User login
Dactylitis, enthesitis, anterior uveitis less frequent in IBD-SpA
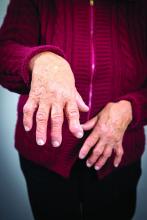
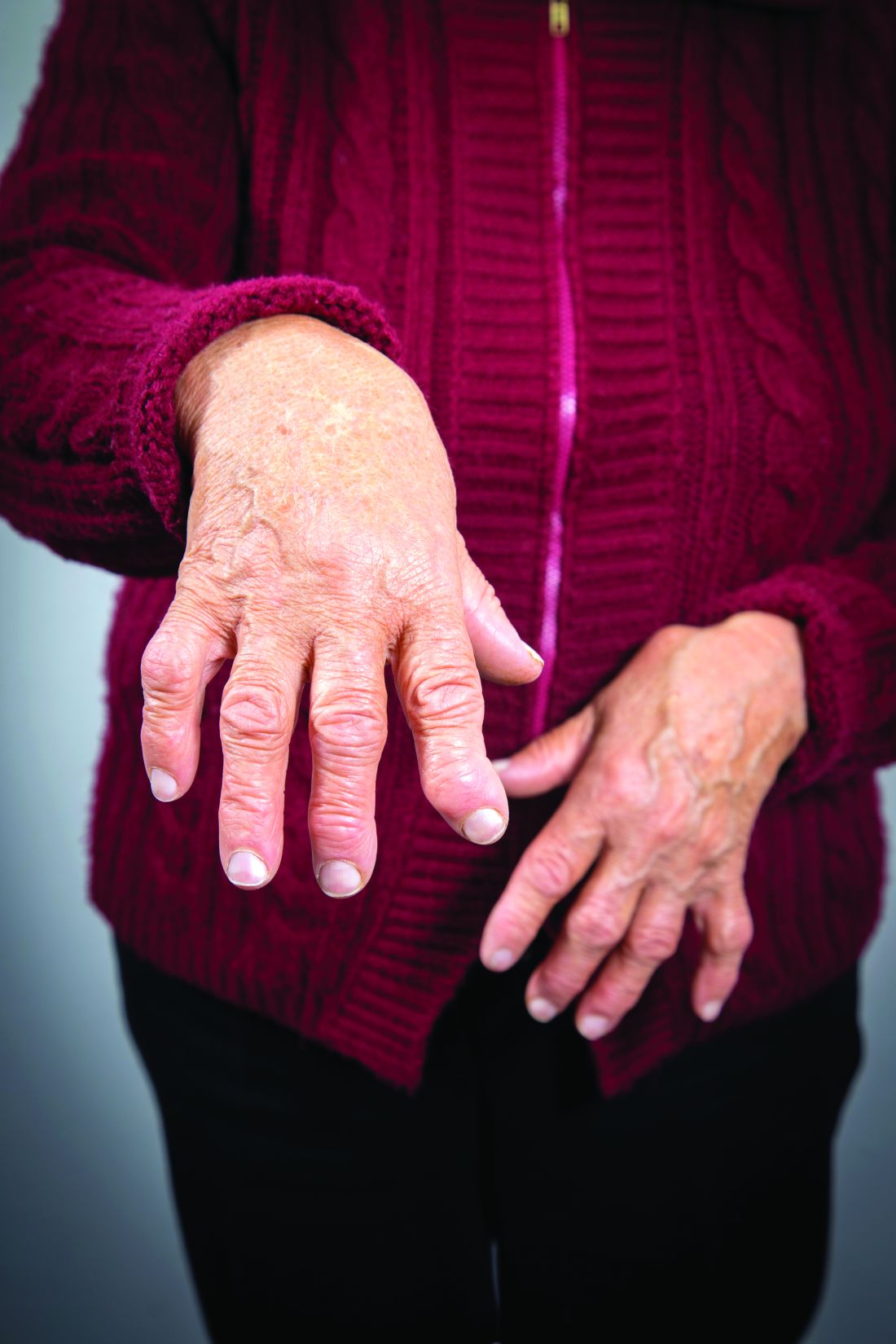
In patients with inflammatory bowel disease and spondyloarthritis (IBD-SpA), dactylitis, enthesitis, and anterior uveitis (AU) are significantly less frequent than in patients with other types of SpA, according to Fabrizio Cantini, MD, and his associates.
In a 12-month, case-control study, 88 patients with IBD-SpA, 29 with ulcerative colitis (UC), and 59 with Crohn’s disease (CD) were examined along with the 176 patients with SpA in the control group. Results showed a significantly lower occurrence of dactylitis in case patients, with 4 episodes (4.5%) in IBD-SpA patients and 30 (17.4%) in controls (P = .008). The comparison of the frequency of dactylitis in patients with UC-SpA and in patients with CD-SpA found no significant differences between the two (3.4% and 5.08%, respectively; P = .843). Enthesitis was significantly lower in IBD-SpA, occurring in 16 out of 88 patients (18.1%), compared with in 78 out of 176 controls (44.3%; P less than .001). AU was also recorded in 3 (3.4%) of the patients with IBD-SpA and in 26 controls (14.7%; P = .010), and B27 positivity was recorded in 10 (11.3%) of patients with IBD-SpA and in 70 (39.8%) of patients with SpA (P less than .001).
There was a significantly lower occurrence of dactylitis reported in IBD-SpA patients without psoriasis (1 case in 74 patients; P = .001) compared with the control group, while dactylitis occurrence was not significantly different in 3 out of 14 patients (21.4%) with coexistent psoriasis (P = .960). Enthesitis was significantly higher in 14 IBD-SpA patients with associated psoriasis (50%), compared with the remaining 74 cases (12.1%; P = .003). It was noted that enthesitis occurrence was not different in patients with UC and in those with CD (P = .103).
“The results of our case-control study show that dactylitis, enthesitis, and AU are significantly less frequent in IBD-SpA, compared with other types of SpA,” researchers concluded. “Owing to the frequent association of psoriasis with IBD, and especially with CD, the coexistence of skin disease should be taken into account when evaluating the prevalence of dactylitis and enthesitis in patients with IBD-SpA.”
Find the full study in the Journal of Rheumatology (doi: 10.3899/jrheum.161518).
In patients with inflammatory bowel disease and spondyloarthritis (IBD-SpA), dactylitis, enthesitis, and anterior uveitis (AU) are significantly less frequent than in patients with other types of SpA, according to Fabrizio Cantini, MD, and his associates.
In a 12-month, case-control study, 88 patients with IBD-SpA, 29 with ulcerative colitis (UC), and 59 with Crohn’s disease (CD) were examined along with the 176 patients with SpA in the control group. Results showed a significantly lower occurrence of dactylitis in case patients, with 4 episodes (4.5%) in IBD-SpA patients and 30 (17.4%) in controls (P = .008). The comparison of the frequency of dactylitis in patients with UC-SpA and in patients with CD-SpA found no significant differences between the two (3.4% and 5.08%, respectively; P = .843). Enthesitis was significantly lower in IBD-SpA, occurring in 16 out of 88 patients (18.1%), compared with in 78 out of 176 controls (44.3%; P less than .001). AU was also recorded in 3 (3.4%) of the patients with IBD-SpA and in 26 controls (14.7%; P = .010), and B27 positivity was recorded in 10 (11.3%) of patients with IBD-SpA and in 70 (39.8%) of patients with SpA (P less than .001).
There was a significantly lower occurrence of dactylitis reported in IBD-SpA patients without psoriasis (1 case in 74 patients; P = .001) compared with the control group, while dactylitis occurrence was not significantly different in 3 out of 14 patients (21.4%) with coexistent psoriasis (P = .960). Enthesitis was significantly higher in 14 IBD-SpA patients with associated psoriasis (50%), compared with the remaining 74 cases (12.1%; P = .003). It was noted that enthesitis occurrence was not different in patients with UC and in those with CD (P = .103).
“The results of our case-control study show that dactylitis, enthesitis, and AU are significantly less frequent in IBD-SpA, compared with other types of SpA,” researchers concluded. “Owing to the frequent association of psoriasis with IBD, and especially with CD, the coexistence of skin disease should be taken into account when evaluating the prevalence of dactylitis and enthesitis in patients with IBD-SpA.”
Find the full study in the Journal of Rheumatology (doi: 10.3899/jrheum.161518).
In patients with inflammatory bowel disease and spondyloarthritis (IBD-SpA), dactylitis, enthesitis, and anterior uveitis (AU) are significantly less frequent than in patients with other types of SpA, according to Fabrizio Cantini, MD, and his associates.
In a 12-month, case-control study, 88 patients with IBD-SpA, 29 with ulcerative colitis (UC), and 59 with Crohn’s disease (CD) were examined along with the 176 patients with SpA in the control group. Results showed a significantly lower occurrence of dactylitis in case patients, with 4 episodes (4.5%) in IBD-SpA patients and 30 (17.4%) in controls (P = .008). The comparison of the frequency of dactylitis in patients with UC-SpA and in patients with CD-SpA found no significant differences between the two (3.4% and 5.08%, respectively; P = .843). Enthesitis was significantly lower in IBD-SpA, occurring in 16 out of 88 patients (18.1%), compared with in 78 out of 176 controls (44.3%; P less than .001). AU was also recorded in 3 (3.4%) of the patients with IBD-SpA and in 26 controls (14.7%; P = .010), and B27 positivity was recorded in 10 (11.3%) of patients with IBD-SpA and in 70 (39.8%) of patients with SpA (P less than .001).
There was a significantly lower occurrence of dactylitis reported in IBD-SpA patients without psoriasis (1 case in 74 patients; P = .001) compared with the control group, while dactylitis occurrence was not significantly different in 3 out of 14 patients (21.4%) with coexistent psoriasis (P = .960). Enthesitis was significantly higher in 14 IBD-SpA patients with associated psoriasis (50%), compared with the remaining 74 cases (12.1%; P = .003). It was noted that enthesitis occurrence was not different in patients with UC and in those with CD (P = .103).
“The results of our case-control study show that dactylitis, enthesitis, and AU are significantly less frequent in IBD-SpA, compared with other types of SpA,” researchers concluded. “Owing to the frequent association of psoriasis with IBD, and especially with CD, the coexistence of skin disease should be taken into account when evaluating the prevalence of dactylitis and enthesitis in patients with IBD-SpA.”
Find the full study in the Journal of Rheumatology (doi: 10.3899/jrheum.161518).
Management of chronic insomnia in adults
Most adults experience problems with sleep from time to time, and 6%-10% meet diagnostic criteria for chronic insomnia. Many of these patients present to their primary care clinicians looking for help. This clinical practice guideline from the American College of Physicians provides recommendations based on a review of studies published during the previous decade, which were assessed in terms of the strength of the recommendation and the quality of evidence. The guideline resulted in two recommendations:
1: All adult patients should receive cognitive behavioral therapy for insomnia (CBT-I) as the initial treatment for chronic insomnia. (strong recommendation)
2: Clinicians should use a shared decision-making approach discussing the benefits, harms, and costs of short-term use of medications, to decide whether to add pharmacological therapy in adults with chronic insomnia in whom cognitive behavioral therapy for insomnia (CBT-I) alone was unsuccessful. (weak recommendation)
Cognitive behavioral therapy for insomnia (CBT-I)
Cognitive behavioral therapy for insomnia encompasses a variety of measures that aim to change patients’ habits and beliefs associated with sleep. These measures include general “sleep hygiene” interventions, as well as stimulus control, sleep restriction, relaxation training, and cognitive reframing. With sleep hygiene, patients are educated about environmental factors that affect sleep, such as avoiding caffeine late in the day, limiting alcohol intake, having a regular sleep schedule, avoiding napping, the importance of exercise, and the importance of a quiet dark room in which to sleep. Examples of stimulus control include going to bed only when sleepy, and avoiding reading and watching TV in the bedroom. Sleep restriction limits the time in bed with strict sleep and wake-up times, gradually increasing time in bed as sleep efficiency improves.
Clinicians may find it surprising that this guideline makes such a strong, clear case for the primacy of behavioral measures in the treatment of chronic insomnia. The authors make a number of points in support of this position.
First, the effects of behavioral interventions appear to be robust – at least comparable to the short-term effects of medications – and often significantly better. For example, various studies of CBT-I show a decrease in sleep onset latency (how long it takes to fall asleep after going to bed) of between 12 and 31 minutes and an increase in total sleep time of 40 minutes. This compares favorably to the short-term effects of commonly used sleep medications.
Second, the effects of behavioral interventions are long-lasting compared with medications, which are usually approved for only short-term use, lose effectiveness over time, and have no benefit at all once they’re no longer being taken. Finally, there appear to be no harms associated with CBT-I, compared with significant adverse effects of medications.
One challenge is that access to effective behavioral interventions for insomnia can be an issue. On the other hand, a number of behavioral delivery methods were examined, and found to be effective, including in-person individual or group therapy, telephone- or Web-based modules or apps, and self-help books. An editorial accompanying the guidelines calls for efforts to increase the availability of behavioral modalities for insomnia.
Pharmacologic therapy
The recommendation to use pharmacologic therapy for insomnia is much more qualified than that for CBT-I, with language about shared decision-making, discussion of risks and benefits, emphasis on short-term use, and a provision that it be used only after an unsatisfactory trial of CBT-I alone. In addition, this recommendation is classified as “weak,” and the associated evidence “low-quality.” Medications reviewed included eszopiclone, zaleplon, zolpidem, orexin receptor antagonist, melatonin, ramelteon, and benzodiazepines.
There are several reasons why pharmacologic therapy is deemphasized. First, as noted above, the effects of commonly used medications are modest. As an example, typical patients with chronic insomnia will have sleep-onset latency of 60-70 minutes. Medications reviewed for this guideline decreased this time by approximately 10-20 minutes in short-term studies, so patients still took 40-60 minutes to fall asleep. Similar modest short-term effects were seen in terms of increasing total sleep time.
A second issue with pharmacologic therapy is that while many patients with chronic insomnia seek to use medications long term, the available studies have tended to look only at short-term use, and those studies with longer duration show a diminution of medication effect over time.
Finally, there are significant adverse effects associated with sedative-hypnotic medications, including somnolence, anxiety, confusion, and disturbance in attention. This is problematic, considering that these are precisely the symptoms that patients may be hoping to avoid when they take medications to help them sleep. Even patients who may not feel impaired often show demonstrable deficits in attention and performance following use of sleep medications; this issue is reflected in the boxed warnings that accompany several commonly prescribed agents.
It is noted in the evidence reviews that there are differences among the available medications. The nonbenzodiazepine hypnotics eszopiclone and zolpidem as well as the orexin receptor antagonist suvorexant improved short-term sleep quality, though the effect was small and there was significant evidence of harm as described above. Benzodiazepine hypnotics, melatonin agonists, and antidepressants studied had little or low-quality evidence to support efficacy on improving sleep. For melatonin and ramelteon, the evidence review notes that adverse effects did not differ between the medication and the placebo groups, though two open-label longer-term studies showed evidence of adverse effects with ramelteon. It is also important to note that patients studied in medication trials were mostly healthy middle-aged individuals; it is possible that the side effects of sleep medications may be greater in those who are older or more infirm.
Bottom line
This guideline from the American College of Physicians strongly endorses the use of tailored cognitive behavioral therapy modalities for the initial treatment of patients with chronic insomnia. Medications are given a weak recommendation for a limited back-up role.
Dr. Clark is associate director of the family medicine residency program at Abington (Pa.) Jefferson Health. Dr. Skolnik is professor of family and community medicine at Sidney Kimmel Medical College, Thomas Jefferson University, Philadelphia, and associate director of the family medicine residency program at Abington Jefferson Health.
References
Qaseem A, et al. Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2016;165:125-33.
Brasure M. Psychological and Behavioral Interventions for Managing Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. 2016;165:113-24.
Wilt TJ, et al. Pharmacologic Treatment of Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. 2016;165:103-12.
Most adults experience problems with sleep from time to time, and 6%-10% meet diagnostic criteria for chronic insomnia. Many of these patients present to their primary care clinicians looking for help. This clinical practice guideline from the American College of Physicians provides recommendations based on a review of studies published during the previous decade, which were assessed in terms of the strength of the recommendation and the quality of evidence. The guideline resulted in two recommendations:
1: All adult patients should receive cognitive behavioral therapy for insomnia (CBT-I) as the initial treatment for chronic insomnia. (strong recommendation)
2: Clinicians should use a shared decision-making approach discussing the benefits, harms, and costs of short-term use of medications, to decide whether to add pharmacological therapy in adults with chronic insomnia in whom cognitive behavioral therapy for insomnia (CBT-I) alone was unsuccessful. (weak recommendation)
Cognitive behavioral therapy for insomnia (CBT-I)
Cognitive behavioral therapy for insomnia encompasses a variety of measures that aim to change patients’ habits and beliefs associated with sleep. These measures include general “sleep hygiene” interventions, as well as stimulus control, sleep restriction, relaxation training, and cognitive reframing. With sleep hygiene, patients are educated about environmental factors that affect sleep, such as avoiding caffeine late in the day, limiting alcohol intake, having a regular sleep schedule, avoiding napping, the importance of exercise, and the importance of a quiet dark room in which to sleep. Examples of stimulus control include going to bed only when sleepy, and avoiding reading and watching TV in the bedroom. Sleep restriction limits the time in bed with strict sleep and wake-up times, gradually increasing time in bed as sleep efficiency improves.
Clinicians may find it surprising that this guideline makes such a strong, clear case for the primacy of behavioral measures in the treatment of chronic insomnia. The authors make a number of points in support of this position.
First, the effects of behavioral interventions appear to be robust – at least comparable to the short-term effects of medications – and often significantly better. For example, various studies of CBT-I show a decrease in sleep onset latency (how long it takes to fall asleep after going to bed) of between 12 and 31 minutes and an increase in total sleep time of 40 minutes. This compares favorably to the short-term effects of commonly used sleep medications.
Second, the effects of behavioral interventions are long-lasting compared with medications, which are usually approved for only short-term use, lose effectiveness over time, and have no benefit at all once they’re no longer being taken. Finally, there appear to be no harms associated with CBT-I, compared with significant adverse effects of medications.
One challenge is that access to effective behavioral interventions for insomnia can be an issue. On the other hand, a number of behavioral delivery methods were examined, and found to be effective, including in-person individual or group therapy, telephone- or Web-based modules or apps, and self-help books. An editorial accompanying the guidelines calls for efforts to increase the availability of behavioral modalities for insomnia.
Pharmacologic therapy
The recommendation to use pharmacologic therapy for insomnia is much more qualified than that for CBT-I, with language about shared decision-making, discussion of risks and benefits, emphasis on short-term use, and a provision that it be used only after an unsatisfactory trial of CBT-I alone. In addition, this recommendation is classified as “weak,” and the associated evidence “low-quality.” Medications reviewed included eszopiclone, zaleplon, zolpidem, orexin receptor antagonist, melatonin, ramelteon, and benzodiazepines.
There are several reasons why pharmacologic therapy is deemphasized. First, as noted above, the effects of commonly used medications are modest. As an example, typical patients with chronic insomnia will have sleep-onset latency of 60-70 minutes. Medications reviewed for this guideline decreased this time by approximately 10-20 minutes in short-term studies, so patients still took 40-60 minutes to fall asleep. Similar modest short-term effects were seen in terms of increasing total sleep time.
A second issue with pharmacologic therapy is that while many patients with chronic insomnia seek to use medications long term, the available studies have tended to look only at short-term use, and those studies with longer duration show a diminution of medication effect over time.
Finally, there are significant adverse effects associated with sedative-hypnotic medications, including somnolence, anxiety, confusion, and disturbance in attention. This is problematic, considering that these are precisely the symptoms that patients may be hoping to avoid when they take medications to help them sleep. Even patients who may not feel impaired often show demonstrable deficits in attention and performance following use of sleep medications; this issue is reflected in the boxed warnings that accompany several commonly prescribed agents.
It is noted in the evidence reviews that there are differences among the available medications. The nonbenzodiazepine hypnotics eszopiclone and zolpidem as well as the orexin receptor antagonist suvorexant improved short-term sleep quality, though the effect was small and there was significant evidence of harm as described above. Benzodiazepine hypnotics, melatonin agonists, and antidepressants studied had little or low-quality evidence to support efficacy on improving sleep. For melatonin and ramelteon, the evidence review notes that adverse effects did not differ between the medication and the placebo groups, though two open-label longer-term studies showed evidence of adverse effects with ramelteon. It is also important to note that patients studied in medication trials were mostly healthy middle-aged individuals; it is possible that the side effects of sleep medications may be greater in those who are older or more infirm.
Bottom line
This guideline from the American College of Physicians strongly endorses the use of tailored cognitive behavioral therapy modalities for the initial treatment of patients with chronic insomnia. Medications are given a weak recommendation for a limited back-up role.
Dr. Clark is associate director of the family medicine residency program at Abington (Pa.) Jefferson Health. Dr. Skolnik is professor of family and community medicine at Sidney Kimmel Medical College, Thomas Jefferson University, Philadelphia, and associate director of the family medicine residency program at Abington Jefferson Health.
References
Qaseem A, et al. Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2016;165:125-33.
Brasure M. Psychological and Behavioral Interventions for Managing Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. 2016;165:113-24.
Wilt TJ, et al. Pharmacologic Treatment of Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. 2016;165:103-12.
Most adults experience problems with sleep from time to time, and 6%-10% meet diagnostic criteria for chronic insomnia. Many of these patients present to their primary care clinicians looking for help. This clinical practice guideline from the American College of Physicians provides recommendations based on a review of studies published during the previous decade, which were assessed in terms of the strength of the recommendation and the quality of evidence. The guideline resulted in two recommendations:
1: All adult patients should receive cognitive behavioral therapy for insomnia (CBT-I) as the initial treatment for chronic insomnia. (strong recommendation)
2: Clinicians should use a shared decision-making approach discussing the benefits, harms, and costs of short-term use of medications, to decide whether to add pharmacological therapy in adults with chronic insomnia in whom cognitive behavioral therapy for insomnia (CBT-I) alone was unsuccessful. (weak recommendation)
Cognitive behavioral therapy for insomnia (CBT-I)
Cognitive behavioral therapy for insomnia encompasses a variety of measures that aim to change patients’ habits and beliefs associated with sleep. These measures include general “sleep hygiene” interventions, as well as stimulus control, sleep restriction, relaxation training, and cognitive reframing. With sleep hygiene, patients are educated about environmental factors that affect sleep, such as avoiding caffeine late in the day, limiting alcohol intake, having a regular sleep schedule, avoiding napping, the importance of exercise, and the importance of a quiet dark room in which to sleep. Examples of stimulus control include going to bed only when sleepy, and avoiding reading and watching TV in the bedroom. Sleep restriction limits the time in bed with strict sleep and wake-up times, gradually increasing time in bed as sleep efficiency improves.
Clinicians may find it surprising that this guideline makes such a strong, clear case for the primacy of behavioral measures in the treatment of chronic insomnia. The authors make a number of points in support of this position.
First, the effects of behavioral interventions appear to be robust – at least comparable to the short-term effects of medications – and often significantly better. For example, various studies of CBT-I show a decrease in sleep onset latency (how long it takes to fall asleep after going to bed) of between 12 and 31 minutes and an increase in total sleep time of 40 minutes. This compares favorably to the short-term effects of commonly used sleep medications.
Second, the effects of behavioral interventions are long-lasting compared with medications, which are usually approved for only short-term use, lose effectiveness over time, and have no benefit at all once they’re no longer being taken. Finally, there appear to be no harms associated with CBT-I, compared with significant adverse effects of medications.
One challenge is that access to effective behavioral interventions for insomnia can be an issue. On the other hand, a number of behavioral delivery methods were examined, and found to be effective, including in-person individual or group therapy, telephone- or Web-based modules or apps, and self-help books. An editorial accompanying the guidelines calls for efforts to increase the availability of behavioral modalities for insomnia.
Pharmacologic therapy
The recommendation to use pharmacologic therapy for insomnia is much more qualified than that for CBT-I, with language about shared decision-making, discussion of risks and benefits, emphasis on short-term use, and a provision that it be used only after an unsatisfactory trial of CBT-I alone. In addition, this recommendation is classified as “weak,” and the associated evidence “low-quality.” Medications reviewed included eszopiclone, zaleplon, zolpidem, orexin receptor antagonist, melatonin, ramelteon, and benzodiazepines.
There are several reasons why pharmacologic therapy is deemphasized. First, as noted above, the effects of commonly used medications are modest. As an example, typical patients with chronic insomnia will have sleep-onset latency of 60-70 minutes. Medications reviewed for this guideline decreased this time by approximately 10-20 minutes in short-term studies, so patients still took 40-60 minutes to fall asleep. Similar modest short-term effects were seen in terms of increasing total sleep time.
A second issue with pharmacologic therapy is that while many patients with chronic insomnia seek to use medications long term, the available studies have tended to look only at short-term use, and those studies with longer duration show a diminution of medication effect over time.
Finally, there are significant adverse effects associated with sedative-hypnotic medications, including somnolence, anxiety, confusion, and disturbance in attention. This is problematic, considering that these are precisely the symptoms that patients may be hoping to avoid when they take medications to help them sleep. Even patients who may not feel impaired often show demonstrable deficits in attention and performance following use of sleep medications; this issue is reflected in the boxed warnings that accompany several commonly prescribed agents.
It is noted in the evidence reviews that there are differences among the available medications. The nonbenzodiazepine hypnotics eszopiclone and zolpidem as well as the orexin receptor antagonist suvorexant improved short-term sleep quality, though the effect was small and there was significant evidence of harm as described above. Benzodiazepine hypnotics, melatonin agonists, and antidepressants studied had little or low-quality evidence to support efficacy on improving sleep. For melatonin and ramelteon, the evidence review notes that adverse effects did not differ between the medication and the placebo groups, though two open-label longer-term studies showed evidence of adverse effects with ramelteon. It is also important to note that patients studied in medication trials were mostly healthy middle-aged individuals; it is possible that the side effects of sleep medications may be greater in those who are older or more infirm.
Bottom line
This guideline from the American College of Physicians strongly endorses the use of tailored cognitive behavioral therapy modalities for the initial treatment of patients with chronic insomnia. Medications are given a weak recommendation for a limited back-up role.
Dr. Clark is associate director of the family medicine residency program at Abington (Pa.) Jefferson Health. Dr. Skolnik is professor of family and community medicine at Sidney Kimmel Medical College, Thomas Jefferson University, Philadelphia, and associate director of the family medicine residency program at Abington Jefferson Health.
References
Qaseem A, et al. Management of Chronic Insomnia Disorder in Adults: A Clinical Practice Guideline From the American College of Physicians. Ann Intern Med. 2016;165:125-33.
Brasure M. Psychological and Behavioral Interventions for Managing Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. 2016;165:113-24.
Wilt TJ, et al. Pharmacologic Treatment of Insomnia Disorder: An Evidence Report for a Clinical Practice Guideline by the American College of Physicians. Ann Intern Med. 2016;165:103-12.
As some holdout states revisit Medicaid expansion, new data show it pays off
Although the GOP-controlled Congress is pledging its continued interest – despite stalls and snags – in dismantling Obamacare, some “red state” legislatures are changing course and showing a newfound interest in embracing the health law’s Medicaid expansion.
And a study published April 12 in Health Affairs adds to these discussions, percolating in places such as Kansas, Georgia, Virginia, North Carolina, and Maine. Thirty-one states plus the District of Columbia already opted to pursue the expansion, which provided federal funding to broaden eligibility to include most low-income adults with incomes up to 138 percent of the federal poverty level (about $16,000 for an individual).
Researchers analyzed data from the National Association of State Budget Officers for fiscal years 2010-2015 to assess the fiscal effects of expansion’s first 2 years.
Their findings address arguments put forth by some GOP lawmakers, who say the expansion will add to the nation’s budget deficit and saddle states with additional coverage costs, forcing them to skimp on other budget priorities like education or transportation.
The researchers concluded that when states expanded eligibility for the low-income health insurance program they did see larger health care expenditures – but those costs were covered with federal funding. In addition, expansion states didn’t have to skimp on other policy priorities – such as environment, housing, and other public health initiatives – to make ends meet.
“This is a potential big benefit, not only to people who get coverage, but to state economies,” said Benjamin Sommers, MD, PhD, an associate professor of health policy and economics at Harvard University’s public health school, and the study’s first author.
This finding – that states expanding Medicaid didn’t encounter unforeseen budget problems – shouldn’t be surprising.
“Expansion is basically free” to the states, agreed Massachusetts Institute of Technology economist Jonathan Gruber, PhD, one of Obamacare’s architects who worked with Dr. Sommers to systematically compare the budgets of all 50 states to examine Medicaid expansion’s impact. “That’s the big insight,” he said. “There’s no sort of hidden downside.”
And that may be part of what’s fueling this renewed interest, said Edwin Park, vice president for health policy at the left-leaning Center for Budget and Policy Priorities. These states are seeing the federal windfall their neighbors received while trying to navigate public health concerns like opioid addiction, he said. They “are looking at how their neighbors or expansion states have done and see the benefits,” Mr. Park said. “The primary argument against the expansion on the state level has been it’s going to break the bank. The research demonstrates that’s not the case.”
But a caveat: The data used in this analysis reflected only years during which the federal government picked up 100% of the tab for expanding Medicaid eligibility and therefore could overestimate the benefit to state budgets. That’s because in 2017 that federal support begins to taper off, and by 2020 states have to pay 10 percent of the expansion costs themselves.
That means policymakers should exert caution in reading too much into this study, said Tom Miller, a resident fellow at the conservative American Enterprise Institute. Because states will eventually shoulder more of the cost, he said, studies that assess its budgetary impact are preliminary at best. Plus, Miller said, other factors such as relative economic growth could have padded state budgets in the years studied – masking any unintended costs with a bigger Medicaid program. It’s unclear whether in times of downturn Medicaid would take a bigger bite out of state budgets.
“It’s just the beginning of this – it’s an early snapshot,” he said.
Dr. Sommers argued the limited data set means researchers should continue to track how state budgets compare between expansion and nonexpansion states. But even when states do take on more of Medicaid’s cost, that may not pose such a burden, suggested Sara Rosenbaum, a professor of health law and policy at George Washington University. Expanding Medicaid brings in other potential economic benefits that this paper doesn’t account for – less uncompensated care in hospitals, for instance – that could offset the expenditures states ultimately take up.
A bigger concern, some experts say, is that – even without the Obamacare repeal – some GOP health proposals would change the federal government’s Medicaid funding mechanism from being an open-ended match to a block grant or per-capita cap in an effort to curb national spending. Those proposals would take away at least some of the federal dollars that have insulated state budgets.
“Ironically, all the arguments that have been made against expansion for years – like creating a hole in the state budget or breaking the bank – that’s exactly what a per-capita grant or block grant does,” Park said.
As more states take on the Medicaid debate, those consequences matter, both Dr. Sommers and Dr. Gruber said. And not just for state budgets – for consumers, too.
“The main lesson is there’s no sort of big hidden cost of expanding Medicaid. What you see is what you get,” Dr. Gruber said. “You get free health insurance for your citizens.”
Kaiser Health News is a national health policy news service that is part of the nonpartisan Henry J. Kaiser Family Foundation.
Although the GOP-controlled Congress is pledging its continued interest – despite stalls and snags – in dismantling Obamacare, some “red state” legislatures are changing course and showing a newfound interest in embracing the health law’s Medicaid expansion.
And a study published April 12 in Health Affairs adds to these discussions, percolating in places such as Kansas, Georgia, Virginia, North Carolina, and Maine. Thirty-one states plus the District of Columbia already opted to pursue the expansion, which provided federal funding to broaden eligibility to include most low-income adults with incomes up to 138 percent of the federal poverty level (about $16,000 for an individual).
Researchers analyzed data from the National Association of State Budget Officers for fiscal years 2010-2015 to assess the fiscal effects of expansion’s first 2 years.
Their findings address arguments put forth by some GOP lawmakers, who say the expansion will add to the nation’s budget deficit and saddle states with additional coverage costs, forcing them to skimp on other budget priorities like education or transportation.
The researchers concluded that when states expanded eligibility for the low-income health insurance program they did see larger health care expenditures – but those costs were covered with federal funding. In addition, expansion states didn’t have to skimp on other policy priorities – such as environment, housing, and other public health initiatives – to make ends meet.
“This is a potential big benefit, not only to people who get coverage, but to state economies,” said Benjamin Sommers, MD, PhD, an associate professor of health policy and economics at Harvard University’s public health school, and the study’s first author.
This finding – that states expanding Medicaid didn’t encounter unforeseen budget problems – shouldn’t be surprising.
“Expansion is basically free” to the states, agreed Massachusetts Institute of Technology economist Jonathan Gruber, PhD, one of Obamacare’s architects who worked with Dr. Sommers to systematically compare the budgets of all 50 states to examine Medicaid expansion’s impact. “That’s the big insight,” he said. “There’s no sort of hidden downside.”
And that may be part of what’s fueling this renewed interest, said Edwin Park, vice president for health policy at the left-leaning Center for Budget and Policy Priorities. These states are seeing the federal windfall their neighbors received while trying to navigate public health concerns like opioid addiction, he said. They “are looking at how their neighbors or expansion states have done and see the benefits,” Mr. Park said. “The primary argument against the expansion on the state level has been it’s going to break the bank. The research demonstrates that’s not the case.”
But a caveat: The data used in this analysis reflected only years during which the federal government picked up 100% of the tab for expanding Medicaid eligibility and therefore could overestimate the benefit to state budgets. That’s because in 2017 that federal support begins to taper off, and by 2020 states have to pay 10 percent of the expansion costs themselves.
That means policymakers should exert caution in reading too much into this study, said Tom Miller, a resident fellow at the conservative American Enterprise Institute. Because states will eventually shoulder more of the cost, he said, studies that assess its budgetary impact are preliminary at best. Plus, Miller said, other factors such as relative economic growth could have padded state budgets in the years studied – masking any unintended costs with a bigger Medicaid program. It’s unclear whether in times of downturn Medicaid would take a bigger bite out of state budgets.
“It’s just the beginning of this – it’s an early snapshot,” he said.
Dr. Sommers argued the limited data set means researchers should continue to track how state budgets compare between expansion and nonexpansion states. But even when states do take on more of Medicaid’s cost, that may not pose such a burden, suggested Sara Rosenbaum, a professor of health law and policy at George Washington University. Expanding Medicaid brings in other potential economic benefits that this paper doesn’t account for – less uncompensated care in hospitals, for instance – that could offset the expenditures states ultimately take up.
A bigger concern, some experts say, is that – even without the Obamacare repeal – some GOP health proposals would change the federal government’s Medicaid funding mechanism from being an open-ended match to a block grant or per-capita cap in an effort to curb national spending. Those proposals would take away at least some of the federal dollars that have insulated state budgets.
“Ironically, all the arguments that have been made against expansion for years – like creating a hole in the state budget or breaking the bank – that’s exactly what a per-capita grant or block grant does,” Park said.
As more states take on the Medicaid debate, those consequences matter, both Dr. Sommers and Dr. Gruber said. And not just for state budgets – for consumers, too.
“The main lesson is there’s no sort of big hidden cost of expanding Medicaid. What you see is what you get,” Dr. Gruber said. “You get free health insurance for your citizens.”
Kaiser Health News is a national health policy news service that is part of the nonpartisan Henry J. Kaiser Family Foundation.
Although the GOP-controlled Congress is pledging its continued interest – despite stalls and snags – in dismantling Obamacare, some “red state” legislatures are changing course and showing a newfound interest in embracing the health law’s Medicaid expansion.
And a study published April 12 in Health Affairs adds to these discussions, percolating in places such as Kansas, Georgia, Virginia, North Carolina, and Maine. Thirty-one states plus the District of Columbia already opted to pursue the expansion, which provided federal funding to broaden eligibility to include most low-income adults with incomes up to 138 percent of the federal poverty level (about $16,000 for an individual).
Researchers analyzed data from the National Association of State Budget Officers for fiscal years 2010-2015 to assess the fiscal effects of expansion’s first 2 years.
Their findings address arguments put forth by some GOP lawmakers, who say the expansion will add to the nation’s budget deficit and saddle states with additional coverage costs, forcing them to skimp on other budget priorities like education or transportation.
The researchers concluded that when states expanded eligibility for the low-income health insurance program they did see larger health care expenditures – but those costs were covered with federal funding. In addition, expansion states didn’t have to skimp on other policy priorities – such as environment, housing, and other public health initiatives – to make ends meet.
“This is a potential big benefit, not only to people who get coverage, but to state economies,” said Benjamin Sommers, MD, PhD, an associate professor of health policy and economics at Harvard University’s public health school, and the study’s first author.
This finding – that states expanding Medicaid didn’t encounter unforeseen budget problems – shouldn’t be surprising.
“Expansion is basically free” to the states, agreed Massachusetts Institute of Technology economist Jonathan Gruber, PhD, one of Obamacare’s architects who worked with Dr. Sommers to systematically compare the budgets of all 50 states to examine Medicaid expansion’s impact. “That’s the big insight,” he said. “There’s no sort of hidden downside.”
And that may be part of what’s fueling this renewed interest, said Edwin Park, vice president for health policy at the left-leaning Center for Budget and Policy Priorities. These states are seeing the federal windfall their neighbors received while trying to navigate public health concerns like opioid addiction, he said. They “are looking at how their neighbors or expansion states have done and see the benefits,” Mr. Park said. “The primary argument against the expansion on the state level has been it’s going to break the bank. The research demonstrates that’s not the case.”
But a caveat: The data used in this analysis reflected only years during which the federal government picked up 100% of the tab for expanding Medicaid eligibility and therefore could overestimate the benefit to state budgets. That’s because in 2017 that federal support begins to taper off, and by 2020 states have to pay 10 percent of the expansion costs themselves.
That means policymakers should exert caution in reading too much into this study, said Tom Miller, a resident fellow at the conservative American Enterprise Institute. Because states will eventually shoulder more of the cost, he said, studies that assess its budgetary impact are preliminary at best. Plus, Miller said, other factors such as relative economic growth could have padded state budgets in the years studied – masking any unintended costs with a bigger Medicaid program. It’s unclear whether in times of downturn Medicaid would take a bigger bite out of state budgets.
“It’s just the beginning of this – it’s an early snapshot,” he said.
Dr. Sommers argued the limited data set means researchers should continue to track how state budgets compare between expansion and nonexpansion states. But even when states do take on more of Medicaid’s cost, that may not pose such a burden, suggested Sara Rosenbaum, a professor of health law and policy at George Washington University. Expanding Medicaid brings in other potential economic benefits that this paper doesn’t account for – less uncompensated care in hospitals, for instance – that could offset the expenditures states ultimately take up.
A bigger concern, some experts say, is that – even without the Obamacare repeal – some GOP health proposals would change the federal government’s Medicaid funding mechanism from being an open-ended match to a block grant or per-capita cap in an effort to curb national spending. Those proposals would take away at least some of the federal dollars that have insulated state budgets.
“Ironically, all the arguments that have been made against expansion for years – like creating a hole in the state budget or breaking the bank – that’s exactly what a per-capita grant or block grant does,” Park said.
As more states take on the Medicaid debate, those consequences matter, both Dr. Sommers and Dr. Gruber said. And not just for state budgets – for consumers, too.
“The main lesson is there’s no sort of big hidden cost of expanding Medicaid. What you see is what you get,” Dr. Gruber said. “You get free health insurance for your citizens.”
Kaiser Health News is a national health policy news service that is part of the nonpartisan Henry J. Kaiser Family Foundation.
Physical frailty may lengthen late-life depression
Physical frailty negatively affects the course of late-life depression and requires multifaceted interventions, according to a new analysis from a study of depression in seniors.
Researchers in the Netherlands worked with participants from the Netherlands Study of Depression in Older Persons, an ongoing cohort study of people aged 60-93 years who have been diagnosed with a depressive disorder.
From the cohort, the researchers examined 285 participants for a 2-year period with physical tests (such as a walking test and a hand grip strength test) and questionnaires aimed at assessing the course of participants’ depression and their physical health.
“The present study, to our knowledge, is the first to examine the longitudinal association between physical frailty and the course of depression in a sample of clinically depressed older persons,” wrote Rose M. Collard, PhD, of the department of psychiatry at Radboud University Medical Center, Nijmegen, the Netherlands, and her coauthors (Eur Psychiatry. 2017 Jan 24;43:66-72). “Our results confirm that late-life depression is a highly persisting disorder, with half of the patients not achieving remission at 2-year follow-up.”
More “performance-based” frailty was associated with nonremission of depression, while “vitality-based” frailty was associated with remission.
The authors commented that “this latter result puzzled us, but a possible explanation might be that the vitality-based dimension of frailty reflects a classic, uncomplicated clinical depression,” which is more treatable.
Physical frailty negatively affects the course of late-life depression and requires multifaceted interventions, according to a new analysis from a study of depression in seniors.
Researchers in the Netherlands worked with participants from the Netherlands Study of Depression in Older Persons, an ongoing cohort study of people aged 60-93 years who have been diagnosed with a depressive disorder.
From the cohort, the researchers examined 285 participants for a 2-year period with physical tests (such as a walking test and a hand grip strength test) and questionnaires aimed at assessing the course of participants’ depression and their physical health.
“The present study, to our knowledge, is the first to examine the longitudinal association between physical frailty and the course of depression in a sample of clinically depressed older persons,” wrote Rose M. Collard, PhD, of the department of psychiatry at Radboud University Medical Center, Nijmegen, the Netherlands, and her coauthors (Eur Psychiatry. 2017 Jan 24;43:66-72). “Our results confirm that late-life depression is a highly persisting disorder, with half of the patients not achieving remission at 2-year follow-up.”
More “performance-based” frailty was associated with nonremission of depression, while “vitality-based” frailty was associated with remission.
The authors commented that “this latter result puzzled us, but a possible explanation might be that the vitality-based dimension of frailty reflects a classic, uncomplicated clinical depression,” which is more treatable.
Physical frailty negatively affects the course of late-life depression and requires multifaceted interventions, according to a new analysis from a study of depression in seniors.
Researchers in the Netherlands worked with participants from the Netherlands Study of Depression in Older Persons, an ongoing cohort study of people aged 60-93 years who have been diagnosed with a depressive disorder.
From the cohort, the researchers examined 285 participants for a 2-year period with physical tests (such as a walking test and a hand grip strength test) and questionnaires aimed at assessing the course of participants’ depression and their physical health.
“The present study, to our knowledge, is the first to examine the longitudinal association between physical frailty and the course of depression in a sample of clinically depressed older persons,” wrote Rose M. Collard, PhD, of the department of psychiatry at Radboud University Medical Center, Nijmegen, the Netherlands, and her coauthors (Eur Psychiatry. 2017 Jan 24;43:66-72). “Our results confirm that late-life depression is a highly persisting disorder, with half of the patients not achieving remission at 2-year follow-up.”
More “performance-based” frailty was associated with nonremission of depression, while “vitality-based” frailty was associated with remission.
The authors commented that “this latter result puzzled us, but a possible explanation might be that the vitality-based dimension of frailty reflects a classic, uncomplicated clinical depression,” which is more treatable.
FROM EUROPEAN PSYCHIATRY
RA treatment delays raise risk of long-term disability
Initiating disease-modifying antirheumatic drugs within 6 months of a diagnosis of rheumatoid arthritis is associated with significantly lower disability scores over the long term, new research suggests.
Better diagnosis and access to early treatment has also likely played a role in a global decline in mortality from rheumatoid arthritis over a recent 25-year period, according to an analysis of World Health Organization and United Nations data, but the decline has occurred unequally across countries.
Impact of early treatment on disability
In the first of two separate studies published online April 20 in Arthritis & Rheumatology, U.K. researchers followed 602 patients from the Norfolk Arthritis Register for 20 years, starting in 1990-1994, and collected clinical data at baseline and years 1-3, 5, 7, 10, 15, and 20.
However, patients who began treatment within 6 months of diagnosis had disability scores similar to those of patients who were never initiated on treatment (Arthritis Rheumatol. 2017 April 20. doi: 10.1002/art.40090).
“This supports the importance of the “window of opportunity” construct for treatment, showing that early treatment leads to improved outcomes even into the second decade following symptom onset,” wrote first author James M. Gwinnutt, a PhD candidate at the University of Manchester (England), and his coauthors. “Increased functional disability over time could be due to worse joint damage, and it has been shown that those who receive later treatment have higher radiological scores at follow-up than those treated early.”
There were 88 deaths in the early treatment group (55%) during the follow-up period, 99 deaths (39.8%) in the late treatment group, and 78 deaths (40.4%) in the never-treated group.
When the researchers adjusted for disease severity in a comparison of mortality across the groups, they found a trend toward a reduced risk of mortality in patients treated early, compared with those who began treatment later, although this did not reach statistical significance.
However, patients in both the early treatment and late treatment groups showed significantly elevated standardized mortality rates, compared with the general population of Norfolk, while the never-treated group showed slightly – but not significantly – elevated mortality.
Overall, around one-quarter of patients (26.6%) began treatment within 6 months of the onset of symptoms, 19.9% were started on treatment within 6-12 months, 17.4% started within 1-2 years, 19% did not start treatment until more than 2 years after symptom onset, and 43.7% of the cohort never received treatment but still attended follow-up.
Patients who began earlier treatment had worse clinical characteristics than did those who began treatment later, except for tender joint counts and autoantibody status.
Researchers saw an overall decline in median swollen joint count and tender joint count in the first year after baseline, and this remained low throughout the course of the study.
Median Health Assessment Questionnaire scores also fell after baseline but then increased steadily from year 2 to year 20, exceeding baseline levels by year 7.
“This paper has two important messages, firstly about the long-term outcome of patients with RA in the modern era treated according to best practice at the time of presentation; secondly about the benefit of early treatment which is still apparent into the second decade after symptom onset with respect to functional disability,” the authors wrote.
An uneven global decline in mortality from RA
Meanwhile, a second study showed that mortality from rheumatoid arthritis declined globally across 31 countries from 1987 to 2011, according to data from the World Health Organization mortality database and the United Nations.
The absolute number of deaths where rheumatoid arthritis was registered as the underlying cause of death declined from 0.12% of all-cause deaths in 1987 to 0.09% of all-cause deaths in 2011 (Arthritis Rheumatol. 2017 April 20. doi: 10.1002/art.40091).
The mean age-standardized mortality rate declined by 48.2%, from 7.1 per million person-years in 1987-1989 to 3.7 in 2009-2011.
However, there was considerable variation between countries; the greatest reduction was seen in Finland, which had an absolute reduction of 20.6 fewer deaths per million person-years, while Croatia had an increase of 3.7 deaths per million person-years.
Younger people with rheumatoid arthritis showed the greatest reductions in mortality, while those in older age groups had smaller reductions in mortality.
“It has been suggested that changes in the management of RA toward early and aggressive treatment with disease-modifying antirheumatic drugs and subsequent biologic therapies has led to better health status and lower mortality for most people with RA over time,” wrote first author Aliasghar A. Kiadaliri, PhD, of Lund (Sweden) University, and his coauthors.
“These findings alongside aging of the population and fall in mortality may lead to an increase in the number of people with RA. Given that it appears that people with RA are now living longer, increase in burden of RA on health care systems is expected and policy makers should be made aware about to appropriately plan for this anticipated increase.”
The first study was supported by Arthritis Research UK. The second study was supported by the Swedish Research Council, Crafoord Foundation, Greta and Johan Kocks Foundation, the Faculty of Medicine Lund University, governmental funding of clinical research within Sweden’s National Health Service. No conflicts of interest were declared for either paper.
Initiating disease-modifying antirheumatic drugs within 6 months of a diagnosis of rheumatoid arthritis is associated with significantly lower disability scores over the long term, new research suggests.
Better diagnosis and access to early treatment has also likely played a role in a global decline in mortality from rheumatoid arthritis over a recent 25-year period, according to an analysis of World Health Organization and United Nations data, but the decline has occurred unequally across countries.
Impact of early treatment on disability
In the first of two separate studies published online April 20 in Arthritis & Rheumatology, U.K. researchers followed 602 patients from the Norfolk Arthritis Register for 20 years, starting in 1990-1994, and collected clinical data at baseline and years 1-3, 5, 7, 10, 15, and 20.
However, patients who began treatment within 6 months of diagnosis had disability scores similar to those of patients who were never initiated on treatment (Arthritis Rheumatol. 2017 April 20. doi: 10.1002/art.40090).
“This supports the importance of the “window of opportunity” construct for treatment, showing that early treatment leads to improved outcomes even into the second decade following symptom onset,” wrote first author James M. Gwinnutt, a PhD candidate at the University of Manchester (England), and his coauthors. “Increased functional disability over time could be due to worse joint damage, and it has been shown that those who receive later treatment have higher radiological scores at follow-up than those treated early.”
There were 88 deaths in the early treatment group (55%) during the follow-up period, 99 deaths (39.8%) in the late treatment group, and 78 deaths (40.4%) in the never-treated group.
When the researchers adjusted for disease severity in a comparison of mortality across the groups, they found a trend toward a reduced risk of mortality in patients treated early, compared with those who began treatment later, although this did not reach statistical significance.
However, patients in both the early treatment and late treatment groups showed significantly elevated standardized mortality rates, compared with the general population of Norfolk, while the never-treated group showed slightly – but not significantly – elevated mortality.
Overall, around one-quarter of patients (26.6%) began treatment within 6 months of the onset of symptoms, 19.9% were started on treatment within 6-12 months, 17.4% started within 1-2 years, 19% did not start treatment until more than 2 years after symptom onset, and 43.7% of the cohort never received treatment but still attended follow-up.
Patients who began earlier treatment had worse clinical characteristics than did those who began treatment later, except for tender joint counts and autoantibody status.
Researchers saw an overall decline in median swollen joint count and tender joint count in the first year after baseline, and this remained low throughout the course of the study.
Median Health Assessment Questionnaire scores also fell after baseline but then increased steadily from year 2 to year 20, exceeding baseline levels by year 7.
“This paper has two important messages, firstly about the long-term outcome of patients with RA in the modern era treated according to best practice at the time of presentation; secondly about the benefit of early treatment which is still apparent into the second decade after symptom onset with respect to functional disability,” the authors wrote.
An uneven global decline in mortality from RA
Meanwhile, a second study showed that mortality from rheumatoid arthritis declined globally across 31 countries from 1987 to 2011, according to data from the World Health Organization mortality database and the United Nations.
The absolute number of deaths where rheumatoid arthritis was registered as the underlying cause of death declined from 0.12% of all-cause deaths in 1987 to 0.09% of all-cause deaths in 2011 (Arthritis Rheumatol. 2017 April 20. doi: 10.1002/art.40091).
The mean age-standardized mortality rate declined by 48.2%, from 7.1 per million person-years in 1987-1989 to 3.7 in 2009-2011.
However, there was considerable variation between countries; the greatest reduction was seen in Finland, which had an absolute reduction of 20.6 fewer deaths per million person-years, while Croatia had an increase of 3.7 deaths per million person-years.
Younger people with rheumatoid arthritis showed the greatest reductions in mortality, while those in older age groups had smaller reductions in mortality.
“It has been suggested that changes in the management of RA toward early and aggressive treatment with disease-modifying antirheumatic drugs and subsequent biologic therapies has led to better health status and lower mortality for most people with RA over time,” wrote first author Aliasghar A. Kiadaliri, PhD, of Lund (Sweden) University, and his coauthors.
“These findings alongside aging of the population and fall in mortality may lead to an increase in the number of people with RA. Given that it appears that people with RA are now living longer, increase in burden of RA on health care systems is expected and policy makers should be made aware about to appropriately plan for this anticipated increase.”
The first study was supported by Arthritis Research UK. The second study was supported by the Swedish Research Council, Crafoord Foundation, Greta and Johan Kocks Foundation, the Faculty of Medicine Lund University, governmental funding of clinical research within Sweden’s National Health Service. No conflicts of interest were declared for either paper.
Initiating disease-modifying antirheumatic drugs within 6 months of a diagnosis of rheumatoid arthritis is associated with significantly lower disability scores over the long term, new research suggests.
Better diagnosis and access to early treatment has also likely played a role in a global decline in mortality from rheumatoid arthritis over a recent 25-year period, according to an analysis of World Health Organization and United Nations data, but the decline has occurred unequally across countries.
Impact of early treatment on disability
In the first of two separate studies published online April 20 in Arthritis & Rheumatology, U.K. researchers followed 602 patients from the Norfolk Arthritis Register for 20 years, starting in 1990-1994, and collected clinical data at baseline and years 1-3, 5, 7, 10, 15, and 20.
However, patients who began treatment within 6 months of diagnosis had disability scores similar to those of patients who were never initiated on treatment (Arthritis Rheumatol. 2017 April 20. doi: 10.1002/art.40090).
“This supports the importance of the “window of opportunity” construct for treatment, showing that early treatment leads to improved outcomes even into the second decade following symptom onset,” wrote first author James M. Gwinnutt, a PhD candidate at the University of Manchester (England), and his coauthors. “Increased functional disability over time could be due to worse joint damage, and it has been shown that those who receive later treatment have higher radiological scores at follow-up than those treated early.”
There were 88 deaths in the early treatment group (55%) during the follow-up period, 99 deaths (39.8%) in the late treatment group, and 78 deaths (40.4%) in the never-treated group.
When the researchers adjusted for disease severity in a comparison of mortality across the groups, they found a trend toward a reduced risk of mortality in patients treated early, compared with those who began treatment later, although this did not reach statistical significance.
However, patients in both the early treatment and late treatment groups showed significantly elevated standardized mortality rates, compared with the general population of Norfolk, while the never-treated group showed slightly – but not significantly – elevated mortality.
Overall, around one-quarter of patients (26.6%) began treatment within 6 months of the onset of symptoms, 19.9% were started on treatment within 6-12 months, 17.4% started within 1-2 years, 19% did not start treatment until more than 2 years after symptom onset, and 43.7% of the cohort never received treatment but still attended follow-up.
Patients who began earlier treatment had worse clinical characteristics than did those who began treatment later, except for tender joint counts and autoantibody status.
Researchers saw an overall decline in median swollen joint count and tender joint count in the first year after baseline, and this remained low throughout the course of the study.
Median Health Assessment Questionnaire scores also fell after baseline but then increased steadily from year 2 to year 20, exceeding baseline levels by year 7.
“This paper has two important messages, firstly about the long-term outcome of patients with RA in the modern era treated according to best practice at the time of presentation; secondly about the benefit of early treatment which is still apparent into the second decade after symptom onset with respect to functional disability,” the authors wrote.
An uneven global decline in mortality from RA
Meanwhile, a second study showed that mortality from rheumatoid arthritis declined globally across 31 countries from 1987 to 2011, according to data from the World Health Organization mortality database and the United Nations.
The absolute number of deaths where rheumatoid arthritis was registered as the underlying cause of death declined from 0.12% of all-cause deaths in 1987 to 0.09% of all-cause deaths in 2011 (Arthritis Rheumatol. 2017 April 20. doi: 10.1002/art.40091).
The mean age-standardized mortality rate declined by 48.2%, from 7.1 per million person-years in 1987-1989 to 3.7 in 2009-2011.
However, there was considerable variation between countries; the greatest reduction was seen in Finland, which had an absolute reduction of 20.6 fewer deaths per million person-years, while Croatia had an increase of 3.7 deaths per million person-years.
Younger people with rheumatoid arthritis showed the greatest reductions in mortality, while those in older age groups had smaller reductions in mortality.
“It has been suggested that changes in the management of RA toward early and aggressive treatment with disease-modifying antirheumatic drugs and subsequent biologic therapies has led to better health status and lower mortality for most people with RA over time,” wrote first author Aliasghar A. Kiadaliri, PhD, of Lund (Sweden) University, and his coauthors.
“These findings alongside aging of the population and fall in mortality may lead to an increase in the number of people with RA. Given that it appears that people with RA are now living longer, increase in burden of RA on health care systems is expected and policy makers should be made aware about to appropriately plan for this anticipated increase.”
The first study was supported by Arthritis Research UK. The second study was supported by the Swedish Research Council, Crafoord Foundation, Greta and Johan Kocks Foundation, the Faculty of Medicine Lund University, governmental funding of clinical research within Sweden’s National Health Service. No conflicts of interest were declared for either paper.
FROM ARTHRITIS & RHEUMATOLOGY
Key clinical point:
Major finding: Patients who began treatment with disease-modifying antirheumatic drugs or steroids within 6 months of the onset of symptoms have significantly reduced disability scores up to 20 years later. Also, across 31 countries, the mean age-standardized mortality rate due to RA declined by 48.2%, from 7.1 per million person-years in 1987-1989 to 3.7 in 2009-2011.
Data source: Inception cohort study of 602 patients with rheumatoid arthritis, and a study of World Health Organization and United Nations data from 31 countries.
Disclosures: The first study was supported by Arthritis Research UK. The second study was supported by the Swedish Research Council, Crafoord Foundation, Greta and Johan Kocks Foundation, the Faculty of Medicine Lund University, governmental funding of clinical research within Sweden’s National Health Service. No conflicts of interest were declared for either paper.
Culture change key in adopting an oncology alternative payment model
SAN DIEGO – If you consider participating in an alternative payment model for your practice, expect to devote a lot of time to work flow changes, according to Blase N. Polite, MD.
“The culture change is one of the hardest things people face as they go into alternative payment models,” Dr. Polite, deputy section chief of clinical operations at the University of Chicago Medical Center, said at the annual meeting of the American College of Physicians.
“You want work flow changes designed to enable you to take better care of your patients in a consistent manner,” he noted. “It has to be designed with a busy clinic and a busy clinician in mind. You want to be able to share the work flow burden among different groups in the system, so it’s important to allow individuals to work at the upper end of their training.”
“We are paid $160 per month throughout the 6-month episode, and you can have as many recurring 6-month episodes as needed, assuming the patient continued to receive chemotherapy in IV or oral format,” Dr. Polite said.
“Our management fees are contingent on documented adherence to care processes,” he added. “We are held accountable to cost of care, quality metrics, and care processes. The shared savings are subject to bringing down costs while maintaining quality. If by year three you have not achieved shared savings, you have two choices: either drop out of the model, or agree to two-sided risk.”
CMS also is collecting detailed stage, molecular data, and recurrence/progression data on each patient.
The ability to perform risk adjustment in your patient population is a cornerstone of any alternative payment model, he said. These include variables such as cancer type, age, sex, selected noncancer comorbidities, receipt of radiation, and participation in a clinical trial.
As an example, Dr. Polite discussed the hypothetical case of a 65-year-old man with lymphoma, Medicare Part D coverage, and no Medicaid.
“If that patient has no comorbidities, the target treatment price is $23,657.80,” he said. “If that patient has been coded for three comorbidities, our target price goes up to $32,090.28. So, you see an almost $10,000 difference in our target price based on whether or not you appropriately coded and accounted for comorbidities in your patient.”
In a 6-month period, about one-third of costs in the university’s oncology care model are related to chemotherapy, another one-third are inpatient costs, “and everything else comes out as rounding error on the back end, such as evaluation and management coding, imaging, and radiation therapy,” Dr. Polite said.
CMS periodically sends national data such as the number of inpatient admissions per 100 patients and ED visits per 100 patients, so the center can compare itself with other practices in the model.
“You have to have a way to think through those data,” he said. “We can look at our drug expenditures and see where it is we’re spending the most money. Are there places where we can save money? Another key area: How do you identify your high-risk patients?”
Currently, Dr. Polite and his associates conduct risk assessments with every new patient, including the Vulnerable Elders Survey (VES-13), the Mini-Cog, the Patient Health Questionnaire–4 (PHQ-4), as well as questions intended to gauge the patient’s social support, financial situation, and health literacy.
“This is triggering within the medical record a best practices alert that is telling the physician there is a recommendation that this patient ought to be referred to social work or geriatric oncology, or psycho-oncology or physical therapy depending on their needs,” he said. “What remains a difficulty is we have about 18% of our patients who have a positive screen. But only in 23% of the cases so far do we have physicians who are actually acting on that screen.”
Clinicians considering adoption of an oncology care model should expect to devote time and resources to additional cancer registry abstraction and data entry, and make electronic medical record changes for data capture and identifying high-risk patients.
“You also want to invest in care coordination and navigation, staffing for after-hours urgent care to avoid emergency department costs, hospitalizations, and readmissions, staffing for pharmacists to manage high-risk patients on complex medications, staffing of additional palliative care providers, and system tools to make sure referral loops are closed,” Dr. Polite said.
“Those are places where money can help you,” he added. “But at the end of the day, money cannot help getting all the staff to collect and act upon the information provided to them.”
Dr. Polite disclosed that he has received research grants from Merck and is a consultant for GLG and Pfizer.
SAN DIEGO – If you consider participating in an alternative payment model for your practice, expect to devote a lot of time to work flow changes, according to Blase N. Polite, MD.
“The culture change is one of the hardest things people face as they go into alternative payment models,” Dr. Polite, deputy section chief of clinical operations at the University of Chicago Medical Center, said at the annual meeting of the American College of Physicians.
“You want work flow changes designed to enable you to take better care of your patients in a consistent manner,” he noted. “It has to be designed with a busy clinic and a busy clinician in mind. You want to be able to share the work flow burden among different groups in the system, so it’s important to allow individuals to work at the upper end of their training.”
“We are paid $160 per month throughout the 6-month episode, and you can have as many recurring 6-month episodes as needed, assuming the patient continued to receive chemotherapy in IV or oral format,” Dr. Polite said.
“Our management fees are contingent on documented adherence to care processes,” he added. “We are held accountable to cost of care, quality metrics, and care processes. The shared savings are subject to bringing down costs while maintaining quality. If by year three you have not achieved shared savings, you have two choices: either drop out of the model, or agree to two-sided risk.”
CMS also is collecting detailed stage, molecular data, and recurrence/progression data on each patient.
The ability to perform risk adjustment in your patient population is a cornerstone of any alternative payment model, he said. These include variables such as cancer type, age, sex, selected noncancer comorbidities, receipt of radiation, and participation in a clinical trial.
As an example, Dr. Polite discussed the hypothetical case of a 65-year-old man with lymphoma, Medicare Part D coverage, and no Medicaid.
“If that patient has no comorbidities, the target treatment price is $23,657.80,” he said. “If that patient has been coded for three comorbidities, our target price goes up to $32,090.28. So, you see an almost $10,000 difference in our target price based on whether or not you appropriately coded and accounted for comorbidities in your patient.”
In a 6-month period, about one-third of costs in the university’s oncology care model are related to chemotherapy, another one-third are inpatient costs, “and everything else comes out as rounding error on the back end, such as evaluation and management coding, imaging, and radiation therapy,” Dr. Polite said.
CMS periodically sends national data such as the number of inpatient admissions per 100 patients and ED visits per 100 patients, so the center can compare itself with other practices in the model.
“You have to have a way to think through those data,” he said. “We can look at our drug expenditures and see where it is we’re spending the most money. Are there places where we can save money? Another key area: How do you identify your high-risk patients?”
Currently, Dr. Polite and his associates conduct risk assessments with every new patient, including the Vulnerable Elders Survey (VES-13), the Mini-Cog, the Patient Health Questionnaire–4 (PHQ-4), as well as questions intended to gauge the patient’s social support, financial situation, and health literacy.
“This is triggering within the medical record a best practices alert that is telling the physician there is a recommendation that this patient ought to be referred to social work or geriatric oncology, or psycho-oncology or physical therapy depending on their needs,” he said. “What remains a difficulty is we have about 18% of our patients who have a positive screen. But only in 23% of the cases so far do we have physicians who are actually acting on that screen.”
Clinicians considering adoption of an oncology care model should expect to devote time and resources to additional cancer registry abstraction and data entry, and make electronic medical record changes for data capture and identifying high-risk patients.
“You also want to invest in care coordination and navigation, staffing for after-hours urgent care to avoid emergency department costs, hospitalizations, and readmissions, staffing for pharmacists to manage high-risk patients on complex medications, staffing of additional palliative care providers, and system tools to make sure referral loops are closed,” Dr. Polite said.
“Those are places where money can help you,” he added. “But at the end of the day, money cannot help getting all the staff to collect and act upon the information provided to them.”
Dr. Polite disclosed that he has received research grants from Merck and is a consultant for GLG and Pfizer.
SAN DIEGO – If you consider participating in an alternative payment model for your practice, expect to devote a lot of time to work flow changes, according to Blase N. Polite, MD.
“The culture change is one of the hardest things people face as they go into alternative payment models,” Dr. Polite, deputy section chief of clinical operations at the University of Chicago Medical Center, said at the annual meeting of the American College of Physicians.
“You want work flow changes designed to enable you to take better care of your patients in a consistent manner,” he noted. “It has to be designed with a busy clinic and a busy clinician in mind. You want to be able to share the work flow burden among different groups in the system, so it’s important to allow individuals to work at the upper end of their training.”
“We are paid $160 per month throughout the 6-month episode, and you can have as many recurring 6-month episodes as needed, assuming the patient continued to receive chemotherapy in IV or oral format,” Dr. Polite said.
“Our management fees are contingent on documented adherence to care processes,” he added. “We are held accountable to cost of care, quality metrics, and care processes. The shared savings are subject to bringing down costs while maintaining quality. If by year three you have not achieved shared savings, you have two choices: either drop out of the model, or agree to two-sided risk.”
CMS also is collecting detailed stage, molecular data, and recurrence/progression data on each patient.
The ability to perform risk adjustment in your patient population is a cornerstone of any alternative payment model, he said. These include variables such as cancer type, age, sex, selected noncancer comorbidities, receipt of radiation, and participation in a clinical trial.
As an example, Dr. Polite discussed the hypothetical case of a 65-year-old man with lymphoma, Medicare Part D coverage, and no Medicaid.
“If that patient has no comorbidities, the target treatment price is $23,657.80,” he said. “If that patient has been coded for three comorbidities, our target price goes up to $32,090.28. So, you see an almost $10,000 difference in our target price based on whether or not you appropriately coded and accounted for comorbidities in your patient.”
In a 6-month period, about one-third of costs in the university’s oncology care model are related to chemotherapy, another one-third are inpatient costs, “and everything else comes out as rounding error on the back end, such as evaluation and management coding, imaging, and radiation therapy,” Dr. Polite said.
CMS periodically sends national data such as the number of inpatient admissions per 100 patients and ED visits per 100 patients, so the center can compare itself with other practices in the model.
“You have to have a way to think through those data,” he said. “We can look at our drug expenditures and see where it is we’re spending the most money. Are there places where we can save money? Another key area: How do you identify your high-risk patients?”
Currently, Dr. Polite and his associates conduct risk assessments with every new patient, including the Vulnerable Elders Survey (VES-13), the Mini-Cog, the Patient Health Questionnaire–4 (PHQ-4), as well as questions intended to gauge the patient’s social support, financial situation, and health literacy.
“This is triggering within the medical record a best practices alert that is telling the physician there is a recommendation that this patient ought to be referred to social work or geriatric oncology, or psycho-oncology or physical therapy depending on their needs,” he said. “What remains a difficulty is we have about 18% of our patients who have a positive screen. But only in 23% of the cases so far do we have physicians who are actually acting on that screen.”
Clinicians considering adoption of an oncology care model should expect to devote time and resources to additional cancer registry abstraction and data entry, and make electronic medical record changes for data capture and identifying high-risk patients.
“You also want to invest in care coordination and navigation, staffing for after-hours urgent care to avoid emergency department costs, hospitalizations, and readmissions, staffing for pharmacists to manage high-risk patients on complex medications, staffing of additional palliative care providers, and system tools to make sure referral loops are closed,” Dr. Polite said.
“Those are places where money can help you,” he added. “But at the end of the day, money cannot help getting all the staff to collect and act upon the information provided to them.”
Dr. Polite disclosed that he has received research grants from Merck and is a consultant for GLG and Pfizer.
EXPERT ANALYSIS AT ACP INTERNAL MEDICINE
Severe Refractory Atopic Dermatitis With Elevated Serum IgE Treated With Omalizumab
To the Editor:
Atopic dermatitis (AD) is a common skin condition with an increasing prevalence, affecting up to 20% of children and 3% of adults.1,2 More than 80% of patients with AD have elevated IgE levels.3,4 IgE modulates the inflammatory response in AD in several ways including “a biphasic immediate/late phase reaction, allergen presentation by IgE-bearing Langerhans cells, allergen-induced activation of IgE-bearing macrophages, and IgE autoreactivity to human proteins.”5 Historically, most therapies have focused on mitigating the allergic symptoms caused by degranulated effector cells, such as antihistamines. However, a new class of biologically engineered medications (eg, anti-IgE [omalizumab]) aim to prevent the initiation of the allergic response.6 Variable success has been reported using omalizumab in the treatment of AD, though the majority of studies have shown improvement, especially when used in combination with conventional therapies.4,5,7-22 Omalizumab dosage is determined by body weight and pretreatment serum total IgE levels and is administered via subcutaneous injections every 2 to 4 weeks.6,7,23-26 However, the dosing tables are based on asthma therapy, in which serum IgE levels may be much lower than chronic AD,7,24 and the appropriate dosage in AD patients with markedly elevated IgE is unclear. We report an interesting case of a 57-year-old man with erythroderma from long-standing severe chronic AD that was unresponsive to conventional therapy as well as an associated serum IgE level of 17,183 IU/mL who dramatically improved when omalizumab was added to his treatment regimen.
A 57-year-old man presented with essentially 100% body surface area involvement of AD with erythroderma and pruritus. Severe AD developed at infancy and cleared at 5 years of age; childhood onset of asthma was responsive to theophylline and oral inhalers. He developed recurrent AD and asthma at 38 years of age, which was progressive and developed into severe recalcitrant erythroderma by 50 years of age. His AD was unresponsive to multiple therapies, including topical steroids, antibiotics, tacrolimus, bleach baths, antihistamines, methotrexate (15 mg weekly for 1 year, then 12.5 mg weekly for 6 months), UVB phototherapy, and psoralen plus UVA photochemotherapy. He had minimal improvement with cyclosporine (200 mg daily for 4 weeks) and mycophenolate mofetil (3 g daily), and required systemic steroids for relief. The skin was violaceous and lichenified (Figure, A). Laboratory studies were normal, except for a serum IgE level of 17,183 IU/mL (reference range, <150 IU/mL) and peripheral blood eosinophilia up to 29.8% (reference range, 1%–5%) of the differential. Skin biopsies showed AD progressing to lichen simplex chronicus. Omalizumab was added to the therapeutic regimen at a dose of 375 mg every 2 weeks, with noticeable improvement after 3 months. The patient had approximately 80% to 90% clearing with resolution of erythroderma and pruritus, and only limited residual lichenification (Figure, B). The mycophenolate was tapered slowly, and the patient experienced a mild flare at 1 g daily. He is presently on 1 g of mycophenolate daily and omalizumab (375 mg every 2 weeks) and remains remarkably improved. His IgE level decreased to 11,983 IU/mL.
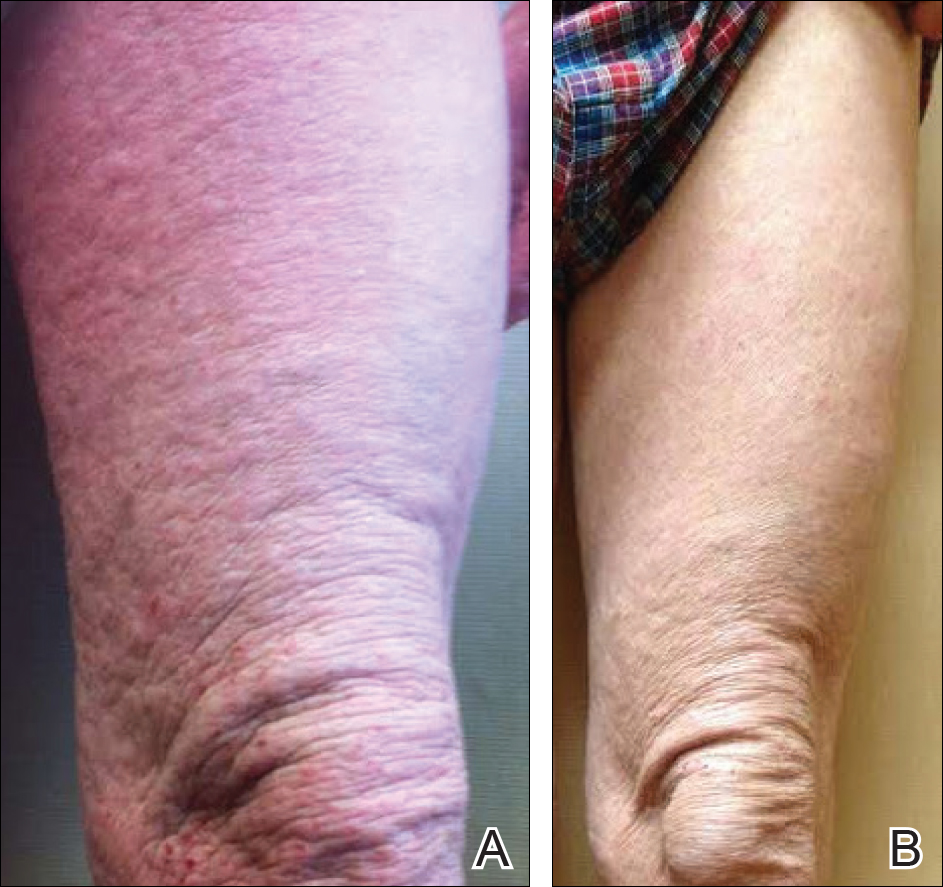
Omalizumab is a monoclonal IgG1 antibody that specifically binds to the FcεRI domain of serum IgE. It blocks binding to high-affinity receptors on effector cells, primarily mast cells, basophils, macrophages, and dendritic cells; it also decreases free IgE serum levels and downregulates the IgE receptor.4,6-10,23-25,27,28 Currently, omalizumab is US Food and Drug Administration approved for moderate to severe persistent asthma in patients 6 years or older with a positive aeroallergen skin test and IgE levels up to 700 IU/mL.6,7,23-25,27,28
However, scattered case reports and small case series have described variable success in the treatment of severe AD that is unresponsive to conventional therapy in patients with markedly elevated serum IgE levels.4,5,7-22 The majority of patients (approximately 80% of published cases yielded by a PubMed search of articles indexed for MEDLINE using the search terms omalizumab and atopic dermatitis) showed improvement when measured by clinical severity scores and quality of life improvement, especially when used in conjunction with conventional therapy. Possible reasons for reported treatment failure include insufficient dosage, lack of established treatment guidelines for markedly elevated serum IgE levels, severity of disease, or variable response with failure to lower IgE level below a required threshold.7,9,23,24,27
Krathen and Hsu9 reported treatment failure with omalizumab for AD in 3 patients with serum IgE levels ranging from 5440 and 24,400 IU/mL, and one review indicated omalizumab may work best in patients with only moderately elevated serum IgE levels.21 However, Toledo et al18 reported efficacy of low-dose omalizumab for pretreatment IgE levels up to 30,000 IU/mL in 6 of 11 reported cases. The pretreatment serum IgE level is not predictive of response, and lowering the serum IgE level without normalization can be efficacious,12,23 as in the current case. Serum IgE levels are not used for monitoring therapeutic response or calculating future dosing, given potential increases in serum IgE levels during and after therapy (for up to 12 months) secondary to the formation of anti-IgE:IgE complexes.6,28 Omalizumab appears most effective when used in combination with conventional therapies. Hopefully ongoing studies will further elucidate the role of omalizumab in recalcitrant AD with elevated serum IgE levels.
- Schultz-Larsen F, Diepgen T, Svennson A. The occurrence of atopic dermatitis in north Europe: an international questionnaire study. J Am Acad Dermatol. 1996;34:760-764.
- Laughter D, Istvan JA, Tofte SJ, et al. The presence of atopic dermatitis in Oregon schoolchildren. J Am Acad Dermatol. 2000;43:649-655.
- Jones HE, Inouye JC, McGerity JL, et al. Atopic disease and serum immunoglobulin-E. Br J Dermatol. 1975;92:17-25.
- Abramovits W. A clinician’s paradigm in the treatment of atopic dermatitis. J Am Acad Dermatol. 2005;53(1, suppl 1):570-577.
- Leung D, Soter N. Cellular and immunologic mechanisms in atopic dermatitis. J Am Acad Dermatol. 2001;44(suppl):S1-S12.
- US Food and Drug Administration. Briefing document on safety. Omalizumab (Xolair) (recombinant humanized monoclonal antibody to IgE) for treatment of allergic asthma. http://www.fda.gov/ohrms/dockets/ac/03/briefing/3952B1_02_FDA-Xolair-Safety.pdf. Published April 18, 2003. Accessed June 23, 2014.
- Lane JE, Cheyney JM, Lane TN, et al. Treatment of recalcitrant atopic dermatitis with omalizumab. J Am Acad Dermatol. 2006;54:68-72.
- Caruso C, Gaeta F, Valluzzi RL, et al. Omalizumab efficacy in a girl with atopic eczema. Allergy. 2010;65:278-279.
- Krathen RA, Hsu S. Failure of omalizumab for the treatment of severe atopic dermatitis. J Am Dermatol. 2005;53:338-340.
- Fernández-Antón Martínez MC, Leis-Dosil V, Alfageme-Roldán F, et al. Omalizumab for the treatment of Atopic Dermatitis. Actas Dermosifiliogr. 2012;103:624-628.
- Pelaia G, Gallelli L, Romeo P, et al. Omalizumab decreases exacerbation frequency, oral intake of corticosteroids and peripheral blood eosinophils in atopic patients with uncontrolled asthma. Int J Clin Pharmacol Ther. 2011;49:713-721.
- Belloni B, Ziai M, Lim A, et al. Low-dose anti-IgE therapy in patients with atopic eczema with high serum IgE levels. J Allergy Clin Immunol. 2007;120:1223-1225.
- Park SY, Choi MR, Na JI, et al. Recalcitrant atopic dermatitis treated with omalizumab. Ann Dermatol. 2010;22:349-352.
- Velling P, Skowasch D, Pabst S. Improvement of quality of life in patients with concomitant allergic asthma and atopic dermatitis: one year follow-up of omalizumab therapy. Eur J Med Res. 2011;15:407-410.
- Amrol D. Anti-immunoglobulin E in the treatment of refractory atopic dermatitis. South Med J. 2010;103:554-558.
- Heil PM, Maurer D, Klein B, et al. Omalizumab therapy in atopic dermatitis: depletion of IgE does not improve the clinical course-a randomized, placebo-controlled and double blind study. J Dtsch Dermatol Ges. 2010;8:990-998.
- Ramírez del Pozo ME, Contreras Contreras E, López Tiro J, et al. Omalizumab (anti-IgE antibody) in the treatment of severe atopic dermatitis. J Investig Allergol Clin Immunol. 2011;21:416-417.
- Toledo F, Silvestre JF, Muñoz C. Combined therapy with low-dose omalizumab and intravenous immunoglobulin for severe atopic dermatitis: report of four cases. J Eur Acad Dermatol Venereol. 2012;26:1325-1327.
- Sheinkopf LE, Rafi AW, Katz RM. Efficacy of omalizumab in the treatment of atopic dermatitis: a pilot study. Allergy Asthma Proc. 2008;29:530-537.
- Incorvia C, Pravettoni C, Mauro M, et al. Effectiveness of omalizumab in a patient with severe asthma and atopic dermatitis. Monaldi Arch Chest Dis. 2008:69:78-80.
- Schmitt J, Schäkel K. Omalizumab as a therapeutic option in atopic eczema. Current evidence and potential benefit [in German]. Hautarzt. 2007;58:130-132.
- Thaiwat S, Sangasapaviliya A. Omalizumab treatment in severe atopic dermatitis. Asian Pac J Allergy Immunol. 2011;29:357-360.
- Kopp MV. Omalizumab: anti-IgE therapy in allergy. Curr Allergy Asthma Rep. 2011;11:101-106.
- Vichyanond P. Omalizumab in allergic diseases, a recent review. Asian Pc J Allergy Immunol. 2011;29:209-219.
- Scheinfeld N. Omalizumab. A recombinant humanized monoclonal IgE-blocking antibody. Dermatol Online J. 2005;11:2.
- Lowe PJ, Georgiou P, Canvin J. Revision of omalizumab dosing table for dosing every 4 instead of 2 weeks for specific ranges of bodyweight and baseline IgE [published online ahead of print December 8, 2014]. Regul Toxicol Pharmacol. 2015;71:68-77.
- Vigo PG, Girgis KR, Pfuetze BL, et al. Efficacy of anti-IgE therapy in patients with atopic dermatitis. J Am Acad Dermatol. 2006;55:168-170.
- Hanifin J, Chan S. Biochemical and immunologic mechanisms in atopic dermatitis: new targets for emerging therapies. J Am Acad Dermatol. 1999;41:72-77.
To the Editor:
Atopic dermatitis (AD) is a common skin condition with an increasing prevalence, affecting up to 20% of children and 3% of adults.1,2 More than 80% of patients with AD have elevated IgE levels.3,4 IgE modulates the inflammatory response in AD in several ways including “a biphasic immediate/late phase reaction, allergen presentation by IgE-bearing Langerhans cells, allergen-induced activation of IgE-bearing macrophages, and IgE autoreactivity to human proteins.”5 Historically, most therapies have focused on mitigating the allergic symptoms caused by degranulated effector cells, such as antihistamines. However, a new class of biologically engineered medications (eg, anti-IgE [omalizumab]) aim to prevent the initiation of the allergic response.6 Variable success has been reported using omalizumab in the treatment of AD, though the majority of studies have shown improvement, especially when used in combination with conventional therapies.4,5,7-22 Omalizumab dosage is determined by body weight and pretreatment serum total IgE levels and is administered via subcutaneous injections every 2 to 4 weeks.6,7,23-26 However, the dosing tables are based on asthma therapy, in which serum IgE levels may be much lower than chronic AD,7,24 and the appropriate dosage in AD patients with markedly elevated IgE is unclear. We report an interesting case of a 57-year-old man with erythroderma from long-standing severe chronic AD that was unresponsive to conventional therapy as well as an associated serum IgE level of 17,183 IU/mL who dramatically improved when omalizumab was added to his treatment regimen.
A 57-year-old man presented with essentially 100% body surface area involvement of AD with erythroderma and pruritus. Severe AD developed at infancy and cleared at 5 years of age; childhood onset of asthma was responsive to theophylline and oral inhalers. He developed recurrent AD and asthma at 38 years of age, which was progressive and developed into severe recalcitrant erythroderma by 50 years of age. His AD was unresponsive to multiple therapies, including topical steroids, antibiotics, tacrolimus, bleach baths, antihistamines, methotrexate (15 mg weekly for 1 year, then 12.5 mg weekly for 6 months), UVB phototherapy, and psoralen plus UVA photochemotherapy. He had minimal improvement with cyclosporine (200 mg daily for 4 weeks) and mycophenolate mofetil (3 g daily), and required systemic steroids for relief. The skin was violaceous and lichenified (Figure, A). Laboratory studies were normal, except for a serum IgE level of 17,183 IU/mL (reference range, <150 IU/mL) and peripheral blood eosinophilia up to 29.8% (reference range, 1%–5%) of the differential. Skin biopsies showed AD progressing to lichen simplex chronicus. Omalizumab was added to the therapeutic regimen at a dose of 375 mg every 2 weeks, with noticeable improvement after 3 months. The patient had approximately 80% to 90% clearing with resolution of erythroderma and pruritus, and only limited residual lichenification (Figure, B). The mycophenolate was tapered slowly, and the patient experienced a mild flare at 1 g daily. He is presently on 1 g of mycophenolate daily and omalizumab (375 mg every 2 weeks) and remains remarkably improved. His IgE level decreased to 11,983 IU/mL.

Omalizumab is a monoclonal IgG1 antibody that specifically binds to the FcεRI domain of serum IgE. It blocks binding to high-affinity receptors on effector cells, primarily mast cells, basophils, macrophages, and dendritic cells; it also decreases free IgE serum levels and downregulates the IgE receptor.4,6-10,23-25,27,28 Currently, omalizumab is US Food and Drug Administration approved for moderate to severe persistent asthma in patients 6 years or older with a positive aeroallergen skin test and IgE levels up to 700 IU/mL.6,7,23-25,27,28
However, scattered case reports and small case series have described variable success in the treatment of severe AD that is unresponsive to conventional therapy in patients with markedly elevated serum IgE levels.4,5,7-22 The majority of patients (approximately 80% of published cases yielded by a PubMed search of articles indexed for MEDLINE using the search terms omalizumab and atopic dermatitis) showed improvement when measured by clinical severity scores and quality of life improvement, especially when used in conjunction with conventional therapy. Possible reasons for reported treatment failure include insufficient dosage, lack of established treatment guidelines for markedly elevated serum IgE levels, severity of disease, or variable response with failure to lower IgE level below a required threshold.7,9,23,24,27
Krathen and Hsu9 reported treatment failure with omalizumab for AD in 3 patients with serum IgE levels ranging from 5440 and 24,400 IU/mL, and one review indicated omalizumab may work best in patients with only moderately elevated serum IgE levels.21 However, Toledo et al18 reported efficacy of low-dose omalizumab for pretreatment IgE levels up to 30,000 IU/mL in 6 of 11 reported cases. The pretreatment serum IgE level is not predictive of response, and lowering the serum IgE level without normalization can be efficacious,12,23 as in the current case. Serum IgE levels are not used for monitoring therapeutic response or calculating future dosing, given potential increases in serum IgE levels during and after therapy (for up to 12 months) secondary to the formation of anti-IgE:IgE complexes.6,28 Omalizumab appears most effective when used in combination with conventional therapies. Hopefully ongoing studies will further elucidate the role of omalizumab in recalcitrant AD with elevated serum IgE levels.
To the Editor:
Atopic dermatitis (AD) is a common skin condition with an increasing prevalence, affecting up to 20% of children and 3% of adults.1,2 More than 80% of patients with AD have elevated IgE levels.3,4 IgE modulates the inflammatory response in AD in several ways including “a biphasic immediate/late phase reaction, allergen presentation by IgE-bearing Langerhans cells, allergen-induced activation of IgE-bearing macrophages, and IgE autoreactivity to human proteins.”5 Historically, most therapies have focused on mitigating the allergic symptoms caused by degranulated effector cells, such as antihistamines. However, a new class of biologically engineered medications (eg, anti-IgE [omalizumab]) aim to prevent the initiation of the allergic response.6 Variable success has been reported using omalizumab in the treatment of AD, though the majority of studies have shown improvement, especially when used in combination with conventional therapies.4,5,7-22 Omalizumab dosage is determined by body weight and pretreatment serum total IgE levels and is administered via subcutaneous injections every 2 to 4 weeks.6,7,23-26 However, the dosing tables are based on asthma therapy, in which serum IgE levels may be much lower than chronic AD,7,24 and the appropriate dosage in AD patients with markedly elevated IgE is unclear. We report an interesting case of a 57-year-old man with erythroderma from long-standing severe chronic AD that was unresponsive to conventional therapy as well as an associated serum IgE level of 17,183 IU/mL who dramatically improved when omalizumab was added to his treatment regimen.
A 57-year-old man presented with essentially 100% body surface area involvement of AD with erythroderma and pruritus. Severe AD developed at infancy and cleared at 5 years of age; childhood onset of asthma was responsive to theophylline and oral inhalers. He developed recurrent AD and asthma at 38 years of age, which was progressive and developed into severe recalcitrant erythroderma by 50 years of age. His AD was unresponsive to multiple therapies, including topical steroids, antibiotics, tacrolimus, bleach baths, antihistamines, methotrexate (15 mg weekly for 1 year, then 12.5 mg weekly for 6 months), UVB phototherapy, and psoralen plus UVA photochemotherapy. He had minimal improvement with cyclosporine (200 mg daily for 4 weeks) and mycophenolate mofetil (3 g daily), and required systemic steroids for relief. The skin was violaceous and lichenified (Figure, A). Laboratory studies were normal, except for a serum IgE level of 17,183 IU/mL (reference range, <150 IU/mL) and peripheral blood eosinophilia up to 29.8% (reference range, 1%–5%) of the differential. Skin biopsies showed AD progressing to lichen simplex chronicus. Omalizumab was added to the therapeutic regimen at a dose of 375 mg every 2 weeks, with noticeable improvement after 3 months. The patient had approximately 80% to 90% clearing with resolution of erythroderma and pruritus, and only limited residual lichenification (Figure, B). The mycophenolate was tapered slowly, and the patient experienced a mild flare at 1 g daily. He is presently on 1 g of mycophenolate daily and omalizumab (375 mg every 2 weeks) and remains remarkably improved. His IgE level decreased to 11,983 IU/mL.

Omalizumab is a monoclonal IgG1 antibody that specifically binds to the FcεRI domain of serum IgE. It blocks binding to high-affinity receptors on effector cells, primarily mast cells, basophils, macrophages, and dendritic cells; it also decreases free IgE serum levels and downregulates the IgE receptor.4,6-10,23-25,27,28 Currently, omalizumab is US Food and Drug Administration approved for moderate to severe persistent asthma in patients 6 years or older with a positive aeroallergen skin test and IgE levels up to 700 IU/mL.6,7,23-25,27,28
However, scattered case reports and small case series have described variable success in the treatment of severe AD that is unresponsive to conventional therapy in patients with markedly elevated serum IgE levels.4,5,7-22 The majority of patients (approximately 80% of published cases yielded by a PubMed search of articles indexed for MEDLINE using the search terms omalizumab and atopic dermatitis) showed improvement when measured by clinical severity scores and quality of life improvement, especially when used in conjunction with conventional therapy. Possible reasons for reported treatment failure include insufficient dosage, lack of established treatment guidelines for markedly elevated serum IgE levels, severity of disease, or variable response with failure to lower IgE level below a required threshold.7,9,23,24,27
Krathen and Hsu9 reported treatment failure with omalizumab for AD in 3 patients with serum IgE levels ranging from 5440 and 24,400 IU/mL, and one review indicated omalizumab may work best in patients with only moderately elevated serum IgE levels.21 However, Toledo et al18 reported efficacy of low-dose omalizumab for pretreatment IgE levels up to 30,000 IU/mL in 6 of 11 reported cases. The pretreatment serum IgE level is not predictive of response, and lowering the serum IgE level without normalization can be efficacious,12,23 as in the current case. Serum IgE levels are not used for monitoring therapeutic response or calculating future dosing, given potential increases in serum IgE levels during and after therapy (for up to 12 months) secondary to the formation of anti-IgE:IgE complexes.6,28 Omalizumab appears most effective when used in combination with conventional therapies. Hopefully ongoing studies will further elucidate the role of omalizumab in recalcitrant AD with elevated serum IgE levels.
- Schultz-Larsen F, Diepgen T, Svennson A. The occurrence of atopic dermatitis in north Europe: an international questionnaire study. J Am Acad Dermatol. 1996;34:760-764.
- Laughter D, Istvan JA, Tofte SJ, et al. The presence of atopic dermatitis in Oregon schoolchildren. J Am Acad Dermatol. 2000;43:649-655.
- Jones HE, Inouye JC, McGerity JL, et al. Atopic disease and serum immunoglobulin-E. Br J Dermatol. 1975;92:17-25.
- Abramovits W. A clinician’s paradigm in the treatment of atopic dermatitis. J Am Acad Dermatol. 2005;53(1, suppl 1):570-577.
- Leung D, Soter N. Cellular and immunologic mechanisms in atopic dermatitis. J Am Acad Dermatol. 2001;44(suppl):S1-S12.
- US Food and Drug Administration. Briefing document on safety. Omalizumab (Xolair) (recombinant humanized monoclonal antibody to IgE) for treatment of allergic asthma. http://www.fda.gov/ohrms/dockets/ac/03/briefing/3952B1_02_FDA-Xolair-Safety.pdf. Published April 18, 2003. Accessed June 23, 2014.
- Lane JE, Cheyney JM, Lane TN, et al. Treatment of recalcitrant atopic dermatitis with omalizumab. J Am Acad Dermatol. 2006;54:68-72.
- Caruso C, Gaeta F, Valluzzi RL, et al. Omalizumab efficacy in a girl with atopic eczema. Allergy. 2010;65:278-279.
- Krathen RA, Hsu S. Failure of omalizumab for the treatment of severe atopic dermatitis. J Am Dermatol. 2005;53:338-340.
- Fernández-Antón Martínez MC, Leis-Dosil V, Alfageme-Roldán F, et al. Omalizumab for the treatment of Atopic Dermatitis. Actas Dermosifiliogr. 2012;103:624-628.
- Pelaia G, Gallelli L, Romeo P, et al. Omalizumab decreases exacerbation frequency, oral intake of corticosteroids and peripheral blood eosinophils in atopic patients with uncontrolled asthma. Int J Clin Pharmacol Ther. 2011;49:713-721.
- Belloni B, Ziai M, Lim A, et al. Low-dose anti-IgE therapy in patients with atopic eczema with high serum IgE levels. J Allergy Clin Immunol. 2007;120:1223-1225.
- Park SY, Choi MR, Na JI, et al. Recalcitrant atopic dermatitis treated with omalizumab. Ann Dermatol. 2010;22:349-352.
- Velling P, Skowasch D, Pabst S. Improvement of quality of life in patients with concomitant allergic asthma and atopic dermatitis: one year follow-up of omalizumab therapy. Eur J Med Res. 2011;15:407-410.
- Amrol D. Anti-immunoglobulin E in the treatment of refractory atopic dermatitis. South Med J. 2010;103:554-558.
- Heil PM, Maurer D, Klein B, et al. Omalizumab therapy in atopic dermatitis: depletion of IgE does not improve the clinical course-a randomized, placebo-controlled and double blind study. J Dtsch Dermatol Ges. 2010;8:990-998.
- Ramírez del Pozo ME, Contreras Contreras E, López Tiro J, et al. Omalizumab (anti-IgE antibody) in the treatment of severe atopic dermatitis. J Investig Allergol Clin Immunol. 2011;21:416-417.
- Toledo F, Silvestre JF, Muñoz C. Combined therapy with low-dose omalizumab and intravenous immunoglobulin for severe atopic dermatitis: report of four cases. J Eur Acad Dermatol Venereol. 2012;26:1325-1327.
- Sheinkopf LE, Rafi AW, Katz RM. Efficacy of omalizumab in the treatment of atopic dermatitis: a pilot study. Allergy Asthma Proc. 2008;29:530-537.
- Incorvia C, Pravettoni C, Mauro M, et al. Effectiveness of omalizumab in a patient with severe asthma and atopic dermatitis. Monaldi Arch Chest Dis. 2008:69:78-80.
- Schmitt J, Schäkel K. Omalizumab as a therapeutic option in atopic eczema. Current evidence and potential benefit [in German]. Hautarzt. 2007;58:130-132.
- Thaiwat S, Sangasapaviliya A. Omalizumab treatment in severe atopic dermatitis. Asian Pac J Allergy Immunol. 2011;29:357-360.
- Kopp MV. Omalizumab: anti-IgE therapy in allergy. Curr Allergy Asthma Rep. 2011;11:101-106.
- Vichyanond P. Omalizumab in allergic diseases, a recent review. Asian Pc J Allergy Immunol. 2011;29:209-219.
- Scheinfeld N. Omalizumab. A recombinant humanized monoclonal IgE-blocking antibody. Dermatol Online J. 2005;11:2.
- Lowe PJ, Georgiou P, Canvin J. Revision of omalizumab dosing table for dosing every 4 instead of 2 weeks for specific ranges of bodyweight and baseline IgE [published online ahead of print December 8, 2014]. Regul Toxicol Pharmacol. 2015;71:68-77.
- Vigo PG, Girgis KR, Pfuetze BL, et al. Efficacy of anti-IgE therapy in patients with atopic dermatitis. J Am Acad Dermatol. 2006;55:168-170.
- Hanifin J, Chan S. Biochemical and immunologic mechanisms in atopic dermatitis: new targets for emerging therapies. J Am Acad Dermatol. 1999;41:72-77.
- Schultz-Larsen F, Diepgen T, Svennson A. The occurrence of atopic dermatitis in north Europe: an international questionnaire study. J Am Acad Dermatol. 1996;34:760-764.
- Laughter D, Istvan JA, Tofte SJ, et al. The presence of atopic dermatitis in Oregon schoolchildren. J Am Acad Dermatol. 2000;43:649-655.
- Jones HE, Inouye JC, McGerity JL, et al. Atopic disease and serum immunoglobulin-E. Br J Dermatol. 1975;92:17-25.
- Abramovits W. A clinician’s paradigm in the treatment of atopic dermatitis. J Am Acad Dermatol. 2005;53(1, suppl 1):570-577.
- Leung D, Soter N. Cellular and immunologic mechanisms in atopic dermatitis. J Am Acad Dermatol. 2001;44(suppl):S1-S12.
- US Food and Drug Administration. Briefing document on safety. Omalizumab (Xolair) (recombinant humanized monoclonal antibody to IgE) for treatment of allergic asthma. http://www.fda.gov/ohrms/dockets/ac/03/briefing/3952B1_02_FDA-Xolair-Safety.pdf. Published April 18, 2003. Accessed June 23, 2014.
- Lane JE, Cheyney JM, Lane TN, et al. Treatment of recalcitrant atopic dermatitis with omalizumab. J Am Acad Dermatol. 2006;54:68-72.
- Caruso C, Gaeta F, Valluzzi RL, et al. Omalizumab efficacy in a girl with atopic eczema. Allergy. 2010;65:278-279.
- Krathen RA, Hsu S. Failure of omalizumab for the treatment of severe atopic dermatitis. J Am Dermatol. 2005;53:338-340.
- Fernández-Antón Martínez MC, Leis-Dosil V, Alfageme-Roldán F, et al. Omalizumab for the treatment of Atopic Dermatitis. Actas Dermosifiliogr. 2012;103:624-628.
- Pelaia G, Gallelli L, Romeo P, et al. Omalizumab decreases exacerbation frequency, oral intake of corticosteroids and peripheral blood eosinophils in atopic patients with uncontrolled asthma. Int J Clin Pharmacol Ther. 2011;49:713-721.
- Belloni B, Ziai M, Lim A, et al. Low-dose anti-IgE therapy in patients with atopic eczema with high serum IgE levels. J Allergy Clin Immunol. 2007;120:1223-1225.
- Park SY, Choi MR, Na JI, et al. Recalcitrant atopic dermatitis treated with omalizumab. Ann Dermatol. 2010;22:349-352.
- Velling P, Skowasch D, Pabst S. Improvement of quality of life in patients with concomitant allergic asthma and atopic dermatitis: one year follow-up of omalizumab therapy. Eur J Med Res. 2011;15:407-410.
- Amrol D. Anti-immunoglobulin E in the treatment of refractory atopic dermatitis. South Med J. 2010;103:554-558.
- Heil PM, Maurer D, Klein B, et al. Omalizumab therapy in atopic dermatitis: depletion of IgE does not improve the clinical course-a randomized, placebo-controlled and double blind study. J Dtsch Dermatol Ges. 2010;8:990-998.
- Ramírez del Pozo ME, Contreras Contreras E, López Tiro J, et al. Omalizumab (anti-IgE antibody) in the treatment of severe atopic dermatitis. J Investig Allergol Clin Immunol. 2011;21:416-417.
- Toledo F, Silvestre JF, Muñoz C. Combined therapy with low-dose omalizumab and intravenous immunoglobulin for severe atopic dermatitis: report of four cases. J Eur Acad Dermatol Venereol. 2012;26:1325-1327.
- Sheinkopf LE, Rafi AW, Katz RM. Efficacy of omalizumab in the treatment of atopic dermatitis: a pilot study. Allergy Asthma Proc. 2008;29:530-537.
- Incorvia C, Pravettoni C, Mauro M, et al. Effectiveness of omalizumab in a patient with severe asthma and atopic dermatitis. Monaldi Arch Chest Dis. 2008:69:78-80.
- Schmitt J, Schäkel K. Omalizumab as a therapeutic option in atopic eczema. Current evidence and potential benefit [in German]. Hautarzt. 2007;58:130-132.
- Thaiwat S, Sangasapaviliya A. Omalizumab treatment in severe atopic dermatitis. Asian Pac J Allergy Immunol. 2011;29:357-360.
- Kopp MV. Omalizumab: anti-IgE therapy in allergy. Curr Allergy Asthma Rep. 2011;11:101-106.
- Vichyanond P. Omalizumab in allergic diseases, a recent review. Asian Pc J Allergy Immunol. 2011;29:209-219.
- Scheinfeld N. Omalizumab. A recombinant humanized monoclonal IgE-blocking antibody. Dermatol Online J. 2005;11:2.
- Lowe PJ, Georgiou P, Canvin J. Revision of omalizumab dosing table for dosing every 4 instead of 2 weeks for specific ranges of bodyweight and baseline IgE [published online ahead of print December 8, 2014]. Regul Toxicol Pharmacol. 2015;71:68-77.
- Vigo PG, Girgis KR, Pfuetze BL, et al. Efficacy of anti-IgE therapy in patients with atopic dermatitis. J Am Acad Dermatol. 2006;55:168-170.
- Hanifin J, Chan S. Biochemical and immunologic mechanisms in atopic dermatitis: new targets for emerging therapies. J Am Acad Dermatol. 1999;41:72-77.
Practice Points
- Omalizumab can be effective in treating patients with severe recalcitrant atopic dermatitis with markedly elevated serum IgE.
- Omalizumab appears most effective when used in combination with conventional therapies.
Nitrous oxide linked to less pain in tattoo removal
SAN DIEGO – The results of a small, single-site study suggest that nitrous oxide (NO) can play a significant role in reducing pain during laser tattoo removal.
“Nitrous oxide is a safe and effective option for patients, particularly those who have large tattoos that can’t be adequately numbed with injections or topical numbing,” the study’s lead author, Jared Mallalieu, DO, said in an interview. “NO has allowed us to treat larger tattoos – full sleeve or large back tattoos – in a single setting, which has made treatment more convenient for patients.”
Patients fared better on pain measures when they received NO, compared with topical and injectable anesthetics, according to Dr. Mallalieu, a cosmetic surgeon at the Laser Center of Maryland, Severna Park. The results were so dramatic that EMLA cream is now rarely used for patients in his clinic, although injectable lidocaine is used on smaller tattoos (smaller than 5 inches by 5 inches), he said.
The use of NO comes with challenges, however, in terms of the extra time and patient monitoring required, he said.
Dr. Mallalieu and his associates reported the results in an e-poster at the annual meeting of the American Society for Laser Medicine and Surgery.
Laser tattoo removal can be an agonizing process. “Patients describe it as being significantly more painful than getting a tattoo,” Dr. Mallalieu said. “The intense pain only lasts during the treatment,” he said, “though many patients will note some discomfort for a few hours after a treatment session.”
Most clinics use a topical cream, such as lidocaine/prilocaine (EMLA) or topical benzocaine/lidocaine/tetracaine (BLT), as an anesthetic for these procedures. “Our center has also used 1% lidocaine with epinephrine in small doses of up to 7 mg/kg,” he said. “The injections are much better than the cream.”
Sometimes the clinic uses a device that blows cold air on the skin, which “helps a little,” he added.
For the study, conducted in 2014, 23 laser tattoo removal patients were surveyed about their pain levels using a 1-10 scale, after undergoing a total of 41 single-location procedures.
The average pain rating during the procedure was 9.1 for those treated only with lidocaine/prilocaine, 5.4 for injections of lidocaine with epinephrine alone, and 6.8 for both lidocaine/prilocaine and lidocaine with epinephrine injections.
The average pain rating for NO alone was 2.6, and was 3.6 for those who received both the injection treatment and lidocaine/prilocaine. Three of 12 NO patients reported anxiety.
Another benefit is that patients can drive after receiving NO, unlike other anesthetics, which leave patients sedated, he said. “Levels of NO are titrated to keep the patient sedated, but breathing on their own,” and patients can be easily woken up within moments of stopping the NO.
However, the use of NO requires more time to set up and more monitoring, he added. The average treatment time for procedures with NO was 27 minutes compared with 4 minutes for the other procedure, and “the patient is put on a monitor that measures pulse rate and oxygenation levels,” which not only takes more time, but requires additional staff to watch the patient. “Also, it takes about 3-5 minutes to slowly the titrate the NO to a perfect level.”
The study points out that physicians at the clinic are the only ones who perform the procedures that use NO, but at many clinics, nonphysicians perform tattoo removals.
As for cost, “NO and oxygen tanks are rather inexpensive to purchase and maintain, and there are various small units which serve to titrate the gas,” Dr. Mallalieu said. “We do charge our patients a small fee because of the added personnel and time cost associated with the procedure. As tattoo removal is considered a cosmetic procedure, insurance doesn’t come into play.”
Training to administer NO brings up the issue of what is allowed in the state, he said. Physicians can give sedation to patients, “but some states may limit the degree to which a patient can be sedated in an office. If the physician has a certified operating room, this is not a problem,” he added. “Because dentists commonly use NO, we followed the American Dental Association guidelines ... As we employ an anesthesiologist, we were quite familiar with it. That said, the administration of NO is not complex and [is] easily mastered.”
Dr. Mallalieu reported no relevant disclosures.
SAN DIEGO – The results of a small, single-site study suggest that nitrous oxide (NO) can play a significant role in reducing pain during laser tattoo removal.
“Nitrous oxide is a safe and effective option for patients, particularly those who have large tattoos that can’t be adequately numbed with injections or topical numbing,” the study’s lead author, Jared Mallalieu, DO, said in an interview. “NO has allowed us to treat larger tattoos – full sleeve or large back tattoos – in a single setting, which has made treatment more convenient for patients.”
Patients fared better on pain measures when they received NO, compared with topical and injectable anesthetics, according to Dr. Mallalieu, a cosmetic surgeon at the Laser Center of Maryland, Severna Park. The results were so dramatic that EMLA cream is now rarely used for patients in his clinic, although injectable lidocaine is used on smaller tattoos (smaller than 5 inches by 5 inches), he said.
The use of NO comes with challenges, however, in terms of the extra time and patient monitoring required, he said.
Dr. Mallalieu and his associates reported the results in an e-poster at the annual meeting of the American Society for Laser Medicine and Surgery.
Laser tattoo removal can be an agonizing process. “Patients describe it as being significantly more painful than getting a tattoo,” Dr. Mallalieu said. “The intense pain only lasts during the treatment,” he said, “though many patients will note some discomfort for a few hours after a treatment session.”
Most clinics use a topical cream, such as lidocaine/prilocaine (EMLA) or topical benzocaine/lidocaine/tetracaine (BLT), as an anesthetic for these procedures. “Our center has also used 1% lidocaine with epinephrine in small doses of up to 7 mg/kg,” he said. “The injections are much better than the cream.”
Sometimes the clinic uses a device that blows cold air on the skin, which “helps a little,” he added.
For the study, conducted in 2014, 23 laser tattoo removal patients were surveyed about their pain levels using a 1-10 scale, after undergoing a total of 41 single-location procedures.
The average pain rating during the procedure was 9.1 for those treated only with lidocaine/prilocaine, 5.4 for injections of lidocaine with epinephrine alone, and 6.8 for both lidocaine/prilocaine and lidocaine with epinephrine injections.
The average pain rating for NO alone was 2.6, and was 3.6 for those who received both the injection treatment and lidocaine/prilocaine. Three of 12 NO patients reported anxiety.
Another benefit is that patients can drive after receiving NO, unlike other anesthetics, which leave patients sedated, he said. “Levels of NO are titrated to keep the patient sedated, but breathing on their own,” and patients can be easily woken up within moments of stopping the NO.
However, the use of NO requires more time to set up and more monitoring, he added. The average treatment time for procedures with NO was 27 minutes compared with 4 minutes for the other procedure, and “the patient is put on a monitor that measures pulse rate and oxygenation levels,” which not only takes more time, but requires additional staff to watch the patient. “Also, it takes about 3-5 minutes to slowly the titrate the NO to a perfect level.”
The study points out that physicians at the clinic are the only ones who perform the procedures that use NO, but at many clinics, nonphysicians perform tattoo removals.
As for cost, “NO and oxygen tanks are rather inexpensive to purchase and maintain, and there are various small units which serve to titrate the gas,” Dr. Mallalieu said. “We do charge our patients a small fee because of the added personnel and time cost associated with the procedure. As tattoo removal is considered a cosmetic procedure, insurance doesn’t come into play.”
Training to administer NO brings up the issue of what is allowed in the state, he said. Physicians can give sedation to patients, “but some states may limit the degree to which a patient can be sedated in an office. If the physician has a certified operating room, this is not a problem,” he added. “Because dentists commonly use NO, we followed the American Dental Association guidelines ... As we employ an anesthesiologist, we were quite familiar with it. That said, the administration of NO is not complex and [is] easily mastered.”
Dr. Mallalieu reported no relevant disclosures.
SAN DIEGO – The results of a small, single-site study suggest that nitrous oxide (NO) can play a significant role in reducing pain during laser tattoo removal.
“Nitrous oxide is a safe and effective option for patients, particularly those who have large tattoos that can’t be adequately numbed with injections or topical numbing,” the study’s lead author, Jared Mallalieu, DO, said in an interview. “NO has allowed us to treat larger tattoos – full sleeve or large back tattoos – in a single setting, which has made treatment more convenient for patients.”
Patients fared better on pain measures when they received NO, compared with topical and injectable anesthetics, according to Dr. Mallalieu, a cosmetic surgeon at the Laser Center of Maryland, Severna Park. The results were so dramatic that EMLA cream is now rarely used for patients in his clinic, although injectable lidocaine is used on smaller tattoos (smaller than 5 inches by 5 inches), he said.
The use of NO comes with challenges, however, in terms of the extra time and patient monitoring required, he said.
Dr. Mallalieu and his associates reported the results in an e-poster at the annual meeting of the American Society for Laser Medicine and Surgery.
Laser tattoo removal can be an agonizing process. “Patients describe it as being significantly more painful than getting a tattoo,” Dr. Mallalieu said. “The intense pain only lasts during the treatment,” he said, “though many patients will note some discomfort for a few hours after a treatment session.”
Most clinics use a topical cream, such as lidocaine/prilocaine (EMLA) or topical benzocaine/lidocaine/tetracaine (BLT), as an anesthetic for these procedures. “Our center has also used 1% lidocaine with epinephrine in small doses of up to 7 mg/kg,” he said. “The injections are much better than the cream.”
Sometimes the clinic uses a device that blows cold air on the skin, which “helps a little,” he added.
For the study, conducted in 2014, 23 laser tattoo removal patients were surveyed about their pain levels using a 1-10 scale, after undergoing a total of 41 single-location procedures.
The average pain rating during the procedure was 9.1 for those treated only with lidocaine/prilocaine, 5.4 for injections of lidocaine with epinephrine alone, and 6.8 for both lidocaine/prilocaine and lidocaine with epinephrine injections.
The average pain rating for NO alone was 2.6, and was 3.6 for those who received both the injection treatment and lidocaine/prilocaine. Three of 12 NO patients reported anxiety.
Another benefit is that patients can drive after receiving NO, unlike other anesthetics, which leave patients sedated, he said. “Levels of NO are titrated to keep the patient sedated, but breathing on their own,” and patients can be easily woken up within moments of stopping the NO.
However, the use of NO requires more time to set up and more monitoring, he added. The average treatment time for procedures with NO was 27 minutes compared with 4 minutes for the other procedure, and “the patient is put on a monitor that measures pulse rate and oxygenation levels,” which not only takes more time, but requires additional staff to watch the patient. “Also, it takes about 3-5 minutes to slowly the titrate the NO to a perfect level.”
The study points out that physicians at the clinic are the only ones who perform the procedures that use NO, but at many clinics, nonphysicians perform tattoo removals.
As for cost, “NO and oxygen tanks are rather inexpensive to purchase and maintain, and there are various small units which serve to titrate the gas,” Dr. Mallalieu said. “We do charge our patients a small fee because of the added personnel and time cost associated with the procedure. As tattoo removal is considered a cosmetic procedure, insurance doesn’t come into play.”
Training to administer NO brings up the issue of what is allowed in the state, he said. Physicians can give sedation to patients, “but some states may limit the degree to which a patient can be sedated in an office. If the physician has a certified operating room, this is not a problem,” he added. “Because dentists commonly use NO, we followed the American Dental Association guidelines ... As we employ an anesthesiologist, we were quite familiar with it. That said, the administration of NO is not complex and [is] easily mastered.”
Dr. Mallalieu reported no relevant disclosures.
Thousands expected to get CAR T-cells by 2018
NEW YORK – Should the first chimeric antigen receptor (CAR) T-cell treatment receive Food and Drug Administration approval for refractory, aggressive non-Hodgkin lymphoma, possibly before the end of 2017, several thousand U.S. patients will be potential candidates for the treatment, Jeremy S. Abramson, MD, predicted at a conference held by Imedex.
Dr. Abramson has led studies using a CAR T cell that differs from the one furthest along in development. He based his predicted timetable for an approved biologics license of the process, with which he can engineer patient-specific T cells that are under development by Kite Pharma, on the “remarkable” level of complete responses the intervention produced in a pivotal phase II study.
“Seeing a complete response rate of close to 40% that is sustained for more than 3 months and a complete response rate of close to a third at 6 months is light years beyond what is now available for patients” with these chemotherapy refractory B-cell lymphomas, said Dr. Abramson, clinical director of the Center for Lymphoma at Massachusetts General Hospital in Boston. “This is the first treatment to show a significant impact on large B-cell lymphoma, and that makes me optimistic” that the FDA will grant license approval later in 2017, he said in an interview.
Dr. Abramson acknowledged that some patients developed grade 3 or 4 cytokine-release syndrome and neurologic events, but the events were reversible and manageable if treated with the immunosuppressant tocilizumab (Actemra) or a corticosteroid.
At the end of March, Kite reported the completion of its FDA application, and, on April 2, the ZUMA-1 investigators presented an updated report on their results, with a 36% complete response rate across all enrolled patients at 6 month follow-up and a 39% complete response rate in all patients out to a median follow-up of 8.7 months.
Annually, in U.S. practice, perhaps 3,000 new patients with diffuse large B-cell lymphoma would meet the enrollment criteria for ZUMA-1, Dr. Abramson estimated. Once axicabtagene ciloleucel becomes commercially available in the United States, several thousand U.S. patients might initially seek the treatment.
Dr. Abramson has been a consultant to Kite Pharma and to AbbVie, Genentech, Gilead, and Seattle Genetics.
[email protected]
On Twitter @mitchelzoler
NEW YORK – Should the first chimeric antigen receptor (CAR) T-cell treatment receive Food and Drug Administration approval for refractory, aggressive non-Hodgkin lymphoma, possibly before the end of 2017, several thousand U.S. patients will be potential candidates for the treatment, Jeremy S. Abramson, MD, predicted at a conference held by Imedex.
Dr. Abramson has led studies using a CAR T cell that differs from the one furthest along in development. He based his predicted timetable for an approved biologics license of the process, with which he can engineer patient-specific T cells that are under development by Kite Pharma, on the “remarkable” level of complete responses the intervention produced in a pivotal phase II study.
“Seeing a complete response rate of close to 40% that is sustained for more than 3 months and a complete response rate of close to a third at 6 months is light years beyond what is now available for patients” with these chemotherapy refractory B-cell lymphomas, said Dr. Abramson, clinical director of the Center for Lymphoma at Massachusetts General Hospital in Boston. “This is the first treatment to show a significant impact on large B-cell lymphoma, and that makes me optimistic” that the FDA will grant license approval later in 2017, he said in an interview.
Dr. Abramson acknowledged that some patients developed grade 3 or 4 cytokine-release syndrome and neurologic events, but the events were reversible and manageable if treated with the immunosuppressant tocilizumab (Actemra) or a corticosteroid.
At the end of March, Kite reported the completion of its FDA application, and, on April 2, the ZUMA-1 investigators presented an updated report on their results, with a 36% complete response rate across all enrolled patients at 6 month follow-up and a 39% complete response rate in all patients out to a median follow-up of 8.7 months.
Annually, in U.S. practice, perhaps 3,000 new patients with diffuse large B-cell lymphoma would meet the enrollment criteria for ZUMA-1, Dr. Abramson estimated. Once axicabtagene ciloleucel becomes commercially available in the United States, several thousand U.S. patients might initially seek the treatment.
Dr. Abramson has been a consultant to Kite Pharma and to AbbVie, Genentech, Gilead, and Seattle Genetics.
[email protected]
On Twitter @mitchelzoler
NEW YORK – Should the first chimeric antigen receptor (CAR) T-cell treatment receive Food and Drug Administration approval for refractory, aggressive non-Hodgkin lymphoma, possibly before the end of 2017, several thousand U.S. patients will be potential candidates for the treatment, Jeremy S. Abramson, MD, predicted at a conference held by Imedex.
Dr. Abramson has led studies using a CAR T cell that differs from the one furthest along in development. He based his predicted timetable for an approved biologics license of the process, with which he can engineer patient-specific T cells that are under development by Kite Pharma, on the “remarkable” level of complete responses the intervention produced in a pivotal phase II study.
“Seeing a complete response rate of close to 40% that is sustained for more than 3 months and a complete response rate of close to a third at 6 months is light years beyond what is now available for patients” with these chemotherapy refractory B-cell lymphomas, said Dr. Abramson, clinical director of the Center for Lymphoma at Massachusetts General Hospital in Boston. “This is the first treatment to show a significant impact on large B-cell lymphoma, and that makes me optimistic” that the FDA will grant license approval later in 2017, he said in an interview.
Dr. Abramson acknowledged that some patients developed grade 3 or 4 cytokine-release syndrome and neurologic events, but the events were reversible and manageable if treated with the immunosuppressant tocilizumab (Actemra) or a corticosteroid.
At the end of March, Kite reported the completion of its FDA application, and, on April 2, the ZUMA-1 investigators presented an updated report on their results, with a 36% complete response rate across all enrolled patients at 6 month follow-up and a 39% complete response rate in all patients out to a median follow-up of 8.7 months.
Annually, in U.S. practice, perhaps 3,000 new patients with diffuse large B-cell lymphoma would meet the enrollment criteria for ZUMA-1, Dr. Abramson estimated. Once axicabtagene ciloleucel becomes commercially available in the United States, several thousand U.S. patients might initially seek the treatment.
Dr. Abramson has been a consultant to Kite Pharma and to AbbVie, Genentech, Gilead, and Seattle Genetics.
[email protected]
On Twitter @mitchelzoler
EXPERT ANALYSIS FROM A MEETING ON HEMATOLOGIC MALIGNANCIES
Study finds psoriasis link to melanoma and hematologic cancers
Patients with psoriasis may be at a greater risk of melanoma and hematologic cancers, compared with the general population, but treatments do not appear to increase risk, according to Shivani P. Reddy of the University of Illinois at Chicago, and associates.
In a retrospective cohort study, they identified 815,765 patients at Kaiser Permanente Southern California who had at least one medical encounter from January 2004 through December 2013. Of these patients, 8,161 (1%) met the diagnostic and inclusion criteria for psoriasis, and there were 7,167 (0.89%) cases of melanoma and 5,399 (0.66%) cases of lymphoma or leukemia.
Among the patients with psoriasis, there were 62 (0.87%) melanoma cases and 47 (0.87%) cases of lymphoma or leukemia.
Of the 109 patients with psoriasis who went on to develop melanoma or lymphoma, the time to diagnosis of melanoma or hematologic cancers was significantly less for patients with psoriasis than for patients without psoriasis (P = .01). The patients with psoriasis had a 1.53 times higher risk of developing a malignancy compared with patients without psoriasis (P less than .01) in the multivariable Cox proportional hazards model.
“There were no differences between patients with melanoma and hematologic cancer by treatment type,” which were phototherapy, tumor necrosis factor inhibitor therapy, and topical medications, they wrote.
“Our study demonstrates that the risk of hematologic cancer and melanoma is increased in patients with psoriasis over time, although this risk is not impacted by psoriasis therapies,” the researchers concluded. “Defining the risk of malignancy in these patients is important for proper workup and management.”
Read the study in the Journal of the American Academy of Dermatology (doi: 10.1016/j.jaad.2016.09.047).
Patients with psoriasis may be at a greater risk of melanoma and hematologic cancers, compared with the general population, but treatments do not appear to increase risk, according to Shivani P. Reddy of the University of Illinois at Chicago, and associates.
In a retrospective cohort study, they identified 815,765 patients at Kaiser Permanente Southern California who had at least one medical encounter from January 2004 through December 2013. Of these patients, 8,161 (1%) met the diagnostic and inclusion criteria for psoriasis, and there were 7,167 (0.89%) cases of melanoma and 5,399 (0.66%) cases of lymphoma or leukemia.
Among the patients with psoriasis, there were 62 (0.87%) melanoma cases and 47 (0.87%) cases of lymphoma or leukemia.
Of the 109 patients with psoriasis who went on to develop melanoma or lymphoma, the time to diagnosis of melanoma or hematologic cancers was significantly less for patients with psoriasis than for patients without psoriasis (P = .01). The patients with psoriasis had a 1.53 times higher risk of developing a malignancy compared with patients without psoriasis (P less than .01) in the multivariable Cox proportional hazards model.
“There were no differences between patients with melanoma and hematologic cancer by treatment type,” which were phototherapy, tumor necrosis factor inhibitor therapy, and topical medications, they wrote.
“Our study demonstrates that the risk of hematologic cancer and melanoma is increased in patients with psoriasis over time, although this risk is not impacted by psoriasis therapies,” the researchers concluded. “Defining the risk of malignancy in these patients is important for proper workup and management.”
Read the study in the Journal of the American Academy of Dermatology (doi: 10.1016/j.jaad.2016.09.047).
Patients with psoriasis may be at a greater risk of melanoma and hematologic cancers, compared with the general population, but treatments do not appear to increase risk, according to Shivani P. Reddy of the University of Illinois at Chicago, and associates.
In a retrospective cohort study, they identified 815,765 patients at Kaiser Permanente Southern California who had at least one medical encounter from January 2004 through December 2013. Of these patients, 8,161 (1%) met the diagnostic and inclusion criteria for psoriasis, and there were 7,167 (0.89%) cases of melanoma and 5,399 (0.66%) cases of lymphoma or leukemia.
Among the patients with psoriasis, there were 62 (0.87%) melanoma cases and 47 (0.87%) cases of lymphoma or leukemia.
Of the 109 patients with psoriasis who went on to develop melanoma or lymphoma, the time to diagnosis of melanoma or hematologic cancers was significantly less for patients with psoriasis than for patients without psoriasis (P = .01). The patients with psoriasis had a 1.53 times higher risk of developing a malignancy compared with patients without psoriasis (P less than .01) in the multivariable Cox proportional hazards model.
“There were no differences between patients with melanoma and hematologic cancer by treatment type,” which were phototherapy, tumor necrosis factor inhibitor therapy, and topical medications, they wrote.
“Our study demonstrates that the risk of hematologic cancer and melanoma is increased in patients with psoriasis over time, although this risk is not impacted by psoriasis therapies,” the researchers concluded. “Defining the risk of malignancy in these patients is important for proper workup and management.”
Read the study in the Journal of the American Academy of Dermatology (doi: 10.1016/j.jaad.2016.09.047).
FROM THE JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY