User login
European Association of Percutaneous Cardiovascular Interventions (EAPCI): EuroPCR 2014
Bioabsorbable coronary scaffold use soars despite missing evidence
PARIS – Bioabsorbable vascular scaffolds have caught on in Europe and elsewhere in the world as an alternative to conventional metal stents for percutaneous coronary interventions in a wide spectrum of patient types.
By May 2014, more than 50,000 bioabsorbable vascular scaffolds (BVS) of the first brand to enter the European market – the Absorb stent made by Abbott Vascular – had gone into patients since the first placement in 2007, with the vast majority placed since this scaffold entered the European market in September 2012. Use of BVS in the United States remains investigational, while in the 20-plus months since BVS first became available in Europe other brands of BVS also have entered that market.
Despite growing BVS use in Europe, as well as in Asia and Central and South America, where they are also available, large-scale data on the consequences, especially long-term consequences, of BVS placement are mostly lacking, particularly data on how BVS perform when directly compared with drug-eluting metallic stents.
"Today we have uncontrolled dissemination of the technology without comparative data," Dr. Patrick W. Serruys, a pioneer in using BVS, said during a session at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
"We need evidence to know exactly what to do" with BVS, which patients to use them in, and when they are preferable to metallic stents, said Dr. Serruys, an interventional cardiologist and professor of medicine at the Thoraxcenter of Erasmus University in Rotterdam, the Netherlands.
"In the 7 years I’ve used them, in patients with 5-year follow-up, there have been no negative signals," he said in an interview, discussing his part of the sizeable anecdotal experience that BVS are safe and effective.
Several large trials comparing BVS with metal stents are in progress, including U.S. pivotal trials, but until these results are out, all that interventionalists have to gauge BVS performance are results from registries and uncontrolled trials. Given that limitation, so far the data look uniformly excellent.
"It is clear that emerging data from real-world, expanded-use registries suggest that use of the Absorb BVS is feasible and safe in a variety of patients, from low to high risk, and from simple to complex lesions," said Dr. Gregg W. Stone in a talk at the meeting. "But attention to procedural detail and technique is essential to optimize the outcomes. BVS are a little more complicated than metallic drug-eluting stents," said Dr. Stone, professor and director of cardiovascular research and education at Columbia University in New York.
"Data from large, randomized controlled trials are necessary to demonstrate whether BVS truly improve outcomes compared with best-in-class metallic stents. We are still early in the technology," he said. Dr. Stone is a lead investigator for one of the large U.S. randomized trials comparing the Absorb BVS to the current standard for percutaneous coronary interventions, a second-generation drug-eluting metallic stent.
Hints of what BVS may deliver
Hints of some of the potential benefits that BVS might provide appeared in results from a post-hoc, across-studies analysis that Dr. Stone presented in his talk. He compared the incidence of angina during the first year following PCI in 287 patients from the Absorb EXTEND study and 602 patients who received coronary stenting with the Xience second-generation everolimus-eluting metallic stent in the SPIRIT IV trial. The analysis matched patients in the Absorb arm with those in the Xience arm by propensity scoring.
The 1-year angina rates were 28% for the patients who received a metallic stent and 16% for those who received an absorbable scaffold, a 12% absolute difference, with a hazard ratio showing a 47% relative reduction in angina in patients who received the BVS, Dr. Stone reported. "There are a variety of mechanisms" by which BVS might reduce the rate of angina compared with metallic stents, including restoration of cyclic pulsatility in the treated arteries and improved vasomotion, he said.
The two outstanding clinical issues that dog PCI with second-generation drug-eluting metallic stents are the accrual of "very late" adverse events and the slow return of angina, with an average rate of target lesion failure with second-generation stents of about 1.8% year that continues out for at least 5 years, he said. "Can BVS flatten out the ongoing event rate" and improve measures like recurrent angina? Dr. Stone asked.
In another cross-study comparison, Dr. Serruys cited a recent, still unpublished analysis on which he collaborated that compared the 1-year outcomes of 102 patients with diabetes who received a BVS and 172 patients with diabetes who received a second-generation drug-eluting metallic stent. The 12-month cumulative rate of cardiovascular death, myocardial infarction, or ischemia-driven target lesion revascularization was 34.9% in the BVS recipients and 6.4% in patients who received state-of-the-art drug-eluting stents.
The working hypothesis behind BVS is that, by dissolving during a period of 12-24 months, the scaffold provides temporary bracing against restenosis but then disappears, allowing improved endovascular healing. During a separate session at EuroPCR, Dr. Charles A. Simonton, an interventional cardiologist and chief medical officer for Abbott Vascular, described the hypothesized impact that bioabsorbable coronary stents might have.
"Our vision is to convert interventional cardiology from mechanically oriented, plumbing-type interventions where you do mechanical things to open arteries" to a focus on tissue regeneration. "What we see when scaffolds resorb is that, at 3-5 years, the arteries look very different from what we see with a metal stent. The vessels show a highly functional neointimal layer that is functioning smooth muscle cells that protect against rupture in underlying plaque," he said.
Having BVS will allow interventional cardiologists to "transition from being mechanical plumbers to really being medical doctors. Not just opening lesions but putting in a treatment that can improve patients long term," Dr. Simonton said, presenting his best-case prediction of what BVS might achieve. "We need to generate a lot of data to make sure this is real," he added, in something of an understatement.
"There is late lumen enlargement with BVS. That is a clear fact," said Dr. Serruys.
The BVS experience
With data from studies that directly compared BVS and metallic stents still a few years off, the only indications of BVS performance now available come from either single- or multicenter registries. The thrust of much of these data presented at EuroPCR was that BVS have performed well as interventionalists have moved in the months since BVS became available for routine use to placing them in sicker patients and in patients with more complex coronary lesions.
The largest registry is ABSORB First, a voluntary-reporting registry that began in January 2013 and involves about 90 centers in countries where Absorb is commercially available in Europe, Asia, New Zealand, and Columbia. Dr. Eric Eeckhout, a cardiologist at Batiment Hospital in Lausanne, Switzerland, reported procedural and 30-day outcome data for the first 800 of the 1,305 patients enrolled in the registry as of May 2014.
Unlike previously reported multicenter series of patients getting BVS, these patients included 46% with at least two affected coronary arteries, 29% with stable angina, 15% with unstable angina, and 35% with an acute or recent MI. Significant calcification was present in 20% of the treated coronaries, 12% of the treated coronary stenoses were located at bifurcations, 12% of the coronaries featured extensive tortuosity, 11% had total occlusions, and 6% had ostial lesions. Lesion complexity scoring based on the American Heart Association and American College of Cardiology method rated 24% of the stenoses type C lesions and another 23% rated as B2 lesions. In addition, 38% of the lesions were at least 20 mm long.
Despite the challenging anatomy that many patients featured, device success occurred in 99% of the patients and procedure success in 98%, reported Dr. Eeckhout. Bailout treatment with a metal stent was needed in five patients (0.6%). During the 30 days following treatment the 800 patients had no deaths, and two cases (0.3%) of definite or probably stent thrombosis with both episodes occurring 1-30 days after scaffold placement – low rates given the complexity of the patients and lesions treated.
"These findings suggest the early safety and performance of Absorb in complex, real-world patients in daily PCI use," Dr. Eeckhout said. "Probably the operators [who treated these 800 patients] knew how to handle a BVS and they were able to expand to more complex pathology without an impact on safety or efficacy," he noted, adding that the "excellent results reflect the increasing experience of interventional cardiologists who use BVS; complexity did not impact efficacy or safety."
"These were "extraordinarily good outcomes in very complex patients," commented Dr. Stone, but he cautioned that the follow-up so far has been brief and that this was a "self-reported" registry, so it is possible that some operators failed to report some of their complications.
Other registry data reported at EuroPCR had longer follow-up, in some cases out to as long as 1 year, but in smaller patient sets and at fewer centers. These series represent "real world" use of BVS at these centers since Absorb came onto the European market in September 2012. Soon after BVS became commercially available, the interventionalists at these centers decided to use them in whichever patients they could regardless of their clinical status – in patients with acute coronary syndrome as well as stable patients, and regardless of lesion type or location. This contrasted with the initial, preapproval trials of BVS that excluded unstable patients and patients with complex coronary lesions or lesions in challenging sites, such as bifurcations or at an arterial ostium.
Findings from several ongoing registries were reported at EuroPCR:
• A group of six German centers had 1-year follow-up on 181 patients. Two thirds had class B2 or C lesions, 16% of lesions were calcified, and 14% involved side branches. These patients had a 5% rate of major adverse coronary events in the first year with no episodes of stent thrombosis, a result comparable with the pivotal trials for second-generation drug-eluting metallic stents as well as the early BVS studies that enrolled patients with simpler lesions, noted Dr. Thomas Schmitz, a cardiologist at the Contilla Heart and Vascular Center in Essen, Germany.
• Single-center experience at the Thoraxcenter in Rotterdam included 6-month follow-up on the first 180 of what are now more than 600 patients who have received BVS at the Thoraxcenter since it came onto the market. The series featured 48% of patients with calcified lesions, 41% with type B2 or C lesions, 38% of patients with multivessel disease, and lesion lengths up to 25 mm. Many patients received a BVS acutely after a ST-segment MI. Device success occurred in 98% of patients. The 6-month rate of major adverse coronary events was 3.3%, with definite or probable stent thrombosis in 2%, and 2% required target-lesion revascularization during 6 months of follow-up. "We had very good results in a complex group of patients that is getting closer to the real world by including patients with unstable and stable angina and ST-elevation myocardial infarction," said Dr. Robert-Jan van Geuns, a cardiologist at the Thoraxcenter. "We got stentlike results using a temporary scaffold. But we want to improve the flexibility of the BVS, reduce strut thickness, and make the procedures easier," he said.
• Interventionalists at Ferrarotto University Hospital in Catania, Italy, decided in March 2013 to start placing BVS when they could "regardless of lesion location or complexity." By this past May they had treated 367 lesions in 289 patients with BVS and had 6-month follow-up on 169 patients and 12-month follow-up on 48, said Dr. Corrado Tamburino, professor of cardiology and director of clinical cardiology at Ferrarotto. Half of their BVS patients had acute coronary syndrome, including 18% with ST-elevation MI, 17% with unstable angina, and 15% with non-STEMI. Half the treated lesions were class C or B2, 27% of patients had two or more lesions, 16% were at bifurcations, 9% were chronic total occlusions, and the mean lesion length was 21 mm. The operators successfully delivered BVS into 98% of patients. Among patients with 6-months’ follow-up, the incidence of major adverse coronary events was 2%, with no episodes of stent thrombosis after 30 days. The series included two deaths: one in a patient who stopped dual-antiplatelet therapy (DAPT) after 25 days and another in a patient who had an arterial dissection. All the BVS thromboses occurred within the first 30 days, "meaning it’s a technical issue. You need to always do lesion preparation, proper sizing [of the BVS for the artery it is entering], and post dilatation. If you do all that, you reduce the risk of thrombosis," he explained. The findings showed that placing "BVS is feasible and safe in the real world, and is effective at midterm follow-up. Stent thrombosis is not an issue if the procedural steps are respected. We expect similar results after 1 and 2 years, but we need to wait and be cautious," Dr. Tamburino said.
• Several centers in Poland began last year to enroll consecutive patients with acute coronary syndrome and culprit lesions that were amenable to BVS treatment. By May they had 1-year follow-up data on 94 BVS recipients, mostly patients with unstable angina or non–ST-elevation MI (NSTEMI) but also several with STEMI. The series had 100% success for BVS delivery and device success, with a 3% rate of major adverse coronary events while the patients remained initially hospitalized. After 12 months the patients had no deaths, three MIs, one target vessel revascularization, and one non–target vessel revascularization. Stent thrombosis occurred in one patient who prematurely stopped DAPT. The series so far has had no need for target-lesion revascularization. The 1-year results "show excellent outcomes. I’m amazed the results have been so good," said Dr. Dariusz Dudek, a cardiologist at University Hospital in Krakow, Poland.
• Interventionalists at two centers in Prague saw 311 consecutive patients with STEMI from December 2012 through the end of April 2014, and among these patients 79 (25%) met the group’s criteria for treatment with BVS. The operators excluded patients with a high likelihood of dying during the 2-3 year period for full BVS disappearance, with a Killip class of III or IV. They also excluded patients with an infarct-related artery less than 2.3 mm in diameter or more than 3.7 mm because of the limited size availability of BVS and because of the dangers from using incorrectly sized BVS. The 79 patients who received a BVS were a third of all patients in the series who received some form of PCI. An analysis presented by Dr. Petr Widimský, professor and head of the department of cardiology at Vinohrady Teaching Hospital in Prague, compared 9-month outcomes for these 79 patients who received BVS and 184 patients from the same series who also had Killip class I or II disease at the time of PCI. The remaining 48 patients from the series had Killip class III or IV disease and were excluded. After 9 months, event-free survival rate was 95% in the BVS recipients and 90% in the patients who received PCI with metallic stents, a nonsignificant difference. In the BVS group, 76 of the 79 patients successfully received a total of 85 BVS. Seventy-two of the 76 who received a BVS had an "ideal" procedural result, with no dissections and achievement of full blood flow through the treated lesion; the other four patients had slightly compromised blood flow after BVS placement. The 76 patients who successfully received a BVS had one death 4 hours after PCI as a result of septal rupture, and another BVS thrombosis 3 days after the patient stopped DAPT. A stroke or transient ischemic attack occurred in three patients. "We conclude that using BVS to treat acute STEMI is feasible and safe, and with currently available BVS sizes can be done in 25%-33% of STEMI patients. Having a 4.0-mm diameter BVS would substantially increase the number of patients we could treat," Dr. Widimský said.
• Cardiologists at one center in Barcelona treated 67 chronic total occlusions (CTO) since BVS became available, 49 of which could be crossed with a guidewire. Of these, the interventionalists could place a BVS in 38 patients; they excluded the other 11 patients because of excessive coronary-artery tortuosity, bifurcated lesions, or inappropriate vessel size. Among the 38 CTO patients who received BVS, three required bail-out PCI with a metallic stent because of a dissection. Average CTO length was 19 mm, and the average total lesion length was 36 mm. At 1-month follow-up, there were no deaths, no MI, no need for additional revascularization, and no BVS thrombosis. The same pattern held among the 33 patients from this group who had 6-months’ follow-up. "These surprising, extremely good results seem too good to be true," said Dr. Antonio Serra, an interventional cardiologist at Hospital Sant Pau in Barcelona. Results from the series so far "show that BVS is extremely feasible and safe for treating complex CTO. We report excellent patency and safety. The results at 6 months were outstanding."
Limits on BVS use
BVS are not for everyone. They get ruled out by substantial tortuosity of the route from the catheterization site to the affected coronary because BVS are stiffer than metallic stents and less amenable to pass through a winding arterial route. Patients need to be good candidates to remain on DAPT for at least 12 months, and the target-vessel diameter cannot veer too far from the currently available BVS diameters of 2.5, 3.0, or 3.5 mm. In most centers, these and other exclusion criteria usually rule out 75%-85% of patients, said several experienced BVS interventionalists at the meeting.
"I want patients who are healthy enough so they stay on DAPT. A BVS is not where you try 3 or 6 months of DAPT," said Dr. van Geuns. He also said that he would not use BVS for treating venous grafts, nor for in-stent restenosis because the existing metal likely would prevent late-lumen enlargement. And in some patients BVS cannot reach the lesion site despite aggressive predilation and vessel preparation.
"We’ve seen increasing breadth of use in the real world. It’s not yet true 100% all-comers, because appropriately people are learning where to use this technology," commented Dr. Stone.
"Our data represent a bias because it is not 100% of our patient population. They are the patients whom we think it is possible to implant a BVS," Dr. Tamburino said.
BVS "technology is not forgiving," Dr. van Guens pointed out. "If you leave a small lumen you will get a small lumen, and that can cause flow disturbances and perhaps a thrombus. Sometimes we are too eager with this technology. I think we can get to 100% in the future, but we should go slow because we are not there yet." He added that the number of BVS recipients and the rate of stent thrombosis were so far too small to allow meaningful analysis of which BVS recipients faced the greatest risk of stent thrombosis. Possible factors include inadequate post dilitation of the BVS, overexpansion of a BVS, and premature halt of DAPT.
"BVS is now feasible to use for every case" as long as the target vessel is no more than 10% smaller than the available BVS, Dr. Julinda Mehilli, an interventional cardiologist at the German Heart Center in Munich, said in a talk at the meeting. Preferred locations are long lesions in distal segments. Operators should be cautious using BVS to treat bifurcations, arteries with pronounced tortuosity, or arteries with moderate to severe calcification. When two BVS are needed in tandem, they should be placed as close to edge to edge as possible. She also stressed the need for systematic attention to every phase of BVS preparation and delivery, starting from selecting the appropriate BVS diameter to match the target vessel, predilation of the lesion and vessel and removal of calcium, gradual inflation of the BVS itself, and then followed by post dilitation of the BVS with a noncompliant balloon, ideally for at least 20 seconds.
"Now that we have BVS, it is the device of choice for chronic total occlusions because long term there is healing of the vessel walls when we use BVS. We often see long-term malopposition of stent struts in chronic total occlusions. With BVS the scaffold will disappear," eliminating the malopposition risk, Dr. Mehilli said.
Dr. Stone had no relevant disclosures, but he is lead investigator for an ongoing trial studying Abbot Vascular’s Absorb BVS. Dr. Serruys, Dr. Eeckhout, Dr. Schmitz, Dr. Dudek, and Dr. Serra had no disclosures. Dr. Tamburino is a consultant to Abbott Vascular and three other companies. Dr. Simonton is an employee of Abbott Vascular. Dr. van Geuns has received honoraria and research support from Abbott Vascular and other companies. Dr. Widimský has received honoraria from Abbott Vascular and other companies. Dr. Mehilli has received lecture fees from Abbott Vascular and other companies.
On Twitter @mitchelzoler
PARIS – Bioabsorbable vascular scaffolds have caught on in Europe and elsewhere in the world as an alternative to conventional metal stents for percutaneous coronary interventions in a wide spectrum of patient types.
By May 2014, more than 50,000 bioabsorbable vascular scaffolds (BVS) of the first brand to enter the European market – the Absorb stent made by Abbott Vascular – had gone into patients since the first placement in 2007, with the vast majority placed since this scaffold entered the European market in September 2012. Use of BVS in the United States remains investigational, while in the 20-plus months since BVS first became available in Europe other brands of BVS also have entered that market.
Despite growing BVS use in Europe, as well as in Asia and Central and South America, where they are also available, large-scale data on the consequences, especially long-term consequences, of BVS placement are mostly lacking, particularly data on how BVS perform when directly compared with drug-eluting metallic stents.
"Today we have uncontrolled dissemination of the technology without comparative data," Dr. Patrick W. Serruys, a pioneer in using BVS, said during a session at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
"We need evidence to know exactly what to do" with BVS, which patients to use them in, and when they are preferable to metallic stents, said Dr. Serruys, an interventional cardiologist and professor of medicine at the Thoraxcenter of Erasmus University in Rotterdam, the Netherlands.
"In the 7 years I’ve used them, in patients with 5-year follow-up, there have been no negative signals," he said in an interview, discussing his part of the sizeable anecdotal experience that BVS are safe and effective.
Several large trials comparing BVS with metal stents are in progress, including U.S. pivotal trials, but until these results are out, all that interventionalists have to gauge BVS performance are results from registries and uncontrolled trials. Given that limitation, so far the data look uniformly excellent.
"It is clear that emerging data from real-world, expanded-use registries suggest that use of the Absorb BVS is feasible and safe in a variety of patients, from low to high risk, and from simple to complex lesions," said Dr. Gregg W. Stone in a talk at the meeting. "But attention to procedural detail and technique is essential to optimize the outcomes. BVS are a little more complicated than metallic drug-eluting stents," said Dr. Stone, professor and director of cardiovascular research and education at Columbia University in New York.
"Data from large, randomized controlled trials are necessary to demonstrate whether BVS truly improve outcomes compared with best-in-class metallic stents. We are still early in the technology," he said. Dr. Stone is a lead investigator for one of the large U.S. randomized trials comparing the Absorb BVS to the current standard for percutaneous coronary interventions, a second-generation drug-eluting metallic stent.
Hints of what BVS may deliver
Hints of some of the potential benefits that BVS might provide appeared in results from a post-hoc, across-studies analysis that Dr. Stone presented in his talk. He compared the incidence of angina during the first year following PCI in 287 patients from the Absorb EXTEND study and 602 patients who received coronary stenting with the Xience second-generation everolimus-eluting metallic stent in the SPIRIT IV trial. The analysis matched patients in the Absorb arm with those in the Xience arm by propensity scoring.
The 1-year angina rates were 28% for the patients who received a metallic stent and 16% for those who received an absorbable scaffold, a 12% absolute difference, with a hazard ratio showing a 47% relative reduction in angina in patients who received the BVS, Dr. Stone reported. "There are a variety of mechanisms" by which BVS might reduce the rate of angina compared with metallic stents, including restoration of cyclic pulsatility in the treated arteries and improved vasomotion, he said.
The two outstanding clinical issues that dog PCI with second-generation drug-eluting metallic stents are the accrual of "very late" adverse events and the slow return of angina, with an average rate of target lesion failure with second-generation stents of about 1.8% year that continues out for at least 5 years, he said. "Can BVS flatten out the ongoing event rate" and improve measures like recurrent angina? Dr. Stone asked.
In another cross-study comparison, Dr. Serruys cited a recent, still unpublished analysis on which he collaborated that compared the 1-year outcomes of 102 patients with diabetes who received a BVS and 172 patients with diabetes who received a second-generation drug-eluting metallic stent. The 12-month cumulative rate of cardiovascular death, myocardial infarction, or ischemia-driven target lesion revascularization was 34.9% in the BVS recipients and 6.4% in patients who received state-of-the-art drug-eluting stents.
The working hypothesis behind BVS is that, by dissolving during a period of 12-24 months, the scaffold provides temporary bracing against restenosis but then disappears, allowing improved endovascular healing. During a separate session at EuroPCR, Dr. Charles A. Simonton, an interventional cardiologist and chief medical officer for Abbott Vascular, described the hypothesized impact that bioabsorbable coronary stents might have.
"Our vision is to convert interventional cardiology from mechanically oriented, plumbing-type interventions where you do mechanical things to open arteries" to a focus on tissue regeneration. "What we see when scaffolds resorb is that, at 3-5 years, the arteries look very different from what we see with a metal stent. The vessels show a highly functional neointimal layer that is functioning smooth muscle cells that protect against rupture in underlying plaque," he said.
Having BVS will allow interventional cardiologists to "transition from being mechanical plumbers to really being medical doctors. Not just opening lesions but putting in a treatment that can improve patients long term," Dr. Simonton said, presenting his best-case prediction of what BVS might achieve. "We need to generate a lot of data to make sure this is real," he added, in something of an understatement.
"There is late lumen enlargement with BVS. That is a clear fact," said Dr. Serruys.
The BVS experience
With data from studies that directly compared BVS and metallic stents still a few years off, the only indications of BVS performance now available come from either single- or multicenter registries. The thrust of much of these data presented at EuroPCR was that BVS have performed well as interventionalists have moved in the months since BVS became available for routine use to placing them in sicker patients and in patients with more complex coronary lesions.
The largest registry is ABSORB First, a voluntary-reporting registry that began in January 2013 and involves about 90 centers in countries where Absorb is commercially available in Europe, Asia, New Zealand, and Columbia. Dr. Eric Eeckhout, a cardiologist at Batiment Hospital in Lausanne, Switzerland, reported procedural and 30-day outcome data for the first 800 of the 1,305 patients enrolled in the registry as of May 2014.
Unlike previously reported multicenter series of patients getting BVS, these patients included 46% with at least two affected coronary arteries, 29% with stable angina, 15% with unstable angina, and 35% with an acute or recent MI. Significant calcification was present in 20% of the treated coronaries, 12% of the treated coronary stenoses were located at bifurcations, 12% of the coronaries featured extensive tortuosity, 11% had total occlusions, and 6% had ostial lesions. Lesion complexity scoring based on the American Heart Association and American College of Cardiology method rated 24% of the stenoses type C lesions and another 23% rated as B2 lesions. In addition, 38% of the lesions were at least 20 mm long.
Despite the challenging anatomy that many patients featured, device success occurred in 99% of the patients and procedure success in 98%, reported Dr. Eeckhout. Bailout treatment with a metal stent was needed in five patients (0.6%). During the 30 days following treatment the 800 patients had no deaths, and two cases (0.3%) of definite or probably stent thrombosis with both episodes occurring 1-30 days after scaffold placement – low rates given the complexity of the patients and lesions treated.
"These findings suggest the early safety and performance of Absorb in complex, real-world patients in daily PCI use," Dr. Eeckhout said. "Probably the operators [who treated these 800 patients] knew how to handle a BVS and they were able to expand to more complex pathology without an impact on safety or efficacy," he noted, adding that the "excellent results reflect the increasing experience of interventional cardiologists who use BVS; complexity did not impact efficacy or safety."
"These were "extraordinarily good outcomes in very complex patients," commented Dr. Stone, but he cautioned that the follow-up so far has been brief and that this was a "self-reported" registry, so it is possible that some operators failed to report some of their complications.
Other registry data reported at EuroPCR had longer follow-up, in some cases out to as long as 1 year, but in smaller patient sets and at fewer centers. These series represent "real world" use of BVS at these centers since Absorb came onto the European market in September 2012. Soon after BVS became commercially available, the interventionalists at these centers decided to use them in whichever patients they could regardless of their clinical status – in patients with acute coronary syndrome as well as stable patients, and regardless of lesion type or location. This contrasted with the initial, preapproval trials of BVS that excluded unstable patients and patients with complex coronary lesions or lesions in challenging sites, such as bifurcations or at an arterial ostium.
Findings from several ongoing registries were reported at EuroPCR:
• A group of six German centers had 1-year follow-up on 181 patients. Two thirds had class B2 or C lesions, 16% of lesions were calcified, and 14% involved side branches. These patients had a 5% rate of major adverse coronary events in the first year with no episodes of stent thrombosis, a result comparable with the pivotal trials for second-generation drug-eluting metallic stents as well as the early BVS studies that enrolled patients with simpler lesions, noted Dr. Thomas Schmitz, a cardiologist at the Contilla Heart and Vascular Center in Essen, Germany.
• Single-center experience at the Thoraxcenter in Rotterdam included 6-month follow-up on the first 180 of what are now more than 600 patients who have received BVS at the Thoraxcenter since it came onto the market. The series featured 48% of patients with calcified lesions, 41% with type B2 or C lesions, 38% of patients with multivessel disease, and lesion lengths up to 25 mm. Many patients received a BVS acutely after a ST-segment MI. Device success occurred in 98% of patients. The 6-month rate of major adverse coronary events was 3.3%, with definite or probable stent thrombosis in 2%, and 2% required target-lesion revascularization during 6 months of follow-up. "We had very good results in a complex group of patients that is getting closer to the real world by including patients with unstable and stable angina and ST-elevation myocardial infarction," said Dr. Robert-Jan van Geuns, a cardiologist at the Thoraxcenter. "We got stentlike results using a temporary scaffold. But we want to improve the flexibility of the BVS, reduce strut thickness, and make the procedures easier," he said.
• Interventionalists at Ferrarotto University Hospital in Catania, Italy, decided in March 2013 to start placing BVS when they could "regardless of lesion location or complexity." By this past May they had treated 367 lesions in 289 patients with BVS and had 6-month follow-up on 169 patients and 12-month follow-up on 48, said Dr. Corrado Tamburino, professor of cardiology and director of clinical cardiology at Ferrarotto. Half of their BVS patients had acute coronary syndrome, including 18% with ST-elevation MI, 17% with unstable angina, and 15% with non-STEMI. Half the treated lesions were class C or B2, 27% of patients had two or more lesions, 16% were at bifurcations, 9% were chronic total occlusions, and the mean lesion length was 21 mm. The operators successfully delivered BVS into 98% of patients. Among patients with 6-months’ follow-up, the incidence of major adverse coronary events was 2%, with no episodes of stent thrombosis after 30 days. The series included two deaths: one in a patient who stopped dual-antiplatelet therapy (DAPT) after 25 days and another in a patient who had an arterial dissection. All the BVS thromboses occurred within the first 30 days, "meaning it’s a technical issue. You need to always do lesion preparation, proper sizing [of the BVS for the artery it is entering], and post dilatation. If you do all that, you reduce the risk of thrombosis," he explained. The findings showed that placing "BVS is feasible and safe in the real world, and is effective at midterm follow-up. Stent thrombosis is not an issue if the procedural steps are respected. We expect similar results after 1 and 2 years, but we need to wait and be cautious," Dr. Tamburino said.
• Several centers in Poland began last year to enroll consecutive patients with acute coronary syndrome and culprit lesions that were amenable to BVS treatment. By May they had 1-year follow-up data on 94 BVS recipients, mostly patients with unstable angina or non–ST-elevation MI (NSTEMI) but also several with STEMI. The series had 100% success for BVS delivery and device success, with a 3% rate of major adverse coronary events while the patients remained initially hospitalized. After 12 months the patients had no deaths, three MIs, one target vessel revascularization, and one non–target vessel revascularization. Stent thrombosis occurred in one patient who prematurely stopped DAPT. The series so far has had no need for target-lesion revascularization. The 1-year results "show excellent outcomes. I’m amazed the results have been so good," said Dr. Dariusz Dudek, a cardiologist at University Hospital in Krakow, Poland.
• Interventionalists at two centers in Prague saw 311 consecutive patients with STEMI from December 2012 through the end of April 2014, and among these patients 79 (25%) met the group’s criteria for treatment with BVS. The operators excluded patients with a high likelihood of dying during the 2-3 year period for full BVS disappearance, with a Killip class of III or IV. They also excluded patients with an infarct-related artery less than 2.3 mm in diameter or more than 3.7 mm because of the limited size availability of BVS and because of the dangers from using incorrectly sized BVS. The 79 patients who received a BVS were a third of all patients in the series who received some form of PCI. An analysis presented by Dr. Petr Widimský, professor and head of the department of cardiology at Vinohrady Teaching Hospital in Prague, compared 9-month outcomes for these 79 patients who received BVS and 184 patients from the same series who also had Killip class I or II disease at the time of PCI. The remaining 48 patients from the series had Killip class III or IV disease and were excluded. After 9 months, event-free survival rate was 95% in the BVS recipients and 90% in the patients who received PCI with metallic stents, a nonsignificant difference. In the BVS group, 76 of the 79 patients successfully received a total of 85 BVS. Seventy-two of the 76 who received a BVS had an "ideal" procedural result, with no dissections and achievement of full blood flow through the treated lesion; the other four patients had slightly compromised blood flow after BVS placement. The 76 patients who successfully received a BVS had one death 4 hours after PCI as a result of septal rupture, and another BVS thrombosis 3 days after the patient stopped DAPT. A stroke or transient ischemic attack occurred in three patients. "We conclude that using BVS to treat acute STEMI is feasible and safe, and with currently available BVS sizes can be done in 25%-33% of STEMI patients. Having a 4.0-mm diameter BVS would substantially increase the number of patients we could treat," Dr. Widimský said.
• Cardiologists at one center in Barcelona treated 67 chronic total occlusions (CTO) since BVS became available, 49 of which could be crossed with a guidewire. Of these, the interventionalists could place a BVS in 38 patients; they excluded the other 11 patients because of excessive coronary-artery tortuosity, bifurcated lesions, or inappropriate vessel size. Among the 38 CTO patients who received BVS, three required bail-out PCI with a metallic stent because of a dissection. Average CTO length was 19 mm, and the average total lesion length was 36 mm. At 1-month follow-up, there were no deaths, no MI, no need for additional revascularization, and no BVS thrombosis. The same pattern held among the 33 patients from this group who had 6-months’ follow-up. "These surprising, extremely good results seem too good to be true," said Dr. Antonio Serra, an interventional cardiologist at Hospital Sant Pau in Barcelona. Results from the series so far "show that BVS is extremely feasible and safe for treating complex CTO. We report excellent patency and safety. The results at 6 months were outstanding."
Limits on BVS use
BVS are not for everyone. They get ruled out by substantial tortuosity of the route from the catheterization site to the affected coronary because BVS are stiffer than metallic stents and less amenable to pass through a winding arterial route. Patients need to be good candidates to remain on DAPT for at least 12 months, and the target-vessel diameter cannot veer too far from the currently available BVS diameters of 2.5, 3.0, or 3.5 mm. In most centers, these and other exclusion criteria usually rule out 75%-85% of patients, said several experienced BVS interventionalists at the meeting.
"I want patients who are healthy enough so they stay on DAPT. A BVS is not where you try 3 or 6 months of DAPT," said Dr. van Geuns. He also said that he would not use BVS for treating venous grafts, nor for in-stent restenosis because the existing metal likely would prevent late-lumen enlargement. And in some patients BVS cannot reach the lesion site despite aggressive predilation and vessel preparation.
"We’ve seen increasing breadth of use in the real world. It’s not yet true 100% all-comers, because appropriately people are learning where to use this technology," commented Dr. Stone.
"Our data represent a bias because it is not 100% of our patient population. They are the patients whom we think it is possible to implant a BVS," Dr. Tamburino said.
BVS "technology is not forgiving," Dr. van Guens pointed out. "If you leave a small lumen you will get a small lumen, and that can cause flow disturbances and perhaps a thrombus. Sometimes we are too eager with this technology. I think we can get to 100% in the future, but we should go slow because we are not there yet." He added that the number of BVS recipients and the rate of stent thrombosis were so far too small to allow meaningful analysis of which BVS recipients faced the greatest risk of stent thrombosis. Possible factors include inadequate post dilitation of the BVS, overexpansion of a BVS, and premature halt of DAPT.
"BVS is now feasible to use for every case" as long as the target vessel is no more than 10% smaller than the available BVS, Dr. Julinda Mehilli, an interventional cardiologist at the German Heart Center in Munich, said in a talk at the meeting. Preferred locations are long lesions in distal segments. Operators should be cautious using BVS to treat bifurcations, arteries with pronounced tortuosity, or arteries with moderate to severe calcification. When two BVS are needed in tandem, they should be placed as close to edge to edge as possible. She also stressed the need for systematic attention to every phase of BVS preparation and delivery, starting from selecting the appropriate BVS diameter to match the target vessel, predilation of the lesion and vessel and removal of calcium, gradual inflation of the BVS itself, and then followed by post dilitation of the BVS with a noncompliant balloon, ideally for at least 20 seconds.
"Now that we have BVS, it is the device of choice for chronic total occlusions because long term there is healing of the vessel walls when we use BVS. We often see long-term malopposition of stent struts in chronic total occlusions. With BVS the scaffold will disappear," eliminating the malopposition risk, Dr. Mehilli said.
Dr. Stone had no relevant disclosures, but he is lead investigator for an ongoing trial studying Abbot Vascular’s Absorb BVS. Dr. Serruys, Dr. Eeckhout, Dr. Schmitz, Dr. Dudek, and Dr. Serra had no disclosures. Dr. Tamburino is a consultant to Abbott Vascular and three other companies. Dr. Simonton is an employee of Abbott Vascular. Dr. van Geuns has received honoraria and research support from Abbott Vascular and other companies. Dr. Widimský has received honoraria from Abbott Vascular and other companies. Dr. Mehilli has received lecture fees from Abbott Vascular and other companies.
On Twitter @mitchelzoler
PARIS – Bioabsorbable vascular scaffolds have caught on in Europe and elsewhere in the world as an alternative to conventional metal stents for percutaneous coronary interventions in a wide spectrum of patient types.
By May 2014, more than 50,000 bioabsorbable vascular scaffolds (BVS) of the first brand to enter the European market – the Absorb stent made by Abbott Vascular – had gone into patients since the first placement in 2007, with the vast majority placed since this scaffold entered the European market in September 2012. Use of BVS in the United States remains investigational, while in the 20-plus months since BVS first became available in Europe other brands of BVS also have entered that market.
Despite growing BVS use in Europe, as well as in Asia and Central and South America, where they are also available, large-scale data on the consequences, especially long-term consequences, of BVS placement are mostly lacking, particularly data on how BVS perform when directly compared with drug-eluting metallic stents.
"Today we have uncontrolled dissemination of the technology without comparative data," Dr. Patrick W. Serruys, a pioneer in using BVS, said during a session at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
"We need evidence to know exactly what to do" with BVS, which patients to use them in, and when they are preferable to metallic stents, said Dr. Serruys, an interventional cardiologist and professor of medicine at the Thoraxcenter of Erasmus University in Rotterdam, the Netherlands.
"In the 7 years I’ve used them, in patients with 5-year follow-up, there have been no negative signals," he said in an interview, discussing his part of the sizeable anecdotal experience that BVS are safe and effective.
Several large trials comparing BVS with metal stents are in progress, including U.S. pivotal trials, but until these results are out, all that interventionalists have to gauge BVS performance are results from registries and uncontrolled trials. Given that limitation, so far the data look uniformly excellent.
"It is clear that emerging data from real-world, expanded-use registries suggest that use of the Absorb BVS is feasible and safe in a variety of patients, from low to high risk, and from simple to complex lesions," said Dr. Gregg W. Stone in a talk at the meeting. "But attention to procedural detail and technique is essential to optimize the outcomes. BVS are a little more complicated than metallic drug-eluting stents," said Dr. Stone, professor and director of cardiovascular research and education at Columbia University in New York.
"Data from large, randomized controlled trials are necessary to demonstrate whether BVS truly improve outcomes compared with best-in-class metallic stents. We are still early in the technology," he said. Dr. Stone is a lead investigator for one of the large U.S. randomized trials comparing the Absorb BVS to the current standard for percutaneous coronary interventions, a second-generation drug-eluting metallic stent.
Hints of what BVS may deliver
Hints of some of the potential benefits that BVS might provide appeared in results from a post-hoc, across-studies analysis that Dr. Stone presented in his talk. He compared the incidence of angina during the first year following PCI in 287 patients from the Absorb EXTEND study and 602 patients who received coronary stenting with the Xience second-generation everolimus-eluting metallic stent in the SPIRIT IV trial. The analysis matched patients in the Absorb arm with those in the Xience arm by propensity scoring.
The 1-year angina rates were 28% for the patients who received a metallic stent and 16% for those who received an absorbable scaffold, a 12% absolute difference, with a hazard ratio showing a 47% relative reduction in angina in patients who received the BVS, Dr. Stone reported. "There are a variety of mechanisms" by which BVS might reduce the rate of angina compared with metallic stents, including restoration of cyclic pulsatility in the treated arteries and improved vasomotion, he said.
The two outstanding clinical issues that dog PCI with second-generation drug-eluting metallic stents are the accrual of "very late" adverse events and the slow return of angina, with an average rate of target lesion failure with second-generation stents of about 1.8% year that continues out for at least 5 years, he said. "Can BVS flatten out the ongoing event rate" and improve measures like recurrent angina? Dr. Stone asked.
In another cross-study comparison, Dr. Serruys cited a recent, still unpublished analysis on which he collaborated that compared the 1-year outcomes of 102 patients with diabetes who received a BVS and 172 patients with diabetes who received a second-generation drug-eluting metallic stent. The 12-month cumulative rate of cardiovascular death, myocardial infarction, or ischemia-driven target lesion revascularization was 34.9% in the BVS recipients and 6.4% in patients who received state-of-the-art drug-eluting stents.
The working hypothesis behind BVS is that, by dissolving during a period of 12-24 months, the scaffold provides temporary bracing against restenosis but then disappears, allowing improved endovascular healing. During a separate session at EuroPCR, Dr. Charles A. Simonton, an interventional cardiologist and chief medical officer for Abbott Vascular, described the hypothesized impact that bioabsorbable coronary stents might have.
"Our vision is to convert interventional cardiology from mechanically oriented, plumbing-type interventions where you do mechanical things to open arteries" to a focus on tissue regeneration. "What we see when scaffolds resorb is that, at 3-5 years, the arteries look very different from what we see with a metal stent. The vessels show a highly functional neointimal layer that is functioning smooth muscle cells that protect against rupture in underlying plaque," he said.
Having BVS will allow interventional cardiologists to "transition from being mechanical plumbers to really being medical doctors. Not just opening lesions but putting in a treatment that can improve patients long term," Dr. Simonton said, presenting his best-case prediction of what BVS might achieve. "We need to generate a lot of data to make sure this is real," he added, in something of an understatement.
"There is late lumen enlargement with BVS. That is a clear fact," said Dr. Serruys.
The BVS experience
With data from studies that directly compared BVS and metallic stents still a few years off, the only indications of BVS performance now available come from either single- or multicenter registries. The thrust of much of these data presented at EuroPCR was that BVS have performed well as interventionalists have moved in the months since BVS became available for routine use to placing them in sicker patients and in patients with more complex coronary lesions.
The largest registry is ABSORB First, a voluntary-reporting registry that began in January 2013 and involves about 90 centers in countries where Absorb is commercially available in Europe, Asia, New Zealand, and Columbia. Dr. Eric Eeckhout, a cardiologist at Batiment Hospital in Lausanne, Switzerland, reported procedural and 30-day outcome data for the first 800 of the 1,305 patients enrolled in the registry as of May 2014.
Unlike previously reported multicenter series of patients getting BVS, these patients included 46% with at least two affected coronary arteries, 29% with stable angina, 15% with unstable angina, and 35% with an acute or recent MI. Significant calcification was present in 20% of the treated coronaries, 12% of the treated coronary stenoses were located at bifurcations, 12% of the coronaries featured extensive tortuosity, 11% had total occlusions, and 6% had ostial lesions. Lesion complexity scoring based on the American Heart Association and American College of Cardiology method rated 24% of the stenoses type C lesions and another 23% rated as B2 lesions. In addition, 38% of the lesions were at least 20 mm long.
Despite the challenging anatomy that many patients featured, device success occurred in 99% of the patients and procedure success in 98%, reported Dr. Eeckhout. Bailout treatment with a metal stent was needed in five patients (0.6%). During the 30 days following treatment the 800 patients had no deaths, and two cases (0.3%) of definite or probably stent thrombosis with both episodes occurring 1-30 days after scaffold placement – low rates given the complexity of the patients and lesions treated.
"These findings suggest the early safety and performance of Absorb in complex, real-world patients in daily PCI use," Dr. Eeckhout said. "Probably the operators [who treated these 800 patients] knew how to handle a BVS and they were able to expand to more complex pathology without an impact on safety or efficacy," he noted, adding that the "excellent results reflect the increasing experience of interventional cardiologists who use BVS; complexity did not impact efficacy or safety."
"These were "extraordinarily good outcomes in very complex patients," commented Dr. Stone, but he cautioned that the follow-up so far has been brief and that this was a "self-reported" registry, so it is possible that some operators failed to report some of their complications.
Other registry data reported at EuroPCR had longer follow-up, in some cases out to as long as 1 year, but in smaller patient sets and at fewer centers. These series represent "real world" use of BVS at these centers since Absorb came onto the European market in September 2012. Soon after BVS became commercially available, the interventionalists at these centers decided to use them in whichever patients they could regardless of their clinical status – in patients with acute coronary syndrome as well as stable patients, and regardless of lesion type or location. This contrasted with the initial, preapproval trials of BVS that excluded unstable patients and patients with complex coronary lesions or lesions in challenging sites, such as bifurcations or at an arterial ostium.
Findings from several ongoing registries were reported at EuroPCR:
• A group of six German centers had 1-year follow-up on 181 patients. Two thirds had class B2 or C lesions, 16% of lesions were calcified, and 14% involved side branches. These patients had a 5% rate of major adverse coronary events in the first year with no episodes of stent thrombosis, a result comparable with the pivotal trials for second-generation drug-eluting metallic stents as well as the early BVS studies that enrolled patients with simpler lesions, noted Dr. Thomas Schmitz, a cardiologist at the Contilla Heart and Vascular Center in Essen, Germany.
• Single-center experience at the Thoraxcenter in Rotterdam included 6-month follow-up on the first 180 of what are now more than 600 patients who have received BVS at the Thoraxcenter since it came onto the market. The series featured 48% of patients with calcified lesions, 41% with type B2 or C lesions, 38% of patients with multivessel disease, and lesion lengths up to 25 mm. Many patients received a BVS acutely after a ST-segment MI. Device success occurred in 98% of patients. The 6-month rate of major adverse coronary events was 3.3%, with definite or probable stent thrombosis in 2%, and 2% required target-lesion revascularization during 6 months of follow-up. "We had very good results in a complex group of patients that is getting closer to the real world by including patients with unstable and stable angina and ST-elevation myocardial infarction," said Dr. Robert-Jan van Geuns, a cardiologist at the Thoraxcenter. "We got stentlike results using a temporary scaffold. But we want to improve the flexibility of the BVS, reduce strut thickness, and make the procedures easier," he said.
• Interventionalists at Ferrarotto University Hospital in Catania, Italy, decided in March 2013 to start placing BVS when they could "regardless of lesion location or complexity." By this past May they had treated 367 lesions in 289 patients with BVS and had 6-month follow-up on 169 patients and 12-month follow-up on 48, said Dr. Corrado Tamburino, professor of cardiology and director of clinical cardiology at Ferrarotto. Half of their BVS patients had acute coronary syndrome, including 18% with ST-elevation MI, 17% with unstable angina, and 15% with non-STEMI. Half the treated lesions were class C or B2, 27% of patients had two or more lesions, 16% were at bifurcations, 9% were chronic total occlusions, and the mean lesion length was 21 mm. The operators successfully delivered BVS into 98% of patients. Among patients with 6-months’ follow-up, the incidence of major adverse coronary events was 2%, with no episodes of stent thrombosis after 30 days. The series included two deaths: one in a patient who stopped dual-antiplatelet therapy (DAPT) after 25 days and another in a patient who had an arterial dissection. All the BVS thromboses occurred within the first 30 days, "meaning it’s a technical issue. You need to always do lesion preparation, proper sizing [of the BVS for the artery it is entering], and post dilatation. If you do all that, you reduce the risk of thrombosis," he explained. The findings showed that placing "BVS is feasible and safe in the real world, and is effective at midterm follow-up. Stent thrombosis is not an issue if the procedural steps are respected. We expect similar results after 1 and 2 years, but we need to wait and be cautious," Dr. Tamburino said.
• Several centers in Poland began last year to enroll consecutive patients with acute coronary syndrome and culprit lesions that were amenable to BVS treatment. By May they had 1-year follow-up data on 94 BVS recipients, mostly patients with unstable angina or non–ST-elevation MI (NSTEMI) but also several with STEMI. The series had 100% success for BVS delivery and device success, with a 3% rate of major adverse coronary events while the patients remained initially hospitalized. After 12 months the patients had no deaths, three MIs, one target vessel revascularization, and one non–target vessel revascularization. Stent thrombosis occurred in one patient who prematurely stopped DAPT. The series so far has had no need for target-lesion revascularization. The 1-year results "show excellent outcomes. I’m amazed the results have been so good," said Dr. Dariusz Dudek, a cardiologist at University Hospital in Krakow, Poland.
• Interventionalists at two centers in Prague saw 311 consecutive patients with STEMI from December 2012 through the end of April 2014, and among these patients 79 (25%) met the group’s criteria for treatment with BVS. The operators excluded patients with a high likelihood of dying during the 2-3 year period for full BVS disappearance, with a Killip class of III or IV. They also excluded patients with an infarct-related artery less than 2.3 mm in diameter or more than 3.7 mm because of the limited size availability of BVS and because of the dangers from using incorrectly sized BVS. The 79 patients who received a BVS were a third of all patients in the series who received some form of PCI. An analysis presented by Dr. Petr Widimský, professor and head of the department of cardiology at Vinohrady Teaching Hospital in Prague, compared 9-month outcomes for these 79 patients who received BVS and 184 patients from the same series who also had Killip class I or II disease at the time of PCI. The remaining 48 patients from the series had Killip class III or IV disease and were excluded. After 9 months, event-free survival rate was 95% in the BVS recipients and 90% in the patients who received PCI with metallic stents, a nonsignificant difference. In the BVS group, 76 of the 79 patients successfully received a total of 85 BVS. Seventy-two of the 76 who received a BVS had an "ideal" procedural result, with no dissections and achievement of full blood flow through the treated lesion; the other four patients had slightly compromised blood flow after BVS placement. The 76 patients who successfully received a BVS had one death 4 hours after PCI as a result of septal rupture, and another BVS thrombosis 3 days after the patient stopped DAPT. A stroke or transient ischemic attack occurred in three patients. "We conclude that using BVS to treat acute STEMI is feasible and safe, and with currently available BVS sizes can be done in 25%-33% of STEMI patients. Having a 4.0-mm diameter BVS would substantially increase the number of patients we could treat," Dr. Widimský said.
• Cardiologists at one center in Barcelona treated 67 chronic total occlusions (CTO) since BVS became available, 49 of which could be crossed with a guidewire. Of these, the interventionalists could place a BVS in 38 patients; they excluded the other 11 patients because of excessive coronary-artery tortuosity, bifurcated lesions, or inappropriate vessel size. Among the 38 CTO patients who received BVS, three required bail-out PCI with a metallic stent because of a dissection. Average CTO length was 19 mm, and the average total lesion length was 36 mm. At 1-month follow-up, there were no deaths, no MI, no need for additional revascularization, and no BVS thrombosis. The same pattern held among the 33 patients from this group who had 6-months’ follow-up. "These surprising, extremely good results seem too good to be true," said Dr. Antonio Serra, an interventional cardiologist at Hospital Sant Pau in Barcelona. Results from the series so far "show that BVS is extremely feasible and safe for treating complex CTO. We report excellent patency and safety. The results at 6 months were outstanding."
Limits on BVS use
BVS are not for everyone. They get ruled out by substantial tortuosity of the route from the catheterization site to the affected coronary because BVS are stiffer than metallic stents and less amenable to pass through a winding arterial route. Patients need to be good candidates to remain on DAPT for at least 12 months, and the target-vessel diameter cannot veer too far from the currently available BVS diameters of 2.5, 3.0, or 3.5 mm. In most centers, these and other exclusion criteria usually rule out 75%-85% of patients, said several experienced BVS interventionalists at the meeting.
"I want patients who are healthy enough so they stay on DAPT. A BVS is not where you try 3 or 6 months of DAPT," said Dr. van Geuns. He also said that he would not use BVS for treating venous grafts, nor for in-stent restenosis because the existing metal likely would prevent late-lumen enlargement. And in some patients BVS cannot reach the lesion site despite aggressive predilation and vessel preparation.
"We’ve seen increasing breadth of use in the real world. It’s not yet true 100% all-comers, because appropriately people are learning where to use this technology," commented Dr. Stone.
"Our data represent a bias because it is not 100% of our patient population. They are the patients whom we think it is possible to implant a BVS," Dr. Tamburino said.
BVS "technology is not forgiving," Dr. van Guens pointed out. "If you leave a small lumen you will get a small lumen, and that can cause flow disturbances and perhaps a thrombus. Sometimes we are too eager with this technology. I think we can get to 100% in the future, but we should go slow because we are not there yet." He added that the number of BVS recipients and the rate of stent thrombosis were so far too small to allow meaningful analysis of which BVS recipients faced the greatest risk of stent thrombosis. Possible factors include inadequate post dilitation of the BVS, overexpansion of a BVS, and premature halt of DAPT.
"BVS is now feasible to use for every case" as long as the target vessel is no more than 10% smaller than the available BVS, Dr. Julinda Mehilli, an interventional cardiologist at the German Heart Center in Munich, said in a talk at the meeting. Preferred locations are long lesions in distal segments. Operators should be cautious using BVS to treat bifurcations, arteries with pronounced tortuosity, or arteries with moderate to severe calcification. When two BVS are needed in tandem, they should be placed as close to edge to edge as possible. She also stressed the need for systematic attention to every phase of BVS preparation and delivery, starting from selecting the appropriate BVS diameter to match the target vessel, predilation of the lesion and vessel and removal of calcium, gradual inflation of the BVS itself, and then followed by post dilitation of the BVS with a noncompliant balloon, ideally for at least 20 seconds.
"Now that we have BVS, it is the device of choice for chronic total occlusions because long term there is healing of the vessel walls when we use BVS. We often see long-term malopposition of stent struts in chronic total occlusions. With BVS the scaffold will disappear," eliminating the malopposition risk, Dr. Mehilli said.
Dr. Stone had no relevant disclosures, but he is lead investigator for an ongoing trial studying Abbot Vascular’s Absorb BVS. Dr. Serruys, Dr. Eeckhout, Dr. Schmitz, Dr. Dudek, and Dr. Serra had no disclosures. Dr. Tamburino is a consultant to Abbott Vascular and three other companies. Dr. Simonton is an employee of Abbott Vascular. Dr. van Geuns has received honoraria and research support from Abbott Vascular and other companies. Dr. Widimský has received honoraria from Abbott Vascular and other companies. Dr. Mehilli has received lecture fees from Abbott Vascular and other companies.
On Twitter @mitchelzoler
EXPERT ANALYSIS FROM EUROPCR 2014
Transcatheter mitral valve replacement reboots
PARIS – Transcatheter mitral valve replacement finally took off this year, but it may keep a low profile short-term as investigators gain more clinical experience with transcatheter systems and slowly start to define the right types of patients for this procedure.
Transcatheter mitral valve replacement (TMVR) had something of a false start 2 years ago when CardiAQ announced the first clinical case of a patient with severe mitral valve regurgitation who underwent valve replacement using a transcatheter system at the Heart Centre of Rigshospitalet University Hospital, Copenhagen. Further details of that first case have not yet been reported. It was not until this past May that a second patient underwent TMVR performed by the same Danish team, using a second-generation CardiAQ system.
Also this year came reports on two new TMVR systems, each used for the first time clinically, with five patients treated with the Fortis system made by Edwards Lifesciences, and two treated with the Tiara system made by Neovasc.
"We are finally on the journey of assessment of multiple transcatheter mitral valves. We’ve been saying that for a number of years, but it seems like now we truly will see progress in the mitral space," Dr. Martyn Thomas said during a talk at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
At the meeting, Dr. Thomas, an interventional cardiologist at St. Thomas’ Hospital, London, and his associate Vinayak Bapat, a cardiac surgeon, reported the experience with five patients treated with the Fortis valve system, including three patients treated by them and their colleagues in London, one patient in Bern, Switzerland, and a fifth who had been treated in Toronto just 4 days before their report at the meeting.
"We have shown that we can deploy the valve, that the valve functions; and we have one patient who is gradually improving, so I believe that the principle is now there as long as we can find the patients" best suited to TMVR, Dr. Thomas said.
"Patient selection is everything," he noted. The selection process is "perhaps more difficult than for transcatheter aortic valve replacement." Patients with severe mitral valve regurgitation often have substantial comorbidities such as left ventricular dysfunction, pulmonary disease, and renal disease, and these may mean a much longer delay to see patient improvement following TMVR compared with after an aortic valve is replaced, he noted.
"Valve replacement seeks to eliminate mitral regurgitation, while clip systems attempt to reduce regurgitation by about one grade. We need to do both, and the difficulty will be determining which patients should get what treatment," Dr. Thomas said in an interview. "Perhaps the highest-risk patients should undergo repair" with a clip, he suggested.
"We need to select patients who will survive the [TMVR] procedure and get through the following 3 months because we may not see any benefit for 3-6 months, in contrast to aortic valve patients who recover and improve very quickly. I believe we will develop a complex algorithm based on each patient’s anatomy that will address the procedure’s risk and its potential to eliminate mitral regurgitation. The mitral clip is a relatively safe procedure, so it will be a much more complex algorithm than for the aortic valve."
A second report at the meeting reviewed experience with the first two patients who received the Tiara TMVR system, both at St. Paul’s Hospital in Vancouver, B.C. Like the Fortis valve, the Tiara is delivered by a transapical approach. The Tiara system delivers a mitral valve via a 32F catheter; the size of the Fortis catheter has not been reported, but a spokeswoman for Edwards acknowledged that it was a similarly large catheter and that efforts are ongoing to try to cut the catheter size. The Fortis mitral valve is 29 mm in diameter, while the size of the Tiara valve has not been reported. Procedure times for the two Tiara cases were 20 minutes for the first patient and 12 minutes for the second, reported Dr. Anson W. Cheung, surgical director of cardiac transplantation at St. Paul’s. The Fortis valve cases showed a learning curve similar to that of the Tiara cases, with the Fortis procedure time falling from 93 minutes for the first patient to 34 minutes for the fourth.
"The key is to catch patients before their left ventricle burns out, and to prevent the vicious cycle of high afterloading" that can occur when the mitral valve is replaced, Dr. Cheung said. He reported that his two cases had no complications or left ventricular outflow tract obstruction, and that one patient has now survived more than 3 months and has shown improved heart function and a halving of her baseline blood level of brain natriuretic peptide.
"In patients with aortic stenosis, when you remove the obstructed [aortic] valve, they improve. In patients with mitral regurgitation, who develop very severely depressed left ventricular function, once you correct the regurgitation it increases stress on the ventricle and they can get into trouble," commented Dr. William Wijns, codirector of the Cardiovascular Center in Aalst, Belgium. "The complexity of the mitral valve problem is several orders of magnitude greater than with transcatheter aortic valve replacement," Dr. Wijns said.
Dr. Thomas has been a consultant to and has received research support from Edwards, the company developing the Fortis valve. Mr. Bapat has been a consultant to Edwards, Medtronic, and St. Jude and has received research support from Edwards. Dr. Cheung has been a consultant to and received honoraria from Neovasc, the company developing the Tiara valve. Dr. Wijns has received grant support to his institution from Edwards and 15 other companies, and he owns stock in two health care companies and a biotechnology company.
On Twitter @mitchelzoler
We had a phase of several years when the mitral valve programs were working hard to figure out how to get started. There has been a sort of critical mass of learning that has now launched the field, with reports on clinical use of three different systems coming out this year.
The procedural understanding that developed during a decade of work on transcatheter aortic valve replacement has helped us figure out how to do mitral valves by generating a broad base of technique development, for example, an understanding of how to percutaneously deliver prosthetic devices more coaxially. It sounds simple, but it had been a critical obstacle for treating the mitral valve.

|
|
Other technical challenges of transcatheter mitral valve replacement have been designing replacement valves to fit the noncircular mitral orifice, and the absence of calcium deposits on the mitral valve to help anchor a prosthesis. There has also been improving understanding of patient selection, including which patients are best suited to transcatheter mitral valve replacement and when is the best time in the course of mitral valve disease to intervene.
Although the safety and efficacy of the mitral clip as a transcatheter approach to mitral valve repair are now established, at least half and perhaps as many as three-quarters of patients with severe mitral regurgitation are not good candidates for clip repair. This includes patients with commissural mitral regurgitation because clip placement in corners can be difficult, patients with large jet origins that can be too big to grab with a clip, and patients with calcified mitral valve leaflets that can’t be clipped, so there are plenty of patients for whom transcatheter valve replacement would be better than clipping.
D. Ted Feldman, M.D., is director of cardiac catheterization at North Shore University Health System in Evanston, Ill. He was lead investigator for the EVEREST II trial that established the safety and efficacy of the mitral clip (N. Engl. J. Med 2011;364:1395-1406). He has been a consultant to Abbott Vascular, Boston Scientific, Edwards, and Jenavalve. He made these comments in an interview.
We had a phase of several years when the mitral valve programs were working hard to figure out how to get started. There has been a sort of critical mass of learning that has now launched the field, with reports on clinical use of three different systems coming out this year.
The procedural understanding that developed during a decade of work on transcatheter aortic valve replacement has helped us figure out how to do mitral valves by generating a broad base of technique development, for example, an understanding of how to percutaneously deliver prosthetic devices more coaxially. It sounds simple, but it had been a critical obstacle for treating the mitral valve.

|
|
Other technical challenges of transcatheter mitral valve replacement have been designing replacement valves to fit the noncircular mitral orifice, and the absence of calcium deposits on the mitral valve to help anchor a prosthesis. There has also been improving understanding of patient selection, including which patients are best suited to transcatheter mitral valve replacement and when is the best time in the course of mitral valve disease to intervene.
Although the safety and efficacy of the mitral clip as a transcatheter approach to mitral valve repair are now established, at least half and perhaps as many as three-quarters of patients with severe mitral regurgitation are not good candidates for clip repair. This includes patients with commissural mitral regurgitation because clip placement in corners can be difficult, patients with large jet origins that can be too big to grab with a clip, and patients with calcified mitral valve leaflets that can’t be clipped, so there are plenty of patients for whom transcatheter valve replacement would be better than clipping.
D. Ted Feldman, M.D., is director of cardiac catheterization at North Shore University Health System in Evanston, Ill. He was lead investigator for the EVEREST II trial that established the safety and efficacy of the mitral clip (N. Engl. J. Med 2011;364:1395-1406). He has been a consultant to Abbott Vascular, Boston Scientific, Edwards, and Jenavalve. He made these comments in an interview.
We had a phase of several years when the mitral valve programs were working hard to figure out how to get started. There has been a sort of critical mass of learning that has now launched the field, with reports on clinical use of three different systems coming out this year.
The procedural understanding that developed during a decade of work on transcatheter aortic valve replacement has helped us figure out how to do mitral valves by generating a broad base of technique development, for example, an understanding of how to percutaneously deliver prosthetic devices more coaxially. It sounds simple, but it had been a critical obstacle for treating the mitral valve.

|
|
Other technical challenges of transcatheter mitral valve replacement have been designing replacement valves to fit the noncircular mitral orifice, and the absence of calcium deposits on the mitral valve to help anchor a prosthesis. There has also been improving understanding of patient selection, including which patients are best suited to transcatheter mitral valve replacement and when is the best time in the course of mitral valve disease to intervene.
Although the safety and efficacy of the mitral clip as a transcatheter approach to mitral valve repair are now established, at least half and perhaps as many as three-quarters of patients with severe mitral regurgitation are not good candidates for clip repair. This includes patients with commissural mitral regurgitation because clip placement in corners can be difficult, patients with large jet origins that can be too big to grab with a clip, and patients with calcified mitral valve leaflets that can’t be clipped, so there are plenty of patients for whom transcatheter valve replacement would be better than clipping.
D. Ted Feldman, M.D., is director of cardiac catheterization at North Shore University Health System in Evanston, Ill. He was lead investigator for the EVEREST II trial that established the safety and efficacy of the mitral clip (N. Engl. J. Med 2011;364:1395-1406). He has been a consultant to Abbott Vascular, Boston Scientific, Edwards, and Jenavalve. He made these comments in an interview.
PARIS – Transcatheter mitral valve replacement finally took off this year, but it may keep a low profile short-term as investigators gain more clinical experience with transcatheter systems and slowly start to define the right types of patients for this procedure.
Transcatheter mitral valve replacement (TMVR) had something of a false start 2 years ago when CardiAQ announced the first clinical case of a patient with severe mitral valve regurgitation who underwent valve replacement using a transcatheter system at the Heart Centre of Rigshospitalet University Hospital, Copenhagen. Further details of that first case have not yet been reported. It was not until this past May that a second patient underwent TMVR performed by the same Danish team, using a second-generation CardiAQ system.
Also this year came reports on two new TMVR systems, each used for the first time clinically, with five patients treated with the Fortis system made by Edwards Lifesciences, and two treated with the Tiara system made by Neovasc.
"We are finally on the journey of assessment of multiple transcatheter mitral valves. We’ve been saying that for a number of years, but it seems like now we truly will see progress in the mitral space," Dr. Martyn Thomas said during a talk at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
At the meeting, Dr. Thomas, an interventional cardiologist at St. Thomas’ Hospital, London, and his associate Vinayak Bapat, a cardiac surgeon, reported the experience with five patients treated with the Fortis valve system, including three patients treated by them and their colleagues in London, one patient in Bern, Switzerland, and a fifth who had been treated in Toronto just 4 days before their report at the meeting.
"We have shown that we can deploy the valve, that the valve functions; and we have one patient who is gradually improving, so I believe that the principle is now there as long as we can find the patients" best suited to TMVR, Dr. Thomas said.
"Patient selection is everything," he noted. The selection process is "perhaps more difficult than for transcatheter aortic valve replacement." Patients with severe mitral valve regurgitation often have substantial comorbidities such as left ventricular dysfunction, pulmonary disease, and renal disease, and these may mean a much longer delay to see patient improvement following TMVR compared with after an aortic valve is replaced, he noted.
"Valve replacement seeks to eliminate mitral regurgitation, while clip systems attempt to reduce regurgitation by about one grade. We need to do both, and the difficulty will be determining which patients should get what treatment," Dr. Thomas said in an interview. "Perhaps the highest-risk patients should undergo repair" with a clip, he suggested.
"We need to select patients who will survive the [TMVR] procedure and get through the following 3 months because we may not see any benefit for 3-6 months, in contrast to aortic valve patients who recover and improve very quickly. I believe we will develop a complex algorithm based on each patient’s anatomy that will address the procedure’s risk and its potential to eliminate mitral regurgitation. The mitral clip is a relatively safe procedure, so it will be a much more complex algorithm than for the aortic valve."
A second report at the meeting reviewed experience with the first two patients who received the Tiara TMVR system, both at St. Paul’s Hospital in Vancouver, B.C. Like the Fortis valve, the Tiara is delivered by a transapical approach. The Tiara system delivers a mitral valve via a 32F catheter; the size of the Fortis catheter has not been reported, but a spokeswoman for Edwards acknowledged that it was a similarly large catheter and that efforts are ongoing to try to cut the catheter size. The Fortis mitral valve is 29 mm in diameter, while the size of the Tiara valve has not been reported. Procedure times for the two Tiara cases were 20 minutes for the first patient and 12 minutes for the second, reported Dr. Anson W. Cheung, surgical director of cardiac transplantation at St. Paul’s. The Fortis valve cases showed a learning curve similar to that of the Tiara cases, with the Fortis procedure time falling from 93 minutes for the first patient to 34 minutes for the fourth.
"The key is to catch patients before their left ventricle burns out, and to prevent the vicious cycle of high afterloading" that can occur when the mitral valve is replaced, Dr. Cheung said. He reported that his two cases had no complications or left ventricular outflow tract obstruction, and that one patient has now survived more than 3 months and has shown improved heart function and a halving of her baseline blood level of brain natriuretic peptide.
"In patients with aortic stenosis, when you remove the obstructed [aortic] valve, they improve. In patients with mitral regurgitation, who develop very severely depressed left ventricular function, once you correct the regurgitation it increases stress on the ventricle and they can get into trouble," commented Dr. William Wijns, codirector of the Cardiovascular Center in Aalst, Belgium. "The complexity of the mitral valve problem is several orders of magnitude greater than with transcatheter aortic valve replacement," Dr. Wijns said.
Dr. Thomas has been a consultant to and has received research support from Edwards, the company developing the Fortis valve. Mr. Bapat has been a consultant to Edwards, Medtronic, and St. Jude and has received research support from Edwards. Dr. Cheung has been a consultant to and received honoraria from Neovasc, the company developing the Tiara valve. Dr. Wijns has received grant support to his institution from Edwards and 15 other companies, and he owns stock in two health care companies and a biotechnology company.
On Twitter @mitchelzoler
PARIS – Transcatheter mitral valve replacement finally took off this year, but it may keep a low profile short-term as investigators gain more clinical experience with transcatheter systems and slowly start to define the right types of patients for this procedure.
Transcatheter mitral valve replacement (TMVR) had something of a false start 2 years ago when CardiAQ announced the first clinical case of a patient with severe mitral valve regurgitation who underwent valve replacement using a transcatheter system at the Heart Centre of Rigshospitalet University Hospital, Copenhagen. Further details of that first case have not yet been reported. It was not until this past May that a second patient underwent TMVR performed by the same Danish team, using a second-generation CardiAQ system.
Also this year came reports on two new TMVR systems, each used for the first time clinically, with five patients treated with the Fortis system made by Edwards Lifesciences, and two treated with the Tiara system made by Neovasc.
"We are finally on the journey of assessment of multiple transcatheter mitral valves. We’ve been saying that for a number of years, but it seems like now we truly will see progress in the mitral space," Dr. Martyn Thomas said during a talk at the annual congress of the European Association of Percutaneous Cardiovascular Interventions.
At the meeting, Dr. Thomas, an interventional cardiologist at St. Thomas’ Hospital, London, and his associate Vinayak Bapat, a cardiac surgeon, reported the experience with five patients treated with the Fortis valve system, including three patients treated by them and their colleagues in London, one patient in Bern, Switzerland, and a fifth who had been treated in Toronto just 4 days before their report at the meeting.
"We have shown that we can deploy the valve, that the valve functions; and we have one patient who is gradually improving, so I believe that the principle is now there as long as we can find the patients" best suited to TMVR, Dr. Thomas said.
"Patient selection is everything," he noted. The selection process is "perhaps more difficult than for transcatheter aortic valve replacement." Patients with severe mitral valve regurgitation often have substantial comorbidities such as left ventricular dysfunction, pulmonary disease, and renal disease, and these may mean a much longer delay to see patient improvement following TMVR compared with after an aortic valve is replaced, he noted.
"Valve replacement seeks to eliminate mitral regurgitation, while clip systems attempt to reduce regurgitation by about one grade. We need to do both, and the difficulty will be determining which patients should get what treatment," Dr. Thomas said in an interview. "Perhaps the highest-risk patients should undergo repair" with a clip, he suggested.
"We need to select patients who will survive the [TMVR] procedure and get through the following 3 months because we may not see any benefit for 3-6 months, in contrast to aortic valve patients who recover and improve very quickly. I believe we will develop a complex algorithm based on each patient’s anatomy that will address the procedure’s risk and its potential to eliminate mitral regurgitation. The mitral clip is a relatively safe procedure, so it will be a much more complex algorithm than for the aortic valve."
A second report at the meeting reviewed experience with the first two patients who received the Tiara TMVR system, both at St. Paul’s Hospital in Vancouver, B.C. Like the Fortis valve, the Tiara is delivered by a transapical approach. The Tiara system delivers a mitral valve via a 32F catheter; the size of the Fortis catheter has not been reported, but a spokeswoman for Edwards acknowledged that it was a similarly large catheter and that efforts are ongoing to try to cut the catheter size. The Fortis mitral valve is 29 mm in diameter, while the size of the Tiara valve has not been reported. Procedure times for the two Tiara cases were 20 minutes for the first patient and 12 minutes for the second, reported Dr. Anson W. Cheung, surgical director of cardiac transplantation at St. Paul’s. The Fortis valve cases showed a learning curve similar to that of the Tiara cases, with the Fortis procedure time falling from 93 minutes for the first patient to 34 minutes for the fourth.
"The key is to catch patients before their left ventricle burns out, and to prevent the vicious cycle of high afterloading" that can occur when the mitral valve is replaced, Dr. Cheung said. He reported that his two cases had no complications or left ventricular outflow tract obstruction, and that one patient has now survived more than 3 months and has shown improved heart function and a halving of her baseline blood level of brain natriuretic peptide.
"In patients with aortic stenosis, when you remove the obstructed [aortic] valve, they improve. In patients with mitral regurgitation, who develop very severely depressed left ventricular function, once you correct the regurgitation it increases stress on the ventricle and they can get into trouble," commented Dr. William Wijns, codirector of the Cardiovascular Center in Aalst, Belgium. "The complexity of the mitral valve problem is several orders of magnitude greater than with transcatheter aortic valve replacement," Dr. Wijns said.
Dr. Thomas has been a consultant to and has received research support from Edwards, the company developing the Fortis valve. Mr. Bapat has been a consultant to Edwards, Medtronic, and St. Jude and has received research support from Edwards. Dr. Cheung has been a consultant to and received honoraria from Neovasc, the company developing the Tiara valve. Dr. Wijns has received grant support to his institution from Edwards and 15 other companies, and he owns stock in two health care companies and a biotechnology company.
On Twitter @mitchelzoler
AT EUROPCR 2014
Renal denervation proceeds as U.S. trial’s flaws emerge
PARIS – At least three different factors undermined the SYMPLICITY HTN-3 trial that earlier this year did not show a significant difference in blood pressure lowering between renal denervation and a sham-control procedure, most notably the failure of the vast majority of operators in the study to follow ablation instructions and produce thorough and reliable interruptions of sympathetic innervation of the kidneys, according to new data released by the trial’s investigators.
As the full range of problems with the U.S.-based SYMPLICITY HTN-3 trial, which had its main results reported in April (N. Engl. J. Med. 2014;370:1393-1401), became apparent in a report at the annual congress of the European Association of Percutaneous Cardiovascular Interventions, many top European practitioners and supporters of renal denervation voiced their belief that the treatment is an effective and safe option for many patients with true drug-resistant, severe hypertension.
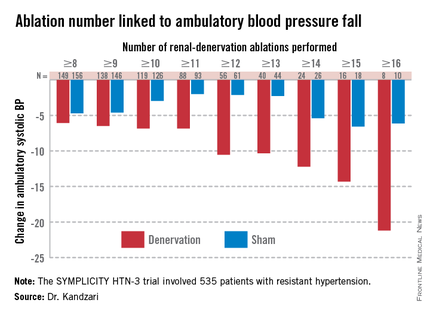
The only qualifications they now add are that renal denervation is not easily performed and must be done carefully and in a more targeted way, with an ongoing need to find the patients best suited for treatment and the best methods for delivering treatment.
During the meeting, Dr. Felix Mahfoud, an interventional cardiologist at the University Hospital of Saarland in Homburg/Saar, Germany, joined with hypertension specialist Dr. Konstantinos Tsioufis of the University of Athens and Dr. William Wijns, codirector of EuroPCR, in an official statement from the meeting that despite the SYMPLICITY HTN-3 results they continued to support renal denervation as a treatment option for selected patients with drug-resistant, severe hypertension.
Their sentiment echoed another endorsement made a few weeks earlier for continued use and study of renal denervation from the European Society of Hypertension (ESH) in reaction to the SYMPLICITY HTN-3 results.
The ESH "sticks to its statement" from 2013 on using renal denervation in appropriate patients with treatment-resistant, severe hypertension (Eurointervention 2013;9:R58-R66), said Dr. Roland E. Schmieder, first author for the 2013 ESH position paper and a leader in European use of renal denervation.
"We need more studies to prove that renal denervation works, and in particular to get more precise information on which patients get the greatest benefit," Dr. Schmieder said in a separate talk at the meeting. For the time being, he said he was comfortable with routine use of renal denervation in patients with an office systolic BP of at least 160 mm Hg that remains at this level despite maximally tolerated treatment with at least three antihypertensive drugs, including a diuretic, the use endorsed by current European guidelines. It remains appropriate to investigate the impact of renal denervation on other disorders, such as heart failure, arrhythmia, metabolic syndrome, and depressed renal function, said Dr. Schmieder, professor and head of hypertension and vascular medicine research at University Hospital in Erlangen, Germany.
The problems with SYMPLICITY HTN-3
While much speculation swirled around what had gone wrong in the SYMPLICITY HTN-3 trial after researchers on the study gave their first report on the results early in the spring, the full extent of the study’s problems didn’t flesh out until a follow-up report during EuroPCR by coinvestigator Dr. David E. Kandzari. In his analysis, Dr. Kandzari highlighted three distinct problems with the trial that he and his associates identified in a series of post hoc analyses:
• The failure of a large minority of enrolled patients in both arms of the study to remain on a stable medical regimen during the 6 months of follow-up before the primary efficacy outcomes were measured.
• The inexplicably large reduction in BP among the sham-control patients, especially among African American patients, who made up a quarter of the trial’s population.
• The vastly incomplete nerve-ablation treatment that most patients received, treatments that usually failed to meet the standards specified in the trial’s protocol.
The background medical regimens that patients received proved unstable during SYMPLICITY HTN-3 even though the study design mandated that patients be on a stable regimen for at least 2 weeks before entering the study. Roughly 80% of enrolled patients in both the denervation and sham-control arms of the study had been on a stable regimen for at least 6 weeks before they entered. Despite that, during the 6 months of follow-up, 211 (39%) of patients in the study underwent a change in their medication regimen. The changes occurred at virtually identical rates in both study arms, and in more than two-thirds of cases were driven by medical necessity.
"The pattern of drug changes challenges the notion of maximally tolerated therapy," Dr. Kandzari said during his report. "Can this [maximally tolerated therapy] be sustained in a randomized, controlled trial?" It also raised the issues of how trial design can better limit drug changes.
Even though it remains unclear why blood pressure reduction was so pronounced among the African Americans in the sham-control group, the impact of this unexpected effect substantially upended the trial’s endpoints. Among the 49 African Americans randomized to sham treatment, office-measured systolic pressure dropped by an average of 17.8 mm Hg, far exceeding the 8.6–mm Hg decline seen among the non–African Americans in the control arm and even exceeding the average 15.5–mm Hg drop in office systolic BP among African Americans treated with renal denervation.
"The absolute reduction in blood pressure by renal denervation in African Americans was identical to non–African Americans." The problem that arose "related more to what happened in the sham-control group of African Americans, who had a nearly 18–mm Hg reduction in blood pressure," said Dr. Kandzari, chief scientific officer and director of interventional cardiology at Piedmont Heart Institute in Atlanta.
The low rate at which patients assigned to receive renal denervation actually received the type of treatment spelled out in the study’s protocol may have been the biggest problem of all, although Dr. Kandzari stressed that, in his opinion "no single factor led to the neutral efficacy seen in the study."
The supplementary methods section of the SYMPLICITY HTN-3 report published in April explicitly called for patients to receive "4-6 ablations" per side, delivering them in a spiral, circumferential pattern starting distally in each renal artery. That meant each patient was to receive a minimum of eight total ablations.
But analysis of data recorded independently by the research nurse and by the proctor during each procedure, as well as cineangiography films made and submitted by the operator for each ablation, clearly showed that many patients did not receive the treatment that the protocol spelled out. Synthesis of the data collected by the three methods showed that about half of the 364 patients randomized to renal denervation received at least eight ablations, while the other half did not receive this minimum number.
The three separate sets of ablation records also contained information on whether ablations occurred in the anterior, posterior, superior, or inferior quadrants of each renal artery. Full circumferential ablation, what the protocol prescribed, required an ablation in at least one of each of these quadrants per side. What actually happened was that 253 patients (70%) received no circumferential ablations, 68 patients (19%) received circumferential ablation on just one side, and 19 patients (5%) received the bilateral circumferential ablations that the protocol called for. Data for the remaining 24 patients treated with renal denervation were not amenable to analysis for this parameter.
As might be expected, greater ablation number and completeness strongly linked with a robust blood pressure effect.
Among patients who received at least eight ablations, office systolic pressure fell by an average 13.1 mm Hg. But among the nine patients who received 16 or more ablations, the average systolic BP reduction at 6 months was 30.9 mm Hg. Among the 18 patients who received at least 15 ablations, the average systolic pressure reduction was 25.4 mm Hg. A very similar relationship occurred for BPs measured by ambulatory monitoring (see graphic), and the data also suggested a positive link between an increasing number of ablations and an increased effect on heart rate. The consistency of the association across all three measures lent further support to this as a real relationship, Dr. Kandzari noted.
Circumferentiality of the ablations showed a similar pattern. The average office systolic pressure fall in patients with no circumferential ablations was 14.2 mm Hg, and it was 16.1 mm Hg in patients who received just one circumferential ablation. But in the 19 patients who received circumferential ablations bilaterally, the average office systolic pressure reduction was 24.3 mm Hg, with a similar pattern seen for ambulatory measures as well as for home-based BP measurements.
"All patients randomized to renal denervation received renal denervation, but they may not have received it in a fashion that seemed to translate into a greater blood pressure reduction," Dr. Kandzari concluded.
Who to treat, where to treat, how to treat
"One result of the neutral HTN-3 result was a call to revisit the basic science behind renal denervation. The clinical enthusiasm had exceeded the science behind renal denervation," Dr. Kandzari observed.
Renal denervation’s many European advocates seem to agree, and have begun the process of determining characteristics of the best patients to receive renal denervation and where and how ablations are best delivered within the renal artery to achieve interruption of sympathetic innervation, although the targeting information they have right now is rudimentary.
"Probably most important is patient selection. You must be sure to get the right patient, one with high sympathetic activity, because the treatment lowers sympathetic activity," said Dr. Atul Pathak, an interventional cardiologist at Paul Sabatier University in Toulouse, France.
Some clues for patient selection have come from the Global SYMPLICITY Registry, which is enrolling patients treated with renal denervation at more than 200 experienced centers worldwide, many of them in Germany but also elsewhere in Europe, Australia, Canada, Korea, and other locations. Initial findings from the first 1,000 patients entered into the registry and followed for 6 months came out in March at the annual meeting of the American College of Cardiology, and Dr. Mahfoud presented new analyses of the data at EuroPCR.
"The major concern we had when we started renal denervation was its safety. I believe the safety issue is now answered," especially with the data collected in the global registry as well as in the SYMPLICITY HTN-3 trial, by far the largest trial completed for the procedure, said Dr. Thomas Zeller, professor and head of clinical and interventional angiology at the Heart Center in Bad Krozingen, Germany. "I was concerned that we might harm the renal arteries with long-lasting stenosis or embolic showers, but this does not happen, at least with the Symplicity catheter," he said during a talk at the meeting.
"The number of patients suitable for renal denervation is potentially much smaller than we initially expected. Real drug resistance is rare, poor adherence is common, and the Symplicity catheter is technically challenging and not effective in every patient. It is hard to rotate the catheter in the tortuous iliac arteries that some patients with hypertension have; the anatomic conditions of hypertension may not be suited to the Symplicity flex catheter," said Dr. Zeller, who added that he has performed renal denervations with the Symplicity catheter since 2009.
"We should focus on the patients that the HTN-3 trial identified as responders, including patients younger than 65, and patients on an aldosterone antagonist," he suggested in a talk at the meeting.
Finding the right patients and the right ablation targets
In the SYMPLICITY HTN-3 trial, 123 (23%) of the 535 patients remained severely hypertensive despite treatment with an aldosterone antagonist such as spironolactone at the time of entry into the study. In this subgroup, renal denervation produced an average 8.1–mm Hg additional reduction in office systolic BP compared with the average reduction seen among the sham-control patients, a much larger effect than the average 3.2–mm Hg incremental reduction by renal denervation over control seen in the patients who were not on an aldosterone antagonist at baseline, Dr. Manesh Patel reported in a talk at the meeting.
One possible explanation for this effect is that "these patients were resistant to an aldosterone antagonist and hence have a good chance of having high sympathetic activity," explained Dr. Patel, director of interventional cardiology at Duke University in Durham, N.C., and a coinvestigator on the SYMPLICITY HTN-3 trial. Another possibility is that "aldosterone antagonist use is a marker for patients who have been treated in a hypertension clinic to receive this fourth-line agent," and hence are more likely to have true drug-resistant hypertension, he added. More recent analyses of the HTN-3 results also showed that the 38% of patients who entered the study while on treatment with a vasodilator had absolutely no added benefit from renal denervation compared with the sham controls, while in the patients not on a vasodilator renal denervation produced an average 6.7–mm Hg reduction in office systolic BP compared with control patients, a statistically significant difference.
"We must accept that currently denervation is a ‘black box’ procedure. You deliver energy and you hope blood pressure goes down, but the main confounder is we are not sure if we have damaged the nerve fibers," Dr. Mahfoud said.
According to data he compiled, the depth of ablation penetration varies by device, with several devices including the Symplicity producing an ablation depth of 3 mm, while a few other systems produce ablation depths of 4 mm or even 6 mm.
Results from autopsy studies he analyzed suggested that afferent nerve density closer to the renal-artery lumen is highest in the distal section of the renal artery compared with the more proximal side, and that the posterior and anterior quadrants of the distal renal artery harbor a higher concentration of nerve fibers closer to the lumen than the superior and inferior quadrants.
This information begins to define the "sweet spot" for applying denervation energy, Dr. Mahfoud said. When he performs renal denervation today "we go even more distally, into the branches [off the distal renal arteries] if they are large enough" to accommodate the catheter. "Nerves are not equally distributed over the entire renal artery," and ideally this information should help guide ablation placements, he said.
The global divide in renal denervation use
The inability of the SYMPLICITY HTN-3 trial to prove the treatment’s efficacy has further divided use of renal denervation by geography. The technology remains unapproved for U.S. use, and will remain that way until another large, sham-controlled trial finishes and shows a clear benefit for BP reduction. In contrast, the procedure’s use in Europe seems on track to continue and grow further, although European thought leaders urge caution and further research to identify the best denervation techniques and optimal patients.
European leaders such as Dr. Mahfoud and Dr. Schmieder also see great promise in using renal denervation for other types of patients, such as those with heart failure or arrhythmias. Just one example of the wide-ranging effects examined for renal denervation was a report Dr. Mahfoud cited published earlier this year that focused on changes in left ventricular mass in 55 patients with resistant hypertension who underwent renal denervation. The results collected by Dr. Mahfoud and his associates showed that even when patients experienced little or no change in their systolic BP they often had substantial reductions in left ventricular mass (Eur. Heart J. 2014 March 6 [doi:10.1093/eurheartj/ehu093]).
"Reducing systolic blood pressure by 10 mm Hg [in patients with severe, drug-resistant hypertension] would have a massive impact, so renal denervation remains an important tool for potentially benefiting patients with uncontrolled hypertension," Dr. Wijns, codirector of the Cardiovascular Center in Aalst, Belgium, said in an interview.
But the renal denervation tool that is increasingly seen as important by the cardiovascular disease leadership in Europe will remain beyond the reach of U.S. physicians for some time to come.
The SYMPLICITY HTN-3 trial and the Global SYMPLICITY Registry were sponsored by Medtronic, which markets the Symplicity catheter. All of the sources for this article have received speaker fees, consulting fees, and/or research grants from Medtronic and numerous other medical device, drug, or biotechnology companies.
On Twitter @mitchelzoler
PARIS – At least three different factors undermined the SYMPLICITY HTN-3 trial that earlier this year did not show a significant difference in blood pressure lowering between renal denervation and a sham-control procedure, most notably the failure of the vast majority of operators in the study to follow ablation instructions and produce thorough and reliable interruptions of sympathetic innervation of the kidneys, according to new data released by the trial’s investigators.
As the full range of problems with the U.S.-based SYMPLICITY HTN-3 trial, which had its main results reported in April (N. Engl. J. Med. 2014;370:1393-1401), became apparent in a report at the annual congress of the European Association of Percutaneous Cardiovascular Interventions, many top European practitioners and supporters of renal denervation voiced their belief that the treatment is an effective and safe option for many patients with true drug-resistant, severe hypertension.

The only qualifications they now add are that renal denervation is not easily performed and must be done carefully and in a more targeted way, with an ongoing need to find the patients best suited for treatment and the best methods for delivering treatment.
During the meeting, Dr. Felix Mahfoud, an interventional cardiologist at the University Hospital of Saarland in Homburg/Saar, Germany, joined with hypertension specialist Dr. Konstantinos Tsioufis of the University of Athens and Dr. William Wijns, codirector of EuroPCR, in an official statement from the meeting that despite the SYMPLICITY HTN-3 results they continued to support renal denervation as a treatment option for selected patients with drug-resistant, severe hypertension.
Their sentiment echoed another endorsement made a few weeks earlier for continued use and study of renal denervation from the European Society of Hypertension (ESH) in reaction to the SYMPLICITY HTN-3 results.
The ESH "sticks to its statement" from 2013 on using renal denervation in appropriate patients with treatment-resistant, severe hypertension (Eurointervention 2013;9:R58-R66), said Dr. Roland E. Schmieder, first author for the 2013 ESH position paper and a leader in European use of renal denervation.
"We need more studies to prove that renal denervation works, and in particular to get more precise information on which patients get the greatest benefit," Dr. Schmieder said in a separate talk at the meeting. For the time being, he said he was comfortable with routine use of renal denervation in patients with an office systolic BP of at least 160 mm Hg that remains at this level despite maximally tolerated treatment with at least three antihypertensive drugs, including a diuretic, the use endorsed by current European guidelines. It remains appropriate to investigate the impact of renal denervation on other disorders, such as heart failure, arrhythmia, metabolic syndrome, and depressed renal function, said Dr. Schmieder, professor and head of hypertension and vascular medicine research at University Hospital in Erlangen, Germany.
The problems with SYMPLICITY HTN-3
While much speculation swirled around what had gone wrong in the SYMPLICITY HTN-3 trial after researchers on the study gave their first report on the results early in the spring, the full extent of the study’s problems didn’t flesh out until a follow-up report during EuroPCR by coinvestigator Dr. David E. Kandzari. In his analysis, Dr. Kandzari highlighted three distinct problems with the trial that he and his associates identified in a series of post hoc analyses:
• The failure of a large minority of enrolled patients in both arms of the study to remain on a stable medical regimen during the 6 months of follow-up before the primary efficacy outcomes were measured.
• The inexplicably large reduction in BP among the sham-control patients, especially among African American patients, who made up a quarter of the trial’s population.
• The vastly incomplete nerve-ablation treatment that most patients received, treatments that usually failed to meet the standards specified in the trial’s protocol.
The background medical regimens that patients received proved unstable during SYMPLICITY HTN-3 even though the study design mandated that patients be on a stable regimen for at least 2 weeks before entering the study. Roughly 80% of enrolled patients in both the denervation and sham-control arms of the study had been on a stable regimen for at least 6 weeks before they entered. Despite that, during the 6 months of follow-up, 211 (39%) of patients in the study underwent a change in their medication regimen. The changes occurred at virtually identical rates in both study arms, and in more than two-thirds of cases were driven by medical necessity.
"The pattern of drug changes challenges the notion of maximally tolerated therapy," Dr. Kandzari said during his report. "Can this [maximally tolerated therapy] be sustained in a randomized, controlled trial?" It also raised the issues of how trial design can better limit drug changes.
Even though it remains unclear why blood pressure reduction was so pronounced among the African Americans in the sham-control group, the impact of this unexpected effect substantially upended the trial’s endpoints. Among the 49 African Americans randomized to sham treatment, office-measured systolic pressure dropped by an average of 17.8 mm Hg, far exceeding the 8.6–mm Hg decline seen among the non–African Americans in the control arm and even exceeding the average 15.5–mm Hg drop in office systolic BP among African Americans treated with renal denervation.
"The absolute reduction in blood pressure by renal denervation in African Americans was identical to non–African Americans." The problem that arose "related more to what happened in the sham-control group of African Americans, who had a nearly 18–mm Hg reduction in blood pressure," said Dr. Kandzari, chief scientific officer and director of interventional cardiology at Piedmont Heart Institute in Atlanta.
The low rate at which patients assigned to receive renal denervation actually received the type of treatment spelled out in the study’s protocol may have been the biggest problem of all, although Dr. Kandzari stressed that, in his opinion "no single factor led to the neutral efficacy seen in the study."
The supplementary methods section of the SYMPLICITY HTN-3 report published in April explicitly called for patients to receive "4-6 ablations" per side, delivering them in a spiral, circumferential pattern starting distally in each renal artery. That meant each patient was to receive a minimum of eight total ablations.
But analysis of data recorded independently by the research nurse and by the proctor during each procedure, as well as cineangiography films made and submitted by the operator for each ablation, clearly showed that many patients did not receive the treatment that the protocol spelled out. Synthesis of the data collected by the three methods showed that about half of the 364 patients randomized to renal denervation received at least eight ablations, while the other half did not receive this minimum number.
The three separate sets of ablation records also contained information on whether ablations occurred in the anterior, posterior, superior, or inferior quadrants of each renal artery. Full circumferential ablation, what the protocol prescribed, required an ablation in at least one of each of these quadrants per side. What actually happened was that 253 patients (70%) received no circumferential ablations, 68 patients (19%) received circumferential ablation on just one side, and 19 patients (5%) received the bilateral circumferential ablations that the protocol called for. Data for the remaining 24 patients treated with renal denervation were not amenable to analysis for this parameter.
As might be expected, greater ablation number and completeness strongly linked with a robust blood pressure effect.
Among patients who received at least eight ablations, office systolic pressure fell by an average 13.1 mm Hg. But among the nine patients who received 16 or more ablations, the average systolic BP reduction at 6 months was 30.9 mm Hg. Among the 18 patients who received at least 15 ablations, the average systolic pressure reduction was 25.4 mm Hg. A very similar relationship occurred for BPs measured by ambulatory monitoring (see graphic), and the data also suggested a positive link between an increasing number of ablations and an increased effect on heart rate. The consistency of the association across all three measures lent further support to this as a real relationship, Dr. Kandzari noted.
Circumferentiality of the ablations showed a similar pattern. The average office systolic pressure fall in patients with no circumferential ablations was 14.2 mm Hg, and it was 16.1 mm Hg in patients who received just one circumferential ablation. But in the 19 patients who received circumferential ablations bilaterally, the average office systolic pressure reduction was 24.3 mm Hg, with a similar pattern seen for ambulatory measures as well as for home-based BP measurements.
"All patients randomized to renal denervation received renal denervation, but they may not have received it in a fashion that seemed to translate into a greater blood pressure reduction," Dr. Kandzari concluded.
Who to treat, where to treat, how to treat
"One result of the neutral HTN-3 result was a call to revisit the basic science behind renal denervation. The clinical enthusiasm had exceeded the science behind renal denervation," Dr. Kandzari observed.
Renal denervation’s many European advocates seem to agree, and have begun the process of determining characteristics of the best patients to receive renal denervation and where and how ablations are best delivered within the renal artery to achieve interruption of sympathetic innervation, although the targeting information they have right now is rudimentary.
"Probably most important is patient selection. You must be sure to get the right patient, one with high sympathetic activity, because the treatment lowers sympathetic activity," said Dr. Atul Pathak, an interventional cardiologist at Paul Sabatier University in Toulouse, France.
Some clues for patient selection have come from the Global SYMPLICITY Registry, which is enrolling patients treated with renal denervation at more than 200 experienced centers worldwide, many of them in Germany but also elsewhere in Europe, Australia, Canada, Korea, and other locations. Initial findings from the first 1,000 patients entered into the registry and followed for 6 months came out in March at the annual meeting of the American College of Cardiology, and Dr. Mahfoud presented new analyses of the data at EuroPCR.
"The major concern we had when we started renal denervation was its safety. I believe the safety issue is now answered," especially with the data collected in the global registry as well as in the SYMPLICITY HTN-3 trial, by far the largest trial completed for the procedure, said Dr. Thomas Zeller, professor and head of clinical and interventional angiology at the Heart Center in Bad Krozingen, Germany. "I was concerned that we might harm the renal arteries with long-lasting stenosis or embolic showers, but this does not happen, at least with the Symplicity catheter," he said during a talk at the meeting.
"The number of patients suitable for renal denervation is potentially much smaller than we initially expected. Real drug resistance is rare, poor adherence is common, and the Symplicity catheter is technically challenging and not effective in every patient. It is hard to rotate the catheter in the tortuous iliac arteries that some patients with hypertension have; the anatomic conditions of hypertension may not be suited to the Symplicity flex catheter," said Dr. Zeller, who added that he has performed renal denervations with the Symplicity catheter since 2009.
"We should focus on the patients that the HTN-3 trial identified as responders, including patients younger than 65, and patients on an aldosterone antagonist," he suggested in a talk at the meeting.
Finding the right patients and the right ablation targets
In the SYMPLICITY HTN-3 trial, 123 (23%) of the 535 patients remained severely hypertensive despite treatment with an aldosterone antagonist such as spironolactone at the time of entry into the study. In this subgroup, renal denervation produced an average 8.1–mm Hg additional reduction in office systolic BP compared with the average reduction seen among the sham-control patients, a much larger effect than the average 3.2–mm Hg incremental reduction by renal denervation over control seen in the patients who were not on an aldosterone antagonist at baseline, Dr. Manesh Patel reported in a talk at the meeting.
One possible explanation for this effect is that "these patients were resistant to an aldosterone antagonist and hence have a good chance of having high sympathetic activity," explained Dr. Patel, director of interventional cardiology at Duke University in Durham, N.C., and a coinvestigator on the SYMPLICITY HTN-3 trial. Another possibility is that "aldosterone antagonist use is a marker for patients who have been treated in a hypertension clinic to receive this fourth-line agent," and hence are more likely to have true drug-resistant hypertension, he added. More recent analyses of the HTN-3 results also showed that the 38% of patients who entered the study while on treatment with a vasodilator had absolutely no added benefit from renal denervation compared with the sham controls, while in the patients not on a vasodilator renal denervation produced an average 6.7–mm Hg reduction in office systolic BP compared with control patients, a statistically significant difference.
"We must accept that currently denervation is a ‘black box’ procedure. You deliver energy and you hope blood pressure goes down, but the main confounder is we are not sure if we have damaged the nerve fibers," Dr. Mahfoud said.
According to data he compiled, the depth of ablation penetration varies by device, with several devices including the Symplicity producing an ablation depth of 3 mm, while a few other systems produce ablation depths of 4 mm or even 6 mm.
Results from autopsy studies he analyzed suggested that afferent nerve density closer to the renal-artery lumen is highest in the distal section of the renal artery compared with the more proximal side, and that the posterior and anterior quadrants of the distal renal artery harbor a higher concentration of nerve fibers closer to the lumen than the superior and inferior quadrants.
This information begins to define the "sweet spot" for applying denervation energy, Dr. Mahfoud said. When he performs renal denervation today "we go even more distally, into the branches [off the distal renal arteries] if they are large enough" to accommodate the catheter. "Nerves are not equally distributed over the entire renal artery," and ideally this information should help guide ablation placements, he said.
The global divide in renal denervation use
The inability of the SYMPLICITY HTN-3 trial to prove the treatment’s efficacy has further divided use of renal denervation by geography. The technology remains unapproved for U.S. use, and will remain that way until another large, sham-controlled trial finishes and shows a clear benefit for BP reduction. In contrast, the procedure’s use in Europe seems on track to continue and grow further, although European thought leaders urge caution and further research to identify the best denervation techniques and optimal patients.
European leaders such as Dr. Mahfoud and Dr. Schmieder also see great promise in using renal denervation for other types of patients, such as those with heart failure or arrhythmias. Just one example of the wide-ranging effects examined for renal denervation was a report Dr. Mahfoud cited published earlier this year that focused on changes in left ventricular mass in 55 patients with resistant hypertension who underwent renal denervation. The results collected by Dr. Mahfoud and his associates showed that even when patients experienced little or no change in their systolic BP they often had substantial reductions in left ventricular mass (Eur. Heart J. 2014 March 6 [doi:10.1093/eurheartj/ehu093]).
"Reducing systolic blood pressure by 10 mm Hg [in patients with severe, drug-resistant hypertension] would have a massive impact, so renal denervation remains an important tool for potentially benefiting patients with uncontrolled hypertension," Dr. Wijns, codirector of the Cardiovascular Center in Aalst, Belgium, said in an interview.
But the renal denervation tool that is increasingly seen as important by the cardiovascular disease leadership in Europe will remain beyond the reach of U.S. physicians for some time to come.
The SYMPLICITY HTN-3 trial and the Global SYMPLICITY Registry were sponsored by Medtronic, which markets the Symplicity catheter. All of the sources for this article have received speaker fees, consulting fees, and/or research grants from Medtronic and numerous other medical device, drug, or biotechnology companies.
On Twitter @mitchelzoler
PARIS – At least three different factors undermined the SYMPLICITY HTN-3 trial that earlier this year did not show a significant difference in blood pressure lowering between renal denervation and a sham-control procedure, most notably the failure of the vast majority of operators in the study to follow ablation instructions and produce thorough and reliable interruptions of sympathetic innervation of the kidneys, according to new data released by the trial’s investigators.
As the full range of problems with the U.S.-based SYMPLICITY HTN-3 trial, which had its main results reported in April (N. Engl. J. Med. 2014;370:1393-1401), became apparent in a report at the annual congress of the European Association of Percutaneous Cardiovascular Interventions, many top European practitioners and supporters of renal denervation voiced their belief that the treatment is an effective and safe option for many patients with true drug-resistant, severe hypertension.

The only qualifications they now add are that renal denervation is not easily performed and must be done carefully and in a more targeted way, with an ongoing need to find the patients best suited for treatment and the best methods for delivering treatment.
During the meeting, Dr. Felix Mahfoud, an interventional cardiologist at the University Hospital of Saarland in Homburg/Saar, Germany, joined with hypertension specialist Dr. Konstantinos Tsioufis of the University of Athens and Dr. William Wijns, codirector of EuroPCR, in an official statement from the meeting that despite the SYMPLICITY HTN-3 results they continued to support renal denervation as a treatment option for selected patients with drug-resistant, severe hypertension.
Their sentiment echoed another endorsement made a few weeks earlier for continued use and study of renal denervation from the European Society of Hypertension (ESH) in reaction to the SYMPLICITY HTN-3 results.
The ESH "sticks to its statement" from 2013 on using renal denervation in appropriate patients with treatment-resistant, severe hypertension (Eurointervention 2013;9:R58-R66), said Dr. Roland E. Schmieder, first author for the 2013 ESH position paper and a leader in European use of renal denervation.
"We need more studies to prove that renal denervation works, and in particular to get more precise information on which patients get the greatest benefit," Dr. Schmieder said in a separate talk at the meeting. For the time being, he said he was comfortable with routine use of renal denervation in patients with an office systolic BP of at least 160 mm Hg that remains at this level despite maximally tolerated treatment with at least three antihypertensive drugs, including a diuretic, the use endorsed by current European guidelines. It remains appropriate to investigate the impact of renal denervation on other disorders, such as heart failure, arrhythmia, metabolic syndrome, and depressed renal function, said Dr. Schmieder, professor and head of hypertension and vascular medicine research at University Hospital in Erlangen, Germany.
The problems with SYMPLICITY HTN-3
While much speculation swirled around what had gone wrong in the SYMPLICITY HTN-3 trial after researchers on the study gave their first report on the results early in the spring, the full extent of the study’s problems didn’t flesh out until a follow-up report during EuroPCR by coinvestigator Dr. David E. Kandzari. In his analysis, Dr. Kandzari highlighted three distinct problems with the trial that he and his associates identified in a series of post hoc analyses:
• The failure of a large minority of enrolled patients in both arms of the study to remain on a stable medical regimen during the 6 months of follow-up before the primary efficacy outcomes were measured.
• The inexplicably large reduction in BP among the sham-control patients, especially among African American patients, who made up a quarter of the trial’s population.
• The vastly incomplete nerve-ablation treatment that most patients received, treatments that usually failed to meet the standards specified in the trial’s protocol.
The background medical regimens that patients received proved unstable during SYMPLICITY HTN-3 even though the study design mandated that patients be on a stable regimen for at least 2 weeks before entering the study. Roughly 80% of enrolled patients in both the denervation and sham-control arms of the study had been on a stable regimen for at least 6 weeks before they entered. Despite that, during the 6 months of follow-up, 211 (39%) of patients in the study underwent a change in their medication regimen. The changes occurred at virtually identical rates in both study arms, and in more than two-thirds of cases were driven by medical necessity.
"The pattern of drug changes challenges the notion of maximally tolerated therapy," Dr. Kandzari said during his report. "Can this [maximally tolerated therapy] be sustained in a randomized, controlled trial?" It also raised the issues of how trial design can better limit drug changes.
Even though it remains unclear why blood pressure reduction was so pronounced among the African Americans in the sham-control group, the impact of this unexpected effect substantially upended the trial’s endpoints. Among the 49 African Americans randomized to sham treatment, office-measured systolic pressure dropped by an average of 17.8 mm Hg, far exceeding the 8.6–mm Hg decline seen among the non–African Americans in the control arm and even exceeding the average 15.5–mm Hg drop in office systolic BP among African Americans treated with renal denervation.
"The absolute reduction in blood pressure by renal denervation in African Americans was identical to non–African Americans." The problem that arose "related more to what happened in the sham-control group of African Americans, who had a nearly 18–mm Hg reduction in blood pressure," said Dr. Kandzari, chief scientific officer and director of interventional cardiology at Piedmont Heart Institute in Atlanta.
The low rate at which patients assigned to receive renal denervation actually received the type of treatment spelled out in the study’s protocol may have been the biggest problem of all, although Dr. Kandzari stressed that, in his opinion "no single factor led to the neutral efficacy seen in the study."
The supplementary methods section of the SYMPLICITY HTN-3 report published in April explicitly called for patients to receive "4-6 ablations" per side, delivering them in a spiral, circumferential pattern starting distally in each renal artery. That meant each patient was to receive a minimum of eight total ablations.
But analysis of data recorded independently by the research nurse and by the proctor during each procedure, as well as cineangiography films made and submitted by the operator for each ablation, clearly showed that many patients did not receive the treatment that the protocol spelled out. Synthesis of the data collected by the three methods showed that about half of the 364 patients randomized to renal denervation received at least eight ablations, while the other half did not receive this minimum number.
The three separate sets of ablation records also contained information on whether ablations occurred in the anterior, posterior, superior, or inferior quadrants of each renal artery. Full circumferential ablation, what the protocol prescribed, required an ablation in at least one of each of these quadrants per side. What actually happened was that 253 patients (70%) received no circumferential ablations, 68 patients (19%) received circumferential ablation on just one side, and 19 patients (5%) received the bilateral circumferential ablations that the protocol called for. Data for the remaining 24 patients treated with renal denervation were not amenable to analysis for this parameter.
As might be expected, greater ablation number and completeness strongly linked with a robust blood pressure effect.
Among patients who received at least eight ablations, office systolic pressure fell by an average 13.1 mm Hg. But among the nine patients who received 16 or more ablations, the average systolic BP reduction at 6 months was 30.9 mm Hg. Among the 18 patients who received at least 15 ablations, the average systolic pressure reduction was 25.4 mm Hg. A very similar relationship occurred for BPs measured by ambulatory monitoring (see graphic), and the data also suggested a positive link between an increasing number of ablations and an increased effect on heart rate. The consistency of the association across all three measures lent further support to this as a real relationship, Dr. Kandzari noted.
Circumferentiality of the ablations showed a similar pattern. The average office systolic pressure fall in patients with no circumferential ablations was 14.2 mm Hg, and it was 16.1 mm Hg in patients who received just one circumferential ablation. But in the 19 patients who received circumferential ablations bilaterally, the average office systolic pressure reduction was 24.3 mm Hg, with a similar pattern seen for ambulatory measures as well as for home-based BP measurements.
"All patients randomized to renal denervation received renal denervation, but they may not have received it in a fashion that seemed to translate into a greater blood pressure reduction," Dr. Kandzari concluded.
Who to treat, where to treat, how to treat
"One result of the neutral HTN-3 result was a call to revisit the basic science behind renal denervation. The clinical enthusiasm had exceeded the science behind renal denervation," Dr. Kandzari observed.
Renal denervation’s many European advocates seem to agree, and have begun the process of determining characteristics of the best patients to receive renal denervation and where and how ablations are best delivered within the renal artery to achieve interruption of sympathetic innervation, although the targeting information they have right now is rudimentary.
"Probably most important is patient selection. You must be sure to get the right patient, one with high sympathetic activity, because the treatment lowers sympathetic activity," said Dr. Atul Pathak, an interventional cardiologist at Paul Sabatier University in Toulouse, France.
Some clues for patient selection have come from the Global SYMPLICITY Registry, which is enrolling patients treated with renal denervation at more than 200 experienced centers worldwide, many of them in Germany but also elsewhere in Europe, Australia, Canada, Korea, and other locations. Initial findings from the first 1,000 patients entered into the registry and followed for 6 months came out in March at the annual meeting of the American College of Cardiology, and Dr. Mahfoud presented new analyses of the data at EuroPCR.
"The major concern we had when we started renal denervation was its safety. I believe the safety issue is now answered," especially with the data collected in the global registry as well as in the SYMPLICITY HTN-3 trial, by far the largest trial completed for the procedure, said Dr. Thomas Zeller, professor and head of clinical and interventional angiology at the Heart Center in Bad Krozingen, Germany. "I was concerned that we might harm the renal arteries with long-lasting stenosis or embolic showers, but this does not happen, at least with the Symplicity catheter," he said during a talk at the meeting.
"The number of patients suitable for renal denervation is potentially much smaller than we initially expected. Real drug resistance is rare, poor adherence is common, and the Symplicity catheter is technically challenging and not effective in every patient. It is hard to rotate the catheter in the tortuous iliac arteries that some patients with hypertension have; the anatomic conditions of hypertension may not be suited to the Symplicity flex catheter," said Dr. Zeller, who added that he has performed renal denervations with the Symplicity catheter since 2009.
"We should focus on the patients that the HTN-3 trial identified as responders, including patients younger than 65, and patients on an aldosterone antagonist," he suggested in a talk at the meeting.
Finding the right patients and the right ablation targets
In the SYMPLICITY HTN-3 trial, 123 (23%) of the 535 patients remained severely hypertensive despite treatment with an aldosterone antagonist such as spironolactone at the time of entry into the study. In this subgroup, renal denervation produced an average 8.1–mm Hg additional reduction in office systolic BP compared with the average reduction seen among the sham-control patients, a much larger effect than the average 3.2–mm Hg incremental reduction by renal denervation over control seen in the patients who were not on an aldosterone antagonist at baseline, Dr. Manesh Patel reported in a talk at the meeting.
One possible explanation for this effect is that "these patients were resistant to an aldosterone antagonist and hence have a good chance of having high sympathetic activity," explained Dr. Patel, director of interventional cardiology at Duke University in Durham, N.C., and a coinvestigator on the SYMPLICITY HTN-3 trial. Another possibility is that "aldosterone antagonist use is a marker for patients who have been treated in a hypertension clinic to receive this fourth-line agent," and hence are more likely to have true drug-resistant hypertension, he added. More recent analyses of the HTN-3 results also showed that the 38% of patients who entered the study while on treatment with a vasodilator had absolutely no added benefit from renal denervation compared with the sham controls, while in the patients not on a vasodilator renal denervation produced an average 6.7–mm Hg reduction in office systolic BP compared with control patients, a statistically significant difference.
"We must accept that currently denervation is a ‘black box’ procedure. You deliver energy and you hope blood pressure goes down, but the main confounder is we are not sure if we have damaged the nerve fibers," Dr. Mahfoud said.
According to data he compiled, the depth of ablation penetration varies by device, with several devices including the Symplicity producing an ablation depth of 3 mm, while a few other systems produce ablation depths of 4 mm or even 6 mm.
Results from autopsy studies he analyzed suggested that afferent nerve density closer to the renal-artery lumen is highest in the distal section of the renal artery compared with the more proximal side, and that the posterior and anterior quadrants of the distal renal artery harbor a higher concentration of nerve fibers closer to the lumen than the superior and inferior quadrants.
This information begins to define the "sweet spot" for applying denervation energy, Dr. Mahfoud said. When he performs renal denervation today "we go even more distally, into the branches [off the distal renal arteries] if they are large enough" to accommodate the catheter. "Nerves are not equally distributed over the entire renal artery," and ideally this information should help guide ablation placements, he said.
The global divide in renal denervation use
The inability of the SYMPLICITY HTN-3 trial to prove the treatment’s efficacy has further divided use of renal denervation by geography. The technology remains unapproved for U.S. use, and will remain that way until another large, sham-controlled trial finishes and shows a clear benefit for BP reduction. In contrast, the procedure’s use in Europe seems on track to continue and grow further, although European thought leaders urge caution and further research to identify the best denervation techniques and optimal patients.
European leaders such as Dr. Mahfoud and Dr. Schmieder also see great promise in using renal denervation for other types of patients, such as those with heart failure or arrhythmias. Just one example of the wide-ranging effects examined for renal denervation was a report Dr. Mahfoud cited published earlier this year that focused on changes in left ventricular mass in 55 patients with resistant hypertension who underwent renal denervation. The results collected by Dr. Mahfoud and his associates showed that even when patients experienced little or no change in their systolic BP they often had substantial reductions in left ventricular mass (Eur. Heart J. 2014 March 6 [doi:10.1093/eurheartj/ehu093]).
"Reducing systolic blood pressure by 10 mm Hg [in patients with severe, drug-resistant hypertension] would have a massive impact, so renal denervation remains an important tool for potentially benefiting patients with uncontrolled hypertension," Dr. Wijns, codirector of the Cardiovascular Center in Aalst, Belgium, said in an interview.
But the renal denervation tool that is increasingly seen as important by the cardiovascular disease leadership in Europe will remain beyond the reach of U.S. physicians for some time to come.
The SYMPLICITY HTN-3 trial and the Global SYMPLICITY Registry were sponsored by Medtronic, which markets the Symplicity catheter. All of the sources for this article have received speaker fees, consulting fees, and/or research grants from Medtronic and numerous other medical device, drug, or biotechnology companies.
On Twitter @mitchelzoler
EXPERT ANALYSIS FROM EUROPCR 2014
Upcoming ESC revascularization guidelines cement heart team’s role
PARIS – A joint European Society of Cardiology and European Association for Cardio-Thoracic Surgery task force that will publish revised revascularization guidelines in late August gave a sneak peak of some important elements of the revision, including renewed endorsement of and a refinement to the heart team concept that was first introduced in the prior, 2010 version of the guidelines.
"One of the most important aspects of the 2010 guidelines was the introduction of the heart team (Eur. Heart J. 2010;31:2501-55) said Dr. Philippe H. Kolh. "In 2010, the heart team concept was still controversial, but I think now it is well accepted. We are further supporting and emphasizing the importance of the heart team," he said of the revised guidelines that will be released in August, during a session that previewed selected parts of the new guidelines at the annual congress of the European Association of Percutaneous Cardiovascular Interventions, an organization that also collaborated on the guidelines.
The revision also calls on each institution where operators perform revascularization to establish local protocols to guide the choice in routine cases between percutaneous coronary interventions (PCIs) or coronary artery bypass grafting (CABG), said Dr. Kolh, a cardiac surgeon at University Hospital in Liège, Belgium, and cochairman of the guideline-writing panel.
"The 2010 guidelines produced a misconception that every patient needs to be discussed by a heart team; the 2014 revision makes it clear that the heart team should develop institutional protocols for appropriate revascularization strategies for different types of patients. So if a patient has single-vessel disease, you can go ahead and do PCI and not wait for a heart-team decision," said Dr. Ulf Landmesser, professor and head of the acute cardiology clinic at University Hospital, Zurich, and a member of the 2014 panel. "Hopefully, it will now be clear that the heart team only needs to discuss complex patients that involve difficult decisions, and that institutional protocols can handle routine cases," Dr. Landmesser said.
The revision comes at a time when "the competition today is not so much between CABG and PCI; the more burning question is who should have revascularization, and how do patients get to the cath lab," noted Dr. Spencer B. King III, an interventional cardiologist at St. Joseph’s Medical Group in Atlanta who was invited to the session to comment on the new revision.
Results from a new meta-analysis highlight the critical role of revascularization relative to medical therapy alone in improving outcomes of patients with coronary artery disease. This finding is especially relevant in 2014, because it marks the 50th anniversary of the launch of revascularization with the first successful CABG performed, observed Dr. Stephan Windecker, professor and chief of cardiology at University Hospital in Bern, Switzerland, and cochairman of the guidelines-writing panel.
He presented an analysis of results from 100 randomized, controlled trials that compared some form of revascularization against medical therapy in 93,553 randomized patients followed for more than 260,000 patient-years. The results showed that CABG cut the rate of all-cause mortality by 20%, compared with medical therapy, a statistically significant difference, and that treatment with new-generation drug-eluting stents produced a significant reduction of more than 25%, according to an as-yet unpublished report by members of the European Myocardial Revascularization Collaborative. Dr. Windecker also noted that all the recommendations in the new revision were approved with 100% consensus by the panel, which included cardiac surgeons, interventional cardiologists, and noninterventional cardiologists in equal numbers.
The session highlighted several other notable new elements in the revised guidelines, although Dr. Windecker stressed several times during the session that everything presented remained pending until the final version is released later this summer. The changes include:
• An "upgrade" of the recommendation for PCI use in patients with left main disease and a SYNTAX score of 23-32 to a IIa, "should be considered" class recommendation, boosted from class III "not recommended" status in 2010. Five-year outcomes from the SYNTAX trial showed "no difference in outcomes between PCI and CABG, a major reason to upgrade the recommendation for PCI," said Dr. Landmesser (Lancet 2013;381:629-38). "The guidelines put a lot of weight on SYNTAX score."
• When performing PCI in patients with non–ST-elevation myocardial infarction (NSTEMI), bivalirudin (Angiomax) is recommended exclusively as the anticoagulant to use during and immediately following PCI – with unfractionated heparin recommended only for patients who cannot receive bivalirudin – based on bivalirudin’s proven reduced risk for causing major bleeds, said Dr. Franz-Josef Neumann, professor and director of the University Heart Center in Bad Krozingen, Germany.
• But for patients with ST-elevation MI (STEMI) undergoing primary PCI, unfractionated heparin received the only unqualified, level I recommendation for anticoagulation, with bivalirudin receiving a level IIa, "should be considered" recommendation. This repositioning of the two options occurred, based to some extent on yet unpublished results from a very large, single-center study in Liverpool, HEAT-PPCI, reported at the annual meeting of the American College of Cardiology meeting in March that showed unfractionated heparin outperformed bivalirudin for 28-day outcomes, Dr. Neumann said. "I was very pleased and sort of amazed that results from HEAT-PPCI jumped into the guidelines, and it’s not even published yet. That [recommendation] will have an impact, I suspect," commented Dr. King.
• For patients with either STEMI or NSTEMI, the preferred antiplatelet P2Y12 inhibitors are prasugrel (Effient) and ticagrelor (Brilinta), with clopidogrel reduced to a back-up role "only when prasugrel or ticagrelor are not available," said Dr. Neumann. "I was a little surprised that clopidogrel has fallen off the charts. With the new stents having a low stent thrombosis rate, U.S. physicians tend to stick with clopidogrel; there has been more of a shift in Europe," commented Dr. King. "For elective cases, we still have a clear statement in favor of clopidogrel," countered Dr. Neumann. "It is only for higher risk, acute coronary syndrome and STEMI patients where the guidelines recommend the new agents."
Dr. Kolh said that he has received honoraria from Astra Zeneca and Braun, and research support from Edwards. Dr. Landmesser said that he had no disclosures. Dr. King said that he had no disclosures. Dr. Windecker said that he had received honoraria from, had been a consultant to, or had been a speaker for nine companies and had received research grants from seven companies. Dr. Neumann said that his institution had received research grants from 15 companies.
On Twitter @mitchelzoler
PARIS – A joint European Society of Cardiology and European Association for Cardio-Thoracic Surgery task force that will publish revised revascularization guidelines in late August gave a sneak peak of some important elements of the revision, including renewed endorsement of and a refinement to the heart team concept that was first introduced in the prior, 2010 version of the guidelines.
"One of the most important aspects of the 2010 guidelines was the introduction of the heart team (Eur. Heart J. 2010;31:2501-55) said Dr. Philippe H. Kolh. "In 2010, the heart team concept was still controversial, but I think now it is well accepted. We are further supporting and emphasizing the importance of the heart team," he said of the revised guidelines that will be released in August, during a session that previewed selected parts of the new guidelines at the annual congress of the European Association of Percutaneous Cardiovascular Interventions, an organization that also collaborated on the guidelines.
The revision also calls on each institution where operators perform revascularization to establish local protocols to guide the choice in routine cases between percutaneous coronary interventions (PCIs) or coronary artery bypass grafting (CABG), said Dr. Kolh, a cardiac surgeon at University Hospital in Liège, Belgium, and cochairman of the guideline-writing panel.
"The 2010 guidelines produced a misconception that every patient needs to be discussed by a heart team; the 2014 revision makes it clear that the heart team should develop institutional protocols for appropriate revascularization strategies for different types of patients. So if a patient has single-vessel disease, you can go ahead and do PCI and not wait for a heart-team decision," said Dr. Ulf Landmesser, professor and head of the acute cardiology clinic at University Hospital, Zurich, and a member of the 2014 panel. "Hopefully, it will now be clear that the heart team only needs to discuss complex patients that involve difficult decisions, and that institutional protocols can handle routine cases," Dr. Landmesser said.
The revision comes at a time when "the competition today is not so much between CABG and PCI; the more burning question is who should have revascularization, and how do patients get to the cath lab," noted Dr. Spencer B. King III, an interventional cardiologist at St. Joseph’s Medical Group in Atlanta who was invited to the session to comment on the new revision.
Results from a new meta-analysis highlight the critical role of revascularization relative to medical therapy alone in improving outcomes of patients with coronary artery disease. This finding is especially relevant in 2014, because it marks the 50th anniversary of the launch of revascularization with the first successful CABG performed, observed Dr. Stephan Windecker, professor and chief of cardiology at University Hospital in Bern, Switzerland, and cochairman of the guidelines-writing panel.
He presented an analysis of results from 100 randomized, controlled trials that compared some form of revascularization against medical therapy in 93,553 randomized patients followed for more than 260,000 patient-years. The results showed that CABG cut the rate of all-cause mortality by 20%, compared with medical therapy, a statistically significant difference, and that treatment with new-generation drug-eluting stents produced a significant reduction of more than 25%, according to an as-yet unpublished report by members of the European Myocardial Revascularization Collaborative. Dr. Windecker also noted that all the recommendations in the new revision were approved with 100% consensus by the panel, which included cardiac surgeons, interventional cardiologists, and noninterventional cardiologists in equal numbers.
The session highlighted several other notable new elements in the revised guidelines, although Dr. Windecker stressed several times during the session that everything presented remained pending until the final version is released later this summer. The changes include:
• An "upgrade" of the recommendation for PCI use in patients with left main disease and a SYNTAX score of 23-32 to a IIa, "should be considered" class recommendation, boosted from class III "not recommended" status in 2010. Five-year outcomes from the SYNTAX trial showed "no difference in outcomes between PCI and CABG, a major reason to upgrade the recommendation for PCI," said Dr. Landmesser (Lancet 2013;381:629-38). "The guidelines put a lot of weight on SYNTAX score."
• When performing PCI in patients with non–ST-elevation myocardial infarction (NSTEMI), bivalirudin (Angiomax) is recommended exclusively as the anticoagulant to use during and immediately following PCI – with unfractionated heparin recommended only for patients who cannot receive bivalirudin – based on bivalirudin’s proven reduced risk for causing major bleeds, said Dr. Franz-Josef Neumann, professor and director of the University Heart Center in Bad Krozingen, Germany.
• But for patients with ST-elevation MI (STEMI) undergoing primary PCI, unfractionated heparin received the only unqualified, level I recommendation for anticoagulation, with bivalirudin receiving a level IIa, "should be considered" recommendation. This repositioning of the two options occurred, based to some extent on yet unpublished results from a very large, single-center study in Liverpool, HEAT-PPCI, reported at the annual meeting of the American College of Cardiology meeting in March that showed unfractionated heparin outperformed bivalirudin for 28-day outcomes, Dr. Neumann said. "I was very pleased and sort of amazed that results from HEAT-PPCI jumped into the guidelines, and it’s not even published yet. That [recommendation] will have an impact, I suspect," commented Dr. King.
• For patients with either STEMI or NSTEMI, the preferred antiplatelet P2Y12 inhibitors are prasugrel (Effient) and ticagrelor (Brilinta), with clopidogrel reduced to a back-up role "only when prasugrel or ticagrelor are not available," said Dr. Neumann. "I was a little surprised that clopidogrel has fallen off the charts. With the new stents having a low stent thrombosis rate, U.S. physicians tend to stick with clopidogrel; there has been more of a shift in Europe," commented Dr. King. "For elective cases, we still have a clear statement in favor of clopidogrel," countered Dr. Neumann. "It is only for higher risk, acute coronary syndrome and STEMI patients where the guidelines recommend the new agents."
Dr. Kolh said that he has received honoraria from Astra Zeneca and Braun, and research support from Edwards. Dr. Landmesser said that he had no disclosures. Dr. King said that he had no disclosures. Dr. Windecker said that he had received honoraria from, had been a consultant to, or had been a speaker for nine companies and had received research grants from seven companies. Dr. Neumann said that his institution had received research grants from 15 companies.
On Twitter @mitchelzoler
PARIS – A joint European Society of Cardiology and European Association for Cardio-Thoracic Surgery task force that will publish revised revascularization guidelines in late August gave a sneak peak of some important elements of the revision, including renewed endorsement of and a refinement to the heart team concept that was first introduced in the prior, 2010 version of the guidelines.
"One of the most important aspects of the 2010 guidelines was the introduction of the heart team (Eur. Heart J. 2010;31:2501-55) said Dr. Philippe H. Kolh. "In 2010, the heart team concept was still controversial, but I think now it is well accepted. We are further supporting and emphasizing the importance of the heart team," he said of the revised guidelines that will be released in August, during a session that previewed selected parts of the new guidelines at the annual congress of the European Association of Percutaneous Cardiovascular Interventions, an organization that also collaborated on the guidelines.
The revision also calls on each institution where operators perform revascularization to establish local protocols to guide the choice in routine cases between percutaneous coronary interventions (PCIs) or coronary artery bypass grafting (CABG), said Dr. Kolh, a cardiac surgeon at University Hospital in Liège, Belgium, and cochairman of the guideline-writing panel.
"The 2010 guidelines produced a misconception that every patient needs to be discussed by a heart team; the 2014 revision makes it clear that the heart team should develop institutional protocols for appropriate revascularization strategies for different types of patients. So if a patient has single-vessel disease, you can go ahead and do PCI and not wait for a heart-team decision," said Dr. Ulf Landmesser, professor and head of the acute cardiology clinic at University Hospital, Zurich, and a member of the 2014 panel. "Hopefully, it will now be clear that the heart team only needs to discuss complex patients that involve difficult decisions, and that institutional protocols can handle routine cases," Dr. Landmesser said.
The revision comes at a time when "the competition today is not so much between CABG and PCI; the more burning question is who should have revascularization, and how do patients get to the cath lab," noted Dr. Spencer B. King III, an interventional cardiologist at St. Joseph’s Medical Group in Atlanta who was invited to the session to comment on the new revision.
Results from a new meta-analysis highlight the critical role of revascularization relative to medical therapy alone in improving outcomes of patients with coronary artery disease. This finding is especially relevant in 2014, because it marks the 50th anniversary of the launch of revascularization with the first successful CABG performed, observed Dr. Stephan Windecker, professor and chief of cardiology at University Hospital in Bern, Switzerland, and cochairman of the guidelines-writing panel.
He presented an analysis of results from 100 randomized, controlled trials that compared some form of revascularization against medical therapy in 93,553 randomized patients followed for more than 260,000 patient-years. The results showed that CABG cut the rate of all-cause mortality by 20%, compared with medical therapy, a statistically significant difference, and that treatment with new-generation drug-eluting stents produced a significant reduction of more than 25%, according to an as-yet unpublished report by members of the European Myocardial Revascularization Collaborative. Dr. Windecker also noted that all the recommendations in the new revision were approved with 100% consensus by the panel, which included cardiac surgeons, interventional cardiologists, and noninterventional cardiologists in equal numbers.
The session highlighted several other notable new elements in the revised guidelines, although Dr. Windecker stressed several times during the session that everything presented remained pending until the final version is released later this summer. The changes include:
• An "upgrade" of the recommendation for PCI use in patients with left main disease and a SYNTAX score of 23-32 to a IIa, "should be considered" class recommendation, boosted from class III "not recommended" status in 2010. Five-year outcomes from the SYNTAX trial showed "no difference in outcomes between PCI and CABG, a major reason to upgrade the recommendation for PCI," said Dr. Landmesser (Lancet 2013;381:629-38). "The guidelines put a lot of weight on SYNTAX score."
• When performing PCI in patients with non–ST-elevation myocardial infarction (NSTEMI), bivalirudin (Angiomax) is recommended exclusively as the anticoagulant to use during and immediately following PCI – with unfractionated heparin recommended only for patients who cannot receive bivalirudin – based on bivalirudin’s proven reduced risk for causing major bleeds, said Dr. Franz-Josef Neumann, professor and director of the University Heart Center in Bad Krozingen, Germany.
• But for patients with ST-elevation MI (STEMI) undergoing primary PCI, unfractionated heparin received the only unqualified, level I recommendation for anticoagulation, with bivalirudin receiving a level IIa, "should be considered" recommendation. This repositioning of the two options occurred, based to some extent on yet unpublished results from a very large, single-center study in Liverpool, HEAT-PPCI, reported at the annual meeting of the American College of Cardiology meeting in March that showed unfractionated heparin outperformed bivalirudin for 28-day outcomes, Dr. Neumann said. "I was very pleased and sort of amazed that results from HEAT-PPCI jumped into the guidelines, and it’s not even published yet. That [recommendation] will have an impact, I suspect," commented Dr. King.
• For patients with either STEMI or NSTEMI, the preferred antiplatelet P2Y12 inhibitors are prasugrel (Effient) and ticagrelor (Brilinta), with clopidogrel reduced to a back-up role "only when prasugrel or ticagrelor are not available," said Dr. Neumann. "I was a little surprised that clopidogrel has fallen off the charts. With the new stents having a low stent thrombosis rate, U.S. physicians tend to stick with clopidogrel; there has been more of a shift in Europe," commented Dr. King. "For elective cases, we still have a clear statement in favor of clopidogrel," countered Dr. Neumann. "It is only for higher risk, acute coronary syndrome and STEMI patients where the guidelines recommend the new agents."
Dr. Kolh said that he has received honoraria from Astra Zeneca and Braun, and research support from Edwards. Dr. Landmesser said that he had no disclosures. Dr. King said that he had no disclosures. Dr. Windecker said that he had received honoraria from, had been a consultant to, or had been a speaker for nine companies and had received research grants from seven companies. Dr. Neumann said that his institution had received research grants from 15 companies.
On Twitter @mitchelzoler
EXPERT ANALYSIS FROM EUROPCR 2014
Paclitaxel-eluting balloon shows high claudication efficacy
PARIS – A drug-eluting balloon produced a stentlike rate of primary patency and need for target vessel revascularization in a multinational, controlled trial with 331 patients with claudication.
The results showed that the paclitaxel-eluting angioplasty balloon used in the study, the IN.PACT model made by Medtronic, has the "potential to become the standard of care" for treating stenoses in the superficial femoral and popliteal arteries, Dr. Marianne Brodmann said at the annual congress of the European Association of Percutaneous Cardiovascular Interventions. After 1 year, the rate of clinically driven target-vessel revascularizations was 2% in the 220 patients treated with the drug-eluting balloon and 21% in 111 control patients treated with plain balloon angioplasty, a statistically significant difference, reported Dr. Brodmann, professor of angiology at the Medical University of Graz (Austria).*
The results seen in this trial contrast with results from studies of other types of drug-eluting balloons in these arteries, said Dr. Marc Bosiers, head of the department of vascular surgery at St. Blasius Hospital in Dendermonde, Belgium, and a coinvestigator in the study. "What we’ve learned from this trial, if you look at the results from other trials [of drug-eluting balloons], is that not all drug-eluting balloons are equal, just as not all stents are equal," Dr. Bosiers said.
The IN.PACT SFA Trial enrolled 150 patients at 13 centers in Europe and 181 patients at 44 U.S. centers. All patients were adults with Rutherford stage 2, 3, or 4 disease; claudication and rest pain; and a single or closely tandem lesion in the superficial femoral or popliteal arteries with a total length of no more than 18 cm. Their average age was 68, and about 40% had diabetes. The trial protocol allowed provisional stenting, which occurred in 7% of the patients treated with a paclitaxel-eluting balloon and in 13% of those treated with a plain balloon. The average lesion length treated was about 9 cm in both arms of the study.
The study’s primary endpoint was the rate of primary patency at 12 months, defined as freedom from clinically driven target-vessel revascularization and freedom from restenosis assessed by Doppler ultrasound at 12 months, which was 82% in patients treated with the drug-eluting balloon and 52% among patients in the control arm, a statistically significant difference.
The study’s primary safety endpoint was the combined rate of procedure- and device-related death at 30 days, freedom from target-limb major amputation at 1 year, and freedom from clinically driven target-vessel revascularization at 1 year, which occurred in 96% of patients treated with the paclitaxel-eluting balloon and in 77% of the control patients, a statistically significant difference.
These outcomes included "the lowest target-vessel revascularization rates and the highest patency rates ever reported" in this setting, and provide "robust, level 1 evidence" for the safety and efficacy of the paclitaxel-eluting balloon for this indication, Dr. Brodmann concluded.
If restenosis were to occur in the target vessel following treatment with the paclitaxel-eluting balloon, it would be possible to retreat the same vessel with a second paclitaxel-eluting balloon, although that scenario was not tested in the trial, Dr. Brodmann said in an interview. The paclitaxel essentially disappears within a few months of treatment, which should allow safe retreatment.
A written statement from Medtronic said that the company has an application pending with the Food and Drug Administration for U.S. marketing approval of the IN.PACT balloon for this indication. The balloon has been available in Europe since 2009.
The IN.PACT SFA Trial was sponsored by Medtronic, which markets the IN.PACT drug-eluting balloon. Dr. Brodmann said she is a consultant to Medtronic. Dr. Bosiers said that he had no disclosures.
On Twitter @mitchelzoler
*Correction, 6/24/2014: A previous version of this article misstated the number of patients in the control arm, the number of study centers, the name of the study, and two references to the device.

|
Mitchel L. Zoler/Frontline Medical News
|
The results from this trial change the way we think about treating stenoses in the superficial femoral and popliteal arteries. These results are probably the first to show with such robust, level 1 evidence that a drug-eluting balloon works at least as well as the best stent available today.
The results mean that the concept of "leave nothing behind" when treating vascular disease in the superficial femoral artery will be the best approach going forward. The 82% 1-year patency rate and the 2.4% rate of clinically driven target-vessel revascularizations were absolutely outstanding results.
Dr. Alberto Cremonesi, director of the interventional cardioangiology unit at Villa Maria Cecilia Hospital in Cotignola-Ravenna, Italy, made these comments in an interview. He said he had no relevant financial disclosures.

|
Mitchel L. Zoler/Frontline Medical News
|
The results from this trial change the way we think about treating stenoses in the superficial femoral and popliteal arteries. These results are probably the first to show with such robust, level 1 evidence that a drug-eluting balloon works at least as well as the best stent available today.
The results mean that the concept of "leave nothing behind" when treating vascular disease in the superficial femoral artery will be the best approach going forward. The 82% 1-year patency rate and the 2.4% rate of clinically driven target-vessel revascularizations were absolutely outstanding results.
Dr. Alberto Cremonesi, director of the interventional cardioangiology unit at Villa Maria Cecilia Hospital in Cotignola-Ravenna, Italy, made these comments in an interview. He said he had no relevant financial disclosures.

|
Mitchel L. Zoler/Frontline Medical News
|
The results from this trial change the way we think about treating stenoses in the superficial femoral and popliteal arteries. These results are probably the first to show with such robust, level 1 evidence that a drug-eluting balloon works at least as well as the best stent available today.
The results mean that the concept of "leave nothing behind" when treating vascular disease in the superficial femoral artery will be the best approach going forward. The 82% 1-year patency rate and the 2.4% rate of clinically driven target-vessel revascularizations were absolutely outstanding results.
Dr. Alberto Cremonesi, director of the interventional cardioangiology unit at Villa Maria Cecilia Hospital in Cotignola-Ravenna, Italy, made these comments in an interview. He said he had no relevant financial disclosures.
PARIS – A drug-eluting balloon produced a stentlike rate of primary patency and need for target vessel revascularization in a multinational, controlled trial with 331 patients with claudication.
The results showed that the paclitaxel-eluting angioplasty balloon used in the study, the IN.PACT model made by Medtronic, has the "potential to become the standard of care" for treating stenoses in the superficial femoral and popliteal arteries, Dr. Marianne Brodmann said at the annual congress of the European Association of Percutaneous Cardiovascular Interventions. After 1 year, the rate of clinically driven target-vessel revascularizations was 2% in the 220 patients treated with the drug-eluting balloon and 21% in 111 control patients treated with plain balloon angioplasty, a statistically significant difference, reported Dr. Brodmann, professor of angiology at the Medical University of Graz (Austria).*
The results seen in this trial contrast with results from studies of other types of drug-eluting balloons in these arteries, said Dr. Marc Bosiers, head of the department of vascular surgery at St. Blasius Hospital in Dendermonde, Belgium, and a coinvestigator in the study. "What we’ve learned from this trial, if you look at the results from other trials [of drug-eluting balloons], is that not all drug-eluting balloons are equal, just as not all stents are equal," Dr. Bosiers said.
The IN.PACT SFA Trial enrolled 150 patients at 13 centers in Europe and 181 patients at 44 U.S. centers. All patients were adults with Rutherford stage 2, 3, or 4 disease; claudication and rest pain; and a single or closely tandem lesion in the superficial femoral or popliteal arteries with a total length of no more than 18 cm. Their average age was 68, and about 40% had diabetes. The trial protocol allowed provisional stenting, which occurred in 7% of the patients treated with a paclitaxel-eluting balloon and in 13% of those treated with a plain balloon. The average lesion length treated was about 9 cm in both arms of the study.
The study’s primary endpoint was the rate of primary patency at 12 months, defined as freedom from clinically driven target-vessel revascularization and freedom from restenosis assessed by Doppler ultrasound at 12 months, which was 82% in patients treated with the drug-eluting balloon and 52% among patients in the control arm, a statistically significant difference.
The study’s primary safety endpoint was the combined rate of procedure- and device-related death at 30 days, freedom from target-limb major amputation at 1 year, and freedom from clinically driven target-vessel revascularization at 1 year, which occurred in 96% of patients treated with the paclitaxel-eluting balloon and in 77% of the control patients, a statistically significant difference.
These outcomes included "the lowest target-vessel revascularization rates and the highest patency rates ever reported" in this setting, and provide "robust, level 1 evidence" for the safety and efficacy of the paclitaxel-eluting balloon for this indication, Dr. Brodmann concluded.
If restenosis were to occur in the target vessel following treatment with the paclitaxel-eluting balloon, it would be possible to retreat the same vessel with a second paclitaxel-eluting balloon, although that scenario was not tested in the trial, Dr. Brodmann said in an interview. The paclitaxel essentially disappears within a few months of treatment, which should allow safe retreatment.
A written statement from Medtronic said that the company has an application pending with the Food and Drug Administration for U.S. marketing approval of the IN.PACT balloon for this indication. The balloon has been available in Europe since 2009.
The IN.PACT SFA Trial was sponsored by Medtronic, which markets the IN.PACT drug-eluting balloon. Dr. Brodmann said she is a consultant to Medtronic. Dr. Bosiers said that he had no disclosures.
On Twitter @mitchelzoler
*Correction, 6/24/2014: A previous version of this article misstated the number of patients in the control arm, the number of study centers, the name of the study, and two references to the device.
PARIS – A drug-eluting balloon produced a stentlike rate of primary patency and need for target vessel revascularization in a multinational, controlled trial with 331 patients with claudication.
The results showed that the paclitaxel-eluting angioplasty balloon used in the study, the IN.PACT model made by Medtronic, has the "potential to become the standard of care" for treating stenoses in the superficial femoral and popliteal arteries, Dr. Marianne Brodmann said at the annual congress of the European Association of Percutaneous Cardiovascular Interventions. After 1 year, the rate of clinically driven target-vessel revascularizations was 2% in the 220 patients treated with the drug-eluting balloon and 21% in 111 control patients treated with plain balloon angioplasty, a statistically significant difference, reported Dr. Brodmann, professor of angiology at the Medical University of Graz (Austria).*
The results seen in this trial contrast with results from studies of other types of drug-eluting balloons in these arteries, said Dr. Marc Bosiers, head of the department of vascular surgery at St. Blasius Hospital in Dendermonde, Belgium, and a coinvestigator in the study. "What we’ve learned from this trial, if you look at the results from other trials [of drug-eluting balloons], is that not all drug-eluting balloons are equal, just as not all stents are equal," Dr. Bosiers said.
The IN.PACT SFA Trial enrolled 150 patients at 13 centers in Europe and 181 patients at 44 U.S. centers. All patients were adults with Rutherford stage 2, 3, or 4 disease; claudication and rest pain; and a single or closely tandem lesion in the superficial femoral or popliteal arteries with a total length of no more than 18 cm. Their average age was 68, and about 40% had diabetes. The trial protocol allowed provisional stenting, which occurred in 7% of the patients treated with a paclitaxel-eluting balloon and in 13% of those treated with a plain balloon. The average lesion length treated was about 9 cm in both arms of the study.
The study’s primary endpoint was the rate of primary patency at 12 months, defined as freedom from clinically driven target-vessel revascularization and freedom from restenosis assessed by Doppler ultrasound at 12 months, which was 82% in patients treated with the drug-eluting balloon and 52% among patients in the control arm, a statistically significant difference.
The study’s primary safety endpoint was the combined rate of procedure- and device-related death at 30 days, freedom from target-limb major amputation at 1 year, and freedom from clinically driven target-vessel revascularization at 1 year, which occurred in 96% of patients treated with the paclitaxel-eluting balloon and in 77% of the control patients, a statistically significant difference.
These outcomes included "the lowest target-vessel revascularization rates and the highest patency rates ever reported" in this setting, and provide "robust, level 1 evidence" for the safety and efficacy of the paclitaxel-eluting balloon for this indication, Dr. Brodmann concluded.
If restenosis were to occur in the target vessel following treatment with the paclitaxel-eluting balloon, it would be possible to retreat the same vessel with a second paclitaxel-eluting balloon, although that scenario was not tested in the trial, Dr. Brodmann said in an interview. The paclitaxel essentially disappears within a few months of treatment, which should allow safe retreatment.
A written statement from Medtronic said that the company has an application pending with the Food and Drug Administration for U.S. marketing approval of the IN.PACT balloon for this indication. The balloon has been available in Europe since 2009.
The IN.PACT SFA Trial was sponsored by Medtronic, which markets the IN.PACT drug-eluting balloon. Dr. Brodmann said she is a consultant to Medtronic. Dr. Bosiers said that he had no disclosures.
On Twitter @mitchelzoler
*Correction, 6/24/2014: A previous version of this article misstated the number of patients in the control arm, the number of study centers, the name of the study, and two references to the device.
AT EUROPCR 2014
Key clinical point: A drug-eluting balloon produced stentlike patency after 1 year in superficial femoral and popliteal arteries.
Major finding: Angioplasty with a paclitaxel-eluting balloon produced a 1-year 82% primary patency rate, compared with 52% in controls.
Data source: A multicenter, randomized controlled trial with 331 patients with claudication and rest pain treated at 57 international sites.
Disclosures: The IN.PACT SFA Trial was sponsored by Medtronic, which markets the IN.PACT drug-eluting balloon. Dr. Brodmann said she is a consultant to Medtronic. Dr. Bosiers said he had no disclosures.
VIDEO: In SYMPLICITY, operator inexperience produced incomplete ablations
PARIS – A central problem with the SYMPLICITY HTN-3 trial of renal denervation was that the operators were inexperienced with the denervation procedure – and thus a majority of the renal denervations they carried out were not properly performed and left intact too many of the nerves that surround the renal arteries, commented Dr. Richard R. Heuser during the annual congress of the European Association of Percutaneous Cardiovascular Intervention.
"If you don’t get to the nerves and denervate them, you’re not going to have an effect," said Dr. Heuser, professor of medicine at the University of Arizona and chief of cardiology at St. Luke’s Medical Center in Phoenix.
Another limitation of the SYMPLICITY HTN-3 trial (N. Engl. J. Med. 2014;370:1393-1401) was that 25% of its enrolled patients were African Americans, and the trial’s results suggest that this patient subgroup does not respond to renal denervation with a significant fall in blood pressure.
In a video interview at the meeting, Dr. Heuser discussed the trial's potential limitations and renal denervation’s post-SYMPLICITY future.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
On Twitter @mitchelzoler
PARIS – A central problem with the SYMPLICITY HTN-3 trial of renal denervation was that the operators were inexperienced with the denervation procedure – and thus a majority of the renal denervations they carried out were not properly performed and left intact too many of the nerves that surround the renal arteries, commented Dr. Richard R. Heuser during the annual congress of the European Association of Percutaneous Cardiovascular Intervention.
"If you don’t get to the nerves and denervate them, you’re not going to have an effect," said Dr. Heuser, professor of medicine at the University of Arizona and chief of cardiology at St. Luke’s Medical Center in Phoenix.
Another limitation of the SYMPLICITY HTN-3 trial (N. Engl. J. Med. 2014;370:1393-1401) was that 25% of its enrolled patients were African Americans, and the trial’s results suggest that this patient subgroup does not respond to renal denervation with a significant fall in blood pressure.
In a video interview at the meeting, Dr. Heuser discussed the trial's potential limitations and renal denervation’s post-SYMPLICITY future.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
On Twitter @mitchelzoler
PARIS – A central problem with the SYMPLICITY HTN-3 trial of renal denervation was that the operators were inexperienced with the denervation procedure – and thus a majority of the renal denervations they carried out were not properly performed and left intact too many of the nerves that surround the renal arteries, commented Dr. Richard R. Heuser during the annual congress of the European Association of Percutaneous Cardiovascular Intervention.
"If you don’t get to the nerves and denervate them, you’re not going to have an effect," said Dr. Heuser, professor of medicine at the University of Arizona and chief of cardiology at St. Luke’s Medical Center in Phoenix.
Another limitation of the SYMPLICITY HTN-3 trial (N. Engl. J. Med. 2014;370:1393-1401) was that 25% of its enrolled patients were African Americans, and the trial’s results suggest that this patient subgroup does not respond to renal denervation with a significant fall in blood pressure.
In a video interview at the meeting, Dr. Heuser discussed the trial's potential limitations and renal denervation’s post-SYMPLICITY future.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
On Twitter @mitchelzoler
AT EUROPCR 2014