User login
Damian McNamara is a journalist for Medscape Medical News and MDedge. He worked full-time for MDedge as the Miami Bureau covering a dozen medical specialties during 2001-2012, then as a freelancer for Medscape and MDedge, before being hired on staff by Medscape in 2018. Now the two companies are one. He uses what he learned in school – Damian has a BS in chemistry and an MS in science, health and environmental reporting/journalism. He works out of a home office in Miami, with a 100-pound chocolate lab known to snore under his desk during work hours.
Suicide Prevention Tool Geared to Primary Care
ORLANDO — A new Web-based toolkit provides guidance and information for primary care physicians in the screening, management, and referral of patients at risk of suicide.
The overall aim of using the kit is to optimize interactions between physicians and at-risk patients. It includes advice on when and how to question patients about their risks, how to refer them to mental health specialists, and how to find community resources. It also emphasizes the importance of training all practice staff to recognize the relevant signs and risk factors for suicide.
“Our data tell us that primary care is an important setting” for the early detection of suicide risk, said David A. Litts, O.D., associate director of the Suicide Prevention Resource Center (SPRC), at the Education Development Center, Newton, Mass., and one of the developers of the kit.
“Why primary care?” asked session moderator, Guy S. Diamond, Ph.D. “Because 70% of adolescents see a physician once a year for a well visit or school check-up—[that's] an opportunity to touch a lot of lives.”
In addition, most adolescents report a willingness to talk with a primary care physician about emotional distress, particularly with a physician they know well, said Dr. Diamond, who is on the psychiatry and behavioral science faculty at Children's Hospital of Pittsburgh.
Matthew B. Wintersteen, Ph.D., emphasized during another presentation that primary care is “the sole source of mental health treatment for most Americans.”
The Suicide Prevention Toolkit for Rural Primary Care includes a user-friendly starter guide and sections on educating the practice staff; developing partnerships with mental health providers; tools for managing patients; patient education tools; and resources.
Although its title includes the word “rural,” the kit is just as useful and easily applicable in the nonrural primary care setting, said Dr. Peggy West, a senior adviser at SPRC, who was also involved in developing the kit.
Dr. Litts stressed the importance of first developing an office protocol on suicide prevention. “Make sure you have [it] in place” before you implement the rest of the prevention protocol, he said.
The component on initiating collaborative partnerships with mental health service providers includes a template letter that can be easily modified depending on a patient's circumstances, as well as a mental health service locator and information about veterans' services and telemental health services, which is particularly important in remote rural areas.
Other components include universal screening for depression and substance abuse and instructions on safe storage of firearms for all patients, especially adolescents. A safety planning guide helps a physician decide whether patients can manage themselves and when they should call a physician for help.
Although there are considerable challenges in the primary care setting, such as time constraints, reimbursement issues, and knowing how to intervene when a patient endorses suicidal ideation, primary care physicians can make a difference, said Dr. Wintersteen, who is director of research, division of child and adolescent psychiatry, Thomas Jefferson University, Philadelphia.
“Be approachable, flexible, and persistent,” he advised.
Suicidal ideation screening in a busy primary care practice should be brief. “You want to keep it short,” said Dr. Litts. He recommended asking a question such as: “Mr. Jones, a lot of people who have had pain as long as you have sometimes think about killing themselves. Have you had any thoughts like that?”
“The bottom line with screening is: Ask and they will tell,” said Dr. Wintersteen, who recently published findings that demonstrate the effectiveness of screening adolescents for suicide risk in primary care (Pediatrics 2010;125:938-44).
The importance of state-specific information in the toolkit—such as state hospital locations, regional resources, and local hotline numbers—are lessons learned from early adopters of the toolkit, Dr. West said.
The SPRC is a federally funded entity that is managed through the Substance Abuse and Mental Health Services Administration. It supports suicide preventionwto advance the National Strategy for Suicide. Funding for the toolkit came from a grant from the Western Interstate Commission for Higher Education (WICHE) Center for Rural Mental Health Research.
The kit is available at www.sprc.org/pctoolkit/index.asp
ORLANDO — A new Web-based toolkit provides guidance and information for primary care physicians in the screening, management, and referral of patients at risk of suicide.
The overall aim of using the kit is to optimize interactions between physicians and at-risk patients. It includes advice on when and how to question patients about their risks, how to refer them to mental health specialists, and how to find community resources. It also emphasizes the importance of training all practice staff to recognize the relevant signs and risk factors for suicide.
“Our data tell us that primary care is an important setting” for the early detection of suicide risk, said David A. Litts, O.D., associate director of the Suicide Prevention Resource Center (SPRC), at the Education Development Center, Newton, Mass., and one of the developers of the kit.
“Why primary care?” asked session moderator, Guy S. Diamond, Ph.D. “Because 70% of adolescents see a physician once a year for a well visit or school check-up—[that's] an opportunity to touch a lot of lives.”
In addition, most adolescents report a willingness to talk with a primary care physician about emotional distress, particularly with a physician they know well, said Dr. Diamond, who is on the psychiatry and behavioral science faculty at Children's Hospital of Pittsburgh.
Matthew B. Wintersteen, Ph.D., emphasized during another presentation that primary care is “the sole source of mental health treatment for most Americans.”
The Suicide Prevention Toolkit for Rural Primary Care includes a user-friendly starter guide and sections on educating the practice staff; developing partnerships with mental health providers; tools for managing patients; patient education tools; and resources.
Although its title includes the word “rural,” the kit is just as useful and easily applicable in the nonrural primary care setting, said Dr. Peggy West, a senior adviser at SPRC, who was also involved in developing the kit.
Dr. Litts stressed the importance of first developing an office protocol on suicide prevention. “Make sure you have [it] in place” before you implement the rest of the prevention protocol, he said.
The component on initiating collaborative partnerships with mental health service providers includes a template letter that can be easily modified depending on a patient's circumstances, as well as a mental health service locator and information about veterans' services and telemental health services, which is particularly important in remote rural areas.
Other components include universal screening for depression and substance abuse and instructions on safe storage of firearms for all patients, especially adolescents. A safety planning guide helps a physician decide whether patients can manage themselves and when they should call a physician for help.
Although there are considerable challenges in the primary care setting, such as time constraints, reimbursement issues, and knowing how to intervene when a patient endorses suicidal ideation, primary care physicians can make a difference, said Dr. Wintersteen, who is director of research, division of child and adolescent psychiatry, Thomas Jefferson University, Philadelphia.
“Be approachable, flexible, and persistent,” he advised.
Suicidal ideation screening in a busy primary care practice should be brief. “You want to keep it short,” said Dr. Litts. He recommended asking a question such as: “Mr. Jones, a lot of people who have had pain as long as you have sometimes think about killing themselves. Have you had any thoughts like that?”
“The bottom line with screening is: Ask and they will tell,” said Dr. Wintersteen, who recently published findings that demonstrate the effectiveness of screening adolescents for suicide risk in primary care (Pediatrics 2010;125:938-44).
The importance of state-specific information in the toolkit—such as state hospital locations, regional resources, and local hotline numbers—are lessons learned from early adopters of the toolkit, Dr. West said.
The SPRC is a federally funded entity that is managed through the Substance Abuse and Mental Health Services Administration. It supports suicide preventionwto advance the National Strategy for Suicide. Funding for the toolkit came from a grant from the Western Interstate Commission for Higher Education (WICHE) Center for Rural Mental Health Research.
The kit is available at www.sprc.org/pctoolkit/index.asp
ORLANDO — A new Web-based toolkit provides guidance and information for primary care physicians in the screening, management, and referral of patients at risk of suicide.
The overall aim of using the kit is to optimize interactions between physicians and at-risk patients. It includes advice on when and how to question patients about their risks, how to refer them to mental health specialists, and how to find community resources. It also emphasizes the importance of training all practice staff to recognize the relevant signs and risk factors for suicide.
“Our data tell us that primary care is an important setting” for the early detection of suicide risk, said David A. Litts, O.D., associate director of the Suicide Prevention Resource Center (SPRC), at the Education Development Center, Newton, Mass., and one of the developers of the kit.
“Why primary care?” asked session moderator, Guy S. Diamond, Ph.D. “Because 70% of adolescents see a physician once a year for a well visit or school check-up—[that's] an opportunity to touch a lot of lives.”
In addition, most adolescents report a willingness to talk with a primary care physician about emotional distress, particularly with a physician they know well, said Dr. Diamond, who is on the psychiatry and behavioral science faculty at Children's Hospital of Pittsburgh.
Matthew B. Wintersteen, Ph.D., emphasized during another presentation that primary care is “the sole source of mental health treatment for most Americans.”
The Suicide Prevention Toolkit for Rural Primary Care includes a user-friendly starter guide and sections on educating the practice staff; developing partnerships with mental health providers; tools for managing patients; patient education tools; and resources.
Although its title includes the word “rural,” the kit is just as useful and easily applicable in the nonrural primary care setting, said Dr. Peggy West, a senior adviser at SPRC, who was also involved in developing the kit.
Dr. Litts stressed the importance of first developing an office protocol on suicide prevention. “Make sure you have [it] in place” before you implement the rest of the prevention protocol, he said.
The component on initiating collaborative partnerships with mental health service providers includes a template letter that can be easily modified depending on a patient's circumstances, as well as a mental health service locator and information about veterans' services and telemental health services, which is particularly important in remote rural areas.
Other components include universal screening for depression and substance abuse and instructions on safe storage of firearms for all patients, especially adolescents. A safety planning guide helps a physician decide whether patients can manage themselves and when they should call a physician for help.
Although there are considerable challenges in the primary care setting, such as time constraints, reimbursement issues, and knowing how to intervene when a patient endorses suicidal ideation, primary care physicians can make a difference, said Dr. Wintersteen, who is director of research, division of child and adolescent psychiatry, Thomas Jefferson University, Philadelphia.
“Be approachable, flexible, and persistent,” he advised.
Suicidal ideation screening in a busy primary care practice should be brief. “You want to keep it short,” said Dr. Litts. He recommended asking a question such as: “Mr. Jones, a lot of people who have had pain as long as you have sometimes think about killing themselves. Have you had any thoughts like that?”
“The bottom line with screening is: Ask and they will tell,” said Dr. Wintersteen, who recently published findings that demonstrate the effectiveness of screening adolescents for suicide risk in primary care (Pediatrics 2010;125:938-44).
The importance of state-specific information in the toolkit—such as state hospital locations, regional resources, and local hotline numbers—are lessons learned from early adopters of the toolkit, Dr. West said.
The SPRC is a federally funded entity that is managed through the Substance Abuse and Mental Health Services Administration. It supports suicide preventionwto advance the National Strategy for Suicide. Funding for the toolkit came from a grant from the Western Interstate Commission for Higher Education (WICHE) Center for Rural Mental Health Research.
The kit is available at www.sprc.org/pctoolkit/index.asp
Rate of HIV Likely to Rise in Older Adults
ORLANDO — Physicians will see more elderly people with HIV, because of both more new infections among the population and prolonged survival of people with HIV, according to a physician epidemiologist.
Physicians should be screening their senior patients for HIV risk. Ask about sexual activity and counsel them about prevention of sexually transmitted diseases, Dr. Kelly A. Gebo advised.
Older people, in general, have a lack of awareness about HIV risk factors, said Dr. Gebo, associate professor and director of undergraduate research studies at John Hopkins Bloomberg School of Public Health in Baltimore. A lack of HIV prevention targeted at seniors is partly to blame, she said.
As a result, seniors with HIV infection often are diagnosed late in the disease. “The average CD4 count is about 250 in our practice at time of diagnosis. We'd like to diagnose them earlier,” she said.
Many older people are newly single and believe that HIV affects only younger people—two additional challenges to HIV prevention in this population. Erectile dysfunction drugs that increase senior sexual activity may play a role, and some older women stop using condoms once the risk of pregnancy passes with menopause, Dr. Gebo noted.
“I ask everyone from 12 to 112 about alcohol, sexual history, and drug use,” she said, while acknowledging that some physicians aren't as comfortable as she asking seniors about these delicate issues.
In a subsequent presentation, Dr. Kevin P. High suggested how doctors could phrase a recommendation for HIV testing: “I don't believe this is likely, but I would not be doing my job in 2010 if I did not test you for HIV. It's a very treatable illness and we ought to test.” He added, “I've never had anyone say no.”
Almost 18% of HIV diagnoses in 2007 were made in people older than 50 years, according to the Centers for Disease Control and Prevention. This proportion is expected to grow, Dr. Gebo added.
Compared with younger people, elderly people with HIV get less immunologic boost from some treatments and have shorter survivals. In addition, seniors with HIV can experience an acceleration of the effects of normal aging, including greater bone loss, muscle mass decreases, and memory loss, Dr. Gebo said.
Inflammation could be at the root of seniors' HIV vulnerability. “We all know inflammation is bad in cardiovascular disease,” said Dr. High, professor of infectious diseases at Wake Forest University, Winston-Salem, N.C. Inflammation “is more present in HIV than in age-matched, HIV-negative adults. We think that is the reason for the disease acceleration in older patients with HIV,” he added.
On the plus side, older people are generally more compliant than younger people with their medication regimens. Adherence to prescriptions is particularly important to combat HIV infection because of an elevated risk for viral resistance, Dr. Gebo said.
Another plus, she added, is that older patients tend to experience better virologic suppression following treatment. In response to an audience question, she said that the improved suppression reported in this population was independent of their better medication compliance.
“Unfortunately, it is not all good news for these older patients,” Dr. Gebo said. Evidence suggests that the decrease in immune system strength that comes with normal aging can diminish the efficacy of antiretroviral agents.
Frailty is another factor working against older people with HIV, Dr. High pointed out. The risk for frailty is increased ninefold by HIV infection, he said. For example, only 1%-2% of 55-year-old HIV-negative men will meet the definition for frailty (J. Acquir. Immune Defic. Syndr. 2009;50:299-306). In contrast, 14% of men of the same age with an 8-year-old HIV diagnosis will meet the definition.
Disclosures: Dr. Gebo and Dr. High reported no financial conflicts of interest.
ORLANDO — Physicians will see more elderly people with HIV, because of both more new infections among the population and prolonged survival of people with HIV, according to a physician epidemiologist.
Physicians should be screening their senior patients for HIV risk. Ask about sexual activity and counsel them about prevention of sexually transmitted diseases, Dr. Kelly A. Gebo advised.
Older people, in general, have a lack of awareness about HIV risk factors, said Dr. Gebo, associate professor and director of undergraduate research studies at John Hopkins Bloomberg School of Public Health in Baltimore. A lack of HIV prevention targeted at seniors is partly to blame, she said.
As a result, seniors with HIV infection often are diagnosed late in the disease. “The average CD4 count is about 250 in our practice at time of diagnosis. We'd like to diagnose them earlier,” she said.
Many older people are newly single and believe that HIV affects only younger people—two additional challenges to HIV prevention in this population. Erectile dysfunction drugs that increase senior sexual activity may play a role, and some older women stop using condoms once the risk of pregnancy passes with menopause, Dr. Gebo noted.
“I ask everyone from 12 to 112 about alcohol, sexual history, and drug use,” she said, while acknowledging that some physicians aren't as comfortable as she asking seniors about these delicate issues.
In a subsequent presentation, Dr. Kevin P. High suggested how doctors could phrase a recommendation for HIV testing: “I don't believe this is likely, but I would not be doing my job in 2010 if I did not test you for HIV. It's a very treatable illness and we ought to test.” He added, “I've never had anyone say no.”
Almost 18% of HIV diagnoses in 2007 were made in people older than 50 years, according to the Centers for Disease Control and Prevention. This proportion is expected to grow, Dr. Gebo added.
Compared with younger people, elderly people with HIV get less immunologic boost from some treatments and have shorter survivals. In addition, seniors with HIV can experience an acceleration of the effects of normal aging, including greater bone loss, muscle mass decreases, and memory loss, Dr. Gebo said.
Inflammation could be at the root of seniors' HIV vulnerability. “We all know inflammation is bad in cardiovascular disease,” said Dr. High, professor of infectious diseases at Wake Forest University, Winston-Salem, N.C. Inflammation “is more present in HIV than in age-matched, HIV-negative adults. We think that is the reason for the disease acceleration in older patients with HIV,” he added.
On the plus side, older people are generally more compliant than younger people with their medication regimens. Adherence to prescriptions is particularly important to combat HIV infection because of an elevated risk for viral resistance, Dr. Gebo said.
Another plus, she added, is that older patients tend to experience better virologic suppression following treatment. In response to an audience question, she said that the improved suppression reported in this population was independent of their better medication compliance.
“Unfortunately, it is not all good news for these older patients,” Dr. Gebo said. Evidence suggests that the decrease in immune system strength that comes with normal aging can diminish the efficacy of antiretroviral agents.
Frailty is another factor working against older people with HIV, Dr. High pointed out. The risk for frailty is increased ninefold by HIV infection, he said. For example, only 1%-2% of 55-year-old HIV-negative men will meet the definition for frailty (J. Acquir. Immune Defic. Syndr. 2009;50:299-306). In contrast, 14% of men of the same age with an 8-year-old HIV diagnosis will meet the definition.
Disclosures: Dr. Gebo and Dr. High reported no financial conflicts of interest.
ORLANDO — Physicians will see more elderly people with HIV, because of both more new infections among the population and prolonged survival of people with HIV, according to a physician epidemiologist.
Physicians should be screening their senior patients for HIV risk. Ask about sexual activity and counsel them about prevention of sexually transmitted diseases, Dr. Kelly A. Gebo advised.
Older people, in general, have a lack of awareness about HIV risk factors, said Dr. Gebo, associate professor and director of undergraduate research studies at John Hopkins Bloomberg School of Public Health in Baltimore. A lack of HIV prevention targeted at seniors is partly to blame, she said.
As a result, seniors with HIV infection often are diagnosed late in the disease. “The average CD4 count is about 250 in our practice at time of diagnosis. We'd like to diagnose them earlier,” she said.
Many older people are newly single and believe that HIV affects only younger people—two additional challenges to HIV prevention in this population. Erectile dysfunction drugs that increase senior sexual activity may play a role, and some older women stop using condoms once the risk of pregnancy passes with menopause, Dr. Gebo noted.
“I ask everyone from 12 to 112 about alcohol, sexual history, and drug use,” she said, while acknowledging that some physicians aren't as comfortable as she asking seniors about these delicate issues.
In a subsequent presentation, Dr. Kevin P. High suggested how doctors could phrase a recommendation for HIV testing: “I don't believe this is likely, but I would not be doing my job in 2010 if I did not test you for HIV. It's a very treatable illness and we ought to test.” He added, “I've never had anyone say no.”
Almost 18% of HIV diagnoses in 2007 were made in people older than 50 years, according to the Centers for Disease Control and Prevention. This proportion is expected to grow, Dr. Gebo added.
Compared with younger people, elderly people with HIV get less immunologic boost from some treatments and have shorter survivals. In addition, seniors with HIV can experience an acceleration of the effects of normal aging, including greater bone loss, muscle mass decreases, and memory loss, Dr. Gebo said.
Inflammation could be at the root of seniors' HIV vulnerability. “We all know inflammation is bad in cardiovascular disease,” said Dr. High, professor of infectious diseases at Wake Forest University, Winston-Salem, N.C. Inflammation “is more present in HIV than in age-matched, HIV-negative adults. We think that is the reason for the disease acceleration in older patients with HIV,” he added.
On the plus side, older people are generally more compliant than younger people with their medication regimens. Adherence to prescriptions is particularly important to combat HIV infection because of an elevated risk for viral resistance, Dr. Gebo said.
Another plus, she added, is that older patients tend to experience better virologic suppression following treatment. In response to an audience question, she said that the improved suppression reported in this population was independent of their better medication compliance.
“Unfortunately, it is not all good news for these older patients,” Dr. Gebo said. Evidence suggests that the decrease in immune system strength that comes with normal aging can diminish the efficacy of antiretroviral agents.
Frailty is another factor working against older people with HIV, Dr. High pointed out. The risk for frailty is increased ninefold by HIV infection, he said. For example, only 1%-2% of 55-year-old HIV-negative men will meet the definition for frailty (J. Acquir. Immune Defic. Syndr. 2009;50:299-306). In contrast, 14% of men of the same age with an 8-year-old HIV diagnosis will meet the definition.
Disclosures: Dr. Gebo and Dr. High reported no financial conflicts of interest.
Cultural Competence Key to Treating Skin of Color
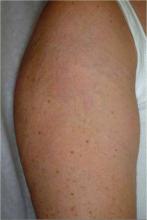
NAPLES, Fla. — Vitiligo, keloids, acne keloidalis nuchae, and hair and scalp concerns are among the challenges dermatologists face when treating darker skin, Dr. George Cohen said.
Black skin is prone to adverse pigmentary or hyperproliferative responses to cryotherapy, lasers, and chemical skin treatments. Because of these and other concerns in a growing population of patients with skin types IV through VI, Dr. Cohen suggested dermatologists learn more about recognition and treatment of these important differences.
"We are a more diverse society. Become culturally competent and learn as much as you can," Dr. Cohen said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons. Respect, inquire, and do not make assumptions—those are the three pillars of cultural competence, he said.
Cultural competence is not only good for patients; it can be good for your practice as well. "Access and acceptance are good for us—this creates more demand for services," said Dr. Cohen, of the department of dermatology and cutaneous surgery at the University of South Florida in Tampa.
Vitiligo
Vitiligo is the prototypic pigmentary challenge for patients with skin of color, Dr. Cohen said. Although the etiology is not completely understood, it may be related to the immune system. The challenge for dermatologists is that "some people respond to some things some of the time, so we don't always know who is going to respond," Dr. Cohen said.
The myriad of treatments available for vitiligo include:
- Narrow-band UVB therapy.
- Targeted laser treatment with the XeCL Excimer (308 nm).
- Topical steroids.
- Calcineurin inhibitors.
- Surgery.
- Depigmentation (using medications or 694-nm Q-switched Ruby laser).
- Makeup.
Unfortunately, "none of these work perfectly," he said.
He cited the case of a patient with vitiligo who tried steroids, psoralen and UVA (PUVA), and other treatments to no avail. "He was desperate. He came to me with his family and asked: 'Doctor, can you make me one color?' I told him we can only make him one color—white—that is all we are able to do.
"Sometimes you cannot repigment the patient, and you have to know how to judiciously offer depigmentation. Some might say I robbed him of his culture. I say, no, I didn't, I robbed him of a disfiguring condition," said Dr. Cohen.
More research is clearly warranted to improve treatment options for vitiligo, such as studies to assess the biology of melanocytes, he said.
Keloids
Keloids are another challenge in skin of color patients. The therapeutic approach depends in part on the extent of the patient's condition. For example, a single keloid on the earlobe would be treated differently than more widespread presentation.
Again, more research is warranted on optimal treatments, Dr. Cohen said, because studies in the literature are contradictory and provide no consensus.
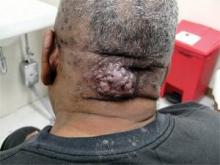
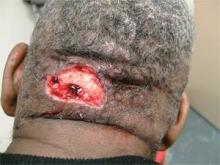
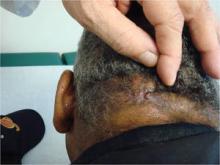
Acne keloidalis nuchae, "the keloids' cousin," most often occur in black men, he said. These nuchae can advance to plaque and form tumors, "and at the very least will need intralesional therapy." One clinical tip is to make an incision only within the keloid, he said.
If a patient presents with an acne keloidalis tumor, simply excise it. Once you get hemostasis, dress the wound with petroleum jelly only, and let it close by the magic of second intention
"I monitor these people. If I see any evidence of regrowth, I treat with triamcinolone early and often," he said.
Hair and Scalp Challenges
Hair and scalp concerns are common in patients with skin of color, Dr. Cohen said. A scalp biopsy is recommended to determine or confirm a diagnosis and to guide the course of clinical treatment.
These presentations can have a great psychosocial impact. "Do not underestimate the effect on patients," he said. Know your limitations and the limitations of therapy, and make sure you communicate those effectively to the patient. Otherwise, both the patient and provider can become frustrated.
Be honest with genetically-susceptible patients who present with scarring on the scalp from physical insult. In this population, scarring results when fibrous tissue replaces hair follicles. "Let them know up front that creams and other nonsense are not going to work," he said.
Contrary to popular belief, Dr. Cohen said, hair transplants are an option in patients with skin of color. "Hair transplants in black patients are not scary— I've been doing them for years and never had keloids," he said.
Black hair is heterogenous, so not everyone has curved follicles. If a skin of color patient has straight follicles, standard hair transplant procedures—for example, with 4-mm donor grafts—would be an option.
Dr. Cohen said that he did not have any relevant financial disclosures.
NAPLES, Fla. — Vitiligo, keloids, acne keloidalis nuchae, and hair and scalp concerns are among the challenges dermatologists face when treating darker skin, Dr. George Cohen said.
Black skin is prone to adverse pigmentary or hyperproliferative responses to cryotherapy, lasers, and chemical skin treatments. Because of these and other concerns in a growing population of patients with skin types IV through VI, Dr. Cohen suggested dermatologists learn more about recognition and treatment of these important differences.
"We are a more diverse society. Become culturally competent and learn as much as you can," Dr. Cohen said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons. Respect, inquire, and do not make assumptions—those are the three pillars of cultural competence, he said.
Cultural competence is not only good for patients; it can be good for your practice as well. "Access and acceptance are good for us—this creates more demand for services," said Dr. Cohen, of the department of dermatology and cutaneous surgery at the University of South Florida in Tampa.
Vitiligo
Vitiligo is the prototypic pigmentary challenge for patients with skin of color, Dr. Cohen said. Although the etiology is not completely understood, it may be related to the immune system. The challenge for dermatologists is that "some people respond to some things some of the time, so we don't always know who is going to respond," Dr. Cohen said.
The myriad of treatments available for vitiligo include:
- Narrow-band UVB therapy.
- Targeted laser treatment with the XeCL Excimer (308 nm).
- Topical steroids.
- Calcineurin inhibitors.
- Surgery.
- Depigmentation (using medications or 694-nm Q-switched Ruby laser).
- Makeup.
Unfortunately, "none of these work perfectly," he said.
He cited the case of a patient with vitiligo who tried steroids, psoralen and UVA (PUVA), and other treatments to no avail. "He was desperate. He came to me with his family and asked: 'Doctor, can you make me one color?' I told him we can only make him one color—white—that is all we are able to do.
"Sometimes you cannot repigment the patient, and you have to know how to judiciously offer depigmentation. Some might say I robbed him of his culture. I say, no, I didn't, I robbed him of a disfiguring condition," said Dr. Cohen.
More research is clearly warranted to improve treatment options for vitiligo, such as studies to assess the biology of melanocytes, he said.
Keloids
Keloids are another challenge in skin of color patients. The therapeutic approach depends in part on the extent of the patient's condition. For example, a single keloid on the earlobe would be treated differently than more widespread presentation.
Again, more research is warranted on optimal treatments, Dr. Cohen said, because studies in the literature are contradictory and provide no consensus.
Acne keloidalis nuchae, "the keloids' cousin," most often occur in black men, he said. These nuchae can advance to plaque and form tumors, "and at the very least will need intralesional therapy." One clinical tip is to make an incision only within the keloid, he said.
If a patient presents with an acne keloidalis tumor, simply excise it. Once you get hemostasis, dress the wound with petroleum jelly only, and let it close by the magic of second intention
"I monitor these people. If I see any evidence of regrowth, I treat with triamcinolone early and often," he said.
Hair and Scalp Challenges
Hair and scalp concerns are common in patients with skin of color, Dr. Cohen said. A scalp biopsy is recommended to determine or confirm a diagnosis and to guide the course of clinical treatment.
These presentations can have a great psychosocial impact. "Do not underestimate the effect on patients," he said. Know your limitations and the limitations of therapy, and make sure you communicate those effectively to the patient. Otherwise, both the patient and provider can become frustrated.
Be honest with genetically-susceptible patients who present with scarring on the scalp from physical insult. In this population, scarring results when fibrous tissue replaces hair follicles. "Let them know up front that creams and other nonsense are not going to work," he said.
Contrary to popular belief, Dr. Cohen said, hair transplants are an option in patients with skin of color. "Hair transplants in black patients are not scary— I've been doing them for years and never had keloids," he said.
Black hair is heterogenous, so not everyone has curved follicles. If a skin of color patient has straight follicles, standard hair transplant procedures—for example, with 4-mm donor grafts—would be an option.
Dr. Cohen said that he did not have any relevant financial disclosures.
NAPLES, Fla. — Vitiligo, keloids, acne keloidalis nuchae, and hair and scalp concerns are among the challenges dermatologists face when treating darker skin, Dr. George Cohen said.
Black skin is prone to adverse pigmentary or hyperproliferative responses to cryotherapy, lasers, and chemical skin treatments. Because of these and other concerns in a growing population of patients with skin types IV through VI, Dr. Cohen suggested dermatologists learn more about recognition and treatment of these important differences.
"We are a more diverse society. Become culturally competent and learn as much as you can," Dr. Cohen said at the annual meeting of the Florida Society of Dermatology & Dermatologic Surgeons. Respect, inquire, and do not make assumptions—those are the three pillars of cultural competence, he said.
Cultural competence is not only good for patients; it can be good for your practice as well. "Access and acceptance are good for us—this creates more demand for services," said Dr. Cohen, of the department of dermatology and cutaneous surgery at the University of South Florida in Tampa.
Vitiligo
Vitiligo is the prototypic pigmentary challenge for patients with skin of color, Dr. Cohen said. Although the etiology is not completely understood, it may be related to the immune system. The challenge for dermatologists is that "some people respond to some things some of the time, so we don't always know who is going to respond," Dr. Cohen said.
The myriad of treatments available for vitiligo include:
- Narrow-band UVB therapy.
- Targeted laser treatment with the XeCL Excimer (308 nm).
- Topical steroids.
- Calcineurin inhibitors.
- Surgery.
- Depigmentation (using medications or 694-nm Q-switched Ruby laser).
- Makeup.
Unfortunately, "none of these work perfectly," he said.
He cited the case of a patient with vitiligo who tried steroids, psoralen and UVA (PUVA), and other treatments to no avail. "He was desperate. He came to me with his family and asked: 'Doctor, can you make me one color?' I told him we can only make him one color—white—that is all we are able to do.
"Sometimes you cannot repigment the patient, and you have to know how to judiciously offer depigmentation. Some might say I robbed him of his culture. I say, no, I didn't, I robbed him of a disfiguring condition," said Dr. Cohen.
More research is clearly warranted to improve treatment options for vitiligo, such as studies to assess the biology of melanocytes, he said.
Keloids
Keloids are another challenge in skin of color patients. The therapeutic approach depends in part on the extent of the patient's condition. For example, a single keloid on the earlobe would be treated differently than more widespread presentation.
Again, more research is warranted on optimal treatments, Dr. Cohen said, because studies in the literature are contradictory and provide no consensus.
Acne keloidalis nuchae, "the keloids' cousin," most often occur in black men, he said. These nuchae can advance to plaque and form tumors, "and at the very least will need intralesional therapy." One clinical tip is to make an incision only within the keloid, he said.
If a patient presents with an acne keloidalis tumor, simply excise it. Once you get hemostasis, dress the wound with petroleum jelly only, and let it close by the magic of second intention
"I monitor these people. If I see any evidence of regrowth, I treat with triamcinolone early and often," he said.
Hair and Scalp Challenges
Hair and scalp concerns are common in patients with skin of color, Dr. Cohen said. A scalp biopsy is recommended to determine or confirm a diagnosis and to guide the course of clinical treatment.
These presentations can have a great psychosocial impact. "Do not underestimate the effect on patients," he said. Know your limitations and the limitations of therapy, and make sure you communicate those effectively to the patient. Otherwise, both the patient and provider can become frustrated.
Be honest with genetically-susceptible patients who present with scarring on the scalp from physical insult. In this population, scarring results when fibrous tissue replaces hair follicles. "Let them know up front that creams and other nonsense are not going to work," he said.
Contrary to popular belief, Dr. Cohen said, hair transplants are an option in patients with skin of color. "Hair transplants in black patients are not scary— I've been doing them for years and never had keloids," he said.
Black hair is heterogenous, so not everyone has curved follicles. If a skin of color patient has straight follicles, standard hair transplant procedures—for example, with 4-mm donor grafts—would be an option.
Dr. Cohen said that he did not have any relevant financial disclosures.
Evidence Backs Imiquimod Tx for Melanoma in Situ
MIAMI — The topical immune response modulator imiquimod has a role in the treatment of melanoma in situ, particularly if patients refuse or fail surgery.
There are several concerns. The agent is only recommended for thinner lesions, and "failures do occur," said Dr. M. Shane Chapman of Darmouth-Hitchcock Medical Center in Lebanon, N.H. Also, "the 5-year follow-up data is not great—it's sparse. We are just not there yet."
Despite this, he said, imiquimod 5% cream (Aldara, Graceway) can have a role in the management of melanoma in situ, also known as lentigo maligna. Dr. Chapman acknowledged the controversial nature of his stance, and based his position on small case series, one "good prospective study" in the literature, and his own experience with more than 60 patients.
As an example, he discussed a 36-year-old man with metastatic melanoma. The patient had multiple surgeries and radiation therapy "and nothing seemed to work," he said. "I basically bathed him in imiquimod over several months." Six years later, the patient is doing well with no signs of nodal or metastatic disease. As with all melanoma patients, regardless of the therapy, they should be followed continuously for a lifetime, he said at the annual meeting of the American Academy of Dermatology.
In his regimen, imiquimod 5% cream is applied five times per week for 12 weeks, with a rest period on weekends. Inflammation can be intense with this aggressive protocol, so it is important to educate patients beforehand. Pretreatment with retinoids—such as tazarotene (Tazarac, Allergan) for 2 weeks—can increase the effectiveness of imiquimod in this setting, he added.
"The only good prospective study to date," Dr. Chapman said, is an open-label trial in which participants received daily treatment with topical 5% imiquimod for 3 months, followed by a biopsy 1 month post therapy (Br. J. Dermatol. 2003;149:66-70). The complete response rate was 93% in 28 patients with histologically confirmed lentigo maligna. Two patients were treatment failures.
Because of potential failures, "always go back and do a biopsy after clearance," he said.
For example, in a retrospective study of 40 patients pretreated with imiquimod (Dermatol. Surg. 2008;34:147-51), 30 appeared clinically clear after staged excision "but three of these had histologic evidence of disease—that is why I always do a follow-up biopsy."
One of his own patients failed after initial clearance of his lesion, Dr. Chapman said. The man had a large scalp lesion that cleared following use of topical imiquimod without retinoid treatment. "For 8 months, we thought he was cleared. He came back and had a node in middle of the lesion site—his third recurrence over 5 years." Dr. Chapman added, "He's doing well, but failures do occur."
It is important to realize that "we think we know when something is in situ, but we don't always know the entire lesion is in situ when we do this," Dr. Chapman said.
Even though surgical excision remains the first-line choice for most patients with melanoma in situ or thin melanoma lesions, surgery nonresponders or those who refuse resection can benefit from imiquimod. He cited three examples: a woman who did not want to have repeat surgery and whose lesion cleared with imiquimod; a man who did not want further surgery following two melanoma lesion excisions close together on his temple, who was treated well with imiquimod; and a patient with recurrent melanoma in situ at the forehead flap of the nose who is doing well 4 years out after imiquimod treatment.
In response to a question from the audience, Dr. Chapman said, "I don't think just any inflammatory response is going to make melanoma go away. Imiquimod is one of those serendipitous chemicals that is useful for a lot of skin tumors for some reason."
Dr. Chapman is a consultant for, and receives honoraria from, Graceway. He also receives honoraria from Abbott.
MIAMI — The topical immune response modulator imiquimod has a role in the treatment of melanoma in situ, particularly if patients refuse or fail surgery.
There are several concerns. The agent is only recommended for thinner lesions, and "failures do occur," said Dr. M. Shane Chapman of Darmouth-Hitchcock Medical Center in Lebanon, N.H. Also, "the 5-year follow-up data is not great—it's sparse. We are just not there yet."
Despite this, he said, imiquimod 5% cream (Aldara, Graceway) can have a role in the management of melanoma in situ, also known as lentigo maligna. Dr. Chapman acknowledged the controversial nature of his stance, and based his position on small case series, one "good prospective study" in the literature, and his own experience with more than 60 patients.
As an example, he discussed a 36-year-old man with metastatic melanoma. The patient had multiple surgeries and radiation therapy "and nothing seemed to work," he said. "I basically bathed him in imiquimod over several months." Six years later, the patient is doing well with no signs of nodal or metastatic disease. As with all melanoma patients, regardless of the therapy, they should be followed continuously for a lifetime, he said at the annual meeting of the American Academy of Dermatology.
In his regimen, imiquimod 5% cream is applied five times per week for 12 weeks, with a rest period on weekends. Inflammation can be intense with this aggressive protocol, so it is important to educate patients beforehand. Pretreatment with retinoids—such as tazarotene (Tazarac, Allergan) for 2 weeks—can increase the effectiveness of imiquimod in this setting, he added.
"The only good prospective study to date," Dr. Chapman said, is an open-label trial in which participants received daily treatment with topical 5% imiquimod for 3 months, followed by a biopsy 1 month post therapy (Br. J. Dermatol. 2003;149:66-70). The complete response rate was 93% in 28 patients with histologically confirmed lentigo maligna. Two patients were treatment failures.
Because of potential failures, "always go back and do a biopsy after clearance," he said.
For example, in a retrospective study of 40 patients pretreated with imiquimod (Dermatol. Surg. 2008;34:147-51), 30 appeared clinically clear after staged excision "but three of these had histologic evidence of disease—that is why I always do a follow-up biopsy."
One of his own patients failed after initial clearance of his lesion, Dr. Chapman said. The man had a large scalp lesion that cleared following use of topical imiquimod without retinoid treatment. "For 8 months, we thought he was cleared. He came back and had a node in middle of the lesion site—his third recurrence over 5 years." Dr. Chapman added, "He's doing well, but failures do occur."
It is important to realize that "we think we know when something is in situ, but we don't always know the entire lesion is in situ when we do this," Dr. Chapman said.
Even though surgical excision remains the first-line choice for most patients with melanoma in situ or thin melanoma lesions, surgery nonresponders or those who refuse resection can benefit from imiquimod. He cited three examples: a woman who did not want to have repeat surgery and whose lesion cleared with imiquimod; a man who did not want further surgery following two melanoma lesion excisions close together on his temple, who was treated well with imiquimod; and a patient with recurrent melanoma in situ at the forehead flap of the nose who is doing well 4 years out after imiquimod treatment.
In response to a question from the audience, Dr. Chapman said, "I don't think just any inflammatory response is going to make melanoma go away. Imiquimod is one of those serendipitous chemicals that is useful for a lot of skin tumors for some reason."
Dr. Chapman is a consultant for, and receives honoraria from, Graceway. He also receives honoraria from Abbott.
MIAMI — The topical immune response modulator imiquimod has a role in the treatment of melanoma in situ, particularly if patients refuse or fail surgery.
There are several concerns. The agent is only recommended for thinner lesions, and "failures do occur," said Dr. M. Shane Chapman of Darmouth-Hitchcock Medical Center in Lebanon, N.H. Also, "the 5-year follow-up data is not great—it's sparse. We are just not there yet."
Despite this, he said, imiquimod 5% cream (Aldara, Graceway) can have a role in the management of melanoma in situ, also known as lentigo maligna. Dr. Chapman acknowledged the controversial nature of his stance, and based his position on small case series, one "good prospective study" in the literature, and his own experience with more than 60 patients.
As an example, he discussed a 36-year-old man with metastatic melanoma. The patient had multiple surgeries and radiation therapy "and nothing seemed to work," he said. "I basically bathed him in imiquimod over several months." Six years later, the patient is doing well with no signs of nodal or metastatic disease. As with all melanoma patients, regardless of the therapy, they should be followed continuously for a lifetime, he said at the annual meeting of the American Academy of Dermatology.
In his regimen, imiquimod 5% cream is applied five times per week for 12 weeks, with a rest period on weekends. Inflammation can be intense with this aggressive protocol, so it is important to educate patients beforehand. Pretreatment with retinoids—such as tazarotene (Tazarac, Allergan) for 2 weeks—can increase the effectiveness of imiquimod in this setting, he added.
"The only good prospective study to date," Dr. Chapman said, is an open-label trial in which participants received daily treatment with topical 5% imiquimod for 3 months, followed by a biopsy 1 month post therapy (Br. J. Dermatol. 2003;149:66-70). The complete response rate was 93% in 28 patients with histologically confirmed lentigo maligna. Two patients were treatment failures.
Because of potential failures, "always go back and do a biopsy after clearance," he said.
For example, in a retrospective study of 40 patients pretreated with imiquimod (Dermatol. Surg. 2008;34:147-51), 30 appeared clinically clear after staged excision "but three of these had histologic evidence of disease—that is why I always do a follow-up biopsy."
One of his own patients failed after initial clearance of his lesion, Dr. Chapman said. The man had a large scalp lesion that cleared following use of topical imiquimod without retinoid treatment. "For 8 months, we thought he was cleared. He came back and had a node in middle of the lesion site—his third recurrence over 5 years." Dr. Chapman added, "He's doing well, but failures do occur."
It is important to realize that "we think we know when something is in situ, but we don't always know the entire lesion is in situ when we do this," Dr. Chapman said.
Even though surgical excision remains the first-line choice for most patients with melanoma in situ or thin melanoma lesions, surgery nonresponders or those who refuse resection can benefit from imiquimod. He cited three examples: a woman who did not want to have repeat surgery and whose lesion cleared with imiquimod; a man who did not want further surgery following two melanoma lesion excisions close together on his temple, who was treated well with imiquimod; and a patient with recurrent melanoma in situ at the forehead flap of the nose who is doing well 4 years out after imiquimod treatment.
In response to a question from the audience, Dr. Chapman said, "I don't think just any inflammatory response is going to make melanoma go away. Imiquimod is one of those serendipitous chemicals that is useful for a lot of skin tumors for some reason."
Dr. Chapman is a consultant for, and receives honoraria from, Graceway. He also receives honoraria from Abbott.
Expertise Is Essential for Effective Laser Tattoo Removal
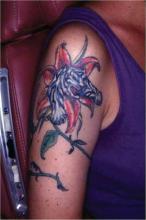
NAPLES, Fla. — Patients present with different reasons for tattoo removal—such as regret following a crazy night or a change in relationship status. The number of options for laser tattoo removal, however, is more limited, Dr. Albert J. Nemeth said.
Specific Q-switched Nd:YAG laser wavelengths are good at shattering tattoo ink but must be applied specific to the ink color. Also, do not use non-Q-switched Nd:YAG lasers or other lasers designed for different dermatologic indications, Dr. Nemeth said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
In general, 95% of amateur tattoos take one to three laser treatment sessions for removal. In contrast, six or more sessions are often required to remove most professional tattoos. Variables include the depth at which pigment was placed and type of ink. "Tattoo depth can vary. That is important to conceptualize when treating these tattoos," Dr. Nemeth said.
Tattoos applied by a friend or family member and those inked professionally share a common challenge for dermatologists—a lack of regulation on what can be used for pigment. "It's really quite interesting in terms of the secret concoctions that I've heard … cigarette ash; for some reason Crest toothpaste seems to be a magic ingredient; and—I don't understand why—but urine seems to be important in there also," Dr. Nemeth said in an interview.
|
An important caveat: If the patient reports or displays any symptoms of allergic dermatitis to the ink (constant oozing or crusting), lasers can worsen those symptoms. Physical removal of the tattoo is the only option for these patients, said Dr. Nemeth, a private-practice dermatologist in Clearwater, Fla., and FSDDS president. Dermabrasion, for example, is an option "if you are extraordinarily proficient at that."
An estimated 14% of all adults in the United States have at least one tattoo, according to a Harris Poll by Harris Interactive in 2008. A predominance of tattooing among a younger segment of the population means dermatologists are likely to see more and more patients with tattoos.
Removal of tattoos via laser can be life changing and/or life saving for some patients. For example, former gang members might feel safer after removal of an identifying tattoo, said Dr. Nemeth, also of the department of dermatology and cutaneous surgery at the University of South Florida, Tampa.
For removal of green tattoo inks, Dr. Nemeth uses a 694-nm Q-switched ruby or 755-nm Q-switched alexandrite laser. To shatter black, blue, sky blue, or darker inks, he employs a 1064-nm Q switched Nd:YAG laser. If a patient's tattoo features red, orange, or purple inks, these can be effectively treated with a 532-nm Q-switched Nd:YAG laser, he said. Also be aware that laser therapy can darken tattoo inks if they contain iron oxide or titanium oxide.
Avoid the temptation to use lasers for other indications. "An EpiTouch ruby laser made for hair removal should not be used for tattoo removal," Dr. Nemeth said. "This is an important take-home message: Just because the wavelength is close, it does not mean the indications are the same."
Also, intense pulsed light systems are not appropriate for this indication, Dr. Nemeth said. "If your salesperson told you IPL can be used to remove tattoos, [he] lied to you. IPL cannot be used to remove a tattoo, in my humble opinion."
The Q-switched lasers have afforded patients a much better aesthetic outcome following tattoo removal. "It used to be every patient knew they were switching their tattoo for a scar, "Dr. Nemeth said. "Now you can get some very, very nice results."
Dr. Nemeth had no relevant financial disclosures.
NAPLES, Fla. — Patients present with different reasons for tattoo removal—such as regret following a crazy night or a change in relationship status. The number of options for laser tattoo removal, however, is more limited, Dr. Albert J. Nemeth said.
Specific Q-switched Nd:YAG laser wavelengths are good at shattering tattoo ink but must be applied specific to the ink color. Also, do not use non-Q-switched Nd:YAG lasers or other lasers designed for different dermatologic indications, Dr. Nemeth said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
In general, 95% of amateur tattoos take one to three laser treatment sessions for removal. In contrast, six or more sessions are often required to remove most professional tattoos. Variables include the depth at which pigment was placed and type of ink. "Tattoo depth can vary. That is important to conceptualize when treating these tattoos," Dr. Nemeth said.
Tattoos applied by a friend or family member and those inked professionally share a common challenge for dermatologists—a lack of regulation on what can be used for pigment. "It's really quite interesting in terms of the secret concoctions that I've heard … cigarette ash; for some reason Crest toothpaste seems to be a magic ingredient; and—I don't understand why—but urine seems to be important in there also," Dr. Nemeth said in an interview.
|
An important caveat: If the patient reports or displays any symptoms of allergic dermatitis to the ink (constant oozing or crusting), lasers can worsen those symptoms. Physical removal of the tattoo is the only option for these patients, said Dr. Nemeth, a private-practice dermatologist in Clearwater, Fla., and FSDDS president. Dermabrasion, for example, is an option "if you are extraordinarily proficient at that."
An estimated 14% of all adults in the United States have at least one tattoo, according to a Harris Poll by Harris Interactive in 2008. A predominance of tattooing among a younger segment of the population means dermatologists are likely to see more and more patients with tattoos.
Removal of tattoos via laser can be life changing and/or life saving for some patients. For example, former gang members might feel safer after removal of an identifying tattoo, said Dr. Nemeth, also of the department of dermatology and cutaneous surgery at the University of South Florida, Tampa.
For removal of green tattoo inks, Dr. Nemeth uses a 694-nm Q-switched ruby or 755-nm Q-switched alexandrite laser. To shatter black, blue, sky blue, or darker inks, he employs a 1064-nm Q switched Nd:YAG laser. If a patient's tattoo features red, orange, or purple inks, these can be effectively treated with a 532-nm Q-switched Nd:YAG laser, he said. Also be aware that laser therapy can darken tattoo inks if they contain iron oxide or titanium oxide.
Avoid the temptation to use lasers for other indications. "An EpiTouch ruby laser made for hair removal should not be used for tattoo removal," Dr. Nemeth said. "This is an important take-home message: Just because the wavelength is close, it does not mean the indications are the same."
Also, intense pulsed light systems are not appropriate for this indication, Dr. Nemeth said. "If your salesperson told you IPL can be used to remove tattoos, [he] lied to you. IPL cannot be used to remove a tattoo, in my humble opinion."
The Q-switched lasers have afforded patients a much better aesthetic outcome following tattoo removal. "It used to be every patient knew they were switching their tattoo for a scar, "Dr. Nemeth said. "Now you can get some very, very nice results."
Dr. Nemeth had no relevant financial disclosures.
NAPLES, Fla. — Patients present with different reasons for tattoo removal—such as regret following a crazy night or a change in relationship status. The number of options for laser tattoo removal, however, is more limited, Dr. Albert J. Nemeth said.
Specific Q-switched Nd:YAG laser wavelengths are good at shattering tattoo ink but must be applied specific to the ink color. Also, do not use non-Q-switched Nd:YAG lasers or other lasers designed for different dermatologic indications, Dr. Nemeth said at the annual meeting of the Florida Society of Dermatology and Dermatologic Surgery.
In general, 95% of amateur tattoos take one to three laser treatment sessions for removal. In contrast, six or more sessions are often required to remove most professional tattoos. Variables include the depth at which pigment was placed and type of ink. "Tattoo depth can vary. That is important to conceptualize when treating these tattoos," Dr. Nemeth said.
Tattoos applied by a friend or family member and those inked professionally share a common challenge for dermatologists—a lack of regulation on what can be used for pigment. "It's really quite interesting in terms of the secret concoctions that I've heard … cigarette ash; for some reason Crest toothpaste seems to be a magic ingredient; and—I don't understand why—but urine seems to be important in there also," Dr. Nemeth said in an interview.
|
An important caveat: If the patient reports or displays any symptoms of allergic dermatitis to the ink (constant oozing or crusting), lasers can worsen those symptoms. Physical removal of the tattoo is the only option for these patients, said Dr. Nemeth, a private-practice dermatologist in Clearwater, Fla., and FSDDS president. Dermabrasion, for example, is an option "if you are extraordinarily proficient at that."
An estimated 14% of all adults in the United States have at least one tattoo, according to a Harris Poll by Harris Interactive in 2008. A predominance of tattooing among a younger segment of the population means dermatologists are likely to see more and more patients with tattoos.
Removal of tattoos via laser can be life changing and/or life saving for some patients. For example, former gang members might feel safer after removal of an identifying tattoo, said Dr. Nemeth, also of the department of dermatology and cutaneous surgery at the University of South Florida, Tampa.
For removal of green tattoo inks, Dr. Nemeth uses a 694-nm Q-switched ruby or 755-nm Q-switched alexandrite laser. To shatter black, blue, sky blue, or darker inks, he employs a 1064-nm Q switched Nd:YAG laser. If a patient's tattoo features red, orange, or purple inks, these can be effectively treated with a 532-nm Q-switched Nd:YAG laser, he said. Also be aware that laser therapy can darken tattoo inks if they contain iron oxide or titanium oxide.
Avoid the temptation to use lasers for other indications. "An EpiTouch ruby laser made for hair removal should not be used for tattoo removal," Dr. Nemeth said. "This is an important take-home message: Just because the wavelength is close, it does not mean the indications are the same."
Also, intense pulsed light systems are not appropriate for this indication, Dr. Nemeth said. "If your salesperson told you IPL can be used to remove tattoos, [he] lied to you. IPL cannot be used to remove a tattoo, in my humble opinion."
The Q-switched lasers have afforded patients a much better aesthetic outcome following tattoo removal. "It used to be every patient knew they were switching their tattoo for a scar, "Dr. Nemeth said. "Now you can get some very, very nice results."
Dr. Nemeth had no relevant financial disclosures.
Emergency Department Use High During Last Months of Life
Major Finding: Of 3,224 seniors reviewed, 74% visited hospital emergency departments during their last 6 months of life and 51% visited during their last month.
Data Source: A cohort of people aged 65 years and older from the Health and Retirement Study and Medicare utilization data.
Disclosures: Dr. Smith had no relevant financial disclosures.
ORLANDO — Almost three-quarters of people aged 65 years and older visit emergency departments in their last 6 months of life, and just more than half do so during their last month, according to a study of 3,224 seniors.
These high utilization rates suggest that emergency department (ED) clinicians should be included in initiatives to improve end-of-life care, such as hospice and better patient-provider communication, Dr. Alexander K. Smith said. “When people come to the ED … it may be an opportunity to change the trajectory of care,” said Dr. Smith of the division of geriatrics at the University of California, San Francisco, and the San Francisco Veterans Affairs Medical Center.
Nursing home residents were less likely than were community-dwelling elders to visit an emergency department. During the last month of life, 41% of the former group and 54% of the latter did so, Dr. Smith said.
Use of ED services also varied considerably in the study by hospice enrollment, ethnicity, and whether the death was expected, which was ascertained through next-of-kin interviews.
Dr. Smith and his associates created a cohort of elderly decedents using data from the Health and Retirement Study, a nationally representative longitudinal survey. During that study, the eventual decedents had been interviewed every 2 years, and Dr. Smith's team focused on the last response prior to death. The study cohort of 3,224 adults included 22% who were 65–74 years old at the time of death between 1995 and 2006, 40% aged 75–85, and 38% older than 85 years at death.
Dr. Smith and his colleagues linked the survey participants' names to Medicare utilization data to find how many had visited EDs in their last months of life. They also looked at visit frequency in this group: 33% visited an ED once, 20% two times, 10% three times, 6% four times, and 5% five times or more.
The researchers compared the figure for how many people went to EDs in their last 1 month of life, 51%, with data for an age-, gender-, and race/ethnicity–matched cohort of elders who did not die in 2006. The researchers found that only 2% of these matched elders visited the ED in a 1-month period.
One aim of the study was to determine factors associated with ED use by dying elders. For example, 3% of hospice enrollees versus 56% of seniors not enrolled in hospice care visited an ED during the last month of life.
Also, 46% of the elders for whom death was expected visited the ED in the last month of life, while 61% of those with unexpected deaths had gone to EDs in that time frame.
“We did not have data on whether or not they had a primary care physician. But we were able to look at whether they visited the doctor frequently, and it was not associated with ED visits,” he said.
'When people come to the ED … it may be an opportunity to change the trajectory of care.'
Source DR. SMITH
Major Finding: Of 3,224 seniors reviewed, 74% visited hospital emergency departments during their last 6 months of life and 51% visited during their last month.
Data Source: A cohort of people aged 65 years and older from the Health and Retirement Study and Medicare utilization data.
Disclosures: Dr. Smith had no relevant financial disclosures.
ORLANDO — Almost three-quarters of people aged 65 years and older visit emergency departments in their last 6 months of life, and just more than half do so during their last month, according to a study of 3,224 seniors.
These high utilization rates suggest that emergency department (ED) clinicians should be included in initiatives to improve end-of-life care, such as hospice and better patient-provider communication, Dr. Alexander K. Smith said. “When people come to the ED … it may be an opportunity to change the trajectory of care,” said Dr. Smith of the division of geriatrics at the University of California, San Francisco, and the San Francisco Veterans Affairs Medical Center.
Nursing home residents were less likely than were community-dwelling elders to visit an emergency department. During the last month of life, 41% of the former group and 54% of the latter did so, Dr. Smith said.
Use of ED services also varied considerably in the study by hospice enrollment, ethnicity, and whether the death was expected, which was ascertained through next-of-kin interviews.
Dr. Smith and his associates created a cohort of elderly decedents using data from the Health and Retirement Study, a nationally representative longitudinal survey. During that study, the eventual decedents had been interviewed every 2 years, and Dr. Smith's team focused on the last response prior to death. The study cohort of 3,224 adults included 22% who were 65–74 years old at the time of death between 1995 and 2006, 40% aged 75–85, and 38% older than 85 years at death.
Dr. Smith and his colleagues linked the survey participants' names to Medicare utilization data to find how many had visited EDs in their last months of life. They also looked at visit frequency in this group: 33% visited an ED once, 20% two times, 10% three times, 6% four times, and 5% five times or more.
The researchers compared the figure for how many people went to EDs in their last 1 month of life, 51%, with data for an age-, gender-, and race/ethnicity–matched cohort of elders who did not die in 2006. The researchers found that only 2% of these matched elders visited the ED in a 1-month period.
One aim of the study was to determine factors associated with ED use by dying elders. For example, 3% of hospice enrollees versus 56% of seniors not enrolled in hospice care visited an ED during the last month of life.
Also, 46% of the elders for whom death was expected visited the ED in the last month of life, while 61% of those with unexpected deaths had gone to EDs in that time frame.
“We did not have data on whether or not they had a primary care physician. But we were able to look at whether they visited the doctor frequently, and it was not associated with ED visits,” he said.
'When people come to the ED … it may be an opportunity to change the trajectory of care.'
Source DR. SMITH
Major Finding: Of 3,224 seniors reviewed, 74% visited hospital emergency departments during their last 6 months of life and 51% visited during their last month.
Data Source: A cohort of people aged 65 years and older from the Health and Retirement Study and Medicare utilization data.
Disclosures: Dr. Smith had no relevant financial disclosures.
ORLANDO — Almost three-quarters of people aged 65 years and older visit emergency departments in their last 6 months of life, and just more than half do so during their last month, according to a study of 3,224 seniors.
These high utilization rates suggest that emergency department (ED) clinicians should be included in initiatives to improve end-of-life care, such as hospice and better patient-provider communication, Dr. Alexander K. Smith said. “When people come to the ED … it may be an opportunity to change the trajectory of care,” said Dr. Smith of the division of geriatrics at the University of California, San Francisco, and the San Francisco Veterans Affairs Medical Center.
Nursing home residents were less likely than were community-dwelling elders to visit an emergency department. During the last month of life, 41% of the former group and 54% of the latter did so, Dr. Smith said.
Use of ED services also varied considerably in the study by hospice enrollment, ethnicity, and whether the death was expected, which was ascertained through next-of-kin interviews.
Dr. Smith and his associates created a cohort of elderly decedents using data from the Health and Retirement Study, a nationally representative longitudinal survey. During that study, the eventual decedents had been interviewed every 2 years, and Dr. Smith's team focused on the last response prior to death. The study cohort of 3,224 adults included 22% who were 65–74 years old at the time of death between 1995 and 2006, 40% aged 75–85, and 38% older than 85 years at death.
Dr. Smith and his colleagues linked the survey participants' names to Medicare utilization data to find how many had visited EDs in their last months of life. They also looked at visit frequency in this group: 33% visited an ED once, 20% two times, 10% three times, 6% four times, and 5% five times or more.
The researchers compared the figure for how many people went to EDs in their last 1 month of life, 51%, with data for an age-, gender-, and race/ethnicity–matched cohort of elders who did not die in 2006. The researchers found that only 2% of these matched elders visited the ED in a 1-month period.
One aim of the study was to determine factors associated with ED use by dying elders. For example, 3% of hospice enrollees versus 56% of seniors not enrolled in hospice care visited an ED during the last month of life.
Also, 46% of the elders for whom death was expected visited the ED in the last month of life, while 61% of those with unexpected deaths had gone to EDs in that time frame.
“We did not have data on whether or not they had a primary care physician. But we were able to look at whether they visited the doctor frequently, and it was not associated with ED visits,” he said.
'When people come to the ED … it may be an opportunity to change the trajectory of care.'
Source DR. SMITH
Primary Care Docs Can Help Prevent Suicide in Veterans
ORLANDO, FLA. — Primary care physicians and psychiatrists outside the military health care system have a pivotal role to play in helping to lower suicide rates, which have been on the rise across all components of the U.S. Army, according to according to Col. Elspeth Cameron Ritchie, MC USA.
There were about 166 suicides in the Army in 2009, a rate of approximately 21 suicides per 100,000 people, or more than twice the rate in 2001.
“We have had difficulties with access to care, we have stigma … and our services are only partially integrated,” said Dr. Ritchie, medical director of the Army Medical Department's Office of Strategic Communications.
A lack of providers who accept the military health plan, TRICARE, is a barrier to those seeking care, Dr. Ritchie said. “The best way you as a provider can help is to sign up for TRICARE.” Physicians who register for the program (www.tricare.mil
Although most active and veteran military personnel receive health care services through institutions such as Walter Reed Army Medical Center and the Veterans Affairs system, there are exceptions. For example, some soldiers are students, have private insurance, or are members of the Reserves. This is where private sector physicians come in, she said.
Risk factors for suicide among a military population can differ from those in the general population. The typical solider at risk of suicide does not have a long history of mental health issues. “What we don't see is major mental illness,” such as schizophrenia or bipolar disorder, that is disabling. Only about 5% of military suicides are associated with a diagnosis of personality disorders, which is “lower than I would have expected,” said Dr. Ritchie, who also is a professor of psychiatry at Uniformed Services University of the Health Sciences, Bethesda, Md.
“We are seeing more and more” suicides spurred by relationship breakups and legal problems, she said. Under such circumstances, “unfortunately, screening does not work very well. They could screen just fine but get the 'Dear John' or 'Dear Jane' letter, buy a 12-pack, and go out and shoot themselves.”
Effective interventions in a military population will require a comprehensive look at all the elements around suicide, including posttraumatic stress disorder (PTSD), mild traumatic brain injury (TBI), and depression. “This is not going to be an issue for just 1 or 2 years; these are going to be issues for 20 years or 40 years,” Dr. Ritchie said. “So we all need to work on this together.”
The type of warfare many soldiers see when deployed in Afghanistan or Iraq increases their risk for mild TBI and associated symptoms. “The signature weapon of this war is the blast. And that causes a lot of symptoms.” Reexperiencing the trauma, numbing/avoidance, and physiologic arousal (“flight or fight” response) are the three main PTSD symptom clusters.
Army research suggests that soldiers need at least 2 years of noncombat time before their symptoms of anxiety and depression begin to wane. Reintegration can be a time of elevated risk for self-harm. “They have this high adrenaline from being in theater, and they don't know what to do with it. They take out a motorcycle and drive it at 120 mph.
“2009 was extraordinary year for suicide—highest they have been,” Dr. Ritchie said. “It seems lower so far this year. We are holding our breath.”
ORLANDO, FLA. — Primary care physicians and psychiatrists outside the military health care system have a pivotal role to play in helping to lower suicide rates, which have been on the rise across all components of the U.S. Army, according to according to Col. Elspeth Cameron Ritchie, MC USA.
There were about 166 suicides in the Army in 2009, a rate of approximately 21 suicides per 100,000 people, or more than twice the rate in 2001.
“We have had difficulties with access to care, we have stigma … and our services are only partially integrated,” said Dr. Ritchie, medical director of the Army Medical Department's Office of Strategic Communications.
A lack of providers who accept the military health plan, TRICARE, is a barrier to those seeking care, Dr. Ritchie said. “The best way you as a provider can help is to sign up for TRICARE.” Physicians who register for the program (www.tricare.mil
Although most active and veteran military personnel receive health care services through institutions such as Walter Reed Army Medical Center and the Veterans Affairs system, there are exceptions. For example, some soldiers are students, have private insurance, or are members of the Reserves. This is where private sector physicians come in, she said.
Risk factors for suicide among a military population can differ from those in the general population. The typical solider at risk of suicide does not have a long history of mental health issues. “What we don't see is major mental illness,” such as schizophrenia or bipolar disorder, that is disabling. Only about 5% of military suicides are associated with a diagnosis of personality disorders, which is “lower than I would have expected,” said Dr. Ritchie, who also is a professor of psychiatry at Uniformed Services University of the Health Sciences, Bethesda, Md.
“We are seeing more and more” suicides spurred by relationship breakups and legal problems, she said. Under such circumstances, “unfortunately, screening does not work very well. They could screen just fine but get the 'Dear John' or 'Dear Jane' letter, buy a 12-pack, and go out and shoot themselves.”
Effective interventions in a military population will require a comprehensive look at all the elements around suicide, including posttraumatic stress disorder (PTSD), mild traumatic brain injury (TBI), and depression. “This is not going to be an issue for just 1 or 2 years; these are going to be issues for 20 years or 40 years,” Dr. Ritchie said. “So we all need to work on this together.”
The type of warfare many soldiers see when deployed in Afghanistan or Iraq increases their risk for mild TBI and associated symptoms. “The signature weapon of this war is the blast. And that causes a lot of symptoms.” Reexperiencing the trauma, numbing/avoidance, and physiologic arousal (“flight or fight” response) are the three main PTSD symptom clusters.
Army research suggests that soldiers need at least 2 years of noncombat time before their symptoms of anxiety and depression begin to wane. Reintegration can be a time of elevated risk for self-harm. “They have this high adrenaline from being in theater, and they don't know what to do with it. They take out a motorcycle and drive it at 120 mph.
“2009 was extraordinary year for suicide—highest they have been,” Dr. Ritchie said. “It seems lower so far this year. We are holding our breath.”
ORLANDO, FLA. — Primary care physicians and psychiatrists outside the military health care system have a pivotal role to play in helping to lower suicide rates, which have been on the rise across all components of the U.S. Army, according to according to Col. Elspeth Cameron Ritchie, MC USA.
There were about 166 suicides in the Army in 2009, a rate of approximately 21 suicides per 100,000 people, or more than twice the rate in 2001.
“We have had difficulties with access to care, we have stigma … and our services are only partially integrated,” said Dr. Ritchie, medical director of the Army Medical Department's Office of Strategic Communications.
A lack of providers who accept the military health plan, TRICARE, is a barrier to those seeking care, Dr. Ritchie said. “The best way you as a provider can help is to sign up for TRICARE.” Physicians who register for the program (www.tricare.mil
Although most active and veteran military personnel receive health care services through institutions such as Walter Reed Army Medical Center and the Veterans Affairs system, there are exceptions. For example, some soldiers are students, have private insurance, or are members of the Reserves. This is where private sector physicians come in, she said.
Risk factors for suicide among a military population can differ from those in the general population. The typical solider at risk of suicide does not have a long history of mental health issues. “What we don't see is major mental illness,” such as schizophrenia or bipolar disorder, that is disabling. Only about 5% of military suicides are associated with a diagnosis of personality disorders, which is “lower than I would have expected,” said Dr. Ritchie, who also is a professor of psychiatry at Uniformed Services University of the Health Sciences, Bethesda, Md.
“We are seeing more and more” suicides spurred by relationship breakups and legal problems, she said. Under such circumstances, “unfortunately, screening does not work very well. They could screen just fine but get the 'Dear John' or 'Dear Jane' letter, buy a 12-pack, and go out and shoot themselves.”
Effective interventions in a military population will require a comprehensive look at all the elements around suicide, including posttraumatic stress disorder (PTSD), mild traumatic brain injury (TBI), and depression. “This is not going to be an issue for just 1 or 2 years; these are going to be issues for 20 years or 40 years,” Dr. Ritchie said. “So we all need to work on this together.”
The type of warfare many soldiers see when deployed in Afghanistan or Iraq increases their risk for mild TBI and associated symptoms. “The signature weapon of this war is the blast. And that causes a lot of symptoms.” Reexperiencing the trauma, numbing/avoidance, and physiologic arousal (“flight or fight” response) are the three main PTSD symptom clusters.
Army research suggests that soldiers need at least 2 years of noncombat time before their symptoms of anxiety and depression begin to wane. Reintegration can be a time of elevated risk for self-harm. “They have this high adrenaline from being in theater, and they don't know what to do with it. They take out a motorcycle and drive it at 120 mph.
“2009 was extraordinary year for suicide—highest they have been,” Dr. Ritchie said. “It seems lower so far this year. We are holding our breath.”
Gender, Abuse Influence Teen Suicidal Behavior
Major Finding: Girls in high school are more likely than boys to report depression and having seriously considered suicide, made a suicide plan, or attempted suicide in the previous 12 months. Boys are more likely to report injury with a suicide attempt.
Data Source: Analysis of five Youth Risk Behavior Surveillance System Surveys between 1999 and 2007.
Disclosures: None was reported.
ORLANDO — Girls in high school are more likely than are boys, regardless of age or race/ethnicity, to report being depressed, having seriously considered suicide, making a suicide plan, or attempting suicide in the past 12 months.
However, “when there is a suicide attempt, males are more likely to be injured than are females,” according to Robert M. Fernquist, Ph.D., “Males, when they do it, tend to do it more severely.”
In addition, a history of abuse emerged as the greatest predictor of suicidal behavior in these children.
“Rarely is suicide spontaneous—often there is a plan,” said Dr. Fernquist, professor of sociology at the University of Central Missouri in Warrensburg. “If there is a trajectory, there is probably depression first, then considering it, then making a plan.”
For that reason, Dr. Fernquist focused on specific questions asked in five Youth Risk Behavior Surveillance System (YRBSS) surveys conducted between 1999 and 2007. He assessed answers to five questions that asked whether, during the last 12 months, the responder had been depressed, considered suicide, made a suicide plan, and/or attempted suicide; and of those who had attempted suicide, if they had been injured as a result (defined as requiring medical attention).
An average of 154 high schools and 14,424 students in grades 9-12 participated in the survey, for a total of approximately 70,000 responses. The Centers for Disease Control and Prevention established the YRBSS to assess health-related behaviors in youth. Every other year, YRBSS researchers survey a nationally representative sample of public and private high school students.
Dr. Fernquist classified the students by sex as well as by age and race or ethnicity. For example, he compared responses from students aged 13-15 years with those aged 16-18 years because “younger teens … are mentally different than older, more mature teens.”
The percentage of high school students who had felt depressed in the previous 12 months was higher among girls across all groupings. “In every case, females were significantly more depressed than males,” Dr. Fernquist said.
For example, among students aged 13-15 years, 33% of black girls and 20% of black boys reported depression, as did 30% of Asian girls and 18% of Asian boys.
“Certainly not everyone who is depressed attempts suicide,” Dr. Fernquist said. Overall, a weighted average of 14.5% of high school students said they had seriously considered attempting suicide during the previous 12 months.
Again, there was a female predominance for consideration of suicide across all age and racial or ethnic comparisons. Among students aged 16-18 years, 25% of American Indian girls and 17% of American Indian boys said they had considered suicide, as did 22% of Hispanic girls and 13% of Hispanic boys.
Girls also were more likely than were boys in all groups to report they had made a suicide plan. For example, among 13- to 15-year-olds, 19% of white girls and 11% of white boys said they had made a plan, as did 15% of girls and 9% of boys in the Hawaiian and Pacific Islander group.
Dr. Fernquist also assessed the percentage of high school students who made at least one suicide attempt. “For the most part, females are more likely, regardless of age and ethnicity … to attempt.”
To assess the responses to the question about injury as a result of a suicide attempt, Dr. Fernquist grouped all the students into one age category because the numbers were small.
“Black, Hispanic, Hawaiian and Pacific Islander, and white males were all significantly more likely to attempt with injury [than were females].” The only exception was among Asian students, where girls were more likely to report injury with a suicide attempt than were their male counterparts.
Dr. Fernquist also assessed the data to determine variables associated with increased risk of suicide. “Regardless of the suicidal type of behavior involved, using drugs, being abused, or having a poor body image increase risk of suicidal behavior,” he said.
However, abuse dominated the regression models. In every case, it was abuse that had the biggest effect on a person's depression or likelihood of having a suicide plan, Dr. Fernquist said.
“One thing I will come away with from this study is that if you have a history of abuse—being hit by a boyfriend or girlfriend or being abused at school—you will have increased risk of suicidal behavior,” he said.
Major Finding: Girls in high school are more likely than boys to report depression and having seriously considered suicide, made a suicide plan, or attempted suicide in the previous 12 months. Boys are more likely to report injury with a suicide attempt.
Data Source: Analysis of five Youth Risk Behavior Surveillance System Surveys between 1999 and 2007.
Disclosures: None was reported.
ORLANDO — Girls in high school are more likely than are boys, regardless of age or race/ethnicity, to report being depressed, having seriously considered suicide, making a suicide plan, or attempting suicide in the past 12 months.
However, “when there is a suicide attempt, males are more likely to be injured than are females,” according to Robert M. Fernquist, Ph.D., “Males, when they do it, tend to do it more severely.”
In addition, a history of abuse emerged as the greatest predictor of suicidal behavior in these children.
“Rarely is suicide spontaneous—often there is a plan,” said Dr. Fernquist, professor of sociology at the University of Central Missouri in Warrensburg. “If there is a trajectory, there is probably depression first, then considering it, then making a plan.”
For that reason, Dr. Fernquist focused on specific questions asked in five Youth Risk Behavior Surveillance System (YRBSS) surveys conducted between 1999 and 2007. He assessed answers to five questions that asked whether, during the last 12 months, the responder had been depressed, considered suicide, made a suicide plan, and/or attempted suicide; and of those who had attempted suicide, if they had been injured as a result (defined as requiring medical attention).
An average of 154 high schools and 14,424 students in grades 9-12 participated in the survey, for a total of approximately 70,000 responses. The Centers for Disease Control and Prevention established the YRBSS to assess health-related behaviors in youth. Every other year, YRBSS researchers survey a nationally representative sample of public and private high school students.
Dr. Fernquist classified the students by sex as well as by age and race or ethnicity. For example, he compared responses from students aged 13-15 years with those aged 16-18 years because “younger teens … are mentally different than older, more mature teens.”
The percentage of high school students who had felt depressed in the previous 12 months was higher among girls across all groupings. “In every case, females were significantly more depressed than males,” Dr. Fernquist said.
For example, among students aged 13-15 years, 33% of black girls and 20% of black boys reported depression, as did 30% of Asian girls and 18% of Asian boys.
“Certainly not everyone who is depressed attempts suicide,” Dr. Fernquist said. Overall, a weighted average of 14.5% of high school students said they had seriously considered attempting suicide during the previous 12 months.
Again, there was a female predominance for consideration of suicide across all age and racial or ethnic comparisons. Among students aged 16-18 years, 25% of American Indian girls and 17% of American Indian boys said they had considered suicide, as did 22% of Hispanic girls and 13% of Hispanic boys.
Girls also were more likely than were boys in all groups to report they had made a suicide plan. For example, among 13- to 15-year-olds, 19% of white girls and 11% of white boys said they had made a plan, as did 15% of girls and 9% of boys in the Hawaiian and Pacific Islander group.
Dr. Fernquist also assessed the percentage of high school students who made at least one suicide attempt. “For the most part, females are more likely, regardless of age and ethnicity … to attempt.”
To assess the responses to the question about injury as a result of a suicide attempt, Dr. Fernquist grouped all the students into one age category because the numbers were small.
“Black, Hispanic, Hawaiian and Pacific Islander, and white males were all significantly more likely to attempt with injury [than were females].” The only exception was among Asian students, where girls were more likely to report injury with a suicide attempt than were their male counterparts.
Dr. Fernquist also assessed the data to determine variables associated with increased risk of suicide. “Regardless of the suicidal type of behavior involved, using drugs, being abused, or having a poor body image increase risk of suicidal behavior,” he said.
However, abuse dominated the regression models. In every case, it was abuse that had the biggest effect on a person's depression or likelihood of having a suicide plan, Dr. Fernquist said.
“One thing I will come away with from this study is that if you have a history of abuse—being hit by a boyfriend or girlfriend or being abused at school—you will have increased risk of suicidal behavior,” he said.
Major Finding: Girls in high school are more likely than boys to report depression and having seriously considered suicide, made a suicide plan, or attempted suicide in the previous 12 months. Boys are more likely to report injury with a suicide attempt.
Data Source: Analysis of five Youth Risk Behavior Surveillance System Surveys between 1999 and 2007.
Disclosures: None was reported.
ORLANDO — Girls in high school are more likely than are boys, regardless of age or race/ethnicity, to report being depressed, having seriously considered suicide, making a suicide plan, or attempting suicide in the past 12 months.
However, “when there is a suicide attempt, males are more likely to be injured than are females,” according to Robert M. Fernquist, Ph.D., “Males, when they do it, tend to do it more severely.”
In addition, a history of abuse emerged as the greatest predictor of suicidal behavior in these children.
“Rarely is suicide spontaneous—often there is a plan,” said Dr. Fernquist, professor of sociology at the University of Central Missouri in Warrensburg. “If there is a trajectory, there is probably depression first, then considering it, then making a plan.”
For that reason, Dr. Fernquist focused on specific questions asked in five Youth Risk Behavior Surveillance System (YRBSS) surveys conducted between 1999 and 2007. He assessed answers to five questions that asked whether, during the last 12 months, the responder had been depressed, considered suicide, made a suicide plan, and/or attempted suicide; and of those who had attempted suicide, if they had been injured as a result (defined as requiring medical attention).
An average of 154 high schools and 14,424 students in grades 9-12 participated in the survey, for a total of approximately 70,000 responses. The Centers for Disease Control and Prevention established the YRBSS to assess health-related behaviors in youth. Every other year, YRBSS researchers survey a nationally representative sample of public and private high school students.
Dr. Fernquist classified the students by sex as well as by age and race or ethnicity. For example, he compared responses from students aged 13-15 years with those aged 16-18 years because “younger teens … are mentally different than older, more mature teens.”
The percentage of high school students who had felt depressed in the previous 12 months was higher among girls across all groupings. “In every case, females were significantly more depressed than males,” Dr. Fernquist said.
For example, among students aged 13-15 years, 33% of black girls and 20% of black boys reported depression, as did 30% of Asian girls and 18% of Asian boys.
“Certainly not everyone who is depressed attempts suicide,” Dr. Fernquist said. Overall, a weighted average of 14.5% of high school students said they had seriously considered attempting suicide during the previous 12 months.
Again, there was a female predominance for consideration of suicide across all age and racial or ethnic comparisons. Among students aged 16-18 years, 25% of American Indian girls and 17% of American Indian boys said they had considered suicide, as did 22% of Hispanic girls and 13% of Hispanic boys.
Girls also were more likely than were boys in all groups to report they had made a suicide plan. For example, among 13- to 15-year-olds, 19% of white girls and 11% of white boys said they had made a plan, as did 15% of girls and 9% of boys in the Hawaiian and Pacific Islander group.
Dr. Fernquist also assessed the percentage of high school students who made at least one suicide attempt. “For the most part, females are more likely, regardless of age and ethnicity … to attempt.”
To assess the responses to the question about injury as a result of a suicide attempt, Dr. Fernquist grouped all the students into one age category because the numbers were small.
“Black, Hispanic, Hawaiian and Pacific Islander, and white males were all significantly more likely to attempt with injury [than were females].” The only exception was among Asian students, where girls were more likely to report injury with a suicide attempt than were their male counterparts.
Dr. Fernquist also assessed the data to determine variables associated with increased risk of suicide. “Regardless of the suicidal type of behavior involved, using drugs, being abused, or having a poor body image increase risk of suicidal behavior,” he said.
However, abuse dominated the regression models. In every case, it was abuse that had the biggest effect on a person's depression or likelihood of having a suicide plan, Dr. Fernquist said.
“One thing I will come away with from this study is that if you have a history of abuse—being hit by a boyfriend or girlfriend or being abused at school—you will have increased risk of suicidal behavior,” he said.
Probiotic Reduced Diarrhea Due to Antibiotics, C. difficile
MIAMI — A proprietary probiotic combination of two live Lactobacillus organisms significantly reduced the incidence and severity of antibiotic-associated diarrhea, as well as the incidence of Clostridium difficile–associated diarrhea, compared with placebo in a prospective, double-blind study.
Researchers at Shanghai Jiao Tong University in China randomized 255 hospitalized patients, aged 50–70 years, within 36 hours of antibiotic initiation to one of three groups: 86 patients took two probiotic capsules daily, 85 took one probiotic capsule plus one placebo capsule daily, and 84 took two placebo capsules daily. Each capsule contained 50 billion colony forming units (c.f.u.) of L. acidophilus CL1285 and L. casei LBC80R (made by Bio-K Plus International, which funded the trial). The regimen continued for 5 days after the usual course of antibiotics, then patients were monitored for another 21days.
The incidence of antibiotic-associated diarrhea–the primary study outcome—was 29% overall, affecting 74 patients. Specifically, diarrhea occurred in 16% of the patients who took two active capsules, 28% of those who took one active and one placebo capsule, and 44% of those who took two placebo capsules. Controlled comparisons were statistically significant between the groups, suggesting a dose-response relationship, Kerry Diaz said in an interview at a poster presentation.
The second outcome, severity of diarrhea, was likewise lower with the 100 billion c.f.u. daily dose. The researchers tracked the mean number of days that patients reported three or more episodes of liquid to soft stool. Patients in the high-dose probiotic group had a mean 2.8 days of severe diarrhea, compared with 4.1 days for those in the low-dose group and 6.4 days in the placebo group. Again, the differences were statistically different.
The researchers also found a significant difference in the incidence of C. difficile—associated diarrhea: 1% in the high-dose probiotic group, 9% in the low-dose group, and 24% in the placebo cohort—a “huge difference,” Ms. Diaz said. The full study findings were published earlier this year (Am. J. Gastroenterol. 2010 Feb. 9 [doi:10.1038/ajg.2010.11
The product is sold as a supplement in the United States, Ms. Diaz said, and has been available for more than a decade in Quebec, where Bio-K Plus is based. The product has not been reviewed by the U.S. Food and Drug Administration for antibiotic-associated and C. difficile—associated diarrhea, she added.
Disclosures: Ms. Diaz is a clinical research manager at Bio-K Plus International.
MIAMI — A proprietary probiotic combination of two live Lactobacillus organisms significantly reduced the incidence and severity of antibiotic-associated diarrhea, as well as the incidence of Clostridium difficile–associated diarrhea, compared with placebo in a prospective, double-blind study.
Researchers at Shanghai Jiao Tong University in China randomized 255 hospitalized patients, aged 50–70 years, within 36 hours of antibiotic initiation to one of three groups: 86 patients took two probiotic capsules daily, 85 took one probiotic capsule plus one placebo capsule daily, and 84 took two placebo capsules daily. Each capsule contained 50 billion colony forming units (c.f.u.) of L. acidophilus CL1285 and L. casei LBC80R (made by Bio-K Plus International, which funded the trial). The regimen continued for 5 days after the usual course of antibiotics, then patients were monitored for another 21days.
The incidence of antibiotic-associated diarrhea–the primary study outcome—was 29% overall, affecting 74 patients. Specifically, diarrhea occurred in 16% of the patients who took two active capsules, 28% of those who took one active and one placebo capsule, and 44% of those who took two placebo capsules. Controlled comparisons were statistically significant between the groups, suggesting a dose-response relationship, Kerry Diaz said in an interview at a poster presentation.
The second outcome, severity of diarrhea, was likewise lower with the 100 billion c.f.u. daily dose. The researchers tracked the mean number of days that patients reported three or more episodes of liquid to soft stool. Patients in the high-dose probiotic group had a mean 2.8 days of severe diarrhea, compared with 4.1 days for those in the low-dose group and 6.4 days in the placebo group. Again, the differences were statistically different.
The researchers also found a significant difference in the incidence of C. difficile—associated diarrhea: 1% in the high-dose probiotic group, 9% in the low-dose group, and 24% in the placebo cohort—a “huge difference,” Ms. Diaz said. The full study findings were published earlier this year (Am. J. Gastroenterol. 2010 Feb. 9 [doi:10.1038/ajg.2010.11
The product is sold as a supplement in the United States, Ms. Diaz said, and has been available for more than a decade in Quebec, where Bio-K Plus is based. The product has not been reviewed by the U.S. Food and Drug Administration for antibiotic-associated and C. difficile—associated diarrhea, she added.
Disclosures: Ms. Diaz is a clinical research manager at Bio-K Plus International.
MIAMI — A proprietary probiotic combination of two live Lactobacillus organisms significantly reduced the incidence and severity of antibiotic-associated diarrhea, as well as the incidence of Clostridium difficile–associated diarrhea, compared with placebo in a prospective, double-blind study.
Researchers at Shanghai Jiao Tong University in China randomized 255 hospitalized patients, aged 50–70 years, within 36 hours of antibiotic initiation to one of three groups: 86 patients took two probiotic capsules daily, 85 took one probiotic capsule plus one placebo capsule daily, and 84 took two placebo capsules daily. Each capsule contained 50 billion colony forming units (c.f.u.) of L. acidophilus CL1285 and L. casei LBC80R (made by Bio-K Plus International, which funded the trial). The regimen continued for 5 days after the usual course of antibiotics, then patients were monitored for another 21days.
The incidence of antibiotic-associated diarrhea–the primary study outcome—was 29% overall, affecting 74 patients. Specifically, diarrhea occurred in 16% of the patients who took two active capsules, 28% of those who took one active and one placebo capsule, and 44% of those who took two placebo capsules. Controlled comparisons were statistically significant between the groups, suggesting a dose-response relationship, Kerry Diaz said in an interview at a poster presentation.
The second outcome, severity of diarrhea, was likewise lower with the 100 billion c.f.u. daily dose. The researchers tracked the mean number of days that patients reported three or more episodes of liquid to soft stool. Patients in the high-dose probiotic group had a mean 2.8 days of severe diarrhea, compared with 4.1 days for those in the low-dose group and 6.4 days in the placebo group. Again, the differences were statistically different.
The researchers also found a significant difference in the incidence of C. difficile—associated diarrhea: 1% in the high-dose probiotic group, 9% in the low-dose group, and 24% in the placebo cohort—a “huge difference,” Ms. Diaz said. The full study findings were published earlier this year (Am. J. Gastroenterol. 2010 Feb. 9 [doi:10.1038/ajg.2010.11
The product is sold as a supplement in the United States, Ms. Diaz said, and has been available for more than a decade in Quebec, where Bio-K Plus is based. The product has not been reviewed by the U.S. Food and Drug Administration for antibiotic-associated and C. difficile—associated diarrhea, she added.
Disclosures: Ms. Diaz is a clinical research manager at Bio-K Plus International.
Ustekinumab Aided Sexual Function in Psoriasis
MIAMI — Treatment with ustekinumab significantly improved sexual function in patients with moderate to severe psoriasis, according to a secondary analysis of phase III study data.
“It has become really clear that psoriasis has an influence on sexual function in our patients,” Dr. Lyn Guenther said during a poster discussion session.
There is, however, a paucity of published data—with only a few researchers quantifying sexual function and none examining possible benefits of medical treatment in this patient population.
To find out if ustekinumab could improve sexual function, Dr. Guenther and her colleagues assessed quality-of-life data from the phase III PHOENIX I (Lancet 2008;371:1665-74) and PHOENIX II (Lancet 2008;371:1675-84) trials.
At baseline, 23% of the combined 1,996 study patients reported that psoriasis affected their sexual function. Impaired function was defined by a patient response of “very much” or “a lot” of sexual difficulties related to their skin disease on the Dermatology Life Quality Index (DLQI). All participants had moderate to severe psoriasis, and 69% were men; 28% of women and 21% of men reported impaired sexual function.
DLQI scores range from 0 to 30. Mean DLQI patient score at baseline was 12, “indicating a very large negative effect on patients' lives,” said Dr. Guenther, professor of dermatology at the University of Western Ontario, London. The mean Psoriasis Area and Severity Index (PASI) score was a “fairly significant” 20, she said, and mean percentage of body surface area affected by psoriasis was 26%.
Worse sexual dysfunction was significantly associated with increased psoriasis disease severity. As an example, 54% of the women with a PASI score greater than 30 reported a significant impact of their condition on sexuality. “At each of the PASI severity cutoff points, it's almost a linear increase,” Dr. Guenther said.
“Can we make a difference?” she asked. After 12 weeks, the percentage of patients who reported sexual function impairment dropped from 23% to 3% in both ustekinumab dosage groups, with no change observed in the control group. “It was surprising to me to see how quickly we could improve the impairment,” she said.
Similarly, at week 12, DLQI scores in the treatment groups decreased by a mean of 9.1 points versus a 0.5-point decrease in controls, a statistically significant difference. Both men and women “improved dramatically,” Dr. Guenther said.
The PHOENIX I and II trial investigators randomized 1,334 patients to ustekinumab (45 mg or 90 mg) at weeks 0, 4, and every 12 weeks thereafter. They also randomized another 662 patients to placebo at weeks 0 and 4, with crossover to ustekinumab (45 mg or 90 mg) at week 12. Placebo patients who crossed over to ustekinumab experienced similar benefits. “The lessening of the sexual dysfunction continued to week 24,” she said.
The mechanism of action for improved sexual function is unknown, but patients treated with ustekinumab might experience less fatigue and more hope about their condition improving, she suggested. “Why these people have [sexual function] problems is not clear. Future trials will be done to identify the reasons,” Dr. Guenther said. She added that further research using validated sexual dysfunction instruments is warranted.
Disclosures: Dr. Guenther was a consultant for Johnson & Johnson, sponsor of the study. Ustekinumab (Stelara) is manufactured by Centocor Ortho Biotech, a wholly owned subsidiary of Johnson & Johnson.
MIAMI — Treatment with ustekinumab significantly improved sexual function in patients with moderate to severe psoriasis, according to a secondary analysis of phase III study data.
“It has become really clear that psoriasis has an influence on sexual function in our patients,” Dr. Lyn Guenther said during a poster discussion session.
There is, however, a paucity of published data—with only a few researchers quantifying sexual function and none examining possible benefits of medical treatment in this patient population.
To find out if ustekinumab could improve sexual function, Dr. Guenther and her colleagues assessed quality-of-life data from the phase III PHOENIX I (Lancet 2008;371:1665-74) and PHOENIX II (Lancet 2008;371:1675-84) trials.
At baseline, 23% of the combined 1,996 study patients reported that psoriasis affected their sexual function. Impaired function was defined by a patient response of “very much” or “a lot” of sexual difficulties related to their skin disease on the Dermatology Life Quality Index (DLQI). All participants had moderate to severe psoriasis, and 69% were men; 28% of women and 21% of men reported impaired sexual function.
DLQI scores range from 0 to 30. Mean DLQI patient score at baseline was 12, “indicating a very large negative effect on patients' lives,” said Dr. Guenther, professor of dermatology at the University of Western Ontario, London. The mean Psoriasis Area and Severity Index (PASI) score was a “fairly significant” 20, she said, and mean percentage of body surface area affected by psoriasis was 26%.
Worse sexual dysfunction was significantly associated with increased psoriasis disease severity. As an example, 54% of the women with a PASI score greater than 30 reported a significant impact of their condition on sexuality. “At each of the PASI severity cutoff points, it's almost a linear increase,” Dr. Guenther said.
“Can we make a difference?” she asked. After 12 weeks, the percentage of patients who reported sexual function impairment dropped from 23% to 3% in both ustekinumab dosage groups, with no change observed in the control group. “It was surprising to me to see how quickly we could improve the impairment,” she said.
Similarly, at week 12, DLQI scores in the treatment groups decreased by a mean of 9.1 points versus a 0.5-point decrease in controls, a statistically significant difference. Both men and women “improved dramatically,” Dr. Guenther said.
The PHOENIX I and II trial investigators randomized 1,334 patients to ustekinumab (45 mg or 90 mg) at weeks 0, 4, and every 12 weeks thereafter. They also randomized another 662 patients to placebo at weeks 0 and 4, with crossover to ustekinumab (45 mg or 90 mg) at week 12. Placebo patients who crossed over to ustekinumab experienced similar benefits. “The lessening of the sexual dysfunction continued to week 24,” she said.
The mechanism of action for improved sexual function is unknown, but patients treated with ustekinumab might experience less fatigue and more hope about their condition improving, she suggested. “Why these people have [sexual function] problems is not clear. Future trials will be done to identify the reasons,” Dr. Guenther said. She added that further research using validated sexual dysfunction instruments is warranted.
Disclosures: Dr. Guenther was a consultant for Johnson & Johnson, sponsor of the study. Ustekinumab (Stelara) is manufactured by Centocor Ortho Biotech, a wholly owned subsidiary of Johnson & Johnson.
MIAMI — Treatment with ustekinumab significantly improved sexual function in patients with moderate to severe psoriasis, according to a secondary analysis of phase III study data.
“It has become really clear that psoriasis has an influence on sexual function in our patients,” Dr. Lyn Guenther said during a poster discussion session.
There is, however, a paucity of published data—with only a few researchers quantifying sexual function and none examining possible benefits of medical treatment in this patient population.
To find out if ustekinumab could improve sexual function, Dr. Guenther and her colleagues assessed quality-of-life data from the phase III PHOENIX I (Lancet 2008;371:1665-74) and PHOENIX II (Lancet 2008;371:1675-84) trials.
At baseline, 23% of the combined 1,996 study patients reported that psoriasis affected their sexual function. Impaired function was defined by a patient response of “very much” or “a lot” of sexual difficulties related to their skin disease on the Dermatology Life Quality Index (DLQI). All participants had moderate to severe psoriasis, and 69% were men; 28% of women and 21% of men reported impaired sexual function.
DLQI scores range from 0 to 30. Mean DLQI patient score at baseline was 12, “indicating a very large negative effect on patients' lives,” said Dr. Guenther, professor of dermatology at the University of Western Ontario, London. The mean Psoriasis Area and Severity Index (PASI) score was a “fairly significant” 20, she said, and mean percentage of body surface area affected by psoriasis was 26%.
Worse sexual dysfunction was significantly associated with increased psoriasis disease severity. As an example, 54% of the women with a PASI score greater than 30 reported a significant impact of their condition on sexuality. “At each of the PASI severity cutoff points, it's almost a linear increase,” Dr. Guenther said.
“Can we make a difference?” she asked. After 12 weeks, the percentage of patients who reported sexual function impairment dropped from 23% to 3% in both ustekinumab dosage groups, with no change observed in the control group. “It was surprising to me to see how quickly we could improve the impairment,” she said.
Similarly, at week 12, DLQI scores in the treatment groups decreased by a mean of 9.1 points versus a 0.5-point decrease in controls, a statistically significant difference. Both men and women “improved dramatically,” Dr. Guenther said.
The PHOENIX I and II trial investigators randomized 1,334 patients to ustekinumab (45 mg or 90 mg) at weeks 0, 4, and every 12 weeks thereafter. They also randomized another 662 patients to placebo at weeks 0 and 4, with crossover to ustekinumab (45 mg or 90 mg) at week 12. Placebo patients who crossed over to ustekinumab experienced similar benefits. “The lessening of the sexual dysfunction continued to week 24,” she said.
The mechanism of action for improved sexual function is unknown, but patients treated with ustekinumab might experience less fatigue and more hope about their condition improving, she suggested. “Why these people have [sexual function] problems is not clear. Future trials will be done to identify the reasons,” Dr. Guenther said. She added that further research using validated sexual dysfunction instruments is warranted.
Disclosures: Dr. Guenther was a consultant for Johnson & Johnson, sponsor of the study. Ustekinumab (Stelara) is manufactured by Centocor Ortho Biotech, a wholly owned subsidiary of Johnson & Johnson.