User login
Low-dose steroids may not increase cardiovascular risk in rheumatoid arthritis
A daily prednisolone dose of 5 mg or higher is associated with increased risk for major adverse cardiovascular events (MACE) among patients with rheumatoid arthritis (RA), data suggest. Patients taking daily doses below this threshold did not appear to have an increased risk of MACE, compared with those not taking glucocorticoids (GCs).
Other studies of GCs and CV risk among RA patients have yielded conflicting results, especially for low-dose GCs. Findings from a 2020 study published in PLOS Medicine suggested that patients who had several immune-mediated inflammatory diseases – including RA – and who took less than a 5-mg prednisolone-equivalent dose daily had 74% higher risk for all-cause CVD, compared with nonusers. But results from a 2021 study published in Annals of the Rheumatic Diseases suggested that a daily prednisone dose of 4 mg or less did not increase cardiovascular events over a period of 6 months to 1 year.
These contradictory results were “primarily due to incomplete control of confounding variables, such as failure to adjust for C-reactive protein (CRP) levels,” Dr. Tam said. “Our study aimed to use a big data analytical approach to determine the effect of systemic GC dose and duration on the risk of major adverse cardiovascular events in patients with RA, while controlling for systemic inflammation, traditional CV risk factors, and other therapies.”
Is there a ‘safe’ dose for glucocorticoids?
To analyze this relationship, Dr. Lam and colleagues used the Hospital Authority Data Collaboration Laboratory, a citywide health care database. The investigators recruited patients with RA who had no history of MACE from 2006 to 2015 and followed them until the end of 2018. The primary outcome was the first occurrence of a MACE, defined as a composite of myocardial infarction (MI), unstable angina, ischemic or hemorrhagic cerebrovascular accident, transient ischemic attack, and CV death.
The study was published in Annals of the Rheumatic Diseases.
The analysis included 12,233 patients with RA and had over 105,826 person-years of follow-up. The average follow-up time was 8.7 years. During the study period, 860 patients had their first MACE. After controlling for confounding factors, a daily prednisolone dose of 5 mg or higher doubled the risk for MACE, compared with GC nonusers. MACE risk increased by 7% per month.
Long-term glucocorticoid use discouraged
Daily doses of less than 5 mg were not associated with higher MACE risk, but more research is necessary to understand whether these low doses are clinically efficacious, Dr. Tam said. “The study results suggest that a very-low-dose GC (less than 5 mg prednisolone daily) may be cardiovascular risk–neutral. However, further evaluation is needed to determine whether this dose is therapeutic. Other potential side effects, such as bone loss, increased infection risk, dyslipidemia, and hyperglycemia, should also be considered.”
Both the American College of Rheumatology and the European Alliance of Associations for Rheumatology acknowledge that short-term GCs may be necessary for some RA patients, but they emphasize using the smallest necessary dose for the shortest period possible because of the known toxicity of GCs.
“We recommend stopping GCs as soon as it is clinically feasible, in line with previous recommendations, until these issues are investigated further,” Dr. Tam added.
Dr. Bartels agreed that long-term use of GCs should be avoided if possible, even at lower doses, because although CV risk may be less of an issue, studies have shown an increased risk for infection even at GC doses of less than 5 mg a day.
How might risk increase with dose?
While the study showed a distinct difference in risk with doses of prednisolone higher and lower than 5 mg, more information on how risk increases with dose could be useful, said Beth Wallace, MD, an assistant professor in internal medicine at the University of Michigan, Ann Arbor, and a staff rheumatologist at the VA Ann Arbor Healthcare Center. She was also unaffiliated with the research. “If someone is on 5-10 mg ... how much better is that than being on 10-20 mg or being on 20-30 mg?” she asked. While these study findings are “very important,” she said, it would be useful to know the risk associated with 7.5 mg vs. a higher dose.
But even in this relatively healthy population in Hong Kong, “taking more than 5 mg of prednisolone doubles the risk of cardiovascular disease,” Dr. Wallace added. This is important for clinicians to know, especially if they are more cautious about prescribing steroids to older or sicker patients but are “using [the drugs] a little more indiscriminately in younger people and healthier people.”
The study did not receive outside funding. Dr. Tam and Dr. Bartels report no relevant financial relationships. Dr. Wallace has received a grant from the Department of Veterans Affairs Administration to study steroid tapering in RA.
A version of this article first appeared on Medscape.com.
A daily prednisolone dose of 5 mg or higher is associated with increased risk for major adverse cardiovascular events (MACE) among patients with rheumatoid arthritis (RA), data suggest. Patients taking daily doses below this threshold did not appear to have an increased risk of MACE, compared with those not taking glucocorticoids (GCs).
Other studies of GCs and CV risk among RA patients have yielded conflicting results, especially for low-dose GCs. Findings from a 2020 study published in PLOS Medicine suggested that patients who had several immune-mediated inflammatory diseases – including RA – and who took less than a 5-mg prednisolone-equivalent dose daily had 74% higher risk for all-cause CVD, compared with nonusers. But results from a 2021 study published in Annals of the Rheumatic Diseases suggested that a daily prednisone dose of 4 mg or less did not increase cardiovascular events over a period of 6 months to 1 year.
These contradictory results were “primarily due to incomplete control of confounding variables, such as failure to adjust for C-reactive protein (CRP) levels,” Dr. Tam said. “Our study aimed to use a big data analytical approach to determine the effect of systemic GC dose and duration on the risk of major adverse cardiovascular events in patients with RA, while controlling for systemic inflammation, traditional CV risk factors, and other therapies.”
Is there a ‘safe’ dose for glucocorticoids?
To analyze this relationship, Dr. Lam and colleagues used the Hospital Authority Data Collaboration Laboratory, a citywide health care database. The investigators recruited patients with RA who had no history of MACE from 2006 to 2015 and followed them until the end of 2018. The primary outcome was the first occurrence of a MACE, defined as a composite of myocardial infarction (MI), unstable angina, ischemic or hemorrhagic cerebrovascular accident, transient ischemic attack, and CV death.
The study was published in Annals of the Rheumatic Diseases.
The analysis included 12,233 patients with RA and had over 105,826 person-years of follow-up. The average follow-up time was 8.7 years. During the study period, 860 patients had their first MACE. After controlling for confounding factors, a daily prednisolone dose of 5 mg or higher doubled the risk for MACE, compared with GC nonusers. MACE risk increased by 7% per month.
Long-term glucocorticoid use discouraged
Daily doses of less than 5 mg were not associated with higher MACE risk, but more research is necessary to understand whether these low doses are clinically efficacious, Dr. Tam said. “The study results suggest that a very-low-dose GC (less than 5 mg prednisolone daily) may be cardiovascular risk–neutral. However, further evaluation is needed to determine whether this dose is therapeutic. Other potential side effects, such as bone loss, increased infection risk, dyslipidemia, and hyperglycemia, should also be considered.”
Both the American College of Rheumatology and the European Alliance of Associations for Rheumatology acknowledge that short-term GCs may be necessary for some RA patients, but they emphasize using the smallest necessary dose for the shortest period possible because of the known toxicity of GCs.
“We recommend stopping GCs as soon as it is clinically feasible, in line with previous recommendations, until these issues are investigated further,” Dr. Tam added.
Dr. Bartels agreed that long-term use of GCs should be avoided if possible, even at lower doses, because although CV risk may be less of an issue, studies have shown an increased risk for infection even at GC doses of less than 5 mg a day.
How might risk increase with dose?
While the study showed a distinct difference in risk with doses of prednisolone higher and lower than 5 mg, more information on how risk increases with dose could be useful, said Beth Wallace, MD, an assistant professor in internal medicine at the University of Michigan, Ann Arbor, and a staff rheumatologist at the VA Ann Arbor Healthcare Center. She was also unaffiliated with the research. “If someone is on 5-10 mg ... how much better is that than being on 10-20 mg or being on 20-30 mg?” she asked. While these study findings are “very important,” she said, it would be useful to know the risk associated with 7.5 mg vs. a higher dose.
But even in this relatively healthy population in Hong Kong, “taking more than 5 mg of prednisolone doubles the risk of cardiovascular disease,” Dr. Wallace added. This is important for clinicians to know, especially if they are more cautious about prescribing steroids to older or sicker patients but are “using [the drugs] a little more indiscriminately in younger people and healthier people.”
The study did not receive outside funding. Dr. Tam and Dr. Bartels report no relevant financial relationships. Dr. Wallace has received a grant from the Department of Veterans Affairs Administration to study steroid tapering in RA.
A version of this article first appeared on Medscape.com.
A daily prednisolone dose of 5 mg or higher is associated with increased risk for major adverse cardiovascular events (MACE) among patients with rheumatoid arthritis (RA), data suggest. Patients taking daily doses below this threshold did not appear to have an increased risk of MACE, compared with those not taking glucocorticoids (GCs).
Other studies of GCs and CV risk among RA patients have yielded conflicting results, especially for low-dose GCs. Findings from a 2020 study published in PLOS Medicine suggested that patients who had several immune-mediated inflammatory diseases – including RA – and who took less than a 5-mg prednisolone-equivalent dose daily had 74% higher risk for all-cause CVD, compared with nonusers. But results from a 2021 study published in Annals of the Rheumatic Diseases suggested that a daily prednisone dose of 4 mg or less did not increase cardiovascular events over a period of 6 months to 1 year.
These contradictory results were “primarily due to incomplete control of confounding variables, such as failure to adjust for C-reactive protein (CRP) levels,” Dr. Tam said. “Our study aimed to use a big data analytical approach to determine the effect of systemic GC dose and duration on the risk of major adverse cardiovascular events in patients with RA, while controlling for systemic inflammation, traditional CV risk factors, and other therapies.”
Is there a ‘safe’ dose for glucocorticoids?
To analyze this relationship, Dr. Lam and colleagues used the Hospital Authority Data Collaboration Laboratory, a citywide health care database. The investigators recruited patients with RA who had no history of MACE from 2006 to 2015 and followed them until the end of 2018. The primary outcome was the first occurrence of a MACE, defined as a composite of myocardial infarction (MI), unstable angina, ischemic or hemorrhagic cerebrovascular accident, transient ischemic attack, and CV death.
The study was published in Annals of the Rheumatic Diseases.
The analysis included 12,233 patients with RA and had over 105,826 person-years of follow-up. The average follow-up time was 8.7 years. During the study period, 860 patients had their first MACE. After controlling for confounding factors, a daily prednisolone dose of 5 mg or higher doubled the risk for MACE, compared with GC nonusers. MACE risk increased by 7% per month.
Long-term glucocorticoid use discouraged
Daily doses of less than 5 mg were not associated with higher MACE risk, but more research is necessary to understand whether these low doses are clinically efficacious, Dr. Tam said. “The study results suggest that a very-low-dose GC (less than 5 mg prednisolone daily) may be cardiovascular risk–neutral. However, further evaluation is needed to determine whether this dose is therapeutic. Other potential side effects, such as bone loss, increased infection risk, dyslipidemia, and hyperglycemia, should also be considered.”
Both the American College of Rheumatology and the European Alliance of Associations for Rheumatology acknowledge that short-term GCs may be necessary for some RA patients, but they emphasize using the smallest necessary dose for the shortest period possible because of the known toxicity of GCs.
“We recommend stopping GCs as soon as it is clinically feasible, in line with previous recommendations, until these issues are investigated further,” Dr. Tam added.
Dr. Bartels agreed that long-term use of GCs should be avoided if possible, even at lower doses, because although CV risk may be less of an issue, studies have shown an increased risk for infection even at GC doses of less than 5 mg a day.
How might risk increase with dose?
While the study showed a distinct difference in risk with doses of prednisolone higher and lower than 5 mg, more information on how risk increases with dose could be useful, said Beth Wallace, MD, an assistant professor in internal medicine at the University of Michigan, Ann Arbor, and a staff rheumatologist at the VA Ann Arbor Healthcare Center. She was also unaffiliated with the research. “If someone is on 5-10 mg ... how much better is that than being on 10-20 mg or being on 20-30 mg?” she asked. While these study findings are “very important,” she said, it would be useful to know the risk associated with 7.5 mg vs. a higher dose.
But even in this relatively healthy population in Hong Kong, “taking more than 5 mg of prednisolone doubles the risk of cardiovascular disease,” Dr. Wallace added. This is important for clinicians to know, especially if they are more cautious about prescribing steroids to older or sicker patients but are “using [the drugs] a little more indiscriminately in younger people and healthier people.”
The study did not receive outside funding. Dr. Tam and Dr. Bartels report no relevant financial relationships. Dr. Wallace has received a grant from the Department of Veterans Affairs Administration to study steroid tapering in RA.
A version of this article first appeared on Medscape.com.
FROM ANNALS OF THE RHEUMATIC DISEASES
Tools may predict inflammatory arthritis in at-risk patients
, according to new research from England.
If validated in further studies, a new simple score using common biomarkers may help identify individuals who can be managed in primary care as well as higher-risk patients who should be referred to a rheumatologist.
The researchers designed a second comprehensive score adding genetics and ultrasound as a tool to identify patients at highest risk for IA for intervention studies and to guide clinical monitoring and care by specialists.
Though there are blood markers and early symptoms in patients that may signal a higher risk for IA, “we don’t know what to do with those people yet,” said Kevin D. Deane, MD, PhD, associate professor of medicine and chair in rheumatology research at the University of Colorado at Denver, Aurora.
“Understanding how to assess these people and predict who’s going to go on to get full blown IA that we should actually treat is very beneficial to the field,” Dr. Deane said. He was not involved with the research but had reviewed an early draft of the paper.
Study seeks to stratify at-risk population
For the study, researchers recruited 455 participants from June 2008 to November 2021, primarily through the UK Primary Care Clinical Research Network. All individuals had new musculoskeletal symptoms, a positive test for anticitrullinated protein antibodies (anti-CCP), and no clinical synovitis.
The researchers selected for anti-CCP positivity because these antibodies are associated with a more aggressive arthritis phenotype. Interventional trials have also found that these anti-CCP–positive individuals are the most responsive to disease-modifying antirheumatic therapy prior to IA development. Patients were followed for at least 48 weeks or until an IA diagnosis.
Using data from this cohort, the team ran statistical analyses guided by potential clinical impact. For the simple score, they aimed to ensure that most people who would go on to develop IA would be identified earlier in clinical practice. For the comprehensive score, they wanted to balance the potential harm of giving preventive treatment to someone who would not develop IA with failing to provide preventive treatment to someone who would develop IA, the authors write.
They developed two scores: a simple score to identify people at lower risk for IA and a comprehensive score to stratify high-risk individuals. The simple score used anti-CCP level, rheumatoid factor value, early morning stiffness, and erythrocyte sedimentation rate to calculate risk.
In addition to these factors, the comprehensive score added smoking history, ultrasound abnormalities, genetic markers for the rheumatoid arthritis shared epitope, as well as patient-reported outcomes from the Health Assessment Questionnaire and the visual analogue scale for global pain.
The study was published in the Annals of Internal Medicine.
Simple score rates more than half as low risk
The simple score identified 249 low-risk individuals, defined as having a less than 10% chance of developing IA within 1 year, with a 5% false-negative rate. This score can help determine which individuals do not need to be referred to a specialist even though they have some known risk factors, said Paul Emery, MD, director of the Leeds Biomedical Research Centre and clinical professor at the University of Leeds in England. He is a co–senior author of the research.
“If you had unlimited resources, you’d refer everyone. But in the real world, we would be overloaded in secondary care, and it just wouldn’t work,” he said. “This is a way of making sure the right people are referred into secondary care.”
The comprehensive score identified 119 high-risk individuals, defined as having a 50% chance or greater of developing IA in 5 years, with a false-positive rate of 29%. Of this high-risk group, 40% developed IA within 1 year, and 71% developed IA in 5 years.
Beyond identifying those who should be referred to specialist care, Dr. Emery noted, this score could be used in research studies to find patients for experimental clinical trials aimed at delaying or preventing the onset of IA.
Both Dr. Emery and Dr. Deane agreed that further research is needed to validate these findings in different patient populations as well as to understand how the scores could be integrated into clinical practice.
What is the role of anti-CCP tests in primary care?
The study also brings up additional questions about the use of anti-CCP tests in primary care, Dr. Deane said. Though previously considered a “specialty test” 10-15 years ago, “now, we really want primary care to do this test along with the rheumatoid factor test,” he noted.
Because the study only included individuals with anti-CCP antibodies, it did not touch on which patients should be getting tested in the first place. Would all patients coming into primary care with joint pain benefit from these blood-marker tests, Deane asked, or would only certain patients qualify? “I think that’s uncertain, and we need to learn more,” he said.
An additional caveat is that the researchers used abnormal ultrasound findings as a predictor of future IA in the comprehensive model, but many clinicians already use ultrasound to identify arthritis, Dr. Deane said.
“If a rheumatologist sees power Doppler signal or erosions, even if the physical examination of a joint didn’t find swelling or inflammation, then they are likely to say that this person has IA now,” and will start treatment, he said. “Because of that, it could be challenging to use ultrasound as a ‘predictive’ marker in clinical practice,” he added, but additional research could help elucidate when to wait on treatment even with abnormal ultrasound findings.
This study was funded by the UK National Institute for Health and Care Research Leeds Biomedical Research Centre. Dr. Emery disclosed financial relationships with AbbVie, AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Galapagos, Gilead, Novartis, and Samsung Bioepis. Dr. Deane reports receiving consulting fees from Werfen.
A version of this article appeared on Medscape.com.
, according to new research from England.
If validated in further studies, a new simple score using common biomarkers may help identify individuals who can be managed in primary care as well as higher-risk patients who should be referred to a rheumatologist.
The researchers designed a second comprehensive score adding genetics and ultrasound as a tool to identify patients at highest risk for IA for intervention studies and to guide clinical monitoring and care by specialists.
Though there are blood markers and early symptoms in patients that may signal a higher risk for IA, “we don’t know what to do with those people yet,” said Kevin D. Deane, MD, PhD, associate professor of medicine and chair in rheumatology research at the University of Colorado at Denver, Aurora.
“Understanding how to assess these people and predict who’s going to go on to get full blown IA that we should actually treat is very beneficial to the field,” Dr. Deane said. He was not involved with the research but had reviewed an early draft of the paper.
Study seeks to stratify at-risk population
For the study, researchers recruited 455 participants from June 2008 to November 2021, primarily through the UK Primary Care Clinical Research Network. All individuals had new musculoskeletal symptoms, a positive test for anticitrullinated protein antibodies (anti-CCP), and no clinical synovitis.
The researchers selected for anti-CCP positivity because these antibodies are associated with a more aggressive arthritis phenotype. Interventional trials have also found that these anti-CCP–positive individuals are the most responsive to disease-modifying antirheumatic therapy prior to IA development. Patients were followed for at least 48 weeks or until an IA diagnosis.
Using data from this cohort, the team ran statistical analyses guided by potential clinical impact. For the simple score, they aimed to ensure that most people who would go on to develop IA would be identified earlier in clinical practice. For the comprehensive score, they wanted to balance the potential harm of giving preventive treatment to someone who would not develop IA with failing to provide preventive treatment to someone who would develop IA, the authors write.
They developed two scores: a simple score to identify people at lower risk for IA and a comprehensive score to stratify high-risk individuals. The simple score used anti-CCP level, rheumatoid factor value, early morning stiffness, and erythrocyte sedimentation rate to calculate risk.
In addition to these factors, the comprehensive score added smoking history, ultrasound abnormalities, genetic markers for the rheumatoid arthritis shared epitope, as well as patient-reported outcomes from the Health Assessment Questionnaire and the visual analogue scale for global pain.
The study was published in the Annals of Internal Medicine.
Simple score rates more than half as low risk
The simple score identified 249 low-risk individuals, defined as having a less than 10% chance of developing IA within 1 year, with a 5% false-negative rate. This score can help determine which individuals do not need to be referred to a specialist even though they have some known risk factors, said Paul Emery, MD, director of the Leeds Biomedical Research Centre and clinical professor at the University of Leeds in England. He is a co–senior author of the research.
“If you had unlimited resources, you’d refer everyone. But in the real world, we would be overloaded in secondary care, and it just wouldn’t work,” he said. “This is a way of making sure the right people are referred into secondary care.”
The comprehensive score identified 119 high-risk individuals, defined as having a 50% chance or greater of developing IA in 5 years, with a false-positive rate of 29%. Of this high-risk group, 40% developed IA within 1 year, and 71% developed IA in 5 years.
Beyond identifying those who should be referred to specialist care, Dr. Emery noted, this score could be used in research studies to find patients for experimental clinical trials aimed at delaying or preventing the onset of IA.
Both Dr. Emery and Dr. Deane agreed that further research is needed to validate these findings in different patient populations as well as to understand how the scores could be integrated into clinical practice.
What is the role of anti-CCP tests in primary care?
The study also brings up additional questions about the use of anti-CCP tests in primary care, Dr. Deane said. Though previously considered a “specialty test” 10-15 years ago, “now, we really want primary care to do this test along with the rheumatoid factor test,” he noted.
Because the study only included individuals with anti-CCP antibodies, it did not touch on which patients should be getting tested in the first place. Would all patients coming into primary care with joint pain benefit from these blood-marker tests, Deane asked, or would only certain patients qualify? “I think that’s uncertain, and we need to learn more,” he said.
An additional caveat is that the researchers used abnormal ultrasound findings as a predictor of future IA in the comprehensive model, but many clinicians already use ultrasound to identify arthritis, Dr. Deane said.
“If a rheumatologist sees power Doppler signal or erosions, even if the physical examination of a joint didn’t find swelling or inflammation, then they are likely to say that this person has IA now,” and will start treatment, he said. “Because of that, it could be challenging to use ultrasound as a ‘predictive’ marker in clinical practice,” he added, but additional research could help elucidate when to wait on treatment even with abnormal ultrasound findings.
This study was funded by the UK National Institute for Health and Care Research Leeds Biomedical Research Centre. Dr. Emery disclosed financial relationships with AbbVie, AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Galapagos, Gilead, Novartis, and Samsung Bioepis. Dr. Deane reports receiving consulting fees from Werfen.
A version of this article appeared on Medscape.com.
, according to new research from England.
If validated in further studies, a new simple score using common biomarkers may help identify individuals who can be managed in primary care as well as higher-risk patients who should be referred to a rheumatologist.
The researchers designed a second comprehensive score adding genetics and ultrasound as a tool to identify patients at highest risk for IA for intervention studies and to guide clinical monitoring and care by specialists.
Though there are blood markers and early symptoms in patients that may signal a higher risk for IA, “we don’t know what to do with those people yet,” said Kevin D. Deane, MD, PhD, associate professor of medicine and chair in rheumatology research at the University of Colorado at Denver, Aurora.
“Understanding how to assess these people and predict who’s going to go on to get full blown IA that we should actually treat is very beneficial to the field,” Dr. Deane said. He was not involved with the research but had reviewed an early draft of the paper.
Study seeks to stratify at-risk population
For the study, researchers recruited 455 participants from June 2008 to November 2021, primarily through the UK Primary Care Clinical Research Network. All individuals had new musculoskeletal symptoms, a positive test for anticitrullinated protein antibodies (anti-CCP), and no clinical synovitis.
The researchers selected for anti-CCP positivity because these antibodies are associated with a more aggressive arthritis phenotype. Interventional trials have also found that these anti-CCP–positive individuals are the most responsive to disease-modifying antirheumatic therapy prior to IA development. Patients were followed for at least 48 weeks or until an IA diagnosis.
Using data from this cohort, the team ran statistical analyses guided by potential clinical impact. For the simple score, they aimed to ensure that most people who would go on to develop IA would be identified earlier in clinical practice. For the comprehensive score, they wanted to balance the potential harm of giving preventive treatment to someone who would not develop IA with failing to provide preventive treatment to someone who would develop IA, the authors write.
They developed two scores: a simple score to identify people at lower risk for IA and a comprehensive score to stratify high-risk individuals. The simple score used anti-CCP level, rheumatoid factor value, early morning stiffness, and erythrocyte sedimentation rate to calculate risk.
In addition to these factors, the comprehensive score added smoking history, ultrasound abnormalities, genetic markers for the rheumatoid arthritis shared epitope, as well as patient-reported outcomes from the Health Assessment Questionnaire and the visual analogue scale for global pain.
The study was published in the Annals of Internal Medicine.
Simple score rates more than half as low risk
The simple score identified 249 low-risk individuals, defined as having a less than 10% chance of developing IA within 1 year, with a 5% false-negative rate. This score can help determine which individuals do not need to be referred to a specialist even though they have some known risk factors, said Paul Emery, MD, director of the Leeds Biomedical Research Centre and clinical professor at the University of Leeds in England. He is a co–senior author of the research.
“If you had unlimited resources, you’d refer everyone. But in the real world, we would be overloaded in secondary care, and it just wouldn’t work,” he said. “This is a way of making sure the right people are referred into secondary care.”
The comprehensive score identified 119 high-risk individuals, defined as having a 50% chance or greater of developing IA in 5 years, with a false-positive rate of 29%. Of this high-risk group, 40% developed IA within 1 year, and 71% developed IA in 5 years.
Beyond identifying those who should be referred to specialist care, Dr. Emery noted, this score could be used in research studies to find patients for experimental clinical trials aimed at delaying or preventing the onset of IA.
Both Dr. Emery and Dr. Deane agreed that further research is needed to validate these findings in different patient populations as well as to understand how the scores could be integrated into clinical practice.
What is the role of anti-CCP tests in primary care?
The study also brings up additional questions about the use of anti-CCP tests in primary care, Dr. Deane said. Though previously considered a “specialty test” 10-15 years ago, “now, we really want primary care to do this test along with the rheumatoid factor test,” he noted.
Because the study only included individuals with anti-CCP antibodies, it did not touch on which patients should be getting tested in the first place. Would all patients coming into primary care with joint pain benefit from these blood-marker tests, Deane asked, or would only certain patients qualify? “I think that’s uncertain, and we need to learn more,” he said.
An additional caveat is that the researchers used abnormal ultrasound findings as a predictor of future IA in the comprehensive model, but many clinicians already use ultrasound to identify arthritis, Dr. Deane said.
“If a rheumatologist sees power Doppler signal or erosions, even if the physical examination of a joint didn’t find swelling or inflammation, then they are likely to say that this person has IA now,” and will start treatment, he said. “Because of that, it could be challenging to use ultrasound as a ‘predictive’ marker in clinical practice,” he added, but additional research could help elucidate when to wait on treatment even with abnormal ultrasound findings.
This study was funded by the UK National Institute for Health and Care Research Leeds Biomedical Research Centre. Dr. Emery disclosed financial relationships with AbbVie, AstraZeneca, Bristol-Myers Squibb, Eli Lilly, Galapagos, Gilead, Novartis, and Samsung Bioepis. Dr. Deane reports receiving consulting fees from Werfen.
A version of this article appeared on Medscape.com.
FROM ANNALS OF INTERNAL MEDICINE
Could risk stratifying methotrexate users lead to less frequent testing?
A new model can predict which patients are more likely to experience side effects from long-term methotrexate (MTX) use, research suggests. Patients with a lower risk profile may benefit from less frequent testing, the authors hypothesize.
Most recommendations advise that patients initiating MTX therapy should get blood testing every 2-4 weeks to monitor for full blood count, liver function, urea electrolytes, and creatinine. After 6 months taking MTX, monitoring can be tapered to every 3 months. But Abhishek Abhishek, MD, PhD, professor of rheumatology and honorary consultant rheumatologist at Nottingham (England) University Hospitals NHS Trust and colleagues argue that abnormal results after the initial 6 months of treatment are “infrequent,” and patients may benefit from fewer tests throughout the year.
“Unnecessary blood tests waste patients’ time and health care resources, including the time of general practitioners and phlebotomists,” Dr. Abhishek and associates write. “It would be beneficial to predict the risk of clinically significant abnormal blood test results during long-term methotrexate treatment to inform the frequency of testing for individuals.”
Stratifying risk
In the study, published in the BMJ, researchers used the UK’s Clinical Practice Research Datalink (CPRD) to identify the electronic medical records of over 37,000 adult patients with an immune-mediated inflammatory disease who were prescribed MTX during 2007-2019. All included patients were prescribed MTX for at least 6 months. The main outcome was discontinuation of methotrexate because of abnormal blood test results. Around 62% of patients had rheumatoid arthritis and 22% had psoriasis or psoriatic arthritis.
Using these anonymized data, the group developed a risk stratification model using 11 clinical predictors. “The factors that went in the model are simple things that most patients can self-report or doctors can get from their patient’s medical records,” Dr. Abhishek told this news organization, including methotrexate dose, age, sex, and comorbidities. Dr. Abhishek emphasized that the model should be used only in patients who have continued taking MTX for at least 6 months and have already undergone more frequent initial testing.
The strongest individual predictors were diabetes (hazard ratio, 1.25), chronic kidney disease stage 3 (HR, 2.01), and previous cytopenia or raised liver enzyme levels during the first 6 months of MTX therapy (HR, 2.97). However, Dr. Abhishek emphasized that the individual factors were less important, noting that the model sums the risks to predict outcomes more accurately. Most patients (68.4%) were sorted into the low-risk cohort, with a less than 10% estimated risk of discontinuing MTX over the next 5 years. About one-fifth (20.9%) were categorized as moderate risk (10%-20% estimated risk over 5 years), and 10.7% were high risk, with a greater than 20% estimated risk of discontinuing the drug over 5 years.
The authors argue that low-risk patients could receive less frequent testing – perhaps every 6 months or annually, while moderate-risk patients would continue to be tested every 3 months. High-risk patients could potentially be tested with even greater frequently.
More research needed
The research involved “incredibly sophisticated statistical analysis,” said Daniel E. Furst, MD, professor emeritus of medicine at the University of California, Los Angeles, who was not involved with the study. However, the data do not yet support altering blood testing frequency based on this model.
“The hypothesis that not all patients have to be examined so frequently is a very reasonable hypothesis,” Dr. Furst said in an interview, and additional research is needed to corroborate it. The model also needs to be validated in patient populations outside of the United Kingdom, he added.
Dr. Abhishek agreed that validating the model in other patient populations is an important next step. “When we develop a tool [using] a one-nation data set, we want other researchers to then validate it in other countries’ data sets to make sure there is nothing odd about patients in the U.K. that makes the tool work well here but not in [the] U.S., Europe, or Asia, for example,” he said. Doing so should be relatively easy, he said, as the model is publicly available, and the information required is routinely collected during clinic visits.
To understand if less frequent testing might be appropriate for some patients, researchers would need to look at data registries like the Brigham and Women’s Hospital Rheumatoid Arthritis Sequential Study (BRASS) registry or CorEvitas registries “where the testing is done in a very regular way over the long haul,” Dr. Furst said. Analyzing these datasets, researchers could determine the testing intervals that would be most efficient for low- and high-risk patients.
A word of caution
While less frequent testing for long-term MTX therapy could likely have benefits, there is still some risk involved, cautioned Prabha Ranganathan, MD, professor of medicine at Washington University in St. Louis.
“Although most methotrexate toxicity occurs within the first 6 months of starting treatment, rare idiosyncratic toxicity can occur that does not correlate with the dose, duration, or method of how methotrexate is administered,” she wrote in an accompanying editorial. “Most rheumatologists can identify a handful of patients who receive methotrexate in their practice who develop sudden leukopenia or thrombocytopenia or transaminitis that is severe enough to warrant drug discontinuation.” While tools like this prediction model can be useful, clinicians need to consider each patient individually and use shared decision-making when monitoring for MTX toxicity, she advised.
“As in most of areas of medicine, the one-size-fits-all approach does not work for methotrexate users,” she noted.
This study was funded by the U.K. National Institute for Health and Care Research and Health Technology Assessment. Dr. Abhishek has received institutional research grants from AstraZeneca and Oxford Immunotech and personal fees from UpToDate, Springer, Cadila Pharmaceuticals, NGM Bio, Limbic, and Inflazome. Dr. Furst and Dr. Ranganathan report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new model can predict which patients are more likely to experience side effects from long-term methotrexate (MTX) use, research suggests. Patients with a lower risk profile may benefit from less frequent testing, the authors hypothesize.
Most recommendations advise that patients initiating MTX therapy should get blood testing every 2-4 weeks to monitor for full blood count, liver function, urea electrolytes, and creatinine. After 6 months taking MTX, monitoring can be tapered to every 3 months. But Abhishek Abhishek, MD, PhD, professor of rheumatology and honorary consultant rheumatologist at Nottingham (England) University Hospitals NHS Trust and colleagues argue that abnormal results after the initial 6 months of treatment are “infrequent,” and patients may benefit from fewer tests throughout the year.
“Unnecessary blood tests waste patients’ time and health care resources, including the time of general practitioners and phlebotomists,” Dr. Abhishek and associates write. “It would be beneficial to predict the risk of clinically significant abnormal blood test results during long-term methotrexate treatment to inform the frequency of testing for individuals.”
Stratifying risk
In the study, published in the BMJ, researchers used the UK’s Clinical Practice Research Datalink (CPRD) to identify the electronic medical records of over 37,000 adult patients with an immune-mediated inflammatory disease who were prescribed MTX during 2007-2019. All included patients were prescribed MTX for at least 6 months. The main outcome was discontinuation of methotrexate because of abnormal blood test results. Around 62% of patients had rheumatoid arthritis and 22% had psoriasis or psoriatic arthritis.
Using these anonymized data, the group developed a risk stratification model using 11 clinical predictors. “The factors that went in the model are simple things that most patients can self-report or doctors can get from their patient’s medical records,” Dr. Abhishek told this news organization, including methotrexate dose, age, sex, and comorbidities. Dr. Abhishek emphasized that the model should be used only in patients who have continued taking MTX for at least 6 months and have already undergone more frequent initial testing.
The strongest individual predictors were diabetes (hazard ratio, 1.25), chronic kidney disease stage 3 (HR, 2.01), and previous cytopenia or raised liver enzyme levels during the first 6 months of MTX therapy (HR, 2.97). However, Dr. Abhishek emphasized that the individual factors were less important, noting that the model sums the risks to predict outcomes more accurately. Most patients (68.4%) were sorted into the low-risk cohort, with a less than 10% estimated risk of discontinuing MTX over the next 5 years. About one-fifth (20.9%) were categorized as moderate risk (10%-20% estimated risk over 5 years), and 10.7% were high risk, with a greater than 20% estimated risk of discontinuing the drug over 5 years.
The authors argue that low-risk patients could receive less frequent testing – perhaps every 6 months or annually, while moderate-risk patients would continue to be tested every 3 months. High-risk patients could potentially be tested with even greater frequently.
More research needed
The research involved “incredibly sophisticated statistical analysis,” said Daniel E. Furst, MD, professor emeritus of medicine at the University of California, Los Angeles, who was not involved with the study. However, the data do not yet support altering blood testing frequency based on this model.
“The hypothesis that not all patients have to be examined so frequently is a very reasonable hypothesis,” Dr. Furst said in an interview, and additional research is needed to corroborate it. The model also needs to be validated in patient populations outside of the United Kingdom, he added.
Dr. Abhishek agreed that validating the model in other patient populations is an important next step. “When we develop a tool [using] a one-nation data set, we want other researchers to then validate it in other countries’ data sets to make sure there is nothing odd about patients in the U.K. that makes the tool work well here but not in [the] U.S., Europe, or Asia, for example,” he said. Doing so should be relatively easy, he said, as the model is publicly available, and the information required is routinely collected during clinic visits.
To understand if less frequent testing might be appropriate for some patients, researchers would need to look at data registries like the Brigham and Women’s Hospital Rheumatoid Arthritis Sequential Study (BRASS) registry or CorEvitas registries “where the testing is done in a very regular way over the long haul,” Dr. Furst said. Analyzing these datasets, researchers could determine the testing intervals that would be most efficient for low- and high-risk patients.
A word of caution
While less frequent testing for long-term MTX therapy could likely have benefits, there is still some risk involved, cautioned Prabha Ranganathan, MD, professor of medicine at Washington University in St. Louis.
“Although most methotrexate toxicity occurs within the first 6 months of starting treatment, rare idiosyncratic toxicity can occur that does not correlate with the dose, duration, or method of how methotrexate is administered,” she wrote in an accompanying editorial. “Most rheumatologists can identify a handful of patients who receive methotrexate in their practice who develop sudden leukopenia or thrombocytopenia or transaminitis that is severe enough to warrant drug discontinuation.” While tools like this prediction model can be useful, clinicians need to consider each patient individually and use shared decision-making when monitoring for MTX toxicity, she advised.
“As in most of areas of medicine, the one-size-fits-all approach does not work for methotrexate users,” she noted.
This study was funded by the U.K. National Institute for Health and Care Research and Health Technology Assessment. Dr. Abhishek has received institutional research grants from AstraZeneca and Oxford Immunotech and personal fees from UpToDate, Springer, Cadila Pharmaceuticals, NGM Bio, Limbic, and Inflazome. Dr. Furst and Dr. Ranganathan report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new model can predict which patients are more likely to experience side effects from long-term methotrexate (MTX) use, research suggests. Patients with a lower risk profile may benefit from less frequent testing, the authors hypothesize.
Most recommendations advise that patients initiating MTX therapy should get blood testing every 2-4 weeks to monitor for full blood count, liver function, urea electrolytes, and creatinine. After 6 months taking MTX, monitoring can be tapered to every 3 months. But Abhishek Abhishek, MD, PhD, professor of rheumatology and honorary consultant rheumatologist at Nottingham (England) University Hospitals NHS Trust and colleagues argue that abnormal results after the initial 6 months of treatment are “infrequent,” and patients may benefit from fewer tests throughout the year.
“Unnecessary blood tests waste patients’ time and health care resources, including the time of general practitioners and phlebotomists,” Dr. Abhishek and associates write. “It would be beneficial to predict the risk of clinically significant abnormal blood test results during long-term methotrexate treatment to inform the frequency of testing for individuals.”
Stratifying risk
In the study, published in the BMJ, researchers used the UK’s Clinical Practice Research Datalink (CPRD) to identify the electronic medical records of over 37,000 adult patients with an immune-mediated inflammatory disease who were prescribed MTX during 2007-2019. All included patients were prescribed MTX for at least 6 months. The main outcome was discontinuation of methotrexate because of abnormal blood test results. Around 62% of patients had rheumatoid arthritis and 22% had psoriasis or psoriatic arthritis.
Using these anonymized data, the group developed a risk stratification model using 11 clinical predictors. “The factors that went in the model are simple things that most patients can self-report or doctors can get from their patient’s medical records,” Dr. Abhishek told this news organization, including methotrexate dose, age, sex, and comorbidities. Dr. Abhishek emphasized that the model should be used only in patients who have continued taking MTX for at least 6 months and have already undergone more frequent initial testing.
The strongest individual predictors were diabetes (hazard ratio, 1.25), chronic kidney disease stage 3 (HR, 2.01), and previous cytopenia or raised liver enzyme levels during the first 6 months of MTX therapy (HR, 2.97). However, Dr. Abhishek emphasized that the individual factors were less important, noting that the model sums the risks to predict outcomes more accurately. Most patients (68.4%) were sorted into the low-risk cohort, with a less than 10% estimated risk of discontinuing MTX over the next 5 years. About one-fifth (20.9%) were categorized as moderate risk (10%-20% estimated risk over 5 years), and 10.7% were high risk, with a greater than 20% estimated risk of discontinuing the drug over 5 years.
The authors argue that low-risk patients could receive less frequent testing – perhaps every 6 months or annually, while moderate-risk patients would continue to be tested every 3 months. High-risk patients could potentially be tested with even greater frequently.
More research needed
The research involved “incredibly sophisticated statistical analysis,” said Daniel E. Furst, MD, professor emeritus of medicine at the University of California, Los Angeles, who was not involved with the study. However, the data do not yet support altering blood testing frequency based on this model.
“The hypothesis that not all patients have to be examined so frequently is a very reasonable hypothesis,” Dr. Furst said in an interview, and additional research is needed to corroborate it. The model also needs to be validated in patient populations outside of the United Kingdom, he added.
Dr. Abhishek agreed that validating the model in other patient populations is an important next step. “When we develop a tool [using] a one-nation data set, we want other researchers to then validate it in other countries’ data sets to make sure there is nothing odd about patients in the U.K. that makes the tool work well here but not in [the] U.S., Europe, or Asia, for example,” he said. Doing so should be relatively easy, he said, as the model is publicly available, and the information required is routinely collected during clinic visits.
To understand if less frequent testing might be appropriate for some patients, researchers would need to look at data registries like the Brigham and Women’s Hospital Rheumatoid Arthritis Sequential Study (BRASS) registry or CorEvitas registries “where the testing is done in a very regular way over the long haul,” Dr. Furst said. Analyzing these datasets, researchers could determine the testing intervals that would be most efficient for low- and high-risk patients.
A word of caution
While less frequent testing for long-term MTX therapy could likely have benefits, there is still some risk involved, cautioned Prabha Ranganathan, MD, professor of medicine at Washington University in St. Louis.
“Although most methotrexate toxicity occurs within the first 6 months of starting treatment, rare idiosyncratic toxicity can occur that does not correlate with the dose, duration, or method of how methotrexate is administered,” she wrote in an accompanying editorial. “Most rheumatologists can identify a handful of patients who receive methotrexate in their practice who develop sudden leukopenia or thrombocytopenia or transaminitis that is severe enough to warrant drug discontinuation.” While tools like this prediction model can be useful, clinicians need to consider each patient individually and use shared decision-making when monitoring for MTX toxicity, she advised.
“As in most of areas of medicine, the one-size-fits-all approach does not work for methotrexate users,” she noted.
This study was funded by the U.K. National Institute for Health and Care Research and Health Technology Assessment. Dr. Abhishek has received institutional research grants from AstraZeneca and Oxford Immunotech and personal fees from UpToDate, Springer, Cadila Pharmaceuticals, NGM Bio, Limbic, and Inflazome. Dr. Furst and Dr. Ranganathan report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM THE BMJ
Could GLP-1 receptor agonists ease knee osteoarthritis pain, slow progression?
Could glucagon-like peptide-1 receptor agonists, such as liraglutide and semaglutide, also be potential disease-modifying treatments for knee osteoarthritis (KOA)?
Weight loss is recommended for patients with KOA, and GLP-1 receptor agonists are approved for weight loss. New early research suggests these drugs might have a disease-modifying effect for KOA.
Three recently published studies investigated this:
- The LOSEIT phase 4, randomized controlled trial of liraglutide vs. placebo in patients with obesity/overweight and KOA.
- A large observational study out of China in patients with KOA and type 2 diabetes.
- A preclinical trial of liraglutide in mouse models of KOA.
The preclinical trial and the observational study report promising results, and the lack of KOA pain relief in patients in the phase 4 trial may be explained by the trial design. Three other trials are in the works.
This news organization invited two researchers and two outside experts to discuss these studies and potential future treatment of KOA with GLP-1 receptor agonists.
The big picture, as seen by two experts
The GLP-1 receptor agonists liraglutide (Victoza) and semaglutide (Ozempic) are approved for type 2 diabetes, and, in higher doses, liraglutide (Saxenda) and semaglutide (Wegovy) are approved for weight loss in patients with obesity (or overweight with comorbidities), and given as weekly injections.
Victoza and Saxenda are expected to come off patent in December 2023, and in 2026, respectively.
Lauren King, MD, PhD, a rheumatologist and clinician scientist who was not involved with the recent investigational studies of GLP-1 receptor agonists for KOA, noted that obesity is the most important, guideline-recommended, modifiable risk factor for KOA.
“In people with overweight and obesity, losing weight can improve knee osteoarthritis symptoms, and some evidence supports that it may also slow joint structural changes,” Dr. King, of the department of medicine at the University of Toronto, said in an interview.
Large trials of GLP-1 receptor agonists in people with overweight and obesity, such as the STEP trials of semaglutide, she noted, “provide evidence that these medications are safe and effective, facilitating clinically relevant and sustained weight loss.”
Further research is needed, she said, to better understand disease-modifying effects of GLP-1 receptor agonists in patients with KOA.
Similarly, W. Timothy Garvey, MD, professor in the department of nutrition sciences at the University of Alabama at Birmingham and director of the UAB Diabetes Research Center, who was not involved with this research, noted that weight loss improves KOA symptoms.
Dr. Garvey was lead investigator in the STEP 5 trial of semaglutide and lead author of the American Association of Clinical Endocrinologists 2016 Obesity Management guidelines.
“The question is whether these GLP-1 receptor agonists have anything to offer over and above weight loss per se, and we don’t know for sure,” he said.
They “do have anti-inflammatory actions,” and “there are GLP-1 receptors in locations where you think GLP-1 receptor agonism may help inflammation in the knee, in joints, and in other tissues,” he noted.
He looks forward to results of the phase 3 trial of semaglutide in patients with KOA, expected this fall.
Three published studies
LOSEIT: RCT of liraglutide for pain and weight control in KOA
Henrik Rindel Gudbergsen, MD, PhD, and colleagues published results of the only randomized controlled trial of a GLP-1 receptor agonist (liraglutide, Saxenda) vs. placebo in patients with overweight/obesity and KOA, the LOSEIT trial.
All patients first entered an 8-week, pre-randomization phase where they had strict caloric restriction (and ate meal replacements) and lost at least 5% of their initial weight. They also had less knee pain at the end of this phase.
Then they were randomly assigned to receive 3 mg liraglutide or placebo daily injections for 1 year.
From randomization until week 52, the liraglutide group had greater mean weight loss than the placebo group (but this was < 5% of their weight). They did not have greater reduction in knee pain than patients in the placebo group.
“Our interpretation was that dieting results in weight loss and diminishes knee pain (which we knew), and that the impact of liraglutide following severe calorie restriction and weight loss and improvement of pain was limited,” Dr. Gudbergsen, a physician and associate professor at The Parker Institute, University of Copenhagen, told this news organization.
“That was the surprise for us as investigators,” he said, “and, I assume, why Novo Nordisk is now pursuing the investigation of semaglutide for KOA, as this is expected to create a larger effect on body weight and knee symptoms.”
The weight loss was about 12.5 kg (27.5 pounds) prior to randomization, and the subsequent weight loss with liraglutide was about 2.8 kg (6 pounds; about 4% of their weight). “Thus, it could seem that the participants’ potential for weight loss as well as symptom reduction was fully exploited in the pre–random assignment dietary intervention period,” according to the researchers.
“It seems highly relevant to use liraglutide or semaglutide for patients impacted by obesity and KOA, as it is in line with guidelines suggesting weight loss for this group,” Dr. Gudbergsen said. “However, whether liraglutide and/or semaglutide, acting via an anti-inflammatory effect, for example, has an added positive impact on cartilage quality remains to be clarified,” he said.
Others who were not involved in this study suggest that the lack of pain-reduction benefit with liraglutide vs. placebo can be explained by the short-term use of liraglutide (1 year), small weight loss (< 5%), and systemic rather than intraarticular injection.
The LOSEIT trial design “is problematic and could not provide a confirmative conclusion,” Hongyi Zhu, MD, PhD, Shanghai Sixth People’s Hospital, China, and colleagues wrote in their observational study. The small weight loss of < 5% in the liraglutide group may explain why the pain relief was not better than with placebo. A longer study duration with significant weight loss/maintenance may be needed, they noted.
Francis Berenbaum, MD, PhD, senior author of a preclinical study of liraglutide, said that in the LOSEIT trial, “daily systemic injections of liraglutide did not ameliorate OA-related pain, probably because of poor access and hence poor local concentrations of liraglutide in the knee joint.”
Dr. Berenbaum is professor of rheumatology at Sorbonne University and director of the department of rheumatology at AP-HP Saint-Antoine Hospital in Paris. He is cofounder and CEO of 4Moving Biotech (a subsidiary of 4P Pharma, an innovator accelerator biotech company), which is testing liraglutide for KOA.
In experiments in mice, systemic injections of liraglutide did not lead to high enough concentration in synovial fluid to show efficacy for pain relief, he told this news organization. “In order to get the direct effect of liraglutide, it should be injected intraarticularly,” he said.
Observational study of patients with diabetes and KOA
Dr. Zhu and colleagues recently published results of the first clinical investigation of long-term effects of GLP-1 receptor agonists on KOA in patients with comorbid type 2 diabetes.
They analyzed data from a subset of patients with KOA and type 2 diabetes from the Shanghai Osteoarthritis Cohort, including 233 patients who received a GLP-1 receptor agonist (semaglutide, liraglutide, or dulaglutide [Trulicity]) for at least 2 years and 1,574 patients who did not receive this therapy.
The patients had a mean weight of 66 kg (145 pounds), a mean body mass index of 27 kg/m2, and a mean A1c of 7.3%.
“According to conventional wisdom, a weight change greater than 5% is considered clinically relevant for KOA,” the researchers wrote. They found that patients had substantial weight loss after GLP-1 receptor agonist therapy.
The primary outcome, the incidence of knee surgery, was lower in the patients who received a GLP-1 receptor agonist than in the other patients (1.7% vs. 5.9%; adjusted P = .014).
Patients who received a GLP-1 receptor agonist also had greater improvements in secondary outcomes than did other patients, including pain subscale scores and cartilage-loss velocity of the medial femorotibial joint in patients with predominantly lateral OA.
“The effects of GLP-1 receptor agonists on arthritic knees were largely mediated by weight loss instead of glycemic control,” Dr. Zhu and colleagues reported.
They concluded that with long-enough treatment, “GLP-1 receptor agonist therapies might be disease-modifying for KOA patients with comorbid [type 2 diabetes mellitus].”
They called for further research to elucidate the effects of GLP-1 receptor agonists on the disease process, joint structure, and patient-reported outcomes of OA.
Dr. Garvey noted that “whether your BMI is 30 or 40, if there are complications, that tells you that degree of adiposity is sufficient to impair health.” So, if a patient in southeast China has a BMI of 27 kg/m2 and has osteoarthritis, he or she could still benefit from weight loss, he said.
Liraglutide and pain-related behavior in mouse models of OA
Dr. Berenbaum and colleagues reported that liraglutide alleviated pain-related behavior in sodium monoiodoacetate mouse models of KOA.
In addition, liraglutide had anti-inflammatory and anticatabolic effects in synovial fluid from the knees of six patients with OA of varying severity.
The researchers analyzed generic liraglutide (from Hybio Pharmaceuticals, Shenzhen, China) and nongeneric liraglutide (from Novo Nordisk, Bagsværd, Denmark).
They found that “when injected intra-articularly, liraglutide blunts the inflammatory process that is present in OA synovial tissue, explaining the acute analgesic effect,” Dr. Berenbaum said.
“Liraglutide could be a game-changer,” he said, “by demonstrating not only an effect on joint structures like synovial tissue and cartilage, but also on symptoms in a short-term period.”
Dr. Garvey said the symptom improvements after intrasynovial infusion of liraglutide in this trial were “impressive.” This study “adds credence to the hypothesis that these GLP-1 receptor agonists could have effects above and beyond weight loss,” he said.
Two trials near completion, one is upcoming
Phase 1 and 2 trials of 4P-004
“We are now in a phase 1 clinical trial [of 4P-004/liraglutide] in patients suffering from knee OA and should start a large phase 2 trial next year,” said Dr. Berenbaum.
The phase 1 LASARE trial, sponsored by 4Moving Biotech, planned to enroll 32 patients with KOA.
The primary outcome is safety and tolerability of single IA administration of 4P-004 at escalating doses in patients with KOA. Secondary outcomes include plasma concentration of liraglutide when administered this way.
Phase 3 trial of semaglutide for KOA
Novo Nordisk is performing a phase 3 study, “Effect of Subcutaneous Semaglutide 2.4 mg Once-weekly Compared to Placebo in Subjects With Obesity and Knee Osteoarthritis,” with an expected enrollment of 407 patients with KOA and estimated trial completion in September.
Eligible patients were aged 18 and older, with BMI > 30 kg/m2 and KOA with Kellgren-Lawrence grades 2 or 3. The co-primary outcomes are change in body weight and change in WOMAC pain score, from baseline to 68 weeks.
The LOSEIT trial was supported by Novo Nordisk and the Cambridge Weight Plan. The observational study in China was supported by the Shanghai Shenkang Hospital Development Centre, the Clinical Research Plan of SHDC, and the National Natural Science Foundation of China. The preclinical trial was supported by 4P Pharma/4Moving Biotech.
Dr. Berenbaum is CEO of 4Moving Biotech and chair of the scientific advisory board of 4P Pharma. He has received personal fees from 4P Pharma as well as numerous other pharmaceutical companies. Dr. Garvey has reported being a consultant to Boehringer Ingelheim, Novo Nordisk, Eli Lilly, Merck, Fractyl Health, and Alnylam Pharmaceuticals, and reported being an investigator for studies sponsored by Novo Nordisk, Eli Lilly, Pfizer, and Epitomee. Dr. Gudbergsen, Dr. King, and Dr. Zhu report no relevant financial relationships.
A version of this article appeared on Medscape.com.
Could glucagon-like peptide-1 receptor agonists, such as liraglutide and semaglutide, also be potential disease-modifying treatments for knee osteoarthritis (KOA)?
Weight loss is recommended for patients with KOA, and GLP-1 receptor agonists are approved for weight loss. New early research suggests these drugs might have a disease-modifying effect for KOA.
Three recently published studies investigated this:
- The LOSEIT phase 4, randomized controlled trial of liraglutide vs. placebo in patients with obesity/overweight and KOA.
- A large observational study out of China in patients with KOA and type 2 diabetes.
- A preclinical trial of liraglutide in mouse models of KOA.
The preclinical trial and the observational study report promising results, and the lack of KOA pain relief in patients in the phase 4 trial may be explained by the trial design. Three other trials are in the works.
This news organization invited two researchers and two outside experts to discuss these studies and potential future treatment of KOA with GLP-1 receptor agonists.
The big picture, as seen by two experts
The GLP-1 receptor agonists liraglutide (Victoza) and semaglutide (Ozempic) are approved for type 2 diabetes, and, in higher doses, liraglutide (Saxenda) and semaglutide (Wegovy) are approved for weight loss in patients with obesity (or overweight with comorbidities), and given as weekly injections.
Victoza and Saxenda are expected to come off patent in December 2023, and in 2026, respectively.
Lauren King, MD, PhD, a rheumatologist and clinician scientist who was not involved with the recent investigational studies of GLP-1 receptor agonists for KOA, noted that obesity is the most important, guideline-recommended, modifiable risk factor for KOA.
“In people with overweight and obesity, losing weight can improve knee osteoarthritis symptoms, and some evidence supports that it may also slow joint structural changes,” Dr. King, of the department of medicine at the University of Toronto, said in an interview.
Large trials of GLP-1 receptor agonists in people with overweight and obesity, such as the STEP trials of semaglutide, she noted, “provide evidence that these medications are safe and effective, facilitating clinically relevant and sustained weight loss.”
Further research is needed, she said, to better understand disease-modifying effects of GLP-1 receptor agonists in patients with KOA.
Similarly, W. Timothy Garvey, MD, professor in the department of nutrition sciences at the University of Alabama at Birmingham and director of the UAB Diabetes Research Center, who was not involved with this research, noted that weight loss improves KOA symptoms.
Dr. Garvey was lead investigator in the STEP 5 trial of semaglutide and lead author of the American Association of Clinical Endocrinologists 2016 Obesity Management guidelines.
“The question is whether these GLP-1 receptor agonists have anything to offer over and above weight loss per se, and we don’t know for sure,” he said.
They “do have anti-inflammatory actions,” and “there are GLP-1 receptors in locations where you think GLP-1 receptor agonism may help inflammation in the knee, in joints, and in other tissues,” he noted.
He looks forward to results of the phase 3 trial of semaglutide in patients with KOA, expected this fall.
Three published studies
LOSEIT: RCT of liraglutide for pain and weight control in KOA
Henrik Rindel Gudbergsen, MD, PhD, and colleagues published results of the only randomized controlled trial of a GLP-1 receptor agonist (liraglutide, Saxenda) vs. placebo in patients with overweight/obesity and KOA, the LOSEIT trial.
All patients first entered an 8-week, pre-randomization phase where they had strict caloric restriction (and ate meal replacements) and lost at least 5% of their initial weight. They also had less knee pain at the end of this phase.
Then they were randomly assigned to receive 3 mg liraglutide or placebo daily injections for 1 year.
From randomization until week 52, the liraglutide group had greater mean weight loss than the placebo group (but this was < 5% of their weight). They did not have greater reduction in knee pain than patients in the placebo group.
“Our interpretation was that dieting results in weight loss and diminishes knee pain (which we knew), and that the impact of liraglutide following severe calorie restriction and weight loss and improvement of pain was limited,” Dr. Gudbergsen, a physician and associate professor at The Parker Institute, University of Copenhagen, told this news organization.
“That was the surprise for us as investigators,” he said, “and, I assume, why Novo Nordisk is now pursuing the investigation of semaglutide for KOA, as this is expected to create a larger effect on body weight and knee symptoms.”
The weight loss was about 12.5 kg (27.5 pounds) prior to randomization, and the subsequent weight loss with liraglutide was about 2.8 kg (6 pounds; about 4% of their weight). “Thus, it could seem that the participants’ potential for weight loss as well as symptom reduction was fully exploited in the pre–random assignment dietary intervention period,” according to the researchers.
“It seems highly relevant to use liraglutide or semaglutide for patients impacted by obesity and KOA, as it is in line with guidelines suggesting weight loss for this group,” Dr. Gudbergsen said. “However, whether liraglutide and/or semaglutide, acting via an anti-inflammatory effect, for example, has an added positive impact on cartilage quality remains to be clarified,” he said.
Others who were not involved in this study suggest that the lack of pain-reduction benefit with liraglutide vs. placebo can be explained by the short-term use of liraglutide (1 year), small weight loss (< 5%), and systemic rather than intraarticular injection.
The LOSEIT trial design “is problematic and could not provide a confirmative conclusion,” Hongyi Zhu, MD, PhD, Shanghai Sixth People’s Hospital, China, and colleagues wrote in their observational study. The small weight loss of < 5% in the liraglutide group may explain why the pain relief was not better than with placebo. A longer study duration with significant weight loss/maintenance may be needed, they noted.
Francis Berenbaum, MD, PhD, senior author of a preclinical study of liraglutide, said that in the LOSEIT trial, “daily systemic injections of liraglutide did not ameliorate OA-related pain, probably because of poor access and hence poor local concentrations of liraglutide in the knee joint.”
Dr. Berenbaum is professor of rheumatology at Sorbonne University and director of the department of rheumatology at AP-HP Saint-Antoine Hospital in Paris. He is cofounder and CEO of 4Moving Biotech (a subsidiary of 4P Pharma, an innovator accelerator biotech company), which is testing liraglutide for KOA.
In experiments in mice, systemic injections of liraglutide did not lead to high enough concentration in synovial fluid to show efficacy for pain relief, he told this news organization. “In order to get the direct effect of liraglutide, it should be injected intraarticularly,” he said.
Observational study of patients with diabetes and KOA
Dr. Zhu and colleagues recently published results of the first clinical investigation of long-term effects of GLP-1 receptor agonists on KOA in patients with comorbid type 2 diabetes.
They analyzed data from a subset of patients with KOA and type 2 diabetes from the Shanghai Osteoarthritis Cohort, including 233 patients who received a GLP-1 receptor agonist (semaglutide, liraglutide, or dulaglutide [Trulicity]) for at least 2 years and 1,574 patients who did not receive this therapy.
The patients had a mean weight of 66 kg (145 pounds), a mean body mass index of 27 kg/m2, and a mean A1c of 7.3%.
“According to conventional wisdom, a weight change greater than 5% is considered clinically relevant for KOA,” the researchers wrote. They found that patients had substantial weight loss after GLP-1 receptor agonist therapy.
The primary outcome, the incidence of knee surgery, was lower in the patients who received a GLP-1 receptor agonist than in the other patients (1.7% vs. 5.9%; adjusted P = .014).
Patients who received a GLP-1 receptor agonist also had greater improvements in secondary outcomes than did other patients, including pain subscale scores and cartilage-loss velocity of the medial femorotibial joint in patients with predominantly lateral OA.
“The effects of GLP-1 receptor agonists on arthritic knees were largely mediated by weight loss instead of glycemic control,” Dr. Zhu and colleagues reported.
They concluded that with long-enough treatment, “GLP-1 receptor agonist therapies might be disease-modifying for KOA patients with comorbid [type 2 diabetes mellitus].”
They called for further research to elucidate the effects of GLP-1 receptor agonists on the disease process, joint structure, and patient-reported outcomes of OA.
Dr. Garvey noted that “whether your BMI is 30 or 40, if there are complications, that tells you that degree of adiposity is sufficient to impair health.” So, if a patient in southeast China has a BMI of 27 kg/m2 and has osteoarthritis, he or she could still benefit from weight loss, he said.
Liraglutide and pain-related behavior in mouse models of OA
Dr. Berenbaum and colleagues reported that liraglutide alleviated pain-related behavior in sodium monoiodoacetate mouse models of KOA.
In addition, liraglutide had anti-inflammatory and anticatabolic effects in synovial fluid from the knees of six patients with OA of varying severity.
The researchers analyzed generic liraglutide (from Hybio Pharmaceuticals, Shenzhen, China) and nongeneric liraglutide (from Novo Nordisk, Bagsværd, Denmark).
They found that “when injected intra-articularly, liraglutide blunts the inflammatory process that is present in OA synovial tissue, explaining the acute analgesic effect,” Dr. Berenbaum said.
“Liraglutide could be a game-changer,” he said, “by demonstrating not only an effect on joint structures like synovial tissue and cartilage, but also on symptoms in a short-term period.”
Dr. Garvey said the symptom improvements after intrasynovial infusion of liraglutide in this trial were “impressive.” This study “adds credence to the hypothesis that these GLP-1 receptor agonists could have effects above and beyond weight loss,” he said.
Two trials near completion, one is upcoming
Phase 1 and 2 trials of 4P-004
“We are now in a phase 1 clinical trial [of 4P-004/liraglutide] in patients suffering from knee OA and should start a large phase 2 trial next year,” said Dr. Berenbaum.
The phase 1 LASARE trial, sponsored by 4Moving Biotech, planned to enroll 32 patients with KOA.
The primary outcome is safety and tolerability of single IA administration of 4P-004 at escalating doses in patients with KOA. Secondary outcomes include plasma concentration of liraglutide when administered this way.
Phase 3 trial of semaglutide for KOA
Novo Nordisk is performing a phase 3 study, “Effect of Subcutaneous Semaglutide 2.4 mg Once-weekly Compared to Placebo in Subjects With Obesity and Knee Osteoarthritis,” with an expected enrollment of 407 patients with KOA and estimated trial completion in September.
Eligible patients were aged 18 and older, with BMI > 30 kg/m2 and KOA with Kellgren-Lawrence grades 2 or 3. The co-primary outcomes are change in body weight and change in WOMAC pain score, from baseline to 68 weeks.
The LOSEIT trial was supported by Novo Nordisk and the Cambridge Weight Plan. The observational study in China was supported by the Shanghai Shenkang Hospital Development Centre, the Clinical Research Plan of SHDC, and the National Natural Science Foundation of China. The preclinical trial was supported by 4P Pharma/4Moving Biotech.
Dr. Berenbaum is CEO of 4Moving Biotech and chair of the scientific advisory board of 4P Pharma. He has received personal fees from 4P Pharma as well as numerous other pharmaceutical companies. Dr. Garvey has reported being a consultant to Boehringer Ingelheim, Novo Nordisk, Eli Lilly, Merck, Fractyl Health, and Alnylam Pharmaceuticals, and reported being an investigator for studies sponsored by Novo Nordisk, Eli Lilly, Pfizer, and Epitomee. Dr. Gudbergsen, Dr. King, and Dr. Zhu report no relevant financial relationships.
A version of this article appeared on Medscape.com.
Could glucagon-like peptide-1 receptor agonists, such as liraglutide and semaglutide, also be potential disease-modifying treatments for knee osteoarthritis (KOA)?
Weight loss is recommended for patients with KOA, and GLP-1 receptor agonists are approved for weight loss. New early research suggests these drugs might have a disease-modifying effect for KOA.
Three recently published studies investigated this:
- The LOSEIT phase 4, randomized controlled trial of liraglutide vs. placebo in patients with obesity/overweight and KOA.
- A large observational study out of China in patients with KOA and type 2 diabetes.
- A preclinical trial of liraglutide in mouse models of KOA.
The preclinical trial and the observational study report promising results, and the lack of KOA pain relief in patients in the phase 4 trial may be explained by the trial design. Three other trials are in the works.
This news organization invited two researchers and two outside experts to discuss these studies and potential future treatment of KOA with GLP-1 receptor agonists.
The big picture, as seen by two experts
The GLP-1 receptor agonists liraglutide (Victoza) and semaglutide (Ozempic) are approved for type 2 diabetes, and, in higher doses, liraglutide (Saxenda) and semaglutide (Wegovy) are approved for weight loss in patients with obesity (or overweight with comorbidities), and given as weekly injections.
Victoza and Saxenda are expected to come off patent in December 2023, and in 2026, respectively.
Lauren King, MD, PhD, a rheumatologist and clinician scientist who was not involved with the recent investigational studies of GLP-1 receptor agonists for KOA, noted that obesity is the most important, guideline-recommended, modifiable risk factor for KOA.
“In people with overweight and obesity, losing weight can improve knee osteoarthritis symptoms, and some evidence supports that it may also slow joint structural changes,” Dr. King, of the department of medicine at the University of Toronto, said in an interview.
Large trials of GLP-1 receptor agonists in people with overweight and obesity, such as the STEP trials of semaglutide, she noted, “provide evidence that these medications are safe and effective, facilitating clinically relevant and sustained weight loss.”
Further research is needed, she said, to better understand disease-modifying effects of GLP-1 receptor agonists in patients with KOA.
Similarly, W. Timothy Garvey, MD, professor in the department of nutrition sciences at the University of Alabama at Birmingham and director of the UAB Diabetes Research Center, who was not involved with this research, noted that weight loss improves KOA symptoms.
Dr. Garvey was lead investigator in the STEP 5 trial of semaglutide and lead author of the American Association of Clinical Endocrinologists 2016 Obesity Management guidelines.
“The question is whether these GLP-1 receptor agonists have anything to offer over and above weight loss per se, and we don’t know for sure,” he said.
They “do have anti-inflammatory actions,” and “there are GLP-1 receptors in locations where you think GLP-1 receptor agonism may help inflammation in the knee, in joints, and in other tissues,” he noted.
He looks forward to results of the phase 3 trial of semaglutide in patients with KOA, expected this fall.
Three published studies
LOSEIT: RCT of liraglutide for pain and weight control in KOA
Henrik Rindel Gudbergsen, MD, PhD, and colleagues published results of the only randomized controlled trial of a GLP-1 receptor agonist (liraglutide, Saxenda) vs. placebo in patients with overweight/obesity and KOA, the LOSEIT trial.
All patients first entered an 8-week, pre-randomization phase where they had strict caloric restriction (and ate meal replacements) and lost at least 5% of their initial weight. They also had less knee pain at the end of this phase.
Then they were randomly assigned to receive 3 mg liraglutide or placebo daily injections for 1 year.
From randomization until week 52, the liraglutide group had greater mean weight loss than the placebo group (but this was < 5% of their weight). They did not have greater reduction in knee pain than patients in the placebo group.
“Our interpretation was that dieting results in weight loss and diminishes knee pain (which we knew), and that the impact of liraglutide following severe calorie restriction and weight loss and improvement of pain was limited,” Dr. Gudbergsen, a physician and associate professor at The Parker Institute, University of Copenhagen, told this news organization.
“That was the surprise for us as investigators,” he said, “and, I assume, why Novo Nordisk is now pursuing the investigation of semaglutide for KOA, as this is expected to create a larger effect on body weight and knee symptoms.”
The weight loss was about 12.5 kg (27.5 pounds) prior to randomization, and the subsequent weight loss with liraglutide was about 2.8 kg (6 pounds; about 4% of their weight). “Thus, it could seem that the participants’ potential for weight loss as well as symptom reduction was fully exploited in the pre–random assignment dietary intervention period,” according to the researchers.
“It seems highly relevant to use liraglutide or semaglutide for patients impacted by obesity and KOA, as it is in line with guidelines suggesting weight loss for this group,” Dr. Gudbergsen said. “However, whether liraglutide and/or semaglutide, acting via an anti-inflammatory effect, for example, has an added positive impact on cartilage quality remains to be clarified,” he said.
Others who were not involved in this study suggest that the lack of pain-reduction benefit with liraglutide vs. placebo can be explained by the short-term use of liraglutide (1 year), small weight loss (< 5%), and systemic rather than intraarticular injection.
The LOSEIT trial design “is problematic and could not provide a confirmative conclusion,” Hongyi Zhu, MD, PhD, Shanghai Sixth People’s Hospital, China, and colleagues wrote in their observational study. The small weight loss of < 5% in the liraglutide group may explain why the pain relief was not better than with placebo. A longer study duration with significant weight loss/maintenance may be needed, they noted.
Francis Berenbaum, MD, PhD, senior author of a preclinical study of liraglutide, said that in the LOSEIT trial, “daily systemic injections of liraglutide did not ameliorate OA-related pain, probably because of poor access and hence poor local concentrations of liraglutide in the knee joint.”
Dr. Berenbaum is professor of rheumatology at Sorbonne University and director of the department of rheumatology at AP-HP Saint-Antoine Hospital in Paris. He is cofounder and CEO of 4Moving Biotech (a subsidiary of 4P Pharma, an innovator accelerator biotech company), which is testing liraglutide for KOA.
In experiments in mice, systemic injections of liraglutide did not lead to high enough concentration in synovial fluid to show efficacy for pain relief, he told this news organization. “In order to get the direct effect of liraglutide, it should be injected intraarticularly,” he said.
Observational study of patients with diabetes and KOA
Dr. Zhu and colleagues recently published results of the first clinical investigation of long-term effects of GLP-1 receptor agonists on KOA in patients with comorbid type 2 diabetes.
They analyzed data from a subset of patients with KOA and type 2 diabetes from the Shanghai Osteoarthritis Cohort, including 233 patients who received a GLP-1 receptor agonist (semaglutide, liraglutide, or dulaglutide [Trulicity]) for at least 2 years and 1,574 patients who did not receive this therapy.
The patients had a mean weight of 66 kg (145 pounds), a mean body mass index of 27 kg/m2, and a mean A1c of 7.3%.
“According to conventional wisdom, a weight change greater than 5% is considered clinically relevant for KOA,” the researchers wrote. They found that patients had substantial weight loss after GLP-1 receptor agonist therapy.
The primary outcome, the incidence of knee surgery, was lower in the patients who received a GLP-1 receptor agonist than in the other patients (1.7% vs. 5.9%; adjusted P = .014).
Patients who received a GLP-1 receptor agonist also had greater improvements in secondary outcomes than did other patients, including pain subscale scores and cartilage-loss velocity of the medial femorotibial joint in patients with predominantly lateral OA.
“The effects of GLP-1 receptor agonists on arthritic knees were largely mediated by weight loss instead of glycemic control,” Dr. Zhu and colleagues reported.
They concluded that with long-enough treatment, “GLP-1 receptor agonist therapies might be disease-modifying for KOA patients with comorbid [type 2 diabetes mellitus].”
They called for further research to elucidate the effects of GLP-1 receptor agonists on the disease process, joint structure, and patient-reported outcomes of OA.
Dr. Garvey noted that “whether your BMI is 30 or 40, if there are complications, that tells you that degree of adiposity is sufficient to impair health.” So, if a patient in southeast China has a BMI of 27 kg/m2 and has osteoarthritis, he or she could still benefit from weight loss, he said.
Liraglutide and pain-related behavior in mouse models of OA
Dr. Berenbaum and colleagues reported that liraglutide alleviated pain-related behavior in sodium monoiodoacetate mouse models of KOA.
In addition, liraglutide had anti-inflammatory and anticatabolic effects in synovial fluid from the knees of six patients with OA of varying severity.
The researchers analyzed generic liraglutide (from Hybio Pharmaceuticals, Shenzhen, China) and nongeneric liraglutide (from Novo Nordisk, Bagsværd, Denmark).
They found that “when injected intra-articularly, liraglutide blunts the inflammatory process that is present in OA synovial tissue, explaining the acute analgesic effect,” Dr. Berenbaum said.
“Liraglutide could be a game-changer,” he said, “by demonstrating not only an effect on joint structures like synovial tissue and cartilage, but also on symptoms in a short-term period.”
Dr. Garvey said the symptom improvements after intrasynovial infusion of liraglutide in this trial were “impressive.” This study “adds credence to the hypothesis that these GLP-1 receptor agonists could have effects above and beyond weight loss,” he said.
Two trials near completion, one is upcoming
Phase 1 and 2 trials of 4P-004
“We are now in a phase 1 clinical trial [of 4P-004/liraglutide] in patients suffering from knee OA and should start a large phase 2 trial next year,” said Dr. Berenbaum.
The phase 1 LASARE trial, sponsored by 4Moving Biotech, planned to enroll 32 patients with KOA.
The primary outcome is safety and tolerability of single IA administration of 4P-004 at escalating doses in patients with KOA. Secondary outcomes include plasma concentration of liraglutide when administered this way.
Phase 3 trial of semaglutide for KOA
Novo Nordisk is performing a phase 3 study, “Effect of Subcutaneous Semaglutide 2.4 mg Once-weekly Compared to Placebo in Subjects With Obesity and Knee Osteoarthritis,” with an expected enrollment of 407 patients with KOA and estimated trial completion in September.
Eligible patients were aged 18 and older, with BMI > 30 kg/m2 and KOA with Kellgren-Lawrence grades 2 or 3. The co-primary outcomes are change in body weight and change in WOMAC pain score, from baseline to 68 weeks.
The LOSEIT trial was supported by Novo Nordisk and the Cambridge Weight Plan. The observational study in China was supported by the Shanghai Shenkang Hospital Development Centre, the Clinical Research Plan of SHDC, and the National Natural Science Foundation of China. The preclinical trial was supported by 4P Pharma/4Moving Biotech.
Dr. Berenbaum is CEO of 4Moving Biotech and chair of the scientific advisory board of 4P Pharma. He has received personal fees from 4P Pharma as well as numerous other pharmaceutical companies. Dr. Garvey has reported being a consultant to Boehringer Ingelheim, Novo Nordisk, Eli Lilly, Merck, Fractyl Health, and Alnylam Pharmaceuticals, and reported being an investigator for studies sponsored by Novo Nordisk, Eli Lilly, Pfizer, and Epitomee. Dr. Gudbergsen, Dr. King, and Dr. Zhu report no relevant financial relationships.
A version of this article appeared on Medscape.com.
SGLT2 inhibitors linked with fewer gout flares in diabetes
TOPLINE:
compared with matched patients treated with a dipeptidyl peptidase–4 (DPP-4) inhibitor.
METHODOLOGY:
- The study used observational data collected from the entire population of British Columbia that included 15,067 adults with both gout and type 2 diabetes in 2014-2020.
- The group included 8,318 patients who initiated an SGLT2 inhibitor and 6,749 patients who initiated a DPP-4 inhibitor during the study period after at least 1 year of continuous enrollment.
- Using propensity-score matching, 4,075 matched pairs were identified, where one person initiated an SGLT2 inhibitor and the other started a DPP-4 inhibitor.
- Primary outcome was recurrent gout flare counts during follow-up that required an ED visit, hospital admission, or an outpatient visit for a gout flare coupled with appropriate treatment, tallied from the first day of drug receipt until June 30, 2022, with an average follow-up of 1.6 years.
- Secondary endpoints included the incidence of myocardial infarction and stroke.
TAKEAWAY:
- Total gout-flare rates after SGLT2 inhibitor initiation were 52.4/1000 person-years and after DPP-4 inhibitor initiation were 79.7/1,000 person-years, an adjusted rate ratio of 0.66, a reduction significantly linked with SGLT2 inhibitor use.
- For flares that required an ED visit or hospitalization, initiation of an SGLT2 inhibitor was linked with a significant, reduced aRR of 0.52, compared with DPP-4 inhibitor initiation.
- The flare-rate reduction linked with SGLT2 inhibitor use was consistent regardless of sex, age, baseline diuretic use, prior treatment with a urate-lowering agent, and baseline gout intensity.
- SGLT2 inhibitor initiation was also significantly linked with an adjusted reduced hazard ratio of 0.69 in the incidence of myocardial infarction, compared with DPP-4 inhibitor initiation, but stroke incidence was not significantly different between the groups.
IN PRACTICE:
These findings suggest that SGLT2 inhibitors could have a much-needed ability to simultaneously reduce the burden of recurrent gout flares and coronary sequelae in patients with gout and type 2 diabetes, indicating that “SGLT2 inhibitors may offer distinct benefits,” making the drug class “a particularly attractive addition to current urate-lowering therapies,” the researchers write.
SOURCE:
The study was primarily conducted by researchers at Massachusetts General Hospital in Boston. The study was published online July 24 in Annals of Internal Medicine.
LIMITATIONS:
The data used in the study did not include gout flares that did not require medical attention and did not include laboratory findings for study participants. Because the data were observational the findings may be susceptible to unmeasured confounding.
DISCLOSURES:
The study received no commercial funding. One author has reported receiving consulting fees from ANI and LG Chem.
A version of this article first appeared on Medscape.com.
TOPLINE:
compared with matched patients treated with a dipeptidyl peptidase–4 (DPP-4) inhibitor.
METHODOLOGY:
- The study used observational data collected from the entire population of British Columbia that included 15,067 adults with both gout and type 2 diabetes in 2014-2020.
- The group included 8,318 patients who initiated an SGLT2 inhibitor and 6,749 patients who initiated a DPP-4 inhibitor during the study period after at least 1 year of continuous enrollment.
- Using propensity-score matching, 4,075 matched pairs were identified, where one person initiated an SGLT2 inhibitor and the other started a DPP-4 inhibitor.
- Primary outcome was recurrent gout flare counts during follow-up that required an ED visit, hospital admission, or an outpatient visit for a gout flare coupled with appropriate treatment, tallied from the first day of drug receipt until June 30, 2022, with an average follow-up of 1.6 years.
- Secondary endpoints included the incidence of myocardial infarction and stroke.
TAKEAWAY:
- Total gout-flare rates after SGLT2 inhibitor initiation were 52.4/1000 person-years and after DPP-4 inhibitor initiation were 79.7/1,000 person-years, an adjusted rate ratio of 0.66, a reduction significantly linked with SGLT2 inhibitor use.
- For flares that required an ED visit or hospitalization, initiation of an SGLT2 inhibitor was linked with a significant, reduced aRR of 0.52, compared with DPP-4 inhibitor initiation.
- The flare-rate reduction linked with SGLT2 inhibitor use was consistent regardless of sex, age, baseline diuretic use, prior treatment with a urate-lowering agent, and baseline gout intensity.
- SGLT2 inhibitor initiation was also significantly linked with an adjusted reduced hazard ratio of 0.69 in the incidence of myocardial infarction, compared with DPP-4 inhibitor initiation, but stroke incidence was not significantly different between the groups.
IN PRACTICE:
These findings suggest that SGLT2 inhibitors could have a much-needed ability to simultaneously reduce the burden of recurrent gout flares and coronary sequelae in patients with gout and type 2 diabetes, indicating that “SGLT2 inhibitors may offer distinct benefits,” making the drug class “a particularly attractive addition to current urate-lowering therapies,” the researchers write.
SOURCE:
The study was primarily conducted by researchers at Massachusetts General Hospital in Boston. The study was published online July 24 in Annals of Internal Medicine.
LIMITATIONS:
The data used in the study did not include gout flares that did not require medical attention and did not include laboratory findings for study participants. Because the data were observational the findings may be susceptible to unmeasured confounding.
DISCLOSURES:
The study received no commercial funding. One author has reported receiving consulting fees from ANI and LG Chem.
A version of this article first appeared on Medscape.com.
TOPLINE:
compared with matched patients treated with a dipeptidyl peptidase–4 (DPP-4) inhibitor.
METHODOLOGY:
- The study used observational data collected from the entire population of British Columbia that included 15,067 adults with both gout and type 2 diabetes in 2014-2020.
- The group included 8,318 patients who initiated an SGLT2 inhibitor and 6,749 patients who initiated a DPP-4 inhibitor during the study period after at least 1 year of continuous enrollment.
- Using propensity-score matching, 4,075 matched pairs were identified, where one person initiated an SGLT2 inhibitor and the other started a DPP-4 inhibitor.
- Primary outcome was recurrent gout flare counts during follow-up that required an ED visit, hospital admission, or an outpatient visit for a gout flare coupled with appropriate treatment, tallied from the first day of drug receipt until June 30, 2022, with an average follow-up of 1.6 years.
- Secondary endpoints included the incidence of myocardial infarction and stroke.
TAKEAWAY:
- Total gout-flare rates after SGLT2 inhibitor initiation were 52.4/1000 person-years and after DPP-4 inhibitor initiation were 79.7/1,000 person-years, an adjusted rate ratio of 0.66, a reduction significantly linked with SGLT2 inhibitor use.
- For flares that required an ED visit or hospitalization, initiation of an SGLT2 inhibitor was linked with a significant, reduced aRR of 0.52, compared with DPP-4 inhibitor initiation.
- The flare-rate reduction linked with SGLT2 inhibitor use was consistent regardless of sex, age, baseline diuretic use, prior treatment with a urate-lowering agent, and baseline gout intensity.
- SGLT2 inhibitor initiation was also significantly linked with an adjusted reduced hazard ratio of 0.69 in the incidence of myocardial infarction, compared with DPP-4 inhibitor initiation, but stroke incidence was not significantly different between the groups.
IN PRACTICE:
These findings suggest that SGLT2 inhibitors could have a much-needed ability to simultaneously reduce the burden of recurrent gout flares and coronary sequelae in patients with gout and type 2 diabetes, indicating that “SGLT2 inhibitors may offer distinct benefits,” making the drug class “a particularly attractive addition to current urate-lowering therapies,” the researchers write.
SOURCE:
The study was primarily conducted by researchers at Massachusetts General Hospital in Boston. The study was published online July 24 in Annals of Internal Medicine.
LIMITATIONS:
The data used in the study did not include gout flares that did not require medical attention and did not include laboratory findings for study participants. Because the data were observational the findings may be susceptible to unmeasured confounding.
DISCLOSURES:
The study received no commercial funding. One author has reported receiving consulting fees from ANI and LG Chem.
A version of this article first appeared on Medscape.com.
FROM ANNALS OF INTERNAL MEDICINE
Rheumatology summit tackles racial disparities in lupus trials
Clinical research in lupus has a mammoth diversity problem: Black individuals are most likely to develop the disease, but they’re the least likely to take part in studies. By the numbers, a 2018 analysis of randomized controlled trials in systemic lupus erythematosus from the years 1997 to 2017 found that 51% of trial participants were White and 14% were Black, even though an estimated 33% of patients with lupus were White and 43% were Black.
Are there ways to fix this disparity? The topic is getting plenty of attention, and speakers at a July 21 online conference touted research projects that aim to boost the numbers of non-White participants in lupus trials.
So far there doesn’t seem to be anything like a magic bullet. Still, the stakes are high. “While race is a social construct, genetic polymorphisms as well as environmental and social differences may influence drugs, safety, and efficacy,” Joy Buie, PhD, MSCR, research director for the Lupus Foundation of America, said at the “Engaging Diverse Participants in Lupus Clinical Trials: The Path Forward” summit held by the American College of Rheumatology (ACR).
As African American patients explained, minority populations often don’t trust the medical system and feel burned by their lengthy struggles to get diagnosed. In some cases, they don’t have full faith in their clinicians and feel unheard.
In a video presentation developed as part of a federal education campaign, Shanelle Gabriel, a poet and musician diagnosed with lupus, described her first reaction when her physician suggested she join a clinical trial. “My first reaction was no. I know my history,” she said, apparently referring to the infamous Tuskegee study that withheld proper treatment from Black men with syphilis for decades. “As an African American woman, I was scared. I didn’t want to be a guinea pig.”
Stacey Kennedy-Conner, a Chicago-area patient and advocate, told the summit audience about how patients can feel that clinical trial information can add “an extra layer of confusion” to their experience. “There’s also the mentality of, ‘If it’s not broke, don’t fix it’: If this medication regimen is working, I don’t want anybody to touch me.”
Monique Gore-Massy, a New York City patient and advocate, added that there can be a perception that patients with lupus “are stuck at home in bed.” In reality, she said, “we have jobs, we have families. Think about that, and consider everything that you’re asking from us: Is this taking me away from my family? Am I going to have to take off work? There may be incentives, but is that worth me taking time off work that I may not get paid for? These are some of the realities that we have to look at in terms of the whole entire clinical trial process.”
It’s also important to keep patients informed of progress being made in trials, she said. “You don’t want to say you just felt like a number and then not get any kind of follow-up.”
In the big picture, “there has to be something that builds up the confidence of individuals so that they are more mindful to participate in these clinical trials,” said Aleta McLean, an Atlanta patient who was diagnosed with lupus 14 years ago.
Several researchers highlighted ongoing projects at the summit. The ACR, for example, has launched a $500,000 initiative called Training to Increase Minority Enrollment in Lupus Clinical Trials with Community Engagement (TIMELY). The federally funded project aims to evaluate whether training of health care professionals can boost clinical trial participation among Black and Hispanic patients.
“We hope to disseminate the results of our project to the scientific community through abstracts, manuscripts, presentations at national meetings,” said rheumatologist Saira Z. Sheikh, MD, of the University of North Carolina at Chapel Hill. “Overall, our goal is to establish new partnerships to support the TIMELY model and advance the education and engagement of providers and community health workers.”
Pamela Payne-Foster, MD, MPH, preventive medicine/public health physician at the University of Alabama College of Community Health Sciences, Tuscaloosa, spoke about the federally funded Deep South Health Equity Project, which is paying patients to take part in an online education program and attend an online regional conference.
Other efforts are underway. The Lupus Research Alliance and its clinical affiliate Lupus Therapeutics have launched two initiatives. One is a program called Project Change (Community-based Health Action Network to Generate Trial Participation and Eliminate Disparities), and the Diversity in Lupus Research Program aims to fund scientists’ work.
Will any of this work boost diversity in clinical trials? As one audience member noted in a Q&A session, health care disparities – and knowledge about them – are nothing new: “Why are we not able to narrow the gap?”
Rear Admiral Richardae Araojo, PharmD, MS, director of the FDA’s Office of Minority Health and Health Equity and associate commissioner for minority health, replied that waves of interest in disparities come and go. “That contributes to why we may not see solutions. But ultimately, there are a lot of people doing a lot of work trying to solve the issues.”
The summit was sponsored by Bristol-Myers Squibb, Genentech, and RemeGen.
A version of this article appeared on Medscape.com.
Clinical research in lupus has a mammoth diversity problem: Black individuals are most likely to develop the disease, but they’re the least likely to take part in studies. By the numbers, a 2018 analysis of randomized controlled trials in systemic lupus erythematosus from the years 1997 to 2017 found that 51% of trial participants were White and 14% were Black, even though an estimated 33% of patients with lupus were White and 43% were Black.
Are there ways to fix this disparity? The topic is getting plenty of attention, and speakers at a July 21 online conference touted research projects that aim to boost the numbers of non-White participants in lupus trials.
So far there doesn’t seem to be anything like a magic bullet. Still, the stakes are high. “While race is a social construct, genetic polymorphisms as well as environmental and social differences may influence drugs, safety, and efficacy,” Joy Buie, PhD, MSCR, research director for the Lupus Foundation of America, said at the “Engaging Diverse Participants in Lupus Clinical Trials: The Path Forward” summit held by the American College of Rheumatology (ACR).
As African American patients explained, minority populations often don’t trust the medical system and feel burned by their lengthy struggles to get diagnosed. In some cases, they don’t have full faith in their clinicians and feel unheard.
In a video presentation developed as part of a federal education campaign, Shanelle Gabriel, a poet and musician diagnosed with lupus, described her first reaction when her physician suggested she join a clinical trial. “My first reaction was no. I know my history,” she said, apparently referring to the infamous Tuskegee study that withheld proper treatment from Black men with syphilis for decades. “As an African American woman, I was scared. I didn’t want to be a guinea pig.”
Stacey Kennedy-Conner, a Chicago-area patient and advocate, told the summit audience about how patients can feel that clinical trial information can add “an extra layer of confusion” to their experience. “There’s also the mentality of, ‘If it’s not broke, don’t fix it’: If this medication regimen is working, I don’t want anybody to touch me.”
Monique Gore-Massy, a New York City patient and advocate, added that there can be a perception that patients with lupus “are stuck at home in bed.” In reality, she said, “we have jobs, we have families. Think about that, and consider everything that you’re asking from us: Is this taking me away from my family? Am I going to have to take off work? There may be incentives, but is that worth me taking time off work that I may not get paid for? These are some of the realities that we have to look at in terms of the whole entire clinical trial process.”
It’s also important to keep patients informed of progress being made in trials, she said. “You don’t want to say you just felt like a number and then not get any kind of follow-up.”
In the big picture, “there has to be something that builds up the confidence of individuals so that they are more mindful to participate in these clinical trials,” said Aleta McLean, an Atlanta patient who was diagnosed with lupus 14 years ago.
Several researchers highlighted ongoing projects at the summit. The ACR, for example, has launched a $500,000 initiative called Training to Increase Minority Enrollment in Lupus Clinical Trials with Community Engagement (TIMELY). The federally funded project aims to evaluate whether training of health care professionals can boost clinical trial participation among Black and Hispanic patients.
“We hope to disseminate the results of our project to the scientific community through abstracts, manuscripts, presentations at national meetings,” said rheumatologist Saira Z. Sheikh, MD, of the University of North Carolina at Chapel Hill. “Overall, our goal is to establish new partnerships to support the TIMELY model and advance the education and engagement of providers and community health workers.”
Pamela Payne-Foster, MD, MPH, preventive medicine/public health physician at the University of Alabama College of Community Health Sciences, Tuscaloosa, spoke about the federally funded Deep South Health Equity Project, which is paying patients to take part in an online education program and attend an online regional conference.
Other efforts are underway. The Lupus Research Alliance and its clinical affiliate Lupus Therapeutics have launched two initiatives. One is a program called Project Change (Community-based Health Action Network to Generate Trial Participation and Eliminate Disparities), and the Diversity in Lupus Research Program aims to fund scientists’ work.
Will any of this work boost diversity in clinical trials? As one audience member noted in a Q&A session, health care disparities – and knowledge about them – are nothing new: “Why are we not able to narrow the gap?”
Rear Admiral Richardae Araojo, PharmD, MS, director of the FDA’s Office of Minority Health and Health Equity and associate commissioner for minority health, replied that waves of interest in disparities come and go. “That contributes to why we may not see solutions. But ultimately, there are a lot of people doing a lot of work trying to solve the issues.”
The summit was sponsored by Bristol-Myers Squibb, Genentech, and RemeGen.
A version of this article appeared on Medscape.com.
Clinical research in lupus has a mammoth diversity problem: Black individuals are most likely to develop the disease, but they’re the least likely to take part in studies. By the numbers, a 2018 analysis of randomized controlled trials in systemic lupus erythematosus from the years 1997 to 2017 found that 51% of trial participants were White and 14% were Black, even though an estimated 33% of patients with lupus were White and 43% were Black.
Are there ways to fix this disparity? The topic is getting plenty of attention, and speakers at a July 21 online conference touted research projects that aim to boost the numbers of non-White participants in lupus trials.
So far there doesn’t seem to be anything like a magic bullet. Still, the stakes are high. “While race is a social construct, genetic polymorphisms as well as environmental and social differences may influence drugs, safety, and efficacy,” Joy Buie, PhD, MSCR, research director for the Lupus Foundation of America, said at the “Engaging Diverse Participants in Lupus Clinical Trials: The Path Forward” summit held by the American College of Rheumatology (ACR).
As African American patients explained, minority populations often don’t trust the medical system and feel burned by their lengthy struggles to get diagnosed. In some cases, they don’t have full faith in their clinicians and feel unheard.
In a video presentation developed as part of a federal education campaign, Shanelle Gabriel, a poet and musician diagnosed with lupus, described her first reaction when her physician suggested she join a clinical trial. “My first reaction was no. I know my history,” she said, apparently referring to the infamous Tuskegee study that withheld proper treatment from Black men with syphilis for decades. “As an African American woman, I was scared. I didn’t want to be a guinea pig.”
Stacey Kennedy-Conner, a Chicago-area patient and advocate, told the summit audience about how patients can feel that clinical trial information can add “an extra layer of confusion” to their experience. “There’s also the mentality of, ‘If it’s not broke, don’t fix it’: If this medication regimen is working, I don’t want anybody to touch me.”
Monique Gore-Massy, a New York City patient and advocate, added that there can be a perception that patients with lupus “are stuck at home in bed.” In reality, she said, “we have jobs, we have families. Think about that, and consider everything that you’re asking from us: Is this taking me away from my family? Am I going to have to take off work? There may be incentives, but is that worth me taking time off work that I may not get paid for? These are some of the realities that we have to look at in terms of the whole entire clinical trial process.”
It’s also important to keep patients informed of progress being made in trials, she said. “You don’t want to say you just felt like a number and then not get any kind of follow-up.”
In the big picture, “there has to be something that builds up the confidence of individuals so that they are more mindful to participate in these clinical trials,” said Aleta McLean, an Atlanta patient who was diagnosed with lupus 14 years ago.
Several researchers highlighted ongoing projects at the summit. The ACR, for example, has launched a $500,000 initiative called Training to Increase Minority Enrollment in Lupus Clinical Trials with Community Engagement (TIMELY). The federally funded project aims to evaluate whether training of health care professionals can boost clinical trial participation among Black and Hispanic patients.
“We hope to disseminate the results of our project to the scientific community through abstracts, manuscripts, presentations at national meetings,” said rheumatologist Saira Z. Sheikh, MD, of the University of North Carolina at Chapel Hill. “Overall, our goal is to establish new partnerships to support the TIMELY model and advance the education and engagement of providers and community health workers.”
Pamela Payne-Foster, MD, MPH, preventive medicine/public health physician at the University of Alabama College of Community Health Sciences, Tuscaloosa, spoke about the federally funded Deep South Health Equity Project, which is paying patients to take part in an online education program and attend an online regional conference.
Other efforts are underway. The Lupus Research Alliance and its clinical affiliate Lupus Therapeutics have launched two initiatives. One is a program called Project Change (Community-based Health Action Network to Generate Trial Participation and Eliminate Disparities), and the Diversity in Lupus Research Program aims to fund scientists’ work.
Will any of this work boost diversity in clinical trials? As one audience member noted in a Q&A session, health care disparities – and knowledge about them – are nothing new: “Why are we not able to narrow the gap?”
Rear Admiral Richardae Araojo, PharmD, MS, director of the FDA’s Office of Minority Health and Health Equity and associate commissioner for minority health, replied that waves of interest in disparities come and go. “That contributes to why we may not see solutions. But ultimately, there are a lot of people doing a lot of work trying to solve the issues.”
The summit was sponsored by Bristol-Myers Squibb, Genentech, and RemeGen.
A version of this article appeared on Medscape.com.
FROM AN ACR CLINICAL TRIAL SUMMIT
New clues arise to consequences of calcium crystal deposition in knee OA
Intra-articular calcium crystal deposition is commonly seen in knee osteoarthritis, but its significance has been debated.
Now, a new study that relied on knee radiographs and bilateral knee CT imaging to evaluate 2,093 participants, including some with and without knee mineralization, has provided some new insights.
The study has addressed the longstanding question: Is the calcium deposition a cause or a consequence of the OA? “If it’s a cause, targeting it might be helpful,” Jean Liew, MD, MS, the study’s lead author and assistant professor of medicine at Boston University, said in an interview. “If a consequence of the OA, targeting is not going to help.”
In this new study, because of the use of advanced imaging, the researchers demonstrated a strong relationship of the presence of this calcification with different pain characteristics, said Tuhina Neogi, MD, PhD, professor of medicine and epidemiology at Boston University, the corresponding author of the study who has focused on this research for many years. “This indicates this mineralization is not inconsequential.”
The bottom line? “Calcification in the knee may not be simply inert and an innocent bystander of longstanding OA,” Dr. Neogi said in an interview.
Study details
Dr. Neogi and colleagues evaluated 2,093 participants (mean age, 61 years; 57% female) with a mean body mass index of 28.8 kg/m2. In all, 10.2% of knees had intra-articular mineralization. The data came from the National Institutes of Health–funded longitudinal Multicenter Osteoarthritis Study. At baseline, participants had knee radiographs and bilateral knee CT scans, and pain assessments every 8 months for 2 years. The Boston University Calcium Knee Score was used to score the CT imaging. The researchers longitudinally examined the relationship of the CT-detected intra-articular mineralization to the risk of frequent knee pain, intermittent or constant knee pain worsening, and pain severity worsening. All analyses were adjusted for age, sex, body mass index, race, site, and Kellgren-Lawrence grade.
Having any mineralization in the cartilage was associated with a doubling of odds for having frequent knee pain (95% confidence interval, 1.38-2.78), and 1.86 times greater likelihood of more frequent intermittent or constant knee pain (95% CI, 1.20-2.78) over the 2 years of follow-up. Similar results were seen for the presence of any intra-articular mineralization in the meniscus or joint capsule. The higher the burden of mineralization anywhere within the knee was linked with higher odds for all pain outcomes, with odds ratios ranging from 2.14 to 2.21.
Perspective
“Because we used more sensitive imaging to pick up the calcification, we are able to more confidently evaluate this association,” Dr. Neogi said in an interview. The problem with prior studies was their reliance on plain radiographs, which are not sensitive enough to pick up this calcification.
Among the other strengths of the new research, she said, is that it was longitudinal, included more than 2,000 people and used multiple ways to look at the pain experience, getting consistent results.
“Here we are saying there seems to be clinical relevance [to the mineralization]. That’s not so surprising. We know there are other medical conditions in which calcium calcification can cause severe pain and inflammation.” The old term, pseudogout, is now called calcium pyrophosphate deposition disease.
The next steps of research, Dr. Neogi said, are to investigate the link of the mineralization to inflammation and its association to cartilage damage.
Could colchicine help?
In another recent study, researchers conducted a post hoc analysis of a randomized clinical trial of the anti-inflammatory drug colchicine, finding that the use of colchicine at 0.5 mg daily was associated with a lower incidence of total knee and hip replacements (TKR, THR). In that study, 2,762 participants received colchicine, while 2,760 received placebo during the median follow-up of 28.6 months. During the trial, TKR or THR was done in 68 patients (2.5%) of those in the treated group and 97 patients (3.5%) in the placebo groups. That resulted in an incidence rate difference of –0.40 [95% CI, –0.74 to –0.06 ] per 100 person-years.
The authors wrote that the results suggest that “colchicine may slow the progression of OA, but this needs to be confirmed in an appropriately designed prospective placebo-controlled trial.”
Independent perspective
The new Boston University study supports the idea that there may be a larger subset of patients that may have a calcium mineralization component, said C. Kent Kwoh, MD, professor of medicine and medical imaging at the University of Arizona, Tucson. He reviewed both studies and provided perspective. He is an editorial advisory board member for MDedge Rheumatology.
The study by Dr. Liew and colleagues shows that “there is an association of crystal deposition not just in the cartilage, but various parts of the joint.” He emphasized the study found only an association and that more study is needed.
As for the colchicine study, he said, it “really shows there is potential at least within some individuals where it may decrease symptoms to the point where people are less likely to need joint replacement.” That analysis follows some previous research, some of it shorter term, finding that colchicine was not beneficial.
Takeaways
Would colchicine be worth a try in patients who have knee pain and calcium mineral deposits?
Dr. Neogi noted that a formulation of colchicine (Lodoco) was recently approved by the Food and Drug Administration to reduce the risk of myocardial infarction and other cardiovascular disease. While she does not advocate adopting a practice without evidence, she suggested if someone has both mineralization and cardiovascular disease, along with difficulty managing symptoms with established treatments, it might be worth a try, if no contraindications exist.
Dr. Kwoh agreed it may be worth a try, given that it is “relatively safe and relatively inexpensive.”
On one point all agreed: More research is needed.
Dr. Kwoh, Dr. Neogi and Dr. Liew have no relevant disclosures.
Intra-articular calcium crystal deposition is commonly seen in knee osteoarthritis, but its significance has been debated.
Now, a new study that relied on knee radiographs and bilateral knee CT imaging to evaluate 2,093 participants, including some with and without knee mineralization, has provided some new insights.
The study has addressed the longstanding question: Is the calcium deposition a cause or a consequence of the OA? “If it’s a cause, targeting it might be helpful,” Jean Liew, MD, MS, the study’s lead author and assistant professor of medicine at Boston University, said in an interview. “If a consequence of the OA, targeting is not going to help.”
In this new study, because of the use of advanced imaging, the researchers demonstrated a strong relationship of the presence of this calcification with different pain characteristics, said Tuhina Neogi, MD, PhD, professor of medicine and epidemiology at Boston University, the corresponding author of the study who has focused on this research for many years. “This indicates this mineralization is not inconsequential.”
The bottom line? “Calcification in the knee may not be simply inert and an innocent bystander of longstanding OA,” Dr. Neogi said in an interview.
Study details
Dr. Neogi and colleagues evaluated 2,093 participants (mean age, 61 years; 57% female) with a mean body mass index of 28.8 kg/m2. In all, 10.2% of knees had intra-articular mineralization. The data came from the National Institutes of Health–funded longitudinal Multicenter Osteoarthritis Study. At baseline, participants had knee radiographs and bilateral knee CT scans, and pain assessments every 8 months for 2 years. The Boston University Calcium Knee Score was used to score the CT imaging. The researchers longitudinally examined the relationship of the CT-detected intra-articular mineralization to the risk of frequent knee pain, intermittent or constant knee pain worsening, and pain severity worsening. All analyses were adjusted for age, sex, body mass index, race, site, and Kellgren-Lawrence grade.
Having any mineralization in the cartilage was associated with a doubling of odds for having frequent knee pain (95% confidence interval, 1.38-2.78), and 1.86 times greater likelihood of more frequent intermittent or constant knee pain (95% CI, 1.20-2.78) over the 2 years of follow-up. Similar results were seen for the presence of any intra-articular mineralization in the meniscus or joint capsule. The higher the burden of mineralization anywhere within the knee was linked with higher odds for all pain outcomes, with odds ratios ranging from 2.14 to 2.21.
Perspective
“Because we used more sensitive imaging to pick up the calcification, we are able to more confidently evaluate this association,” Dr. Neogi said in an interview. The problem with prior studies was their reliance on plain radiographs, which are not sensitive enough to pick up this calcification.
Among the other strengths of the new research, she said, is that it was longitudinal, included more than 2,000 people and used multiple ways to look at the pain experience, getting consistent results.
“Here we are saying there seems to be clinical relevance [to the mineralization]. That’s not so surprising. We know there are other medical conditions in which calcium calcification can cause severe pain and inflammation.” The old term, pseudogout, is now called calcium pyrophosphate deposition disease.
The next steps of research, Dr. Neogi said, are to investigate the link of the mineralization to inflammation and its association to cartilage damage.
Could colchicine help?
In another recent study, researchers conducted a post hoc analysis of a randomized clinical trial of the anti-inflammatory drug colchicine, finding that the use of colchicine at 0.5 mg daily was associated with a lower incidence of total knee and hip replacements (TKR, THR). In that study, 2,762 participants received colchicine, while 2,760 received placebo during the median follow-up of 28.6 months. During the trial, TKR or THR was done in 68 patients (2.5%) of those in the treated group and 97 patients (3.5%) in the placebo groups. That resulted in an incidence rate difference of –0.40 [95% CI, –0.74 to –0.06 ] per 100 person-years.
The authors wrote that the results suggest that “colchicine may slow the progression of OA, but this needs to be confirmed in an appropriately designed prospective placebo-controlled trial.”
Independent perspective
The new Boston University study supports the idea that there may be a larger subset of patients that may have a calcium mineralization component, said C. Kent Kwoh, MD, professor of medicine and medical imaging at the University of Arizona, Tucson. He reviewed both studies and provided perspective. He is an editorial advisory board member for MDedge Rheumatology.
The study by Dr. Liew and colleagues shows that “there is an association of crystal deposition not just in the cartilage, but various parts of the joint.” He emphasized the study found only an association and that more study is needed.
As for the colchicine study, he said, it “really shows there is potential at least within some individuals where it may decrease symptoms to the point where people are less likely to need joint replacement.” That analysis follows some previous research, some of it shorter term, finding that colchicine was not beneficial.
Takeaways
Would colchicine be worth a try in patients who have knee pain and calcium mineral deposits?
Dr. Neogi noted that a formulation of colchicine (Lodoco) was recently approved by the Food and Drug Administration to reduce the risk of myocardial infarction and other cardiovascular disease. While she does not advocate adopting a practice without evidence, she suggested if someone has both mineralization and cardiovascular disease, along with difficulty managing symptoms with established treatments, it might be worth a try, if no contraindications exist.
Dr. Kwoh agreed it may be worth a try, given that it is “relatively safe and relatively inexpensive.”
On one point all agreed: More research is needed.
Dr. Kwoh, Dr. Neogi and Dr. Liew have no relevant disclosures.
Intra-articular calcium crystal deposition is commonly seen in knee osteoarthritis, but its significance has been debated.
Now, a new study that relied on knee radiographs and bilateral knee CT imaging to evaluate 2,093 participants, including some with and without knee mineralization, has provided some new insights.
The study has addressed the longstanding question: Is the calcium deposition a cause or a consequence of the OA? “If it’s a cause, targeting it might be helpful,” Jean Liew, MD, MS, the study’s lead author and assistant professor of medicine at Boston University, said in an interview. “If a consequence of the OA, targeting is not going to help.”
In this new study, because of the use of advanced imaging, the researchers demonstrated a strong relationship of the presence of this calcification with different pain characteristics, said Tuhina Neogi, MD, PhD, professor of medicine and epidemiology at Boston University, the corresponding author of the study who has focused on this research for many years. “This indicates this mineralization is not inconsequential.”
The bottom line? “Calcification in the knee may not be simply inert and an innocent bystander of longstanding OA,” Dr. Neogi said in an interview.
Study details
Dr. Neogi and colleagues evaluated 2,093 participants (mean age, 61 years; 57% female) with a mean body mass index of 28.8 kg/m2. In all, 10.2% of knees had intra-articular mineralization. The data came from the National Institutes of Health–funded longitudinal Multicenter Osteoarthritis Study. At baseline, participants had knee radiographs and bilateral knee CT scans, and pain assessments every 8 months for 2 years. The Boston University Calcium Knee Score was used to score the CT imaging. The researchers longitudinally examined the relationship of the CT-detected intra-articular mineralization to the risk of frequent knee pain, intermittent or constant knee pain worsening, and pain severity worsening. All analyses were adjusted for age, sex, body mass index, race, site, and Kellgren-Lawrence grade.
Having any mineralization in the cartilage was associated with a doubling of odds for having frequent knee pain (95% confidence interval, 1.38-2.78), and 1.86 times greater likelihood of more frequent intermittent or constant knee pain (95% CI, 1.20-2.78) over the 2 years of follow-up. Similar results were seen for the presence of any intra-articular mineralization in the meniscus or joint capsule. The higher the burden of mineralization anywhere within the knee was linked with higher odds for all pain outcomes, with odds ratios ranging from 2.14 to 2.21.
Perspective
“Because we used more sensitive imaging to pick up the calcification, we are able to more confidently evaluate this association,” Dr. Neogi said in an interview. The problem with prior studies was their reliance on plain radiographs, which are not sensitive enough to pick up this calcification.
Among the other strengths of the new research, she said, is that it was longitudinal, included more than 2,000 people and used multiple ways to look at the pain experience, getting consistent results.
“Here we are saying there seems to be clinical relevance [to the mineralization]. That’s not so surprising. We know there are other medical conditions in which calcium calcification can cause severe pain and inflammation.” The old term, pseudogout, is now called calcium pyrophosphate deposition disease.
The next steps of research, Dr. Neogi said, are to investigate the link of the mineralization to inflammation and its association to cartilage damage.
Could colchicine help?
In another recent study, researchers conducted a post hoc analysis of a randomized clinical trial of the anti-inflammatory drug colchicine, finding that the use of colchicine at 0.5 mg daily was associated with a lower incidence of total knee and hip replacements (TKR, THR). In that study, 2,762 participants received colchicine, while 2,760 received placebo during the median follow-up of 28.6 months. During the trial, TKR or THR was done in 68 patients (2.5%) of those in the treated group and 97 patients (3.5%) in the placebo groups. That resulted in an incidence rate difference of –0.40 [95% CI, –0.74 to –0.06 ] per 100 person-years.
The authors wrote that the results suggest that “colchicine may slow the progression of OA, but this needs to be confirmed in an appropriately designed prospective placebo-controlled trial.”
Independent perspective
The new Boston University study supports the idea that there may be a larger subset of patients that may have a calcium mineralization component, said C. Kent Kwoh, MD, professor of medicine and medical imaging at the University of Arizona, Tucson. He reviewed both studies and provided perspective. He is an editorial advisory board member for MDedge Rheumatology.
The study by Dr. Liew and colleagues shows that “there is an association of crystal deposition not just in the cartilage, but various parts of the joint.” He emphasized the study found only an association and that more study is needed.
As for the colchicine study, he said, it “really shows there is potential at least within some individuals where it may decrease symptoms to the point where people are less likely to need joint replacement.” That analysis follows some previous research, some of it shorter term, finding that colchicine was not beneficial.
Takeaways
Would colchicine be worth a try in patients who have knee pain and calcium mineral deposits?
Dr. Neogi noted that a formulation of colchicine (Lodoco) was recently approved by the Food and Drug Administration to reduce the risk of myocardial infarction and other cardiovascular disease. While she does not advocate adopting a practice without evidence, she suggested if someone has both mineralization and cardiovascular disease, along with difficulty managing symptoms with established treatments, it might be worth a try, if no contraindications exist.
Dr. Kwoh agreed it may be worth a try, given that it is “relatively safe and relatively inexpensive.”
On one point all agreed: More research is needed.
Dr. Kwoh, Dr. Neogi and Dr. Liew have no relevant disclosures.
FROM ARTHRITIS & RHEUMATOLOGY
Transcutaneous vagus nerve stimulation on the ear proves ineffective in RA treatment
Noninvasive auricular vagus nerve stimulation (VNS) is no more effective than placebo at controlling symptoms of rheumatoid arthritis, according to a new study. But experts emphasize that these results do not mean trials of different forms of VNS will have the same fate.
VNS offers a potential additional therapy for autoimmune disease beyond disease-modifying antirheumatic drugs, explained first author Matthew Baker, MD, clinical chief, division of immunology and rheumatology, Stanford (Calif.) University, and colleagues.
“The principle of VNS is based upon the inflammatory reflex, which describes a primitive connection between the nervous system and immune system,” the authors write. Signals sent down the vagus nerve to the splenic nerve stimulate immune cells in the spleen, which ultimately results in blocking production of inflammatory cytokines such as tumor necrosis factor. “It is hypothesized that this reduction in systemic inflammation can be harnessed for the treatment of diseases such as RA,” they continue, and smaller studies suggest this treatment could benefit patients.
In a previous 12-week, open-label trial, 17 patients with RA who were implanted with a VNS device on the left cervical vagus nerve saw improvement in RA symptoms, as well as a decrease in TNF production. Noninvasive devices that stimulate the auricular branch of the vagus nerve have also shown some promise. A sham-controlled study of 18 patients with systemic lupus erythematosus (SLE) found that patients who received transcutaneous auricular VNS reported reduced musculoskeletal pain over just 4 days. An open-label study of 30 patients with RA showed clinically significant reductions in disease activity score of 28 joints with C-reactive protein (DAS28-CRP) and clinical improvement in American College of Rheumatology responses over 12 weeks. Additional trials have also demonstrated this positive effect of noninvasive VNS on RA symptoms, but all studies conducted thus far have been relatively small or uncontrolled, Dr. Baker said.
Results of latest trial
In this new trial, published online in Arthritis & Rheumatology, researchers enrolled 113 patients with active RA who had inadequate responses or intolerance to conventional synthetic DMARDs and were naïve to biologic or targeted synthetic DMARDs. All patients were given an auricular vagus nerve stimulator via a custom-molded earpiece that was controlled by a smartphone app. Patients wore the device for 15 minutes each day. When worn and turned on, the device generated electrical signals delivered transcutaneously to the cymba concha, a region of the ear connected to the auricular branch of the vagus nerve. This stimulation is imperceptible to patients, Dr. Baker explained. “For the sham arm, we simply did not turn the device on at all,” he said. A subject in the sham arm would use the same device on a 15-minute timer, but no stimulation was given.
After 12 weeks, researchers found no statistically significant difference between the treatment and sham arms in achieving 20% improvement in ACR response criteria or mean change in DAS28-CRP. A total of 17 patients, including 12 in the treatment arm, reported adverse events during the study, and all events were categorized as mild to moderate.
While the research team was “obviously disappointed” about the results, Dr. Baker said, negative findings in trials also are important. “The real value of our study is pointing out the need for large controlled, sham-controlled studies,” he said, especially for potential treatments with a lot of enthusiasm behind them.
Results don’t seal the fate of other VNS approaches
“As a properly controlled trial, the results are impressively negative,” writes Roy Fleischmann, MD, clinical professor of medicine, University of Texas Southwestern Medical Center, and codirector, Metroplex Clinical Research Center, both in Dallas, in an editorial about the study. Many of the previous studies looking at this therapy in RA were open label, which could bias the results, he argued. The biggest question, he noted, is if other blinded, sham-controlled trials looking at VNS devices will show similar results.
By itself, this finding does not imply that other VNS devices will be unsuccessful, argued Jonathan Kay, MD, the Timothy S. and Elaine L. Peterson chair in rheumatology, and professor of medicine and population and quantitative health sciences, UMass Chan Medical School and UMass Memorial Medical Center, both in Worcester, Mass. He is also an investigator for the RESET-RA trial, a randomized, sham-controlled trial that will assess the safety and efficacy of an implantable VNS device in an estimated 250 patients with RA. He was not involved with Dr. Baker’s work.
“Auricular VNS is delivered more distally than cervical or splenic nerve stimulation,” Dr. Kay said, and the potential effect of these other forms of VNS may have different outcomes.
Cynthia Aranow, MD, rheumatologist and director of the Clinical Autoimmunity Center of Excellence at Feinstein Institutes for Medical Research, Manhasset, New York, agreed with Dr. Kay, noting that direct VNS stimulation via implantable device and transcutaneous stimulation through the skin are not comparable. She also is unaffiliated with the study.
“This group conducted a well-designed, sham-controlled study of a reasonable number of patients and over a reasonable period of time and observed no significant differences between those participants receiving true and those participants receiving sham stimulation,” she wrote in an email. “However, it’s important to point out that the stimulation settings used in this study were kHz (kilohertz) which is 1,000 times greater than the settings used in multiple other studies in which transauricular VNS has been shown to be clinically effective, including studies in long COVID, tinnitus, SLE, cluster headaches, erosive hand osteoarthritis, pediatric kidney disease, among others,” she said.
The role for VNS treatment, whether direct stimulation via implantable device or transcutaneous, in autoimmune and inflammatory diseases “remains to be determined by future studies,” she said.
The study was funded by Nesos. Dr. Baker received personal fees from Nesos during the study. Dr. Kay has received consulting fees from AbbVie, Boehringer Ingelheim, Celltrion Healthcare, and several other pharmaceutical companies. Dr. Aranow reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Noninvasive auricular vagus nerve stimulation (VNS) is no more effective than placebo at controlling symptoms of rheumatoid arthritis, according to a new study. But experts emphasize that these results do not mean trials of different forms of VNS will have the same fate.
VNS offers a potential additional therapy for autoimmune disease beyond disease-modifying antirheumatic drugs, explained first author Matthew Baker, MD, clinical chief, division of immunology and rheumatology, Stanford (Calif.) University, and colleagues.
“The principle of VNS is based upon the inflammatory reflex, which describes a primitive connection between the nervous system and immune system,” the authors write. Signals sent down the vagus nerve to the splenic nerve stimulate immune cells in the spleen, which ultimately results in blocking production of inflammatory cytokines such as tumor necrosis factor. “It is hypothesized that this reduction in systemic inflammation can be harnessed for the treatment of diseases such as RA,” they continue, and smaller studies suggest this treatment could benefit patients.
In a previous 12-week, open-label trial, 17 patients with RA who were implanted with a VNS device on the left cervical vagus nerve saw improvement in RA symptoms, as well as a decrease in TNF production. Noninvasive devices that stimulate the auricular branch of the vagus nerve have also shown some promise. A sham-controlled study of 18 patients with systemic lupus erythematosus (SLE) found that patients who received transcutaneous auricular VNS reported reduced musculoskeletal pain over just 4 days. An open-label study of 30 patients with RA showed clinically significant reductions in disease activity score of 28 joints with C-reactive protein (DAS28-CRP) and clinical improvement in American College of Rheumatology responses over 12 weeks. Additional trials have also demonstrated this positive effect of noninvasive VNS on RA symptoms, but all studies conducted thus far have been relatively small or uncontrolled, Dr. Baker said.
Results of latest trial
In this new trial, published online in Arthritis & Rheumatology, researchers enrolled 113 patients with active RA who had inadequate responses or intolerance to conventional synthetic DMARDs and were naïve to biologic or targeted synthetic DMARDs. All patients were given an auricular vagus nerve stimulator via a custom-molded earpiece that was controlled by a smartphone app. Patients wore the device for 15 minutes each day. When worn and turned on, the device generated electrical signals delivered transcutaneously to the cymba concha, a region of the ear connected to the auricular branch of the vagus nerve. This stimulation is imperceptible to patients, Dr. Baker explained. “For the sham arm, we simply did not turn the device on at all,” he said. A subject in the sham arm would use the same device on a 15-minute timer, but no stimulation was given.
After 12 weeks, researchers found no statistically significant difference between the treatment and sham arms in achieving 20% improvement in ACR response criteria or mean change in DAS28-CRP. A total of 17 patients, including 12 in the treatment arm, reported adverse events during the study, and all events were categorized as mild to moderate.
While the research team was “obviously disappointed” about the results, Dr. Baker said, negative findings in trials also are important. “The real value of our study is pointing out the need for large controlled, sham-controlled studies,” he said, especially for potential treatments with a lot of enthusiasm behind them.
Results don’t seal the fate of other VNS approaches
“As a properly controlled trial, the results are impressively negative,” writes Roy Fleischmann, MD, clinical professor of medicine, University of Texas Southwestern Medical Center, and codirector, Metroplex Clinical Research Center, both in Dallas, in an editorial about the study. Many of the previous studies looking at this therapy in RA were open label, which could bias the results, he argued. The biggest question, he noted, is if other blinded, sham-controlled trials looking at VNS devices will show similar results.
By itself, this finding does not imply that other VNS devices will be unsuccessful, argued Jonathan Kay, MD, the Timothy S. and Elaine L. Peterson chair in rheumatology, and professor of medicine and population and quantitative health sciences, UMass Chan Medical School and UMass Memorial Medical Center, both in Worcester, Mass. He is also an investigator for the RESET-RA trial, a randomized, sham-controlled trial that will assess the safety and efficacy of an implantable VNS device in an estimated 250 patients with RA. He was not involved with Dr. Baker’s work.
“Auricular VNS is delivered more distally than cervical or splenic nerve stimulation,” Dr. Kay said, and the potential effect of these other forms of VNS may have different outcomes.
Cynthia Aranow, MD, rheumatologist and director of the Clinical Autoimmunity Center of Excellence at Feinstein Institutes for Medical Research, Manhasset, New York, agreed with Dr. Kay, noting that direct VNS stimulation via implantable device and transcutaneous stimulation through the skin are not comparable. She also is unaffiliated with the study.
“This group conducted a well-designed, sham-controlled study of a reasonable number of patients and over a reasonable period of time and observed no significant differences between those participants receiving true and those participants receiving sham stimulation,” she wrote in an email. “However, it’s important to point out that the stimulation settings used in this study were kHz (kilohertz) which is 1,000 times greater than the settings used in multiple other studies in which transauricular VNS has been shown to be clinically effective, including studies in long COVID, tinnitus, SLE, cluster headaches, erosive hand osteoarthritis, pediatric kidney disease, among others,” she said.
The role for VNS treatment, whether direct stimulation via implantable device or transcutaneous, in autoimmune and inflammatory diseases “remains to be determined by future studies,” she said.
The study was funded by Nesos. Dr. Baker received personal fees from Nesos during the study. Dr. Kay has received consulting fees from AbbVie, Boehringer Ingelheim, Celltrion Healthcare, and several other pharmaceutical companies. Dr. Aranow reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Noninvasive auricular vagus nerve stimulation (VNS) is no more effective than placebo at controlling symptoms of rheumatoid arthritis, according to a new study. But experts emphasize that these results do not mean trials of different forms of VNS will have the same fate.
VNS offers a potential additional therapy for autoimmune disease beyond disease-modifying antirheumatic drugs, explained first author Matthew Baker, MD, clinical chief, division of immunology and rheumatology, Stanford (Calif.) University, and colleagues.
“The principle of VNS is based upon the inflammatory reflex, which describes a primitive connection between the nervous system and immune system,” the authors write. Signals sent down the vagus nerve to the splenic nerve stimulate immune cells in the spleen, which ultimately results in blocking production of inflammatory cytokines such as tumor necrosis factor. “It is hypothesized that this reduction in systemic inflammation can be harnessed for the treatment of diseases such as RA,” they continue, and smaller studies suggest this treatment could benefit patients.
In a previous 12-week, open-label trial, 17 patients with RA who were implanted with a VNS device on the left cervical vagus nerve saw improvement in RA symptoms, as well as a decrease in TNF production. Noninvasive devices that stimulate the auricular branch of the vagus nerve have also shown some promise. A sham-controlled study of 18 patients with systemic lupus erythematosus (SLE) found that patients who received transcutaneous auricular VNS reported reduced musculoskeletal pain over just 4 days. An open-label study of 30 patients with RA showed clinically significant reductions in disease activity score of 28 joints with C-reactive protein (DAS28-CRP) and clinical improvement in American College of Rheumatology responses over 12 weeks. Additional trials have also demonstrated this positive effect of noninvasive VNS on RA symptoms, but all studies conducted thus far have been relatively small or uncontrolled, Dr. Baker said.
Results of latest trial
In this new trial, published online in Arthritis & Rheumatology, researchers enrolled 113 patients with active RA who had inadequate responses or intolerance to conventional synthetic DMARDs and were naïve to biologic or targeted synthetic DMARDs. All patients were given an auricular vagus nerve stimulator via a custom-molded earpiece that was controlled by a smartphone app. Patients wore the device for 15 minutes each day. When worn and turned on, the device generated electrical signals delivered transcutaneously to the cymba concha, a region of the ear connected to the auricular branch of the vagus nerve. This stimulation is imperceptible to patients, Dr. Baker explained. “For the sham arm, we simply did not turn the device on at all,” he said. A subject in the sham arm would use the same device on a 15-minute timer, but no stimulation was given.
After 12 weeks, researchers found no statistically significant difference between the treatment and sham arms in achieving 20% improvement in ACR response criteria or mean change in DAS28-CRP. A total of 17 patients, including 12 in the treatment arm, reported adverse events during the study, and all events were categorized as mild to moderate.
While the research team was “obviously disappointed” about the results, Dr. Baker said, negative findings in trials also are important. “The real value of our study is pointing out the need for large controlled, sham-controlled studies,” he said, especially for potential treatments with a lot of enthusiasm behind them.
Results don’t seal the fate of other VNS approaches
“As a properly controlled trial, the results are impressively negative,” writes Roy Fleischmann, MD, clinical professor of medicine, University of Texas Southwestern Medical Center, and codirector, Metroplex Clinical Research Center, both in Dallas, in an editorial about the study. Many of the previous studies looking at this therapy in RA were open label, which could bias the results, he argued. The biggest question, he noted, is if other blinded, sham-controlled trials looking at VNS devices will show similar results.
By itself, this finding does not imply that other VNS devices will be unsuccessful, argued Jonathan Kay, MD, the Timothy S. and Elaine L. Peterson chair in rheumatology, and professor of medicine and population and quantitative health sciences, UMass Chan Medical School and UMass Memorial Medical Center, both in Worcester, Mass. He is also an investigator for the RESET-RA trial, a randomized, sham-controlled trial that will assess the safety and efficacy of an implantable VNS device in an estimated 250 patients with RA. He was not involved with Dr. Baker’s work.
“Auricular VNS is delivered more distally than cervical or splenic nerve stimulation,” Dr. Kay said, and the potential effect of these other forms of VNS may have different outcomes.
Cynthia Aranow, MD, rheumatologist and director of the Clinical Autoimmunity Center of Excellence at Feinstein Institutes for Medical Research, Manhasset, New York, agreed with Dr. Kay, noting that direct VNS stimulation via implantable device and transcutaneous stimulation through the skin are not comparable. She also is unaffiliated with the study.
“This group conducted a well-designed, sham-controlled study of a reasonable number of patients and over a reasonable period of time and observed no significant differences between those participants receiving true and those participants receiving sham stimulation,” she wrote in an email. “However, it’s important to point out that the stimulation settings used in this study were kHz (kilohertz) which is 1,000 times greater than the settings used in multiple other studies in which transauricular VNS has been shown to be clinically effective, including studies in long COVID, tinnitus, SLE, cluster headaches, erosive hand osteoarthritis, pediatric kidney disease, among others,” she said.
The role for VNS treatment, whether direct stimulation via implantable device or transcutaneous, in autoimmune and inflammatory diseases “remains to be determined by future studies,” she said.
The study was funded by Nesos. Dr. Baker received personal fees from Nesos during the study. Dr. Kay has received consulting fees from AbbVie, Boehringer Ingelheim, Celltrion Healthcare, and several other pharmaceutical companies. Dr. Aranow reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM ARTHRITIS & RHEUMATOLOGY
Humira biosimilars: Five things to know
The best-selling drug Humira (adalimumab) now faces competition in the United States after a 20-year monopoly. The first adalimumab biosimilar, Amjevita, launched in the United States on January 31, and in July, seven additional biosimilars became available. These drugs have the potential to lower prescription drug prices, but when and by how much remains to be seen.
Here’s what you need to know about adalimumab biosimilars.
What Humira biosimilars are now available?
Eight different biosimilars have launched in 2023 with discounts as large at 85% from Humira’s list price of $6,922. A few companies also offer two price points.
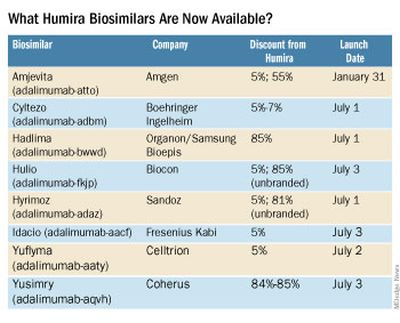
Three of these biosimilars – Hadlima, Hyrimoz, and Yuflyma – are available in high concentration formulations. This high concentration formulation makes up 85% of Humira prescriptions, according to a report from Goodroot, a collection of companies focused on lowering health care costs.
Cyltezo is currently the only adalimumab biosimilar with an interchangeability designation, meaning that a pharmacist can substitute the biosimilar for an equivalent Humira prescription without the intervention of a clinician. A total of 47 states allow for these substitutions without prior approval from a clinician, according to Goodroot, and the clinician must be notified of the switch within a certain time frame. A total of 40 states require that patients be notified of the switch before substitution.
However, it’s not clear if this interchangeability designation will prove an advantage for Cyltezo, as it is interchangeable with the lower concentration version of Humira that makes up just 15% of prescriptions.
Most of the companies behind these biosimilars are pursuing interchangeability designations for their drugs, except for Fresenius Kabi (Idacio) and Coherus (Yusimry).
A ninth biosimilar, Pfizer’s adalimumab-afzb (Abrilada), is not yet on the market and is currently awaiting an approval decision from the Food and Drug Administration to add an interchangeability designation to its prior approval for a low-concentration formulation.
Why are they priced differently?
The two price points offer different deals to payers. Pharmacy benefit managers make confidential agreements with drug manufacturers to get a discount – called a rebate – to get the drug on the PBM’s formulary. The PBM keeps a portion of that rebate, and the rest is passed on to the insurance company and patients. Biosimilars at a higher price point will likely offer larger rebates. Biosimilars offered at lower price points incorporate this discount up front in their list pricing and likely will not offer large rebates.
Will biosimilars be covered by payers?
Currently, biosimilars are being offered on formularies at parity with Humira, meaning they are on the same tier. The PBM companies OptumRx and Cigna Group’s Express Scripts will offer Amjevita (at both price points), Cyltezo, and Hyrimoz (at both price points).
“This decision allows our clients flexibility to provide access to the lower list price, so members in high-deductible plans and benefit designs with coinsurance can experience lower out-of-pocket costs,” said OptumRx spokesperson Isaac Sorensen in an email.
Mark Cuban Cost Plus Drug Company, which uses a direct-to-consumer model, will offer Yusimry for $567.27 on its website. SmithRx, a PBM based in San Francisco, announced it would partner with Cost Plus Drugs to offer Yusimry, adding that SmithRx members can use their insurance benefits to further reduce out-of-pocket costs. RxPreferred, another PBM, will also offer Yusimry through its partnership with Cuban’s company.
The news website Formulary Watch previously reported that CVS Caremark, another of the biggest PBMs, will be offering Amjevita, but as a nonpreferred brand, while Humira remains the preferred brand. CVS Caremark did not respond to a request for comment.
Will patients pay less?
Biosimilars have been touted as a potential solution to lower spending on biologic drugs, but it’s unknown if patients will ultimately benefit with lower out-of-pocket costs. It’s “impossible to predict” if the discount that third-party payers pay will be passed on to consumers, said Mark Fendrick, MD, who directs the University of Michigan Center for Value-based Insurance Design in Ann Arbor.
Generally, a consumer’s copay is a percentage of a drug’s list price, so it stands to reason that a low drug price would result in lower out-of-pocket payments. While this is mostly true, Humira has a successful copay assistance program to lower prescription costs for consumers. According to a 2022 IQVIA report, 82% of commercial prescriptions cost patients less than $10 for Humira because of this program.
To appeal to patients, biosimilar companies will need to offer similar savings, Dr. Fendrick added. “There will be some discontent if patients are actually asked to pay more out-of-pocket for a less expensive drug,” he said.
All eight companies behind these biosimilars are offering or will be launching copay saving programs, many which advertise copays as low as $0 per month for eligible patients.
How will Humira respond?
Marta Wosińska, PhD, a health care economist at the Brookings Institute, Washington, predicts payers will use these lower biosimilar prices to negotiate better deals with AbbVie, Humira’s manufacturer. “We have a lot of players coming into [the market] right now, so the competition is really fierce,” she said. In response, AbbVie will need to increase rebates on Humira and/or lower its price to compete with these biosimilars.
“The ball is in AbbVie’s court,” she said. “If [the company] is not willing to drop price sufficiently, then payers will start switching to biosimilars.”
Dr. Fendrick reported past financial relationships and consulting arrangements with AbbVie, Amgen, Arnold Ventures, Bayer, CareFirst, BlueCross BlueShield, and many other companies. Dr. Wosińska has received funding from Arnold Ventures and serves as an expert witness on antitrust cases involving generic medication.
A version of this article first appeared on Medscape.com.
The best-selling drug Humira (adalimumab) now faces competition in the United States after a 20-year monopoly. The first adalimumab biosimilar, Amjevita, launched in the United States on January 31, and in July, seven additional biosimilars became available. These drugs have the potential to lower prescription drug prices, but when and by how much remains to be seen.
Here’s what you need to know about adalimumab biosimilars.
What Humira biosimilars are now available?
Eight different biosimilars have launched in 2023 with discounts as large at 85% from Humira’s list price of $6,922. A few companies also offer two price points.

Three of these biosimilars – Hadlima, Hyrimoz, and Yuflyma – are available in high concentration formulations. This high concentration formulation makes up 85% of Humira prescriptions, according to a report from Goodroot, a collection of companies focused on lowering health care costs.
Cyltezo is currently the only adalimumab biosimilar with an interchangeability designation, meaning that a pharmacist can substitute the biosimilar for an equivalent Humira prescription without the intervention of a clinician. A total of 47 states allow for these substitutions without prior approval from a clinician, according to Goodroot, and the clinician must be notified of the switch within a certain time frame. A total of 40 states require that patients be notified of the switch before substitution.
However, it’s not clear if this interchangeability designation will prove an advantage for Cyltezo, as it is interchangeable with the lower concentration version of Humira that makes up just 15% of prescriptions.
Most of the companies behind these biosimilars are pursuing interchangeability designations for their drugs, except for Fresenius Kabi (Idacio) and Coherus (Yusimry).
A ninth biosimilar, Pfizer’s adalimumab-afzb (Abrilada), is not yet on the market and is currently awaiting an approval decision from the Food and Drug Administration to add an interchangeability designation to its prior approval for a low-concentration formulation.
Why are they priced differently?
The two price points offer different deals to payers. Pharmacy benefit managers make confidential agreements with drug manufacturers to get a discount – called a rebate – to get the drug on the PBM’s formulary. The PBM keeps a portion of that rebate, and the rest is passed on to the insurance company and patients. Biosimilars at a higher price point will likely offer larger rebates. Biosimilars offered at lower price points incorporate this discount up front in their list pricing and likely will not offer large rebates.
Will biosimilars be covered by payers?
Currently, biosimilars are being offered on formularies at parity with Humira, meaning they are on the same tier. The PBM companies OptumRx and Cigna Group’s Express Scripts will offer Amjevita (at both price points), Cyltezo, and Hyrimoz (at both price points).
“This decision allows our clients flexibility to provide access to the lower list price, so members in high-deductible plans and benefit designs with coinsurance can experience lower out-of-pocket costs,” said OptumRx spokesperson Isaac Sorensen in an email.
Mark Cuban Cost Plus Drug Company, which uses a direct-to-consumer model, will offer Yusimry for $567.27 on its website. SmithRx, a PBM based in San Francisco, announced it would partner with Cost Plus Drugs to offer Yusimry, adding that SmithRx members can use their insurance benefits to further reduce out-of-pocket costs. RxPreferred, another PBM, will also offer Yusimry through its partnership with Cuban’s company.
The news website Formulary Watch previously reported that CVS Caremark, another of the biggest PBMs, will be offering Amjevita, but as a nonpreferred brand, while Humira remains the preferred brand. CVS Caremark did not respond to a request for comment.
Will patients pay less?
Biosimilars have been touted as a potential solution to lower spending on biologic drugs, but it’s unknown if patients will ultimately benefit with lower out-of-pocket costs. It’s “impossible to predict” if the discount that third-party payers pay will be passed on to consumers, said Mark Fendrick, MD, who directs the University of Michigan Center for Value-based Insurance Design in Ann Arbor.
Generally, a consumer’s copay is a percentage of a drug’s list price, so it stands to reason that a low drug price would result in lower out-of-pocket payments. While this is mostly true, Humira has a successful copay assistance program to lower prescription costs for consumers. According to a 2022 IQVIA report, 82% of commercial prescriptions cost patients less than $10 for Humira because of this program.
To appeal to patients, biosimilar companies will need to offer similar savings, Dr. Fendrick added. “There will be some discontent if patients are actually asked to pay more out-of-pocket for a less expensive drug,” he said.
All eight companies behind these biosimilars are offering or will be launching copay saving programs, many which advertise copays as low as $0 per month for eligible patients.
How will Humira respond?
Marta Wosińska, PhD, a health care economist at the Brookings Institute, Washington, predicts payers will use these lower biosimilar prices to negotiate better deals with AbbVie, Humira’s manufacturer. “We have a lot of players coming into [the market] right now, so the competition is really fierce,” she said. In response, AbbVie will need to increase rebates on Humira and/or lower its price to compete with these biosimilars.
“The ball is in AbbVie’s court,” she said. “If [the company] is not willing to drop price sufficiently, then payers will start switching to biosimilars.”
Dr. Fendrick reported past financial relationships and consulting arrangements with AbbVie, Amgen, Arnold Ventures, Bayer, CareFirst, BlueCross BlueShield, and many other companies. Dr. Wosińska has received funding from Arnold Ventures and serves as an expert witness on antitrust cases involving generic medication.
A version of this article first appeared on Medscape.com.
The best-selling drug Humira (adalimumab) now faces competition in the United States after a 20-year monopoly. The first adalimumab biosimilar, Amjevita, launched in the United States on January 31, and in July, seven additional biosimilars became available. These drugs have the potential to lower prescription drug prices, but when and by how much remains to be seen.
Here’s what you need to know about adalimumab biosimilars.
What Humira biosimilars are now available?
Eight different biosimilars have launched in 2023 with discounts as large at 85% from Humira’s list price of $6,922. A few companies also offer two price points.

Three of these biosimilars – Hadlima, Hyrimoz, and Yuflyma – are available in high concentration formulations. This high concentration formulation makes up 85% of Humira prescriptions, according to a report from Goodroot, a collection of companies focused on lowering health care costs.
Cyltezo is currently the only adalimumab biosimilar with an interchangeability designation, meaning that a pharmacist can substitute the biosimilar for an equivalent Humira prescription without the intervention of a clinician. A total of 47 states allow for these substitutions without prior approval from a clinician, according to Goodroot, and the clinician must be notified of the switch within a certain time frame. A total of 40 states require that patients be notified of the switch before substitution.
However, it’s not clear if this interchangeability designation will prove an advantage for Cyltezo, as it is interchangeable with the lower concentration version of Humira that makes up just 15% of prescriptions.
Most of the companies behind these biosimilars are pursuing interchangeability designations for their drugs, except for Fresenius Kabi (Idacio) and Coherus (Yusimry).
A ninth biosimilar, Pfizer’s adalimumab-afzb (Abrilada), is not yet on the market and is currently awaiting an approval decision from the Food and Drug Administration to add an interchangeability designation to its prior approval for a low-concentration formulation.
Why are they priced differently?
The two price points offer different deals to payers. Pharmacy benefit managers make confidential agreements with drug manufacturers to get a discount – called a rebate – to get the drug on the PBM’s formulary. The PBM keeps a portion of that rebate, and the rest is passed on to the insurance company and patients. Biosimilars at a higher price point will likely offer larger rebates. Biosimilars offered at lower price points incorporate this discount up front in their list pricing and likely will not offer large rebates.
Will biosimilars be covered by payers?
Currently, biosimilars are being offered on formularies at parity with Humira, meaning they are on the same tier. The PBM companies OptumRx and Cigna Group’s Express Scripts will offer Amjevita (at both price points), Cyltezo, and Hyrimoz (at both price points).
“This decision allows our clients flexibility to provide access to the lower list price, so members in high-deductible plans and benefit designs with coinsurance can experience lower out-of-pocket costs,” said OptumRx spokesperson Isaac Sorensen in an email.
Mark Cuban Cost Plus Drug Company, which uses a direct-to-consumer model, will offer Yusimry for $567.27 on its website. SmithRx, a PBM based in San Francisco, announced it would partner with Cost Plus Drugs to offer Yusimry, adding that SmithRx members can use their insurance benefits to further reduce out-of-pocket costs. RxPreferred, another PBM, will also offer Yusimry through its partnership with Cuban’s company.
The news website Formulary Watch previously reported that CVS Caremark, another of the biggest PBMs, will be offering Amjevita, but as a nonpreferred brand, while Humira remains the preferred brand. CVS Caremark did not respond to a request for comment.
Will patients pay less?
Biosimilars have been touted as a potential solution to lower spending on biologic drugs, but it’s unknown if patients will ultimately benefit with lower out-of-pocket costs. It’s “impossible to predict” if the discount that third-party payers pay will be passed on to consumers, said Mark Fendrick, MD, who directs the University of Michigan Center for Value-based Insurance Design in Ann Arbor.
Generally, a consumer’s copay is a percentage of a drug’s list price, so it stands to reason that a low drug price would result in lower out-of-pocket payments. While this is mostly true, Humira has a successful copay assistance program to lower prescription costs for consumers. According to a 2022 IQVIA report, 82% of commercial prescriptions cost patients less than $10 for Humira because of this program.
To appeal to patients, biosimilar companies will need to offer similar savings, Dr. Fendrick added. “There will be some discontent if patients are actually asked to pay more out-of-pocket for a less expensive drug,” he said.
All eight companies behind these biosimilars are offering or will be launching copay saving programs, many which advertise copays as low as $0 per month for eligible patients.
How will Humira respond?
Marta Wosińska, PhD, a health care economist at the Brookings Institute, Washington, predicts payers will use these lower biosimilar prices to negotiate better deals with AbbVie, Humira’s manufacturer. “We have a lot of players coming into [the market] right now, so the competition is really fierce,” she said. In response, AbbVie will need to increase rebates on Humira and/or lower its price to compete with these biosimilars.
“The ball is in AbbVie’s court,” she said. “If [the company] is not willing to drop price sufficiently, then payers will start switching to biosimilars.”
Dr. Fendrick reported past financial relationships and consulting arrangements with AbbVie, Amgen, Arnold Ventures, Bayer, CareFirst, BlueCross BlueShield, and many other companies. Dr. Wosińska has received funding from Arnold Ventures and serves as an expert witness on antitrust cases involving generic medication.
A version of this article first appeared on Medscape.com.
Remote teams offer chance to improve difficult-to-treat PsA
DUBLIN – according to presenters at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
In the same session at the meeting, GRAPPA also announced a new initiative to define difficult-to-treat PsA.
Deepak Jadon, MBBCh, PhD, a rheumatologist with Cambridge (England) University Hospitals NHS Foundation Trust, described his experience of running a clinic for patients with difficult-to-treat PsA in eastern England, covering a catchment area of approximately 6 million people between six and seven hospitals. He discussed how the MDT in his region operates to discuss the management of such patients, whose treatment options may also have indications for comorbidities such as inflammatory bowel disease or uveitis, or have complicating factors such as metabolic syndrome.
“You have to have an interested and engaged colleague to form that collaboration,” Dr. Jadon said. “If you are working in isolation, without your colleagues in the same building, that becomes harder. We have been running remote multispecialty meetings without the patient being present, and I have had the good fortune of having medical students brought into our practice. We discussed approximately 220 patients, initially in our psoriasis-spondyloarthritis MDT and subsequently in our inflammatory bowel disease–spondyloarthritis MDT.”
There are also MDTs with hepatologist colleagues carried out on an ad hoc basis to discuss patients with nonalcoholic fatty liver disease, as well as patients with hepatitis or a transplanted liver, who have psoriatic disease.
This difficult-to-treat cohort is discussed in MDT meetings conducted on Zoom. At MDT meetings, carried out with frequencies ranging from monthly to bimonthly, Dr. Jadon said there would be two dermatologists, two rheumatologists, one to four dermatology and rheumatology trainees and fellows, one to four specialist nurses, one to three research nurses, and one biologics pharmacist. They record the meetings and discuss anywhere from 4 to 18 patients, reviewing items in their electronic medical record, calling or writing patients and/or their primary care clinician as needed. They take about an hour to meet, with a half hour of prep time and another 1.5 hours to undertake necessary actions.
“Generally, the question is, how can we change treatment to best cover the domains of disease?” Dr. Jadon said. “Progressively, more patients are being put onto biologics as a result of these conversations, and I do feel that it has helped our patients and us to consolidate their management plan. Naturally, as all clinicians do, we doubt ourselves and wonder if we are missing something. Is there an aspect of the disease [being missed]? Is there a treatment that I haven’t been using? [The meetings have] been reassuring in that regard. I also learn from my colleagues who have earlier access to treatments, especially in dermatology.”
In a small number of patients, some combinations of advanced therapies, such as combining a Janus kinase inhibitor with a biologic, have been used as a result of these collaborations, “and to discuss this in an MDT has been reassuring, including from a medico-legal perspective,” Dr. Jadon said. “One of the main things we found to be useful is having a brief referral pro forma. Usually, by the time patients reach this forum, they have used a lot of treatments, and it can be difficult to remember that on the spot. It is also important to focus on what the actual question is. Naturally, in these discussions, where you talk about the complexities and various facets of disease, you can get a bit lost and sometimes you actually don’t address the original question.”
He also said it has been very beneficial to use screen sharing in the remote MDTs so that different disciplines can review images together, such as with radiology colleagues. “There are varying skill sets among our colleagues, especially in radiology, and it has been quite nice to review their peripheral imaging, their axial imaging, laboratory markers, and skin lesions together.”
New GRAPPA project to provide clarity
A new GRAPPA project has been devised to help physicians identify and define difficult-to-treat and difficult-to-manage PsA in order to help physicians to categorize and treat these patients.
“We have a growing treatment armamentarium ... but we still do not reach all the patients that we would like to,” said Fabian Proft, MD, of Charité University Medicine, Berlin. “We set our targets, but we see in the real world that we are only reaching them in 40% or 50% of our patients. So, we need to do better, and in order to do better, we need to understand better.”
“We should not only make a definition of difficult-to-treat PsA, which is nonresponse to treatment with objective signs of inflammation, but also we need to address and acknowledge difficult-to-manage [patients],” Dr. Proft said. “We should not stop as soon as we come up with a definition. This will be a working definition and will need to be validated.”
The speakers reported no relevant financial relationships.
A version of this article appeared on Medscape.com.
DUBLIN – according to presenters at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
In the same session at the meeting, GRAPPA also announced a new initiative to define difficult-to-treat PsA.
Deepak Jadon, MBBCh, PhD, a rheumatologist with Cambridge (England) University Hospitals NHS Foundation Trust, described his experience of running a clinic for patients with difficult-to-treat PsA in eastern England, covering a catchment area of approximately 6 million people between six and seven hospitals. He discussed how the MDT in his region operates to discuss the management of such patients, whose treatment options may also have indications for comorbidities such as inflammatory bowel disease or uveitis, or have complicating factors such as metabolic syndrome.
“You have to have an interested and engaged colleague to form that collaboration,” Dr. Jadon said. “If you are working in isolation, without your colleagues in the same building, that becomes harder. We have been running remote multispecialty meetings without the patient being present, and I have had the good fortune of having medical students brought into our practice. We discussed approximately 220 patients, initially in our psoriasis-spondyloarthritis MDT and subsequently in our inflammatory bowel disease–spondyloarthritis MDT.”
There are also MDTs with hepatologist colleagues carried out on an ad hoc basis to discuss patients with nonalcoholic fatty liver disease, as well as patients with hepatitis or a transplanted liver, who have psoriatic disease.
This difficult-to-treat cohort is discussed in MDT meetings conducted on Zoom. At MDT meetings, carried out with frequencies ranging from monthly to bimonthly, Dr. Jadon said there would be two dermatologists, two rheumatologists, one to four dermatology and rheumatology trainees and fellows, one to four specialist nurses, one to three research nurses, and one biologics pharmacist. They record the meetings and discuss anywhere from 4 to 18 patients, reviewing items in their electronic medical record, calling or writing patients and/or their primary care clinician as needed. They take about an hour to meet, with a half hour of prep time and another 1.5 hours to undertake necessary actions.
“Generally, the question is, how can we change treatment to best cover the domains of disease?” Dr. Jadon said. “Progressively, more patients are being put onto biologics as a result of these conversations, and I do feel that it has helped our patients and us to consolidate their management plan. Naturally, as all clinicians do, we doubt ourselves and wonder if we are missing something. Is there an aspect of the disease [being missed]? Is there a treatment that I haven’t been using? [The meetings have] been reassuring in that regard. I also learn from my colleagues who have earlier access to treatments, especially in dermatology.”
In a small number of patients, some combinations of advanced therapies, such as combining a Janus kinase inhibitor with a biologic, have been used as a result of these collaborations, “and to discuss this in an MDT has been reassuring, including from a medico-legal perspective,” Dr. Jadon said. “One of the main things we found to be useful is having a brief referral pro forma. Usually, by the time patients reach this forum, they have used a lot of treatments, and it can be difficult to remember that on the spot. It is also important to focus on what the actual question is. Naturally, in these discussions, where you talk about the complexities and various facets of disease, you can get a bit lost and sometimes you actually don’t address the original question.”
He also said it has been very beneficial to use screen sharing in the remote MDTs so that different disciplines can review images together, such as with radiology colleagues. “There are varying skill sets among our colleagues, especially in radiology, and it has been quite nice to review their peripheral imaging, their axial imaging, laboratory markers, and skin lesions together.”
New GRAPPA project to provide clarity
A new GRAPPA project has been devised to help physicians identify and define difficult-to-treat and difficult-to-manage PsA in order to help physicians to categorize and treat these patients.
“We have a growing treatment armamentarium ... but we still do not reach all the patients that we would like to,” said Fabian Proft, MD, of Charité University Medicine, Berlin. “We set our targets, but we see in the real world that we are only reaching them in 40% or 50% of our patients. So, we need to do better, and in order to do better, we need to understand better.”
“We should not only make a definition of difficult-to-treat PsA, which is nonresponse to treatment with objective signs of inflammation, but also we need to address and acknowledge difficult-to-manage [patients],” Dr. Proft said. “We should not stop as soon as we come up with a definition. This will be a working definition and will need to be validated.”
The speakers reported no relevant financial relationships.
A version of this article appeared on Medscape.com.
DUBLIN – according to presenters at the annual meeting of the Group for Research and Assessment of Psoriasis and Psoriatic Arthritis.
In the same session at the meeting, GRAPPA also announced a new initiative to define difficult-to-treat PsA.
Deepak Jadon, MBBCh, PhD, a rheumatologist with Cambridge (England) University Hospitals NHS Foundation Trust, described his experience of running a clinic for patients with difficult-to-treat PsA in eastern England, covering a catchment area of approximately 6 million people between six and seven hospitals. He discussed how the MDT in his region operates to discuss the management of such patients, whose treatment options may also have indications for comorbidities such as inflammatory bowel disease or uveitis, or have complicating factors such as metabolic syndrome.
“You have to have an interested and engaged colleague to form that collaboration,” Dr. Jadon said. “If you are working in isolation, without your colleagues in the same building, that becomes harder. We have been running remote multispecialty meetings without the patient being present, and I have had the good fortune of having medical students brought into our practice. We discussed approximately 220 patients, initially in our psoriasis-spondyloarthritis MDT and subsequently in our inflammatory bowel disease–spondyloarthritis MDT.”
There are also MDTs with hepatologist colleagues carried out on an ad hoc basis to discuss patients with nonalcoholic fatty liver disease, as well as patients with hepatitis or a transplanted liver, who have psoriatic disease.
This difficult-to-treat cohort is discussed in MDT meetings conducted on Zoom. At MDT meetings, carried out with frequencies ranging from monthly to bimonthly, Dr. Jadon said there would be two dermatologists, two rheumatologists, one to four dermatology and rheumatology trainees and fellows, one to four specialist nurses, one to three research nurses, and one biologics pharmacist. They record the meetings and discuss anywhere from 4 to 18 patients, reviewing items in their electronic medical record, calling or writing patients and/or their primary care clinician as needed. They take about an hour to meet, with a half hour of prep time and another 1.5 hours to undertake necessary actions.
“Generally, the question is, how can we change treatment to best cover the domains of disease?” Dr. Jadon said. “Progressively, more patients are being put onto biologics as a result of these conversations, and I do feel that it has helped our patients and us to consolidate their management plan. Naturally, as all clinicians do, we doubt ourselves and wonder if we are missing something. Is there an aspect of the disease [being missed]? Is there a treatment that I haven’t been using? [The meetings have] been reassuring in that regard. I also learn from my colleagues who have earlier access to treatments, especially in dermatology.”
In a small number of patients, some combinations of advanced therapies, such as combining a Janus kinase inhibitor with a biologic, have been used as a result of these collaborations, “and to discuss this in an MDT has been reassuring, including from a medico-legal perspective,” Dr. Jadon said. “One of the main things we found to be useful is having a brief referral pro forma. Usually, by the time patients reach this forum, they have used a lot of treatments, and it can be difficult to remember that on the spot. It is also important to focus on what the actual question is. Naturally, in these discussions, where you talk about the complexities and various facets of disease, you can get a bit lost and sometimes you actually don’t address the original question.”
He also said it has been very beneficial to use screen sharing in the remote MDTs so that different disciplines can review images together, such as with radiology colleagues. “There are varying skill sets among our colleagues, especially in radiology, and it has been quite nice to review their peripheral imaging, their axial imaging, laboratory markers, and skin lesions together.”
New GRAPPA project to provide clarity
A new GRAPPA project has been devised to help physicians identify and define difficult-to-treat and difficult-to-manage PsA in order to help physicians to categorize and treat these patients.
“We have a growing treatment armamentarium ... but we still do not reach all the patients that we would like to,” said Fabian Proft, MD, of Charité University Medicine, Berlin. “We set our targets, but we see in the real world that we are only reaching them in 40% or 50% of our patients. So, we need to do better, and in order to do better, we need to understand better.”
“We should not only make a definition of difficult-to-treat PsA, which is nonresponse to treatment with objective signs of inflammation, but also we need to address and acknowledge difficult-to-manage [patients],” Dr. Proft said. “We should not stop as soon as we come up with a definition. This will be a working definition and will need to be validated.”
The speakers reported no relevant financial relationships.
A version of this article appeared on Medscape.com.
AT GRAPPA 2023