User login
Uninsured cancer patients pay more

Photo by Rhoda Baer
Uninsured patients are asked to pay much more for cancer treatments than Medicare and private insurers pay, according to research published in Health Affairs.
Researchers reviewed newly available Medicare data on what physicians charged for intravenous chemotherapy drugs in 2012.
And the results showed that uninsured cancer patients were asked to pay anywhere from 2 to 43 times what Medicare would pay and 2 to 5 times as
much as private insurance would pay.
For example, uninsured patients who did not negotiate the billed amounts could expect to pay $6711 for an infusion of the colorectal cancer drug oxaliplatin. But Medicare and private health plans only pay $3090 and $3616, respectively.
“Patients with Medicare and private insurance don’t pay the sticker price of healthcare,” said study author Stacie Dusetzina, PhD, of the University of North Carolina at Chapel Hill.
“They pay a discounted rate. However, uninsured patients don’t have the bargaining power, or they may not try to negotiate for a better price.”
In addition to estimating costs for infused chemotherapy drugs, Dr Dusetzina and her colleagues looked at what cancer patients were asked to pay for a doctor visit.
Uninsured patients were billed between $129 and $391, depending on the complexity of the visit. Medicare paid between $65 and $188, and private insurance paid $78 to $246 for the same visits.
“This is unreasonable,” Dr Dusetzina said. “There needs to be more transparency and less variability in healthcare pricing.”
Under the Affordable Care Act, everyone in the US must be insured or face a tax penalty. However, many Americans remain without insurance. So differences in what the uninsured are charged really matter, Dr Dusetzina said.
“In states like North Carolina that didn’t expand Medicaid, there is a large group of people who can get insurance on the federal exchange but cannot get subsidies because the law assumed they would be covered by Medicaid,” she noted.
This population earns at or near the federal poverty level. Without subsidies to help pay for private insurance, many are likely to remain uninsured.
These drug pricing discrepancies could become even more important depending on the outcome of the pending Supreme Court case King vs Burwell, which challenges the legitimacy of federal healthcare subsidies and could leave as many as 8 million Americans without subsidies and uninsured in 2016. ![]()

Photo by Rhoda Baer
Uninsured patients are asked to pay much more for cancer treatments than Medicare and private insurers pay, according to research published in Health Affairs.
Researchers reviewed newly available Medicare data on what physicians charged for intravenous chemotherapy drugs in 2012.
And the results showed that uninsured cancer patients were asked to pay anywhere from 2 to 43 times what Medicare would pay and 2 to 5 times as
much as private insurance would pay.
For example, uninsured patients who did not negotiate the billed amounts could expect to pay $6711 for an infusion of the colorectal cancer drug oxaliplatin. But Medicare and private health plans only pay $3090 and $3616, respectively.
“Patients with Medicare and private insurance don’t pay the sticker price of healthcare,” said study author Stacie Dusetzina, PhD, of the University of North Carolina at Chapel Hill.
“They pay a discounted rate. However, uninsured patients don’t have the bargaining power, or they may not try to negotiate for a better price.”
In addition to estimating costs for infused chemotherapy drugs, Dr Dusetzina and her colleagues looked at what cancer patients were asked to pay for a doctor visit.
Uninsured patients were billed between $129 and $391, depending on the complexity of the visit. Medicare paid between $65 and $188, and private insurance paid $78 to $246 for the same visits.
“This is unreasonable,” Dr Dusetzina said. “There needs to be more transparency and less variability in healthcare pricing.”
Under the Affordable Care Act, everyone in the US must be insured or face a tax penalty. However, many Americans remain without insurance. So differences in what the uninsured are charged really matter, Dr Dusetzina said.
“In states like North Carolina that didn’t expand Medicaid, there is a large group of people who can get insurance on the federal exchange but cannot get subsidies because the law assumed they would be covered by Medicaid,” she noted.
This population earns at or near the federal poverty level. Without subsidies to help pay for private insurance, many are likely to remain uninsured.
These drug pricing discrepancies could become even more important depending on the outcome of the pending Supreme Court case King vs Burwell, which challenges the legitimacy of federal healthcare subsidies and could leave as many as 8 million Americans without subsidies and uninsured in 2016. ![]()

Photo by Rhoda Baer
Uninsured patients are asked to pay much more for cancer treatments than Medicare and private insurers pay, according to research published in Health Affairs.
Researchers reviewed newly available Medicare data on what physicians charged for intravenous chemotherapy drugs in 2012.
And the results showed that uninsured cancer patients were asked to pay anywhere from 2 to 43 times what Medicare would pay and 2 to 5 times as
much as private insurance would pay.
For example, uninsured patients who did not negotiate the billed amounts could expect to pay $6711 for an infusion of the colorectal cancer drug oxaliplatin. But Medicare and private health plans only pay $3090 and $3616, respectively.
“Patients with Medicare and private insurance don’t pay the sticker price of healthcare,” said study author Stacie Dusetzina, PhD, of the University of North Carolina at Chapel Hill.
“They pay a discounted rate. However, uninsured patients don’t have the bargaining power, or they may not try to negotiate for a better price.”
In addition to estimating costs for infused chemotherapy drugs, Dr Dusetzina and her colleagues looked at what cancer patients were asked to pay for a doctor visit.
Uninsured patients were billed between $129 and $391, depending on the complexity of the visit. Medicare paid between $65 and $188, and private insurance paid $78 to $246 for the same visits.
“This is unreasonable,” Dr Dusetzina said. “There needs to be more transparency and less variability in healthcare pricing.”
Under the Affordable Care Act, everyone in the US must be insured or face a tax penalty. However, many Americans remain without insurance. So differences in what the uninsured are charged really matter, Dr Dusetzina said.
“In states like North Carolina that didn’t expand Medicaid, there is a large group of people who can get insurance on the federal exchange but cannot get subsidies because the law assumed they would be covered by Medicaid,” she noted.
This population earns at or near the federal poverty level. Without subsidies to help pay for private insurance, many are likely to remain uninsured.
These drug pricing discrepancies could become even more important depending on the outcome of the pending Supreme Court case King vs Burwell, which challenges the legitimacy of federal healthcare subsidies and could leave as many as 8 million Americans without subsidies and uninsured in 2016. ![]()
Environmental factors affect bloodstream infections

New research suggests environmental factors can affect the development of catheter-related bloodstream infections (CRBSIs) in patients who
receive parenteral nutrition therapy at home.
Using a peripherally inserted central venous catheter (PICC) for 1 additional infusion day per week significantly reduced the amount of time before a first CRBSI, and using a tunneled vascular access device managed by a home care nurse increased the mean incidence of CRBSIs.
Laura Fuglsang Bech, of Aalborg University in Denmark, and her colleagues reported these results in the Journal of Parenteral and Enteral Nutrition.
The researchers set out to determine if environmental factors play a role in the development of bloodstream infections among patients receiving parenteral nutrition therapy via vascular access devices or PICCs, the 2 most commonly used catheters.
The team looked at factors such as smoking, catheter management by a home care nurse, colectomy with stoma, number of infusion days per week, and C-reactive protein values at catheter insertion day.
Adult patients suffering from intestinal failure and receiving home parenteral nutrition were included in the study. There were 295 catheters—169 tunneled vascular access devices and 126 PICCs—used in 136 patients.
The researchers found that using a PICC for 1 additional infusion day per week significantly reduced the amount of time before a first bloodstream infection. The time to first CRBSI decreased by a factor of 2.47 with 1 additional infusion day per week (P=0.04).
The team also found that using a tunneled vascular access device managed by a home care nurse increased the mean incidence of bloodstream infections. The mean CRBSI incidence per 1000 catheter days was 1.45± 0.68 for catheters managed by a home care nurse and 0.56 ± 0.24 for catheters that were not (P<0.001).
None of the other factors the researchers analyzed had any significant impact on the timing or incidence of CRBSIs.
Based on these results, the researchers recommended revisions to current home care guidelines. They advised using PICCs only for short-term home therapy and when few infusion days per week are needed. And they said management of tunneled vascular access devices by home care nurses should be further specialized. ![]()

New research suggests environmental factors can affect the development of catheter-related bloodstream infections (CRBSIs) in patients who
receive parenteral nutrition therapy at home.
Using a peripherally inserted central venous catheter (PICC) for 1 additional infusion day per week significantly reduced the amount of time before a first CRBSI, and using a tunneled vascular access device managed by a home care nurse increased the mean incidence of CRBSIs.
Laura Fuglsang Bech, of Aalborg University in Denmark, and her colleagues reported these results in the Journal of Parenteral and Enteral Nutrition.
The researchers set out to determine if environmental factors play a role in the development of bloodstream infections among patients receiving parenteral nutrition therapy via vascular access devices or PICCs, the 2 most commonly used catheters.
The team looked at factors such as smoking, catheter management by a home care nurse, colectomy with stoma, number of infusion days per week, and C-reactive protein values at catheter insertion day.
Adult patients suffering from intestinal failure and receiving home parenteral nutrition were included in the study. There were 295 catheters—169 tunneled vascular access devices and 126 PICCs—used in 136 patients.
The researchers found that using a PICC for 1 additional infusion day per week significantly reduced the amount of time before a first bloodstream infection. The time to first CRBSI decreased by a factor of 2.47 with 1 additional infusion day per week (P=0.04).
The team also found that using a tunneled vascular access device managed by a home care nurse increased the mean incidence of bloodstream infections. The mean CRBSI incidence per 1000 catheter days was 1.45± 0.68 for catheters managed by a home care nurse and 0.56 ± 0.24 for catheters that were not (P<0.001).
None of the other factors the researchers analyzed had any significant impact on the timing or incidence of CRBSIs.
Based on these results, the researchers recommended revisions to current home care guidelines. They advised using PICCs only for short-term home therapy and when few infusion days per week are needed. And they said management of tunneled vascular access devices by home care nurses should be further specialized. ![]()

New research suggests environmental factors can affect the development of catheter-related bloodstream infections (CRBSIs) in patients who
receive parenteral nutrition therapy at home.
Using a peripherally inserted central venous catheter (PICC) for 1 additional infusion day per week significantly reduced the amount of time before a first CRBSI, and using a tunneled vascular access device managed by a home care nurse increased the mean incidence of CRBSIs.
Laura Fuglsang Bech, of Aalborg University in Denmark, and her colleagues reported these results in the Journal of Parenteral and Enteral Nutrition.
The researchers set out to determine if environmental factors play a role in the development of bloodstream infections among patients receiving parenteral nutrition therapy via vascular access devices or PICCs, the 2 most commonly used catheters.
The team looked at factors such as smoking, catheter management by a home care nurse, colectomy with stoma, number of infusion days per week, and C-reactive protein values at catheter insertion day.
Adult patients suffering from intestinal failure and receiving home parenteral nutrition were included in the study. There were 295 catheters—169 tunneled vascular access devices and 126 PICCs—used in 136 patients.
The researchers found that using a PICC for 1 additional infusion day per week significantly reduced the amount of time before a first bloodstream infection. The time to first CRBSI decreased by a factor of 2.47 with 1 additional infusion day per week (P=0.04).
The team also found that using a tunneled vascular access device managed by a home care nurse increased the mean incidence of bloodstream infections. The mean CRBSI incidence per 1000 catheter days was 1.45± 0.68 for catheters managed by a home care nurse and 0.56 ± 0.24 for catheters that were not (P<0.001).
None of the other factors the researchers analyzed had any significant impact on the timing or incidence of CRBSIs.
Based on these results, the researchers recommended revisions to current home care guidelines. They advised using PICCs only for short-term home therapy and when few infusion days per week are needed. And they said management of tunneled vascular access devices by home care nurses should be further specialized. ![]()
Low doses of imatinib promote hematopoiesis

Image by Volker Brinkmann
Low doses of the tyrosine kinase inhibitor imatinib can promote hematopoiesis, according to research published in PLOS Pathogens.
Preclinical experiments revealed that the drug can induce differentiation in hematopoietic stem cells (HSCs) and progenitors in the bone marrow,
augment myelopoiesis, and increase the number of myeloid cells in the blood and spleen.
Researchers said these findings suggest imatinib or related drugs could be used to treat infections.
“We think that low doses of imatinib are mimicking ‘emergency hematopoiesis,’ a normal early response to infection,” said study author Daniel Kalman, PhD, of the Emory University School of Medicine in Atlanta, Georgia.
“This was surprising because there are reports that imatinib can be immunosuppressive in some patients. Our data suggest that, at subclinical doses, imatinib can stimulate bone marrow stem cells to produce several types of myeloid cells, such as neutrophils and macrophages, and trigger their exodus from the bone marrow. However, higher doses appear to inhibit this process.”
Dr Kalman and his colleagues observed a 4-fold increase of neutrophils and a 3-fold increase of monocytes in the bone marrow of imatinib-treated mice. However, these mice did not see a significant change in the number of mature B cells, T cells, dendritic cells, eosinophils, or natural killer cells.
Imatinib did not induce the accumulation of HSCs, but it did regulate the accumulation of multipotent progenitors. The drug also reduced the accumulation of HSCs upon infection, which suggests it may increase the flux of HSCs to progenitors.
Imatinib did not increase the number of transplantable HSCs, but it did induce an irreversible commitment of HSCs into progenitors that could differentiate into myeloid cells ex vivo.
Imatinib induced an irreversible differentiation of HSCs or progenitors into myeloid cells in a dose-dependent manner. The drug facilitated the exodus of myeloid cells from the bone marrow only at lower doses. It inhibited this same process at higher doses.
Despite increasing the number of neutrophils, low doses of imatinib did not activate neutrophils. However, the cells retained the capacity to activate upon infection.
In fact, an increase in the number of neutrophils was sufficient to reduce Mycobacterium marinum bacterial load. And imatinib reduced the bacterial load in mice infected with pathogenic Francisella species.
The researchers said these results suggest low doses of imatinib could potentially be used to treat a variety of infections and might prove particularly useful in immunocompromised patients. ![]()

Image by Volker Brinkmann
Low doses of the tyrosine kinase inhibitor imatinib can promote hematopoiesis, according to research published in PLOS Pathogens.
Preclinical experiments revealed that the drug can induce differentiation in hematopoietic stem cells (HSCs) and progenitors in the bone marrow,
augment myelopoiesis, and increase the number of myeloid cells in the blood and spleen.
Researchers said these findings suggest imatinib or related drugs could be used to treat infections.
“We think that low doses of imatinib are mimicking ‘emergency hematopoiesis,’ a normal early response to infection,” said study author Daniel Kalman, PhD, of the Emory University School of Medicine in Atlanta, Georgia.
“This was surprising because there are reports that imatinib can be immunosuppressive in some patients. Our data suggest that, at subclinical doses, imatinib can stimulate bone marrow stem cells to produce several types of myeloid cells, such as neutrophils and macrophages, and trigger their exodus from the bone marrow. However, higher doses appear to inhibit this process.”
Dr Kalman and his colleagues observed a 4-fold increase of neutrophils and a 3-fold increase of monocytes in the bone marrow of imatinib-treated mice. However, these mice did not see a significant change in the number of mature B cells, T cells, dendritic cells, eosinophils, or natural killer cells.
Imatinib did not induce the accumulation of HSCs, but it did regulate the accumulation of multipotent progenitors. The drug also reduced the accumulation of HSCs upon infection, which suggests it may increase the flux of HSCs to progenitors.
Imatinib did not increase the number of transplantable HSCs, but it did induce an irreversible commitment of HSCs into progenitors that could differentiate into myeloid cells ex vivo.
Imatinib induced an irreversible differentiation of HSCs or progenitors into myeloid cells in a dose-dependent manner. The drug facilitated the exodus of myeloid cells from the bone marrow only at lower doses. It inhibited this same process at higher doses.
Despite increasing the number of neutrophils, low doses of imatinib did not activate neutrophils. However, the cells retained the capacity to activate upon infection.
In fact, an increase in the number of neutrophils was sufficient to reduce Mycobacterium marinum bacterial load. And imatinib reduced the bacterial load in mice infected with pathogenic Francisella species.
The researchers said these results suggest low doses of imatinib could potentially be used to treat a variety of infections and might prove particularly useful in immunocompromised patients. ![]()

Image by Volker Brinkmann
Low doses of the tyrosine kinase inhibitor imatinib can promote hematopoiesis, according to research published in PLOS Pathogens.
Preclinical experiments revealed that the drug can induce differentiation in hematopoietic stem cells (HSCs) and progenitors in the bone marrow,
augment myelopoiesis, and increase the number of myeloid cells in the blood and spleen.
Researchers said these findings suggest imatinib or related drugs could be used to treat infections.
“We think that low doses of imatinib are mimicking ‘emergency hematopoiesis,’ a normal early response to infection,” said study author Daniel Kalman, PhD, of the Emory University School of Medicine in Atlanta, Georgia.
“This was surprising because there are reports that imatinib can be immunosuppressive in some patients. Our data suggest that, at subclinical doses, imatinib can stimulate bone marrow stem cells to produce several types of myeloid cells, such as neutrophils and macrophages, and trigger their exodus from the bone marrow. However, higher doses appear to inhibit this process.”
Dr Kalman and his colleagues observed a 4-fold increase of neutrophils and a 3-fold increase of monocytes in the bone marrow of imatinib-treated mice. However, these mice did not see a significant change in the number of mature B cells, T cells, dendritic cells, eosinophils, or natural killer cells.
Imatinib did not induce the accumulation of HSCs, but it did regulate the accumulation of multipotent progenitors. The drug also reduced the accumulation of HSCs upon infection, which suggests it may increase the flux of HSCs to progenitors.
Imatinib did not increase the number of transplantable HSCs, but it did induce an irreversible commitment of HSCs into progenitors that could differentiate into myeloid cells ex vivo.
Imatinib induced an irreversible differentiation of HSCs or progenitors into myeloid cells in a dose-dependent manner. The drug facilitated the exodus of myeloid cells from the bone marrow only at lower doses. It inhibited this same process at higher doses.
Despite increasing the number of neutrophils, low doses of imatinib did not activate neutrophils. However, the cells retained the capacity to activate upon infection.
In fact, an increase in the number of neutrophils was sufficient to reduce Mycobacterium marinum bacterial load. And imatinib reduced the bacterial load in mice infected with pathogenic Francisella species.
The researchers said these results suggest low doses of imatinib could potentially be used to treat a variety of infections and might prove particularly useful in immunocompromised patients. ![]()
Collaboration may help prevent CLABSIs
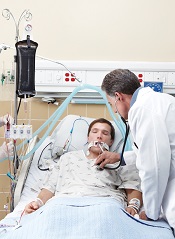
Collaborative relationships between nurses and physicians may help reduce the rates of healthcare-associated infections in critical care, according to research published in Critical Care Nurse.
Study investigators found lower rates of central line-associated bloodstream infections (CLABSIs) and ventilator-associated pneumonia (VAP) in critical care units in which nurses reported a more favorable perception of nurse-physician collaboration.
“Our findings suggest that raising the quality of collaboration and communication among nurses and physicians has the potential to improve patient safety,” said study author Christine Boev, RN, PhD, CCRN, of Wegmans School of Nursing at St John Fisher College in Rochester, New York.
Dr Boev and her colleagues analyzed 5 years of data from 671 surveys of nurses in 4 specialized intensive care units (ICUs) at a 750-bed New York hospital.
The investigators also collected patient outcome data from those units for the same period, focusing on patients with CLABSIs or VAP. And the team analyzed unit-level variables such as nurses’ skill mix, nursing hours per patient day, and voluntary turnover.
Results revealed a significant association between nurse-physician collaboration and both CLABSIs and VAP. For every 0.5 unit increase in collaboration, the rate of CLABSIs decreased by 2.98 (P=0.005), and the rate of VAP decreased by 1.13 (P=0.005).
In addition, ICUs with a higher proportion of certified nurses had significantly lower incidences of both CLABSIs and VAP—0.43 (P=0.02) and 0.17 (P=0.01), respectively. And ICUs with higher numbers of nursing hours per patient day had significantly lower rates of CLABSIs—0.42 (P=0.05).
However, there was no significant difference in VAP rates according to nursing hours. And there was no significant difference in the rate of either type of infection according to nurses’ skill mix or voluntary turnover.
Dr Boev said these results suggest that efforts to prevent healthcare-associated infections should include interventions to improve nurse-physician collaboration. Such interventions might include multidisciplinary daily patient rounds and interprofessional educational programs, such as shared simulation training. ![]()

Collaborative relationships between nurses and physicians may help reduce the rates of healthcare-associated infections in critical care, according to research published in Critical Care Nurse.
Study investigators found lower rates of central line-associated bloodstream infections (CLABSIs) and ventilator-associated pneumonia (VAP) in critical care units in which nurses reported a more favorable perception of nurse-physician collaboration.
“Our findings suggest that raising the quality of collaboration and communication among nurses and physicians has the potential to improve patient safety,” said study author Christine Boev, RN, PhD, CCRN, of Wegmans School of Nursing at St John Fisher College in Rochester, New York.
Dr Boev and her colleagues analyzed 5 years of data from 671 surveys of nurses in 4 specialized intensive care units (ICUs) at a 750-bed New York hospital.
The investigators also collected patient outcome data from those units for the same period, focusing on patients with CLABSIs or VAP. And the team analyzed unit-level variables such as nurses’ skill mix, nursing hours per patient day, and voluntary turnover.
Results revealed a significant association between nurse-physician collaboration and both CLABSIs and VAP. For every 0.5 unit increase in collaboration, the rate of CLABSIs decreased by 2.98 (P=0.005), and the rate of VAP decreased by 1.13 (P=0.005).
In addition, ICUs with a higher proportion of certified nurses had significantly lower incidences of both CLABSIs and VAP—0.43 (P=0.02) and 0.17 (P=0.01), respectively. And ICUs with higher numbers of nursing hours per patient day had significantly lower rates of CLABSIs—0.42 (P=0.05).
However, there was no significant difference in VAP rates according to nursing hours. And there was no significant difference in the rate of either type of infection according to nurses’ skill mix or voluntary turnover.
Dr Boev said these results suggest that efforts to prevent healthcare-associated infections should include interventions to improve nurse-physician collaboration. Such interventions might include multidisciplinary daily patient rounds and interprofessional educational programs, such as shared simulation training. ![]()

Collaborative relationships between nurses and physicians may help reduce the rates of healthcare-associated infections in critical care, according to research published in Critical Care Nurse.
Study investigators found lower rates of central line-associated bloodstream infections (CLABSIs) and ventilator-associated pneumonia (VAP) in critical care units in which nurses reported a more favorable perception of nurse-physician collaboration.
“Our findings suggest that raising the quality of collaboration and communication among nurses and physicians has the potential to improve patient safety,” said study author Christine Boev, RN, PhD, CCRN, of Wegmans School of Nursing at St John Fisher College in Rochester, New York.
Dr Boev and her colleagues analyzed 5 years of data from 671 surveys of nurses in 4 specialized intensive care units (ICUs) at a 750-bed New York hospital.
The investigators also collected patient outcome data from those units for the same period, focusing on patients with CLABSIs or VAP. And the team analyzed unit-level variables such as nurses’ skill mix, nursing hours per patient day, and voluntary turnover.
Results revealed a significant association between nurse-physician collaboration and both CLABSIs and VAP. For every 0.5 unit increase in collaboration, the rate of CLABSIs decreased by 2.98 (P=0.005), and the rate of VAP decreased by 1.13 (P=0.005).
In addition, ICUs with a higher proportion of certified nurses had significantly lower incidences of both CLABSIs and VAP—0.43 (P=0.02) and 0.17 (P=0.01), respectively. And ICUs with higher numbers of nursing hours per patient day had significantly lower rates of CLABSIs—0.42 (P=0.05).
However, there was no significant difference in VAP rates according to nursing hours. And there was no significant difference in the rate of either type of infection according to nurses’ skill mix or voluntary turnover.
Dr Boev said these results suggest that efforts to prevent healthcare-associated infections should include interventions to improve nurse-physician collaboration. Such interventions might include multidisciplinary daily patient rounds and interprofessional educational programs, such as shared simulation training. ![]()
Mouse model could aid study of malaria
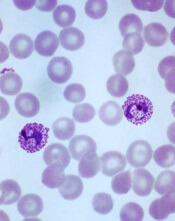
Plasmodium vivax infection
Image by Mae Melvin
Researchers say they have developed a human-chimeric mouse model that can advance the study of the malaria parasite Plasmodium vivax.
The model is engineered to grow human livers that can be infected with P vivax and used for investigations into parasite development, dormancy, and activation, as well as the effect certain drugs have on each aspect of the infection.
The researchers described this model in Cell Host & Microbe.
Stefan Kappe, PhD, of Seattle Biomedical Research Institute in Washington, and his colleagues noted that P vivax malaria parasites are more resistant to control and elimination than other malaria parasites because, after infection, they fall dormant within the liver for months to years.
When these dormant parasites eventually become activated, they replicate, infect the bloodstream, and cause relapsing malaria.
The lack of tractable P vivax animal models has made it difficult to examine P vivax liver-stage infection, but Dr Kappe and his colleagues found a solution in a model known as FRG KO huHep.
To create the FRG KO huHep model, the team transplanted human hepatocytes in the severely immunocompromised FRG KO mouse, which has deletions in fumarylacetoacetate hydrolase (FAH), recombinationactivating gene 2 (Rag2), and interleukin-2 receptor subunit gamma (Il2rg).
The researchers found that FRG KO huHep mice support P vivax sporozoite infection, liver-stage development, and the formation and persistence of dormant liver-stage parasites.
In addition, experiments with this model revealed that the antimalarial drug primaquine could prevent and eliminate liver-stage infection.
The researchers therefore concluded that P vivax-infected FRG KO huHep mice are a suitable model for studying liver-stage development and dormancy and may facilitate the discovery of drugs targeting relapsing malaria.
“This model is a real game-changer,” said Ivo Mueller, PhD, a malaria expert at the Walter and Eliza Hall Institute in Melbourne, Victoria, Australia, who was not involved in this research.
“For the first time, we now have a realistic opportunity that not only allows us to directly study this normally hidden P vivax life-stage, but also to test new drugs and vaccines. This new model is an essential resource in our quest to develop the new anti-vivax interventions that we will need to eliminate P vivax malaria.” ![]()

Plasmodium vivax infection
Image by Mae Melvin
Researchers say they have developed a human-chimeric mouse model that can advance the study of the malaria parasite Plasmodium vivax.
The model is engineered to grow human livers that can be infected with P vivax and used for investigations into parasite development, dormancy, and activation, as well as the effect certain drugs have on each aspect of the infection.
The researchers described this model in Cell Host & Microbe.
Stefan Kappe, PhD, of Seattle Biomedical Research Institute in Washington, and his colleagues noted that P vivax malaria parasites are more resistant to control and elimination than other malaria parasites because, after infection, they fall dormant within the liver for months to years.
When these dormant parasites eventually become activated, they replicate, infect the bloodstream, and cause relapsing malaria.
The lack of tractable P vivax animal models has made it difficult to examine P vivax liver-stage infection, but Dr Kappe and his colleagues found a solution in a model known as FRG KO huHep.
To create the FRG KO huHep model, the team transplanted human hepatocytes in the severely immunocompromised FRG KO mouse, which has deletions in fumarylacetoacetate hydrolase (FAH), recombinationactivating gene 2 (Rag2), and interleukin-2 receptor subunit gamma (Il2rg).
The researchers found that FRG KO huHep mice support P vivax sporozoite infection, liver-stage development, and the formation and persistence of dormant liver-stage parasites.
In addition, experiments with this model revealed that the antimalarial drug primaquine could prevent and eliminate liver-stage infection.
The researchers therefore concluded that P vivax-infected FRG KO huHep mice are a suitable model for studying liver-stage development and dormancy and may facilitate the discovery of drugs targeting relapsing malaria.
“This model is a real game-changer,” said Ivo Mueller, PhD, a malaria expert at the Walter and Eliza Hall Institute in Melbourne, Victoria, Australia, who was not involved in this research.
“For the first time, we now have a realistic opportunity that not only allows us to directly study this normally hidden P vivax life-stage, but also to test new drugs and vaccines. This new model is an essential resource in our quest to develop the new anti-vivax interventions that we will need to eliminate P vivax malaria.” ![]()

Plasmodium vivax infection
Image by Mae Melvin
Researchers say they have developed a human-chimeric mouse model that can advance the study of the malaria parasite Plasmodium vivax.
The model is engineered to grow human livers that can be infected with P vivax and used for investigations into parasite development, dormancy, and activation, as well as the effect certain drugs have on each aspect of the infection.
The researchers described this model in Cell Host & Microbe.
Stefan Kappe, PhD, of Seattle Biomedical Research Institute in Washington, and his colleagues noted that P vivax malaria parasites are more resistant to control and elimination than other malaria parasites because, after infection, they fall dormant within the liver for months to years.
When these dormant parasites eventually become activated, they replicate, infect the bloodstream, and cause relapsing malaria.
The lack of tractable P vivax animal models has made it difficult to examine P vivax liver-stage infection, but Dr Kappe and his colleagues found a solution in a model known as FRG KO huHep.
To create the FRG KO huHep model, the team transplanted human hepatocytes in the severely immunocompromised FRG KO mouse, which has deletions in fumarylacetoacetate hydrolase (FAH), recombinationactivating gene 2 (Rag2), and interleukin-2 receptor subunit gamma (Il2rg).
The researchers found that FRG KO huHep mice support P vivax sporozoite infection, liver-stage development, and the formation and persistence of dormant liver-stage parasites.
In addition, experiments with this model revealed that the antimalarial drug primaquine could prevent and eliminate liver-stage infection.
The researchers therefore concluded that P vivax-infected FRG KO huHep mice are a suitable model for studying liver-stage development and dormancy and may facilitate the discovery of drugs targeting relapsing malaria.
“This model is a real game-changer,” said Ivo Mueller, PhD, a malaria expert at the Walter and Eliza Hall Institute in Melbourne, Victoria, Australia, who was not involved in this research.
“For the first time, we now have a realistic opportunity that not only allows us to directly study this normally hidden P vivax life-stage, but also to test new drugs and vaccines. This new model is an essential resource in our quest to develop the new anti-vivax interventions that we will need to eliminate P vivax malaria.” ![]()
Fish oil may cause chemoresistance

Consuming certain types of fish and taking fish oil supplements may induce chemoresistance, according to research published in JAMA Oncology.
Researchers found that herring and mackerel, as well as 6 different types of fish oil supplements, raised blood levels of the fatty acid 16:4(n-3).
And experiments in mice showed that small amounts of either purified 16:4(n-3) or fish oil induced resistance to the chemotherapy drug cisplatin.
Emile E. Voest, MD, PhD, of the Netherlands Cancer Institute in Amsterdam, and his colleagues conducted this multi-part study.
In one part, the team conducted a survey to determine the rate of fish oil use among patients undergoing cancer treatment (n=118). Thirty-five patients (30%) reported regular use of nutritional supplements, and 13 (11%) said they used supplements containing omega-3 fatty acids.
For another part of the study, the researchers evaluated 6 types of fish oil supplements. All of them contained relevant amounts of 16:4(n-3), ranging from 0.2 µM to 5.7 µM.
The team also recruited healthy volunteers to examine blood levels of 16:4(n-3) after the ingestion of fish oil supplements (n=30) and fish (n=20).
Volunteers had increased blood levels of 16:4(n-3) after the recommended daily amount of 10 mL of fish oil and after a 50 mL dose. Subjects had an almost-complete normalization of blood levels 8 hours after a 10 mL fish oil dose, but they had a more prolonged elevation of fatty acid levels after a 50 mL dose.
Eating 100 grams of herring and mackerel also increased blood levels of 16:4(n-3) compared with tuna, which did not affect blood levels, and salmon,
which resulted in a small, short-lived peak.
Finally, experiments in mice showed that as little as 2.5 pmol of purified 16:4(n-3) or 1 µL of fish oil was sufficient to induce resistance to the chemotherapy drug cisplatin.
The fish oil/cisplatin combination had no significant impact on mouse tumors when compared to vehicle control treatment. The estimated tumor volume difference was 44.1 mm3 (P >0.99).
When the researchers compared cisplatin alone to cisplatin plus 16:4(n-3), the estimated tumor volume difference was 95.5 mm3 (P=0 .04). When they compared vehicle control to cisplatin alone, there was an estimated tumor volume difference of 142.4 mm3 (P=0.001).
The team said these results suggest that simultaneous exposure to chemotherapy and fish oil may be detrimental to cancer patients. So until further data become available, patients should avoid consuming fish oil from the day before chemotherapy until the day after. ![]()

Consuming certain types of fish and taking fish oil supplements may induce chemoresistance, according to research published in JAMA Oncology.
Researchers found that herring and mackerel, as well as 6 different types of fish oil supplements, raised blood levels of the fatty acid 16:4(n-3).
And experiments in mice showed that small amounts of either purified 16:4(n-3) or fish oil induced resistance to the chemotherapy drug cisplatin.
Emile E. Voest, MD, PhD, of the Netherlands Cancer Institute in Amsterdam, and his colleagues conducted this multi-part study.
In one part, the team conducted a survey to determine the rate of fish oil use among patients undergoing cancer treatment (n=118). Thirty-five patients (30%) reported regular use of nutritional supplements, and 13 (11%) said they used supplements containing omega-3 fatty acids.
For another part of the study, the researchers evaluated 6 types of fish oil supplements. All of them contained relevant amounts of 16:4(n-3), ranging from 0.2 µM to 5.7 µM.
The team also recruited healthy volunteers to examine blood levels of 16:4(n-3) after the ingestion of fish oil supplements (n=30) and fish (n=20).
Volunteers had increased blood levels of 16:4(n-3) after the recommended daily amount of 10 mL of fish oil and after a 50 mL dose. Subjects had an almost-complete normalization of blood levels 8 hours after a 10 mL fish oil dose, but they had a more prolonged elevation of fatty acid levels after a 50 mL dose.
Eating 100 grams of herring and mackerel also increased blood levels of 16:4(n-3) compared with tuna, which did not affect blood levels, and salmon,
which resulted in a small, short-lived peak.
Finally, experiments in mice showed that as little as 2.5 pmol of purified 16:4(n-3) or 1 µL of fish oil was sufficient to induce resistance to the chemotherapy drug cisplatin.
The fish oil/cisplatin combination had no significant impact on mouse tumors when compared to vehicle control treatment. The estimated tumor volume difference was 44.1 mm3 (P >0.99).
When the researchers compared cisplatin alone to cisplatin plus 16:4(n-3), the estimated tumor volume difference was 95.5 mm3 (P=0 .04). When they compared vehicle control to cisplatin alone, there was an estimated tumor volume difference of 142.4 mm3 (P=0.001).
The team said these results suggest that simultaneous exposure to chemotherapy and fish oil may be detrimental to cancer patients. So until further data become available, patients should avoid consuming fish oil from the day before chemotherapy until the day after. ![]()

Consuming certain types of fish and taking fish oil supplements may induce chemoresistance, according to research published in JAMA Oncology.
Researchers found that herring and mackerel, as well as 6 different types of fish oil supplements, raised blood levels of the fatty acid 16:4(n-3).
And experiments in mice showed that small amounts of either purified 16:4(n-3) or fish oil induced resistance to the chemotherapy drug cisplatin.
Emile E. Voest, MD, PhD, of the Netherlands Cancer Institute in Amsterdam, and his colleagues conducted this multi-part study.
In one part, the team conducted a survey to determine the rate of fish oil use among patients undergoing cancer treatment (n=118). Thirty-five patients (30%) reported regular use of nutritional supplements, and 13 (11%) said they used supplements containing omega-3 fatty acids.
For another part of the study, the researchers evaluated 6 types of fish oil supplements. All of them contained relevant amounts of 16:4(n-3), ranging from 0.2 µM to 5.7 µM.
The team also recruited healthy volunteers to examine blood levels of 16:4(n-3) after the ingestion of fish oil supplements (n=30) and fish (n=20).
Volunteers had increased blood levels of 16:4(n-3) after the recommended daily amount of 10 mL of fish oil and after a 50 mL dose. Subjects had an almost-complete normalization of blood levels 8 hours after a 10 mL fish oil dose, but they had a more prolonged elevation of fatty acid levels after a 50 mL dose.
Eating 100 grams of herring and mackerel also increased blood levels of 16:4(n-3) compared with tuna, which did not affect blood levels, and salmon,
which resulted in a small, short-lived peak.
Finally, experiments in mice showed that as little as 2.5 pmol of purified 16:4(n-3) or 1 µL of fish oil was sufficient to induce resistance to the chemotherapy drug cisplatin.
The fish oil/cisplatin combination had no significant impact on mouse tumors when compared to vehicle control treatment. The estimated tumor volume difference was 44.1 mm3 (P >0.99).
When the researchers compared cisplatin alone to cisplatin plus 16:4(n-3), the estimated tumor volume difference was 95.5 mm3 (P=0 .04). When they compared vehicle control to cisplatin alone, there was an estimated tumor volume difference of 142.4 mm3 (P=0.001).
The team said these results suggest that simultaneous exposure to chemotherapy and fish oil may be detrimental to cancer patients. So until further data become available, patients should avoid consuming fish oil from the day before chemotherapy until the day after. ![]()
Patients want more info about medical imaging risks

Photo by Rhoda Baer
Patients want more information about medical imaging tests that use radiation, according to research published in Radiology.
Most of the 30 subjects involved in this study said their healthcare providers did not initiate a discussion about the risks and benefits of imaging tests.
So a majority of participants obtained information from the Internet. Researchers said these findings highlight a need for better communication between patients and providers.
“This may not be what we in the medical field want to hear, but I think it’s important that we hear it,” said study author Jennifer Hay, PhD, of Memorial Sloan Kettering Cancer Center in New York, New York.
“Patients want this information, and they prefer to receive it from doctors they know and trust.”
Dr Hay and her colleagues analyzed over 9 hours of transcribed conversations with 30 people who had undergone medical imaging exams or consented for their children to undergo such exams.
The goal was to determine the subjects’ understanding of the benefits and risks associated with various medical imaging procedures and their expectations regarding communication of those benefits and risks.
The study group was divided into 6 focus groups, including 5 groups of cancer patients (or parents of young cancer patients) and 1 group of participants in a lung cancer screening program.
Quantifying subjects’ knowledge
The researchers found that participants perceived clear benefits from imaging tests like X-rays, computed tomography (CT) scans, and nuclear medicine examinations.
And most subjects were highly aware of the risks associated with ionizing radiation exposure, including the potential risk of future cancer. But their knowledge regarding which imaging tests use ionizing radiation varied.
In general, participants were more likely to understand that X-rays, CTs, and positron emission tomography (PET) scans deliver ionizing radiation and less likely to know about mammography, bone scanning, or stress tests. Many subjects did not know if magnetic resonance imaging (MRI) involved ionizing radiation.
Some participants did not know how tests differed, and some believed there was a “best” imaging test. Occasionally, subjects confused ionizing radiation from diagnostic medical imaging with radiation therapy.
Desire for information
Participants considered the availability of basic benefit-risk information to be a fundamental component of care. And they expressed a desire for a wide range of information about medical imaging tests.
Most subjects wanted basic education about which imaging tests use ionizing radiation and how doses compare among them. Nearly all subjects wanted to understand how tests differ, what governs selection of one over another, and why multiple tests are sometimes ordered.
A majority of participants met their needs for more information through self-directed Internet searches.
Concern about risks
Most subjects agreed that learning about possible future risks was important, but having this information would probably not alter their decision to proceed with a recommended test.
The desire for information about risks was strongest among cancer patients who had made the transition from treatment to survivorship.
These patients wanted to know how risk accumulates from multiple exams over time, whether additional ionizing radiation exposure could be avoided by substituting MRI for CT, and if longer intervals between follow-up examinations could be negotiated.
“Interest in having more information and participating in decision-making about medical imaging clearly increased as patients transitioned from active cancer treatment to survivorship,” said study author Raymond H. Thornton, MD, of Memorial Sloan Kettering Cancer Center.
“Cancer survivors typically focus on healthful living and risk-factor reduction, so they were particularly eager to participate in discussions about potential long-term risks of radiation.”
The different levels of desire for information among the study subjects lend support to a tiered approach for patient-centered communication, according to Dr Hay.
“A tiered approach would provide all patients with information and offer additional options to those who want to dig deeper and find out more,” she said.
Presenting information
Subjects expressed interest in 2 different modes of information exchange. Many participants said the ideal situation would be a face-to-face discussion with their personal physician, a medical physicist, or radiologist.
Others expressed an interest in written resources, especially hospital-endorsed Internet sites and printed materials. ![]()

Photo by Rhoda Baer
Patients want more information about medical imaging tests that use radiation, according to research published in Radiology.
Most of the 30 subjects involved in this study said their healthcare providers did not initiate a discussion about the risks and benefits of imaging tests.
So a majority of participants obtained information from the Internet. Researchers said these findings highlight a need for better communication between patients and providers.
“This may not be what we in the medical field want to hear, but I think it’s important that we hear it,” said study author Jennifer Hay, PhD, of Memorial Sloan Kettering Cancer Center in New York, New York.
“Patients want this information, and they prefer to receive it from doctors they know and trust.”
Dr Hay and her colleagues analyzed over 9 hours of transcribed conversations with 30 people who had undergone medical imaging exams or consented for their children to undergo such exams.
The goal was to determine the subjects’ understanding of the benefits and risks associated with various medical imaging procedures and their expectations regarding communication of those benefits and risks.
The study group was divided into 6 focus groups, including 5 groups of cancer patients (or parents of young cancer patients) and 1 group of participants in a lung cancer screening program.
Quantifying subjects’ knowledge
The researchers found that participants perceived clear benefits from imaging tests like X-rays, computed tomography (CT) scans, and nuclear medicine examinations.
And most subjects were highly aware of the risks associated with ionizing radiation exposure, including the potential risk of future cancer. But their knowledge regarding which imaging tests use ionizing radiation varied.
In general, participants were more likely to understand that X-rays, CTs, and positron emission tomography (PET) scans deliver ionizing radiation and less likely to know about mammography, bone scanning, or stress tests. Many subjects did not know if magnetic resonance imaging (MRI) involved ionizing radiation.
Some participants did not know how tests differed, and some believed there was a “best” imaging test. Occasionally, subjects confused ionizing radiation from diagnostic medical imaging with radiation therapy.
Desire for information
Participants considered the availability of basic benefit-risk information to be a fundamental component of care. And they expressed a desire for a wide range of information about medical imaging tests.
Most subjects wanted basic education about which imaging tests use ionizing radiation and how doses compare among them. Nearly all subjects wanted to understand how tests differ, what governs selection of one over another, and why multiple tests are sometimes ordered.
A majority of participants met their needs for more information through self-directed Internet searches.
Concern about risks
Most subjects agreed that learning about possible future risks was important, but having this information would probably not alter their decision to proceed with a recommended test.
The desire for information about risks was strongest among cancer patients who had made the transition from treatment to survivorship.
These patients wanted to know how risk accumulates from multiple exams over time, whether additional ionizing radiation exposure could be avoided by substituting MRI for CT, and if longer intervals between follow-up examinations could be negotiated.
“Interest in having more information and participating in decision-making about medical imaging clearly increased as patients transitioned from active cancer treatment to survivorship,” said study author Raymond H. Thornton, MD, of Memorial Sloan Kettering Cancer Center.
“Cancer survivors typically focus on healthful living and risk-factor reduction, so they were particularly eager to participate in discussions about potential long-term risks of radiation.”
The different levels of desire for information among the study subjects lend support to a tiered approach for patient-centered communication, according to Dr Hay.
“A tiered approach would provide all patients with information and offer additional options to those who want to dig deeper and find out more,” she said.
Presenting information
Subjects expressed interest in 2 different modes of information exchange. Many participants said the ideal situation would be a face-to-face discussion with their personal physician, a medical physicist, or radiologist.
Others expressed an interest in written resources, especially hospital-endorsed Internet sites and printed materials. ![]()

Photo by Rhoda Baer
Patients want more information about medical imaging tests that use radiation, according to research published in Radiology.
Most of the 30 subjects involved in this study said their healthcare providers did not initiate a discussion about the risks and benefits of imaging tests.
So a majority of participants obtained information from the Internet. Researchers said these findings highlight a need for better communication between patients and providers.
“This may not be what we in the medical field want to hear, but I think it’s important that we hear it,” said study author Jennifer Hay, PhD, of Memorial Sloan Kettering Cancer Center in New York, New York.
“Patients want this information, and they prefer to receive it from doctors they know and trust.”
Dr Hay and her colleagues analyzed over 9 hours of transcribed conversations with 30 people who had undergone medical imaging exams or consented for their children to undergo such exams.
The goal was to determine the subjects’ understanding of the benefits and risks associated with various medical imaging procedures and their expectations regarding communication of those benefits and risks.
The study group was divided into 6 focus groups, including 5 groups of cancer patients (or parents of young cancer patients) and 1 group of participants in a lung cancer screening program.
Quantifying subjects’ knowledge
The researchers found that participants perceived clear benefits from imaging tests like X-rays, computed tomography (CT) scans, and nuclear medicine examinations.
And most subjects were highly aware of the risks associated with ionizing radiation exposure, including the potential risk of future cancer. But their knowledge regarding which imaging tests use ionizing radiation varied.
In general, participants were more likely to understand that X-rays, CTs, and positron emission tomography (PET) scans deliver ionizing radiation and less likely to know about mammography, bone scanning, or stress tests. Many subjects did not know if magnetic resonance imaging (MRI) involved ionizing radiation.
Some participants did not know how tests differed, and some believed there was a “best” imaging test. Occasionally, subjects confused ionizing radiation from diagnostic medical imaging with radiation therapy.
Desire for information
Participants considered the availability of basic benefit-risk information to be a fundamental component of care. And they expressed a desire for a wide range of information about medical imaging tests.
Most subjects wanted basic education about which imaging tests use ionizing radiation and how doses compare among them. Nearly all subjects wanted to understand how tests differ, what governs selection of one over another, and why multiple tests are sometimes ordered.
A majority of participants met their needs for more information through self-directed Internet searches.
Concern about risks
Most subjects agreed that learning about possible future risks was important, but having this information would probably not alter their decision to proceed with a recommended test.
The desire for information about risks was strongest among cancer patients who had made the transition from treatment to survivorship.
These patients wanted to know how risk accumulates from multiple exams over time, whether additional ionizing radiation exposure could be avoided by substituting MRI for CT, and if longer intervals between follow-up examinations could be negotiated.
“Interest in having more information and participating in decision-making about medical imaging clearly increased as patients transitioned from active cancer treatment to survivorship,” said study author Raymond H. Thornton, MD, of Memorial Sloan Kettering Cancer Center.
“Cancer survivors typically focus on healthful living and risk-factor reduction, so they were particularly eager to participate in discussions about potential long-term risks of radiation.”
The different levels of desire for information among the study subjects lend support to a tiered approach for patient-centered communication, according to Dr Hay.
“A tiered approach would provide all patients with information and offer additional options to those who want to dig deeper and find out more,” she said.
Presenting information
Subjects expressed interest in 2 different modes of information exchange. Many participants said the ideal situation would be a face-to-face discussion with their personal physician, a medical physicist, or radiologist.
Others expressed an interest in written resources, especially hospital-endorsed Internet sites and printed materials.
Studies investigate risk of DVT, infection with PICCs
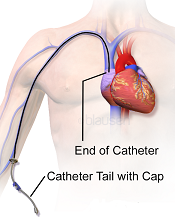
Image courtesy of Blausen
Medical Communications, Inc.
Three recently published papers may help ensure the appropriate use of peripherally inserted central catheters (PICCs).
A case-control study uncovered several factors that appear to affect the risk of deep vein thrombosis (DVT) associated with PICCs.
A retrospective study revealed the “prevalence, patterns, and predictors” of PICC-associated bloodstream infections.
And a literature review informed the creation of a guide to help hospitalists choose the right intravenous device.
“[PICCs] are very popular, but in an under-the-radar way, because they make care more convenient and can be placed relatively easily,” said Vineet Chopra, MD, an author on all 3 articles and a hospitalist at the University of Michigan Health System in Ann Arbor.
“But our new results, and review of research on the topic, show it’s important for physicians to think hard about both the risks and the benefits.”
Case-control study
In the study of PICC-DVT, published in Thrombosis Research, the investigators looked at records from 909 patients who received PICCs at the University of Michigan Health System in 2012 and 2013.
Patients had PICCs placed so they could receive long-term intravenous antibiotic therapy (n=447; 49.1%) or total parenteral nutrition (n=120; 6.7%). They also required PICCs for in-hospital venous access for blood draws or infusion of medications (n=342; 44.2%).
In all, 268 patients developed a DVT associated with their PICC. The median time to DVT development was 12.4 days from PICC placement.
Patients who were already taking aspirin and statins before their PICC was placed had a significantly lower risk of DVT-PICC (odds ratio [OR]=0.31). Patients who received pharmacological DVT prophylaxis had a lower risk of DVT-PICC than patients who were not on prophylaxis, although the difference was not statistically significant (OR=0.72).
Patients had a significantly greater risk of PICC-DVT if they underwent surgery during their hospital stay (OR=2.17) or had a prior history of venous thromboembolism (OR=1.70). And, compared to patients who received 4-Fr PICCs, those who had 5-Fr or 6-Fr PICCs had a significantly greater risk of DVT (ORs=2.74 and 7.40, respectively).
Retrospective study
In The American Journal of Medicine, Dr Chopra and his colleagues described a retrospective study of bloodstream infections associated with PICCs.
The investigators analyzed data from 747 patients who received 966 PICCs for a total of 26,887 catheter days. Patients had PICCs for long-term antibiotic administration (n=503; 52%), venous access (n=201; 21%), total parenteral nutrition (n=155; 16%), and chemotherapy (n=107; 11%).
There were 58 cases (6%) of PICC-bloodstream infection over 1156 catheter days, for an infection rate of 2.16 per 1000 catheter days. The median time to infection was 10 days.
Bivariate analysis revealed several factors associated with PICC-bloodstream infections. These included intensive care unit status (ICU; OR=3.23), mechanical ventilation (OR=4.39), length of stay (hospital, OR=1.04; ICU, OR=1.03), PowerPICCs (OR=2.58), devices placed by interventional radiology (OR=2.57), double lumens (OR=5.21), and triple lumens (OR=10.84).
In multivariable analysis, only some of these factors remained significantly associated with PICC-bloodstream infection. These included hospital length of stay (OR=1.04), ICU status (OR=1.02), double lumens (OR=3.99), and triple lumens (OR=6.34).
Dr Chopra said the results of these 2 studies suggest hospitalists should tread carefully when considering PICCs.
“These are not innocuous devices,” he said. “The time has come to stop thinking of them as a device of convenience and rather one with clear risks and benefits.”
Review and guide
In the Journal of Hospital Medicine, Dr Chopra and his colleagues offered advice on choosing vascular access devices. After reviewing the literature, the investigators designed a flow chart that can help hospitalists decide which device is appropriate for each patient.
For instance, different devices will work best depending on whether access to the bloodstream is needed urgently or less urgently, whether the patient will likely need the device for more or less than a week, what kind of drug or nutrition the doctor will order, and whether the patient’s kidneys are functioning normally.

Image courtesy of Blausen
Medical Communications, Inc.
Three recently published papers may help ensure the appropriate use of peripherally inserted central catheters (PICCs).
A case-control study uncovered several factors that appear to affect the risk of deep vein thrombosis (DVT) associated with PICCs.
A retrospective study revealed the “prevalence, patterns, and predictors” of PICC-associated bloodstream infections.
And a literature review informed the creation of a guide to help hospitalists choose the right intravenous device.
“[PICCs] are very popular, but in an under-the-radar way, because they make care more convenient and can be placed relatively easily,” said Vineet Chopra, MD, an author on all 3 articles and a hospitalist at the University of Michigan Health System in Ann Arbor.
“But our new results, and review of research on the topic, show it’s important for physicians to think hard about both the risks and the benefits.”
Case-control study
In the study of PICC-DVT, published in Thrombosis Research, the investigators looked at records from 909 patients who received PICCs at the University of Michigan Health System in 2012 and 2013.
Patients had PICCs placed so they could receive long-term intravenous antibiotic therapy (n=447; 49.1%) or total parenteral nutrition (n=120; 6.7%). They also required PICCs for in-hospital venous access for blood draws or infusion of medications (n=342; 44.2%).
In all, 268 patients developed a DVT associated with their PICC. The median time to DVT development was 12.4 days from PICC placement.
Patients who were already taking aspirin and statins before their PICC was placed had a significantly lower risk of DVT-PICC (odds ratio [OR]=0.31). Patients who received pharmacological DVT prophylaxis had a lower risk of DVT-PICC than patients who were not on prophylaxis, although the difference was not statistically significant (OR=0.72).
Patients had a significantly greater risk of PICC-DVT if they underwent surgery during their hospital stay (OR=2.17) or had a prior history of venous thromboembolism (OR=1.70). And, compared to patients who received 4-Fr PICCs, those who had 5-Fr or 6-Fr PICCs had a significantly greater risk of DVT (ORs=2.74 and 7.40, respectively).
Retrospective study
In The American Journal of Medicine, Dr Chopra and his colleagues described a retrospective study of bloodstream infections associated with PICCs.
The investigators analyzed data from 747 patients who received 966 PICCs for a total of 26,887 catheter days. Patients had PICCs for long-term antibiotic administration (n=503; 52%), venous access (n=201; 21%), total parenteral nutrition (n=155; 16%), and chemotherapy (n=107; 11%).
There were 58 cases (6%) of PICC-bloodstream infection over 1156 catheter days, for an infection rate of 2.16 per 1000 catheter days. The median time to infection was 10 days.
Bivariate analysis revealed several factors associated with PICC-bloodstream infections. These included intensive care unit status (ICU; OR=3.23), mechanical ventilation (OR=4.39), length of stay (hospital, OR=1.04; ICU, OR=1.03), PowerPICCs (OR=2.58), devices placed by interventional radiology (OR=2.57), double lumens (OR=5.21), and triple lumens (OR=10.84).
In multivariable analysis, only some of these factors remained significantly associated with PICC-bloodstream infection. These included hospital length of stay (OR=1.04), ICU status (OR=1.02), double lumens (OR=3.99), and triple lumens (OR=6.34).
Dr Chopra said the results of these 2 studies suggest hospitalists should tread carefully when considering PICCs.
“These are not innocuous devices,” he said. “The time has come to stop thinking of them as a device of convenience and rather one with clear risks and benefits.”
Review and guide
In the Journal of Hospital Medicine, Dr Chopra and his colleagues offered advice on choosing vascular access devices. After reviewing the literature, the investigators designed a flow chart that can help hospitalists decide which device is appropriate for each patient.
For instance, different devices will work best depending on whether access to the bloodstream is needed urgently or less urgently, whether the patient will likely need the device for more or less than a week, what kind of drug or nutrition the doctor will order, and whether the patient’s kidneys are functioning normally.

Image courtesy of Blausen
Medical Communications, Inc.
Three recently published papers may help ensure the appropriate use of peripherally inserted central catheters (PICCs).
A case-control study uncovered several factors that appear to affect the risk of deep vein thrombosis (DVT) associated with PICCs.
A retrospective study revealed the “prevalence, patterns, and predictors” of PICC-associated bloodstream infections.
And a literature review informed the creation of a guide to help hospitalists choose the right intravenous device.
“[PICCs] are very popular, but in an under-the-radar way, because they make care more convenient and can be placed relatively easily,” said Vineet Chopra, MD, an author on all 3 articles and a hospitalist at the University of Michigan Health System in Ann Arbor.
“But our new results, and review of research on the topic, show it’s important for physicians to think hard about both the risks and the benefits.”
Case-control study
In the study of PICC-DVT, published in Thrombosis Research, the investigators looked at records from 909 patients who received PICCs at the University of Michigan Health System in 2012 and 2013.
Patients had PICCs placed so they could receive long-term intravenous antibiotic therapy (n=447; 49.1%) or total parenteral nutrition (n=120; 6.7%). They also required PICCs for in-hospital venous access for blood draws or infusion of medications (n=342; 44.2%).
In all, 268 patients developed a DVT associated with their PICC. The median time to DVT development was 12.4 days from PICC placement.
Patients who were already taking aspirin and statins before their PICC was placed had a significantly lower risk of DVT-PICC (odds ratio [OR]=0.31). Patients who received pharmacological DVT prophylaxis had a lower risk of DVT-PICC than patients who were not on prophylaxis, although the difference was not statistically significant (OR=0.72).
Patients had a significantly greater risk of PICC-DVT if they underwent surgery during their hospital stay (OR=2.17) or had a prior history of venous thromboembolism (OR=1.70). And, compared to patients who received 4-Fr PICCs, those who had 5-Fr or 6-Fr PICCs had a significantly greater risk of DVT (ORs=2.74 and 7.40, respectively).
Retrospective study
In The American Journal of Medicine, Dr Chopra and his colleagues described a retrospective study of bloodstream infections associated with PICCs.
The investigators analyzed data from 747 patients who received 966 PICCs for a total of 26,887 catheter days. Patients had PICCs for long-term antibiotic administration (n=503; 52%), venous access (n=201; 21%), total parenteral nutrition (n=155; 16%), and chemotherapy (n=107; 11%).
There were 58 cases (6%) of PICC-bloodstream infection over 1156 catheter days, for an infection rate of 2.16 per 1000 catheter days. The median time to infection was 10 days.
Bivariate analysis revealed several factors associated with PICC-bloodstream infections. These included intensive care unit status (ICU; OR=3.23), mechanical ventilation (OR=4.39), length of stay (hospital, OR=1.04; ICU, OR=1.03), PowerPICCs (OR=2.58), devices placed by interventional radiology (OR=2.57), double lumens (OR=5.21), and triple lumens (OR=10.84).
In multivariable analysis, only some of these factors remained significantly associated with PICC-bloodstream infection. These included hospital length of stay (OR=1.04), ICU status (OR=1.02), double lumens (OR=3.99), and triple lumens (OR=6.34).
Dr Chopra said the results of these 2 studies suggest hospitalists should tread carefully when considering PICCs.
“These are not innocuous devices,” he said. “The time has come to stop thinking of them as a device of convenience and rather one with clear risks and benefits.”
Review and guide
In the Journal of Hospital Medicine, Dr Chopra and his colleagues offered advice on choosing vascular access devices. After reviewing the literature, the investigators designed a flow chart that can help hospitalists decide which device is appropriate for each patient.
For instance, different devices will work best depending on whether access to the bloodstream is needed urgently or less urgently, whether the patient will likely need the device for more or less than a week, what kind of drug or nutrition the doctor will order, and whether the patient’s kidneys are functioning normally.
Pathway appears critical to HSC aging

in the bone marrow
Scientists say they’ve identified a molecular pathway that is critical to hematopoietic stem cell (HSC) aging and can be manipulated to rejuvenate blood.
The researchers found that HSCs’ ability to repair damage caused by inappropriate protein folding in the mitochondria is essential for the cells’ survival and regenerative capacity.
The discovery has implications for research on reversing the signs of aging, a process thought to be caused by increased cellular stress and damage.
“Ultimately, a cell dies when it can’t deal well with stress,” said study author Danica Chen, PhD, of the University of California, Berkeley.
“We found that by slowing down the activity of mitochondria in the blood stem cells of mice, we were able to enhance their capacity to handle stress and rejuvenate old blood. This confirms the significance of this pathway in the aging process.”
Mitochondria host a multitude of proteins that must be folded properly to function correctly. When the folding goes awry, the mitochondrial unfolded-protein response (UPRmt) kicks in to boost the production of specific proteins to fix or remove the misfolded protein.
There has been little research on the UPRmt pathway, but studies in roundworms suggest its activity increases when there is a burst of mitochondrial growth.
Dr Chen and her colleagues noted that adult stem cells are normally in a quiescent state with little mitochondrial activity. They are activated only when needed to replenish tissue.
At that time, the mitochondrial activity increases, and stem cells proliferate and differentiate. When protein-folding problems occur, this fast growth could lead to more harm.
Dr Chen’s lab stumbled upon the importance of UPRmt in HSC aging while studying sirtuins, a class of proteins recognized as stress-resistance regulators.
The researchers noticed that levels of one particular sirtuin, SIRT7, increase as a way to help cells cope with stress from misfolded proteins in the mitochondria. But SIRT7 levels decline with age.
“We isolated blood stem cells from aged mice and found that when we increased the levels of SIRT7, we were able to reduce mitochondrial protein-folding stress,” Dr Chen said. “We then transplanted the blood stem cells back into mice, and SIRT7 improved the blood stem cells’ regenerative capacity.”
The researchers also found that HSCs deficient in SIRT7 proliferate more. This faster growth is due to increased protein production and increased activity of the mitochondria, and slowing things down appears to be a critical step in giving cells time to recover from stress.
Dr Chen likened this to an auto accident or stalled car stopping traffic on a freeway.
“When there’s a mitochondrial protein-folding problem, there is a traffic jam in the mitochondria,” she said. “If you prevent more proteins from being created and added to the mitochondria, you are helping to reduce the jam.”
Until this study, it was unclear which stress signals regulate HSCs’ transition to and from the quiescent state and how that related to tissue regeneration during aging.
“Identifying the role of this mitochondrial pathway in blood stem cells gives us a new target for controlling the aging process,” Dr Chen said.
She and her colleagues described this work in Science.

in the bone marrow
Scientists say they’ve identified a molecular pathway that is critical to hematopoietic stem cell (HSC) aging and can be manipulated to rejuvenate blood.
The researchers found that HSCs’ ability to repair damage caused by inappropriate protein folding in the mitochondria is essential for the cells’ survival and regenerative capacity.
The discovery has implications for research on reversing the signs of aging, a process thought to be caused by increased cellular stress and damage.
“Ultimately, a cell dies when it can’t deal well with stress,” said study author Danica Chen, PhD, of the University of California, Berkeley.
“We found that by slowing down the activity of mitochondria in the blood stem cells of mice, we were able to enhance their capacity to handle stress and rejuvenate old blood. This confirms the significance of this pathway in the aging process.”
Mitochondria host a multitude of proteins that must be folded properly to function correctly. When the folding goes awry, the mitochondrial unfolded-protein response (UPRmt) kicks in to boost the production of specific proteins to fix or remove the misfolded protein.
There has been little research on the UPRmt pathway, but studies in roundworms suggest its activity increases when there is a burst of mitochondrial growth.
Dr Chen and her colleagues noted that adult stem cells are normally in a quiescent state with little mitochondrial activity. They are activated only when needed to replenish tissue.
At that time, the mitochondrial activity increases, and stem cells proliferate and differentiate. When protein-folding problems occur, this fast growth could lead to more harm.
Dr Chen’s lab stumbled upon the importance of UPRmt in HSC aging while studying sirtuins, a class of proteins recognized as stress-resistance regulators.
The researchers noticed that levels of one particular sirtuin, SIRT7, increase as a way to help cells cope with stress from misfolded proteins in the mitochondria. But SIRT7 levels decline with age.
“We isolated blood stem cells from aged mice and found that when we increased the levels of SIRT7, we were able to reduce mitochondrial protein-folding stress,” Dr Chen said. “We then transplanted the blood stem cells back into mice, and SIRT7 improved the blood stem cells’ regenerative capacity.”
The researchers also found that HSCs deficient in SIRT7 proliferate more. This faster growth is due to increased protein production and increased activity of the mitochondria, and slowing things down appears to be a critical step in giving cells time to recover from stress.
Dr Chen likened this to an auto accident or stalled car stopping traffic on a freeway.
“When there’s a mitochondrial protein-folding problem, there is a traffic jam in the mitochondria,” she said. “If you prevent more proteins from being created and added to the mitochondria, you are helping to reduce the jam.”
Until this study, it was unclear which stress signals regulate HSCs’ transition to and from the quiescent state and how that related to tissue regeneration during aging.
“Identifying the role of this mitochondrial pathway in blood stem cells gives us a new target for controlling the aging process,” Dr Chen said.
She and her colleagues described this work in Science.

in the bone marrow
Scientists say they’ve identified a molecular pathway that is critical to hematopoietic stem cell (HSC) aging and can be manipulated to rejuvenate blood.
The researchers found that HSCs’ ability to repair damage caused by inappropriate protein folding in the mitochondria is essential for the cells’ survival and regenerative capacity.
The discovery has implications for research on reversing the signs of aging, a process thought to be caused by increased cellular stress and damage.
“Ultimately, a cell dies when it can’t deal well with stress,” said study author Danica Chen, PhD, of the University of California, Berkeley.
“We found that by slowing down the activity of mitochondria in the blood stem cells of mice, we were able to enhance their capacity to handle stress and rejuvenate old blood. This confirms the significance of this pathway in the aging process.”
Mitochondria host a multitude of proteins that must be folded properly to function correctly. When the folding goes awry, the mitochondrial unfolded-protein response (UPRmt) kicks in to boost the production of specific proteins to fix or remove the misfolded protein.
There has been little research on the UPRmt pathway, but studies in roundworms suggest its activity increases when there is a burst of mitochondrial growth.
Dr Chen and her colleagues noted that adult stem cells are normally in a quiescent state with little mitochondrial activity. They are activated only when needed to replenish tissue.
At that time, the mitochondrial activity increases, and stem cells proliferate and differentiate. When protein-folding problems occur, this fast growth could lead to more harm.
Dr Chen’s lab stumbled upon the importance of UPRmt in HSC aging while studying sirtuins, a class of proteins recognized as stress-resistance regulators.
The researchers noticed that levels of one particular sirtuin, SIRT7, increase as a way to help cells cope with stress from misfolded proteins in the mitochondria. But SIRT7 levels decline with age.
“We isolated blood stem cells from aged mice and found that when we increased the levels of SIRT7, we were able to reduce mitochondrial protein-folding stress,” Dr Chen said. “We then transplanted the blood stem cells back into mice, and SIRT7 improved the blood stem cells’ regenerative capacity.”
The researchers also found that HSCs deficient in SIRT7 proliferate more. This faster growth is due to increased protein production and increased activity of the mitochondria, and slowing things down appears to be a critical step in giving cells time to recover from stress.
Dr Chen likened this to an auto accident or stalled car stopping traffic on a freeway.
“When there’s a mitochondrial protein-folding problem, there is a traffic jam in the mitochondria,” she said. “If you prevent more proteins from being created and added to the mitochondria, you are helping to reduce the jam.”
Until this study, it was unclear which stress signals regulate HSCs’ transition to and from the quiescent state and how that related to tissue regeneration during aging.
“Identifying the role of this mitochondrial pathway in blood stem cells gives us a new target for controlling the aging process,” Dr Chen said.
She and her colleagues described this work in Science.
Discovery may aid malaria vaccine development

a red blood cell
Image courtesy of St. Jude
Children’s Research Hospital
Researchers say they have made a major advance in the quest toward a viable malaria vaccine—by uncovering a strategy the immune system employs to protect against malaria infection.
The team discovered how antibodies work in partnership with complement proteins to block Plasmodium falciparum infection.
And they believe this finding will aid the development of vaccine candidates that are already under investigation.
“We have known that antibodies on their own are not highly effective at blocking malaria, so they must be getting help from other parts of the immune system,” said James Beeson, MBBS, PhD, of the Burnet Institute in Melbourne, Victoria, Australia.
“This new research provides evidence that complement plays a key role in antibody-mediated immunity to blood-stage replication of Plasmodium falciparum malaria in humans.”
Dr Beeson and his colleagues described their research in Immunity.
The team found that acquired and vaccine-induced human antibodies recruited complement to block red blood cell infection and blood-stage replication of P falciparum.
Without complement, many of the antibodies were not functional, and P falciparum merozoites invaded red blood cells. But when the antibodies interacted with complement factors, they were able to prevent invasion and lyse merozoites.
Further investigation revealed that inhibitory activity was mediated predominately by C1q fixation, and merozoite surface proteins (MSPs) 1 and 2 were major targets of antibody-mediated complement-dependent (Ab-C’) inhibition.
To examine the importance of antibody-mediated complement fixation in acquired immunity to malaria, the researchers tested antibodies for C1q fixation in 206 children (ages 5 to 14) living in a malaria-endemic region.
This revealed that complement fixation was strongly associated with protection from clinical malaria and high-density parasitemia.
The researchers also investigated whether Ab-C′ inhibitory activity could be induced by human immunization with a candidate MSP vaccine. They studied 10 immunoglobulin G (IgG) samples from a phase 1 trial of the MSP2-C1 vaccine.
Eight of the IgG samples showed substantial inhibition in normal serum, but not in heat-inactivated serum, which suggests vaccination induced Ab-C’ inhibition. The researchers did not observe inhibition in IgG from pre-vaccinated individuals or placebo-vaccinated samples.
The team said this suggests that MSP2 antibodies induced by vaccination can inhibit P falciparum invasion via Ab-C’ inhibition.
“We have shown that it is possible to effectively generate this protective immune response by immunizing humans with a candidate vaccine,” Dr Beeson said, noting that this “may prove a valuable strategy to prevent the devastating effects of malaria.”

a red blood cell
Image courtesy of St. Jude
Children’s Research Hospital
Researchers say they have made a major advance in the quest toward a viable malaria vaccine—by uncovering a strategy the immune system employs to protect against malaria infection.
The team discovered how antibodies work in partnership with complement proteins to block Plasmodium falciparum infection.
And they believe this finding will aid the development of vaccine candidates that are already under investigation.
“We have known that antibodies on their own are not highly effective at blocking malaria, so they must be getting help from other parts of the immune system,” said James Beeson, MBBS, PhD, of the Burnet Institute in Melbourne, Victoria, Australia.
“This new research provides evidence that complement plays a key role in antibody-mediated immunity to blood-stage replication of Plasmodium falciparum malaria in humans.”
Dr Beeson and his colleagues described their research in Immunity.
The team found that acquired and vaccine-induced human antibodies recruited complement to block red blood cell infection and blood-stage replication of P falciparum.
Without complement, many of the antibodies were not functional, and P falciparum merozoites invaded red blood cells. But when the antibodies interacted with complement factors, they were able to prevent invasion and lyse merozoites.
Further investigation revealed that inhibitory activity was mediated predominately by C1q fixation, and merozoite surface proteins (MSPs) 1 and 2 were major targets of antibody-mediated complement-dependent (Ab-C’) inhibition.
To examine the importance of antibody-mediated complement fixation in acquired immunity to malaria, the researchers tested antibodies for C1q fixation in 206 children (ages 5 to 14) living in a malaria-endemic region.
This revealed that complement fixation was strongly associated with protection from clinical malaria and high-density parasitemia.
The researchers also investigated whether Ab-C′ inhibitory activity could be induced by human immunization with a candidate MSP vaccine. They studied 10 immunoglobulin G (IgG) samples from a phase 1 trial of the MSP2-C1 vaccine.
Eight of the IgG samples showed substantial inhibition in normal serum, but not in heat-inactivated serum, which suggests vaccination induced Ab-C’ inhibition. The researchers did not observe inhibition in IgG from pre-vaccinated individuals or placebo-vaccinated samples.
The team said this suggests that MSP2 antibodies induced by vaccination can inhibit P falciparum invasion via Ab-C’ inhibition.
“We have shown that it is possible to effectively generate this protective immune response by immunizing humans with a candidate vaccine,” Dr Beeson said, noting that this “may prove a valuable strategy to prevent the devastating effects of malaria.”

a red blood cell
Image courtesy of St. Jude
Children’s Research Hospital
Researchers say they have made a major advance in the quest toward a viable malaria vaccine—by uncovering a strategy the immune system employs to protect against malaria infection.
The team discovered how antibodies work in partnership with complement proteins to block Plasmodium falciparum infection.
And they believe this finding will aid the development of vaccine candidates that are already under investigation.
“We have known that antibodies on their own are not highly effective at blocking malaria, so they must be getting help from other parts of the immune system,” said James Beeson, MBBS, PhD, of the Burnet Institute in Melbourne, Victoria, Australia.
“This new research provides evidence that complement plays a key role in antibody-mediated immunity to blood-stage replication of Plasmodium falciparum malaria in humans.”
Dr Beeson and his colleagues described their research in Immunity.
The team found that acquired and vaccine-induced human antibodies recruited complement to block red blood cell infection and blood-stage replication of P falciparum.
Without complement, many of the antibodies were not functional, and P falciparum merozoites invaded red blood cells. But when the antibodies interacted with complement factors, they were able to prevent invasion and lyse merozoites.
Further investigation revealed that inhibitory activity was mediated predominately by C1q fixation, and merozoite surface proteins (MSPs) 1 and 2 were major targets of antibody-mediated complement-dependent (Ab-C’) inhibition.
To examine the importance of antibody-mediated complement fixation in acquired immunity to malaria, the researchers tested antibodies for C1q fixation in 206 children (ages 5 to 14) living in a malaria-endemic region.
This revealed that complement fixation was strongly associated with protection from clinical malaria and high-density parasitemia.
The researchers also investigated whether Ab-C′ inhibitory activity could be induced by human immunization with a candidate MSP vaccine. They studied 10 immunoglobulin G (IgG) samples from a phase 1 trial of the MSP2-C1 vaccine.
Eight of the IgG samples showed substantial inhibition in normal serum, but not in heat-inactivated serum, which suggests vaccination induced Ab-C’ inhibition. The researchers did not observe inhibition in IgG from pre-vaccinated individuals or placebo-vaccinated samples.
The team said this suggests that MSP2 antibodies induced by vaccination can inhibit P falciparum invasion via Ab-C’ inhibition.
“We have shown that it is possible to effectively generate this protective immune response by immunizing humans with a candidate vaccine,” Dr Beeson said, noting that this “may prove a valuable strategy to prevent the devastating effects of malaria.”