User login
Collaborative depression care model offers promise in rural practice
An ob.gyn. practice in rural Washington state has successfully implemented a collaborative care model for depression management that relies on “depression care managers” and a consulting psychiatrist to aid ob.gyns. in providing effective depression care.
The initiative was a rural test run of the DAWN (Depression Attention for Women Now) intervention that was shown in a randomized controlled trial 2 years ago to improve depression outcomes for women in two urban ob.gyn. clinics affiliated with the University of Washington in Seattle. Both the trial and the pilot project were funded by the National Institute of Mental Health.
Nearly 75% of the 25 women enrolled in the rural pilot project had a significant improvement in their Patient Health Questionnaire-9 (PHQ-9) scores, and more than half improved their depression symptoms by at least 50%, Roger Rowles, MD, of the Generations practice in Yakima, Wash., and Susan D. Reed, MD, a coinvestigator of the original DAWN trial, reported at the annual meeting of the American College of Obstetricians and Gynecologists.
They urged others to consider taking a similar collaborative approach to depression care, especially now that the U.S. Preventive Services Task Force has recommended depression screening for all adults, including pregnant and postpartum women.
Previously, “when we identified someone with perinatal depression, we’d need a 30-minute initial consultation and then 15-20 minutes on a regular basis,” Dr. Rowles said. “We didn’t have the time to do that. ... And I had no training. Most of us felt we weren’t capable [of providing quality depression care].”
In the DAWN model, a social worker, nurse, medical assistant, or other staff member is trained to provide collaborative depression care and takes charge of this care, regularly meeting in-person or by phone with the patient to promote engagement and to closely monitor treatment progress.
Patients choose their initial treatment, including medication and Problem-Solving Treatment in Primary Care (PST-PC) therapy, an evidence-based brief behavioral intervention that helps identify stressors and improve problem solving. The depression care manager delivers the PST-PC therapy, tracks treatment response and compliance, and participates in weekly structured case reviews with the ob.gyn. and a consulting psychiatrist.
Results then and now
The original DAWN trial randomized women at two urban clinics to either 12 months of collaborative depression care or to usual care. Usual care included educational material, access to the clinic social worker, and possible psychiatry referral and prescriptions from the ob.gyn.
At 6 months, the reduction in depression scores as measured by the 20-item Hopkins Symptom Checklist was similar between the two groups, but at 12 months and at 18 months follow-up, the intervention group had significantly lower scores. They were more likely to have at least a 50% decrease in depressive symptoms at 12 months and were significantly more satisfied with their depression care (Obstet Gynecol. 2014 Jun;123[6]:1237-46).
The pilot project in Yakima, a farming community of 80,000 people, was of shorter duration than the randomized trial and focused on women coming for periconception, pregnancy, and postpartum care.
The majority – 74% – had significant improvement in their PHQ scores (a final score of less than 10), and almost one-third had a final score of less than 5. A score of 10 or more indicates the likelihood of having major depression. More than half – 59% – had at least a 50% improvement in depressive symptoms.
Unlike in the original DAWN trial, depression care managers in the Yakima project used text messaging in addition to phone calls to stay engaged with patients and monitor treatment. Almost all of the 25 enrolled women received PST-PC, and approximately 56% received antidepressants, for a mean treatment time of 14 weeks.
“Given that short duration of follow-up, the improvement we saw was very good,” said Amritha Bhat, MD, MBBS, the University of Washington psychiatrist who served as the consulting psychiatrist for the project.
Without a placebo-controlled arm, the researchers don’t know how much of the improvement was due to the collaborative care, Dr. Bhat said in an interview. “But we know now that it’s feasible in a rural setting.”
Depression care needs
Women have two times the rate of major depression as men, with prevalence rates of 13% annually and 21% over a lifetime, and low-income and minority women are at highest risk of depression and are also more likely to seek routine care from ob.gyns., according to Dr. Reed, who is a professor of ob.gyn at the University of Washington, Seattle, and chief of ob.gyn. at Harborview Medical Center.
Dr. Rowles said he was “astounded” that 30% of the screened patients in his practice had positive results. Many “either didn’t want to participate in the project or had exclusions, but even so we enrolled [our cohort] quickly,” he said.
The DAWN model stipulates that depression care managers support women as much as possible with social service interventions, facilitating financial assistance for medications, and serving as a “point person” for assistance with housing, food, domestic abuse, and other issues.
The task of integrating a social service element into depression care is necessary but can be daunting, Dr. Rowles said. In Yakima, he said, the significant need for basic assistance was a “big frustration” to the depression care managers involved in the project. “They wanted to do more, because they’d identified these problems and had a rapport [with the women], but our resources in Yakima are not that great.”
To prepare the Yakima practice for the intervention, a University of Washington team visited the clinic to educate staff about collaborative care, and three depression care managers were trained to deliver PST-PC and manage care. The depression care managers – a nurse employed by the local hospital, a nurse employed by another clinic for farm workers, and a local psychologist – “were the glue for this program,” Dr. Rowles said.
In other settings, depression care managers might more likely be clinic social workers or other members of the practice.
A psychiatrist’s involvement is also crucial, particularly when it comes to prescribing antidepressant medications at their full effective doses, Dr. Reed stressed. “You won’t feel comfortable pushing those doses to the max without [a psychiatrist to consult with],” Dr. Reed said at the ACOG meeting.
In the DAWN trial, similar numbers of patients in the collaborative care group and the usual care group were prescribed antidepressants, but more patients in the intervention group had their doses increased to an effective therapeutic range, and more patients adhered to their medication regimens, she said.
The 12-month DAWN intervention was provided at a cost per patient of up to $1,000.
Dr. Reed’s clinic has sustained funding for the intervention since the National Institute of Mental Health grant expired, and Dr. Rowles said he was seeking funding to continue DAWN at his Yakima clinic. Funding sources for ob.gyn. practices interested in implementing the model may include state funding agencies and organizations such as the March of Dimes, Dr. Reed said, noting that some states offer maternal services support that could be helpful for integrating collaborative depression care.
While the pilot project focused on pregnancy care, Dr. Reed urged ob.gyns. to think broadly. “Do you know when you catch these women? When they come in for their Pap smears and their routine care, before they become pregnant,” she said. “If you help them with their mood disorder early, they’ll do so much better with pregnancy.”
Information about DAWN – including resources on PST-PC and antidepressant medication, and an intervention manual – can be found at www.dawncare.org.
An ob.gyn. practice in rural Washington state has successfully implemented a collaborative care model for depression management that relies on “depression care managers” and a consulting psychiatrist to aid ob.gyns. in providing effective depression care.
The initiative was a rural test run of the DAWN (Depression Attention for Women Now) intervention that was shown in a randomized controlled trial 2 years ago to improve depression outcomes for women in two urban ob.gyn. clinics affiliated with the University of Washington in Seattle. Both the trial and the pilot project were funded by the National Institute of Mental Health.
Nearly 75% of the 25 women enrolled in the rural pilot project had a significant improvement in their Patient Health Questionnaire-9 (PHQ-9) scores, and more than half improved their depression symptoms by at least 50%, Roger Rowles, MD, of the Generations practice in Yakima, Wash., and Susan D. Reed, MD, a coinvestigator of the original DAWN trial, reported at the annual meeting of the American College of Obstetricians and Gynecologists.
They urged others to consider taking a similar collaborative approach to depression care, especially now that the U.S. Preventive Services Task Force has recommended depression screening for all adults, including pregnant and postpartum women.
Previously, “when we identified someone with perinatal depression, we’d need a 30-minute initial consultation and then 15-20 minutes on a regular basis,” Dr. Rowles said. “We didn’t have the time to do that. ... And I had no training. Most of us felt we weren’t capable [of providing quality depression care].”
In the DAWN model, a social worker, nurse, medical assistant, or other staff member is trained to provide collaborative depression care and takes charge of this care, regularly meeting in-person or by phone with the patient to promote engagement and to closely monitor treatment progress.
Patients choose their initial treatment, including medication and Problem-Solving Treatment in Primary Care (PST-PC) therapy, an evidence-based brief behavioral intervention that helps identify stressors and improve problem solving. The depression care manager delivers the PST-PC therapy, tracks treatment response and compliance, and participates in weekly structured case reviews with the ob.gyn. and a consulting psychiatrist.
Results then and now
The original DAWN trial randomized women at two urban clinics to either 12 months of collaborative depression care or to usual care. Usual care included educational material, access to the clinic social worker, and possible psychiatry referral and prescriptions from the ob.gyn.
At 6 months, the reduction in depression scores as measured by the 20-item Hopkins Symptom Checklist was similar between the two groups, but at 12 months and at 18 months follow-up, the intervention group had significantly lower scores. They were more likely to have at least a 50% decrease in depressive symptoms at 12 months and were significantly more satisfied with their depression care (Obstet Gynecol. 2014 Jun;123[6]:1237-46).
The pilot project in Yakima, a farming community of 80,000 people, was of shorter duration than the randomized trial and focused on women coming for periconception, pregnancy, and postpartum care.
The majority – 74% – had significant improvement in their PHQ scores (a final score of less than 10), and almost one-third had a final score of less than 5. A score of 10 or more indicates the likelihood of having major depression. More than half – 59% – had at least a 50% improvement in depressive symptoms.
Unlike in the original DAWN trial, depression care managers in the Yakima project used text messaging in addition to phone calls to stay engaged with patients and monitor treatment. Almost all of the 25 enrolled women received PST-PC, and approximately 56% received antidepressants, for a mean treatment time of 14 weeks.
“Given that short duration of follow-up, the improvement we saw was very good,” said Amritha Bhat, MD, MBBS, the University of Washington psychiatrist who served as the consulting psychiatrist for the project.
Without a placebo-controlled arm, the researchers don’t know how much of the improvement was due to the collaborative care, Dr. Bhat said in an interview. “But we know now that it’s feasible in a rural setting.”
Depression care needs
Women have two times the rate of major depression as men, with prevalence rates of 13% annually and 21% over a lifetime, and low-income and minority women are at highest risk of depression and are also more likely to seek routine care from ob.gyns., according to Dr. Reed, who is a professor of ob.gyn at the University of Washington, Seattle, and chief of ob.gyn. at Harborview Medical Center.
Dr. Rowles said he was “astounded” that 30% of the screened patients in his practice had positive results. Many “either didn’t want to participate in the project or had exclusions, but even so we enrolled [our cohort] quickly,” he said.
The DAWN model stipulates that depression care managers support women as much as possible with social service interventions, facilitating financial assistance for medications, and serving as a “point person” for assistance with housing, food, domestic abuse, and other issues.
The task of integrating a social service element into depression care is necessary but can be daunting, Dr. Rowles said. In Yakima, he said, the significant need for basic assistance was a “big frustration” to the depression care managers involved in the project. “They wanted to do more, because they’d identified these problems and had a rapport [with the women], but our resources in Yakima are not that great.”
To prepare the Yakima practice for the intervention, a University of Washington team visited the clinic to educate staff about collaborative care, and three depression care managers were trained to deliver PST-PC and manage care. The depression care managers – a nurse employed by the local hospital, a nurse employed by another clinic for farm workers, and a local psychologist – “were the glue for this program,” Dr. Rowles said.
In other settings, depression care managers might more likely be clinic social workers or other members of the practice.
A psychiatrist’s involvement is also crucial, particularly when it comes to prescribing antidepressant medications at their full effective doses, Dr. Reed stressed. “You won’t feel comfortable pushing those doses to the max without [a psychiatrist to consult with],” Dr. Reed said at the ACOG meeting.
In the DAWN trial, similar numbers of patients in the collaborative care group and the usual care group were prescribed antidepressants, but more patients in the intervention group had their doses increased to an effective therapeutic range, and more patients adhered to their medication regimens, she said.
The 12-month DAWN intervention was provided at a cost per patient of up to $1,000.
Dr. Reed’s clinic has sustained funding for the intervention since the National Institute of Mental Health grant expired, and Dr. Rowles said he was seeking funding to continue DAWN at his Yakima clinic. Funding sources for ob.gyn. practices interested in implementing the model may include state funding agencies and organizations such as the March of Dimes, Dr. Reed said, noting that some states offer maternal services support that could be helpful for integrating collaborative depression care.
While the pilot project focused on pregnancy care, Dr. Reed urged ob.gyns. to think broadly. “Do you know when you catch these women? When they come in for their Pap smears and their routine care, before they become pregnant,” she said. “If you help them with their mood disorder early, they’ll do so much better with pregnancy.”
Information about DAWN – including resources on PST-PC and antidepressant medication, and an intervention manual – can be found at www.dawncare.org.
An ob.gyn. practice in rural Washington state has successfully implemented a collaborative care model for depression management that relies on “depression care managers” and a consulting psychiatrist to aid ob.gyns. in providing effective depression care.
The initiative was a rural test run of the DAWN (Depression Attention for Women Now) intervention that was shown in a randomized controlled trial 2 years ago to improve depression outcomes for women in two urban ob.gyn. clinics affiliated with the University of Washington in Seattle. Both the trial and the pilot project were funded by the National Institute of Mental Health.
Nearly 75% of the 25 women enrolled in the rural pilot project had a significant improvement in their Patient Health Questionnaire-9 (PHQ-9) scores, and more than half improved their depression symptoms by at least 50%, Roger Rowles, MD, of the Generations practice in Yakima, Wash., and Susan D. Reed, MD, a coinvestigator of the original DAWN trial, reported at the annual meeting of the American College of Obstetricians and Gynecologists.
They urged others to consider taking a similar collaborative approach to depression care, especially now that the U.S. Preventive Services Task Force has recommended depression screening for all adults, including pregnant and postpartum women.
Previously, “when we identified someone with perinatal depression, we’d need a 30-minute initial consultation and then 15-20 minutes on a regular basis,” Dr. Rowles said. “We didn’t have the time to do that. ... And I had no training. Most of us felt we weren’t capable [of providing quality depression care].”
In the DAWN model, a social worker, nurse, medical assistant, or other staff member is trained to provide collaborative depression care and takes charge of this care, regularly meeting in-person or by phone with the patient to promote engagement and to closely monitor treatment progress.
Patients choose their initial treatment, including medication and Problem-Solving Treatment in Primary Care (PST-PC) therapy, an evidence-based brief behavioral intervention that helps identify stressors and improve problem solving. The depression care manager delivers the PST-PC therapy, tracks treatment response and compliance, and participates in weekly structured case reviews with the ob.gyn. and a consulting psychiatrist.
Results then and now
The original DAWN trial randomized women at two urban clinics to either 12 months of collaborative depression care or to usual care. Usual care included educational material, access to the clinic social worker, and possible psychiatry referral and prescriptions from the ob.gyn.
At 6 months, the reduction in depression scores as measured by the 20-item Hopkins Symptom Checklist was similar between the two groups, but at 12 months and at 18 months follow-up, the intervention group had significantly lower scores. They were more likely to have at least a 50% decrease in depressive symptoms at 12 months and were significantly more satisfied with their depression care (Obstet Gynecol. 2014 Jun;123[6]:1237-46).
The pilot project in Yakima, a farming community of 80,000 people, was of shorter duration than the randomized trial and focused on women coming for periconception, pregnancy, and postpartum care.
The majority – 74% – had significant improvement in their PHQ scores (a final score of less than 10), and almost one-third had a final score of less than 5. A score of 10 or more indicates the likelihood of having major depression. More than half – 59% – had at least a 50% improvement in depressive symptoms.
Unlike in the original DAWN trial, depression care managers in the Yakima project used text messaging in addition to phone calls to stay engaged with patients and monitor treatment. Almost all of the 25 enrolled women received PST-PC, and approximately 56% received antidepressants, for a mean treatment time of 14 weeks.
“Given that short duration of follow-up, the improvement we saw was very good,” said Amritha Bhat, MD, MBBS, the University of Washington psychiatrist who served as the consulting psychiatrist for the project.
Without a placebo-controlled arm, the researchers don’t know how much of the improvement was due to the collaborative care, Dr. Bhat said in an interview. “But we know now that it’s feasible in a rural setting.”
Depression care needs
Women have two times the rate of major depression as men, with prevalence rates of 13% annually and 21% over a lifetime, and low-income and minority women are at highest risk of depression and are also more likely to seek routine care from ob.gyns., according to Dr. Reed, who is a professor of ob.gyn at the University of Washington, Seattle, and chief of ob.gyn. at Harborview Medical Center.
Dr. Rowles said he was “astounded” that 30% of the screened patients in his practice had positive results. Many “either didn’t want to participate in the project or had exclusions, but even so we enrolled [our cohort] quickly,” he said.
The DAWN model stipulates that depression care managers support women as much as possible with social service interventions, facilitating financial assistance for medications, and serving as a “point person” for assistance with housing, food, domestic abuse, and other issues.
The task of integrating a social service element into depression care is necessary but can be daunting, Dr. Rowles said. In Yakima, he said, the significant need for basic assistance was a “big frustration” to the depression care managers involved in the project. “They wanted to do more, because they’d identified these problems and had a rapport [with the women], but our resources in Yakima are not that great.”
To prepare the Yakima practice for the intervention, a University of Washington team visited the clinic to educate staff about collaborative care, and three depression care managers were trained to deliver PST-PC and manage care. The depression care managers – a nurse employed by the local hospital, a nurse employed by another clinic for farm workers, and a local psychologist – “were the glue for this program,” Dr. Rowles said.
In other settings, depression care managers might more likely be clinic social workers or other members of the practice.
A psychiatrist’s involvement is also crucial, particularly when it comes to prescribing antidepressant medications at their full effective doses, Dr. Reed stressed. “You won’t feel comfortable pushing those doses to the max without [a psychiatrist to consult with],” Dr. Reed said at the ACOG meeting.
In the DAWN trial, similar numbers of patients in the collaborative care group and the usual care group were prescribed antidepressants, but more patients in the intervention group had their doses increased to an effective therapeutic range, and more patients adhered to their medication regimens, she said.
The 12-month DAWN intervention was provided at a cost per patient of up to $1,000.
Dr. Reed’s clinic has sustained funding for the intervention since the National Institute of Mental Health grant expired, and Dr. Rowles said he was seeking funding to continue DAWN at his Yakima clinic. Funding sources for ob.gyn. practices interested in implementing the model may include state funding agencies and organizations such as the March of Dimes, Dr. Reed said, noting that some states offer maternal services support that could be helpful for integrating collaborative depression care.
While the pilot project focused on pregnancy care, Dr. Reed urged ob.gyns. to think broadly. “Do you know when you catch these women? When they come in for their Pap smears and their routine care, before they become pregnant,” she said. “If you help them with their mood disorder early, they’ll do so much better with pregnancy.”
Information about DAWN – including resources on PST-PC and antidepressant medication, and an intervention manual – can be found at www.dawncare.org.
VIDEO: Expert roundtable explores 50 years of contraception
WASHINGTON – What has the increased access to contraception over the last 50 years meant for American women?
We asked Ob.Gyn. News editorial advisory board member Dr. Eve Espey, professor and chair of the department of obstetrics and gynecology at the University of New Mexico, Albuquerque, along with three experts in family planning, to explore how expanded contraception options have affected public health, what barriers still remain, and what new products are in the pipeline.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Perhaps the biggest impact for women has been the ability to participate in the workforce, and that includes women entering medical school.
“Over the last 50 years, we’ve seen a big increase in the number of women who are professionals, who are physicians,” Dr. Espey said during the roundtable. “And during that same period of time, we’ve seen the growth of more focus on family planning.”
“I think that really would not be possible without the ability to control our fertility,” said Dr. Sarah W. Prager, associate professor of obstetrics and gynecology and director of the Ryan Family Planning Program at the University of Washington, Seattle.
And the widespread availability of contraception has translated into a decrease in maternal mortality as a result of fewer unintended pregnancies. “The implications for public health – for women and children in this country – is huge,” Dr. Prager said.
LARCs
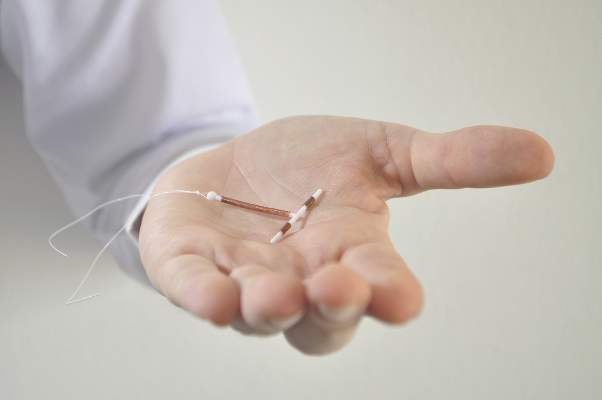
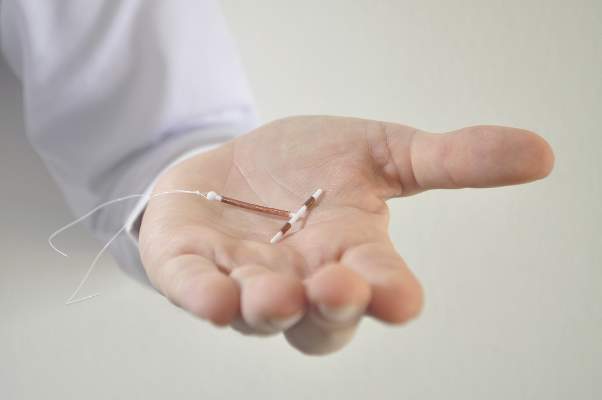
One of the big shifts in contraceptive trends has been the slow but increasing uptake of long-acting reversible contraceptives (LARCs), such as IUDs and implants. After a drop-off in the 1970s following safety problems with the Dalkon Shield, there has been a resurgence in interest.
In the last decade, the rate of LARC use has grown from about 2% to 10%, corresponding to a slight drop in rates of unintended pregnancy, said Dr. Nikki B. Zite, professor and residency program director in the department of obstetrics and gynecology at the University of Tennessee, Knoxville.
The Contraceptive CHOICE Project, which enrolled more than 9,000 women who were provided with the no-cost reversible contraceptive method of their choice, found that about three-quarters of the women chose an IUD or an implant, which was associated with significant reductions in unintended and teen pregnancies.
“What we saw was that when we removed barriers to contraception in general, that uptake of IUDs and implants really went up,” said Dr. Tessa Madden, director of the division of family planning and associate professor in the department of obstetrics and gynecology at Washington University, St. Louis.
There is no “best” contraceptive method, Dr. Madden said. “Contraception really needs to be tailored to the individual woman [ensuring] that her values and preferences about contraception are taken into consideration during counseling, to help her choose the method that’s going to be the best fit for her.”
Resources
There are resources available to aid in tailoring contraception methods to the needs of patients.
U.S. Medical Eligibility Criteria for Contraceptive Use, guidance that is available through the Centers for Disease Control and Prevention, allows physicians to tailor the method to a patient’s comorbid medical conditions, Dr. Zite said. Physicians can search by contraceptive method or patient characteristic to determine the risk for a given patient, rated on a scale of 1-4 (where 1 or 2 means generally safe, 3 means that the risks may outweigh the benefits, and 4 means that the risks clearly outweigh the benefits).
“It’s a really easy starting-off point to use with patients and physicians when trying to decide what contraceptive method is safe for their patient,” Dr. Zite said.
Common medical comorbidities, including obesity, diabetes, thyroid disease, and hypertension, are all addressed in the medical eligibility criteria.
Another resource is the U.S. Selected Practice Recommendations for Contraceptive Use, which can help in deciding when it is appropriate to start a contraceptive method, what exams and tests are needed before initiation, what follow-up is needed, and how to handle problems such as missed pills or potential side effects.
Barriers
Over the years, many of the barriers to contraceptive access have been reduced. Some forms of emergency contraception are now available over the counter to women of all ages; more states are considering laws allowing women to access up to a year’s supply of hormonal contraceptives at one time; and a few states have passed laws allowing pharmacists to prescribe hormonal birth control directly. In addition, the Affordable Care Act’s mandate for insurers to cover approved methods of contraception without cost sharing has eliminated some cost barriers.
But other systems barriers still remain, such as making women return for multiple visits for the insertion of an IUD or implant, or limiting LARC use only to women who have already had a child. “There’s not a reason to avoid use of IUDs in women that have not had babies but there are still providers out there who will not insert an IUD, so we need to still do a better job to increase access even more,” Dr. Zite said.
Future trends
What new contraceptive options are in the pipeline? Dr. Prager predicted more development in the area of longer-acting injectables and implants, potentially even biodegradable implants. Also likely is the development of nonsurgical sterilization methods for women that eliminate some of the risk and cost barriers. And male contraceptive methods are in the works, both hormonal and nonhormonal, Dr. Prager said.
There’s an increasing interested in nonhormonal longer-acting methods, beyond just the copper IUD, Dr. Madden said, and there are new products on the horizon in that area. Researchers are exploring new methods to protect against HIV and other sexually transmitted infections, while offering contraception, Dr. Zite said.
Dr. Espey reported having no relevant financial disclosures. Dr. Prager is an unpaid trainer for Nexplanon (Merck). Dr. Zite is an unpaid trainer for Nexplanon and serves on an international IUD advisory board for Bayer. Dr. Madden serves on a scientific advisory board for Bayer and on a data safety monitoring board for phase IV safety studies of Bayer contraceptive products.
Throughout 2016, Ob.Gyn. News is celebrating its 50th anniversary with exclusive articles looking at the evolution of the specialty, including the history of infertility treatment, changes in gynecologic surgery, and the transformation of the well-woman visit. Look for these articles and more special features in the pages of Ob.Gyn. News and online at obgynnews.com.
On Twitter @maryellenny
WASHINGTON – What has the increased access to contraception over the last 50 years meant for American women?
We asked Ob.Gyn. News editorial advisory board member Dr. Eve Espey, professor and chair of the department of obstetrics and gynecology at the University of New Mexico, Albuquerque, along with three experts in family planning, to explore how expanded contraception options have affected public health, what barriers still remain, and what new products are in the pipeline.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Perhaps the biggest impact for women has been the ability to participate in the workforce, and that includes women entering medical school.
“Over the last 50 years, we’ve seen a big increase in the number of women who are professionals, who are physicians,” Dr. Espey said during the roundtable. “And during that same period of time, we’ve seen the growth of more focus on family planning.”
“I think that really would not be possible without the ability to control our fertility,” said Dr. Sarah W. Prager, associate professor of obstetrics and gynecology and director of the Ryan Family Planning Program at the University of Washington, Seattle.
And the widespread availability of contraception has translated into a decrease in maternal mortality as a result of fewer unintended pregnancies. “The implications for public health – for women and children in this country – is huge,” Dr. Prager said.
LARCs
One of the big shifts in contraceptive trends has been the slow but increasing uptake of long-acting reversible contraceptives (LARCs), such as IUDs and implants. After a drop-off in the 1970s following safety problems with the Dalkon Shield, there has been a resurgence in interest.
In the last decade, the rate of LARC use has grown from about 2% to 10%, corresponding to a slight drop in rates of unintended pregnancy, said Dr. Nikki B. Zite, professor and residency program director in the department of obstetrics and gynecology at the University of Tennessee, Knoxville.
The Contraceptive CHOICE Project, which enrolled more than 9,000 women who were provided with the no-cost reversible contraceptive method of their choice, found that about three-quarters of the women chose an IUD or an implant, which was associated with significant reductions in unintended and teen pregnancies.
“What we saw was that when we removed barriers to contraception in general, that uptake of IUDs and implants really went up,” said Dr. Tessa Madden, director of the division of family planning and associate professor in the department of obstetrics and gynecology at Washington University, St. Louis.
There is no “best” contraceptive method, Dr. Madden said. “Contraception really needs to be tailored to the individual woman [ensuring] that her values and preferences about contraception are taken into consideration during counseling, to help her choose the method that’s going to be the best fit for her.”
Resources
There are resources available to aid in tailoring contraception methods to the needs of patients.
U.S. Medical Eligibility Criteria for Contraceptive Use, guidance that is available through the Centers for Disease Control and Prevention, allows physicians to tailor the method to a patient’s comorbid medical conditions, Dr. Zite said. Physicians can search by contraceptive method or patient characteristic to determine the risk for a given patient, rated on a scale of 1-4 (where 1 or 2 means generally safe, 3 means that the risks may outweigh the benefits, and 4 means that the risks clearly outweigh the benefits).
“It’s a really easy starting-off point to use with patients and physicians when trying to decide what contraceptive method is safe for their patient,” Dr. Zite said.
Common medical comorbidities, including obesity, diabetes, thyroid disease, and hypertension, are all addressed in the medical eligibility criteria.
Another resource is the U.S. Selected Practice Recommendations for Contraceptive Use, which can help in deciding when it is appropriate to start a contraceptive method, what exams and tests are needed before initiation, what follow-up is needed, and how to handle problems such as missed pills or potential side effects.
Barriers
Over the years, many of the barriers to contraceptive access have been reduced. Some forms of emergency contraception are now available over the counter to women of all ages; more states are considering laws allowing women to access up to a year’s supply of hormonal contraceptives at one time; and a few states have passed laws allowing pharmacists to prescribe hormonal birth control directly. In addition, the Affordable Care Act’s mandate for insurers to cover approved methods of contraception without cost sharing has eliminated some cost barriers.
But other systems barriers still remain, such as making women return for multiple visits for the insertion of an IUD or implant, or limiting LARC use only to women who have already had a child. “There’s not a reason to avoid use of IUDs in women that have not had babies but there are still providers out there who will not insert an IUD, so we need to still do a better job to increase access even more,” Dr. Zite said.
Future trends
What new contraceptive options are in the pipeline? Dr. Prager predicted more development in the area of longer-acting injectables and implants, potentially even biodegradable implants. Also likely is the development of nonsurgical sterilization methods for women that eliminate some of the risk and cost barriers. And male contraceptive methods are in the works, both hormonal and nonhormonal, Dr. Prager said.
There’s an increasing interested in nonhormonal longer-acting methods, beyond just the copper IUD, Dr. Madden said, and there are new products on the horizon in that area. Researchers are exploring new methods to protect against HIV and other sexually transmitted infections, while offering contraception, Dr. Zite said.
Dr. Espey reported having no relevant financial disclosures. Dr. Prager is an unpaid trainer for Nexplanon (Merck). Dr. Zite is an unpaid trainer for Nexplanon and serves on an international IUD advisory board for Bayer. Dr. Madden serves on a scientific advisory board for Bayer and on a data safety monitoring board for phase IV safety studies of Bayer contraceptive products.
Throughout 2016, Ob.Gyn. News is celebrating its 50th anniversary with exclusive articles looking at the evolution of the specialty, including the history of infertility treatment, changes in gynecologic surgery, and the transformation of the well-woman visit. Look for these articles and more special features in the pages of Ob.Gyn. News and online at obgynnews.com.
On Twitter @maryellenny
WASHINGTON – What has the increased access to contraception over the last 50 years meant for American women?
We asked Ob.Gyn. News editorial advisory board member Dr. Eve Espey, professor and chair of the department of obstetrics and gynecology at the University of New Mexico, Albuquerque, along with three experts in family planning, to explore how expanded contraception options have affected public health, what barriers still remain, and what new products are in the pipeline.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Perhaps the biggest impact for women has been the ability to participate in the workforce, and that includes women entering medical school.
“Over the last 50 years, we’ve seen a big increase in the number of women who are professionals, who are physicians,” Dr. Espey said during the roundtable. “And during that same period of time, we’ve seen the growth of more focus on family planning.”
“I think that really would not be possible without the ability to control our fertility,” said Dr. Sarah W. Prager, associate professor of obstetrics and gynecology and director of the Ryan Family Planning Program at the University of Washington, Seattle.
And the widespread availability of contraception has translated into a decrease in maternal mortality as a result of fewer unintended pregnancies. “The implications for public health – for women and children in this country – is huge,” Dr. Prager said.
LARCs
One of the big shifts in contraceptive trends has been the slow but increasing uptake of long-acting reversible contraceptives (LARCs), such as IUDs and implants. After a drop-off in the 1970s following safety problems with the Dalkon Shield, there has been a resurgence in interest.
In the last decade, the rate of LARC use has grown from about 2% to 10%, corresponding to a slight drop in rates of unintended pregnancy, said Dr. Nikki B. Zite, professor and residency program director in the department of obstetrics and gynecology at the University of Tennessee, Knoxville.
The Contraceptive CHOICE Project, which enrolled more than 9,000 women who were provided with the no-cost reversible contraceptive method of their choice, found that about three-quarters of the women chose an IUD or an implant, which was associated with significant reductions in unintended and teen pregnancies.
“What we saw was that when we removed barriers to contraception in general, that uptake of IUDs and implants really went up,” said Dr. Tessa Madden, director of the division of family planning and associate professor in the department of obstetrics and gynecology at Washington University, St. Louis.
There is no “best” contraceptive method, Dr. Madden said. “Contraception really needs to be tailored to the individual woman [ensuring] that her values and preferences about contraception are taken into consideration during counseling, to help her choose the method that’s going to be the best fit for her.”
Resources
There are resources available to aid in tailoring contraception methods to the needs of patients.
U.S. Medical Eligibility Criteria for Contraceptive Use, guidance that is available through the Centers for Disease Control and Prevention, allows physicians to tailor the method to a patient’s comorbid medical conditions, Dr. Zite said. Physicians can search by contraceptive method or patient characteristic to determine the risk for a given patient, rated on a scale of 1-4 (where 1 or 2 means generally safe, 3 means that the risks may outweigh the benefits, and 4 means that the risks clearly outweigh the benefits).
“It’s a really easy starting-off point to use with patients and physicians when trying to decide what contraceptive method is safe for their patient,” Dr. Zite said.
Common medical comorbidities, including obesity, diabetes, thyroid disease, and hypertension, are all addressed in the medical eligibility criteria.
Another resource is the U.S. Selected Practice Recommendations for Contraceptive Use, which can help in deciding when it is appropriate to start a contraceptive method, what exams and tests are needed before initiation, what follow-up is needed, and how to handle problems such as missed pills or potential side effects.
Barriers
Over the years, many of the barriers to contraceptive access have been reduced. Some forms of emergency contraception are now available over the counter to women of all ages; more states are considering laws allowing women to access up to a year’s supply of hormonal contraceptives at one time; and a few states have passed laws allowing pharmacists to prescribe hormonal birth control directly. In addition, the Affordable Care Act’s mandate for insurers to cover approved methods of contraception without cost sharing has eliminated some cost barriers.
But other systems barriers still remain, such as making women return for multiple visits for the insertion of an IUD or implant, or limiting LARC use only to women who have already had a child. “There’s not a reason to avoid use of IUDs in women that have not had babies but there are still providers out there who will not insert an IUD, so we need to still do a better job to increase access even more,” Dr. Zite said.
Future trends
What new contraceptive options are in the pipeline? Dr. Prager predicted more development in the area of longer-acting injectables and implants, potentially even biodegradable implants. Also likely is the development of nonsurgical sterilization methods for women that eliminate some of the risk and cost barriers. And male contraceptive methods are in the works, both hormonal and nonhormonal, Dr. Prager said.
There’s an increasing interested in nonhormonal longer-acting methods, beyond just the copper IUD, Dr. Madden said, and there are new products on the horizon in that area. Researchers are exploring new methods to protect against HIV and other sexually transmitted infections, while offering contraception, Dr. Zite said.
Dr. Espey reported having no relevant financial disclosures. Dr. Prager is an unpaid trainer for Nexplanon (Merck). Dr. Zite is an unpaid trainer for Nexplanon and serves on an international IUD advisory board for Bayer. Dr. Madden serves on a scientific advisory board for Bayer and on a data safety monitoring board for phase IV safety studies of Bayer contraceptive products.
Throughout 2016, Ob.Gyn. News is celebrating its 50th anniversary with exclusive articles looking at the evolution of the specialty, including the history of infertility treatment, changes in gynecologic surgery, and the transformation of the well-woman visit. Look for these articles and more special features in the pages of Ob.Gyn. News and online at obgynnews.com.
On Twitter @maryellenny
Immediate Postpartum IUD Insertion Causes Little Pain, Distress
WASHINGTON – Many women who underwent post-placental IUD insertion reported little or no pain, regardless of whether they had an epidural during childbirth, according to the findings of a small pilot study.
Dr. Shannon Carr and her colleagues at the University of New Mexico, Albuquerque, assessed 66 women using both a 100-mm visual analog pain scale (VAS) and a four-point Likert verbal rating scale (VRS). They also interviewed a subset of the participants to gather qualitative data about the experience. About half the group received an epidural (36 women) and half did not (30 women).
The VAS scores did not reveal normal distributions and the standard deviations were large, which was not statistically meaningful, according to Dr. Carr. The median scores were 40.5 mm and 2.8 mm in the no-epidural and epidural groups, respectively. But using the four-point pain scale – none, mild, moderate, and severe – the researchers found that 53% of women in the no-epidural group reported pain ranging from none to mild, while 89% of women in the epidural group reported pain in the none-to-mild range.
“What I saw basically reflected what we call the floor effect of the VAS scores in the epidural group. Most of the women hardly had any pain,” Dr. Carr said at the annual meeting of the American College of Obstetricians and Gynecologists. “Women who did not have an epidural reported scores that were all over the map.”
The results help to shed light on what is probably the most common question asked by women considering post-placental IUD insertion – Will it hurt?
“The more we learn about it, the more we can reassure women and counsel them appropriately about what to expect, not only clinically but on a personal level with their labor experience,” Dr. Carr said. “I think that’s really important, and it might promote uptake of the procedure and more women getting really effective contraception before leaving the hospital.”
Qualitative data, based on interviews with 9 women in the no-epidural group and 12 in the epidural group, showed that they had no regrets about the procedure, and most reported that it didn’t detract from their overall labor experience. Instead, most of the women in the study said that holding their newborn baby was a pleasant distraction from the placement of the IUD.
The primary driver for undergoing IUD insertion immediately post partum was convenience. “They wanted to have really good birth control on board before they left the hospital,” Dr. Carr said. “They recognize those logistical barriers to getting to that 6-week postpartum visit.”
The researchers did not report having any financial disclosures.
WASHINGTON – Many women who underwent post-placental IUD insertion reported little or no pain, regardless of whether they had an epidural during childbirth, according to the findings of a small pilot study.
Dr. Shannon Carr and her colleagues at the University of New Mexico, Albuquerque, assessed 66 women using both a 100-mm visual analog pain scale (VAS) and a four-point Likert verbal rating scale (VRS). They also interviewed a subset of the participants to gather qualitative data about the experience. About half the group received an epidural (36 women) and half did not (30 women).
The VAS scores did not reveal normal distributions and the standard deviations were large, which was not statistically meaningful, according to Dr. Carr. The median scores were 40.5 mm and 2.8 mm in the no-epidural and epidural groups, respectively. But using the four-point pain scale – none, mild, moderate, and severe – the researchers found that 53% of women in the no-epidural group reported pain ranging from none to mild, while 89% of women in the epidural group reported pain in the none-to-mild range.
“What I saw basically reflected what we call the floor effect of the VAS scores in the epidural group. Most of the women hardly had any pain,” Dr. Carr said at the annual meeting of the American College of Obstetricians and Gynecologists. “Women who did not have an epidural reported scores that were all over the map.”
The results help to shed light on what is probably the most common question asked by women considering post-placental IUD insertion – Will it hurt?
“The more we learn about it, the more we can reassure women and counsel them appropriately about what to expect, not only clinically but on a personal level with their labor experience,” Dr. Carr said. “I think that’s really important, and it might promote uptake of the procedure and more women getting really effective contraception before leaving the hospital.”
Qualitative data, based on interviews with 9 women in the no-epidural group and 12 in the epidural group, showed that they had no regrets about the procedure, and most reported that it didn’t detract from their overall labor experience. Instead, most of the women in the study said that holding their newborn baby was a pleasant distraction from the placement of the IUD.
The primary driver for undergoing IUD insertion immediately post partum was convenience. “They wanted to have really good birth control on board before they left the hospital,” Dr. Carr said. “They recognize those logistical barriers to getting to that 6-week postpartum visit.”
The researchers did not report having any financial disclosures.
WASHINGTON – Many women who underwent post-placental IUD insertion reported little or no pain, regardless of whether they had an epidural during childbirth, according to the findings of a small pilot study.
Dr. Shannon Carr and her colleagues at the University of New Mexico, Albuquerque, assessed 66 women using both a 100-mm visual analog pain scale (VAS) and a four-point Likert verbal rating scale (VRS). They also interviewed a subset of the participants to gather qualitative data about the experience. About half the group received an epidural (36 women) and half did not (30 women).
The VAS scores did not reveal normal distributions and the standard deviations were large, which was not statistically meaningful, according to Dr. Carr. The median scores were 40.5 mm and 2.8 mm in the no-epidural and epidural groups, respectively. But using the four-point pain scale – none, mild, moderate, and severe – the researchers found that 53% of women in the no-epidural group reported pain ranging from none to mild, while 89% of women in the epidural group reported pain in the none-to-mild range.
“What I saw basically reflected what we call the floor effect of the VAS scores in the epidural group. Most of the women hardly had any pain,” Dr. Carr said at the annual meeting of the American College of Obstetricians and Gynecologists. “Women who did not have an epidural reported scores that were all over the map.”
The results help to shed light on what is probably the most common question asked by women considering post-placental IUD insertion – Will it hurt?
“The more we learn about it, the more we can reassure women and counsel them appropriately about what to expect, not only clinically but on a personal level with their labor experience,” Dr. Carr said. “I think that’s really important, and it might promote uptake of the procedure and more women getting really effective contraception before leaving the hospital.”
Qualitative data, based on interviews with 9 women in the no-epidural group and 12 in the epidural group, showed that they had no regrets about the procedure, and most reported that it didn’t detract from their overall labor experience. Instead, most of the women in the study said that holding their newborn baby was a pleasant distraction from the placement of the IUD.
The primary driver for undergoing IUD insertion immediately post partum was convenience. “They wanted to have really good birth control on board before they left the hospital,” Dr. Carr said. “They recognize those logistical barriers to getting to that 6-week postpartum visit.”
The researchers did not report having any financial disclosures.
AT ACOG 2016
Immediate postpartum IUD insertion causes little pain, distress
WASHINGTON – Many women who underwent post-placental IUD insertion reported little or no pain, regardless of whether they had an epidural during childbirth, according to the findings of a small pilot study.
Dr. Shannon Carr and her colleagues at the University of New Mexico, Albuquerque, assessed 66 women using both a 100-mm visual analog pain scale (VAS) and a four-point Likert verbal rating scale (VRS). They also interviewed a subset of the participants to gather qualitative data about the experience. About half the group received an epidural (36 women) and half did not (30 women).
The VAS scores did not reveal normal distributions and the standard deviations were large, which was not statistically meaningful, according to Dr. Carr. The median scores were 40.5 mm and 2.8 mm in the no-epidural and epidural groups, respectively. But using the four-point pain scale – none, mild, moderate, and severe – the researchers found that 53% of women in the no-epidural group reported pain ranging from none to mild, while 89% of women in the epidural group reported pain in the none-to-mild range.
“What I saw basically reflected what we call the floor effect of the VAS scores in the epidural group. Most of the women hardly had any pain,” Dr. Carr said at the annual meeting of the American College of Obstetricians and Gynecologists. “Women who did not have an epidural reported scores that were all over the map.”
The results help to shed light on what is probably the most common question asked by women considering post-placental IUD insertion – Will it hurt?
“The more we learn about it, the more we can reassure women and counsel them appropriately about what to expect, not only clinically but on a personal level with their labor experience,” Dr. Carr said. “I think that’s really important, and it might promote uptake of the procedure and more women getting really effective contraception before leaving the hospital.”
Qualitative data, based on interviews with 9 women in the no-epidural group and 12 in the epidural group, showed that they had no regrets about the procedure, and most reported that it didn’t detract from their overall labor experience. Instead, most of the women in the study said that holding their newborn baby was a pleasant distraction from the placement of the IUD.
The primary driver for undergoing IUD insertion immediately post partum was convenience. “They wanted to have really good birth control on board before they left the hospital,” Dr. Carr said. “They recognize those logistical barriers to getting to that 6-week postpartum visit.”
The researchers did not report having any financial disclosures.
On Twitter @maryellenny
WASHINGTON – Many women who underwent post-placental IUD insertion reported little or no pain, regardless of whether they had an epidural during childbirth, according to the findings of a small pilot study.
Dr. Shannon Carr and her colleagues at the University of New Mexico, Albuquerque, assessed 66 women using both a 100-mm visual analog pain scale (VAS) and a four-point Likert verbal rating scale (VRS). They also interviewed a subset of the participants to gather qualitative data about the experience. About half the group received an epidural (36 women) and half did not (30 women).
The VAS scores did not reveal normal distributions and the standard deviations were large, which was not statistically meaningful, according to Dr. Carr. The median scores were 40.5 mm and 2.8 mm in the no-epidural and epidural groups, respectively. But using the four-point pain scale – none, mild, moderate, and severe – the researchers found that 53% of women in the no-epidural group reported pain ranging from none to mild, while 89% of women in the epidural group reported pain in the none-to-mild range.
“What I saw basically reflected what we call the floor effect of the VAS scores in the epidural group. Most of the women hardly had any pain,” Dr. Carr said at the annual meeting of the American College of Obstetricians and Gynecologists. “Women who did not have an epidural reported scores that were all over the map.”
The results help to shed light on what is probably the most common question asked by women considering post-placental IUD insertion – Will it hurt?
“The more we learn about it, the more we can reassure women and counsel them appropriately about what to expect, not only clinically but on a personal level with their labor experience,” Dr. Carr said. “I think that’s really important, and it might promote uptake of the procedure and more women getting really effective contraception before leaving the hospital.”
Qualitative data, based on interviews with 9 women in the no-epidural group and 12 in the epidural group, showed that they had no regrets about the procedure, and most reported that it didn’t detract from their overall labor experience. Instead, most of the women in the study said that holding their newborn baby was a pleasant distraction from the placement of the IUD.
The primary driver for undergoing IUD insertion immediately post partum was convenience. “They wanted to have really good birth control on board before they left the hospital,” Dr. Carr said. “They recognize those logistical barriers to getting to that 6-week postpartum visit.”
The researchers did not report having any financial disclosures.
On Twitter @maryellenny
WASHINGTON – Many women who underwent post-placental IUD insertion reported little or no pain, regardless of whether they had an epidural during childbirth, according to the findings of a small pilot study.
Dr. Shannon Carr and her colleagues at the University of New Mexico, Albuquerque, assessed 66 women using both a 100-mm visual analog pain scale (VAS) and a four-point Likert verbal rating scale (VRS). They also interviewed a subset of the participants to gather qualitative data about the experience. About half the group received an epidural (36 women) and half did not (30 women).
The VAS scores did not reveal normal distributions and the standard deviations were large, which was not statistically meaningful, according to Dr. Carr. The median scores were 40.5 mm and 2.8 mm in the no-epidural and epidural groups, respectively. But using the four-point pain scale – none, mild, moderate, and severe – the researchers found that 53% of women in the no-epidural group reported pain ranging from none to mild, while 89% of women in the epidural group reported pain in the none-to-mild range.
“What I saw basically reflected what we call the floor effect of the VAS scores in the epidural group. Most of the women hardly had any pain,” Dr. Carr said at the annual meeting of the American College of Obstetricians and Gynecologists. “Women who did not have an epidural reported scores that were all over the map.”
The results help to shed light on what is probably the most common question asked by women considering post-placental IUD insertion – Will it hurt?
“The more we learn about it, the more we can reassure women and counsel them appropriately about what to expect, not only clinically but on a personal level with their labor experience,” Dr. Carr said. “I think that’s really important, and it might promote uptake of the procedure and more women getting really effective contraception before leaving the hospital.”
Qualitative data, based on interviews with 9 women in the no-epidural group and 12 in the epidural group, showed that they had no regrets about the procedure, and most reported that it didn’t detract from their overall labor experience. Instead, most of the women in the study said that holding their newborn baby was a pleasant distraction from the placement of the IUD.
The primary driver for undergoing IUD insertion immediately post partum was convenience. “They wanted to have really good birth control on board before they left the hospital,” Dr. Carr said. “They recognize those logistical barriers to getting to that 6-week postpartum visit.”
The researchers did not report having any financial disclosures.
On Twitter @maryellenny
AT ACOG 2016
Key clinical point: Many women felt little to no pain during post-placental IUD insertion.
Major finding: More than half of women (53%) who did not have an epidural, and 89% of women who did, reported experiencing little to no pain during post-placental IUD insertion.
Data source: A mixed-methods pilot study of 66 women.
Disclosures: The researchers did not report having any financial disclosures.
Study helps set upper boundary for leukocytosis after prenatal corticosteroids
WASHINGTON – Maternal leukocytosis after prenatal corticosteroid administration peaks at up to 24 hours after therapy, with the highest second standard deviation from the mean being 18.3 x 109/L, according to a systematic review and meta-analysis.
There has been limited data available on the magnitude and timing of leukocytosis after corticosteroid administration, making it difficult to interpret the significance of elevated white blood cell counts, Dr. Samuel Bauer, of Beaumont Health, Royal Oak, Mich., said at the annual meeting of the American College of Obstetricians and Gynecologists.
“We know corticosteroids cause leukocytosis, but we haven’t really known what the upper boundary is,” he said.
Driven by concerns about maternal sepsis and the ability to recognize early signs, Dr. Bauer and his colleagues identified six studies that reported white blood cell counts prior to corticosteroid administration, and between 24 and 96 hours afterward in healthy women with singleton gestations. The studies also met the inclusion criterion of having “excluded infected parturients between 23 and 34 weeks of gestation,” he said.
Mean maternal white blood cell count values prior to corticosteroid administration and up to 24 hours, 48 hours, 72 hours, and 96 hours after corticosteroid administration were 10.2, 13.7, 12.8, 11.5, and 11.1 x 109/L, respectively.
The highest second standard deviation from the mean of 18.3 x 109/L did not occur after 24 hours, he emphasized, and by 72 hours, mean values had returned to 11.5 x 109/L.
The findings need to be applied “cautiously” in practice, Dr. Bauer said, since the analysis did not include women with signs of infection and because some women who develop serious infections “have a very low white blood cell count.”
Still, the findings “establish a temporal trend and give us an upper boundary” for the level of leukocytosis that can be expected with prenatal corticosteroids. This can be helpful – along with other considerations – in determining whether an infectious workup is needed when white blood cell counts are high, he said in an interview.
It is not uncommon in clinical practice for maternal leukocytosis at 5-6 days or a week after corticosteroid administration to be attributed to the corticosteroids, he said. But the parameters drawn by this analysis of healthy, non-infected patients show this is a faulty assumption, he added.
The analysis covered 524 patients and 1,406 observations. Dr. Bauer and his coinvestigators did not report any financial disclosures.
WASHINGTON – Maternal leukocytosis after prenatal corticosteroid administration peaks at up to 24 hours after therapy, with the highest second standard deviation from the mean being 18.3 x 109/L, according to a systematic review and meta-analysis.
There has been limited data available on the magnitude and timing of leukocytosis after corticosteroid administration, making it difficult to interpret the significance of elevated white blood cell counts, Dr. Samuel Bauer, of Beaumont Health, Royal Oak, Mich., said at the annual meeting of the American College of Obstetricians and Gynecologists.
“We know corticosteroids cause leukocytosis, but we haven’t really known what the upper boundary is,” he said.
Driven by concerns about maternal sepsis and the ability to recognize early signs, Dr. Bauer and his colleagues identified six studies that reported white blood cell counts prior to corticosteroid administration, and between 24 and 96 hours afterward in healthy women with singleton gestations. The studies also met the inclusion criterion of having “excluded infected parturients between 23 and 34 weeks of gestation,” he said.
Mean maternal white blood cell count values prior to corticosteroid administration and up to 24 hours, 48 hours, 72 hours, and 96 hours after corticosteroid administration were 10.2, 13.7, 12.8, 11.5, and 11.1 x 109/L, respectively.
The highest second standard deviation from the mean of 18.3 x 109/L did not occur after 24 hours, he emphasized, and by 72 hours, mean values had returned to 11.5 x 109/L.
The findings need to be applied “cautiously” in practice, Dr. Bauer said, since the analysis did not include women with signs of infection and because some women who develop serious infections “have a very low white blood cell count.”
Still, the findings “establish a temporal trend and give us an upper boundary” for the level of leukocytosis that can be expected with prenatal corticosteroids. This can be helpful – along with other considerations – in determining whether an infectious workup is needed when white blood cell counts are high, he said in an interview.
It is not uncommon in clinical practice for maternal leukocytosis at 5-6 days or a week after corticosteroid administration to be attributed to the corticosteroids, he said. But the parameters drawn by this analysis of healthy, non-infected patients show this is a faulty assumption, he added.
The analysis covered 524 patients and 1,406 observations. Dr. Bauer and his coinvestigators did not report any financial disclosures.
WASHINGTON – Maternal leukocytosis after prenatal corticosteroid administration peaks at up to 24 hours after therapy, with the highest second standard deviation from the mean being 18.3 x 109/L, according to a systematic review and meta-analysis.
There has been limited data available on the magnitude and timing of leukocytosis after corticosteroid administration, making it difficult to interpret the significance of elevated white blood cell counts, Dr. Samuel Bauer, of Beaumont Health, Royal Oak, Mich., said at the annual meeting of the American College of Obstetricians and Gynecologists.
“We know corticosteroids cause leukocytosis, but we haven’t really known what the upper boundary is,” he said.
Driven by concerns about maternal sepsis and the ability to recognize early signs, Dr. Bauer and his colleagues identified six studies that reported white blood cell counts prior to corticosteroid administration, and between 24 and 96 hours afterward in healthy women with singleton gestations. The studies also met the inclusion criterion of having “excluded infected parturients between 23 and 34 weeks of gestation,” he said.
Mean maternal white blood cell count values prior to corticosteroid administration and up to 24 hours, 48 hours, 72 hours, and 96 hours after corticosteroid administration were 10.2, 13.7, 12.8, 11.5, and 11.1 x 109/L, respectively.
The highest second standard deviation from the mean of 18.3 x 109/L did not occur after 24 hours, he emphasized, and by 72 hours, mean values had returned to 11.5 x 109/L.
The findings need to be applied “cautiously” in practice, Dr. Bauer said, since the analysis did not include women with signs of infection and because some women who develop serious infections “have a very low white blood cell count.”
Still, the findings “establish a temporal trend and give us an upper boundary” for the level of leukocytosis that can be expected with prenatal corticosteroids. This can be helpful – along with other considerations – in determining whether an infectious workup is needed when white blood cell counts are high, he said in an interview.
It is not uncommon in clinical practice for maternal leukocytosis at 5-6 days or a week after corticosteroid administration to be attributed to the corticosteroids, he said. But the parameters drawn by this analysis of healthy, non-infected patients show this is a faulty assumption, he added.
The analysis covered 524 patients and 1,406 observations. Dr. Bauer and his coinvestigators did not report any financial disclosures.
AT ACOG 2016
Key clinical point: Leukocytosis attributable to prenatal corticosteroids, rather than infection, has a definable upper boundary.
Major finding: Maternal leukocytosis peaks at up to 24 hours after administration of antenatal corticosteroids. The highest second standard deviation from the mean was 18.3 x 109/L.
Data source: A systematic review and meta-analysis.
Disclosures: Dr. Bauer reported that he and his coinvestigators had no financial disclosures.
Remote prenatal care monitoring is a hit with patients
WASHINGTON – Is it time to reconsider the standard prenatal care model of 12-14 in-office prenatal visits?
As pregnant women increasingly use digital technology, and as the array of available health monitoring tools grows larger and smarter, the question looms.
Research findings reported at the annual meeting of the American College of Obstetricians and Gynecologists suggest that women with low-risk pregnancies have equivalent outcomes but are more satisfied with models that reduce the number of office visits and utilize remote monitoring.
At the Mayo Clinic in Rochester, Minn., 300 women deemed to have low-risk pregnancies were randomized to either 12 planned office visits with a physician or midwife, or to the clinic’s “OB Nest” model of care consisting of 8 planned clinic visits with a physician or midwife, 6 virtual visits with a nurse (by phone or email), home monitoring with an automatic blood pressure cuff and a hand-held fetal Doppler monitor, and access to an online prenatal care community.
The clinic’s OB Nest model “was born out of concern that the traditional model no longer met the needs of our patients,” said Dr. Yvonne S. Butler Tobah, a senior associate consultant to the department of obstetrics and gynecology at Mayo.
The goal, she said, is to “shift our prenatal clinic’s culture … to a wellness care model and to strengthen the autonomy, confidence, self-awareness and empowerment of our patients.”
Patients in the OB Nest group were encouraged to get blood pressure readings once a week, and weekly Doppler readings of fetal heart rate between weeks 12 and 28. They could use the cuff and monitor anytime they chose, however.
Values were recorded in a pregnancy journal – along with weight – and reported during the scheduled virtual visits. The patients could send in concerning readings or otherwise communicate with dedicated OB Nest nurses at any time they chose by phone or via an online portal. Emergencies were to be reported immediately.
The online prenatal care community is an invitation-only, Mayo-specific social platform, monitored by the OB Nest nurses, which gave patients the opportunity to share and discuss issues.
Patient satisfaction, as measured at 36 weeks with a 16-item validated satisfaction scale, was significantly higher in the OB Nest group; these patients had a mean score of 93.9 on a 1-100 point scale, compared with a mean score of 78.9 in the usual care group.
Levels of pregnancy-related stress – measured at three points in time with a 9-item prenatal maternal stress survey – were also significantly lower at 14 weeks and lower at 36 weeks in the OB Nest group compared with usual care. Stress levels were similar in both groups at 24 weeks.
Perceived quality of care was assessed at 36 weeks using a modified version of a prenatal processes-of-care scale that addressed communication and decision making, and no differences were observed.
“OB Nest significantly improved patient satisfaction with care and reduced maternal stress,” Dr. Tobah said. “And it did this while maintaining perceived quality of care and maintaining [safe] outcomes.”
The study was not sufficiently powered to detect statistically significant differences in clinical outcomes, which were the study’s secondary outcomes. However, there were no differences observed in maternal-fetal events or delivery outcomes, with the exception of a 4.5% rate of gestational diabetes in the OB Nest group, compared with none in the usual care group, Dr. Tobah explained.
Of the 150 patients randomized to each group, 19 and 20 were lost to follow-up in the OB Nest group and usual care group, respectively. Patients in the study had a mean age of 29, and the majority were white and married. “It was a highly educated, low-risk group,” she said. “Patients said [at the end] that they liked the general accessibility and consistent communication with a provider on an ongoing basis.”
While patients in the OB Nest group ultimately had 3.4 fewer in-office appointments than did usual care patients, they required more out-of-office nursing time and the length of in-office visits was significantly higher, Dr. Tobah noted.
In another study of remote prenatal care monitoring reported at the ACOG meeting, low-risk patients assigned to an alternative prenatal care schedule of 8 in-office visits supplemented with digital monitoring of blood pressure and weight similarly had higher patient satisfaction scores than did low-risk patients assigned to 14 prenatal visits.
Patient satisfaction was measured several times during pregnancy. Scores were significantly higher at 20 weeks in the 49-patient alternative care group “and evened out [with the 41-patient usual-care group] at the tail end of pregnancy,” said Dr. Nihar Ganju of George Washington University, Washington. “And there was no difference in pregnancy outcomes.”
This study used the Babyscripts mobile app connected to a wireless weight scale and a wireless blood pressure cuff. Patients were instructed to check their weight and blood pressure at least once a week.
They were “highly engaged,” Dr. Ganju said, checking their blood pressure a mean of 1.4 times weekly and their weight almost twice weekly. Providers received “four notifications of abnormal values,” he said.
Dr. Ganju and his colleagues are hopeful that the digital health tool “can really be effective in addressing the issue of excessive weight gain,” he said at the ACOG meeting. They are also beginning a study on remote monitoring for patients with chronic hypertension.
Findings on the effectiveness of remote personalized weight management are also expected to come from the soon-to-be-completed LIFE-Moms study, a national project looking at how overweight and obese women can best manage weight gain in pregnancy and improve their maternal and fetal outcomes.
Dr. Ganju reported having no disclosures. Two coauthors reported a nonfinancial advisory relationship with 1Eq Inc., the mobile app company that developed Babyscripts and helped fund the study. Another author is an employee of 1Eq. Dr. Tobah reported that she had no disclosures.
WASHINGTON – Is it time to reconsider the standard prenatal care model of 12-14 in-office prenatal visits?
As pregnant women increasingly use digital technology, and as the array of available health monitoring tools grows larger and smarter, the question looms.
Research findings reported at the annual meeting of the American College of Obstetricians and Gynecologists suggest that women with low-risk pregnancies have equivalent outcomes but are more satisfied with models that reduce the number of office visits and utilize remote monitoring.
At the Mayo Clinic in Rochester, Minn., 300 women deemed to have low-risk pregnancies were randomized to either 12 planned office visits with a physician or midwife, or to the clinic’s “OB Nest” model of care consisting of 8 planned clinic visits with a physician or midwife, 6 virtual visits with a nurse (by phone or email), home monitoring with an automatic blood pressure cuff and a hand-held fetal Doppler monitor, and access to an online prenatal care community.
The clinic’s OB Nest model “was born out of concern that the traditional model no longer met the needs of our patients,” said Dr. Yvonne S. Butler Tobah, a senior associate consultant to the department of obstetrics and gynecology at Mayo.
The goal, she said, is to “shift our prenatal clinic’s culture … to a wellness care model and to strengthen the autonomy, confidence, self-awareness and empowerment of our patients.”
Patients in the OB Nest group were encouraged to get blood pressure readings once a week, and weekly Doppler readings of fetal heart rate between weeks 12 and 28. They could use the cuff and monitor anytime they chose, however.
Values were recorded in a pregnancy journal – along with weight – and reported during the scheduled virtual visits. The patients could send in concerning readings or otherwise communicate with dedicated OB Nest nurses at any time they chose by phone or via an online portal. Emergencies were to be reported immediately.
The online prenatal care community is an invitation-only, Mayo-specific social platform, monitored by the OB Nest nurses, which gave patients the opportunity to share and discuss issues.
Patient satisfaction, as measured at 36 weeks with a 16-item validated satisfaction scale, was significantly higher in the OB Nest group; these patients had a mean score of 93.9 on a 1-100 point scale, compared with a mean score of 78.9 in the usual care group.
Levels of pregnancy-related stress – measured at three points in time with a 9-item prenatal maternal stress survey – were also significantly lower at 14 weeks and lower at 36 weeks in the OB Nest group compared with usual care. Stress levels were similar in both groups at 24 weeks.
Perceived quality of care was assessed at 36 weeks using a modified version of a prenatal processes-of-care scale that addressed communication and decision making, and no differences were observed.
“OB Nest significantly improved patient satisfaction with care and reduced maternal stress,” Dr. Tobah said. “And it did this while maintaining perceived quality of care and maintaining [safe] outcomes.”
The study was not sufficiently powered to detect statistically significant differences in clinical outcomes, which were the study’s secondary outcomes. However, there were no differences observed in maternal-fetal events or delivery outcomes, with the exception of a 4.5% rate of gestational diabetes in the OB Nest group, compared with none in the usual care group, Dr. Tobah explained.
Of the 150 patients randomized to each group, 19 and 20 were lost to follow-up in the OB Nest group and usual care group, respectively. Patients in the study had a mean age of 29, and the majority were white and married. “It was a highly educated, low-risk group,” she said. “Patients said [at the end] that they liked the general accessibility and consistent communication with a provider on an ongoing basis.”
While patients in the OB Nest group ultimately had 3.4 fewer in-office appointments than did usual care patients, they required more out-of-office nursing time and the length of in-office visits was significantly higher, Dr. Tobah noted.
In another study of remote prenatal care monitoring reported at the ACOG meeting, low-risk patients assigned to an alternative prenatal care schedule of 8 in-office visits supplemented with digital monitoring of blood pressure and weight similarly had higher patient satisfaction scores than did low-risk patients assigned to 14 prenatal visits.
Patient satisfaction was measured several times during pregnancy. Scores were significantly higher at 20 weeks in the 49-patient alternative care group “and evened out [with the 41-patient usual-care group] at the tail end of pregnancy,” said Dr. Nihar Ganju of George Washington University, Washington. “And there was no difference in pregnancy outcomes.”
This study used the Babyscripts mobile app connected to a wireless weight scale and a wireless blood pressure cuff. Patients were instructed to check their weight and blood pressure at least once a week.
They were “highly engaged,” Dr. Ganju said, checking their blood pressure a mean of 1.4 times weekly and their weight almost twice weekly. Providers received “four notifications of abnormal values,” he said.
Dr. Ganju and his colleagues are hopeful that the digital health tool “can really be effective in addressing the issue of excessive weight gain,” he said at the ACOG meeting. They are also beginning a study on remote monitoring for patients with chronic hypertension.
Findings on the effectiveness of remote personalized weight management are also expected to come from the soon-to-be-completed LIFE-Moms study, a national project looking at how overweight and obese women can best manage weight gain in pregnancy and improve their maternal and fetal outcomes.
Dr. Ganju reported having no disclosures. Two coauthors reported a nonfinancial advisory relationship with 1Eq Inc., the mobile app company that developed Babyscripts and helped fund the study. Another author is an employee of 1Eq. Dr. Tobah reported that she had no disclosures.
WASHINGTON – Is it time to reconsider the standard prenatal care model of 12-14 in-office prenatal visits?
As pregnant women increasingly use digital technology, and as the array of available health monitoring tools grows larger and smarter, the question looms.
Research findings reported at the annual meeting of the American College of Obstetricians and Gynecologists suggest that women with low-risk pregnancies have equivalent outcomes but are more satisfied with models that reduce the number of office visits and utilize remote monitoring.
At the Mayo Clinic in Rochester, Minn., 300 women deemed to have low-risk pregnancies were randomized to either 12 planned office visits with a physician or midwife, or to the clinic’s “OB Nest” model of care consisting of 8 planned clinic visits with a physician or midwife, 6 virtual visits with a nurse (by phone or email), home monitoring with an automatic blood pressure cuff and a hand-held fetal Doppler monitor, and access to an online prenatal care community.
The clinic’s OB Nest model “was born out of concern that the traditional model no longer met the needs of our patients,” said Dr. Yvonne S. Butler Tobah, a senior associate consultant to the department of obstetrics and gynecology at Mayo.
The goal, she said, is to “shift our prenatal clinic’s culture … to a wellness care model and to strengthen the autonomy, confidence, self-awareness and empowerment of our patients.”
Patients in the OB Nest group were encouraged to get blood pressure readings once a week, and weekly Doppler readings of fetal heart rate between weeks 12 and 28. They could use the cuff and monitor anytime they chose, however.
Values were recorded in a pregnancy journal – along with weight – and reported during the scheduled virtual visits. The patients could send in concerning readings or otherwise communicate with dedicated OB Nest nurses at any time they chose by phone or via an online portal. Emergencies were to be reported immediately.
The online prenatal care community is an invitation-only, Mayo-specific social platform, monitored by the OB Nest nurses, which gave patients the opportunity to share and discuss issues.
Patient satisfaction, as measured at 36 weeks with a 16-item validated satisfaction scale, was significantly higher in the OB Nest group; these patients had a mean score of 93.9 on a 1-100 point scale, compared with a mean score of 78.9 in the usual care group.
Levels of pregnancy-related stress – measured at three points in time with a 9-item prenatal maternal stress survey – were also significantly lower at 14 weeks and lower at 36 weeks in the OB Nest group compared with usual care. Stress levels were similar in both groups at 24 weeks.
Perceived quality of care was assessed at 36 weeks using a modified version of a prenatal processes-of-care scale that addressed communication and decision making, and no differences were observed.
“OB Nest significantly improved patient satisfaction with care and reduced maternal stress,” Dr. Tobah said. “And it did this while maintaining perceived quality of care and maintaining [safe] outcomes.”
The study was not sufficiently powered to detect statistically significant differences in clinical outcomes, which were the study’s secondary outcomes. However, there were no differences observed in maternal-fetal events or delivery outcomes, with the exception of a 4.5% rate of gestational diabetes in the OB Nest group, compared with none in the usual care group, Dr. Tobah explained.
Of the 150 patients randomized to each group, 19 and 20 were lost to follow-up in the OB Nest group and usual care group, respectively. Patients in the study had a mean age of 29, and the majority were white and married. “It was a highly educated, low-risk group,” she said. “Patients said [at the end] that they liked the general accessibility and consistent communication with a provider on an ongoing basis.”
While patients in the OB Nest group ultimately had 3.4 fewer in-office appointments than did usual care patients, they required more out-of-office nursing time and the length of in-office visits was significantly higher, Dr. Tobah noted.
In another study of remote prenatal care monitoring reported at the ACOG meeting, low-risk patients assigned to an alternative prenatal care schedule of 8 in-office visits supplemented with digital monitoring of blood pressure and weight similarly had higher patient satisfaction scores than did low-risk patients assigned to 14 prenatal visits.
Patient satisfaction was measured several times during pregnancy. Scores were significantly higher at 20 weeks in the 49-patient alternative care group “and evened out [with the 41-patient usual-care group] at the tail end of pregnancy,” said Dr. Nihar Ganju of George Washington University, Washington. “And there was no difference in pregnancy outcomes.”
This study used the Babyscripts mobile app connected to a wireless weight scale and a wireless blood pressure cuff. Patients were instructed to check their weight and blood pressure at least once a week.
They were “highly engaged,” Dr. Ganju said, checking their blood pressure a mean of 1.4 times weekly and their weight almost twice weekly. Providers received “four notifications of abnormal values,” he said.
Dr. Ganju and his colleagues are hopeful that the digital health tool “can really be effective in addressing the issue of excessive weight gain,” he said at the ACOG meeting. They are also beginning a study on remote monitoring for patients with chronic hypertension.
Findings on the effectiveness of remote personalized weight management are also expected to come from the soon-to-be-completed LIFE-Moms study, a national project looking at how overweight and obese women can best manage weight gain in pregnancy and improve their maternal and fetal outcomes.
Dr. Ganju reported having no disclosures. Two coauthors reported a nonfinancial advisory relationship with 1Eq Inc., the mobile app company that developed Babyscripts and helped fund the study. Another author is an employee of 1Eq. Dr. Tobah reported that she had no disclosures.
AT ACOG 2016
Key clinical point: Patient satisfaction improves with reduced clinic visits supplemented with remote monitoring.
Major finding: Patient satisfaction scores were significantly higher in alternative care groups, compared with usual care groups (12-14 in-office visits) in two studies.
Data source: A 300-patient randomized controlled trial of the OB Nest model at the Mayo Clinic, Rochester, Minn., and a 90-patient controlled study involving the Babyscripts tool at George Washington University, Washington.
Disclosures: Dr. Ganju reported having no disclosures. Two coauthors reported a nonfinancial advisory relationship with 1Eq Inc., the mobile app company that developed Babyscripts and helped fund the study. Another author is an employee of 1Eq. Dr. Tobah reported that she had no disclosures.
Women prescribed opioids during pregnancy have outcomes similar to those of illicit users
WASHINGTON – Women using chronic prescription opioids while pregnant have obstetrics outcomes similar to those of women chronically using illegal opioids and/or other forms of opioid substitution therapy.
Dr. Kaitlin Hanmer of Brigham & Women’s Hospital and Massachusetts General Hospital, Boston, analyzed 76 women who presented to the medical center for care between 2000 and 2015, comparing 22 women in the prescription opioid group and 54 women in the illicit opioid/opioid substitution therapy group. Among the 22 women in the prescription group, 13.6% of those pregnancies had a neonatal intensive care unit (NICU) consult, compared with 44.4% of the 54 women in the illicit opioid/opioid substitution therapy. She presented the findings at the annual meeting of the American College of Obstetricians and Gynecologists.
“The surprising finding was that women who used prescription opioids were less likely to be offered, or to have, an NICU consult during their pregnancy – prior to the birth – than were the women in the illicit opioid/opioid substitution therapy group, even though infants from both groups were significantly more likely to have longer hospital stays than their mothers,” Dr. Hanmer said in an interview.
In both groups, the hospital stays for the infants were significantly longer than for their mothers. Among infants born to mothers in the prescribed opioids group, 54.5% were hospitalized for more than 4 days longer than their mothers. This was true for 83.3% of infants born to mothers in the illicit opioid/opioid substitution therapy group.
The study also examined neonatal abstinence syndrome and found that 50% of infants of mothers using prescribed opioids were likely to be diagnosed with neonatal abstinence syndrome, compared with 81.5% of the infants of mothers in the illicit opioid/opioid substitution therapy group.
“Regardless of type of opioid use in pregnancy or preconceived notions about certain patients, we as practicing doctors need to use our points of care during the antenatal period to maximize the success of transition to the post partum period for both mom and baby,” Dr. Hanmer said. “At the end of the day, the goal is healthy mom and healthy baby.”
Dr. Hanmer reported having no financial disclosures.
WASHINGTON – Women using chronic prescription opioids while pregnant have obstetrics outcomes similar to those of women chronically using illegal opioids and/or other forms of opioid substitution therapy.
Dr. Kaitlin Hanmer of Brigham & Women’s Hospital and Massachusetts General Hospital, Boston, analyzed 76 women who presented to the medical center for care between 2000 and 2015, comparing 22 women in the prescription opioid group and 54 women in the illicit opioid/opioid substitution therapy group. Among the 22 women in the prescription group, 13.6% of those pregnancies had a neonatal intensive care unit (NICU) consult, compared with 44.4% of the 54 women in the illicit opioid/opioid substitution therapy. She presented the findings at the annual meeting of the American College of Obstetricians and Gynecologists.
“The surprising finding was that women who used prescription opioids were less likely to be offered, or to have, an NICU consult during their pregnancy – prior to the birth – than were the women in the illicit opioid/opioid substitution therapy group, even though infants from both groups were significantly more likely to have longer hospital stays than their mothers,” Dr. Hanmer said in an interview.
In both groups, the hospital stays for the infants were significantly longer than for their mothers. Among infants born to mothers in the prescribed opioids group, 54.5% were hospitalized for more than 4 days longer than their mothers. This was true for 83.3% of infants born to mothers in the illicit opioid/opioid substitution therapy group.
The study also examined neonatal abstinence syndrome and found that 50% of infants of mothers using prescribed opioids were likely to be diagnosed with neonatal abstinence syndrome, compared with 81.5% of the infants of mothers in the illicit opioid/opioid substitution therapy group.
“Regardless of type of opioid use in pregnancy or preconceived notions about certain patients, we as practicing doctors need to use our points of care during the antenatal period to maximize the success of transition to the post partum period for both mom and baby,” Dr. Hanmer said. “At the end of the day, the goal is healthy mom and healthy baby.”
Dr. Hanmer reported having no financial disclosures.
WASHINGTON – Women using chronic prescription opioids while pregnant have obstetrics outcomes similar to those of women chronically using illegal opioids and/or other forms of opioid substitution therapy.
Dr. Kaitlin Hanmer of Brigham & Women’s Hospital and Massachusetts General Hospital, Boston, analyzed 76 women who presented to the medical center for care between 2000 and 2015, comparing 22 women in the prescription opioid group and 54 women in the illicit opioid/opioid substitution therapy group. Among the 22 women in the prescription group, 13.6% of those pregnancies had a neonatal intensive care unit (NICU) consult, compared with 44.4% of the 54 women in the illicit opioid/opioid substitution therapy. She presented the findings at the annual meeting of the American College of Obstetricians and Gynecologists.
“The surprising finding was that women who used prescription opioids were less likely to be offered, or to have, an NICU consult during their pregnancy – prior to the birth – than were the women in the illicit opioid/opioid substitution therapy group, even though infants from both groups were significantly more likely to have longer hospital stays than their mothers,” Dr. Hanmer said in an interview.
In both groups, the hospital stays for the infants were significantly longer than for their mothers. Among infants born to mothers in the prescribed opioids group, 54.5% were hospitalized for more than 4 days longer than their mothers. This was true for 83.3% of infants born to mothers in the illicit opioid/opioid substitution therapy group.
The study also examined neonatal abstinence syndrome and found that 50% of infants of mothers using prescribed opioids were likely to be diagnosed with neonatal abstinence syndrome, compared with 81.5% of the infants of mothers in the illicit opioid/opioid substitution therapy group.
“Regardless of type of opioid use in pregnancy or preconceived notions about certain patients, we as practicing doctors need to use our points of care during the antenatal period to maximize the success of transition to the post partum period for both mom and baby,” Dr. Hanmer said. “At the end of the day, the goal is healthy mom and healthy baby.”
Dr. Hanmer reported having no financial disclosures.
AT ACOG 2016
Key clinical point: Use of chronic prescription opioids in pregnancy results in similar obstetrics outcomes, compared with use of illegal opioids and other forms of opioid substitution therapy.
Major finding: Half of infants whose mothers used prescribed opioids were likely to be diagnosed with neonatal abstinence syndrome, compared with 81.5% of the infants of mothers using illicit opioid and/or opioid substitution therapy.
Data source: A retrospective chart review of 76 pregnancies between 2000 and 2015.
Disclosures: Dr. Hanmer reported having no financial disclosures.
Sodium fluorescein emerges as alternative to indigo carmine in cystoscopy
WASHINGTON – Sodium fluorescein is proving to be an excellent agent for helping to verify ureteral efflux during intraoperative cystoscopy, Dr. Jay Goldberg said at the annual meeting of the American College of Obstetricians and Gynecologists.
Dr. Goldberg said he first read about the use of the dye as an alternative to indigo carmine, which is no longer available, in a study published in 2015; the study reported good results with a 10% preparation of sodium fluorescein administered at 0.25-1 mL intravenously during intraoperative cystoscopy (Obstet Gynecol. 2015 Mar;125[3]:548-50).
Since then, he and his colleagues at Einstein Medical Center, Philadelphia, have been evaluating the use of 0.1 mL of 10% sodium fluorescein IV during cystoscopies performed at the end of gynecologic surgeries, measuring the time to visualization and the level of satisfaction with the dye.
Thus far, in more than 50 cases, the average time until colored ureteral jets were seen has been 4.3 minutes (a range of 2-6.8 minutes, consistent with the 2015 study). And according to questionnaires completed by each surgeon, the degree of certainty for visualizing the ureteral jets was improved with fluorescein (a rating of 5 on a 5-point scale, compared with 2.9 without the dye).
Compared with both indigo carmine and methylene blue, fluorescein was preferred, Dr. Goldberg reported, with surgeons citing quicker onset, better color contrast, cheaper cost, and fewer side effects.
“Given that it’s at least equivalent and probably better, and that it’s 50 times cheaper [than indigo carmine], even if indigo carmine comes back again, I’m certainly not going to be switching back,” Dr. Goldberg said during a seminar on cystoscopy after hysterectomy.
Intravenous sodium fluorescein is routinely used in ophthalmology in retinal angiography, at a dosage of 5 mL of 10% fluorescein, he said. The most common complications reported in the literature are nausea, vomiting, and flushing or rash (rates of 2.9%, 1.2%, and 0.5%, respectively, according to a 1991 report). None of their patients has experienced any complications, Dr. Goldberg said.
Methylene blue (50 mg IV over a period of 5 minutes) appears to have been a common go-to dye for gynecologic surgeons, along with pyridium (a 200-mg oral dose prior to surgery), ever since production of indigo carmine was discontinued because of a lack of raw material.
“But with methylene blue, it may take longer to see the blue urine efflux from the ureteral orifices,” Dr. Goldberg said. And with pyridium, “by the time cystoscopy is performed, the bladder will have already been stained orange, making it more difficult to see the same colored urine jets.”
“Sodium fluorescein is very quick in onset. I wait [to have it administered] until I am actually ready to insert the cystoscope,” he said.
And at 60 cents per dose, fluorescein is less expensive than methylene blue ($1.50) and significantly less expensive than indigo carmine ($30 a dose), he said.
Dr. Goldberg reported having no relevant financial conflicts.
WASHINGTON – Sodium fluorescein is proving to be an excellent agent for helping to verify ureteral efflux during intraoperative cystoscopy, Dr. Jay Goldberg said at the annual meeting of the American College of Obstetricians and Gynecologists.
Dr. Goldberg said he first read about the use of the dye as an alternative to indigo carmine, which is no longer available, in a study published in 2015; the study reported good results with a 10% preparation of sodium fluorescein administered at 0.25-1 mL intravenously during intraoperative cystoscopy (Obstet Gynecol. 2015 Mar;125[3]:548-50).
Since then, he and his colleagues at Einstein Medical Center, Philadelphia, have been evaluating the use of 0.1 mL of 10% sodium fluorescein IV during cystoscopies performed at the end of gynecologic surgeries, measuring the time to visualization and the level of satisfaction with the dye.
Thus far, in more than 50 cases, the average time until colored ureteral jets were seen has been 4.3 minutes (a range of 2-6.8 minutes, consistent with the 2015 study). And according to questionnaires completed by each surgeon, the degree of certainty for visualizing the ureteral jets was improved with fluorescein (a rating of 5 on a 5-point scale, compared with 2.9 without the dye).
Compared with both indigo carmine and methylene blue, fluorescein was preferred, Dr. Goldberg reported, with surgeons citing quicker onset, better color contrast, cheaper cost, and fewer side effects.
“Given that it’s at least equivalent and probably better, and that it’s 50 times cheaper [than indigo carmine], even if indigo carmine comes back again, I’m certainly not going to be switching back,” Dr. Goldberg said during a seminar on cystoscopy after hysterectomy.
Intravenous sodium fluorescein is routinely used in ophthalmology in retinal angiography, at a dosage of 5 mL of 10% fluorescein, he said. The most common complications reported in the literature are nausea, vomiting, and flushing or rash (rates of 2.9%, 1.2%, and 0.5%, respectively, according to a 1991 report). None of their patients has experienced any complications, Dr. Goldberg said.
Methylene blue (50 mg IV over a period of 5 minutes) appears to have been a common go-to dye for gynecologic surgeons, along with pyridium (a 200-mg oral dose prior to surgery), ever since production of indigo carmine was discontinued because of a lack of raw material.
“But with methylene blue, it may take longer to see the blue urine efflux from the ureteral orifices,” Dr. Goldberg said. And with pyridium, “by the time cystoscopy is performed, the bladder will have already been stained orange, making it more difficult to see the same colored urine jets.”
“Sodium fluorescein is very quick in onset. I wait [to have it administered] until I am actually ready to insert the cystoscope,” he said.
And at 60 cents per dose, fluorescein is less expensive than methylene blue ($1.50) and significantly less expensive than indigo carmine ($30 a dose), he said.
Dr. Goldberg reported having no relevant financial conflicts.
WASHINGTON – Sodium fluorescein is proving to be an excellent agent for helping to verify ureteral efflux during intraoperative cystoscopy, Dr. Jay Goldberg said at the annual meeting of the American College of Obstetricians and Gynecologists.
Dr. Goldberg said he first read about the use of the dye as an alternative to indigo carmine, which is no longer available, in a study published in 2015; the study reported good results with a 10% preparation of sodium fluorescein administered at 0.25-1 mL intravenously during intraoperative cystoscopy (Obstet Gynecol. 2015 Mar;125[3]:548-50).
Since then, he and his colleagues at Einstein Medical Center, Philadelphia, have been evaluating the use of 0.1 mL of 10% sodium fluorescein IV during cystoscopies performed at the end of gynecologic surgeries, measuring the time to visualization and the level of satisfaction with the dye.
Thus far, in more than 50 cases, the average time until colored ureteral jets were seen has been 4.3 minutes (a range of 2-6.8 minutes, consistent with the 2015 study). And according to questionnaires completed by each surgeon, the degree of certainty for visualizing the ureteral jets was improved with fluorescein (a rating of 5 on a 5-point scale, compared with 2.9 without the dye).
Compared with both indigo carmine and methylene blue, fluorescein was preferred, Dr. Goldberg reported, with surgeons citing quicker onset, better color contrast, cheaper cost, and fewer side effects.
“Given that it’s at least equivalent and probably better, and that it’s 50 times cheaper [than indigo carmine], even if indigo carmine comes back again, I’m certainly not going to be switching back,” Dr. Goldberg said during a seminar on cystoscopy after hysterectomy.
Intravenous sodium fluorescein is routinely used in ophthalmology in retinal angiography, at a dosage of 5 mL of 10% fluorescein, he said. The most common complications reported in the literature are nausea, vomiting, and flushing or rash (rates of 2.9%, 1.2%, and 0.5%, respectively, according to a 1991 report). None of their patients has experienced any complications, Dr. Goldberg said.
Methylene blue (50 mg IV over a period of 5 minutes) appears to have been a common go-to dye for gynecologic surgeons, along with pyridium (a 200-mg oral dose prior to surgery), ever since production of indigo carmine was discontinued because of a lack of raw material.
“But with methylene blue, it may take longer to see the blue urine efflux from the ureteral orifices,” Dr. Goldberg said. And with pyridium, “by the time cystoscopy is performed, the bladder will have already been stained orange, making it more difficult to see the same colored urine jets.”
“Sodium fluorescein is very quick in onset. I wait [to have it administered] until I am actually ready to insert the cystoscope,” he said.
And at 60 cents per dose, fluorescein is less expensive than methylene blue ($1.50) and significantly less expensive than indigo carmine ($30 a dose), he said.
Dr. Goldberg reported having no relevant financial conflicts.
AT ACOG 2016
Key clinical point: Sodium fluorescein is an effective, and possibly superior, alternative to the unavailable indigo carmine.Major finding: In more than 50 cases of intraoperative cystoscopy, the average time from intravenous administration of the dye to visualization of colored ureteral jets has been 4.3 minutes.
Data source: An observational study of more than 50 cystoscopies.
Disclosures: Dr. Goldberg and his colleagues reported having no relevant financial conflicts.
Cystoscopy after hysterectomy: Consider more frequent use
WASHINGTON – Universal cystoscopy at the time of hysterectomy – or at least more frequent use of the procedure – is worth considering since delayed diagnosis of urinary tract injury causes increased morbidity for patients, and in all likelihood increases litigation, Dr. Jay Goldberg and Dr. Cheung Kim suggested at the annual meeting of the American College of Obstetricians and Gynecologists.
“We’re often hesitant to do cystoscopy because we don’t want to add time,” said Dr. Kim. “But I always feel that no matter how much time it takes, I’ll be happier in the end if I do it. [And] if you have [experience], a routine, and readily available equipment, it can take as little as 10 minutes.”
Universal cystoscopy to confirm ureteral patency is “fairly straightforward, low risk, and more likely to detect most injuries [than visual inspection alone], particularly ureteral injuries,” Dr. Kim said. On the other hand, it adds to operating time and increases procedure cost, and there is some research suggesting it may be relatively “low yield” and lead to some false positives.
Dr. Kim and Dr. Goldberg both practice at the Einstein Healthcare Network in Philadelphia. Here are some of the findings they shared, and advice they gave, on the use of cystoscopy – universal or selective – after hysterectomy.
Conflicting findings
There is conflicting opinion as to whether universal or selective cystoscopy after hysterectomy is best, and “there’s data on both sides,” said Dr. Goldberg, vice chairman of ob.gyn. and director of the Philadelphia Fibroid Center at Einstein.
A prospective study done at Louisiana State University, New Orleans, to evaluate the impact of a universal approach, for instance, showed an incidence of urinary tract injury of 4.3% (2.9% bladder injury, 1.8% ureteral injury, plus cases of simultaneous injury) in 839 hysterectomies for benign disease. The injury detection rate using intraoperative cystoscopy was 97.4%, and the majority of injuries – 76% – were not suspected prior to cystoscopy being performed (Obstet Gynecol. 2009 Jan;113[1]:6-10).
But researchers in Boston who looked retrospectively at 1,982 hysterectomies performed for any gynecologic indication found a much lower incidence of complications, and reported that cystoscopy did not detect any of the bladder injuries (0.71%) or ureteral injuries (0.25%) incurred in the group. Cystoscopy was performed selectively, however, in 250 of the patients, and was either normal or omitted in the patients who had complications (Obstet Gynecol. 2012 Dec;120[6]:1363-70).
Cystoscopy failed to detect any of the bladder injuries, but “all five of the ureteral injuries occurred in patients who had not undergone cystoscopy,” said Dr. Kim, chairman of ob.gyn. at Einstein Medical Center Montgomery in East Norriton, Pa.
Possible false-positives
Cystoscopy may lead on occasion to an incorrect presumption of a ureteral injury in patients with a pre-existing nonfunctional kidney, Dr. Goldberg noted.
He relayed the case of a 42-year-old patient who underwent a total abdominal hysterectomy without apparent complication. Cystoscopy was then performed with indigo carmine. An efflux of dye was seen from the left ureteral orifice but not from the right orifice.
Urology was consulted and investigated the presumed ureteral injury with additional surgical exploration. An intraoperative intravenous pyelogram (IVP) was eventually performed and was unable to identify the right kidney. A CT then showed an atrophic right kidney with compensatory hypertrophy of the left kidney, probably due to congenital right multicystic dysplastic kidney.
An estimated 0.2% of the population – 1 in 500 – will have a unilateral nonfunctional kidney, the majority of which have not been previously diagnosed. Etiologies include multicystic dysplastic kidney, congenital unilateral renal agenesis, and vascular events. “As we do more and more cystoscopies, this scenario is going to come up every so often,” said Dr. Goldberg, who reported on two such cases last year (Obstet Gynecol. 2015 Sep;126[3]:635-7).
It is also possible, Dr. Kim noted, that a weak urine jet observed on cystoscopy may not necessarily reflect injury. In the LSU study evaluating a universal approach, there was no injury detected on further evaluation in each of the 21 cases of low, subnormal dye efflux from the ureteral orifices. “So it’s not a benign process to undergo cystoscopy in terms of what the ramifications might be,” Dr. Kim said.
Increasing use
Ob.gyn. residents are required by the Accreditation Council for Graduate Medical Education to have completed 15 cystoscopies by the time they graduate, and according to recent survey findings, residents are more likely to utilize universal cystoscopy at the time of hysterectomy than currently practicing gynecologic surgeons.
The survey of ob.gyn residents (n = 56) shows universal cystoscopy (defined as greater than 90%) was performed in only a minority of cases during residency: 27% of total laparoscopic hysterectomies (TLH), 14% of laparoscopically assisted vaginal hysterectomies (LAVH), 12% of vaginal hysterectomies (VH), 2% of total abdominal hysterectomies (TAH), and 0% of supracervical hysterectomies (SCH), for instance.
Yet for every hysterectomy type, residents planned to perform universal cystoscopy post-residency more often than they had during their training (49% TLH, 34% LAVH, 34% VH, 15% TAH, 12% SCH), and “residents familiar with the literature on cystoscopy were statistically more likely to plan to perform universal cystoscopy,” said Dr. Goldberg, the senior author of the paper (Womens Health (Lond Engl). 2015 Nov;11[6]:825-31).
Litigation possible
Failure to detect a urinary tract injury at the time of hysterectomy may result in the need for future additional surgeries. Litigation in the Philadelphia market suggests that “if you have an injury that’s missed, there’s a chance that litigation may result,” Dr. Kim said.
Plaintiff’s attorneys have argued that not recognizing ureteral injury during surgery is a deviation from acceptable practice, while defense attorneys have contended that unavoidable complications occur and that no evaluation is required, or supported by the medical literature, when injury is not intraoperatively suspected. Currently, as cystoscopy is performed less than 25% of the time for all types of hysterectomy, the standard of care does not require the procedure intraoperatively if no injury is suspected, Dr. Goldberg said.
Primary prevention of urinary tract injury is most important, both physicians emphasized. The best way to accomplish this is to meticulously identify the anatomy and know the path of the ureter, and to document that the ureter has been identified and viewed as outside of the operative area, they said.
Dr. Kim and Dr. Goldberg reported having no relevant financial disclosures.
WASHINGTON – Universal cystoscopy at the time of hysterectomy – or at least more frequent use of the procedure – is worth considering since delayed diagnosis of urinary tract injury causes increased morbidity for patients, and in all likelihood increases litigation, Dr. Jay Goldberg and Dr. Cheung Kim suggested at the annual meeting of the American College of Obstetricians and Gynecologists.
“We’re often hesitant to do cystoscopy because we don’t want to add time,” said Dr. Kim. “But I always feel that no matter how much time it takes, I’ll be happier in the end if I do it. [And] if you have [experience], a routine, and readily available equipment, it can take as little as 10 minutes.”
Universal cystoscopy to confirm ureteral patency is “fairly straightforward, low risk, and more likely to detect most injuries [than visual inspection alone], particularly ureteral injuries,” Dr. Kim said. On the other hand, it adds to operating time and increases procedure cost, and there is some research suggesting it may be relatively “low yield” and lead to some false positives.
Dr. Kim and Dr. Goldberg both practice at the Einstein Healthcare Network in Philadelphia. Here are some of the findings they shared, and advice they gave, on the use of cystoscopy – universal or selective – after hysterectomy.
Conflicting findings
There is conflicting opinion as to whether universal or selective cystoscopy after hysterectomy is best, and “there’s data on both sides,” said Dr. Goldberg, vice chairman of ob.gyn. and director of the Philadelphia Fibroid Center at Einstein.
A prospective study done at Louisiana State University, New Orleans, to evaluate the impact of a universal approach, for instance, showed an incidence of urinary tract injury of 4.3% (2.9% bladder injury, 1.8% ureteral injury, plus cases of simultaneous injury) in 839 hysterectomies for benign disease. The injury detection rate using intraoperative cystoscopy was 97.4%, and the majority of injuries – 76% – were not suspected prior to cystoscopy being performed (Obstet Gynecol. 2009 Jan;113[1]:6-10).
But researchers in Boston who looked retrospectively at 1,982 hysterectomies performed for any gynecologic indication found a much lower incidence of complications, and reported that cystoscopy did not detect any of the bladder injuries (0.71%) or ureteral injuries (0.25%) incurred in the group. Cystoscopy was performed selectively, however, in 250 of the patients, and was either normal or omitted in the patients who had complications (Obstet Gynecol. 2012 Dec;120[6]:1363-70).
Cystoscopy failed to detect any of the bladder injuries, but “all five of the ureteral injuries occurred in patients who had not undergone cystoscopy,” said Dr. Kim, chairman of ob.gyn. at Einstein Medical Center Montgomery in East Norriton, Pa.
Possible false-positives
Cystoscopy may lead on occasion to an incorrect presumption of a ureteral injury in patients with a pre-existing nonfunctional kidney, Dr. Goldberg noted.
He relayed the case of a 42-year-old patient who underwent a total abdominal hysterectomy without apparent complication. Cystoscopy was then performed with indigo carmine. An efflux of dye was seen from the left ureteral orifice but not from the right orifice.
Urology was consulted and investigated the presumed ureteral injury with additional surgical exploration. An intraoperative intravenous pyelogram (IVP) was eventually performed and was unable to identify the right kidney. A CT then showed an atrophic right kidney with compensatory hypertrophy of the left kidney, probably due to congenital right multicystic dysplastic kidney.
An estimated 0.2% of the population – 1 in 500 – will have a unilateral nonfunctional kidney, the majority of which have not been previously diagnosed. Etiologies include multicystic dysplastic kidney, congenital unilateral renal agenesis, and vascular events. “As we do more and more cystoscopies, this scenario is going to come up every so often,” said Dr. Goldberg, who reported on two such cases last year (Obstet Gynecol. 2015 Sep;126[3]:635-7).
It is also possible, Dr. Kim noted, that a weak urine jet observed on cystoscopy may not necessarily reflect injury. In the LSU study evaluating a universal approach, there was no injury detected on further evaluation in each of the 21 cases of low, subnormal dye efflux from the ureteral orifices. “So it’s not a benign process to undergo cystoscopy in terms of what the ramifications might be,” Dr. Kim said.
Increasing use
Ob.gyn. residents are required by the Accreditation Council for Graduate Medical Education to have completed 15 cystoscopies by the time they graduate, and according to recent survey findings, residents are more likely to utilize universal cystoscopy at the time of hysterectomy than currently practicing gynecologic surgeons.
The survey of ob.gyn residents (n = 56) shows universal cystoscopy (defined as greater than 90%) was performed in only a minority of cases during residency: 27% of total laparoscopic hysterectomies (TLH), 14% of laparoscopically assisted vaginal hysterectomies (LAVH), 12% of vaginal hysterectomies (VH), 2% of total abdominal hysterectomies (TAH), and 0% of supracervical hysterectomies (SCH), for instance.
Yet for every hysterectomy type, residents planned to perform universal cystoscopy post-residency more often than they had during their training (49% TLH, 34% LAVH, 34% VH, 15% TAH, 12% SCH), and “residents familiar with the literature on cystoscopy were statistically more likely to plan to perform universal cystoscopy,” said Dr. Goldberg, the senior author of the paper (Womens Health (Lond Engl). 2015 Nov;11[6]:825-31).
Litigation possible
Failure to detect a urinary tract injury at the time of hysterectomy may result in the need for future additional surgeries. Litigation in the Philadelphia market suggests that “if you have an injury that’s missed, there’s a chance that litigation may result,” Dr. Kim said.
Plaintiff’s attorneys have argued that not recognizing ureteral injury during surgery is a deviation from acceptable practice, while defense attorneys have contended that unavoidable complications occur and that no evaluation is required, or supported by the medical literature, when injury is not intraoperatively suspected. Currently, as cystoscopy is performed less than 25% of the time for all types of hysterectomy, the standard of care does not require the procedure intraoperatively if no injury is suspected, Dr. Goldberg said.
Primary prevention of urinary tract injury is most important, both physicians emphasized. The best way to accomplish this is to meticulously identify the anatomy and know the path of the ureter, and to document that the ureter has been identified and viewed as outside of the operative area, they said.
Dr. Kim and Dr. Goldberg reported having no relevant financial disclosures.
WASHINGTON – Universal cystoscopy at the time of hysterectomy – or at least more frequent use of the procedure – is worth considering since delayed diagnosis of urinary tract injury causes increased morbidity for patients, and in all likelihood increases litigation, Dr. Jay Goldberg and Dr. Cheung Kim suggested at the annual meeting of the American College of Obstetricians and Gynecologists.
“We’re often hesitant to do cystoscopy because we don’t want to add time,” said Dr. Kim. “But I always feel that no matter how much time it takes, I’ll be happier in the end if I do it. [And] if you have [experience], a routine, and readily available equipment, it can take as little as 10 minutes.”
Universal cystoscopy to confirm ureteral patency is “fairly straightforward, low risk, and more likely to detect most injuries [than visual inspection alone], particularly ureteral injuries,” Dr. Kim said. On the other hand, it adds to operating time and increases procedure cost, and there is some research suggesting it may be relatively “low yield” and lead to some false positives.
Dr. Kim and Dr. Goldberg both practice at the Einstein Healthcare Network in Philadelphia. Here are some of the findings they shared, and advice they gave, on the use of cystoscopy – universal or selective – after hysterectomy.
Conflicting findings
There is conflicting opinion as to whether universal or selective cystoscopy after hysterectomy is best, and “there’s data on both sides,” said Dr. Goldberg, vice chairman of ob.gyn. and director of the Philadelphia Fibroid Center at Einstein.
A prospective study done at Louisiana State University, New Orleans, to evaluate the impact of a universal approach, for instance, showed an incidence of urinary tract injury of 4.3% (2.9% bladder injury, 1.8% ureteral injury, plus cases of simultaneous injury) in 839 hysterectomies for benign disease. The injury detection rate using intraoperative cystoscopy was 97.4%, and the majority of injuries – 76% – were not suspected prior to cystoscopy being performed (Obstet Gynecol. 2009 Jan;113[1]:6-10).
But researchers in Boston who looked retrospectively at 1,982 hysterectomies performed for any gynecologic indication found a much lower incidence of complications, and reported that cystoscopy did not detect any of the bladder injuries (0.71%) or ureteral injuries (0.25%) incurred in the group. Cystoscopy was performed selectively, however, in 250 of the patients, and was either normal or omitted in the patients who had complications (Obstet Gynecol. 2012 Dec;120[6]:1363-70).
Cystoscopy failed to detect any of the bladder injuries, but “all five of the ureteral injuries occurred in patients who had not undergone cystoscopy,” said Dr. Kim, chairman of ob.gyn. at Einstein Medical Center Montgomery in East Norriton, Pa.
Possible false-positives
Cystoscopy may lead on occasion to an incorrect presumption of a ureteral injury in patients with a pre-existing nonfunctional kidney, Dr. Goldberg noted.
He relayed the case of a 42-year-old patient who underwent a total abdominal hysterectomy without apparent complication. Cystoscopy was then performed with indigo carmine. An efflux of dye was seen from the left ureteral orifice but not from the right orifice.
Urology was consulted and investigated the presumed ureteral injury with additional surgical exploration. An intraoperative intravenous pyelogram (IVP) was eventually performed and was unable to identify the right kidney. A CT then showed an atrophic right kidney with compensatory hypertrophy of the left kidney, probably due to congenital right multicystic dysplastic kidney.
An estimated 0.2% of the population – 1 in 500 – will have a unilateral nonfunctional kidney, the majority of which have not been previously diagnosed. Etiologies include multicystic dysplastic kidney, congenital unilateral renal agenesis, and vascular events. “As we do more and more cystoscopies, this scenario is going to come up every so often,” said Dr. Goldberg, who reported on two such cases last year (Obstet Gynecol. 2015 Sep;126[3]:635-7).
It is also possible, Dr. Kim noted, that a weak urine jet observed on cystoscopy may not necessarily reflect injury. In the LSU study evaluating a universal approach, there was no injury detected on further evaluation in each of the 21 cases of low, subnormal dye efflux from the ureteral orifices. “So it’s not a benign process to undergo cystoscopy in terms of what the ramifications might be,” Dr. Kim said.
Increasing use
Ob.gyn. residents are required by the Accreditation Council for Graduate Medical Education to have completed 15 cystoscopies by the time they graduate, and according to recent survey findings, residents are more likely to utilize universal cystoscopy at the time of hysterectomy than currently practicing gynecologic surgeons.
The survey of ob.gyn residents (n = 56) shows universal cystoscopy (defined as greater than 90%) was performed in only a minority of cases during residency: 27% of total laparoscopic hysterectomies (TLH), 14% of laparoscopically assisted vaginal hysterectomies (LAVH), 12% of vaginal hysterectomies (VH), 2% of total abdominal hysterectomies (TAH), and 0% of supracervical hysterectomies (SCH), for instance.
Yet for every hysterectomy type, residents planned to perform universal cystoscopy post-residency more often than they had during their training (49% TLH, 34% LAVH, 34% VH, 15% TAH, 12% SCH), and “residents familiar with the literature on cystoscopy were statistically more likely to plan to perform universal cystoscopy,” said Dr. Goldberg, the senior author of the paper (Womens Health (Lond Engl). 2015 Nov;11[6]:825-31).
Litigation possible
Failure to detect a urinary tract injury at the time of hysterectomy may result in the need for future additional surgeries. Litigation in the Philadelphia market suggests that “if you have an injury that’s missed, there’s a chance that litigation may result,” Dr. Kim said.
Plaintiff’s attorneys have argued that not recognizing ureteral injury during surgery is a deviation from acceptable practice, while defense attorneys have contended that unavoidable complications occur and that no evaluation is required, or supported by the medical literature, when injury is not intraoperatively suspected. Currently, as cystoscopy is performed less than 25% of the time for all types of hysterectomy, the standard of care does not require the procedure intraoperatively if no injury is suspected, Dr. Goldberg said.
Primary prevention of urinary tract injury is most important, both physicians emphasized. The best way to accomplish this is to meticulously identify the anatomy and know the path of the ureter, and to document that the ureter has been identified and viewed as outside of the operative area, they said.
Dr. Kim and Dr. Goldberg reported having no relevant financial disclosures.
EXPERT ANALYSIS FROM ACOG 2016
Maternal flu shot offers far-reaching protection
WASHINGTON – The influenza vaccine is highly recommended for pregnant women, protecting the woman, the newborn, and even the fetus, according to Dr. Sonja Rasmussen.
Multiple prospective and retrospective studies have shown that the inactivated influenza shot is safe and effective for pregnant women. And not only does it confer a transient passive immunity upon the newborn, the vaccine also guards against the dangers the flu poses to fetuses, she said at the annual meeting of the American College of Obstetricians and Gynecologists.
Among the benefits seen with the flu shot are healthier birth weights, less preterm birth, and a much lower risk of birth defects that are associated with maternal fever in the first trimester, said Dr. Rasmussen, director of public health information dissemination at the Centers for Disease Control and Prevention.
“Fever in the first trimester doubles the risk of neural tube defects in the fetus,” said Dr. Rasmussen. She cited a 2014 meta-analysis that found increased risks of other fetal anomalies associated with first trimester flu: hydrocephaly (odds ratio, 5.74), congenital heart defects (OR, 1.56), cleft lip (OR, 3.12), limb abnormalities (OR, 2.03) and digestive system defects (OR, 1.72) (Hum Reprod. 2014 Apr;29[4]:809-23).
“We don’t know if these are more due to the hyperthermia of fever or to the flu virus crossing the placenta,” she said. “But we do know these are real risks.”
Newborns come with an immature immune system that takes a while to get ramped up. In the first 6 months of life, they’re especially vulnerable to communicable illnesses, and they can become severely ill and even die from flu, Dr. Rasmussen said. A new study of nearly 250,000 mother-child pairs confirmed that maternal vaccination reduces the risks of flu hospitalization by more than 80% in infants younger than 6 months (Pediatrics. 2016 May 2. doi: 10.1542/peds.2015-2360).
For most women, the understanding that a flu shot protects their baby before and after birth is good enough reason to get one, Dr. Rasmussen said, but the benefits for the woman are extremely important. “Pregnant women experience a lot of changes in immune function and heart and lung function that increase the risk for complications from influenza. In prior pandemics, we have seen pregnant women at an increased risk of severe illness, hospitalization, and death.”
She cited data from the 2009 H1N1 epidemic that showed that 5% of those who died from H1N1 flu were pregnant women, despite the fact that they represented only 1% of the U.S. population (JAMA. 2010;303[15]:1517-25).
Despite the well-documented benefits and reassuring safety data, flu vaccine coverage remains suboptimal for pregnant women, Dr. Rasmussen said. The most recent CDC data suggest that just half of pregnant women were immunized in 2014-2015, a rate that has remained steady since 2012.
The most effective way to boost this number, Dr. Rasmussen suggested, is to stress to women that the vaccine protects both the fetus and newborn from a potentially fatal illness. “We know that a large number of babies and children die of influenza every year,” she said. “The biggest motivator for moms is their desire to protect their baby – much more so than protecting themselves.”
Dr. Rasmussen reported having no relevant financial disclosures.
WASHINGTON – The influenza vaccine is highly recommended for pregnant women, protecting the woman, the newborn, and even the fetus, according to Dr. Sonja Rasmussen.
Multiple prospective and retrospective studies have shown that the inactivated influenza shot is safe and effective for pregnant women. And not only does it confer a transient passive immunity upon the newborn, the vaccine also guards against the dangers the flu poses to fetuses, she said at the annual meeting of the American College of Obstetricians and Gynecologists.
Among the benefits seen with the flu shot are healthier birth weights, less preterm birth, and a much lower risk of birth defects that are associated with maternal fever in the first trimester, said Dr. Rasmussen, director of public health information dissemination at the Centers for Disease Control and Prevention.
“Fever in the first trimester doubles the risk of neural tube defects in the fetus,” said Dr. Rasmussen. She cited a 2014 meta-analysis that found increased risks of other fetal anomalies associated with first trimester flu: hydrocephaly (odds ratio, 5.74), congenital heart defects (OR, 1.56), cleft lip (OR, 3.12), limb abnormalities (OR, 2.03) and digestive system defects (OR, 1.72) (Hum Reprod. 2014 Apr;29[4]:809-23).
“We don’t know if these are more due to the hyperthermia of fever or to the flu virus crossing the placenta,” she said. “But we do know these are real risks.”
Newborns come with an immature immune system that takes a while to get ramped up. In the first 6 months of life, they’re especially vulnerable to communicable illnesses, and they can become severely ill and even die from flu, Dr. Rasmussen said. A new study of nearly 250,000 mother-child pairs confirmed that maternal vaccination reduces the risks of flu hospitalization by more than 80% in infants younger than 6 months (Pediatrics. 2016 May 2. doi: 10.1542/peds.2015-2360).
For most women, the understanding that a flu shot protects their baby before and after birth is good enough reason to get one, Dr. Rasmussen said, but the benefits for the woman are extremely important. “Pregnant women experience a lot of changes in immune function and heart and lung function that increase the risk for complications from influenza. In prior pandemics, we have seen pregnant women at an increased risk of severe illness, hospitalization, and death.”
She cited data from the 2009 H1N1 epidemic that showed that 5% of those who died from H1N1 flu were pregnant women, despite the fact that they represented only 1% of the U.S. population (JAMA. 2010;303[15]:1517-25).
Despite the well-documented benefits and reassuring safety data, flu vaccine coverage remains suboptimal for pregnant women, Dr. Rasmussen said. The most recent CDC data suggest that just half of pregnant women were immunized in 2014-2015, a rate that has remained steady since 2012.
The most effective way to boost this number, Dr. Rasmussen suggested, is to stress to women that the vaccine protects both the fetus and newborn from a potentially fatal illness. “We know that a large number of babies and children die of influenza every year,” she said. “The biggest motivator for moms is their desire to protect their baby – much more so than protecting themselves.”
Dr. Rasmussen reported having no relevant financial disclosures.
WASHINGTON – The influenza vaccine is highly recommended for pregnant women, protecting the woman, the newborn, and even the fetus, according to Dr. Sonja Rasmussen.
Multiple prospective and retrospective studies have shown that the inactivated influenza shot is safe and effective for pregnant women. And not only does it confer a transient passive immunity upon the newborn, the vaccine also guards against the dangers the flu poses to fetuses, she said at the annual meeting of the American College of Obstetricians and Gynecologists.
Among the benefits seen with the flu shot are healthier birth weights, less preterm birth, and a much lower risk of birth defects that are associated with maternal fever in the first trimester, said Dr. Rasmussen, director of public health information dissemination at the Centers for Disease Control and Prevention.
“Fever in the first trimester doubles the risk of neural tube defects in the fetus,” said Dr. Rasmussen. She cited a 2014 meta-analysis that found increased risks of other fetal anomalies associated with first trimester flu: hydrocephaly (odds ratio, 5.74), congenital heart defects (OR, 1.56), cleft lip (OR, 3.12), limb abnormalities (OR, 2.03) and digestive system defects (OR, 1.72) (Hum Reprod. 2014 Apr;29[4]:809-23).
“We don’t know if these are more due to the hyperthermia of fever or to the flu virus crossing the placenta,” she said. “But we do know these are real risks.”
Newborns come with an immature immune system that takes a while to get ramped up. In the first 6 months of life, they’re especially vulnerable to communicable illnesses, and they can become severely ill and even die from flu, Dr. Rasmussen said. A new study of nearly 250,000 mother-child pairs confirmed that maternal vaccination reduces the risks of flu hospitalization by more than 80% in infants younger than 6 months (Pediatrics. 2016 May 2. doi: 10.1542/peds.2015-2360).
For most women, the understanding that a flu shot protects their baby before and after birth is good enough reason to get one, Dr. Rasmussen said, but the benefits for the woman are extremely important. “Pregnant women experience a lot of changes in immune function and heart and lung function that increase the risk for complications from influenza. In prior pandemics, we have seen pregnant women at an increased risk of severe illness, hospitalization, and death.”
She cited data from the 2009 H1N1 epidemic that showed that 5% of those who died from H1N1 flu were pregnant women, despite the fact that they represented only 1% of the U.S. population (JAMA. 2010;303[15]:1517-25).
Despite the well-documented benefits and reassuring safety data, flu vaccine coverage remains suboptimal for pregnant women, Dr. Rasmussen said. The most recent CDC data suggest that just half of pregnant women were immunized in 2014-2015, a rate that has remained steady since 2012.
The most effective way to boost this number, Dr. Rasmussen suggested, is to stress to women that the vaccine protects both the fetus and newborn from a potentially fatal illness. “We know that a large number of babies and children die of influenza every year,” she said. “The biggest motivator for moms is their desire to protect their baby – much more so than protecting themselves.”
Dr. Rasmussen reported having no relevant financial disclosures.
EXPERT ANALYSIS FROM ACOG 2016