User login
Long-term safety, efficacy of hemophilia B therapy
Interim results from the B-YOND trial suggest prophylactic treatment with a recombinant factor IX Fc fusion protein (rFIXFc) can provide long-term safety and efficacy, according to researchers.
B-YOND is an extension study for adults and adolescents who completed the B-LONG study and children who completed the Kids B-LONG study.
In both trials, researchers tested rFIXFc in patients with hemophilia B.
The median duration of rFIXFc treatment has surpassed 3 years for the adults and adolescents enrolled in B-YOND and exceeded 1.5 years for children in this trial.
Researchers said the median annualized bleeding rates (ABRs) have been low in these patients, and none of the patients have developed inhibitors.
“The interim data from B-YOND confirm the safety profile of [rFIXFc] and show that adult, adolescent, and pediatric subjects maintained low annual bleed rates with prophylactic dosing of [rFIXFc] every 1 to 2 weeks,” said principal investigator John Pasi, MD, PhD, of Barts and the London School of Medicine and Dentistry in London, UK.
“These results come from the longest-term study of an extended half-life therapy for hemophilia B and provide physicians across the globe with important insights and information about the treatment of hemophilia B.”
The results were published in Thrombosis and Haemostasis.
The research was sponsored by Bioverativ Therapeutics Inc., the company developing rFIXFc (also known as eftrenonacog alfa and by the brand name Alprolix) in collaboration with Sobi. rFIXFc is approved to treat hemophilia B in the US, European Union, and other countries.
Treatment
B-YOND has enrolled 116 patients with hemophilia B who completed B-LONG (n=93) or Kids B-LONG (n=23). The patients were placed in 1 of 4 treatment groups (but could change at any point):
- Weekly prophylaxis—20 to 100 IU/kg every 7 days (50 adults/adolescents, 19 children)
- Individualized prophylaxis—100 IU/kg every 8 to 16 days (30 adults/adolescents, 5 children)
- Modified prophylaxis, which was defined as further dosing personalization to optimize prophylaxis (13 adults/adolescents, 1 child)
- Episodic treatment, which was available only to adults and adolescents (n=15).
In the weekly prophylaxis group, the median dosing interval was 7.0 days for adults, adolescents, and children. The average weekly prophylactic dose was 49.5 IU/kg in adults/adolescents, 64.4 IU/kg in kids younger than 6, and 63.1 IU/kg in kids ages 6 to 11.
In the individualized prophylaxis group, the median dosing interval was 13.7 days for adults and adolescents and 10.0 days in pediatric patients (ages 6 to 11 only). The average weekly prophylactic dose was 50.2 IU/kg in adults/adolescents, and 66.6 IU/kg in kids ages 6 to 11.
In the modified prophylaxis group, the median dosing interval was 6.9 days for adults and adolescents and 4.1 days in the single pediatric patient (who was older than 6). The average weekly prophylactic dose was 61.7 IU/kg in adults/adolescents and 157.9 IU/kg in the pediatric patient.
From the start of B-LONG to the B-YOND interim data cut, adults/adolescents had a median of 39.5 months of cumulative rFIXFc treatment and a median of 162 cumulative exposure days.
From the start of Kids B-LONG to the data cut, pediatric patients had a median of 21.9 months of cumulative rFIXFc treatment and a median of 94 cumulative exposure days.
ABRs
As of the interim data cut, the overall median ABR was 2.3 for adults/adolescents in both the weekly and individualized prophylaxis groups.
The median ABR was 2.4 for adults/adolescents in the modified prophylaxis group and 11.3 for those receiving on-demand treatment.
Among children under age 6 (n=9), the median ABR in the weekly prophylaxis group was 0. (None of the younger children had individualized or modified prophylaxis.)
For children ages 6 to 11, the median ABR was 2.7 in the weekly prophylaxis group (n=10) and 2.4 in the individualized prophylaxis group (n=5). The patient in the modified prophylaxis group had an ABR of 3.1.
Safety
The researchers said rFIXFc was well-tolerated, and the adverse events (AEs) reported were typical of the population studied.
AEs were reported in 75.9% of patients. The most common were headache (n=14, 12.1%) and common cold (n=13, 11.2%), and the majority of AEs were considered unrelated to rFIXFc.
Three adult/adolescent patients experienced AEs during B-YOND that were considered treatment-related, including noncardiac chest pain, hematuria, and obstructive uropathy. All 3 events resolved.
One patient experienced breath odor during B-LONG that was considered treatment-related. And 1 patient reported decreased appetite during Kids B-LONG that was considered treatment-related. Neither of these events resolved.
There were 39 serious AEs in 23 patients (19.8%). All but 1 of these events were considered unrelated to rFIXFc.
The treatment-related serious AE was renal colic in a patient originally enrolled in the B-LONG study. The patient had a medical history of previous clot colic. The event resolved and did not lead to study discontinuation.
There have been no reports of serious allergic reactions or anaphylaxis associated with rFIXFc, no vascular thrombotic events, and no deaths. ![]()
Interim results from the B-YOND trial suggest prophylactic treatment with a recombinant factor IX Fc fusion protein (rFIXFc) can provide long-term safety and efficacy, according to researchers.
B-YOND is an extension study for adults and adolescents who completed the B-LONG study and children who completed the Kids B-LONG study.
In both trials, researchers tested rFIXFc in patients with hemophilia B.
The median duration of rFIXFc treatment has surpassed 3 years for the adults and adolescents enrolled in B-YOND and exceeded 1.5 years for children in this trial.
Researchers said the median annualized bleeding rates (ABRs) have been low in these patients, and none of the patients have developed inhibitors.
“The interim data from B-YOND confirm the safety profile of [rFIXFc] and show that adult, adolescent, and pediatric subjects maintained low annual bleed rates with prophylactic dosing of [rFIXFc] every 1 to 2 weeks,” said principal investigator John Pasi, MD, PhD, of Barts and the London School of Medicine and Dentistry in London, UK.
“These results come from the longest-term study of an extended half-life therapy for hemophilia B and provide physicians across the globe with important insights and information about the treatment of hemophilia B.”
The results were published in Thrombosis and Haemostasis.
The research was sponsored by Bioverativ Therapeutics Inc., the company developing rFIXFc (also known as eftrenonacog alfa and by the brand name Alprolix) in collaboration with Sobi. rFIXFc is approved to treat hemophilia B in the US, European Union, and other countries.
Treatment
B-YOND has enrolled 116 patients with hemophilia B who completed B-LONG (n=93) or Kids B-LONG (n=23). The patients were placed in 1 of 4 treatment groups (but could change at any point):
- Weekly prophylaxis—20 to 100 IU/kg every 7 days (50 adults/adolescents, 19 children)
- Individualized prophylaxis—100 IU/kg every 8 to 16 days (30 adults/adolescents, 5 children)
- Modified prophylaxis, which was defined as further dosing personalization to optimize prophylaxis (13 adults/adolescents, 1 child)
- Episodic treatment, which was available only to adults and adolescents (n=15).
In the weekly prophylaxis group, the median dosing interval was 7.0 days for adults, adolescents, and children. The average weekly prophylactic dose was 49.5 IU/kg in adults/adolescents, 64.4 IU/kg in kids younger than 6, and 63.1 IU/kg in kids ages 6 to 11.
In the individualized prophylaxis group, the median dosing interval was 13.7 days for adults and adolescents and 10.0 days in pediatric patients (ages 6 to 11 only). The average weekly prophylactic dose was 50.2 IU/kg in adults/adolescents, and 66.6 IU/kg in kids ages 6 to 11.
In the modified prophylaxis group, the median dosing interval was 6.9 days for adults and adolescents and 4.1 days in the single pediatric patient (who was older than 6). The average weekly prophylactic dose was 61.7 IU/kg in adults/adolescents and 157.9 IU/kg in the pediatric patient.
From the start of B-LONG to the B-YOND interim data cut, adults/adolescents had a median of 39.5 months of cumulative rFIXFc treatment and a median of 162 cumulative exposure days.
From the start of Kids B-LONG to the data cut, pediatric patients had a median of 21.9 months of cumulative rFIXFc treatment and a median of 94 cumulative exposure days.
ABRs
As of the interim data cut, the overall median ABR was 2.3 for adults/adolescents in both the weekly and individualized prophylaxis groups.
The median ABR was 2.4 for adults/adolescents in the modified prophylaxis group and 11.3 for those receiving on-demand treatment.
Among children under age 6 (n=9), the median ABR in the weekly prophylaxis group was 0. (None of the younger children had individualized or modified prophylaxis.)
For children ages 6 to 11, the median ABR was 2.7 in the weekly prophylaxis group (n=10) and 2.4 in the individualized prophylaxis group (n=5). The patient in the modified prophylaxis group had an ABR of 3.1.
Safety
The researchers said rFIXFc was well-tolerated, and the adverse events (AEs) reported were typical of the population studied.
AEs were reported in 75.9% of patients. The most common were headache (n=14, 12.1%) and common cold (n=13, 11.2%), and the majority of AEs were considered unrelated to rFIXFc.
Three adult/adolescent patients experienced AEs during B-YOND that were considered treatment-related, including noncardiac chest pain, hematuria, and obstructive uropathy. All 3 events resolved.
One patient experienced breath odor during B-LONG that was considered treatment-related. And 1 patient reported decreased appetite during Kids B-LONG that was considered treatment-related. Neither of these events resolved.
There were 39 serious AEs in 23 patients (19.8%). All but 1 of these events were considered unrelated to rFIXFc.
The treatment-related serious AE was renal colic in a patient originally enrolled in the B-LONG study. The patient had a medical history of previous clot colic. The event resolved and did not lead to study discontinuation.
There have been no reports of serious allergic reactions or anaphylaxis associated with rFIXFc, no vascular thrombotic events, and no deaths. ![]()
Interim results from the B-YOND trial suggest prophylactic treatment with a recombinant factor IX Fc fusion protein (rFIXFc) can provide long-term safety and efficacy, according to researchers.
B-YOND is an extension study for adults and adolescents who completed the B-LONG study and children who completed the Kids B-LONG study.
In both trials, researchers tested rFIXFc in patients with hemophilia B.
The median duration of rFIXFc treatment has surpassed 3 years for the adults and adolescents enrolled in B-YOND and exceeded 1.5 years for children in this trial.
Researchers said the median annualized bleeding rates (ABRs) have been low in these patients, and none of the patients have developed inhibitors.
“The interim data from B-YOND confirm the safety profile of [rFIXFc] and show that adult, adolescent, and pediatric subjects maintained low annual bleed rates with prophylactic dosing of [rFIXFc] every 1 to 2 weeks,” said principal investigator John Pasi, MD, PhD, of Barts and the London School of Medicine and Dentistry in London, UK.
“These results come from the longest-term study of an extended half-life therapy for hemophilia B and provide physicians across the globe with important insights and information about the treatment of hemophilia B.”
The results were published in Thrombosis and Haemostasis.
The research was sponsored by Bioverativ Therapeutics Inc., the company developing rFIXFc (also known as eftrenonacog alfa and by the brand name Alprolix) in collaboration with Sobi. rFIXFc is approved to treat hemophilia B in the US, European Union, and other countries.
Treatment
B-YOND has enrolled 116 patients with hemophilia B who completed B-LONG (n=93) or Kids B-LONG (n=23). The patients were placed in 1 of 4 treatment groups (but could change at any point):
- Weekly prophylaxis—20 to 100 IU/kg every 7 days (50 adults/adolescents, 19 children)
- Individualized prophylaxis—100 IU/kg every 8 to 16 days (30 adults/adolescents, 5 children)
- Modified prophylaxis, which was defined as further dosing personalization to optimize prophylaxis (13 adults/adolescents, 1 child)
- Episodic treatment, which was available only to adults and adolescents (n=15).
In the weekly prophylaxis group, the median dosing interval was 7.0 days for adults, adolescents, and children. The average weekly prophylactic dose was 49.5 IU/kg in adults/adolescents, 64.4 IU/kg in kids younger than 6, and 63.1 IU/kg in kids ages 6 to 11.
In the individualized prophylaxis group, the median dosing interval was 13.7 days for adults and adolescents and 10.0 days in pediatric patients (ages 6 to 11 only). The average weekly prophylactic dose was 50.2 IU/kg in adults/adolescents, and 66.6 IU/kg in kids ages 6 to 11.
In the modified prophylaxis group, the median dosing interval was 6.9 days for adults and adolescents and 4.1 days in the single pediatric patient (who was older than 6). The average weekly prophylactic dose was 61.7 IU/kg in adults/adolescents and 157.9 IU/kg in the pediatric patient.
From the start of B-LONG to the B-YOND interim data cut, adults/adolescents had a median of 39.5 months of cumulative rFIXFc treatment and a median of 162 cumulative exposure days.
From the start of Kids B-LONG to the data cut, pediatric patients had a median of 21.9 months of cumulative rFIXFc treatment and a median of 94 cumulative exposure days.
ABRs
As of the interim data cut, the overall median ABR was 2.3 for adults/adolescents in both the weekly and individualized prophylaxis groups.
The median ABR was 2.4 for adults/adolescents in the modified prophylaxis group and 11.3 for those receiving on-demand treatment.
Among children under age 6 (n=9), the median ABR in the weekly prophylaxis group was 0. (None of the younger children had individualized or modified prophylaxis.)
For children ages 6 to 11, the median ABR was 2.7 in the weekly prophylaxis group (n=10) and 2.4 in the individualized prophylaxis group (n=5). The patient in the modified prophylaxis group had an ABR of 3.1.
Safety
The researchers said rFIXFc was well-tolerated, and the adverse events (AEs) reported were typical of the population studied.
AEs were reported in 75.9% of patients. The most common were headache (n=14, 12.1%) and common cold (n=13, 11.2%), and the majority of AEs were considered unrelated to rFIXFc.
Three adult/adolescent patients experienced AEs during B-YOND that were considered treatment-related, including noncardiac chest pain, hematuria, and obstructive uropathy. All 3 events resolved.
One patient experienced breath odor during B-LONG that was considered treatment-related. And 1 patient reported decreased appetite during Kids B-LONG that was considered treatment-related. Neither of these events resolved.
There were 39 serious AEs in 23 patients (19.8%). All but 1 of these events were considered unrelated to rFIXFc.
The treatment-related serious AE was renal colic in a patient originally enrolled in the B-LONG study. The patient had a medical history of previous clot colic. The event resolved and did not lead to study discontinuation.
There have been no reports of serious allergic reactions or anaphylaxis associated with rFIXFc, no vascular thrombotic events, and no deaths. ![]()
Group reports rejuvenation of aging HSCs
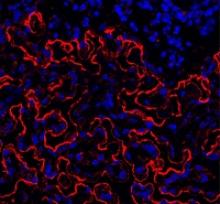
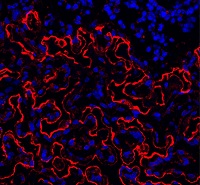
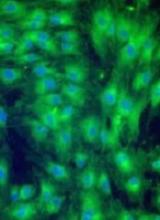
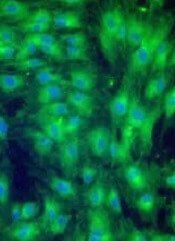
Preclinical research suggests osteopontin, a protein made by osteoblasts, plays a role in hematopoietic stem cell (HSC) aging.
Experiments in mice revealed that, with age, there is a reduction in the expression of osteopontin in the bone marrow stroma.
A lack of osteopontin induced young HSCs to “act” older, while treating older HSCs with recombinant osteopontin restored youthful properties.
Hartmut Geiger, PhD, of the University of Ulm in Germany, and his colleagues reported these findings in EMBO.
“We show that the place where HSCs form in the bone marrow loses osteopontin upon aging, but if you give back the missing protein to the blood-forming cells, they suddenly rejuvenate and act younger,” Dr Geiger said.
“Our study points to exciting, novel ways to have a better immune system and possibly less blood cancer upon aging by therapeutically targeting the place where blood stem cells form.”
The researchers conducted a number of experiments to test the formation and vitality of cells in and near the bone marrow microenvironment.
The team looked at the formation of endosteum stroma cells in aging mice and monitored levels of osteopontin and other proteins linked to distinct cells in the bone marrow during the aging process.
The researchers said they observed reduced production of osteoblasts and other stroma cells in the endosteum of older mice. They also saw decreased osteopontin levels in the bone marrow of older animals, which was associated with reduced vigor and function of HSCs.
The team followed up these experiments by transplanting bone marrow cells from older mice (19 to 21 months) into young mice (8 to 10 weeks).
The researchers also transplanted aged HSCs from older mice into younger mice, and the team treated aged HSCs with a recombinant form of the osteopontin protein.
Transplantation into the younger animals caused HSCs to behave in a younger, more vital manner, the researchers said. This meant smaller numbers of HSCs with greater potential for forming different blood cells, which included larger populations of B and T cells and decreased production of myeloid cells.
The researchers also saw aged HSCs treated with recombinant osteopontin regain their youthful characteristics and capacity to form different blood cell types. Also observed was diminished signaling of Cdc42, a protein previously shown to cause aging in HSCs.
Osteopontin levels are not only low in the bone marrow niche but also in the blood upon aging. As a follow-up to the current study, the researchers are investigating the possibility of using osteopontin replacement therapy in mice to counter the influence of an aging niche directly in the animals. ![]()
Preclinical research suggests osteopontin, a protein made by osteoblasts, plays a role in hematopoietic stem cell (HSC) aging.
Experiments in mice revealed that, with age, there is a reduction in the expression of osteopontin in the bone marrow stroma.
A lack of osteopontin induced young HSCs to “act” older, while treating older HSCs with recombinant osteopontin restored youthful properties.
Hartmut Geiger, PhD, of the University of Ulm in Germany, and his colleagues reported these findings in EMBO.
“We show that the place where HSCs form in the bone marrow loses osteopontin upon aging, but if you give back the missing protein to the blood-forming cells, they suddenly rejuvenate and act younger,” Dr Geiger said.
“Our study points to exciting, novel ways to have a better immune system and possibly less blood cancer upon aging by therapeutically targeting the place where blood stem cells form.”
The researchers conducted a number of experiments to test the formation and vitality of cells in and near the bone marrow microenvironment.
The team looked at the formation of endosteum stroma cells in aging mice and monitored levels of osteopontin and other proteins linked to distinct cells in the bone marrow during the aging process.
The researchers said they observed reduced production of osteoblasts and other stroma cells in the endosteum of older mice. They also saw decreased osteopontin levels in the bone marrow of older animals, which was associated with reduced vigor and function of HSCs.
The team followed up these experiments by transplanting bone marrow cells from older mice (19 to 21 months) into young mice (8 to 10 weeks).
The researchers also transplanted aged HSCs from older mice into younger mice, and the team treated aged HSCs with a recombinant form of the osteopontin protein.
Transplantation into the younger animals caused HSCs to behave in a younger, more vital manner, the researchers said. This meant smaller numbers of HSCs with greater potential for forming different blood cells, which included larger populations of B and T cells and decreased production of myeloid cells.
The researchers also saw aged HSCs treated with recombinant osteopontin regain their youthful characteristics and capacity to form different blood cell types. Also observed was diminished signaling of Cdc42, a protein previously shown to cause aging in HSCs.
Osteopontin levels are not only low in the bone marrow niche but also in the blood upon aging. As a follow-up to the current study, the researchers are investigating the possibility of using osteopontin replacement therapy in mice to counter the influence of an aging niche directly in the animals. ![]()
Preclinical research suggests osteopontin, a protein made by osteoblasts, plays a role in hematopoietic stem cell (HSC) aging.
Experiments in mice revealed that, with age, there is a reduction in the expression of osteopontin in the bone marrow stroma.
A lack of osteopontin induced young HSCs to “act” older, while treating older HSCs with recombinant osteopontin restored youthful properties.
Hartmut Geiger, PhD, of the University of Ulm in Germany, and his colleagues reported these findings in EMBO.
“We show that the place where HSCs form in the bone marrow loses osteopontin upon aging, but if you give back the missing protein to the blood-forming cells, they suddenly rejuvenate and act younger,” Dr Geiger said.
“Our study points to exciting, novel ways to have a better immune system and possibly less blood cancer upon aging by therapeutically targeting the place where blood stem cells form.”
The researchers conducted a number of experiments to test the formation and vitality of cells in and near the bone marrow microenvironment.
The team looked at the formation of endosteum stroma cells in aging mice and monitored levels of osteopontin and other proteins linked to distinct cells in the bone marrow during the aging process.
The researchers said they observed reduced production of osteoblasts and other stroma cells in the endosteum of older mice. They also saw decreased osteopontin levels in the bone marrow of older animals, which was associated with reduced vigor and function of HSCs.
The team followed up these experiments by transplanting bone marrow cells from older mice (19 to 21 months) into young mice (8 to 10 weeks).
The researchers also transplanted aged HSCs from older mice into younger mice, and the team treated aged HSCs with a recombinant form of the osteopontin protein.
Transplantation into the younger animals caused HSCs to behave in a younger, more vital manner, the researchers said. This meant smaller numbers of HSCs with greater potential for forming different blood cells, which included larger populations of B and T cells and decreased production of myeloid cells.
The researchers also saw aged HSCs treated with recombinant osteopontin regain their youthful characteristics and capacity to form different blood cell types. Also observed was diminished signaling of Cdc42, a protein previously shown to cause aging in HSCs.
Osteopontin levels are not only low in the bone marrow niche but also in the blood upon aging. As a follow-up to the current study, the researchers are investigating the possibility of using osteopontin replacement therapy in mice to counter the influence of an aging niche directly in the animals. ![]()
MSC product granted fast track designation
The US Food and Drug Administration (FDA) has granted fast track designation to a mesenchymal stem cell (MSC) product, MSC-100-IV, as a treatment for children with steroid-refractory acute graft-vs-host disease (aGVHD).
MSC-100-IV consists of human MSCs derived from donor bone marrow and expanded in culture.
Fast track designation has the potential to shorten the time to FDA approval for MSC-100-IV through priority review, which reduces the FDA review process from 10 months to 6 months.
The designation also allows for a rolling review process, whereby completed sections of the Biologics License Application can be submitted for FDA review as they become available, instead of waiting for all sections to be completed.
In addition, fast track designation provides product developers with opportunities for more frequent meetings and written communications with the FDA.
MSC-100-IV is being developed by Mesoblast Limited in partnership with Mallinckrodt Pharmaceuticals.
Trial results
The application for fast track designation for MSC-100-IV was supported by a trial of 241 pediatric patients with steroid-refractory aGVHD. Results from this trial were presented at the 2016 BMT Tandem Meetings.
Patients initially received 2 million MSCs/kg twice a week for 4 weeks, at least 3 days apart. If they achieved a partial or mixed response (improvement in one organ with deterioration in another) at the day-28 assessment, patients then received 2 million MSCs/kg once a week for 4 weeks.
The patients received a total of 2434 infusions—a median of 11 (range, 1-24)—and had a median treatment duration of 46 days (range, 1-186).
Fifty-seven percent of patients (n=138) had at least 1 serious adverse event. About 5% (n=11) were considered treatment-related, and 1.7% (n=4) led to study discontinuation. There was 1 infusion reaction.
The overall response rate at day 28 was 65%, and the complete response rate was 14%. Responses were observed for all aGVHD grades and did not differ by baseline organ involvement.
Day 100 survival was significantly better in children who achieved a response at day 28—82%, compared to 39% for non-responders (P<0.0001).
In November 2016, Mesoblast reported success in an ongoing, phase 3 registration trial of MSC-100-IV in 60 children with steroid-refractory aGVHD.
The company said the trial was successful in a pre-specified interim futility analysis using the primary endpoint of day-28 overall response. Enrollment in this trial is expected to be complete in mid-2017. ![]()
The US Food and Drug Administration (FDA) has granted fast track designation to a mesenchymal stem cell (MSC) product, MSC-100-IV, as a treatment for children with steroid-refractory acute graft-vs-host disease (aGVHD).
MSC-100-IV consists of human MSCs derived from donor bone marrow and expanded in culture.
Fast track designation has the potential to shorten the time to FDA approval for MSC-100-IV through priority review, which reduces the FDA review process from 10 months to 6 months.
The designation also allows for a rolling review process, whereby completed sections of the Biologics License Application can be submitted for FDA review as they become available, instead of waiting for all sections to be completed.
In addition, fast track designation provides product developers with opportunities for more frequent meetings and written communications with the FDA.
MSC-100-IV is being developed by Mesoblast Limited in partnership with Mallinckrodt Pharmaceuticals.
Trial results
The application for fast track designation for MSC-100-IV was supported by a trial of 241 pediatric patients with steroid-refractory aGVHD. Results from this trial were presented at the 2016 BMT Tandem Meetings.
Patients initially received 2 million MSCs/kg twice a week for 4 weeks, at least 3 days apart. If they achieved a partial or mixed response (improvement in one organ with deterioration in another) at the day-28 assessment, patients then received 2 million MSCs/kg once a week for 4 weeks.
The patients received a total of 2434 infusions—a median of 11 (range, 1-24)—and had a median treatment duration of 46 days (range, 1-186).
Fifty-seven percent of patients (n=138) had at least 1 serious adverse event. About 5% (n=11) were considered treatment-related, and 1.7% (n=4) led to study discontinuation. There was 1 infusion reaction.
The overall response rate at day 28 was 65%, and the complete response rate was 14%. Responses were observed for all aGVHD grades and did not differ by baseline organ involvement.
Day 100 survival was significantly better in children who achieved a response at day 28—82%, compared to 39% for non-responders (P<0.0001).
In November 2016, Mesoblast reported success in an ongoing, phase 3 registration trial of MSC-100-IV in 60 children with steroid-refractory aGVHD.
The company said the trial was successful in a pre-specified interim futility analysis using the primary endpoint of day-28 overall response. Enrollment in this trial is expected to be complete in mid-2017. ![]()
The US Food and Drug Administration (FDA) has granted fast track designation to a mesenchymal stem cell (MSC) product, MSC-100-IV, as a treatment for children with steroid-refractory acute graft-vs-host disease (aGVHD).
MSC-100-IV consists of human MSCs derived from donor bone marrow and expanded in culture.
Fast track designation has the potential to shorten the time to FDA approval for MSC-100-IV through priority review, which reduces the FDA review process from 10 months to 6 months.
The designation also allows for a rolling review process, whereby completed sections of the Biologics License Application can be submitted for FDA review as they become available, instead of waiting for all sections to be completed.
In addition, fast track designation provides product developers with opportunities for more frequent meetings and written communications with the FDA.
MSC-100-IV is being developed by Mesoblast Limited in partnership with Mallinckrodt Pharmaceuticals.
Trial results
The application for fast track designation for MSC-100-IV was supported by a trial of 241 pediatric patients with steroid-refractory aGVHD. Results from this trial were presented at the 2016 BMT Tandem Meetings.
Patients initially received 2 million MSCs/kg twice a week for 4 weeks, at least 3 days apart. If they achieved a partial or mixed response (improvement in one organ with deterioration in another) at the day-28 assessment, patients then received 2 million MSCs/kg once a week for 4 weeks.
The patients received a total of 2434 infusions—a median of 11 (range, 1-24)—and had a median treatment duration of 46 days (range, 1-186).
Fifty-seven percent of patients (n=138) had at least 1 serious adverse event. About 5% (n=11) were considered treatment-related, and 1.7% (n=4) led to study discontinuation. There was 1 infusion reaction.
The overall response rate at day 28 was 65%, and the complete response rate was 14%. Responses were observed for all aGVHD grades and did not differ by baseline organ involvement.
Day 100 survival was significantly better in children who achieved a response at day 28—82%, compared to 39% for non-responders (P<0.0001).
In November 2016, Mesoblast reported success in an ongoing, phase 3 registration trial of MSC-100-IV in 60 children with steroid-refractory aGVHD.
The company said the trial was successful in a pre-specified interim futility analysis using the primary endpoint of day-28 overall response. Enrollment in this trial is expected to be complete in mid-2017. ![]()
Survey: Patients largely unaware of docs’ industry ties
A survey of nearly 2000 people suggests many Americans may not know if their physician receives industry payments.
A majority of the individuals surveyed were treated by a doctor who received some form of industry payment in the last year, but few of the patients were aware of these payments.
In fact, more than half of the patients did not know that accepting industry payments is something physicians may do.
“The findings suggest that although physicians who accept industry payments are in the minority, they are caring for a very substantial portion of America’s adult patient population,” said Genevieve Pham-Kanter, PhD, of Drexel University’s Dornsife School of Public Health in Philadelphia, Pennsylvania.
She and her colleagues reported these findings in the Journal of General Internal Medicine.
Since 2013, the Sunshine Act, part of the Patient Protection and Affordable Care Act, has required pharmaceutical and medical device manufacturers to report gifts and payments they make to healthcare providers. This information is publicly available on the Centers for Medicare and Medicaid Services’ Open Payments website.
Dr Pham-Kanter and her colleagues conducted their survey shortly before the first release of the Open Payments data in September 2014. However, payment data were already publicly available in certain states, nationwide via the Pro Publica website, and through disclosures made by pharmaceutical and medical device firms themselves (who had been required to release payment information as part of legal settlements or did so voluntarily).
Survey results
The researchers conducted their online survey in 3542 adults. Respondents were asked whether they were aware of industry payments and to name the physicians they had seen most frequently in the previous year.
Physician names were then linked to the Open Payment data to ascertain how often patients saw doctors who accepted industry payments.
There were 1987 respondents who could be matched to a specific physician. Sixty-five percent of these individuals had visited a physician who accepted an industry payment in the last 12 months, but only 5% of the respondents actually knew if their doctors received industry payments.
Forty-five percent of respondents said they knew about the practice of doctors receiving industry payments, and 12% said information about such payments was publicly available.
“These findings tell us that if you thought that your doctor was not receiving any money from industry, you’re most likely mistaken,” Dr Pham-Kanter said. “Patients should be aware of the incentives that their physicians face that may lead them to not always act in their patients’ best interest.”
In Open Payments, all physicians averaged $193 in yearly payments and gifts. But when measuring only the doctors visited by participants in the survey, the median payment amount over the last year was $510, more than 2.5 times the US average.
“We may be lulled into thinking this isn’t a big deal because the average payment amount across all doctors is low,” Dr Pham-Kanter said. “But that obscures the fact that most people are seeing doctors who receive the largest payments.”
“Drug companies have long known that even small gifts to physicians can be influential,” added study author Michelle Mello, JD, PhD, of Stanford University School of Medicine and Stanford Law School in California. “And research validates the notion that they tend to induce feelings of reciprocity.” ![]()
A survey of nearly 2000 people suggests many Americans may not know if their physician receives industry payments.
A majority of the individuals surveyed were treated by a doctor who received some form of industry payment in the last year, but few of the patients were aware of these payments.
In fact, more than half of the patients did not know that accepting industry payments is something physicians may do.
“The findings suggest that although physicians who accept industry payments are in the minority, they are caring for a very substantial portion of America’s adult patient population,” said Genevieve Pham-Kanter, PhD, of Drexel University’s Dornsife School of Public Health in Philadelphia, Pennsylvania.
She and her colleagues reported these findings in the Journal of General Internal Medicine.
Since 2013, the Sunshine Act, part of the Patient Protection and Affordable Care Act, has required pharmaceutical and medical device manufacturers to report gifts and payments they make to healthcare providers. This information is publicly available on the Centers for Medicare and Medicaid Services’ Open Payments website.
Dr Pham-Kanter and her colleagues conducted their survey shortly before the first release of the Open Payments data in September 2014. However, payment data were already publicly available in certain states, nationwide via the Pro Publica website, and through disclosures made by pharmaceutical and medical device firms themselves (who had been required to release payment information as part of legal settlements or did so voluntarily).
Survey results
The researchers conducted their online survey in 3542 adults. Respondents were asked whether they were aware of industry payments and to name the physicians they had seen most frequently in the previous year.
Physician names were then linked to the Open Payment data to ascertain how often patients saw doctors who accepted industry payments.
There were 1987 respondents who could be matched to a specific physician. Sixty-five percent of these individuals had visited a physician who accepted an industry payment in the last 12 months, but only 5% of the respondents actually knew if their doctors received industry payments.
Forty-five percent of respondents said they knew about the practice of doctors receiving industry payments, and 12% said information about such payments was publicly available.
“These findings tell us that if you thought that your doctor was not receiving any money from industry, you’re most likely mistaken,” Dr Pham-Kanter said. “Patients should be aware of the incentives that their physicians face that may lead them to not always act in their patients’ best interest.”
In Open Payments, all physicians averaged $193 in yearly payments and gifts. But when measuring only the doctors visited by participants in the survey, the median payment amount over the last year was $510, more than 2.5 times the US average.
“We may be lulled into thinking this isn’t a big deal because the average payment amount across all doctors is low,” Dr Pham-Kanter said. “But that obscures the fact that most people are seeing doctors who receive the largest payments.”
“Drug companies have long known that even small gifts to physicians can be influential,” added study author Michelle Mello, JD, PhD, of Stanford University School of Medicine and Stanford Law School in California. “And research validates the notion that they tend to induce feelings of reciprocity.” ![]()
A survey of nearly 2000 people suggests many Americans may not know if their physician receives industry payments.
A majority of the individuals surveyed were treated by a doctor who received some form of industry payment in the last year, but few of the patients were aware of these payments.
In fact, more than half of the patients did not know that accepting industry payments is something physicians may do.
“The findings suggest that although physicians who accept industry payments are in the minority, they are caring for a very substantial portion of America’s adult patient population,” said Genevieve Pham-Kanter, PhD, of Drexel University’s Dornsife School of Public Health in Philadelphia, Pennsylvania.
She and her colleagues reported these findings in the Journal of General Internal Medicine.
Since 2013, the Sunshine Act, part of the Patient Protection and Affordable Care Act, has required pharmaceutical and medical device manufacturers to report gifts and payments they make to healthcare providers. This information is publicly available on the Centers for Medicare and Medicaid Services’ Open Payments website.
Dr Pham-Kanter and her colleagues conducted their survey shortly before the first release of the Open Payments data in September 2014. However, payment data were already publicly available in certain states, nationwide via the Pro Publica website, and through disclosures made by pharmaceutical and medical device firms themselves (who had been required to release payment information as part of legal settlements or did so voluntarily).
Survey results
The researchers conducted their online survey in 3542 adults. Respondents were asked whether they were aware of industry payments and to name the physicians they had seen most frequently in the previous year.
Physician names were then linked to the Open Payment data to ascertain how often patients saw doctors who accepted industry payments.
There were 1987 respondents who could be matched to a specific physician. Sixty-five percent of these individuals had visited a physician who accepted an industry payment in the last 12 months, but only 5% of the respondents actually knew if their doctors received industry payments.
Forty-five percent of respondents said they knew about the practice of doctors receiving industry payments, and 12% said information about such payments was publicly available.
“These findings tell us that if you thought that your doctor was not receiving any money from industry, you’re most likely mistaken,” Dr Pham-Kanter said. “Patients should be aware of the incentives that their physicians face that may lead them to not always act in their patients’ best interest.”
In Open Payments, all physicians averaged $193 in yearly payments and gifts. But when measuring only the doctors visited by participants in the survey, the median payment amount over the last year was $510, more than 2.5 times the US average.
“We may be lulled into thinking this isn’t a big deal because the average payment amount across all doctors is low,” Dr Pham-Kanter said. “But that obscures the fact that most people are seeing doctors who receive the largest payments.”
“Drug companies have long known that even small gifts to physicians can be influential,” added study author Michelle Mello, JD, PhD, of Stanford University School of Medicine and Stanford Law School in California. “And research validates the notion that they tend to induce feelings of reciprocity.” ![]()
Genetic variants linked to HSCT outcomes in ALL
ORLANDO, FL—Results of a genome-wide association study suggest that several genetic variants are associated with outcomes of allogeneic hematopoietic stem cell transplant (HSCT) in patients with acute lymphoblastic leukemia (ALL).
Investigators identified several single-nucleotide polymorphisms (SNPs) in ALL patients and their unrelated donors that were associated with disease-related death or progression-free survival (PFS) within 1 year of HSCT.
“We believe that these findings will lead to a better understanding of the biology of this disease,” said investigator Theresa Hahn, PhD, of Roswell Park Cancer Institute in Buffalo, New York.
“Additionally, we expect that this work will eventually help clinical teams to identify unrelated donors with genotypes that yield better survival in transplant patients and enhance the chances for successful blood and marrow transplants.”
Dr Hahn presented this work as a “Best Abstract” at the 2017 BMT Tandem Meetings (abstract 1).
For this study, she and her colleagues analyzed data on patients treated at more than 150 US transplant centers between 2000 and 2011. The investigators evaluated data on more than 3000 patients with acute leukemias or myelodysplastic syndromes, but Dr Hahn only presented findings in the ALL patients and their donors.
The patients and donors were divided into 2 cohorts. Cohort 1 included 483 ALL patients who underwent HSCT from 2000 to 2008 and 466 unrelated donors who were a 10/10 HLA match for the patients.
Cohort 2 included 94 ALL patients who received a transplant from a 10/10 HLA-matched donor between 2009 and 2011 or from an 8/8 HLA-matched donor between 2000 and 2011. There were 92 donors in this cohort.
The investigators sequenced blood samples from the recipients and donors to identify SNPs. The SNPs were then measured for association with disease-related death and PFS using Cox proportional hazards models adjusted for recipient age, disease status at HSCT (early, intermediate, or advanced), graft source (blood or marrow), and year of transplant.
SNPs in donors
The top 2 SNPs in donors that were associated with a significant increase in disease-related death were:
- rs79503405 in LRP2 on chromosome 2.
- rs77618918 in ASIC2 on chromosome 17.
Dr Hahn noted that rs79503405 is in complete linkage disequilibrium (r2=1.0) with a genotyped missense variant (rs17848149) and a synonymous coding variant (rs35114151) in LRP2.
She also pointed out that the other top SNP (rs77618918) associated with disease-related death is not in linkage disequilibrium with other SNPs of functional importance, so the significance of this SNP is unknown.
There were no SNPs in donors that were significantly associated with PFS.
SNPs in recipients
In HSCT recipients, there were 3 linked variants in NRG1 on chromosome 8 (rs79853417, rs6990973, and rs145488394) that were significantly associated with disease-related death.
Another SNP (rs60640657) on chromosome 2 (CTNNA3/LOC101928961/LRRTM3) was also significantly associated with ALL-related death.
In addition, Dr Hahn and her colleagues found that 1 region in recipient genomes contains multiple variants (rs113263921 and others) associated with PFS. The SNPs are located on chromosome 3 in MLH1 and TRANK1.
“The donor and recipient genetic variants contributed independently to death due to ALL,” Dr Hahn said in closing. “Genetic variants for PFS do not overlap with death due to ALL, and this is probably due to the inclusion of both non-fatal disease progression as well as transplant-related mortality in the definition of PFS.”
“Constitutional genetic variants in recipients and donors increase the risk of death due to ALL, and they warrant further study into the impact of these genes on disease and transplant-related biology.” ![]()
ORLANDO, FL—Results of a genome-wide association study suggest that several genetic variants are associated with outcomes of allogeneic hematopoietic stem cell transplant (HSCT) in patients with acute lymphoblastic leukemia (ALL).
Investigators identified several single-nucleotide polymorphisms (SNPs) in ALL patients and their unrelated donors that were associated with disease-related death or progression-free survival (PFS) within 1 year of HSCT.
“We believe that these findings will lead to a better understanding of the biology of this disease,” said investigator Theresa Hahn, PhD, of Roswell Park Cancer Institute in Buffalo, New York.
“Additionally, we expect that this work will eventually help clinical teams to identify unrelated donors with genotypes that yield better survival in transplant patients and enhance the chances for successful blood and marrow transplants.”
Dr Hahn presented this work as a “Best Abstract” at the 2017 BMT Tandem Meetings (abstract 1).
For this study, she and her colleagues analyzed data on patients treated at more than 150 US transplant centers between 2000 and 2011. The investigators evaluated data on more than 3000 patients with acute leukemias or myelodysplastic syndromes, but Dr Hahn only presented findings in the ALL patients and their donors.
The patients and donors were divided into 2 cohorts. Cohort 1 included 483 ALL patients who underwent HSCT from 2000 to 2008 and 466 unrelated donors who were a 10/10 HLA match for the patients.
Cohort 2 included 94 ALL patients who received a transplant from a 10/10 HLA-matched donor between 2009 and 2011 or from an 8/8 HLA-matched donor between 2000 and 2011. There were 92 donors in this cohort.
The investigators sequenced blood samples from the recipients and donors to identify SNPs. The SNPs were then measured for association with disease-related death and PFS using Cox proportional hazards models adjusted for recipient age, disease status at HSCT (early, intermediate, or advanced), graft source (blood or marrow), and year of transplant.
SNPs in donors
The top 2 SNPs in donors that were associated with a significant increase in disease-related death were:
- rs79503405 in LRP2 on chromosome 2.
- rs77618918 in ASIC2 on chromosome 17.
Dr Hahn noted that rs79503405 is in complete linkage disequilibrium (r2=1.0) with a genotyped missense variant (rs17848149) and a synonymous coding variant (rs35114151) in LRP2.
She also pointed out that the other top SNP (rs77618918) associated with disease-related death is not in linkage disequilibrium with other SNPs of functional importance, so the significance of this SNP is unknown.
There were no SNPs in donors that were significantly associated with PFS.
SNPs in recipients
In HSCT recipients, there were 3 linked variants in NRG1 on chromosome 8 (rs79853417, rs6990973, and rs145488394) that were significantly associated with disease-related death.
Another SNP (rs60640657) on chromosome 2 (CTNNA3/LOC101928961/LRRTM3) was also significantly associated with ALL-related death.
In addition, Dr Hahn and her colleagues found that 1 region in recipient genomes contains multiple variants (rs113263921 and others) associated with PFS. The SNPs are located on chromosome 3 in MLH1 and TRANK1.
“The donor and recipient genetic variants contributed independently to death due to ALL,” Dr Hahn said in closing. “Genetic variants for PFS do not overlap with death due to ALL, and this is probably due to the inclusion of both non-fatal disease progression as well as transplant-related mortality in the definition of PFS.”
“Constitutional genetic variants in recipients and donors increase the risk of death due to ALL, and they warrant further study into the impact of these genes on disease and transplant-related biology.” ![]()
ORLANDO, FL—Results of a genome-wide association study suggest that several genetic variants are associated with outcomes of allogeneic hematopoietic stem cell transplant (HSCT) in patients with acute lymphoblastic leukemia (ALL).
Investigators identified several single-nucleotide polymorphisms (SNPs) in ALL patients and their unrelated donors that were associated with disease-related death or progression-free survival (PFS) within 1 year of HSCT.
“We believe that these findings will lead to a better understanding of the biology of this disease,” said investigator Theresa Hahn, PhD, of Roswell Park Cancer Institute in Buffalo, New York.
“Additionally, we expect that this work will eventually help clinical teams to identify unrelated donors with genotypes that yield better survival in transplant patients and enhance the chances for successful blood and marrow transplants.”
Dr Hahn presented this work as a “Best Abstract” at the 2017 BMT Tandem Meetings (abstract 1).
For this study, she and her colleagues analyzed data on patients treated at more than 150 US transplant centers between 2000 and 2011. The investigators evaluated data on more than 3000 patients with acute leukemias or myelodysplastic syndromes, but Dr Hahn only presented findings in the ALL patients and their donors.
The patients and donors were divided into 2 cohorts. Cohort 1 included 483 ALL patients who underwent HSCT from 2000 to 2008 and 466 unrelated donors who were a 10/10 HLA match for the patients.
Cohort 2 included 94 ALL patients who received a transplant from a 10/10 HLA-matched donor between 2009 and 2011 or from an 8/8 HLA-matched donor between 2000 and 2011. There were 92 donors in this cohort.
The investigators sequenced blood samples from the recipients and donors to identify SNPs. The SNPs were then measured for association with disease-related death and PFS using Cox proportional hazards models adjusted for recipient age, disease status at HSCT (early, intermediate, or advanced), graft source (blood or marrow), and year of transplant.
SNPs in donors
The top 2 SNPs in donors that were associated with a significant increase in disease-related death were:
- rs79503405 in LRP2 on chromosome 2.
- rs77618918 in ASIC2 on chromosome 17.
Dr Hahn noted that rs79503405 is in complete linkage disequilibrium (r2=1.0) with a genotyped missense variant (rs17848149) and a synonymous coding variant (rs35114151) in LRP2.
She also pointed out that the other top SNP (rs77618918) associated with disease-related death is not in linkage disequilibrium with other SNPs of functional importance, so the significance of this SNP is unknown.
There were no SNPs in donors that were significantly associated with PFS.
SNPs in recipients
In HSCT recipients, there were 3 linked variants in NRG1 on chromosome 8 (rs79853417, rs6990973, and rs145488394) that were significantly associated with disease-related death.
Another SNP (rs60640657) on chromosome 2 (CTNNA3/LOC101928961/LRRTM3) was also significantly associated with ALL-related death.
In addition, Dr Hahn and her colleagues found that 1 region in recipient genomes contains multiple variants (rs113263921 and others) associated with PFS. The SNPs are located on chromosome 3 in MLH1 and TRANK1.
“The donor and recipient genetic variants contributed independently to death due to ALL,” Dr Hahn said in closing. “Genetic variants for PFS do not overlap with death due to ALL, and this is probably due to the inclusion of both non-fatal disease progression as well as transplant-related mortality in the definition of PFS.”
“Constitutional genetic variants in recipients and donors increase the risk of death due to ALL, and they warrant further study into the impact of these genes on disease and transplant-related biology.” ![]()
Combo prolongs OS in relapsed/refractory MM
NEW DEHLI—A 2-drug combination previously shown to prolong progression-free survival (PFS) in patients with relapsed/refractory multiple myeloma (MM) can prolong overall survival (OS) as well, according to researchers.
Updated results of the phase 3 ENDEAVOR trial showed that patients who received treatment with carfilzomib and dexamethasone had a 7.6-month benefit in median OS when compared to patients who received bortezomib and dexamethasone.
Previous results from this trial showed a 9.3-month benefit in median PFS with carfilzomib and dexamethasone.
“Based on these data, we now know that [carfilzomib] not only significantly extended progression-free survival compared to [bortezomib] but also overall survival, making it a clinically meaningful advance in the treatment of relapsed or refractory multiple myeloma,” said Meletios A. Dimopoulos, MD, of the University of Athens in Greece.
Dr Dimopoulos presented OS results from ENDEAVOR at the 16th International Myeloma Workshop. The trial was funded by Onyx Pharmaceuticals, Inc., a subsidiary of Amgen.
ENDEAVOR included 929 MM patients who had received 1 to 3 prior treatment regimens. The patients were randomized to receive carfilzomib and low-dose dexamethasone (n=464) or bortezomib and low-dose dexamethasone (n=465) until disease progression.
Baseline characteristics were similar between the treatment arms.
Detailed patient and treatment characteristics, as well as response and PFS data, have been previously reported.
OS and safety
The median OS was 47.6 months in the carfilzomib arm and 40.0 months in the bortezomib arm. All-cause mortality was significantly lower with the carfilzomib combination than the bortezomib combination (hazard ratio [HR]=0.791, 1-sided P=0.0100).
Researchers said there was an OS benefit with the carfilzomib combination whether or not patients received prior treatment with bortezomib and regardless of patients’ age, ECOG performance status at baseline, cytogenetic risk group, or the number of previous therapies they received.
The HR was 0.75 (carfilzomib vs bortezomib) for patients with no prior bortezomib and 0.84 for patients who received prior bortezomib. The HR was 0.85 for patients younger than 65, 0.71 for those ages 65 to 74, and 0.84 for patients age 75 and older.
The HR was 0.81 for patients with an ECOG status of 0, 0.80 for those with a status of 1, and 0.50 for those with a status of 2. The HR was 0.83 for patients with high-risk cytogenetics and 0.85 for those with standard-risk cytogenetics.
The HR was 0.83 for patients with 1 prior line of therapy and 0.76 for those with 2 to 3 prior lines of therapy.
The researchers said safety results in this analysis were comparable with previously reported results. The incidence of grade 3 or higher adverse events was 81.4% in the carfilzomib arm and 71.1% in the bortezomib arm.
The most common adverse events of any grade (in the carfilzomib and bortezomib arms, respectively) were anemia (42.5% and 28.3%), diarrhea (36.3% and 40.6%), pyrexia (32.4% and 15.4%), dyspnea (32.2% and 13.6%), fatigue (32.2% and 30.7%), and hypertension (32.2% and 9.9%). ![]()
NEW DEHLI—A 2-drug combination previously shown to prolong progression-free survival (PFS) in patients with relapsed/refractory multiple myeloma (MM) can prolong overall survival (OS) as well, according to researchers.
Updated results of the phase 3 ENDEAVOR trial showed that patients who received treatment with carfilzomib and dexamethasone had a 7.6-month benefit in median OS when compared to patients who received bortezomib and dexamethasone.
Previous results from this trial showed a 9.3-month benefit in median PFS with carfilzomib and dexamethasone.
“Based on these data, we now know that [carfilzomib] not only significantly extended progression-free survival compared to [bortezomib] but also overall survival, making it a clinically meaningful advance in the treatment of relapsed or refractory multiple myeloma,” said Meletios A. Dimopoulos, MD, of the University of Athens in Greece.
Dr Dimopoulos presented OS results from ENDEAVOR at the 16th International Myeloma Workshop. The trial was funded by Onyx Pharmaceuticals, Inc., a subsidiary of Amgen.
ENDEAVOR included 929 MM patients who had received 1 to 3 prior treatment regimens. The patients were randomized to receive carfilzomib and low-dose dexamethasone (n=464) or bortezomib and low-dose dexamethasone (n=465) until disease progression.
Baseline characteristics were similar between the treatment arms.
Detailed patient and treatment characteristics, as well as response and PFS data, have been previously reported.
OS and safety
The median OS was 47.6 months in the carfilzomib arm and 40.0 months in the bortezomib arm. All-cause mortality was significantly lower with the carfilzomib combination than the bortezomib combination (hazard ratio [HR]=0.791, 1-sided P=0.0100).
Researchers said there was an OS benefit with the carfilzomib combination whether or not patients received prior treatment with bortezomib and regardless of patients’ age, ECOG performance status at baseline, cytogenetic risk group, or the number of previous therapies they received.
The HR was 0.75 (carfilzomib vs bortezomib) for patients with no prior bortezomib and 0.84 for patients who received prior bortezomib. The HR was 0.85 for patients younger than 65, 0.71 for those ages 65 to 74, and 0.84 for patients age 75 and older.
The HR was 0.81 for patients with an ECOG status of 0, 0.80 for those with a status of 1, and 0.50 for those with a status of 2. The HR was 0.83 for patients with high-risk cytogenetics and 0.85 for those with standard-risk cytogenetics.
The HR was 0.83 for patients with 1 prior line of therapy and 0.76 for those with 2 to 3 prior lines of therapy.
The researchers said safety results in this analysis were comparable with previously reported results. The incidence of grade 3 or higher adverse events was 81.4% in the carfilzomib arm and 71.1% in the bortezomib arm.
The most common adverse events of any grade (in the carfilzomib and bortezomib arms, respectively) were anemia (42.5% and 28.3%), diarrhea (36.3% and 40.6%), pyrexia (32.4% and 15.4%), dyspnea (32.2% and 13.6%), fatigue (32.2% and 30.7%), and hypertension (32.2% and 9.9%). ![]()
NEW DEHLI—A 2-drug combination previously shown to prolong progression-free survival (PFS) in patients with relapsed/refractory multiple myeloma (MM) can prolong overall survival (OS) as well, according to researchers.
Updated results of the phase 3 ENDEAVOR trial showed that patients who received treatment with carfilzomib and dexamethasone had a 7.6-month benefit in median OS when compared to patients who received bortezomib and dexamethasone.
Previous results from this trial showed a 9.3-month benefit in median PFS with carfilzomib and dexamethasone.
“Based on these data, we now know that [carfilzomib] not only significantly extended progression-free survival compared to [bortezomib] but also overall survival, making it a clinically meaningful advance in the treatment of relapsed or refractory multiple myeloma,” said Meletios A. Dimopoulos, MD, of the University of Athens in Greece.
Dr Dimopoulos presented OS results from ENDEAVOR at the 16th International Myeloma Workshop. The trial was funded by Onyx Pharmaceuticals, Inc., a subsidiary of Amgen.
ENDEAVOR included 929 MM patients who had received 1 to 3 prior treatment regimens. The patients were randomized to receive carfilzomib and low-dose dexamethasone (n=464) or bortezomib and low-dose dexamethasone (n=465) until disease progression.
Baseline characteristics were similar between the treatment arms.
Detailed patient and treatment characteristics, as well as response and PFS data, have been previously reported.
OS and safety
The median OS was 47.6 months in the carfilzomib arm and 40.0 months in the bortezomib arm. All-cause mortality was significantly lower with the carfilzomib combination than the bortezomib combination (hazard ratio [HR]=0.791, 1-sided P=0.0100).
Researchers said there was an OS benefit with the carfilzomib combination whether or not patients received prior treatment with bortezomib and regardless of patients’ age, ECOG performance status at baseline, cytogenetic risk group, or the number of previous therapies they received.
The HR was 0.75 (carfilzomib vs bortezomib) for patients with no prior bortezomib and 0.84 for patients who received prior bortezomib. The HR was 0.85 for patients younger than 65, 0.71 for those ages 65 to 74, and 0.84 for patients age 75 and older.
The HR was 0.81 for patients with an ECOG status of 0, 0.80 for those with a status of 1, and 0.50 for those with a status of 2. The HR was 0.83 for patients with high-risk cytogenetics and 0.85 for those with standard-risk cytogenetics.
The HR was 0.83 for patients with 1 prior line of therapy and 0.76 for those with 2 to 3 prior lines of therapy.
The researchers said safety results in this analysis were comparable with previously reported results. The incidence of grade 3 or higher adverse events was 81.4% in the carfilzomib arm and 71.1% in the bortezomib arm.
The most common adverse events of any grade (in the carfilzomib and bortezomib arms, respectively) were anemia (42.5% and 28.3%), diarrhea (36.3% and 40.6%), pyrexia (32.4% and 15.4%), dyspnea (32.2% and 13.6%), fatigue (32.2% and 30.7%), and hypertension (32.2% and 9.9%). ![]()
Chlormethine gel approved to treat mycosis fungoides
The European Commission has granted marketing authorization for chlormethine gel (Ledaga®) as a treatment for adults with mycosis fungoides (MF), but the product is not expected to be available until next year.
Ledaga is a hybrid medicine of Caryolysine, which has been approved for use in the European Union since 1946.
Hybrid medicines have a different strength, are administered differently, or have a different indication from the reference medicine.
Ledaga contains the same active substance as Caryolysine—chlormethine, a bifunctional alkylating agent that inhibits rapidly proliferating cells—but Ledaga is a gel intended for cutaneous use.
Actelion Pharmaceuticals Ltd, the company developing Ledaga, has agreed to fulfill a list of post-approval measures for the product proposed by the European Medicines Agency’s Committee for Medicinal Products for Human Use.
Subject to fulfilling the agreed commitments and achieving market access in various countries, a potential first European launch of Ledaga is not expected before January 2018. When it is launched, Ledaga will be available as a 160 μg/g gel.
Phase 2 study
The authorization of hybrid medicines depends partly on the results of tests on the reference medicine and partly on new data from clinical trials.
The marketing authorization for Ledaga is based, in part, on results of a multicenter, randomized, observer-blinded, active-controlled study of patients with stage I and IIA MF. Results from this phase 2 study were published in JAMA Dermatology.
The study enrolled 260 MF patients who were randomized 1:1 to receive topical treatment with 0.02% chlormethine gel (Ledaga) or compounded control—0.02% chlormethine compounded in Aquaphor® ointment—once daily for up to 12 months.
A response was defined as at least a 50% improvement in the baseline Composite Assessment of Index Lesion Severity score.
In the intent-to-treat population, 59% (76/130) of patients who received Ledaga achieved a clinical response, compared to 48% (62/130) of patients treated with the compounded control. The rate of complete response was 14% (n=18) and 12% (n=15), respectively.
Patients who were treated for at least 6 months were included in the efficacy-evaluable population. In this population, 77% (69/90) of patients who received Ledaga achieved a clinical response, compared to 59% (56/95) of patients treated with the compounded control. The rate of complete response was 19% (n=17) and 15% (n=14), respectively.
Reductions in mean lesion severity were seen as early as 4 weeks into the study, with further reductions observed with continuing therapy. The time to first confirmed response favored Ledaga.
The most frequent adverse reactions reported with Ledaga were skin-related—dermatitis (55%; eg, skin irritation, erythema, rash, urticaria, skin-burning sensation, skin pain), pruritus (20%), skin infections (12%), skin ulceration and blistering (6%), and skin hyperpigmentation (6%).
No systemic absorption of chlormethine was detected with treatment. ![]()
The European Commission has granted marketing authorization for chlormethine gel (Ledaga®) as a treatment for adults with mycosis fungoides (MF), but the product is not expected to be available until next year.
Ledaga is a hybrid medicine of Caryolysine, which has been approved for use in the European Union since 1946.
Hybrid medicines have a different strength, are administered differently, or have a different indication from the reference medicine.
Ledaga contains the same active substance as Caryolysine—chlormethine, a bifunctional alkylating agent that inhibits rapidly proliferating cells—but Ledaga is a gel intended for cutaneous use.
Actelion Pharmaceuticals Ltd, the company developing Ledaga, has agreed to fulfill a list of post-approval measures for the product proposed by the European Medicines Agency’s Committee for Medicinal Products for Human Use.
Subject to fulfilling the agreed commitments and achieving market access in various countries, a potential first European launch of Ledaga is not expected before January 2018. When it is launched, Ledaga will be available as a 160 μg/g gel.
Phase 2 study
The authorization of hybrid medicines depends partly on the results of tests on the reference medicine and partly on new data from clinical trials.
The marketing authorization for Ledaga is based, in part, on results of a multicenter, randomized, observer-blinded, active-controlled study of patients with stage I and IIA MF. Results from this phase 2 study were published in JAMA Dermatology.
The study enrolled 260 MF patients who were randomized 1:1 to receive topical treatment with 0.02% chlormethine gel (Ledaga) or compounded control—0.02% chlormethine compounded in Aquaphor® ointment—once daily for up to 12 months.
A response was defined as at least a 50% improvement in the baseline Composite Assessment of Index Lesion Severity score.
In the intent-to-treat population, 59% (76/130) of patients who received Ledaga achieved a clinical response, compared to 48% (62/130) of patients treated with the compounded control. The rate of complete response was 14% (n=18) and 12% (n=15), respectively.
Patients who were treated for at least 6 months were included in the efficacy-evaluable population. In this population, 77% (69/90) of patients who received Ledaga achieved a clinical response, compared to 59% (56/95) of patients treated with the compounded control. The rate of complete response was 19% (n=17) and 15% (n=14), respectively.
Reductions in mean lesion severity were seen as early as 4 weeks into the study, with further reductions observed with continuing therapy. The time to first confirmed response favored Ledaga.
The most frequent adverse reactions reported with Ledaga were skin-related—dermatitis (55%; eg, skin irritation, erythema, rash, urticaria, skin-burning sensation, skin pain), pruritus (20%), skin infections (12%), skin ulceration and blistering (6%), and skin hyperpigmentation (6%).
No systemic absorption of chlormethine was detected with treatment. ![]()
The European Commission has granted marketing authorization for chlormethine gel (Ledaga®) as a treatment for adults with mycosis fungoides (MF), but the product is not expected to be available until next year.
Ledaga is a hybrid medicine of Caryolysine, which has been approved for use in the European Union since 1946.
Hybrid medicines have a different strength, are administered differently, or have a different indication from the reference medicine.
Ledaga contains the same active substance as Caryolysine—chlormethine, a bifunctional alkylating agent that inhibits rapidly proliferating cells—but Ledaga is a gel intended for cutaneous use.
Actelion Pharmaceuticals Ltd, the company developing Ledaga, has agreed to fulfill a list of post-approval measures for the product proposed by the European Medicines Agency’s Committee for Medicinal Products for Human Use.
Subject to fulfilling the agreed commitments and achieving market access in various countries, a potential first European launch of Ledaga is not expected before January 2018. When it is launched, Ledaga will be available as a 160 μg/g gel.
Phase 2 study
The authorization of hybrid medicines depends partly on the results of tests on the reference medicine and partly on new data from clinical trials.
The marketing authorization for Ledaga is based, in part, on results of a multicenter, randomized, observer-blinded, active-controlled study of patients with stage I and IIA MF. Results from this phase 2 study were published in JAMA Dermatology.
The study enrolled 260 MF patients who were randomized 1:1 to receive topical treatment with 0.02% chlormethine gel (Ledaga) or compounded control—0.02% chlormethine compounded in Aquaphor® ointment—once daily for up to 12 months.
A response was defined as at least a 50% improvement in the baseline Composite Assessment of Index Lesion Severity score.
In the intent-to-treat population, 59% (76/130) of patients who received Ledaga achieved a clinical response, compared to 48% (62/130) of patients treated with the compounded control. The rate of complete response was 14% (n=18) and 12% (n=15), respectively.
Patients who were treated for at least 6 months were included in the efficacy-evaluable population. In this population, 77% (69/90) of patients who received Ledaga achieved a clinical response, compared to 59% (56/95) of patients treated with the compounded control. The rate of complete response was 19% (n=17) and 15% (n=14), respectively.
Reductions in mean lesion severity were seen as early as 4 weeks into the study, with further reductions observed with continuing therapy. The time to first confirmed response favored Ledaga.
The most frequent adverse reactions reported with Ledaga were skin-related—dermatitis (55%; eg, skin irritation, erythema, rash, urticaria, skin-burning sensation, skin pain), pruritus (20%), skin infections (12%), skin ulceration and blistering (6%), and skin hyperpigmentation (6%).
No systemic absorption of chlormethine was detected with treatment.
Study reveals higher rate of early death in kids with cancer
New research suggests that, in the US, early deaths from childhood cancer may be more common than clinical trials suggest.
Researchers found the rate of death within 1 month of diagnosis was higher among patients included in a large national database than among patients enrolled in phase 3 trials.
The data also indicated that early death is more likely in cancer patients under the age of 1 and those belonging to minority racial and ethnic groups.
Adam Green, MD, of the University of Colorado Anschutz Medical Campus in Aurora, and his colleagues conducted this research and reported the results in the Journal of Clinical Oncology.
The researchers analyzed data from the Surveillance, Epidemiology and End Results (SEER) database, which collects about 15% of all cancer outcomes across the US (representing a geographic and socioeconomic cross-section).
The team identified 36,337 patients with pediatric cancer (ages 0 to 19) diagnosed between 1992 and 2011. Of these patients, 555 (1.5%) died within 1 month of diagnosis.
Young age
Overall, the strongest predictor of early death was age below 1 year. The odds ratio (OR) was 4.36 for these patients (P<0.001), 0.75 for patients age 1 to 4, 0.78 for patients age 5 to 9, 1.00 (reference) for those age 10 to 14, and 1.69 for those age 15 to 19.
For hematologic malignancies, the adjusted OR (adjusted by poverty, unemployment, education, and year of diagnosis) was 4.32 for patients younger than 1 (P<0.001), 0.76 for patients age 1 to 4, 0.79 for patients age 5 to 9, 1.00 for those age 10 to 14, and 1.76 for those age 15 to 19 (P=0.002).
“In general, babies are just challenging, clinically, because they can’t tell you what they’re feeling,” Dr Green noted. “Parents and physicians have to pick the ones with cancer from the ones with a cold, without the patient being able to tell you about symptoms that could be diagnostic.”
“Babies tend to get aggressive cancers, it’s hard to tell when they’re getting sick, and some are even born with cancers that have already progressed. These factors combine to make very young age the strongest predictor of early death in our study.”
Race/ethnicity
Black race and Hispanic ethnicity also predicted early death. The OR was 1.48 for black race, 1.00 for white race (reference), and 1.09 for “other” races (P=0.102). The OR was 1.39 for Hispanic patients and 1.00 (reference) for non-Hispanic patients (P=0.007).
For hematologic malignancies, the adjusted OR was 1.68 for black patients (P=0.01) and 1.44 for patients of other, non-white races. The adjusted OR was 1.48 for Hispanic patients (P=0.009).
Dr Green said he hopes future studies will be able to determine the factors responsible for these disparities.
Higher death rates
Dr Green and his colleagues also found the rate of early death due to pediatric cancers is higher than reported in clinical trials, and this was true for all cancer subtypes assessed.
“Most of what we know about outcomes for cancer patients come from clinical trials, which have much more thorough reporting rules than cancer treated outside trials,” Dr Green said. “However, these kids in our study aren’t surviving long enough to join clinical trials.”
The researchers looked at a phase 3 trial (COG AAML0531) of pediatric patients with acute myeloid leukemia (AML) who were studied from August 2006 to June 2010. The early death rate in this trial was 1.6% (16/1022).
In contrast, the SEER database showed an early death rate for pediatric AML patients of 5.9% (15/256) during the same period as the trial and 6.2% (106/1698) for the period from 1992 to 2011. This is almost 4 times as high as the death rate in the trial.
The same effect was observed for acute lymphoblastic leukemia (ALL).
The early death rate for non-infant ALL was 0.7% (13/1790) in a trial (POG 9900) conducted from April 2000 to April 2005, 1.6% (30/1823) in the SEER data covering the same time period, and 1.3% (94/7353) in the SEER data from 1992 to 2011.
For infant ALL, the rates were 2.0% (3/149) in a trial (COG AALL0631) conducted from January 2008 to June 2014, 5.0% (2/40) in the SEER data during the trial period, and 5.4% (12/223) in the SEER data from 1992 to 2011.
“I had a hunch this was a bigger problem than we thought,” Dr Green said. “Now we see that is indeed the case.”
New research suggests that, in the US, early deaths from childhood cancer may be more common than clinical trials suggest.
Researchers found the rate of death within 1 month of diagnosis was higher among patients included in a large national database than among patients enrolled in phase 3 trials.
The data also indicated that early death is more likely in cancer patients under the age of 1 and those belonging to minority racial and ethnic groups.
Adam Green, MD, of the University of Colorado Anschutz Medical Campus in Aurora, and his colleagues conducted this research and reported the results in the Journal of Clinical Oncology.
The researchers analyzed data from the Surveillance, Epidemiology and End Results (SEER) database, which collects about 15% of all cancer outcomes across the US (representing a geographic and socioeconomic cross-section).
The team identified 36,337 patients with pediatric cancer (ages 0 to 19) diagnosed between 1992 and 2011. Of these patients, 555 (1.5%) died within 1 month of diagnosis.
Young age
Overall, the strongest predictor of early death was age below 1 year. The odds ratio (OR) was 4.36 for these patients (P<0.001), 0.75 for patients age 1 to 4, 0.78 for patients age 5 to 9, 1.00 (reference) for those age 10 to 14, and 1.69 for those age 15 to 19.
For hematologic malignancies, the adjusted OR (adjusted by poverty, unemployment, education, and year of diagnosis) was 4.32 for patients younger than 1 (P<0.001), 0.76 for patients age 1 to 4, 0.79 for patients age 5 to 9, 1.00 for those age 10 to 14, and 1.76 for those age 15 to 19 (P=0.002).
“In general, babies are just challenging, clinically, because they can’t tell you what they’re feeling,” Dr Green noted. “Parents and physicians have to pick the ones with cancer from the ones with a cold, without the patient being able to tell you about symptoms that could be diagnostic.”
“Babies tend to get aggressive cancers, it’s hard to tell when they’re getting sick, and some are even born with cancers that have already progressed. These factors combine to make very young age the strongest predictor of early death in our study.”
Race/ethnicity
Black race and Hispanic ethnicity also predicted early death. The OR was 1.48 for black race, 1.00 for white race (reference), and 1.09 for “other” races (P=0.102). The OR was 1.39 for Hispanic patients and 1.00 (reference) for non-Hispanic patients (P=0.007).
For hematologic malignancies, the adjusted OR was 1.68 for black patients (P=0.01) and 1.44 for patients of other, non-white races. The adjusted OR was 1.48 for Hispanic patients (P=0.009).
Dr Green said he hopes future studies will be able to determine the factors responsible for these disparities.
Higher death rates
Dr Green and his colleagues also found the rate of early death due to pediatric cancers is higher than reported in clinical trials, and this was true for all cancer subtypes assessed.
“Most of what we know about outcomes for cancer patients come from clinical trials, which have much more thorough reporting rules than cancer treated outside trials,” Dr Green said. “However, these kids in our study aren’t surviving long enough to join clinical trials.”
The researchers looked at a phase 3 trial (COG AAML0531) of pediatric patients with acute myeloid leukemia (AML) who were studied from August 2006 to June 2010. The early death rate in this trial was 1.6% (16/1022).
In contrast, the SEER database showed an early death rate for pediatric AML patients of 5.9% (15/256) during the same period as the trial and 6.2% (106/1698) for the period from 1992 to 2011. This is almost 4 times as high as the death rate in the trial.
The same effect was observed for acute lymphoblastic leukemia (ALL).
The early death rate for non-infant ALL was 0.7% (13/1790) in a trial (POG 9900) conducted from April 2000 to April 2005, 1.6% (30/1823) in the SEER data covering the same time period, and 1.3% (94/7353) in the SEER data from 1992 to 2011.
For infant ALL, the rates were 2.0% (3/149) in a trial (COG AALL0631) conducted from January 2008 to June 2014, 5.0% (2/40) in the SEER data during the trial period, and 5.4% (12/223) in the SEER data from 1992 to 2011.
“I had a hunch this was a bigger problem than we thought,” Dr Green said. “Now we see that is indeed the case.”
New research suggests that, in the US, early deaths from childhood cancer may be more common than clinical trials suggest.
Researchers found the rate of death within 1 month of diagnosis was higher among patients included in a large national database than among patients enrolled in phase 3 trials.
The data also indicated that early death is more likely in cancer patients under the age of 1 and those belonging to minority racial and ethnic groups.
Adam Green, MD, of the University of Colorado Anschutz Medical Campus in Aurora, and his colleagues conducted this research and reported the results in the Journal of Clinical Oncology.
The researchers analyzed data from the Surveillance, Epidemiology and End Results (SEER) database, which collects about 15% of all cancer outcomes across the US (representing a geographic and socioeconomic cross-section).
The team identified 36,337 patients with pediatric cancer (ages 0 to 19) diagnosed between 1992 and 2011. Of these patients, 555 (1.5%) died within 1 month of diagnosis.
Young age
Overall, the strongest predictor of early death was age below 1 year. The odds ratio (OR) was 4.36 for these patients (P<0.001), 0.75 for patients age 1 to 4, 0.78 for patients age 5 to 9, 1.00 (reference) for those age 10 to 14, and 1.69 for those age 15 to 19.
For hematologic malignancies, the adjusted OR (adjusted by poverty, unemployment, education, and year of diagnosis) was 4.32 for patients younger than 1 (P<0.001), 0.76 for patients age 1 to 4, 0.79 for patients age 5 to 9, 1.00 for those age 10 to 14, and 1.76 for those age 15 to 19 (P=0.002).
“In general, babies are just challenging, clinically, because they can’t tell you what they’re feeling,” Dr Green noted. “Parents and physicians have to pick the ones with cancer from the ones with a cold, without the patient being able to tell you about symptoms that could be diagnostic.”
“Babies tend to get aggressive cancers, it’s hard to tell when they’re getting sick, and some are even born with cancers that have already progressed. These factors combine to make very young age the strongest predictor of early death in our study.”
Race/ethnicity
Black race and Hispanic ethnicity also predicted early death. The OR was 1.48 for black race, 1.00 for white race (reference), and 1.09 for “other” races (P=0.102). The OR was 1.39 for Hispanic patients and 1.00 (reference) for non-Hispanic patients (P=0.007).
For hematologic malignancies, the adjusted OR was 1.68 for black patients (P=0.01) and 1.44 for patients of other, non-white races. The adjusted OR was 1.48 for Hispanic patients (P=0.009).
Dr Green said he hopes future studies will be able to determine the factors responsible for these disparities.
Higher death rates
Dr Green and his colleagues also found the rate of early death due to pediatric cancers is higher than reported in clinical trials, and this was true for all cancer subtypes assessed.
“Most of what we know about outcomes for cancer patients come from clinical trials, which have much more thorough reporting rules than cancer treated outside trials,” Dr Green said. “However, these kids in our study aren’t surviving long enough to join clinical trials.”
The researchers looked at a phase 3 trial (COG AAML0531) of pediatric patients with acute myeloid leukemia (AML) who were studied from August 2006 to June 2010. The early death rate in this trial was 1.6% (16/1022).
In contrast, the SEER database showed an early death rate for pediatric AML patients of 5.9% (15/256) during the same period as the trial and 6.2% (106/1698) for the period from 1992 to 2011. This is almost 4 times as high as the death rate in the trial.
The same effect was observed for acute lymphoblastic leukemia (ALL).
The early death rate for non-infant ALL was 0.7% (13/1790) in a trial (POG 9900) conducted from April 2000 to April 2005, 1.6% (30/1823) in the SEER data covering the same time period, and 1.3% (94/7353) in the SEER data from 1992 to 2011.
For infant ALL, the rates were 2.0% (3/149) in a trial (COG AALL0631) conducted from January 2008 to June 2014, 5.0% (2/40) in the SEER data during the trial period, and 5.4% (12/223) in the SEER data from 1992 to 2011.
“I had a hunch this was a bigger problem than we thought,” Dr Green said. “Now we see that is indeed the case.”
Gene therapy proves effective in SCD patient
Researchers have reported a favorable outcome in the first patient with severe sickle cell disease (SCD) to receive gene therapy in the HGB-205 study.
The subject, known as Patient 1204, was treated with LentiGlobin BB305, a product consisting of his own manipulated hematopoietic stem cells (HSCs).
A functional human β-globin gene was inserted into the patient’s HSCs ex vivo, and the cells were returned to him via transplant.
Fifteen months after receiving this treatment, Patient 1204 had high levels of anti-sickling hemoglobin (HbAT87Q), and there were no adverse events thought to be related to LentiGlobin BB305.
These results were published in NEJM. The research was supported by bluebird bio, the company developing LentiGlobin BB305.
Patient 1204 is a male with βS/βS genotype. In May 2014, at 13 years of age, the patient was enrolled in the HGB-205 study at Hôpital Necker-Enfants Malades in Paris, France.
The patient had received hydroxyurea from age 2 to 9 and had both a cholecystectomy and a splenectomy. He received regular transfusions (plus iron chelation with deferasirox) for 4 years prior to this study.
The patient had an average of 1.6 SCD-related events annually in the 9 years prior to starting transfusions. His complications from SCD included vaso-occlusive crises, acute-chest syndrome, bilateral hip osteonecrosis, and cerebral vasculopathy.
The patient underwent 2 bone marrow harvests to collect HSCs for gene transfer and back-up (6.2×108 and 5.4×108 total nucleated cells/kg harvested).
CD34+ cells were enriched from the harvested marrow and then transduced with LentiGlobin BB305 lentiviral vector.
The patient underwent myeloablation with intravenous busulfan (2.3 to 4.8 mg/kg per day for 4 days) with daily pharmacokinetic studies and dose adjustment. Total busulfan area under the curve was 19,363 μmol/min.
After a 2-day washout, the patient received LentiGlobin BB305 in October 2014 at a post-thaw total dose of 5.6×106 CD34+ cells/kg. Neutrophil and platelet engraftment were achieved on day 38 and day 91 post-transplant, respectively.
Red blood cell transfusions were to be continued after transplant until a sufficient proportion of HbAT87Q (25% to 30% of total hemoglobin) was detected. Transfusions were discontinued after day 88 post-transplant.
HbAT87Q reached 5.5 g/dL (46% of total hemoglobin) at month 9 and continued to increase to 5.7 g/dL at month 15 (48%). Hemoglobin S levels were 5.5 g/dL (46%) at month 9 and 5.8 g/dL (49%) at month 15.
Total hemoglobin levels were stable, between 10.6 and 12.0 g/dL, from months 6 to 15. Fetal hemoglobin levels remained below 1.0 g/dL.
No adverse events related to LentiGlobin BB305 were reported. There were, however, adverse events related to busulfan conditioning (grade 3 anemia, thrombocytopenia, and infection; grade 4 neutropenia).
During 15 months of follow-up, there were no SCD-related clinical events or hospitalizations. The patient was able to stop all medications, including pain medication.
The patient resumed regular school attendance and reported full participation in normal physical activities.
“We have managed this patient at Necker for more than 10 years, and standard treatments were not able to control his SCD symptoms,” said Marina Cavazzana, MD, PhD, of Hôpital Necker-Enfants Malades.
“He had to receive blood transfusions every month to prevent severe pain crises. Since receiving the autologous stem cell transplant with LentiGlobin, he has been free from severe symptoms and has resumed normal activities, without the need for further transfusions.”
Researchers have reported a favorable outcome in the first patient with severe sickle cell disease (SCD) to receive gene therapy in the HGB-205 study.
The subject, known as Patient 1204, was treated with LentiGlobin BB305, a product consisting of his own manipulated hematopoietic stem cells (HSCs).
A functional human β-globin gene was inserted into the patient’s HSCs ex vivo, and the cells were returned to him via transplant.
Fifteen months after receiving this treatment, Patient 1204 had high levels of anti-sickling hemoglobin (HbAT87Q), and there were no adverse events thought to be related to LentiGlobin BB305.
These results were published in NEJM. The research was supported by bluebird bio, the company developing LentiGlobin BB305.
Patient 1204 is a male with βS/βS genotype. In May 2014, at 13 years of age, the patient was enrolled in the HGB-205 study at Hôpital Necker-Enfants Malades in Paris, France.
The patient had received hydroxyurea from age 2 to 9 and had both a cholecystectomy and a splenectomy. He received regular transfusions (plus iron chelation with deferasirox) for 4 years prior to this study.
The patient had an average of 1.6 SCD-related events annually in the 9 years prior to starting transfusions. His complications from SCD included vaso-occlusive crises, acute-chest syndrome, bilateral hip osteonecrosis, and cerebral vasculopathy.
The patient underwent 2 bone marrow harvests to collect HSCs for gene transfer and back-up (6.2×108 and 5.4×108 total nucleated cells/kg harvested).
CD34+ cells were enriched from the harvested marrow and then transduced with LentiGlobin BB305 lentiviral vector.
The patient underwent myeloablation with intravenous busulfan (2.3 to 4.8 mg/kg per day for 4 days) with daily pharmacokinetic studies and dose adjustment. Total busulfan area under the curve was 19,363 μmol/min.
After a 2-day washout, the patient received LentiGlobin BB305 in October 2014 at a post-thaw total dose of 5.6×106 CD34+ cells/kg. Neutrophil and platelet engraftment were achieved on day 38 and day 91 post-transplant, respectively.
Red blood cell transfusions were to be continued after transplant until a sufficient proportion of HbAT87Q (25% to 30% of total hemoglobin) was detected. Transfusions were discontinued after day 88 post-transplant.
HbAT87Q reached 5.5 g/dL (46% of total hemoglobin) at month 9 and continued to increase to 5.7 g/dL at month 15 (48%). Hemoglobin S levels were 5.5 g/dL (46%) at month 9 and 5.8 g/dL (49%) at month 15.
Total hemoglobin levels were stable, between 10.6 and 12.0 g/dL, from months 6 to 15. Fetal hemoglobin levels remained below 1.0 g/dL.
No adverse events related to LentiGlobin BB305 were reported. There were, however, adverse events related to busulfan conditioning (grade 3 anemia, thrombocytopenia, and infection; grade 4 neutropenia).
During 15 months of follow-up, there were no SCD-related clinical events or hospitalizations. The patient was able to stop all medications, including pain medication.
The patient resumed regular school attendance and reported full participation in normal physical activities.
“We have managed this patient at Necker for more than 10 years, and standard treatments were not able to control his SCD symptoms,” said Marina Cavazzana, MD, PhD, of Hôpital Necker-Enfants Malades.
“He had to receive blood transfusions every month to prevent severe pain crises. Since receiving the autologous stem cell transplant with LentiGlobin, he has been free from severe symptoms and has resumed normal activities, without the need for further transfusions.”
Researchers have reported a favorable outcome in the first patient with severe sickle cell disease (SCD) to receive gene therapy in the HGB-205 study.
The subject, known as Patient 1204, was treated with LentiGlobin BB305, a product consisting of his own manipulated hematopoietic stem cells (HSCs).
A functional human β-globin gene was inserted into the patient’s HSCs ex vivo, and the cells were returned to him via transplant.
Fifteen months after receiving this treatment, Patient 1204 had high levels of anti-sickling hemoglobin (HbAT87Q), and there were no adverse events thought to be related to LentiGlobin BB305.
These results were published in NEJM. The research was supported by bluebird bio, the company developing LentiGlobin BB305.
Patient 1204 is a male with βS/βS genotype. In May 2014, at 13 years of age, the patient was enrolled in the HGB-205 study at Hôpital Necker-Enfants Malades in Paris, France.
The patient had received hydroxyurea from age 2 to 9 and had both a cholecystectomy and a splenectomy. He received regular transfusions (plus iron chelation with deferasirox) for 4 years prior to this study.
The patient had an average of 1.6 SCD-related events annually in the 9 years prior to starting transfusions. His complications from SCD included vaso-occlusive crises, acute-chest syndrome, bilateral hip osteonecrosis, and cerebral vasculopathy.
The patient underwent 2 bone marrow harvests to collect HSCs for gene transfer and back-up (6.2×108 and 5.4×108 total nucleated cells/kg harvested).
CD34+ cells were enriched from the harvested marrow and then transduced with LentiGlobin BB305 lentiviral vector.
The patient underwent myeloablation with intravenous busulfan (2.3 to 4.8 mg/kg per day for 4 days) with daily pharmacokinetic studies and dose adjustment. Total busulfan area under the curve was 19,363 μmol/min.
After a 2-day washout, the patient received LentiGlobin BB305 in October 2014 at a post-thaw total dose of 5.6×106 CD34+ cells/kg. Neutrophil and platelet engraftment were achieved on day 38 and day 91 post-transplant, respectively.
Red blood cell transfusions were to be continued after transplant until a sufficient proportion of HbAT87Q (25% to 30% of total hemoglobin) was detected. Transfusions were discontinued after day 88 post-transplant.
HbAT87Q reached 5.5 g/dL (46% of total hemoglobin) at month 9 and continued to increase to 5.7 g/dL at month 15 (48%). Hemoglobin S levels were 5.5 g/dL (46%) at month 9 and 5.8 g/dL (49%) at month 15.
Total hemoglobin levels were stable, between 10.6 and 12.0 g/dL, from months 6 to 15. Fetal hemoglobin levels remained below 1.0 g/dL.
No adverse events related to LentiGlobin BB305 were reported. There were, however, adverse events related to busulfan conditioning (grade 3 anemia, thrombocytopenia, and infection; grade 4 neutropenia).
During 15 months of follow-up, there were no SCD-related clinical events or hospitalizations. The patient was able to stop all medications, including pain medication.
The patient resumed regular school attendance and reported full participation in normal physical activities.
“We have managed this patient at Necker for more than 10 years, and standard treatments were not able to control his SCD symptoms,” said Marina Cavazzana, MD, PhD, of Hôpital Necker-Enfants Malades.
“He had to receive blood transfusions every month to prevent severe pain crises. Since receiving the autologous stem cell transplant with LentiGlobin, he has been free from severe symptoms and has resumed normal activities, without the need for further transfusions.”
Hemophilia B therapy granted access to PRIME program
SPK-9001, an investigational therapy intended to treat hemophilia B, has been granted access to the European Medicines Agency’s (EMA) PRIority MEdicines (PRIME) program.
The goal of the EMA’s PRIME program is to accelerate the development of therapies that may offer a major advantage over existing treatments or benefit patients with no treatment options.
Through PRIME, the EMA offers early and enhanced support to developers in order to optimize development plans and speed regulatory evaluations to potentially bring therapies to patients more quickly.
To be accepted for PRIME, a therapy must demonstrate the potential to benefit patients with unmet medical need through early clinical or nonclinical data.
About SPK-9001
SPK-9001 is a bio-engineered adeno-associated virus capsid expressing a codon-optimized, high-activity human factor IX variant enabling endogenous production of factor IX. The therapy is being developed by Spark Therapeutics and Pfizer Inc.
SPK-9001 is under investigation in a phase 1/2 trial. Results from this trial were presented at the 2016 ASH Annual Meeting.
The presentation included data on 9 patients who received a single intravenous infusion of SPK-9001 at 5 x 1011 vg/kg. The patients were followed for 52 weeks, with a long-term follow-up of 14 years.
Before their SPK-9001 infusion, the patients required anywhere from 0 to 159 factor IX infusions each year. Three patients had annualized bleeding rates (ABRs) of 0, and the remaining 6 patients had ABRs of 1, 2, 4, 10, 12, and 49.
After SPK-9001, 8 patients were able to stop receiving factor IX infusions and achieved an ABR of 0. One patient had an ABR of 2 and required on-demand factor IX therapy. (All patients stopped receiving factor IX prophylaxis).
The researchers said there were no unexpected vector or procedure-related adverse events, and none of the patients developed factor IX alloinhibitory antibodies.
SPK-9001, an investigational therapy intended to treat hemophilia B, has been granted access to the European Medicines Agency’s (EMA) PRIority MEdicines (PRIME) program.
The goal of the EMA’s PRIME program is to accelerate the development of therapies that may offer a major advantage over existing treatments or benefit patients with no treatment options.
Through PRIME, the EMA offers early and enhanced support to developers in order to optimize development plans and speed regulatory evaluations to potentially bring therapies to patients more quickly.
To be accepted for PRIME, a therapy must demonstrate the potential to benefit patients with unmet medical need through early clinical or nonclinical data.
About SPK-9001
SPK-9001 is a bio-engineered adeno-associated virus capsid expressing a codon-optimized, high-activity human factor IX variant enabling endogenous production of factor IX. The therapy is being developed by Spark Therapeutics and Pfizer Inc.
SPK-9001 is under investigation in a phase 1/2 trial. Results from this trial were presented at the 2016 ASH Annual Meeting.
The presentation included data on 9 patients who received a single intravenous infusion of SPK-9001 at 5 x 1011 vg/kg. The patients were followed for 52 weeks, with a long-term follow-up of 14 years.
Before their SPK-9001 infusion, the patients required anywhere from 0 to 159 factor IX infusions each year. Three patients had annualized bleeding rates (ABRs) of 0, and the remaining 6 patients had ABRs of 1, 2, 4, 10, 12, and 49.
After SPK-9001, 8 patients were able to stop receiving factor IX infusions and achieved an ABR of 0. One patient had an ABR of 2 and required on-demand factor IX therapy. (All patients stopped receiving factor IX prophylaxis).
The researchers said there were no unexpected vector or procedure-related adverse events, and none of the patients developed factor IX alloinhibitory antibodies.
SPK-9001, an investigational therapy intended to treat hemophilia B, has been granted access to the European Medicines Agency’s (EMA) PRIority MEdicines (PRIME) program.
The goal of the EMA’s PRIME program is to accelerate the development of therapies that may offer a major advantage over existing treatments or benefit patients with no treatment options.
Through PRIME, the EMA offers early and enhanced support to developers in order to optimize development plans and speed regulatory evaluations to potentially bring therapies to patients more quickly.
To be accepted for PRIME, a therapy must demonstrate the potential to benefit patients with unmet medical need through early clinical or nonclinical data.
About SPK-9001
SPK-9001 is a bio-engineered adeno-associated virus capsid expressing a codon-optimized, high-activity human factor IX variant enabling endogenous production of factor IX. The therapy is being developed by Spark Therapeutics and Pfizer Inc.
SPK-9001 is under investigation in a phase 1/2 trial. Results from this trial were presented at the 2016 ASH Annual Meeting.
The presentation included data on 9 patients who received a single intravenous infusion of SPK-9001 at 5 x 1011 vg/kg. The patients were followed for 52 weeks, with a long-term follow-up of 14 years.
Before their SPK-9001 infusion, the patients required anywhere from 0 to 159 factor IX infusions each year. Three patients had annualized bleeding rates (ABRs) of 0, and the remaining 6 patients had ABRs of 1, 2, 4, 10, 12, and 49.
After SPK-9001, 8 patients were able to stop receiving factor IX infusions and achieved an ABR of 0. One patient had an ABR of 2 and required on-demand factor IX therapy. (All patients stopped receiving factor IX prophylaxis).
The researchers said there were no unexpected vector or procedure-related adverse events, and none of the patients developed factor IX alloinhibitory antibodies.