User login
ANSWER
The correct diagnosis is relapsing polychondritis (RP; choice “a”). The lack of surface changes in the affected skin rules out contact dermatitis, while the lack of a positive response to antibiotics and absence of an entrance wound eliminate the possibility of an infectious etiology.
DISCUSSION
There are no tests to confirm the diagnosis of RP. It is a rare autoimmune condition that usually manifests in the later decades of life and equally affects men and women.
RP’s ability to appear in cartilage anywhere in the body and in a variety of forms makes timely diagnosis almost impossible. But this case illustrates some diagnostically useful signs to watch for.
The unexplained erythema in the ear, which very obviously spared the cartilage-free lobe, prompted a biopsy of the cartilage; this showed changes consistent with RP. A subsequent review of the patient’s ophthalmology records indicated a chronic episcleritis, most likely due to inflammation of eyelid cartilage.
Further testing was performed to rule out other explanations, such as gout, or autoimmune diseases, such as lupus. Results were negative.
The patient was then referred to a pulmonologist, who found no respiratory involvement, and a rheumatologist, for further evaluation (including blood work) to rule out other conditions and end-organ (eg, renal) involvement.
On follow-up, the patient was responding well to prednisone prescribed by her rheumatologist. Given her limited disease, her prognosis is fairly good.
ANSWER
The correct diagnosis is relapsing polychondritis (RP; choice “a”). The lack of surface changes in the affected skin rules out contact dermatitis, while the lack of a positive response to antibiotics and absence of an entrance wound eliminate the possibility of an infectious etiology.
DISCUSSION
There are no tests to confirm the diagnosis of RP. It is a rare autoimmune condition that usually manifests in the later decades of life and equally affects men and women.
RP’s ability to appear in cartilage anywhere in the body and in a variety of forms makes timely diagnosis almost impossible. But this case illustrates some diagnostically useful signs to watch for.
The unexplained erythema in the ear, which very obviously spared the cartilage-free lobe, prompted a biopsy of the cartilage; this showed changes consistent with RP. A subsequent review of the patient’s ophthalmology records indicated a chronic episcleritis, most likely due to inflammation of eyelid cartilage.
Further testing was performed to rule out other explanations, such as gout, or autoimmune diseases, such as lupus. Results were negative.
The patient was then referred to a pulmonologist, who found no respiratory involvement, and a rheumatologist, for further evaluation (including blood work) to rule out other conditions and end-organ (eg, renal) involvement.
On follow-up, the patient was responding well to prednisone prescribed by her rheumatologist. Given her limited disease, her prognosis is fairly good.
ANSWER
The correct diagnosis is relapsing polychondritis (RP; choice “a”). The lack of surface changes in the affected skin rules out contact dermatitis, while the lack of a positive response to antibiotics and absence of an entrance wound eliminate the possibility of an infectious etiology.
DISCUSSION
There are no tests to confirm the diagnosis of RP. It is a rare autoimmune condition that usually manifests in the later decades of life and equally affects men and women.
RP’s ability to appear in cartilage anywhere in the body and in a variety of forms makes timely diagnosis almost impossible. But this case illustrates some diagnostically useful signs to watch for.
The unexplained erythema in the ear, which very obviously spared the cartilage-free lobe, prompted a biopsy of the cartilage; this showed changes consistent with RP. A subsequent review of the patient’s ophthalmology records indicated a chronic episcleritis, most likely due to inflammation of eyelid cartilage.
Further testing was performed to rule out other explanations, such as gout, or autoimmune diseases, such as lupus. Results were negative.
The patient was then referred to a pulmonologist, who found no respiratory involvement, and a rheumatologist, for further evaluation (including blood work) to rule out other conditions and end-organ (eg, renal) involvement.
On follow-up, the patient was responding well to prednisone prescribed by her rheumatologist. Given her limited disease, her prognosis is fairly good.
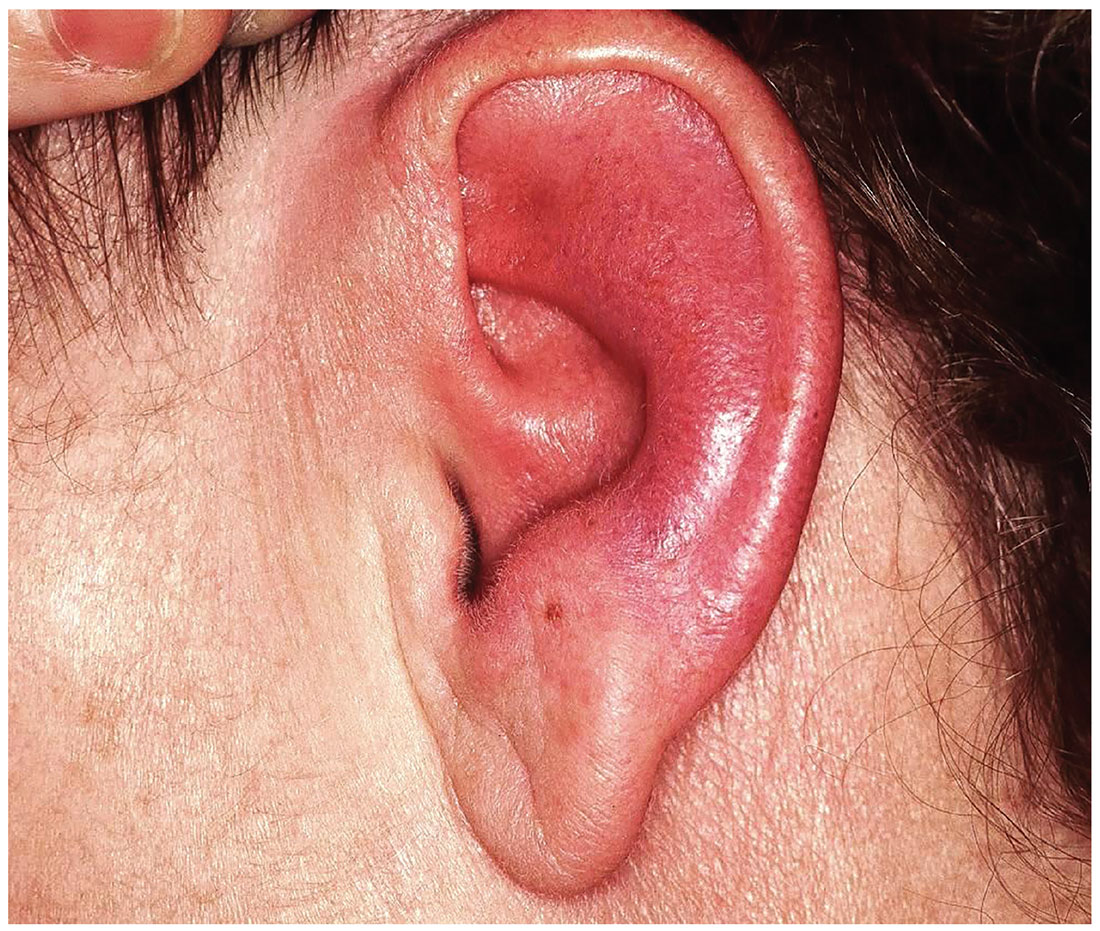
Several months ago, family members pointed out that this 60-year-old woman’s left ear was red. She consulted her primary care provider, who prescribed antibiotics. But when these failed to clear the problem, she was referred to dermatology.
Today, the patient complains of some discomfort in the ear but denies actual pain; she is, for example, able to sleep despite the problem. She reports that the redness manifested slowly but has spread over time to encompass most of her ear.
Uniformly distributed, bright red erythema on the left ear spares only the lobe. No wound or epidermal component (eg, scaling or blistering) is noted. However, there is increased warmth and tenderness on palpation of the erythematous portion. No nodes can be felt in the vicinity, nor are any abnormalities observed in the other ear.
The patient denies other skin problems, joint pain, and breathing difficulty. But she does have an ongoing history of irritation in both eyes. She has been seeing an ophthalmologist for months without relief. On examination, both eyes appear injected, with slightly swollen eyelids. Inspection and palpation of the nose reveal no abnormalities.
