User login
Screen pregnant women for OSA, given known risks
Pregnant women who have even mild sleep apnea should be treated for their sleep-disordered breathing given what is known about associated risks for hypertensive disorders of pregnancy and gestational diabetes, Carolyn M. D’Ambrosio, MS, MD, FCCP, said at the virtual annual meeting of the Associated Professional Sleep Societies.
“This is the current standard of care,” Dr. D’Ambrosio said. “Although guidelines on this issue are not hard and fast, I’d say that knowing what we know about the risk of adverse [maternal] outcomes, we should all try to treat these problems as soon as they’re identified” and then repeat polysomnography or home sleep testing 3-6 months post partum to “be sure the sleep-disordered breathing has resolved.”
Estimates of obstructive sleep apnea (OSA) prevalence range from approximately 9% in the first trimester to 20% in the third trimester. Yet recognizing the significance of OSA in pregnant women and identifying women for testing remains a major challenge. “Most women won’t [report sleep problems] because it’s pretty much common folklore that you don’t sleep well when you’re pregnant,” said Dr. D’Ambrosio, associate professor of medicine at Harvard Medical School, Boston, and current past-chair of the Women’s Lung Health Network for CHEST.
Many obstetricians and obstetrics providers, meanwhile, do not adequately screen. Typical screening tools like the Epworth Sleepiness Scale have low sensitivity and specificity during pregnancy, which means that inquiries about sleepiness, snoring, and disruptions in sleep are important, as is attention to potential risks for OSA posed by obesity, chronic hypertension, and neck circumference.
Only about a quarter of women in the United States snore during pregnancy, she noted. Snoring prevalence does increase as pregnancy progresses, reaching up to almost 50% in during the third trimester in some studies.
A four-variable screening tool reported almost 10 years ago for pregnant women is reliable for gauging risk, Dr. D’Ambrosio said. The model considers self-reported frequent snoring (more than three times/week), chronic hypertension, advanced maternal age, and a pregestational body mass index of at least 30 kg/m2. “If these [factors] are present, the patient is at significant risk for OSA and should be strongly considered for testing,” she said.
Home sleep apnea testing (HSAT) is validated for pregnant women but “it can underestimate,” she said. “If you get a negative result and [have clinical suspicion], then don’t stop there.”
And considering that the prevalence of OSA – at all levels of severity – increases as pregnancy progresses, it’s important to continue talking about sleep with patients who have frequent snoring, for instance, but negative sleep test results early in pregnancy. “They could develop [OSA] as time goes on,” she said.
Associated risk factors
Independent associations between sleep-disordered breathing and adverse maternal outcomes were demonstrated in a prospective cohort study published several years ago of 3,705 women who underwent HSAT in early and mid-pregnancy. The adjusted odds ratios for preeclampsia when sleep-disordered breathing (an apnea-hypopnea index of ≥5) was present early in pregnancy and in mid-pregnancy were 1.94 and 1.95, respectively.
For hypertensive disorders of pregnancy more broadly, the ORs were 1.46 and 1.73, and for gestational diabetes, the ORs were 3.47 and 2.79.
“Faced with the question about why it’s important to diagnosis and treat OSA [during pregnancy] since the pregnancy will be over in a few months, I go to this study,” Dr. D’Ambrosio said. “Waiting until the end of pregnancy is not safe. There are increased risks of very serious conditions if sleep apnea is there and it’s not treated.”
Another study demonstrating a link between OSA and maternal outcomes looked over 1.5 million deliveries in the United States and found a significantly higher prevalence of gestational diabetes (OR, 2.08), gestational hypertension (OR, 1.77), preeclampsia (OR, 2.07), and eclampsia (OR, 2.70) in pregnant women with OSA than without, after adjusting for maternal obesity. Associations remained significant after adjusting for a more comprehensive list of covariates.
Multiple potential casual pathways are at play, Dr. D’Ambrosio said. Short sleep duration decreases leptin and increases ghrelin levels, for instance, and sleep fragmentation activates the HPA axis and increases cortisol. Intermittent hypoxemia affects sympathetic activity, and intrathoracic pressure swings cause increased oxidative stress and systemic inflammation.
The resulting endothelial dysfunction, glucose dysfunction, and dyslipidemia can drive the adverse maternal outcomes documented in these studies, she said, noting that the adverse outcomes can have long-term cardiovascular consequences.
Continuous positive airway pressure therapy is well tolerated in pregnancy, and given pregnancy’s continual weight change, auto-titrating CPAP may be the best option, she said.
There is “some limited data that treatment improves maternal outcomes, and we’re still working on trying to get better data and more solid recommendations,” Dr. D’Ambrosio said. There currently are no guidelines covering the diagnosis and management of OSA during pregnancy.
“We’ve come a long way ... but we still have more to do,” she said. “We have a long way to go to getting [OSA in pregnant women] well recognized, with screening techniques and diagnosis.”
Asked after the meeting about Dr. D’Ambrosio’s messages, Anita Rajagopal, MD, said that OSA screening during pregnancy needs to be improved through more collaboration “with our ob.gyn. and primary care colleagues.”
Too often, she said, “the signs and symptoms of OSA in pregnancy are written off as ‘just harmless snoring’ while in fact the patient has treatable sleep disordered breathing with potential adverse effects.” Dr. Rajagopal is department medical director for sleep medicine at Community Physician Network and medical director of the Community Health Network Sleep-Wake Disorders Center, both in Indianapolis.
Dr. D’Ambrosio reported that she has no potential conflicts of interest related to the material she presented, and Dr. Rajagopal stated she has no potential conflicts of interest.
Pregnant women who have even mild sleep apnea should be treated for their sleep-disordered breathing given what is known about associated risks for hypertensive disorders of pregnancy and gestational diabetes, Carolyn M. D’Ambrosio, MS, MD, FCCP, said at the virtual annual meeting of the Associated Professional Sleep Societies.
“This is the current standard of care,” Dr. D’Ambrosio said. “Although guidelines on this issue are not hard and fast, I’d say that knowing what we know about the risk of adverse [maternal] outcomes, we should all try to treat these problems as soon as they’re identified” and then repeat polysomnography or home sleep testing 3-6 months post partum to “be sure the sleep-disordered breathing has resolved.”
Estimates of obstructive sleep apnea (OSA) prevalence range from approximately 9% in the first trimester to 20% in the third trimester. Yet recognizing the significance of OSA in pregnant women and identifying women for testing remains a major challenge. “Most women won’t [report sleep problems] because it’s pretty much common folklore that you don’t sleep well when you’re pregnant,” said Dr. D’Ambrosio, associate professor of medicine at Harvard Medical School, Boston, and current past-chair of the Women’s Lung Health Network for CHEST.
Many obstetricians and obstetrics providers, meanwhile, do not adequately screen. Typical screening tools like the Epworth Sleepiness Scale have low sensitivity and specificity during pregnancy, which means that inquiries about sleepiness, snoring, and disruptions in sleep are important, as is attention to potential risks for OSA posed by obesity, chronic hypertension, and neck circumference.
Only about a quarter of women in the United States snore during pregnancy, she noted. Snoring prevalence does increase as pregnancy progresses, reaching up to almost 50% in during the third trimester in some studies.
A four-variable screening tool reported almost 10 years ago for pregnant women is reliable for gauging risk, Dr. D’Ambrosio said. The model considers self-reported frequent snoring (more than three times/week), chronic hypertension, advanced maternal age, and a pregestational body mass index of at least 30 kg/m2. “If these [factors] are present, the patient is at significant risk for OSA and should be strongly considered for testing,” she said.
Home sleep apnea testing (HSAT) is validated for pregnant women but “it can underestimate,” she said. “If you get a negative result and [have clinical suspicion], then don’t stop there.”
And considering that the prevalence of OSA – at all levels of severity – increases as pregnancy progresses, it’s important to continue talking about sleep with patients who have frequent snoring, for instance, but negative sleep test results early in pregnancy. “They could develop [OSA] as time goes on,” she said.
Associated risk factors
Independent associations between sleep-disordered breathing and adverse maternal outcomes were demonstrated in a prospective cohort study published several years ago of 3,705 women who underwent HSAT in early and mid-pregnancy. The adjusted odds ratios for preeclampsia when sleep-disordered breathing (an apnea-hypopnea index of ≥5) was present early in pregnancy and in mid-pregnancy were 1.94 and 1.95, respectively.
For hypertensive disorders of pregnancy more broadly, the ORs were 1.46 and 1.73, and for gestational diabetes, the ORs were 3.47 and 2.79.
“Faced with the question about why it’s important to diagnosis and treat OSA [during pregnancy] since the pregnancy will be over in a few months, I go to this study,” Dr. D’Ambrosio said. “Waiting until the end of pregnancy is not safe. There are increased risks of very serious conditions if sleep apnea is there and it’s not treated.”
Another study demonstrating a link between OSA and maternal outcomes looked over 1.5 million deliveries in the United States and found a significantly higher prevalence of gestational diabetes (OR, 2.08), gestational hypertension (OR, 1.77), preeclampsia (OR, 2.07), and eclampsia (OR, 2.70) in pregnant women with OSA than without, after adjusting for maternal obesity. Associations remained significant after adjusting for a more comprehensive list of covariates.
Multiple potential casual pathways are at play, Dr. D’Ambrosio said. Short sleep duration decreases leptin and increases ghrelin levels, for instance, and sleep fragmentation activates the HPA axis and increases cortisol. Intermittent hypoxemia affects sympathetic activity, and intrathoracic pressure swings cause increased oxidative stress and systemic inflammation.
The resulting endothelial dysfunction, glucose dysfunction, and dyslipidemia can drive the adverse maternal outcomes documented in these studies, she said, noting that the adverse outcomes can have long-term cardiovascular consequences.
Continuous positive airway pressure therapy is well tolerated in pregnancy, and given pregnancy’s continual weight change, auto-titrating CPAP may be the best option, she said.
There is “some limited data that treatment improves maternal outcomes, and we’re still working on trying to get better data and more solid recommendations,” Dr. D’Ambrosio said. There currently are no guidelines covering the diagnosis and management of OSA during pregnancy.
“We’ve come a long way ... but we still have more to do,” she said. “We have a long way to go to getting [OSA in pregnant women] well recognized, with screening techniques and diagnosis.”
Asked after the meeting about Dr. D’Ambrosio’s messages, Anita Rajagopal, MD, said that OSA screening during pregnancy needs to be improved through more collaboration “with our ob.gyn. and primary care colleagues.”
Too often, she said, “the signs and symptoms of OSA in pregnancy are written off as ‘just harmless snoring’ while in fact the patient has treatable sleep disordered breathing with potential adverse effects.” Dr. Rajagopal is department medical director for sleep medicine at Community Physician Network and medical director of the Community Health Network Sleep-Wake Disorders Center, both in Indianapolis.
Dr. D’Ambrosio reported that she has no potential conflicts of interest related to the material she presented, and Dr. Rajagopal stated she has no potential conflicts of interest.
Pregnant women who have even mild sleep apnea should be treated for their sleep-disordered breathing given what is known about associated risks for hypertensive disorders of pregnancy and gestational diabetes, Carolyn M. D’Ambrosio, MS, MD, FCCP, said at the virtual annual meeting of the Associated Professional Sleep Societies.
“This is the current standard of care,” Dr. D’Ambrosio said. “Although guidelines on this issue are not hard and fast, I’d say that knowing what we know about the risk of adverse [maternal] outcomes, we should all try to treat these problems as soon as they’re identified” and then repeat polysomnography or home sleep testing 3-6 months post partum to “be sure the sleep-disordered breathing has resolved.”
Estimates of obstructive sleep apnea (OSA) prevalence range from approximately 9% in the first trimester to 20% in the third trimester. Yet recognizing the significance of OSA in pregnant women and identifying women for testing remains a major challenge. “Most women won’t [report sleep problems] because it’s pretty much common folklore that you don’t sleep well when you’re pregnant,” said Dr. D’Ambrosio, associate professor of medicine at Harvard Medical School, Boston, and current past-chair of the Women’s Lung Health Network for CHEST.
Many obstetricians and obstetrics providers, meanwhile, do not adequately screen. Typical screening tools like the Epworth Sleepiness Scale have low sensitivity and specificity during pregnancy, which means that inquiries about sleepiness, snoring, and disruptions in sleep are important, as is attention to potential risks for OSA posed by obesity, chronic hypertension, and neck circumference.
Only about a quarter of women in the United States snore during pregnancy, she noted. Snoring prevalence does increase as pregnancy progresses, reaching up to almost 50% in during the third trimester in some studies.
A four-variable screening tool reported almost 10 years ago for pregnant women is reliable for gauging risk, Dr. D’Ambrosio said. The model considers self-reported frequent snoring (more than three times/week), chronic hypertension, advanced maternal age, and a pregestational body mass index of at least 30 kg/m2. “If these [factors] are present, the patient is at significant risk for OSA and should be strongly considered for testing,” she said.
Home sleep apnea testing (HSAT) is validated for pregnant women but “it can underestimate,” she said. “If you get a negative result and [have clinical suspicion], then don’t stop there.”
And considering that the prevalence of OSA – at all levels of severity – increases as pregnancy progresses, it’s important to continue talking about sleep with patients who have frequent snoring, for instance, but negative sleep test results early in pregnancy. “They could develop [OSA] as time goes on,” she said.
Associated risk factors
Independent associations between sleep-disordered breathing and adverse maternal outcomes were demonstrated in a prospective cohort study published several years ago of 3,705 women who underwent HSAT in early and mid-pregnancy. The adjusted odds ratios for preeclampsia when sleep-disordered breathing (an apnea-hypopnea index of ≥5) was present early in pregnancy and in mid-pregnancy were 1.94 and 1.95, respectively.
For hypertensive disorders of pregnancy more broadly, the ORs were 1.46 and 1.73, and for gestational diabetes, the ORs were 3.47 and 2.79.
“Faced with the question about why it’s important to diagnosis and treat OSA [during pregnancy] since the pregnancy will be over in a few months, I go to this study,” Dr. D’Ambrosio said. “Waiting until the end of pregnancy is not safe. There are increased risks of very serious conditions if sleep apnea is there and it’s not treated.”
Another study demonstrating a link between OSA and maternal outcomes looked over 1.5 million deliveries in the United States and found a significantly higher prevalence of gestational diabetes (OR, 2.08), gestational hypertension (OR, 1.77), preeclampsia (OR, 2.07), and eclampsia (OR, 2.70) in pregnant women with OSA than without, after adjusting for maternal obesity. Associations remained significant after adjusting for a more comprehensive list of covariates.
Multiple potential casual pathways are at play, Dr. D’Ambrosio said. Short sleep duration decreases leptin and increases ghrelin levels, for instance, and sleep fragmentation activates the HPA axis and increases cortisol. Intermittent hypoxemia affects sympathetic activity, and intrathoracic pressure swings cause increased oxidative stress and systemic inflammation.
The resulting endothelial dysfunction, glucose dysfunction, and dyslipidemia can drive the adverse maternal outcomes documented in these studies, she said, noting that the adverse outcomes can have long-term cardiovascular consequences.
Continuous positive airway pressure therapy is well tolerated in pregnancy, and given pregnancy’s continual weight change, auto-titrating CPAP may be the best option, she said.
There is “some limited data that treatment improves maternal outcomes, and we’re still working on trying to get better data and more solid recommendations,” Dr. D’Ambrosio said. There currently are no guidelines covering the diagnosis and management of OSA during pregnancy.
“We’ve come a long way ... but we still have more to do,” she said. “We have a long way to go to getting [OSA in pregnant women] well recognized, with screening techniques and diagnosis.”
Asked after the meeting about Dr. D’Ambrosio’s messages, Anita Rajagopal, MD, said that OSA screening during pregnancy needs to be improved through more collaboration “with our ob.gyn. and primary care colleagues.”
Too often, she said, “the signs and symptoms of OSA in pregnancy are written off as ‘just harmless snoring’ while in fact the patient has treatable sleep disordered breathing with potential adverse effects.” Dr. Rajagopal is department medical director for sleep medicine at Community Physician Network and medical director of the Community Health Network Sleep-Wake Disorders Center, both in Indianapolis.
Dr. D’Ambrosio reported that she has no potential conflicts of interest related to the material she presented, and Dr. Rajagopal stated she has no potential conflicts of interest.
FROM SLEEP 2021
‘Praise Diabetes’: Support programs in Black churches yield lasting A1c changes
A church-based diabetes self-management support intervention that incorporated parish nurses and peer leaders is feasible and may help improve diabetes-related outcomes in participants.
Sustained reductions in hemoglobin A1c and diabetes distress were seen in the Praise Diabetes Project, a 33-month study that piloted several different approaches to parish nurse and peer leader support at 21 urban churches in Michigan and Ohio, said Gretchen Piatt, MPH, PhD, associate professor in the department of learning health sciences at the University of Michigan, Ann Arbor, reported at the annual scientific sessions of the American Diabetes Association.
“Of the participants who achieved glycemic control following diabetes self-management education, a really large proportion – upward of 77% of participants across all the groups– achieved sustained glycemic control at 33 months,” Dr. Piatt said.
Findings from this study has helped diabetes educators better understand how to design effective support approaches that may have a long-term impact on glycemic control and diabetes distress, Dr. Piatt said.
The Praise Diabetes Project represents a “very smart strategy” of leveraging institutions that already exist in the African American community that are trusted and provide emotional support, said Tracey D. Brown, CEO of the ADA.
“This is about behavior change, really, at its crux,” Ms. Brown said in an interview. “To get there, you’ve got to have trust, and you have to have an emotional connection. If you don’t get either one of those things, then you really are not going to do anything in terms of changing behavior.”
Long-term solutions needed
Many studies show that diabetes self-management education can improve clinical and psychosocial outcomes, and reduce health care utilization and cost, at least in the short term, Dr. Piatt said. However, it’s less clear how those improvements can be sustained over longer periods of time.
“This then presents a critical need to develop and evaluate diabetes self-management support models that are ongoing, patient driven, and embedded within existing community infrastructures,” Dr. Piatt said in her presentation.
Working with churches is one approach to working within existing community infrastructures: “Churches are embedded in the community, they have the personnel oftentimes to facilitate these types of health programs, and most importantly, they have the established relationships with the community that brings about sustained changes,” Dr. Piatt said in her presentation.
Addressing diabetes education needs in urban, low-resource communities
The Praise Diabetes Project was a randomized, 33-month clinical trial conducted in 21 predominantly Black churches in Detroit; Flint, Mich.; and Toledo, Ohio, which are all urban, low-resource communities where diabetes is a significant public health problem, according to Dr. Piatt.
The study was designed to evaluate the relative effectiveness of three different approaches to diabetes self-management support at improving A1c and levels of diabetes distress, according to the investigators.
The churches were randomized to one of the support arms, including parish nurse plus peer leader support, parish nurse support by itself, or peer leader support by itself.
A total of 47 individuals were trained, including 31 peer leaders and 16 parish nurses.
All three interventions included an initial 6-month period of “enhanced usual care” during which biweekly newsletters that were distributed, according to Dr. Piatt. That was followed by 12 months of diabetes self-management support, and an additional 12 months of ongoing support facilitated by parish nurses and peer leaders on their own, without input from the research team or health care providers.
Participants in the program had to be at least 21 years old and under the care of a physician for their diabetes, according to Dr. Piatt. The parish nurses had to be registered nurses in Michigan or Ohio. Peer leaders had to be at least 21 years old, had at least an eighth-grade education, and had to commit to a 30-hour training program.
Peer leaders also had to be individuals living with diabetes: “Prior studies have found that, when peer leaders are actively working on their own self-management goals, they tend to be much more successful in helping others,” Dr. Piatt explained.
In addition to facilitating diabetes self-management education, the parish nurses and peer leaders in these interventions were responsible for recruitment, church announcements, room reservations, follow-up calls to participants, according to Dr. Piatt. Parish nurses also provided clinical content knowledge and supervised the peer leaders in the combined model.
Sustained reductions in A1c and diabetes distress
These diabetes self-management support approaches led to significant changes over time in A1c and diabetes distress, the primary outcomes of the study, Dr. Piatt said.
The peer leader support approach resulted in a statistically significant decline in A1c, from a mean of 8.0% at baseline to 7.7% at 33 months (P = .04), while nonsignificant declines were observed in the parish nurse and combined parish nurse–peer leader approach, according to the researcher.
Reductions in A1c persisted despite the COVID-19 pandemic, which began roughly 21 months into the study, she said.
Glycemic control remained steady over the course of the study, as illustrated by similar proportions of participants with A1c below 7% from baseline to 33 months, she added.
Sustained glycemic control was seen in all three groups, according to Dr. Piatt. For example, 42.7% of individuals in the parish nurse and peer leader support group achieved glycemic control following the intervention, and 88.5% of them sustained it at 33 months.
“I think this is one of the longest diabetes self-management education and diabetes self-management support interventions that’s out there right now, so we were so happy to see that sustained by glycemic control that far into the future,” she said.
Diabetes distress levels decreased steadily over time in all three groups, with declines that were statistically significant from baseline to 33 months in the parish nurse–only and peer leader–only groups, the investigator said.
The proportion of participants reporting moderate levels of diabetes distress dropped over time, especially in the peer leader support group, where there was a 50% reduction, she added.
Despite these findings, the study had limitations, according to Dr. Piatt, including some “burnout” that impacted participants, parish nurses, and peer leaders, especially after the pandemic started.
In addition, this type of intervention may have limited impact in the community at large: “We probably didn’t reach people who did not have good connection to the church,” Dr. Piatt said.
Dr. Piatt reported no conflicts of interest related to the research.
A church-based diabetes self-management support intervention that incorporated parish nurses and peer leaders is feasible and may help improve diabetes-related outcomes in participants.
Sustained reductions in hemoglobin A1c and diabetes distress were seen in the Praise Diabetes Project, a 33-month study that piloted several different approaches to parish nurse and peer leader support at 21 urban churches in Michigan and Ohio, said Gretchen Piatt, MPH, PhD, associate professor in the department of learning health sciences at the University of Michigan, Ann Arbor, reported at the annual scientific sessions of the American Diabetes Association.
“Of the participants who achieved glycemic control following diabetes self-management education, a really large proportion – upward of 77% of participants across all the groups– achieved sustained glycemic control at 33 months,” Dr. Piatt said.
Findings from this study has helped diabetes educators better understand how to design effective support approaches that may have a long-term impact on glycemic control and diabetes distress, Dr. Piatt said.
The Praise Diabetes Project represents a “very smart strategy” of leveraging institutions that already exist in the African American community that are trusted and provide emotional support, said Tracey D. Brown, CEO of the ADA.
“This is about behavior change, really, at its crux,” Ms. Brown said in an interview. “To get there, you’ve got to have trust, and you have to have an emotional connection. If you don’t get either one of those things, then you really are not going to do anything in terms of changing behavior.”
Long-term solutions needed
Many studies show that diabetes self-management education can improve clinical and psychosocial outcomes, and reduce health care utilization and cost, at least in the short term, Dr. Piatt said. However, it’s less clear how those improvements can be sustained over longer periods of time.
“This then presents a critical need to develop and evaluate diabetes self-management support models that are ongoing, patient driven, and embedded within existing community infrastructures,” Dr. Piatt said in her presentation.
Working with churches is one approach to working within existing community infrastructures: “Churches are embedded in the community, they have the personnel oftentimes to facilitate these types of health programs, and most importantly, they have the established relationships with the community that brings about sustained changes,” Dr. Piatt said in her presentation.
Addressing diabetes education needs in urban, low-resource communities
The Praise Diabetes Project was a randomized, 33-month clinical trial conducted in 21 predominantly Black churches in Detroit; Flint, Mich.; and Toledo, Ohio, which are all urban, low-resource communities where diabetes is a significant public health problem, according to Dr. Piatt.
The study was designed to evaluate the relative effectiveness of three different approaches to diabetes self-management support at improving A1c and levels of diabetes distress, according to the investigators.
The churches were randomized to one of the support arms, including parish nurse plus peer leader support, parish nurse support by itself, or peer leader support by itself.
A total of 47 individuals were trained, including 31 peer leaders and 16 parish nurses.
All three interventions included an initial 6-month period of “enhanced usual care” during which biweekly newsletters that were distributed, according to Dr. Piatt. That was followed by 12 months of diabetes self-management support, and an additional 12 months of ongoing support facilitated by parish nurses and peer leaders on their own, without input from the research team or health care providers.
Participants in the program had to be at least 21 years old and under the care of a physician for their diabetes, according to Dr. Piatt. The parish nurses had to be registered nurses in Michigan or Ohio. Peer leaders had to be at least 21 years old, had at least an eighth-grade education, and had to commit to a 30-hour training program.
Peer leaders also had to be individuals living with diabetes: “Prior studies have found that, when peer leaders are actively working on their own self-management goals, they tend to be much more successful in helping others,” Dr. Piatt explained.
In addition to facilitating diabetes self-management education, the parish nurses and peer leaders in these interventions were responsible for recruitment, church announcements, room reservations, follow-up calls to participants, according to Dr. Piatt. Parish nurses also provided clinical content knowledge and supervised the peer leaders in the combined model.
Sustained reductions in A1c and diabetes distress
These diabetes self-management support approaches led to significant changes over time in A1c and diabetes distress, the primary outcomes of the study, Dr. Piatt said.
The peer leader support approach resulted in a statistically significant decline in A1c, from a mean of 8.0% at baseline to 7.7% at 33 months (P = .04), while nonsignificant declines were observed in the parish nurse and combined parish nurse–peer leader approach, according to the researcher.
Reductions in A1c persisted despite the COVID-19 pandemic, which began roughly 21 months into the study, she said.
Glycemic control remained steady over the course of the study, as illustrated by similar proportions of participants with A1c below 7% from baseline to 33 months, she added.
Sustained glycemic control was seen in all three groups, according to Dr. Piatt. For example, 42.7% of individuals in the parish nurse and peer leader support group achieved glycemic control following the intervention, and 88.5% of them sustained it at 33 months.
“I think this is one of the longest diabetes self-management education and diabetes self-management support interventions that’s out there right now, so we were so happy to see that sustained by glycemic control that far into the future,” she said.
Diabetes distress levels decreased steadily over time in all three groups, with declines that were statistically significant from baseline to 33 months in the parish nurse–only and peer leader–only groups, the investigator said.
The proportion of participants reporting moderate levels of diabetes distress dropped over time, especially in the peer leader support group, where there was a 50% reduction, she added.
Despite these findings, the study had limitations, according to Dr. Piatt, including some “burnout” that impacted participants, parish nurses, and peer leaders, especially after the pandemic started.
In addition, this type of intervention may have limited impact in the community at large: “We probably didn’t reach people who did not have good connection to the church,” Dr. Piatt said.
Dr. Piatt reported no conflicts of interest related to the research.
A church-based diabetes self-management support intervention that incorporated parish nurses and peer leaders is feasible and may help improve diabetes-related outcomes in participants.
Sustained reductions in hemoglobin A1c and diabetes distress were seen in the Praise Diabetes Project, a 33-month study that piloted several different approaches to parish nurse and peer leader support at 21 urban churches in Michigan and Ohio, said Gretchen Piatt, MPH, PhD, associate professor in the department of learning health sciences at the University of Michigan, Ann Arbor, reported at the annual scientific sessions of the American Diabetes Association.
“Of the participants who achieved glycemic control following diabetes self-management education, a really large proportion – upward of 77% of participants across all the groups– achieved sustained glycemic control at 33 months,” Dr. Piatt said.
Findings from this study has helped diabetes educators better understand how to design effective support approaches that may have a long-term impact on glycemic control and diabetes distress, Dr. Piatt said.
The Praise Diabetes Project represents a “very smart strategy” of leveraging institutions that already exist in the African American community that are trusted and provide emotional support, said Tracey D. Brown, CEO of the ADA.
“This is about behavior change, really, at its crux,” Ms. Brown said in an interview. “To get there, you’ve got to have trust, and you have to have an emotional connection. If you don’t get either one of those things, then you really are not going to do anything in terms of changing behavior.”
Long-term solutions needed
Many studies show that diabetes self-management education can improve clinical and psychosocial outcomes, and reduce health care utilization and cost, at least in the short term, Dr. Piatt said. However, it’s less clear how those improvements can be sustained over longer periods of time.
“This then presents a critical need to develop and evaluate diabetes self-management support models that are ongoing, patient driven, and embedded within existing community infrastructures,” Dr. Piatt said in her presentation.
Working with churches is one approach to working within existing community infrastructures: “Churches are embedded in the community, they have the personnel oftentimes to facilitate these types of health programs, and most importantly, they have the established relationships with the community that brings about sustained changes,” Dr. Piatt said in her presentation.
Addressing diabetes education needs in urban, low-resource communities
The Praise Diabetes Project was a randomized, 33-month clinical trial conducted in 21 predominantly Black churches in Detroit; Flint, Mich.; and Toledo, Ohio, which are all urban, low-resource communities where diabetes is a significant public health problem, according to Dr. Piatt.
The study was designed to evaluate the relative effectiveness of three different approaches to diabetes self-management support at improving A1c and levels of diabetes distress, according to the investigators.
The churches were randomized to one of the support arms, including parish nurse plus peer leader support, parish nurse support by itself, or peer leader support by itself.
A total of 47 individuals were trained, including 31 peer leaders and 16 parish nurses.
All three interventions included an initial 6-month period of “enhanced usual care” during which biweekly newsletters that were distributed, according to Dr. Piatt. That was followed by 12 months of diabetes self-management support, and an additional 12 months of ongoing support facilitated by parish nurses and peer leaders on their own, without input from the research team or health care providers.
Participants in the program had to be at least 21 years old and under the care of a physician for their diabetes, according to Dr. Piatt. The parish nurses had to be registered nurses in Michigan or Ohio. Peer leaders had to be at least 21 years old, had at least an eighth-grade education, and had to commit to a 30-hour training program.
Peer leaders also had to be individuals living with diabetes: “Prior studies have found that, when peer leaders are actively working on their own self-management goals, they tend to be much more successful in helping others,” Dr. Piatt explained.
In addition to facilitating diabetes self-management education, the parish nurses and peer leaders in these interventions were responsible for recruitment, church announcements, room reservations, follow-up calls to participants, according to Dr. Piatt. Parish nurses also provided clinical content knowledge and supervised the peer leaders in the combined model.
Sustained reductions in A1c and diabetes distress
These diabetes self-management support approaches led to significant changes over time in A1c and diabetes distress, the primary outcomes of the study, Dr. Piatt said.
The peer leader support approach resulted in a statistically significant decline in A1c, from a mean of 8.0% at baseline to 7.7% at 33 months (P = .04), while nonsignificant declines were observed in the parish nurse and combined parish nurse–peer leader approach, according to the researcher.
Reductions in A1c persisted despite the COVID-19 pandemic, which began roughly 21 months into the study, she said.
Glycemic control remained steady over the course of the study, as illustrated by similar proportions of participants with A1c below 7% from baseline to 33 months, she added.
Sustained glycemic control was seen in all three groups, according to Dr. Piatt. For example, 42.7% of individuals in the parish nurse and peer leader support group achieved glycemic control following the intervention, and 88.5% of them sustained it at 33 months.
“I think this is one of the longest diabetes self-management education and diabetes self-management support interventions that’s out there right now, so we were so happy to see that sustained by glycemic control that far into the future,” she said.
Diabetes distress levels decreased steadily over time in all three groups, with declines that were statistically significant from baseline to 33 months in the parish nurse–only and peer leader–only groups, the investigator said.
The proportion of participants reporting moderate levels of diabetes distress dropped over time, especially in the peer leader support group, where there was a 50% reduction, she added.
Despite these findings, the study had limitations, according to Dr. Piatt, including some “burnout” that impacted participants, parish nurses, and peer leaders, especially after the pandemic started.
In addition, this type of intervention may have limited impact in the community at large: “We probably didn’t reach people who did not have good connection to the church,” Dr. Piatt said.
Dr. Piatt reported no conflicts of interest related to the research.
FROM ADA 2020
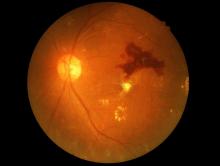
Anti-VEGF injections for diabetic retinopathy linked to mortality risk
The use of anti–vascular endothelial growth factor injections has been linked to an increased risk of mortality in patients with diabetic retinopathy in a new study, sounding a note of caution regarding the cardiovascular safety of these agents in clinical practice, an investigator said.
There was no increased risk of MI or stroke risk associated with intravitreal anti-VEGF injections versus steroid injections or laser photocoagulation in the study, which was based on analysis of health records for more than 60,000 treated individuals.
However, a “signal” was observed for increased risk of death from any cause among patients receiving anti-VEGF injections, and especially so in those with a history of cardiovascular events, said investigator Miin Roh, MD, PhD, a retina surgeon and instructor in ophthalmology at Harvard Medical School, Boston.
“This study suggests that we would have to be very careful in giving anti-VEGF injections in patients for diabetic retinopathy, especially when you’re giving it for a long-term period,” Dr. Roh said in a virtual presentation at the annual scientific sessions of the American Diabetes Association.
Report of a mortality signal
The study by Dr. Roh and colleagues included patients with type 1 or 2 diabetes, identified in health claims databases who started intravitreal anti-VEGF injections, intravitreal steroid injections, or laser photocoagulation between 2009 and 2017.
Their analysis included 30,741 patients who received anti-VEGF injections and 30,741 matched controls who received laser or steroid treatment.
There were no differences in the primary composite outcome of MI or stroke, with 674 events in the anti-VEGF group and 708 events in the laser or steroid group over a 365-day treatment period, Dr. Roh reported.
By contrast, the investigator said she saw a signal for increased risk of all-cause mortality in analyses of secondary outcomes.
Over a 180-day treatment period, there was a “slight numerical increase” in all-cause mortality, with 144 deaths in the anti-VEGF group and 115 in the control group. That translated into a hazard ratio of 1.26 (95% confidence interval, 0.99-1.60).
Looking at a 365-day treatment period, there was an increase in all-cause mortality in the anti-VEGF group that this time was statistically significant, she said, with 311 and 236 events, respectively (HR, 1.32; 95% CI, 1.12-1.57).
The mortality signal was especially strong among individuals who had a prior history of a cardiovascular event, according to Dr. Roh.
In patients with cardiovascular disease history, there were 219 deaths from any cause in the anti-VEGF group and 153 in the laser or steroid group (HR, 1.44, 95% CI, 3.10-11.22) over a 365-day period, the investigator reported. By comparison, in patients with no cardiovascular disease history, there were 95 and 96 deaths (HR, 1.00; 95% CI, 0.75-1.33).
More research needed
Although these findings are “hypothesis generating,” exploration of other datasets would be warranted to measure mortality risk among patients receiving treatment for diabetic neuropathy, said Robert Gabbay, MD, PhD, chief scientific and medical officer of the ADA.
“It’s something that we need now to study more rigorously,” Dr. Gabbay said in an interview. “It doesn’t prove that there’s a connection, but it tells us that this is worth studying.”
The current study is not a randomized comparison, which means that the people chosen to receive anti-VEGF therapy, as opposed to steroid injections or laser treatment, may differ in other ways that are associated with mortality, he said.
“It’s always good to monitor these patients,” Dr. Gabbay added. “The good news is that these individuals typically are coming in, oftentimes monthly for repeated injections, and so there’s an opportunity to monitor any changes.”
Dr. Roh reported that she is a coinvestigator in a Boehringer Ingelheim–initiated study that is not directly related to the topic of this research.
The use of anti–vascular endothelial growth factor injections has been linked to an increased risk of mortality in patients with diabetic retinopathy in a new study, sounding a note of caution regarding the cardiovascular safety of these agents in clinical practice, an investigator said.
There was no increased risk of MI or stroke risk associated with intravitreal anti-VEGF injections versus steroid injections or laser photocoagulation in the study, which was based on analysis of health records for more than 60,000 treated individuals.
However, a “signal” was observed for increased risk of death from any cause among patients receiving anti-VEGF injections, and especially so in those with a history of cardiovascular events, said investigator Miin Roh, MD, PhD, a retina surgeon and instructor in ophthalmology at Harvard Medical School, Boston.
“This study suggests that we would have to be very careful in giving anti-VEGF injections in patients for diabetic retinopathy, especially when you’re giving it for a long-term period,” Dr. Roh said in a virtual presentation at the annual scientific sessions of the American Diabetes Association.
Report of a mortality signal
The study by Dr. Roh and colleagues included patients with type 1 or 2 diabetes, identified in health claims databases who started intravitreal anti-VEGF injections, intravitreal steroid injections, or laser photocoagulation between 2009 and 2017.
Their analysis included 30,741 patients who received anti-VEGF injections and 30,741 matched controls who received laser or steroid treatment.
There were no differences in the primary composite outcome of MI or stroke, with 674 events in the anti-VEGF group and 708 events in the laser or steroid group over a 365-day treatment period, Dr. Roh reported.
By contrast, the investigator said she saw a signal for increased risk of all-cause mortality in analyses of secondary outcomes.
Over a 180-day treatment period, there was a “slight numerical increase” in all-cause mortality, with 144 deaths in the anti-VEGF group and 115 in the control group. That translated into a hazard ratio of 1.26 (95% confidence interval, 0.99-1.60).
Looking at a 365-day treatment period, there was an increase in all-cause mortality in the anti-VEGF group that this time was statistically significant, she said, with 311 and 236 events, respectively (HR, 1.32; 95% CI, 1.12-1.57).
The mortality signal was especially strong among individuals who had a prior history of a cardiovascular event, according to Dr. Roh.
In patients with cardiovascular disease history, there were 219 deaths from any cause in the anti-VEGF group and 153 in the laser or steroid group (HR, 1.44, 95% CI, 3.10-11.22) over a 365-day period, the investigator reported. By comparison, in patients with no cardiovascular disease history, there were 95 and 96 deaths (HR, 1.00; 95% CI, 0.75-1.33).
More research needed
Although these findings are “hypothesis generating,” exploration of other datasets would be warranted to measure mortality risk among patients receiving treatment for diabetic neuropathy, said Robert Gabbay, MD, PhD, chief scientific and medical officer of the ADA.
“It’s something that we need now to study more rigorously,” Dr. Gabbay said in an interview. “It doesn’t prove that there’s a connection, but it tells us that this is worth studying.”
The current study is not a randomized comparison, which means that the people chosen to receive anti-VEGF therapy, as opposed to steroid injections or laser treatment, may differ in other ways that are associated with mortality, he said.
“It’s always good to monitor these patients,” Dr. Gabbay added. “The good news is that these individuals typically are coming in, oftentimes monthly for repeated injections, and so there’s an opportunity to monitor any changes.”
Dr. Roh reported that she is a coinvestigator in a Boehringer Ingelheim–initiated study that is not directly related to the topic of this research.
The use of anti–vascular endothelial growth factor injections has been linked to an increased risk of mortality in patients with diabetic retinopathy in a new study, sounding a note of caution regarding the cardiovascular safety of these agents in clinical practice, an investigator said.
There was no increased risk of MI or stroke risk associated with intravitreal anti-VEGF injections versus steroid injections or laser photocoagulation in the study, which was based on analysis of health records for more than 60,000 treated individuals.
However, a “signal” was observed for increased risk of death from any cause among patients receiving anti-VEGF injections, and especially so in those with a history of cardiovascular events, said investigator Miin Roh, MD, PhD, a retina surgeon and instructor in ophthalmology at Harvard Medical School, Boston.
“This study suggests that we would have to be very careful in giving anti-VEGF injections in patients for diabetic retinopathy, especially when you’re giving it for a long-term period,” Dr. Roh said in a virtual presentation at the annual scientific sessions of the American Diabetes Association.
Report of a mortality signal
The study by Dr. Roh and colleagues included patients with type 1 or 2 diabetes, identified in health claims databases who started intravitreal anti-VEGF injections, intravitreal steroid injections, or laser photocoagulation between 2009 and 2017.
Their analysis included 30,741 patients who received anti-VEGF injections and 30,741 matched controls who received laser or steroid treatment.
There were no differences in the primary composite outcome of MI or stroke, with 674 events in the anti-VEGF group and 708 events in the laser or steroid group over a 365-day treatment period, Dr. Roh reported.
By contrast, the investigator said she saw a signal for increased risk of all-cause mortality in analyses of secondary outcomes.
Over a 180-day treatment period, there was a “slight numerical increase” in all-cause mortality, with 144 deaths in the anti-VEGF group and 115 in the control group. That translated into a hazard ratio of 1.26 (95% confidence interval, 0.99-1.60).
Looking at a 365-day treatment period, there was an increase in all-cause mortality in the anti-VEGF group that this time was statistically significant, she said, with 311 and 236 events, respectively (HR, 1.32; 95% CI, 1.12-1.57).
The mortality signal was especially strong among individuals who had a prior history of a cardiovascular event, according to Dr. Roh.
In patients with cardiovascular disease history, there were 219 deaths from any cause in the anti-VEGF group and 153 in the laser or steroid group (HR, 1.44, 95% CI, 3.10-11.22) over a 365-day period, the investigator reported. By comparison, in patients with no cardiovascular disease history, there were 95 and 96 deaths (HR, 1.00; 95% CI, 0.75-1.33).
More research needed
Although these findings are “hypothesis generating,” exploration of other datasets would be warranted to measure mortality risk among patients receiving treatment for diabetic neuropathy, said Robert Gabbay, MD, PhD, chief scientific and medical officer of the ADA.
“It’s something that we need now to study more rigorously,” Dr. Gabbay said in an interview. “It doesn’t prove that there’s a connection, but it tells us that this is worth studying.”
The current study is not a randomized comparison, which means that the people chosen to receive anti-VEGF therapy, as opposed to steroid injections or laser treatment, may differ in other ways that are associated with mortality, he said.
“It’s always good to monitor these patients,” Dr. Gabbay added. “The good news is that these individuals typically are coming in, oftentimes monthly for repeated injections, and so there’s an opportunity to monitor any changes.”
Dr. Roh reported that she is a coinvestigator in a Boehringer Ingelheim–initiated study that is not directly related to the topic of this research.
FROM ADA 2021
AMPLITUDE-O: Efpeglenatide benefits in high-risk diabetes
The AMPLITUDE-O phase 3 trial showed that investigational drug efpeglenatide (Sanofi/Hanmi Pharmaceutical) – an exendin-based glucagonlike peptide-1 receptor agonist – was safe and reduced the risk of worsening renal and cardiovascular outcomes in patients with type 2 diabetes at high cardiovascular risk.
That is, in patients with type 2 diabetes and a high prevalence of cardiovascular and kidney disease with a high hemoglobin A1c and moderate use of a sodium-glucose cotransporter 2 inhibitor, subcutaneous efpeglenatide (4 or 6 mg/week) significantly and safely reduced cardiovascular and renal outcomes, said study investigator Naveed Sattar, MD.
Dr. Sattar, of the University of Glasgow, summarized the results during a symposium at the annual scientific sessions of the American Diabetes Association. The study was simultaneously published online in the New England Journal of Medicine.
AMPLITUDE-O was a cardiovascular outcome trial (CVOT) in more than 4,000 high-risk patients with type 2 diabetes followed for a mean of 1.8 years.
Compared with patients who received placebo, those who received either dose of efpeglenatide had a 27% lower risk of a major adverse cardiovascular event, defined as nonfatal myocardial infarction, nonfatal stroke, or death from cardiovascular or undetermined causes; a 21% lower risk of expanded MACE (MACE, coronary revascularization, or hospitalization for unstable angina); a 32% lower risk of a composite renal outcome (decrease in kidney function or macroalbuminuria); and a 27% lower risk of MACE or noncardiovascular death.
And “these effects were independent of baseline SGLT2 inhibitors, estimated glomerular filtration rate (eGFR), or metformin use,” Dr. Sattar pointed out.
New and important findings, but Sanofi no longer developing drug
The trial’s primary investigator, Hertzel C. Gerstein, MD, pointed out several new and important findings of the drug and study, compared with CVOTs of seven other GLP-1 receptor agonists.
The trial included more patients (32%) with renal disease (eGFR, 25-60 mL/min) than the other trials.
There were enough patients taking SGLT2 inhibitors at baseline (15%) to show no difference in the effect of a GLP-1 receptor agonist in the presence/absence of an SGLT2 inhibitor.
So this is the first clearly positive GLP-1 receptor agonist CVOT with an exendin-4–based GLP-1 receptor agonist showing that the GLP-1 receptor agonist class is cardioprotective whether or not it is based on a human or animal GLP-1 structure.
And there was a significant reduction in MACE or noncardiovascular death.
“This would be good for people with type 2 diabetes and either cardiovascular or renal disease at high risk for cardiovascular and/or renal outcomes,” said Dr. Gerstein, professor of medicine at McMaster University, Hamilton, Ont.
However, the trial sponsor, Sanofi, is no longer developing the drug. The company returned the rights back to Hanmi, which had started this line of research. “Hopefully” Hanmi or another company will develop the drug further, said Dr. Gerstein.
Sicker patients than in 7 other GLP-1 agonist CVOTs
Efpeglenatide – like two other drugs in the class, exenatide and lixisenatide – is an exendin-based GLP-1 agonist. (Exendin-4 is a peptide found in the saliva of the Gila monster lizard.) In contrast, liraglutide, dulaglutide, albiglutide, and semaglutide are human-analog GLP-1 agonists.
A meta-analysis of the seven CVOTs of these other drugs in this class reported, among other things, that “overall, GLP-1 agonist treatment reduced MACE by 12%.”
Amanda I. Adler, MD, PhD, professor of diabetic medicine and health policy, University of Oxford, (England), and the assigned independent commenter at the symposium, cited many things “the investigators did well.”
Compared with the CVOTs of the other GLP-1 receptor agonists – ELIXA (lixisenatide), LEADER (liraglutide), SUSTAIN-6 (semaglutide), EXSCEL (exenatide), Harmony Outcomes (albiglutide), REWIND (dulaglutide), and PIONEER 6 (oral semaglutide) – patients in the AMPLITUDE-O trial were sicker, she noted.
AMPLITUDE-O participants had the longest duration of diabetes (15 years), lowest mean eGFR of 72 ml/min per 1.73 m2, highest A1c (8.9%), and highest percentage of insulin use (62%), she noted.
The study was primarily a safety and noninferiority trial, she pointed out, although a series of superiority analyses were prespecified that would be conducted if the drug was found to be noninferior to placebo for the primary outcome of 3-point MACE.
It was good that patients were stratified according to SGLT2 inhibitor use – into current user, likely future user, and not likely future user – although “likely future user” may have misclassified some patients.
The various stakeholders – patients, regulators, doctors, payers, statisticians, and the marketing department of any company providing the drug – would want to know more, such as quality of life, long-term effects, and cost, she observed.
Meta-analysis of 8 CVOTs shows stronger class benefit
Dr. Sattar presented an eight-trial meta-analysis (an update of the seven-trial meta-analysis that included data from AMPLITUDE-O), which showed patients with type 2 diabetes who received GLP-1 agonists had a decreased rate of the 3-component MACE and decreased individual components (stroke more so than MI) – regardless of the structure of these drugs (exenatide or human analogs).
The updated meta-analysis also showed that, overall, GLP-1 agonists decreased all-cause mortality and possibly reduced the risk of heart failure hospitalization (perhaps linked to atherosclerotic benefits) as well as renal dysfunction.
There was no increase in risk of severe hypoglycemia, retinopathy, or pancreatic adverse effects.
AMPLITUDE-O: Design and findings
AMPLITUDE-O included 4,076 adults with type 2 diabetes from 344 sites in 28 countries who were screened from May 2018 to April 2019. Participants also had cardiovascular disease or kidney disease (eGFR, 25-60 mL/min) plus at least one other cardiovascular risk factor. They were randomized 1:1:1 to receive subcutaneous efpeglenatide (4 or 6 mg/week) or placebo.
Patients were a mean age of 65, most (87%) were White, and 33% were female. They had a mean A1c of 8.9%. Most (90%) had a history of cardiovascular disease and 31% had current kidney disease.
MACE occurred in 189 participants (7.0%) assigned to efpeglenatide and 125 participants (9.2%) assigned to receive placebo (3.9 vs. 5.3 events/100 person-years) (hazard ratio, 0.73; 95% confidence interval, 0.58-0.92; P < .001 for noninferiority; P = .007 for superiority).
The composite renal outcome event (decreased kidney function or macroalbuminuria) occurred in 353 participants (13.0%) assigned to receive efpeglenatide and in 250 participants (18.4%) assigned to receive placebo (HR, 0.68; 95% CI, 0.57-0.79; P < .001).
Diarrhea, constipation, nausea, vomiting, or bloating occurred more frequently with efpeglenatide than placebo.
The study was funded by Sanofi. Dr. Sattar has reported being on advisory panels for Amgen, AstraZeneca, Boehringer Ingelheim, Eli Lilly, Merck, Novartis, Novo Nordisk, Pfizer, and Sanofi, and receiving research support from Boehringer Ingelheim. Dr. Gerstein has reported being a member of advisory panels for Novo Nordisk, Pfizer, and Sanofi, and a consultant for Abbott, Covance, Eli Lilly, Kowa, and Sanofi. He reported receiving research support from AstraZeneca, Eli Lilly, Merck, Novo Nordisk, and Sanofi, and having other relationships with Boehringer Ingelheim, DKSH, Eli Lilly, Sanofi, and Zuellig Pharma. Dr. Adler has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The AMPLITUDE-O phase 3 trial showed that investigational drug efpeglenatide (Sanofi/Hanmi Pharmaceutical) – an exendin-based glucagonlike peptide-1 receptor agonist – was safe and reduced the risk of worsening renal and cardiovascular outcomes in patients with type 2 diabetes at high cardiovascular risk.
That is, in patients with type 2 diabetes and a high prevalence of cardiovascular and kidney disease with a high hemoglobin A1c and moderate use of a sodium-glucose cotransporter 2 inhibitor, subcutaneous efpeglenatide (4 or 6 mg/week) significantly and safely reduced cardiovascular and renal outcomes, said study investigator Naveed Sattar, MD.
Dr. Sattar, of the University of Glasgow, summarized the results during a symposium at the annual scientific sessions of the American Diabetes Association. The study was simultaneously published online in the New England Journal of Medicine.
AMPLITUDE-O was a cardiovascular outcome trial (CVOT) in more than 4,000 high-risk patients with type 2 diabetes followed for a mean of 1.8 years.
Compared with patients who received placebo, those who received either dose of efpeglenatide had a 27% lower risk of a major adverse cardiovascular event, defined as nonfatal myocardial infarction, nonfatal stroke, or death from cardiovascular or undetermined causes; a 21% lower risk of expanded MACE (MACE, coronary revascularization, or hospitalization for unstable angina); a 32% lower risk of a composite renal outcome (decrease in kidney function or macroalbuminuria); and a 27% lower risk of MACE or noncardiovascular death.
And “these effects were independent of baseline SGLT2 inhibitors, estimated glomerular filtration rate (eGFR), or metformin use,” Dr. Sattar pointed out.
New and important findings, but Sanofi no longer developing drug
The trial’s primary investigator, Hertzel C. Gerstein, MD, pointed out several new and important findings of the drug and study, compared with CVOTs of seven other GLP-1 receptor agonists.
The trial included more patients (32%) with renal disease (eGFR, 25-60 mL/min) than the other trials.
There were enough patients taking SGLT2 inhibitors at baseline (15%) to show no difference in the effect of a GLP-1 receptor agonist in the presence/absence of an SGLT2 inhibitor.
So this is the first clearly positive GLP-1 receptor agonist CVOT with an exendin-4–based GLP-1 receptor agonist showing that the GLP-1 receptor agonist class is cardioprotective whether or not it is based on a human or animal GLP-1 structure.
And there was a significant reduction in MACE or noncardiovascular death.
“This would be good for people with type 2 diabetes and either cardiovascular or renal disease at high risk for cardiovascular and/or renal outcomes,” said Dr. Gerstein, professor of medicine at McMaster University, Hamilton, Ont.
However, the trial sponsor, Sanofi, is no longer developing the drug. The company returned the rights back to Hanmi, which had started this line of research. “Hopefully” Hanmi or another company will develop the drug further, said Dr. Gerstein.
Sicker patients than in 7 other GLP-1 agonist CVOTs
Efpeglenatide – like two other drugs in the class, exenatide and lixisenatide – is an exendin-based GLP-1 agonist. (Exendin-4 is a peptide found in the saliva of the Gila monster lizard.) In contrast, liraglutide, dulaglutide, albiglutide, and semaglutide are human-analog GLP-1 agonists.
A meta-analysis of the seven CVOTs of these other drugs in this class reported, among other things, that “overall, GLP-1 agonist treatment reduced MACE by 12%.”
Amanda I. Adler, MD, PhD, professor of diabetic medicine and health policy, University of Oxford, (England), and the assigned independent commenter at the symposium, cited many things “the investigators did well.”
Compared with the CVOTs of the other GLP-1 receptor agonists – ELIXA (lixisenatide), LEADER (liraglutide), SUSTAIN-6 (semaglutide), EXSCEL (exenatide), Harmony Outcomes (albiglutide), REWIND (dulaglutide), and PIONEER 6 (oral semaglutide) – patients in the AMPLITUDE-O trial were sicker, she noted.
AMPLITUDE-O participants had the longest duration of diabetes (15 years), lowest mean eGFR of 72 ml/min per 1.73 m2, highest A1c (8.9%), and highest percentage of insulin use (62%), she noted.
The study was primarily a safety and noninferiority trial, she pointed out, although a series of superiority analyses were prespecified that would be conducted if the drug was found to be noninferior to placebo for the primary outcome of 3-point MACE.
It was good that patients were stratified according to SGLT2 inhibitor use – into current user, likely future user, and not likely future user – although “likely future user” may have misclassified some patients.
The various stakeholders – patients, regulators, doctors, payers, statisticians, and the marketing department of any company providing the drug – would want to know more, such as quality of life, long-term effects, and cost, she observed.
Meta-analysis of 8 CVOTs shows stronger class benefit
Dr. Sattar presented an eight-trial meta-analysis (an update of the seven-trial meta-analysis that included data from AMPLITUDE-O), which showed patients with type 2 diabetes who received GLP-1 agonists had a decreased rate of the 3-component MACE and decreased individual components (stroke more so than MI) – regardless of the structure of these drugs (exenatide or human analogs).
The updated meta-analysis also showed that, overall, GLP-1 agonists decreased all-cause mortality and possibly reduced the risk of heart failure hospitalization (perhaps linked to atherosclerotic benefits) as well as renal dysfunction.
There was no increase in risk of severe hypoglycemia, retinopathy, or pancreatic adverse effects.
AMPLITUDE-O: Design and findings
AMPLITUDE-O included 4,076 adults with type 2 diabetes from 344 sites in 28 countries who were screened from May 2018 to April 2019. Participants also had cardiovascular disease or kidney disease (eGFR, 25-60 mL/min) plus at least one other cardiovascular risk factor. They were randomized 1:1:1 to receive subcutaneous efpeglenatide (4 or 6 mg/week) or placebo.
Patients were a mean age of 65, most (87%) were White, and 33% were female. They had a mean A1c of 8.9%. Most (90%) had a history of cardiovascular disease and 31% had current kidney disease.
MACE occurred in 189 participants (7.0%) assigned to efpeglenatide and 125 participants (9.2%) assigned to receive placebo (3.9 vs. 5.3 events/100 person-years) (hazard ratio, 0.73; 95% confidence interval, 0.58-0.92; P < .001 for noninferiority; P = .007 for superiority).
The composite renal outcome event (decreased kidney function or macroalbuminuria) occurred in 353 participants (13.0%) assigned to receive efpeglenatide and in 250 participants (18.4%) assigned to receive placebo (HR, 0.68; 95% CI, 0.57-0.79; P < .001).
Diarrhea, constipation, nausea, vomiting, or bloating occurred more frequently with efpeglenatide than placebo.
The study was funded by Sanofi. Dr. Sattar has reported being on advisory panels for Amgen, AstraZeneca, Boehringer Ingelheim, Eli Lilly, Merck, Novartis, Novo Nordisk, Pfizer, and Sanofi, and receiving research support from Boehringer Ingelheim. Dr. Gerstein has reported being a member of advisory panels for Novo Nordisk, Pfizer, and Sanofi, and a consultant for Abbott, Covance, Eli Lilly, Kowa, and Sanofi. He reported receiving research support from AstraZeneca, Eli Lilly, Merck, Novo Nordisk, and Sanofi, and having other relationships with Boehringer Ingelheim, DKSH, Eli Lilly, Sanofi, and Zuellig Pharma. Dr. Adler has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The AMPLITUDE-O phase 3 trial showed that investigational drug efpeglenatide (Sanofi/Hanmi Pharmaceutical) – an exendin-based glucagonlike peptide-1 receptor agonist – was safe and reduced the risk of worsening renal and cardiovascular outcomes in patients with type 2 diabetes at high cardiovascular risk.
That is, in patients with type 2 diabetes and a high prevalence of cardiovascular and kidney disease with a high hemoglobin A1c and moderate use of a sodium-glucose cotransporter 2 inhibitor, subcutaneous efpeglenatide (4 or 6 mg/week) significantly and safely reduced cardiovascular and renal outcomes, said study investigator Naveed Sattar, MD.
Dr. Sattar, of the University of Glasgow, summarized the results during a symposium at the annual scientific sessions of the American Diabetes Association. The study was simultaneously published online in the New England Journal of Medicine.
AMPLITUDE-O was a cardiovascular outcome trial (CVOT) in more than 4,000 high-risk patients with type 2 diabetes followed for a mean of 1.8 years.
Compared with patients who received placebo, those who received either dose of efpeglenatide had a 27% lower risk of a major adverse cardiovascular event, defined as nonfatal myocardial infarction, nonfatal stroke, or death from cardiovascular or undetermined causes; a 21% lower risk of expanded MACE (MACE, coronary revascularization, or hospitalization for unstable angina); a 32% lower risk of a composite renal outcome (decrease in kidney function or macroalbuminuria); and a 27% lower risk of MACE or noncardiovascular death.
And “these effects were independent of baseline SGLT2 inhibitors, estimated glomerular filtration rate (eGFR), or metformin use,” Dr. Sattar pointed out.
New and important findings, but Sanofi no longer developing drug
The trial’s primary investigator, Hertzel C. Gerstein, MD, pointed out several new and important findings of the drug and study, compared with CVOTs of seven other GLP-1 receptor agonists.
The trial included more patients (32%) with renal disease (eGFR, 25-60 mL/min) than the other trials.
There were enough patients taking SGLT2 inhibitors at baseline (15%) to show no difference in the effect of a GLP-1 receptor agonist in the presence/absence of an SGLT2 inhibitor.
So this is the first clearly positive GLP-1 receptor agonist CVOT with an exendin-4–based GLP-1 receptor agonist showing that the GLP-1 receptor agonist class is cardioprotective whether or not it is based on a human or animal GLP-1 structure.
And there was a significant reduction in MACE or noncardiovascular death.
“This would be good for people with type 2 diabetes and either cardiovascular or renal disease at high risk for cardiovascular and/or renal outcomes,” said Dr. Gerstein, professor of medicine at McMaster University, Hamilton, Ont.
However, the trial sponsor, Sanofi, is no longer developing the drug. The company returned the rights back to Hanmi, which had started this line of research. “Hopefully” Hanmi or another company will develop the drug further, said Dr. Gerstein.
Sicker patients than in 7 other GLP-1 agonist CVOTs
Efpeglenatide – like two other drugs in the class, exenatide and lixisenatide – is an exendin-based GLP-1 agonist. (Exendin-4 is a peptide found in the saliva of the Gila monster lizard.) In contrast, liraglutide, dulaglutide, albiglutide, and semaglutide are human-analog GLP-1 agonists.
A meta-analysis of the seven CVOTs of these other drugs in this class reported, among other things, that “overall, GLP-1 agonist treatment reduced MACE by 12%.”
Amanda I. Adler, MD, PhD, professor of diabetic medicine and health policy, University of Oxford, (England), and the assigned independent commenter at the symposium, cited many things “the investigators did well.”
Compared with the CVOTs of the other GLP-1 receptor agonists – ELIXA (lixisenatide), LEADER (liraglutide), SUSTAIN-6 (semaglutide), EXSCEL (exenatide), Harmony Outcomes (albiglutide), REWIND (dulaglutide), and PIONEER 6 (oral semaglutide) – patients in the AMPLITUDE-O trial were sicker, she noted.
AMPLITUDE-O participants had the longest duration of diabetes (15 years), lowest mean eGFR of 72 ml/min per 1.73 m2, highest A1c (8.9%), and highest percentage of insulin use (62%), she noted.
The study was primarily a safety and noninferiority trial, she pointed out, although a series of superiority analyses were prespecified that would be conducted if the drug was found to be noninferior to placebo for the primary outcome of 3-point MACE.
It was good that patients were stratified according to SGLT2 inhibitor use – into current user, likely future user, and not likely future user – although “likely future user” may have misclassified some patients.
The various stakeholders – patients, regulators, doctors, payers, statisticians, and the marketing department of any company providing the drug – would want to know more, such as quality of life, long-term effects, and cost, she observed.
Meta-analysis of 8 CVOTs shows stronger class benefit
Dr. Sattar presented an eight-trial meta-analysis (an update of the seven-trial meta-analysis that included data from AMPLITUDE-O), which showed patients with type 2 diabetes who received GLP-1 agonists had a decreased rate of the 3-component MACE and decreased individual components (stroke more so than MI) – regardless of the structure of these drugs (exenatide or human analogs).
The updated meta-analysis also showed that, overall, GLP-1 agonists decreased all-cause mortality and possibly reduced the risk of heart failure hospitalization (perhaps linked to atherosclerotic benefits) as well as renal dysfunction.
There was no increase in risk of severe hypoglycemia, retinopathy, or pancreatic adverse effects.
AMPLITUDE-O: Design and findings
AMPLITUDE-O included 4,076 adults with type 2 diabetes from 344 sites in 28 countries who were screened from May 2018 to April 2019. Participants also had cardiovascular disease or kidney disease (eGFR, 25-60 mL/min) plus at least one other cardiovascular risk factor. They were randomized 1:1:1 to receive subcutaneous efpeglenatide (4 or 6 mg/week) or placebo.
Patients were a mean age of 65, most (87%) were White, and 33% were female. They had a mean A1c of 8.9%. Most (90%) had a history of cardiovascular disease and 31% had current kidney disease.
MACE occurred in 189 participants (7.0%) assigned to efpeglenatide and 125 participants (9.2%) assigned to receive placebo (3.9 vs. 5.3 events/100 person-years) (hazard ratio, 0.73; 95% confidence interval, 0.58-0.92; P < .001 for noninferiority; P = .007 for superiority).
The composite renal outcome event (decreased kidney function or macroalbuminuria) occurred in 353 participants (13.0%) assigned to receive efpeglenatide and in 250 participants (18.4%) assigned to receive placebo (HR, 0.68; 95% CI, 0.57-0.79; P < .001).
Diarrhea, constipation, nausea, vomiting, or bloating occurred more frequently with efpeglenatide than placebo.
The study was funded by Sanofi. Dr. Sattar has reported being on advisory panels for Amgen, AstraZeneca, Boehringer Ingelheim, Eli Lilly, Merck, Novartis, Novo Nordisk, Pfizer, and Sanofi, and receiving research support from Boehringer Ingelheim. Dr. Gerstein has reported being a member of advisory panels for Novo Nordisk, Pfizer, and Sanofi, and a consultant for Abbott, Covance, Eli Lilly, Kowa, and Sanofi. He reported receiving research support from AstraZeneca, Eli Lilly, Merck, Novo Nordisk, and Sanofi, and having other relationships with Boehringer Ingelheim, DKSH, Eli Lilly, Sanofi, and Zuellig Pharma. Dr. Adler has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Semaglutide 2.4 mg ‘likely to usher in a new era’ in obesity treatment
The recently licensed weight-loss drug semaglutide 2.4 mg/week (Wegovy, Novo Nordisk) “is likely to usher in a new era in the medical treatment of obesity,” Lee M. Kaplan, MD, PhD, stated at the annual scientific sessions of the American Diabetes Association, held virtually.
Dr. Kaplan discussed the clinical implications of caring for patients with obesity now that the glucagon-like peptide-1 (GLP-1) receptor agonist is approved in the United States for weight loss.
Weight loss with semaglutide 2.4 mg was twice that achieved with liraglutide 3 mg (Saxenda, Novo Nordisk) – that is, roughly a 10%-15% weight loss at 68 weeks, said Dr. Kaplan, who was not involved in the pivotal STEP clinical trials of the agent.
“I think as we start to see more data come in over the next couple of years,” including from the cardiovascular outcome trial SELECT, he continued, “we’ll be able to use the data to create a nuanced [individualized patient treatment] approach, but we’ll also be able to use our clinical experience, which will grow rapidly over the next few years.”
In the future, semaglutide is likely to be combined with other drugs to provide even greater weight loss, predicts Dr. Kaplan, director of the Obesity, Metabolism, and Nutrition Institute at Massachusetts General Hospital in Boston.
In the meantime, “to be effective, semaglutide needs to be used,” he stressed, while noting that responses to the drug vary by individual, and so this will need to be taken into account.
“Obesity needs to be recognized as a disease in its own right, as well as a risk factor for numerous other diseases, [and] equitable access to obesity treatment needs to be broadened,” he emphasized.
Four pivotal phase 3 trials
As previously reported, four pivotal 68-week, phase 3 clinical trials in the Semaglutide Treatment Effect in People With Obesity (STEP) program tested the safety and efficacy of subcutaneous semaglutide 2.4 mg/week in more than 4,500 adults with overweight or obesity.
The trials have been published in high profile journals – the New England Journal of Medicine (STEP 1), The Lancet (STEP 2), and JAMA (STEP 3 and STEP 4) – said Robert F. Kushner, MD.
“I would encourage all of you to download and read each of these trials on your own,” Dr. Kushner, professor of medicine and medicine education at Northwestern University, Chicago, and coauthor of STEP 1, said before presenting a top-level review of key results.
STEP 1 examined weight management, STEP 3 added a background of intensive behavioral therapy, STEP 4 investigated sustained weight management, and STEP 2 (unlike the others) investigated weight management in patients with type 2 diabetes, he summarized.
In STEP 1, patients who received semaglutide had an average 15% weight loss, and those who stayed on the drug had a 17% weight loss, compared with the 2.4% weight loss in the placebo group.
“One-third of individuals in the trial achieved at least a 20% weight loss or more,” Dr. Kushner said, which is “really phenomenal.”
The results of STEP 3 “suggest that semaglutide with monthly brief lifestyle counseling alone is sufficient to produce a mean weight loss of 15%,” he noted, as adding a low-calorie diet and intensive behavior therapy sped up the initial weight loss but did not increase the final weight loss.
A post hoc analysis of STEP 2 showed “it’s clear that improvement in A1c” is greater with at least a 10% weight loss versus a smaller weight loss, Dr. Kushner said. A1c dropped by 2.2% versus 1.3%, with these two weight losses, respectively.
In STEP 4, after dose escalation to 2.4 mg at 20 weeks, patients had lost 10.6% of their initial weight. At 68 weeks, those who were switched to placebo at 20 weeks had lost 5.4% of their initial weight, whereas those who remained on semaglutide had lost 17.7% of their initial weight.
This shows that “if you remove the drug, the disease starts to come back,” Dr. Kushner pointed out.
Nausea, the most common side effect, occurred in 20% of patients, but was mostly mild or moderate, and gastrointestinal effects including constipation, vomiting, and diarrhea were transient and occurred early in the dose escalation phase.
Large individual variability, combination therapies on horizon
Dr. Kaplan pointed out, however, that “like [with] other antiobesity therapies ... there’s a large patient-to-patient variability.”
A third of patients exhibit more than 20% weight loss, and 10% exhibit more than 30% weight loss – approaching the efficacy of bariatric surgery.
However, nearly 10% of patients without diabetes and upwards of 30% of patients with diabetes will experience less than 5% weight loss, he said.
Therefore, “success or failure in one patient doesn’t predict response in another, and we should always remember that as we treat different patients with these medications,” Dr. Kaplan advised.
A recent phase 1b study suggests that combination therapy with semaglutide and the amylin agonist cagrilintide ups weight loss, as previously reported.
In this short trial with no lifestyle modification, it took 16 weeks for patients to reach full dosing, and at 20 weeks, patients on semaglutide had lost 8% of their initial weight, whereas those on combination therapy had lost 17% of their initial weight.
“There’s hope that, in combination with cagrilintide and probably with several other agents that are still in early development, we’ll be seeing average weight loss that is in the range of that seen with bariatric surgery,” Dr. Kushner said.
Doctors discuss two hypothetical cases
Session moderator Julio Rosenstock, MD, of the University of Texas, Dallas, a coinvestigator in several of the STEP trials, invited Dr. Kaplan and two other panelists to explain how they would manage two hypothetical patients.
Case 1
You have a patient with type 2 diabetes, a body mass index of 32, 33 kg/m2, and an A1c of 7.5% or 8% on metformin. Would you use semaglutide 1 mg (Ozempic, Novo Nordisk) that is indicated for type 2 diabetes, or would you use semaglutide 2.4 mg that is indicated for obesity and risk factors?
“We have the answer to that from STEP 2,” said Melanie J. Davies, MB ChB, MD, professor of diabetes medicine at the University of Leicester, England, who led the STEP 2 trial.
“For some patients, the 1-mg dose, which we use routinely in the clinic, may be reasonable to get good glycemic control for cardiovascular protection and will obviously achieve some weight loss. But if you really want to go for the weight-related comorbidities, then the 2.4-mg dose is what you need,” she said.
“A lot of [clinicians] might say: ‘I’ll see how [the patient goes] with the 1-mg dose, and then maybe if they’re not losing the weight and not getting to glycemic target, then maybe I’ll switch to 2.4 mg,’” said John Wilding, MD, who leads clinical research into obesity, diabetes, and endocrinology at the University of Liverpool, England, and led the STEP 1 trial.
“But the STEP 2 data show very clearly that you get almost the same A1c,” Dr. Rosenstock interjected. “I would go for 2.4 mg. The patient has a BMI of 32, 33 kg/m2. I would hit hard the BMI. We need to change that paradigm.”
“For other diseases we don’t always go to the maximum dose that’s available. We go to the dose that’s necessary to achieve the clinical endpoint that we want,” Dr. Kaplan noted. “I think one of the challenges is going to be to learn how to clinically nuance our therapy the way we do for other diseases.”
“That is the usual thinking,” Dr. Rosenstock agreed. But “with the 2.4-mg dose, one third get a 20% reduction of BMI, and 10% get almost a 30% reduction – and you [aren’t] going to see that with semaglutide 1 mg!”
“That’s true,” Dr. Kaplan conceded. However, a patient with a relatively low BMI of 32, 33 kg/m2 may not need the higher dose, unlike a patient who has a BMI of 45 kg/m2 and diabetes. But we’re going to find that out over the next couple of years, he expects.
Case 2
You have a patient with a BMI of 31 kg/m2 who is newly diagnosed with type 2 diabetes. Why should you start that patient with metformin? Why won’t you start with something that will directly tackle obesity and get the patient to lose 20 pounds and for sure the blood sugar is going to be better?
“I think if I have someone who is really keen to put their diabetes into remission,” Dr. Wilding said, “this would be a fantastic approach because they would have a really high chance of doing that.”
The prediabetes data from STEP showed that “we can put a lot of people from prediabetes back to normal glucose tolerance,” Dr. Wilding noted. “Maybe we can put people with early diabetes back to normal as well. I think that’s a trial that really does need to be done,” he said.
“We’re going to have to figure out the best pathway forward,” Dr. Kaplan observed, noting that multiple stakeholders, including payers, patients, and providers, play a role in the uptake of new obesity drugs.
“Do you think we will see less bariatric surgery with these drugs?” Dr. Rosenstock asked Dr. Kaplan.
“I think you have to remember that of the millions and millions of people with obesity, a very small portion are currently treated with antiobesity medication, and an even smaller portion are getting bariatric surgery,” Dr. Kaplan replied.
“In the United States, 90% of people who get bariatric surgery are self-referred,” he said, so, “I think initially we are not going to see much of a change” in rates of bariatric surgery.
Dr. Rosenstock, Dr. Kaplan, Dr. Wilding, and Dr. Davies disclosed ties with Novo Nordisk and numerous other companies.
A version of this article first appeared on Medscape.com.
The recently licensed weight-loss drug semaglutide 2.4 mg/week (Wegovy, Novo Nordisk) “is likely to usher in a new era in the medical treatment of obesity,” Lee M. Kaplan, MD, PhD, stated at the annual scientific sessions of the American Diabetes Association, held virtually.
Dr. Kaplan discussed the clinical implications of caring for patients with obesity now that the glucagon-like peptide-1 (GLP-1) receptor agonist is approved in the United States for weight loss.
Weight loss with semaglutide 2.4 mg was twice that achieved with liraglutide 3 mg (Saxenda, Novo Nordisk) – that is, roughly a 10%-15% weight loss at 68 weeks, said Dr. Kaplan, who was not involved in the pivotal STEP clinical trials of the agent.
“I think as we start to see more data come in over the next couple of years,” including from the cardiovascular outcome trial SELECT, he continued, “we’ll be able to use the data to create a nuanced [individualized patient treatment] approach, but we’ll also be able to use our clinical experience, which will grow rapidly over the next few years.”
In the future, semaglutide is likely to be combined with other drugs to provide even greater weight loss, predicts Dr. Kaplan, director of the Obesity, Metabolism, and Nutrition Institute at Massachusetts General Hospital in Boston.
In the meantime, “to be effective, semaglutide needs to be used,” he stressed, while noting that responses to the drug vary by individual, and so this will need to be taken into account.
“Obesity needs to be recognized as a disease in its own right, as well as a risk factor for numerous other diseases, [and] equitable access to obesity treatment needs to be broadened,” he emphasized.
Four pivotal phase 3 trials
As previously reported, four pivotal 68-week, phase 3 clinical trials in the Semaglutide Treatment Effect in People With Obesity (STEP) program tested the safety and efficacy of subcutaneous semaglutide 2.4 mg/week in more than 4,500 adults with overweight or obesity.
The trials have been published in high profile journals – the New England Journal of Medicine (STEP 1), The Lancet (STEP 2), and JAMA (STEP 3 and STEP 4) – said Robert F. Kushner, MD.
“I would encourage all of you to download and read each of these trials on your own,” Dr. Kushner, professor of medicine and medicine education at Northwestern University, Chicago, and coauthor of STEP 1, said before presenting a top-level review of key results.
STEP 1 examined weight management, STEP 3 added a background of intensive behavioral therapy, STEP 4 investigated sustained weight management, and STEP 2 (unlike the others) investigated weight management in patients with type 2 diabetes, he summarized.
In STEP 1, patients who received semaglutide had an average 15% weight loss, and those who stayed on the drug had a 17% weight loss, compared with the 2.4% weight loss in the placebo group.
“One-third of individuals in the trial achieved at least a 20% weight loss or more,” Dr. Kushner said, which is “really phenomenal.”
The results of STEP 3 “suggest that semaglutide with monthly brief lifestyle counseling alone is sufficient to produce a mean weight loss of 15%,” he noted, as adding a low-calorie diet and intensive behavior therapy sped up the initial weight loss but did not increase the final weight loss.
A post hoc analysis of STEP 2 showed “it’s clear that improvement in A1c” is greater with at least a 10% weight loss versus a smaller weight loss, Dr. Kushner said. A1c dropped by 2.2% versus 1.3%, with these two weight losses, respectively.
In STEP 4, after dose escalation to 2.4 mg at 20 weeks, patients had lost 10.6% of their initial weight. At 68 weeks, those who were switched to placebo at 20 weeks had lost 5.4% of their initial weight, whereas those who remained on semaglutide had lost 17.7% of their initial weight.
This shows that “if you remove the drug, the disease starts to come back,” Dr. Kushner pointed out.
Nausea, the most common side effect, occurred in 20% of patients, but was mostly mild or moderate, and gastrointestinal effects including constipation, vomiting, and diarrhea were transient and occurred early in the dose escalation phase.
Large individual variability, combination therapies on horizon
Dr. Kaplan pointed out, however, that “like [with] other antiobesity therapies ... there’s a large patient-to-patient variability.”
A third of patients exhibit more than 20% weight loss, and 10% exhibit more than 30% weight loss – approaching the efficacy of bariatric surgery.
However, nearly 10% of patients without diabetes and upwards of 30% of patients with diabetes will experience less than 5% weight loss, he said.
Therefore, “success or failure in one patient doesn’t predict response in another, and we should always remember that as we treat different patients with these medications,” Dr. Kaplan advised.
A recent phase 1b study suggests that combination therapy with semaglutide and the amylin agonist cagrilintide ups weight loss, as previously reported.
In this short trial with no lifestyle modification, it took 16 weeks for patients to reach full dosing, and at 20 weeks, patients on semaglutide had lost 8% of their initial weight, whereas those on combination therapy had lost 17% of their initial weight.
“There’s hope that, in combination with cagrilintide and probably with several other agents that are still in early development, we’ll be seeing average weight loss that is in the range of that seen with bariatric surgery,” Dr. Kushner said.
Doctors discuss two hypothetical cases
Session moderator Julio Rosenstock, MD, of the University of Texas, Dallas, a coinvestigator in several of the STEP trials, invited Dr. Kaplan and two other panelists to explain how they would manage two hypothetical patients.
Case 1
You have a patient with type 2 diabetes, a body mass index of 32, 33 kg/m2, and an A1c of 7.5% or 8% on metformin. Would you use semaglutide 1 mg (Ozempic, Novo Nordisk) that is indicated for type 2 diabetes, or would you use semaglutide 2.4 mg that is indicated for obesity and risk factors?
“We have the answer to that from STEP 2,” said Melanie J. Davies, MB ChB, MD, professor of diabetes medicine at the University of Leicester, England, who led the STEP 2 trial.
“For some patients, the 1-mg dose, which we use routinely in the clinic, may be reasonable to get good glycemic control for cardiovascular protection and will obviously achieve some weight loss. But if you really want to go for the weight-related comorbidities, then the 2.4-mg dose is what you need,” she said.
“A lot of [clinicians] might say: ‘I’ll see how [the patient goes] with the 1-mg dose, and then maybe if they’re not losing the weight and not getting to glycemic target, then maybe I’ll switch to 2.4 mg,’” said John Wilding, MD, who leads clinical research into obesity, diabetes, and endocrinology at the University of Liverpool, England, and led the STEP 1 trial.
“But the STEP 2 data show very clearly that you get almost the same A1c,” Dr. Rosenstock interjected. “I would go for 2.4 mg. The patient has a BMI of 32, 33 kg/m2. I would hit hard the BMI. We need to change that paradigm.”
“For other diseases we don’t always go to the maximum dose that’s available. We go to the dose that’s necessary to achieve the clinical endpoint that we want,” Dr. Kaplan noted. “I think one of the challenges is going to be to learn how to clinically nuance our therapy the way we do for other diseases.”
“That is the usual thinking,” Dr. Rosenstock agreed. But “with the 2.4-mg dose, one third get a 20% reduction of BMI, and 10% get almost a 30% reduction – and you [aren’t] going to see that with semaglutide 1 mg!”
“That’s true,” Dr. Kaplan conceded. However, a patient with a relatively low BMI of 32, 33 kg/m2 may not need the higher dose, unlike a patient who has a BMI of 45 kg/m2 and diabetes. But we’re going to find that out over the next couple of years, he expects.
Case 2
You have a patient with a BMI of 31 kg/m2 who is newly diagnosed with type 2 diabetes. Why should you start that patient with metformin? Why won’t you start with something that will directly tackle obesity and get the patient to lose 20 pounds and for sure the blood sugar is going to be better?
“I think if I have someone who is really keen to put their diabetes into remission,” Dr. Wilding said, “this would be a fantastic approach because they would have a really high chance of doing that.”
The prediabetes data from STEP showed that “we can put a lot of people from prediabetes back to normal glucose tolerance,” Dr. Wilding noted. “Maybe we can put people with early diabetes back to normal as well. I think that’s a trial that really does need to be done,” he said.
“We’re going to have to figure out the best pathway forward,” Dr. Kaplan observed, noting that multiple stakeholders, including payers, patients, and providers, play a role in the uptake of new obesity drugs.
“Do you think we will see less bariatric surgery with these drugs?” Dr. Rosenstock asked Dr. Kaplan.
“I think you have to remember that of the millions and millions of people with obesity, a very small portion are currently treated with antiobesity medication, and an even smaller portion are getting bariatric surgery,” Dr. Kaplan replied.
“In the United States, 90% of people who get bariatric surgery are self-referred,” he said, so, “I think initially we are not going to see much of a change” in rates of bariatric surgery.
Dr. Rosenstock, Dr. Kaplan, Dr. Wilding, and Dr. Davies disclosed ties with Novo Nordisk and numerous other companies.
A version of this article first appeared on Medscape.com.
The recently licensed weight-loss drug semaglutide 2.4 mg/week (Wegovy, Novo Nordisk) “is likely to usher in a new era in the medical treatment of obesity,” Lee M. Kaplan, MD, PhD, stated at the annual scientific sessions of the American Diabetes Association, held virtually.
Dr. Kaplan discussed the clinical implications of caring for patients with obesity now that the glucagon-like peptide-1 (GLP-1) receptor agonist is approved in the United States for weight loss.
Weight loss with semaglutide 2.4 mg was twice that achieved with liraglutide 3 mg (Saxenda, Novo Nordisk) – that is, roughly a 10%-15% weight loss at 68 weeks, said Dr. Kaplan, who was not involved in the pivotal STEP clinical trials of the agent.
“I think as we start to see more data come in over the next couple of years,” including from the cardiovascular outcome trial SELECT, he continued, “we’ll be able to use the data to create a nuanced [individualized patient treatment] approach, but we’ll also be able to use our clinical experience, which will grow rapidly over the next few years.”
In the future, semaglutide is likely to be combined with other drugs to provide even greater weight loss, predicts Dr. Kaplan, director of the Obesity, Metabolism, and Nutrition Institute at Massachusetts General Hospital in Boston.
In the meantime, “to be effective, semaglutide needs to be used,” he stressed, while noting that responses to the drug vary by individual, and so this will need to be taken into account.
“Obesity needs to be recognized as a disease in its own right, as well as a risk factor for numerous other diseases, [and] equitable access to obesity treatment needs to be broadened,” he emphasized.
Four pivotal phase 3 trials
As previously reported, four pivotal 68-week, phase 3 clinical trials in the Semaglutide Treatment Effect in People With Obesity (STEP) program tested the safety and efficacy of subcutaneous semaglutide 2.4 mg/week in more than 4,500 adults with overweight or obesity.
The trials have been published in high profile journals – the New England Journal of Medicine (STEP 1), The Lancet (STEP 2), and JAMA (STEP 3 and STEP 4) – said Robert F. Kushner, MD.
“I would encourage all of you to download and read each of these trials on your own,” Dr. Kushner, professor of medicine and medicine education at Northwestern University, Chicago, and coauthor of STEP 1, said before presenting a top-level review of key results.
STEP 1 examined weight management, STEP 3 added a background of intensive behavioral therapy, STEP 4 investigated sustained weight management, and STEP 2 (unlike the others) investigated weight management in patients with type 2 diabetes, he summarized.
In STEP 1, patients who received semaglutide had an average 15% weight loss, and those who stayed on the drug had a 17% weight loss, compared with the 2.4% weight loss in the placebo group.
“One-third of individuals in the trial achieved at least a 20% weight loss or more,” Dr. Kushner said, which is “really phenomenal.”
The results of STEP 3 “suggest that semaglutide with monthly brief lifestyle counseling alone is sufficient to produce a mean weight loss of 15%,” he noted, as adding a low-calorie diet and intensive behavior therapy sped up the initial weight loss but did not increase the final weight loss.
A post hoc analysis of STEP 2 showed “it’s clear that improvement in A1c” is greater with at least a 10% weight loss versus a smaller weight loss, Dr. Kushner said. A1c dropped by 2.2% versus 1.3%, with these two weight losses, respectively.
In STEP 4, after dose escalation to 2.4 mg at 20 weeks, patients had lost 10.6% of their initial weight. At 68 weeks, those who were switched to placebo at 20 weeks had lost 5.4% of their initial weight, whereas those who remained on semaglutide had lost 17.7% of their initial weight.
This shows that “if you remove the drug, the disease starts to come back,” Dr. Kushner pointed out.
Nausea, the most common side effect, occurred in 20% of patients, but was mostly mild or moderate, and gastrointestinal effects including constipation, vomiting, and diarrhea were transient and occurred early in the dose escalation phase.
Large individual variability, combination therapies on horizon
Dr. Kaplan pointed out, however, that “like [with] other antiobesity therapies ... there’s a large patient-to-patient variability.”
A third of patients exhibit more than 20% weight loss, and 10% exhibit more than 30% weight loss – approaching the efficacy of bariatric surgery.
However, nearly 10% of patients without diabetes and upwards of 30% of patients with diabetes will experience less than 5% weight loss, he said.
Therefore, “success or failure in one patient doesn’t predict response in another, and we should always remember that as we treat different patients with these medications,” Dr. Kaplan advised.
A recent phase 1b study suggests that combination therapy with semaglutide and the amylin agonist cagrilintide ups weight loss, as previously reported.
In this short trial with no lifestyle modification, it took 16 weeks for patients to reach full dosing, and at 20 weeks, patients on semaglutide had lost 8% of their initial weight, whereas those on combination therapy had lost 17% of their initial weight.
“There’s hope that, in combination with cagrilintide and probably with several other agents that are still in early development, we’ll be seeing average weight loss that is in the range of that seen with bariatric surgery,” Dr. Kushner said.
Doctors discuss two hypothetical cases
Session moderator Julio Rosenstock, MD, of the University of Texas, Dallas, a coinvestigator in several of the STEP trials, invited Dr. Kaplan and two other panelists to explain how they would manage two hypothetical patients.
Case 1
You have a patient with type 2 diabetes, a body mass index of 32, 33 kg/m2, and an A1c of 7.5% or 8% on metformin. Would you use semaglutide 1 mg (Ozempic, Novo Nordisk) that is indicated for type 2 diabetes, or would you use semaglutide 2.4 mg that is indicated for obesity and risk factors?
“We have the answer to that from STEP 2,” said Melanie J. Davies, MB ChB, MD, professor of diabetes medicine at the University of Leicester, England, who led the STEP 2 trial.
“For some patients, the 1-mg dose, which we use routinely in the clinic, may be reasonable to get good glycemic control for cardiovascular protection and will obviously achieve some weight loss. But if you really want to go for the weight-related comorbidities, then the 2.4-mg dose is what you need,” she said.
“A lot of [clinicians] might say: ‘I’ll see how [the patient goes] with the 1-mg dose, and then maybe if they’re not losing the weight and not getting to glycemic target, then maybe I’ll switch to 2.4 mg,’” said John Wilding, MD, who leads clinical research into obesity, diabetes, and endocrinology at the University of Liverpool, England, and led the STEP 1 trial.
“But the STEP 2 data show very clearly that you get almost the same A1c,” Dr. Rosenstock interjected. “I would go for 2.4 mg. The patient has a BMI of 32, 33 kg/m2. I would hit hard the BMI. We need to change that paradigm.”
“For other diseases we don’t always go to the maximum dose that’s available. We go to the dose that’s necessary to achieve the clinical endpoint that we want,” Dr. Kaplan noted. “I think one of the challenges is going to be to learn how to clinically nuance our therapy the way we do for other diseases.”
“That is the usual thinking,” Dr. Rosenstock agreed. But “with the 2.4-mg dose, one third get a 20% reduction of BMI, and 10% get almost a 30% reduction – and you [aren’t] going to see that with semaglutide 1 mg!”
“That’s true,” Dr. Kaplan conceded. However, a patient with a relatively low BMI of 32, 33 kg/m2 may not need the higher dose, unlike a patient who has a BMI of 45 kg/m2 and diabetes. But we’re going to find that out over the next couple of years, he expects.
Case 2
You have a patient with a BMI of 31 kg/m2 who is newly diagnosed with type 2 diabetes. Why should you start that patient with metformin? Why won’t you start with something that will directly tackle obesity and get the patient to lose 20 pounds and for sure the blood sugar is going to be better?
“I think if I have someone who is really keen to put their diabetes into remission,” Dr. Wilding said, “this would be a fantastic approach because they would have a really high chance of doing that.”
The prediabetes data from STEP showed that “we can put a lot of people from prediabetes back to normal glucose tolerance,” Dr. Wilding noted. “Maybe we can put people with early diabetes back to normal as well. I think that’s a trial that really does need to be done,” he said.
“We’re going to have to figure out the best pathway forward,” Dr. Kaplan observed, noting that multiple stakeholders, including payers, patients, and providers, play a role in the uptake of new obesity drugs.
“Do you think we will see less bariatric surgery with these drugs?” Dr. Rosenstock asked Dr. Kaplan.
“I think you have to remember that of the millions and millions of people with obesity, a very small portion are currently treated with antiobesity medication, and an even smaller portion are getting bariatric surgery,” Dr. Kaplan replied.
“In the United States, 90% of people who get bariatric surgery are self-referred,” he said, so, “I think initially we are not going to see much of a change” in rates of bariatric surgery.
Dr. Rosenstock, Dr. Kaplan, Dr. Wilding, and Dr. Davies disclosed ties with Novo Nordisk and numerous other companies.
A version of this article first appeared on Medscape.com.
'Full throttle': 'Diabetes Garage' workshops boost Mexican American men's self-management
Automotive-themed workshops that refer to doctor visits as “tune-ups” and nutritious food as “high-performance fuel” are showing promise as a strategy to better explain diabetes self-management to Mexican American men, an investigator has reported.
The workshops, which started out in person and transitioned online because of the COVID-19 pandemic, have improved self-care behaviors among Mexican American men with diabetes, said Jeannie Belinda Concha, PhD, MPH, of the University of Texas, El Paso.
After participating in the workshops, known as The Diabetes Garage, men more often measured food portions and counted carbohydrates, and had improved confidence in their ability to self-manage their diabetes, Dr. Concha said in a virtual presentation on the study.
Although those improvements in self-care behaviors didn’t translate into significant improvements in blood pressure or hemoglobin A1c, she said, they could be predecessors to improved physical health outcomes with longer follow-up.
”We know it takes some time to move those numbers, but they are going in the right direction,” Dr. Concha said in her presentation, which took place during the annual scientific sessions of the American Diabetes Association.
Meeting Mexican American men where they’re at
Robert Gabbay, MD, PhD, chief scientific and medical officer of the ADA, said The Diabetes Garage is an “innovative” approach to tailoring diabetes self-care message for a specific of individuals.
“It’s such a wonderful example of something that we believe so strongly, which is that you’ve got to meet people where they’re at,” Dr. Gabbay said in an interview.
“We know that people learn in different ways, and people and with different backgrounds have different things that resonate with them,” he continued. “For better or worse, one size doesn’t fit all, and that in a sense is one of the challenges around diabetes, because we’re really trying to help everybody.”
Unmet needs for diabetes education
The prevalence of diabetes in the United States is high among Hispanics, higher among Mexican Americans, and even higher still among Mexican-American men, according to Dr. Concha.
The age-adjusted prevalence of diabetes is 16.2% among Mexican-American men, as compared with 12.8% for Mexican American women, and 8.6% for White non-Hispanic men, according to 2018 data from the Centers for Disease Control and Prevention that Dr. Concha highlighted in her presentation.
Moreover, only 25% of participants in diabetes education are men, highlighting another disparity that needs to be addressed, she said.
Infusing diabetes self-management with car culture
The Diabetes Garage leverages a positive “car culture” that is prevalent in Mexican American communities in general, and cities like El Paso in particular, Dr. Concha said.
This culture brings Mexican American people together at numerous car shows, and is viewed as a form of family identification for enthusiasts, who will illustrate their own pride by customizing their cars with cultural symbols, according to Dr. Concha.
The diabetes education intervention consists of four workshops delivered as 2-hour weekly sessions that include a diabetes educator and an automotive instructor:
In the first session, men learn about “starting and operating” their body with diabetes, and checking their “gauges” when it comes to blood pressure, cholesterol, and other measures, according to Dr. Concha.
The second session stresses the importance of physical activity (“using all your gears”) and of managing stress (“full throttle”).
The third session highlights medication as a tool (“to keep your battery charged”) and the importance of diabetes complications (“catastrophic failure”) as well as visiting the doctor (“tune ups and inspections”).
Finally, men learn about nutrition (high-performance fuel) in a workshop on eating well with diabetes. “We ask them to invite their family and friends, and they do,” said Dr. Concha.
Rubber hits the road
Since 2018, 16 workshops have been completed in El Paso, San Antonio, and Harlingen, Tex., of which 9 were in English, 5 were in Spanish, and 2 were bilingual. Due to the COVID-19 pandemic, 10 of the workshops were completed online, Dr. Concha said.
In total, 97 men engaged in the workshops, of whom 91% were Hispanic/Latino; 71% were employed, 71% were married, and 84% had health insurance. Eighty-six percent completed all four workshops, while 89% completed at least three workshops.
The number of days men measured food portions increased significantly from pre- to postworkshop assessment, from a mean of 2.1 days to 2.74 days, Dr. Concha reported. Similarly, the mean number of days counting carbohydrate portions increased significantly, from 1.92 to 2.64 days.
The proportion of men agreeing or strongly agreeing they were confident they could manage diabetes increased from 74% before the intervention to 93% afterward, according to Dr. Concha’s presentation.
By contrast, there were no statistically significant increases in physical outcomes including physical activity, weight, waist circumference, A1c, or blood pressure from before the workshop to after, though outcomes trended in an improved direction, according to Dr. Concha.
Postactivity satisfaction survey results showed that 86%of men said the automotive analogies in the program helped them understand the importance of diabetes management. “I am looking forward to better managing my human-mobile for a long, long time with a good quality of life,” one of the men wrote in survey feedback.
Dr. Concha and coauthors reported no conflicts of interest related to the study.
Automotive-themed workshops that refer to doctor visits as “tune-ups” and nutritious food as “high-performance fuel” are showing promise as a strategy to better explain diabetes self-management to Mexican American men, an investigator has reported.
The workshops, which started out in person and transitioned online because of the COVID-19 pandemic, have improved self-care behaviors among Mexican American men with diabetes, said Jeannie Belinda Concha, PhD, MPH, of the University of Texas, El Paso.
After participating in the workshops, known as The Diabetes Garage, men more often measured food portions and counted carbohydrates, and had improved confidence in their ability to self-manage their diabetes, Dr. Concha said in a virtual presentation on the study.
Although those improvements in self-care behaviors didn’t translate into significant improvements in blood pressure or hemoglobin A1c, she said, they could be predecessors to improved physical health outcomes with longer follow-up.
”We know it takes some time to move those numbers, but they are going in the right direction,” Dr. Concha said in her presentation, which took place during the annual scientific sessions of the American Diabetes Association.
Meeting Mexican American men where they’re at
Robert Gabbay, MD, PhD, chief scientific and medical officer of the ADA, said The Diabetes Garage is an “innovative” approach to tailoring diabetes self-care message for a specific of individuals.
“It’s such a wonderful example of something that we believe so strongly, which is that you’ve got to meet people where they’re at,” Dr. Gabbay said in an interview.
“We know that people learn in different ways, and people and with different backgrounds have different things that resonate with them,” he continued. “For better or worse, one size doesn’t fit all, and that in a sense is one of the challenges around diabetes, because we’re really trying to help everybody.”
Unmet needs for diabetes education
The prevalence of diabetes in the United States is high among Hispanics, higher among Mexican Americans, and even higher still among Mexican-American men, according to Dr. Concha.
The age-adjusted prevalence of diabetes is 16.2% among Mexican-American men, as compared with 12.8% for Mexican American women, and 8.6% for White non-Hispanic men, according to 2018 data from the Centers for Disease Control and Prevention that Dr. Concha highlighted in her presentation.
Moreover, only 25% of participants in diabetes education are men, highlighting another disparity that needs to be addressed, she said.
Infusing diabetes self-management with car culture
The Diabetes Garage leverages a positive “car culture” that is prevalent in Mexican American communities in general, and cities like El Paso in particular, Dr. Concha said.
This culture brings Mexican American people together at numerous car shows, and is viewed as a form of family identification for enthusiasts, who will illustrate their own pride by customizing their cars with cultural symbols, according to Dr. Concha.
The diabetes education intervention consists of four workshops delivered as 2-hour weekly sessions that include a diabetes educator and an automotive instructor:
In the first session, men learn about “starting and operating” their body with diabetes, and checking their “gauges” when it comes to blood pressure, cholesterol, and other measures, according to Dr. Concha.
The second session stresses the importance of physical activity (“using all your gears”) and of managing stress (“full throttle”).
The third session highlights medication as a tool (“to keep your battery charged”) and the importance of diabetes complications (“catastrophic failure”) as well as visiting the doctor (“tune ups and inspections”).
Finally, men learn about nutrition (high-performance fuel) in a workshop on eating well with diabetes. “We ask them to invite their family and friends, and they do,” said Dr. Concha.
Rubber hits the road
Since 2018, 16 workshops have been completed in El Paso, San Antonio, and Harlingen, Tex., of which 9 were in English, 5 were in Spanish, and 2 were bilingual. Due to the COVID-19 pandemic, 10 of the workshops were completed online, Dr. Concha said.
In total, 97 men engaged in the workshops, of whom 91% were Hispanic/Latino; 71% were employed, 71% were married, and 84% had health insurance. Eighty-six percent completed all four workshops, while 89% completed at least three workshops.
The number of days men measured food portions increased significantly from pre- to postworkshop assessment, from a mean of 2.1 days to 2.74 days, Dr. Concha reported. Similarly, the mean number of days counting carbohydrate portions increased significantly, from 1.92 to 2.64 days.
The proportion of men agreeing or strongly agreeing they were confident they could manage diabetes increased from 74% before the intervention to 93% afterward, according to Dr. Concha’s presentation.
By contrast, there were no statistically significant increases in physical outcomes including physical activity, weight, waist circumference, A1c, or blood pressure from before the workshop to after, though outcomes trended in an improved direction, according to Dr. Concha.
Postactivity satisfaction survey results showed that 86%of men said the automotive analogies in the program helped them understand the importance of diabetes management. “I am looking forward to better managing my human-mobile for a long, long time with a good quality of life,” one of the men wrote in survey feedback.
Dr. Concha and coauthors reported no conflicts of interest related to the study.
Automotive-themed workshops that refer to doctor visits as “tune-ups” and nutritious food as “high-performance fuel” are showing promise as a strategy to better explain diabetes self-management to Mexican American men, an investigator has reported.
The workshops, which started out in person and transitioned online because of the COVID-19 pandemic, have improved self-care behaviors among Mexican American men with diabetes, said Jeannie Belinda Concha, PhD, MPH, of the University of Texas, El Paso.
After participating in the workshops, known as The Diabetes Garage, men more often measured food portions and counted carbohydrates, and had improved confidence in their ability to self-manage their diabetes, Dr. Concha said in a virtual presentation on the study.
Although those improvements in self-care behaviors didn’t translate into significant improvements in blood pressure or hemoglobin A1c, she said, they could be predecessors to improved physical health outcomes with longer follow-up.
”We know it takes some time to move those numbers, but they are going in the right direction,” Dr. Concha said in her presentation, which took place during the annual scientific sessions of the American Diabetes Association.
Meeting Mexican American men where they’re at
Robert Gabbay, MD, PhD, chief scientific and medical officer of the ADA, said The Diabetes Garage is an “innovative” approach to tailoring diabetes self-care message for a specific of individuals.
“It’s such a wonderful example of something that we believe so strongly, which is that you’ve got to meet people where they’re at,” Dr. Gabbay said in an interview.
“We know that people learn in different ways, and people and with different backgrounds have different things that resonate with them,” he continued. “For better or worse, one size doesn’t fit all, and that in a sense is one of the challenges around diabetes, because we’re really trying to help everybody.”
Unmet needs for diabetes education
The prevalence of diabetes in the United States is high among Hispanics, higher among Mexican Americans, and even higher still among Mexican-American men, according to Dr. Concha.
The age-adjusted prevalence of diabetes is 16.2% among Mexican-American men, as compared with 12.8% for Mexican American women, and 8.6% for White non-Hispanic men, according to 2018 data from the Centers for Disease Control and Prevention that Dr. Concha highlighted in her presentation.
Moreover, only 25% of participants in diabetes education are men, highlighting another disparity that needs to be addressed, she said.
Infusing diabetes self-management with car culture
The Diabetes Garage leverages a positive “car culture” that is prevalent in Mexican American communities in general, and cities like El Paso in particular, Dr. Concha said.
This culture brings Mexican American people together at numerous car shows, and is viewed as a form of family identification for enthusiasts, who will illustrate their own pride by customizing their cars with cultural symbols, according to Dr. Concha.
The diabetes education intervention consists of four workshops delivered as 2-hour weekly sessions that include a diabetes educator and an automotive instructor:
In the first session, men learn about “starting and operating” their body with diabetes, and checking their “gauges” when it comes to blood pressure, cholesterol, and other measures, according to Dr. Concha.
The second session stresses the importance of physical activity (“using all your gears”) and of managing stress (“full throttle”).
The third session highlights medication as a tool (“to keep your battery charged”) and the importance of diabetes complications (“catastrophic failure”) as well as visiting the doctor (“tune ups and inspections”).
Finally, men learn about nutrition (high-performance fuel) in a workshop on eating well with diabetes. “We ask them to invite their family and friends, and they do,” said Dr. Concha.
Rubber hits the road
Since 2018, 16 workshops have been completed in El Paso, San Antonio, and Harlingen, Tex., of which 9 were in English, 5 were in Spanish, and 2 were bilingual. Due to the COVID-19 pandemic, 10 of the workshops were completed online, Dr. Concha said.
In total, 97 men engaged in the workshops, of whom 91% were Hispanic/Latino; 71% were employed, 71% were married, and 84% had health insurance. Eighty-six percent completed all four workshops, while 89% completed at least three workshops.
The number of days men measured food portions increased significantly from pre- to postworkshop assessment, from a mean of 2.1 days to 2.74 days, Dr. Concha reported. Similarly, the mean number of days counting carbohydrate portions increased significantly, from 1.92 to 2.64 days.
The proportion of men agreeing or strongly agreeing they were confident they could manage diabetes increased from 74% before the intervention to 93% afterward, according to Dr. Concha’s presentation.
By contrast, there were no statistically significant increases in physical outcomes including physical activity, weight, waist circumference, A1c, or blood pressure from before the workshop to after, though outcomes trended in an improved direction, according to Dr. Concha.
Postactivity satisfaction survey results showed that 86%of men said the automotive analogies in the program helped them understand the importance of diabetes management. “I am looking forward to better managing my human-mobile for a long, long time with a good quality of life,” one of the men wrote in survey feedback.
Dr. Concha and coauthors reported no conflicts of interest related to the study.
FROM ADA 2021
Nocturnal hypoglycemia halved with insulin degludec vs. glargine
Patients with type 1 diabetes who used insulin degludec as their basal insulin had fewer than half the number of nocturnal hypoglycemia events, compared with patients who used insulin glargine U100, in a head-to-head crossover study with 51 patients who had a history of nighttime hypoglycemia episodes.
Patients with type 1 diabetes who are “struggling with nocturnal hypoglycemia would benefit from insulin degludec treatment,” said Julie M. Brøsen, MD, at the annual scientific sessions of the American Diabetes Association.
Accumulating evidence for less hypoglycemia with insulin degludec
Results from several studies comparing insulin degludec (Tresiba), a second-generation, longer-acting insulin with more stable steady-state performance, with the first-generation basal insulin analogue glargine (Lantus), have built the case that degludec produces fewer hypoglycemia events.
The landmark SWITCH 1 crossover study published in 2017 showed in about 500 patients with type 1 diabetes and a risk factor for hypoglycemia that treatment with insulin degludec led to significantly few total hypoglycemia episodes and significantly fewer nocturnal episodes, compared with insulin glargine.
Next came similar findings from ReFLeCT, a multicenter observational study that followed 556 unselected patients with type 1 diabetes in routine practice settings who switched to insulin degludec following treatment with a different basal insulin. The results again showed a significant drop-off in total, nonsevere, severe, and nocturnal hypoglycemia events.
Homing in on higher-risk patients
The current study, HypoDeg (Insulin Degludec and Symptomatic Nocturnal Hypoglycaemia), ran at 10 Danish centers and enrolled 149 adults with type 1 diabetes who had at least one episode of severe nocturnal hypoglycemia within the prior 2 years, focusing on patients most at risk for future nocturnal hypoglycemia events. In an unusual study design, researchers identified nocturnal hypoglycemic episodes with hourly venous blood samples drawn from a subcutaneous line.
They randomized the patients to basal insulin treatment with either insulin degludec or to insulin glargine U100, allowed their treatment to stabilize for 3 months, and then tallied nocturnal hypoglycemia events for 9 months. They then crossed patients to the alternative basal insulin and repeated the process.
Results from the full study have not yet appeared in published form but were in a pair of reports at the 2020 scientific sessions of the ADA.
One report included findings based on 136 episodes of severe hypoglycemia identified clinically and showed these events occurred 35% less often during treatment with insulin degludec, a significant difference. The overall finding was primarily driven by 48% fewer episodes of severe nocturnal hypoglycemia, but this difference was not significant.
The second report identified hypoglycemia events with continuous glucose monitoring in 74 of the study participants, which identified 193 episodes of nonsevere nocturnal hypoglycemia and found that treatment with insulin degludec cut the rate by 47%, primarily by reducing asymptomatic episodes.
Hourly blood draws track overnight hypoglycemia
The current study included 51 of the 149 HypoDeg patients who agreed to undergo overnight blood sampling and had this done at least once while treated with each of the two study insulins. (The study design called for two blood sampling nights for each willing patient during each of the two treatment periods.) The 51 patients had type 1 diabetes for an average of 28 years and an average age of 58 years. Two-thirds were men, their baseline A1c was 7.8%, and on average had 2.6 episodes of severe nocturnal hypoglycemia during the prior 2 years.
The researchers drew hourly blood specimens on a total of 196 nights from the 51 participating patients and identified 57 nights when blood glucose levels reached hypoglycemia thresholds in 33 patients. One-third of the events occurred when patients were on insulin degludec treatment, and two-thirds when they were on insulin glargine, reported Dr. Brøsen.
She presented three separate analyses of the data. One analysis focused on level 1 hypoglycemia events, when blood glucose dips to 70 mg/dL or less, which occurred 54% less often when patients were on insulin degludec. A second analysis looked at level 2 events, when blood glucose falls below 54 mg/dL, and treatment with insulin degludec cut this by 64% compared with insulin glargine. The third analysis focused on symptomatic events when blood glucose was 70 mg/dL or less, and treatment with insulin degludec linked with a 62% cut in this metric. All three between-group differences were significant.
Evidence supports already-changed practice
This new evidence “supports recommending” insulin degludec over insulin glargine, commented Bastiaan E. de Galan, MD, PhD, an endocrinologist and professor at Maastrict (the Netherlands) University Medical Center. The new results “extend those from previous trials in populations with type 1 diabetes that were unselected for the risk of hypoglycemia. In clinical practice, insulin degludec is already considered for patients who reported nocturnal hypoglycemia while on insulin glargine U100, but it’s great this study provides the scientific evidence,” said Dr. de Galan in an interview.
“The lower rate of nocturnal hypoglycemia with degludec, compared with glargine U100 is well established. Inpatient assessment of hypoglycemia with measurement of hourly plasma glucose allowed HypoDeg to provide stronger evidence than prior studies. The benefit of delgudec versus glargine U100 was significant and clinically meaningful, in hypo-prone patients who would benefit the most” by using insulin degludec, commented Gian Paolo Fadini, MD, an endocrinologist at the University of Padova (Italy), and a lead investigator on the ReFLeCT study.
But insulin degludec is not a completely silver bullet. Its prolonged duration of action and stability that may in part explain why it limits hypoglycemia events can also be a drawback: “It probably offers fewer options for flexibility. Any change in dose takes at least a day or 2 to settle, which may be unfavorable in certain circumstances,” noted Dr. de Galan.
“I wouldn’t recommend insulin degludec for all patients with type 1 diabetes. It’s an individual evaluation in each patient,” said Dr. Brøsen. “We will be looking into whether some patients are better off on insulin glargine.”
Cost makes a difference
Another, potentially more consequential flaw is insulin degludec’s relative expense.
“To date, use of degludec in routine practice has been limited by its cost, compared with older basal insulins,” observed Dr. Fadini in an interview. “In several countries, including the United States, degludec is substantially more expensive than glargine.”
The ADA’s Standards of Medical Care in Diabetes–2021 includes table 9.3 that lists the costs of various insulins and shows the median average wholesale price of insulin glargine U100 follow-on products as $190/vial, compared with a $407 price for a similar vial of insulin degludec.
Insulin degludec “is clearly superior from a hypoglycemia standpoint. Patients with type 1 diabetes like the reduction because hypoglycemia is scary, and dangerous. The main issue is cost, and the extent to which it may be covered by insurance,” commented Lisa Chow, MD, an endocrinologist at the University of Minnesota, Minneapolis. “We generally won’t prescribe degludec unless it is at a price affordable to the patient. We try to use patient assistance programs sponsored by the company [that markets insulin degludec: Novo Nordisk] to try to make it more affordable.”
Dr. Chow also highlighted that a new wrinkle has been introduction of a more concentrated formulation of insulin glargine, U300, which appears to cause less hypoglycemia than insulin glargine U100. Recent study results indicated that no significant difference exists in the incidence of hypoglycemia among patients treated with insulin glargine U300 and those treated with insulin degludec, such as findings from the BRIGHT trial, which included just over 900 patients, and in the CONCLUDE trial, which randomized more than 1,600 patients.
The HypoDeg study was sponsored by Novo Nordisk, the company that markets insulin degludec. Dr. Brøsen had no personal disclosures, but several of her coauthors were either Novo Nordisk employees or had financial relationships with the company. Dr. de Galan has received research funding from Novo Nordisk. Dr. Fadini has received lecture fees and research funding from Novo Nordisk, from Sanofi, the company that markets insulin glargine, and from several other companies. Dr. Chow has received research funding from Dexcom.
Patients with type 1 diabetes who used insulin degludec as their basal insulin had fewer than half the number of nocturnal hypoglycemia events, compared with patients who used insulin glargine U100, in a head-to-head crossover study with 51 patients who had a history of nighttime hypoglycemia episodes.
Patients with type 1 diabetes who are “struggling with nocturnal hypoglycemia would benefit from insulin degludec treatment,” said Julie M. Brøsen, MD, at the annual scientific sessions of the American Diabetes Association.
Accumulating evidence for less hypoglycemia with insulin degludec
Results from several studies comparing insulin degludec (Tresiba), a second-generation, longer-acting insulin with more stable steady-state performance, with the first-generation basal insulin analogue glargine (Lantus), have built the case that degludec produces fewer hypoglycemia events.
The landmark SWITCH 1 crossover study published in 2017 showed in about 500 patients with type 1 diabetes and a risk factor for hypoglycemia that treatment with insulin degludec led to significantly few total hypoglycemia episodes and significantly fewer nocturnal episodes, compared with insulin glargine.
Next came similar findings from ReFLeCT, a multicenter observational study that followed 556 unselected patients with type 1 diabetes in routine practice settings who switched to insulin degludec following treatment with a different basal insulin. The results again showed a significant drop-off in total, nonsevere, severe, and nocturnal hypoglycemia events.
Homing in on higher-risk patients
The current study, HypoDeg (Insulin Degludec and Symptomatic Nocturnal Hypoglycaemia), ran at 10 Danish centers and enrolled 149 adults with type 1 diabetes who had at least one episode of severe nocturnal hypoglycemia within the prior 2 years, focusing on patients most at risk for future nocturnal hypoglycemia events. In an unusual study design, researchers identified nocturnal hypoglycemic episodes with hourly venous blood samples drawn from a subcutaneous line.
They randomized the patients to basal insulin treatment with either insulin degludec or to insulin glargine U100, allowed their treatment to stabilize for 3 months, and then tallied nocturnal hypoglycemia events for 9 months. They then crossed patients to the alternative basal insulin and repeated the process.
Results from the full study have not yet appeared in published form but were in a pair of reports at the 2020 scientific sessions of the ADA.
One report included findings based on 136 episodes of severe hypoglycemia identified clinically and showed these events occurred 35% less often during treatment with insulin degludec, a significant difference. The overall finding was primarily driven by 48% fewer episodes of severe nocturnal hypoglycemia, but this difference was not significant.
The second report identified hypoglycemia events with continuous glucose monitoring in 74 of the study participants, which identified 193 episodes of nonsevere nocturnal hypoglycemia and found that treatment with insulin degludec cut the rate by 47%, primarily by reducing asymptomatic episodes.
Hourly blood draws track overnight hypoglycemia
The current study included 51 of the 149 HypoDeg patients who agreed to undergo overnight blood sampling and had this done at least once while treated with each of the two study insulins. (The study design called for two blood sampling nights for each willing patient during each of the two treatment periods.) The 51 patients had type 1 diabetes for an average of 28 years and an average age of 58 years. Two-thirds were men, their baseline A1c was 7.8%, and on average had 2.6 episodes of severe nocturnal hypoglycemia during the prior 2 years.
The researchers drew hourly blood specimens on a total of 196 nights from the 51 participating patients and identified 57 nights when blood glucose levels reached hypoglycemia thresholds in 33 patients. One-third of the events occurred when patients were on insulin degludec treatment, and two-thirds when they were on insulin glargine, reported Dr. Brøsen.
She presented three separate analyses of the data. One analysis focused on level 1 hypoglycemia events, when blood glucose dips to 70 mg/dL or less, which occurred 54% less often when patients were on insulin degludec. A second analysis looked at level 2 events, when blood glucose falls below 54 mg/dL, and treatment with insulin degludec cut this by 64% compared with insulin glargine. The third analysis focused on symptomatic events when blood glucose was 70 mg/dL or less, and treatment with insulin degludec linked with a 62% cut in this metric. All three between-group differences were significant.
Evidence supports already-changed practice
This new evidence “supports recommending” insulin degludec over insulin glargine, commented Bastiaan E. de Galan, MD, PhD, an endocrinologist and professor at Maastrict (the Netherlands) University Medical Center. The new results “extend those from previous trials in populations with type 1 diabetes that were unselected for the risk of hypoglycemia. In clinical practice, insulin degludec is already considered for patients who reported nocturnal hypoglycemia while on insulin glargine U100, but it’s great this study provides the scientific evidence,” said Dr. de Galan in an interview.
“The lower rate of nocturnal hypoglycemia with degludec, compared with glargine U100 is well established. Inpatient assessment of hypoglycemia with measurement of hourly plasma glucose allowed HypoDeg to provide stronger evidence than prior studies. The benefit of delgudec versus glargine U100 was significant and clinically meaningful, in hypo-prone patients who would benefit the most” by using insulin degludec, commented Gian Paolo Fadini, MD, an endocrinologist at the University of Padova (Italy), and a lead investigator on the ReFLeCT study.
But insulin degludec is not a completely silver bullet. Its prolonged duration of action and stability that may in part explain why it limits hypoglycemia events can also be a drawback: “It probably offers fewer options for flexibility. Any change in dose takes at least a day or 2 to settle, which may be unfavorable in certain circumstances,” noted Dr. de Galan.
“I wouldn’t recommend insulin degludec for all patients with type 1 diabetes. It’s an individual evaluation in each patient,” said Dr. Brøsen. “We will be looking into whether some patients are better off on insulin glargine.”
Cost makes a difference
Another, potentially more consequential flaw is insulin degludec’s relative expense.
“To date, use of degludec in routine practice has been limited by its cost, compared with older basal insulins,” observed Dr. Fadini in an interview. “In several countries, including the United States, degludec is substantially more expensive than glargine.”
The ADA’s Standards of Medical Care in Diabetes–2021 includes table 9.3 that lists the costs of various insulins and shows the median average wholesale price of insulin glargine U100 follow-on products as $190/vial, compared with a $407 price for a similar vial of insulin degludec.
Insulin degludec “is clearly superior from a hypoglycemia standpoint. Patients with type 1 diabetes like the reduction because hypoglycemia is scary, and dangerous. The main issue is cost, and the extent to which it may be covered by insurance,” commented Lisa Chow, MD, an endocrinologist at the University of Minnesota, Minneapolis. “We generally won’t prescribe degludec unless it is at a price affordable to the patient. We try to use patient assistance programs sponsored by the company [that markets insulin degludec: Novo Nordisk] to try to make it more affordable.”
Dr. Chow also highlighted that a new wrinkle has been introduction of a more concentrated formulation of insulin glargine, U300, which appears to cause less hypoglycemia than insulin glargine U100. Recent study results indicated that no significant difference exists in the incidence of hypoglycemia among patients treated with insulin glargine U300 and those treated with insulin degludec, such as findings from the BRIGHT trial, which included just over 900 patients, and in the CONCLUDE trial, which randomized more than 1,600 patients.
The HypoDeg study was sponsored by Novo Nordisk, the company that markets insulin degludec. Dr. Brøsen had no personal disclosures, but several of her coauthors were either Novo Nordisk employees or had financial relationships with the company. Dr. de Galan has received research funding from Novo Nordisk. Dr. Fadini has received lecture fees and research funding from Novo Nordisk, from Sanofi, the company that markets insulin glargine, and from several other companies. Dr. Chow has received research funding from Dexcom.
Patients with type 1 diabetes who used insulin degludec as their basal insulin had fewer than half the number of nocturnal hypoglycemia events, compared with patients who used insulin glargine U100, in a head-to-head crossover study with 51 patients who had a history of nighttime hypoglycemia episodes.
Patients with type 1 diabetes who are “struggling with nocturnal hypoglycemia would benefit from insulin degludec treatment,” said Julie M. Brøsen, MD, at the annual scientific sessions of the American Diabetes Association.
Accumulating evidence for less hypoglycemia with insulin degludec
Results from several studies comparing insulin degludec (Tresiba), a second-generation, longer-acting insulin with more stable steady-state performance, with the first-generation basal insulin analogue glargine (Lantus), have built the case that degludec produces fewer hypoglycemia events.
The landmark SWITCH 1 crossover study published in 2017 showed in about 500 patients with type 1 diabetes and a risk factor for hypoglycemia that treatment with insulin degludec led to significantly few total hypoglycemia episodes and significantly fewer nocturnal episodes, compared with insulin glargine.
Next came similar findings from ReFLeCT, a multicenter observational study that followed 556 unselected patients with type 1 diabetes in routine practice settings who switched to insulin degludec following treatment with a different basal insulin. The results again showed a significant drop-off in total, nonsevere, severe, and nocturnal hypoglycemia events.
Homing in on higher-risk patients
The current study, HypoDeg (Insulin Degludec and Symptomatic Nocturnal Hypoglycaemia), ran at 10 Danish centers and enrolled 149 adults with type 1 diabetes who had at least one episode of severe nocturnal hypoglycemia within the prior 2 years, focusing on patients most at risk for future nocturnal hypoglycemia events. In an unusual study design, researchers identified nocturnal hypoglycemic episodes with hourly venous blood samples drawn from a subcutaneous line.
They randomized the patients to basal insulin treatment with either insulin degludec or to insulin glargine U100, allowed their treatment to stabilize for 3 months, and then tallied nocturnal hypoglycemia events for 9 months. They then crossed patients to the alternative basal insulin and repeated the process.
Results from the full study have not yet appeared in published form but were in a pair of reports at the 2020 scientific sessions of the ADA.
One report included findings based on 136 episodes of severe hypoglycemia identified clinically and showed these events occurred 35% less often during treatment with insulin degludec, a significant difference. The overall finding was primarily driven by 48% fewer episodes of severe nocturnal hypoglycemia, but this difference was not significant.
The second report identified hypoglycemia events with continuous glucose monitoring in 74 of the study participants, which identified 193 episodes of nonsevere nocturnal hypoglycemia and found that treatment with insulin degludec cut the rate by 47%, primarily by reducing asymptomatic episodes.
Hourly blood draws track overnight hypoglycemia
The current study included 51 of the 149 HypoDeg patients who agreed to undergo overnight blood sampling and had this done at least once while treated with each of the two study insulins. (The study design called for two blood sampling nights for each willing patient during each of the two treatment periods.) The 51 patients had type 1 diabetes for an average of 28 years and an average age of 58 years. Two-thirds were men, their baseline A1c was 7.8%, and on average had 2.6 episodes of severe nocturnal hypoglycemia during the prior 2 years.
The researchers drew hourly blood specimens on a total of 196 nights from the 51 participating patients and identified 57 nights when blood glucose levels reached hypoglycemia thresholds in 33 patients. One-third of the events occurred when patients were on insulin degludec treatment, and two-thirds when they were on insulin glargine, reported Dr. Brøsen.
She presented three separate analyses of the data. One analysis focused on level 1 hypoglycemia events, when blood glucose dips to 70 mg/dL or less, which occurred 54% less often when patients were on insulin degludec. A second analysis looked at level 2 events, when blood glucose falls below 54 mg/dL, and treatment with insulin degludec cut this by 64% compared with insulin glargine. The third analysis focused on symptomatic events when blood glucose was 70 mg/dL or less, and treatment with insulin degludec linked with a 62% cut in this metric. All three between-group differences were significant.
Evidence supports already-changed practice
This new evidence “supports recommending” insulin degludec over insulin glargine, commented Bastiaan E. de Galan, MD, PhD, an endocrinologist and professor at Maastrict (the Netherlands) University Medical Center. The new results “extend those from previous trials in populations with type 1 diabetes that were unselected for the risk of hypoglycemia. In clinical practice, insulin degludec is already considered for patients who reported nocturnal hypoglycemia while on insulin glargine U100, but it’s great this study provides the scientific evidence,” said Dr. de Galan in an interview.
“The lower rate of nocturnal hypoglycemia with degludec, compared with glargine U100 is well established. Inpatient assessment of hypoglycemia with measurement of hourly plasma glucose allowed HypoDeg to provide stronger evidence than prior studies. The benefit of delgudec versus glargine U100 was significant and clinically meaningful, in hypo-prone patients who would benefit the most” by using insulin degludec, commented Gian Paolo Fadini, MD, an endocrinologist at the University of Padova (Italy), and a lead investigator on the ReFLeCT study.
But insulin degludec is not a completely silver bullet. Its prolonged duration of action and stability that may in part explain why it limits hypoglycemia events can also be a drawback: “It probably offers fewer options for flexibility. Any change in dose takes at least a day or 2 to settle, which may be unfavorable in certain circumstances,” noted Dr. de Galan.
“I wouldn’t recommend insulin degludec for all patients with type 1 diabetes. It’s an individual evaluation in each patient,” said Dr. Brøsen. “We will be looking into whether some patients are better off on insulin glargine.”
Cost makes a difference
Another, potentially more consequential flaw is insulin degludec’s relative expense.
“To date, use of degludec in routine practice has been limited by its cost, compared with older basal insulins,” observed Dr. Fadini in an interview. “In several countries, including the United States, degludec is substantially more expensive than glargine.”
The ADA’s Standards of Medical Care in Diabetes–2021 includes table 9.3 that lists the costs of various insulins and shows the median average wholesale price of insulin glargine U100 follow-on products as $190/vial, compared with a $407 price for a similar vial of insulin degludec.
Insulin degludec “is clearly superior from a hypoglycemia standpoint. Patients with type 1 diabetes like the reduction because hypoglycemia is scary, and dangerous. The main issue is cost, and the extent to which it may be covered by insurance,” commented Lisa Chow, MD, an endocrinologist at the University of Minnesota, Minneapolis. “We generally won’t prescribe degludec unless it is at a price affordable to the patient. We try to use patient assistance programs sponsored by the company [that markets insulin degludec: Novo Nordisk] to try to make it more affordable.”
Dr. Chow also highlighted that a new wrinkle has been introduction of a more concentrated formulation of insulin glargine, U300, which appears to cause less hypoglycemia than insulin glargine U100. Recent study results indicated that no significant difference exists in the incidence of hypoglycemia among patients treated with insulin glargine U300 and those treated with insulin degludec, such as findings from the BRIGHT trial, which included just over 900 patients, and in the CONCLUDE trial, which randomized more than 1,600 patients.
The HypoDeg study was sponsored by Novo Nordisk, the company that markets insulin degludec. Dr. Brøsen had no personal disclosures, but several of her coauthors were either Novo Nordisk employees or had financial relationships with the company. Dr. de Galan has received research funding from Novo Nordisk. Dr. Fadini has received lecture fees and research funding from Novo Nordisk, from Sanofi, the company that markets insulin glargine, and from several other companies. Dr. Chow has received research funding from Dexcom.
FROM ADA 2021
Diabetes plus frequent sleep disturbances tied to higher mortality
A single, simple question about sleep habits asked to people with diabetes in the UK Biobank database identified a subgroup with a nearly doubled mortality rate during almost 9 years of follow-up: those who said they usually had sleep disturbances.
The question was: Do you never, rarely, sometimes, or usually have trouble falling asleep, or waking in the middle of the night?
Adults in the UK Biobank with any form of self-reported diabetes or insulin use who answered that they usually have sleep disturbances had a significant 87% higher mortality rate than did those without diabetes who said they never or rarely had sleep disturbances, in a fully adjusted model with an average follow-up of 8.9 years, Kristen L. Knutson, PhD, and coauthors reported in the Journal of Sleep Research.
Mortality was 11% higher in respondents who reported frequent sleep disturbances but had no diabetes than in those without frequent sleep disturbances. Furthermore, those with diabetes but without frequent sleep disturbances had a 67% higher mortality rate, compared with those without diabetes. Both differences were statistically significant in a model that adjusted for age, sex, ethnicity, smoking, sleep duration, body mass index, and other covariates.
The findings suggest that diabetes and frequent sleep disturbances act in a roughly additive way to raise mortality risk, said Dr. Knutson, an epidemiologist and neurologist who specializes in sleep medicine at Northwestern University, Chicago.
She suggested that, based on these findings, clinicians should consider annually asking patients with diabetes this key question about the frequency of their sleep disturbances. They should then follow up with patients who report usual disturbances by referring them to a sleep clinic to test for a sleep disorders such as insomnia or sleep apnea. Sleep apnea especially is “particularly common in patients with type 2 diabetes,” Dr. Knutson noted in an interview.
A need to ‘spread awareness’ about diabetes and disturbed sleep.
The study run by Dr. Knutson and associates “is one of the largest population-based studies” to examine the relationship between sleep disturbances, diabetes, and mortality, commented Sirimon Reutrakul, MD, an endocrinologist and diabetes specialist at the University of Illinois Hospital in Chicago.
“This study highlights the detrimental effects of sleep disturbances in people with or without diabetes, and adds to the effects of sleep disturbances such as insomnia symptoms. People with diabetes often have sleep disturbances. Obstructive sleep apnea is very common in people with diabetes, and insomnia symptoms could be present in people with obstructive sleep apnea or it could be a separate problem,” Dr. Reutrakul said in an interview. Sleep disturbances can arise from direct effects of diabetes, such as nocturia, worry about glucose levels, pain, depressive symptoms, and anxiety, or can result from comorbidities that interfere with sleep.
“It is prudent to ask patients with diabetes about sleep patterns,” said Dr. Reutrakul, and she endorsed the specific question that Dr. Knutson recommended asking patients. Other aspects of sleep quality that could be helpful for a diagnosis include sleep duration, sleep timing, and snoring. “Some physicians ask these questions, but we need to spread awareness,” she added.
Prior to referring patients to a sleep clinic, Dr. Reutrakul suggested that clinicians could also assess possible triggers such as inadequate glucose control, pain, and anxiety, and they could also recommend good sleep hygiene strategies such as what’s recommended by the Sleep Foundation.
Sleep disturbances ‘highly prevalent’ among U.K. adults.
The UK Biobank enrolled just over 500,000 people aged 37-73 years during 2006-2010, and 487,728 of these people had data available that allowed their inclusion in the analysis. That group averaged about 57 years of age, 54% were women, 94% were White, and their average body mass index was 27-28 kg/m2.
More than a quarter of these people reported having “usual” sleep disturbances, showing that sleep disturbances are “highly prevalent” among U.K. residents, noted the authors. Just under a quarter of the subjects reported they never or rarely had sleep disturbances, and the remaining half of subjects said they “sometimes” had sleep disturbances.
In addition, 69% reported neither diabetes nor frequent sleep disturbances, 26% had frequent sleep disturbances but no diabetes, 3% had diabetes but not frequent sleep disturbances, and 2% had both diabetes and frequent sleep disturbances.
During the average 8.9-year follow-up, 19,177 people died from any cause (4%), and 3,874 of these deaths involved cardiovascular disease causes. Despite the significant association of diabetes and frequent sleep disturbances with an increased rate of all-cause mortality, the same combination showed no significant link with cardiovascular mortality in the study’s full-adjusted model. This may be because “frequent sleep disturbances can lead to a variety of causes of death,” Dr. Knutson suggested.
The information collected by the UK Biobank did not allow the researchers to distinguish between type 1 and type 2 diabetes.
The findings “suggest that regardless of the cause of sleep disturbance, reporting sleep disturbances on a frequent basis is an important signal of elevated risk of mortality. Such symptoms should therefore be investigated further by physicians, particularly in patients who have also been diagnosed with diabetes,” wrote Dr. Knutson and coauthors. “This is the first study to examine the effect of the combination of insomnia and diabetes on mortality risk.”
But Dr. Knutson highlighted that “sleep problems are important for everyone, not just people with diabetes.
Neither Dr. Knutson and coauthors nor Dr. Reutrakul had no disclosures.
A single, simple question about sleep habits asked to people with diabetes in the UK Biobank database identified a subgroup with a nearly doubled mortality rate during almost 9 years of follow-up: those who said they usually had sleep disturbances.
The question was: Do you never, rarely, sometimes, or usually have trouble falling asleep, or waking in the middle of the night?
Adults in the UK Biobank with any form of self-reported diabetes or insulin use who answered that they usually have sleep disturbances had a significant 87% higher mortality rate than did those without diabetes who said they never or rarely had sleep disturbances, in a fully adjusted model with an average follow-up of 8.9 years, Kristen L. Knutson, PhD, and coauthors reported in the Journal of Sleep Research.
Mortality was 11% higher in respondents who reported frequent sleep disturbances but had no diabetes than in those without frequent sleep disturbances. Furthermore, those with diabetes but without frequent sleep disturbances had a 67% higher mortality rate, compared with those without diabetes. Both differences were statistically significant in a model that adjusted for age, sex, ethnicity, smoking, sleep duration, body mass index, and other covariates.
The findings suggest that diabetes and frequent sleep disturbances act in a roughly additive way to raise mortality risk, said Dr. Knutson, an epidemiologist and neurologist who specializes in sleep medicine at Northwestern University, Chicago.
She suggested that, based on these findings, clinicians should consider annually asking patients with diabetes this key question about the frequency of their sleep disturbances. They should then follow up with patients who report usual disturbances by referring them to a sleep clinic to test for a sleep disorders such as insomnia or sleep apnea. Sleep apnea especially is “particularly common in patients with type 2 diabetes,” Dr. Knutson noted in an interview.
A need to ‘spread awareness’ about diabetes and disturbed sleep.
The study run by Dr. Knutson and associates “is one of the largest population-based studies” to examine the relationship between sleep disturbances, diabetes, and mortality, commented Sirimon Reutrakul, MD, an endocrinologist and diabetes specialist at the University of Illinois Hospital in Chicago.
“This study highlights the detrimental effects of sleep disturbances in people with or without diabetes, and adds to the effects of sleep disturbances such as insomnia symptoms. People with diabetes often have sleep disturbances. Obstructive sleep apnea is very common in people with diabetes, and insomnia symptoms could be present in people with obstructive sleep apnea or it could be a separate problem,” Dr. Reutrakul said in an interview. Sleep disturbances can arise from direct effects of diabetes, such as nocturia, worry about glucose levels, pain, depressive symptoms, and anxiety, or can result from comorbidities that interfere with sleep.
“It is prudent to ask patients with diabetes about sleep patterns,” said Dr. Reutrakul, and she endorsed the specific question that Dr. Knutson recommended asking patients. Other aspects of sleep quality that could be helpful for a diagnosis include sleep duration, sleep timing, and snoring. “Some physicians ask these questions, but we need to spread awareness,” she added.
Prior to referring patients to a sleep clinic, Dr. Reutrakul suggested that clinicians could also assess possible triggers such as inadequate glucose control, pain, and anxiety, and they could also recommend good sleep hygiene strategies such as what’s recommended by the Sleep Foundation.
Sleep disturbances ‘highly prevalent’ among U.K. adults.
The UK Biobank enrolled just over 500,000 people aged 37-73 years during 2006-2010, and 487,728 of these people had data available that allowed their inclusion in the analysis. That group averaged about 57 years of age, 54% were women, 94% were White, and their average body mass index was 27-28 kg/m2.
More than a quarter of these people reported having “usual” sleep disturbances, showing that sleep disturbances are “highly prevalent” among U.K. residents, noted the authors. Just under a quarter of the subjects reported they never or rarely had sleep disturbances, and the remaining half of subjects said they “sometimes” had sleep disturbances.
In addition, 69% reported neither diabetes nor frequent sleep disturbances, 26% had frequent sleep disturbances but no diabetes, 3% had diabetes but not frequent sleep disturbances, and 2% had both diabetes and frequent sleep disturbances.
During the average 8.9-year follow-up, 19,177 people died from any cause (4%), and 3,874 of these deaths involved cardiovascular disease causes. Despite the significant association of diabetes and frequent sleep disturbances with an increased rate of all-cause mortality, the same combination showed no significant link with cardiovascular mortality in the study’s full-adjusted model. This may be because “frequent sleep disturbances can lead to a variety of causes of death,” Dr. Knutson suggested.
The information collected by the UK Biobank did not allow the researchers to distinguish between type 1 and type 2 diabetes.
The findings “suggest that regardless of the cause of sleep disturbance, reporting sleep disturbances on a frequent basis is an important signal of elevated risk of mortality. Such symptoms should therefore be investigated further by physicians, particularly in patients who have also been diagnosed with diabetes,” wrote Dr. Knutson and coauthors. “This is the first study to examine the effect of the combination of insomnia and diabetes on mortality risk.”
But Dr. Knutson highlighted that “sleep problems are important for everyone, not just people with diabetes.
Neither Dr. Knutson and coauthors nor Dr. Reutrakul had no disclosures.
A single, simple question about sleep habits asked to people with diabetes in the UK Biobank database identified a subgroup with a nearly doubled mortality rate during almost 9 years of follow-up: those who said they usually had sleep disturbances.
The question was: Do you never, rarely, sometimes, or usually have trouble falling asleep, or waking in the middle of the night?
Adults in the UK Biobank with any form of self-reported diabetes or insulin use who answered that they usually have sleep disturbances had a significant 87% higher mortality rate than did those without diabetes who said they never or rarely had sleep disturbances, in a fully adjusted model with an average follow-up of 8.9 years, Kristen L. Knutson, PhD, and coauthors reported in the Journal of Sleep Research.
Mortality was 11% higher in respondents who reported frequent sleep disturbances but had no diabetes than in those without frequent sleep disturbances. Furthermore, those with diabetes but without frequent sleep disturbances had a 67% higher mortality rate, compared with those without diabetes. Both differences were statistically significant in a model that adjusted for age, sex, ethnicity, smoking, sleep duration, body mass index, and other covariates.
The findings suggest that diabetes and frequent sleep disturbances act in a roughly additive way to raise mortality risk, said Dr. Knutson, an epidemiologist and neurologist who specializes in sleep medicine at Northwestern University, Chicago.
She suggested that, based on these findings, clinicians should consider annually asking patients with diabetes this key question about the frequency of their sleep disturbances. They should then follow up with patients who report usual disturbances by referring them to a sleep clinic to test for a sleep disorders such as insomnia or sleep apnea. Sleep apnea especially is “particularly common in patients with type 2 diabetes,” Dr. Knutson noted in an interview.
A need to ‘spread awareness’ about diabetes and disturbed sleep.
The study run by Dr. Knutson and associates “is one of the largest population-based studies” to examine the relationship between sleep disturbances, diabetes, and mortality, commented Sirimon Reutrakul, MD, an endocrinologist and diabetes specialist at the University of Illinois Hospital in Chicago.
“This study highlights the detrimental effects of sleep disturbances in people with or without diabetes, and adds to the effects of sleep disturbances such as insomnia symptoms. People with diabetes often have sleep disturbances. Obstructive sleep apnea is very common in people with diabetes, and insomnia symptoms could be present in people with obstructive sleep apnea or it could be a separate problem,” Dr. Reutrakul said in an interview. Sleep disturbances can arise from direct effects of diabetes, such as nocturia, worry about glucose levels, pain, depressive symptoms, and anxiety, or can result from comorbidities that interfere with sleep.
“It is prudent to ask patients with diabetes about sleep patterns,” said Dr. Reutrakul, and she endorsed the specific question that Dr. Knutson recommended asking patients. Other aspects of sleep quality that could be helpful for a diagnosis include sleep duration, sleep timing, and snoring. “Some physicians ask these questions, but we need to spread awareness,” she added.
Prior to referring patients to a sleep clinic, Dr. Reutrakul suggested that clinicians could also assess possible triggers such as inadequate glucose control, pain, and anxiety, and they could also recommend good sleep hygiene strategies such as what’s recommended by the Sleep Foundation.
Sleep disturbances ‘highly prevalent’ among U.K. adults.
The UK Biobank enrolled just over 500,000 people aged 37-73 years during 2006-2010, and 487,728 of these people had data available that allowed their inclusion in the analysis. That group averaged about 57 years of age, 54% were women, 94% were White, and their average body mass index was 27-28 kg/m2.
More than a quarter of these people reported having “usual” sleep disturbances, showing that sleep disturbances are “highly prevalent” among U.K. residents, noted the authors. Just under a quarter of the subjects reported they never or rarely had sleep disturbances, and the remaining half of subjects said they “sometimes” had sleep disturbances.
In addition, 69% reported neither diabetes nor frequent sleep disturbances, 26% had frequent sleep disturbances but no diabetes, 3% had diabetes but not frequent sleep disturbances, and 2% had both diabetes and frequent sleep disturbances.
During the average 8.9-year follow-up, 19,177 people died from any cause (4%), and 3,874 of these deaths involved cardiovascular disease causes. Despite the significant association of diabetes and frequent sleep disturbances with an increased rate of all-cause mortality, the same combination showed no significant link with cardiovascular mortality in the study’s full-adjusted model. This may be because “frequent sleep disturbances can lead to a variety of causes of death,” Dr. Knutson suggested.
The information collected by the UK Biobank did not allow the researchers to distinguish between type 1 and type 2 diabetes.
The findings “suggest that regardless of the cause of sleep disturbance, reporting sleep disturbances on a frequent basis is an important signal of elevated risk of mortality. Such symptoms should therefore be investigated further by physicians, particularly in patients who have also been diagnosed with diabetes,” wrote Dr. Knutson and coauthors. “This is the first study to examine the effect of the combination of insomnia and diabetes on mortality risk.”
But Dr. Knutson highlighted that “sleep problems are important for everyone, not just people with diabetes.
Neither Dr. Knutson and coauthors nor Dr. Reutrakul had no disclosures.
FROM THE JOURNAL OF SLEEP RESEARCH
Omnipod 5 ‘artificial pancreas’ shows benefit in type 1 diabetes
Insulet’s investigational Omnipod 5 automated insulin delivery system improves glycemic control in people with type 1 diabetes aged as young as 2 years, new data suggest.
The Omnipod 5 system combines a tubing-free insulin-filled delivery “Pod” with the Dexcom G6 continuous glucose monitor and an algorithm built into the Pod connecting the two devices via a smartphone app to semiautomate insulin delivery. It is currently under review by the Food and Drug Administration. The company expects to launch it in limited release during the second half of 2021.
Results from a pivotal trial of the system in children aged 2-5.9 years with type 1 diabetes were presented during the annual scientific sessions of the American Diabetes Association.
Follow-up data at 6 months were also presented for another pivotal study of 112 children aged 6-13.9 years and 129 adults aged 14-70 years. Those primary 3-month data were reported earlier this year at the Endocrine Society’s annual meeting and subsequently published online June 7, 2021, in Diabetes Care. Another study presented at ADA looked at quality of life in children using Omnipod 5 and their caregivers.
If approved by the FDA, the Omnipod 5 would be the third commercially available automated insulin delivery system – also called hybrid closed-loop or artificial pancreas systems – in the United States. It would be the second approved for children as young as 2 years of age and the first to deliver insulin subcutaneously without tubing.
‘No-tubing’ feature will be a draw for parents of young children
Asked to comment, pediatric endocrinologist Laura M. Jacobsen, MD, of the University of Florida, Gainesville, said in an interview: “I think the big advantage for the Omnipod 5 is that [if approved it will be] the only tubeless automated insulin delivery system in the U.S.”
“The automated delivery systems have just been wonderful for helping patients achieve time in range, especially overnight. And the fact that this goes down to such a young age where that can be very difficult is wonderful.”
Another difference between the Omnipod 5 and other systems is the ability to adjust glucose targets (from 110 to 150 mg/dL), although newer versions of the currently available hybrid closed-loop systems are expected to include that feature as well. “They’re all slightly different in the way the algorithms work, but I think the end result is similar,” Dr. Jacobsen said.
But, she said, the no-tubing feature might be particularly helpful for some very active young kids. “A lot of small kids do use the tubed pumps, and you can make it work with a lot of kids, but with some kids it just won’t ... the tubing gets caught. I think this really helps parents make the step. A lot of them don’t want to try the tubing whereas they see the Omnipod and might feel a little more confidence to try a pump.”
Overall, said Dr. Jacobsen, who has no financial disclosures with Insulet, Dexcom, or any of their competitors, “I think any addition to the technology field to improve quality of life for people with type 1 diabetes is important and people need choices.”
Pivotal data show benefit in ‘difficult-to-manage’ preschool children
Pivotal 3-month data for the Omnipod 5 in children aged 2-5.9 years with type 1 diabetes were presented on June 26 by pediatric endocrinologist Jennifer Sherr, MD, PhD, Yale University, New Haven, Conn.
“As a pediatric endocrinologist, I can attest to the difficulty of managing this age group, due to grazing eating patterns and erratic physical activity. Oftentimes, care providers may fear hypoglycemia as these youth can not verbalize or self-treat lows,” she remarked.
A total of 80 children were enrolled at 10 institutions across the United Sates. There was a single 14-day standard therapy phase (baseline), followed by 3 months of automated insulin delivery during which the children’s eating and exercise were unrestricted.
At 3 months, average hemoglobin A1c had fallen from 7.4% at baseline to 6.9%, a significant difference (P < .05). The proportions achieving the target A1c of less than 7% were 54% at 3 months versus 31% at baseline. The reduction was even greater among the 25 with baseline A1c of 8% or greater, although it was significant even among the 55 who started with a lower A1c (–1.06 vs. –0.31 percentage points; both P < .05).
Time in range rose from 57.2% at baseline to 68.1% at 3 months (P < .05).
“These youngsters are spending an average of 2.6 more hours/day in range,” Dr. Sherr commented, noting that the difference became apparent shortly after study start and was maintained during the 3 months.
Dr. Sherr noted that this 10.9% improvement in time in range with Omnipod 5 was similar to improvements in the previously reported pivotal study of older children and adults. Data from that study showed improvement in time in range from a gain of 15.6% for the 6 to 13.9 year olds to 8.0% for those aged 26-49 years. Interestingly, improvements in time in range were seen even in the oldest group, aged 50-70, who increased from an already high baseline of 69.9% to 79.1% with Omnipod 5 after 3 months.
In her current study, in the youngest age group, the improvement in time in range was achieved primarily by a reduction of time above range, from 2.4 fewer hours/day above 180 mg/dL, while time below 70 mg/dL was reduced by 4 minutes/day. Overnight time in range improved by 1.4 hours/night, with most of the improvements in reduction of hyperglycemia.
The proportions meeting the combined goals of less than 4% time below range and greater than 60% time in range rose from 29% to 65%.
There were no episodes of severe hypoglycemia or diabetic ketoacidosis during the 3-month study phase.
Another important related metric, sleep quality for parents/caregivers, also improved. The percentage reporting overall sleep quality of “very good” or “fairly good” increased from 65% at baseline to 90% with Omnipod 5, while “very bad” sleep quality fell from 8.8% to 0%.
All 80 patients completed the study and elected to continue in a 12-month extension phase.
Ongoing benefit seen in older children and adults
In a late-breaking poster presented on June 25, Anders L. Carlson, MD, medical director at the International Diabetes Center at Park Nicollet, Minneapolis, presented more follow-up data to the previously reported 3-month pivotal study, including 108 older children and 109 adults from the original study.
A1c remained lower after 6 months than at baseline for both children and adults (P < .001). In the children, A1c levels weren’t significantly different at the end of 6 versus 3 months, while in the adults there was an additional 0.1 percentage point decrease (P < .01).
There was one episode of diabetic ketoacidosis and no severe hypoglycemic episodes in the 3-month extension. “Sustained reduction of A1c indicates the potential long-term benefit of the Omnipod 5 System,” Dr. Carlson and colleagues concluded.
Reduced diabetes distress, don’t forget parents’ quality of life
Meanwhile, psychologist Korey K. Hood, PhD, of Stanford (Calif.) University, presented quality of life data at the meeting for 83 children aged 6-11.9 years and 42 teens aged 12-17.9 years using the Omnipod 5 from the larger study population and their parents.
Significant improvements were seen for both the youth and their caregivers in the Problem Areas in Diabetes score, a measure of diabetes-related emotional distress. Changes were less dramatic on the Hypoglycemic Confidence Scale, although improvements were significant for the caregivers of the younger children.
“We know this is a group that is really worried about hypoglycemia across a lot of situations, not just sleep but also school and outside of the home. So, to increase their confidence to this extent I think is a pretty important finding,” Dr. Hood commented.
There were nonsignificant trends in improvement across groups on the Pittsburgh Sleep Quality Index, but overall sleep quality did significantly improve among parents of the younger children. And on the World Health Organization–5 quality of life survey, significant improvements again were seen among the caregivers of young children.
“Reduced diabetes distress and improved quality of life are key benefits of using the Omnipod 5 [automated insulin delivery] system that are complementary to the glycemic benefits achieved,” Dr. Hood said.
Dr. Jacobsen has reported no relevant financial relationships. Dr. Sherr has reported being an adviser for, consultant for, and/or grant recipient from Bigfoot Biomedical, Cecelia Health, Insulet, Medtronic Diabetes, Eli Lilly, Lexicon, Sanofi, and the National Institute of Diabetes and Digestive and Kidney Diseases. Dr. Hood has reported being a consultant for Cecelia Health, Havas, and Cercacor.
A version of this article first appeared on Medscape.com.
Insulet’s investigational Omnipod 5 automated insulin delivery system improves glycemic control in people with type 1 diabetes aged as young as 2 years, new data suggest.
The Omnipod 5 system combines a tubing-free insulin-filled delivery “Pod” with the Dexcom G6 continuous glucose monitor and an algorithm built into the Pod connecting the two devices via a smartphone app to semiautomate insulin delivery. It is currently under review by the Food and Drug Administration. The company expects to launch it in limited release during the second half of 2021.
Results from a pivotal trial of the system in children aged 2-5.9 years with type 1 diabetes were presented during the annual scientific sessions of the American Diabetes Association.
Follow-up data at 6 months were also presented for another pivotal study of 112 children aged 6-13.9 years and 129 adults aged 14-70 years. Those primary 3-month data were reported earlier this year at the Endocrine Society’s annual meeting and subsequently published online June 7, 2021, in Diabetes Care. Another study presented at ADA looked at quality of life in children using Omnipod 5 and their caregivers.
If approved by the FDA, the Omnipod 5 would be the third commercially available automated insulin delivery system – also called hybrid closed-loop or artificial pancreas systems – in the United States. It would be the second approved for children as young as 2 years of age and the first to deliver insulin subcutaneously without tubing.
‘No-tubing’ feature will be a draw for parents of young children
Asked to comment, pediatric endocrinologist Laura M. Jacobsen, MD, of the University of Florida, Gainesville, said in an interview: “I think the big advantage for the Omnipod 5 is that [if approved it will be] the only tubeless automated insulin delivery system in the U.S.”
“The automated delivery systems have just been wonderful for helping patients achieve time in range, especially overnight. And the fact that this goes down to such a young age where that can be very difficult is wonderful.”
Another difference between the Omnipod 5 and other systems is the ability to adjust glucose targets (from 110 to 150 mg/dL), although newer versions of the currently available hybrid closed-loop systems are expected to include that feature as well. “They’re all slightly different in the way the algorithms work, but I think the end result is similar,” Dr. Jacobsen said.
But, she said, the no-tubing feature might be particularly helpful for some very active young kids. “A lot of small kids do use the tubed pumps, and you can make it work with a lot of kids, but with some kids it just won’t ... the tubing gets caught. I think this really helps parents make the step. A lot of them don’t want to try the tubing whereas they see the Omnipod and might feel a little more confidence to try a pump.”
Overall, said Dr. Jacobsen, who has no financial disclosures with Insulet, Dexcom, or any of their competitors, “I think any addition to the technology field to improve quality of life for people with type 1 diabetes is important and people need choices.”
Pivotal data show benefit in ‘difficult-to-manage’ preschool children
Pivotal 3-month data for the Omnipod 5 in children aged 2-5.9 years with type 1 diabetes were presented on June 26 by pediatric endocrinologist Jennifer Sherr, MD, PhD, Yale University, New Haven, Conn.
“As a pediatric endocrinologist, I can attest to the difficulty of managing this age group, due to grazing eating patterns and erratic physical activity. Oftentimes, care providers may fear hypoglycemia as these youth can not verbalize or self-treat lows,” she remarked.
A total of 80 children were enrolled at 10 institutions across the United Sates. There was a single 14-day standard therapy phase (baseline), followed by 3 months of automated insulin delivery during which the children’s eating and exercise were unrestricted.
At 3 months, average hemoglobin A1c had fallen from 7.4% at baseline to 6.9%, a significant difference (P < .05). The proportions achieving the target A1c of less than 7% were 54% at 3 months versus 31% at baseline. The reduction was even greater among the 25 with baseline A1c of 8% or greater, although it was significant even among the 55 who started with a lower A1c (–1.06 vs. –0.31 percentage points; both P < .05).
Time in range rose from 57.2% at baseline to 68.1% at 3 months (P < .05).
“These youngsters are spending an average of 2.6 more hours/day in range,” Dr. Sherr commented, noting that the difference became apparent shortly after study start and was maintained during the 3 months.
Dr. Sherr noted that this 10.9% improvement in time in range with Omnipod 5 was similar to improvements in the previously reported pivotal study of older children and adults. Data from that study showed improvement in time in range from a gain of 15.6% for the 6 to 13.9 year olds to 8.0% for those aged 26-49 years. Interestingly, improvements in time in range were seen even in the oldest group, aged 50-70, who increased from an already high baseline of 69.9% to 79.1% with Omnipod 5 after 3 months.
In her current study, in the youngest age group, the improvement in time in range was achieved primarily by a reduction of time above range, from 2.4 fewer hours/day above 180 mg/dL, while time below 70 mg/dL was reduced by 4 minutes/day. Overnight time in range improved by 1.4 hours/night, with most of the improvements in reduction of hyperglycemia.
The proportions meeting the combined goals of less than 4% time below range and greater than 60% time in range rose from 29% to 65%.
There were no episodes of severe hypoglycemia or diabetic ketoacidosis during the 3-month study phase.
Another important related metric, sleep quality for parents/caregivers, also improved. The percentage reporting overall sleep quality of “very good” or “fairly good” increased from 65% at baseline to 90% with Omnipod 5, while “very bad” sleep quality fell from 8.8% to 0%.
All 80 patients completed the study and elected to continue in a 12-month extension phase.
Ongoing benefit seen in older children and adults
In a late-breaking poster presented on June 25, Anders L. Carlson, MD, medical director at the International Diabetes Center at Park Nicollet, Minneapolis, presented more follow-up data to the previously reported 3-month pivotal study, including 108 older children and 109 adults from the original study.
A1c remained lower after 6 months than at baseline for both children and adults (P < .001). In the children, A1c levels weren’t significantly different at the end of 6 versus 3 months, while in the adults there was an additional 0.1 percentage point decrease (P < .01).
There was one episode of diabetic ketoacidosis and no severe hypoglycemic episodes in the 3-month extension. “Sustained reduction of A1c indicates the potential long-term benefit of the Omnipod 5 System,” Dr. Carlson and colleagues concluded.
Reduced diabetes distress, don’t forget parents’ quality of life
Meanwhile, psychologist Korey K. Hood, PhD, of Stanford (Calif.) University, presented quality of life data at the meeting for 83 children aged 6-11.9 years and 42 teens aged 12-17.9 years using the Omnipod 5 from the larger study population and their parents.
Significant improvements were seen for both the youth and their caregivers in the Problem Areas in Diabetes score, a measure of diabetes-related emotional distress. Changes were less dramatic on the Hypoglycemic Confidence Scale, although improvements were significant for the caregivers of the younger children.
“We know this is a group that is really worried about hypoglycemia across a lot of situations, not just sleep but also school and outside of the home. So, to increase their confidence to this extent I think is a pretty important finding,” Dr. Hood commented.
There were nonsignificant trends in improvement across groups on the Pittsburgh Sleep Quality Index, but overall sleep quality did significantly improve among parents of the younger children. And on the World Health Organization–5 quality of life survey, significant improvements again were seen among the caregivers of young children.
“Reduced diabetes distress and improved quality of life are key benefits of using the Omnipod 5 [automated insulin delivery] system that are complementary to the glycemic benefits achieved,” Dr. Hood said.
Dr. Jacobsen has reported no relevant financial relationships. Dr. Sherr has reported being an adviser for, consultant for, and/or grant recipient from Bigfoot Biomedical, Cecelia Health, Insulet, Medtronic Diabetes, Eli Lilly, Lexicon, Sanofi, and the National Institute of Diabetes and Digestive and Kidney Diseases. Dr. Hood has reported being a consultant for Cecelia Health, Havas, and Cercacor.
A version of this article first appeared on Medscape.com.
Insulet’s investigational Omnipod 5 automated insulin delivery system improves glycemic control in people with type 1 diabetes aged as young as 2 years, new data suggest.
The Omnipod 5 system combines a tubing-free insulin-filled delivery “Pod” with the Dexcom G6 continuous glucose monitor and an algorithm built into the Pod connecting the two devices via a smartphone app to semiautomate insulin delivery. It is currently under review by the Food and Drug Administration. The company expects to launch it in limited release during the second half of 2021.
Results from a pivotal trial of the system in children aged 2-5.9 years with type 1 diabetes were presented during the annual scientific sessions of the American Diabetes Association.
Follow-up data at 6 months were also presented for another pivotal study of 112 children aged 6-13.9 years and 129 adults aged 14-70 years. Those primary 3-month data were reported earlier this year at the Endocrine Society’s annual meeting and subsequently published online June 7, 2021, in Diabetes Care. Another study presented at ADA looked at quality of life in children using Omnipod 5 and their caregivers.
If approved by the FDA, the Omnipod 5 would be the third commercially available automated insulin delivery system – also called hybrid closed-loop or artificial pancreas systems – in the United States. It would be the second approved for children as young as 2 years of age and the first to deliver insulin subcutaneously without tubing.
‘No-tubing’ feature will be a draw for parents of young children
Asked to comment, pediatric endocrinologist Laura M. Jacobsen, MD, of the University of Florida, Gainesville, said in an interview: “I think the big advantage for the Omnipod 5 is that [if approved it will be] the only tubeless automated insulin delivery system in the U.S.”
“The automated delivery systems have just been wonderful for helping patients achieve time in range, especially overnight. And the fact that this goes down to such a young age where that can be very difficult is wonderful.”
Another difference between the Omnipod 5 and other systems is the ability to adjust glucose targets (from 110 to 150 mg/dL), although newer versions of the currently available hybrid closed-loop systems are expected to include that feature as well. “They’re all slightly different in the way the algorithms work, but I think the end result is similar,” Dr. Jacobsen said.
But, she said, the no-tubing feature might be particularly helpful for some very active young kids. “A lot of small kids do use the tubed pumps, and you can make it work with a lot of kids, but with some kids it just won’t ... the tubing gets caught. I think this really helps parents make the step. A lot of them don’t want to try the tubing whereas they see the Omnipod and might feel a little more confidence to try a pump.”
Overall, said Dr. Jacobsen, who has no financial disclosures with Insulet, Dexcom, or any of their competitors, “I think any addition to the technology field to improve quality of life for people with type 1 diabetes is important and people need choices.”
Pivotal data show benefit in ‘difficult-to-manage’ preschool children
Pivotal 3-month data for the Omnipod 5 in children aged 2-5.9 years with type 1 diabetes were presented on June 26 by pediatric endocrinologist Jennifer Sherr, MD, PhD, Yale University, New Haven, Conn.
“As a pediatric endocrinologist, I can attest to the difficulty of managing this age group, due to grazing eating patterns and erratic physical activity. Oftentimes, care providers may fear hypoglycemia as these youth can not verbalize or self-treat lows,” she remarked.
A total of 80 children were enrolled at 10 institutions across the United Sates. There was a single 14-day standard therapy phase (baseline), followed by 3 months of automated insulin delivery during which the children’s eating and exercise were unrestricted.
At 3 months, average hemoglobin A1c had fallen from 7.4% at baseline to 6.9%, a significant difference (P < .05). The proportions achieving the target A1c of less than 7% were 54% at 3 months versus 31% at baseline. The reduction was even greater among the 25 with baseline A1c of 8% or greater, although it was significant even among the 55 who started with a lower A1c (–1.06 vs. –0.31 percentage points; both P < .05).
Time in range rose from 57.2% at baseline to 68.1% at 3 months (P < .05).
“These youngsters are spending an average of 2.6 more hours/day in range,” Dr. Sherr commented, noting that the difference became apparent shortly after study start and was maintained during the 3 months.
Dr. Sherr noted that this 10.9% improvement in time in range with Omnipod 5 was similar to improvements in the previously reported pivotal study of older children and adults. Data from that study showed improvement in time in range from a gain of 15.6% for the 6 to 13.9 year olds to 8.0% for those aged 26-49 years. Interestingly, improvements in time in range were seen even in the oldest group, aged 50-70, who increased from an already high baseline of 69.9% to 79.1% with Omnipod 5 after 3 months.
In her current study, in the youngest age group, the improvement in time in range was achieved primarily by a reduction of time above range, from 2.4 fewer hours/day above 180 mg/dL, while time below 70 mg/dL was reduced by 4 minutes/day. Overnight time in range improved by 1.4 hours/night, with most of the improvements in reduction of hyperglycemia.
The proportions meeting the combined goals of less than 4% time below range and greater than 60% time in range rose from 29% to 65%.
There were no episodes of severe hypoglycemia or diabetic ketoacidosis during the 3-month study phase.
Another important related metric, sleep quality for parents/caregivers, also improved. The percentage reporting overall sleep quality of “very good” or “fairly good” increased from 65% at baseline to 90% with Omnipod 5, while “very bad” sleep quality fell from 8.8% to 0%.
All 80 patients completed the study and elected to continue in a 12-month extension phase.
Ongoing benefit seen in older children and adults
In a late-breaking poster presented on June 25, Anders L. Carlson, MD, medical director at the International Diabetes Center at Park Nicollet, Minneapolis, presented more follow-up data to the previously reported 3-month pivotal study, including 108 older children and 109 adults from the original study.
A1c remained lower after 6 months than at baseline for both children and adults (P < .001). In the children, A1c levels weren’t significantly different at the end of 6 versus 3 months, while in the adults there was an additional 0.1 percentage point decrease (P < .01).
There was one episode of diabetic ketoacidosis and no severe hypoglycemic episodes in the 3-month extension. “Sustained reduction of A1c indicates the potential long-term benefit of the Omnipod 5 System,” Dr. Carlson and colleagues concluded.
Reduced diabetes distress, don’t forget parents’ quality of life
Meanwhile, psychologist Korey K. Hood, PhD, of Stanford (Calif.) University, presented quality of life data at the meeting for 83 children aged 6-11.9 years and 42 teens aged 12-17.9 years using the Omnipod 5 from the larger study population and their parents.
Significant improvements were seen for both the youth and their caregivers in the Problem Areas in Diabetes score, a measure of diabetes-related emotional distress. Changes were less dramatic on the Hypoglycemic Confidence Scale, although improvements were significant for the caregivers of the younger children.
“We know this is a group that is really worried about hypoglycemia across a lot of situations, not just sleep but also school and outside of the home. So, to increase their confidence to this extent I think is a pretty important finding,” Dr. Hood commented.
There were nonsignificant trends in improvement across groups on the Pittsburgh Sleep Quality Index, but overall sleep quality did significantly improve among parents of the younger children. And on the World Health Organization–5 quality of life survey, significant improvements again were seen among the caregivers of young children.
“Reduced diabetes distress and improved quality of life are key benefits of using the Omnipod 5 [automated insulin delivery] system that are complementary to the glycemic benefits achieved,” Dr. Hood said.
Dr. Jacobsen has reported no relevant financial relationships. Dr. Sherr has reported being an adviser for, consultant for, and/or grant recipient from Bigfoot Biomedical, Cecelia Health, Insulet, Medtronic Diabetes, Eli Lilly, Lexicon, Sanofi, and the National Institute of Diabetes and Digestive and Kidney Diseases. Dr. Hood has reported being a consultant for Cecelia Health, Havas, and Cercacor.
A version of this article first appeared on Medscape.com.
Intervention opens access to care for minority youths with type 1 diabetes
For racial or ethnic minority youths with type 1 diabetes, participating in an interventional program improves access to care, new research shows.
Youth categorized as Black, Indigenous, and other people of color (BIPOC) had significantly improved outpatient attendance during and after participating in Novel Interventions in Children’s Healthcare (NICH), a systems intervention for children with chronic health conditions and their families.
By comparison, no improvements in care access were observed among BIPOC children who were not able to access the program because of insurance or other reasons, David V. Wagner, PhD, Associate Professor and NICH research director at Oregon Health & Science University, Portland, reported at the annual scientific sessions of the American Diabetes Association.
The findings demonstrate a need for intensive, home-based services that aim to correct health inequities, said Dr. Wagner, who presented the findings along with Winniebhelle Cadiz, a scholar in the BUILD EXITO undergraduate research training program at Portland (Ore.) State University.
The NICH program hinges on trained interventionists who visit families at home, attend clinic visits, and work with schools and other contacts to help solve problems that keep children from following medical instructions, according to a program description.
“Families report having somebody by their side to help them navigate the system, address the transportation difficulties experienced, and help them and build that relationship with their health care provider seems to be hugely influential in terms of helping them navigate and access care,” Dr. Wagner said in a presentation of the study.
A NICH for youths with chronic health conditions
The NICH program differs from some other programs that have been developed in an attempt to improve health outcomes among youths in the community, according to Dr. Wagner.
“Many of the programs that exist out there are often piloted on, and seemingly built for, those who have more resources,” he said in his presentation. “Those who are in greatest need often have difficulty accessing and responding to the services.”
NICH doesn’t take the place of existing services, but is “an addition to the continuum of care” for youths and families who are struggling because of lack of resources or marginalization in the health care system, Dr. Wagner said.
While NICH is not specific to any one chronic health condition, several previous investigations have specifically looked at the impact of the NICH program on access to care in youths with type 1 diabetes.
Youths participating in the program for a year had fewer ED visits, including fewer visits with diabetic ketoacidosis (DKA), as well as fewer and shorter admissions as compared with the year prior to participating in the program, Dr. Wagner said.
In another study, youths had fewer admissions for diabetes or DKA and less frequent pediatric ICU contact during the NICH program, as compared with before the program.
Another study showed that, while NICH had no impact overall on access to care among youths with type 1 diabetes, BIPOC youths had an improvement in the mean number of outpatient visits as compared with preprogram levels. However, because none of those studies included a control group, Dr. Wagner said, it remained unclear whether this systems intervention might improve outpatient access among youths with type 1 diabetes as compared with those who did not participate.
Intervention linked to increased BIPOC care access
The latest study includes 144 youths with type 1 diabetes referred for the program. The mean age was 13.7 years, 58% were female, and 81% were non-Hispanic White. While 51 youths were able to participate in NICH, the remaining 93 were not served by the program because of insurance denial or nonresponse, according to investigators.
While participation in the program made no difference in access to care overall, results of this study suggest NICH reduced access disparities among BIPOC youths, the investigators said.
Those BIPOC youth, 28 in total, had significantly worse access to care prior to referral. However, BIPOC youth participation in NICH was associated with improved attendance at endocrinology appointments and outpatient attendance overall.
A mean change of 1.9 more appointments per year was seen among BIPOC youth who participated in NICH, compared with a mean decrease of 0.5 appointments per year among BIPOC youth not served by the program (P = .03), according to the study abstract.
Prior to NICH participation, outpatient attendance among BIPOC youths was about 2.5 visits per year, data presented by the investigators show.
Systemic changes needed
This study is representative of systemic changes that are needed to improve access to quality care for BIPOC youth, according Cynthia E. Muñoz, PhD, MPH, ADA’s president of health care and education.
“We know that there are increased risks for poor health outcomes for these children and youths, and we know that there is a risk for mental health and psychosocial challenges for youth from these communities,” said Dr. Muñoz, a bilingual licensed psychologist and assistant professor of clinical pediatrics at the University of Southern California, Los Angeles.
In his presentation, Dr. Wagner said lumping racial and ethnic minority participants under a single BIPOC header probably wasn’t ideal because of the diversity and differences among racial and ethnic minorities. However, it was necessary in this particular study because of limited sample size.
Dr. Wagner and coauthors disclosed no conflicts of interest related to the research, which was supported by the Leona M. and Harry B. Helmsley Charitable Trust.
For racial or ethnic minority youths with type 1 diabetes, participating in an interventional program improves access to care, new research shows.
Youth categorized as Black, Indigenous, and other people of color (BIPOC) had significantly improved outpatient attendance during and after participating in Novel Interventions in Children’s Healthcare (NICH), a systems intervention for children with chronic health conditions and their families.
By comparison, no improvements in care access were observed among BIPOC children who were not able to access the program because of insurance or other reasons, David V. Wagner, PhD, Associate Professor and NICH research director at Oregon Health & Science University, Portland, reported at the annual scientific sessions of the American Diabetes Association.
The findings demonstrate a need for intensive, home-based services that aim to correct health inequities, said Dr. Wagner, who presented the findings along with Winniebhelle Cadiz, a scholar in the BUILD EXITO undergraduate research training program at Portland (Ore.) State University.
The NICH program hinges on trained interventionists who visit families at home, attend clinic visits, and work with schools and other contacts to help solve problems that keep children from following medical instructions, according to a program description.
“Families report having somebody by their side to help them navigate the system, address the transportation difficulties experienced, and help them and build that relationship with their health care provider seems to be hugely influential in terms of helping them navigate and access care,” Dr. Wagner said in a presentation of the study.
A NICH for youths with chronic health conditions
The NICH program differs from some other programs that have been developed in an attempt to improve health outcomes among youths in the community, according to Dr. Wagner.
“Many of the programs that exist out there are often piloted on, and seemingly built for, those who have more resources,” he said in his presentation. “Those who are in greatest need often have difficulty accessing and responding to the services.”
NICH doesn’t take the place of existing services, but is “an addition to the continuum of care” for youths and families who are struggling because of lack of resources or marginalization in the health care system, Dr. Wagner said.
While NICH is not specific to any one chronic health condition, several previous investigations have specifically looked at the impact of the NICH program on access to care in youths with type 1 diabetes.
Youths participating in the program for a year had fewer ED visits, including fewer visits with diabetic ketoacidosis (DKA), as well as fewer and shorter admissions as compared with the year prior to participating in the program, Dr. Wagner said.
In another study, youths had fewer admissions for diabetes or DKA and less frequent pediatric ICU contact during the NICH program, as compared with before the program.
Another study showed that, while NICH had no impact overall on access to care among youths with type 1 diabetes, BIPOC youths had an improvement in the mean number of outpatient visits as compared with preprogram levels. However, because none of those studies included a control group, Dr. Wagner said, it remained unclear whether this systems intervention might improve outpatient access among youths with type 1 diabetes as compared with those who did not participate.
Intervention linked to increased BIPOC care access
The latest study includes 144 youths with type 1 diabetes referred for the program. The mean age was 13.7 years, 58% were female, and 81% were non-Hispanic White. While 51 youths were able to participate in NICH, the remaining 93 were not served by the program because of insurance denial or nonresponse, according to investigators.
While participation in the program made no difference in access to care overall, results of this study suggest NICH reduced access disparities among BIPOC youths, the investigators said.
Those BIPOC youth, 28 in total, had significantly worse access to care prior to referral. However, BIPOC youth participation in NICH was associated with improved attendance at endocrinology appointments and outpatient attendance overall.
A mean change of 1.9 more appointments per year was seen among BIPOC youth who participated in NICH, compared with a mean decrease of 0.5 appointments per year among BIPOC youth not served by the program (P = .03), according to the study abstract.
Prior to NICH participation, outpatient attendance among BIPOC youths was about 2.5 visits per year, data presented by the investigators show.
Systemic changes needed
This study is representative of systemic changes that are needed to improve access to quality care for BIPOC youth, according Cynthia E. Muñoz, PhD, MPH, ADA’s president of health care and education.
“We know that there are increased risks for poor health outcomes for these children and youths, and we know that there is a risk for mental health and psychosocial challenges for youth from these communities,” said Dr. Muñoz, a bilingual licensed psychologist and assistant professor of clinical pediatrics at the University of Southern California, Los Angeles.
In his presentation, Dr. Wagner said lumping racial and ethnic minority participants under a single BIPOC header probably wasn’t ideal because of the diversity and differences among racial and ethnic minorities. However, it was necessary in this particular study because of limited sample size.
Dr. Wagner and coauthors disclosed no conflicts of interest related to the research, which was supported by the Leona M. and Harry B. Helmsley Charitable Trust.
For racial or ethnic minority youths with type 1 diabetes, participating in an interventional program improves access to care, new research shows.
Youth categorized as Black, Indigenous, and other people of color (BIPOC) had significantly improved outpatient attendance during and after participating in Novel Interventions in Children’s Healthcare (NICH), a systems intervention for children with chronic health conditions and their families.
By comparison, no improvements in care access were observed among BIPOC children who were not able to access the program because of insurance or other reasons, David V. Wagner, PhD, Associate Professor and NICH research director at Oregon Health & Science University, Portland, reported at the annual scientific sessions of the American Diabetes Association.
The findings demonstrate a need for intensive, home-based services that aim to correct health inequities, said Dr. Wagner, who presented the findings along with Winniebhelle Cadiz, a scholar in the BUILD EXITO undergraduate research training program at Portland (Ore.) State University.
The NICH program hinges on trained interventionists who visit families at home, attend clinic visits, and work with schools and other contacts to help solve problems that keep children from following medical instructions, according to a program description.
“Families report having somebody by their side to help them navigate the system, address the transportation difficulties experienced, and help them and build that relationship with their health care provider seems to be hugely influential in terms of helping them navigate and access care,” Dr. Wagner said in a presentation of the study.
A NICH for youths with chronic health conditions
The NICH program differs from some other programs that have been developed in an attempt to improve health outcomes among youths in the community, according to Dr. Wagner.
“Many of the programs that exist out there are often piloted on, and seemingly built for, those who have more resources,” he said in his presentation. “Those who are in greatest need often have difficulty accessing and responding to the services.”
NICH doesn’t take the place of existing services, but is “an addition to the continuum of care” for youths and families who are struggling because of lack of resources or marginalization in the health care system, Dr. Wagner said.
While NICH is not specific to any one chronic health condition, several previous investigations have specifically looked at the impact of the NICH program on access to care in youths with type 1 diabetes.
Youths participating in the program for a year had fewer ED visits, including fewer visits with diabetic ketoacidosis (DKA), as well as fewer and shorter admissions as compared with the year prior to participating in the program, Dr. Wagner said.
In another study, youths had fewer admissions for diabetes or DKA and less frequent pediatric ICU contact during the NICH program, as compared with before the program.
Another study showed that, while NICH had no impact overall on access to care among youths with type 1 diabetes, BIPOC youths had an improvement in the mean number of outpatient visits as compared with preprogram levels. However, because none of those studies included a control group, Dr. Wagner said, it remained unclear whether this systems intervention might improve outpatient access among youths with type 1 diabetes as compared with those who did not participate.
Intervention linked to increased BIPOC care access
The latest study includes 144 youths with type 1 diabetes referred for the program. The mean age was 13.7 years, 58% were female, and 81% were non-Hispanic White. While 51 youths were able to participate in NICH, the remaining 93 were not served by the program because of insurance denial or nonresponse, according to investigators.
While participation in the program made no difference in access to care overall, results of this study suggest NICH reduced access disparities among BIPOC youths, the investigators said.
Those BIPOC youth, 28 in total, had significantly worse access to care prior to referral. However, BIPOC youth participation in NICH was associated with improved attendance at endocrinology appointments and outpatient attendance overall.
A mean change of 1.9 more appointments per year was seen among BIPOC youth who participated in NICH, compared with a mean decrease of 0.5 appointments per year among BIPOC youth not served by the program (P = .03), according to the study abstract.
Prior to NICH participation, outpatient attendance among BIPOC youths was about 2.5 visits per year, data presented by the investigators show.
Systemic changes needed
This study is representative of systemic changes that are needed to improve access to quality care for BIPOC youth, according Cynthia E. Muñoz, PhD, MPH, ADA’s president of health care and education.
“We know that there are increased risks for poor health outcomes for these children and youths, and we know that there is a risk for mental health and psychosocial challenges for youth from these communities,” said Dr. Muñoz, a bilingual licensed psychologist and assistant professor of clinical pediatrics at the University of Southern California, Los Angeles.
In his presentation, Dr. Wagner said lumping racial and ethnic minority participants under a single BIPOC header probably wasn’t ideal because of the diversity and differences among racial and ethnic minorities. However, it was necessary in this particular study because of limited sample size.
Dr. Wagner and coauthors disclosed no conflicts of interest related to the research, which was supported by the Leona M. and Harry B. Helmsley Charitable Trust.
FROM ADA 2021