User login
Questionnaire for patients with psoriasis might identify risk of axial involvement
Preliminary findings are encouraging
NEW YORK – A questionnaire-based screening tool appears to accelerate the time to diagnosis of axial involvement in patients presenting with psoriasis but no clinical signs of joint pain, according to a study called ATTRACT that was presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
The risk of a delayed diagnosis of an axial component in patients with psoriasis, meaning a delay in the underlying diagnosis of psoriatic arthritis (PsA), is substantial, according to Devis Benfaremo, MD, of the department of clinical and molecular science at Marche Polytechnic University, Ancona, Italy.
There is “no consensus for the best strategy to achieve early detection of joint disease” in patients presenting with psoriasis, but Dr. Benfaremo pointed out that missing axial involvement is a particular problem because it is far more likely than swollen joints to be missed on clinical examination.
While about one in three patients with psoriasis have or will develop psoriatic arthritis, according to the National Psoriasis Foundation, delays in diagnosis are common, according to Dr. Benfaremo. In patients with undiagnosed PsA characterized by axial involvement alone, subtle symptoms can be overlooked or attributed to other causes.
There are several screening questionnaires to detect joint symptoms in patients presenting with psoriasis, such as the five-question Psoriasis Epidemiology Screening Tool, but the questionnaire tested in the ATTRACT trial is focused on detecting axial involvement specifically. It was characterized as the first to do so.
In the ongoing ATTRACT study, 253 patients with psoriasis but no history of PsA or axial disease have been enrolled so far. In the study, patients are screened for PsA based on a patient-completed yes-or-no questionnaire, which takes only a few minutes to complete.
“It is a validated questionnaire for axial [spondyloarthritis], but we have adopted it for detection of psoriasis patients with PsA,” Dr. Benfaremo explained.
The questionnaire for axial spondyloarthritis (axSpA) was initially evaluated and validated by Fabian Proft, MD, head of the clinical trials unit at Charité Hospital, Berlin. In addition to a patient self-completed questionnaire, Dr. Proft and coinvestigators have also created a related questionnaire to be administered by physicians.
In the ATTRACT study, patients completed the questionnaire on an electronic device in the waiting room. Positive answers to specific questions about symptoms, which addressed back pain and joint function as well as joint symptoms, divided patients into three groups:
- Group A patients did not respond positively to any of the symptom questions that would prompt suspicion of axial disease. These represented about one-third of those screened so far.
- Group B patients were those who answered positively to at least two questions that related to a high suspicion of axial involvement. These represented 45% of patients.
- The remaining patients were placed in Group C, a category of intermediate risk based on positive responses to some, but not all, questions relating to axial symptoms.
Those in group B are being referred to rheumatology. Patients in group C are given “conditional” eligibility based on the presence of additional risk factors.
AxSpA screening tool ‘makes sense’ for potential use in PsA
The primary outcome of the ATTRACT trial is early identification of axial PsA. Correctly identifying patients with or without peripheral joint involvement is one of several secondary outcomes. The identification of patients who fulfill Assessment Spondyloarthritis International Society (ASAS) criteria for axSpA is another secondary outcome.
Of the 114 patients placed in group B and analyzed so far, 87 have completed an assessment by a rheumatologist with laboratory analyses and imaging, as well as a clinical examination.
Of those 87 assessed by a rheumatologist, 17 did not have either axial or peripheral inflammation. Another 19 were diagnosed with axial disease, including 14 who met ASAS criteria. A total of 10 were classified as having PsA with peripheral inflammation, according to Classification for Psoriatic Arthritis criteria, and 41 are still being considered for a diagnosis of axial or peripheral PsA on the basis of further workup.
“Among the patients with axial PsA, only 10% had elevated C-reactive protein levels,” according to Dr. Benfaremo, echoing previous evidence that inflammatory biomarkers by themselves have limited value for identifying psoriasis patients at high risk of joint involvement.
The findings are preliminary, but Dr. Benfaremo reported that the questionnaire is showing promise for the routine stratification of patients who should be considered for a rheumatology consultation.
If further analyses validate the clinical utility of these stratifications, there is the potential for a substantial acceleration to the diagnosis of PsA.
When contacted to comment about this work, Dr. Proft said that there is an important need for new strategies reduce delay in the diagnosis of PsA among patients presenting with psoriasis. He thinks the screening tool he developed for axSpA “makes sense” as a potential tool in PsA.
“If validated, this could be a very useful for earlier identification of PsA,” Dr. Proft said. He reiterated the importance of focusing on axial involvement.
“Previous screening tools have focused on symptoms of PsA more generally, but inflammation in the peripheral joints is something that you can easily see in most patients,” he said.
In addition to the patient-completed questionnaire and the physician-administered questionnaire, Dr. Proft has also evaluated an online self-referral tool for patients.
“If we can diagnose PsA earlier in the course of disease, we can start treatment earlier, prevent or delay joint damage, and potentially improve outcomes for patients,” Dr. Proft said. He considers this an important direction of research.
Dr. Benfaremo and Dr. Proft reported no potential conflicts of interest.
Preliminary findings are encouraging
Preliminary findings are encouraging
NEW YORK – A questionnaire-based screening tool appears to accelerate the time to diagnosis of axial involvement in patients presenting with psoriasis but no clinical signs of joint pain, according to a study called ATTRACT that was presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
The risk of a delayed diagnosis of an axial component in patients with psoriasis, meaning a delay in the underlying diagnosis of psoriatic arthritis (PsA), is substantial, according to Devis Benfaremo, MD, of the department of clinical and molecular science at Marche Polytechnic University, Ancona, Italy.
There is “no consensus for the best strategy to achieve early detection of joint disease” in patients presenting with psoriasis, but Dr. Benfaremo pointed out that missing axial involvement is a particular problem because it is far more likely than swollen joints to be missed on clinical examination.
While about one in three patients with psoriasis have or will develop psoriatic arthritis, according to the National Psoriasis Foundation, delays in diagnosis are common, according to Dr. Benfaremo. In patients with undiagnosed PsA characterized by axial involvement alone, subtle symptoms can be overlooked or attributed to other causes.
There are several screening questionnaires to detect joint symptoms in patients presenting with psoriasis, such as the five-question Psoriasis Epidemiology Screening Tool, but the questionnaire tested in the ATTRACT trial is focused on detecting axial involvement specifically. It was characterized as the first to do so.
In the ongoing ATTRACT study, 253 patients with psoriasis but no history of PsA or axial disease have been enrolled so far. In the study, patients are screened for PsA based on a patient-completed yes-or-no questionnaire, which takes only a few minutes to complete.
“It is a validated questionnaire for axial [spondyloarthritis], but we have adopted it for detection of psoriasis patients with PsA,” Dr. Benfaremo explained.
The questionnaire for axial spondyloarthritis (axSpA) was initially evaluated and validated by Fabian Proft, MD, head of the clinical trials unit at Charité Hospital, Berlin. In addition to a patient self-completed questionnaire, Dr. Proft and coinvestigators have also created a related questionnaire to be administered by physicians.
In the ATTRACT study, patients completed the questionnaire on an electronic device in the waiting room. Positive answers to specific questions about symptoms, which addressed back pain and joint function as well as joint symptoms, divided patients into three groups:
- Group A patients did not respond positively to any of the symptom questions that would prompt suspicion of axial disease. These represented about one-third of those screened so far.
- Group B patients were those who answered positively to at least two questions that related to a high suspicion of axial involvement. These represented 45% of patients.
- The remaining patients were placed in Group C, a category of intermediate risk based on positive responses to some, but not all, questions relating to axial symptoms.
Those in group B are being referred to rheumatology. Patients in group C are given “conditional” eligibility based on the presence of additional risk factors.
AxSpA screening tool ‘makes sense’ for potential use in PsA
The primary outcome of the ATTRACT trial is early identification of axial PsA. Correctly identifying patients with or without peripheral joint involvement is one of several secondary outcomes. The identification of patients who fulfill Assessment Spondyloarthritis International Society (ASAS) criteria for axSpA is another secondary outcome.
Of the 114 patients placed in group B and analyzed so far, 87 have completed an assessment by a rheumatologist with laboratory analyses and imaging, as well as a clinical examination.
Of those 87 assessed by a rheumatologist, 17 did not have either axial or peripheral inflammation. Another 19 were diagnosed with axial disease, including 14 who met ASAS criteria. A total of 10 were classified as having PsA with peripheral inflammation, according to Classification for Psoriatic Arthritis criteria, and 41 are still being considered for a diagnosis of axial or peripheral PsA on the basis of further workup.
“Among the patients with axial PsA, only 10% had elevated C-reactive protein levels,” according to Dr. Benfaremo, echoing previous evidence that inflammatory biomarkers by themselves have limited value for identifying psoriasis patients at high risk of joint involvement.
The findings are preliminary, but Dr. Benfaremo reported that the questionnaire is showing promise for the routine stratification of patients who should be considered for a rheumatology consultation.
If further analyses validate the clinical utility of these stratifications, there is the potential for a substantial acceleration to the diagnosis of PsA.
When contacted to comment about this work, Dr. Proft said that there is an important need for new strategies reduce delay in the diagnosis of PsA among patients presenting with psoriasis. He thinks the screening tool he developed for axSpA “makes sense” as a potential tool in PsA.
“If validated, this could be a very useful for earlier identification of PsA,” Dr. Proft said. He reiterated the importance of focusing on axial involvement.
“Previous screening tools have focused on symptoms of PsA more generally, but inflammation in the peripheral joints is something that you can easily see in most patients,” he said.
In addition to the patient-completed questionnaire and the physician-administered questionnaire, Dr. Proft has also evaluated an online self-referral tool for patients.
“If we can diagnose PsA earlier in the course of disease, we can start treatment earlier, prevent or delay joint damage, and potentially improve outcomes for patients,” Dr. Proft said. He considers this an important direction of research.
Dr. Benfaremo and Dr. Proft reported no potential conflicts of interest.
NEW YORK – A questionnaire-based screening tool appears to accelerate the time to diagnosis of axial involvement in patients presenting with psoriasis but no clinical signs of joint pain, according to a study called ATTRACT that was presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
The risk of a delayed diagnosis of an axial component in patients with psoriasis, meaning a delay in the underlying diagnosis of psoriatic arthritis (PsA), is substantial, according to Devis Benfaremo, MD, of the department of clinical and molecular science at Marche Polytechnic University, Ancona, Italy.
There is “no consensus for the best strategy to achieve early detection of joint disease” in patients presenting with psoriasis, but Dr. Benfaremo pointed out that missing axial involvement is a particular problem because it is far more likely than swollen joints to be missed on clinical examination.
While about one in three patients with psoriasis have or will develop psoriatic arthritis, according to the National Psoriasis Foundation, delays in diagnosis are common, according to Dr. Benfaremo. In patients with undiagnosed PsA characterized by axial involvement alone, subtle symptoms can be overlooked or attributed to other causes.
There are several screening questionnaires to detect joint symptoms in patients presenting with psoriasis, such as the five-question Psoriasis Epidemiology Screening Tool, but the questionnaire tested in the ATTRACT trial is focused on detecting axial involvement specifically. It was characterized as the first to do so.
In the ongoing ATTRACT study, 253 patients with psoriasis but no history of PsA or axial disease have been enrolled so far. In the study, patients are screened for PsA based on a patient-completed yes-or-no questionnaire, which takes only a few minutes to complete.
“It is a validated questionnaire for axial [spondyloarthritis], but we have adopted it for detection of psoriasis patients with PsA,” Dr. Benfaremo explained.
The questionnaire for axial spondyloarthritis (axSpA) was initially evaluated and validated by Fabian Proft, MD, head of the clinical trials unit at Charité Hospital, Berlin. In addition to a patient self-completed questionnaire, Dr. Proft and coinvestigators have also created a related questionnaire to be administered by physicians.
In the ATTRACT study, patients completed the questionnaire on an electronic device in the waiting room. Positive answers to specific questions about symptoms, which addressed back pain and joint function as well as joint symptoms, divided patients into three groups:
- Group A patients did not respond positively to any of the symptom questions that would prompt suspicion of axial disease. These represented about one-third of those screened so far.
- Group B patients were those who answered positively to at least two questions that related to a high suspicion of axial involvement. These represented 45% of patients.
- The remaining patients were placed in Group C, a category of intermediate risk based on positive responses to some, but not all, questions relating to axial symptoms.
Those in group B are being referred to rheumatology. Patients in group C are given “conditional” eligibility based on the presence of additional risk factors.
AxSpA screening tool ‘makes sense’ for potential use in PsA
The primary outcome of the ATTRACT trial is early identification of axial PsA. Correctly identifying patients with or without peripheral joint involvement is one of several secondary outcomes. The identification of patients who fulfill Assessment Spondyloarthritis International Society (ASAS) criteria for axSpA is another secondary outcome.
Of the 114 patients placed in group B and analyzed so far, 87 have completed an assessment by a rheumatologist with laboratory analyses and imaging, as well as a clinical examination.
Of those 87 assessed by a rheumatologist, 17 did not have either axial or peripheral inflammation. Another 19 were diagnosed with axial disease, including 14 who met ASAS criteria. A total of 10 were classified as having PsA with peripheral inflammation, according to Classification for Psoriatic Arthritis criteria, and 41 are still being considered for a diagnosis of axial or peripheral PsA on the basis of further workup.
“Among the patients with axial PsA, only 10% had elevated C-reactive protein levels,” according to Dr. Benfaremo, echoing previous evidence that inflammatory biomarkers by themselves have limited value for identifying psoriasis patients at high risk of joint involvement.
The findings are preliminary, but Dr. Benfaremo reported that the questionnaire is showing promise for the routine stratification of patients who should be considered for a rheumatology consultation.
If further analyses validate the clinical utility of these stratifications, there is the potential for a substantial acceleration to the diagnosis of PsA.
When contacted to comment about this work, Dr. Proft said that there is an important need for new strategies reduce delay in the diagnosis of PsA among patients presenting with psoriasis. He thinks the screening tool he developed for axSpA “makes sense” as a potential tool in PsA.
“If validated, this could be a very useful for earlier identification of PsA,” Dr. Proft said. He reiterated the importance of focusing on axial involvement.
“Previous screening tools have focused on symptoms of PsA more generally, but inflammation in the peripheral joints is something that you can easily see in most patients,” he said.
In addition to the patient-completed questionnaire and the physician-administered questionnaire, Dr. Proft has also evaluated an online self-referral tool for patients.
“If we can diagnose PsA earlier in the course of disease, we can start treatment earlier, prevent or delay joint damage, and potentially improve outcomes for patients,” Dr. Proft said. He considers this an important direction of research.
Dr. Benfaremo and Dr. Proft reported no potential conflicts of interest.
AT GRAPPA 2022
NAFLD strongly correlated with psoriasis, PsA; risk linked to severity
NEW YORK – – and probably in those with psoriatic arthritis (PsA) as well, according to a systematic review and meta-analysis presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
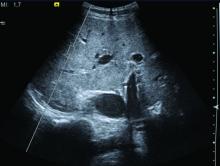
“Our findings imply that psoriatic patients should be screened with an ultrasonographic exam in cases where there are metabolic features that are associated with NAFLD,” reported Francesco Bellinato, MD, a researcher in the section of dermatology and venereology, University of Verona (Italy).
The data are strong. Of 76 nonduplicate publications found in the literature, the 11 observational studies included in the meta-analysis met stringent criteria, including a diagnosis of psoriasis and PsA based on objective criteria, NAFLD confirmed with liver biopsy or imaging, and odds rates calculated with 95% confidence intervals.
From these 11 studies, aggregate data were available for 249,333 psoriatic patients, of which 49% had NAFLD, and 1,491,402 were healthy controls. Among the controls, 36% had NAFLD. Four of the studies were from North America, four from Europe, and three from Asia.
In the pooled data, the risk of NAFLD among those with psoriasis relative to healthy controls fell just short of a twofold increase (odds ratio, 1.96; 95% CI, 1.70-2.26; P < .001). When stratified by studies that confirmed NAFLD by biopsy relative to ultrasonography, there was no significant heterogeneity.
Eight of the studies included an analysis of relative risk in the context of skin lesion severity defined by Psoriasis Area and Severity Index (PASI) score. Relative to those without NAFLD, psoriatic patients with NAFLD had a significant greater mean PASI score on a pooled weighted mean difference analysis (OR, 3.93; 95% CI, 2.01-5.84; P < .0001).
For PsA relative to no PsA in the five studies that compared risk between these two groups, the risk of NAFLD was again nearly twofold higher. This fell short of conventional definition of statistical significance, but it was associated with a strong trend (OR, 1.83; 95% CI, 0.98-3.43; P = .06).
The risk of NAFLD among patients with psoriasis was not found to vary significantly when assessed by univariable meta-regressions across numerous characteristics, such as sex and body mass index.
In one of the largest of the observational studies included in the meta-analysis by Alexis Ogdie, MD, associate professor of medicine and epidemiology at the University of Pennsylvania, Philadelphia, and colleagues, data were analyzed in more than 1.5 million patients, which included 54,251 patients with rheumatoid arthritis. While the hazard ratio of NAFLD was increased for both psoriasis (HR, 2.23) and PsA (HR, 2.11), it was not elevated in those with RA (HR, 0.96).
Risk by severity, possible mechanisms
This study also included an analysis of NAFLD risk according to psoriasis severity. While risk was still significant among those with mild disease (HR, 1.18; 95% CI, 1.07-1.30), it was almost twofold greater in those with moderate to severe psoriasis (HR, 2.23; 95% CI, 1.73-2.87).
Dr. Bellinato conceded that the mechanisms underlying the association between psoriasis and NAFLD are unknown, but he said “metaflammation” is suspected.
“The secretion of proinflammatory, prothrombotic, and oxidative stress mediators in both psoriatic skin and adipose tissue might act systemically and promote insulin resistance and other metabolic derangements that promote the development and progression of NAFLD,” Dr. Bellinato explained.
He thinks that noninvasive screening methods, such as currently used methods to calculate fibrosis score, might be useful for evaluating patients with psoriasis for NAFLD and referring them to a hepatologist when appropriate.
Given the strong association with NAFLD, Dr. Bellinato suggested that “the findings of this meta-analysis pave the way for novel, large, prospective, and histologically based studies.”
The association between psoriasis and NAFLD is clinically relevant, agreed Joel M. Gelfand, MD, vice-chair of clinical research and medical director of the clinical studies unit, department of dermatology, University of Pennsylvania, Philadelphia.
“It is not clear if psoriasis causes fatty liver disease or vice versa, but clinicians should be aware of this association,” he said in an interview. Dr. Gelfand was a coauthor of the study by Dr. Ogdie and colleagues and led another more recent population-based study that implicated methotrexate as a factor in psoriasis-related hepatotoxicity.
If NAFLD is identified in a patient with psoriasis, treatments are limited, but Dr. Gelfand suggested that patients should be made aware of the risk. “Clinicians should encourage patients with psoriasis to take measures to protect their liver, such as avoiding drinking alcohol to excess and trying to maintain a healthy body weight,” he said.
Dr. Bellinato reported no conflicts of interest. Dr. Gelfand has financial relationships with more than 10 pharmaceutical companies, including those that make therapies for psoriasis.
NEW YORK – – and probably in those with psoriatic arthritis (PsA) as well, according to a systematic review and meta-analysis presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
“Our findings imply that psoriatic patients should be screened with an ultrasonographic exam in cases where there are metabolic features that are associated with NAFLD,” reported Francesco Bellinato, MD, a researcher in the section of dermatology and venereology, University of Verona (Italy).
The data are strong. Of 76 nonduplicate publications found in the literature, the 11 observational studies included in the meta-analysis met stringent criteria, including a diagnosis of psoriasis and PsA based on objective criteria, NAFLD confirmed with liver biopsy or imaging, and odds rates calculated with 95% confidence intervals.
From these 11 studies, aggregate data were available for 249,333 psoriatic patients, of which 49% had NAFLD, and 1,491,402 were healthy controls. Among the controls, 36% had NAFLD. Four of the studies were from North America, four from Europe, and three from Asia.
In the pooled data, the risk of NAFLD among those with psoriasis relative to healthy controls fell just short of a twofold increase (odds ratio, 1.96; 95% CI, 1.70-2.26; P < .001). When stratified by studies that confirmed NAFLD by biopsy relative to ultrasonography, there was no significant heterogeneity.
Eight of the studies included an analysis of relative risk in the context of skin lesion severity defined by Psoriasis Area and Severity Index (PASI) score. Relative to those without NAFLD, psoriatic patients with NAFLD had a significant greater mean PASI score on a pooled weighted mean difference analysis (OR, 3.93; 95% CI, 2.01-5.84; P < .0001).
For PsA relative to no PsA in the five studies that compared risk between these two groups, the risk of NAFLD was again nearly twofold higher. This fell short of conventional definition of statistical significance, but it was associated with a strong trend (OR, 1.83; 95% CI, 0.98-3.43; P = .06).
The risk of NAFLD among patients with psoriasis was not found to vary significantly when assessed by univariable meta-regressions across numerous characteristics, such as sex and body mass index.
In one of the largest of the observational studies included in the meta-analysis by Alexis Ogdie, MD, associate professor of medicine and epidemiology at the University of Pennsylvania, Philadelphia, and colleagues, data were analyzed in more than 1.5 million patients, which included 54,251 patients with rheumatoid arthritis. While the hazard ratio of NAFLD was increased for both psoriasis (HR, 2.23) and PsA (HR, 2.11), it was not elevated in those with RA (HR, 0.96).
Risk by severity, possible mechanisms
This study also included an analysis of NAFLD risk according to psoriasis severity. While risk was still significant among those with mild disease (HR, 1.18; 95% CI, 1.07-1.30), it was almost twofold greater in those with moderate to severe psoriasis (HR, 2.23; 95% CI, 1.73-2.87).
Dr. Bellinato conceded that the mechanisms underlying the association between psoriasis and NAFLD are unknown, but he said “metaflammation” is suspected.
“The secretion of proinflammatory, prothrombotic, and oxidative stress mediators in both psoriatic skin and adipose tissue might act systemically and promote insulin resistance and other metabolic derangements that promote the development and progression of NAFLD,” Dr. Bellinato explained.
He thinks that noninvasive screening methods, such as currently used methods to calculate fibrosis score, might be useful for evaluating patients with psoriasis for NAFLD and referring them to a hepatologist when appropriate.
Given the strong association with NAFLD, Dr. Bellinato suggested that “the findings of this meta-analysis pave the way for novel, large, prospective, and histologically based studies.”
The association between psoriasis and NAFLD is clinically relevant, agreed Joel M. Gelfand, MD, vice-chair of clinical research and medical director of the clinical studies unit, department of dermatology, University of Pennsylvania, Philadelphia.
“It is not clear if psoriasis causes fatty liver disease or vice versa, but clinicians should be aware of this association,” he said in an interview. Dr. Gelfand was a coauthor of the study by Dr. Ogdie and colleagues and led another more recent population-based study that implicated methotrexate as a factor in psoriasis-related hepatotoxicity.
If NAFLD is identified in a patient with psoriasis, treatments are limited, but Dr. Gelfand suggested that patients should be made aware of the risk. “Clinicians should encourage patients with psoriasis to take measures to protect their liver, such as avoiding drinking alcohol to excess and trying to maintain a healthy body weight,” he said.
Dr. Bellinato reported no conflicts of interest. Dr. Gelfand has financial relationships with more than 10 pharmaceutical companies, including those that make therapies for psoriasis.
NEW YORK – – and probably in those with psoriatic arthritis (PsA) as well, according to a systematic review and meta-analysis presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
“Our findings imply that psoriatic patients should be screened with an ultrasonographic exam in cases where there are metabolic features that are associated with NAFLD,” reported Francesco Bellinato, MD, a researcher in the section of dermatology and venereology, University of Verona (Italy).
The data are strong. Of 76 nonduplicate publications found in the literature, the 11 observational studies included in the meta-analysis met stringent criteria, including a diagnosis of psoriasis and PsA based on objective criteria, NAFLD confirmed with liver biopsy or imaging, and odds rates calculated with 95% confidence intervals.
From these 11 studies, aggregate data were available for 249,333 psoriatic patients, of which 49% had NAFLD, and 1,491,402 were healthy controls. Among the controls, 36% had NAFLD. Four of the studies were from North America, four from Europe, and three from Asia.
In the pooled data, the risk of NAFLD among those with psoriasis relative to healthy controls fell just short of a twofold increase (odds ratio, 1.96; 95% CI, 1.70-2.26; P < .001). When stratified by studies that confirmed NAFLD by biopsy relative to ultrasonography, there was no significant heterogeneity.
Eight of the studies included an analysis of relative risk in the context of skin lesion severity defined by Psoriasis Area and Severity Index (PASI) score. Relative to those without NAFLD, psoriatic patients with NAFLD had a significant greater mean PASI score on a pooled weighted mean difference analysis (OR, 3.93; 95% CI, 2.01-5.84; P < .0001).
For PsA relative to no PsA in the five studies that compared risk between these two groups, the risk of NAFLD was again nearly twofold higher. This fell short of conventional definition of statistical significance, but it was associated with a strong trend (OR, 1.83; 95% CI, 0.98-3.43; P = .06).
The risk of NAFLD among patients with psoriasis was not found to vary significantly when assessed by univariable meta-regressions across numerous characteristics, such as sex and body mass index.
In one of the largest of the observational studies included in the meta-analysis by Alexis Ogdie, MD, associate professor of medicine and epidemiology at the University of Pennsylvania, Philadelphia, and colleagues, data were analyzed in more than 1.5 million patients, which included 54,251 patients with rheumatoid arthritis. While the hazard ratio of NAFLD was increased for both psoriasis (HR, 2.23) and PsA (HR, 2.11), it was not elevated in those with RA (HR, 0.96).
Risk by severity, possible mechanisms
This study also included an analysis of NAFLD risk according to psoriasis severity. While risk was still significant among those with mild disease (HR, 1.18; 95% CI, 1.07-1.30), it was almost twofold greater in those with moderate to severe psoriasis (HR, 2.23; 95% CI, 1.73-2.87).
Dr. Bellinato conceded that the mechanisms underlying the association between psoriasis and NAFLD are unknown, but he said “metaflammation” is suspected.
“The secretion of proinflammatory, prothrombotic, and oxidative stress mediators in both psoriatic skin and adipose tissue might act systemically and promote insulin resistance and other metabolic derangements that promote the development and progression of NAFLD,” Dr. Bellinato explained.
He thinks that noninvasive screening methods, such as currently used methods to calculate fibrosis score, might be useful for evaluating patients with psoriasis for NAFLD and referring them to a hepatologist when appropriate.
Given the strong association with NAFLD, Dr. Bellinato suggested that “the findings of this meta-analysis pave the way for novel, large, prospective, and histologically based studies.”
The association between psoriasis and NAFLD is clinically relevant, agreed Joel M. Gelfand, MD, vice-chair of clinical research and medical director of the clinical studies unit, department of dermatology, University of Pennsylvania, Philadelphia.
“It is not clear if psoriasis causes fatty liver disease or vice versa, but clinicians should be aware of this association,” he said in an interview. Dr. Gelfand was a coauthor of the study by Dr. Ogdie and colleagues and led another more recent population-based study that implicated methotrexate as a factor in psoriasis-related hepatotoxicity.
If NAFLD is identified in a patient with psoriasis, treatments are limited, but Dr. Gelfand suggested that patients should be made aware of the risk. “Clinicians should encourage patients with psoriasis to take measures to protect their liver, such as avoiding drinking alcohol to excess and trying to maintain a healthy body weight,” he said.
Dr. Bellinato reported no conflicts of interest. Dr. Gelfand has financial relationships with more than 10 pharmaceutical companies, including those that make therapies for psoriasis.
AT GRAPPA 2022
Neural networks can distinguish PsA from rheumatoid arthritis on MRI
Hand images are sufficient
NEW YORK – On the basis of MRI images of the hand, a neural network has been trained to distinguish seronegative and seropositive rheumatoid arthritis (RA) from psoriatic arthritis (PsA) as well as from each other, according to a study that was presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
In the work so far, the neural network was correct about 70% of the time in the absence of any further clinical analyses, according to David Simon, MD, a rheumatologist in the department of internal medicine at Friedrich-Alexander University, Erlangen, Germany.
Previous to this work, “there has been no study that has exclusively used hand MRI data and deep learning without requiring further expert input for the classification of arthritides,” Dr. Simon said.
In fact, when demographic and clinical data were added, there was no improvement in the performance of patient classification relative to the deep learning classification alone, according to the data presented by Dr. Simon.
The images were evaluated with residual neural networks (ResNet), which represents a sophisticated form of deep learning to facilitate the flow of information across the network layers as they form to improve accuracy in their ability to distinguish one form of disease from the other. The training was performed on images from the T1 coronal, T2 corona1, T1 coronal fat suppressed with contrast, T1 axial fat suppressed with contrast, and T2 fat suppressed axial sequences.
The study included hand MRI scans from 135 patients with seronegative RA, 190 with seropositive RA, 177 with PsA, and 147 with psoriasis. The performance was judged on the basis of area under the receiver operating characteristics curve (AUROC) with and without input of clinical characteristics. Patients who had psoriasis without clinical arthritis were included as a control population.
The AUROC for accuracy was 75% for seropositive RA relative to PsA, 74% for seronegative RA relative to PsA, and 67% for seropositive relative to seronegative RA. Of the patients who had psoriasis without arthritis, 98% were classified as PsA and 2% as RA.
Subsequent to the classification of the patients with psoriasis, 14 of the 147 (9.5%) have developed PsA so far over a relatively short follow-up. All of these were among those identified as PsA by neural network evaluation of the hand MRIs.
This suggests that “a PsA-like pattern may be present early in the course of psoriatic disease,” Dr. Simon said.
In the groups with joint disease, who had mean ages ranging from 56 to 65, the mean disease durations were 2.6 years for those with seropositive RA, 1.3 years for those with seronegative RA, and 0.8 years for those with PsA. The patients with psoriasis were younger (mean age, 40.5 years) but had a longer disease duration (mean 4.2 years).
All of the MRI sequences were relevant for classification, but contrast did not appear to help with accuracy.
“If the images with contrast enhancement were deleted, the loss of performance was only marginal,” Dr. Simon reported.
The accuracy of neural networks increases with data, making it likely that further refinements in methodology will lead to a greater degree of accuracy, according to Dr. Simon. While the methodology is not yet ready for routine use in the clinic, the study demonstrates that neural network analysis of hand MRI to distinguish forms of arthritis “is possible.” Further studies are planned toward the goal of creating a viable clinical tool.
“Of course, if we could create an accurate tool with ultrasound, this would be even more practical,” said Dr. Simon, recognizing the value of an office tool, but he cautioned that this would be far more challenging.
“The precision of MRI is an important factor for effective neural network training,” he said.
Utility: ‘In challenging cases if the accuracy improves’?
A viable method for objectively and rapidly distinguishing inflammatory joint diseases, particularly in patients with an ambiguous clinical presentation, is an unmet need, according to Philip J. Mease, MD, director of rheumatology research at Swedish Medical Center, Seattle.
Although the data presented are promising, Dr. Mease said in an interview that he believes there is a fair amount of work to be done before imaging analysis based on deep learning makes its way into routine clinical care. He is also hoping for methods to distinguish RA from PsA that are easier and less expensive, such as serum biomarkers. However, he agreed that a MRI-based tool could be useful when differentiating disease that is challenging.
“MRI is an expensive way for routine classification of disease, but this approach could be useful in challenging cases if the accuracy improves,” he said.
Meanwhile, other clinical researchers might want to test the principle. “You can try it,” said Dr. Simon, who reported that his team has made the methodology publicly available.
Dr. Simon reported no conflicts of interest. Dr. Mease reported financial relationships with more than 10 pharmaceutical companies, most of which make products used for the treatment of inflammatory joint diseases.
Hand images are sufficient
Hand images are sufficient
NEW YORK – On the basis of MRI images of the hand, a neural network has been trained to distinguish seronegative and seropositive rheumatoid arthritis (RA) from psoriatic arthritis (PsA) as well as from each other, according to a study that was presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
In the work so far, the neural network was correct about 70% of the time in the absence of any further clinical analyses, according to David Simon, MD, a rheumatologist in the department of internal medicine at Friedrich-Alexander University, Erlangen, Germany.
Previous to this work, “there has been no study that has exclusively used hand MRI data and deep learning without requiring further expert input for the classification of arthritides,” Dr. Simon said.
In fact, when demographic and clinical data were added, there was no improvement in the performance of patient classification relative to the deep learning classification alone, according to the data presented by Dr. Simon.
The images were evaluated with residual neural networks (ResNet), which represents a sophisticated form of deep learning to facilitate the flow of information across the network layers as they form to improve accuracy in their ability to distinguish one form of disease from the other. The training was performed on images from the T1 coronal, T2 corona1, T1 coronal fat suppressed with contrast, T1 axial fat suppressed with contrast, and T2 fat suppressed axial sequences.
The study included hand MRI scans from 135 patients with seronegative RA, 190 with seropositive RA, 177 with PsA, and 147 with psoriasis. The performance was judged on the basis of area under the receiver operating characteristics curve (AUROC) with and without input of clinical characteristics. Patients who had psoriasis without clinical arthritis were included as a control population.
The AUROC for accuracy was 75% for seropositive RA relative to PsA, 74% for seronegative RA relative to PsA, and 67% for seropositive relative to seronegative RA. Of the patients who had psoriasis without arthritis, 98% were classified as PsA and 2% as RA.
Subsequent to the classification of the patients with psoriasis, 14 of the 147 (9.5%) have developed PsA so far over a relatively short follow-up. All of these were among those identified as PsA by neural network evaluation of the hand MRIs.
This suggests that “a PsA-like pattern may be present early in the course of psoriatic disease,” Dr. Simon said.
In the groups with joint disease, who had mean ages ranging from 56 to 65, the mean disease durations were 2.6 years for those with seropositive RA, 1.3 years for those with seronegative RA, and 0.8 years for those with PsA. The patients with psoriasis were younger (mean age, 40.5 years) but had a longer disease duration (mean 4.2 years).
All of the MRI sequences were relevant for classification, but contrast did not appear to help with accuracy.
“If the images with contrast enhancement were deleted, the loss of performance was only marginal,” Dr. Simon reported.
The accuracy of neural networks increases with data, making it likely that further refinements in methodology will lead to a greater degree of accuracy, according to Dr. Simon. While the methodology is not yet ready for routine use in the clinic, the study demonstrates that neural network analysis of hand MRI to distinguish forms of arthritis “is possible.” Further studies are planned toward the goal of creating a viable clinical tool.
“Of course, if we could create an accurate tool with ultrasound, this would be even more practical,” said Dr. Simon, recognizing the value of an office tool, but he cautioned that this would be far more challenging.
“The precision of MRI is an important factor for effective neural network training,” he said.
Utility: ‘In challenging cases if the accuracy improves’?
A viable method for objectively and rapidly distinguishing inflammatory joint diseases, particularly in patients with an ambiguous clinical presentation, is an unmet need, according to Philip J. Mease, MD, director of rheumatology research at Swedish Medical Center, Seattle.
Although the data presented are promising, Dr. Mease said in an interview that he believes there is a fair amount of work to be done before imaging analysis based on deep learning makes its way into routine clinical care. He is also hoping for methods to distinguish RA from PsA that are easier and less expensive, such as serum biomarkers. However, he agreed that a MRI-based tool could be useful when differentiating disease that is challenging.
“MRI is an expensive way for routine classification of disease, but this approach could be useful in challenging cases if the accuracy improves,” he said.
Meanwhile, other clinical researchers might want to test the principle. “You can try it,” said Dr. Simon, who reported that his team has made the methodology publicly available.
Dr. Simon reported no conflicts of interest. Dr. Mease reported financial relationships with more than 10 pharmaceutical companies, most of which make products used for the treatment of inflammatory joint diseases.
NEW YORK – On the basis of MRI images of the hand, a neural network has been trained to distinguish seronegative and seropositive rheumatoid arthritis (RA) from psoriatic arthritis (PsA) as well as from each other, according to a study that was presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
In the work so far, the neural network was correct about 70% of the time in the absence of any further clinical analyses, according to David Simon, MD, a rheumatologist in the department of internal medicine at Friedrich-Alexander University, Erlangen, Germany.
Previous to this work, “there has been no study that has exclusively used hand MRI data and deep learning without requiring further expert input for the classification of arthritides,” Dr. Simon said.
In fact, when demographic and clinical data were added, there was no improvement in the performance of patient classification relative to the deep learning classification alone, according to the data presented by Dr. Simon.
The images were evaluated with residual neural networks (ResNet), which represents a sophisticated form of deep learning to facilitate the flow of information across the network layers as they form to improve accuracy in their ability to distinguish one form of disease from the other. The training was performed on images from the T1 coronal, T2 corona1, T1 coronal fat suppressed with contrast, T1 axial fat suppressed with contrast, and T2 fat suppressed axial sequences.
The study included hand MRI scans from 135 patients with seronegative RA, 190 with seropositive RA, 177 with PsA, and 147 with psoriasis. The performance was judged on the basis of area under the receiver operating characteristics curve (AUROC) with and without input of clinical characteristics. Patients who had psoriasis without clinical arthritis were included as a control population.
The AUROC for accuracy was 75% for seropositive RA relative to PsA, 74% for seronegative RA relative to PsA, and 67% for seropositive relative to seronegative RA. Of the patients who had psoriasis without arthritis, 98% were classified as PsA and 2% as RA.
Subsequent to the classification of the patients with psoriasis, 14 of the 147 (9.5%) have developed PsA so far over a relatively short follow-up. All of these were among those identified as PsA by neural network evaluation of the hand MRIs.
This suggests that “a PsA-like pattern may be present early in the course of psoriatic disease,” Dr. Simon said.
In the groups with joint disease, who had mean ages ranging from 56 to 65, the mean disease durations were 2.6 years for those with seropositive RA, 1.3 years for those with seronegative RA, and 0.8 years for those with PsA. The patients with psoriasis were younger (mean age, 40.5 years) but had a longer disease duration (mean 4.2 years).
All of the MRI sequences were relevant for classification, but contrast did not appear to help with accuracy.
“If the images with contrast enhancement were deleted, the loss of performance was only marginal,” Dr. Simon reported.
The accuracy of neural networks increases with data, making it likely that further refinements in methodology will lead to a greater degree of accuracy, according to Dr. Simon. While the methodology is not yet ready for routine use in the clinic, the study demonstrates that neural network analysis of hand MRI to distinguish forms of arthritis “is possible.” Further studies are planned toward the goal of creating a viable clinical tool.
“Of course, if we could create an accurate tool with ultrasound, this would be even more practical,” said Dr. Simon, recognizing the value of an office tool, but he cautioned that this would be far more challenging.
“The precision of MRI is an important factor for effective neural network training,” he said.
Utility: ‘In challenging cases if the accuracy improves’?
A viable method for objectively and rapidly distinguishing inflammatory joint diseases, particularly in patients with an ambiguous clinical presentation, is an unmet need, according to Philip J. Mease, MD, director of rheumatology research at Swedish Medical Center, Seattle.
Although the data presented are promising, Dr. Mease said in an interview that he believes there is a fair amount of work to be done before imaging analysis based on deep learning makes its way into routine clinical care. He is also hoping for methods to distinguish RA from PsA that are easier and less expensive, such as serum biomarkers. However, he agreed that a MRI-based tool could be useful when differentiating disease that is challenging.
“MRI is an expensive way for routine classification of disease, but this approach could be useful in challenging cases if the accuracy improves,” he said.
Meanwhile, other clinical researchers might want to test the principle. “You can try it,” said Dr. Simon, who reported that his team has made the methodology publicly available.
Dr. Simon reported no conflicts of interest. Dr. Mease reported financial relationships with more than 10 pharmaceutical companies, most of which make products used for the treatment of inflammatory joint diseases.
AT GRAPPA 2022
New algorithm for initial PsA treatment choice is driven by T-cell behavior
T-cell behavior
Biologic selection is cytokine based
NEW YORK – An algorithm in development for psoriatic arthritis (PsA) is showing promise for directing patients to the biologic with the greatest likelihood of producing disease control, according to a proof-of-concept study presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
“Our technique involves a more precise functional assay showing exact T-cell behavior, compared to the previous assessments that only analyzed cellular phenotypes,” reported Gizem Ayan, MD, a fellow in rheumatology at Hacettepe University Faculty of Medicine, Ankara, Turkey.
The concept of precision medicine in PsA as well as other autoimmune diseases is not new. Phenotypes and biomarkers have already shown potential for guiding treatment, according to Dr. Ayan, but she said none are yet guideline recommended or proven to improve patient outcomes.
The principle of the new algorithm that she and her coinvestigators are pursing is based on immunophenotype analysis conducted with a flow-cytometric cytokine secretion assay (FCCSA). In the protocol, monocytes obtained from peripheral blood undergo activation before an FCCSA to distinguish patients by their T-cell behavior.
The treatment decision tree is based on median ratios of tumor necrosis factor (TNF)-alpha, interleukin (IL)–22, IL-17, and interferon-gamma expression among CD4+ and CD8+ cells. Based on a yes-or-no response to specific immune patterns, the patient is funneled to a biologic that inhibits a dominant cytokine.
The proof-of-concept study, which enrolled 8 patients with PsA who were naive to conventional synthetic disease-modifying antirheumatic drugs (csDMARDs) and 11 patients with PsA who were naive to biologic DMARDs (bDMARDs), was designed to demonstrate feasibility. It did not test clinical benefit, but it did show that immunophenotyping with this methodology can be performed efficiently.
“From the time a blood sample is obtained, the method provided results within 24 hours,” according to Dr. Ayan, who is now planning a randomized trial to test the ability of the algorithm to improve clinical outcomes.
In the decision tree, there are five yes-no pathways to a treatment choice. The first step of the algorithm is to test the ratio of TNF-alpha to interferon-gamma CD4+ T cells. A “yes’ response is produced if the ratio is greater than or equal to 2. These patients are then evaluated for the ratio of TNF-alpha to interferon-gamma CD8+ T cells. A yes response is produced if the ratio is greater than or equal to 0.5. If yes, they are candidates for a TNF-alpha inhibitor. If no, they are directed to an IL-12/23 inhibitor.
If the answer at the first decision point in the algorithm is a “no,” meaning they do not have a TNF-alpha to interferon-gamma CD4+ ratio of 2 or higher, they are evaluated for percentage of CD4+ T cells expressing IL-22 or IL-17. Is it greater than or equal to 2%? If the answer is “no,” they are candidates for an IL-12/23 inhibitor.
If “yes,” they are evaluated for percentage of IL-22 to IL-17 CD4+. If the IL-22 CD4+ percentage is lower than the IL-17 CD4+ percentage, meaning a “yes” to this decision point, they are directed to an IL-17 inhibitor. If the answer at this decision point is “no,” they are directed to an IL-12/23 inhibitor.
Prior to enrollment in this proof-of-concept study, 10 of the bDMARD patients were scheduled to receive an anti-TNF drug and 1 was scheduled to receive an IL-12/23 inhibitor. On the basis of this algorithm, only 5 patients were directed to an anti-TNF drug. Of the remaining, 5 were directed to an IL-17 inhibitor, and 1 was directed to an IL-12/23 inhibitor.
All 19 participants in the proof-of-concept study had peripheral arthritis; their median age was 45 years. Approximately 90% had skin lesions. Axial involvement was present in only one patient. Based on these and other characteristics and the median ratios of the cytokines measured, Dr. Ayan called this a representative population.
Based on the feasibility of this method for subtyping patients by T-cell behavior to guide drug selection, Dr. Ayan anticipates pursuing the additional steps that would show the algorithm makes a difference to patient care, including such adjunctive benefits as more cost-effective treatment selection.
“We aim to develop a treatment decision algorithm that can be implemented in daily practice,” Dr. Ayan said.
Is peripheral blood sampling adequate?
In addition to saying that the algorithm will need to prove that it alters outcomes, Samuel Tzen-yue Hwang, MD, PhD, professor and chair of the department of dermatology at the University of California, Davis, Sacramento, pointed out some potential practical issues.
“Flow cytometry is not typically available as a rapid throughput, and the cost is high,” he said. Moreover, he remains skeptical about performing this algorithm on the basis of peripheral blood samples.
“It is debatable that looking at peripheral cells would provide adequate information about what is taking place at sites of inflammation,” he said. Although it would “be fantastic” to develop an algorithm that required only a peripheral blood sample, he pointed out that “only a fraction of these cells is relevant” to disease activity.
Aspirating fluid from an involved joint “might be more useful,” but it is more work, he added. Yet, Dr. Hwang acknowledged that this approach is intriguing. He agreed that there is considerable heterogeneity among patients with PsA in their response to specific biologics, and a method to better direct patients to the treatment most likely to elicit a response is needed.
Dr. Ayan and Dr. Hwang reported no potential conflicts of interest.
Biologic selection is cytokine based
Biologic selection is cytokine based
NEW YORK – An algorithm in development for psoriatic arthritis (PsA) is showing promise for directing patients to the biologic with the greatest likelihood of producing disease control, according to a proof-of-concept study presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
“Our technique involves a more precise functional assay showing exact T-cell behavior, compared to the previous assessments that only analyzed cellular phenotypes,” reported Gizem Ayan, MD, a fellow in rheumatology at Hacettepe University Faculty of Medicine, Ankara, Turkey.
The concept of precision medicine in PsA as well as other autoimmune diseases is not new. Phenotypes and biomarkers have already shown potential for guiding treatment, according to Dr. Ayan, but she said none are yet guideline recommended or proven to improve patient outcomes.
The principle of the new algorithm that she and her coinvestigators are pursing is based on immunophenotype analysis conducted with a flow-cytometric cytokine secretion assay (FCCSA). In the protocol, monocytes obtained from peripheral blood undergo activation before an FCCSA to distinguish patients by their T-cell behavior.
The treatment decision tree is based on median ratios of tumor necrosis factor (TNF)-alpha, interleukin (IL)–22, IL-17, and interferon-gamma expression among CD4+ and CD8+ cells. Based on a yes-or-no response to specific immune patterns, the patient is funneled to a biologic that inhibits a dominant cytokine.
The proof-of-concept study, which enrolled 8 patients with PsA who were naive to conventional synthetic disease-modifying antirheumatic drugs (csDMARDs) and 11 patients with PsA who were naive to biologic DMARDs (bDMARDs), was designed to demonstrate feasibility. It did not test clinical benefit, but it did show that immunophenotyping with this methodology can be performed efficiently.
“From the time a blood sample is obtained, the method provided results within 24 hours,” according to Dr. Ayan, who is now planning a randomized trial to test the ability of the algorithm to improve clinical outcomes.
In the decision tree, there are five yes-no pathways to a treatment choice. The first step of the algorithm is to test the ratio of TNF-alpha to interferon-gamma CD4+ T cells. A “yes’ response is produced if the ratio is greater than or equal to 2. These patients are then evaluated for the ratio of TNF-alpha to interferon-gamma CD8+ T cells. A yes response is produced if the ratio is greater than or equal to 0.5. If yes, they are candidates for a TNF-alpha inhibitor. If no, they are directed to an IL-12/23 inhibitor.
If the answer at the first decision point in the algorithm is a “no,” meaning they do not have a TNF-alpha to interferon-gamma CD4+ ratio of 2 or higher, they are evaluated for percentage of CD4+ T cells expressing IL-22 or IL-17. Is it greater than or equal to 2%? If the answer is “no,” they are candidates for an IL-12/23 inhibitor.
If “yes,” they are evaluated for percentage of IL-22 to IL-17 CD4+. If the IL-22 CD4+ percentage is lower than the IL-17 CD4+ percentage, meaning a “yes” to this decision point, they are directed to an IL-17 inhibitor. If the answer at this decision point is “no,” they are directed to an IL-12/23 inhibitor.
Prior to enrollment in this proof-of-concept study, 10 of the bDMARD patients were scheduled to receive an anti-TNF drug and 1 was scheduled to receive an IL-12/23 inhibitor. On the basis of this algorithm, only 5 patients were directed to an anti-TNF drug. Of the remaining, 5 were directed to an IL-17 inhibitor, and 1 was directed to an IL-12/23 inhibitor.
All 19 participants in the proof-of-concept study had peripheral arthritis; their median age was 45 years. Approximately 90% had skin lesions. Axial involvement was present in only one patient. Based on these and other characteristics and the median ratios of the cytokines measured, Dr. Ayan called this a representative population.
Based on the feasibility of this method for subtyping patients by T-cell behavior to guide drug selection, Dr. Ayan anticipates pursuing the additional steps that would show the algorithm makes a difference to patient care, including such adjunctive benefits as more cost-effective treatment selection.
“We aim to develop a treatment decision algorithm that can be implemented in daily practice,” Dr. Ayan said.
Is peripheral blood sampling adequate?
In addition to saying that the algorithm will need to prove that it alters outcomes, Samuel Tzen-yue Hwang, MD, PhD, professor and chair of the department of dermatology at the University of California, Davis, Sacramento, pointed out some potential practical issues.
“Flow cytometry is not typically available as a rapid throughput, and the cost is high,” he said. Moreover, he remains skeptical about performing this algorithm on the basis of peripheral blood samples.
“It is debatable that looking at peripheral cells would provide adequate information about what is taking place at sites of inflammation,” he said. Although it would “be fantastic” to develop an algorithm that required only a peripheral blood sample, he pointed out that “only a fraction of these cells is relevant” to disease activity.
Aspirating fluid from an involved joint “might be more useful,” but it is more work, he added. Yet, Dr. Hwang acknowledged that this approach is intriguing. He agreed that there is considerable heterogeneity among patients with PsA in their response to specific biologics, and a method to better direct patients to the treatment most likely to elicit a response is needed.
Dr. Ayan and Dr. Hwang reported no potential conflicts of interest.
NEW YORK – An algorithm in development for psoriatic arthritis (PsA) is showing promise for directing patients to the biologic with the greatest likelihood of producing disease control, according to a proof-of-concept study presented at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
“Our technique involves a more precise functional assay showing exact T-cell behavior, compared to the previous assessments that only analyzed cellular phenotypes,” reported Gizem Ayan, MD, a fellow in rheumatology at Hacettepe University Faculty of Medicine, Ankara, Turkey.
The concept of precision medicine in PsA as well as other autoimmune diseases is not new. Phenotypes and biomarkers have already shown potential for guiding treatment, according to Dr. Ayan, but she said none are yet guideline recommended or proven to improve patient outcomes.
The principle of the new algorithm that she and her coinvestigators are pursing is based on immunophenotype analysis conducted with a flow-cytometric cytokine secretion assay (FCCSA). In the protocol, monocytes obtained from peripheral blood undergo activation before an FCCSA to distinguish patients by their T-cell behavior.
The treatment decision tree is based on median ratios of tumor necrosis factor (TNF)-alpha, interleukin (IL)–22, IL-17, and interferon-gamma expression among CD4+ and CD8+ cells. Based on a yes-or-no response to specific immune patterns, the patient is funneled to a biologic that inhibits a dominant cytokine.
The proof-of-concept study, which enrolled 8 patients with PsA who were naive to conventional synthetic disease-modifying antirheumatic drugs (csDMARDs) and 11 patients with PsA who were naive to biologic DMARDs (bDMARDs), was designed to demonstrate feasibility. It did not test clinical benefit, but it did show that immunophenotyping with this methodology can be performed efficiently.
“From the time a blood sample is obtained, the method provided results within 24 hours,” according to Dr. Ayan, who is now planning a randomized trial to test the ability of the algorithm to improve clinical outcomes.
In the decision tree, there are five yes-no pathways to a treatment choice. The first step of the algorithm is to test the ratio of TNF-alpha to interferon-gamma CD4+ T cells. A “yes’ response is produced if the ratio is greater than or equal to 2. These patients are then evaluated for the ratio of TNF-alpha to interferon-gamma CD8+ T cells. A yes response is produced if the ratio is greater than or equal to 0.5. If yes, they are candidates for a TNF-alpha inhibitor. If no, they are directed to an IL-12/23 inhibitor.
If the answer at the first decision point in the algorithm is a “no,” meaning they do not have a TNF-alpha to interferon-gamma CD4+ ratio of 2 or higher, they are evaluated for percentage of CD4+ T cells expressing IL-22 or IL-17. Is it greater than or equal to 2%? If the answer is “no,” they are candidates for an IL-12/23 inhibitor.
If “yes,” they are evaluated for percentage of IL-22 to IL-17 CD4+. If the IL-22 CD4+ percentage is lower than the IL-17 CD4+ percentage, meaning a “yes” to this decision point, they are directed to an IL-17 inhibitor. If the answer at this decision point is “no,” they are directed to an IL-12/23 inhibitor.
Prior to enrollment in this proof-of-concept study, 10 of the bDMARD patients were scheduled to receive an anti-TNF drug and 1 was scheduled to receive an IL-12/23 inhibitor. On the basis of this algorithm, only 5 patients were directed to an anti-TNF drug. Of the remaining, 5 were directed to an IL-17 inhibitor, and 1 was directed to an IL-12/23 inhibitor.
All 19 participants in the proof-of-concept study had peripheral arthritis; their median age was 45 years. Approximately 90% had skin lesions. Axial involvement was present in only one patient. Based on these and other characteristics and the median ratios of the cytokines measured, Dr. Ayan called this a representative population.
Based on the feasibility of this method for subtyping patients by T-cell behavior to guide drug selection, Dr. Ayan anticipates pursuing the additional steps that would show the algorithm makes a difference to patient care, including such adjunctive benefits as more cost-effective treatment selection.
“We aim to develop a treatment decision algorithm that can be implemented in daily practice,” Dr. Ayan said.
Is peripheral blood sampling adequate?
In addition to saying that the algorithm will need to prove that it alters outcomes, Samuel Tzen-yue Hwang, MD, PhD, professor and chair of the department of dermatology at the University of California, Davis, Sacramento, pointed out some potential practical issues.
“Flow cytometry is not typically available as a rapid throughput, and the cost is high,” he said. Moreover, he remains skeptical about performing this algorithm on the basis of peripheral blood samples.
“It is debatable that looking at peripheral cells would provide adequate information about what is taking place at sites of inflammation,” he said. Although it would “be fantastic” to develop an algorithm that required only a peripheral blood sample, he pointed out that “only a fraction of these cells is relevant” to disease activity.
Aspirating fluid from an involved joint “might be more useful,” but it is more work, he added. Yet, Dr. Hwang acknowledged that this approach is intriguing. He agreed that there is considerable heterogeneity among patients with PsA in their response to specific biologics, and a method to better direct patients to the treatment most likely to elicit a response is needed.
Dr. Ayan and Dr. Hwang reported no potential conflicts of interest.
T-cell behavior
T-cell behavior
AT GRAPPA 2022