User login
Dose-related Increase in Mortality With Antipsychotics in Dementia
Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, compared with antidepressants or nonuse, a retrospective case-control study involving 90,786 patients has found.
Patients taking haloperidol had a 3.8% increase in mortality, and those taking risperidone had a 3.7% increase relative to nonusers, while olanzapine and quetiapine also were associated with significant increases in mortality risk, according to a study published online March 18 in JAMA Psychiatry.
When compared with individuals on antidepressants, haloperidol was associated with a 12.3% increase in mortality, representing a number-needed-to-harm of 8, while antidepressants alone were associated with a small but statistically significant increase in mortality risk.
“Prescribing a medication that increases mortality risk seems contrary to the tenet ‘first, do no harm,’ yet for patients who pose a danger to themselves and others and are in profound distress, use of such medications may still be appropriate,” wrote Dr. Donovan T. Maust of the department of psychiatry at the University of Michigan, Ann Arbor, and his coauthors (JAMA Psychiatry 2015 March 18 [doi:10.1001/jamapsychiatry.2014.3018]). “These new data can help physicians minimize the potential harm associated with antipsychotic treatment.”
The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, compared with antidepressants or nonuse, a retrospective case-control study involving 90,786 patients has found.
Patients taking haloperidol had a 3.8% increase in mortality, and those taking risperidone had a 3.7% increase relative to nonusers, while olanzapine and quetiapine also were associated with significant increases in mortality risk, according to a study published online March 18 in JAMA Psychiatry.
When compared with individuals on antidepressants, haloperidol was associated with a 12.3% increase in mortality, representing a number-needed-to-harm of 8, while antidepressants alone were associated with a small but statistically significant increase in mortality risk.
“Prescribing a medication that increases mortality risk seems contrary to the tenet ‘first, do no harm,’ yet for patients who pose a danger to themselves and others and are in profound distress, use of such medications may still be appropriate,” wrote Dr. Donovan T. Maust of the department of psychiatry at the University of Michigan, Ann Arbor, and his coauthors (JAMA Psychiatry 2015 March 18 [doi:10.1001/jamapsychiatry.2014.3018]). “These new data can help physicians minimize the potential harm associated with antipsychotic treatment.”
The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, compared with antidepressants or nonuse, a retrospective case-control study involving 90,786 patients has found.
Patients taking haloperidol had a 3.8% increase in mortality, and those taking risperidone had a 3.7% increase relative to nonusers, while olanzapine and quetiapine also were associated with significant increases in mortality risk, according to a study published online March 18 in JAMA Psychiatry.
When compared with individuals on antidepressants, haloperidol was associated with a 12.3% increase in mortality, representing a number-needed-to-harm of 8, while antidepressants alone were associated with a small but statistically significant increase in mortality risk.
“Prescribing a medication that increases mortality risk seems contrary to the tenet ‘first, do no harm,’ yet for patients who pose a danger to themselves and others and are in profound distress, use of such medications may still be appropriate,” wrote Dr. Donovan T. Maust of the department of psychiatry at the University of Michigan, Ann Arbor, and his coauthors (JAMA Psychiatry 2015 March 18 [doi:10.1001/jamapsychiatry.2014.3018]). “These new data can help physicians minimize the potential harm associated with antipsychotic treatment.”
The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
FROM JAMA PSYCHIATRY
Dose-related increase in mortality with antipsychotics in dementia
Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, compared with antidepressants or nonuse, a retrospective case-control study involving 90,786 patients has found.
Patients taking haloperidol had a 3.8% increase in mortality, and those taking risperidone had a 3.7% increase relative to nonusers, while olanzapine and quetiapine also were associated with significant increases in mortality risk, according to a study published online March 18 in JAMA Psychiatry.
When compared with individuals on antidepressants, haloperidol was associated with a 12.3% increase in mortality, representing a number-needed-to-harm of 8, while antidepressants alone were associated with a small but statistically significant increase in mortality risk.
“Prescribing a medication that increases mortality risk seems contrary to the tenet ‘first, do no harm,’ yet for patients who pose a danger to themselves and others and are in profound distress, use of such medications may still be appropriate,” wrote Dr. Donovan T. Maust of the department of psychiatry at the University of Michigan, Ann Arbor, and his coauthors (JAMA Psychiatry 2015 March 18 [doi:10.1001/jamapsychiatry.2014.3018]). “These new data can help physicians minimize the potential harm associated with antipsychotic treatment.”
The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, compared with antidepressants or nonuse, a retrospective case-control study involving 90,786 patients has found.
Patients taking haloperidol had a 3.8% increase in mortality, and those taking risperidone had a 3.7% increase relative to nonusers, while olanzapine and quetiapine also were associated with significant increases in mortality risk, according to a study published online March 18 in JAMA Psychiatry.
When compared with individuals on antidepressants, haloperidol was associated with a 12.3% increase in mortality, representing a number-needed-to-harm of 8, while antidepressants alone were associated with a small but statistically significant increase in mortality risk.
“Prescribing a medication that increases mortality risk seems contrary to the tenet ‘first, do no harm,’ yet for patients who pose a danger to themselves and others and are in profound distress, use of such medications may still be appropriate,” wrote Dr. Donovan T. Maust of the department of psychiatry at the University of Michigan, Ann Arbor, and his coauthors (JAMA Psychiatry 2015 March 18 [doi:10.1001/jamapsychiatry.2014.3018]). “These new data can help physicians minimize the potential harm associated with antipsychotic treatment.”
The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, compared with antidepressants or nonuse, a retrospective case-control study involving 90,786 patients has found.
Patients taking haloperidol had a 3.8% increase in mortality, and those taking risperidone had a 3.7% increase relative to nonusers, while olanzapine and quetiapine also were associated with significant increases in mortality risk, according to a study published online March 18 in JAMA Psychiatry.
When compared with individuals on antidepressants, haloperidol was associated with a 12.3% increase in mortality, representing a number-needed-to-harm of 8, while antidepressants alone were associated with a small but statistically significant increase in mortality risk.
“Prescribing a medication that increases mortality risk seems contrary to the tenet ‘first, do no harm,’ yet for patients who pose a danger to themselves and others and are in profound distress, use of such medications may still be appropriate,” wrote Dr. Donovan T. Maust of the department of psychiatry at the University of Michigan, Ann Arbor, and his coauthors (JAMA Psychiatry 2015 March 18 [doi:10.1001/jamapsychiatry.2014.3018]). “These new data can help physicians minimize the potential harm associated with antipsychotic treatment.”
The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
FROM JAMA PSYCHIATRY
Key clinical point: Antipsychotics such as haloperidol and risperidone are associated with a significant and dose-related increase in mortality in elderly patients with dementia, which “should raise the threshold for prescribing further.”
Major finding: Patients taking haloperidol had a 3.8% increase in mortality risk, and those taking risperidone had a 3.7% increase in mortality risk, compared with nonusers.
Data source: A retrospective case-control study conducted in the Veterans Health Administration among 90,786 patients with dementia.
Disclosures: The study was supported by the National Institute of Mental Health, the National Institute on Aging, the American Federation for Aging Research, the John A. Hartford Foundation, and the Atlantic Philanthropies. One author reported grants, research support, and consultancies with several pharmaceutical companies, and others reported receiving grants from the study’s supporters.
Achieving Diabetes Treatment Goals Rarely Influenced By Provider Beliefs
Primary care providers’ beliefs about diabetic treatment and glycated hemoglobin goals have a relatively small impact on patients achieving their diabetes treatment goals, researchers said.
A study linking the survey responses from 149 primary care providers to the health records of their 18,346 patients with diabetes showed that only two survey responses bore any significant relationship to patients’ glycemic control.
The 21% of responders who agreed with the statement that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement (odds ratio, 0.87; 95% confidence interval, 0.78-0.97; P = .02), according to Dr. Erin S. LeBlanc of the Kaiser Permanente Center for Health Research in Portland, Ore., and her coauthors.
Similarly, the 21% of providers who disagreed with the statement that “some patients will have an HbA1c greater than 9% no matter what I do” were 16% more likely to have patients achieving an HbA1cbelow 7% (OR, 1.16; 95%CI 1.03-1.30; P= .01) than those providers who were neutral about the statement.
“To the best of our knowledge, no previous research has linked what clinicians identify as patient and care setting barriers to the documented glycemic control of their patients,” they wrote (BMJ Open Diab. Res. Care 2015 Feb. 24).
The survey highlighted psychosocial issues, resistance to lifestyle change, and noncompliance as the most common patient-related barriers to achieving optimal control.
On the question of what factors might delay pharmacologic intensification, providers singled out patients’ resistance to lifestyle change and noncompliance as two factors that came into play at least 25% of the time, while unwillingness to consider insulin and psychosocial issues also played a key role.
Side effects, cost, cultural issues, and a lack of established patient-provider relationship played relatively minor roles in influencing pharmacologic intensification.
“These data suggest that patient and system barriers play a larger role than clinician beliefs and behaviors in prolonged poor control and delayed treatment intensification,” Dr. LeBlanc and her associates wrote.
“HbA1clevels were consistent across patients despite differences in their providers’ treatment behaviors, HbA1c goals, and diabetic treatment opinions,” they said.
The survey also revealed that 80% of primary care providers gave patients who were above their glycemic goals 3-6 months to work on lifestyle changes before resorting to pharmacologic therapy, while a similar percentage agreed that older patients needed less-stringent glycemic goals.
The majority also agreed that weight loss was a key component of diabetes care, but only 40% agreed that the impact of a diabetes medication on weight influenced their therapy decisions.
“Taken together, it seems that intervention to reduce barriers to glycemic control directed at providers would not produce much benefit, and that addressing these barriers may be most fruitful at the health system level,” the authors suggested.
The authors acknowledged that the survey was limited by a lack of variation in provider attitudes – possibly the result of conducting it within a single organization – as well as being of an insured population restricted to a range of treatments that did not include newer medications.
“This could affect the relative importance of cost issues in prescribing and intensification practices, and may also constrain our ability to assess the value of more therapeutic options,” they wrote.
The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.
Primary care providers’ beliefs about diabetic treatment and glycated hemoglobin goals have a relatively small impact on patients achieving their diabetes treatment goals, researchers said.
A study linking the survey responses from 149 primary care providers to the health records of their 18,346 patients with diabetes showed that only two survey responses bore any significant relationship to patients’ glycemic control.
The 21% of responders who agreed with the statement that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement (odds ratio, 0.87; 95% confidence interval, 0.78-0.97; P = .02), according to Dr. Erin S. LeBlanc of the Kaiser Permanente Center for Health Research in Portland, Ore., and her coauthors.
Similarly, the 21% of providers who disagreed with the statement that “some patients will have an HbA1c greater than 9% no matter what I do” were 16% more likely to have patients achieving an HbA1cbelow 7% (OR, 1.16; 95%CI 1.03-1.30; P= .01) than those providers who were neutral about the statement.
“To the best of our knowledge, no previous research has linked what clinicians identify as patient and care setting barriers to the documented glycemic control of their patients,” they wrote (BMJ Open Diab. Res. Care 2015 Feb. 24).
The survey highlighted psychosocial issues, resistance to lifestyle change, and noncompliance as the most common patient-related barriers to achieving optimal control.
On the question of what factors might delay pharmacologic intensification, providers singled out patients’ resistance to lifestyle change and noncompliance as two factors that came into play at least 25% of the time, while unwillingness to consider insulin and psychosocial issues also played a key role.
Side effects, cost, cultural issues, and a lack of established patient-provider relationship played relatively minor roles in influencing pharmacologic intensification.
“These data suggest that patient and system barriers play a larger role than clinician beliefs and behaviors in prolonged poor control and delayed treatment intensification,” Dr. LeBlanc and her associates wrote.
“HbA1clevels were consistent across patients despite differences in their providers’ treatment behaviors, HbA1c goals, and diabetic treatment opinions,” they said.
The survey also revealed that 80% of primary care providers gave patients who were above their glycemic goals 3-6 months to work on lifestyle changes before resorting to pharmacologic therapy, while a similar percentage agreed that older patients needed less-stringent glycemic goals.
The majority also agreed that weight loss was a key component of diabetes care, but only 40% agreed that the impact of a diabetes medication on weight influenced their therapy decisions.
“Taken together, it seems that intervention to reduce barriers to glycemic control directed at providers would not produce much benefit, and that addressing these barriers may be most fruitful at the health system level,” the authors suggested.
The authors acknowledged that the survey was limited by a lack of variation in provider attitudes – possibly the result of conducting it within a single organization – as well as being of an insured population restricted to a range of treatments that did not include newer medications.
“This could affect the relative importance of cost issues in prescribing and intensification practices, and may also constrain our ability to assess the value of more therapeutic options,” they wrote.
The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.
Primary care providers’ beliefs about diabetic treatment and glycated hemoglobin goals have a relatively small impact on patients achieving their diabetes treatment goals, researchers said.
A study linking the survey responses from 149 primary care providers to the health records of their 18,346 patients with diabetes showed that only two survey responses bore any significant relationship to patients’ glycemic control.
The 21% of responders who agreed with the statement that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement (odds ratio, 0.87; 95% confidence interval, 0.78-0.97; P = .02), according to Dr. Erin S. LeBlanc of the Kaiser Permanente Center for Health Research in Portland, Ore., and her coauthors.
Similarly, the 21% of providers who disagreed with the statement that “some patients will have an HbA1c greater than 9% no matter what I do” were 16% more likely to have patients achieving an HbA1cbelow 7% (OR, 1.16; 95%CI 1.03-1.30; P= .01) than those providers who were neutral about the statement.
“To the best of our knowledge, no previous research has linked what clinicians identify as patient and care setting barriers to the documented glycemic control of their patients,” they wrote (BMJ Open Diab. Res. Care 2015 Feb. 24).
The survey highlighted psychosocial issues, resistance to lifestyle change, and noncompliance as the most common patient-related barriers to achieving optimal control.
On the question of what factors might delay pharmacologic intensification, providers singled out patients’ resistance to lifestyle change and noncompliance as two factors that came into play at least 25% of the time, while unwillingness to consider insulin and psychosocial issues also played a key role.
Side effects, cost, cultural issues, and a lack of established patient-provider relationship played relatively minor roles in influencing pharmacologic intensification.
“These data suggest that patient and system barriers play a larger role than clinician beliefs and behaviors in prolonged poor control and delayed treatment intensification,” Dr. LeBlanc and her associates wrote.
“HbA1clevels were consistent across patients despite differences in their providers’ treatment behaviors, HbA1c goals, and diabetic treatment opinions,” they said.
The survey also revealed that 80% of primary care providers gave patients who were above their glycemic goals 3-6 months to work on lifestyle changes before resorting to pharmacologic therapy, while a similar percentage agreed that older patients needed less-stringent glycemic goals.
The majority also agreed that weight loss was a key component of diabetes care, but only 40% agreed that the impact of a diabetes medication on weight influenced their therapy decisions.
“Taken together, it seems that intervention to reduce barriers to glycemic control directed at providers would not produce much benefit, and that addressing these barriers may be most fruitful at the health system level,” the authors suggested.
The authors acknowledged that the survey was limited by a lack of variation in provider attitudes – possibly the result of conducting it within a single organization – as well as being of an insured population restricted to a range of treatments that did not include newer medications.
“This could affect the relative importance of cost issues in prescribing and intensification practices, and may also constrain our ability to assess the value of more therapeutic options,” they wrote.
The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.
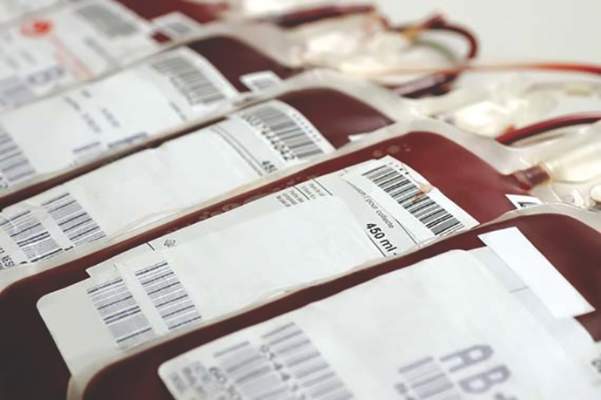
Fresh red blood cells add no advantages for critically ill
The use of fresh red blood cells for transfusion did not reduce mortality or improve other outcomes, compared with older standard-issue red cells, according to results of a multicenter, blinded, randomized prospective study presented at the annual meeting of the International Society on Intensive Care and Emergency Medicine.
In the Age of Blood Evaluation (ABLE) study, researchers randomized 1,211 critically ill patients to red blood cells stored for less than 8 days and 1,219 patients to standard-issue cells stored for a mean of 22.4 days. The study was conducted at 64 centers in Europe and Canada, where all blood units were leukoreduced and SAGM (saline-adenine-glucose-mannitol) suspended. Similar products are supplied in the United States, but red cells are suspended in additive solution 3 (AS3) rather than SAGM.
At 90 days, 37% of patients in the fresh-blood group and 35.3% of patients in the standard blood group had died. The survival analysis of the time to death showed a hazard ratio of those in the fresh-blood group was 1.1, compared with those in the standard blood group (95% confidence interval, 0.9-1.2; P = .38).
There were no significant differences in the rates of death, organ failure, acute respiratory distress, cardiovascular complications, thrombosis, infection, or acute transfusion reaction.
There also were no significant differences between the two groups in length of hospital stay or duration of supportive care such as mechanical ventilation, as was simultaneously reported in the March 17 edition of the New England Journal of Medicine (doi:10.1056/NEJMoa1500704).
“Although [other] initial studies showed an association between longer red-cell storage and adverse outcomes, these associations may have been spurious owing to sicker patients receiving more units with longer storage, the overlap between comparison groups in the age of the red cells transfused, and the inclusion of transfusions that occurred after the clinical events,” Dr. Jacque Lacroix of University of Montreal and his coauthors wrote.
The study was supported by the Canadian Institutes of Health Research, Fonds de Recherche du Québec–Santé, the National Institute for Health Research Evaluation, the French Ministry of Health, and the Etablissement Français du Sang, and Sanquin Blood Supply. Two authors reported grants and personal fees from pharmaceutical companies outside the submitted work, while others reported financial support from the study funding sources.
The use of fresh red blood cells for transfusion did not reduce mortality or improve other outcomes, compared with older standard-issue red cells, according to results of a multicenter, blinded, randomized prospective study presented at the annual meeting of the International Society on Intensive Care and Emergency Medicine.
In the Age of Blood Evaluation (ABLE) study, researchers randomized 1,211 critically ill patients to red blood cells stored for less than 8 days and 1,219 patients to standard-issue cells stored for a mean of 22.4 days. The study was conducted at 64 centers in Europe and Canada, where all blood units were leukoreduced and SAGM (saline-adenine-glucose-mannitol) suspended. Similar products are supplied in the United States, but red cells are suspended in additive solution 3 (AS3) rather than SAGM.
At 90 days, 37% of patients in the fresh-blood group and 35.3% of patients in the standard blood group had died. The survival analysis of the time to death showed a hazard ratio of those in the fresh-blood group was 1.1, compared with those in the standard blood group (95% confidence interval, 0.9-1.2; P = .38).
There were no significant differences in the rates of death, organ failure, acute respiratory distress, cardiovascular complications, thrombosis, infection, or acute transfusion reaction.
There also were no significant differences between the two groups in length of hospital stay or duration of supportive care such as mechanical ventilation, as was simultaneously reported in the March 17 edition of the New England Journal of Medicine (doi:10.1056/NEJMoa1500704).
“Although [other] initial studies showed an association between longer red-cell storage and adverse outcomes, these associations may have been spurious owing to sicker patients receiving more units with longer storage, the overlap between comparison groups in the age of the red cells transfused, and the inclusion of transfusions that occurred after the clinical events,” Dr. Jacque Lacroix of University of Montreal and his coauthors wrote.
The study was supported by the Canadian Institutes of Health Research, Fonds de Recherche du Québec–Santé, the National Institute for Health Research Evaluation, the French Ministry of Health, and the Etablissement Français du Sang, and Sanquin Blood Supply. Two authors reported grants and personal fees from pharmaceutical companies outside the submitted work, while others reported financial support from the study funding sources.
The use of fresh red blood cells for transfusion did not reduce mortality or improve other outcomes, compared with older standard-issue red cells, according to results of a multicenter, blinded, randomized prospective study presented at the annual meeting of the International Society on Intensive Care and Emergency Medicine.
In the Age of Blood Evaluation (ABLE) study, researchers randomized 1,211 critically ill patients to red blood cells stored for less than 8 days and 1,219 patients to standard-issue cells stored for a mean of 22.4 days. The study was conducted at 64 centers in Europe and Canada, where all blood units were leukoreduced and SAGM (saline-adenine-glucose-mannitol) suspended. Similar products are supplied in the United States, but red cells are suspended in additive solution 3 (AS3) rather than SAGM.
At 90 days, 37% of patients in the fresh-blood group and 35.3% of patients in the standard blood group had died. The survival analysis of the time to death showed a hazard ratio of those in the fresh-blood group was 1.1, compared with those in the standard blood group (95% confidence interval, 0.9-1.2; P = .38).
There were no significant differences in the rates of death, organ failure, acute respiratory distress, cardiovascular complications, thrombosis, infection, or acute transfusion reaction.
There also were no significant differences between the two groups in length of hospital stay or duration of supportive care such as mechanical ventilation, as was simultaneously reported in the March 17 edition of the New England Journal of Medicine (doi:10.1056/NEJMoa1500704).
“Although [other] initial studies showed an association between longer red-cell storage and adverse outcomes, these associations may have been spurious owing to sicker patients receiving more units with longer storage, the overlap between comparison groups in the age of the red cells transfused, and the inclusion of transfusions that occurred after the clinical events,” Dr. Jacque Lacroix of University of Montreal and his coauthors wrote.
The study was supported by the Canadian Institutes of Health Research, Fonds de Recherche du Québec–Santé, the National Institute for Health Research Evaluation, the French Ministry of Health, and the Etablissement Français du Sang, and Sanquin Blood Supply. Two authors reported grants and personal fees from pharmaceutical companies outside the submitted work, while others reported financial support from the study funding sources.
Key clinical point: Fresh red blood cells didn’t provide any additional gains in outcomes or reduce mortality at 90 days.
Major finding: The survival analysis of the time to death showed a hazard ratio of those in the fresh-blood group was 1.1, compared to those in the standard blood group (95% confidence interval, 0.9-1.2) (P = .38).
Data source: A multicenter, blinded, randomized prospective study in 2,430 patients receiving red blood cell transfusions.
Disclosures: The study was supported by the Canadian Institutes of Health Research, Fonds de Recherche du Québec–Santé, the National Institute for Health Research Evaluation, the French Ministry of Health, and the Etablissement Français du Sang, and Sanquin Blood Supply. Two authors reported grants and personal fees from pharmaceutical companies outside the submitted work, while others reported financial support from the study funding sources.
Everolimus-eluting stents linked to higher MI risk than CABG
Percutaneous coronary intervention with second-generation everolimus-eluting stents is associated with a similar risk of death but a higher risk of myocardial infarction and repeat revascularization than is coronary-artery bypass grafting.
An observational registry study of 34,819 patients with multivessel coronary artery disease who underwent one or the other procedure showed a similar risk of death at a mean follow-up of 2.9 years between patients who underwent PCI with everolimus-eluting stents and those who underwent CABG (3.1% and 2.9% per year, hazard ratio, 1.04; P = .50).
However, those in the percutaneous coronary intervention (PCI) group had a 51% greater risk of MI (95% confidence interval, 1.29-1.77; P < .001).
This increase in risk was significant only in patients who had incomplete revascularization and not in those with complete revascularization. In addition, the increase in risk largely was tied to spontaneous myocardial infarction, according to the findings.
“Randomized trials comparing PCI with CABG have not been typically powered to evaluate differences in the rates of myocardial infarction, stroke, and death from any cause; instead, they have been based on composite outcomes that include repeat revascularization,” wrote Dr. Sripal Bangalore of the cardiovascular clinical research center at the New York University, and his coauthors.
Patients undergoing PCI with everolimus-eluting stents also had a greater than twofold increase in the risk of repeat revascularization (hazard ratio, 2.35; 95% CI, 2.14-2.58; P < .001), but particularly in patients with three-vessel as opposed to two-vessel disease.
However, those in the PCI group also had a 58% lower risk of stroke than did those in the CABG group (95% CI, 0.50-0.76; P < .001), which was driven largely by a reduced risk in the first 30 days after the procedure (N. Engl. J. Med. 2015 March 16 [doi:10.1056/NEJMoa1412168]).
In the short term – in the hospital or within 30 days of the procedure – patients who underwent PCI showed significantly lower risk of death and stroke but no significant differences in MI risk.
“Thus, the choice between CABG and PCI with everolimus-eluting stents may depend on whether complete revascularization can be achieved with PCI,” the authors wrote. “If the answer is yes, the choice between PCI and CABG should be made on the basis of weighing the short-term risk of death and stroke against the long-term risk of revascularization with PCI.”
The authors acknowledged limitations of the study. It was a nonrandomized, observational trial; it did not examine variables such as smoking and other comorbidities; and it did not capture other neurologic events, such as transient ischemic attack.
The study was supported by Abbott Vascular. Dr. Bangalore has received consultant fees or honoraria from Abbott Vascular, Boehringer Ingelheim, Daiichi Sankyo, Gilead Sciences, Pfizer, and Unique Pharmaceuticals.
CABG previously has been shown to be associated with fewer repeat vascularizations than has PCI, but questions have been raised about incremental improvements in stent technology that might narrow this gap.

|
Dr. Robert A. Harrington |
However, data from this and the BEST study show there are clearly trade-offs between the two revascularization strategies that need to be discussed with patients as part of the shared decision-making process.
The early risk of stroke with CABG may be unacceptable to some, while others may want to avoid the risk of a later myocardial infarction or repeat procedure associated with PCI.
Dr. Robert A. Harrington is Arthur L. Bloomfield Professor of Medicine at Stanford (Calif.) University. These comments are taken from an editorial (N. Engl. J. Med. 2015 March 16 [doi:10.1056/NEJMe1501045]) accompanying this and the BEST study, which was also presented at the annual meeting of the American College of Cardiology in San Diego (N. Engl. J. Med. 2015 March 15 [doi:10.1056/NEJMoa1415447]). Dr. Harrington has received consultant fees and/or research grants from numerous pharmaceutical and device companies, including Amgen, Medtronic, Merck, Novartis, GlaxoSmithKline, and the Medicines Company. He is a principal or has ownership interest in Element Science and MyoKardia.
CABG previously has been shown to be associated with fewer repeat vascularizations than has PCI, but questions have been raised about incremental improvements in stent technology that might narrow this gap.

|
Dr. Robert A. Harrington |
However, data from this and the BEST study show there are clearly trade-offs between the two revascularization strategies that need to be discussed with patients as part of the shared decision-making process.
The early risk of stroke with CABG may be unacceptable to some, while others may want to avoid the risk of a later myocardial infarction or repeat procedure associated with PCI.
Dr. Robert A. Harrington is Arthur L. Bloomfield Professor of Medicine at Stanford (Calif.) University. These comments are taken from an editorial (N. Engl. J. Med. 2015 March 16 [doi:10.1056/NEJMe1501045]) accompanying this and the BEST study, which was also presented at the annual meeting of the American College of Cardiology in San Diego (N. Engl. J. Med. 2015 March 15 [doi:10.1056/NEJMoa1415447]). Dr. Harrington has received consultant fees and/or research grants from numerous pharmaceutical and device companies, including Amgen, Medtronic, Merck, Novartis, GlaxoSmithKline, and the Medicines Company. He is a principal or has ownership interest in Element Science and MyoKardia.
CABG previously has been shown to be associated with fewer repeat vascularizations than has PCI, but questions have been raised about incremental improvements in stent technology that might narrow this gap.

|
Dr. Robert A. Harrington |
However, data from this and the BEST study show there are clearly trade-offs between the two revascularization strategies that need to be discussed with patients as part of the shared decision-making process.
The early risk of stroke with CABG may be unacceptable to some, while others may want to avoid the risk of a later myocardial infarction or repeat procedure associated with PCI.
Dr. Robert A. Harrington is Arthur L. Bloomfield Professor of Medicine at Stanford (Calif.) University. These comments are taken from an editorial (N. Engl. J. Med. 2015 March 16 [doi:10.1056/NEJMe1501045]) accompanying this and the BEST study, which was also presented at the annual meeting of the American College of Cardiology in San Diego (N. Engl. J. Med. 2015 March 15 [doi:10.1056/NEJMoa1415447]). Dr. Harrington has received consultant fees and/or research grants from numerous pharmaceutical and device companies, including Amgen, Medtronic, Merck, Novartis, GlaxoSmithKline, and the Medicines Company. He is a principal or has ownership interest in Element Science and MyoKardia.
Percutaneous coronary intervention with second-generation everolimus-eluting stents is associated with a similar risk of death but a higher risk of myocardial infarction and repeat revascularization than is coronary-artery bypass grafting.
An observational registry study of 34,819 patients with multivessel coronary artery disease who underwent one or the other procedure showed a similar risk of death at a mean follow-up of 2.9 years between patients who underwent PCI with everolimus-eluting stents and those who underwent CABG (3.1% and 2.9% per year, hazard ratio, 1.04; P = .50).
However, those in the percutaneous coronary intervention (PCI) group had a 51% greater risk of MI (95% confidence interval, 1.29-1.77; P < .001).
This increase in risk was significant only in patients who had incomplete revascularization and not in those with complete revascularization. In addition, the increase in risk largely was tied to spontaneous myocardial infarction, according to the findings.
“Randomized trials comparing PCI with CABG have not been typically powered to evaluate differences in the rates of myocardial infarction, stroke, and death from any cause; instead, they have been based on composite outcomes that include repeat revascularization,” wrote Dr. Sripal Bangalore of the cardiovascular clinical research center at the New York University, and his coauthors.
Patients undergoing PCI with everolimus-eluting stents also had a greater than twofold increase in the risk of repeat revascularization (hazard ratio, 2.35; 95% CI, 2.14-2.58; P < .001), but particularly in patients with three-vessel as opposed to two-vessel disease.
However, those in the PCI group also had a 58% lower risk of stroke than did those in the CABG group (95% CI, 0.50-0.76; P < .001), which was driven largely by a reduced risk in the first 30 days after the procedure (N. Engl. J. Med. 2015 March 16 [doi:10.1056/NEJMoa1412168]).
In the short term – in the hospital or within 30 days of the procedure – patients who underwent PCI showed significantly lower risk of death and stroke but no significant differences in MI risk.
“Thus, the choice between CABG and PCI with everolimus-eluting stents may depend on whether complete revascularization can be achieved with PCI,” the authors wrote. “If the answer is yes, the choice between PCI and CABG should be made on the basis of weighing the short-term risk of death and stroke against the long-term risk of revascularization with PCI.”
The authors acknowledged limitations of the study. It was a nonrandomized, observational trial; it did not examine variables such as smoking and other comorbidities; and it did not capture other neurologic events, such as transient ischemic attack.
The study was supported by Abbott Vascular. Dr. Bangalore has received consultant fees or honoraria from Abbott Vascular, Boehringer Ingelheim, Daiichi Sankyo, Gilead Sciences, Pfizer, and Unique Pharmaceuticals.
Percutaneous coronary intervention with second-generation everolimus-eluting stents is associated with a similar risk of death but a higher risk of myocardial infarction and repeat revascularization than is coronary-artery bypass grafting.
An observational registry study of 34,819 patients with multivessel coronary artery disease who underwent one or the other procedure showed a similar risk of death at a mean follow-up of 2.9 years between patients who underwent PCI with everolimus-eluting stents and those who underwent CABG (3.1% and 2.9% per year, hazard ratio, 1.04; P = .50).
However, those in the percutaneous coronary intervention (PCI) group had a 51% greater risk of MI (95% confidence interval, 1.29-1.77; P < .001).
This increase in risk was significant only in patients who had incomplete revascularization and not in those with complete revascularization. In addition, the increase in risk largely was tied to spontaneous myocardial infarction, according to the findings.
“Randomized trials comparing PCI with CABG have not been typically powered to evaluate differences in the rates of myocardial infarction, stroke, and death from any cause; instead, they have been based on composite outcomes that include repeat revascularization,” wrote Dr. Sripal Bangalore of the cardiovascular clinical research center at the New York University, and his coauthors.
Patients undergoing PCI with everolimus-eluting stents also had a greater than twofold increase in the risk of repeat revascularization (hazard ratio, 2.35; 95% CI, 2.14-2.58; P < .001), but particularly in patients with three-vessel as opposed to two-vessel disease.
However, those in the PCI group also had a 58% lower risk of stroke than did those in the CABG group (95% CI, 0.50-0.76; P < .001), which was driven largely by a reduced risk in the first 30 days after the procedure (N. Engl. J. Med. 2015 March 16 [doi:10.1056/NEJMoa1412168]).
In the short term – in the hospital or within 30 days of the procedure – patients who underwent PCI showed significantly lower risk of death and stroke but no significant differences in MI risk.
“Thus, the choice between CABG and PCI with everolimus-eluting stents may depend on whether complete revascularization can be achieved with PCI,” the authors wrote. “If the answer is yes, the choice between PCI and CABG should be made on the basis of weighing the short-term risk of death and stroke against the long-term risk of revascularization with PCI.”
The authors acknowledged limitations of the study. It was a nonrandomized, observational trial; it did not examine variables such as smoking and other comorbidities; and it did not capture other neurologic events, such as transient ischemic attack.
The study was supported by Abbott Vascular. Dr. Bangalore has received consultant fees or honoraria from Abbott Vascular, Boehringer Ingelheim, Daiichi Sankyo, Gilead Sciences, Pfizer, and Unique Pharmaceuticals.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: PCI with second-generation everolimus-eluting stents is associated with a similar risk of death but a higher risk of MI and repeat revascularization than does CABG.
Major finding: PCI was associated with a 51% greater risk of MI at 2.9 years of follow-up, compared with CABG.
Data source: An observational registry study of 34,819 patients with multivessel coronary artery disease.
Disclosures: The study was supported by Abbott Vascular. Dr. Bangalore has received consultant fees or honoraria from Abbott Vascular, Boehringer Ingelheim, Daiichi Sankyo, Gilead Sciences, Pfizer, and Unique Pharmaceuticals.
PCI linked to higher rate of cardiovascular events than CABG
SAN DIEGO– Percutaneous coronary intervention with everolimus-eluting stents is associated with significantly higher major adverse cardiovascular events than is coronary artery bypass grafting in patients with multivessel coronary artery disease, according to results of the BEST trial.
In the randomized noninferiority trial of 880 patients, there was a 47% higher rate of the primary endpoint of death, myocardial infarction, or target vessel revascularization among patients randomized to percutaneous coronary intervention (PCI) with the new-generation drug-eluting stent than among those randomized to coronary artery bypass grafting (CABG), after a median of 4.6 years follow-up.
However, the differences in primary endpoint were not significant for noninferiority between the two groups at the 2-year follow-up mark, Dr. Seung-Jung Park said at the annual meeting of the American College of Cardiology.
The Xience everolimus-eluting stent used in BEST (Randomized Comparison of Coronary Artery Bypass Surgery and Everolimus-Eluting Stent Implantation in the Treatment of Patients with Multivessel Coronary Artery Disease) is one of several bioabsorbable vascular scaffolds that have caught on in recent years. The working hypothesis behind the device is that by dissolving during a period of 12-24 months, the scaffold provides temporary bracing against restenosis but then disappears, allowing improved endovascular healing.
Patients were randomized after diagnostic coronary angiography to PCI (438 patients) or to CABG (442).
The study, which was terminated early because of slow enrollment, also found a significantly greater rate of the composite secondary endpoint of death, myocardial infarction, stroke, or repeat revascularization in the PCI group compared to the CABG group (19.9% vs. 13.3%, P = .01).
There were no significant differences between the two groups in the rate of the other secondary safety endpoint: a composite of death, MI, and stroke.
In total, 29 patients assigned to PCI died, compared with 22 assigned to CABG (6.6% vs. 5%, P = .30).
The rate of spontaneous myocardial infarction was significantly higher in the PCI group (4.3% vs. 1.6%, P = .02), as was the rate of repeat revascularization (11% vs. 5.4%, P = .003).
There were fewer incidences of major bleeding in the PCI group compared to the CABG group, although the rate of fatal major bleeding was similar for both arms of the study.
Diabetes status had a major negative impact on outcome for patients undergoing PCI, increasing the rate of the primary endpoint to 19.2%, compared to 9.1% in patients undergoing CABG (P = .007).
“In the BEST trial, PCI with everolimus-eluting stents was not shown to be noninferior to CABG with respect to the primary endpoint of death, myocardial infarction, or target vessel revascularization at 2 years,” wrote Dr. Park of the University of Ulsan College of Medicine, and his coauthors. The article was published online simultaneously with his presentation (N. Engl. J. Med. 2015 March 15 [doi:10.1056/NEJMoa1415447]).
“At longer-term follow-up (median 4.6 years), PCI was associated with a significant increase in the incidence of the primary endpoint, as compared to the incidence with CABG.”
The authors suggested this difference was largely attributable to the higher rate of repeat target-vessel revascularization in patients who had undergone PCI, as well as the spontaneous myocardial infarction and new lesion revascularization.
In contrast to previous studies, the researchers did not find a significant difference in the rate of stroke between the two groups.
“The reason for this discrepancy is not clear, but the use of off-pump CABG can avoid excessive manipulation of the aorta, and may have contributed to a reduced rate of stroke in the CABG group in our study,” the authors noted.
The researchers acknowledged that the trial was not powered to detect differences in individual endpoints and that they did experience enrollment difficulties.
The CardioVascular Research Foundation, Abbott Vascular, and the Korea Healthcare Technology Research and Development Project supported the study. Dr. Park disclosed ties with Abbott, Cordis, Boston Scientific, and Medtronic, and has an ownership interest in the Cardiovascular Research Foundation.
SAN DIEGO– Percutaneous coronary intervention with everolimus-eluting stents is associated with significantly higher major adverse cardiovascular events than is coronary artery bypass grafting in patients with multivessel coronary artery disease, according to results of the BEST trial.
In the randomized noninferiority trial of 880 patients, there was a 47% higher rate of the primary endpoint of death, myocardial infarction, or target vessel revascularization among patients randomized to percutaneous coronary intervention (PCI) with the new-generation drug-eluting stent than among those randomized to coronary artery bypass grafting (CABG), after a median of 4.6 years follow-up.
However, the differences in primary endpoint were not significant for noninferiority between the two groups at the 2-year follow-up mark, Dr. Seung-Jung Park said at the annual meeting of the American College of Cardiology.
The Xience everolimus-eluting stent used in BEST (Randomized Comparison of Coronary Artery Bypass Surgery and Everolimus-Eluting Stent Implantation in the Treatment of Patients with Multivessel Coronary Artery Disease) is one of several bioabsorbable vascular scaffolds that have caught on in recent years. The working hypothesis behind the device is that by dissolving during a period of 12-24 months, the scaffold provides temporary bracing against restenosis but then disappears, allowing improved endovascular healing.
Patients were randomized after diagnostic coronary angiography to PCI (438 patients) or to CABG (442).
The study, which was terminated early because of slow enrollment, also found a significantly greater rate of the composite secondary endpoint of death, myocardial infarction, stroke, or repeat revascularization in the PCI group compared to the CABG group (19.9% vs. 13.3%, P = .01).
There were no significant differences between the two groups in the rate of the other secondary safety endpoint: a composite of death, MI, and stroke.
In total, 29 patients assigned to PCI died, compared with 22 assigned to CABG (6.6% vs. 5%, P = .30).
The rate of spontaneous myocardial infarction was significantly higher in the PCI group (4.3% vs. 1.6%, P = .02), as was the rate of repeat revascularization (11% vs. 5.4%, P = .003).
There were fewer incidences of major bleeding in the PCI group compared to the CABG group, although the rate of fatal major bleeding was similar for both arms of the study.
Diabetes status had a major negative impact on outcome for patients undergoing PCI, increasing the rate of the primary endpoint to 19.2%, compared to 9.1% in patients undergoing CABG (P = .007).
“In the BEST trial, PCI with everolimus-eluting stents was not shown to be noninferior to CABG with respect to the primary endpoint of death, myocardial infarction, or target vessel revascularization at 2 years,” wrote Dr. Park of the University of Ulsan College of Medicine, and his coauthors. The article was published online simultaneously with his presentation (N. Engl. J. Med. 2015 March 15 [doi:10.1056/NEJMoa1415447]).
“At longer-term follow-up (median 4.6 years), PCI was associated with a significant increase in the incidence of the primary endpoint, as compared to the incidence with CABG.”
The authors suggested this difference was largely attributable to the higher rate of repeat target-vessel revascularization in patients who had undergone PCI, as well as the spontaneous myocardial infarction and new lesion revascularization.
In contrast to previous studies, the researchers did not find a significant difference in the rate of stroke between the two groups.
“The reason for this discrepancy is not clear, but the use of off-pump CABG can avoid excessive manipulation of the aorta, and may have contributed to a reduced rate of stroke in the CABG group in our study,” the authors noted.
The researchers acknowledged that the trial was not powered to detect differences in individual endpoints and that they did experience enrollment difficulties.
The CardioVascular Research Foundation, Abbott Vascular, and the Korea Healthcare Technology Research and Development Project supported the study. Dr. Park disclosed ties with Abbott, Cordis, Boston Scientific, and Medtronic, and has an ownership interest in the Cardiovascular Research Foundation.
SAN DIEGO– Percutaneous coronary intervention with everolimus-eluting stents is associated with significantly higher major adverse cardiovascular events than is coronary artery bypass grafting in patients with multivessel coronary artery disease, according to results of the BEST trial.
In the randomized noninferiority trial of 880 patients, there was a 47% higher rate of the primary endpoint of death, myocardial infarction, or target vessel revascularization among patients randomized to percutaneous coronary intervention (PCI) with the new-generation drug-eluting stent than among those randomized to coronary artery bypass grafting (CABG), after a median of 4.6 years follow-up.
However, the differences in primary endpoint were not significant for noninferiority between the two groups at the 2-year follow-up mark, Dr. Seung-Jung Park said at the annual meeting of the American College of Cardiology.
The Xience everolimus-eluting stent used in BEST (Randomized Comparison of Coronary Artery Bypass Surgery and Everolimus-Eluting Stent Implantation in the Treatment of Patients with Multivessel Coronary Artery Disease) is one of several bioabsorbable vascular scaffolds that have caught on in recent years. The working hypothesis behind the device is that by dissolving during a period of 12-24 months, the scaffold provides temporary bracing against restenosis but then disappears, allowing improved endovascular healing.
Patients were randomized after diagnostic coronary angiography to PCI (438 patients) or to CABG (442).
The study, which was terminated early because of slow enrollment, also found a significantly greater rate of the composite secondary endpoint of death, myocardial infarction, stroke, or repeat revascularization in the PCI group compared to the CABG group (19.9% vs. 13.3%, P = .01).
There were no significant differences between the two groups in the rate of the other secondary safety endpoint: a composite of death, MI, and stroke.
In total, 29 patients assigned to PCI died, compared with 22 assigned to CABG (6.6% vs. 5%, P = .30).
The rate of spontaneous myocardial infarction was significantly higher in the PCI group (4.3% vs. 1.6%, P = .02), as was the rate of repeat revascularization (11% vs. 5.4%, P = .003).
There were fewer incidences of major bleeding in the PCI group compared to the CABG group, although the rate of fatal major bleeding was similar for both arms of the study.
Diabetes status had a major negative impact on outcome for patients undergoing PCI, increasing the rate of the primary endpoint to 19.2%, compared to 9.1% in patients undergoing CABG (P = .007).
“In the BEST trial, PCI with everolimus-eluting stents was not shown to be noninferior to CABG with respect to the primary endpoint of death, myocardial infarction, or target vessel revascularization at 2 years,” wrote Dr. Park of the University of Ulsan College of Medicine, and his coauthors. The article was published online simultaneously with his presentation (N. Engl. J. Med. 2015 March 15 [doi:10.1056/NEJMoa1415447]).
“At longer-term follow-up (median 4.6 years), PCI was associated with a significant increase in the incidence of the primary endpoint, as compared to the incidence with CABG.”
The authors suggested this difference was largely attributable to the higher rate of repeat target-vessel revascularization in patients who had undergone PCI, as well as the spontaneous myocardial infarction and new lesion revascularization.
In contrast to previous studies, the researchers did not find a significant difference in the rate of stroke between the two groups.
“The reason for this discrepancy is not clear, but the use of off-pump CABG can avoid excessive manipulation of the aorta, and may have contributed to a reduced rate of stroke in the CABG group in our study,” the authors noted.
The researchers acknowledged that the trial was not powered to detect differences in individual endpoints and that they did experience enrollment difficulties.
The CardioVascular Research Foundation, Abbott Vascular, and the Korea Healthcare Technology Research and Development Project supported the study. Dr. Park disclosed ties with Abbott, Cordis, Boston Scientific, and Medtronic, and has an ownership interest in the Cardiovascular Research Foundation.
AT ACC 15
Key clinical point: PCI with everolimus-eluting stents is associated with significantly higher major adverse cardiovascular events than is CABG in patients with multivessel coronary artery disease.
Major finding: Patients undergoing PCI had a 47% higher rate of the primary endpoint of death, myocardial infarction, or target vessel revascularization among patients compared to those undergoing CABG.
Data source: BEST, a randomized noninferiority trial of 880 patients.
Disclosures: The CardioVascular Research Foundation, Abbott Vascular, and the Korea Healthcare Technology Research and Development Project supported the study. Dr. Park disclosed ties with Abbott, Cordis, Boston Scientific, and Medtronic, and has an ownership interest in the Cardiovascular Research Foundation.
Cardiovascular event rates similar in PCI and CABG after 5 years
Percutaneous coronary intervention with a sirolimus-eluting stent showed comparable rates of death, myocardial infarction and stroke to coronary artery bypass grafting in patients with coronary artery stenosis after 5 years in a randomized trial.
The PRECOMBAT (Premier of Randomized Comparison of Bypass Surgery versus Angioplasty Using Sirolimus-Eluting Stent in Patients with Left Main Coronary Artery Disease) study randomized trial in 600 patients with unprotected left main coronary artery stenosis – 300 of whom were randomized to PCI and the rest to CABG – showed no significant difference in major adverse cardiac or cerebrovascular events (hazard ratio, 1.27; 95% confidence interval, 0.84-1.90; P = 0.26), according to a presentation at the American College of Cardiology meeting in San Diego.
However, the study did observe a twofold increase in the rate of ischemia-driven target vessel revascularization among patients treated with PCI, compared to those who underwent CABG (HR, 2.11; 95% CI, 1.16-3.84; P = 0.012), although the authors pointed out that this did not appear to impact the study’s harder endpoints.
“Given a higher rate of repeat revascularization even after the use of second-generation drug-eluting stents for unprotected left main coronary artery stenosis, frequent repeat revascularization could be an inherent weakness of stent-related treatments,” wrote Dr. Jung-Min Ahn, from the Asan Medical Center, Seoul, and coauthors (J. Am. Coll. Cardiol. 2015; March 15 [doi:10.1016/j.jacc.2015.03.033]).
The study was supported by the CardioVascular Research Foundation, Cordis, Johnson and Johnson, and the Korean Ministry of Health & Welfare. No conflicts of interest were disclosed.
Percutaneous coronary intervention with a sirolimus-eluting stent showed comparable rates of death, myocardial infarction and stroke to coronary artery bypass grafting in patients with coronary artery stenosis after 5 years in a randomized trial.
The PRECOMBAT (Premier of Randomized Comparison of Bypass Surgery versus Angioplasty Using Sirolimus-Eluting Stent in Patients with Left Main Coronary Artery Disease) study randomized trial in 600 patients with unprotected left main coronary artery stenosis – 300 of whom were randomized to PCI and the rest to CABG – showed no significant difference in major adverse cardiac or cerebrovascular events (hazard ratio, 1.27; 95% confidence interval, 0.84-1.90; P = 0.26), according to a presentation at the American College of Cardiology meeting in San Diego.
However, the study did observe a twofold increase in the rate of ischemia-driven target vessel revascularization among patients treated with PCI, compared to those who underwent CABG (HR, 2.11; 95% CI, 1.16-3.84; P = 0.012), although the authors pointed out that this did not appear to impact the study’s harder endpoints.
“Given a higher rate of repeat revascularization even after the use of second-generation drug-eluting stents for unprotected left main coronary artery stenosis, frequent repeat revascularization could be an inherent weakness of stent-related treatments,” wrote Dr. Jung-Min Ahn, from the Asan Medical Center, Seoul, and coauthors (J. Am. Coll. Cardiol. 2015; March 15 [doi:10.1016/j.jacc.2015.03.033]).
The study was supported by the CardioVascular Research Foundation, Cordis, Johnson and Johnson, and the Korean Ministry of Health & Welfare. No conflicts of interest were disclosed.
Percutaneous coronary intervention with a sirolimus-eluting stent showed comparable rates of death, myocardial infarction and stroke to coronary artery bypass grafting in patients with coronary artery stenosis after 5 years in a randomized trial.
The PRECOMBAT (Premier of Randomized Comparison of Bypass Surgery versus Angioplasty Using Sirolimus-Eluting Stent in Patients with Left Main Coronary Artery Disease) study randomized trial in 600 patients with unprotected left main coronary artery stenosis – 300 of whom were randomized to PCI and the rest to CABG – showed no significant difference in major adverse cardiac or cerebrovascular events (hazard ratio, 1.27; 95% confidence interval, 0.84-1.90; P = 0.26), according to a presentation at the American College of Cardiology meeting in San Diego.
However, the study did observe a twofold increase in the rate of ischemia-driven target vessel revascularization among patients treated with PCI, compared to those who underwent CABG (HR, 2.11; 95% CI, 1.16-3.84; P = 0.012), although the authors pointed out that this did not appear to impact the study’s harder endpoints.
“Given a higher rate of repeat revascularization even after the use of second-generation drug-eluting stents for unprotected left main coronary artery stenosis, frequent repeat revascularization could be an inherent weakness of stent-related treatments,” wrote Dr. Jung-Min Ahn, from the Asan Medical Center, Seoul, and coauthors (J. Am. Coll. Cardiol. 2015; March 15 [doi:10.1016/j.jacc.2015.03.033]).
The study was supported by the CardioVascular Research Foundation, Cordis, Johnson and Johnson, and the Korean Ministry of Health & Welfare. No conflicts of interest were disclosed.
FROM ACC 2015
Key clinical point: Percutaneous coronary intervention with sirolimus-eluting stents shows comparable rates of death, myocardial infarction and stroke to coronary artery bypass grafting after 5 years.
Major finding: There were no significant differences in major adverse cardiac or cerebrovascular events between PCI and CABG in patients with unprotected left main coronary artery stenosis.
Data source: PRECOMBAT, A randomized trial in 600 patients with unprotected left main coronary artery stenosis.
Disclosures: The study was supported by the CardioVascular Research Foundation, Cordis, Johnson&Johnson, and the Korean Ministry of Health & Welfare. No conflicts of interest were disclosed.
Type 1 Diabetes Doubles Infection and Hospitalization Risk
Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls, according to a prospective cohort study.
Finnish researchers found the rate of hospitalization for bacterial infections was 2.3 times higher in patients with diabetes compared with nondiabetic controls (relative risk, 2.3; 95% confidence interval, 2.11-2.51), and nearly 7 times higher in patients who had received a kidney transplant (RR, 11.2; 95% CI 8.1-15.5) compared with those with diabetes and normal urinary albumin excretion rate (AER).
Data from 4,748 patients enrolled in the Finnish Diabetic Nephropathy (FinnDiane) Study, and 12,954 matched nondiabetic controls, showed the rate of hospitalization was linked with the severity of diabetic nephropathy, ranging from a 23% increase in risk with microalbuminuria to an 11-fold increase in risk for dialysis patients, compared to a normal AER.
“Even in patients with normal AER, each unit increase in hemoglobin A1c increased hospitalizations by 26%,” wrote Dr. Johan R Simonsen of the Folkhälsan Institute of Genetics, Helsinki, Finland, and coauthors. The study was published online March 5 in BMJ Open Diabetes Research & Care (doi:10.1136/bmjdrc-2014-000067).
Individuals with type 1 diabetes also purchased significantly greater numbers of antibiotics than did nondiabetic controls, and each unit of increase in glycated hemoglobin was associated with a 6%-10% increase in annual antibiotic purchases.
Annual antibiotic purchases were 1.18-fold more frequent in patients with microalbuminuria, 1.29-fold with macroalbuminuria, 2.43-fold with dialysis, and 2.74-fold with kidney transplant, compared with patients who had normal AER, according to the investigators.
Patients with normal urinary AER had a 48% greater rate of antibiotic purchase than that of healthy controls, even after the researchers controlled for comorbidities.
Researchers also examined whether frequent antibiotic use was associated with the progression of nephropathy. They found that the mean number of antibiotic purchases was higher among patients who developed microalbuminuria compared with diabetic patients with normal urinary AER.
“In patients with incident microalbuminuria, the number of antibiotic purchases was higher at the time of nephropathy diagnosis (year 0) compared with 4 years before the progression (year −4; P = .04 for time effect),” they wrote, finding no differences in antibiotic purchases in patients with normal urinary AER during follow-up.
The impact of comorbidities on hospitalization and antibiotic prescribing varied with the type of comorbidity; hypertension significantly increased the rate of hospitalization in patients with diabetes compared with those without, while cancer was associated with much higher hospitalization rates in those without diabetes.
Antibiotic purchases were significantly higher in patients with diabetes and atherosclerosis compared with those without diabetes, but lower in diabetic patients with respiratory diseases such as COPD compared to nondiabetic patients with the same conditions.
The rate of hospitalization for infection was similar in men and women with diabetes, whereas women with diabetes purchased significantly more antibiotics than did men.
While hyperglycemia is known to cause immunosuppression, and therefore to increase susceptibility to bacterial infection, infections themselves may also cause hyperglycemia, the authors suggested.
“Hence, a vicious cycle may arise as frequent infections can worsen the glycemic control in patients with diabetes, and conversely, chronic hyperglycemia may facilitate the development of infections,” they wrote.
“As chronic hyperglycemia remains the primary cause of metabolic, biochemical, and vascular abnormalities in diabetic nephropathy, it could be argued that poor glycemic control may be the link between the progression of diabetic nephropathy and the higher incidence of bacterial infections.”
The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls, according to a prospective cohort study.
Finnish researchers found the rate of hospitalization for bacterial infections was 2.3 times higher in patients with diabetes compared with nondiabetic controls (relative risk, 2.3; 95% confidence interval, 2.11-2.51), and nearly 7 times higher in patients who had received a kidney transplant (RR, 11.2; 95% CI 8.1-15.5) compared with those with diabetes and normal urinary albumin excretion rate (AER).
Data from 4,748 patients enrolled in the Finnish Diabetic Nephropathy (FinnDiane) Study, and 12,954 matched nondiabetic controls, showed the rate of hospitalization was linked with the severity of diabetic nephropathy, ranging from a 23% increase in risk with microalbuminuria to an 11-fold increase in risk for dialysis patients, compared to a normal AER.
“Even in patients with normal AER, each unit increase in hemoglobin A1c increased hospitalizations by 26%,” wrote Dr. Johan R Simonsen of the Folkhälsan Institute of Genetics, Helsinki, Finland, and coauthors. The study was published online March 5 in BMJ Open Diabetes Research & Care (doi:10.1136/bmjdrc-2014-000067).
Individuals with type 1 diabetes also purchased significantly greater numbers of antibiotics than did nondiabetic controls, and each unit of increase in glycated hemoglobin was associated with a 6%-10% increase in annual antibiotic purchases.
Annual antibiotic purchases were 1.18-fold more frequent in patients with microalbuminuria, 1.29-fold with macroalbuminuria, 2.43-fold with dialysis, and 2.74-fold with kidney transplant, compared with patients who had normal AER, according to the investigators.
Patients with normal urinary AER had a 48% greater rate of antibiotic purchase than that of healthy controls, even after the researchers controlled for comorbidities.
Researchers also examined whether frequent antibiotic use was associated with the progression of nephropathy. They found that the mean number of antibiotic purchases was higher among patients who developed microalbuminuria compared with diabetic patients with normal urinary AER.
“In patients with incident microalbuminuria, the number of antibiotic purchases was higher at the time of nephropathy diagnosis (year 0) compared with 4 years before the progression (year −4; P = .04 for time effect),” they wrote, finding no differences in antibiotic purchases in patients with normal urinary AER during follow-up.
The impact of comorbidities on hospitalization and antibiotic prescribing varied with the type of comorbidity; hypertension significantly increased the rate of hospitalization in patients with diabetes compared with those without, while cancer was associated with much higher hospitalization rates in those without diabetes.
Antibiotic purchases were significantly higher in patients with diabetes and atherosclerosis compared with those without diabetes, but lower in diabetic patients with respiratory diseases such as COPD compared to nondiabetic patients with the same conditions.
The rate of hospitalization for infection was similar in men and women with diabetes, whereas women with diabetes purchased significantly more antibiotics than did men.
While hyperglycemia is known to cause immunosuppression, and therefore to increase susceptibility to bacterial infection, infections themselves may also cause hyperglycemia, the authors suggested.
“Hence, a vicious cycle may arise as frequent infections can worsen the glycemic control in patients with diabetes, and conversely, chronic hyperglycemia may facilitate the development of infections,” they wrote.
“As chronic hyperglycemia remains the primary cause of metabolic, biochemical, and vascular abnormalities in diabetic nephropathy, it could be argued that poor glycemic control may be the link between the progression of diabetic nephropathy and the higher incidence of bacterial infections.”
The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls, according to a prospective cohort study.
Finnish researchers found the rate of hospitalization for bacterial infections was 2.3 times higher in patients with diabetes compared with nondiabetic controls (relative risk, 2.3; 95% confidence interval, 2.11-2.51), and nearly 7 times higher in patients who had received a kidney transplant (RR, 11.2; 95% CI 8.1-15.5) compared with those with diabetes and normal urinary albumin excretion rate (AER).
Data from 4,748 patients enrolled in the Finnish Diabetic Nephropathy (FinnDiane) Study, and 12,954 matched nondiabetic controls, showed the rate of hospitalization was linked with the severity of diabetic nephropathy, ranging from a 23% increase in risk with microalbuminuria to an 11-fold increase in risk for dialysis patients, compared to a normal AER.
“Even in patients with normal AER, each unit increase in hemoglobin A1c increased hospitalizations by 26%,” wrote Dr. Johan R Simonsen of the Folkhälsan Institute of Genetics, Helsinki, Finland, and coauthors. The study was published online March 5 in BMJ Open Diabetes Research & Care (doi:10.1136/bmjdrc-2014-000067).
Individuals with type 1 diabetes also purchased significantly greater numbers of antibiotics than did nondiabetic controls, and each unit of increase in glycated hemoglobin was associated with a 6%-10% increase in annual antibiotic purchases.
Annual antibiotic purchases were 1.18-fold more frequent in patients with microalbuminuria, 1.29-fold with macroalbuminuria, 2.43-fold with dialysis, and 2.74-fold with kidney transplant, compared with patients who had normal AER, according to the investigators.
Patients with normal urinary AER had a 48% greater rate of antibiotic purchase than that of healthy controls, even after the researchers controlled for comorbidities.
Researchers also examined whether frequent antibiotic use was associated with the progression of nephropathy. They found that the mean number of antibiotic purchases was higher among patients who developed microalbuminuria compared with diabetic patients with normal urinary AER.
“In patients with incident microalbuminuria, the number of antibiotic purchases was higher at the time of nephropathy diagnosis (year 0) compared with 4 years before the progression (year −4; P = .04 for time effect),” they wrote, finding no differences in antibiotic purchases in patients with normal urinary AER during follow-up.
The impact of comorbidities on hospitalization and antibiotic prescribing varied with the type of comorbidity; hypertension significantly increased the rate of hospitalization in patients with diabetes compared with those without, while cancer was associated with much higher hospitalization rates in those without diabetes.
Antibiotic purchases were significantly higher in patients with diabetes and atherosclerosis compared with those without diabetes, but lower in diabetic patients with respiratory diseases such as COPD compared to nondiabetic patients with the same conditions.
The rate of hospitalization for infection was similar in men and women with diabetes, whereas women with diabetes purchased significantly more antibiotics than did men.
While hyperglycemia is known to cause immunosuppression, and therefore to increase susceptibility to bacterial infection, infections themselves may also cause hyperglycemia, the authors suggested.
“Hence, a vicious cycle may arise as frequent infections can worsen the glycemic control in patients with diabetes, and conversely, chronic hyperglycemia may facilitate the development of infections,” they wrote.
“As chronic hyperglycemia remains the primary cause of metabolic, biochemical, and vascular abnormalities in diabetic nephropathy, it could be argued that poor glycemic control may be the link between the progression of diabetic nephropathy and the higher incidence of bacterial infections.”
The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
FROM BMJ OPEN DIABETES RESEARCH & CARE
Type 1 diabetes doubles infection and hospitalization risk
Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls, according to a prospective cohort study.
Finnish researchers found the rate of hospitalization for bacterial infections was 2.3 times higher in patients with diabetes compared with nondiabetic controls (relative risk, 2.3; 95% confidence interval, 2.11-2.51), and nearly 7 times higher in patients who had received a kidney transplant (RR, 11.2; 95% CI 8.1-15.5) compared with those with diabetes and normal urinary albumin excretion rate (AER).
Data from 4,748 patients enrolled in the Finnish Diabetic Nephropathy (FinnDiane) Study, and 12,954 matched nondiabetic controls, showed the rate of hospitalization was linked with the severity of diabetic nephropathy, ranging from a 23% increase in risk with microalbuminuria to an 11-fold increase in risk for dialysis patients, compared to a normal AER.
“Even in patients with normal AER, each unit increase in hemoglobin A1c increased hospitalizations by 26%,” wrote Dr. Johan R Simonsen of the Folkhälsan Institute of Genetics, Helsinki, Finland, and coauthors. The study was published online March 5 in BMJ Open Diabetes Research & Care (doi:10.1136/bmjdrc-2014-000067).
Individuals with type 1 diabetes also purchased significantly greater numbers of antibiotics than did nondiabetic controls, and each unit of increase in glycated hemoglobin was associated with a 6%-10% increase in annual antibiotic purchases.
Annual antibiotic purchases were 1.18-fold more frequent in patients with microalbuminuria, 1.29-fold with macroalbuminuria, 2.43-fold with dialysis, and 2.74-fold with kidney transplant, compared with patients who had normal AER, according to the investigators.
Patients with normal urinary AER had a 48% greater rate of antibiotic purchase than that of healthy controls, even after the researchers controlled for comorbidities.
Researchers also examined whether frequent antibiotic use was associated with the progression of nephropathy. They found that the mean number of antibiotic purchases was higher among patients who developed microalbuminuria compared with diabetic patients with normal urinary AER.
“In patients with incident microalbuminuria, the number of antibiotic purchases was higher at the time of nephropathy diagnosis (year 0) compared with 4 years before the progression (year −4; P = .04 for time effect),” they wrote, finding no differences in antibiotic purchases in patients with normal urinary AER during follow-up.
The impact of comorbidities on hospitalization and antibiotic prescribing varied with the type of comorbidity; hypertension significantly increased the rate of hospitalization in patients with diabetes compared with those without, while cancer was associated with much higher hospitalization rates in those without diabetes.
Antibiotic purchases were significantly higher in patients with diabetes and atherosclerosis compared with those without diabetes, but lower in diabetic patients with respiratory diseases such as COPD compared to nondiabetic patients with the same conditions.
The rate of hospitalization for infection was similar in men and women with diabetes, whereas women with diabetes purchased significantly more antibiotics than did men.
While hyperglycemia is known to cause immunosuppression, and therefore to increase susceptibility to bacterial infection, infections themselves may also cause hyperglycemia, the authors suggested.
“Hence, a vicious cycle may arise as frequent infections can worsen the glycemic control in patients with diabetes, and conversely, chronic hyperglycemia may facilitate the development of infections,” they wrote.
“As chronic hyperglycemia remains the primary cause of metabolic, biochemical, and vascular abnormalities in diabetic nephropathy, it could be argued that poor glycemic control may be the link between the progression of diabetic nephropathy and the higher incidence of bacterial infections.”
The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls, according to a prospective cohort study.
Finnish researchers found the rate of hospitalization for bacterial infections was 2.3 times higher in patients with diabetes compared with nondiabetic controls (relative risk, 2.3; 95% confidence interval, 2.11-2.51), and nearly 7 times higher in patients who had received a kidney transplant (RR, 11.2; 95% CI 8.1-15.5) compared with those with diabetes and normal urinary albumin excretion rate (AER).
Data from 4,748 patients enrolled in the Finnish Diabetic Nephropathy (FinnDiane) Study, and 12,954 matched nondiabetic controls, showed the rate of hospitalization was linked with the severity of diabetic nephropathy, ranging from a 23% increase in risk with microalbuminuria to an 11-fold increase in risk for dialysis patients, compared to a normal AER.
“Even in patients with normal AER, each unit increase in hemoglobin A1c increased hospitalizations by 26%,” wrote Dr. Johan R Simonsen of the Folkhälsan Institute of Genetics, Helsinki, Finland, and coauthors. The study was published online March 5 in BMJ Open Diabetes Research & Care (doi:10.1136/bmjdrc-2014-000067).
Individuals with type 1 diabetes also purchased significantly greater numbers of antibiotics than did nondiabetic controls, and each unit of increase in glycated hemoglobin was associated with a 6%-10% increase in annual antibiotic purchases.
Annual antibiotic purchases were 1.18-fold more frequent in patients with microalbuminuria, 1.29-fold with macroalbuminuria, 2.43-fold with dialysis, and 2.74-fold with kidney transplant, compared with patients who had normal AER, according to the investigators.
Patients with normal urinary AER had a 48% greater rate of antibiotic purchase than that of healthy controls, even after the researchers controlled for comorbidities.
Researchers also examined whether frequent antibiotic use was associated with the progression of nephropathy. They found that the mean number of antibiotic purchases was higher among patients who developed microalbuminuria compared with diabetic patients with normal urinary AER.
“In patients with incident microalbuminuria, the number of antibiotic purchases was higher at the time of nephropathy diagnosis (year 0) compared with 4 years before the progression (year −4; P = .04 for time effect),” they wrote, finding no differences in antibiotic purchases in patients with normal urinary AER during follow-up.
The impact of comorbidities on hospitalization and antibiotic prescribing varied with the type of comorbidity; hypertension significantly increased the rate of hospitalization in patients with diabetes compared with those without, while cancer was associated with much higher hospitalization rates in those without diabetes.
Antibiotic purchases were significantly higher in patients with diabetes and atherosclerosis compared with those without diabetes, but lower in diabetic patients with respiratory diseases such as COPD compared to nondiabetic patients with the same conditions.
The rate of hospitalization for infection was similar in men and women with diabetes, whereas women with diabetes purchased significantly more antibiotics than did men.
While hyperglycemia is known to cause immunosuppression, and therefore to increase susceptibility to bacterial infection, infections themselves may also cause hyperglycemia, the authors suggested.
“Hence, a vicious cycle may arise as frequent infections can worsen the glycemic control in patients with diabetes, and conversely, chronic hyperglycemia may facilitate the development of infections,” they wrote.
“As chronic hyperglycemia remains the primary cause of metabolic, biochemical, and vascular abnormalities in diabetic nephropathy, it could be argued that poor glycemic control may be the link between the progression of diabetic nephropathy and the higher incidence of bacterial infections.”
The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls, according to a prospective cohort study.
Finnish researchers found the rate of hospitalization for bacterial infections was 2.3 times higher in patients with diabetes compared with nondiabetic controls (relative risk, 2.3; 95% confidence interval, 2.11-2.51), and nearly 7 times higher in patients who had received a kidney transplant (RR, 11.2; 95% CI 8.1-15.5) compared with those with diabetes and normal urinary albumin excretion rate (AER).
Data from 4,748 patients enrolled in the Finnish Diabetic Nephropathy (FinnDiane) Study, and 12,954 matched nondiabetic controls, showed the rate of hospitalization was linked with the severity of diabetic nephropathy, ranging from a 23% increase in risk with microalbuminuria to an 11-fold increase in risk for dialysis patients, compared to a normal AER.
“Even in patients with normal AER, each unit increase in hemoglobin A1c increased hospitalizations by 26%,” wrote Dr. Johan R Simonsen of the Folkhälsan Institute of Genetics, Helsinki, Finland, and coauthors. The study was published online March 5 in BMJ Open Diabetes Research & Care (doi:10.1136/bmjdrc-2014-000067).
Individuals with type 1 diabetes also purchased significantly greater numbers of antibiotics than did nondiabetic controls, and each unit of increase in glycated hemoglobin was associated with a 6%-10% increase in annual antibiotic purchases.
Annual antibiotic purchases were 1.18-fold more frequent in patients with microalbuminuria, 1.29-fold with macroalbuminuria, 2.43-fold with dialysis, and 2.74-fold with kidney transplant, compared with patients who had normal AER, according to the investigators.
Patients with normal urinary AER had a 48% greater rate of antibiotic purchase than that of healthy controls, even after the researchers controlled for comorbidities.
Researchers also examined whether frequent antibiotic use was associated with the progression of nephropathy. They found that the mean number of antibiotic purchases was higher among patients who developed microalbuminuria compared with diabetic patients with normal urinary AER.
“In patients with incident microalbuminuria, the number of antibiotic purchases was higher at the time of nephropathy diagnosis (year 0) compared with 4 years before the progression (year −4; P = .04 for time effect),” they wrote, finding no differences in antibiotic purchases in patients with normal urinary AER during follow-up.
The impact of comorbidities on hospitalization and antibiotic prescribing varied with the type of comorbidity; hypertension significantly increased the rate of hospitalization in patients with diabetes compared with those without, while cancer was associated with much higher hospitalization rates in those without diabetes.
Antibiotic purchases were significantly higher in patients with diabetes and atherosclerosis compared with those without diabetes, but lower in diabetic patients with respiratory diseases such as COPD compared to nondiabetic patients with the same conditions.
The rate of hospitalization for infection was similar in men and women with diabetes, whereas women with diabetes purchased significantly more antibiotics than did men.
While hyperglycemia is known to cause immunosuppression, and therefore to increase susceptibility to bacterial infection, infections themselves may also cause hyperglycemia, the authors suggested.
“Hence, a vicious cycle may arise as frequent infections can worsen the glycemic control in patients with diabetes, and conversely, chronic hyperglycemia may facilitate the development of infections,” they wrote.
“As chronic hyperglycemia remains the primary cause of metabolic, biochemical, and vascular abnormalities in diabetic nephropathy, it could be argued that poor glycemic control may be the link between the progression of diabetic nephropathy and the higher incidence of bacterial infections.”
The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
FROM BMJ OPEN DIABETES RESEARCH & CARE
Key clinical point: Individuals with type 1 diabetes are at significantly higher risk of bacterial infections compared with nondiabetic controls.
Major finding: The rate of hospitalization for bacterial infections was 2.3 times higher in patients with type 1 diabetes compared to nondiabetic controls.
Data source: A prospective cohort study of 4,748 individuals with type 1 diabetes and 12,954 age- and sex-matched controls.
Disclosures: The Folkhälsan Research Foundation, the Wilhelm and Else Stockmann Foundation, the Livoch Hälsa Foundation, the Päivikki and Sakari Sohlberg Foundation, the Academy of Finland, the Diabetes Research Foundation, and the Novo Nordisk Foundation supported the study. One author disclosed ties to several pharmaceutical companies, including Novo Nordisk. There were no other conflicts of interest declared.
Achieving diabetes treatment goals rarely influenced by provider beliefs
Primary care providers’ beliefs about diabetic treatment and glycated hemoglobin goals have a relatively small impact on patients achieving their diabetes treatment goals, researchers said.
A study linking the survey responses from 149 primary care providers to the health records of their 18,346 patients with diabetes showed that only two survey responses bore any significant relationship to patients’ glycemic control.
The 21% of responders who agreed with the statement that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement (odds ratio, 0.87; 95% confidence interval, 0.78-0.97; P = .02), according to Dr. Erin S. LeBlanc of the Kaiser Permanente Center for Health Research in Portland, Ore., and her coauthors.
Similarly, the 21% of providers who disagreed with the statement that “some patients will have an HbA1c greater than 9% no matter what I do” were 16% more likely to have patients achieving an HbA1cbelow 7% (OR, 1.16; 95%CI 1.03-1.30; P= .01) than those providers who were neutral about the statement.
“To the best of our knowledge, no previous research has linked what clinicians identify as patient and care setting barriers to the documented glycemic control of their patients,” they wrote (BMJ Open Diab. Res. Care 2015 Feb. 24).
The survey highlighted psychosocial issues, resistance to lifestyle change, and noncompliance as the most common patient-related barriers to achieving optimal control.
On the question of what factors might delay pharmacologic intensification, providers singled out patients’ resistance to lifestyle change and noncompliance as two factors that came into play at least 25% of the time, while unwillingness to consider insulin and psychosocial issues also played a key role.
Side effects, cost, cultural issues, and a lack of established patient-provider relationship played relatively minor roles in influencing pharmacologic intensification.
“These data suggest that patient and system barriers play a larger role than clinician beliefs and behaviors in prolonged poor control and delayed treatment intensification,” Dr. LeBlanc and her associates wrote.
“HbA1clevels were consistent across patients despite differences in their providers’ treatment behaviors, HbA1c goals, and diabetic treatment opinions,” they said.
The survey also revealed that 80% of primary care providers gave patients who were above their glycemic goals 3-6 months to work on lifestyle changes before resorting to pharmacologic therapy, while a similar percentage agreed that older patients needed less-stringent glycemic goals.
The majority also agreed that weight loss was a key component of diabetes care, but only 40% agreed that the impact of a diabetes medication on weight influenced their therapy decisions.
“Taken together, it seems that intervention to reduce barriers to glycemic control directed at providers would not produce much benefit, and that addressing these barriers may be most fruitful at the health system level,” the authors suggested.
The authors acknowledged that the survey was limited by a lack of variation in provider attitudes – possibly the result of conducting it within a single organization – as well as being of an insured population restricted to a range of treatments that did not include newer medications.
“This could affect the relative importance of cost issues in prescribing and intensification practices, and may also constrain our ability to assess the value of more therapeutic options,” they wrote.
The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.
Primary care providers’ beliefs about diabetic treatment and glycated hemoglobin goals have a relatively small impact on patients achieving their diabetes treatment goals, researchers said.
A study linking the survey responses from 149 primary care providers to the health records of their 18,346 patients with diabetes showed that only two survey responses bore any significant relationship to patients’ glycemic control.
The 21% of responders who agreed with the statement that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement (odds ratio, 0.87; 95% confidence interval, 0.78-0.97; P = .02), according to Dr. Erin S. LeBlanc of the Kaiser Permanente Center for Health Research in Portland, Ore., and her coauthors.
Similarly, the 21% of providers who disagreed with the statement that “some patients will have an HbA1c greater than 9% no matter what I do” were 16% more likely to have patients achieving an HbA1cbelow 7% (OR, 1.16; 95%CI 1.03-1.30; P= .01) than those providers who were neutral about the statement.
“To the best of our knowledge, no previous research has linked what clinicians identify as patient and care setting barriers to the documented glycemic control of their patients,” they wrote (BMJ Open Diab. Res. Care 2015 Feb. 24).
The survey highlighted psychosocial issues, resistance to lifestyle change, and noncompliance as the most common patient-related barriers to achieving optimal control.
On the question of what factors might delay pharmacologic intensification, providers singled out patients’ resistance to lifestyle change and noncompliance as two factors that came into play at least 25% of the time, while unwillingness to consider insulin and psychosocial issues also played a key role.
Side effects, cost, cultural issues, and a lack of established patient-provider relationship played relatively minor roles in influencing pharmacologic intensification.
“These data suggest that patient and system barriers play a larger role than clinician beliefs and behaviors in prolonged poor control and delayed treatment intensification,” Dr. LeBlanc and her associates wrote.
“HbA1clevels were consistent across patients despite differences in their providers’ treatment behaviors, HbA1c goals, and diabetic treatment opinions,” they said.
The survey also revealed that 80% of primary care providers gave patients who were above their glycemic goals 3-6 months to work on lifestyle changes before resorting to pharmacologic therapy, while a similar percentage agreed that older patients needed less-stringent glycemic goals.
The majority also agreed that weight loss was a key component of diabetes care, but only 40% agreed that the impact of a diabetes medication on weight influenced their therapy decisions.
“Taken together, it seems that intervention to reduce barriers to glycemic control directed at providers would not produce much benefit, and that addressing these barriers may be most fruitful at the health system level,” the authors suggested.
The authors acknowledged that the survey was limited by a lack of variation in provider attitudes – possibly the result of conducting it within a single organization – as well as being of an insured population restricted to a range of treatments that did not include newer medications.
“This could affect the relative importance of cost issues in prescribing and intensification practices, and may also constrain our ability to assess the value of more therapeutic options,” they wrote.
The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.
Primary care providers’ beliefs about diabetic treatment and glycated hemoglobin goals have a relatively small impact on patients achieving their diabetes treatment goals, researchers said.
A study linking the survey responses from 149 primary care providers to the health records of their 18,346 patients with diabetes showed that only two survey responses bore any significant relationship to patients’ glycemic control.
The 21% of responders who agreed with the statement that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement (odds ratio, 0.87; 95% confidence interval, 0.78-0.97; P = .02), according to Dr. Erin S. LeBlanc of the Kaiser Permanente Center for Health Research in Portland, Ore., and her coauthors.
Similarly, the 21% of providers who disagreed with the statement that “some patients will have an HbA1c greater than 9% no matter what I do” were 16% more likely to have patients achieving an HbA1cbelow 7% (OR, 1.16; 95%CI 1.03-1.30; P= .01) than those providers who were neutral about the statement.
“To the best of our knowledge, no previous research has linked what clinicians identify as patient and care setting barriers to the documented glycemic control of their patients,” they wrote (BMJ Open Diab. Res. Care 2015 Feb. 24).
The survey highlighted psychosocial issues, resistance to lifestyle change, and noncompliance as the most common patient-related barriers to achieving optimal control.
On the question of what factors might delay pharmacologic intensification, providers singled out patients’ resistance to lifestyle change and noncompliance as two factors that came into play at least 25% of the time, while unwillingness to consider insulin and psychosocial issues also played a key role.
Side effects, cost, cultural issues, and a lack of established patient-provider relationship played relatively minor roles in influencing pharmacologic intensification.
“These data suggest that patient and system barriers play a larger role than clinician beliefs and behaviors in prolonged poor control and delayed treatment intensification,” Dr. LeBlanc and her associates wrote.
“HbA1clevels were consistent across patients despite differences in their providers’ treatment behaviors, HbA1c goals, and diabetic treatment opinions,” they said.
The survey also revealed that 80% of primary care providers gave patients who were above their glycemic goals 3-6 months to work on lifestyle changes before resorting to pharmacologic therapy, while a similar percentage agreed that older patients needed less-stringent glycemic goals.
The majority also agreed that weight loss was a key component of diabetes care, but only 40% agreed that the impact of a diabetes medication on weight influenced their therapy decisions.
“Taken together, it seems that intervention to reduce barriers to glycemic control directed at providers would not produce much benefit, and that addressing these barriers may be most fruitful at the health system level,” the authors suggested.
The authors acknowledged that the survey was limited by a lack of variation in provider attitudes – possibly the result of conducting it within a single organization – as well as being of an insured population restricted to a range of treatments that did not include newer medications.
“This could affect the relative importance of cost issues in prescribing and intensification practices, and may also constrain our ability to assess the value of more therapeutic options,” they wrote.
The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.
FROM BMJ OPEN DIABETES RESEARCH AND CARE
Key clinical point: Primary care providers’ beliefs about diabetes treatment have a relatively small impact on patients achieving treatment goals.
Major finding: Responders who agreed that “current research did not support HbA1c levels below 7%” were 13% less likely to have patients with HbA1c levels below 7%, compared with responders who were neutral about that statement.
Data source: Survey of 149 health care providers and their 18,346 patients with diabetes.
Disclosures: The study was funded by AstraZeneca and Bristol-Myers Squibb. Two authors declared additional research funding from other pharmaceutical companies, while two authors were employees of Bristol-Myers Squibb.