User login
Cognitive Behavioral Therapy for Veterans With Tinnitus
Chronic tinnitus is defined as nonsensical, persistent sound in the head or ears with no external sound source that persists for more than 6 months.1 It is most commonly associated with sound trauma, aging, head injury, and damage to the ear structures.2 Tinnitus affects up to 30% of military veterans, a prevalence rate that is twice that of the nonveteran population.3 It also is the most common service-connected disability for veterans.4 In 2016, more than 1.6 million veterans had service-connected tinnitus.
Clinical management of tinnitus is the purview of audiologists, although their role in providing this service is not well defined.5 Following an audiologic evaluation for hearing loss, devices such as hearing aids, ear-level sound generators, or sounds played through speakers may be prescribed. However, effectiveness of these devices has been shown only when coupled with counseling.6 Counseling provided by audiologists often includes education about tinnitus etiology, maintaining hearing health, and use of sound to manage tinnitus. Length, content of care, and follow-up services vary among audiologists.
Given the importance of counseling and the added complexities of mental health and behavioral health comorbidities (eg, depression, anxiety, sleep disorders), various psychological therapies delivered by mental health specialists for tinnitus management have been explored.7-11 In fact, only psychological therapies have been documented to be efficacious for mitigating the negative effects of tinnitus on sleep, concentration, communication, and emotions.12 Among these approaches, cognitive behavioral therapy (CBT) has the strongest empirical support, particularly in terms of improving quality of life (QOL) and reducing depressive symptoms.11,12 Cognitive behavioral therapy for tinnitus is derived from social cognitive theory (SCT) and modeled after CBT for depression, anxiety, pain, and insomnia.11,13-15
Cognitive behavioral therapy helps patients with tinnitus reconceptualize the auditory problem as manageable and encourages acquisition, practice, and use of a range of specific tinnitus coping strategies to enhance perceptions of self-control and self-efficacy. Cognitive behavioral therapy involves a number of distinct therapeutic components, and there is no consensus about the efficacious components of CBT for tinnitus. For example, use of sound and purposeful exposure to tinnitus varies among providers.16 Additional questions about CBT pertain to its clinical implementation (eg, group vs individual sessions, frequency and length of sessions, in-person sessions vs delivery via telephone or Internet).
Programs offered at the Department of Veterans Affairs (VA) facilities take veteran-specific factors into account to promote optimal engagement and outcomes. Factors that differentiate veterans from civilians include (1) increased probability of low health literacy and low socioeconomic status among seniors17; (2) increased likelihood of acoustic and/or psychological trauma3,18; (3) overrepresentation of males; and (4) increased probability of mental health diagnoses.19,20 At the same time, veterans are highly diverse with respect to age, academic achievement, cultural background, medical and mental health comorbidities, and economic resources.17 In spite of this diversity, most veterans are unified by their sense of camaraderie, loyalty to country, and adherence to discipline and order.21 Peer support and other variables such as compassionate understanding of their military experiences may be especially important to consider when designing behavioral interventions for veterans.
The present phenomenologic study was motivated by the need to develop and test a veteran-specific CBT for tinnitus protocol (VET CBT-T). To examine veterans’ experiences with VET CBT-T, we designed a small pilot randomized controlled trial (RCT) of VET CBT-T comparing it to structured audiologist counseling (AC). A mixed quantitative and qualitative approach was employed, including assessing veterans’ acceptance of care, identifying aspects that can be modified to improve outcomes, and obtaining feasibility data to guide refinements to VET CBT-T to inform a larger RCT.
Methods
The study used a single-blind, randomized, parallel treatment (VET CBT-T vs AC) concurrent design complemented by collection of qualitative data. This study was approved by the institutional review board at the VA Connecticut Healthcare System (VACHS) and was registered at ClinicalTrials.gov (NCT00724152).
Measures
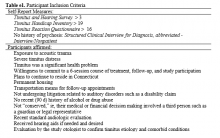
Four standardized measures were administered to potential participants. Callers were screened for eligibility by the research coordinator using Section A of the Tinnitus and Hearing Survey (THS), which had been developed to screen candidates for tinnitus studies by phone.22 The THS contains 3 sections to identify problems related to tinnitus (Section A), hearing (Section B), and sound tolerance (Section C). Section A contains 4 items, each with a possible score of 0 to 4, which identifies tinnitus problems. Callers who were veterans and who met the necessary cutoff of 4 out of 16 possible points on Section A were invited to meet in-person with the research coordinator to obtain written informed consent and conduct a thorough assessment of eligibility.23
Three additional assessment measures were then administered sequentially to determine eligibility. The first 2 of these measures were readministered to eligible candidates who agreed to participate in the study and were used to examine outcomes:
(1) Tinnitus Handicap Inventory (THI): The 25-item THI provides an index score (0-100), with higher scores reflecting poorer QOL and more perceived functional limitations due to tinnitus.24 Candidates with scores of ≤ 19 were excluded.
(2) Tinnitus Reaction Questionnaire (TRQ): The TRQ measures perceived impact of tinnitus on QOL with emphasis on emotional consequences of tinnitus.25 Higher scores indicate more severe impact. Scores of ≥ 17 points purportedly indicate significant tinnitus disturbance. Candidates scoring < 17 were excluded.
(3) Structured Clinical Interview for Diagnosis, Abbreviated-Interview/Nonpatient (SCIDa-I/NP): The SCIDa-I/NP is a measure used to assess symptoms of psychopathology.26 Candidates with a lifetime history of psychosis were excluded.
Interventions
Each of the interventions was offered using 6 group sessions, with 2 or more participants, on an approximate weekly schedule.
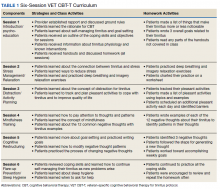
VET CBT-T. Two primary texts served as resources for developing the VET CBT-T protocol: (1) the Psychological Management of Chronic Tinnitus: A Cognitive-Behavioral Approach14; and (2) a manual for providing CBT for the treatment of chronic pain.27,28 Draft materials were developed by the clinical psychologist, including a clinician’s manual for providing VET CBT-T. Handouts were provided to each veteran. Components were compared to another unpublished CBT for tinnitus workbook.10
Key components targeted psychological difficulties including sleep disturbance, reduced functioning, low mood, nervousness, reduced pleasure from activities, and negative changes in relationships. The protocol emphasized basic information about tinnitus; relationships among tinnitus, acoustic trauma, and mental health symptoms; veterans’ sense of camaraderie and loyalty; and goal setting, making use of discipline and order veterans may desire.
To build rapport, the psychologist used reflective listening, encouraged interactive dialogue, and promoted participant understanding. Since tinnitus is thought to be exacerbated by stress, participants learned ways to manage stress and practiced relaxation exercises. Participants learned to create individualized, intersession goals that were realistic, specific, and measurable to promote self-efficacy. They also learned to list and increase pleasant activities to distract from tinnitus, improve QOL, and enable behavioral activation. Motivational interviewing addressed readiness, ambivalence, and resistance to achieving these specific goals. Participants also learned to identify and modify unhelpful thoughts about tinnitus (ie, cognitive restructuring).
Audiologist Counseling (AC). To control for patient contact in VET CBT-T, the study audiologist created a 6-session counseling protocol. The AC emphasized education about tinnitus and available tinnitus interventions. Participants were encouraged to ask questions, share their tinnitus experiences, and cope with tinnitus by avoiding silence.
Quantitative Analysis
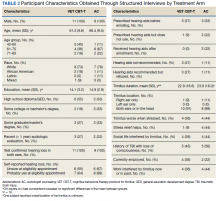
To assess baseline between-group differences, pretreatment (t1;immediately prior to attending the first group session) administrations of the THI and TRQ were compared using t tests. Demographics between groups were compared using the chi-square test.
The THI and TRQ were readministered following completion of the last group session (t2) and about 8 weeks after the last group session (t3). Because of the small sample size, required assumptions for analyzing parametric tests of linear effects were not met. Thus, only descriptive results and mean differences in scores on the THI and TRQ between these 3 assessment periods are presented. SPSS PASW Statistics 18.0 (Hong Kong, China) was used for analyses.
Qualitative Analysis
VET CBT-T. After each VET CBT-T session, veterans’ acceptance of the protocol was assessed using 4 questions: (1) Was the information presented to you today easy to understand? Yes/No. If no, why not? (2) Were the examples (if there were any) useful? Yes/No. If no, why not? (3) Was the way the information was presented by the group leader helpful? Yes/No. If no, why not? and (4) Please tell us what you thought about today’s group. Participants were encouraged to be honest and provide detailed feedback. To facilitate unbiased responding, the group leader left the room while a research assistant collected the comments.
Participants’ experiences and acceptance of the interventions were explored using a stepwise content analysis approach.29,30First, the feedback data were prepared for analysis by entering verbatim responses into a spreadsheet. Next, these responses were reviewed by the clinical psychologist who identified themes. Examination of data involved qualitative analyses in which the phenomenon of interest was veterans’ acceptance of the interventions. This process presumed that most veterans would respond favorably to the intervention and, thus, acknowledged that the clinical psychologist designed and delivered the intervention.
Any contrary or negative comments were flagged. However, neutral and positive comments also were analyzed and tallied. Notations within each comment were used to calculate the number of occurrences of themes. Similar themes with few responses were collapsed into a single theme when appropriate. Final themes and tallies were shared with an auditor familiar with tinnitus, psychology, and qualitative methods who made comments and checked tallies within each theme. The themes were revised based on this audit and retallied. The clinical psychologist then summarized the themes in text, which was reviewed by the auditor for accuracy in capturing the important emergent themes.
Next, themes were used to examine typed verbatim transcripts from the second and fifth sessions of the intervention. Thematic content derived from the above feedback was extracted from the transcripts by the clinical psychologist. Then the study audiologist read the transcripts to confirm or reject these comments as relevant to the themes. Additional comments were nominated by the study audiologist and reviewed by the clinical psychologist who finalized feedback thought to best represent the themes.
Results
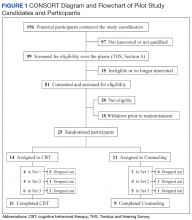
One hundred ninety-six persons inquired about the study (Figure 1).
After being deemed eligible by the otologist as having tinnitus associated with sound trauma, the remaining 25 eligible and interested candidates were randomized into the 2 treatment arms. To reduce attrition, formation of groups took into account participants’ preferred appointment days and times. When 3 or more participants were allocated to a treatment arm, group sessions were scheduled. Five (20%) participants were lost to attrition, including 1 randomized to VET CBT-T and 2 to AC who dropped out prior to receiving any intervention, and 2 randomized to VET CBT-T who dropped out after attending 1 session. Reasons stated for dropping out included concerns they would not learn new information, inability to tolerate sound in a group, unexpected moves out of the area, lack of time, loss of interest, and family emergencies.
Quantitative Analysis
Participants in the 2 treatment arms did not differ significantly on the pretreatment (t1) THI (t = 1.39, df = 18, P = .18) or TRQ (t = 0.99, df = 18, P = .33) scores. Differences in THI scores were computed from pre- to posttreatment (VET CBT-Tt1−t2 = 6.2; ACt1−t2 = 10.0) and from pretreatment to 8-week follow-up (VET CBT-Tt1−t3 = 4.4; ACt1−t3 = 9.1). Similarly, differences in mean TRQ index scores were computed from pre- to posttreatment (VET CBT-Tt1−t2 = 5.3; ACt1−t2 = 7.6) and from pretreatment to 8 weeks follow-up (VET CBT-Tt1−t3 = 1.5; ACt1−t3 = 5.6). These mean differences reveal consistent reductions in mean index scores (improved tinnitus-related QOL) between time points for each treatment arm, but do not indicate statistically or clinically significant reductions of distress.
Qualitative Analysis
The 89 comments that participants provided after the 18 VET CBT-T sessions (3 series of 6 sessions each) were mostly positive (67 responses, 75%) (eTable 2).
Components of VET CBT-T and Number of Sessions (n = 53)
Psychoeducation and Sound Enrichment. Participants generally appreciated the psychoeducation component of VET CBT-T, including basic information about the prevalence of tinnitus, mechanics of the ear and hearing, and how an enriched sound environment may assist with coping (5 comments).
Stress Reduction. Two of the 14 participants who commented on the stress reduction session (via relaxation exercises) noted that it was helpful in their lives overall but “had no effect on tinnitus.”
Goal Setting. Nine participants noted that they valued the goal-setting strategies and long-term relapse planning, one writing that he was “…glad to be encouraged to document and set specific, documented goals each week.”
Cognitive Restructuring and Acceptance. Participants reported that the cognitive restructuring session was important for “accepting” their tinnitus (9 comments). Overall cognitive restructuring appeared to be well received by participants as a concept when learning ways to cope with tinnitus.
Distraction. Of the 8 comments that regarded the increasing-pleasant-activities session, 1 participant reported that the pleasant activities worksheet had a female bias and that activities on one of the worksheets “were not helpful and overlapped too much.” A participant suggested that group leaders allow participants to brainstorm pleasant activities using an open-ended format instead of using categories of pleasant activities. Participants generally found the increasing-pleasant-activities component very beneficial for managing tinnitus.
Self-Hypnosis and Exposure Therapy. Two components not presented during VET CBT-T were identified by participants as potentially desirable. One participant suggested providing information on self-hypnosis and another stated that he focuses on his tinnitus to cope, much like exposure therapy for tinnitus.
Number of Sessions. One participant wrote after the last (sixth) session that he was “glad it’s over” possibly suggesting the intervention was too long. Another participant stated at the fifth session, “I basically want to get out of here—out of this, out of these meetings.” Conversely a participant stated, “I was kind of hoping there was one more after next week.” Another participant explained the intervention itself can be in conflict with its own stated goals of attending less to tinnitus.
Leader, Materials, and Presentations (n = 16).
Overall, the participants had positive experiences (15 comments) with their study therapist. They noted that the group leader was “flexible” and “did a great job of facilitating discussion.” One participant commented on the need for better visual presentations of the information and the need for the group leader to “use her own words” rather than reading the content.
Previous Use of CBT Skills (n = 5).
Five participants noted that information presented was “not new” and that they had acquired the coping skills spontaneously years earlier. Two expressed relief that some of the ways they had been dealing with their tinnitus prior to the intervention were actually recommended. One discussed that reviewing skills that he had already implemented was helpful.
Hope, Anger, and Mental Health (n = 8).
Three participants indicated the intervention gave them “hope” that they will learn ways to cope with tinnitus. One noted that the discussion regarding depression as a commonly co-occurring condition with tinnitus should include a better description of depressive symptoms. Two expressed relief to receive help for their frustration and anger resulting from tinnitus, and 1 participant discussed the added frustration of hearing loss with tinnitus. Excessive alcohol use to cope with tinnitus and the comorbidity of tinnitus and PTSD also were discussed.
Group Cohesiveness (n = 8)/Discord (n = 2).
Many group members commented that they enjoyed listening to information about tinnitus and sharing their experiences. There was friendly interaction and discussion among most of the participants. They commented that it was informative to see that others were coming forward for help and were interested to hear others’ experiences. The group format was mostly welcomed and appreciated. However, group discord occurred when topics other than tinnitus were shared, such as recovery from substance abuse. Two feedback comments indicated that this discussion was unwelcomed.
Discussion
This pilot study provides evidence that at least some of the veterans who were eligible and participated accrued benefit from either AC or VET CBT-T. There also is evidence that a structured and intensive counseling approach by an audiologist that does not include sound therapy is beneficial. Participants generally found that the interventions were acceptable for understanding basic information about tinnitus, and those in the VET CBT-T treatment arm reported improvements in problem solving and coping.
The planned qualitative analyses enabled in-depth examination of intervention feedback from participants and revealed important themes for modifying the VET CBT-T intervention, which occurred following completion of this pilot study. Further, these themes echo the success in creating a unique, veteran-centric, CBT intervention for tinnitus management.
Primarily, participants indicated that education about tinnitus prevalence, etiology, and sound enrichment assisted in coping with tinnitus. This theme also reflects the protocol’s emphasis on health literacy. The wide availability of misinformation on tinnitus, along with the potential for monetary scams, underlies the need for well-designed and research-informed tinnitus education programs. Helping veterans distinguish facts and myths is a potentially important element of tinnitus management. Experiences coping with trauma were salient as participants diverged in their opinions regarding the appropriateness of discussing these issues during a tinnitus management group.
Specific themes emerged regarding the relevance of posttraumatic stress disorder (PTSD) symptoms and substance use to cope with tinnitus. Comfort levels when hearing and discussing these symptoms varied among participants. Due to the high comorbidities of mental health disorders and tinnitus, this theme is important to consider when designing tinnitus management programs. Other qualitative themes served to validate peer support and that the veteran-centric protocol was acceptable, including positive regard for goal setting, indicating that adherence to discipline and order had been addressed.
Identified VET CBT-T Modifications
There were multiple indicators that the rationale for sessions needed to be clarified. Participants highlighted the need to hear clear expectations about what the coping skills would address and multiple reminders regarding the goals of relaxation exercises for tinnitus. Some expressed concern about their lack of concentration during the relaxation exercises. A concern that was discussed with participants only during the informed consent process was the possibility that the intervention could increase focus on tinnitus and, thus, temporarily increase tinnitus distress while receiving the intervention.
Need for Interdisciplinary Care
Perhaps the fact that both interventions were beneficial is not surprising since AC as delivered in this study was designed to be an active intervention that incorporated education and support, including some components similar to those included in VET CBT-T. It appears that AC designed to match the CBT intervention in terms of number of sessions among other enhancements suggests that this intervention may be efficacious. The AC intervention offered support and education about tinnitus; however, sound therapy was not provided despite some empirical support for its use.31 Future research should examine whether sound therapy adds benefit to an intensive and structured AC approach.
It has been proposed that a combination of CBT delivered by a mental health provider and AC should be implemented as an optimal tinnitus management protocol.31,32 Results of this and a number of other recent studies 16,32,33 encourage an integrated, interdisciplinary approach.
Findings of the present study were applied toward development of a hierarchical and interdisciplinary tinnitus management protocol, Progressive Tinnitus Management (PTM).22,34 Components of VET CBT-T were selected for the intervention provided with PTM, modified as per the feedback from participants in this study. This approach was combined with components of the AC intervention, further complemented by sound therapy. The new combined protocol was tested in a pilot telephone study of PTM for veterans and military members with positive results.32 Two VA-supported RCTs of PTM have since been completed.35,36 Results indicate that relative to wait list control, PTM is effective in mitigating negative effects of tinnitus.
Last, after this pilot study, the protocol was modified to address participants’ concerns that their primary care and other providers were unaware that interventions for tinnitus exist. Providers offering tinnitus care are now encouraged to share its availability with veterans and other clinicians. This study provides compelling evidence that veterans respond to messages of hope from providers that they do not needlessly have to suffer alone. Rather than telling veterans to “just live with it,” primary care providers should be able to offer ideas and services for learning how to live with tinnitus.
Future Directions
Future revisions of VET CBT-T could incorporate “acceptance” as a concept for coping with tinnitus, components such as self-hypnosis and exposure therapy, and strategies for coping with hearing loss and communication difficulties. Reexamination of the number and length of sessions also is encouraged, as well as integration of evidence-based interventions for comorbid conditions such as PTSD, substance use disorders, and insomnia. Perhaps increasing the use of peer support services would help reach veterans concerned by the stigma of receiving mental health care. Some veterans were dissatisfied with hearing about others’ mental health concerns. It may be beneficial to offer tinnitus interventions to cohorts of veterans identified with specific comorbid mental health or substance use disorders. However, peer support may be more important than protecting veterans from hearing about others’ mental health concerns as social cognitive theory suggests.
Limitations
This feasibility study’s strict inclusion criteria resulted in a small but well-defined sample that may not be representative of the larger population of veterans who could potentially benefit from these interventions. The extensive evaluation requirements and eligibility requirements likely enhanced the internal validity of the trial but may have compromised the external validity and generalizability of the study findings.
While a few women were assessed during the eligibility process, unfortunately, only men were deemed eligible. It is therefore unknown how women veterans would receive this protocol. Currently there is a bias in selecting male participants for tinnitus research. It is hoped that in the future a sample of women veterans could also provide feedback on this tinnitus management protocol developed by the VHA.
The fact that a large proportion of those who made initial contact about the study decided not to follow up is not inconsistent with studies of similar psychological interventions.37 Challenges related to engaging otherwise appropriate candidates in psychological interventions for a range of chronic health concerns have been well described and may apply to tinnitus management.
Conclusion
The qualitative feedback from participants was generally positive for both protocols. Emergent themes confirmed the need for a veteran-specific intervention while highlighting individual veterans’ needs. Transcripts from sessions provided additional descriptive information that identified changes to the protocols that would improve veterans’ receipt of care. Due to the abundance of veterans with tinnitus and the needs of veterans in terms of health care delivery and receipt, an interdisciplinary CBT-plus-AC protocol was created that is specific to and accepted by veterans with tinnitus.
Refinements to the VET CBT-T protocol were identified that led to development of PTM that was the subject of another small study, which then led to the authors’ 2 larger RCTs. Attempts were made to include greater attention to the mental health concerns of veterans both in terms of education and in offering sensitive delivery of the protocol. Session content was used to create an organized, visual presentation that follows an organized workbook.22,35 Refinements to the protocol are ongoing.
Acknowledgments
This material was based on work supported by US Department of Veterans Affairs, Rehabilitation Research and Development (RR&D): (1) R.D. Kerns’ Pilot Merit Grant #C6324P and (2) C.J. (Kendall) Schmidt’s Career Development Award-1 #D6848M. The authors would like to acknowledge the assistance from Rebecca Czlapinski, MA; Kathryn LaChappelle, MPH; and Emily Thielman, MS, for the conduct of the study, data collection and management, and preparation of this manuscript.
1. Henry JA. “Measurement” of tinnitus. Otol Neurotol. 2016;37(8):e276-e285.
2. Hoffman HJ, Reed GW. Epidemiology of tinnitus. In Snow JB, ed. Tinnitus: Theory and Management. Hamilton, Canada: BC Becker; 2004:16-41.
3. Folmer RL, Theodoroff SM, Martin WH, Shi Y. Experimental, controversial, and futuristic treatments for chronic tinnitus. J Am Acad Audiol. 2014;25(1):106-125.
4. US Department of Veterans Affairs. Veterans Benefits Administration annual benefits report fiscal year 2016. https://www.benefits.va.gov/REPORTS/abr/ABR-All_Sec tions_FY16_06292017.pdf . Accessed June 19, 2018.
5. Henry JA, Zaugg TL, Myers PJ, Schechter MA. The role of audiologic evaluation in progressive audiologic tinnitus management. Trends Amplif. 2008;12(3):170-187.
6. Hoare DJ, Searchfield GD, El Refaie A, Henry JA. Sound therapy for tinnitus management: practicable options. J Am Acad Audiol. 2014;25(1):62-75.
7. Andersson G, Porsaeus D, Wiklund M, Kaldo V, Larsen HC. Treatment of tinnitus in the elderly: a controlled trial of cognitive behavior therapy. Int J Audiol. 2005;44(11):671-675.
8. Henry JL, Wilson PH. Coping with tinnitus: two studies of psychological and audiological characteristics of patients with high and low tinnitus-related distress. Int Tinnitus J. 1995;1(2):85-92.
9. Henry JL, Wilson PH. The psychological management of tinnitus: comparison of a combined cognitive educational program, education alone and a waiting-list control. Int Tinnitus J. 1996;2:9-20.
10. Robinson SK, Viirre ES, Bailey KA, et al. A randomized controlled trial of cognitive-behavior therapy for tinnitus. Int Tinnitus J. 2008;14(2):119-126.
11. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2010(9):CD005233.
12. Tunkel DE, Bauer CA, Sun GH, et al. Clinical practice guideline: tinnitus. Otolaryngol Head Neck Surg. 2014;151(Suppl)(2):S1-S40.
13. Beck JS. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, NY: Guilford Press; 2011.
14. Henry JL, Wilson PH. The Psychological Management of Chronic Tinnitus : A Cognitive-Behavioral Approach. Boston, MA: Allyn and Bacon; 2001.
15. Bandura A. Health promotion by social cognitive means. Health Educ Behav. 2004;31(2):143-164.
16. Cima RF, Andersson G, Schmidt CJ, Henry JA. Cognitive-behavioral treatments for tinnitus: a review of the literature. J Am Acad Audiol. 2014;25(1):29-61.
17. Rodriguez V, Andrade AD, García-Retamero R, et al. Health literacy, numeracy, and graphical literacy among veterans in primary care and their effect on shared decision making and trust in physicians. J Health Commun. 2013;18(suppl 1):273-289.
18. Seal KH, Metzler TJ, Gima KS, Bertenthal D, Maguen S, Marmar CR. Trends and risk factors for mental health diagnoses among Iraq and Afghanistan veterans using Department of Veterans Affairs health care, 2002-2008. Am J Public Health. 2009;99(9):1651-1658.
19. Thomas JL, Wilk JE, Riviere LA, et al. Prevalence of mental health problems and functional impairment among active component and National Guard soldiers 3 and 12 months following combat in Iraq. Arch Gen Psychiatry. 2010;67(6):614-623.
20. Zivin K, McCarthy JF, McCammon RJ, et al. Health-related quality of life and utilities among patients with depression in the Department of Veterans Affairs. Psychiatr Serv. 2008;59(11):1331-1334.
21. Costa DL, Kahn ME. Health, wartime stress, and unit cohesion: evidence from Union Army veterans. Demography. 2010;47(1):45-66.
22. Henry JA, Zaugg TL, Myers PJ, Kendall (Schmidt) CJ. Progressive Tinnitus Management: Clinical Handbook for Audiologists. San Diego, CA: Plural Publishing; 2010.
23. Henry JA, Schechter MA, Loovis CL, et al. Clinical management of tinnitus using a “progressive intervention” approach. J Rehabil Res Dev. 2005;42(4 suppl 2):95-116.
24. Newman CW, Jacobson GP, Spitzer JB. Development of the Tinnitus Handicap Inventory. Arch Otolaryngol Head Neck Surg. 1996;122(2):143-148.
25. Wilson PH, Henry JL, Bowen M, Haralambous G. Tinnitus Reaction Questionnaire: psychometric properties of a measure of distress associated with tinnitus. J Speech Hear Res. 1991;34(1):197-201.
26. First MB, Spitzer RL, Gibbon M, Williams JBW. Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I) Clinical Version, Administration Booklet. Washington, DC: American Psychiatric Press; 2012.
27. Kerns RD, Thorn BE, Dixon KE. Psychological treatments for persistent pain: an introduction. J Clin Psychol. 2006;62(11):1327-1331.
28. Otis JD. Managing Chronic Pain: A Cognitive-Behavioral Therapy Approach. New York, NY: Oxford; 2007.
29. Sandelowski M. Whatever happened to qualitative description? Res Nurs Health. 2000;23(4):334-340.
30. Mertens DM. Research and Evaluation in Education and Psychology: Integrating Diversity With Quantitative, Qualitative, and Mixed Methods. 3rd ed. Los Angeles, CA: Sage; 2009 .
31. Hobson J, Chisholm E, El Refaie A. Sound therapy (masking) in the management of tinnitus in adults. Cochrane Database Syst Rev. 2010;(12):CD006371.
32. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehabil Res Dev. 2012;49(7):1025-1042.
33. Weise C, Heinecke K, Rief W. Biofeedback-based behavioral treatment for chronic tinnitus: results of a randomized controlled trial. J Consult Clin Psychol. 2008;76(6):1046-1057.
34. Henry JA, Zaugg TL, Myers PJ, Kendall (Schmidt) CJ. How to Manage Your Tinnitus: A Step-by-Step Workbook, 3rd ed. San Diego, CA: Plural Publishing; 2010.
35. Henry JA, Thielman EJ, Zaugg TL, et al. Randomized controlled trial in clinical settings to evaluate effectiveness of coping skills education used with Progressive Tinnitus Management. J Speech Lang Hear Res. 2017;60(5):1378-1397.
36. Henry, JA, Thielman, E, Zaugg, et al. Telephone-based progressive tinnitus management for persons with and without traumatic brain injury: a randomized controlled trial. Ear Hear. 2018. [Epub ahead of print.]
37. Chang MW, Nitzke S, Brown R, et al. Recruitment challenges and enrollment observations from a community based intervention (Mothers In Motion) for low-income overweight and obese women. Contemp Clin Trials Commun. 2017;5:26-33.
Chronic tinnitus is defined as nonsensical, persistent sound in the head or ears with no external sound source that persists for more than 6 months.1 It is most commonly associated with sound trauma, aging, head injury, and damage to the ear structures.2 Tinnitus affects up to 30% of military veterans, a prevalence rate that is twice that of the nonveteran population.3 It also is the most common service-connected disability for veterans.4 In 2016, more than 1.6 million veterans had service-connected tinnitus.
Clinical management of tinnitus is the purview of audiologists, although their role in providing this service is not well defined.5 Following an audiologic evaluation for hearing loss, devices such as hearing aids, ear-level sound generators, or sounds played through speakers may be prescribed. However, effectiveness of these devices has been shown only when coupled with counseling.6 Counseling provided by audiologists often includes education about tinnitus etiology, maintaining hearing health, and use of sound to manage tinnitus. Length, content of care, and follow-up services vary among audiologists.
Given the importance of counseling and the added complexities of mental health and behavioral health comorbidities (eg, depression, anxiety, sleep disorders), various psychological therapies delivered by mental health specialists for tinnitus management have been explored.7-11 In fact, only psychological therapies have been documented to be efficacious for mitigating the negative effects of tinnitus on sleep, concentration, communication, and emotions.12 Among these approaches, cognitive behavioral therapy (CBT) has the strongest empirical support, particularly in terms of improving quality of life (QOL) and reducing depressive symptoms.11,12 Cognitive behavioral therapy for tinnitus is derived from social cognitive theory (SCT) and modeled after CBT for depression, anxiety, pain, and insomnia.11,13-15
Cognitive behavioral therapy helps patients with tinnitus reconceptualize the auditory problem as manageable and encourages acquisition, practice, and use of a range of specific tinnitus coping strategies to enhance perceptions of self-control and self-efficacy. Cognitive behavioral therapy involves a number of distinct therapeutic components, and there is no consensus about the efficacious components of CBT for tinnitus. For example, use of sound and purposeful exposure to tinnitus varies among providers.16 Additional questions about CBT pertain to its clinical implementation (eg, group vs individual sessions, frequency and length of sessions, in-person sessions vs delivery via telephone or Internet).
Programs offered at the Department of Veterans Affairs (VA) facilities take veteran-specific factors into account to promote optimal engagement and outcomes. Factors that differentiate veterans from civilians include (1) increased probability of low health literacy and low socioeconomic status among seniors17; (2) increased likelihood of acoustic and/or psychological trauma3,18; (3) overrepresentation of males; and (4) increased probability of mental health diagnoses.19,20 At the same time, veterans are highly diverse with respect to age, academic achievement, cultural background, medical and mental health comorbidities, and economic resources.17 In spite of this diversity, most veterans are unified by their sense of camaraderie, loyalty to country, and adherence to discipline and order.21 Peer support and other variables such as compassionate understanding of their military experiences may be especially important to consider when designing behavioral interventions for veterans.
The present phenomenologic study was motivated by the need to develop and test a veteran-specific CBT for tinnitus protocol (VET CBT-T). To examine veterans’ experiences with VET CBT-T, we designed a small pilot randomized controlled trial (RCT) of VET CBT-T comparing it to structured audiologist counseling (AC). A mixed quantitative and qualitative approach was employed, including assessing veterans’ acceptance of care, identifying aspects that can be modified to improve outcomes, and obtaining feasibility data to guide refinements to VET CBT-T to inform a larger RCT.
Methods
The study used a single-blind, randomized, parallel treatment (VET CBT-T vs AC) concurrent design complemented by collection of qualitative data. This study was approved by the institutional review board at the VA Connecticut Healthcare System (VACHS) and was registered at ClinicalTrials.gov (NCT00724152).
Measures
Four standardized measures were administered to potential participants. Callers were screened for eligibility by the research coordinator using Section A of the Tinnitus and Hearing Survey (THS), which had been developed to screen candidates for tinnitus studies by phone.22 The THS contains 3 sections to identify problems related to tinnitus (Section A), hearing (Section B), and sound tolerance (Section C). Section A contains 4 items, each with a possible score of 0 to 4, which identifies tinnitus problems. Callers who were veterans and who met the necessary cutoff of 4 out of 16 possible points on Section A were invited to meet in-person with the research coordinator to obtain written informed consent and conduct a thorough assessment of eligibility.23
Three additional assessment measures were then administered sequentially to determine eligibility. The first 2 of these measures were readministered to eligible candidates who agreed to participate in the study and were used to examine outcomes:
(1) Tinnitus Handicap Inventory (THI): The 25-item THI provides an index score (0-100), with higher scores reflecting poorer QOL and more perceived functional limitations due to tinnitus.24 Candidates with scores of ≤ 19 were excluded.
(2) Tinnitus Reaction Questionnaire (TRQ): The TRQ measures perceived impact of tinnitus on QOL with emphasis on emotional consequences of tinnitus.25 Higher scores indicate more severe impact. Scores of ≥ 17 points purportedly indicate significant tinnitus disturbance. Candidates scoring < 17 were excluded.
(3) Structured Clinical Interview for Diagnosis, Abbreviated-Interview/Nonpatient (SCIDa-I/NP): The SCIDa-I/NP is a measure used to assess symptoms of psychopathology.26 Candidates with a lifetime history of psychosis were excluded.
Interventions
Each of the interventions was offered using 6 group sessions, with 2 or more participants, on an approximate weekly schedule.
VET CBT-T. Two primary texts served as resources for developing the VET CBT-T protocol: (1) the Psychological Management of Chronic Tinnitus: A Cognitive-Behavioral Approach14; and (2) a manual for providing CBT for the treatment of chronic pain.27,28 Draft materials were developed by the clinical psychologist, including a clinician’s manual for providing VET CBT-T. Handouts were provided to each veteran. Components were compared to another unpublished CBT for tinnitus workbook.10
Key components targeted psychological difficulties including sleep disturbance, reduced functioning, low mood, nervousness, reduced pleasure from activities, and negative changes in relationships. The protocol emphasized basic information about tinnitus; relationships among tinnitus, acoustic trauma, and mental health symptoms; veterans’ sense of camaraderie and loyalty; and goal setting, making use of discipline and order veterans may desire.
To build rapport, the psychologist used reflective listening, encouraged interactive dialogue, and promoted participant understanding. Since tinnitus is thought to be exacerbated by stress, participants learned ways to manage stress and practiced relaxation exercises. Participants learned to create individualized, intersession goals that were realistic, specific, and measurable to promote self-efficacy. They also learned to list and increase pleasant activities to distract from tinnitus, improve QOL, and enable behavioral activation. Motivational interviewing addressed readiness, ambivalence, and resistance to achieving these specific goals. Participants also learned to identify and modify unhelpful thoughts about tinnitus (ie, cognitive restructuring).
Audiologist Counseling (AC). To control for patient contact in VET CBT-T, the study audiologist created a 6-session counseling protocol. The AC emphasized education about tinnitus and available tinnitus interventions. Participants were encouraged to ask questions, share their tinnitus experiences, and cope with tinnitus by avoiding silence.
Quantitative Analysis
To assess baseline between-group differences, pretreatment (t1;immediately prior to attending the first group session) administrations of the THI and TRQ were compared using t tests. Demographics between groups were compared using the chi-square test.
The THI and TRQ were readministered following completion of the last group session (t2) and about 8 weeks after the last group session (t3). Because of the small sample size, required assumptions for analyzing parametric tests of linear effects were not met. Thus, only descriptive results and mean differences in scores on the THI and TRQ between these 3 assessment periods are presented. SPSS PASW Statistics 18.0 (Hong Kong, China) was used for analyses.
Qualitative Analysis
VET CBT-T. After each VET CBT-T session, veterans’ acceptance of the protocol was assessed using 4 questions: (1) Was the information presented to you today easy to understand? Yes/No. If no, why not? (2) Were the examples (if there were any) useful? Yes/No. If no, why not? (3) Was the way the information was presented by the group leader helpful? Yes/No. If no, why not? and (4) Please tell us what you thought about today’s group. Participants were encouraged to be honest and provide detailed feedback. To facilitate unbiased responding, the group leader left the room while a research assistant collected the comments.
Participants’ experiences and acceptance of the interventions were explored using a stepwise content analysis approach.29,30First, the feedback data were prepared for analysis by entering verbatim responses into a spreadsheet. Next, these responses were reviewed by the clinical psychologist who identified themes. Examination of data involved qualitative analyses in which the phenomenon of interest was veterans’ acceptance of the interventions. This process presumed that most veterans would respond favorably to the intervention and, thus, acknowledged that the clinical psychologist designed and delivered the intervention.
Any contrary or negative comments were flagged. However, neutral and positive comments also were analyzed and tallied. Notations within each comment were used to calculate the number of occurrences of themes. Similar themes with few responses were collapsed into a single theme when appropriate. Final themes and tallies were shared with an auditor familiar with tinnitus, psychology, and qualitative methods who made comments and checked tallies within each theme. The themes were revised based on this audit and retallied. The clinical psychologist then summarized the themes in text, which was reviewed by the auditor for accuracy in capturing the important emergent themes.
Next, themes were used to examine typed verbatim transcripts from the second and fifth sessions of the intervention. Thematic content derived from the above feedback was extracted from the transcripts by the clinical psychologist. Then the study audiologist read the transcripts to confirm or reject these comments as relevant to the themes. Additional comments were nominated by the study audiologist and reviewed by the clinical psychologist who finalized feedback thought to best represent the themes.
Results
One hundred ninety-six persons inquired about the study (Figure 1).
After being deemed eligible by the otologist as having tinnitus associated with sound trauma, the remaining 25 eligible and interested candidates were randomized into the 2 treatment arms. To reduce attrition, formation of groups took into account participants’ preferred appointment days and times. When 3 or more participants were allocated to a treatment arm, group sessions were scheduled. Five (20%) participants were lost to attrition, including 1 randomized to VET CBT-T and 2 to AC who dropped out prior to receiving any intervention, and 2 randomized to VET CBT-T who dropped out after attending 1 session. Reasons stated for dropping out included concerns they would not learn new information, inability to tolerate sound in a group, unexpected moves out of the area, lack of time, loss of interest, and family emergencies.
Quantitative Analysis
Participants in the 2 treatment arms did not differ significantly on the pretreatment (t1) THI (t = 1.39, df = 18, P = .18) or TRQ (t = 0.99, df = 18, P = .33) scores. Differences in THI scores were computed from pre- to posttreatment (VET CBT-Tt1−t2 = 6.2; ACt1−t2 = 10.0) and from pretreatment to 8-week follow-up (VET CBT-Tt1−t3 = 4.4; ACt1−t3 = 9.1). Similarly, differences in mean TRQ index scores were computed from pre- to posttreatment (VET CBT-Tt1−t2 = 5.3; ACt1−t2 = 7.6) and from pretreatment to 8 weeks follow-up (VET CBT-Tt1−t3 = 1.5; ACt1−t3 = 5.6). These mean differences reveal consistent reductions in mean index scores (improved tinnitus-related QOL) between time points for each treatment arm, but do not indicate statistically or clinically significant reductions of distress.
Qualitative Analysis
The 89 comments that participants provided after the 18 VET CBT-T sessions (3 series of 6 sessions each) were mostly positive (67 responses, 75%) (eTable 2).
Components of VET CBT-T and Number of Sessions (n = 53)
Psychoeducation and Sound Enrichment. Participants generally appreciated the psychoeducation component of VET CBT-T, including basic information about the prevalence of tinnitus, mechanics of the ear and hearing, and how an enriched sound environment may assist with coping (5 comments).
Stress Reduction. Two of the 14 participants who commented on the stress reduction session (via relaxation exercises) noted that it was helpful in their lives overall but “had no effect on tinnitus.”
Goal Setting. Nine participants noted that they valued the goal-setting strategies and long-term relapse planning, one writing that he was “…glad to be encouraged to document and set specific, documented goals each week.”
Cognitive Restructuring and Acceptance. Participants reported that the cognitive restructuring session was important for “accepting” their tinnitus (9 comments). Overall cognitive restructuring appeared to be well received by participants as a concept when learning ways to cope with tinnitus.
Distraction. Of the 8 comments that regarded the increasing-pleasant-activities session, 1 participant reported that the pleasant activities worksheet had a female bias and that activities on one of the worksheets “were not helpful and overlapped too much.” A participant suggested that group leaders allow participants to brainstorm pleasant activities using an open-ended format instead of using categories of pleasant activities. Participants generally found the increasing-pleasant-activities component very beneficial for managing tinnitus.
Self-Hypnosis and Exposure Therapy. Two components not presented during VET CBT-T were identified by participants as potentially desirable. One participant suggested providing information on self-hypnosis and another stated that he focuses on his tinnitus to cope, much like exposure therapy for tinnitus.
Number of Sessions. One participant wrote after the last (sixth) session that he was “glad it’s over” possibly suggesting the intervention was too long. Another participant stated at the fifth session, “I basically want to get out of here—out of this, out of these meetings.” Conversely a participant stated, “I was kind of hoping there was one more after next week.” Another participant explained the intervention itself can be in conflict with its own stated goals of attending less to tinnitus.
Leader, Materials, and Presentations (n = 16).
Overall, the participants had positive experiences (15 comments) with their study therapist. They noted that the group leader was “flexible” and “did a great job of facilitating discussion.” One participant commented on the need for better visual presentations of the information and the need for the group leader to “use her own words” rather than reading the content.
Previous Use of CBT Skills (n = 5).
Five participants noted that information presented was “not new” and that they had acquired the coping skills spontaneously years earlier. Two expressed relief that some of the ways they had been dealing with their tinnitus prior to the intervention were actually recommended. One discussed that reviewing skills that he had already implemented was helpful.
Hope, Anger, and Mental Health (n = 8).
Three participants indicated the intervention gave them “hope” that they will learn ways to cope with tinnitus. One noted that the discussion regarding depression as a commonly co-occurring condition with tinnitus should include a better description of depressive symptoms. Two expressed relief to receive help for their frustration and anger resulting from tinnitus, and 1 participant discussed the added frustration of hearing loss with tinnitus. Excessive alcohol use to cope with tinnitus and the comorbidity of tinnitus and PTSD also were discussed.
Group Cohesiveness (n = 8)/Discord (n = 2).
Many group members commented that they enjoyed listening to information about tinnitus and sharing their experiences. There was friendly interaction and discussion among most of the participants. They commented that it was informative to see that others were coming forward for help and were interested to hear others’ experiences. The group format was mostly welcomed and appreciated. However, group discord occurred when topics other than tinnitus were shared, such as recovery from substance abuse. Two feedback comments indicated that this discussion was unwelcomed.
Discussion
This pilot study provides evidence that at least some of the veterans who were eligible and participated accrued benefit from either AC or VET CBT-T. There also is evidence that a structured and intensive counseling approach by an audiologist that does not include sound therapy is beneficial. Participants generally found that the interventions were acceptable for understanding basic information about tinnitus, and those in the VET CBT-T treatment arm reported improvements in problem solving and coping.
The planned qualitative analyses enabled in-depth examination of intervention feedback from participants and revealed important themes for modifying the VET CBT-T intervention, which occurred following completion of this pilot study. Further, these themes echo the success in creating a unique, veteran-centric, CBT intervention for tinnitus management.
Primarily, participants indicated that education about tinnitus prevalence, etiology, and sound enrichment assisted in coping with tinnitus. This theme also reflects the protocol’s emphasis on health literacy. The wide availability of misinformation on tinnitus, along with the potential for monetary scams, underlies the need for well-designed and research-informed tinnitus education programs. Helping veterans distinguish facts and myths is a potentially important element of tinnitus management. Experiences coping with trauma were salient as participants diverged in their opinions regarding the appropriateness of discussing these issues during a tinnitus management group.
Specific themes emerged regarding the relevance of posttraumatic stress disorder (PTSD) symptoms and substance use to cope with tinnitus. Comfort levels when hearing and discussing these symptoms varied among participants. Due to the high comorbidities of mental health disorders and tinnitus, this theme is important to consider when designing tinnitus management programs. Other qualitative themes served to validate peer support and that the veteran-centric protocol was acceptable, including positive regard for goal setting, indicating that adherence to discipline and order had been addressed.
Identified VET CBT-T Modifications
There were multiple indicators that the rationale for sessions needed to be clarified. Participants highlighted the need to hear clear expectations about what the coping skills would address and multiple reminders regarding the goals of relaxation exercises for tinnitus. Some expressed concern about their lack of concentration during the relaxation exercises. A concern that was discussed with participants only during the informed consent process was the possibility that the intervention could increase focus on tinnitus and, thus, temporarily increase tinnitus distress while receiving the intervention.
Need for Interdisciplinary Care
Perhaps the fact that both interventions were beneficial is not surprising since AC as delivered in this study was designed to be an active intervention that incorporated education and support, including some components similar to those included in VET CBT-T. It appears that AC designed to match the CBT intervention in terms of number of sessions among other enhancements suggests that this intervention may be efficacious. The AC intervention offered support and education about tinnitus; however, sound therapy was not provided despite some empirical support for its use.31 Future research should examine whether sound therapy adds benefit to an intensive and structured AC approach.
It has been proposed that a combination of CBT delivered by a mental health provider and AC should be implemented as an optimal tinnitus management protocol.31,32 Results of this and a number of other recent studies 16,32,33 encourage an integrated, interdisciplinary approach.
Findings of the present study were applied toward development of a hierarchical and interdisciplinary tinnitus management protocol, Progressive Tinnitus Management (PTM).22,34 Components of VET CBT-T were selected for the intervention provided with PTM, modified as per the feedback from participants in this study. This approach was combined with components of the AC intervention, further complemented by sound therapy. The new combined protocol was tested in a pilot telephone study of PTM for veterans and military members with positive results.32 Two VA-supported RCTs of PTM have since been completed.35,36 Results indicate that relative to wait list control, PTM is effective in mitigating negative effects of tinnitus.
Last, after this pilot study, the protocol was modified to address participants’ concerns that their primary care and other providers were unaware that interventions for tinnitus exist. Providers offering tinnitus care are now encouraged to share its availability with veterans and other clinicians. This study provides compelling evidence that veterans respond to messages of hope from providers that they do not needlessly have to suffer alone. Rather than telling veterans to “just live with it,” primary care providers should be able to offer ideas and services for learning how to live with tinnitus.
Future Directions
Future revisions of VET CBT-T could incorporate “acceptance” as a concept for coping with tinnitus, components such as self-hypnosis and exposure therapy, and strategies for coping with hearing loss and communication difficulties. Reexamination of the number and length of sessions also is encouraged, as well as integration of evidence-based interventions for comorbid conditions such as PTSD, substance use disorders, and insomnia. Perhaps increasing the use of peer support services would help reach veterans concerned by the stigma of receiving mental health care. Some veterans were dissatisfied with hearing about others’ mental health concerns. It may be beneficial to offer tinnitus interventions to cohorts of veterans identified with specific comorbid mental health or substance use disorders. However, peer support may be more important than protecting veterans from hearing about others’ mental health concerns as social cognitive theory suggests.
Limitations
This feasibility study’s strict inclusion criteria resulted in a small but well-defined sample that may not be representative of the larger population of veterans who could potentially benefit from these interventions. The extensive evaluation requirements and eligibility requirements likely enhanced the internal validity of the trial but may have compromised the external validity and generalizability of the study findings.
While a few women were assessed during the eligibility process, unfortunately, only men were deemed eligible. It is therefore unknown how women veterans would receive this protocol. Currently there is a bias in selecting male participants for tinnitus research. It is hoped that in the future a sample of women veterans could also provide feedback on this tinnitus management protocol developed by the VHA.
The fact that a large proportion of those who made initial contact about the study decided not to follow up is not inconsistent with studies of similar psychological interventions.37 Challenges related to engaging otherwise appropriate candidates in psychological interventions for a range of chronic health concerns have been well described and may apply to tinnitus management.
Conclusion
The qualitative feedback from participants was generally positive for both protocols. Emergent themes confirmed the need for a veteran-specific intervention while highlighting individual veterans’ needs. Transcripts from sessions provided additional descriptive information that identified changes to the protocols that would improve veterans’ receipt of care. Due to the abundance of veterans with tinnitus and the needs of veterans in terms of health care delivery and receipt, an interdisciplinary CBT-plus-AC protocol was created that is specific to and accepted by veterans with tinnitus.
Refinements to the VET CBT-T protocol were identified that led to development of PTM that was the subject of another small study, which then led to the authors’ 2 larger RCTs. Attempts were made to include greater attention to the mental health concerns of veterans both in terms of education and in offering sensitive delivery of the protocol. Session content was used to create an organized, visual presentation that follows an organized workbook.22,35 Refinements to the protocol are ongoing.
Acknowledgments
This material was based on work supported by US Department of Veterans Affairs, Rehabilitation Research and Development (RR&D): (1) R.D. Kerns’ Pilot Merit Grant #C6324P and (2) C.J. (Kendall) Schmidt’s Career Development Award-1 #D6848M. The authors would like to acknowledge the assistance from Rebecca Czlapinski, MA; Kathryn LaChappelle, MPH; and Emily Thielman, MS, for the conduct of the study, data collection and management, and preparation of this manuscript.
Chronic tinnitus is defined as nonsensical, persistent sound in the head or ears with no external sound source that persists for more than 6 months.1 It is most commonly associated with sound trauma, aging, head injury, and damage to the ear structures.2 Tinnitus affects up to 30% of military veterans, a prevalence rate that is twice that of the nonveteran population.3 It also is the most common service-connected disability for veterans.4 In 2016, more than 1.6 million veterans had service-connected tinnitus.
Clinical management of tinnitus is the purview of audiologists, although their role in providing this service is not well defined.5 Following an audiologic evaluation for hearing loss, devices such as hearing aids, ear-level sound generators, or sounds played through speakers may be prescribed. However, effectiveness of these devices has been shown only when coupled with counseling.6 Counseling provided by audiologists often includes education about tinnitus etiology, maintaining hearing health, and use of sound to manage tinnitus. Length, content of care, and follow-up services vary among audiologists.
Given the importance of counseling and the added complexities of mental health and behavioral health comorbidities (eg, depression, anxiety, sleep disorders), various psychological therapies delivered by mental health specialists for tinnitus management have been explored.7-11 In fact, only psychological therapies have been documented to be efficacious for mitigating the negative effects of tinnitus on sleep, concentration, communication, and emotions.12 Among these approaches, cognitive behavioral therapy (CBT) has the strongest empirical support, particularly in terms of improving quality of life (QOL) and reducing depressive symptoms.11,12 Cognitive behavioral therapy for tinnitus is derived from social cognitive theory (SCT) and modeled after CBT for depression, anxiety, pain, and insomnia.11,13-15
Cognitive behavioral therapy helps patients with tinnitus reconceptualize the auditory problem as manageable and encourages acquisition, practice, and use of a range of specific tinnitus coping strategies to enhance perceptions of self-control and self-efficacy. Cognitive behavioral therapy involves a number of distinct therapeutic components, and there is no consensus about the efficacious components of CBT for tinnitus. For example, use of sound and purposeful exposure to tinnitus varies among providers.16 Additional questions about CBT pertain to its clinical implementation (eg, group vs individual sessions, frequency and length of sessions, in-person sessions vs delivery via telephone or Internet).
Programs offered at the Department of Veterans Affairs (VA) facilities take veteran-specific factors into account to promote optimal engagement and outcomes. Factors that differentiate veterans from civilians include (1) increased probability of low health literacy and low socioeconomic status among seniors17; (2) increased likelihood of acoustic and/or psychological trauma3,18; (3) overrepresentation of males; and (4) increased probability of mental health diagnoses.19,20 At the same time, veterans are highly diverse with respect to age, academic achievement, cultural background, medical and mental health comorbidities, and economic resources.17 In spite of this diversity, most veterans are unified by their sense of camaraderie, loyalty to country, and adherence to discipline and order.21 Peer support and other variables such as compassionate understanding of their military experiences may be especially important to consider when designing behavioral interventions for veterans.
The present phenomenologic study was motivated by the need to develop and test a veteran-specific CBT for tinnitus protocol (VET CBT-T). To examine veterans’ experiences with VET CBT-T, we designed a small pilot randomized controlled trial (RCT) of VET CBT-T comparing it to structured audiologist counseling (AC). A mixed quantitative and qualitative approach was employed, including assessing veterans’ acceptance of care, identifying aspects that can be modified to improve outcomes, and obtaining feasibility data to guide refinements to VET CBT-T to inform a larger RCT.
Methods
The study used a single-blind, randomized, parallel treatment (VET CBT-T vs AC) concurrent design complemented by collection of qualitative data. This study was approved by the institutional review board at the VA Connecticut Healthcare System (VACHS) and was registered at ClinicalTrials.gov (NCT00724152).
Measures
Four standardized measures were administered to potential participants. Callers were screened for eligibility by the research coordinator using Section A of the Tinnitus and Hearing Survey (THS), which had been developed to screen candidates for tinnitus studies by phone.22 The THS contains 3 sections to identify problems related to tinnitus (Section A), hearing (Section B), and sound tolerance (Section C). Section A contains 4 items, each with a possible score of 0 to 4, which identifies tinnitus problems. Callers who were veterans and who met the necessary cutoff of 4 out of 16 possible points on Section A were invited to meet in-person with the research coordinator to obtain written informed consent and conduct a thorough assessment of eligibility.23
Three additional assessment measures were then administered sequentially to determine eligibility. The first 2 of these measures were readministered to eligible candidates who agreed to participate in the study and were used to examine outcomes:
(1) Tinnitus Handicap Inventory (THI): The 25-item THI provides an index score (0-100), with higher scores reflecting poorer QOL and more perceived functional limitations due to tinnitus.24 Candidates with scores of ≤ 19 were excluded.
(2) Tinnitus Reaction Questionnaire (TRQ): The TRQ measures perceived impact of tinnitus on QOL with emphasis on emotional consequences of tinnitus.25 Higher scores indicate more severe impact. Scores of ≥ 17 points purportedly indicate significant tinnitus disturbance. Candidates scoring < 17 were excluded.
(3) Structured Clinical Interview for Diagnosis, Abbreviated-Interview/Nonpatient (SCIDa-I/NP): The SCIDa-I/NP is a measure used to assess symptoms of psychopathology.26 Candidates with a lifetime history of psychosis were excluded.
Interventions
Each of the interventions was offered using 6 group sessions, with 2 or more participants, on an approximate weekly schedule.
VET CBT-T. Two primary texts served as resources for developing the VET CBT-T protocol: (1) the Psychological Management of Chronic Tinnitus: A Cognitive-Behavioral Approach14; and (2) a manual for providing CBT for the treatment of chronic pain.27,28 Draft materials were developed by the clinical psychologist, including a clinician’s manual for providing VET CBT-T. Handouts were provided to each veteran. Components were compared to another unpublished CBT for tinnitus workbook.10
Key components targeted psychological difficulties including sleep disturbance, reduced functioning, low mood, nervousness, reduced pleasure from activities, and negative changes in relationships. The protocol emphasized basic information about tinnitus; relationships among tinnitus, acoustic trauma, and mental health symptoms; veterans’ sense of camaraderie and loyalty; and goal setting, making use of discipline and order veterans may desire.
To build rapport, the psychologist used reflective listening, encouraged interactive dialogue, and promoted participant understanding. Since tinnitus is thought to be exacerbated by stress, participants learned ways to manage stress and practiced relaxation exercises. Participants learned to create individualized, intersession goals that were realistic, specific, and measurable to promote self-efficacy. They also learned to list and increase pleasant activities to distract from tinnitus, improve QOL, and enable behavioral activation. Motivational interviewing addressed readiness, ambivalence, and resistance to achieving these specific goals. Participants also learned to identify and modify unhelpful thoughts about tinnitus (ie, cognitive restructuring).
Audiologist Counseling (AC). To control for patient contact in VET CBT-T, the study audiologist created a 6-session counseling protocol. The AC emphasized education about tinnitus and available tinnitus interventions. Participants were encouraged to ask questions, share their tinnitus experiences, and cope with tinnitus by avoiding silence.
Quantitative Analysis
To assess baseline between-group differences, pretreatment (t1;immediately prior to attending the first group session) administrations of the THI and TRQ were compared using t tests. Demographics between groups were compared using the chi-square test.
The THI and TRQ were readministered following completion of the last group session (t2) and about 8 weeks after the last group session (t3). Because of the small sample size, required assumptions for analyzing parametric tests of linear effects were not met. Thus, only descriptive results and mean differences in scores on the THI and TRQ between these 3 assessment periods are presented. SPSS PASW Statistics 18.0 (Hong Kong, China) was used for analyses.
Qualitative Analysis
VET CBT-T. After each VET CBT-T session, veterans’ acceptance of the protocol was assessed using 4 questions: (1) Was the information presented to you today easy to understand? Yes/No. If no, why not? (2) Were the examples (if there were any) useful? Yes/No. If no, why not? (3) Was the way the information was presented by the group leader helpful? Yes/No. If no, why not? and (4) Please tell us what you thought about today’s group. Participants were encouraged to be honest and provide detailed feedback. To facilitate unbiased responding, the group leader left the room while a research assistant collected the comments.
Participants’ experiences and acceptance of the interventions were explored using a stepwise content analysis approach.29,30First, the feedback data were prepared for analysis by entering verbatim responses into a spreadsheet. Next, these responses were reviewed by the clinical psychologist who identified themes. Examination of data involved qualitative analyses in which the phenomenon of interest was veterans’ acceptance of the interventions. This process presumed that most veterans would respond favorably to the intervention and, thus, acknowledged that the clinical psychologist designed and delivered the intervention.
Any contrary or negative comments were flagged. However, neutral and positive comments also were analyzed and tallied. Notations within each comment were used to calculate the number of occurrences of themes. Similar themes with few responses were collapsed into a single theme when appropriate. Final themes and tallies were shared with an auditor familiar with tinnitus, psychology, and qualitative methods who made comments and checked tallies within each theme. The themes were revised based on this audit and retallied. The clinical psychologist then summarized the themes in text, which was reviewed by the auditor for accuracy in capturing the important emergent themes.
Next, themes were used to examine typed verbatim transcripts from the second and fifth sessions of the intervention. Thematic content derived from the above feedback was extracted from the transcripts by the clinical psychologist. Then the study audiologist read the transcripts to confirm or reject these comments as relevant to the themes. Additional comments were nominated by the study audiologist and reviewed by the clinical psychologist who finalized feedback thought to best represent the themes.
Results
One hundred ninety-six persons inquired about the study (Figure 1).
After being deemed eligible by the otologist as having tinnitus associated with sound trauma, the remaining 25 eligible and interested candidates were randomized into the 2 treatment arms. To reduce attrition, formation of groups took into account participants’ preferred appointment days and times. When 3 or more participants were allocated to a treatment arm, group sessions were scheduled. Five (20%) participants were lost to attrition, including 1 randomized to VET CBT-T and 2 to AC who dropped out prior to receiving any intervention, and 2 randomized to VET CBT-T who dropped out after attending 1 session. Reasons stated for dropping out included concerns they would not learn new information, inability to tolerate sound in a group, unexpected moves out of the area, lack of time, loss of interest, and family emergencies.
Quantitative Analysis
Participants in the 2 treatment arms did not differ significantly on the pretreatment (t1) THI (t = 1.39, df = 18, P = .18) or TRQ (t = 0.99, df = 18, P = .33) scores. Differences in THI scores were computed from pre- to posttreatment (VET CBT-Tt1−t2 = 6.2; ACt1−t2 = 10.0) and from pretreatment to 8-week follow-up (VET CBT-Tt1−t3 = 4.4; ACt1−t3 = 9.1). Similarly, differences in mean TRQ index scores were computed from pre- to posttreatment (VET CBT-Tt1−t2 = 5.3; ACt1−t2 = 7.6) and from pretreatment to 8 weeks follow-up (VET CBT-Tt1−t3 = 1.5; ACt1−t3 = 5.6). These mean differences reveal consistent reductions in mean index scores (improved tinnitus-related QOL) between time points for each treatment arm, but do not indicate statistically or clinically significant reductions of distress.
Qualitative Analysis
The 89 comments that participants provided after the 18 VET CBT-T sessions (3 series of 6 sessions each) were mostly positive (67 responses, 75%) (eTable 2).
Components of VET CBT-T and Number of Sessions (n = 53)
Psychoeducation and Sound Enrichment. Participants generally appreciated the psychoeducation component of VET CBT-T, including basic information about the prevalence of tinnitus, mechanics of the ear and hearing, and how an enriched sound environment may assist with coping (5 comments).
Stress Reduction. Two of the 14 participants who commented on the stress reduction session (via relaxation exercises) noted that it was helpful in their lives overall but “had no effect on tinnitus.”
Goal Setting. Nine participants noted that they valued the goal-setting strategies and long-term relapse planning, one writing that he was “…glad to be encouraged to document and set specific, documented goals each week.”
Cognitive Restructuring and Acceptance. Participants reported that the cognitive restructuring session was important for “accepting” their tinnitus (9 comments). Overall cognitive restructuring appeared to be well received by participants as a concept when learning ways to cope with tinnitus.
Distraction. Of the 8 comments that regarded the increasing-pleasant-activities session, 1 participant reported that the pleasant activities worksheet had a female bias and that activities on one of the worksheets “were not helpful and overlapped too much.” A participant suggested that group leaders allow participants to brainstorm pleasant activities using an open-ended format instead of using categories of pleasant activities. Participants generally found the increasing-pleasant-activities component very beneficial for managing tinnitus.
Self-Hypnosis and Exposure Therapy. Two components not presented during VET CBT-T were identified by participants as potentially desirable. One participant suggested providing information on self-hypnosis and another stated that he focuses on his tinnitus to cope, much like exposure therapy for tinnitus.
Number of Sessions. One participant wrote after the last (sixth) session that he was “glad it’s over” possibly suggesting the intervention was too long. Another participant stated at the fifth session, “I basically want to get out of here—out of this, out of these meetings.” Conversely a participant stated, “I was kind of hoping there was one more after next week.” Another participant explained the intervention itself can be in conflict with its own stated goals of attending less to tinnitus.
Leader, Materials, and Presentations (n = 16).
Overall, the participants had positive experiences (15 comments) with their study therapist. They noted that the group leader was “flexible” and “did a great job of facilitating discussion.” One participant commented on the need for better visual presentations of the information and the need for the group leader to “use her own words” rather than reading the content.
Previous Use of CBT Skills (n = 5).
Five participants noted that information presented was “not new” and that they had acquired the coping skills spontaneously years earlier. Two expressed relief that some of the ways they had been dealing with their tinnitus prior to the intervention were actually recommended. One discussed that reviewing skills that he had already implemented was helpful.
Hope, Anger, and Mental Health (n = 8).
Three participants indicated the intervention gave them “hope” that they will learn ways to cope with tinnitus. One noted that the discussion regarding depression as a commonly co-occurring condition with tinnitus should include a better description of depressive symptoms. Two expressed relief to receive help for their frustration and anger resulting from tinnitus, and 1 participant discussed the added frustration of hearing loss with tinnitus. Excessive alcohol use to cope with tinnitus and the comorbidity of tinnitus and PTSD also were discussed.
Group Cohesiveness (n = 8)/Discord (n = 2).
Many group members commented that they enjoyed listening to information about tinnitus and sharing their experiences. There was friendly interaction and discussion among most of the participants. They commented that it was informative to see that others were coming forward for help and were interested to hear others’ experiences. The group format was mostly welcomed and appreciated. However, group discord occurred when topics other than tinnitus were shared, such as recovery from substance abuse. Two feedback comments indicated that this discussion was unwelcomed.
Discussion
This pilot study provides evidence that at least some of the veterans who were eligible and participated accrued benefit from either AC or VET CBT-T. There also is evidence that a structured and intensive counseling approach by an audiologist that does not include sound therapy is beneficial. Participants generally found that the interventions were acceptable for understanding basic information about tinnitus, and those in the VET CBT-T treatment arm reported improvements in problem solving and coping.
The planned qualitative analyses enabled in-depth examination of intervention feedback from participants and revealed important themes for modifying the VET CBT-T intervention, which occurred following completion of this pilot study. Further, these themes echo the success in creating a unique, veteran-centric, CBT intervention for tinnitus management.
Primarily, participants indicated that education about tinnitus prevalence, etiology, and sound enrichment assisted in coping with tinnitus. This theme also reflects the protocol’s emphasis on health literacy. The wide availability of misinformation on tinnitus, along with the potential for monetary scams, underlies the need for well-designed and research-informed tinnitus education programs. Helping veterans distinguish facts and myths is a potentially important element of tinnitus management. Experiences coping with trauma were salient as participants diverged in their opinions regarding the appropriateness of discussing these issues during a tinnitus management group.
Specific themes emerged regarding the relevance of posttraumatic stress disorder (PTSD) symptoms and substance use to cope with tinnitus. Comfort levels when hearing and discussing these symptoms varied among participants. Due to the high comorbidities of mental health disorders and tinnitus, this theme is important to consider when designing tinnitus management programs. Other qualitative themes served to validate peer support and that the veteran-centric protocol was acceptable, including positive regard for goal setting, indicating that adherence to discipline and order had been addressed.
Identified VET CBT-T Modifications
There were multiple indicators that the rationale for sessions needed to be clarified. Participants highlighted the need to hear clear expectations about what the coping skills would address and multiple reminders regarding the goals of relaxation exercises for tinnitus. Some expressed concern about their lack of concentration during the relaxation exercises. A concern that was discussed with participants only during the informed consent process was the possibility that the intervention could increase focus on tinnitus and, thus, temporarily increase tinnitus distress while receiving the intervention.
Need for Interdisciplinary Care
Perhaps the fact that both interventions were beneficial is not surprising since AC as delivered in this study was designed to be an active intervention that incorporated education and support, including some components similar to those included in VET CBT-T. It appears that AC designed to match the CBT intervention in terms of number of sessions among other enhancements suggests that this intervention may be efficacious. The AC intervention offered support and education about tinnitus; however, sound therapy was not provided despite some empirical support for its use.31 Future research should examine whether sound therapy adds benefit to an intensive and structured AC approach.
It has been proposed that a combination of CBT delivered by a mental health provider and AC should be implemented as an optimal tinnitus management protocol.31,32 Results of this and a number of other recent studies 16,32,33 encourage an integrated, interdisciplinary approach.
Findings of the present study were applied toward development of a hierarchical and interdisciplinary tinnitus management protocol, Progressive Tinnitus Management (PTM).22,34 Components of VET CBT-T were selected for the intervention provided with PTM, modified as per the feedback from participants in this study. This approach was combined with components of the AC intervention, further complemented by sound therapy. The new combined protocol was tested in a pilot telephone study of PTM for veterans and military members with positive results.32 Two VA-supported RCTs of PTM have since been completed.35,36 Results indicate that relative to wait list control, PTM is effective in mitigating negative effects of tinnitus.
Last, after this pilot study, the protocol was modified to address participants’ concerns that their primary care and other providers were unaware that interventions for tinnitus exist. Providers offering tinnitus care are now encouraged to share its availability with veterans and other clinicians. This study provides compelling evidence that veterans respond to messages of hope from providers that they do not needlessly have to suffer alone. Rather than telling veterans to “just live with it,” primary care providers should be able to offer ideas and services for learning how to live with tinnitus.
Future Directions
Future revisions of VET CBT-T could incorporate “acceptance” as a concept for coping with tinnitus, components such as self-hypnosis and exposure therapy, and strategies for coping with hearing loss and communication difficulties. Reexamination of the number and length of sessions also is encouraged, as well as integration of evidence-based interventions for comorbid conditions such as PTSD, substance use disorders, and insomnia. Perhaps increasing the use of peer support services would help reach veterans concerned by the stigma of receiving mental health care. Some veterans were dissatisfied with hearing about others’ mental health concerns. It may be beneficial to offer tinnitus interventions to cohorts of veterans identified with specific comorbid mental health or substance use disorders. However, peer support may be more important than protecting veterans from hearing about others’ mental health concerns as social cognitive theory suggests.
Limitations
This feasibility study’s strict inclusion criteria resulted in a small but well-defined sample that may not be representative of the larger population of veterans who could potentially benefit from these interventions. The extensive evaluation requirements and eligibility requirements likely enhanced the internal validity of the trial but may have compromised the external validity and generalizability of the study findings.
While a few women were assessed during the eligibility process, unfortunately, only men were deemed eligible. It is therefore unknown how women veterans would receive this protocol. Currently there is a bias in selecting male participants for tinnitus research. It is hoped that in the future a sample of women veterans could also provide feedback on this tinnitus management protocol developed by the VHA.
The fact that a large proportion of those who made initial contact about the study decided not to follow up is not inconsistent with studies of similar psychological interventions.37 Challenges related to engaging otherwise appropriate candidates in psychological interventions for a range of chronic health concerns have been well described and may apply to tinnitus management.
Conclusion
The qualitative feedback from participants was generally positive for both protocols. Emergent themes confirmed the need for a veteran-specific intervention while highlighting individual veterans’ needs. Transcripts from sessions provided additional descriptive information that identified changes to the protocols that would improve veterans’ receipt of care. Due to the abundance of veterans with tinnitus and the needs of veterans in terms of health care delivery and receipt, an interdisciplinary CBT-plus-AC protocol was created that is specific to and accepted by veterans with tinnitus.
Refinements to the VET CBT-T protocol were identified that led to development of PTM that was the subject of another small study, which then led to the authors’ 2 larger RCTs. Attempts were made to include greater attention to the mental health concerns of veterans both in terms of education and in offering sensitive delivery of the protocol. Session content was used to create an organized, visual presentation that follows an organized workbook.22,35 Refinements to the protocol are ongoing.
Acknowledgments
This material was based on work supported by US Department of Veterans Affairs, Rehabilitation Research and Development (RR&D): (1) R.D. Kerns’ Pilot Merit Grant #C6324P and (2) C.J. (Kendall) Schmidt’s Career Development Award-1 #D6848M. The authors would like to acknowledge the assistance from Rebecca Czlapinski, MA; Kathryn LaChappelle, MPH; and Emily Thielman, MS, for the conduct of the study, data collection and management, and preparation of this manuscript.
1. Henry JA. “Measurement” of tinnitus. Otol Neurotol. 2016;37(8):e276-e285.
2. Hoffman HJ, Reed GW. Epidemiology of tinnitus. In Snow JB, ed. Tinnitus: Theory and Management. Hamilton, Canada: BC Becker; 2004:16-41.
3. Folmer RL, Theodoroff SM, Martin WH, Shi Y. Experimental, controversial, and futuristic treatments for chronic tinnitus. J Am Acad Audiol. 2014;25(1):106-125.
4. US Department of Veterans Affairs. Veterans Benefits Administration annual benefits report fiscal year 2016. https://www.benefits.va.gov/REPORTS/abr/ABR-All_Sec tions_FY16_06292017.pdf . Accessed June 19, 2018.
5. Henry JA, Zaugg TL, Myers PJ, Schechter MA. The role of audiologic evaluation in progressive audiologic tinnitus management. Trends Amplif. 2008;12(3):170-187.
6. Hoare DJ, Searchfield GD, El Refaie A, Henry JA. Sound therapy for tinnitus management: practicable options. J Am Acad Audiol. 2014;25(1):62-75.
7. Andersson G, Porsaeus D, Wiklund M, Kaldo V, Larsen HC. Treatment of tinnitus in the elderly: a controlled trial of cognitive behavior therapy. Int J Audiol. 2005;44(11):671-675.
8. Henry JL, Wilson PH. Coping with tinnitus: two studies of psychological and audiological characteristics of patients with high and low tinnitus-related distress. Int Tinnitus J. 1995;1(2):85-92.
9. Henry JL, Wilson PH. The psychological management of tinnitus: comparison of a combined cognitive educational program, education alone and a waiting-list control. Int Tinnitus J. 1996;2:9-20.
10. Robinson SK, Viirre ES, Bailey KA, et al. A randomized controlled trial of cognitive-behavior therapy for tinnitus. Int Tinnitus J. 2008;14(2):119-126.
11. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2010(9):CD005233.
12. Tunkel DE, Bauer CA, Sun GH, et al. Clinical practice guideline: tinnitus. Otolaryngol Head Neck Surg. 2014;151(Suppl)(2):S1-S40.
13. Beck JS. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, NY: Guilford Press; 2011.
14. Henry JL, Wilson PH. The Psychological Management of Chronic Tinnitus : A Cognitive-Behavioral Approach. Boston, MA: Allyn and Bacon; 2001.
15. Bandura A. Health promotion by social cognitive means. Health Educ Behav. 2004;31(2):143-164.
16. Cima RF, Andersson G, Schmidt CJ, Henry JA. Cognitive-behavioral treatments for tinnitus: a review of the literature. J Am Acad Audiol. 2014;25(1):29-61.
17. Rodriguez V, Andrade AD, García-Retamero R, et al. Health literacy, numeracy, and graphical literacy among veterans in primary care and their effect on shared decision making and trust in physicians. J Health Commun. 2013;18(suppl 1):273-289.
18. Seal KH, Metzler TJ, Gima KS, Bertenthal D, Maguen S, Marmar CR. Trends and risk factors for mental health diagnoses among Iraq and Afghanistan veterans using Department of Veterans Affairs health care, 2002-2008. Am J Public Health. 2009;99(9):1651-1658.
19. Thomas JL, Wilk JE, Riviere LA, et al. Prevalence of mental health problems and functional impairment among active component and National Guard soldiers 3 and 12 months following combat in Iraq. Arch Gen Psychiatry. 2010;67(6):614-623.
20. Zivin K, McCarthy JF, McCammon RJ, et al. Health-related quality of life and utilities among patients with depression in the Department of Veterans Affairs. Psychiatr Serv. 2008;59(11):1331-1334.
21. Costa DL, Kahn ME. Health, wartime stress, and unit cohesion: evidence from Union Army veterans. Demography. 2010;47(1):45-66.
22. Henry JA, Zaugg TL, Myers PJ, Kendall (Schmidt) CJ. Progressive Tinnitus Management: Clinical Handbook for Audiologists. San Diego, CA: Plural Publishing; 2010.
23. Henry JA, Schechter MA, Loovis CL, et al. Clinical management of tinnitus using a “progressive intervention” approach. J Rehabil Res Dev. 2005;42(4 suppl 2):95-116.
24. Newman CW, Jacobson GP, Spitzer JB. Development of the Tinnitus Handicap Inventory. Arch Otolaryngol Head Neck Surg. 1996;122(2):143-148.
25. Wilson PH, Henry JL, Bowen M, Haralambous G. Tinnitus Reaction Questionnaire: psychometric properties of a measure of distress associated with tinnitus. J Speech Hear Res. 1991;34(1):197-201.
26. First MB, Spitzer RL, Gibbon M, Williams JBW. Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I) Clinical Version, Administration Booklet. Washington, DC: American Psychiatric Press; 2012.
27. Kerns RD, Thorn BE, Dixon KE. Psychological treatments for persistent pain: an introduction. J Clin Psychol. 2006;62(11):1327-1331.
28. Otis JD. Managing Chronic Pain: A Cognitive-Behavioral Therapy Approach. New York, NY: Oxford; 2007.
29. Sandelowski M. Whatever happened to qualitative description? Res Nurs Health. 2000;23(4):334-340.
30. Mertens DM. Research and Evaluation in Education and Psychology: Integrating Diversity With Quantitative, Qualitative, and Mixed Methods. 3rd ed. Los Angeles, CA: Sage; 2009 .
31. Hobson J, Chisholm E, El Refaie A. Sound therapy (masking) in the management of tinnitus in adults. Cochrane Database Syst Rev. 2010;(12):CD006371.
32. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehabil Res Dev. 2012;49(7):1025-1042.
33. Weise C, Heinecke K, Rief W. Biofeedback-based behavioral treatment for chronic tinnitus: results of a randomized controlled trial. J Consult Clin Psychol. 2008;76(6):1046-1057.
34. Henry JA, Zaugg TL, Myers PJ, Kendall (Schmidt) CJ. How to Manage Your Tinnitus: A Step-by-Step Workbook, 3rd ed. San Diego, CA: Plural Publishing; 2010.
35. Henry JA, Thielman EJ, Zaugg TL, et al. Randomized controlled trial in clinical settings to evaluate effectiveness of coping skills education used with Progressive Tinnitus Management. J Speech Lang Hear Res. 2017;60(5):1378-1397.
36. Henry, JA, Thielman, E, Zaugg, et al. Telephone-based progressive tinnitus management for persons with and without traumatic brain injury: a randomized controlled trial. Ear Hear. 2018. [Epub ahead of print.]
37. Chang MW, Nitzke S, Brown R, et al. Recruitment challenges and enrollment observations from a community based intervention (Mothers In Motion) for low-income overweight and obese women. Contemp Clin Trials Commun. 2017;5:26-33.
1. Henry JA. “Measurement” of tinnitus. Otol Neurotol. 2016;37(8):e276-e285.
2. Hoffman HJ, Reed GW. Epidemiology of tinnitus. In Snow JB, ed. Tinnitus: Theory and Management. Hamilton, Canada: BC Becker; 2004:16-41.
3. Folmer RL, Theodoroff SM, Martin WH, Shi Y. Experimental, controversial, and futuristic treatments for chronic tinnitus. J Am Acad Audiol. 2014;25(1):106-125.
4. US Department of Veterans Affairs. Veterans Benefits Administration annual benefits report fiscal year 2016. https://www.benefits.va.gov/REPORTS/abr/ABR-All_Sec tions_FY16_06292017.pdf . Accessed June 19, 2018.
5. Henry JA, Zaugg TL, Myers PJ, Schechter MA. The role of audiologic evaluation in progressive audiologic tinnitus management. Trends Amplif. 2008;12(3):170-187.
6. Hoare DJ, Searchfield GD, El Refaie A, Henry JA. Sound therapy for tinnitus management: practicable options. J Am Acad Audiol. 2014;25(1):62-75.
7. Andersson G, Porsaeus D, Wiklund M, Kaldo V, Larsen HC. Treatment of tinnitus in the elderly: a controlled trial of cognitive behavior therapy. Int J Audiol. 2005;44(11):671-675.
8. Henry JL, Wilson PH. Coping with tinnitus: two studies of psychological and audiological characteristics of patients with high and low tinnitus-related distress. Int Tinnitus J. 1995;1(2):85-92.
9. Henry JL, Wilson PH. The psychological management of tinnitus: comparison of a combined cognitive educational program, education alone and a waiting-list control. Int Tinnitus J. 1996;2:9-20.
10. Robinson SK, Viirre ES, Bailey KA, et al. A randomized controlled trial of cognitive-behavior therapy for tinnitus. Int Tinnitus J. 2008;14(2):119-126.
11. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2010(9):CD005233.
12. Tunkel DE, Bauer CA, Sun GH, et al. Clinical practice guideline: tinnitus. Otolaryngol Head Neck Surg. 2014;151(Suppl)(2):S1-S40.
13. Beck JS. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, NY: Guilford Press; 2011.
14. Henry JL, Wilson PH. The Psychological Management of Chronic Tinnitus : A Cognitive-Behavioral Approach. Boston, MA: Allyn and Bacon; 2001.
15. Bandura A. Health promotion by social cognitive means. Health Educ Behav. 2004;31(2):143-164.
16. Cima RF, Andersson G, Schmidt CJ, Henry JA. Cognitive-behavioral treatments for tinnitus: a review of the literature. J Am Acad Audiol. 2014;25(1):29-61.
17. Rodriguez V, Andrade AD, García-Retamero R, et al. Health literacy, numeracy, and graphical literacy among veterans in primary care and their effect on shared decision making and trust in physicians. J Health Commun. 2013;18(suppl 1):273-289.
18. Seal KH, Metzler TJ, Gima KS, Bertenthal D, Maguen S, Marmar CR. Trends and risk factors for mental health diagnoses among Iraq and Afghanistan veterans using Department of Veterans Affairs health care, 2002-2008. Am J Public Health. 2009;99(9):1651-1658.
19. Thomas JL, Wilk JE, Riviere LA, et al. Prevalence of mental health problems and functional impairment among active component and National Guard soldiers 3 and 12 months following combat in Iraq. Arch Gen Psychiatry. 2010;67(6):614-623.
20. Zivin K, McCarthy JF, McCammon RJ, et al. Health-related quality of life and utilities among patients with depression in the Department of Veterans Affairs. Psychiatr Serv. 2008;59(11):1331-1334.
21. Costa DL, Kahn ME. Health, wartime stress, and unit cohesion: evidence from Union Army veterans. Demography. 2010;47(1):45-66.
22. Henry JA, Zaugg TL, Myers PJ, Kendall (Schmidt) CJ. Progressive Tinnitus Management: Clinical Handbook for Audiologists. San Diego, CA: Plural Publishing; 2010.
23. Henry JA, Schechter MA, Loovis CL, et al. Clinical management of tinnitus using a “progressive intervention” approach. J Rehabil Res Dev. 2005;42(4 suppl 2):95-116.
24. Newman CW, Jacobson GP, Spitzer JB. Development of the Tinnitus Handicap Inventory. Arch Otolaryngol Head Neck Surg. 1996;122(2):143-148.
25. Wilson PH, Henry JL, Bowen M, Haralambous G. Tinnitus Reaction Questionnaire: psychometric properties of a measure of distress associated with tinnitus. J Speech Hear Res. 1991;34(1):197-201.
26. First MB, Spitzer RL, Gibbon M, Williams JBW. Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I) Clinical Version, Administration Booklet. Washington, DC: American Psychiatric Press; 2012.
27. Kerns RD, Thorn BE, Dixon KE. Psychological treatments for persistent pain: an introduction. J Clin Psychol. 2006;62(11):1327-1331.
28. Otis JD. Managing Chronic Pain: A Cognitive-Behavioral Therapy Approach. New York, NY: Oxford; 2007.
29. Sandelowski M. Whatever happened to qualitative description? Res Nurs Health. 2000;23(4):334-340.
30. Mertens DM. Research and Evaluation in Education and Psychology: Integrating Diversity With Quantitative, Qualitative, and Mixed Methods. 3rd ed. Los Angeles, CA: Sage; 2009 .
31. Hobson J, Chisholm E, El Refaie A. Sound therapy (masking) in the management of tinnitus in adults. Cochrane Database Syst Rev. 2010;(12):CD006371.
32. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehabil Res Dev. 2012;49(7):1025-1042.
33. Weise C, Heinecke K, Rief W. Biofeedback-based behavioral treatment for chronic tinnitus: results of a randomized controlled trial. J Consult Clin Psychol. 2008;76(6):1046-1057.
34. Henry JA, Zaugg TL, Myers PJ, Kendall (Schmidt) CJ. How to Manage Your Tinnitus: A Step-by-Step Workbook, 3rd ed. San Diego, CA: Plural Publishing; 2010.
35. Henry JA, Thielman EJ, Zaugg TL, et al. Randomized controlled trial in clinical settings to evaluate effectiveness of coping skills education used with Progressive Tinnitus Management. J Speech Lang Hear Res. 2017;60(5):1378-1397.
36. Henry, JA, Thielman, E, Zaugg, et al. Telephone-based progressive tinnitus management for persons with and without traumatic brain injury: a randomized controlled trial. Ear Hear. 2018. [Epub ahead of print.]
37. Chang MW, Nitzke S, Brown R, et al. Recruitment challenges and enrollment observations from a community based intervention (Mothers In Motion) for low-income overweight and obese women. Contemp Clin Trials Commun. 2017;5:26-33.
Need for Mental Health Providers in Progressive Tinnitus Management
Hearing loss and tinnitus (ringing or other noises in the ears or head) have been problematic for military service members and veterans for many years. Military personnel are exposed to high levels of noise in operational and training settings. In spite of hearing conservation efforts, hearing loss and auditory injuries (including tinnitus) continue to occur. Although current military leadership teaches the importance of hearing protection, that was not usually the case until the past few decades. Military leadership provides the means for hearing protection and monitors risk through conservation and hearing readiness programs. Unfortunately, the need for hearing during battle often overrides the expediency of using hearing protective devices.
Military members often equate hearing protection with increased vulnerability, widening the gap between preventive efforts and hearing preservation. It is therefore not surprising that tinnitus and hearing loss have been the 2 most common service-connected disabilities for veterans for a decade.1 These conditions are irreversible; affected service members and veterans need strategies to cope with distress associated with these chronic conditions. Clinical care often is essential to manage the associated distress and mental health (MH) symptoms, such as sleep disturbance, irritability, isolation, tension, and low mood.
There is no cure for tinnitus, meaning there is no proven method to permanently eliminate or even reduce the perception of tinnitus. Intervention for tinnitus therefore is limited to methods intended to mitigate reactions to tinnitus, with the ultimate goal to facilitate good quality of life in spite of the perception of this unwanted auditory anomaly. These methods include numerous means of utilizing therapeutic sound.2 Sound therapy, however, has been shown in controlled trials to be effective only when accompanied by counseling, which often focuses on teaching different coping skills.3 In such instances, MH providers can become an integral part of the hearing health team to assist patients in the management of their tinnitus.
Evidence-Based Practice
Evidence-based research should guide clinical services that are offered for tinnitus. Randomized controlled trials (RCTs) comprise the most important source for such evidence.4 Cochrane Reviews uses meta-analyses to examine rigorous RCTs to determine which methods have credible evidence. One of these reviews conducted in 2007 and updated in 2010 concluded that cognitive behavioral therapy (CBT) can improve depression scores and reduce distress for many people with bothersome tinnitus.5,6 Another Cochrane Review concluded that sound therapy combined with counseling can be beneficial, but on its own, sound therapy has not been shown to result in significant benefit.3 Yet another Cochrane Review focused on using hearing aids with patients who have both hearing loss and bothersome tinnitus; the researchers concluded that “there is currently no evidence to support or refute their use as a more routine intervention for tinnitus.”7 However, many patients and clinicians report hearing aids are helpful for coping with tinnitus.
The American Academy of Otolaryngology–Head and Neck Surgery Foundation (AAO-HNSF) published a clinical practice guideline (CPG) for the management of tinnitus.8 Developing the CPG involved a comprehensive evaluation of the peer-reviewed literature, including the available Cochrane Reviews, to identify appropriate RCTs to inform evidence-based recommendations. Cognitive behavioral therapy was the only intervention for tinnitus recommended in the CPG. Cognitive behavioral therapy targets emotional response by identifying behaviors, thoughts, and beliefs that may be altered.9 For tinnitus, CBT typically includes stress management including relaxation exercises, purposeful distraction, and changing how individuals view and appraise their tinnitus.
Both the CPG and Cochrane Reviews concluded that CBT has the strongest evidence base for reducing effects of tinnitus. It should be noted that the CPG recommended teaching patients basic information about tinnitus management and stated that it was optional (due to limited research evidence) to use sound therapy to augment coping skills training.
Progressive Tinnitus Management
Tinnitus research at the VA National Center for Rehabilitative Auditory Research (NCRAR) has led to the development and refinement of an interdisciplinary program called Progressive Tinnitus Management (PTM). Audiologists and MH providers work together to deliver portions of the protocol. In addition, otolaryngologists are important for patients requiring a medical examination. Audiologists, MH providers, and otolaryngologists comprise the hearing health team for tinnitus management. The PTM program involves 5 stepped-care levels of management, and patients receive only the levels they need.
Level 1 is the referral level, which specifies guidelines for any clinician who encounters patients experiencing tinnitus. The “standard” referral is to audiology for a hearing evaluation (PTM level 2)—every patient reporting tinnitus should have a hearing evaluation and brief tinnitus assessment. Less typical would be an urgent referral to a different provider for certain symptoms such as referral to ENT for sudden hearing loss.
Patients who desire intervention for bothersome tinnitus are offered PTM skills education (level 3). At this level, patients are taught facts and skills that they need to self-manage their tinnitus-related problems. Ideally, the audiologist and MH provider collaborate to deliver the level 3 intervention, which utilizes a 5-session (2 with an audiologist and 3 with a MH provider) problem-solving method. Audiologists explain different forms of sound therapy, and MH providers deliver brief CBT. The research studies and clinics that use PTM have shown that the majority of patients who receive the level 3 skills education interventions have their tinnitus needs met to the degree that they do not desire further services.
Those relatively few patients who desire further services are invited for a PTM interdisciplinary evaluation (level 4), which involves a more in-depth needs evaluation by both an audiologist and a MH provider. Based on the outcome of the level 4 evaluation, clear treatment goals are discussed with the patient. If the patient and providers mutually agree that further intervention is needed, then the patient is offered PTM individualized support (level 5), which involves one-on-one services by an audiologist and/or a MH provider. The providers then build on the lessons taught during level 3 and address barriers to enacting the already discussed skills. The MH provider also may expand on CBT skills that were provided in level 3, offering care such as CBT for insomnia during level 5, depending on the specific needs and desires of the patient.
At the NCRAR, a pilot study and 2 RCTs of PTM have been completed.10 The first of these 2 RCTs was a clinical effectiveness study of PTM that was conducted in 2 VA audiology clinics: Memphis, Tennessee, and West Haven, Connecticut.11 Patients who came to the clinics signed up for the study if they felt that the PTM level 3 intervention might be helpful. Half of the 300 veterans in the study were enrolled to receive PTM right away, and half were put on a 6-month wait list. The PTM group showed significantly greater benefit than that of the wait-list group.
The second RCT of PTM was motivated by the high number of service members and veterans with a history of traumatic brain injury (TBI), which is strongly associated with tinnitus.12 The PTM level 3 skills education was administered to participants individually over the telephone by both an audiologist and a psychologist. Participants, located all over the U.S., had bothersome tinnitus, and some had experienced ≥ 1 TBI. They were randomized to receive either Tele-PTM immediately for 6 months or to be put on a 6-month wait list. The Tele-PTM group showed much greater improvement than that of the wait-list group.
Both of these recent RCTs have validated the effectiveness of PTM and demonstrated that PTM should be considered for the practice of evidence-based tinnitus management. PTM is mostly consistent with the AAO-HNSF CPG and provides a structured and defined framework for implementing both assessment and intervention services for patients who report tinnitus. As such, VA Central Office has endorsed PTM as an effective intervention for tinnitus management and has recommended its use at VAMCs. The NCRAR researchers have provided PTM training to hundreds of VA audiologists and MH providers, yet the level of implementation across the VA system of care varies widely.
VA Survey
In 2015, in partnership with the VA Offices of Audiology and Speech Pathology and Mental Health Services, and the Health Services Research & Development/Quality Enhancement Research Initiative (HSR&D/QUERI), the NCRAR conducted a study to examine PTM variation across sites via surveys and/or interviews of VA Audiology and MH programs nationwide.13,14 The objectives of this study were to: (1) describe current tinnitus-management practices in VAMCs; (2) identify barriers and facilitators to PTM program implementation based on clinics that have fully, partially, or not implemented PTM; and (3) determine readiness to implement PTM within VISN 20 (Northwest states and Alaska).
Clinicians at VAMCs nationwide were surveyed regarding current provision of tinnitus clinical services. Requests were sent to audiology programs and MH programs at 142 major VAMCs along with instructions to complete the online survey. Responses were received from 87 audiologists and 66 MH providers. Clinicians at VAMCs with full PTM, partial PTM, and no-PTM (based on survey results) were then interviewed regarding site-specific barriers and facilitators to implementing and providing PTM, readiness to adopt PTM, and strategies for full PTM implementation.
Key findings from the study demonstrated the following: (1) There is considerable between-site variability in how PTM is implemented, particularly with the delivery of the MH portion of the protocol; (2) audiologists show higher levels of readiness to provide tinnitus services than do MH providers (7% of MH survey respondents vs 62% of audiologists reported their site implementing PTM); (3) 66% of MH survey respondents were interested in receiving training in tinnitus management (note that online PTM training for MH does not yet exist); (4) PTM implementation barriers include audio-visual technology issues, room scheduling, as well as lack of collaboration and colocation between MH and audiology departments, administrative time/support, group facilitator skills, and availability of PTM materials.
Overall, results of this HSR&D/QUERI-funded study suggested the need to develop MH-specific training to support the necessary interdisciplinary engagement. Although a patient workbook is available to order and visual presentation aids may be accessed online, it became clear that lack of MH participation in the inherently interdisciplinary PTM skills education was the most common deviation from PTM.
DoD an VA Questionnaire
In 2014 the DoD Hearing Center of Excellence (HCE) conducted the DoD and VA Tinnitus Evaluation, Management, and Treatment Assessment.13 The HCE conducted this questionnaire under the Tinnitus Care Quality Improvement, Process Development, and Implementation Plan, to develop, establish, and implement an interdisciplinary and ongoing process to continually assess and improve the quality and continuum of tinnitus care delivered to service members and veterans at a consistent, enterprise-wide level. The HCE developed the questionnaire to: (1) identify DoD and VA audiologists and otolaryngologists and their institutions providing comprehensive tinnitus care; (2) assess current tinnitus evaluation and management/treatment protocols used; (3) disseminate common practice improvements to all providers for enhancing overall tinnitus evaluation and management/treatment; and (4) evaluate implementation of improvements to include efficiency of implementation and efficacy of improvements.
The questionnaire was administered using SurveyMonkey (San Mateo, CA) and was disseminated by the otolaryngology and audiology consultants to the Army, Navy, and Air Force surgeons general and specialty leaders as well as through VA specialty leaders. Also, the HCE posted the link for the questionnaire on its website for 11 months. A total of 200 providers responded to the questionnaire, of which 13 did not indicate their specialty (eg, otolaryngology) or classification (eg, DoD active duty) and were excluded from data analysis. The 187 qualified respondents included 66 DoD audiologists, 120 VA audiologists, and 1 DoD otolaryngologist.
The questionnaire results indicated that DoD and VA respondents provided tinnitus services for their patients at similar rates (72% of DoD providers and 79% of VA providers). The use of PTM by those same providers, however, was far more widespread in VA (66%) than it was in DoD (37%). Of the providers indicating they did not offer tinnitus clinical services, the main reasons given were lack of necessary training/expertise, lack of time, and insufficient clinical support. The majority of respondents indicated they had training on tinnitus evaluation and/or management and that they were comfortable providing these services; despite this, most providers indicated a need or desire for tinnitus-specific training and education. These results suggested that more support and education for hearing health care providers were needed to implement PTM in VA and, especially, in DoD.
About half of the respondents indicated that psychological/behavioral treatment services, which would correspond to PTM levels 3 and 5, are available for patients at their facility who have tinnitus. It is encouraging to know that some patients with problematic tinnitus are receiving MH services. However, it is essential that patients with any degree of bothersome tinnitus have access to evidence-based clinical services, which would require CBT delivered by a qualified MH provider.
Conclusion
Numerous VA and DoD clinics have begun providing PTM. Individual sites, however, typically adapt the program during the process of implementation.13,14 The most common adaptation that sites make to PTM is to proceed with level 3 skills education without the assistance of MH, and thus CBT, due to the lack of provider availability. It is unknown what impact this has on the effectiveness of PTM. Skills education forms the heart of PTM and addresses the needs of the majority of patients who seek intervention.
Collaboration with MH is integral to the delivery of PTM. Mental health providers partner in PTM levels 3 and 5 by providing CBT, which has the strongest evidence for reducing tinnitus distress among all interventions and always will be critical to the provision of PTM. Clearly VA MH programs need to increase involvement in veterans’ tinnitus management. Increased involvement may be accomplished by (1) developing training or other materials that increase understanding of MH’s role in addressing tinnitus; (2) developing pathways for coordination of care between audiology and MH providers, including different models of coordination based on individual site needs; and (3) documenting the prevalence of tinnitus-MH comorbidities to empirically justify the need for such coordination between audiology and MH providers.
To address gaps identified in the VA survey and in a similar questionnaire conducted by HCE regarding tinnitus care in VA and DoD, the NCRAR, HCE, and Walter Reed National Military Medical Center are collaborating on several initiatives to improve tinnitus services for service members and veterans.13-15 These efforts include enhancing service member and veteran access to VA and DoD MH services in PTM.
1. U.S. Department of Veterans Affairs. Veterans Benefits Administration reports: annual benefits report. http://www.benefits.va.gov/REPORTS/abr/index.asp. Updated December 19, 2016. Accessed April 13, 2017.
2. Hoare DJ, Searchfield GD, El Refaie A, Henry JA. Sound therapy for tinnitus management: practicable options. J Am Acad Audiol. 2014;25(1):62-75.
3. Hobson J, Chisholm E, El Refaie A. Sound therapy (masking) in the management of tinnitus in adults. Cochrane Database Syst Rev. 2010;(12):CD006371.
4. Keech A, Gebski V, Pike R. Interpreting and Reporting Clinical Trials. A Guide to the CONSORT Statement and the Principles of Randomised Controlled Trials. Sydney: MJA Books, Australasian Medical Publishing Company; 2007.
5. Martinez Devesa P, Waddell A, Perera R, Theodoulou M. Cognitive behavioural therapy for tinnitus (review). Cochrane Database Syst Rev. 2007;(1):CD005233.
6. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2010;(9):CD005233.
7. Hoare DJ, Edmondson-Jones M, Sereda M, Akeroyd MA, Hall D. Amplification with hearing aids for patients with tinnitus and co-existing hearing loss. Cochrane Database Syst Rev. 2014;(1):CD010151.
8. Tunkel DE, Bauer CA, Rosenfeld RM, et al. Clinical practice guideline: tinnitus. Otolaryngol Head Neck Surg. 2014;151(suppl 2):S1-S40.
9. Beck JS, Beck AT. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, New York: Guilford Press; 2011.
10. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehab Res Dev. 2012;49(7):1025-1042.
11. Henry JA, Thielman EJ, Zaugg TL, et al. Randomized controlled trial in clinical settings to evaluate effectiveness of coping skills education used with progressive tinnitus management. J Speech Lang Hear Res. 2017;1-20. [Epub ahead of print]
12. Henry JA, Griest S, Thielman E, McMillan G, Kaelin C, Carlson K. The tinnitus functional index: development, validation, outcomes research, and clinical application. Hear Res. 2016;334:58-64.
13. Boudin A, Carlson KC, Elnitsky C, et al. Online Surveys of Tinnitus Management Practices in VA and DoD: Results and Clinical Implications. Joint Defense Veterans Audiology Conference (JDVAC), St Louis, MO, February 22-24, 2016.
14. Carlson KC, Thielman E, Zaugg TL, Elnitsky C, Tuepker A, Kaelin C, Henry JA. “VA Clinician Surveys and Interviews Reveal Need for Increased Mental Health Involvement in Tinnitus Management.” Joint Defense Veterans Audiology Conference (JDVAC), St Louis, MO, February 22-24, 2016.
15. Carlson K, Thielman E, Zaugg T, et al. Factors affecting the provision of evidence-based progressive tinnitus management in Department of Veterans Affairs medical centers. Paper presented at: Academy Health Annual Research Meeting; June 26-28, 2016;
Hearing loss and tinnitus (ringing or other noises in the ears or head) have been problematic for military service members and veterans for many years. Military personnel are exposed to high levels of noise in operational and training settings. In spite of hearing conservation efforts, hearing loss and auditory injuries (including tinnitus) continue to occur. Although current military leadership teaches the importance of hearing protection, that was not usually the case until the past few decades. Military leadership provides the means for hearing protection and monitors risk through conservation and hearing readiness programs. Unfortunately, the need for hearing during battle often overrides the expediency of using hearing protective devices.
Military members often equate hearing protection with increased vulnerability, widening the gap between preventive efforts and hearing preservation. It is therefore not surprising that tinnitus and hearing loss have been the 2 most common service-connected disabilities for veterans for a decade.1 These conditions are irreversible; affected service members and veterans need strategies to cope with distress associated with these chronic conditions. Clinical care often is essential to manage the associated distress and mental health (MH) symptoms, such as sleep disturbance, irritability, isolation, tension, and low mood.
There is no cure for tinnitus, meaning there is no proven method to permanently eliminate or even reduce the perception of tinnitus. Intervention for tinnitus therefore is limited to methods intended to mitigate reactions to tinnitus, with the ultimate goal to facilitate good quality of life in spite of the perception of this unwanted auditory anomaly. These methods include numerous means of utilizing therapeutic sound.2 Sound therapy, however, has been shown in controlled trials to be effective only when accompanied by counseling, which often focuses on teaching different coping skills.3 In such instances, MH providers can become an integral part of the hearing health team to assist patients in the management of their tinnitus.
Evidence-Based Practice
Evidence-based research should guide clinical services that are offered for tinnitus. Randomized controlled trials (RCTs) comprise the most important source for such evidence.4 Cochrane Reviews uses meta-analyses to examine rigorous RCTs to determine which methods have credible evidence. One of these reviews conducted in 2007 and updated in 2010 concluded that cognitive behavioral therapy (CBT) can improve depression scores and reduce distress for many people with bothersome tinnitus.5,6 Another Cochrane Review concluded that sound therapy combined with counseling can be beneficial, but on its own, sound therapy has not been shown to result in significant benefit.3 Yet another Cochrane Review focused on using hearing aids with patients who have both hearing loss and bothersome tinnitus; the researchers concluded that “there is currently no evidence to support or refute their use as a more routine intervention for tinnitus.”7 However, many patients and clinicians report hearing aids are helpful for coping with tinnitus.
The American Academy of Otolaryngology–Head and Neck Surgery Foundation (AAO-HNSF) published a clinical practice guideline (CPG) for the management of tinnitus.8 Developing the CPG involved a comprehensive evaluation of the peer-reviewed literature, including the available Cochrane Reviews, to identify appropriate RCTs to inform evidence-based recommendations. Cognitive behavioral therapy was the only intervention for tinnitus recommended in the CPG. Cognitive behavioral therapy targets emotional response by identifying behaviors, thoughts, and beliefs that may be altered.9 For tinnitus, CBT typically includes stress management including relaxation exercises, purposeful distraction, and changing how individuals view and appraise their tinnitus.
Both the CPG and Cochrane Reviews concluded that CBT has the strongest evidence base for reducing effects of tinnitus. It should be noted that the CPG recommended teaching patients basic information about tinnitus management and stated that it was optional (due to limited research evidence) to use sound therapy to augment coping skills training.
Progressive Tinnitus Management
Tinnitus research at the VA National Center for Rehabilitative Auditory Research (NCRAR) has led to the development and refinement of an interdisciplinary program called Progressive Tinnitus Management (PTM). Audiologists and MH providers work together to deliver portions of the protocol. In addition, otolaryngologists are important for patients requiring a medical examination. Audiologists, MH providers, and otolaryngologists comprise the hearing health team for tinnitus management. The PTM program involves 5 stepped-care levels of management, and patients receive only the levels they need.
Level 1 is the referral level, which specifies guidelines for any clinician who encounters patients experiencing tinnitus. The “standard” referral is to audiology for a hearing evaluation (PTM level 2)—every patient reporting tinnitus should have a hearing evaluation and brief tinnitus assessment. Less typical would be an urgent referral to a different provider for certain symptoms such as referral to ENT for sudden hearing loss.
Patients who desire intervention for bothersome tinnitus are offered PTM skills education (level 3). At this level, patients are taught facts and skills that they need to self-manage their tinnitus-related problems. Ideally, the audiologist and MH provider collaborate to deliver the level 3 intervention, which utilizes a 5-session (2 with an audiologist and 3 with a MH provider) problem-solving method. Audiologists explain different forms of sound therapy, and MH providers deliver brief CBT. The research studies and clinics that use PTM have shown that the majority of patients who receive the level 3 skills education interventions have their tinnitus needs met to the degree that they do not desire further services.
Those relatively few patients who desire further services are invited for a PTM interdisciplinary evaluation (level 4), which involves a more in-depth needs evaluation by both an audiologist and a MH provider. Based on the outcome of the level 4 evaluation, clear treatment goals are discussed with the patient. If the patient and providers mutually agree that further intervention is needed, then the patient is offered PTM individualized support (level 5), which involves one-on-one services by an audiologist and/or a MH provider. The providers then build on the lessons taught during level 3 and address barriers to enacting the already discussed skills. The MH provider also may expand on CBT skills that were provided in level 3, offering care such as CBT for insomnia during level 5, depending on the specific needs and desires of the patient.
At the NCRAR, a pilot study and 2 RCTs of PTM have been completed.10 The first of these 2 RCTs was a clinical effectiveness study of PTM that was conducted in 2 VA audiology clinics: Memphis, Tennessee, and West Haven, Connecticut.11 Patients who came to the clinics signed up for the study if they felt that the PTM level 3 intervention might be helpful. Half of the 300 veterans in the study were enrolled to receive PTM right away, and half were put on a 6-month wait list. The PTM group showed significantly greater benefit than that of the wait-list group.
The second RCT of PTM was motivated by the high number of service members and veterans with a history of traumatic brain injury (TBI), which is strongly associated with tinnitus.12 The PTM level 3 skills education was administered to participants individually over the telephone by both an audiologist and a psychologist. Participants, located all over the U.S., had bothersome tinnitus, and some had experienced ≥ 1 TBI. They were randomized to receive either Tele-PTM immediately for 6 months or to be put on a 6-month wait list. The Tele-PTM group showed much greater improvement than that of the wait-list group.
Both of these recent RCTs have validated the effectiveness of PTM and demonstrated that PTM should be considered for the practice of evidence-based tinnitus management. PTM is mostly consistent with the AAO-HNSF CPG and provides a structured and defined framework for implementing both assessment and intervention services for patients who report tinnitus. As such, VA Central Office has endorsed PTM as an effective intervention for tinnitus management and has recommended its use at VAMCs. The NCRAR researchers have provided PTM training to hundreds of VA audiologists and MH providers, yet the level of implementation across the VA system of care varies widely.
VA Survey
In 2015, in partnership with the VA Offices of Audiology and Speech Pathology and Mental Health Services, and the Health Services Research & Development/Quality Enhancement Research Initiative (HSR&D/QUERI), the NCRAR conducted a study to examine PTM variation across sites via surveys and/or interviews of VA Audiology and MH programs nationwide.13,14 The objectives of this study were to: (1) describe current tinnitus-management practices in VAMCs; (2) identify barriers and facilitators to PTM program implementation based on clinics that have fully, partially, or not implemented PTM; and (3) determine readiness to implement PTM within VISN 20 (Northwest states and Alaska).
Clinicians at VAMCs nationwide were surveyed regarding current provision of tinnitus clinical services. Requests were sent to audiology programs and MH programs at 142 major VAMCs along with instructions to complete the online survey. Responses were received from 87 audiologists and 66 MH providers. Clinicians at VAMCs with full PTM, partial PTM, and no-PTM (based on survey results) were then interviewed regarding site-specific barriers and facilitators to implementing and providing PTM, readiness to adopt PTM, and strategies for full PTM implementation.
Key findings from the study demonstrated the following: (1) There is considerable between-site variability in how PTM is implemented, particularly with the delivery of the MH portion of the protocol; (2) audiologists show higher levels of readiness to provide tinnitus services than do MH providers (7% of MH survey respondents vs 62% of audiologists reported their site implementing PTM); (3) 66% of MH survey respondents were interested in receiving training in tinnitus management (note that online PTM training for MH does not yet exist); (4) PTM implementation barriers include audio-visual technology issues, room scheduling, as well as lack of collaboration and colocation between MH and audiology departments, administrative time/support, group facilitator skills, and availability of PTM materials.
Overall, results of this HSR&D/QUERI-funded study suggested the need to develop MH-specific training to support the necessary interdisciplinary engagement. Although a patient workbook is available to order and visual presentation aids may be accessed online, it became clear that lack of MH participation in the inherently interdisciplinary PTM skills education was the most common deviation from PTM.
DoD an VA Questionnaire
In 2014 the DoD Hearing Center of Excellence (HCE) conducted the DoD and VA Tinnitus Evaluation, Management, and Treatment Assessment.13 The HCE conducted this questionnaire under the Tinnitus Care Quality Improvement, Process Development, and Implementation Plan, to develop, establish, and implement an interdisciplinary and ongoing process to continually assess and improve the quality and continuum of tinnitus care delivered to service members and veterans at a consistent, enterprise-wide level. The HCE developed the questionnaire to: (1) identify DoD and VA audiologists and otolaryngologists and their institutions providing comprehensive tinnitus care; (2) assess current tinnitus evaluation and management/treatment protocols used; (3) disseminate common practice improvements to all providers for enhancing overall tinnitus evaluation and management/treatment; and (4) evaluate implementation of improvements to include efficiency of implementation and efficacy of improvements.
The questionnaire was administered using SurveyMonkey (San Mateo, CA) and was disseminated by the otolaryngology and audiology consultants to the Army, Navy, and Air Force surgeons general and specialty leaders as well as through VA specialty leaders. Also, the HCE posted the link for the questionnaire on its website for 11 months. A total of 200 providers responded to the questionnaire, of which 13 did not indicate their specialty (eg, otolaryngology) or classification (eg, DoD active duty) and were excluded from data analysis. The 187 qualified respondents included 66 DoD audiologists, 120 VA audiologists, and 1 DoD otolaryngologist.
The questionnaire results indicated that DoD and VA respondents provided tinnitus services for their patients at similar rates (72% of DoD providers and 79% of VA providers). The use of PTM by those same providers, however, was far more widespread in VA (66%) than it was in DoD (37%). Of the providers indicating they did not offer tinnitus clinical services, the main reasons given were lack of necessary training/expertise, lack of time, and insufficient clinical support. The majority of respondents indicated they had training on tinnitus evaluation and/or management and that they were comfortable providing these services; despite this, most providers indicated a need or desire for tinnitus-specific training and education. These results suggested that more support and education for hearing health care providers were needed to implement PTM in VA and, especially, in DoD.
About half of the respondents indicated that psychological/behavioral treatment services, which would correspond to PTM levels 3 and 5, are available for patients at their facility who have tinnitus. It is encouraging to know that some patients with problematic tinnitus are receiving MH services. However, it is essential that patients with any degree of bothersome tinnitus have access to evidence-based clinical services, which would require CBT delivered by a qualified MH provider.
Conclusion
Numerous VA and DoD clinics have begun providing PTM. Individual sites, however, typically adapt the program during the process of implementation.13,14 The most common adaptation that sites make to PTM is to proceed with level 3 skills education without the assistance of MH, and thus CBT, due to the lack of provider availability. It is unknown what impact this has on the effectiveness of PTM. Skills education forms the heart of PTM and addresses the needs of the majority of patients who seek intervention.
Collaboration with MH is integral to the delivery of PTM. Mental health providers partner in PTM levels 3 and 5 by providing CBT, which has the strongest evidence for reducing tinnitus distress among all interventions and always will be critical to the provision of PTM. Clearly VA MH programs need to increase involvement in veterans’ tinnitus management. Increased involvement may be accomplished by (1) developing training or other materials that increase understanding of MH’s role in addressing tinnitus; (2) developing pathways for coordination of care between audiology and MH providers, including different models of coordination based on individual site needs; and (3) documenting the prevalence of tinnitus-MH comorbidities to empirically justify the need for such coordination between audiology and MH providers.
To address gaps identified in the VA survey and in a similar questionnaire conducted by HCE regarding tinnitus care in VA and DoD, the NCRAR, HCE, and Walter Reed National Military Medical Center are collaborating on several initiatives to improve tinnitus services for service members and veterans.13-15 These efforts include enhancing service member and veteran access to VA and DoD MH services in PTM.
Hearing loss and tinnitus (ringing or other noises in the ears or head) have been problematic for military service members and veterans for many years. Military personnel are exposed to high levels of noise in operational and training settings. In spite of hearing conservation efforts, hearing loss and auditory injuries (including tinnitus) continue to occur. Although current military leadership teaches the importance of hearing protection, that was not usually the case until the past few decades. Military leadership provides the means for hearing protection and monitors risk through conservation and hearing readiness programs. Unfortunately, the need for hearing during battle often overrides the expediency of using hearing protective devices.
Military members often equate hearing protection with increased vulnerability, widening the gap between preventive efforts and hearing preservation. It is therefore not surprising that tinnitus and hearing loss have been the 2 most common service-connected disabilities for veterans for a decade.1 These conditions are irreversible; affected service members and veterans need strategies to cope with distress associated with these chronic conditions. Clinical care often is essential to manage the associated distress and mental health (MH) symptoms, such as sleep disturbance, irritability, isolation, tension, and low mood.
There is no cure for tinnitus, meaning there is no proven method to permanently eliminate or even reduce the perception of tinnitus. Intervention for tinnitus therefore is limited to methods intended to mitigate reactions to tinnitus, with the ultimate goal to facilitate good quality of life in spite of the perception of this unwanted auditory anomaly. These methods include numerous means of utilizing therapeutic sound.2 Sound therapy, however, has been shown in controlled trials to be effective only when accompanied by counseling, which often focuses on teaching different coping skills.3 In such instances, MH providers can become an integral part of the hearing health team to assist patients in the management of their tinnitus.
Evidence-Based Practice
Evidence-based research should guide clinical services that are offered for tinnitus. Randomized controlled trials (RCTs) comprise the most important source for such evidence.4 Cochrane Reviews uses meta-analyses to examine rigorous RCTs to determine which methods have credible evidence. One of these reviews conducted in 2007 and updated in 2010 concluded that cognitive behavioral therapy (CBT) can improve depression scores and reduce distress for many people with bothersome tinnitus.5,6 Another Cochrane Review concluded that sound therapy combined with counseling can be beneficial, but on its own, sound therapy has not been shown to result in significant benefit.3 Yet another Cochrane Review focused on using hearing aids with patients who have both hearing loss and bothersome tinnitus; the researchers concluded that “there is currently no evidence to support or refute their use as a more routine intervention for tinnitus.”7 However, many patients and clinicians report hearing aids are helpful for coping with tinnitus.
The American Academy of Otolaryngology–Head and Neck Surgery Foundation (AAO-HNSF) published a clinical practice guideline (CPG) for the management of tinnitus.8 Developing the CPG involved a comprehensive evaluation of the peer-reviewed literature, including the available Cochrane Reviews, to identify appropriate RCTs to inform evidence-based recommendations. Cognitive behavioral therapy was the only intervention for tinnitus recommended in the CPG. Cognitive behavioral therapy targets emotional response by identifying behaviors, thoughts, and beliefs that may be altered.9 For tinnitus, CBT typically includes stress management including relaxation exercises, purposeful distraction, and changing how individuals view and appraise their tinnitus.
Both the CPG and Cochrane Reviews concluded that CBT has the strongest evidence base for reducing effects of tinnitus. It should be noted that the CPG recommended teaching patients basic information about tinnitus management and stated that it was optional (due to limited research evidence) to use sound therapy to augment coping skills training.
Progressive Tinnitus Management
Tinnitus research at the VA National Center for Rehabilitative Auditory Research (NCRAR) has led to the development and refinement of an interdisciplinary program called Progressive Tinnitus Management (PTM). Audiologists and MH providers work together to deliver portions of the protocol. In addition, otolaryngologists are important for patients requiring a medical examination. Audiologists, MH providers, and otolaryngologists comprise the hearing health team for tinnitus management. The PTM program involves 5 stepped-care levels of management, and patients receive only the levels they need.
Level 1 is the referral level, which specifies guidelines for any clinician who encounters patients experiencing tinnitus. The “standard” referral is to audiology for a hearing evaluation (PTM level 2)—every patient reporting tinnitus should have a hearing evaluation and brief tinnitus assessment. Less typical would be an urgent referral to a different provider for certain symptoms such as referral to ENT for sudden hearing loss.
Patients who desire intervention for bothersome tinnitus are offered PTM skills education (level 3). At this level, patients are taught facts and skills that they need to self-manage their tinnitus-related problems. Ideally, the audiologist and MH provider collaborate to deliver the level 3 intervention, which utilizes a 5-session (2 with an audiologist and 3 with a MH provider) problem-solving method. Audiologists explain different forms of sound therapy, and MH providers deliver brief CBT. The research studies and clinics that use PTM have shown that the majority of patients who receive the level 3 skills education interventions have their tinnitus needs met to the degree that they do not desire further services.
Those relatively few patients who desire further services are invited for a PTM interdisciplinary evaluation (level 4), which involves a more in-depth needs evaluation by both an audiologist and a MH provider. Based on the outcome of the level 4 evaluation, clear treatment goals are discussed with the patient. If the patient and providers mutually agree that further intervention is needed, then the patient is offered PTM individualized support (level 5), which involves one-on-one services by an audiologist and/or a MH provider. The providers then build on the lessons taught during level 3 and address barriers to enacting the already discussed skills. The MH provider also may expand on CBT skills that were provided in level 3, offering care such as CBT for insomnia during level 5, depending on the specific needs and desires of the patient.
At the NCRAR, a pilot study and 2 RCTs of PTM have been completed.10 The first of these 2 RCTs was a clinical effectiveness study of PTM that was conducted in 2 VA audiology clinics: Memphis, Tennessee, and West Haven, Connecticut.11 Patients who came to the clinics signed up for the study if they felt that the PTM level 3 intervention might be helpful. Half of the 300 veterans in the study were enrolled to receive PTM right away, and half were put on a 6-month wait list. The PTM group showed significantly greater benefit than that of the wait-list group.
The second RCT of PTM was motivated by the high number of service members and veterans with a history of traumatic brain injury (TBI), which is strongly associated with tinnitus.12 The PTM level 3 skills education was administered to participants individually over the telephone by both an audiologist and a psychologist. Participants, located all over the U.S., had bothersome tinnitus, and some had experienced ≥ 1 TBI. They were randomized to receive either Tele-PTM immediately for 6 months or to be put on a 6-month wait list. The Tele-PTM group showed much greater improvement than that of the wait-list group.
Both of these recent RCTs have validated the effectiveness of PTM and demonstrated that PTM should be considered for the practice of evidence-based tinnitus management. PTM is mostly consistent with the AAO-HNSF CPG and provides a structured and defined framework for implementing both assessment and intervention services for patients who report tinnitus. As such, VA Central Office has endorsed PTM as an effective intervention for tinnitus management and has recommended its use at VAMCs. The NCRAR researchers have provided PTM training to hundreds of VA audiologists and MH providers, yet the level of implementation across the VA system of care varies widely.
VA Survey
In 2015, in partnership with the VA Offices of Audiology and Speech Pathology and Mental Health Services, and the Health Services Research & Development/Quality Enhancement Research Initiative (HSR&D/QUERI), the NCRAR conducted a study to examine PTM variation across sites via surveys and/or interviews of VA Audiology and MH programs nationwide.13,14 The objectives of this study were to: (1) describe current tinnitus-management practices in VAMCs; (2) identify barriers and facilitators to PTM program implementation based on clinics that have fully, partially, or not implemented PTM; and (3) determine readiness to implement PTM within VISN 20 (Northwest states and Alaska).
Clinicians at VAMCs nationwide were surveyed regarding current provision of tinnitus clinical services. Requests were sent to audiology programs and MH programs at 142 major VAMCs along with instructions to complete the online survey. Responses were received from 87 audiologists and 66 MH providers. Clinicians at VAMCs with full PTM, partial PTM, and no-PTM (based on survey results) were then interviewed regarding site-specific barriers and facilitators to implementing and providing PTM, readiness to adopt PTM, and strategies for full PTM implementation.
Key findings from the study demonstrated the following: (1) There is considerable between-site variability in how PTM is implemented, particularly with the delivery of the MH portion of the protocol; (2) audiologists show higher levels of readiness to provide tinnitus services than do MH providers (7% of MH survey respondents vs 62% of audiologists reported their site implementing PTM); (3) 66% of MH survey respondents were interested in receiving training in tinnitus management (note that online PTM training for MH does not yet exist); (4) PTM implementation barriers include audio-visual technology issues, room scheduling, as well as lack of collaboration and colocation between MH and audiology departments, administrative time/support, group facilitator skills, and availability of PTM materials.
Overall, results of this HSR&D/QUERI-funded study suggested the need to develop MH-specific training to support the necessary interdisciplinary engagement. Although a patient workbook is available to order and visual presentation aids may be accessed online, it became clear that lack of MH participation in the inherently interdisciplinary PTM skills education was the most common deviation from PTM.
DoD an VA Questionnaire
In 2014 the DoD Hearing Center of Excellence (HCE) conducted the DoD and VA Tinnitus Evaluation, Management, and Treatment Assessment.13 The HCE conducted this questionnaire under the Tinnitus Care Quality Improvement, Process Development, and Implementation Plan, to develop, establish, and implement an interdisciplinary and ongoing process to continually assess and improve the quality and continuum of tinnitus care delivered to service members and veterans at a consistent, enterprise-wide level. The HCE developed the questionnaire to: (1) identify DoD and VA audiologists and otolaryngologists and their institutions providing comprehensive tinnitus care; (2) assess current tinnitus evaluation and management/treatment protocols used; (3) disseminate common practice improvements to all providers for enhancing overall tinnitus evaluation and management/treatment; and (4) evaluate implementation of improvements to include efficiency of implementation and efficacy of improvements.
The questionnaire was administered using SurveyMonkey (San Mateo, CA) and was disseminated by the otolaryngology and audiology consultants to the Army, Navy, and Air Force surgeons general and specialty leaders as well as through VA specialty leaders. Also, the HCE posted the link for the questionnaire on its website for 11 months. A total of 200 providers responded to the questionnaire, of which 13 did not indicate their specialty (eg, otolaryngology) or classification (eg, DoD active duty) and were excluded from data analysis. The 187 qualified respondents included 66 DoD audiologists, 120 VA audiologists, and 1 DoD otolaryngologist.
The questionnaire results indicated that DoD and VA respondents provided tinnitus services for their patients at similar rates (72% of DoD providers and 79% of VA providers). The use of PTM by those same providers, however, was far more widespread in VA (66%) than it was in DoD (37%). Of the providers indicating they did not offer tinnitus clinical services, the main reasons given were lack of necessary training/expertise, lack of time, and insufficient clinical support. The majority of respondents indicated they had training on tinnitus evaluation and/or management and that they were comfortable providing these services; despite this, most providers indicated a need or desire for tinnitus-specific training and education. These results suggested that more support and education for hearing health care providers were needed to implement PTM in VA and, especially, in DoD.
About half of the respondents indicated that psychological/behavioral treatment services, which would correspond to PTM levels 3 and 5, are available for patients at their facility who have tinnitus. It is encouraging to know that some patients with problematic tinnitus are receiving MH services. However, it is essential that patients with any degree of bothersome tinnitus have access to evidence-based clinical services, which would require CBT delivered by a qualified MH provider.
Conclusion
Numerous VA and DoD clinics have begun providing PTM. Individual sites, however, typically adapt the program during the process of implementation.13,14 The most common adaptation that sites make to PTM is to proceed with level 3 skills education without the assistance of MH, and thus CBT, due to the lack of provider availability. It is unknown what impact this has on the effectiveness of PTM. Skills education forms the heart of PTM and addresses the needs of the majority of patients who seek intervention.
Collaboration with MH is integral to the delivery of PTM. Mental health providers partner in PTM levels 3 and 5 by providing CBT, which has the strongest evidence for reducing tinnitus distress among all interventions and always will be critical to the provision of PTM. Clearly VA MH programs need to increase involvement in veterans’ tinnitus management. Increased involvement may be accomplished by (1) developing training or other materials that increase understanding of MH’s role in addressing tinnitus; (2) developing pathways for coordination of care between audiology and MH providers, including different models of coordination based on individual site needs; and (3) documenting the prevalence of tinnitus-MH comorbidities to empirically justify the need for such coordination between audiology and MH providers.
To address gaps identified in the VA survey and in a similar questionnaire conducted by HCE regarding tinnitus care in VA and DoD, the NCRAR, HCE, and Walter Reed National Military Medical Center are collaborating on several initiatives to improve tinnitus services for service members and veterans.13-15 These efforts include enhancing service member and veteran access to VA and DoD MH services in PTM.
1. U.S. Department of Veterans Affairs. Veterans Benefits Administration reports: annual benefits report. http://www.benefits.va.gov/REPORTS/abr/index.asp. Updated December 19, 2016. Accessed April 13, 2017.
2. Hoare DJ, Searchfield GD, El Refaie A, Henry JA. Sound therapy for tinnitus management: practicable options. J Am Acad Audiol. 2014;25(1):62-75.
3. Hobson J, Chisholm E, El Refaie A. Sound therapy (masking) in the management of tinnitus in adults. Cochrane Database Syst Rev. 2010;(12):CD006371.
4. Keech A, Gebski V, Pike R. Interpreting and Reporting Clinical Trials. A Guide to the CONSORT Statement and the Principles of Randomised Controlled Trials. Sydney: MJA Books, Australasian Medical Publishing Company; 2007.
5. Martinez Devesa P, Waddell A, Perera R, Theodoulou M. Cognitive behavioural therapy for tinnitus (review). Cochrane Database Syst Rev. 2007;(1):CD005233.
6. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2010;(9):CD005233.
7. Hoare DJ, Edmondson-Jones M, Sereda M, Akeroyd MA, Hall D. Amplification with hearing aids for patients with tinnitus and co-existing hearing loss. Cochrane Database Syst Rev. 2014;(1):CD010151.
8. Tunkel DE, Bauer CA, Rosenfeld RM, et al. Clinical practice guideline: tinnitus. Otolaryngol Head Neck Surg. 2014;151(suppl 2):S1-S40.
9. Beck JS, Beck AT. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, New York: Guilford Press; 2011.
10. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehab Res Dev. 2012;49(7):1025-1042.
11. Henry JA, Thielman EJ, Zaugg TL, et al. Randomized controlled trial in clinical settings to evaluate effectiveness of coping skills education used with progressive tinnitus management. J Speech Lang Hear Res. 2017;1-20. [Epub ahead of print]
12. Henry JA, Griest S, Thielman E, McMillan G, Kaelin C, Carlson K. The tinnitus functional index: development, validation, outcomes research, and clinical application. Hear Res. 2016;334:58-64.
13. Boudin A, Carlson KC, Elnitsky C, et al. Online Surveys of Tinnitus Management Practices in VA and DoD: Results and Clinical Implications. Joint Defense Veterans Audiology Conference (JDVAC), St Louis, MO, February 22-24, 2016.
14. Carlson KC, Thielman E, Zaugg TL, Elnitsky C, Tuepker A, Kaelin C, Henry JA. “VA Clinician Surveys and Interviews Reveal Need for Increased Mental Health Involvement in Tinnitus Management.” Joint Defense Veterans Audiology Conference (JDVAC), St Louis, MO, February 22-24, 2016.
15. Carlson K, Thielman E, Zaugg T, et al. Factors affecting the provision of evidence-based progressive tinnitus management in Department of Veterans Affairs medical centers. Paper presented at: Academy Health Annual Research Meeting; June 26-28, 2016;
1. U.S. Department of Veterans Affairs. Veterans Benefits Administration reports: annual benefits report. http://www.benefits.va.gov/REPORTS/abr/index.asp. Updated December 19, 2016. Accessed April 13, 2017.
2. Hoare DJ, Searchfield GD, El Refaie A, Henry JA. Sound therapy for tinnitus management: practicable options. J Am Acad Audiol. 2014;25(1):62-75.
3. Hobson J, Chisholm E, El Refaie A. Sound therapy (masking) in the management of tinnitus in adults. Cochrane Database Syst Rev. 2010;(12):CD006371.
4. Keech A, Gebski V, Pike R. Interpreting and Reporting Clinical Trials. A Guide to the CONSORT Statement and the Principles of Randomised Controlled Trials. Sydney: MJA Books, Australasian Medical Publishing Company; 2007.
5. Martinez Devesa P, Waddell A, Perera R, Theodoulou M. Cognitive behavioural therapy for tinnitus (review). Cochrane Database Syst Rev. 2007;(1):CD005233.
6. Martinez-Devesa P, Perera R, Theodoulou M, Waddell A. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2010;(9):CD005233.
7. Hoare DJ, Edmondson-Jones M, Sereda M, Akeroyd MA, Hall D. Amplification with hearing aids for patients with tinnitus and co-existing hearing loss. Cochrane Database Syst Rev. 2014;(1):CD010151.
8. Tunkel DE, Bauer CA, Rosenfeld RM, et al. Clinical practice guideline: tinnitus. Otolaryngol Head Neck Surg. 2014;151(suppl 2):S1-S40.
9. Beck JS, Beck AT. Cognitive Behavior Therapy: Basics and Beyond. 2nd ed. New York, New York: Guilford Press; 2011.
10. Henry JA, Zaugg TL, Myers PJ, et al. Pilot study to develop telehealth tinnitus management for persons with and without traumatic brain injury. J Rehab Res Dev. 2012;49(7):1025-1042.
11. Henry JA, Thielman EJ, Zaugg TL, et al. Randomized controlled trial in clinical settings to evaluate effectiveness of coping skills education used with progressive tinnitus management. J Speech Lang Hear Res. 2017;1-20. [Epub ahead of print]
12. Henry JA, Griest S, Thielman E, McMillan G, Kaelin C, Carlson K. The tinnitus functional index: development, validation, outcomes research, and clinical application. Hear Res. 2016;334:58-64.
13. Boudin A, Carlson KC, Elnitsky C, et al. Online Surveys of Tinnitus Management Practices in VA and DoD: Results and Clinical Implications. Joint Defense Veterans Audiology Conference (JDVAC), St Louis, MO, February 22-24, 2016.
14. Carlson KC, Thielman E, Zaugg TL, Elnitsky C, Tuepker A, Kaelin C, Henry JA. “VA Clinician Surveys and Interviews Reveal Need for Increased Mental Health Involvement in Tinnitus Management.” Joint Defense Veterans Audiology Conference (JDVAC), St Louis, MO, February 22-24, 2016.
15. Carlson K, Thielman E, Zaugg T, et al. Factors affecting the provision of evidence-based progressive tinnitus management in Department of Veterans Affairs medical centers. Paper presented at: Academy Health Annual Research Meeting; June 26-28, 2016;
A triage guide for tinnitus
• Let patients know that they can learn to manage their reactions to tinnitus with methods that include stress reduction, therapeutic sound, and coping skills. A
• Refer patients with tinnitus to an audiologist for a hearing evaluation, assessment of the tinnitus, and, if indicated, support in learning to manage reactions to tinnitus. A
• Give patients with suicidal ideation or extreme anxiety or depression in response to tinnitus a same-day referral to a mental health professional. A
• Provide an urgent referral to an otolaryngologist or emergency care if you suspect sudden sensorineural hearing loss or another urgent medical condition. A
Strength of recommendation (SOR)
A Good-quality patient-oriented evidence
B Inconsistent or limited-quality patient-oriented evidence
C Consensus, usual practice, opinion, disease-oriented evidence, case series
“Doctor, I have this ringing in my ears.”
With an estimated 10% to 15% of adults experiencing chronic tinnitus,1 most primary care physicians are familiar with this complaint. The prevalence of tinnitus increases with age and with exposure to high levels of noise—the most commonly reported cause.1 With people living longer and such “toxic” noise levels on the rise, tinnitus is a condition you can expect to encounter even more frequently.
Despite the prevalence of tinnitus, however, there are no clinical standards or best practice guidelines for managing it. Thus, many physicians are uncertain about what to tell patients with this distressing disorder, and when (or whether) to refer them to specialists. So patients are sometimes told that “nothing can be done” and that they simply must “learn to live with” tinnitus.
Such negative messages from a trusted physician can have a detrimental effect, causing some patients to stop seeking help and to become increasingly disturbed by tinnitus.2 What’s more, these messages are untrue. Some conditions that result in tinnitus can be treated. And, although tinnitus itself cannot normally be cured, there are numerous interventions and educational strategies that can help patients change their reactions to—and learn to cope with—the ringing in their ears. We developed this evidence-based review and tinnitus triage guide (TABLE 1) to help family physicians respond appropriately to this distressing, but common, condition.
TABLE 1
Tinnitus triage guide27
| If the patient | Refer to | Status/considerations |
|---|---|---|
| Has neural deficits such as facial weakness, head trauma, or other urgent medical condition | Otolaryngology or ED | Emergency |
| Has unexplained sudden hearing loss | Audiology and otolaryngology | Emergency; must see audiologist prior to otolaryngologist on same day |
| Expresses suicidal ideation or manifests obvious mental illness | Mental health or ED | May be emergency; report suicide ideation; provide escort, if necessary |
Has any of the following:
| Otolaryngology and audiology | Urgent; schedule otolaryngology exam as soon as possible |
Has symptoms that suggest a neurophysiologic origin of tinnitus without:
| Audiology and otolaryngology | Nonurgent; schedule audiology exam before patient sees otolaryngologist |
| ED, emergency department. | ||
Is it transient noise, or tinnitus?
Virtually everyone experiences “transient ear noise,” which is usually described as a whistling sound accompanied by a sensation of sudden temporary hearing loss.3,4 These idiopathic episodes are usually unilateral, and often accompanied by a feeling of ear blockage.
To distinguish between tinnitus—the perception of sound that is produced internally, rather than by an external stimulus—and transient ear noise, consider the duration and frequency. Transient ear noise generally disappears within seconds (and does not require diagnostic testing or treatment). Tinnitus, which can have a variety of underlying pathologies, is defined as ear or head noise that lasts at least 5 minutes and occurs at least twice a week.5
Neurophysiologic tinnitus is most common
Neurophysiologic (sensorineural) tinnitus, which originates within the auditory nervous system, accounts for the vast majority of cases. The pathology exists anywhere between the cochlea and the auditory cortex, and excludes any sounds generated by mechanical (somatic) processes.6
The ringing may be relatively soft; in some cases, it can be heard only in quiet environments or while the patient is trying to sleep. In others, the tinnitus may be constant, interfering with concentration and daily activities, as well as sleep. In the most severe cases, tinnitus may be associated with severe depression and anxiety, even to the point of suicidal ideation.7
Notably, however, the loudness or other perceptual characteristics of tinnitus do not necessarily indicate the degree to which it is a problem for the patient.7 Although patients often report that tinnitus interferes with their hearing, they usually also have hearing loss, which an audiologic evaluation will reveal.7-9
Certain medications can trigger or exacerbate tinnitus, including aspirin, nonsteroidal anti-inflammatory drugs, loop diuretics, and quinine.2 Fairly high doses are usually required to cause tinnitus, however, and the effects are typically temporary. Patients have also reported exacerbation of tinnitus due to alcohol, salt, and caffeine intake. Ototoxicity from aminoglycosides and platinum-containing chemotherapeutic drugs is a well-known cause of hearing loss and tinnitus, but these effects are often irreversible.10,11
Neurophysiologic tinnitus is generally not serious from a medical standpoint. While all patients with this condition should undergo an audiologic exam and hearing evaluation, only about 20% of adults who experience tinnitus require intervention.12-14 Although there is no cure, patients with clinically significant tinnitus can be taught stress management and therapeutic use of sound techniques, as well as lifestyle modifications (TABLE 2) to minimize its detrimental effects.
TABLE 2
Managing neurophysiologic tinnitus: A range of options2,5,25-27
| Cognitive-behavioral therapy |
| Elimination of tinnitus-inducing medications (eg, NSAIDs, loop diuretics, and quinine) |
| Hearing aids, sound generators, or other sound devices |
| Lifestyle modifications (eg, improve sleep hygiene, exercise regularly, limit salt intake) |
| Medication (antidepressants or anxiolytics) |
| Patient education that stresses that there are numerous techniques that can be used to manage reactions to tinnitus |
| Stress reduction techniques (eg, imagery, meditation, and deep breathing techniques) |
| Therapeutic sound (eg, using interesting sound to direct attention away from tinnitus, low-level background sound to reduce auditory contrast, and soothing sound for relief) |
| NSAIDs, nonsteroidal anti-inflammatory drugs. |
Somatic tinnitus may be serious
Somatic tinnitus, also known as somato-sound, refers to the perception of sound that originates within the body—in vascular, muscular, skeletal, or respiratory structures, or in the temporomandibular joint.4 These “body sounds” have an internal acoustic source.9
Pulsatile tinnitus, which pulses in synchrony with the heartbeat, is the most common somatosound.15,16 Most patients with pulsatile tinnitus have benign venous “hums,” but serious conditions such as arteriovenous malformations, glomus tumors, and carotid stenosis must be considered. Auscultation over the neck and temporal bone may reveal bruits that can help localize the lesion. We recommend either magnetic resonance imaging (MRI) of the head or computed tomography (CT) angiography, accompanied by timely referral to an otolaryngologist for a focused evaluation.15,17,18
Somatosounds can also be nonpulsatile, indicating a nonvascular source. Examples of nonvascular somatosounds include middle-ear muscle spasms and eustachian tube dysfunction. Nonpulsatile somatic tinnitus is rarely progressive or dangerous. It is reasonable to offer reassurance to patients with nonpulsatile tinnitus, followed by a referral to an otolaryngologist if the symptoms interfere with daily activities.
Unilateral tinnitus is a red flag
In most cases, tinnitus is bilateral. Unilateral tinnitus may indicate a more serious medical condition. It is a common presenting sign of both vestibular schwannoma (also known as acoustic neuroma) and Meniere’s disease.
Patients with unilateral tinnitus should receive a hearing test as soon as possible; if asymmetric hearing loss is found, MRI is indicated, both with and without contrast of the internal auditory canal, to rule out vestibular schwannoma.
Idiopathic sudden sensorineural hearing loss (ISSNHL), which may be associated with new onset unilateral tinnitus, should be considered an otologic emergency. When you suspect ISSNHL, you’ll need to make a same-day referral for an otologic examination.
If left untreated, the ISSNHL and associated tinnitus will resolve partially or completely at least 50% of the time. This recovery rate may be improved with glucocorticoid treatments.19 Prompt initiation of corticosteroid therapy can be a factor in the chances of recovery—the more rapidly such patients are seen and treated, the better their prognosis.20
Tinnitus triage: Key points
Following our triage guide (TABLE 1) should result in appropriate care in most cases. Here are some considerations to keep in mind:
Urgent medical referral. Any patient with tinnitus and symptoms suggestive of serious underlying treatable pathology requires an urgent otolaryngology referral. That includes ISSNHL, which you should suspect whenever a patient reports an unexplained decrease in hearing, as well as pulsatile tinnitus, vestibular symptoms, and long-standing ear pain, drainage, or malodor that does not resolve with routine treatment. If possible, such patients should undergo an audiologic assessment prior to the otolaryngology visit; however, the otolaryngology exam is the primary concern.
Facial paralysis, severe vertigo, or sudden onset pulsatile tinnitus can indicate a serious intracranial condition. These symptoms may point to cerebrovascular disease or neoplasm, and should be treated as an otologic emergency.
Mental health referral. Some tinnitus patients require a mental health assessment, either because of obvious manifestations of a mental illness or because of expressed suicidal ideation. If there’s a question about the patient’s mental health, consider consulting with a mental health provider or using basic screening tools for anxiety and depression to help determine the need for referral, as well as the urgency.12
Some patients experience extreme anxiety or depression in response to tinnitus and should be referred to a mental health professional on the day they present with symptoms. Suicidal ideation warrants special attention, of course—possibly including the need to escort the patient to the emergency department or to a behavioral specialist.21-23
Nonurgent medical referral. Ideally, all patients who present with tinnitus should see an audiologist and an otolaryngologist, but those who have no serious symptoms should be referred on a nonurgent basis. Such patients need to have a comprehensive hearing evaluation—ideally, before they see the otolaryngologist so the test results are available at the time of the exam. The audiologist should also assess the severity of the tinnitus, using a validated questionnaire such as the Tinnitus Handicap Inventory, for the initial assessment and to monitor changes in the severity of the tinnitus as an outcome measure of therapy.24
Enlist an interdisciplinary team
For patients with somatic tinnitus, the treatment—and the specialist who provides it—depends on the underlying cause. A patient who has unilateral tinnitus may be referred by an audiologist or otolaryngologist to a neurologist, for example, if he or she is found to have Meniere’s disease; a patient with pulsatile tinnitus may be sent back to his or her primary care physician after diagnostic testing has ruled out serious causes.
For patients with neurophysiologic tinnitus (and any patient with untreatable somatic tinnitus), a well-organized interdisciplinary team that includes the family physician, an audiologist, and a psychologist is the best approach. The variety of available management options (TABLE 2) incorporate medical approaches, complementary and alternative treatments, psychological interventions, and sound-based methods. Lifestyle modifications, such as improved sleep hygiene, regular exercise, and dietary modifications, may help, as well.25-27 First-line strategies include:
Adjusting medications. Eliminating tinnitus-inducing medications, if medically safe, is a common starting point. No prescription drug has been developed specifically for tinnitus. But some antidepressants or anxiolytics (eg, amitriptyline or lorazepam) are commonly used to address coexisting sleep and mental health disorders—primarily depression and anxiety—that may be associated with, or exacerbated by, tinnitus.28-30
Addressing hearing problems. Patients should undergo a hearing evaluation and receive help in managing a hearing problem, if necessary. Hearing aids improve hearing and reduce the perception of tinnitus.31
Using therapeutic sound. Some audiologists are trained to implement various forms of sound-based therapy. Tinnitus retraining therapy involves the use of background sound to facilitate habituation to tinnitus; tinnitus masking involves the use of soothing sound to provide a sense of relief. Progressive tinnitus management is a more recent method that educates patients in the use of all types of therapeutic sound.32 These sound-based methods often include the use of hearing aids, sound generators, and other devices.
Circling in a mental health professional. It is essential to involve psychologists or other mental health specialists in the care of patients with clinically significant tinnitus to ensure that psychological and other barriers to successful management of the condition are identified and addressed. Cognitive-behavioral therapy (CBT) has been shown to be helpful for patients with tinnitus.33 In fact, we have been successful in teaching patients to manage their reactions to tinnitus—resulting in a better quality of life—using a combination of educational counseling, therapeutic sound, and CBT. JFP
Acknowledgments
Funding for this work was provided by Veterans Health Administration, and Veterans Affairs Rehabilitation Research and Development (RR&D) Service (C4488R). Thanks to Robert Folmer, PhD, William Martin, PhD, Dennis Trune, PhD, and Baker Shi, MD, PhD, for advice that contributed to this manuscript. Special thanks to Martin Schechter, PhD, for his significant contributions to our research. The authors also wish to thank Stephen Fausti, PhD, and Sara Ruth Oliver, AuD, for their consistent support of our research.
CORRESPONDENCE James A. Henry, PhD, VA Medical Center (NCRAR), Post Office Box 1034, Portland, OR 97207; [email protected]
1. Hoffman HJ, Reed GW. Epidemiology of tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:16-41.
2. Jastreboff PJ, Hazell JWP. Tinnitus Retraining Therapy: Implementing the Neurophysiological Model. New York: Cambridge University Press; 2004.
3. Kiang NYS, Moxon EC, Levine RA. Auditory-nerve activity in cats with normal and abnormal cochleas. In: Wolstenholme GEW, Knight J, eds. Sensorineural Hearing Loss. London: J. & A. Churchill; 1970:241-273.
4. Henry JA, Dennis K, Schechter MA. General review of tinnitus: prevalence, mechanisms, effects, and management. J Speech Lang Hear Res. 2005;48:1204-1235.
5. Dauman R, Tyler RS. Some considerations on the classification of tinnitus. In: Aran J-M, Dauman R, eds. Proceedings of the Fourth International Tinnitus Seminar. Amsterdam/New York: Kugler Publications; 1992:225-229.
6. Hazell J. Incidence, classification, and models of tinnitus. In: Ludman H, Wright T, eds. Diseases of the Ear. London: Arnold; 1998:185-195.
7. Dobie RA. Overview: suffering from tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:1-7.
8. Zaugg TL, et al. Difficulties caused by patients’ misconceptions that hearing problems are due to tinnitus. In: Patuzzi R, ed. Proceedings of the Seventh International Tinnitus Seminar. Perth: University of Western Australia; 2002:226-228.
9. Coles RRA. Classification of causes, mechanisms of patient disturbance, and associated counseling. In: Vernon JA, Moller AR, eds. Mechanisms of Tinnitus. Needham Heights, Mass: Allyn & Bacon; 1995:11-19.
10. Fausti SA, et al. Ototoxicity. In: Northern JL, ed. Hearing Disorders. Needham Heights, Mass: Allyn & Bacon; 1995:149-164.
11. Rachel JD, Kaltenbach JA, Janisse J. Increases in spontaneous neural activity in the hamster dorsal cochlear nucleus following cisplatin treatment: a possible basis for cisplatin-induced tinnitus. Hear Res. 2002;164:206-214.
12. Henry JA, Zaugg TL, Myers PJ, et al. The role of audiologic evaluation in progressive audiologic tinnitus management. Trends Amplif. 2008;12:170-187.
13. Jastreboff PJ, Hazell JWP. Treatment of tinnitus based on a neurophysiological model. In: Vernon JA, ed. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998:201-217.
14. Davis A, Refaie AE. Epidemiology of tinnitus. In: Tyler R, ed. Tinnitus Handbook. San Diego: Singular Publishing Group; 2000:1-23.
15. Lockwood AH, Burkard RF, Salvi RJ. Imaging tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:253-264.
16. Sismanis A. Pulsatile tinnitus. Otolaryngol Clin North Am. 2003;36:389-402.
17. Sismanis A. Pulsatile tinnitus. In: Vernon JA, ed. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998:28-33.
18. Wackym PA, Friedland DR. Otologic evaluation. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:205-219.
19. Hamid M, Trune D. Issues, indications, and controversies regarding intratympanic steroid perfusion. Curr Opin Otolaryngol Head Neck Surg. 2008;16:434-440.
20. Jeyakumar A, et al. Treatment of idiopathic sudden sensorineural hearing loss. Acta Otolaryngol. 2006;126:708-713.
21. Brown GK, et al. Suicide intent and accurate expectations of lethality: predictors of medical lethality of suicide attempts. J Consult Clin Psychol. 2004;72:1170-1174.
22. Hawton K. Studying survivors of nearly lethal suicide attempts: an important strategy in suicide research. Suicide Life Threat Behav. 2001;32(1 suppl):76-84.
23. Kessler RC, Borges G, Walters EE. Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56:617-626.
24. Newman CW, Sandridge SA, Jacobson GP. Psychometric adequacy of the Tinnitus Handicap Inventory (THI) for evaluating treatment outcome. J Am Acad Audiol. 1998;9:153-160.
25. Tyler RS, ed. Tinnitus Treatment: Clinical Protocols. New York: Thieme Medical Publishers, Inc; 2005.
26. Vernon JA. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998.
27. Henry JA, Zaugg TL, Myers PM, et al. Progressive Tinnitus Management: Clinical Handbook for Audiologists. San Diego, Calif: Plural Publishing; 2010.
28. Robinson SK, Viirre ES, Stein MB. Antidepressant therapy for tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:278-293.
29. Dobie RA. Clinical trials and drug therapy for tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:266-277.
30. Henry JA, Zaugg TL, Schechter MA. Clinical guide for audiologic tinnitus management I: assessment. Am J Audiol. 2005;14:21-48.
31. Surr RK, Montgomery AA, Mueller HG. Effect of amplification on tinnitus among new hearing aid users. Ear Hear. 1985;6:71-75.
32. Henry JA, et al. Using therapeutic sound with progressive audiologic tinnitus management. Trends Amplif. 2008;12:185-206.
33. Martinez Devesa P, Waddell A, Perera R, et al. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2007;(1):CD005233.-
• Let patients know that they can learn to manage their reactions to tinnitus with methods that include stress reduction, therapeutic sound, and coping skills. A
• Refer patients with tinnitus to an audiologist for a hearing evaluation, assessment of the tinnitus, and, if indicated, support in learning to manage reactions to tinnitus. A
• Give patients with suicidal ideation or extreme anxiety or depression in response to tinnitus a same-day referral to a mental health professional. A
• Provide an urgent referral to an otolaryngologist or emergency care if you suspect sudden sensorineural hearing loss or another urgent medical condition. A
Strength of recommendation (SOR)
A Good-quality patient-oriented evidence
B Inconsistent or limited-quality patient-oriented evidence
C Consensus, usual practice, opinion, disease-oriented evidence, case series
“Doctor, I have this ringing in my ears.”
With an estimated 10% to 15% of adults experiencing chronic tinnitus,1 most primary care physicians are familiar with this complaint. The prevalence of tinnitus increases with age and with exposure to high levels of noise—the most commonly reported cause.1 With people living longer and such “toxic” noise levels on the rise, tinnitus is a condition you can expect to encounter even more frequently.
Despite the prevalence of tinnitus, however, there are no clinical standards or best practice guidelines for managing it. Thus, many physicians are uncertain about what to tell patients with this distressing disorder, and when (or whether) to refer them to specialists. So patients are sometimes told that “nothing can be done” and that they simply must “learn to live with” tinnitus.
Such negative messages from a trusted physician can have a detrimental effect, causing some patients to stop seeking help and to become increasingly disturbed by tinnitus.2 What’s more, these messages are untrue. Some conditions that result in tinnitus can be treated. And, although tinnitus itself cannot normally be cured, there are numerous interventions and educational strategies that can help patients change their reactions to—and learn to cope with—the ringing in their ears. We developed this evidence-based review and tinnitus triage guide (TABLE 1) to help family physicians respond appropriately to this distressing, but common, condition.
TABLE 1
Tinnitus triage guide27
| If the patient | Refer to | Status/considerations |
|---|---|---|
| Has neural deficits such as facial weakness, head trauma, or other urgent medical condition | Otolaryngology or ED | Emergency |
| Has unexplained sudden hearing loss | Audiology and otolaryngology | Emergency; must see audiologist prior to otolaryngologist on same day |
| Expresses suicidal ideation or manifests obvious mental illness | Mental health or ED | May be emergency; report suicide ideation; provide escort, if necessary |
Has any of the following:
| Otolaryngology and audiology | Urgent; schedule otolaryngology exam as soon as possible |
Has symptoms that suggest a neurophysiologic origin of tinnitus without:
| Audiology and otolaryngology | Nonurgent; schedule audiology exam before patient sees otolaryngologist |
| ED, emergency department. | ||
Is it transient noise, or tinnitus?
Virtually everyone experiences “transient ear noise,” which is usually described as a whistling sound accompanied by a sensation of sudden temporary hearing loss.3,4 These idiopathic episodes are usually unilateral, and often accompanied by a feeling of ear blockage.
To distinguish between tinnitus—the perception of sound that is produced internally, rather than by an external stimulus—and transient ear noise, consider the duration and frequency. Transient ear noise generally disappears within seconds (and does not require diagnostic testing or treatment). Tinnitus, which can have a variety of underlying pathologies, is defined as ear or head noise that lasts at least 5 minutes and occurs at least twice a week.5
Neurophysiologic tinnitus is most common
Neurophysiologic (sensorineural) tinnitus, which originates within the auditory nervous system, accounts for the vast majority of cases. The pathology exists anywhere between the cochlea and the auditory cortex, and excludes any sounds generated by mechanical (somatic) processes.6
The ringing may be relatively soft; in some cases, it can be heard only in quiet environments or while the patient is trying to sleep. In others, the tinnitus may be constant, interfering with concentration and daily activities, as well as sleep. In the most severe cases, tinnitus may be associated with severe depression and anxiety, even to the point of suicidal ideation.7
Notably, however, the loudness or other perceptual characteristics of tinnitus do not necessarily indicate the degree to which it is a problem for the patient.7 Although patients often report that tinnitus interferes with their hearing, they usually also have hearing loss, which an audiologic evaluation will reveal.7-9
Certain medications can trigger or exacerbate tinnitus, including aspirin, nonsteroidal anti-inflammatory drugs, loop diuretics, and quinine.2 Fairly high doses are usually required to cause tinnitus, however, and the effects are typically temporary. Patients have also reported exacerbation of tinnitus due to alcohol, salt, and caffeine intake. Ototoxicity from aminoglycosides and platinum-containing chemotherapeutic drugs is a well-known cause of hearing loss and tinnitus, but these effects are often irreversible.10,11
Neurophysiologic tinnitus is generally not serious from a medical standpoint. While all patients with this condition should undergo an audiologic exam and hearing evaluation, only about 20% of adults who experience tinnitus require intervention.12-14 Although there is no cure, patients with clinically significant tinnitus can be taught stress management and therapeutic use of sound techniques, as well as lifestyle modifications (TABLE 2) to minimize its detrimental effects.
TABLE 2
Managing neurophysiologic tinnitus: A range of options2,5,25-27
| Cognitive-behavioral therapy |
| Elimination of tinnitus-inducing medications (eg, NSAIDs, loop diuretics, and quinine) |
| Hearing aids, sound generators, or other sound devices |
| Lifestyle modifications (eg, improve sleep hygiene, exercise regularly, limit salt intake) |
| Medication (antidepressants or anxiolytics) |
| Patient education that stresses that there are numerous techniques that can be used to manage reactions to tinnitus |
| Stress reduction techniques (eg, imagery, meditation, and deep breathing techniques) |
| Therapeutic sound (eg, using interesting sound to direct attention away from tinnitus, low-level background sound to reduce auditory contrast, and soothing sound for relief) |
| NSAIDs, nonsteroidal anti-inflammatory drugs. |
Somatic tinnitus may be serious
Somatic tinnitus, also known as somato-sound, refers to the perception of sound that originates within the body—in vascular, muscular, skeletal, or respiratory structures, or in the temporomandibular joint.4 These “body sounds” have an internal acoustic source.9
Pulsatile tinnitus, which pulses in synchrony with the heartbeat, is the most common somatosound.15,16 Most patients with pulsatile tinnitus have benign venous “hums,” but serious conditions such as arteriovenous malformations, glomus tumors, and carotid stenosis must be considered. Auscultation over the neck and temporal bone may reveal bruits that can help localize the lesion. We recommend either magnetic resonance imaging (MRI) of the head or computed tomography (CT) angiography, accompanied by timely referral to an otolaryngologist for a focused evaluation.15,17,18
Somatosounds can also be nonpulsatile, indicating a nonvascular source. Examples of nonvascular somatosounds include middle-ear muscle spasms and eustachian tube dysfunction. Nonpulsatile somatic tinnitus is rarely progressive or dangerous. It is reasonable to offer reassurance to patients with nonpulsatile tinnitus, followed by a referral to an otolaryngologist if the symptoms interfere with daily activities.
Unilateral tinnitus is a red flag
In most cases, tinnitus is bilateral. Unilateral tinnitus may indicate a more serious medical condition. It is a common presenting sign of both vestibular schwannoma (also known as acoustic neuroma) and Meniere’s disease.
Patients with unilateral tinnitus should receive a hearing test as soon as possible; if asymmetric hearing loss is found, MRI is indicated, both with and without contrast of the internal auditory canal, to rule out vestibular schwannoma.
Idiopathic sudden sensorineural hearing loss (ISSNHL), which may be associated with new onset unilateral tinnitus, should be considered an otologic emergency. When you suspect ISSNHL, you’ll need to make a same-day referral for an otologic examination.
If left untreated, the ISSNHL and associated tinnitus will resolve partially or completely at least 50% of the time. This recovery rate may be improved with glucocorticoid treatments.19 Prompt initiation of corticosteroid therapy can be a factor in the chances of recovery—the more rapidly such patients are seen and treated, the better their prognosis.20
Tinnitus triage: Key points
Following our triage guide (TABLE 1) should result in appropriate care in most cases. Here are some considerations to keep in mind:
Urgent medical referral. Any patient with tinnitus and symptoms suggestive of serious underlying treatable pathology requires an urgent otolaryngology referral. That includes ISSNHL, which you should suspect whenever a patient reports an unexplained decrease in hearing, as well as pulsatile tinnitus, vestibular symptoms, and long-standing ear pain, drainage, or malodor that does not resolve with routine treatment. If possible, such patients should undergo an audiologic assessment prior to the otolaryngology visit; however, the otolaryngology exam is the primary concern.
Facial paralysis, severe vertigo, or sudden onset pulsatile tinnitus can indicate a serious intracranial condition. These symptoms may point to cerebrovascular disease or neoplasm, and should be treated as an otologic emergency.
Mental health referral. Some tinnitus patients require a mental health assessment, either because of obvious manifestations of a mental illness or because of expressed suicidal ideation. If there’s a question about the patient’s mental health, consider consulting with a mental health provider or using basic screening tools for anxiety and depression to help determine the need for referral, as well as the urgency.12
Some patients experience extreme anxiety or depression in response to tinnitus and should be referred to a mental health professional on the day they present with symptoms. Suicidal ideation warrants special attention, of course—possibly including the need to escort the patient to the emergency department or to a behavioral specialist.21-23
Nonurgent medical referral. Ideally, all patients who present with tinnitus should see an audiologist and an otolaryngologist, but those who have no serious symptoms should be referred on a nonurgent basis. Such patients need to have a comprehensive hearing evaluation—ideally, before they see the otolaryngologist so the test results are available at the time of the exam. The audiologist should also assess the severity of the tinnitus, using a validated questionnaire such as the Tinnitus Handicap Inventory, for the initial assessment and to monitor changes in the severity of the tinnitus as an outcome measure of therapy.24
Enlist an interdisciplinary team
For patients with somatic tinnitus, the treatment—and the specialist who provides it—depends on the underlying cause. A patient who has unilateral tinnitus may be referred by an audiologist or otolaryngologist to a neurologist, for example, if he or she is found to have Meniere’s disease; a patient with pulsatile tinnitus may be sent back to his or her primary care physician after diagnostic testing has ruled out serious causes.
For patients with neurophysiologic tinnitus (and any patient with untreatable somatic tinnitus), a well-organized interdisciplinary team that includes the family physician, an audiologist, and a psychologist is the best approach. The variety of available management options (TABLE 2) incorporate medical approaches, complementary and alternative treatments, psychological interventions, and sound-based methods. Lifestyle modifications, such as improved sleep hygiene, regular exercise, and dietary modifications, may help, as well.25-27 First-line strategies include:
Adjusting medications. Eliminating tinnitus-inducing medications, if medically safe, is a common starting point. No prescription drug has been developed specifically for tinnitus. But some antidepressants or anxiolytics (eg, amitriptyline or lorazepam) are commonly used to address coexisting sleep and mental health disorders—primarily depression and anxiety—that may be associated with, or exacerbated by, tinnitus.28-30
Addressing hearing problems. Patients should undergo a hearing evaluation and receive help in managing a hearing problem, if necessary. Hearing aids improve hearing and reduce the perception of tinnitus.31
Using therapeutic sound. Some audiologists are trained to implement various forms of sound-based therapy. Tinnitus retraining therapy involves the use of background sound to facilitate habituation to tinnitus; tinnitus masking involves the use of soothing sound to provide a sense of relief. Progressive tinnitus management is a more recent method that educates patients in the use of all types of therapeutic sound.32 These sound-based methods often include the use of hearing aids, sound generators, and other devices.
Circling in a mental health professional. It is essential to involve psychologists or other mental health specialists in the care of patients with clinically significant tinnitus to ensure that psychological and other barriers to successful management of the condition are identified and addressed. Cognitive-behavioral therapy (CBT) has been shown to be helpful for patients with tinnitus.33 In fact, we have been successful in teaching patients to manage their reactions to tinnitus—resulting in a better quality of life—using a combination of educational counseling, therapeutic sound, and CBT. JFP
Acknowledgments
Funding for this work was provided by Veterans Health Administration, and Veterans Affairs Rehabilitation Research and Development (RR&D) Service (C4488R). Thanks to Robert Folmer, PhD, William Martin, PhD, Dennis Trune, PhD, and Baker Shi, MD, PhD, for advice that contributed to this manuscript. Special thanks to Martin Schechter, PhD, for his significant contributions to our research. The authors also wish to thank Stephen Fausti, PhD, and Sara Ruth Oliver, AuD, for their consistent support of our research.
CORRESPONDENCE James A. Henry, PhD, VA Medical Center (NCRAR), Post Office Box 1034, Portland, OR 97207; [email protected]
• Let patients know that they can learn to manage their reactions to tinnitus with methods that include stress reduction, therapeutic sound, and coping skills. A
• Refer patients with tinnitus to an audiologist for a hearing evaluation, assessment of the tinnitus, and, if indicated, support in learning to manage reactions to tinnitus. A
• Give patients with suicidal ideation or extreme anxiety or depression in response to tinnitus a same-day referral to a mental health professional. A
• Provide an urgent referral to an otolaryngologist or emergency care if you suspect sudden sensorineural hearing loss or another urgent medical condition. A
Strength of recommendation (SOR)
A Good-quality patient-oriented evidence
B Inconsistent or limited-quality patient-oriented evidence
C Consensus, usual practice, opinion, disease-oriented evidence, case series
“Doctor, I have this ringing in my ears.”
With an estimated 10% to 15% of adults experiencing chronic tinnitus,1 most primary care physicians are familiar with this complaint. The prevalence of tinnitus increases with age and with exposure to high levels of noise—the most commonly reported cause.1 With people living longer and such “toxic” noise levels on the rise, tinnitus is a condition you can expect to encounter even more frequently.
Despite the prevalence of tinnitus, however, there are no clinical standards or best practice guidelines for managing it. Thus, many physicians are uncertain about what to tell patients with this distressing disorder, and when (or whether) to refer them to specialists. So patients are sometimes told that “nothing can be done” and that they simply must “learn to live with” tinnitus.
Such negative messages from a trusted physician can have a detrimental effect, causing some patients to stop seeking help and to become increasingly disturbed by tinnitus.2 What’s more, these messages are untrue. Some conditions that result in tinnitus can be treated. And, although tinnitus itself cannot normally be cured, there are numerous interventions and educational strategies that can help patients change their reactions to—and learn to cope with—the ringing in their ears. We developed this evidence-based review and tinnitus triage guide (TABLE 1) to help family physicians respond appropriately to this distressing, but common, condition.
TABLE 1
Tinnitus triage guide27
| If the patient | Refer to | Status/considerations |
|---|---|---|
| Has neural deficits such as facial weakness, head trauma, or other urgent medical condition | Otolaryngology or ED | Emergency |
| Has unexplained sudden hearing loss | Audiology and otolaryngology | Emergency; must see audiologist prior to otolaryngologist on same day |
| Expresses suicidal ideation or manifests obvious mental illness | Mental health or ED | May be emergency; report suicide ideation; provide escort, if necessary |
Has any of the following:
| Otolaryngology and audiology | Urgent; schedule otolaryngology exam as soon as possible |
Has symptoms that suggest a neurophysiologic origin of tinnitus without:
| Audiology and otolaryngology | Nonurgent; schedule audiology exam before patient sees otolaryngologist |
| ED, emergency department. | ||
Is it transient noise, or tinnitus?
Virtually everyone experiences “transient ear noise,” which is usually described as a whistling sound accompanied by a sensation of sudden temporary hearing loss.3,4 These idiopathic episodes are usually unilateral, and often accompanied by a feeling of ear blockage.
To distinguish between tinnitus—the perception of sound that is produced internally, rather than by an external stimulus—and transient ear noise, consider the duration and frequency. Transient ear noise generally disappears within seconds (and does not require diagnostic testing or treatment). Tinnitus, which can have a variety of underlying pathologies, is defined as ear or head noise that lasts at least 5 minutes and occurs at least twice a week.5
Neurophysiologic tinnitus is most common
Neurophysiologic (sensorineural) tinnitus, which originates within the auditory nervous system, accounts for the vast majority of cases. The pathology exists anywhere between the cochlea and the auditory cortex, and excludes any sounds generated by mechanical (somatic) processes.6
The ringing may be relatively soft; in some cases, it can be heard only in quiet environments or while the patient is trying to sleep. In others, the tinnitus may be constant, interfering with concentration and daily activities, as well as sleep. In the most severe cases, tinnitus may be associated with severe depression and anxiety, even to the point of suicidal ideation.7
Notably, however, the loudness or other perceptual characteristics of tinnitus do not necessarily indicate the degree to which it is a problem for the patient.7 Although patients often report that tinnitus interferes with their hearing, they usually also have hearing loss, which an audiologic evaluation will reveal.7-9
Certain medications can trigger or exacerbate tinnitus, including aspirin, nonsteroidal anti-inflammatory drugs, loop diuretics, and quinine.2 Fairly high doses are usually required to cause tinnitus, however, and the effects are typically temporary. Patients have also reported exacerbation of tinnitus due to alcohol, salt, and caffeine intake. Ototoxicity from aminoglycosides and platinum-containing chemotherapeutic drugs is a well-known cause of hearing loss and tinnitus, but these effects are often irreversible.10,11
Neurophysiologic tinnitus is generally not serious from a medical standpoint. While all patients with this condition should undergo an audiologic exam and hearing evaluation, only about 20% of adults who experience tinnitus require intervention.12-14 Although there is no cure, patients with clinically significant tinnitus can be taught stress management and therapeutic use of sound techniques, as well as lifestyle modifications (TABLE 2) to minimize its detrimental effects.
TABLE 2
Managing neurophysiologic tinnitus: A range of options2,5,25-27
| Cognitive-behavioral therapy |
| Elimination of tinnitus-inducing medications (eg, NSAIDs, loop diuretics, and quinine) |
| Hearing aids, sound generators, or other sound devices |
| Lifestyle modifications (eg, improve sleep hygiene, exercise regularly, limit salt intake) |
| Medication (antidepressants or anxiolytics) |
| Patient education that stresses that there are numerous techniques that can be used to manage reactions to tinnitus |
| Stress reduction techniques (eg, imagery, meditation, and deep breathing techniques) |
| Therapeutic sound (eg, using interesting sound to direct attention away from tinnitus, low-level background sound to reduce auditory contrast, and soothing sound for relief) |
| NSAIDs, nonsteroidal anti-inflammatory drugs. |
Somatic tinnitus may be serious
Somatic tinnitus, also known as somato-sound, refers to the perception of sound that originates within the body—in vascular, muscular, skeletal, or respiratory structures, or in the temporomandibular joint.4 These “body sounds” have an internal acoustic source.9
Pulsatile tinnitus, which pulses in synchrony with the heartbeat, is the most common somatosound.15,16 Most patients with pulsatile tinnitus have benign venous “hums,” but serious conditions such as arteriovenous malformations, glomus tumors, and carotid stenosis must be considered. Auscultation over the neck and temporal bone may reveal bruits that can help localize the lesion. We recommend either magnetic resonance imaging (MRI) of the head or computed tomography (CT) angiography, accompanied by timely referral to an otolaryngologist for a focused evaluation.15,17,18
Somatosounds can also be nonpulsatile, indicating a nonvascular source. Examples of nonvascular somatosounds include middle-ear muscle spasms and eustachian tube dysfunction. Nonpulsatile somatic tinnitus is rarely progressive or dangerous. It is reasonable to offer reassurance to patients with nonpulsatile tinnitus, followed by a referral to an otolaryngologist if the symptoms interfere with daily activities.
Unilateral tinnitus is a red flag
In most cases, tinnitus is bilateral. Unilateral tinnitus may indicate a more serious medical condition. It is a common presenting sign of both vestibular schwannoma (also known as acoustic neuroma) and Meniere’s disease.
Patients with unilateral tinnitus should receive a hearing test as soon as possible; if asymmetric hearing loss is found, MRI is indicated, both with and without contrast of the internal auditory canal, to rule out vestibular schwannoma.
Idiopathic sudden sensorineural hearing loss (ISSNHL), which may be associated with new onset unilateral tinnitus, should be considered an otologic emergency. When you suspect ISSNHL, you’ll need to make a same-day referral for an otologic examination.
If left untreated, the ISSNHL and associated tinnitus will resolve partially or completely at least 50% of the time. This recovery rate may be improved with glucocorticoid treatments.19 Prompt initiation of corticosteroid therapy can be a factor in the chances of recovery—the more rapidly such patients are seen and treated, the better their prognosis.20
Tinnitus triage: Key points
Following our triage guide (TABLE 1) should result in appropriate care in most cases. Here are some considerations to keep in mind:
Urgent medical referral. Any patient with tinnitus and symptoms suggestive of serious underlying treatable pathology requires an urgent otolaryngology referral. That includes ISSNHL, which you should suspect whenever a patient reports an unexplained decrease in hearing, as well as pulsatile tinnitus, vestibular symptoms, and long-standing ear pain, drainage, or malodor that does not resolve with routine treatment. If possible, such patients should undergo an audiologic assessment prior to the otolaryngology visit; however, the otolaryngology exam is the primary concern.
Facial paralysis, severe vertigo, or sudden onset pulsatile tinnitus can indicate a serious intracranial condition. These symptoms may point to cerebrovascular disease or neoplasm, and should be treated as an otologic emergency.
Mental health referral. Some tinnitus patients require a mental health assessment, either because of obvious manifestations of a mental illness or because of expressed suicidal ideation. If there’s a question about the patient’s mental health, consider consulting with a mental health provider or using basic screening tools for anxiety and depression to help determine the need for referral, as well as the urgency.12
Some patients experience extreme anxiety or depression in response to tinnitus and should be referred to a mental health professional on the day they present with symptoms. Suicidal ideation warrants special attention, of course—possibly including the need to escort the patient to the emergency department or to a behavioral specialist.21-23
Nonurgent medical referral. Ideally, all patients who present with tinnitus should see an audiologist and an otolaryngologist, but those who have no serious symptoms should be referred on a nonurgent basis. Such patients need to have a comprehensive hearing evaluation—ideally, before they see the otolaryngologist so the test results are available at the time of the exam. The audiologist should also assess the severity of the tinnitus, using a validated questionnaire such as the Tinnitus Handicap Inventory, for the initial assessment and to monitor changes in the severity of the tinnitus as an outcome measure of therapy.24
Enlist an interdisciplinary team
For patients with somatic tinnitus, the treatment—and the specialist who provides it—depends on the underlying cause. A patient who has unilateral tinnitus may be referred by an audiologist or otolaryngologist to a neurologist, for example, if he or she is found to have Meniere’s disease; a patient with pulsatile tinnitus may be sent back to his or her primary care physician after diagnostic testing has ruled out serious causes.
For patients with neurophysiologic tinnitus (and any patient with untreatable somatic tinnitus), a well-organized interdisciplinary team that includes the family physician, an audiologist, and a psychologist is the best approach. The variety of available management options (TABLE 2) incorporate medical approaches, complementary and alternative treatments, psychological interventions, and sound-based methods. Lifestyle modifications, such as improved sleep hygiene, regular exercise, and dietary modifications, may help, as well.25-27 First-line strategies include:
Adjusting medications. Eliminating tinnitus-inducing medications, if medically safe, is a common starting point. No prescription drug has been developed specifically for tinnitus. But some antidepressants or anxiolytics (eg, amitriptyline or lorazepam) are commonly used to address coexisting sleep and mental health disorders—primarily depression and anxiety—that may be associated with, or exacerbated by, tinnitus.28-30
Addressing hearing problems. Patients should undergo a hearing evaluation and receive help in managing a hearing problem, if necessary. Hearing aids improve hearing and reduce the perception of tinnitus.31
Using therapeutic sound. Some audiologists are trained to implement various forms of sound-based therapy. Tinnitus retraining therapy involves the use of background sound to facilitate habituation to tinnitus; tinnitus masking involves the use of soothing sound to provide a sense of relief. Progressive tinnitus management is a more recent method that educates patients in the use of all types of therapeutic sound.32 These sound-based methods often include the use of hearing aids, sound generators, and other devices.
Circling in a mental health professional. It is essential to involve psychologists or other mental health specialists in the care of patients with clinically significant tinnitus to ensure that psychological and other barriers to successful management of the condition are identified and addressed. Cognitive-behavioral therapy (CBT) has been shown to be helpful for patients with tinnitus.33 In fact, we have been successful in teaching patients to manage their reactions to tinnitus—resulting in a better quality of life—using a combination of educational counseling, therapeutic sound, and CBT. JFP
Acknowledgments
Funding for this work was provided by Veterans Health Administration, and Veterans Affairs Rehabilitation Research and Development (RR&D) Service (C4488R). Thanks to Robert Folmer, PhD, William Martin, PhD, Dennis Trune, PhD, and Baker Shi, MD, PhD, for advice that contributed to this manuscript. Special thanks to Martin Schechter, PhD, for his significant contributions to our research. The authors also wish to thank Stephen Fausti, PhD, and Sara Ruth Oliver, AuD, for their consistent support of our research.
CORRESPONDENCE James A. Henry, PhD, VA Medical Center (NCRAR), Post Office Box 1034, Portland, OR 97207; [email protected]
1. Hoffman HJ, Reed GW. Epidemiology of tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:16-41.
2. Jastreboff PJ, Hazell JWP. Tinnitus Retraining Therapy: Implementing the Neurophysiological Model. New York: Cambridge University Press; 2004.
3. Kiang NYS, Moxon EC, Levine RA. Auditory-nerve activity in cats with normal and abnormal cochleas. In: Wolstenholme GEW, Knight J, eds. Sensorineural Hearing Loss. London: J. & A. Churchill; 1970:241-273.
4. Henry JA, Dennis K, Schechter MA. General review of tinnitus: prevalence, mechanisms, effects, and management. J Speech Lang Hear Res. 2005;48:1204-1235.
5. Dauman R, Tyler RS. Some considerations on the classification of tinnitus. In: Aran J-M, Dauman R, eds. Proceedings of the Fourth International Tinnitus Seminar. Amsterdam/New York: Kugler Publications; 1992:225-229.
6. Hazell J. Incidence, classification, and models of tinnitus. In: Ludman H, Wright T, eds. Diseases of the Ear. London: Arnold; 1998:185-195.
7. Dobie RA. Overview: suffering from tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:1-7.
8. Zaugg TL, et al. Difficulties caused by patients’ misconceptions that hearing problems are due to tinnitus. In: Patuzzi R, ed. Proceedings of the Seventh International Tinnitus Seminar. Perth: University of Western Australia; 2002:226-228.
9. Coles RRA. Classification of causes, mechanisms of patient disturbance, and associated counseling. In: Vernon JA, Moller AR, eds. Mechanisms of Tinnitus. Needham Heights, Mass: Allyn & Bacon; 1995:11-19.
10. Fausti SA, et al. Ototoxicity. In: Northern JL, ed. Hearing Disorders. Needham Heights, Mass: Allyn & Bacon; 1995:149-164.
11. Rachel JD, Kaltenbach JA, Janisse J. Increases in spontaneous neural activity in the hamster dorsal cochlear nucleus following cisplatin treatment: a possible basis for cisplatin-induced tinnitus. Hear Res. 2002;164:206-214.
12. Henry JA, Zaugg TL, Myers PJ, et al. The role of audiologic evaluation in progressive audiologic tinnitus management. Trends Amplif. 2008;12:170-187.
13. Jastreboff PJ, Hazell JWP. Treatment of tinnitus based on a neurophysiological model. In: Vernon JA, ed. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998:201-217.
14. Davis A, Refaie AE. Epidemiology of tinnitus. In: Tyler R, ed. Tinnitus Handbook. San Diego: Singular Publishing Group; 2000:1-23.
15. Lockwood AH, Burkard RF, Salvi RJ. Imaging tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:253-264.
16. Sismanis A. Pulsatile tinnitus. Otolaryngol Clin North Am. 2003;36:389-402.
17. Sismanis A. Pulsatile tinnitus. In: Vernon JA, ed. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998:28-33.
18. Wackym PA, Friedland DR. Otologic evaluation. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:205-219.
19. Hamid M, Trune D. Issues, indications, and controversies regarding intratympanic steroid perfusion. Curr Opin Otolaryngol Head Neck Surg. 2008;16:434-440.
20. Jeyakumar A, et al. Treatment of idiopathic sudden sensorineural hearing loss. Acta Otolaryngol. 2006;126:708-713.
21. Brown GK, et al. Suicide intent and accurate expectations of lethality: predictors of medical lethality of suicide attempts. J Consult Clin Psychol. 2004;72:1170-1174.
22. Hawton K. Studying survivors of nearly lethal suicide attempts: an important strategy in suicide research. Suicide Life Threat Behav. 2001;32(1 suppl):76-84.
23. Kessler RC, Borges G, Walters EE. Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56:617-626.
24. Newman CW, Sandridge SA, Jacobson GP. Psychometric adequacy of the Tinnitus Handicap Inventory (THI) for evaluating treatment outcome. J Am Acad Audiol. 1998;9:153-160.
25. Tyler RS, ed. Tinnitus Treatment: Clinical Protocols. New York: Thieme Medical Publishers, Inc; 2005.
26. Vernon JA. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998.
27. Henry JA, Zaugg TL, Myers PM, et al. Progressive Tinnitus Management: Clinical Handbook for Audiologists. San Diego, Calif: Plural Publishing; 2010.
28. Robinson SK, Viirre ES, Stein MB. Antidepressant therapy for tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:278-293.
29. Dobie RA. Clinical trials and drug therapy for tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:266-277.
30. Henry JA, Zaugg TL, Schechter MA. Clinical guide for audiologic tinnitus management I: assessment. Am J Audiol. 2005;14:21-48.
31. Surr RK, Montgomery AA, Mueller HG. Effect of amplification on tinnitus among new hearing aid users. Ear Hear. 1985;6:71-75.
32. Henry JA, et al. Using therapeutic sound with progressive audiologic tinnitus management. Trends Amplif. 2008;12:185-206.
33. Martinez Devesa P, Waddell A, Perera R, et al. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2007;(1):CD005233.-
1. Hoffman HJ, Reed GW. Epidemiology of tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:16-41.
2. Jastreboff PJ, Hazell JWP. Tinnitus Retraining Therapy: Implementing the Neurophysiological Model. New York: Cambridge University Press; 2004.
3. Kiang NYS, Moxon EC, Levine RA. Auditory-nerve activity in cats with normal and abnormal cochleas. In: Wolstenholme GEW, Knight J, eds. Sensorineural Hearing Loss. London: J. & A. Churchill; 1970:241-273.
4. Henry JA, Dennis K, Schechter MA. General review of tinnitus: prevalence, mechanisms, effects, and management. J Speech Lang Hear Res. 2005;48:1204-1235.
5. Dauman R, Tyler RS. Some considerations on the classification of tinnitus. In: Aran J-M, Dauman R, eds. Proceedings of the Fourth International Tinnitus Seminar. Amsterdam/New York: Kugler Publications; 1992:225-229.
6. Hazell J. Incidence, classification, and models of tinnitus. In: Ludman H, Wright T, eds. Diseases of the Ear. London: Arnold; 1998:185-195.
7. Dobie RA. Overview: suffering from tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:1-7.
8. Zaugg TL, et al. Difficulties caused by patients’ misconceptions that hearing problems are due to tinnitus. In: Patuzzi R, ed. Proceedings of the Seventh International Tinnitus Seminar. Perth: University of Western Australia; 2002:226-228.
9. Coles RRA. Classification of causes, mechanisms of patient disturbance, and associated counseling. In: Vernon JA, Moller AR, eds. Mechanisms of Tinnitus. Needham Heights, Mass: Allyn & Bacon; 1995:11-19.
10. Fausti SA, et al. Ototoxicity. In: Northern JL, ed. Hearing Disorders. Needham Heights, Mass: Allyn & Bacon; 1995:149-164.
11. Rachel JD, Kaltenbach JA, Janisse J. Increases in spontaneous neural activity in the hamster dorsal cochlear nucleus following cisplatin treatment: a possible basis for cisplatin-induced tinnitus. Hear Res. 2002;164:206-214.
12. Henry JA, Zaugg TL, Myers PJ, et al. The role of audiologic evaluation in progressive audiologic tinnitus management. Trends Amplif. 2008;12:170-187.
13. Jastreboff PJ, Hazell JWP. Treatment of tinnitus based on a neurophysiological model. In: Vernon JA, ed. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998:201-217.
14. Davis A, Refaie AE. Epidemiology of tinnitus. In: Tyler R, ed. Tinnitus Handbook. San Diego: Singular Publishing Group; 2000:1-23.
15. Lockwood AH, Burkard RF, Salvi RJ. Imaging tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:253-264.
16. Sismanis A. Pulsatile tinnitus. Otolaryngol Clin North Am. 2003;36:389-402.
17. Sismanis A. Pulsatile tinnitus. In: Vernon JA, ed. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998:28-33.
18. Wackym PA, Friedland DR. Otologic evaluation. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:205-219.
19. Hamid M, Trune D. Issues, indications, and controversies regarding intratympanic steroid perfusion. Curr Opin Otolaryngol Head Neck Surg. 2008;16:434-440.
20. Jeyakumar A, et al. Treatment of idiopathic sudden sensorineural hearing loss. Acta Otolaryngol. 2006;126:708-713.
21. Brown GK, et al. Suicide intent and accurate expectations of lethality: predictors of medical lethality of suicide attempts. J Consult Clin Psychol. 2004;72:1170-1174.
22. Hawton K. Studying survivors of nearly lethal suicide attempts: an important strategy in suicide research. Suicide Life Threat Behav. 2001;32(1 suppl):76-84.
23. Kessler RC, Borges G, Walters EE. Prevalence of and risk factors for lifetime suicide attempts in the National Comorbidity Survey. Arch Gen Psychiatry. 1999;56:617-626.
24. Newman CW, Sandridge SA, Jacobson GP. Psychometric adequacy of the Tinnitus Handicap Inventory (THI) for evaluating treatment outcome. J Am Acad Audiol. 1998;9:153-160.
25. Tyler RS, ed. Tinnitus Treatment: Clinical Protocols. New York: Thieme Medical Publishers, Inc; 2005.
26. Vernon JA. Tinnitus Treatment and Relief. Needham Heights, Mass: Allyn & Bacon; 1998.
27. Henry JA, Zaugg TL, Myers PM, et al. Progressive Tinnitus Management: Clinical Handbook for Audiologists. San Diego, Calif: Plural Publishing; 2010.
28. Robinson SK, Viirre ES, Stein MB. Antidepressant therapy for tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:278-293.
29. Dobie RA. Clinical trials and drug therapy for tinnitus. In: Snow JB, ed. Tinnitus: Theory and Management. Lewiston, NY: BC Decker Inc; 2004:266-277.
30. Henry JA, Zaugg TL, Schechter MA. Clinical guide for audiologic tinnitus management I: assessment. Am J Audiol. 2005;14:21-48.
31. Surr RK, Montgomery AA, Mueller HG. Effect of amplification on tinnitus among new hearing aid users. Ear Hear. 1985;6:71-75.
32. Henry JA, et al. Using therapeutic sound with progressive audiologic tinnitus management. Trends Amplif. 2008;12:185-206.
33. Martinez Devesa P, Waddell A, Perera R, et al. Cognitive behavioural therapy for tinnitus. Cochrane Database Syst Rev. 2007;(1):CD005233.-