User login
Prostatectomy vs. radiotherapy: 15-year functional outcomes are same
Fifteen years after treatment for localized prostate cancer, men who underwent radical prostatectomy reported no differences in urinary, bowel, or sexual function compared with men who underwent external-beam radiation, according to a report published online Jan. 30 in the New England Journal of Medicine.
Using data from the Prostate Cancer Outcomes Study (PCOS), a population-based cohort of men across the United States diagnosed as having prostate cancer in the mid-1990s, researchers tracked the long-term disease-specific outcomes of 1,655 men who underwent radical prostatectomy (70.3% of patients) or radiotherapy (29.7%), with or without androgen-deprivation therapy.
Source: American Gastroenterological Association (www.youtube.com/AmerGastroAssn)
"Since the median life expectancy after treatment for prostate cancer is 13.8 years, a careful evaluation of long-term functional outcomes is critical to an understanding of the comprehensive experience of men living with a diagnosis of prostate cancer," said Dr. Matthew J. Resnick of the department of urologic surgery and the Center for Surgical Quality and Outcomes Research, Vanderbilt University, Nashville, Tenn., and his associates.
Even though men who had radical prostatectomy were more likely to be bothered by such difficulties as urinary incontinence, bowel urgency, and erectile dysfunction at 2 years and 5 years after treatment, those differences disappeared by the 15-year mark. At that time, the prevalence of ED was "nearly universal," affecting 87% of men in the prostatectomy group and 94% of those in the radiotherapy group; yet only 43% and 38%, respectively, reported that this bothered them.
"Long-term follow-up reveals consistent functional declines after 5 years. It remains unknown whether this continued decline is due to prostate cancer and its treatment, the normal aging process, or a combination of factors," the investigators said (N. Engl. J. Med. 2013 [doi10.1056/NEJMoa1209978]).
This study was funded by the National Cancer Institute. Dr. Resnick was supported by the VA National Quality Scholars Program and the T. J. Martell Foundation. Dr. Resnick reported ties to Dendreon and Bayer Healthcare, and his associates reported ties to Ferring and Johnson & Johnson.
Fifteen years after treatment for localized prostate cancer, men who underwent radical prostatectomy reported no differences in urinary, bowel, or sexual function compared with men who underwent external-beam radiation, according to a report published online Jan. 30 in the New England Journal of Medicine.
Using data from the Prostate Cancer Outcomes Study (PCOS), a population-based cohort of men across the United States diagnosed as having prostate cancer in the mid-1990s, researchers tracked the long-term disease-specific outcomes of 1,655 men who underwent radical prostatectomy (70.3% of patients) or radiotherapy (29.7%), with or without androgen-deprivation therapy.
Source: American Gastroenterological Association (www.youtube.com/AmerGastroAssn)
"Since the median life expectancy after treatment for prostate cancer is 13.8 years, a careful evaluation of long-term functional outcomes is critical to an understanding of the comprehensive experience of men living with a diagnosis of prostate cancer," said Dr. Matthew J. Resnick of the department of urologic surgery and the Center for Surgical Quality and Outcomes Research, Vanderbilt University, Nashville, Tenn., and his associates.
Even though men who had radical prostatectomy were more likely to be bothered by such difficulties as urinary incontinence, bowel urgency, and erectile dysfunction at 2 years and 5 years after treatment, those differences disappeared by the 15-year mark. At that time, the prevalence of ED was "nearly universal," affecting 87% of men in the prostatectomy group and 94% of those in the radiotherapy group; yet only 43% and 38%, respectively, reported that this bothered them.
"Long-term follow-up reveals consistent functional declines after 5 years. It remains unknown whether this continued decline is due to prostate cancer and its treatment, the normal aging process, or a combination of factors," the investigators said (N. Engl. J. Med. 2013 [doi10.1056/NEJMoa1209978]).
This study was funded by the National Cancer Institute. Dr. Resnick was supported by the VA National Quality Scholars Program and the T. J. Martell Foundation. Dr. Resnick reported ties to Dendreon and Bayer Healthcare, and his associates reported ties to Ferring and Johnson & Johnson.
Fifteen years after treatment for localized prostate cancer, men who underwent radical prostatectomy reported no differences in urinary, bowel, or sexual function compared with men who underwent external-beam radiation, according to a report published online Jan. 30 in the New England Journal of Medicine.
Using data from the Prostate Cancer Outcomes Study (PCOS), a population-based cohort of men across the United States diagnosed as having prostate cancer in the mid-1990s, researchers tracked the long-term disease-specific outcomes of 1,655 men who underwent radical prostatectomy (70.3% of patients) or radiotherapy (29.7%), with or without androgen-deprivation therapy.
Source: American Gastroenterological Association (www.youtube.com/AmerGastroAssn)
"Since the median life expectancy after treatment for prostate cancer is 13.8 years, a careful evaluation of long-term functional outcomes is critical to an understanding of the comprehensive experience of men living with a diagnosis of prostate cancer," said Dr. Matthew J. Resnick of the department of urologic surgery and the Center for Surgical Quality and Outcomes Research, Vanderbilt University, Nashville, Tenn., and his associates.
Even though men who had radical prostatectomy were more likely to be bothered by such difficulties as urinary incontinence, bowel urgency, and erectile dysfunction at 2 years and 5 years after treatment, those differences disappeared by the 15-year mark. At that time, the prevalence of ED was "nearly universal," affecting 87% of men in the prostatectomy group and 94% of those in the radiotherapy group; yet only 43% and 38%, respectively, reported that this bothered them.
"Long-term follow-up reveals consistent functional declines after 5 years. It remains unknown whether this continued decline is due to prostate cancer and its treatment, the normal aging process, or a combination of factors," the investigators said (N. Engl. J. Med. 2013 [doi10.1056/NEJMoa1209978]).
This study was funded by the National Cancer Institute. Dr. Resnick was supported by the VA National Quality Scholars Program and the T. J. Martell Foundation. Dr. Resnick reported ties to Dendreon and Bayer Healthcare, and his associates reported ties to Ferring and Johnson & Johnson.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Major Finding: At 15-year follow-up, there were no significant differences in urinary, bowel, or sexual function between 1,164 men who had undergone radical prostatectomy and 491 who had undergone radiotherapy for localized prostate cancer.
Data Source: Long-term follow-up of 1,655 men participating in the Prostate Cancer Outcomes Study, a population-based prospective study of men in six states who were diagnosed as having localized prostate cancer in the mid-1990s.
Disclosures: This study was funded by the National Cancer Institute. Dr. Resnick was supported by the VA National Quality Scholars Program and the T. J. Martell Foundation. Dr. Resnick reported ties to Dendreon and Bayer Healthcare, and his associates reported ties to Ferring and Johnson & Johnson.
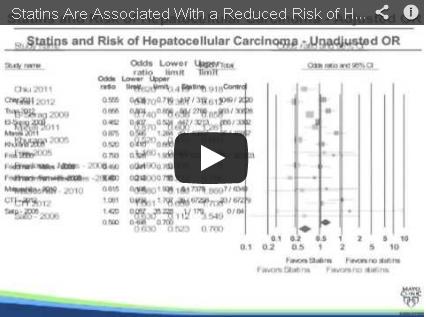
Statins cut risk of hepatocellular carcinoma
Statin therapy taken to prevent cardiovascular events also appears to protect against hepatocellular carcinoma, reducing the overall risk for the cancer by 37%, according to the results of a systematic review and meta-analysis.
In a meta-analysis of all the studies in the literature that have examined statins’ effect on HCC risk, use of the drugs was associated with a pronounced and consistent risk reduction (48%) in Asian populations, as well as a still-significant reduction (33%) in Western populations, reported Dr. Siddharth Singh and his associates at the Mayo Clinic, Rochester, Minn.
Video source: American Gastroenterological Association's YouTube page
At present, "it does not seem prudent to prescribe statins for chemoprevention" of HCC in the general population, mainly because of the high number of people who would need to be treated to prevent a single case of HCC. "However, in patients with multiple risk factors, such as East Asian men who have chronic HBV [hepatitis B virus] infection, statins may have a clinically relevant chemoprotective effect against HCC, the investigators said (Gastroenterology 2012 Oct. 15 [doi: 10.1053/j.gastro.2012.10.005]).
Prospective cohort studies or randomized clinical trials of the issue are warranted in populations at high risk for HCC, they noted.
The results of preclinical studies have suggested that statins may decrease the risk of cancers, perhaps because their antiproliferative, proapoptotic, antiangiogenic, immunomodulatory, and anti-infective effects may prevent cancer growth. But clinical studies have produced conflicting results.
Dr. Singh and his colleagues performed a systematic review of the literature for studies that clearly defined statin exposure, reported HCC risk, and either reported relative risks or odds ratios for the development of HCC or provided the data so those risks could be calculated. They then performed a meta-analysis of 10 studies: 7 observational studies and 3 that reported pooled data from 26 randomized clinical trials.
Most of the studies were considered to be of high quality. Most of them accounted for various potential confounders such as patient age; sex; medication use; and the presence of viral hepatitis, cirrhosis, diabetes, or alcoholic liver disease. The likelihood of selection bias and of publication bias in the included studies was judged to be very low.
Altogether the 10 studies included 1,459,417 subjects and 4,298 cases of HCC.
In an initial analysis of the data, the use of statins was associated with a significant 41% reduction in the rate of HCC. After the data were adjusted to account for several potential confounders, the risk reduction was altered slightly, but a robust 37% reduction in HCC rate remained.
The investigators also performed an analysis of the data based on the location of the studies, because the epidemiology of HCC is so different between Western and Asian populations. They found that statin use correlated with a 48% reduction in the rate of HCC in Asian populations, where viral hepatitis is the primary risk factor for the disease, and a 33% reduction in the rate of HCC in Western populations, where the metabolic syndrome, nonalcoholic fatty liver disease, and alcohol-related cirrhosis are the primary risk factors.
The researchers also performed sensitivity analyses according to the studies’ design (cohort vs. case control) and quality (high vs. low). Both cohort and case-control studies confirmed a protective effect of statins against the development of HCC, as did both high-quality and low-quality studies.
In a final sensitivity analysis, each study was serially excluded from the meta-analysis to determine whether any one study was having a dominant effect on the odds ratios. None of the studies was found to markedly affect the outcomes of the analyses.
The study design didn’t permit separate analyses of the protective effects of statins by drug type or by dose or duration of therapy.
The studies included in this meta-analysis were too heterogeneous to allow the investigators to calculate an overall number needed to treat. But the studies restricted to Asian patients were homogeneous and did allow this calculation for men of Asian ethnicity.
Dr. Singh and his associates determined that 5,209 East Asian men would need to be treated with statins to prevent 1 case of HCC per year. For very-high-risk Asian men with chronic HBV-associated cirrhosis, the number needed to treat with statins to prevent 1 case of HCC per year would be 57.
No financial conflicts of interest were reported.
Statin therapy taken to prevent cardiovascular events also appears to protect against hepatocellular carcinoma, reducing the overall risk for the cancer by 37%, according to the results of a systematic review and meta-analysis.
In a meta-analysis of all the studies in the literature that have examined statins’ effect on HCC risk, use of the drugs was associated with a pronounced and consistent risk reduction (48%) in Asian populations, as well as a still-significant reduction (33%) in Western populations, reported Dr. Siddharth Singh and his associates at the Mayo Clinic, Rochester, Minn.
Video source: American Gastroenterological Association's YouTube page
At present, "it does not seem prudent to prescribe statins for chemoprevention" of HCC in the general population, mainly because of the high number of people who would need to be treated to prevent a single case of HCC. "However, in patients with multiple risk factors, such as East Asian men who have chronic HBV [hepatitis B virus] infection, statins may have a clinically relevant chemoprotective effect against HCC, the investigators said (Gastroenterology 2012 Oct. 15 [doi: 10.1053/j.gastro.2012.10.005]).
Prospective cohort studies or randomized clinical trials of the issue are warranted in populations at high risk for HCC, they noted.
The results of preclinical studies have suggested that statins may decrease the risk of cancers, perhaps because their antiproliferative, proapoptotic, antiangiogenic, immunomodulatory, and anti-infective effects may prevent cancer growth. But clinical studies have produced conflicting results.
Dr. Singh and his colleagues performed a systematic review of the literature for studies that clearly defined statin exposure, reported HCC risk, and either reported relative risks or odds ratios for the development of HCC or provided the data so those risks could be calculated. They then performed a meta-analysis of 10 studies: 7 observational studies and 3 that reported pooled data from 26 randomized clinical trials.
Most of the studies were considered to be of high quality. Most of them accounted for various potential confounders such as patient age; sex; medication use; and the presence of viral hepatitis, cirrhosis, diabetes, or alcoholic liver disease. The likelihood of selection bias and of publication bias in the included studies was judged to be very low.
Altogether the 10 studies included 1,459,417 subjects and 4,298 cases of HCC.
In an initial analysis of the data, the use of statins was associated with a significant 41% reduction in the rate of HCC. After the data were adjusted to account for several potential confounders, the risk reduction was altered slightly, but a robust 37% reduction in HCC rate remained.
The investigators also performed an analysis of the data based on the location of the studies, because the epidemiology of HCC is so different between Western and Asian populations. They found that statin use correlated with a 48% reduction in the rate of HCC in Asian populations, where viral hepatitis is the primary risk factor for the disease, and a 33% reduction in the rate of HCC in Western populations, where the metabolic syndrome, nonalcoholic fatty liver disease, and alcohol-related cirrhosis are the primary risk factors.
The researchers also performed sensitivity analyses according to the studies’ design (cohort vs. case control) and quality (high vs. low). Both cohort and case-control studies confirmed a protective effect of statins against the development of HCC, as did both high-quality and low-quality studies.
In a final sensitivity analysis, each study was serially excluded from the meta-analysis to determine whether any one study was having a dominant effect on the odds ratios. None of the studies was found to markedly affect the outcomes of the analyses.
The study design didn’t permit separate analyses of the protective effects of statins by drug type or by dose or duration of therapy.
The studies included in this meta-analysis were too heterogeneous to allow the investigators to calculate an overall number needed to treat. But the studies restricted to Asian patients were homogeneous and did allow this calculation for men of Asian ethnicity.
Dr. Singh and his associates determined that 5,209 East Asian men would need to be treated with statins to prevent 1 case of HCC per year. For very-high-risk Asian men with chronic HBV-associated cirrhosis, the number needed to treat with statins to prevent 1 case of HCC per year would be 57.
No financial conflicts of interest were reported.
Statin therapy taken to prevent cardiovascular events also appears to protect against hepatocellular carcinoma, reducing the overall risk for the cancer by 37%, according to the results of a systematic review and meta-analysis.
In a meta-analysis of all the studies in the literature that have examined statins’ effect on HCC risk, use of the drugs was associated with a pronounced and consistent risk reduction (48%) in Asian populations, as well as a still-significant reduction (33%) in Western populations, reported Dr. Siddharth Singh and his associates at the Mayo Clinic, Rochester, Minn.
Video source: American Gastroenterological Association's YouTube page
At present, "it does not seem prudent to prescribe statins for chemoprevention" of HCC in the general population, mainly because of the high number of people who would need to be treated to prevent a single case of HCC. "However, in patients with multiple risk factors, such as East Asian men who have chronic HBV [hepatitis B virus] infection, statins may have a clinically relevant chemoprotective effect against HCC, the investigators said (Gastroenterology 2012 Oct. 15 [doi: 10.1053/j.gastro.2012.10.005]).
Prospective cohort studies or randomized clinical trials of the issue are warranted in populations at high risk for HCC, they noted.
The results of preclinical studies have suggested that statins may decrease the risk of cancers, perhaps because their antiproliferative, proapoptotic, antiangiogenic, immunomodulatory, and anti-infective effects may prevent cancer growth. But clinical studies have produced conflicting results.
Dr. Singh and his colleagues performed a systematic review of the literature for studies that clearly defined statin exposure, reported HCC risk, and either reported relative risks or odds ratios for the development of HCC or provided the data so those risks could be calculated. They then performed a meta-analysis of 10 studies: 7 observational studies and 3 that reported pooled data from 26 randomized clinical trials.
Most of the studies were considered to be of high quality. Most of them accounted for various potential confounders such as patient age; sex; medication use; and the presence of viral hepatitis, cirrhosis, diabetes, or alcoholic liver disease. The likelihood of selection bias and of publication bias in the included studies was judged to be very low.
Altogether the 10 studies included 1,459,417 subjects and 4,298 cases of HCC.
In an initial analysis of the data, the use of statins was associated with a significant 41% reduction in the rate of HCC. After the data were adjusted to account for several potential confounders, the risk reduction was altered slightly, but a robust 37% reduction in HCC rate remained.
The investigators also performed an analysis of the data based on the location of the studies, because the epidemiology of HCC is so different between Western and Asian populations. They found that statin use correlated with a 48% reduction in the rate of HCC in Asian populations, where viral hepatitis is the primary risk factor for the disease, and a 33% reduction in the rate of HCC in Western populations, where the metabolic syndrome, nonalcoholic fatty liver disease, and alcohol-related cirrhosis are the primary risk factors.
The researchers also performed sensitivity analyses according to the studies’ design (cohort vs. case control) and quality (high vs. low). Both cohort and case-control studies confirmed a protective effect of statins against the development of HCC, as did both high-quality and low-quality studies.
In a final sensitivity analysis, each study was serially excluded from the meta-analysis to determine whether any one study was having a dominant effect on the odds ratios. None of the studies was found to markedly affect the outcomes of the analyses.
The study design didn’t permit separate analyses of the protective effects of statins by drug type or by dose or duration of therapy.
The studies included in this meta-analysis were too heterogeneous to allow the investigators to calculate an overall number needed to treat. But the studies restricted to Asian patients were homogeneous and did allow this calculation for men of Asian ethnicity.
Dr. Singh and his associates determined that 5,209 East Asian men would need to be treated with statins to prevent 1 case of HCC per year. For very-high-risk Asian men with chronic HBV-associated cirrhosis, the number needed to treat with statins to prevent 1 case of HCC per year would be 57.
No financial conflicts of interest were reported.
FROM GASTROENTEROLOGY
Major Finding: Statin therapy reduced the risk of developing hepatocellular carcinoma by 37% overall; the risk reduction was stronger (48%) in Asian populations but still significant (33%) in Western populations.
Data Source: A systematic review and meta-analysis of 10 observational studies or randomized clinical trials involving 1,459,417 subjects, of whom 4,298 developed HCC during follow-up.
Disclosures: No financial conflicts of interest were reported.
Anesthesia assistance used in 9% of routine colonoscopies
Nearly 9% of all routine outpatient colonoscopies that were performed in 1 year in a nationally representative sample of Medicare beneficiaries used anesthesia assistance – an anesthesiologist or nurse-anesthetist – to administer deep sedation using propofol.
The American Society for Gastrointestinal Endoscopy recommends against anesthesia assistance for such average-risk patients because it isn’t warranted and is cost-prohibitive. Nevertheless, in this retrospective cohort study using a nationally representative sample of 328,177 Medicare patients who underwent routine outpatient colonoscopy during 2003, anesthesia assistance was used in 8.7% of the procedures. This included 8.2% of procedures done in patients who had no comorbidities (Gastroenterology 2012 Oct. 29 [doi: 10.1053/j.gastro.2012.10.038]).
The researchers, led by Dr. Jason A. Dominitz of the VA Puget Sound Health Care System in Seattle, found that the use of anesthesia assistance varied dramatically by geographic location and by the endoscopist’s specialty. A very small proportion of the endoscopists in this study, 4.5%, accounted for more than 40% of the procedures performed using anesthesia assistance.
"Those endoscopists with very high rates of anesthesia assistance overwhelmingly practiced in an urban setting (95%) and were disproportionately represented by gastroenterologists (76%) and colorectal surgeons (10%)," as compared with general surgeons, internists, family physicians, or others.
"This practice has enormous economic implications for society, as the use of an anesthesia provider adds a considerable cost to each procedure and is at variance with recommendations from professional societies. In 2003, charges to Medicare for sedation by anesthesia professionals during colonoscopy were nearly $80 million," said Dr. Dominitz, who is also with the division of gastroenterology at the University of Washington, Seattle, and his associates.
"If the projected growth in the use of anesthesia assistance does reach 53% by 2015, the total national expenditure for this service could range from approximately $800 million to $3.8 billion annually," they noted.
The investigators studied this issue because the use of propofol for deep sedation during routine colonoscopies has increased markedly.
The study sample included only colonoscopies performed in hospital outpatient clinics, ambulatory surgery centers, private offices, and other outpatient settings by 18,578 physicians.
Among the study’s findings:
• Use of anesthesia assistance didn’t alter the rate of detection of colonic polyps or the rate of complications such as GI bleeding, perforation, and hospital/ED visits within 30 days.
• Use of anesthesia assistance varied widely among the states, and even between states that bordered each other. The lowest rates of use were in Montana (0.1%) and South Dakota (0.2%); the highest were in New Jersey (48.1%), New York (27.9%), and Nevada (26.0%). "This variation is most likely attributable to variation in reimbursement practices by different carriers," Dr. Dominitz and his associates said.
• Younger endoscopists and those with fewer years in practice were more likely than older endoscopists and those with more years in practice to use anesthesia assistance.
• The volume of patients seen by the endoscopist did not correlate with use of anesthesia assistance.
• More than 80% of general surgeons, internists, and family physicians performed no colonoscopies with anesthesia assistance.
• Anesthesia assistance was more frequently used in black than in white patients, perhaps because of the very high rates of use in urban settings, where there is more racial diversity. Urban patients were more than twice as likely to receive anesthesia assistance as rural patients.
In a sensitivity analysis excluding patients with comorbidities, the findings confirmed those of the main analysis.
This study was not designed to determine the reasons for these variations in the use of anesthesia assistance. However, the researchers speculated that because propofol has a faster onset and more rapid recovery time than opiates and benzodiazepines, it improves practice efficiency, allowing more procedures to be performed per day.
In addition, employing anesthesia providers can generate an extra income stream for endoscopy practices. And if endoscopists who practice outside of hospitals already employ anesthesia providers for higher-risk or hard-to-sedate patients, "it may be prudent business practice to utilize these providers for more routine cases as well," Dr. Dominitz and his colleagues said.
This study was supported by the American College of Gastroenterology, the American Society for Gastrointestinal Endoscopy, and the VA Puget Sound Health Care System. No financial conflicts of interest were reported.
Nearly 9% of all routine outpatient colonoscopies that were performed in 1 year in a nationally representative sample of Medicare beneficiaries used anesthesia assistance – an anesthesiologist or nurse-anesthetist – to administer deep sedation using propofol.
The American Society for Gastrointestinal Endoscopy recommends against anesthesia assistance for such average-risk patients because it isn’t warranted and is cost-prohibitive. Nevertheless, in this retrospective cohort study using a nationally representative sample of 328,177 Medicare patients who underwent routine outpatient colonoscopy during 2003, anesthesia assistance was used in 8.7% of the procedures. This included 8.2% of procedures done in patients who had no comorbidities (Gastroenterology 2012 Oct. 29 [doi: 10.1053/j.gastro.2012.10.038]).
The researchers, led by Dr. Jason A. Dominitz of the VA Puget Sound Health Care System in Seattle, found that the use of anesthesia assistance varied dramatically by geographic location and by the endoscopist’s specialty. A very small proportion of the endoscopists in this study, 4.5%, accounted for more than 40% of the procedures performed using anesthesia assistance.
"Those endoscopists with very high rates of anesthesia assistance overwhelmingly practiced in an urban setting (95%) and were disproportionately represented by gastroenterologists (76%) and colorectal surgeons (10%)," as compared with general surgeons, internists, family physicians, or others.
"This practice has enormous economic implications for society, as the use of an anesthesia provider adds a considerable cost to each procedure and is at variance with recommendations from professional societies. In 2003, charges to Medicare for sedation by anesthesia professionals during colonoscopy were nearly $80 million," said Dr. Dominitz, who is also with the division of gastroenterology at the University of Washington, Seattle, and his associates.
"If the projected growth in the use of anesthesia assistance does reach 53% by 2015, the total national expenditure for this service could range from approximately $800 million to $3.8 billion annually," they noted.
The investigators studied this issue because the use of propofol for deep sedation during routine colonoscopies has increased markedly.
The study sample included only colonoscopies performed in hospital outpatient clinics, ambulatory surgery centers, private offices, and other outpatient settings by 18,578 physicians.
Among the study’s findings:
• Use of anesthesia assistance didn’t alter the rate of detection of colonic polyps or the rate of complications such as GI bleeding, perforation, and hospital/ED visits within 30 days.
• Use of anesthesia assistance varied widely among the states, and even between states that bordered each other. The lowest rates of use were in Montana (0.1%) and South Dakota (0.2%); the highest were in New Jersey (48.1%), New York (27.9%), and Nevada (26.0%). "This variation is most likely attributable to variation in reimbursement practices by different carriers," Dr. Dominitz and his associates said.
• Younger endoscopists and those with fewer years in practice were more likely than older endoscopists and those with more years in practice to use anesthesia assistance.
• The volume of patients seen by the endoscopist did not correlate with use of anesthesia assistance.
• More than 80% of general surgeons, internists, and family physicians performed no colonoscopies with anesthesia assistance.
• Anesthesia assistance was more frequently used in black than in white patients, perhaps because of the very high rates of use in urban settings, where there is more racial diversity. Urban patients were more than twice as likely to receive anesthesia assistance as rural patients.
In a sensitivity analysis excluding patients with comorbidities, the findings confirmed those of the main analysis.
This study was not designed to determine the reasons for these variations in the use of anesthesia assistance. However, the researchers speculated that because propofol has a faster onset and more rapid recovery time than opiates and benzodiazepines, it improves practice efficiency, allowing more procedures to be performed per day.
In addition, employing anesthesia providers can generate an extra income stream for endoscopy practices. And if endoscopists who practice outside of hospitals already employ anesthesia providers for higher-risk or hard-to-sedate patients, "it may be prudent business practice to utilize these providers for more routine cases as well," Dr. Dominitz and his colleagues said.
This study was supported by the American College of Gastroenterology, the American Society for Gastrointestinal Endoscopy, and the VA Puget Sound Health Care System. No financial conflicts of interest were reported.
Nearly 9% of all routine outpatient colonoscopies that were performed in 1 year in a nationally representative sample of Medicare beneficiaries used anesthesia assistance – an anesthesiologist or nurse-anesthetist – to administer deep sedation using propofol.
The American Society for Gastrointestinal Endoscopy recommends against anesthesia assistance for such average-risk patients because it isn’t warranted and is cost-prohibitive. Nevertheless, in this retrospective cohort study using a nationally representative sample of 328,177 Medicare patients who underwent routine outpatient colonoscopy during 2003, anesthesia assistance was used in 8.7% of the procedures. This included 8.2% of procedures done in patients who had no comorbidities (Gastroenterology 2012 Oct. 29 [doi: 10.1053/j.gastro.2012.10.038]).
The researchers, led by Dr. Jason A. Dominitz of the VA Puget Sound Health Care System in Seattle, found that the use of anesthesia assistance varied dramatically by geographic location and by the endoscopist’s specialty. A very small proportion of the endoscopists in this study, 4.5%, accounted for more than 40% of the procedures performed using anesthesia assistance.
"Those endoscopists with very high rates of anesthesia assistance overwhelmingly practiced in an urban setting (95%) and were disproportionately represented by gastroenterologists (76%) and colorectal surgeons (10%)," as compared with general surgeons, internists, family physicians, or others.
"This practice has enormous economic implications for society, as the use of an anesthesia provider adds a considerable cost to each procedure and is at variance with recommendations from professional societies. In 2003, charges to Medicare for sedation by anesthesia professionals during colonoscopy were nearly $80 million," said Dr. Dominitz, who is also with the division of gastroenterology at the University of Washington, Seattle, and his associates.
"If the projected growth in the use of anesthesia assistance does reach 53% by 2015, the total national expenditure for this service could range from approximately $800 million to $3.8 billion annually," they noted.
The investigators studied this issue because the use of propofol for deep sedation during routine colonoscopies has increased markedly.
The study sample included only colonoscopies performed in hospital outpatient clinics, ambulatory surgery centers, private offices, and other outpatient settings by 18,578 physicians.
Among the study’s findings:
• Use of anesthesia assistance didn’t alter the rate of detection of colonic polyps or the rate of complications such as GI bleeding, perforation, and hospital/ED visits within 30 days.
• Use of anesthesia assistance varied widely among the states, and even between states that bordered each other. The lowest rates of use were in Montana (0.1%) and South Dakota (0.2%); the highest were in New Jersey (48.1%), New York (27.9%), and Nevada (26.0%). "This variation is most likely attributable to variation in reimbursement practices by different carriers," Dr. Dominitz and his associates said.
• Younger endoscopists and those with fewer years in practice were more likely than older endoscopists and those with more years in practice to use anesthesia assistance.
• The volume of patients seen by the endoscopist did not correlate with use of anesthesia assistance.
• More than 80% of general surgeons, internists, and family physicians performed no colonoscopies with anesthesia assistance.
• Anesthesia assistance was more frequently used in black than in white patients, perhaps because of the very high rates of use in urban settings, where there is more racial diversity. Urban patients were more than twice as likely to receive anesthesia assistance as rural patients.
In a sensitivity analysis excluding patients with comorbidities, the findings confirmed those of the main analysis.
This study was not designed to determine the reasons for these variations in the use of anesthesia assistance. However, the researchers speculated that because propofol has a faster onset and more rapid recovery time than opiates and benzodiazepines, it improves practice efficiency, allowing more procedures to be performed per day.
In addition, employing anesthesia providers can generate an extra income stream for endoscopy practices. And if endoscopists who practice outside of hospitals already employ anesthesia providers for higher-risk or hard-to-sedate patients, "it may be prudent business practice to utilize these providers for more routine cases as well," Dr. Dominitz and his colleagues said.
This study was supported by the American College of Gastroenterology, the American Society for Gastrointestinal Endoscopy, and the VA Puget Sound Health Care System. No financial conflicts of interest were reported.
FROM GASTROENTEROLOGY
Major Finding: The use of anesthesia assistance for routine outpatient colonoscopies was 8.7%, and the rate of use varied dramatically by practice location and physician specialty.
Data Source: A retrospective cohort study involving a nationally representative sample of 328,177 Medicare patients who saw 18,578 physicians for routine outpatient colonoscopy in 2003.
Disclosures: This study was supported by the American College of Gastroenterology, the American Society for Gastrointestinal Endoscopy, and the VA Puget Sound Health Care System. No financial conflicts of interest were reported.
Manometry, esophagram combo detects achalasia posttreatment problems
High-resolution manometry with esophageal pressure topography is known to improve the accuracy of manometry for detecting achalasia and defined clinically relevant subtypes prior to treatment, but new data demonstrate that the procedure also is useful for evaluating treatment efficacy.
In a study of 31 men and 19 women aged 20-79 years, resolution of the achalasia pattern on high-resolution manometry with esophageal pressure topography (HRM-EPT) after treatment was associated with symptom improvement and reduced bolus retention, reported Dr. Frédéric Nicodème of Northwestern University, Chicago, and his colleagues.
Video source: American Gastroenterological Association's YouTube Channel
Study participants included one cohort of 25 patients who underwent endoscopy, HRM, timed barium esophagram (TBE) following a 200-mL barium swallow, and symptom assessment before treatment, and a second cohort of 25 treated patients who had pretreatment type 1 or 2 achalasia and who were undergoing a posttreatment study protocol including HRM, TBE, endoscopy, and symptom assessment. The investigators assessed dysphagia, regurgitation, retrosternal pain, and weight loss and used them to calculate an Eckardt score (ES) for both cohorts.
In the untreated cohort, which included 10 patients with type 1 achalasia and 15 with type 2 achalasia, the key EPT metric of integrated relaxation pressure (IRP) was significantly greater in the type 2 patients, as was the nadir-relaxation pressure. No differences were seen based on disease type with respect to resting esophagogastric junction (EGJ) pressure, barium column height, barium column width, or ES (Clin. Gastroenterol. Hepatol. 2012 Oct. 12 [doi: 10.1016/j.cgh.2012.10.015]).
No correlation was found between TBE column height at 5 minutes and IRP, resting EGJ pressure, nadir-EGJ relaxation pressure, or ES, and no correlation was seen between ES and IRP, resting EGJ pressure, or nadir-EGJ relaxation pressure.
In the posttreatment cohort, 10 patients, including 6 with type 1 disease and 4 with type 2 disease, had EPT findings of persistent achalasia pattern, and 15 had resolution of the achalasia pattern. Of these 15 patients, 8 converted to absent peristalsis and 7 to weak peristalsis.
"The IRP, resting EGJ pressure, and nadir-EGJ were all significantly correlated with posttreatment ES," the investigators noted.
Furthermore, TBE column height at 5 minutes, IRP, and ES were significantly lower in patients with resolved achalasia patterns on HRM than in those with a persistent achalasia pattern; the subgroup of 7 patients with weak peristalsis appeared to have the best outcome.
"The median TBE column height at 5 minutes was significantly lower [in those with weak peristalsis] than the three other groups, and ES showed a trend toward a lower value compared to the other 3 groups," they explained.
No significant correlations between TBE column height at 5 minutes and resting EGJ pressure or nadir-EGJ relaxation pressure were noted in the posttreatment patients. Only the IRP showed a weak correlation.
"The correlation between TBE column height at 5 minutes and ES after treatment was also not significant. However, the median TBE column height at 5 minutes for patients with an ES of 3 or greater was significantly greater than that for patients with an ES less than 3," they wrote.
"Our findings suggest that resolution of the achalasia pattern on EPT after treatment was associated with an improvement in symptoms and reduced bolus retention. Although the IRP was not strongly linearly correlated with symptom severity, when analyzed dichotomously patients with an IRP greater than or equal to 15 mm Hg had worse symptom scores and greater bolus retention on TBE compared to those with normal IRP values," the investigators wrote.
In contrast, no EPT pattern or metric, and no TBE variable predicted symptom severity in the untreated cohort, and barium height on TBE did not distinguish achalasia EPT subtypes, they noted.
"These findings suggest that in addition to its proven utility in detecting pretreatment achalasia, EPT also has utility in the management of posttreatment achalasia that can complement TBE," they said.
Although TBE did not distinguish disease subtypes, it does complement EPT, especially when the disease has progressed to an anatomic-dominant disorder, they said. Additional studies in larger series of patients are needed before and after therapy to confidently establish the relative merits of each evaluation with respect to the prediction of long-term outcomes and cost-effectiveness, they said.
This study was supported by the Public Health Service. The authors reported having no disclosures.
Most patients with achalasia do well in the postoperative period after either pneumatic dilation (PD) or laparoscopic surgical myotomy, with an initial success rate as high as 90% after 2 years. However, predicting failure based on symptom recurrence is problematic, as symptoms are often underreported or absent due to esophageal dilation or impaired esophageal sensation. Thus, a strategy of avoiding esophageal decompensation due to delayed diagnosis cannot solely rely on patient report of symptom recurrence. Objective testing by barium esophagram or esophageal manometry may be needed.

|
|
This study adds new knowledge regarding the benefit of high-resolution manometry (HRM) in the management of posttreatment achalasia. The novelty of the study is in its use of timed barium esophagram (TBE), HRM, and symptoms in a group of patients with achalasia pre- and posttherapy. TBE was previously advocated as the objective test of choice; however, this study suggests that TBE and HRM may be complementary in this regard.
What is clear from this report as well as others regarding objective testing in achalasia is that patients’ symptoms alone are a poor marker of esophageal emptying. Posttherapy testing with HRM and/or TBE with special emphasis on bolus emptying should be employed in order to avoid long-term complications with achalasia. The choice between the tests may depend on the expertise and availability of each of the proposed test modalities.
Dr. Vaezi is clinical director of the division of gastroenterology, hepatology, and nutrition, and director of the Center for Swallowing and Esophageal Disorders and Clinical Research at Vanderbilt University Medical Center, Nashville, Tenn. He said he had no conflicts of interest to disclose.
Most patients with achalasia do well in the postoperative period after either pneumatic dilation (PD) or laparoscopic surgical myotomy, with an initial success rate as high as 90% after 2 years. However, predicting failure based on symptom recurrence is problematic, as symptoms are often underreported or absent due to esophageal dilation or impaired esophageal sensation. Thus, a strategy of avoiding esophageal decompensation due to delayed diagnosis cannot solely rely on patient report of symptom recurrence. Objective testing by barium esophagram or esophageal manometry may be needed.

|
|
This study adds new knowledge regarding the benefit of high-resolution manometry (HRM) in the management of posttreatment achalasia. The novelty of the study is in its use of timed barium esophagram (TBE), HRM, and symptoms in a group of patients with achalasia pre- and posttherapy. TBE was previously advocated as the objective test of choice; however, this study suggests that TBE and HRM may be complementary in this regard.
What is clear from this report as well as others regarding objective testing in achalasia is that patients’ symptoms alone are a poor marker of esophageal emptying. Posttherapy testing with HRM and/or TBE with special emphasis on bolus emptying should be employed in order to avoid long-term complications with achalasia. The choice between the tests may depend on the expertise and availability of each of the proposed test modalities.
Dr. Vaezi is clinical director of the division of gastroenterology, hepatology, and nutrition, and director of the Center for Swallowing and Esophageal Disorders and Clinical Research at Vanderbilt University Medical Center, Nashville, Tenn. He said he had no conflicts of interest to disclose.
Most patients with achalasia do well in the postoperative period after either pneumatic dilation (PD) or laparoscopic surgical myotomy, with an initial success rate as high as 90% after 2 years. However, predicting failure based on symptom recurrence is problematic, as symptoms are often underreported or absent due to esophageal dilation or impaired esophageal sensation. Thus, a strategy of avoiding esophageal decompensation due to delayed diagnosis cannot solely rely on patient report of symptom recurrence. Objective testing by barium esophagram or esophageal manometry may be needed.

|
|
This study adds new knowledge regarding the benefit of high-resolution manometry (HRM) in the management of posttreatment achalasia. The novelty of the study is in its use of timed barium esophagram (TBE), HRM, and symptoms in a group of patients with achalasia pre- and posttherapy. TBE was previously advocated as the objective test of choice; however, this study suggests that TBE and HRM may be complementary in this regard.
What is clear from this report as well as others regarding objective testing in achalasia is that patients’ symptoms alone are a poor marker of esophageal emptying. Posttherapy testing with HRM and/or TBE with special emphasis on bolus emptying should be employed in order to avoid long-term complications with achalasia. The choice between the tests may depend on the expertise and availability of each of the proposed test modalities.
Dr. Vaezi is clinical director of the division of gastroenterology, hepatology, and nutrition, and director of the Center for Swallowing and Esophageal Disorders and Clinical Research at Vanderbilt University Medical Center, Nashville, Tenn. He said he had no conflicts of interest to disclose.
High-resolution manometry with esophageal pressure topography is known to improve the accuracy of manometry for detecting achalasia and defined clinically relevant subtypes prior to treatment, but new data demonstrate that the procedure also is useful for evaluating treatment efficacy.
In a study of 31 men and 19 women aged 20-79 years, resolution of the achalasia pattern on high-resolution manometry with esophageal pressure topography (HRM-EPT) after treatment was associated with symptom improvement and reduced bolus retention, reported Dr. Frédéric Nicodème of Northwestern University, Chicago, and his colleagues.
Video source: American Gastroenterological Association's YouTube Channel
Study participants included one cohort of 25 patients who underwent endoscopy, HRM, timed barium esophagram (TBE) following a 200-mL barium swallow, and symptom assessment before treatment, and a second cohort of 25 treated patients who had pretreatment type 1 or 2 achalasia and who were undergoing a posttreatment study protocol including HRM, TBE, endoscopy, and symptom assessment. The investigators assessed dysphagia, regurgitation, retrosternal pain, and weight loss and used them to calculate an Eckardt score (ES) for both cohorts.
In the untreated cohort, which included 10 patients with type 1 achalasia and 15 with type 2 achalasia, the key EPT metric of integrated relaxation pressure (IRP) was significantly greater in the type 2 patients, as was the nadir-relaxation pressure. No differences were seen based on disease type with respect to resting esophagogastric junction (EGJ) pressure, barium column height, barium column width, or ES (Clin. Gastroenterol. Hepatol. 2012 Oct. 12 [doi: 10.1016/j.cgh.2012.10.015]).
No correlation was found between TBE column height at 5 minutes and IRP, resting EGJ pressure, nadir-EGJ relaxation pressure, or ES, and no correlation was seen between ES and IRP, resting EGJ pressure, or nadir-EGJ relaxation pressure.
In the posttreatment cohort, 10 patients, including 6 with type 1 disease and 4 with type 2 disease, had EPT findings of persistent achalasia pattern, and 15 had resolution of the achalasia pattern. Of these 15 patients, 8 converted to absent peristalsis and 7 to weak peristalsis.
"The IRP, resting EGJ pressure, and nadir-EGJ were all significantly correlated with posttreatment ES," the investigators noted.
Furthermore, TBE column height at 5 minutes, IRP, and ES were significantly lower in patients with resolved achalasia patterns on HRM than in those with a persistent achalasia pattern; the subgroup of 7 patients with weak peristalsis appeared to have the best outcome.
"The median TBE column height at 5 minutes was significantly lower [in those with weak peristalsis] than the three other groups, and ES showed a trend toward a lower value compared to the other 3 groups," they explained.
No significant correlations between TBE column height at 5 minutes and resting EGJ pressure or nadir-EGJ relaxation pressure were noted in the posttreatment patients. Only the IRP showed a weak correlation.
"The correlation between TBE column height at 5 minutes and ES after treatment was also not significant. However, the median TBE column height at 5 minutes for patients with an ES of 3 or greater was significantly greater than that for patients with an ES less than 3," they wrote.
"Our findings suggest that resolution of the achalasia pattern on EPT after treatment was associated with an improvement in symptoms and reduced bolus retention. Although the IRP was not strongly linearly correlated with symptom severity, when analyzed dichotomously patients with an IRP greater than or equal to 15 mm Hg had worse symptom scores and greater bolus retention on TBE compared to those with normal IRP values," the investigators wrote.
In contrast, no EPT pattern or metric, and no TBE variable predicted symptom severity in the untreated cohort, and barium height on TBE did not distinguish achalasia EPT subtypes, they noted.
"These findings suggest that in addition to its proven utility in detecting pretreatment achalasia, EPT also has utility in the management of posttreatment achalasia that can complement TBE," they said.
Although TBE did not distinguish disease subtypes, it does complement EPT, especially when the disease has progressed to an anatomic-dominant disorder, they said. Additional studies in larger series of patients are needed before and after therapy to confidently establish the relative merits of each evaluation with respect to the prediction of long-term outcomes and cost-effectiveness, they said.
This study was supported by the Public Health Service. The authors reported having no disclosures.
High-resolution manometry with esophageal pressure topography is known to improve the accuracy of manometry for detecting achalasia and defined clinically relevant subtypes prior to treatment, but new data demonstrate that the procedure also is useful for evaluating treatment efficacy.
In a study of 31 men and 19 women aged 20-79 years, resolution of the achalasia pattern on high-resolution manometry with esophageal pressure topography (HRM-EPT) after treatment was associated with symptom improvement and reduced bolus retention, reported Dr. Frédéric Nicodème of Northwestern University, Chicago, and his colleagues.
Video source: American Gastroenterological Association's YouTube Channel
Study participants included one cohort of 25 patients who underwent endoscopy, HRM, timed barium esophagram (TBE) following a 200-mL barium swallow, and symptom assessment before treatment, and a second cohort of 25 treated patients who had pretreatment type 1 or 2 achalasia and who were undergoing a posttreatment study protocol including HRM, TBE, endoscopy, and symptom assessment. The investigators assessed dysphagia, regurgitation, retrosternal pain, and weight loss and used them to calculate an Eckardt score (ES) for both cohorts.
In the untreated cohort, which included 10 patients with type 1 achalasia and 15 with type 2 achalasia, the key EPT metric of integrated relaxation pressure (IRP) was significantly greater in the type 2 patients, as was the nadir-relaxation pressure. No differences were seen based on disease type with respect to resting esophagogastric junction (EGJ) pressure, barium column height, barium column width, or ES (Clin. Gastroenterol. Hepatol. 2012 Oct. 12 [doi: 10.1016/j.cgh.2012.10.015]).
No correlation was found between TBE column height at 5 minutes and IRP, resting EGJ pressure, nadir-EGJ relaxation pressure, or ES, and no correlation was seen between ES and IRP, resting EGJ pressure, or nadir-EGJ relaxation pressure.
In the posttreatment cohort, 10 patients, including 6 with type 1 disease and 4 with type 2 disease, had EPT findings of persistent achalasia pattern, and 15 had resolution of the achalasia pattern. Of these 15 patients, 8 converted to absent peristalsis and 7 to weak peristalsis.
"The IRP, resting EGJ pressure, and nadir-EGJ were all significantly correlated with posttreatment ES," the investigators noted.
Furthermore, TBE column height at 5 minutes, IRP, and ES were significantly lower in patients with resolved achalasia patterns on HRM than in those with a persistent achalasia pattern; the subgroup of 7 patients with weak peristalsis appeared to have the best outcome.
"The median TBE column height at 5 minutes was significantly lower [in those with weak peristalsis] than the three other groups, and ES showed a trend toward a lower value compared to the other 3 groups," they explained.
No significant correlations between TBE column height at 5 minutes and resting EGJ pressure or nadir-EGJ relaxation pressure were noted in the posttreatment patients. Only the IRP showed a weak correlation.
"The correlation between TBE column height at 5 minutes and ES after treatment was also not significant. However, the median TBE column height at 5 minutes for patients with an ES of 3 or greater was significantly greater than that for patients with an ES less than 3," they wrote.
"Our findings suggest that resolution of the achalasia pattern on EPT after treatment was associated with an improvement in symptoms and reduced bolus retention. Although the IRP was not strongly linearly correlated with symptom severity, when analyzed dichotomously patients with an IRP greater than or equal to 15 mm Hg had worse symptom scores and greater bolus retention on TBE compared to those with normal IRP values," the investigators wrote.
In contrast, no EPT pattern or metric, and no TBE variable predicted symptom severity in the untreated cohort, and barium height on TBE did not distinguish achalasia EPT subtypes, they noted.
"These findings suggest that in addition to its proven utility in detecting pretreatment achalasia, EPT also has utility in the management of posttreatment achalasia that can complement TBE," they said.
Although TBE did not distinguish disease subtypes, it does complement EPT, especially when the disease has progressed to an anatomic-dominant disorder, they said. Additional studies in larger series of patients are needed before and after therapy to confidently establish the relative merits of each evaluation with respect to the prediction of long-term outcomes and cost-effectiveness, they said.
This study was supported by the Public Health Service. The authors reported having no disclosures.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Major Finding: In a study of 31 men and 19 women aged 20-79 years, resolution of the achalasia pattern on HRM-EPT after treatment was associated with symptom improvement and reduced bolus retention.
Data Source: A prospective study of 50 achalasia patients.
Disclosures: This study was supported by the Public Health Service. The authors reported having no disclosures.
Futility rules defined for telaprevir-based HCV therapy
Therapy with telaprevir, peginterferon, and ribavirin should be stopped in both treatment-naive and treatment-experienced patients with hepatitis C virus infection if HCV RNA levels are greater than 1,000 IU/mL at week 4 or 12 of treatment, according to new futility rules developed using phase II and III trial data.
The rules are important for preventing needless drug exposure and to minimize the development of drug-resistant variants in patients with little or no chance of achieving sustained virologic response, reported Dr. Nathalie Adda of Vertex Pharmaceuticals Inc., Cambridge, Mass., and her colleagues.
The futility rules were initially developed during clinical trials of telaprevir combination therapy and were instituted along with standard peginterferon/ribavirin (Peg-IFN/RBV) futility rules; phase II trial data were analyzed to determine whether the telaprevir rules could differentiate patients likely to experience viral breakthrough and patients likely to achieve sustained virologic response, and it was found that the majority of viral breakthroughs occurred within the first 4 weeks of treatment. Thus, a futility rule was implemented at week 4 in studies of telaprevir combination therapy as has long been the case for studies of Peg-IFN/RBV therapy (Clin. Gastroenterol. Hepatol. 2012 Nov. 16 [doi: 10.1016/j.cgh.2012.10.045]).
For treatment-naive patients, a level of 1,000 IU/mL at week 4 was used; for treatment-experienced patients, a more conservative level of 100 IU/mL at week 4 (and at weeks 6 and 8) was used.
These rules were further analyzed based on phase III studies of patients who were treated with 12 weeks of telaprevir, Peg-IFN/RBV followed by 12 or 36 weeks of Peg-IFN/RBV alone. This allowed for refinement of the optimal thresholds and time points for identifying patients unlikely to achieve sustained virologic response.
"In this analysis, we also sought to harmonize the futility rules for all patient populations (treatment-naive and -experienced)," the investigators wrote.
They found that 1.7% of 844 treatment-naive patients, 0.7% of 138 prior relapsers, and 0% of 46 prior partial responders had HCV RNA levels greater than 1,000 IU/mL at week 4, compared with 14% of 70 prior nonresponders. None of the 25 patients with HCV RNA levels above the 1,000 IU/mL level at week 4 achieved sustained virologic response with continued therapy. Among those who had HCV RNA levels between 100 and 1,000 IU/mL at week 4, a small subset achieved sustained virologic response with continued treatment: 25% of treatment-naive and 14% of treatment-experienced patients.
The 1,000 IU/mL threshold was retained, as it was found to maximize the likelihood of achieving sustained virologic response, they said.
"Furthermore, 13/14 (93%) treatment-naive and 10/11 (91%) treatment-experienced patients with HCV RNA levels greater than 1,000 IU/mL at week 4 reached their HCV RNA nadir prior to week 4, typically by week 2, with subsequent increase in HCV RNA by week 4, meeting the definition of viral breakthrough," they wrote.
Additionally, the investigators reassessed previously-established Peg-IFN/RBV treatment futility rule of a 2 log10 decrease or greater in HCV RNA at week 12 in the context of a telaprevir-based regimen, and implemented a futility rule for treatment-naive patients of greater than 1,000 IU/mL HCV RNA at the end of the telaprevir dosing period to avoid unnecessary Peg-IFN/RBV exposure in those unlikely to achieve SVR.
This rule was met by 1.5% of 605 treatment naive patients who completed week 12. Similar rules were implemented at weeks 6, 8, and 12 for treatment-experienced patients, but few patients met the week 6 and 8 futility rules (5 and 2 of 266 patients, respectively), and the HCV RNA assessment at these time points was replaced by the week 12 assessment.
"In conclusion, data from phase II and III trials confirmed that a futility rule of greater than 1,000 IU/mL at week 4 accurately and specifically identified patients unlikely to achieve sustained virologic response. Less than 2% of treatment-naive, prior relapse, and prior partial response, and 14% of prior null response patients met the above criterion, and none achieved sustained virologic response after stopping telaprevir, with continued Peg-IFN/RBV," the investigators wrote, noting that the vast majority of these patients were already experiencing viral breakthrough by week 4.
The new rules prevent unnecessary drug exposure in those unlikely to achieve sustained virologic response, and, importantly, they minimize additional HCV RNA testing, because the futility time points coincide with those used to guide total treatment duration.
"This strategy will avoid additional adverse effects of continued treatment and will help minimize the evolution, enrichment, or protracted persistence of resistant variants, which could adversely impact patient candidacy for potential treatment with subsequent antiviral regimens," they concluded.
Several authors are employees of Janssen Pharmaceuticals and stock owners of Johnson and Johnson. One author reported receiving consulting fees, lecture fees, and/or grant/research support from many companies involved in hepatitis C virus therapeutics.
Therapy with telaprevir, peginterferon, and ribavirin should be stopped in both treatment-naive and treatment-experienced patients with hepatitis C virus infection if HCV RNA levels are greater than 1,000 IU/mL at week 4 or 12 of treatment, according to new futility rules developed using phase II and III trial data.
The rules are important for preventing needless drug exposure and to minimize the development of drug-resistant variants in patients with little or no chance of achieving sustained virologic response, reported Dr. Nathalie Adda of Vertex Pharmaceuticals Inc., Cambridge, Mass., and her colleagues.
The futility rules were initially developed during clinical trials of telaprevir combination therapy and were instituted along with standard peginterferon/ribavirin (Peg-IFN/RBV) futility rules; phase II trial data were analyzed to determine whether the telaprevir rules could differentiate patients likely to experience viral breakthrough and patients likely to achieve sustained virologic response, and it was found that the majority of viral breakthroughs occurred within the first 4 weeks of treatment. Thus, a futility rule was implemented at week 4 in studies of telaprevir combination therapy as has long been the case for studies of Peg-IFN/RBV therapy (Clin. Gastroenterol. Hepatol. 2012 Nov. 16 [doi: 10.1016/j.cgh.2012.10.045]).
For treatment-naive patients, a level of 1,000 IU/mL at week 4 was used; for treatment-experienced patients, a more conservative level of 100 IU/mL at week 4 (and at weeks 6 and 8) was used.
These rules were further analyzed based on phase III studies of patients who were treated with 12 weeks of telaprevir, Peg-IFN/RBV followed by 12 or 36 weeks of Peg-IFN/RBV alone. This allowed for refinement of the optimal thresholds and time points for identifying patients unlikely to achieve sustained virologic response.
"In this analysis, we also sought to harmonize the futility rules for all patient populations (treatment-naive and -experienced)," the investigators wrote.
They found that 1.7% of 844 treatment-naive patients, 0.7% of 138 prior relapsers, and 0% of 46 prior partial responders had HCV RNA levels greater than 1,000 IU/mL at week 4, compared with 14% of 70 prior nonresponders. None of the 25 patients with HCV RNA levels above the 1,000 IU/mL level at week 4 achieved sustained virologic response with continued therapy. Among those who had HCV RNA levels between 100 and 1,000 IU/mL at week 4, a small subset achieved sustained virologic response with continued treatment: 25% of treatment-naive and 14% of treatment-experienced patients.
The 1,000 IU/mL threshold was retained, as it was found to maximize the likelihood of achieving sustained virologic response, they said.
"Furthermore, 13/14 (93%) treatment-naive and 10/11 (91%) treatment-experienced patients with HCV RNA levels greater than 1,000 IU/mL at week 4 reached their HCV RNA nadir prior to week 4, typically by week 2, with subsequent increase in HCV RNA by week 4, meeting the definition of viral breakthrough," they wrote.
Additionally, the investigators reassessed previously-established Peg-IFN/RBV treatment futility rule of a 2 log10 decrease or greater in HCV RNA at week 12 in the context of a telaprevir-based regimen, and implemented a futility rule for treatment-naive patients of greater than 1,000 IU/mL HCV RNA at the end of the telaprevir dosing period to avoid unnecessary Peg-IFN/RBV exposure in those unlikely to achieve SVR.
This rule was met by 1.5% of 605 treatment naive patients who completed week 12. Similar rules were implemented at weeks 6, 8, and 12 for treatment-experienced patients, but few patients met the week 6 and 8 futility rules (5 and 2 of 266 patients, respectively), and the HCV RNA assessment at these time points was replaced by the week 12 assessment.
"In conclusion, data from phase II and III trials confirmed that a futility rule of greater than 1,000 IU/mL at week 4 accurately and specifically identified patients unlikely to achieve sustained virologic response. Less than 2% of treatment-naive, prior relapse, and prior partial response, and 14% of prior null response patients met the above criterion, and none achieved sustained virologic response after stopping telaprevir, with continued Peg-IFN/RBV," the investigators wrote, noting that the vast majority of these patients were already experiencing viral breakthrough by week 4.
The new rules prevent unnecessary drug exposure in those unlikely to achieve sustained virologic response, and, importantly, they minimize additional HCV RNA testing, because the futility time points coincide with those used to guide total treatment duration.
"This strategy will avoid additional adverse effects of continued treatment and will help minimize the evolution, enrichment, or protracted persistence of resistant variants, which could adversely impact patient candidacy for potential treatment with subsequent antiviral regimens," they concluded.
Several authors are employees of Janssen Pharmaceuticals and stock owners of Johnson and Johnson. One author reported receiving consulting fees, lecture fees, and/or grant/research support from many companies involved in hepatitis C virus therapeutics.
Therapy with telaprevir, peginterferon, and ribavirin should be stopped in both treatment-naive and treatment-experienced patients with hepatitis C virus infection if HCV RNA levels are greater than 1,000 IU/mL at week 4 or 12 of treatment, according to new futility rules developed using phase II and III trial data.
The rules are important for preventing needless drug exposure and to minimize the development of drug-resistant variants in patients with little or no chance of achieving sustained virologic response, reported Dr. Nathalie Adda of Vertex Pharmaceuticals Inc., Cambridge, Mass., and her colleagues.
The futility rules were initially developed during clinical trials of telaprevir combination therapy and were instituted along with standard peginterferon/ribavirin (Peg-IFN/RBV) futility rules; phase II trial data were analyzed to determine whether the telaprevir rules could differentiate patients likely to experience viral breakthrough and patients likely to achieve sustained virologic response, and it was found that the majority of viral breakthroughs occurred within the first 4 weeks of treatment. Thus, a futility rule was implemented at week 4 in studies of telaprevir combination therapy as has long been the case for studies of Peg-IFN/RBV therapy (Clin. Gastroenterol. Hepatol. 2012 Nov. 16 [doi: 10.1016/j.cgh.2012.10.045]).
For treatment-naive patients, a level of 1,000 IU/mL at week 4 was used; for treatment-experienced patients, a more conservative level of 100 IU/mL at week 4 (and at weeks 6 and 8) was used.
These rules were further analyzed based on phase III studies of patients who were treated with 12 weeks of telaprevir, Peg-IFN/RBV followed by 12 or 36 weeks of Peg-IFN/RBV alone. This allowed for refinement of the optimal thresholds and time points for identifying patients unlikely to achieve sustained virologic response.
"In this analysis, we also sought to harmonize the futility rules for all patient populations (treatment-naive and -experienced)," the investigators wrote.
They found that 1.7% of 844 treatment-naive patients, 0.7% of 138 prior relapsers, and 0% of 46 prior partial responders had HCV RNA levels greater than 1,000 IU/mL at week 4, compared with 14% of 70 prior nonresponders. None of the 25 patients with HCV RNA levels above the 1,000 IU/mL level at week 4 achieved sustained virologic response with continued therapy. Among those who had HCV RNA levels between 100 and 1,000 IU/mL at week 4, a small subset achieved sustained virologic response with continued treatment: 25% of treatment-naive and 14% of treatment-experienced patients.
The 1,000 IU/mL threshold was retained, as it was found to maximize the likelihood of achieving sustained virologic response, they said.
"Furthermore, 13/14 (93%) treatment-naive and 10/11 (91%) treatment-experienced patients with HCV RNA levels greater than 1,000 IU/mL at week 4 reached their HCV RNA nadir prior to week 4, typically by week 2, with subsequent increase in HCV RNA by week 4, meeting the definition of viral breakthrough," they wrote.
Additionally, the investigators reassessed previously-established Peg-IFN/RBV treatment futility rule of a 2 log10 decrease or greater in HCV RNA at week 12 in the context of a telaprevir-based regimen, and implemented a futility rule for treatment-naive patients of greater than 1,000 IU/mL HCV RNA at the end of the telaprevir dosing period to avoid unnecessary Peg-IFN/RBV exposure in those unlikely to achieve SVR.
This rule was met by 1.5% of 605 treatment naive patients who completed week 12. Similar rules were implemented at weeks 6, 8, and 12 for treatment-experienced patients, but few patients met the week 6 and 8 futility rules (5 and 2 of 266 patients, respectively), and the HCV RNA assessment at these time points was replaced by the week 12 assessment.
"In conclusion, data from phase II and III trials confirmed that a futility rule of greater than 1,000 IU/mL at week 4 accurately and specifically identified patients unlikely to achieve sustained virologic response. Less than 2% of treatment-naive, prior relapse, and prior partial response, and 14% of prior null response patients met the above criterion, and none achieved sustained virologic response after stopping telaprevir, with continued Peg-IFN/RBV," the investigators wrote, noting that the vast majority of these patients were already experiencing viral breakthrough by week 4.
The new rules prevent unnecessary drug exposure in those unlikely to achieve sustained virologic response, and, importantly, they minimize additional HCV RNA testing, because the futility time points coincide with those used to guide total treatment duration.
"This strategy will avoid additional adverse effects of continued treatment and will help minimize the evolution, enrichment, or protracted persistence of resistant variants, which could adversely impact patient candidacy for potential treatment with subsequent antiviral regimens," they concluded.
Several authors are employees of Janssen Pharmaceuticals and stock owners of Johnson and Johnson. One author reported receiving consulting fees, lecture fees, and/or grant/research support from many companies involved in hepatitis C virus therapeutics.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Major Finding: Telaprevir, peginterferon, and ribavirin for the treatment of hepatitis C should be stopped in both treatment-naive and treatment-experienced patients if HCV RNA levels are greater than 1,000 IU/mL at week 4 or 12 of treatment.
Data Source: A retrospective review of clinical trial data.
Disclosures: Several authors are employees of Janssen Pharmaceuticals and stock owners of Johnson and Johnson. One author reported receiving consulting fees, lecture fees, and/or grant/research support from many companies involved in hepatitis C virus therapeutics.
Ten percent of neoplastic polyps may be incompletely resected
Approximately 10% of neoplastic polyps that were 5-20 mm in size were not completely resected in a series of 1,427 patients undergoing colonoscopy, Dr. Heiko Pohl and his colleagues reported in the January issue of Gastroenterology.
Biopsies from the resection margins of 346 neoplastic polyps showed that some neoplastic tissue had been left behind in 35 cases in the Complete Adenoma Resection (CARE) study, which involved 11 experienced gastroenterologists practicing at two large academic medical centers.
Video source: American Gastroenterological Association YouTube channel
The rate of incomplete resections varied widely across the different endoscopists, from 6.5% to 22.7%. Moreover, these physicians were aware that they were participating in the study and may have been more careful than usual to accomplish complete resection.
"Our study provides plausible data that incomplete polyp resection in daily clinical practice is relatively common and may contribute to future interval cancers," said Dr. Pohl of White River Junction (Vt.) VA Medical Center and Dartmouth-Hitchcock Medical Center, Lebanon, N.H., and his associates.
The findings also suggest that quality measures for colonoscopy, which to date have focused primarily on detection rates, should now include the completeness of the resection. "The performance of high-quality and effective colonoscopy not only requires expertise in finding neoplastic polyps, but also removing them," the investigators noted (Gastroenterology 2013;144:74-80).
Until now, there has been "surprisingly little direct information on the adequacy of polyp resection. It is generally assumed that resection is complete if no apparent polyp tissue is visible after resection. Using a snare with electrocautery should further destroy any remaining polyp tissue," but whether it actually does so has never been tested, they said.
Dr. Pohl and his colleagues reviewed the cases of all adults aged 40-85 years who presented for outpatient colonoscopy at the two study centers, had no history of inflammatory bowel disease, had no coagulopathies, and were found to have at least one polyp that was 5-20 mm in size.
The board-certified gastroenterologists participating in the study used standard colonoscopes and polypectomy snares to remove the lesions, along with standard electrocautery equipment. The polyps were measured and resected, then the gastroenterologists inspected the resection margins macroscopically, obtained forceps biopsies of the resection margins, and attested that the removal was complete.
They also recorded whether the resection had been easy, moderately difficult, or difficult.
The use of narrow band imaging, chromoendoscopy, or argon plasma coagulation was not required by the study protocol but was allowed at the discretion of each gastroenterologist.
An expert gastrointestinal pathologist independently examined all the biopsies for residual adenomatous tissue, as well as to classify the polyps.
A total of 346 polyps (83%) were neoplastic.
Sixty-eight percent of these polyps were classified as tubular, tubulovillous, or villous adenomas. Twelve percent had a serrated histology, including 42 (10%) that were sessile serrated adenomas/polyps.
The expert reviewer found that overall, 10% of the neoplastic polyps were incompletely resected.
Large (10- to 20-mm) growths were more than twice as likely to be incompletely resected (17.3%) than were small (5- to 9-mm) growths (6.8%). Sessile serrated adenomas/polyps were four times more likely than other types to be incompletely resected (31% vs. 7%).
As a result, almost half (48%) of all large sessile serrated adenomas/polyps were incompletely resected.
"Because adenoma size is associated with both a higher prevalence of advanced histology and greater near-term risk of transition to cancer, incomplete resection of large neoplastic polyps is concerning," Dr. Pohl and his colleagues wrote.
No other factors were found to correspond with incomplete removal, including whether the resection was rated as difficult rather than easy, whether the polyps had to be removed piecemeal rather than all at once, whether the polyps were located in the right or left colon, and whether they had flat or other morphology.
"Our results raise questions regarding the quality of polyp resection and call for efforts to improve resection of neoplastic polyps, especially large polyps and sessile serrated adenomas/polyps," the researchers wrote.
In particular, increased attention to the polyp margin using special imaging may be warranted. Outlining and marking the margin before resection also might improve the completeness of the removal. And in some cases, adjunctive ablation of the margins after resection may be useful, they added.
The authors reported no relevant financial conflicts.
Colonoscopy can achieve significant levels of protection against colorectal cancer (CRC), but its effectiveness depends on performance quality, which is operator dependent, according to Dr. Charles J. Kahi.
Studies have shown that patients are best protected against CRC when they undergo colonoscopy by endoscopists with high adenoma detection and cecal intubation rates, and high rates of polypectomy in the case of proximal CRC. Provider specialty also is associated with the risk of postcolonoscopy CRC, with gastroenterologists achieving higher levels of protection than other specialists.
Colonoscopic polypectomy is a cornerstone of effective CRC prevention; however, polypectomy technique and quality have been understudied, compared with other colonoscopy quality metrics, despite the known variability in polypectomy technique among U.S. endoscopists, and the estimation that one in every four interval CRCs may be due to inadequate polypectomy. The CARE study by Dr. Pohl and his colleagues is an important addition to the literature: It is focused on nonpedunculated polyps 5-20 mm in size, which are commonly detected and are most relevant to general endoscopy practice, and it provides information regarding the prevalence and factors associated with incomplete polypectomy.
The CARE study shows that incomplete polypectomy is likely a common phenomenon, and that colonoscopy’s operator dependency with regard to neoplasm detection also applies to resection. Additional study is warranted to determine and standardize the technique components required to achieve complete polypectomy, and thus decrease operator variability and optimize colonoscopic polypectomy quality.
Dr. Kahi is chief of the GI section at the Richard L. Roudebush VA Medical Center, Indianapolis. He said he had no relevant financial disclosures.
Colonoscopy can achieve significant levels of protection against colorectal cancer (CRC), but its effectiveness depends on performance quality, which is operator dependent, according to Dr. Charles J. Kahi.
Studies have shown that patients are best protected against CRC when they undergo colonoscopy by endoscopists with high adenoma detection and cecal intubation rates, and high rates of polypectomy in the case of proximal CRC. Provider specialty also is associated with the risk of postcolonoscopy CRC, with gastroenterologists achieving higher levels of protection than other specialists.
Colonoscopic polypectomy is a cornerstone of effective CRC prevention; however, polypectomy technique and quality have been understudied, compared with other colonoscopy quality metrics, despite the known variability in polypectomy technique among U.S. endoscopists, and the estimation that one in every four interval CRCs may be due to inadequate polypectomy. The CARE study by Dr. Pohl and his colleagues is an important addition to the literature: It is focused on nonpedunculated polyps 5-20 mm in size, which are commonly detected and are most relevant to general endoscopy practice, and it provides information regarding the prevalence and factors associated with incomplete polypectomy.
The CARE study shows that incomplete polypectomy is likely a common phenomenon, and that colonoscopy’s operator dependency with regard to neoplasm detection also applies to resection. Additional study is warranted to determine and standardize the technique components required to achieve complete polypectomy, and thus decrease operator variability and optimize colonoscopic polypectomy quality.
Dr. Kahi is chief of the GI section at the Richard L. Roudebush VA Medical Center, Indianapolis. He said he had no relevant financial disclosures.
Colonoscopy can achieve significant levels of protection against colorectal cancer (CRC), but its effectiveness depends on performance quality, which is operator dependent, according to Dr. Charles J. Kahi.
Studies have shown that patients are best protected against CRC when they undergo colonoscopy by endoscopists with high adenoma detection and cecal intubation rates, and high rates of polypectomy in the case of proximal CRC. Provider specialty also is associated with the risk of postcolonoscopy CRC, with gastroenterologists achieving higher levels of protection than other specialists.
Colonoscopic polypectomy is a cornerstone of effective CRC prevention; however, polypectomy technique and quality have been understudied, compared with other colonoscopy quality metrics, despite the known variability in polypectomy technique among U.S. endoscopists, and the estimation that one in every four interval CRCs may be due to inadequate polypectomy. The CARE study by Dr. Pohl and his colleagues is an important addition to the literature: It is focused on nonpedunculated polyps 5-20 mm in size, which are commonly detected and are most relevant to general endoscopy practice, and it provides information regarding the prevalence and factors associated with incomplete polypectomy.
The CARE study shows that incomplete polypectomy is likely a common phenomenon, and that colonoscopy’s operator dependency with regard to neoplasm detection also applies to resection. Additional study is warranted to determine and standardize the technique components required to achieve complete polypectomy, and thus decrease operator variability and optimize colonoscopic polypectomy quality.
Dr. Kahi is chief of the GI section at the Richard L. Roudebush VA Medical Center, Indianapolis. He said he had no relevant financial disclosures.
Approximately 10% of neoplastic polyps that were 5-20 mm in size were not completely resected in a series of 1,427 patients undergoing colonoscopy, Dr. Heiko Pohl and his colleagues reported in the January issue of Gastroenterology.
Biopsies from the resection margins of 346 neoplastic polyps showed that some neoplastic tissue had been left behind in 35 cases in the Complete Adenoma Resection (CARE) study, which involved 11 experienced gastroenterologists practicing at two large academic medical centers.
Video source: American Gastroenterological Association YouTube channel
The rate of incomplete resections varied widely across the different endoscopists, from 6.5% to 22.7%. Moreover, these physicians were aware that they were participating in the study and may have been more careful than usual to accomplish complete resection.
"Our study provides plausible data that incomplete polyp resection in daily clinical practice is relatively common and may contribute to future interval cancers," said Dr. Pohl of White River Junction (Vt.) VA Medical Center and Dartmouth-Hitchcock Medical Center, Lebanon, N.H., and his associates.
The findings also suggest that quality measures for colonoscopy, which to date have focused primarily on detection rates, should now include the completeness of the resection. "The performance of high-quality and effective colonoscopy not only requires expertise in finding neoplastic polyps, but also removing them," the investigators noted (Gastroenterology 2013;144:74-80).
Until now, there has been "surprisingly little direct information on the adequacy of polyp resection. It is generally assumed that resection is complete if no apparent polyp tissue is visible after resection. Using a snare with electrocautery should further destroy any remaining polyp tissue," but whether it actually does so has never been tested, they said.
Dr. Pohl and his colleagues reviewed the cases of all adults aged 40-85 years who presented for outpatient colonoscopy at the two study centers, had no history of inflammatory bowel disease, had no coagulopathies, and were found to have at least one polyp that was 5-20 mm in size.
The board-certified gastroenterologists participating in the study used standard colonoscopes and polypectomy snares to remove the lesions, along with standard electrocautery equipment. The polyps were measured and resected, then the gastroenterologists inspected the resection margins macroscopically, obtained forceps biopsies of the resection margins, and attested that the removal was complete.
They also recorded whether the resection had been easy, moderately difficult, or difficult.
The use of narrow band imaging, chromoendoscopy, or argon plasma coagulation was not required by the study protocol but was allowed at the discretion of each gastroenterologist.
An expert gastrointestinal pathologist independently examined all the biopsies for residual adenomatous tissue, as well as to classify the polyps.
A total of 346 polyps (83%) were neoplastic.
Sixty-eight percent of these polyps were classified as tubular, tubulovillous, or villous adenomas. Twelve percent had a serrated histology, including 42 (10%) that were sessile serrated adenomas/polyps.
The expert reviewer found that overall, 10% of the neoplastic polyps were incompletely resected.
Large (10- to 20-mm) growths were more than twice as likely to be incompletely resected (17.3%) than were small (5- to 9-mm) growths (6.8%). Sessile serrated adenomas/polyps were four times more likely than other types to be incompletely resected (31% vs. 7%).
As a result, almost half (48%) of all large sessile serrated adenomas/polyps were incompletely resected.
"Because adenoma size is associated with both a higher prevalence of advanced histology and greater near-term risk of transition to cancer, incomplete resection of large neoplastic polyps is concerning," Dr. Pohl and his colleagues wrote.
No other factors were found to correspond with incomplete removal, including whether the resection was rated as difficult rather than easy, whether the polyps had to be removed piecemeal rather than all at once, whether the polyps were located in the right or left colon, and whether they had flat or other morphology.
"Our results raise questions regarding the quality of polyp resection and call for efforts to improve resection of neoplastic polyps, especially large polyps and sessile serrated adenomas/polyps," the researchers wrote.
In particular, increased attention to the polyp margin using special imaging may be warranted. Outlining and marking the margin before resection also might improve the completeness of the removal. And in some cases, adjunctive ablation of the margins after resection may be useful, they added.
The authors reported no relevant financial conflicts.
Approximately 10% of neoplastic polyps that were 5-20 mm in size were not completely resected in a series of 1,427 patients undergoing colonoscopy, Dr. Heiko Pohl and his colleagues reported in the January issue of Gastroenterology.
Biopsies from the resection margins of 346 neoplastic polyps showed that some neoplastic tissue had been left behind in 35 cases in the Complete Adenoma Resection (CARE) study, which involved 11 experienced gastroenterologists practicing at two large academic medical centers.
Video source: American Gastroenterological Association YouTube channel
The rate of incomplete resections varied widely across the different endoscopists, from 6.5% to 22.7%. Moreover, these physicians were aware that they were participating in the study and may have been more careful than usual to accomplish complete resection.
"Our study provides plausible data that incomplete polyp resection in daily clinical practice is relatively common and may contribute to future interval cancers," said Dr. Pohl of White River Junction (Vt.) VA Medical Center and Dartmouth-Hitchcock Medical Center, Lebanon, N.H., and his associates.
The findings also suggest that quality measures for colonoscopy, which to date have focused primarily on detection rates, should now include the completeness of the resection. "The performance of high-quality and effective colonoscopy not only requires expertise in finding neoplastic polyps, but also removing them," the investigators noted (Gastroenterology 2013;144:74-80).
Until now, there has been "surprisingly little direct information on the adequacy of polyp resection. It is generally assumed that resection is complete if no apparent polyp tissue is visible after resection. Using a snare with electrocautery should further destroy any remaining polyp tissue," but whether it actually does so has never been tested, they said.
Dr. Pohl and his colleagues reviewed the cases of all adults aged 40-85 years who presented for outpatient colonoscopy at the two study centers, had no history of inflammatory bowel disease, had no coagulopathies, and were found to have at least one polyp that was 5-20 mm in size.
The board-certified gastroenterologists participating in the study used standard colonoscopes and polypectomy snares to remove the lesions, along with standard electrocautery equipment. The polyps were measured and resected, then the gastroenterologists inspected the resection margins macroscopically, obtained forceps biopsies of the resection margins, and attested that the removal was complete.
They also recorded whether the resection had been easy, moderately difficult, or difficult.
The use of narrow band imaging, chromoendoscopy, or argon plasma coagulation was not required by the study protocol but was allowed at the discretion of each gastroenterologist.
An expert gastrointestinal pathologist independently examined all the biopsies for residual adenomatous tissue, as well as to classify the polyps.
A total of 346 polyps (83%) were neoplastic.
Sixty-eight percent of these polyps were classified as tubular, tubulovillous, or villous adenomas. Twelve percent had a serrated histology, including 42 (10%) that were sessile serrated adenomas/polyps.
The expert reviewer found that overall, 10% of the neoplastic polyps were incompletely resected.
Large (10- to 20-mm) growths were more than twice as likely to be incompletely resected (17.3%) than were small (5- to 9-mm) growths (6.8%). Sessile serrated adenomas/polyps were four times more likely than other types to be incompletely resected (31% vs. 7%).
As a result, almost half (48%) of all large sessile serrated adenomas/polyps were incompletely resected.
"Because adenoma size is associated with both a higher prevalence of advanced histology and greater near-term risk of transition to cancer, incomplete resection of large neoplastic polyps is concerning," Dr. Pohl and his colleagues wrote.
No other factors were found to correspond with incomplete removal, including whether the resection was rated as difficult rather than easy, whether the polyps had to be removed piecemeal rather than all at once, whether the polyps were located in the right or left colon, and whether they had flat or other morphology.
"Our results raise questions regarding the quality of polyp resection and call for efforts to improve resection of neoplastic polyps, especially large polyps and sessile serrated adenomas/polyps," the researchers wrote.
In particular, increased attention to the polyp margin using special imaging may be warranted. Outlining and marking the margin before resection also might improve the completeness of the removal. And in some cases, adjunctive ablation of the margins after resection may be useful, they added.
The authors reported no relevant financial conflicts.
FROM GASTROENTEROLOGY
Major Finding: Ten percent of neoplastic polyps (5-20 mm) were not resected completely, as evidenced by neoplastic tissue in biopsies from the margins of the lesions.
Data Source: An analysis of biopsies from the margins of 346 neoplastic polyps removed via colonoscopy from adult outpatients at two academic medical centers.
Disclosures: No relevant financial conflicts were reported.
Poor performance seen after optical biopsy training
Only 3 of 12 gastroenterologists in a community practice were able to assess colon polyps 5 mm or less in size with 90% accuracy after completing a computer-based self-training program for "optical biopsy" using narrow band imaging, Dr. Uri Ladabaum and his colleagues reported in the January issue of Gastroenterology.
This performance was not as good as that reported for experts evaluated in clinical studies, but it was similar to that reported for students at academic medical centers.
Video Source: American Gastroenterological Association YouTube channel
Although it is "promising" that three gastroenterologists learned how to perform optical biopsy using this method, "better results in community practice must be achieved before NBI [narrow band imaging]-based optical biopsy methods can be used routinely to evaluate polyps," wrote Dr. Ladabaum of Stanford (Calif.) University and his associates (Gastroenterology 2013;144:81-91).
The American Society of Gastrointestinal Endoscopy recommends a negative predictive value threshold of 90% or greater for adenomatous histology of diminutive colorectal polyps using optical biopsy.
The investigators evaluated a self-training program that was designed to be practical to implement in a busy community gastroenterology practice. None of the study subjects had significant experience or formal training with NBI, which uses narrow band light filters to highlight colonic mucosal architecture and vasculature.
Participants first completed three self-administered units at their own pace during the first week of the program: a pretest, a learning module instructing them on using narrow band imaging to help distinguish adenomas from hyperplastic polyps, and a posttest. The two tests featured different sets of 25 endoscopic images of polyps and asked the study subjects to judge whether they were adenomas or hyperplastic, or to indicate that they couldn’t decide.
Next, the participants put their learning into practice, using optical biopsy with NBI on all colonoscopies they performed in which at least one polyp was removed. They noted the location, size, and morphology of each lesion; took photographs under white light and under NBI; classified the features they observed; predicted whether the lesions would prove to be adenomas or hyperplastic on pathologic examination; and recorded their level of confidence (high or low) in their predictions.
After the specimens were examined and classified by fellowship-trained GI pathologists, the study gastroenterologists were required to record the actual diagnosis for each lesion and encouraged to compare that with their own optical diagnoses. They received ongoing confidential feedback as to the accuracy of their work every 1-2 weeks.
Polyps were classified by size as diminutive (5 mm or smaller), small (6-9 mm), or large (10 mm or larger). The primary analysis focused on the study subjects’ success in optical diagnosis of diminutive polyps only, and each subject’s final evaluation was performed after he or she assessed at least 90 such lesions.
The 12 gastroenterologists who participated in both the ex vivo and in vivo study phases of the training program performed a total of 1,673 colonoscopies and removed 2,596 polyps. This included 1,858 diminutive, 547 small, and 177 large polyps; the size was not recorded for the remaining 14 polyps.
All 12 study subjects scored 90% or greater accuracy on the posttests they took after training.
However, only three of them performed that well in their real world practice. The other nine gastroenterologists did not achieve 90% or greater accuracy in assessing the histology of diminutive polyps using NBI.
The participants did not show typical learning curves with the technique over time. "There was no clear pattern of early learning with later stabilization of performance at a higher level," Dr. Ladabaum and his colleagues wrote.
Many factors that might have influenced subjects’ accuracy in distinguishing adenomas from hyperplasia actually proved to have no such effect. The location of the polyp within the colon, the endoscopists’ years in practice and colonoscopy volume, and the changes in subjects’ scores from pretest to posttest all showed no association with their final accuracy in optical biopsy.
One factor that predicted such accuracy was the participant’s confidence in each of his or her predictions.
Finally, there was some attrition over the course of the study, as some subjects who took part in the initial computer-based training did not proceed to the in vivo phase, "and not all participants remained engaged in the in vivo phase. Incentives may need to be developed for busy clinicians to learn and use optical biopsy techniques," the investigators wrote.
Overall, the study findings show that "high accuracy can be achieved ex vivo by community gastroenterologists after self-paced training with a computerized module." However, it remains to be seen whether a gastroenterologist’s ultimate proficiency in optical diagnosis "is determined by technical issues, dedication, motivation, or innate skill," they added.
This study was supported by Stanford University. One author reported receiving research support from and serving on the speakers bureau for Olympus Corp.
Only 3 of 12 gastroenterologists in a community practice were able to assess colon polyps 5 mm or less in size with 90% accuracy after completing a computer-based self-training program for "optical biopsy" using narrow band imaging, Dr. Uri Ladabaum and his colleagues reported in the January issue of Gastroenterology.
This performance was not as good as that reported for experts evaluated in clinical studies, but it was similar to that reported for students at academic medical centers.
Video Source: American Gastroenterological Association YouTube channel
Although it is "promising" that three gastroenterologists learned how to perform optical biopsy using this method, "better results in community practice must be achieved before NBI [narrow band imaging]-based optical biopsy methods can be used routinely to evaluate polyps," wrote Dr. Ladabaum of Stanford (Calif.) University and his associates (Gastroenterology 2013;144:81-91).
The American Society of Gastrointestinal Endoscopy recommends a negative predictive value threshold of 90% or greater for adenomatous histology of diminutive colorectal polyps using optical biopsy.
The investigators evaluated a self-training program that was designed to be practical to implement in a busy community gastroenterology practice. None of the study subjects had significant experience or formal training with NBI, which uses narrow band light filters to highlight colonic mucosal architecture and vasculature.
Participants first completed three self-administered units at their own pace during the first week of the program: a pretest, a learning module instructing them on using narrow band imaging to help distinguish adenomas from hyperplastic polyps, and a posttest. The two tests featured different sets of 25 endoscopic images of polyps and asked the study subjects to judge whether they were adenomas or hyperplastic, or to indicate that they couldn’t decide.
Next, the participants put their learning into practice, using optical biopsy with NBI on all colonoscopies they performed in which at least one polyp was removed. They noted the location, size, and morphology of each lesion; took photographs under white light and under NBI; classified the features they observed; predicted whether the lesions would prove to be adenomas or hyperplastic on pathologic examination; and recorded their level of confidence (high or low) in their predictions.
After the specimens were examined and classified by fellowship-trained GI pathologists, the study gastroenterologists were required to record the actual diagnosis for each lesion and encouraged to compare that with their own optical diagnoses. They received ongoing confidential feedback as to the accuracy of their work every 1-2 weeks.
Polyps were classified by size as diminutive (5 mm or smaller), small (6-9 mm), or large (10 mm or larger). The primary analysis focused on the study subjects’ success in optical diagnosis of diminutive polyps only, and each subject’s final evaluation was performed after he or she assessed at least 90 such lesions.
The 12 gastroenterologists who participated in both the ex vivo and in vivo study phases of the training program performed a total of 1,673 colonoscopies and removed 2,596 polyps. This included 1,858 diminutive, 547 small, and 177 large polyps; the size was not recorded for the remaining 14 polyps.
All 12 study subjects scored 90% or greater accuracy on the posttests they took after training.
However, only three of them performed that well in their real world practice. The other nine gastroenterologists did not achieve 90% or greater accuracy in assessing the histology of diminutive polyps using NBI.
The participants did not show typical learning curves with the technique over time. "There was no clear pattern of early learning with later stabilization of performance at a higher level," Dr. Ladabaum and his colleagues wrote.
Many factors that might have influenced subjects’ accuracy in distinguishing adenomas from hyperplasia actually proved to have no such effect. The location of the polyp within the colon, the endoscopists’ years in practice and colonoscopy volume, and the changes in subjects’ scores from pretest to posttest all showed no association with their final accuracy in optical biopsy.
One factor that predicted such accuracy was the participant’s confidence in each of his or her predictions.
Finally, there was some attrition over the course of the study, as some subjects who took part in the initial computer-based training did not proceed to the in vivo phase, "and not all participants remained engaged in the in vivo phase. Incentives may need to be developed for busy clinicians to learn and use optical biopsy techniques," the investigators wrote.
Overall, the study findings show that "high accuracy can be achieved ex vivo by community gastroenterologists after self-paced training with a computerized module." However, it remains to be seen whether a gastroenterologist’s ultimate proficiency in optical diagnosis "is determined by technical issues, dedication, motivation, or innate skill," they added.
This study was supported by Stanford University. One author reported receiving research support from and serving on the speakers bureau for Olympus Corp.
Only 3 of 12 gastroenterologists in a community practice were able to assess colon polyps 5 mm or less in size with 90% accuracy after completing a computer-based self-training program for "optical biopsy" using narrow band imaging, Dr. Uri Ladabaum and his colleagues reported in the January issue of Gastroenterology.
This performance was not as good as that reported for experts evaluated in clinical studies, but it was similar to that reported for students at academic medical centers.
Video Source: American Gastroenterological Association YouTube channel
Although it is "promising" that three gastroenterologists learned how to perform optical biopsy using this method, "better results in community practice must be achieved before NBI [narrow band imaging]-based optical biopsy methods can be used routinely to evaluate polyps," wrote Dr. Ladabaum of Stanford (Calif.) University and his associates (Gastroenterology 2013;144:81-91).
The American Society of Gastrointestinal Endoscopy recommends a negative predictive value threshold of 90% or greater for adenomatous histology of diminutive colorectal polyps using optical biopsy.
The investigators evaluated a self-training program that was designed to be practical to implement in a busy community gastroenterology practice. None of the study subjects had significant experience or formal training with NBI, which uses narrow band light filters to highlight colonic mucosal architecture and vasculature.
Participants first completed three self-administered units at their own pace during the first week of the program: a pretest, a learning module instructing them on using narrow band imaging to help distinguish adenomas from hyperplastic polyps, and a posttest. The two tests featured different sets of 25 endoscopic images of polyps and asked the study subjects to judge whether they were adenomas or hyperplastic, or to indicate that they couldn’t decide.
Next, the participants put their learning into practice, using optical biopsy with NBI on all colonoscopies they performed in which at least one polyp was removed. They noted the location, size, and morphology of each lesion; took photographs under white light and under NBI; classified the features they observed; predicted whether the lesions would prove to be adenomas or hyperplastic on pathologic examination; and recorded their level of confidence (high or low) in their predictions.
After the specimens were examined and classified by fellowship-trained GI pathologists, the study gastroenterologists were required to record the actual diagnosis for each lesion and encouraged to compare that with their own optical diagnoses. They received ongoing confidential feedback as to the accuracy of their work every 1-2 weeks.
Polyps were classified by size as diminutive (5 mm or smaller), small (6-9 mm), or large (10 mm or larger). The primary analysis focused on the study subjects’ success in optical diagnosis of diminutive polyps only, and each subject’s final evaluation was performed after he or she assessed at least 90 such lesions.
The 12 gastroenterologists who participated in both the ex vivo and in vivo study phases of the training program performed a total of 1,673 colonoscopies and removed 2,596 polyps. This included 1,858 diminutive, 547 small, and 177 large polyps; the size was not recorded for the remaining 14 polyps.
All 12 study subjects scored 90% or greater accuracy on the posttests they took after training.
However, only three of them performed that well in their real world practice. The other nine gastroenterologists did not achieve 90% or greater accuracy in assessing the histology of diminutive polyps using NBI.
The participants did not show typical learning curves with the technique over time. "There was no clear pattern of early learning with later stabilization of performance at a higher level," Dr. Ladabaum and his colleagues wrote.
Many factors that might have influenced subjects’ accuracy in distinguishing adenomas from hyperplasia actually proved to have no such effect. The location of the polyp within the colon, the endoscopists’ years in practice and colonoscopy volume, and the changes in subjects’ scores from pretest to posttest all showed no association with their final accuracy in optical biopsy.
One factor that predicted such accuracy was the participant’s confidence in each of his or her predictions.
Finally, there was some attrition over the course of the study, as some subjects who took part in the initial computer-based training did not proceed to the in vivo phase, "and not all participants remained engaged in the in vivo phase. Incentives may need to be developed for busy clinicians to learn and use optical biopsy techniques," the investigators wrote.
Overall, the study findings show that "high accuracy can be achieved ex vivo by community gastroenterologists after self-paced training with a computerized module." However, it remains to be seen whether a gastroenterologist’s ultimate proficiency in optical diagnosis "is determined by technical issues, dedication, motivation, or innate skill," they added.
This study was supported by Stanford University. One author reported receiving research support from and serving on the speakers bureau for Olympus Corp.
FROM GASTROENTEROLOGY
Major Finding: Three of 12 community gastroenterologists learned to distinguish adenomatous from hyperplastic colon polyps 5 mm in size or smaller with 90% accuracy using optical biopsy techniques.
Data Source: An analysis of the success of a computer-based self-training program to teach 12 gastroenterologists in a community practice to perform optical biopsy.
Disclosures: This study was supported by Stanford University. One author reported receiving research support from and serving on the speakers bureau for Olympus Corp.
Depressive symptoms doubled risk of Crohn's disease in women
Depressive symptoms were associated with a doubling of the risk of Crohn’s disease in two large prospective cohorts of women, Dr. Ashwin N. Ananthakrishnan and his colleagues reported in the January issue of Clinical Gastroenterology and Hepatology (2013;11:57-62).
For women with recent and past episodes of depressive symptoms, the associations with the development of Crohn’s disease were significant, and were stronger for those with recent depression. The effect sizes were "in the same range we found for current smoking, oral contraceptive use, and NSAID use," all of which are known risk factors for Crohn’s disease, said Dr. Ananthakrishnan of Massachusetts General Hospital and Harvard Medical School, both in Boston, and his associates.
Video Source: American Gastroenterological Association YouTube channe
"Our findings support the potential importance of a biopsychosocial model in the pathogenesis of Crohn’s disease, and suggest the need for further studies on the effect of depression and stress on immune function and regulation," they noted.
Depression and life stress long have been thought to contribute to immune dysfunction and to influence both the risk for and the course of immune-mediated disorders such as Crohn’s. But until now, few studies have examined the role of mood in the onset of Crohn’s disease and ulcerative colitis, and those that did so were retrospective, failed to adjust for possible confounders, and assessed only the occurrence of major life stressors rather than the presence of depressive symptoms.
To address these shortcomings, the investigators examined the link between depressive symptoms and later onset of Crohn’s disease and ulcerative colitis using data from the prospective Nurses Health Study I and II. NHS I enrolled 121,700 female registered nurses who were 30-55 years old at baseline in 1976, and NHS II enrolled 116,686 female RNs aged 25-42 years at baseline in 1989.
For this study, Dr. Ananthakrishnan and his colleagues analyzed data for 152,461 of these participants in the two NHS cohorts. A total of 170 developed incident Crohn’s disease and 203 developed incident ulcerative colitis during follow-up.
Depressive symptoms were assessed several times in both the NHS I and II subjects using the five-question Mental Health Index (MHI-5), a subscale of the Short Form 36 health status survey. The participants received scores ranging from 1 to 100; 16,986 women (11% of the study population) received scores of 0-52, indicating the presence of depressive symptoms.
Subjects who scored from 86 to 100 composed the reference group.
The data were adjusted to account for numerous covariates that might influence risk for Crohn’s disease and ulcerative colitis, including the subjects’ race/ethnicity; smoking status; weight; menopausal status; and use of oral contraceptives, hormone therapy, and aspirin or NSAIDs.
There was a significant and linear increase in the risk of developing Crohn’s disease as MHI-5 scores decreased. Compared with the reference group, women with an MHI-5 score of 76-85 had a hazard ratio for Crohn’s disease of 1.38, those with an MHI-5 score of 53-75 had an HR of 1.59, and women with depressive symptoms and a score of 0-52 had an HR of 2.36.
No such association was seen between depressive symptoms and ulcerative colitis.
To account for the possibility that the study subjects’ depressed mood might be due to as-yet undiagnosed GI symptoms, the researchers performed a "lag" analysis excluding all cases of Crohn’s and ulcerative colitis that developed within 2 years of MHI-5 assessment. The results were unchanged in this analysis, they said.
The investigators also performed a sensitivity analysis restricted only to cases of Crohn’s disease that developed after 1996, when the NHS subjects first were routinely questioned about their use of antidepressant medications. Adjusting for the use of these drugs only slightly attenuated the strong association between depressive symptoms and Crohn’s disease.
"Preliminary animal and human studies suggest that treating depression through administration of antidepressants, or through improvement in coping mechanisms, could reduce risk of disease relapse. Whether similar interventions can also influence risk of disease onset, particularly among individuals with genetic susceptibility for Crohn’s disease or ulcerative colitis, merits further study," Dr. Ananthakrishnan and his associates said.
This study was supported by the American Gastroenterological Association, the Crohn’s and Colitis Foundation of America, the Broad Foundation, and the National Institutes of Health. Dr. Ananthakrishnan reported no potential financial conflicts of interest; his associates reported ties to Policy Analysis, Bayer HealthCare, Millennium Pharmaceuticals, and Pfizer.
Depressive symptoms were associated with a doubling of the risk of Crohn’s disease in two large prospective cohorts of women, Dr. Ashwin N. Ananthakrishnan and his colleagues reported in the January issue of Clinical Gastroenterology and Hepatology (2013;11:57-62).
For women with recent and past episodes of depressive symptoms, the associations with the development of Crohn’s disease were significant, and were stronger for those with recent depression. The effect sizes were "in the same range we found for current smoking, oral contraceptive use, and NSAID use," all of which are known risk factors for Crohn’s disease, said Dr. Ananthakrishnan of Massachusetts General Hospital and Harvard Medical School, both in Boston, and his associates.
Video Source: American Gastroenterological Association YouTube channe
"Our findings support the potential importance of a biopsychosocial model in the pathogenesis of Crohn’s disease, and suggest the need for further studies on the effect of depression and stress on immune function and regulation," they noted.
Depression and life stress long have been thought to contribute to immune dysfunction and to influence both the risk for and the course of immune-mediated disorders such as Crohn’s. But until now, few studies have examined the role of mood in the onset of Crohn’s disease and ulcerative colitis, and those that did so were retrospective, failed to adjust for possible confounders, and assessed only the occurrence of major life stressors rather than the presence of depressive symptoms.
To address these shortcomings, the investigators examined the link between depressive symptoms and later onset of Crohn’s disease and ulcerative colitis using data from the prospective Nurses Health Study I and II. NHS I enrolled 121,700 female registered nurses who were 30-55 years old at baseline in 1976, and NHS II enrolled 116,686 female RNs aged 25-42 years at baseline in 1989.
For this study, Dr. Ananthakrishnan and his colleagues analyzed data for 152,461 of these participants in the two NHS cohorts. A total of 170 developed incident Crohn’s disease and 203 developed incident ulcerative colitis during follow-up.
Depressive symptoms were assessed several times in both the NHS I and II subjects using the five-question Mental Health Index (MHI-5), a subscale of the Short Form 36 health status survey. The participants received scores ranging from 1 to 100; 16,986 women (11% of the study population) received scores of 0-52, indicating the presence of depressive symptoms.
Subjects who scored from 86 to 100 composed the reference group.
The data were adjusted to account for numerous covariates that might influence risk for Crohn’s disease and ulcerative colitis, including the subjects’ race/ethnicity; smoking status; weight; menopausal status; and use of oral contraceptives, hormone therapy, and aspirin or NSAIDs.
There was a significant and linear increase in the risk of developing Crohn’s disease as MHI-5 scores decreased. Compared with the reference group, women with an MHI-5 score of 76-85 had a hazard ratio for Crohn’s disease of 1.38, those with an MHI-5 score of 53-75 had an HR of 1.59, and women with depressive symptoms and a score of 0-52 had an HR of 2.36.
No such association was seen between depressive symptoms and ulcerative colitis.
To account for the possibility that the study subjects’ depressed mood might be due to as-yet undiagnosed GI symptoms, the researchers performed a "lag" analysis excluding all cases of Crohn’s and ulcerative colitis that developed within 2 years of MHI-5 assessment. The results were unchanged in this analysis, they said.
The investigators also performed a sensitivity analysis restricted only to cases of Crohn’s disease that developed after 1996, when the NHS subjects first were routinely questioned about their use of antidepressant medications. Adjusting for the use of these drugs only slightly attenuated the strong association between depressive symptoms and Crohn’s disease.
"Preliminary animal and human studies suggest that treating depression through administration of antidepressants, or through improvement in coping mechanisms, could reduce risk of disease relapse. Whether similar interventions can also influence risk of disease onset, particularly among individuals with genetic susceptibility for Crohn’s disease or ulcerative colitis, merits further study," Dr. Ananthakrishnan and his associates said.
This study was supported by the American Gastroenterological Association, the Crohn’s and Colitis Foundation of America, the Broad Foundation, and the National Institutes of Health. Dr. Ananthakrishnan reported no potential financial conflicts of interest; his associates reported ties to Policy Analysis, Bayer HealthCare, Millennium Pharmaceuticals, and Pfizer.
Depressive symptoms were associated with a doubling of the risk of Crohn’s disease in two large prospective cohorts of women, Dr. Ashwin N. Ananthakrishnan and his colleagues reported in the January issue of Clinical Gastroenterology and Hepatology (2013;11:57-62).
For women with recent and past episodes of depressive symptoms, the associations with the development of Crohn’s disease were significant, and were stronger for those with recent depression. The effect sizes were "in the same range we found for current smoking, oral contraceptive use, and NSAID use," all of which are known risk factors for Crohn’s disease, said Dr. Ananthakrishnan of Massachusetts General Hospital and Harvard Medical School, both in Boston, and his associates.
Video Source: American Gastroenterological Association YouTube channe
"Our findings support the potential importance of a biopsychosocial model in the pathogenesis of Crohn’s disease, and suggest the need for further studies on the effect of depression and stress on immune function and regulation," they noted.
Depression and life stress long have been thought to contribute to immune dysfunction and to influence both the risk for and the course of immune-mediated disorders such as Crohn’s. But until now, few studies have examined the role of mood in the onset of Crohn’s disease and ulcerative colitis, and those that did so were retrospective, failed to adjust for possible confounders, and assessed only the occurrence of major life stressors rather than the presence of depressive symptoms.
To address these shortcomings, the investigators examined the link between depressive symptoms and later onset of Crohn’s disease and ulcerative colitis using data from the prospective Nurses Health Study I and II. NHS I enrolled 121,700 female registered nurses who were 30-55 years old at baseline in 1976, and NHS II enrolled 116,686 female RNs aged 25-42 years at baseline in 1989.
For this study, Dr. Ananthakrishnan and his colleagues analyzed data for 152,461 of these participants in the two NHS cohorts. A total of 170 developed incident Crohn’s disease and 203 developed incident ulcerative colitis during follow-up.
Depressive symptoms were assessed several times in both the NHS I and II subjects using the five-question Mental Health Index (MHI-5), a subscale of the Short Form 36 health status survey. The participants received scores ranging from 1 to 100; 16,986 women (11% of the study population) received scores of 0-52, indicating the presence of depressive symptoms.
Subjects who scored from 86 to 100 composed the reference group.
The data were adjusted to account for numerous covariates that might influence risk for Crohn’s disease and ulcerative colitis, including the subjects’ race/ethnicity; smoking status; weight; menopausal status; and use of oral contraceptives, hormone therapy, and aspirin or NSAIDs.
There was a significant and linear increase in the risk of developing Crohn’s disease as MHI-5 scores decreased. Compared with the reference group, women with an MHI-5 score of 76-85 had a hazard ratio for Crohn’s disease of 1.38, those with an MHI-5 score of 53-75 had an HR of 1.59, and women with depressive symptoms and a score of 0-52 had an HR of 2.36.
No such association was seen between depressive symptoms and ulcerative colitis.
To account for the possibility that the study subjects’ depressed mood might be due to as-yet undiagnosed GI symptoms, the researchers performed a "lag" analysis excluding all cases of Crohn’s and ulcerative colitis that developed within 2 years of MHI-5 assessment. The results were unchanged in this analysis, they said.
The investigators also performed a sensitivity analysis restricted only to cases of Crohn’s disease that developed after 1996, when the NHS subjects first were routinely questioned about their use of antidepressant medications. Adjusting for the use of these drugs only slightly attenuated the strong association between depressive symptoms and Crohn’s disease.
"Preliminary animal and human studies suggest that treating depression through administration of antidepressants, or through improvement in coping mechanisms, could reduce risk of disease relapse. Whether similar interventions can also influence risk of disease onset, particularly among individuals with genetic susceptibility for Crohn’s disease or ulcerative colitis, merits further study," Dr. Ananthakrishnan and his associates said.
This study was supported by the American Gastroenterological Association, the Crohn’s and Colitis Foundation of America, the Broad Foundation, and the National Institutes of Health. Dr. Ananthakrishnan reported no potential financial conflicts of interest; his associates reported ties to Policy Analysis, Bayer HealthCare, Millennium Pharmaceuticals, and Pfizer.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Major Finding: Women with depressive symptoms and an MHI-5 score of 0-52 had a hazard ratio of 2.36 for Crohn’s disease.
Data Source: An analysis of data on 152,461 subjects in the Nurses Health Study I and II.
Disclosures: This study was supported by the American Gastroenterological Association, the Crohn’s and Colitis Foundation of America, the Broad Foundation, and the National Institutes of Health. Dr. Ananthakrishnan reported no potential financial conflicts of interest; his associates reported ties to Policy Analysis, Bayer HealthCare, Millennium Pharmaceuticals, and Pfizer.
Stopping aspirin after bleeding ulcer raises CV death rate sixfold
Aspirin therapy should be continued at the time of hospital discharge in patients with cardiovascular comorbidities treated for peptic ulcer bleeding, researchers say.
Among patients taking low-dose aspirin therapy who were hospitalized for bleeding of peptic ulcers, those who stopped aspirin altogether were more than six times as likely to die or have a cardiovascular event in the near future as were patients who resumed aspirin therapy after discharge, according to a database analysis. Researcher Maryam Derogar of the Karolinska Institute, Stockholm, and her associates reported their findings in the January issue of Clinical Gastroenterology and Hepatology.
Video Source: American Gastroenterological Association YouTube channel
"Balancing between the cardioprotective effect of aspirin and the increased risk of rebleeding associated with aspirin use requires a careful clinical tradeoff," the investigators wrote (Clin. Gastroenterol. Hepatol. 2013;11:38-42).
They noted that all deaths or acute CV events in the study were among patients at least 64 years old. The study findings indicate that aspirin therapy should not be permanently discontinued in older patients at cardiovascular risk who develop bleeding peptic ulcer, but should resume after the bleeding episode is treated, they wrote.
Given the ulcerogenic properties of aspirin, "concomitant prescription of acid suppressants in the form of proton pump inhibitors is highly recommended," the researchers added.
Only one randomized clinical trial has examined the consequences of discontinuing aspirin therapy in this patient population, and it found a substantially higher risk of short-term mortality in patients who didn’t resume taking aspirin after treatment of the bleeding ulcer (Ann. Intern. Med. 2010;152:1-9). However, that trial had methodological flaws and a short follow-up of only 8 weeks, the investigators said.
They used an administrative database at their hospital to examine this issue, reviewing the medical records of 118 adults treated in 2007-2010 for upper GI bleeding. All the study subjects had endoscopically verified peptic ulcer and were taking low-dose aspirin therapy (75 mg or 160 mg daily) at the time of hospitalization.
Patients who had bleeding from sources other than peptic ulcer, such as esophageal varices or angiodysplasia, were excluded from the study.
Aspirin therapy was permanently discontinued in 40% (47) of the study subjects. Forty percent of patients (48) restarted aspirin therapy immediately after hospital discharge, and the remaining 20% (23) restarted aspirin therapy a median of 1 week later (range, 2 days to 2 months).
During a median follow-up of 2 years, 37% (44) of study subjects either died or had acute cardiovascular events.
The rate of death or acute CV events during the first 6 months of follow-up was more than sixfold higher in patients who discontinued aspirin therapy than in those who resumed aspirin therapy, with a hazard ratio of 6.8, the investigators said. The investigators adjusted the comparison to account for numerous potential confounders, such as alcohol abuse, chronic ischemic heart disease (angina), chronic heart failure, previous MI, atrial fibrillation, previous stroke or TIA, chronic renal failure, diabetes, COPD, and cancer.
Further analysis showed that the rate of mortality and acute CV events during the first 6 months of follow-up rose only in study subjects who had existing cardiovascular comorbidities at hospitalization, and did not rise in those who had no CV comorbidities. This rate was 31% in the 26 such patients who stopped aspirin therapy, compared with only 8% in the 50 who resumed aspirin therapy.
After 6 months of follow-up, the rate of mortality and acute CV events was not significantly different between patients who stopped and patients who resumed aspirin therapy.
Six percent of patients required rehospitalization for recurrent peptic ulcer bleeding during follow-up. No patients died from such rebleeding.
These findings confirm and extend those of the previous randomized clinical trial, which reported an eightfold increase in mortality during 2 months of follow-up for patients who permanently discontinued aspirin therapy, Ms. Derogar and her colleagues said.
No patients in their study who were under age 64 died or developed an acute CV event. "The results are therefore not fully applicable to younger patients and might imply that the elderly are more susceptible to discontinuation of aspirin therapy," they wrote.
Ms. Derogar reported no potential financial conflicts of interest. One of her associates reported receiving a scholarship from the Olle Engkvist Byggmastare Foundation.
When patients with coronary artery disease or cerebrovascular disease develop GI bleeding and undergo endoscopic therapy, a question that most gastroenterologists face is whether aspirin, clopidogrel, or both should be restarted, and if so, when. Many of these patients are at high risk for bleeding-related complications due to advanced age and comorbidities and are also at increased risk for cardiovascular or cerebrovascular complications due to advanced vascular disease.
There are four possible courses of action for the practitioner: Discontinue the aspirin and clopidogrel with no intent to resume them, discontinue aspirin and resume clopidogrel, resume both antiplatelet drugs after endoscopic hemostasis is achieved, or withhold antiplatelet drugs for 7-10 days after endoscopic hemostasis has been achieved.
Although we do not have a complete and valid evidence base to guide our current practice, several important points can be made from recent studies. Ms. Derogar and her colleagues show us that discontinuing aspirin completely is associated with a high rate of death or cardiovascular complications. Rebleeding, on the other hand, was rare patients in whom aspirin was continued. In a recent randomized controlled trial, patients on low-dose aspirin who developed a GI bleed were randomized to continued aspirin or no aspirin after endoscopic hemostasis (Ann. Intern. Med. 2010;152:1-9). Recurrent ulcer bleeding within 30 days was 10.3% in the aspirin group and 5.4% in the placebo group. Patients who received aspirin had lower all-cause mortality rates than patients who received placebo (1.3% vs. 12.9%). Other studies have shown that resuming aspirin with a proton pump inhibitor is superior to administering clopidogrel alone.
There is little evidence to guide us as to whether aspirin or clopidogrel should be held for a short period of time or resumed immediately after endoscopic hemostasis is achieved. This decision should probably be individualized based on the magnitude of the bleeding, the severity of the underlying cardiovascular and cerebrovascular disease, and concurrent comorbid illnesses. The available evidence is clear that it is unwise to discontinue aspirin in patients receiving this agent for cardiovascular or cerebrovascular disease due to the high rate of adverse outcomes.
Nimish Vakil, M.D., AGAF, is a clinical professor of medicine at the University of Wisconsin School of Medicine and Public Health, Madison. He is a consultant to AstraZeneca, Takeda, Otsuka, Xenoport, Orexo, Ironwood, and Restech, and has stock options in Orexo and Meridian Bioscience.
When patients with coronary artery disease or cerebrovascular disease develop GI bleeding and undergo endoscopic therapy, a question that most gastroenterologists face is whether aspirin, clopidogrel, or both should be restarted, and if so, when. Many of these patients are at high risk for bleeding-related complications due to advanced age and comorbidities and are also at increased risk for cardiovascular or cerebrovascular complications due to advanced vascular disease.
There are four possible courses of action for the practitioner: Discontinue the aspirin and clopidogrel with no intent to resume them, discontinue aspirin and resume clopidogrel, resume both antiplatelet drugs after endoscopic hemostasis is achieved, or withhold antiplatelet drugs for 7-10 days after endoscopic hemostasis has been achieved.
Although we do not have a complete and valid evidence base to guide our current practice, several important points can be made from recent studies. Ms. Derogar and her colleagues show us that discontinuing aspirin completely is associated with a high rate of death or cardiovascular complications. Rebleeding, on the other hand, was rare patients in whom aspirin was continued. In a recent randomized controlled trial, patients on low-dose aspirin who developed a GI bleed were randomized to continued aspirin or no aspirin after endoscopic hemostasis (Ann. Intern. Med. 2010;152:1-9). Recurrent ulcer bleeding within 30 days was 10.3% in the aspirin group and 5.4% in the placebo group. Patients who received aspirin had lower all-cause mortality rates than patients who received placebo (1.3% vs. 12.9%). Other studies have shown that resuming aspirin with a proton pump inhibitor is superior to administering clopidogrel alone.
There is little evidence to guide us as to whether aspirin or clopidogrel should be held for a short period of time or resumed immediately after endoscopic hemostasis is achieved. This decision should probably be individualized based on the magnitude of the bleeding, the severity of the underlying cardiovascular and cerebrovascular disease, and concurrent comorbid illnesses. The available evidence is clear that it is unwise to discontinue aspirin in patients receiving this agent for cardiovascular or cerebrovascular disease due to the high rate of adverse outcomes.
Nimish Vakil, M.D., AGAF, is a clinical professor of medicine at the University of Wisconsin School of Medicine and Public Health, Madison. He is a consultant to AstraZeneca, Takeda, Otsuka, Xenoport, Orexo, Ironwood, and Restech, and has stock options in Orexo and Meridian Bioscience.
When patients with coronary artery disease or cerebrovascular disease develop GI bleeding and undergo endoscopic therapy, a question that most gastroenterologists face is whether aspirin, clopidogrel, or both should be restarted, and if so, when. Many of these patients are at high risk for bleeding-related complications due to advanced age and comorbidities and are also at increased risk for cardiovascular or cerebrovascular complications due to advanced vascular disease.
There are four possible courses of action for the practitioner: Discontinue the aspirin and clopidogrel with no intent to resume them, discontinue aspirin and resume clopidogrel, resume both antiplatelet drugs after endoscopic hemostasis is achieved, or withhold antiplatelet drugs for 7-10 days after endoscopic hemostasis has been achieved.
Although we do not have a complete and valid evidence base to guide our current practice, several important points can be made from recent studies. Ms. Derogar and her colleagues show us that discontinuing aspirin completely is associated with a high rate of death or cardiovascular complications. Rebleeding, on the other hand, was rare patients in whom aspirin was continued. In a recent randomized controlled trial, patients on low-dose aspirin who developed a GI bleed were randomized to continued aspirin or no aspirin after endoscopic hemostasis (Ann. Intern. Med. 2010;152:1-9). Recurrent ulcer bleeding within 30 days was 10.3% in the aspirin group and 5.4% in the placebo group. Patients who received aspirin had lower all-cause mortality rates than patients who received placebo (1.3% vs. 12.9%). Other studies have shown that resuming aspirin with a proton pump inhibitor is superior to administering clopidogrel alone.
There is little evidence to guide us as to whether aspirin or clopidogrel should be held for a short period of time or resumed immediately after endoscopic hemostasis is achieved. This decision should probably be individualized based on the magnitude of the bleeding, the severity of the underlying cardiovascular and cerebrovascular disease, and concurrent comorbid illnesses. The available evidence is clear that it is unwise to discontinue aspirin in patients receiving this agent for cardiovascular or cerebrovascular disease due to the high rate of adverse outcomes.
Nimish Vakil, M.D., AGAF, is a clinical professor of medicine at the University of Wisconsin School of Medicine and Public Health, Madison. He is a consultant to AstraZeneca, Takeda, Otsuka, Xenoport, Orexo, Ironwood, and Restech, and has stock options in Orexo and Meridian Bioscience.
Aspirin therapy should be continued at the time of hospital discharge in patients with cardiovascular comorbidities treated for peptic ulcer bleeding, researchers say.
Among patients taking low-dose aspirin therapy who were hospitalized for bleeding of peptic ulcers, those who stopped aspirin altogether were more than six times as likely to die or have a cardiovascular event in the near future as were patients who resumed aspirin therapy after discharge, according to a database analysis. Researcher Maryam Derogar of the Karolinska Institute, Stockholm, and her associates reported their findings in the January issue of Clinical Gastroenterology and Hepatology.
Video Source: American Gastroenterological Association YouTube channel
"Balancing between the cardioprotective effect of aspirin and the increased risk of rebleeding associated with aspirin use requires a careful clinical tradeoff," the investigators wrote (Clin. Gastroenterol. Hepatol. 2013;11:38-42).
They noted that all deaths or acute CV events in the study were among patients at least 64 years old. The study findings indicate that aspirin therapy should not be permanently discontinued in older patients at cardiovascular risk who develop bleeding peptic ulcer, but should resume after the bleeding episode is treated, they wrote.
Given the ulcerogenic properties of aspirin, "concomitant prescription of acid suppressants in the form of proton pump inhibitors is highly recommended," the researchers added.
Only one randomized clinical trial has examined the consequences of discontinuing aspirin therapy in this patient population, and it found a substantially higher risk of short-term mortality in patients who didn’t resume taking aspirin after treatment of the bleeding ulcer (Ann. Intern. Med. 2010;152:1-9). However, that trial had methodological flaws and a short follow-up of only 8 weeks, the investigators said.
They used an administrative database at their hospital to examine this issue, reviewing the medical records of 118 adults treated in 2007-2010 for upper GI bleeding. All the study subjects had endoscopically verified peptic ulcer and were taking low-dose aspirin therapy (75 mg or 160 mg daily) at the time of hospitalization.
Patients who had bleeding from sources other than peptic ulcer, such as esophageal varices or angiodysplasia, were excluded from the study.
Aspirin therapy was permanently discontinued in 40% (47) of the study subjects. Forty percent of patients (48) restarted aspirin therapy immediately after hospital discharge, and the remaining 20% (23) restarted aspirin therapy a median of 1 week later (range, 2 days to 2 months).
During a median follow-up of 2 years, 37% (44) of study subjects either died or had acute cardiovascular events.
The rate of death or acute CV events during the first 6 months of follow-up was more than sixfold higher in patients who discontinued aspirin therapy than in those who resumed aspirin therapy, with a hazard ratio of 6.8, the investigators said. The investigators adjusted the comparison to account for numerous potential confounders, such as alcohol abuse, chronic ischemic heart disease (angina), chronic heart failure, previous MI, atrial fibrillation, previous stroke or TIA, chronic renal failure, diabetes, COPD, and cancer.
Further analysis showed that the rate of mortality and acute CV events during the first 6 months of follow-up rose only in study subjects who had existing cardiovascular comorbidities at hospitalization, and did not rise in those who had no CV comorbidities. This rate was 31% in the 26 such patients who stopped aspirin therapy, compared with only 8% in the 50 who resumed aspirin therapy.
After 6 months of follow-up, the rate of mortality and acute CV events was not significantly different between patients who stopped and patients who resumed aspirin therapy.
Six percent of patients required rehospitalization for recurrent peptic ulcer bleeding during follow-up. No patients died from such rebleeding.
These findings confirm and extend those of the previous randomized clinical trial, which reported an eightfold increase in mortality during 2 months of follow-up for patients who permanently discontinued aspirin therapy, Ms. Derogar and her colleagues said.
No patients in their study who were under age 64 died or developed an acute CV event. "The results are therefore not fully applicable to younger patients and might imply that the elderly are more susceptible to discontinuation of aspirin therapy," they wrote.
Ms. Derogar reported no potential financial conflicts of interest. One of her associates reported receiving a scholarship from the Olle Engkvist Byggmastare Foundation.
Aspirin therapy should be continued at the time of hospital discharge in patients with cardiovascular comorbidities treated for peptic ulcer bleeding, researchers say.
Among patients taking low-dose aspirin therapy who were hospitalized for bleeding of peptic ulcers, those who stopped aspirin altogether were more than six times as likely to die or have a cardiovascular event in the near future as were patients who resumed aspirin therapy after discharge, according to a database analysis. Researcher Maryam Derogar of the Karolinska Institute, Stockholm, and her associates reported their findings in the January issue of Clinical Gastroenterology and Hepatology.
Video Source: American Gastroenterological Association YouTube channel
"Balancing between the cardioprotective effect of aspirin and the increased risk of rebleeding associated with aspirin use requires a careful clinical tradeoff," the investigators wrote (Clin. Gastroenterol. Hepatol. 2013;11:38-42).
They noted that all deaths or acute CV events in the study were among patients at least 64 years old. The study findings indicate that aspirin therapy should not be permanently discontinued in older patients at cardiovascular risk who develop bleeding peptic ulcer, but should resume after the bleeding episode is treated, they wrote.
Given the ulcerogenic properties of aspirin, "concomitant prescription of acid suppressants in the form of proton pump inhibitors is highly recommended," the researchers added.
Only one randomized clinical trial has examined the consequences of discontinuing aspirin therapy in this patient population, and it found a substantially higher risk of short-term mortality in patients who didn’t resume taking aspirin after treatment of the bleeding ulcer (Ann. Intern. Med. 2010;152:1-9). However, that trial had methodological flaws and a short follow-up of only 8 weeks, the investigators said.
They used an administrative database at their hospital to examine this issue, reviewing the medical records of 118 adults treated in 2007-2010 for upper GI bleeding. All the study subjects had endoscopically verified peptic ulcer and were taking low-dose aspirin therapy (75 mg or 160 mg daily) at the time of hospitalization.
Patients who had bleeding from sources other than peptic ulcer, such as esophageal varices or angiodysplasia, were excluded from the study.
Aspirin therapy was permanently discontinued in 40% (47) of the study subjects. Forty percent of patients (48) restarted aspirin therapy immediately after hospital discharge, and the remaining 20% (23) restarted aspirin therapy a median of 1 week later (range, 2 days to 2 months).
During a median follow-up of 2 years, 37% (44) of study subjects either died or had acute cardiovascular events.
The rate of death or acute CV events during the first 6 months of follow-up was more than sixfold higher in patients who discontinued aspirin therapy than in those who resumed aspirin therapy, with a hazard ratio of 6.8, the investigators said. The investigators adjusted the comparison to account for numerous potential confounders, such as alcohol abuse, chronic ischemic heart disease (angina), chronic heart failure, previous MI, atrial fibrillation, previous stroke or TIA, chronic renal failure, diabetes, COPD, and cancer.
Further analysis showed that the rate of mortality and acute CV events during the first 6 months of follow-up rose only in study subjects who had existing cardiovascular comorbidities at hospitalization, and did not rise in those who had no CV comorbidities. This rate was 31% in the 26 such patients who stopped aspirin therapy, compared with only 8% in the 50 who resumed aspirin therapy.
After 6 months of follow-up, the rate of mortality and acute CV events was not significantly different between patients who stopped and patients who resumed aspirin therapy.
Six percent of patients required rehospitalization for recurrent peptic ulcer bleeding during follow-up. No patients died from such rebleeding.
These findings confirm and extend those of the previous randomized clinical trial, which reported an eightfold increase in mortality during 2 months of follow-up for patients who permanently discontinued aspirin therapy, Ms. Derogar and her colleagues said.
No patients in their study who were under age 64 died or developed an acute CV event. "The results are therefore not fully applicable to younger patients and might imply that the elderly are more susceptible to discontinuation of aspirin therapy," they wrote.
Ms. Derogar reported no potential financial conflicts of interest. One of her associates reported receiving a scholarship from the Olle Engkvist Byggmastare Foundation.
FROM CLINICAL GASTROENTEROLOGY AND HEPATOLOGY
Major Finding: The combined rate of death or acute CV events during the first 6 months of follow-up was more than sixfold higher in patients who discontinued aspirin therapy than in those who resumed aspirin therapy, with a hazard ratio of 6.8.
Data Source: An analysis of 6-month and 12-month mortality in 118 adults on aspirin therapy who were hospitalized at a single institution for bleeding peptic ulcer in 2007-2010.
Disclosures: Ms. Derogar reported no potential financial conflicts of interest. One of her associates reported receiving a scholarship from the Olle Engkvist Byggmastare Foundation.
FDA approves teduglutide for short bowel syndrome
The Food and Drug Administration on Dec. 21 approved teduglutide, to be marketed under the trade name Gattex, to treat adults with short bowel syndrome (SBS) who need parenteral nutrition.
Teduglutide, a recombinant analogue of human glucagon-like peptide-2 (GLP-2), was unanimously recommended for approval by an FDA advisory panel in October. It is a once-daily subcutaneous injection that helps improve intestinal absorption of fluids and nutrients, reducing the frequency and volume of parenteral nutrition.
"Considering Gattex has been shown to significantly reduce or in some cases even eliminate the requirement for parenteral support, it may become a cornerstone therapy in the management of short bowel syndrome." Dr. Ken Fujioka of the Nutrition and Metabolic Research Center, Scripps Clinic, Del Mar, Calif., said in a statement issued by Gattex’s maker, NPA Pharmaceuticals.
It is the third drug to be approved by the FDA for SBS patients who are dependent on parenteral nutrition. Somatropin (Zorbtive) was approved in 2003 and glutamine (Nutrestore) in 2004.
"Today’s approval expands the available treatment options for patients with this life-threatening condition," Dr. Victoria Kusiak, deputy director of the Office of Drug Evaluation III in the FDA Center for Drug Evaluation and Research, said in a statement. "Because Gattex may cause other serious health conditions, it is critical that patients and health care professionals understand the drug’s potential and known safety risks."
Teduglutide therapy increases the risk of developing cancer and polyps in the intestine, obstructions in the intestine, gallbladder disease, biliary tract disease, and pancreatic disease. The drug will have a Risk Evaluation and Mitigation Strategy, consisting of a communication plan and training for prescribers, according to the FDA.
Pivotal data on the drug were published in September in Gastroenterology (Gastroenterology 2012 Sept. 13 [doi:10.1053/j.gastro.2012.09.007]).
The Food and Drug Administration on Dec. 21 approved teduglutide, to be marketed under the trade name Gattex, to treat adults with short bowel syndrome (SBS) who need parenteral nutrition.
Teduglutide, a recombinant analogue of human glucagon-like peptide-2 (GLP-2), was unanimously recommended for approval by an FDA advisory panel in October. It is a once-daily subcutaneous injection that helps improve intestinal absorption of fluids and nutrients, reducing the frequency and volume of parenteral nutrition.
"Considering Gattex has been shown to significantly reduce or in some cases even eliminate the requirement for parenteral support, it may become a cornerstone therapy in the management of short bowel syndrome." Dr. Ken Fujioka of the Nutrition and Metabolic Research Center, Scripps Clinic, Del Mar, Calif., said in a statement issued by Gattex’s maker, NPA Pharmaceuticals.
It is the third drug to be approved by the FDA for SBS patients who are dependent on parenteral nutrition. Somatropin (Zorbtive) was approved in 2003 and glutamine (Nutrestore) in 2004.
"Today’s approval expands the available treatment options for patients with this life-threatening condition," Dr. Victoria Kusiak, deputy director of the Office of Drug Evaluation III in the FDA Center for Drug Evaluation and Research, said in a statement. "Because Gattex may cause other serious health conditions, it is critical that patients and health care professionals understand the drug’s potential and known safety risks."
Teduglutide therapy increases the risk of developing cancer and polyps in the intestine, obstructions in the intestine, gallbladder disease, biliary tract disease, and pancreatic disease. The drug will have a Risk Evaluation and Mitigation Strategy, consisting of a communication plan and training for prescribers, according to the FDA.
Pivotal data on the drug were published in September in Gastroenterology (Gastroenterology 2012 Sept. 13 [doi:10.1053/j.gastro.2012.09.007]).
The Food and Drug Administration on Dec. 21 approved teduglutide, to be marketed under the trade name Gattex, to treat adults with short bowel syndrome (SBS) who need parenteral nutrition.
Teduglutide, a recombinant analogue of human glucagon-like peptide-2 (GLP-2), was unanimously recommended for approval by an FDA advisory panel in October. It is a once-daily subcutaneous injection that helps improve intestinal absorption of fluids and nutrients, reducing the frequency and volume of parenteral nutrition.
"Considering Gattex has been shown to significantly reduce or in some cases even eliminate the requirement for parenteral support, it may become a cornerstone therapy in the management of short bowel syndrome." Dr. Ken Fujioka of the Nutrition and Metabolic Research Center, Scripps Clinic, Del Mar, Calif., said in a statement issued by Gattex’s maker, NPA Pharmaceuticals.
It is the third drug to be approved by the FDA for SBS patients who are dependent on parenteral nutrition. Somatropin (Zorbtive) was approved in 2003 and glutamine (Nutrestore) in 2004.
"Today’s approval expands the available treatment options for patients with this life-threatening condition," Dr. Victoria Kusiak, deputy director of the Office of Drug Evaluation III in the FDA Center for Drug Evaluation and Research, said in a statement. "Because Gattex may cause other serious health conditions, it is critical that patients and health care professionals understand the drug’s potential and known safety risks."
Teduglutide therapy increases the risk of developing cancer and polyps in the intestine, obstructions in the intestine, gallbladder disease, biliary tract disease, and pancreatic disease. The drug will have a Risk Evaluation and Mitigation Strategy, consisting of a communication plan and training for prescribers, according to the FDA.
Pivotal data on the drug were published in September in Gastroenterology (Gastroenterology 2012 Sept. 13 [doi:10.1053/j.gastro.2012.09.007]).