-blind ANNEXA-A study was to evaluate the safety and efficacy of andexanet alfa in reversing apixaban-induced anticoagulation in healthy volunteers ages 50 to 75.
In part 1, 33 healthy volunteers received apixaban at 5 mg twice daily for 4 days and were then randomized in a 3:1 ratio to andexanet alfa administered as a 400 mg intravenous bolus (n=24) or to placebo (n=9). Results from this part of the study were presented at the American Heart Association 2014 Scientific Sessions.
In the second part of the study, 32 healthy volunteers received apixaban at 5 mg twice daily for 4 days and were then randomized in a 3:1 ratio to andexanet alfa administered as a 400 mg intravenous bolus followed by a continuous infusion of 4 mg/min for 120 minutes (n=24) or to placebo (n=8).
Safety
One subject in the andexanet alfa arm discontinued treatment during the infusion due to mild hives. The subject did not have any other allergic
manifestations or cardiorespiratory effects.
Six subjects had mild infusion-related reactions, 4 (16.7%) in the andexanet alfa arm and 2 (25%) in the placebo arm.
None of the subjects had an increase in D-dimer (more than 2 times the upper limit of normal) on more than 1 day.
The majority of andexanet-alfa-treated subjects had transient elevation of F1 and F2, but, in all cases, levels returned to less than or equal to 2 times the upper limit of normal by the fourth day.
Efficacy
Twenty-three subjects in the andexanet alfa arm and all 8 subjects in the placebo arm were evaluable for efficacy.
All evaluable subjects in the andexanet alfa arm had an 80% or greater reduction in anti-factor Xa activity post-infusion nadir, compared to none of the subjects on placebo (P<0.0001).
The mean percent change in anti-factor Xa activity from baseline to post-infusion nadir was 92% in the andexanet alfa arm (P<0.0001 vs placebo). And the mean percent change from baseline to post-bolus nadir was 93% (P<0.0001 vs placebo).
The mean change in free apixaban concentration from baseline to post-infusion nadir was 1.39 ng/mL in the andexanet alfa arm (P=0.0002 vs placebo).
Thrombin generation was restored to the day 1, pre-apixaban baseline range in all 23 subjects on andexanet alfa (P<0.0001). And there was no long-term effect on thrombin generation.
The researchers said andexanet alfa demonstrated rapid onset and offset of action. Furthermore, it seems that either a bolus dose alone or a bolus plus infusion can reverse apixaban’s anticoagulant activity, which could provide flexibility for bleeding patients.
Andexanet alfa is also under investigation as an antidote to rivaroxaban, edoxaban, enoxaparin, and betrixaban. ![]()
Cord milking better than delayed clamping for some preterm infants
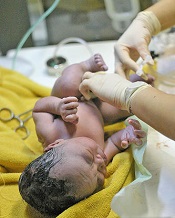
Photo courtesy of Meutia
Chaerani & Indradi Soemardjan
Umbilical cord milking may be more beneficial than delayed cord clamping for preterm infants delivered by Cesarean section, according to new research.
The study showed that cord milking produced greater blood circulation, higher hemoglobin levels, and higher blood pressure, but only in preterm infants delivered by Cesarean.
For preterm infants delivered vaginally, there was no significant difference between the milking and delayed clamping groups.
Anup C. Katheria, MD, of the Neonatal Research Institute at the Sharp Mary Birch Hospital in San Diego, California, and his colleagues reported these findings in Pediatrics.
The researchers noted that, in 2012, the American College of Obstetricians and Gynecologists recommended a 30- to 60-second delay before clamping the umbilical cord in all preterm deliveries.
This is thought to allow sufficient time for blood from the umbilical cord to fill the blood vessels in the infant’s lungs and to protect infants from intraventricular hemorrhage. However, some previous studies failed to find a reduction in intraventricular hemorrhage from delayed cord clamping among preterm infants delivered by Cesarean.
Dr Katheria and his colleagues theorized that the use of an anesthetic in Cesarean delivery reduces uterine contractions and therefore hinders the exodus of blood from the umbilical cord.
They reasoned that cord milking—encircling the cord with thumb and forefingers, gently squeezing, and slowly pushing the blood through the cord to the infant’s abdomen—might compensate for diminished blood flow through the umbilical cord and increase the amount of blood available to the infant.
To test this theory, the researchers enrolled 197 infants in a prospective study. Mothers went into labor at or before the 32nd week of pregnancy.
Of the 154 infants delivered by Cesarean, 75 were randomized to the umbilical cord milking (UCM) group and 79 to the delayed cord clamping (DCC) group.
Infants in the UCM group had significantly higher blood flow in the superior vena cava than those in the DCC group—93 ± 24 mL/kg per min vs 81 ± 29 mL/kg per min (P<0.05)—and a significantly higher output of blood from the right ventricle—261 ± 80 mL/kg per min vs 216 ±73 mL/kg per min (P<0.001).
These measures, taken together, are an indication of blood circulation in the brain and body.
Infants in the UCM group had significantly higher hemoglobin levels at birth than infants in the DCC group—16.3 ± 2.4 g/dL vs 15.6 ± 2.2 g/dL (P<0.05). And mean arterial pressure in the first 15 hours of life was significantly higher in the UCM group than the DCC group (P=0.02).
Among the 43 infants who were delivered vaginally, the researchers found no significant differences in outcomes between infants randomized to UCM or DCC. ![]()

Photo courtesy of Meutia
Chaerani & Indradi Soemardjan
Umbilical cord milking may be more beneficial than delayed cord clamping for preterm infants delivered by Cesarean section, according to new research.
The study showed that cord milking produced greater blood circulation, higher hemoglobin levels, and higher blood pressure, but only in preterm infants delivered by Cesarean.
For preterm infants delivered vaginally, there was no significant difference between the milking and delayed clamping groups.
Anup C. Katheria, MD, of the Neonatal Research Institute at the Sharp Mary Birch Hospital in San Diego, California, and his colleagues reported these findings in Pediatrics.
The researchers noted that, in 2012, the American College of Obstetricians and Gynecologists recommended a 30- to 60-second delay before clamping the umbilical cord in all preterm deliveries.
This is thought to allow sufficient time for blood from the umbilical cord to fill the blood vessels in the infant’s lungs and to protect infants from intraventricular hemorrhage. However, some previous studies failed to find a reduction in intraventricular hemorrhage from delayed cord clamping among preterm infants delivered by Cesarean.
Dr Katheria and his colleagues theorized that the use of an anesthetic in Cesarean delivery reduces uterine contractions and therefore hinders the exodus of blood from the umbilical cord.
They reasoned that cord milking—encircling the cord with thumb and forefingers, gently squeezing, and slowly pushing the blood through the cord to the infant’s abdomen—might compensate for diminished blood flow through the umbilical cord and increase the amount of blood available to the infant.
To test this theory, the researchers enrolled 197 infants in a prospective study. Mothers went into labor at or before the 32nd week of pregnancy.
Of the 154 infants delivered by Cesarean, 75 were randomized to the umbilical cord milking (UCM) group and 79 to the delayed cord clamping (DCC) group.
Infants in the UCM group had significantly higher blood flow in the superior vena cava than those in the DCC group—93 ± 24 mL/kg per min vs 81 ± 29 mL/kg per min (P<0.05)—and a significantly higher output of blood from the right ventricle—261 ± 80 mL/kg per min vs 216 ±73 mL/kg per min (P<0.001).
These measures, taken together, are an indication of blood circulation in the brain and body.
Infants in the UCM group had significantly higher hemoglobin levels at birth than infants in the DCC group—16.3 ± 2.4 g/dL vs 15.6 ± 2.2 g/dL (P<0.05). And mean arterial pressure in the first 15 hours of life was significantly higher in the UCM group than the DCC group (P=0.02).
Among the 43 infants who were delivered vaginally, the researchers found no significant differences in outcomes between infants randomized to UCM or DCC. ![]()

Photo courtesy of Meutia
Chaerani & Indradi Soemardjan
Umbilical cord milking may be more beneficial than delayed cord clamping for preterm infants delivered by Cesarean section, according to new research.
The study showed that cord milking produced greater blood circulation, higher hemoglobin levels, and higher blood pressure, but only in preterm infants delivered by Cesarean.
For preterm infants delivered vaginally, there was no significant difference between the milking and delayed clamping groups.
Anup C. Katheria, MD, of the Neonatal Research Institute at the Sharp Mary Birch Hospital in San Diego, California, and his colleagues reported these findings in Pediatrics.
The researchers noted that, in 2012, the American College of Obstetricians and Gynecologists recommended a 30- to 60-second delay before clamping the umbilical cord in all preterm deliveries.
This is thought to allow sufficient time for blood from the umbilical cord to fill the blood vessels in the infant’s lungs and to protect infants from intraventricular hemorrhage. However, some previous studies failed to find a reduction in intraventricular hemorrhage from delayed cord clamping among preterm infants delivered by Cesarean.
Dr Katheria and his colleagues theorized that the use of an anesthetic in Cesarean delivery reduces uterine contractions and therefore hinders the exodus of blood from the umbilical cord.
They reasoned that cord milking—encircling the cord with thumb and forefingers, gently squeezing, and slowly pushing the blood through the cord to the infant’s abdomen—might compensate for diminished blood flow through the umbilical cord and increase the amount of blood available to the infant.
To test this theory, the researchers enrolled 197 infants in a prospective study. Mothers went into labor at or before the 32nd week of pregnancy.
Of the 154 infants delivered by Cesarean, 75 were randomized to the umbilical cord milking (UCM) group and 79 to the delayed cord clamping (DCC) group.
Infants in the UCM group had significantly higher blood flow in the superior vena cava than those in the DCC group—93 ± 24 mL/kg per min vs 81 ± 29 mL/kg per min (P<0.05)—and a significantly higher output of blood from the right ventricle—261 ± 80 mL/kg per min vs 216 ±73 mL/kg per min (P<0.001).
These measures, taken together, are an indication of blood circulation in the brain and body.
Infants in the UCM group had significantly higher hemoglobin levels at birth than infants in the DCC group—16.3 ± 2.4 g/dL vs 15.6 ± 2.2 g/dL (P<0.05). And mean arterial pressure in the first 15 hours of life was significantly higher in the UCM group than the DCC group (P=0.02).
Among the 43 infants who were delivered vaginally, the researchers found no significant differences in outcomes between infants randomized to UCM or DCC. ![]()
Long-term data support use of FVIII treatment
TORONTO—The antihemophilic factor turoctocog alfa is safe and effective long-term, according to interim data from the phase 3 guardian 2 trial.
With more than 4 years of safety data, researchers have found turoctocog alfa to be well-tolerated in patients with hemophilia A.
The median annualized bleeding rate for patients on prophylactic treatment was 1.56 bleeds per patient per year. For patients who received turoctocog alfa on demand, a single injection stopped all bleeds.
And none of the patients developed factor VIII (FVIII) inhibitors.
Margareth Ozelo, MD, PhD, of the University of Campinas in Sao Paulo, Brazil and her colleagues presented these data at the ISTH 2015 Congress (abstract PO251-WED). The research is sponsored by Novo Nordisk, the company developing turoctocog alfa (as NovoEight).
Turoctocog alfa is a B-domain truncated recombinant human coagulation FVIII product indicated for the treatment and prevention of bleeding in patients with hemophilia A. The ongoing guardian 2 trial is a prospective safety and efficacy extension trial of the guardian 1 and guardian 3 studies.
Two hundred patients received turoctocog alfa in guardian 2. They had severe hemophilia A (FVIII activity ≤ 1%), no history of inhibitors, and had completed guardian 1, guardian 3, or a third pharmacokinetics trial. The patients’ mean age at first turoctocog alfa injection was 22.3 ± 14.4 years.
In guardian 1 and guardian 3, all patients switched from other FVIII products to turoctocog alfa prophylaxis every second day (adults/adolescents, 20–40 IU/kg; children, 25–50 IU/kg), or 3 times weekly (adults/adolescents, 20–50 IU/kg; children 25–60 IU/kg). Patients also received turoctocog alfa when bleeds arose.
Of the 200 patients enrolled on guardian 2, 133 were still participating in the trial at the interim cutoff date, December 31, 2013.
The interim analysis includes data for 451.6 patient-years and 72,320 days of exposure to turoctocog alfa. The total number of exposure days was 364.5
(range, 1-762) per patient for prophylaxis and 23.8 (range, 1-90) per patient for on-demand treatment.
The mean number of turoctocog alfa doses was 368.3 (range, 1-766) per patient for prophylaxis and 24.2 (range, 1-90) per patient for on-demand treatment.
Safety results
At the interim cutoff, none of the patients had developed FVIII inhibitors. Adverse events occurred in 84% of patients (n=168). The most common were
headache, nasopharyngitis, upper respiratory tract infection, and arthralgia.
Eight adverse events were considered possibly or probably related to turoctocog alfa in 5 patients (2.5%). These events were mild or moderate and included local swelling (n=1), increased aspartate aminotransferase (n=1), increased alanine aminotransferase (n=1), pain in extremity (n=1), musculoskeletal pain (n=1), lichenoid keratosis (n=1), and arthropathy (n=2).
There were 29 serious adverse events that were considered unlikely to be treatment-related. This included a death from subdural hemorrhage.
Efficacy results
For patients on prophylactic treatment (n=197), the median annualized bleeding rate was 1.56 bleeds per patient per year for all bleeds. It was 0.50 for
spontaneous bleeds, 0.49 for traumatic bleeds, 0.93 for joint bleeds, and 0.35 for nonjoint bleeds.
The success rate for treating bleeds during prophylaxis was 89.4%, and 90% of all bleeding episodes were successfully treated with 1 or 2 infusions of
turoctocog alfa. As for on-demand treatment, a single injection stopped all 73 bleeds.
“These interim results provide an extension to the body of evidence supporting the long-term use of NovoEight,” Dr Ozelo said. “For people with hemophilia A, finding treatments that are effective at preventing bleeding episodes long-term is essential.” ![]()

TORONTO—The antihemophilic factor turoctocog alfa is safe and effective long-term, according to interim data from the phase 3 guardian 2 trial.
With more than 4 years of safety data, researchers have found turoctocog alfa to be well-tolerated in patients with hemophilia A.
The median annualized bleeding rate for patients on prophylactic treatment was 1.56 bleeds per patient per year. For patients who received turoctocog alfa on demand, a single injection stopped all bleeds.
And none of the patients developed factor VIII (FVIII) inhibitors.
Margareth Ozelo, MD, PhD, of the University of Campinas in Sao Paulo, Brazil and her colleagues presented these data at the ISTH 2015 Congress (abstract PO251-WED). The research is sponsored by Novo Nordisk, the company developing turoctocog alfa (as NovoEight).
Turoctocog alfa is a B-domain truncated recombinant human coagulation FVIII product indicated for the treatment and prevention of bleeding in patients with hemophilia A. The ongoing guardian 2 trial is a prospective safety and efficacy extension trial of the guardian 1 and guardian 3 studies.
Two hundred patients received turoctocog alfa in guardian 2. They had severe hemophilia A (FVIII activity ≤ 1%), no history of inhibitors, and had completed guardian 1, guardian 3, or a third pharmacokinetics trial. The patients’ mean age at first turoctocog alfa injection was 22.3 ± 14.4 years.
In guardian 1 and guardian 3, all patients switched from other FVIII products to turoctocog alfa prophylaxis every second day (adults/adolescents, 20–40 IU/kg; children, 25–50 IU/kg), or 3 times weekly (adults/adolescents, 20–50 IU/kg; children 25–60 IU/kg). Patients also received turoctocog alfa when bleeds arose.
Of the 200 patients enrolled on guardian 2, 133 were still participating in the trial at the interim cutoff date, December 31, 2013.
The interim analysis includes data for 451.6 patient-years and 72,320 days of exposure to turoctocog alfa. The total number of exposure days was 364.5
(range, 1-762) per patient for prophylaxis and 23.8 (range, 1-90) per patient for on-demand treatment.
The mean number of turoctocog alfa doses was 368.3 (range, 1-766) per patient for prophylaxis and 24.2 (range, 1-90) per patient for on-demand treatment.
Safety results
At the interim cutoff, none of the patients had developed FVIII inhibitors. Adverse events occurred in 84% of patients (n=168). The most common were
headache, nasopharyngitis, upper respiratory tract infection, and arthralgia.
Eight adverse events were considered possibly or probably related to turoctocog alfa in 5 patients (2.5%). These events were mild or moderate and included local swelling (n=1), increased aspartate aminotransferase (n=1), increased alanine aminotransferase (n=1), pain in extremity (n=1), musculoskeletal pain (n=1), lichenoid keratosis (n=1), and arthropathy (n=2).
There were 29 serious adverse events that were considered unlikely to be treatment-related. This included a death from subdural hemorrhage.
Efficacy results
For patients on prophylactic treatment (n=197), the median annualized bleeding rate was 1.56 bleeds per patient per year for all bleeds. It was 0.50 for
spontaneous bleeds, 0.49 for traumatic bleeds, 0.93 for joint bleeds, and 0.35 for nonjoint bleeds.
The success rate for treating bleeds during prophylaxis was 89.4%, and 90% of all bleeding episodes were successfully treated with 1 or 2 infusions of
turoctocog alfa. As for on-demand treatment, a single injection stopped all 73 bleeds.
“These interim results provide an extension to the body of evidence supporting the long-term use of NovoEight,” Dr Ozelo said. “For people with hemophilia A, finding treatments that are effective at preventing bleeding episodes long-term is essential.” ![]()

TORONTO—The antihemophilic factor turoctocog alfa is safe and effective long-term, according to interim data from the phase 3 guardian 2 trial.
With more than 4 years of safety data, researchers have found turoctocog alfa to be well-tolerated in patients with hemophilia A.
The median annualized bleeding rate for patients on prophylactic treatment was 1.56 bleeds per patient per year. For patients who received turoctocog alfa on demand, a single injection stopped all bleeds.
And none of the patients developed factor VIII (FVIII) inhibitors.
Margareth Ozelo, MD, PhD, of the University of Campinas in Sao Paulo, Brazil and her colleagues presented these data at the ISTH 2015 Congress (abstract PO251-WED). The research is sponsored by Novo Nordisk, the company developing turoctocog alfa (as NovoEight).
Turoctocog alfa is a B-domain truncated recombinant human coagulation FVIII product indicated for the treatment and prevention of bleeding in patients with hemophilia A. The ongoing guardian 2 trial is a prospective safety and efficacy extension trial of the guardian 1 and guardian 3 studies.
Two hundred patients received turoctocog alfa in guardian 2. They had severe hemophilia A (FVIII activity ≤ 1%), no history of inhibitors, and had completed guardian 1, guardian 3, or a third pharmacokinetics trial. The patients’ mean age at first turoctocog alfa injection was 22.3 ± 14.4 years.
In guardian 1 and guardian 3, all patients switched from other FVIII products to turoctocog alfa prophylaxis every second day (adults/adolescents, 20–40 IU/kg; children, 25–50 IU/kg), or 3 times weekly (adults/adolescents, 20–50 IU/kg; children 25–60 IU/kg). Patients also received turoctocog alfa when bleeds arose.
Of the 200 patients enrolled on guardian 2, 133 were still participating in the trial at the interim cutoff date, December 31, 2013.
The interim analysis includes data for 451.6 patient-years and 72,320 days of exposure to turoctocog alfa. The total number of exposure days was 364.5
(range, 1-762) per patient for prophylaxis and 23.8 (range, 1-90) per patient for on-demand treatment.
The mean number of turoctocog alfa doses was 368.3 (range, 1-766) per patient for prophylaxis and 24.2 (range, 1-90) per patient for on-demand treatment.
Safety results
At the interim cutoff, none of the patients had developed FVIII inhibitors. Adverse events occurred in 84% of patients (n=168). The most common were
headache, nasopharyngitis, upper respiratory tract infection, and arthralgia.
Eight adverse events were considered possibly or probably related to turoctocog alfa in 5 patients (2.5%). These events were mild or moderate and included local swelling (n=1), increased aspartate aminotransferase (n=1), increased alanine aminotransferase (n=1), pain in extremity (n=1), musculoskeletal pain (n=1), lichenoid keratosis (n=1), and arthropathy (n=2).
There were 29 serious adverse events that were considered unlikely to be treatment-related. This included a death from subdural hemorrhage.
Efficacy results
For patients on prophylactic treatment (n=197), the median annualized bleeding rate was 1.56 bleeds per patient per year for all bleeds. It was 0.50 for
spontaneous bleeds, 0.49 for traumatic bleeds, 0.93 for joint bleeds, and 0.35 for nonjoint bleeds.
The success rate for treating bleeds during prophylaxis was 89.4%, and 90% of all bleeding episodes were successfully treated with 1 or 2 infusions of
turoctocog alfa. As for on-demand treatment, a single injection stopped all 73 bleeds.
“These interim results provide an extension to the body of evidence supporting the long-term use of NovoEight,” Dr Ozelo said. “For people with hemophilia A, finding treatments that are effective at preventing bleeding episodes long-term is essential.” ![]()
Insecticide can cause NHL, experts say

Photo by John Messina
The insecticide gamma-hexachlorocyclohexane (lindane) is carcinogenic, according to experts from the International Agency for Research on Cancer (IARC), the specialized cancer agency of the World Health Organization.
The experts said they found sufficient evidence that lindane, which is banned or restricted in most countries, can cause non-Hodgkin lymphoma (NHL).
The group also discovered that 2 other chemicals might cause NHL.
The evidence suggests the insecticide dichlorodiphenyltrichloroethane (DDT) is probably carcinogenic, and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) is possibly carcinogenic.
A summary of these findings is available in The Lancet Oncology, and the experts’ detailed assessments will be published as Volume 113 of the IARC Monographs.
The group, which consisted of 26 experts convened by the IARC Monographs Programme, reviewed the latest scientific literature on lindane, DDT, and 2,4-D and used their findings to classify these 3 chemicals according to carcinogenicity.
The classification (Group 1, Group 2A, etc.) indicates the strength of the evidence that a substance causes cancer, not the level of risk associated with exposure. The Monographs Programme identifies cancer hazards even when risks are very low at current exposure levels, because new uses or unforeseen exposures could engender risks that are significantly higher.
Lindane
The experts classified lindane as carcinogenic to humans (Group 1), saying they found sufficient evidence that it can cause NHL. Large epidemiological studies of agricultural exposures in the US and Canada showed a 60% increased risk of NHL in people exposed to lindane.
Lindane has been used extensively for insect control, including in agriculture and for the treatment of human lice and scabies. High exposures have occurred among agricultural workers and pesticide applicators. However, the use of lindane is now banned or restricted in most countries.
DDT
The experts classified DDT as probably carcinogenic to humans (Group 2A), saying they found sufficient evidence that DDT causes cancer in experimental animals and limited evidence of DDT’s carcinogenicity in humans.
Epidemiological studies have shown positive associations between exposure to DDT and NHL, testicular cancer, and liver cancer.
There was also strong experimental evidence that DDT can suppress the immune system and disrupt sex hormones. However, overall, there was no association between breast cancer and DDT levels measured in samples of blood or fat.
DDT was introduced for the control of insect-borne diseases during World War II and was later applied widely to eradicate malaria and in agriculture. Most uses of DDT were banned in the 1970s. However, DDT and its breakdown products are highly persistent and can be found in the environment and in animal and human tissues throughout the world.
Exposure to DDT still occurs, mainly through diet. The remaining and essential use of DDT is for disease vector control, mainly for malaria. This use is strictly restricted under the Stockholm Convention.
2,4-D
The experts classified 2,4-D as possibly carcinogenic to humans (Group 2B), saying they had inadequate evidence in humans and limited evidence in experimental animals.
There is strong evidence that 2,4-D induces oxidative stress and moderate evidence that 2,4-D causes immunosuppression, based on in vivo and in vitro studies. However, epidemiological studies did not show strong or consistent increases in the risk of NHL or other cancers in relation to 2,4-D exposure.
Since its introduction in 1945, 2,4-D has been widely used to control weeds in agriculture, forestry, and urban and residential settings. Occupational exposures to 2,4-D can occur during manufacturing and application, and the general population can be exposed through food, water, dust, or residential application, and during spraying. ![]()

Photo by John Messina
The insecticide gamma-hexachlorocyclohexane (lindane) is carcinogenic, according to experts from the International Agency for Research on Cancer (IARC), the specialized cancer agency of the World Health Organization.
The experts said they found sufficient evidence that lindane, which is banned or restricted in most countries, can cause non-Hodgkin lymphoma (NHL).
The group also discovered that 2 other chemicals might cause NHL.
The evidence suggests the insecticide dichlorodiphenyltrichloroethane (DDT) is probably carcinogenic, and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) is possibly carcinogenic.
A summary of these findings is available in The Lancet Oncology, and the experts’ detailed assessments will be published as Volume 113 of the IARC Monographs.
The group, which consisted of 26 experts convened by the IARC Monographs Programme, reviewed the latest scientific literature on lindane, DDT, and 2,4-D and used their findings to classify these 3 chemicals according to carcinogenicity.
The classification (Group 1, Group 2A, etc.) indicates the strength of the evidence that a substance causes cancer, not the level of risk associated with exposure. The Monographs Programme identifies cancer hazards even when risks are very low at current exposure levels, because new uses or unforeseen exposures could engender risks that are significantly higher.
Lindane
The experts classified lindane as carcinogenic to humans (Group 1), saying they found sufficient evidence that it can cause NHL. Large epidemiological studies of agricultural exposures in the US and Canada showed a 60% increased risk of NHL in people exposed to lindane.
Lindane has been used extensively for insect control, including in agriculture and for the treatment of human lice and scabies. High exposures have occurred among agricultural workers and pesticide applicators. However, the use of lindane is now banned or restricted in most countries.
DDT
The experts classified DDT as probably carcinogenic to humans (Group 2A), saying they found sufficient evidence that DDT causes cancer in experimental animals and limited evidence of DDT’s carcinogenicity in humans.
Epidemiological studies have shown positive associations between exposure to DDT and NHL, testicular cancer, and liver cancer.
There was also strong experimental evidence that DDT can suppress the immune system and disrupt sex hormones. However, overall, there was no association between breast cancer and DDT levels measured in samples of blood or fat.
DDT was introduced for the control of insect-borne diseases during World War II and was later applied widely to eradicate malaria and in agriculture. Most uses of DDT were banned in the 1970s. However, DDT and its breakdown products are highly persistent and can be found in the environment and in animal and human tissues throughout the world.
Exposure to DDT still occurs, mainly through diet. The remaining and essential use of DDT is for disease vector control, mainly for malaria. This use is strictly restricted under the Stockholm Convention.
2,4-D
The experts classified 2,4-D as possibly carcinogenic to humans (Group 2B), saying they had inadequate evidence in humans and limited evidence in experimental animals.
There is strong evidence that 2,4-D induces oxidative stress and moderate evidence that 2,4-D causes immunosuppression, based on in vivo and in vitro studies. However, epidemiological studies did not show strong or consistent increases in the risk of NHL or other cancers in relation to 2,4-D exposure.
Since its introduction in 1945, 2,4-D has been widely used to control weeds in agriculture, forestry, and urban and residential settings. Occupational exposures to 2,4-D can occur during manufacturing and application, and the general population can be exposed through food, water, dust, or residential application, and during spraying. ![]()

Photo by John Messina
The insecticide gamma-hexachlorocyclohexane (lindane) is carcinogenic, according to experts from the International Agency for Research on Cancer (IARC), the specialized cancer agency of the World Health Organization.
The experts said they found sufficient evidence that lindane, which is banned or restricted in most countries, can cause non-Hodgkin lymphoma (NHL).
The group also discovered that 2 other chemicals might cause NHL.
The evidence suggests the insecticide dichlorodiphenyltrichloroethane (DDT) is probably carcinogenic, and the herbicide 2,4-dichlorophenoxyacetic acid (2,4-D) is possibly carcinogenic.
A summary of these findings is available in The Lancet Oncology, and the experts’ detailed assessments will be published as Volume 113 of the IARC Monographs.
The group, which consisted of 26 experts convened by the IARC Monographs Programme, reviewed the latest scientific literature on lindane, DDT, and 2,4-D and used their findings to classify these 3 chemicals according to carcinogenicity.
The classification (Group 1, Group 2A, etc.) indicates the strength of the evidence that a substance causes cancer, not the level of risk associated with exposure. The Monographs Programme identifies cancer hazards even when risks are very low at current exposure levels, because new uses or unforeseen exposures could engender risks that are significantly higher.
Lindane
The experts classified lindane as carcinogenic to humans (Group 1), saying they found sufficient evidence that it can cause NHL. Large epidemiological studies of agricultural exposures in the US and Canada showed a 60% increased risk of NHL in people exposed to lindane.
Lindane has been used extensively for insect control, including in agriculture and for the treatment of human lice and scabies. High exposures have occurred among agricultural workers and pesticide applicators. However, the use of lindane is now banned or restricted in most countries.
DDT
The experts classified DDT as probably carcinogenic to humans (Group 2A), saying they found sufficient evidence that DDT causes cancer in experimental animals and limited evidence of DDT’s carcinogenicity in humans.
Epidemiological studies have shown positive associations between exposure to DDT and NHL, testicular cancer, and liver cancer.
There was also strong experimental evidence that DDT can suppress the immune system and disrupt sex hormones. However, overall, there was no association between breast cancer and DDT levels measured in samples of blood or fat.
DDT was introduced for the control of insect-borne diseases during World War II and was later applied widely to eradicate malaria and in agriculture. Most uses of DDT were banned in the 1970s. However, DDT and its breakdown products are highly persistent and can be found in the environment and in animal and human tissues throughout the world.
Exposure to DDT still occurs, mainly through diet. The remaining and essential use of DDT is for disease vector control, mainly for malaria. This use is strictly restricted under the Stockholm Convention.
2,4-D
The experts classified 2,4-D as possibly carcinogenic to humans (Group 2B), saying they had inadequate evidence in humans and limited evidence in experimental animals.
There is strong evidence that 2,4-D induces oxidative stress and moderate evidence that 2,4-D causes immunosuppression, based on in vivo and in vitro studies. However, epidemiological studies did not show strong or consistent increases in the risk of NHL or other cancers in relation to 2,4-D exposure.
Since its introduction in 1945, 2,4-D has been widely used to control weeds in agriculture, forestry, and urban and residential settings. Occupational exposures to 2,4-D can occur during manufacturing and application, and the general population can be exposed through food, water, dust, or residential application, and during spraying. ![]()
EC approves edoxaban for patients with VTE, NVAF

Image by Andre E.X. Brown
The European Commission (EC) has approved edoxaban (Lixiana), an oral factor Xa inhibitor, for use in patients with venous thromboembolism (VTE) or nonvalvular atrial fibrillation (NVAF).
The drug can now be used to treat and prevent the recurrence of deep vein thrombosis (DVT) and pulmonary embolism (PE).
It can also be used to prevent stroke and systemic embolism in adults with NVAF who have one or more risk factors for stroke or systemic embolism, such as congestive heart failure, hypertension, age ≥ 75 years, diabetes mellitus, prior stroke, or transient ischemic attack.
The EC’s decision affects all 28 European Union member states, plus Iceland, Norway, and Liechtenstein. Edoxaban is already approved for use in the US, Japan, and Switzerland.
The EC based its approval of edoxaban on results of 2 phase 3 clinical trials, ENGAGE AF-TIMI 48 and Hokusai-VTE.
Hokusai-VTE
In the Hokusai-VTE trial, researchers evaluated edoxaban in 4921 patients with DVT and 3319 with PE. Patients received initial treatment with low-molecular-weight heparin and were then randomized to receive edoxaban or warfarin daily for 3 to 12 months.
Overall, edoxaban proved as effective as warfarin. Recurrent, symptomatic VTE occurred in 3.2% and 3.5% of patients, respectively (P<0.001 for non-inferiority).
In addition, the incidence of clinically relevant bleeding was significantly lower in the edoxaban arm than the warfarin arm—8.5% and 10.3%, respectively (P=0.004 for superiority).
ENGAGE-AF TIMI 48
In the ENGAGE AF-TIMI 48 trial, researchers compared edoxaban and warfarin as prophylaxis for stroke or systemic embolism in patients with NVAF.
The trial included 21,105 patients who were randomized to receive warfarin (n=7036), edoxaban at 60 mg (n=7035), or edoxaban at 30 mg (n=7034).
Edoxaban was at least non-inferior to warfarin with regard to efficacy. The annual incidence of stroke or systemic embolism was 1.50% with warfarin, 1.18% with edoxaban at 60 mg (P<0.001 for non-inferiority), and 1.61% with edoxaban at 30 mg (P=0.005 for non-inferiority).
In addition, edoxaban was associated with a significantly lower rate of major and fatal bleeding. The annual incidence of major bleeding was 3.43% with warfarin, 2.75% with edoxaban at 60 mg (P<0.001), and 1.61% with edoxaban at 30 mg (P<0.001).
Fatal bleeds occurred at an annual rate of 0.38% with warfarin, 0.21% with edoxaban at 60 mg (P=0.006), and 0.13% with edoxaban at 30 mg (P<0.001).
Edoxaban is under development by Daiichi Sankyo Co., Ltd. ![]()

Image by Andre E.X. Brown
The European Commission (EC) has approved edoxaban (Lixiana), an oral factor Xa inhibitor, for use in patients with venous thromboembolism (VTE) or nonvalvular atrial fibrillation (NVAF).
The drug can now be used to treat and prevent the recurrence of deep vein thrombosis (DVT) and pulmonary embolism (PE).
It can also be used to prevent stroke and systemic embolism in adults with NVAF who have one or more risk factors for stroke or systemic embolism, such as congestive heart failure, hypertension, age ≥ 75 years, diabetes mellitus, prior stroke, or transient ischemic attack.
The EC’s decision affects all 28 European Union member states, plus Iceland, Norway, and Liechtenstein. Edoxaban is already approved for use in the US, Japan, and Switzerland.
The EC based its approval of edoxaban on results of 2 phase 3 clinical trials, ENGAGE AF-TIMI 48 and Hokusai-VTE.
Hokusai-VTE
In the Hokusai-VTE trial, researchers evaluated edoxaban in 4921 patients with DVT and 3319 with PE. Patients received initial treatment with low-molecular-weight heparin and were then randomized to receive edoxaban or warfarin daily for 3 to 12 months.
Overall, edoxaban proved as effective as warfarin. Recurrent, symptomatic VTE occurred in 3.2% and 3.5% of patients, respectively (P<0.001 for non-inferiority).
In addition, the incidence of clinically relevant bleeding was significantly lower in the edoxaban arm than the warfarin arm—8.5% and 10.3%, respectively (P=0.004 for superiority).
ENGAGE-AF TIMI 48
In the ENGAGE AF-TIMI 48 trial, researchers compared edoxaban and warfarin as prophylaxis for stroke or systemic embolism in patients with NVAF.
The trial included 21,105 patients who were randomized to receive warfarin (n=7036), edoxaban at 60 mg (n=7035), or edoxaban at 30 mg (n=7034).
Edoxaban was at least non-inferior to warfarin with regard to efficacy. The annual incidence of stroke or systemic embolism was 1.50% with warfarin, 1.18% with edoxaban at 60 mg (P<0.001 for non-inferiority), and 1.61% with edoxaban at 30 mg (P=0.005 for non-inferiority).
In addition, edoxaban was associated with a significantly lower rate of major and fatal bleeding. The annual incidence of major bleeding was 3.43% with warfarin, 2.75% with edoxaban at 60 mg (P<0.001), and 1.61% with edoxaban at 30 mg (P<0.001).
Fatal bleeds occurred at an annual rate of 0.38% with warfarin, 0.21% with edoxaban at 60 mg (P=0.006), and 0.13% with edoxaban at 30 mg (P<0.001).
Edoxaban is under development by Daiichi Sankyo Co., Ltd. ![]()

Image by Andre E.X. Brown
The European Commission (EC) has approved edoxaban (Lixiana), an oral factor Xa inhibitor, for use in patients with venous thromboembolism (VTE) or nonvalvular atrial fibrillation (NVAF).
The drug can now be used to treat and prevent the recurrence of deep vein thrombosis (DVT) and pulmonary embolism (PE).
It can also be used to prevent stroke and systemic embolism in adults with NVAF who have one or more risk factors for stroke or systemic embolism, such as congestive heart failure, hypertension, age ≥ 75 years, diabetes mellitus, prior stroke, or transient ischemic attack.
The EC’s decision affects all 28 European Union member states, plus Iceland, Norway, and Liechtenstein. Edoxaban is already approved for use in the US, Japan, and Switzerland.
The EC based its approval of edoxaban on results of 2 phase 3 clinical trials, ENGAGE AF-TIMI 48 and Hokusai-VTE.
Hokusai-VTE
In the Hokusai-VTE trial, researchers evaluated edoxaban in 4921 patients with DVT and 3319 with PE. Patients received initial treatment with low-molecular-weight heparin and were then randomized to receive edoxaban or warfarin daily for 3 to 12 months.
Overall, edoxaban proved as effective as warfarin. Recurrent, symptomatic VTE occurred in 3.2% and 3.5% of patients, respectively (P<0.001 for non-inferiority).
In addition, the incidence of clinically relevant bleeding was significantly lower in the edoxaban arm than the warfarin arm—8.5% and 10.3%, respectively (P=0.004 for superiority).
ENGAGE-AF TIMI 48
In the ENGAGE AF-TIMI 48 trial, researchers compared edoxaban and warfarin as prophylaxis for stroke or systemic embolism in patients with NVAF.
The trial included 21,105 patients who were randomized to receive warfarin (n=7036), edoxaban at 60 mg (n=7035), or edoxaban at 30 mg (n=7034).
Edoxaban was at least non-inferior to warfarin with regard to efficacy. The annual incidence of stroke or systemic embolism was 1.50% with warfarin, 1.18% with edoxaban at 60 mg (P<0.001 for non-inferiority), and 1.61% with edoxaban at 30 mg (P=0.005 for non-inferiority).
In addition, edoxaban was associated with a significantly lower rate of major and fatal bleeding. The annual incidence of major bleeding was 3.43% with warfarin, 2.75% with edoxaban at 60 mg (P<0.001), and 1.61% with edoxaban at 30 mg (P<0.001).
Fatal bleeds occurred at an annual rate of 0.38% with warfarin, 0.21% with edoxaban at 60 mg (P=0.006), and 0.13% with edoxaban at 30 mg (P<0.001).
Edoxaban is under development by Daiichi Sankyo Co., Ltd. ![]()
CHMP recommends panobinostat for MM

Photo courtesy of the CDC
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) is recommending regulatory approval for panobinostat (Farydak) to treat relapsed and/or refractory multiple myeloma (MM).
The drug is indicated for use in combination with bortezomib and dexamethasone to treat adults with MM who have received at least 2 prior treatment regimens, including bortezomib and an immunomodulatory agent (IMiD).
Panobinostat is already approved for this indication in the US and Chile.
If the European Commission follows the CHMP’s recommendation, panobinostat will be the first histone deacetylase (HDAC) inhibitor approved to treat MM in the European Union.
The European Commission generally follows CHMP recommendations and delivers its final decision within 3 months of the recommendation. The decision will be applicable to all 28 European Union member states, plus Iceland, Norway, and Liechtenstein.
“Panobinostat is the first and only HDAC inhibitor recommended by the CHMP for the treatment of patients living with multiple myeloma who have progressed after standard-of-care therapy with bortezomib and an IMiD,” said Alessandro Riva, MD, Global Head of Oncology Development and Medical Affairs at Novartis Oncology, the company developing panobinostat.
“We are pleased with the positive CHMP opinion on panobinostat for previously treated patients because it brings us one step closer to providing a new treatment option for patients in need in Europe.”
The CHMP’s recommendation is based on efficacy and safety data in a subgroup analysis of 147 patients on the phase 3 PANORAMA-1 trial. Results from this analysis were recently presented at the 2015 ASCO Annual Meeting.
PANORAMA-1 was designed to compare panobinostat in combination with bortezomib and dexamethasone to bortezomib and dexamethasone alone in patients who had relapsed or relapsed and refractory MM.
At ASCO, researchers presented results in 147 patients who had received 2 or more prior treatment regimens, including bortezomib and an IMiD.
The patients who received panobinostat, bortezomib, and dexamethasone had a longer median progression-free survival than patients who received bortezomib and dexamethasone alone—12.5 months and 4.7 months, respectively (hazard ratio=0.47).
Common grade 3/4 adverse events in both treatment arms were thrombocytopenia, lymphopenia, neutropenia, diarrhea, asthenia/fatigue, and peripheral neuropathy. About 7% of patients in both arms died while on treatment. ![]()

Photo courtesy of the CDC
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) is recommending regulatory approval for panobinostat (Farydak) to treat relapsed and/or refractory multiple myeloma (MM).
The drug is indicated for use in combination with bortezomib and dexamethasone to treat adults with MM who have received at least 2 prior treatment regimens, including bortezomib and an immunomodulatory agent (IMiD).
Panobinostat is already approved for this indication in the US and Chile.
If the European Commission follows the CHMP’s recommendation, panobinostat will be the first histone deacetylase (HDAC) inhibitor approved to treat MM in the European Union.
The European Commission generally follows CHMP recommendations and delivers its final decision within 3 months of the recommendation. The decision will be applicable to all 28 European Union member states, plus Iceland, Norway, and Liechtenstein.
“Panobinostat is the first and only HDAC inhibitor recommended by the CHMP for the treatment of patients living with multiple myeloma who have progressed after standard-of-care therapy with bortezomib and an IMiD,” said Alessandro Riva, MD, Global Head of Oncology Development and Medical Affairs at Novartis Oncology, the company developing panobinostat.
“We are pleased with the positive CHMP opinion on panobinostat for previously treated patients because it brings us one step closer to providing a new treatment option for patients in need in Europe.”
The CHMP’s recommendation is based on efficacy and safety data in a subgroup analysis of 147 patients on the phase 3 PANORAMA-1 trial. Results from this analysis were recently presented at the 2015 ASCO Annual Meeting.
PANORAMA-1 was designed to compare panobinostat in combination with bortezomib and dexamethasone to bortezomib and dexamethasone alone in patients who had relapsed or relapsed and refractory MM.
At ASCO, researchers presented results in 147 patients who had received 2 or more prior treatment regimens, including bortezomib and an IMiD.
The patients who received panobinostat, bortezomib, and dexamethasone had a longer median progression-free survival than patients who received bortezomib and dexamethasone alone—12.5 months and 4.7 months, respectively (hazard ratio=0.47).
Common grade 3/4 adverse events in both treatment arms were thrombocytopenia, lymphopenia, neutropenia, diarrhea, asthenia/fatigue, and peripheral neuropathy. About 7% of patients in both arms died while on treatment. ![]()

Photo courtesy of the CDC
The European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) is recommending regulatory approval for panobinostat (Farydak) to treat relapsed and/or refractory multiple myeloma (MM).
The drug is indicated for use in combination with bortezomib and dexamethasone to treat adults with MM who have received at least 2 prior treatment regimens, including bortezomib and an immunomodulatory agent (IMiD).
Panobinostat is already approved for this indication in the US and Chile.
If the European Commission follows the CHMP’s recommendation, panobinostat will be the first histone deacetylase (HDAC) inhibitor approved to treat MM in the European Union.
The European Commission generally follows CHMP recommendations and delivers its final decision within 3 months of the recommendation. The decision will be applicable to all 28 European Union member states, plus Iceland, Norway, and Liechtenstein.
“Panobinostat is the first and only HDAC inhibitor recommended by the CHMP for the treatment of patients living with multiple myeloma who have progressed after standard-of-care therapy with bortezomib and an IMiD,” said Alessandro Riva, MD, Global Head of Oncology Development and Medical Affairs at Novartis Oncology, the company developing panobinostat.
“We are pleased with the positive CHMP opinion on panobinostat for previously treated patients because it brings us one step closer to providing a new treatment option for patients in need in Europe.”
The CHMP’s recommendation is based on efficacy and safety data in a subgroup analysis of 147 patients on the phase 3 PANORAMA-1 trial. Results from this analysis were recently presented at the 2015 ASCO Annual Meeting.
PANORAMA-1 was designed to compare panobinostat in combination with bortezomib and dexamethasone to bortezomib and dexamethasone alone in patients who had relapsed or relapsed and refractory MM.
At ASCO, researchers presented results in 147 patients who had received 2 or more prior treatment regimens, including bortezomib and an IMiD.
The patients who received panobinostat, bortezomib, and dexamethasone had a longer median progression-free survival than patients who received bortezomib and dexamethasone alone—12.5 months and 4.7 months, respectively (hazard ratio=0.47).
Common grade 3/4 adverse events in both treatment arms were thrombocytopenia, lymphopenia, neutropenia, diarrhea, asthenia/fatigue, and peripheral neuropathy. About 7% of patients in both arms died while on treatment.
Approach could build bridge to HSCT in T-PLL

Photo by Chad McNeeley
A treatment approach that combines epigenetics and immunotherapy could provide a bridge to transplant in patients with T-cell prolymphocytic leukemia (T-PLL), according to researchers.
In a pilot study, the team found that combining alemtuzumab with epigenetic agents could override alemtuzumab resistance in T-PLL.
The approach produced complete responses (CRs) in 7 of 8 patients. The eighth patient achieved a partial response (PR).
However, 5 of the patients ultimately died of persistent disease, and 2 are alive in early relapse. One patient remains in remission after allogeneic hematopoietic stem cell transplant (HSCT).
“There’s been a revolution in the last few years seeing success with immunotherapy, and people speculated that, perhaps, if you combined epigenetic and immunotherapy, that might be even more spectacular,” said Thomas P. Loughran Jr, MD, of the University of Virginia Cancer Center in Charlottesville. “This is proof of principle that this might be true.”
Dr Loughran and his colleagues described this research in Science Translational Medicine.
The researchers evaluated 8 patients with T-PLL, 4 of whom were previously untreated (patients 3, 4, 5, and 6).
Patient 2 presented with alemtuzumab-resistant disease but achieved a CR after receiving the drug along with cladribine and vorinostat. He achieved PRs with the same regimen after a second and third relapse but ultimately progressed and died.
“It was unbelievable, really, seeing a patient who had already failed [alemtuzumab] literally going back into remission,” Dr Loughran said.
Patients 1, 4, 6, and 8 achieved a CR with cladribine and alemtuzumab, and patient 3 achieved a PR on the same regimen.
Patient 7 received cladribine and alemtuzumab as well but only achieved a CR with the addition of valproic acid. Patient 5 achieved a CR with cladribine, alemtuzumab, and vorinostat.
Patients 3, 4, and 5 ultimately died. Patient 4 experienced a grade 5 intracranial hemorrhage that may have been treatment-related.
Patients 7 and 8 are in relapse, but they are receiving treatment and are under consideration for HSCT. Patient 6 went on to HSCT after achieving a CR and has been in remission for 4 years.
Major adverse events in this study include neutropenia (5 grade 4, 3 grade 3), thrombocytopenia (2 grade 4, 1 grade 3), anemia (1 grade 2, 2 grade 3), grade 3 febrile neutropenia (n=2), grade 2 lung infection (n=2), grade 1 CMV reactivation (n=1), grade 3 oral mucositis (n=1), grade 3 skin infection (n=1), and grade 5 intracranial hemorrhage (n=1).

Photo by Chad McNeeley
A treatment approach that combines epigenetics and immunotherapy could provide a bridge to transplant in patients with T-cell prolymphocytic leukemia (T-PLL), according to researchers.
In a pilot study, the team found that combining alemtuzumab with epigenetic agents could override alemtuzumab resistance in T-PLL.
The approach produced complete responses (CRs) in 7 of 8 patients. The eighth patient achieved a partial response (PR).
However, 5 of the patients ultimately died of persistent disease, and 2 are alive in early relapse. One patient remains in remission after allogeneic hematopoietic stem cell transplant (HSCT).
“There’s been a revolution in the last few years seeing success with immunotherapy, and people speculated that, perhaps, if you combined epigenetic and immunotherapy, that might be even more spectacular,” said Thomas P. Loughran Jr, MD, of the University of Virginia Cancer Center in Charlottesville. “This is proof of principle that this might be true.”
Dr Loughran and his colleagues described this research in Science Translational Medicine.
The researchers evaluated 8 patients with T-PLL, 4 of whom were previously untreated (patients 3, 4, 5, and 6).
Patient 2 presented with alemtuzumab-resistant disease but achieved a CR after receiving the drug along with cladribine and vorinostat. He achieved PRs with the same regimen after a second and third relapse but ultimately progressed and died.
“It was unbelievable, really, seeing a patient who had already failed [alemtuzumab] literally going back into remission,” Dr Loughran said.
Patients 1, 4, 6, and 8 achieved a CR with cladribine and alemtuzumab, and patient 3 achieved a PR on the same regimen.
Patient 7 received cladribine and alemtuzumab as well but only achieved a CR with the addition of valproic acid. Patient 5 achieved a CR with cladribine, alemtuzumab, and vorinostat.
Patients 3, 4, and 5 ultimately died. Patient 4 experienced a grade 5 intracranial hemorrhage that may have been treatment-related.
Patients 7 and 8 are in relapse, but they are receiving treatment and are under consideration for HSCT. Patient 6 went on to HSCT after achieving a CR and has been in remission for 4 years.
Major adverse events in this study include neutropenia (5 grade 4, 3 grade 3), thrombocytopenia (2 grade 4, 1 grade 3), anemia (1 grade 2, 2 grade 3), grade 3 febrile neutropenia (n=2), grade 2 lung infection (n=2), grade 1 CMV reactivation (n=1), grade 3 oral mucositis (n=1), grade 3 skin infection (n=1), and grade 5 intracranial hemorrhage (n=1).

Photo by Chad McNeeley
A treatment approach that combines epigenetics and immunotherapy could provide a bridge to transplant in patients with T-cell prolymphocytic leukemia (T-PLL), according to researchers.
In a pilot study, the team found that combining alemtuzumab with epigenetic agents could override alemtuzumab resistance in T-PLL.
The approach produced complete responses (CRs) in 7 of 8 patients. The eighth patient achieved a partial response (PR).
However, 5 of the patients ultimately died of persistent disease, and 2 are alive in early relapse. One patient remains in remission after allogeneic hematopoietic stem cell transplant (HSCT).
“There’s been a revolution in the last few years seeing success with immunotherapy, and people speculated that, perhaps, if you combined epigenetic and immunotherapy, that might be even more spectacular,” said Thomas P. Loughran Jr, MD, of the University of Virginia Cancer Center in Charlottesville. “This is proof of principle that this might be true.”
Dr Loughran and his colleagues described this research in Science Translational Medicine.
The researchers evaluated 8 patients with T-PLL, 4 of whom were previously untreated (patients 3, 4, 5, and 6).
Patient 2 presented with alemtuzumab-resistant disease but achieved a CR after receiving the drug along with cladribine and vorinostat. He achieved PRs with the same regimen after a second and third relapse but ultimately progressed and died.
“It was unbelievable, really, seeing a patient who had already failed [alemtuzumab] literally going back into remission,” Dr Loughran said.
Patients 1, 4, 6, and 8 achieved a CR with cladribine and alemtuzumab, and patient 3 achieved a PR on the same regimen.
Patient 7 received cladribine and alemtuzumab as well but only achieved a CR with the addition of valproic acid. Patient 5 achieved a CR with cladribine, alemtuzumab, and vorinostat.
Patients 3, 4, and 5 ultimately died. Patient 4 experienced a grade 5 intracranial hemorrhage that may have been treatment-related.
Patients 7 and 8 are in relapse, but they are receiving treatment and are under consideration for HSCT. Patient 6 went on to HSCT after achieving a CR and has been in remission for 4 years.
Major adverse events in this study include neutropenia (5 grade 4, 3 grade 3), thrombocytopenia (2 grade 4, 1 grade 3), anemia (1 grade 2, 2 grade 3), grade 3 febrile neutropenia (n=2), grade 2 lung infection (n=2), grade 1 CMV reactivation (n=1), grade 3 oral mucositis (n=1), grade 3 skin infection (n=1), and grade 5 intracranial hemorrhage (n=1).
Agent reduces fibrosis, improves platelet counts in MF

VIENNA—The immunotherapeutic agent PRM-151, when given alone or in combination with ruxolitinib, can reduce bone marrow fibrosis and improve platelet counts in patients with myelofibrosis (MF), results of a phase 2 trial suggest.
Using a novel assessment technique known as computer-assisted image analysis (CIA), researchers found that PRM-151, with or without ruxolitinib, prompted fibrosis responses in nearly three-quarters of patients studied.
And nearly 60% of thrombocytopenic patients saw improvements in their platelet counts.
“Thrombocytopenia remains a significant problem for many patients with myelofibrosis, and a new treatment that is not myelosuppressive and actually increases platelet counts would be of great benefit to patients,” said Srdan Verstovsek, MD, PhD, of the University of Texas MD Anderson Cancer Center in Houston.
He and his colleagues presented this research—the first part of a 2-stage study—at the 20th Congress of the European Hematology Association (abstract P677*). The trial is sponsored by Promedior, the company developing PRM-151.
Stage 1 of the study included 27 patients with a median age of 67 (range, 51-85). They had been diagnosed with primary MF, post-polycythemia vera MF, or post-essential thrombocythemia MF.
The patients received PRM-151 at 10 mg/kg IV dosed weekly (n=8) or monthly (n=7), or ruxolitinib plus PRM-151 at 10 mg/kg IV dosed weekly (n=6) or monthly (n=6). The patients who received ruxolitinib were already taking the drug, and doses varied. The mean duration of ruxolitinib treatment was 1.6 years (range, 0.6-3 years).
Patients were set to receive study treatment for 24 weeks but could continue beyond that if they experienced clinical improvement.
Response assessment: Using CIA
Hematopathologists who were blinded to the patient, treatment, and time point performed morphologic analysis on bone marrow specimens taken at baseline and at 12, 24, and 36 weeks (if available).
The pathologists also performed CIA on whole-slide scans from specimens taken at the same time points. The idea to use CIA came after morphologic analyses revealed some surprising findings.
“[The pathologists] were really struck by the fact that, in the patients who had reductions in fibrosis, there were other elements in the bone marrow that showed improvements,” said Beth Trehu, MD, Chief Medical Officer at Promedior. “There were trends toward normalization of the red cells and of the megakaryocytes.”
“They also remarked that, whereas the baseline samples were totally homogeneous—a grade 3 was a grade 3 throughout the bone marrow—after treatment, the samples became very heterogeneous. There were areas of grade 3, grade 2, grade 1, and 0, all in one sample.”
To solve this problem, the pathologists decided that a sample’s WHO grade would be defined as whatever grade was present in at least 50% of the sample. But the team still thought these grades weren’t accurately quantifying the effects of PRM-151.
So they turned to CIA, which allowed them to quantify the volume of collagen or reticulin fibers in the bone marrow.
Fibrosis and platelet responses
According to CIA, 73% of evaluable patients (19/26) experienced reductions in bone marrow fibrosis at any time during the trial.
Of the 23 evaluable patients who had grade 2 or 3 fibrosis at baseline, 11 patients had a reduction of 1 grade or more during the study period, according to morphologic analysis. Nine patients had a fibrosis response by morphology at the last time point they were assessed.
Reductions in fibrosis correlated with increased platelet counts in thrombocytopenic patients. Fifty-seven percent of thrombocytopenic patients (8/14) saw an improvement in platelet counts after treatment.
Results across treatment groups were as follows:
| Treatment group (n) | WHO fibrosis
response at any time |
CIA fibrosis
response at any time |
Platelet
improvement |
| PRM-151 QW (7) | 3 | 4 | 2 |
| PRM-151 Q4W (7) | 3 | 6 | 4 |
| PRM-151 QW + RUX (6) | 2 | 4 | 1 |
| PRM-151 Q4W + RUX (6) | 3 | 5 | 1 |
“The responses we saw with single-agent PRM-151, in particular, give us a lot of confidence that this drug is absolutely reversing fibrosis in the bone marrow,” Dr Trehu said. “And that is very nicely correlated with improvements in platelets, which are much harder to see in patients who are getting ruxolitinib because it’s a myelosuppressive agent.”
Dr Trehu added that these data suggest a monthly dose of PRM-151 is sufficient to treat MF patients, and there is a path forward for PRM-151 both alone and in combination with ruxolitinib.
Hemoglobin and spleen responses
The researchers also observed some improvements in hemoglobin levels and spleen size after treatment.
Of the 15 patients who had hemoglobin levels below 100 g/L at baseline, 3 met criteria for hemoglobin improvement. This included becoming transfusion independent, having a 50% reduction in the need for transfusion, or experiencing a 2 g/L increase in hemoglobin.
“Other patients had a nice trend toward hemoglobin improvement,” Dr Trehu noted.
Of the 20 patients with palpable spleen at baseline, reductions occurred in all but 1 patient. Four patients had a 50% or greater reduction in spleen size, but this response did not last beyond 12 weeks.
Adverse events
Forty-eight percent of patients (13/27) had at least 1 treatment-related adverse event (AE). Grade 1 AEs included diarrhea (n=3), fatigue (n=2), bruising at the infusion site (n=2), oral herpes (n=1), joint swelling (n=2), and headache (n=2). One patient had grade 2 oral herpes.
There were 5 serious AEs that were possibly treatment-related. Three events, from which patients recovered, were abdominal pain, sialadenitis, and pneumonia. The other 2 serious AEs were gastroenteritis and pneumonia, which resulted in death in an 85-year-old patient.
There were 2 deaths unrelated to treatment. One was due to pneumonia, and the other was a result of multi-organ failure and cardiac arrest.
*Information in the abstract differs from that presented at the meeting.

VIENNA—The immunotherapeutic agent PRM-151, when given alone or in combination with ruxolitinib, can reduce bone marrow fibrosis and improve platelet counts in patients with myelofibrosis (MF), results of a phase 2 trial suggest.
Using a novel assessment technique known as computer-assisted image analysis (CIA), researchers found that PRM-151, with or without ruxolitinib, prompted fibrosis responses in nearly three-quarters of patients studied.
And nearly 60% of thrombocytopenic patients saw improvements in their platelet counts.
“Thrombocytopenia remains a significant problem for many patients with myelofibrosis, and a new treatment that is not myelosuppressive and actually increases platelet counts would be of great benefit to patients,” said Srdan Verstovsek, MD, PhD, of the University of Texas MD Anderson Cancer Center in Houston.
He and his colleagues presented this research—the first part of a 2-stage study—at the 20th Congress of the European Hematology Association (abstract P677*). The trial is sponsored by Promedior, the company developing PRM-151.
Stage 1 of the study included 27 patients with a median age of 67 (range, 51-85). They had been diagnosed with primary MF, post-polycythemia vera MF, or post-essential thrombocythemia MF.
The patients received PRM-151 at 10 mg/kg IV dosed weekly (n=8) or monthly (n=7), or ruxolitinib plus PRM-151 at 10 mg/kg IV dosed weekly (n=6) or monthly (n=6). The patients who received ruxolitinib were already taking the drug, and doses varied. The mean duration of ruxolitinib treatment was 1.6 years (range, 0.6-3 years).
Patients were set to receive study treatment for 24 weeks but could continue beyond that if they experienced clinical improvement.
Response assessment: Using CIA
Hematopathologists who were blinded to the patient, treatment, and time point performed morphologic analysis on bone marrow specimens taken at baseline and at 12, 24, and 36 weeks (if available).
The pathologists also performed CIA on whole-slide scans from specimens taken at the same time points. The idea to use CIA came after morphologic analyses revealed some surprising findings.
“[The pathologists] were really struck by the fact that, in the patients who had reductions in fibrosis, there were other elements in the bone marrow that showed improvements,” said Beth Trehu, MD, Chief Medical Officer at Promedior. “There were trends toward normalization of the red cells and of the megakaryocytes.”
“They also remarked that, whereas the baseline samples were totally homogeneous—a grade 3 was a grade 3 throughout the bone marrow—after treatment, the samples became very heterogeneous. There were areas of grade 3, grade 2, grade 1, and 0, all in one sample.”
To solve this problem, the pathologists decided that a sample’s WHO grade would be defined as whatever grade was present in at least 50% of the sample. But the team still thought these grades weren’t accurately quantifying the effects of PRM-151.
So they turned to CIA, which allowed them to quantify the volume of collagen or reticulin fibers in the bone marrow.
Fibrosis and platelet responses
According to CIA, 73% of evaluable patients (19/26) experienced reductions in bone marrow fibrosis at any time during the trial.
Of the 23 evaluable patients who had grade 2 or 3 fibrosis at baseline, 11 patients had a reduction of 1 grade or more during the study period, according to morphologic analysis. Nine patients had a fibrosis response by morphology at the last time point they were assessed.
Reductions in fibrosis correlated with increased platelet counts in thrombocytopenic patients. Fifty-seven percent of thrombocytopenic patients (8/14) saw an improvement in platelet counts after treatment.
Results across treatment groups were as follows:
| Treatment group (n) | WHO fibrosis
response at any time |
CIA fibrosis
response at any time |
Platelet
improvement |
| PRM-151 QW (7) | 3 | 4 | 2 |
| PRM-151 Q4W (7) | 3 | 6 | 4 |
| PRM-151 QW + RUX (6) | 2 | 4 | 1 |
| PRM-151 Q4W + RUX (6) | 3 | 5 | 1 |
“The responses we saw with single-agent PRM-151, in particular, give us a lot of confidence that this drug is absolutely reversing fibrosis in the bone marrow,” Dr Trehu said. “And that is very nicely correlated with improvements in platelets, which are much harder to see in patients who are getting ruxolitinib because it’s a myelosuppressive agent.”
Dr Trehu added that these data suggest a monthly dose of PRM-151 is sufficient to treat MF patients, and there is a path forward for PRM-151 both alone and in combination with ruxolitinib.
Hemoglobin and spleen responses
The researchers also observed some improvements in hemoglobin levels and spleen size after treatment.
Of the 15 patients who had hemoglobin levels below 100 g/L at baseline, 3 met criteria for hemoglobin improvement. This included becoming transfusion independent, having a 50% reduction in the need for transfusion, or experiencing a 2 g/L increase in hemoglobin.
“Other patients had a nice trend toward hemoglobin improvement,” Dr Trehu noted.
Of the 20 patients with palpable spleen at baseline, reductions occurred in all but 1 patient. Four patients had a 50% or greater reduction in spleen size, but this response did not last beyond 12 weeks.
Adverse events
Forty-eight percent of patients (13/27) had at least 1 treatment-related adverse event (AE). Grade 1 AEs included diarrhea (n=3), fatigue (n=2), bruising at the infusion site (n=2), oral herpes (n=1), joint swelling (n=2), and headache (n=2). One patient had grade 2 oral herpes.
There were 5 serious AEs that were possibly treatment-related. Three events, from which patients recovered, were abdominal pain, sialadenitis, and pneumonia. The other 2 serious AEs were gastroenteritis and pneumonia, which resulted in death in an 85-year-old patient.
There were 2 deaths unrelated to treatment. One was due to pneumonia, and the other was a result of multi-organ failure and cardiac arrest.
*Information in the abstract differs from that presented at the meeting.

VIENNA—The immunotherapeutic agent PRM-151, when given alone or in combination with ruxolitinib, can reduce bone marrow fibrosis and improve platelet counts in patients with myelofibrosis (MF), results of a phase 2 trial suggest.
Using a novel assessment technique known as computer-assisted image analysis (CIA), researchers found that PRM-151, with or without ruxolitinib, prompted fibrosis responses in nearly three-quarters of patients studied.
And nearly 60% of thrombocytopenic patients saw improvements in their platelet counts.
“Thrombocytopenia remains a significant problem for many patients with myelofibrosis, and a new treatment that is not myelosuppressive and actually increases platelet counts would be of great benefit to patients,” said Srdan Verstovsek, MD, PhD, of the University of Texas MD Anderson Cancer Center in Houston.
He and his colleagues presented this research—the first part of a 2-stage study—at the 20th Congress of the European Hematology Association (abstract P677*). The trial is sponsored by Promedior, the company developing PRM-151.
Stage 1 of the study included 27 patients with a median age of 67 (range, 51-85). They had been diagnosed with primary MF, post-polycythemia vera MF, or post-essential thrombocythemia MF.
The patients received PRM-151 at 10 mg/kg IV dosed weekly (n=8) or monthly (n=7), or ruxolitinib plus PRM-151 at 10 mg/kg IV dosed weekly (n=6) or monthly (n=6). The patients who received ruxolitinib were already taking the drug, and doses varied. The mean duration of ruxolitinib treatment was 1.6 years (range, 0.6-3 years).
Patients were set to receive study treatment for 24 weeks but could continue beyond that if they experienced clinical improvement.
Response assessment: Using CIA
Hematopathologists who were blinded to the patient, treatment, and time point performed morphologic analysis on bone marrow specimens taken at baseline and at 12, 24, and 36 weeks (if available).
The pathologists also performed CIA on whole-slide scans from specimens taken at the same time points. The idea to use CIA came after morphologic analyses revealed some surprising findings.
“[The pathologists] were really struck by the fact that, in the patients who had reductions in fibrosis, there were other elements in the bone marrow that showed improvements,” said Beth Trehu, MD, Chief Medical Officer at Promedior. “There were trends toward normalization of the red cells and of the megakaryocytes.”
“They also remarked that, whereas the baseline samples were totally homogeneous—a grade 3 was a grade 3 throughout the bone marrow—after treatment, the samples became very heterogeneous. There were areas of grade 3, grade 2, grade 1, and 0, all in one sample.”
To solve this problem, the pathologists decided that a sample’s WHO grade would be defined as whatever grade was present in at least 50% of the sample. But the team still thought these grades weren’t accurately quantifying the effects of PRM-151.
So they turned to CIA, which allowed them to quantify the volume of collagen or reticulin fibers in the bone marrow.
Fibrosis and platelet responses
According to CIA, 73% of evaluable patients (19/26) experienced reductions in bone marrow fibrosis at any time during the trial.
Of the 23 evaluable patients who had grade 2 or 3 fibrosis at baseline, 11 patients had a reduction of 1 grade or more during the study period, according to morphologic analysis. Nine patients had a fibrosis response by morphology at the last time point they were assessed.
Reductions in fibrosis correlated with increased platelet counts in thrombocytopenic patients. Fifty-seven percent of thrombocytopenic patients (8/14) saw an improvement in platelet counts after treatment.
Results across treatment groups were as follows:
| Treatment group (n) | WHO fibrosis
response at any time |
CIA fibrosis
response at any time |
Platelet
improvement |
| PRM-151 QW (7) | 3 | 4 | 2 |
| PRM-151 Q4W (7) | 3 | 6 | 4 |
| PRM-151 QW + RUX (6) | 2 | 4 | 1 |
| PRM-151 Q4W + RUX (6) | 3 | 5 | 1 |
“The responses we saw with single-agent PRM-151, in particular, give us a lot of confidence that this drug is absolutely reversing fibrosis in the bone marrow,” Dr Trehu said. “And that is very nicely correlated with improvements in platelets, which are much harder to see in patients who are getting ruxolitinib because it’s a myelosuppressive agent.”
Dr Trehu added that these data suggest a monthly dose of PRM-151 is sufficient to treat MF patients, and there is a path forward for PRM-151 both alone and in combination with ruxolitinib.
Hemoglobin and spleen responses
The researchers also observed some improvements in hemoglobin levels and spleen size after treatment.
Of the 15 patients who had hemoglobin levels below 100 g/L at baseline, 3 met criteria for hemoglobin improvement. This included becoming transfusion independent, having a 50% reduction in the need for transfusion, or experiencing a 2 g/L increase in hemoglobin.
“Other patients had a nice trend toward hemoglobin improvement,” Dr Trehu noted.
Of the 20 patients with palpable spleen at baseline, reductions occurred in all but 1 patient. Four patients had a 50% or greater reduction in spleen size, but this response did not last beyond 12 weeks.
Adverse events
Forty-eight percent of patients (13/27) had at least 1 treatment-related adverse event (AE). Grade 1 AEs included diarrhea (n=3), fatigue (n=2), bruising at the infusion site (n=2), oral herpes (n=1), joint swelling (n=2), and headache (n=2). One patient had grade 2 oral herpes.
There were 5 serious AEs that were possibly treatment-related. Three events, from which patients recovered, were abdominal pain, sialadenitis, and pneumonia. The other 2 serious AEs were gastroenteritis and pneumonia, which resulted in death in an 85-year-old patient.
There were 2 deaths unrelated to treatment. One was due to pneumonia, and the other was a result of multi-organ failure and cardiac arrest.
*Information in the abstract differs from that presented at the meeting.
Nanobody can help treat acquired TTP
Image by Erhabor Osaro
TORONTO—Adding the anti-von Willebrand factor nanobody caplacizumab to standard therapy can provide clinical benefits for patients with
acquired thrombotic thrombocytopenic purpura (TTP), according to research presented at the 2015 ISTH Congress.
In the phase 2 TITAN trial, patients who received caplacizumab and standard therapy had a significantly shorter time to platelet normalization than patients who received standard therapy and placebo.
Caplacizumab was also associated with a shorter time to troponin, creatinine, and lactate dehydrogenase (LDH) normalization, as well as a reduced need for plasma exchange (PE).
However, some patients relapsed after stopping caplacizumab, and the majority of these relapses could be linked to unresolved disease activity. The drug also increased the risk of mild-to-moderate bleeding compared to placebo.
Flora Peyvandi, MD, PhD, of the University of Milan in Italy, presented data from the TITAN trial at ISTH as abstract LB006. Information on using ADAMTS13 activity for treatment monitoring in the TITAN trial was also presented at the meeting, as abstract OR363.
TITAN was sponsored by Ablynx, the company developing caplacizumab.
The study enrolled 75 patients with acquired TTP from January 2011 to January 2014. Patients were randomized to receive caplacizumab (n=36) or placebo (n=39).
All patients also received the current standard of care, which is, primarily, multiple PEs. The protocol for the study was adapted in September 2013 to allow 1 day of PE prior to study enrollment.
Patients in the caplacizumab arm immediately received an intravenous bolus dose of 10 mg and then a 10 mg subcutaneous dose of the drug daily until 30 days had elapsed after the final PE. Patients in the control arm received placebo at the same time points.
Platelet responses and relapse
The study’s primary endpoint was the time to platelet normalization. And patients in the caplacizumab arm achieved platelet normalization at more than twice the rate of patients in the placebo arm (overall hazard rate ratio=2.2, P=0.005).
Among patients with no prior PE, the median time to platelet normalization was 3 days in caplacizumab-treated patients (n=34) and 4.9 days in controls (n=35). Among patients with 1 prior PE, the median time to platelet normalization was 2.4 days in the caplacizumab arm (n=2) and 4.3 days in the placebo arm (n=4).
In the caplacizumab arm, a higher proportion of patients achieved a complete remission, and fewer patients had exacerbations of TTP. The complete remission rates were 81% and 46%, respectively. And the exacerbation rates were 8% and 28%, respectively.
However, the rate of exacerbation and/or relapse at up to 1 month of follow-up was the same in both arms, at 28%.
Seven patients relapsed within 10 days of stopping caplacizumab. All of these patients had continuous low ADAMTS13 activity (<10%) during and near the end of treatment.
Cardiac, renal, and tissue responses
Additional analyses revealed that patients in the caplacizumab arm had a faster time to troponin normalization than those in the placebo arm. At baseline, 53% of caplacizumab-treated patients and 46% of controls had elevated troponin. The median time to normalization was 9 days and 27 days, respectively.
Patients in the caplacizumab arm also had a faster time to creatinine normalization than those in the placebo arm. At baseline, 31% of caplacizumab-treated patients and 41% of controls had elevated creatinine. The median time to normalization was 4 days and 6 days, respectively.
And patients in the caplacizumab arm had a faster time to LDH normalization than those in the placebo arm. At baseline, 91% of caplacizumab-treated patients and 87% of controls had elevated LDH. The median time to normalization was 3 days and 4 days, respectively.
However, the investigators said they could not rule out a possible effect of PE therapy on LDH, creatinine, and troponin levels.
Need for PE
Results showed that caplacizumab could reduce the need for PE, at least while patients continued to receive the drug.
Patients in the caplacizumab arm required fewer PEs during the daily PE treatment period and the overall treatment period. But this benefit was lost during the 1-month follow-up period, which is reflective of the increased number of relapses, according to the investigators.
During the daily PE treatment period, the mean number of PE days was 5.9 in the caplacizumab arm and 7.9 in the placebo arm. During the overall treatment period, it was 7.7 and 11.7 days, respectively. And during the overall treatment and follow-up period, it was 10.2 and 11.7 days, respectively.
Adverse events
The investigators said caplacizumab increased the risk of bleeding events, but these were readily managed.
Treatment-emergent adverse events (AEs) occurred in 97% of patients in the caplacizumab arm and 100% of patients in the placebo arm. Eight percent of caplacizumab-treated patients discontinued treatment due to AEs, but none of the controls did.
Fifty-four percent of patients in the caplacizumab arm had a bleeding event, as did 38% of patients in the placebo arm. Eighty percent of the bleeding events in the caplacizumab arm were mild. Three patients required drug treatment. None required von Willebrand factor or factor VIII substitution.
Serious AEs occurred in 57% of caplacizumab-treated patients and 51% of controls. Serious bleeding events occurred in 6% and 5%, respectively.

Image by Erhabor Osaro
TORONTO—Adding the anti-von Willebrand factor nanobody caplacizumab to standard therapy can provide clinical benefits for patients with
acquired thrombotic thrombocytopenic purpura (TTP), according to research presented at the 2015 ISTH Congress.
In the phase 2 TITAN trial, patients who received caplacizumab and standard therapy had a significantly shorter time to platelet normalization than patients who received standard therapy and placebo.
Caplacizumab was also associated with a shorter time to troponin, creatinine, and lactate dehydrogenase (LDH) normalization, as well as a reduced need for plasma exchange (PE).
However, some patients relapsed after stopping caplacizumab, and the majority of these relapses could be linked to unresolved disease activity. The drug also increased the risk of mild-to-moderate bleeding compared to placebo.
Flora Peyvandi, MD, PhD, of the University of Milan in Italy, presented data from the TITAN trial at ISTH as abstract LB006. Information on using ADAMTS13 activity for treatment monitoring in the TITAN trial was also presented at the meeting, as abstract OR363.
TITAN was sponsored by Ablynx, the company developing caplacizumab.
The study enrolled 75 patients with acquired TTP from January 2011 to January 2014. Patients were randomized to receive caplacizumab (n=36) or placebo (n=39).
All patients also received the current standard of care, which is, primarily, multiple PEs. The protocol for the study was adapted in September 2013 to allow 1 day of PE prior to study enrollment.
Patients in the caplacizumab arm immediately received an intravenous bolus dose of 10 mg and then a 10 mg subcutaneous dose of the drug daily until 30 days had elapsed after the final PE. Patients in the control arm received placebo at the same time points.
Platelet responses and relapse
The study’s primary endpoint was the time to platelet normalization. And patients in the caplacizumab arm achieved platelet normalization at more than twice the rate of patients in the placebo arm (overall hazard rate ratio=2.2, P=0.005).
Among patients with no prior PE, the median time to platelet normalization was 3 days in caplacizumab-treated patients (n=34) and 4.9 days in controls (n=35). Among patients with 1 prior PE, the median time to platelet normalization was 2.4 days in the caplacizumab arm (n=2) and 4.3 days in the placebo arm (n=4).
In the caplacizumab arm, a higher proportion of patients achieved a complete remission, and fewer patients had exacerbations of TTP. The complete remission rates were 81% and 46%, respectively. And the exacerbation rates were 8% and 28%, respectively.
However, the rate of exacerbation and/or relapse at up to 1 month of follow-up was the same in both arms, at 28%.
Seven patients relapsed within 10 days of stopping caplacizumab. All of these patients had continuous low ADAMTS13 activity (<10%) during and near the end of treatment.
Cardiac, renal, and tissue responses
Additional analyses revealed that patients in the caplacizumab arm had a faster time to troponin normalization than those in the placebo arm. At baseline, 53% of caplacizumab-treated patients and 46% of controls had elevated troponin. The median time to normalization was 9 days and 27 days, respectively.
Patients in the caplacizumab arm also had a faster time to creatinine normalization than those in the placebo arm. At baseline, 31% of caplacizumab-treated patients and 41% of controls had elevated creatinine. The median time to normalization was 4 days and 6 days, respectively.
And patients in the caplacizumab arm had a faster time to LDH normalization than those in the placebo arm. At baseline, 91% of caplacizumab-treated patients and 87% of controls had elevated LDH. The median time to normalization was 3 days and 4 days, respectively.
However, the investigators said they could not rule out a possible effect of PE therapy on LDH, creatinine, and troponin levels.
Need for PE
Results showed that caplacizumab could reduce the need for PE, at least while patients continued to receive the drug.
Patients in the caplacizumab arm required fewer PEs during the daily PE treatment period and the overall treatment period. But this benefit was lost during the 1-month follow-up period, which is reflective of the increased number of relapses, according to the investigators.
During the daily PE treatment period, the mean number of PE days was 5.9 in the caplacizumab arm and 7.9 in the placebo arm. During the overall treatment period, it was 7.7 and 11.7 days, respectively. And during the overall treatment and follow-up period, it was 10.2 and 11.7 days, respectively.
Adverse events
The investigators said caplacizumab increased the risk of bleeding events, but these were readily managed.
Treatment-emergent adverse events (AEs) occurred in 97% of patients in the caplacizumab arm and 100% of patients in the placebo arm. Eight percent of caplacizumab-treated patients discontinued treatment due to AEs, but none of the controls did.
Fifty-four percent of patients in the caplacizumab arm had a bleeding event, as did 38% of patients in the placebo arm. Eighty percent of the bleeding events in the caplacizumab arm were mild. Three patients required drug treatment. None required von Willebrand factor or factor VIII substitution.
Serious AEs occurred in 57% of caplacizumab-treated patients and 51% of controls. Serious bleeding events occurred in 6% and 5%, respectively.

Image by Erhabor Osaro
TORONTO—Adding the anti-von Willebrand factor nanobody caplacizumab to standard therapy can provide clinical benefits for patients with
acquired thrombotic thrombocytopenic purpura (TTP), according to research presented at the 2015 ISTH Congress.
In the phase 2 TITAN trial, patients who received caplacizumab and standard therapy had a significantly shorter time to platelet normalization than patients who received standard therapy and placebo.
Caplacizumab was also associated with a shorter time to troponin, creatinine, and lactate dehydrogenase (LDH) normalization, as well as a reduced need for plasma exchange (PE).
However, some patients relapsed after stopping caplacizumab, and the majority of these relapses could be linked to unresolved disease activity. The drug also increased the risk of mild-to-moderate bleeding compared to placebo.
Flora Peyvandi, MD, PhD, of the University of Milan in Italy, presented data from the TITAN trial at ISTH as abstract LB006. Information on using ADAMTS13 activity for treatment monitoring in the TITAN trial was also presented at the meeting, as abstract OR363.
TITAN was sponsored by Ablynx, the company developing caplacizumab.
The study enrolled 75 patients with acquired TTP from January 2011 to January 2014. Patients were randomized to receive caplacizumab (n=36) or placebo (n=39).
All patients also received the current standard of care, which is, primarily, multiple PEs. The protocol for the study was adapted in September 2013 to allow 1 day of PE prior to study enrollment.
Patients in the caplacizumab arm immediately received an intravenous bolus dose of 10 mg and then a 10 mg subcutaneous dose of the drug daily until 30 days had elapsed after the final PE. Patients in the control arm received placebo at the same time points.
Platelet responses and relapse
The study’s primary endpoint was the time to platelet normalization. And patients in the caplacizumab arm achieved platelet normalization at more than twice the rate of patients in the placebo arm (overall hazard rate ratio=2.2, P=0.005).
Among patients with no prior PE, the median time to platelet normalization was 3 days in caplacizumab-treated patients (n=34) and 4.9 days in controls (n=35). Among patients with 1 prior PE, the median time to platelet normalization was 2.4 days in the caplacizumab arm (n=2) and 4.3 days in the placebo arm (n=4).
In the caplacizumab arm, a higher proportion of patients achieved a complete remission, and fewer patients had exacerbations of TTP. The complete remission rates were 81% and 46%, respectively. And the exacerbation rates were 8% and 28%, respectively.
However, the rate of exacerbation and/or relapse at up to 1 month of follow-up was the same in both arms, at 28%.
Seven patients relapsed within 10 days of stopping caplacizumab. All of these patients had continuous low ADAMTS13 activity (<10%) during and near the end of treatment.
Cardiac, renal, and tissue responses
Additional analyses revealed that patients in the caplacizumab arm had a faster time to troponin normalization than those in the placebo arm. At baseline, 53% of caplacizumab-treated patients and 46% of controls had elevated troponin. The median time to normalization was 9 days and 27 days, respectively.
Patients in the caplacizumab arm also had a faster time to creatinine normalization than those in the placebo arm. At baseline, 31% of caplacizumab-treated patients and 41% of controls had elevated creatinine. The median time to normalization was 4 days and 6 days, respectively.
And patients in the caplacizumab arm had a faster time to LDH normalization than those in the placebo arm. At baseline, 91% of caplacizumab-treated patients and 87% of controls had elevated LDH. The median time to normalization was 3 days and 4 days, respectively.
However, the investigators said they could not rule out a possible effect of PE therapy on LDH, creatinine, and troponin levels.
Need for PE
Results showed that caplacizumab could reduce the need for PE, at least while patients continued to receive the drug.
Patients in the caplacizumab arm required fewer PEs during the daily PE treatment period and the overall treatment period. But this benefit was lost during the 1-month follow-up period, which is reflective of the increased number of relapses, according to the investigators.
During the daily PE treatment period, the mean number of PE days was 5.9 in the caplacizumab arm and 7.9 in the placebo arm. During the overall treatment period, it was 7.7 and 11.7 days, respectively. And during the overall treatment and follow-up period, it was 10.2 and 11.7 days, respectively.
Adverse events
The investigators said caplacizumab increased the risk of bleeding events, but these were readily managed.
Treatment-emergent adverse events (AEs) occurred in 97% of patients in the caplacizumab arm and 100% of patients in the placebo arm. Eight percent of caplacizumab-treated patients discontinued treatment due to AEs, but none of the controls did.
Fifty-four percent of patients in the caplacizumab arm had a bleeding event, as did 38% of patients in the placebo arm. Eighty percent of the bleeding events in the caplacizumab arm were mild. Three patients required drug treatment. None required von Willebrand factor or factor VIII substitution.
Serious AEs occurred in 57% of caplacizumab-treated patients and 51% of controls. Serious bleeding events occurred in 6% and 5%, respectively.