User login
FDA gives nod to first mobile app for substance use disorders
The Food and Drug Administration has permitted marketing of the first mobile medical application aimed at helping to treat substance use disorders (SUDs) in adults, the agency announced Sept. 14.
“This is an example of how innovative digital technologies can help provide patients access to additional tools during their treatment,” said Carlos Peña, PhD, director of the division of neurological and physical medicine devices in the FDA’s Center for Devices and Radiological Health, in a statement.
“More therapy tools means a greater potential to help improve outcomes ... for patients with substance use disorder,” Dr. Peña added.
The agency’s permission is based on data reviewed from a multisite, unblinded 12-week clinical trial sponsored by the National Institute on Drug Abuse of 399 patients who received either standard treatment or standard treatment with the addition of a desktop-based version of reSET. According to the data, adherence to abstinence for patients with alcohol, cocaine, marijuana, and stimulant SUD who used reSET increased 40.3%, compared with an increase of 17.6% in adherence to abstinence for patients who did not use the system.
No side effects are associated with the reSET application. Adverse events reported in clinical trials were in line with those found in patients with SUD, including cardiovascular disease, gastrointestinal events, depression, mania, suicidal behavior and ideation, and suicide attempts.
Edward V. Nunes, MD, said in a statement issued by the company that developed reSET, Pear Therapeutics, that the clinical outcomes found in the pivotal study were remarkable. “Clinically validated digital therapeutics may become a cornerstone of future treatment,” said Dr. Nunes, lead investigator in the study submitted to the FDA and a professor of psychiatry at Columbia University in New York.
For more information about the reSET medical application system, click here.
[email protected]
On Twitter @abbbbeeeyyy
The Food and Drug Administration has permitted marketing of the first mobile medical application aimed at helping to treat substance use disorders (SUDs) in adults, the agency announced Sept. 14.
“This is an example of how innovative digital technologies can help provide patients access to additional tools during their treatment,” said Carlos Peña, PhD, director of the division of neurological and physical medicine devices in the FDA’s Center for Devices and Radiological Health, in a statement.
“More therapy tools means a greater potential to help improve outcomes ... for patients with substance use disorder,” Dr. Peña added.
The agency’s permission is based on data reviewed from a multisite, unblinded 12-week clinical trial sponsored by the National Institute on Drug Abuse of 399 patients who received either standard treatment or standard treatment with the addition of a desktop-based version of reSET. According to the data, adherence to abstinence for patients with alcohol, cocaine, marijuana, and stimulant SUD who used reSET increased 40.3%, compared with an increase of 17.6% in adherence to abstinence for patients who did not use the system.
No side effects are associated with the reSET application. Adverse events reported in clinical trials were in line with those found in patients with SUD, including cardiovascular disease, gastrointestinal events, depression, mania, suicidal behavior and ideation, and suicide attempts.
Edward V. Nunes, MD, said in a statement issued by the company that developed reSET, Pear Therapeutics, that the clinical outcomes found in the pivotal study were remarkable. “Clinically validated digital therapeutics may become a cornerstone of future treatment,” said Dr. Nunes, lead investigator in the study submitted to the FDA and a professor of psychiatry at Columbia University in New York.
For more information about the reSET medical application system, click here.
[email protected]
On Twitter @abbbbeeeyyy
The Food and Drug Administration has permitted marketing of the first mobile medical application aimed at helping to treat substance use disorders (SUDs) in adults, the agency announced Sept. 14.
“This is an example of how innovative digital technologies can help provide patients access to additional tools during their treatment,” said Carlos Peña, PhD, director of the division of neurological and physical medicine devices in the FDA’s Center for Devices and Radiological Health, in a statement.
“More therapy tools means a greater potential to help improve outcomes ... for patients with substance use disorder,” Dr. Peña added.
The agency’s permission is based on data reviewed from a multisite, unblinded 12-week clinical trial sponsored by the National Institute on Drug Abuse of 399 patients who received either standard treatment or standard treatment with the addition of a desktop-based version of reSET. According to the data, adherence to abstinence for patients with alcohol, cocaine, marijuana, and stimulant SUD who used reSET increased 40.3%, compared with an increase of 17.6% in adherence to abstinence for patients who did not use the system.
No side effects are associated with the reSET application. Adverse events reported in clinical trials were in line with those found in patients with SUD, including cardiovascular disease, gastrointestinal events, depression, mania, suicidal behavior and ideation, and suicide attempts.
Edward V. Nunes, MD, said in a statement issued by the company that developed reSET, Pear Therapeutics, that the clinical outcomes found in the pivotal study were remarkable. “Clinically validated digital therapeutics may become a cornerstone of future treatment,” said Dr. Nunes, lead investigator in the study submitted to the FDA and a professor of psychiatry at Columbia University in New York.
For more information about the reSET medical application system, click here.
[email protected]
On Twitter @abbbbeeeyyy
Postpartum depression screening in well-child care appears promising
, according to results of a study from the Netherlands.
“This promising finding warrants wider implementation of screening for postpartum depression,” said Dr. Angarath I. Van der Zee-van den Berg of the University of Twente, Enschede, the Netherlands, and associates.
Results showed significantly fewer mothers in the intervention group were depressed at 9 months post partum, compared with the CAU group (0.6% of 1,843 vs. 2.5% 1,246 for major depression), with an adjusted odds ratio of 0.28 (95% confidence interval, 0.12-0.63). The difference also was significant for minor and major depression, with 3.0% of the intervention group affected vs. 8.4% of the CAU group, and the adjusted odds ratio was 0.40 (95% confidence interval, 0.27-0.58). For parenting, anxiety symptoms, and mental health functioning, the intervention resulted in effect sizes ranging from 0.23 to 0.27.
“We found screening for postpartum depression to have a negligible effect on socioemotional development of the child with no former evidence to compare with,” Dr. Van der Zee-van den Berg and his associates said. “Attention for the mother-child interaction in the trajectory after screening may improve child outcomes; this evidently requires further study.”
To find out more information see Pediatrics (2017;140[4]:e20170110).
, according to results of a study from the Netherlands.
“This promising finding warrants wider implementation of screening for postpartum depression,” said Dr. Angarath I. Van der Zee-van den Berg of the University of Twente, Enschede, the Netherlands, and associates.
Results showed significantly fewer mothers in the intervention group were depressed at 9 months post partum, compared with the CAU group (0.6% of 1,843 vs. 2.5% 1,246 for major depression), with an adjusted odds ratio of 0.28 (95% confidence interval, 0.12-0.63). The difference also was significant for minor and major depression, with 3.0% of the intervention group affected vs. 8.4% of the CAU group, and the adjusted odds ratio was 0.40 (95% confidence interval, 0.27-0.58). For parenting, anxiety symptoms, and mental health functioning, the intervention resulted in effect sizes ranging from 0.23 to 0.27.
“We found screening for postpartum depression to have a negligible effect on socioemotional development of the child with no former evidence to compare with,” Dr. Van der Zee-van den Berg and his associates said. “Attention for the mother-child interaction in the trajectory after screening may improve child outcomes; this evidently requires further study.”
To find out more information see Pediatrics (2017;140[4]:e20170110).
, according to results of a study from the Netherlands.
“This promising finding warrants wider implementation of screening for postpartum depression,” said Dr. Angarath I. Van der Zee-van den Berg of the University of Twente, Enschede, the Netherlands, and associates.
Results showed significantly fewer mothers in the intervention group were depressed at 9 months post partum, compared with the CAU group (0.6% of 1,843 vs. 2.5% 1,246 for major depression), with an adjusted odds ratio of 0.28 (95% confidence interval, 0.12-0.63). The difference also was significant for minor and major depression, with 3.0% of the intervention group affected vs. 8.4% of the CAU group, and the adjusted odds ratio was 0.40 (95% confidence interval, 0.27-0.58). For parenting, anxiety symptoms, and mental health functioning, the intervention resulted in effect sizes ranging from 0.23 to 0.27.
“We found screening for postpartum depression to have a negligible effect on socioemotional development of the child with no former evidence to compare with,” Dr. Van der Zee-van den Berg and his associates said. “Attention for the mother-child interaction in the trajectory after screening may improve child outcomes; this evidently requires further study.”
To find out more information see Pediatrics (2017;140[4]:e20170110).
FROM PEDIATRICS
Mental health courts tied to ‘modest’ drop in recidivism
Participation in mental health courts appears to reduce some measures of recidivism among adults with mental illness – but the impact is modest, according to a meta-analysis conducted by Evan M. Lowder, PhD, and his associates.
“Our findings inform the overall effectiveness of [mental health courts] as a judicial strategy to reduce the number of adults with mental illnesses who are returning to the criminal justice system,” wrote Dr. Lowder, formerly with the department of psychology at North Carolina State University, Raleigh, and now with the school of public and environmental affairs at Indiana University, Indianapolis (Psychiatr Serv. 2017 Aug 15. doi: 10.1176/appi.ps.201700107).
The growing numbers of adults with mental illnesses in the U.S. criminal justice system led to the development of mental health courts in the 1990s. Mental health courts allow defendants to agree on a voluntary basis to mental health treatment in the community, “often in exchange for a reduced or dismissed index charge upon successful completion,” the investigators wrote. Previous research has shown that graduation from mental health courts, rather than participation, is tied to better outcomes (Law Hum Behav. 2016 Apr;40[2]:118-27) and (Int J Psychiatry. 2014 Sep-Oct;37[5]:448-54).
Overall, the meta-analysis showed a “significant, negative, and small effect of mental health court participation on recidivism” (d, –.20; 95% confidence interval, –2.9 to –.10; P less than .001), compared with traditional processing, Dr. Lowder and his associates reported. Specifically, they found that participation lowered two measures of recidivism: charge and jail time. But the impact of participation on the measures of arrest and conviction were not significantly affected. When they looked at the subset of studies that were based on defendants who completed their mental health court participation, however, the impact proved broader, and included lower rates of arrest and conviction.
“Given the already high rates of reoffending in this population, it may not be realistic to expect complete distance from criminal activity among [mental health court] participants,” the researchers wrote. “Rather, [mental health court] participation may be a means to mitigate the severity of future offending (that is, jail time associated with a new offense).”
Dr. Lowder and his associates cited several limitations related to the data they chose to include and how those numbers were analyzed. “These are important directions for future research,” they wrote. They added that future research should look at components of mental health courts that are associated with better outcomes in participation.
The investigators reported no financial disclosures.
[email protected]
On Twitter @ Abbbbeeeyyy
Participation in mental health courts appears to reduce some measures of recidivism among adults with mental illness – but the impact is modest, according to a meta-analysis conducted by Evan M. Lowder, PhD, and his associates.
“Our findings inform the overall effectiveness of [mental health courts] as a judicial strategy to reduce the number of adults with mental illnesses who are returning to the criminal justice system,” wrote Dr. Lowder, formerly with the department of psychology at North Carolina State University, Raleigh, and now with the school of public and environmental affairs at Indiana University, Indianapolis (Psychiatr Serv. 2017 Aug 15. doi: 10.1176/appi.ps.201700107).
The growing numbers of adults with mental illnesses in the U.S. criminal justice system led to the development of mental health courts in the 1990s. Mental health courts allow defendants to agree on a voluntary basis to mental health treatment in the community, “often in exchange for a reduced or dismissed index charge upon successful completion,” the investigators wrote. Previous research has shown that graduation from mental health courts, rather than participation, is tied to better outcomes (Law Hum Behav. 2016 Apr;40[2]:118-27) and (Int J Psychiatry. 2014 Sep-Oct;37[5]:448-54).
Overall, the meta-analysis showed a “significant, negative, and small effect of mental health court participation on recidivism” (d, –.20; 95% confidence interval, –2.9 to –.10; P less than .001), compared with traditional processing, Dr. Lowder and his associates reported. Specifically, they found that participation lowered two measures of recidivism: charge and jail time. But the impact of participation on the measures of arrest and conviction were not significantly affected. When they looked at the subset of studies that were based on defendants who completed their mental health court participation, however, the impact proved broader, and included lower rates of arrest and conviction.
“Given the already high rates of reoffending in this population, it may not be realistic to expect complete distance from criminal activity among [mental health court] participants,” the researchers wrote. “Rather, [mental health court] participation may be a means to mitigate the severity of future offending (that is, jail time associated with a new offense).”
Dr. Lowder and his associates cited several limitations related to the data they chose to include and how those numbers were analyzed. “These are important directions for future research,” they wrote. They added that future research should look at components of mental health courts that are associated with better outcomes in participation.
The investigators reported no financial disclosures.
[email protected]
On Twitter @ Abbbbeeeyyy
Participation in mental health courts appears to reduce some measures of recidivism among adults with mental illness – but the impact is modest, according to a meta-analysis conducted by Evan M. Lowder, PhD, and his associates.
“Our findings inform the overall effectiveness of [mental health courts] as a judicial strategy to reduce the number of adults with mental illnesses who are returning to the criminal justice system,” wrote Dr. Lowder, formerly with the department of psychology at North Carolina State University, Raleigh, and now with the school of public and environmental affairs at Indiana University, Indianapolis (Psychiatr Serv. 2017 Aug 15. doi: 10.1176/appi.ps.201700107).
The growing numbers of adults with mental illnesses in the U.S. criminal justice system led to the development of mental health courts in the 1990s. Mental health courts allow defendants to agree on a voluntary basis to mental health treatment in the community, “often in exchange for a reduced or dismissed index charge upon successful completion,” the investigators wrote. Previous research has shown that graduation from mental health courts, rather than participation, is tied to better outcomes (Law Hum Behav. 2016 Apr;40[2]:118-27) and (Int J Psychiatry. 2014 Sep-Oct;37[5]:448-54).
Overall, the meta-analysis showed a “significant, negative, and small effect of mental health court participation on recidivism” (d, –.20; 95% confidence interval, –2.9 to –.10; P less than .001), compared with traditional processing, Dr. Lowder and his associates reported. Specifically, they found that participation lowered two measures of recidivism: charge and jail time. But the impact of participation on the measures of arrest and conviction were not significantly affected. When they looked at the subset of studies that were based on defendants who completed their mental health court participation, however, the impact proved broader, and included lower rates of arrest and conviction.
“Given the already high rates of reoffending in this population, it may not be realistic to expect complete distance from criminal activity among [mental health court] participants,” the researchers wrote. “Rather, [mental health court] participation may be a means to mitigate the severity of future offending (that is, jail time associated with a new offense).”
Dr. Lowder and his associates cited several limitations related to the data they chose to include and how those numbers were analyzed. “These are important directions for future research,” they wrote. They added that future research should look at components of mental health courts that are associated with better outcomes in participation.
The investigators reported no financial disclosures.
[email protected]
On Twitter @ Abbbbeeeyyy
FROM PSYCHIATRIC SERVICES
Ibrutinib and bleeding complications in Mohs surgery
Clinically significant bleeding events occurred in two elderly men who were taking ibrutinib and underwent Mohs micrographic surgery for squamous cell carcinomas, Cindy E. Parra and her colleagues reported in JAMA Dermatology.
On day 3 after his Mohs procedure, one 73-year-old man taking ibrutinib for Waldenstrom macroglobulinemia developed extensive bilateral periorbital ecchymosis that extended down to his upper chest. The other patient, an 88-year-old man taking ibrutinib for chronic lymphocytic leukemia, developed ecchymosis down to the chin. The first patient discontinued ibrutinib 3 days before his surgery; the second patient was taking ibrutinib at the time of his surgery.
“The increased incidence of nonmelanoma skin cancer and poorer outcomes in patients with non-Hodgkin lymphoma and CLL is well recognized, as is the importance of aggressive dermatologic management,” the researchers wrote (JAMA Dermatol. 2017 Jul 12. doi: 10.1001/jamadermatol.2017.1877). “It may be prudent to withhold ibrutinib treatment prior to dermatologic surgery to avoid potential bleeding complications.”
The findings argue for close collaboration between the dermatologic surgeon and the patient’s hematologist when scheduling extended-duration dermatologic procedures in patients taking ibrutinib.
Find the full summary here.
Clinically significant bleeding events occurred in two elderly men who were taking ibrutinib and underwent Mohs micrographic surgery for squamous cell carcinomas, Cindy E. Parra and her colleagues reported in JAMA Dermatology.
On day 3 after his Mohs procedure, one 73-year-old man taking ibrutinib for Waldenstrom macroglobulinemia developed extensive bilateral periorbital ecchymosis that extended down to his upper chest. The other patient, an 88-year-old man taking ibrutinib for chronic lymphocytic leukemia, developed ecchymosis down to the chin. The first patient discontinued ibrutinib 3 days before his surgery; the second patient was taking ibrutinib at the time of his surgery.
“The increased incidence of nonmelanoma skin cancer and poorer outcomes in patients with non-Hodgkin lymphoma and CLL is well recognized, as is the importance of aggressive dermatologic management,” the researchers wrote (JAMA Dermatol. 2017 Jul 12. doi: 10.1001/jamadermatol.2017.1877). “It may be prudent to withhold ibrutinib treatment prior to dermatologic surgery to avoid potential bleeding complications.”
The findings argue for close collaboration between the dermatologic surgeon and the patient’s hematologist when scheduling extended-duration dermatologic procedures in patients taking ibrutinib.
Find the full summary here.
Clinically significant bleeding events occurred in two elderly men who were taking ibrutinib and underwent Mohs micrographic surgery for squamous cell carcinomas, Cindy E. Parra and her colleagues reported in JAMA Dermatology.
On day 3 after his Mohs procedure, one 73-year-old man taking ibrutinib for Waldenstrom macroglobulinemia developed extensive bilateral periorbital ecchymosis that extended down to his upper chest. The other patient, an 88-year-old man taking ibrutinib for chronic lymphocytic leukemia, developed ecchymosis down to the chin. The first patient discontinued ibrutinib 3 days before his surgery; the second patient was taking ibrutinib at the time of his surgery.
“The increased incidence of nonmelanoma skin cancer and poorer outcomes in patients with non-Hodgkin lymphoma and CLL is well recognized, as is the importance of aggressive dermatologic management,” the researchers wrote (JAMA Dermatol. 2017 Jul 12. doi: 10.1001/jamadermatol.2017.1877). “It may be prudent to withhold ibrutinib treatment prior to dermatologic surgery to avoid potential bleeding complications.”
The findings argue for close collaboration between the dermatologic surgeon and the patient’s hematologist when scheduling extended-duration dermatologic procedures in patients taking ibrutinib.
Find the full summary here.
FROM JAMA DERMATOLOGY
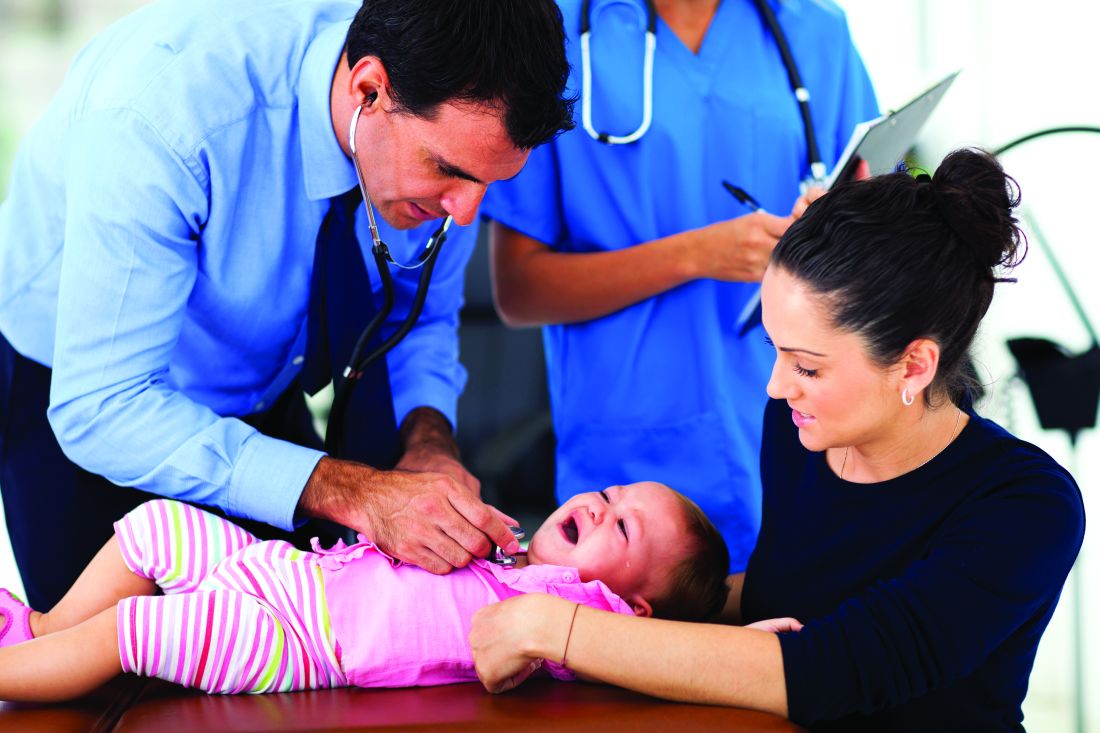
Maternal Tdap vaccination highly protective against infant pertussis
, results of a study show.
From 2010 to 2015, researchers collected data from a cohort study of full-term infants born at Kaiser Permanente of Northern California. “We estimated the effectiveness of maternal pertussis vaccination for protecting newborns against pertussis in the first 2 months of life and in the first year of life, accounting for each infant DTaP dose,” said Roger Baxter, MD, and his associates at Kaiser Permanente Vaccine Study Center, Oakland, Calif.
The vaccine effectiveness was an estimated 88% before infants had any DTaP vaccine doses, 81% between doses 1 and 2, 6% between doses 2 and 3, and 66% after infants had 3 DTaP doses.
“This result is consistent with 2 earlier studies in the United Kingdom” showing protection in infants less than 3 months of age, and a U.S. study showing maternal Tdap vaccination conferring protection to infants in the first 8 weeks of life, the researchers said.
In conclusion, even after infant DTaP dosing, there was evidence of additional protection from maternal Tdap vaccination for the first year of life (Pediatrics. 2017 Apr 3. doi: 10.1542/peds.2016-4091).
, results of a study show.
From 2010 to 2015, researchers collected data from a cohort study of full-term infants born at Kaiser Permanente of Northern California. “We estimated the effectiveness of maternal pertussis vaccination for protecting newborns against pertussis in the first 2 months of life and in the first year of life, accounting for each infant DTaP dose,” said Roger Baxter, MD, and his associates at Kaiser Permanente Vaccine Study Center, Oakland, Calif.
The vaccine effectiveness was an estimated 88% before infants had any DTaP vaccine doses, 81% between doses 1 and 2, 6% between doses 2 and 3, and 66% after infants had 3 DTaP doses.
“This result is consistent with 2 earlier studies in the United Kingdom” showing protection in infants less than 3 months of age, and a U.S. study showing maternal Tdap vaccination conferring protection to infants in the first 8 weeks of life, the researchers said.
In conclusion, even after infant DTaP dosing, there was evidence of additional protection from maternal Tdap vaccination for the first year of life (Pediatrics. 2017 Apr 3. doi: 10.1542/peds.2016-4091).
, results of a study show.
From 2010 to 2015, researchers collected data from a cohort study of full-term infants born at Kaiser Permanente of Northern California. “We estimated the effectiveness of maternal pertussis vaccination for protecting newborns against pertussis in the first 2 months of life and in the first year of life, accounting for each infant DTaP dose,” said Roger Baxter, MD, and his associates at Kaiser Permanente Vaccine Study Center, Oakland, Calif.
The vaccine effectiveness was an estimated 88% before infants had any DTaP vaccine doses, 81% between doses 1 and 2, 6% between doses 2 and 3, and 66% after infants had 3 DTaP doses.
“This result is consistent with 2 earlier studies in the United Kingdom” showing protection in infants less than 3 months of age, and a U.S. study showing maternal Tdap vaccination conferring protection to infants in the first 8 weeks of life, the researchers said.
In conclusion, even after infant DTaP dosing, there was evidence of additional protection from maternal Tdap vaccination for the first year of life (Pediatrics. 2017 Apr 3. doi: 10.1542/peds.2016-4091).
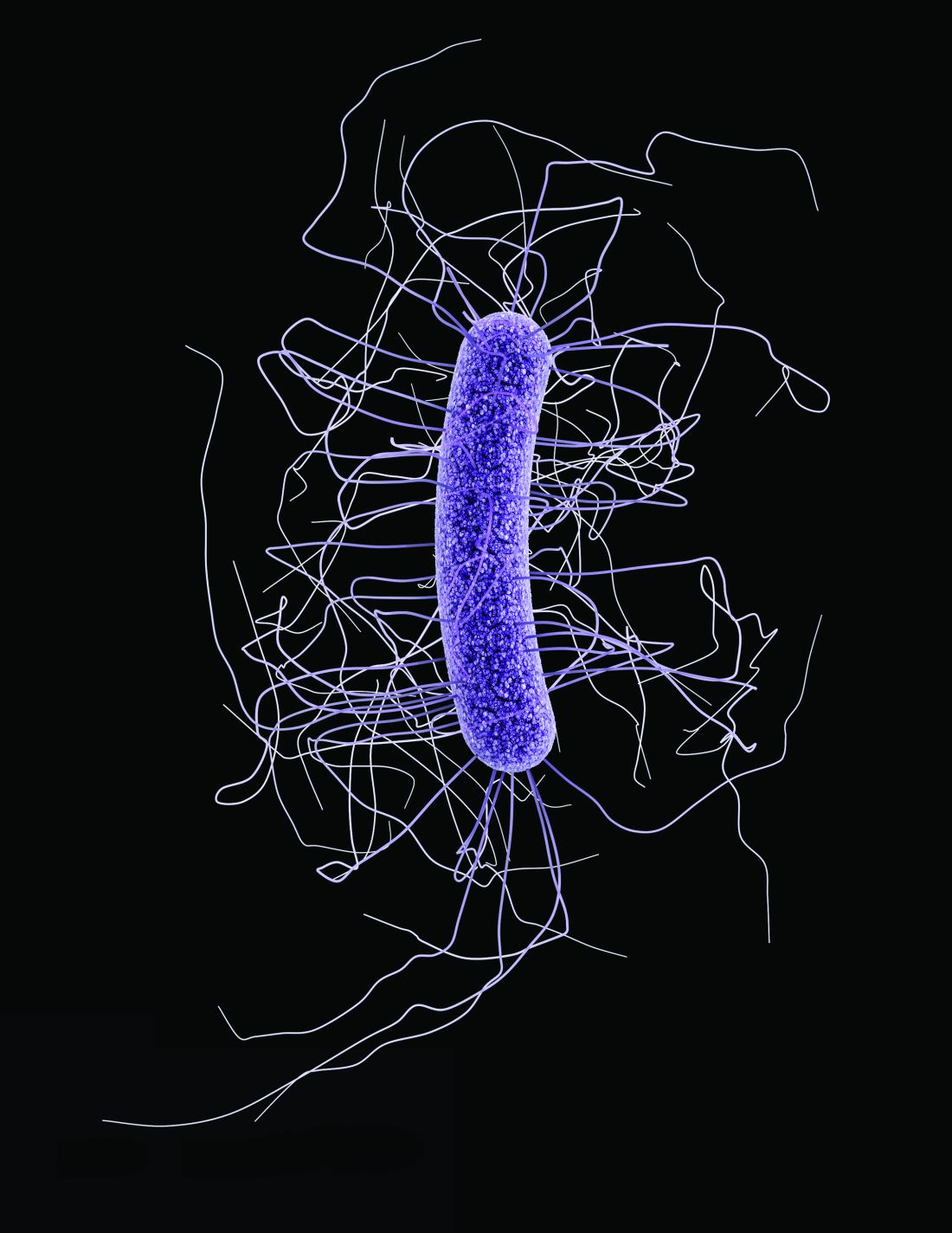
Avoid laxatives or stool softeners prior to C. difficile test in ped in patients
Improved education could keep clinicians from ordering laxatives and stool softeners just prior to ordering Clostridium difficile tests, improving the specificity of such testing.
In a 4-month prospective cohort study of pediatric inpatients, most clinicians were aware that their patients were receiving laxatives or stool softeners before they were sent for C. difficile tests.
Misclassifying colonized patients as having CDI reduces the utility of interfacility data comparison and may potentially result in inappropriate penalties for hospitals, they added.
From August to November 2015, 217 pediatric inpatients underwent 278 C. difficile tests that were eligible for inclusion in the study. There were 48 episodes of CDI in 44 patients in which bowel medications were administered prior to the test.
Of the 48 tests sent after receipt of bowel medications, either the ordering clinician or the bedside nurse completed the qualitative survey in 42 instances (88%). The response rate was higher among nurses (71%) than clinicians (48%). Awareness of bowel medication administration before testing was acknowledged by 78% of ordering providers and 88% bedside nurses. A majority of nurses (70%) and providers (71%) reported the medical team wanted the test.
“The main reasons for testing included a change in stool quality from baseline, other changes in clinical status, and the presence of risk factors for CDI,” Ms. Kinlay and Dr. Sandora said.
Read more in the American Journal of Infection Control (2017 Mar 13. doi: 10.1016/j.ajic.2017.01.035).
Improved education could keep clinicians from ordering laxatives and stool softeners just prior to ordering Clostridium difficile tests, improving the specificity of such testing.
In a 4-month prospective cohort study of pediatric inpatients, most clinicians were aware that their patients were receiving laxatives or stool softeners before they were sent for C. difficile tests.
Misclassifying colonized patients as having CDI reduces the utility of interfacility data comparison and may potentially result in inappropriate penalties for hospitals, they added.
From August to November 2015, 217 pediatric inpatients underwent 278 C. difficile tests that were eligible for inclusion in the study. There were 48 episodes of CDI in 44 patients in which bowel medications were administered prior to the test.
Of the 48 tests sent after receipt of bowel medications, either the ordering clinician or the bedside nurse completed the qualitative survey in 42 instances (88%). The response rate was higher among nurses (71%) than clinicians (48%). Awareness of bowel medication administration before testing was acknowledged by 78% of ordering providers and 88% bedside nurses. A majority of nurses (70%) and providers (71%) reported the medical team wanted the test.
“The main reasons for testing included a change in stool quality from baseline, other changes in clinical status, and the presence of risk factors for CDI,” Ms. Kinlay and Dr. Sandora said.
Read more in the American Journal of Infection Control (2017 Mar 13. doi: 10.1016/j.ajic.2017.01.035).
Improved education could keep clinicians from ordering laxatives and stool softeners just prior to ordering Clostridium difficile tests, improving the specificity of such testing.
In a 4-month prospective cohort study of pediatric inpatients, most clinicians were aware that their patients were receiving laxatives or stool softeners before they were sent for C. difficile tests.
Misclassifying colonized patients as having CDI reduces the utility of interfacility data comparison and may potentially result in inappropriate penalties for hospitals, they added.
From August to November 2015, 217 pediatric inpatients underwent 278 C. difficile tests that were eligible for inclusion in the study. There were 48 episodes of CDI in 44 patients in which bowel medications were administered prior to the test.
Of the 48 tests sent after receipt of bowel medications, either the ordering clinician or the bedside nurse completed the qualitative survey in 42 instances (88%). The response rate was higher among nurses (71%) than clinicians (48%). Awareness of bowel medication administration before testing was acknowledged by 78% of ordering providers and 88% bedside nurses. A majority of nurses (70%) and providers (71%) reported the medical team wanted the test.
“The main reasons for testing included a change in stool quality from baseline, other changes in clinical status, and the presence of risk factors for CDI,” Ms. Kinlay and Dr. Sandora said.
Read more in the American Journal of Infection Control (2017 Mar 13. doi: 10.1016/j.ajic.2017.01.035).
FROM THE JOURNAL OF INFECTION CONTROL
Grandparents aid in early diagnosis of autism
Family members other than parents can play a key role in initial recognition of problems prior to diagnosis of autism, which may lead to earlier diagnosis and potentially better outcomes, a study found.
Of 477 parents of children with autism who were surveyed online, 25% of parents reported that other individuals indicated their child might have a serious condition before they themselves suspected it. “The two most common categories of individuals are maternal grandmothers (27%) and teachers (24%),” Nachum Sicherman, PhD, of Columbia Business School, New York, and associates said. “If one adds maternal and paternal grandmothers and grandfathers together, then 59% of respondents who reported that anyone had raised concerns before they were aware that their child had a problem identified grandparents as having done so” (Autism. 2017. doi: 10.1177/1362361316679632)”
Children with no siblings were diagnosed 6-8 months earlier than children with siblings (P less than .01).Children with an older sibling were diagnosed approximately 10 months earlier, relative to those with only younger siblings. (P less than .01).
Thus, the presence of grandparents and siblings significantly affects age of diagnosis in autistic children, Dr. Sicherman and associates said.
*This article was update 3/27/2018
Family members other than parents can play a key role in initial recognition of problems prior to diagnosis of autism, which may lead to earlier diagnosis and potentially better outcomes, a study found.
Of 477 parents of children with autism who were surveyed online, 25% of parents reported that other individuals indicated their child might have a serious condition before they themselves suspected it. “The two most common categories of individuals are maternal grandmothers (27%) and teachers (24%),” Nachum Sicherman, PhD, of Columbia Business School, New York, and associates said. “If one adds maternal and paternal grandmothers and grandfathers together, then 59% of respondents who reported that anyone had raised concerns before they were aware that their child had a problem identified grandparents as having done so” (Autism. 2017. doi: 10.1177/1362361316679632)”
Children with no siblings were diagnosed 6-8 months earlier than children with siblings (P less than .01).Children with an older sibling were diagnosed approximately 10 months earlier, relative to those with only younger siblings. (P less than .01).
Thus, the presence of grandparents and siblings significantly affects age of diagnosis in autistic children, Dr. Sicherman and associates said.
*This article was update 3/27/2018
Family members other than parents can play a key role in initial recognition of problems prior to diagnosis of autism, which may lead to earlier diagnosis and potentially better outcomes, a study found.
Of 477 parents of children with autism who were surveyed online, 25% of parents reported that other individuals indicated their child might have a serious condition before they themselves suspected it. “The two most common categories of individuals are maternal grandmothers (27%) and teachers (24%),” Nachum Sicherman, PhD, of Columbia Business School, New York, and associates said. “If one adds maternal and paternal grandmothers and grandfathers together, then 59% of respondents who reported that anyone had raised concerns before they were aware that their child had a problem identified grandparents as having done so” (Autism. 2017. doi: 10.1177/1362361316679632)”
Children with no siblings were diagnosed 6-8 months earlier than children with siblings (P less than .01).Children with an older sibling were diagnosed approximately 10 months earlier, relative to those with only younger siblings. (P less than .01).
Thus, the presence of grandparents and siblings significantly affects age of diagnosis in autistic children, Dr. Sicherman and associates said.
*This article was update 3/27/2018
Factors may flag kids at high risk for C. difficile recurrence
The identification of risk factors associated with recurrent Clostridium difficile infection (rCDI) might allow early recognition of those children at highest risk, said Dr. Maribeth Nicholson of Vanderbilt University, Nashville, Tenn., and her associates.
In a small study, results showed that fecal lactoferrin, calprotectin, and interleukin-8 (IL-8) should be further studied to determine their value in predicting the risk of rCDI in children.
Of the 28 pediatric patients enrolled, 27 completed follow-up and 8 (30%) experienced rCDI. There were higher initial median fecal lactoferrin, calprotectin, and IL-8 values in those with recurrent disease, although there was a notably wide range of results in these patients. These values were lower in children with malignancy, the investigators said.
This study was partially supported by the Thrasher Early Career Award and two National Institutes of Health grants. The investigators had no relevant financial disclosures.
The identification of risk factors associated with recurrent Clostridium difficile infection (rCDI) might allow early recognition of those children at highest risk, said Dr. Maribeth Nicholson of Vanderbilt University, Nashville, Tenn., and her associates.
In a small study, results showed that fecal lactoferrin, calprotectin, and interleukin-8 (IL-8) should be further studied to determine their value in predicting the risk of rCDI in children.
Of the 28 pediatric patients enrolled, 27 completed follow-up and 8 (30%) experienced rCDI. There were higher initial median fecal lactoferrin, calprotectin, and IL-8 values in those with recurrent disease, although there was a notably wide range of results in these patients. These values were lower in children with malignancy, the investigators said.
This study was partially supported by the Thrasher Early Career Award and two National Institutes of Health grants. The investigators had no relevant financial disclosures.
The identification of risk factors associated with recurrent Clostridium difficile infection (rCDI) might allow early recognition of those children at highest risk, said Dr. Maribeth Nicholson of Vanderbilt University, Nashville, Tenn., and her associates.
In a small study, results showed that fecal lactoferrin, calprotectin, and interleukin-8 (IL-8) should be further studied to determine their value in predicting the risk of rCDI in children.
Of the 28 pediatric patients enrolled, 27 completed follow-up and 8 (30%) experienced rCDI. There were higher initial median fecal lactoferrin, calprotectin, and IL-8 values in those with recurrent disease, although there was a notably wide range of results in these patients. These values were lower in children with malignancy, the investigators said.
This study was partially supported by the Thrasher Early Career Award and two National Institutes of Health grants. The investigators had no relevant financial disclosures.
FROM THE PEDIATRIC INFECTIOUS DISEASE JOURNAL
Pertussis susceptibility estimates call for public health push
, according to results of research by Lana Childs and Robert A. Bednarczyk, PhD.
There were 32,971 pertussis cases reported in 2014, a 15% increase over 2013; most cases occurred in children who were too young to be fully vaccinated and in preadolescents with waning immunity from their vaccines. In the United States, vaccine coverage during childhood tends to be high overall, but DTaP coverage (84% in 2014) “remains lower than coverage for other childhood vaccinations,” they noted.
“These findings emphasize the need for public health professionals to continue efforts to increase DTaP vaccine coverage in children and Tdap coverage in pregnant women, plan for potential outbreaks, and maintain immunity levels needed to prevent the spread of pertussis.” the investigators concluded.
Read more at (Ped Inf Dis J. 2017. doi: 10.1097/INF.0000000000001537).
, according to results of research by Lana Childs and Robert A. Bednarczyk, PhD.
There were 32,971 pertussis cases reported in 2014, a 15% increase over 2013; most cases occurred in children who were too young to be fully vaccinated and in preadolescents with waning immunity from their vaccines. In the United States, vaccine coverage during childhood tends to be high overall, but DTaP coverage (84% in 2014) “remains lower than coverage for other childhood vaccinations,” they noted.
“These findings emphasize the need for public health professionals to continue efforts to increase DTaP vaccine coverage in children and Tdap coverage in pregnant women, plan for potential outbreaks, and maintain immunity levels needed to prevent the spread of pertussis.” the investigators concluded.
Read more at (Ped Inf Dis J. 2017. doi: 10.1097/INF.0000000000001537).
, according to results of research by Lana Childs and Robert A. Bednarczyk, PhD.
There were 32,971 pertussis cases reported in 2014, a 15% increase over 2013; most cases occurred in children who were too young to be fully vaccinated and in preadolescents with waning immunity from their vaccines. In the United States, vaccine coverage during childhood tends to be high overall, but DTaP coverage (84% in 2014) “remains lower than coverage for other childhood vaccinations,” they noted.
“These findings emphasize the need for public health professionals to continue efforts to increase DTaP vaccine coverage in children and Tdap coverage in pregnant women, plan for potential outbreaks, and maintain immunity levels needed to prevent the spread of pertussis.” the investigators concluded.
Read more at (Ped Inf Dis J. 2017. doi: 10.1097/INF.0000000000001537).
FROM THE PEDIATRIC INFECTIOUS DISEASE JOURNAL
E-cigarette ‘dripping’ is up among teens
Use of electronic cigarettes among young people is on the rise, and one in four high school students report using these devices for dripping, according to a study by Suchitra Krishnan-Sarin, PhD, of Yale University, New Haven, and associates.
In the spring of 2015, 7,045 students from eight Connecticut high schools completed anonymous surveys that examined tobacco use behaviors and perceptions. Among 1,080 ever e-cigarette users, 26% of students reported ever using e-cigarettes for dripping, which involves “vaporizing the e-liquid at high temperatures by dripping a couple of drops of e-liquid directly onto an atomizer’s coil and then immediately inhaling the vapor.”
Students use dripping because it produces thicker clouds of vapor (according to 64% of respondents); because they get a stronger throat hit (28%); and because it makes the flavors taste better (39%). Curiosity was cited by 22% of the students.
These results suggest that youth who use dripping may be those who are more familiar with and have experience with using multiple tobacco products, including e-cigarettes Pediatrics. 2017. doi: 10.1542/peds.2016-3224).
“Importantly, risk assessment models for e-cigarettes must take into consideration the prevalence rates and toxicities of these alternative e-cigarette use behaviors, especially among vulnerable youth. There is also a critical need for regulatory efforts that consider restrictions on the e-cigarette device so it cannot be easily manipulated for behaviors such as dripping,” the researchers noted. “Finally, there is an urgent need for prevention programs that educate youth about the potential dangers and toxicity of the use of e-cigarettes for dripping.”
Use of electronic cigarettes among young people is on the rise, and one in four high school students report using these devices for dripping, according to a study by Suchitra Krishnan-Sarin, PhD, of Yale University, New Haven, and associates.
In the spring of 2015, 7,045 students from eight Connecticut high schools completed anonymous surveys that examined tobacco use behaviors and perceptions. Among 1,080 ever e-cigarette users, 26% of students reported ever using e-cigarettes for dripping, which involves “vaporizing the e-liquid at high temperatures by dripping a couple of drops of e-liquid directly onto an atomizer’s coil and then immediately inhaling the vapor.”
Students use dripping because it produces thicker clouds of vapor (according to 64% of respondents); because they get a stronger throat hit (28%); and because it makes the flavors taste better (39%). Curiosity was cited by 22% of the students.
These results suggest that youth who use dripping may be those who are more familiar with and have experience with using multiple tobacco products, including e-cigarettes Pediatrics. 2017. doi: 10.1542/peds.2016-3224).
“Importantly, risk assessment models for e-cigarettes must take into consideration the prevalence rates and toxicities of these alternative e-cigarette use behaviors, especially among vulnerable youth. There is also a critical need for regulatory efforts that consider restrictions on the e-cigarette device so it cannot be easily manipulated for behaviors such as dripping,” the researchers noted. “Finally, there is an urgent need for prevention programs that educate youth about the potential dangers and toxicity of the use of e-cigarettes for dripping.”
Use of electronic cigarettes among young people is on the rise, and one in four high school students report using these devices for dripping, according to a study by Suchitra Krishnan-Sarin, PhD, of Yale University, New Haven, and associates.
In the spring of 2015, 7,045 students from eight Connecticut high schools completed anonymous surveys that examined tobacco use behaviors and perceptions. Among 1,080 ever e-cigarette users, 26% of students reported ever using e-cigarettes for dripping, which involves “vaporizing the e-liquid at high temperatures by dripping a couple of drops of e-liquid directly onto an atomizer’s coil and then immediately inhaling the vapor.”
Students use dripping because it produces thicker clouds of vapor (according to 64% of respondents); because they get a stronger throat hit (28%); and because it makes the flavors taste better (39%). Curiosity was cited by 22% of the students.
These results suggest that youth who use dripping may be those who are more familiar with and have experience with using multiple tobacco products, including e-cigarettes Pediatrics. 2017. doi: 10.1542/peds.2016-3224).
“Importantly, risk assessment models for e-cigarettes must take into consideration the prevalence rates and toxicities of these alternative e-cigarette use behaviors, especially among vulnerable youth. There is also a critical need for regulatory efforts that consider restrictions on the e-cigarette device so it cannot be easily manipulated for behaviors such as dripping,” the researchers noted. “Finally, there is an urgent need for prevention programs that educate youth about the potential dangers and toxicity of the use of e-cigarettes for dripping.”
FROM PEDIATRICS